User login
One fish, two fish, are good fish for you ... fish
Good news for pregnant women; bad news for fish
As soon as women find out they’re pregnant, doctors recommend they give up smoking, drinking, and eating certain types of fish. That last item may need to be reconsidered, since a recent study supports the idea that it doesn’t matter what type of fish pregnant women are eating, as long as they’re eating it.
Researchers collected data from two different studies that reviewed the mercury levels of mothers from Bristol, England, and the Seychelles, a island chain off East Africa where “fish consumption is high and prenatal mercury levels are 10 times higher than in the [United States],” they said in NeuroToxicology.
Those data showed that the mercury levels had no adverse effects on child development as long as the mother ate fish. The nutrients and vitamins in the fish – vitamin D, long-chain fatty acids, selenium, and iodine – provide protection against mercury. There’s also the already-known benefits to eyesight and intellectual abilities that have been associated with fish consumption.
This analysis goes starkly against the grain of what is commonly recommended to expectant mothers, which is to cut out fish altogether. The researchers suggested that governments should review and change those recommendations to focus on the benefits instead.
As long as women follow the researchers’ recommendation to eat “at least two portions of fish a week, one of which should be oily,” they may not have to lay off on the sushi after all.
We’ll show our gut worms the world
Never let it be said that mankind is not a generous species. Sure, we could maybe be kinder to our fellow human beings, maybe declare a little less war on each other, but for the past 50,000 years, we’ve been giving a free ride to millions upon millions to one of mankind’s closest companions: the whipworm.
This revelation into human kindness comes from Denmark, where researchers from Copenhagen conducted a genetic analysis of ancient preserved whipworm eggs found in old Viking and Norse settlements, some of which date back over 2,000 years. In normal conditions genetic material wouldn’t last very long, but these were Viking whipworms eggs with tiny little horned helmets, so the DNA within has remained unchanged. Or it may be the tough chitinous exterior of the eggs protecting the DNA from degrading, combined with their preservation in moist soil.
Once they had their Viking whipworm DNA, the researchers compared it with whipworm DNA from all over the world, tracing its history as it followed mankind from Africa. And it’s been a while: We brought whipworms with us during our initial migration into Asia and Europe over 50,000 years ago. When the Bering land bridge opened up and humanity moved into the Americas, the worms came as well.
This is all possible because the whipworm goes about its parasitic business quietly and cleverly. It mostly sits harmlessly in our digestive systems, producing thousands of eggs a day that get expelled through poop and picked up by another host (human or otherwise); whipworms only cause disease in those with compromised immune systems.
The researchers noted that their study, the first complete genetic analysis of the whipworm, could help combat the parasite, which to this day infects hundred of millions who don’t have access to modern medicine or sanitary conditions. Hopefully, though, the days of free rides will soon be over for the whipworm. After all, if we have to pay hundreds or thousands of dollars to visit other countries, it’s only fair that our parasites do as well.
From zero to vasectomy in 6.7 seconds
There’s an old saying that you’ve probably heard: When life gives you lemons, make lemonade. It’s meant to encourage optimism in the face of adversity. Then there’s the new saying we just made up: When life gives you a power outage, plug your surgical instruments into an electric pickup.
That’s what Dr. Christopher Yang did, and now we’re making the urologist from Austin, Tex., famous by sharing his surgical/electrical adventure with all 17 of LOTME’s regular readers. That’s some serious lemonade.
Dr. Yang’s tale begins when the electricity went out at his clinic, seemingly forcing him to cancel or reschedule several surgical procedures. Not so fast. Dr. Yang happens to own a Rivian R1T, an electric pickup truck that has four power outlets. A staff member suggested plugging the surgical instruments into the truck and, surprisingly, one of the day’s patients agreed to go ahead with his vasectomy.
“We were fortunate that my normal parking spot is close enough to a patient room to run an extension cord,” Dr. Yang said on TheDrive.com. That extension cord was attached to an electrocautery device, with a handheld device available as backup, and “after we were done, I told his family. We all had a good laugh together too,” Dr. Yang told radio station WGLT in Normal, Ill.
To us, anyway, this opens up all sorts of alternative energy possibilities. Can a windmill power a liposuction? Is a gerbil running in a wheel enough to do a colonoscopy? How many potatoes do you need to keep an EHR going?
Learning through random acts of not-exactly noisiness
First things first. Transcranial random noise stimulation (tRNS) is not really noise in the auditory sense of the word. For some people with learning disabilities, though, it can actually be very helpful. The technology, which uses electrodes attached to the head so a weak current can pass through specific parts of the brain, may help those with learning disabilities, perhaps even those with brain injuries and visual deficits, learn, said Dr. Onno van der Groen of Edith Cowan University in Perth, Australia.
“When you add this type of stimulation during learning, you get better performance, faster learning and better attention afterwards as well,” he said in a statement from the university.
The researchers say that tRNS can allow the brain to form new connections and pathways, which in turn help a person learn more effectively. “If you do 10 sessions of a visual perception task with the tRNS and then come back and do it again without it, you’ll find you perform better than the control group who hasn’t used it,” Dr. van der Groen noted.
Can this also work for the average person? It’s possible, but tRNS didn’t seem to improve the math skills of a top-level mathematician who underwent the process, according to a case study that Dr. van der Groen mentioned.
This line of work is still pretty new, though, so researchers don’t have all the answers yet. As always, we’re rooting for you, science!
Good news for pregnant women; bad news for fish
As soon as women find out they’re pregnant, doctors recommend they give up smoking, drinking, and eating certain types of fish. That last item may need to be reconsidered, since a recent study supports the idea that it doesn’t matter what type of fish pregnant women are eating, as long as they’re eating it.
Researchers collected data from two different studies that reviewed the mercury levels of mothers from Bristol, England, and the Seychelles, a island chain off East Africa where “fish consumption is high and prenatal mercury levels are 10 times higher than in the [United States],” they said in NeuroToxicology.
Those data showed that the mercury levels had no adverse effects on child development as long as the mother ate fish. The nutrients and vitamins in the fish – vitamin D, long-chain fatty acids, selenium, and iodine – provide protection against mercury. There’s also the already-known benefits to eyesight and intellectual abilities that have been associated with fish consumption.
This analysis goes starkly against the grain of what is commonly recommended to expectant mothers, which is to cut out fish altogether. The researchers suggested that governments should review and change those recommendations to focus on the benefits instead.
As long as women follow the researchers’ recommendation to eat “at least two portions of fish a week, one of which should be oily,” they may not have to lay off on the sushi after all.
We’ll show our gut worms the world
Never let it be said that mankind is not a generous species. Sure, we could maybe be kinder to our fellow human beings, maybe declare a little less war on each other, but for the past 50,000 years, we’ve been giving a free ride to millions upon millions to one of mankind’s closest companions: the whipworm.
This revelation into human kindness comes from Denmark, where researchers from Copenhagen conducted a genetic analysis of ancient preserved whipworm eggs found in old Viking and Norse settlements, some of which date back over 2,000 years. In normal conditions genetic material wouldn’t last very long, but these were Viking whipworms eggs with tiny little horned helmets, so the DNA within has remained unchanged. Or it may be the tough chitinous exterior of the eggs protecting the DNA from degrading, combined with their preservation in moist soil.
Once they had their Viking whipworm DNA, the researchers compared it with whipworm DNA from all over the world, tracing its history as it followed mankind from Africa. And it’s been a while: We brought whipworms with us during our initial migration into Asia and Europe over 50,000 years ago. When the Bering land bridge opened up and humanity moved into the Americas, the worms came as well.
This is all possible because the whipworm goes about its parasitic business quietly and cleverly. It mostly sits harmlessly in our digestive systems, producing thousands of eggs a day that get expelled through poop and picked up by another host (human or otherwise); whipworms only cause disease in those with compromised immune systems.
The researchers noted that their study, the first complete genetic analysis of the whipworm, could help combat the parasite, which to this day infects hundred of millions who don’t have access to modern medicine or sanitary conditions. Hopefully, though, the days of free rides will soon be over for the whipworm. After all, if we have to pay hundreds or thousands of dollars to visit other countries, it’s only fair that our parasites do as well.
From zero to vasectomy in 6.7 seconds
There’s an old saying that you’ve probably heard: When life gives you lemons, make lemonade. It’s meant to encourage optimism in the face of adversity. Then there’s the new saying we just made up: When life gives you a power outage, plug your surgical instruments into an electric pickup.
That’s what Dr. Christopher Yang did, and now we’re making the urologist from Austin, Tex., famous by sharing his surgical/electrical adventure with all 17 of LOTME’s regular readers. That’s some serious lemonade.
Dr. Yang’s tale begins when the electricity went out at his clinic, seemingly forcing him to cancel or reschedule several surgical procedures. Not so fast. Dr. Yang happens to own a Rivian R1T, an electric pickup truck that has four power outlets. A staff member suggested plugging the surgical instruments into the truck and, surprisingly, one of the day’s patients agreed to go ahead with his vasectomy.
“We were fortunate that my normal parking spot is close enough to a patient room to run an extension cord,” Dr. Yang said on TheDrive.com. That extension cord was attached to an electrocautery device, with a handheld device available as backup, and “after we were done, I told his family. We all had a good laugh together too,” Dr. Yang told radio station WGLT in Normal, Ill.
To us, anyway, this opens up all sorts of alternative energy possibilities. Can a windmill power a liposuction? Is a gerbil running in a wheel enough to do a colonoscopy? How many potatoes do you need to keep an EHR going?
Learning through random acts of not-exactly noisiness
First things first. Transcranial random noise stimulation (tRNS) is not really noise in the auditory sense of the word. For some people with learning disabilities, though, it can actually be very helpful. The technology, which uses electrodes attached to the head so a weak current can pass through specific parts of the brain, may help those with learning disabilities, perhaps even those with brain injuries and visual deficits, learn, said Dr. Onno van der Groen of Edith Cowan University in Perth, Australia.
“When you add this type of stimulation during learning, you get better performance, faster learning and better attention afterwards as well,” he said in a statement from the university.
The researchers say that tRNS can allow the brain to form new connections and pathways, which in turn help a person learn more effectively. “If you do 10 sessions of a visual perception task with the tRNS and then come back and do it again without it, you’ll find you perform better than the control group who hasn’t used it,” Dr. van der Groen noted.
Can this also work for the average person? It’s possible, but tRNS didn’t seem to improve the math skills of a top-level mathematician who underwent the process, according to a case study that Dr. van der Groen mentioned.
This line of work is still pretty new, though, so researchers don’t have all the answers yet. As always, we’re rooting for you, science!
Good news for pregnant women; bad news for fish
As soon as women find out they’re pregnant, doctors recommend they give up smoking, drinking, and eating certain types of fish. That last item may need to be reconsidered, since a recent study supports the idea that it doesn’t matter what type of fish pregnant women are eating, as long as they’re eating it.
Researchers collected data from two different studies that reviewed the mercury levels of mothers from Bristol, England, and the Seychelles, a island chain off East Africa where “fish consumption is high and prenatal mercury levels are 10 times higher than in the [United States],” they said in NeuroToxicology.
Those data showed that the mercury levels had no adverse effects on child development as long as the mother ate fish. The nutrients and vitamins in the fish – vitamin D, long-chain fatty acids, selenium, and iodine – provide protection against mercury. There’s also the already-known benefits to eyesight and intellectual abilities that have been associated with fish consumption.
This analysis goes starkly against the grain of what is commonly recommended to expectant mothers, which is to cut out fish altogether. The researchers suggested that governments should review and change those recommendations to focus on the benefits instead.
As long as women follow the researchers’ recommendation to eat “at least two portions of fish a week, one of which should be oily,” they may not have to lay off on the sushi after all.
We’ll show our gut worms the world
Never let it be said that mankind is not a generous species. Sure, we could maybe be kinder to our fellow human beings, maybe declare a little less war on each other, but for the past 50,000 years, we’ve been giving a free ride to millions upon millions to one of mankind’s closest companions: the whipworm.
This revelation into human kindness comes from Denmark, where researchers from Copenhagen conducted a genetic analysis of ancient preserved whipworm eggs found in old Viking and Norse settlements, some of which date back over 2,000 years. In normal conditions genetic material wouldn’t last very long, but these were Viking whipworms eggs with tiny little horned helmets, so the DNA within has remained unchanged. Or it may be the tough chitinous exterior of the eggs protecting the DNA from degrading, combined with their preservation in moist soil.
Once they had their Viking whipworm DNA, the researchers compared it with whipworm DNA from all over the world, tracing its history as it followed mankind from Africa. And it’s been a while: We brought whipworms with us during our initial migration into Asia and Europe over 50,000 years ago. When the Bering land bridge opened up and humanity moved into the Americas, the worms came as well.
This is all possible because the whipworm goes about its parasitic business quietly and cleverly. It mostly sits harmlessly in our digestive systems, producing thousands of eggs a day that get expelled through poop and picked up by another host (human or otherwise); whipworms only cause disease in those with compromised immune systems.
The researchers noted that their study, the first complete genetic analysis of the whipworm, could help combat the parasite, which to this day infects hundred of millions who don’t have access to modern medicine or sanitary conditions. Hopefully, though, the days of free rides will soon be over for the whipworm. After all, if we have to pay hundreds or thousands of dollars to visit other countries, it’s only fair that our parasites do as well.
From zero to vasectomy in 6.7 seconds
There’s an old saying that you’ve probably heard: When life gives you lemons, make lemonade. It’s meant to encourage optimism in the face of adversity. Then there’s the new saying we just made up: When life gives you a power outage, plug your surgical instruments into an electric pickup.
That’s what Dr. Christopher Yang did, and now we’re making the urologist from Austin, Tex., famous by sharing his surgical/electrical adventure with all 17 of LOTME’s regular readers. That’s some serious lemonade.
Dr. Yang’s tale begins when the electricity went out at his clinic, seemingly forcing him to cancel or reschedule several surgical procedures. Not so fast. Dr. Yang happens to own a Rivian R1T, an electric pickup truck that has four power outlets. A staff member suggested plugging the surgical instruments into the truck and, surprisingly, one of the day’s patients agreed to go ahead with his vasectomy.
“We were fortunate that my normal parking spot is close enough to a patient room to run an extension cord,” Dr. Yang said on TheDrive.com. That extension cord was attached to an electrocautery device, with a handheld device available as backup, and “after we were done, I told his family. We all had a good laugh together too,” Dr. Yang told radio station WGLT in Normal, Ill.
To us, anyway, this opens up all sorts of alternative energy possibilities. Can a windmill power a liposuction? Is a gerbil running in a wheel enough to do a colonoscopy? How many potatoes do you need to keep an EHR going?
Learning through random acts of not-exactly noisiness
First things first. Transcranial random noise stimulation (tRNS) is not really noise in the auditory sense of the word. For some people with learning disabilities, though, it can actually be very helpful. The technology, which uses electrodes attached to the head so a weak current can pass through specific parts of the brain, may help those with learning disabilities, perhaps even those with brain injuries and visual deficits, learn, said Dr. Onno van der Groen of Edith Cowan University in Perth, Australia.
“When you add this type of stimulation during learning, you get better performance, faster learning and better attention afterwards as well,” he said in a statement from the university.
The researchers say that tRNS can allow the brain to form new connections and pathways, which in turn help a person learn more effectively. “If you do 10 sessions of a visual perception task with the tRNS and then come back and do it again without it, you’ll find you perform better than the control group who hasn’t used it,” Dr. van der Groen noted.
Can this also work for the average person? It’s possible, but tRNS didn’t seem to improve the math skills of a top-level mathematician who underwent the process, according to a case study that Dr. van der Groen mentioned.
This line of work is still pretty new, though, so researchers don’t have all the answers yet. As always, we’re rooting for you, science!
Commentary: Better Migraine Outcomes Measures, September 2022
The theme of this month's commentary is alternative outcomes measures for future migraine studies. The traditional outcomes measures, such as headache frequency measured in headache days, have long been considered gold standards when evaluating the efficacy of preventive interventions. When headache conditions are complicated by interictal pain or other symptoms, or when medication overuse adds a higher frequency or greater severity, those traditional measures are somewhat less exact and specific. Meaningful change for patients with higher frequency of attacks, near-continuous pain, or other migraine symptoms is quite different from that for those without these complications.
Ailani and colleagues reviewed post hoc data from the CONQUER trial, a prior study evaluating the safety and efficacy of galcanezumab vs placebo in patients who had previously not benefited from two to four categories of migraine preventive medication. This refractory population was initially noted to have 4.1 fewer headache days per month than patients taking placebo, but the authors now attempted to review these data with a focus on a different measure: total pain burden (TPB). They defined daily TPB as a single composite measure assessing the frequency, duration, and severity of migraine, calculated by multiplying the number of hours of migraine by the maximum daily migraine pain severity score. The monthly TPB was calculated by adding the daily pain burden over the entire month. The Migraine Disability Assessment questionnaire (MIDAS) and Migraine-Specific Quality of Life Questionnaire (MSQ) scores were also included to compare migraine-related disability and quality of life.
The patients who received galcanezumab were noted to have a significantly lower TPB, both in episodic and chronic migraine. Significantly greater reductions in monthly TPB relative to placebo were observed at each individual month as well. The change from baseline TPB was also noted to be significantly improved in the galcanezumab group compared with the placebo group. The reduction in TPB was noted even when migraine-day reductions were accounted for as part of a sensitivity analysis.
Preventive trials for migraine treatment focus primarily on migraine-day reduction, and for many patients with higher-frequency migraine, this measure does not adequately account for their disease-related disability. This unique way of looking at pain as part of a bigger picture is much more significant and meaningful for this patient population. Migraine frequency is still a very important outcomes measure, but it would be wise to add TBP or another measure that looks more globally at disease-related disability, especially when investigating preventive options in patients with chronic migraine.
When considering whether an intervention is helpful, most patients and clinicians follow the headache frequency, severity, or quality-of-life factors. As most patients will readily report, not all "headache-free days" are created equal. Although most people with migraine will experience days with absolutely no headache pain or other migraine-associated symptoms, on many days they will still have some symptoms of migraine. Lee and colleagues attempted to quantify the difference between headache-free days and crystal-clear days.
Most headache studies use the frequency of headache days as a primary or secondary outcome. This study collected data on both headache days and crystal-clear days, using data from a questionnaire-based large South Korean nationwide population study that evaluated headache and sleep. The study questions were validated for migraine and aura, and included: "How many days have you had a headache during the previous 30 days?" and "How many days have you had crystal-clear days without headache during the previous 30 days?" The data were then analyzed and compared with the widespread pain index (criteria for fibromyalgia) as well as sleep duration, sleep quality, depression and anxiety scales, and an allodynia checklist.
A little over 3000 respondents completed the surveys; 1938 had experienced headache over the past year, 170 were classified as having a diagnosis of migraine, and 50 of those were diagnosed with aura as well. Out of the patients with migraine, 97% had "unclear days." This was higher than the rate of those with non-migraine headaches (91%). Nearly all people surveyed had some crystal-clear days (99.4%).
The number of crystal-clear days per 30 days was significantly lower in participants with migraine than in those with non-migraine headache. Participants with migraine also had higher frequencies of cutaneous allodynia, anxiety, and depression. The weekly average sleep duration in participants with migraine did not significantly differ from that in participants with non-migraine headaches. The widespread pain index rate was much higher in those with migraine as well.
Most patients will definitely understand the difference between crystal-clear and unclear headache days. Many of the newer outcomes studies in migraine have started focusing on the most bothersome symptom, as headache pain is far from the only significant or disabling symptom associated with migraine. This study makes clear that further outcomes changes are necessary, and that a potentially more meaningful result in migraine studies may actually be crystal-clear days rather than simply headache-free days.
