User login
Interventions to Prevent and Correct Antiretroviral Medication Errors in Patients with HIV
From the University of North Carolina Medical Center (Dr. Daniels) and Renovion (Dr. Durham), Chapel Hill, NC.
To Download a PDF of the Full Article:
ABSTRACT
• Objective: To examine common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
• Methods: Review of the literature.
• Results: The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in patients with HIV place these patients at risk for medication errors and adverse drug events. Many studies of hospitalized patients with HIV have reported high rates of medication errors in this population. The consequences of antiretroviral therapy errors can range from minimal harm to life-threatening toxicities and the possibility of resistance and treatment failure. This review discusses the factors contributing to the high rates of error associated with antiretroviral therapy and details strategies to reduce and prevent errors in these patients.
• Conclusion: A comprehensive approach combining multiple interventions can be used to reduce and prevent antiretroviral medication errors in patients with HIV in order to improve the quality of care for this population.
Great progress has been made in the treatment of HIV over the past several decades. With the advancements in treatment options for HIV, considerable reductions in the morbidity and mortality associated with HIV and HIV-related complications have been realized [1,2]. Antiretroviral therapy (ART) has rapidly evolved, offering different mechanisms of action, improved potency, increased tolerability and reduced pill burdens. As a result, HIV infection has transformed from a terminal illness to a manageable chronic disease.
The success of HIV treatment has created a new set of challenges for health care professionals. Patients with successfully treated HIV can expect to live a nearly normal lifespan [3]. With this extended life expectancy, the number of older adults infected with HIV continues to rise, and care for these patients requires a broader and more comprehensive approach. Although HIV-related illnesses such as opportunistic infections have declined, the rate of non–HIV-related comorbidities among patients with HIV has increased [4]. Large cohort studies have shown an association between the risk for HIV-associated non–AIDS-related conditions and CD4 counts [5,6]. HIV-associated non–AIDS-related conditions include cardiovascular disease, kidney disease, liver disease, central nervous system disease, osteoporosis, and non–AIDS-associated malignancies. These conditions occur either more frequently or are more severe in patients with lower CD4 counts or detectable viral loads, but can also arise or persist in virologically suppressed patients with high CD4 counts [4].
The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in this population place these patients at risk for experiencing medication errors and adverse drug events. Patients with HIV often receive care by many providers in many different settings. Clinicians caring for patients with HIV must be familiar not only with the treatment of HIV but also with the management and integration of their patients’ primary care needs. In addition, the rates of hospitalization for HIV-infected patients have declined substantially since the mid-1990s [7]. Of the patients with HIV requiring hospitalization, the proportion of hospitalizations due to opportunistic infections has decreased and the proportion of hospitalizations due to other conditions has increased [7]. For many of these patients, the treatment of HIV has retreated to the background as a stable condition, while the management of other acute illness requires more attention.
An estimated 1.5 million adverse drug events occur each year in the United States due to medication errors [8]. Medication errors are common and can occur at any point during the medication use process, including procurement, prescribing, transcribing, preparing or compounding, dispensing, administration, and monitoring. Any time a patient moves from one setting of health care to another, the risk for medication errors is increased. Several reports have highlighted the increased risk for medication errors and adverse effects that can occur during these transitions of care. In fact, up to 70% of patients have an unintentional medication discrepancy at hospital discharge [9]. Errors during hospital admission are common as well, affecting up to two-thirds of patients admitted to hospitals [10,11].
As HIV care becomes more complex, concerns have been raised regarding increases in the number of medication errors in these patients, especially during transitions of care. Most studies of hospitalized patients with HIV have reported error rates of 5% to 30% [12–15]. One study demonstrated that the risk for a medication error at admission for patients with HIV was 3.8 errors per patient, whereas for patients without HIV the rate was 2.8 errors per patient [16]. Because of the potential for the emergence of resistance mutations, adherence to ART is essential for successful treatment and sustained viral suppression. Thus, medication errors of omission could have particularly detrimental effects for the long-term treatment of patients with HIV. Furthermore, as this population ages, polypharmacy becomes common, placing these patients at risk for errors related to dosing and drug interactions [17]. Because medication errors can lead to patient harm and death as well as increased health care costs, elucidating the reasons for errors associated with HIV management and exploring strategies aimed at the reduction and prevention of errors is essential.
The goal of this review is to examine the common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
Incidence of ART Errors
Several studies have indicated that the incidence of ART errors in hospitalized patients is rising. The rate of ART errors detected at admission among hospitalized patients increased from 2% in 1996 to 12% in 1998 according to one study [13]. Studies conducted from 2004 to 2007 report ART error rates at hospital admission ranging from 17% to 26% [12,15,18]. In more recent studies, high ART error rates ranging from 35% to 55% have been reported [19–23]. Two studies have reported ART error rates occurring at hospital admission to be as high as 70% [24,25].
Various types of ART medication errors can occur. Commonly reported errors include those related to drug interactions, incorrect dosing, incorrect scheduling, and incomplete regimens. Errors occurring at the time of hospital admission appear to be more common than errors occurring at other time points [20,24,26]. A comprehensive systematic review of studies regarding medication errors in hospitalized patients with HIV found that errors at the point of prescribing encompass the majority of errors [27]. One study identified 82 ART errors occurring at admission in 68 hospitalized patients. Of these errors, 37% occurred at the point of prescribing, 27% were attributed to dispensing, and 18% were attributed to inaccuracies in outpatient clinic documentation [24].
Several authors have drawn associations between the rate of errors and the class of antiretroviral prescribed. Protease inhibitors have been the most frequently implicated drug class [13,18,20,27,28]. In an analysis of 145 ART errors in one hospital, 70% of dosing errors involved protease inhibitors and 30% involved nucleoside/nucleotide reverse transcriptase inhibitors (NRTIs). In addition, scheduling errors occurred most often with protease inhibitors, and errors due to drug interactions were also most likely to involve protease inhibitors [28]. Conversely, another study did not find an association between protease inhibitors and the risk for error compared to other classes of drugs. In fact, this study showed that the NRTI class was associated with an increased risk of prescribing error compared to protease inhibitors and that the use of co-formulated drugs that were available on the hospital formulary protected against error [20]. These findings highlight the various factors contributing to error among different institutions, especially related to hospital formulary selections and availability of specific drugs.
Fewer studies have evaluated ART errors in outpatient settings. One report evaluated the NRTI medication records from an outpatient electronic medical record system from August 2004 to September 2005. A total of 902 NRTI records for 603 patients were analyzed. The overall error rate was 6% (53/902), with renal dosing errors being most common (75% of errors) [29]. Another evaluation of ART errors among privately insured patients with HIV found that the probability of a patient with HIV receiving an inappropriate drug combination in a given year was higher in 2005 (5.9%) compared to 1999 and 2000 (1.9%). Many of the increased errors seen in 2005 compared to 1999–2000 in this study were attributed to errors related to protease inhibitor boosting [30].
Harms and Consequences of ART Errors
Because of the potential for the emergence of drug resistance, adherence to an ART regimen is essential for successful treatment and sustained viral suppression. ART medication errors causing disrupted therapy, omitted drugs, or suboptimal dosing can lead to the development of viral resistance mutations and ultimately treatment failure placing patients at risk for HIV-related complications such as opportunistic infections as well as non–HIV-related complications [31]. Health care providers should recognize the importance of appropriate uninterrupted therapy for this population and should assist in facilitating this effort. On a community level, patients with elevated plasma HIV RNA levels due to untreated disease or treatment failure have a greater risk of transmitting HIV to others [32]. Effective ART on a population basis will have important public health advantages.
In addition to the potential consequences of ART error relating to treatment failure and resistance, ART errors may also lead to drug toxicities and drug intolerance, increasing the risk of nonadherence, and further exacerbating the aforementioned consequences.
ART errors also carry the same consequences as errors involving other non-ART medications, such as loss of patient trust, civil and criminal legal consequences, professional board discipline, and increased health care costs [33]. One study reported a cost avoidance of $24,000 annually for inpatient and $124,000 annually for outpatient through the use of pharmacists’ interventions to prevent errors [34]. Another study found that patients experiencing an ART error related to protease inhibitor boosting incurred claims costing 21.5% more than patients not experiencing a boosting error [30].
Contributing Factors
Health care professional–associated factors can also contribute to ART errors. The increasing complexity and specialization of HIV care and the rapidly evolving nature of medication management in this population have created an environment in which many providers without extensive experience in the treatment of HIV are responsible for managing HIV in settings beyond the HIV clinic. A survey of non-HIV specialized physicians conducted in 2007 revealed a poor knowledge base of common ART regimens among these physicians [37]. Likewise, HIV providers may be uncomfortable serving a primary care role for patients with HIV due to their own lack of experience and knowledge of primary care [38]. This issue is becoming more relevant, as non-AIDS comorbidities are emerging as the main health concerns for patients with HIV [39]. Health care professionals’ knowledge of HIV care also contributes to ART errors at other points in the medication use process beyond prescribing. Pharmacists lacking experience in identifying appropriate ART regimens may not recognize errors, and, therefore, may not be able to intervene and prevent errors from occurring.
Medication factors contributing to the risk for errors include risks related to the pharmacologic properties of certain drugs as well as drug naming and labeling factors. Certain antiretroviral classes are known to interact with many medications due to inhibition or induction of metabolic pathways responsible for drug metabolism, such as the cytochrome P-450 pathways. In addition, many antiretroviral medications require “boosting” with another drug to increase systemic exposure of the antiretroviral. Boosting is required for most protease inhibitors and for the integrase inhibitor elvitegravir. For some of these medications, the boosting agent is provided in a co-formulated product. However, for others, a separate prescription for the boosting medication is required. These factors contribute to the risks for drug interactions as well as drug and dosing errors.
Errors may also occur due to drug naming and labeling factors. Confusion due to look-alike/sound-alike medications is common, especially with handwritten or verbally transcribed orders. Examples of look-alike/sound-alike medications include lamivudine/lamotrigine, Viramune/Viread/Viracept, and ritonavir/Retrovir. The use of abbreviations can also lead to error. Reports have described errors associated with zidovudine, which is often abbreviated AZT, being confused with azathioprine [40,41]. An evaluation of ART errors reported to a national medication error reporting program found that look-alike/sound-alike medication names contributed to 19% (77/400) of the errors reported during the 48-month time period evaluated [15].
Several antiretroviral medications are co-formulated into single tablets to decrease pill burden and increase adherence. The use of co-formulated products has the potential to either increase or decrease the risk of errors. Prescribing one co-formulated product rather than its individual components simplifies the prescribing process, allowing the prescriber to become familiar with one product and one dosing scheme in place of 2 or more drugs with different dosing recommendations. The risk of inadvertent omission of a drug and the risk of improper dosing is reduced with the use of co-formulated products. On the other hand, when patients are transitioned from one health care setting to another (such as admission to a hospital), these products may require conversion to the individual components of the drug due to formulary availability and/or cost concerns. Studies have shown that formulary conversions from co-formulated products to individual components are frequently associated with ART errors and that the use of co-formulated products in the inpatient setting reduces these errors [20,22,24,26].
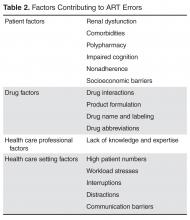
Finally, factors related to the health care setting can influence the risk for errors. High patient numbers, time constraints, and workload stresses can all increase the likelihood that an error will occur [36]. Interruptions and distractions occurring at any point in the medication use process can lead to error.
Transitioning from one health care setting to another also places patients at risk for being harmed by medication errors. Up to 70% of patients may have an unintentional medication discrepancy at hospital discharge, and errors occurring at hospital admission have been reported to affect two-thirds of admitted patients [42]. Many of these errors hold the potential to cause harm to the patient, especially if the errors are carried forward throughout the patient’s admission and after discharge. One study found that 22% of ART errors occurring at hospital admission were attributable to outpatient clinic documentation errors [24]. This highlights the need for improved documentation processes and draws attention to the element of communication at transitional points of care. Lack of adequate resources for medication reconciliation is a widely recognized challenge. This includes resources of personnel as well as electronic medical record systems that can facilitate the reconciliation process. The importance of accurately documenting a patient’s medication history and the ability to easily communicate this information to other health care settings cannot be underestimated. Electronic medical record systems should be developed to facilitate and enhance the processes of reconciliation, documentation, and communication.
Interventions to Address ART Errors
The causes of ART errors are multifactorial and should be addressed using comprehensive approaches tailored to the specific health care setting. Several types of interventions aimed at reducing and preventing ART errors have been evaluated in the literature [12,18,26,27]. In general, these interventions have focused on provider education, use of technology and clinical decision support systems, pharmacist-led medication review and intervention, and hospital formulary changes. Other interventions that may lead to a reduction in ART errors include minimizing polypharmacy, improving medication reconciliation processes during transitions of care, and multidisciplinary follow-up clinic visits after hospital discharge.
Because the sources of ART errors are multifactorial, the optimal strategy to prevent and reduce errors is likely to be a comprehensive approach combining several of the aforementioned interventions. One study showed that a combined approach that included updates to the institution’s computerized physician order entry (CPOE) system, education for the pharmacy and ID departments, and daily review of patients’ medications by pharmacists was successful in reducing the percentage of admissions with an ART error from 50% to 34%. In addition, the time to error resolution decreased from 180 hours to 23 hours, and the error resolution rate increased from 32% to 68% [21]. Another study demonstrated benefits using a comprehensive approach including the dissemination of educational pocket cards for physicians, pharmacists and nurses; CPOE alerts; hospital formulary updates to include co-formulated products; and a daily review of medications by an ID-specialized pharmacist for patients receiving ART. These strategies resulted in a reduced ART error rate from 72% to 15% in 7 months [26]. These studies demonstrate the benefit of multifaceted strategies to reduce ART error rates.
Education
Given the complexity of HIV care and overall lack of antiretroviral medication knowledge among non-ID specialized health care professionals, educational programs aimed at increasing the comfort level and familiarity of ART is important [16,37]. Frequent training to update health care professionals on the newest recommendations for HIV management can help achieve this goal [19,27]. Educational interventions aimed at reducing medication errors have been shown to be transiently effective but may lack sustained effects [43]. Educational programs for health care professionals should be designed to provide frequent brief updates, and are likely to be more successful when combined with other approaches [19,26].
Education directed toward patients, families, and caregivers can also play a pivotal role in error prevention. Patients should be encouraged to use one pharmacy, if possible, to ensure that one complete, accurate, and current profile is maintained. The use of one pharmacy can also assist in the identification of therapeutic duplications and drug interactions. Counseling patients with visual aids, such as charts with pictures of drugs, can also be used as a tool for education. Patients who are familiar with the names and the appearances of their drugs are more likely to recognize errors. In addition, patients should be advised to maintain their own current medication list so that they will be able to provide this information to all of the health care professionals involved in their care [33,44].
Technology and Clinical Decision Support Systems
Overall, the increasing use of technology such as CPOE, decision support systems, and barcoding systems has been shown to decrease the risk of medication error [19,45,46]. Guo et al observed a 35% decrease in ART error rates after the integration of customized order entry sets into an existing CPOE program [19]. Another study reported a 50% decrease in the ART error rate after the introduction of an electronic medical record system [45]. On the other hand, some reports evaluating the role of CPOE systems to reduce medication error rates are conflicting [15,19,23,48]. Differences in system capabilities and programming and differing needs and challenges of institutions may account for the varying results reported in the literature. CPOE systems can serve as valuable tools for assisting in medication prescribing. Confusion due to abbreviations, illegible writing and look-alike/sound-alike drugs should be eliminated or greatly reduced with the use of CPOE. However, the limitations of these systems, which may differ among different systems, should be appreciated. As ART regimens and dosing recommendations change, clinical decision support systems can quickly become out-of-date and require frequent updating. One study identified fields that pre-populated drug names and frequencies within a CPOE system to be the cause of several medication errors [16]. Studies have also identified errors related to disregarded alerts from decision support software [15,16]. “Alert fatigue” is a well-recognized phenomenon that occurs when clinicians are exposed to a large volume of clinical decision support alerts of varying clinical significance. Over time, clinicians begin to become desensitized to the alerts, and they may eventually stop responding to them.
Some limitations of CPOE systems arise from the individual system capabilities. Some systems have the ability to check for appropriate dosing, recommend adjustments in renal dysfunction, and provide alerts for drug interactions, but some systems lack these capabilities. In addition, CPOE systems are often not able to prevent errors of omission, delays in continuation of therapy, and medication scheduling errors [15,45].
Given the limitations of CPOE and clinical decision support technologies, it is unlikely that these interventions alone will be sufficient to fully address the problem of ART errors. These technologies can, however, serve as a powerful tool in the prevention and reduction of ART errors, especially when used in combination with other strategies.
Pharmacist Intervention
Multiple studies have shown that clinical pharmacists are effective at decreasing ART medication errors in the inpatient setting [12,18,23,25,28,45,49,50]. One institution implemented an HIV-specialized pharmacist review strategy that decreased the median time to error correction from 84 hours to 15.5 hours among hospitalized patients [12]. Corrigan et al showed that a review of medications by an HIV-specialized pharmacist 48 hours after hospital admission decreased error rates from 52% to 5% [50]. Another study showed that with the use of an electronic medical record, errors among hospitalized patients with HIV were 9.4 times more likely to be corrected within 24 hours when an HIV-specialized pharmacist was consulted [45].
The majority of studies evaluating the effect of pharmacist interventions have utilized the services of a pharmacist with specialized training in HIV. Few studies have evaluated the impact of interventions by pharmacists without this specialized training. One study retrospectively evaluated and characterized ART errors among hospitalized patients. Medication reconciliation was performed within 24 hours of admission by unit-based pharmacists without specialized training in HIV. Overall, 30.8% of errors were corrected within 24 hours and 14.2% were corrected after 24 hours. However, 54.7% of the errors were not recognized and were never corrected [20]. Just as physicians trained in general medicine lack knowledge of antiretroviral medications, pharmacists without HIV-specialized training may also be less familiar with current ART recommendations [16,37].
Overall, the studies evaluating the impact of pharmacist intervention on reducing ART error rates have shown significant reductions in time to error corrections. The nature of this type of intervention however, lends itself to correction of errors rather than prevention of errors. Indeed, one hospital reported an ART error rate of 29% on the first day of admission compared to 7% on the second day of admission, a decrease that was attributed to retrospective review of medication orders by clinical pharmacists. This study also noted the occurrences of additional errors identified on the second day of admission, highlighting the importance of daily review and follow-up throughout the hospital stay [28].
Hospital Formulary Selections
Several studies have documented an association between hospital formulary options and ART errors [20,22,24,26]. The prescribing of ART medications that are not available on hospital formulary is consistently associated with higher rates of error. Many hospitals minimize the numbers of different medications offered through the maintenance of a formulary. Formularies assist in reducing costs, preserving storage space, and simplifying prescribing. Because some hospitals choose to exclude co-formulated products from the formulary, several ART medications may not be included. In addition, some ART medications may be excluded from formulary due to their infrequent use or higher costs. The extra step of converting a co-formulated product to its individual components increases the risk for errors. In one study, the addition of all co-formulated ART medications to the hospital formulary in combination with several other interventions had a significant effect on reducing the ART error rate [26].
Transitions of Care Interventions
Patients with HIV are at risk for experiencing medication errors and discrepancies any time they transition from one health care setting to another. Hospitalization poses the highest risk as it often disrupts continuity of care and corresponds with a comparatively larger number of medication changes [16,51]. This risk is present on admission, throughout hospitalization, and upon discharge. Perhaps the errors of greatest concern are those that are carried forward after discharge on to the outpatient setting. Medication discrepancies at transitions of care have been associated with increases in adverse events and increased hospital readmission rates [52,53]. One study evaluating adverse events in geriatric patients transitioning from hospital to home found that the most frequently reported adverse events after discharge were related to incorrect drugs or dosages of medication regimens [54]. Tools that can assist in integration and coordination during transitions of care are greatly needed.
One of the most important strategies to prevent and correct medication discrepancies during transitions of care is medication reconciliation. Several studies have demonstrated the efficacy of medication reconciliation in decreasing medication errors [55]. Medication reconciliation is especially important for patients taking many medications. An estimated 14% of patients with HIV older than age 65 take 4 or more medications [56]. This population often requires treatment for other chronic conditions such as hypertension, diabetes, and depression, further increasing the risk for adverse drug events including medication error. Because of the complexities associated with the treatment of HIV and the increased risk for errors, routine medication reconciliation among this population should be a priority.
In addition to medication reconciliation, several studies have evaluated the effects of coordinated pharmacist or multidisciplinary post-discharge follow-up visits for medication therapy management as a strategy to reduce preventable medication-related adverse events [57–59]. Patients receiving clinic-based medication therapy management by a clinical pharmacist after hospital discharge had a lower 60-day hospital readmission rate compared to those who did not have a clinic visit with a pharmacist (18.2% vs. 43.1%) [59]. Another study compared 2 models of post-discharge follow-up, a multidisciplinary team model led by a clinical pharmacist compared to a standard physician-only model. The goal of the multi-disciplinary team model was to complete a thorough medication review, address lifestyle interventions, and address barriers to care. Overall, patients seen by the multidisciplinary team had a 30-day hospital readmission rate of 14.3% compared with a 34.3% readmission rate in the physician-only team [58]. Many different care models have been proposed to improve continuity of care for patients with HIV. The ideal model is not known, and it is likely that several different models would be effective. Optimal models should integrate the patient-physician relationship with multidisciplinary team approaches [60].
Conclusion
The rapidly evolving nature of HIV management and the increase in non–HIV-related comorbidities among this population has created a landscape that places these patients at risk for medication errors. Although ART has improved survival, medication errors place these patients at risk for adverse events and treatment failure. Medication errors are particularly likely to occur during transitions of care. Several interventions to prevent and decrease ART errors have been evaluated including educational strategies, hospital formulary changes, use of technology, and medication review and intervention by clinical pharmacists. However more research is needed to determine optimal strategies to address ART medication errors. Successful approaches have implemented comprehensive methods combining multiple interventions aimed at addressing several distinct sources of error. Promotion of a culture of safety is also an important component of medication error management. Health care professionals should be encouraged to report errors, and lessons learned from errors should be used to guide efforts to prevent future errors. Finally, improved integration of care with a focus on systematic initiatives for medication reconciliation as well as multidisciplinary approaches to transitions of care will be essential for reducing the rate of medication error among patients with HIV.
Corresponding author: Lindsay M. Daniels, PharmD, [email protected].
Financial disclosures: None.
References
1. Egger M, May M, Chene G, et al. Prognosis of HIV-1 infected patients starting highly active, antiretroviral therapy: a collaborative analysis of prospective studies. Lancet 2002;360:119–29.
2. Palella FJ, Delaney KM, Moorman AC, et al. Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. N Engl J Med 1998;338:853–60.
3. May MT, Gompels M, Delpech V, et al. Impact on life expectancy of HIV-1 positive individuals of CD4 cell count and viral load response to antiretroviral therapy. AIDS 2014; 28:1193–202.
4. Greene M, Justice AC, Lampiris HW, Valcour V. Management of HIV infection in advanced age. JAMA 2013;309:1397–1405.
5. Baker JV, Peng G, Rapkin J, et al. CD4+ count and risk of non-AIDS diseases following initial treatment of HIV infection. AIDS 2008;22:841–8.
6. Monforte A, Abrams D, Pradier C, et al. HIV-induced immunodeficiency and mortality from AIDS-defining and non-AIDS-defining malignancies. AIDS 2008;22:2143–53.
7. Buchacz K, Baker RK, Moorman AC, et al. Rates of hospitalizations and associated diagnoses in a large multisite cohort of HIV patients in the United States, 1994-2005. AIDS 2008;22:1345–54.
8. Aspden P, Wolcott J, Bootman JL, et al. Preventing medication errors: quality chasm series. Washington DC: National Academies Press; 2007.
9. Kripalani S, Roumie CL, Dalal AK, et al. Effect of a pharmacist intervention on clinically important medication errors after hospital discharge: a randomized trial. Ann Intern Med 2012;157:1–10.
10. Tam VC, Knowles SR, Cornish PL, et al. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ 2005;173:510–515.
11. Bell CM, Brener SS, Gunraj N, et al. Association of ICU or hospital admission with unintentional discontinuation of medications for chonic diseases. JAMA 2011;306:840–7.
12. Heelon M, Skiest D, Tereso G, et al. Effect of a clinical pharmacist’s interventions on duration of antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2007;64:2064–8.
13. Purdy BD, Raymond AM, Lesar TS. Antiretroviral prescribing errors in hospitalized patients. Ann Pharmacother 2000;34:833–8.
14. Gray J, Hicks RW, Hutchings C. Antiretroviral medication errors in a national medication error database. AIDS Patient Care STDS 2005;19:803–12.
15. Rastegar DA, Knight AM, Monolakis JS. Antiretroviral medication errors among patients with HIV infection. Clin Infect Dis 2006;43:933–8.
16. Snyder AM, Klinker K, Orrick JJ, et al. An in-depth analysis of medication errors in hospitalized patients with HIV. Ann Pharmacother 2011;45:459–68.
17. Edelman EJ, Gordon KS, Glover J, et al. The next therapeutic challenge in HIV: polypharmacy. Drugs Aging 2013;30:613–28.
18. Carcelero E, Tuset M, Martin M, et al. Evaluation of antiretroviral-related errors and interventions by the clinical pharmacist in hospitalized HIV-infected patients. HIV Medicine 2011;12:494–9.
19. Guo Y, Chung P, Weiss C, et al. Customized order-entry sets can prevent antiretroviral prescribing errors: a novel opportunity for antimicrobial stewardship. P T 2015;40:353–8.
20. Commers T, Swindells S, Sayles H, et al. Antiretroviral medication prescribing errors are common with hospitalization of HIV-infected patients. J Antimicrob Chemother 2014;69:262–7.
21. Sanders J, Pallotta A, Bauer S, et al. Antimicrobial stewardship program to reduce antiretroviral medication errors in hospitalized patients with HIV infection. Infect Control Hosp Epidemiol 2014;35:272–7.
22. Chiampas TD, Kim H, Badowski M. Evaluation of the occurrence and type of antiretroviral and opportunistic infection medication errors within the inpatient setting. Pharm Pract 2015;13:512.
23. Eginger KH, Yarborough LL, Inge LD, et al. Medication errors in HIV-infected hospitalized patients: a pharmacist’s impact. Ann Pharmacother 2013;47:953–60.
24. Pastakia SD, Corbett AH, Raasch RH, et al. Frequency of HIV-related medication errors and associated risk factors in hospitalized patients. Ann Pharmacother 2008;42:491–7.
25. Garey KW, Teichner P. Pharmacist intervention program for hospitalized patients with HIV infection. Am J Health Syst Pharm 2000;57:2283–4.
26. Daniels LM, Raasch RH, Corbett AH. Implementation of targeted interventions to decrease antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2012;69:422–30.
27. Li EH, Foisy MM. Antiretroviral and medication errors in hospitalized HIV-positive patients. Ann Pharmacother 2014;48:998–1010.
28. Yehia BR, Mehta JM, Ciuffetelli D, et al. Antiretroviral medication errors remain high but are quickly corrected among hospitalized HIV-infected adults. Clin Infect Dis 2012;55:593–99.
29. Willig JH, Westfall AO, Allison J, et al. Nucleoside reverse-transcriptase inhibitor dosing errors in an outpatient HIV clinic in the electronic medical record era. Clin Infect Dis 2007;45:658–61.
30. Hellinger FJ, Encinosa WE. The cost and incidence of prescribing errors among privately insured HIV patients. Pharmacoeconomics 2010;28:23–34.
31. Deeks SG, Gange SJ, Kitahata MM, et al. Trends in multidrug treatment failure and subsequent mortality among antiretroviral therapy-experienced patients with HIV infection in North America. Clin Infect Dis 2009;49:1582–90.
32. Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med 2011;365:493–505.
33. Wittich CM, Burkle CM, Lanier WL. Medication errors: an overview for clinicians. Mayo Clin Proc 2014;89:1116–25.
34. Merchen BA, Gerzenshtein L, Scarsi KK, et al. Evaluation of HIV-specialized pharmacists’ impact on prescribing errors in hospitalized patients on antiretroviral therapy. 51st Interscience Conference on Antimicrobial Agents and Chemotherapy; 2011 Sep 17-20; Chicago IL. Abstract H2–794.
35. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997;277:312–17.
36. Agu KA, Oqua D, Adeyanju Z, et al. The incidence and types of medication errors in patients receiving antiretroviral therapy in resource constrained settings. PLoS ONE 2014;9:e87338.
37. Arshad S, Rothberg M, Rastegar DA, et al. Survey of physician knowledge regarding antiretroviral medications in hospitalized HIV-infected patients. J Int AIDS Soc 2009;12:1.
38. Fultz SL, Goulet JL, Weissman S, et al. Differences between infectious diseases-certified physicians and general medicine-certified physicians in the level of comfort with providing primary care to patients. Clin Infect Dis 2005;41:738–43.
39. Cheng QJ, Engelage EM, Grogan TR, et al. Who provides primary care? An assessment of HIV patient and provider practices and preferences. J AIDS Clin Res 2014;5:366.
40. Cohen MR, Davis NM. AZT is a dangerous abbreviation. Am Pharm 1992;32:26.
41. Ambrosini MT, Mandler HD, Wood CA. AZT: zidovudine or azathioprine? Lancet 1992;339:935.
42. Sponsler KC, Neal EB, Kripalani S. Improving medication safety during hospital-based transitions of care. Cleve Clin J Med 2015;82:351–60.
43. Peeters MJ, Pinto SL. Assessing the impact of an educational program on decreasing prescribing errors at a university hospital. J Hosp Med 2009;4:97–101.
44. Faragon JJ, Lesar TS. Update on prescribing errors with HAART. AIDS Read 2003;13:268–78.
45. Batra R, Wolbach-Lowes J, Swindells S, et al. Impact of an electronic medical record on the incidence of antiretroviral prescription errors and HIV pharmacist reconciliation on error correction among hospitalized HIV-infected patients. Antivir Ther 2015:2040–58.
46. Keers RN, Williams SD, Cooke J, et al. Impact of interventions designed to reduce medication administration errors in hospitals: a systematic review. Drug Saf 2014;37:317–32.
47. Reckmann MH, Westbrook JI, Koh Y, et al. Does computerized provider order entry reduce prescribing errors for hospital inpatients? A systematic review. J Am Med Inform Assoc 2009;16:613–23.
48. Bozek PS, Perdue BE, Bar-Din M, Weidle PJ. Effect of pharmacist interventions on medication use and cost in hospitalized patients with or without HIV infection. Am J Health Syst Pharm 1998;55:1151–5.
49. De Maat MM, de Boer A, Koks CH, et al. Evaluation of clinical pharmacist interventions on drug interactions in outpatient pharmaceutical HIV care. J Clin Pharm Ther 2004;29:121–30.
50. Corrigan MA, Atkinson KM, Sha BE, Crank CW. Evaluation of pharmacy-implemented medication reconciliation directed at antiretroviral therapy in hospitalized HIV/AIDS patients. Ann Pharmacother 2010;44:222–3.
51. Rao N, Patel V, Grigoriu A, et al. Antiretroviral therapy prescribing in hospitalized HIV clinic patients. HIV Med 2012;13:367–71.
52. Coleman EA, Smith JD, Raha D, Min S. Posthospital medication discrepancies. Arch Intern Med 2005;165:1842–7.
53. Forster AJ, Murff HJ, Peterson JF, et al. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med 2003;138:161–7.
54. Mesteig M, Helbostad JL, Sletvold O, et al. Unwanted incidents during transition of geriatric patients from hospital to home: a prospective observational study. BMC Health Serv Res 2010;10:1.
55. Mueller SK, Sponsler KC, Kripalani S, Schnipper JL. Hospital-based medication reconciliation practices: a systematic review. Arch Intern Med 2012;172:1057–69.
56. Hasse B, Ledergerber B, Furrer H, et al. Morbidity and aging in HIV-infected persons: the Swiss HIV Cohort Study. Clin Infect Dis 2011;53:1130–9.
57. Downes JM, O’Neal KS, Miller MJ, et al. Identifying opportunities to improve medication management in transitions of care. Am J Health Syst Pharm 2015;72:S58–69.
58. Cavanaugh JJ, Lindsey KN, Shilliday BB, Ratner SP. Pharmacist-coordinated multidisciplinary hospital follow-up visits improve patient outcomes. J Manag Care Spec Pharm 2015;21:256–60.
59. Bellone JM, Barner JC, Lopez DA. Postdischarge interventions by pharmacists and impact on hospital readmission rates. J Am Pharm Assoc 2012;52:358–62.
60. Handford CD, Tynan AM, Rackal JM, Glazier RH. Setting and organization of care for persons living with HIV/AIDS. Cochrane Database Syst Rev 2006;19:CD004348.
From the University of North Carolina Medical Center (Dr. Daniels) and Renovion (Dr. Durham), Chapel Hill, NC.
To Download a PDF of the Full Article:
ABSTRACT
• Objective: To examine common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
• Methods: Review of the literature.
• Results: The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in patients with HIV place these patients at risk for medication errors and adverse drug events. Many studies of hospitalized patients with HIV have reported high rates of medication errors in this population. The consequences of antiretroviral therapy errors can range from minimal harm to life-threatening toxicities and the possibility of resistance and treatment failure. This review discusses the factors contributing to the high rates of error associated with antiretroviral therapy and details strategies to reduce and prevent errors in these patients.
• Conclusion: A comprehensive approach combining multiple interventions can be used to reduce and prevent antiretroviral medication errors in patients with HIV in order to improve the quality of care for this population.
Great progress has been made in the treatment of HIV over the past several decades. With the advancements in treatment options for HIV, considerable reductions in the morbidity and mortality associated with HIV and HIV-related complications have been realized [1,2]. Antiretroviral therapy (ART) has rapidly evolved, offering different mechanisms of action, improved potency, increased tolerability and reduced pill burdens. As a result, HIV infection has transformed from a terminal illness to a manageable chronic disease.
The success of HIV treatment has created a new set of challenges for health care professionals. Patients with successfully treated HIV can expect to live a nearly normal lifespan [3]. With this extended life expectancy, the number of older adults infected with HIV continues to rise, and care for these patients requires a broader and more comprehensive approach. Although HIV-related illnesses such as opportunistic infections have declined, the rate of non–HIV-related comorbidities among patients with HIV has increased [4]. Large cohort studies have shown an association between the risk for HIV-associated non–AIDS-related conditions and CD4 counts [5,6]. HIV-associated non–AIDS-related conditions include cardiovascular disease, kidney disease, liver disease, central nervous system disease, osteoporosis, and non–AIDS-associated malignancies. These conditions occur either more frequently or are more severe in patients with lower CD4 counts or detectable viral loads, but can also arise or persist in virologically suppressed patients with high CD4 counts [4].
The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in this population place these patients at risk for experiencing medication errors and adverse drug events. Patients with HIV often receive care by many providers in many different settings. Clinicians caring for patients with HIV must be familiar not only with the treatment of HIV but also with the management and integration of their patients’ primary care needs. In addition, the rates of hospitalization for HIV-infected patients have declined substantially since the mid-1990s [7]. Of the patients with HIV requiring hospitalization, the proportion of hospitalizations due to opportunistic infections has decreased and the proportion of hospitalizations due to other conditions has increased [7]. For many of these patients, the treatment of HIV has retreated to the background as a stable condition, while the management of other acute illness requires more attention.
An estimated 1.5 million adverse drug events occur each year in the United States due to medication errors [8]. Medication errors are common and can occur at any point during the medication use process, including procurement, prescribing, transcribing, preparing or compounding, dispensing, administration, and monitoring. Any time a patient moves from one setting of health care to another, the risk for medication errors is increased. Several reports have highlighted the increased risk for medication errors and adverse effects that can occur during these transitions of care. In fact, up to 70% of patients have an unintentional medication discrepancy at hospital discharge [9]. Errors during hospital admission are common as well, affecting up to two-thirds of patients admitted to hospitals [10,11].
As HIV care becomes more complex, concerns have been raised regarding increases in the number of medication errors in these patients, especially during transitions of care. Most studies of hospitalized patients with HIV have reported error rates of 5% to 30% [12–15]. One study demonstrated that the risk for a medication error at admission for patients with HIV was 3.8 errors per patient, whereas for patients without HIV the rate was 2.8 errors per patient [16]. Because of the potential for the emergence of resistance mutations, adherence to ART is essential for successful treatment and sustained viral suppression. Thus, medication errors of omission could have particularly detrimental effects for the long-term treatment of patients with HIV. Furthermore, as this population ages, polypharmacy becomes common, placing these patients at risk for errors related to dosing and drug interactions [17]. Because medication errors can lead to patient harm and death as well as increased health care costs, elucidating the reasons for errors associated with HIV management and exploring strategies aimed at the reduction and prevention of errors is essential.
The goal of this review is to examine the common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
Incidence of ART Errors
Several studies have indicated that the incidence of ART errors in hospitalized patients is rising. The rate of ART errors detected at admission among hospitalized patients increased from 2% in 1996 to 12% in 1998 according to one study [13]. Studies conducted from 2004 to 2007 report ART error rates at hospital admission ranging from 17% to 26% [12,15,18]. In more recent studies, high ART error rates ranging from 35% to 55% have been reported [19–23]. Two studies have reported ART error rates occurring at hospital admission to be as high as 70% [24,25].
Various types of ART medication errors can occur. Commonly reported errors include those related to drug interactions, incorrect dosing, incorrect scheduling, and incomplete regimens. Errors occurring at the time of hospital admission appear to be more common than errors occurring at other time points [20,24,26]. A comprehensive systematic review of studies regarding medication errors in hospitalized patients with HIV found that errors at the point of prescribing encompass the majority of errors [27]. One study identified 82 ART errors occurring at admission in 68 hospitalized patients. Of these errors, 37% occurred at the point of prescribing, 27% were attributed to dispensing, and 18% were attributed to inaccuracies in outpatient clinic documentation [24].
Several authors have drawn associations between the rate of errors and the class of antiretroviral prescribed. Protease inhibitors have been the most frequently implicated drug class [13,18,20,27,28]. In an analysis of 145 ART errors in one hospital, 70% of dosing errors involved protease inhibitors and 30% involved nucleoside/nucleotide reverse transcriptase inhibitors (NRTIs). In addition, scheduling errors occurred most often with protease inhibitors, and errors due to drug interactions were also most likely to involve protease inhibitors [28]. Conversely, another study did not find an association between protease inhibitors and the risk for error compared to other classes of drugs. In fact, this study showed that the NRTI class was associated with an increased risk of prescribing error compared to protease inhibitors and that the use of co-formulated drugs that were available on the hospital formulary protected against error [20]. These findings highlight the various factors contributing to error among different institutions, especially related to hospital formulary selections and availability of specific drugs.
Fewer studies have evaluated ART errors in outpatient settings. One report evaluated the NRTI medication records from an outpatient electronic medical record system from August 2004 to September 2005. A total of 902 NRTI records for 603 patients were analyzed. The overall error rate was 6% (53/902), with renal dosing errors being most common (75% of errors) [29]. Another evaluation of ART errors among privately insured patients with HIV found that the probability of a patient with HIV receiving an inappropriate drug combination in a given year was higher in 2005 (5.9%) compared to 1999 and 2000 (1.9%). Many of the increased errors seen in 2005 compared to 1999–2000 in this study were attributed to errors related to protease inhibitor boosting [30].
Harms and Consequences of ART Errors
Because of the potential for the emergence of drug resistance, adherence to an ART regimen is essential for successful treatment and sustained viral suppression. ART medication errors causing disrupted therapy, omitted drugs, or suboptimal dosing can lead to the development of viral resistance mutations and ultimately treatment failure placing patients at risk for HIV-related complications such as opportunistic infections as well as non–HIV-related complications [31]. Health care providers should recognize the importance of appropriate uninterrupted therapy for this population and should assist in facilitating this effort. On a community level, patients with elevated plasma HIV RNA levels due to untreated disease or treatment failure have a greater risk of transmitting HIV to others [32]. Effective ART on a population basis will have important public health advantages.
In addition to the potential consequences of ART error relating to treatment failure and resistance, ART errors may also lead to drug toxicities and drug intolerance, increasing the risk of nonadherence, and further exacerbating the aforementioned consequences.
ART errors also carry the same consequences as errors involving other non-ART medications, such as loss of patient trust, civil and criminal legal consequences, professional board discipline, and increased health care costs [33]. One study reported a cost avoidance of $24,000 annually for inpatient and $124,000 annually for outpatient through the use of pharmacists’ interventions to prevent errors [34]. Another study found that patients experiencing an ART error related to protease inhibitor boosting incurred claims costing 21.5% more than patients not experiencing a boosting error [30].
Contributing Factors
Health care professional–associated factors can also contribute to ART errors. The increasing complexity and specialization of HIV care and the rapidly evolving nature of medication management in this population have created an environment in which many providers without extensive experience in the treatment of HIV are responsible for managing HIV in settings beyond the HIV clinic. A survey of non-HIV specialized physicians conducted in 2007 revealed a poor knowledge base of common ART regimens among these physicians [37]. Likewise, HIV providers may be uncomfortable serving a primary care role for patients with HIV due to their own lack of experience and knowledge of primary care [38]. This issue is becoming more relevant, as non-AIDS comorbidities are emerging as the main health concerns for patients with HIV [39]. Health care professionals’ knowledge of HIV care also contributes to ART errors at other points in the medication use process beyond prescribing. Pharmacists lacking experience in identifying appropriate ART regimens may not recognize errors, and, therefore, may not be able to intervene and prevent errors from occurring.
Medication factors contributing to the risk for errors include risks related to the pharmacologic properties of certain drugs as well as drug naming and labeling factors. Certain antiretroviral classes are known to interact with many medications due to inhibition or induction of metabolic pathways responsible for drug metabolism, such as the cytochrome P-450 pathways. In addition, many antiretroviral medications require “boosting” with another drug to increase systemic exposure of the antiretroviral. Boosting is required for most protease inhibitors and for the integrase inhibitor elvitegravir. For some of these medications, the boosting agent is provided in a co-formulated product. However, for others, a separate prescription for the boosting medication is required. These factors contribute to the risks for drug interactions as well as drug and dosing errors.
Errors may also occur due to drug naming and labeling factors. Confusion due to look-alike/sound-alike medications is common, especially with handwritten or verbally transcribed orders. Examples of look-alike/sound-alike medications include lamivudine/lamotrigine, Viramune/Viread/Viracept, and ritonavir/Retrovir. The use of abbreviations can also lead to error. Reports have described errors associated with zidovudine, which is often abbreviated AZT, being confused with azathioprine [40,41]. An evaluation of ART errors reported to a national medication error reporting program found that look-alike/sound-alike medication names contributed to 19% (77/400) of the errors reported during the 48-month time period evaluated [15].
Several antiretroviral medications are co-formulated into single tablets to decrease pill burden and increase adherence. The use of co-formulated products has the potential to either increase or decrease the risk of errors. Prescribing one co-formulated product rather than its individual components simplifies the prescribing process, allowing the prescriber to become familiar with one product and one dosing scheme in place of 2 or more drugs with different dosing recommendations. The risk of inadvertent omission of a drug and the risk of improper dosing is reduced with the use of co-formulated products. On the other hand, when patients are transitioned from one health care setting to another (such as admission to a hospital), these products may require conversion to the individual components of the drug due to formulary availability and/or cost concerns. Studies have shown that formulary conversions from co-formulated products to individual components are frequently associated with ART errors and that the use of co-formulated products in the inpatient setting reduces these errors [20,22,24,26].
Finally, factors related to the health care setting can influence the risk for errors. High patient numbers, time constraints, and workload stresses can all increase the likelihood that an error will occur [36]. Interruptions and distractions occurring at any point in the medication use process can lead to error.
Transitioning from one health care setting to another also places patients at risk for being harmed by medication errors. Up to 70% of patients may have an unintentional medication discrepancy at hospital discharge, and errors occurring at hospital admission have been reported to affect two-thirds of admitted patients [42]. Many of these errors hold the potential to cause harm to the patient, especially if the errors are carried forward throughout the patient’s admission and after discharge. One study found that 22% of ART errors occurring at hospital admission were attributable to outpatient clinic documentation errors [24]. This highlights the need for improved documentation processes and draws attention to the element of communication at transitional points of care. Lack of adequate resources for medication reconciliation is a widely recognized challenge. This includes resources of personnel as well as electronic medical record systems that can facilitate the reconciliation process. The importance of accurately documenting a patient’s medication history and the ability to easily communicate this information to other health care settings cannot be underestimated. Electronic medical record systems should be developed to facilitate and enhance the processes of reconciliation, documentation, and communication.
Interventions to Address ART Errors
The causes of ART errors are multifactorial and should be addressed using comprehensive approaches tailored to the specific health care setting. Several types of interventions aimed at reducing and preventing ART errors have been evaluated in the literature [12,18,26,27]. In general, these interventions have focused on provider education, use of technology and clinical decision support systems, pharmacist-led medication review and intervention, and hospital formulary changes. Other interventions that may lead to a reduction in ART errors include minimizing polypharmacy, improving medication reconciliation processes during transitions of care, and multidisciplinary follow-up clinic visits after hospital discharge.
Because the sources of ART errors are multifactorial, the optimal strategy to prevent and reduce errors is likely to be a comprehensive approach combining several of the aforementioned interventions. One study showed that a combined approach that included updates to the institution’s computerized physician order entry (CPOE) system, education for the pharmacy and ID departments, and daily review of patients’ medications by pharmacists was successful in reducing the percentage of admissions with an ART error from 50% to 34%. In addition, the time to error resolution decreased from 180 hours to 23 hours, and the error resolution rate increased from 32% to 68% [21]. Another study demonstrated benefits using a comprehensive approach including the dissemination of educational pocket cards for physicians, pharmacists and nurses; CPOE alerts; hospital formulary updates to include co-formulated products; and a daily review of medications by an ID-specialized pharmacist for patients receiving ART. These strategies resulted in a reduced ART error rate from 72% to 15% in 7 months [26]. These studies demonstrate the benefit of multifaceted strategies to reduce ART error rates.
Education
Given the complexity of HIV care and overall lack of antiretroviral medication knowledge among non-ID specialized health care professionals, educational programs aimed at increasing the comfort level and familiarity of ART is important [16,37]. Frequent training to update health care professionals on the newest recommendations for HIV management can help achieve this goal [19,27]. Educational interventions aimed at reducing medication errors have been shown to be transiently effective but may lack sustained effects [43]. Educational programs for health care professionals should be designed to provide frequent brief updates, and are likely to be more successful when combined with other approaches [19,26].
Education directed toward patients, families, and caregivers can also play a pivotal role in error prevention. Patients should be encouraged to use one pharmacy, if possible, to ensure that one complete, accurate, and current profile is maintained. The use of one pharmacy can also assist in the identification of therapeutic duplications and drug interactions. Counseling patients with visual aids, such as charts with pictures of drugs, can also be used as a tool for education. Patients who are familiar with the names and the appearances of their drugs are more likely to recognize errors. In addition, patients should be advised to maintain their own current medication list so that they will be able to provide this information to all of the health care professionals involved in their care [33,44].
Technology and Clinical Decision Support Systems
Overall, the increasing use of technology such as CPOE, decision support systems, and barcoding systems has been shown to decrease the risk of medication error [19,45,46]. Guo et al observed a 35% decrease in ART error rates after the integration of customized order entry sets into an existing CPOE program [19]. Another study reported a 50% decrease in the ART error rate after the introduction of an electronic medical record system [45]. On the other hand, some reports evaluating the role of CPOE systems to reduce medication error rates are conflicting [15,19,23,48]. Differences in system capabilities and programming and differing needs and challenges of institutions may account for the varying results reported in the literature. CPOE systems can serve as valuable tools for assisting in medication prescribing. Confusion due to abbreviations, illegible writing and look-alike/sound-alike drugs should be eliminated or greatly reduced with the use of CPOE. However, the limitations of these systems, which may differ among different systems, should be appreciated. As ART regimens and dosing recommendations change, clinical decision support systems can quickly become out-of-date and require frequent updating. One study identified fields that pre-populated drug names and frequencies within a CPOE system to be the cause of several medication errors [16]. Studies have also identified errors related to disregarded alerts from decision support software [15,16]. “Alert fatigue” is a well-recognized phenomenon that occurs when clinicians are exposed to a large volume of clinical decision support alerts of varying clinical significance. Over time, clinicians begin to become desensitized to the alerts, and they may eventually stop responding to them.
Some limitations of CPOE systems arise from the individual system capabilities. Some systems have the ability to check for appropriate dosing, recommend adjustments in renal dysfunction, and provide alerts for drug interactions, but some systems lack these capabilities. In addition, CPOE systems are often not able to prevent errors of omission, delays in continuation of therapy, and medication scheduling errors [15,45].
Given the limitations of CPOE and clinical decision support technologies, it is unlikely that these interventions alone will be sufficient to fully address the problem of ART errors. These technologies can, however, serve as a powerful tool in the prevention and reduction of ART errors, especially when used in combination with other strategies.
Pharmacist Intervention
Multiple studies have shown that clinical pharmacists are effective at decreasing ART medication errors in the inpatient setting [12,18,23,25,28,45,49,50]. One institution implemented an HIV-specialized pharmacist review strategy that decreased the median time to error correction from 84 hours to 15.5 hours among hospitalized patients [12]. Corrigan et al showed that a review of medications by an HIV-specialized pharmacist 48 hours after hospital admission decreased error rates from 52% to 5% [50]. Another study showed that with the use of an electronic medical record, errors among hospitalized patients with HIV were 9.4 times more likely to be corrected within 24 hours when an HIV-specialized pharmacist was consulted [45].
The majority of studies evaluating the effect of pharmacist interventions have utilized the services of a pharmacist with specialized training in HIV. Few studies have evaluated the impact of interventions by pharmacists without this specialized training. One study retrospectively evaluated and characterized ART errors among hospitalized patients. Medication reconciliation was performed within 24 hours of admission by unit-based pharmacists without specialized training in HIV. Overall, 30.8% of errors were corrected within 24 hours and 14.2% were corrected after 24 hours. However, 54.7% of the errors were not recognized and were never corrected [20]. Just as physicians trained in general medicine lack knowledge of antiretroviral medications, pharmacists without HIV-specialized training may also be less familiar with current ART recommendations [16,37].
Overall, the studies evaluating the impact of pharmacist intervention on reducing ART error rates have shown significant reductions in time to error corrections. The nature of this type of intervention however, lends itself to correction of errors rather than prevention of errors. Indeed, one hospital reported an ART error rate of 29% on the first day of admission compared to 7% on the second day of admission, a decrease that was attributed to retrospective review of medication orders by clinical pharmacists. This study also noted the occurrences of additional errors identified on the second day of admission, highlighting the importance of daily review and follow-up throughout the hospital stay [28].
Hospital Formulary Selections
Several studies have documented an association between hospital formulary options and ART errors [20,22,24,26]. The prescribing of ART medications that are not available on hospital formulary is consistently associated with higher rates of error. Many hospitals minimize the numbers of different medications offered through the maintenance of a formulary. Formularies assist in reducing costs, preserving storage space, and simplifying prescribing. Because some hospitals choose to exclude co-formulated products from the formulary, several ART medications may not be included. In addition, some ART medications may be excluded from formulary due to their infrequent use or higher costs. The extra step of converting a co-formulated product to its individual components increases the risk for errors. In one study, the addition of all co-formulated ART medications to the hospital formulary in combination with several other interventions had a significant effect on reducing the ART error rate [26].
Transitions of Care Interventions
Patients with HIV are at risk for experiencing medication errors and discrepancies any time they transition from one health care setting to another. Hospitalization poses the highest risk as it often disrupts continuity of care and corresponds with a comparatively larger number of medication changes [16,51]. This risk is present on admission, throughout hospitalization, and upon discharge. Perhaps the errors of greatest concern are those that are carried forward after discharge on to the outpatient setting. Medication discrepancies at transitions of care have been associated with increases in adverse events and increased hospital readmission rates [52,53]. One study evaluating adverse events in geriatric patients transitioning from hospital to home found that the most frequently reported adverse events after discharge were related to incorrect drugs or dosages of medication regimens [54]. Tools that can assist in integration and coordination during transitions of care are greatly needed.
One of the most important strategies to prevent and correct medication discrepancies during transitions of care is medication reconciliation. Several studies have demonstrated the efficacy of medication reconciliation in decreasing medication errors [55]. Medication reconciliation is especially important for patients taking many medications. An estimated 14% of patients with HIV older than age 65 take 4 or more medications [56]. This population often requires treatment for other chronic conditions such as hypertension, diabetes, and depression, further increasing the risk for adverse drug events including medication error. Because of the complexities associated with the treatment of HIV and the increased risk for errors, routine medication reconciliation among this population should be a priority.
In addition to medication reconciliation, several studies have evaluated the effects of coordinated pharmacist or multidisciplinary post-discharge follow-up visits for medication therapy management as a strategy to reduce preventable medication-related adverse events [57–59]. Patients receiving clinic-based medication therapy management by a clinical pharmacist after hospital discharge had a lower 60-day hospital readmission rate compared to those who did not have a clinic visit with a pharmacist (18.2% vs. 43.1%) [59]. Another study compared 2 models of post-discharge follow-up, a multidisciplinary team model led by a clinical pharmacist compared to a standard physician-only model. The goal of the multi-disciplinary team model was to complete a thorough medication review, address lifestyle interventions, and address barriers to care. Overall, patients seen by the multidisciplinary team had a 30-day hospital readmission rate of 14.3% compared with a 34.3% readmission rate in the physician-only team [58]. Many different care models have been proposed to improve continuity of care for patients with HIV. The ideal model is not known, and it is likely that several different models would be effective. Optimal models should integrate the patient-physician relationship with multidisciplinary team approaches [60].
Conclusion
The rapidly evolving nature of HIV management and the increase in non–HIV-related comorbidities among this population has created a landscape that places these patients at risk for medication errors. Although ART has improved survival, medication errors place these patients at risk for adverse events and treatment failure. Medication errors are particularly likely to occur during transitions of care. Several interventions to prevent and decrease ART errors have been evaluated including educational strategies, hospital formulary changes, use of technology, and medication review and intervention by clinical pharmacists. However more research is needed to determine optimal strategies to address ART medication errors. Successful approaches have implemented comprehensive methods combining multiple interventions aimed at addressing several distinct sources of error. Promotion of a culture of safety is also an important component of medication error management. Health care professionals should be encouraged to report errors, and lessons learned from errors should be used to guide efforts to prevent future errors. Finally, improved integration of care with a focus on systematic initiatives for medication reconciliation as well as multidisciplinary approaches to transitions of care will be essential for reducing the rate of medication error among patients with HIV.
Corresponding author: Lindsay M. Daniels, PharmD, [email protected].
Financial disclosures: None.
References
1. Egger M, May M, Chene G, et al. Prognosis of HIV-1 infected patients starting highly active, antiretroviral therapy: a collaborative analysis of prospective studies. Lancet 2002;360:119–29.
2. Palella FJ, Delaney KM, Moorman AC, et al. Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. N Engl J Med 1998;338:853–60.
3. May MT, Gompels M, Delpech V, et al. Impact on life expectancy of HIV-1 positive individuals of CD4 cell count and viral load response to antiretroviral therapy. AIDS 2014; 28:1193–202.
4. Greene M, Justice AC, Lampiris HW, Valcour V. Management of HIV infection in advanced age. JAMA 2013;309:1397–1405.
5. Baker JV, Peng G, Rapkin J, et al. CD4+ count and risk of non-AIDS diseases following initial treatment of HIV infection. AIDS 2008;22:841–8.
6. Monforte A, Abrams D, Pradier C, et al. HIV-induced immunodeficiency and mortality from AIDS-defining and non-AIDS-defining malignancies. AIDS 2008;22:2143–53.
7. Buchacz K, Baker RK, Moorman AC, et al. Rates of hospitalizations and associated diagnoses in a large multisite cohort of HIV patients in the United States, 1994-2005. AIDS 2008;22:1345–54.
8. Aspden P, Wolcott J, Bootman JL, et al. Preventing medication errors: quality chasm series. Washington DC: National Academies Press; 2007.
9. Kripalani S, Roumie CL, Dalal AK, et al. Effect of a pharmacist intervention on clinically important medication errors after hospital discharge: a randomized trial. Ann Intern Med 2012;157:1–10.
10. Tam VC, Knowles SR, Cornish PL, et al. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ 2005;173:510–515.
11. Bell CM, Brener SS, Gunraj N, et al. Association of ICU or hospital admission with unintentional discontinuation of medications for chonic diseases. JAMA 2011;306:840–7.
12. Heelon M, Skiest D, Tereso G, et al. Effect of a clinical pharmacist’s interventions on duration of antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2007;64:2064–8.
13. Purdy BD, Raymond AM, Lesar TS. Antiretroviral prescribing errors in hospitalized patients. Ann Pharmacother 2000;34:833–8.
14. Gray J, Hicks RW, Hutchings C. Antiretroviral medication errors in a national medication error database. AIDS Patient Care STDS 2005;19:803–12.
15. Rastegar DA, Knight AM, Monolakis JS. Antiretroviral medication errors among patients with HIV infection. Clin Infect Dis 2006;43:933–8.
16. Snyder AM, Klinker K, Orrick JJ, et al. An in-depth analysis of medication errors in hospitalized patients with HIV. Ann Pharmacother 2011;45:459–68.
17. Edelman EJ, Gordon KS, Glover J, et al. The next therapeutic challenge in HIV: polypharmacy. Drugs Aging 2013;30:613–28.
18. Carcelero E, Tuset M, Martin M, et al. Evaluation of antiretroviral-related errors and interventions by the clinical pharmacist in hospitalized HIV-infected patients. HIV Medicine 2011;12:494–9.
19. Guo Y, Chung P, Weiss C, et al. Customized order-entry sets can prevent antiretroviral prescribing errors: a novel opportunity for antimicrobial stewardship. P T 2015;40:353–8.
20. Commers T, Swindells S, Sayles H, et al. Antiretroviral medication prescribing errors are common with hospitalization of HIV-infected patients. J Antimicrob Chemother 2014;69:262–7.
21. Sanders J, Pallotta A, Bauer S, et al. Antimicrobial stewardship program to reduce antiretroviral medication errors in hospitalized patients with HIV infection. Infect Control Hosp Epidemiol 2014;35:272–7.
22. Chiampas TD, Kim H, Badowski M. Evaluation of the occurrence and type of antiretroviral and opportunistic infection medication errors within the inpatient setting. Pharm Pract 2015;13:512.
23. Eginger KH, Yarborough LL, Inge LD, et al. Medication errors in HIV-infected hospitalized patients: a pharmacist’s impact. Ann Pharmacother 2013;47:953–60.
24. Pastakia SD, Corbett AH, Raasch RH, et al. Frequency of HIV-related medication errors and associated risk factors in hospitalized patients. Ann Pharmacother 2008;42:491–7.
25. Garey KW, Teichner P. Pharmacist intervention program for hospitalized patients with HIV infection. Am J Health Syst Pharm 2000;57:2283–4.
26. Daniels LM, Raasch RH, Corbett AH. Implementation of targeted interventions to decrease antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2012;69:422–30.
27. Li EH, Foisy MM. Antiretroviral and medication errors in hospitalized HIV-positive patients. Ann Pharmacother 2014;48:998–1010.
28. Yehia BR, Mehta JM, Ciuffetelli D, et al. Antiretroviral medication errors remain high but are quickly corrected among hospitalized HIV-infected adults. Clin Infect Dis 2012;55:593–99.
29. Willig JH, Westfall AO, Allison J, et al. Nucleoside reverse-transcriptase inhibitor dosing errors in an outpatient HIV clinic in the electronic medical record era. Clin Infect Dis 2007;45:658–61.
30. Hellinger FJ, Encinosa WE. The cost and incidence of prescribing errors among privately insured HIV patients. Pharmacoeconomics 2010;28:23–34.
31. Deeks SG, Gange SJ, Kitahata MM, et al. Trends in multidrug treatment failure and subsequent mortality among antiretroviral therapy-experienced patients with HIV infection in North America. Clin Infect Dis 2009;49:1582–90.
32. Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med 2011;365:493–505.
33. Wittich CM, Burkle CM, Lanier WL. Medication errors: an overview for clinicians. Mayo Clin Proc 2014;89:1116–25.
34. Merchen BA, Gerzenshtein L, Scarsi KK, et al. Evaluation of HIV-specialized pharmacists’ impact on prescribing errors in hospitalized patients on antiretroviral therapy. 51st Interscience Conference on Antimicrobial Agents and Chemotherapy; 2011 Sep 17-20; Chicago IL. Abstract H2–794.
35. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997;277:312–17.
36. Agu KA, Oqua D, Adeyanju Z, et al. The incidence and types of medication errors in patients receiving antiretroviral therapy in resource constrained settings. PLoS ONE 2014;9:e87338.
37. Arshad S, Rothberg M, Rastegar DA, et al. Survey of physician knowledge regarding antiretroviral medications in hospitalized HIV-infected patients. J Int AIDS Soc 2009;12:1.
38. Fultz SL, Goulet JL, Weissman S, et al. Differences between infectious diseases-certified physicians and general medicine-certified physicians in the level of comfort with providing primary care to patients. Clin Infect Dis 2005;41:738–43.
39. Cheng QJ, Engelage EM, Grogan TR, et al. Who provides primary care? An assessment of HIV patient and provider practices and preferences. J AIDS Clin Res 2014;5:366.
40. Cohen MR, Davis NM. AZT is a dangerous abbreviation. Am Pharm 1992;32:26.
41. Ambrosini MT, Mandler HD, Wood CA. AZT: zidovudine or azathioprine? Lancet 1992;339:935.
42. Sponsler KC, Neal EB, Kripalani S. Improving medication safety during hospital-based transitions of care. Cleve Clin J Med 2015;82:351–60.
43. Peeters MJ, Pinto SL. Assessing the impact of an educational program on decreasing prescribing errors at a university hospital. J Hosp Med 2009;4:97–101.
44. Faragon JJ, Lesar TS. Update on prescribing errors with HAART. AIDS Read 2003;13:268–78.
45. Batra R, Wolbach-Lowes J, Swindells S, et al. Impact of an electronic medical record on the incidence of antiretroviral prescription errors and HIV pharmacist reconciliation on error correction among hospitalized HIV-infected patients. Antivir Ther 2015:2040–58.
46. Keers RN, Williams SD, Cooke J, et al. Impact of interventions designed to reduce medication administration errors in hospitals: a systematic review. Drug Saf 2014;37:317–32.
47. Reckmann MH, Westbrook JI, Koh Y, et al. Does computerized provider order entry reduce prescribing errors for hospital inpatients? A systematic review. J Am Med Inform Assoc 2009;16:613–23.
48. Bozek PS, Perdue BE, Bar-Din M, Weidle PJ. Effect of pharmacist interventions on medication use and cost in hospitalized patients with or without HIV infection. Am J Health Syst Pharm 1998;55:1151–5.
49. De Maat MM, de Boer A, Koks CH, et al. Evaluation of clinical pharmacist interventions on drug interactions in outpatient pharmaceutical HIV care. J Clin Pharm Ther 2004;29:121–30.
50. Corrigan MA, Atkinson KM, Sha BE, Crank CW. Evaluation of pharmacy-implemented medication reconciliation directed at antiretroviral therapy in hospitalized HIV/AIDS patients. Ann Pharmacother 2010;44:222–3.
51. Rao N, Patel V, Grigoriu A, et al. Antiretroviral therapy prescribing in hospitalized HIV clinic patients. HIV Med 2012;13:367–71.
52. Coleman EA, Smith JD, Raha D, Min S. Posthospital medication discrepancies. Arch Intern Med 2005;165:1842–7.
53. Forster AJ, Murff HJ, Peterson JF, et al. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med 2003;138:161–7.
54. Mesteig M, Helbostad JL, Sletvold O, et al. Unwanted incidents during transition of geriatric patients from hospital to home: a prospective observational study. BMC Health Serv Res 2010;10:1.
55. Mueller SK, Sponsler KC, Kripalani S, Schnipper JL. Hospital-based medication reconciliation practices: a systematic review. Arch Intern Med 2012;172:1057–69.
56. Hasse B, Ledergerber B, Furrer H, et al. Morbidity and aging in HIV-infected persons: the Swiss HIV Cohort Study. Clin Infect Dis 2011;53:1130–9.
57. Downes JM, O’Neal KS, Miller MJ, et al. Identifying opportunities to improve medication management in transitions of care. Am J Health Syst Pharm 2015;72:S58–69.
58. Cavanaugh JJ, Lindsey KN, Shilliday BB, Ratner SP. Pharmacist-coordinated multidisciplinary hospital follow-up visits improve patient outcomes. J Manag Care Spec Pharm 2015;21:256–60.
59. Bellone JM, Barner JC, Lopez DA. Postdischarge interventions by pharmacists and impact on hospital readmission rates. J Am Pharm Assoc 2012;52:358–62.
60. Handford CD, Tynan AM, Rackal JM, Glazier RH. Setting and organization of care for persons living with HIV/AIDS. Cochrane Database Syst Rev 2006;19:CD004348.
From the University of North Carolina Medical Center (Dr. Daniels) and Renovion (Dr. Durham), Chapel Hill, NC.
To Download a PDF of the Full Article:
ABSTRACT
• Objective: To examine common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
• Methods: Review of the literature.
• Results: The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in patients with HIV place these patients at risk for medication errors and adverse drug events. Many studies of hospitalized patients with HIV have reported high rates of medication errors in this population. The consequences of antiretroviral therapy errors can range from minimal harm to life-threatening toxicities and the possibility of resistance and treatment failure. This review discusses the factors contributing to the high rates of error associated with antiretroviral therapy and details strategies to reduce and prevent errors in these patients.
• Conclusion: A comprehensive approach combining multiple interventions can be used to reduce and prevent antiretroviral medication errors in patients with HIV in order to improve the quality of care for this population.
Great progress has been made in the treatment of HIV over the past several decades. With the advancements in treatment options for HIV, considerable reductions in the morbidity and mortality associated with HIV and HIV-related complications have been realized [1,2]. Antiretroviral therapy (ART) has rapidly evolved, offering different mechanisms of action, improved potency, increased tolerability and reduced pill burdens. As a result, HIV infection has transformed from a terminal illness to a manageable chronic disease.
The success of HIV treatment has created a new set of challenges for health care professionals. Patients with successfully treated HIV can expect to live a nearly normal lifespan [3]. With this extended life expectancy, the number of older adults infected with HIV continues to rise, and care for these patients requires a broader and more comprehensive approach. Although HIV-related illnesses such as opportunistic infections have declined, the rate of non–HIV-related comorbidities among patients with HIV has increased [4]. Large cohort studies have shown an association between the risk for HIV-associated non–AIDS-related conditions and CD4 counts [5,6]. HIV-associated non–AIDS-related conditions include cardiovascular disease, kidney disease, liver disease, central nervous system disease, osteoporosis, and non–AIDS-associated malignancies. These conditions occur either more frequently or are more severe in patients with lower CD4 counts or detectable viral loads, but can also arise or persist in virologically suppressed patients with high CD4 counts [4].
The increased complexity and specialization of HIV care, the presence of comorbidities, and the evolving nature of medication management in this population place these patients at risk for experiencing medication errors and adverse drug events. Patients with HIV often receive care by many providers in many different settings. Clinicians caring for patients with HIV must be familiar not only with the treatment of HIV but also with the management and integration of their patients’ primary care needs. In addition, the rates of hospitalization for HIV-infected patients have declined substantially since the mid-1990s [7]. Of the patients with HIV requiring hospitalization, the proportion of hospitalizations due to opportunistic infections has decreased and the proportion of hospitalizations due to other conditions has increased [7]. For many of these patients, the treatment of HIV has retreated to the background as a stable condition, while the management of other acute illness requires more attention.
An estimated 1.5 million adverse drug events occur each year in the United States due to medication errors [8]. Medication errors are common and can occur at any point during the medication use process, including procurement, prescribing, transcribing, preparing or compounding, dispensing, administration, and monitoring. Any time a patient moves from one setting of health care to another, the risk for medication errors is increased. Several reports have highlighted the increased risk for medication errors and adverse effects that can occur during these transitions of care. In fact, up to 70% of patients have an unintentional medication discrepancy at hospital discharge [9]. Errors during hospital admission are common as well, affecting up to two-thirds of patients admitted to hospitals [10,11].
As HIV care becomes more complex, concerns have been raised regarding increases in the number of medication errors in these patients, especially during transitions of care. Most studies of hospitalized patients with HIV have reported error rates of 5% to 30% [12–15]. One study demonstrated that the risk for a medication error at admission for patients with HIV was 3.8 errors per patient, whereas for patients without HIV the rate was 2.8 errors per patient [16]. Because of the potential for the emergence of resistance mutations, adherence to ART is essential for successful treatment and sustained viral suppression. Thus, medication errors of omission could have particularly detrimental effects for the long-term treatment of patients with HIV. Furthermore, as this population ages, polypharmacy becomes common, placing these patients at risk for errors related to dosing and drug interactions [17]. Because medication errors can lead to patient harm and death as well as increased health care costs, elucidating the reasons for errors associated with HIV management and exploring strategies aimed at the reduction and prevention of errors is essential.
The goal of this review is to examine the common types of medication errors occurring in patients with HIV, with a focus on patient risk, contributing factors, and interventions that can be employed to address the problem of medication errors in this population.
Incidence of ART Errors
Several studies have indicated that the incidence of ART errors in hospitalized patients is rising. The rate of ART errors detected at admission among hospitalized patients increased from 2% in 1996 to 12% in 1998 according to one study [13]. Studies conducted from 2004 to 2007 report ART error rates at hospital admission ranging from 17% to 26% [12,15,18]. In more recent studies, high ART error rates ranging from 35% to 55% have been reported [19–23]. Two studies have reported ART error rates occurring at hospital admission to be as high as 70% [24,25].
Various types of ART medication errors can occur. Commonly reported errors include those related to drug interactions, incorrect dosing, incorrect scheduling, and incomplete regimens. Errors occurring at the time of hospital admission appear to be more common than errors occurring at other time points [20,24,26]. A comprehensive systematic review of studies regarding medication errors in hospitalized patients with HIV found that errors at the point of prescribing encompass the majority of errors [27]. One study identified 82 ART errors occurring at admission in 68 hospitalized patients. Of these errors, 37% occurred at the point of prescribing, 27% were attributed to dispensing, and 18% were attributed to inaccuracies in outpatient clinic documentation [24].
Several authors have drawn associations between the rate of errors and the class of antiretroviral prescribed. Protease inhibitors have been the most frequently implicated drug class [13,18,20,27,28]. In an analysis of 145 ART errors in one hospital, 70% of dosing errors involved protease inhibitors and 30% involved nucleoside/nucleotide reverse transcriptase inhibitors (NRTIs). In addition, scheduling errors occurred most often with protease inhibitors, and errors due to drug interactions were also most likely to involve protease inhibitors [28]. Conversely, another study did not find an association between protease inhibitors and the risk for error compared to other classes of drugs. In fact, this study showed that the NRTI class was associated with an increased risk of prescribing error compared to protease inhibitors and that the use of co-formulated drugs that were available on the hospital formulary protected against error [20]. These findings highlight the various factors contributing to error among different institutions, especially related to hospital formulary selections and availability of specific drugs.
Fewer studies have evaluated ART errors in outpatient settings. One report evaluated the NRTI medication records from an outpatient electronic medical record system from August 2004 to September 2005. A total of 902 NRTI records for 603 patients were analyzed. The overall error rate was 6% (53/902), with renal dosing errors being most common (75% of errors) [29]. Another evaluation of ART errors among privately insured patients with HIV found that the probability of a patient with HIV receiving an inappropriate drug combination in a given year was higher in 2005 (5.9%) compared to 1999 and 2000 (1.9%). Many of the increased errors seen in 2005 compared to 1999–2000 in this study were attributed to errors related to protease inhibitor boosting [30].
Harms and Consequences of ART Errors
Because of the potential for the emergence of drug resistance, adherence to an ART regimen is essential for successful treatment and sustained viral suppression. ART medication errors causing disrupted therapy, omitted drugs, or suboptimal dosing can lead to the development of viral resistance mutations and ultimately treatment failure placing patients at risk for HIV-related complications such as opportunistic infections as well as non–HIV-related complications [31]. Health care providers should recognize the importance of appropriate uninterrupted therapy for this population and should assist in facilitating this effort. On a community level, patients with elevated plasma HIV RNA levels due to untreated disease or treatment failure have a greater risk of transmitting HIV to others [32]. Effective ART on a population basis will have important public health advantages.
In addition to the potential consequences of ART error relating to treatment failure and resistance, ART errors may also lead to drug toxicities and drug intolerance, increasing the risk of nonadherence, and further exacerbating the aforementioned consequences.
ART errors also carry the same consequences as errors involving other non-ART medications, such as loss of patient trust, civil and criminal legal consequences, professional board discipline, and increased health care costs [33]. One study reported a cost avoidance of $24,000 annually for inpatient and $124,000 annually for outpatient through the use of pharmacists’ interventions to prevent errors [34]. Another study found that patients experiencing an ART error related to protease inhibitor boosting incurred claims costing 21.5% more than patients not experiencing a boosting error [30].
Contributing Factors
Health care professional–associated factors can also contribute to ART errors. The increasing complexity and specialization of HIV care and the rapidly evolving nature of medication management in this population have created an environment in which many providers without extensive experience in the treatment of HIV are responsible for managing HIV in settings beyond the HIV clinic. A survey of non-HIV specialized physicians conducted in 2007 revealed a poor knowledge base of common ART regimens among these physicians [37]. Likewise, HIV providers may be uncomfortable serving a primary care role for patients with HIV due to their own lack of experience and knowledge of primary care [38]. This issue is becoming more relevant, as non-AIDS comorbidities are emerging as the main health concerns for patients with HIV [39]. Health care professionals’ knowledge of HIV care also contributes to ART errors at other points in the medication use process beyond prescribing. Pharmacists lacking experience in identifying appropriate ART regimens may not recognize errors, and, therefore, may not be able to intervene and prevent errors from occurring.
Medication factors contributing to the risk for errors include risks related to the pharmacologic properties of certain drugs as well as drug naming and labeling factors. Certain antiretroviral classes are known to interact with many medications due to inhibition or induction of metabolic pathways responsible for drug metabolism, such as the cytochrome P-450 pathways. In addition, many antiretroviral medications require “boosting” with another drug to increase systemic exposure of the antiretroviral. Boosting is required for most protease inhibitors and for the integrase inhibitor elvitegravir. For some of these medications, the boosting agent is provided in a co-formulated product. However, for others, a separate prescription for the boosting medication is required. These factors contribute to the risks for drug interactions as well as drug and dosing errors.
Errors may also occur due to drug naming and labeling factors. Confusion due to look-alike/sound-alike medications is common, especially with handwritten or verbally transcribed orders. Examples of look-alike/sound-alike medications include lamivudine/lamotrigine, Viramune/Viread/Viracept, and ritonavir/Retrovir. The use of abbreviations can also lead to error. Reports have described errors associated with zidovudine, which is often abbreviated AZT, being confused with azathioprine [40,41]. An evaluation of ART errors reported to a national medication error reporting program found that look-alike/sound-alike medication names contributed to 19% (77/400) of the errors reported during the 48-month time period evaluated [15].
Several antiretroviral medications are co-formulated into single tablets to decrease pill burden and increase adherence. The use of co-formulated products has the potential to either increase or decrease the risk of errors. Prescribing one co-formulated product rather than its individual components simplifies the prescribing process, allowing the prescriber to become familiar with one product and one dosing scheme in place of 2 or more drugs with different dosing recommendations. The risk of inadvertent omission of a drug and the risk of improper dosing is reduced with the use of co-formulated products. On the other hand, when patients are transitioned from one health care setting to another (such as admission to a hospital), these products may require conversion to the individual components of the drug due to formulary availability and/or cost concerns. Studies have shown that formulary conversions from co-formulated products to individual components are frequently associated with ART errors and that the use of co-formulated products in the inpatient setting reduces these errors [20,22,24,26].
Finally, factors related to the health care setting can influence the risk for errors. High patient numbers, time constraints, and workload stresses can all increase the likelihood that an error will occur [36]. Interruptions and distractions occurring at any point in the medication use process can lead to error.
Transitioning from one health care setting to another also places patients at risk for being harmed by medication errors. Up to 70% of patients may have an unintentional medication discrepancy at hospital discharge, and errors occurring at hospital admission have been reported to affect two-thirds of admitted patients [42]. Many of these errors hold the potential to cause harm to the patient, especially if the errors are carried forward throughout the patient’s admission and after discharge. One study found that 22% of ART errors occurring at hospital admission were attributable to outpatient clinic documentation errors [24]. This highlights the need for improved documentation processes and draws attention to the element of communication at transitional points of care. Lack of adequate resources for medication reconciliation is a widely recognized challenge. This includes resources of personnel as well as electronic medical record systems that can facilitate the reconciliation process. The importance of accurately documenting a patient’s medication history and the ability to easily communicate this information to other health care settings cannot be underestimated. Electronic medical record systems should be developed to facilitate and enhance the processes of reconciliation, documentation, and communication.
Interventions to Address ART Errors
The causes of ART errors are multifactorial and should be addressed using comprehensive approaches tailored to the specific health care setting. Several types of interventions aimed at reducing and preventing ART errors have been evaluated in the literature [12,18,26,27]. In general, these interventions have focused on provider education, use of technology and clinical decision support systems, pharmacist-led medication review and intervention, and hospital formulary changes. Other interventions that may lead to a reduction in ART errors include minimizing polypharmacy, improving medication reconciliation processes during transitions of care, and multidisciplinary follow-up clinic visits after hospital discharge.
Because the sources of ART errors are multifactorial, the optimal strategy to prevent and reduce errors is likely to be a comprehensive approach combining several of the aforementioned interventions. One study showed that a combined approach that included updates to the institution’s computerized physician order entry (CPOE) system, education for the pharmacy and ID departments, and daily review of patients’ medications by pharmacists was successful in reducing the percentage of admissions with an ART error from 50% to 34%. In addition, the time to error resolution decreased from 180 hours to 23 hours, and the error resolution rate increased from 32% to 68% [21]. Another study demonstrated benefits using a comprehensive approach including the dissemination of educational pocket cards for physicians, pharmacists and nurses; CPOE alerts; hospital formulary updates to include co-formulated products; and a daily review of medications by an ID-specialized pharmacist for patients receiving ART. These strategies resulted in a reduced ART error rate from 72% to 15% in 7 months [26]. These studies demonstrate the benefit of multifaceted strategies to reduce ART error rates.
Education
Given the complexity of HIV care and overall lack of antiretroviral medication knowledge among non-ID specialized health care professionals, educational programs aimed at increasing the comfort level and familiarity of ART is important [16,37]. Frequent training to update health care professionals on the newest recommendations for HIV management can help achieve this goal [19,27]. Educational interventions aimed at reducing medication errors have been shown to be transiently effective but may lack sustained effects [43]. Educational programs for health care professionals should be designed to provide frequent brief updates, and are likely to be more successful when combined with other approaches [19,26].
Education directed toward patients, families, and caregivers can also play a pivotal role in error prevention. Patients should be encouraged to use one pharmacy, if possible, to ensure that one complete, accurate, and current profile is maintained. The use of one pharmacy can also assist in the identification of therapeutic duplications and drug interactions. Counseling patients with visual aids, such as charts with pictures of drugs, can also be used as a tool for education. Patients who are familiar with the names and the appearances of their drugs are more likely to recognize errors. In addition, patients should be advised to maintain their own current medication list so that they will be able to provide this information to all of the health care professionals involved in their care [33,44].
Technology and Clinical Decision Support Systems
Overall, the increasing use of technology such as CPOE, decision support systems, and barcoding systems has been shown to decrease the risk of medication error [19,45,46]. Guo et al observed a 35% decrease in ART error rates after the integration of customized order entry sets into an existing CPOE program [19]. Another study reported a 50% decrease in the ART error rate after the introduction of an electronic medical record system [45]. On the other hand, some reports evaluating the role of CPOE systems to reduce medication error rates are conflicting [15,19,23,48]. Differences in system capabilities and programming and differing needs and challenges of institutions may account for the varying results reported in the literature. CPOE systems can serve as valuable tools for assisting in medication prescribing. Confusion due to abbreviations, illegible writing and look-alike/sound-alike drugs should be eliminated or greatly reduced with the use of CPOE. However, the limitations of these systems, which may differ among different systems, should be appreciated. As ART regimens and dosing recommendations change, clinical decision support systems can quickly become out-of-date and require frequent updating. One study identified fields that pre-populated drug names and frequencies within a CPOE system to be the cause of several medication errors [16]. Studies have also identified errors related to disregarded alerts from decision support software [15,16]. “Alert fatigue” is a well-recognized phenomenon that occurs when clinicians are exposed to a large volume of clinical decision support alerts of varying clinical significance. Over time, clinicians begin to become desensitized to the alerts, and they may eventually stop responding to them.
Some limitations of CPOE systems arise from the individual system capabilities. Some systems have the ability to check for appropriate dosing, recommend adjustments in renal dysfunction, and provide alerts for drug interactions, but some systems lack these capabilities. In addition, CPOE systems are often not able to prevent errors of omission, delays in continuation of therapy, and medication scheduling errors [15,45].
Given the limitations of CPOE and clinical decision support technologies, it is unlikely that these interventions alone will be sufficient to fully address the problem of ART errors. These technologies can, however, serve as a powerful tool in the prevention and reduction of ART errors, especially when used in combination with other strategies.
Pharmacist Intervention
Multiple studies have shown that clinical pharmacists are effective at decreasing ART medication errors in the inpatient setting [12,18,23,25,28,45,49,50]. One institution implemented an HIV-specialized pharmacist review strategy that decreased the median time to error correction from 84 hours to 15.5 hours among hospitalized patients [12]. Corrigan et al showed that a review of medications by an HIV-specialized pharmacist 48 hours after hospital admission decreased error rates from 52% to 5% [50]. Another study showed that with the use of an electronic medical record, errors among hospitalized patients with HIV were 9.4 times more likely to be corrected within 24 hours when an HIV-specialized pharmacist was consulted [45].
The majority of studies evaluating the effect of pharmacist interventions have utilized the services of a pharmacist with specialized training in HIV. Few studies have evaluated the impact of interventions by pharmacists without this specialized training. One study retrospectively evaluated and characterized ART errors among hospitalized patients. Medication reconciliation was performed within 24 hours of admission by unit-based pharmacists without specialized training in HIV. Overall, 30.8% of errors were corrected within 24 hours and 14.2% were corrected after 24 hours. However, 54.7% of the errors were not recognized and were never corrected [20]. Just as physicians trained in general medicine lack knowledge of antiretroviral medications, pharmacists without HIV-specialized training may also be less familiar with current ART recommendations [16,37].
Overall, the studies evaluating the impact of pharmacist intervention on reducing ART error rates have shown significant reductions in time to error corrections. The nature of this type of intervention however, lends itself to correction of errors rather than prevention of errors. Indeed, one hospital reported an ART error rate of 29% on the first day of admission compared to 7% on the second day of admission, a decrease that was attributed to retrospective review of medication orders by clinical pharmacists. This study also noted the occurrences of additional errors identified on the second day of admission, highlighting the importance of daily review and follow-up throughout the hospital stay [28].
Hospital Formulary Selections
Several studies have documented an association between hospital formulary options and ART errors [20,22,24,26]. The prescribing of ART medications that are not available on hospital formulary is consistently associated with higher rates of error. Many hospitals minimize the numbers of different medications offered through the maintenance of a formulary. Formularies assist in reducing costs, preserving storage space, and simplifying prescribing. Because some hospitals choose to exclude co-formulated products from the formulary, several ART medications may not be included. In addition, some ART medications may be excluded from formulary due to their infrequent use or higher costs. The extra step of converting a co-formulated product to its individual components increases the risk for errors. In one study, the addition of all co-formulated ART medications to the hospital formulary in combination with several other interventions had a significant effect on reducing the ART error rate [26].
Transitions of Care Interventions
Patients with HIV are at risk for experiencing medication errors and discrepancies any time they transition from one health care setting to another. Hospitalization poses the highest risk as it often disrupts continuity of care and corresponds with a comparatively larger number of medication changes [16,51]. This risk is present on admission, throughout hospitalization, and upon discharge. Perhaps the errors of greatest concern are those that are carried forward after discharge on to the outpatient setting. Medication discrepancies at transitions of care have been associated with increases in adverse events and increased hospital readmission rates [52,53]. One study evaluating adverse events in geriatric patients transitioning from hospital to home found that the most frequently reported adverse events after discharge were related to incorrect drugs or dosages of medication regimens [54]. Tools that can assist in integration and coordination during transitions of care are greatly needed.
One of the most important strategies to prevent and correct medication discrepancies during transitions of care is medication reconciliation. Several studies have demonstrated the efficacy of medication reconciliation in decreasing medication errors [55]. Medication reconciliation is especially important for patients taking many medications. An estimated 14% of patients with HIV older than age 65 take 4 or more medications [56]. This population often requires treatment for other chronic conditions such as hypertension, diabetes, and depression, further increasing the risk for adverse drug events including medication error. Because of the complexities associated with the treatment of HIV and the increased risk for errors, routine medication reconciliation among this population should be a priority.
In addition to medication reconciliation, several studies have evaluated the effects of coordinated pharmacist or multidisciplinary post-discharge follow-up visits for medication therapy management as a strategy to reduce preventable medication-related adverse events [57–59]. Patients receiving clinic-based medication therapy management by a clinical pharmacist after hospital discharge had a lower 60-day hospital readmission rate compared to those who did not have a clinic visit with a pharmacist (18.2% vs. 43.1%) [59]. Another study compared 2 models of post-discharge follow-up, a multidisciplinary team model led by a clinical pharmacist compared to a standard physician-only model. The goal of the multi-disciplinary team model was to complete a thorough medication review, address lifestyle interventions, and address barriers to care. Overall, patients seen by the multidisciplinary team had a 30-day hospital readmission rate of 14.3% compared with a 34.3% readmission rate in the physician-only team [58]. Many different care models have been proposed to improve continuity of care for patients with HIV. The ideal model is not known, and it is likely that several different models would be effective. Optimal models should integrate the patient-physician relationship with multidisciplinary team approaches [60].
Conclusion
The rapidly evolving nature of HIV management and the increase in non–HIV-related comorbidities among this population has created a landscape that places these patients at risk for medication errors. Although ART has improved survival, medication errors place these patients at risk for adverse events and treatment failure. Medication errors are particularly likely to occur during transitions of care. Several interventions to prevent and decrease ART errors have been evaluated including educational strategies, hospital formulary changes, use of technology, and medication review and intervention by clinical pharmacists. However more research is needed to determine optimal strategies to address ART medication errors. Successful approaches have implemented comprehensive methods combining multiple interventions aimed at addressing several distinct sources of error. Promotion of a culture of safety is also an important component of medication error management. Health care professionals should be encouraged to report errors, and lessons learned from errors should be used to guide efforts to prevent future errors. Finally, improved integration of care with a focus on systematic initiatives for medication reconciliation as well as multidisciplinary approaches to transitions of care will be essential for reducing the rate of medication error among patients with HIV.
Corresponding author: Lindsay M. Daniels, PharmD, [email protected].
Financial disclosures: None.
References
1. Egger M, May M, Chene G, et al. Prognosis of HIV-1 infected patients starting highly active, antiretroviral therapy: a collaborative analysis of prospective studies. Lancet 2002;360:119–29.
2. Palella FJ, Delaney KM, Moorman AC, et al. Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. N Engl J Med 1998;338:853–60.
3. May MT, Gompels M, Delpech V, et al. Impact on life expectancy of HIV-1 positive individuals of CD4 cell count and viral load response to antiretroviral therapy. AIDS 2014; 28:1193–202.
4. Greene M, Justice AC, Lampiris HW, Valcour V. Management of HIV infection in advanced age. JAMA 2013;309:1397–1405.
5. Baker JV, Peng G, Rapkin J, et al. CD4+ count and risk of non-AIDS diseases following initial treatment of HIV infection. AIDS 2008;22:841–8.
6. Monforte A, Abrams D, Pradier C, et al. HIV-induced immunodeficiency and mortality from AIDS-defining and non-AIDS-defining malignancies. AIDS 2008;22:2143–53.
7. Buchacz K, Baker RK, Moorman AC, et al. Rates of hospitalizations and associated diagnoses in a large multisite cohort of HIV patients in the United States, 1994-2005. AIDS 2008;22:1345–54.
8. Aspden P, Wolcott J, Bootman JL, et al. Preventing medication errors: quality chasm series. Washington DC: National Academies Press; 2007.
9. Kripalani S, Roumie CL, Dalal AK, et al. Effect of a pharmacist intervention on clinically important medication errors after hospital discharge: a randomized trial. Ann Intern Med 2012;157:1–10.
10. Tam VC, Knowles SR, Cornish PL, et al. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ 2005;173:510–515.
11. Bell CM, Brener SS, Gunraj N, et al. Association of ICU or hospital admission with unintentional discontinuation of medications for chonic diseases. JAMA 2011;306:840–7.
12. Heelon M, Skiest D, Tereso G, et al. Effect of a clinical pharmacist’s interventions on duration of antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2007;64:2064–8.
13. Purdy BD, Raymond AM, Lesar TS. Antiretroviral prescribing errors in hospitalized patients. Ann Pharmacother 2000;34:833–8.
14. Gray J, Hicks RW, Hutchings C. Antiretroviral medication errors in a national medication error database. AIDS Patient Care STDS 2005;19:803–12.
15. Rastegar DA, Knight AM, Monolakis JS. Antiretroviral medication errors among patients with HIV infection. Clin Infect Dis 2006;43:933–8.
16. Snyder AM, Klinker K, Orrick JJ, et al. An in-depth analysis of medication errors in hospitalized patients with HIV. Ann Pharmacother 2011;45:459–68.
17. Edelman EJ, Gordon KS, Glover J, et al. The next therapeutic challenge in HIV: polypharmacy. Drugs Aging 2013;30:613–28.
18. Carcelero E, Tuset M, Martin M, et al. Evaluation of antiretroviral-related errors and interventions by the clinical pharmacist in hospitalized HIV-infected patients. HIV Medicine 2011;12:494–9.
19. Guo Y, Chung P, Weiss C, et al. Customized order-entry sets can prevent antiretroviral prescribing errors: a novel opportunity for antimicrobial stewardship. P T 2015;40:353–8.
20. Commers T, Swindells S, Sayles H, et al. Antiretroviral medication prescribing errors are common with hospitalization of HIV-infected patients. J Antimicrob Chemother 2014;69:262–7.
21. Sanders J, Pallotta A, Bauer S, et al. Antimicrobial stewardship program to reduce antiretroviral medication errors in hospitalized patients with HIV infection. Infect Control Hosp Epidemiol 2014;35:272–7.
22. Chiampas TD, Kim H, Badowski M. Evaluation of the occurrence and type of antiretroviral and opportunistic infection medication errors within the inpatient setting. Pharm Pract 2015;13:512.
23. Eginger KH, Yarborough LL, Inge LD, et al. Medication errors in HIV-infected hospitalized patients: a pharmacist’s impact. Ann Pharmacother 2013;47:953–60.
24. Pastakia SD, Corbett AH, Raasch RH, et al. Frequency of HIV-related medication errors and associated risk factors in hospitalized patients. Ann Pharmacother 2008;42:491–7.
25. Garey KW, Teichner P. Pharmacist intervention program for hospitalized patients with HIV infection. Am J Health Syst Pharm 2000;57:2283–4.
26. Daniels LM, Raasch RH, Corbett AH. Implementation of targeted interventions to decrease antiretroviral-related errors in hospitalized patients. Am J Health Syst Pharm 2012;69:422–30.
27. Li EH, Foisy MM. Antiretroviral and medication errors in hospitalized HIV-positive patients. Ann Pharmacother 2014;48:998–1010.
28. Yehia BR, Mehta JM, Ciuffetelli D, et al. Antiretroviral medication errors remain high but are quickly corrected among hospitalized HIV-infected adults. Clin Infect Dis 2012;55:593–99.
29. Willig JH, Westfall AO, Allison J, et al. Nucleoside reverse-transcriptase inhibitor dosing errors in an outpatient HIV clinic in the electronic medical record era. Clin Infect Dis 2007;45:658–61.
30. Hellinger FJ, Encinosa WE. The cost and incidence of prescribing errors among privately insured HIV patients. Pharmacoeconomics 2010;28:23–34.
31. Deeks SG, Gange SJ, Kitahata MM, et al. Trends in multidrug treatment failure and subsequent mortality among antiretroviral therapy-experienced patients with HIV infection in North America. Clin Infect Dis 2009;49:1582–90.
32. Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med 2011;365:493–505.
33. Wittich CM, Burkle CM, Lanier WL. Medication errors: an overview for clinicians. Mayo Clin Proc 2014;89:1116–25.
34. Merchen BA, Gerzenshtein L, Scarsi KK, et al. Evaluation of HIV-specialized pharmacists’ impact on prescribing errors in hospitalized patients on antiretroviral therapy. 51st Interscience Conference on Antimicrobial Agents and Chemotherapy; 2011 Sep 17-20; Chicago IL. Abstract H2–794.
35. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997;277:312–17.
36. Agu KA, Oqua D, Adeyanju Z, et al. The incidence and types of medication errors in patients receiving antiretroviral therapy in resource constrained settings. PLoS ONE 2014;9:e87338.
37. Arshad S, Rothberg M, Rastegar DA, et al. Survey of physician knowledge regarding antiretroviral medications in hospitalized HIV-infected patients. J Int AIDS Soc 2009;12:1.
38. Fultz SL, Goulet JL, Weissman S, et al. Differences between infectious diseases-certified physicians and general medicine-certified physicians in the level of comfort with providing primary care to patients. Clin Infect Dis 2005;41:738–43.
39. Cheng QJ, Engelage EM, Grogan TR, et al. Who provides primary care? An assessment of HIV patient and provider practices and preferences. J AIDS Clin Res 2014;5:366.
40. Cohen MR, Davis NM. AZT is a dangerous abbreviation. Am Pharm 1992;32:26.
41. Ambrosini MT, Mandler HD, Wood CA. AZT: zidovudine or azathioprine? Lancet 1992;339:935.
42. Sponsler KC, Neal EB, Kripalani S. Improving medication safety during hospital-based transitions of care. Cleve Clin J Med 2015;82:351–60.
43. Peeters MJ, Pinto SL. Assessing the impact of an educational program on decreasing prescribing errors at a university hospital. J Hosp Med 2009;4:97–101.
44. Faragon JJ, Lesar TS. Update on prescribing errors with HAART. AIDS Read 2003;13:268–78.
45. Batra R, Wolbach-Lowes J, Swindells S, et al. Impact of an electronic medical record on the incidence of antiretroviral prescription errors and HIV pharmacist reconciliation on error correction among hospitalized HIV-infected patients. Antivir Ther 2015:2040–58.
46. Keers RN, Williams SD, Cooke J, et al. Impact of interventions designed to reduce medication administration errors in hospitals: a systematic review. Drug Saf 2014;37:317–32.
47. Reckmann MH, Westbrook JI, Koh Y, et al. Does computerized provider order entry reduce prescribing errors for hospital inpatients? A systematic review. J Am Med Inform Assoc 2009;16:613–23.
48. Bozek PS, Perdue BE, Bar-Din M, Weidle PJ. Effect of pharmacist interventions on medication use and cost in hospitalized patients with or without HIV infection. Am J Health Syst Pharm 1998;55:1151–5.
49. De Maat MM, de Boer A, Koks CH, et al. Evaluation of clinical pharmacist interventions on drug interactions in outpatient pharmaceutical HIV care. J Clin Pharm Ther 2004;29:121–30.
50. Corrigan MA, Atkinson KM, Sha BE, Crank CW. Evaluation of pharmacy-implemented medication reconciliation directed at antiretroviral therapy in hospitalized HIV/AIDS patients. Ann Pharmacother 2010;44:222–3.
51. Rao N, Patel V, Grigoriu A, et al. Antiretroviral therapy prescribing in hospitalized HIV clinic patients. HIV Med 2012;13:367–71.
52. Coleman EA, Smith JD, Raha D, Min S. Posthospital medication discrepancies. Arch Intern Med 2005;165:1842–7.
53. Forster AJ, Murff HJ, Peterson JF, et al. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med 2003;138:161–7.
54. Mesteig M, Helbostad JL, Sletvold O, et al. Unwanted incidents during transition of geriatric patients from hospital to home: a prospective observational study. BMC Health Serv Res 2010;10:1.
55. Mueller SK, Sponsler KC, Kripalani S, Schnipper JL. Hospital-based medication reconciliation practices: a systematic review. Arch Intern Med 2012;172:1057–69.
56. Hasse B, Ledergerber B, Furrer H, et al. Morbidity and aging in HIV-infected persons: the Swiss HIV Cohort Study. Clin Infect Dis 2011;53:1130–9.
57. Downes JM, O’Neal KS, Miller MJ, et al. Identifying opportunities to improve medication management in transitions of care. Am J Health Syst Pharm 2015;72:S58–69.
58. Cavanaugh JJ, Lindsey KN, Shilliday BB, Ratner SP. Pharmacist-coordinated multidisciplinary hospital follow-up visits improve patient outcomes. J Manag Care Spec Pharm 2015;21:256–60.
59. Bellone JM, Barner JC, Lopez DA. Postdischarge interventions by pharmacists and impact on hospital readmission rates. J Am Pharm Assoc 2012;52:358–62.
60. Handford CD, Tynan AM, Rackal JM, Glazier RH. Setting and organization of care for persons living with HIV/AIDS. Cochrane Database Syst Rev 2006;19:CD004348.
Standing Linked to Reduced Obesity
Study Overview
Objective. To examine the cross-sectional relationships between standing time, obesity, and metabolic syndrome.
Design. Cross-sectional study.
Setting and participants. Participants were patients aged 20–79 years old attending Cooper Clinic in Dallas for a preventive medicine visit who enrolled in the Cooper Center Longitudinal Study, an ongoing prospective investigation established in 1970 to explore the effects of physical activity on morbidity and mortality [1]. Included in the analysis were those enrolled starting in 2010, when questions pertaining to standing patterns began to be included in the medical history. Patients who did not have complete information or who had a history of myocardial infarction, stroke, or cancer were excluded.
Measures. Obesity was directly measured using body mass index (≥ 30), waist circumference (men: ≥ 102 cm; women: ≥ 88 cm), and body fat percentage (men: ≥ 25%; women ≥ 30%) and was adjusted for history of diabetes and hypertension. Metabolic syndrome, a clustering of risk factors that increase the risk for heart disease, stroke, and diabetes, was assessed. Participants’ standing patterns were ascertained from responses to survey questions derived from the Canada Fitness Survey Questionnaire (“For those activities that you do most days of the week, such as work, school, and housework, how much time do you spend standing: Almost all of the time, ¾ of the time, ½ of the time, ¼ of the time, almost none of the time?”). Leisure-time physical activity was determined based on responses to survey questions, and answers were used to categorize participants as either meeting or not meeting the Physical Activity Guidelines for Americans.
Results. The study sample consisted of 7075 participants, who were primarily white and college educated. Over two-thirds were men and the mean age was 50.0 ± 10.1 years. Multivariable analysis showed that in men, increased standing was significantly associated with a lower likelihood of elevated body fat percentage. Specifically, standing a quarter of the time was linked to a 32% reduced likelihood of obesity (body fat percentage), standing half the time was associated with a 59% reduced likelihood of obesity, but standing more than three-quarters of the time was not associated with a lower risk of obesity. In women, standing a quarter, half, and three-quarters of the time was associated with 35%, 47%, and 57% respective reductions in the likelihood of abdominal obesity (waist circumference). No relationship between standing and metabolic syndrome was found among women or men.
The study also examined whether physical activity in conjunction with standing provided additional reduction risk for obesity. The study showed that 150 minutes of moderate activity and/or 75 minutes of vigorous activity per week added to standing time was associated with significant reduction in the probability of obesity and metabolic syndrome in both women and men.
Conclusion. Standing a quarter of the time per day or more is associated with reduced odds of obesity. The inverse relationship of standing to obesity and metabolic syndrome is more robust when combined with health-promoting leisure-time physical activity.
Commentary
Obesity is considered one of the main risk factors for cardiovascular diseases worldwide. Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer, some of the leading causes of preventable death. The effects of obesity among Americans add more than $147 billion in medical costs to the U.S. economy annually [2].
Obesity is a national epidemic, with more than 78.9 million obese adults in the United States [2]. Studies have shown that Americans are currently less active as compared to past decades [3]. This decline in physical activity combined with other factors, such as the ubiquity of low-cost high-energy foods and beverages, has likely contributed to the high rate of obesity.
This cross-sectional study aimed to assess the relationship between standing time, obesity, and metabolic syndrome alongside and independent of leisure-time physical activity. The researchers found that standing for at least one quarter of the day is linked to lower odds of obesity, which was directly assessed through 3 measures: BMI, body fat percentage, and waist circumference. The apparent benefit of standing is an important finding in light of obesity being such an important public health concern.
The large sample size is a strength of this study in terms of statistical power; however, there are important limitations that must be acknowledged. First, given the cross-sectional design, no causal inferences can be made. Moreover, while obesity and metabolic syndrome were objectively measured, standing and physical activity were based on self-report, which may lead to over- or underestimation of these behaviors. In addition, due to the survey measure used in the study, it is unclear whether study participants were standing still or standing and moving. More information in this regard would be helpful. Longitudinal research is encouraged in order to provide better evidence of these relationships and their effects.
In addition, cultural aspects were not assessed in this study. Racial and ethnic differences may influence the relationship between the variables of physical activity and obesity reduction.
Applications for Clinical Practice
Obesity is a complex but preventable health problem commonly associated with sedentary lifestyle. Physical activity is recommended as a component of weight management for prevention of weight gain and for weight loss [4]. Whether standing more often will aid in reducing obesity cannot be determined from this study.
—Paloma Cesar de Sales, BS, RN, MS
1. Shuval K, Finley CE, Barlow CE, et al. Sedentary behavior, cardiorespiratory fitness, physical activity, and cardiometabolic risk in men: the cooper center longitudinal study. Mayo Clin Proc 2014;89:1052–62.
2. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA 2014;311:806–14.
3. Ng SW, Popkin BM. Time use and physical activity: a shift away from movement across the globe. Obes Rev 2012;13:659–80.
4. Jensen MD, Ryan DH, Apovian CM, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 2014;129(25 Suppl 2):S102–38.
Study Overview
Objective. To examine the cross-sectional relationships between standing time, obesity, and metabolic syndrome.
Design. Cross-sectional study.
Setting and participants. Participants were patients aged 20–79 years old attending Cooper Clinic in Dallas for a preventive medicine visit who enrolled in the Cooper Center Longitudinal Study, an ongoing prospective investigation established in 1970 to explore the effects of physical activity on morbidity and mortality [1]. Included in the analysis were those enrolled starting in 2010, when questions pertaining to standing patterns began to be included in the medical history. Patients who did not have complete information or who had a history of myocardial infarction, stroke, or cancer were excluded.
Measures. Obesity was directly measured using body mass index (≥ 30), waist circumference (men: ≥ 102 cm; women: ≥ 88 cm), and body fat percentage (men: ≥ 25%; women ≥ 30%) and was adjusted for history of diabetes and hypertension. Metabolic syndrome, a clustering of risk factors that increase the risk for heart disease, stroke, and diabetes, was assessed. Participants’ standing patterns were ascertained from responses to survey questions derived from the Canada Fitness Survey Questionnaire (“For those activities that you do most days of the week, such as work, school, and housework, how much time do you spend standing: Almost all of the time, ¾ of the time, ½ of the time, ¼ of the time, almost none of the time?”). Leisure-time physical activity was determined based on responses to survey questions, and answers were used to categorize participants as either meeting or not meeting the Physical Activity Guidelines for Americans.
Results. The study sample consisted of 7075 participants, who were primarily white and college educated. Over two-thirds were men and the mean age was 50.0 ± 10.1 years. Multivariable analysis showed that in men, increased standing was significantly associated with a lower likelihood of elevated body fat percentage. Specifically, standing a quarter of the time was linked to a 32% reduced likelihood of obesity (body fat percentage), standing half the time was associated with a 59% reduced likelihood of obesity, but standing more than three-quarters of the time was not associated with a lower risk of obesity. In women, standing a quarter, half, and three-quarters of the time was associated with 35%, 47%, and 57% respective reductions in the likelihood of abdominal obesity (waist circumference). No relationship between standing and metabolic syndrome was found among women or men.
The study also examined whether physical activity in conjunction with standing provided additional reduction risk for obesity. The study showed that 150 minutes of moderate activity and/or 75 minutes of vigorous activity per week added to standing time was associated with significant reduction in the probability of obesity and metabolic syndrome in both women and men.
Conclusion. Standing a quarter of the time per day or more is associated with reduced odds of obesity. The inverse relationship of standing to obesity and metabolic syndrome is more robust when combined with health-promoting leisure-time physical activity.
Commentary
Obesity is considered one of the main risk factors for cardiovascular diseases worldwide. Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer, some of the leading causes of preventable death. The effects of obesity among Americans add more than $147 billion in medical costs to the U.S. economy annually [2].
Obesity is a national epidemic, with more than 78.9 million obese adults in the United States [2]. Studies have shown that Americans are currently less active as compared to past decades [3]. This decline in physical activity combined with other factors, such as the ubiquity of low-cost high-energy foods and beverages, has likely contributed to the high rate of obesity.
This cross-sectional study aimed to assess the relationship between standing time, obesity, and metabolic syndrome alongside and independent of leisure-time physical activity. The researchers found that standing for at least one quarter of the day is linked to lower odds of obesity, which was directly assessed through 3 measures: BMI, body fat percentage, and waist circumference. The apparent benefit of standing is an important finding in light of obesity being such an important public health concern.
The large sample size is a strength of this study in terms of statistical power; however, there are important limitations that must be acknowledged. First, given the cross-sectional design, no causal inferences can be made. Moreover, while obesity and metabolic syndrome were objectively measured, standing and physical activity were based on self-report, which may lead to over- or underestimation of these behaviors. In addition, due to the survey measure used in the study, it is unclear whether study participants were standing still or standing and moving. More information in this regard would be helpful. Longitudinal research is encouraged in order to provide better evidence of these relationships and their effects.
In addition, cultural aspects were not assessed in this study. Racial and ethnic differences may influence the relationship between the variables of physical activity and obesity reduction.
Applications for Clinical Practice
Obesity is a complex but preventable health problem commonly associated with sedentary lifestyle. Physical activity is recommended as a component of weight management for prevention of weight gain and for weight loss [4]. Whether standing more often will aid in reducing obesity cannot be determined from this study.
—Paloma Cesar de Sales, BS, RN, MS
Study Overview
Objective. To examine the cross-sectional relationships between standing time, obesity, and metabolic syndrome.
Design. Cross-sectional study.
Setting and participants. Participants were patients aged 20–79 years old attending Cooper Clinic in Dallas for a preventive medicine visit who enrolled in the Cooper Center Longitudinal Study, an ongoing prospective investigation established in 1970 to explore the effects of physical activity on morbidity and mortality [1]. Included in the analysis were those enrolled starting in 2010, when questions pertaining to standing patterns began to be included in the medical history. Patients who did not have complete information or who had a history of myocardial infarction, stroke, or cancer were excluded.
Measures. Obesity was directly measured using body mass index (≥ 30), waist circumference (men: ≥ 102 cm; women: ≥ 88 cm), and body fat percentage (men: ≥ 25%; women ≥ 30%) and was adjusted for history of diabetes and hypertension. Metabolic syndrome, a clustering of risk factors that increase the risk for heart disease, stroke, and diabetes, was assessed. Participants’ standing patterns were ascertained from responses to survey questions derived from the Canada Fitness Survey Questionnaire (“For those activities that you do most days of the week, such as work, school, and housework, how much time do you spend standing: Almost all of the time, ¾ of the time, ½ of the time, ¼ of the time, almost none of the time?”). Leisure-time physical activity was determined based on responses to survey questions, and answers were used to categorize participants as either meeting or not meeting the Physical Activity Guidelines for Americans.
Results. The study sample consisted of 7075 participants, who were primarily white and college educated. Over two-thirds were men and the mean age was 50.0 ± 10.1 years. Multivariable analysis showed that in men, increased standing was significantly associated with a lower likelihood of elevated body fat percentage. Specifically, standing a quarter of the time was linked to a 32% reduced likelihood of obesity (body fat percentage), standing half the time was associated with a 59% reduced likelihood of obesity, but standing more than three-quarters of the time was not associated with a lower risk of obesity. In women, standing a quarter, half, and three-quarters of the time was associated with 35%, 47%, and 57% respective reductions in the likelihood of abdominal obesity (waist circumference). No relationship between standing and metabolic syndrome was found among women or men.
The study also examined whether physical activity in conjunction with standing provided additional reduction risk for obesity. The study showed that 150 minutes of moderate activity and/or 75 minutes of vigorous activity per week added to standing time was associated with significant reduction in the probability of obesity and metabolic syndrome in both women and men.
Conclusion. Standing a quarter of the time per day or more is associated with reduced odds of obesity. The inverse relationship of standing to obesity and metabolic syndrome is more robust when combined with health-promoting leisure-time physical activity.
Commentary
Obesity is considered one of the main risk factors for cardiovascular diseases worldwide. Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer, some of the leading causes of preventable death. The effects of obesity among Americans add more than $147 billion in medical costs to the U.S. economy annually [2].
Obesity is a national epidemic, with more than 78.9 million obese adults in the United States [2]. Studies have shown that Americans are currently less active as compared to past decades [3]. This decline in physical activity combined with other factors, such as the ubiquity of low-cost high-energy foods and beverages, has likely contributed to the high rate of obesity.
This cross-sectional study aimed to assess the relationship between standing time, obesity, and metabolic syndrome alongside and independent of leisure-time physical activity. The researchers found that standing for at least one quarter of the day is linked to lower odds of obesity, which was directly assessed through 3 measures: BMI, body fat percentage, and waist circumference. The apparent benefit of standing is an important finding in light of obesity being such an important public health concern.
The large sample size is a strength of this study in terms of statistical power; however, there are important limitations that must be acknowledged. First, given the cross-sectional design, no causal inferences can be made. Moreover, while obesity and metabolic syndrome were objectively measured, standing and physical activity were based on self-report, which may lead to over- or underestimation of these behaviors. In addition, due to the survey measure used in the study, it is unclear whether study participants were standing still or standing and moving. More information in this regard would be helpful. Longitudinal research is encouraged in order to provide better evidence of these relationships and their effects.
In addition, cultural aspects were not assessed in this study. Racial and ethnic differences may influence the relationship between the variables of physical activity and obesity reduction.
Applications for Clinical Practice
Obesity is a complex but preventable health problem commonly associated with sedentary lifestyle. Physical activity is recommended as a component of weight management for prevention of weight gain and for weight loss [4]. Whether standing more often will aid in reducing obesity cannot be determined from this study.
—Paloma Cesar de Sales, BS, RN, MS
1. Shuval K, Finley CE, Barlow CE, et al. Sedentary behavior, cardiorespiratory fitness, physical activity, and cardiometabolic risk in men: the cooper center longitudinal study. Mayo Clin Proc 2014;89:1052–62.
2. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA 2014;311:806–14.
3. Ng SW, Popkin BM. Time use and physical activity: a shift away from movement across the globe. Obes Rev 2012;13:659–80.
4. Jensen MD, Ryan DH, Apovian CM, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 2014;129(25 Suppl 2):S102–38.
1. Shuval K, Finley CE, Barlow CE, et al. Sedentary behavior, cardiorespiratory fitness, physical activity, and cardiometabolic risk in men: the cooper center longitudinal study. Mayo Clin Proc 2014;89:1052–62.
2. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA 2014;311:806–14.
3. Ng SW, Popkin BM. Time use and physical activity: a shift away from movement across the globe. Obes Rev 2012;13:659–80.
4. Jensen MD, Ryan DH, Apovian CM, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 2014;129(25 Suppl 2):S102–38.
Hodgkin lymphoma going untreated in patients with HIV

