User login
What Is Your Diagnosis? Argyria
PDL Versus PDT for Port-wine Stains

In the May 2013 issue of the British Journal of Dermatology (2013;168:1040-1046) Gao et al reported on a side-by-side comparison of the use of photodynamic therapy (PDT) versus the pulsed dye laser (PDL) for the treatment of 9 red and 6 purple port-wine stains (PWSs). Fifteen patients (age range, 11–36 years) with PWSs were chosen and 2 adjacent areas of the lesion were randomly assigned to receive either a single PDL treatment or a single PDT session. Eleven lesions were on the neck area, 3 on the upper arm, and 1 on the upper leg. The PDL had a wavelength of 585 nm, and PDT was performed with intravenous hematoporphyrin monomethyl ether and a low-power copper vapor laser (510.6 and 578.2 nm, respectively). The PDT-treated area was done 30 minutes after the PDL-treated area with the other areas being covered. The clinical outcome was measured colorimetrically (blanching rates) and visually.
For the red PWSs the blanching rates at 2 months with the PDL were 11% to 24% and 22% to 55% with PDT (P=.006). For the purple PWSs, blanching rates ranged from 8% to 33% with PDL and 30% to 45% with PDT (P=.0313). Two patients with purple PWSs showed no response to either PDT or PDL. All PDT sites developed localized edema, and all PDL sites developed edema, blistering, purpura, and crusts. Four patients with red PWSs developed hyperpigmentation at the PDL sites.
What’s the issue?
Although there have been studies showing that PDT is an effective treatment of PWSs, this study is a side-by-side quantitative comparison of PDL versus PDT. This study showed that PDT is as effective and as safe as PDL and possibly superior for the treatment of red and purple flat PWSs. This study represents promising steps forward in PDT treatment of dermatologic conditions.
Even though PDL therapy is considered the current standard for treatment of PWSs, this study does show good clearance with PDT. Pulsed dye laser therapy has been more readily available in North America and Europe, though in China, where this study took place, it is not common. The PDT in this study utilized an intravenous photosensitizer, which may not be suitable for all patients. Other limitations of this study include the small sample size and the possibility that treating the lesion halves in close proximity to each other may compound adverse effects. Because each half of the lesion (close proximity to one another) was treated, the effects of each treatment may have been compounded.
Could PDT become an adjuvant treatment in the armamentarium for resistant port-wine stains?

In the May 2013 issue of the British Journal of Dermatology (2013;168:1040-1046) Gao et al reported on a side-by-side comparison of the use of photodynamic therapy (PDT) versus the pulsed dye laser (PDL) for the treatment of 9 red and 6 purple port-wine stains (PWSs). Fifteen patients (age range, 11–36 years) with PWSs were chosen and 2 adjacent areas of the lesion were randomly assigned to receive either a single PDL treatment or a single PDT session. Eleven lesions were on the neck area, 3 on the upper arm, and 1 on the upper leg. The PDL had a wavelength of 585 nm, and PDT was performed with intravenous hematoporphyrin monomethyl ether and a low-power copper vapor laser (510.6 and 578.2 nm, respectively). The PDT-treated area was done 30 minutes after the PDL-treated area with the other areas being covered. The clinical outcome was measured colorimetrically (blanching rates) and visually.
For the red PWSs the blanching rates at 2 months with the PDL were 11% to 24% and 22% to 55% with PDT (P=.006). For the purple PWSs, blanching rates ranged from 8% to 33% with PDL and 30% to 45% with PDT (P=.0313). Two patients with purple PWSs showed no response to either PDT or PDL. All PDT sites developed localized edema, and all PDL sites developed edema, blistering, purpura, and crusts. Four patients with red PWSs developed hyperpigmentation at the PDL sites.
What’s the issue?
Although there have been studies showing that PDT is an effective treatment of PWSs, this study is a side-by-side quantitative comparison of PDL versus PDT. This study showed that PDT is as effective and as safe as PDL and possibly superior for the treatment of red and purple flat PWSs. This study represents promising steps forward in PDT treatment of dermatologic conditions.
Even though PDL therapy is considered the current standard for treatment of PWSs, this study does show good clearance with PDT. Pulsed dye laser therapy has been more readily available in North America and Europe, though in China, where this study took place, it is not common. The PDT in this study utilized an intravenous photosensitizer, which may not be suitable for all patients. Other limitations of this study include the small sample size and the possibility that treating the lesion halves in close proximity to each other may compound adverse effects. Because each half of the lesion (close proximity to one another) was treated, the effects of each treatment may have been compounded.
Could PDT become an adjuvant treatment in the armamentarium for resistant port-wine stains?

In the May 2013 issue of the British Journal of Dermatology (2013;168:1040-1046) Gao et al reported on a side-by-side comparison of the use of photodynamic therapy (PDT) versus the pulsed dye laser (PDL) for the treatment of 9 red and 6 purple port-wine stains (PWSs). Fifteen patients (age range, 11–36 years) with PWSs were chosen and 2 adjacent areas of the lesion were randomly assigned to receive either a single PDL treatment or a single PDT session. Eleven lesions were on the neck area, 3 on the upper arm, and 1 on the upper leg. The PDL had a wavelength of 585 nm, and PDT was performed with intravenous hematoporphyrin monomethyl ether and a low-power copper vapor laser (510.6 and 578.2 nm, respectively). The PDT-treated area was done 30 minutes after the PDL-treated area with the other areas being covered. The clinical outcome was measured colorimetrically (blanching rates) and visually.
