User login
Ultraviolet Radiation and Melanoma
Holly E. Kanavy, DO, and Meg R. Gerstenblith, MD
Melanoma is a particularly aggressive type of skin cancer, and its incidence has been increasing steadily since the 1970s. This article will review the extensive epidemiologic data demonstrating that ultraviolet radiation (UVR) exposure, from the sun or artificial tanning beds, is the most important environmental risk factor for melanoma; the multiple detrimental effects of UVR on human skin, including DNA damage through the formation of dimeric photoproducts, gene mutations, oxidative stress, inflammation, and immunosuppression, all of which contribute to melanomagenesis; and the evidence that protection from UVR exposure, whether by melanin or by sunscreen, reduces the risk of developing melanoma.
*For a PDF of the full article, click on the link to the left of this introduction.
Holly E. Kanavy, DO, and Meg R. Gerstenblith, MD
Melanoma is a particularly aggressive type of skin cancer, and its incidence has been increasing steadily since the 1970s. This article will review the extensive epidemiologic data demonstrating that ultraviolet radiation (UVR) exposure, from the sun or artificial tanning beds, is the most important environmental risk factor for melanoma; the multiple detrimental effects of UVR on human skin, including DNA damage through the formation of dimeric photoproducts, gene mutations, oxidative stress, inflammation, and immunosuppression, all of which contribute to melanomagenesis; and the evidence that protection from UVR exposure, whether by melanin or by sunscreen, reduces the risk of developing melanoma.
*For a PDF of the full article, click on the link to the left of this introduction.
Holly E. Kanavy, DO, and Meg R. Gerstenblith, MD
Melanoma is a particularly aggressive type of skin cancer, and its incidence has been increasing steadily since the 1970s. This article will review the extensive epidemiologic data demonstrating that ultraviolet radiation (UVR) exposure, from the sun or artificial tanning beds, is the most important environmental risk factor for melanoma; the multiple detrimental effects of UVR on human skin, including DNA damage through the formation of dimeric photoproducts, gene mutations, oxidative stress, inflammation, and immunosuppression, all of which contribute to melanomagenesis; and the evidence that protection from UVR exposure, whether by melanin or by sunscreen, reduces the risk of developing melanoma.
*For a PDF of the full article, click on the link to the left of this introduction.
Update on Photodermatoses
Frank A. Santoro, MD, and Henry W. Lim, MD
Interactions with ultraviolet radiation (UVR) and chromophores in the skin happen on a daily basis. Photodermatoses, which are abnormal responses to UV exposure, can be classified into subgroups based on pathogenesis. This review will discuss the clinical features, pathogenesis, photobiologic evaluation, prognosis and therapies of the most common photodermatoses.
*For a PDF of the full article, click on the link to the left of this introduction.
Frank A. Santoro, MD, and Henry W. Lim, MD
Interactions with ultraviolet radiation (UVR) and chromophores in the skin happen on a daily basis. Photodermatoses, which are abnormal responses to UV exposure, can be classified into subgroups based on pathogenesis. This review will discuss the clinical features, pathogenesis, photobiologic evaluation, prognosis and therapies of the most common photodermatoses.
*For a PDF of the full article, click on the link to the left of this introduction.
Frank A. Santoro, MD, and Henry W. Lim, MD
Interactions with ultraviolet radiation (UVR) and chromophores in the skin happen on a daily basis. Photodermatoses, which are abnormal responses to UV exposure, can be classified into subgroups based on pathogenesis. This review will discuss the clinical features, pathogenesis, photobiologic evaluation, prognosis and therapies of the most common photodermatoses.
*For a PDF of the full article, click on the link to the left of this introduction.
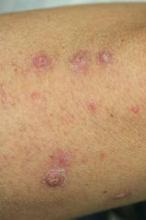
In this review we will discuss the clinical features, pathogenesis, photobiologic evaluation, prognosis, and therapies of the more commonly encountered photodermatoses: polymorphous light eruption, chronic actinic dermatitis, solar urticarial, phototoxicity, photoallergy, porphyria cutanea tarda, and erythropoietic protoporphyria.
