User login
Liquid biopsy–based test detects BRAF mutations
Analysis of plasma-derived cell-free DNA can identify BRAF mutations as accurately as formalin-fixed paraffin-embedded tumor sample analysis, investigators report.
Of 160 patients with advanced solid tumors, BRAF V600 mutations were detected in 62 (39%) archival formalin-fixed paraffin-embedded (FFPE) tumor samples and 47 (29%) plasma cell-free (cf) DNA samples. The two methods had overall agreement in 141 patients (88%; kappa coefficient, 0.74; SE, 0.06; 95% confidence interval, 0.63-0.85), Dr. Filip Janku of the University of Texas and his associates reported (Mol Cancer Ther. 2016 May 20. doi: 10.1158/1535-7163.MCT-15-0712).
BRAF mutations are prevalent in many types of advanced cancers, and targeting these mutations has demonstrated efficacy, but current assessment of BRAF mutations is limited by a lack of tissue samples and complicated by constantly changing mutation status.
cfDNA is secreted into the circulation by tumor cells and cells in the tumor microenvironment that are undergoing apoptosis or necroptosis and might serve as an alternate source for determining BRAF mutation.
“Collecting plasma cfDNA is a minimally invasive procedure that can be repeated at multiple times for diagnostic and disease-monitoring purposes,” Dr. Janku and associates said.
The investigators analyzed plasma samples from 160 patients with advanced solid tumors – most commonly colorectal cancer and melanoma –who had available archival FFPE tumor samples. cfDNA was isolated and extracted from whole blood and analyzed using the Idylla BRAF Mutation Test, a fully integrated real-time polymerase chain reaction–based test with a turnaround time of about 90 minutes.
Dr. Janku and associates found that a higher amount of mutant cfDNA was associated with shorter overall survival. Mean overall survival for patients with a BRAF-mutant cfDNA percentage of less than 2% (10.7 months; 95% CI, 9-12.4) was significantly longer than patients with a BRAF-mutant cfDNA percentage of greater than 2% (4.4 months; 95% CI, 3.2-5.6). Similar results were observed using different percentage cutoffs.
“Our study shows that the Idylla system can detect BRAF V600 mutations in plasma-derived cfDNA from patients with advanced cancers and has acceptable concordance (baseline, 88%; any time point, 90%); sensitivity (baseline, 73%; any time, 77%); and specificity (baseline, 98%; any time, 98%), compared with CLIA-certified laboratory testing of FFPE tumor tissue obtained at different times during routine care,” investigators wrote.
This study was supported by Biocartis, the Elsa U. Pardee Foundation, and the Sidney Kimmel Foundation for Cancer Research. Five of the investigators reported serving in an advisory role for, having ownership interest in, or receiving financial compensation or honoraria from multiple companies. The other investigators reported having no disclosures.
On Twitter @JessCraig_OP
Analysis of plasma-derived cell-free DNA can identify BRAF mutations as accurately as formalin-fixed paraffin-embedded tumor sample analysis, investigators report.
Of 160 patients with advanced solid tumors, BRAF V600 mutations were detected in 62 (39%) archival formalin-fixed paraffin-embedded (FFPE) tumor samples and 47 (29%) plasma cell-free (cf) DNA samples. The two methods had overall agreement in 141 patients (88%; kappa coefficient, 0.74; SE, 0.06; 95% confidence interval, 0.63-0.85), Dr. Filip Janku of the University of Texas and his associates reported (Mol Cancer Ther. 2016 May 20. doi: 10.1158/1535-7163.MCT-15-0712).
BRAF mutations are prevalent in many types of advanced cancers, and targeting these mutations has demonstrated efficacy, but current assessment of BRAF mutations is limited by a lack of tissue samples and complicated by constantly changing mutation status.
cfDNA is secreted into the circulation by tumor cells and cells in the tumor microenvironment that are undergoing apoptosis or necroptosis and might serve as an alternate source for determining BRAF mutation.
“Collecting plasma cfDNA is a minimally invasive procedure that can be repeated at multiple times for diagnostic and disease-monitoring purposes,” Dr. Janku and associates said.
The investigators analyzed plasma samples from 160 patients with advanced solid tumors – most commonly colorectal cancer and melanoma –who had available archival FFPE tumor samples. cfDNA was isolated and extracted from whole blood and analyzed using the Idylla BRAF Mutation Test, a fully integrated real-time polymerase chain reaction–based test with a turnaround time of about 90 minutes.
Dr. Janku and associates found that a higher amount of mutant cfDNA was associated with shorter overall survival. Mean overall survival for patients with a BRAF-mutant cfDNA percentage of less than 2% (10.7 months; 95% CI, 9-12.4) was significantly longer than patients with a BRAF-mutant cfDNA percentage of greater than 2% (4.4 months; 95% CI, 3.2-5.6). Similar results were observed using different percentage cutoffs.
“Our study shows that the Idylla system can detect BRAF V600 mutations in plasma-derived cfDNA from patients with advanced cancers and has acceptable concordance (baseline, 88%; any time point, 90%); sensitivity (baseline, 73%; any time, 77%); and specificity (baseline, 98%; any time, 98%), compared with CLIA-certified laboratory testing of FFPE tumor tissue obtained at different times during routine care,” investigators wrote.
This study was supported by Biocartis, the Elsa U. Pardee Foundation, and the Sidney Kimmel Foundation for Cancer Research. Five of the investigators reported serving in an advisory role for, having ownership interest in, or receiving financial compensation or honoraria from multiple companies. The other investigators reported having no disclosures.
On Twitter @JessCraig_OP
Analysis of plasma-derived cell-free DNA can identify BRAF mutations as accurately as formalin-fixed paraffin-embedded tumor sample analysis, investigators report.
Of 160 patients with advanced solid tumors, BRAF V600 mutations were detected in 62 (39%) archival formalin-fixed paraffin-embedded (FFPE) tumor samples and 47 (29%) plasma cell-free (cf) DNA samples. The two methods had overall agreement in 141 patients (88%; kappa coefficient, 0.74; SE, 0.06; 95% confidence interval, 0.63-0.85), Dr. Filip Janku of the University of Texas and his associates reported (Mol Cancer Ther. 2016 May 20. doi: 10.1158/1535-7163.MCT-15-0712).
BRAF mutations are prevalent in many types of advanced cancers, and targeting these mutations has demonstrated efficacy, but current assessment of BRAF mutations is limited by a lack of tissue samples and complicated by constantly changing mutation status.
cfDNA is secreted into the circulation by tumor cells and cells in the tumor microenvironment that are undergoing apoptosis or necroptosis and might serve as an alternate source for determining BRAF mutation.
“Collecting plasma cfDNA is a minimally invasive procedure that can be repeated at multiple times for diagnostic and disease-monitoring purposes,” Dr. Janku and associates said.
The investigators analyzed plasma samples from 160 patients with advanced solid tumors – most commonly colorectal cancer and melanoma –who had available archival FFPE tumor samples. cfDNA was isolated and extracted from whole blood and analyzed using the Idylla BRAF Mutation Test, a fully integrated real-time polymerase chain reaction–based test with a turnaround time of about 90 minutes.
Dr. Janku and associates found that a higher amount of mutant cfDNA was associated with shorter overall survival. Mean overall survival for patients with a BRAF-mutant cfDNA percentage of less than 2% (10.7 months; 95% CI, 9-12.4) was significantly longer than patients with a BRAF-mutant cfDNA percentage of greater than 2% (4.4 months; 95% CI, 3.2-5.6). Similar results were observed using different percentage cutoffs.
“Our study shows that the Idylla system can detect BRAF V600 mutations in plasma-derived cfDNA from patients with advanced cancers and has acceptable concordance (baseline, 88%; any time point, 90%); sensitivity (baseline, 73%; any time, 77%); and specificity (baseline, 98%; any time, 98%), compared with CLIA-certified laboratory testing of FFPE tumor tissue obtained at different times during routine care,” investigators wrote.
This study was supported by Biocartis, the Elsa U. Pardee Foundation, and the Sidney Kimmel Foundation for Cancer Research. Five of the investigators reported serving in an advisory role for, having ownership interest in, or receiving financial compensation or honoraria from multiple companies. The other investigators reported having no disclosures.
On Twitter @JessCraig_OP
FROM MOLECULAR CANCER THERAPEUTICS
Key clinical point: Analysis of plasma-derived cfDNA can identify BRAF mutations as accurately as FFPE tumor sample analysis.
Major finding: Concordance between mutation analysis of FFPE tumor samples and plasma cfDNA was in overall agreement (88%; kappa, 0.74; SE, 0.06; 95% CI, 0.63-0.85).
Data source: Analysis of FFPE tumor samples and plasma-derived cfDNA for 160 patients with advanced cancers.
Disclosures: This study was supported by Biocartis, the Elsa U. Pardee Foundation, and the Sidney Kimmel Foundation for Cancer Research. Five of the investigators reported serving in an advisory role for, having ownership interest in, or receiving financial compensation or honoraria from multiple companies. The other investigators reported having no disclosures.
Pembrolizumab benefit holds long-term for some melanoma patients
The anti–PD-1 immunotherapy pembrolizumab increases long-term survival in some patients with advanced melanoma, according to updated results of KEYNOTE-001.
Among the 655 patients studied in the phase 1b trial, the 3-year overall survival rate for advanced melanoma patients treated with pembrolizumab was 40%, Dr. Caroline Robert reported in a presscast leading up to the annual meeting of the American Society of Clinical Oncology.
Median overall survival was 24.4 months. Before 2011, patients with advanced melanoma had a median overall survival of less than one year, said Dr. Robert, head of the dermatology unit at the Institut Gustave-Roussy in Paris.
Study participants received pembrolizumab at either 2 or 10 mg/kg every 3 weeks. During the trial, 2 mg/kg every 3 weeks was determined to be the optimal dosing regimen. Patients remained on the treatment until disease progression, intolerable toxicity, or investigator decision. Eight percent of patients stopped treatment due to drug-related symptoms, and there were no drug-related deaths.
Survival rates differed slightly based on prior melanoma treatment. Of the 655 patients in the study, 75% had received previous treatments; patients who had not received prior treatment had slightly higher survival at 45%.
Overall response rate was 33%. Responses were durable as 73% of patients had a response rate of two or more years. Ninety-five patients had a complete response, and 61 of those patients stopped treatment following the complete response.
“I really hope for a cure for these people,” Dr. Robert said.
Pembrolizumab was generally well tolerated with the most common adverse events being fatigue (40%), itchiness (28%), and rash (23%).
ASCO spokesperson and moderator, Dr. Don Dizon, said the results of this study are “incredibly exciting given they came from a phase I trial. This is a new treatment and the longest follow-up of people [with melanoma] who have received pembrolizumab.” Dr. Dizon hopes to “potentially see a cure [for] melanoma” given the reported durability and response rate to the drug.
On Twitter @JessCraig_OP
The anti–PD-1 immunotherapy pembrolizumab increases long-term survival in some patients with advanced melanoma, according to updated results of KEYNOTE-001.
Among the 655 patients studied in the phase 1b trial, the 3-year overall survival rate for advanced melanoma patients treated with pembrolizumab was 40%, Dr. Caroline Robert reported in a presscast leading up to the annual meeting of the American Society of Clinical Oncology.
Median overall survival was 24.4 months. Before 2011, patients with advanced melanoma had a median overall survival of less than one year, said Dr. Robert, head of the dermatology unit at the Institut Gustave-Roussy in Paris.
Study participants received pembrolizumab at either 2 or 10 mg/kg every 3 weeks. During the trial, 2 mg/kg every 3 weeks was determined to be the optimal dosing regimen. Patients remained on the treatment until disease progression, intolerable toxicity, or investigator decision. Eight percent of patients stopped treatment due to drug-related symptoms, and there were no drug-related deaths.
Survival rates differed slightly based on prior melanoma treatment. Of the 655 patients in the study, 75% had received previous treatments; patients who had not received prior treatment had slightly higher survival at 45%.
Overall response rate was 33%. Responses were durable as 73% of patients had a response rate of two or more years. Ninety-five patients had a complete response, and 61 of those patients stopped treatment following the complete response.
“I really hope for a cure for these people,” Dr. Robert said.
Pembrolizumab was generally well tolerated with the most common adverse events being fatigue (40%), itchiness (28%), and rash (23%).
ASCO spokesperson and moderator, Dr. Don Dizon, said the results of this study are “incredibly exciting given they came from a phase I trial. This is a new treatment and the longest follow-up of people [with melanoma] who have received pembrolizumab.” Dr. Dizon hopes to “potentially see a cure [for] melanoma” given the reported durability and response rate to the drug.
On Twitter @JessCraig_OP
The anti–PD-1 immunotherapy pembrolizumab increases long-term survival in some patients with advanced melanoma, according to updated results of KEYNOTE-001.
Among the 655 patients studied in the phase 1b trial, the 3-year overall survival rate for advanced melanoma patients treated with pembrolizumab was 40%, Dr. Caroline Robert reported in a presscast leading up to the annual meeting of the American Society of Clinical Oncology.
