User login
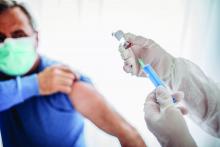
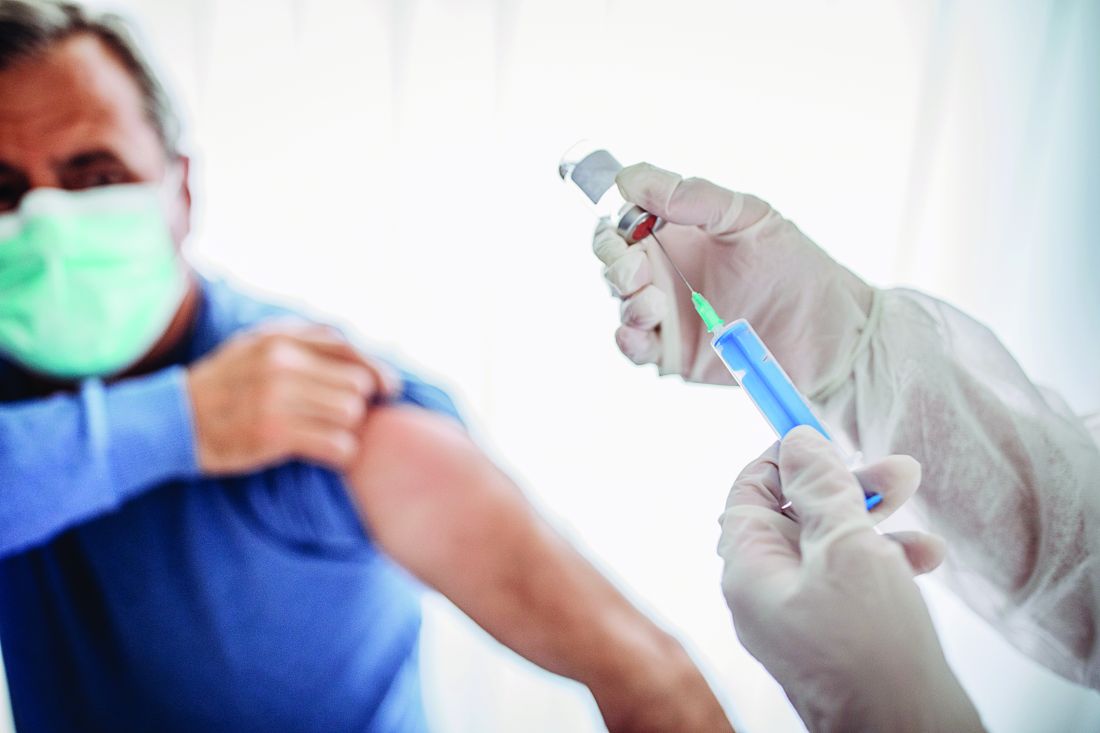
Updated guidance for COVID vaccination in rheumatology patients arrives amid continued hesitancy
As rheumatologists contend with vaccine hesitancy among certain subsets of patients, the American College of Rheumatology has released updated clinical guidelines on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases (RMDs), including new recommendations on supplemental and booster doses.
The revised guidance from this fifth version of the ACR guidelines includes strongly recommending that all RMD patients receive a booster after their primary vaccine series, regardless of whether they have been naturally infected with COVID-19. In addition, they strongly recommend third supplemental doses for patients with autoimmune inflammatory rheumatic diseases (AIIRDs) who likely mounted an inadequate vaccine response, which would then be followed by a fourth booster dose as advised by the Centers for Disease Control and Prevention for immunocompromised individuals.
Other recommendations include pre-exposure prophylaxis monoclonal antibody treatment for high-risk AIIRD patients, defined as those with moderate to severely compromised immune systems who may not mount an adequate immune response to COVID-19 vaccination, when it is available and authorized for emergency use by the Food and Drug Administration, as well as monoclonal antibody therapy for postexposure prophylaxis of asymptomatic, recently exposed high-risk AIIRD patients or as treatment for newly symptomatic, high-risk AIIRD patients. The ACR guidance notes that, currently, neither the monoclonal antibodies bamlanivimab and etesevimab (administered together) nor casirivimab and imdevimab (REGEN-COV), are licensed or available under an emergency use authorization given their lack of activity against the Omicron variant, the dominant strain of SARS-CoV-2 circulating in the United States.
Finally, the guidance clarified that the timing of intravenous immunoglobulin doses does not need to be modified around the administration of COVID vaccine doses, based on moderate consensus among task force members.
Vaccine hesitancy in community rheumatology practices
The revised guidelines were released just as Arthritis & Rheumatology published a new study that assessed vaccine hesitancy among rheumatology patients on immunomodulatory therapies. A three-item electronic survey was conducted at 101 offices within a community practice–based rheumatology research network and ultimately collected responses from 58,529 patients, 20,987 of whom had an AIIRD and were receiving targeted therapies like biologics or Janus kinase inhibitors.
Of the total respondents, 77% (n = 43,675) had been vaccinated, 16.9% were not vaccinated and did not plan to be, and 6.1% were not vaccinated but planned to be. However, AIIRD patients were 16% less likely to be vaccinated, compared with the other patients, such as those with osteoarthritis or osteoporosis who were not receiving disease-modifying antirheumatic drugs (76.9% vs. 87%; odds ratio, 0.84; 95% confidence interval, 0.77-0.92; P < .001). Multivariable analysis also found that older patients (OR, 1.49 per 10 years) and Asians (OR, 2.42; 95% CI, 1.77-3.33) were more likely to be vaccinated.
“Rheumatologists need to be asking their patients more than just: ‘Are you vaccinated?’ ” Jeffrey Curtis, MD, MPH, head of the ACR COVID-19 vaccine task force and a coauthor of the vaccine hesitancy study, said in an interview. “A year ago, that was a fine approach, but now they need to be asking whether you’ve been vaccinated, and with what, and how many times, and how recently. There are a whole lot of subtleties there; ‘vaccinated: yes or no’ is just the tip of the iceberg.”
His research into the vaccine hesitant includes recent anecdotal data from thousands of patients treated in local rheumatology community practices, many of whom cited long-term safety data and potential side effects as reasons why they were unwilling to get vaccinated. But despite their on-paper responses, he cautioned rheumatologists to think critically when determining which patients may truly be open to vaccination.
“If you’re designing strategies to affect vaccine hesitancy, you may be wasting your time with some people,” said Dr. Curtis, professor of medicine at the University of Alabama at Birmingham. “A critical need is to figure out who are the patients who may be amendable to more information or an intervention or a little bit more time and care, and who are the people where you know, this is a lost cause: You don’t get a flu shot, you haven’t been vaccinated for shingles, [and] you’re not going to get this one either.
“In terms of a research agenda, how do we develop efficient, simple, short screening tools?” he added. “Something with a few helpful questions, on a patient portal or an iPad, that will do a good job identifying your patients at risk who haven’t had vaccination but that you might be able to spend time with, intervene, and actually change their mind. If you spend gobs of time with everyone, you’ll help some people, but clinicians don’t have an infinite amount of time.”
One of the authors of the vaccine hesitancy study acknowledged being employed by the rheumatology research network that hosted the survey. Several others, including Dr. Curtis, reported receiving grants and consulting fees from various pharmaceutical companies.
As rheumatologists contend with vaccine hesitancy among certain subsets of patients, the American College of Rheumatology has released updated clinical guidelines on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases (RMDs), including new recommendations on supplemental and booster doses.
The revised guidance from this fifth version of the ACR guidelines includes strongly recommending that all RMD patients receive a booster after their primary vaccine series, regardless of whether they have been naturally infected with COVID-19. In addition, they strongly recommend third supplemental doses for patients with autoimmune inflammatory rheumatic diseases (AIIRDs) who likely mounted an inadequate vaccine response, which would then be followed by a fourth booster dose as advised by the Centers for Disease Control and Prevention for immunocompromised individuals.
Other recommendations include pre-exposure prophylaxis monoclonal antibody treatment for high-risk AIIRD patients, defined as those with moderate to severely compromised immune systems who may not mount an adequate immune response to COVID-19 vaccination, when it is available and authorized for emergency use by the Food and Drug Administration, as well as monoclonal antibody therapy for postexposure prophylaxis of asymptomatic, recently exposed high-risk AIIRD patients or as treatment for newly symptomatic, high-risk AIIRD patients. The ACR guidance notes that, currently, neither the monoclonal antibodies bamlanivimab and etesevimab (administered together) nor casirivimab and imdevimab (REGEN-COV), are licensed or available under an emergency use authorization given their lack of activity against the Omicron variant, the dominant strain of SARS-CoV-2 circulating in the United States.
Finally, the guidance clarified that the timing of intravenous immunoglobulin doses does not need to be modified around the administration of COVID vaccine doses, based on moderate consensus among task force members.
Vaccine hesitancy in community rheumatology practices
The revised guidelines were released just as Arthritis & Rheumatology published a new study that assessed vaccine hesitancy among rheumatology patients on immunomodulatory therapies. A three-item electronic survey was conducted at 101 offices within a community practice–based rheumatology research network and ultimately collected responses from 58,529 patients, 20,987 of whom had an AIIRD and were receiving targeted therapies like biologics or Janus kinase inhibitors.
Of the total respondents, 77% (n = 43,675) had been vaccinated, 16.9% were not vaccinated and did not plan to be, and 6.1% were not vaccinated but planned to be. However, AIIRD patients were 16% less likely to be vaccinated, compared with the other patients, such as those with osteoarthritis or osteoporosis who were not receiving disease-modifying antirheumatic drugs (76.9% vs. 87%; odds ratio, 0.84; 95% confidence interval, 0.77-0.92; P < .001). Multivariable analysis also found that older patients (OR, 1.49 per 10 years) and Asians (OR, 2.42; 95% CI, 1.77-3.33) were more likely to be vaccinated.
“Rheumatologists need to be asking their patients more than just: ‘Are you vaccinated?’ ” Jeffrey Curtis, MD, MPH, head of the ACR COVID-19 vaccine task force and a coauthor of the vaccine hesitancy study, said in an interview. “A year ago, that was a fine approach, but now they need to be asking whether you’ve been vaccinated, and with what, and how many times, and how recently. There are a whole lot of subtleties there; ‘vaccinated: yes or no’ is just the tip of the iceberg.”
His research into the vaccine hesitant includes recent anecdotal data from thousands of patients treated in local rheumatology community practices, many of whom cited long-term safety data and potential side effects as reasons why they were unwilling to get vaccinated. But despite their on-paper responses, he cautioned rheumatologists to think critically when determining which patients may truly be open to vaccination.
“If you’re designing strategies to affect vaccine hesitancy, you may be wasting your time with some people,” said Dr. Curtis, professor of medicine at the University of Alabama at Birmingham. “A critical need is to figure out who are the patients who may be amendable to more information or an intervention or a little bit more time and care, and who are the people where you know, this is a lost cause: You don’t get a flu shot, you haven’t been vaccinated for shingles, [and] you’re not going to get this one either.
“In terms of a research agenda, how do we develop efficient, simple, short screening tools?” he added. “Something with a few helpful questions, on a patient portal or an iPad, that will do a good job identifying your patients at risk who haven’t had vaccination but that you might be able to spend time with, intervene, and actually change their mind. If you spend gobs of time with everyone, you’ll help some people, but clinicians don’t have an infinite amount of time.”
One of the authors of the vaccine hesitancy study acknowledged being employed by the rheumatology research network that hosted the survey. Several others, including Dr. Curtis, reported receiving grants and consulting fees from various pharmaceutical companies.
As rheumatologists contend with vaccine hesitancy among certain subsets of patients, the American College of Rheumatology has released updated clinical guidelines on COVID-19 vaccination for patients with rheumatic and musculoskeletal diseases (RMDs), including new recommendations on supplemental and booster doses.
The revised guidance from this fifth version of the ACR guidelines includes strongly recommending that all RMD patients receive a booster after their primary vaccine series, regardless of whether they have been naturally infected with COVID-19. In addition, they strongly recommend third supplemental doses for patients with autoimmune inflammatory rheumatic diseases (AIIRDs) who likely mounted an inadequate vaccine response, which would then be followed by a fourth booster dose as advised by the Centers for Disease Control and Prevention for immunocompromised individuals.
Other recommendations include pre-exposure prophylaxis monoclonal antibody treatment for high-risk AIIRD patients, defined as those with moderate to severely compromised immune systems who may not mount an adequate immune response to COVID-19 vaccination, when it is available and authorized for emergency use by the Food and Drug Administration, as well as monoclonal antibody therapy for postexposure prophylaxis of asymptomatic, recently exposed high-risk AIIRD patients or as treatment for newly symptomatic, high-risk AIIRD patients. The ACR guidance notes that, currently, neither the monoclonal antibodies bamlanivimab and etesevimab (administered together) nor casirivimab and imdevimab (REGEN-COV), are licensed or available under an emergency use authorization given their lack of activity against the Omicron variant, the dominant strain of SARS-CoV-2 circulating in the United States.
Finally, the guidance clarified that the timing of intravenous immunoglobulin doses does not need to be modified around the administration of COVID vaccine doses, based on moderate consensus among task force members.
Vaccine hesitancy in community rheumatology practices
The revised guidelines were released just as Arthritis & Rheumatology published a new study that assessed vaccine hesitancy among rheumatology patients on immunomodulatory therapies. A three-item electronic survey was conducted at 101 offices within a community practice–based rheumatology research network and ultimately collected responses from 58,529 patients, 20,987 of whom had an AIIRD and were receiving targeted therapies like biologics or Janus kinase inhibitors.
Of the total respondents, 77% (n = 43,675) had been vaccinated, 16.9% were not vaccinated and did not plan to be, and 6.1% were not vaccinated but planned to be. However, AIIRD patients were 16% less likely to be vaccinated, compared with the other patients, such as those with osteoarthritis or osteoporosis who were not receiving disease-modifying antirheumatic drugs (76.9% vs. 87%; odds ratio, 0.84; 95% confidence interval, 0.77-0.92; P < .001). Multivariable analysis also found that older patients (OR, 1.49 per 10 years) and Asians (OR, 2.42; 95% CI, 1.77-3.33) were more likely to be vaccinated.
“Rheumatologists need to be asking their patients more than just: ‘Are you vaccinated?’ ” Jeffrey Curtis, MD, MPH, head of the ACR COVID-19 vaccine task force and a coauthor of the vaccine hesitancy study, said in an interview. “A year ago, that was a fine approach, but now they need to be asking whether you’ve been vaccinated, and with what, and how many times, and how recently. There are a whole lot of subtleties there; ‘vaccinated: yes or no’ is just the tip of the iceberg.”
His research into the vaccine hesitant includes recent anecdotal data from thousands of patients treated in local rheumatology community practices, many of whom cited long-term safety data and potential side effects as reasons why they were unwilling to get vaccinated. But despite their on-paper responses, he cautioned rheumatologists to think critically when determining which patients may truly be open to vaccination.