For the red PWSs the blanching rates at 2 months with the PDL were 11% to 24% and 22% to 55% with PDT (P=.006). For the purple PWSs, blanching rates ranged from 8% to 33% with PDL and 30% to 45% with PDT (P=.0313). Two patients with purple PWSs showed no response to either PDT or PDL. All PDT sites developed localized edema, and all PDL sites developed edema, blistering, purpura, and crusts. Four patients with red PWSs developed hyperpigmentation at the PDL sites.
What’s the issue?
Although there have been studies showing that PDT is an effective treatment of PWSs, this study is a side-by-side quantitative comparison of PDL versus PDT. This study showed that PDT is as effective and as safe as PDL and possibly superior for the treatment of red and purple flat PWSs. This study represents promising steps forward in PDT treatment of dermatologic conditions.
Even though PDL therapy is considered the current standard for treatment of PWSs, this study does show good clearance with PDT. Pulsed dye laser therapy has been more readily available in North America and Europe, though in China, where this study took place, it is not common. The PDT in this study utilized an intravenous photosensitizer, which may not be suitable for all patients. Other limitations of this study include the small sample size and the possibility that treating the lesion halves in close proximity to each other may compound adverse effects. Because each half of the lesion (close proximity to one another) was treated, the effects of each treatment may have been compounded.
Could PDT become an adjuvant treatment in the armamentarium for resistant port-wine stains?
Technique is key for filler injection in darker skin
MIAMI BEACH – When considering dermal fillers for skin of color patients, remember that fewer injections can help reduce the risk of keloid formation and pigmentary changes, Dr. Valerie D. Callender said at the annual meeting of the American Academy of Dermatology.
People with skin of color made up 20% of the patient population seeking cosmetic procedures in 2011, and they are the fastest-growing demographic group in the U.S. population, Dr. Callender said. Dermatologists can expect to see more patients with ethnic skin in their practices, and it’s important for them to remember that not all aging skin is created equal, and that different techniques come into play for different skin types, she added.
Aging in ethnic facial skin differs from aging in lighter skin, mainly because of the photoprotective effect of melanin against UV radiation, said Dr. Callender. The effects of photodamage usually appear 10-20 years later in skin of color patients and with less severity.
"Your typical skin of color patient is 45 years old, has some volume loss, some infraorbital hollowing, and is definitely concerned about laugh lines," said Dr. Callender.
"The No. 1 tip is to minimize the number of injections to minimize the risk of postinflammatory hyperpigmentation," she emphasized. "If there is erythema, apply a topical corticosteroid."
Hyaluronic acid fillers are among the top five nonsurgical cosmetic procedures in the United States, but there is a paucity of published studies in skin of color patients, said Dr. Callender of Howard University, Washington. The population included in large, pivotal clinical studies is composed mainly of white patients, and even if these studies include a subset of skin of color patients, they don’t specifically report on treatment and safety outcomes in those patients, Dr. Callender said.
Dr. Callender listed several published and unpublished studies including data on the use of fillers in patients with Fitzpatrick Skin Types IV to VI. The products studied included Restylane, Perlane, Juvéderm Ultra and Ultra Plus, Hylaform, Hylaform Plus, Captique, Belotero Balance, and Radiesse.
Pigmentary changes were common throughout the studies, but they did not affected more than 9% of the study population, according to Dr. Callender. In the Radiesse study, the authors concluded that lack of pigmentary changes may have occurred from a deeper injection level, compared with HA fillers, she noted. No keloids or scarring were reported at 6 months’ follow-up and the investigators used a 25- to 27-gauge needle (Dermatol. Surg. 2009; 35:1641-5).
There have been no formal clinical trials evaluating safety of Sculptra in skin of color patients, said Dr. Callender, director of Callender Dermatology & Cosmetic Center, Glenn Dale, Md. However, the investigators in a 2010 study advised clinicians to lower the injection time, use proper product reconstitution and proper produce placement, perform immediate and postoperative massage, and avoid Sculptra on patients with a history of keloids in order to reduce the risk of adverse events (J. Drugs Dermatol. 2010;9:451-6).
Dr. Callender has been a consultant and investigator for Allergan, Galderma, Medicis, and Merz.
On Twitter @NaseemSMiller
MIAMI BEACH – When considering dermal fillers for skin of color patients, remember that fewer injections can help reduce the risk of keloid formation and pigmentary changes, Dr. Valerie D. Callender said at the annual meeting of the American Academy of Dermatology.
People with skin of color made up 20% of the patient population seeking cosmetic procedures in 2011, and they are the fastest-growing demographic group in the U.S. population, Dr. Callender said. Dermatologists can expect to see more patients with ethnic skin in their practices, and it’s important for them to remember that not all aging skin is created equal, and that different techniques come into play for different skin types, she added.
Aging in ethnic facial skin differs from aging in lighter skin, mainly because of the photoprotective effect of melanin against UV radiation, said Dr. Callender. The effects of photodamage usually appear 10-20 years later in skin of color patients and with less severity.
"Your typical skin of color patient is 45 years old, has some volume loss, some infraorbital hollowing, and is definitely concerned about laugh lines," said Dr. Callender.
"The No. 1 tip is to minimize the number of injections to minimize the risk of postinflammatory hyperpigmentation," she emphasized. "If there is erythema, apply a topical corticosteroid."
Hyaluronic acid fillers are among the top five nonsurgical cosmetic procedures in the United States, but there is a paucity of published studies in skin of color patients, said Dr. Callender of Howard University, Washington. The population included in large, pivotal clinical studies is composed mainly of white patients, and even if these studies include a subset of skin of color patients, they don’t specifically report on treatment and safety outcomes in those patients, Dr. Callender said.
Dr. Callender listed several published and unpublished studies including data on the use of fillers in patients with Fitzpatrick Skin Types IV to VI. The products studied included Restylane, Perlane, Juvéderm Ultra and Ultra Plus, Hylaform, Hylaform Plus, Captique, Belotero Balance, and Radiesse.