Median overall survival was 24.4 months. Before 2011, patients with advanced melanoma had a median overall survival of less than one year, said Dr. Robert, head of the dermatology unit at the Institut Gustave-Roussy in Paris.
Study participants received pembrolizumab at either 2 or 10 mg/kg every 3 weeks. During the trial, 2 mg/kg every 3 weeks was determined to be the optimal dosing regimen. Patients remained on the treatment until disease progression, intolerable toxicity, or investigator decision. Eight percent of patients stopped treatment due to drug-related symptoms, and there were no drug-related deaths.
Survival rates differed slightly based on prior melanoma treatment. Of the 655 patients in the study, 75% had received previous treatments; patients who had not received prior treatment had slightly higher survival at 45%.
Overall response rate was 33%. Responses were durable as 73% of patients had a response rate of two or more years. Ninety-five patients had a complete response, and 61 of those patients stopped treatment following the complete response.
“I really hope for a cure for these people,” Dr. Robert said.
Pembrolizumab was generally well tolerated with the most common adverse events being fatigue (40%), itchiness (28%), and rash (23%).
ASCO spokesperson and moderator, Dr. Don Dizon, said the results of this study are “incredibly exciting given they came from a phase I trial. This is a new treatment and the longest follow-up of people [with melanoma] who have received pembrolizumab.” Dr. Dizon hopes to “potentially see a cure [for] melanoma” given the reported durability and response rate to the drug.
On Twitter @JessCraig_OP
FROM THE 2016 ASCO ANNUAL MEETING
Key clinical point: Pembrolizumab increases long-term survival in some patients with advanced melanoma.
Major finding: The 3-year overall survival rate for advanced melanoma patients treated with pembrolizumab was 40%. The median overall survival was 24.4 months.
Data source: A phase Ib clinical trial of 655 patients with advanced melanoma.
Disclosures: This study was funded by Merck. All of the investigators reported serving in advisory/consultatory roles for, having stock in, or receiving financial compensation or honoraria from several companies.
Early Detection of Melanoma in Men
Men do not know as much about skin cancer prevention and detection techniques as women, according to a recent survey conducted by the American Academy of Dermatology (AAD). This lack of knowledge may delay or prevent early diagnosis and treatment of melanoma and other nonmelanoma skin cancers in this patient population.
The survey results showed that only 56% of men versus 76% of women know there is no such thing as a healthy tan, and only 54% of men versus 70% of women know that getting a base tan is not a healthy way to protect skin from the sun. Furthermore, only 56% of men surveyed were aware that skin cancer could occur on areas of the skin not typically exposed to the sun compared to 65% of women.
“While our survey results indicate that men don’t know as much about skin cancer prevention and detection as women, men over 50 have a higher risk of developing melanoma, so it’s especially important for them to be vigilant about protecting and monitoring their skin,” said AAD President Abel Torres, MD, JD.
May is skin cancer awareness month and the AAD is encouraging patients to make sure their skin is “Looking Good in 2016” by using sun protection and regularly examining skin for signs of skin cancer. The campaign features a public service announcement encouraging men to check their skin for signs of skin cancer and find a partner to help. The AAD also released a new infographic with tips on performing a skin cancer self-examination that dermatologists can share with patients to promote early detection of skin cancer.
Dermatologist intervention in catching skin cancers when they are easier to treat also is key. At the 74th Annual Meeting of the American Academy of Dermatology in Washington, DC, Dr. Orit Markowitz discussed noninvasive imaging tools that can help dermatologists diagnose skin cancers earlier. She noted that even when a lesion looks very small, tools such as dermoscopy can reveal features that indicate it already has depth and therefore may progress to a more serious malignancy. Early detection is particularly crucial in cases of rare aggressive tumors such as amelanotic melanoma. “If something is very pink clinically and then suddenly has pigmentation dermoscopically, you really have to be considering biopsying that lesion because you may be looking at an early amelanotic melanoma,” Dr. Markowitz explained. By the time the lesion develops more obvious clinical features suggesting malignancy, the tumor progression may be far more advanced.
Men do not know as much about skin cancer prevention and detection techniques as women, according to a recent survey conducted by the American Academy of Dermatology (AAD). This lack of knowledge may delay or prevent early diagnosis and treatment of melanoma and other nonmelanoma skin cancers in this patient population.
The survey results showed that only 56% of men versus 76% of women know there is no such thing as a healthy tan, and only 54% of men versus 70% of women know that getting a base tan is not a healthy way to protect skin from the sun. Furthermore, only 56% of men surveyed were aware that skin cancer could occur on areas of the skin not typically exposed to the sun compared to 65% of women.
“While our survey results indicate that men don’t know as much about skin cancer prevention and detection as women, men over 50 have a higher risk of developing melanoma, so it’s especially important for them to be vigilant about protecting and monitoring their skin,” said AAD President Abel Torres, MD, JD.
May is skin cancer awareness month and the AAD is encouraging patients to make sure their skin is “Looking Good in 2016” by using sun protection and regularly examining skin for signs of skin cancer. The campaign features a public service announcement encouraging men to check their skin for signs of skin cancer and find a partner to help. The AAD also released a new infographic with tips on performing a skin cancer self-examination that dermatologists can share with patients to promote early detection of skin cancer.
Dermatologist intervention in catching skin cancers when they are easier to treat also is key. At the 74th Annual Meeting of the American Academy of Dermatology in Washington, DC, Dr. Orit Markowitz discussed noninvasive imaging tools that can help dermatologists diagnose skin cancers earlier. She noted that even when a lesion looks very small, tools such as dermoscopy can reveal features that indicate it already has depth and therefore may progress to a more serious malignancy. Early detection is particularly crucial in cases of rare aggressive tumors such as amelanotic melanoma. “If something is very pink clinically and then suddenly has pigmentation dermoscopically, you really have to be considering biopsying that lesion because you may be looking at an early amelanotic melanoma,” Dr. Markowitz explained. By the time the lesion develops more obvious clinical features suggesting malignancy, the tumor progression may be far more advanced.
Men do not know as much about skin cancer prevention and detection techniques as women, according to a recent survey conducted by the American Academy of Dermatology (AAD). This lack of knowledge may delay or prevent early diagnosis and treatment of melanoma and other nonmelanoma skin cancers in this patient population.
The survey results showed that only 56% of men versus 76% of women know there is no such thing as a healthy tan, and only 54% of men versus 70% of women know that getting a base tan is not a healthy way to protect skin from the sun. Furthermore, only 56% of men surveyed were aware that skin cancer could occur on areas of the skin not typically exposed to the sun compared to 65% of women.
“While our survey results indicate that men don’t know as much about skin cancer prevention and detection as women, men over 50 have a higher risk of developing melanoma, so it’s especially important for them to be vigilant about protecting and monitoring their skin,” said AAD President Abel Torres, MD, JD.
May is skin cancer awareness month and the AAD is encouraging patients to make sure their skin is “Looking Good in 2016” by using sun protection and regularly examining skin for signs of skin cancer. The campaign features a public service announcement encouraging men to check their skin for signs of skin cancer and find a partner to help. The AAD also released a new infographic with tips on performing a skin cancer self-examination that dermatologists can share with patients to promote early detection of skin cancer.
Dermatologist intervention in catching skin cancers when they are easier to treat also is key. At the 74th Annual Meeting of the American Academy of Dermatology in Washington, DC, Dr. Orit Markowitz discussed noninvasive imaging tools that can help dermatologists diagnose skin cancers earlier. She noted that even when a lesion looks very small, tools such as dermoscopy can reveal features that indicate it already has depth and therefore may progress to a more serious malignancy. Early detection is particularly crucial in cases of rare aggressive tumors such as amelanotic melanoma. “If something is very pink clinically and then suddenly has pigmentation dermoscopically, you really have to be considering biopsying that lesion because you may be looking at an early amelanotic melanoma,” Dr. Markowitz explained. By the time the lesion develops more obvious clinical features suggesting malignancy, the tumor progression may be far more advanced.
Mohs surgeons, dermatopathologists nearly always agree on frozen section analysis
ORLANDO – Mohs fellowship–trained surgeons are highly skilled at reading frozen section slides obtained during surgery, agreeing with the dermatopathologist’s assessment more than 99% of the time, according to a review of more than 4,000 cases.
Among 4,145 slides in five datasets, only 28 were discordant. The concordance of surgeons’ and dermatopathologists’ assessments was quite consistent, ranging from 95%-of 99.7%.
“There is absolutely no detriment to our interpretation of these frozen section slides,” Dr. James Highsmith said at the annual meeting of the American College of Mohs Surgery. “These numbers give credence as to why we have these good cure rates. We can say with 99% accuracy that yes, we are removing these tumors from our patients.”
Dr. Highsmith, a Mohs surgeon in Birmingham, Ala., reviewed 10 years of his own data (1,720 cases), as well as four published cohorts comprising another 2,425 cases. All of the studies examined the concordance of frozen section assessments between fellowship-trained Mohs surgeons and the dermatopathologists working with them. All of the series reported concordance, discordance, sensitivity, and specificity.
His own database is the largest one yet compiled, spanning the longest period of time. Of 1,720 cases, there were eight discrepancies: one in which the surgeon identified tumor that was not supported by dermatopathology, and seven in which the surgeon missed tumor that dermatopathology confirmed was present. The concordance rate was 99.5%. This worked out to a 99.4% sensitivity and 99.8% specificity, Dr. Highsmith said.
Results were similar with the other four studies.
The largest was a 2009 retrospective review of 1,156 slides collected over 10 years; they were part of a preexisting randomized, blinded study. Of these, 32 slides (2.8%) were discordant between the Mohs surgeon and the dermatopathologist, for a 99.7% concordance rate (J Am Acad Dermatol. 2009 Jan;[1]: 94-8).
The second largest cohort was published in 1989. It comprised 1,000 slides that were evaluated by the Mohs surgeon and a general pathologist; disputed slides were read by two other Mohs surgeons, two pathologists, and a dermatopathologist. The overall concordance rate was 98.9% (J Am Acad Dermatol. 1989;20[4]:670-4).
In 2013, a Mohs surgeon published a set of 170 slides that had been randomly selected from his cases as part of a quality assurance audit. There was one discordant interpretation, for an overall concordance rate of 99.4% (Dermatol Surg. 2013;39[11]:1648-52).
The smallest study, published in 2011, reviewed 99 slides assessed by a single Mohs surgeon. The concordance rate with dermatopathology was 95%.
An overall analysis of these four cohorts determined a sensitivity of 99.4%, specificity of 99.2% and negative predictive value of 99.2%, Dr. Highsmith said.
“When a fellowship-trained Mohs surgeon looks at a slide and says there’s no more tumor present, then there’s a greater-than-99% chance that is accurate,” he said.
Dr. Highsmith had no financial disclosures.
ORLANDO – Mohs fellowship–trained surgeons are highly skilled at reading frozen section slides obtained during surgery, agreeing with the dermatopathologist’s assessment more than 99% of the time, according to a review of more than 4,000 cases.
Among 4,145 slides in five datasets, only 28 were discordant. The concordance of surgeons’ and dermatopathologists’ assessments was quite consistent, ranging from 95%-of 99.7%.
“There is absolutely no detriment to our interpretation of these frozen section slides,” Dr. James Highsmith said at the annual meeting of the American College of Mohs Surgery. “These numbers give credence as to why we have these good cure rates. We can say with 99% accuracy that yes, we are removing these tumors from our patients.”
Dr. Highsmith, a Mohs surgeon in Birmingham, Ala., reviewed 10 years of his own data (1,720 cases), as well as four published cohorts comprising another 2,425 cases. All of the studies examined the concordance of frozen section assessments between fellowship-trained Mohs surgeons and the dermatopathologists working with them. All of the series reported concordance, discordance, sensitivity, and specificity.
His own database is the largest one yet compiled, spanning the longest period of time. Of 1,720 cases, there were eight discrepancies: one in which the surgeon identified tumor that was not supported by dermatopathology, and seven in which the surgeon missed tumor that dermatopathology confirmed was present. The concordance rate was 99.5%. This worked out to a 99.4% sensitivity and 99.8% specificity, Dr. Highsmith said.
Results were similar with the other four studies.
The largest was a 2009 retrospective review of 1,156 slides collected over 10 years; they were part of a preexisting randomized, blinded study. Of these, 32 slides (2.8%) were discordant between the Mohs surgeon and the dermatopathologist, for a 99.7% concordance rate (J Am Acad Dermatol. 2009 Jan;[1]: 94-8).
The second largest cohort was published in 1989. It comprised 1,000 slides that were evaluated by the Mohs surgeon and a general pathologist; disputed slides were read by two other Mohs surgeons, two pathologists, and a dermatopathologist. The overall concordance rate was 98.9% (J Am Acad Dermatol. 1989;20[4]:670-4).
In 2013, a Mohs surgeon published a set of 170 slides that had been randomly selected from his cases as part of a quality assurance audit. There was one discordant interpretation, for an overall concordance rate of 99.4% (Dermatol Surg. 2013;39[11]:1648-52).
