User login
FDA approves nilotinib for kids with CML
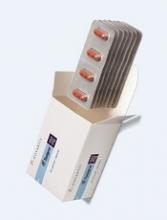
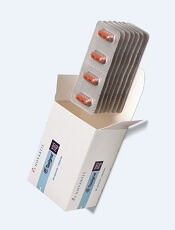
The US Food and Drug Administration (FDA) has expanded the approved indication for nilotinib (Tasigna®) to include the treatment of children.
The drug is now approved to treat patients age 1 and older who have newly diagnosed Philadelphia chromosome-positive (Ph+) chronic myeloid leukemia (CML) in the chronic phase.
Nilotinib is also approved to treat pediatric patients age 1 and older who have chronic phase, Ph+ CML that is resistant or intolerant to prior tyrosine kinase inhibitor (TKI) therapy, as well as adults with Ph+ CML in chronic phase and accelerated phase that is resistant or intolerant to prior therapy including imatinib.
The new pediatric indications for nilotinib, granted under the FDA’s priority review designation, are based on results from 2 studies of the drug—a phase 1 and phase 2.
According to Novartis, the studies included 69 CML patients who ranged in age from 2 to 17. They had either newly diagnosed, chronic phase, Ph+ CML or chronic phase, Ph+ CML with resistance or intolerance to prior TKI therapy.
In the newly diagnosed patients, the major molecular response (MMR) rate was 60.0% at 12 cycles, with 15 patients achieving MMR.
In patients with resistance or intolerance to prior therapy, the MMR rate was 40.9% at 12 cycles, with 18 patients being in MMR.
In newly diagnosed patients, the cumulative MMR rate was 64.0% by cycle 12. In patients with resistance or intolerance to prior therapy, the cumulative MMR rate was 47.7% by cycle 12.
Adverse events were generally consistent with those observed in adults, with the exception of hyperbilirubinemia and transaminase elevation, which were reported at a higher frequency than in adults.
The rate of grade 3/4 hyperbilirubinemia was 13.0%, the rate of grade 3/4 AST elevation was 1.4%, and the rate of grade 3/4 ALT elevation was 8.7%.
There were no deaths on treatment or after treatment discontinuation.
There was 1 patient with resistant/intolerant CML who progressed to advance phase/blast crisis after about 10 months on nilotinib.
The US Food and Drug Administration (FDA) has expanded the approved indication for nilotinib (Tasigna®) to include the treatment of children.
The drug is now approved to treat patients age 1 and older who have newly diagnosed Philadelphia chromosome-positive (Ph+) chronic myeloid leukemia (CML) in the chronic phase.
Nilotinib is also approved to treat pediatric patients age 1 and older who have chronic phase, Ph+ CML that is resistant or intolerant to prior tyrosine kinase inhibitor (TKI) therapy, as well as adults with Ph+ CML in chronic phase and accelerated phase that is resistant or intolerant to prior therapy including imatinib.
The new pediatric indications for nilotinib, granted under the FDA’s priority review designation, are based on results from 2 studies of the drug—a phase 1 and phase 2.
According to Novartis, the studies included 69 CML patients who ranged in age from 2 to 17. They had either newly diagnosed, chronic phase, Ph+ CML or chronic phase, Ph+ CML with resistance or intolerance to prior TKI therapy.
In the newly diagnosed patients, the major molecular response (MMR) rate was 60.0% at 12 cycles, with 15 patients achieving MMR.
In patients with resistance or intolerance to prior therapy, the MMR rate was 40.9% at 12 cycles, with 18 patients being in MMR.
In newly diagnosed patients, the cumulative MMR rate was 64.0% by cycle 12. In patients with resistance or intolerance to prior therapy, the cumulative MMR rate was 47.7% by cycle 12.
Adverse events were generally consistent with those observed in adults, with the exception of hyperbilirubinemia and transaminase elevation, which were reported at a higher frequency than in adults.
The rate of grade 3/4 hyperbilirubinemia was 13.0%, the rate of grade 3/4 AST elevation was 1.4%, and the rate of grade 3/4 ALT elevation was 8.7%.
There were no deaths on treatment or after treatment discontinuation.
There was 1 patient with resistant/intolerant CML who progressed to advance phase/blast crisis after about 10 months on nilotinib.
The US Food and Drug Administration (FDA) has expanded the approved indication for nilotinib (Tasigna®) to include the treatment of children.
The drug is now approved to treat patients age 1 and older who have newly diagnosed Philadelphia chromosome-positive (Ph+) chronic myeloid leukemia (CML) in the chronic phase.
Nilotinib is also approved to treat pediatric patients age 1 and older who have chronic phase, Ph+ CML that is resistant or intolerant to prior tyrosine kinase inhibitor (TKI) therapy, as well as adults with Ph+ CML in chronic phase and accelerated phase that is resistant or intolerant to prior therapy including imatinib.
The new pediatric indications for nilotinib, granted under the FDA’s priority review designation, are based on results from 2 studies of the drug—a phase 1 and phase 2.
According to Novartis, the studies included 69 CML patients who ranged in age from 2 to 17. They had either newly diagnosed, chronic phase, Ph+ CML or chronic phase, Ph+ CML with resistance or intolerance to prior TKI therapy.
In the newly diagnosed patients, the major molecular response (MMR) rate was 60.0% at 12 cycles, with 15 patients achieving MMR.
In patients with resistance or intolerance to prior therapy, the MMR rate was 40.9% at 12 cycles, with 18 patients being in MMR.
In newly diagnosed patients, the cumulative MMR rate was 64.0% by cycle 12. In patients with resistance or intolerance to prior therapy, the cumulative MMR rate was 47.7% by cycle 12.
Adverse events were generally consistent with those observed in adults, with the exception of hyperbilirubinemia and transaminase elevation, which were reported at a higher frequency than in adults.
The rate of grade 3/4 hyperbilirubinemia was 13.0%, the rate of grade 3/4 AST elevation was 1.4%, and the rate of grade 3/4 ALT elevation was 8.7%.
There were no deaths on treatment or after treatment discontinuation.
There was 1 patient with resistant/intolerant CML who progressed to advance phase/blast crisis after about 10 months on nilotinib.
Health Canada approves SC rituximab for CLL
Health Canada has approved a subcutaneous (SC) formulation of rituximab (Rituxan®) to treat patients with chronic lymphocytic leukemia (CLL).
The product is now approved for use in combination with fludarabine and cyclophosphamide to treat patients with previously treated or untreated CLL, Binet Stage B or C.
The SC formulation is intended to provide a more convenient delivery method than intravenous (IV) rituximab. The SC formulation enables administration of the drug in large volumes under the skin.
“The approval of Rituxan SC is exciting news and a meaningful advancement for those living with CLL, as intravenous treatments can take around 4 hours to receive, requiring patients to spend up to a half day sitting in the chemo suite,” said Robin Markowitz, chief executive officer of Lymphoma Canada.
“The administration of Rituxan SC only takes 7 minutes, giving patients valuable time back in their day.”
SAWYER study
Health Canada’s approval of SC rituximab is based on data from the phase 1b SAWYER study. This randomized study was conducted in patients with previously untreated CLL to investigate the pharmacokinetic profile, safety, and efficacy of SC rituximab in combination with chemotherapy.
Results from this study were published in The Lancet Haematology in March 2016.
The trial included 176 patients who were randomized to receive SC rituximab (1600 mg, n=88) or IV rituximab (500 mg/m2, n=88) on day 1 from cycles 2 to 6. In cycle 1, both groups received IV rituximab (375 mg/m2) on day 0.
All patients also received fludarabine (IV 25 mg/m2 on days 1-3 of all cycles or orally at either 25 mg/m2 on days 1-5 of all cycles or 30-40 mg/m2 on days 1-3 of all cycles) and cyclophosphamide (IV at 250 mg/m2 on days 1-3 of all cycles or orally at either 150 mg/m2 on days 1-5 of all cycles or 200-250 mg/m2 on days 1-3 of all cycles) every 4 weeks for up to 6 cycles.
The primary endpoint was pharmacokinetic noninferiority of SC to IV rituximab assessed at cycle 5. At that time, the geometric mean trough serum concentration in the SC rituximab arm was noninferior to that in the IV arm—97.5 µg/mL and 61.5 µg/mL, respectively—with an adjusted geometric mean ratio of 1.53 (90% CI, 1.27 to 1.85).
Safety was a secondary endpoint, and efficacy was an exploratory endpoint.
The overall response rate was 85% in the SC arm and 81% in the IV arm. Complete response rates were 26% and 33%, respectively.
Rates of adverse events (AEs) were 96% in the SC arm and 91% in the IV arm. Rates of grade 3 or higher AEs were 69% and 71%, respectively, and rates of serious AEs were 29% and 33%, respectively.
The most common serious AE overall was febrile neutropenia, which occurred in 11% of patients in the SC arm and 4% in the IV arm.
The most common AEs of any grade (occurring in >20% of patients in either arm) were:
- Neutropenia—65% with SC and 58% with IV
- Thrombocytopenia—24% with SC and 26% with IV
- Anemia—13% with SC and 24% with IV
- Nausea—38% with SC and 35% with IV
- Vomiting—21% with SC and 22% with IV
- Pyrexia—32% with SC and 25% with IV
- Injection-site erythema—26% with SC and 0% with IV.
Local cutaneous reactions were reported in 42% of patients in the SC arm. The most common of these were injection-site erythema (26%) and injection-site pain (16%).
Health Canada has approved a subcutaneous (SC) formulation of rituximab (Rituxan®) to treat patients with chronic lymphocytic leukemia (CLL).
The product is now approved for use in combination with fludarabine and cyclophosphamide to treat patients with previously treated or untreated CLL, Binet Stage B or C.
The SC formulation is intended to provide a more convenient delivery method than intravenous (IV) rituximab. The SC formulation enables administration of the drug in large volumes under the skin.
“The approval of Rituxan SC is exciting news and a meaningful advancement for those living with CLL, as intravenous treatments can take around 4 hours to receive, requiring patients to spend up to a half day sitting in the chemo suite,” said Robin Markowitz, chief executive officer of Lymphoma Canada.
“The administration of Rituxan SC only takes 7 minutes, giving patients valuable time back in their day.”
SAWYER study
Health Canada’s approval of SC rituximab is based on data from the phase 1b SAWYER study. This randomized study was conducted in patients with previously untreated CLL to investigate the pharmacokinetic profile, safety, and efficacy of SC rituximab in combination with chemotherapy.
Results from this study were published in The Lancet Haematology in March 2016.
The trial included 176 patients who were randomized to receive SC rituximab (1600 mg, n=88) or IV rituximab (500 mg/m2, n=88) on day 1 from cycles 2 to 6. In cycle 1, both groups received IV rituximab (375 mg/m2) on day 0.
All patients also received fludarabine (IV 25 mg/m2 on days 1-3 of all cycles or orally at either 25 mg/m2 on days 1-5 of all cycles or 30-40 mg/m2 on days 1-3 of all cycles) and cyclophosphamide (IV at 250 mg/m2 on days 1-3 of all cycles or orally at either 150 mg/m2 on days 1-5 of all cycles or 200-250 mg/m2 on days 1-3 of all cycles) every 4 weeks for up to 6 cycles.
The primary endpoint was pharmacokinetic noninferiority of SC to IV rituximab assessed at cycle 5. At that time, the geometric mean trough serum concentration in the SC rituximab arm was noninferior to that in the IV arm—97.5 µg/mL and 61.5 µg/mL, respectively—with an adjusted geometric mean ratio of 1.53 (90% CI, 1.27 to 1.85).
Safety was a secondary endpoint, and efficacy was an exploratory endpoint.
The overall response rate was 85% in the SC arm and 81% in the IV arm. Complete response rates were 26% and 33%, respectively.
Rates of adverse events (AEs) were 96% in the SC arm and 91% in the IV arm. Rates of grade 3 or higher AEs were 69% and 71%, respectively, and rates of serious AEs were 29% and 33%, respectively.
The most common serious AE overall was febrile neutropenia, which occurred in 11% of patients in the SC arm and 4% in the IV arm.
The most common AEs of any grade (occurring in >20% of patients in either arm) were:
- Neutropenia—65% with SC and 58% with IV
- Thrombocytopenia—24% with SC and 26% with IV
- Anemia—13% with SC and 24% with IV
- Nausea—38% with SC and 35% with IV
- Vomiting—21% with SC and 22% with IV
- Pyrexia—32% with SC and 25% with IV
- Injection-site erythema—26% with SC and 0% with IV.
Local cutaneous reactions were reported in 42% of patients in the SC arm. The most common of these were injection-site erythema (26%) and injection-site pain (16%).