cultured lymphocyte
Image courtesy of the CDC
Patients with HIV-associated Hodgkin lymphoma may not be getting potentially curative treatment, according to a study published in the journal AIDS.
The study showed that 16% of HIV-positive patients did not receive treatment for their lymphoma, compared to 9% of Hodgkin lymphoma patients who were HIV-negative.
“Hodgkin lymphoma is generally believed to be highly curable,” said study author Adam Olszewski, MD, of Brown University in Providence, Rhode Island.
“We have an expectation to cure over 90% of early stage patients and even 70% to 80% of quite advanced cases.”
It hasn’t been clear whether HIV-positive patients with Hodgkin lymphoma survive the cancer as well as people who are HIV-negative. While some small studies, particularly in Europe, have shown that HIV status makes no difference to survival, observations in the US population suggest that being HIV-positive makes survival less likely.
The new study, which is the largest of its kind to date, may reconcile that conflict. It suggests that, in the US, the reason people with HIV seem to fare worse with the cancer is because they are less likely to be treated for it.
The study included 2090 cases of HIV-associated Hodgkin lymphoma recorded in the National Cancer Data Base between 2004 and 2012, as well as 41,846 cases of Hodgkin lymphoma in patients who were HIV-negative.
The unadjusted 5-year overall survival was 66% for HIV-positive patients and 80% for the HIV-negative population.
Among the HIV-positive patients, 81% received chemotherapy (12% in combination with radiation), 13% received any radiation therapy, and 16% received no treatment for their lymphoma. The corresponding numbers for HIV-negative patients were 87%, 31%, and 9%, respectively (P<0.00001 for all comparisons).
The researchers assessed patient- and disease-related factors associated with the risk of not receiving chemotherapy in the HIV-positive population.
And they found the risk was significantly higher for patients who were older than 40, male, “nonwhite” (black, Hispanic, or Asian/”other”), did not have health insurance, lived in areas with the lowest median income, and had early stage Hodgkin lymphoma or an undetermined histology.
Dr Olszewski said the lack of treatment among HIV-positive patients could be due to a lingering assumption that they won’t tolerate the treatment well. Or some patients may be declining treatment, either for HIV (thereby making them seem more vulnerable) or for the lymphoma itself.
He noted, however, that lymphoma treatment can be effective for and tolerated by HIV-positive patients, especially when the lymphoma subtype is known.
Among the patients who received chemotherapy in this study, there was no significant difference in the hazard of death between HIV-positive and HIV-negative patients who had one of the defined classical histologic subtypes: nodular sclerosis, mixed cellularity, lymphocyte-rich, or lymphocyte-depleted Hodgkin lymphoma. However, mortality was significantly higher for HIV-positive patients with an undetermined histologic subtype. ![]()