Although there are more acute options available for headache treatment, medication overuse headache remains a major complicating factor for most clinicians who treat headache. When educating patients, there is always a strong emphasis on guidelines for acute medication use. Many patients struggle with knowing when to use an acute treatment and when to alternate with a different treatment, and often they will withhold treatment completely due to fear of medication overuse. The new class of calcitonin gene-related peptide (CGRP) antagonist medications has shown some potential benefit as a preventive option for both medication overuse headache and migraine.
The prospective study by Curone and colleagues enrolled 300 patients with confirmed medication overuse headache who did not undergo withdrawal of the overused acute medication. Patients who are already taking preventive medications were excluded, as were patients with diagnoses other than chronic migraine or medication overuse. Patients were given one of the three injectable CGRP antagonist medications for prevention and were followed up at 3, 6, 9, and 12 months. The primary outcome was MIDAS score as well as monthly headache days and analgesic consumption.
Out of 303 patients, 242 (80%) showed both a ≥50% reduction of monthly headache days and ≥50% reduction in analgesic intake at 3-month follow-up visit. At 9 months, 198 (65%) were still responders. Monthly analgesic intake decreased ≥50% in 268 of 303 patients (88%) at 3 months and in 241 of 303 patients (79%) at the 6-month follow-up.
For years there has been a debate regarding whether withdrawal of an overused medication is necessary for effective treatment of medication overuse headache. Many preventive treatments are less effective when medication overuse is ongoing. The CGRP class of medications does appear to be effective even with ongoing acute medication overuse. This class of medications should definitely be considered when withdrawing an overused medication is complicated, or when a patient needs to continue to take analgesic medications for another condition.
The theme of this month's commentary is alternative outcomes measures for future migraine studies. The traditional outcomes measures, such as headache frequency measured in headache days, have long been considered gold standards when evaluating the efficacy of preventive interventions. When headache conditions are complicated by interictal pain or other symptoms, or when medication overuse adds a higher frequency or greater severity, those traditional measures are somewhat less exact and specific. Meaningful change for patients with higher frequency of attacks, near-continuous pain, or other migraine symptoms is quite different from that for those without these complications.
Ailani and colleagues reviewed post hoc data from the CONQUER trial, a prior study evaluating the safety and efficacy of galcanezumab vs placebo in patients who had previously not benefited from two to four categories of migraine preventive medication. This refractory population was initially noted to have 4.1 fewer headache days per month than patients taking placebo, but the authors now attempted to review these data with a focus on a different measure: total pain burden (TPB). They defined daily TPB as a single composite measure assessing the frequency, duration, and severity of migraine, calculated by multiplying the number of hours of migraine by the maximum daily migraine pain severity score. The monthly TPB was calculated by adding the daily pain burden over the entire month. The Migraine Disability Assessment questionnaire (MIDAS) and Migraine-Specific Quality of Life Questionnaire (MSQ) scores were also included to compare migraine-related disability and quality of life.
The patients who received galcanezumab were noted to have a significantly lower TPB, both in episodic and chronic migraine. Significantly greater reductions in monthly TPB relative to placebo were observed at each individual month as well. The change from baseline TPB was also noted to be significantly improved in the galcanezumab group compared with the placebo group. The reduction in TPB was noted even when migraine-day reductions were accounted for as part of a sensitivity analysis.
Preventive trials for migraine treatment focus primarily on migraine-day reduction, and for many patients with higher-frequency migraine, this measure does not adequately account for their disease-related disability. This unique way of looking at pain as part of a bigger picture is much more significant and meaningful for this patient population. Migraine frequency is still a very important outcomes measure, but it would be wise to add TBP or another measure that looks more globally at disease-related disability, especially when investigating preventive options in patients with chronic migraine.
When considering whether an intervention is helpful, most patients and clinicians follow the headache frequency, severity, or quality-of-life factors. As most patients will readily report, not all "headache-free days" are created equal. Although most people with migraine will experience days with absolutely no headache pain or other migraine-associated symptoms, on many days they will still have some symptoms of migraine. Lee and colleagues attempted to quantify the difference between headache-free days and crystal-clear days.
Most headache studies use the frequency of headache days as a primary or secondary outcome. This study collected data on both headache days and crystal-clear days, using data from a questionnaire-based large South Korean nationwide population study that evaluated headache and sleep. The study questions were validated for migraine and aura, and included: "How many days have you had a headache during the previous 30 days?" and "How many days have you had crystal-clear days without headache during the previous 30 days?" The data were then analyzed and compared with the widespread pain index (criteria for fibromyalgia) as well as sleep duration, sleep quality, depression and anxiety scales, and an allodynia checklist.
A little over 3000 respondents completed the surveys; 1938 had experienced headache over the past year, 170 were classified as having a diagnosis of migraine, and 50 of those were diagnosed with aura as well. Out of the patients with migraine, 97% had "unclear days." This was higher than the rate of those with non-migraine headaches (91%). Nearly all people surveyed had some crystal-clear days (99.4%).
The number of crystal-clear days per 30 days was significantly lower in participants with migraine than in those with non-migraine headache. Participants with migraine also had higher frequencies of cutaneous allodynia, anxiety, and depression. The weekly average sleep duration in participants with migraine did not significantly differ from that in participants with non-migraine headaches. The widespread pain index rate was much higher in those with migraine as well.
Most patients will definitely understand the difference between crystal-clear and unclear headache days. Many of the newer outcomes studies in migraine have started focusing on the most bothersome symptom, as headache pain is far from the only significant or disabling symptom associated with migraine. This study makes clear that further outcomes changes are necessary, and that a potentially more meaningful result in migraine studies may actually be crystal-clear days rather than simply headache-free days.
Although there are more acute options available for headache treatment, medication overuse headache remains a major complicating factor for most clinicians who treat headache. When educating patients, there is always a strong emphasis on guidelines for acute medication use. Many patients struggle with knowing when to use an acute treatment and when to alternate with a different treatment, and often they will withhold treatment completely due to fear of medication overuse. The new class of calcitonin gene-related peptide (CGRP) antagonist medications has shown some potential benefit as a preventive option for both medication overuse headache and migraine.
The prospective study by Curone and colleagues enrolled 300 patients with confirmed medication overuse headache who did not undergo withdrawal of the overused acute medication. Patients who are already taking preventive medications were excluded, as were patients with diagnoses other than chronic migraine or medication overuse. Patients were given one of the three injectable CGRP antagonist medications for prevention and were followed up at 3, 6, 9, and 12 months. The primary outcome was MIDAS score as well as monthly headache days and analgesic consumption.
Out of 303 patients, 242 (80%) showed both a ≥50% reduction of monthly headache days and ≥50% reduction in analgesic intake at 3-month follow-up visit. At 9 months, 198 (65%) were still responders. Monthly analgesic intake decreased ≥50% in 268 of 303 patients (88%) at 3 months and in 241 of 303 patients (79%) at the 6-month follow-up.
For years there has been a debate regarding whether withdrawal of an overused medication is necessary for effective treatment of medication overuse headache. Many preventive treatments are less effective when medication overuse is ongoing. The CGRP class of medications does appear to be effective even with ongoing acute medication overuse. This class of medications should definitely be considered when withdrawing an overused medication is complicated, or when a patient needs to continue to take analgesic medications for another condition.
The theme of this month's commentary is alternative outcomes measures for future migraine studies. The traditional outcomes measures, such as headache frequency measured in headache days, have long been considered gold standards when evaluating the efficacy of preventive interventions. When headache conditions are complicated by interictal pain or other symptoms, or when medication overuse adds a higher frequency or greater severity, those traditional measures are somewhat less exact and specific. Meaningful change for patients with higher frequency of attacks, near-continuous pain, or other migraine symptoms is quite different from that for those without these complications.
Ailani and colleagues reviewed post hoc data from the CONQUER trial, a prior study evaluating the safety and efficacy of galcanezumab vs placebo in patients who had previously not benefited from two to four categories of migraine preventive medication. This refractory population was initially noted to have 4.1 fewer headache days per month than patients taking placebo, but the authors now attempted to review these data with a focus on a different measure: total pain burden (TPB). They defined daily TPB as a single composite measure assessing the frequency, duration, and severity of migraine, calculated by multiplying the number of hours of migraine by the maximum daily migraine pain severity score. The monthly TPB was calculated by adding the daily pain burden over the entire month. The Migraine Disability Assessment questionnaire (MIDAS) and Migraine-Specific Quality of Life Questionnaire (MSQ) scores were also included to compare migraine-related disability and quality of life.
The patients who received galcanezumab were noted to have a significantly lower TPB, both in episodic and chronic migraine. Significantly greater reductions in monthly TPB relative to placebo were observed at each individual month as well. The change from baseline TPB was also noted to be significantly improved in the galcanezumab group compared with the placebo group. The reduction in TPB was noted even when migraine-day reductions were accounted for as part of a sensitivity analysis.
Preventive trials for migraine treatment focus primarily on migraine-day reduction, and for many patients with higher-frequency migraine, this measure does not adequately account for their disease-related disability. This unique way of looking at pain as part of a bigger picture is much more significant and meaningful for this patient population. Migraine frequency is still a very important outcomes measure, but it would be wise to add TBP or another measure that looks more globally at disease-related disability, especially when investigating preventive options in patients with chronic migraine.
When considering whether an intervention is helpful, most patients and clinicians follow the headache frequency, severity, or quality-of-life factors. As most patients will readily report, not all "headache-free days" are created equal. Although most people with migraine will experience days with absolutely no headache pain or other migraine-associated symptoms, on many days they will still have some symptoms of migraine. Lee and colleagues attempted to quantify the difference between headache-free days and crystal-clear days.
Most headache studies use the frequency of headache days as a primary or secondary outcome. This study collected data on both headache days and crystal-clear days, using data from a questionnaire-based large South Korean nationwide population study that evaluated headache and sleep. The study questions were validated for migraine and aura, and included: "How many days have you had a headache during the previous 30 days?" and "How many days have you had crystal-clear days without headache during the previous 30 days?" The data were then analyzed and compared with the widespread pain index (criteria for fibromyalgia) as well as sleep duration, sleep quality, depression and anxiety scales, and an allodynia checklist.
A little over 3000 respondents completed the surveys; 1938 had experienced headache over the past year, 170 were classified as having a diagnosis of migraine, and 50 of those were diagnosed with aura as well. Out of the patients with migraine, 97% had "unclear days." This was higher than the rate of those with non-migraine headaches (91%). Nearly all people surveyed had some crystal-clear days (99.4%).
The number of crystal-clear days per 30 days was significantly lower in participants with migraine than in those with non-migraine headache. Participants with migraine also had higher frequencies of cutaneous allodynia, anxiety, and depression. The weekly average sleep duration in participants with migraine did not significantly differ from that in participants with non-migraine headaches. The widespread pain index rate was much higher in those with migraine as well.
Most patients will definitely understand the difference between crystal-clear and unclear headache days. Many of the newer outcomes studies in migraine have started focusing on the most bothersome symptom, as headache pain is far from the only significant or disabling symptom associated with migraine. This study makes clear that further outcomes changes are necessary, and that a potentially more meaningful result in migraine studies may actually be crystal-clear days rather than simply headache-free days.
Although there are more acute options available for headache treatment, medication overuse headache remains a major complicating factor for most clinicians who treat headache. When educating patients, there is always a strong emphasis on guidelines for acute medication use. Many patients struggle with knowing when to use an acute treatment and when to alternate with a different treatment, and often they will withhold treatment completely due to fear of medication overuse. The new class of calcitonin gene-related peptide (CGRP) antagonist medications has shown some potential benefit as a preventive option for both medication overuse headache and migraine.
The prospective study by Curone and colleagues enrolled 300 patients with confirmed medication overuse headache who did not undergo withdrawal of the overused acute medication. Patients who are already taking preventive medications were excluded, as were patients with diagnoses other than chronic migraine or medication overuse. Patients were given one of the three injectable CGRP antagonist medications for prevention and were followed up at 3, 6, 9, and 12 months. The primary outcome was MIDAS score as well as monthly headache days and analgesic consumption.
Out of 303 patients, 242 (80%) showed both a ≥50% reduction of monthly headache days and ≥50% reduction in analgesic intake at 3-month follow-up visit. At 9 months, 198 (65%) were still responders. Monthly analgesic intake decreased ≥50% in 268 of 303 patients (88%) at 3 months and in 241 of 303 patients (79%) at the 6-month follow-up.
For years there has been a debate regarding whether withdrawal of an overused medication is necessary for effective treatment of medication overuse headache. Many preventive treatments are less effective when medication overuse is ongoing. The CGRP class of medications does appear to be effective even with ongoing acute medication overuse. This class of medications should definitely be considered when withdrawing an overused medication is complicated, or when a patient needs to continue to take analgesic medications for another condition.
Where a child eats breakfast is important
We’ve been told for decades that a child who doesn’t start the day with a good breakfast is entering school at a serious disadvantage. The brain needs a good supply of energy to learn optimally. So the standard wisdom goes. Subsidized school breakfast programs have been built around this chestnut. But, is there solid evidence to support the notion that simply adding a morning meal to a child’s schedule will improve his or her school performance? It sounds like common sense, but is it just one of those old grandmother’s nuggets that doesn’t stand up under close scrutiny?
A recent study from Spain suggests that the relationship between breakfast and school performance is not merely related to the nutritional needs of a growing brain. Using data from nearly 4,000 Spanish children aged 4-14 collected in a 2017 national health survey, the investigators found “skipping breakfast and eating breakfast out of the home were linked to greater odds of psychosocial behavioral problems than eating breakfast at home.” And, we already know that, in general, children who misbehave in school don’t thrive academically.
There were also associations between the absence or presence of certain food groups in the morning meal with behavioral problems. But the data lacked the granularity to draw any firm conclusions – although the authors felt that what they consider a healthy Spanish diet may have had a positive influence on behavior.
The findings in this study may simply be another example of the many positive influences that have been associated with family meals and have little to do with what is actually consumed. The association may not have much to do with the family gathering together at a single Norman Rockwell sitting, a reality that I suspect seldom occurs. The apparent positive influence of breakfast may be that it reflects a family’s priorities: that food is important, that sleep is important, and that school is important – so important that scheduling the morning should focus on sending the child off well prepared. The child who is allowed to stay up to an unhealthy hour is likely to be difficult to arouse in the morning for breakfast and getting off to school.
It may be that the child’s behavior problems are so disruptive and taxing for the family that even with their best efforts, the parents can’t find the time and energy to provide a breakfast in the home.
On the other hand, the study doesn’t tell us how many children aren’t offered breakfast at home because their families simply can’t afford it. Obviously, the answer depends on the socioeconomic mix of a given community. In some localities this may represent a sizable percentage of the population.
So where does this leave us? Unfortunately, as I read through the discussion at the end of this paper I felt that the authors were leaning too much toward further research based on the potential associations between behavior and specific food groups their data suggested.
For me, the take-home message from this paper is that our existing efforts to improve academic success with food offered in school should also include strategies that promote eating breakfast at home. For example, the backpack take-home food distribution programs that seem to have been effective could include breakfast-targeted items packaged in a way that encourage families to provide breakfast at home.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
We’ve been told for decades that a child who doesn’t start the day with a good breakfast is entering school at a serious disadvantage. The brain needs a good supply of energy to learn optimally. So the standard wisdom goes. Subsidized school breakfast programs have been built around this chestnut. But, is there solid evidence to support the notion that simply adding a morning meal to a child’s schedule will improve his or her school performance? It sounds like common sense, but is it just one of those old grandmother’s nuggets that doesn’t stand up under close scrutiny?
A recent study from Spain suggests that the relationship between breakfast and school performance is not merely related to the nutritional needs of a growing brain. Using data from nearly 4,000 Spanish children aged 4-14 collected in a 2017 national health survey, the investigators found “skipping breakfast and eating breakfast out of the home were linked to greater odds of psychosocial behavioral problems than eating breakfast at home.” And, we already know that, in general, children who misbehave in school don’t thrive academically.
There were also associations between the absence or presence of certain food groups in the morning meal with behavioral problems. But the data lacked the granularity to draw any firm conclusions – although the authors felt that what they consider a healthy Spanish diet may have had a positive influence on behavior.
The findings in this study may simply be another example of the many positive influences that have been associated with family meals and have little to do with what is actually consumed. The association may not have much to do with the family gathering together at a single Norman Rockwell sitting, a reality that I suspect seldom occurs. The apparent positive influence of breakfast may be that it reflects a family’s priorities: that food is important, that sleep is important, and that school is important – so important that scheduling the morning should focus on sending the child off well prepared. The child who is allowed to stay up to an unhealthy hour is likely to be difficult to arouse in the morning for breakfast and getting off to school.
It may be that the child’s behavior problems are so disruptive and taxing for the family that even with their best efforts, the parents can’t find the time and energy to provide a breakfast in the home.
On the other hand, the study doesn’t tell us how many children aren’t offered breakfast at home because their families simply can’t afford it. Obviously, the answer depends on the socioeconomic mix of a given community. In some localities this may represent a sizable percentage of the population.
So where does this leave us? Unfortunately, as I read through the discussion at the end of this paper I felt that the authors were leaning too much toward further research based on the potential associations between behavior and specific food groups their data suggested.
For me, the take-home message from this paper is that our existing efforts to improve academic success with food offered in school should also include strategies that promote eating breakfast at home. For example, the backpack take-home food distribution programs that seem to have been effective could include breakfast-targeted items packaged in a way that encourage families to provide breakfast at home.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
We’ve been told for decades that a child who doesn’t start the day with a good breakfast is entering school at a serious disadvantage. The brain needs a good supply of energy to learn optimally. So the standard wisdom goes. Subsidized school breakfast programs have been built around this chestnut. But, is there solid evidence to support the notion that simply adding a morning meal to a child’s schedule will improve his or her school performance? It sounds like common sense, but is it just one of those old grandmother’s nuggets that doesn’t stand up under close scrutiny?
A recent study from Spain suggests that the relationship between breakfast and school performance is not merely related to the nutritional needs of a growing brain. Using data from nearly 4,000 Spanish children aged 4-14 collected in a 2017 national health survey, the investigators found “skipping breakfast and eating breakfast out of the home were linked to greater odds of psychosocial behavioral problems than eating breakfast at home.” And, we already know that, in general, children who misbehave in school don’t thrive academically.
There were also associations between the absence or presence of certain food groups in the morning meal with behavioral problems. But the data lacked the granularity to draw any firm conclusions – although the authors felt that what they consider a healthy Spanish diet may have had a positive influence on behavior.
The findings in this study may simply be another example of the many positive influences that have been associated with family meals and have little to do with what is actually consumed. The association may not have much to do with the family gathering together at a single Norman Rockwell sitting, a reality that I suspect seldom occurs. The apparent positive influence of breakfast may be that it reflects a family’s priorities: that food is important, that sleep is important, and that school is important – so important that scheduling the morning should focus on sending the child off well prepared. The child who is allowed to stay up to an unhealthy hour is likely to be difficult to arouse in the morning for breakfast and getting off to school.
It may be that the child’s behavior problems are so disruptive and taxing for the family that even with their best efforts, the parents can’t find the time and energy to provide a breakfast in the home.
On the other hand, the study doesn’t tell us how many children aren’t offered breakfast at home because their families simply can’t afford it. Obviously, the answer depends on the socioeconomic mix of a given community. In some localities this may represent a sizable percentage of the population.
So where does this leave us? Unfortunately, as I read through the discussion at the end of this paper I felt that the authors were leaning too much toward further research based on the potential associations between behavior and specific food groups their data suggested.