“If you’re designing strategies to affect vaccine hesitancy, you may be wasting your time with some people,” said Dr. Curtis, professor of medicine at the University of Alabama at Birmingham. “A critical need is to figure out who are the patients who may be amendable to more information or an intervention or a little bit more time and care, and who are the people where you know, this is a lost cause: You don’t get a flu shot, you haven’t been vaccinated for shingles, [and] you’re not going to get this one either.
“In terms of a research agenda, how do we develop efficient, simple, short screening tools?” he added. “Something with a few helpful questions, on a patient portal or an iPad, that will do a good job identifying your patients at risk who haven’t had vaccination but that you might be able to spend time with, intervene, and actually change their mind. If you spend gobs of time with everyone, you’ll help some people, but clinicians don’t have an infinite amount of time.”
One of the authors of the vaccine hesitancy study acknowledged being employed by the rheumatology research network that hosted the survey. Several others, including Dr. Curtis, reported receiving grants and consulting fees from various pharmaceutical companies.
FROM ARTHRITIS & RHEUMATOLOGY
New AAD guidelines eye comorbidities in adults with atopic dermatitis
While it’s well established that atopic dermatitis (AD) in adults is associated with asthma, allergic rhinitis, and other atopic conditions, the links between AD and other comorbidities are coming into clearer focus.
, published evidence supports an association between AD and comorbidities that may not be on the radar of clinicians and patients, including substance use, attention-deficit/hyperactivity disorder (ADHD), elements of metabolic syndrome, and various cardiovascular conditions.
“There are more comorbidities with AD than we anticipated, that are supported by data in the literature,” Dawn M.R. Davis, MD, cochair and an author of the guidelines, told this news organization. “We are learning more about the interconnectivity of various medical conditions,” she continued. “Many skin diseases over time have been noted to be impactful to the whole person and not only the skin. A classic example of that is psoriasis. We now understand that psoriasis is a multisystem inflammatory disorder.”
As for AD, “we’ve always appreciated that AD patients tend to be at higher risk for other atopic diseases such as asthma, allergic rhinoconjunctivitis, and food allergies,” said Dr. Davis, of the departments of dermatology and pediatrics at the Mayo Clinic, Rochester, Minn. “With further research, we are now able to delineate those associations more intimately and have data to support our suspicions. Additionally, we’re now understanding that these inflammatory conditions can impact more than the end organ involved, such as the skin and AD. We wanted to look at how AD can affect the whole patient.”
For the guidelines, which are the first of their kind and were published online in the Journal of the American Academy of Dermatology, Dr. Davis and project cochair Robert Sidbury, MD, MPH, chief of dermatology at Seattle Children’s Hospital, led a multidisciplinary group of 12 experts to review the association between AD and selected comorbidities. They applied the Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) for prognosis approach for assessing the certainty of the evidence and provided statements of association based on the available evidence.
With respect to highlights for atopic and allergic conditions, the guideline authors found high-quality evidence that AD in adults is associated with food allergies, moderate-quality evidence that AD is associated with asthma, and low-quality evidence that AD in adults may be associated with eosinophilic esophagitis.
In the realm of mental health and substance use, ample evidence exists to support an association between AD and mental health conditions such as depression and anxiety, the guidelines state. “For many patients, low mood may be driven by the symptoms of AD, including chronic itch and poor sleep,” Dr. Davis and her coauthors wrote. “Successfully treating AD may alleviate depressive symptoms for some patients; for others, assessment and treatment specific to their mental health may be needed.”
The guidelines also state that low-quality evidence exists to suggest that AD in adults may be associated with alcohol abuse disorders and cigarette smoking.
The authors noted “limited but consistent evidence” supporting a link between AD and adverse bone health, including osteoporosis and fractures, while associations between AD and cardiovascular risk factors and comorbidities, including hypertension, myocardial infarction, and stroke, are more controversial.
“I have published on bone health and AD so that was not as surprising to me,” Dr. Davis said in the interview. “I found a lot of the evidence in the guidelines to be validating of patterns that we see in our patients. The most significant learning point for me was [the link to] cardiovascular disease and the link to specific mental health and substance use disorders. It validates how impactful AD is to the individual.”
According to the guidelines, moderate-quality evidence exists linking AD in adults to both alopecia areata and urticaria. “Because we are dermatologists and take care of both of those diseases, be mindful of that in your daily practice,” Dr. Davis advised. “I would also encourage our colleagues to remember to educate patients on the comorbidities of AD so that they are empowered, and to screen for those comorbidities in your office based on the patient and their history and physical exam, to the level that you think is appropriate for that person’s individual’s care.”
Christine Ko, MD, who was asked to comment on the guidelines, characterized some of the reported comorbidity associations as predictable, such as asthma, food allergy, allergic rhinitis, and skin infections. “As the authors comment, ‘associations between AD and other atopic and allergic conditions have been recognized for decades and even contribute to diagnostic criteria for AD,’ ” said Dr. Ko, professor of dermatology and pathology at Yale University, New Haven, Conn, who was not involved with the guidelines. “I was a bit surprised to see that atopic dermatitis in adults is associated with osteoporosis and fractures. As the authors suggest, this could be secondary to treatment with oral prednisone, and it is possible that use of dupilumab and JAK inhibitors may lessen this association.”
Shawn G. Kwatra, MD, of the department of dermatology at Johns Hopkins University, Baltimore, who was not involved with the guidelines, and was also asked to comment, said that the guidelines underscore the importance of informing adults with AD “of the risks of unchecked inflammation and the potential for multiple disease comorbidities.” Dr. Kwatra, who has AD, added that “these results make me want to be more proactive in treating my eczema to reduce the potential for development of these comorbidities.”
He pointed out that the guidelines did not address racial and ethnic differences in the observed comorbidities. “Unfortunately, minority populations have a greater comorbidity burden in many inflammatory skin diseases so this will be another area needing further investigation,” he said. “As an example, our group found from multicenter data that black patients with atopic dermatitis have higher levels of C-reactive protein, blood eosinophils, and other inflammatory biomarkers.”
The AAD guidelines are the first in a four-part series on AD expected to be published over the next 1-2 years, Dr. Davis said. The subsequent guidelines will address topicals, phototherapy/systemics, and pediatrics.
The study was funded by internal funds from the AAD. Dr. Davis reported having no financial disclosures. Dr. Sidbury disclosed that he serves as an advisory board member for Pfizer, a principal investigator for Regeneron, and an investigator for Brickell Biotech and Galderma. He is also a consultant for Galderma Global and Microes. Dr. Ko reported having no financial disclosures. Dr. Kwatra is a member of the board of directors of the Skin of Color Society. He is also an advisory board member/consultant for AbbVie, Galderma, Incyte, Pfizer, Regeneron Pharmaceuticals, and Sanofi, and has served as an investigator for Galderma, Pfizer, and Sanofi.
While it’s well established that atopic dermatitis (AD) in adults is associated with asthma, allergic rhinitis, and other atopic conditions, the links between AD and other comorbidities are coming into clearer focus.
, published evidence supports an association between AD and comorbidities that may not be on the radar of clinicians and patients, including substance use, attention-deficit/hyperactivity disorder (ADHD), elements of metabolic syndrome, and various cardiovascular conditions.
“There are more comorbidities with AD than we anticipated, that are supported by data in the literature,” Dawn M.R. Davis, MD, cochair and an author of the guidelines, told this news organization. “We are learning more about the interconnectivity of various medical conditions,” she continued. “Many skin diseases over time have been noted to be impactful to the whole person and not only the skin. A classic example of that is psoriasis. We now understand that psoriasis is a multisystem inflammatory disorder.”
As for AD, “we’ve always appreciated that AD patients tend to be at higher risk for other atopic diseases such as asthma, allergic rhinoconjunctivitis, and food allergies,” said Dr. Davis, of the departments of dermatology and pediatrics at the Mayo Clinic, Rochester, Minn. “With further research, we are now able to delineate those associations more intimately and have data to support our suspicions. Additionally, we’re now understanding that these inflammatory conditions can impact more than the end organ involved, such as the skin and AD. We wanted to look at how AD can affect the whole patient.”
For the guidelines, which are the first of their kind and were published online in the Journal of the American Academy of Dermatology, Dr. Davis and project cochair Robert Sidbury, MD, MPH, chief of dermatology at Seattle Children’s Hospital, led a multidisciplinary group of 12 experts to review the association between AD and selected comorbidities. They applied the Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) for prognosis approach for assessing the certainty of the evidence and provided statements of association based on the available evidence.
With respect to highlights for atopic and allergic conditions, the guideline authors found high-quality evidence that AD in adults is associated with food allergies, moderate-quality evidence that AD is associated with asthma, and low-quality evidence that AD in adults may be associated with eosinophilic esophagitis.
In the realm of mental health and substance use, ample evidence exists to support an association between AD and mental health conditions such as depression and anxiety, the guidelines state. “For many patients, low mood may be driven by the symptoms of AD, including chronic itch and poor sleep,” Dr. Davis and her coauthors wrote. “Successfully treating AD may alleviate depressive symptoms for some patients; for others, assessment and treatment specific to their mental health may be needed.”
The guidelines also state that low-quality evidence exists to suggest that AD in adults may be associated with alcohol abuse disorders and cigarette smoking.
The authors noted “limited but consistent evidence” supporting a link between AD and adverse bone health, including osteoporosis and fractures, while associations between AD and cardiovascular risk factors and comorbidities, including hypertension, myocardial infarction, and stroke, are more controversial.
“I have published on bone health and AD so that was not as surprising to me,” Dr. Davis said in the interview. “I found a lot of the evidence in the guidelines to be validating of patterns that we see in our patients. The most significant learning point for me was [the link to] cardiovascular disease and the link to specific mental health and substance use disorders. It validates how impactful AD is to the individual.”
According to the guidelines, moderate-quality evidence exists linking AD in adults to both alopecia areata and urticaria. “Because we are dermatologists and take care of both of those diseases, be mindful of that in your daily practice,” Dr. Davis advised. “I would also encourage our colleagues to remember to educate patients on the comorbidities of AD so that they are empowered, and to screen for those comorbidities in your office based on the patient and their history and physical exam, to the level that you think is appropriate for that person’s individual’s care.”
Christine Ko, MD, who was asked to comment on the guidelines, characterized some of the reported comorbidity associations as predictable, such as asthma, food allergy, allergic rhinitis, and skin infections. “As the authors comment, ‘associations between AD and other atopic and allergic conditions have been recognized for decades and even contribute to diagnostic criteria for AD,’ ” said Dr. Ko, professor of dermatology and pathology at Yale University, New Haven, Conn, who was not involved with the guidelines. “I was a bit surprised to see that atopic dermatitis in adults is associated with osteoporosis and fractures. As the authors suggest, this could be secondary to treatment with oral prednisone, and it is possible that use of dupilumab and JAK inhibitors may lessen this association.”
Shawn G. Kwatra, MD, of the department of dermatology at Johns Hopkins University, Baltimore, who was not involved with the guidelines, and was also asked to comment, said that the guidelines underscore the importance of informing adults with AD “of the risks of unchecked inflammation and the potential for multiple disease comorbidities.” Dr. Kwatra, who has AD, added that “these results make me want to be more proactive in treating my eczema to reduce the potential for development of these comorbidities.”
He pointed out that the guidelines did not address racial and ethnic differences in the observed comorbidities. “Unfortunately, minority populations have a greater comorbidity burden in many inflammatory skin diseases so this will be another area needing further investigation,” he said. “As an example, our group found from multicenter data that black patients with atopic dermatitis have higher levels of C-reactive protein, blood eosinophils, and other inflammatory biomarkers.”
The AAD guidelines are the first in a four-part series on AD expected to be published over the next 1-2 years, Dr. Davis said. The subsequent guidelines will address topicals, phototherapy/systemics, and pediatrics.
The study was funded by internal funds from the AAD. Dr. Davis reported having no financial disclosures. Dr. Sidbury disclosed that he serves as an advisory board member for Pfizer, a principal investigator for Regeneron, and an investigator for Brickell Biotech and Galderma. He is also a consultant for Galderma Global and Microes. Dr. Ko reported having no financial disclosures. Dr. Kwatra is a member of the board of directors of the Skin of Color Society. He is also an advisory board member/consultant for AbbVie, Galderma, Incyte, Pfizer, Regeneron Pharmaceuticals, and Sanofi, and has served as an investigator for Galderma, Pfizer, and Sanofi.
While it’s well established that atopic dermatitis (AD) in adults is associated with asthma, allergic rhinitis, and other atopic conditions, the links between AD and other comorbidities are coming into clearer focus.
, published evidence supports an association between AD and comorbidities that may not be on the radar of clinicians and patients, including substance use, attention-deficit/hyperactivity disorder (ADHD), elements of metabolic syndrome, and various cardiovascular conditions.
“There are more comorbidities with AD than we anticipated, that are supported by data in the literature,” Dawn M.R. Davis, MD, cochair and an author of the guidelines, told this news organization. “We are learning more about the interconnectivity of various medical conditions,” she continued. “Many skin diseases over time have been noted to be impactful to the whole person and not only the skin. A classic example of that is psoriasis. We now understand that psoriasis is a multisystem inflammatory disorder.”
As for AD, “we’ve always appreciated that AD patients tend to be at higher risk for other atopic diseases such as asthma, allergic rhinoconjunctivitis, and food allergies,” said Dr. Davis, of the departments of dermatology and pediatrics at the Mayo Clinic, Rochester, Minn. “With further research, we are now able to delineate those associations more intimately and have data to support our suspicions. Additionally, we’re now understanding that these inflammatory conditions can impact more than the end organ involved, such as the skin and AD. We wanted to look at how AD can affect the whole patient.”
For the guidelines, which are the first of their kind and were published online in the Journal of the American Academy of Dermatology, Dr. Davis and project cochair Robert Sidbury, MD, MPH, chief of dermatology at Seattle Children’s Hospital, led a multidisciplinary group of 12 experts to review the association between AD and selected comorbidities. They applied the Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) for prognosis approach for assessing the certainty of the evidence and provided statements of association based on the available evidence.
With respect to highlights for atopic and allergic conditions, the guideline authors found high-quality evidence that AD in adults is associated with food allergies, moderate-quality evidence that AD is associated with asthma, and low-quality evidence that AD in adults may be associated with eosinophilic esophagitis.
In the realm of mental health and substance use, ample evidence exists to support an association between AD and mental health conditions such as depression and anxiety, the guidelines state. “For many patients, low mood may be driven by the symptoms of AD, including chronic itch and poor sleep,” Dr. Davis and her coauthors wrote. “Successfully treating AD may alleviate depressive symptoms for some patients; for others, assessment and treatment specific to their mental health may be needed.”
The guidelines also state that low-quality evidence exists to suggest that AD in adults may be associated with alcohol abuse disorders and cigarette smoking.
The authors noted “limited but consistent evidence” supporting a link between AD and adverse bone health, including osteoporosis and fractures, while associations between AD and cardiovascular risk factors and comorbidities, including hypertension, myocardial infarction, and stroke, are more controversial.
“I have published on bone health and AD so that was not as surprising to me,” Dr. Davis said in the interview. “I found a lot of the evidence in the guidelines to be validating of patterns that we see in our patients. The most significant learning point for me was [the link to] cardiovascular disease and the link to specific mental health and substance use disorders. It validates how impactful AD is to the individual.”