Health Canada has approved a subcutaneous (SC) formulation of rituximab (Rituxan®) to treat patients with chronic lymphocytic leukemia (CLL).
The product is now approved for use in combination with fludarabine and cyclophosphamide to treat patients with previously treated or untreated CLL, Binet Stage B or C.
The SC formulation is intended to provide a more convenient delivery method than intravenous (IV) rituximab. The SC formulation enables administration of the drug in large volumes under the skin.
“The approval of Rituxan SC is exciting news and a meaningful advancement for those living with CLL, as intravenous treatments can take around 4 hours to receive, requiring patients to spend up to a half day sitting in the chemo suite,” said Robin Markowitz, chief executive officer of Lymphoma Canada.
“The administration of Rituxan SC only takes 7 minutes, giving patients valuable time back in their day.”
SAWYER study
Health Canada’s approval of SC rituximab is based on data from the phase 1b SAWYER study. This randomized study was conducted in patients with previously untreated CLL to investigate the pharmacokinetic profile, safety, and efficacy of SC rituximab in combination with chemotherapy.
Results from this study were published in The Lancet Haematology in March 2016.
The trial included 176 patients who were randomized to receive SC rituximab (1600 mg, n=88) or IV rituximab (500 mg/m2, n=88) on day 1 from cycles 2 to 6. In cycle 1, both groups received IV rituximab (375 mg/m2) on day 0.
All patients also received fludarabine (IV 25 mg/m2 on days 1-3 of all cycles or orally at either 25 mg/m2 on days 1-5 of all cycles or 30-40 mg/m2 on days 1-3 of all cycles) and cyclophosphamide (IV at 250 mg/m2 on days 1-3 of all cycles or orally at either 150 mg/m2 on days 1-5 of all cycles or 200-250 mg/m2 on days 1-3 of all cycles) every 4 weeks for up to 6 cycles.
The primary endpoint was pharmacokinetic noninferiority of SC to IV rituximab assessed at cycle 5. At that time, the geometric mean trough serum concentration in the SC rituximab arm was noninferior to that in the IV arm—97.5 µg/mL and 61.5 µg/mL, respectively—with an adjusted geometric mean ratio of 1.53 (90% CI, 1.27 to 1.85).
Safety was a secondary endpoint, and efficacy was an exploratory endpoint.
The overall response rate was 85% in the SC arm and 81% in the IV arm. Complete response rates were 26% and 33%, respectively.
Rates of adverse events (AEs) were 96% in the SC arm and 91% in the IV arm. Rates of grade 3 or higher AEs were 69% and 71%, respectively, and rates of serious AEs were 29% and 33%, respectively.
The most common serious AE overall was febrile neutropenia, which occurred in 11% of patients in the SC arm and 4% in the IV arm.
The most common AEs of any grade (occurring in >20% of patients in either arm) were:
- Neutropenia—65% with SC and 58% with IV
- Thrombocytopenia—24% with SC and 26% with IV
- Anemia—13% with SC and 24% with IV
- Nausea—38% with SC and 35% with IV
- Vomiting—21% with SC and 22% with IV
- Pyrexia—32% with SC and 25% with IV
- Injection-site erythema—26% with SC and 0% with IV.
Local cutaneous reactions were reported in 42% of patients in the SC arm. The most common of these were injection-site erythema (26%) and injection-site pain (16%).
Ponatinib efficacy maintained despite dose reductions
Final results from the phase 2 PACE trial suggest dose reductions did not have an effect on the efficacy of ponatinib in patients with chronic phase (CP) chronic myeloid leukemia (CML).
Trial investigators began reducing ponatinib doses after the drug was linked to arterial occlusive events (AOEs).
Most patients who achieved a major molecular response (MMR) or major cytogenetic response (MCyR) on higher doses of ponatinib maintained those responses after dose reductions.
These results were published in Blood. The trial was sponsored by Ariad Pharmaceuticals, Inc., a wholly owned subsidiary of Takeda Pharmaceutical Company Limited.
Earlier results from the PACE trial indicated that ponatinib increased a patient’s risk of vascular occlusive events (VOEs), including AOEs.
Therefore, in October 2013, a phase 3 trial of ponatinib was discontinued, and all other ponatinib trials were put on partial clinical hold. Trial enrollment was halted temporarily, and investigators began reducing ponatinib doses.
Then, the US Food and Drug Administration suspended sales and marketing of ponatinib, pending results of a safety evaluation.
However, in December 2013, the agency decided ponatinib could return to the market if new safety measures were implemented. In January 2014, the drug was back on the market.
Patients
The PACE trial included 449 patients with CML or acute lymphoblastic leukemia, but the results published in Blood focused only on patients with CP-CML. All of these patients were resistant or intolerant to dasatinib or nilotinib, or they had the BCR-ABLT315I mutation.
There were 270 patients with CP-CML. They had a median age of 60 (range, 18-94), and 47% were female.
Ninety-three percent had received at least 2 prior approved tyrosine kinase inhibitors (TKIs), and 57% had received at least 3. The median duration of prior TKI treatment was 5.4 years (range, 0.4-13.3).
Eighty percent of patients were resistant to dasatinib or nilotinib, 14% were intolerant to either drug, and 19% were both resistant and intolerant. Twenty-four percent of patients had the T315I mutation.
Treatment
The starting dose of ponatinib was 45 mg once daily. Doses were reduced to 30 mg or 15 mg once daily to manage adverse events (AEs), or reductions were implemented proactively (starting on October 10, 2013) due to concerns about VOEs.
Unless a benefit-risk analysis justified use of a higher dose, the recommendation for CP-CML patients was a 15 mg daily dose for those with an MCyR and a 30 mg daily dose for those without an MCyR.
Patients received ponatinib until disease progression, intolerance, or the patient or investigator decided to stop treatment.
The median duration of treatment was 32.1 months (range, 0.1-73.0), and the median follow-up was 56.8 months (range, 0.1-73.1).
Efficacy
Of the 267 evaluable patients, 60% achieved an MCyR at any time, with 54% achieving a complete cytogenetic response. Forty-eight percent of patients were still in MCyR at the last response assessment, and 82% of patients who achieved an MCyR were estimated to remain in MCyR at 5 years.
There were 69 patients in MCyR as of October 10, 2013, when pre-emptive dose reduction began, who had their dose reduced. Ninety-six percent of these patients (n=66) maintained MCyR after dose reduction. Of the 34 patients in MCyR who did not have pre-emptive dose reductions, 94% (n=32) maintained MCyR.
Forty percent of patients attained a major molecular response (MMR) at any time during the study, with 30% achieving MR4 and 24% achieving MR4.5. Thirty percent of patients were in MMR at the last response assessment, and 59% of patients who achieved MMR were estimated to remain in MMR at 5 years.
There were 52 patients in MMR as of October 10, 2013, who had their dose reduced. Ninety percent (n=47) of these patients maintained MMR following dose reduction. Of the 19 patients in MMR who did not have pre-emptive dose reductions, 95% (n=18) maintained MMR.
“The PACE trial is among the longest and largest studies of patients with CP-CML who have received 2 or 3 prior TKIs, and the findings provide treating physicians with important updated information . . . ,” said study author Jorge Eduardo Cortes, MD, of MD Anderson Cancer Center in Houston, Texas.
“These final PACE results demonstrate that [ponatinib] provides lasting clinically meaningful responses, irrespective of dose reductions, in this population.”
At 5 years, the progression-free survival rate was 53%, and the overall survival rate was 73%.
AOEs
The incidence of AOEs was 31%, and the incidence of serious AOEs was 26%. This included cardiovascular AOEs (16%, 12% serious), cerebrovascular (13%, 10% serious), and peripheral vascular AOEs (14%, 11% serious). The exposure-adjusted incidence of AOEs was 14.1 per 100 patient-years.
Among patients without AOEs prior to October 2013 when pre-emptive dose reductions began, the incidence of AOEs was 19% in patients who had dose reductions and 18% in patients who did not.
The cumulative incidence of AOEs increased over time, but the exposure-adjusted incidence of new AOEs did not. It was 15.8 per 100 patient-years in year 1 and 4.9 per 100 patient-years in year 5.
The investigators said the lack of increase in exposure-adjusted AOE incidence could be due to the natural history or etiology of AOEs, dose reductions, or a change in the patient population (ie, an enrichment of patients who may have a lower risk of vascular events).
Therefore, it is unclear whether lower doses of ponatinib reduce the risk of AOEs in patients with risk factors. However, AOEs appear to be dose-related and modified by pre-existing cardiovascular disease and other risk factors.
Venous thromboembolism (VTE), on the other hand, does not seem to be dose-related. The investigators said the rate of VTE in this study was consistent with rates typically observed in cancer patients.
The incidence of VTE was 6%, and 5% of patients had serious VTEs. The exposure-adjusted incidence of VTEs was 2.1 per 100 patient-years.
Other AEs
The most common any-grade treatment-emergent AEs (≥40%) were rash (47%), abdominal pain (46%), thrombocytopenia (46%), headache (43%), dry skin (42%), and constipation (41%).
The most common grade 3/4 treatment-emergent AEs (≥10%) were thrombocytopenia (35%), neutropenia (17%), hypertension (14%), increased lipase (13%), abdominal pain (10%), and anemia (10%).
Serious AEs (≥5%) included pancreatitis (7%), atrial fibrillation (6%), pneumonia (6%), and angina pectoris (5%).
There were 12 deaths (4%) that occurred on study or within 30 days of the end of study treatment. Two deaths were considered possibly or probably related to ponatinib, 1 due to pneumonia and 1 due to acute myocardial infarction.
Final results from the phase 2 PACE trial suggest dose reductions did not have an effect on the efficacy of ponatinib in patients with chronic phase (CP) chronic myeloid leukemia (CML).
Trial investigators began reducing ponatinib doses after the drug was linked to arterial occlusive events (AOEs).
Most patients who achieved a major molecular response (MMR) or major cytogenetic response (MCyR) on higher doses of ponatinib maintained those responses after dose reductions.
These results were published in Blood. The trial was sponsored by Ariad Pharmaceuticals, Inc., a wholly owned subsidiary of Takeda Pharmaceutical Company Limited.
Earlier results from the PACE trial indicated that ponatinib increased a patient’s risk of vascular occlusive events (VOEs), including AOEs.
Therefore, in October 2013, a phase 3 trial of ponatinib was discontinued, and all other ponatinib trials were put on partial clinical hold. Trial enrollment was halted temporarily, and investigators began reducing ponatinib doses.
Then, the US Food and Drug Administration suspended sales and marketing of ponatinib, pending results of a safety evaluation.
However, in December 2013, the agency decided ponatinib could return to the market if new safety measures were implemented. In January 2014, the drug was back on the market.
Patients
The PACE trial included 449 patients with CML or acute lymphoblastic leukemia, but the results published in Blood focused only on patients with CP-CML. All of these patients were resistant or intolerant to dasatinib or nilotinib, or they had the BCR-ABLT315I mutation.
There were 270 patients with CP-CML. They had a median age of 60 (range, 18-94), and 47% were female.
Ninety-three percent had received at least 2 prior approved tyrosine kinase inhibitors (TKIs), and 57% had received at least 3. The median duration of prior TKI treatment was 5.4 years (range, 0.4-13.3).
Eighty percent of patients were resistant to dasatinib or nilotinib, 14% were intolerant to either drug, and 19% were both resistant and intolerant. Twenty-four percent of patients had the T315I mutation.
Treatment
The starting dose of ponatinib was 45 mg once daily. Doses were reduced to 30 mg or 15 mg once daily to manage adverse events (AEs), or reductions were implemented proactively (starting on October 10, 2013) due to concerns about VOEs.
Unless a benefit-risk analysis justified use of a higher dose, the recommendation for CP-CML patients was a 15 mg daily dose for those with an MCyR and a 30 mg daily dose for those without an MCyR.
Patients received ponatinib until disease progression, intolerance, or the patient or investigator decided to stop treatment.
The median duration of treatment was 32.1 months (range, 0.1-73.0), and the median follow-up was 56.8 months (range, 0.1-73.1).
Efficacy
Of the 267 evaluable patients, 60% achieved an MCyR at any time, with 54% achieving a complete cytogenetic response. Forty-eight percent of patients were still in MCyR at the last response assessment, and 82% of patients who achieved an MCyR were estimated to remain in MCyR at 5 years.
There were 69 patients in MCyR as of October 10, 2013, when pre-emptive dose reduction began, who had their dose reduced. Ninety-six percent of these patients (n=66) maintained MCyR after dose reduction. Of the 34 patients in MCyR who did not have pre-emptive dose reductions, 94% (n=32) maintained MCyR.
