User login
VIDEO: When to turn to surgery in postpartum uterine infection
PARK CITY, UTAH – When postpartum infections don’t respond to antibiotics, doctors and surgeons need to move fast; surgery – often hysterectomy – is the only thing that will save the woman’s life.
The problem is that with today’s antibiotics, doctors may have never encountered the situation, and sometimes continue to treat with antibiotics until it’s too late.
In Seattle, physicians turn to David Eschenbach, MD, chair of the department of obstetrics and gynecology at the University of Washington, for advice on when it’s time to give up on antibiotics and go to the OR. It’s a difficult decision, especially when patients are young.
In an interview at the annual scientific meeting of the Infectious Diseases Society for Obstetrics and Gynecology, Dr. Eschenbach shared what he’s learned from decades of experience in dealing with one of the most devastating postpartum complications.
PARK CITY, UTAH – When postpartum infections don’t respond to antibiotics, doctors and surgeons need to move fast; surgery – often hysterectomy – is the only thing that will save the woman’s life.
The problem is that with today’s antibiotics, doctors may have never encountered the situation, and sometimes continue to treat with antibiotics until it’s too late.
In Seattle, physicians turn to David Eschenbach, MD, chair of the department of obstetrics and gynecology at the University of Washington, for advice on when it’s time to give up on antibiotics and go to the OR. It’s a difficult decision, especially when patients are young.
In an interview at the annual scientific meeting of the Infectious Diseases Society for Obstetrics and Gynecology, Dr. Eschenbach shared what he’s learned from decades of experience in dealing with one of the most devastating postpartum complications.
PARK CITY, UTAH – When postpartum infections don’t respond to antibiotics, doctors and surgeons need to move fast; surgery – often hysterectomy – is the only thing that will save the woman’s life.
The problem is that with today’s antibiotics, doctors may have never encountered the situation, and sometimes continue to treat with antibiotics until it’s too late.
In Seattle, physicians turn to David Eschenbach, MD, chair of the department of obstetrics and gynecology at the University of Washington, for advice on when it’s time to give up on antibiotics and go to the OR. It’s a difficult decision, especially when patients are young.
In an interview at the annual scientific meeting of the Infectious Diseases Society for Obstetrics and Gynecology, Dr. Eschenbach shared what he’s learned from decades of experience in dealing with one of the most devastating postpartum complications.
AT IDSOG
Fewer severe hypoglycemia episodes seen over time in patients on tight control
Episodes of severe hypoglycemia became less frequent over a period of 26 years in patients with type 1 diabetes whose glucose was initially intensively managed to a hemoglobin A1c target of 7%, but, conversely, these problems increased in patients who had been managed to a conventional target of 9%, .
At the end of the 20-year-long Epidemiology of Diabetes Interventions and Complications (EDIC) study, which used an 8% HbA1c target for everyone, rates of severe hypoglycemia were 37 cases per 100 patient-years in patients managed intensively in the preceding Diabetes Control and Complications Trial (DCCT) – a significant decrease from the 61 cases per 100 patient-years observed when the DCCT concluded. However, rates of severe hypoglycemia also increased in the conventionally managed group, from 19 to 41 cases per 100 patient-years, according to Rose A. Gubitosi-Klug, MD, PhD, and her coauthors (Diab Care. 2017;40[8]:1010-6).
“The equalization of rates between the two original treatment groups is largely attributable to their similar HbA1c levels during EDIC,” wrote Dr. Gubitosi-Klug, who is division chief of pediatric endocrinology at University Hospital, Cleveland Medical Center, and her coauthors. “[There was] a 13%-15% rise in severe hypoglycemia risk for every 10% decrement in HbA1c.”
The DCCT enrolled 1,441 patients with type 1 diabetes from 1983 to 1989. They were either managed intensively, with a target HbA1c of 7%, or, conventionally, with a 9% target. Specifically, during the DCCT, participants in the intensive group had lower current and mean HbA1c levels (~2% mean difference; P less than .001) as well as higher insulin doses than those in the conventional group (mean difference, 0.04 units/kg per day; P less than .001). During the DCCT, pump use across all quarterly visits averaged 35.7% in the intensive group versus 0.7% in the conventional group and rose to 41% and 1.6%, respectively, by the DCCT closeout (P less than .001).
Almost everyone in the DCCT then enrolled in the EDIC study, which ran from 1995 to 2013. EDIC used an 8% HbA1c target. During EDIC, diabetes management has evolved dramatically, with the introduction of rapid- and long-acting insulins and improved insulin pumps and blood glucose meters. Dr. Gubitosi-Klug and her colleagues examined how rates of severe hypoglycemia have changed with those advances.
During the DCCT, intensively managed patients were three times more likely than those conventionally managed to experience an episode of severe hypoglycemia, including seizure or coma. During EDIC, the frequency of severe hypoglycemia increased in patients who had been conventionally managed but decreased among those who had been intensively managed.
When the DCCT ended with an average 6.5 years follow-up, 65% of the intensive group and 35% of the conventional group had experienced at least one episode of severe hypoglycemia. But when the 20-year EDIC study ended, about half of everyone in the group had experienced at least one episode. Many experienced multiple events. In the DCCT, 54% of the intensive group and 30% of the conventional group had experienced at least four episodes. In EDIC, 37% of the intensive group and 33% of the conventional group had experienced at least four.
But the repeat events seemed to occur in a subset of patients, with 14% in the DCCT experiencing about half of the study’s severe hypoglycemic events, and 7% in EDIC experiencing about a third of them in that study.
The biggest risk factor for severe hypoglycemia was similar for both groups. A first incident doubled the risk for another in the conventional therapy group and tripled it in the intensive therapy group.
“The current data support the clinical perception that a small subset of individuals is more susceptible to severe hypoglycemia,” with 7% of patients with 11 or more episodes during EDIC representing 32% all the events in that study.
These events impart a risk of serious consequences, the authors said. There were 51 major accidents during the 6.5 years of the DCCT and 143 during the 20 years of EDIC, and these were similar between treatment groups. Most of these were motor vehicle accidents, and hypoglycemia was the possible, probable, or principal cause of 18 of the 28 in the DCCT and 23 of the 54 in EDIC.
Nevertheless, the finding that intensively managed patients did better over the years is encouraging, the authors noted. “Advancements in the tools for diabetes management and additional clinical trials have also demonstrated the importance of educational programs to support intensive diabetes therapy. Thus, with increasing years of experience, participants have likely benefitted from tailored educational efforts provided by treating physicians and certified diabetes educators to minimize hypoglycemia.”
None of the study authors reported any financial conflicts.
[email protected]
On Twitter @Alz_gal
Episodes of severe hypoglycemia became less frequent over a period of 26 years in patients with type 1 diabetes whose glucose was initially intensively managed to a hemoglobin A1c target of 7%, but, conversely, these problems increased in patients who had been managed to a conventional target of 9%, .
At the end of the 20-year-long Epidemiology of Diabetes Interventions and Complications (EDIC) study, which used an 8% HbA1c target for everyone, rates of severe hypoglycemia were 37 cases per 100 patient-years in patients managed intensively in the preceding Diabetes Control and Complications Trial (DCCT) – a significant decrease from the 61 cases per 100 patient-years observed when the DCCT concluded. However, rates of severe hypoglycemia also increased in the conventionally managed group, from 19 to 41 cases per 100 patient-years, according to Rose A. Gubitosi-Klug, MD, PhD, and her coauthors (Diab Care. 2017;40[8]:1010-6).
“The equalization of rates between the two original treatment groups is largely attributable to their similar HbA1c levels during EDIC,” wrote Dr. Gubitosi-Klug, who is division chief of pediatric endocrinology at University Hospital, Cleveland Medical Center, and her coauthors. “[There was] a 13%-15% rise in severe hypoglycemia risk for every 10% decrement in HbA1c.”
The DCCT enrolled 1,441 patients with type 1 diabetes from 1983 to 1989. They were either managed intensively, with a target HbA1c of 7%, or, conventionally, with a 9% target. Specifically, during the DCCT, participants in the intensive group had lower current and mean HbA1c levels (~2% mean difference; P less than .001) as well as higher insulin doses than those in the conventional group (mean difference, 0.04 units/kg per day; P less than .001). During the DCCT, pump use across all quarterly visits averaged 35.7% in the intensive group versus 0.7% in the conventional group and rose to 41% and 1.6%, respectively, by the DCCT closeout (P less than .001).
Almost everyone in the DCCT then enrolled in the EDIC study, which ran from 1995 to 2013. EDIC used an 8% HbA1c target. During EDIC, diabetes management has evolved dramatically, with the introduction of rapid- and long-acting insulins and improved insulin pumps and blood glucose meters. Dr. Gubitosi-Klug and her colleagues examined how rates of severe hypoglycemia have changed with those advances.
During the DCCT, intensively managed patients were three times more likely than those conventionally managed to experience an episode of severe hypoglycemia, including seizure or coma. During EDIC, the frequency of severe hypoglycemia increased in patients who had been conventionally managed but decreased among those who had been intensively managed.
When the DCCT ended with an average 6.5 years follow-up, 65% of the intensive group and 35% of the conventional group had experienced at least one episode of severe hypoglycemia. But when the 20-year EDIC study ended, about half of everyone in the group had experienced at least one episode. Many experienced multiple events. In the DCCT, 54% of the intensive group and 30% of the conventional group had experienced at least four episodes. In EDIC, 37% of the intensive group and 33% of the conventional group had experienced at least four.
But the repeat events seemed to occur in a subset of patients, with 14% in the DCCT experiencing about half of the study’s severe hypoglycemic events, and 7% in EDIC experiencing about a third of them in that study.
The biggest risk factor for severe hypoglycemia was similar for both groups. A first incident doubled the risk for another in the conventional therapy group and tripled it in the intensive therapy group.
“The current data support the clinical perception that a small subset of individuals is more susceptible to severe hypoglycemia,” with 7% of patients with 11 or more episodes during EDIC representing 32% all the events in that study.
These events impart a risk of serious consequences, the authors said. There were 51 major accidents during the 6.5 years of the DCCT and 143 during the 20 years of EDIC, and these were similar between treatment groups. Most of these were motor vehicle accidents, and hypoglycemia was the possible, probable, or principal cause of 18 of the 28 in the DCCT and 23 of the 54 in EDIC.
Nevertheless, the finding that intensively managed patients did better over the years is encouraging, the authors noted. “Advancements in the tools for diabetes management and additional clinical trials have also demonstrated the importance of educational programs to support intensive diabetes therapy. Thus, with increasing years of experience, participants have likely benefitted from tailored educational efforts provided by treating physicians and certified diabetes educators to minimize hypoglycemia.”
None of the study authors reported any financial conflicts.
[email protected]
On Twitter @Alz_gal
Episodes of severe hypoglycemia became less frequent over a period of 26 years in patients with type 1 diabetes whose glucose was initially intensively managed to a hemoglobin A1c target of 7%, but, conversely, these problems increased in patients who had been managed to a conventional target of 9%, .
At the end of the 20-year-long Epidemiology of Diabetes Interventions and Complications (EDIC) study, which used an 8% HbA1c target for everyone, rates of severe hypoglycemia were 37 cases per 100 patient-years in patients managed intensively in the preceding Diabetes Control and Complications Trial (DCCT) – a significant decrease from the 61 cases per 100 patient-years observed when the DCCT concluded. However, rates of severe hypoglycemia also increased in the conventionally managed group, from 19 to 41 cases per 100 patient-years, according to Rose A. Gubitosi-Klug, MD, PhD, and her coauthors (Diab Care. 2017;40[8]:1010-6).
“The equalization of rates between the two original treatment groups is largely attributable to their similar HbA1c levels during EDIC,” wrote Dr. Gubitosi-Klug, who is division chief of pediatric endocrinology at University Hospital, Cleveland Medical Center, and her coauthors. “[There was] a 13%-15% rise in severe hypoglycemia risk for every 10% decrement in HbA1c.”
The DCCT enrolled 1,441 patients with type 1 diabetes from 1983 to 1989. They were either managed intensively, with a target HbA1c of 7%, or, conventionally, with a 9% target. Specifically, during the DCCT, participants in the intensive group had lower current and mean HbA1c levels (~2% mean difference; P less than .001) as well as higher insulin doses than those in the conventional group (mean difference, 0.04 units/kg per day; P less than .001). During the DCCT, pump use across all quarterly visits averaged 35.7% in the intensive group versus 0.7% in the conventional group and rose to 41% and 1.6%, respectively, by the DCCT closeout (P less than .001).
Almost everyone in the DCCT then enrolled in the EDIC study, which ran from 1995 to 2013. EDIC used an 8% HbA1c target. During EDIC, diabetes management has evolved dramatically, with the introduction of rapid- and long-acting insulins and improved insulin pumps and blood glucose meters. Dr. Gubitosi-Klug and her colleagues examined how rates of severe hypoglycemia have changed with those advances.
During the DCCT, intensively managed patients were three times more likely than those conventionally managed to experience an episode of severe hypoglycemia, including seizure or coma. During EDIC, the frequency of severe hypoglycemia increased in patients who had been conventionally managed but decreased among those who had been intensively managed.
When the DCCT ended with an average 6.5 years follow-up, 65% of the intensive group and 35% of the conventional group had experienced at least one episode of severe hypoglycemia. But when the 20-year EDIC study ended, about half of everyone in the group had experienced at least one episode. Many experienced multiple events. In the DCCT, 54% of the intensive group and 30% of the conventional group had experienced at least four episodes. In EDIC, 37% of the intensive group and 33% of the conventional group had experienced at least four.
But the repeat events seemed to occur in a subset of patients, with 14% in the DCCT experiencing about half of the study’s severe hypoglycemic events, and 7% in EDIC experiencing about a third of them in that study.
The biggest risk factor for severe hypoglycemia was similar for both groups. A first incident doubled the risk for another in the conventional therapy group and tripled it in the intensive therapy group.
“The current data support the clinical perception that a small subset of individuals is more susceptible to severe hypoglycemia,” with 7% of patients with 11 or more episodes during EDIC representing 32% all the events in that study.
These events impart a risk of serious consequences, the authors said. There were 51 major accidents during the 6.5 years of the DCCT and 143 during the 20 years of EDIC, and these were similar between treatment groups. Most of these were motor vehicle accidents, and hypoglycemia was the possible, probable, or principal cause of 18 of the 28 in the DCCT and 23 of the 54 in EDIC.
Nevertheless, the finding that intensively managed patients did better over the years is encouraging, the authors noted. “Advancements in the tools for diabetes management and additional clinical trials have also demonstrated the importance of educational programs to support intensive diabetes therapy. Thus, with increasing years of experience, participants have likely benefitted from tailored educational efforts provided by treating physicians and certified diabetes educators to minimize hypoglycemia.”
None of the study authors reported any financial conflicts.
[email protected]
On Twitter @Alz_gal
FROM DIABETES CARE
Key clinical point:
Major finding: About half of the patients in the follow-up study, the Epidemiology of Diabetes Interventions and Complications trial, experienced at least one severe hypoglycemia event, regardless of their initial management.
Data source: The Diabetes Control and Complications Trial involving 1,441 patients, 97% of whom enrolled in the Epidemiology of Diabetes Interventions and Complications trial.
Disclosures: The authors had no financial disclosures.
Crizotinib shows responses in pediatric ALCL and IMT
Treatment with the ALK-inhibitor crizotinib produced high response rates in pediatric patients with ALK-positive anaplastic large cell lymphoma (ALCL) and inflammatory myofibroblastic tumors (IMTs), according to phase 2 trial results.
“The robust and sustained clinical responses to crizotinib in patients with relapsed or refractory ALK-driven ALCL and IMT highlight the importance of this oncogene and the sensitivity to ALK inhibition in these diseases,” said Yaël P. Mossé, MD, of Children’s Hospital of Philadelphia, and her associates.
Twenty-six patients with recurrent ALCL and 14 with unresectable IMTs – not older than 22 years – were enrolled. Six of the ALCL patients were treated at 165 mg/m2 (ALCL165) and 20 at 280 mg/m2 (ALCL280), which was found to be the recommended phase 2 dose. Ten of the ALCL280 patients had been treated at an equivalent to this dose in phase 1 and they were included in the phase 2 analysis. Those in the ALCL280 group tended to be older, at a median age of 12.2 years, than the other patients in the study, the investigators reported (J Clin Oncol. 2017 Aug 8 doi: 10.1200/JCO.2017.73.4830).
Eight of the IMT patients were enrolled in a dose-escalation portion of the study, with one receiving a 100 mg/m2 dose, one receiving 165 mg/m2, and the other six receiving 280 mg/m2. The other six were treated at 280 mg/m2. All of the IMT patient results are presented as one pool because those at the lower doses had toxicity and responses similar to those in patients given the higher dose.