The smallest study, published in 2011, reviewed 99 slides assessed by a single Mohs surgeon. The concordance rate with dermatopathology was 95%.
An overall analysis of these four cohorts determined a sensitivity of 99.4%, specificity of 99.2% and negative predictive value of 99.2%, Dr. Highsmith said.
“When a fellowship-trained Mohs surgeon looks at a slide and says there’s no more tumor present, then there’s a greater-than-99% chance that is accurate,” he said.
Dr. Highsmith had no financial disclosures.
ORLANDO – Mohs fellowship–trained surgeons are highly skilled at reading frozen section slides obtained during surgery, agreeing with the dermatopathologist’s assessment more than 99% of the time, according to a review of more than 4,000 cases.
Among 4,145 slides in five datasets, only 28 were discordant. The concordance of surgeons’ and dermatopathologists’ assessments was quite consistent, ranging from 95%-of 99.7%.
“There is absolutely no detriment to our interpretation of these frozen section slides,” Dr. James Highsmith said at the annual meeting of the American College of Mohs Surgery. “These numbers give credence as to why we have these good cure rates. We can say with 99% accuracy that yes, we are removing these tumors from our patients.”
Dr. Highsmith, a Mohs surgeon in Birmingham, Ala., reviewed 10 years of his own data (1,720 cases), as well as four published cohorts comprising another 2,425 cases. All of the studies examined the concordance of frozen section assessments between fellowship-trained Mohs surgeons and the dermatopathologists working with them. All of the series reported concordance, discordance, sensitivity, and specificity.
His own database is the largest one yet compiled, spanning the longest period of time. Of 1,720 cases, there were eight discrepancies: one in which the surgeon identified tumor that was not supported by dermatopathology, and seven in which the surgeon missed tumor that dermatopathology confirmed was present. The concordance rate was 99.5%. This worked out to a 99.4% sensitivity and 99.8% specificity, Dr. Highsmith said.
Results were similar with the other four studies.
The largest was a 2009 retrospective review of 1,156 slides collected over 10 years; they were part of a preexisting randomized, blinded study. Of these, 32 slides (2.8%) were discordant between the Mohs surgeon and the dermatopathologist, for a 99.7% concordance rate (J Am Acad Dermatol. 2009 Jan;[1]: 94-8).
The second largest cohort was published in 1989. It comprised 1,000 slides that were evaluated by the Mohs surgeon and a general pathologist; disputed slides were read by two other Mohs surgeons, two pathologists, and a dermatopathologist. The overall concordance rate was 98.9% (J Am Acad Dermatol. 1989;20[4]:670-4).
In 2013, a Mohs surgeon published a set of 170 slides that had been randomly selected from his cases as part of a quality assurance audit. There was one discordant interpretation, for an overall concordance rate of 99.4% (Dermatol Surg. 2013;39[11]:1648-52).
The smallest study, published in 2011, reviewed 99 slides assessed by a single Mohs surgeon. The concordance rate with dermatopathology was 95%.
An overall analysis of these four cohorts determined a sensitivity of 99.4%, specificity of 99.2% and negative predictive value of 99.2%, Dr. Highsmith said.
“When a fellowship-trained Mohs surgeon looks at a slide and says there’s no more tumor present, then there’s a greater-than-99% chance that is accurate,” he said.
Dr. Highsmith had no financial disclosures.
AT THE ACMS ANNUAL MEETING
Key clinical point: Fellowship-trained Mohs surgeons and dermatopathologists almost always agree on slide interpretation.
Major finding: The concordance rate between surgeons and dermatopathologists was over 99% in a pooled review of studies.
Data source: A review of 4,145 frozen section slides analyzed for concordance rates between Mohs surgeons and dermatopathologists.
Disclosures: Dr. James Highsmith had no financial disclosures.
En bloc excision may be viable amputation alternative for nail melanoma
ORLANDO – En bloc excision can cure melanoma in situ of the nail apparatus without amputation, while also preserving function and quality of life, according to the results of a retrospective study of patients treated with this approach.
At 3 years’ follow-up, there were no melanoma recurrences in any of 29 patients treated with the digit-sparing excision, Dr. Thomas Knackstedt said at the annual meeting of the American College of Mohs Surgery. Follow-up telephone interviews found that patients retained full function of the affected finger, and reported virtually no quality of life impairment.
“Because treatment without disarticulation or amputation can provide these excellent long-term cure rates in nail apparatus melanoma in situ, it should be the first-line treatment whenever possible,” said Dr. Knackstedt, a Mohs surgeon in East Greenwich, R.I.
Although similar excellent outcomes have been reported with wide local excision, Dr. Knackstedt said it remains a controversial treatment for nail apparatus melanoma in situ (NAMis).
He reviewed his institution’s experience with treating 29 cases of NAMis with en bloc excision: removal of nail folds, matrix, bed, hyponychium, and margins. All of the surgeries were performed between 2005 and 2015. The current mean follow-up time is 35.5 months for clinic visits and 39 months for telephone contact. The longest follow-up is 103 months. There have been no melanoma recurrences.
The patients were a mean of 39 years old. Melanoma appeared most often on the thumb (seven patients) and hallux (six). The average duration of the lesion was almost 5 years, although that varied from 6 months to 13 years.
Twenty-four patients (83%) presented with longitudinal melanonychia, with an average diameter of 4.1 mm. Four patients (14%) had complete melanonychia, and one patient had erythronychia.
Most of the cases were repaired with a full-thickness skin graft. One was left to heal by second intention, and one case was repaired by a dorsal metacarpal artery flap.
There were two wound infections, one case of delayed graft necrosis, seven nail spicules, and two cysts. There were no cases of tendon injury. One patient complained about temperature sensitivity in the affected finger. There were no cases of disease recurrence, although one patient with a nail spicule did show disease persistence. The spicule was excised, and that patient remains disease free 5 years later, Dr. Knackstedt said.
The telephone survey collected data from 23 patients (79%). Patients were unanimous in reporting that they were “very satisfied” with their treatment. In an 11-question quality of life survey, 78% said that the surgery affected their quality of life “only a little” or “not at all.” On a 10-point Likert scale with 10 being most affected by the surgery, the mean rating was 1.3.
“In light of these results, and when we consider that even a distal joint amputation can reduce the functionality of a finger by 40%-80%, we conclude that en bloc excision must be considered as a viable alternative to amputation for NAMis,” Dr. Knackstedt said.
He had no relevant financial disclosures.
ORLANDO – En bloc excision can cure melanoma in situ of the nail apparatus without amputation, while also preserving function and quality of life, according to the results of a retrospective study of patients treated with this approach.
At 3 years’ follow-up, there were no melanoma recurrences in any of 29 patients treated with the digit-sparing excision, Dr. Thomas Knackstedt said at the annual meeting of the American College of Mohs Surgery. Follow-up telephone interviews found that patients retained full function of the affected finger, and reported virtually no quality of life impairment.
“Because treatment without disarticulation or amputation can provide these excellent long-term cure rates in nail apparatus melanoma in situ, it should be the first-line treatment whenever possible,” said Dr. Knackstedt, a Mohs surgeon in East Greenwich, R.I.
Although similar excellent outcomes have been reported with wide local excision, Dr. Knackstedt said it remains a controversial treatment for nail apparatus melanoma in situ (NAMis).
He reviewed his institution’s experience with treating 29 cases of NAMis with en bloc excision: removal of nail folds, matrix, bed, hyponychium, and margins. All of the surgeries were performed between 2005 and 2015. The current mean follow-up time is 35.5 months for clinic visits and 39 months for telephone contact. The longest follow-up is 103 months. There have been no melanoma recurrences.
The patients were a mean of 39 years old. Melanoma appeared most often on the thumb (seven patients) and hallux (six). The average duration of the lesion was almost 5 years, although that varied from 6 months to 13 years.
Twenty-four patients (83%) presented with longitudinal melanonychia, with an average diameter of 4.1 mm. Four patients (14%) had complete melanonychia, and one patient had erythronychia.
Most of the cases were repaired with a full-thickness skin graft. One was left to heal by second intention, and one case was repaired by a dorsal metacarpal artery flap.
There were two wound infections, one case of delayed graft necrosis, seven nail spicules, and two cysts. There were no cases of tendon injury. One patient complained about temperature sensitivity in the affected finger. There were no cases of disease recurrence, although one patient with a nail spicule did show disease persistence. The spicule was excised, and that patient remains disease free 5 years later, Dr. Knackstedt said.
The telephone survey collected data from 23 patients (79%). Patients were unanimous in reporting that they were “very satisfied” with their treatment. In an 11-question quality of life survey, 78% said that the surgery affected their quality of life “only a little” or “not at all.” On a 10-point Likert scale with 10 being most affected by the surgery, the mean rating was 1.3.
“In light of these results, and when we consider that even a distal joint amputation can reduce the functionality of a finger by 40%-80%, we conclude that en bloc excision must be considered as a viable alternative to amputation for NAMis,” Dr. Knackstedt said.
He had no relevant financial disclosures.
ORLANDO – En bloc excision can cure melanoma in situ of the nail apparatus without amputation, while also preserving function and quality of life, according to the results of a retrospective study of patients treated with this approach.
At 3 years’ follow-up, there were no melanoma recurrences in any of 29 patients treated with the digit-sparing excision, Dr. Thomas Knackstedt said at the annual meeting of the American College of Mohs Surgery. Follow-up telephone interviews found that patients retained full function of the affected finger, and reported virtually no quality of life impairment.
“Because treatment without disarticulation or amputation can provide these excellent long-term cure rates in nail apparatus melanoma in situ, it should be the first-line treatment whenever possible,” said Dr. Knackstedt, a Mohs surgeon in East Greenwich, R.I.
Although similar excellent outcomes have been reported with wide local excision, Dr. Knackstedt said it remains a controversial treatment for nail apparatus melanoma in situ (NAMis).
He reviewed his institution’s experience with treating 29 cases of NAMis with en bloc excision: removal of nail folds, matrix, bed, hyponychium, and margins. All of the surgeries were performed between 2005 and 2015. The current mean follow-up time is 35.5 months for clinic visits and 39 months for telephone contact. The longest follow-up is 103 months. There have been no melanoma recurrences.
The patients were a mean of 39 years old. Melanoma appeared most often on the thumb (seven patients) and hallux (six). The average duration of the lesion was almost 5 years, although that varied from 6 months to 13 years.
Twenty-four patients (83%) presented with longitudinal melanonychia, with an average diameter of 4.1 mm. Four patients (14%) had complete melanonychia, and one patient had erythronychia.
Most of the cases were repaired with a full-thickness skin graft. One was left to heal by second intention, and one case was repaired by a dorsal metacarpal artery flap.
There were two wound infections, one case of delayed graft necrosis, seven nail spicules, and two cysts. There were no cases of tendon injury. One patient complained about temperature sensitivity in the affected finger. There were no cases of disease recurrence, although one patient with a nail spicule did show disease persistence. The spicule was excised, and that patient remains disease free 5 years later, Dr. Knackstedt said.
The telephone survey collected data from 23 patients (79%). Patients were unanimous in reporting that they were “very satisfied” with their treatment. In an 11-question quality of life survey, 78% said that the surgery affected their quality of life “only a little” or “not at all.” On a 10-point Likert scale with 10 being most affected by the surgery, the mean rating was 1.3.
“In light of these results, and when we consider that even a distal joint amputation can reduce the functionality of a finger by 40%-80%, we conclude that en bloc excision must be considered as a viable alternative to amputation for NAMis,” Dr. Knackstedt said.
He had no relevant financial disclosures.
AT THE ACMS ANNUAL MEETING
Key clinical point: En bloc removal of the nail apparatus effected good clinical and quality of life outcomes in nail melanoma.
Major finding: There have been no recurrences of melanoma over a mean follow-up of 39 months.
Data source: A review evaluated 29 cases of nail apparatus melanoma in situ treated with en bloc excision at one institution.
Disclosures: Dr. Knackstedt had no relevant financial disclosures.
What’s Less Noticeable: A Straight Scar or a Zigzag Scar?
One of the determinants of a successful surgical outcome is the perception, on the part of the patient, of the cosmesis of a scar. The use of Z-plasty is an accepted means by which to break a scar up into smaller geometric segments. In some instances, a Z-plasty is used for scar revision to elongate a scar that may be pulling. However, a study published online in JAMA Facial Plastic Surgery on April 7 mentions the lack of studies measuring the perception of these scars among the normal population after surgery.
Ratnarathorn et al designed a prospective Internet-based survey with a goal of 580 responses to give a power of 90%. The survey was distributed to a diverse sample of the US population. Using editing software, Ratnarathorn et al superimposed a mature linear scar and a mature zigzag scar onto the faces of standardized headshots from 4 individuals (2 males, 2 females). Each individual had 1 image of the linear scar and 1 image of the zigzag scars superimposed onto each of 3 anatomical areas—forehead (flat surface), cheek (convex surface), and temple (concave surface)—yielding 24 images for the respondents to assess.