Forty percent of patients attained a major molecular response (MMR) at any time during the study, with 30% achieving MR4 and 24% achieving MR4.5. Thirty percent of patients were in MMR at the last response assessment, and 59% of patients who achieved MMR were estimated to remain in MMR at 5 years.
There were 52 patients in MMR as of October 10, 2013, who had their dose reduced. Ninety percent (n=47) of these patients maintained MMR following dose reduction. Of the 19 patients in MMR who did not have pre-emptive dose reductions, 95% (n=18) maintained MMR.
“The PACE trial is among the longest and largest studies of patients with CP-CML who have received 2 or 3 prior TKIs, and the findings provide treating physicians with important updated information . . . ,” said study author Jorge Eduardo Cortes, MD, of MD Anderson Cancer Center in Houston, Texas.
“These final PACE results demonstrate that [ponatinib] provides lasting clinically meaningful responses, irrespective of dose reductions, in this population.”
At 5 years, the progression-free survival rate was 53%, and the overall survival rate was 73%.
AOEs
The incidence of AOEs was 31%, and the incidence of serious AOEs was 26%. This included cardiovascular AOEs (16%, 12% serious), cerebrovascular (13%, 10% serious), and peripheral vascular AOEs (14%, 11% serious). The exposure-adjusted incidence of AOEs was 14.1 per 100 patient-years.
Among patients without AOEs prior to October 2013 when pre-emptive dose reductions began, the incidence of AOEs was 19% in patients who had dose reductions and 18% in patients who did not.
The cumulative incidence of AOEs increased over time, but the exposure-adjusted incidence of new AOEs did not. It was 15.8 per 100 patient-years in year 1 and 4.9 per 100 patient-years in year 5.
The investigators said the lack of increase in exposure-adjusted AOE incidence could be due to the natural history or etiology of AOEs, dose reductions, or a change in the patient population (ie, an enrichment of patients who may have a lower risk of vascular events).
Therefore, it is unclear whether lower doses of ponatinib reduce the risk of AOEs in patients with risk factors. However, AOEs appear to be dose-related and modified by pre-existing cardiovascular disease and other risk factors.
Venous thromboembolism (VTE), on the other hand, does not seem to be dose-related. The investigators said the rate of VTE in this study was consistent with rates typically observed in cancer patients.
The incidence of VTE was 6%, and 5% of patients had serious VTEs. The exposure-adjusted incidence of VTEs was 2.1 per 100 patient-years.
Other AEs
The most common any-grade treatment-emergent AEs (≥40%) were rash (47%), abdominal pain (46%), thrombocytopenia (46%), headache (43%), dry skin (42%), and constipation (41%).
The most common grade 3/4 treatment-emergent AEs (≥10%) were thrombocytopenia (35%), neutropenia (17%), hypertension (14%), increased lipase (13%), abdominal pain (10%), and anemia (10%).
Serious AEs (≥5%) included pancreatitis (7%), atrial fibrillation (6%), pneumonia (6%), and angina pectoris (5%).
There were 12 deaths (4%) that occurred on study or within 30 days of the end of study treatment. Two deaths were considered possibly or probably related to ponatinib, 1 due to pneumonia and 1 due to acute myocardial infarction.
Final results from the phase 2 PACE trial suggest dose reductions did not have an effect on the efficacy of ponatinib in patients with chronic phase (CP) chronic myeloid leukemia (CML).
Trial investigators began reducing ponatinib doses after the drug was linked to arterial occlusive events (AOEs).
Most patients who achieved a major molecular response (MMR) or major cytogenetic response (MCyR) on higher doses of ponatinib maintained those responses after dose reductions.
These results were published in Blood. The trial was sponsored by Ariad Pharmaceuticals, Inc., a wholly owned subsidiary of Takeda Pharmaceutical Company Limited.
Earlier results from the PACE trial indicated that ponatinib increased a patient’s risk of vascular occlusive events (VOEs), including AOEs.
Therefore, in October 2013, a phase 3 trial of ponatinib was discontinued, and all other ponatinib trials were put on partial clinical hold. Trial enrollment was halted temporarily, and investigators began reducing ponatinib doses.
Then, the US Food and Drug Administration suspended sales and marketing of ponatinib, pending results of a safety evaluation.
However, in December 2013, the agency decided ponatinib could return to the market if new safety measures were implemented. In January 2014, the drug was back on the market.
Patients
The PACE trial included 449 patients with CML or acute lymphoblastic leukemia, but the results published in Blood focused only on patients with CP-CML. All of these patients were resistant or intolerant to dasatinib or nilotinib, or they had the BCR-ABLT315I mutation.
There were 270 patients with CP-CML. They had a median age of 60 (range, 18-94), and 47% were female.
Ninety-three percent had received at least 2 prior approved tyrosine kinase inhibitors (TKIs), and 57% had received at least 3. The median duration of prior TKI treatment was 5.4 years (range, 0.4-13.3).
Eighty percent of patients were resistant to dasatinib or nilotinib, 14% were intolerant to either drug, and 19% were both resistant and intolerant. Twenty-four percent of patients had the T315I mutation.
Treatment
The starting dose of ponatinib was 45 mg once daily. Doses were reduced to 30 mg or 15 mg once daily to manage adverse events (AEs), or reductions were implemented proactively (starting on October 10, 2013) due to concerns about VOEs.
Unless a benefit-risk analysis justified use of a higher dose, the recommendation for CP-CML patients was a 15 mg daily dose for those with an MCyR and a 30 mg daily dose for those without an MCyR.
Patients received ponatinib until disease progression, intolerance, or the patient or investigator decided to stop treatment.
The median duration of treatment was 32.1 months (range, 0.1-73.0), and the median follow-up was 56.8 months (range, 0.1-73.1).
Efficacy
Of the 267 evaluable patients, 60% achieved an MCyR at any time, with 54% achieving a complete cytogenetic response. Forty-eight percent of patients were still in MCyR at the last response assessment, and 82% of patients who achieved an MCyR were estimated to remain in MCyR at 5 years.
There were 69 patients in MCyR as of October 10, 2013, when pre-emptive dose reduction began, who had their dose reduced. Ninety-six percent of these patients (n=66) maintained MCyR after dose reduction. Of the 34 patients in MCyR who did not have pre-emptive dose reductions, 94% (n=32) maintained MCyR.
Forty percent of patients attained a major molecular response (MMR) at any time during the study, with 30% achieving MR4 and 24% achieving MR4.5. Thirty percent of patients were in MMR at the last response assessment, and 59% of patients who achieved MMR were estimated to remain in MMR at 5 years.
There were 52 patients in MMR as of October 10, 2013, who had their dose reduced. Ninety percent (n=47) of these patients maintained MMR following dose reduction. Of the 19 patients in MMR who did not have pre-emptive dose reductions, 95% (n=18) maintained MMR.
“The PACE trial is among the longest and largest studies of patients with CP-CML who have received 2 or 3 prior TKIs, and the findings provide treating physicians with important updated information . . . ,” said study author Jorge Eduardo Cortes, MD, of MD Anderson Cancer Center in Houston, Texas.
“These final PACE results demonstrate that [ponatinib] provides lasting clinically meaningful responses, irrespective of dose reductions, in this population.”
At 5 years, the progression-free survival rate was 53%, and the overall survival rate was 73%.
AOEs
The incidence of AOEs was 31%, and the incidence of serious AOEs was 26%. This included cardiovascular AOEs (16%, 12% serious), cerebrovascular (13%, 10% serious), and peripheral vascular AOEs (14%, 11% serious). The exposure-adjusted incidence of AOEs was 14.1 per 100 patient-years.
Among patients without AOEs prior to October 2013 when pre-emptive dose reductions began, the incidence of AOEs was 19% in patients who had dose reductions and 18% in patients who did not.
The cumulative incidence of AOEs increased over time, but the exposure-adjusted incidence of new AOEs did not. It was 15.8 per 100 patient-years in year 1 and 4.9 per 100 patient-years in year 5.
The investigators said the lack of increase in exposure-adjusted AOE incidence could be due to the natural history or etiology of AOEs, dose reductions, or a change in the patient population (ie, an enrichment of patients who may have a lower risk of vascular events).
Therefore, it is unclear whether lower doses of ponatinib reduce the risk of AOEs in patients with risk factors. However, AOEs appear to be dose-related and modified by pre-existing cardiovascular disease and other risk factors.
Venous thromboembolism (VTE), on the other hand, does not seem to be dose-related. The investigators said the rate of VTE in this study was consistent with rates typically observed in cancer patients.
The incidence of VTE was 6%, and 5% of patients had serious VTEs. The exposure-adjusted incidence of VTEs was 2.1 per 100 patient-years.
Other AEs
The most common any-grade treatment-emergent AEs (≥40%) were rash (47%), abdominal pain (46%), thrombocytopenia (46%), headache (43%), dry skin (42%), and constipation (41%).
The most common grade 3/4 treatment-emergent AEs (≥10%) were thrombocytopenia (35%), neutropenia (17%), hypertension (14%), increased lipase (13%), abdominal pain (10%), and anemia (10%).
Serious AEs (≥5%) included pancreatitis (7%), atrial fibrillation (6%), pneumonia (6%), and angina pectoris (5%).
There were 12 deaths (4%) that occurred on study or within 30 days of the end of study treatment. Two deaths were considered possibly or probably related to ponatinib, 1 due to pneumonia and 1 due to acute myocardial infarction.
Cannabis users at highest psychosis risk may elect to quit
Cannabis users who experience symptoms suggestive of psychosis are more likely to stop using the drug – or report wanting to stop – than are those who report more pleasurable experiences.
This finding, published March 23 in Psychological Medicine, might help explain an epidemiological conundrum related to cannabis use.
Yet, despite evidence of increasing cannabis potency and cannabis use over the last 15 years, levels of psychotic disorders, such as schizophrenia, “are stable and have remained stable over time,” said Musa Basseer Sami, MD, the study’s lead author, in an interview. “This is a big stumbling block for anyone who says pot is associated with psychosis.”
Dr. Sami’s findings suggest that people who report psychosis-like experiences with cannabis might be those most likely to stop consuming it, in turn reducing their risk. “If people are discontinuing after bad experiences, and if such experiences are a risk factor for developing a psychotic disorder, they may be deselecting themselves” out of the cannabis-using population, said Dr. Sami of King’s College London.
For their research, the investigators conducted a cross-sectional online survey study of more than 1,200 current or previous cannabis users, about three-quarters of whom reported current use. To do this, they modified a validated survey tool called the Cannabis Experiences Questionnaire, which measures the euphoric and paranoid-dysphoric effects of cannabis. They also collected qualitative data from respondents explaining how their experiences shaped their attitudes on whether to continue using.
Current users who said they intended to quit cannabis reported greater psychosis-like experiences (OR, 1.131; 95% CI, 1.044-1.225; P less than 0.003). People who expressed a desire to continue, meanwhile, reported increased pleasurable experiences (OR, 0.892; 95% CI, 0.814-0.978; P less than 0.015).
The differences remained statistically significant across groups when age, sex, frequency of use, age of first use, and other drug use were accounted for.
Dr. Sami said. “And even if you continue using, you’re more likely to say you’re going to stop using in the future.”
Dr. Sami noted that nearly 40% of survey respondents reported having been treated for, or sought treatment for, a mental health complaint but cautioned against assuming these were attributable to cannabis use. “It’s very difficult to tease out whether they were using cannabis to self-medicate,” he said.
The new findings could help guide clinicians whose patients express a desire to quit and report psychosis-like experiences associated with cannabis. Helping patients elucidate those experiences could help inform conversations about risk and plans to quit, he said.
Currently, “we don’t really treat people who have these kind of experiences. If you came to me, as a psychiatrist, and asked me why I’m getting paranoid when I use cannabis, I’d tell you to stop using cannabis,” he said.
“But people who continue to use cannabis have a higher risk of psychotic disorder. And we’re now finding out that people who have psychotic-like experiences when they use cannabis tend to be more likely to develop psychotic disorders. So if I smoke weed and I start hearing voices and become suspicious, it might be a marker for me to develop schizophrenia.”
Dr. Sami and his colleagues are continuing to examine, by way of an online survey, why people might have very different experiences with the same drug. The survey is open to all adults whether they use cannabis or not at thecannabissurvey.com.
The research group declared support from the U.K. National Institute for Health Research, King’s College London, the Medical Research Council, and the U.K. Society for the Study of Addiction. The researchers reported no financial conflicts of interest.
SOURCE: Sami MB et al. Psychol Med. 2018 Mar 23. doi: 10.1017/S0033291718000569.
Cannabis users who experience symptoms suggestive of psychosis are more likely to stop using the drug – or report wanting to stop – than are those who report more pleasurable experiences.
This finding, published March 23 in Psychological Medicine, might help explain an epidemiological conundrum related to cannabis use.
