User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
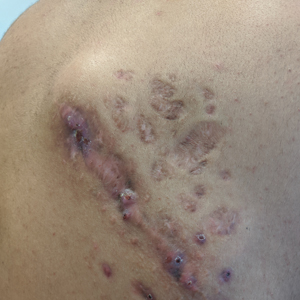
Indurated Mass on the Right Central Back
The Diagnosis: Actinomycetoma
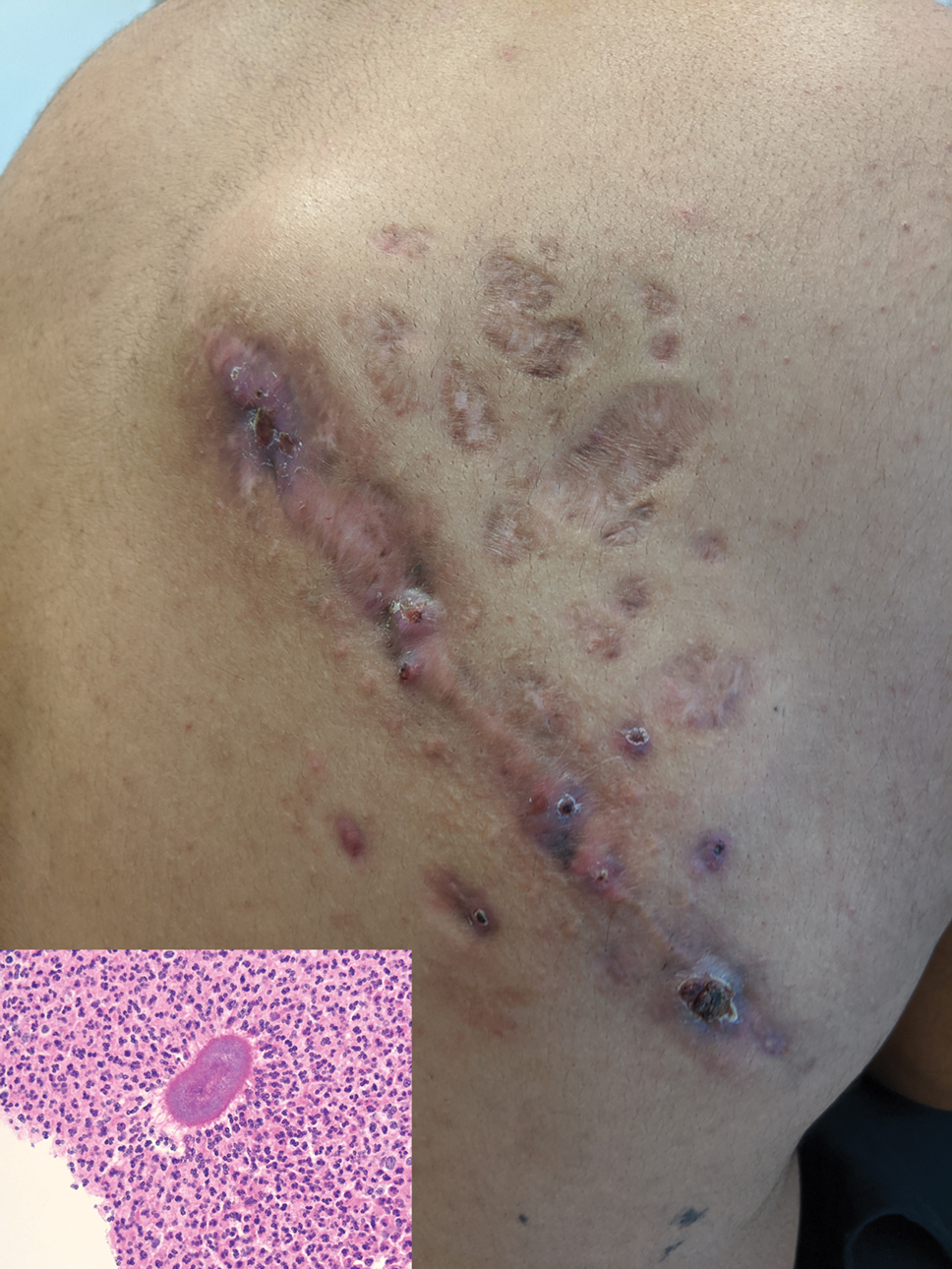
Histopathology revealed evidence of an actinomycete organism within the suppuration, consistent with actinomycosis (quiz image [inset]). Given the clinical presentation and histopathologic findings, our patient was diagnosed with actinomycetoma.
Actinomycetoma is an indolent, progressive, subcutaneous infection characterized by a well-known clinical triad of tumefaction/subcutaneous mass, draining sinuses, and an exudate containing grains on microscopy. The sinus tracts are formed from the chronic infectious process that destroys tissue, creating tunnels. This infectious disease of soft tissue is a clinical subset of mycetoma, which is categorized as eumycetoma (fungal) and actinomycetoma (bacterial). Actinomycetoma resembles the behavior of insidious and chronic fungal infections; however, most mycetoma infections are bacterial.1,2 Actinomycetoma may be confused with actinomycosis, which is caused by Actinomycoses species, commensal organisms commonly located on the teeth and oral mucosa in association with other microorganisms that may pathogenically cause cervicofacial actinomycosis.3,4 Actinomycetoma can be caused by Nocardia, Streptomyces, and Actinomadura. 2,5 The foot is the most common location of involvement followed by the thoracic region. It is more common in tropical or equatorial locations and may be contracted through exposure to soil or wood.5 Mycetoma is considered a neglected tropical disease by the World Health Organization.1 In tropical countries, this disease may go undiagnosed or untreated for so long that surgical amputation may be the only effective treatment.
Actinomycetoma commonly is identifiable by direct microscopy, Gram stain, or bacterial culture, with Gram stain being more sensitive than bacterial culture.3 It is important to indicate the suspected organism to the microbiology laboratory because common bacterial pathogens are detected within 24 to 48 hours, but the causative microorganism in actinomycetoma may require up to 4 weeks for culture,2 leading to possible false negatives due to inadequate culture time.3 Histopathology of actinomycotic infections will demonstrate granulomatous inflammation, focal suppuration, and the presence of grains (ie, a colony of filamentous bacteria in a stellate shaped mass)(quiz image [inset]).
The gold standard of treatment is trimethoprim-sulfamethoxazole for up to several years.4,5 Amoxicillin–clavulanic acid, dapsone, amikacin, streptomycin, and beta-lactams have been used successfully.2,5 The treatment course is dependent on clinical severity and location of the disease. The cure rate with appropriate antibiotics can be as high as 90%,2,5 and thus surgical intervention can be avoided.
In the differential, cutaneous tuberculosis would show tuberculoid granulomas with epithelioid histiocytes with possible caseation on histopathology, typically alongside positive tuberculosis screening. Botryomycosis has a similar clinical presentation of a swollen or indurated lesion with draining sinus tracts, but it less commonly occurs on the trunk. Histopathology also is a close mimic of actinomycetoma with a small grain inside a suppurative infiltrate; however, it has no filamentous bacteria. A foreign body reaction would not histologically present with suppuration or grains, and draining sinuses typically would not be seen on clinical presentation. Sarcoma is a neoplastic process and most commonly would show a proliferation of cells with soft tissue or bone origin on histopathology and not primarily an inflammatory cell process.6
- Verma P, Jha A. Mycetoma: reviewing a neglected disease. Clin Exp Dermatol. 2019;44:123-129.
- Valour F, Sénéchal A, Dupieux C, et al. Actinomycosis: etiology, clinical features, diagnosis, treatment, and management. Infect Drug Resist. 2014;7:183-197.
- Bennhoff DF. Actinomycosis: diagnostic and therapeutic considerations and a review of 32 cases. Laryngoscope. 1984;94:1198-1217.
- Welsh O, Vera-Cabrera L, Welsh E, et al. Actinomycetoma and advances in its treatment. Clin Dermatol. 2012;30:372-381.
- Arenas R, Fernandez Martinez RF, Torres-Guerrero E, et al. Actinomycetoma: an update on diagnosis and treatment. Cutis. 2017;99:E11-E15.
- Weedon D. Weedon’s Skin Pathology. 3rd ed. Churchill Livingstone Elsevier; 2010.
The Diagnosis: Actinomycetoma
Histopathology revealed evidence of an actinomycete organism within the suppuration, consistent with actinomycosis (quiz image [inset]). Given the clinical presentation and histopathologic findings, our patient was diagnosed with actinomycetoma.
Actinomycetoma is an indolent, progressive, subcutaneous infection characterized by a well-known clinical triad of tumefaction/subcutaneous mass, draining sinuses, and an exudate containing grains on microscopy. The sinus tracts are formed from the chronic infectious process that destroys tissue, creating tunnels. This infectious disease of soft tissue is a clinical subset of mycetoma, which is categorized as eumycetoma (fungal) and actinomycetoma (bacterial). Actinomycetoma resembles the behavior of insidious and chronic fungal infections; however, most mycetoma infections are bacterial.1,2 Actinomycetoma may be confused with actinomycosis, which is caused by Actinomycoses species, commensal organisms commonly located on the teeth and oral mucosa in association with other microorganisms that may pathogenically cause cervicofacial actinomycosis.3,4 Actinomycetoma can be caused by Nocardia, Streptomyces, and Actinomadura. 2,5 The foot is the most common location of involvement followed by the thoracic region. It is more common in tropical or equatorial locations and may be contracted through exposure to soil or wood.5 Mycetoma is considered a neglected tropical disease by the World Health Organization.1 In tropical countries, this disease may go undiagnosed or untreated for so long that surgical amputation may be the only effective treatment.
Actinomycetoma commonly is identifiable by direct microscopy, Gram stain, or bacterial culture, with Gram stain being more sensitive than bacterial culture.3 It is important to indicate the suspected organism to the microbiology laboratory because common bacterial pathogens are detected within 24 to 48 hours, but the causative microorganism in actinomycetoma may require up to 4 weeks for culture,2 leading to possible false negatives due to inadequate culture time.3 Histopathology of actinomycotic infections will demonstrate granulomatous inflammation, focal suppuration, and the presence of grains (ie, a colony of filamentous bacteria in a stellate shaped mass)(quiz image [inset]).
The gold standard of treatment is trimethoprim-sulfamethoxazole for up to several years.4,5 Amoxicillin–clavulanic acid, dapsone, amikacin, streptomycin, and beta-lactams have been used successfully.2,5 The treatment course is dependent on clinical severity and location of the disease. The cure rate with appropriate antibiotics can be as high as 90%,2,5 and thus surgical intervention can be avoided.
In the differential, cutaneous tuberculosis would show tuberculoid granulomas with epithelioid histiocytes with possible caseation on histopathology, typically alongside positive tuberculosis screening. Botryomycosis has a similar clinical presentation of a swollen or indurated lesion with draining sinus tracts, but it less commonly occurs on the trunk. Histopathology also is a close mimic of actinomycetoma with a small grain inside a suppurative infiltrate; however, it has no filamentous bacteria. A foreign body reaction would not histologically present with suppuration or grains, and draining sinuses typically would not be seen on clinical presentation. Sarcoma is a neoplastic process and most commonly would show a proliferation of cells with soft tissue or bone origin on histopathology and not primarily an inflammatory cell process.6
The Diagnosis: Actinomycetoma
Histopathology revealed evidence of an actinomycete organism within the suppuration, consistent with actinomycosis (quiz image [inset]). Given the clinical presentation and histopathologic findings, our patient was diagnosed with actinomycetoma.
Actinomycetoma is an indolent, progressive, subcutaneous infection characterized by a well-known clinical triad of tumefaction/subcutaneous mass, draining sinuses, and an exudate containing grains on microscopy. The sinus tracts are formed from the chronic infectious process that destroys tissue, creating tunnels. This infectious disease of soft tissue is a clinical subset of mycetoma, which is categorized as eumycetoma (fungal) and actinomycetoma (bacterial). Actinomycetoma resembles the behavior of insidious and chronic fungal infections; however, most mycetoma infections are bacterial.1,2 Actinomycetoma may be confused with actinomycosis, which is caused by Actinomycoses species, commensal organisms commonly located on the teeth and oral mucosa in association with other microorganisms that may pathogenically cause cervicofacial actinomycosis.3,4 Actinomycetoma can be caused by Nocardia, Streptomyces, and Actinomadura. 2,5 The foot is the most common location of involvement followed by the thoracic region. It is more common in tropical or equatorial locations and may be contracted through exposure to soil or wood.5 Mycetoma is considered a neglected tropical disease by the World Health Organization.1 In tropical countries, this disease may go undiagnosed or untreated for so long that surgical amputation may be the only effective treatment.
Actinomycetoma commonly is identifiable by direct microscopy, Gram stain, or bacterial culture, with Gram stain being more sensitive than bacterial culture.3 It is important to indicate the suspected organism to the microbiology laboratory because common bacterial pathogens are detected within 24 to 48 hours, but the causative microorganism in actinomycetoma may require up to 4 weeks for culture,2 leading to possible false negatives due to inadequate culture time.3 Histopathology of actinomycotic infections will demonstrate granulomatous inflammation, focal suppuration, and the presence of grains (ie, a colony of filamentous bacteria in a stellate shaped mass)(quiz image [inset]).
The gold standard of treatment is trimethoprim-sulfamethoxazole for up to several years.4,5 Amoxicillin–clavulanic acid, dapsone, amikacin, streptomycin, and beta-lactams have been used successfully.2,5 The treatment course is dependent on clinical severity and location of the disease. The cure rate with appropriate antibiotics can be as high as 90%,2,5 and thus surgical intervention can be avoided.
In the differential, cutaneous tuberculosis would show tuberculoid granulomas with epithelioid histiocytes with possible caseation on histopathology, typically alongside positive tuberculosis screening. Botryomycosis has a similar clinical presentation of a swollen or indurated lesion with draining sinus tracts, but it less commonly occurs on the trunk. Histopathology also is a close mimic of actinomycetoma with a small grain inside a suppurative infiltrate; however, it has no filamentous bacteria. A foreign body reaction would not histologically present with suppuration or grains, and draining sinuses typically would not be seen on clinical presentation. Sarcoma is a neoplastic process and most commonly would show a proliferation of cells with soft tissue or bone origin on histopathology and not primarily an inflammatory cell process.6
- Verma P, Jha A. Mycetoma: reviewing a neglected disease. Clin Exp Dermatol. 2019;44:123-129.
- Valour F, Sénéchal A, Dupieux C, et al. Actinomycosis: etiology, clinical features, diagnosis, treatment, and management. Infect Drug Resist. 2014;7:183-197.
- Bennhoff DF. Actinomycosis: diagnostic and therapeutic considerations and a review of 32 cases. Laryngoscope. 1984;94:1198-1217.
- Welsh O, Vera-Cabrera L, Welsh E, et al. Actinomycetoma and advances in its treatment. Clin Dermatol. 2012;30:372-381.
- Arenas R, Fernandez Martinez RF, Torres-Guerrero E, et al. Actinomycetoma: an update on diagnosis and treatment. Cutis. 2017;99:E11-E15.
- Weedon D. Weedon’s Skin Pathology. 3rd ed. Churchill Livingstone Elsevier; 2010.
- Verma P, Jha A. Mycetoma: reviewing a neglected disease. Clin Exp Dermatol. 2019;44:123-129.
- Valour F, Sénéchal A, Dupieux C, et al. Actinomycosis: etiology, clinical features, diagnosis, treatment, and management. Infect Drug Resist. 2014;7:183-197.
- Bennhoff DF. Actinomycosis: diagnostic and therapeutic considerations and a review of 32 cases. Laryngoscope. 1984;94:1198-1217.
- Welsh O, Vera-Cabrera L, Welsh E, et al. Actinomycetoma and advances in its treatment. Clin Dermatol. 2012;30:372-381.
- Arenas R, Fernandez Martinez RF, Torres-Guerrero E, et al. Actinomycetoma: an update on diagnosis and treatment. Cutis. 2017;99:E11-E15.
- Weedon D. Weedon’s Skin Pathology. 3rd ed. Churchill Livingstone Elsevier; 2010.
A 26-year-old Guatemalan man who was a former carpenter presented with an indurated, nontender, nonpruritic, subcutaneous mass on the right central back with multiple draining sinus tracts on the surface and several depressed circular atrophic scars on the periphery of the mass. He noticed that the lesion began as a pustule 1.5 years prior and gradually enlarged. He denied any trauma, insect bites, fever, chills, headaches, weight loss, or travel history (he relocated to the United States 3.5 years ago) prior to the skin eruption. A biopsy was performed by an outside dermatologist 1 year prior to the current presentation, with a diagnosis of Pityrosporum folliculitis. Throughout his clinical course, treatment with oral antifungals, oral doxycycline, and topical clindamycin all failed. The mass was removed by plastic surgery 1 year prior.
A tissue biopsy for histology and culture was obtained at presentation to our institution. Laboratory findings showed that the basic metabolic panel was within reference range. Chest radiography indicated no active disease. A tuberculosis screening was negative. A bacterial culture of the lesion identified no growth after 48 hours. Our tissue biopsy revealed fibrosing granulation tissue, but the surgical pathology from a prior mass excision revealed sinus tracts with suppuration, evidence of scarring, foreign body giant cell reaction, and a characteristic finding (inset: H&E, original magnification ×200).
Atopic dermatitis can be especially burdensome in the elderly
During the Revolutionizing Atopic Dermatitis virtual symposium, Katrina Abuabara, MD, highlighted the epidemiology and burden of AD among older adults. She began by noting that the disease peaks in infancy and older adulthood. In an analysis that she and her colleagues made of physician-diagnosed AD among more than 8.6 million patients in the United Kingdom between 1994 and 2013, the mean prevalence in a given year was 12.3% among those aged 0-17 years, 5.1% among those age 18-74 years, and 8.7% among those age 75 and older.