Pigmentary changes were common throughout the studies, but they did not affected more than 9% of the study population, according to Dr. Callender. In the Radiesse study, the authors concluded that lack of pigmentary changes may have occurred from a deeper injection level, compared with HA fillers, she noted. No keloids or scarring were reported at 6 months’ follow-up and the investigators used a 25- to 27-gauge needle (Dermatol. Surg. 2009; 35:1641-5).
There have been no formal clinical trials evaluating safety of Sculptra in skin of color patients, said Dr. Callender, director of Callender Dermatology & Cosmetic Center, Glenn Dale, Md. However, the investigators in a 2010 study advised clinicians to lower the injection time, use proper product reconstitution and proper produce placement, perform immediate and postoperative massage, and avoid Sculptra on patients with a history of keloids in order to reduce the risk of adverse events (J. Drugs Dermatol. 2010;9:451-6).
Dr. Callender has been a consultant and investigator for Allergan, Galderma, Medicis, and Merz.
On Twitter @NaseemSMiller
MIAMI BEACH – When considering dermal fillers for skin of color patients, remember that fewer injections can help reduce the risk of keloid formation and pigmentary changes, Dr. Valerie D. Callender said at the annual meeting of the American Academy of Dermatology.
People with skin of color made up 20% of the patient population seeking cosmetic procedures in 2011, and they are the fastest-growing demographic group in the U.S. population, Dr. Callender said. Dermatologists can expect to see more patients with ethnic skin in their practices, and it’s important for them to remember that not all aging skin is created equal, and that different techniques come into play for different skin types, she added.
Aging in ethnic facial skin differs from aging in lighter skin, mainly because of the photoprotective effect of melanin against UV radiation, said Dr. Callender. The effects of photodamage usually appear 10-20 years later in skin of color patients and with less severity.
"Your typical skin of color patient is 45 years old, has some volume loss, some infraorbital hollowing, and is definitely concerned about laugh lines," said Dr. Callender.
"The No. 1 tip is to minimize the number of injections to minimize the risk of postinflammatory hyperpigmentation," she emphasized. "If there is erythema, apply a topical corticosteroid."
Hyaluronic acid fillers are among the top five nonsurgical cosmetic procedures in the United States, but there is a paucity of published studies in skin of color patients, said Dr. Callender of Howard University, Washington. The population included in large, pivotal clinical studies is composed mainly of white patients, and even if these studies include a subset of skin of color patients, they don’t specifically report on treatment and safety outcomes in those patients, Dr. Callender said.
Dr. Callender listed several published and unpublished studies including data on the use of fillers in patients with Fitzpatrick Skin Types IV to VI. The products studied included Restylane, Perlane, Juvéderm Ultra and Ultra Plus, Hylaform, Hylaform Plus, Captique, Belotero Balance, and Radiesse.
Pigmentary changes were common throughout the studies, but they did not affected more than 9% of the study population, according to Dr. Callender. In the Radiesse study, the authors concluded that lack of pigmentary changes may have occurred from a deeper injection level, compared with HA fillers, she noted. No keloids or scarring were reported at 6 months’ follow-up and the investigators used a 25- to 27-gauge needle (Dermatol. Surg. 2009; 35:1641-5).
There have been no formal clinical trials evaluating safety of Sculptra in skin of color patients, said Dr. Callender, director of Callender Dermatology & Cosmetic Center, Glenn Dale, Md. However, the investigators in a 2010 study advised clinicians to lower the injection time, use proper product reconstitution and proper produce placement, perform immediate and postoperative massage, and avoid Sculptra on patients with a history of keloids in order to reduce the risk of adverse events (J. Drugs Dermatol. 2010;9:451-6).
Dr. Callender has been a consultant and investigator for Allergan, Galderma, Medicis, and Merz.
On Twitter @NaseemSMiller
EXPERT ANALYSIS FROM THE AAD ANNUAL MEETING
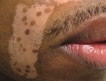
Chemical Leukoderma Induced by Amyl Nitrite
Safety First: Fractional Nonablative Laser Resurfacing in Fitzpatrick Skin Types IV to VI

In the April 2013 issue of the Journal of Drugs in Dermatology (2013;12:428-431), Clark et al retrospectively reviewed 115 laser sessions with the 1550-nm erbium-doped fractional nonablative laser (Fraxel Re:Store SR 1550, Solta Medical) in 45 patients with Fitzpatrick skin types IV to VI to assess the rate of postinflammatory hyperpigmentation and the associated laser parameters. The fluence, treatment level, and number of passes were all reviewed, as well as any posttreatment complications (ie, erythema, blistering, edema, bruising, pain) and long-term (1 month) complications (ie, hypopigmentation, hyperpigmentation). All patients were pretreated with hydroquinone cream 4% 2 weeks before, stopping 7 days before treatment and then continuing 4 weeks thereafter. Also, continuous forced-air cooling was used during treatment as well as posttreatment ice packs. Fifty-eight percent (26/45) of treatments were performed in patients with Fitzpatrick skin type IV, 24% (11/45) with type V, and 18% (8/45) with type VI. Laser parameters ranged from 4 to 70 mJ, treatment level 2 to 9, and 4 to 8 passes. Of 115 sessions, 5 (4%) were associated with postinflammatory hyperpigmentation; 2 of these instances occurred in 1 patient. The occurrence of postinflammatory hyperpigmentation was found to be statistically significant (P=.05), correlating with higher mean energy levels compared to those without hyperpigmentation (60.8 vs 44.7 mJ). Only 1 episode of postinflammatory hyperpigmentation lasted longer than 1 month, and 2 of 5 cases had only transient (<7 days) hyperpigmentation. All 5 cases resolved.
What’s the issue?