Yet, despite evidence of increasing cannabis potency and cannabis use over the last 15 years, levels of psychotic disorders, such as schizophrenia, “are stable and have remained stable over time,” said Musa Basseer Sami, MD, the study’s lead author, in an interview. “This is a big stumbling block for anyone who says pot is associated with psychosis.”
Dr. Sami’s findings suggest that people who report psychosis-like experiences with cannabis might be those most likely to stop consuming it, in turn reducing their risk. “If people are discontinuing after bad experiences, and if such experiences are a risk factor for developing a psychotic disorder, they may be deselecting themselves” out of the cannabis-using population, said Dr. Sami of King’s College London.
For their research, the investigators conducted a cross-sectional online survey study of more than 1,200 current or previous cannabis users, about three-quarters of whom reported current use. To do this, they modified a validated survey tool called the Cannabis Experiences Questionnaire, which measures the euphoric and paranoid-dysphoric effects of cannabis. They also collected qualitative data from respondents explaining how their experiences shaped their attitudes on whether to continue using.
Current users who said they intended to quit cannabis reported greater psychosis-like experiences (OR, 1.131; 95% CI, 1.044-1.225; P less than 0.003). People who expressed a desire to continue, meanwhile, reported increased pleasurable experiences (OR, 0.892; 95% CI, 0.814-0.978; P less than 0.015).
The differences remained statistically significant across groups when age, sex, frequency of use, age of first use, and other drug use were accounted for.
Dr. Sami said. “And even if you continue using, you’re more likely to say you’re going to stop using in the future.”
Dr. Sami noted that nearly 40% of survey respondents reported having been treated for, or sought treatment for, a mental health complaint but cautioned against assuming these were attributable to cannabis use. “It’s very difficult to tease out whether they were using cannabis to self-medicate,” he said.
The new findings could help guide clinicians whose patients express a desire to quit and report psychosis-like experiences associated with cannabis. Helping patients elucidate those experiences could help inform conversations about risk and plans to quit, he said.
Currently, “we don’t really treat people who have these kind of experiences. If you came to me, as a psychiatrist, and asked me why I’m getting paranoid when I use cannabis, I’d tell you to stop using cannabis,” he said.
“But people who continue to use cannabis have a higher risk of psychotic disorder. And we’re now finding out that people who have psychotic-like experiences when they use cannabis tend to be more likely to develop psychotic disorders. So if I smoke weed and I start hearing voices and become suspicious, it might be a marker for me to develop schizophrenia.”
Dr. Sami and his colleagues are continuing to examine, by way of an online survey, why people might have very different experiences with the same drug. The survey is open to all adults whether they use cannabis or not at thecannabissurvey.com.
The research group declared support from the U.K. National Institute for Health Research, King’s College London, the Medical Research Council, and the U.K. Society for the Study of Addiction. The researchers reported no financial conflicts of interest.
SOURCE: Sami MB et al. Psychol Med. 2018 Mar 23. doi: 10.1017/S0033291718000569.
Cannabis users who experience symptoms suggestive of psychosis are more likely to stop using the drug – or report wanting to stop – than are those who report more pleasurable experiences.
This finding, published March 23 in Psychological Medicine, might help explain an epidemiological conundrum related to cannabis use.
Yet, despite evidence of increasing cannabis potency and cannabis use over the last 15 years, levels of psychotic disorders, such as schizophrenia, “are stable and have remained stable over time,” said Musa Basseer Sami, MD, the study’s lead author, in an interview. “This is a big stumbling block for anyone who says pot is associated with psychosis.”
Dr. Sami’s findings suggest that people who report psychosis-like experiences with cannabis might be those most likely to stop consuming it, in turn reducing their risk. “If people are discontinuing after bad experiences, and if such experiences are a risk factor for developing a psychotic disorder, they may be deselecting themselves” out of the cannabis-using population, said Dr. Sami of King’s College London.
For their research, the investigators conducted a cross-sectional online survey study of more than 1,200 current or previous cannabis users, about three-quarters of whom reported current use. To do this, they modified a validated survey tool called the Cannabis Experiences Questionnaire, which measures the euphoric and paranoid-dysphoric effects of cannabis. They also collected qualitative data from respondents explaining how their experiences shaped their attitudes on whether to continue using.
Current users who said they intended to quit cannabis reported greater psychosis-like experiences (OR, 1.131; 95% CI, 1.044-1.225; P less than 0.003). People who expressed a desire to continue, meanwhile, reported increased pleasurable experiences (OR, 0.892; 95% CI, 0.814-0.978; P less than 0.015).
The differences remained statistically significant across groups when age, sex, frequency of use, age of first use, and other drug use were accounted for.
Dr. Sami said. “And even if you continue using, you’re more likely to say you’re going to stop using in the future.”
Dr. Sami noted that nearly 40% of survey respondents reported having been treated for, or sought treatment for, a mental health complaint but cautioned against assuming these were attributable to cannabis use. “It’s very difficult to tease out whether they were using cannabis to self-medicate,” he said.
The new findings could help guide clinicians whose patients express a desire to quit and report psychosis-like experiences associated with cannabis. Helping patients elucidate those experiences could help inform conversations about risk and plans to quit, he said.
Currently, “we don’t really treat people who have these kind of experiences. If you came to me, as a psychiatrist, and asked me why I’m getting paranoid when I use cannabis, I’d tell you to stop using cannabis,” he said.
“But people who continue to use cannabis have a higher risk of psychotic disorder. And we’re now finding out that people who have psychotic-like experiences when they use cannabis tend to be more likely to develop psychotic disorders. So if I smoke weed and I start hearing voices and become suspicious, it might be a marker for me to develop schizophrenia.”
Dr. Sami and his colleagues are continuing to examine, by way of an online survey, why people might have very different experiences with the same drug. The survey is open to all adults whether they use cannabis or not at thecannabissurvey.com.
The research group declared support from the U.K. National Institute for Health Research, King’s College London, the Medical Research Council, and the U.K. Society for the Study of Addiction. The researchers reported no financial conflicts of interest.
SOURCE: Sami MB et al. Psychol Med. 2018 Mar 23. doi: 10.1017/S0033291718000569.
FROM PSYCHOLOGICAL MEDICINE
Key clinical point: Psychosis-like experiences with cannabis use predict cannabis cessation and the desire to quit.
Major finding: Cessation of cannabis use was associated with having greater self-reported psychosis-like experiences (odds ratio, 1.262; 95% confidence interval, 1.179-1.351; P less than 0.001).
Study details: An online survey of 1,231 cannabis users (69% male; n = 926 current users) measuring the effects of psychosis-like and pleasurable experiences on quitting or intending to quit.
Disclosures: The research group declared support from the U.K. National Institute for Health Research, King’s College London, the Medical Research Council, and the U.K. Society for the Study of Addiction. The researchers reported no financial conflicts of interest.
Source: Sami MB et al. Psychol Med. 2018 Mar 23. doi: 10.1017/S0033291718000569.
Abstract: The Opioid Crisis and the Need for Compassion in Pain Management
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Rothstein, M.A., Am J Publ Health 107(8):1253, August 2017
The author, from the University of Louisville School of Medicine, comments on the unintended consequences of restricting opioid prescribing. Causes and outcomes of the opioid addiction epidemic are well documented, including aggressive marketing by pharmaceutical companies without full disclosure of risk and a four-fold increase in US opioid-related deaths between 1999 and 2014 alone. Countermeasures include prescription drug monitoring programs to restrict use, legal limits on pill numbers per prescription, opioid patient “contracts,” and drug testing to ensure compliance. For fear of medicolegal risk, many physicians have decided to stop prescribing opioids for patients with chronic pain, limiting use to postoperative pain, cancer pain and terminal illness. In some cases, patients with severe pain turn to illicit drugs as the only alternative, leading to diseases such as HIV and hepatitis, as well as more overdose deaths. Eliminating opioids entirely as an option for chronic pain shows a lack of compassion and violates both standards of care and medical ethics. Many patients with severe pain due to chronic conditions legitimately need potent analgesics such as opioids, especially during acute episodes, because over-the-counter analgesics are completely ineffective. Patients who became addicted after using a lawful prescription also cannot be abandoned but need proper management. Stakeholders at all levels must address the undertreatment of pain with research, education and policy changes to acknowledge both the problem of opioid abuse and the needs of patients with chronic pain. After all, policies “should not presume that all physicians are reckless prescribers or that all patients are deceitful drug seekers.” 7 references ([email protected] – no reprints)
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Rothstein, M.A., Am J Publ Health 107(8):1253, August 2017
The author, from the University of Louisville School of Medicine, comments on the unintended consequences of restricting opioid prescribing. Causes and outcomes of the opioid addiction epidemic are well documented, including aggressive marketing by pharmaceutical companies without full disclosure of risk and a four-fold increase in US opioid-related deaths between 1999 and 2014 alone. Countermeasures include prescription drug monitoring programs to restrict use, legal limits on pill numbers per prescription, opioid patient “contracts,” and drug testing to ensure compliance. For fear of medicolegal risk, many physicians have decided to stop prescribing opioids for patients with chronic pain, limiting use to postoperative pain, cancer pain and terminal illness. In some cases, patients with severe pain turn to illicit drugs as the only alternative, leading to diseases such as HIV and hepatitis, as well as more overdose deaths. Eliminating opioids entirely as an option for chronic pain shows a lack of compassion and violates both standards of care and medical ethics. Many patients with severe pain due to chronic conditions legitimately need potent analgesics such as opioids, especially during acute episodes, because over-the-counter analgesics are completely ineffective. Patients who became addicted after using a lawful prescription also cannot be abandoned but need proper management. Stakeholders at all levels must address the undertreatment of pain with research, education and policy changes to acknowledge both the problem of opioid abuse and the needs of patients with chronic pain. After all, policies “should not presume that all physicians are reckless prescribers or that all patients are deceitful drug seekers.” 7 references ([email protected] – no reprints)
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Rothstein, M.A., Am J Publ Health 107(8):1253, August 2017
The author, from the University of Louisville School of Medicine, comments on the unintended consequences of restricting opioid prescribing. Causes and outcomes of the opioid addiction epidemic are well documented, including aggressive marketing by pharmaceutical companies without full disclosure of risk and a four-fold increase in US opioid-related deaths between 1999 and 2014 alone. Countermeasures include prescription drug monitoring programs to restrict use, legal limits on pill numbers per prescription, opioid patient “contracts,” and drug testing to ensure compliance. For fear of medicolegal risk, many physicians have decided to stop prescribing opioids for patients with chronic pain, limiting use to postoperative pain, cancer pain and terminal illness. In some cases, patients with severe pain turn to illicit drugs as the only alternative, leading to diseases such as HIV and hepatitis, as well as more overdose deaths. Eliminating opioids entirely as an option for chronic pain shows a lack of compassion and violates both standards of care and medical ethics. Many patients with severe pain due to chronic conditions legitimately need potent analgesics such as opioids, especially during acute episodes, because over-the-counter analgesics are completely ineffective. Patients who became addicted after using a lawful prescription also cannot be abandoned but need proper management. Stakeholders at all levels must address the undertreatment of pain with research, education and policy changes to acknowledge both the problem of opioid abuse and the needs of patients with chronic pain. After all, policies “should not presume that all physicians are reckless prescribers or that all patients are deceitful drug seekers.” 7 references ([email protected] – no reprints)
Learn more about the Primary Care Medical Abstracts and podcasts, for which you can earn up to 9 CME credits per month.
Copyright © The Center for Medical Education
Interventions urged to stop rising NAS, stem Medicaid costs
The incidence of neonatal abstinence syndrome (NAS) and the corresponding costs to Medicaid are unlikely to decline unless interventions focus on stopping opioid use by low-income mothers, said Tyler N.A. Winkelman, MD, of Hennepin County Medical Center, Minneapolis, and his associates.
Dr. Winkelman and his associates conducted a serial cross-sectional analysis that used 9,115,457 birth discharge records from the 2004-2014 National Inpatient Sample (NIS), which were representative of 43.6 million weighted births. Overall, 3,991,336 infants were covered by Medicaid, which were representative of 19.1 million weighted births. There were 35,629 (0.89%) infants with a diagnosis of NAS, which were representative of 173,384 weighted births. Medicaid was the primary payer for 74% (95% confidence interval, 68.9%-77.9%) of NAS-related births in 2004 and 82% (95% CI, 80.5%-83.5%) of NAS-related births in 2014.
Infants with NAS who were enrolled in Medicaid were significantly more likely to be male, live in a rural county, and have comorbidities reflective of the syndrome than were infants without NAS who were enrolled in Medicaid, the researchers wrote in Pediatrics.
from 1.5 per 1,000 hospital births (95% CI, 1.2-1.9) to 8 per 1,000 hospital births (95% CI, 7.2-8.7), as the opioid epidemic worsened in the country.