According to the guidelines, moderate-quality evidence exists linking AD in adults to both alopecia areata and urticaria. “Because we are dermatologists and take care of both of those diseases, be mindful of that in your daily practice,” Dr. Davis advised. “I would also encourage our colleagues to remember to educate patients on the comorbidities of AD so that they are empowered, and to screen for those comorbidities in your office based on the patient and their history and physical exam, to the level that you think is appropriate for that person’s individual’s care.”
Christine Ko, MD, who was asked to comment on the guidelines, characterized some of the reported comorbidity associations as predictable, such as asthma, food allergy, allergic rhinitis, and skin infections. “As the authors comment, ‘associations between AD and other atopic and allergic conditions have been recognized for decades and even contribute to diagnostic criteria for AD,’ ” said Dr. Ko, professor of dermatology and pathology at Yale University, New Haven, Conn, who was not involved with the guidelines. “I was a bit surprised to see that atopic dermatitis in adults is associated with osteoporosis and fractures. As the authors suggest, this could be secondary to treatment with oral prednisone, and it is possible that use of dupilumab and JAK inhibitors may lessen this association.”
Shawn G. Kwatra, MD, of the department of dermatology at Johns Hopkins University, Baltimore, who was not involved with the guidelines, and was also asked to comment, said that the guidelines underscore the importance of informing adults with AD “of the risks of unchecked inflammation and the potential for multiple disease comorbidities.” Dr. Kwatra, who has AD, added that “these results make me want to be more proactive in treating my eczema to reduce the potential for development of these comorbidities.”
He pointed out that the guidelines did not address racial and ethnic differences in the observed comorbidities. “Unfortunately, minority populations have a greater comorbidity burden in many inflammatory skin diseases so this will be another area needing further investigation,” he said. “As an example, our group found from multicenter data that black patients with atopic dermatitis have higher levels of C-reactive protein, blood eosinophils, and other inflammatory biomarkers.”
The AAD guidelines are the first in a four-part series on AD expected to be published over the next 1-2 years, Dr. Davis said. The subsequent guidelines will address topicals, phototherapy/systemics, and pediatrics.
The study was funded by internal funds from the AAD. Dr. Davis reported having no financial disclosures. Dr. Sidbury disclosed that he serves as an advisory board member for Pfizer, a principal investigator for Regeneron, and an investigator for Brickell Biotech and Galderma. He is also a consultant for Galderma Global and Microes. Dr. Ko reported having no financial disclosures. Dr. Kwatra is a member of the board of directors of the Skin of Color Society. He is also an advisory board member/consultant for AbbVie, Galderma, Incyte, Pfizer, Regeneron Pharmaceuticals, and Sanofi, and has served as an investigator for Galderma, Pfizer, and Sanofi.
FROM JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY
USPSTF says evidence still lacking for AFib screening in asymptomatic patients
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
ACP advocates outpatient treatment of uncomplicated diverticulitis
The estimated prevalence of acute colonic diverticulitis in the United States appears to be on the rise, wrote Amir Qaseem, MD, and members of the ACP Clinical Guidelines Committee. “Approximately 200,000 hospitalizations for acute left-sided colonic diverticulitis occur in the United States each year, with annual costs of more than $8 billion. Timely and correct diagnosis of acute left-sided colonic diverticulitis is essential for the selection of the most appropriate management options.”
Diverticulitis is becoming increasingly common in patients treated by internal medicine physicians, according to the ACP, and the new clinical guidelines specify a course of treatment focused on outpatient management and minimal medications.
The guidelines, published in Annals of Internal Medicine, were based on a systematic review of evidence from studies published between Jan. 1, 1990, and June 1, 2020. Notably, right-sided diverticulitis was excluded because it is rare in Western countries and involves a different natural history and management options, the authors wrote.
In the guidelines, uncomplicated diverticulitis refers to localized inflammation, and complicated diverticulitis refers to “inflammation associated with an abscess, a phlegmon, a fistula, an obstruction, bleeding, or perforation.”
Guidance on diagnosis and management
In the first guideline, “Diagnosis and Management of Acute Left-Sided Colonic Diverticulitis”, the authors provided three recommendations. First, they recommended that clinicians use abdominal CT imaging in cases of diagnostic uncertainty for patients with suspected acute left-sided colonic diverticulitis. The evidence showed that abdominal CT was associated with appropriate management in patients with suspected acute left-sided colonic diverticulitis, and that misdiagnosis with CT was rare.
Second, the authors of this guidance recommended management of most patients with acute left-sided colonic diverticulitis in an outpatient setting. Evidence showed that the risk for elective surgery and for recurrence were not significantly different based on inpatient or outpatient management.
The third recommendation advised clinicians to manage most patients without antibiotics. This recommendation was based on data showing no significant difference in quality of life at 3, 6, 12, or 24 months; no difference in diverticulitis-related complications; and no difference in the need for surgery in patients treated with antibiotics and those not treated with antibiotics.
All three recommendations are conditional, with low-certainty evidence, according to the authors.
Colonoscopy for diagnostic evaluation and interventions
In the second guideline, “Colonoscopy for Diagnostic Evaluation and Interventions to Prevent Recurrence After Acute Left-Sided Colonic Diverticulitis, the authors advised clinicians to refer patients for a colonoscopy after an initial episode of complicated left-sided colonic diverticulitis if they have not had a recent colonoscopy.
Although acute diverticulitis is usually uncomplicated, approximately 12% of cases are considered complicated, and these patients may have a higher prevalence of colorectal cancer, the authors noted. This recommendation was conditional, with low-certainty evidence. Additional diagnostic colonoscopy is not needed for patients who are up to date on recommended colorectal cancer screening, according to this guideline.
A second recommendation, given as a strong recommendation with high-certainty evidence, advised against using mesalamine to prevent recurrent diverticulitis. Evidence showed that use of mesalamine at doses ranging from 1.2 g/day to 4.8 g/day made no difference in recurrent diverticulitis risk compared with placebo. Mesalamine has no demonstrated clinical benefits, and has been associated with epigastric pain, nausea, diarrhea, dizziness, rash, and renal and hepatic impairment, the authors wrote.
The third recommendation advised the discussion of elective surgery with patients with a history of uncomplicated diverticulitis that persists or recurs frequently. Surgery also may be an option for patients with complicated diverticulitis, according to the guideline. However, “this recommendation does not apply to patients with uncomplicated diverticulitis that is not persistent or frequently recurring,” the authors wrote.
The decision to pursue elective surgery should be informed and personalized according to potential benefits, harms, costs, and patient preferences, they said. This recommendation is conditional, with low-certainty evidence.
This new guideline was designed “to guide care based on the best available evidence and may not apply to all patients or individual clinical situations,” the authors emphasized. “It should not be used as a replacement for a clinician’s judgment.”
Update confirms best practices
“Concerns about inappropriate antimicrobial therapy use and the delay in seeking preventative care such as a colonoscopy have led to poorer outcomes for patients,” ACP president George Abraham, MD, said in an interview. These concerns about a lack of antimicrobial stewardship and of care not being representative of ‘high value care’ “supported the need to reinforce best practices.”
Although most clinicians are aware of the nature of the recommendations in their own clinical practices, “a systematic review helped confirm and codify best practice that everyone can confidently incorporate into their daily decision-making,” Dr. Abraham said.
Compared with previous guidelines, “the single biggest difference is the fact that antimicrobial therapy is not indicated in mild, uncomplicated diverticulitis; we hope this will lead to lesser and more judicious antimicrobial prescribing,” Dr. Abraham emphasized.
Like all guidelines, the current guidelines are meant to be advisory, not mandatory; “they do not replace good clinical judgment and individual patient care decision-making,” Dr. Abraham said. “These guidelines are useful when they are widely read by clinicians, including physicians and advanced practice clinicians, and incorporated into their daily practice.”
Curbing antibiotic use
It is important for clinicians to recognize that uncomplicated diverticulitis in selected patients does not require initial antibiotics, David A. Johnson, MD, chief of gastroenterology at Eastern Virginia School of Medicine, Norfolk, said in an interview. “This paradigm shift began with the AGA guidelines in 2015, and was more recently updated with the 2021 best practice recommendations,” first published in Gastroenterology.
“I was surprised to see this current guideline not mentioning that, if antibiotics are to be used, that amoxicillin-clavulanate alone should be favored over combination of fluoroquinolones and metronidazole,” Dr. Johnson noted. “Furthermore, the U.S. Food and Drug Administration has advised that fluoroquinolones should be reserved for conditions with no alternative treatment options.”
“The initial management approach for the AGA guidelines and best practice are comparable with these most recent ACP recommendations,” said Dr. Johnson. However, “I would suggest that clinicians treating diverticulitis also review the AGA best practice recommendations, which build out important other important points for diverticulitis management including timeframes for colonoscopy, strong effect of genetics, dietary effects, recurrence rates, and the role of surgery.”
As for research gaps, “further data on cost savings would be helpful,” as savings may be likely with significant reduction without antibiotics and imaging in select patients, Dr. Johnson said. “Cost savings and risk reduction of adverse implications of antibiotic and radiation risks should be included in these analyses.”
The guidelines were based on systematic reviews conducted by the Evidence-based Practice Center at Brown University, Providence, R.I., funded by the Agency for Healthcare Research and Quality. The development of the guidelines was supported by the ACP operating budget. The authors, Dr. Abraham, and Dr. Johnson had no financial conflicts to disclose.
The estimated prevalence of acute colonic diverticulitis in the United States appears to be on the rise, wrote Amir Qaseem, MD, and members of the ACP Clinical Guidelines Committee. “Approximately 200,000 hospitalizations for acute left-sided colonic diverticulitis occur in the United States each year, with annual costs of more than $8 billion. Timely and correct diagnosis of acute left-sided colonic diverticulitis is essential for the selection of the most appropriate management options.”
Diverticulitis is becoming increasingly common in patients treated by internal medicine physicians, according to the ACP, and the new clinical guidelines specify a course of treatment focused on outpatient management and minimal medications.
The guidelines, published in Annals of Internal Medicine, were based on a systematic review of evidence from studies published between Jan. 1, 1990, and June 1, 2020. Notably, right-sided diverticulitis was excluded because it is rare in Western countries and involves a different natural history and management options, the authors wrote.
In the guidelines, uncomplicated diverticulitis refers to localized inflammation, and complicated diverticulitis refers to “inflammation associated with an abscess, a phlegmon, a fistula, an obstruction, bleeding, or perforation.”
Guidance on diagnosis and management
In the first guideline, “Diagnosis and Management of Acute Left-Sided Colonic Diverticulitis”, the authors provided three recommendations. First, they recommended that clinicians use abdominal CT imaging in cases of diagnostic uncertainty for patients with suspected acute left-sided colonic diverticulitis. The evidence showed that abdominal CT was associated with appropriate management in patients with suspected acute left-sided colonic diverticulitis, and that misdiagnosis with CT was rare.
Second, the authors of this guidance recommended management of most patients with acute left-sided colonic diverticulitis in an outpatient setting. Evidence showed that the risk for elective surgery and for recurrence were not significantly different based on inpatient or outpatient management.
The third recommendation advised clinicians to manage most patients without antibiotics. This recommendation was based on data showing no significant difference in quality of life at 3, 6, 12, or 24 months; no difference in diverticulitis-related complications; and no difference in the need for surgery in patients treated with antibiotics and those not treated with antibiotics.
All three recommendations are conditional, with low-certainty evidence, according to the authors.
Colonoscopy for diagnostic evaluation and interventions
In the second guideline, “Colonoscopy for Diagnostic Evaluation and Interventions to Prevent Recurrence After Acute Left-Sided Colonic Diverticulitis, the authors advised clinicians to refer patients for a colonoscopy after an initial episode of complicated left-sided colonic diverticulitis if they have not had a recent colonoscopy.
Although acute diverticulitis is usually uncomplicated, approximately 12% of cases are considered complicated, and these patients may have a higher prevalence of colorectal cancer, the authors noted. This recommendation was conditional, with low-certainty evidence. Additional diagnostic colonoscopy is not needed for patients who are up to date on recommended colorectal cancer screening, according to this guideline.
A second recommendation, given as a strong recommendation with high-certainty evidence, advised against using mesalamine to prevent recurrent diverticulitis. Evidence showed that use of mesalamine at doses ranging from 1.2 g/day to 4.8 g/day made no difference in recurrent diverticulitis risk compared with placebo. Mesalamine has no demonstrated clinical benefits, and has been associated with epigastric pain, nausea, diarrhea, dizziness, rash, and renal and hepatic impairment, the authors wrote.
The third recommendation advised the discussion of elective surgery with patients with a history of uncomplicated diverticulitis that persists or recurs frequently. Surgery also may be an option for patients with complicated diverticulitis, according to the guideline. However, “this recommendation does not apply to patients with uncomplicated diverticulitis that is not persistent or frequently recurring,” the authors wrote.
The decision to pursue elective surgery should be informed and personalized according to potential benefits, harms, costs, and patient preferences, they said. This recommendation is conditional, with low-certainty evidence.
This new guideline was designed “to guide care based on the best available evidence and may not apply to all patients or individual clinical situations,” the authors emphasized. “It should not be used as a replacement for a clinician’s judgment.”
Update confirms best practices
“Concerns about inappropriate antimicrobial therapy use and the delay in seeking preventative care such as a colonoscopy have led to poorer outcomes for patients,” ACP president George Abraham, MD, said in an interview. These concerns about a lack of antimicrobial stewardship and of care not being representative of ‘high value care’ “supported the need to reinforce best practices.”
Although most clinicians are aware of the nature of the recommendations in their own clinical practices, “a systematic review helped confirm and codify best practice that everyone can confidently incorporate into their daily decision-making,” Dr. Abraham said.
Compared with previous guidelines, “the single biggest difference is the fact that antimicrobial therapy is not indicated in mild, uncomplicated diverticulitis; we hope this will lead to lesser and more judicious antimicrobial prescribing,” Dr. Abraham emphasized.
Like all guidelines, the current guidelines are meant to be advisory, not mandatory; “they do not replace good clinical judgment and individual patient care decision-making,” Dr. Abraham said. “These guidelines are useful when they are widely read by clinicians, including physicians and advanced practice clinicians, and incorporated into their daily practice.”
Curbing antibiotic use
It is important for clinicians to recognize that uncomplicated diverticulitis in selected patients does not require initial antibiotics, David A. Johnson, MD, chief of gastroenterology at Eastern Virginia School of Medicine, Norfolk, said in an interview. “This paradigm shift began with the AGA guidelines in 2015, and was more recently updated with the 2021 best practice recommendations,” first published in Gastroenterology.
“I was surprised to see this current guideline not mentioning that, if antibiotics are to be used, that amoxicillin-clavulanate alone should be favored over combination of fluoroquinolones and metronidazole,” Dr. Johnson noted. “Furthermore, the U.S. Food and Drug Administration has advised that fluoroquinolones should be reserved for conditions with no alternative treatment options.”
“The initial management approach for the AGA guidelines and best practice are comparable with these most recent ACP recommendations,” said Dr. Johnson. However, “I would suggest that clinicians treating diverticulitis also review the AGA best practice recommendations, which build out important other important points for diverticulitis management including timeframes for colonoscopy, strong effect of genetics, dietary effects, recurrence rates, and the role of surgery.”