cultured lymphocyte
Image courtesy of the CDC
Patients with HIV-associated Hodgkin lymphoma may not be getting potentially curative treatment, according to a study published in the journal AIDS.
The study showed that 16% of HIV-positive patients did not receive treatment for their lymphoma, compared to 9% of Hodgkin lymphoma patients who were HIV-negative.
“Hodgkin lymphoma is generally believed to be highly curable,” said study author Adam Olszewski, MD, of Brown University in Providence, Rhode Island.
“We have an expectation to cure over 90% of early stage patients and even 70% to 80% of quite advanced cases.”
It hasn’t been clear whether HIV-positive patients with Hodgkin lymphoma survive the cancer as well as people who are HIV-negative. While some small studies, particularly in Europe, have shown that HIV status makes no difference to survival, observations in the US population suggest that being HIV-positive makes survival less likely.
The new study, which is the largest of its kind to date, may reconcile that conflict. It suggests that, in the US, the reason people with HIV seem to fare worse with the cancer is because they are less likely to be treated for it.
The study included 2090 cases of HIV-associated Hodgkin lymphoma recorded in the National Cancer Data Base between 2004 and 2012, as well as 41,846 cases of Hodgkin lymphoma in patients who were HIV-negative.
The unadjusted 5-year overall survival was 66% for HIV-positive patients and 80% for the HIV-negative population.
Among the HIV-positive patients, 81% received chemotherapy (12% in combination with radiation), 13% received any radiation therapy, and 16% received no treatment for their lymphoma. The corresponding numbers for HIV-negative patients were 87%, 31%, and 9%, respectively (P<0.00001 for all comparisons).
The researchers assessed patient- and disease-related factors associated with the risk of not receiving chemotherapy in the HIV-positive population.
And they found the risk was significantly higher for patients who were older than 40, male, “nonwhite” (black, Hispanic, or Asian/”other”), did not have health insurance, lived in areas with the lowest median income, and had early stage Hodgkin lymphoma or an undetermined histology.
Dr Olszewski said the lack of treatment among HIV-positive patients could be due to a lingering assumption that they won’t tolerate the treatment well. Or some patients may be declining treatment, either for HIV (thereby making them seem more vulnerable) or for the lymphoma itself.
He noted, however, that lymphoma treatment can be effective for and tolerated by HIV-positive patients, especially when the lymphoma subtype is known.
Among the patients who received chemotherapy in this study, there was no significant difference in the hazard of death between HIV-positive and HIV-negative patients who had one of the defined classical histologic subtypes: nodular sclerosis, mixed cellularity, lymphocyte-rich, or lymphocyte-depleted Hodgkin lymphoma. However, mortality was significantly higher for HIV-positive patients with an undetermined histologic subtype. ![]()