Infants with NAS who were covered by Medicaid had a greater chance of being transferred to another hospital for care (9% vs. 7%; P = .02) and stay in the hospital longer (17 days vs. 15 days; P less than .001), compared with infants with NAS who were covered by private insurance.
NAS is costly. In the 2011-2014 era, mean hospital costs for a NAS infant covered by Medicaid were more than fivefold higher than for an infant without NAS ($19,340/birth vs. $3,700/birth; P less than .001). After adjustment for inflation, mean hospital costs for infants with NAS who were covered by Medicaid increased 26% between 2004-2006 and 2011-2014 ($15,350 vs. $19,340; P less than .001), the researchers reported. Annual hospital costs, which were adjusted for inflation to 2014 U.S. dollars, for all infants with NAS who were covered by Medicaid rose from $65.4 million in 2004 to $462 million in 2014.
“With the disproportionate impact of NAS on the Medicaid population, we suggest that NAS incidence rates are unlikely to improve without interventions targeted at low-income mothers and infants,” Dr. Winkelman and his associates concluded.
Nonpharmacologic interventions are available to help NAS infants. “Systematic implementation of policies that support rooming-in, breastfeeding, swaddling, on-demand feeding schedules, and minimization of sleep disruption may reduce symptoms of NAS and reduce the duration of, or even eliminate the need for, pharmacologic treatment of NAS,” the researchers said. “Pharmacologic treatment with buprenorphine, for example, has been shown to reduce hospital length of stay by 35%.”
Another intervention is medication-assisted treatment during pregnancy, which studies have shown “improves outcomes and reduces costs associated with NAS, compared with attempted abstinence,” Dr. Winkelman and his associates said. It does not necessarily reduce NAS incidence, but “it may prevent prolonged hospital stays due to preterm birth, reduce NICU [neonatal intensive care unit] admissions, decrease the severity of NAS symptoms, and improve birth outcomes for some infants.”
The researchers also endorsed screening, referral, and treatment for substance abuse and mental health disorders among reproductive age women, including adolescents, because these are risk factors for opioid abuse.
One author was supported by an award from the National Institute on Drug Abuse. None of the other authors had relevant financial disclosures.
SOURCE: Winkelman TNA et al. Pediatrics. 2018;141(4):e20173520.
The incidence of neonatal abstinence syndrome (NAS) and the corresponding costs to Medicaid are unlikely to decline unless interventions focus on stopping opioid use by low-income mothers, said Tyler N.A. Winkelman, MD, of Hennepin County Medical Center, Minneapolis, and his associates.
Dr. Winkelman and his associates conducted a serial cross-sectional analysis that used 9,115,457 birth discharge records from the 2004-2014 National Inpatient Sample (NIS), which were representative of 43.6 million weighted births. Overall, 3,991,336 infants were covered by Medicaid, which were representative of 19.1 million weighted births. There were 35,629 (0.89%) infants with a diagnosis of NAS, which were representative of 173,384 weighted births. Medicaid was the primary payer for 74% (95% confidence interval, 68.9%-77.9%) of NAS-related births in 2004 and 82% (95% CI, 80.5%-83.5%) of NAS-related births in 2014.
Infants with NAS who were enrolled in Medicaid were significantly more likely to be male, live in a rural county, and have comorbidities reflective of the syndrome than were infants without NAS who were enrolled in Medicaid, the researchers wrote in Pediatrics.
from 1.5 per 1,000 hospital births (95% CI, 1.2-1.9) to 8 per 1,000 hospital births (95% CI, 7.2-8.7), as the opioid epidemic worsened in the country.
Infants with NAS who were covered by Medicaid had a greater chance of being transferred to another hospital for care (9% vs. 7%; P = .02) and stay in the hospital longer (17 days vs. 15 days; P less than .001), compared with infants with NAS who were covered by private insurance.
NAS is costly. In the 2011-2014 era, mean hospital costs for a NAS infant covered by Medicaid were more than fivefold higher than for an infant without NAS ($19,340/birth vs. $3,700/birth; P less than .001). After adjustment for inflation, mean hospital costs for infants with NAS who were covered by Medicaid increased 26% between 2004-2006 and 2011-2014 ($15,350 vs. $19,340; P less than .001), the researchers reported. Annual hospital costs, which were adjusted for inflation to 2014 U.S. dollars, for all infants with NAS who were covered by Medicaid rose from $65.4 million in 2004 to $462 million in 2014.
“With the disproportionate impact of NAS on the Medicaid population, we suggest that NAS incidence rates are unlikely to improve without interventions targeted at low-income mothers and infants,” Dr. Winkelman and his associates concluded.
Nonpharmacologic interventions are available to help NAS infants. “Systematic implementation of policies that support rooming-in, breastfeeding, swaddling, on-demand feeding schedules, and minimization of sleep disruption may reduce symptoms of NAS and reduce the duration of, or even eliminate the need for, pharmacologic treatment of NAS,” the researchers said. “Pharmacologic treatment with buprenorphine, for example, has been shown to reduce hospital length of stay by 35%.”
Another intervention is medication-assisted treatment during pregnancy, which studies have shown “improves outcomes and reduces costs associated with NAS, compared with attempted abstinence,” Dr. Winkelman and his associates said. It does not necessarily reduce NAS incidence, but “it may prevent prolonged hospital stays due to preterm birth, reduce NICU [neonatal intensive care unit] admissions, decrease the severity of NAS symptoms, and improve birth outcomes for some infants.”
The researchers also endorsed screening, referral, and treatment for substance abuse and mental health disorders among reproductive age women, including adolescents, because these are risk factors for opioid abuse.
One author was supported by an award from the National Institute on Drug Abuse. None of the other authors had relevant financial disclosures.
SOURCE: Winkelman TNA et al. Pediatrics. 2018;141(4):e20173520.
The incidence of neonatal abstinence syndrome (NAS) and the corresponding costs to Medicaid are unlikely to decline unless interventions focus on stopping opioid use by low-income mothers, said Tyler N.A. Winkelman, MD, of Hennepin County Medical Center, Minneapolis, and his associates.
Dr. Winkelman and his associates conducted a serial cross-sectional analysis that used 9,115,457 birth discharge records from the 2004-2014 National Inpatient Sample (NIS), which were representative of 43.6 million weighted births. Overall, 3,991,336 infants were covered by Medicaid, which were representative of 19.1 million weighted births. There were 35,629 (0.89%) infants with a diagnosis of NAS, which were representative of 173,384 weighted births. Medicaid was the primary payer for 74% (95% confidence interval, 68.9%-77.9%) of NAS-related births in 2004 and 82% (95% CI, 80.5%-83.5%) of NAS-related births in 2014.
Infants with NAS who were enrolled in Medicaid were significantly more likely to be male, live in a rural county, and have comorbidities reflective of the syndrome than were infants without NAS who were enrolled in Medicaid, the researchers wrote in Pediatrics.
from 1.5 per 1,000 hospital births (95% CI, 1.2-1.9) to 8 per 1,000 hospital births (95% CI, 7.2-8.7), as the opioid epidemic worsened in the country.
Infants with NAS who were covered by Medicaid had a greater chance of being transferred to another hospital for care (9% vs. 7%; P = .02) and stay in the hospital longer (17 days vs. 15 days; P less than .001), compared with infants with NAS who were covered by private insurance.
NAS is costly. In the 2011-2014 era, mean hospital costs for a NAS infant covered by Medicaid were more than fivefold higher than for an infant without NAS ($19,340/birth vs. $3,700/birth; P less than .001). After adjustment for inflation, mean hospital costs for infants with NAS who were covered by Medicaid increased 26% between 2004-2006 and 2011-2014 ($15,350 vs. $19,340; P less than .001), the researchers reported. Annual hospital costs, which were adjusted for inflation to 2014 U.S. dollars, for all infants with NAS who were covered by Medicaid rose from $65.4 million in 2004 to $462 million in 2014.
“With the disproportionate impact of NAS on the Medicaid population, we suggest that NAS incidence rates are unlikely to improve without interventions targeted at low-income mothers and infants,” Dr. Winkelman and his associates concluded.
Nonpharmacologic interventions are available to help NAS infants. “Systematic implementation of policies that support rooming-in, breastfeeding, swaddling, on-demand feeding schedules, and minimization of sleep disruption may reduce symptoms of NAS and reduce the duration of, or even eliminate the need for, pharmacologic treatment of NAS,” the researchers said. “Pharmacologic treatment with buprenorphine, for example, has been shown to reduce hospital length of stay by 35%.”
Another intervention is medication-assisted treatment during pregnancy, which studies have shown “improves outcomes and reduces costs associated with NAS, compared with attempted abstinence,” Dr. Winkelman and his associates said. It does not necessarily reduce NAS incidence, but “it may prevent prolonged hospital stays due to preterm birth, reduce NICU [neonatal intensive care unit] admissions, decrease the severity of NAS symptoms, and improve birth outcomes for some infants.”
The researchers also endorsed screening, referral, and treatment for substance abuse and mental health disorders among reproductive age women, including adolescents, because these are risk factors for opioid abuse.
One author was supported by an award from the National Institute on Drug Abuse. None of the other authors had relevant financial disclosures.
SOURCE: Winkelman TNA et al. Pediatrics. 2018;141(4):e20173520.
FROM PEDIATRICS
Key clinical point:
Major finding: In 2011-2014, mean hospital costs for NAS infants covered by Medicaid were more than fivefold higher than for infants without NAS ($19,340/birth vs. $3,700/birth).
Study details: A serial cross-sectional analysis that usd data from the 2004-2014 National Inpatient Sample (NIS) of 9,115,457 birth discharge records.
Disclosures: Stephen W. Patrick, MD, was supported by an award from the National Institute on Drug Abuse. None of the other authors had relevant financial disclosures.
Source: Winkelman TNA et al. Pediatrics. 2018;141(4):e20173520.
Siponimod trial ‘first’ to show delayed disability in secondary progressive MS
Phase 3 data with siponimod, Novartis’ investigational treatment for multiple sclerosis, show a 21% reduction in the time to disease progression versus placebo in patients with the secondary progressive subtype of the disease.
A significantly lower percentage of patients with secondary progressive multiple sclerosis (SPMS) treated with siponimod met the primary endpoint of confirmed disease progression (CDP) at 3 months, compared with those who received placebo in the EXPAND trial (26% vs. 32% of patients; hazard ratio [HR], 0.79; 95% confidence interval [CI], 0.65–0.95; P = .013).
No significant difference between siponimod and placebo was seen in one of the two main secondary outcomes of the study – the time to 3-month confirmed worsening of the timed 25-foot walk test (T25FW). This result led Luanne Metz, MD, and Wei-Qiao Liu, MD, both of the department of clinical neurosciences and the Hotchkiss Brain Institute at the University of Calgary (Alta.), to take a cautionary view of the findings in an editorial about the trial’s results.
“Although siponimod seems to reduce the time to confirmed disability in SPMS, the treatment effect was small,” Dr. Metz and Dr. Liu argued.
“In our opinion, the reduction in the proportion of participants reaching the primary endpoint of only 6% and the absence of a significant difference for the key secondary clinical outcome [T25FW] are disappointing results and do not suggest that siponimod is an effective treatment for SPMS,” the two wrote.
“Confidence in the treatment benefit of siponimod in progressive MS will, in our opinion, require confirmation in a second trial. Trials of other novel treatments that target noninflammatory mechanisms are still needed,” they said.
EXPAND (Exploring the efficacy and safety of siponimod in patients with secondary progressive multiple sclerosis) was an event- and exposure-driven double-blind trial that recruited patients with SPMS over a 2-year period starting in February 2013. Of 1,651 patients who were recruited, randomized, and actually received treatment, 1,099 were treated with oral siponimod, 2 mg once daily, and 546 were given a matching placebo.
Treatment was for up to 3 years or until 374 CDP events assessed via the Expanded Disability Status Scale (EDSS) had occurred. Patients who had CDP after 6 months in the double-blind trial could be re-consented and continue with double-blind treatment, switch to open-label siponimod, or stop study treatment and either remain on no treatment or receive another disease-modifying treatment.
On average, the patients had been diagnosed with SPMS for a mean of 3.8 years and had been first diagnosed with MS around 17 years prior to this.
The primary endpoint of the trial – CDP at 3 months – was first reported in 2016 at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS). CDP was defined as a 0.5- to 1-point increase in EDSS depending on the baseline score.
A host of additional secondary endpoints were studied, with the risk of 6-month CDP being significantly reduced by siponimod versus placebo (HR, 0.74; 95% CI, 0.60-0.92; P = .0058).
