User login
Methylphenidate is overprescribed to children in France
The prevalence of attention-deficit/hyperactivity disorder is difficult to evaluate, and the diagnosis is based primarily on clinical criteria. In 2008, a French study estimated the prevalence to be between 3.5% and 5.6%, but the study’s design was questionable.
Treatment of this disorder consists first and foremost of educational, social, and psychotherapeutic management. Only if such treatment fails is methylphenidate (MPH), the only drug that has been approved in France for this indication, to be considered, according to the recommendations.
The drug’s short-term efficacy has been proven, but it has not shown any effect on the long-term risks for academic failure, delinquency, and drug addiction associated with ADHD. In contrast, its adverse effects are numerous. Cases of nervousness, sleep disorders, headaches, weight loss, risk for aggravation of psychiatric conditions, and progression to violent or suicidal behavior have all been documented extensively, as well as cases of cardiovascular and cerebrovascular disease. Moreover, MPH is classified as a narcotic.
Inappropriate prescribing conditions
A study that appeared in the French journal of neuropsychiatry in minors, Neuropsychiatrie de l’Enfance et de l’Adolescence, investigated the prescribing procedures for this drug in France. Researchers examined Social Security data for 144,509 patients between the ages of 0 and 17 years who had received at least one prescription between 2010 and 2019. The researchers made the following observations about prescribing patterns and usage during this period:
- New MPH prescriptions increased by 56% per year, and the total number of annual prescriptions increased by 116%. In 3- to 17-year-olds, the prevalence was estimated at 0.61% to 0.75% of the pediatric population in 2019. Boys accounted for most of this consumption (82.5% to 80.8% over this period).
- In 2011, the median duration of consumption by children 6 years of age and older was 5.5 years. For 25% of those children, it was more than 8 years.
- Contrary to the labeling, some prescriptions were written for children younger than 6 years.
- Twenty-five percent of initial prescriptions and 50% of annual renewals were not written by a hospital specialist, in violation of the regulatory requirements in effect until Sept. 13, 2021. On that date, the French National Authority for Health (HAS) decided that initial hospital prescription of MPH should end.
- Eighty-four percent of children did not have any medical consultations at the prescribing hospital department in the 13 months after starting MPH. While the prevalence of ADHD has more than doubled, the number of consultations at specialist French medical, psychological, and educational centers for minors (CMPPs) is now less than a fourth of what it was – a drop from 4.1% to 0.8%.
- The prescribing of MPH is not always associated with an ADHD diagnosis, even though ADHD is its only indication.
- Of children and adolescents who use MPH, 22.8% received one or more other psychotropic drugs in the year following the initial prescription, including the following: neuroleptics (64.5%), anxiolytics (35.5%), antidepressants (16.2%), antiepileptics (11%), hypnotics (4.8%), and antiparkinsonian drugs (3%). “These co-prescriptions are often way off-label and are not within HAS recommendations,” according to the authors.
- For the youngest children in school classes (those born in December rather than in January), between 2010 and 2019, there was on average a 54% increased risk of being medicated.
- In 2019, 21.7% of children who received MPH lived in families with Universal Health Coverage or a similar plan. Yet, according to the French National Institute of Statistics and Economic Studies, only 7.8% of the French population had this type of assistance.
A minority of practitioners
The authors of this article state that “the distribution of consumption suggests a predominant role of a minority of practitioners and hospital departments in the prescription of methylphenidate.” They note that “in European countries and in North America, the prescription rate of psychotropic drugs for ADHD has stabilized or shown a clear trend toward stabilization since 2008. The same cannot be said for France, where this rate is continuously increasing; so much so that in 2019, it reached a higher level than in other European countries like Great Britain.” The reasons for this are disputed.
A version of this article first appeared on Medscape.com.
The prevalence of attention-deficit/hyperactivity disorder is difficult to evaluate, and the diagnosis is based primarily on clinical criteria. In 2008, a French study estimated the prevalence to be between 3.5% and 5.6%, but the study’s design was questionable.
Treatment of this disorder consists first and foremost of educational, social, and psychotherapeutic management. Only if such treatment fails is methylphenidate (MPH), the only drug that has been approved in France for this indication, to be considered, according to the recommendations.
The drug’s short-term efficacy has been proven, but it has not shown any effect on the long-term risks for academic failure, delinquency, and drug addiction associated with ADHD. In contrast, its adverse effects are numerous. Cases of nervousness, sleep disorders, headaches, weight loss, risk for aggravation of psychiatric conditions, and progression to violent or suicidal behavior have all been documented extensively, as well as cases of cardiovascular and cerebrovascular disease. Moreover, MPH is classified as a narcotic.
Inappropriate prescribing conditions
A study that appeared in the French journal of neuropsychiatry in minors, Neuropsychiatrie de l’Enfance et de l’Adolescence, investigated the prescribing procedures for this drug in France. Researchers examined Social Security data for 144,509 patients between the ages of 0 and 17 years who had received at least one prescription between 2010 and 2019. The researchers made the following observations about prescribing patterns and usage during this period:
- New MPH prescriptions increased by 56% per year, and the total number of annual prescriptions increased by 116%. In 3- to 17-year-olds, the prevalence was estimated at 0.61% to 0.75% of the pediatric population in 2019. Boys accounted for most of this consumption (82.5% to 80.8% over this period).
- In 2011, the median duration of consumption by children 6 years of age and older was 5.5 years. For 25% of those children, it was more than 8 years.
- Contrary to the labeling, some prescriptions were written for children younger than 6 years.
- Twenty-five percent of initial prescriptions and 50% of annual renewals were not written by a hospital specialist, in violation of the regulatory requirements in effect until Sept. 13, 2021. On that date, the French National Authority for Health (HAS) decided that initial hospital prescription of MPH should end.
- Eighty-four percent of children did not have any medical consultations at the prescribing hospital department in the 13 months after starting MPH. While the prevalence of ADHD has more than doubled, the number of consultations at specialist French medical, psychological, and educational centers for minors (CMPPs) is now less than a fourth of what it was – a drop from 4.1% to 0.8%.
- The prescribing of MPH is not always associated with an ADHD diagnosis, even though ADHD is its only indication.
- Of children and adolescents who use MPH, 22.8% received one or more other psychotropic drugs in the year following the initial prescription, including the following: neuroleptics (64.5%), anxiolytics (35.5%), antidepressants (16.2%), antiepileptics (11%), hypnotics (4.8%), and antiparkinsonian drugs (3%). “These co-prescriptions are often way off-label and are not within HAS recommendations,” according to the authors.
- For the youngest children in school classes (those born in December rather than in January), between 2010 and 2019, there was on average a 54% increased risk of being medicated.
- In 2019, 21.7% of children who received MPH lived in families with Universal Health Coverage or a similar plan. Yet, according to the French National Institute of Statistics and Economic Studies, only 7.8% of the French population had this type of assistance.
A minority of practitioners
The authors of this article state that “the distribution of consumption suggests a predominant role of a minority of practitioners and hospital departments in the prescription of methylphenidate.” They note that “in European countries and in North America, the prescription rate of psychotropic drugs for ADHD has stabilized or shown a clear trend toward stabilization since 2008. The same cannot be said for France, where this rate is continuously increasing; so much so that in 2019, it reached a higher level than in other European countries like Great Britain.” The reasons for this are disputed.
A version of this article first appeared on Medscape.com.
The prevalence of attention-deficit/hyperactivity disorder is difficult to evaluate, and the diagnosis is based primarily on clinical criteria. In 2008, a French study estimated the prevalence to be between 3.5% and 5.6%, but the study’s design was questionable.
Treatment of this disorder consists first and foremost of educational, social, and psychotherapeutic management. Only if such treatment fails is methylphenidate (MPH), the only drug that has been approved in France for this indication, to be considered, according to the recommendations.
The drug’s short-term efficacy has been proven, but it has not shown any effect on the long-term risks for academic failure, delinquency, and drug addiction associated with ADHD. In contrast, its adverse effects are numerous. Cases of nervousness, sleep disorders, headaches, weight loss, risk for aggravation of psychiatric conditions, and progression to violent or suicidal behavior have all been documented extensively, as well as cases of cardiovascular and cerebrovascular disease. Moreover, MPH is classified as a narcotic.
Inappropriate prescribing conditions
A study that appeared in the French journal of neuropsychiatry in minors, Neuropsychiatrie de l’Enfance et de l’Adolescence, investigated the prescribing procedures for this drug in France. Researchers examined Social Security data for 144,509 patients between the ages of 0 and 17 years who had received at least one prescription between 2010 and 2019. The researchers made the following observations about prescribing patterns and usage during this period:
- New MPH prescriptions increased by 56% per year, and the total number of annual prescriptions increased by 116%. In 3- to 17-year-olds, the prevalence was estimated at 0.61% to 0.75% of the pediatric population in 2019. Boys accounted for most of this consumption (82.5% to 80.8% over this period).
- In 2011, the median duration of consumption by children 6 years of age and older was 5.5 years. For 25% of those children, it was more than 8 years.
- Contrary to the labeling, some prescriptions were written for children younger than 6 years.
- Twenty-five percent of initial prescriptions and 50% of annual renewals were not written by a hospital specialist, in violation of the regulatory requirements in effect until Sept. 13, 2021. On that date, the French National Authority for Health (HAS) decided that initial hospital prescription of MPH should end.
- Eighty-four percent of children did not have any medical consultations at the prescribing hospital department in the 13 months after starting MPH. While the prevalence of ADHD has more than doubled, the number of consultations at specialist French medical, psychological, and educational centers for minors (CMPPs) is now less than a fourth of what it was – a drop from 4.1% to 0.8%.
- The prescribing of MPH is not always associated with an ADHD diagnosis, even though ADHD is its only indication.
- Of children and adolescents who use MPH, 22.8% received one or more other psychotropic drugs in the year following the initial prescription, including the following: neuroleptics (64.5%), anxiolytics (35.5%), antidepressants (16.2%), antiepileptics (11%), hypnotics (4.8%), and antiparkinsonian drugs (3%). “These co-prescriptions are often way off-label and are not within HAS recommendations,” according to the authors.
- For the youngest children in school classes (those born in December rather than in January), between 2010 and 2019, there was on average a 54% increased risk of being medicated.
- In 2019, 21.7% of children who received MPH lived in families with Universal Health Coverage or a similar plan. Yet, according to the French National Institute of Statistics and Economic Studies, only 7.8% of the French population had this type of assistance.
A minority of practitioners
The authors of this article state that “the distribution of consumption suggests a predominant role of a minority of practitioners and hospital departments in the prescription of methylphenidate.” They note that “in European countries and in North America, the prescription rate of psychotropic drugs for ADHD has stabilized or shown a clear trend toward stabilization since 2008. The same cannot be said for France, where this rate is continuously increasing; so much so that in 2019, it reached a higher level than in other European countries like Great Britain.” The reasons for this are disputed.
A version of this article first appeared on Medscape.com.
Adolescent overdose deaths nearly doubled in 2020 and spiked again in 2021
The number of overdose deaths in adolescents nearly doubled in 2020 from the year before and increased substantially again in 2021 after nearly a decade of fairly stable rates, according to data published in a JAMA research letter.
Most of the deaths involved fentanyl, the researchers found.
Joseph Friedman, MPH, of the Center for Social Medicine and Humanities at the University of California, Los Angeles, led the study, which analyzed adolescent (14-18 years old) overdose deaths in the United States from 2010 to June 2021 in light of increasing contamination in the supply of illicit drugs.
The researchers found there were 518 deaths among adolescents (2.40 per 100,000 population) in 2010, and the rates remained stable through 2019 with 492 deaths (2.36 per 100,000).
In 2020, however, deaths spiked to 954 (4.57 per 100 000), increasing by 94.3%, compared with 2019. In 2021, they increased another 20%.
The rise in fentanyl-involved deaths was particularly striking. Fentanyl-involved deaths increased from 253 (1.21 per 100,000) in 2019 to 680 (3.26 per 100,000) in 2020. The numbers through June 2021 were annualized for 2021 and calculations predicted 884 deaths (4.23 per 100,000) for the year.
Numbers point to fentanyl potency
In 2021, more than three-fourths (77.14%) of adolescent overdose deaths involved fentanyl, compared with 13.26% for benzodiazepines, 9.77% for methamphetamine, 7.33% for cocaine, 5.76% for prescription opioids, and 2.27% for heroin.
American Indian and Alaska Native adolescents had the highest overdose rate in 2021 (n = 24; 11.79 per 100,000), followed by Latinx adolescents (n = 354; 6.98 per 100,000).
“These adolescent trends fit a wider pattern of increasing racial and ethnic inequalities in overdose that deserve further investigation and intervention efforts,” the authors wrote.
Pandemic’s role unclear
The spikes in adolescent overdoses overlap the COVID-19 pandemic, but Dr. Friedman said in an interview the pandemic “may or may not have been a big factor. “
The authors wrote that drug use had generally been stable among adolescents between 2010 and 2020. The number of 10th graders reporting any illicit drug use was 30.2% in 2010 and 30.4% in 2020.
“So it’s not that more teens are using drugs. It’s just that drug use is becoming more dangerous due to the spread of counterfeit pills containing fentanyls,” Dr. Friedman said.
The authors noted that “the illicit drug supply has increasingly become contaminated with illicitly manufactured fentanyls and other synthetic opioid and benzodiazepine analogues.”
Mr. Friedman said the pandemic may have accelerated the spread of more dangerous forms of drugs as supply chains were disrupted.
Benjamin Brady, DrPH, an assistant professor at the University of Arizona, Tucson, who also has an appointment in the university’s Comprehensive Pain and Addiction Center, said in an interview the numbers that Dr. Friedman and colleagues present represent “worst fears coming true.”
He said he and his colleagues in the field “were anticipating a rise in overdose deaths for the next 5-10 years because of the way the supply-and-demand environment exists in the U.S.”
Dr. Brady explained that restricting access to prescription opioids has had an unfortunate side effect in decreasing access to a safer supply of drugs.
“Without having solutions that would reduce demand at the same rate, supply of the safer form of the drug has been reduced; that has pushed people toward heroin and street drugs and from 2016 on those have been adulterated with fentanyl,” he said.
He said the United States, compared with other developed nations, has been slower to embrace longer-term harm-reduction strategies and to improve access to treatment and care.
COVID likely also has exacerbated the problem in terms of isolation and reduction in quality of life that has adolescents seeking to fill that void with drugs, Dr. Brady said. They may be completely unaware that the drugs they are seeking are commonly cut with counterfeit fentanyl.
“Fentanyl can be up to 50 times stronger than heroin,” he noted. “Even just a little bit of fentanyl dramatically changes the risk profile on an overdose.”
Increasing rates of mental health concerns among adolescents over decades also contribute to drug-seeking trends, Dr. Brady noted.
Overdose increases in the overall population were smaller
In the overall population, the percentage increases were not nearly as large in 2020 and 2021 as they were for adolescents.
Rates of overdose deaths in the overall population increased steadily from 2010 and reached 70,630 in 2019. In 2020, the deaths increased to 91,799 (an increase of 29.48% from 2019) and increased 11.48% in 2021.
The researchers analyzed numbers from the Centers for Disease Control and Prevention WONDER (Wide-Ranging Online Data for Epidemiologic Research) database, which has records of all U.S. deaths for which drug overdose was listed as the underlying cause.
The authors and Dr. Brady report no relevant financial relationships.
The number of overdose deaths in adolescents nearly doubled in 2020 from the year before and increased substantially again in 2021 after nearly a decade of fairly stable rates, according to data published in a JAMA research letter.
Most of the deaths involved fentanyl, the researchers found.
Joseph Friedman, MPH, of the Center for Social Medicine and Humanities at the University of California, Los Angeles, led the study, which analyzed adolescent (14-18 years old) overdose deaths in the United States from 2010 to June 2021 in light of increasing contamination in the supply of illicit drugs.
The researchers found there were 518 deaths among adolescents (2.40 per 100,000 population) in 2010, and the rates remained stable through 2019 with 492 deaths (2.36 per 100,000).
In 2020, however, deaths spiked to 954 (4.57 per 100 000), increasing by 94.3%, compared with 2019. In 2021, they increased another 20%.
The rise in fentanyl-involved deaths was particularly striking. Fentanyl-involved deaths increased from 253 (1.21 per 100,000) in 2019 to 680 (3.26 per 100,000) in 2020. The numbers through June 2021 were annualized for 2021 and calculations predicted 884 deaths (4.23 per 100,000) for the year.
Numbers point to fentanyl potency
In 2021, more than three-fourths (77.14%) of adolescent overdose deaths involved fentanyl, compared with 13.26% for benzodiazepines, 9.77% for methamphetamine, 7.33% for cocaine, 5.76% for prescription opioids, and 2.27% for heroin.
American Indian and Alaska Native adolescents had the highest overdose rate in 2021 (n = 24; 11.79 per 100,000), followed by Latinx adolescents (n = 354; 6.98 per 100,000).
“These adolescent trends fit a wider pattern of increasing racial and ethnic inequalities in overdose that deserve further investigation and intervention efforts,” the authors wrote.
Pandemic’s role unclear
The spikes in adolescent overdoses overlap the COVID-19 pandemic, but Dr. Friedman said in an interview the pandemic “may or may not have been a big factor. “
The authors wrote that drug use had generally been stable among adolescents between 2010 and 2020. The number of 10th graders reporting any illicit drug use was 30.2% in 2010 and 30.4% in 2020.
“So it’s not that more teens are using drugs. It’s just that drug use is becoming more dangerous due to the spread of counterfeit pills containing fentanyls,” Dr. Friedman said.