A 24.5% (n=876) response rate was achieved with 3575 surveys distributed. Of the 876 respondents, 810 (92.5%) completed the survey (46.1% male, 53.9% female). Respondents were asked to rate the scars on a scale of 1 to 10 (1=normal skin; 10=worst scar imaginable).
Results were statistically significantly lower (better) for the linear scars compared to the zigzag scars in all 3 anatomic areas and across both male and female groups with a mean score of 2.9 versus 4.5 (P<.001). A multivariable regression model of respondent age, sex, educational level, and income showed no statistically significant effect on the rating of the scars.
What’s the issue?
This study highlights some interesting points. Coming from an academic practice, we oftentimes find ourselves teaching residents a variety of skin closure techniques to deal with defects from skin cancer excisions. It is both challenging and fun to design complex closures; however, we must keep in mind what is in the best interest of the patient. One of the points I try to emphasize is that we must understand that there are no true straight lines on the face. In fact, when scars from procedures appear as geometric shapes on the face, our eyes tend to be drawn to them. For this reason, it often is best to use curvilinear lines wherever possible. Ratnarathorn et al highlights that point exactly. More studies of this nature are needed to assess what is perceived as a successful outcome, by both physicians and patients.
As you follow your patients for the long-term, have you noticed that you perform more or fewer zigzag scars?
One of the determinants of a successful surgical outcome is the perception, on the part of the patient, of the cosmesis of a scar. The use of Z-plasty is an accepted means by which to break a scar up into smaller geometric segments. In some instances, a Z-plasty is used for scar revision to elongate a scar that may be pulling. However, a study published online in JAMA Facial Plastic Surgery on April 7 mentions the lack of studies measuring the perception of these scars among the normal population after surgery.
Ratnarathorn et al designed a prospective Internet-based survey with a goal of 580 responses to give a power of 90%. The survey was distributed to a diverse sample of the US population. Using editing software, Ratnarathorn et al superimposed a mature linear scar and a mature zigzag scar onto the faces of standardized headshots from 4 individuals (2 males, 2 females). Each individual had 1 image of the linear scar and 1 image of the zigzag scars superimposed onto each of 3 anatomical areas—forehead (flat surface), cheek (convex surface), and temple (concave surface)—yielding 24 images for the respondents to assess.
A 24.5% (n=876) response rate was achieved with 3575 surveys distributed. Of the 876 respondents, 810 (92.5%) completed the survey (46.1% male, 53.9% female). Respondents were asked to rate the scars on a scale of 1 to 10 (1=normal skin; 10=worst scar imaginable).
Results were statistically significantly lower (better) for the linear scars compared to the zigzag scars in all 3 anatomic areas and across both male and female groups with a mean score of 2.9 versus 4.5 (P<.001). A multivariable regression model of respondent age, sex, educational level, and income showed no statistically significant effect on the rating of the scars.
What’s the issue?
This study highlights some interesting points. Coming from an academic practice, we oftentimes find ourselves teaching residents a variety of skin closure techniques to deal with defects from skin cancer excisions. It is both challenging and fun to design complex closures; however, we must keep in mind what is in the best interest of the patient. One of the points I try to emphasize is that we must understand that there are no true straight lines on the face. In fact, when scars from procedures appear as geometric shapes on the face, our eyes tend to be drawn to them. For this reason, it often is best to use curvilinear lines wherever possible. Ratnarathorn et al highlights that point exactly. More studies of this nature are needed to assess what is perceived as a successful outcome, by both physicians and patients.
As you follow your patients for the long-term, have you noticed that you perform more or fewer zigzag scars?
One of the determinants of a successful surgical outcome is the perception, on the part of the patient, of the cosmesis of a scar. The use of Z-plasty is an accepted means by which to break a scar up into smaller geometric segments. In some instances, a Z-plasty is used for scar revision to elongate a scar that may be pulling. However, a study published online in JAMA Facial Plastic Surgery on April 7 mentions the lack of studies measuring the perception of these scars among the normal population after surgery.
Ratnarathorn et al designed a prospective Internet-based survey with a goal of 580 responses to give a power of 90%. The survey was distributed to a diverse sample of the US population. Using editing software, Ratnarathorn et al superimposed a mature linear scar and a mature zigzag scar onto the faces of standardized headshots from 4 individuals (2 males, 2 females). Each individual had 1 image of the linear scar and 1 image of the zigzag scars superimposed onto each of 3 anatomical areas—forehead (flat surface), cheek (convex surface), and temple (concave surface)—yielding 24 images for the respondents to assess.
A 24.5% (n=876) response rate was achieved with 3575 surveys distributed. Of the 876 respondents, 810 (92.5%) completed the survey (46.1% male, 53.9% female). Respondents were asked to rate the scars on a scale of 1 to 10 (1=normal skin; 10=worst scar imaginable).
Results were statistically significantly lower (better) for the linear scars compared to the zigzag scars in all 3 anatomic areas and across both male and female groups with a mean score of 2.9 versus 4.5 (P<.001). A multivariable regression model of respondent age, sex, educational level, and income showed no statistically significant effect on the rating of the scars.
What’s the issue?
This study highlights some interesting points. Coming from an academic practice, we oftentimes find ourselves teaching residents a variety of skin closure techniques to deal with defects from skin cancer excisions. It is both challenging and fun to design complex closures; however, we must keep in mind what is in the best interest of the patient. One of the points I try to emphasize is that we must understand that there are no true straight lines on the face. In fact, when scars from procedures appear as geometric shapes on the face, our eyes tend to be drawn to them. For this reason, it often is best to use curvilinear lines wherever possible. Ratnarathorn et al highlights that point exactly. More studies of this nature are needed to assess what is perceived as a successful outcome, by both physicians and patients.
As you follow your patients for the long-term, have you noticed that you perform more or fewer zigzag scars?
Search is on for cases of aggressive, ruxolitinib-associated skin cancers
ORLANDO – The hematologic cancer drug ruxolitinib seems to be associated with cases of aggressive nonmelanoma skin cancer.
After treating a very aggressive squamous cell carcinoma in a 55-year-old man treated with ruxolitinib for polycythemia vera, and hearing firsthand of three other similar cases, Dr. Fiona Zwald is collecting additional data on the association. She intends to publish these cases in a monograph as a warning to dermatologists, hematologists, oncologists, and other physicians who manage patients with hematologic malignancies, she said at the annual meeting of the American College of Mohs Surgery.
The prescribing information for ruxolitinib (Jakafi, Incyte Pharmaceuticals; Jakavi, Novartis) was updated in 2014 to warn that patients taking the drug face an increased risk of nonmelanoma skin cancers. The label also recommends that physicians inspect the skin regularly and urge patients to be alert for and report any new or changing lesions.
Despite the warnings and recommendations, cases are occurring – and some are quite serious, said Dr. Zwald, a Mohs surgeon in Atlanta.
“People should know this is actually happening. If you have experience with this medication, please let us know so we can compile this report. We are trying to assess the number of skin cancers before and after initiating this medication,” she said.
Ruxolitinib is an inhibitor of Janus kinase with a special affinity for the JAK1 and JAK2 subtypes. Like other cytokine-signaling molecules, their function depends on cell context; it may inhibit cell growth in one setting, and, in another, stimulate it. Ruxolitinib was initially approved in 2011 for the treatment of intermediate- and high-risk myelofibrosis, including primary myelofibrosis, post–polycythemia vera myelofibrosis, and post–essential thrombocythemia myelofibrosis.
In 2014, indications for ruxolitinib were expanded to include treatment of patients with polycythemia vera who have had an inadequate response to or are intolerant of hydroxyurea.
Dr. Zwald’s patient had a 10-year history of polycythemia vera. He was initially well controlled on the standard hydroxyurea treatment. In the meantime, he began working as a caddy at a major U.S. golf club. He developed many facial squamous cell carcinomas that were treated with excision and radiation. A year before he presented to Dr. Zwald, he stopped responding to hydroxyurea and was placed on ruxolitinib.
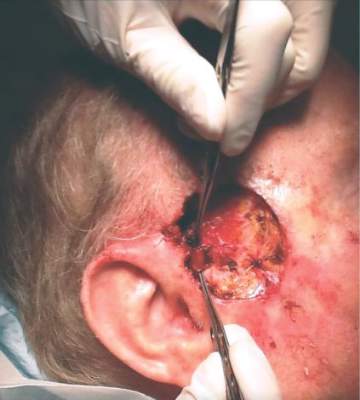
The patient presented with a 4-cm ulcerated lesion over part of his right temple and to the right helical crus; the lesion had developed over 3 months. Dr. Zwald consulted with the patient’s medical oncologist; treatment with ruxolitinib continued, albeit at a reduced dosage in light of recent events.
She performed Mohs surgery on the patient. It was a challenging case, she said, not the least because adequate anesthesia could not be achieved with local anesthetic. Preoperative staging showed no nodal spread.
“He did, unfortunately demonstrate a large, indurated mass located over one branch of the superficial temporal artery. At the helical crus there was an area of bound-down, fixed tumor. Knowing that I would not be able to fully resect this, I passed him on to the operating room,” Dr. Zwald said. “This tumor was found to extend down to the parotid capsule, but margins were clear.” The surgical defect was successfully repaired with a split-thickness skin graft.
The tumor recurred about 3 months later, and the patient underwent another surgery.
“This time we could not get clear surgical margins, and the tumor was approaching the external auditory meatus. Surgery was abandoned due to fears of complications to that area,” she said.
She presented the case at tumor board, during which she and her colleagues discussed adjuvant radiation. They initially abandoned this idea because he had already had so much radiation to his face. After the second surgery, they decide to proceed with radiation. “The next conversation we have will be whether to add another adjuvant therapy to treatment.”
She sent out the case and requests for feedback to the International Transplant Skin Cancer Collaborative, an 800-member consortium of dermatologists and Mohs surgeons who take care of transplant patients. She received information on three additional cases of aggressive squamous cell carcinoma (SCC) associated with ruxolitinib treatment:
• A patient with myelodysplastic syndrome with aggressive scalp SCC with cutaneous metastases.
• A patient with undifferentiated pleomorphic sarcoma of the scalp, several cutaneous SCCs.
• A patient with a myelodysplastic syndrome with in-transit metastases and explosive cutaneous SCCs. The patient has had the ruxolitinib dose reduced and may be switched to capecitabine.
Dr. Zwald noted that her patient was at risk for aggressive skin cancers for reasons in addition to ruxolitinib treatment.
“He was already immunosuppressed from his malignancy. He was on hydroxyurea, a drug that’s a cumulative phototoxin, and he’s out in the sun playing golf every day, and then was put on ruxolitinib. But the question we face now is how to try and stop this medication so we can get better treatment for him which will, of course, be very difficult.”
To contribute to Dr. Zwald’s case series, please email her at [email protected].
She had no relevant financial disclosures.
On Twitter @Alz_Gal
ORLANDO – The hematologic cancer drug ruxolitinib seems to be associated with cases of aggressive nonmelanoma skin cancer.
After treating a very aggressive squamous cell carcinoma in a 55-year-old man treated with ruxolitinib for polycythemia vera, and hearing firsthand of three other similar cases, Dr. Fiona Zwald is collecting additional data on the association. She intends to publish these cases in a monograph as a warning to dermatologists, hematologists, oncologists, and other physicians who manage patients with hematologic malignancies, she said at the annual meeting of the American College of Mohs Surgery.
The prescribing information for ruxolitinib (Jakafi, Incyte Pharmaceuticals; Jakavi, Novartis) was updated in 2014 to warn that patients taking the drug face an increased risk of nonmelanoma skin cancers. The label also recommends that physicians inspect the skin regularly and urge patients to be alert for and report any new or changing lesions.
Despite the warnings and recommendations, cases are occurring – and some are quite serious, said Dr. Zwald, a Mohs surgeon in Atlanta.
“People should know this is actually happening. If you have experience with this medication, please let us know so we can compile this report. We are trying to assess the number of skin cancers before and after initiating this medication,” she said.
Ruxolitinib is an inhibitor of Janus kinase with a special affinity for the JAK1 and JAK2 subtypes. Like other cytokine-signaling molecules, their function depends on cell context; it may inhibit cell growth in one setting, and, in another, stimulate it. Ruxolitinib was initially approved in 2011 for the treatment of intermediate- and high-risk myelofibrosis, including primary myelofibrosis, post–polycythemia vera myelofibrosis, and post–essential thrombocythemia myelofibrosis.
In 2014, indications for ruxolitinib were expanded to include treatment of patients with polycythemia vera who have had an inadequate response to or are intolerant of hydroxyurea.
Dr. Zwald’s patient had a 10-year history of polycythemia vera. He was initially well controlled on the standard hydroxyurea treatment. In the meantime, he began working as a caddy at a major U.S. golf club. He developed many facial squamous cell carcinomas that were treated with excision and radiation. A year before he presented to Dr. Zwald, he stopped responding to hydroxyurea and was placed on ruxolitinib.