Sixteen of 20 patients in the ALCL280 group – 80% – had a complete response, two had a partial response, and two were found to have stable disease. The median duration of treatment in this group was 0.4 years, and the median time to the first partial or complete response was 27 days. In the ALCL165 group, five of six, or 83%, had a complete response, along with one found to have stable disease. This group had a median treatment duration of 2.79 years, and the median time to the first partial or complete response was 26.5 days.
In the IMT group, 5 of 14, or 36%, had a complete response; 7, or 50%, had a partial response, and 2 had stable disease. They received treatment for a median of 1.63 years, and the median time to the first partial or complete response was 28.5 days.
Investigators reported that at least one grade 3 or 4 adverse event occurred in 83% of patients in the ALCL165 group, in all of the patients in the ALCL280 group, and in 71% in the IMT group. Adverse events considered possibly, probably, or definitely related to the study treatment occurred in 33% of the ALCL165 group, in 85% of the ALCL280 group, and in 57% of the IMT group. The most common adverse event was a decreased neutrophil count.
“Notable objective and sustained responses were observed in patients with ALK fusion-positive ALCL and IMT,” the investigators wrote, “establishing a precedent in pediatric oncology for studying the early-phase activity of a targeted agent in a biomarker-selected and histology-independent cohort of patients.
“In the cohort of patients with ALK-positive unresectable IMTs,” they continued, “ALK inhibition was a highly effective therapy and supports consideration of frontline therapy with crizotinib, a strategy that could also be relevant to adults with this rare disease.”
Treatment with the ALK-inhibitor crizotinib produced high response rates in pediatric patients with ALK-positive anaplastic large cell lymphoma (ALCL) and inflammatory myofibroblastic tumors (IMTs), according to phase 2 trial results.
“The robust and sustained clinical responses to crizotinib in patients with relapsed or refractory ALK-driven ALCL and IMT highlight the importance of this oncogene and the sensitivity to ALK inhibition in these diseases,” said Yaël P. Mossé, MD, of Children’s Hospital of Philadelphia, and her associates.
Twenty-six patients with recurrent ALCL and 14 with unresectable IMTs – not older than 22 years – were enrolled. Six of the ALCL patients were treated at 165 mg/m2 (ALCL165) and 20 at 280 mg/m2 (ALCL280), which was found to be the recommended phase 2 dose. Ten of the ALCL280 patients had been treated at an equivalent to this dose in phase 1 and they were included in the phase 2 analysis. Those in the ALCL280 group tended to be older, at a median age of 12.2 years, than the other patients in the study, the investigators reported (J Clin Oncol. 2017 Aug 8 doi: 10.1200/JCO.2017.73.4830).
Eight of the IMT patients were enrolled in a dose-escalation portion of the study, with one receiving a 100 mg/m2 dose, one receiving 165 mg/m2, and the other six receiving 280 mg/m2. The other six were treated at 280 mg/m2. All of the IMT patient results are presented as one pool because those at the lower doses had toxicity and responses similar to those in patients given the higher dose.
Sixteen of 20 patients in the ALCL280 group – 80% – had a complete response, two had a partial response, and two were found to have stable disease. The median duration of treatment in this group was 0.4 years, and the median time to the first partial or complete response was 27 days. In the ALCL165 group, five of six, or 83%, had a complete response, along with one found to have stable disease. This group had a median treatment duration of 2.79 years, and the median time to the first partial or complete response was 26.5 days.
In the IMT group, 5 of 14, or 36%, had a complete response; 7, or 50%, had a partial response, and 2 had stable disease. They received treatment for a median of 1.63 years, and the median time to the first partial or complete response was 28.5 days.
Investigators reported that at least one grade 3 or 4 adverse event occurred in 83% of patients in the ALCL165 group, in all of the patients in the ALCL280 group, and in 71% in the IMT group. Adverse events considered possibly, probably, or definitely related to the study treatment occurred in 33% of the ALCL165 group, in 85% of the ALCL280 group, and in 57% of the IMT group. The most common adverse event was a decreased neutrophil count.
“Notable objective and sustained responses were observed in patients with ALK fusion-positive ALCL and IMT,” the investigators wrote, “establishing a precedent in pediatric oncology for studying the early-phase activity of a targeted agent in a biomarker-selected and histology-independent cohort of patients.
“In the cohort of patients with ALK-positive unresectable IMTs,” they continued, “ALK inhibition was a highly effective therapy and supports consideration of frontline therapy with crizotinib, a strategy that could also be relevant to adults with this rare disease.”
Treatment with the ALK-inhibitor crizotinib produced high response rates in pediatric patients with ALK-positive anaplastic large cell lymphoma (ALCL) and inflammatory myofibroblastic tumors (IMTs), according to phase 2 trial results.
“The robust and sustained clinical responses to crizotinib in patients with relapsed or refractory ALK-driven ALCL and IMT highlight the importance of this oncogene and the sensitivity to ALK inhibition in these diseases,” said Yaël P. Mossé, MD, of Children’s Hospital of Philadelphia, and her associates.
Twenty-six patients with recurrent ALCL and 14 with unresectable IMTs – not older than 22 years – were enrolled. Six of the ALCL patients were treated at 165 mg/m2 (ALCL165) and 20 at 280 mg/m2 (ALCL280), which was found to be the recommended phase 2 dose. Ten of the ALCL280 patients had been treated at an equivalent to this dose in phase 1 and they were included in the phase 2 analysis. Those in the ALCL280 group tended to be older, at a median age of 12.2 years, than the other patients in the study, the investigators reported (J Clin Oncol. 2017 Aug 8 doi: 10.1200/JCO.2017.73.4830).
Eight of the IMT patients were enrolled in a dose-escalation portion of the study, with one receiving a 100 mg/m2 dose, one receiving 165 mg/m2, and the other six receiving 280 mg/m2. The other six were treated at 280 mg/m2. All of the IMT patient results are presented as one pool because those at the lower doses had toxicity and responses similar to those in patients given the higher dose.
Sixteen of 20 patients in the ALCL280 group – 80% – had a complete response, two had a partial response, and two were found to have stable disease. The median duration of treatment in this group was 0.4 years, and the median time to the first partial or complete response was 27 days. In the ALCL165 group, five of six, or 83%, had a complete response, along with one found to have stable disease. This group had a median treatment duration of 2.79 years, and the median time to the first partial or complete response was 26.5 days.
In the IMT group, 5 of 14, or 36%, had a complete response; 7, or 50%, had a partial response, and 2 had stable disease. They received treatment for a median of 1.63 years, and the median time to the first partial or complete response was 28.5 days.
Investigators reported that at least one grade 3 or 4 adverse event occurred in 83% of patients in the ALCL165 group, in all of the patients in the ALCL280 group, and in 71% in the IMT group. Adverse events considered possibly, probably, or definitely related to the study treatment occurred in 33% of the ALCL165 group, in 85% of the ALCL280 group, and in 57% of the IMT group. The most common adverse event was a decreased neutrophil count.
“Notable objective and sustained responses were observed in patients with ALK fusion-positive ALCL and IMT,” the investigators wrote, “establishing a precedent in pediatric oncology for studying the early-phase activity of a targeted agent in a biomarker-selected and histology-independent cohort of patients.
“In the cohort of patients with ALK-positive unresectable IMTs,” they continued, “ALK inhibition was a highly effective therapy and supports consideration of frontline therapy with crizotinib, a strategy that could also be relevant to adults with this rare disease.”
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: The ALK-inhibitor crizotinib produced good responses in pediatric, relapsed/refractory ALK-positive anaplastic large cell lymphoma and unresectable inflammatory myofibroblastic tumors.
Major finding: Eighty percent of ALCL patients in the high-dose group had a complete response, along with 83% given the lower dose. In the IMT group, 36%, had a complete response.
Data source: A 26-patient trial with a two-stage design, including phase 2 results as well as some data from phase 1, conducted across four U.S. centers.
Disclosures: Several study authors reported financial conflicts, including stock or other ownership, speaking fees, or institutional research funding from Pfizer, Novartis, Johnson & Johnson and other companies.
Lenalidomide maintenance boosts survival in de novo myeloma after ASCT
Patients with newly diagnosed multiple myeloma who received lenalidomide as maintenance therapy following an autologous stem cell transplant (ASCT) had significantly better progression-free and overall survival, compared with patients who received placebo or observation after transplant, results of a meta-analysis showed.
Among 1,208 patients in an intention-to-treat analysis, the median progression-free survival (PFS) for patients who received lenalidomide maintenance was nearly double that of patients treated with placebo or observation alone after ASCT, and the median overall survival for patients on maintenance had not been reached after a median follow-up of 79.5 months, reported Phillip J McCarthy, MD, of Roswell Park Cancer Institute in Buffalo, N.Y., and his colleagues.
“This study demonstrates a statistically significant and clinically meaningful improvement in OS with lenalidomide maintenance. With new, highly active, triplet induction regimens enhancing depth and duration of response, as well as ongoing studies evaluating the optimal timing of ASCT, the use of lenalidomide maintenance for transplantation-eligible patients can be considered a standard of care,” they wrote in the Journal of Clinical Oncology.
The authors drew on data from three randomized controlled trials in which patients with newly diagnosed multiple myeloma underwent ASCT followed by lenalidomide maintenance, placebo, or observation. The trials were the Cancer and Leukemia Group B (CALGB) 100104, Gruppo Italiano Malattie Ematologiche dell’Adulto (GIMEMA) RV-MM-PI-209, and Intergroupe Francophone du Myelome (IFM) 2005-02.
Because all three studies had PFS as the primary endpoint and were not powered to detect an overall survival (OS) benefit, the investigators conducted a meta-analysis to get a better sense of the effect of maintenance on both PFS and OS.
The meta-analysis included 605 patients randomized to lenalidomide maintenance and 603 to placebo or observation.
The median PFS was 52.8 months with lenalidomide, vs. 23.5 months for placebo or observation (hazard ratio [HR] 0.48; 95% confidence interval, 0.41-0.55).
After a median follow-up of 79.5 months for all survivors, the median OS for patients on lenalidomide was not reached, compared with 86.0 months for placebo/observation (HR, 0.75, P = .001).
An analysis of safety data from the CALGB and IFM studies (GIMEMA data were not available) showed that second primary malignancies occurring before disease progression were more frequent in the lenalidomide maintenance group, at 5.3%, compared with 0.8%. In contrast, the cumulative incidence rates of progression, death, or myeloma-specific death were all higher with placebo or observation versus lenalidomide maintenance, the investigators found.
Although lenalidomide maintenance adds to the cost of care, the “costs of maintenance therapy should be weighed against the costs of shorter survival, earlier progression, and earlier use of subsequent lines of therapies for patients without maintenance,” the researchers wrote.
The study was supported by Celgene. Dr. McCarthy and multiple coauthors reported consulting/advisory roles, honoraria, travel support, and/or research support from the company.
Patients with newly diagnosed multiple myeloma who received lenalidomide as maintenance therapy following an autologous stem cell transplant (ASCT) had significantly better progression-free and overall survival, compared with patients who received placebo or observation after transplant, results of a meta-analysis showed.
Among 1,208 patients in an intention-to-treat analysis, the median progression-free survival (PFS) for patients who received lenalidomide maintenance was nearly double that of patients treated with placebo or observation alone after ASCT, and the median overall survival for patients on maintenance had not been reached after a median follow-up of 79.5 months, reported Phillip J McCarthy, MD, of Roswell Park Cancer Institute in Buffalo, N.Y., and his colleagues.
“This study demonstrates a statistically significant and clinically meaningful improvement in OS with lenalidomide maintenance. With new, highly active, triplet induction regimens enhancing depth and duration of response, as well as ongoing studies evaluating the optimal timing of ASCT, the use of lenalidomide maintenance for transplantation-eligible patients can be considered a standard of care,” they wrote in the Journal of Clinical Oncology.
The authors drew on data from three randomized controlled trials in which patients with newly diagnosed multiple myeloma underwent ASCT followed by lenalidomide maintenance, placebo, or observation. The trials were the Cancer and Leukemia Group B (CALGB) 100104, Gruppo Italiano Malattie Ematologiche dell’Adulto (GIMEMA) RV-MM-PI-209, and Intergroupe Francophone du Myelome (IFM) 2005-02.
Because all three studies had PFS as the primary endpoint and were not powered to detect an overall survival (OS) benefit, the investigators conducted a meta-analysis to get a better sense of the effect of maintenance on both PFS and OS.
The meta-analysis included 605 patients randomized to lenalidomide maintenance and 603 to placebo or observation.
The median PFS was 52.8 months with lenalidomide, vs. 23.5 months for placebo or observation (hazard ratio [HR] 0.48; 95% confidence interval, 0.41-0.55).
After a median follow-up of 79.5 months for all survivors, the median OS for patients on lenalidomide was not reached, compared with 86.0 months for placebo/observation (HR, 0.75, P = .001).
An analysis of safety data from the CALGB and IFM studies (GIMEMA data were not available) showed that second primary malignancies occurring before disease progression were more frequent in the lenalidomide maintenance group, at 5.3%, compared with 0.8%. In contrast, the cumulative incidence rates of progression, death, or myeloma-specific death were all higher with placebo or observation versus lenalidomide maintenance, the investigators found.
Although lenalidomide maintenance adds to the cost of care, the “costs of maintenance therapy should be weighed against the costs of shorter survival, earlier progression, and earlier use of subsequent lines of therapies for patients without maintenance,” the researchers wrote.
The study was supported by Celgene. Dr. McCarthy and multiple coauthors reported consulting/advisory roles, honoraria, travel support, and/or research support from the company.
Patients with newly diagnosed multiple myeloma who received lenalidomide as maintenance therapy following an autologous stem cell transplant (ASCT) had significantly better progression-free and overall survival, compared with patients who received placebo or observation after transplant, results of a meta-analysis showed.
Among 1,208 patients in an intention-to-treat analysis, the median progression-free survival (PFS) for patients who received lenalidomide maintenance was nearly double that of patients treated with placebo or observation alone after ASCT, and the median overall survival for patients on maintenance had not been reached after a median follow-up of 79.5 months, reported Phillip J McCarthy, MD, of Roswell Park Cancer Institute in Buffalo, N.Y., and his colleagues.
“This study demonstrates a statistically significant and clinically meaningful improvement in OS with lenalidomide maintenance. With new, highly active, triplet induction regimens enhancing depth and duration of response, as well as ongoing studies evaluating the optimal timing of ASCT, the use of lenalidomide maintenance for transplantation-eligible patients can be considered a standard of care,” they wrote in the Journal of Clinical Oncology.
The authors drew on data from three randomized controlled trials in which patients with newly diagnosed multiple myeloma underwent ASCT followed by lenalidomide maintenance, placebo, or observation. The trials were the Cancer and Leukemia Group B (CALGB) 100104, Gruppo Italiano Malattie Ematologiche dell’Adulto (GIMEMA) RV-MM-PI-209, and Intergroupe Francophone du Myelome (IFM) 2005-02.
Because all three studies had PFS as the primary endpoint and were not powered to detect an overall survival (OS) benefit, the investigators conducted a meta-analysis to get a better sense of the effect of maintenance on both PFS and OS.
The meta-analysis included 605 patients randomized to lenalidomide maintenance and 603 to placebo or observation.
The median PFS was 52.8 months with lenalidomide, vs. 23.5 months for placebo or observation (hazard ratio [HR] 0.48; 95% confidence interval, 0.41-0.55).
After a median follow-up of 79.5 months for all survivors, the median OS for patients on lenalidomide was not reached, compared with 86.0 months for placebo/observation (HR, 0.75, P = .001).
An analysis of safety data from the CALGB and IFM studies (GIMEMA data were not available) showed that second primary malignancies occurring before disease progression were more frequent in the lenalidomide maintenance group, at 5.3%, compared with 0.8%. In contrast, the cumulative incidence rates of progression, death, or myeloma-specific death were all higher with placebo or observation versus lenalidomide maintenance, the investigators found.
Although lenalidomide maintenance adds to the cost of care, the “costs of maintenance therapy should be weighed against the costs of shorter survival, earlier progression, and earlier use of subsequent lines of therapies for patients without maintenance,” the researchers wrote.
The study was supported by Celgene. Dr. McCarthy and multiple coauthors reported consulting/advisory roles, honoraria, travel support, and/or research support from the company.
FROM JCO
Key clinical point: Lenalidomide maintenance after stem cell transplant in patients with newly diagnosed multiple myeloma is associated with better progression-free and overall survival.
Major finding: Median overall survival was not reached with lenalidomide after a median 79.5 months’ follow-up, vs. 86 months for placebo/observation.
Data source: A meta-analysis of data from three randomized controlled trials, with a total of 1,208 patients with newly diagnosed multiple myeloma.
Disclosures: The study was supported by Celgene. Dr. McCarthy and multiple coauthors reported consulting/advisory roles, honoraria, travel support, and/or research support from the company.
Pertussis resurgence is real, but possible solutions exist
MADRID – The explanation for the ongoing resurgence in pertussis in adolescents and adults in the United States and other developed countries lies largely in the waning effectiveness of current acellular pertussis vaccines as early as 2-3 years post boosters, according to Stanley A. Plotkin, MD, chair of the steering committee for the Global Pertussis Initiative.
“The problem seems to lie in the lack of persistence of immunity after vaccination using the acellular pertussis vaccines. To say that this is not controversial would clearly be wrong, but that is my view,” he declared at the annual meeting of the European Society for Paediatric Infectious Diseases.
It’s a view supported by persuasive evidence, added Dr. Plotkin, emeritus professor of pediatrics at the University of Pennsylvania, Philadelphia.
In the United States, investigators at Northern California Kaiser Permanente have shown that the effectiveness of acellular pertussis in the Tdap vaccine wanes rapidly in adolescents. Indeed, it plunged from 69% effectiveness in the first year after vaccination to less than 9% by year 4 (Pediatrics. 2016 Mar;137[3]:e20153326).
In contrast, whole-cell pertussis vaccines provide roughly 6-10 years of protection against infection, and native infection provides persistent protection against reinfection for 7-20 years, Dr. Plotkin noted.
He was senior coauthor of a recent study that addresses why acellular pertussis vaccine immunity wanes so quickly. He and his coinvestigators demonstrated that while whole-cell pertussis vaccines promote vigorous Th1 and Th17 responses, which discourage pharyngeal colonization, acellular pertussis vaccines orient the immune system toward a less salutary Th1/Th2 response (Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029454).
In addition, other investigators have shown that repeated booster doses of acellular pertussis vaccine generate higher levels of antigen-specific IgG4, which doesn’t bind complement and results in impaired phagocytosis and a suboptimal inflammatory response. In contrast, priming of the immune system via administration of a whole-cell pertussis vaccine at birth followed by acellular pertussis boosters results in improved phagocytosis and complement-mediated microbial killing via preferential induction of IgG1(Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029553).
Possible solutions to the pertussis problem
Infants don’t need a new vaccine; that’s not where the vaccine failures are occurring. “Again, I stress that the problem so far has not been in infants, it has been in adolescents and adults,” he said.
A new vaccine is a daunting prospect. Given the huge investment vaccine manufacturers made in the 1990s to bring the current acellular vaccines to the market, they are hardly eager to launch development programs for new pertussis vaccines. They have other vaccine development priorities.
Moreover, the regulatory challenges are huge unless the Food and Drug Administration and other licensing authorities are willing to forgo the large, long, and expensive clinical trials that have traditionally been required. In lieu of such efficacy studies, they would need to consider studies demonstrating better immunogenicity based upon antibody titers, or animal studies.
“The possibility of a human challenge study in adults is an idea I like; I’m not sure about the FDA,” the pediatrician said.
Until a new or improved vaccine becomes available, the most important strategy to control the resurgence of pertussis is acellular vaccination of pregnant women in their third trimester to provide passive protection to the newborn via transplacental antibody. That practice is already recommended in the United States and many other countries. And while it reduces the risk of pertussis in early infancy – the most serious form of the disease – that strategy won’t have any real impact on the adult burden of disease, which Dr. Plotkin estimated at more than 600,000 cases annually.
Cocooning – a strategy of vaccinating all of a newborn’s family contacts – has been promoted in guidelines but has proved difficult to implement. “I think cocooning strategies by and large have been a failure,” he declared.
More frequent boosters of current acellular pertussis vaccines would presumably increase effectiveness, but that would be costly and tough to put in place on a public health scale.
A return to using conventional whole-cell pertussis vaccines would be a tough sell to the public and is probably flat out unacceptable. Developing a less reactogenic whole-cell vaccine might be a work-around, but it hasn’t been done yet.
The easiest way to improve acellular pertussis vaccine for adolescents and adults is to improve the pertussis toxin antigen component. Increasing the dose of pertussis toxin could generate more and longer-lasting antibodies to it. An even more exciting possibility is based upon evidence more than a decade old that genetic inactivation of pertussis toxin results in antibody levels far higher and presumably more bactericidal than the formalin-inactivated pertussis toxin included in current vaccines, according to Dr. Plotkin.
Adding stronger adjuvants to a Tdap vaccine for adolescents is another appealing strategy. There are plenty to choose from, including some that would presumably have an easier pathway to regulatory approval because they are already contained in licensed vaccines. This beefed-up adjuvant strategy, like the notion of changing the antigens in acellular pertussis vaccines to those from currently circulating strains, is feasible albeit more difficult than simply improving the pertussis toxin component of existing vaccines, he said.
The Global Pertussis Initiative is sponsored by Sanofi Pasteur. Dr. Plotkin reported serving as a consultant to that vaccine manufacturer and numerous others but declared he had no financial conflicts regarding his presentation.
MADRID – The explanation for the ongoing resurgence in pertussis in adolescents and adults in the United States and other developed countries lies largely in the waning effectiveness of current acellular pertussis vaccines as early as 2-3 years post boosters, according to Stanley A. Plotkin, MD, chair of the steering committee for the Global Pertussis Initiative.
“The problem seems to lie in the lack of persistence of immunity after vaccination using the acellular pertussis vaccines. To say that this is not controversial would clearly be wrong, but that is my view,” he declared at the annual meeting of the European Society for Paediatric Infectious Diseases.
It’s a view supported by persuasive evidence, added Dr. Plotkin, emeritus professor of pediatrics at the University of Pennsylvania, Philadelphia.
In the United States, investigators at Northern California Kaiser Permanente have shown that the effectiveness of acellular pertussis in the Tdap vaccine wanes rapidly in adolescents. Indeed, it plunged from 69% effectiveness in the first year after vaccination to less than 9% by year 4 (Pediatrics. 2016 Mar;137[3]:e20153326).
In contrast, whole-cell pertussis vaccines provide roughly 6-10 years of protection against infection, and native infection provides persistent protection against reinfection for 7-20 years, Dr. Plotkin noted.
He was senior coauthor of a recent study that addresses why acellular pertussis vaccine immunity wanes so quickly. He and his coinvestigators demonstrated that while whole-cell pertussis vaccines promote vigorous Th1 and Th17 responses, which discourage pharyngeal colonization, acellular pertussis vaccines orient the immune system toward a less salutary Th1/Th2 response (Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029454).
In addition, other investigators have shown that repeated booster doses of acellular pertussis vaccine generate higher levels of antigen-specific IgG4, which doesn’t bind complement and results in impaired phagocytosis and a suboptimal inflammatory response. In contrast, priming of the immune system via administration of a whole-cell pertussis vaccine at birth followed by acellular pertussis boosters results in improved phagocytosis and complement-mediated microbial killing via preferential induction of IgG1(Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029553).
Possible solutions to the pertussis problem
Infants don’t need a new vaccine; that’s not where the vaccine failures are occurring. “Again, I stress that the problem so far has not been in infants, it has been in adolescents and adults,” he said.
A new vaccine is a daunting prospect. Given the huge investment vaccine manufacturers made in the 1990s to bring the current acellular vaccines to the market, they are hardly eager to launch development programs for new pertussis vaccines. They have other vaccine development priorities.
Moreover, the regulatory challenges are huge unless the Food and Drug Administration and other licensing authorities are willing to forgo the large, long, and expensive clinical trials that have traditionally been required. In lieu of such efficacy studies, they would need to consider studies demonstrating better immunogenicity based upon antibody titers, or animal studies.
“The possibility of a human challenge study in adults is an idea I like; I’m not sure about the FDA,” the pediatrician said.
Until a new or improved vaccine becomes available, the most important strategy to control the resurgence of pertussis is acellular vaccination of pregnant women in their third trimester to provide passive protection to the newborn via transplacental antibody. That practice is already recommended in the United States and many other countries. And while it reduces the risk of pertussis in early infancy – the most serious form of the disease – that strategy won’t have any real impact on the adult burden of disease, which Dr. Plotkin estimated at more than 600,000 cases annually.
Cocooning – a strategy of vaccinating all of a newborn’s family contacts – has been promoted in guidelines but has proved difficult to implement. “I think cocooning strategies by and large have been a failure,” he declared.
More frequent boosters of current acellular pertussis vaccines would presumably increase effectiveness, but that would be costly and tough to put in place on a public health scale.
A return to using conventional whole-cell pertussis vaccines would be a tough sell to the public and is probably flat out unacceptable. Developing a less reactogenic whole-cell vaccine might be a work-around, but it hasn’t been done yet.
The easiest way to improve acellular pertussis vaccine for adolescents and adults is to improve the pertussis toxin antigen component. Increasing the dose of pertussis toxin could generate more and longer-lasting antibodies to it. An even more exciting possibility is based upon evidence more than a decade old that genetic inactivation of pertussis toxin results in antibody levels far higher and presumably more bactericidal than the formalin-inactivated pertussis toxin included in current vaccines, according to Dr. Plotkin.
Adding stronger adjuvants to a Tdap vaccine for adolescents is another appealing strategy. There are plenty to choose from, including some that would presumably have an easier pathway to regulatory approval because they are already contained in licensed vaccines. This beefed-up adjuvant strategy, like the notion of changing the antigens in acellular pertussis vaccines to those from currently circulating strains, is feasible albeit more difficult than simply improving the pertussis toxin component of existing vaccines, he said.
The Global Pertussis Initiative is sponsored by Sanofi Pasteur. Dr. Plotkin reported serving as a consultant to that vaccine manufacturer and numerous others but declared he had no financial conflicts regarding his presentation.
MADRID – The explanation for the ongoing resurgence in pertussis in adolescents and adults in the United States and other developed countries lies largely in the waning effectiveness of current acellular pertussis vaccines as early as 2-3 years post boosters, according to Stanley A. Plotkin, MD, chair of the steering committee for the Global Pertussis Initiative.
“The problem seems to lie in the lack of persistence of immunity after vaccination using the acellular pertussis vaccines. To say that this is not controversial would clearly be wrong, but that is my view,” he declared at the annual meeting of the European Society for Paediatric Infectious Diseases.
It’s a view supported by persuasive evidence, added Dr. Plotkin, emeritus professor of pediatrics at the University of Pennsylvania, Philadelphia.
In the United States, investigators at Northern California Kaiser Permanente have shown that the effectiveness of acellular pertussis in the Tdap vaccine wanes rapidly in adolescents. Indeed, it plunged from 69% effectiveness in the first year after vaccination to less than 9% by year 4 (Pediatrics. 2016 Mar;137[3]:e20153326).
In contrast, whole-cell pertussis vaccines provide roughly 6-10 years of protection against infection, and native infection provides persistent protection against reinfection for 7-20 years, Dr. Plotkin noted.
He was senior coauthor of a recent study that addresses why acellular pertussis vaccine immunity wanes so quickly. He and his coinvestigators demonstrated that while whole-cell pertussis vaccines promote vigorous Th1 and Th17 responses, which discourage pharyngeal colonization, acellular pertussis vaccines orient the immune system toward a less salutary Th1/Th2 response (Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029454).
In addition, other investigators have shown that repeated booster doses of acellular pertussis vaccine generate higher levels of antigen-specific IgG4, which doesn’t bind complement and results in impaired phagocytosis and a suboptimal inflammatory response. In contrast, priming of the immune system via administration of a whole-cell pertussis vaccine at birth followed by acellular pertussis boosters results in improved phagocytosis and complement-mediated microbial killing via preferential induction of IgG1(Cold Spring Harb Perspect Biol. 2017 Mar 13. doi: 10.1101/cshperspect.a029553).
Possible solutions to the pertussis problem
Infants don’t need a new vaccine; that’s not where the vaccine failures are occurring. “Again, I stress that the problem so far has not been in infants, it has been in adolescents and adults,” he said.
A new vaccine is a daunting prospect. Given the huge investment vaccine manufacturers made in the 1990s to bring the current acellular vaccines to the market, they are hardly eager to launch development programs for new pertussis vaccines. They have other vaccine development priorities.
Moreover, the regulatory challenges are huge unless the Food and Drug Administration and other licensing authorities are willing to forgo the large, long, and expensive clinical trials that have traditionally been required. In lieu of such efficacy studies, they would need to consider studies demonstrating better immunogenicity based upon antibody titers, or animal studies.
“The possibility of a human challenge study in adults is an idea I like; I’m not sure about the FDA,” the pediatrician said.
Until a new or improved vaccine becomes available, the most important strategy to control the resurgence of pertussis is acellular vaccination of pregnant women in their third trimester to provide passive protection to the newborn via transplacental antibody. That practice is already recommended in the United States and many other countries. And while it reduces the risk of pertussis in early infancy – the most serious form of the disease – that strategy won’t have any real impact on the adult burden of disease, which Dr. Plotkin estimated at more than 600,000 cases annually.
Cocooning – a strategy of vaccinating all of a newborn’s family contacts – has been promoted in guidelines but has proved difficult to implement. “I think cocooning strategies by and large have been a failure,” he declared.
More frequent boosters of current acellular pertussis vaccines would presumably increase effectiveness, but that would be costly and tough to put in place on a public health scale.
A return to using conventional whole-cell pertussis vaccines would be a tough sell to the public and is probably flat out unacceptable. Developing a less reactogenic whole-cell vaccine might be a work-around, but it hasn’t been done yet.
The easiest way to improve acellular pertussis vaccine for adolescents and adults is to improve the pertussis toxin antigen component. Increasing the dose of pertussis toxin could generate more and longer-lasting antibodies to it. An even more exciting possibility is based upon evidence more than a decade old that genetic inactivation of pertussis toxin results in antibody levels far higher and presumably more bactericidal than the formalin-inactivated pertussis toxin included in current vaccines, according to Dr. Plotkin.
Adding stronger adjuvants to a Tdap vaccine for adolescents is another appealing strategy. There are plenty to choose from, including some that would presumably have an easier pathway to regulatory approval because they are already contained in licensed vaccines. This beefed-up adjuvant strategy, like the notion of changing the antigens in acellular pertussis vaccines to those from currently circulating strains, is feasible albeit more difficult than simply improving the pertussis toxin component of existing vaccines, he said.
The Global Pertussis Initiative is sponsored by Sanofi Pasteur. Dr. Plotkin reported serving as a consultant to that vaccine manufacturer and numerous others but declared he had no financial conflicts regarding his presentation.
EXPERT ANALYSIS FROM ESPID 2017
Referral Patterns for Chronic Groin Pain and Athletic Pubalgia/Sports Hernia: Magnetic Resonance Imaging Findings, Treatment, and Outcomes
The past 3 decades have seen an evolution in the understanding, diagnosis, and treatment of groin pain, both chronic and acute, in athletes and non-athletes alike. Groin pain and groin injury are common. Most cases are transient, with patients returning to their activities within weeks or months. There has also been increasing awareness of a definitive population of patients who do not get better, or who improve and plateau before reaching preinjury level of performance.1-3 Several authors have brought more attention to the injury, introducing vocabulary, theories, diagnostic testing, and diagnoses, which now constitute a knowledge base.1,3-5
As stated in almost every article on groin pain and diagnosis, lack of cohesive agreement and vocabulary, and consistent protocols and procedures, has abounded, making general understanding and agreement in this area inconsistent.1,6-8In this article, members of a tertiary-care group specializing in chronic groin pain, athletic pubalgia (sports hernia), and inguinal herniorrhaphy outline their clinical examination, diagnostic algorithm, imaging protocol, treatment strategy, and outcomes for a population of patients referred by physicians and allied health professionals for a suspected diagnosis of athletic pubalgia.
Background
The pubic symphysis acts as a stabilizing central anchor with elaborate involvement of the anterior structures, including the rectus abdominis, adductor longus, and inguinal ligaments.3,7,9 Literature from Europe, Australia, and the United States has described groin pain, mostly in professional athletes, involving these pubic structures and attachments. Several publications have been addressing chronic groin pain, and each has its own diagnostic algorithm, imaging protocol, and treatment strategy.3,6,9-18
Terminology specific to groin pain in athletes is not new, and has a varied history dating to the early 20th century. Terms such as sportsman hernia19 and subsequently sports hernia20, have recently been embraced by the lay population. In 1999, Gibbon21 described shearing of the common adductor–rectus abdominis anatomical and functional unit and referenced a 1902 anatomical text that describes vertical ligamentous fibers contiguous with rectus sheath and adductor muscles, both attaching to the pubis. Injury to this region is the basis of pubalgia, a term originally used in 1984 by Brunet to describe a pain syndrome at the pubis.22
Many authors have proposed replacing sports hernia with athletic pubalgia.1,3,6,7,10,14,18,23 These terms refer to a group of musculoskeletal processes that occur in and around the pubic symphysis and that share similar mechanisms of injury and common clinical manifestations. The condition was originally described in high-performance athletes, and at one point the term sports hernia was reserved for this patient population.5 According to many authors, presence of an inguinal hernia excludes the diagnosis.1,2,5Magnetic resonance imaging (MRI) has helped to advance and define our understanding of the injury.10 As the history of the literature suggests, earlier concepts of chronic pain focused either on the medial aspect of the inguinal canal and its structures or on the pubic attachments. Many specialists in the area have concluded that the chronic groin pain injury can and often does embody both elements.3,9 Correlation with MRI findings, injury seen during surgical procedures, and cadaveric studies have directed our understanding to a structure, the pre-pubic aponeurotic complex (P-PAC), or rectus aponeurotic plate.12,24,25 Anatomically, the P-PAC, which has several fascial components, attaches posteriorly to the pubic bone and, to a degree, the pubic symphyseal cartilaginous disc. Major contributions to the P-PAC are fibers from the rectus abdominis tendon, the medial aspect of the transversalis and internal oblique muscles (the conjoint tendon, according to some), the inguinal ligament, and the adductor longus tendon.26When communicating with referring physicians, we use the term athletic pubalgia to indicate a specific injury. The athletic pubalgia injury can be defined as serial microtearing,1 or complete tearing, of the posterior attachment of the P-PAC off the anterior pubis.3,10 Complete tearing or displacement can occur unilaterally or across the midline to the other side. As athletic pubalgia is a specific anatomical injury rather than a broad category of findings, an additional pathologic diagnosis, such as inguinal hernia, does not exclude the diagnosis of athletic pubalgia. Unfortunately, the terms sports hernia and sportsman hernia, commonly used in the media and in professional communities, have largely confused the broader understanding of nuances and of the differences between the specific injuries and MRI findings.18
Our Experience
In our practice, we see groin pain patients referred by internists, physiatrists, physical therapists, trainers, general surgeons, urologists, gynecologists, and orthopedic surgeons. In many cases, patients have been through several consultations and work-ups, as their pain syndrome does not fall under a specific category. Patients without inguinal hernia, hip injury, urologic, or gynecologic issues typically are referred to a physiatrist or a physical therapist. Often, there are marginal improvements with physical therapy, but in some cases the injury never completely resolves, and the patient continues to have pain with activity or return to sports.
Most of our patients are nonprofessional athletes, men and women who range widely in age and participate casually or regularly in sporting events. Most lack the rigorous training, conditioning, and close supervision that professional athletes receive. Many other patients are nonprofessional but elite athletes who train 7 days a week for marathons, ultramarathons, triathlons, obstacle course races (“mudders”), and similar events.
Work-Up
A single algorithm is used for all patients initially referred to the surgeon’s office for pelvic or groin pain. The initial interview directs attention to injury onset and mechanism, duration of rest or physical therapy after surgery, pain quality and pain levels, and antagonistic movements and positions. Examination starts with assessment for inguinal, femoral, and umbilical hernias. Resisted sit-up, leg-raise, adduction, and hip assessment tests are performed. The P-PAC is examined with a maneuver similar to the one used for inguinal hernia, as it allows for better assessment of the transversalis fascia (over the direct space) to determine if the inguinal canal floor is attenuated and bulges forward with the Valsalva maneuver. Then, the lateral aspect of the rectus muscle is assessed for pain, usually with the head raised to contract the muscle, to determine tenderness along the lateral border. The rectus edge is traced down to the pubis at its attachment, the superolateral border of the P-PAC. Examination proceeds medially, over the rectus attachment, toward the pubic symphysis, continuing the assessment for tenderness. Laterally, the conjoint tendon and inguinal ligament medial attachments are assessed at the level of the pubic tubercle, which represents the lateral border of the P-PAC. Finally, the examination continues to the inferior border with assessment of the adductor longus attachment, which is best performed with the leg in an adducted position. In the acute or semiacute setting (pain within 1 year of injury onset), tenderness is often elicited. With long-standing injuries, pain is often not elicited, but the patient experiences pain along this axis during activity or afterward.
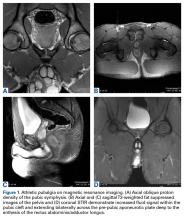
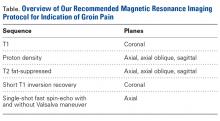
Patients with positive history and physical examination findings proceed through an MRI protocol designed to detect pathology of the pubic symphysis, hips, and inguinal canals (Figures 1A-1D).
Treatment
Patients who report sustaining an acute groin injury within the previous 6 months are treated nonoperatively. A combination of rest, nonsteroidal anti-inflammatory drugs, and physical therapy is generally recommended.2,10 In cases of failed nonoperative management, patients are evaluated for surgery. No single operation is recommended for all patients.1,6,14,27,28 (Larson26 recently reviewed results from several trials involving a variety of surgical repairs and found return-to-sports rates ranging from 80% to 100%.) Findings from the physical examination and from the properly protocolled MRI examination are used in planning surgery to correct any pathology that could be contributing to symptoms or destabilization of the structures attaching to the pubis. Disruption of the P-PAC from the pubis would be repaired, for example. Additional injuries, such as partial or complete detachment of the conjoint tendon or inguinal ligament, may be repaired as well. If the transversalis fascia is attenuated and bulging forward, the inguinal floor is closed. Adductor longus tendon pathology is addressed, most commonly with partial tendinolysis. Often, concomitant inguinal hernias are found, and these may be repaired in open fashion while other maneuvers are being performed, or laparoscopically.
Materials and Methods
After receiving study approval from our Institutional Review Board, we retrospectively searched for all MRIs performed by our radiology department between March 1, 2011 and March 31, 2013 on patients referred for an indication of groin pain, sports hernia, or athletic pubalgia. Patients were excluded if they were younger than 18 years any time during their care. Some patients previously or subsequently underwent computed tomography or ultrasonography. MRIs were reviewed and positive findings were compiled in a database. Charts were reviewed to identify which patients in the dataset underwent surgery, after MRI, to address their presenting chief complaint. Surgery date and procedure(s) performed were recorded. Patients were interviewed by telephone as part of the in-office postoperative follow-up.
Results
One hundred nineteen MRIs were performed on 117 patients (97 men, 83%). Mean age was 39.8 years. Seventy-nine patients (68%) had an MRI finding of athletic pubalgia, 67 (57%) had an acetabular labral tear in one or both hip joints, and 41 (35%) had a true inguinal hernia. Concomitant findings were common: 47 cases of athletic pubalgia and labral tear(s), 28 cases of athletic pubalgia and inguinal hernia, and 15 cases of all 3 (athletic pubalgia, labral tear, inguinal hernia).
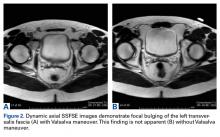
Use of breath-hold axial single-shot fast spin-echo sequences with and without the Valsalva maneuver increased sensitivity in detecting pathologies—inguinal hernia and Gilmore groin in particular. On 24 of the 119 MRIs, the Valsalva maneuver either revealed the finding or made it significantly more apparent.
Of all patients referred for MRI for chronic groin pain, 48 (41%) subsequently underwent surgery. In 29 surgeries, the rectus abdominis, adductor longus, and/or pre-pubic aponeurotic plate were repaired; in 13 cases, herniorrhaphy was performed as well; in 2 cases, masses involving the spermatic cord were removed.
The most common surgery (30 cases) was herniorrhaphy, which was performed as a single procedure, multiple procedures, or in combination with procedures not related to a true hernia. Eighteen patients underwent surgery only for hernia repair.
Of the 79 patients with MRI-positive athletic pubalgia, 39 subsequently underwent surgery, and 31 (79%) of these were followed up by telephone. Mean duration of rest after surgery was 6.2 weeks. Twelve patients (39%) had physical therapy after surgery, some as early as 4 weeks, and some have continued their therapy since surgery. Of the 31 patients who were followed up after surgery, 23 (74%) resumed previous activity levels. Return to previous activity level took these patients a mean of 17.9 weeks. When asked if outcomes satisfied their expectations, 28 patients (90%) said yes, and 3 said no.
Forty patients with MRI-positive athletic pubalgia were nonoperatively treated, and 28 (70%) of these patients were followed up. In this group, mean duration of rest after surgery was 6.9 weeks. Thirteen patients (46%) participated in physical therapy, for a mean duration of 10.8 weeks. Of the patients followed up, 19 (68%) returned to previous activity level. Twenty-one patients (75%) were satisfied with their outcome.
Discussion
Diagnosis and treatment of chronic groin pain have had a long, confusing, and frustrating history for both patients and the medical professionals who provide them with care.3,6,7,10 Historically, the problem has been, in part, the lack of diagnostic capabilities. Currently, however, pubalgia MRI protocol allows the exact pathology to be demonstrated.3 As already noted, concomitant hip pathology or inguinal hernia is not unusual8; any structural abnormality in the area is a potential destabilizer of the structures attached to the pubis.18 Solving only one of these issues may offer only partial resolution of symptoms and thereby reduce the rate of successful treatment of groin pain.
Diagnostic algorithms are being developed. In addition, nonoperative treatments are being tried for some of the issues. Physicians are giving diagnostic and therapeutic steroid injections in the pubic cleft, along the rectus abdominis/adductor longus complex, or posterior to the P-PAC. Platelet-rich plasma injection therapy has had limited success.29This article provides a snapshot of what a tertiary-care group of physicians specializing in chronic groin pain sees in an unfiltered setting. We think this is instructive for several reasons.
First, many patients in our population have visited a multitude of specialists without receiving a diagnosis or being referred appropriately. Simply, many specialists do not know the next step in treating groin pain and thus do not make the appropriate referral. Until recently, the literature has not been helpful. It has poorly described the constellation of injuries comprising chronic groin pain. More significantly, groin injuries have been presented as ambiguous injuries lacking effective treatment. Over the past decade, however, abundant literature on the correlation of these injuries with specific MRI findings has made the case otherwise.
Second, a specific MRI pubalgia protocol is needed. Inability to make a correct diagnosis, because of improper MRI, continues to add to the confusion surrounding the injury and undoubtedly prolongs the general medical community’s thinking that diagnosis and treatment of chronic groin pain are elusive. Our data support this point in many ways. Although all patients in this study were seen by a medical professional before coming to our office, none had received a diagnosis of occult hernia or attenuated transversalis fascia; nevertheless, we identified inguinal hernia, Gilmore groin, or both in 44% of these patients. These findings are not surprising, as MRI was the crucial link in diagnosis. In addition, the point made by other groin pain specialists—that a hernia precludes a pubalgia diagnosis1,2,5—is not supported by our data. Inguinal hernia can and does exist in conjunction with pubalgia. More than half the patients in our study had a combined diagnosis. We contend that, much as hip labral pathology occurs concomitantly with pubalgia,23 inguinal hernia may be a predisposing factor as well. A defect in the direct or indirect space can destabilize the area and place additional strain on the pubic attachments.
In our experience, the dynamic Valsalva sequence improves detection of true hernias and anterior abdominal wall deficiencies and should be included in each protocol for the evaluation of acute or chronic groin pain.
Shear forces and injury at the pubis can occur outside professional athletics. Our patient population is nonprofessional athletes, teenagers to retirees, and all can develop athletic pubalgia. Ninety percent of surveyed patients who received a diagnosis and were treated surgically were satisfied with their outcomes.
Am J Orthop. 2017;46(4):E251-E256. Copyright Frontline Medical Communications Inc. 2017. All rights reserved.
1. Meyers WC, Lanfranco A, Castellanos A. Surgical management of chronic lower abdominal and groin pain in high-performance athletes. Curr Sports Med Rep. 2002;1(5):301-305.
2. Ahumada LA, Ashruf S, Espinosa-de-los-Monteros A, et al. Athletic pubalgia: definition and surgical treatment. Ann Plast Surg. 2005;55(4):393-396.
3. Omar IM, Zoga AC, Kavanagh EC, et al. Athletic pubalgia and “sports hernia”: optimal MR imaging technique and findings. Radiographics. 2008;28(5):1415-1438.
4. Gilmore OJA. Gilmore’s groin: ten years experience of groin disruption—a previously unsolved problem in sportsmen. Sports Med Soft Tissue Trauma. 1991;3:12-14.
5. Meyers WC, Foley DP, Garrett WE, Lohnes JH, Mandlebaum BR. Management of severe lower abdominal or inguinal pain in high-performance athletes. PAIN (Performing Athletes with Abdominal or Inguinal Neuromuscular Pain Study Group). Am J Sports Med. 2000;28(1):2-8.
6. Kavanagh EC, Koulouris G, Ford S, McMahon P, Johnson C, Eustace SJ. MR imaging of groin pain in the athlete. Semin Musculoskelet Radiol. 2006;10(3):197-207.
7. Cunningham PM, Brennan D, O’Connell M, MacMahon P, O’Neill P, Eustace S. Patterns of bone and soft-tissue injury at the symphysis pubis in soccer players: observations at MRI. AJR Am J Roentgenol. 2007;188(3):W291-W296.
8. Zoga AC, Kavanagh EC, Omar IM, et al. Athletic pubalgia and the “sports hernia”: MR imaging findings. Radiology. 2008;247(3):797-807.
9. Koulouris G. Imaging review of groin pain in elite athletes: an anatomic approach to imaging findings. AJR Am J Roentgenol. 2008;191(4):962-972.
10. Albers SL, Spritzer CE, Garrett WE Jr, Meyers WC. MR findings in athletes with pubalgia. Skeletal Radiol. 2001;30(5):270-277.
11. Brennan D, O’Connell MJ, Ryan M, et al. Secondary cleft sign as a marker of injury in athletes with groin pain: MR image appearance and interpretation. Radiology. 2005;235(1):162-167.
12. Robinson P, Salehi F, Grainger A, et al. Cadaveric and MRI study of the musculotendinous contributions to the capsule of the symphysis pubis. AJR Am J Roentgenol. 2007;188(5):W440-W445.
13. Schilders E, Talbot JC, Robinson P, Dimitrakopoulou A, Gibbon WW, Bismil Q. Adductor-related groin pain in recreational athletes. J Bone Joint Surg Am. 2009;91(10):2455-2460.
14. Davies AG, Clarke AW, Gilmore J, Wotherspoon M, Connell DA. Review: imaging of groin pain in the athlete. Skeletal Radiol. 2010;39(7):629-644.
15. Mullens FE, Zoga AC, Morrison WB, Meyers WC. Review of MRI technique and imaging findings in athletic pubalgia and the “sports hernia.” Eur J Radiol. 2012;81(12):3780-3792.
16. Zoga AC, Meyers WC. Magnetic resonance imaging for pain after surgical treatment for athletic pubalgia and the “sports hernia.” Semin Musculoskelet Radiol. 2011;15(4):372-382.
17. Beer E. Periostitis of symphysis and descending rami of pubes following suprapubic operations. Int J Med Surg. 1924;37(5):224-225.
18. MacMahon PJ, Hogan BA, Shelly MJ, Eustace SJ, Kavanagh EC. Imaging of groin pain. Magn Reson Imaging Clin N Am. 2009;17(4):655-666.
19. Malycha P, Lovell G. Inguinal surgery in athletes with chronic groin pain: the ‘sportsman’s’ hernia. Aust N Z J Surg. 1992;62(2):123-125.
20. Hackney RG. The sports hernia: a cause of chronic groin pain. Br J Sports Med. 1993;27(1):58-62.
21. Gibbon WW. Groin pain in athletes. Lancet. 1999;353(9162):1444-1445.
22. Brunet B, Brunet-Geudj E, Genety J. La pubalgie: syndrome “fourre-tout” pur une plus grande riguer diagnostique et therapeutique. Intantanes Medicaux. 1984;55:25-30.
23. Lischuk AW, Dorantes TM, Wong W, Haims AH. Imaging of sports-related hip and groin injuries. Sports Health. 2010;2(3):252-261.
24. Gibbon WW, Hession PR. Diseases of the pubis and pubic symphysis: MR imaging appearances. AJR Am J Roentgenol. 1997;169(3):849-853.
25. Gamble JG, Simmons SC, Freedman M. The symphysis pubis. Anatomic and pathologic considerations. Clin Orthop Relat Res. 1986;(203):261-272.
26. Larson CM. Sports hernia/athletic pubalgia: evaluation and management. Sports Health. 2014;6(2):139-144.
27. Maffulli N, Loppini M, Longo UG, Denaro V. Bilateral mini-invasive adductor tenotomy for the management of chronic unilateral adductor longus tendinopathy in athletes. Am J Sports Med. 2012;40(8):1880-1886.
28. Schilders E, Dimitrakopoulou A, Cooke M, Bismil Q, Cooke C. Effectiveness of a selective partial adductor release for chronic adductor-related groin pain in professional athletes. Am J Sports Med. 2013;41(3):603-607.
29. Scholten PM, Massimi S, Dahmen N, Diamond J, Wyss J. Successful treatment of athletic pubalgia in a lacrosse player with ultrasound-guided needle tenotomy and platelet-rich plasma injection: a case report. PM R. 2015;7(1):79-83.
The past 3 decades have seen an evolution in the understanding, diagnosis, and treatment of groin pain, both chronic and acute, in athletes and non-athletes alike. Groin pain and groin injury are common. Most cases are transient, with patients returning to their activities within weeks or months. There has also been increasing awareness of a definitive population of patients who do not get better, or who improve and plateau before reaching preinjury level of performance.1-3 Several authors have brought more attention to the injury, introducing vocabulary, theories, diagnostic testing, and diagnoses, which now constitute a knowledge base.1,3-5
As stated in almost every article on groin pain and diagnosis, lack of cohesive agreement and vocabulary, and consistent protocols and procedures, has abounded, making general understanding and agreement in this area inconsistent.1,6-8In this article, members of a tertiary-care group specializing in chronic groin pain, athletic pubalgia (sports hernia), and inguinal herniorrhaphy outline their clinical examination, diagnostic algorithm, imaging protocol, treatment strategy, and outcomes for a population of patients referred by physicians and allied health professionals for a suspected diagnosis of athletic pubalgia.
Background
The pubic symphysis acts as a stabilizing central anchor with elaborate involvement of the anterior structures, including the rectus abdominis, adductor longus, and inguinal ligaments.3,7,9 Literature from Europe, Australia, and the United States has described groin pain, mostly in professional athletes, involving these pubic structures and attachments. Several publications have been addressing chronic groin pain, and each has its own diagnostic algorithm, imaging protocol, and treatment strategy.3,6,9-18
Terminology specific to groin pain in athletes is not new, and has a varied history dating to the early 20th century. Terms such as sportsman hernia19 and subsequently sports hernia20, have recently been embraced by the lay population. In 1999, Gibbon21 described shearing of the common adductor–rectus abdominis anatomical and functional unit and referenced a 1902 anatomical text that describes vertical ligamentous fibers contiguous with rectus sheath and adductor muscles, both attaching to the pubis. Injury to this region is the basis of pubalgia, a term originally used in 1984 by Brunet to describe a pain syndrome at the pubis.22
Many authors have proposed replacing sports hernia with athletic pubalgia.1,3,6,7,10,14,18,23 These terms refer to a group of musculoskeletal processes that occur in and around the pubic symphysis and that share similar mechanisms of injury and common clinical manifestations. The condition was originally described in high-performance athletes, and at one point the term sports hernia was reserved for this patient population.5 According to many authors, presence of an inguinal hernia excludes the diagnosis.1,2,5Magnetic resonance imaging (MRI) has helped to advance and define our understanding of the injury.10 As the history of the literature suggests, earlier concepts of chronic pain focused either on the medial aspect of the inguinal canal and its structures or on the pubic attachments. Many specialists in the area have concluded that the chronic groin pain injury can and often does embody both elements.3,9 Correlation with MRI findings, injury seen during surgical procedures, and cadaveric studies have directed our understanding to a structure, the pre-pubic aponeurotic complex (P-PAC), or rectus aponeurotic plate.12,24,25 Anatomically, the P-PAC, which has several fascial components, attaches posteriorly to the pubic bone and, to a degree, the pubic symphyseal cartilaginous disc. Major contributions to the P-PAC are fibers from the rectus abdominis tendon, the medial aspect of the transversalis and internal oblique muscles (the conjoint tendon, according to some), the inguinal ligament, and the adductor longus tendon.26When communicating with referring physicians, we use the term athletic pubalgia to indicate a specific injury. The athletic pubalgia injury can be defined as serial microtearing,1 or complete tearing, of the posterior attachment of the P-PAC off the anterior pubis.3,10 Complete tearing or displacement can occur unilaterally or across the midline to the other side. As athletic pubalgia is a specific anatomical injury rather than a broad category of findings, an additional pathologic diagnosis, such as inguinal hernia, does not exclude the diagnosis of athletic pubalgia. Unfortunately, the terms sports hernia and sportsman hernia, commonly used in the media and in professional communities, have largely confused the broader understanding of nuances and of the differences between the specific injuries and MRI findings.18
Our Experience
In our practice, we see groin pain patients referred by internists, physiatrists, physical therapists, trainers, general surgeons, urologists, gynecologists, and orthopedic surgeons. In many cases, patients have been through several consultations and work-ups, as their pain syndrome does not fall under a specific category. Patients without inguinal hernia, hip injury, urologic, or gynecologic issues typically are referred to a physiatrist or a physical therapist. Often, there are marginal improvements with physical therapy, but in some cases the injury never completely resolves, and the patient continues to have pain with activity or return to sports.
Most of our patients are nonprofessional athletes, men and women who range widely in age and participate casually or regularly in sporting events. Most lack the rigorous training, conditioning, and close supervision that professional athletes receive. Many other patients are nonprofessional but elite athletes who train 7 days a week for marathons, ultramarathons, triathlons, obstacle course races (“mudders”), and similar events.
Work-Up
A single algorithm is used for all patients initially referred to the surgeon’s office for pelvic or groin pain. The initial interview directs attention to injury onset and mechanism, duration of rest or physical therapy after surgery, pain quality and pain levels, and antagonistic movements and positions. Examination starts with assessment for inguinal, femoral, and umbilical hernias. Resisted sit-up, leg-raise, adduction, and hip assessment tests are performed. The P-PAC is examined with a maneuver similar to the one used for inguinal hernia, as it allows for better assessment of the transversalis fascia (over the direct space) to determine if the inguinal canal floor is attenuated and bulges forward with the Valsalva maneuver. Then, the lateral aspect of the rectus muscle is assessed for pain, usually with the head raised to contract the muscle, to determine tenderness along the lateral border. The rectus edge is traced down to the pubis at its attachment, the superolateral border of the P-PAC. Examination proceeds medially, over the rectus attachment, toward the pubic symphysis, continuing the assessment for tenderness. Laterally, the conjoint tendon and inguinal ligament medial attachments are assessed at the level of the pubic tubercle, which represents the lateral border of the P-PAC. Finally, the examination continues to the inferior border with assessment of the adductor longus attachment, which is best performed with the leg in an adducted position. In the acute or semiacute setting (pain within 1 year of injury onset), tenderness is often elicited. With long-standing injuries, pain is often not elicited, but the patient experiences pain along this axis during activity or afterward.
Patients with positive history and physical examination findings proceed through an MRI protocol designed to detect pathology of the pubic symphysis, hips, and inguinal canals (Figures 1A-1D).
Treatment
Patients who report sustaining an acute groin injury within the previous 6 months are treated nonoperatively. A combination of rest, nonsteroidal anti-inflammatory drugs, and physical therapy is generally recommended.2,10 In cases of failed nonoperative management, patients are evaluated for surgery. No single operation is recommended for all patients.1,6,14,27,28 (Larson26 recently reviewed results from several trials involving a variety of surgical repairs and found return-to-sports rates ranging from 80% to 100%.) Findings from the physical examination and from the properly protocolled MRI examination are used in planning surgery to correct any pathology that could be contributing to symptoms or destabilization of the structures attaching to the pubis. Disruption of the P-PAC from the pubis would be repaired, for example. Additional injuries, such as partial or complete detachment of the conjoint tendon or inguinal ligament, may be repaired as well. If the transversalis fascia is attenuated and bulging forward, the inguinal floor is closed. Adductor longus tendon pathology is addressed, most commonly with partial tendinolysis. Often, concomitant inguinal hernias are found, and these may be repaired in open fashion while other maneuvers are being performed, or laparoscopically.
Materials and Methods
After receiving study approval from our Institutional Review Board, we retrospectively searched for all MRIs performed by our radiology department between March 1, 2011 and March 31, 2013 on patients referred for an indication of groin pain, sports hernia, or athletic pubalgia. Patients were excluded if they were younger than 18 years any time during their care. Some patients previously or subsequently underwent computed tomography or ultrasonography. MRIs were reviewed and positive findings were compiled in a database. Charts were reviewed to identify which patients in the dataset underwent surgery, after MRI, to address their presenting chief complaint. Surgery date and procedure(s) performed were recorded. Patients were interviewed by telephone as part of the in-office postoperative follow-up.
Results
One hundred nineteen MRIs were performed on 117 patients (97 men, 83%). Mean age was 39.8 years. Seventy-nine patients (68%) had an MRI finding of athletic pubalgia, 67 (57%) had an acetabular labral tear in one or both hip joints, and 41 (35%) had a true inguinal hernia. Concomitant findings were common: 47 cases of athletic pubalgia and labral tear(s), 28 cases of athletic pubalgia and inguinal hernia, and 15 cases of all 3 (athletic pubalgia, labral tear, inguinal hernia).
Use of breath-hold axial single-shot fast spin-echo sequences with and without the Valsalva maneuver increased sensitivity in detecting pathologies—inguinal hernia and Gilmore groin in particular. On 24 of the 119 MRIs, the Valsalva maneuver either revealed the finding or made it significantly more apparent.
Of all patients referred for MRI for chronic groin pain, 48 (41%) subsequently underwent surgery. In 29 surgeries, the rectus abdominis, adductor longus, and/or pre-pubic aponeurotic plate were repaired; in 13 cases, herniorrhaphy was performed as well; in 2 cases, masses involving the spermatic cord were removed.
The most common surgery (30 cases) was herniorrhaphy, which was performed as a single procedure, multiple procedures, or in combination with procedures not related to a true hernia. Eighteen patients underwent surgery only for hernia repair.
Of the 79 patients with MRI-positive athletic pubalgia, 39 subsequently underwent surgery, and 31 (79%) of these were followed up by telephone. Mean duration of rest after surgery was 6.2 weeks. Twelve patients (39%) had physical therapy after surgery, some as early as 4 weeks, and some have continued their therapy since surgery. Of the 31 patients who were followed up after surgery, 23 (74%) resumed previous activity levels. Return to previous activity level took these patients a mean of 17.9 weeks. When asked if outcomes satisfied their expectations, 28 patients (90%) said yes, and 3 said no.
Forty patients with MRI-positive athletic pubalgia were nonoperatively treated, and 28 (70%) of these patients were followed up. In this group, mean duration of rest after surgery was 6.9 weeks. Thirteen patients (46%) participated in physical therapy, for a mean duration of 10.8 weeks. Of the patients followed up, 19 (68%) returned to previous activity level. Twenty-one patients (75%) were satisfied with their outcome.
Discussion
Diagnosis and treatment of chronic groin pain have had a long, confusing, and frustrating history for both patients and the medical professionals who provide them with care.3,6,7,10 Historically, the problem has been, in part, the lack of diagnostic capabilities. Currently, however, pubalgia MRI protocol allows the exact pathology to be demonstrated.3 As already noted, concomitant hip pathology or inguinal hernia is not unusual8; any structural abnormality in the area is a potential destabilizer of the structures attached to the pubis.18 Solving only one of these issues may offer only partial resolution of symptoms and thereby reduce the rate of successful treatment of groin pain.
Diagnostic algorithms are being developed. In addition, nonoperative treatments are being tried for some of the issues. Physicians are giving diagnostic and therapeutic steroid injections in the pubic cleft, along the rectus abdominis/adductor longus complex, or posterior to the P-PAC. Platelet-rich plasma injection therapy has had limited success.29This article provides a snapshot of what a tertiary-care group of physicians specializing in chronic groin pain sees in an unfiltered setting. We think this is instructive for several reasons.
First, many patients in our population have visited a multitude of specialists without receiving a diagnosis or being referred appropriately. Simply, many specialists do not know the next step in treating groin pain and thus do not make the appropriate referral. Until recently, the literature has not been helpful. It has poorly described the constellation of injuries comprising chronic groin pain. More significantly, groin injuries have been presented as ambiguous injuries lacking effective treatment. Over the past decade, however, abundant literature on the correlation of these injuries with specific MRI findings has made the case otherwise.
Second, a specific MRI pubalgia protocol is needed. Inability to make a correct diagnosis, because of improper MRI, continues to add to the confusion surrounding the injury and undoubtedly prolongs the general medical community’s thinking that diagnosis and treatment of chronic groin pain are elusive. Our data support this point in many ways. Although all patients in this study were seen by a medical professional before coming to our office, none had received a diagnosis of occult hernia or attenuated transversalis fascia; nevertheless, we identified inguinal hernia, Gilmore groin, or both in 44% of these patients. These findings are not surprising, as MRI was the crucial link in diagnosis. In addition, the point made by other groin pain specialists—that a hernia precludes a pubalgia diagnosis1,2,5—is not supported by our data. Inguinal hernia can and does exist in conjunction with pubalgia. More than half the patients in our study had a combined diagnosis. We contend that, much as hip labral pathology occurs concomitantly with pubalgia,23 inguinal hernia may be a predisposing factor as well. A defect in the direct or indirect space can destabilize the area and place additional strain on the pubic attachments.
In our experience, the dynamic Valsalva sequence improves detection of true hernias and anterior abdominal wall deficiencies and should be included in each protocol for the evaluation of acute or chronic groin pain.
Shear forces and injury at the pubis can occur outside professional athletics. Our patient population is nonprofessional athletes, teenagers to retirees, and all can develop athletic pubalgia. Ninety percent of surveyed patients who received a diagnosis and were treated surgically were satisfied with their outcomes.
Am J Orthop. 2017;46(4):E251-E256. Copyright Frontline Medical Communications Inc. 2017. All rights reserved.
The past 3 decades have seen an evolution in the understanding, diagnosis, and treatment of groin pain, both chronic and acute, in athletes and non-athletes alike. Groin pain and groin injury are common. Most cases are transient, with patients returning to their activities within weeks or months. There has also been increasing awareness of a definitive population of patients who do not get better, or who improve and plateau before reaching preinjury level of performance.1-3 Several authors have brought more attention to the injury, introducing vocabulary, theories, diagnostic testing, and diagnoses, which now constitute a knowledge base.1,3-5
As stated in almost every article on groin pain and diagnosis, lack of cohesive agreement and vocabulary, and consistent protocols and procedures, has abounded, making general understanding and agreement in this area inconsistent.1,6-8In this article, members of a tertiary-care group specializing in chronic groin pain, athletic pubalgia (sports hernia), and inguinal herniorrhaphy outline their clinical examination, diagnostic algorithm, imaging protocol, treatment strategy, and outcomes for a population of patients referred by physicians and allied health professionals for a suspected diagnosis of athletic pubalgia.
Background
The pubic symphysis acts as a stabilizing central anchor with elaborate involvement of the anterior structures, including the rectus abdominis, adductor longus, and inguinal ligaments.3,7,9 Literature from Europe, Australia, and the United States has described groin pain, mostly in professional athletes, involving these pubic structures and attachments. Several publications have been addressing chronic groin pain, and each has its own diagnostic algorithm, imaging protocol, and treatment strategy.3,6,9-18
Terminology specific to groin pain in athletes is not new, and has a varied history dating to the early 20th century. Terms such as sportsman hernia19 and subsequently sports hernia20, have recently been embraced by the lay population. In 1999, Gibbon21 described shearing of the common adductor–rectus abdominis anatomical and functional unit and referenced a 1902 anatomical text that describes vertical ligamentous fibers contiguous with rectus sheath and adductor muscles, both attaching to the pubis. Injury to this region is the basis of pubalgia, a term originally used in 1984 by Brunet to describe a pain syndrome at the pubis.22
Many authors have proposed replacing sports hernia with athletic pubalgia.1,3,6,7,10,14,18,23 These terms refer to a group of musculoskeletal processes that occur in and around the pubic symphysis and that share similar mechanisms of injury and common clinical manifestations. The condition was originally described in high-performance athletes, and at one point the term sports hernia was reserved for this patient population.5 According to many authors, presence of an inguinal hernia excludes the diagnosis.1,2,5Magnetic resonance imaging (MRI) has helped to advance and define our understanding of the injury.10 As the history of the literature suggests, earlier concepts of chronic pain focused either on the medial aspect of the inguinal canal and its structures or on the pubic attachments. Many specialists in the area have concluded that the chronic groin pain injury can and often does embody both elements.3,9 Correlation with MRI findings, injury seen during surgical procedures, and cadaveric studies have directed our understanding to a structure, the pre-pubic aponeurotic complex (P-PAC), or rectus aponeurotic plate.12,24,25 Anatomically, the P-PAC, which has several fascial components, attaches posteriorly to the pubic bone and, to a degree, the pubic symphyseal cartilaginous disc. Major contributions to the P-PAC are fibers from the rectus abdominis tendon, the medial aspect of the transversalis and internal oblique muscles (the conjoint tendon, according to some), the inguinal ligament, and the adductor longus tendon.26When communicating with referring physicians, we use the term athletic pubalgia to indicate a specific injury. The athletic pubalgia injury can be defined as serial microtearing,1 or complete tearing, of the posterior attachment of the P-PAC off the anterior pubis.3,10 Complete tearing or displacement can occur unilaterally or across the midline to the other side. As athletic pubalgia is a specific anatomical injury rather than a broad category of findings, an additional pathologic diagnosis, such as inguinal hernia, does not exclude the diagnosis of athletic pubalgia. Unfortunately, the terms sports hernia and sportsman hernia, commonly used in the media and in professional communities, have largely confused the broader understanding of nuances and of the differences between the specific injuries and MRI findings.18
Our Experience
In our practice, we see groin pain patients referred by internists, physiatrists, physical therapists, trainers, general surgeons, urologists, gynecologists, and orthopedic surgeons. In many cases, patients have been through several consultations and work-ups, as their pain syndrome does not fall under a specific category. Patients without inguinal hernia, hip injury, urologic, or gynecologic issues typically are referred to a physiatrist or a physical therapist. Often, there are marginal improvements with physical therapy, but in some cases the injury never completely resolves, and the patient continues to have pain with activity or return to sports.
Most of our patients are nonprofessional athletes, men and women who range widely in age and participate casually or regularly in sporting events. Most lack the rigorous training, conditioning, and close supervision that professional athletes receive. Many other patients are nonprofessional but elite athletes who train 7 days a week for marathons, ultramarathons, triathlons, obstacle course races (“mudders”), and similar events.
Work-Up
A single algorithm is used for all patients initially referred to the surgeon’s office for pelvic or groin pain. The initial interview directs attention to injury onset and mechanism, duration of rest or physical therapy after surgery, pain quality and pain levels, and antagonistic movements and positions. Examination starts with assessment for inguinal, femoral, and umbilical hernias. Resisted sit-up, leg-raise, adduction, and hip assessment tests are performed. The P-PAC is examined with a maneuver similar to the one used for inguinal hernia, as it allows for better assessment of the transversalis fascia (over the direct space) to determine if the inguinal canal floor is attenuated and bulges forward with the Valsalva maneuver. Then, the lateral aspect of the rectus muscle is assessed for pain, usually with the head raised to contract the muscle, to determine tenderness along the lateral border. The rectus edge is traced down to the pubis at its attachment, the superolateral border of the P-PAC. Examination proceeds medially, over the rectus attachment, toward the pubic symphysis, continuing the assessment for tenderness. Laterally, the conjoint tendon and inguinal ligament medial attachments are assessed at the level of the pubic tubercle, which represents the lateral border of the P-PAC. Finally, the examination continues to the inferior border with assessment of the adductor longus attachment, which is best performed with the leg in an adducted position. In the acute or semiacute setting (pain within 1 year of injury onset), tenderness is often elicited. With long-standing injuries, pain is often not elicited, but the patient experiences pain along this axis during activity or afterward.
Patients with positive history and physical examination findings proceed through an MRI protocol designed to detect pathology of the pubic symphysis, hips, and inguinal canals (Figures 1A-1D).
Treatment
Patients who report sustaining an acute groin injury within the previous 6 months are treated nonoperatively. A combination of rest, nonsteroidal anti-inflammatory drugs, and physical therapy is generally recommended.2,10 In cases of failed nonoperative management, patients are evaluated for surgery. No single operation is recommended for all patients.1,6,14,27,28 (Larson26 recently reviewed results from several trials involving a variety of surgical repairs and found return-to-sports rates ranging from 80% to 100%.) Findings from the physical examination and from the properly protocolled MRI examination are used in planning surgery to correct any pathology that could be contributing to symptoms or destabilization of the structures attaching to the pubis. Disruption of the P-PAC from the pubis would be repaired, for example. Additional injuries, such as partial or complete detachment of the conjoint tendon or inguinal ligament, may be repaired as well. If the transversalis fascia is attenuated and bulging forward, the inguinal floor is closed. Adductor longus tendon pathology is addressed, most commonly with partial tendinolysis. Often, concomitant inguinal hernias are found, and these may be repaired in open fashion while other maneuvers are being performed, or laparoscopically.
Materials and Methods
After receiving study approval from our Institutional Review Board, we retrospectively searched for all MRIs performed by our radiology department between March 1, 2011 and March 31, 2013 on patients referred for an indication of groin pain, sports hernia, or athletic pubalgia. Patients were excluded if they were younger than 18 years any time during their care. Some patients previously or subsequently underwent computed tomography or ultrasonography. MRIs were reviewed and positive findings were compiled in a database. Charts were reviewed to identify which patients in the dataset underwent surgery, after MRI, to address their presenting chief complaint. Surgery date and procedure(s) performed were recorded. Patients were interviewed by telephone as part of the in-office postoperative follow-up.
Results
One hundred nineteen MRIs were performed on 117 patients (97 men, 83%). Mean age was 39.8 years. Seventy-nine patients (68%) had an MRI finding of athletic pubalgia, 67 (57%) had an acetabular labral tear in one or both hip joints, and 41 (35%) had a true inguinal hernia. Concomitant findings were common: 47 cases of athletic pubalgia and labral tear(s), 28 cases of athletic pubalgia and inguinal hernia, and 15 cases of all 3 (athletic pubalgia, labral tear, inguinal hernia).
Use of breath-hold axial single-shot fast spin-echo sequences with and without the Valsalva maneuver increased sensitivity in detecting pathologies—inguinal hernia and Gilmore groin in particular. On 24 of the 119 MRIs, the Valsalva maneuver either revealed the finding or made it significantly more apparent.
Of all patients referred for MRI for chronic groin pain, 48 (41%) subsequently underwent surgery. In 29 surgeries, the rectus abdominis, adductor longus, and/or pre-pubic aponeurotic plate were repaired; in 13 cases, herniorrhaphy was performed as well; in 2 cases, masses involving the spermatic cord were removed.
The most common surgery (30 cases) was herniorrhaphy, which was performed as a single procedure, multiple procedures, or in combination with procedures not related to a true hernia. Eighteen patients underwent surgery only for hernia repair.
Of the 79 patients with MRI-positive athletic pubalgia, 39 subsequently underwent surgery, and 31 (79%) of these were followed up by telephone. Mean duration of rest after surgery was 6.2 weeks. Twelve patients (39%) had physical therapy after surgery, some as early as 4 weeks, and some have continued their therapy since surgery. Of the 31 patients who were followed up after surgery, 23 (74%) resumed previous activity levels. Return to previous activity level took these patients a mean of 17.9 weeks. When asked if outcomes satisfied their expectations, 28 patients (90%) said yes, and 3 said no.
Forty patients with MRI-positive athletic pubalgia were nonoperatively treated, and 28 (70%) of these patients were followed up. In this group, mean duration of rest after surgery was 6.9 weeks. Thirteen patients (46%) participated in physical therapy, for a mean duration of 10.8 weeks. Of the patients followed up, 19 (68%) returned to previous activity level. Twenty-one patients (75%) were satisfied with their outcome.
Discussion
Diagnosis and treatment of chronic groin pain have had a long, confusing, and frustrating history for both patients and the medical professionals who provide them with care.3,6,7,10 Historically, the problem has been, in part, the lack of diagnostic capabilities. Currently, however, pubalgia MRI protocol allows the exact pathology to be demonstrated.3 As already noted, concomitant hip pathology or inguinal hernia is not unusual8; any structural abnormality in the area is a potential destabilizer of the structures attached to the pubis.18 Solving only one of these issues may offer only partial resolution of symptoms and thereby reduce the rate of successful treatment of groin pain.
Diagnostic algorithms are being developed. In addition, nonoperative treatments are being tried for some of the issues. Physicians are giving diagnostic and therapeutic steroid injections in the pubic cleft, along the rectus abdominis/adductor longus complex, or posterior to the P-PAC. Platelet-rich plasma injection therapy has had limited success.29This article provides a snapshot of what a tertiary-care group of physicians specializing in chronic groin pain sees in an unfiltered setting. We think this is instructive for several reasons.
First, many patients in our population have visited a multitude of specialists without receiving a diagnosis or being referred appropriately. Simply, many specialists do not know the next step in treating groin pain and thus do not make the appropriate referral. Until recently, the literature has not been helpful. It has poorly described the constellation of injuries comprising chronic groin pain. More significantly, groin injuries have been presented as ambiguous injuries lacking effective treatment. Over the past decade, however, abundant literature on the correlation of these injuries with specific MRI findings has made the case otherwise.
Second, a specific MRI pubalgia protocol is needed. Inability to make a correct diagnosis, because of improper MRI, continues to add to the confusion surrounding the injury and undoubtedly prolongs the general medical community’s thinking that diagnosis and treatment of chronic groin pain are elusive. Our data support this point in many ways. Although all patients in this study were seen by a medical professional before coming to our office, none had received a diagnosis of occult hernia or attenuated transversalis fascia; nevertheless, we identified inguinal hernia, Gilmore groin, or both in 44% of these patients. These findings are not surprising, as MRI was the crucial link in diagnosis. In addition, the point made by other groin pain specialists—that a hernia precludes a pubalgia diagnosis1,2,5—is not supported by our data. Inguinal hernia can and does exist in conjunction with pubalgia. More than half the patients in our study had a combined diagnosis. We contend that, much as hip labral pathology occurs concomitantly with pubalgia,23 inguinal hernia may be a predisposing factor as well. A defect in the direct or indirect space can destabilize the area and place additional strain on the pubic attachments.
In our experience, the dynamic Valsalva sequence improves detection of true hernias and anterior abdominal wall deficiencies and should be included in each protocol for the evaluation of acute or chronic groin pain.
Shear forces and injury at the pubis can occur outside professional athletics. Our patient population is nonprofessional athletes, teenagers to retirees, and all can develop athletic pubalgia. Ninety percent of surveyed patients who received a diagnosis and were treated surgically were satisfied with their outcomes.
Am J Orthop. 2017;46(4):E251-E256. Copyright Frontline Medical Communications Inc. 2017. All rights reserved.
1. Meyers WC, Lanfranco A, Castellanos A. Surgical management of chronic lower abdominal and groin pain in high-performance athletes. Curr Sports Med Rep. 2002;1(5):301-305.
2. Ahumada LA, Ashruf S, Espinosa-de-los-Monteros A, et al. Athletic pubalgia: definition and surgical treatment. Ann Plast Surg. 2005;55(4):393-396.
3. Omar IM, Zoga AC, Kavanagh EC, et al. Athletic pubalgia and “sports hernia”: optimal MR imaging technique and findings. Radiographics. 2008;28(5):1415-1438.
4. Gilmore OJA. Gilmore’s groin: ten years experience of groin disruption—a previously unsolved problem in sportsmen. Sports Med Soft Tissue Trauma. 1991;3:12-14.
5. Meyers WC, Foley DP, Garrett WE, Lohnes JH, Mandlebaum BR. Management of severe lower abdominal or inguinal pain in high-performance athletes. PAIN (Performing Athletes with Abdominal or Inguinal Neuromuscular Pain Study Group). Am J Sports Med. 2000;28(1):2-8.
6. Kavanagh EC, Koulouris G, Ford S, McMahon P, Johnson C, Eustace SJ. MR imaging of groin pain in the athlete. Semin Musculoskelet Radiol. 2006;10(3):197-207.
7. Cunningham PM, Brennan D, O’Connell M, MacMahon P, O’Neill P, Eustace S. Patterns of bone and soft-tissue injury at the symphysis pubis in soccer players: observations at MRI. AJR Am J Roentgenol. 2007;188(3):W291-W296.
8. Zoga AC, Kavanagh EC, Omar IM, et al. Athletic pubalgia and the “sports hernia”: MR imaging findings. Radiology. 2008;247(3):797-807.
9. Koulouris G. Imaging review of groin pain in elite athletes: an anatomic approach to imaging findings. AJR Am J Roentgenol. 2008;191(4):962-972.
10. Albers SL, Spritzer CE, Garrett WE Jr, Meyers WC. MR findings in athletes with pubalgia. Skeletal Radiol. 2001;30(5):270-277.
11. Brennan D, O’Connell MJ, Ryan M, et al. Secondary cleft sign as a marker of injury in athletes with groin pain: MR image appearance and interpretation. Radiology. 2005;235(1):162-167.
12. Robinson P, Salehi F, Grainger A, et al. Cadaveric and MRI study of the musculotendinous contributions to the capsule of the symphysis pubis. AJR Am J Roentgenol. 2007;188(5):W440-W445.
13. Schilders E, Talbot JC, Robinson P, Dimitrakopoulou A, Gibbon WW, Bismil Q. Adductor-related groin pain in recreational athletes. J Bone Joint Surg Am. 2009;91(10):2455-2460.
14. Davies AG, Clarke AW, Gilmore J, Wotherspoon M, Connell DA. Review: imaging of groin pain in the athlete. Skeletal Radiol. 2010;39(7):629-644.
15. Mullens FE, Zoga AC, Morrison WB, Meyers WC. Review of MRI technique and imaging findings in athletic pubalgia and the “sports hernia.” Eur J Radiol. 2012;81(12):3780-3792.
16. Zoga AC, Meyers WC. Magnetic resonance imaging for pain after surgical treatment for athletic pubalgia and the “sports hernia.” Semin Musculoskelet Radiol. 2011;15(4):372-382.
17. Beer E. Periostitis of symphysis and descending rami of pubes following suprapubic operations. Int J Med Surg. 1924;37(5):224-225.
18. MacMahon PJ, Hogan BA, Shelly MJ, Eustace SJ, Kavanagh EC. Imaging of groin pain. Magn Reson Imaging Clin N Am. 2009;17(4):655-666.
19. Malycha P, Lovell G. Inguinal surgery in athletes with chronic groin pain: the ‘sportsman’s’ hernia. Aust N Z J Surg. 1992;62(2):123-125.
20. Hackney RG. The sports hernia: a cause of chronic groin pain. Br J Sports Med. 1993;27(1):58-62.
21. Gibbon WW. Groin pain in athletes. Lancet. 1999;353(9162):1444-1445.
22. Brunet B, Brunet-Geudj E, Genety J. La pubalgie: syndrome “fourre-tout” pur une plus grande riguer diagnostique et therapeutique. Intantanes Medicaux. 1984;55:25-30.
23. Lischuk AW, Dorantes TM, Wong W, Haims AH. Imaging of sports-related hip and groin injuries. Sports Health. 2010;2(3):252-261.
24. Gibbon WW, Hession PR. Diseases of the pubis and pubic symphysis: MR imaging appearances. AJR Am J Roentgenol. 1997;169(3):849-853.
25. Gamble JG, Simmons SC, Freedman M. The symphysis pubis. Anatomic and pathologic considerations. Clin Orthop Relat Res. 1986;(203):261-272.
26. Larson CM. Sports hernia/athletic pubalgia: evaluation and management. Sports Health. 2014;6(2):139-144.
27. Maffulli N, Loppini M, Longo UG, Denaro V. Bilateral mini-invasive adductor tenotomy for the management of chronic unilateral adductor longus tendinopathy in athletes. Am J Sports Med. 2012;40(8):1880-1886.
28. Schilders E, Dimitrakopoulou A, Cooke M, Bismil Q, Cooke C. Effectiveness of a selective partial adductor release for chronic adductor-related groin pain in professional athletes. Am J Sports Med. 2013;41(3):603-607.
29. Scholten PM, Massimi S, Dahmen N, Diamond J, Wyss J. Successful treatment of athletic pubalgia in a lacrosse player with ultrasound-guided needle tenotomy and platelet-rich plasma injection: a case report. PM R. 2015;7(1):79-83.
1. Meyers WC, Lanfranco A, Castellanos A. Surgical management of chronic lower abdominal and groin pain in high-performance athletes. Curr Sports Med Rep. 2002;1(5):301-305.
2. Ahumada LA, Ashruf S, Espinosa-de-los-Monteros A, et al. Athletic pubalgia: definition and surgical treatment. Ann Plast Surg. 2005;55(4):393-396.
3. Omar IM, Zoga AC, Kavanagh EC, et al. Athletic pubalgia and “sports hernia”: optimal MR imaging technique and findings. Radiographics. 2008;28(5):1415-1438.
4. Gilmore OJA. Gilmore’s groin: ten years experience of groin disruption—a previously unsolved problem in sportsmen. Sports Med Soft Tissue Trauma. 1991;3:12-14.
5. Meyers WC, Foley DP, Garrett WE, Lohnes JH, Mandlebaum BR. Management of severe lower abdominal or inguinal pain in high-performance athletes. PAIN (Performing Athletes with Abdominal or Inguinal Neuromuscular Pain Study Group). Am J Sports Med. 2000;28(1):2-8.
6. Kavanagh EC, Koulouris G, Ford S, McMahon P, Johnson C, Eustace SJ. MR imaging of groin pain in the athlete. Semin Musculoskelet Radiol. 2006;10(3):197-207.
7. Cunningham PM, Brennan D, O’Connell M, MacMahon P, O’Neill P, Eustace S. Patterns of bone and soft-tissue injury at the symphysis pubis in soccer players: observations at MRI. AJR Am J Roentgenol. 2007;188(3):W291-W296.
8. Zoga AC, Kavanagh EC, Omar IM, et al. Athletic pubalgia and the “sports hernia”: MR imaging findings. Radiology. 2008;247(3):797-807.
9. Koulouris G. Imaging review of groin pain in elite athletes: an anatomic approach to imaging findings. AJR Am J Roentgenol. 2008;191(4):962-972.
10. Albers SL, Spritzer CE, Garrett WE Jr, Meyers WC. MR findings in athletes with pubalgia. Skeletal Radiol. 2001;30(5):270-277.
11. Brennan D, O’Connell MJ, Ryan M, et al. Secondary cleft sign as a marker of injury in athletes with groin pain: MR image appearance and interpretation. Radiology. 2005;235(1):162-167.
12. Robinson P, Salehi F, Grainger A, et al. Cadaveric and MRI study of the musculotendinous contributions to the capsule of the symphysis pubis. AJR Am J Roentgenol. 2007;188(5):W440-W445.
13. Schilders E, Talbot JC, Robinson P, Dimitrakopoulou A, Gibbon WW, Bismil Q. Adductor-related groin pain in recreational athletes. J Bone Joint Surg Am. 2009;91(10):2455-2460.
14. Davies AG, Clarke AW, Gilmore J, Wotherspoon M, Connell DA. Review: imaging of groin pain in the athlete. Skeletal Radiol. 2010;39(7):629-644.
15. Mullens FE, Zoga AC, Morrison WB, Meyers WC. Review of MRI technique and imaging findings in athletic pubalgia and the “sports hernia.” Eur J Radiol. 2012;81(12):3780-3792.
16. Zoga AC, Meyers WC. Magnetic resonance imaging for pain after surgical treatment for athletic pubalgia and the “sports hernia.” Semin Musculoskelet Radiol. 2011;15(4):372-382.
17. Beer E. Periostitis of symphysis and descending rami of pubes following suprapubic operations. Int J Med Surg. 1924;37(5):224-225.
18. MacMahon PJ, Hogan BA, Shelly MJ, Eustace SJ, Kavanagh EC. Imaging of groin pain. Magn Reson Imaging Clin N Am. 2009;17(4):655-666.
19. Malycha P, Lovell G. Inguinal surgery in athletes with chronic groin pain: the ‘sportsman’s’ hernia. Aust N Z J Surg. 1992;62(2):123-125.
20. Hackney RG. The sports hernia: a cause of chronic groin pain. Br J Sports Med. 1993;27(1):58-62.
21. Gibbon WW. Groin pain in athletes. Lancet. 1999;353(9162):1444-1445.
22. Brunet B, Brunet-Geudj E, Genety J. La pubalgie: syndrome “fourre-tout” pur une plus grande riguer diagnostique et therapeutique. Intantanes Medicaux. 1984;55:25-30.
23. Lischuk AW, Dorantes TM, Wong W, Haims AH. Imaging of sports-related hip and groin injuries. Sports Health. 2010;2(3):252-261.
24. Gibbon WW, Hession PR. Diseases of the pubis and pubic symphysis: MR imaging appearances. AJR Am J Roentgenol. 1997;169(3):849-853.
25. Gamble JG, Simmons SC, Freedman M. The symphysis pubis. Anatomic and pathologic considerations. Clin Orthop Relat Res. 1986;(203):261-272.
26. Larson CM. Sports hernia/athletic pubalgia: evaluation and management. Sports Health. 2014;6(2):139-144.
27. Maffulli N, Loppini M, Longo UG, Denaro V. Bilateral mini-invasive adductor tenotomy for the management of chronic unilateral adductor longus tendinopathy in athletes. Am J Sports Med. 2012;40(8):1880-1886.
28. Schilders E, Dimitrakopoulou A, Cooke M, Bismil Q, Cooke C. Effectiveness of a selective partial adductor release for chronic adductor-related groin pain in professional athletes. Am J Sports Med. 2013;41(3):603-607.
29. Scholten PM, Massimi S, Dahmen N, Diamond J, Wyss J. Successful treatment of athletic pubalgia in a lacrosse player with ultrasound-guided needle tenotomy and platelet-rich plasma injection: a case report. PM R. 2015;7(1):79-83.
Avoiding Disasters With Injectables: Tips From Charlene Lam at the Summer AAD
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”
New findings from first all-female TAVR registry
Paris – A history of pregnancy did not protect against adverse outcomes at 1 year in the Women’s International Transcatheter Aortic Valve Implantation Registry (WIN-TAVI), even though it did within the first 30 days, Alaide Chieffo, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
One year ago, at EuroPCR 2016, she reported that in WIN-TAVI, a history of pregnancy – albeit typically more than half a century previously – was independently associated with a 43% reduction in the Valve Academic Research Consortium-2 (VARC-2) 30-day composite endpoint, including death, stroke, major vascular complications, life-threatening bleeding, stage 2 or 3 acute kidney injury, coronary artery obstruction, or repeat transcatheter aortic valve replacement (TAVR) done because of valve-related dysfunction. Those early findings, first reported in this publication, were later published (JACC Cardiovasc Interv. 2016 Aug 8;9[15]:1589-600).
At 1 year of follow-up, however, the rate of the VARC-2 composite endpoint was no longer significantly different in women with or without a history of pregnancy. Nor was a history of pregnancy associated with a significantly reduced risk of the secondary endpoint of death or stroke: The 27% reduction in risk of this secondary endpoint in women with a history of pregnancy, compared with that of nulliparous women, didn’t achieve statistical significance in multivariate analysis, according to Dr. Chieffo of the San Raffaele Scientific Institute in Milan.
She speculated that pregnancy earlier in life provided strong protection against poor 30-day outcomes and a similar trend – albeit not statistically significant – at 1 year because women without children may have less family support.
“They are old women, left alone, without the family taking care of them. This is socially important, I think, because we are investing quite a lot of money in a procedure, and then maybe we’re adding adverse events because these patients are not properly taken care of when they are out of the hospital,” the interventional cardiologist said.
Neither of the other two female-specific characteristics evaluated in WIN-TAVI – having a history of osteoporosis or age at menopause – turned out to be related to the risk of bad outcomes at 1 year, she added.
WIN-TAVI is the first all-female registry of patients undergoing TAVR for severe aortic stenosis. The prospective, observational registry includes 1,019 women treated at 19 highly experienced European and North American TAVR centers. They averaged 82.5 years of age with a mean Society of Thoracic Surgeons score of 8.3%, putting them at intermediate or high surgical risk. A percutaneous transfemoral approach was used in 91% of cases. TAVR was performed under conscious sedation in 28% of the women and under local anesthesia in another 37%. Of the women in the registry, 42% received a newer-generation device.
In addition to the lack of significant impact of prior pregnancy on 1-year outcomes, another noteworthy finding at 1 year of follow-up was that preprocedural atrial fibrillation was independently associated with a 58% increase in the risk of death or stroke (P = .02). Prior percutaneous coronary intervention and EuroSCORE (European System for Cardiac Operative Risk Evaluation) were the only other independent predictors.
This observation suggests the need for a women-only randomized trial of TAVR versus surgical aortic valve replacement in women with intermediate surgical risk, Dr. Chieffo suggested. It will be important to learn whether the ability to surgically ablate preoperative atrial fibrillation in women during surgical valve replacement results in a lower 1-year risk of death or stroke than is achieved with TAVR.
Overall, the 1-year clinical outcomes seen in WIN-TAVI are “very good,” she noted. The VARC-2 composite endpoint occurred in 16.5% of women, all-cause mortality in 12.5%, cardiovascular mortality in 10.8%, and stroke in 2.2%. Only 3.2% of women were hospitalized for heart failure or valve-related symptoms. A new pacemaker was implanted in 12.7% of participants. At baseline 74% of women were New York Heart Association functional class III or IV; at 1 year, only 8.1% were. Moderate paravalvular aortic regurgitation was present in 6% of patients at 6 months and in 9.7% at 1 year
The WIN-TAVI registry is entirely self-funded. Dr. Chieffo reported having no financial conflicts regarding her presentation.
Paris – A history of pregnancy did not protect against adverse outcomes at 1 year in the Women’s International Transcatheter Aortic Valve Implantation Registry (WIN-TAVI), even though it did within the first 30 days, Alaide Chieffo, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
One year ago, at EuroPCR 2016, she reported that in WIN-TAVI, a history of pregnancy – albeit typically more than half a century previously – was independently associated with a 43% reduction in the Valve Academic Research Consortium-2 (VARC-2) 30-day composite endpoint, including death, stroke, major vascular complications, life-threatening bleeding, stage 2 or 3 acute kidney injury, coronary artery obstruction, or repeat transcatheter aortic valve replacement (TAVR) done because of valve-related dysfunction. Those early findings, first reported in this publication, were later published (JACC Cardiovasc Interv. 2016 Aug 8;9[15]:1589-600).
At 1 year of follow-up, however, the rate of the VARC-2 composite endpoint was no longer significantly different in women with or without a history of pregnancy. Nor was a history of pregnancy associated with a significantly reduced risk of the secondary endpoint of death or stroke: The 27% reduction in risk of this secondary endpoint in women with a history of pregnancy, compared with that of nulliparous women, didn’t achieve statistical significance in multivariate analysis, according to Dr. Chieffo of the San Raffaele Scientific Institute in Milan.
She speculated that pregnancy earlier in life provided strong protection against poor 30-day outcomes and a similar trend – albeit not statistically significant – at 1 year because women without children may have less family support.
“They are old women, left alone, without the family taking care of them. This is socially important, I think, because we are investing quite a lot of money in a procedure, and then maybe we’re adding adverse events because these patients are not properly taken care of when they are out of the hospital,” the interventional cardiologist said.
Neither of the other two female-specific characteristics evaluated in WIN-TAVI – having a history of osteoporosis or age at menopause – turned out to be related to the risk of bad outcomes at 1 year, she added.
WIN-TAVI is the first all-female registry of patients undergoing TAVR for severe aortic stenosis. The prospective, observational registry includes 1,019 women treated at 19 highly experienced European and North American TAVR centers. They averaged 82.5 years of age with a mean Society of Thoracic Surgeons score of 8.3%, putting them at intermediate or high surgical risk. A percutaneous transfemoral approach was used in 91% of cases. TAVR was performed under conscious sedation in 28% of the women and under local anesthesia in another 37%. Of the women in the registry, 42% received a newer-generation device.
In addition to the lack of significant impact of prior pregnancy on 1-year outcomes, another noteworthy finding at 1 year of follow-up was that preprocedural atrial fibrillation was independently associated with a 58% increase in the risk of death or stroke (P = .02). Prior percutaneous coronary intervention and EuroSCORE (European System for Cardiac Operative Risk Evaluation) were the only other independent predictors.
This observation suggests the need for a women-only randomized trial of TAVR versus surgical aortic valve replacement in women with intermediate surgical risk, Dr. Chieffo suggested. It will be important to learn whether the ability to surgically ablate preoperative atrial fibrillation in women during surgical valve replacement results in a lower 1-year risk of death or stroke than is achieved with TAVR.
Overall, the 1-year clinical outcomes seen in WIN-TAVI are “very good,” she noted. The VARC-2 composite endpoint occurred in 16.5% of women, all-cause mortality in 12.5%, cardiovascular mortality in 10.8%, and stroke in 2.2%. Only 3.2% of women were hospitalized for heart failure or valve-related symptoms. A new pacemaker was implanted in 12.7% of participants. At baseline 74% of women were New York Heart Association functional class III or IV; at 1 year, only 8.1% were. Moderate paravalvular aortic regurgitation was present in 6% of patients at 6 months and in 9.7% at 1 year
The WIN-TAVI registry is entirely self-funded. Dr. Chieffo reported having no financial conflicts regarding her presentation.
Paris – A history of pregnancy did not protect against adverse outcomes at 1 year in the Women’s International Transcatheter Aortic Valve Implantation Registry (WIN-TAVI), even though it did within the first 30 days, Alaide Chieffo, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
One year ago, at EuroPCR 2016, she reported that in WIN-TAVI, a history of pregnancy – albeit typically more than half a century previously – was independently associated with a 43% reduction in the Valve Academic Research Consortium-2 (VARC-2) 30-day composite endpoint, including death, stroke, major vascular complications, life-threatening bleeding, stage 2 or 3 acute kidney injury, coronary artery obstruction, or repeat transcatheter aortic valve replacement (TAVR) done because of valve-related dysfunction. Those early findings, first reported in this publication, were later published (JACC Cardiovasc Interv. 2016 Aug 8;9[15]:1589-600).
At 1 year of follow-up, however, the rate of the VARC-2 composite endpoint was no longer significantly different in women with or without a history of pregnancy. Nor was a history of pregnancy associated with a significantly reduced risk of the secondary endpoint of death or stroke: The 27% reduction in risk of this secondary endpoint in women with a history of pregnancy, compared with that of nulliparous women, didn’t achieve statistical significance in multivariate analysis, according to Dr. Chieffo of the San Raffaele Scientific Institute in Milan.
She speculated that pregnancy earlier in life provided strong protection against poor 30-day outcomes and a similar trend – albeit not statistically significant – at 1 year because women without children may have less family support.
“They are old women, left alone, without the family taking care of them. This is socially important, I think, because we are investing quite a lot of money in a procedure, and then maybe we’re adding adverse events because these patients are not properly taken care of when they are out of the hospital,” the interventional cardiologist said.
Neither of the other two female-specific characteristics evaluated in WIN-TAVI – having a history of osteoporosis or age at menopause – turned out to be related to the risk of bad outcomes at 1 year, she added.
WIN-TAVI is the first all-female registry of patients undergoing TAVR for severe aortic stenosis. The prospective, observational registry includes 1,019 women treated at 19 highly experienced European and North American TAVR centers. They averaged 82.5 years of age with a mean Society of Thoracic Surgeons score of 8.3%, putting them at intermediate or high surgical risk. A percutaneous transfemoral approach was used in 91% of cases. TAVR was performed under conscious sedation in 28% of the women and under local anesthesia in another 37%. Of the women in the registry, 42% received a newer-generation device.
In addition to the lack of significant impact of prior pregnancy on 1-year outcomes, another noteworthy finding at 1 year of follow-up was that preprocedural atrial fibrillation was independently associated with a 58% increase in the risk of death or stroke (P = .02). Prior percutaneous coronary intervention and EuroSCORE (European System for Cardiac Operative Risk Evaluation) were the only other independent predictors.
This observation suggests the need for a women-only randomized trial of TAVR versus surgical aortic valve replacement in women with intermediate surgical risk, Dr. Chieffo suggested. It will be important to learn whether the ability to surgically ablate preoperative atrial fibrillation in women during surgical valve replacement results in a lower 1-year risk of death or stroke than is achieved with TAVR.
Overall, the 1-year clinical outcomes seen in WIN-TAVI are “very good,” she noted. The VARC-2 composite endpoint occurred in 16.5% of women, all-cause mortality in 12.5%, cardiovascular mortality in 10.8%, and stroke in 2.2%. Only 3.2% of women were hospitalized for heart failure or valve-related symptoms. A new pacemaker was implanted in 12.7% of participants. At baseline 74% of women were New York Heart Association functional class III or IV; at 1 year, only 8.1% were. Moderate paravalvular aortic regurgitation was present in 6% of patients at 6 months and in 9.7% at 1 year
The WIN-TAVI registry is entirely self-funded. Dr. Chieffo reported having no financial conflicts regarding her presentation.
AT EuroPCR
Key clinical point:
Major finding: Prior pregnancy didn’t protect women against death or stroke at 1 year post TAVR.
Data source: WIN-TAVI, a prospective, multicenter, observational registry includes 1,019 women who underwent TAVR.
Disclosures: WIN-TAVI is entirely self-funded. The presenter reported having no financial conflicts.
Student Hospitalist Scholars: First experiences with clinical research
Editor’s Note: The Society of Hospital Medicine’s (SHM’s) Physician in Training Committee launched a scholarship program in 2015 for medical students to help transform health care and revolutionize patient care. The program has been expanded for the 2017-2018 year, offering two options for students to receive funding and engage in scholarly work during their first, second, and third years of medical school. As a part of the program, recipients are required to write about their experience on a biweekly basis.
The work on my summer project is moving along. Right now, I am collecting data from patients who had clinical deterioration events and unplanned transfers to the PICU in Cincinnati Children’s Hospital over the past year or so.
My mentor has been very helpful in this process by setting up regular meetings with me and keeping communications open. He has provided me with some data from Cincinnati Children’s Hospital that identifies emergency transfer cases, as well as clinical deterioration cases. This saves me a significant amount of time and decreases the potential for errors in the data, because I don’t have to go back and decide which cases were emergency transfers on my own. We are discussing some of the exclusion criteria for the study at this point as well.
I’m enjoying this project, as it is one of my first experiences with clinical research. In addition to the research experience, I am also learning a good amount of medicine as I learn about the care given to these complex patients.
Farah Hussain is a 2nd-year medical student at University of Cincinnati College of Medicine and student researcher at Cincinnati Children’s Hospital Medical Center. Her research interests involve bettering patient care to vulnerable populations.
Editor’s Note: The Society of Hospital Medicine’s (SHM’s) Physician in Training Committee launched a scholarship program in 2015 for medical students to help transform health care and revolutionize patient care. The program has been expanded for the 2017-2018 year, offering two options for students to receive funding and engage in scholarly work during their first, second, and third years of medical school. As a part of the program, recipients are required to write about their experience on a biweekly basis.
The work on my summer project is moving along. Right now, I am collecting data from patients who had clinical deterioration events and unplanned transfers to the PICU in Cincinnati Children’s Hospital over the past year or so.
My mentor has been very helpful in this process by setting up regular meetings with me and keeping communications open. He has provided me with some data from Cincinnati Children’s Hospital that identifies emergency transfer cases, as well as clinical deterioration cases. This saves me a significant amount of time and decreases the potential for errors in the data, because I don’t have to go back and decide which cases were emergency transfers on my own. We are discussing some of the exclusion criteria for the study at this point as well.
I’m enjoying this project, as it is one of my first experiences with clinical research. In addition to the research experience, I am also learning a good amount of medicine as I learn about the care given to these complex patients.
Farah Hussain is a 2nd-year medical student at University of Cincinnati College of Medicine and student researcher at Cincinnati Children’s Hospital Medical Center. Her research interests involve bettering patient care to vulnerable populations.
Editor’s Note: The Society of Hospital Medicine’s (SHM’s) Physician in Training Committee launched a scholarship program in 2015 for medical students to help transform health care and revolutionize patient care. The program has been expanded for the 2017-2018 year, offering two options for students to receive funding and engage in scholarly work during their first, second, and third years of medical school. As a part of the program, recipients are required to write about their experience on a biweekly basis.
The work on my summer project is moving along. Right now, I am collecting data from patients who had clinical deterioration events and unplanned transfers to the PICU in Cincinnati Children’s Hospital over the past year or so.
My mentor has been very helpful in this process by setting up regular meetings with me and keeping communications open. He has provided me with some data from Cincinnati Children’s Hospital that identifies emergency transfer cases, as well as clinical deterioration cases. This saves me a significant amount of time and decreases the potential for errors in the data, because I don’t have to go back and decide which cases were emergency transfers on my own. We are discussing some of the exclusion criteria for the study at this point as well.
I’m enjoying this project, as it is one of my first experiences with clinical research. In addition to the research experience, I am also learning a good amount of medicine as I learn about the care given to these complex patients.
Farah Hussain is a 2nd-year medical student at University of Cincinnati College of Medicine and student researcher at Cincinnati Children’s Hospital Medical Center. Her research interests involve bettering patient care to vulnerable populations.
A passion for education: Lonika Sood, MD
On top of her role as a hospitalist at the Aurora BayCare Medical Center in Green Bay, Wis., Lonika Sood, MD, FACP, is currently a candidate for a Masters in health professions education.
From her earliest training to the present day, she has maintained her passion for education, both as a student and an educator.
“I am a part of a community of practice, if you will, of other health professionals who do just this – medical education on a higher level.” Dr. Sood said. “Not only on the front lines of care, but also in designing curricula, undertaking medical education research, and holding leadership positions at medical schools and hospitals around the world.”
As one of the eight new members of The Hospitalist editorial advisory board, Dr. Sood is excited to use her role to help inform and to learn. She told us more about herself in a recent interview.
Q: How did you choose a career in medicine?
A: I grew up in India. I come from a family of doctors. When I was in high school, we found that we had close to 60 physicians in our family, and that number has grown quite a bit since then. At home, being around physicians, that was the language that I grew into. It was a big part of who I wanted to become when I grew up. The other part of it was that I’ve always wanted to help people and do something in one of the science fields, so this seemed like a natural choice for me.
Q: What made you choose hospital medicine?
A: I’ll be very honest – when I came to the United States for my residency, I wanted to become a subspecialist. I used to joke with my mentors in my residency program that every month I wanted to be a different subspecialist depending on which rotation I had or which physician really did a great job on the wards. After moving to Green Bay, Wis., I thought, “We’ll keep residency on hold for a couple of years.” Then I realized that I really liked medical education. I knew that I wanted to be a "specialist" in medical education, yet keep practicing internal medicine, which is something that I’ve always wanted to do. Being a hospitalist is like a marriage of those two passions.
Q: What about medical education draws you?
A: I think a large part of it was that my mother is a physician. My dad is in the merchant navy. In their midlife, they kind of fine-tuned their career paths by going into teaching, so both of them are educators, and very well accomplished in their own right. Growing up, that was a big part of what I saw myself becoming. I did not realize until later in my residency that it was my calling. Additionally, my experience of going into medicine and learning from good teachers is, in my mind, one of the things that really makes me comfortable, and happy being a doctor. I want to be able to leave that legacy for the coming generation.
Q: Tell us how your skills as a teacher help you when you’re working with your patients?
A: To give you an example, we have an adult internal medicine hospital, so we frequently have patients who come to the hospital for the first time. Some of our patients have not seen a physician in over 30 or 40 years. There may be many reasons for that, but they’re scared. They’re sick. They’re in a new environment. They are placing their trust in somebody else’s hands. As teachers and as doctors, it’s important for us to be compassionate, kind, and relatable to patients. We must also be able to explain to patients in their own words what is going on with their body, what might happen, and how can we help. We’re not telling patients what to do or forcing them to take our treatment recommendations, but we are helping them make informed choices. I think hospital medicine really is an incredibly powerful field that can help us relate to our patients.
Q: What is the best professional advice you have received in medicine?
A: I think the advice that I try to follow every day is to be humble. Try to be the best that you can be, yet stay humble, because there’s so much more that you can accomplish if you stay grounded. I think that has stuck with me. It’s come from my parents. It’s come from my mentors. And sometimes it comes from my patients, too.
Q: What is the worst advice you have received?
A: That’s a hard question, but an important one as well, I think. Sometimes there is a push – from society or your colleagues – to be as efficient as you can be, which is great, but we have to look at the downside of it. We sometimes don’t stop and think, or stop and be human. We’re kind of mechanical if data are all we follow.
Q: So where do you see yourself in the next 10 years?
A: That’s a question I try to answer daily, and I get a different answer each time. I think I do see myself continuing to provide clinical care for hospitalized patients. I see myself doing a little more in educational leadership, working with medical students and medical residents. I’m just completing my master’s in health professions education, so I’m excited to also start a career in medical education research.
Q: What’s the best book that you’ve read recently, and why was it the best?
A: Oh, well, it’s not a new book, and I’ve read this before, but I keep coming back to it. I don’t know if you’ve heard of Jim Corbett. He was a wildlife enthusiast in the early 20th century. He wrote a lot of books on man-eating tigers and leopards in India. My brother and I and my dad used to read these books growing up. That’s something that I’m going back to and rereading. There is a lot of rich description about Indian wildlife, and it’s something that brings back good memories.
On top of her role as a hospitalist at the Aurora BayCare Medical Center in Green Bay, Wis., Lonika Sood, MD, FACP, is currently a candidate for a Masters in health professions education.
From her earliest training to the present day, she has maintained her passion for education, both as a student and an educator.
“I am a part of a community of practice, if you will, of other health professionals who do just this – medical education on a higher level.” Dr. Sood said. “Not only on the front lines of care, but also in designing curricula, undertaking medical education research, and holding leadership positions at medical schools and hospitals around the world.”
As one of the eight new members of The Hospitalist editorial advisory board, Dr. Sood is excited to use her role to help inform and to learn. She told us more about herself in a recent interview.
Q: How did you choose a career in medicine?
A: I grew up in India. I come from a family of doctors. When I was in high school, we found that we had close to 60 physicians in our family, and that number has grown quite a bit since then. At home, being around physicians, that was the language that I grew into. It was a big part of who I wanted to become when I grew up. The other part of it was that I’ve always wanted to help people and do something in one of the science fields, so this seemed like a natural choice for me.
Q: What made you choose hospital medicine?
A: I’ll be very honest – when I came to the United States for my residency, I wanted to become a subspecialist. I used to joke with my mentors in my residency program that every month I wanted to be a different subspecialist depending on which rotation I had or which physician really did a great job on the wards. After moving to Green Bay, Wis., I thought, “We’ll keep residency on hold for a couple of years.” Then I realized that I really liked medical education. I knew that I wanted to be a "specialist" in medical education, yet keep practicing internal medicine, which is something that I’ve always wanted to do. Being a hospitalist is like a marriage of those two passions.
Q: What about medical education draws you?
A: I think a large part of it was that my mother is a physician. My dad is in the merchant navy. In their midlife, they kind of fine-tuned their career paths by going into teaching, so both of them are educators, and very well accomplished in their own right. Growing up, that was a big part of what I saw myself becoming. I did not realize until later in my residency that it was my calling. Additionally, my experience of going into medicine and learning from good teachers is, in my mind, one of the things that really makes me comfortable, and happy being a doctor. I want to be able to leave that legacy for the coming generation.
Q: Tell us how your skills as a teacher help you when you’re working with your patients?
A: To give you an example, we have an adult internal medicine hospital, so we frequently have patients who come to the hospital for the first time. Some of our patients have not seen a physician in over 30 or 40 years. There may be many reasons for that, but they’re scared. They’re sick. They’re in a new environment. They are placing their trust in somebody else’s hands. As teachers and as doctors, it’s important for us to be compassionate, kind, and relatable to patients. We must also be able to explain to patients in their own words what is going on with their body, what might happen, and how can we help. We’re not telling patients what to do or forcing them to take our treatment recommendations, but we are helping them make informed choices. I think hospital medicine really is an incredibly powerful field that can help us relate to our patients.
Q: What is the best professional advice you have received in medicine?
A: I think the advice that I try to follow every day is to be humble. Try to be the best that you can be, yet stay humble, because there’s so much more that you can accomplish if you stay grounded. I think that has stuck with me. It’s come from my parents. It’s come from my mentors. And sometimes it comes from my patients, too.
Q: What is the worst advice you have received?
A: That’s a hard question, but an important one as well, I think. Sometimes there is a push – from society or your colleagues – to be as efficient as you can be, which is great, but we have to look at the downside of it. We sometimes don’t stop and think, or stop and be human. We’re kind of mechanical if data are all we follow.
Q: So where do you see yourself in the next 10 years?
A: That’s a question I try to answer daily, and I get a different answer each time. I think I do see myself continuing to provide clinical care for hospitalized patients. I see myself doing a little more in educational leadership, working with medical students and medical residents. I’m just completing my master’s in health professions education, so I’m excited to also start a career in medical education research.
Q: What’s the best book that you’ve read recently, and why was it the best?
A: Oh, well, it’s not a new book, and I’ve read this before, but I keep coming back to it. I don’t know if you’ve heard of Jim Corbett. He was a wildlife enthusiast in the early 20th century. He wrote a lot of books on man-eating tigers and leopards in India. My brother and I and my dad used to read these books growing up. That’s something that I’m going back to and rereading. There is a lot of rich description about Indian wildlife, and it’s something that brings back good memories.
On top of her role as a hospitalist at the Aurora BayCare Medical Center in Green Bay, Wis., Lonika Sood, MD, FACP, is currently a candidate for a Masters in health professions education.
From her earliest training to the present day, she has maintained her passion for education, both as a student and an educator.
“I am a part of a community of practice, if you will, of other health professionals who do just this – medical education on a higher level.” Dr. Sood said. “Not only on the front lines of care, but also in designing curricula, undertaking medical education research, and holding leadership positions at medical schools and hospitals around the world.”
As one of the eight new members of The Hospitalist editorial advisory board, Dr. Sood is excited to use her role to help inform and to learn. She told us more about herself in a recent interview.
Q: How did you choose a career in medicine?
A: I grew up in India. I come from a family of doctors. When I was in high school, we found that we had close to 60 physicians in our family, and that number has grown quite a bit since then. At home, being around physicians, that was the language that I grew into. It was a big part of who I wanted to become when I grew up. The other part of it was that I’ve always wanted to help people and do something in one of the science fields, so this seemed like a natural choice for me.
Q: What made you choose hospital medicine?
A: I’ll be very honest – when I came to the United States for my residency, I wanted to become a subspecialist. I used to joke with my mentors in my residency program that every month I wanted to be a different subspecialist depending on which rotation I had or which physician really did a great job on the wards. After moving to Green Bay, Wis., I thought, “We’ll keep residency on hold for a couple of years.” Then I realized that I really liked medical education. I knew that I wanted to be a "specialist" in medical education, yet keep practicing internal medicine, which is something that I’ve always wanted to do. Being a hospitalist is like a marriage of those two passions.
Q: What about medical education draws you?
A: I think a large part of it was that my mother is a physician. My dad is in the merchant navy. In their midlife, they kind of fine-tuned their career paths by going into teaching, so both of them are educators, and very well accomplished in their own right. Growing up, that was a big part of what I saw myself becoming. I did not realize until later in my residency that it was my calling. Additionally, my experience of going into medicine and learning from good teachers is, in my mind, one of the things that really makes me comfortable, and happy being a doctor. I want to be able to leave that legacy for the coming generation.
Q: Tell us how your skills as a teacher help you when you’re working with your patients?
A: To give you an example, we have an adult internal medicine hospital, so we frequently have patients who come to the hospital for the first time. Some of our patients have not seen a physician in over 30 or 40 years. There may be many reasons for that, but they’re scared. They’re sick. They’re in a new environment. They are placing their trust in somebody else’s hands. As teachers and as doctors, it’s important for us to be compassionate, kind, and relatable to patients. We must also be able to explain to patients in their own words what is going on with their body, what might happen, and how can we help. We’re not telling patients what to do or forcing them to take our treatment recommendations, but we are helping them make informed choices. I think hospital medicine really is an incredibly powerful field that can help us relate to our patients.
Q: What is the best professional advice you have received in medicine?
A: I think the advice that I try to follow every day is to be humble. Try to be the best that you can be, yet stay humble, because there’s so much more that you can accomplish if you stay grounded. I think that has stuck with me. It’s come from my parents. It’s come from my mentors. And sometimes it comes from my patients, too.
Q: What is the worst advice you have received?
A: That’s a hard question, but an important one as well, I think. Sometimes there is a push – from society or your colleagues – to be as efficient as you can be, which is great, but we have to look at the downside of it. We sometimes don’t stop and think, or stop and be human. We’re kind of mechanical if data are all we follow.
Q: So where do you see yourself in the next 10 years?
A: That’s a question I try to answer daily, and I get a different answer each time. I think I do see myself continuing to provide clinical care for hospitalized patients. I see myself doing a little more in educational leadership, working with medical students and medical residents. I’m just completing my master’s in health professions education, so I’m excited to also start a career in medical education research.
Q: What’s the best book that you’ve read recently, and why was it the best?
A: Oh, well, it’s not a new book, and I’ve read this before, but I keep coming back to it. I don’t know if you’ve heard of Jim Corbett. He was a wildlife enthusiast in the early 20th century. He wrote a lot of books on man-eating tigers and leopards in India. My brother and I and my dad used to read these books growing up. That’s something that I’m going back to and rereading. There is a lot of rich description about Indian wildlife, and it’s something that brings back good memories.