What's on the Horizon in Tanning Bed Legislation? It Depends on You!
Protein Kinase Inhibitors Spur Keratoacanthomalike Growths
SAN DIEGO – Sorafenib, an oral agent used to treat advanced kidney cancer and unresectable liver cancer, works like "fertilizer" for lesions resembling keratoacanthomas, producing a multitude of the horny epithelial tumors in oncology patients, according to Dr. Ronald P. Rapini.
Marketed as Nexavar by Onyx Pharmaceuticals and Bayer HealthCare, sorafenib is one of many new protein kinase inhibitors approved and in development for the treatment of various forms of cancer, including leukemia.
The agents have been called "smart drugs" for their ability to mediate signaling pathways that underlie many functions of malignant cells, including growth, differentiation, and apoptosis.
"You will see this," Dr. Rapini said at a meeting sponsored by the American Society for Mohs Surgery. Medical oncologists "are using these [drugs] like crazy."
Other examples of protein kinase inhibitors are imatinib, a tyrosine-kinase inhibitor (TKI) marketed by Novartis as Gleevec, for chronic myeloid leukemia and gastrointestinal stromal tumors (GISTs), and sunitinib, marketed by Pfizer as Sutent, for GISTs, advanced kidney cancer, and pancreatic neuroendocrine tumors, noted Dr. Rapini, professor and chair of dermatology at the University of Texas Health Science Center and M.D. Anderson Cancer Center in Houston.
No keratoacanthomatous lesions have been reported to date with bosutinib, a third-generation TKI under investigation by Pfizer for the treatment of various forms of cancer, including leukemia, he said.
The initiation of benign tumor growth is likely secondary to the multikinase inhibitor mechanism of action of the oncologic drugs.
Management of the keratoacanthomalike lesions is not clear; Dr. Rapini said the role of retinoids in such cases is "questionable," with "believers and nonbelievers."
The lesions may regress upon discontinuation of the protein kinase inhibitor; otherwise, they "relentlessly" continue to develop.
Other reported skin reactions seen in conjunction with protein kinase inhibitor therapy include skin rashes, pruritus, blistering, peeling skin, hand-foot skin reaction, and difficulties with wound healing.
Dr. Rapini said he had no relevant financial disclosures.
SAN DIEGO – Sorafenib, an oral agent used to treat advanced kidney cancer and unresectable liver cancer, works like "fertilizer" for lesions resembling keratoacanthomas, producing a multitude of the horny epithelial tumors in oncology patients, according to Dr. Ronald P. Rapini.
Marketed as Nexavar by Onyx Pharmaceuticals and Bayer HealthCare, sorafenib is one of many new protein kinase inhibitors approved and in development for the treatment of various forms of cancer, including leukemia.
The agents have been called "smart drugs" for their ability to mediate signaling pathways that underlie many functions of malignant cells, including growth, differentiation, and apoptosis.
"You will see this," Dr. Rapini said at a meeting sponsored by the American Society for Mohs Surgery. Medical oncologists "are using these [drugs] like crazy."
Other examples of protein kinase inhibitors are imatinib, a tyrosine-kinase inhibitor (TKI) marketed by Novartis as Gleevec, for chronic myeloid leukemia and gastrointestinal stromal tumors (GISTs), and sunitinib, marketed by Pfizer as Sutent, for GISTs, advanced kidney cancer, and pancreatic neuroendocrine tumors, noted Dr. Rapini, professor and chair of dermatology at the University of Texas Health Science Center and M.D. Anderson Cancer Center in Houston.
No keratoacanthomatous lesions have been reported to date with bosutinib, a third-generation TKI under investigation by Pfizer for the treatment of various forms of cancer, including leukemia, he said.