As for research gaps, “further data on cost savings would be helpful,” as savings may be likely with significant reduction without antibiotics and imaging in select patients, Dr. Johnson said. “Cost savings and risk reduction of adverse implications of antibiotic and radiation risks should be included in these analyses.”
The guidelines were based on systematic reviews conducted by the Evidence-based Practice Center at Brown University, Providence, R.I., funded by the Agency for Healthcare Research and Quality. The development of the guidelines was supported by the ACP operating budget. The authors, Dr. Abraham, and Dr. Johnson had no financial conflicts to disclose.
The estimated prevalence of acute colonic diverticulitis in the United States appears to be on the rise, wrote Amir Qaseem, MD, and members of the ACP Clinical Guidelines Committee. “Approximately 200,000 hospitalizations for acute left-sided colonic diverticulitis occur in the United States each year, with annual costs of more than $8 billion. Timely and correct diagnosis of acute left-sided colonic diverticulitis is essential for the selection of the most appropriate management options.”
Diverticulitis is becoming increasingly common in patients treated by internal medicine physicians, according to the ACP, and the new clinical guidelines specify a course of treatment focused on outpatient management and minimal medications.
The guidelines, published in Annals of Internal Medicine, were based on a systematic review of evidence from studies published between Jan. 1, 1990, and June 1, 2020. Notably, right-sided diverticulitis was excluded because it is rare in Western countries and involves a different natural history and management options, the authors wrote.
In the guidelines, uncomplicated diverticulitis refers to localized inflammation, and complicated diverticulitis refers to “inflammation associated with an abscess, a phlegmon, a fistula, an obstruction, bleeding, or perforation.”
Guidance on diagnosis and management
In the first guideline, “Diagnosis and Management of Acute Left-Sided Colonic Diverticulitis”, the authors provided three recommendations. First, they recommended that clinicians use abdominal CT imaging in cases of diagnostic uncertainty for patients with suspected acute left-sided colonic diverticulitis. The evidence showed that abdominal CT was associated with appropriate management in patients with suspected acute left-sided colonic diverticulitis, and that misdiagnosis with CT was rare.
Second, the authors of this guidance recommended management of most patients with acute left-sided colonic diverticulitis in an outpatient setting. Evidence showed that the risk for elective surgery and for recurrence were not significantly different based on inpatient or outpatient management.
The third recommendation advised clinicians to manage most patients without antibiotics. This recommendation was based on data showing no significant difference in quality of life at 3, 6, 12, or 24 months; no difference in diverticulitis-related complications; and no difference in the need for surgery in patients treated with antibiotics and those not treated with antibiotics.
All three recommendations are conditional, with low-certainty evidence, according to the authors.
Colonoscopy for diagnostic evaluation and interventions
In the second guideline, “Colonoscopy for Diagnostic Evaluation and Interventions to Prevent Recurrence After Acute Left-Sided Colonic Diverticulitis, the authors advised clinicians to refer patients for a colonoscopy after an initial episode of complicated left-sided colonic diverticulitis if they have not had a recent colonoscopy.
Although acute diverticulitis is usually uncomplicated, approximately 12% of cases are considered complicated, and these patients may have a higher prevalence of colorectal cancer, the authors noted. This recommendation was conditional, with low-certainty evidence. Additional diagnostic colonoscopy is not needed for patients who are up to date on recommended colorectal cancer screening, according to this guideline.
A second recommendation, given as a strong recommendation with high-certainty evidence, advised against using mesalamine to prevent recurrent diverticulitis. Evidence showed that use of mesalamine at doses ranging from 1.2 g/day to 4.8 g/day made no difference in recurrent diverticulitis risk compared with placebo. Mesalamine has no demonstrated clinical benefits, and has been associated with epigastric pain, nausea, diarrhea, dizziness, rash, and renal and hepatic impairment, the authors wrote.
The third recommendation advised the discussion of elective surgery with patients with a history of uncomplicated diverticulitis that persists or recurs frequently. Surgery also may be an option for patients with complicated diverticulitis, according to the guideline. However, “this recommendation does not apply to patients with uncomplicated diverticulitis that is not persistent or frequently recurring,” the authors wrote.
The decision to pursue elective surgery should be informed and personalized according to potential benefits, harms, costs, and patient preferences, they said. This recommendation is conditional, with low-certainty evidence.
This new guideline was designed “to guide care based on the best available evidence and may not apply to all patients or individual clinical situations,” the authors emphasized. “It should not be used as a replacement for a clinician’s judgment.”
Update confirms best practices
“Concerns about inappropriate antimicrobial therapy use and the delay in seeking preventative care such as a colonoscopy have led to poorer outcomes for patients,” ACP president George Abraham, MD, said in an interview. These concerns about a lack of antimicrobial stewardship and of care not being representative of ‘high value care’ “supported the need to reinforce best practices.”
Although most clinicians are aware of the nature of the recommendations in their own clinical practices, “a systematic review helped confirm and codify best practice that everyone can confidently incorporate into their daily decision-making,” Dr. Abraham said.
Compared with previous guidelines, “the single biggest difference is the fact that antimicrobial therapy is not indicated in mild, uncomplicated diverticulitis; we hope this will lead to lesser and more judicious antimicrobial prescribing,” Dr. Abraham emphasized.
Like all guidelines, the current guidelines are meant to be advisory, not mandatory; “they do not replace good clinical judgment and individual patient care decision-making,” Dr. Abraham said. “These guidelines are useful when they are widely read by clinicians, including physicians and advanced practice clinicians, and incorporated into their daily practice.”
Curbing antibiotic use
It is important for clinicians to recognize that uncomplicated diverticulitis in selected patients does not require initial antibiotics, David A. Johnson, MD, chief of gastroenterology at Eastern Virginia School of Medicine, Norfolk, said in an interview. “This paradigm shift began with the AGA guidelines in 2015, and was more recently updated with the 2021 best practice recommendations,” first published in Gastroenterology.
“I was surprised to see this current guideline not mentioning that, if antibiotics are to be used, that amoxicillin-clavulanate alone should be favored over combination of fluoroquinolones and metronidazole,” Dr. Johnson noted. “Furthermore, the U.S. Food and Drug Administration has advised that fluoroquinolones should be reserved for conditions with no alternative treatment options.”
“The initial management approach for the AGA guidelines and best practice are comparable with these most recent ACP recommendations,” said Dr. Johnson. However, “I would suggest that clinicians treating diverticulitis also review the AGA best practice recommendations, which build out important other important points for diverticulitis management including timeframes for colonoscopy, strong effect of genetics, dietary effects, recurrence rates, and the role of surgery.”
As for research gaps, “further data on cost savings would be helpful,” as savings may be likely with significant reduction without antibiotics and imaging in select patients, Dr. Johnson said. “Cost savings and risk reduction of adverse implications of antibiotic and radiation risks should be included in these analyses.”
The guidelines were based on systematic reviews conducted by the Evidence-based Practice Center at Brown University, Providence, R.I., funded by the Agency for Healthcare Research and Quality. The development of the guidelines was supported by the ACP operating budget. The authors, Dr. Abraham, and Dr. Johnson had no financial conflicts to disclose.
FROM ANNALS OF INTERNAL MEDICINE
Private insurers must cover follow-up colonoscopies
Private insurers are now required to cover the cost of follow-up colonoscopies after a positive stool-based test, according to updated guidance from the Biden administration cited in a press release from the American Gastroenterological Association.
“Now patients can choose the best colorectal cancer screening test for them without fear of a surprise bill. Patients have full coverage of the full screening continuum – from an initial stool or endoscopic test to a follow-up colonoscopy. Now that the financial barriers have been eliminated, we can focus on increasing screening so we can prevent cancer deaths,” John Inadomi, MD, president of the AGA, said in the press release.
The updated guidance, issued on Jan. 10, 2022, “will prevent patients from receiving surprise bills for a colonoscopy when they receive a positive result from a stool-based test,” according to the AGA press release.
In 2016, the U.S. Preventive Services Task Force recommended colorectal cancer screening for all adults starting at age 50 years and continuing to age 75 years, with an “A” rating. Because the Affordable Care Act (ACA) mandated coverage for preventive screenings without cost-sharing that receive an “A” or “B” grade from the USPSTF, previous statements have confirmed that cost sharing may not be imposed on patients for screening in accordance with the USPSTF recommendation, which included specialist consultation prior to the procedure, bowel prep medications, anesthesia services in conjunction with a preventive colonoscopy, polyp removal performed during the screening procedure, and any pathology exam on a polyp biopsy performed as part of the screening. By adding colonoscopies following positive stool tests to that list, the updated guidance means that all aspects of the screening procedure are now covered without cost sharing.
In May 2021, an update to the USPSTF recommendations called for a follow-up colonoscopy in the wake of a positive test: “Positive results on stool-based screening tests require follow-up with colonoscopy for the screening benefits to be achieved.” The 2021 update also extended the screening recommendation to adults aged 45-49 years with a “B” rating.
Private insurers must now pay for follow-up colonoscopy as needed in addition to the initial noninvasive screening, according to the guidance.
The updated guidance is presented as part of a series of frequently asked questions regarding implementation of the Families First Coronavirus Response Act, the Coronavirus Aid, Relief, and Economic Security Act, and the Affordable Care Act. The colonoscopy guidance falls under the heading of “Coverage of Preventive Services,” which includes evidence-based recommendations given an A or B rating by the USPSTF.
Coverage without cost sharing must begin on or after May 31, 2022, which is 1 year after the date of the latest recommendations, according to the FAQ.
Representatives of multiple organizations, including the AGA, American Cancer Society, American Cancer Society Cancer Action Network, and Fight CRC collaborated to promote the additional coverage. “We applaud the administration for supporting coverage of the full colorectal cancer screening continuum, which will improve access to lifesaving screening,” the collaborators said in the press release.
Colorectal cancer remains the second leading cancer killer in the United States, but only two-thirds of eligible individuals were screened in 2018, according to the AGA, and screening challenges were exacerbated by the arrival of the COVID-19 pandemic. The AGA estimates that colorectal cancer screening declined by 86% during the first few months of the COVID-19 pandemic in 2020.
The full Jan. 10 FAQ is available here.
This article was updated Jan. 14, 2022.
Private insurers are now required to cover the cost of follow-up colonoscopies after a positive stool-based test, according to updated guidance from the Biden administration cited in a press release from the American Gastroenterological Association.
“Now patients can choose the best colorectal cancer screening test for them without fear of a surprise bill. Patients have full coverage of the full screening continuum – from an initial stool or endoscopic test to a follow-up colonoscopy. Now that the financial barriers have been eliminated, we can focus on increasing screening so we can prevent cancer deaths,” John Inadomi, MD, president of the AGA, said in the press release.
The updated guidance, issued on Jan. 10, 2022, “will prevent patients from receiving surprise bills for a colonoscopy when they receive a positive result from a stool-based test,” according to the AGA press release.
In 2016, the U.S. Preventive Services Task Force recommended colorectal cancer screening for all adults starting at age 50 years and continuing to age 75 years, with an “A” rating. Because the Affordable Care Act (ACA) mandated coverage for preventive screenings without cost-sharing that receive an “A” or “B” grade from the USPSTF, previous statements have confirmed that cost sharing may not be imposed on patients for screening in accordance with the USPSTF recommendation, which included specialist consultation prior to the procedure, bowel prep medications, anesthesia services in conjunction with a preventive colonoscopy, polyp removal performed during the screening procedure, and any pathology exam on a polyp biopsy performed as part of the screening. By adding colonoscopies following positive stool tests to that list, the updated guidance means that all aspects of the screening procedure are now covered without cost sharing.
In May 2021, an update to the USPSTF recommendations called for a follow-up colonoscopy in the wake of a positive test: “Positive results on stool-based screening tests require follow-up with colonoscopy for the screening benefits to be achieved.” The 2021 update also extended the screening recommendation to adults aged 45-49 years with a “B” rating.
Private insurers must now pay for follow-up colonoscopy as needed in addition to the initial noninvasive screening, according to the guidance.
The updated guidance is presented as part of a series of frequently asked questions regarding implementation of the Families First Coronavirus Response Act, the Coronavirus Aid, Relief, and Economic Security Act, and the Affordable Care Act. The colonoscopy guidance falls under the heading of “Coverage of Preventive Services,” which includes evidence-based recommendations given an A or B rating by the USPSTF.
Coverage without cost sharing must begin on or after May 31, 2022, which is 1 year after the date of the latest recommendations, according to the FAQ.
Representatives of multiple organizations, including the AGA, American Cancer Society, American Cancer Society Cancer Action Network, and Fight CRC collaborated to promote the additional coverage. “We applaud the administration for supporting coverage of the full colorectal cancer screening continuum, which will improve access to lifesaving screening,” the collaborators said in the press release.
Colorectal cancer remains the second leading cancer killer in the United States, but only two-thirds of eligible individuals were screened in 2018, according to the AGA, and screening challenges were exacerbated by the arrival of the COVID-19 pandemic. The AGA estimates that colorectal cancer screening declined by 86% during the first few months of the COVID-19 pandemic in 2020.
The full Jan. 10 FAQ is available here.
This article was updated Jan. 14, 2022.
Private insurers are now required to cover the cost of follow-up colonoscopies after a positive stool-based test, according to updated guidance from the Biden administration cited in a press release from the American Gastroenterological Association.
“Now patients can choose the best colorectal cancer screening test for them without fear of a surprise bill. Patients have full coverage of the full screening continuum – from an initial stool or endoscopic test to a follow-up colonoscopy. Now that the financial barriers have been eliminated, we can focus on increasing screening so we can prevent cancer deaths,” John Inadomi, MD, president of the AGA, said in the press release.
The updated guidance, issued on Jan. 10, 2022, “will prevent patients from receiving surprise bills for a colonoscopy when they receive a positive result from a stool-based test,” according to the AGA press release.
In 2016, the U.S. Preventive Services Task Force recommended colorectal cancer screening for all adults starting at age 50 years and continuing to age 75 years, with an “A” rating. Because the Affordable Care Act (ACA) mandated coverage for preventive screenings without cost-sharing that receive an “A” or “B” grade from the USPSTF, previous statements have confirmed that cost sharing may not be imposed on patients for screening in accordance with the USPSTF recommendation, which included specialist consultation prior to the procedure, bowel prep medications, anesthesia services in conjunction with a preventive colonoscopy, polyp removal performed during the screening procedure, and any pathology exam on a polyp biopsy performed as part of the screening. By adding colonoscopies following positive stool tests to that list, the updated guidance means that all aspects of the screening procedure are now covered without cost sharing.
In May 2021, an update to the USPSTF recommendations called for a follow-up colonoscopy in the wake of a positive test: “Positive results on stool-based screening tests require follow-up with colonoscopy for the screening benefits to be achieved.” The 2021 update also extended the screening recommendation to adults aged 45-49 years with a “B” rating.
Private insurers must now pay for follow-up colonoscopy as needed in addition to the initial noninvasive screening, according to the guidance.