The change from baseline in T2 lesion volume – the second of the two main secondary endpoints studied – showed a potential benefit of siponimod treatment over placebo, with a lower mean-adjusted increase in lesion volume over months 12 and 24 (183.9 mm3 vs. 879.2 mm3; P less than .0001).
More patients receiving siponimod than placebo were free from new or enlarging T2 lesions (57% vs. 37%) or T1 gadolinium-enhancing lesions (89% vs. 67%), and brain volume decreased at a lower rate with siponimod than with placebo.
Adverse events occurred at a higher rate with siponimod than with placebo (89% of patients vs. 82%), of which 18% and 15%, respectively, were defined as serious.
Adverse events seen more commonly in siponimod- than in placebo-treated patients were lymphopenia (1% vs. 0%), abnormal liver-related investigations (12% vs. 4%), hypertension (10% vs. 8%), and bradycardia (4% vs. 3%) and bradyarrhythmia (3% vs. 0.4%) at the start of treatment, which were mitigated by dose titration. Other adverse events that occurred less often but more frequently with siponimod included macular edema (2% vs. less than 1%), reactivation of varicella zoster (2% vs. 1%), and convulsions (2% vs. less than 1%).
“The safety profile of siponimod in EXPAND was generally aligned with that of other drugs in the class,” Dr. Kappos and his colleagues observed.
Siponimod, also known as BAF312, is a selective sphingosine 1-phosphate (S1P) receptor modulator that targets the targets the S1P 1 and 5 receptor subtypes; the other currently approved drug in its class is fingolimod (Gilenya), which is currently indicated for treating the relapsing-remitting form of multiple sclerosis (RRMS).
Phase 2 data have shown that siponimod could also be a promising treatment for RRMS, with reduced relapse rates and fewer brain lesions seen versus placebo (JAMA Neurol. 2016;73[9]:1089-98).
The EXPAND study was funded by Novartis. The lead author Dr. Kappos has received research and educational support funding via his institution from Novartis and multiple other pharmaceutical companies. Editorial author Dr. Metz has received grants from Roche and Biogen and personal fees from EMD Serono. The other editorial author, Dr. Liu, reported receiving personal fees from Novartis and personal fees and grants from EMD Serono. Dr. Liu was a back-up treating neurologist in the EXPAND trial.
SOURCE: Kappos L et al. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30475-6, and Metz L and Liu W. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30426-4.
Phase 3 data with siponimod, Novartis’ investigational treatment for multiple sclerosis, show a 21% reduction in the time to disease progression versus placebo in patients with the secondary progressive subtype of the disease.
A significantly lower percentage of patients with secondary progressive multiple sclerosis (SPMS) treated with siponimod met the primary endpoint of confirmed disease progression (CDP) at 3 months, compared with those who received placebo in the EXPAND trial (26% vs. 32% of patients; hazard ratio [HR], 0.79; 95% confidence interval [CI], 0.65–0.95; P = .013).
No significant difference between siponimod and placebo was seen in one of the two main secondary outcomes of the study – the time to 3-month confirmed worsening of the timed 25-foot walk test (T25FW). This result led Luanne Metz, MD, and Wei-Qiao Liu, MD, both of the department of clinical neurosciences and the Hotchkiss Brain Institute at the University of Calgary (Alta.), to take a cautionary view of the findings in an editorial about the trial’s results.
“Although siponimod seems to reduce the time to confirmed disability in SPMS, the treatment effect was small,” Dr. Metz and Dr. Liu argued.
“In our opinion, the reduction in the proportion of participants reaching the primary endpoint of only 6% and the absence of a significant difference for the key secondary clinical outcome [T25FW] are disappointing results and do not suggest that siponimod is an effective treatment for SPMS,” the two wrote.
“Confidence in the treatment benefit of siponimod in progressive MS will, in our opinion, require confirmation in a second trial. Trials of other novel treatments that target noninflammatory mechanisms are still needed,” they said.
EXPAND (Exploring the efficacy and safety of siponimod in patients with secondary progressive multiple sclerosis) was an event- and exposure-driven double-blind trial that recruited patients with SPMS over a 2-year period starting in February 2013. Of 1,651 patients who were recruited, randomized, and actually received treatment, 1,099 were treated with oral siponimod, 2 mg once daily, and 546 were given a matching placebo.
Treatment was for up to 3 years or until 374 CDP events assessed via the Expanded Disability Status Scale (EDSS) had occurred. Patients who had CDP after 6 months in the double-blind trial could be re-consented and continue with double-blind treatment, switch to open-label siponimod, or stop study treatment and either remain on no treatment or receive another disease-modifying treatment.
On average, the patients had been diagnosed with SPMS for a mean of 3.8 years and had been first diagnosed with MS around 17 years prior to this.
The primary endpoint of the trial – CDP at 3 months – was first reported in 2016 at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS). CDP was defined as a 0.5- to 1-point increase in EDSS depending on the baseline score.
A host of additional secondary endpoints were studied, with the risk of 6-month CDP being significantly reduced by siponimod versus placebo (HR, 0.74; 95% CI, 0.60-0.92; P = .0058).
The change from baseline in T2 lesion volume – the second of the two main secondary endpoints studied – showed a potential benefit of siponimod treatment over placebo, with a lower mean-adjusted increase in lesion volume over months 12 and 24 (183.9 mm3 vs. 879.2 mm3; P less than .0001).
More patients receiving siponimod than placebo were free from new or enlarging T2 lesions (57% vs. 37%) or T1 gadolinium-enhancing lesions (89% vs. 67%), and brain volume decreased at a lower rate with siponimod than with placebo.
Adverse events occurred at a higher rate with siponimod than with placebo (89% of patients vs. 82%), of which 18% and 15%, respectively, were defined as serious.
Adverse events seen more commonly in siponimod- than in placebo-treated patients were lymphopenia (1% vs. 0%), abnormal liver-related investigations (12% vs. 4%), hypertension (10% vs. 8%), and bradycardia (4% vs. 3%) and bradyarrhythmia (3% vs. 0.4%) at the start of treatment, which were mitigated by dose titration. Other adverse events that occurred less often but more frequently with siponimod included macular edema (2% vs. less than 1%), reactivation of varicella zoster (2% vs. 1%), and convulsions (2% vs. less than 1%).
“The safety profile of siponimod in EXPAND was generally aligned with that of other drugs in the class,” Dr. Kappos and his colleagues observed.
Siponimod, also known as BAF312, is a selective sphingosine 1-phosphate (S1P) receptor modulator that targets the targets the S1P 1 and 5 receptor subtypes; the other currently approved drug in its class is fingolimod (Gilenya), which is currently indicated for treating the relapsing-remitting form of multiple sclerosis (RRMS).
Phase 2 data have shown that siponimod could also be a promising treatment for RRMS, with reduced relapse rates and fewer brain lesions seen versus placebo (JAMA Neurol. 2016;73[9]:1089-98).
The EXPAND study was funded by Novartis. The lead author Dr. Kappos has received research and educational support funding via his institution from Novartis and multiple other pharmaceutical companies. Editorial author Dr. Metz has received grants from Roche and Biogen and personal fees from EMD Serono. The other editorial author, Dr. Liu, reported receiving personal fees from Novartis and personal fees and grants from EMD Serono. Dr. Liu was a back-up treating neurologist in the EXPAND trial.
SOURCE: Kappos L et al. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30475-6, and Metz L and Liu W. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30426-4.
Phase 3 data with siponimod, Novartis’ investigational treatment for multiple sclerosis, show a 21% reduction in the time to disease progression versus placebo in patients with the secondary progressive subtype of the disease.
A significantly lower percentage of patients with secondary progressive multiple sclerosis (SPMS) treated with siponimod met the primary endpoint of confirmed disease progression (CDP) at 3 months, compared with those who received placebo in the EXPAND trial (26% vs. 32% of patients; hazard ratio [HR], 0.79; 95% confidence interval [CI], 0.65–0.95; P = .013).
No significant difference between siponimod and placebo was seen in one of the two main secondary outcomes of the study – the time to 3-month confirmed worsening of the timed 25-foot walk test (T25FW). This result led Luanne Metz, MD, and Wei-Qiao Liu, MD, both of the department of clinical neurosciences and the Hotchkiss Brain Institute at the University of Calgary (Alta.), to take a cautionary view of the findings in an editorial about the trial’s results.
“Although siponimod seems to reduce the time to confirmed disability in SPMS, the treatment effect was small,” Dr. Metz and Dr. Liu argued.
“In our opinion, the reduction in the proportion of participants reaching the primary endpoint of only 6% and the absence of a significant difference for the key secondary clinical outcome [T25FW] are disappointing results and do not suggest that siponimod is an effective treatment for SPMS,” the two wrote.
“Confidence in the treatment benefit of siponimod in progressive MS will, in our opinion, require confirmation in a second trial. Trials of other novel treatments that target noninflammatory mechanisms are still needed,” they said.
EXPAND (Exploring the efficacy and safety of siponimod in patients with secondary progressive multiple sclerosis) was an event- and exposure-driven double-blind trial that recruited patients with SPMS over a 2-year period starting in February 2013. Of 1,651 patients who were recruited, randomized, and actually received treatment, 1,099 were treated with oral siponimod, 2 mg once daily, and 546 were given a matching placebo.
Treatment was for up to 3 years or until 374 CDP events assessed via the Expanded Disability Status Scale (EDSS) had occurred. Patients who had CDP after 6 months in the double-blind trial could be re-consented and continue with double-blind treatment, switch to open-label siponimod, or stop study treatment and either remain on no treatment or receive another disease-modifying treatment.
On average, the patients had been diagnosed with SPMS for a mean of 3.8 years and had been first diagnosed with MS around 17 years prior to this.
The primary endpoint of the trial – CDP at 3 months – was first reported in 2016 at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS). CDP was defined as a 0.5- to 1-point increase in EDSS depending on the baseline score.
A host of additional secondary endpoints were studied, with the risk of 6-month CDP being significantly reduced by siponimod versus placebo (HR, 0.74; 95% CI, 0.60-0.92; P = .0058).
The change from baseline in T2 lesion volume – the second of the two main secondary endpoints studied – showed a potential benefit of siponimod treatment over placebo, with a lower mean-adjusted increase in lesion volume over months 12 and 24 (183.9 mm3 vs. 879.2 mm3; P less than .0001).
More patients receiving siponimod than placebo were free from new or enlarging T2 lesions (57% vs. 37%) or T1 gadolinium-enhancing lesions (89% vs. 67%), and brain volume decreased at a lower rate with siponimod than with placebo.
Adverse events occurred at a higher rate with siponimod than with placebo (89% of patients vs. 82%), of which 18% and 15%, respectively, were defined as serious.
Adverse events seen more commonly in siponimod- than in placebo-treated patients were lymphopenia (1% vs. 0%), abnormal liver-related investigations (12% vs. 4%), hypertension (10% vs. 8%), and bradycardia (4% vs. 3%) and bradyarrhythmia (3% vs. 0.4%) at the start of treatment, which were mitigated by dose titration. Other adverse events that occurred less often but more frequently with siponimod included macular edema (2% vs. less than 1%), reactivation of varicella zoster (2% vs. 1%), and convulsions (2% vs. less than 1%).
“The safety profile of siponimod in EXPAND was generally aligned with that of other drugs in the class,” Dr. Kappos and his colleagues observed.
Siponimod, also known as BAF312, is a selective sphingosine 1-phosphate (S1P) receptor modulator that targets the targets the S1P 1 and 5 receptor subtypes; the other currently approved drug in its class is fingolimod (Gilenya), which is currently indicated for treating the relapsing-remitting form of multiple sclerosis (RRMS).
Phase 2 data have shown that siponimod could also be a promising treatment for RRMS, with reduced relapse rates and fewer brain lesions seen versus placebo (JAMA Neurol. 2016;73[9]:1089-98).
The EXPAND study was funded by Novartis. The lead author Dr. Kappos has received research and educational support funding via his institution from Novartis and multiple other pharmaceutical companies. Editorial author Dr. Metz has received grants from Roche and Biogen and personal fees from EMD Serono. The other editorial author, Dr. Liu, reported receiving personal fees from Novartis and personal fees and grants from EMD Serono. Dr. Liu was a back-up treating neurologist in the EXPAND trial.
SOURCE: Kappos L et al. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30475-6, and Metz L and Liu W. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30426-4.
FROM THE LANCET
Key clinical point:
Major finding: A significantly lower percentage of patients had confirmed disease progression at 3 months if treated with siponimod (26% vs. 32% with placebo; hazard ratio, 0.79; 95% confidence interval, 0.65–0.95; P = .013).
Study details: A double-blind, randomized, multicenter, placebo-controlled, phase 3 study of siponimod involving 1,651 patients with SPMS.