The patient presented with a 4-cm ulcerated lesion over part of his right temple and to the right helical crus; the lesion had developed over 3 months. Dr. Zwald consulted with the patient’s medical oncologist; treatment with ruxolitinib continued, albeit at a reduced dosage in light of recent events.
She performed Mohs surgery on the patient. It was a challenging case, she said, not the least because adequate anesthesia could not be achieved with local anesthetic. Preoperative staging showed no nodal spread.
“He did, unfortunately demonstrate a large, indurated mass located over one branch of the superficial temporal artery. At the helical crus there was an area of bound-down, fixed tumor. Knowing that I would not be able to fully resect this, I passed him on to the operating room,” Dr. Zwald said. “This tumor was found to extend down to the parotid capsule, but margins were clear.” The surgical defect was successfully repaired with a split-thickness skin graft.
The tumor recurred about 3 months later, and the patient underwent another surgery.
“This time we could not get clear surgical margins, and the tumor was approaching the external auditory meatus. Surgery was abandoned due to fears of complications to that area,” she said.
She presented the case at tumor board, during which she and her colleagues discussed adjuvant radiation. They initially abandoned this idea because he had already had so much radiation to his face. After the second surgery, they decide to proceed with radiation. “The next conversation we have will be whether to add another adjuvant therapy to treatment.”
She sent out the case and requests for feedback to the International Transplant Skin Cancer Collaborative, an 800-member consortium of dermatologists and Mohs surgeons who take care of transplant patients. She received information on three additional cases of aggressive squamous cell carcinoma (SCC) associated with ruxolitinib treatment:
• A patient with myelodysplastic syndrome with aggressive scalp SCC with cutaneous metastases.
• A patient with undifferentiated pleomorphic sarcoma of the scalp, several cutaneous SCCs.
• A patient with a myelodysplastic syndrome with in-transit metastases and explosive cutaneous SCCs. The patient has had the ruxolitinib dose reduced and may be switched to capecitabine.
Dr. Zwald noted that her patient was at risk for aggressive skin cancers for reasons in addition to ruxolitinib treatment.
“He was already immunosuppressed from his malignancy. He was on hydroxyurea, a drug that’s a cumulative phototoxin, and he’s out in the sun playing golf every day, and then was put on ruxolitinib. But the question we face now is how to try and stop this medication so we can get better treatment for him which will, of course, be very difficult.”
To contribute to Dr. Zwald’s case series, please email her at [email protected].
She had no relevant financial disclosures.
On Twitter @Alz_Gal
ORLANDO – The hematologic cancer drug ruxolitinib seems to be associated with cases of aggressive nonmelanoma skin cancer.
After treating a very aggressive squamous cell carcinoma in a 55-year-old man treated with ruxolitinib for polycythemia vera, and hearing firsthand of three other similar cases, Dr. Fiona Zwald is collecting additional data on the association. She intends to publish these cases in a monograph as a warning to dermatologists, hematologists, oncologists, and other physicians who manage patients with hematologic malignancies, she said at the annual meeting of the American College of Mohs Surgery.
The prescribing information for ruxolitinib (Jakafi, Incyte Pharmaceuticals; Jakavi, Novartis) was updated in 2014 to warn that patients taking the drug face an increased risk of nonmelanoma skin cancers. The label also recommends that physicians inspect the skin regularly and urge patients to be alert for and report any new or changing lesions.
Despite the warnings and recommendations, cases are occurring – and some are quite serious, said Dr. Zwald, a Mohs surgeon in Atlanta.
“People should know this is actually happening. If you have experience with this medication, please let us know so we can compile this report. We are trying to assess the number of skin cancers before and after initiating this medication,” she said.
Ruxolitinib is an inhibitor of Janus kinase with a special affinity for the JAK1 and JAK2 subtypes. Like other cytokine-signaling molecules, their function depends on cell context; it may inhibit cell growth in one setting, and, in another, stimulate it. Ruxolitinib was initially approved in 2011 for the treatment of intermediate- and high-risk myelofibrosis, including primary myelofibrosis, post–polycythemia vera myelofibrosis, and post–essential thrombocythemia myelofibrosis.
In 2014, indications for ruxolitinib were expanded to include treatment of patients with polycythemia vera who have had an inadequate response to or are intolerant of hydroxyurea.
Dr. Zwald’s patient had a 10-year history of polycythemia vera. He was initially well controlled on the standard hydroxyurea treatment. In the meantime, he began working as a caddy at a major U.S. golf club. He developed many facial squamous cell carcinomas that were treated with excision and radiation. A year before he presented to Dr. Zwald, he stopped responding to hydroxyurea and was placed on ruxolitinib.
The patient presented with a 4-cm ulcerated lesion over part of his right temple and to the right helical crus; the lesion had developed over 3 months. Dr. Zwald consulted with the patient’s medical oncologist; treatment with ruxolitinib continued, albeit at a reduced dosage in light of recent events.
She performed Mohs surgery on the patient. It was a challenging case, she said, not the least because adequate anesthesia could not be achieved with local anesthetic. Preoperative staging showed no nodal spread.
“He did, unfortunately demonstrate a large, indurated mass located over one branch of the superficial temporal artery. At the helical crus there was an area of bound-down, fixed tumor. Knowing that I would not be able to fully resect this, I passed him on to the operating room,” Dr. Zwald said. “This tumor was found to extend down to the parotid capsule, but margins were clear.” The surgical defect was successfully repaired with a split-thickness skin graft.
The tumor recurred about 3 months later, and the patient underwent another surgery.
“This time we could not get clear surgical margins, and the tumor was approaching the external auditory meatus. Surgery was abandoned due to fears of complications to that area,” she said.
She presented the case at tumor board, during which she and her colleagues discussed adjuvant radiation. They initially abandoned this idea because he had already had so much radiation to his face. After the second surgery, they decide to proceed with radiation. “The next conversation we have will be whether to add another adjuvant therapy to treatment.”
She sent out the case and requests for feedback to the International Transplant Skin Cancer Collaborative, an 800-member consortium of dermatologists and Mohs surgeons who take care of transplant patients. She received information on three additional cases of aggressive squamous cell carcinoma (SCC) associated with ruxolitinib treatment:
• A patient with myelodysplastic syndrome with aggressive scalp SCC with cutaneous metastases.
• A patient with undifferentiated pleomorphic sarcoma of the scalp, several cutaneous SCCs.
• A patient with a myelodysplastic syndrome with in-transit metastases and explosive cutaneous SCCs. The patient has had the ruxolitinib dose reduced and may be switched to capecitabine.
Dr. Zwald noted that her patient was at risk for aggressive skin cancers for reasons in addition to ruxolitinib treatment.
“He was already immunosuppressed from his malignancy. He was on hydroxyurea, a drug that’s a cumulative phototoxin, and he’s out in the sun playing golf every day, and then was put on ruxolitinib. But the question we face now is how to try and stop this medication so we can get better treatment for him which will, of course, be very difficult.”
To contribute to Dr. Zwald’s case series, please email her at [email protected].
She had no relevant financial disclosures.
On Twitter @Alz_Gal
AT THE ACMS ANNUAL MEETING
Mohs with CK-7 staining: 98% 5-year cure rate for extramammary Paget disease
ORLANDO – Mohs surgery with cytokeratin-7 immunohistochemistry staining effected complete removal of extramammary Paget disease and resulted in a 5-year, 95% recurrence-free cure rate.
The results are significantly better than the often-cited 77% cure rate seen with Mohs surgery alone, Dr. Ali Alexander Damavandy said at the annual meeting of the American College of Mohs Surgery.
“These are statistically significant and clinically substantial results,” said Dr. Damavandy, a procedural dermatology fellow at the University of Pennsylvania, Philadelphia. “With this method you can tell a patient that in 5 years, he has a 95% chance of still not having the tumor. The high recurrence-free rate we have seen supports the view that Mohs surgery with cytokeratin-7 [CK-7] immunohistochemistry should be considered the curative treatment of choice for both primary and recurrent extramammary Paget disease of the skin.”
Dr. Damavandy’s retrospective review of 49 cases may seem small, he said, but it is “far and away the biggest cohort that exists, and the only substantial cohort with immunohistochemistry staining of CK-7.” The 5-year follow-up is also a strength of the study, he added.
Extramammary Paget disease (EMPD) remains an “extraordinarily hard tumor to treat. It typically presents with widespread intraepithelial islands of disease that are not clinically apparent. Local recurrence rates range from 33% to 60%, “leaving a lot of room for improvement,” Dr. Damavandy said.
“The explanations for recurrence are twofold,” he added. “First there is difficulty visualizing tumor cells in frozen sections. Second, it is a multifocal tumor that grows in a discontinuous fashion.”
Although one simply has to deal with the tumor spread, improvements can be made in reading the histopathology. Immunohistochemistry staining with CK-7 allows highly accurate visualization of individual Paget tumor cells, which express a very high level of the protein.
“Our hypothesis was that combining this improved tumor cell visualization with Mohs total excision would really make a dent in the recurrence rates of this disease,” Dr. Damavandy said.
He conducted a review of patients who were treated at four practices from 2004 to 2012. The cohort comprised 49 patients with 62 tumors; 43 were primary and the rest were recurrences. The majority (90%) occurred in the urogenital and anogenital region; the rest were axial or facial. All were treated with Mohs microsurgery enhanced by CK-7 staining of frozen sections. Recurrences were biopsy proven.
The typical Mohs technique for EMPD is to delineate a tumor-free area peripherally, and then excise the central tumor and tumor-bearing islands. The procedure can be long and arduous. Many cases are multiday efforts with large areas of excision.
“These can be very difficult wounds to manage even in a hospital. It’s resource-intense surgery,” Dr. Damavandy said.
The mean margin necessary to clear the lesions in this cohort was 2.6 cm. A 4-cm margin cleared almost 80%; 10% required a 7-cm margin.
“If we were going to make a recommendation to a nonMohs surgeon, it would be that 7 cm are needed to clear 98% of the tumors. That seems to me not reasonable for these anatomically complex and delicate regions. At the same time, the most commonly reported margin in the literature is 2 cm. In this cohort that would only have cleared 40% of the tumors.”
A mean of 3.4 Mohs stages were needed to obtain clear margins, although the range was wide (1-14 stages). Surgery took a mean of 1.5 days (range 1-5 days). Four patients could not be cleared and needed multidisciplinary care. These included two with vaginal invasion and two with invasion of the anal canal.
By 5 years, the overall tumor-free survival rate was 97%; the tumor-free survival rate was slightly better for primary than recurrent tumors (98% vs. 95%). When these rates were compared with Mohs without CK-7 staining, “primary Mohs doesn’t compare very well,” Dr. Damavandy said. At 5 years, the literature-reported recurrence rate for primary tumors treated with Mohs alone was 16% vs. Dr. Damavandy’s report of 2.3% for Mohs plus CK-7 staining. For recurrent tumors, the recurrence rates were 50% vs. 5.3%.
Two tumors recurred; the mean time to recurrence was 31 months. One recurrence was of a primary tumor treated by peripheral Mohs surgery, which was an uncommon approach in this cohort. This patient had a deep recurrence at 16 months.
The other case was a recurrence of a vulvar tumor that extended into the vaginal epithelium and across the cervix. Despite a vaginectomy and vaginal hysterectomy with clear margins, the patient had a recurrence at 46 months.
The patients were retreated and at last follow-up were free of disease.
Dr. Damavandy had no financial disclosures.
ORLANDO – Mohs surgery with cytokeratin-7 immunohistochemistry staining effected complete removal of extramammary Paget disease and resulted in a 5-year, 95% recurrence-free cure rate.
The results are significantly better than the often-cited 77% cure rate seen with Mohs surgery alone, Dr. Ali Alexander Damavandy said at the annual meeting of the American College of Mohs Surgery.
“These are statistically significant and clinically substantial results,” said Dr. Damavandy, a procedural dermatology fellow at the University of Pennsylvania, Philadelphia. “With this method you can tell a patient that in 5 years, he has a 95% chance of still not having the tumor. The high recurrence-free rate we have seen supports the view that Mohs surgery with cytokeratin-7 [CK-7] immunohistochemistry should be considered the curative treatment of choice for both primary and recurrent extramammary Paget disease of the skin.”
Dr. Damavandy’s retrospective review of 49 cases may seem small, he said, but it is “far and away the biggest cohort that exists, and the only substantial cohort with immunohistochemistry staining of CK-7.” The 5-year follow-up is also a strength of the study, he added.
Extramammary Paget disease (EMPD) remains an “extraordinarily hard tumor to treat. It typically presents with widespread intraepithelial islands of disease that are not clinically apparent. Local recurrence rates range from 33% to 60%, “leaving a lot of room for improvement,” Dr. Damavandy said.
“The explanations for recurrence are twofold,” he added. “First there is difficulty visualizing tumor cells in frozen sections. Second, it is a multifocal tumor that grows in a discontinuous fashion.”
Although one simply has to deal with the tumor spread, improvements can be made in reading the histopathology. Immunohistochemistry staining with CK-7 allows highly accurate visualization of individual Paget tumor cells, which express a very high level of the protein.