The authors noted that “the illicit drug supply has increasingly become contaminated with illicitly manufactured fentanyls and other synthetic opioid and benzodiazepine analogues.”
Mr. Friedman said the pandemic may have accelerated the spread of more dangerous forms of drugs as supply chains were disrupted.
Benjamin Brady, DrPH, an assistant professor at the University of Arizona, Tucson, who also has an appointment in the university’s Comprehensive Pain and Addiction Center, said in an interview the numbers that Dr. Friedman and colleagues present represent “worst fears coming true.”
He said he and his colleagues in the field “were anticipating a rise in overdose deaths for the next 5-10 years because of the way the supply-and-demand environment exists in the U.S.”
Dr. Brady explained that restricting access to prescription opioids has had an unfortunate side effect in decreasing access to a safer supply of drugs.
“Without having solutions that would reduce demand at the same rate, supply of the safer form of the drug has been reduced; that has pushed people toward heroin and street drugs and from 2016 on those have been adulterated with fentanyl,” he said.
He said the United States, compared with other developed nations, has been slower to embrace longer-term harm-reduction strategies and to improve access to treatment and care.
COVID likely also has exacerbated the problem in terms of isolation and reduction in quality of life that has adolescents seeking to fill that void with drugs, Dr. Brady said. They may be completely unaware that the drugs they are seeking are commonly cut with counterfeit fentanyl.
“Fentanyl can be up to 50 times stronger than heroin,” he noted. “Even just a little bit of fentanyl dramatically changes the risk profile on an overdose.”
Increasing rates of mental health concerns among adolescents over decades also contribute to drug-seeking trends, Dr. Brady noted.
Overdose increases in the overall population were smaller
In the overall population, the percentage increases were not nearly as large in 2020 and 2021 as they were for adolescents.
Rates of overdose deaths in the overall population increased steadily from 2010 and reached 70,630 in 2019. In 2020, the deaths increased to 91,799 (an increase of 29.48% from 2019) and increased 11.48% in 2021.
The researchers analyzed numbers from the Centers for Disease Control and Prevention WONDER (Wide-Ranging Online Data for Epidemiologic Research) database, which has records of all U.S. deaths for which drug overdose was listed as the underlying cause.
The authors and Dr. Brady report no relevant financial relationships.
The number of overdose deaths in adolescents nearly doubled in 2020 from the year before and increased substantially again in 2021 after nearly a decade of fairly stable rates, according to data published in a JAMA research letter.
Most of the deaths involved fentanyl, the researchers found.
Joseph Friedman, MPH, of the Center for Social Medicine and Humanities at the University of California, Los Angeles, led the study, which analyzed adolescent (14-18 years old) overdose deaths in the United States from 2010 to June 2021 in light of increasing contamination in the supply of illicit drugs.
The researchers found there were 518 deaths among adolescents (2.40 per 100,000 population) in 2010, and the rates remained stable through 2019 with 492 deaths (2.36 per 100,000).
In 2020, however, deaths spiked to 954 (4.57 per 100 000), increasing by 94.3%, compared with 2019. In 2021, they increased another 20%.
The rise in fentanyl-involved deaths was particularly striking. Fentanyl-involved deaths increased from 253 (1.21 per 100,000) in 2019 to 680 (3.26 per 100,000) in 2020. The numbers through June 2021 were annualized for 2021 and calculations predicted 884 deaths (4.23 per 100,000) for the year.
Numbers point to fentanyl potency
In 2021, more than three-fourths (77.14%) of adolescent overdose deaths involved fentanyl, compared with 13.26% for benzodiazepines, 9.77% for methamphetamine, 7.33% for cocaine, 5.76% for prescription opioids, and 2.27% for heroin.
American Indian and Alaska Native adolescents had the highest overdose rate in 2021 (n = 24; 11.79 per 100,000), followed by Latinx adolescents (n = 354; 6.98 per 100,000).
“These adolescent trends fit a wider pattern of increasing racial and ethnic inequalities in overdose that deserve further investigation and intervention efforts,” the authors wrote.
Pandemic’s role unclear
The spikes in adolescent overdoses overlap the COVID-19 pandemic, but Dr. Friedman said in an interview the pandemic “may or may not have been a big factor. “
The authors wrote that drug use had generally been stable among adolescents between 2010 and 2020. The number of 10th graders reporting any illicit drug use was 30.2% in 2010 and 30.4% in 2020.
“So it’s not that more teens are using drugs. It’s just that drug use is becoming more dangerous due to the spread of counterfeit pills containing fentanyls,” Dr. Friedman said.
The authors noted that “the illicit drug supply has increasingly become contaminated with illicitly manufactured fentanyls and other synthetic opioid and benzodiazepine analogues.”
Mr. Friedman said the pandemic may have accelerated the spread of more dangerous forms of drugs as supply chains were disrupted.
Benjamin Brady, DrPH, an assistant professor at the University of Arizona, Tucson, who also has an appointment in the university’s Comprehensive Pain and Addiction Center, said in an interview the numbers that Dr. Friedman and colleagues present represent “worst fears coming true.”
He said he and his colleagues in the field “were anticipating a rise in overdose deaths for the next 5-10 years because of the way the supply-and-demand environment exists in the U.S.”
Dr. Brady explained that restricting access to prescription opioids has had an unfortunate side effect in decreasing access to a safer supply of drugs.
“Without having solutions that would reduce demand at the same rate, supply of the safer form of the drug has been reduced; that has pushed people toward heroin and street drugs and from 2016 on those have been adulterated with fentanyl,” he said.
He said the United States, compared with other developed nations, has been slower to embrace longer-term harm-reduction strategies and to improve access to treatment and care.
COVID likely also has exacerbated the problem in terms of isolation and reduction in quality of life that has adolescents seeking to fill that void with drugs, Dr. Brady said. They may be completely unaware that the drugs they are seeking are commonly cut with counterfeit fentanyl.
“Fentanyl can be up to 50 times stronger than heroin,” he noted. “Even just a little bit of fentanyl dramatically changes the risk profile on an overdose.”
Increasing rates of mental health concerns among adolescents over decades also contribute to drug-seeking trends, Dr. Brady noted.
Overdose increases in the overall population were smaller
In the overall population, the percentage increases were not nearly as large in 2020 and 2021 as they were for adolescents.
Rates of overdose deaths in the overall population increased steadily from 2010 and reached 70,630 in 2019. In 2020, the deaths increased to 91,799 (an increase of 29.48% from 2019) and increased 11.48% in 2021.
The researchers analyzed numbers from the Centers for Disease Control and Prevention WONDER (Wide-Ranging Online Data for Epidemiologic Research) database, which has records of all U.S. deaths for which drug overdose was listed as the underlying cause.
The authors and Dr. Brady report no relevant financial relationships.
FROM JAMA
Adolescents are undertested for STIs
Approximately 20% of sexually active high schoolers reported testing for a sexually transmitted infection in the previous year, based on data from 2,501 respondents to the 2019 national Youth Risk Behavior Survey.
Data suggest that half of all new STIs in the United States occur in youth aged 15-24 years, and that 25% of sexually active young women in the United States have an STI, wrote Nicole Liddon, PhD, of the Centers for Disease Control and Prevention, Atlanta, and colleagues.
Although organizations including the American Academy of Pediatrics and the U.S. Preventive Services Task Force recommend varying degrees of routine STI screening for adolescents, data on the prevalence of testing in this population are limited, the researchers said.
However, the addition in 2019 of a question on STI testing to the national Youth Risk Behavior Survey (YRBS) provided an opportunity to assess prevalence of STI testing, identify potential barriers, and increase screening rates, they wrote.
In a study published in Pediatrics, the researchers reviewed data from the 2019 national YRBS, an anonymous survey administered biannually to public and private high school students across the United States.
The study population included 2,501 individuals who reported sexual activity with at least one person during the 3 months prior to the survey.
Overall, 20.4% of the respondents reported being tested for an STI in the previous year, including significantly more females than males (26.1% vs. 13.7%).
The prevalence of testing among females was not significantly different according to race/ethnicity, sexual identity, or the sex of sexual contacts, but the prevalence increased with age; 12.6%, 22.8%, 28.5%, and 36.9% for females aged 15 years and younger, 16 years, 17 years, and 18 years, respectively.
Among males, no significant differences in STI testing were noted according to race/ethnicity, age, sexual identity, or sex of sexual contacts.
The researchers also analyzed prevalence of STI tested based on sexual behaviors. Among female students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: nonuse of condoms at last sexual intercourse (34.1% vs. 18.2%), substance use at last sexual intercourse (32.0% vs. 24.7%), and having four or more lifetime sex partners (31.9% vs. 24.7%).
Among male students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: sex before age 13 years (27.1% vs. 12.1%), having two or more recent sex partners (22.4% vs. 10.4%), having four or more lifetime sex partners (22.3% vs. 9.5%), and substance use at last sexual intercourse (19.2% vs. 12.1%).
The low prevalence of STI testing in teens has become more urgent in the wake of the coronavirus pandemic, the researchers wrote. “These prevalence estimates were derived before the possible profound impacts of the pandemic on adolescent sexual behavior and access to and use of health care services.”
Current guidelines allow health care providers the options for opt-out STI screening as a strategy to improve screening rates and testing; however, this option does not eliminate the need for conversations with adolescent patients about sexual activity, they emphasized.
The study findings were limited by several other factors including the inability to directly assess adherence to screening recommendations specifically, the inability to determine whether low testing rates resulted from limited access to health care or missed screening opportunities at visits, and the inclusion only of high school students but not out-of-school youth who may have more limited access to testing.
However, the results highlight the need to improve STI testing services for adolescents, and to address barriers at the individual and clinic level, they said. The addition of a question about past-year STI testing to the 2019 and future YRBS survey will promote ongoing monitoring of efforts to increase testing rates.
Teen sexual health goes beyond testing
The current study shows that routine testing for STIs according to published guidelines is low, Cynthia Holland-Hall, MD, and Andrea E. Bonny, MD, of Nationwide Children’s Hospital and Ohio State University, both in Columbus, wrote in an accompanying editorial.
Notably, sexually active females and males who had sex with male partners, two groups for whom annual testing is specifically recommended by multiple organizations, had testing rates of less than 30%, they said. The authors highlighted the study’s lack of information on which specific barriers, such as lack of access to the health care system, lack of knowledge, and fear of disclosure, contributed to overall low rates of testing.
However, STI testing is only one element of sexual and reproductive health care. Although opt-out testing may improve detection rates, the editorialists emphasized the need for patient-provider conversations about sex, citing recent studies showing that adolescents who spent some time alone with providers were more likely to receive sexual and reproductive health (SRH) services in the past year.
“Resources such as confidentiality policies, checklists, and written screening tools may facilitate SRH discussions,” Dr. Holland-Hall and Dr. Bonny said. “With a little practice, respect, and intention, a caring provider can take the awkward out of discussing sexual health but must not opt out of the conversation.”
Privacy and time issues exacerbate low testing rates
The current study is especially important at this time because many adolescents have likely missed well visits, and therefore important STI screens, because of disruptions caused by the COVID-19 pandemic, Karalyn Kinsella, MD, a pediatrician in private practice in Cheshire, Conn., said in an interview.
“I was surprised that the rate of screening was only one in five,” said Dr. Kinsella. “I knew it would be suboptimal, but not that low.”
According to Dr. Kinsella, there are two major barriers to increasing STI testing in adolescents in primary care. One barrier is that insurance companies will often state on the bill what the testing was for, which will lead to an uncomfortable conversation at a later date for the adolescent and parent when the bill arrives in the mail. A second barrier is when to test during a visit,. “If we obtain urine samples on all adolescents and many of them are not sexually active, we are wasting a lot of time in the short visit to obtain urine,” she explained. “If testing is scheduled for the end of the visit, they often leave without providing a urine sample.”
Overall, the study is an important reminder to general pediatricians about STI testing for sexually active teens, she emphasized.
The study received no outside funding. The researchers had no financial conflicts to disclose. The editorialists had no financial conflicts to disclose. Dr. Kinsella had no financial conflicts to disclose and serves on the editorial advisory board of Pediatric News.
Approximately 20% of sexually active high schoolers reported testing for a sexually transmitted infection in the previous year, based on data from 2,501 respondents to the 2019 national Youth Risk Behavior Survey.
Data suggest that half of all new STIs in the United States occur in youth aged 15-24 years, and that 25% of sexually active young women in the United States have an STI, wrote Nicole Liddon, PhD, of the Centers for Disease Control and Prevention, Atlanta, and colleagues.
Although organizations including the American Academy of Pediatrics and the U.S. Preventive Services Task Force recommend varying degrees of routine STI screening for adolescents, data on the prevalence of testing in this population are limited, the researchers said.
However, the addition in 2019 of a question on STI testing to the national Youth Risk Behavior Survey (YRBS) provided an opportunity to assess prevalence of STI testing, identify potential barriers, and increase screening rates, they wrote.
In a study published in Pediatrics, the researchers reviewed data from the 2019 national YRBS, an anonymous survey administered biannually to public and private high school students across the United States.
The study population included 2,501 individuals who reported sexual activity with at least one person during the 3 months prior to the survey.
Overall, 20.4% of the respondents reported being tested for an STI in the previous year, including significantly more females than males (26.1% vs. 13.7%).
The prevalence of testing among females was not significantly different according to race/ethnicity, sexual identity, or the sex of sexual contacts, but the prevalence increased with age; 12.6%, 22.8%, 28.5%, and 36.9% for females aged 15 years and younger, 16 years, 17 years, and 18 years, respectively.
Among males, no significant differences in STI testing were noted according to race/ethnicity, age, sexual identity, or sex of sexual contacts.
The researchers also analyzed prevalence of STI tested based on sexual behaviors. Among female students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: nonuse of condoms at last sexual intercourse (34.1% vs. 18.2%), substance use at last sexual intercourse (32.0% vs. 24.7%), and having four or more lifetime sex partners (31.9% vs. 24.7%).
Among male students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: sex before age 13 years (27.1% vs. 12.1%), having two or more recent sex partners (22.4% vs. 10.4%), having four or more lifetime sex partners (22.3% vs. 9.5%), and substance use at last sexual intercourse (19.2% vs. 12.1%).
The low prevalence of STI testing in teens has become more urgent in the wake of the coronavirus pandemic, the researchers wrote. “These prevalence estimates were derived before the possible profound impacts of the pandemic on adolescent sexual behavior and access to and use of health care services.”
Current guidelines allow health care providers the options for opt-out STI screening as a strategy to improve screening rates and testing; however, this option does not eliminate the need for conversations with adolescent patients about sexual activity, they emphasized.
The study findings were limited by several other factors including the inability to directly assess adherence to screening recommendations specifically, the inability to determine whether low testing rates resulted from limited access to health care or missed screening opportunities at visits, and the inclusion only of high school students but not out-of-school youth who may have more limited access to testing.
However, the results highlight the need to improve STI testing services for adolescents, and to address barriers at the individual and clinic level, they said. The addition of a question about past-year STI testing to the 2019 and future YRBS survey will promote ongoing monitoring of efforts to increase testing rates.
Teen sexual health goes beyond testing
The current study shows that routine testing for STIs according to published guidelines is low, Cynthia Holland-Hall, MD, and Andrea E. Bonny, MD, of Nationwide Children’s Hospital and Ohio State University, both in Columbus, wrote in an accompanying editorial.
Notably, sexually active females and males who had sex with male partners, two groups for whom annual testing is specifically recommended by multiple organizations, had testing rates of less than 30%, they said. The authors highlighted the study’s lack of information on which specific barriers, such as lack of access to the health care system, lack of knowledge, and fear of disclosure, contributed to overall low rates of testing.
However, STI testing is only one element of sexual and reproductive health care. Although opt-out testing may improve detection rates, the editorialists emphasized the need for patient-provider conversations about sex, citing recent studies showing that adolescents who spent some time alone with providers were more likely to receive sexual and reproductive health (SRH) services in the past year.
“Resources such as confidentiality policies, checklists, and written screening tools may facilitate SRH discussions,” Dr. Holland-Hall and Dr. Bonny said. “With a little practice, respect, and intention, a caring provider can take the awkward out of discussing sexual health but must not opt out of the conversation.”
Privacy and time issues exacerbate low testing rates
The current study is especially important at this time because many adolescents have likely missed well visits, and therefore important STI screens, because of disruptions caused by the COVID-19 pandemic, Karalyn Kinsella, MD, a pediatrician in private practice in Cheshire, Conn., said in an interview.
“I was surprised that the rate of screening was only one in five,” said Dr. Kinsella. “I knew it would be suboptimal, but not that low.”
According to Dr. Kinsella, there are two major barriers to increasing STI testing in adolescents in primary care. One barrier is that insurance companies will often state on the bill what the testing was for, which will lead to an uncomfortable conversation at a later date for the adolescent and parent when the bill arrives in the mail. A second barrier is when to test during a visit,. “If we obtain urine samples on all adolescents and many of them are not sexually active, we are wasting a lot of time in the short visit to obtain urine,” she explained. “If testing is scheduled for the end of the visit, they often leave without providing a urine sample.”
Overall, the study is an important reminder to general pediatricians about STI testing for sexually active teens, she emphasized.
The study received no outside funding. The researchers had no financial conflicts to disclose. The editorialists had no financial conflicts to disclose. Dr. Kinsella had no financial conflicts to disclose and serves on the editorial advisory board of Pediatric News.
Approximately 20% of sexually active high schoolers reported testing for a sexually transmitted infection in the previous year, based on data from 2,501 respondents to the 2019 national Youth Risk Behavior Survey.
Data suggest that half of all new STIs in the United States occur in youth aged 15-24 years, and that 25% of sexually active young women in the United States have an STI, wrote Nicole Liddon, PhD, of the Centers for Disease Control and Prevention, Atlanta, and colleagues.