Disclosures: The EXPAND study was funded by Novartis. The lead author Dr. Kappos has received research and educational support funding via his institution from Novartis and multiple other pharmaceutical companies. Editorial author Dr. Metz has received grants from Roche and Biogen and personal fees from EMD Serono. The other editorial author, Dr. Liu, reported receiving personal fees from Novartis and personal fees and grants from EMD Serono. Dr. Liu was a back-up treating neurologist in the EXPAND trial.
Source: Kappos L et al. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30475-6, and Metz L and Liu W. Lancet. 2018 Mar 22. doi: 10.1016/S0140-6736(18)30426-4.
Adapting consumer technology into GI practice
BOSTON – You can command Alexa to order pizza and spool up your favorite flick, but accessing digital health data remains a struggle. Michael Docktor, MD, wants to change that.
A pediatric gastroenterologist and the clinical director of innovation at Boston Children’s Hospital, Dr. Docktor believes that it’s just a matter of time before consumer-driven digital technology fundamentally changes the way physicians and patients interact.
“In medicine, we are often in the habit of trying to recreate the wheel,” he said during the “Digital Health in GI Disease” session at the 2018 AGA Tech Summit, sponsored by the AGA Center for GI Innovation and Technology. “My hope and belief is that we can borrow from the best of the consumer technology world and apply that to our world in health care and GI specifically.”
Dr. Docktor shared some of the “tools and toys” that have come of his group’s program and also “exposed folks to things that they may not be thinking about traditionally in medicine.”
In particular, one area he focused on was how certain voice technologies are enhancing health care delivery, such as integration of Amazon’s Alexa. Consider Alexa a nurse on call.
he said. “We have placed a fairly large bet on voice in health care and built some skills for Alexa.”
He also highlighted a new virtual reality tool that was recently launched by Boston Children’s Hospital to help gastroenterologists better educate their patients.
HealthVoyager was developed in conjunction with Klick Health. The kid-friendly app lets children take a virtual ride through their GI tract. Clinicians draw in abnormal findings on a simplified template. The app then recreates those findings – lesions, polyps, or inflammatory changes – in the positions they actually occupy in the patient. It generates a QR code that’s given to the patient, allowing the child to access her imaging in a HIPAA-compliant manner.
It’s cool, sure, Dr. Docktor said. But does it bring any value to the physician-patient interaction?
“The challenge of digital health is to prove that there’s actual value, it’s not just a bunch of snazzy tech. Are patients really using it? Sharing it? Are they educating themselves and their family and their community? We want to study this clinically and validate whether or not it results in improved adherence and improved patient satisfaction.”
He covered other technologies, such as Chatbox and blockchain, and the roles they can play in health care.
In the not-too-distant future, Dr. Docktor envisions voice assistants integrated into daily medical practice. Amazon’s Alexa provides an aspirational goal, he said.
“We are seeing the rise of the voice assistant. By 2020, researchers predict that 50% of all Internet searches will happen just by voice. Voice interface, I believe, will be driving health care by interfacing with patients at home. I predict that over the next 5 years, most of us will have a medical encounter on a device like this. Technology is not a limiting factor in this scenario. It’s just red tape on the payer and provider side at this point.”
Dr. Docktor’s colleague, Carla E. Small, senior director of the Innovation & Digital Health Accelerator at Boston Children’s Hospital, provided another real-life example of his digital vision. The Innovation & Digital Health Accelerator is a division within the hospital devoted to identifying, nurturing, and implementing digital health care solutions.
“The world has moved to a technology-enabled health care environment, and we all have to be there along with it,” she said. “That also creates a great opportunity for those who have an interest in innovation. There is a lot of ground for changing the way we do things and really leveraging that creativity and innovation.”
One Accelerator product that’s up and running is Thermia. The online tool guides parents through the anxiety of managing a child’s fever.
Thermia quickly and easily allows concerned parents to interpret a child’s temperature and understand which steps they should consider taking. Parents enter their child’s age, temperature, weight, any associated symptoms like rash, sore throat, or GI upset, as well as comorbid medical conditions. An algorithm issues advice for treatment at home or, if the data suggest a risk or serious problem, suggests a visit to the pediatrician or the emergency room. Thermia also automatically calculates the dosage of over-the-counter antipyretic medications based on age and weight.
The Accelerator is investigating a host of other digital health products in different stages of concept, design, and execution. Health care simply has to embrace the digital trends that are changing the way people interact with their world.
The AGA Center for GI Innovation and Technology wants to hear the unique ways gastroenterologists are leveraging consumer technology in their practices. Send us an email at [email protected].
[email protected]
[email protected]
BOSTON – You can command Alexa to order pizza and spool up your favorite flick, but accessing digital health data remains a struggle. Michael Docktor, MD, wants to change that.
A pediatric gastroenterologist and the clinical director of innovation at Boston Children’s Hospital, Dr. Docktor believes that it’s just a matter of time before consumer-driven digital technology fundamentally changes the way physicians and patients interact.
“In medicine, we are often in the habit of trying to recreate the wheel,” he said during the “Digital Health in GI Disease” session at the 2018 AGA Tech Summit, sponsored by the AGA Center for GI Innovation and Technology. “My hope and belief is that we can borrow from the best of the consumer technology world and apply that to our world in health care and GI specifically.”
Dr. Docktor shared some of the “tools and toys” that have come of his group’s program and also “exposed folks to things that they may not be thinking about traditionally in medicine.”
In particular, one area he focused on was how certain voice technologies are enhancing health care delivery, such as integration of Amazon’s Alexa. Consider Alexa a nurse on call.
he said. “We have placed a fairly large bet on voice in health care and built some skills for Alexa.”
He also highlighted a new virtual reality tool that was recently launched by Boston Children’s Hospital to help gastroenterologists better educate their patients.
HealthVoyager was developed in conjunction with Klick Health. The kid-friendly app lets children take a virtual ride through their GI tract. Clinicians draw in abnormal findings on a simplified template. The app then recreates those findings – lesions, polyps, or inflammatory changes – in the positions they actually occupy in the patient. It generates a QR code that’s given to the patient, allowing the child to access her imaging in a HIPAA-compliant manner.
It’s cool, sure, Dr. Docktor said. But does it bring any value to the physician-patient interaction?
“The challenge of digital health is to prove that there’s actual value, it’s not just a bunch of snazzy tech. Are patients really using it? Sharing it? Are they educating themselves and their family and their community? We want to study this clinically and validate whether or not it results in improved adherence and improved patient satisfaction.”
He covered other technologies, such as Chatbox and blockchain, and the roles they can play in health care.
In the not-too-distant future, Dr. Docktor envisions voice assistants integrated into daily medical practice. Amazon’s Alexa provides an aspirational goal, he said.
“We are seeing the rise of the voice assistant. By 2020, researchers predict that 50% of all Internet searches will happen just by voice. Voice interface, I believe, will be driving health care by interfacing with patients at home. I predict that over the next 5 years, most of us will have a medical encounter on a device like this. Technology is not a limiting factor in this scenario. It’s just red tape on the payer and provider side at this point.”
Dr. Docktor’s colleague, Carla E. Small, senior director of the Innovation & Digital Health Accelerator at Boston Children’s Hospital, provided another real-life example of his digital vision. The Innovation & Digital Health Accelerator is a division within the hospital devoted to identifying, nurturing, and implementing digital health care solutions.
“The world has moved to a technology-enabled health care environment, and we all have to be there along with it,” she said. “That also creates a great opportunity for those who have an interest in innovation. There is a lot of ground for changing the way we do things and really leveraging that creativity and innovation.”
One Accelerator product that’s up and running is Thermia. The online tool guides parents through the anxiety of managing a child’s fever.
Thermia quickly and easily allows concerned parents to interpret a child’s temperature and understand which steps they should consider taking. Parents enter their child’s age, temperature, weight, any associated symptoms like rash, sore throat, or GI upset, as well as comorbid medical conditions. An algorithm issues advice for treatment at home or, if the data suggest a risk or serious problem, suggests a visit to the pediatrician or the emergency room. Thermia also automatically calculates the dosage of over-the-counter antipyretic medications based on age and weight.
The Accelerator is investigating a host of other digital health products in different stages of concept, design, and execution. Health care simply has to embrace the digital trends that are changing the way people interact with their world.
The AGA Center for GI Innovation and Technology wants to hear the unique ways gastroenterologists are leveraging consumer technology in their practices. Send us an email at [email protected].
[email protected]
[email protected]
BOSTON – You can command Alexa to order pizza and spool up your favorite flick, but accessing digital health data remains a struggle. Michael Docktor, MD, wants to change that.
A pediatric gastroenterologist and the clinical director of innovation at Boston Children’s Hospital, Dr. Docktor believes that it’s just a matter of time before consumer-driven digital technology fundamentally changes the way physicians and patients interact.
“In medicine, we are often in the habit of trying to recreate the wheel,” he said during the “Digital Health in GI Disease” session at the 2018 AGA Tech Summit, sponsored by the AGA Center for GI Innovation and Technology. “My hope and belief is that we can borrow from the best of the consumer technology world and apply that to our world in health care and GI specifically.”
Dr. Docktor shared some of the “tools and toys” that have come of his group’s program and also “exposed folks to things that they may not be thinking about traditionally in medicine.”
In particular, one area he focused on was how certain voice technologies are enhancing health care delivery, such as integration of Amazon’s Alexa. Consider Alexa a nurse on call.
he said. “We have placed a fairly large bet on voice in health care and built some skills for Alexa.”
He also highlighted a new virtual reality tool that was recently launched by Boston Children’s Hospital to help gastroenterologists better educate their patients.
HealthVoyager was developed in conjunction with Klick Health. The kid-friendly app lets children take a virtual ride through their GI tract. Clinicians draw in abnormal findings on a simplified template. The app then recreates those findings – lesions, polyps, or inflammatory changes – in the positions they actually occupy in the patient. It generates a QR code that’s given to the patient, allowing the child to access her imaging in a HIPAA-compliant manner.
It’s cool, sure, Dr. Docktor said. But does it bring any value to the physician-patient interaction?
“The challenge of digital health is to prove that there’s actual value, it’s not just a bunch of snazzy tech. Are patients really using it? Sharing it? Are they educating themselves and their family and their community? We want to study this clinically and validate whether or not it results in improved adherence and improved patient satisfaction.”
He covered other technologies, such as Chatbox and blockchain, and the roles they can play in health care.
In the not-too-distant future, Dr. Docktor envisions voice assistants integrated into daily medical practice. Amazon’s Alexa provides an aspirational goal, he said.
“We are seeing the rise of the voice assistant. By 2020, researchers predict that 50% of all Internet searches will happen just by voice. Voice interface, I believe, will be driving health care by interfacing with patients at home. I predict that over the next 5 years, most of us will have a medical encounter on a device like this. Technology is not a limiting factor in this scenario. It’s just red tape on the payer and provider side at this point.”
Dr. Docktor’s colleague, Carla E. Small, senior director of the Innovation & Digital Health Accelerator at Boston Children’s Hospital, provided another real-life example of his digital vision. The Innovation & Digital Health Accelerator is a division within the hospital devoted to identifying, nurturing, and implementing digital health care solutions.
“The world has moved to a technology-enabled health care environment, and we all have to be there along with it,” she said. “That also creates a great opportunity for those who have an interest in innovation. There is a lot of ground for changing the way we do things and really leveraging that creativity and innovation.”
One Accelerator product that’s up and running is Thermia. The online tool guides parents through the anxiety of managing a child’s fever.
Thermia quickly and easily allows concerned parents to interpret a child’s temperature and understand which steps they should consider taking. Parents enter their child’s age, temperature, weight, any associated symptoms like rash, sore throat, or GI upset, as well as comorbid medical conditions. An algorithm issues advice for treatment at home or, if the data suggest a risk or serious problem, suggests a visit to the pediatrician or the emergency room. Thermia also automatically calculates the dosage of over-the-counter antipyretic medications based on age and weight.
The Accelerator is investigating a host of other digital health products in different stages of concept, design, and execution. Health care simply has to embrace the digital trends that are changing the way people interact with their world.
The AGA Center for GI Innovation and Technology wants to hear the unique ways gastroenterologists are leveraging consumer technology in their practices. Send us an email at [email protected].
[email protected]
[email protected]
REPORTING FROM THE 2018 AGA TECH SUMMIT
Cost, coverage concerns cited as barriers to acne medication adherence
Patients with acne who did not follow through with treatment cited high prices and insurance barriers as their main reasons for medication nonadherence, in a study published in JAMA Dermatology.
In the study, more than half of the 26 participants interviewed reported that they intended to fill the acne prescriptions but were not able to do so because of cost- or insurance-related concerns, reported Kira L. Ryskina, MD, of the Leonard Davis Institute of Health Economics at the University of Pennsylvania, Philadelphia, and her coauthors.