The initiation of benign tumor growth is likely secondary to the multikinase inhibitor mechanism of action of the oncologic drugs.
Management of the keratoacanthomalike lesions is not clear; Dr. Rapini said the role of retinoids in such cases is "questionable," with "believers and nonbelievers."
The lesions may regress upon discontinuation of the protein kinase inhibitor; otherwise, they "relentlessly" continue to develop.
Other reported skin reactions seen in conjunction with protein kinase inhibitor therapy include skin rashes, pruritus, blistering, peeling skin, hand-foot skin reaction, and difficulties with wound healing.
Dr. Rapini said he had no relevant financial disclosures.
SAN DIEGO – Sorafenib, an oral agent used to treat advanced kidney cancer and unresectable liver cancer, works like "fertilizer" for lesions resembling keratoacanthomas, producing a multitude of the horny epithelial tumors in oncology patients, according to Dr. Ronald P. Rapini.
Marketed as Nexavar by Onyx Pharmaceuticals and Bayer HealthCare, sorafenib is one of many new protein kinase inhibitors approved and in development for the treatment of various forms of cancer, including leukemia.
The agents have been called "smart drugs" for their ability to mediate signaling pathways that underlie many functions of malignant cells, including growth, differentiation, and apoptosis.
"You will see this," Dr. Rapini said at a meeting sponsored by the American Society for Mohs Surgery. Medical oncologists "are using these [drugs] like crazy."
Other examples of protein kinase inhibitors are imatinib, a tyrosine-kinase inhibitor (TKI) marketed by Novartis as Gleevec, for chronic myeloid leukemia and gastrointestinal stromal tumors (GISTs), and sunitinib, marketed by Pfizer as Sutent, for GISTs, advanced kidney cancer, and pancreatic neuroendocrine tumors, noted Dr. Rapini, professor and chair of dermatology at the University of Texas Health Science Center and M.D. Anderson Cancer Center in Houston.
No keratoacanthomatous lesions have been reported to date with bosutinib, a third-generation TKI under investigation by Pfizer for the treatment of various forms of cancer, including leukemia, he said.
The initiation of benign tumor growth is likely secondary to the multikinase inhibitor mechanism of action of the oncologic drugs.
Management of the keratoacanthomalike lesions is not clear; Dr. Rapini said the role of retinoids in such cases is "questionable," with "believers and nonbelievers."
The lesions may regress upon discontinuation of the protein kinase inhibitor; otherwise, they "relentlessly" continue to develop.
Other reported skin reactions seen in conjunction with protein kinase inhibitor therapy include skin rashes, pruritus, blistering, peeling skin, hand-foot skin reaction, and difficulties with wound healing.
Dr. Rapini said he had no relevant financial disclosures.
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY
Mohs Emergency Preparedness Starts Before the Appointment
SAN DIEGO – A man goes into full cardiopulmonary arrest in the waiting room. A patient coughs up pink frothy sputum during a Mohs surgical procedure. Another pops two ibuprofen 20 minutes before a biopsy and goes into anaphylaxis once the procedure is underway.
These aren’t scenarios concocted for an emergency training film, but real-life events that transpired in the private practice of Dr. Alexander Miller, a Mohs surgeon in private practice in Yorba Linda, Calif.
"Stuff happens," he said during the meeting sponsored by the American Society for Mohs Surgery. "You’ve got to be prepared."
Preparedness begins with a preoperative consultation, said Dr. Edward H. Yob, a Mohs surgeon in private practice in Tulsa, Okla., who noted that it’s an "odd week" when he doesn’t find at least one prospective patient with a systolic blood pressure well over 200 mm Hg.
Mohs surgeons who meet their patients for the first time during the surgical appointment might never realize that the patient in his 50s with nitroglycerine on his medication list actually requires the medication 1-2 times a day. Dr. Yob sent this patient for a cardiac consultation, eventually deciding to schedule his procedure in a hospital operating room.