Although organizations including the American Academy of Pediatrics and the U.S. Preventive Services Task Force recommend varying degrees of routine STI screening for adolescents, data on the prevalence of testing in this population are limited, the researchers said.
However, the addition in 2019 of a question on STI testing to the national Youth Risk Behavior Survey (YRBS) provided an opportunity to assess prevalence of STI testing, identify potential barriers, and increase screening rates, they wrote.
In a study published in Pediatrics, the researchers reviewed data from the 2019 national YRBS, an anonymous survey administered biannually to public and private high school students across the United States.
The study population included 2,501 individuals who reported sexual activity with at least one person during the 3 months prior to the survey.
Overall, 20.4% of the respondents reported being tested for an STI in the previous year, including significantly more females than males (26.1% vs. 13.7%).
The prevalence of testing among females was not significantly different according to race/ethnicity, sexual identity, or the sex of sexual contacts, but the prevalence increased with age; 12.6%, 22.8%, 28.5%, and 36.9% for females aged 15 years and younger, 16 years, 17 years, and 18 years, respectively.
Among males, no significant differences in STI testing were noted according to race/ethnicity, age, sexual identity, or sex of sexual contacts.
The researchers also analyzed prevalence of STI tested based on sexual behaviors. Among female students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: nonuse of condoms at last sexual intercourse (34.1% vs. 18.2%), substance use at last sexual intercourse (32.0% vs. 24.7%), and having four or more lifetime sex partners (31.9% vs. 24.7%).
Among male students, the prevalence of STI testing was higher among those who reported the following behaviors, compared with those who did not: sex before age 13 years (27.1% vs. 12.1%), having two or more recent sex partners (22.4% vs. 10.4%), having four or more lifetime sex partners (22.3% vs. 9.5%), and substance use at last sexual intercourse (19.2% vs. 12.1%).
The low prevalence of STI testing in teens has become more urgent in the wake of the coronavirus pandemic, the researchers wrote. “These prevalence estimates were derived before the possible profound impacts of the pandemic on adolescent sexual behavior and access to and use of health care services.”
Current guidelines allow health care providers the options for opt-out STI screening as a strategy to improve screening rates and testing; however, this option does not eliminate the need for conversations with adolescent patients about sexual activity, they emphasized.
The study findings were limited by several other factors including the inability to directly assess adherence to screening recommendations specifically, the inability to determine whether low testing rates resulted from limited access to health care or missed screening opportunities at visits, and the inclusion only of high school students but not out-of-school youth who may have more limited access to testing.
However, the results highlight the need to improve STI testing services for adolescents, and to address barriers at the individual and clinic level, they said. The addition of a question about past-year STI testing to the 2019 and future YRBS survey will promote ongoing monitoring of efforts to increase testing rates.
Teen sexual health goes beyond testing
The current study shows that routine testing for STIs according to published guidelines is low, Cynthia Holland-Hall, MD, and Andrea E. Bonny, MD, of Nationwide Children’s Hospital and Ohio State University, both in Columbus, wrote in an accompanying editorial.
Notably, sexually active females and males who had sex with male partners, two groups for whom annual testing is specifically recommended by multiple organizations, had testing rates of less than 30%, they said. The authors highlighted the study’s lack of information on which specific barriers, such as lack of access to the health care system, lack of knowledge, and fear of disclosure, contributed to overall low rates of testing.
However, STI testing is only one element of sexual and reproductive health care. Although opt-out testing may improve detection rates, the editorialists emphasized the need for patient-provider conversations about sex, citing recent studies showing that adolescents who spent some time alone with providers were more likely to receive sexual and reproductive health (SRH) services in the past year.
“Resources such as confidentiality policies, checklists, and written screening tools may facilitate SRH discussions,” Dr. Holland-Hall and Dr. Bonny said. “With a little practice, respect, and intention, a caring provider can take the awkward out of discussing sexual health but must not opt out of the conversation.”
Privacy and time issues exacerbate low testing rates
The current study is especially important at this time because many adolescents have likely missed well visits, and therefore important STI screens, because of disruptions caused by the COVID-19 pandemic, Karalyn Kinsella, MD, a pediatrician in private practice in Cheshire, Conn., said in an interview.
“I was surprised that the rate of screening was only one in five,” said Dr. Kinsella. “I knew it would be suboptimal, but not that low.”
According to Dr. Kinsella, there are two major barriers to increasing STI testing in adolescents in primary care. One barrier is that insurance companies will often state on the bill what the testing was for, which will lead to an uncomfortable conversation at a later date for the adolescent and parent when the bill arrives in the mail. A second barrier is when to test during a visit,. “If we obtain urine samples on all adolescents and many of them are not sexually active, we are wasting a lot of time in the short visit to obtain urine,” she explained. “If testing is scheduled for the end of the visit, they often leave without providing a urine sample.”
Overall, the study is an important reminder to general pediatricians about STI testing for sexually active teens, she emphasized.
The study received no outside funding. The researchers had no financial conflicts to disclose. The editorialists had no financial conflicts to disclose. Dr. Kinsella had no financial conflicts to disclose and serves on the editorial advisory board of Pediatric News.
FROM PEDIATRICS
Rapper sings about living with sickle cell disease
MANCHESTER, ENGLAND – A London-based rapper known for his gospel-inspired music has now given a voice to patients with sickle cell disease. He is using one of his music videos to raise awareness and educate health care professionals about living with the condition.
One important aim of the video, he says, is to help educate health care professionals, some of whom have not come across this condition, he explained at a session during the annual meeting of the British Society for Haematology, held recently in Manchester, England.
“It’s kind of frustrating to feel like your safe space, when you’re in front of doctors and nurses and paramedics who are supposed to know what it is and react with treatment, [and they] don’t know what it is,” Mr. Gaspar said.
He recalled an occasion in which he was experiencing a crisis, and his wife called for an ambulance. The paramedics arrived and his wife asked them for “gas and air and morphine, and they were, like, no, we don’t want to give that to him.” She tried to explain that he has sickle cell disease, but the paramedics had not heard of the condition and were suspicious that the request for morphine was a sign of drug addiction.
Mr. Gaspar expressed his frustration over “constantly having to prove that you have something serious enough to need the treatment you are asking for.”
At the meeting, Mr. Gaspar was talking on the stage with hematologist Dr. Stephen Hibbs from Barts Health NHS Trust, London.
Mr. Gaspar explained that it took years before he eventually reached “a point where I understood that it’s something that affects me and affects many other people, and I didn’t want to hide it any more.”
Sickle cell disease, which occurs primarily in people of Afro-Caribbean background, is a taboo subject in his community, Mr. Gaspar elaborated in an interview.
The condition has been associated with a great deal of stigma, with young sufferers traditionally seen as “demonically possessed,” he commented.
“So there was always a shameful aspect around it when it came to African families speaking about it, especially back in Africa.”
But after his parents came to the United Kingdom, he was able to “do his research and understand that it’s just genetics.”
This knowledge, Mr. Gaspar said, “takes away the spiritual aspect” and allows people to “have the conversation about sickle cell with potential partners” and ask them to find out their genotype, which in turn helps to “break down the barriers and the stigma.”
Mr. Gaspar emphasizes that there is much more work still to do.
In the video, he appeals to the Black community to make blood donations.
He said that something that “haunts” him is that currently, only 1% of Black people in the United Kingdom give blood, “so I really want the song to move my community to take a step forward and make that difference.”
He has been in contact with NHS Blood and Transplant, which provides blood and transplantation service to the National Health Service. They “really liked” the song, Mr. Gaspar said, and helped him get access to a hospital ward in University College Hospital, London, for the video.
“I really wanted to make a video that made people uncomfortable when watching it,” he said. It shows him hospitalized for pain and breathlessness and recalling having to use a Zimmer frame at the age of 25.
“This is a side of sickle cell that normally people don’t know,” he said.
Since releasing the song and the video, Mr. Gaspar says he has been contacted by many fellow patients. They have told him that he is now their “voice”; when they are asked how the condition affects them, “they can show someone the Hidden Pain video and say: This is how it feels.”
Clinicians have also approached him, asking if they can show his video to illustrate to patients and their families how having the condition may affect their lives.
Preventable deaths
At the meeting, Dr. Hibbs highlighted the 2021 report No One’s Listening, which was issued by the Sickle Cell Society following an inquiry into avoidable deaths and failures of care for sickle cell patients.
The inquiry, published by an All-Party Parliamentary group, found “serious care failings” in acute services and evidence of attitudes underpinned by racism. There was evidence of substandard care for sickle cell patients who were admitted to general wards or to hospital accident and emergency departments, as well as low awareness of the condition among health care professionals.
The report noted that the care failings have led to patient deaths, some which could have been prevented, and that there have been many “near misses.”
Many patients with sickle cell disease said they are “not being listened to” or are not being understood, especially during that vulnerable period when they are “in a crisis.”
Mr. Gaspar said that the report, and also the deaths, really struck a chord with him and many in his community. “We felt like that was us. ... We’ve all been in that same position where we’ve been misunderstood and not heard by nurses, doctors, or paramedics.”
He emphasized the need for awareness of the condition and the need for timely treatment. Just 3 weeks ago, Mr. Gaspar attended the funeral of one of his friends who is in the Hidden Pain video, a fellow sickle cell disease patient, who died at 30 years of age.
Ignorance about the condition ‘all too common’
The lack of awareness about sickle cell disease, even among health care professionals, is “all too common,” says Dr. Subarna Chakravorty, consultant pediatric hematologist, King’s College Hospital, London.
Even in London, where there is a large Black community and the teaching hospitals have world-class expertise, patients with sickle cell disease are “still facing a lot of problems with knowledge” among health care professionals, she said in an interview.
“Often people are having to speak for their own condition; which is fine, except that sometimes they are not believed,” she commented.
“On the one hand, you rely on the patient to provide information about their disease, and then when you receive it, you don’t do anything about it. So [they’re] between a rock and a hard place.”
Why are sickle cell patients treated in this way?
For Dr. Chakravorty, there is “a lot to be said about racism and disparities” in treating patients “as morphine-seekers, opiate addicts, even in children.”
“So we really need to improve the knowledge and perceptions among nonspecialist staff,” she said, “and even among specialists.”
Mr. Gaspar aims to help with this effort and hopes that his song and video will be useful to health care professionals. Sickle cell disease “needs to be spoken about,” and more doctors and nurses need to “know what it is,” he said.
He said it is a relief to encounter health care professionals who are knowledgeable about his condition. There have been times when he has been “having a crisis at home, calling the ambulance, and the paramedic comes and says: ‘Mr. Gaspar, you have sickle cell...we believe that you usually have gas and air and morphine, is that correct?’”
“That gives me a sense of peace, to know that I don’t have to fight my case or convince someone I have sickle cell, and I need to start treatment. They already know.”
No relevant financial relationships have been disclosed.
A version of this article first appeared on Medscape.com.
MANCHESTER, ENGLAND – A London-based rapper known for his gospel-inspired music has now given a voice to patients with sickle cell disease. He is using one of his music videos to raise awareness and educate health care professionals about living with the condition.
One important aim of the video, he says, is to help educate health care professionals, some of whom have not come across this condition, he explained at a session during the annual meeting of the British Society for Haematology, held recently in Manchester, England.
“It’s kind of frustrating to feel like your safe space, when you’re in front of doctors and nurses and paramedics who are supposed to know what it is and react with treatment, [and they] don’t know what it is,” Mr. Gaspar said.
He recalled an occasion in which he was experiencing a crisis, and his wife called for an ambulance. The paramedics arrived and his wife asked them for “gas and air and morphine, and they were, like, no, we don’t want to give that to him.” She tried to explain that he has sickle cell disease, but the paramedics had not heard of the condition and were suspicious that the request for morphine was a sign of drug addiction.
Mr. Gaspar expressed his frustration over “constantly having to prove that you have something serious enough to need the treatment you are asking for.”
At the meeting, Mr. Gaspar was talking on the stage with hematologist Dr. Stephen Hibbs from Barts Health NHS Trust, London.
Mr. Gaspar explained that it took years before he eventually reached “a point where I understood that it’s something that affects me and affects many other people, and I didn’t want to hide it any more.”
Sickle cell disease, which occurs primarily in people of Afro-Caribbean background, is a taboo subject in his community, Mr. Gaspar elaborated in an interview.
The condition has been associated with a great deal of stigma, with young sufferers traditionally seen as “demonically possessed,” he commented.
“So there was always a shameful aspect around it when it came to African families speaking about it, especially back in Africa.”
But after his parents came to the United Kingdom, he was able to “do his research and understand that it’s just genetics.”
This knowledge, Mr. Gaspar said, “takes away the spiritual aspect” and allows people to “have the conversation about sickle cell with potential partners” and ask them to find out their genotype, which in turn helps to “break down the barriers and the stigma.”
Mr. Gaspar emphasizes that there is much more work still to do.
In the video, he appeals to the Black community to make blood donations.
He said that something that “haunts” him is that currently, only 1% of Black people in the United Kingdom give blood, “so I really want the song to move my community to take a step forward and make that difference.”
He has been in contact with NHS Blood and Transplant, which provides blood and transplantation service to the National Health Service. They “really liked” the song, Mr. Gaspar said, and helped him get access to a hospital ward in University College Hospital, London, for the video.
“I really wanted to make a video that made people uncomfortable when watching it,” he said. It shows him hospitalized for pain and breathlessness and recalling having to use a Zimmer frame at the age of 25.
“This is a side of sickle cell that normally people don’t know,” he said.
Since releasing the song and the video, Mr. Gaspar says he has been contacted by many fellow patients. They have told him that he is now their “voice”; when they are asked how the condition affects them, “they can show someone the Hidden Pain video and say: This is how it feels.”
Clinicians have also approached him, asking if they can show his video to illustrate to patients and their families how having the condition may affect their lives.
Preventable deaths
At the meeting, Dr. Hibbs highlighted the 2021 report No One’s Listening, which was issued by the Sickle Cell Society following an inquiry into avoidable deaths and failures of care for sickle cell patients.
The inquiry, published by an All-Party Parliamentary group, found “serious care failings” in acute services and evidence of attitudes underpinned by racism. There was evidence of substandard care for sickle cell patients who were admitted to general wards or to hospital accident and emergency departments, as well as low awareness of the condition among health care professionals.
The report noted that the care failings have led to patient deaths, some which could have been prevented, and that there have been many “near misses.”
Many patients with sickle cell disease said they are “not being listened to” or are not being understood, especially during that vulnerable period when they are “in a crisis.”
Mr. Gaspar said that the report, and also the deaths, really struck a chord with him and many in his community. “We felt like that was us. ... We’ve all been in that same position where we’ve been misunderstood and not heard by nurses, doctors, or paramedics.”
He emphasized the need for awareness of the condition and the need for timely treatment. Just 3 weeks ago, Mr. Gaspar attended the funeral of one of his friends who is in the Hidden Pain video, a fellow sickle cell disease patient, who died at 30 years of age.
Ignorance about the condition ‘all too common’
The lack of awareness about sickle cell disease, even among health care professionals, is “all too common,” says Dr. Subarna Chakravorty, consultant pediatric hematologist, King’s College Hospital, London.
Even in London, where there is a large Black community and the teaching hospitals have world-class expertise, patients with sickle cell disease are “still facing a lot of problems with knowledge” among health care professionals, she said in an interview.
“Often people are having to speak for their own condition; which is fine, except that sometimes they are not believed,” she commented.
“On the one hand, you rely on the patient to provide information about their disease, and then when you receive it, you don’t do anything about it. So [they’re] between a rock and a hard place.”
Why are sickle cell patients treated in this way?
For Dr. Chakravorty, there is “a lot to be said about racism and disparities” in treating patients “as morphine-seekers, opiate addicts, even in children.”
“So we really need to improve the knowledge and perceptions among nonspecialist staff,” she said, “and even among specialists.”
Mr. Gaspar aims to help with this effort and hopes that his song and video will be useful to health care professionals. Sickle cell disease “needs to be spoken about,” and more doctors and nurses need to “know what it is,” he said.
He said it is a relief to encounter health care professionals who are knowledgeable about his condition. There have been times when he has been “having a crisis at home, calling the ambulance, and the paramedic comes and says: ‘Mr. Gaspar, you have sickle cell...we believe that you usually have gas and air and morphine, is that correct?’”
“That gives me a sense of peace, to know that I don’t have to fight my case or convince someone I have sickle cell, and I need to start treatment. They already know.”
No relevant financial relationships have been disclosed.
A version of this article first appeared on Medscape.com.
MANCHESTER, ENGLAND – A London-based rapper known for his gospel-inspired music has now given a voice to patients with sickle cell disease. He is using one of his music videos to raise awareness and educate health care professionals about living with the condition.
One important aim of the video, he says, is to help educate health care professionals, some of whom have not come across this condition, he explained at a session during the annual meeting of the British Society for Haematology, held recently in Manchester, England.
“It’s kind of frustrating to feel like your safe space, when you’re in front of doctors and nurses and paramedics who are supposed to know what it is and react with treatment, [and they] don’t know what it is,” Mr. Gaspar said.
He recalled an occasion in which he was experiencing a crisis, and his wife called for an ambulance. The paramedics arrived and his wife asked them for “gas and air and morphine, and they were, like, no, we don’t want to give that to him.” She tried to explain that he has sickle cell disease, but the paramedics had not heard of the condition and were suspicious that the request for morphine was a sign of drug addiction.
Mr. Gaspar expressed his frustration over “constantly having to prove that you have something serious enough to need the treatment you are asking for.”