For me, the take-home message from this paper is that our existing efforts to improve academic success with food offered in school should also include strategies that promote eating breakfast at home. For example, the backpack take-home food distribution programs that seem to have been effective could include breakfast-targeted items packaged in a way that encourage families to provide breakfast at home.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
Pediatricians urge flu vaccine for children
Attention parents: The nation’s leading pediatric medical society is urging you to make sure your children get a flu shot this fall to prevent and control the spread of the illness.
The American Academy of Pediatrics recently called on parents and caregivers to seek flu vaccines for their children as soon as they are available in the fall. The group is encouraging parents to catch up on all other vaccines for their children, too.
“As a pediatrician and a parent, I consider the flu vaccine as critical for all family members,” Kristina A. Bryant, MD, said in a statement about the academy’s recommendations. “We should not underestimate the flu, especially when other respiratory viruses like COVID-19 are circulating within our communities. Besides making your child miserable and wreaking havoc on your family’s routine, influenza can also be serious and even deadly in children.”
Only 55% of children aged 6 months to 17 years had been vaccinated against influenza as of early April – down 2% from the previous April – and coverage levels were 8.1% lower for Black children compared with non-Hispanic White children, according to the CDC. In the 2019-2020 flu season, 188 children in the United States died of the infection, equaling the high mark for deaths set in the 2017-2018 season, the agency reported.
American Academy of Pediatrics guidelines recommend children aged 6 months and older be vaccinated with the flu vaccine every year. Depending on the child’s age and health, they may receive either a shot, which has an inactive version of the flu virus, or the nasal spray, which has a weakened form of the virus. The academy has more information about the different vaccines.
Children aged 6-8 months who are getting flu vaccines for the first time should receive two doses at least 4 weeks apart. Pregnant women can get the flu vaccine any time in their pregnancy. Influenza vaccines are safe for developing fetuses, according to the academy.
The group stressed the importance of flu vaccines for high-risk and medically vulnerable children and acknowledged the need to end barriers to immunizations for all people, regardless of income or insurance coverage. In 2020, an estimated 16.1% of children in the United States were living in poverty, up from 14.4% in 2019, according to the U.S. Census Bureau.
A version of this article first appeared on WebMD.com.
Attention parents: The nation’s leading pediatric medical society is urging you to make sure your children get a flu shot this fall to prevent and control the spread of the illness.
The American Academy of Pediatrics recently called on parents and caregivers to seek flu vaccines for their children as soon as they are available in the fall. The group is encouraging parents to catch up on all other vaccines for their children, too.
“As a pediatrician and a parent, I consider the flu vaccine as critical for all family members,” Kristina A. Bryant, MD, said in a statement about the academy’s recommendations. “We should not underestimate the flu, especially when other respiratory viruses like COVID-19 are circulating within our communities. Besides making your child miserable and wreaking havoc on your family’s routine, influenza can also be serious and even deadly in children.”
Only 55% of children aged 6 months to 17 years had been vaccinated against influenza as of early April – down 2% from the previous April – and coverage levels were 8.1% lower for Black children compared with non-Hispanic White children, according to the CDC. In the 2019-2020 flu season, 188 children in the United States died of the infection, equaling the high mark for deaths set in the 2017-2018 season, the agency reported.
American Academy of Pediatrics guidelines recommend children aged 6 months and older be vaccinated with the flu vaccine every year. Depending on the child’s age and health, they may receive either a shot, which has an inactive version of the flu virus, or the nasal spray, which has a weakened form of the virus. The academy has more information about the different vaccines.
Children aged 6-8 months who are getting flu vaccines for the first time should receive two doses at least 4 weeks apart. Pregnant women can get the flu vaccine any time in their pregnancy. Influenza vaccines are safe for developing fetuses, according to the academy.
The group stressed the importance of flu vaccines for high-risk and medically vulnerable children and acknowledged the need to end barriers to immunizations for all people, regardless of income or insurance coverage. In 2020, an estimated 16.1% of children in the United States were living in poverty, up from 14.4% in 2019, according to the U.S. Census Bureau.
A version of this article first appeared on WebMD.com.
Attention parents: The nation’s leading pediatric medical society is urging you to make sure your children get a flu shot this fall to prevent and control the spread of the illness.
The American Academy of Pediatrics recently called on parents and caregivers to seek flu vaccines for their children as soon as they are available in the fall. The group is encouraging parents to catch up on all other vaccines for their children, too.
“As a pediatrician and a parent, I consider the flu vaccine as critical for all family members,” Kristina A. Bryant, MD, said in a statement about the academy’s recommendations. “We should not underestimate the flu, especially when other respiratory viruses like COVID-19 are circulating within our communities. Besides making your child miserable and wreaking havoc on your family’s routine, influenza can also be serious and even deadly in children.”
Only 55% of children aged 6 months to 17 years had been vaccinated against influenza as of early April – down 2% from the previous April – and coverage levels were 8.1% lower for Black children compared with non-Hispanic White children, according to the CDC. In the 2019-2020 flu season, 188 children in the United States died of the infection, equaling the high mark for deaths set in the 2017-2018 season, the agency reported.
American Academy of Pediatrics guidelines recommend children aged 6 months and older be vaccinated with the flu vaccine every year. Depending on the child’s age and health, they may receive either a shot, which has an inactive version of the flu virus, or the nasal spray, which has a weakened form of the virus. The academy has more information about the different vaccines.
Children aged 6-8 months who are getting flu vaccines for the first time should receive two doses at least 4 weeks apart. Pregnant women can get the flu vaccine any time in their pregnancy. Influenza vaccines are safe for developing fetuses, according to the academy.
The group stressed the importance of flu vaccines for high-risk and medically vulnerable children and acknowledged the need to end barriers to immunizations for all people, regardless of income or insurance coverage. In 2020, an estimated 16.1% of children in the United States were living in poverty, up from 14.4% in 2019, according to the U.S. Census Bureau.
A version of this article first appeared on WebMD.com.
Punked By the Punctum: Domestically Acquired Cutaneous Myiasis
To the Editor:
Cutaneous myiasis is a skin infestation with dipterous larvae that feed on the host’s tissue and cause a wide range of manifestations depending on the location of infestation. Cutaneous myiasis, which includes furuncular, wound, and migratory types, is the most common clinical form of this condition.1 It is endemic to tropical and subtropical areas and is not common in the United States, thus it can pose a diagnostic challenge when presenting in nonendemic areas. We present the case of a woman from Michigan who acquired furuncular myiasis without travel history to a tropical or subtropical locale.
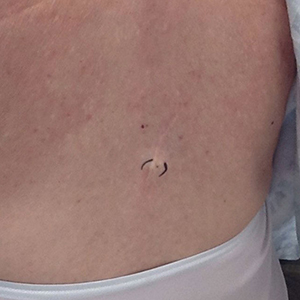
A 72-year-old woman presented to our clinic with a chief concern of a burning, pruritic, migratory skin lesion on the left arm of approximately 1 week’s duration. She had a medical history of squamous cell carcinoma, keratoacanthoma, and multiple tick bites. She reported that the lesion started on the distal aspect of the left arm as an eraser-sized, perfectly round, raised bruise with a dark pepperlike bump in the center. The lesion then spread proximally over the course of 1 week, creating 3 more identical lesions. As one lesion resolved, a new lesion appeared approximately 2 to 4 cm proximal to the preceding lesion. The patient had traveled to England, Scotland, and Ireland 2 months prior but otherwise denied leaving the state of Michigan. She reported frequent exposure to gardens, meadows, and wetlands in search of milkweed and monarch butterfly larvae that she raises in northeast Michigan. She denied any recent illness or associated systemic symptoms. Initial evaluation by a primary care physician resulted in a diagnosis of a furuncle or tick bite; she completed a 10-day course of amoxicillin and a methylprednisolone dose pack without improvement.
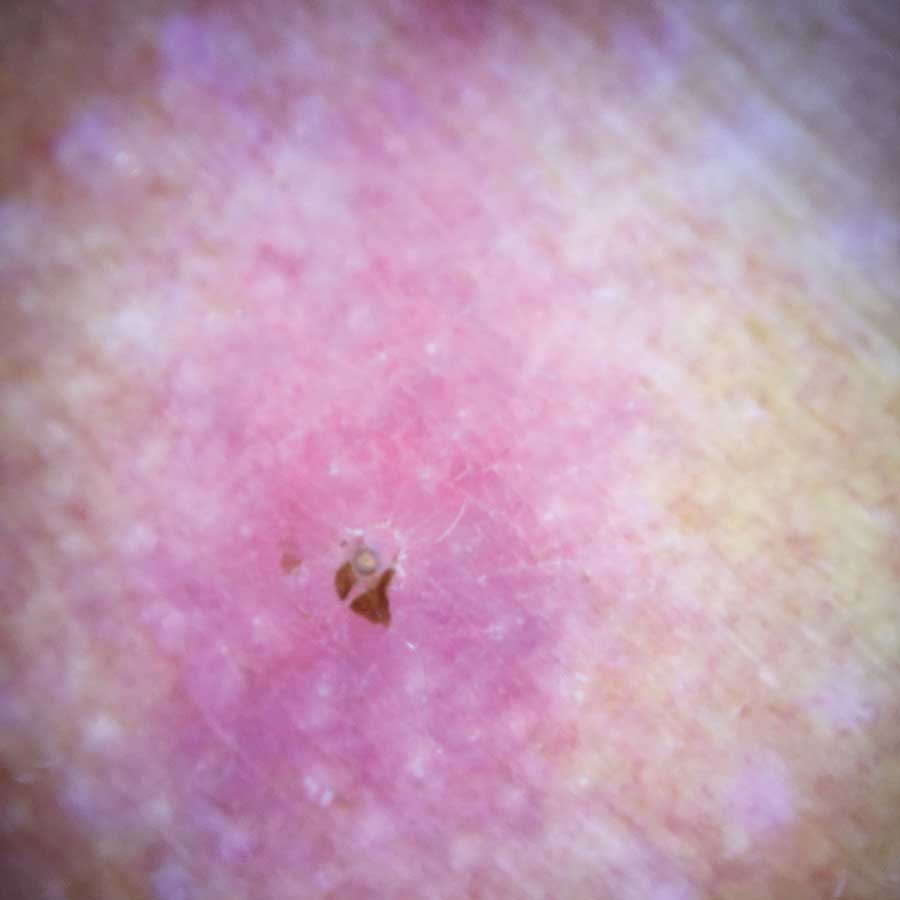
Physical examination revealed a 1-cm, firm, violaceous nodule with a small distinct central punctum and surrounding erythema on the proximal aspect of the left arm. Dermoscopy revealed a pulsating motion and expulsion of serosanguineous fluid from the central punctum (Figure 1). Further inspection of the patient’s left arm exposed several noninflammatory puncta distal to the primary lesion spaced at 2- to 4-cm intervals.
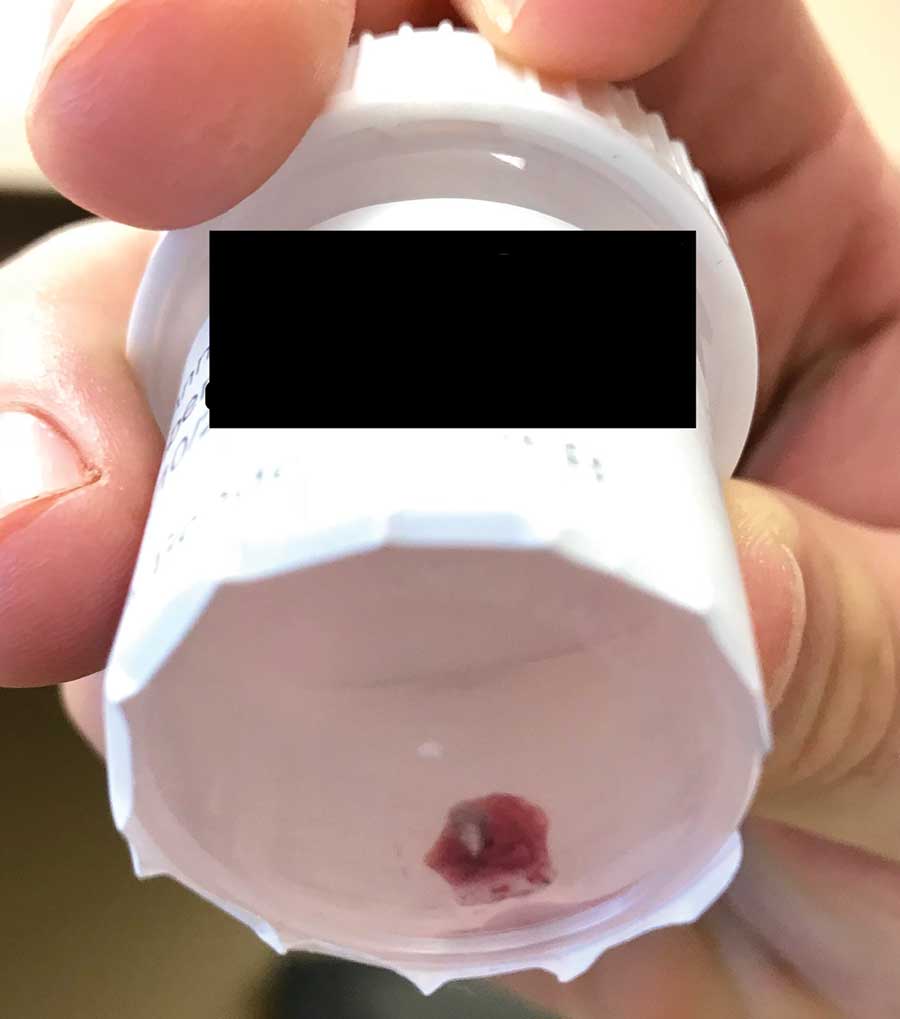
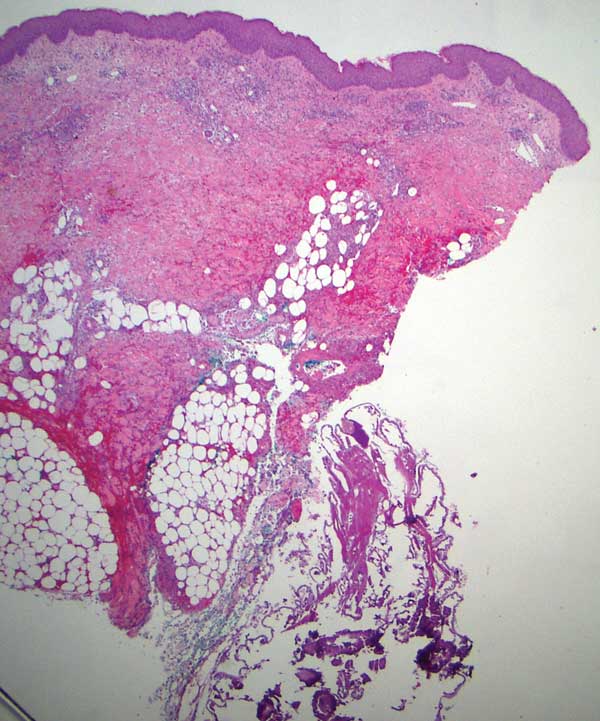
Gross examination of a 6-mm punch biopsy from the primary inflammatory nodule uncovered a small, motile, gray-white larval organism in the inferior portion of the specimen (Figure 2). Histopathology revealed superficial and deep eosinophil-rich inflammation, fibrosis, and hemorrhage. There was a complex wedge-shaped organism with extensive internal muscle bounded by a thin cuticle bearing rows of chitinous hooklets located at one side within the deep dermis (Figure 3). The findings were consistent with a diagnosis of cutaneous myiasis. No further treatment was required, as the organism was completely excised with the biopsy.
The most common causative agents of furuncular myiasis obtained from travelers returning from Mexico and Central and South America are Dermatobia hominis and Cordylobia anthropophaga. Cases of furuncular myiasis acquired in the United States without recent foreign travel are rare. Most of these cases are caused by larvae of the Cuterebra species (also known as the rabbit botfly or rodent botfly).2 In a 2003 literature review by Safdar et al3 on 56 cases of furuncular myiasis in the United States, the median age of patients was 14 years, 87% of cases occurred in August and September, and most involved exposure in rural or suburban settings; 53% of cases presented in the northeastern United States.
Furuncular myiasis occurs when the organism’s ova are deposited on the skin of a human host by the parent organism or a mosquito vector. The heat of the skin causes the eggs to hatch and the dipteran larvae must penetrate the skin within 20 days.1 Signs of infection typically are seen 6 to 10 days after infestation.3 The larvae then feed on human tissue and burrow deep in the dermis, forming an erythematous furunculoid nodule containing one or multiple maggots. After 5 to 10 weeks, the adult larvae drop to the ground, where they mature into adult organisms in the soil.1
The most reported symptoms of furuncular myiasis include pruritus, pain, and movement sensation, typically occurring suddenly at night.4 The most common presentation is a furunclelike lesion that exudes serosanguineous or purulent fluid,1 but there have been reports of vesicular, bullous, pustular, erosive, ecchymotic, and ulcerative lesions.5Dermatobia hominis usually presents on an exposed site, such as the scalp, face, and extremities. It may present with paroxysmal episodes of lancinating pain. Over time, the lesion usually heals without a scar, though hyperpigmentation and scarring can occur. The most reported complication is secondary bacterial infection.4 Local lymphadenopathy or systemic symptoms should raise concern for infection. Staphylococcus aureus and group B Streptococcus have been cultured from lesions.6,7
The differential diagnosis for myiasis should include furuncle, insect bite, insect prurigo, pyoderma, inflamed cyst, and tungiasis. Myiasis also can present similarly to severe soft tissue infections or cellulitis. If located on the breasts, it can be mistaken for periductal mastitis, a benign mass with microcalcification, or inflammatory carcinoma. Lastly, due to pain, erythema, pruritus, small vesicles, and crusting, it may be confused for herpes simplex virus.1
Furuncular myiasis typically is diagnosed based on clinical presentation, especially in endemic regions. In nonendemic areas, the patient’s history may reveal recent travel or predisposition to myiasis. In cases where there is uncertainty, dermoscopy may be used to identify the maggot in the lesion, or ultrasonography can be used to confirm myiasis through the detection of larval movement.8 Dermoscopy will reveal a furuncular lesion with a central opening surrounded by dilated blood vessels and a yellowish structure with black barblike spines.9 Within the dermis is a fibrous cystic sinus tract containing the dipteran larva. Laboratory studies typically are unremarkable. In chronic cases, a complete blood cell count and other laboratory tests may show systemic inflammation, peripheral eosinophilia, and elevated IgE.10 Biopsies of furuncular myiasis are not necessary for diagnosis. Histopathology reveals an ulcerated epidermis with or without hyperkeratosis and an inflammatory infiltrate composed of lymphocytes and neutrophils with eosinophils, fibroblasts, histiocytes, basophils, mast cells, plasma cells, and Langerhans cells within the dermis and subcutis.11
There are various approaches to treating furuncular myiasis, with the goal of complete removal of the larva and prevention of secondary infection. One treatment option is to apply a toxic substance to the larva, effectively killing it. Another approach is to force the larva to emerge via localized hypoxia, which can be done by occluding the punctum of the lesion for at least 24 hours. A complication of this method is suffocation of the larva without migration, leading to incomplete extraction and secondary infection.1 A third method is to surgically remove the larva, which allows for debridement of necrotic tissue surrounding the lesion if present.12 Ultrasonography also can be used therapeutically to aid in the removal of the larvae. The last method is to inject lidocaine into the base of the lesion, forcing the larva out of the punctum via fluid pressure.13 Oral treatments such as ivermectin are not recommended because they can result in the death of larvae within the lesion, leading to an inflammatory response.8
Furuncular myiasis is a form of cutaneous larvae infestation not commonly seen in individuals who do not live or travel in endemic, tropical, and subtropical regions. Diagnosis is based on clinical presentation, with imaging and laboratory studies available to supplement in unclear or atypical manifestations. Treatment involves complete removal of the larva, typically through forced evacuation via hypoxia or through surgical removal. Most cases resolve without notable scarring or other sequelae; however, in those who do have complications, the most common is secondary bacterial infection. Our patient’s absence of notable travel history and frequent environmental exposure in Michigan led us to believe the organism was from a domestic source. Our case underlines the importance of a thorough history and clinical examination of furuncular lesions including the use of dermoscopy to yield an appropriate diagnosis and treatment plan.