cultured lymphocyte
Image courtesy of the CDC
Patients with HIV-associated Hodgkin lymphoma may not be getting potentially curative treatment, according to a study published in the journal AIDS.
The study showed that 16% of HIV-positive patients did not receive treatment for their lymphoma, compared to 9% of Hodgkin lymphoma patients who were HIV-negative.
“Hodgkin lymphoma is generally believed to be highly curable,” said study author Adam Olszewski, MD, of Brown University in Providence, Rhode Island.
“We have an expectation to cure over 90% of early stage patients and even 70% to 80% of quite advanced cases.”
It hasn’t been clear whether HIV-positive patients with Hodgkin lymphoma survive the cancer as well as people who are HIV-negative. While some small studies, particularly in Europe, have shown that HIV status makes no difference to survival, observations in the US population suggest that being HIV-positive makes survival less likely.
The new study, which is the largest of its kind to date, may reconcile that conflict. It suggests that, in the US, the reason people with HIV seem to fare worse with the cancer is because they are less likely to be treated for it.
The study included 2090 cases of HIV-associated Hodgkin lymphoma recorded in the National Cancer Data Base between 2004 and 2012, as well as 41,846 cases of Hodgkin lymphoma in patients who were HIV-negative.
The unadjusted 5-year overall survival was 66% for HIV-positive patients and 80% for the HIV-negative population.
Among the HIV-positive patients, 81% received chemotherapy (12% in combination with radiation), 13% received any radiation therapy, and 16% received no treatment for their lymphoma. The corresponding numbers for HIV-negative patients were 87%, 31%, and 9%, respectively (P<0.00001 for all comparisons).
The researchers assessed patient- and disease-related factors associated with the risk of not receiving chemotherapy in the HIV-positive population.
And they found the risk was significantly higher for patients who were older than 40, male, “nonwhite” (black, Hispanic, or Asian/”other”), did not have health insurance, lived in areas with the lowest median income, and had early stage Hodgkin lymphoma or an undetermined histology.
Dr Olszewski said the lack of treatment among HIV-positive patients could be due to a lingering assumption that they won’t tolerate the treatment well. Or some patients may be declining treatment, either for HIV (thereby making them seem more vulnerable) or for the lymphoma itself.
He noted, however, that lymphoma treatment can be effective for and tolerated by HIV-positive patients, especially when the lymphoma subtype is known.
Among the patients who received chemotherapy in this study, there was no significant difference in the hazard of death between HIV-positive and HIV-negative patients who had one of the defined classical histologic subtypes: nodular sclerosis, mixed cellularity, lymphocyte-rich, or lymphocyte-depleted Hodgkin lymphoma. However, mortality was significantly higher for HIV-positive patients with an undetermined histologic subtype. ![]()
Watchdog says trial was unethical
Photo courtesy of
The Medicines Company
The watchdog group Public Citizen is alleging that ethics violations were made during the CHAMPION PHOENIX trial, in which researchers compared cangrelor and clopidogrel as thromboprophylaxis for patients undergoing coronary stent procedures.
Public Citizen said the trial “needlessly threatened” the lives of subjects assigned to the control group, and trial participants may not have been informed about the potential risks of enrollment.
Public Citizen sent a letter to the Office of Research Oversight (ORO) at the US Department of Veterans Affairs (VA) asserting that the CHAMPION PHOENIX trial unnecessarily increased the risk of death, heart attack, and other adverse cardiac events for subjects placed in the control group.
The trial was conducted at 153 institutions around the world, including 3 VA facilities: the Dallas VA Medical Center, the Jesse Brown VA Medical Center in Chicago, and the VA Boston Healthcare System. The study involved more than 11,000 subjects, 84 of whom were patients at the 3 VA medical centers.
The primary goal of the trial was to determine whether cangrelor is more effective than clopidogrel at preventing death, heart attacks, and other serious cardiac complications in patients undergoing coronary artery stent procedures.
Public Citizen said the increased risk to subjects in the control group resulted from failure to ensure they were treated with clopidogrel prior to their coronary stent procedures.
An analysis by a senior medical reviewer at the US Food and Drug Administration revealed that failure to administer the necessary antiplatelet treatment occurred in 89% of subjects enrolled at the 3 VA facilities, compared with 30% of subjects enrolled at non-VA facilities.
“The seriously flawed trial protocol paved the way for inappropriate and shocking delays in antiplatelet therapy for subjects enrolled in the control group at all trial institutions,” said Michael Carome, MD, director of Public Citizen’s Health Research Group.
“Inexplicably, the rate of such delays was extraordinarily high at the VA trial sites, making participation in the trial even more hazardous for subjects randomized to the control group at those sites compared with other sites.”
Public Citizen’s complaint contends that the trial’s research protocol was unethical because it failed to require that control group subjects receive lifesaving antiplatelet medications as soon as possible prior to undergoing coronary artery stent procedures.
Prior research conducted by the same research team, expert clinical practice guidelines, and other data available to the researchers established that withholding clopidogrel until after the coronary stent procedures constitutes substandard care.
Indeed, one of the two lead researchers for the trial stated publicly before the trial’s initiation, “If you ask the experts, they will all tell you to give antiplatelet therapy upfront before the PCI [coronary stent] procedure.”
Public Citizen is calling on the ORO to investigate why the institutional review boards responsible for reviewing human research at the 3 VA medical facilities approved the trial given a design that was unethical and failed to minimize the risks to the control group subjects.
The complaint also urges the ORO to investigate whether proper consent of the subjects was obtained in light of the risks, as required by the VA’s human subjects protection rules.
Public Citizen said another issue that requires further inquiry—but falls outside the scope of the ORO’s jurisdiction—is whether inappropriate delays in antiplatelet therapy were more widespread at VA healthcare facilities for patients who did not participate in the trial.
In a separate letter, Public Citizen urged the VA’s Office of Inspector General to launch an investigation to find out. ![]()