At the meeting, Mr. Gaspar was talking on the stage with hematologist Dr. Stephen Hibbs from Barts Health NHS Trust, London.
Mr. Gaspar explained that it took years before he eventually reached “a point where I understood that it’s something that affects me and affects many other people, and I didn’t want to hide it any more.”
Sickle cell disease, which occurs primarily in people of Afro-Caribbean background, is a taboo subject in his community, Mr. Gaspar elaborated in an interview.
The condition has been associated with a great deal of stigma, with young sufferers traditionally seen as “demonically possessed,” he commented.
“So there was always a shameful aspect around it when it came to African families speaking about it, especially back in Africa.”
But after his parents came to the United Kingdom, he was able to “do his research and understand that it’s just genetics.”
This knowledge, Mr. Gaspar said, “takes away the spiritual aspect” and allows people to “have the conversation about sickle cell with potential partners” and ask them to find out their genotype, which in turn helps to “break down the barriers and the stigma.”
Mr. Gaspar emphasizes that there is much more work still to do.
In the video, he appeals to the Black community to make blood donations.
He said that something that “haunts” him is that currently, only 1% of Black people in the United Kingdom give blood, “so I really want the song to move my community to take a step forward and make that difference.”
He has been in contact with NHS Blood and Transplant, which provides blood and transplantation service to the National Health Service. They “really liked” the song, Mr. Gaspar said, and helped him get access to a hospital ward in University College Hospital, London, for the video.
“I really wanted to make a video that made people uncomfortable when watching it,” he said. It shows him hospitalized for pain and breathlessness and recalling having to use a Zimmer frame at the age of 25.
“This is a side of sickle cell that normally people don’t know,” he said.
Since releasing the song and the video, Mr. Gaspar says he has been contacted by many fellow patients. They have told him that he is now their “voice”; when they are asked how the condition affects them, “they can show someone the Hidden Pain video and say: This is how it feels.”
Clinicians have also approached him, asking if they can show his video to illustrate to patients and their families how having the condition may affect their lives.
Preventable deaths
At the meeting, Dr. Hibbs highlighted the 2021 report No One’s Listening, which was issued by the Sickle Cell Society following an inquiry into avoidable deaths and failures of care for sickle cell patients.
The inquiry, published by an All-Party Parliamentary group, found “serious care failings” in acute services and evidence of attitudes underpinned by racism. There was evidence of substandard care for sickle cell patients who were admitted to general wards or to hospital accident and emergency departments, as well as low awareness of the condition among health care professionals.
The report noted that the care failings have led to patient deaths, some which could have been prevented, and that there have been many “near misses.”
Many patients with sickle cell disease said they are “not being listened to” or are not being understood, especially during that vulnerable period when they are “in a crisis.”
Mr. Gaspar said that the report, and also the deaths, really struck a chord with him and many in his community. “We felt like that was us. ... We’ve all been in that same position where we’ve been misunderstood and not heard by nurses, doctors, or paramedics.”
He emphasized the need for awareness of the condition and the need for timely treatment. Just 3 weeks ago, Mr. Gaspar attended the funeral of one of his friends who is in the Hidden Pain video, a fellow sickle cell disease patient, who died at 30 years of age.
Ignorance about the condition ‘all too common’
The lack of awareness about sickle cell disease, even among health care professionals, is “all too common,” says Dr. Subarna Chakravorty, consultant pediatric hematologist, King’s College Hospital, London.
Even in London, where there is a large Black community and the teaching hospitals have world-class expertise, patients with sickle cell disease are “still facing a lot of problems with knowledge” among health care professionals, she said in an interview.
“Often people are having to speak for their own condition; which is fine, except that sometimes they are not believed,” she commented.
“On the one hand, you rely on the patient to provide information about their disease, and then when you receive it, you don’t do anything about it. So [they’re] between a rock and a hard place.”
Why are sickle cell patients treated in this way?
For Dr. Chakravorty, there is “a lot to be said about racism and disparities” in treating patients “as morphine-seekers, opiate addicts, even in children.”
“So we really need to improve the knowledge and perceptions among nonspecialist staff,” she said, “and even among specialists.”
Mr. Gaspar aims to help with this effort and hopes that his song and video will be useful to health care professionals. Sickle cell disease “needs to be spoken about,” and more doctors and nurses need to “know what it is,” he said.
He said it is a relief to encounter health care professionals who are knowledgeable about his condition. There have been times when he has been “having a crisis at home, calling the ambulance, and the paramedic comes and says: ‘Mr. Gaspar, you have sickle cell...we believe that you usually have gas and air and morphine, is that correct?’”
“That gives me a sense of peace, to know that I don’t have to fight my case or convince someone I have sickle cell, and I need to start treatment. They already know.”
No relevant financial relationships have been disclosed.
A version of this article first appeared on Medscape.com.
Study finds social media use negatively affects male and female adolescents at different ages
A cross-sectional study in the United Kingdom has revealed an association between social media use and lower life satisfaction among children and adolescents aged 10-21 years.
“[Our] study provides evidence for age- and sex-specific windows of sensitivity to social media use in adolescence,” lead author Amy Orben, PhD, of the University of Cambridge (England), and colleagues wrote. The findings were published in Nature Communications.
The researchers analyzed cross-sectional and longitudinal data from the Understanding Society dataset and the Millennium Cohort Study. The cross-sectional data was used to investigate the existence of developmental windows of sensitivity to social media, while the longitudinal data was used to evaluate whether sex-specific windows of sensitivity to social media were present during the adolescence period.
These two datasets comprised 84,011 participants aged 10-80 years old. After applying the modeling framework, 17,409 participants aged 10-21 years were included in the analysis.
Longitudinal analyses revealed different developmental windows of sensitivity to social media during adolescence, with higher estimated social media use predicting lower life satisfaction scores 1 year later (regression coefficient [beta], −0.02; 95% confidence interval, −0.03 to −0.01; P = .004).
Among females, the researchers observed a window of sensitivity to social media between the ages of 11 and 13, with higher estimated social media use predicting lower life satisfaction ratings 1 year later (age 11: beta, −0.11; 95% CI, −0.21 to −0.02; P = .020; age 12: beta, −0.14; 95% CI, −0.22 to −0.07; P < .001; age 13: beta, −0.08; 95% CI, −0.15 to −0.01; P = .019).
Among males, a similar window was observed between the ages of 14 and 15 (age 14: beta, −0.10; 95% CI, −0.17 to −0.03; P = .005; age 15: beta, –0.18; 95% CI, −0.29 to −0.08; P = .001).
Furthermore, they showed that a later increase in sensitivity to social media, which was present at age 19 for both females and males, suggested a different underlying process was present in late adolescence (females: beta, −0.16; 95% CI, −0.25 to −0.07; P < .001; males: beta, −0.16; 95% CI, −0.26 to −0.07; P = .001).
“Speculatively, this might be related to changes in the social environment such as a move away from home and subsequent disruptions in social networks,” the researchers wrote.
Importantly, Dr. Orben and colleagues noted that these results should be interpreted with caution. Owing to the cross-sectional nature of the data, causality cannot be inferred from these findings.
“The findings reported here may enable investigation of potential mechanisms of interest, for example, in datasets with pubertal or additional social measurements,” they wrote. “One could also carry out more targeted investigations, for example, by examining the mental health measures only completed by select age ranges in the datasets.”
Digital literacy is important, expert says
“Digital literacy and education about social media use is warranted for all ages, starting young,” Yalda T. Uhls, MBA, PhD, of the department of psychology at the University of California, Los Angeles, said in an interview. “Attending to underlying issues for vulnerable ages, such as anxiety, as well as parental support is critical.”
“I would urge social media platforms to pay attention to what kinds of content they are making available to ensure the highest possible quality, and to embed things like suggestions for pauses and other ways to check in on someone who may be experiencing distress when on socials,” Dr. Uhls said. “We also need to increase access to mental health resources for young people and social media could help provide information for those experiencing issues.”
This study was supported by the University of Cambridge and the UK Medical Research Council. The authors reported no relevant disclosures. Dr. Uhls had no relevant disclosures.
A cross-sectional study in the United Kingdom has revealed an association between social media use and lower life satisfaction among children and adolescents aged 10-21 years.
“[Our] study provides evidence for age- and sex-specific windows of sensitivity to social media use in adolescence,” lead author Amy Orben, PhD, of the University of Cambridge (England), and colleagues wrote. The findings were published in Nature Communications.
The researchers analyzed cross-sectional and longitudinal data from the Understanding Society dataset and the Millennium Cohort Study. The cross-sectional data was used to investigate the existence of developmental windows of sensitivity to social media, while the longitudinal data was used to evaluate whether sex-specific windows of sensitivity to social media were present during the adolescence period.
These two datasets comprised 84,011 participants aged 10-80 years old. After applying the modeling framework, 17,409 participants aged 10-21 years were included in the analysis.
Longitudinal analyses revealed different developmental windows of sensitivity to social media during adolescence, with higher estimated social media use predicting lower life satisfaction scores 1 year later (regression coefficient [beta], −0.02; 95% confidence interval, −0.03 to −0.01; P = .004).
Among females, the researchers observed a window of sensitivity to social media between the ages of 11 and 13, with higher estimated social media use predicting lower life satisfaction ratings 1 year later (age 11: beta, −0.11; 95% CI, −0.21 to −0.02; P = .020; age 12: beta, −0.14; 95% CI, −0.22 to −0.07; P < .001; age 13: beta, −0.08; 95% CI, −0.15 to −0.01; P = .019).
Among males, a similar window was observed between the ages of 14 and 15 (age 14: beta, −0.10; 95% CI, −0.17 to −0.03; P = .005; age 15: beta, –0.18; 95% CI, −0.29 to −0.08; P = .001).
Furthermore, they showed that a later increase in sensitivity to social media, which was present at age 19 for both females and males, suggested a different underlying process was present in late adolescence (females: beta, −0.16; 95% CI, −0.25 to −0.07; P < .001; males: beta, −0.16; 95% CI, −0.26 to −0.07; P = .001).
“Speculatively, this might be related to changes in the social environment such as a move away from home and subsequent disruptions in social networks,” the researchers wrote.
Importantly, Dr. Orben and colleagues noted that these results should be interpreted with caution. Owing to the cross-sectional nature of the data, causality cannot be inferred from these findings.
“The findings reported here may enable investigation of potential mechanisms of interest, for example, in datasets with pubertal or additional social measurements,” they wrote. “One could also carry out more targeted investigations, for example, by examining the mental health measures only completed by select age ranges in the datasets.”
Digital literacy is important, expert says
“Digital literacy and education about social media use is warranted for all ages, starting young,” Yalda T. Uhls, MBA, PhD, of the department of psychology at the University of California, Los Angeles, said in an interview. “Attending to underlying issues for vulnerable ages, such as anxiety, as well as parental support is critical.”
“I would urge social media platforms to pay attention to what kinds of content they are making available to ensure the highest possible quality, and to embed things like suggestions for pauses and other ways to check in on someone who may be experiencing distress when on socials,” Dr. Uhls said. “We also need to increase access to mental health resources for young people and social media could help provide information for those experiencing issues.”
This study was supported by the University of Cambridge and the UK Medical Research Council. The authors reported no relevant disclosures. Dr. Uhls had no relevant disclosures.
A cross-sectional study in the United Kingdom has revealed an association between social media use and lower life satisfaction among children and adolescents aged 10-21 years.
“[Our] study provides evidence for age- and sex-specific windows of sensitivity to social media use in adolescence,” lead author Amy Orben, PhD, of the University of Cambridge (England), and colleagues wrote. The findings were published in Nature Communications.
The researchers analyzed cross-sectional and longitudinal data from the Understanding Society dataset and the Millennium Cohort Study. The cross-sectional data was used to investigate the existence of developmental windows of sensitivity to social media, while the longitudinal data was used to evaluate whether sex-specific windows of sensitivity to social media were present during the adolescence period.
These two datasets comprised 84,011 participants aged 10-80 years old. After applying the modeling framework, 17,409 participants aged 10-21 years were included in the analysis.
Longitudinal analyses revealed different developmental windows of sensitivity to social media during adolescence, with higher estimated social media use predicting lower life satisfaction scores 1 year later (regression coefficient [beta], −0.02; 95% confidence interval, −0.03 to −0.01; P = .004).
Among females, the researchers observed a window of sensitivity to social media between the ages of 11 and 13, with higher estimated social media use predicting lower life satisfaction ratings 1 year later (age 11: beta, −0.11; 95% CI, −0.21 to −0.02; P = .020; age 12: beta, −0.14; 95% CI, −0.22 to −0.07; P < .001; age 13: beta, −0.08; 95% CI, −0.15 to −0.01; P = .019).
Among males, a similar window was observed between the ages of 14 and 15 (age 14: beta, −0.10; 95% CI, −0.17 to −0.03; P = .005; age 15: beta, –0.18; 95% CI, −0.29 to −0.08; P = .001).
Furthermore, they showed that a later increase in sensitivity to social media, which was present at age 19 for both females and males, suggested a different underlying process was present in late adolescence (females: beta, −0.16; 95% CI, −0.25 to −0.07; P < .001; males: beta, −0.16; 95% CI, −0.26 to −0.07; P = .001).
“Speculatively, this might be related to changes in the social environment such as a move away from home and subsequent disruptions in social networks,” the researchers wrote.
Importantly, Dr. Orben and colleagues noted that these results should be interpreted with caution. Owing to the cross-sectional nature of the data, causality cannot be inferred from these findings.
“The findings reported here may enable investigation of potential mechanisms of interest, for example, in datasets with pubertal or additional social measurements,” they wrote. “One could also carry out more targeted investigations, for example, by examining the mental health measures only completed by select age ranges in the datasets.”
Digital literacy is important, expert says
“Digital literacy and education about social media use is warranted for all ages, starting young,” Yalda T. Uhls, MBA, PhD, of the department of psychology at the University of California, Los Angeles, said in an interview. “Attending to underlying issues for vulnerable ages, such as anxiety, as well as parental support is critical.”
“I would urge social media platforms to pay attention to what kinds of content they are making available to ensure the highest possible quality, and to embed things like suggestions for pauses and other ways to check in on someone who may be experiencing distress when on socials,” Dr. Uhls said. “We also need to increase access to mental health resources for young people and social media could help provide information for those experiencing issues.”
This study was supported by the University of Cambridge and the UK Medical Research Council. The authors reported no relevant disclosures. Dr. Uhls had no relevant disclosures.
FROM NATURE COMMUNICATIONS
Jury is out on universal screening for eating disorders
Eating disorders (binge eating disorder, bulimia nervosa, and anorexia nervosa) can cause “serious harms to physical and psychosocial health and take a tremendous toll on individuals and families,” task force member Lori Pbert, PhD, told this news organization.
“Screening for eating disorders has the potential to improve health by leading to early detection and effective treatment,” said Dr. Pbert, with the department of population and quantitative health sciences, University of Massachusetts, Worcester.
However, a “deep dive” into the available literature failed to turn up adequate evidence to recommend for or against routine screening for eating disorders for children and adolescents aged 10 years and older and for adults who have no signs or symptoms of an eating disorder or concerns about their eating and who have not previously been diagnosed with an eating disorder, Dr. Pbert said.
The task force, therefore, issued an “I” statement (insufficient evidence), meaning it cannot at this time recommend for or against screening for eating disorders.
An “I” statement is “fundamentally a call for more research,” Dr. Pbert noted.
Adolescents and adults who have signs and symptoms of an eating disorder – which include rapid weight loss; weight gain or pronounced deviation from growth trajectory; pubertal delay; bradycardia; oligomenorrhea; and amenorrhea – are not included in this recommendation.
The USPSTF recommendation statement and accompanying evidence report were published online March 15 in JAMA.
Clinical judgment key
In the absence of evidence, clinicians should use their judgment when determining whether or not to screen an individual patient for an eating disorder, Dr. Pbert advised.
One thing to consider is whether the patient is in a group at higher risk for eating disorders, such as athletes, females, young adults aged 18-29, and transgender individuals.
Another is whether the patient reports engaging in unhealthy weight control behaviors, such as fasting or skipping meals, Dr. Pbert said.
Importantly, any patient who has signs or symptoms of an eating disorder or is expressing concerns about their eating should be assessed and referred for appropriate care, Dr. Pbert said.
“The good news is that eating disorders can be treated,” she said.
Several organizations currently recommend screening in the context of monitoring changes in weight and other vital signs or signs and symptoms to determine whether a patient might have an eating disorder.
Dr. Pbert said it’s important to recognize that the USPSTF statement “doesn’t really conflict” with the recommendations of other organizations. “We all agree that patients who present with signs or symptoms of an eating disorder should be assessed further.”
Evidence gaps
The authors of an invited commentary in JAMA) say the task force has identified several “notable deficiencies” in the available data on screening for eating disorders.
“Directing attention to rigorous research to close this evidence gap will be important to find optimal approaches to identify patients with these complex disorders and improve their health outcomes,” write Evelyn Attia, MD, with Weill Cornell Medicine in New York, and Angela Guarda, MD, with Johns Hopkins University, Baltimore.
This “I” statement, they say, “highlights the need to prioritize research aimed at closing the evidence gap identified by USPSTF in a timely manner and underscores the need for new studies that address screening for eating disorders, treatment trials that enroll screen-detected populations from primary care settings, and screening in specific populations.
“Research on screening in primary care also should be paired with development and assessment of early brief intervention strategies for those individuals who screen positive, especially adolescents,” Dr. Attia and Dr. Guarda say.
Members of the USPSTF have disclosed no relevant financial relationships. Dr. Attia has received research support from the National Institute of Mental Health and the Hilda & Preston David Foundation; royalties from UpToDate; and has served as a clinical advisor to Equip Health. Dr. Guarda has received support from the Stephen and Jean Robinson Fund and research funding from the Klarman Family Foundation.