The updated guidance is presented as part of a series of frequently asked questions regarding implementation of the Families First Coronavirus Response Act, the Coronavirus Aid, Relief, and Economic Security Act, and the Affordable Care Act. The colonoscopy guidance falls under the heading of “Coverage of Preventive Services,” which includes evidence-based recommendations given an A or B rating by the USPSTF.
Coverage without cost sharing must begin on or after May 31, 2022, which is 1 year after the date of the latest recommendations, according to the FAQ.
Representatives of multiple organizations, including the AGA, American Cancer Society, American Cancer Society Cancer Action Network, and Fight CRC collaborated to promote the additional coverage. “We applaud the administration for supporting coverage of the full colorectal cancer screening continuum, which will improve access to lifesaving screening,” the collaborators said in the press release.
Colorectal cancer remains the second leading cancer killer in the United States, but only two-thirds of eligible individuals were screened in 2018, according to the AGA, and screening challenges were exacerbated by the arrival of the COVID-19 pandemic. The AGA estimates that colorectal cancer screening declined by 86% during the first few months of the COVID-19 pandemic in 2020.
The full Jan. 10 FAQ is available here.
This article was updated Jan. 14, 2022.
Wilderness Medical Society issues clinical guidelines for tick-borne illness
The recently published “Clinical Practice Guidelines for the Prevention and Management of Tick-Borne Illness,” from the Wilderness Medical Society, are a good compilation of treatment suggestions but are not, in fact, new recommendations, lead author Benjamin Ho, MD, of Southern Wisconsin Emergency Associates in Janesville, acknowledged in an interview.
Dr. Ho emphasized that the focus of the report was on “practitioners who practice in resource-limited settings” and are “the group’s way of solidifying a ... standard of practice” for such physicians. Dr. Ho also said that, while “a lot of the recommendations aren’t well supported, the risk-benefit ratio, we believe, supports the recommendations.”
The article first reviewed the different types of ticks and their distribution in the United States, the specific pathogen associated with each, the disease it causes, and comments about seasonal variations in biting behavior. Another table outlines the most common clinical syndromes, typical lab findings, recommended diagnostic testing, and antibiotic treatments. A third section contains images of different types of ticks and photos of ticks in various life-cycle stages and different levels of engorgement.
The authors were careful to note: “Several tick species are able to carry multiple pathogens. In one study, nearly 25% of Ixodes were coinfected with some combination of the bacteria or parasites causing Lyme disease, anaplasmosis, or babesiosis. Although TBI [tick-borne illness] diagnosis is not the focus of this [clinical practice guideline], providers should be aware of high rates of coinfection; the presence of one TBI should in many instances prompt testing for others.”
In terms of recommendations for preventing TBIs, the authors challenge the suggestion of wearing light-colored clothing. For repellents, they recommend DEET, picaridin, and permethrin. And they also give instructions for laundering clothing and removing ticks.
One recommendation is controversial: that of providing single-dose doxycycline as prophylaxis against Lyme disease. Dr. Ho stresses that this was only for “high-risk” tick bites, defined as a tick bite from an identified Ixodes vector species in which the tick was attached for at least 36 hours and that occurred in an endemic area.
The recommendation for prophylactic doxycycline originated with an article by Robert Nadelman and colleagues in the New England Journal of Medicine and has been strongly challenged by ILADS (International Lyme and Associated Diseases Society) physicians, including Daniel Cameron, MD, and others.
Sam Donta, MD, a recent member of the Department of Health & Human Services Tick-borne Working Group and a member of the Infectious Disease Society of America, said in an interview: “The problem with the one-dose doxycycline is you may not begin to develop symptoms until 2 months later.” It might mask the early symptoms of Lyme. “My impression is that the doxycycline – even the single dose – might have abrogated the ability to see an immune response. The idea, though, if you’ve had a tick bite, is to do nothing and to wait for symptoms to develop. That becomes a little bit more complex. But even then, you could choose to follow the patient and see the patient in 2 weeks and then get blood testing.”
Dr. Donta added: “I think the screening test is inadequate. So you have to go directly to the Western blot. And you have to do both the IgM and IgG” and look for specific bands.
Dr. Donta emphasized that patients should be encouraged to save any ticks that were attached and that, if at all possible, ticks should be sent to a reference lab for testing before committing a patient to a course of antibiotics. There is no harm in that brief delay, he said, and most labs can identify an array of pathogens.
The Wilderness Society guidelines on TBIs provide a good overview for clinicians practicing in limited resource settings and mirror those from the IDSA.
Dr. Ho and Dr. Donta reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The recently published “Clinical Practice Guidelines for the Prevention and Management of Tick-Borne Illness,” from the Wilderness Medical Society, are a good compilation of treatment suggestions but are not, in fact, new recommendations, lead author Benjamin Ho, MD, of Southern Wisconsin Emergency Associates in Janesville, acknowledged in an interview.
Dr. Ho emphasized that the focus of the report was on “practitioners who practice in resource-limited settings” and are “the group’s way of solidifying a ... standard of practice” for such physicians. Dr. Ho also said that, while “a lot of the recommendations aren’t well supported, the risk-benefit ratio, we believe, supports the recommendations.”
The article first reviewed the different types of ticks and their distribution in the United States, the specific pathogen associated with each, the disease it causes, and comments about seasonal variations in biting behavior. Another table outlines the most common clinical syndromes, typical lab findings, recommended diagnostic testing, and antibiotic treatments. A third section contains images of different types of ticks and photos of ticks in various life-cycle stages and different levels of engorgement.
The authors were careful to note: “Several tick species are able to carry multiple pathogens. In one study, nearly 25% of Ixodes were coinfected with some combination of the bacteria or parasites causing Lyme disease, anaplasmosis, or babesiosis. Although TBI [tick-borne illness] diagnosis is not the focus of this [clinical practice guideline], providers should be aware of high rates of coinfection; the presence of one TBI should in many instances prompt testing for others.”
In terms of recommendations for preventing TBIs, the authors challenge the suggestion of wearing light-colored clothing. For repellents, they recommend DEET, picaridin, and permethrin. And they also give instructions for laundering clothing and removing ticks.
One recommendation is controversial: that of providing single-dose doxycycline as prophylaxis against Lyme disease. Dr. Ho stresses that this was only for “high-risk” tick bites, defined as a tick bite from an identified Ixodes vector species in which the tick was attached for at least 36 hours and that occurred in an endemic area.
The recommendation for prophylactic doxycycline originated with an article by Robert Nadelman and colleagues in the New England Journal of Medicine and has been strongly challenged by ILADS (International Lyme and Associated Diseases Society) physicians, including Daniel Cameron, MD, and others.
Sam Donta, MD, a recent member of the Department of Health & Human Services Tick-borne Working Group and a member of the Infectious Disease Society of America, said in an interview: “The problem with the one-dose doxycycline is you may not begin to develop symptoms until 2 months later.” It might mask the early symptoms of Lyme. “My impression is that the doxycycline – even the single dose – might have abrogated the ability to see an immune response. The idea, though, if you’ve had a tick bite, is to do nothing and to wait for symptoms to develop. That becomes a little bit more complex. But even then, you could choose to follow the patient and see the patient in 2 weeks and then get blood testing.”
Dr. Donta added: “I think the screening test is inadequate. So you have to go directly to the Western blot. And you have to do both the IgM and IgG” and look for specific bands.
Dr. Donta emphasized that patients should be encouraged to save any ticks that were attached and that, if at all possible, ticks should be sent to a reference lab for testing before committing a patient to a course of antibiotics. There is no harm in that brief delay, he said, and most labs can identify an array of pathogens.
The Wilderness Society guidelines on TBIs provide a good overview for clinicians practicing in limited resource settings and mirror those from the IDSA.
Dr. Ho and Dr. Donta reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The recently published “Clinical Practice Guidelines for the Prevention and Management of Tick-Borne Illness,” from the Wilderness Medical Society, are a good compilation of treatment suggestions but are not, in fact, new recommendations, lead author Benjamin Ho, MD, of Southern Wisconsin Emergency Associates in Janesville, acknowledged in an interview.
Dr. Ho emphasized that the focus of the report was on “practitioners who practice in resource-limited settings” and are “the group’s way of solidifying a ... standard of practice” for such physicians. Dr. Ho also said that, while “a lot of the recommendations aren’t well supported, the risk-benefit ratio, we believe, supports the recommendations.”
The article first reviewed the different types of ticks and their distribution in the United States, the specific pathogen associated with each, the disease it causes, and comments about seasonal variations in biting behavior. Another table outlines the most common clinical syndromes, typical lab findings, recommended diagnostic testing, and antibiotic treatments. A third section contains images of different types of ticks and photos of ticks in various life-cycle stages and different levels of engorgement.
The authors were careful to note: “Several tick species are able to carry multiple pathogens. In one study, nearly 25% of Ixodes were coinfected with some combination of the bacteria or parasites causing Lyme disease, anaplasmosis, or babesiosis. Although TBI [tick-borne illness] diagnosis is not the focus of this [clinical practice guideline], providers should be aware of high rates of coinfection; the presence of one TBI should in many instances prompt testing for others.”
In terms of recommendations for preventing TBIs, the authors challenge the suggestion of wearing light-colored clothing. For repellents, they recommend DEET, picaridin, and permethrin. And they also give instructions for laundering clothing and removing ticks.
One recommendation is controversial: that of providing single-dose doxycycline as prophylaxis against Lyme disease. Dr. Ho stresses that this was only for “high-risk” tick bites, defined as a tick bite from an identified Ixodes vector species in which the tick was attached for at least 36 hours and that occurred in an endemic area.
The recommendation for prophylactic doxycycline originated with an article by Robert Nadelman and colleagues in the New England Journal of Medicine and has been strongly challenged by ILADS (International Lyme and Associated Diseases Society) physicians, including Daniel Cameron, MD, and others.
Sam Donta, MD, a recent member of the Department of Health & Human Services Tick-borne Working Group and a member of the Infectious Disease Society of America, said in an interview: “The problem with the one-dose doxycycline is you may not begin to develop symptoms until 2 months later.” It might mask the early symptoms of Lyme. “My impression is that the doxycycline – even the single dose – might have abrogated the ability to see an immune response. The idea, though, if you’ve had a tick bite, is to do nothing and to wait for symptoms to develop. That becomes a little bit more complex. But even then, you could choose to follow the patient and see the patient in 2 weeks and then get blood testing.”
Dr. Donta added: “I think the screening test is inadequate. So you have to go directly to the Western blot. And you have to do both the IgM and IgG” and look for specific bands.
Dr. Donta emphasized that patients should be encouraged to save any ticks that were attached and that, if at all possible, ticks should be sent to a reference lab for testing before committing a patient to a course of antibiotics. There is no harm in that brief delay, he said, and most labs can identify an array of pathogens.
The Wilderness Society guidelines on TBIs provide a good overview for clinicians practicing in limited resource settings and mirror those from the IDSA.
Dr. Ho and Dr. Donta reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM WILDERNESS ENVIRONMENTAL MEDICINE
AHA advice for diabetes patients to stay heart healthy
A new document from the American Heart Association summarizes the latest research on cardiovascular risk factor management in type 2 diabetes, including medications, lifestyle, and social determinants of health.
Despite the availability of effective therapies for improving cardiovascular risk, in the United States fewer than one in five people with type 2 diabetes and without known cardiovascular disease meet control targets for a combination of A1c, blood pressure, LDL cholesterol, and nonsmoking status.
That proportion drops to less than 1 in 10 if body mass index less than 30 kg/m2 is included among the targets, and even less than that among individuals with established atherosclerotic cardiovascular disease, Joshua J. Joseph, MD, and colleagues point out in their paper, published online Jan. 10 in Circulation.
“This new scientific statement is an urgent call to action to follow the latest evidence-based approaches and to develop new best practices to advance type 2 diabetes treatment and care and reduce cardiovascular disease risk,” wrote Dr. Joseph, assistant professor of medicine in the division of endocrinology, diabetes, and metabolism at The Ohio State University, Columbus, Ohio, and coauthors.
The statement is not a guideline but an expert analysis that may inform future clinical practice guidelines, according to a press release from the AHA.
The new statement reviews evidence through June 2020 for lifestyle management of diabetes and weight, glycemic targets and control, blood pressure management, lipid management, antithrombotic therapy, and screening for cardiovascular and renal complications, including imaging. It also discusses the clinical implications of recent cardiovascular outcomes trials of newer glucose-lowering medications.
However, Dr. Joseph and colleagues point out, clinical care and treatment account for just 10%-20% of modifiable contributors to health outcomes. The other 80%-90% relate to social determinants of health, including health-related behaviors, socioeconomic factors, environmental factors, and racism.
“If we are to continue to advance the management of cardiovascular risk factors, we must also address the [social determinants of health] in the delivery of health care,” they noted.
Overall, they advise a patient-centered approach, meaning “reframing our clinical encounters to think about patients as people who live in families, communities, and societies that must be considered in their cardiovascular risk management.”
“People with [type 2 diabetes] face numerous barriers to health including access to care and equitable care, which must be considered when developing individualized care plans with our patients,” Dr. Joseph said in the AHA press release.
Lifestyle, medications for lowering A1c, BP, lipids
For lifestyle management, the authors say, “culturally appropriate recommendations through diabetes self-management education and support and medical nutrition therapy are key to meeting individualized goals for behavioral change and diabetes self-management.”
The document summarizes recommendations from other professional societies regarding glycemic targets and glucose lowering medications, i.e., target A1c levels of either < 7% or < 6.5% for the majority, with adjustments based on individual factors, such as life expectancy. It advises on use of metformin as first-line therapy followed by a sodium-glucose cotransporter-2 inhibitor or a glucagon-like peptide-1 agonist for those with established cardiovascular disease or risk factors.
“Cost may be a barrier to taking some [type 2 diabetes] medications as prescribed; however, many of these medications are now more commonly covered by more health insurance plans,” Dr. Joseph said.
“Another barrier is recognition by patients that these newer [type 2 diabetes] medications are also effective in reducing the risk of heart disease, stroke, heart failure, and kidney disease.”
Blood pressure treatment guidelines differ between those of the AHA/American College of Cardiology (ACC) and the American Diabetes Association (ADA), most notably that the AHA/ACC guidelines advise a general target of < 130/80 mm Hg, whereas ADA advises < 140/90 mm Hg or < 130/80 mm Hg for those with high risk if it can be safely achieved.
The decision should be “patient-centered with shared decision-making,” Dr. Joseph and colleagues advised.
For lipid-lowering, the document cites the 2018 ACC/AHA cholesterol guidelines, which include advising statins as first-line therapy for both primary and secondary prevention in diabetes, with highest intensity statins used in those at highest risk. But again, treatment should be individualized, and other agents should be used for patients in whom statins don’t work or aren’t tolerated.
And while use of antiplatelets – that is, aspirin – is well established as secondary prevention in type 2 diabetes, given new data suggesting that the risk for major bleeding could outweigh the benefits for primary prevention, “the relative benefits of antithrombotic approaches need to be weighed carefully against risks using a patient-centered approach,” the authors advised.
Among the many imaging tests available to facilitate cardiovascular risk stratification in type 2 diabetes, coronary artery calcification (CAC) CT screening is one of the few with sufficient data to support routine use in selected patients. The National Lipid Association, for example, recommends escalation to high-intensity statin for CAC > 100.