Photo courtesy of
The Medicines Company
The watchdog group Public Citizen is alleging that ethics violations were made during the CHAMPION PHOENIX trial, in which researchers compared cangrelor and clopidogrel as thromboprophylaxis for patients undergoing coronary stent procedures.
Public Citizen said the trial “needlessly threatened” the lives of subjects assigned to the control group, and trial participants may not have been informed about the potential risks of enrollment.
Public Citizen sent a letter to the Office of Research Oversight (ORO) at the US Department of Veterans Affairs (VA) asserting that the CHAMPION PHOENIX trial unnecessarily increased the risk of death, heart attack, and other adverse cardiac events for subjects placed in the control group.
The trial was conducted at 153 institutions around the world, including 3 VA facilities: the Dallas VA Medical Center, the Jesse Brown VA Medical Center in Chicago, and the VA Boston Healthcare System. The study involved more than 11,000 subjects, 84 of whom were patients at the 3 VA medical centers.
The primary goal of the trial was to determine whether cangrelor is more effective than clopidogrel at preventing death, heart attacks, and other serious cardiac complications in patients undergoing coronary artery stent procedures.
Public Citizen said the increased risk to subjects in the control group resulted from failure to ensure they were treated with clopidogrel prior to their coronary stent procedures.
An analysis by a senior medical reviewer at the US Food and Drug Administration revealed that failure to administer the necessary antiplatelet treatment occurred in 89% of subjects enrolled at the 3 VA facilities, compared with 30% of subjects enrolled at non-VA facilities.
“The seriously flawed trial protocol paved the way for inappropriate and shocking delays in antiplatelet therapy for subjects enrolled in the control group at all trial institutions,” said Michael Carome, MD, director of Public Citizen’s Health Research Group.
“Inexplicably, the rate of such delays was extraordinarily high at the VA trial sites, making participation in the trial even more hazardous for subjects randomized to the control group at those sites compared with other sites.”
Public Citizen’s complaint contends that the trial’s research protocol was unethical because it failed to require that control group subjects receive lifesaving antiplatelet medications as soon as possible prior to undergoing coronary artery stent procedures.
Prior research conducted by the same research team, expert clinical practice guidelines, and other data available to the researchers established that withholding clopidogrel until after the coronary stent procedures constitutes substandard care.
Indeed, one of the two lead researchers for the trial stated publicly before the trial’s initiation, “If you ask the experts, they will all tell you to give antiplatelet therapy upfront before the PCI [coronary stent] procedure.”
Public Citizen is calling on the ORO to investigate why the institutional review boards responsible for reviewing human research at the 3 VA medical facilities approved the trial given a design that was unethical and failed to minimize the risks to the control group subjects.
The complaint also urges the ORO to investigate whether proper consent of the subjects was obtained in light of the risks, as required by the VA’s human subjects protection rules.
Public Citizen said another issue that requires further inquiry—but falls outside the scope of the ORO’s jurisdiction—is whether inappropriate delays in antiplatelet therapy were more widespread at VA healthcare facilities for patients who did not participate in the trial.
In a separate letter, Public Citizen urged the VA’s Office of Inspector General to launch an investigation to find out. ![]()

Photo courtesy of
The Medicines Company
The watchdog group Public Citizen is alleging that ethics violations were made during the CHAMPION PHOENIX trial, in which researchers compared cangrelor and clopidogrel as thromboprophylaxis for patients undergoing coronary stent procedures.
Public Citizen said the trial “needlessly threatened” the lives of subjects assigned to the control group, and trial participants may not have been informed about the potential risks of enrollment.
Public Citizen sent a letter to the Office of Research Oversight (ORO) at the US Department of Veterans Affairs (VA) asserting that the CHAMPION PHOENIX trial unnecessarily increased the risk of death, heart attack, and other adverse cardiac events for subjects placed in the control group.
The trial was conducted at 153 institutions around the world, including 3 VA facilities: the Dallas VA Medical Center, the Jesse Brown VA Medical Center in Chicago, and the VA Boston Healthcare System. The study involved more than 11,000 subjects, 84 of whom were patients at the 3 VA medical centers.
The primary goal of the trial was to determine whether cangrelor is more effective than clopidogrel at preventing death, heart attacks, and other serious cardiac complications in patients undergoing coronary artery stent procedures.
Public Citizen said the increased risk to subjects in the control group resulted from failure to ensure they were treated with clopidogrel prior to their coronary stent procedures.
An analysis by a senior medical reviewer at the US Food and Drug Administration revealed that failure to administer the necessary antiplatelet treatment occurred in 89% of subjects enrolled at the 3 VA facilities, compared with 30% of subjects enrolled at non-VA facilities.
“The seriously flawed trial protocol paved the way for inappropriate and shocking delays in antiplatelet therapy for subjects enrolled in the control group at all trial institutions,” said Michael Carome, MD, director of Public Citizen’s Health Research Group.
“Inexplicably, the rate of such delays was extraordinarily high at the VA trial sites, making participation in the trial even more hazardous for subjects randomized to the control group at those sites compared with other sites.”
Public Citizen’s complaint contends that the trial’s research protocol was unethical because it failed to require that control group subjects receive lifesaving antiplatelet medications as soon as possible prior to undergoing coronary artery stent procedures.
Prior research conducted by the same research team, expert clinical practice guidelines, and other data available to the researchers established that withholding clopidogrel until after the coronary stent procedures constitutes substandard care.
Indeed, one of the two lead researchers for the trial stated publicly before the trial’s initiation, “If you ask the experts, they will all tell you to give antiplatelet therapy upfront before the PCI [coronary stent] procedure.”
Public Citizen is calling on the ORO to investigate why the institutional review boards responsible for reviewing human research at the 3 VA medical facilities approved the trial given a design that was unethical and failed to minimize the risks to the control group subjects.
The complaint also urges the ORO to investigate whether proper consent of the subjects was obtained in light of the risks, as required by the VA’s human subjects protection rules.
Public Citizen said another issue that requires further inquiry—but falls outside the scope of the ORO’s jurisdiction—is whether inappropriate delays in antiplatelet therapy were more widespread at VA healthcare facilities for patients who did not participate in the trial.
In a separate letter, Public Citizen urged the VA’s Office of Inspector General to launch an investigation to find out. ![]()
Concomitant Sensitization to Inhaled Budesonide and Oral Nystatin Presenting as Allergic Contact Stomatitis and Systemic Allergic Contact Dermatitis
The development of concomitant allergic reactions to multiple drugs is uncommon. Dermatitis induced by topical or inhaled corticosteroids (eg, budesonide) is rare,1 and allergic reactions associated with oral nystatin, a macrolide antifungal drug, also are unusual.2 We present the case of concomitant sensitization to inhaled budesonide and oral nystatin presenting as allergic contact stomatitis and systemic allergic contact dermatitis. Concomitant allergic reactions to these treatments are rare and may result in diagnostic challenges for the physician.
Case Report
A 66-year-old woman presented to the Allergy Department for evaluation of painful erosions on the oral mucosa that had developed 72 hours after she started treatment with inhaled budesonide (400 mcg every 12 hours) prescribed by her general practitioner for a nonproductive cough. Budesonide inhalation was discontinued due to suspected oral candidiasis and treatment with oral nystatin (500,000 IU every 8 hours) was started, but the erosions did not resolve. After 2 days of treatment with oral nystatin, the patient presented with erythematous macules on the abdomen and thighs as well as a larger erythematous and edematous lesion with papules and vesicles on the hypothenar eminence of the right hand. Nystatin was discontinued and the lesions turned desquamative and healed spontaneously 7 days later. The oral lesions resolved after 15 days with no further treatment.
Patch testing was conducted using a commercially standard series of contact allergens, all of which showed negative results at 48 and 96 hours except for budesonide and triamcinolone, which led to the diagnosis of allergic contact stomatitis from the inhaled budesonide. Patch testing with other corticosteroids was negative. Challenge tests with alternative corticosteroids (ie, oral methylprednisolone, parenteral betamethasone, topical mometasone furoate, inhaled fluticasone) were negative.
In order to rule out involvement of oral nystatin, a single-blind, placebo-controlled oral challenge test was performed. Eight hours after taking oral nystatin (500,000 IU), erythematous macules developed on the patient’s abdomen along with an erythematous, 3×4-cm lesion with papules on the hypothenar eminence of the right hand that was similar in appearance to the original presentation. The lesion on the hand was biopsied and histologic examination revealed spongiosis, edema of the superficial dermis, perivascular lymphocytic infiltrates, and extravasated erythrocytes with no vasculitis. Further patch testing subsequently was conducted with antifungal and antibiotic macrolides in different vehicles (ie, petrolatum, water, polyethylene glycol), as well as with excipients of the oral nystatin formulation that had been tested (Figure). Patch testing was positive with nystatin 10% in petrolatum and nystatin 30,000 IU and 90,000 IU in polyethylene glycol. Testing also were conducted in 7 healthy volunteers to rule out an irritant reaction and showed negative results. Finally, challenge tests conducted in our patient with another antifungal macrolide (parenteral amphotericin B) and antibiotic macrolides (oral clarithromycin, erythromycin, and azithromycin) were negative.
Patch and challenge test results along with the histologic findings led to diagnosis of concomitant systemic allergic contact dermatitis from oral nystatin.
Comment
Our patient presented with 2 unusual delayed hypersensitivity reactions that occurred in the same medical episode: allergic contact stomatitis from inhaled budesonide and systemic allergic contact dermatitis from oral nystatin. It is noteworthy that, despite the poor intestinal absorption of nystatin, systemic contact dermatitis to this drug has been previously described.3 Patch testing with macrolides proved useful for diagnosis in our patient, and based on the results we concluded that polyethylene glycol seemed to be the optimal vehicle for patch testing macrolide drugs versus water or petrolatum, as has been previously suggested.4
When a diagnosis of drug allergy is established, it is important to rule out cross-reactivity with other similar drugs by assessing if they produce the same reaction despite differences in chemical structure. Possible cross-reactivity of nystatin with other macrolides (validated on patch testing) has been reported but the tolerability was not evaluated.5 Our patient showed good tolerability to other macrolide drugs, both antibiotics and antifungals. Therefore, nystatin does not seem to cross-react with other structurally related drugs belonging to the macrolide group based on our results.
Corticosteroid allergies are more common than those associated with macrolides, especially contact dermatitis. Nonhalogenated corticosteroids (eg, hydrocortisone, budesonide) are most frequently associated with allergic reactions,6 and patch testing remains the diagnostic method of choice for the detection of delayed hypersensitivity to corticosteroids. In Europe, standard series include budesonide and tixocortol pivalate, and in the United States they include hydrocortisone 17–butyrate, triamcinolone acetonide, and clobetasol 17–propionate.6
To assess cross-reactivity among topical corticosteroids, patch testing with other steroids should be performed. In 1989, Coopman et al7 established a classification system for corticosteroids based on molecular structure, thus dividing them into 4 empirical groups: group A, hydrocortisone type; group B, acetonide type; group C, betamethasone type; and group D, ester type. The investigators hypothesized that allergic contact reactions occurred more frequently with corticosteroids belonging to the same group, while cross-reactions were uncommon between groups; however, cross-reactivity is known to occur among corticosteroids belonging to different groups in standard clinical practice, which conflicts with this claim.
Due to distinctively different behaviors among certain compounds in group D, Matura et al8 proposed subdividing the ester steroids into 2 groups: group D1, containing C16 methyl substitution and halogenation on the B ring, and group D2, comprising the labile ester steroids that lack both substitutions. A modified classification system including these subdivided groups is presented in the Table.8