A version of this article first appeared on Medscape.com.
Eating disorders (binge eating disorder, bulimia nervosa, and anorexia nervosa) can cause “serious harms to physical and psychosocial health and take a tremendous toll on individuals and families,” task force member Lori Pbert, PhD, told this news organization.
“Screening for eating disorders has the potential to improve health by leading to early detection and effective treatment,” said Dr. Pbert, with the department of population and quantitative health sciences, University of Massachusetts, Worcester.
However, a “deep dive” into the available literature failed to turn up adequate evidence to recommend for or against routine screening for eating disorders for children and adolescents aged 10 years and older and for adults who have no signs or symptoms of an eating disorder or concerns about their eating and who have not previously been diagnosed with an eating disorder, Dr. Pbert said.
The task force, therefore, issued an “I” statement (insufficient evidence), meaning it cannot at this time recommend for or against screening for eating disorders.
An “I” statement is “fundamentally a call for more research,” Dr. Pbert noted.
Adolescents and adults who have signs and symptoms of an eating disorder – which include rapid weight loss; weight gain or pronounced deviation from growth trajectory; pubertal delay; bradycardia; oligomenorrhea; and amenorrhea – are not included in this recommendation.
The USPSTF recommendation statement and accompanying evidence report were published online March 15 in JAMA.
Clinical judgment key
In the absence of evidence, clinicians should use their judgment when determining whether or not to screen an individual patient for an eating disorder, Dr. Pbert advised.
One thing to consider is whether the patient is in a group at higher risk for eating disorders, such as athletes, females, young adults aged 18-29, and transgender individuals.
Another is whether the patient reports engaging in unhealthy weight control behaviors, such as fasting or skipping meals, Dr. Pbert said.
Importantly, any patient who has signs or symptoms of an eating disorder or is expressing concerns about their eating should be assessed and referred for appropriate care, Dr. Pbert said.
“The good news is that eating disorders can be treated,” she said.
Several organizations currently recommend screening in the context of monitoring changes in weight and other vital signs or signs and symptoms to determine whether a patient might have an eating disorder.
Dr. Pbert said it’s important to recognize that the USPSTF statement “doesn’t really conflict” with the recommendations of other organizations. “We all agree that patients who present with signs or symptoms of an eating disorder should be assessed further.”
Evidence gaps
The authors of an invited commentary in JAMA) say the task force has identified several “notable deficiencies” in the available data on screening for eating disorders.
“Directing attention to rigorous research to close this evidence gap will be important to find optimal approaches to identify patients with these complex disorders and improve their health outcomes,” write Evelyn Attia, MD, with Weill Cornell Medicine in New York, and Angela Guarda, MD, with Johns Hopkins University, Baltimore.
This “I” statement, they say, “highlights the need to prioritize research aimed at closing the evidence gap identified by USPSTF in a timely manner and underscores the need for new studies that address screening for eating disorders, treatment trials that enroll screen-detected populations from primary care settings, and screening in specific populations.
“Research on screening in primary care also should be paired with development and assessment of early brief intervention strategies for those individuals who screen positive, especially adolescents,” Dr. Attia and Dr. Guarda say.
Members of the USPSTF have disclosed no relevant financial relationships. Dr. Attia has received research support from the National Institute of Mental Health and the Hilda & Preston David Foundation; royalties from UpToDate; and has served as a clinical advisor to Equip Health. Dr. Guarda has received support from the Stephen and Jean Robinson Fund and research funding from the Klarman Family Foundation.
A version of this article first appeared on Medscape.com.
Eating disorders (binge eating disorder, bulimia nervosa, and anorexia nervosa) can cause “serious harms to physical and psychosocial health and take a tremendous toll on individuals and families,” task force member Lori Pbert, PhD, told this news organization.
“Screening for eating disorders has the potential to improve health by leading to early detection and effective treatment,” said Dr. Pbert, with the department of population and quantitative health sciences, University of Massachusetts, Worcester.
However, a “deep dive” into the available literature failed to turn up adequate evidence to recommend for or against routine screening for eating disorders for children and adolescents aged 10 years and older and for adults who have no signs or symptoms of an eating disorder or concerns about their eating and who have not previously been diagnosed with an eating disorder, Dr. Pbert said.
The task force, therefore, issued an “I” statement (insufficient evidence), meaning it cannot at this time recommend for or against screening for eating disorders.
An “I” statement is “fundamentally a call for more research,” Dr. Pbert noted.
Adolescents and adults who have signs and symptoms of an eating disorder – which include rapid weight loss; weight gain or pronounced deviation from growth trajectory; pubertal delay; bradycardia; oligomenorrhea; and amenorrhea – are not included in this recommendation.
The USPSTF recommendation statement and accompanying evidence report were published online March 15 in JAMA.
Clinical judgment key
In the absence of evidence, clinicians should use their judgment when determining whether or not to screen an individual patient for an eating disorder, Dr. Pbert advised.
One thing to consider is whether the patient is in a group at higher risk for eating disorders, such as athletes, females, young adults aged 18-29, and transgender individuals.
Another is whether the patient reports engaging in unhealthy weight control behaviors, such as fasting or skipping meals, Dr. Pbert said.
Importantly, any patient who has signs or symptoms of an eating disorder or is expressing concerns about their eating should be assessed and referred for appropriate care, Dr. Pbert said.
“The good news is that eating disorders can be treated,” she said.
Several organizations currently recommend screening in the context of monitoring changes in weight and other vital signs or signs and symptoms to determine whether a patient might have an eating disorder.
Dr. Pbert said it’s important to recognize that the USPSTF statement “doesn’t really conflict” with the recommendations of other organizations. “We all agree that patients who present with signs or symptoms of an eating disorder should be assessed further.”
Evidence gaps
The authors of an invited commentary in JAMA) say the task force has identified several “notable deficiencies” in the available data on screening for eating disorders.
“Directing attention to rigorous research to close this evidence gap will be important to find optimal approaches to identify patients with these complex disorders and improve their health outcomes,” write Evelyn Attia, MD, with Weill Cornell Medicine in New York, and Angela Guarda, MD, with Johns Hopkins University, Baltimore.
This “I” statement, they say, “highlights the need to prioritize research aimed at closing the evidence gap identified by USPSTF in a timely manner and underscores the need for new studies that address screening for eating disorders, treatment trials that enroll screen-detected populations from primary care settings, and screening in specific populations.
“Research on screening in primary care also should be paired with development and assessment of early brief intervention strategies for those individuals who screen positive, especially adolescents,” Dr. Attia and Dr. Guarda say.
Members of the USPSTF have disclosed no relevant financial relationships. Dr. Attia has received research support from the National Institute of Mental Health and the Hilda & Preston David Foundation; royalties from UpToDate; and has served as a clinical advisor to Equip Health. Dr. Guarda has received support from the Stephen and Jean Robinson Fund and research funding from the Klarman Family Foundation.
A version of this article first appeared on Medscape.com.
‘Alarming’ worldwide decline in mental health
The Mental Health Million project of Sapien Labs issued its second report, published online March 15, encompassing 34 countries and over 220,000 Internet-enabled adults. It found a continued decline in mental health in all age groups and genders, with English-speaking countries having the lowest mental well-being.
The decline was significantly correlated with the stringency of COVID-19 lockdown measures in each country and was directionally correlated to the cases and deaths per million.
The youngest age group (18-24 years) reported the poorest mental well-being, with better mental health scores rising in every successively older age group.
“Some of our findings, especially regarding mental health in young adults, are alarming,” Tara Thiagarajan, PhD, Sapien Labs founder and chief scientist, told this news organization.
“Our data, which are continually updated in real time, are freely available for nonprofit, noncommercial use and research, and we hope that researchers will get involved in an interdisciplinary way that spans sociology, economics, psychiatry, and other fields,” she said.
Pioneering research
Dr. Thiagarajan and her team pioneered the Mental Health Million project, an ongoing research initiative utilizing a “free and anonymous assessment tool,” the Mental Health Quotient (MHQ), which “encompasses a comprehensive view of our emotional, social, and cognitive function and capability.”
The MHQ consists of 47 “elements of mental well-being,” with scores ranging from –100 to +200. (Negative scores indicate poorer mental well-being.) The MHQ categorizes respondents as “clinical, at-risk, enduring, managing, succeeding, and thriving” and computes scores on the basis of six broad dimensions of mental health: core cognition, complex cognition, mood and outlook, drive and motivation, social self, and mind-body connection.
As reported by this news organization, Sapien Lab’s first Mental Health State of the World report (n = 49,000 adults) was conducted in eight English-speaking countries in 2020. Participants were compared to a smaller sample of people from the same countries polled in 2019.
In this year’s report, “we expanded quite substantially,” Dr. Thiagarajan said. The project added Spanish, French, and Arabic and recruited participants from 34 countries on six continents (n = 223,087) via advertising on Google and Facebook.
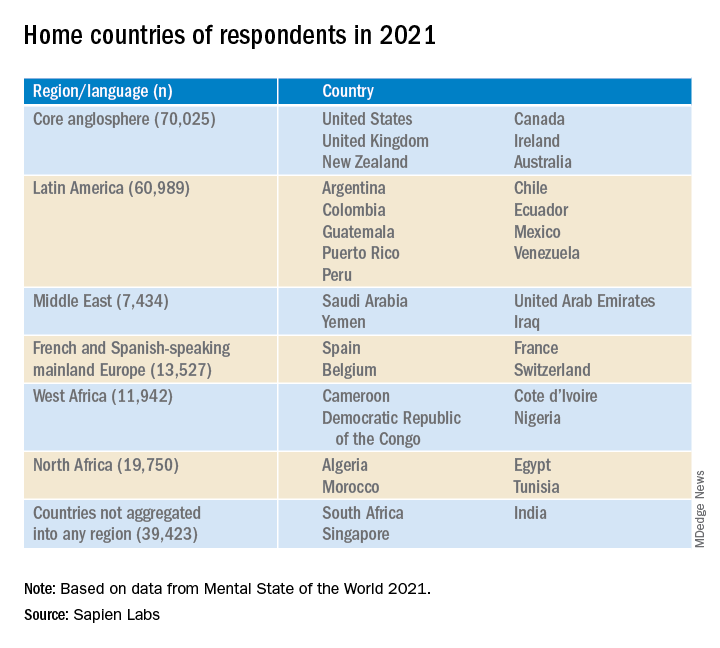
Economic prosperity not protective
Across the eight English-speaking countries, there was a decline in mental well-being of 3% from 2020 to 2021, which was smaller than the 8% decline from 2019 to 2020. The percentage of people who were “distressed or struggling” increased from 26% to 30% in 2021.
“Now that a lot of pandemic issue seems to be easing up, I hope we’ll see mental well-being coming back up, but at least it’s a smaller decline than we saw between 2019 and 2020,” said Dr. Thiagarajan.
The decline across countries from 2019 to 2021 was significantly correlated with the stringency of governmental COVID-19-related measures (based on the Oxford COVID-19 Government Response Tracker, 2022; r = .54) and directionally correlated to the cases and deaths per million.
In total, 30% of respondents in English-speaking countries had mental well-being scores in the “distressed” or “struggling” range – higher than the Middle Eastern countries, North Africa, Latin America, and Europe (23%, 23%, 24%, and 18%, respectively).
Only 36% of participants in the English-speaking countries, the Middle East, and North Africa reported “thriving or succeeding,” vs. 45% and 46% in Latin America and Europe, respectively. Venezuela topped the list with an average MHQ of 91, while the United Kingdom and South Africa had the lowest scores, at 46 each.
Mental well-being was slightly higher in males than in females but was dramatically lower in nonbinary/third-gender respondents. In fact, those identifying as nonbinary/third gender had the lowest mental well-being of any group.
Across all countries and languages, higher education was associated with better mental well-being. Employment was also associated with superior mental well-being, compared with being unemployed – particularly in core English-speaking countries.
However, “country indicators of economic prosperity were negatively correlated with mental well-being, particularly for young adults and males, belying the commonly held belief that national economic prosperity translates into greater mental well-being,” said Dr. Thiagarajan.
‘Stark’ contrast
The most dramatic finding was the difference in mental well-being between younger and older adults, which was two- to threefold larger than differences in other dimensions (for example, age, gender, employment). Even the maximum difference between countries overall (15%) was still smaller than the generational gap within any region.
While only 7% (6%- 9%) of participants aged ≥65 years were “distressed and struggling” with their mental well-being to a “clinical” extent, 44% (38%-50%) of those aged 18-24 years reported mental well-being scores in the “distressed or struggling” range – representing a “growing gap between generations that, while present prior to the COVID-19 pandemic, has since been exacerbated,” the authors state.
With every successive decrement in age group, mental well-being “plummeted,” Dr. Thiagarajan said. She noted that research conducted prior to 2010 in several regions of the world showed that young adults typically had the highest well-being. “Our findings stand in stark contrast to these previous patterns.”
The relationship between lockdown stringency and poorer mental health could play a role. “The impact of social isolation may be most strongly felt in younger people,” she said.
Internet a culprit?
“Within almost every region, scores for cognition and drive and motivation were highest while mood and outlook and social self were the lowest,” the authors report.
The aggregate percentage of respondents who reported being “distressed or struggling” in the various MHQ dimensions is shown in the following table.
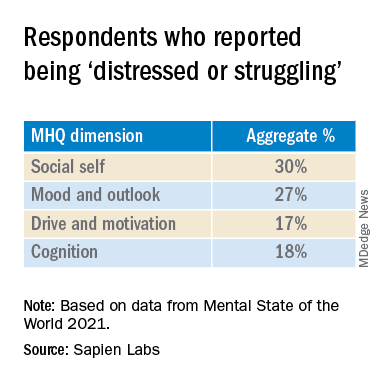
In particular, English-speaking countries scored lowest on the social self scale.
The sense of social self is “how you see yourself with respect to others, how you relate to others and the ability to form strong, stable relationships and maintain them with other people,” said Dr. Thiagarajan.
Internet use might account for the “massive” difference between the youngest and the oldest generations, she suggested. “Following 2010, mobile phone penetration picked up and rose rapidly. ... Mobile phones took over the world.”
Time spent on the Internet – an estimated 7-10 hours per day – “eats into the time people in older generations used in building the social self. Kids who grow up on the Internet are losing thousands of hours in social interactions, which is challenging their ability to form relationships, how they see themselves, and how they fit into the social fabric,” Dr. Thiagarajan added
Sedentary time
Commenting for this news organization, Bernardo Ng, MD, a member of the American Psychiatric Association’s Council on International Psychiatry and Global Health and medical director of Sun Valley Research Center, Imperial, Calif., called the report “interesting, with an impressive sample size” and an “impressive geographic distribution.”
Dr. Ng, who was not involved in the report, said, “I did not think the impact of Internet use on mental health was as dramatic before looking at this report.
“On the other hand, I have personally been interested in the impact of sedentarism in mental health – not only emotionally but also biologically. Sedentarism, which is directly related to screen use time, produces inflammation that worsens brain function.”
Also commenting, Ken Duckworth, MD, chief medical officer of the National Alliance of Mental Illness, called the survey “extremely well timed and creative, although it looked only at Internet-enabled populations, so one cannot make too many overall pronouncements, because a lot of people don’t have access to the Internet.”
The data regarding young people are particularly powerful. “The idea that young people are having a decrease in their experience of mental health across the world is something I haven’t seen before.”
Dr. Duckworth suggested the reason might “have to do with the impact of the COVID lockdown on normal development that young people go through, while older people don’t struggle with these developmental challenges in the same way.”
A version of this article first appeared on Medscape.com.
The Mental Health Million project of Sapien Labs issued its second report, published online March 15, encompassing 34 countries and over 220,000 Internet-enabled adults. It found a continued decline in mental health in all age groups and genders, with English-speaking countries having the lowest mental well-being.
The decline was significantly correlated with the stringency of COVID-19 lockdown measures in each country and was directionally correlated to the cases and deaths per million.
The youngest age group (18-24 years) reported the poorest mental well-being, with better mental health scores rising in every successively older age group.
“Some of our findings, especially regarding mental health in young adults, are alarming,” Tara Thiagarajan, PhD, Sapien Labs founder and chief scientist, told this news organization.
“Our data, which are continually updated in real time, are freely available for nonprofit, noncommercial use and research, and we hope that researchers will get involved in an interdisciplinary way that spans sociology, economics, psychiatry, and other fields,” she said.
Pioneering research
Dr. Thiagarajan and her team pioneered the Mental Health Million project, an ongoing research initiative utilizing a “free and anonymous assessment tool,” the Mental Health Quotient (MHQ), which “encompasses a comprehensive view of our emotional, social, and cognitive function and capability.”
The MHQ consists of 47 “elements of mental well-being,” with scores ranging from –100 to +200. (Negative scores indicate poorer mental well-being.) The MHQ categorizes respondents as “clinical, at-risk, enduring, managing, succeeding, and thriving” and computes scores on the basis of six broad dimensions of mental health: core cognition, complex cognition, mood and outlook, drive and motivation, social self, and mind-body connection.
As reported by this news organization, Sapien Lab’s first Mental Health State of the World report (n = 49,000 adults) was conducted in eight English-speaking countries in 2020. Participants were compared to a smaller sample of people from the same countries polled in 2019.
In this year’s report, “we expanded quite substantially,” Dr. Thiagarajan said. The project added Spanish, French, and Arabic and recruited participants from 34 countries on six continents (n = 223,087) via advertising on Google and Facebook.