- Francesconi F, Lupi O. Myiasis. Clin Microbiol Rev. 2012;25:79-105. doi:10.1128/CMR.00010-11
- Schiff TA. Furuncular cutaneous myiasis caused by Cuterebra larva. J Am Acad Dermatol 1993;28:261-263.
- Safdar N, Young DK, Andes D. Autochthonous furuncular myiasis in the United States: case report and literature review. Clin Infect Dis. 2003;26:73-80.
- Mahal JJ, Sperling JD. Furuncular myiasis from Dermatobia hominus: a case of human botfly infestation. J Emerg Med. 2012;43:618-621.
- Francesconi F, Lupi O. Myiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. Elsevier; 2006:232-239.
- Gordon PM, Hepburn NC, Williams AE, et al. Cutaneous myiasis due to Dermatobia hominis: a report of six cases. Br J Dermatol. 1995;132:811-814.
- Hubler WR Jr, Rudolph AH, Dougherty EF. Dermal myiasis. Arch Dermatol. 1974;110:109-110.
- Quintanilla-Cedillo MR, León-Ureña H, Contreras-Ruiz J, et al. The value of Doppler ultrasound in diagnosis in 25 cases of furunculoid myiasis. Int J Dermatol. 2005;44:34-37.
- Bakos RM, Bakos L. Dermoscopic diagnosis of furuncular myiasis. Arch Dermatol. 2007;143:123-124.
- Varani S, Tassinari D, Elleri D, et al. A case of furuncular myiasis associated with systemic inflammation. Parasitol Int. 2007;56:330-333.
- Grogan TM, Payne CM, Spier C, et al. Cutaneous myiasis. immunohistologic and ultrastructural morphometric features of a human botfly lesion. Am J Dermatopathol. 1987;9:232-239.
- Krajewski A, Allen B, Hoss D, et al. Cutaneous myiasis. J Plast Reconstr Aesthet Surg. 2009;62:383-386.
- Lebwohl MG, Heymann WR, Berth-Jones J, et al. Myiasis: Treatment of Skin Diseases. Comprehensive Therapeutic Strategies. 2nd ed. Elsevier-Mosby; 2006.
To the Editor:
Cutaneous myiasis is a skin infestation with dipterous larvae that feed on the host’s tissue and cause a wide range of manifestations depending on the location of infestation. Cutaneous myiasis, which includes furuncular, wound, and migratory types, is the most common clinical form of this condition.1 It is endemic to tropical and subtropical areas and is not common in the United States, thus it can pose a diagnostic challenge when presenting in nonendemic areas. We present the case of a woman from Michigan who acquired furuncular myiasis without travel history to a tropical or subtropical locale.
A 72-year-old woman presented to our clinic with a chief concern of a burning, pruritic, migratory skin lesion on the left arm of approximately 1 week’s duration. She had a medical history of squamous cell carcinoma, keratoacanthoma, and multiple tick bites. She reported that the lesion started on the distal aspect of the left arm as an eraser-sized, perfectly round, raised bruise with a dark pepperlike bump in the center. The lesion then spread proximally over the course of 1 week, creating 3 more identical lesions. As one lesion resolved, a new lesion appeared approximately 2 to 4 cm proximal to the preceding lesion. The patient had traveled to England, Scotland, and Ireland 2 months prior but otherwise denied leaving the state of Michigan. She reported frequent exposure to gardens, meadows, and wetlands in search of milkweed and monarch butterfly larvae that she raises in northeast Michigan. She denied any recent illness or associated systemic symptoms. Initial evaluation by a primary care physician resulted in a diagnosis of a furuncle or tick bite; she completed a 10-day course of amoxicillin and a methylprednisolone dose pack without improvement.
Physical examination revealed a 1-cm, firm, violaceous nodule with a small distinct central punctum and surrounding erythema on the proximal aspect of the left arm. Dermoscopy revealed a pulsating motion and expulsion of serosanguineous fluid from the central punctum (Figure 1). Further inspection of the patient’s left arm exposed several noninflammatory puncta distal to the primary lesion spaced at 2- to 4-cm intervals.

Gross examination of a 6-mm punch biopsy from the primary inflammatory nodule uncovered a small, motile, gray-white larval organism in the inferior portion of the specimen (Figure 2). Histopathology revealed superficial and deep eosinophil-rich inflammation, fibrosis, and hemorrhage. There was a complex wedge-shaped organism with extensive internal muscle bounded by a thin cuticle bearing rows of chitinous hooklets located at one side within the deep dermis (Figure 3). The findings were consistent with a diagnosis of cutaneous myiasis. No further treatment was required, as the organism was completely excised with the biopsy.

The most common causative agents of furuncular myiasis obtained from travelers returning from Mexico and Central and South America are Dermatobia hominis and Cordylobia anthropophaga. Cases of furuncular myiasis acquired in the United States without recent foreign travel are rare. Most of these cases are caused by larvae of the Cuterebra species (also known as the rabbit botfly or rodent botfly).2 In a 2003 literature review by Safdar et al3 on 56 cases of furuncular myiasis in the United States, the median age of patients was 14 years, 87% of cases occurred in August and September, and most involved exposure in rural or suburban settings; 53% of cases presented in the northeastern United States.

Furuncular myiasis occurs when the organism’s ova are deposited on the skin of a human host by the parent organism or a mosquito vector. The heat of the skin causes the eggs to hatch and the dipteran larvae must penetrate the skin within 20 days.1 Signs of infection typically are seen 6 to 10 days after infestation.3 The larvae then feed on human tissue and burrow deep in the dermis, forming an erythematous furunculoid nodule containing one or multiple maggots. After 5 to 10 weeks, the adult larvae drop to the ground, where they mature into adult organisms in the soil.1
The most reported symptoms of furuncular myiasis include pruritus, pain, and movement sensation, typically occurring suddenly at night.4 The most common presentation is a furunclelike lesion that exudes serosanguineous or purulent fluid,1 but there have been reports of vesicular, bullous, pustular, erosive, ecchymotic, and ulcerative lesions.5Dermatobia hominis usually presents on an exposed site, such as the scalp, face, and extremities. It may present with paroxysmal episodes of lancinating pain. Over time, the lesion usually heals without a scar, though hyperpigmentation and scarring can occur. The most reported complication is secondary bacterial infection.4 Local lymphadenopathy or systemic symptoms should raise concern for infection. Staphylococcus aureus and group B Streptococcus have been cultured from lesions.6,7
The differential diagnosis for myiasis should include furuncle, insect bite, insect prurigo, pyoderma, inflamed cyst, and tungiasis. Myiasis also can present similarly to severe soft tissue infections or cellulitis. If located on the breasts, it can be mistaken for periductal mastitis, a benign mass with microcalcification, or inflammatory carcinoma. Lastly, due to pain, erythema, pruritus, small vesicles, and crusting, it may be confused for herpes simplex virus.1
Furuncular myiasis typically is diagnosed based on clinical presentation, especially in endemic regions. In nonendemic areas, the patient’s history may reveal recent travel or predisposition to myiasis. In cases where there is uncertainty, dermoscopy may be used to identify the maggot in the lesion, or ultrasonography can be used to confirm myiasis through the detection of larval movement.8 Dermoscopy will reveal a furuncular lesion with a central opening surrounded by dilated blood vessels and a yellowish structure with black barblike spines.9 Within the dermis is a fibrous cystic sinus tract containing the dipteran larva. Laboratory studies typically are unremarkable. In chronic cases, a complete blood cell count and other laboratory tests may show systemic inflammation, peripheral eosinophilia, and elevated IgE.10 Biopsies of furuncular myiasis are not necessary for diagnosis. Histopathology reveals an ulcerated epidermis with or without hyperkeratosis and an inflammatory infiltrate composed of lymphocytes and neutrophils with eosinophils, fibroblasts, histiocytes, basophils, mast cells, plasma cells, and Langerhans cells within the dermis and subcutis.11
There are various approaches to treating furuncular myiasis, with the goal of complete removal of the larva and prevention of secondary infection. One treatment option is to apply a toxic substance to the larva, effectively killing it. Another approach is to force the larva to emerge via localized hypoxia, which can be done by occluding the punctum of the lesion for at least 24 hours. A complication of this method is suffocation of the larva without migration, leading to incomplete extraction and secondary infection.1 A third method is to surgically remove the larva, which allows for debridement of necrotic tissue surrounding the lesion if present.12 Ultrasonography also can be used therapeutically to aid in the removal of the larvae. The last method is to inject lidocaine into the base of the lesion, forcing the larva out of the punctum via fluid pressure.13 Oral treatments such as ivermectin are not recommended because they can result in the death of larvae within the lesion, leading to an inflammatory response.8
Furuncular myiasis is a form of cutaneous larvae infestation not commonly seen in individuals who do not live or travel in endemic, tropical, and subtropical regions. Diagnosis is based on clinical presentation, with imaging and laboratory studies available to supplement in unclear or atypical manifestations. Treatment involves complete removal of the larva, typically through forced evacuation via hypoxia or through surgical removal. Most cases resolve without notable scarring or other sequelae; however, in those who do have complications, the most common is secondary bacterial infection. Our patient’s absence of notable travel history and frequent environmental exposure in Michigan led us to believe the organism was from a domestic source. Our case underlines the importance of a thorough history and clinical examination of furuncular lesions including the use of dermoscopy to yield an appropriate diagnosis and treatment plan.
To the Editor:
Cutaneous myiasis is a skin infestation with dipterous larvae that feed on the host’s tissue and cause a wide range of manifestations depending on the location of infestation. Cutaneous myiasis, which includes furuncular, wound, and migratory types, is the most common clinical form of this condition.1 It is endemic to tropical and subtropical areas and is not common in the United States, thus it can pose a diagnostic challenge when presenting in nonendemic areas. We present the case of a woman from Michigan who acquired furuncular myiasis without travel history to a tropical or subtropical locale.
A 72-year-old woman presented to our clinic with a chief concern of a burning, pruritic, migratory skin lesion on the left arm of approximately 1 week’s duration. She had a medical history of squamous cell carcinoma, keratoacanthoma, and multiple tick bites. She reported that the lesion started on the distal aspect of the left arm as an eraser-sized, perfectly round, raised bruise with a dark pepperlike bump in the center. The lesion then spread proximally over the course of 1 week, creating 3 more identical lesions. As one lesion resolved, a new lesion appeared approximately 2 to 4 cm proximal to the preceding lesion. The patient had traveled to England, Scotland, and Ireland 2 months prior but otherwise denied leaving the state of Michigan. She reported frequent exposure to gardens, meadows, and wetlands in search of milkweed and monarch butterfly larvae that she raises in northeast Michigan. She denied any recent illness or associated systemic symptoms. Initial evaluation by a primary care physician resulted in a diagnosis of a furuncle or tick bite; she completed a 10-day course of amoxicillin and a methylprednisolone dose pack without improvement.
Physical examination revealed a 1-cm, firm, violaceous nodule with a small distinct central punctum and surrounding erythema on the proximal aspect of the left arm. Dermoscopy revealed a pulsating motion and expulsion of serosanguineous fluid from the central punctum (Figure 1). Further inspection of the patient’s left arm exposed several noninflammatory puncta distal to the primary lesion spaced at 2- to 4-cm intervals.

Gross examination of a 6-mm punch biopsy from the primary inflammatory nodule uncovered a small, motile, gray-white larval organism in the inferior portion of the specimen (Figure 2). Histopathology revealed superficial and deep eosinophil-rich inflammation, fibrosis, and hemorrhage. There was a complex wedge-shaped organism with extensive internal muscle bounded by a thin cuticle bearing rows of chitinous hooklets located at one side within the deep dermis (Figure 3). The findings were consistent with a diagnosis of cutaneous myiasis. No further treatment was required, as the organism was completely excised with the biopsy.

The most common causative agents of furuncular myiasis obtained from travelers returning from Mexico and Central and South America are Dermatobia hominis and Cordylobia anthropophaga. Cases of furuncular myiasis acquired in the United States without recent foreign travel are rare. Most of these cases are caused by larvae of the Cuterebra species (also known as the rabbit botfly or rodent botfly).2 In a 2003 literature review by Safdar et al3 on 56 cases of furuncular myiasis in the United States, the median age of patients was 14 years, 87% of cases occurred in August and September, and most involved exposure in rural or suburban settings; 53% of cases presented in the northeastern United States.

Furuncular myiasis occurs when the organism’s ova are deposited on the skin of a human host by the parent organism or a mosquito vector. The heat of the skin causes the eggs to hatch and the dipteran larvae must penetrate the skin within 20 days.1 Signs of infection typically are seen 6 to 10 days after infestation.3 The larvae then feed on human tissue and burrow deep in the dermis, forming an erythematous furunculoid nodule containing one or multiple maggots. After 5 to 10 weeks, the adult larvae drop to the ground, where they mature into adult organisms in the soil.1
The most reported symptoms of furuncular myiasis include pruritus, pain, and movement sensation, typically occurring suddenly at night.4 The most common presentation is a furunclelike lesion that exudes serosanguineous or purulent fluid,1 but there have been reports of vesicular, bullous, pustular, erosive, ecchymotic, and ulcerative lesions.5Dermatobia hominis usually presents on an exposed site, such as the scalp, face, and extremities. It may present with paroxysmal episodes of lancinating pain. Over time, the lesion usually heals without a scar, though hyperpigmentation and scarring can occur. The most reported complication is secondary bacterial infection.4 Local lymphadenopathy or systemic symptoms should raise concern for infection. Staphylococcus aureus and group B Streptococcus have been cultured from lesions.6,7
The differential diagnosis for myiasis should include furuncle, insect bite, insect prurigo, pyoderma, inflamed cyst, and tungiasis. Myiasis also can present similarly to severe soft tissue infections or cellulitis. If located on the breasts, it can be mistaken for periductal mastitis, a benign mass with microcalcification, or inflammatory carcinoma. Lastly, due to pain, erythema, pruritus, small vesicles, and crusting, it may be confused for herpes simplex virus.1
Furuncular myiasis typically is diagnosed based on clinical presentation, especially in endemic regions. In nonendemic areas, the patient’s history may reveal recent travel or predisposition to myiasis. In cases where there is uncertainty, dermoscopy may be used to identify the maggot in the lesion, or ultrasonography can be used to confirm myiasis through the detection of larval movement.8 Dermoscopy will reveal a furuncular lesion with a central opening surrounded by dilated blood vessels and a yellowish structure with black barblike spines.9 Within the dermis is a fibrous cystic sinus tract containing the dipteran larva. Laboratory studies typically are unremarkable. In chronic cases, a complete blood cell count and other laboratory tests may show systemic inflammation, peripheral eosinophilia, and elevated IgE.10 Biopsies of furuncular myiasis are not necessary for diagnosis. Histopathology reveals an ulcerated epidermis with or without hyperkeratosis and an inflammatory infiltrate composed of lymphocytes and neutrophils with eosinophils, fibroblasts, histiocytes, basophils, mast cells, plasma cells, and Langerhans cells within the dermis and subcutis.11
There are various approaches to treating furuncular myiasis, with the goal of complete removal of the larva and prevention of secondary infection. One treatment option is to apply a toxic substance to the larva, effectively killing it. Another approach is to force the larva to emerge via localized hypoxia, which can be done by occluding the punctum of the lesion for at least 24 hours. A complication of this method is suffocation of the larva without migration, leading to incomplete extraction and secondary infection.1 A third method is to surgically remove the larva, which allows for debridement of necrotic tissue surrounding the lesion if present.12 Ultrasonography also can be used therapeutically to aid in the removal of the larvae. The last method is to inject lidocaine into the base of the lesion, forcing the larva out of the punctum via fluid pressure.13 Oral treatments such as ivermectin are not recommended because they can result in the death of larvae within the lesion, leading to an inflammatory response.8
Furuncular myiasis is a form of cutaneous larvae infestation not commonly seen in individuals who do not live or travel in endemic, tropical, and subtropical regions. Diagnosis is based on clinical presentation, with imaging and laboratory studies available to supplement in unclear or atypical manifestations. Treatment involves complete removal of the larva, typically through forced evacuation via hypoxia or through surgical removal. Most cases resolve without notable scarring or other sequelae; however, in those who do have complications, the most common is secondary bacterial infection. Our patient’s absence of notable travel history and frequent environmental exposure in Michigan led us to believe the organism was from a domestic source. Our case underlines the importance of a thorough history and clinical examination of furuncular lesions including the use of dermoscopy to yield an appropriate diagnosis and treatment plan.
- Francesconi F, Lupi O. Myiasis. Clin Microbiol Rev. 2012;25:79-105. doi:10.1128/CMR.00010-11
- Schiff TA. Furuncular cutaneous myiasis caused by Cuterebra larva. J Am Acad Dermatol 1993;28:261-263.
- Safdar N, Young DK, Andes D. Autochthonous furuncular myiasis in the United States: case report and literature review. Clin Infect Dis. 2003;26:73-80.
- Mahal JJ, Sperling JD. Furuncular myiasis from Dermatobia hominus: a case of human botfly infestation. J Emerg Med. 2012;43:618-621.
- Francesconi F, Lupi O. Myiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. Elsevier; 2006:232-239.
- Gordon PM, Hepburn NC, Williams AE, et al. Cutaneous myiasis due to Dermatobia hominis: a report of six cases. Br J Dermatol. 1995;132:811-814.
- Hubler WR Jr, Rudolph AH, Dougherty EF. Dermal myiasis. Arch Dermatol. 1974;110:109-110.
- Quintanilla-Cedillo MR, León-Ureña H, Contreras-Ruiz J, et al. The value of Doppler ultrasound in diagnosis in 25 cases of furunculoid myiasis. Int J Dermatol. 2005;44:34-37.
- Bakos RM, Bakos L. Dermoscopic diagnosis of furuncular myiasis. Arch Dermatol. 2007;143:123-124.
- Varani S, Tassinari D, Elleri D, et al. A case of furuncular myiasis associated with systemic inflammation. Parasitol Int. 2007;56:330-333.
- Grogan TM, Payne CM, Spier C, et al. Cutaneous myiasis. immunohistologic and ultrastructural morphometric features of a human botfly lesion. Am J Dermatopathol. 1987;9:232-239.
- Krajewski A, Allen B, Hoss D, et al. Cutaneous myiasis. J Plast Reconstr Aesthet Surg. 2009;62:383-386.
- Lebwohl MG, Heymann WR, Berth-Jones J, et al. Myiasis: Treatment of Skin Diseases. Comprehensive Therapeutic Strategies. 2nd ed. Elsevier-Mosby; 2006.
- Francesconi F, Lupi O. Myiasis. Clin Microbiol Rev. 2012;25:79-105. doi:10.1128/CMR.00010-11
- Schiff TA. Furuncular cutaneous myiasis caused by Cuterebra larva. J Am Acad Dermatol 1993;28:261-263.
- Safdar N, Young DK, Andes D. Autochthonous furuncular myiasis in the United States: case report and literature review. Clin Infect Dis. 2003;26:73-80.
- Mahal JJ, Sperling JD. Furuncular myiasis from Dermatobia hominus: a case of human botfly infestation. J Emerg Med. 2012;43:618-621.
