User login
Parental bias about a doctor can’t trump a patient’s health
This transcript has been edited for clarity.
I’d like to present you today with a case that raised a large amount of discussion and debate. I got involved as an ethics consultant on the case. I think you’ll find it very interesting and I also think there are going to be some differences of opinion about how to manage the case. I’ll be looking forward to getting comments and feedback on this.
The case involved a 14-year-old boy who had been brought into the hospital by his parents, suffering from severe bouts of anxiety that were just almost overwhelming to him. When he was brought in, he was assigned a health care provider who had a West African last name. Prior to meeting the patient, I have to say that the father of this kid told the intake department nurse that he requested someone else. He saw the name – he hadn’t even met the provider – and he said he wanted someone who might be Catholic.
The parents are both from the Dominican Republic. They identified as White, but they appeared to be non-White Latinx to the nurse who was doing some of the initial intake. They got reassigned to a different provider in the department who identified as African American.
The first month of treatment for the young boy went very well, and he seemed to be getting along extremely well with his provider. He was reporting relief to both parents of some of his anxiety, and the provider felt very connected to the child. A good doctor-patient alliance had been formed.
Nevertheless, at the end of the first month, the father connected back to one of the administrators at the hospital and complained, saying he still wanted a different provider. When asked why, he said, “Well, I don’t really want to answer that,” but getting pressed, he basically said he wasn’t comfortable with having an African American doctor take care of his child. He eventually went back to the argument that what he wanted was someone with a Catholic background, although I don’t know that he knew whether this particular provider was religious – Catholic or anything else.
Some people felt that, as the father in charge of the child’s care, if we could accommodate what he wanted in terms of the parents being comfortable, then that’s something we should do. I absolutely did not agree.
My view is that in a situation where a strong provider-patient relationship has been established, where trust is going both ways, where there are no issues coming up between this 14-year-old and the provider, and when a serious mental health issue is being adequately addressed, the patient’s interest must come first.
Once that therapeutic alliance had been established and both the patient and the provider felt satisfied, I don’t think the father’s wishes made any sense. He may have been acting more out of bigotry or just discomfort about difference in terms of who the provider was. I don’t think that’s something that any health system should have to accommodate unless it is getting in the way of patient care.
I hope that we treat all physicians as properly trained to deal with all kinds of patients, regardless of their religion, ethnicity, or skin color. They should have the skills to manage and do well with any patient. There may be situations where it just doesn’t work or where people don’t get along. Yes, I think we then should try, perhaps, to shift the doctor, get a different nurse, or have a different person do an exam. That’s because of the inability to get the patient’s health interests addressed.
Listening to this dad about what he preferred in terms of religion or ethnicity seemed to me to be interfering with medical success. Could I stop him from moving this patient out entirely from the care setting? Probably not, but I think the way to manage this is to try to talk to him – and, by the way, to talk to the mother.
When we did bring the mom into the situation, she was very happy with the health care provider. She didn’t agree with the dad and wanted to have a meeting with the social worker, the dad, and her to get him to get over the worries, concerns, and maybe even biases he was bringing in about the kind of provider he wanted. That’s exactly what we did.
I know that there are many instances where patients may say, “I don’t want a particular doctor or a particular type.” My view is that we shouldn’t accommodate that. We should say that our doctors are trained to help and care for all manner of people. Unless we can think of some reason that there might be a gap or a problem in the actual delivery of the quality of care, we are not going to accommodate racism, bigotry, or bias.
We certainly shouldn’t be accommodating that once a successful therapeutic relationship is established. Even when it’s a child, I would argue that the patient’s best interest has to trump parental desires, parental worries, and parental concerns about the background, ethnicity, and religion of the provider.
Dr. Caplan is director of the division of medical ethics at NYU Langone Medical Center, New York. He disclosed a conflict of interest with Johnson & Johnson.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I’d like to present you today with a case that raised a large amount of discussion and debate. I got involved as an ethics consultant on the case. I think you’ll find it very interesting and I also think there are going to be some differences of opinion about how to manage the case. I’ll be looking forward to getting comments and feedback on this.
The case involved a 14-year-old boy who had been brought into the hospital by his parents, suffering from severe bouts of anxiety that were just almost overwhelming to him. When he was brought in, he was assigned a health care provider who had a West African last name. Prior to meeting the patient, I have to say that the father of this kid told the intake department nurse that he requested someone else. He saw the name – he hadn’t even met the provider – and he said he wanted someone who might be Catholic.
The parents are both from the Dominican Republic. They identified as White, but they appeared to be non-White Latinx to the nurse who was doing some of the initial intake. They got reassigned to a different provider in the department who identified as African American.
The first month of treatment for the young boy went very well, and he seemed to be getting along extremely well with his provider. He was reporting relief to both parents of some of his anxiety, and the provider felt very connected to the child. A good doctor-patient alliance had been formed.
Nevertheless, at the end of the first month, the father connected back to one of the administrators at the hospital and complained, saying he still wanted a different provider. When asked why, he said, “Well, I don’t really want to answer that,” but getting pressed, he basically said he wasn’t comfortable with having an African American doctor take care of his child. He eventually went back to the argument that what he wanted was someone with a Catholic background, although I don’t know that he knew whether this particular provider was religious – Catholic or anything else.
Some people felt that, as the father in charge of the child’s care, if we could accommodate what he wanted in terms of the parents being comfortable, then that’s something we should do. I absolutely did not agree.
My view is that in a situation where a strong provider-patient relationship has been established, where trust is going both ways, where there are no issues coming up between this 14-year-old and the provider, and when a serious mental health issue is being adequately addressed, the patient’s interest must come first.
Once that therapeutic alliance had been established and both the patient and the provider felt satisfied, I don’t think the father’s wishes made any sense. He may have been acting more out of bigotry or just discomfort about difference in terms of who the provider was. I don’t think that’s something that any health system should have to accommodate unless it is getting in the way of patient care.
I hope that we treat all physicians as properly trained to deal with all kinds of patients, regardless of their religion, ethnicity, or skin color. They should have the skills to manage and do well with any patient. There may be situations where it just doesn’t work or where people don’t get along. Yes, I think we then should try, perhaps, to shift the doctor, get a different nurse, or have a different person do an exam. That’s because of the inability to get the patient’s health interests addressed.
Listening to this dad about what he preferred in terms of religion or ethnicity seemed to me to be interfering with medical success. Could I stop him from moving this patient out entirely from the care setting? Probably not, but I think the way to manage this is to try to talk to him – and, by the way, to talk to the mother.
When we did bring the mom into the situation, she was very happy with the health care provider. She didn’t agree with the dad and wanted to have a meeting with the social worker, the dad, and her to get him to get over the worries, concerns, and maybe even biases he was bringing in about the kind of provider he wanted. That’s exactly what we did.
I know that there are many instances where patients may say, “I don’t want a particular doctor or a particular type.” My view is that we shouldn’t accommodate that. We should say that our doctors are trained to help and care for all manner of people. Unless we can think of some reason that there might be a gap or a problem in the actual delivery of the quality of care, we are not going to accommodate racism, bigotry, or bias.
We certainly shouldn’t be accommodating that once a successful therapeutic relationship is established. Even when it’s a child, I would argue that the patient’s best interest has to trump parental desires, parental worries, and parental concerns about the background, ethnicity, and religion of the provider.
Dr. Caplan is director of the division of medical ethics at NYU Langone Medical Center, New York. He disclosed a conflict of interest with Johnson & Johnson.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I’d like to present you today with a case that raised a large amount of discussion and debate. I got involved as an ethics consultant on the case. I think you’ll find it very interesting and I also think there are going to be some differences of opinion about how to manage the case. I’ll be looking forward to getting comments and feedback on this.
The case involved a 14-year-old boy who had been brought into the hospital by his parents, suffering from severe bouts of anxiety that were just almost overwhelming to him. When he was brought in, he was assigned a health care provider who had a West African last name. Prior to meeting the patient, I have to say that the father of this kid told the intake department nurse that he requested someone else. He saw the name – he hadn’t even met the provider – and he said he wanted someone who might be Catholic.
The parents are both from the Dominican Republic. They identified as White, but they appeared to be non-White Latinx to the nurse who was doing some of the initial intake. They got reassigned to a different provider in the department who identified as African American.
The first month of treatment for the young boy went very well, and he seemed to be getting along extremely well with his provider. He was reporting relief to both parents of some of his anxiety, and the provider felt very connected to the child. A good doctor-patient alliance had been formed.
Nevertheless, at the end of the first month, the father connected back to one of the administrators at the hospital and complained, saying he still wanted a different provider. When asked why, he said, “Well, I don’t really want to answer that,” but getting pressed, he basically said he wasn’t comfortable with having an African American doctor take care of his child. He eventually went back to the argument that what he wanted was someone with a Catholic background, although I don’t know that he knew whether this particular provider was religious – Catholic or anything else.
Some people felt that, as the father in charge of the child’s care, if we could accommodate what he wanted in terms of the parents being comfortable, then that’s something we should do. I absolutely did not agree.
My view is that in a situation where a strong provider-patient relationship has been established, where trust is going both ways, where there are no issues coming up between this 14-year-old and the provider, and when a serious mental health issue is being adequately addressed, the patient’s interest must come first.
Once that therapeutic alliance had been established and both the patient and the provider felt satisfied, I don’t think the father’s wishes made any sense. He may have been acting more out of bigotry or just discomfort about difference in terms of who the provider was. I don’t think that’s something that any health system should have to accommodate unless it is getting in the way of patient care.
I hope that we treat all physicians as properly trained to deal with all kinds of patients, regardless of their religion, ethnicity, or skin color. They should have the skills to manage and do well with any patient. There may be situations where it just doesn’t work or where people don’t get along. Yes, I think we then should try, perhaps, to shift the doctor, get a different nurse, or have a different person do an exam. That’s because of the inability to get the patient’s health interests addressed.
Listening to this dad about what he preferred in terms of religion or ethnicity seemed to me to be interfering with medical success. Could I stop him from moving this patient out entirely from the care setting? Probably not, but I think the way to manage this is to try to talk to him – and, by the way, to talk to the mother.
When we did bring the mom into the situation, she was very happy with the health care provider. She didn’t agree with the dad and wanted to have a meeting with the social worker, the dad, and her to get him to get over the worries, concerns, and maybe even biases he was bringing in about the kind of provider he wanted. That’s exactly what we did.
I know that there are many instances where patients may say, “I don’t want a particular doctor or a particular type.” My view is that we shouldn’t accommodate that. We should say that our doctors are trained to help and care for all manner of people. Unless we can think of some reason that there might be a gap or a problem in the actual delivery of the quality of care, we are not going to accommodate racism, bigotry, or bias.
We certainly shouldn’t be accommodating that once a successful therapeutic relationship is established. Even when it’s a child, I would argue that the patient’s best interest has to trump parental desires, parental worries, and parental concerns about the background, ethnicity, and religion of the provider.
Dr. Caplan is director of the division of medical ethics at NYU Langone Medical Center, New York. He disclosed a conflict of interest with Johnson & Johnson.
A version of this article first appeared on Medscape.com.
Delayed introduction of allergens increases allergy risk
These findings were published in Allergy.
Launched in April 2011, the French ELFE study aims to monitor children from birth to adulthood to better understand the factors from the intrauterine period to adolescence that affect their development, health, social skills, and school career. Thanks to this cohort, a team of scientists has reviewed the relationship between complementary feeding practices and allergies in French children.
The study focused on 6,662 children who had no signs of an allergic reaction before 2 months of age. Data on feeding practices were collected monthly from ages 3 months to 10 months. Their age at complementary feeding introduction was calculated, and a food diversity score was determined at 8 and 10 months. The number of major allergenic foods (out of eggs, fish, wheat, and dairy products) not introduced at 8 and 10 months was also determined. Allergic diseases (food allergy, eczema, asthma, and rhinoconjunctivitis) were reported by parents at 2 months and at 1, 2, 3.5, and 5.5 years.
Initially, scientists determined that just 62% of children began complementary feeding in the recommended age window, which is between ages 4 months and 6 months. They then closely studied the link between delayed introduction of major allergenic foods and the risk of food allergies. They saw that for 1 in 10 children, at least two major allergens, from eggs, fish, wheat, and dairy products, had still not been introduced into the diet of infants by the age of 10 months. Now, these children have a risk of developing a food allergy before the age of 5.5 years that is two times greater than that of children in whom the four major allergens were introduced before the age of 10 months.
These findings therefore confirm the importance of not delaying the introduction of major food allergens to prevent the occurrence of childhood allergic diseases. They provide convincing arguments in support of new recommendations made by the French pediatric and allergy societies as well as those issued by Public Health France.
ELFE: The first cohort to follow children from birth to adulthood
ELFE is the first longitudinal nationwide French study dedicated to monitoring children from birth to adulthood. More than 18,000 children born in metropolitan France in 2011 were included in this study, which represents 1 in 50 children born in 2011. From the time that researchers first met the families in the maternity ward, the parents who agreed to participate in this great scientific adventure have been questioned at regular intervals to better understand how environment, family members, and living conditions affect the development, health, and socialization of children.
This article was translated from the Medscape French Edition. A version of this article first appeared on Medscape.com.
These findings were published in Allergy.
Launched in April 2011, the French ELFE study aims to monitor children from birth to adulthood to better understand the factors from the intrauterine period to adolescence that affect their development, health, social skills, and school career. Thanks to this cohort, a team of scientists has reviewed the relationship between complementary feeding practices and allergies in French children.
The study focused on 6,662 children who had no signs of an allergic reaction before 2 months of age. Data on feeding practices were collected monthly from ages 3 months to 10 months. Their age at complementary feeding introduction was calculated, and a food diversity score was determined at 8 and 10 months. The number of major allergenic foods (out of eggs, fish, wheat, and dairy products) not introduced at 8 and 10 months was also determined. Allergic diseases (food allergy, eczema, asthma, and rhinoconjunctivitis) were reported by parents at 2 months and at 1, 2, 3.5, and 5.5 years.
Initially, scientists determined that just 62% of children began complementary feeding in the recommended age window, which is between ages 4 months and 6 months. They then closely studied the link between delayed introduction of major allergenic foods and the risk of food allergies. They saw that for 1 in 10 children, at least two major allergens, from eggs, fish, wheat, and dairy products, had still not been introduced into the diet of infants by the age of 10 months. Now, these children have a risk of developing a food allergy before the age of 5.5 years that is two times greater than that of children in whom the four major allergens were introduced before the age of 10 months.
These findings therefore confirm the importance of not delaying the introduction of major food allergens to prevent the occurrence of childhood allergic diseases. They provide convincing arguments in support of new recommendations made by the French pediatric and allergy societies as well as those issued by Public Health France.