“We saw what we expected in early infancy with very high rates of active disease,” said Dr. Abuabara, associate professor of dermatology and epidemiology at the University of California, San Francisco. “We also saw a second peak in older adulthood. This was more surprising to us because the disease hadn’t been as well studied in this population.” Researchers who analyzed data from the Global Burden of Disease Study, which evaluates disease-related morbidity and mortality worldwide, found a somewhat attenuated peak but a similar trend around the world. Its authors ranked AD as 15th among all nonfatal diseases.
In a separate analysis, Dr. Abuabara and colleagues evaluated records of more than 9.1 million primary care patients in the United Kingdom between 1994 and 2013, and who were followed for an average of 6 years. They examined AD activity and found that, based on doctor visits and prescriptions, AD appeared to be active in 48% of those aged 0-17 years, compared with 42% of those aged 18-74 years, and 60% of those aged 75 years and older. “Also, when we looked at the distribution of active disease in older adults, we saw that those who were older had more severe disease,” she said. When they evaluated the prevalence of AD by sociodemographic factors, AD increased with age among older adults (adjusted odd ratio, 1.06), while it decreased by 14% annually among children. In addition, female older adults had about three-fourths the odds of prevalent disease as their male counterparts (aOR, 0.73).
“We also looked at rural and urban differences and found that across ages it was more common in urban as compared to rural populations,” she said. “As for socioeconomic status, it tends to be more common among those of higher socioeconomic status in children and in the older adult group.”
In a study that drew from medical records of 3.85 million primary care patients in the United Kingdom, AD was more common in Asian and Black ethnic groups than in people of White ethnicity. In addition, higher socioeconomic status was associated with a greater incidence of eczema in infants aged younger than 2 years, but the reverse was seen for all other age groups.
To identify subtypes of atopic eczema based on patterns of disease activity through mid-adulthood, Dr. Abuabara and colleagues evaluated members of two population-based birth cohorts: the 1958 National Childhood Development Study and the 1970 British Cohort Study. The patients were classified into one of four patters of disease activity followed to age 50: rare/none, increasing, decreasing, and high. “We found that there was the early-onset decreasing subgroup, which tend to have a lower probability of AD over time,” Dr. Abuabara said. “We also found that there was a small subgroup that had a constant high probability of AD over time. But we were surprised to find a subgroup with increasing probability over time. This was a fairly sizable subgroup.”
In an earlier study, she and her colleagues examined whether there were differences based on whether people had adult-onset or childhood-onset disease in the same two cohorts of U.K. patients. Those with childhood-onset disease had stronger associations with known genetic risk factors and they tended to be of higher socioeconomic status. “They also tended to have more asthma and other allergic comorbidities,” Dr. Abuabara said. “On the other hand, the adult-onset group [after age 23] were more likely to be female, more likely to be smokers, and tended to have lower childhood socioeconomic status.”
According to the best available evidence, she continued, there is good data on higher relative risk of osteoporosis/fractures and dementia specifically among older adults with AD, and good data on associations with cardiometabolic disease and atopic disease among adults overall, as well as data showing that AD does not seem to be associated with cancer overall. In a study conducted by Jonathan I. Silverberg, MD, PhD, MPH, and Mohammed S. Shaheen, JD, the researchers used physician-diagnosed AD to investigate the associations of osteopenia and osteoporosis in two large U.S. databases: the 2006-2012 Nationwide Emergency Department Sample (NEDS) database and 2002-2012 National Inpatient Sample (NIS). Among patients aged 50 years and older, AD was associated with a higher odds of osteoporosis in NEDS (aOR, 1.31) and NIS (aOR, 1.25) and osteopenia in NEDS (aOR, 1.86).
In a separate matched cohort study, Dr. Abuabara and colleagues used U.K. primary care patient data to evaluate the association between AD and fracture and whether fracture risk varies with AD severity. Overall, they observed a 10% increase in fracture risk among people with AD, compared with those without, especially those of the hip, spine, pelvis, and wrist. “We found that there was a dose-response effect,” she said. “Those with more severe eczema had a much higher risk of fractures. When we looked at different age groups, we found a similar increased risk in the oldest adults as in younger adults.”
In a longitudinal cohort study of primary care medical records from more than 1.1 million individuals in the United Kingdom, AD was associated with an increased risk of vascular dementia (hazard ratio, 1.88), Alzheimer’s disease (HR, 1.69, and other/unspecified dementia (HR, 1.48; .269). “We found a nice dose response, where people with more severe AD had higher rates of dementia,” Dr. Abuabara said. Results from a more recent, smaller study of patients in Taiwan also found an increased risk between AD and the risk of dementia, but not a dose-response effect, likely because of a much smaller sample size.
Mounting research suggests that the risk for cardiovascular disease is also elevated in patients with AD. “There is some variability in the literature, but I think it’s important that when we’re talking about atopic dermatitis to think about the heterogeneity of the disease,” Dr. Abuabara said. In a meta-analysis and systematic review of 19 studies on the topic, she and her colleagues found that AD was associated with an increased risk of myocardial infarction (relative risk, 1.12), stroke (RR, 1.10), ischemic stroke (RR, 1.17), angina (RR, 1.18), and heart failure (RR, 1.26). “For all the different [cardiovascular disease] outcomes there was increasing risk with increasing disease severity,” she said.
She reported that UCSF receives research funding from Pfizer and Cosmetique Active International. She also receives consulting fees from Target RWE.
During the Revolutionizing Atopic Dermatitis virtual symposium, Katrina Abuabara, MD, highlighted the epidemiology and burden of AD among older adults. She began by noting that the disease peaks in infancy and older adulthood. In an analysis that she and her colleagues made of physician-diagnosed AD among more than 8.6 million patients in the United Kingdom between 1994 and 2013, the mean prevalence in a given year was 12.3% among those aged 0-17 years, 5.1% among those age 18-74 years, and 8.7% among those age 75 and older.
“We saw what we expected in early infancy with very high rates of active disease,” said Dr. Abuabara, associate professor of dermatology and epidemiology at the University of California, San Francisco. “We also saw a second peak in older adulthood. This was more surprising to us because the disease hadn’t been as well studied in this population.” Researchers who analyzed data from the Global Burden of Disease Study, which evaluates disease-related morbidity and mortality worldwide, found a somewhat attenuated peak but a similar trend around the world. Its authors ranked AD as 15th among all nonfatal diseases.
In a separate analysis, Dr. Abuabara and colleagues evaluated records of more than 9.1 million primary care patients in the United Kingdom between 1994 and 2013, and who were followed for an average of 6 years. They examined AD activity and found that, based on doctor visits and prescriptions, AD appeared to be active in 48% of those aged 0-17 years, compared with 42% of those aged 18-74 years, and 60% of those aged 75 years and older. “Also, when we looked at the distribution of active disease in older adults, we saw that those who were older had more severe disease,” she said. When they evaluated the prevalence of AD by sociodemographic factors, AD increased with age among older adults (adjusted odd ratio, 1.06), while it decreased by 14% annually among children. In addition, female older adults had about three-fourths the odds of prevalent disease as their male counterparts (aOR, 0.73).
“We also looked at rural and urban differences and found that across ages it was more common in urban as compared to rural populations,” she said. “As for socioeconomic status, it tends to be more common among those of higher socioeconomic status in children and in the older adult group.”
In a study that drew from medical records of 3.85 million primary care patients in the United Kingdom, AD was more common in Asian and Black ethnic groups than in people of White ethnicity. In addition, higher socioeconomic status was associated with a greater incidence of eczema in infants aged younger than 2 years, but the reverse was seen for all other age groups.
To identify subtypes of atopic eczema based on patterns of disease activity through mid-adulthood, Dr. Abuabara and colleagues evaluated members of two population-based birth cohorts: the 1958 National Childhood Development Study and the 1970 British Cohort Study. The patients were classified into one of four patters of disease activity followed to age 50: rare/none, increasing, decreasing, and high. “We found that there was the early-onset decreasing subgroup, which tend to have a lower probability of AD over time,” Dr. Abuabara said. “We also found that there was a small subgroup that had a constant high probability of AD over time. But we were surprised to find a subgroup with increasing probability over time. This was a fairly sizable subgroup.”
In an earlier study, she and her colleagues examined whether there were differences based on whether people had adult-onset or childhood-onset disease in the same two cohorts of U.K. patients. Those with childhood-onset disease had stronger associations with known genetic risk factors and they tended to be of higher socioeconomic status. “They also tended to have more asthma and other allergic comorbidities,” Dr. Abuabara said. “On the other hand, the adult-onset group [after age 23] were more likely to be female, more likely to be smokers, and tended to have lower childhood socioeconomic status.”
According to the best available evidence, she continued, there is good data on higher relative risk of osteoporosis/fractures and dementia specifically among older adults with AD, and good data on associations with cardiometabolic disease and atopic disease among adults overall, as well as data showing that AD does not seem to be associated with cancer overall. In a study conducted by Jonathan I. Silverberg, MD, PhD, MPH, and Mohammed S. Shaheen, JD, the researchers used physician-diagnosed AD to investigate the associations of osteopenia and osteoporosis in two large U.S. databases: the 2006-2012 Nationwide Emergency Department Sample (NEDS) database and 2002-2012 National Inpatient Sample (NIS). Among patients aged 50 years and older, AD was associated with a higher odds of osteoporosis in NEDS (aOR, 1.31) and NIS (aOR, 1.25) and osteopenia in NEDS (aOR, 1.86).
In a separate matched cohort study, Dr. Abuabara and colleagues used U.K. primary care patient data to evaluate the association between AD and fracture and whether fracture risk varies with AD severity. Overall, they observed a 10% increase in fracture risk among people with AD, compared with those without, especially those of the hip, spine, pelvis, and wrist. “We found that there was a dose-response effect,” she said. “Those with more severe eczema had a much higher risk of fractures. When we looked at different age groups, we found a similar increased risk in the oldest adults as in younger adults.”
In a longitudinal cohort study of primary care medical records from more than 1.1 million individuals in the United Kingdom, AD was associated with an increased risk of vascular dementia (hazard ratio, 1.88), Alzheimer’s disease (HR, 1.69, and other/unspecified dementia (HR, 1.48; .269). “We found a nice dose response, where people with more severe AD had higher rates of dementia,” Dr. Abuabara said. Results from a more recent, smaller study of patients in Taiwan also found an increased risk between AD and the risk of dementia, but not a dose-response effect, likely because of a much smaller sample size.
Mounting research suggests that the risk for cardiovascular disease is also elevated in patients with AD. “There is some variability in the literature, but I think it’s important that when we’re talking about atopic dermatitis to think about the heterogeneity of the disease,” Dr. Abuabara said. In a meta-analysis and systematic review of 19 studies on the topic, she and her colleagues found that AD was associated with an increased risk of myocardial infarction (relative risk, 1.12), stroke (RR, 1.10), ischemic stroke (RR, 1.17), angina (RR, 1.18), and heart failure (RR, 1.26). “For all the different [cardiovascular disease] outcomes there was increasing risk with increasing disease severity,” she said.
She reported that UCSF receives research funding from Pfizer and Cosmetique Active International. She also receives consulting fees from Target RWE.
During the Revolutionizing Atopic Dermatitis virtual symposium, Katrina Abuabara, MD, highlighted the epidemiology and burden of AD among older adults. She began by noting that the disease peaks in infancy and older adulthood. In an analysis that she and her colleagues made of physician-diagnosed AD among more than 8.6 million patients in the United Kingdom between 1994 and 2013, the mean prevalence in a given year was 12.3% among those aged 0-17 years, 5.1% among those age 18-74 years, and 8.7% among those age 75 and older.
“We saw what we expected in early infancy with very high rates of active disease,” said Dr. Abuabara, associate professor of dermatology and epidemiology at the University of California, San Francisco. “We also saw a second peak in older adulthood. This was more surprising to us because the disease hadn’t been as well studied in this population.” Researchers who analyzed data from the Global Burden of Disease Study, which evaluates disease-related morbidity and mortality worldwide, found a somewhat attenuated peak but a similar trend around the world. Its authors ranked AD as 15th among all nonfatal diseases.
In a separate analysis, Dr. Abuabara and colleagues evaluated records of more than 9.1 million primary care patients in the United Kingdom between 1994 and 2013, and who were followed for an average of 6 years. They examined AD activity and found that, based on doctor visits and prescriptions, AD appeared to be active in 48% of those aged 0-17 years, compared with 42% of those aged 18-74 years, and 60% of those aged 75 years and older. “Also, when we looked at the distribution of active disease in older adults, we saw that those who were older had more severe disease,” she said. When they evaluated the prevalence of AD by sociodemographic factors, AD increased with age among older adults (adjusted odd ratio, 1.06), while it decreased by 14% annually among children. In addition, female older adults had about three-fourths the odds of prevalent disease as their male counterparts (aOR, 0.73).
“We also looked at rural and urban differences and found that across ages it was more common in urban as compared to rural populations,” she said. “As for socioeconomic status, it tends to be more common among those of higher socioeconomic status in children and in the older adult group.”
In a study that drew from medical records of 3.85 million primary care patients in the United Kingdom, AD was more common in Asian and Black ethnic groups than in people of White ethnicity. In addition, higher socioeconomic status was associated with a greater incidence of eczema in infants aged younger than 2 years, but the reverse was seen for all other age groups.
To identify subtypes of atopic eczema based on patterns of disease activity through mid-adulthood, Dr. Abuabara and colleagues evaluated members of two population-based birth cohorts: the 1958 National Childhood Development Study and the 1970 British Cohort Study. The patients were classified into one of four patters of disease activity followed to age 50: rare/none, increasing, decreasing, and high. “We found that there was the early-onset decreasing subgroup, which tend to have a lower probability of AD over time,” Dr. Abuabara said. “We also found that there was a small subgroup that had a constant high probability of AD over time. But we were surprised to find a subgroup with increasing probability over time. This was a fairly sizable subgroup.”
In an earlier study, she and her colleagues examined whether there were differences based on whether people had adult-onset or childhood-onset disease in the same two cohorts of U.K. patients. Those with childhood-onset disease had stronger associations with known genetic risk factors and they tended to be of higher socioeconomic status. “They also tended to have more asthma and other allergic comorbidities,” Dr. Abuabara said. “On the other hand, the adult-onset group [after age 23] were more likely to be female, more likely to be smokers, and tended to have lower childhood socioeconomic status.”
According to the best available evidence, she continued, there is good data on higher relative risk of osteoporosis/fractures and dementia specifically among older adults with AD, and good data on associations with cardiometabolic disease and atopic disease among adults overall, as well as data showing that AD does not seem to be associated with cancer overall. In a study conducted by Jonathan I. Silverberg, MD, PhD, MPH, and Mohammed S. Shaheen, JD, the researchers used physician-diagnosed AD to investigate the associations of osteopenia and osteoporosis in two large U.S. databases: the 2006-2012 Nationwide Emergency Department Sample (NEDS) database and 2002-2012 National Inpatient Sample (NIS). Among patients aged 50 years and older, AD was associated with a higher odds of osteoporosis in NEDS (aOR, 1.31) and NIS (aOR, 1.25) and osteopenia in NEDS (aOR, 1.86).
In a separate matched cohort study, Dr. Abuabara and colleagues used U.K. primary care patient data to evaluate the association between AD and fracture and whether fracture risk varies with AD severity. Overall, they observed a 10% increase in fracture risk among people with AD, compared with those without, especially those of the hip, spine, pelvis, and wrist. “We found that there was a dose-response effect,” she said. “Those with more severe eczema had a much higher risk of fractures. When we looked at different age groups, we found a similar increased risk in the oldest adults as in younger adults.”
In a longitudinal cohort study of primary care medical records from more than 1.1 million individuals in the United Kingdom, AD was associated with an increased risk of vascular dementia (hazard ratio, 1.88), Alzheimer’s disease (HR, 1.69, and other/unspecified dementia (HR, 1.48; .269). “We found a nice dose response, where people with more severe AD had higher rates of dementia,” Dr. Abuabara said. Results from a more recent, smaller study of patients in Taiwan also found an increased risk between AD and the risk of dementia, but not a dose-response effect, likely because of a much smaller sample size.
Mounting research suggests that the risk for cardiovascular disease is also elevated in patients with AD. “There is some variability in the literature, but I think it’s important that when we’re talking about atopic dermatitis to think about the heterogeneity of the disease,” Dr. Abuabara said. In a meta-analysis and systematic review of 19 studies on the topic, she and her colleagues found that AD was associated with an increased risk of myocardial infarction (relative risk, 1.12), stroke (RR, 1.10), ischemic stroke (RR, 1.17), angina (RR, 1.18), and heart failure (RR, 1.26). “For all the different [cardiovascular disease] outcomes there was increasing risk with increasing disease severity,” she said.
She reported that UCSF receives research funding from Pfizer and Cosmetique Active International. She also receives consulting fees from Target RWE.
FROM REVOLUTIONIZING AD 2021
FDA backs Pfizer booster for 12- to 15-year-olds
Besides updating the authorization for the Pfizer COVID-19 vaccine, the agency also shortened the recommended time between a second dose and the booster to 5 months or more, based on new evidence. In addition, a third primary series dose is now authorized for certain immunocompromised children 5 years to 11 years old. Full details are available in an FDA news release.
The amended emergency use authorization (EUA) only applies to the Pfizer vaccine, said acting FDA Commissioner Janet Woodcock, MD.