Economic prosperity not protective
Across the eight English-speaking countries, there was a decline in mental well-being of 3% from 2020 to 2021, which was smaller than the 8% decline from 2019 to 2020. The percentage of people who were “distressed or struggling” increased from 26% to 30% in 2021.
“Now that a lot of pandemic issue seems to be easing up, I hope we’ll see mental well-being coming back up, but at least it’s a smaller decline than we saw between 2019 and 2020,” said Dr. Thiagarajan.
The decline across countries from 2019 to 2021 was significantly correlated with the stringency of governmental COVID-19-related measures (based on the Oxford COVID-19 Government Response Tracker, 2022; r = .54) and directionally correlated to the cases and deaths per million.
In total, 30% of respondents in English-speaking countries had mental well-being scores in the “distressed” or “struggling” range – higher than the Middle Eastern countries, North Africa, Latin America, and Europe (23%, 23%, 24%, and 18%, respectively).
Only 36% of participants in the English-speaking countries, the Middle East, and North Africa reported “thriving or succeeding,” vs. 45% and 46% in Latin America and Europe, respectively. Venezuela topped the list with an average MHQ of 91, while the United Kingdom and South Africa had the lowest scores, at 46 each.
Mental well-being was slightly higher in males than in females but was dramatically lower in nonbinary/third-gender respondents. In fact, those identifying as nonbinary/third gender had the lowest mental well-being of any group.
Across all countries and languages, higher education was associated with better mental well-being. Employment was also associated with superior mental well-being, compared with being unemployed – particularly in core English-speaking countries.
However, “country indicators of economic prosperity were negatively correlated with mental well-being, particularly for young adults and males, belying the commonly held belief that national economic prosperity translates into greater mental well-being,” said Dr. Thiagarajan.
‘Stark’ contrast
The most dramatic finding was the difference in mental well-being between younger and older adults, which was two- to threefold larger than differences in other dimensions (for example, age, gender, employment). Even the maximum difference between countries overall (15%) was still smaller than the generational gap within any region.
While only 7% (6%- 9%) of participants aged ≥65 years were “distressed and struggling” with their mental well-being to a “clinical” extent, 44% (38%-50%) of those aged 18-24 years reported mental well-being scores in the “distressed or struggling” range – representing a “growing gap between generations that, while present prior to the COVID-19 pandemic, has since been exacerbated,” the authors state.
With every successive decrement in age group, mental well-being “plummeted,” Dr. Thiagarajan said. She noted that research conducted prior to 2010 in several regions of the world showed that young adults typically had the highest well-being. “Our findings stand in stark contrast to these previous patterns.”
The relationship between lockdown stringency and poorer mental health could play a role. “The impact of social isolation may be most strongly felt in younger people,” she said.
Internet a culprit?
“Within almost every region, scores for cognition and drive and motivation were highest while mood and outlook and social self were the lowest,” the authors report.
The aggregate percentage of respondents who reported being “distressed or struggling” in the various MHQ dimensions is shown in the following table.

In particular, English-speaking countries scored lowest on the social self scale.
The sense of social self is “how you see yourself with respect to others, how you relate to others and the ability to form strong, stable relationships and maintain them with other people,” said Dr. Thiagarajan.
Internet use might account for the “massive” difference between the youngest and the oldest generations, she suggested. “Following 2010, mobile phone penetration picked up and rose rapidly. ... Mobile phones took over the world.”
Time spent on the Internet – an estimated 7-10 hours per day – “eats into the time people in older generations used in building the social self. Kids who grow up on the Internet are losing thousands of hours in social interactions, which is challenging their ability to form relationships, how they see themselves, and how they fit into the social fabric,” Dr. Thiagarajan added
Sedentary time
Commenting for this news organization, Bernardo Ng, MD, a member of the American Psychiatric Association’s Council on International Psychiatry and Global Health and medical director of Sun Valley Research Center, Imperial, Calif., called the report “interesting, with an impressive sample size” and an “impressive geographic distribution.”
Dr. Ng, who was not involved in the report, said, “I did not think the impact of Internet use on mental health was as dramatic before looking at this report.
“On the other hand, I have personally been interested in the impact of sedentarism in mental health – not only emotionally but also biologically. Sedentarism, which is directly related to screen use time, produces inflammation that worsens brain function.”
Also commenting, Ken Duckworth, MD, chief medical officer of the National Alliance of Mental Illness, called the survey “extremely well timed and creative, although it looked only at Internet-enabled populations, so one cannot make too many overall pronouncements, because a lot of people don’t have access to the Internet.”
The data regarding young people are particularly powerful. “The idea that young people are having a decrease in their experience of mental health across the world is something I haven’t seen before.”
Dr. Duckworth suggested the reason might “have to do with the impact of the COVID lockdown on normal development that young people go through, while older people don’t struggle with these developmental challenges in the same way.”
A version of this article first appeared on Medscape.com.
The Mental Health Million project of Sapien Labs issued its second report, published online March 15, encompassing 34 countries and over 220,000 Internet-enabled adults. It found a continued decline in mental health in all age groups and genders, with English-speaking countries having the lowest mental well-being.
The decline was significantly correlated with the stringency of COVID-19 lockdown measures in each country and was directionally correlated to the cases and deaths per million.
The youngest age group (18-24 years) reported the poorest mental well-being, with better mental health scores rising in every successively older age group.
“Some of our findings, especially regarding mental health in young adults, are alarming,” Tara Thiagarajan, PhD, Sapien Labs founder and chief scientist, told this news organization.
“Our data, which are continually updated in real time, are freely available for nonprofit, noncommercial use and research, and we hope that researchers will get involved in an interdisciplinary way that spans sociology, economics, psychiatry, and other fields,” she said.
Pioneering research
Dr. Thiagarajan and her team pioneered the Mental Health Million project, an ongoing research initiative utilizing a “free and anonymous assessment tool,” the Mental Health Quotient (MHQ), which “encompasses a comprehensive view of our emotional, social, and cognitive function and capability.”
The MHQ consists of 47 “elements of mental well-being,” with scores ranging from –100 to +200. (Negative scores indicate poorer mental well-being.) The MHQ categorizes respondents as “clinical, at-risk, enduring, managing, succeeding, and thriving” and computes scores on the basis of six broad dimensions of mental health: core cognition, complex cognition, mood and outlook, drive and motivation, social self, and mind-body connection.
As reported by this news organization, Sapien Lab’s first Mental Health State of the World report (n = 49,000 adults) was conducted in eight English-speaking countries in 2020. Participants were compared to a smaller sample of people from the same countries polled in 2019.
In this year’s report, “we expanded quite substantially,” Dr. Thiagarajan said. The project added Spanish, French, and Arabic and recruited participants from 34 countries on six continents (n = 223,087) via advertising on Google and Facebook.

Economic prosperity not protective
Across the eight English-speaking countries, there was a decline in mental well-being of 3% from 2020 to 2021, which was smaller than the 8% decline from 2019 to 2020. The percentage of people who were “distressed or struggling” increased from 26% to 30% in 2021.
“Now that a lot of pandemic issue seems to be easing up, I hope we’ll see mental well-being coming back up, but at least it’s a smaller decline than we saw between 2019 and 2020,” said Dr. Thiagarajan.
The decline across countries from 2019 to 2021 was significantly correlated with the stringency of governmental COVID-19-related measures (based on the Oxford COVID-19 Government Response Tracker, 2022; r = .54) and directionally correlated to the cases and deaths per million.
In total, 30% of respondents in English-speaking countries had mental well-being scores in the “distressed” or “struggling” range – higher than the Middle Eastern countries, North Africa, Latin America, and Europe (23%, 23%, 24%, and 18%, respectively).
Only 36% of participants in the English-speaking countries, the Middle East, and North Africa reported “thriving or succeeding,” vs. 45% and 46% in Latin America and Europe, respectively. Venezuela topped the list with an average MHQ of 91, while the United Kingdom and South Africa had the lowest scores, at 46 each.
Mental well-being was slightly higher in males than in females but was dramatically lower in nonbinary/third-gender respondents. In fact, those identifying as nonbinary/third gender had the lowest mental well-being of any group.
Across all countries and languages, higher education was associated with better mental well-being. Employment was also associated with superior mental well-being, compared with being unemployed – particularly in core English-speaking countries.
However, “country indicators of economic prosperity were negatively correlated with mental well-being, particularly for young adults and males, belying the commonly held belief that national economic prosperity translates into greater mental well-being,” said Dr. Thiagarajan.
‘Stark’ contrast
The most dramatic finding was the difference in mental well-being between younger and older adults, which was two- to threefold larger than differences in other dimensions (for example, age, gender, employment). Even the maximum difference between countries overall (15%) was still smaller than the generational gap within any region.
While only 7% (6%- 9%) of participants aged ≥65 years were “distressed and struggling” with their mental well-being to a “clinical” extent, 44% (38%-50%) of those aged 18-24 years reported mental well-being scores in the “distressed or struggling” range – representing a “growing gap between generations that, while present prior to the COVID-19 pandemic, has since been exacerbated,” the authors state.
With every successive decrement in age group, mental well-being “plummeted,” Dr. Thiagarajan said. She noted that research conducted prior to 2010 in several regions of the world showed that young adults typically had the highest well-being. “Our findings stand in stark contrast to these previous patterns.”
The relationship between lockdown stringency and poorer mental health could play a role. “The impact of social isolation may be most strongly felt in younger people,” she said.
Internet a culprit?
“Within almost every region, scores for cognition and drive and motivation were highest while mood and outlook and social self were the lowest,” the authors report.
The aggregate percentage of respondents who reported being “distressed or struggling” in the various MHQ dimensions is shown in the following table.

In particular, English-speaking countries scored lowest on the social self scale.
The sense of social self is “how you see yourself with respect to others, how you relate to others and the ability to form strong, stable relationships and maintain them with other people,” said Dr. Thiagarajan.
Internet use might account for the “massive” difference between the youngest and the oldest generations, she suggested. “Following 2010, mobile phone penetration picked up and rose rapidly. ... Mobile phones took over the world.”
Time spent on the Internet – an estimated 7-10 hours per day – “eats into the time people in older generations used in building the social self. Kids who grow up on the Internet are losing thousands of hours in social interactions, which is challenging their ability to form relationships, how they see themselves, and how they fit into the social fabric,” Dr. Thiagarajan added
Sedentary time
Commenting for this news organization, Bernardo Ng, MD, a member of the American Psychiatric Association’s Council on International Psychiatry and Global Health and medical director of Sun Valley Research Center, Imperial, Calif., called the report “interesting, with an impressive sample size” and an “impressive geographic distribution.”
Dr. Ng, who was not involved in the report, said, “I did not think the impact of Internet use on mental health was as dramatic before looking at this report.
“On the other hand, I have personally been interested in the impact of sedentarism in mental health – not only emotionally but also biologically. Sedentarism, which is directly related to screen use time, produces inflammation that worsens brain function.”
Also commenting, Ken Duckworth, MD, chief medical officer of the National Alliance of Mental Illness, called the survey “extremely well timed and creative, although it looked only at Internet-enabled populations, so one cannot make too many overall pronouncements, because a lot of people don’t have access to the Internet.”
The data regarding young people are particularly powerful. “The idea that young people are having a decrease in their experience of mental health across the world is something I haven’t seen before.”
Dr. Duckworth suggested the reason might “have to do with the impact of the COVID lockdown on normal development that young people go through, while older people don’t struggle with these developmental challenges in the same way.”
A version of this article first appeared on Medscape.com.
Diagnosing adolescent ADHD
Pediatricians are increasingly expert in the assessment and treatment of attention-deficit/hyperactivity disorder. But what do you do when adolescents present to your office saying they think they have ADHD? While ADHD is a common and treatable disorder of youth, it is important to take special care when assessing an adolescent. Difficulties with attention and concentration are common symptoms for many different challenges of adolescence, and for ADHD to be the underlying cause, those symptoms must have started prior to adolescence (according to DSM-5, prior to the age of 12). When your adolescent patients or their parents come to your office complaining of inattention, it is important to consider the full range of possible explanations.
Sleep
We have written in this column previously about the challenges that adolescents face in getting adequate sleep consistently. Teenagers, on average, need more than 9 hours of sleep nightly and American teenagers get fewer than 6. This mismatch is because of physiologic shifts that move their natural sleep onset time significantly later, while school still starts early. It’s often compounded by other demands on their time, including homework, extracurricular activities, and the gravitational pull of social connections. Independent teenagers make their own decisions about how to manage their time and may feel sleep is optional, or manage their fatigue with naps and caffeine, both of which will further compromise the quality and efficiency of sleep.
Chronic sleep deprivation will present with difficulties with focus, attention, memory, and cognitive performance. Treatment of this problem with stimulants is likely to make the underlying poor sleep habits even worse. When your patient presents complaining of difficulty concentrating and worsening school performance, be sure to start with a thorough sleep history, and always provide guidance about the body’s need for sleep and healthy sleep habits.
Anxiety
Anxiety disorders are the most common psychiatric illnesses of youth, with estimates of as many as 30% of children and adolescents experiencing one. The true prevalence of ADHD is estimated to be about 4% of the population. Whether social phobia, generalized anxiety disorder, or even posttraumatic stress disorder, anxiety disorders interfere with attention as ruminative worry tends to distract those experiencing it. It can also affect attention and focus indirectly by interfering with restful sleep. Anxiety disorders can be difficult to identify, as the sufferers typically internalize their symptoms. But inquire about specific worries (such as speaking in front of others, meeting new people, or an illness or accident striking themselves or a loved one) and how much time they take up. Explore if worries fill their thoughts during quiet or downtime, and explore more about their worries. You may use a screening instrument such as the Pediatric Symptom Checklist or the SCARED, both of which will indicate a likely problem with anxiety. While it is possible to have comorbid ADHD with an anxiety disorder, the anxiety disorder will likely worsen with stimulants and should be treated first. These are usually curable illnesses and you may find that remission of anxiety symptoms resolves the attentional problems.
Depression
Mood disorders are less common than anxiety disorders in youth, but far more prevalent than ADHD. And depression is usually marked by serious difficulty concentrating across settings (including for things that were previously very interesting). A sullen teenager who is deeply self-critical about school performance would benefit from exploration of associated changes in mood, interests, energy, appetite, sleep, and for feelings of worthlessness, guilt, and suicidal thoughts. The PHQ9A is a simple, free screening instrument that is reasonable to use with every sick visit (and well-check) with your adolescent patients, given the risks of undetected and untreated depression. If your patient presents complaining of poor school performance, always screen for depression. As with anxiety disorders, comorbid ADHD is possible, but it is always recommended to treat the mood disorder first and then to assess for residual ADHD symptoms once the mood disorder is in remission.
Substance abuse
Adolescence is a time of exploration, and drug and alcohol use is common. While attentional impairment will happen with intoxication, occasional or rare use should not lead to consistent impairment in school. But when parents are more worried than their children about a significant change in school performance, it is important to screen for substance abuse. A child with a secret substance use disorder will often present with behavioral changes and deteriorating school performance and might deny any drug or alcohol use to parents. Indeed, stimulants have some street value and some patients may be seeking a stimulant prescription to sell or trade for other drugs. Regular marijuana use may present with only deteriorating school performance and no irritability or other noticeable behavioral changes. Marijuana is seen as safe and even healthy by many teenagers (and even many parents), and some youth may be using it recreationally or to manage difficulties with sleep, anxiety, or mood symptoms.
But there is compelling evidence that marijuana use causes cognitive impairment, including difficulty with sustaining attention, short-term memory, and processing speed, for as long as 24 hours after use. If a teenager is using marijuana daily after school, it is certainly going to interfere, in a dose-dependent manner, with attention and cognitive function. Sustained heavy use can lead to permanent cognitive deficits. It can also trigger or worsen anxiety or mood symptoms (contrary to much popular opinion).
Gathering a thorough substance use history is essential when assessing a teenager for difficulties with focus or attention, especially when these are accompanied by change in behavior and school performance. Remember, it is critical to interview these children without their parents present to invite them to be forthcoming with you.
History
While true ADHD should have been present throughout childhood, it is possible that the symptoms have become noticeable only in adolescence. For patients with very high intelligence and lower levels of impulsivity and hyperactivity, they might easily have “flown under the radar” during their elementary and even middle school years. Their difficulties with attention and focus might become apparent only when the volume and difficulty of schoolwork both are great enough that their intelligence is not enough to get good grades. That is, their problems with executive function, prioritizing, shifting sets, and completing tasks in a timely way make it impossible to keep up good grades when the work gets harder.
Your history should reveal a long history of dreaminess or distractibility, a tendency to lose and forget things, and the other symptoms of inattention. Did they often seem to not be listening when they were younger? Forget to hand in homework? Leave chores unfinished? Leave messes behind everywhere they went? These will not be definitive, but they do reassure that symptoms may have been present for a long time, even if school performance was considered fine until the workload got too large. If such problems were not present before puberty, consider whether a subtle learning disability could be impairing them as they face more challenging academic subjects.
If you have ruled out anxiety, mood, and substance use concerns, and helped them to address a sleep deficit, then you can proceed. It is worthwhile to get Vanderbilt Assessments as you would for a younger child. If they meet criteria, discuss the risks and benefits of medication, executive skills coaching, and environmental adjustments (extra time for tests, a less stimulating environment) that can help them explore academic challenges without the discouragement that ADHD can bring.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at [email protected].
Pediatricians are increasingly expert in the assessment and treatment of attention-deficit/hyperactivity disorder. But what do you do when adolescents present to your office saying they think they have ADHD? While ADHD is a common and treatable disorder of youth, it is important to take special care when assessing an adolescent. Difficulties with attention and concentration are common symptoms for many different challenges of adolescence, and for ADHD to be the underlying cause, those symptoms must have started prior to adolescence (according to DSM-5, prior to the age of 12). When your adolescent patients or their parents come to your office complaining of inattention, it is important to consider the full range of possible explanations.