In recent years, new corticosteroid drugs such as deflazacort, fluticasone propionate, and mometasone furoate have been developed, but classification of these agents has been difficult due to differences in their chemical structure, although mometasone furoate and fluticasone propionate have been included in group D1.9 Futhermore, the structural differences of these new steroids may mean less cross-reactivity with other steroids, which would facilitate their use in patients who are allergic to classic steroids. However, cross-reactivity between mometasone furoate and corticosteroids belonging to group B has already been described,10 which may restrict its use in patients who are allergic to other corticosteroids.
The classification of corticosteroids can provide useful information about cross-reactivity, which may help physicians in choosing an alternative drug in patients with an allergy to topical corticosteroids, but this advice about cross-reactivity does not seem to apply to systemic allergic dermatitis or immediate-type reactions to corticosteroids.11 Therefore, in these types of reactions, an individualized evaluation of the sensitization profile is needed, performing wider studies with alternative corticosteroids by skin tests with late readings and challenge tests.
It is important to emphasize that hypersensitivity to corticosteroids should always be considered in the differential diagnosis along with oral candidiasis when oropharyngeal symptoms appear during inhaled corticosteroid along with oral candidiasis. We recommend that all drugs involved in a presumed allergic reaction must be systematically evaluated because an unexpected concomitant sensitization to multiple drugs could be present.
- English JS. Corticosteroid-induced contact dermatitis: a pragmatic approach. Clin Exp Dermatol. 2000;25:261-264.
- Martínez FV, Muñoz Pamplona MP, García EC, et al. Delayed hypersensitivity to oral nystatin. Contact Dermatitis. 2007;57:200-201.
- Quirce S, Parra F, Lázaro M, et al. Generalized dermatitis due to oral nystatin. Contact Dermatitis. 1991;25:197-198.
- de Groot AC, Conemans JM. Nystatin allergy: petrolatum is not the optimal vehicle for patch testing. Dermatol Clin. 1990;8:153-155.
- Barranco R, Tornero P, de Barrio M, et al. Type IV hypersensitivity to oral nystatin. Contact Dermatitis. 2001;45:60.
- Jacob SE, Steele T. Corticosteroid classes: a quick reference guide including patch test substances and cross-reactivity. J Am Acad Dermatol. 2006;54:723-727.
- Coopman S, Degreef H, Dooms-Goossens A. Identification of cross-reaction patterns in allergic contact dermatitis from topical corticosteroids. Br J Dermatol. 1989;121:27-34.
- Matura M, Goossens A. Contact allergy to corticosteroids. Allergy. 2000;55:698-704.
- Baeck M, Chamelle JA, Goossens A, et al. Corticosteroid cross-reactivity: clinical and molecular modeling tools. Allergy. 2011;66:1367-1374.
- Seyfarth F, Elsner P, Tittelbach J, et al. Contact allergy to mometasone furoate with cross-reactivity to group B corticosteroids. Contact Dermatitis. 2008;58:180-181.
- Torres MJ, Canto G. Hypersensitivity reactions to corticosteroids. Curr Opin Allergy Clin Immunol. 2010;10:273-279.
The development of concomitant allergic reactions to multiple drugs is uncommon. Dermatitis induced by topical or inhaled corticosteroids (eg, budesonide) is rare,1 and allergic reactions associated with oral nystatin, a macrolide antifungal drug, also are unusual.2 We present the case of concomitant sensitization to inhaled budesonide and oral nystatin presenting as allergic contact stomatitis and systemic allergic contact dermatitis. Concomitant allergic reactions to these treatments are rare and may result in diagnostic challenges for the physician.
Case Report
A 66-year-old woman presented to the Allergy Department for evaluation of painful erosions on the oral mucosa that had developed 72 hours after she started treatment with inhaled budesonide (400 mcg every 12 hours) prescribed by her general practitioner for a nonproductive cough. Budesonide inhalation was discontinued due to suspected oral candidiasis and treatment with oral nystatin (500,000 IU every 8 hours) was started, but the erosions did not resolve. After 2 days of treatment with oral nystatin, the patient presented with erythematous macules on the abdomen and thighs as well as a larger erythematous and edematous lesion with papules and vesicles on the hypothenar eminence of the right hand. Nystatin was discontinued and the lesions turned desquamative and healed spontaneously 7 days later. The oral lesions resolved after 15 days with no further treatment.
Patch testing was conducted using a commercially standard series of contact allergens, all of which showed negative results at 48 and 96 hours except for budesonide and triamcinolone, which led to the diagnosis of allergic contact stomatitis from the inhaled budesonide. Patch testing with other corticosteroids was negative. Challenge tests with alternative corticosteroids (ie, oral methylprednisolone, parenteral betamethasone, topical mometasone furoate, inhaled fluticasone) were negative.
In order to rule out involvement of oral nystatin, a single-blind, placebo-controlled oral challenge test was performed. Eight hours after taking oral nystatin (500,000 IU), erythematous macules developed on the patient’s abdomen along with an erythematous, 3×4-cm lesion with papules on the hypothenar eminence of the right hand that was similar in appearance to the original presentation. The lesion on the hand was biopsied and histologic examination revealed spongiosis, edema of the superficial dermis, perivascular lymphocytic infiltrates, and extravasated erythrocytes with no vasculitis. Further patch testing subsequently was conducted with antifungal and antibiotic macrolides in different vehicles (ie, petrolatum, water, polyethylene glycol), as well as with excipients of the oral nystatin formulation that had been tested (Figure). Patch testing was positive with nystatin 10% in petrolatum and nystatin 30,000 IU and 90,000 IU in polyethylene glycol. Testing also were conducted in 7 healthy volunteers to rule out an irritant reaction and showed negative results. Finally, challenge tests conducted in our patient with another antifungal macrolide (parenteral amphotericin B) and antibiotic macrolides (oral clarithromycin, erythromycin, and azithromycin) were negative.

Patch and challenge test results along with the histologic findings led to diagnosis of concomitant systemic allergic contact dermatitis from oral nystatin.
Comment
Our patient presented with 2 unusual delayed hypersensitivity reactions that occurred in the same medical episode: allergic contact stomatitis from inhaled budesonide and systemic allergic contact dermatitis from oral nystatin. It is noteworthy that, despite the poor intestinal absorption of nystatin, systemic contact dermatitis to this drug has been previously described.3 Patch testing with macrolides proved useful for diagnosis in our patient, and based on the results we concluded that polyethylene glycol seemed to be the optimal vehicle for patch testing macrolide drugs versus water or petrolatum, as has been previously suggested.4
When a diagnosis of drug allergy is established, it is important to rule out cross-reactivity with other similar drugs by assessing if they produce the same reaction despite differences in chemical structure. Possible cross-reactivity of nystatin with other macrolides (validated on patch testing) has been reported but the tolerability was not evaluated.5 Our patient showed good tolerability to other macrolide drugs, both antibiotics and antifungals. Therefore, nystatin does not seem to cross-react with other structurally related drugs belonging to the macrolide group based on our results.
Corticosteroid allergies are more common than those associated with macrolides, especially contact dermatitis. Nonhalogenated corticosteroids (eg, hydrocortisone, budesonide) are most frequently associated with allergic reactions,6 and patch testing remains the diagnostic method of choice for the detection of delayed hypersensitivity to corticosteroids. In Europe, standard series include budesonide and tixocortol pivalate, and in the United States they include hydrocortisone 17–butyrate, triamcinolone acetonide, and clobetasol 17–propionate.6
To assess cross-reactivity among topical corticosteroids, patch testing with other steroids should be performed. In 1989, Coopman et al7 established a classification system for corticosteroids based on molecular structure, thus dividing them into 4 empirical groups: group A, hydrocortisone type; group B, acetonide type; group C, betamethasone type; and group D, ester type. The investigators hypothesized that allergic contact reactions occurred more frequently with corticosteroids belonging to the same group, while cross-reactions were uncommon between groups; however, cross-reactivity is known to occur among corticosteroids belonging to different groups in standard clinical practice, which conflicts with this claim.
Due to distinctively different behaviors among certain compounds in group D, Matura et al8 proposed subdividing the ester steroids into 2 groups: group D1, containing C16 methyl substitution and halogenation on the B ring, and group D2, comprising the labile ester steroids that lack both substitutions. A modified classification system including these subdivided groups is presented in the Table.8

In recent years, new corticosteroid drugs such as deflazacort, fluticasone propionate, and mometasone furoate have been developed, but classification of these agents has been difficult due to differences in their chemical structure, although mometasone furoate and fluticasone propionate have been included in group D1.9 Futhermore, the structural differences of these new steroids may mean less cross-reactivity with other steroids, which would facilitate their use in patients who are allergic to classic steroids. However, cross-reactivity between mometasone furoate and corticosteroids belonging to group B has already been described,10 which may restrict its use in patients who are allergic to other corticosteroids.
The classification of corticosteroids can provide useful information about cross-reactivity, which may help physicians in choosing an alternative drug in patients with an allergy to topical corticosteroids, but this advice about cross-reactivity does not seem to apply to systemic allergic dermatitis or immediate-type reactions to corticosteroids.11 Therefore, in these types of reactions, an individualized evaluation of the sensitization profile is needed, performing wider studies with alternative corticosteroids by skin tests with late readings and challenge tests.
It is important to emphasize that hypersensitivity to corticosteroids should always be considered in the differential diagnosis along with oral candidiasis when oropharyngeal symptoms appear during inhaled corticosteroid along with oral candidiasis. We recommend that all drugs involved in a presumed allergic reaction must be systematically evaluated because an unexpected concomitant sensitization to multiple drugs could be present.
The development of concomitant allergic reactions to multiple drugs is uncommon. Dermatitis induced by topical or inhaled corticosteroids (eg, budesonide) is rare,1 and allergic reactions associated with oral nystatin, a macrolide antifungal drug, also are unusual.2 We present the case of concomitant sensitization to inhaled budesonide and oral nystatin presenting as allergic contact stomatitis and systemic allergic contact dermatitis. Concomitant allergic reactions to these treatments are rare and may result in diagnostic challenges for the physician.
Case Report
A 66-year-old woman presented to the Allergy Department for evaluation of painful erosions on the oral mucosa that had developed 72 hours after she started treatment with inhaled budesonide (400 mcg every 12 hours) prescribed by her general practitioner for a nonproductive cough. Budesonide inhalation was discontinued due to suspected oral candidiasis and treatment with oral nystatin (500,000 IU every 8 hours) was started, but the erosions did not resolve. After 2 days of treatment with oral nystatin, the patient presented with erythematous macules on the abdomen and thighs as well as a larger erythematous and edematous lesion with papules and vesicles on the hypothenar eminence of the right hand. Nystatin was discontinued and the lesions turned desquamative and healed spontaneously 7 days later. The oral lesions resolved after 15 days with no further treatment.
Patch testing was conducted using a commercially standard series of contact allergens, all of which showed negative results at 48 and 96 hours except for budesonide and triamcinolone, which led to the diagnosis of allergic contact stomatitis from the inhaled budesonide. Patch testing with other corticosteroids was negative. Challenge tests with alternative corticosteroids (ie, oral methylprednisolone, parenteral betamethasone, topical mometasone furoate, inhaled fluticasone) were negative.
In order to rule out involvement of oral nystatin, a single-blind, placebo-controlled oral challenge test was performed. Eight hours after taking oral nystatin (500,000 IU), erythematous macules developed on the patient’s abdomen along with an erythematous, 3×4-cm lesion with papules on the hypothenar eminence of the right hand that was similar in appearance to the original presentation. The lesion on the hand was biopsied and histologic examination revealed spongiosis, edema of the superficial dermis, perivascular lymphocytic infiltrates, and extravasated erythrocytes with no vasculitis. Further patch testing subsequently was conducted with antifungal and antibiotic macrolides in different vehicles (ie, petrolatum, water, polyethylene glycol), as well as with excipients of the oral nystatin formulation that had been tested (Figure). Patch testing was positive with nystatin 10% in petrolatum and nystatin 30,000 IU and 90,000 IU in polyethylene glycol. Testing also were conducted in 7 healthy volunteers to rule out an irritant reaction and showed negative results. Finally, challenge tests conducted in our patient with another antifungal macrolide (parenteral amphotericin B) and antibiotic macrolides (oral clarithromycin, erythromycin, and azithromycin) were negative.

Patch and challenge test results along with the histologic findings led to diagnosis of concomitant systemic allergic contact dermatitis from oral nystatin.
Comment
Our patient presented with 2 unusual delayed hypersensitivity reactions that occurred in the same medical episode: allergic contact stomatitis from inhaled budesonide and systemic allergic contact dermatitis from oral nystatin. It is noteworthy that, despite the poor intestinal absorption of nystatin, systemic contact dermatitis to this drug has been previously described.3 Patch testing with macrolides proved useful for diagnosis in our patient, and based on the results we concluded that polyethylene glycol seemed to be the optimal vehicle for patch testing macrolide drugs versus water or petrolatum, as has been previously suggested.4
When a diagnosis of drug allergy is established, it is important to rule out cross-reactivity with other similar drugs by assessing if they produce the same reaction despite differences in chemical structure. Possible cross-reactivity of nystatin with other macrolides (validated on patch testing) has been reported but the tolerability was not evaluated.5 Our patient showed good tolerability to other macrolide drugs, both antibiotics and antifungals. Therefore, nystatin does not seem to cross-react with other structurally related drugs belonging to the macrolide group based on our results.
Corticosteroid allergies are more common than those associated with macrolides, especially contact dermatitis. Nonhalogenated corticosteroids (eg, hydrocortisone, budesonide) are most frequently associated with allergic reactions,6 and patch testing remains the diagnostic method of choice for the detection of delayed hypersensitivity to corticosteroids. In Europe, standard series include budesonide and tixocortol pivalate, and in the United States they include hydrocortisone 17–butyrate, triamcinolone acetonide, and clobetasol 17–propionate.6
To assess cross-reactivity among topical corticosteroids, patch testing with other steroids should be performed. In 1989, Coopman et al7 established a classification system for corticosteroids based on molecular structure, thus dividing them into 4 empirical groups: group A, hydrocortisone type; group B, acetonide type; group C, betamethasone type; and group D, ester type. The investigators hypothesized that allergic contact reactions occurred more frequently with corticosteroids belonging to the same group, while cross-reactions were uncommon between groups; however, cross-reactivity is known to occur among corticosteroids belonging to different groups in standard clinical practice, which conflicts with this claim.
Due to distinctively different behaviors among certain compounds in group D, Matura et al8 proposed subdividing the ester steroids into 2 groups: group D1, containing C16 methyl substitution and halogenation on the B ring, and group D2, comprising the labile ester steroids that lack both substitutions. A modified classification system including these subdivided groups is presented in the Table.8

In recent years, new corticosteroid drugs such as deflazacort, fluticasone propionate, and mometasone furoate have been developed, but classification of these agents has been difficult due to differences in their chemical structure, although mometasone furoate and fluticasone propionate have been included in group D1.9 Futhermore, the structural differences of these new steroids may mean less cross-reactivity with other steroids, which would facilitate their use in patients who are allergic to classic steroids. However, cross-reactivity between mometasone furoate and corticosteroids belonging to group B has already been described,10 which may restrict its use in patients who are allergic to other corticosteroids.
The classification of corticosteroids can provide useful information about cross-reactivity, which may help physicians in choosing an alternative drug in patients with an allergy to topical corticosteroids, but this advice about cross-reactivity does not seem to apply to systemic allergic dermatitis or immediate-type reactions to corticosteroids.11 Therefore, in these types of reactions, an individualized evaluation of the sensitization profile is needed, performing wider studies with alternative corticosteroids by skin tests with late readings and challenge tests.
It is important to emphasize that hypersensitivity to corticosteroids should always be considered in the differential diagnosis along with oral candidiasis when oropharyngeal symptoms appear during inhaled corticosteroid along with oral candidiasis. We recommend that all drugs involved in a presumed allergic reaction must be systematically evaluated because an unexpected concomitant sensitization to multiple drugs could be present.
- English JS. Corticosteroid-induced contact dermatitis: a pragmatic approach. Clin Exp Dermatol. 2000;25:261-264.
- Martínez FV, Muñoz Pamplona MP, García EC, et al. Delayed hypersensitivity to oral nystatin. Contact Dermatitis. 2007;57:200-201.
- Quirce S, Parra F, Lázaro M, et al. Generalized dermatitis due to oral nystatin. Contact Dermatitis. 1991;25:197-198.
- de Groot AC, Conemans JM. Nystatin allergy: petrolatum is not the optimal vehicle for patch testing. Dermatol Clin. 1990;8:153-155.
- Barranco R, Tornero P, de Barrio M, et al. Type IV hypersensitivity to oral nystatin. Contact Dermatitis. 2001;45:60.
- Jacob SE, Steele T. Corticosteroid classes: a quick reference guide including patch test substances and cross-reactivity. J Am Acad Dermatol. 2006;54:723-727.
- Coopman S, Degreef H, Dooms-Goossens A. Identification of cross-reaction patterns in allergic contact dermatitis from topical corticosteroids. Br J Dermatol. 1989;121:27-34.
- Matura M, Goossens A. Contact allergy to corticosteroids. Allergy. 2000;55:698-704.
- Baeck M, Chamelle JA, Goossens A, et al. Corticosteroid cross-reactivity: clinical and molecular modeling tools. Allergy. 2011;66:1367-1374.
- Seyfarth F, Elsner P, Tittelbach J, et al. Contact allergy to mometasone furoate with cross-reactivity to group B corticosteroids. Contact Dermatitis. 2008;58:180-181.
- Torres MJ, Canto G. Hypersensitivity reactions to corticosteroids. Curr Opin Allergy Clin Immunol. 2010;10:273-279.
- English JS. Corticosteroid-induced contact dermatitis: a pragmatic approach. Clin Exp Dermatol. 2000;25:261-264.
- Martínez FV, Muñoz Pamplona MP, García EC, et al. Delayed hypersensitivity to oral nystatin. Contact Dermatitis. 2007;57:200-201.
- Quirce S, Parra F, Lázaro M, et al. Generalized dermatitis due to oral nystatin. Contact Dermatitis. 1991;25:197-198.
- de Groot AC, Conemans JM. Nystatin allergy: petrolatum is not the optimal vehicle for patch testing. Dermatol Clin. 1990;8:153-155.
- Barranco R, Tornero P, de Barrio M, et al. Type IV hypersensitivity to oral nystatin. Contact Dermatitis. 2001;45:60.
- Jacob SE, Steele T. Corticosteroid classes: a quick reference guide including patch test substances and cross-reactivity. J Am Acad Dermatol. 2006;54:723-727.
- Coopman S, Degreef H, Dooms-Goossens A. Identification of cross-reaction patterns in allergic contact dermatitis from topical corticosteroids. Br J Dermatol. 1989;121:27-34.
- Matura M, Goossens A. Contact allergy to corticosteroids. Allergy. 2000;55:698-704.
- Baeck M, Chamelle JA, Goossens A, et al. Corticosteroid cross-reactivity: clinical and molecular modeling tools. Allergy. 2011;66:1367-1374.
- Seyfarth F, Elsner P, Tittelbach J, et al. Contact allergy to mometasone furoate with cross-reactivity to group B corticosteroids. Contact Dermatitis. 2008;58:180-181.
- Torres MJ, Canto G. Hypersensitivity reactions to corticosteroids. Curr Opin Allergy Clin Immunol. 2010;10:273-279.
Practice Points
- When lesions develop in the oral cavity during treatment with inhaled corticosteroids, delayed contact allergy should be considered in the differential diagnosis along with fungal infection.
- Although it generally is not considered to be allergenic due to its poor intestinal absorption, oral nystatin may induce systemic allergic disorders.
- All drugs involved in a presumed allergic reaction must be evaluated since concomitant sensitization to multiple drugs could be present. Patch and challenge testing should be conducted to diagnose allergic contact dermatitis and assess drug cross-reactivity.
Recalcitrant Hailey-Hailey Disease Responds to Oral Tacrolimus and Botulinum Toxin Type A
To the Editor:
Hailey-Hailey disease, also known as familial benign pemphigus, is a chronic blistering skin disorder that typically presents as a recurrent vesicular or bullous dermatitis found predominantly in the intertriginous regions of the body. Because current treatment regimens for Hailey-Hailey disease are fairly limited, novel treatments may be explored in intractable cases.
A 71-year-old woman presented with well-demarcated erythematous plaques with erosions and white verrucous regions in the perivulvar, vaginal, and perianal areas of 1 month’s duration (Figure 1). The lesions were excruciatingly pruritic and excoriated. The patient reported no personal or family history of similar lesions.

Histopathologic examination of multiple biopsies from the periphery of the plaques showed acantholysis of the epidermis and surface necrosis with negative direct immunofluorescence. A diagnosis of Hailey-Hailey disease was made. Over several months following the initial presentation, the patient was treated with regimens of corticosteroids, antibiotics, antifungals, acitretin, and topical tacrolimus (which showed minimal response), but the condition continued to progress and thus warranted a more aggressive approach. After a 4-week course of oral cyclosporine 1.25 mg/kg twice daily, some healthy granulation tissue had formed, but new erosions continued to develop on the vulva, labia, and intergluteal cleft (Figure 2). Subsequently, a 2-month course of methotrexate yielded similar results with minimal healing and new necrotic areas (Figure 3).
Following methotrexate therapy, treatment with several other oral agents was considered such as azathioprine, mycophenolate mofetil, and oral tacrolimus. Since the patient had previously shown minimal response to topical tacrolimus, a course of oral treatment (0.05 mg/kg twice daily) was initiated. At 4 weeks’ follow-up, extensive healing of the lesions was noted (Figure 4) and the patient reported that the painful pruritus had improved.
After 6 weeks of treatment, there still were a few small lesions in the intergluteal cleft, which were treated with botulinum toxin type A (100 U diluted with 5 cc of bacteriostatic saline per cm2). After 3 separate injections with botulinum toxin type A and oral tacrolimus for 9 months, complete resolution of the lesions was obtained (Figure 5). After more than 6 months of remission, oral tacrolimus slowly was decreased by 1 mg every 6 weeks until treatment was stopped completely. She has remained in remission without oral treatment. After tapering the tacrolimus, botulinum toxin A injections were continued every 6 months for maintenance with the use of topical tacrolimus 3 to 4 times weekly (Figure 6).
The inheritance of Hailey-Hailey disease is autosomal dominant with incomplete penetrance, although spontaneous mutations are implicated in up to 30% of patients.1,2 The pathogenesis of Hailey-Hailey disease involves a mutation in the ATPase, Ca++ transporting, type 2C, member 1 gene (ATP2C1), which encodes for the hSPCA1 protein.1-2 The malfunction of this ATPase leads to inadequacy of the keratinocyte adhesive barrier resulting in acantholysis and intraepidermal vesicle formation. Macerated plaques also may be found instead of intact vesicles.3
Initial presentation of lesions in Hailey-Hailey disease typically occurs in the third or fourth decades of life but may present at any age.4 Areas exposed to increased amounts of friction (eg, axillae, groin, neck, perineum) commonly are involved.5 Lesions may occur in a relapsing and remitting course and usually are more prominent in summer months because they are exacerbated by sunburn and frictional trauma. Secondary bacterial or fungal infections are common and antibiotics and antifungals often are necessary to prevent progression of the lesions.5,6
Various treatment regimens for Hailey-Hailey disease include topical and oral corticosteroids and antibiotics.5 Topical and oral retinoids, calcitriol, topical tacrolimus, cyclosporin, methotrexate, and even botulinum toxin A have been reported to be effective for refractory cases.7-12 Our case describes a novel regimen of oral tacrolimus in conjunction with botulinum toxin A used in the successful treatment of recalcitrant Hailey-Hailey disease.
Tacrolimus binds to the immunophilin FK506 binding protein, which inhibits calcineurin. Calcineurin, a protein phosphatase, is necessary for T-cell activation through the nuclear factor of activated T cells.This inhibition of calcineurin blocks the expression of several cytokines.13 The efficacy of oral tacrolimus demonstrates that cellular immunity could play a role in the pathogenic mechanism of Hailey-Hailey disease.
Contraindications to oral tacrolimus therapy include renal or hepatic impairment, breast-feeding, pregnancy, and certain neoplastic diseases. There also is an increased risk of patients developing malignancies such as lymphoma or skin cancer due to immunosuppression. Use of oral tacrolimus also requires routine laboratory monitoring of renal and hepatic function, potassium, and blood glucose levels.13
Botulinum toxin A injections augmented the therapeutic approach in our patient possibly by controlling secretions of sweat and mucous, which may cause maceration and lead to exacerbation of Hailey-Hailey disease. Control of secretions may help in creating an environment that is less prone to exacerbation of lesions and secondary infection.14 The combination of oral tacrolimus and botulinum toxin A injections provided a safe therapeutic option for recalcitrant Hailey-Hailey disease in our patient.
- Fairclough RJ, Dode L, Vanoevelen J, et al. Effect of Hailey-Hailey Disease mutations on the function of a new variant of human secretory pathway Ca2+/Mn2+-ATPase (hSPCA1). J Biol Chem. 2003; 278:24721-24730.
- Dobson-Stone C, Fairclough R, Dunne E, et al. Hailey-Hailey disease: molecular and clinical characterization of novel mutations in the ATP2C1 gene. J Invest Dermatol. 2002;118:338-343.
- Warycha M, Patel R, Meehan S, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2009;15:15.
- Tchernev GJ, Cardosa C. Familial benign chronic pemphigus (Hailey-Hailey Disease): use of topical immunomodulators as a modern treatment option. Rev Med Chil. 2011;139:633-637.
- Hunt R, O’Reilly K, Ralston J, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2010;16:14.
- Berger EM, Galadari HI, Gottlieb AB. Successful treatment of Hailey-Hailey with acitretin. J Drugs Dermatol. 2007;6:734-736.
- Rabeni EJ, Cunningham NM. Effective treatment of Hailey-Hailey disease with topical tacrolimus. J Am Acad Dermatol. 2002;47:797-798.
- Sand C, Thomsen HK. Topical tacrolimus ointment is an effective therapy for Hailey-Hailey disease. Arch Dermatol. 2003;139:1401-1402.
- Bianchi L, Chimenti MS, Giunta A. Treatment of Hailey-Hailey with topical calcitriol. J Am Acad of Dermatol. 2004;51:475-476.
- Berth-Jones J, Smith SG, Graham-Brown RA. Benign familial chronic pemphigus (Hailey-Hailey disease) responds to cyclosporin. Clin Exp Dermatol. 1995;20:70-72.
- Vilarinho CF, Ventura F, Brito C. Methotrexate for refractory Hailey-Hailey disease. J Eur Acad Dermatol Venereol. 2010;24:106.
- Koeyers WJ, Van Der Geer S, Krekels G. Botulinum toxin type A as an adjuvant treatment modality for extensive Hailey-Hailey disease. J Dermatolog Treatment. 2008;19:251-254.
- Katzung BG, Masters SB, Trevor AJ, eds. Basic and Clinical Pharmacology. 11th ed. New York, NY: McGraw-Hill; 2009.14. Lapiere JC, Hirsh A, Gordon KB, et al. Botulinum toxin type A for the treatment of axillary Hailey-Hailey disease. Dermatol Surg. 2000;26:371-374.
To the Editor:
Hailey-Hailey disease, also known as familial benign pemphigus, is a chronic blistering skin disorder that typically presents as a recurrent vesicular or bullous dermatitis found predominantly in the intertriginous regions of the body. Because current treatment regimens for Hailey-Hailey disease are fairly limited, novel treatments may be explored in intractable cases.
A 71-year-old woman presented with well-demarcated erythematous plaques with erosions and white verrucous regions in the perivulvar, vaginal, and perianal areas of 1 month’s duration (Figure 1). The lesions were excruciatingly pruritic and excoriated. The patient reported no personal or family history of similar lesions.