The 1550-nm erbium-doped fractional nonablative laser is being used for many skin conditions and has a low incidence of adverse effects when appropriate laser parameters are chosen. When treating darker skin phototypes with this technology, the concern for postinflammatory pigmentary alteration is more concerning. Higher treatment densities used in darker phototypes have been associated with a greater risk for postinflammatory hyperpigmentation. In their review, the authors showed that higher energy levels were associated with their cases of postinflammatory hyperpigmentation, with the caveat that they were careful not to use higher density or treatment levels than they would have used in lighter phototypes. Importantly, all 5 cases of hyperpigmentation did resolve and only 1 lasted longer than 1 month (2 months in total). This analysis reinforces that the 1550-nm erbium-doped fractional nonablative laser is quite safe in Fitzpatrick skin types IV to VI when appropriate parameters are utilized, as well as methodical pretreatment and posttreatment with hydroquinone, concomitant cooling, and strict posttreatment sun protection. With the right parameters, the treatment is quite safe; however, what are the optimal treatment parameters to provide efficacious and lasting results?

In the April 2013 issue of the Journal of Drugs in Dermatology (2013;12:428-431), Clark et al retrospectively reviewed 115 laser sessions with the 1550-nm erbium-doped fractional nonablative laser (Fraxel Re:Store SR 1550, Solta Medical) in 45 patients with Fitzpatrick skin types IV to VI to assess the rate of postinflammatory hyperpigmentation and the associated laser parameters. The fluence, treatment level, and number of passes were all reviewed, as well as any posttreatment complications (ie, erythema, blistering, edema, bruising, pain) and long-term (1 month) complications (ie, hypopigmentation, hyperpigmentation). All patients were pretreated with hydroquinone cream 4% 2 weeks before, stopping 7 days before treatment and then continuing 4 weeks thereafter. Also, continuous forced-air cooling was used during treatment as well as posttreatment ice packs. Fifty-eight percent (26/45) of treatments were performed in patients with Fitzpatrick skin type IV, 24% (11/45) with type V, and 18% (8/45) with type VI. Laser parameters ranged from 4 to 70 mJ, treatment level 2 to 9, and 4 to 8 passes. Of 115 sessions, 5 (4%) were associated with postinflammatory hyperpigmentation; 2 of these instances occurred in 1 patient. The occurrence of postinflammatory hyperpigmentation was found to be statistically significant (P=.05), correlating with higher mean energy levels compared to those without hyperpigmentation (60.8 vs 44.7 mJ). Only 1 episode of postinflammatory hyperpigmentation lasted longer than 1 month, and 2 of 5 cases had only transient (<7 days) hyperpigmentation. All 5 cases resolved.
What’s the issue?
The 1550-nm erbium-doped fractional nonablative laser is being used for many skin conditions and has a low incidence of adverse effects when appropriate laser parameters are chosen. When treating darker skin phototypes with this technology, the concern for postinflammatory pigmentary alteration is more concerning. Higher treatment densities used in darker phototypes have been associated with a greater risk for postinflammatory hyperpigmentation. In their review, the authors showed that higher energy levels were associated with their cases of postinflammatory hyperpigmentation, with the caveat that they were careful not to use higher density or treatment levels than they would have used in lighter phototypes. Importantly, all 5 cases of hyperpigmentation did resolve and only 1 lasted longer than 1 month (2 months in total). This analysis reinforces that the 1550-nm erbium-doped fractional nonablative laser is quite safe in Fitzpatrick skin types IV to VI when appropriate parameters are utilized, as well as methodical pretreatment and posttreatment with hydroquinone, concomitant cooling, and strict posttreatment sun protection. With the right parameters, the treatment is quite safe; however, what are the optimal treatment parameters to provide efficacious and lasting results?

In the April 2013 issue of the Journal of Drugs in Dermatology (2013;12:428-431), Clark et al retrospectively reviewed 115 laser sessions with the 1550-nm erbium-doped fractional nonablative laser (Fraxel Re:Store SR 1550, Solta Medical) in 45 patients with Fitzpatrick skin types IV to VI to assess the rate of postinflammatory hyperpigmentation and the associated laser parameters. The fluence, treatment level, and number of passes were all reviewed, as well as any posttreatment complications (ie, erythema, blistering, edema, bruising, pain) and long-term (1 month) complications (ie, hypopigmentation, hyperpigmentation). All patients were pretreated with hydroquinone cream 4% 2 weeks before, stopping 7 days before treatment and then continuing 4 weeks thereafter. Also, continuous forced-air cooling was used during treatment as well as posttreatment ice packs. Fifty-eight percent (26/45) of treatments were performed in patients with Fitzpatrick skin type IV, 24% (11/45) with type V, and 18% (8/45) with type VI. Laser parameters ranged from 4 to 70 mJ, treatment level 2 to 9, and 4 to 8 passes. Of 115 sessions, 5 (4%) were associated with postinflammatory hyperpigmentation; 2 of these instances occurred in 1 patient. The occurrence of postinflammatory hyperpigmentation was found to be statistically significant (P=.05), correlating with higher mean energy levels compared to those without hyperpigmentation (60.8 vs 44.7 mJ). Only 1 episode of postinflammatory hyperpigmentation lasted longer than 1 month, and 2 of 5 cases had only transient (<7 days) hyperpigmentation. All 5 cases resolved.
What’s the issue?