“Our hypothesis was that combining this improved tumor cell visualization with Mohs total excision would really make a dent in the recurrence rates of this disease,” Dr. Damavandy said.
He conducted a review of patients who were treated at four practices from 2004 to 2012. The cohort comprised 49 patients with 62 tumors; 43 were primary and the rest were recurrences. The majority (90%) occurred in the urogenital and anogenital region; the rest were axial or facial. All were treated with Mohs microsurgery enhanced by CK-7 staining of frozen sections. Recurrences were biopsy proven.
The typical Mohs technique for EMPD is to delineate a tumor-free area peripherally, and then excise the central tumor and tumor-bearing islands. The procedure can be long and arduous. Many cases are multiday efforts with large areas of excision.
“These can be very difficult wounds to manage even in a hospital. It’s resource-intense surgery,” Dr. Damavandy said.
The mean margin necessary to clear the lesions in this cohort was 2.6 cm. A 4-cm margin cleared almost 80%; 10% required a 7-cm margin.
“If we were going to make a recommendation to a nonMohs surgeon, it would be that 7 cm are needed to clear 98% of the tumors. That seems to me not reasonable for these anatomically complex and delicate regions. At the same time, the most commonly reported margin in the literature is 2 cm. In this cohort that would only have cleared 40% of the tumors.”
A mean of 3.4 Mohs stages were needed to obtain clear margins, although the range was wide (1-14 stages). Surgery took a mean of 1.5 days (range 1-5 days). Four patients could not be cleared and needed multidisciplinary care. These included two with vaginal invasion and two with invasion of the anal canal.
By 5 years, the overall tumor-free survival rate was 97%; the tumor-free survival rate was slightly better for primary than recurrent tumors (98% vs. 95%). When these rates were compared with Mohs without CK-7 staining, “primary Mohs doesn’t compare very well,” Dr. Damavandy said. At 5 years, the literature-reported recurrence rate for primary tumors treated with Mohs alone was 16% vs. Dr. Damavandy’s report of 2.3% for Mohs plus CK-7 staining. For recurrent tumors, the recurrence rates were 50% vs. 5.3%.
Two tumors recurred; the mean time to recurrence was 31 months. One recurrence was of a primary tumor treated by peripheral Mohs surgery, which was an uncommon approach in this cohort. This patient had a deep recurrence at 16 months.
The other case was a recurrence of a vulvar tumor that extended into the vaginal epithelium and across the cervix. Despite a vaginectomy and vaginal hysterectomy with clear margins, the patient had a recurrence at 46 months.
The patients were retreated and at last follow-up were free of disease.
Dr. Damavandy had no financial disclosures.
ORLANDO – Mohs surgery with cytokeratin-7 immunohistochemistry staining effected complete removal of extramammary Paget disease and resulted in a 5-year, 95% recurrence-free cure rate.
The results are significantly better than the often-cited 77% cure rate seen with Mohs surgery alone, Dr. Ali Alexander Damavandy said at the annual meeting of the American College of Mohs Surgery.
“These are statistically significant and clinically substantial results,” said Dr. Damavandy, a procedural dermatology fellow at the University of Pennsylvania, Philadelphia. “With this method you can tell a patient that in 5 years, he has a 95% chance of still not having the tumor. The high recurrence-free rate we have seen supports the view that Mohs surgery with cytokeratin-7 [CK-7] immunohistochemistry should be considered the curative treatment of choice for both primary and recurrent extramammary Paget disease of the skin.”
Dr. Damavandy’s retrospective review of 49 cases may seem small, he said, but it is “far and away the biggest cohort that exists, and the only substantial cohort with immunohistochemistry staining of CK-7.” The 5-year follow-up is also a strength of the study, he added.
Extramammary Paget disease (EMPD) remains an “extraordinarily hard tumor to treat. It typically presents with widespread intraepithelial islands of disease that are not clinically apparent. Local recurrence rates range from 33% to 60%, “leaving a lot of room for improvement,” Dr. Damavandy said.
“The explanations for recurrence are twofold,” he added. “First there is difficulty visualizing tumor cells in frozen sections. Second, it is a multifocal tumor that grows in a discontinuous fashion.”
Although one simply has to deal with the tumor spread, improvements can be made in reading the histopathology. Immunohistochemistry staining with CK-7 allows highly accurate visualization of individual Paget tumor cells, which express a very high level of the protein.
“Our hypothesis was that combining this improved tumor cell visualization with Mohs total excision would really make a dent in the recurrence rates of this disease,” Dr. Damavandy said.
He conducted a review of patients who were treated at four practices from 2004 to 2012. The cohort comprised 49 patients with 62 tumors; 43 were primary and the rest were recurrences. The majority (90%) occurred in the urogenital and anogenital region; the rest were axial or facial. All were treated with Mohs microsurgery enhanced by CK-7 staining of frozen sections. Recurrences were biopsy proven.
The typical Mohs technique for EMPD is to delineate a tumor-free area peripherally, and then excise the central tumor and tumor-bearing islands. The procedure can be long and arduous. Many cases are multiday efforts with large areas of excision.
“These can be very difficult wounds to manage even in a hospital. It’s resource-intense surgery,” Dr. Damavandy said.
The mean margin necessary to clear the lesions in this cohort was 2.6 cm. A 4-cm margin cleared almost 80%; 10% required a 7-cm margin.
“If we were going to make a recommendation to a nonMohs surgeon, it would be that 7 cm are needed to clear 98% of the tumors. That seems to me not reasonable for these anatomically complex and delicate regions. At the same time, the most commonly reported margin in the literature is 2 cm. In this cohort that would only have cleared 40% of the tumors.”
A mean of 3.4 Mohs stages were needed to obtain clear margins, although the range was wide (1-14 stages). Surgery took a mean of 1.5 days (range 1-5 days). Four patients could not be cleared and needed multidisciplinary care. These included two with vaginal invasion and two with invasion of the anal canal.
By 5 years, the overall tumor-free survival rate was 97%; the tumor-free survival rate was slightly better for primary than recurrent tumors (98% vs. 95%). When these rates were compared with Mohs without CK-7 staining, “primary Mohs doesn’t compare very well,” Dr. Damavandy said. At 5 years, the literature-reported recurrence rate for primary tumors treated with Mohs alone was 16% vs. Dr. Damavandy’s report of 2.3% for Mohs plus CK-7 staining. For recurrent tumors, the recurrence rates were 50% vs. 5.3%.
Two tumors recurred; the mean time to recurrence was 31 months. One recurrence was of a primary tumor treated by peripheral Mohs surgery, which was an uncommon approach in this cohort. This patient had a deep recurrence at 16 months.
The other case was a recurrence of a vulvar tumor that extended into the vaginal epithelium and across the cervix. Despite a vaginectomy and vaginal hysterectomy with clear margins, the patient had a recurrence at 46 months.
The patients were retreated and at last follow-up were free of disease.
Dr. Damavandy had no financial disclosures.
AT THE ACMS ANNUAL MEETING
Key clinical point: Mohs surgery enhanced with cytokeratin-7 immunohistochemistry appears to be very effective for extamammaory Paget disease.
Major finding: The 5-year recurrence rate was less than 5%.
Data source: The case review comprised 49 patients with 62 tumors.
Disclosures: Dr. Damavandy had no financial disclosures
Detecting morphologically difficult-to-diagnose melanomas
WAIKOLOA, HAWAII – Nodular melanoma is one of a handful of morphologic subtypes of melanoma that are difficult to diagnose in a timely way because they lack the conventional features associated with melanoma. But certain clinical and dermoscopic clues are helpful in avoiding misdiagnosis, Dr. Ashfaq A. Marghoob said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
He provided tips on how to recognize nodular melanoma and other difficult-to-diagnose morphologic subtypes, including desmoplastic, amelanotic, nevoid, and epidermotropic metastatic melanoma.
These diagnostically challenging melanoma subtypes have several things in common: clinically, they don’t look like melanomas, and dermoscopically, they display specific tell-tale features that speak of malignancy, including atypical polymorphous blood vessels and crystalline structures. Dermoscopy can be a big help in deciding whether to biopsy a clinically unremarkable-looking lesion, observed Dr. Marghoob of Memorial Sloan Kettering Cancer Center in New York.
Here’s the rundown on how to avoid delayed diagnosis of these melanomas:
Nodular melanoma: The big challenge posed by nodular melanoma is that it grows at a very high rate, a median of 0.5 mm per month, “so it’s really not a subtype of melanoma that’s amenable to screening,” the dermatologist said.
“Think about this: A patient comes in for screening today and you see nothing on their skin. Then a month from today they start a nodular melanoma. Their next appointment with you is a year from now. By the time they come back, that nodular melanoma is going to be a life-threatening cancer,” he explained. “It requires patient engagement in self-examination to bring these lesions to our attention, and we have to be perceptive enough to see these patients in a timely manner when they call. Otherwise these are melanomas that are really the killer tumors.”
Nodular melanomas often lack the “ABCD” features associated with most melanomas: asymmetry, border irregularity, color, and diameter greater than one-quarter of an inch. Instead, the lesions may exhibit the modified ABCDs described in pediatric melanoma: amelanotic, bump showing symmetry, color homogeneity in a shade of either pink or blue-black, and de novo, meaning the lesion didn’t arise in association with a nevus, Dr. Marghoob continued.
Roughly 60% of nodular melanomas are pigmented, the other 40% amelanotic. Dermoscopically, pigmented nodular melanomas are characterized by a greater degree of symmetry than that seen with other melanomas. Atypical vessels that exhibit tortuosity, a cork screw pattern, or an irregular hairpin shape are prominently visible. The lesions are multicolored, often blue-black, and may exhibit a blue-white veil. Notably absent are regression structures, streaks, and networks.
An amelanotic nodular melanoma also features prominent atypical vessels, symmetry, and sometimes crystalline structures, which appear as shiny white lines. Comma vessels and arborizing vessels are absent.
A more detailed description of the dermoscopic findings in nodular melanoma is available in a study coauthored by Dr. Marghoob (JAMA Dermatol. 2013;149[6]:699-709).
Desmoplastic melanoma: Seventy percent of desmoplastic melanomas are amelanotic. They often present as an unremarkable firm subcutaneous papule or nodule. Indeed, desmoplastic melanomas often have such a banal clinical appearance that in one-third of cases, melanoma is not even in the differential diagnosis.
“You’re thinking cyst, lipoma, dermatofibroma ... something other than a malignancy,” Dr. Marghoob said.
Suspicion is raised by a benign-looking lesion that’s symptomatic and/or exhibiting growth on chronically sun-damaged skin in an older patient. A scar with no history of trauma that’s located on chronically sun-damaged skin is another tipoff. Also, desmoplastic melanoma can arise in association with a lentigo maligna component.
“It is this knowledge of the association between lentigo maligna and desmoplastic melanoma that for the first time has enabled us to diagnose desmoplastic melanomas that are thin – not 5 or 10 mm, but more like 0.6 mm in thickness,” Dr. Marghoob said.
The main dermoscopic clue is the presence of atypical vascular structures.
For a fuller account of the dermoscopic characteristics of desmoplastic melanomas, Dr. Marghoob recommended a study he coauthored (JAMA Dermatol. 2013;149[4]:413-21).
Amelanotic melanoma: An indication of how difficult these cancers are to diagnose was provided by the international Genes, Environment, and Melanoma Study of nearly 3,500 invasive melanomas, 8% of which were amelanotic. They were at a more advanced tumor stage at diagnosis. As a result, the mortality risk during a median 7.6 years of follow-up was an adjusted twofold greater for patients with amelanotic as compared with pigmented melanomas (JAMA Dermatol. 2014;150[12]:1306-314).
Dr. Marghoob coauthored a retrospective review of 20 consecutively diagnosed amelanotic melanomas. The lesions lacked any of the classic ABCD features. Most were symmetric, oval to round in shape, had regular borders, and were pink in color. Dermoscopically, a consistent finding was a polymorphous vascular pattern (J Eur Acad Dermatol Venereol. 2012;26[5]:591-6).
In an earlier five-continent study comparing dermoscopic features of 222 amelanotic melanomas, 105 pigmented melanomas, and 170 benign melanocytic lesions, investigators came up with a simple model that distinguished melanomas from nonmelanomas with 70% sensitivity and 56% specificity. The take-home message: Amelanotic melanomas often feature more than one shade of pink upon dermoscopic examination, along with dotted and linear irregular vessels and predominant central vessels (Arch Dermatol. 2008;144[9]:1120-7).
Nevoid melanoma: Clinically they often resemble an intradermal nevus, and they’re often amelanotic. Dermoscopically, however, an intradermal nevus displays a mammillated surface, with each individual mammillated area being associated with an isolated comma or hairpin vessel. In contrast, the surface of a nevoid melanoma is more undulating in appearance and lacks the classic vascular pattern seen in intradermal nevi. If there’s pigmentation present in a nevoid melanoma it will be distributed heterogeneously. The dermoscopic finding of irregular blood vessels and/or crystalline structures tips the balance in favor of biopsy.