“One avenue to continue to address and advance diabetes management is through breaking down the four walls of the clinic or hospital through community engagement, clinic-to-community connections, and academic-community-government partnerships that may help address and support modifiable lifestyle behaviors such as physical activity, nutrition, smoking cessation and stress management,” Dr. Joseph concluded.
The AHA receives funding primarily from individuals. Foundations and corporations, including pharmaceutical, device manufacturers, and other companies, also make donations and fund AHA programs and events. The AHA’s strict policies prevent these relationships from influencing the science content. Revenues from pharmaceutical and biotech companies, device manufacturers, and health insurance providers and the AHA’s financial information are available on the association’s website. Dr. Joseph has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new document from the American Heart Association summarizes the latest research on cardiovascular risk factor management in type 2 diabetes, including medications, lifestyle, and social determinants of health.
Despite the availability of effective therapies for improving cardiovascular risk, in the United States fewer than one in five people with type 2 diabetes and without known cardiovascular disease meet control targets for a combination of A1c, blood pressure, LDL cholesterol, and nonsmoking status.
That proportion drops to less than 1 in 10 if body mass index less than 30 kg/m2 is included among the targets, and even less than that among individuals with established atherosclerotic cardiovascular disease, Joshua J. Joseph, MD, and colleagues point out in their paper, published online Jan. 10 in Circulation.
“This new scientific statement is an urgent call to action to follow the latest evidence-based approaches and to develop new best practices to advance type 2 diabetes treatment and care and reduce cardiovascular disease risk,” wrote Dr. Joseph, assistant professor of medicine in the division of endocrinology, diabetes, and metabolism at The Ohio State University, Columbus, Ohio, and coauthors.
The statement is not a guideline but an expert analysis that may inform future clinical practice guidelines, according to a press release from the AHA.
The new statement reviews evidence through June 2020 for lifestyle management of diabetes and weight, glycemic targets and control, blood pressure management, lipid management, antithrombotic therapy, and screening for cardiovascular and renal complications, including imaging. It also discusses the clinical implications of recent cardiovascular outcomes trials of newer glucose-lowering medications.
However, Dr. Joseph and colleagues point out, clinical care and treatment account for just 10%-20% of modifiable contributors to health outcomes. The other 80%-90% relate to social determinants of health, including health-related behaviors, socioeconomic factors, environmental factors, and racism.
“If we are to continue to advance the management of cardiovascular risk factors, we must also address the [social determinants of health] in the delivery of health care,” they noted.
Overall, they advise a patient-centered approach, meaning “reframing our clinical encounters to think about patients as people who live in families, communities, and societies that must be considered in their cardiovascular risk management.”
“People with [type 2 diabetes] face numerous barriers to health including access to care and equitable care, which must be considered when developing individualized care plans with our patients,” Dr. Joseph said in the AHA press release.
Lifestyle, medications for lowering A1c, BP, lipids
For lifestyle management, the authors say, “culturally appropriate recommendations through diabetes self-management education and support and medical nutrition therapy are key to meeting individualized goals for behavioral change and diabetes self-management.”
The document summarizes recommendations from other professional societies regarding glycemic targets and glucose lowering medications, i.e., target A1c levels of either < 7% or < 6.5% for the majority, with adjustments based on individual factors, such as life expectancy. It advises on use of metformin as first-line therapy followed by a sodium-glucose cotransporter-2 inhibitor or a glucagon-like peptide-1 agonist for those with established cardiovascular disease or risk factors.
“Cost may be a barrier to taking some [type 2 diabetes] medications as prescribed; however, many of these medications are now more commonly covered by more health insurance plans,” Dr. Joseph said.
“Another barrier is recognition by patients that these newer [type 2 diabetes] medications are also effective in reducing the risk of heart disease, stroke, heart failure, and kidney disease.”
Blood pressure treatment guidelines differ between those of the AHA/American College of Cardiology (ACC) and the American Diabetes Association (ADA), most notably that the AHA/ACC guidelines advise a general target of < 130/80 mm Hg, whereas ADA advises < 140/90 mm Hg or < 130/80 mm Hg for those with high risk if it can be safely achieved.
The decision should be “patient-centered with shared decision-making,” Dr. Joseph and colleagues advised.
For lipid-lowering, the document cites the 2018 ACC/AHA cholesterol guidelines, which include advising statins as first-line therapy for both primary and secondary prevention in diabetes, with highest intensity statins used in those at highest risk. But again, treatment should be individualized, and other agents should be used for patients in whom statins don’t work or aren’t tolerated.
And while use of antiplatelets – that is, aspirin – is well established as secondary prevention in type 2 diabetes, given new data suggesting that the risk for major bleeding could outweigh the benefits for primary prevention, “the relative benefits of antithrombotic approaches need to be weighed carefully against risks using a patient-centered approach,” the authors advised.
Among the many imaging tests available to facilitate cardiovascular risk stratification in type 2 diabetes, coronary artery calcification (CAC) CT screening is one of the few with sufficient data to support routine use in selected patients. The National Lipid Association, for example, recommends escalation to high-intensity statin for CAC > 100.
“One avenue to continue to address and advance diabetes management is through breaking down the four walls of the clinic or hospital through community engagement, clinic-to-community connections, and academic-community-government partnerships that may help address and support modifiable lifestyle behaviors such as physical activity, nutrition, smoking cessation and stress management,” Dr. Joseph concluded.
The AHA receives funding primarily from individuals. Foundations and corporations, including pharmaceutical, device manufacturers, and other companies, also make donations and fund AHA programs and events. The AHA’s strict policies prevent these relationships from influencing the science content. Revenues from pharmaceutical and biotech companies, device manufacturers, and health insurance providers and the AHA’s financial information are available on the association’s website. Dr. Joseph has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new document from the American Heart Association summarizes the latest research on cardiovascular risk factor management in type 2 diabetes, including medications, lifestyle, and social determinants of health.
Despite the availability of effective therapies for improving cardiovascular risk, in the United States fewer than one in five people with type 2 diabetes and without known cardiovascular disease meet control targets for a combination of A1c, blood pressure, LDL cholesterol, and nonsmoking status.
That proportion drops to less than 1 in 10 if body mass index less than 30 kg/m2 is included among the targets, and even less than that among individuals with established atherosclerotic cardiovascular disease, Joshua J. Joseph, MD, and colleagues point out in their paper, published online Jan. 10 in Circulation.
“This new scientific statement is an urgent call to action to follow the latest evidence-based approaches and to develop new best practices to advance type 2 diabetes treatment and care and reduce cardiovascular disease risk,” wrote Dr. Joseph, assistant professor of medicine in the division of endocrinology, diabetes, and metabolism at The Ohio State University, Columbus, Ohio, and coauthors.
The statement is not a guideline but an expert analysis that may inform future clinical practice guidelines, according to a press release from the AHA.
The new statement reviews evidence through June 2020 for lifestyle management of diabetes and weight, glycemic targets and control, blood pressure management, lipid management, antithrombotic therapy, and screening for cardiovascular and renal complications, including imaging. It also discusses the clinical implications of recent cardiovascular outcomes trials of newer glucose-lowering medications.
However, Dr. Joseph and colleagues point out, clinical care and treatment account for just 10%-20% of modifiable contributors to health outcomes. The other 80%-90% relate to social determinants of health, including health-related behaviors, socioeconomic factors, environmental factors, and racism.
“If we are to continue to advance the management of cardiovascular risk factors, we must also address the [social determinants of health] in the delivery of health care,” they noted.
Overall, they advise a patient-centered approach, meaning “reframing our clinical encounters to think about patients as people who live in families, communities, and societies that must be considered in their cardiovascular risk management.”
“People with [type 2 diabetes] face numerous barriers to health including access to care and equitable care, which must be considered when developing individualized care plans with our patients,” Dr. Joseph said in the AHA press release.
Lifestyle, medications for lowering A1c, BP, lipids
For lifestyle management, the authors say, “culturally appropriate recommendations through diabetes self-management education and support and medical nutrition therapy are key to meeting individualized goals for behavioral change and diabetes self-management.”
The document summarizes recommendations from other professional societies regarding glycemic targets and glucose lowering medications, i.e., target A1c levels of either < 7% or < 6.5% for the majority, with adjustments based on individual factors, such as life expectancy. It advises on use of metformin as first-line therapy followed by a sodium-glucose cotransporter-2 inhibitor or a glucagon-like peptide-1 agonist for those with established cardiovascular disease or risk factors.
“Cost may be a barrier to taking some [type 2 diabetes] medications as prescribed; however, many of these medications are now more commonly covered by more health insurance plans,” Dr. Joseph said.
“Another barrier is recognition by patients that these newer [type 2 diabetes] medications are also effective in reducing the risk of heart disease, stroke, heart failure, and kidney disease.”
Blood pressure treatment guidelines differ between those of the AHA/American College of Cardiology (ACC) and the American Diabetes Association (ADA), most notably that the AHA/ACC guidelines advise a general target of < 130/80 mm Hg, whereas ADA advises < 140/90 mm Hg or < 130/80 mm Hg for those with high risk if it can be safely achieved.
The decision should be “patient-centered with shared decision-making,” Dr. Joseph and colleagues advised.
For lipid-lowering, the document cites the 2018 ACC/AHA cholesterol guidelines, which include advising statins as first-line therapy for both primary and secondary prevention in diabetes, with highest intensity statins used in those at highest risk. But again, treatment should be individualized, and other agents should be used for patients in whom statins don’t work or aren’t tolerated.
And while use of antiplatelets – that is, aspirin – is well established as secondary prevention in type 2 diabetes, given new data suggesting that the risk for major bleeding could outweigh the benefits for primary prevention, “the relative benefits of antithrombotic approaches need to be weighed carefully against risks using a patient-centered approach,” the authors advised.
Among the many imaging tests available to facilitate cardiovascular risk stratification in type 2 diabetes, coronary artery calcification (CAC) CT screening is one of the few with sufficient data to support routine use in selected patients. The National Lipid Association, for example, recommends escalation to high-intensity statin for CAC > 100.
“One avenue to continue to address and advance diabetes management is through breaking down the four walls of the clinic or hospital through community engagement, clinic-to-community connections, and academic-community-government partnerships that may help address and support modifiable lifestyle behaviors such as physical activity, nutrition, smoking cessation and stress management,” Dr. Joseph concluded.
The AHA receives funding primarily from individuals. Foundations and corporations, including pharmaceutical, device manufacturers, and other companies, also make donations and fund AHA programs and events. The AHA’s strict policies prevent these relationships from influencing the science content. Revenues from pharmaceutical and biotech companies, device manufacturers, and health insurance providers and the AHA’s financial information are available on the association’s website. Dr. Joseph has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
AAN updates treatment guidance on painful diabetic neuropathy
Painful diabetic neuropathy is very common and can greatly affect an individual’s quality of life, guideline author Brian Callaghan, MD, University of Michigan, Ann Arbor, noted in a news release.
“This guideline aims to help neurologists and other doctors provide the highest quality patient care based on the latest evidence,” Dr. Callaghan said.
The recommendations update the 2011 AAN guideline on the treatment of painful diabetic neuropathy. The new guidance was published online Dec. 27, 2021, in Neurology and has been endorsed by the American Association of Neuromuscular & Electrodiagnostic Medicine.
Multiple options
To update the guideline, an expert panel reviewed data from more than 100 randomized controlled trials published from January 2008 to April 2020.
The panel noted that more than 16% of individuals with diabetes experience painful diabetic neuropathy, but it often goes unrecognized and untreated. The guideline recommends clinicians assess patients with diabetes for peripheral neuropathic pain and its effect on their function and quality of life.
Before prescribing treatment, health providers should determine if the patient also has mood or sleep problems as both can influence pain perception.
The guideline recommends offering one of four classes of oral medications found to be effective for neuropathic pain: tricyclic antidepressants such as amitriptyline, nortriptyline, or imipramine; serotonin norepinephrine reuptake inhibitors such as duloxetine, venlafaxine, or desvenlafaxine; gabapentinoids such as gabapentin or pregabalin; and/or sodium channel blockers such as carbamazepine, oxcarbazepine, lamotrigine, or lacosamide.
All four classes of medications have “comparable effect sizes just above or just below our cutoff for a medium effect size” (standardized median difference, 0.5), the panel noted.
In addition, “new studies on sodium channel blockers published since the last guideline have resulted in these drugs now being recommended and considered as effective at providing pain relief as the other drug classes recommended in this guideline,” said Dr. Callaghan.
When an initial medication fails to provide meaningful improvement in pain, or produces significant side effects, a trial of another medication from a different class is recommended.
Pain reduction, not elimination
Opioids are not recommended for painful diabetic neuropathy. Not only do they come with risks, there is also no strong evidence they are effective for painful diabetic neuropathy in the long term, the panel wrote. Tramadol and tapentadol are also not recommended for the treatment of painful diabetic neuropathy.
“Current evidence suggests that the risks of the use of opioids for painful diabetic neuropathy therapy outweigh the benefits, so they should not be prescribed,” Dr. Callaghan said.
For patients interested in trying topical, nontraditional, or nondrug interventions to reduce pain, the guideline recommends a number of options including capsaicin, glyceryl trinitrate spray, and Citrullus colocynthis. Ginkgo biloba, exercise, mindfulness, cognitive-behavioral therapy, and tai chi are also suggested.
“It is important to note that the recommended drugs and topical treatments in this guideline may not eliminate pain, but they have been shown to reduce pain,” Dr. Callaghan said. “The good news is there are many treatment options for painful diabetic neuropathy, so a treatment plan can be tailored specifically to each person living with this condition.”
Along with the updated guideline, the AAN has also published a new Polyneuropathy Quality Measurement Set to assist neurologists and other health care providers in treating patients with painful diabetic neuropathy.
The updated guideline was developed with financial support from the AAN.
A version of this article first appeared on Medscape.com.
Painful diabetic neuropathy is very common and can greatly affect an individual’s quality of life, guideline author Brian Callaghan, MD, University of Michigan, Ann Arbor, noted in a news release.
“This guideline aims to help neurologists and other doctors provide the highest quality patient care based on the latest evidence,” Dr. Callaghan said.
The recommendations update the 2011 AAN guideline on the treatment of painful diabetic neuropathy. The new guidance was published online Dec. 27, 2021, in Neurology and has been endorsed by the American Association of Neuromuscular & Electrodiagnostic Medicine.
Multiple options
To update the guideline, an expert panel reviewed data from more than 100 randomized controlled trials published from January 2008 to April 2020.
The panel noted that more than 16% of individuals with diabetes experience painful diabetic neuropathy, but it often goes unrecognized and untreated. The guideline recommends clinicians assess patients with diabetes for peripheral neuropathic pain and its effect on their function and quality of life.
Before prescribing treatment, health providers should determine if the patient also has mood or sleep problems as both can influence pain perception.
The guideline recommends offering one of four classes of oral medications found to be effective for neuropathic pain: tricyclic antidepressants such as amitriptyline, nortriptyline, or imipramine; serotonin norepinephrine reuptake inhibitors such as duloxetine, venlafaxine, or desvenlafaxine; gabapentinoids such as gabapentin or pregabalin; and/or sodium channel blockers such as carbamazepine, oxcarbazepine, lamotrigine, or lacosamide.