“Just to make sure every everyone is clear on this, right now: If you got [Johnson & Johnson’s one-dose vaccine], you get a booster after 2 months. If you got Moderna, you can get a booster at 6 months or beyond,” she said during a media briefing.
What is new, she said, is “if you got Pfizer as your primary series, you can get a booster at 5 months or beyond.”
A lower risk of myocarditis?
Asked about concerns about the risk of myocarditis with vaccination in the 12- to 15-year age group, Dr. Woodcock said they expect it would be “extremely rare with the third dose.”
“We have the real-world evidence from the Israeli experience to help us with that analysis,” she said.
The data so far consistently points to a higher risk of myocarditis after a second mRNA vaccine dose among males, from teenagers to 30-year-olds, with a peak at about 16 to 17 years of age, Peter Marks, MD, PhD, director of the FDA’s Center for Biologics Evaluation and Research, said during the media call.
The risk of myocarditis is about 2 to 3 times higher after a second vaccine dose, compared to a booster shot, Dr. Marks said, based on available data. It may be related to the closer dose timing of the second dose versus a third, he added.
“The inference here is that on the risk of myocarditis with third doses in the 12- to 15-year age range is likely to be quite acceptable,” he said.
Dr. Marks also pointed out that most cases of myocarditis clear up quickly.
“We’re not seeing long-lasting effects. That’s not to say that we don’t care about this and that it’s not important,” he said.
“But what it is saying is that in the setting of a tremendous number of Omicron and Delta cases in this country, the potential benefits of getting vaccinated in this age group outweigh that risk,” Dr. Marks said. “We can look at that risk-benefit and still feel comfortable.”
He said that “the really overwhelming majority of these cases, 98%, have been mild” -- shown by a 1-day median hospital stay.
Even so, the FDA plans to continue monitoring for the risk of myocarditis “very closely,” he said.
Interestingly, swollen underarm lymph nodes were seen more frequently after the booster dose than after the second dose of a two-dose primary series, the FDA said.
Reducing the time between primary vaccination with the Pfizer vaccine -- two initial doses -- and the booster shot from 6 months to 5 months is based on decreasing efficacy data that the drugmaker submitted to the FDA.
The 5-month interval was evaluated in a study from Israel published Dec. 21 in the New England Journal of Medicine .
Mixing and matching vaccines
Less clear at the moment is guidance about boosters for people who opted to mix and match their primary vaccine series.
“There was a mix-and-match study that was done which showed that in some cases, the mixing and matching … of an adenoviral record vaccine and an mRNA vaccine seem to give a very good immune response,” Dr. Marks said.
Once more data comes in on mixing and matching, “we’ll analyze them and then potentially make recommendations,” he said.
‘It’s not too late’
No federal government media briefing on COVID-19 would be complete without a plea for the unvaccinated to get immunized.
“We’re talking a lot about boosters right now, but it’s not too late for those who have not gotten a vaccine to get a vaccine,” Dr. Marks said, referring to the tens of millions of Americans who remain unvaccinated at the beginning of 2022.
“We know from our previous studies that even a single dose of the vaccine -- and probably two doses -- can help prevent the worst outcomes from COVID-19, including hospitalization and death.”
A version of this article first appeared on WebMD.com.
Besides updating the authorization for the Pfizer COVID-19 vaccine, the agency also shortened the recommended time between a second dose and the booster to 5 months or more, based on new evidence. In addition, a third primary series dose is now authorized for certain immunocompromised children 5 years to 11 years old. Full details are available in an FDA news release.
The amended emergency use authorization (EUA) only applies to the Pfizer vaccine, said acting FDA Commissioner Janet Woodcock, MD.
“Just to make sure every everyone is clear on this, right now: If you got [Johnson & Johnson’s one-dose vaccine], you get a booster after 2 months. If you got Moderna, you can get a booster at 6 months or beyond,” she said during a media briefing.
What is new, she said, is “if you got Pfizer as your primary series, you can get a booster at 5 months or beyond.”
A lower risk of myocarditis?
Asked about concerns about the risk of myocarditis with vaccination in the 12- to 15-year age group, Dr. Woodcock said they expect it would be “extremely rare with the third dose.”
“We have the real-world evidence from the Israeli experience to help us with that analysis,” she said.
The data so far consistently points to a higher risk of myocarditis after a second mRNA vaccine dose among males, from teenagers to 30-year-olds, with a peak at about 16 to 17 years of age, Peter Marks, MD, PhD, director of the FDA’s Center for Biologics Evaluation and Research, said during the media call.
The risk of myocarditis is about 2 to 3 times higher after a second vaccine dose, compared to a booster shot, Dr. Marks said, based on available data. It may be related to the closer dose timing of the second dose versus a third, he added.
“The inference here is that on the risk of myocarditis with third doses in the 12- to 15-year age range is likely to be quite acceptable,” he said.
Dr. Marks also pointed out that most cases of myocarditis clear up quickly.
“We’re not seeing long-lasting effects. That’s not to say that we don’t care about this and that it’s not important,” he said.
“But what it is saying is that in the setting of a tremendous number of Omicron and Delta cases in this country, the potential benefits of getting vaccinated in this age group outweigh that risk,” Dr. Marks said. “We can look at that risk-benefit and still feel comfortable.”
He said that “the really overwhelming majority of these cases, 98%, have been mild” -- shown by a 1-day median hospital stay.
Even so, the FDA plans to continue monitoring for the risk of myocarditis “very closely,” he said.
Interestingly, swollen underarm lymph nodes were seen more frequently after the booster dose than after the second dose of a two-dose primary series, the FDA said.
Reducing the time between primary vaccination with the Pfizer vaccine -- two initial doses -- and the booster shot from 6 months to 5 months is based on decreasing efficacy data that the drugmaker submitted to the FDA.
The 5-month interval was evaluated in a study from Israel published Dec. 21 in the New England Journal of Medicine .
Mixing and matching vaccines
Less clear at the moment is guidance about boosters for people who opted to mix and match their primary vaccine series.
“There was a mix-and-match study that was done which showed that in some cases, the mixing and matching … of an adenoviral record vaccine and an mRNA vaccine seem to give a very good immune response,” Dr. Marks said.
Once more data comes in on mixing and matching, “we’ll analyze them and then potentially make recommendations,” he said.
‘It’s not too late’
No federal government media briefing on COVID-19 would be complete without a plea for the unvaccinated to get immunized.
“We’re talking a lot about boosters right now, but it’s not too late for those who have not gotten a vaccine to get a vaccine,” Dr. Marks said, referring to the tens of millions of Americans who remain unvaccinated at the beginning of 2022.
“We know from our previous studies that even a single dose of the vaccine -- and probably two doses -- can help prevent the worst outcomes from COVID-19, including hospitalization and death.”
A version of this article first appeared on WebMD.com.
Besides updating the authorization for the Pfizer COVID-19 vaccine, the agency also shortened the recommended time between a second dose and the booster to 5 months or more, based on new evidence. In addition, a third primary series dose is now authorized for certain immunocompromised children 5 years to 11 years old. Full details are available in an FDA news release.
The amended emergency use authorization (EUA) only applies to the Pfizer vaccine, said acting FDA Commissioner Janet Woodcock, MD.
“Just to make sure every everyone is clear on this, right now: If you got [Johnson & Johnson’s one-dose vaccine], you get a booster after 2 months. If you got Moderna, you can get a booster at 6 months or beyond,” she said during a media briefing.
What is new, she said, is “if you got Pfizer as your primary series, you can get a booster at 5 months or beyond.”
A lower risk of myocarditis?
Asked about concerns about the risk of myocarditis with vaccination in the 12- to 15-year age group, Dr. Woodcock said they expect it would be “extremely rare with the third dose.”
“We have the real-world evidence from the Israeli experience to help us with that analysis,” she said.
The data so far consistently points to a higher risk of myocarditis after a second mRNA vaccine dose among males, from teenagers to 30-year-olds, with a peak at about 16 to 17 years of age, Peter Marks, MD, PhD, director of the FDA’s Center for Biologics Evaluation and Research, said during the media call.
The risk of myocarditis is about 2 to 3 times higher after a second vaccine dose, compared to a booster shot, Dr. Marks said, based on available data. It may be related to the closer dose timing of the second dose versus a third, he added.
“The inference here is that on the risk of myocarditis with third doses in the 12- to 15-year age range is likely to be quite acceptable,” he said.
Dr. Marks also pointed out that most cases of myocarditis clear up quickly.
“We’re not seeing long-lasting effects. That’s not to say that we don’t care about this and that it’s not important,” he said.
“But what it is saying is that in the setting of a tremendous number of Omicron and Delta cases in this country, the potential benefits of getting vaccinated in this age group outweigh that risk,” Dr. Marks said. “We can look at that risk-benefit and still feel comfortable.”
He said that “the really overwhelming majority of these cases, 98%, have been mild” -- shown by a 1-day median hospital stay.
Even so, the FDA plans to continue monitoring for the risk of myocarditis “very closely,” he said.
Interestingly, swollen underarm lymph nodes were seen more frequently after the booster dose than after the second dose of a two-dose primary series, the FDA said.
Reducing the time between primary vaccination with the Pfizer vaccine -- two initial doses -- and the booster shot from 6 months to 5 months is based on decreasing efficacy data that the drugmaker submitted to the FDA.
The 5-month interval was evaluated in a study from Israel published Dec. 21 in the New England Journal of Medicine .
Mixing and matching vaccines
Less clear at the moment is guidance about boosters for people who opted to mix and match their primary vaccine series.
“There was a mix-and-match study that was done which showed that in some cases, the mixing and matching … of an adenoviral record vaccine and an mRNA vaccine seem to give a very good immune response,” Dr. Marks said.
Once more data comes in on mixing and matching, “we’ll analyze them and then potentially make recommendations,” he said.
‘It’s not too late’
No federal government media briefing on COVID-19 would be complete without a plea for the unvaccinated to get immunized.
“We’re talking a lot about boosters right now, but it’s not too late for those who have not gotten a vaccine to get a vaccine,” Dr. Marks said, referring to the tens of millions of Americans who remain unvaccinated at the beginning of 2022.
“We know from our previous studies that even a single dose of the vaccine -- and probably two doses -- can help prevent the worst outcomes from COVID-19, including hospitalization and death.”
A version of this article first appeared on WebMD.com.
Travel/school disruptions as COVID-19 cases grow in 2022
As the United States enters a third year of the COVID-19 pandemic,
The United States is reporting a 7-day average of more than 386,000 cases after several record-breaking days, according to the data tracker by the New York Times. The United States surpassed 585,000 cases on Dec. 30, setting a new record before the New Year’s holiday.
New York, Washington, D.C., and other states along the East Coast are leading the national surge. New York reported more than 85,000 new cases on the last day of 2021, marking the highest 1-day total in the state since the pandemic began.
“As we fight the winter surge, we need to keep the most vulnerable among us in mind – do what you can to keep others in your community safe from COVID-19,” New York Gov. Kathy Hochul said in a statement on Jan. 1, 2022.
“Wear a mask, wash your hands, and take advantage of the best tool we have at our disposal – the vaccine,” she said.
The 2021 winter surge in the United States peaked around Jan. 12, which may suggest that the country has a week or so before the current wave reaches its height and begins to drop, the newspaper reported.
In the meantime, people are dealing with disruptions as they return from holiday travel and begin the new year. Airlines canceled more than 2,700 flights on Jan. 1 and more than 1,900 flights on Jan. 2, bringing the total since Christmas Eve to more than 14,000 canceled flights.
About half of cancellations were connected to wintry weather at key airline hubs in Chicago and Denver, the newspaper reported, as well as ongoing flight crew shortages caused by the Omicron variant.
More disruptions could continue, the Federal Aviation Administration warned, as an increasing number of its air-traffic control employees test positive for COVID-19.
“To maintain safety, traffic volumes at some facilities could be reduced, which might result in delays during busy periods,” an FAA spokesman told The Wall Street Journal.
The current COVID-19 surge will also affect businesses and schools as the new year begins. A growing number of universities are opting to start the next semester with remote instruction.
American University, Duke University, and Michigan State University announced in recent days that they would delay in-person classes to slow the spread of the coronavirus on campus. They will begin classes online on Jan. 10 and return to campus the following week or later.
“I realize that students prefer to be in person, and so do I. But it is important that we do so in a safe manner,” Samuel Stanley Jr., MD, president of Michigan State University, said in a statement on New Year’s Eve.
K-12 school districts are deciding how to adapt as well. Some districts are bringing back mask requirements, and some are ramping up testing. Others are moving to remote learning – and signaling the need for flexibility as the Omicron variant brings new surprises.
“Change has been the only constant in this fight,” Roger Leon, the superintendent for Newark (N.J.) Public Schools, wrote in a note to parents. He announced on Dec. 30, 2021, that students would learn remotely for at least the first 2 weeks of the new year.
This continues “to be a brutal, relentless, and ruthless virus that rears its ugly head at inopportune times,” he said.
A version of this article first appeared on WebMD.com.
As the United States enters a third year of the COVID-19 pandemic,
The United States is reporting a 7-day average of more than 386,000 cases after several record-breaking days, according to the data tracker by the New York Times. The United States surpassed 585,000 cases on Dec. 30, setting a new record before the New Year’s holiday.
New York, Washington, D.C., and other states along the East Coast are leading the national surge. New York reported more than 85,000 new cases on the last day of 2021, marking the highest 1-day total in the state since the pandemic began.
“As we fight the winter surge, we need to keep the most vulnerable among us in mind – do what you can to keep others in your community safe from COVID-19,” New York Gov. Kathy Hochul said in a statement on Jan. 1, 2022.
“Wear a mask, wash your hands, and take advantage of the best tool we have at our disposal – the vaccine,” she said.
The 2021 winter surge in the United States peaked around Jan. 12, which may suggest that the country has a week or so before the current wave reaches its height and begins to drop, the newspaper reported.
In the meantime, people are dealing with disruptions as they return from holiday travel and begin the new year. Airlines canceled more than 2,700 flights on Jan. 1 and more than 1,900 flights on Jan. 2, bringing the total since Christmas Eve to more than 14,000 canceled flights.
About half of cancellations were connected to wintry weather at key airline hubs in Chicago and Denver, the newspaper reported, as well as ongoing flight crew shortages caused by the Omicron variant.
More disruptions could continue, the Federal Aviation Administration warned, as an increasing number of its air-traffic control employees test positive for COVID-19.
“To maintain safety, traffic volumes at some facilities could be reduced, which might result in delays during busy periods,” an FAA spokesman told The Wall Street Journal.
The current COVID-19 surge will also affect businesses and schools as the new year begins. A growing number of universities are opting to start the next semester with remote instruction.
American University, Duke University, and Michigan State University announced in recent days that they would delay in-person classes to slow the spread of the coronavirus on campus. They will begin classes online on Jan. 10 and return to campus the following week or later.
“I realize that students prefer to be in person, and so do I. But it is important that we do so in a safe manner,” Samuel Stanley Jr., MD, president of Michigan State University, said in a statement on New Year’s Eve.
K-12 school districts are deciding how to adapt as well. Some districts are bringing back mask requirements, and some are ramping up testing. Others are moving to remote learning – and signaling the need for flexibility as the Omicron variant brings new surprises.
“Change has been the only constant in this fight,” Roger Leon, the superintendent for Newark (N.J.) Public Schools, wrote in a note to parents. He announced on Dec. 30, 2021, that students would learn remotely for at least the first 2 weeks of the new year.
This continues “to be a brutal, relentless, and ruthless virus that rears its ugly head at inopportune times,” he said.
A version of this article first appeared on WebMD.com.
As the United States enters a third year of the COVID-19 pandemic,
The United States is reporting a 7-day average of more than 386,000 cases after several record-breaking days, according to the data tracker by the New York Times. The United States surpassed 585,000 cases on Dec. 30, setting a new record before the New Year’s holiday.
New York, Washington, D.C., and other states along the East Coast are leading the national surge. New York reported more than 85,000 new cases on the last day of 2021, marking the highest 1-day total in the state since the pandemic began.
“As we fight the winter surge, we need to keep the most vulnerable among us in mind – do what you can to keep others in your community safe from COVID-19,” New York Gov. Kathy Hochul said in a statement on Jan. 1, 2022.
“Wear a mask, wash your hands, and take advantage of the best tool we have at our disposal – the vaccine,” she said.
The 2021 winter surge in the United States peaked around Jan. 12, which may suggest that the country has a week or so before the current wave reaches its height and begins to drop, the newspaper reported.
In the meantime, people are dealing with disruptions as they return from holiday travel and begin the new year. Airlines canceled more than 2,700 flights on Jan. 1 and more than 1,900 flights on Jan. 2, bringing the total since Christmas Eve to more than 14,000 canceled flights.
About half of cancellations were connected to wintry weather at key airline hubs in Chicago and Denver, the newspaper reported, as well as ongoing flight crew shortages caused by the Omicron variant.
More disruptions could continue, the Federal Aviation Administration warned, as an increasing number of its air-traffic control employees test positive for COVID-19.
“To maintain safety, traffic volumes at some facilities could be reduced, which might result in delays during busy periods,” an FAA spokesman told The Wall Street Journal.
The current COVID-19 surge will also affect businesses and schools as the new year begins. A growing number of universities are opting to start the next semester with remote instruction.
American University, Duke University, and Michigan State University announced in recent days that they would delay in-person classes to slow the spread of the coronavirus on campus. They will begin classes online on Jan. 10 and return to campus the following week or later.
“I realize that students prefer to be in person, and so do I. But it is important that we do so in a safe manner,” Samuel Stanley Jr., MD, president of Michigan State University, said in a statement on New Year’s Eve.
K-12 school districts are deciding how to adapt as well. Some districts are bringing back mask requirements, and some are ramping up testing. Others are moving to remote learning – and signaling the need for flexibility as the Omicron variant brings new surprises.
“Change has been the only constant in this fight,” Roger Leon, the superintendent for Newark (N.J.) Public Schools, wrote in a note to parents. He announced on Dec. 30, 2021, that students would learn remotely for at least the first 2 weeks of the new year.
This continues “to be a brutal, relentless, and ruthless virus that rears its ugly head at inopportune times,” he said.
A version of this article first appeared on WebMD.com.
Medicaid implements waivers for some clinical trial coverage
Federal officials will allow some flexibility in meeting new requirements on covering the costs of clinical trials for people enrolled in Medicaid, seeking to accommodate states where legislatures will not meet in time to make needed changes in rules.
Congress in 2020 ordered U.S. states to have their Medicaid programs cover expenses related to participation in certain clinical trials, a move that was hailed by the American Society of Clinical Oncology (ASCO) and other groups as a boost to trials as well as to patients with serious illness who have lower incomes.
The mandate went into effect on Jan. 1, but the Centers for Medicare & Medicaid Services will allow accommodations in terms of implementation time for states that have not yet been able to make needed legislative changes, Daniel Tsai, deputy administrator and director of the Center for Medicaid and CHIP Services, wrote in a Dec. 7 letter. Mr. Tsai’s letter doesn’t mention specific states. The CMS did not immediately respond to a request seeking information on the states expected to apply for waivers.
Medicaid has in recent years been a rare large U.S. insurance program that does not cover the costs of clinical trials. The Affordable Care Act of 2010 mandated this coverage for people in private insurance plans. The federal government in 2000 decided that Medicare would do so.
‘A hidden opportunity’
A perspective article last May in the New England Journal of Medicine referred to the new Medicaid mandate on clinical trials as a “hidden opportunity,” referring to its genesis as an add-on in a massive federal spending package enacted in December 2020.
In the article, Samuel U. Takvorian, MD, MSHP, of the University of Pennsylvania, Philadelphia, and coauthors noted that rates of participation in clinical trials remain low for racial and ethnic minority groups, due in part to the lack of Medicaid coverage.
“For example, non-Hispanic White patients are nearly twice as likely as Black patients and three times as likely as Hispanic patients to enroll in cancer clinical trials – a gap that has widened over time,” Dr. Takvorian and coauthors wrote. “Inequities in enrollment have also manifested during the COVID-19 pandemic, which has disproportionately affected non-White patients, without their commensurate representation in trials of COVID-19 therapeutics.”
In October, researchers from the Arthur G. James Cancer Hospital and Ohio State University, Columbus, published results of a retrospective study of patients with stage I-IV pancreatic cancer that also found inequities in enrollment. Mariam F. Eskander, MD, MPH, and coauthors reported what they found by examining records for 1,127 patients (0.4%) enrolled in clinical trials and 301,340 (99.6%) who did not enroll. They found that enrollment in trials increased over the study period, but not for Black patients or patients on Medicaid.
In an interview, Dr. Eskander said the new Medicaid policy will remove a major obstacle to participation in clinical trials. An oncologist, Dr. Eskander said she is looking forward to being able to help more of her patients get access to experimental medicines and treatments.
But that may not be enough to draw more people with low incomes into these studies, said Dr. Eskander, who is now at Rutgers Cancer Institute of New Jersey in New Brunswick. She urges greater use of patient navigators to help people on Medicaid understand the resources available to them, as well as broad use of Medicaid’s nonemergency medical transportation (NEMT) benefit.
“Some patients will be offered clinical trial enrollment and some will accept, but I really worry about the challenges low-income people face with things like transportation and getting time off work,” she said.
A version of this article first appeared on Medscape.com.
Federal officials will allow some flexibility in meeting new requirements on covering the costs of clinical trials for people enrolled in Medicaid, seeking to accommodate states where legislatures will not meet in time to make needed changes in rules.
Congress in 2020 ordered U.S. states to have their Medicaid programs cover expenses related to participation in certain clinical trials, a move that was hailed by the American Society of Clinical Oncology (ASCO) and other groups as a boost to trials as well as to patients with serious illness who have lower incomes.
The mandate went into effect on Jan. 1, but the Centers for Medicare & Medicaid Services will allow accommodations in terms of implementation time for states that have not yet been able to make needed legislative changes, Daniel Tsai, deputy administrator and director of the Center for Medicaid and CHIP Services, wrote in a Dec. 7 letter. Mr. Tsai’s letter doesn’t mention specific states. The CMS did not immediately respond to a request seeking information on the states expected to apply for waivers.
Medicaid has in recent years been a rare large U.S. insurance program that does not cover the costs of clinical trials. The Affordable Care Act of 2010 mandated this coverage for people in private insurance plans. The federal government in 2000 decided that Medicare would do so.
‘A hidden opportunity’
A perspective article last May in the New England Journal of Medicine referred to the new Medicaid mandate on clinical trials as a “hidden opportunity,” referring to its genesis as an add-on in a massive federal spending package enacted in December 2020.
In the article, Samuel U. Takvorian, MD, MSHP, of the University of Pennsylvania, Philadelphia, and coauthors noted that rates of participation in clinical trials remain low for racial and ethnic minority groups, due in part to the lack of Medicaid coverage.
“For example, non-Hispanic White patients are nearly twice as likely as Black patients and three times as likely as Hispanic patients to enroll in cancer clinical trials – a gap that has widened over time,” Dr. Takvorian and coauthors wrote. “Inequities in enrollment have also manifested during the COVID-19 pandemic, which has disproportionately affected non-White patients, without their commensurate representation in trials of COVID-19 therapeutics.”
In October, researchers from the Arthur G. James Cancer Hospital and Ohio State University, Columbus, published results of a retrospective study of patients with stage I-IV pancreatic cancer that also found inequities in enrollment. Mariam F. Eskander, MD, MPH, and coauthors reported what they found by examining records for 1,127 patients (0.4%) enrolled in clinical trials and 301,340 (99.6%) who did not enroll. They found that enrollment in trials increased over the study period, but not for Black patients or patients on Medicaid.
In an interview, Dr. Eskander said the new Medicaid policy will remove a major obstacle to participation in clinical trials. An oncologist, Dr. Eskander said she is looking forward to being able to help more of her patients get access to experimental medicines and treatments.
But that may not be enough to draw more people with low incomes into these studies, said Dr. Eskander, who is now at Rutgers Cancer Institute of New Jersey in New Brunswick. She urges greater use of patient navigators to help people on Medicaid understand the resources available to them, as well as broad use of Medicaid’s nonemergency medical transportation (NEMT) benefit.
“Some patients will be offered clinical trial enrollment and some will accept, but I really worry about the challenges low-income people face with things like transportation and getting time off work,” she said.
A version of this article first appeared on Medscape.com.
Federal officials will allow some flexibility in meeting new requirements on covering the costs of clinical trials for people enrolled in Medicaid, seeking to accommodate states where legislatures will not meet in time to make needed changes in rules.
Congress in 2020 ordered U.S. states to have their Medicaid programs cover expenses related to participation in certain clinical trials, a move that was hailed by the American Society of Clinical Oncology (ASCO) and other groups as a boost to trials as well as to patients with serious illness who have lower incomes.
The mandate went into effect on Jan. 1, but the Centers for Medicare & Medicaid Services will allow accommodations in terms of implementation time for states that have not yet been able to make needed legislative changes, Daniel Tsai, deputy administrator and director of the Center for Medicaid and CHIP Services, wrote in a Dec. 7 letter. Mr. Tsai’s letter doesn’t mention specific states. The CMS did not immediately respond to a request seeking information on the states expected to apply for waivers.
Medicaid has in recent years been a rare large U.S. insurance program that does not cover the costs of clinical trials. The Affordable Care Act of 2010 mandated this coverage for people in private insurance plans. The federal government in 2000 decided that Medicare would do so.
‘A hidden opportunity’
A perspective article last May in the New England Journal of Medicine referred to the new Medicaid mandate on clinical trials as a “hidden opportunity,” referring to its genesis as an add-on in a massive federal spending package enacted in December 2020.
In the article, Samuel U. Takvorian, MD, MSHP, of the University of Pennsylvania, Philadelphia, and coauthors noted that rates of participation in clinical trials remain low for racial and ethnic minority groups, due in part to the lack of Medicaid coverage.
“For example, non-Hispanic White patients are nearly twice as likely as Black patients and three times as likely as Hispanic patients to enroll in cancer clinical trials – a gap that has widened over time,” Dr. Takvorian and coauthors wrote. “Inequities in enrollment have also manifested during the COVID-19 pandemic, which has disproportionately affected non-White patients, without their commensurate representation in trials of COVID-19 therapeutics.”
In October, researchers from the Arthur G. James Cancer Hospital and Ohio State University, Columbus, published results of a retrospective study of patients with stage I-IV pancreatic cancer that also found inequities in enrollment. Mariam F. Eskander, MD, MPH, and coauthors reported what they found by examining records for 1,127 patients (0.4%) enrolled in clinical trials and 301,340 (99.6%) who did not enroll. They found that enrollment in trials increased over the study period, but not for Black patients or patients on Medicaid.
In an interview, Dr. Eskander said the new Medicaid policy will remove a major obstacle to participation in clinical trials. An oncologist, Dr. Eskander said she is looking forward to being able to help more of her patients get access to experimental medicines and treatments.
But that may not be enough to draw more people with low incomes into these studies, said Dr. Eskander, who is now at Rutgers Cancer Institute of New Jersey in New Brunswick. She urges greater use of patient navigators to help people on Medicaid understand the resources available to them, as well as broad use of Medicaid’s nonemergency medical transportation (NEMT) benefit.
“Some patients will be offered clinical trial enrollment and some will accept, but I really worry about the challenges low-income people face with things like transportation and getting time off work,” she said.
A version of this article first appeared on Medscape.com.
Were these true medical miracles? Doctors disagree
It was a freezing December day, and two young brothers were playing outside near a swimming pool when the younger boy, a 3-year-old toddler, fell into the water.
The 7-year-old immediately jumped into the pool to save his brother and was able to pull the toddler to the pool steps where the boy’s head was above water. But the icy temperatures overcame the older brother and he drifted underwater.
“Despite being at the forefront of medicine, what we don’t understand often exceeds what we do understand,” said Harley Rotbart, MD, author of “Miracles We Have Seen” (Health Communications: Deerfield Beach, Fla., 2016).
Paramedics arrived to find both boys unconscious and rushed them to the Children’s Hospital of Philadelphia. The younger boy regained consciousness in the ICU and recovered. The 7-year-old, however, was unresponsive and remained in a coma, said Dr. Rotbart a pediatrician and author based in Denver.
Family members stayed at the boy’s bedside and prayed. But after several weeks, the child’s condition remained unchanged. His parents began to discuss ending life support and organ donation. Then late one night, as Dr. Rotbart sat reading to the unconscious patient, the little boy squeezed his hand. In disbelief, Dr. Rotbart told all of his colleagues about the squeeze the next morning. Everyone attributed the movement to an involuntary muscle spasm, he said. After all, every test and scan showed the boy had no brain function.
But later that day, the child grasped another staff member’s hand. Shortly after that, he squeezed in response to a command. Dr. Rotbart and his staff were stunned, but cautious about feeling too much hope.
Days later, the child opened his eyes. Then, he smiled. His parents were overjoyed.
“When he walked out of the hospital more than 2 months after the near-drowning and his heroic rescue of his little brother, we all cheered and cried,” Dr. Rotbart wrote in his book. “We cried many times in the weeks preceding, and I still cry whenever I recall this story.”
The experience, which happened years ago when Dr. Rotbart was a trainee, has stayed with the pediatrician his entire career.
“His awakening was seemingly impossible – and then it happened,” Dr. Rotbart said. “Despite being at the forefront of medicine and science, what we don’t understand often exceeds what we do understand. And even when we think we understand, we are frequently proven wrong.”
For many, Dr. Rotbart’s experience raises questions about the existence of medical miracles.
Do physicians believe in medical miracles? The answers are diverse.
“I have no doubt that extraordinary outcomes happen where patients who are overwhelmingly expected not to survive, do,” says Eric Beam, MD, a hospitalist based in San Diego. “That’s one of the reasons we choose our words very carefully in our conversations with patients and their families and remember that nothing is 0%, and nothing is 100%. But doctors tend to treat situations that are 99.9% as absolute. I don’t think you can practice medicine with the hope or expectation that every case you see has the potential to beat the odds – or be a medical miracle.”
Disappearing cancer hailed as ‘miracle’
In 2003, physicians projected that Joseph Rick, 40, had just a few months to live. His mucosal melanoma had spread throughout his body, progressing even after several surgeries, radiation therapy, and a combination of chemotherapy agents, recalled Antoni Ribas, MD, PhD, an oncologist and director of the tumor immunology program at Jonsson Comprehensive Cancer Center in Los Angeles.
Mr. Rick’s melanoma had spread to his intestines with traces on his stomach and bladder. Tumors were present on his liver, lungs, and pancreas. Rick bought a grave and prepared for the worst, he recounted in a Cancer Research Institute video. But his fate took a turn when he enrolled in an experimental drug trial in December 2003. The phase 1 trial was for a new immune modulating antibody, called an anti–CTLA-4 antibody, said Dr. Ribas, who conducted the trial.
Over the next few weeks and months, all areas of Rick’s melanoma metastases disappeared. By 2009, he was in remission. He has lived the rest of his life with no evidence of melanoma, according to Dr. Ribas.
Mr. Rick’s case has been referenced throughout literature and news stories as a “medical miracle” and a “cancer miracle.”
Does Dr. Ribas think the case was a medical miracle?
“The response in Joseph Rick was what happened in 10%-15% of patients who received anti-CTLA-4 therapy,” Dr. Ribas said. “These were not miracles. These patients responded because their immune system trying to attack the cancer had been stuck at the CTLA-4 checkpoint. Blocking this checkpoint allowed their immune system to proceed to attack and kill cancer cells anywhere in the body.”
The scientific basis of this therapy was work by University of Texas MD Anderson Cancer Center immunologist James Allison, PhD, that had been done 5 years earlier in mouse models, where giving an anti–CTLA-4 antibody to mice allowed them to reject several implanted cancers, Dr. Ribas explained. Dr. Allison received the 2018 Nobel Prize in Physiology or Medicine for this work, subsequently opening the door for what we now call “immune checkpoint blockade therapy for cancer.” Dr. Ribas added.
“We tend to call miracles good things that we do not understand how they happened,” Dr. Ribas said. “From the human observation perspective, there have been plenty of medical miracles. However, each one has a specific biological mechanism that led to improvement in a patient. In cancer treatment, early studies using the immune system resulted in occasional patients having tumor responses and long-term benefits.
“With the increased understanding of how the immune system interacts with cancers, which is based on remarkable progress in understanding how the immune system works generated over the past several decades, these ‘miracles’ become specific mechanisms leading to response to cancer, which can then be replicated in other patients.”
Patient defies odds after 45 minutes without heartbeat
Florida ob.gyn. Michael Fleischer, MD, had just performed a routine repeat cesarean birth, delivering a healthy baby girl. His patient, Ruby, had a history of high blood pressure but medication taken during the pregnancy had kept her levels stabilized.
In the waiting room, Dr. Fleischer informed Ruby’s large family of the good news. He was planning to head home early that day when he heard his name being called over the hospital’s loudspeaker. Ruby had stopped breathing.
“The anesthesiologist was with her and had immediately intubated her,” Dr. Fleischer said. “We checked to make sure there was no problems or bleeding from the C-section, but everything was completely fine. However, we couldn’t keep her blood pressure stable.”
Dr. Fleischer suspected the respiratory arrest was caused by either an amniotic fluid embolism or a pulmonary embolism. Intubation continued and physicians gave Ruby medication to stabilize her blood pressure. Then suddenly, Ruby’s heart stopped.
Dr. Fleischer and other doctors began compressions, which they continued for 30 minutes. They shocked Ruby with defibrillator paddles multiple times, but there was no change.
“I was already thinking, this is hopeless, there’s nothing we can do,” he said. “The writing is on the wall. She’s going to die.”
Dr. Fleischer spoke to Ruby’s family and explained the tragic turn of events. Relatives were distraught and tearfully visited Ruby to say their goodbyes. They prayed and cried. Eventually, physicians ceased compressions. Ruby had gone 45 minutes without a pulse. The EKG was still showing some irregularity, FDr. leischer said, but no rhythm. Physicians kept Ruby intubated as they waited for the background electrical activity to fade. As they watched the screen in anguish, there was suddenly a blip on the heart rate monitor. Then another and another. Within seconds, Ruby’s heart went back into sinus rhythm.
“We were in disbelief,” Dr. Fleischer said. “We did some tests and put her in the ICU, and she was fine. Usually, after doing compressions on anyone, you’d have bruising or broken ribs. She had nothing. She just woke up and said: ‘What am I doing here? Let me go see my baby.’ ”
Ruby fully recovered, and 3 days later, she went home with her newborn.
While the recovery was unbelievable, Dr. Fleischer stopped short of calling it a medical miracle. There were scientific contributors to her survival: she was immediately intubated when she stopped breathing and compressions were started as soon as her heart stopped.
However, Dr. Fleischer said the fact that lifesaving measures had ended, and Ruby revived on her own was indeed, miraculous.
“It wasn’t like we were doing compressions and brought her back,” he said. “I can scientifically explain things in my mind, except for that. That when we finally stopped and took our hands off her, that’s when something changed. That’s when she came back.”
How do ‘medical miracles’ impact physicians?
When Dr. Rotbart was writing his book, which includes physician essays from across the world, he was struck by how many of the events happened decades earlier.
“This is another testament to the powerful impact these experiences have on those witnessing them,” he said. “In many cases, physicians describing events occurring years ago noted that those early memories served to give them hope as they encountered new, seemingly hopeless cases in subsequent years. Some contributors wrote that the ‘miracle experience’ actually directed them in their choice of specialty and has influenced much of their professional decision-making throughout their careers. Others draw on those miraculous moments at times when they themselves feel hopeless in the face of adversity and tragedy.”
Dr. Fleischer said that, although Ruby’s story has stayed with him, his mindset or practice style didn’t necessarily change after the experience.
“I’m not sure if it’s affected me because I haven’t been in that situation again,” he said. “I’m in the middle. I would never rule out anything, but I’m not going to base how I practice on the hope for a medical miracle.”
In a recent opinion piece for the New York Times, pulmonary and critical care physician, Daniela Lamas, MD, wrote about the sometimes negative effects of miracle cases on physicians. Such experiences for instance, can lead to a greater drive to beat the odds in future cases, which can sometimes lead to false hope, protracted critical care admissions, and futile procedures.
“After all, in most cases in the ICU, our initial prognoses are correct,” she wrote. “So there’s a risk to standing at the bedside, thinking about that one patient who made it home despite our predictions. We can give that experience too much weight in influencing our decisions and recommendations.”
Dr. Beam said unexpected outcomes – particularly in the age of COVID-19 – can certainly make physicians think differently about life-sustaining measures and when to discuss end-of-life care with family members. In his own practice, Dr. Beam has encountered unexpected COVID recoveries. Now, he generally gives extremely ill COVID patients a little more time to see if their bodies recover.
“It remains true that people who are really sick with COVID, who are on ventilated or who are requiring a lot of up respiratory support, they don’t do well on average,” he said. “But it is [also] true that there are a handful of people who get to that point and do come back to 80% or 90% of where they were. It makes you think twice.”
What to do when parents hope for a miracle
In his palliative care practice, Nashville, Tenn., surgeon Myrick Shinall Jr., MD, PhD, regularly encounters families and patients who wish for a medical miracle.
“It happens pretty often from a palliative care perspective,” he said. “What I have experienced the most is a patient with a severe brain injury who we don’t believe is recoverable. The medical team is discussing with the family that it is probably time to discontinue the ventilator. In those situations, families will often talk about wanting us to continue on [our life-sustaining efforts] in the hopes that a miracle will happen.”
Dr. Shinall and Trevor Bibler, PhD, recently authored two articles about best practices for responding to patients who hope for a miracle. The first one, published in the American Journal of Bioethics, is directed toward bioethicists; the second article, in the Journal of Pain and Symptom Management, targets clinicians.
A primary takeaway from the papers is that health professionals should recognize that hope for a miracle may mean different things to different people, said Dr. Bibler, an ethicist and assistant professor at Baylor College of Medicine, Houston. Some patients may have an innocuous hope for a miracle without a religious connotation, whereas others may have a firm conviction in their idea of God, their spirituality, and a concrete vision of the miracle.
“To hear that a family or patient is hoping for a miracle, one shouldn’t assume they already know what the patient or the family might mean by that,” Dr. Bibler said. “If a patient were to say, ‘I hope for a miracle,’ you might ask: ‘What do you mean by a miracle?’ Health professionals should feel empowered to ask that question.”
Health care professionals should explore a patient’s hope for a miracle, be nonjudgmental, ask clarifying questions, restate what the patient has said, and delve into the patient’s world view on death and dying, according to Dr. Bibler’s analyses. In some cases, it may be helpful to include a chaplain or the presence of a theology outsider in discussions.
When his patients and their families raise the subject of miracles, Dr. Shinall said he inquires what a miracle would look like in their opinion and tries to gauge how much of the assertion is a general hope compared with a firm belief.
“I try to work with them to make sure they understand doctors’ decisions and recommendations are based on what we know and can predict from our medical experience,” he said. “And that there’s nothing we’re going to do to prevent a miracle from happening, but that that can’t be our medical plan – to wait for a miracle.”
Despite the many patients and families Dr. Shinall has encountered who hope for a miracle, he has never experienced a case that he would describe as a medical miracle, he said.
Dr. Rotbart believes all physicians struggle with finding balance in how far to push in hope of a miracle and when to let go.
“Miracles, whether they happen to us, or we hear of them from colleagues or we read about them, should humble us as physicians,” he said. “I have come to believe that what we don’t know or don’t understand about medicine, medical miracles, or life in general, isn‘t necessarily cause for fear, and can even be reason for hope.
“Medicine has come a long way since Hippocrates’ theory of The Four Humors and The Four Temperaments, yet we still have much to learn about the workings of the human body. As physicians, we should take comfort in how much we don’t know because that allows us to share hope with our patients and, occasionally, makes medical miracles possible.”
A version of this article first appeared on Medscape.com.
It was a freezing December day, and two young brothers were playing outside near a swimming pool when the younger boy, a 3-year-old toddler, fell into the water.
The 7-year-old immediately jumped into the pool to save his brother and was able to pull the toddler to the pool steps where the boy’s head was above water. But the icy temperatures overcame the older brother and he drifted underwater.
“Despite being at the forefront of medicine, what we don’t understand often exceeds what we do understand,” said Harley Rotbart, MD, author of “Miracles We Have Seen” (Health Communications: Deerfield Beach, Fla., 2016).
Paramedics arrived to find both boys unconscious and rushed them to the Children’s Hospital of Philadelphia. The younger boy regained consciousness in the ICU and recovered. The 7-year-old, however, was unresponsive and remained in a coma, said Dr. Rotbart a pediatrician and author based in Denver.
Family members stayed at the boy’s bedside and prayed. But after several weeks, the child’s condition remained unchanged. His parents began to discuss ending life support and organ donation. Then late one night, as Dr. Rotbart sat reading to the unconscious patient, the little boy squeezed his hand. In disbelief, Dr. Rotbart told all of his colleagues about the squeeze the next morning. Everyone attributed the movement to an involuntary muscle spasm, he said. After all, every test and scan showed the boy had no brain function.
But later that day, the child grasped another staff member’s hand. Shortly after that, he squeezed in response to a command. Dr. Rotbart and his staff were stunned, but cautious about feeling too much hope.
Days later, the child opened his eyes. Then, he smiled. His parents were overjoyed.
“When he walked out of the hospital more than 2 months after the near-drowning and his heroic rescue of his little brother, we all cheered and cried,” Dr. Rotbart wrote in his book. “We cried many times in the weeks preceding, and I still cry whenever I recall this story.”
The experience, which happened years ago when Dr. Rotbart was a trainee, has stayed with the pediatrician his entire career.
“His awakening was seemingly impossible – and then it happened,” Dr. Rotbart said. “Despite being at the forefront of medicine and science, what we don’t understand often exceeds what we do understand. And even when we think we understand, we are frequently proven wrong.”
For many, Dr. Rotbart’s experience raises questions about the existence of medical miracles.
Do physicians believe in medical miracles? The answers are diverse.
“I have no doubt that extraordinary outcomes happen where patients who are overwhelmingly expected not to survive, do,” says Eric Beam, MD, a hospitalist based in San Diego. “That’s one of the reasons we choose our words very carefully in our conversations with patients and their families and remember that nothing is 0%, and nothing is 100%. But doctors tend to treat situations that are 99.9% as absolute. I don’t think you can practice medicine with the hope or expectation that every case you see has the potential to beat the odds – or be a medical miracle.”
Disappearing cancer hailed as ‘miracle’
In 2003, physicians projected that Joseph Rick, 40, had just a few months to live. His mucosal melanoma had spread throughout his body, progressing even after several surgeries, radiation therapy, and a combination of chemotherapy agents, recalled Antoni Ribas, MD, PhD, an oncologist and director of the tumor immunology program at Jonsson Comprehensive Cancer Center in Los Angeles.
Mr. Rick’s melanoma had spread to his intestines with traces on his stomach and bladder. Tumors were present on his liver, lungs, and pancreas. Rick bought a grave and prepared for the worst, he recounted in a Cancer Research Institute video. But his fate took a turn when he enrolled in an experimental drug trial in December 2003. The phase 1 trial was for a new immune modulating antibody, called an anti–CTLA-4 antibody, said Dr. Ribas, who conducted the trial.
Over the next few weeks and months, all areas of Rick’s melanoma metastases disappeared. By 2009, he was in remission. He has lived the rest of his life with no evidence of melanoma, according to Dr. Ribas.
Mr. Rick’s case has been referenced throughout literature and news stories as a “medical miracle” and a “cancer miracle.”
Does Dr. Ribas think the case was a medical miracle?
“The response in Joseph Rick was what happened in 10%-15% of patients who received anti-CTLA-4 therapy,” Dr. Ribas said. “These were not miracles. These patients responded because their immune system trying to attack the cancer had been stuck at the CTLA-4 checkpoint. Blocking this checkpoint allowed their immune system to proceed to attack and kill cancer cells anywhere in the body.”
The scientific basis of this therapy was work by University of Texas MD Anderson Cancer Center immunologist James Allison, PhD, that had been done 5 years earlier in mouse models, where giving an anti–CTLA-4 antibody to mice allowed them to reject several implanted cancers, Dr. Ribas explained. Dr. Allison received the 2018 Nobel Prize in Physiology or Medicine for this work, subsequently opening the door for what we now call “immune checkpoint blockade therapy for cancer.” Dr. Ribas added.
“We tend to call miracles good things that we do not understand how they happened,” Dr. Ribas said. “From the human observation perspective, there have been plenty of medical miracles. However, each one has a specific biological mechanism that led to improvement in a patient. In cancer treatment, early studies using the immune system resulted in occasional patients having tumor responses and long-term benefits.
“With the increased understanding of how the immune system interacts with cancers, which is based on remarkable progress in understanding how the immune system works generated over the past several decades, these ‘miracles’ become specific mechanisms leading to response to cancer, which can then be replicated in other patients.”
Patient defies odds after 45 minutes without heartbeat
Florida ob.gyn. Michael Fleischer, MD, had just performed a routine repeat cesarean birth, delivering a healthy baby girl. His patient, Ruby, had a history of high blood pressure but medication taken during the pregnancy had kept her levels stabilized.
In the waiting room, Dr. Fleischer informed Ruby’s large family of the good news. He was planning to head home early that day when he heard his name being called over the hospital’s loudspeaker. Ruby had stopped breathing.
“The anesthesiologist was with her and had immediately intubated her,” Dr. Fleischer said. “We checked to make sure there was no problems or bleeding from the C-section, but everything was completely fine. However, we couldn’t keep her blood pressure stable.”
Dr. Fleischer suspected the respiratory arrest was caused by either an amniotic fluid embolism or a pulmonary embolism. Intubation continued and physicians gave Ruby medication to stabilize her blood pressure. Then suddenly, Ruby’s heart stopped.
Dr. Fleischer and other doctors began compressions, which they continued for 30 minutes. They shocked Ruby with defibrillator paddles multiple times, but there was no change.
“I was already thinking, this is hopeless, there’s nothing we can do,” he said. “The writing is on the wall. She’s going to die.”
Dr. Fleischer spoke to Ruby’s family and explained the tragic turn of events. Relatives were distraught and tearfully visited Ruby to say their goodbyes. They prayed and cried. Eventually, physicians ceased compressions. Ruby had gone 45 minutes without a pulse. The EKG was still showing some irregularity, FDr. leischer said, but no rhythm. Physicians kept Ruby intubated as they waited for the background electrical activity to fade. As they watched the screen in anguish, there was suddenly a blip on the heart rate monitor. Then another and another. Within seconds, Ruby’s heart went back into sinus rhythm.
“We were in disbelief,” Dr. Fleischer said. “We did some tests and put her in the ICU, and she was fine. Usually, after doing compressions on anyone, you’d have bruising or broken ribs. She had nothing. She just woke up and said: ‘What am I doing here? Let me go see my baby.’ ”
Ruby fully recovered, and 3 days later, she went home with her newborn.
While the recovery was unbelievable, Dr. Fleischer stopped short of calling it a medical miracle. There were scientific contributors to her survival: she was immediately intubated when she stopped breathing and compressions were started as soon as her heart stopped.
However, Dr. Fleischer said the fact that lifesaving measures had ended, and Ruby revived on her own was indeed, miraculous.
“It wasn’t like we were doing compressions and brought her back,” he said. “I can scientifically explain things in my mind, except for that. That when we finally stopped and took our hands off her, that’s when something changed. That’s when she came back.”
How do ‘medical miracles’ impact physicians?
When Dr. Rotbart was writing his book, which includes physician essays from across the world, he was struck by how many of the events happened decades earlier.
“This is another testament to the powerful impact these experiences have on those witnessing them,” he said. “In many cases, physicians describing events occurring years ago noted that those early memories served to give them hope as they encountered new, seemingly hopeless cases in subsequent years. Some contributors wrote that the ‘miracle experience’ actually directed them in their choice of specialty and has influenced much of their professional decision-making throughout their careers. Others draw on those miraculous moments at times when they themselves feel hopeless in the face of adversity and tragedy.”
Dr. Fleischer said that, although Ruby’s story has stayed with him, his mindset or practice style didn’t necessarily change after the experience.
“I’m not sure if it’s affected me because I haven’t been in that situation again,” he said. “I’m in the middle. I would never rule out anything, but I’m not going to base how I practice on the hope for a medical miracle.”
In a recent opinion piece for the New York Times, pulmonary and critical care physician, Daniela Lamas, MD, wrote about the sometimes negative effects of miracle cases on physicians. Such experiences for instance, can lead to a greater drive to beat the odds in future cases, which can sometimes lead to false hope, protracted critical care admissions, and futile procedures.
“After all, in most cases in the ICU, our initial prognoses are correct,” she wrote. “So there’s a risk to standing at the bedside, thinking about that one patient who made it home despite our predictions. We can give that experience too much weight in influencing our decisions and recommendations.”
Dr. Beam said unexpected outcomes – particularly in the age of COVID-19 – can certainly make physicians think differently about life-sustaining measures and when to discuss end-of-life care with family members. In his own practice, Dr. Beam has encountered unexpected COVID recoveries. Now, he generally gives extremely ill COVID patients a little more time to see if their bodies recover.
“It remains true that people who are really sick with COVID, who are on ventilated or who are requiring a lot of up respiratory support, they don’t do well on average,” he said. “But it is [also] true that there are a handful of people who get to that point and do come back to 80% or 90% of where they were. It makes you think twice.”
What to do when parents hope for a miracle
In his palliative care practice, Nashville, Tenn., surgeon Myrick Shinall Jr., MD, PhD, regularly encounters families and patients who wish for a medical miracle.
“It happens pretty often from a palliative care perspective,” he said. “What I have experienced the most is a patient with a severe brain injury who we don’t believe is recoverable. The medical team is discussing with the family that it is probably time to discontinue the ventilator. In those situations, families will often talk about wanting us to continue on [our life-sustaining efforts] in the hopes that a miracle will happen.”
Dr. Shinall and Trevor Bibler, PhD, recently authored two articles about best practices for responding to patients who hope for a miracle. The first one, published in the American Journal of Bioethics, is directed toward bioethicists; the second article, in the Journal of Pain and Symptom Management, targets clinicians.
A primary takeaway from the papers is that health professionals should recognize that hope for a miracle may mean different things to different people, said Dr. Bibler, an ethicist and assistant professor at Baylor College of Medicine, Houston. Some patients may have an innocuous hope for a miracle without a religious connotation, whereas others may have a firm conviction in their idea of God, their spirituality, and a concrete vision of the miracle.
“To hear that a family or patient is hoping for a miracle, one shouldn’t assume they already know what the patient or the family might mean by that,” Dr. Bibler said. “If a patient were to say, ‘I hope for a miracle,’ you might ask: ‘What do you mean by a miracle?’ Health professionals should feel empowered to ask that question.”
Health care professionals should explore a patient’s hope for a miracle, be nonjudgmental, ask clarifying questions, restate what the patient has said, and delve into the patient’s world view on death and dying, according to Dr. Bibler’s analyses. In some cases, it may be helpful to include a chaplain or the presence of a theology outsider in discussions.
When his patients and their families raise the subject of miracles, Dr. Shinall said he inquires what a miracle would look like in their opinion and tries to gauge how much of the assertion is a general hope compared with a firm belief.
“I try to work with them to make sure they understand doctors’ decisions and recommendations are based on what we know and can predict from our medical experience,” he said. “And that there’s nothing we’re going to do to prevent a miracle from happening, but that that can’t be our medical plan – to wait for a miracle.”
Despite the many patients and families Dr. Shinall has encountered who hope for a miracle, he has never experienced a case that he would describe as a medical miracle, he said.
Dr. Rotbart believes all physicians struggle with finding balance in how far to push in hope of a miracle and when to let go.
“Miracles, whether they happen to us, or we hear of them from colleagues or we read about them, should humble us as physicians,” he said. “I have come to believe that what we don’t know or don’t understand about medicine, medical miracles, or life in general, isn‘t necessarily cause for fear, and can even be reason for hope.
“Medicine has come a long way since Hippocrates’ theory of The Four Humors and The Four Temperaments, yet we still have much to learn about the workings of the human body. As physicians, we should take comfort in how much we don’t know because that allows us to share hope with our patients and, occasionally, makes medical miracles possible.”
A version of this article first appeared on Medscape.com.
It was a freezing December day, and two young brothers were playing outside near a swimming pool when the younger boy, a 3-year-old toddler, fell into the water.
The 7-year-old immediately jumped into the pool to save his brother and was able to pull the toddler to the pool steps where the boy’s head was above water. But the icy temperatures overcame the older brother and he drifted underwater.
“Despite being at the forefront of medicine, what we don’t understand often exceeds what we do understand,” said Harley Rotbart, MD, author of “Miracles We Have Seen” (Health Communications: Deerfield Beach, Fla., 2016).
Paramedics arrived to find both boys unconscious and rushed them to the Children’s Hospital of Philadelphia. The younger boy regained consciousness in the ICU and recovered. The 7-year-old, however, was unresponsive and remained in a coma, said Dr. Rotbart a pediatrician and author based in Denver.
Family members stayed at the boy’s bedside and prayed. But after several weeks, the child’s condition remained unchanged. His parents began to discuss ending life support and organ donation. Then late one night, as Dr. Rotbart sat reading to the unconscious patient, the little boy squeezed his hand. In disbelief, Dr. Rotbart told all of his colleagues about the squeeze the next morning. Everyone attributed the movement to an involuntary muscle spasm, he said. After all, every test and scan showed the boy had no brain function.
But later that day, the child grasped another staff member’s hand. Shortly after that, he squeezed in response to a command. Dr. Rotbart and his staff were stunned, but cautious about feeling too much hope.
Days later, the child opened his eyes. Then, he smiled. His parents were overjoyed.
“When he walked out of the hospital more than 2 months after the near-drowning and his heroic rescue of his little brother, we all cheered and cried,” Dr. Rotbart wrote in his book. “We cried many times in the weeks preceding, and I still cry whenever I recall this story.”
The experience, which happened years ago when Dr. Rotbart was a trainee, has stayed with the pediatrician his entire career.
“His awakening was seemingly impossible – and then it happened,” Dr. Rotbart said. “Despite being at the forefront of medicine and science, what we don’t understand often exceeds what we do understand. And even when we think we understand, we are frequently proven wrong.”
For many, Dr. Rotbart’s experience raises questions about the existence of medical miracles.
Do physicians believe in medical miracles? The answers are diverse.
“I have no doubt that extraordinary outcomes happen where patients who are overwhelmingly expected not to survive, do,” says Eric Beam, MD, a hospitalist based in San Diego. “That’s one of the reasons we choose our words very carefully in our conversations with patients and their families and remember that nothing is 0%, and nothing is 100%. But doctors tend to treat situations that are 99.9% as absolute. I don’t think you can practice medicine with the hope or expectation that every case you see has the potential to beat the odds – or be a medical miracle.”
Disappearing cancer hailed as ‘miracle’
In 2003, physicians projected that Joseph Rick, 40, had just a few months to live. His mucosal melanoma had spread throughout his body, progressing even after several surgeries, radiation therapy, and a combination of chemotherapy agents, recalled Antoni Ribas, MD, PhD, an oncologist and director of the tumor immunology program at Jonsson Comprehensive Cancer Center in Los Angeles.
Mr. Rick’s melanoma had spread to his intestines with traces on his stomach and bladder. Tumors were present on his liver, lungs, and pancreas. Rick bought a grave and prepared for the worst, he recounted in a Cancer Research Institute video. But his fate took a turn when he enrolled in an experimental drug trial in December 2003. The phase 1 trial was for a new immune modulating antibody, called an anti–CTLA-4 antibody, said Dr. Ribas, who conducted the trial.
Over the next few weeks and months, all areas of Rick’s melanoma metastases disappeared. By 2009, he was in remission. He has lived the rest of his life with no evidence of melanoma, according to Dr. Ribas.
Mr. Rick’s case has been referenced throughout literature and news stories as a “medical miracle” and a “cancer miracle.”
Does Dr. Ribas think the case was a medical miracle?
“The response in Joseph Rick was what happened in 10%-15% of patients who received anti-CTLA-4 therapy,” Dr. Ribas said. “These were not miracles. These patients responded because their immune system trying to attack the cancer had been stuck at the CTLA-4 checkpoint. Blocking this checkpoint allowed their immune system to proceed to attack and kill cancer cells anywhere in the body.”
The scientific basis of this therapy was work by University of Texas MD Anderson Cancer Center immunologist James Allison, PhD, that had been done 5 years earlier in mouse models, where giving an anti–CTLA-4 antibody to mice allowed them to reject several implanted cancers, Dr. Ribas explained. Dr. Allison received the 2018 Nobel Prize in Physiology or Medicine for this work, subsequently opening the door for what we now call “immune checkpoint blockade therapy for cancer.” Dr. Ribas added.
“We tend to call miracles good things that we do not understand how they happened,” Dr. Ribas said. “From the human observation perspective, there have been plenty of medical miracles. However, each one has a specific biological mechanism that led to improvement in a patient. In cancer treatment, early studies using the immune system resulted in occasional patients having tumor responses and long-term benefits.
“With the increased understanding of how the immune system interacts with cancers, which is based on remarkable progress in understanding how the immune system works generated over the past several decades, these ‘miracles’ become specific mechanisms leading to response to cancer, which can then be replicated in other patients.”
Patient defies odds after 45 minutes without heartbeat
Florida ob.gyn. Michael Fleischer, MD, had just performed a routine repeat cesarean birth, delivering a healthy baby girl. His patient, Ruby, had a history of high blood pressure but medication taken during the pregnancy had kept her levels stabilized.
In the waiting room, Dr. Fleischer informed Ruby’s large family of the good news. He was planning to head home early that day when he heard his name being called over the hospital’s loudspeaker. Ruby had stopped breathing.
“The anesthesiologist was with her and had immediately intubated her,” Dr. Fleischer said. “We checked to make sure there was no problems or bleeding from the C-section, but everything was completely fine. However, we couldn’t keep her blood pressure stable.”
Dr. Fleischer suspected the respiratory arrest was caused by either an amniotic fluid embolism or a pulmonary embolism. Intubation continued and physicians gave Ruby medication to stabilize her blood pressure. Then suddenly, Ruby’s heart stopped.
Dr. Fleischer and other doctors began compressions, which they continued for 30 minutes. They shocked Ruby with defibrillator paddles multiple times, but there was no change.
“I was already thinking, this is hopeless, there’s nothing we can do,” he said. “The writing is on the wall. She’s going to die.”
Dr. Fleischer spoke to Ruby’s family and explained the tragic turn of events. Relatives were distraught and tearfully visited Ruby to say their goodbyes. They prayed and cried. Eventually, physicians ceased compressions. Ruby had gone 45 minutes without a pulse. The EKG was still showing some irregularity, FDr. leischer said, but no rhythm. Physicians kept Ruby intubated as they waited for the background electrical activity to fade. As they watched the screen in anguish, there was suddenly a blip on the heart rate monitor. Then another and another. Within seconds, Ruby’s heart went back into sinus rhythm.
“We were in disbelief,” Dr. Fleischer said. “We did some tests and put her in the ICU, and she was fine. Usually, after doing compressions on anyone, you’d have bruising or broken ribs. She had nothing. She just woke up and said: ‘What am I doing here? Let me go see my baby.’ ”
Ruby fully recovered, and 3 days later, she went home with her newborn.
While the recovery was unbelievable, Dr. Fleischer stopped short of calling it a medical miracle. There were scientific contributors to her survival: she was immediately intubated when she stopped breathing and compressions were started as soon as her heart stopped.
However, Dr. Fleischer said the fact that lifesaving measures had ended, and Ruby revived on her own was indeed, miraculous.
“It wasn’t like we were doing compressions and brought her back,” he said. “I can scientifically explain things in my mind, except for that. That when we finally stopped and took our hands off her, that’s when something changed. That’s when she came back.”
How do ‘medical miracles’ impact physicians?
When Dr. Rotbart was writing his book, which includes physician essays from across the world, he was struck by how many of the events happened decades earlier.
“This is another testament to the powerful impact these experiences have on those witnessing them,” he said. “In many cases, physicians describing events occurring years ago noted that those early memories served to give them hope as they encountered new, seemingly hopeless cases in subsequent years. Some contributors wrote that the ‘miracle experience’ actually directed them in their choice of specialty and has influenced much of their professional decision-making throughout their careers. Others draw on those miraculous moments at times when they themselves feel hopeless in the face of adversity and tragedy.”
Dr. Fleischer said that, although Ruby’s story has stayed with him, his mindset or practice style didn’t necessarily change after the experience.
“I’m not sure if it’s affected me because I haven’t been in that situation again,” he said. “I’m in the middle. I would never rule out anything, but I’m not going to base how I practice on the hope for a medical miracle.”
In a recent opinion piece for the New York Times, pulmonary and critical care physician, Daniela Lamas, MD, wrote about the sometimes negative effects of miracle cases on physicians. Such experiences for instance, can lead to a greater drive to beat the odds in future cases, which can sometimes lead to false hope, protracted critical care admissions, and futile procedures.
“After all, in most cases in the ICU, our initial prognoses are correct,” she wrote. “So there’s a risk to standing at the bedside, thinking about that one patient who made it home despite our predictions. We can give that experience too much weight in influencing our decisions and recommendations.”
Dr. Beam said unexpected outcomes – particularly in the age of COVID-19 – can certainly make physicians think differently about life-sustaining measures and when to discuss end-of-life care with family members. In his own practice, Dr. Beam has encountered unexpected COVID recoveries. Now, he generally gives extremely ill COVID patients a little more time to see if their bodies recover.
“It remains true that people who are really sick with COVID, who are on ventilated or who are requiring a lot of up respiratory support, they don’t do well on average,” he said. “But it is [also] true that there are a handful of people who get to that point and do come back to 80% or 90% of where they were. It makes you think twice.”
What to do when parents hope for a miracle
In his palliative care practice, Nashville, Tenn., surgeon Myrick Shinall Jr., MD, PhD, regularly encounters families and patients who wish for a medical miracle.
“It happens pretty often from a palliative care perspective,” he said. “What I have experienced the most is a patient with a severe brain injury who we don’t believe is recoverable. The medical team is discussing with the family that it is probably time to discontinue the ventilator. In those situations, families will often talk about wanting us to continue on [our life-sustaining efforts] in the hopes that a miracle will happen.”
Dr. Shinall and Trevor Bibler, PhD, recently authored two articles about best practices for responding to patients who hope for a miracle. The first one, published in the American Journal of Bioethics, is directed toward bioethicists; the second article, in the Journal of Pain and Symptom Management, targets clinicians.
A primary takeaway from the papers is that health professionals should recognize that hope for a miracle may mean different things to different people, said Dr. Bibler, an ethicist and assistant professor at Baylor College of Medicine, Houston. Some patients may have an innocuous hope for a miracle without a religious connotation, whereas others may have a firm conviction in their idea of God, their spirituality, and a concrete vision of the miracle.
“To hear that a family or patient is hoping for a miracle, one shouldn’t assume they already know what the patient or the family might mean by that,” Dr. Bibler said. “If a patient were to say, ‘I hope for a miracle,’ you might ask: ‘What do you mean by a miracle?’ Health professionals should feel empowered to ask that question.”
Health care professionals should explore a patient’s hope for a miracle, be nonjudgmental, ask clarifying questions, restate what the patient has said, and delve into the patient’s world view on death and dying, according to Dr. Bibler’s analyses. In some cases, it may be helpful to include a chaplain or the presence of a theology outsider in discussions.
When his patients and their families raise the subject of miracles, Dr. Shinall said he inquires what a miracle would look like in their opinion and tries to gauge how much of the assertion is a general hope compared with a firm belief.
“I try to work with them to make sure they understand doctors’ decisions and recommendations are based on what we know and can predict from our medical experience,” he said. “And that there’s nothing we’re going to do to prevent a miracle from happening, but that that can’t be our medical plan – to wait for a miracle.”
Despite the many patients and families Dr. Shinall has encountered who hope for a miracle, he has never experienced a case that he would describe as a medical miracle, he said.
Dr. Rotbart believes all physicians struggle with finding balance in how far to push in hope of a miracle and when to let go.
“Miracles, whether they happen to us, or we hear of them from colleagues or we read about them, should humble us as physicians,” he said. “I have come to believe that what we don’t know or don’t understand about medicine, medical miracles, or life in general, isn‘t necessarily cause for fear, and can even be reason for hope.
“Medicine has come a long way since Hippocrates’ theory of The Four Humors and The Four Temperaments, yet we still have much to learn about the workings of the human body. As physicians, we should take comfort in how much we don’t know because that allows us to share hope with our patients and, occasionally, makes medical miracles possible.”
A version of this article first appeared on Medscape.com.
Clinical Edge Journal Scan Commentary: Atopic Dermatitis January 2022
George Washington University School of Medicine and Health Sciences
Washington, DC
A new era of evidence-based practice for atopic dermatitis
Atopic dermatitis (AD) is one of the most common diseases of childhood and still very common in adults worldwide. AD is also a very burdensome disease with considerable patient-burden. Despite the enormous population- and patient- burden, there remain many unmet needs in the management of AD. In addition, many treatments commonly used in AD had scant or mixed evidence regarding their efficacy and safety. For example, topical corticosteroids (TCS) are the workhorse for treatment in AD and most other inflammatory skin diseases. Yet, virtually everything we know about the efficacy of TCS comes from vasoconstriction proxy assays with almost no studies formally studying the efficacy of TCS in AD. Similarly, many therapies used off-label to treat more severe AD, such as phototherapy or allergen immunotherapy have inconsistent evidence to guide their use. Well, things are finally changing and the evidence is coming in at a frenzied pace. Development of multiple novel therapeutics in AD led to renewed interest in studying the efficacy and safety of older therapies as well.
- Phototherapy is an important treatment modality in AD patients who have an inadequate response to topical therapy. Many different modalities and devices were used to treat AD over the years, including narrowband ultraviolet B (NBUVB) and ultraviolet A (UVA)-1. NBUVB is the most commonly used approach in the United States and some other regions of the world. Ben Mordehai et al. published the results of a retrospective cohort study of 390 Israeli patients with moderate-severe AD treated with NBUVB therapy between 2000-2017 with ≥3 years of follow-up. Overall, 55.4% achieved an Investigator’s Global Assessment score of clear or almost clear. Facial involvement, occurrence of adverse effects, fewer treatments, and pretreatment immunoglobulin E levels >4000 IU/ml were associated with poorer clinical response to NBUVB. Median duration of response was 12 months with more relapses in children (<18 years).
- House dust mites (HDM) were previously shown to be triggers of AD via Immunoglobulin E dependent and independent mechanisms. Unfortunately, HDM avoidance is challenging for patients and has not proven to be reliably effective in clinical trials. Previous studies examined different approaches for immunotherapy to HDM with mixed results. Langer et al. published the results of a randomized, double-blind, placebo-controlled trial of HDM sublingual immunotherapy (SLIT) or placebo for 18 months in 91 children and adults with AD and positive skin test result and/or Immunoglobulin E to Dermatophagoides pteronyssinus. After 18 months, patients treated with HDM SLIT achieved greater reductions in the SCOring AD (SCORAD) index and were more likely to achieve an Investigator’s Global Assessment score of clear or almost clear compared to placebo. Headache and abdominal pain were the most common adverse events reported by both groups. Efficacy of HDM SLIT in this study was relatively modest. Nevertheless, it appears to be a safe therapy and a reasonable adjunctive therapy in patients with AD whose disease is believed to be triggered by HDM.
- We are fortunate to have multiple non-steroidal topical therapies for atopic dermatitis, including crisaborole ointment, pimecrolimus cream and tacrolimus ointment. A number of questions remain about how these therapies compare with each other and with topical corticosteroids. Some of these questions were answered in two recent studies.
- Thom et al. compared individual data from two phase 3 studies of crisaborole ointment with previously published data for topical pimecrolimus and tacrolimus in patients ≥2 years with mild-to-moderate AD using an approach referred to as unanchored matching-adjusted indirect comparison. By week 6, the odds of achieving Investigator’s Static Global Assessment score of 0/1 was higher for crisaborole ointment vs. pimecrolimus cream and tacrolimus 0.03% ointment.
- Salava et al. followed 152 children age 1-3 years with moderate-severe AD for 36 months. They found no significant differences of topical tacrolimus 0.03% or 0.1% ointment vs. low or mid potency topical corticosteroids on AD severity (as judged by the eczema area and severity index), skin or other infections, and various cytokine levels.
While these data do not replace the need for head-to-head studies, they do provide important context about comparative efficacy and safety of the various topical agents in our toolbox.
References
- Ben Mordehai Y et al. Long-Term Narrowband UV-B Efficacy in Moderate to Severe Atopic Dermatitis. Dermatitis. 2021 (Nov 27).
- Langer SS et al. Efficacy of house dust mite sublingual immunotherapy in patients with atopic dermatitis: a randomized, double-blind, placebo-controlled trial. J Allergy Clin Immunol Pract. 2021 (Nov 9).
- Thom H et al. Matching-Adjusted Indirect Comparison of Crisaborole Ointment 2% vs. Topical Calcineurin Inhibitors in the Treatment of Patients with Mild-to-Moderate Atopic Dermatitis Dermatol Ther (Heidelb). 2021 (Dec 8).
- Salava A et al. Safety of tacrolimus 0.03% and 0.1% ointments in young children with atopic dermatitis - a 36-month follow-up study. Clin Exp Dermatol. 2021 (Nov 19).
George Washington University School of Medicine and Health Sciences
Washington, DC
A new era of evidence-based practice for atopic dermatitis
Atopic dermatitis (AD) is one of the most common diseases of childhood and still very common in adults worldwide. AD is also a very burdensome disease with considerable patient-burden. Despite the enormous population- and patient- burden, there remain many unmet needs in the management of AD. In addition, many treatments commonly used in AD had scant or mixed evidence regarding their efficacy and safety. For example, topical corticosteroids (TCS) are the workhorse for treatment in AD and most other inflammatory skin diseases. Yet, virtually everything we know about the efficacy of TCS comes from vasoconstriction proxy assays with almost no studies formally studying the efficacy of TCS in AD. Similarly, many therapies used off-label to treat more severe AD, such as phototherapy or allergen immunotherapy have inconsistent evidence to guide their use. Well, things are finally changing and the evidence is coming in at a frenzied pace. Development of multiple novel therapeutics in AD led to renewed interest in studying the efficacy and safety of older therapies as well.
- Phototherapy is an important treatment modality in AD patients who have an inadequate response to topical therapy. Many different modalities and devices were used to treat AD over the years, including narrowband ultraviolet B (NBUVB) and ultraviolet A (UVA)-1. NBUVB is the most commonly used approach in the United States and some other regions of the world. Ben Mordehai et al. published the results of a retrospective cohort study of 390 Israeli patients with moderate-severe AD treated with NBUVB therapy between 2000-2017 with ≥3 years of follow-up. Overall, 55.4% achieved an Investigator’s Global Assessment score of clear or almost clear. Facial involvement, occurrence of adverse effects, fewer treatments, and pretreatment immunoglobulin E levels >4000 IU/ml were associated with poorer clinical response to NBUVB. Median duration of response was 12 months with more relapses in children (<18 years).
- House dust mites (HDM) were previously shown to be triggers of AD via Immunoglobulin E dependent and independent mechanisms. Unfortunately, HDM avoidance is challenging for patients and has not proven to be reliably effective in clinical trials. Previous studies examined different approaches for immunotherapy to HDM with mixed results. Langer et al. published the results of a randomized, double-blind, placebo-controlled trial of HDM sublingual immunotherapy (SLIT) or placebo for 18 months in 91 children and adults with AD and positive skin test result and/or Immunoglobulin E to Dermatophagoides pteronyssinus. After 18 months, patients treated with HDM SLIT achieved greater reductions in the SCOring AD (SCORAD) index and were more likely to achieve an Investigator’s Global Assessment score of clear or almost clear compared to placebo. Headache and abdominal pain were the most common adverse events reported by both groups. Efficacy of HDM SLIT in this study was relatively modest. Nevertheless, it appears to be a safe therapy and a reasonable adjunctive therapy in patients with AD whose disease is believed to be triggered by HDM.
- We are fortunate to have multiple non-steroidal topical therapies for atopic dermatitis, including crisaborole ointment, pimecrolimus cream and tacrolimus ointment. A number of questions remain about how these therapies compare with each other and with topical corticosteroids. Some of these questions were answered in two recent studies.
- Thom et al. compared individual data from two phase 3 studies of crisaborole ointment with previously published data for topical pimecrolimus and tacrolimus in patients ≥2 years with mild-to-moderate AD using an approach referred to as unanchored matching-adjusted indirect comparison. By week 6, the odds of achieving Investigator’s Static Global Assessment score of 0/1 was higher for crisaborole ointment vs. pimecrolimus cream and tacrolimus 0.03% ointment.
- Salava et al. followed 152 children age 1-3 years with moderate-severe AD for 36 months. They found no significant differences of topical tacrolimus 0.03% or 0.1% ointment vs. low or mid potency topical corticosteroids on AD severity (as judged by the eczema area and severity index), skin or other infections, and various cytokine levels.
While these data do not replace the need for head-to-head studies, they do provide important context about comparative efficacy and safety of the various topical agents in our toolbox.
References
- Ben Mordehai Y et al. Long-Term Narrowband UV-B Efficacy in Moderate to Severe Atopic Dermatitis. Dermatitis. 2021 (Nov 27).
- Langer SS et al. Efficacy of house dust mite sublingual immunotherapy in patients with atopic dermatitis: a randomized, double-blind, placebo-controlled trial. J Allergy Clin Immunol Pract. 2021 (Nov 9).
- Thom H et al. Matching-Adjusted Indirect Comparison of Crisaborole Ointment 2% vs. Topical Calcineurin Inhibitors in the Treatment of Patients with Mild-to-Moderate Atopic Dermatitis Dermatol Ther (Heidelb). 2021 (Dec 8).
- Salava A et al. Safety of tacrolimus 0.03% and 0.1% ointments in young children with atopic dermatitis - a 36-month follow-up study. Clin Exp Dermatol. 2021 (Nov 19).
George Washington University School of Medicine and Health Sciences
Washington, DC
A new era of evidence-based practice for atopic dermatitis
Atopic dermatitis (AD) is one of the most common diseases of childhood and still very common in adults worldwide. AD is also a very burdensome disease with considerable patient-burden. Despite the enormous population- and patient- burden, there remain many unmet needs in the management of AD. In addition, many treatments commonly used in AD had scant or mixed evidence regarding their efficacy and safety. For example, topical corticosteroids (TCS) are the workhorse for treatment in AD and most other inflammatory skin diseases. Yet, virtually everything we know about the efficacy of TCS comes from vasoconstriction proxy assays with almost no studies formally studying the efficacy of TCS in AD. Similarly, many therapies used off-label to treat more severe AD, such as phototherapy or allergen immunotherapy have inconsistent evidence to guide their use. Well, things are finally changing and the evidence is coming in at a frenzied pace. Development of multiple novel therapeutics in AD led to renewed interest in studying the efficacy and safety of older therapies as well.
- Phototherapy is an important treatment modality in AD patients who have an inadequate response to topical therapy. Many different modalities and devices were used to treat AD over the years, including narrowband ultraviolet B (NBUVB) and ultraviolet A (UVA)-1. NBUVB is the most commonly used approach in the United States and some other regions of the world. Ben Mordehai et al. published the results of a retrospective cohort study of 390 Israeli patients with moderate-severe AD treated with NBUVB therapy between 2000-2017 with ≥3 years of follow-up. Overall, 55.4% achieved an Investigator’s Global Assessment score of clear or almost clear. Facial involvement, occurrence of adverse effects, fewer treatments, and pretreatment immunoglobulin E levels >4000 IU/ml were associated with poorer clinical response to NBUVB. Median duration of response was 12 months with more relapses in children (<18 years).
- House dust mites (HDM) were previously shown to be triggers of AD via Immunoglobulin E dependent and independent mechanisms. Unfortunately, HDM avoidance is challenging for patients and has not proven to be reliably effective in clinical trials. Previous studies examined different approaches for immunotherapy to HDM with mixed results. Langer et al. published the results of a randomized, double-blind, placebo-controlled trial of HDM sublingual immunotherapy (SLIT) or placebo for 18 months in 91 children and adults with AD and positive skin test result and/or Immunoglobulin E to Dermatophagoides pteronyssinus. After 18 months, patients treated with HDM SLIT achieved greater reductions in the SCOring AD (SCORAD) index and were more likely to achieve an Investigator’s Global Assessment score of clear or almost clear compared to placebo. Headache and abdominal pain were the most common adverse events reported by both groups. Efficacy of HDM SLIT in this study was relatively modest. Nevertheless, it appears to be a safe therapy and a reasonable adjunctive therapy in patients with AD whose disease is believed to be triggered by HDM.
- We are fortunate to have multiple non-steroidal topical therapies for atopic dermatitis, including crisaborole ointment, pimecrolimus cream and tacrolimus ointment. A number of questions remain about how these therapies compare with each other and with topical corticosteroids. Some of these questions were answered in two recent studies.
- Thom et al. compared individual data from two phase 3 studies of crisaborole ointment with previously published data for topical pimecrolimus and tacrolimus in patients ≥2 years with mild-to-moderate AD using an approach referred to as unanchored matching-adjusted indirect comparison. By week 6, the odds of achieving Investigator’s Static Global Assessment score of 0/1 was higher for crisaborole ointment vs. pimecrolimus cream and tacrolimus 0.03% ointment.
- Salava et al. followed 152 children age 1-3 years with moderate-severe AD for 36 months. They found no significant differences of topical tacrolimus 0.03% or 0.1% ointment vs. low or mid potency topical corticosteroids on AD severity (as judged by the eczema area and severity index), skin or other infections, and various cytokine levels.
While these data do not replace the need for head-to-head studies, they do provide important context about comparative efficacy and safety of the various topical agents in our toolbox.
References
- Ben Mordehai Y et al. Long-Term Narrowband UV-B Efficacy in Moderate to Severe Atopic Dermatitis. Dermatitis. 2021 (Nov 27).
- Langer SS et al. Efficacy of house dust mite sublingual immunotherapy in patients with atopic dermatitis: a randomized, double-blind, placebo-controlled trial. J Allergy Clin Immunol Pract. 2021 (Nov 9).
- Thom H et al. Matching-Adjusted Indirect Comparison of Crisaborole Ointment 2% vs. Topical Calcineurin Inhibitors in the Treatment of Patients with Mild-to-Moderate Atopic Dermatitis Dermatol Ther (Heidelb). 2021 (Dec 8).
- Salava A et al. Safety of tacrolimus 0.03% and 0.1% ointments in young children with atopic dermatitis - a 36-month follow-up study. Clin Exp Dermatol. 2021 (Nov 19).
FDA to review PDE4-inhibitor roflumilast for psoriasis
The , according to a statement from the manufacturer.
Roflumilast cream (also known as ARQ-151) is a small molecule inhibitor of PDE4, an enzyme that increases proinflammatory mediators and decreases anti-inflammatory mediators. PDE4 is an established treatment target in dermatology: The FDA approved PDE-4 inhibitor crisaborole (Eucrisa) as a topical treatment for mild to moderate atopic dermatitis in 2016, and an oral PDE-4 inhibitor, orismilast, is being studied for the treatment of plaque psoriasis.
Topical roflumilast, if approved, would be the first topical PDE4 inhibitor for psoriasis in particular, according to the Arcutis Biotherapeutics statement. The cream is designed for use on the entire body, including the face and sensitive intertriginous areas.
The NDA is based on data from a pair of phase 3 randomized, double-blind 8-week studies known as DERMIS 1 and DERMIS 2 (Trials of PDE4 Inhibition with Roflumilast for the Management of Plaque Psoriasis” One and Two) and a long-term phase 2b open-label study.
DERMIS 1 and DERMIS 2 were identical multinational, multicenter studies designed to assess the safety and efficacy of 0.3% roflumilast cream. In the studies, roflumilast met its primary endpoint and patients treated with it demonstrated an Investigator Global Assessment (IGA) success rate of 42.4% compared with 6.1% for the vehicle control (P < .0001), and 37.5% compared with 6.9% for the vehicle control (P < .0001), in the DERMIS 1 and 2 trials, respectively, according to Arcutis.
In the phase 2b study, the treatment effect lasted for 52-64 weeks. Roflumilast was well tolerated across the three studies.
Overall, the most common adverse events reported in the studies were diarrhea (3%), headache (2%), insomnia (1%), nausea (1%), upper respiratory tract infections (1%), and urinary tract infections (1%).
Roflumilast also showed statistically significant improvement compared to a vehicle on secondary endpoints including Intertriginous IGA (I-IGA) Success, Psoriasis Area Severity Index-75 (PASI-75), reductions in itch as measured by the Worst Itch-Numerical Rating Scale (WI-NRS), and patient perceptions of symptoms based on the Psoriasis Symptoms Diary (PSD).
The FDA has set a Prescription Drug User Fee Act (PDUFA) target action date of July 29, 2022, according to the manufacturer’s statement. An oral formulation of roflumilast was approved by the FDA in 2011, for reducing the risk of exacerbations of chronic obstructive pulmonary disease (COPD) in patients with severe COPD.
The , according to a statement from the manufacturer.
Roflumilast cream (also known as ARQ-151) is a small molecule inhibitor of PDE4, an enzyme that increases proinflammatory mediators and decreases anti-inflammatory mediators. PDE4 is an established treatment target in dermatology: The FDA approved PDE-4 inhibitor crisaborole (Eucrisa) as a topical treatment for mild to moderate atopic dermatitis in 2016, and an oral PDE-4 inhibitor, orismilast, is being studied for the treatment of plaque psoriasis.
Topical roflumilast, if approved, would be the first topical PDE4 inhibitor for psoriasis in particular, according to the Arcutis Biotherapeutics statement. The cream is designed for use on the entire body, including the face and sensitive intertriginous areas.
The NDA is based on data from a pair of phase 3 randomized, double-blind 8-week studies known as DERMIS 1 and DERMIS 2 (Trials of PDE4 Inhibition with Roflumilast for the Management of Plaque Psoriasis” One and Two) and a long-term phase 2b open-label study.
DERMIS 1 and DERMIS 2 were identical multinational, multicenter studies designed to assess the safety and efficacy of 0.3% roflumilast cream. In the studies, roflumilast met its primary endpoint and patients treated with it demonstrated an Investigator Global Assessment (IGA) success rate of 42.4% compared with 6.1% for the vehicle control (P < .0001), and 37.5% compared with 6.9% for the vehicle control (P < .0001), in the DERMIS 1 and 2 trials, respectively, according to Arcutis.
In the phase 2b study, the treatment effect lasted for 52-64 weeks. Roflumilast was well tolerated across the three studies.
Overall, the most common adverse events reported in the studies were diarrhea (3%), headache (2%), insomnia (1%), nausea (1%), upper respiratory tract infections (1%), and urinary tract infections (1%).
Roflumilast also showed statistically significant improvement compared to a vehicle on secondary endpoints including Intertriginous IGA (I-IGA) Success, Psoriasis Area Severity Index-75 (PASI-75), reductions in itch as measured by the Worst Itch-Numerical Rating Scale (WI-NRS), and patient perceptions of symptoms based on the Psoriasis Symptoms Diary (PSD).
The FDA has set a Prescription Drug User Fee Act (PDUFA) target action date of July 29, 2022, according to the manufacturer’s statement. An oral formulation of roflumilast was approved by the FDA in 2011, for reducing the risk of exacerbations of chronic obstructive pulmonary disease (COPD) in patients with severe COPD.
The , according to a statement from the manufacturer.
Roflumilast cream (also known as ARQ-151) is a small molecule inhibitor of PDE4, an enzyme that increases proinflammatory mediators and decreases anti-inflammatory mediators. PDE4 is an established treatment target in dermatology: The FDA approved PDE-4 inhibitor crisaborole (Eucrisa) as a topical treatment for mild to moderate atopic dermatitis in 2016, and an oral PDE-4 inhibitor, orismilast, is being studied for the treatment of plaque psoriasis.
Topical roflumilast, if approved, would be the first topical PDE4 inhibitor for psoriasis in particular, according to the Arcutis Biotherapeutics statement. The cream is designed for use on the entire body, including the face and sensitive intertriginous areas.
The NDA is based on data from a pair of phase 3 randomized, double-blind 8-week studies known as DERMIS 1 and DERMIS 2 (Trials of PDE4 Inhibition with Roflumilast for the Management of Plaque Psoriasis” One and Two) and a long-term phase 2b open-label study.
DERMIS 1 and DERMIS 2 were identical multinational, multicenter studies designed to assess the safety and efficacy of 0.3% roflumilast cream. In the studies, roflumilast met its primary endpoint and patients treated with it demonstrated an Investigator Global Assessment (IGA) success rate of 42.4% compared with 6.1% for the vehicle control (P < .0001), and 37.5% compared with 6.9% for the vehicle control (P < .0001), in the DERMIS 1 and 2 trials, respectively, according to Arcutis.
In the phase 2b study, the treatment effect lasted for 52-64 weeks. Roflumilast was well tolerated across the three studies.
Overall, the most common adverse events reported in the studies were diarrhea (3%), headache (2%), insomnia (1%), nausea (1%), upper respiratory tract infections (1%), and urinary tract infections (1%).
Roflumilast also showed statistically significant improvement compared to a vehicle on secondary endpoints including Intertriginous IGA (I-IGA) Success, Psoriasis Area Severity Index-75 (PASI-75), reductions in itch as measured by the Worst Itch-Numerical Rating Scale (WI-NRS), and patient perceptions of symptoms based on the Psoriasis Symptoms Diary (PSD).
The FDA has set a Prescription Drug User Fee Act (PDUFA) target action date of July 29, 2022, according to the manufacturer’s statement. An oral formulation of roflumilast was approved by the FDA in 2011, for reducing the risk of exacerbations of chronic obstructive pulmonary disease (COPD) in patients with severe COPD.
COVID-19, sure, but what else will we remember 2021 for?
who answered a recent Medscape Medical News poll. Perhaps no surprise there.
Coming in distant second, at 26%, was the new law requiring that patients be granted electronic access to clinical notes. The controversial Food and Drug Administration approval of aducanumab (Aduhelm, Biogen/Eisai) to treat Alzheimer’s disease was next, cited by almost 16% when asked what they would remember most about 2021.
Coming in at 10% or less were the permanent end to the Step 2 Clinical Skills test, the JAMA deputy editor resignation over controversial comments, and an “other” option that allowed for write-in responses.
It should be noted respondents could choose up to three answers to this and other questions in this survey, except for questions about profession and specialty.
Exciting news in 2021
Widespread availability of COVID-19 vaccines was the No. 1 response – chosen by 85% – when asked what medical news or events excited them in 2021.
FDA clearance of a 5-minute test for early dementia was selected by 22%, followed by almost 16% citing approval in October 2021 of abemaciclib (Verzenio, Lilly) “described as the first advance for early breast cancer in 20 years.”
The resignation of JAMA editors over a podcast on race rounded out the list of exciting medical news or events – coming in fourth at 11%. A total 5% of readers chose “other” and were asked to specify what news or events excited them in 2021.
A frustrating year?
Medscape also asked readers what medical news or events frustrated them in 2021. A majority, 81%, chose COVID-19 vaccine hesitancy or refusal. Almost one-third, 31%, chose the effect of climate change on health worldwide.
Some of the most memorable news or events of 2021 were also selected as frustrating by readers. For example, 22% were frustrated by the law requiring that patients be granted electronic access to clinical notes, followed by 19% who referred to the aducanumab approval in June. Furthermore, about 12% selected the JAMA resignations.
A shocking survey question
Asked what medical news or event from 2021 shocked readers, COVID-19 vaccine hesitancy or refusal was the most common answer, at 69%.
The U.S. Preventive Services Task Force ruling out aspirin in people over age 60 for primary prevention of cardiovascular disease shocked 36% of respondents.
Coming in third and fourth on the survey were the two JAMA editors resigning after a podcast on race, chosen by 19%, and the demise of the Step 2 Clinical Skills test, selected by 18%.
Interestingly, almost 96% of respondents were physicians. Less than 1% were residents, physician assistants, or nurses. Respondents also represented a wide range of specialties. From a list of 29 possible specialties, including “other,” family medicine, internal medicine, and psychiatry were the most common.
For more on the year that was 2021, see the Medscape Year in Medicine 2021: News That Made a Difference slideshow. Read Medscape’s full Year in Medicine report.
Wondering what stood out most to our readers in 2020? Here is a story about the results of a similar survey 1 year ago.
A version of this article first appeared on Medscape.com.
who answered a recent Medscape Medical News poll. Perhaps no surprise there.
Coming in distant second, at 26%, was the new law requiring that patients be granted electronic access to clinical notes. The controversial Food and Drug Administration approval of aducanumab (Aduhelm, Biogen/Eisai) to treat Alzheimer’s disease was next, cited by almost 16% when asked what they would remember most about 2021.
Coming in at 10% or less were the permanent end to the Step 2 Clinical Skills test, the JAMA deputy editor resignation over controversial comments, and an “other” option that allowed for write-in responses.
It should be noted respondents could choose up to three answers to this and other questions in this survey, except for questions about profession and specialty.
Exciting news in 2021
Widespread availability of COVID-19 vaccines was the No. 1 response – chosen by 85% – when asked what medical news or events excited them in 2021.
FDA clearance of a 5-minute test for early dementia was selected by 22%, followed by almost 16% citing approval in October 2021 of abemaciclib (Verzenio, Lilly) “described as the first advance for early breast cancer in 20 years.”
The resignation of JAMA editors over a podcast on race rounded out the list of exciting medical news or events – coming in fourth at 11%. A total 5% of readers chose “other” and were asked to specify what news or events excited them in 2021.
A frustrating year?
Medscape also asked readers what medical news or events frustrated them in 2021. A majority, 81%, chose COVID-19 vaccine hesitancy or refusal. Almost one-third, 31%, chose the effect of climate change on health worldwide.
Some of the most memorable news or events of 2021 were also selected as frustrating by readers. For example, 22% were frustrated by the law requiring that patients be granted electronic access to clinical notes, followed by 19% who referred to the aducanumab approval in June. Furthermore, about 12% selected the JAMA resignations.
A shocking survey question
Asked what medical news or event from 2021 shocked readers, COVID-19 vaccine hesitancy or refusal was the most common answer, at 69%.
The U.S. Preventive Services Task Force ruling out aspirin in people over age 60 for primary prevention of cardiovascular disease shocked 36% of respondents.
Coming in third and fourth on the survey were the two JAMA editors resigning after a podcast on race, chosen by 19%, and the demise of the Step 2 Clinical Skills test, selected by 18%.
Interestingly, almost 96% of respondents were physicians. Less than 1% were residents, physician assistants, or nurses. Respondents also represented a wide range of specialties. From a list of 29 possible specialties, including “other,” family medicine, internal medicine, and psychiatry were the most common.
For more on the year that was 2021, see the Medscape Year in Medicine 2021: News That Made a Difference slideshow. Read Medscape’s full Year in Medicine report.
Wondering what stood out most to our readers in 2020? Here is a story about the results of a similar survey 1 year ago.
A version of this article first appeared on Medscape.com.
who answered a recent Medscape Medical News poll. Perhaps no surprise there.
Coming in distant second, at 26%, was the new law requiring that patients be granted electronic access to clinical notes. The controversial Food and Drug Administration approval of aducanumab (Aduhelm, Biogen/Eisai) to treat Alzheimer’s disease was next, cited by almost 16% when asked what they would remember most about 2021.
Coming in at 10% or less were the permanent end to the Step 2 Clinical Skills test, the JAMA deputy editor resignation over controversial comments, and an “other” option that allowed for write-in responses.
It should be noted respondents could choose up to three answers to this and other questions in this survey, except for questions about profession and specialty.
Exciting news in 2021
Widespread availability of COVID-19 vaccines was the No. 1 response – chosen by 85% – when asked what medical news or events excited them in 2021.
FDA clearance of a 5-minute test for early dementia was selected by 22%, followed by almost 16% citing approval in October 2021 of abemaciclib (Verzenio, Lilly) “described as the first advance for early breast cancer in 20 years.”
The resignation of JAMA editors over a podcast on race rounded out the list of exciting medical news or events – coming in fourth at 11%. A total 5% of readers chose “other” and were asked to specify what news or events excited them in 2021.
A frustrating year?
Medscape also asked readers what medical news or events frustrated them in 2021. A majority, 81%, chose COVID-19 vaccine hesitancy or refusal. Almost one-third, 31%, chose the effect of climate change on health worldwide.
Some of the most memorable news or events of 2021 were also selected as frustrating by readers. For example, 22% were frustrated by the law requiring that patients be granted electronic access to clinical notes, followed by 19% who referred to the aducanumab approval in June. Furthermore, about 12% selected the JAMA resignations.
A shocking survey question
Asked what medical news or event from 2021 shocked readers, COVID-19 vaccine hesitancy or refusal was the most common answer, at 69%.
The U.S. Preventive Services Task Force ruling out aspirin in people over age 60 for primary prevention of cardiovascular disease shocked 36% of respondents.
Coming in third and fourth on the survey were the two JAMA editors resigning after a podcast on race, chosen by 19%, and the demise of the Step 2 Clinical Skills test, selected by 18%.
Interestingly, almost 96% of respondents were physicians. Less than 1% were residents, physician assistants, or nurses. Respondents also represented a wide range of specialties. From a list of 29 possible specialties, including “other,” family medicine, internal medicine, and psychiatry were the most common.
For more on the year that was 2021, see the Medscape Year in Medicine 2021: News That Made a Difference slideshow. Read Medscape’s full Year in Medicine report.
Wondering what stood out most to our readers in 2020? Here is a story about the results of a similar survey 1 year ago.
A version of this article first appeared on Medscape.com.
Why patients should ditch cloth masks
Are you still wearing a cloth face mask?
Amid the rapidly spreading Omicron variant, experts stress that we all should swap cloth masks for N95 respirators or 3-ply surgical masks.
For background: N95 respirators are tightly fitting masks that cover your mouth and nose and help prevent contact with droplets and tiny particles in the air from people talking, coughing, sneezing, and spreading in other ways. Usually worn by health care workers and first responders, these masks can filter up to 95% of air droplets and particles, according to the CDC.
KN95 and KN94 masks are similar but are designed to meet international standards, unlike N95s that are approved by the Centers for Disease Control and Prevention’s National Institute for Occupational Safety and Health.
Meanwhile, a 3-ply surgical mask is a looser-fitting mask that can help prevent contact with infected droplets in the air.
But recommendations to opt for N95 and 3-ply surgical masks over cloth masks are nothing new, says Leana Wen, MD, an emergency doctor and public health professor at George Washington University, Washington.
In fact, public health experts have been urging stronger mask protection for months.
“It’s not just with Omicron that we need better masks, it was with Delta, it was with Alpha before that,” Dr. Wen said. “We have known for many months that COVID-19 is airborne, and therefore, a simple cloth mask is not going to cut it.”
Here’s what to know about these protective masks.
They’re necessary
Omicron is spreading much faster than previous COVID-19 variants. As it’s up to three times as likely to spread as the Delta variant, mask-wearing is paramount right now, says Anita Gupta, DO, an adjunct assistant professor of anesthesiology and critical care medicine and pain medicine at Johns Hopkins University, Baltimore.
The quality of a mask also matters a lot, said Dr. Wen.
“Double masking, including a well-fitting cloth mask on top of a surgical mask, adds additional protection,” she said. “Ideally, though, people should be wearing an N95, KN95, or KF94 when in indoor settings around other people with unknown vaccination status.”
If wearing an N95 mask causes extreme discomfort, wear it in high-risk settings where there are lots of people, like crowded restaurants and busy commuter trains, says Dr. Wen. “If you’re in a grocery store, there’s plenty of space and ventilation. You may not need an N95. I recommend that people obtain different masks and practice with them in low-risk settings before they go out in public in a high-risk setting.”
But people should wear a 3-ply surgical mask at the very least.
Three-ply surgical and N95 mask qualities
With 3-ply surgical masks, the fit of the mask is often more of an issue than its comfort, Dr. Wen said. But there are ways to adjust these masks, especially for those who have smaller heads.
“You can put a rubber band around the ear loops and make them a bit tighter,” said Dr. Wen. “Some people have found that using pins in their hair, that’s another way of keeping the loops in place.”
Another important tip on 3-ply surgical masks and N95s: These masks are reusable.
But how many times you should use them varies, Dr. Wen said. “As an example, if you are sweating a lot, and the mask is now really damp. Or putting it in your purse or backpack, and now it’s misshapen, and you cannot get it back to fit on your face, then it’s time to throw it away.”
Protection first
For some, cloth masks became somewhat of a statement, with people sporting logos of their favorite NFL team, or maybe even a fun animal print.
But you should always keep in mind the purpose of wearing a mask, Dr. Wen said. “Mask wearing is very functional and is about reducing your likelihood of contracting COVID. People should also use whatever methods inspire them, too, but for me, it’s purely a functional exercise.”
Mask wearing is not always enjoyable, but it remains critical in keeping people safe from COVID-19, especially the elderly and other high-risk people, Gupta says.
“There is lots of research and experts working hard to stop COVID-19,” she says. “It is important for all of us to remember that wearing a mask alone doesn’t make us safe.”
“We all need to keep washing our hands frequently and maintaining a distance from people, as well.”
For more information on where to find 3-ply surgical masks and N95s, check here or here to start.
A version of this article first appeared on WebMD.com.
Are you still wearing a cloth face mask?
Amid the rapidly spreading Omicron variant, experts stress that we all should swap cloth masks for N95 respirators or 3-ply surgical masks.
For background: N95 respirators are tightly fitting masks that cover your mouth and nose and help prevent contact with droplets and tiny particles in the air from people talking, coughing, sneezing, and spreading in other ways. Usually worn by health care workers and first responders, these masks can filter up to 95% of air droplets and particles, according to the CDC.
KN95 and KN94 masks are similar but are designed to meet international standards, unlike N95s that are approved by the Centers for Disease Control and Prevention’s National Institute for Occupational Safety and Health.
Meanwhile, a 3-ply surgical mask is a looser-fitting mask that can help prevent contact with infected droplets in the air.
But recommendations to opt for N95 and 3-ply surgical masks over cloth masks are nothing new, says Leana Wen, MD, an emergency doctor and public health professor at George Washington University, Washington.
In fact, public health experts have been urging stronger mask protection for months.
“It’s not just with Omicron that we need better masks, it was with Delta, it was with Alpha before that,” Dr. Wen said. “We have known for many months that COVID-19 is airborne, and therefore, a simple cloth mask is not going to cut it.”
Here’s what to know about these protective masks.
They’re necessary
Omicron is spreading much faster than previous COVID-19 variants. As it’s up to three times as likely to spread as the Delta variant, mask-wearing is paramount right now, says Anita Gupta, DO, an adjunct assistant professor of anesthesiology and critical care medicine and pain medicine at Johns Hopkins University, Baltimore.
The quality of a mask also matters a lot, said Dr. Wen.
“Double masking, including a well-fitting cloth mask on top of a surgical mask, adds additional protection,” she said. “Ideally, though, people should be wearing an N95, KN95, or KF94 when in indoor settings around other people with unknown vaccination status.”
If wearing an N95 mask causes extreme discomfort, wear it in high-risk settings where there are lots of people, like crowded restaurants and busy commuter trains, says Dr. Wen. “If you’re in a grocery store, there’s plenty of space and ventilation. You may not need an N95. I recommend that people obtain different masks and practice with them in low-risk settings before they go out in public in a high-risk setting.”
But people should wear a 3-ply surgical mask at the very least.
Three-ply surgical and N95 mask qualities
With 3-ply surgical masks, the fit of the mask is often more of an issue than its comfort, Dr. Wen said. But there are ways to adjust these masks, especially for those who have smaller heads.
“You can put a rubber band around the ear loops and make them a bit tighter,” said Dr. Wen. “Some people have found that using pins in their hair, that’s another way of keeping the loops in place.”
Another important tip on 3-ply surgical masks and N95s: These masks are reusable.
But how many times you should use them varies, Dr. Wen said. “As an example, if you are sweating a lot, and the mask is now really damp. Or putting it in your purse or backpack, and now it’s misshapen, and you cannot get it back to fit on your face, then it’s time to throw it away.”
Protection first
For some, cloth masks became somewhat of a statement, with people sporting logos of their favorite NFL team, or maybe even a fun animal print.
But you should always keep in mind the purpose of wearing a mask, Dr. Wen said. “Mask wearing is very functional and is about reducing your likelihood of contracting COVID. People should also use whatever methods inspire them, too, but for me, it’s purely a functional exercise.”
Mask wearing is not always enjoyable, but it remains critical in keeping people safe from COVID-19, especially the elderly and other high-risk people, Gupta says.
“There is lots of research and experts working hard to stop COVID-19,” she says. “It is important for all of us to remember that wearing a mask alone doesn’t make us safe.”
“We all need to keep washing our hands frequently and maintaining a distance from people, as well.”
For more information on where to find 3-ply surgical masks and N95s, check here or here to start.
A version of this article first appeared on WebMD.com.
Are you still wearing a cloth face mask?
Amid the rapidly spreading Omicron variant, experts stress that we all should swap cloth masks for N95 respirators or 3-ply surgical masks.
For background: N95 respirators are tightly fitting masks that cover your mouth and nose and help prevent contact with droplets and tiny particles in the air from people talking, coughing, sneezing, and spreading in other ways. Usually worn by health care workers and first responders, these masks can filter up to 95% of air droplets and particles, according to the CDC.
KN95 and KN94 masks are similar but are designed to meet international standards, unlike N95s that are approved by the Centers for Disease Control and Prevention’s National Institute for Occupational Safety and Health.
Meanwhile, a 3-ply surgical mask is a looser-fitting mask that can help prevent contact with infected droplets in the air.
But recommendations to opt for N95 and 3-ply surgical masks over cloth masks are nothing new, says Leana Wen, MD, an emergency doctor and public health professor at George Washington University, Washington.
In fact, public health experts have been urging stronger mask protection for months.
“It’s not just with Omicron that we need better masks, it was with Delta, it was with Alpha before that,” Dr. Wen said. “We have known for many months that COVID-19 is airborne, and therefore, a simple cloth mask is not going to cut it.”
Here’s what to know about these protective masks.
They’re necessary
Omicron is spreading much faster than previous COVID-19 variants. As it’s up to three times as likely to spread as the Delta variant, mask-wearing is paramount right now, says Anita Gupta, DO, an adjunct assistant professor of anesthesiology and critical care medicine and pain medicine at Johns Hopkins University, Baltimore.
The quality of a mask also matters a lot, said Dr. Wen.
“Double masking, including a well-fitting cloth mask on top of a surgical mask, adds additional protection,” she said. “Ideally, though, people should be wearing an N95, KN95, or KF94 when in indoor settings around other people with unknown vaccination status.”
If wearing an N95 mask causes extreme discomfort, wear it in high-risk settings where there are lots of people, like crowded restaurants and busy commuter trains, says Dr. Wen. “If you’re in a grocery store, there’s plenty of space and ventilation. You may not need an N95. I recommend that people obtain different masks and practice with them in low-risk settings before they go out in public in a high-risk setting.”
But people should wear a 3-ply surgical mask at the very least.
Three-ply surgical and N95 mask qualities
With 3-ply surgical masks, the fit of the mask is often more of an issue than its comfort, Dr. Wen said. But there are ways to adjust these masks, especially for those who have smaller heads.
“You can put a rubber band around the ear loops and make them a bit tighter,” said Dr. Wen. “Some people have found that using pins in their hair, that’s another way of keeping the loops in place.”
Another important tip on 3-ply surgical masks and N95s: These masks are reusable.
But how many times you should use them varies, Dr. Wen said. “As an example, if you are sweating a lot, and the mask is now really damp. Or putting it in your purse or backpack, and now it’s misshapen, and you cannot get it back to fit on your face, then it’s time to throw it away.”
Protection first
For some, cloth masks became somewhat of a statement, with people sporting logos of their favorite NFL team, or maybe even a fun animal print.
But you should always keep in mind the purpose of wearing a mask, Dr. Wen said. “Mask wearing is very functional and is about reducing your likelihood of contracting COVID. People should also use whatever methods inspire them, too, but for me, it’s purely a functional exercise.”
Mask wearing is not always enjoyable, but it remains critical in keeping people safe from COVID-19, especially the elderly and other high-risk people, Gupta says.
“There is lots of research and experts working hard to stop COVID-19,” she says. “It is important for all of us to remember that wearing a mask alone doesn’t make us safe.”
“We all need to keep washing our hands frequently and maintaining a distance from people, as well.”
For more information on where to find 3-ply surgical masks and N95s, check here or here to start.
A version of this article first appeared on WebMD.com.