Of the initial 385 patients, 26 agreed to participate and met inclusion criteria. Most (58%) were aged 26-40 years, 19% were over aged 40, and 23% were younger than aged 26; 73% were female. Almost 40% had Medicaid coverage, 54% had commercial insurance, and the rest had “other.” Structured interviews were conducted via telephone between November 30, 2016, and January 31, 2017. Based on recorded interviews, five major themes were identified by investigator consensus: medication costs, poor understanding of prior authorization, physician-patient communication about costs, solutions and back-up plans offered by physicians, and reservations about treatment.
Lack of insurance coverage was a concern for 10 patients (38%), and high out-of-pocket costs were a concern for 11 patients (42%), the authors reported. Additionally, 5 participants (19%) said they had received inconsistent information from physicians, physician’s office staff, and pharmacy staff about the prior authorization process.
Participants reported having discussions with providers about treatment side effects and instructions for use – but not about price concerns. In addition, patients “did not expect physicians to know medication cost or insurance coverage,” the authors said. The patients also described various approaches recommended by providers to address problems obtaining medication, including asking patients to call the office back (7%), shopping around for medication (7%), suggesting alternatives to first-line treatment (7%), and offering coupons (4%). Backup plans (offered when the medication was not available) were received positively by 23% of the patients, as was a candid conversation about cost (19%), whereas shopping around and calling the office back were not, the authors said.
Overall, 10 patients (38%) reported reservations about treatment, which included concerns about possible adverse effects (15%), unwillingness to start a “strong” medication (8%), desire to try homeopathic treatment (3%), and belief that their acne was not serious enough to require medication (12%).
The results suggest that “physician-level interventions to improve primary adherence should incorporate discussion of medication costs and provide specific alternative plans in case the patient is unable to fill the prescription, rather than asking patients to call back,” the authors wrote. “Physicians who discuss medication costs and provide a concrete alternative plan may be able to improve primary adherence among their patients,” they concluded.
Limitations of the study include its qualitative nature and its limited generalizability because all participants were part of the same Philadelphia health system.
The study was funded by a Pfizer grant from the American Academy of Dermatology and was cosponsored by the Pennsylvania Academy of Dermatology and Dermatologic Surgery.
SOURCE: Ryskina K et al. JAMA Dermatol. 2018 Feb 28. doi: 10.1001/jamadermatol.2017.6144.
Patients with acne who did not follow through with treatment cited high prices and insurance barriers as their main reasons for medication nonadherence, in a study published in JAMA Dermatology.
In the study, more than half of the 26 participants interviewed reported that they intended to fill the acne prescriptions but were not able to do so because of cost- or insurance-related concerns, reported Kira L. Ryskina, MD, of the Leonard Davis Institute of Health Economics at the University of Pennsylvania, Philadelphia, and her coauthors.
Of the initial 385 patients, 26 agreed to participate and met inclusion criteria. Most (58%) were aged 26-40 years, 19% were over aged 40, and 23% were younger than aged 26; 73% were female. Almost 40% had Medicaid coverage, 54% had commercial insurance, and the rest had “other.” Structured interviews were conducted via telephone between November 30, 2016, and January 31, 2017. Based on recorded interviews, five major themes were identified by investigator consensus: medication costs, poor understanding of prior authorization, physician-patient communication about costs, solutions and back-up plans offered by physicians, and reservations about treatment.
Lack of insurance coverage was a concern for 10 patients (38%), and high out-of-pocket costs were a concern for 11 patients (42%), the authors reported. Additionally, 5 participants (19%) said they had received inconsistent information from physicians, physician’s office staff, and pharmacy staff about the prior authorization process.
Participants reported having discussions with providers about treatment side effects and instructions for use – but not about price concerns. In addition, patients “did not expect physicians to know medication cost or insurance coverage,” the authors said. The patients also described various approaches recommended by providers to address problems obtaining medication, including asking patients to call the office back (7%), shopping around for medication (7%), suggesting alternatives to first-line treatment (7%), and offering coupons (4%). Backup plans (offered when the medication was not available) were received positively by 23% of the patients, as was a candid conversation about cost (19%), whereas shopping around and calling the office back were not, the authors said.
Overall, 10 patients (38%) reported reservations about treatment, which included concerns about possible adverse effects (15%), unwillingness to start a “strong” medication (8%), desire to try homeopathic treatment (3%), and belief that their acne was not serious enough to require medication (12%).
The results suggest that “physician-level interventions to improve primary adherence should incorporate discussion of medication costs and provide specific alternative plans in case the patient is unable to fill the prescription, rather than asking patients to call back,” the authors wrote. “Physicians who discuss medication costs and provide a concrete alternative plan may be able to improve primary adherence among their patients,” they concluded.
Limitations of the study include its qualitative nature and its limited generalizability because all participants were part of the same Philadelphia health system.
The study was funded by a Pfizer grant from the American Academy of Dermatology and was cosponsored by the Pennsylvania Academy of Dermatology and Dermatologic Surgery.
SOURCE: Ryskina K et al. JAMA Dermatol. 2018 Feb 28. doi: 10.1001/jamadermatol.2017.6144.
Patients with acne who did not follow through with treatment cited high prices and insurance barriers as their main reasons for medication nonadherence, in a study published in JAMA Dermatology.
In the study, more than half of the 26 participants interviewed reported that they intended to fill the acne prescriptions but were not able to do so because of cost- or insurance-related concerns, reported Kira L. Ryskina, MD, of the Leonard Davis Institute of Health Economics at the University of Pennsylvania, Philadelphia, and her coauthors.
Of the initial 385 patients, 26 agreed to participate and met inclusion criteria. Most (58%) were aged 26-40 years, 19% were over aged 40, and 23% were younger than aged 26; 73% were female. Almost 40% had Medicaid coverage, 54% had commercial insurance, and the rest had “other.” Structured interviews were conducted via telephone between November 30, 2016, and January 31, 2017. Based on recorded interviews, five major themes were identified by investigator consensus: medication costs, poor understanding of prior authorization, physician-patient communication about costs, solutions and back-up plans offered by physicians, and reservations about treatment.
Lack of insurance coverage was a concern for 10 patients (38%), and high out-of-pocket costs were a concern for 11 patients (42%), the authors reported. Additionally, 5 participants (19%) said they had received inconsistent information from physicians, physician’s office staff, and pharmacy staff about the prior authorization process.
Participants reported having discussions with providers about treatment side effects and instructions for use – but not about price concerns. In addition, patients “did not expect physicians to know medication cost or insurance coverage,” the authors said. The patients also described various approaches recommended by providers to address problems obtaining medication, including asking patients to call the office back (7%), shopping around for medication (7%), suggesting alternatives to first-line treatment (7%), and offering coupons (4%). Backup plans (offered when the medication was not available) were received positively by 23% of the patients, as was a candid conversation about cost (19%), whereas shopping around and calling the office back were not, the authors said.
Overall, 10 patients (38%) reported reservations about treatment, which included concerns about possible adverse effects (15%), unwillingness to start a “strong” medication (8%), desire to try homeopathic treatment (3%), and belief that their acne was not serious enough to require medication (12%).
The results suggest that “physician-level interventions to improve primary adherence should incorporate discussion of medication costs and provide specific alternative plans in case the patient is unable to fill the prescription, rather than asking patients to call back,” the authors wrote. “Physicians who discuss medication costs and provide a concrete alternative plan may be able to improve primary adherence among their patients,” they concluded.
Limitations of the study include its qualitative nature and its limited generalizability because all participants were part of the same Philadelphia health system.
The study was funded by a Pfizer grant from the American Academy of Dermatology and was cosponsored by the Pennsylvania Academy of Dermatology and Dermatologic Surgery.
SOURCE: Ryskina K et al. JAMA Dermatol. 2018 Feb 28. doi: 10.1001/jamadermatol.2017.6144.
FROM JAMA DERMATOLOGY
Key clinical point: Most patients cited high prescription costs and insurance coverage concerns as reasons for medication nonadherence.
Major finding: Of the patients in the study, 65% reported being unable to fill prescriptions because of price or insurance coverage concerns.
Data source: A qualitative analysis of structured interviews with 26 acne patients in Philadelphia.
Disclosures: The study was funded by a Pfizer grant from the American Academy of Dermatology and was cosponsored by the Pennsylvania Academy of Dermatology and Dermatologic Surgery.
Source: Ryskina K et al. JAMA Dermatol. 2018 Feb 28. doi: 10.1001/jamadermatol.2017.6144.
FDA approves certolizumab label update for pregnancy, breastfeeding
The manufacturer of certolizumab pegol, UCB, announced March 22 that the Food and Drug Administration approved a label update to the biologic that includes pharmacokinetic data showing negligible to low transfer of the biologic through the placenta and minimal mother-to-infant transfer from breast milk.
In the CRIB study, certolizumab levels were below the lower limit of quantification (defined as 0.032 mcg/mL) in 13 out of 15 infant blood samples at birth and in all samples at weeks 4 and 8. No anticertolizumab antibodies were detected in mothers, umbilical cords, or infants.
In the CRADLE study, 56% of 137 breast milk samples from 17 mothers had no measurable certolizumab, and the remaining samples showed minimal levels of the biologic. No serious adverse reactions were noted in the 17 infants in the study.
“It is well recognized that women with chronic inflammatory disease face uncertainty during motherhood given the lack of information on treatment during pregnancy and breastfeeding. Many women with chronic inflammatory disease discontinue their biologic treatment during pregnancy, often when they need disease control the most,” said CRADLE lead study author Megan E. B. Clowse, MD, of Duke University, Durham, N.C., in a press release issued by UCB. “These data for Cimzia provide important information to empower women and healthcare providers making decisions about treatment during pregnancy and breastfeeding.”
UCB said that limited data from an ongoing pregnancy registry regarding the use of certolizumab in pregnant women are not sufficient to inform a risk of major birth defects or other adverse pregnancy outcomes.
The manufacturer of certolizumab pegol, UCB, announced March 22 that the Food and Drug Administration approved a label update to the biologic that includes pharmacokinetic data showing negligible to low transfer of the biologic through the placenta and minimal mother-to-infant transfer from breast milk.
In the CRIB study, certolizumab levels were below the lower limit of quantification (defined as 0.032 mcg/mL) in 13 out of 15 infant blood samples at birth and in all samples at weeks 4 and 8. No anticertolizumab antibodies were detected in mothers, umbilical cords, or infants.
In the CRADLE study, 56% of 137 breast milk samples from 17 mothers had no measurable certolizumab, and the remaining samples showed minimal levels of the biologic. No serious adverse reactions were noted in the 17 infants in the study.
“It is well recognized that women with chronic inflammatory disease face uncertainty during motherhood given the lack of information on treatment during pregnancy and breastfeeding. Many women with chronic inflammatory disease discontinue their biologic treatment during pregnancy, often when they need disease control the most,” said CRADLE lead study author Megan E. B. Clowse, MD, of Duke University, Durham, N.C., in a press release issued by UCB. “These data for Cimzia provide important information to empower women and healthcare providers making decisions about treatment during pregnancy and breastfeeding.”
UCB said that limited data from an ongoing pregnancy registry regarding the use of certolizumab in pregnant women are not sufficient to inform a risk of major birth defects or other adverse pregnancy outcomes.
The manufacturer of certolizumab pegol, UCB, announced March 22 that the Food and Drug Administration approved a label update to the biologic that includes pharmacokinetic data showing negligible to low transfer of the biologic through the placenta and minimal mother-to-infant transfer from breast milk.
In the CRIB study, certolizumab levels were below the lower limit of quantification (defined as 0.032 mcg/mL) in 13 out of 15 infant blood samples at birth and in all samples at weeks 4 and 8. No anticertolizumab antibodies were detected in mothers, umbilical cords, or infants.
In the CRADLE study, 56% of 137 breast milk samples from 17 mothers had no measurable certolizumab, and the remaining samples showed minimal levels of the biologic. No serious adverse reactions were noted in the 17 infants in the study.
“It is well recognized that women with chronic inflammatory disease face uncertainty during motherhood given the lack of information on treatment during pregnancy and breastfeeding. Many women with chronic inflammatory disease discontinue their biologic treatment during pregnancy, often when they need disease control the most,” said CRADLE lead study author Megan E. B. Clowse, MD, of Duke University, Durham, N.C., in a press release issued by UCB. “These data for Cimzia provide important information to empower women and healthcare providers making decisions about treatment during pregnancy and breastfeeding.”
UCB said that limited data from an ongoing pregnancy registry regarding the use of certolizumab in pregnant women are not sufficient to inform a risk of major birth defects or other adverse pregnancy outcomes.