The 1550-nm erbium-doped fractional nonablative laser is being used for many skin conditions and has a low incidence of adverse effects when appropriate laser parameters are chosen. When treating darker skin phototypes with this technology, the concern for postinflammatory pigmentary alteration is more concerning. Higher treatment densities used in darker phototypes have been associated with a greater risk for postinflammatory hyperpigmentation. In their review, the authors showed that higher energy levels were associated with their cases of postinflammatory hyperpigmentation, with the caveat that they were careful not to use higher density or treatment levels than they would have used in lighter phototypes. Importantly, all 5 cases of hyperpigmentation did resolve and only 1 lasted longer than 1 month (2 months in total). This analysis reinforces that the 1550-nm erbium-doped fractional nonablative laser is quite safe in Fitzpatrick skin types IV to VI when appropriate parameters are utilized, as well as methodical pretreatment and posttreatment with hydroquinone, concomitant cooling, and strict posttreatment sun protection. With the right parameters, the treatment is quite safe; however, what are the optimal treatment parameters to provide efficacious and lasting results?
Laser choice enhances hair removal for darker skin
MIAMI BEACH – Choosing the right laser and the correct parameters, along with proper patient selection and counseling, can reduce the risk of complications and promote safe and effective hair removal in skin of color patients, according to Dr. H. Ray Jalian of the University of California, Los Angeles.
Patient selection and counseling come first, Dr. Jalian said at the annual meeting of the American Academy of Dermatology. Explain to darker-skinned patients that they may need more treatments than patients with lighter skin (Fitzpatrick types I to III), he said.
Both the 800-810-nm long-pulsed diode laser and the long-pulsed 1064 Nd:YAG laser have proven safe and effective in laser hair removal in darker skin types, but Dr. Jalian said he prefers the long-pulsed 1064 Nd:YAG.
To improve safety, pay attention to the laser parameters, Dr. Jalian advised. Use longer wavelengths to ensure less melanin absorption, he said. In addition, the pulse duration should to be longer than the thermal relaxation time (TRT) of the epidermal melanosomes. For example, the TRT for a melanosome is 250 ns, and a typical laser pulse duration is 10-100 ns; the TRT for a terminal hair follicle is 100 ms, and a typical pulse duration is 3-100 ms, he said.
Before a procedure, Dr. Jalian advises his patients to use sun protection and to shave the area, because the burning hair can act like a "hot coal." He also puts patients on oral antibiotics if they report a history of pseudofolliculitis barbae flares.
In addition, "perform the procedure on a test spot that’s representative of the area for hair removal, and reevaluate it in 4 weeks before treating the entire area," said Dr. Jalian.
During the procedure, look for desired endpoints, including perifollicular erythema and singed hairs. But also look for undesired endpoints, including epidermal graying, blisters, and excessive pain, Dr. Jalian said.
He also recommended epidermal cooling to minimize epidermal damage caused by the absorption of light by melanin. Cooling strategies include using passive cooling methods such as cold gel, and using the cooling tools available on many lasers, such as the sapphire tip, cryogen spray, and forced chilled air, he added.
"And remember that there can be too much of a good thing," in terms of cooling, said Dr. Jalian. "There should be a balance between heating and cooling of the skin to achieve best results."
After a laser hair removal procedure, he recommends a single application of a midpotency topical steroid, and sun protection.
Common complications of laser hair removal in darker skin types include hyperpigmentation and hypopigmentation, infections and folliculitis, scarring, and eye injury. Dr. Jalian advised against using an Nd:YAG laser close to the orbit of the eye to reduce the odds of such an injury.
Paradoxical hypertrichosis after laser hair removal has been reported, mostly in darker skin types, and with all light sources. Some risk factors include Mediterranean, Middle Eastern, and Indian ethnicities, a low-set frontal hair line, and fine or intermediate hair. Subtherapeutic fluence also may cause induction of hair cycle at the edge of a laser spot, he said.
Dr. Jalian had no financial conflicts to disclose.
On Twitter @naseemsmiller
MIAMI BEACH – Choosing the right laser and the correct parameters, along with proper patient selection and counseling, can reduce the risk of complications and promote safe and effective hair removal in skin of color patients, according to Dr. H. Ray Jalian of the University of California, Los Angeles.
Patient selection and counseling come first, Dr. Jalian said at the annual meeting of the American Academy of Dermatology. Explain to darker-skinned patients that they may need more treatments than patients with lighter skin (Fitzpatrick types I to III), he said.
Both the 800-810-nm long-pulsed diode laser and the long-pulsed 1064 Nd:YAG laser have proven safe and effective in laser hair removal in darker skin types, but Dr. Jalian said he prefers the long-pulsed 1064 Nd:YAG.
To improve safety, pay attention to the laser parameters, Dr. Jalian advised. Use longer wavelengths to ensure less melanin absorption, he said. In addition, the pulse duration should to be longer than the thermal relaxation time (TRT) of the epidermal melanosomes. For example, the TRT for a melanosome is 250 ns, and a typical laser pulse duration is 10-100 ns; the TRT for a terminal hair follicle is 100 ms, and a typical pulse duration is 3-100 ms, he said.
Before a procedure, Dr. Jalian advises his patients to use sun protection and to shave the area, because the burning hair can act like a "hot coal." He also puts patients on oral antibiotics if they report a history of pseudofolliculitis barbae flares.
In addition, "perform the procedure on a test spot that’s representative of the area for hair removal, and reevaluate it in 4 weeks before treating the entire area," said Dr. Jalian.
During the procedure, look for desired endpoints, including perifollicular erythema and singed hairs. But also look for undesired endpoints, including epidermal graying, blisters, and excessive pain, Dr. Jalian said.
He also recommended epidermal cooling to minimize epidermal damage caused by the absorption of light by melanin. Cooling strategies include using passive cooling methods such as cold gel, and using the cooling tools available on many lasers, such as the sapphire tip, cryogen spray, and forced chilled air, he added.
"And remember that there can be too much of a good thing," in terms of cooling, said Dr. Jalian. "There should be a balance between heating and cooling of the skin to achieve best results."
After a laser hair removal procedure, he recommends a single application of a midpotency topical steroid, and sun protection.
Common complications of laser hair removal in darker skin types include hyperpigmentation and hypopigmentation, infections and folliculitis, scarring, and eye injury. Dr. Jalian advised against using an Nd:YAG laser close to the orbit of the eye to reduce the odds of such an injury.
Paradoxical hypertrichosis after laser hair removal has been reported, mostly in darker skin types, and with all light sources. Some risk factors include Mediterranean, Middle Eastern, and Indian ethnicities, a low-set frontal hair line, and fine or intermediate hair. Subtherapeutic fluence also may cause induction of hair cycle at the edge of a laser spot, he said.
Dr. Jalian had no financial conflicts to disclose.
On Twitter @naseemsmiller
MIAMI BEACH – Choosing the right laser and the correct parameters, along with proper patient selection and counseling, can reduce the risk of complications and promote safe and effective hair removal in skin of color patients, according to Dr. H. Ray Jalian of the University of California, Los Angeles.
Patient selection and counseling come first, Dr. Jalian said at the annual meeting of the American Academy of Dermatology. Explain to darker-skinned patients that they may need more treatments than patients with lighter skin (Fitzpatrick types I to III), he said.
Both the 800-810-nm long-pulsed diode laser and the long-pulsed 1064 Nd:YAG laser have proven safe and effective in laser hair removal in darker skin types, but Dr. Jalian said he prefers the long-pulsed 1064 Nd:YAG.
To improve safety, pay attention to the laser parameters, Dr. Jalian advised. Use longer wavelengths to ensure less melanin absorption, he said. In addition, the pulse duration should to be longer than the thermal relaxation time (TRT) of the epidermal melanosomes. For example, the TRT for a melanosome is 250 ns, and a typical laser pulse duration is 10-100 ns; the TRT for a terminal hair follicle is 100 ms, and a typical pulse duration is 3-100 ms, he said.
Before a procedure, Dr. Jalian advises his patients to use sun protection and to shave the area, because the burning hair can act like a "hot coal." He also puts patients on oral antibiotics if they report a history of pseudofolliculitis barbae flares.
In addition, "perform the procedure on a test spot that’s representative of the area for hair removal, and reevaluate it in 4 weeks before treating the entire area," said Dr. Jalian.
During the procedure, look for desired endpoints, including perifollicular erythema and singed hairs. But also look for undesired endpoints, including epidermal graying, blisters, and excessive pain, Dr. Jalian said.
He also recommended epidermal cooling to minimize epidermal damage caused by the absorption of light by melanin. Cooling strategies include using passive cooling methods such as cold gel, and using the cooling tools available on many lasers, such as the sapphire tip, cryogen spray, and forced chilled air, he added.
"And remember that there can be too much of a good thing," in terms of cooling, said Dr. Jalian. "There should be a balance between heating and cooling of the skin to achieve best results."
After a laser hair removal procedure, he recommends a single application of a midpotency topical steroid, and sun protection.
Common complications of laser hair removal in darker skin types include hyperpigmentation and hypopigmentation, infections and folliculitis, scarring, and eye injury. Dr. Jalian advised against using an Nd:YAG laser close to the orbit of the eye to reduce the odds of such an injury.
Paradoxical hypertrichosis after laser hair removal has been reported, mostly in darker skin types, and with all light sources. Some risk factors include Mediterranean, Middle Eastern, and Indian ethnicities, a low-set frontal hair line, and fine or intermediate hair. Subtherapeutic fluence also may cause induction of hair cycle at the edge of a laser spot, he said.
Dr. Jalian had no financial conflicts to disclose.
On Twitter @naseemsmiller
EXPERT ANALYSIS FROM THE AAD ANNUAL MEETING
Prevent pigment problems in skin of color
MIAMI BEACH – When it comes to procedures such as chemical peels, microdermabrasion, and laser therapies, one size doesn’t fit all, and dermatologists should take special precautions when treating patients with darker skin.
Dr. Marta Rendon, a dermatologist in Boca Raton, Florida, said she sees at least two patients a week who are seeking treatment for pigmentary complications that have been caused by prior cosmetic procedures performed by other physicians.
Some she can treat, and some are beyond repair.
"If I were to sum up my presentation, I would tell you that above all, be conservative and don’t be aggressive," especially in patients with ethnic skin, she told her audience at the annual meeting of the American Academy of Dermatology.
Dr. Rendon, who is also the president of the Skin of Color Society, urged physicians to take precautions because with the increasing diversity of the United States, their patient population is only going to get more diverse.
"Do the patient history. Take your time," advised Dr. Rendon. "Find out what their ethnic background is. Ask them about their grandmother, and where they are from."
The second most important part of history, she said, is asking about reaction to prior procedures or surgeries and prior history of postinflammatory hyperpigmentation (PIH).
"Ask them about what they do, what their hobbies are, or if they play a sport," she said. And take into account the season. During warmer temperatures, consider superficial peels and be careful with lasers. Medium peels and laser resurfacing are more appropriate during cooler and cloudier seasons, she said.
Take caution
Dr. Rendon had the following advice for various procedures in ethnic skin:
• Don’t perform chemical peels on patients on tretinoin. Don’t start with a high concentration. Don’t do excessive layers. And don’t combine surgical procedures with peels in the same visit.
• When performing microdermabrasion, don’t be too aggressive to avoid PIH, streaking, and scratch marks. Don\'t perform the procedure too close to the eyes. Avoid extremely sensitive skin and pressure urticaria. And always start with the lowest strength and time interval.
• With fillers, be careful with superficial placement since the colored material can be seen through the skin. Hyaluronic acid is safer, because it’s colorless and less risky to use. Be mindful that severe bruising can lead to hemosiderin. And be sure that all your patients are using sunscreen.