Histopathologic examination of multiple biopsies from the periphery of the plaques showed acantholysis of the epidermis and surface necrosis with negative direct immunofluorescence. A diagnosis of Hailey-Hailey disease was made. Over several months following the initial presentation, the patient was treated with regimens of corticosteroids, antibiotics, antifungals, acitretin, and topical tacrolimus (which showed minimal response), but the condition continued to progress and thus warranted a more aggressive approach. After a 4-week course of oral cyclosporine 1.25 mg/kg twice daily, some healthy granulation tissue had formed, but new erosions continued to develop on the vulva, labia, and intergluteal cleft (Figure 2). Subsequently, a 2-month course of methotrexate yielded similar results with minimal healing and new necrotic areas (Figure 3).


Following methotrexate therapy, treatment with several other oral agents was considered such as azathioprine, mycophenolate mofetil, and oral tacrolimus. Since the patient had previously shown minimal response to topical tacrolimus, a course of oral treatment (0.05 mg/kg twice daily) was initiated. At 4 weeks’ follow-up, extensive healing of the lesions was noted (Figure 4) and the patient reported that the painful pruritus had improved.

After 6 weeks of treatment, there still were a few small lesions in the intergluteal cleft, which were treated with botulinum toxin type A (100 U diluted with 5 cc of bacteriostatic saline per cm2). After 3 separate injections with botulinum toxin type A and oral tacrolimus for 9 months, complete resolution of the lesions was obtained (Figure 5). After more than 6 months of remission, oral tacrolimus slowly was decreased by 1 mg every 6 weeks until treatment was stopped completely. She has remained in remission without oral treatment. After tapering the tacrolimus, botulinum toxin A injections were continued every 6 months for maintenance with the use of topical tacrolimus 3 to 4 times weekly (Figure 6).


The inheritance of Hailey-Hailey disease is autosomal dominant with incomplete penetrance, although spontaneous mutations are implicated in up to 30% of patients.1,2 The pathogenesis of Hailey-Hailey disease involves a mutation in the ATPase, Ca++ transporting, type 2C, member 1 gene (ATP2C1), which encodes for the hSPCA1 protein.1-2 The malfunction of this ATPase leads to inadequacy of the keratinocyte adhesive barrier resulting in acantholysis and intraepidermal vesicle formation. Macerated plaques also may be found instead of intact vesicles.3
Initial presentation of lesions in Hailey-Hailey disease typically occurs in the third or fourth decades of life but may present at any age.4 Areas exposed to increased amounts of friction (eg, axillae, groin, neck, perineum) commonly are involved.5 Lesions may occur in a relapsing and remitting course and usually are more prominent in summer months because they are exacerbated by sunburn and frictional trauma. Secondary bacterial or fungal infections are common and antibiotics and antifungals often are necessary to prevent progression of the lesions.5,6
Various treatment regimens for Hailey-Hailey disease include topical and oral corticosteroids and antibiotics.5 Topical and oral retinoids, calcitriol, topical tacrolimus, cyclosporin, methotrexate, and even botulinum toxin A have been reported to be effective for refractory cases.7-12 Our case describes a novel regimen of oral tacrolimus in conjunction with botulinum toxin A used in the successful treatment of recalcitrant Hailey-Hailey disease.
Tacrolimus binds to the immunophilin FK506 binding protein, which inhibits calcineurin. Calcineurin, a protein phosphatase, is necessary for T-cell activation through the nuclear factor of activated T cells.This inhibition of calcineurin blocks the expression of several cytokines.13 The efficacy of oral tacrolimus demonstrates that cellular immunity could play a role in the pathogenic mechanism of Hailey-Hailey disease.
Contraindications to oral tacrolimus therapy include renal or hepatic impairment, breast-feeding, pregnancy, and certain neoplastic diseases. There also is an increased risk of patients developing malignancies such as lymphoma or skin cancer due to immunosuppression. Use of oral tacrolimus also requires routine laboratory monitoring of renal and hepatic function, potassium, and blood glucose levels.13
Botulinum toxin A injections augmented the therapeutic approach in our patient possibly by controlling secretions of sweat and mucous, which may cause maceration and lead to exacerbation of Hailey-Hailey disease. Control of secretions may help in creating an environment that is less prone to exacerbation of lesions and secondary infection.14 The combination of oral tacrolimus and botulinum toxin A injections provided a safe therapeutic option for recalcitrant Hailey-Hailey disease in our patient.
To the Editor:
Hailey-Hailey disease, also known as familial benign pemphigus, is a chronic blistering skin disorder that typically presents as a recurrent vesicular or bullous dermatitis found predominantly in the intertriginous regions of the body. Because current treatment regimens for Hailey-Hailey disease are fairly limited, novel treatments may be explored in intractable cases.
A 71-year-old woman presented with well-demarcated erythematous plaques with erosions and white verrucous regions in the perivulvar, vaginal, and perianal areas of 1 month’s duration (Figure 1). The lesions were excruciatingly pruritic and excoriated. The patient reported no personal or family history of similar lesions.

Histopathologic examination of multiple biopsies from the periphery of the plaques showed acantholysis of the epidermis and surface necrosis with negative direct immunofluorescence. A diagnosis of Hailey-Hailey disease was made. Over several months following the initial presentation, the patient was treated with regimens of corticosteroids, antibiotics, antifungals, acitretin, and topical tacrolimus (which showed minimal response), but the condition continued to progress and thus warranted a more aggressive approach. After a 4-week course of oral cyclosporine 1.25 mg/kg twice daily, some healthy granulation tissue had formed, but new erosions continued to develop on the vulva, labia, and intergluteal cleft (Figure 2). Subsequently, a 2-month course of methotrexate yielded similar results with minimal healing and new necrotic areas (Figure 3).


Following methotrexate therapy, treatment with several other oral agents was considered such as azathioprine, mycophenolate mofetil, and oral tacrolimus. Since the patient had previously shown minimal response to topical tacrolimus, a course of oral treatment (0.05 mg/kg twice daily) was initiated. At 4 weeks’ follow-up, extensive healing of the lesions was noted (Figure 4) and the patient reported that the painful pruritus had improved.

After 6 weeks of treatment, there still were a few small lesions in the intergluteal cleft, which were treated with botulinum toxin type A (100 U diluted with 5 cc of bacteriostatic saline per cm2). After 3 separate injections with botulinum toxin type A and oral tacrolimus for 9 months, complete resolution of the lesions was obtained (Figure 5). After more than 6 months of remission, oral tacrolimus slowly was decreased by 1 mg every 6 weeks until treatment was stopped completely. She has remained in remission without oral treatment. After tapering the tacrolimus, botulinum toxin A injections were continued every 6 months for maintenance with the use of topical tacrolimus 3 to 4 times weekly (Figure 6).


The inheritance of Hailey-Hailey disease is autosomal dominant with incomplete penetrance, although spontaneous mutations are implicated in up to 30% of patients.1,2 The pathogenesis of Hailey-Hailey disease involves a mutation in the ATPase, Ca++ transporting, type 2C, member 1 gene (ATP2C1), which encodes for the hSPCA1 protein.1-2 The malfunction of this ATPase leads to inadequacy of the keratinocyte adhesive barrier resulting in acantholysis and intraepidermal vesicle formation. Macerated plaques also may be found instead of intact vesicles.3
Initial presentation of lesions in Hailey-Hailey disease typically occurs in the third or fourth decades of life but may present at any age.4 Areas exposed to increased amounts of friction (eg, axillae, groin, neck, perineum) commonly are involved.5 Lesions may occur in a relapsing and remitting course and usually are more prominent in summer months because they are exacerbated by sunburn and frictional trauma. Secondary bacterial or fungal infections are common and antibiotics and antifungals often are necessary to prevent progression of the lesions.5,6
Various treatment regimens for Hailey-Hailey disease include topical and oral corticosteroids and antibiotics.5 Topical and oral retinoids, calcitriol, topical tacrolimus, cyclosporin, methotrexate, and even botulinum toxin A have been reported to be effective for refractory cases.7-12 Our case describes a novel regimen of oral tacrolimus in conjunction with botulinum toxin A used in the successful treatment of recalcitrant Hailey-Hailey disease.
Tacrolimus binds to the immunophilin FK506 binding protein, which inhibits calcineurin. Calcineurin, a protein phosphatase, is necessary for T-cell activation through the nuclear factor of activated T cells.This inhibition of calcineurin blocks the expression of several cytokines.13 The efficacy of oral tacrolimus demonstrates that cellular immunity could play a role in the pathogenic mechanism of Hailey-Hailey disease.
Contraindications to oral tacrolimus therapy include renal or hepatic impairment, breast-feeding, pregnancy, and certain neoplastic diseases. There also is an increased risk of patients developing malignancies such as lymphoma or skin cancer due to immunosuppression. Use of oral tacrolimus also requires routine laboratory monitoring of renal and hepatic function, potassium, and blood glucose levels.13
Botulinum toxin A injections augmented the therapeutic approach in our patient possibly by controlling secretions of sweat and mucous, which may cause maceration and lead to exacerbation of Hailey-Hailey disease. Control of secretions may help in creating an environment that is less prone to exacerbation of lesions and secondary infection.14 The combination of oral tacrolimus and botulinum toxin A injections provided a safe therapeutic option for recalcitrant Hailey-Hailey disease in our patient.
- Fairclough RJ, Dode L, Vanoevelen J, et al. Effect of Hailey-Hailey Disease mutations on the function of a new variant of human secretory pathway Ca2+/Mn2+-ATPase (hSPCA1). J Biol Chem. 2003; 278:24721-24730.
- Dobson-Stone C, Fairclough R, Dunne E, et al. Hailey-Hailey disease: molecular and clinical characterization of novel mutations in the ATP2C1 gene. J Invest Dermatol. 2002;118:338-343.
- Warycha M, Patel R, Meehan S, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2009;15:15.
- Tchernev GJ, Cardosa C. Familial benign chronic pemphigus (Hailey-Hailey Disease): use of topical immunomodulators as a modern treatment option. Rev Med Chil. 2011;139:633-637.
- Hunt R, O’Reilly K, Ralston J, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2010;16:14.
- Berger EM, Galadari HI, Gottlieb AB. Successful treatment of Hailey-Hailey with acitretin. J Drugs Dermatol. 2007;6:734-736.
- Rabeni EJ, Cunningham NM. Effective treatment of Hailey-Hailey disease with topical tacrolimus. J Am Acad Dermatol. 2002;47:797-798.
- Sand C, Thomsen HK. Topical tacrolimus ointment is an effective therapy for Hailey-Hailey disease. Arch Dermatol. 2003;139:1401-1402.
- Bianchi L, Chimenti MS, Giunta A. Treatment of Hailey-Hailey with topical calcitriol. J Am Acad of Dermatol. 2004;51:475-476.
- Berth-Jones J, Smith SG, Graham-Brown RA. Benign familial chronic pemphigus (Hailey-Hailey disease) responds to cyclosporin. Clin Exp Dermatol. 1995;20:70-72.
- Vilarinho CF, Ventura F, Brito C. Methotrexate for refractory Hailey-Hailey disease. J Eur Acad Dermatol Venereol. 2010;24:106.
- Koeyers WJ, Van Der Geer S, Krekels G. Botulinum toxin type A as an adjuvant treatment modality for extensive Hailey-Hailey disease. J Dermatolog Treatment. 2008;19:251-254.
- Katzung BG, Masters SB, Trevor AJ, eds. Basic and Clinical Pharmacology. 11th ed. New York, NY: McGraw-Hill; 2009.14. Lapiere JC, Hirsh A, Gordon KB, et al. Botulinum toxin type A for the treatment of axillary Hailey-Hailey disease. Dermatol Surg. 2000;26:371-374.
- Fairclough RJ, Dode L, Vanoevelen J, et al. Effect of Hailey-Hailey Disease mutations on the function of a new variant of human secretory pathway Ca2+/Mn2+-ATPase (hSPCA1). J Biol Chem. 2003; 278:24721-24730.
- Dobson-Stone C, Fairclough R, Dunne E, et al. Hailey-Hailey disease: molecular and clinical characterization of novel mutations in the ATP2C1 gene. J Invest Dermatol. 2002;118:338-343.
- Warycha M, Patel R, Meehan S, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2009;15:15.
- Tchernev GJ, Cardosa C. Familial benign chronic pemphigus (Hailey-Hailey Disease): use of topical immunomodulators as a modern treatment option. Rev Med Chil. 2011;139:633-637.
- Hunt R, O’Reilly K, Ralston J, et al. Familial benign chronic pemphigus (Hailey-Hailey disease). Dermatol Online J. 2010;16:14.
- Berger EM, Galadari HI, Gottlieb AB. Successful treatment of Hailey-Hailey with acitretin. J Drugs Dermatol. 2007;6:734-736.
- Rabeni EJ, Cunningham NM. Effective treatment of Hailey-Hailey disease with topical tacrolimus. J Am Acad Dermatol. 2002;47:797-798.
- Sand C, Thomsen HK. Topical tacrolimus ointment is an effective therapy for Hailey-Hailey disease. Arch Dermatol. 2003;139:1401-1402.
- Bianchi L, Chimenti MS, Giunta A. Treatment of Hailey-Hailey with topical calcitriol. J Am Acad of Dermatol. 2004;51:475-476.
- Berth-Jones J, Smith SG, Graham-Brown RA. Benign familial chronic pemphigus (Hailey-Hailey disease) responds to cyclosporin. Clin Exp Dermatol. 1995;20:70-72.
- Vilarinho CF, Ventura F, Brito C. Methotrexate for refractory Hailey-Hailey disease. J Eur Acad Dermatol Venereol. 2010;24:106.
- Koeyers WJ, Van Der Geer S, Krekels G. Botulinum toxin type A as an adjuvant treatment modality for extensive Hailey-Hailey disease. J Dermatolog Treatment. 2008;19:251-254.
- Katzung BG, Masters SB, Trevor AJ, eds. Basic and Clinical Pharmacology. 11th ed. New York, NY: McGraw-Hill; 2009.14. Lapiere JC, Hirsh A, Gordon KB, et al. Botulinum toxin type A for the treatment of axillary Hailey-Hailey disease. Dermatol Surg. 2000;26:371-374.
Hong Kong zygomycosis deaths pinned to dirty hospital laundry
Contaminated laundry led to an outbreak of cutaneous and pulmonary zygomycosis that killed three immunocompromised patients and sickened three others at Queen Mary Hospital in Hong Kong.
The contamination was traced to a contract laundry service that was, in short, a microbe Disneyland. It was hot and humid, with sealed windows, dim lights, and a thick layer of dust on just about everything. Washers weren’t hot enough to kill spores; washed items were packed while warm and moist; and dirty linens rich with organic material were transported with clean ones (Clin Infect Dis. 2015 Dec 13. doi:10.1093/cid/civ1006).
Of 195 environmental samples, 119 (61%) were positive for Zygomycetes, as well as 100% of air samples. Freshly laundered items – including clothes and bedding – had bacteria counts of 1,028 colony forming units (CFU)/100 cm2, far exceeding the “hygienically clean” standard of 20 CFU/100 cm2 set by U.S. healthcare textile certification requirements.
Queen Mary didn’t regularly audit its linens for cleanliness and microbe counts. “Our findings [suggest] that such standards should be adopted to prevent similar outbreaks,” said the investigators, led by Dr. Vincent Cheng, an infection control officer at Queen Mary, one of Hong Kong’s largest hospitals and a teaching hospital for the University of Hong Kong.
It has since switched to a new laundry service.
The outbreak ran from June 2 to July 18, 2015, during Hong Kong’s hot and humid season, which didn’t help matters.
The six patients were 42-74 years old; one had interstitial lung disease and the rest were either cancer or transplant patients. Infection was due to the spore-forming mold Rhizopus microsporus. Two pulmonary and one cutaneous infection patient died.
Length of stay was the most significant risk factor for infection; the mean interval from admission to diagnosis was more than 2 months.
“Pulmonary zygomycosis due to contaminated hospital linens has never been reported.” Clinicians need to “maintain a high index of suspicion for early diagnosis and treatment of zygomycosis in immunosuppressed patients,” the investigators said.
The U.S. recently had a cutaneous outbreak in Louisiana; hospital linens contaminated with Rhizopus species killed five immunocompromised children there in 2015.
“Invasive zygomycosis is an emerging infection that is increasingly reported in immunosuppressed hosts;” previously reported sources include adhesive bandages, wooden tongue depressors, ostomy bags, damaged water circuitry, adjacent building construction activity, and, as Queen Mary reported previously, contaminated allopurinol tablets.
Detecting the problem isn’t easy. None of the Replicate Organism Detection and Counting contact plates at Queen Mary recovered zygomycetes from the contaminated linen items. It took sponge swapping to find it; “without the use of sponge swab and selective culture medium, the causative agents in this outbreak would have been overlooked,” the investigators said.
Hong Kong government services helped support the work. The authors did not have any financial conflicts of interest.
Contaminated laundry led to an outbreak of cutaneous and pulmonary zygomycosis that killed three immunocompromised patients and sickened three others at Queen Mary Hospital in Hong Kong.
The contamination was traced to a contract laundry service that was, in short, a microbe Disneyland. It was hot and humid, with sealed windows, dim lights, and a thick layer of dust on just about everything. Washers weren’t hot enough to kill spores; washed items were packed while warm and moist; and dirty linens rich with organic material were transported with clean ones (Clin Infect Dis. 2015 Dec 13. doi:10.1093/cid/civ1006).
Of 195 environmental samples, 119 (61%) were positive for Zygomycetes, as well as 100% of air samples. Freshly laundered items – including clothes and bedding – had bacteria counts of 1,028 colony forming units (CFU)/100 cm2, far exceeding the “hygienically clean” standard of 20 CFU/100 cm2 set by U.S. healthcare textile certification requirements.
Queen Mary didn’t regularly audit its linens for cleanliness and microbe counts. “Our findings [suggest] that such standards should be adopted to prevent similar outbreaks,” said the investigators, led by Dr. Vincent Cheng, an infection control officer at Queen Mary, one of Hong Kong’s largest hospitals and a teaching hospital for the University of Hong Kong.
It has since switched to a new laundry service.
The outbreak ran from June 2 to July 18, 2015, during Hong Kong’s hot and humid season, which didn’t help matters.
The six patients were 42-74 years old; one had interstitial lung disease and the rest were either cancer or transplant patients. Infection was due to the spore-forming mold Rhizopus microsporus. Two pulmonary and one cutaneous infection patient died.
Length of stay was the most significant risk factor for infection; the mean interval from admission to diagnosis was more than 2 months.
“Pulmonary zygomycosis due to contaminated hospital linens has never been reported.” Clinicians need to “maintain a high index of suspicion for early diagnosis and treatment of zygomycosis in immunosuppressed patients,” the investigators said.
The U.S. recently had a cutaneous outbreak in Louisiana; hospital linens contaminated with Rhizopus species killed five immunocompromised children there in 2015.
“Invasive zygomycosis is an emerging infection that is increasingly reported in immunosuppressed hosts;” previously reported sources include adhesive bandages, wooden tongue depressors, ostomy bags, damaged water circuitry, adjacent building construction activity, and, as Queen Mary reported previously, contaminated allopurinol tablets.
Detecting the problem isn’t easy. None of the Replicate Organism Detection and Counting contact plates at Queen Mary recovered zygomycetes from the contaminated linen items. It took sponge swapping to find it; “without the use of sponge swab and selective culture medium, the causative agents in this outbreak would have been overlooked,” the investigators said.
Hong Kong government services helped support the work. The authors did not have any financial conflicts of interest.
Contaminated laundry led to an outbreak of cutaneous and pulmonary zygomycosis that killed three immunocompromised patients and sickened three others at Queen Mary Hospital in Hong Kong.
The contamination was traced to a contract laundry service that was, in short, a microbe Disneyland. It was hot and humid, with sealed windows, dim lights, and a thick layer of dust on just about everything. Washers weren’t hot enough to kill spores; washed items were packed while warm and moist; and dirty linens rich with organic material were transported with clean ones (Clin Infect Dis. 2015 Dec 13. doi:10.1093/cid/civ1006).
Of 195 environmental samples, 119 (61%) were positive for Zygomycetes, as well as 100% of air samples. Freshly laundered items – including clothes and bedding – had bacteria counts of 1,028 colony forming units (CFU)/100 cm2, far exceeding the “hygienically clean” standard of 20 CFU/100 cm2 set by U.S. healthcare textile certification requirements.
Queen Mary didn’t regularly audit its linens for cleanliness and microbe counts. “Our findings [suggest] that such standards should be adopted to prevent similar outbreaks,” said the investigators, led by Dr. Vincent Cheng, an infection control officer at Queen Mary, one of Hong Kong’s largest hospitals and a teaching hospital for the University of Hong Kong.
It has since switched to a new laundry service.
The outbreak ran from June 2 to July 18, 2015, during Hong Kong’s hot and humid season, which didn’t help matters.
The six patients were 42-74 years old; one had interstitial lung disease and the rest were either cancer or transplant patients. Infection was due to the spore-forming mold Rhizopus microsporus. Two pulmonary and one cutaneous infection patient died.
Length of stay was the most significant risk factor for infection; the mean interval from admission to diagnosis was more than 2 months.
“Pulmonary zygomycosis due to contaminated hospital linens has never been reported.” Clinicians need to “maintain a high index of suspicion for early diagnosis and treatment of zygomycosis in immunosuppressed patients,” the investigators said.
The U.S. recently had a cutaneous outbreak in Louisiana; hospital linens contaminated with Rhizopus species killed five immunocompromised children there in 2015.
“Invasive zygomycosis is an emerging infection that is increasingly reported in immunosuppressed hosts;” previously reported sources include adhesive bandages, wooden tongue depressors, ostomy bags, damaged water circuitry, adjacent building construction activity, and, as Queen Mary reported previously, contaminated allopurinol tablets.
Detecting the problem isn’t easy. None of the Replicate Organism Detection and Counting contact plates at Queen Mary recovered zygomycetes from the contaminated linen items. It took sponge swapping to find it; “without the use of sponge swab and selective culture medium, the causative agents in this outbreak would have been overlooked,” the investigators said.
Hong Kong government services helped support the work. The authors did not have any financial conflicts of interest.
FROM CLINICAL INFECTIOUS DISEASES
Key clinical point: Clinicians need to maintain a high index of suspicion for early diagnosis and treatment of zygomycosis in immunosuppressed patients,
Major finding: Of 195 environmental samples at the contaminated laundry, 119 (61%) were positive for Zygomycetes, as well as 100% of air samples.
Data source: Epidemiological study in Hong Kong.
Disclosures: Hong Kong government services helped support the work. The authors do not have any financial conflicts of interest.
Study confirms resistant malaria in Cambodia

Image by Ute Frevert
and Margaret Shear
Results of a new study confirm that dihydroartemisinin-piperaquine, the first-line treatment for Plasmodium falciparum malaria infection in Cambodia, has failed in certain provinces due to parasite resistance to both artemisinin and piperaquine.
Dihydroartemisinin-piperaquine is an artemisinin combination therapy (ACT) that combines fast-acting artemisinin with a long-acting partner drug, piperaquine.
Resistance to artemisinin in parts of Southeast Asia is well-documented, but, until now, only a few studies have presented clear evidence of piperaquine resistance.
Additional results from this study suggest that artesunate, a form of artemisinin, plus mefloquine, a different long-acting partner drug, should be the first-line ACT in areas where dihydroartemisinin-piperaquine treatment has failed.
Chanaki Amaratunga, PhD, of the National Institute of Allergy and Infectious Diseases in Rockville, Maryland, and colleagues reported these results in The Lancet Infectious Diseases.
The researchers assessed the efficacy of dihydroartemisinin-piperaquine treatment in 241 malaria-afflicted participants ages 2 to 65. The subjects lived in 3 different Cambodian provinces with varying levels of artemisinin resistance.
After monitoring parasite levels in the blood for 63 days, the researchers found that parasites had reemerged despite initial clearance in 45.7% of participants in Pursat, 15.9% of participants in Preah Vihear, and 1.67% of participants in Ratanakiri.
The results indicate the ACT is failing in Pursat and Preah Vihear, where artemisinin resistance is common, but remains highly efficacious in Ratanakiri, where resistance is uncommon.
Laboratory tests showed the parasites from dihydroartemisinin-piperaquine failures contained a genetic marker of artemisinin resistance and had a decreased susceptibility to piperaquine, demonstrating that both artemisinin and piperaquine resistance contributed to treatment failures.
However, the parasites also showed an increased susceptibility to mefloquine and completely lacked the molecular marker for mefloquine resistance.
These findings informed new World Health Organization guidelines reinstating artesunate plus mefloquine as the first-line ACT in Cambodia where dihydroartemisinin-piperaquine treatment has failed.
The researchers said the findings also provide evidence to initiate surveillance programs to track the spread of piperaquine resistance and clinical trials to test alternative combination therapies. ![]()

Image by Ute Frevert
and Margaret Shear
Results of a new study confirm that dihydroartemisinin-piperaquine, the first-line treatment for Plasmodium falciparum malaria infection in Cambodia, has failed in certain provinces due to parasite resistance to both artemisinin and piperaquine.
Dihydroartemisinin-piperaquine is an artemisinin combination therapy (ACT) that combines fast-acting artemisinin with a long-acting partner drug, piperaquine.
Resistance to artemisinin in parts of Southeast Asia is well-documented, but, until now, only a few studies have presented clear evidence of piperaquine resistance.
Additional results from this study suggest that artesunate, a form of artemisinin, plus mefloquine, a different long-acting partner drug, should be the first-line ACT in areas where dihydroartemisinin-piperaquine treatment has failed.
Chanaki Amaratunga, PhD, of the National Institute of Allergy and Infectious Diseases in Rockville, Maryland, and colleagues reported these results in The Lancet Infectious Diseases.
The researchers assessed the efficacy of dihydroartemisinin-piperaquine treatment in 241 malaria-afflicted participants ages 2 to 65. The subjects lived in 3 different Cambodian provinces with varying levels of artemisinin resistance.
After monitoring parasite levels in the blood for 63 days, the researchers found that parasites had reemerged despite initial clearance in 45.7% of participants in Pursat, 15.9% of participants in Preah Vihear, and 1.67% of participants in Ratanakiri.
The results indicate the ACT is failing in Pursat and Preah Vihear, where artemisinin resistance is common, but remains highly efficacious in Ratanakiri, where resistance is uncommon.
Laboratory tests showed the parasites from dihydroartemisinin-piperaquine failures contained a genetic marker of artemisinin resistance and had a decreased susceptibility to piperaquine, demonstrating that both artemisinin and piperaquine resistance contributed to treatment failures.
However, the parasites also showed an increased susceptibility to mefloquine and completely lacked the molecular marker for mefloquine resistance.
These findings informed new World Health Organization guidelines reinstating artesunate plus mefloquine as the first-line ACT in Cambodia where dihydroartemisinin-piperaquine treatment has failed.
The researchers said the findings also provide evidence to initiate surveillance programs to track the spread of piperaquine resistance and clinical trials to test alternative combination therapies. ![]()