Sleep
We have written in this column previously about the challenges that adolescents face in getting adequate sleep consistently. Teenagers, on average, need more than 9 hours of sleep nightly and American teenagers get fewer than 6. This mismatch is because of physiologic shifts that move their natural sleep onset time significantly later, while school still starts early. It’s often compounded by other demands on their time, including homework, extracurricular activities, and the gravitational pull of social connections. Independent teenagers make their own decisions about how to manage their time and may feel sleep is optional, or manage their fatigue with naps and caffeine, both of which will further compromise the quality and efficiency of sleep.
Chronic sleep deprivation will present with difficulties with focus, attention, memory, and cognitive performance. Treatment of this problem with stimulants is likely to make the underlying poor sleep habits even worse. When your patient presents complaining of difficulty concentrating and worsening school performance, be sure to start with a thorough sleep history, and always provide guidance about the body’s need for sleep and healthy sleep habits.
Anxiety
Anxiety disorders are the most common psychiatric illnesses of youth, with estimates of as many as 30% of children and adolescents experiencing one. The true prevalence of ADHD is estimated to be about 4% of the population. Whether social phobia, generalized anxiety disorder, or even posttraumatic stress disorder, anxiety disorders interfere with attention as ruminative worry tends to distract those experiencing it. It can also affect attention and focus indirectly by interfering with restful sleep. Anxiety disorders can be difficult to identify, as the sufferers typically internalize their symptoms. But inquire about specific worries (such as speaking in front of others, meeting new people, or an illness or accident striking themselves or a loved one) and how much time they take up. Explore if worries fill their thoughts during quiet or downtime, and explore more about their worries. You may use a screening instrument such as the Pediatric Symptom Checklist or the SCARED, both of which will indicate a likely problem with anxiety. While it is possible to have comorbid ADHD with an anxiety disorder, the anxiety disorder will likely worsen with stimulants and should be treated first. These are usually curable illnesses and you may find that remission of anxiety symptoms resolves the attentional problems.
Depression
Mood disorders are less common than anxiety disorders in youth, but far more prevalent than ADHD. And depression is usually marked by serious difficulty concentrating across settings (including for things that were previously very interesting). A sullen teenager who is deeply self-critical about school performance would benefit from exploration of associated changes in mood, interests, energy, appetite, sleep, and for feelings of worthlessness, guilt, and suicidal thoughts. The PHQ9A is a simple, free screening instrument that is reasonable to use with every sick visit (and well-check) with your adolescent patients, given the risks of undetected and untreated depression. If your patient presents complaining of poor school performance, always screen for depression. As with anxiety disorders, comorbid ADHD is possible, but it is always recommended to treat the mood disorder first and then to assess for residual ADHD symptoms once the mood disorder is in remission.
Substance abuse
Adolescence is a time of exploration, and drug and alcohol use is common. While attentional impairment will happen with intoxication, occasional or rare use should not lead to consistent impairment in school. But when parents are more worried than their children about a significant change in school performance, it is important to screen for substance abuse. A child with a secret substance use disorder will often present with behavioral changes and deteriorating school performance and might deny any drug or alcohol use to parents. Indeed, stimulants have some street value and some patients may be seeking a stimulant prescription to sell or trade for other drugs. Regular marijuana use may present with only deteriorating school performance and no irritability or other noticeable behavioral changes. Marijuana is seen as safe and even healthy by many teenagers (and even many parents), and some youth may be using it recreationally or to manage difficulties with sleep, anxiety, or mood symptoms.
But there is compelling evidence that marijuana use causes cognitive impairment, including difficulty with sustaining attention, short-term memory, and processing speed, for as long as 24 hours after use. If a teenager is using marijuana daily after school, it is certainly going to interfere, in a dose-dependent manner, with attention and cognitive function. Sustained heavy use can lead to permanent cognitive deficits. It can also trigger or worsen anxiety or mood symptoms (contrary to much popular opinion).
Gathering a thorough substance use history is essential when assessing a teenager for difficulties with focus or attention, especially when these are accompanied by change in behavior and school performance. Remember, it is critical to interview these children without their parents present to invite them to be forthcoming with you.
History
While true ADHD should have been present throughout childhood, it is possible that the symptoms have become noticeable only in adolescence. For patients with very high intelligence and lower levels of impulsivity and hyperactivity, they might easily have “flown under the radar” during their elementary and even middle school years. Their difficulties with attention and focus might become apparent only when the volume and difficulty of schoolwork both are great enough that their intelligence is not enough to get good grades. That is, their problems with executive function, prioritizing, shifting sets, and completing tasks in a timely way make it impossible to keep up good grades when the work gets harder.
Your history should reveal a long history of dreaminess or distractibility, a tendency to lose and forget things, and the other symptoms of inattention. Did they often seem to not be listening when they were younger? Forget to hand in homework? Leave chores unfinished? Leave messes behind everywhere they went? These will not be definitive, but they do reassure that symptoms may have been present for a long time, even if school performance was considered fine until the workload got too large. If such problems were not present before puberty, consider whether a subtle learning disability could be impairing them as they face more challenging academic subjects.
If you have ruled out anxiety, mood, and substance use concerns, and helped them to address a sleep deficit, then you can proceed. It is worthwhile to get Vanderbilt Assessments as you would for a younger child. If they meet criteria, discuss the risks and benefits of medication, executive skills coaching, and environmental adjustments (extra time for tests, a less stimulating environment) that can help them explore academic challenges without the discouragement that ADHD can bring.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at [email protected].
Pediatricians are increasingly expert in the assessment and treatment of attention-deficit/hyperactivity disorder. But what do you do when adolescents present to your office saying they think they have ADHD? While ADHD is a common and treatable disorder of youth, it is important to take special care when assessing an adolescent. Difficulties with attention and concentration are common symptoms for many different challenges of adolescence, and for ADHD to be the underlying cause, those symptoms must have started prior to adolescence (according to DSM-5, prior to the age of 12). When your adolescent patients or their parents come to your office complaining of inattention, it is important to consider the full range of possible explanations.
Sleep
We have written in this column previously about the challenges that adolescents face in getting adequate sleep consistently. Teenagers, on average, need more than 9 hours of sleep nightly and American teenagers get fewer than 6. This mismatch is because of physiologic shifts that move their natural sleep onset time significantly later, while school still starts early. It’s often compounded by other demands on their time, including homework, extracurricular activities, and the gravitational pull of social connections. Independent teenagers make their own decisions about how to manage their time and may feel sleep is optional, or manage their fatigue with naps and caffeine, both of which will further compromise the quality and efficiency of sleep.
Chronic sleep deprivation will present with difficulties with focus, attention, memory, and cognitive performance. Treatment of this problem with stimulants is likely to make the underlying poor sleep habits even worse. When your patient presents complaining of difficulty concentrating and worsening school performance, be sure to start with a thorough sleep history, and always provide guidance about the body’s need for sleep and healthy sleep habits.
Anxiety
Anxiety disorders are the most common psychiatric illnesses of youth, with estimates of as many as 30% of children and adolescents experiencing one. The true prevalence of ADHD is estimated to be about 4% of the population. Whether social phobia, generalized anxiety disorder, or even posttraumatic stress disorder, anxiety disorders interfere with attention as ruminative worry tends to distract those experiencing it. It can also affect attention and focus indirectly by interfering with restful sleep. Anxiety disorders can be difficult to identify, as the sufferers typically internalize their symptoms. But inquire about specific worries (such as speaking in front of others, meeting new people, or an illness or accident striking themselves or a loved one) and how much time they take up. Explore if worries fill their thoughts during quiet or downtime, and explore more about their worries. You may use a screening instrument such as the Pediatric Symptom Checklist or the SCARED, both of which will indicate a likely problem with anxiety. While it is possible to have comorbid ADHD with an anxiety disorder, the anxiety disorder will likely worsen with stimulants and should be treated first. These are usually curable illnesses and you may find that remission of anxiety symptoms resolves the attentional problems.
Depression
Mood disorders are less common than anxiety disorders in youth, but far more prevalent than ADHD. And depression is usually marked by serious difficulty concentrating across settings (including for things that were previously very interesting). A sullen teenager who is deeply self-critical about school performance would benefit from exploration of associated changes in mood, interests, energy, appetite, sleep, and for feelings of worthlessness, guilt, and suicidal thoughts. The PHQ9A is a simple, free screening instrument that is reasonable to use with every sick visit (and well-check) with your adolescent patients, given the risks of undetected and untreated depression. If your patient presents complaining of poor school performance, always screen for depression. As with anxiety disorders, comorbid ADHD is possible, but it is always recommended to treat the mood disorder first and then to assess for residual ADHD symptoms once the mood disorder is in remission.
Substance abuse
Adolescence is a time of exploration, and drug and alcohol use is common. While attentional impairment will happen with intoxication, occasional or rare use should not lead to consistent impairment in school. But when parents are more worried than their children about a significant change in school performance, it is important to screen for substance abuse. A child with a secret substance use disorder will often present with behavioral changes and deteriorating school performance and might deny any drug or alcohol use to parents. Indeed, stimulants have some street value and some patients may be seeking a stimulant prescription to sell or trade for other drugs. Regular marijuana use may present with only deteriorating school performance and no irritability or other noticeable behavioral changes. Marijuana is seen as safe and even healthy by many teenagers (and even many parents), and some youth may be using it recreationally or to manage difficulties with sleep, anxiety, or mood symptoms.
But there is compelling evidence that marijuana use causes cognitive impairment, including difficulty with sustaining attention, short-term memory, and processing speed, for as long as 24 hours after use. If a teenager is using marijuana daily after school, it is certainly going to interfere, in a dose-dependent manner, with attention and cognitive function. Sustained heavy use can lead to permanent cognitive deficits. It can also trigger or worsen anxiety or mood symptoms (contrary to much popular opinion).
Gathering a thorough substance use history is essential when assessing a teenager for difficulties with focus or attention, especially when these are accompanied by change in behavior and school performance. Remember, it is critical to interview these children without their parents present to invite them to be forthcoming with you.
History
While true ADHD should have been present throughout childhood, it is possible that the symptoms have become noticeable only in adolescence. For patients with very high intelligence and lower levels of impulsivity and hyperactivity, they might easily have “flown under the radar” during their elementary and even middle school years. Their difficulties with attention and focus might become apparent only when the volume and difficulty of schoolwork both are great enough that their intelligence is not enough to get good grades. That is, their problems with executive function, prioritizing, shifting sets, and completing tasks in a timely way make it impossible to keep up good grades when the work gets harder.
Your history should reveal a long history of dreaminess or distractibility, a tendency to lose and forget things, and the other symptoms of inattention. Did they often seem to not be listening when they were younger? Forget to hand in homework? Leave chores unfinished? Leave messes behind everywhere they went? These will not be definitive, but they do reassure that symptoms may have been present for a long time, even if school performance was considered fine until the workload got too large. If such problems were not present before puberty, consider whether a subtle learning disability could be impairing them as they face more challenging academic subjects.
If you have ruled out anxiety, mood, and substance use concerns, and helped them to address a sleep deficit, then you can proceed. It is worthwhile to get Vanderbilt Assessments as you would for a younger child. If they meet criteria, discuss the risks and benefits of medication, executive skills coaching, and environmental adjustments (extra time for tests, a less stimulating environment) that can help them explore academic challenges without the discouragement that ADHD can bring.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at [email protected].
‘Bigorexia’: Why teenage boys are obsessed with bulking up
Why are teenage boys obsessed with bulking up?
While the effects of Instagram on girls’ body image has long been documented – an article in The Wall Street Journal that was published this fall reported that Facebook knew Instagram was toxic for teen girls – teenage boys are under just as much pressure.
For adolescent boys, the goal is often to get superhero-size buff – and this is leading to anxiety, stress, excessive selfies, and, often, obsessive staring in the mirror to assess their “pec” progress.
So-called “bigorexia” – or extreme gym time, excessive focus on protein diets, and intense muscle-building goals – has hit new and concerning levels, according to a recent New York Times report.
Whether it’s the pandemic or TikTok that’s to blame, teen boys are pushing hard to achieve six-pack abs, with one-third of them in the U.S. trying to bulk up, according to a study published in the Journal of Adolescent Health. What’s more, 22% reported they’re engaging in muscle-enhancing behavior, including excess exercise, taking supplements or steroids, or eating more to bulk up, according to a study published in the International Journal of Eating Disorders.
“The pandemic and social media have been a perfect storm for eating disorders and body image issues for all teens, but this has been under-recognized in boys,” says Jason Nagata, MD, a pediatrician who specializes in adolescent medicine at the University of California, San Francisco. “Both are directly connected to an increase in muscle dysmorphia.”
While “bigorexia” is a newer term coined by mental health professionals, the concept of muscular dysmorphia isn’t, says Jennifer Bahrman, PhD, a licensed psychologist with McGovern Medical School at UTHealth Houston. This may be why about a third of boys ages 11-18 reported that they aren’t enamored with their bodies, according to a small survey published in 2019 in the Californian Journal of Health Promotion.
“When we think of dysmorphia, we think of girls having it, since we see it more in females,” says Dr. Bahrman, who works extensively with adolescents and athletes. “The interesting thing about muscular dysmorphia is that it’s the only body dysmorphic disorder that’s almost exclusively present in males.”
Social media’s role
Unlike other things in boys’ lives, like movies, TV, or even the uber-buff GI Joe doll, social media has created opportunities for young men to put their bodies on display – and become an influencer or get followers because of it.
“An everyday teen can become a celebrity,” Dr. Nagata says. “Then, thanks to social media algorithms, if a teenage boy likes or interacts with a post that features a muscular guy or is all about fitness, they’ll start getting all sorts of related content. They’ll get bombarded with tons of ads for protein shakes, for example, as well as bodybuilding equipment, and that will further distort reality.”
Before-and-after photos are also known to be quite misleading.
“Some of the most popular Instagram posts among teens feature people who have experienced a massive body transformation,” Dr. Nagata says. “It’s usually someone who lost a lot of weight or someone who was scrawny and then got muscular. The most drastic changes tend to get the most likes and are perpetuated the most and shared the most often with friends.”
But as many are aware, photos posted to social media are selected to tell the best story – with the best filters, lighting, and angles possible, however exaggerated.
“A guy will post his worst picture out of a thousand for his before shot and then post the best photo out of a thousand,” Dr. Nagata says. “This, in itself, can really confuse a teenager, because the story of this person’s changed body looks so realistic.”
Worse, these images tend to be damaging to your teenager’s self-esteem.
“When you see images of people you’re aspiring to look like, it can be very upsetting,” Dr. Bahrman says. “After all, it’s easy to think, ‘I’m doing all of these pushups, and I don’t look like this.’ From there, it’s easy to begin internalizing that something is wrong with you.”
Red flags to watch out for
If you’ve noticed that your son is obsessed with his appearance, weight, food, or exercise, take note. Also, notice if he’s asking you to buy protein powder or is spending more time at the gym than with his friends.
“Pay attention if he is withdrawing from friends and family because of his concerns about his appearance,” Dr. Nagata says. “For example, we often hear that a teenager will no longer eat family meals or at a restaurant because the protein content isn’t high enough or the food is too fatty.”
If you’re concerned, always make sure to discuss this with your son’s pediatrician.
“Ultimately, you want to make sure you share your concerns before your teen son becomes even more body-image obsessed,” Dr. Nagata says.
A version of this article first appeared on WebMD.com.
Why are teenage boys obsessed with bulking up?
While the effects of Instagram on girls’ body image has long been documented – an article in The Wall Street Journal that was published this fall reported that Facebook knew Instagram was toxic for teen girls – teenage boys are under just as much pressure.
For adolescent boys, the goal is often to get superhero-size buff – and this is leading to anxiety, stress, excessive selfies, and, often, obsessive staring in the mirror to assess their “pec” progress.
So-called “bigorexia” – or extreme gym time, excessive focus on protein diets, and intense muscle-building goals – has hit new and concerning levels, according to a recent New York Times report.
Whether it’s the pandemic or TikTok that’s to blame, teen boys are pushing hard to achieve six-pack abs, with one-third of them in the U.S. trying to bulk up, according to a study published in the Journal of Adolescent Health. What’s more, 22% reported they’re engaging in muscle-enhancing behavior, including excess exercise, taking supplements or steroids, or eating more to bulk up, according to a study published in the International Journal of Eating Disorders.
“The pandemic and social media have been a perfect storm for eating disorders and body image issues for all teens, but this has been under-recognized in boys,” says Jason Nagata, MD, a pediatrician who specializes in adolescent medicine at the University of California, San Francisco. “Both are directly connected to an increase in muscle dysmorphia.”
While “bigorexia” is a newer term coined by mental health professionals, the concept of muscular dysmorphia isn’t, says Jennifer Bahrman, PhD, a licensed psychologist with McGovern Medical School at UTHealth Houston. This may be why about a third of boys ages 11-18 reported that they aren’t enamored with their bodies, according to a small survey published in 2019 in the Californian Journal of Health Promotion.
“When we think of dysmorphia, we think of girls having it, since we see it more in females,” says Dr. Bahrman, who works extensively with adolescents and athletes. “The interesting thing about muscular dysmorphia is that it’s the only body dysmorphic disorder that’s almost exclusively present in males.”
Social media’s role
Unlike other things in boys’ lives, like movies, TV, or even the uber-buff GI Joe doll, social media has created opportunities for young men to put their bodies on display – and become an influencer or get followers because of it.