Dr. Marghoob referred dermatologists interested in the dermoscopic features of nevoid melanoma to a recent study by members of the International Dermoscopy Society; he was one of the authors (Br J Dermatol. 2015;172[4]:961-7).
Epidermotropic metastatic melanoma: These lesions lack the ABCDs, are often amelanotic, and look like nondescript papules. If such a lesion is new, especially in a patient with a history of melanoma, think epidermotropic metastatic melanoma.
Spanish dermatologists have described five different dermoscopic patterns of melanoma metastases in an informative retrospective study: blue nevus-like, angioma-like, nevus-like, vascular, and unspecific. The vascular type is the most common form, characterized by amelanotic papules 2-3 mm in diameter and tortuous corkscrew vessels within the lesions (Br J Dermatol. 2013;169[1]:91-9).
Dr. Marghoob reported having no financial conflicts of interest regarding his presentation. SDEF and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Nodular melanoma is one of a handful of morphologic subtypes of melanoma that are difficult to diagnose in a timely way because they lack the conventional features associated with melanoma. But certain clinical and dermoscopic clues are helpful in avoiding misdiagnosis, Dr. Ashfaq A. Marghoob said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
He provided tips on how to recognize nodular melanoma and other difficult-to-diagnose morphologic subtypes, including desmoplastic, amelanotic, nevoid, and epidermotropic metastatic melanoma.
These diagnostically challenging melanoma subtypes have several things in common: clinically, they don’t look like melanomas, and dermoscopically, they display specific tell-tale features that speak of malignancy, including atypical polymorphous blood vessels and crystalline structures. Dermoscopy can be a big help in deciding whether to biopsy a clinically unremarkable-looking lesion, observed Dr. Marghoob of Memorial Sloan Kettering Cancer Center in New York.
Here’s the rundown on how to avoid delayed diagnosis of these melanomas:
Nodular melanoma: The big challenge posed by nodular melanoma is that it grows at a very high rate, a median of 0.5 mm per month, “so it’s really not a subtype of melanoma that’s amenable to screening,” the dermatologist said.
“Think about this: A patient comes in for screening today and you see nothing on their skin. Then a month from today they start a nodular melanoma. Their next appointment with you is a year from now. By the time they come back, that nodular melanoma is going to be a life-threatening cancer,” he explained. “It requires patient engagement in self-examination to bring these lesions to our attention, and we have to be perceptive enough to see these patients in a timely manner when they call. Otherwise these are melanomas that are really the killer tumors.”
Nodular melanomas often lack the “ABCD” features associated with most melanomas: asymmetry, border irregularity, color, and diameter greater than one-quarter of an inch. Instead, the lesions may exhibit the modified ABCDs described in pediatric melanoma: amelanotic, bump showing symmetry, color homogeneity in a shade of either pink or blue-black, and de novo, meaning the lesion didn’t arise in association with a nevus, Dr. Marghoob continued.
Roughly 60% of nodular melanomas are pigmented, the other 40% amelanotic. Dermoscopically, pigmented nodular melanomas are characterized by a greater degree of symmetry than that seen with other melanomas. Atypical vessels that exhibit tortuosity, a cork screw pattern, or an irregular hairpin shape are prominently visible. The lesions are multicolored, often blue-black, and may exhibit a blue-white veil. Notably absent are regression structures, streaks, and networks.
An amelanotic nodular melanoma also features prominent atypical vessels, symmetry, and sometimes crystalline structures, which appear as shiny white lines. Comma vessels and arborizing vessels are absent.
A more detailed description of the dermoscopic findings in nodular melanoma is available in a study coauthored by Dr. Marghoob (JAMA Dermatol. 2013;149[6]:699-709).
Desmoplastic melanoma: Seventy percent of desmoplastic melanomas are amelanotic. They often present as an unremarkable firm subcutaneous papule or nodule. Indeed, desmoplastic melanomas often have such a banal clinical appearance that in one-third of cases, melanoma is not even in the differential diagnosis.
“You’re thinking cyst, lipoma, dermatofibroma ... something other than a malignancy,” Dr. Marghoob said.
Suspicion is raised by a benign-looking lesion that’s symptomatic and/or exhibiting growth on chronically sun-damaged skin in an older patient. A scar with no history of trauma that’s located on chronically sun-damaged skin is another tipoff. Also, desmoplastic melanoma can arise in association with a lentigo maligna component.
“It is this knowledge of the association between lentigo maligna and desmoplastic melanoma that for the first time has enabled us to diagnose desmoplastic melanomas that are thin – not 5 or 10 mm, but more like 0.6 mm in thickness,” Dr. Marghoob said.
The main dermoscopic clue is the presence of atypical vascular structures.
For a fuller account of the dermoscopic characteristics of desmoplastic melanomas, Dr. Marghoob recommended a study he coauthored (JAMA Dermatol. 2013;149[4]:413-21).
Amelanotic melanoma: An indication of how difficult these cancers are to diagnose was provided by the international Genes, Environment, and Melanoma Study of nearly 3,500 invasive melanomas, 8% of which were amelanotic. They were at a more advanced tumor stage at diagnosis. As a result, the mortality risk during a median 7.6 years of follow-up was an adjusted twofold greater for patients with amelanotic as compared with pigmented melanomas (JAMA Dermatol. 2014;150[12]:1306-314).
Dr. Marghoob coauthored a retrospective review of 20 consecutively diagnosed amelanotic melanomas. The lesions lacked any of the classic ABCD features. Most were symmetric, oval to round in shape, had regular borders, and were pink in color. Dermoscopically, a consistent finding was a polymorphous vascular pattern (J Eur Acad Dermatol Venereol. 2012;26[5]:591-6).
In an earlier five-continent study comparing dermoscopic features of 222 amelanotic melanomas, 105 pigmented melanomas, and 170 benign melanocytic lesions, investigators came up with a simple model that distinguished melanomas from nonmelanomas with 70% sensitivity and 56% specificity. The take-home message: Amelanotic melanomas often feature more than one shade of pink upon dermoscopic examination, along with dotted and linear irregular vessels and predominant central vessels (Arch Dermatol. 2008;144[9]:1120-7).
Nevoid melanoma: Clinically they often resemble an intradermal nevus, and they’re often amelanotic. Dermoscopically, however, an intradermal nevus displays a mammillated surface, with each individual mammillated area being associated with an isolated comma or hairpin vessel. In contrast, the surface of a nevoid melanoma is more undulating in appearance and lacks the classic vascular pattern seen in intradermal nevi. If there’s pigmentation present in a nevoid melanoma it will be distributed heterogeneously. The dermoscopic finding of irregular blood vessels and/or crystalline structures tips the balance in favor of biopsy.
Dr. Marghoob referred dermatologists interested in the dermoscopic features of nevoid melanoma to a recent study by members of the International Dermoscopy Society; he was one of the authors (Br J Dermatol. 2015;172[4]:961-7).
Epidermotropic metastatic melanoma: These lesions lack the ABCDs, are often amelanotic, and look like nondescript papules. If such a lesion is new, especially in a patient with a history of melanoma, think epidermotropic metastatic melanoma.
Spanish dermatologists have described five different dermoscopic patterns of melanoma metastases in an informative retrospective study: blue nevus-like, angioma-like, nevus-like, vascular, and unspecific. The vascular type is the most common form, characterized by amelanotic papules 2-3 mm in diameter and tortuous corkscrew vessels within the lesions (Br J Dermatol. 2013;169[1]:91-9).
Dr. Marghoob reported having no financial conflicts of interest regarding his presentation. SDEF and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Nodular melanoma is one of a handful of morphologic subtypes of melanoma that are difficult to diagnose in a timely way because they lack the conventional features associated with melanoma. But certain clinical and dermoscopic clues are helpful in avoiding misdiagnosis, Dr. Ashfaq A. Marghoob said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
He provided tips on how to recognize nodular melanoma and other difficult-to-diagnose morphologic subtypes, including desmoplastic, amelanotic, nevoid, and epidermotropic metastatic melanoma.
These diagnostically challenging melanoma subtypes have several things in common: clinically, they don’t look like melanomas, and dermoscopically, they display specific tell-tale features that speak of malignancy, including atypical polymorphous blood vessels and crystalline structures. Dermoscopy can be a big help in deciding whether to biopsy a clinically unremarkable-looking lesion, observed Dr. Marghoob of Memorial Sloan Kettering Cancer Center in New York.
Here’s the rundown on how to avoid delayed diagnosis of these melanomas:
Nodular melanoma: The big challenge posed by nodular melanoma is that it grows at a very high rate, a median of 0.5 mm per month, “so it’s really not a subtype of melanoma that’s amenable to screening,” the dermatologist said.
“Think about this: A patient comes in for screening today and you see nothing on their skin. Then a month from today they start a nodular melanoma. Their next appointment with you is a year from now. By the time they come back, that nodular melanoma is going to be a life-threatening cancer,” he explained. “It requires patient engagement in self-examination to bring these lesions to our attention, and we have to be perceptive enough to see these patients in a timely manner when they call. Otherwise these are melanomas that are really the killer tumors.”
Nodular melanomas often lack the “ABCD” features associated with most melanomas: asymmetry, border irregularity, color, and diameter greater than one-quarter of an inch. Instead, the lesions may exhibit the modified ABCDs described in pediatric melanoma: amelanotic, bump showing symmetry, color homogeneity in a shade of either pink or blue-black, and de novo, meaning the lesion didn’t arise in association with a nevus, Dr. Marghoob continued.
Roughly 60% of nodular melanomas are pigmented, the other 40% amelanotic. Dermoscopically, pigmented nodular melanomas are characterized by a greater degree of symmetry than that seen with other melanomas. Atypical vessels that exhibit tortuosity, a cork screw pattern, or an irregular hairpin shape are prominently visible. The lesions are multicolored, often blue-black, and may exhibit a blue-white veil. Notably absent are regression structures, streaks, and networks.
An amelanotic nodular melanoma also features prominent atypical vessels, symmetry, and sometimes crystalline structures, which appear as shiny white lines. Comma vessels and arborizing vessels are absent.
A more detailed description of the dermoscopic findings in nodular melanoma is available in a study coauthored by Dr. Marghoob (JAMA Dermatol. 2013;149[6]:699-709).
Desmoplastic melanoma: Seventy percent of desmoplastic melanomas are amelanotic. They often present as an unremarkable firm subcutaneous papule or nodule. Indeed, desmoplastic melanomas often have such a banal clinical appearance that in one-third of cases, melanoma is not even in the differential diagnosis.
“You’re thinking cyst, lipoma, dermatofibroma ... something other than a malignancy,” Dr. Marghoob said.
Suspicion is raised by a benign-looking lesion that’s symptomatic and/or exhibiting growth on chronically sun-damaged skin in an older patient. A scar with no history of trauma that’s located on chronically sun-damaged skin is another tipoff. Also, desmoplastic melanoma can arise in association with a lentigo maligna component.
“It is this knowledge of the association between lentigo maligna and desmoplastic melanoma that for the first time has enabled us to diagnose desmoplastic melanomas that are thin – not 5 or 10 mm, but more like 0.6 mm in thickness,” Dr. Marghoob said.
The main dermoscopic clue is the presence of atypical vascular structures.
For a fuller account of the dermoscopic characteristics of desmoplastic melanomas, Dr. Marghoob recommended a study he coauthored (JAMA Dermatol. 2013;149[4]:413-21).
Amelanotic melanoma: An indication of how difficult these cancers are to diagnose was provided by the international Genes, Environment, and Melanoma Study of nearly 3,500 invasive melanomas, 8% of which were amelanotic. They were at a more advanced tumor stage at diagnosis. As a result, the mortality risk during a median 7.6 years of follow-up was an adjusted twofold greater for patients with amelanotic as compared with pigmented melanomas (JAMA Dermatol. 2014;150[12]:1306-314).
Dr. Marghoob coauthored a retrospective review of 20 consecutively diagnosed amelanotic melanomas. The lesions lacked any of the classic ABCD features. Most were symmetric, oval to round in shape, had regular borders, and were pink in color. Dermoscopically, a consistent finding was a polymorphous vascular pattern (J Eur Acad Dermatol Venereol. 2012;26[5]:591-6).
In an earlier five-continent study comparing dermoscopic features of 222 amelanotic melanomas, 105 pigmented melanomas, and 170 benign melanocytic lesions, investigators came up with a simple model that distinguished melanomas from nonmelanomas with 70% sensitivity and 56% specificity. The take-home message: Amelanotic melanomas often feature more than one shade of pink upon dermoscopic examination, along with dotted and linear irregular vessels and predominant central vessels (Arch Dermatol. 2008;144[9]:1120-7).
Nevoid melanoma: Clinically they often resemble an intradermal nevus, and they’re often amelanotic. Dermoscopically, however, an intradermal nevus displays a mammillated surface, with each individual mammillated area being associated with an isolated comma or hairpin vessel. In contrast, the surface of a nevoid melanoma is more undulating in appearance and lacks the classic vascular pattern seen in intradermal nevi. If there’s pigmentation present in a nevoid melanoma it will be distributed heterogeneously. The dermoscopic finding of irregular blood vessels and/or crystalline structures tips the balance in favor of biopsy.