All four classes of medications have “comparable effect sizes just above or just below our cutoff for a medium effect size” (standardized median difference, 0.5), the panel noted.
In addition, “new studies on sodium channel blockers published since the last guideline have resulted in these drugs now being recommended and considered as effective at providing pain relief as the other drug classes recommended in this guideline,” said Dr. Callaghan.
When an initial medication fails to provide meaningful improvement in pain, or produces significant side effects, a trial of another medication from a different class is recommended.
Pain reduction, not elimination
Opioids are not recommended for painful diabetic neuropathy. Not only do they come with risks, there is also no strong evidence they are effective for painful diabetic neuropathy in the long term, the panel wrote. Tramadol and tapentadol are also not recommended for the treatment of painful diabetic neuropathy.
“Current evidence suggests that the risks of the use of opioids for painful diabetic neuropathy therapy outweigh the benefits, so they should not be prescribed,” Dr. Callaghan said.
For patients interested in trying topical, nontraditional, or nondrug interventions to reduce pain, the guideline recommends a number of options including capsaicin, glyceryl trinitrate spray, and Citrullus colocynthis. Ginkgo biloba, exercise, mindfulness, cognitive-behavioral therapy, and tai chi are also suggested.
“It is important to note that the recommended drugs and topical treatments in this guideline may not eliminate pain, but they have been shown to reduce pain,” Dr. Callaghan said. “The good news is there are many treatment options for painful diabetic neuropathy, so a treatment plan can be tailored specifically to each person living with this condition.”
Along with the updated guideline, the AAN has also published a new Polyneuropathy Quality Measurement Set to assist neurologists and other health care providers in treating patients with painful diabetic neuropathy.
The updated guideline was developed with financial support from the AAN.
A version of this article first appeared on Medscape.com.
Painful diabetic neuropathy is very common and can greatly affect an individual’s quality of life, guideline author Brian Callaghan, MD, University of Michigan, Ann Arbor, noted in a news release.
“This guideline aims to help neurologists and other doctors provide the highest quality patient care based on the latest evidence,” Dr. Callaghan said.
The recommendations update the 2011 AAN guideline on the treatment of painful diabetic neuropathy. The new guidance was published online Dec. 27, 2021, in Neurology and has been endorsed by the American Association of Neuromuscular & Electrodiagnostic Medicine.
Multiple options
To update the guideline, an expert panel reviewed data from more than 100 randomized controlled trials published from January 2008 to April 2020.
The panel noted that more than 16% of individuals with diabetes experience painful diabetic neuropathy, but it often goes unrecognized and untreated. The guideline recommends clinicians assess patients with diabetes for peripheral neuropathic pain and its effect on their function and quality of life.
Before prescribing treatment, health providers should determine if the patient also has mood or sleep problems as both can influence pain perception.
The guideline recommends offering one of four classes of oral medications found to be effective for neuropathic pain: tricyclic antidepressants such as amitriptyline, nortriptyline, or imipramine; serotonin norepinephrine reuptake inhibitors such as duloxetine, venlafaxine, or desvenlafaxine; gabapentinoids such as gabapentin or pregabalin; and/or sodium channel blockers such as carbamazepine, oxcarbazepine, lamotrigine, or lacosamide.
All four classes of medications have “comparable effect sizes just above or just below our cutoff for a medium effect size” (standardized median difference, 0.5), the panel noted.
In addition, “new studies on sodium channel blockers published since the last guideline have resulted in these drugs now being recommended and considered as effective at providing pain relief as the other drug classes recommended in this guideline,” said Dr. Callaghan.
When an initial medication fails to provide meaningful improvement in pain, or produces significant side effects, a trial of another medication from a different class is recommended.
Pain reduction, not elimination
Opioids are not recommended for painful diabetic neuropathy. Not only do they come with risks, there is also no strong evidence they are effective for painful diabetic neuropathy in the long term, the panel wrote. Tramadol and tapentadol are also not recommended for the treatment of painful diabetic neuropathy.
“Current evidence suggests that the risks of the use of opioids for painful diabetic neuropathy therapy outweigh the benefits, so they should not be prescribed,” Dr. Callaghan said.
For patients interested in trying topical, nontraditional, or nondrug interventions to reduce pain, the guideline recommends a number of options including capsaicin, glyceryl trinitrate spray, and Citrullus colocynthis. Ginkgo biloba, exercise, mindfulness, cognitive-behavioral therapy, and tai chi are also suggested.
“It is important to note that the recommended drugs and topical treatments in this guideline may not eliminate pain, but they have been shown to reduce pain,” Dr. Callaghan said. “The good news is there are many treatment options for painful diabetic neuropathy, so a treatment plan can be tailored specifically to each person living with this condition.”
Along with the updated guideline, the AAN has also published a new Polyneuropathy Quality Measurement Set to assist neurologists and other health care providers in treating patients with painful diabetic neuropathy.
The updated guideline was developed with financial support from the AAN.
A version of this article first appeared on Medscape.com.
FROM NEUROLOGY
ADA standards of care 2022: Screen more, personalize, use technology
The American Diabetes Association’s updated clinical recommendations for 2022 call for wider population screening, along with furthering the trends toward individualization of care use of diabetes technology.
The summary of changes from 2021 spans four pages. “Diabetes is a really dynamic field so there is a lot to update which is good. It means progress,” ADA chief science and medical officer Robert A. Gabbay, MD, PhD, told this news organization.
The ADA Standards of Medical Care in Diabetes – 2022 was published Dec. 20, 2021, online as a supplement to Diabetes Care.
Screening widened by age, in pregnancy, and for type 1 diabetes
One dramatic change is a drop in age to begin screening all people for prediabetes and diabetes from 45 years to 35 years, regardless of risk factors such as obesity.
“Sadly, there are increasing numbers of people with diabetes and developing diabetes younger,” Dr. Gabbay said.
In August 2021, the U.S. Preventive Services Task Force dropped its recommended age of diabetes screening from 40 to 35 years for people with overweight or obesity, but not universally, as ADA now has.
The ADA made its recommendation independently, Dr. Gabbay noted.
The recommendation for testing pregnant women early in gestation (<15 weeks) for preexisting diabetes was also expanded, from just those with risk factors to consideration of testing all women for undiagnosed diabetes at the time they’re planning pregnancy, and if not then, at the first prenatal visit. Screening for gestational diabetes is then performed at 24-28 weeks.
Again, this is caused by increasing diabetes onset at younger ages, Dr. Gabbay said. “We’re well aware that the number of women who have diabetes and don’t know it and become pregnant is significant and therefore screening early on is important.”
New guidance regarding autoantibody screening in adults suspected of having type 1 diabetes and genetic testing for those who don’t fit typical criteria for either of the two main types are based on the ADA/European Association for the Study of Diabetes joint consensus statement on type 1 diabetes in adults.
Individualization of care based on comorbidities, other factors
The concept of individualization of care in diabetes has been emphasized for several years now, but continues to be enhanced with new data and newly available management tools.
Regarding management of type 2 diabetes, several charts have been included to help guide decision-making.
One lists drug-specific and patient factors, including comorbidities, to consider when selecting glucose-lowering medications. A new table depicts a building with four “pillars,” for complication risk reduction, including management of blood pressure, lipids, and glucose, as well as use of agents with cardiovascular and kidney benefit.
“On the type 2 side, the choice of therapy is really guided by several factors. We lay them out in a nice diagram. ... A lot of useful information there compares classes of drugs in order to help clinicians make decisions on what would be the appropriate therapy for a given individual,” Dr. Gabbay said.
An algorithm for pharmacologic treatment includes considerations of weight, hypoglycemia, and cost. Tables are also provided listing average wholesale prices of insulins and noninsulin medications.
A section now entitled “Obesity and weight management for the prevention and treatment of type 2 diabetes” has added content regarding the importance of addressing obesity in diabetes, particularly in the context of the COVID-19 pandemic, and the addition of semaglutide as an approved obesity treatment.
“What we hope is that this engenders a shared decision-making process with the patient to identify what the goals are and then choose the appropriate therapy for those goals,” Dr. Gabbay said.
New information has also been added about management of nonalcoholic fatty liver disease. “I think that’s one of the unrecognized and unaddressed complications of diabetes that we’ll see in the future, particularly as new therapies come out,” Dr. Gabbay predicted.
The section on cardiovascular disease and risk management, endorsed for the fourth year in a row by the American College of Cardiology, includes several new recommendations, including diagnosis of hypertension at a single visit if blood pressure is 180/110 mm Hg or greater, and individualization of blood pressure targets.
Chronic kidney disease management has now been separated from other microvascular complications into a standalone section, with several new updates. Retinopathy, neuropathy, and foot care remain combined in one section.
Diabetes technology: Rapidly evolving, access an issue
The new technology section “doubles down on the time in [normal glucose] range (TIR) concept,” but also emphasizes the importance of time below range.
“When we see that, we need to make a therapeutic change. We were concerned that as there’s more and more information and numbers, users might not pick up on what’s important,” Dr. Gabbay noted.
The new standards also provides greater affirmation of the value of continuous glucose monitoring (CGM) for people with both type 1 and type 2 diabetes at any age, with individualized choice of devices.
Access to technology is a “big issue, and something the ADA has really been fighting for, particularly in terms of health disparities,” Dr. Gabbay said, noting that ADA has a new Health Equity Now platform, which includes a “bill of rights” calling for all patients with diabetes to have access to state-of-the-art technologies, including CGM.
Overall, he said, “I think the big picture is diabetes continues to evolve and advance. After careful review of the literature, the standards of care identifies at least four big areas where there are some changes that clinicians need to know about: screening, how to individualize treatment, considerations of comorbidities, and the important role that technology plays.”
Dr. Gabbay is an employee of the ADA.
A version of this article first appeared on Medscape.com.
The American Diabetes Association’s updated clinical recommendations for 2022 call for wider population screening, along with furthering the trends toward individualization of care use of diabetes technology.
The summary of changes from 2021 spans four pages. “Diabetes is a really dynamic field so there is a lot to update which is good. It means progress,” ADA chief science and medical officer Robert A. Gabbay, MD, PhD, told this news organization.
The ADA Standards of Medical Care in Diabetes – 2022 was published Dec. 20, 2021, online as a supplement to Diabetes Care.
Screening widened by age, in pregnancy, and for type 1 diabetes
One dramatic change is a drop in age to begin screening all people for prediabetes and diabetes from 45 years to 35 years, regardless of risk factors such as obesity.
“Sadly, there are increasing numbers of people with diabetes and developing diabetes younger,” Dr. Gabbay said.
In August 2021, the U.S. Preventive Services Task Force dropped its recommended age of diabetes screening from 40 to 35 years for people with overweight or obesity, but not universally, as ADA now has.
The ADA made its recommendation independently, Dr. Gabbay noted.
The recommendation for testing pregnant women early in gestation (<15 weeks) for preexisting diabetes was also expanded, from just those with risk factors to consideration of testing all women for undiagnosed diabetes at the time they’re planning pregnancy, and if not then, at the first prenatal visit. Screening for gestational diabetes is then performed at 24-28 weeks.
Again, this is caused by increasing diabetes onset at younger ages, Dr. Gabbay said. “We’re well aware that the number of women who have diabetes and don’t know it and become pregnant is significant and therefore screening early on is important.”
New guidance regarding autoantibody screening in adults suspected of having type 1 diabetes and genetic testing for those who don’t fit typical criteria for either of the two main types are based on the ADA/European Association for the Study of Diabetes joint consensus statement on type 1 diabetes in adults.
Individualization of care based on comorbidities, other factors
The concept of individualization of care in diabetes has been emphasized for several years now, but continues to be enhanced with new data and newly available management tools.
Regarding management of type 2 diabetes, several charts have been included to help guide decision-making.
One lists drug-specific and patient factors, including comorbidities, to consider when selecting glucose-lowering medications. A new table depicts a building with four “pillars,” for complication risk reduction, including management of blood pressure, lipids, and glucose, as well as use of agents with cardiovascular and kidney benefit.
“On the type 2 side, the choice of therapy is really guided by several factors. We lay them out in a nice diagram. ... A lot of useful information there compares classes of drugs in order to help clinicians make decisions on what would be the appropriate therapy for a given individual,” Dr. Gabbay said.
An algorithm for pharmacologic treatment includes considerations of weight, hypoglycemia, and cost. Tables are also provided listing average wholesale prices of insulins and noninsulin medications.
A section now entitled “Obesity and weight management for the prevention and treatment of type 2 diabetes” has added content regarding the importance of addressing obesity in diabetes, particularly in the context of the COVID-19 pandemic, and the addition of semaglutide as an approved obesity treatment.
“What we hope is that this engenders a shared decision-making process with the patient to identify what the goals are and then choose the appropriate therapy for those goals,” Dr. Gabbay said.
New information has also been added about management of nonalcoholic fatty liver disease. “I think that’s one of the unrecognized and unaddressed complications of diabetes that we’ll see in the future, particularly as new therapies come out,” Dr. Gabbay predicted.
The section on cardiovascular disease and risk management, endorsed for the fourth year in a row by the American College of Cardiology, includes several new recommendations, including diagnosis of hypertension at a single visit if blood pressure is 180/110 mm Hg or greater, and individualization of blood pressure targets.
Chronic kidney disease management has now been separated from other microvascular complications into a standalone section, with several new updates. Retinopathy, neuropathy, and foot care remain combined in one section.
Diabetes technology: Rapidly evolving, access an issue
The new technology section “doubles down on the time in [normal glucose] range (TIR) concept,” but also emphasizes the importance of time below range.
“When we see that, we need to make a therapeutic change. We were concerned that as there’s more and more information and numbers, users might not pick up on what’s important,” Dr. Gabbay noted.
The new standards also provides greater affirmation of the value of continuous glucose monitoring (CGM) for people with both type 1 and type 2 diabetes at any age, with individualized choice of devices.
Access to technology is a “big issue, and something the ADA has really been fighting for, particularly in terms of health disparities,” Dr. Gabbay said, noting that ADA has a new Health Equity Now platform, which includes a “bill of rights” calling for all patients with diabetes to have access to state-of-the-art technologies, including CGM.
Overall, he said, “I think the big picture is diabetes continues to evolve and advance. After careful review of the literature, the standards of care identifies at least four big areas where there are some changes that clinicians need to know about: screening, how to individualize treatment, considerations of comorbidities, and the important role that technology plays.”
Dr. Gabbay is an employee of the ADA.
A version of this article first appeared on Medscape.com.
The American Diabetes Association’s updated clinical recommendations for 2022 call for wider population screening, along with furthering the trends toward individualization of care use of diabetes technology.
The summary of changes from 2021 spans four pages. “Diabetes is a really dynamic field so there is a lot to update which is good. It means progress,” ADA chief science and medical officer Robert A. Gabbay, MD, PhD, told this news organization.
The ADA Standards of Medical Care in Diabetes – 2022 was published Dec. 20, 2021, online as a supplement to Diabetes Care.
Screening widened by age, in pregnancy, and for type 1 diabetes
One dramatic change is a drop in age to begin screening all people for prediabetes and diabetes from 45 years to 35 years, regardless of risk factors such as obesity.