ELFE: The first cohort to follow children from birth to adulthood
ELFE is the first longitudinal nationwide French study dedicated to monitoring children from birth to adulthood. More than 18,000 children born in metropolitan France in 2011 were included in this study, which represents 1 in 50 children born in 2011. From the time that researchers first met the families in the maternity ward, the parents who agreed to participate in this great scientific adventure have been questioned at regular intervals to better understand how environment, family members, and living conditions affect the development, health, and socialization of children.
This article was translated from the Medscape French Edition. A version of this article first appeared on Medscape.com.
These findings were published in Allergy.
Launched in April 2011, the French ELFE study aims to monitor children from birth to adulthood to better understand the factors from the intrauterine period to adolescence that affect their development, health, social skills, and school career. Thanks to this cohort, a team of scientists has reviewed the relationship between complementary feeding practices and allergies in French children.
The study focused on 6,662 children who had no signs of an allergic reaction before 2 months of age. Data on feeding practices were collected monthly from ages 3 months to 10 months. Their age at complementary feeding introduction was calculated, and a food diversity score was determined at 8 and 10 months. The number of major allergenic foods (out of eggs, fish, wheat, and dairy products) not introduced at 8 and 10 months was also determined. Allergic diseases (food allergy, eczema, asthma, and rhinoconjunctivitis) were reported by parents at 2 months and at 1, 2, 3.5, and 5.5 years.
Initially, scientists determined that just 62% of children began complementary feeding in the recommended age window, which is between ages 4 months and 6 months. They then closely studied the link between delayed introduction of major allergenic foods and the risk of food allergies. They saw that for 1 in 10 children, at least two major allergens, from eggs, fish, wheat, and dairy products, had still not been introduced into the diet of infants by the age of 10 months. Now, these children have a risk of developing a food allergy before the age of 5.5 years that is two times greater than that of children in whom the four major allergens were introduced before the age of 10 months.
These findings therefore confirm the importance of not delaying the introduction of major food allergens to prevent the occurrence of childhood allergic diseases. They provide convincing arguments in support of new recommendations made by the French pediatric and allergy societies as well as those issued by Public Health France.
ELFE: The first cohort to follow children from birth to adulthood
ELFE is the first longitudinal nationwide French study dedicated to monitoring children from birth to adulthood. More than 18,000 children born in metropolitan France in 2011 were included in this study, which represents 1 in 50 children born in 2011. From the time that researchers first met the families in the maternity ward, the parents who agreed to participate in this great scientific adventure have been questioned at regular intervals to better understand how environment, family members, and living conditions affect the development, health, and socialization of children.
This article was translated from the Medscape French Edition. A version of this article first appeared on Medscape.com.
FROM ALLERGY
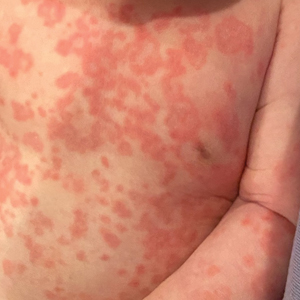
Diffuse Annular Plaques in an Infant
The Diagnosis: Neonatal Lupus Erythematosus
A review of the medical records of the patient’s mother from her first pregnancy revealed positive anti-Ro/SSA (Sjögren syndrome A) (>8.0 U [reference range <1.0 U]) and anti-La/SSB (Sjögren syndrome B) antibodies (>8.0 U [reference range <1.0 U]), which were reconfirmed during her pregnancy with our patient (the second child). The patient’s older brother was diagnosed with neonatal lupus erythematosus (NLE) 2 years prior at 1 month of age; therefore, the mother took hydroxychloroquine during the pregnancy with the second child to help prevent heart block if the child was diagnosed with NLE. Given the family history, positive antibodies in the mother, and clinical presentation, our patient was diagnosed with NLE. He was referred to a pediatric cardiologist and pediatrician to continue the workup of systemic manifestations of NLE and to rule out the presence of congenital heart block. The rash resolved 6 months after the initial presentation, and he did not develop any systemic manifestations of NLE.
Neonatal lupus erythematosus is a rare acquired autoimmune disorder caused by the placental transfer of anti-Ro/SSA and anti-La/SSB antibodies and less commonly anti-U1 ribonucleoprotein antinuclear autoantibodies.1,2 Approximately 1% to 2% of mothers with these positive antibodies will have infants affected with NLE.2 The annual prevalence of NLE in the United States is approximately 1 in 20,000 live births. Mothers of children with NLE most commonly have clinical Sjögren syndrome; however, anti-Ro/SSA and anti-LA/SSB antibodies may be present in 0.1% to 1.5% of healthy women, and 25% to 60% of women with autoimmune disease may be asymptomatic.1 As demonstrated in our case, when there is a family history of NLE in an infant from an earlier pregnancy, the risk for NLE increases to 17% to 20% in subsequent pregnancies1,3 and up to 25% in subsequent pregnancies if the initial child was diagnosed with a congenital heart block in the setting of NLE.1
Neonatal lupus erythematosus classically presents as annular erythematous macules and plaques with central scaling, telangictasia, atrophy, and pigmentary changes. It may start on the scalp and face and spread caudally.1,2 Patients may develop these lesions after UV exposure, and 80% of infants may not have dermatologic findings at birth. Importantly, 40% to 60% of mothers may be asymptomatic at the time of presentation of their child’s NLE.1 The diagnosis can be confirmed via antibody testing in the mother and/or infant. If performed, a punch biopsy shows interface dermatitis, vacuolar degeneration, and possible periadnexal lymphocytic infiltrates on histopathology.1,2
Management of cutaneous NLE includes sun protection (eg, application of sunscreen) and topical corticosteroids. Most dermatologic manifestations of NLE are transient, resolving after clearance of maternal IgG antibodies in 6 to 9 months; however, some telangiectasia, dyspigmentation, and atrophic scarring may persist.1-3
Neonatal lupus erythematosus also may have hepatobiliary, cardiac, hematologic, and less commonly neurologic manifestations. Hepatobiliary manifestations usually present as hepatomegaly or asymptomatic elevated transaminases or γ-glutamyl transferase.1,3 Approximately 10% to 20% of infants with NLE may present with transient anemia and thrombocytopenia.1 Cardiac manifestations are permanent and may require pacemaker implantation.1,3 The incidence of a congenital heart block in infants with NLE is 15% to 30%.3 Cardiac NLE most commonly injures the conductive tissue, leading to a congenital atrioventricular block. The development of a congenital heart block develops in the 18th to 24th week of gestation. Manifestations of a more advanced condition can include dilation of the ascending aorta and dilated cardiomyopathy.1 As such, patients need to be followed by a pediatric cardiologist for monitoring and treatment of any cardiac manifestations.
The overall prognosis of infants affected with NLE varies. Cardiac involvement is associated with a poor prognosis, while isolated cutaneous involvement requires little treatment and portends a favorable prognosis. It is critical for dermatologists to recognize NLE to refer patients to appropriate specialists to investigate and further monitor possible extracutaneous manifestations. With an understanding of the increased risk for a congenital heart block and NLE in subsequent pregnancies, mothers with positive anti-Ro/La antibodies should receive timely counseling and screening. In expectant mothers with suspected autoimmune disease, testing for antinuclear antibodies and SSA and SSB antibodies can be considered, as administration of hydroxychloroquine or prenatal systemic corticosteroids has proven to be effective in preventing a congenital heart block.1 Our patient was followed by pediatric cardiology and was not found to have a congenital heart block.
The differential diagnosis includes other causes of annular erythema in infants, as NLE can mimic several conditions. Tinea corporis may present as scaly annular plaques with central clearing; however, it rarely is encountered fulminantly in neonates.4 Erythema multiforme is a mucocutaneous hypersensitivy reaction distinguished by targetoid morphology.5 It is an exceedingly rare diagnosis in neonates; the average pediatric age of onset is 5.6 years.6 Erythema multiforme often is associated with an infection, most commonly herpes simplex virus,5 and mucosal involvement is common.6 Urticaria multiforme (also known as acute annular urticaria) is a benign disease that appears between 2 months to 3 years of age with blanchable urticarial plaques that likely are triggered by viral or bacterial infections, antibiotics, or vaccines.6 Specific lesions usually will resolve within 24 hours. Annular erythema of infancy is a benign and asymptomatic gyrate erythema that presents as annular plaques with palpable borders that spread centrifugally in patients younger than 1 year. Notably, lesions should periodically fade and may reappear cyclically for months to years. Evaluation for underlying disease usually is negative.6
- Derdulska JM, Rudnicka L, Szykut-Badaczewska A, et al. Neonatal lupus erythematosus—practical guidelines. J Perinat Med. 2021;49:529-538. doi:10.1515/jpm-2020-0543
- Wu J, Berk-Krauss J, Glick SA. Neonatal lupus erythematosus. JAMA Dermatol. 2021;157:590. doi:10.1001/jamadermatol.2021.0041
- Hon KL, Leung AK. Neonatal lupus erythematosus. Autoimmune Dis. 2012;2012:301274. doi:10.1155/2012/301274
- Khare AK, Gupta LK, Mittal A, et al. Neonatal tinea corporis. Indian J Dermatol. 2010;55:201. doi:10.4103/0019-5154.6274
- Ang-Tiu CU, Nicolas ME. Erythema multiforme in a 25-day old neonate. Pediatr Dermatol. 2013;30:E118-E120. doi:10.1111 /j.1525-1470.2012.01873.x
- Agnihotri G, Tsoukas MM. Annular skin lesions in infancy [published online February 3, 2022]. Clin Dermatol. 2022;40:505-512. doi:10.1016/j.clindermatol.2021.12.011
The Diagnosis: Neonatal Lupus Erythematosus
A review of the medical records of the patient’s mother from her first pregnancy revealed positive anti-Ro/SSA (Sjögren syndrome A) (>8.0 U [reference range <1.0 U]) and anti-La/SSB (Sjögren syndrome B) antibodies (>8.0 U [reference range <1.0 U]), which were reconfirmed during her pregnancy with our patient (the second child). The patient’s older brother was diagnosed with neonatal lupus erythematosus (NLE) 2 years prior at 1 month of age; therefore, the mother took hydroxychloroquine during the pregnancy with the second child to help prevent heart block if the child was diagnosed with NLE. Given the family history, positive antibodies in the mother, and clinical presentation, our patient was diagnosed with NLE. He was referred to a pediatric cardiologist and pediatrician to continue the workup of systemic manifestations of NLE and to rule out the presence of congenital heart block. The rash resolved 6 months after the initial presentation, and he did not develop any systemic manifestations of NLE.
Neonatal lupus erythematosus is a rare acquired autoimmune disorder caused by the placental transfer of anti-Ro/SSA and anti-La/SSB antibodies and less commonly anti-U1 ribonucleoprotein antinuclear autoantibodies.1,2 Approximately 1% to 2% of mothers with these positive antibodies will have infants affected with NLE.2 The annual prevalence of NLE in the United States is approximately 1 in 20,000 live births. Mothers of children with NLE most commonly have clinical Sjögren syndrome; however, anti-Ro/SSA and anti-LA/SSB antibodies may be present in 0.1% to 1.5% of healthy women, and 25% to 60% of women with autoimmune disease may be asymptomatic.1 As demonstrated in our case, when there is a family history of NLE in an infant from an earlier pregnancy, the risk for NLE increases to 17% to 20% in subsequent pregnancies1,3 and up to 25% in subsequent pregnancies if the initial child was diagnosed with a congenital heart block in the setting of NLE.1
Neonatal lupus erythematosus classically presents as annular erythematous macules and plaques with central scaling, telangictasia, atrophy, and pigmentary changes. It may start on the scalp and face and spread caudally.1,2 Patients may develop these lesions after UV exposure, and 80% of infants may not have dermatologic findings at birth. Importantly, 40% to 60% of mothers may be asymptomatic at the time of presentation of their child’s NLE.1 The diagnosis can be confirmed via antibody testing in the mother and/or infant. If performed, a punch biopsy shows interface dermatitis, vacuolar degeneration, and possible periadnexal lymphocytic infiltrates on histopathology.1,2
Management of cutaneous NLE includes sun protection (eg, application of sunscreen) and topical corticosteroids. Most dermatologic manifestations of NLE are transient, resolving after clearance of maternal IgG antibodies in 6 to 9 months; however, some telangiectasia, dyspigmentation, and atrophic scarring may persist.1-3
Neonatal lupus erythematosus also may have hepatobiliary, cardiac, hematologic, and less commonly neurologic manifestations. Hepatobiliary manifestations usually present as hepatomegaly or asymptomatic elevated transaminases or γ-glutamyl transferase.1,3 Approximately 10% to 20% of infants with NLE may present with transient anemia and thrombocytopenia.1 Cardiac manifestations are permanent and may require pacemaker implantation.1,3 The incidence of a congenital heart block in infants with NLE is 15% to 30%.3 Cardiac NLE most commonly injures the conductive tissue, leading to a congenital atrioventricular block. The development of a congenital heart block develops in the 18th to 24th week of gestation. Manifestations of a more advanced condition can include dilation of the ascending aorta and dilated cardiomyopathy.1 As such, patients need to be followed by a pediatric cardiologist for monitoring and treatment of any cardiac manifestations.
The overall prognosis of infants affected with NLE varies. Cardiac involvement is associated with a poor prognosis, while isolated cutaneous involvement requires little treatment and portends a favorable prognosis. It is critical for dermatologists to recognize NLE to refer patients to appropriate specialists to investigate and further monitor possible extracutaneous manifestations. With an understanding of the increased risk for a congenital heart block and NLE in subsequent pregnancies, mothers with positive anti-Ro/La antibodies should receive timely counseling and screening. In expectant mothers with suspected autoimmune disease, testing for antinuclear antibodies and SSA and SSB antibodies can be considered, as administration of hydroxychloroquine or prenatal systemic corticosteroids has proven to be effective in preventing a congenital heart block.1 Our patient was followed by pediatric cardiology and was not found to have a congenital heart block.
The differential diagnosis includes other causes of annular erythema in infants, as NLE can mimic several conditions. Tinea corporis may present as scaly annular plaques with central clearing; however, it rarely is encountered fulminantly in neonates.4 Erythema multiforme is a mucocutaneous hypersensitivy reaction distinguished by targetoid morphology.5 It is an exceedingly rare diagnosis in neonates; the average pediatric age of onset is 5.6 years.6 Erythema multiforme often is associated with an infection, most commonly herpes simplex virus,5 and mucosal involvement is common.6 Urticaria multiforme (also known as acute annular urticaria) is a benign disease that appears between 2 months to 3 years of age with blanchable urticarial plaques that likely are triggered by viral or bacterial infections, antibiotics, or vaccines.6 Specific lesions usually will resolve within 24 hours. Annular erythema of infancy is a benign and asymptomatic gyrate erythema that presents as annular plaques with palpable borders that spread centrifugally in patients younger than 1 year. Notably, lesions should periodically fade and may reappear cyclically for months to years. Evaluation for underlying disease usually is negative.6
The Diagnosis: Neonatal Lupus Erythematosus
A review of the medical records of the patient’s mother from her first pregnancy revealed positive anti-Ro/SSA (Sjögren syndrome A) (>8.0 U [reference range <1.0 U]) and anti-La/SSB (Sjögren syndrome B) antibodies (>8.0 U [reference range <1.0 U]), which were reconfirmed during her pregnancy with our patient (the second child). The patient’s older brother was diagnosed with neonatal lupus erythematosus (NLE) 2 years prior at 1 month of age; therefore, the mother took hydroxychloroquine during the pregnancy with the second child to help prevent heart block if the child was diagnosed with NLE. Given the family history, positive antibodies in the mother, and clinical presentation, our patient was diagnosed with NLE. He was referred to a pediatric cardiologist and pediatrician to continue the workup of systemic manifestations of NLE and to rule out the presence of congenital heart block. The rash resolved 6 months after the initial presentation, and he did not develop any systemic manifestations of NLE.
Neonatal lupus erythematosus is a rare acquired autoimmune disorder caused by the placental transfer of anti-Ro/SSA and anti-La/SSB antibodies and less commonly anti-U1 ribonucleoprotein antinuclear autoantibodies.1,2 Approximately 1% to 2% of mothers with these positive antibodies will have infants affected with NLE.2 The annual prevalence of NLE in the United States is approximately 1 in 20,000 live births. Mothers of children with NLE most commonly have clinical Sjögren syndrome; however, anti-Ro/SSA and anti-LA/SSB antibodies may be present in 0.1% to 1.5% of healthy women, and 25% to 60% of women with autoimmune disease may be asymptomatic.1 As demonstrated in our case, when there is a family history of NLE in an infant from an earlier pregnancy, the risk for NLE increases to 17% to 20% in subsequent pregnancies1,3 and up to 25% in subsequent pregnancies if the initial child was diagnosed with a congenital heart block in the setting of NLE.1
Neonatal lupus erythematosus classically presents as annular erythematous macules and plaques with central scaling, telangictasia, atrophy, and pigmentary changes. It may start on the scalp and face and spread caudally.1,2 Patients may develop these lesions after UV exposure, and 80% of infants may not have dermatologic findings at birth. Importantly, 40% to 60% of mothers may be asymptomatic at the time of presentation of their child’s NLE.1 The diagnosis can be confirmed via antibody testing in the mother and/or infant. If performed, a punch biopsy shows interface dermatitis, vacuolar degeneration, and possible periadnexal lymphocytic infiltrates on histopathology.1,2
Management of cutaneous NLE includes sun protection (eg, application of sunscreen) and topical corticosteroids. Most dermatologic manifestations of NLE are transient, resolving after clearance of maternal IgG antibodies in 6 to 9 months; however, some telangiectasia, dyspigmentation, and atrophic scarring may persist.1-3
Neonatal lupus erythematosus also may have hepatobiliary, cardiac, hematologic, and less commonly neurologic manifestations. Hepatobiliary manifestations usually present as hepatomegaly or asymptomatic elevated transaminases or γ-glutamyl transferase.1,3 Approximately 10% to 20% of infants with NLE may present with transient anemia and thrombocytopenia.1 Cardiac manifestations are permanent and may require pacemaker implantation.1,3 The incidence of a congenital heart block in infants with NLE is 15% to 30%.3 Cardiac NLE most commonly injures the conductive tissue, leading to a congenital atrioventricular block. The development of a congenital heart block develops in the 18th to 24th week of gestation. Manifestations of a more advanced condition can include dilation of the ascending aorta and dilated cardiomyopathy.1 As such, patients need to be followed by a pediatric cardiologist for monitoring and treatment of any cardiac manifestations.
The overall prognosis of infants affected with NLE varies. Cardiac involvement is associated with a poor prognosis, while isolated cutaneous involvement requires little treatment and portends a favorable prognosis. It is critical for dermatologists to recognize NLE to refer patients to appropriate specialists to investigate and further monitor possible extracutaneous manifestations. With an understanding of the increased risk for a congenital heart block and NLE in subsequent pregnancies, mothers with positive anti-Ro/La antibodies should receive timely counseling and screening. In expectant mothers with suspected autoimmune disease, testing for antinuclear antibodies and SSA and SSB antibodies can be considered, as administration of hydroxychloroquine or prenatal systemic corticosteroids has proven to be effective in preventing a congenital heart block.1 Our patient was followed by pediatric cardiology and was not found to have a congenital heart block.
The differential diagnosis includes other causes of annular erythema in infants, as NLE can mimic several conditions. Tinea corporis may present as scaly annular plaques with central clearing; however, it rarely is encountered fulminantly in neonates.4 Erythema multiforme is a mucocutaneous hypersensitivy reaction distinguished by targetoid morphology.5 It is an exceedingly rare diagnosis in neonates; the average pediatric age of onset is 5.6 years.6 Erythema multiforme often is associated with an infection, most commonly herpes simplex virus,5 and mucosal involvement is common.6 Urticaria multiforme (also known as acute annular urticaria) is a benign disease that appears between 2 months to 3 years of age with blanchable urticarial plaques that likely are triggered by viral or bacterial infections, antibiotics, or vaccines.6 Specific lesions usually will resolve within 24 hours. Annular erythema of infancy is a benign and asymptomatic gyrate erythema that presents as annular plaques with palpable borders that spread centrifugally in patients younger than 1 year. Notably, lesions should periodically fade and may reappear cyclically for months to years. Evaluation for underlying disease usually is negative.6
- Derdulska JM, Rudnicka L, Szykut-Badaczewska A, et al. Neonatal lupus erythematosus—practical guidelines. J Perinat Med. 2021;49:529-538. doi:10.1515/jpm-2020-0543
- Wu J, Berk-Krauss J, Glick SA. Neonatal lupus erythematosus. JAMA Dermatol. 2021;157:590. doi:10.1001/jamadermatol.2021.0041
- Hon KL, Leung AK. Neonatal lupus erythematosus. Autoimmune Dis. 2012;2012:301274. doi:10.1155/2012/301274
- Khare AK, Gupta LK, Mittal A, et al. Neonatal tinea corporis. Indian J Dermatol. 2010;55:201. doi:10.4103/0019-5154.6274
- Ang-Tiu CU, Nicolas ME. Erythema multiforme in a 25-day old neonate. Pediatr Dermatol. 2013;30:E118-E120. doi:10.1111 /j.1525-1470.2012.01873.x
- Agnihotri G, Tsoukas MM. Annular skin lesions in infancy [published online February 3, 2022]. Clin Dermatol. 2022;40:505-512. doi:10.1016/j.clindermatol.2021.12.011
- Derdulska JM, Rudnicka L, Szykut-Badaczewska A, et al. Neonatal lupus erythematosus—practical guidelines. J Perinat Med. 2021;49:529-538. doi:10.1515/jpm-2020-0543
- Wu J, Berk-Krauss J, Glick SA. Neonatal lupus erythematosus. JAMA Dermatol. 2021;157:590. doi:10.1001/jamadermatol.2021.0041
- Hon KL, Leung AK. Neonatal lupus erythematosus. Autoimmune Dis. 2012;2012:301274. doi:10.1155/2012/301274
- Khare AK, Gupta LK, Mittal A, et al. Neonatal tinea corporis. Indian J Dermatol. 2010;55:201. doi:10.4103/0019-5154.6274
- Ang-Tiu CU, Nicolas ME. Erythema multiforme in a 25-day old neonate. Pediatr Dermatol. 2013;30:E118-E120. doi:10.1111 /j.1525-1470.2012.01873.x
- Agnihotri G, Tsoukas MM. Annular skin lesions in infancy [published online February 3, 2022]. Clin Dermatol. 2022;40:505-512. doi:10.1016/j.clindermatol.2021.12.011
A 5-week-old infant boy presented with a rash at birth (left). The pregnancy was full term without complications, and he was otherwise healthy. A family history revealed that his older brother developed a similar rash 2 weeks after birth (right). Physical examination revealed polycyclic annular patches with an erythematous border and central clearing diffusely located on the trunk, extremities, scalp, and face with periorbital edema.
Child assault tied to triple the risk for mental illness within 1 year
The greatest risk was found in the first year following the assault, increasing to three times the risk of being diagnosed with mental illness, compared with children not assaulted. Mood and anxiety disorders were the most common diagnoses.
“From a clinical and policy perspective, our study highlights that there is a critical opportunity for health care clinicians to support children in the first year following physical assault,” Natasha Saunders, MD, MSc, of the Hospital for Sick Children, Toronto, and colleagues wrote. “There is a need to develop and implement targeted mental illness prevention, screening, and treatment programs for assaulted children.”
The findings were published online in JAMA Network Open.
While it has been well established that children exposed to assault have an increased risk for subsequent mental illness, Dr. Saunders and coinvestigators noted that using an age-matched, population-based cohort study would enable them to obtain detailed information on the patterns and timing of subsequent psychiatric diagnoses.
To that end, the researchers used several medical databases in Ontario to find 5,487 children (infants to age 13 years) who required an ED visit or hospitalization for a physical assault in Ontario between 2006 and 2014.
These children were matched on a 1:4 basis with 21,948 children not exposed to physical assault. The children were followed until their 18th birthday or until the study ended in March 2019.
The researchers found that more than a third of the children (39%) who were exposed to assault received a mental health diagnosis, according to health records, compared with 23% of unexposed children.
Mood and anxiety disorders were the most common diagnoses among children exposed to assault (16.2% vs. 10.6%, respectively); followed by select childhood behavior disorders, such as ADHD, oppositional defiant disorder, or conduct disorder (9.9% vs. 5.2%); and substance use disorders (2.4% vs. 0.4%).
Triple risk of mental illness in first year
The researchers found that the children exposed to assault were nearly twice as likely to be diagnosed with a mental illness over a median follow-up of 7 years, compared with those not exposed to assault (adjusted hazard ratio, 1.96; 95% confidence interval, 1.85,2.08).
In the year following the assault, children exposed to assault bore three times the risk of being diagnosed with a mental illness, compared with unexposed children (aHR, 3.08; 95% CI, 2.68,3.54).
In addition, the children who had been assaulted were more likely to be diagnosed in an acute care setting than those who were not assaulted (14% vs. 2.8%).
The children who had been assaulted were an average age of 7 years and were more often boys (55% vs. 45%). Children who were assaulted were also more likely to have mothers with mental illness (35% vs. 19%).
The investigators noted that the study likely underestimated the number of children exposed to assault, as many do not end up in the ED.
In addition to highlighting the need for medical personnel to support children in the first year following assault, the investigators wrote that “our results also advocate for accessible mental health care outside of the acute setting and for care that addresses the social and health needs of mothers, who themselves have high social and health risks.”
This study received funding from the National Foundation to End Child Abuse and Neglect and the Ontario Ministry of Health and the Ministry of Long-Term Care. Dr. Saunders reported receiving personal fees from The BMJ Group, Archives of Diseases in Childhood outside the submitted work.
A version of this article first appeared on Medscape.com.
The greatest risk was found in the first year following the assault, increasing to three times the risk of being diagnosed with mental illness, compared with children not assaulted. Mood and anxiety disorders were the most common diagnoses.
“From a clinical and policy perspective, our study highlights that there is a critical opportunity for health care clinicians to support children in the first year following physical assault,” Natasha Saunders, MD, MSc, of the Hospital for Sick Children, Toronto, and colleagues wrote. “There is a need to develop and implement targeted mental illness prevention, screening, and treatment programs for assaulted children.”
The findings were published online in JAMA Network Open.
While it has been well established that children exposed to assault have an increased risk for subsequent mental illness, Dr. Saunders and coinvestigators noted that using an age-matched, population-based cohort study would enable them to obtain detailed information on the patterns and timing of subsequent psychiatric diagnoses.
To that end, the researchers used several medical databases in Ontario to find 5,487 children (infants to age 13 years) who required an ED visit or hospitalization for a physical assault in Ontario between 2006 and 2014.
These children were matched on a 1:4 basis with 21,948 children not exposed to physical assault. The children were followed until their 18th birthday or until the study ended in March 2019.
The researchers found that more than a third of the children (39%) who were exposed to assault received a mental health diagnosis, according to health records, compared with 23% of unexposed children.
Mood and anxiety disorders were the most common diagnoses among children exposed to assault (16.2% vs. 10.6%, respectively); followed by select childhood behavior disorders, such as ADHD, oppositional defiant disorder, or conduct disorder (9.9% vs. 5.2%); and substance use disorders (2.4% vs. 0.4%).
Triple risk of mental illness in first year
The researchers found that the children exposed to assault were nearly twice as likely to be diagnosed with a mental illness over a median follow-up of 7 years, compared with those not exposed to assault (adjusted hazard ratio, 1.96; 95% confidence interval, 1.85,2.08).
In the year following the assault, children exposed to assault bore three times the risk of being diagnosed with a mental illness, compared with unexposed children (aHR, 3.08; 95% CI, 2.68,3.54).
In addition, the children who had been assaulted were more likely to be diagnosed in an acute care setting than those who were not assaulted (14% vs. 2.8%).
The children who had been assaulted were an average age of 7 years and were more often boys (55% vs. 45%). Children who were assaulted were also more likely to have mothers with mental illness (35% vs. 19%).
The investigators noted that the study likely underestimated the number of children exposed to assault, as many do not end up in the ED.
In addition to highlighting the need for medical personnel to support children in the first year following assault, the investigators wrote that “our results also advocate for accessible mental health care outside of the acute setting and for care that addresses the social and health needs of mothers, who themselves have high social and health risks.”
This study received funding from the National Foundation to End Child Abuse and Neglect and the Ontario Ministry of Health and the Ministry of Long-Term Care. Dr. Saunders reported receiving personal fees from The BMJ Group, Archives of Diseases in Childhood outside the submitted work.
A version of this article first appeared on Medscape.com.
The greatest risk was found in the first year following the assault, increasing to three times the risk of being diagnosed with mental illness, compared with children not assaulted. Mood and anxiety disorders were the most common diagnoses.
“From a clinical and policy perspective, our study highlights that there is a critical opportunity for health care clinicians to support children in the first year following physical assault,” Natasha Saunders, MD, MSc, of the Hospital for Sick Children, Toronto, and colleagues wrote. “There is a need to develop and implement targeted mental illness prevention, screening, and treatment programs for assaulted children.”
The findings were published online in JAMA Network Open.
While it has been well established that children exposed to assault have an increased risk for subsequent mental illness, Dr. Saunders and coinvestigators noted that using an age-matched, population-based cohort study would enable them to obtain detailed information on the patterns and timing of subsequent psychiatric diagnoses.
To that end, the researchers used several medical databases in Ontario to find 5,487 children (infants to age 13 years) who required an ED visit or hospitalization for a physical assault in Ontario between 2006 and 2014.
These children were matched on a 1:4 basis with 21,948 children not exposed to physical assault. The children were followed until their 18th birthday or until the study ended in March 2019.
The researchers found that more than a third of the children (39%) who were exposed to assault received a mental health diagnosis, according to health records, compared with 23% of unexposed children.
Mood and anxiety disorders were the most common diagnoses among children exposed to assault (16.2% vs. 10.6%, respectively); followed by select childhood behavior disorders, such as ADHD, oppositional defiant disorder, or conduct disorder (9.9% vs. 5.2%); and substance use disorders (2.4% vs. 0.4%).
Triple risk of mental illness in first year
The researchers found that the children exposed to assault were nearly twice as likely to be diagnosed with a mental illness over a median follow-up of 7 years, compared with those not exposed to assault (adjusted hazard ratio, 1.96; 95% confidence interval, 1.85,2.08).
In the year following the assault, children exposed to assault bore three times the risk of being diagnosed with a mental illness, compared with unexposed children (aHR, 3.08; 95% CI, 2.68,3.54).
In addition, the children who had been assaulted were more likely to be diagnosed in an acute care setting than those who were not assaulted (14% vs. 2.8%).
The children who had been assaulted were an average age of 7 years and were more often boys (55% vs. 45%). Children who were assaulted were also more likely to have mothers with mental illness (35% vs. 19%).
The investigators noted that the study likely underestimated the number of children exposed to assault, as many do not end up in the ED.
In addition to highlighting the need for medical personnel to support children in the first year following assault, the investigators wrote that “our results also advocate for accessible mental health care outside of the acute setting and for care that addresses the social and health needs of mothers, who themselves have high social and health risks.”
This study received funding from the National Foundation to End Child Abuse and Neglect and the Ontario Ministry of Health and the Ministry of Long-Term Care. Dr. Saunders reported receiving personal fees from The BMJ Group, Archives of Diseases in Childhood outside the submitted work.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
Healthy babies can still get very sick from RSV
Any parent might naturally assume that their newborn is at little risk from respiratory syncytial virus (RSV), which in healthy infants has been thought to cause mild symptoms similar to having a cold. But a new study challenges the assumption that only infirm children are at risk for the worst outcomes from RSV, finding that
The researchers, who published their study in JAMA Network Open, said the results reinforce the importance of a new preventive injection that can lower the risk for severe RSV infection in babies.
“RSV is the number one cause of hospitalizations in young infants,” said Natasha Halasa, MD, MPH, an infectious disease specialist at Vanderbilt University Medical Center in Nashville, Tenn., and the lead author of the new study. But “the vast majority of kids didn’t have underlying medical conditions” when they got sick.
Every infant in the study was in an intensive care unit for at least 24 hours, Dr. Halasa said, and most babies gave no prior indication that RSV would affect them so profoundly.
“Two to three of every 100 babies in the United States will be hospitalized for RSV in their first year of life,” added study author Angela Campbell, MD, MPH, of the Coronavirus and Other Respiratory Viruses Division of the Centers for Disease Control and Prevention in Atlanta.
Until recently, only one treatment was available for children up to age 2 at high risk for RSV, the monoclonal antibody palivizumab (Synagis). Palivizumab is reserved for children who are born prematurely, are immunocompromised, or have chronic heart or lung disease. The injection is given monthly during the 5-month peak of RSV season, from fall to spring.
In July, the Food and Drug Administration approved, and the CDC has since recommended, a new monoclonal antibody called nirsevimab (Beyfortus) to prevent the worst effects of RSV. Nirsevimab is intended for all newborns under age 8 months who were born during the RSV season, or babies who will be entering that season before reaching 8 months. The injection is given only once and can act for 150 days. The FDA and CDC actions came following a clinical trial showing that nirsevimab lowers the risk for hospitalization from RSV among infants by more than 75%.
“We’re very excited that this product exists now,” Dr. Campbell said.
Chart reviews during the ‘tripledemic’
In fall 2022 the United States experienced a “tripledemic” of elevated hospitalizations for COVID-19, influenza, and RSV. For the new study, Dr. Halasa and her colleagues examined the medical records of 600 infants (under age 1; average age, 2.6 months) admitted to U.S. ICUs for lower respiratory tract infections caused by RSV from October to December 2022, during the height of the tripledemic.
More than 60% of admissions, 361, were boys; 44% were White, 23% were Hispanic, 16% were Black, 10% were unknown race, 5% were multiple race, and 2% were Asian.
Of the 600 infants, 572 (95.3%) required oxygen at the hospital and 487 (81.2%) had no underlying medical conditions linked to higher risk from RSV. The other infants had at least one ailment, such as a cardiac or lung condition, that could result in more severe RSV outcomes.
The 169 preemies in the study population were more likely to be intubated in the ICU than were those born at term. But 90 of the 143 total recorded intubations happened among full-term infants. Two children in the study group died.
Christopher Horvat, MD, MHA, who works in the pediatric ICU at the University of Pittsburgh Medical Center, called the new study “important,” adding that it shows “the RSV burden is substantial for children who are otherwise healthy.” Dr. Horvat, who was not involved in the work, said the new data highlight the value of preventive measures to prevent any repeat of the tripledemic.
On the same day the new study was published, the American Academy of Pediatrics (AAP) released a statement calling for widespread access to nirsevimab.
“The American Academy of Pediatrics recommends that all infants – and especially those at high risk – receive the new preventive antibody, nirsevimab, to protect against severe disease caused by respiratory syncytial virus (RSV), which is common, highly contagious, and sometimes deadly,” the organization said in a statement.
The AAP called for the CDC and the Centers for Medicaid & Medicare Services to work together to ensure that any parent in America can obtain nirsevimab for their children if needed. Anyone who cannot access nirsevimab this year, the AAP said, should rely on the older treatment palivizumab instead.
The sources in this story reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Any parent might naturally assume that their newborn is at little risk from respiratory syncytial virus (RSV), which in healthy infants has been thought to cause mild symptoms similar to having a cold. But a new study challenges the assumption that only infirm children are at risk for the worst outcomes from RSV, finding that
The researchers, who published their study in JAMA Network Open, said the results reinforce the importance of a new preventive injection that can lower the risk for severe RSV infection in babies.
“RSV is the number one cause of hospitalizations in young infants,” said Natasha Halasa, MD, MPH, an infectious disease specialist at Vanderbilt University Medical Center in Nashville, Tenn., and the lead author of the new study. But “the vast majority of kids didn’t have underlying medical conditions” when they got sick.
Every infant in the study was in an intensive care unit for at least 24 hours, Dr. Halasa said, and most babies gave no prior indication that RSV would affect them so profoundly.
“Two to three of every 100 babies in the United States will be hospitalized for RSV in their first year of life,” added study author Angela Campbell, MD, MPH, of the Coronavirus and Other Respiratory Viruses Division of the Centers for Disease Control and Prevention in Atlanta.
Until recently, only one treatment was available for children up to age 2 at high risk for RSV, the monoclonal antibody palivizumab (Synagis). Palivizumab is reserved for children who are born prematurely, are immunocompromised, or have chronic heart or lung disease. The injection is given monthly during the 5-month peak of RSV season, from fall to spring.
In July, the Food and Drug Administration approved, and the CDC has since recommended, a new monoclonal antibody called nirsevimab (Beyfortus) to prevent the worst effects of RSV. Nirsevimab is intended for all newborns under age 8 months who were born during the RSV season, or babies who will be entering that season before reaching 8 months. The injection is given only once and can act for 150 days. The FDA and CDC actions came following a clinical trial showing that nirsevimab lowers the risk for hospitalization from RSV among infants by more than 75%.
“We’re very excited that this product exists now,” Dr. Campbell said.
Chart reviews during the ‘tripledemic’
In fall 2022 the United States experienced a “tripledemic” of elevated hospitalizations for COVID-19, influenza, and RSV. For the new study, Dr. Halasa and her colleagues examined the medical records of 600 infants (under age 1; average age, 2.6 months) admitted to U.S. ICUs for lower respiratory tract infections caused by RSV from October to December 2022, during the height of the tripledemic.
More than 60% of admissions, 361, were boys; 44% were White, 23% were Hispanic, 16% were Black, 10% were unknown race, 5% were multiple race, and 2% were Asian.
Of the 600 infants, 572 (95.3%) required oxygen at the hospital and 487 (81.2%) had no underlying medical conditions linked to higher risk from RSV. The other infants had at least one ailment, such as a cardiac or lung condition, that could result in more severe RSV outcomes.
The 169 preemies in the study population were more likely to be intubated in the ICU than were those born at term. But 90 of the 143 total recorded intubations happened among full-term infants. Two children in the study group died.
Christopher Horvat, MD, MHA, who works in the pediatric ICU at the University of Pittsburgh Medical Center, called the new study “important,” adding that it shows “the RSV burden is substantial for children who are otherwise healthy.” Dr. Horvat, who was not involved in the work, said the new data highlight the value of preventive measures to prevent any repeat of the tripledemic.
On the same day the new study was published, the American Academy of Pediatrics (AAP) released a statement calling for widespread access to nirsevimab.
“The American Academy of Pediatrics recommends that all infants – and especially those at high risk – receive the new preventive antibody, nirsevimab, to protect against severe disease caused by respiratory syncytial virus (RSV), which is common, highly contagious, and sometimes deadly,” the organization said in a statement.
The AAP called for the CDC and the Centers for Medicaid & Medicare Services to work together to ensure that any parent in America can obtain nirsevimab for their children if needed. Anyone who cannot access nirsevimab this year, the AAP said, should rely on the older treatment palivizumab instead.
The sources in this story reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Any parent might naturally assume that their newborn is at little risk from respiratory syncytial virus (RSV), which in healthy infants has been thought to cause mild symptoms similar to having a cold. But a new study challenges the assumption that only infirm children are at risk for the worst outcomes from RSV, finding that
The researchers, who published their study in JAMA Network Open, said the results reinforce the importance of a new preventive injection that can lower the risk for severe RSV infection in babies.
“RSV is the number one cause of hospitalizations in young infants,” said Natasha Halasa, MD, MPH, an infectious disease specialist at Vanderbilt University Medical Center in Nashville, Tenn., and the lead author of the new study. But “the vast majority of kids didn’t have underlying medical conditions” when they got sick.
Every infant in the study was in an intensive care unit for at least 24 hours, Dr. Halasa said, and most babies gave no prior indication that RSV would affect them so profoundly.
“Two to three of every 100 babies in the United States will be hospitalized for RSV in their first year of life,” added study author Angela Campbell, MD, MPH, of the Coronavirus and Other Respiratory Viruses Division of the Centers for Disease Control and Prevention in Atlanta.
Until recently, only one treatment was available for children up to age 2 at high risk for RSV, the monoclonal antibody palivizumab (Synagis). Palivizumab is reserved for children who are born prematurely, are immunocompromised, or have chronic heart or lung disease. The injection is given monthly during the 5-month peak of RSV season, from fall to spring.
In July, the Food and Drug Administration approved, and the CDC has since recommended, a new monoclonal antibody called nirsevimab (Beyfortus) to prevent the worst effects of RSV. Nirsevimab is intended for all newborns under age 8 months who were born during the RSV season, or babies who will be entering that season before reaching 8 months. The injection is given only once and can act for 150 days. The FDA and CDC actions came following a clinical trial showing that nirsevimab lowers the risk for hospitalization from RSV among infants by more than 75%.
“We’re very excited that this product exists now,” Dr. Campbell said.
Chart reviews during the ‘tripledemic’
In fall 2022 the United States experienced a “tripledemic” of elevated hospitalizations for COVID-19, influenza, and RSV. For the new study, Dr. Halasa and her colleagues examined the medical records of 600 infants (under age 1; average age, 2.6 months) admitted to U.S. ICUs for lower respiratory tract infections caused by RSV from October to December 2022, during the height of the tripledemic.
More than 60% of admissions, 361, were boys; 44% were White, 23% were Hispanic, 16% were Black, 10% were unknown race, 5% were multiple race, and 2% were Asian.
Of the 600 infants, 572 (95.3%) required oxygen at the hospital and 487 (81.2%) had no underlying medical conditions linked to higher risk from RSV. The other infants had at least one ailment, such as a cardiac or lung condition, that could result in more severe RSV outcomes.
The 169 preemies in the study population were more likely to be intubated in the ICU than were those born at term. But 90 of the 143 total recorded intubations happened among full-term infants. Two children in the study group died.
Christopher Horvat, MD, MHA, who works in the pediatric ICU at the University of Pittsburgh Medical Center, called the new study “important,” adding that it shows “the RSV burden is substantial for children who are otherwise healthy.” Dr. Horvat, who was not involved in the work, said the new data highlight the value of preventive measures to prevent any repeat of the tripledemic.
On the same day the new study was published, the American Academy of Pediatrics (AAP) released a statement calling for widespread access to nirsevimab.
“The American Academy of Pediatrics recommends that all infants – and especially those at high risk – receive the new preventive antibody, nirsevimab, to protect against severe disease caused by respiratory syncytial virus (RSV), which is common, highly contagious, and sometimes deadly,” the organization said in a statement.
The AAP called for the CDC and the Centers for Medicaid & Medicare Services to work together to ensure that any parent in America can obtain nirsevimab for their children if needed. Anyone who cannot access nirsevimab this year, the AAP said, should rely on the older treatment palivizumab instead.
The sources in this story reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
Analysis reveals recent acne prescribing trends
While.
Notably, isotretinoin prescribing among men and women decreased slightly during the study period, “which may reflect ongoing administrative burdens associated with iPLEDGE,” study author John S. Barbieri, MD, MBA, of the department of dermatology, at Brigham and Women’s Hospital, Boston, told this news organization.
For the cross-sectional study, which was published online as a research letter in JAMA Dermatology, Dr. Barbieri drew from the Truven Health MarketScan Commercial Claims Database from Jan. 1, 2017, to Dec. 31, 2020, to identify individuals with an encounter for acne, prescriptions for oral tetracycline antibiotics (doxycycline, minocycline), other commonly prescribed oral antibiotics (trimethoprim-sulfamethoxazole, amoxicillin, cephalexin), spironolactone, and isotretinoin. Only drug courses greater than 28 days were included in the analysis, and Dr. Barbieri stratified them according to clinician type (dermatologist, nondermatology physician, and nurse-practitioner or physician assistant). To normalize prescribing rates (to address possible changes in the number of patients treated for acne over time), the number of treatment courses prescribed each year was standardized to the number of encounters for acne with that clinician type during the same calendar year.
The study period included a mean of 1.9 million acne encounters per year.
Dr. Barbieri found that dermatologists prescribed more oral antibiotics per clinician for acne than any other major medical specialty and that oral antibiotics remained frequently prescribed for treating acne by both dermatologists and nondermatologists. “Among oral antibiotics, minocycline and trimethoprim-sulfamethoxazole remain relatively commonly prescribed, despite potential safety concerns and a lack of evidence that they are any more effective than doxycycline,” he said in an interview.
“Patient outcomes could likely be improved by reducing use of minocycline and particularly trimethoprim-sulfamethoxazole given its high risk of serious side effects such as SJS/TEN [Stevens-Johnson syndrome/toxic epidermal necrolysis] and acute respiratory failure,” he added.
Dr. Barbieri noted that there are likely opportunities to consider nonantibiotic alternatives such as hormonal therapy (spironolactone, combined oral contraceptives) and isotretinoin. “There is also a need for continued research to identify nonantibiotic treatment options for patients with acne,” he said.
The analysis revealed that for women with acne prescriptions for spironolactone increased about three- to fourfold during the study period among all clinician types. In 2017, oral antibiotics were prescribed about two- to threefold more often than spironolactone, but by 2020 they were being prescribed at about the same frequency. “Given spironolactone may have similar effectiveness to oral antibiotics in the treatment of acne, this shift in practice has the potential to improve outcomes for patients by reducing the risk of antibiotic-associated complications,” Dr. Barbieri wrote. Still, in 2020, oral antibiotics were still slightly more commonly prescribed than spironolactone by nondermatology physicians and NP or PAs.
In other findings, isotretinoin prescribing decreased slightly among male and female patients during the study period. Among antibiotic prescriptions, prescribing for doxycycline increased at a higher rate than prescribing for minocycline, especially among dermatologists and NPs or PAs.
In the interview, Dr. Barbieri acknowledged certain limitations of the study, including the fact that the dataset “does not allow for evaluation of severity of acne and it is not possible to directly link prescriptions to diagnoses, so some prescriptions might not be for acne and others that are for acne might not have been included.”
Lawrence J. Green, MD, of the department of dermatology at George Washington University, Washington, who was asked to comment on the results, said that, while a course of antibiotic therapy was tied to an office visit in the analysis, the duration of each course of therapy was unclear. It would be interesting to see if antibiotic courses became shorter during the time period analyzed, such as 1-3 months versus 4 or more months, he added, “as this should reduce risks associated with long-term use of oral antibiotics.”
Dr. Barbieri reported personal fees from Dexcel Pharma for consulting outside the submitted work. Dr. Green disclosed that he is a speaker, consultant, or investigator for numerous pharmaceutical companies.
While.
Notably, isotretinoin prescribing among men and women decreased slightly during the study period, “which may reflect ongoing administrative burdens associated with iPLEDGE,” study author John S. Barbieri, MD, MBA, of the department of dermatology, at Brigham and Women’s Hospital, Boston, told this news organization.
For the cross-sectional study, which was published online as a research letter in JAMA Dermatology, Dr. Barbieri drew from the Truven Health MarketScan Commercial Claims Database from Jan. 1, 2017, to Dec. 31, 2020, to identify individuals with an encounter for acne, prescriptions for oral tetracycline antibiotics (doxycycline, minocycline), other commonly prescribed oral antibiotics (trimethoprim-sulfamethoxazole, amoxicillin, cephalexin), spironolactone, and isotretinoin. Only drug courses greater than 28 days were included in the analysis, and Dr. Barbieri stratified them according to clinician type (dermatologist, nondermatology physician, and nurse-practitioner or physician assistant). To normalize prescribing rates (to address possible changes in the number of patients treated for acne over time), the number of treatment courses prescribed each year was standardized to the number of encounters for acne with that clinician type during the same calendar year.
The study period included a mean of 1.9 million acne encounters per year.
Dr. Barbieri found that dermatologists prescribed more oral antibiotics per clinician for acne than any other major medical specialty and that oral antibiotics remained frequently prescribed for treating acne by both dermatologists and nondermatologists. “Among oral antibiotics, minocycline and trimethoprim-sulfamethoxazole remain relatively commonly prescribed, despite potential safety concerns and a lack of evidence that they are any more effective than doxycycline,” he said in an interview.
“Patient outcomes could likely be improved by reducing use of minocycline and particularly trimethoprim-sulfamethoxazole given its high risk of serious side effects such as SJS/TEN [Stevens-Johnson syndrome/toxic epidermal necrolysis] and acute respiratory failure,” he added.
Dr. Barbieri noted that there are likely opportunities to consider nonantibiotic alternatives such as hormonal therapy (spironolactone, combined oral contraceptives) and isotretinoin. “There is also a need for continued research to identify nonantibiotic treatment options for patients with acne,” he said.
The analysis revealed that for women with acne prescriptions for spironolactone increased about three- to fourfold during the study period among all clinician types. In 2017, oral antibiotics were prescribed about two- to threefold more often than spironolactone, but by 2020 they were being prescribed at about the same frequency. “Given spironolactone may have similar effectiveness to oral antibiotics in the treatment of acne, this shift in practice has the potential to improve outcomes for patients by reducing the risk of antibiotic-associated complications,” Dr. Barbieri wrote. Still, in 2020, oral antibiotics were still slightly more commonly prescribed than spironolactone by nondermatology physicians and NP or PAs.
In other findings, isotretinoin prescribing decreased slightly among male and female patients during the study period. Among antibiotic prescriptions, prescribing for doxycycline increased at a higher rate than prescribing for minocycline, especially among dermatologists and NPs or PAs.
In the interview, Dr. Barbieri acknowledged certain limitations of the study, including the fact that the dataset “does not allow for evaluation of severity of acne and it is not possible to directly link prescriptions to diagnoses, so some prescriptions might not be for acne and others that are for acne might not have been included.”
Lawrence J. Green, MD, of the department of dermatology at George Washington University, Washington, who was asked to comment on the results, said that, while a course of antibiotic therapy was tied to an office visit in the analysis, the duration of each course of therapy was unclear. It would be interesting to see if antibiotic courses became shorter during the time period analyzed, such as 1-3 months versus 4 or more months, he added, “as this should reduce risks associated with long-term use of oral antibiotics.”
Dr. Barbieri reported personal fees from Dexcel Pharma for consulting outside the submitted work. Dr. Green disclosed that he is a speaker, consultant, or investigator for numerous pharmaceutical companies.
While.
Notably, isotretinoin prescribing among men and women decreased slightly during the study period, “which may reflect ongoing administrative burdens associated with iPLEDGE,” study author John S. Barbieri, MD, MBA, of the department of dermatology, at Brigham and Women’s Hospital, Boston, told this news organization.
For the cross-sectional study, which was published online as a research letter in JAMA Dermatology, Dr. Barbieri drew from the Truven Health MarketScan Commercial Claims Database from Jan. 1, 2017, to Dec. 31, 2020, to identify individuals with an encounter for acne, prescriptions for oral tetracycline antibiotics (doxycycline, minocycline), other commonly prescribed oral antibiotics (trimethoprim-sulfamethoxazole, amoxicillin, cephalexin), spironolactone, and isotretinoin. Only drug courses greater than 28 days were included in the analysis, and Dr. Barbieri stratified them according to clinician type (dermatologist, nondermatology physician, and nurse-practitioner or physician assistant). To normalize prescribing rates (to address possible changes in the number of patients treated for acne over time), the number of treatment courses prescribed each year was standardized to the number of encounters for acne with that clinician type during the same calendar year.
The study period included a mean of 1.9 million acne encounters per year.
Dr. Barbieri found that dermatologists prescribed more oral antibiotics per clinician for acne than any other major medical specialty and that oral antibiotics remained frequently prescribed for treating acne by both dermatologists and nondermatologists. “Among oral antibiotics, minocycline and trimethoprim-sulfamethoxazole remain relatively commonly prescribed, despite potential safety concerns and a lack of evidence that they are any more effective than doxycycline,” he said in an interview.
“Patient outcomes could likely be improved by reducing use of minocycline and particularly trimethoprim-sulfamethoxazole given its high risk of serious side effects such as SJS/TEN [Stevens-Johnson syndrome/toxic epidermal necrolysis] and acute respiratory failure,” he added.
Dr. Barbieri noted that there are likely opportunities to consider nonantibiotic alternatives such as hormonal therapy (spironolactone, combined oral contraceptives) and isotretinoin. “There is also a need for continued research to identify nonantibiotic treatment options for patients with acne,” he said.
The analysis revealed that for women with acne prescriptions for spironolactone increased about three- to fourfold during the study period among all clinician types. In 2017, oral antibiotics were prescribed about two- to threefold more often than spironolactone, but by 2020 they were being prescribed at about the same frequency. “Given spironolactone may have similar effectiveness to oral antibiotics in the treatment of acne, this shift in practice has the potential to improve outcomes for patients by reducing the risk of antibiotic-associated complications,” Dr. Barbieri wrote. Still, in 2020, oral antibiotics were still slightly more commonly prescribed than spironolactone by nondermatology physicians and NP or PAs.
In other findings, isotretinoin prescribing decreased slightly among male and female patients during the study period. Among antibiotic prescriptions, prescribing for doxycycline increased at a higher rate than prescribing for minocycline, especially among dermatologists and NPs or PAs.
In the interview, Dr. Barbieri acknowledged certain limitations of the study, including the fact that the dataset “does not allow for evaluation of severity of acne and it is not possible to directly link prescriptions to diagnoses, so some prescriptions might not be for acne and others that are for acne might not have been included.”
Lawrence J. Green, MD, of the department of dermatology at George Washington University, Washington, who was asked to comment on the results, said that, while a course of antibiotic therapy was tied to an office visit in the analysis, the duration of each course of therapy was unclear. It would be interesting to see if antibiotic courses became shorter during the time period analyzed, such as 1-3 months versus 4 or more months, he added, “as this should reduce risks associated with long-term use of oral antibiotics.”
Dr. Barbieri reported personal fees from Dexcel Pharma for consulting outside the submitted work. Dr. Green disclosed that he is a speaker, consultant, or investigator for numerous pharmaceutical companies.
FROM JAMA DERMATOLOGY
Primary care vision testing rates in children low
In data from the 2018-2020 National Survey of Children’s Health, an annual, nationally representative cross-sectional study, fewer than half of children aged 3-5 with private insurance received vision testing, with rates even lower in those lacking private insurance. The findings point to unmet eye care needs, especially in young children for whom early testing to ward off vision loss is highly recommended.
The report was published online in JAMA Ophthalmology by Olivia J. Killeen MD, MS, an ophthalmologist during the study in the department of ophthalmology and visual sciences at the University of Michigan, Ann Arbor, and colleagues.
Future work should focus on improving primary care provider vision screening rates, especially for the 3- to 5-year age group, the authors wrote.
“Because children often are not aware they have an eye problem, routine vision testing in the primary care setting can help identify those with potential eye disease,” Dr. Killeen said. “We have an opportunity to improve the early detection and treatment of eye disease by improving primary care vision testing.”
Childhood vision testing, which falls into the vital signs section of the wellness check, is critical because undiagnosed problems can cause amblyopia or “lazy eye.” The American Academy of Pediatrics recommends vision testing at well-child visits starting at age 3. Regional studies,however, have suggested low rates of PCP vision testing.
Study findings
In a sample of 89,936 participants, with a mean age of 10 years (51.1% male), an estimated 30.7% overall received vision testing in primary care. Adjusted odds of vision testing in primary care decreased by 41% (odds ratio, 0.59; 95% confidence interval [CI], 0.49-0.72) for uninsured and by 24% (OR, 0.76; 95% CI, 0.70-0.82) for publicly insured participants vs. those with private insurance.
Adjusted estimated probability of vision testing was 22% (95% CI, 18.8%-25.2%) for uninsured participants, 26.6% (95% CI, 25.3%-27.9%) for those publicly insured, and 32.3% (95% CI, 31.4%-33.%) for those privately insured.
In children aged 3-5, estimated probability was 29.7% (95% CI, 25.6%-33.7%) for those uninsured, 35.2% (95% CI, 33.1%-37.3%) for those publicly insured, and 41.6% (95% CI, 39.8%-43.5%) for those privately insured – all well under 50%. The children least likely to be tested, regardless of insurance status, were adolescents aged 12-17.
Commenting on the study but not involved in it, Natalie J. Choi, MD, assistant professor of family medicine at Northwestern Medicine in Chicago, noted that the authors did not address other screening venues such as schools. She also pointed out that it is challenging for primary care physicians to address all the recommended prevention measures in addition to acute issues during an office visit.
“Oftentimes parents are the first to notice a concern about vision, and parental concerns are routinely addressed in primary care,” she said.
According to Dr. Killeen, vision testing should always be worked into the exam flow as a routine part of well-child visits. “There are devices called photoscreeners which provide automated vision tests for young children and can save a lot of time and make vision testing less burdensome for physicians and their staff,” she said. Not all primary care offices, however, offer these testing modalities.
Dr. Choi said low vision screening rates are part of the larger problem of preventive care. “In the study, the percentage of children attending a preventive health visit within the last 12 months varied by insurance coverage and was definitely not 100%,” she said. “Investing in preventive medicine helps us identify things before they become a problem, so I would love to see the number of well-child checks increase.” Identifying this gap in vision care is one of many steps, she said.
This work was supported by the University of Michigan National Clinician Scholars Program and by an unrestricted grant to the University of Michigan Department of Ophthalmology and Visual Sciences from Research to Prevent Blindness. Study coauthor Brian C. Stagg, MD, reported a grant from the National Eye Institute during the conduct of the study. Dr. Choi disclosed no conflicts of interest relevant to her comments.
In data from the 2018-2020 National Survey of Children’s Health, an annual, nationally representative cross-sectional study, fewer than half of children aged 3-5 with private insurance received vision testing, with rates even lower in those lacking private insurance. The findings point to unmet eye care needs, especially in young children for whom early testing to ward off vision loss is highly recommended.
The report was published online in JAMA Ophthalmology by Olivia J. Killeen MD, MS, an ophthalmologist during the study in the department of ophthalmology and visual sciences at the University of Michigan, Ann Arbor, and colleagues.
Future work should focus on improving primary care provider vision screening rates, especially for the 3- to 5-year age group, the authors wrote.
“Because children often are not aware they have an eye problem, routine vision testing in the primary care setting can help identify those with potential eye disease,” Dr. Killeen said. “We have an opportunity to improve the early detection and treatment of eye disease by improving primary care vision testing.”
Childhood vision testing, which falls into the vital signs section of the wellness check, is critical because undiagnosed problems can cause amblyopia or “lazy eye.” The American Academy of Pediatrics recommends vision testing at well-child visits starting at age 3. Regional studies,however, have suggested low rates of PCP vision testing.
Study findings
In a sample of 89,936 participants, with a mean age of 10 years (51.1% male), an estimated 30.7% overall received vision testing in primary care. Adjusted odds of vision testing in primary care decreased by 41% (odds ratio, 0.59; 95% confidence interval [CI], 0.49-0.72) for uninsured and by 24% (OR, 0.76; 95% CI, 0.70-0.82) for publicly insured participants vs. those with private insurance.
Adjusted estimated probability of vision testing was 22% (95% CI, 18.8%-25.2%) for uninsured participants, 26.6% (95% CI, 25.3%-27.9%) for those publicly insured, and 32.3% (95% CI, 31.4%-33.%) for those privately insured.
In children aged 3-5, estimated probability was 29.7% (95% CI, 25.6%-33.7%) for those uninsured, 35.2% (95% CI, 33.1%-37.3%) for those publicly insured, and 41.6% (95% CI, 39.8%-43.5%) for those privately insured – all well under 50%. The children least likely to be tested, regardless of insurance status, were adolescents aged 12-17.
Commenting on the study but not involved in it, Natalie J. Choi, MD, assistant professor of family medicine at Northwestern Medicine in Chicago, noted that the authors did not address other screening venues such as schools. She also pointed out that it is challenging for primary care physicians to address all the recommended prevention measures in addition to acute issues during an office visit.
“Oftentimes parents are the first to notice a concern about vision, and parental concerns are routinely addressed in primary care,” she said.
According to Dr. Killeen, vision testing should always be worked into the exam flow as a routine part of well-child visits. “There are devices called photoscreeners which provide automated vision tests for young children and can save a lot of time and make vision testing less burdensome for physicians and their staff,” she said. Not all primary care offices, however, offer these testing modalities.
Dr. Choi said low vision screening rates are part of the larger problem of preventive care. “In the study, the percentage of children attending a preventive health visit within the last 12 months varied by insurance coverage and was definitely not 100%,” she said. “Investing in preventive medicine helps us identify things before they become a problem, so I would love to see the number of well-child checks increase.” Identifying this gap in vision care is one of many steps, she said.
This work was supported by the University of Michigan National Clinician Scholars Program and by an unrestricted grant to the University of Michigan Department of Ophthalmology and Visual Sciences from Research to Prevent Blindness. Study coauthor Brian C. Stagg, MD, reported a grant from the National Eye Institute during the conduct of the study. Dr. Choi disclosed no conflicts of interest relevant to her comments.
In data from the 2018-2020 National Survey of Children’s Health, an annual, nationally representative cross-sectional study, fewer than half of children aged 3-5 with private insurance received vision testing, with rates even lower in those lacking private insurance. The findings point to unmet eye care needs, especially in young children for whom early testing to ward off vision loss is highly recommended.
The report was published online in JAMA Ophthalmology by Olivia J. Killeen MD, MS, an ophthalmologist during the study in the department of ophthalmology and visual sciences at the University of Michigan, Ann Arbor, and colleagues.
Future work should focus on improving primary care provider vision screening rates, especially for the 3- to 5-year age group, the authors wrote.
“Because children often are not aware they have an eye problem, routine vision testing in the primary care setting can help identify those with potential eye disease,” Dr. Killeen said. “We have an opportunity to improve the early detection and treatment of eye disease by improving primary care vision testing.”
Childhood vision testing, which falls into the vital signs section of the wellness check, is critical because undiagnosed problems can cause amblyopia or “lazy eye.” The American Academy of Pediatrics recommends vision testing at well-child visits starting at age 3. Regional studies,however, have suggested low rates of PCP vision testing.
Study findings
In a sample of 89,936 participants, with a mean age of 10 years (51.1% male), an estimated 30.7% overall received vision testing in primary care. Adjusted odds of vision testing in primary care decreased by 41% (odds ratio, 0.59; 95% confidence interval [CI], 0.49-0.72) for uninsured and by 24% (OR, 0.76; 95% CI, 0.70-0.82) for publicly insured participants vs. those with private insurance.
Adjusted estimated probability of vision testing was 22% (95% CI, 18.8%-25.2%) for uninsured participants, 26.6% (95% CI, 25.3%-27.9%) for those publicly insured, and 32.3% (95% CI, 31.4%-33.%) for those privately insured.
In children aged 3-5, estimated probability was 29.7% (95% CI, 25.6%-33.7%) for those uninsured, 35.2% (95% CI, 33.1%-37.3%) for those publicly insured, and 41.6% (95% CI, 39.8%-43.5%) for those privately insured – all well under 50%. The children least likely to be tested, regardless of insurance status, were adolescents aged 12-17.
Commenting on the study but not involved in it, Natalie J. Choi, MD, assistant professor of family medicine at Northwestern Medicine in Chicago, noted that the authors did not address other screening venues such as schools. She also pointed out that it is challenging for primary care physicians to address all the recommended prevention measures in addition to acute issues during an office visit.
“Oftentimes parents are the first to notice a concern about vision, and parental concerns are routinely addressed in primary care,” she said.
According to Dr. Killeen, vision testing should always be worked into the exam flow as a routine part of well-child visits. “There are devices called photoscreeners which provide automated vision tests for young children and can save a lot of time and make vision testing less burdensome for physicians and their staff,” she said. Not all primary care offices, however, offer these testing modalities.
Dr. Choi said low vision screening rates are part of the larger problem of preventive care. “In the study, the percentage of children attending a preventive health visit within the last 12 months varied by insurance coverage and was definitely not 100%,” she said. “Investing in preventive medicine helps us identify things before they become a problem, so I would love to see the number of well-child checks increase.” Identifying this gap in vision care is one of many steps, she said.
This work was supported by the University of Michigan National Clinician Scholars Program and by an unrestricted grant to the University of Michigan Department of Ophthalmology and Visual Sciences from Research to Prevent Blindness. Study coauthor Brian C. Stagg, MD, reported a grant from the National Eye Institute during the conduct of the study. Dr. Choi disclosed no conflicts of interest relevant to her comments.
FROM JAMA OPHTHALMOLOGY
Telehealth visit helps reconnect adolescents lost to follow-up
A telehealth primary care visit more than doubled the well-visit show rate for a cohort of hard-to-reach adolescents, results of a small pilot study show.
Brian P. Jenssen, MD, MSHP, department of pediatrics, University of Pennsylvania, Philadelphia, led the pilot study and the project team, which included physicians, researchers, and experts in innovation, quality improvement, and data analytics.
Findings were published online in Annals of Family Medicine.
Keeping adolescents in consistent primary care can be challenging for many reasons. The study authors note, “Only 50% of adolescents have had a health supervision visit in the past year, missing a critical opportunity for clinicians to influence health, development, screening, and counseling.”
Interest high in hard-to-reach group
This study included a particularly hard-to-reach group of 18-year-old patients at an urban primary care clinic who were lost to follow-up and had Medicaid insurance. They had not completed a well visit in more than 2 years and had a history of no-show visits.
Interest in the pilot program was high. The authors write: “We contacted patients (or their caregivers) to gauge interest in a virtual well visit with a goal to fill five telehealth slots in one evening block with one clinician. Due to high patient interest and demand, we expanded to 15 slots over three evenings, filling the slots after contacting just 24 patients.”
Professional organizations have recommended a telehealth/in-person hybrid care model to meet hard-to-reach adolescents “wherever they are,” the authors note, but the concept has not been well studied.
Under the hybrid model, the first visit is through telehealth and in-person follow-up is scheduled as needed.
Navigators contacted patients to remind them of the appointment, and helped activate the patient portal and complete previsit screening questions for depression and other health risks.
Telehealth visits were billed as preventive visits and in-person follow-up visits as no-charge nurse visits, and these payments were supported by Medicaid.
Sharp increase in show rate
In the pilot study, of the 15 patients scheduled for the telehealth visit, 11 connected virtually (73% show rate). Of those, nine needed in-person follow-up, and five completed the follow-up.
Before the intervention, the average well-visit show rate for this patient group was 33%.
Clinicians counseled all the patients about substance use and safe sex. One patient screened positive for depression and was then connected to services. Two patients were started on birth control.
During the in-person follow-up, all patients received vaccinations (influenza, meningococcal, and/or COVID-19) and were screened for sexually transmitted infection. Eight patients completed the satisfaction survey and all said they liked the convenience of the telehealth visit.
Telehealth may reduce barriers for teens
Anthony Cheng, MD, a family medicine physician at Oregon Health & Science University in Portland, who was not part of the study, said he found the hybrid model promising.
One reason is that telehealth eliminates the need for transportation to medical appointments, which can be a barrier for adolescents.
Among the top causes of death for young people are mental health issues and addressing those, Dr. Cheng noted, is well-suited to a telehealth visit.
“There’s so much we can do if we can establish a relationship and maintain a relationship with our patients as young adults,” he said. “People do better when they have a regular source of care.”
He added that adolescents also have grown up communicating via screens so it’s often more comfortable for them to communicate with health care providers this way.
Dr. Cheng said adopting such a model may be difficult for providers reluctant to switch from the practice model with which they are most comfortable.
“We prefer to do things we have the most confidence in,” he said. “It does take an investment to train staff and build your own clinical comfort. If that experience wasn’t good over the past 3 years, you may be anxious to get back to your normal way of doing business.”
The authors and Dr. Cheng have no relevant financial relationships to disclose.
A telehealth primary care visit more than doubled the well-visit show rate for a cohort of hard-to-reach adolescents, results of a small pilot study show.
Brian P. Jenssen, MD, MSHP, department of pediatrics, University of Pennsylvania, Philadelphia, led the pilot study and the project team, which included physicians, researchers, and experts in innovation, quality improvement, and data analytics.
Findings were published online in Annals of Family Medicine.
Keeping adolescents in consistent primary care can be challenging for many reasons. The study authors note, “Only 50% of adolescents have had a health supervision visit in the past year, missing a critical opportunity for clinicians to influence health, development, screening, and counseling.”
Interest high in hard-to-reach group
This study included a particularly hard-to-reach group of 18-year-old patients at an urban primary care clinic who were lost to follow-up and had Medicaid insurance. They had not completed a well visit in more than 2 years and had a history of no-show visits.
Interest in the pilot program was high. The authors write: “We contacted patients (or their caregivers) to gauge interest in a virtual well visit with a goal to fill five telehealth slots in one evening block with one clinician. Due to high patient interest and demand, we expanded to 15 slots over three evenings, filling the slots after contacting just 24 patients.”
Professional organizations have recommended a telehealth/in-person hybrid care model to meet hard-to-reach adolescents “wherever they are,” the authors note, but the concept has not been well studied.
Under the hybrid model, the first visit is through telehealth and in-person follow-up is scheduled as needed.
Navigators contacted patients to remind them of the appointment, and helped activate the patient portal and complete previsit screening questions for depression and other health risks.
Telehealth visits were billed as preventive visits and in-person follow-up visits as no-charge nurse visits, and these payments were supported by Medicaid.
Sharp increase in show rate
In the pilot study, of the 15 patients scheduled for the telehealth visit, 11 connected virtually (73% show rate). Of those, nine needed in-person follow-up, and five completed the follow-up.
Before the intervention, the average well-visit show rate for this patient group was 33%.
Clinicians counseled all the patients about substance use and safe sex. One patient screened positive for depression and was then connected to services. Two patients were started on birth control.
During the in-person follow-up, all patients received vaccinations (influenza, meningococcal, and/or COVID-19) and were screened for sexually transmitted infection. Eight patients completed the satisfaction survey and all said they liked the convenience of the telehealth visit.
Telehealth may reduce barriers for teens
Anthony Cheng, MD, a family medicine physician at Oregon Health & Science University in Portland, who was not part of the study, said he found the hybrid model promising.
One reason is that telehealth eliminates the need for transportation to medical appointments, which can be a barrier for adolescents.
Among the top causes of death for young people are mental health issues and addressing those, Dr. Cheng noted, is well-suited to a telehealth visit.
“There’s so much we can do if we can establish a relationship and maintain a relationship with our patients as young adults,” he said. “People do better when they have a regular source of care.”
He added that adolescents also have grown up communicating via screens so it’s often more comfortable for them to communicate with health care providers this way.
Dr. Cheng said adopting such a model may be difficult for providers reluctant to switch from the practice model with which they are most comfortable.
“We prefer to do things we have the most confidence in,” he said. “It does take an investment to train staff and build your own clinical comfort. If that experience wasn’t good over the past 3 years, you may be anxious to get back to your normal way of doing business.”
The authors and Dr. Cheng have no relevant financial relationships to disclose.
A telehealth primary care visit more than doubled the well-visit show rate for a cohort of hard-to-reach adolescents, results of a small pilot study show.
Brian P. Jenssen, MD, MSHP, department of pediatrics, University of Pennsylvania, Philadelphia, led the pilot study and the project team, which included physicians, researchers, and experts in innovation, quality improvement, and data analytics.
Findings were published online in Annals of Family Medicine.
Keeping adolescents in consistent primary care can be challenging for many reasons. The study authors note, “Only 50% of adolescents have had a health supervision visit in the past year, missing a critical opportunity for clinicians to influence health, development, screening, and counseling.”
Interest high in hard-to-reach group
This study included a particularly hard-to-reach group of 18-year-old patients at an urban primary care clinic who were lost to follow-up and had Medicaid insurance. They had not completed a well visit in more than 2 years and had a history of no-show visits.
Interest in the pilot program was high. The authors write: “We contacted patients (or their caregivers) to gauge interest in a virtual well visit with a goal to fill five telehealth slots in one evening block with one clinician. Due to high patient interest and demand, we expanded to 15 slots over three evenings, filling the slots after contacting just 24 patients.”
Professional organizations have recommended a telehealth/in-person hybrid care model to meet hard-to-reach adolescents “wherever they are,” the authors note, but the concept has not been well studied.
Under the hybrid model, the first visit is through telehealth and in-person follow-up is scheduled as needed.
Navigators contacted patients to remind them of the appointment, and helped activate the patient portal and complete previsit screening questions for depression and other health risks.
Telehealth visits were billed as preventive visits and in-person follow-up visits as no-charge nurse visits, and these payments were supported by Medicaid.
Sharp increase in show rate
In the pilot study, of the 15 patients scheduled for the telehealth visit, 11 connected virtually (73% show rate). Of those, nine needed in-person follow-up, and five completed the follow-up.
Before the intervention, the average well-visit show rate for this patient group was 33%.
Clinicians counseled all the patients about substance use and safe sex. One patient screened positive for depression and was then connected to services. Two patients were started on birth control.
During the in-person follow-up, all patients received vaccinations (influenza, meningococcal, and/or COVID-19) and were screened for sexually transmitted infection. Eight patients completed the satisfaction survey and all said they liked the convenience of the telehealth visit.
Telehealth may reduce barriers for teens
Anthony Cheng, MD, a family medicine physician at Oregon Health & Science University in Portland, who was not part of the study, said he found the hybrid model promising.
One reason is that telehealth eliminates the need for transportation to medical appointments, which can be a barrier for adolescents.
Among the top causes of death for young people are mental health issues and addressing those, Dr. Cheng noted, is well-suited to a telehealth visit.
“There’s so much we can do if we can establish a relationship and maintain a relationship with our patients as young adults,” he said. “People do better when they have a regular source of care.”
He added that adolescents also have grown up communicating via screens so it’s often more comfortable for them to communicate with health care providers this way.
Dr. Cheng said adopting such a model may be difficult for providers reluctant to switch from the practice model with which they are most comfortable.
“We prefer to do things we have the most confidence in,” he said. “It does take an investment to train staff and build your own clinical comfort. If that experience wasn’t good over the past 3 years, you may be anxious to get back to your normal way of doing business.”
The authors and Dr. Cheng have no relevant financial relationships to disclose.
FROM ANNALS OF INTERNAL MEDICINE
Nutritional psychiatry: Does it exist?
Matt was diagnosed with ADHD combined type when he was 6 years old. Given his age, the family was reluctant to try medications, but after a couple years of parenting classes and reward charts, the parents requested a stimulant. He had significant improvement in focus and impulsivity but also reduced appetite. Now at age 13, irritability and depressive symptoms have been increasing for 9 months. Skeptical of adding another medication, his parents ask whether nutrition might be an alternative tool to treat his symptoms?
What a healthy diet even consists of seems to be a moving target over decades and years. Trendy research, supplements, and dietary approaches proliferate alongside appealing theories of action. In the end, weighing which intervention is effective for which disorder and at what cost becomes murky.
Yet several fundamental principles seem clear and consistent over time and across studies.
Starting early
There is reliable evidence that in the perinatal environment, nutrition sets the stage for many aspects of healthy development. These effects are likely mediated variously through the hypothalamic-pituitary-adrenal axis, the trillions of gut bacteria that make up the microbiome, gene-environment interactions, and more. Maternal malnutrition and stress prenatally puts infants at risk for not only poor birth outcomes but also psychiatric challenges throughout childhood, such as ADHD, anxiety, depression, and autism.1
Intervening in the perinatal period has long-term benefits. A first step includes assessing food security, beginning with consistent access to nutritious food. It is important to inquire about the role of food and nutrition in the family’s history and culture, as well as identifying resources to support access to affordable nutrition. This can be paired with parenting interventions, such as family meals without screens. This may require scaffolding positive conversations in high-conflict family settings (see The Family Dinner Project).
Healthy diets promote mental health
If food security is achieved, what is next? Clinicians can inquire about the who, what, where, when, and why of nutrition to learn about a family’s eating habits.2 While randomized controlled data is very limited, both cross-sectional and longitudinal studies show that healthy diets in youth correlate with mental health – more healthy foods reducing internalizing and externalizing disorders, and more typical Western diets increasing the risk. On average, dietary interventions include higher levels of fruits and vegetables, fish, and nuts, and lower levels of processed foods.2 There is not evidence that restrictive diets or fasting is appropriate or safe for youth. Additionally, involving children in getting, growing, or preparing food with gradually increasing autonomy fosters self-confidence and skill development.
In those struggling with restrictive eating disorders, food is medicine – helping those with restrictive diets to develop more balanced and adequate intake for metabolic needs. Outside of diagnosable eating disorders, weight or body mass index is less of a goal or marker when it comes to mental health. Instead, look for participation in enjoyable activities, opportunities to move and rest, and a body image that supports self-care and self-confidence (see the National Institutes of Health’s We Can! Program). Creating dissonance with cultural ideals of appearance centered on thinness can prevent future eating disorders.3
Nutraceutical options
Outside of eating disorders, specific foods and plants with health or medicinal properties – variously called nutraceuticals, phytoceuticals, or micronutrients – have emerging evidence in mental health. A 2022 expert academic consensus panel reviewed the literature to create clinical guidelines in this area.4 For major depression, adding omega-3 fatty acids to standard antidepressant treatment or standalone St. John’s wort have adequate evidence to recommend, while adjunctive probiotics, zinc, saffron, and curcumin have sufficient though less robust evidence. S-adenosyl methionine, vitamin D, and methyfolate showed only weak evidence for depression, while vitamin C, magnesium, creatine, N-acetylcysteine, folate, and monotherapy omega-3s do not have sufficient evidence to be recommended. For ADHD there was weak support for vitamin D, but no clear evidence for omega-3s, zinc, gingko, or acetyl L-carnitine. For anxiety, there is moderate evidence for ashwagandha and lavender in adults. A child psychiatry review suggests also trying chamomile for generalized anxiety based on the evidence in young adults, and underscores some data for N-acetylcysteine for OCD in particular.5
Many of these nutraceuticals exhibit small or moderate effects in a limited number of trials, with generally much less data for youth, compared with adults. While the same could be said for many on- and off-label uses of psychiatric medications for kids, clinicians would be wise to consider these highly specific nutritional interventions as items on the menu of treatment options rather than stand-alone treatments.
Revisitng the case study
Reflecting on Matt’s care, his pediatrician first assessed his dietary patterns, noting late-night eating and caffeine use with minimal hydration or fiber across the day. Recommendations for keeping fruit and vegetable snacks easily accessible as well as carrying a water flask are well received. They also discuss adding omega-3 fatty acids and probiotics with his morning stimulant while he awaits a referral for cognitive-behavioral therapy in order to address his depressive symptoms and minimize medication needs.
Beyond addressing food security and balanced family meals, specific interventions may be appropriate as initial treatment adjuncts for mild and some moderate mental illness. For more intense moderate to severe illness, nutritional psychiatry may be considered in combination with treatments with stronger evidence. At a community level, clinicians can help advocate for universal school meal programs to address food security, and so-called salad bar interventions to increase fruit/vegetable uptake among school-age children.
Dr. Rosenfeld is associate professor of psychiatry and pediatrics at University of Vermont and the Vermont Center for Children, Youth, and Families, both in Burlington. He has no disclosures.
References
1 Vohr BR et al. Pediatrics. 2017;139:S38-49.
2. Hosker DK et al. Child Adol Psychiatr Clin N Am. 2019;28(2):171-93.
3. Stice E et al. Int J Eat Disord. 2013;46(5):478-85.
4. Sarris J et al. World J Biol Psychiatry. 2022;23(6):424-55.
5. Simkin DR et al. Child Adolesc Psychiatric Clin N Am. 2023;32:193-216.
Matt was diagnosed with ADHD combined type when he was 6 years old. Given his age, the family was reluctant to try medications, but after a couple years of parenting classes and reward charts, the parents requested a stimulant. He had significant improvement in focus and impulsivity but also reduced appetite. Now at age 13, irritability and depressive symptoms have been increasing for 9 months. Skeptical of adding another medication, his parents ask whether nutrition might be an alternative tool to treat his symptoms?
What a healthy diet even consists of seems to be a moving target over decades and years. Trendy research, supplements, and dietary approaches proliferate alongside appealing theories of action. In the end, weighing which intervention is effective for which disorder and at what cost becomes murky.
Yet several fundamental principles seem clear and consistent over time and across studies.
Starting early
There is reliable evidence that in the perinatal environment, nutrition sets the stage for many aspects of healthy development. These effects are likely mediated variously through the hypothalamic-pituitary-adrenal axis, the trillions of gut bacteria that make up the microbiome, gene-environment interactions, and more. Maternal malnutrition and stress prenatally puts infants at risk for not only poor birth outcomes but also psychiatric challenges throughout childhood, such as ADHD, anxiety, depression, and autism.1
Intervening in the perinatal period has long-term benefits. A first step includes assessing food security, beginning with consistent access to nutritious food. It is important to inquire about the role of food and nutrition in the family’s history and culture, as well as identifying resources to support access to affordable nutrition. This can be paired with parenting interventions, such as family meals without screens. This may require scaffolding positive conversations in high-conflict family settings (see The Family Dinner Project).
Healthy diets promote mental health
If food security is achieved, what is next? Clinicians can inquire about the who, what, where, when, and why of nutrition to learn about a family’s eating habits.2 While randomized controlled data is very limited, both cross-sectional and longitudinal studies show that healthy diets in youth correlate with mental health – more healthy foods reducing internalizing and externalizing disorders, and more typical Western diets increasing the risk. On average, dietary interventions include higher levels of fruits and vegetables, fish, and nuts, and lower levels of processed foods.2 There is not evidence that restrictive diets or fasting is appropriate or safe for youth. Additionally, involving children in getting, growing, or preparing food with gradually increasing autonomy fosters self-confidence and skill development.
In those struggling with restrictive eating disorders, food is medicine – helping those with restrictive diets to develop more balanced and adequate intake for metabolic needs. Outside of diagnosable eating disorders, weight or body mass index is less of a goal or marker when it comes to mental health. Instead, look for participation in enjoyable activities, opportunities to move and rest, and a body image that supports self-care and self-confidence (see the National Institutes of Health’s We Can! Program). Creating dissonance with cultural ideals of appearance centered on thinness can prevent future eating disorders.3
Nutraceutical options
Outside of eating disorders, specific foods and plants with health or medicinal properties – variously called nutraceuticals, phytoceuticals, or micronutrients – have emerging evidence in mental health. A 2022 expert academic consensus panel reviewed the literature to create clinical guidelines in this area.4 For major depression, adding omega-3 fatty acids to standard antidepressant treatment or standalone St. John’s wort have adequate evidence to recommend, while adjunctive probiotics, zinc, saffron, and curcumin have sufficient though less robust evidence. S-adenosyl methionine, vitamin D, and methyfolate showed only weak evidence for depression, while vitamin C, magnesium, creatine, N-acetylcysteine, folate, and monotherapy omega-3s do not have sufficient evidence to be recommended. For ADHD there was weak support for vitamin D, but no clear evidence for omega-3s, zinc, gingko, or acetyl L-carnitine. For anxiety, there is moderate evidence for ashwagandha and lavender in adults. A child psychiatry review suggests also trying chamomile for generalized anxiety based on the evidence in young adults, and underscores some data for N-acetylcysteine for OCD in particular.5
Many of these nutraceuticals exhibit small or moderate effects in a limited number of trials, with generally much less data for youth, compared with adults. While the same could be said for many on- and off-label uses of psychiatric medications for kids, clinicians would be wise to consider these highly specific nutritional interventions as items on the menu of treatment options rather than stand-alone treatments.
Revisitng the case study
Reflecting on Matt’s care, his pediatrician first assessed his dietary patterns, noting late-night eating and caffeine use with minimal hydration or fiber across the day. Recommendations for keeping fruit and vegetable snacks easily accessible as well as carrying a water flask are well received. They also discuss adding omega-3 fatty acids and probiotics with his morning stimulant while he awaits a referral for cognitive-behavioral therapy in order to address his depressive symptoms and minimize medication needs.
Beyond addressing food security and balanced family meals, specific interventions may be appropriate as initial treatment adjuncts for mild and some moderate mental illness. For more intense moderate to severe illness, nutritional psychiatry may be considered in combination with treatments with stronger evidence. At a community level, clinicians can help advocate for universal school meal programs to address food security, and so-called salad bar interventions to increase fruit/vegetable uptake among school-age children.
Dr. Rosenfeld is associate professor of psychiatry and pediatrics at University of Vermont and the Vermont Center for Children, Youth, and Families, both in Burlington. He has no disclosures.
References
1 Vohr BR et al. Pediatrics. 2017;139:S38-49.
2. Hosker DK et al. Child Adol Psychiatr Clin N Am. 2019;28(2):171-93.
3. Stice E et al. Int J Eat Disord. 2013;46(5):478-85.
4. Sarris J et al. World J Biol Psychiatry. 2022;23(6):424-55.
5. Simkin DR et al. Child Adolesc Psychiatric Clin N Am. 2023;32:193-216.
Matt was diagnosed with ADHD combined type when he was 6 years old. Given his age, the family was reluctant to try medications, but after a couple years of parenting classes and reward charts, the parents requested a stimulant. He had significant improvement in focus and impulsivity but also reduced appetite. Now at age 13, irritability and depressive symptoms have been increasing for 9 months. Skeptical of adding another medication, his parents ask whether nutrition might be an alternative tool to treat his symptoms?
What a healthy diet even consists of seems to be a moving target over decades and years. Trendy research, supplements, and dietary approaches proliferate alongside appealing theories of action. In the end, weighing which intervention is effective for which disorder and at what cost becomes murky.
Yet several fundamental principles seem clear and consistent over time and across studies.
Starting early
There is reliable evidence that in the perinatal environment, nutrition sets the stage for many aspects of healthy development. These effects are likely mediated variously through the hypothalamic-pituitary-adrenal axis, the trillions of gut bacteria that make up the microbiome, gene-environment interactions, and more. Maternal malnutrition and stress prenatally puts infants at risk for not only poor birth outcomes but also psychiatric challenges throughout childhood, such as ADHD, anxiety, depression, and autism.1
Intervening in the perinatal period has long-term benefits. A first step includes assessing food security, beginning with consistent access to nutritious food. It is important to inquire about the role of food and nutrition in the family’s history and culture, as well as identifying resources to support access to affordable nutrition. This can be paired with parenting interventions, such as family meals without screens. This may require scaffolding positive conversations in high-conflict family settings (see The Family Dinner Project).
Healthy diets promote mental health
If food security is achieved, what is next? Clinicians can inquire about the who, what, where, when, and why of nutrition to learn about a family’s eating habits.2 While randomized controlled data is very limited, both cross-sectional and longitudinal studies show that healthy diets in youth correlate with mental health – more healthy foods reducing internalizing and externalizing disorders, and more typical Western diets increasing the risk. On average, dietary interventions include higher levels of fruits and vegetables, fish, and nuts, and lower levels of processed foods.2 There is not evidence that restrictive diets or fasting is appropriate or safe for youth. Additionally, involving children in getting, growing, or preparing food with gradually increasing autonomy fosters self-confidence and skill development.
In those struggling with restrictive eating disorders, food is medicine – helping those with restrictive diets to develop more balanced and adequate intake for metabolic needs. Outside of diagnosable eating disorders, weight or body mass index is less of a goal or marker when it comes to mental health. Instead, look for participation in enjoyable activities, opportunities to move and rest, and a body image that supports self-care and self-confidence (see the National Institutes of Health’s We Can! Program). Creating dissonance with cultural ideals of appearance centered on thinness can prevent future eating disorders.3
Nutraceutical options
Outside of eating disorders, specific foods and plants with health or medicinal properties – variously called nutraceuticals, phytoceuticals, or micronutrients – have emerging evidence in mental health. A 2022 expert academic consensus panel reviewed the literature to create clinical guidelines in this area.4 For major depression, adding omega-3 fatty acids to standard antidepressant treatment or standalone St. John’s wort have adequate evidence to recommend, while adjunctive probiotics, zinc, saffron, and curcumin have sufficient though less robust evidence. S-adenosyl methionine, vitamin D, and methyfolate showed only weak evidence for depression, while vitamin C, magnesium, creatine, N-acetylcysteine, folate, and monotherapy omega-3s do not have sufficient evidence to be recommended. For ADHD there was weak support for vitamin D, but no clear evidence for omega-3s, zinc, gingko, or acetyl L-carnitine. For anxiety, there is moderate evidence for ashwagandha and lavender in adults. A child psychiatry review suggests also trying chamomile for generalized anxiety based on the evidence in young adults, and underscores some data for N-acetylcysteine for OCD in particular.5
Many of these nutraceuticals exhibit small or moderate effects in a limited number of trials, with generally much less data for youth, compared with adults. While the same could be said for many on- and off-label uses of psychiatric medications for kids, clinicians would be wise to consider these highly specific nutritional interventions as items on the menu of treatment options rather than stand-alone treatments.
Revisitng the case study
Reflecting on Matt’s care, his pediatrician first assessed his dietary patterns, noting late-night eating and caffeine use with minimal hydration or fiber across the day. Recommendations for keeping fruit and vegetable snacks easily accessible as well as carrying a water flask are well received. They also discuss adding omega-3 fatty acids and probiotics with his morning stimulant while he awaits a referral for cognitive-behavioral therapy in order to address his depressive symptoms and minimize medication needs.
Beyond addressing food security and balanced family meals, specific interventions may be appropriate as initial treatment adjuncts for mild and some moderate mental illness. For more intense moderate to severe illness, nutritional psychiatry may be considered in combination with treatments with stronger evidence. At a community level, clinicians can help advocate for universal school meal programs to address food security, and so-called salad bar interventions to increase fruit/vegetable uptake among school-age children.
Dr. Rosenfeld is associate professor of psychiatry and pediatrics at University of Vermont and the Vermont Center for Children, Youth, and Families, both in Burlington. He has no disclosures.
References
1 Vohr BR et al. Pediatrics. 2017;139:S38-49.
2. Hosker DK et al. Child Adol Psychiatr Clin N Am. 2019;28(2):171-93.
3. Stice E et al. Int J Eat Disord. 2013;46(5):478-85.
4. Sarris J et al. World J Biol Psychiatry. 2022;23(6):424-55.
5. Simkin DR et al. Child Adolesc Psychiatric Clin N Am. 2023;32:193-216.
Children and long COVID: How many are affected?
Long COVID most often strikes seniors and adults, but children are also affected, even though they get less attention, new research shows.
Experts noted that the disease poses particular challenges for children and the doctors who treat them.
Parents and doctors need to be on the lookout for symptoms of long COVID in children and teens that might be easily missed or misdiagnosed, according to physicians and family groups.
Children are at lower risk for contracting COVID and often experience milder symptoms. But the virus is now widespread, and a recent study found that around 16% of pediatric patients with COVID go on to develop symptoms that last more than 3 months – the working definition of long COVID.
Parents and doctors are calling for more studies and more awareness.
Diane Sheehan, who lives outside Charlotte, N.C., says she was an active person and is now permanently disabled from long COVID. Her teenage son has it too and is still recovering.
He contracted COVID after a school event, she said. He had a mild case, but then he started experiencing dizziness and would even experience loss of consciousness when he stood up suddenly. After he contracted the virus a second time, he was bedridden for 8 months.
The staff at Hackensack Meridian Health, a pediatric long COVID clinic in New Jersey, has been working with area schools to help teachers and school nurses recognize possible long COVID in children and young people. The clinic is one of about a dozen in the United States that specializes in pediatric cases.
Katherine Clouser, MD, a pediatric hospital medicine specialist, has been with the clinic since it opened in 2021, and she’s seen a steady flow of patients. Some get better, but she sees a few new cases each week.
“We are seeing children who are having a difficult time returning to school and sports,” she said.
The clinic is having success with a mix of approaches, including intensive rehabilitation, talk therapy, and some off-label use of nirmatrelvir (Paxlovid), an antiviral now being studied as a treatment for long COVID through a National Institutes of Health clinical trials initiative that was announced last month.
Treatment depends on symptoms and is determined on a case-by-case basis, Dr. Clouser said.
Families of her patients are grateful, she added.
“We hear a lot of parents who were desperate for someone to believe them – or someone who knows about it,” she said.
A recent review of more than 30 studies with about 15,000 participants concluded that 16.2% (95% confidence interval, 8.5%-28.6%) of the pediatric participants experienced one or more persistent symptoms of long COVID at least 3 months after acute infection.
Estimates of the number of children and youth with long COVID have varied widely. A 2022 study put the number at more than 25% of cases, but the American Academy of Pediatrics notes that estimates of the percentage of children infected with SARS-CoV-2 who go on to have long COVID range from 2% to 66%.
The federal Recover Initiative has enrolled more than 10,000 children and youth – a number it plans to double – and studies of electronic health records are underway. The Recover pediatric team is also setting up a cohort that they plan to follow into 2025.
Some clinics are having luck treating young people with approaches ranging from special diets to off-label medication.
David W. Miller, MD, who runs the long COVID clinic at the UH Rainbow Babies and Children’s Hospital, Cleveland, said he’s seen about 250 patients.
A warning sign of long COVID in children is profound fatigue, he said.
“It’s the most common symptom,” Dr. Miller said. “They feel like they have the flu all the time.”
Many also experience orthostatic hypotension on standing, triggering dizziness.
He said his team targets symptom groups. Initial management consists of a diet without sugar or refined carbohydrates. Skipping pasta and sweets can be hard for young people, but Dr. Miller said sometimes the diet alone helps.
Many have vitamin D and iron deficiencies. Others need help getting a good night’s sleep. He’s treated 50 with off-label low-dose naltrexone.
Some people with long COVID – both young and old – complain about being misdiagnosed as having depression. Dr. Miller says he see a lot of anxiety – some situational and some biochemical – in pediatric patients. But he cautions doctors not to treat their illness solely as a mental health problem.
His advice: If a young person or child experiences a major change in his or her regular level of functioning or has multiple COVID symptoms that don’t go away after several months, parents and doctors should consider long COVID as a possible cause.
Dr. Miller said most of his patients get better over time with some treatments: “We see improvement in the majority of kids who can stick to the regimen,” such as a sugar-free diet, supplements, and adequate sleep. Recovery has been slow and incomplete for Diane Sheehan and her son. She was training as a permanent make-up artist, she said, but now has hand tremors that make work impossible.
She has found doctors who treat some of her symptoms with antihistamines, and her son has benefited from physical therapy.
But for now, her son is passing on a scholarship he was awarded to attend North Carolina State University this year. Instead, he’s living at home and going to a local college.
Ms. Sheehan urges parents to be on the alert for signs that their children might have long COVID, which can be confused with many other conditions.
A version of this article first appeared on Medscape.com.
Long COVID most often strikes seniors and adults, but children are also affected, even though they get less attention, new research shows.
Experts noted that the disease poses particular challenges for children and the doctors who treat them.
Parents and doctors need to be on the lookout for symptoms of long COVID in children and teens that might be easily missed or misdiagnosed, according to physicians and family groups.
Children are at lower risk for contracting COVID and often experience milder symptoms. But the virus is now widespread, and a recent study found that around 16% of pediatric patients with COVID go on to develop symptoms that last more than 3 months – the working definition of long COVID.
Parents and doctors are calling for more studies and more awareness.
Diane Sheehan, who lives outside Charlotte, N.C., says she was an active person and is now permanently disabled from long COVID. Her teenage son has it too and is still recovering.
He contracted COVID after a school event, she said. He had a mild case, but then he started experiencing dizziness and would even experience loss of consciousness when he stood up suddenly. After he contracted the virus a second time, he was bedridden for 8 months.
The staff at Hackensack Meridian Health, a pediatric long COVID clinic in New Jersey, has been working with area schools to help teachers and school nurses recognize possible long COVID in children and young people. The clinic is one of about a dozen in the United States that specializes in pediatric cases.
Katherine Clouser, MD, a pediatric hospital medicine specialist, has been with the clinic since it opened in 2021, and she’s seen a steady flow of patients. Some get better, but she sees a few new cases each week.
“We are seeing children who are having a difficult time returning to school and sports,” she said.
The clinic is having success with a mix of approaches, including intensive rehabilitation, talk therapy, and some off-label use of nirmatrelvir (Paxlovid), an antiviral now being studied as a treatment for long COVID through a National Institutes of Health clinical trials initiative that was announced last month.
Treatment depends on symptoms and is determined on a case-by-case basis, Dr. Clouser said.
Families of her patients are grateful, she added.
“We hear a lot of parents who were desperate for someone to believe them – or someone who knows about it,” she said.
A recent review of more than 30 studies with about 15,000 participants concluded that 16.2% (95% confidence interval, 8.5%-28.6%) of the pediatric participants experienced one or more persistent symptoms of long COVID at least 3 months after acute infection.
Estimates of the number of children and youth with long COVID have varied widely. A 2022 study put the number at more than 25% of cases, but the American Academy of Pediatrics notes that estimates of the percentage of children infected with SARS-CoV-2 who go on to have long COVID range from 2% to 66%.
The federal Recover Initiative has enrolled more than 10,000 children and youth – a number it plans to double – and studies of electronic health records are underway. The Recover pediatric team is also setting up a cohort that they plan to follow into 2025.
Some clinics are having luck treating young people with approaches ranging from special diets to off-label medication.
David W. Miller, MD, who runs the long COVID clinic at the UH Rainbow Babies and Children’s Hospital, Cleveland, said he’s seen about 250 patients.
A warning sign of long COVID in children is profound fatigue, he said.
“It’s the most common symptom,” Dr. Miller said. “They feel like they have the flu all the time.”
Many also experience orthostatic hypotension on standing, triggering dizziness.
He said his team targets symptom groups. Initial management consists of a diet without sugar or refined carbohydrates. Skipping pasta and sweets can be hard for young people, but Dr. Miller said sometimes the diet alone helps.
Many have vitamin D and iron deficiencies. Others need help getting a good night’s sleep. He’s treated 50 with off-label low-dose naltrexone.
Some people with long COVID – both young and old – complain about being misdiagnosed as having depression. Dr. Miller says he see a lot of anxiety – some situational and some biochemical – in pediatric patients. But he cautions doctors not to treat their illness solely as a mental health problem.
His advice: If a young person or child experiences a major change in his or her regular level of functioning or has multiple COVID symptoms that don’t go away after several months, parents and doctors should consider long COVID as a possible cause.
Dr. Miller said most of his patients get better over time with some treatments: “We see improvement in the majority of kids who can stick to the regimen,” such as a sugar-free diet, supplements, and adequate sleep. Recovery has been slow and incomplete for Diane Sheehan and her son. She was training as a permanent make-up artist, she said, but now has hand tremors that make work impossible.
She has found doctors who treat some of her symptoms with antihistamines, and her son has benefited from physical therapy.
But for now, her son is passing on a scholarship he was awarded to attend North Carolina State University this year. Instead, he’s living at home and going to a local college.
Ms. Sheehan urges parents to be on the alert for signs that their children might have long COVID, which can be confused with many other conditions.
A version of this article first appeared on Medscape.com.
Long COVID most often strikes seniors and adults, but children are also affected, even though they get less attention, new research shows.
Experts noted that the disease poses particular challenges for children and the doctors who treat them.
Parents and doctors need to be on the lookout for symptoms of long COVID in children and teens that might be easily missed or misdiagnosed, according to physicians and family groups.
Children are at lower risk for contracting COVID and often experience milder symptoms. But the virus is now widespread, and a recent study found that around 16% of pediatric patients with COVID go on to develop symptoms that last more than 3 months – the working definition of long COVID.
Parents and doctors are calling for more studies and more awareness.
Diane Sheehan, who lives outside Charlotte, N.C., says she was an active person and is now permanently disabled from long COVID. Her teenage son has it too and is still recovering.
He contracted COVID after a school event, she said. He had a mild case, but then he started experiencing dizziness and would even experience loss of consciousness when he stood up suddenly. After he contracted the virus a second time, he was bedridden for 8 months.
The staff at Hackensack Meridian Health, a pediatric long COVID clinic in New Jersey, has been working with area schools to help teachers and school nurses recognize possible long COVID in children and young people. The clinic is one of about a dozen in the United States that specializes in pediatric cases.
Katherine Clouser, MD, a pediatric hospital medicine specialist, has been with the clinic since it opened in 2021, and she’s seen a steady flow of patients. Some get better, but she sees a few new cases each week.
“We are seeing children who are having a difficult time returning to school and sports,” she said.
The clinic is having success with a mix of approaches, including intensive rehabilitation, talk therapy, and some off-label use of nirmatrelvir (Paxlovid), an antiviral now being studied as a treatment for long COVID through a National Institutes of Health clinical trials initiative that was announced last month.
Treatment depends on symptoms and is determined on a case-by-case basis, Dr. Clouser said.
Families of her patients are grateful, she added.
“We hear a lot of parents who were desperate for someone to believe them – or someone who knows about it,” she said.
A recent review of more than 30 studies with about 15,000 participants concluded that 16.2% (95% confidence interval, 8.5%-28.6%) of the pediatric participants experienced one or more persistent symptoms of long COVID at least 3 months after acute infection.
Estimates of the number of children and youth with long COVID have varied widely. A 2022 study put the number at more than 25% of cases, but the American Academy of Pediatrics notes that estimates of the percentage of children infected with SARS-CoV-2 who go on to have long COVID range from 2% to 66%.
The federal Recover Initiative has enrolled more than 10,000 children and youth – a number it plans to double – and studies of electronic health records are underway. The Recover pediatric team is also setting up a cohort that they plan to follow into 2025.
Some clinics are having luck treating young people with approaches ranging from special diets to off-label medication.
David W. Miller, MD, who runs the long COVID clinic at the UH Rainbow Babies and Children’s Hospital, Cleveland, said he’s seen about 250 patients.
A warning sign of long COVID in children is profound fatigue, he said.
“It’s the most common symptom,” Dr. Miller said. “They feel like they have the flu all the time.”
Many also experience orthostatic hypotension on standing, triggering dizziness.
He said his team targets symptom groups. Initial management consists of a diet without sugar or refined carbohydrates. Skipping pasta and sweets can be hard for young people, but Dr. Miller said sometimes the diet alone helps.
Many have vitamin D and iron deficiencies. Others need help getting a good night’s sleep. He’s treated 50 with off-label low-dose naltrexone.
Some people with long COVID – both young and old – complain about being misdiagnosed as having depression. Dr. Miller says he see a lot of anxiety – some situational and some biochemical – in pediatric patients. But he cautions doctors not to treat their illness solely as a mental health problem.
His advice: If a young person or child experiences a major change in his or her regular level of functioning or has multiple COVID symptoms that don’t go away after several months, parents and doctors should consider long COVID as a possible cause.
Dr. Miller said most of his patients get better over time with some treatments: “We see improvement in the majority of kids who can stick to the regimen,” such as a sugar-free diet, supplements, and adequate sleep. Recovery has been slow and incomplete for Diane Sheehan and her son. She was training as a permanent make-up artist, she said, but now has hand tremors that make work impossible.
She has found doctors who treat some of her symptoms with antihistamines, and her son has benefited from physical therapy.
But for now, her son is passing on a scholarship he was awarded to attend North Carolina State University this year. Instead, he’s living at home and going to a local college.
Ms. Sheehan urges parents to be on the alert for signs that their children might have long COVID, which can be confused with many other conditions.
A version of this article first appeared on Medscape.com.