Dr. Marghoob referred dermatologists interested in the dermoscopic features of nevoid melanoma to a recent study by members of the International Dermoscopy Society; he was one of the authors (Br J Dermatol. 2015;172[4]:961-7).
Epidermotropic metastatic melanoma: These lesions lack the ABCDs, are often amelanotic, and look like nondescript papules. If such a lesion is new, especially in a patient with a history of melanoma, think epidermotropic metastatic melanoma.
Spanish dermatologists have described five different dermoscopic patterns of melanoma metastases in an informative retrospective study: blue nevus-like, angioma-like, nevus-like, vascular, and unspecific. The vascular type is the most common form, characterized by amelanotic papules 2-3 mm in diameter and tortuous corkscrew vessels within the lesions (Br J Dermatol. 2013;169[1]:91-9).
Dr. Marghoob reported having no financial conflicts of interest regarding his presentation. SDEF and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR
Patient-related factors are key to nevus suspiciousness
WAIKOLOA, HAWAII – Some melanomas can be diagnosed from the examination room doorway. Others are evident only upon close visual inspection. But the most challenging cases require integration of information regarding the lesion’s dermoscopic pattern in the context of the clues provided by key patient-specific characteristics, according to Dr. Michael A. Marchetti.
“Consider a melanoma diagnosis when a lesion is wrong for the patient’s age, the anatomic location, or skin type, or if it deviates from the patient’s expected signature pattern of nevi,” noted Dr. Marchetti, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York.
A landmark study that provides guidance in this area was conducted several years ago at dermatology centers in four European countries and at Memorial Sloan-Kettering. The investigators enrolled 480 consecutive children and adults with a total of 5,481 melanocytic nevi. The study showcased significant age- and anatomic site–related differences in the distribution of nevi categorized according to dermoscopic subgroups (Arch Dermatol. 2011;147[6]:663-70).
For example, nevi characterized dermoscopically by a peripheral rim of globules were found to be vastly more common during the first 3 decades of life than later. Based upon this study and other data, Dr. Marchetti’s suggested management strategy for peripheral globular nevus with no other concerning features in patients up to age 30 is reassurance that the lesion is not going to be a problem and doesn’t require careful monitoring or biopsy. In a patient beyond age 30, however, frequent monitoring or biopsy is appropriate – and the older the patient with a peripheral globular nevus, the lower the threshold for biopsy.
A peripheral globular nevus is typically a nevus in its radial growth phase, which can continue for years before the nevus enters senescence. The same is true of a nevus that exhibits a Spitzoid starbust pattern on dermoscopy. It is growing radially, and the pretest probability that it’s malignant is highly age dependent.
“In a child, it’s very likely to be a Spitz nevus. In an adult, it’s very likely to be a melanoma. Based upon morphology alone, you really can’t make a distinction between these lesions,” Dr. Marchetti said.
The importance of age in differentiating these starburst lesions was underscored in a recent Italian study involving 384 symmetric, dermoscopically Spitzoid-looking lesions in patients aged 12 or older. Histopathologically, 13.3% of the lesions were diagnosed as melanoma. The probability increased with advancing age, reaching 50% or more after age 50 years. The investigators concluded that the only safe strategy to avoid missing a melanoma is to excise all Spitzoid-looking lesions in patients aged 12 years or older (J Am Acad Dermatol. 2015;72[1]:47-53).
“That concurs with our practice at Memorial Sloan-Kettering. We tend to biopsy all lesions with this particular morphology because you just can’t tell,” Dr. Marchetti said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
Nevi with a globular dermoscopic pattern occur mostly in children and mainly on the upper back. A globular lesion that develops in an adult or on an extremity is “wrong,” and therefore biopsy should be seriously considered.
In contrast, nevi classified dermoscopically as reticular occur on the trunk and extremities with similar frequency, he continued.
Age and anatomic location are also important considerations in deciding whether a lesion might be a case of nested melanoma of the elderly. This is a form of melanoma first described only a few years ago. It takes the form of a large flat pigmented lesion showing a dermoscopic pattern of irregular globules throughout in a patient over aged 60 years. Notably, three-quarters of cases of nested melanoma of the elderly occur on the extremities (JAMA Dermatol. 2013;149[8]:941-5).
Skin type can raise or diminish the concern that a pigmented lesion is a melanoma. Patients with a lighter skin type tend to have light brown nevi with a patchy reticular network and central hypopigmentation; dark nevi are relatively uncommon in lighter-skinned patients and thus stand out as suspicious outliers. The flip side is also true: Patients with darker skin types tend to have dark nevi with central hyperpigmentation.
A nevus that deviates from a patient’s signature pattern is often referred to as the ugly duckling sign of melanoma.
“It’s the context provided by the background nevi which informs you if there’s an outlier. This can be helpful not only in detecting melanoma, but also in reducing unnecessary biopsies. If a lesion you’re wondering about looks dermoscopically like the patient’s other nevi, that’s reassuring,” Dr. Marchetti said.
He reported having no financial conflicts regarding his presentation. SDEF and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Some melanomas can be diagnosed from the examination room doorway. Others are evident only upon close visual inspection. But the most challenging cases require integration of information regarding the lesion’s dermoscopic pattern in the context of the clues provided by key patient-specific characteristics, according to Dr. Michael A. Marchetti.
“Consider a melanoma diagnosis when a lesion is wrong for the patient’s age, the anatomic location, or skin type, or if it deviates from the patient’s expected signature pattern of nevi,” noted Dr. Marchetti, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York.
A landmark study that provides guidance in this area was conducted several years ago at dermatology centers in four European countries and at Memorial Sloan-Kettering. The investigators enrolled 480 consecutive children and adults with a total of 5,481 melanocytic nevi. The study showcased significant age- and anatomic site–related differences in the distribution of nevi categorized according to dermoscopic subgroups (Arch Dermatol. 2011;147[6]:663-70).
For example, nevi characterized dermoscopically by a peripheral rim of globules were found to be vastly more common during the first 3 decades of life than later. Based upon this study and other data, Dr. Marchetti’s suggested management strategy for peripheral globular nevus with no other concerning features in patients up to age 30 is reassurance that the lesion is not going to be a problem and doesn’t require careful monitoring or biopsy. In a patient beyond age 30, however, frequent monitoring or biopsy is appropriate – and the older the patient with a peripheral globular nevus, the lower the threshold for biopsy.
A peripheral globular nevus is typically a nevus in its radial growth phase, which can continue for years before the nevus enters senescence. The same is true of a nevus that exhibits a Spitzoid starbust pattern on dermoscopy. It is growing radially, and the pretest probability that it’s malignant is highly age dependent.
“In a child, it’s very likely to be a Spitz nevus. In an adult, it’s very likely to be a melanoma. Based upon morphology alone, you really can’t make a distinction between these lesions,” Dr. Marchetti said.
The importance of age in differentiating these starburst lesions was underscored in a recent Italian study involving 384 symmetric, dermoscopically Spitzoid-looking lesions in patients aged 12 or older. Histopathologically, 13.3% of the lesions were diagnosed as melanoma. The probability increased with advancing age, reaching 50% or more after age 50 years. The investigators concluded that the only safe strategy to avoid missing a melanoma is to excise all Spitzoid-looking lesions in patients aged 12 years or older (J Am Acad Dermatol. 2015;72[1]:47-53).
“That concurs with our practice at Memorial Sloan-Kettering. We tend to biopsy all lesions with this particular morphology because you just can’t tell,” Dr. Marchetti said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
Nevi with a globular dermoscopic pattern occur mostly in children and mainly on the upper back. A globular lesion that develops in an adult or on an extremity is “wrong,” and therefore biopsy should be seriously considered.
In contrast, nevi classified dermoscopically as reticular occur on the trunk and extremities with similar frequency, he continued.
Age and anatomic location are also important considerations in deciding whether a lesion might be a case of nested melanoma of the elderly. This is a form of melanoma first described only a few years ago. It takes the form of a large flat pigmented lesion showing a dermoscopic pattern of irregular globules throughout in a patient over aged 60 years. Notably, three-quarters of cases of nested melanoma of the elderly occur on the extremities (JAMA Dermatol. 2013;149[8]:941-5).
Skin type can raise or diminish the concern that a pigmented lesion is a melanoma. Patients with a lighter skin type tend to have light brown nevi with a patchy reticular network and central hypopigmentation; dark nevi are relatively uncommon in lighter-skinned patients and thus stand out as suspicious outliers. The flip side is also true: Patients with darker skin types tend to have dark nevi with central hyperpigmentation.
A nevus that deviates from a patient’s signature pattern is often referred to as the ugly duckling sign of melanoma.
“It’s the context provided by the background nevi which informs you if there’s an outlier. This can be helpful not only in detecting melanoma, but also in reducing unnecessary biopsies. If a lesion you’re wondering about looks dermoscopically like the patient’s other nevi, that’s reassuring,” Dr. Marchetti said.
He reported having no financial conflicts regarding his presentation. SDEF and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Some melanomas can be diagnosed from the examination room doorway. Others are evident only upon close visual inspection. But the most challenging cases require integration of information regarding the lesion’s dermoscopic pattern in the context of the clues provided by key patient-specific characteristics, according to Dr. Michael A. Marchetti.
“Consider a melanoma diagnosis when a lesion is wrong for the patient’s age, the anatomic location, or skin type, or if it deviates from the patient’s expected signature pattern of nevi,” noted Dr. Marchetti, a dermatologist at Memorial Sloan-Kettering Cancer Center in New York.
A landmark study that provides guidance in this area was conducted several years ago at dermatology centers in four European countries and at Memorial Sloan-Kettering. The investigators enrolled 480 consecutive children and adults with a total of 5,481 melanocytic nevi. The study showcased significant age- and anatomic site–related differences in the distribution of nevi categorized according to dermoscopic subgroups (Arch Dermatol. 2011;147[6]:663-70).
For example, nevi characterized dermoscopically by a peripheral rim of globules were found to be vastly more common during the first 3 decades of life than later. Based upon this study and other data, Dr. Marchetti’s suggested management strategy for peripheral globular nevus with no other concerning features in patients up to age 30 is reassurance that the lesion is not going to be a problem and doesn’t require careful monitoring or biopsy. In a patient beyond age 30, however, frequent monitoring or biopsy is appropriate – and the older the patient with a peripheral globular nevus, the lower the threshold for biopsy.
A peripheral globular nevus is typically a nevus in its radial growth phase, which can continue for years before the nevus enters senescence. The same is true of a nevus that exhibits a Spitzoid starbust pattern on dermoscopy. It is growing radially, and the pretest probability that it’s malignant is highly age dependent.
“In a child, it’s very likely to be a Spitz nevus. In an adult, it’s very likely to be a melanoma. Based upon morphology alone, you really can’t make a distinction between these lesions,” Dr. Marchetti said.
The importance of age in differentiating these starburst lesions was underscored in a recent Italian study involving 384 symmetric, dermoscopically Spitzoid-looking lesions in patients aged 12 or older. Histopathologically, 13.3% of the lesions were diagnosed as melanoma. The probability increased with advancing age, reaching 50% or more after age 50 years. The investigators concluded that the only safe strategy to avoid missing a melanoma is to excise all Spitzoid-looking lesions in patients aged 12 years or older (J Am Acad Dermatol. 2015;72[1]:47-53).
“That concurs with our practice at Memorial Sloan-Kettering. We tend to biopsy all lesions with this particular morphology because you just can’t tell,” Dr. Marchetti said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
Nevi with a globular dermoscopic pattern occur mostly in children and mainly on the upper back. A globular lesion that develops in an adult or on an extremity is “wrong,” and therefore biopsy should be seriously considered.
In contrast, nevi classified dermoscopically as reticular occur on the trunk and extremities with similar frequency, he continued.
Age and anatomic location are also important considerations in deciding whether a lesion might be a case of nested melanoma of the elderly. This is a form of melanoma first described only a few years ago. It takes the form of a large flat pigmented lesion showing a dermoscopic pattern of irregular globules throughout in a patient over aged 60 years. Notably, three-quarters of cases of nested melanoma of the elderly occur on the extremities (JAMA Dermatol. 2013;149[8]:941-5).
Skin type can raise or diminish the concern that a pigmented lesion is a melanoma. Patients with a lighter skin type tend to have light brown nevi with a patchy reticular network and central hypopigmentation; dark nevi are relatively uncommon in lighter-skinned patients and thus stand out as suspicious outliers. The flip side is also true: Patients with darker skin types tend to have dark nevi with central hyperpigmentation.
A nevus that deviates from a patient’s signature pattern is often referred to as the ugly duckling sign of melanoma.
“It’s the context provided by the background nevi which informs you if there’s an outlier. This can be helpful not only in detecting melanoma, but also in reducing unnecessary biopsies. If a lesion you’re wondering about looks dermoscopically like the patient’s other nevi, that’s reassuring,” Dr. Marchetti said.
He reported having no financial conflicts regarding his presentation. SDEF and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR