User login
Update and Clinical Use of Imaging Technologies for Pigmented Lesions of the Skin
Allison T. O’Donnell, MPH, and Caroline C. Kim, MD
The incidence of melanoma is on the rise, and early detection of disease is imperative to reduce mortality. Dermatologists are key players in the early detection of melanoma; however, some clinicians rely on their clinical examination without any additional diagnostic tools to make this important diagnosis. Certain patients, such as atypical nevus patients, have more complicated mole examinations, making the diagnosis of melanoma difficult, whereas some melanomas, such as amelanotic melanomas, can be diagnostically challenging. The goal of the clinician is to detect melanoma with the highest accuracy, while avoiding unnecessary biopsies. Using diagnostic melanoma tools as an adjunct to the clinical examination, dermatologists have the opportunity to increase both their sensitivity and specificity for melanoma detection. This article will review current imaging technologies and those in development for pigmented lesions, updating the clinician on basic principals of such modalities and clinical use of such technologies in practice.
*For a PDF of the full article, click on the link to the left of this introduction.
Allison T. O’Donnell, MPH, and Caroline C. Kim, MD
The incidence of melanoma is on the rise, and early detection of disease is imperative to reduce mortality. Dermatologists are key players in the early detection of melanoma; however, some clinicians rely on their clinical examination without any additional diagnostic tools to make this important diagnosis. Certain patients, such as atypical nevus patients, have more complicated mole examinations, making the diagnosis of melanoma difficult, whereas some melanomas, such as amelanotic melanomas, can be diagnostically challenging. The goal of the clinician is to detect melanoma with the highest accuracy, while avoiding unnecessary biopsies. Using diagnostic melanoma tools as an adjunct to the clinical examination, dermatologists have the opportunity to increase both their sensitivity and specificity for melanoma detection. This article will review current imaging technologies and those in development for pigmented lesions, updating the clinician on basic principals of such modalities and clinical use of such technologies in practice.
*For a PDF of the full article, click on the link to the left of this introduction.
Allison T. O’Donnell, MPH, and Caroline C. Kim, MD
The incidence of melanoma is on the rise, and early detection of disease is imperative to reduce mortality. Dermatologists are key players in the early detection of melanoma; however, some clinicians rely on their clinical examination without any additional diagnostic tools to make this important diagnosis. Certain patients, such as atypical nevus patients, have more complicated mole examinations, making the diagnosis of melanoma difficult, whereas some melanomas, such as amelanotic melanomas, can be diagnostically challenging. The goal of the clinician is to detect melanoma with the highest accuracy, while avoiding unnecessary biopsies. Using diagnostic melanoma tools as an adjunct to the clinical examination, dermatologists have the opportunity to increase both their sensitivity and specificity for melanoma detection. This article will review current imaging technologies and those in development for pigmented lesions, updating the clinician on basic principals of such modalities and clinical use of such technologies in practice.
*For a PDF of the full article, click on the link to the left of this introduction.
Malignant Melanoma: Advances in Diagnosis, Prognosis, and Treatment
Michael Krathen, MD
The detection of cutaneous melanoma still largely relies on clinical suspicion, skin biopsy, and histopathologic evaluation. New technologies are being evaluated to bypass the skin biopsy in the detection of melanoma. The quest for reliable biomarkers, with respect to subclinical detection, prognosis, and predicting treatment response, is longstanding and ongoing. New therapies have been developed for metastatic disease, including targeted small molecule inhibitors as well as immune modulators.
*For a PDF of the full article, click on the link to the left of this introduction.
Michael Krathen, MD
The detection of cutaneous melanoma still largely relies on clinical suspicion, skin biopsy, and histopathologic evaluation. New technologies are being evaluated to bypass the skin biopsy in the detection of melanoma. The quest for reliable biomarkers, with respect to subclinical detection, prognosis, and predicting treatment response, is longstanding and ongoing. New therapies have been developed for metastatic disease, including targeted small molecule inhibitors as well as immune modulators.
*For a PDF of the full article, click on the link to the left of this introduction.
Michael Krathen, MD
The detection of cutaneous melanoma still largely relies on clinical suspicion, skin biopsy, and histopathologic evaluation. New technologies are being evaluated to bypass the skin biopsy in the detection of melanoma. The quest for reliable biomarkers, with respect to subclinical detection, prognosis, and predicting treatment response, is longstanding and ongoing. New therapies have been developed for metastatic disease, including targeted small molecule inhibitors as well as immune modulators.
*For a PDF of the full article, click on the link to the left of this introduction.
Molecular Mechanisms of Melanoma
Malignant Melanoma in Transplant Patients: A Case Report and Review of the Literature
Metastatic Melanoma and Melanogenuria
What Is Your Diagnosis? Anal Mucosal Melanoma
New Melanoma Treatments: A Panacea or a Pandora's Box? [editorial]
Vemurafenib in melanoma with the BRAF V600E mutation
Vemurafenib, an oral inhibitor of some mutated forms of the BRAF serine threonine kinase, was recently approved for the treatment of patients with unresectable or metastatic melanoma with the BRAF V600E mutation as detected by an FDA- approved test. It is not recommended for use in patients with wild-type BRAF melanoma. The clinical trial supporting approval of vemurafenib (PLX4032) was performed in treatment-naïve patients with the V600E mutation as detected by the Cobas 4800 BRAF V600 Mutation Test. About 40%-60% of cutaneous melanomas have BRAF mutations that result in constitutive activation of downstream signaling through the MAPK pathway; about 90% of those carry the V600E mutation.
*For a PDF of the full article, click on the link to the left of this introduction.
Vemurafenib, an oral inhibitor of some mutated forms of the BRAF serine threonine kinase, was recently approved for the treatment of patients with unresectable or metastatic melanoma with the BRAF V600E mutation as detected by an FDA- approved test. It is not recommended for use in patients with wild-type BRAF melanoma. The clinical trial supporting approval of vemurafenib (PLX4032) was performed in treatment-naïve patients with the V600E mutation as detected by the Cobas 4800 BRAF V600 Mutation Test. About 40%-60% of cutaneous melanomas have BRAF mutations that result in constitutive activation of downstream signaling through the MAPK pathway; about 90% of those carry the V600E mutation.
*For a PDF of the full article, click on the link to the left of this introduction.
Vemurafenib, an oral inhibitor of some mutated forms of the BRAF serine threonine kinase, was recently approved for the treatment of patients with unresectable or metastatic melanoma with the BRAF V600E mutation as detected by an FDA- approved test. It is not recommended for use in patients with wild-type BRAF melanoma. The clinical trial supporting approval of vemurafenib (PLX4032) was performed in treatment-naïve patients with the V600E mutation as detected by the Cobas 4800 BRAF V600 Mutation Test. About 40%-60% of cutaneous melanomas have BRAF mutations that result in constitutive activation of downstream signaling through the MAPK pathway; about 90% of those carry the V600E mutation.
*For a PDF of the full article, click on the link to the left of this introduction.
'Early, Proactive' Management of Chemo Toxicites Improves QOL
Skin conditions in cancer patients can lead to a decreased quality of life because of the psychosocial impact, financial burden, poor health, and disruption of anticancer treatments, said Dr. Mario E. Lacouture at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Clinical trials are underway to address management, cost, and quality of life, but in the meantime, "an early and proactive approach toward toxicities is advisable," he said.
Dr. Lacouture, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York, discussed common cancer-associated dermatology at the seminar.
• Rashes. A RAF inhibitor–induced rash can occur within 1-2 weeks of starting treatment, Dr. Lacouture noted. This rash is associated with sensations of burning or itching in photo-exposed areas. In most cases, the rash can be managed with topical steroids and oral GABA agonists. Vemurafenib use also has been associated with rashes, as well as with photosensitivity, itching, and alopecia, he said.
In addition, mTOR inhibitor–induced rashes involving erythematous pruritic papules and ulcerlike lesions have been observed in patients on everolimus and temsirolimus.
• Skin cancers. Data from several studies suggest that the incidence of squamous cell carcinomas in patients on RAF inhibitors is 7%, and the incidence of actinic keratoses in these patients is 4%, according to Dr. Lacouture. These conditions usually develop after approximately 6 months of treatment. They can be managed by surgery or destruction; and there have been no reports of metastases.
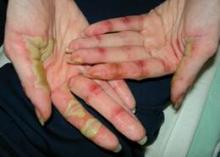
• Hand-foot syndrome. Hand-Foot Syndrome (HFSR) is a common side effect in cancer patients that usually occurs within 45 days of starting treatment, said Dr. Lacouture. HFSR is often associated with the use of sorafenib, sunitinib, and pazopanib, and the histology of these patients shows epidermal necrosis, he noted. Patients who develop HFSR may need to temporarily reduce their medications. Additional management of HFSR includes avoiding excess pressure on the affected areas and keeping them cool and moist to reduce patient discomfort.
• Hair and nail changes. Changes in hair can occur in patients being treated with epidermal growth factor receptor inhibitors (EGFRIs), including a slower hair growth rate and alopecia, Dr. Lacouture said. Changes in hair texture such as increased brittleness and hair curling also have been observed, he said. Other hair-related adverse events can include hirsutism on the face and eyelash trichomegaly. In addition, paronychia has been observed in patients on EGFRIs for more than 6 months.
• Radiation dermatitis. Approximately 50% of cancer patients develop radiation dermatitis, including 87% of breast cancer patients, reported Dr. Lacouture. However, the treatment of radiation dermatitis remains challenging, he said. In several studies, patients who used a nonsteroidal topical, including aloe vera and trolamine, showed no significant improvement in radiation dermatitis, compared with controls. However, studies are ongoing, and significant improvements in radiation dermatitis in breast cancer patients have been seen with topical corticosteroids including mometasone, beclomethasone, and betamethasone.
Dr. Lacouture disclosed financial relationships with multiple companies including Amgen, Bristol-Myers Squibb, Genentech, GlaxoSmithKline, Merck, and Roche. SDEF and this news organization are owned by Elsevier.
Skin conditions in cancer patients can lead to a decreased quality of life because of the psychosocial impact, financial burden, poor health, and disruption of anticancer treatments, said Dr. Mario E. Lacouture at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Clinical trials are underway to address management, cost, and quality of life, but in the meantime, "an early and proactive approach toward toxicities is advisable," he said.
Dr. Lacouture, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York, discussed common cancer-associated dermatology at the seminar.
• Rashes. A RAF inhibitor–induced rash can occur within 1-2 weeks of starting treatment, Dr. Lacouture noted. This rash is associated with sensations of burning or itching in photo-exposed areas. In most cases, the rash can be managed with topical steroids and oral GABA agonists. Vemurafenib use also has been associated with rashes, as well as with photosensitivity, itching, and alopecia, he said.
In addition, mTOR inhibitor–induced rashes involving erythematous pruritic papules and ulcerlike lesions have been observed in patients on everolimus and temsirolimus.
• Skin cancers. Data from several studies suggest that the incidence of squamous cell carcinomas in patients on RAF inhibitors is 7%, and the incidence of actinic keratoses in these patients is 4%, according to Dr. Lacouture. These conditions usually develop after approximately 6 months of treatment. They can be managed by surgery or destruction; and there have been no reports of metastases.
• Hand-foot syndrome. Hand-Foot Syndrome (HFSR) is a common side effect in cancer patients that usually occurs within 45 days of starting treatment, said Dr. Lacouture. HFSR is often associated with the use of sorafenib, sunitinib, and pazopanib, and the histology of these patients shows epidermal necrosis, he noted. Patients who develop HFSR may need to temporarily reduce their medications. Additional management of HFSR includes avoiding excess pressure on the affected areas and keeping them cool and moist to reduce patient discomfort.