“An everyday teen can become a celebrity,” Dr. Nagata says. “Then, thanks to social media algorithms, if a teenage boy likes or interacts with a post that features a muscular guy or is all about fitness, they’ll start getting all sorts of related content. They’ll get bombarded with tons of ads for protein shakes, for example, as well as bodybuilding equipment, and that will further distort reality.”
Before-and-after photos are also known to be quite misleading.
“Some of the most popular Instagram posts among teens feature people who have experienced a massive body transformation,” Dr. Nagata says. “It’s usually someone who lost a lot of weight or someone who was scrawny and then got muscular. The most drastic changes tend to get the most likes and are perpetuated the most and shared the most often with friends.”
But as many are aware, photos posted to social media are selected to tell the best story – with the best filters, lighting, and angles possible, however exaggerated.
“A guy will post his worst picture out of a thousand for his before shot and then post the best photo out of a thousand,” Dr. Nagata says. “This, in itself, can really confuse a teenager, because the story of this person’s changed body looks so realistic.”
Worse, these images tend to be damaging to your teenager’s self-esteem.
“When you see images of people you’re aspiring to look like, it can be very upsetting,” Dr. Bahrman says. “After all, it’s easy to think, ‘I’m doing all of these pushups, and I don’t look like this.’ From there, it’s easy to begin internalizing that something is wrong with you.”
Red flags to watch out for
If you’ve noticed that your son is obsessed with his appearance, weight, food, or exercise, take note. Also, notice if he’s asking you to buy protein powder or is spending more time at the gym than with his friends.
“Pay attention if he is withdrawing from friends and family because of his concerns about his appearance,” Dr. Nagata says. “For example, we often hear that a teenager will no longer eat family meals or at a restaurant because the protein content isn’t high enough or the food is too fatty.”
If you’re concerned, always make sure to discuss this with your son’s pediatrician.
“Ultimately, you want to make sure you share your concerns before your teen son becomes even more body-image obsessed,” Dr. Nagata says.
A version of this article first appeared on WebMD.com.
Why are teenage boys obsessed with bulking up?
While the effects of Instagram on girls’ body image has long been documented – an article in The Wall Street Journal that was published this fall reported that Facebook knew Instagram was toxic for teen girls – teenage boys are under just as much pressure.
For adolescent boys, the goal is often to get superhero-size buff – and this is leading to anxiety, stress, excessive selfies, and, often, obsessive staring in the mirror to assess their “pec” progress.
So-called “bigorexia” – or extreme gym time, excessive focus on protein diets, and intense muscle-building goals – has hit new and concerning levels, according to a recent New York Times report.
Whether it’s the pandemic or TikTok that’s to blame, teen boys are pushing hard to achieve six-pack abs, with one-third of them in the U.S. trying to bulk up, according to a study published in the Journal of Adolescent Health. What’s more, 22% reported they’re engaging in muscle-enhancing behavior, including excess exercise, taking supplements or steroids, or eating more to bulk up, according to a study published in the International Journal of Eating Disorders.
“The pandemic and social media have been a perfect storm for eating disorders and body image issues for all teens, but this has been under-recognized in boys,” says Jason Nagata, MD, a pediatrician who specializes in adolescent medicine at the University of California, San Francisco. “Both are directly connected to an increase in muscle dysmorphia.”
While “bigorexia” is a newer term coined by mental health professionals, the concept of muscular dysmorphia isn’t, says Jennifer Bahrman, PhD, a licensed psychologist with McGovern Medical School at UTHealth Houston. This may be why about a third of boys ages 11-18 reported that they aren’t enamored with their bodies, according to a small survey published in 2019 in the Californian Journal of Health Promotion.
“When we think of dysmorphia, we think of girls having it, since we see it more in females,” says Dr. Bahrman, who works extensively with adolescents and athletes. “The interesting thing about muscular dysmorphia is that it’s the only body dysmorphic disorder that’s almost exclusively present in males.”
Social media’s role
Unlike other things in boys’ lives, like movies, TV, or even the uber-buff GI Joe doll, social media has created opportunities for young men to put their bodies on display – and become an influencer or get followers because of it.
“An everyday teen can become a celebrity,” Dr. Nagata says. “Then, thanks to social media algorithms, if a teenage boy likes or interacts with a post that features a muscular guy or is all about fitness, they’ll start getting all sorts of related content. They’ll get bombarded with tons of ads for protein shakes, for example, as well as bodybuilding equipment, and that will further distort reality.”
Before-and-after photos are also known to be quite misleading.
“Some of the most popular Instagram posts among teens feature people who have experienced a massive body transformation,” Dr. Nagata says. “It’s usually someone who lost a lot of weight or someone who was scrawny and then got muscular. The most drastic changes tend to get the most likes and are perpetuated the most and shared the most often with friends.”
But as many are aware, photos posted to social media are selected to tell the best story – with the best filters, lighting, and angles possible, however exaggerated.
“A guy will post his worst picture out of a thousand for his before shot and then post the best photo out of a thousand,” Dr. Nagata says. “This, in itself, can really confuse a teenager, because the story of this person’s changed body looks so realistic.”
Worse, these images tend to be damaging to your teenager’s self-esteem.
“When you see images of people you’re aspiring to look like, it can be very upsetting,” Dr. Bahrman says. “After all, it’s easy to think, ‘I’m doing all of these pushups, and I don’t look like this.’ From there, it’s easy to begin internalizing that something is wrong with you.”
Red flags to watch out for
If you’ve noticed that your son is obsessed with his appearance, weight, food, or exercise, take note. Also, notice if he’s asking you to buy protein powder or is spending more time at the gym than with his friends.
“Pay attention if he is withdrawing from friends and family because of his concerns about his appearance,” Dr. Nagata says. “For example, we often hear that a teenager will no longer eat family meals or at a restaurant because the protein content isn’t high enough or the food is too fatty.”
If you’re concerned, always make sure to discuss this with your son’s pediatrician.
“Ultimately, you want to make sure you share your concerns before your teen son becomes even more body-image obsessed,” Dr. Nagata says.
A version of this article first appeared on WebMD.com.
Prescription video game focuses attention in ADHD
Investigators found children who used the video game-based therapy (EndeavorRx) experienced increased brain activity related to attention function, as measured by EEG, which correlated with improvements in objective behavioral measures of attention.
“While the previous multicenter trials show attention improvement for children using EndeavorRx, this is the first study to look at the brain activity in children with a primary concern of ADHD,” principal investigator Elysa Marco, MD, clinical executive for neurodevelopmental medicine at Cortica Healthcare, San Rafael, Calif., said in news release.
“It is exciting to see measurable improvement on the EEGs that correlates with the behavioral benefits,” said Dr. Marco.
The study was recently published online in PLOS ONE.
Measurable changes
As previously reported by this news organization, the Food and Drug Administration approved EndeavorRx in June 2020 as a prescription video game–based therapeutic device for children aged 8-12 years with primarily inattentive or combined-type ADHD, who have a demonstrated attention issue.
“The device is intended for use as part of a therapeutic program that may include clinician-directed therapy, medication, and/or educational programs, which further address symptoms of the disorder,” the FDA said upon approval.
In the current unblinded, single-arm study, the researchers assessed 25 children (aged 8-12 years) with a confirmed diagnosis of ADHD on neural, behavioral, and clinical metrics of attention before and after a 4-week at-home intervention.
Participants were instructed to use EndeavorRx for about 25 minutes a day at least 5 days a week for 4 weeks, as recommended by the FDA.
“EndeavorRx enhanced midline frontal theta (MFT) activity, suggesting that patients who used EndeavorRx for 4 weeks showed changes in measurable brain function,” Anil S. Jina, MD, chief medical officer of Akili Interactive, told this news organization. Dr. Jina was not involved with the study.
There was also a correlation between MFT activity and attention functioning, “suggesting that children who experienced the largest gains in MFT activity as measured by EEG also showed the greatest improvements in computerized performance tests designed to measure attention,” Dr. Jina said.
In addition, parents reported significantly fewer inattention symptoms in children after EndeavorRx treatment, as measured by the Vanderbilt ADHD Diagnostic Rating Scale.
‘Not just another video game’
EndeavorRx has been evaluated in five clinical studies involving more than 600 children with ADHD, including the STARS-ADHD trial, a prospective, randomized, controlled study published in The Lancet Digital Health.
The STARS-ADHD trial randomly allocated 348 children to either EndeavorRx treatment or a controlled intervention, which was a word game.
The researchers reported statistically significant improvements in attentional functioning in the EndeavorRx group as rated by test of variables of attention.
“This is not just another video game,” STARS-ADHD trialist Scott H. Kollins, PhD, MS, a clinical psychologist at Duke Health’s ADHD Clinic in Durham, N.C., who helped developed it, previously told this news organization.
The tool’s adaptive algorithms adjust and monitor task difficulty based on performance, using a video game format and rewards to engage users, he explained. EndeavorRx is a challenge to play by design.
“The treatment was programmed into the gameplay experience and designed to challenge a child’s attentional control during gameplay, requiring focus and flexibility to manage tasks at the same time,” Dr. Jina said in an interview.
“Unlike a video game that is designed only for entertainment purposes, to drive efficacy, EndeavorRx is designed to be challenging and can therefore sometimes feel repetitive, and frustrating to some children,” Dr. Jina said.
Commenting on the study, Stephen Faraone, PhD, distinguished professor of psychiatry and vice chair of research, department of psychiatry, State University of New York, Syracuse, said this study “supports the idea that EndeavorRx improves a neural measure of attention.
“The limitation is that we don’t know if this translates into clinically relevant outcomes,” cautioned Dr. Faraone, who was not associated with the current study.
“The main caveat about EndeavorRx is that it was cleared by the FDA for improving a computer-based measure of inattention, not inattentive symptoms as reported by the parents of children with ADHD,” he noted.
Several authors have disclosed financial relationships with Akili Interactive Labs, which funded the study. Dr. Faraone was an investigator on the STARS-ADHD trial.
A version of this article first appeared on Medscape.com.
Investigators found children who used the video game-based therapy (EndeavorRx) experienced increased brain activity related to attention function, as measured by EEG, which correlated with improvements in objective behavioral measures of attention.
“While the previous multicenter trials show attention improvement for children using EndeavorRx, this is the first study to look at the brain activity in children with a primary concern of ADHD,” principal investigator Elysa Marco, MD, clinical executive for neurodevelopmental medicine at Cortica Healthcare, San Rafael, Calif., said in news release.
“It is exciting to see measurable improvement on the EEGs that correlates with the behavioral benefits,” said Dr. Marco.
The study was recently published online in PLOS ONE.
Measurable changes
As previously reported by this news organization, the Food and Drug Administration approved EndeavorRx in June 2020 as a prescription video game–based therapeutic device for children aged 8-12 years with primarily inattentive or combined-type ADHD, who have a demonstrated attention issue.
“The device is intended for use as part of a therapeutic program that may include clinician-directed therapy, medication, and/or educational programs, which further address symptoms of the disorder,” the FDA said upon approval.
In the current unblinded, single-arm study, the researchers assessed 25 children (aged 8-12 years) with a confirmed diagnosis of ADHD on neural, behavioral, and clinical metrics of attention before and after a 4-week at-home intervention.
Participants were instructed to use EndeavorRx for about 25 minutes a day at least 5 days a week for 4 weeks, as recommended by the FDA.
“EndeavorRx enhanced midline frontal theta (MFT) activity, suggesting that patients who used EndeavorRx for 4 weeks showed changes in measurable brain function,” Anil S. Jina, MD, chief medical officer of Akili Interactive, told this news organization. Dr. Jina was not involved with the study.
There was also a correlation between MFT activity and attention functioning, “suggesting that children who experienced the largest gains in MFT activity as measured by EEG also showed the greatest improvements in computerized performance tests designed to measure attention,” Dr. Jina said.
In addition, parents reported significantly fewer inattention symptoms in children after EndeavorRx treatment, as measured by the Vanderbilt ADHD Diagnostic Rating Scale.
‘Not just another video game’
EndeavorRx has been evaluated in five clinical studies involving more than 600 children with ADHD, including the STARS-ADHD trial, a prospective, randomized, controlled study published in The Lancet Digital Health.
The STARS-ADHD trial randomly allocated 348 children to either EndeavorRx treatment or a controlled intervention, which was a word game.
The researchers reported statistically significant improvements in attentional functioning in the EndeavorRx group as rated by test of variables of attention.
“This is not just another video game,” STARS-ADHD trialist Scott H. Kollins, PhD, MS, a clinical psychologist at Duke Health’s ADHD Clinic in Durham, N.C., who helped developed it, previously told this news organization.
The tool’s adaptive algorithms adjust and monitor task difficulty based on performance, using a video game format and rewards to engage users, he explained. EndeavorRx is a challenge to play by design.
“The treatment was programmed into the gameplay experience and designed to challenge a child’s attentional control during gameplay, requiring focus and flexibility to manage tasks at the same time,” Dr. Jina said in an interview.
“Unlike a video game that is designed only for entertainment purposes, to drive efficacy, EndeavorRx is designed to be challenging and can therefore sometimes feel repetitive, and frustrating to some children,” Dr. Jina said.
Commenting on the study, Stephen Faraone, PhD, distinguished professor of psychiatry and vice chair of research, department of psychiatry, State University of New York, Syracuse, said this study “supports the idea that EndeavorRx improves a neural measure of attention.
“The limitation is that we don’t know if this translates into clinically relevant outcomes,” cautioned Dr. Faraone, who was not associated with the current study.
“The main caveat about EndeavorRx is that it was cleared by the FDA for improving a computer-based measure of inattention, not inattentive symptoms as reported by the parents of children with ADHD,” he noted.
Several authors have disclosed financial relationships with Akili Interactive Labs, which funded the study. Dr. Faraone was an investigator on the STARS-ADHD trial.
A version of this article first appeared on Medscape.com.
Investigators found children who used the video game-based therapy (EndeavorRx) experienced increased brain activity related to attention function, as measured by EEG, which correlated with improvements in objective behavioral measures of attention.
“While the previous multicenter trials show attention improvement for children using EndeavorRx, this is the first study to look at the brain activity in children with a primary concern of ADHD,” principal investigator Elysa Marco, MD, clinical executive for neurodevelopmental medicine at Cortica Healthcare, San Rafael, Calif., said in news release.
“It is exciting to see measurable improvement on the EEGs that correlates with the behavioral benefits,” said Dr. Marco.
The study was recently published online in PLOS ONE.
Measurable changes
As previously reported by this news organization, the Food and Drug Administration approved EndeavorRx in June 2020 as a prescription video game–based therapeutic device for children aged 8-12 years with primarily inattentive or combined-type ADHD, who have a demonstrated attention issue.
“The device is intended for use as part of a therapeutic program that may include clinician-directed therapy, medication, and/or educational programs, which further address symptoms of the disorder,” the FDA said upon approval.
In the current unblinded, single-arm study, the researchers assessed 25 children (aged 8-12 years) with a confirmed diagnosis of ADHD on neural, behavioral, and clinical metrics of attention before and after a 4-week at-home intervention.
Participants were instructed to use EndeavorRx for about 25 minutes a day at least 5 days a week for 4 weeks, as recommended by the FDA.
“EndeavorRx enhanced midline frontal theta (MFT) activity, suggesting that patients who used EndeavorRx for 4 weeks showed changes in measurable brain function,” Anil S. Jina, MD, chief medical officer of Akili Interactive, told this news organization. Dr. Jina was not involved with the study.
There was also a correlation between MFT activity and attention functioning, “suggesting that children who experienced the largest gains in MFT activity as measured by EEG also showed the greatest improvements in computerized performance tests designed to measure attention,” Dr. Jina said.
In addition, parents reported significantly fewer inattention symptoms in children after EndeavorRx treatment, as measured by the Vanderbilt ADHD Diagnostic Rating Scale.
‘Not just another video game’
EndeavorRx has been evaluated in five clinical studies involving more than 600 children with ADHD, including the STARS-ADHD trial, a prospective, randomized, controlled study published in The Lancet Digital Health.
The STARS-ADHD trial randomly allocated 348 children to either EndeavorRx treatment or a controlled intervention, which was a word game.
The researchers reported statistically significant improvements in attentional functioning in the EndeavorRx group as rated by test of variables of attention.
“This is not just another video game,” STARS-ADHD trialist Scott H. Kollins, PhD, MS, a clinical psychologist at Duke Health’s ADHD Clinic in Durham, N.C., who helped developed it, previously told this news organization.
The tool’s adaptive algorithms adjust and monitor task difficulty based on performance, using a video game format and rewards to engage users, he explained. EndeavorRx is a challenge to play by design.
“The treatment was programmed into the gameplay experience and designed to challenge a child’s attentional control during gameplay, requiring focus and flexibility to manage tasks at the same time,” Dr. Jina said in an interview.
“Unlike a video game that is designed only for entertainment purposes, to drive efficacy, EndeavorRx is designed to be challenging and can therefore sometimes feel repetitive, and frustrating to some children,” Dr. Jina said.
Commenting on the study, Stephen Faraone, PhD, distinguished professor of psychiatry and vice chair of research, department of psychiatry, State University of New York, Syracuse, said this study “supports the idea that EndeavorRx improves a neural measure of attention.
“The limitation is that we don’t know if this translates into clinically relevant outcomes,” cautioned Dr. Faraone, who was not associated with the current study.
“The main caveat about EndeavorRx is that it was cleared by the FDA for improving a computer-based measure of inattention, not inattentive symptoms as reported by the parents of children with ADHD,” he noted.
Several authors have disclosed financial relationships with Akili Interactive Labs, which funded the study. Dr. Faraone was an investigator on the STARS-ADHD trial.
A version of this article first appeared on Medscape.com.