• For laser and light therapies, always do a test spot. Have a solid understanding of laser-tissue interaction. And be prepared if pigmentation problems develop, so that you can treat them early.
Treatment
Aggressive and early intervention is crucial in treating side effects from cosmetic procedures.
One of the keys to prevent hyperpigmentation is UV protection, whether it’s with sunscreens, cosmetics, antioxidants such as topical vitamin C and E, or systemic agents such as chloroquine, fish oil, or green-tea extract, said Dr. Rendon.
Several topical agents can be used to treat hyperpigmentation. They include hydroquinone, hydroquinone combination, glycolic/retinoid/steroid combination, or antioxidants.
Dr. Rendon also listed several combination bleaching agents including hydroquinone 4%, tretinoin 0.05%, and fluocinolone 0.01%; hydroquinone 4% and retinol 0.3%; hydroquinone microentrapped 4% and retinol 0.15%; hydroquinone and glycolic acid 10%; hydroquinone, glycolic acid 10% + and hyaluronic acid; mequinol and tretinoin 0.01%; retinaldehyde and glycolic acid; and compounded hydroquinone 6%-8%.
Niacinamide is one of the cosmeceutical skin-lightening agents that act as a vitamin exfoliant, reducing melanosome transfer. Soy-protease inhibitors and glutathione also have skin-lightening effects. Dr. Rendon also listed several skin lightening products including Melanozyme, Melaplex, Lumixyl (oligopeptide), retinaldehyde, lactic acid, ferrulic acid, and sunscreen.
She said her favorite method of treating pigmentary complications is to combine treatments. For instance, she combines peels with microdermabrasion; peels with laser; microdermabrasion with IPL; and fractional resurfacing with topical regimens. She added that she maximizes the procedures with topical regimens.
The bottom line is aggressive and early intervention for side effects, Dr. Rendon said.
As a result of growing ethnic population, the treatment options for pigmented skin is expanding, but in the meantime, dermatologists should ensure that their procedures are specific and individualized, Dr. Rendon advised.
"There’s no way of predicting who will hyperpigment, unless you take a good history," she said. And remember two pearls to stay out of trouble: Be conservative, and don’t use aggressive techniques.
Dr. Rendon has performed clinical research for and/or served as a consultant for several companies, including Amgen, Aveeno, Galderma, J&J, Neutrogena, and Sanofi-Aventis. She is a global spokesperson for the H&S brand.
On Twitter @naseemsmiller
MIAMI BEACH – When it comes to procedures such as chemical peels, microdermabrasion, and laser therapies, one size doesn’t fit all, and dermatologists should take special precautions when treating patients with darker skin.
Dr. Marta Rendon, a dermatologist in Boca Raton, Florida, said she sees at least two patients a week who are seeking treatment for pigmentary complications that have been caused by prior cosmetic procedures performed by other physicians.
Some she can treat, and some are beyond repair.
"If I were to sum up my presentation, I would tell you that above all, be conservative and don’t be aggressive," especially in patients with ethnic skin, she told her audience at the annual meeting of the American Academy of Dermatology.
Dr. Rendon, who is also the president of the Skin of Color Society, urged physicians to take precautions because with the increasing diversity of the United States, their patient population is only going to get more diverse.
"Do the patient history. Take your time," advised Dr. Rendon. "Find out what their ethnic background is. Ask them about their grandmother, and where they are from."
The second most important part of history, she said, is asking about reaction to prior procedures or surgeries and prior history of postinflammatory hyperpigmentation (PIH).
"Ask them about what they do, what their hobbies are, or if they play a sport," she said. And take into account the season. During warmer temperatures, consider superficial peels and be careful with lasers. Medium peels and laser resurfacing are more appropriate during cooler and cloudier seasons, she said.
Take caution
Dr. Rendon had the following advice for various procedures in ethnic skin:
• Don’t perform chemical peels on patients on tretinoin. Don’t start with a high concentration. Don’t do excessive layers. And don’t combine surgical procedures with peels in the same visit.
• When performing microdermabrasion, don’t be too aggressive to avoid PIH, streaking, and scratch marks. Don\'t perform the procedure too close to the eyes. Avoid extremely sensitive skin and pressure urticaria. And always start with the lowest strength and time interval.
• With fillers, be careful with superficial placement since the colored material can be seen through the skin. Hyaluronic acid is safer, because it’s colorless and less risky to use. Be mindful that severe bruising can lead to hemosiderin. And be sure that all your patients are using sunscreen.
• For laser and light therapies, always do a test spot. Have a solid understanding of laser-tissue interaction. And be prepared if pigmentation problems develop, so that you can treat them early.
Treatment
Aggressive and early intervention is crucial in treating side effects from cosmetic procedures.
One of the keys to prevent hyperpigmentation is UV protection, whether it’s with sunscreens, cosmetics, antioxidants such as topical vitamin C and E, or systemic agents such as chloroquine, fish oil, or green-tea extract, said Dr. Rendon.
Several topical agents can be used to treat hyperpigmentation. They include hydroquinone, hydroquinone combination, glycolic/retinoid/steroid combination, or antioxidants.
Dr. Rendon also listed several combination bleaching agents including hydroquinone 4%, tretinoin 0.05%, and fluocinolone 0.01%; hydroquinone 4% and retinol 0.3%; hydroquinone microentrapped 4% and retinol 0.15%; hydroquinone and glycolic acid 10%; hydroquinone, glycolic acid 10% + and hyaluronic acid; mequinol and tretinoin 0.01%; retinaldehyde and glycolic acid; and compounded hydroquinone 6%-8%.