• Hair and nail changes. Changes in hair can occur in patients being treated with epidermal growth factor receptor inhibitors (EGFRIs), including a slower hair growth rate and alopecia, Dr. Lacouture said. Changes in hair texture such as increased brittleness and hair curling also have been observed, he said. Other hair-related adverse events can include hirsutism on the face and eyelash trichomegaly. In addition, paronychia has been observed in patients on EGFRIs for more than 6 months.
• Radiation dermatitis. Approximately 50% of cancer patients develop radiation dermatitis, including 87% of breast cancer patients, reported Dr. Lacouture. However, the treatment of radiation dermatitis remains challenging, he said. In several studies, patients who used a nonsteroidal topical, including aloe vera and trolamine, showed no significant improvement in radiation dermatitis, compared with controls. However, studies are ongoing, and significant improvements in radiation dermatitis in breast cancer patients have been seen with topical corticosteroids including mometasone, beclomethasone, and betamethasone.
Dr. Lacouture disclosed financial relationships with multiple companies including Amgen, Bristol-Myers Squibb, Genentech, GlaxoSmithKline, Merck, and Roche. SDEF and this news organization are owned by Elsevier.
Skin conditions in cancer patients can lead to a decreased quality of life because of the psychosocial impact, financial burden, poor health, and disruption of anticancer treatments, said Dr. Mario E. Lacouture at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Clinical trials are underway to address management, cost, and quality of life, but in the meantime, "an early and proactive approach toward toxicities is advisable," he said.
Dr. Lacouture, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York, discussed common cancer-associated dermatology at the seminar.
• Rashes. A RAF inhibitor–induced rash can occur within 1-2 weeks of starting treatment, Dr. Lacouture noted. This rash is associated with sensations of burning or itching in photo-exposed areas. In most cases, the rash can be managed with topical steroids and oral GABA agonists. Vemurafenib use also has been associated with rashes, as well as with photosensitivity, itching, and alopecia, he said.
In addition, mTOR inhibitor–induced rashes involving erythematous pruritic papules and ulcerlike lesions have been observed in patients on everolimus and temsirolimus.
• Skin cancers. Data from several studies suggest that the incidence of squamous cell carcinomas in patients on RAF inhibitors is 7%, and the incidence of actinic keratoses in these patients is 4%, according to Dr. Lacouture. These conditions usually develop after approximately 6 months of treatment. They can be managed by surgery or destruction; and there have been no reports of metastases.
• Hand-foot syndrome. Hand-Foot Syndrome (HFSR) is a common side effect in cancer patients that usually occurs within 45 days of starting treatment, said Dr. Lacouture. HFSR is often associated with the use of sorafenib, sunitinib, and pazopanib, and the histology of these patients shows epidermal necrosis, he noted. Patients who develop HFSR may need to temporarily reduce their medications. Additional management of HFSR includes avoiding excess pressure on the affected areas and keeping them cool and moist to reduce patient discomfort.
• Hair and nail changes. Changes in hair can occur in patients being treated with epidermal growth factor receptor inhibitors (EGFRIs), including a slower hair growth rate and alopecia, Dr. Lacouture said. Changes in hair texture such as increased brittleness and hair curling also have been observed, he said. Other hair-related adverse events can include hirsutism on the face and eyelash trichomegaly. In addition, paronychia has been observed in patients on EGFRIs for more than 6 months.
• Radiation dermatitis. Approximately 50% of cancer patients develop radiation dermatitis, including 87% of breast cancer patients, reported Dr. Lacouture. However, the treatment of radiation dermatitis remains challenging, he said. In several studies, patients who used a nonsteroidal topical, including aloe vera and trolamine, showed no significant improvement in radiation dermatitis, compared with controls. However, studies are ongoing, and significant improvements in radiation dermatitis in breast cancer patients have been seen with topical corticosteroids including mometasone, beclomethasone, and betamethasone.
Dr. Lacouture disclosed financial relationships with multiple companies including Amgen, Bristol-Myers Squibb, Genentech, GlaxoSmithKline, Merck, and Roche. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
VEGF-Targeting Cancer Drugs Raise Risk of Fatal Side Effects
SAN FRANCISCO – Tyrosine kinase inhibitors that target the vascular endothelial growth factor receptor increase the risk of a fatal adverse event in cancer patients, but the absolute rate is still low, investigators concluded from a meta-analysis of 10 randomized trials with a total of 4,679 patients.
Trial participants given sorafenib (Nexavar), sunitinib (Sutent), or pazopanib (Votrient) were more than twice as likely to die from an adverse event as were peers given control treatment, said lead investigator Dr. Christopher J. Richards of the Beth Israel Deaconess Medical Center in Boston. Yet, the rate was still less than 2%.
"Our analysis may underestimate the true incidence of fatal adverse events, as study patients may be healthier than the general population exposed to these drugs," he noted at the Genitourinary Cancers Symposium. But that said, "all three of the study drugs have been shown in various randomized controlled trials to improve clinical outcomes compared to traditional therapies."
Discussant Dr. Thomas E. Hutson of the Baylor Sammons Cancer Center in Dallas commented, "I feel confident that everyone or almost everyone in the room today would agree with me that our current therapy benefit outweighs the risk associated with the treatment."
Moreover, even among the new targeted agents, the 1.5% rate seen with the vascular endothelial growth factor receptor (VEGFR) tyrosine kinase inhibitors (TKIs) in the meta-analysis "compares very favorably" with the rate of 2.9% seen previously with bevacizumab (Avastin), another VEGF-targeted therapy, in a similar analysis (JAMA 2011;305:487-94).
"Targeted therapies have real toxicities, and these toxicities include a low risk of death – a risk of death not much different than other therapies used for kidney and other cancer types," Dr. Hutson asserted. "If anything, this meta-analysis shows us that close monitoring is going to be essential for optimal use of these agents."
In the study, Dr. Richards and his colleagues identified 10 randomized controlled phase II or III trials in which patients received any of three VEGFR TKIs approved by the Food and Drug Administration for cancer treatment as of February 2011: sorafenib, sunitinib, or pazopanib. The control groups were usually treated with a placebo, but in some cases with chemotherapy or immunotherapy.
The enrolled patients had a variety of malignancies: renal cell carcinoma, hepatocellular carcinoma, melanoma, non–small cell lung cancer, breast cancer, and pancreatic neuroendocrine tumor. "All patients included in the studies had good performance status and had adequate baseline cardiac, hematologic, and renal function at the time of study entry," Dr. Richards pointed out.
In a pooled analysis, relative to control treatment, VEGFR TKI treatment was associated with a 2.23-fold increased risk of fatal adverse events (P = .02). But even so, the absolute rate of such events was just 1.5%, compared with 0.7% with the control treatment.
In stratified analyses, there was no significant difference in the relative risks across the three agents or the relative risks for renal cell carcinoma vs. other types of cancer.
The most common fatal adverse events in the trials overall (considering both control and VEGFR TKI arms) were hemorrhage (48% of the total), myocardial infarction (15%), and hepatic failure (10%). These events "occurred in both the placebo and control groups as well as study groups," Dr. Richards noted.
He acknowledged that limitations of the study included the fact that the analysis used study-level instead of patient-level data, which may have resulted in confounding, and that it did not have adequate power to detect differences between the three VEGFR TKIs, although they all have a similar mechanism of action.
The symposium was sponsored by the American Society of Clinical Oncology, the American Society for Radiation Oncology, and the Society of Urologic Oncology.
Dr. Richards disclosed that he had no relevant conflicts of interest. Dr. Hutson disclosed that he is a consultant to and receives honoraria from Bayer, Genentech, GlaxoSmithKline, Novartis, Onyx, Pfizer, and Wyeth, and that he receives research funding from GlaxoSmithKline, Pfizer, and Wyeth.
SAN FRANCISCO – Tyrosine kinase inhibitors that target the vascular endothelial growth factor receptor increase the risk of a fatal adverse event in cancer patients, but the absolute rate is still low, investigators concluded from a meta-analysis of 10 randomized trials with a total of 4,679 patients.
Trial participants given sorafenib (Nexavar), sunitinib (Sutent), or pazopanib (Votrient) were more than twice as likely to die from an adverse event as were peers given control treatment, said lead investigator Dr. Christopher J. Richards of the Beth Israel Deaconess Medical Center in Boston. Yet, the rate was still less than 2%.
"Our analysis may underestimate the true incidence of fatal adverse events, as study patients may be healthier than the general population exposed to these drugs," he noted at the Genitourinary Cancers Symposium. But that said, "all three of the study drugs have been shown in various randomized controlled trials to improve clinical outcomes compared to traditional therapies."
Discussant Dr. Thomas E. Hutson of the Baylor Sammons Cancer Center in Dallas commented, "I feel confident that everyone or almost everyone in the room today would agree with me that our current therapy benefit outweighs the risk associated with the treatment."
Moreover, even among the new targeted agents, the 1.5% rate seen with the vascular endothelial growth factor receptor (VEGFR) tyrosine kinase inhibitors (TKIs) in the meta-analysis "compares very favorably" with the rate of 2.9% seen previously with bevacizumab (Avastin), another VEGF-targeted therapy, in a similar analysis (JAMA 2011;305:487-94).
"Targeted therapies have real toxicities, and these toxicities include a low risk of death – a risk of death not much different than other therapies used for kidney and other cancer types," Dr. Hutson asserted. "If anything, this meta-analysis shows us that close monitoring is going to be essential for optimal use of these agents."
In the study, Dr. Richards and his colleagues identified 10 randomized controlled phase II or III trials in which patients received any of three VEGFR TKIs approved by the Food and Drug Administration for cancer treatment as of February 2011: sorafenib, sunitinib, or pazopanib. The control groups were usually treated with a placebo, but in some cases with chemotherapy or immunotherapy.
The enrolled patients had a variety of malignancies: renal cell carcinoma, hepatocellular carcinoma, melanoma, non–small cell lung cancer, breast cancer, and pancreatic neuroendocrine tumor. "All patients included in the studies had good performance status and had adequate baseline cardiac, hematologic, and renal function at the time of study entry," Dr. Richards pointed out.
In a pooled analysis, relative to control treatment, VEGFR TKI treatment was associated with a 2.23-fold increased risk of fatal adverse events (P = .02). But even so, the absolute rate of such events was just 1.5%, compared with 0.7% with the control treatment.
In stratified analyses, there was no significant difference in the relative risks across the three agents or the relative risks for renal cell carcinoma vs. other types of cancer.
The most common fatal adverse events in the trials overall (considering both control and VEGFR TKI arms) were hemorrhage (48% of the total), myocardial infarction (15%), and hepatic failure (10%). These events "occurred in both the placebo and control groups as well as study groups," Dr. Richards noted.
He acknowledged that limitations of the study included the fact that the analysis used study-level instead of patient-level data, which may have resulted in confounding, and that it did not have adequate power to detect differences between the three VEGFR TKIs, although they all have a similar mechanism of action.
The symposium was sponsored by the American Society of Clinical Oncology, the American Society for Radiation Oncology, and the Society of Urologic Oncology.
Dr. Richards disclosed that he had no relevant conflicts of interest. Dr. Hutson disclosed that he is a consultant to and receives honoraria from Bayer, Genentech, GlaxoSmithKline, Novartis, Onyx, Pfizer, and Wyeth, and that he receives research funding from GlaxoSmithKline, Pfizer, and Wyeth.
SAN FRANCISCO – Tyrosine kinase inhibitors that target the vascular endothelial growth factor receptor increase the risk of a fatal adverse event in cancer patients, but the absolute rate is still low, investigators concluded from a meta-analysis of 10 randomized trials with a total of 4,679 patients.
Trial participants given sorafenib (Nexavar), sunitinib (Sutent), or pazopanib (Votrient) were more than twice as likely to die from an adverse event as were peers given control treatment, said lead investigator Dr. Christopher J. Richards of the Beth Israel Deaconess Medical Center in Boston. Yet, the rate was still less than 2%.
"Our analysis may underestimate the true incidence of fatal adverse events, as study patients may be healthier than the general population exposed to these drugs," he noted at the Genitourinary Cancers Symposium. But that said, "all three of the study drugs have been shown in various randomized controlled trials to improve clinical outcomes compared to traditional therapies."
Discussant Dr. Thomas E. Hutson of the Baylor Sammons Cancer Center in Dallas commented, "I feel confident that everyone or almost everyone in the room today would agree with me that our current therapy benefit outweighs the risk associated with the treatment."
Moreover, even among the new targeted agents, the 1.5% rate seen with the vascular endothelial growth factor receptor (VEGFR) tyrosine kinase inhibitors (TKIs) in the meta-analysis "compares very favorably" with the rate of 2.9% seen previously with bevacizumab (Avastin), another VEGF-targeted therapy, in a similar analysis (JAMA 2011;305:487-94).
"Targeted therapies have real toxicities, and these toxicities include a low risk of death – a risk of death not much different than other therapies used for kidney and other cancer types," Dr. Hutson asserted. "If anything, this meta-analysis shows us that close monitoring is going to be essential for optimal use of these agents."
In the study, Dr. Richards and his colleagues identified 10 randomized controlled phase II or III trials in which patients received any of three VEGFR TKIs approved by the Food and Drug Administration for cancer treatment as of February 2011: sorafenib, sunitinib, or pazopanib. The control groups were usually treated with a placebo, but in some cases with chemotherapy or immunotherapy.
The enrolled patients had a variety of malignancies: renal cell carcinoma, hepatocellular carcinoma, melanoma, non–small cell lung cancer, breast cancer, and pancreatic neuroendocrine tumor. "All patients included in the studies had good performance status and had adequate baseline cardiac, hematologic, and renal function at the time of study entry," Dr. Richards pointed out.
In a pooled analysis, relative to control treatment, VEGFR TKI treatment was associated with a 2.23-fold increased risk of fatal adverse events (P = .02). But even so, the absolute rate of such events was just 1.5%, compared with 0.7% with the control treatment.
In stratified analyses, there was no significant difference in the relative risks across the three agents or the relative risks for renal cell carcinoma vs. other types of cancer.
The most common fatal adverse events in the trials overall (considering both control and VEGFR TKI arms) were hemorrhage (48% of the total), myocardial infarction (15%), and hepatic failure (10%). These events "occurred in both the placebo and control groups as well as study groups," Dr. Richards noted.
He acknowledged that limitations of the study included the fact that the analysis used study-level instead of patient-level data, which may have resulted in confounding, and that it did not have adequate power to detect differences between the three VEGFR TKIs, although they all have a similar mechanism of action.
The symposium was sponsored by the American Society of Clinical Oncology, the American Society for Radiation Oncology, and the Society of Urologic Oncology.
Dr. Richards disclosed that he had no relevant conflicts of interest. Dr. Hutson disclosed that he is a consultant to and receives honoraria from Bayer, Genentech, GlaxoSmithKline, Novartis, Onyx, Pfizer, and Wyeth, and that he receives research funding from GlaxoSmithKline, Pfizer, and Wyeth.
FROM THE GENITOURINARY CANCERS SYMPOSIUM