- Francesconi F, Lupi O. Myiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. Elsevier; 2006:232-239.
- Gordon PM, Hepburn NC, Williams AE, et al. Cutaneous myiasis due to Dermatobia hominis: a report of six cases. Br J Dermatol. 1995;132:811-814.
- Hubler WR Jr, Rudolph AH, Dougherty EF. Dermal myiasis. Arch Dermatol. 1974;110:109-110.
- Quintanilla-Cedillo MR, León-Ureña H, Contreras-Ruiz J, et al. The value of Doppler ultrasound in diagnosis in 25 cases of furunculoid myiasis. Int J Dermatol. 2005;44:34-37.
- Bakos RM, Bakos L. Dermoscopic diagnosis of furuncular myiasis. Arch Dermatol. 2007;143:123-124.
- Varani S, Tassinari D, Elleri D, et al. A case of furuncular myiasis associated with systemic inflammation. Parasitol Int. 2007;56:330-333.
- Grogan TM, Payne CM, Spier C, et al. Cutaneous myiasis. immunohistologic and ultrastructural morphometric features of a human botfly lesion. Am J Dermatopathol. 1987;9:232-239.
- Krajewski A, Allen B, Hoss D, et al. Cutaneous myiasis. J Plast Reconstr Aesthet Surg. 2009;62:383-386.
- Lebwohl MG, Heymann WR, Berth-Jones J, et al. Myiasis: Treatment of Skin Diseases. Comprehensive Therapeutic Strategies. 2nd ed. Elsevier-Mosby; 2006.
Practice Points
- Cutaneous myiasis is a skin infestation with dipterous larvae that feed on the host’s tissue and cause a wide range of manifestations depending on the location of infestation. It consists of 3 types: furuncular, wound, and migratory forms.
- It is uncommon in the United States and not typically seen in patients who have no history of recent travel to tropical or subtropical areas.
- The most common cause of African furuncular myiasis acquired in the United States is larvae of the Cuterebra species (also known as the rabbit botfly or rodent botfly).
Ultra-Late Cutaneous Melanoma Recurrence Following 49 Years of Quiescence
To the Editor:
Ultra-late melanoma recurrence represents a minority of cases in which the quiescent period lasts longer than 15 years, and epidemiologic studies have reported recurrence rates of 6% to 10% during the ultra-late period.1 Even more uncommon are cases that span many decades (eg, >30 years), but all are useful in understanding the cellular behavior leading to the reactivation of fully excised melanomas. Few cases have been reported in which recurrence occurs more than 35 years after the original diagnosis of melanoma. Unfortunately, mechanisms underlying this long stable quiescence and subsequent reactivation are poorly understood, which is why it is important to identify and document cases. We present a case of local recurrence of cutaneous melanoma on the patient’s lower back after a 49-year disease-free period.
A 78-year-old White woman presented to a private dermatology office for a full-body skin examination. She had a medical history of a cutaneous melanoma that had been removed on the lower back 49 years prior; Parkinson disease of 10 years’ duration; and an enlarged thyroid nodule with decreased thyrotropin and hyperthyroidism, atrial fibrillation, mitral valve prolapse, osteoarthritis in the knees, and actinic keratoses, all of which were chronic conditions lasting years to decades. She was taking several medications for these medical conditions. Her surgical history included a hysterectomy, hip replacement, hernia repair, cardioversion, and tonsillectomy in childhood. Her family medical history included breast cancer in her paternal grandmother and aunt; hypertension in her father; and sarcoma in her mother at 78 years of age, which initially was identified in the sacrum and metastasized to the lungs causing death. No family history of melanoma or other skin cancers was reported. Prior to the original diagnosis of melanoma at 29 years of age, she had no history of skin cancer or any other medical condition other than acne. The patient did report spending a great deal of time in the sun during high school.
The patient reported developing the original cutaneous melanoma during her second pregnancy at 29 years of age and recalled that it was excised with wide margins. There had been a mole on her back that was present for years but changed in size during pregnancy, prompting the original visit to the primary care physician for evaluation. Remarkably, the original pathology report was obtained from the patient and revealed a specimen consisting of a 3.7×1.7-cm skin
Physical examination at the current presentation 49 years later revealed an even-bordered 2-mm black macule that was located approximately 1 cm from the original melanoma excision scar line (Figure). A biopsy was performed and sent to a dermatopathologist. Microscopic evaluation revealed nests, islands, and sheets of atypical epithelioid melanocytes extending through the dermis between collagen bundles. The melanocytes varied in size and shape with moderate nuclear pleomorphism present. Scattered mitotic figures and necrotic melanocytes were present, which most likely represented cutaneous satellite metastases of melanoma. Subsequent chest radiography, full-body positron emission tomography, and standard laboratory blood tests were unremarkable except for an enlarged right thyroid gland and moderate cardiomegaly. The patient was sent to a surgical oncologist for excision with wide surgical margins, and she elected not to have a sentinel lymph node biopsy. At follow-up 3, 6, 12, and 24 months later, there were no signs of recurrence based on direct clinical examination. The patient subsequently was lost to follow-up.
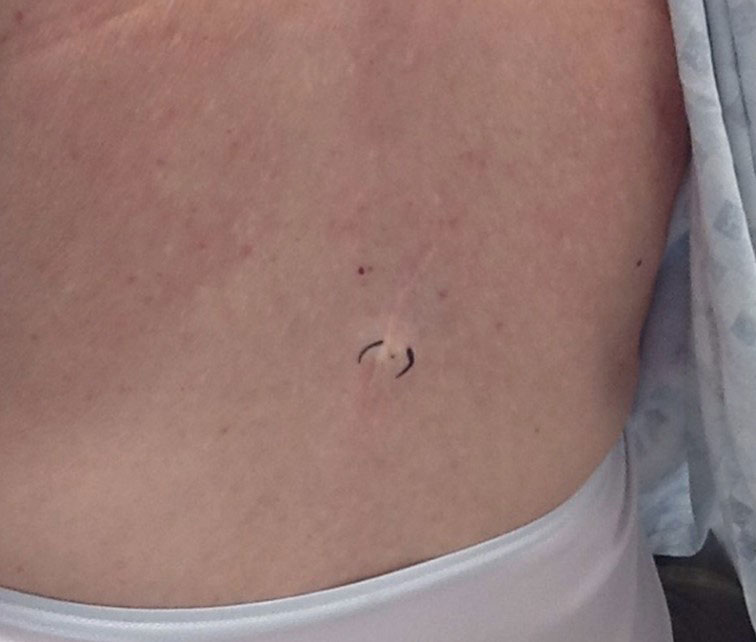
Recurrence rates of melanoma vary by stage and age at diagnosis, but prior studies have reported a recurrence rate of approximately 6% after 10 or more years following the initial diagnosis.2 Ultra-late recurrences of approximately 4 decades or more are extremely rare. A PubMed search of articles indexed for MEDLINE using the terms melanoma and ultra-late recurrence revealed 4 reported cases with a quiescent period of 38 or more years.3-6 All cases were metastatic melanomas in women; spanned 38, 40, 41, and 45 years from the initial melanoma diagnosis to recurrence; and all of the recurrences except one were regional or distal metastatic lesions (eg, lymph node, brain). In one case, both the original and recurrent lesions occurred on the left elbow.6 The original lesions occurred on the legs, elbow, and back of the neck, and there were no notable concomitant medical conditions. The patients were aged 72, 73, 73, and 84 years at recurrence.3-6 However, generalizations from these cases are limited given the potential for selection bias (eg, men may be less likely to visit a clinic for follow-up and nevi examination) and the likelihood that many cases of ultra-late melanoma recurrence are unrecognized or unreported.
More recently, genomic analyses on melanoma lesions occurring 30 years apart confirmed that the second lesion was indeed a recurrence, although with numerous additional mutations.7 The specific mechanisms underlying the dormancy and subsequent reemergence of metastatic lesions are unclear, but
It also is worth highlighting the concomitant diagnosis of Parkinson disease in our patient. In recent years, Parkinson disease has been linked to melanoma in both epidemiologic and genetic studies. For example, one large-scale study found a 50% increased risk for developing Parkinson disease in patients with melanoma (and vice versa), and this finding has been replicated in other studies.10 Moreover, patients with Parkinson disease have a 2-fold increase in their risk for developing melanoma, demonstrating that it is a bidirectional pathway. Not surprisingly, associations between melanin and neuromelanin pathways have been identified as a potential link between these diseases, and scientists are in the process of understanding the genetic components of both.10 It is unknown if specific genetic mutations contributed to both diseases in our case, but follow-up genetic testing on the recurrent melanoma specimen currently is being pursued.
The 49-year quiescent period in our case of recurrent cutaneous malignant melanoma potentially represents the longest ultra-late recurrence of melanoma in the literature to date based on a review of indexed publications. Moreover, it is relatively unique compared to other similar cases in that the recurrence was within a centimeter of the original excisional scar. Most metastases occur in locoregional lymph nodes or the lungs3; therefore, it is unusual to find one so close to the original lesion, especially one that occurred decades later. Factors associated with ultra-late recurrences are unknown, primarily because of the rarity of these cases as well as the biases and other factors that limit existing studies. However, genetic sequencing may provide information regarding these factors and related processes. Genetic sequencing specifically points to a small cell group remaining after excision of the primary tumor, which mutates while proliferating. Low antigenicity and tolerance to immunity during the quiescent period may explain the long duration of dormancy.6 More recently, there have been efforts to identify immunohistochemical signatures that may predict late recurrences, though the data are preliminary in nature.11
Given the latency period and location of the recurrence, our case demonstrates that even fully excised melanomas may recur locally many decades later, hence patients should be aware of the importance of a lifetime of vigilance after being diagnosed with melanoma.
- Tsao H, Cosimi AB, Sober AJ. Ultra-late recurrence (15 years or longer) of cutaneous melanoma. Cancer. 1997;79:2361-2370.
- Faries MB, Steen S, Ye X, et al. Late recurrence in melanoma: clinical implications of lost dormancy. J Am Coll Surg. 2013;217:27-34.
- Mansour D, Kejariwal D. It is never too late: ultra-late recurrence of melanoma with distant metastases [published online March 8, 2012]. BMJ Case Rep. 2012:bcr0120125474. doi:10.1136/bcr.01.2012.5474
- Saleh D, Peach AHS. Ultra-late recurrence of malignant melanoma after 40 years of quiescent disease. J Surg Oncol. 2011;103:290-291.
- Goodenough J, Cozon CL, Liew SH. An incidental finding of a nodal recurrence of cutaneous malignant melanoma after a 45-year disease-free period [published online June 4, 2014]. BMJ Case Rep. 2014:bcr2014204289. doi:10.1136/bcr-2014-204289
- Nakamura M, Obayashi M, Yoshimitsu M, et al. Comparative whole-exome sequencing of an ultra-late recurrent malignant melanoma. Br J Dermatol. 2021;184:762-763.
- Miller JJ, Lofgren KA, Hughes SR, et al. Genomic analysis of melanoma evolution following a 30-year disease-free interval. J Cutan Pathol. 2017;44:805-808.
- North JP, Kageshita T, Pinkel D, et al. Distribution and significance of occult intraepidermal tumor cells surrounding primary melanoma. J Invest Dermatol. 2008;128:2024-2030.
- Massi G, LeBoit PE. Recurrent and persistent melanoma. In: Massi G, LeBoit PE, eds. Histological Diagnosis of Nevi and Melanoma. 2nd ed. Springer-Verlag; 2014:689-698.
- Bose A, Petsko GA, Eliezer D. Parkinson’s disease and melanoma: co-occurrence and mechanisms. J Parkinsons Dis. 2018;8:385-398.
- Reschke R, Dumann K, Ziemer M. Risk stratification and clinical characteristics of patients with late recurrence of melanoma (>10 years).J Clin Med. 2022;11:2026.
To the Editor:
Ultra-late melanoma recurrence represents a minority of cases in which the quiescent period lasts longer than 15 years, and epidemiologic studies have reported recurrence rates of 6% to 10% during the ultra-late period.1 Even more uncommon are cases that span many decades (eg, >30 years), but all are useful in understanding the cellular behavior leading to the reactivation of fully excised melanomas. Few cases have been reported in which recurrence occurs more than 35 years after the original diagnosis of melanoma. Unfortunately, mechanisms underlying this long stable quiescence and subsequent reactivation are poorly understood, which is why it is important to identify and document cases. We present a case of local recurrence of cutaneous melanoma on the patient’s lower back after a 49-year disease-free period.
A 78-year-old White woman presented to a private dermatology office for a full-body skin examination. She had a medical history of a cutaneous melanoma that had been removed on the lower back 49 years prior; Parkinson disease of 10 years’ duration; and an enlarged thyroid nodule with decreased thyrotropin and hyperthyroidism, atrial fibrillation, mitral valve prolapse, osteoarthritis in the knees, and actinic keratoses, all of which were chronic conditions lasting years to decades. She was taking several medications for these medical conditions. Her surgical history included a hysterectomy, hip replacement, hernia repair, cardioversion, and tonsillectomy in childhood. Her family medical history included breast cancer in her paternal grandmother and aunt; hypertension in her father; and sarcoma in her mother at 78 years of age, which initially was identified in the sacrum and metastasized to the lungs causing death. No family history of melanoma or other skin cancers was reported. Prior to the original diagnosis of melanoma at 29 years of age, she had no history of skin cancer or any other medical condition other than acne. The patient did report spending a great deal of time in the sun during high school.
The patient reported developing the original cutaneous melanoma during her second pregnancy at 29 years of age and recalled that it was excised with wide margins. There had been a mole on her back that was present for years but changed in size during pregnancy, prompting the original visit to the primary care physician for evaluation. Remarkably, the original pathology report was obtained from the patient and revealed a specimen consisting of a 3.7×1.7-cm skin
Physical examination at the current presentation 49 years later revealed an even-bordered 2-mm black macule that was located approximately 1 cm from the original melanoma excision scar line (Figure). A biopsy was performed and sent to a dermatopathologist. Microscopic evaluation revealed nests, islands, and sheets of atypical epithelioid melanocytes extending through the dermis between collagen bundles. The melanocytes varied in size and shape with moderate nuclear pleomorphism present. Scattered mitotic figures and necrotic melanocytes were present, which most likely represented cutaneous satellite metastases of melanoma. Subsequent chest radiography, full-body positron emission tomography, and standard laboratory blood tests were unremarkable except for an enlarged right thyroid gland and moderate cardiomegaly. The patient was sent to a surgical oncologist for excision with wide surgical margins, and she elected not to have a sentinel lymph node biopsy. At follow-up 3, 6, 12, and 24 months later, there were no signs of recurrence based on direct clinical examination. The patient subsequently was lost to follow-up.

Recurrence rates of melanoma vary by stage and age at diagnosis, but prior studies have reported a recurrence rate of approximately 6% after 10 or more years following the initial diagnosis.2 Ultra-late recurrences of approximately 4 decades or more are extremely rare. A PubMed search of articles indexed for MEDLINE using the terms melanoma and ultra-late recurrence revealed 4 reported cases with a quiescent period of 38 or more years.3-6 All cases were metastatic melanomas in women; spanned 38, 40, 41, and 45 years from the initial melanoma diagnosis to recurrence; and all of the recurrences except one were regional or distal metastatic lesions (eg, lymph node, brain). In one case, both the original and recurrent lesions occurred on the left elbow.6 The original lesions occurred on the legs, elbow, and back of the neck, and there were no notable concomitant medical conditions. The patients were aged 72, 73, 73, and 84 years at recurrence.3-6 However, generalizations from these cases are limited given the potential for selection bias (eg, men may be less likely to visit a clinic for follow-up and nevi examination) and the likelihood that many cases of ultra-late melanoma recurrence are unrecognized or unreported.
More recently, genomic analyses on melanoma lesions occurring 30 years apart confirmed that the second lesion was indeed a recurrence, although with numerous additional mutations.7 The specific mechanisms underlying the dormancy and subsequent reemergence of metastatic lesions are unclear, but
It also is worth highlighting the concomitant diagnosis of Parkinson disease in our patient. In recent years, Parkinson disease has been linked to melanoma in both epidemiologic and genetic studies. For example, one large-scale study found a 50% increased risk for developing Parkinson disease in patients with melanoma (and vice versa), and this finding has been replicated in other studies.10 Moreover, patients with Parkinson disease have a 2-fold increase in their risk for developing melanoma, demonstrating that it is a bidirectional pathway. Not surprisingly, associations between melanin and neuromelanin pathways have been identified as a potential link between these diseases, and scientists are in the process of understanding the genetic components of both.10 It is unknown if specific genetic mutations contributed to both diseases in our case, but follow-up genetic testing on the recurrent melanoma specimen currently is being pursued.
The 49-year quiescent period in our case of recurrent cutaneous malignant melanoma potentially represents the longest ultra-late recurrence of melanoma in the literature to date based on a review of indexed publications. Moreover, it is relatively unique compared to other similar cases in that the recurrence was within a centimeter of the original excisional scar. Most metastases occur in locoregional lymph nodes or the lungs3; therefore, it is unusual to find one so close to the original lesion, especially one that occurred decades later. Factors associated with ultra-late recurrences are unknown, primarily because of the rarity of these cases as well as the biases and other factors that limit existing studies. However, genetic sequencing may provide information regarding these factors and related processes. Genetic sequencing specifically points to a small cell group remaining after excision of the primary tumor, which mutates while proliferating. Low antigenicity and tolerance to immunity during the quiescent period may explain the long duration of dormancy.6 More recently, there have been efforts to identify immunohistochemical signatures that may predict late recurrences, though the data are preliminary in nature.11
Given the latency period and location of the recurrence, our case demonstrates that even fully excised melanomas may recur locally many decades later, hence patients should be aware of the importance of a lifetime of vigilance after being diagnosed with melanoma.
To the Editor:
Ultra-late melanoma recurrence represents a minority of cases in which the quiescent period lasts longer than 15 years, and epidemiologic studies have reported recurrence rates of 6% to 10% during the ultra-late period.1 Even more uncommon are cases that span many decades (eg, >30 years), but all are useful in understanding the cellular behavior leading to the reactivation of fully excised melanomas. Few cases have been reported in which recurrence occurs more than 35 years after the original diagnosis of melanoma. Unfortunately, mechanisms underlying this long stable quiescence and subsequent reactivation are poorly understood, which is why it is important to identify and document cases. We present a case of local recurrence of cutaneous melanoma on the patient’s lower back after a 49-year disease-free period.
A 78-year-old White woman presented to a private dermatology office for a full-body skin examination. She had a medical history of a cutaneous melanoma that had been removed on the lower back 49 years prior; Parkinson disease of 10 years’ duration; and an enlarged thyroid nodule with decreased thyrotropin and hyperthyroidism, atrial fibrillation, mitral valve prolapse, osteoarthritis in the knees, and actinic keratoses, all of which were chronic conditions lasting years to decades. She was taking several medications for these medical conditions. Her surgical history included a hysterectomy, hip replacement, hernia repair, cardioversion, and tonsillectomy in childhood. Her family medical history included breast cancer in her paternal grandmother and aunt; hypertension in her father; and sarcoma in her mother at 78 years of age, which initially was identified in the sacrum and metastasized to the lungs causing death. No family history of melanoma or other skin cancers was reported. Prior to the original diagnosis of melanoma at 29 years of age, she had no history of skin cancer or any other medical condition other than acne. The patient did report spending a great deal of time in the sun during high school.
The patient reported developing the original cutaneous melanoma during her second pregnancy at 29 years of age and recalled that it was excised with wide margins. There had been a mole on her back that was present for years but changed in size during pregnancy, prompting the original visit to the primary care physician for evaluation. Remarkably, the original pathology report was obtained from the patient and revealed a specimen consisting of a 3.7×1.7-cm skin
Physical examination at the current presentation 49 years later revealed an even-bordered 2-mm black macule that was located approximately 1 cm from the original melanoma excision scar line (Figure). A biopsy was performed and sent to a dermatopathologist. Microscopic evaluation revealed nests, islands, and sheets of atypical epithelioid melanocytes extending through the dermis between collagen bundles. The melanocytes varied in size and shape with moderate nuclear pleomorphism present. Scattered mitotic figures and necrotic melanocytes were present, which most likely represented cutaneous satellite metastases of melanoma. Subsequent chest radiography, full-body positron emission tomography, and standard laboratory blood tests were unremarkable except for an enlarged right thyroid gland and moderate cardiomegaly. The patient was sent to a surgical oncologist for excision with wide surgical margins, and she elected not to have a sentinel lymph node biopsy. At follow-up 3, 6, 12, and 24 months later, there were no signs of recurrence based on direct clinical examination. The patient subsequently was lost to follow-up.

Recurrence rates of melanoma vary by stage and age at diagnosis, but prior studies have reported a recurrence rate of approximately 6% after 10 or more years following the initial diagnosis.2 Ultra-late recurrences of approximately 4 decades or more are extremely rare. A PubMed search of articles indexed for MEDLINE using the terms melanoma and ultra-late recurrence revealed 4 reported cases with a quiescent period of 38 or more years.3-6 All cases were metastatic melanomas in women; spanned 38, 40, 41, and 45 years from the initial melanoma diagnosis to recurrence; and all of the recurrences except one were regional or distal metastatic lesions (eg, lymph node, brain). In one case, both the original and recurrent lesions occurred on the left elbow.6 The original lesions occurred on the legs, elbow, and back of the neck, and there were no notable concomitant medical conditions. The patients were aged 72, 73, 73, and 84 years at recurrence.3-6 However, generalizations from these cases are limited given the potential for selection bias (eg, men may be less likely to visit a clinic for follow-up and nevi examination) and the likelihood that many cases of ultra-late melanoma recurrence are unrecognized or unreported.
More recently, genomic analyses on melanoma lesions occurring 30 years apart confirmed that the second lesion was indeed a recurrence, although with numerous additional mutations.7 The specific mechanisms underlying the dormancy and subsequent reemergence of metastatic lesions are unclear, but
It also is worth highlighting the concomitant diagnosis of Parkinson disease in our patient. In recent years, Parkinson disease has been linked to melanoma in both epidemiologic and genetic studies. For example, one large-scale study found a 50% increased risk for developing Parkinson disease in patients with melanoma (and vice versa), and this finding has been replicated in other studies.10 Moreover, patients with Parkinson disease have a 2-fold increase in their risk for developing melanoma, demonstrating that it is a bidirectional pathway. Not surprisingly, associations between melanin and neuromelanin pathways have been identified as a potential link between these diseases, and scientists are in the process of understanding the genetic components of both.10 It is unknown if specific genetic mutations contributed to both diseases in our case, but follow-up genetic testing on the recurrent melanoma specimen currently is being pursued.
The 49-year quiescent period in our case of recurrent cutaneous malignant melanoma potentially represents the longest ultra-late recurrence of melanoma in the literature to date based on a review of indexed publications. Moreover, it is relatively unique compared to other similar cases in that the recurrence was within a centimeter of the original excisional scar. Most metastases occur in locoregional lymph nodes or the lungs3; therefore, it is unusual to find one so close to the original lesion, especially one that occurred decades later. Factors associated with ultra-late recurrences are unknown, primarily because of the rarity of these cases as well as the biases and other factors that limit existing studies. However, genetic sequencing may provide information regarding these factors and related processes. Genetic sequencing specifically points to a small cell group remaining after excision of the primary tumor, which mutates while proliferating. Low antigenicity and tolerance to immunity during the quiescent period may explain the long duration of dormancy.6 More recently, there have been efforts to identify immunohistochemical signatures that may predict late recurrences, though the data are preliminary in nature.11
Given the latency period and location of the recurrence, our case demonstrates that even fully excised melanomas may recur locally many decades later, hence patients should be aware of the importance of a lifetime of vigilance after being diagnosed with melanoma.
- Tsao H, Cosimi AB, Sober AJ. Ultra-late recurrence (15 years or longer) of cutaneous melanoma. Cancer. 1997;79:2361-2370.
- Faries MB, Steen S, Ye X, et al. Late recurrence in melanoma: clinical implications of lost dormancy. J Am Coll Surg. 2013;217:27-34.
- Mansour D, Kejariwal D. It is never too late: ultra-late recurrence of melanoma with distant metastases [published online March 8, 2012]. BMJ Case Rep. 2012:bcr0120125474. doi:10.1136/bcr.01.2012.5474
- Saleh D, Peach AHS. Ultra-late recurrence of malignant melanoma after 40 years of quiescent disease. J Surg Oncol. 2011;103:290-291.
- Goodenough J, Cozon CL, Liew SH. An incidental finding of a nodal recurrence of cutaneous malignant melanoma after a 45-year disease-free period [published online June 4, 2014]. BMJ Case Rep. 2014:bcr2014204289. doi:10.1136/bcr-2014-204289
- Nakamura M, Obayashi M, Yoshimitsu M, et al. Comparative whole-exome sequencing of an ultra-late recurrent malignant melanoma. Br J Dermatol. 2021;184:762-763.
- Miller JJ, Lofgren KA, Hughes SR, et al. Genomic analysis of melanoma evolution following a 30-year disease-free interval. J Cutan Pathol. 2017;44:805-808.
- North JP, Kageshita T, Pinkel D, et al. Distribution and significance of occult intraepidermal tumor cells surrounding primary melanoma. J Invest Dermatol. 2008;128:2024-2030.
- Massi G, LeBoit PE. Recurrent and persistent melanoma. In: Massi G, LeBoit PE, eds. Histological Diagnosis of Nevi and Melanoma. 2nd ed. Springer-Verlag; 2014:689-698.
- Bose A, Petsko GA, Eliezer D. Parkinson’s disease and melanoma: co-occurrence and mechanisms. J Parkinsons Dis. 2018;8:385-398.
- Reschke R, Dumann K, Ziemer M. Risk stratification and clinical characteristics of patients with late recurrence of melanoma (>10 years).J Clin Med. 2022;11:2026.
- Tsao H, Cosimi AB, Sober AJ. Ultra-late recurrence (15 years or longer) of cutaneous melanoma. Cancer. 1997;79:2361-2370.
- Faries MB, Steen S, Ye X, et al. Late recurrence in melanoma: clinical implications of lost dormancy. J Am Coll Surg. 2013;217:27-34.
- Mansour D, Kejariwal D. It is never too late: ultra-late recurrence of melanoma with distant metastases [published online March 8, 2012]. BMJ Case Rep. 2012:bcr0120125474. doi:10.1136/bcr.01.2012.5474
- Saleh D, Peach AHS. Ultra-late recurrence of malignant melanoma after 40 years of quiescent disease. J Surg Oncol. 2011;103:290-291.
- Goodenough J, Cozon CL, Liew SH. An incidental finding of a nodal recurrence of cutaneous malignant melanoma after a 45-year disease-free period [published online June 4, 2014]. BMJ Case Rep. 2014:bcr2014204289. doi:10.1136/bcr-2014-204289
- Nakamura M, Obayashi M, Yoshimitsu M, et al. Comparative whole-exome sequencing of an ultra-late recurrent malignant melanoma. Br J Dermatol. 2021;184:762-763.
- Miller JJ, Lofgren KA, Hughes SR, et al. Genomic analysis of melanoma evolution following a 30-year disease-free interval. J Cutan Pathol. 2017;44:805-808.
- North JP, Kageshita T, Pinkel D, et al. Distribution and significance of occult intraepidermal tumor cells surrounding primary melanoma. J Invest Dermatol. 2008;128:2024-2030.
- Massi G, LeBoit PE. Recurrent and persistent melanoma. In: Massi G, LeBoit PE, eds. Histological Diagnosis of Nevi and Melanoma. 2nd ed. Springer-Verlag; 2014:689-698.
- Bose A, Petsko GA, Eliezer D. Parkinson’s disease and melanoma: co-occurrence and mechanisms. J Parkinsons Dis. 2018;8:385-398.
- Reschke R, Dumann K, Ziemer M. Risk stratification and clinical characteristics of patients with late recurrence of melanoma (>10 years).J Clin Med. 2022;11:2026.
Practice Points
- In some cases of ultra-late malignant melanoma recurrence, the quiescent period can last more than 30 years.
- There does not appear to be specificity with location since ultra-late melanoma recurrences can occur locally, regionally, and distally, and original lesions appear to be randomly distributed in these cases.
- Mechanisms for ultra-late melanoma recurrence are poorly understood; histologically, unrecognizable aberrations in the skin beyond the histopathologic margins may represent an early phase of disease that lies dormant for many years before reemerging in response to external or immunologic changes.
- Patients with malignant melanoma are at a higher risk for developing Parkinson disease (and vice versa) given the link between melanin and neuromelanin pathways.
Biomarker-guided steroid therapy shown safe for COPD
Eosinophil-guided corticosteroid therapy for patients with chronic obstructive pulmonary disease (COPD) is equivalent in efficacy to standard of care therapy, but the eosinophil-guided therapy may help mitigate the harmful side effects associated with even short courses of corticosteroids, investigators said in a primary care–based randomized trial.
Among patients in 14 primary care practices in the United Kingdom who experienced COPD exacerbations, the proportion of patients who experienced treatment failure at day 28 was 27% for those who were randomized to receive prednisolone only when blood eosinophil counts on a point-of-care assay equaled or exceeded 2%, compared with 34% of all patients randomized to standard of care.
The relative risk for treatment failure using the eosinophil-guided approach was 0.82, which did not reach statistical significance, but indicated noninferiority for the biomarker-based dosing method, Mona Bafadhel, MD, of King’s College London, reported on behalf of colleagues in the Stratified Treatment to Reduce Risk in COPD (STARR2) trial.
This is the largest primary care multicenter trial, and probably adds another 20% to the literature base for exacerbations in COPD,” she said in an oral abstract presentation at the European Respiratory Society 2022 Congress.
“A personalized endotype-based treatment with oral prednisolone is possible in patients with COPD and I think should be now part of clinical guidelines,” she added.
Too much of a good thing
Although systemic corticosteroids are the universal treatment for COPD exacerbations, the drugs are also known to increase harm, with studies showing that cumulative doses of oral corticosteroids in COPD patients is associated with an increased risk for death. In addition, systemic corticosteroids are the third most common cause of adverse events leading to hospitalization, behind only chemotherapy and antibiotic use leading to Clostridioides difficile infections, Dr. Bafadhel said.
“And of course, corticosteroids are associated with significant harmful effects, including a five-times increased risk of sepsis, three-times increased risk of [venous thromboembolism], and a twice-increased risk of fracture,” she said.
Dr. Bafadhel and colleagues had previously shown in the single-center BEAT-COPD study that peripheral blood eosinophils at the time of a moderate COPD exacerbation could be used to safely direct oral corticosteroid therapy. She also pointed to a 2019 multicenter open-label study showing that eosinophil-guided care was noninferior to standard prescribing of oral corticosteroids for patients with severe exacerbations.
Primary care study
The investigators conducted the current study to test whether eosinophil-guided therapy at the point of care in a primary practice setting was efficacious, with the ultimate goal of encouraging changes in guidelines.
They recruited patients with COPD exacerbations from 14 general practices in Oxfordshire and Buckinghamshire in the Thames Valley.
The patients were randomly assigned to receive either standard of care or the biomarker-guided intervention for 14 days. In this arm, patients with eosinophil counts of 2% or greater received matched prednisolone, while patients with counts below 2% received placebo. The patients were blinded to the assigned drug.
A total of 203 exacerbations among 152 patients were evenly allocated to treatment or control groups. The mean patient age was 71. Of the 102 exacerbations allocated to eosinophil-guided therapy, 34 were treated with placebo.
As noted before, in the intention-to-treat analysis the primary outcome of the treatment failure rate, defined as any need for antibiotics and/or steroids at one month, was 27% in the biomarker-guided arm and 34% in the standard care arm.
“In the per-protocol analysis we also demonstrated that there was a suggestion that there is possible superiority of using blood eosinophil-directed oral corticosteroid prescriptions at the time of acute exacerbation using the point-of-care eosinophil test,” Dr. Bafadhel said.
There were no significant differences in the secondary outcomes of mean change in forced expiratory volume in 1 second (FEV1), COPD Assessment Test scores from exacerbation to follow-up, and symptoms according to a visual analog scale.
Invited discussant Dave Singh, MD, of the University of Manchester, England, asked Dr. Bafadhel how the data she presented supported her conclusions about the potential benefits of eosinophil-guided therapy, given that the P values were nonsignificant.
“The primary outcome was powered on noninferiority, and of course what we’ve shown is that it’s not any worse, it’s not any better, but of course it’s the effect of how many courses of steroids you can reduce in that population,” Dr. Bafadhel replied.
She noted that although the investigators have not performed an economic analysis to determine how many adverse events might be avoided using the biomarker-guided approach, “we do know that some of these patients who are given prednisolone, their comorbidities of diabetes worsened, for example.”
In the online Q&A for the presentation, Sohail Ansari, MD, from the Mid and South Essex NHS Foundation Trust in the United Kingdom, said that many patients in primary care practices receive “rescue packs” containing antibiotics and steroids, but may not be equipped to know when they should use the steroids and therefore may overuse them.
“Perhaps community-based, adequately resourced respiratory teams [may] be a way forward, but it will need adequate investment and commitment,” he wrote.
The trial was supported by the University of Oxford and National Institute for Health and Care Research, UK. Dr. Bafadhel reported grant and research support from the National Institute for Health and Care Research, Asthma & Lung UK, AstraZeneca, and Roche, and honoraria or fees from others. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Ansari reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
Eosinophil-guided corticosteroid therapy for patients with chronic obstructive pulmonary disease (COPD) is equivalent in efficacy to standard of care therapy, but the eosinophil-guided therapy may help mitigate the harmful side effects associated with even short courses of corticosteroids, investigators said in a primary care–based randomized trial.
Among patients in 14 primary care practices in the United Kingdom who experienced COPD exacerbations, the proportion of patients who experienced treatment failure at day 28 was 27% for those who were randomized to receive prednisolone only when blood eosinophil counts on a point-of-care assay equaled or exceeded 2%, compared with 34% of all patients randomized to standard of care.
The relative risk for treatment failure using the eosinophil-guided approach was 0.82, which did not reach statistical significance, but indicated noninferiority for the biomarker-based dosing method, Mona Bafadhel, MD, of King’s College London, reported on behalf of colleagues in the Stratified Treatment to Reduce Risk in COPD (STARR2) trial.
This is the largest primary care multicenter trial, and probably adds another 20% to the literature base for exacerbations in COPD,” she said in an oral abstract presentation at the European Respiratory Society 2022 Congress.
“A personalized endotype-based treatment with oral prednisolone is possible in patients with COPD and I think should be now part of clinical guidelines,” she added.
Too much of a good thing
Although systemic corticosteroids are the universal treatment for COPD exacerbations, the drugs are also known to increase harm, with studies showing that cumulative doses of oral corticosteroids in COPD patients is associated with an increased risk for death. In addition, systemic corticosteroids are the third most common cause of adverse events leading to hospitalization, behind only chemotherapy and antibiotic use leading to Clostridioides difficile infections, Dr. Bafadhel said.
“And of course, corticosteroids are associated with significant harmful effects, including a five-times increased risk of sepsis, three-times increased risk of [venous thromboembolism], and a twice-increased risk of fracture,” she said.
Dr. Bafadhel and colleagues had previously shown in the single-center BEAT-COPD study that peripheral blood eosinophils at the time of a moderate COPD exacerbation could be used to safely direct oral corticosteroid therapy. She also pointed to a 2019 multicenter open-label study showing that eosinophil-guided care was noninferior to standard prescribing of oral corticosteroids for patients with severe exacerbations.
Primary care study
The investigators conducted the current study to test whether eosinophil-guided therapy at the point of care in a primary practice setting was efficacious, with the ultimate goal of encouraging changes in guidelines.
They recruited patients with COPD exacerbations from 14 general practices in Oxfordshire and Buckinghamshire in the Thames Valley.
The patients were randomly assigned to receive either standard of care or the biomarker-guided intervention for 14 days. In this arm, patients with eosinophil counts of 2% or greater received matched prednisolone, while patients with counts below 2% received placebo. The patients were blinded to the assigned drug.
A total of 203 exacerbations among 152 patients were evenly allocated to treatment or control groups. The mean patient age was 71. Of the 102 exacerbations allocated to eosinophil-guided therapy, 34 were treated with placebo.
As noted before, in the intention-to-treat analysis the primary outcome of the treatment failure rate, defined as any need for antibiotics and/or steroids at one month, was 27% in the biomarker-guided arm and 34% in the standard care arm.
“In the per-protocol analysis we also demonstrated that there was a suggestion that there is possible superiority of using blood eosinophil-directed oral corticosteroid prescriptions at the time of acute exacerbation using the point-of-care eosinophil test,” Dr. Bafadhel said.
There were no significant differences in the secondary outcomes of mean change in forced expiratory volume in 1 second (FEV1), COPD Assessment Test scores from exacerbation to follow-up, and symptoms according to a visual analog scale.
Invited discussant Dave Singh, MD, of the University of Manchester, England, asked Dr. Bafadhel how the data she presented supported her conclusions about the potential benefits of eosinophil-guided therapy, given that the P values were nonsignificant.
“The primary outcome was powered on noninferiority, and of course what we’ve shown is that it’s not any worse, it’s not any better, but of course it’s the effect of how many courses of steroids you can reduce in that population,” Dr. Bafadhel replied.
She noted that although the investigators have not performed an economic analysis to determine how many adverse events might be avoided using the biomarker-guided approach, “we do know that some of these patients who are given prednisolone, their comorbidities of diabetes worsened, for example.”
In the online Q&A for the presentation, Sohail Ansari, MD, from the Mid and South Essex NHS Foundation Trust in the United Kingdom, said that many patients in primary care practices receive “rescue packs” containing antibiotics and steroids, but may not be equipped to know when they should use the steroids and therefore may overuse them.
“Perhaps community-based, adequately resourced respiratory teams [may] be a way forward, but it will need adequate investment and commitment,” he wrote.
The trial was supported by the University of Oxford and National Institute for Health and Care Research, UK. Dr. Bafadhel reported grant and research support from the National Institute for Health and Care Research, Asthma & Lung UK, AstraZeneca, and Roche, and honoraria or fees from others. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Ansari reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
Eosinophil-guided corticosteroid therapy for patients with chronic obstructive pulmonary disease (COPD) is equivalent in efficacy to standard of care therapy, but the eosinophil-guided therapy may help mitigate the harmful side effects associated with even short courses of corticosteroids, investigators said in a primary care–based randomized trial.
Among patients in 14 primary care practices in the United Kingdom who experienced COPD exacerbations, the proportion of patients who experienced treatment failure at day 28 was 27% for those who were randomized to receive prednisolone only when blood eosinophil counts on a point-of-care assay equaled or exceeded 2%, compared with 34% of all patients randomized to standard of care.
The relative risk for treatment failure using the eosinophil-guided approach was 0.82, which did not reach statistical significance, but indicated noninferiority for the biomarker-based dosing method, Mona Bafadhel, MD, of King’s College London, reported on behalf of colleagues in the Stratified Treatment to Reduce Risk in COPD (STARR2) trial.
This is the largest primary care multicenter trial, and probably adds another 20% to the literature base for exacerbations in COPD,” she said in an oral abstract presentation at the European Respiratory Society 2022 Congress.
“A personalized endotype-based treatment with oral prednisolone is possible in patients with COPD and I think should be now part of clinical guidelines,” she added.
Too much of a good thing
Although systemic corticosteroids are the universal treatment for COPD exacerbations, the drugs are also known to increase harm, with studies showing that cumulative doses of oral corticosteroids in COPD patients is associated with an increased risk for death. In addition, systemic corticosteroids are the third most common cause of adverse events leading to hospitalization, behind only chemotherapy and antibiotic use leading to Clostridioides difficile infections, Dr. Bafadhel said.
“And of course, corticosteroids are associated with significant harmful effects, including a five-times increased risk of sepsis, three-times increased risk of [venous thromboembolism], and a twice-increased risk of fracture,” she said.
Dr. Bafadhel and colleagues had previously shown in the single-center BEAT-COPD study that peripheral blood eosinophils at the time of a moderate COPD exacerbation could be used to safely direct oral corticosteroid therapy. She also pointed to a 2019 multicenter open-label study showing that eosinophil-guided care was noninferior to standard prescribing of oral corticosteroids for patients with severe exacerbations.
Primary care study
The investigators conducted the current study to test whether eosinophil-guided therapy at the point of care in a primary practice setting was efficacious, with the ultimate goal of encouraging changes in guidelines.
They recruited patients with COPD exacerbations from 14 general practices in Oxfordshire and Buckinghamshire in the Thames Valley.
The patients were randomly assigned to receive either standard of care or the biomarker-guided intervention for 14 days. In this arm, patients with eosinophil counts of 2% or greater received matched prednisolone, while patients with counts below 2% received placebo. The patients were blinded to the assigned drug.
A total of 203 exacerbations among 152 patients were evenly allocated to treatment or control groups. The mean patient age was 71. Of the 102 exacerbations allocated to eosinophil-guided therapy, 34 were treated with placebo.
As noted before, in the intention-to-treat analysis the primary outcome of the treatment failure rate, defined as any need for antibiotics and/or steroids at one month, was 27% in the biomarker-guided arm and 34% in the standard care arm.
“In the per-protocol analysis we also demonstrated that there was a suggestion that there is possible superiority of using blood eosinophil-directed oral corticosteroid prescriptions at the time of acute exacerbation using the point-of-care eosinophil test,” Dr. Bafadhel said.
There were no significant differences in the secondary outcomes of mean change in forced expiratory volume in 1 second (FEV1), COPD Assessment Test scores from exacerbation to follow-up, and symptoms according to a visual analog scale.
Invited discussant Dave Singh, MD, of the University of Manchester, England, asked Dr. Bafadhel how the data she presented supported her conclusions about the potential benefits of eosinophil-guided therapy, given that the P values were nonsignificant.
“The primary outcome was powered on noninferiority, and of course what we’ve shown is that it’s not any worse, it’s not any better, but of course it’s the effect of how many courses of steroids you can reduce in that population,” Dr. Bafadhel replied.
She noted that although the investigators have not performed an economic analysis to determine how many adverse events might be avoided using the biomarker-guided approach, “we do know that some of these patients who are given prednisolone, their comorbidities of diabetes worsened, for example.”
In the online Q&A for the presentation, Sohail Ansari, MD, from the Mid and South Essex NHS Foundation Trust in the United Kingdom, said that many patients in primary care practices receive “rescue packs” containing antibiotics and steroids, but may not be equipped to know when they should use the steroids and therefore may overuse them.
“Perhaps community-based, adequately resourced respiratory teams [may] be a way forward, but it will need adequate investment and commitment,” he wrote.
The trial was supported by the University of Oxford and National Institute for Health and Care Research, UK. Dr. Bafadhel reported grant and research support from the National Institute for Health and Care Research, Asthma & Lung UK, AstraZeneca, and Roche, and honoraria or fees from others. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Ansari reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
FROM ERS 2022 CONGRESS
RETHINC takes air out of COPD-like therapy for smokers
Current or former smokers who have clinically significant respiratory symptoms but no spirometric evidence of airway obstruction are often treated with dual bronchodilators commonly prescribed for patients with chronic obstructive pulmonary disease (COPD).
But as results of the randomized RETHINC (Redefining Therapy In Early COPD for the Pulmonary Trials Cooperative) trial showed, bronchodilator therapy was no better than placebo at reducing respiratory symptoms in smokers, reported MeiLan K. Han, MD, from the University of Michigan, Ann Arbor, on behalf of colleagues in the RETHINC study group.
“Many tobacco-exposed symptomatic individuals are currently being treated. We don’t know if this is because physicians just aren’t doing spirometry and assuming COPD or they strongly believe that there’s a benefit, but the bottom line is that we really need to do spirometry to understand who benefits from bronchodilators, and we need further research to understand how to treat this specific group of patients because there truly is pathogenesis and disease burden,” Dr. Han said in an oral abstract presentation at the annual congress of the European Respiratory Society.
The study results were also published online in the New England Journal of Medicine to coincide with the presentation.
In an editorial accompanying the study, Don D. Sin, MD, MPH, from the University of British Columbia, Vancouver, commented that these medications should most likely be reserved for patients with COPD who have clinically significant airflow limitation,” and that “respiratory symptoms in tobacco-exposed persons are common but are highly variable over time.”
Dave Singh, MD, from the University of Manchester (England), the invited discussant, called it “a very important negative study.”
Not up to GOLD standard
Current or former smokers who are symptomatic, with COPD Assessment Test (CAT) scores of at least 10 despite having preserved function on spirometry, have been shown to have higher prospective rates of respiratory disease exacerbations and increased sputum total mucin concentrations. Approximately 43% of such patients are treated with bronchodilators, and 23% are treated with inhaled corticosteroids (ICS), Dr. Han noted.
Her group hypothesized that ever-smokers with spirometric values that fall within the normal range – that is, a postbronchodilator FEV1/FVC ratio of 70 or greater – would still derive benefit from long-acting bronchodilator therapy, even though these patients are currently excluded from Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommendations.
To test this, they conducted a 12-week, multicenter, randomized, parallel-group study in which patients were assigned to receive either indacaterol (27.5 mcg) and glycopyrrolate (15.6 mcg) inhaled twice daily or placebo.
They enrolled adults aged 40-80 years with a minimum of 10 pack-years of smoking history, postbronchodilator FEV1/FVC ratio of 70 or greater, and CAT scores of 10 or greater. Patients with known concomitant lung disease, a primary diagnosis of asthma, or body mass index lower than 15 or higher than 40 and those being concomitantly treated with long-acting beta2-agonists or muscarinic antagonists or a short-acting combination were excluded, although patients were allowed to be on a short-acting beta-agonist.
A total of 535 participants were randomized, but COVID-19 pandemic–imposed obstacles resulted in a modified intention-to-treat population of 277 patients assigned to receive the active treatment and 244 assigned to receive placebo.
There was no difference between the groups for the primary outcome of an at least 4-point decrease in St. George’s Respiratory Questionnaire scores in patients who did not experience treatment failure, defined as an increase in respiratory symptoms requiring treatment with active long-acting bronchodilators or ICS.
The primary endpoint was seen in 56.4% of patients in the bronchodilator group, and 59% of controls.
Although there was greater improvement in pulmonary function from baseline in the treatment group, compared with the placebo group, the improvements did not correlate with similar improvements in symptoms, Dr. Han said.
There were 4 serious adverse events in the bronchodilator group and 11 in the placebo group, but none of the events were deemed to be related to the assigned treatments.
Dr. Han acknowledged limitations of the study, which may have included symptoms driven by other factors such as cardiac disease, suggesting that if such patients had been identified and excluded, a stronger effect might have been seen for the active treatment.
In addition, the study was underpowered to look at the subgroup of participants with chronic bronchitis, and the 12 weeks of the study may have been too short to see improvements in symptoms.
In his editorial, Dr. Sin noted that the study showed that cough and sputum production rather than exertion dyspnea are the primary symptoms among ever-smokers.
“Although bronchodilators are effective in ameliorating breathlessness and improving exercise tolerance, they are generally ineffective for cough,” he wrote. “Existing drugs for the treatment of COPD, such as inhaled glucocorticoids or phosphodiesterase-4 inhibitors, or new therapeutics such as P2X3 receptor antagonists may be more effective for the treatment of cough and sputum production related to smoking and could be considered for future evaluations in this patient population.”
The study was supported by the National Heart, Lung, and Blood Institute, the National Center for Advancing Translational Sciences, and Sunovion Pharmaceuticals. Novartis Pharmaceuticals donated the trial medication and placebo. Dr. Han disclosed grant/research support and honoraria or consulting fees from various companies. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Sin reported having no conflicts of interest to disclose.
A version of this article first appeared on Medscape.com.
Current or former smokers who have clinically significant respiratory symptoms but no spirometric evidence of airway obstruction are often treated with dual bronchodilators commonly prescribed for patients with chronic obstructive pulmonary disease (COPD).
But as results of the randomized RETHINC (Redefining Therapy In Early COPD for the Pulmonary Trials Cooperative) trial showed, bronchodilator therapy was no better than placebo at reducing respiratory symptoms in smokers, reported MeiLan K. Han, MD, from the University of Michigan, Ann Arbor, on behalf of colleagues in the RETHINC study group.
“Many tobacco-exposed symptomatic individuals are currently being treated. We don’t know if this is because physicians just aren’t doing spirometry and assuming COPD or they strongly believe that there’s a benefit, but the bottom line is that we really need to do spirometry to understand who benefits from bronchodilators, and we need further research to understand how to treat this specific group of patients because there truly is pathogenesis and disease burden,” Dr. Han said in an oral abstract presentation at the annual congress of the European Respiratory Society.
The study results were also published online in the New England Journal of Medicine to coincide with the presentation.
In an editorial accompanying the study, Don D. Sin, MD, MPH, from the University of British Columbia, Vancouver, commented that these medications should most likely be reserved for patients with COPD who have clinically significant airflow limitation,” and that “respiratory symptoms in tobacco-exposed persons are common but are highly variable over time.”
Dave Singh, MD, from the University of Manchester (England), the invited discussant, called it “a very important negative study.”
Not up to GOLD standard
Current or former smokers who are symptomatic, with COPD Assessment Test (CAT) scores of at least 10 despite having preserved function on spirometry, have been shown to have higher prospective rates of respiratory disease exacerbations and increased sputum total mucin concentrations. Approximately 43% of such patients are treated with bronchodilators, and 23% are treated with inhaled corticosteroids (ICS), Dr. Han noted.
Her group hypothesized that ever-smokers with spirometric values that fall within the normal range – that is, a postbronchodilator FEV1/FVC ratio of 70 or greater – would still derive benefit from long-acting bronchodilator therapy, even though these patients are currently excluded from Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommendations.
To test this, they conducted a 12-week, multicenter, randomized, parallel-group study in which patients were assigned to receive either indacaterol (27.5 mcg) and glycopyrrolate (15.6 mcg) inhaled twice daily or placebo.
They enrolled adults aged 40-80 years with a minimum of 10 pack-years of smoking history, postbronchodilator FEV1/FVC ratio of 70 or greater, and CAT scores of 10 or greater. Patients with known concomitant lung disease, a primary diagnosis of asthma, or body mass index lower than 15 or higher than 40 and those being concomitantly treated with long-acting beta2-agonists or muscarinic antagonists or a short-acting combination were excluded, although patients were allowed to be on a short-acting beta-agonist.
A total of 535 participants were randomized, but COVID-19 pandemic–imposed obstacles resulted in a modified intention-to-treat population of 277 patients assigned to receive the active treatment and 244 assigned to receive placebo.
There was no difference between the groups for the primary outcome of an at least 4-point decrease in St. George’s Respiratory Questionnaire scores in patients who did not experience treatment failure, defined as an increase in respiratory symptoms requiring treatment with active long-acting bronchodilators or ICS.
The primary endpoint was seen in 56.4% of patients in the bronchodilator group, and 59% of controls.
Although there was greater improvement in pulmonary function from baseline in the treatment group, compared with the placebo group, the improvements did not correlate with similar improvements in symptoms, Dr. Han said.
There were 4 serious adverse events in the bronchodilator group and 11 in the placebo group, but none of the events were deemed to be related to the assigned treatments.
Dr. Han acknowledged limitations of the study, which may have included symptoms driven by other factors such as cardiac disease, suggesting that if such patients had been identified and excluded, a stronger effect might have been seen for the active treatment.
In addition, the study was underpowered to look at the subgroup of participants with chronic bronchitis, and the 12 weeks of the study may have been too short to see improvements in symptoms.
In his editorial, Dr. Sin noted that the study showed that cough and sputum production rather than exertion dyspnea are the primary symptoms among ever-smokers.
“Although bronchodilators are effective in ameliorating breathlessness and improving exercise tolerance, they are generally ineffective for cough,” he wrote. “Existing drugs for the treatment of COPD, such as inhaled glucocorticoids or phosphodiesterase-4 inhibitors, or new therapeutics such as P2X3 receptor antagonists may be more effective for the treatment of cough and sputum production related to smoking and could be considered for future evaluations in this patient population.”
The study was supported by the National Heart, Lung, and Blood Institute, the National Center for Advancing Translational Sciences, and Sunovion Pharmaceuticals. Novartis Pharmaceuticals donated the trial medication and placebo. Dr. Han disclosed grant/research support and honoraria or consulting fees from various companies. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Sin reported having no conflicts of interest to disclose.
A version of this article first appeared on Medscape.com.
Current or former smokers who have clinically significant respiratory symptoms but no spirometric evidence of airway obstruction are often treated with dual bronchodilators commonly prescribed for patients with chronic obstructive pulmonary disease (COPD).
But as results of the randomized RETHINC (Redefining Therapy In Early COPD for the Pulmonary Trials Cooperative) trial showed, bronchodilator therapy was no better than placebo at reducing respiratory symptoms in smokers, reported MeiLan K. Han, MD, from the University of Michigan, Ann Arbor, on behalf of colleagues in the RETHINC study group.
“Many tobacco-exposed symptomatic individuals are currently being treated. We don’t know if this is because physicians just aren’t doing spirometry and assuming COPD or they strongly believe that there’s a benefit, but the bottom line is that we really need to do spirometry to understand who benefits from bronchodilators, and we need further research to understand how to treat this specific group of patients because there truly is pathogenesis and disease burden,” Dr. Han said in an oral abstract presentation at the annual congress of the European Respiratory Society.
The study results were also published online in the New England Journal of Medicine to coincide with the presentation.
In an editorial accompanying the study, Don D. Sin, MD, MPH, from the University of British Columbia, Vancouver, commented that these medications should most likely be reserved for patients with COPD who have clinically significant airflow limitation,” and that “respiratory symptoms in tobacco-exposed persons are common but are highly variable over time.”
Dave Singh, MD, from the University of Manchester (England), the invited discussant, called it “a very important negative study.”
Not up to GOLD standard
Current or former smokers who are symptomatic, with COPD Assessment Test (CAT) scores of at least 10 despite having preserved function on spirometry, have been shown to have higher prospective rates of respiratory disease exacerbations and increased sputum total mucin concentrations. Approximately 43% of such patients are treated with bronchodilators, and 23% are treated with inhaled corticosteroids (ICS), Dr. Han noted.
Her group hypothesized that ever-smokers with spirometric values that fall within the normal range – that is, a postbronchodilator FEV1/FVC ratio of 70 or greater – would still derive benefit from long-acting bronchodilator therapy, even though these patients are currently excluded from Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommendations.
To test this, they conducted a 12-week, multicenter, randomized, parallel-group study in which patients were assigned to receive either indacaterol (27.5 mcg) and glycopyrrolate (15.6 mcg) inhaled twice daily or placebo.
They enrolled adults aged 40-80 years with a minimum of 10 pack-years of smoking history, postbronchodilator FEV1/FVC ratio of 70 or greater, and CAT scores of 10 or greater. Patients with known concomitant lung disease, a primary diagnosis of asthma, or body mass index lower than 15 or higher than 40 and those being concomitantly treated with long-acting beta2-agonists or muscarinic antagonists or a short-acting combination were excluded, although patients were allowed to be on a short-acting beta-agonist.
A total of 535 participants were randomized, but COVID-19 pandemic–imposed obstacles resulted in a modified intention-to-treat population of 277 patients assigned to receive the active treatment and 244 assigned to receive placebo.
There was no difference between the groups for the primary outcome of an at least 4-point decrease in St. George’s Respiratory Questionnaire scores in patients who did not experience treatment failure, defined as an increase in respiratory symptoms requiring treatment with active long-acting bronchodilators or ICS.
The primary endpoint was seen in 56.4% of patients in the bronchodilator group, and 59% of controls.
Although there was greater improvement in pulmonary function from baseline in the treatment group, compared with the placebo group, the improvements did not correlate with similar improvements in symptoms, Dr. Han said.
There were 4 serious adverse events in the bronchodilator group and 11 in the placebo group, but none of the events were deemed to be related to the assigned treatments.
Dr. Han acknowledged limitations of the study, which may have included symptoms driven by other factors such as cardiac disease, suggesting that if such patients had been identified and excluded, a stronger effect might have been seen for the active treatment.
In addition, the study was underpowered to look at the subgroup of participants with chronic bronchitis, and the 12 weeks of the study may have been too short to see improvements in symptoms.
In his editorial, Dr. Sin noted that the study showed that cough and sputum production rather than exertion dyspnea are the primary symptoms among ever-smokers.
“Although bronchodilators are effective in ameliorating breathlessness and improving exercise tolerance, they are generally ineffective for cough,” he wrote. “Existing drugs for the treatment of COPD, such as inhaled glucocorticoids or phosphodiesterase-4 inhibitors, or new therapeutics such as P2X3 receptor antagonists may be more effective for the treatment of cough and sputum production related to smoking and could be considered for future evaluations in this patient population.”
The study was supported by the National Heart, Lung, and Blood Institute, the National Center for Advancing Translational Sciences, and Sunovion Pharmaceuticals. Novartis Pharmaceuticals donated the trial medication and placebo. Dr. Han disclosed grant/research support and honoraria or consulting fees from various companies. Dr. Singh reported speaking fees, honoraria, and research grants from multiple companies. Dr. Sin reported having no conflicts of interest to disclose.
A version of this article first appeared on Medscape.com.
FROM ERS 2022
Five contract red flags every physician should know
Recruiting health care workers is a challenge these days for both private practice and hospital employers, and competition can be fierce. In order to be competitive, employers need to review the package they are offering potential candidates and understand that it’s more than just compensation and benefits that matter.
As someone who reviews physician contracts extensively, there are some common examples of language that may cause a candidate to choose a different position.
Probationary period
Although every employer wants to find out if they like the physician or midlevel employee that they have just hired before fully committing, the inclusion of a probationary period (usually 90 days) is offensive to a candidate, especially one with a choice of contracts.
Essentially, the employer is asking the employee to (potentially) relocate, go through the credentialing process, and turn down other potential offers, all for the possibility that they could easily be terminated. Probationary periods typically allow an employee to be immediately terminated without notice or cause, which can then leave them stranded without a paycheck (and with a new home and/or other recent commitments).
Moreover, contracts with probationary periods tend to terminate the employee without covering any tail costs or clarifying that the employer will not enforce restrictive provisions (even if unlikely to be legally enforceable based on the short relationship).
It is important to understand that the process of a person finding a new position, which includes interviewing, contract negotiation, and credentialing, can take up to 6 months. For this reason, probationary provisions create real job insecurity for a candidate.
Entering into a new affiliation is a leap of faith both for the employer and the employee. If the circumstances do not work out, the employer should fairly compensate the employee for the notice period and ask them not to return to work or otherwise allow them to keep working the notice period while they search for a new position.
Acceleration of notice
Another objectionable provision that employers like to include in their contracts is one which allows the employer to accelerate and immediately terminate an employee who has given proper notice.
The contract will contain a standard notice provision, but when the health care professional submits notice, their last date is suddenly accelerated, and they are released without further compensation, notice, or benefits. This type of provision is particularly offensive to health care employees who take the step of giving proper contractual notice and, similar to the probationary language, can create real job insecurity for an employee who suddenly loses their paycheck and has no new job to start.
Medical workers should be paid for the entire notice period whether or not they are allowed to work. Unfortunately, this type of provision is sometimes hidden in contracts and not noticed by employees, who tend to focus on the notice provision itself. I consider this provision to be a red flag about the employer when I review clients’ contracts.
Malpractice tail
Although many employers will claim it is not unusual for an employee to pay for their own malpractice tail, in the current marketplace, the payment of tail can be a deciding factor in whether a candidate accepts a contract.
At a minimum, employers should consider paying for the tail under circumstances where they non-renew a contract, terminate without cause, or the contract is terminated for the employer’s breach. Similarly, I like to seek out payment of the tail by the employer where the contract is terminated owing to a change in the law, use of a force majeure provision, loss of the employer’s hospital contract, or similar provisions where termination is outside the control of the employee.
Employers should also consider a provision where they share the cost of a tail or cover the entire cost on the basis of years of service in order to stand out to a potential candidate.
Noncompete provisions
I do not find noncompete provisions to be generally unacceptable when properly written; however, employers should reevaluate the reasonableness of their noncompete language frequently, because such language can make the difference in whether a candidate accepts a contract.
A reasonable noncompete that only protects the employer as necessary and does not restrict the reasonable practice of medicine is always preferable and can be the deciding factor for a candidate. Tying enforcement of a noncompete to reasons for termination (similar to the tail) can also make a positive difference in a candidate’s review of a contract.
Egregious noncompetes, where the candidate is simply informed that the language is “not negotiable,” are unlikely to be compelling to a candidate with other options.
Specifics on location, call, schedule
One item potential employees find extremely frustrating about contracts is when it fails to include promises made regarding location, call, and schedule.
These particular items affect a physician’s expectations about a job, including commute time, family life, and lifestyle. An employer or recruiter that makes a lot of promises on these points but won’t commit to the details in writing (or at least offer mutual agreement on these issues) can cause an uncertain candidate to choose the job that offers greater certainty.
There are many provisions of a contract that can make a difference to a particular job applicant. A savvy employer seeking to capture a particular health care professional should find out what the specific goals and needs of the candidate might be and consider adjusting the contract to best satisfy the candidate.
At the end of the day, however, at least for those physicians and others reviewing contracts that are fairly equivalent, it may be the fairness of the contract provisions that end up being the deciding factor.
Ms. Adler is Health Law Group Practice Leader for the law firm Roetzel in Chicago. She reported no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
Recruiting health care workers is a challenge these days for both private practice and hospital employers, and competition can be fierce. In order to be competitive, employers need to review the package they are offering potential candidates and understand that it’s more than just compensation and benefits that matter.
As someone who reviews physician contracts extensively, there are some common examples of language that may cause a candidate to choose a different position.
Probationary period
Although every employer wants to find out if they like the physician or midlevel employee that they have just hired before fully committing, the inclusion of a probationary period (usually 90 days) is offensive to a candidate, especially one with a choice of contracts.
Essentially, the employer is asking the employee to (potentially) relocate, go through the credentialing process, and turn down other potential offers, all for the possibility that they could easily be terminated. Probationary periods typically allow an employee to be immediately terminated without notice or cause, which can then leave them stranded without a paycheck (and with a new home and/or other recent commitments).
Moreover, contracts with probationary periods tend to terminate the employee without covering any tail costs or clarifying that the employer will not enforce restrictive provisions (even if unlikely to be legally enforceable based on the short relationship).
It is important to understand that the process of a person finding a new position, which includes interviewing, contract negotiation, and credentialing, can take up to 6 months. For this reason, probationary provisions create real job insecurity for a candidate.
Entering into a new affiliation is a leap of faith both for the employer and the employee. If the circumstances do not work out, the employer should fairly compensate the employee for the notice period and ask them not to return to work or otherwise allow them to keep working the notice period while they search for a new position.
Acceleration of notice
Another objectionable provision that employers like to include in their contracts is one which allows the employer to accelerate and immediately terminate an employee who has given proper notice.
The contract will contain a standard notice provision, but when the health care professional submits notice, their last date is suddenly accelerated, and they are released without further compensation, notice, or benefits. This type of provision is particularly offensive to health care employees who take the step of giving proper contractual notice and, similar to the probationary language, can create real job insecurity for an employee who suddenly loses their paycheck and has no new job to start.
Medical workers should be paid for the entire notice period whether or not they are allowed to work. Unfortunately, this type of provision is sometimes hidden in contracts and not noticed by employees, who tend to focus on the notice provision itself. I consider this provision to be a red flag about the employer when I review clients’ contracts.
Malpractice tail
Although many employers will claim it is not unusual for an employee to pay for their own malpractice tail, in the current marketplace, the payment of tail can be a deciding factor in whether a candidate accepts a contract.
At a minimum, employers should consider paying for the tail under circumstances where they non-renew a contract, terminate without cause, or the contract is terminated for the employer’s breach. Similarly, I like to seek out payment of the tail by the employer where the contract is terminated owing to a change in the law, use of a force majeure provision, loss of the employer’s hospital contract, or similar provisions where termination is outside the control of the employee.
Employers should also consider a provision where they share the cost of a tail or cover the entire cost on the basis of years of service in order to stand out to a potential candidate.
Noncompete provisions
I do not find noncompete provisions to be generally unacceptable when properly written; however, employers should reevaluate the reasonableness of their noncompete language frequently, because such language can make the difference in whether a candidate accepts a contract.
A reasonable noncompete that only protects the employer as necessary and does not restrict the reasonable practice of medicine is always preferable and can be the deciding factor for a candidate. Tying enforcement of a noncompete to reasons for termination (similar to the tail) can also make a positive difference in a candidate’s review of a contract.
Egregious noncompetes, where the candidate is simply informed that the language is “not negotiable,” are unlikely to be compelling to a candidate with other options.
Specifics on location, call, schedule
One item potential employees find extremely frustrating about contracts is when it fails to include promises made regarding location, call, and schedule.
These particular items affect a physician’s expectations about a job, including commute time, family life, and lifestyle. An employer or recruiter that makes a lot of promises on these points but won’t commit to the details in writing (or at least offer mutual agreement on these issues) can cause an uncertain candidate to choose the job that offers greater certainty.
There are many provisions of a contract that can make a difference to a particular job applicant. A savvy employer seeking to capture a particular health care professional should find out what the specific goals and needs of the candidate might be and consider adjusting the contract to best satisfy the candidate.
At the end of the day, however, at least for those physicians and others reviewing contracts that are fairly equivalent, it may be the fairness of the contract provisions that end up being the deciding factor.
Ms. Adler is Health Law Group Practice Leader for the law firm Roetzel in Chicago. She reported no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
Recruiting health care workers is a challenge these days for both private practice and hospital employers, and competition can be fierce. In order to be competitive, employers need to review the package they are offering potential candidates and understand that it’s more than just compensation and benefits that matter.
As someone who reviews physician contracts extensively, there are some common examples of language that may cause a candidate to choose a different position.
Probationary period
Although every employer wants to find out if they like the physician or midlevel employee that they have just hired before fully committing, the inclusion of a probationary period (usually 90 days) is offensive to a candidate, especially one with a choice of contracts.
Essentially, the employer is asking the employee to (potentially) relocate, go through the credentialing process, and turn down other potential offers, all for the possibility that they could easily be terminated. Probationary periods typically allow an employee to be immediately terminated without notice or cause, which can then leave them stranded without a paycheck (and with a new home and/or other recent commitments).
Moreover, contracts with probationary periods tend to terminate the employee without covering any tail costs or clarifying that the employer will not enforce restrictive provisions (even if unlikely to be legally enforceable based on the short relationship).
It is important to understand that the process of a person finding a new position, which includes interviewing, contract negotiation, and credentialing, can take up to 6 months. For this reason, probationary provisions create real job insecurity for a candidate.
Entering into a new affiliation is a leap of faith both for the employer and the employee. If the circumstances do not work out, the employer should fairly compensate the employee for the notice period and ask them not to return to work or otherwise allow them to keep working the notice period while they search for a new position.
Acceleration of notice
Another objectionable provision that employers like to include in their contracts is one which allows the employer to accelerate and immediately terminate an employee who has given proper notice.
The contract will contain a standard notice provision, but when the health care professional submits notice, their last date is suddenly accelerated, and they are released without further compensation, notice, or benefits. This type of provision is particularly offensive to health care employees who take the step of giving proper contractual notice and, similar to the probationary language, can create real job insecurity for an employee who suddenly loses their paycheck and has no new job to start.
Medical workers should be paid for the entire notice period whether or not they are allowed to work. Unfortunately, this type of provision is sometimes hidden in contracts and not noticed by employees, who tend to focus on the notice provision itself. I consider this provision to be a red flag about the employer when I review clients’ contracts.
Malpractice tail
Although many employers will claim it is not unusual for an employee to pay for their own malpractice tail, in the current marketplace, the payment of tail can be a deciding factor in whether a candidate accepts a contract.
At a minimum, employers should consider paying for the tail under circumstances where they non-renew a contract, terminate without cause, or the contract is terminated for the employer’s breach. Similarly, I like to seek out payment of the tail by the employer where the contract is terminated owing to a change in the law, use of a force majeure provision, loss of the employer’s hospital contract, or similar provisions where termination is outside the control of the employee.
Employers should also consider a provision where they share the cost of a tail or cover the entire cost on the basis of years of service in order to stand out to a potential candidate.
Noncompete provisions
I do not find noncompete provisions to be generally unacceptable when properly written; however, employers should reevaluate the reasonableness of their noncompete language frequently, because such language can make the difference in whether a candidate accepts a contract.
A reasonable noncompete that only protects the employer as necessary and does not restrict the reasonable practice of medicine is always preferable and can be the deciding factor for a candidate. Tying enforcement of a noncompete to reasons for termination (similar to the tail) can also make a positive difference in a candidate’s review of a contract.
Egregious noncompetes, where the candidate is simply informed that the language is “not negotiable,” are unlikely to be compelling to a candidate with other options.
Specifics on location, call, schedule
One item potential employees find extremely frustrating about contracts is when it fails to include promises made regarding location, call, and schedule.
These particular items affect a physician’s expectations about a job, including commute time, family life, and lifestyle. An employer or recruiter that makes a lot of promises on these points but won’t commit to the details in writing (or at least offer mutual agreement on these issues) can cause an uncertain candidate to choose the job that offers greater certainty.
There are many provisions of a contract that can make a difference to a particular job applicant. A savvy employer seeking to capture a particular health care professional should find out what the specific goals and needs of the candidate might be and consider adjusting the contract to best satisfy the candidate.
At the end of the day, however, at least for those physicians and others reviewing contracts that are fairly equivalent, it may be the fairness of the contract provisions that end up being the deciding factor.
Ms. Adler is Health Law Group Practice Leader for the law firm Roetzel in Chicago. She reported no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
Stronger evidence that exercise lowers breast cancer risk
The results of the new study suggest that greater overall physical activity levels, greater vigorous activity, and lower sedentary time are likely to reduce breast cancer risk, said the authors.
“Increasing physical activity and reducing sedentary time are already recommended for cancer prevention. Our study adds further evidence that such behavioral changes are likely to lower the incidence of future breast cancer rates,” Suzanne C. Dixon-Suen, PhD, of Cancer Council Victoria, Melbourne, and colleagues reported on behalf of the Breast Cancer Association Consortium (BCAC).
The findings were published online in the British Journal of Sports Medicine.
The investigators used individual-level BCAC case-control data and performed two-sample Mendelian randomization – a study method that assesses causality by using genetic variants as proxies for particular risk factors. In this case, genetic variants were used as proxies for lifelong physical activity levels and sedentary behaviors.
“[Genetic] instruments were single-nucleotide polymorphisms (SNPs) associated in UK Biobank [genomewide association studies] with overall physical activity (all movement), vigorous physical activity, or sedentary time” as assessed by a wrist-worn accelerometer.
Patients with greater genetic predisposition to higher overall activity levels had a 41% lower overall breast cancer risk (odds ratio, 0.59), the team reported. Genetically predicted vigorous activity was associated with a 38% lower risk of premenopausal and perimenopausal breast cancer (OR, 0.62 for 3 or more days vs. 0 days of self-reported days per week).
Conversely, greater genetically predicted sedentary time was associated with a 77% higher risk of hormone receptor–negative breast cancer risk (OR, 1.77), including triple-negative breast cancer, for which the risk was 104% higher (OR, 2.04).
The findings were generally consistent across disease types and stages, and were unchanged after factoring in “the production by a single gene of two or more apparently unrelated effects (pleiotropy), such as smoking and overweight, for example,” according to a press release from the journal.
The investigators included data from 130,957 women of European ancestry. Of those, 69,838 had invasive disease, 6,667 had in situ tumors, and 54,452 were controls without breast cancer. The case-control groups included 23,999 pre-/perimenopausal women with invasive breast cancer and 17,686 women without, and 45,839 postmenopausal women with breast cancer and 36,766 without.
A number of plausible biological explanations for the findings exist, the authors noted, adding that convincing evidence suggests there are causal pathways between physical activity and breast cancer risk, including overweight and obesity, disordered metabolism, sex hormones, and inflammation.
Furthermore, the researchers reported, “mechanisms linking sedentary time and cancer are likely to at least partially overlap with those underpinning the physical activity relationship.”
For the future, they suggested that “[a] stronger cancer-control focus on physical activity and sedentary time as modifiable cancer risk factors is warranted, given the heavy burden of disease attributed to the most common cancer in women.”
This study was funded by multiple international sources. Dr. Dixon-Suen reported no relevant financial relationships. Several coauthors disclosed relationships with industry.
A version of this article first appeared on Medscape.com.
The results of the new study suggest that greater overall physical activity levels, greater vigorous activity, and lower sedentary time are likely to reduce breast cancer risk, said the authors.
“Increasing physical activity and reducing sedentary time are already recommended for cancer prevention. Our study adds further evidence that such behavioral changes are likely to lower the incidence of future breast cancer rates,” Suzanne C. Dixon-Suen, PhD, of Cancer Council Victoria, Melbourne, and colleagues reported on behalf of the Breast Cancer Association Consortium (BCAC).
The findings were published online in the British Journal of Sports Medicine.
The investigators used individual-level BCAC case-control data and performed two-sample Mendelian randomization – a study method that assesses causality by using genetic variants as proxies for particular risk factors. In this case, genetic variants were used as proxies for lifelong physical activity levels and sedentary behaviors.
“[Genetic] instruments were single-nucleotide polymorphisms (SNPs) associated in UK Biobank [genomewide association studies] with overall physical activity (all movement), vigorous physical activity, or sedentary time” as assessed by a wrist-worn accelerometer.
Patients with greater genetic predisposition to higher overall activity levels had a 41% lower overall breast cancer risk (odds ratio, 0.59), the team reported. Genetically predicted vigorous activity was associated with a 38% lower risk of premenopausal and perimenopausal breast cancer (OR, 0.62 for 3 or more days vs. 0 days of self-reported days per week).
Conversely, greater genetically predicted sedentary time was associated with a 77% higher risk of hormone receptor–negative breast cancer risk (OR, 1.77), including triple-negative breast cancer, for which the risk was 104% higher (OR, 2.04).
The findings were generally consistent across disease types and stages, and were unchanged after factoring in “the production by a single gene of two or more apparently unrelated effects (pleiotropy), such as smoking and overweight, for example,” according to a press release from the journal.
The investigators included data from 130,957 women of European ancestry. Of those, 69,838 had invasive disease, 6,667 had in situ tumors, and 54,452 were controls without breast cancer. The case-control groups included 23,999 pre-/perimenopausal women with invasive breast cancer and 17,686 women without, and 45,839 postmenopausal women with breast cancer and 36,766 without.
A number of plausible biological explanations for the findings exist, the authors noted, adding that convincing evidence suggests there are causal pathways between physical activity and breast cancer risk, including overweight and obesity, disordered metabolism, sex hormones, and inflammation.
Furthermore, the researchers reported, “mechanisms linking sedentary time and cancer are likely to at least partially overlap with those underpinning the physical activity relationship.”
For the future, they suggested that “[a] stronger cancer-control focus on physical activity and sedentary time as modifiable cancer risk factors is warranted, given the heavy burden of disease attributed to the most common cancer in women.”
This study was funded by multiple international sources. Dr. Dixon-Suen reported no relevant financial relationships. Several coauthors disclosed relationships with industry.
A version of this article first appeared on Medscape.com.
The results of the new study suggest that greater overall physical activity levels, greater vigorous activity, and lower sedentary time are likely to reduce breast cancer risk, said the authors.
“Increasing physical activity and reducing sedentary time are already recommended for cancer prevention. Our study adds further evidence that such behavioral changes are likely to lower the incidence of future breast cancer rates,” Suzanne C. Dixon-Suen, PhD, of Cancer Council Victoria, Melbourne, and colleagues reported on behalf of the Breast Cancer Association Consortium (BCAC).
The findings were published online in the British Journal of Sports Medicine.
The investigators used individual-level BCAC case-control data and performed two-sample Mendelian randomization – a study method that assesses causality by using genetic variants as proxies for particular risk factors. In this case, genetic variants were used as proxies for lifelong physical activity levels and sedentary behaviors.
“[Genetic] instruments were single-nucleotide polymorphisms (SNPs) associated in UK Biobank [genomewide association studies] with overall physical activity (all movement), vigorous physical activity, or sedentary time” as assessed by a wrist-worn accelerometer.
Patients with greater genetic predisposition to higher overall activity levels had a 41% lower overall breast cancer risk (odds ratio, 0.59), the team reported. Genetically predicted vigorous activity was associated with a 38% lower risk of premenopausal and perimenopausal breast cancer (OR, 0.62 for 3 or more days vs. 0 days of self-reported days per week).
Conversely, greater genetically predicted sedentary time was associated with a 77% higher risk of hormone receptor–negative breast cancer risk (OR, 1.77), including triple-negative breast cancer, for which the risk was 104% higher (OR, 2.04).
The findings were generally consistent across disease types and stages, and were unchanged after factoring in “the production by a single gene of two or more apparently unrelated effects (pleiotropy), such as smoking and overweight, for example,” according to a press release from the journal.
The investigators included data from 130,957 women of European ancestry. Of those, 69,838 had invasive disease, 6,667 had in situ tumors, and 54,452 were controls without breast cancer. The case-control groups included 23,999 pre-/perimenopausal women with invasive breast cancer and 17,686 women without, and 45,839 postmenopausal women with breast cancer and 36,766 without.
A number of plausible biological explanations for the findings exist, the authors noted, adding that convincing evidence suggests there are causal pathways between physical activity and breast cancer risk, including overweight and obesity, disordered metabolism, sex hormones, and inflammation.
Furthermore, the researchers reported, “mechanisms linking sedentary time and cancer are likely to at least partially overlap with those underpinning the physical activity relationship.”
For the future, they suggested that “[a] stronger cancer-control focus on physical activity and sedentary time as modifiable cancer risk factors is warranted, given the heavy burden of disease attributed to the most common cancer in women.”
This study was funded by multiple international sources. Dr. Dixon-Suen reported no relevant financial relationships. Several coauthors disclosed relationships with industry.
A version of this article first appeared on Medscape.com.
FROM THE BRITISH JOURNAL OF SPORTS MEDICINE