Niacinamide is one of the cosmeceutical skin-lightening agents that act as a vitamin exfoliant, reducing melanosome transfer. Soy-protease inhibitors and glutathione also have skin-lightening effects. Dr. Rendon also listed several skin lightening products including Melanozyme, Melaplex, Lumixyl (oligopeptide), retinaldehyde, lactic acid, ferrulic acid, and sunscreen.
She said her favorite method of treating pigmentary complications is to combine treatments. For instance, she combines peels with microdermabrasion; peels with laser; microdermabrasion with IPL; and fractional resurfacing with topical regimens. She added that she maximizes the procedures with topical regimens.
The bottom line is aggressive and early intervention for side effects, Dr. Rendon said.
As a result of growing ethnic population, the treatment options for pigmented skin is expanding, but in the meantime, dermatologists should ensure that their procedures are specific and individualized, Dr. Rendon advised.
"There’s no way of predicting who will hyperpigment, unless you take a good history," she said. And remember two pearls to stay out of trouble: Be conservative, and don’t use aggressive techniques.
Dr. Rendon has performed clinical research for and/or served as a consultant for several companies, including Amgen, Aveeno, Galderma, J&J, Neutrogena, and Sanofi-Aventis. She is a global spokesperson for the H&S brand.
On Twitter @naseemsmiller
MIAMI BEACH – When it comes to procedures such as chemical peels, microdermabrasion, and laser therapies, one size doesn’t fit all, and dermatologists should take special precautions when treating patients with darker skin.
Dr. Marta Rendon, a dermatologist in Boca Raton, Florida, said she sees at least two patients a week who are seeking treatment for pigmentary complications that have been caused by prior cosmetic procedures performed by other physicians.
Some she can treat, and some are beyond repair.
"If I were to sum up my presentation, I would tell you that above all, be conservative and don’t be aggressive," especially in patients with ethnic skin, she told her audience at the annual meeting of the American Academy of Dermatology.
Dr. Rendon, who is also the president of the Skin of Color Society, urged physicians to take precautions because with the increasing diversity of the United States, their patient population is only going to get more diverse.
"Do the patient history. Take your time," advised Dr. Rendon. "Find out what their ethnic background is. Ask them about their grandmother, and where they are from."
The second most important part of history, she said, is asking about reaction to prior procedures or surgeries and prior history of postinflammatory hyperpigmentation (PIH).
"Ask them about what they do, what their hobbies are, or if they play a sport," she said. And take into account the season. During warmer temperatures, consider superficial peels and be careful with lasers. Medium peels and laser resurfacing are more appropriate during cooler and cloudier seasons, she said.
Take caution
Dr. Rendon had the following advice for various procedures in ethnic skin:
• Don’t perform chemical peels on patients on tretinoin. Don’t start with a high concentration. Don’t do excessive layers. And don’t combine surgical procedures with peels in the same visit.
• When performing microdermabrasion, don’t be too aggressive to avoid PIH, streaking, and scratch marks. Don\'t perform the procedure too close to the eyes. Avoid extremely sensitive skin and pressure urticaria. And always start with the lowest strength and time interval.
• With fillers, be careful with superficial placement since the colored material can be seen through the skin. Hyaluronic acid is safer, because it’s colorless and less risky to use. Be mindful that severe bruising can lead to hemosiderin. And be sure that all your patients are using sunscreen.
• For laser and light therapies, always do a test spot. Have a solid understanding of laser-tissue interaction. And be prepared if pigmentation problems develop, so that you can treat them early.
Treatment
Aggressive and early intervention is crucial in treating side effects from cosmetic procedures.
One of the keys to prevent hyperpigmentation is UV protection, whether it’s with sunscreens, cosmetics, antioxidants such as topical vitamin C and E, or systemic agents such as chloroquine, fish oil, or green-tea extract, said Dr. Rendon.
Several topical agents can be used to treat hyperpigmentation. They include hydroquinone, hydroquinone combination, glycolic/retinoid/steroid combination, or antioxidants.
Dr. Rendon also listed several combination bleaching agents including hydroquinone 4%, tretinoin 0.05%, and fluocinolone 0.01%; hydroquinone 4% and retinol 0.3%; hydroquinone microentrapped 4% and retinol 0.15%; hydroquinone and glycolic acid 10%; hydroquinone, glycolic acid 10% + and hyaluronic acid; mequinol and tretinoin 0.01%; retinaldehyde and glycolic acid; and compounded hydroquinone 6%-8%.
Niacinamide is one of the cosmeceutical skin-lightening agents that act as a vitamin exfoliant, reducing melanosome transfer. Soy-protease inhibitors and glutathione also have skin-lightening effects. Dr. Rendon also listed several skin lightening products including Melanozyme, Melaplex, Lumixyl (oligopeptide), retinaldehyde, lactic acid, ferrulic acid, and sunscreen.
She said her favorite method of treating pigmentary complications is to combine treatments. For instance, she combines peels with microdermabrasion; peels with laser; microdermabrasion with IPL; and fractional resurfacing with topical regimens. She added that she maximizes the procedures with topical regimens.
The bottom line is aggressive and early intervention for side effects, Dr. Rendon said.
As a result of growing ethnic population, the treatment options for pigmented skin is expanding, but in the meantime, dermatologists should ensure that their procedures are specific and individualized, Dr. Rendon advised.
"There’s no way of predicting who will hyperpigment, unless you take a good history," she said. And remember two pearls to stay out of trouble: Be conservative, and don’t use aggressive techniques.
Dr. Rendon has performed clinical research for and/or served as a consultant for several companies, including Amgen, Aveeno, Galderma, J&J, Neutrogena, and Sanofi-Aventis. She is a global spokesperson for the H&S brand.
On Twitter @naseemsmiller
EXPERT ANALYSIS FROM THE AAD ANNUAL MEETING