“Sadly, there are increasing numbers of people with diabetes and developing diabetes younger,” Dr. Gabbay said.
In August 2021, the U.S. Preventive Services Task Force dropped its recommended age of diabetes screening from 40 to 35 years for people with overweight or obesity, but not universally, as ADA now has.
The ADA made its recommendation independently, Dr. Gabbay noted.
The recommendation for testing pregnant women early in gestation (<15 weeks) for preexisting diabetes was also expanded, from just those with risk factors to consideration of testing all women for undiagnosed diabetes at the time they’re planning pregnancy, and if not then, at the first prenatal visit. Screening for gestational diabetes is then performed at 24-28 weeks.
Again, this is caused by increasing diabetes onset at younger ages, Dr. Gabbay said. “We’re well aware that the number of women who have diabetes and don’t know it and become pregnant is significant and therefore screening early on is important.”
New guidance regarding autoantibody screening in adults suspected of having type 1 diabetes and genetic testing for those who don’t fit typical criteria for either of the two main types are based on the ADA/European Association for the Study of Diabetes joint consensus statement on type 1 diabetes in adults.
Individualization of care based on comorbidities, other factors
The concept of individualization of care in diabetes has been emphasized for several years now, but continues to be enhanced with new data and newly available management tools.
Regarding management of type 2 diabetes, several charts have been included to help guide decision-making.
One lists drug-specific and patient factors, including comorbidities, to consider when selecting glucose-lowering medications. A new table depicts a building with four “pillars,” for complication risk reduction, including management of blood pressure, lipids, and glucose, as well as use of agents with cardiovascular and kidney benefit.
“On the type 2 side, the choice of therapy is really guided by several factors. We lay them out in a nice diagram. ... A lot of useful information there compares classes of drugs in order to help clinicians make decisions on what would be the appropriate therapy for a given individual,” Dr. Gabbay said.
An algorithm for pharmacologic treatment includes considerations of weight, hypoglycemia, and cost. Tables are also provided listing average wholesale prices of insulins and noninsulin medications.
A section now entitled “Obesity and weight management for the prevention and treatment of type 2 diabetes” has added content regarding the importance of addressing obesity in diabetes, particularly in the context of the COVID-19 pandemic, and the addition of semaglutide as an approved obesity treatment.
“What we hope is that this engenders a shared decision-making process with the patient to identify what the goals are and then choose the appropriate therapy for those goals,” Dr. Gabbay said.
New information has also been added about management of nonalcoholic fatty liver disease. “I think that’s one of the unrecognized and unaddressed complications of diabetes that we’ll see in the future, particularly as new therapies come out,” Dr. Gabbay predicted.
The section on cardiovascular disease and risk management, endorsed for the fourth year in a row by the American College of Cardiology, includes several new recommendations, including diagnosis of hypertension at a single visit if blood pressure is 180/110 mm Hg or greater, and individualization of blood pressure targets.
Chronic kidney disease management has now been separated from other microvascular complications into a standalone section, with several new updates. Retinopathy, neuropathy, and foot care remain combined in one section.
Diabetes technology: Rapidly evolving, access an issue
The new technology section “doubles down on the time in [normal glucose] range (TIR) concept,” but also emphasizes the importance of time below range.
“When we see that, we need to make a therapeutic change. We were concerned that as there’s more and more information and numbers, users might not pick up on what’s important,” Dr. Gabbay noted.
The new standards also provides greater affirmation of the value of continuous glucose monitoring (CGM) for people with both type 1 and type 2 diabetes at any age, with individualized choice of devices.
Access to technology is a “big issue, and something the ADA has really been fighting for, particularly in terms of health disparities,” Dr. Gabbay said, noting that ADA has a new Health Equity Now platform, which includes a “bill of rights” calling for all patients with diabetes to have access to state-of-the-art technologies, including CGM.
Overall, he said, “I think the big picture is diabetes continues to evolve and advance. After careful review of the literature, the standards of care identifies at least four big areas where there are some changes that clinicians need to know about: screening, how to individualize treatment, considerations of comorbidities, and the important role that technology plays.”
Dr. Gabbay is an employee of the ADA.
A version of this article first appeared on Medscape.com.
US Multi-Society Task Force lowers recommended CRC screening age
The U.S. Multi-Society Task Force on Colorectal Cancer (CRC) has lowered the recommended age to start CRC screening from 50 to 45 years of age for all average-risk individuals.
Although no studies have directly demonstrated the result of lowering the age of screening, lead author Swati G. Patel, MD, of University of Colorado Anschutz Medical Center, Aurora, and colleagues suggested that the increasing incidence of advanced CRC among younger individuals, coupled with the net benefit of screening, warrant a lower age threshold.
“Recent data ... show that CRC incidence rates in individuals ages 50 to 64 have increased by 1% annually between 2011 and 2016,” the authors wrote in Gastroenterology. “Similarly, CRC incidence and mortality rates in persons under age 50, termed early-age onset CRC (EAO-CRC), are also increasing.”
The task force of nine experts, representing the American Gastroenterological Association, the American College of Gastroenterology, and the American Society for Gastrointestinal Endoscopy, conducted a literature review and generated recommendations using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) criteria. In addition to recommending a lower age for initial screening, Dr. Patel and colleagues provided guidance for cessation of screening among older individuals.
Guidance for screening initiation
According to the authors, the present risk of CRC among younger individuals mirrors the historical risk for older individuals before screening was prevalent.
“The current CRC incidence rates in individuals ages 45 to 49 are similar to the incidence rates observed in 50-year-olds in 1992, before widespread CRC screening was performed,” they wrote.
Elevated rates among younger people have been disproportionately driven by rectal cancer, according to the authors. From 2006 to 2015, incidence of rectal cancer among Americans under 50 increased 1.7% per year, compared with 0.7% per year for colon cancer, based on data from the North American Association of Central Cancer Registries.
Associated mortality rates also increased, the authors noted. From 1999-2019, mortality from colon cancer among people 45-49 years increased from 6.4 to 6.6 deaths per 100,000 individuals, while deaths from rectal cancer increased from 1.3 to 1.7 per 100,000, according to the CDC. Concurrently, CRC-associated mortality rates among older individuals generally declined.
While these findings suggest a growing disease burden among the under-50-year age group, controlled data demonstrating the effects of earlier screening are lacking, Dr. Patel and colleagues noted. Still, they predicted that expanded screening would generate a net benefit.
“Although there are no CRC screening safety data for average-risk individuals [younger than] 50, there are ample data that colonoscopy for other indications (screening based on family history, symptom evaluation, etc.) is safer when comparing younger versus older individuals,” they wrote.
Supporting this claim, the authors cited three independently generated microsimulation models from the Agency for Healthcare Research and Quality that “showed a favorable balance of life-years gained compared with adverse events,” given 100% compliance.
Guidance for screening cessation
Like the situation with younger individuals, minimal data are available to determine the best time for screening cessation, according to the task force.
“There are no randomized or observational studies after 2017 that enrolled individuals over age 75 to inform the appropriate time to stop CRC screening,” the authors wrote. “In our search of 37 relevant articles, only one presented primary data for when to stop screening.”
This one available study showed that some individuals older than 74 do in fact gain benefit from screening,
“For example,” Dr. Patel and colleagues wrote, “women without a history of screening and no comorbidities benefitted from annual fecal immunochemical test (FIT) screening until age 90, whereas unscreened men with or without comorbidities benefited from annual FIT screening until age 88. Conversely, screening was not beneficial beyond age 66 in men or women with severe comorbidities.”
The task force therefore recommended personalized screening for individuals 76-85 years of age “based on the balance of benefits and harms and individual patient clinical factors and preferences.”
Screening for individuals 86 years and older, according to the task force, is unnecessary.
The authors disclosed relationships with Olympus America, Bayer Pharmaceuticals, Janssen Pharmaceuticals, and others.
This article was updated on Jan. 3, 2022.
The U.S. Multi-Society Task Force on Colorectal Cancer (CRC) has lowered the recommended age to start CRC screening from 50 to 45 years of age for all average-risk individuals.
Although no studies have directly demonstrated the result of lowering the age of screening, lead author Swati G. Patel, MD, of University of Colorado Anschutz Medical Center, Aurora, and colleagues suggested that the increasing incidence of advanced CRC among younger individuals, coupled with the net benefit of screening, warrant a lower age threshold.
“Recent data ... show that CRC incidence rates in individuals ages 50 to 64 have increased by 1% annually between 2011 and 2016,” the authors wrote in Gastroenterology. “Similarly, CRC incidence and mortality rates in persons under age 50, termed early-age onset CRC (EAO-CRC), are also increasing.”
The task force of nine experts, representing the American Gastroenterological Association, the American College of Gastroenterology, and the American Society for Gastrointestinal Endoscopy, conducted a literature review and generated recommendations using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) criteria. In addition to recommending a lower age for initial screening, Dr. Patel and colleagues provided guidance for cessation of screening among older individuals.
Guidance for screening initiation
According to the authors, the present risk of CRC among younger individuals mirrors the historical risk for older individuals before screening was prevalent.
“The current CRC incidence rates in individuals ages 45 to 49 are similar to the incidence rates observed in 50-year-olds in 1992, before widespread CRC screening was performed,” they wrote.
Elevated rates among younger people have been disproportionately driven by rectal cancer, according to the authors. From 2006 to 2015, incidence of rectal cancer among Americans under 50 increased 1.7% per year, compared with 0.7% per year for colon cancer, based on data from the North American Association of Central Cancer Registries.
Associated mortality rates also increased, the authors noted. From 1999-2019, mortality from colon cancer among people 45-49 years increased from 6.4 to 6.6 deaths per 100,000 individuals, while deaths from rectal cancer increased from 1.3 to 1.7 per 100,000, according to the CDC. Concurrently, CRC-associated mortality rates among older individuals generally declined.
While these findings suggest a growing disease burden among the under-50-year age group, controlled data demonstrating the effects of earlier screening are lacking, Dr. Patel and colleagues noted. Still, they predicted that expanded screening would generate a net benefit.
“Although there are no CRC screening safety data for average-risk individuals [younger than] 50, there are ample data that colonoscopy for other indications (screening based on family history, symptom evaluation, etc.) is safer when comparing younger versus older individuals,” they wrote.
Supporting this claim, the authors cited three independently generated microsimulation models from the Agency for Healthcare Research and Quality that “showed a favorable balance of life-years gained compared with adverse events,” given 100% compliance.
Guidance for screening cessation
Like the situation with younger individuals, minimal data are available to determine the best time for screening cessation, according to the task force.
“There are no randomized or observational studies after 2017 that enrolled individuals over age 75 to inform the appropriate time to stop CRC screening,” the authors wrote. “In our search of 37 relevant articles, only one presented primary data for when to stop screening.”
This one available study showed that some individuals older than 74 do in fact gain benefit from screening,
“For example,” Dr. Patel and colleagues wrote, “women without a history of screening and no comorbidities benefitted from annual fecal immunochemical test (FIT) screening until age 90, whereas unscreened men with or without comorbidities benefited from annual FIT screening until age 88. Conversely, screening was not beneficial beyond age 66 in men or women with severe comorbidities.”
The task force therefore recommended personalized screening for individuals 76-85 years of age “based on the balance of benefits and harms and individual patient clinical factors and preferences.”
Screening for individuals 86 years and older, according to the task force, is unnecessary.
The authors disclosed relationships with Olympus America, Bayer Pharmaceuticals, Janssen Pharmaceuticals, and others.
This article was updated on Jan. 3, 2022.
The U.S. Multi-Society Task Force on Colorectal Cancer (CRC) has lowered the recommended age to start CRC screening from 50 to 45 years of age for all average-risk individuals.
Although no studies have directly demonstrated the result of lowering the age of screening, lead author Swati G. Patel, MD, of University of Colorado Anschutz Medical Center, Aurora, and colleagues suggested that the increasing incidence of advanced CRC among younger individuals, coupled with the net benefit of screening, warrant a lower age threshold.
“Recent data ... show that CRC incidence rates in individuals ages 50 to 64 have increased by 1% annually between 2011 and 2016,” the authors wrote in Gastroenterology. “Similarly, CRC incidence and mortality rates in persons under age 50, termed early-age onset CRC (EAO-CRC), are also increasing.”
The task force of nine experts, representing the American Gastroenterological Association, the American College of Gastroenterology, and the American Society for Gastrointestinal Endoscopy, conducted a literature review and generated recommendations using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) criteria. In addition to recommending a lower age for initial screening, Dr. Patel and colleagues provided guidance for cessation of screening among older individuals.
Guidance for screening initiation
According to the authors, the present risk of CRC among younger individuals mirrors the historical risk for older individuals before screening was prevalent.
“The current CRC incidence rates in individuals ages 45 to 49 are similar to the incidence rates observed in 50-year-olds in 1992, before widespread CRC screening was performed,” they wrote.
Elevated rates among younger people have been disproportionately driven by rectal cancer, according to the authors. From 2006 to 2015, incidence of rectal cancer among Americans under 50 increased 1.7% per year, compared with 0.7% per year for colon cancer, based on data from the North American Association of Central Cancer Registries.
Associated mortality rates also increased, the authors noted. From 1999-2019, mortality from colon cancer among people 45-49 years increased from 6.4 to 6.6 deaths per 100,000 individuals, while deaths from rectal cancer increased from 1.3 to 1.7 per 100,000, according to the CDC. Concurrently, CRC-associated mortality rates among older individuals generally declined.
While these findings suggest a growing disease burden among the under-50-year age group, controlled data demonstrating the effects of earlier screening are lacking, Dr. Patel and colleagues noted. Still, they predicted that expanded screening would generate a net benefit.
“Although there are no CRC screening safety data for average-risk individuals [younger than] 50, there are ample data that colonoscopy for other indications (screening based on family history, symptom evaluation, etc.) is safer when comparing younger versus older individuals,” they wrote.
Supporting this claim, the authors cited three independently generated microsimulation models from the Agency for Healthcare Research and Quality that “showed a favorable balance of life-years gained compared with adverse events,” given 100% compliance.
Guidance for screening cessation
Like the situation with younger individuals, minimal data are available to determine the best time for screening cessation, according to the task force.
“There are no randomized or observational studies after 2017 that enrolled individuals over age 75 to inform the appropriate time to stop CRC screening,” the authors wrote. “In our search of 37 relevant articles, only one presented primary data for when to stop screening.”
This one available study showed that some individuals older than 74 do in fact gain benefit from screening,
“For example,” Dr. Patel and colleagues wrote, “women without a history of screening and no comorbidities benefitted from annual fecal immunochemical test (FIT) screening until age 90, whereas unscreened men with or without comorbidities benefited from annual FIT screening until age 88. Conversely, screening was not beneficial beyond age 66 in men or women with severe comorbidities.”
The task force therefore recommended personalized screening for individuals 76-85 years of age “based on the balance of benefits and harms and individual patient clinical factors and preferences.”
Screening for individuals 86 years and older, according to the task force, is unnecessary.
The authors disclosed relationships with Olympus America, Bayer Pharmaceuticals, Janssen Pharmaceuticals, and others.
This article was updated on Jan. 3, 2022.
FROM GASTROENTEROLOGY