Image by Ute Frevert
and Margaret Shear
Results of a new study confirm that dihydroartemisinin-piperaquine, the first-line treatment for Plasmodium falciparum malaria infection in Cambodia, has failed in certain provinces due to parasite resistance to both artemisinin and piperaquine.
Dihydroartemisinin-piperaquine is an artemisinin combination therapy (ACT) that combines fast-acting artemisinin with a long-acting partner drug, piperaquine.
Resistance to artemisinin in parts of Southeast Asia is well-documented, but, until now, only a few studies have presented clear evidence of piperaquine resistance.
Additional results from this study suggest that artesunate, a form of artemisinin, plus mefloquine, a different long-acting partner drug, should be the first-line ACT in areas where dihydroartemisinin-piperaquine treatment has failed.
Chanaki Amaratunga, PhD, of the National Institute of Allergy and Infectious Diseases in Rockville, Maryland, and colleagues reported these results in The Lancet Infectious Diseases.
The researchers assessed the efficacy of dihydroartemisinin-piperaquine treatment in 241 malaria-afflicted participants ages 2 to 65. The subjects lived in 3 different Cambodian provinces with varying levels of artemisinin resistance.
After monitoring parasite levels in the blood for 63 days, the researchers found that parasites had reemerged despite initial clearance in 45.7% of participants in Pursat, 15.9% of participants in Preah Vihear, and 1.67% of participants in Ratanakiri.
The results indicate the ACT is failing in Pursat and Preah Vihear, where artemisinin resistance is common, but remains highly efficacious in Ratanakiri, where resistance is uncommon.
Laboratory tests showed the parasites from dihydroartemisinin-piperaquine failures contained a genetic marker of artemisinin resistance and had a decreased susceptibility to piperaquine, demonstrating that both artemisinin and piperaquine resistance contributed to treatment failures.
However, the parasites also showed an increased susceptibility to mefloquine and completely lacked the molecular marker for mefloquine resistance.
These findings informed new World Health Organization guidelines reinstating artesunate plus mefloquine as the first-line ACT in Cambodia where dihydroartemisinin-piperaquine treatment has failed.
The researchers said the findings also provide evidence to initiate surveillance programs to track the spread of piperaquine resistance and clinical trials to test alternative combination therapies. ![]()
Antilymphocyte globulin curbs chronic graft-versus-host disease
Antilymphocyte globulin (ATG) added to the myeloablative conditioning regimen of patients undergoing allogeneic stem cell transplantation resulted in a lower incidence of chronic graft-versus-host disease (GVHD) compared with conditioning regimens without ATG.
At two years, the cumulative incidence of chronic GVHD was 32.2% (95% CI, 22.1–46.7) for the ATG group vs 68.7% (58.4-80.7) for the non-ATG group (P < .001). At one year, 91% of the ATG group had discontinued cyclosporine, compared with 39% in the non-ATG group. The difference between groups was most pronounced in rates of the clinical extensive form of chronic GVHD: 7.6% (3.0-19.6) with ATG compared with 52.4% (39.3-69.9) without ATG.
T-cell depletion may cause a loss of graft-versus-leukemia effects, which is cause for concern. This study showed similar rates of relapse-free and overall survival for the ATG and non-ATG groups. Two-year relapse-free survival was 59.4% (47.8-69.2) in the ATG group and 64.6% (50.9-75.3) in the non-ATG group. The composite 2-year survival, free from chronic GVHD and relapse, was 36.6% (25.2-48.0) for the ATG group vs 16.8% (9.2-26.4) for the non-ATG group, according to the study reported in the January 7 issue of the New England Journal of Medicine (2016;374:43-53).
Chronic GVHD is the leading cause of later illness and death after allogeneic hematopoietic stem-cell transplantation, according to the authors. “Even if a modest increase in the rate of relapse in the ATG group cannot be ruled out, the significantly lower incidence of chronic GVHD with ATG resulted in a significantly higher rate of 2-year survival free from chronic GVD among patients who received ATG than among those who did not receive ATG (50% vs. 23%),” wrote Dr. Nicolaus Kröger, Professor and Medical Director of the Department of Stem Cell Transplantation at the University Hospital Hamburg-Eppendorf, Germany, and colleagues.
The prospective, open-label, randomized phase 3 trial evaluated 155 patients at 27 centers from 2006 to 2012. Patients with acute leukemia undergoing allogeneic stem cell transplantation with peripheral blood stem cells were randomized 1:1 to receive myeloablative conditioning with or without ATG.
Post-transplantation lymphoproliferative disorder was not observed in either group. The ATG and non-ATG groups had similar rates of infectious complications (57.8% and 54.2%, respectively), and nonrelapse-related death at 2 years (14.0% and 12.0%, respectively).
The study was funded by the Neovii Biotech and the European Society for Blood and Marrow Transplantation; ClinicalTrials.gov number, NCT00678275. Dr. Kröger reported grant support from Neovii Biotech. Several of his coauthors reported ties to industry.
Antilymphocyte globulin (ATG) added to the myeloablative conditioning regimen of patients undergoing allogeneic stem cell transplantation resulted in a lower incidence of chronic graft-versus-host disease (GVHD) compared with conditioning regimens without ATG.
At two years, the cumulative incidence of chronic GVHD was 32.2% (95% CI, 22.1–46.7) for the ATG group vs 68.7% (58.4-80.7) for the non-ATG group (P < .001). At one year, 91% of the ATG group had discontinued cyclosporine, compared with 39% in the non-ATG group. The difference between groups was most pronounced in rates of the clinical extensive form of chronic GVHD: 7.6% (3.0-19.6) with ATG compared with 52.4% (39.3-69.9) without ATG.
T-cell depletion may cause a loss of graft-versus-leukemia effects, which is cause for concern. This study showed similar rates of relapse-free and overall survival for the ATG and non-ATG groups. Two-year relapse-free survival was 59.4% (47.8-69.2) in the ATG group and 64.6% (50.9-75.3) in the non-ATG group. The composite 2-year survival, free from chronic GVHD and relapse, was 36.6% (25.2-48.0) for the ATG group vs 16.8% (9.2-26.4) for the non-ATG group, according to the study reported in the January 7 issue of the New England Journal of Medicine (2016;374:43-53).
Chronic GVHD is the leading cause of later illness and death after allogeneic hematopoietic stem-cell transplantation, according to the authors. “Even if a modest increase in the rate of relapse in the ATG group cannot be ruled out, the significantly lower incidence of chronic GVHD with ATG resulted in a significantly higher rate of 2-year survival free from chronic GVD among patients who received ATG than among those who did not receive ATG (50% vs. 23%),” wrote Dr. Nicolaus Kröger, Professor and Medical Director of the Department of Stem Cell Transplantation at the University Hospital Hamburg-Eppendorf, Germany, and colleagues.
The prospective, open-label, randomized phase 3 trial evaluated 155 patients at 27 centers from 2006 to 2012. Patients with acute leukemia undergoing allogeneic stem cell transplantation with peripheral blood stem cells were randomized 1:1 to receive myeloablative conditioning with or without ATG.
Post-transplantation lymphoproliferative disorder was not observed in either group. The ATG and non-ATG groups had similar rates of infectious complications (57.8% and 54.2%, respectively), and nonrelapse-related death at 2 years (14.0% and 12.0%, respectively).
The study was funded by the Neovii Biotech and the European Society for Blood and Marrow Transplantation; ClinicalTrials.gov number, NCT00678275. Dr. Kröger reported grant support from Neovii Biotech. Several of his coauthors reported ties to industry.
Antilymphocyte globulin (ATG) added to the myeloablative conditioning regimen of patients undergoing allogeneic stem cell transplantation resulted in a lower incidence of chronic graft-versus-host disease (GVHD) compared with conditioning regimens without ATG.
At two years, the cumulative incidence of chronic GVHD was 32.2% (95% CI, 22.1–46.7) for the ATG group vs 68.7% (58.4-80.7) for the non-ATG group (P < .001). At one year, 91% of the ATG group had discontinued cyclosporine, compared with 39% in the non-ATG group. The difference between groups was most pronounced in rates of the clinical extensive form of chronic GVHD: 7.6% (3.0-19.6) with ATG compared with 52.4% (39.3-69.9) without ATG.
T-cell depletion may cause a loss of graft-versus-leukemia effects, which is cause for concern. This study showed similar rates of relapse-free and overall survival for the ATG and non-ATG groups. Two-year relapse-free survival was 59.4% (47.8-69.2) in the ATG group and 64.6% (50.9-75.3) in the non-ATG group. The composite 2-year survival, free from chronic GVHD and relapse, was 36.6% (25.2-48.0) for the ATG group vs 16.8% (9.2-26.4) for the non-ATG group, according to the study reported in the January 7 issue of the New England Journal of Medicine (2016;374:43-53).
Chronic GVHD is the leading cause of later illness and death after allogeneic hematopoietic stem-cell transplantation, according to the authors. “Even if a modest increase in the rate of relapse in the ATG group cannot be ruled out, the significantly lower incidence of chronic GVHD with ATG resulted in a significantly higher rate of 2-year survival free from chronic GVD among patients who received ATG than among those who did not receive ATG (50% vs. 23%),” wrote Dr. Nicolaus Kröger, Professor and Medical Director of the Department of Stem Cell Transplantation at the University Hospital Hamburg-Eppendorf, Germany, and colleagues.
The prospective, open-label, randomized phase 3 trial evaluated 155 patients at 27 centers from 2006 to 2012. Patients with acute leukemia undergoing allogeneic stem cell transplantation with peripheral blood stem cells were randomized 1:1 to receive myeloablative conditioning with or without ATG.
Post-transplantation lymphoproliferative disorder was not observed in either group. The ATG and non-ATG groups had similar rates of infectious complications (57.8% and 54.2%, respectively), and nonrelapse-related death at 2 years (14.0% and 12.0%, respectively).
The study was funded by the Neovii Biotech and the European Society for Blood and Marrow Transplantation; ClinicalTrials.gov number, NCT00678275. Dr. Kröger reported grant support from Neovii Biotech. Several of his coauthors reported ties to industry.
FROM NEJM
Key clinical point: Chronic graft-versus-host disease (GVHD) after allogeneic stem cell transplantation with peripheral blood stem cells was less than half as frequent with antilymphocyte globulin added to the conditioning regimen.
Major finding: Cumulative incidence of chronic GVHD at 2 years was 32.2% with antilymphocyte globulin vs 68.7% without it.
Data source: The prospective, open-label, randomized phase 3 trial evaluated 155 patients at 27 centers from 2006 to 2012.
Disclosures: Research was supported in part by Neovii Biotech. Dr. Kröger reported grant support from Neovii Biotech. Several of his coauthors reported ties to industry.
Noncompete clauses: Be wary, negotiate early
Noncompete clauses can severely limit a doctor’s business options and create serious financial challenges, so negotiate with employers early and watch out for tricky contract terms that could stifle future opportunities.
That is the advice from health law experts around the country. They point out that when it comes to noncompete clauses – employment contract language that limits where physicians can practice after employment ends or is terminated – doctors should pay close attention, especially to the following:
Geographical limitations
Distance requirements within noncompete provisions are a top issue that can trip up doctors, Bloomfield Hills, Mich., health law attorney Mark S. Kopson said. The clause typically specifies that a physician cannot practice within a certain radius of the former employer. However, if an employer has three offices for instance, that 10-mile radius can quickly become a 30-mile radius or more depending how the provision is worded. Mr. Kopson recalled a recent client who practiced for 5 years in one office and was transferred to an office in another town for 30 days. He was then terminated, and his employer attempted to enforce contract terms that would prevent him from practicing within a 10-mile radius of both offices. A court determined that the employer was acting in bad faith and sought an unfair competitive advantage.
“But No. 1, you don’t want to have to go to court,” Mr. Kopson said. “And No. 2, you can have the best lawyer, but once it’s in the hands of the judge or the jury, anything can happen. That’s why you really want to do the work on this up front.”
When negotiating noncompete clauses, be cognizant of where distances are being measured from and around, the legal experts stress. Also, be clear with employers about what defines a reasonable distance, based on the geographic spread of their patient base.
“What’s reasonable for a family practice physician is probably not going to be reasonable for a pediatric neurosurgeon, as they draw their patients from varying distances,” he said. “Also, negotiate to ensure that the length of time of the restriction is reasonable. Taking into account, both the distance and time period, the physician must still be able to earn a living.”
Time frame restrictions
Negotiate the shortest duration that you can, advises Greenbelt, Md., labor and employment attorney Jay P. Holland. Noncompete provisions typically limit a doctor from practicing around a certain radius for 1-5 years, but some employers may try to enforce longer time periods.
“Consider your career and lifestyle goals carefully prior to entering into a noncompete,” Mr. Holland said. “The first approach should always be an attempt to exclude the noncompete from your prospective agreement if you are joining a practice. If a noncompete is unavoidable, then strive to make it the least onerous possible. Ask yourself prior to signing an agreement, ‘If I were to leave this practice, what are the restrictions I could live with? Are the restrictions reasonable?’ ”
Knowing your state’s law is key. State regulation of noncompete provisions widely differ. States such as California broadly hold that noncompete contracts are per se invalid – even if narrowly tailored – unless necessary to protect trade secrets. States such as Maryland allow the provisions only if area and duration restrictions are reasonable and do not impose undue hardship on employees. Three states – Colorado, Delaware, and Massachusetts – have laws that strictly prohibit noncompete clauses in physician contracts.
“Most other states will generally enforce noncompete clauses so long as their terms are reasonable in light of the interests of the employer, the employee, and the general public,” Mr. Holland said. “Therefore, noncompete clauses should be no greater in scope than is necessary to protect the business or goodwill of the employer.”
Patient retention problems
Watch out for contract language referring to “trade secrets,” adds Los Angeles health law attorney Andrew H. Selesnick. Trade secret clauses are often lengthy and typically state that physicians cannot use or retain information from the employer that is considered confidential. Because patient lists are usually considered confidential, these terms could potentially prohibit patients from following their doctor.
“If you want to leave and take your patients with you, there may be some trade secret implications associated with that,” Mr. Selesnick said. “The ability to be able to move patients is significant and can have significant financial impacts. Know what you’re getting into.”
If bringing patients with them to a new practice, doctors should make sure the employment agreement excludes these patients from any nonsolicitation provision at the time the doctor leaves, notes Mr. Holland. Include language that states physicians can retain patients they originally brought to the practice when they depart without violating the agreement.
Make sure to review any proposed noncompete clauses in relation to proposed termination provisions, Mr. Kopson said. Doctors should negotiate language that ensures noncompete obligations will be null and void if physicians are terminated without cause (if such terminations are permitted by the contract), or if the employer breaches the contract.
Seeking the advice of an experienced contract attorney before signing a noncompete clause can save doctors significant time, money, and heartache in the long run, Mr. Kopson notes.
“The biggest risk is signing a contract that has such a clause with an expectation that it will not be enforced,” he said. “If [clauses are] properly drafted, they’re going to be binding. If you get the help up front, it’s going to be a lot less expensive than having your life turned upside down because you’re stuck with a noncompete that has bad terms in it.”
Unreasonable terms
Once signed, getting out of non-compete clauses can be tricky, Mr. Selesnick said. However, doctors can usually escape them if they can prove the terms are unreasonable.
“You can get out of them, especially if they’re very restrictive and say you can’t practice within an area that may prevent you from earning your livelihood,” Mr. Selesnick said. “Courts [generally] think that employees should be able to leave and be able to get a job elsewhere, even if it’s across the street.”
Courts are typically more favorable to physician-employees than independent contractors when it comes to noncompete clauses, Mr. Selesnick said. Independent contractors are generally viewed as having more power over their work than physician-employees. They may have a tougher time convincing a court that such provisions will harm their employment options.
When seeking to enforce a disputed noncompete agreement, employers frequently will request a court-ordered temporary restraining order or injunction to enforce the clause, Mr. Holland said. Judges consider general principles of fairness and equity, and balance the relative harm to the employer and the employee, when deciding whether to issue the injunction. The employee-physician can also try to beat the employer to the courthouse steps by filing a “declaratory judgment” lawsuit that seeks guidance from the court on the contract’s enforceability.
“Typically, employers attempt to do that which is in their best economic interest,” Mr. Holland said. “If a proposal can be negotiated where the employer’s economic well-being is not threatened, then the employer should have a strong interest in a compromise.”
On Twitter @legal_med
Noncompete clauses can severely limit a doctor’s business options and create serious financial challenges, so negotiate with employers early and watch out for tricky contract terms that could stifle future opportunities.
That is the advice from health law experts around the country. They point out that when it comes to noncompete clauses – employment contract language that limits where physicians can practice after employment ends or is terminated – doctors should pay close attention, especially to the following:
Geographical limitations
Distance requirements within noncompete provisions are a top issue that can trip up doctors, Bloomfield Hills, Mich., health law attorney Mark S. Kopson said. The clause typically specifies that a physician cannot practice within a certain radius of the former employer. However, if an employer has three offices for instance, that 10-mile radius can quickly become a 30-mile radius or more depending how the provision is worded. Mr. Kopson recalled a recent client who practiced for 5 years in one office and was transferred to an office in another town for 30 days. He was then terminated, and his employer attempted to enforce contract terms that would prevent him from practicing within a 10-mile radius of both offices. A court determined that the employer was acting in bad faith and sought an unfair competitive advantage.
“But No. 1, you don’t want to have to go to court,” Mr. Kopson said. “And No. 2, you can have the best lawyer, but once it’s in the hands of the judge or the jury, anything can happen. That’s why you really want to do the work on this up front.”
When negotiating noncompete clauses, be cognizant of where distances are being measured from and around, the legal experts stress. Also, be clear with employers about what defines a reasonable distance, based on the geographic spread of their patient base.
“What’s reasonable for a family practice physician is probably not going to be reasonable for a pediatric neurosurgeon, as they draw their patients from varying distances,” he said. “Also, negotiate to ensure that the length of time of the restriction is reasonable. Taking into account, both the distance and time period, the physician must still be able to earn a living.”
Time frame restrictions
Negotiate the shortest duration that you can, advises Greenbelt, Md., labor and employment attorney Jay P. Holland. Noncompete provisions typically limit a doctor from practicing around a certain radius for 1-5 years, but some employers may try to enforce longer time periods.
“Consider your career and lifestyle goals carefully prior to entering into a noncompete,” Mr. Holland said. “The first approach should always be an attempt to exclude the noncompete from your prospective agreement if you are joining a practice. If a noncompete is unavoidable, then strive to make it the least onerous possible. Ask yourself prior to signing an agreement, ‘If I were to leave this practice, what are the restrictions I could live with? Are the restrictions reasonable?’ ”
Knowing your state’s law is key. State regulation of noncompete provisions widely differ. States such as California broadly hold that noncompete contracts are per se invalid – even if narrowly tailored – unless necessary to protect trade secrets. States such as Maryland allow the provisions only if area and duration restrictions are reasonable and do not impose undue hardship on employees. Three states – Colorado, Delaware, and Massachusetts – have laws that strictly prohibit noncompete clauses in physician contracts.
“Most other states will generally enforce noncompete clauses so long as their terms are reasonable in light of the interests of the employer, the employee, and the general public,” Mr. Holland said. “Therefore, noncompete clauses should be no greater in scope than is necessary to protect the business or goodwill of the employer.”
Patient retention problems
Watch out for contract language referring to “trade secrets,” adds Los Angeles health law attorney Andrew H. Selesnick. Trade secret clauses are often lengthy and typically state that physicians cannot use or retain information from the employer that is considered confidential. Because patient lists are usually considered confidential, these terms could potentially prohibit patients from following their doctor.
“If you want to leave and take your patients with you, there may be some trade secret implications associated with that,” Mr. Selesnick said. “The ability to be able to move patients is significant and can have significant financial impacts. Know what you’re getting into.”
If bringing patients with them to a new practice, doctors should make sure the employment agreement excludes these patients from any nonsolicitation provision at the time the doctor leaves, notes Mr. Holland. Include language that states physicians can retain patients they originally brought to the practice when they depart without violating the agreement.
Make sure to review any proposed noncompete clauses in relation to proposed termination provisions, Mr. Kopson said. Doctors should negotiate language that ensures noncompete obligations will be null and void if physicians are terminated without cause (if such terminations are permitted by the contract), or if the employer breaches the contract.
Seeking the advice of an experienced contract attorney before signing a noncompete clause can save doctors significant time, money, and heartache in the long run, Mr. Kopson notes.
“The biggest risk is signing a contract that has such a clause with an expectation that it will not be enforced,” he said. “If [clauses are] properly drafted, they’re going to be binding. If you get the help up front, it’s going to be a lot less expensive than having your life turned upside down because you’re stuck with a noncompete that has bad terms in it.”
Unreasonable terms
Once signed, getting out of non-compete clauses can be tricky, Mr. Selesnick said. However, doctors can usually escape them if they can prove the terms are unreasonable.
“You can get out of them, especially if they’re very restrictive and say you can’t practice within an area that may prevent you from earning your livelihood,” Mr. Selesnick said. “Courts [generally] think that employees should be able to leave and be able to get a job elsewhere, even if it’s across the street.”
Courts are typically more favorable to physician-employees than independent contractors when it comes to noncompete clauses, Mr. Selesnick said. Independent contractors are generally viewed as having more power over their work than physician-employees. They may have a tougher time convincing a court that such provisions will harm their employment options.
When seeking to enforce a disputed noncompete agreement, employers frequently will request a court-ordered temporary restraining order or injunction to enforce the clause, Mr. Holland said. Judges consider general principles of fairness and equity, and balance the relative harm to the employer and the employee, when deciding whether to issue the injunction. The employee-physician can also try to beat the employer to the courthouse steps by filing a “declaratory judgment” lawsuit that seeks guidance from the court on the contract’s enforceability.
“Typically, employers attempt to do that which is in their best economic interest,” Mr. Holland said. “If a proposal can be negotiated where the employer’s economic well-being is not threatened, then the employer should have a strong interest in a compromise.”
On Twitter @legal_med
Noncompete clauses can severely limit a doctor’s business options and create serious financial challenges, so negotiate with employers early and watch out for tricky contract terms that could stifle future opportunities.
That is the advice from health law experts around the country. They point out that when it comes to noncompete clauses – employment contract language that limits where physicians can practice after employment ends or is terminated – doctors should pay close attention, especially to the following:
Geographical limitations
Distance requirements within noncompete provisions are a top issue that can trip up doctors, Bloomfield Hills, Mich., health law attorney Mark S. Kopson said. The clause typically specifies that a physician cannot practice within a certain radius of the former employer. However, if an employer has three offices for instance, that 10-mile radius can quickly become a 30-mile radius or more depending how the provision is worded. Mr. Kopson recalled a recent client who practiced for 5 years in one office and was transferred to an office in another town for 30 days. He was then terminated, and his employer attempted to enforce contract terms that would prevent him from practicing within a 10-mile radius of both offices. A court determined that the employer was acting in bad faith and sought an unfair competitive advantage.
“But No. 1, you don’t want to have to go to court,” Mr. Kopson said. “And No. 2, you can have the best lawyer, but once it’s in the hands of the judge or the jury, anything can happen. That’s why you really want to do the work on this up front.”
When negotiating noncompete clauses, be cognizant of where distances are being measured from and around, the legal experts stress. Also, be clear with employers about what defines a reasonable distance, based on the geographic spread of their patient base.
“What’s reasonable for a family practice physician is probably not going to be reasonable for a pediatric neurosurgeon, as they draw their patients from varying distances,” he said. “Also, negotiate to ensure that the length of time of the restriction is reasonable. Taking into account, both the distance and time period, the physician must still be able to earn a living.”
Time frame restrictions
Negotiate the shortest duration that you can, advises Greenbelt, Md., labor and employment attorney Jay P. Holland. Noncompete provisions typically limit a doctor from practicing around a certain radius for 1-5 years, but some employers may try to enforce longer time periods.
“Consider your career and lifestyle goals carefully prior to entering into a noncompete,” Mr. Holland said. “The first approach should always be an attempt to exclude the noncompete from your prospective agreement if you are joining a practice. If a noncompete is unavoidable, then strive to make it the least onerous possible. Ask yourself prior to signing an agreement, ‘If I were to leave this practice, what are the restrictions I could live with? Are the restrictions reasonable?’ ”
Knowing your state’s law is key. State regulation of noncompete provisions widely differ. States such as California broadly hold that noncompete contracts are per se invalid – even if narrowly tailored – unless necessary to protect trade secrets. States such as Maryland allow the provisions only if area and duration restrictions are reasonable and do not impose undue hardship on employees. Three states – Colorado, Delaware, and Massachusetts – have laws that strictly prohibit noncompete clauses in physician contracts.
“Most other states will generally enforce noncompete clauses so long as their terms are reasonable in light of the interests of the employer, the employee, and the general public,” Mr. Holland said. “Therefore, noncompete clauses should be no greater in scope than is necessary to protect the business or goodwill of the employer.”
Patient retention problems
Watch out for contract language referring to “trade secrets,” adds Los Angeles health law attorney Andrew H. Selesnick. Trade secret clauses are often lengthy and typically state that physicians cannot use or retain information from the employer that is considered confidential. Because patient lists are usually considered confidential, these terms could potentially prohibit patients from following their doctor.
“If you want to leave and take your patients with you, there may be some trade secret implications associated with that,” Mr. Selesnick said. “The ability to be able to move patients is significant and can have significant financial impacts. Know what you’re getting into.”
If bringing patients with them to a new practice, doctors should make sure the employment agreement excludes these patients from any nonsolicitation provision at the time the doctor leaves, notes Mr. Holland. Include language that states physicians can retain patients they originally brought to the practice when they depart without violating the agreement.
Make sure to review any proposed noncompete clauses in relation to proposed termination provisions, Mr. Kopson said. Doctors should negotiate language that ensures noncompete obligations will be null and void if physicians are terminated without cause (if such terminations are permitted by the contract), or if the employer breaches the contract.
Seeking the advice of an experienced contract attorney before signing a noncompete clause can save doctors significant time, money, and heartache in the long run, Mr. Kopson notes.
“The biggest risk is signing a contract that has such a clause with an expectation that it will not be enforced,” he said. “If [clauses are] properly drafted, they’re going to be binding. If you get the help up front, it’s going to be a lot less expensive than having your life turned upside down because you’re stuck with a noncompete that has bad terms in it.”
Unreasonable terms
Once signed, getting out of non-compete clauses can be tricky, Mr. Selesnick said. However, doctors can usually escape them if they can prove the terms are unreasonable.
“You can get out of them, especially if they’re very restrictive and say you can’t practice within an area that may prevent you from earning your livelihood,” Mr. Selesnick said. “Courts [generally] think that employees should be able to leave and be able to get a job elsewhere, even if it’s across the street.”
Courts are typically more favorable to physician-employees than independent contractors when it comes to noncompete clauses, Mr. Selesnick said. Independent contractors are generally viewed as having more power over their work than physician-employees. They may have a tougher time convincing a court that such provisions will harm their employment options.
When seeking to enforce a disputed noncompete agreement, employers frequently will request a court-ordered temporary restraining order or injunction to enforce the clause, Mr. Holland said. Judges consider general principles of fairness and equity, and balance the relative harm to the employer and the employee, when deciding whether to issue the injunction. The employee-physician can also try to beat the employer to the courthouse steps by filing a “declaratory judgment” lawsuit that seeks guidance from the court on the contract’s enforceability.
“Typically, employers attempt to do that which is in their best economic interest,” Mr. Holland said. “If a proposal can be negotiated where the employer’s economic well-being is not threatened, then the employer should have a strong interest in a compromise.”
On Twitter @legal_med