"You have to decide how far you’re going to take this, whether you’re going to monitor patients. In our office, we don’t monitor. We take blood pressure, pulse oximetry, and pulse. [Beyond that], we have our cutoff and say, ‘We won’t operate on this patient in the office,’ " he said.
However, an occasional medical emergency is bound to strike, regardless of how thorough the preoperative workup might be, both surgeons agreed.
For that, planning is the key.
"Designate a 911 caller," suggested Dr. Miller. "[While the staff is] sort of scared and wide-eyed and gaga, [someone needs] to actually call 911."
Likewise, he said, "Train yourself to maintain composure and calmness, and do the steps that are required."
Maintain CPR certification and proficiency, and have the right equipment on hand, he recommended.
Dr. Yob said the extent of equipment required will depend not only on the complexity level of patients accepted for Mohs surgery, but also the practice’s proximity to the hospital.
"How long does it take for an ambulance to get there?" he asked.
At a minimum, an office performing Mohs surgery should have available oxygen, Benadryl, atropine, epinephrine, intravenous supplies, and oral and intravenous dextrose.
An automated external defibrillator is an element of state-of-the-art care, said Dr. Yob.
A review of internet sites found that such units are available for about $2,400 and up, and come with simple instructions designed to be easily followed even in the pressure of an emergency.
Dr. Yob and Dr. Miller reported no disclosures pertaining to their talks.
SAN DIEGO – A man goes into full cardiopulmonary arrest in the waiting room. A patient coughs up pink frothy sputum during a Mohs surgical procedure. Another pops two ibuprofen 20 minutes before a biopsy and goes into anaphylaxis once the procedure is underway.
These aren’t scenarios concocted for an emergency training film, but real-life events that transpired in the private practice of Dr. Alexander Miller, a Mohs surgeon in private practice in Yorba Linda, Calif.
"Stuff happens," he said during the meeting sponsored by the American Society for Mohs Surgery. "You’ve got to be prepared."
Preparedness begins with a preoperative consultation, said Dr. Edward H. Yob, a Mohs surgeon in private practice in Tulsa, Okla., who noted that it’s an "odd week" when he doesn’t find at least one prospective patient with a systolic blood pressure well over 200 mm Hg.
Mohs surgeons who meet their patients for the first time during the surgical appointment might never realize that the patient in his 50s with nitroglycerine on his medication list actually requires the medication 1-2 times a day. Dr. Yob sent this patient for a cardiac consultation, eventually deciding to schedule his procedure in a hospital operating room.
"You have to decide how far you’re going to take this, whether you’re going to monitor patients. In our office, we don’t monitor. We take blood pressure, pulse oximetry, and pulse. [Beyond that], we have our cutoff and say, ‘We won’t operate on this patient in the office,’ " he said.
However, an occasional medical emergency is bound to strike, regardless of how thorough the preoperative workup might be, both surgeons agreed.
For that, planning is the key.
"Designate a 911 caller," suggested Dr. Miller. "[While the staff is] sort of scared and wide-eyed and gaga, [someone needs] to actually call 911."
Likewise, he said, "Train yourself to maintain composure and calmness, and do the steps that are required."
Maintain CPR certification and proficiency, and have the right equipment on hand, he recommended.
Dr. Yob said the extent of equipment required will depend not only on the complexity level of patients accepted for Mohs surgery, but also the practice’s proximity to the hospital.
"How long does it take for an ambulance to get there?" he asked.
At a minimum, an office performing Mohs surgery should have available oxygen, Benadryl, atropine, epinephrine, intravenous supplies, and oral and intravenous dextrose.
An automated external defibrillator is an element of state-of-the-art care, said Dr. Yob.
A review of internet sites found that such units are available for about $2,400 and up, and come with simple instructions designed to be easily followed even in the pressure of an emergency.
Dr. Yob and Dr. Miller reported no disclosures pertaining to their talks.
SAN DIEGO – A man goes into full cardiopulmonary arrest in the waiting room. A patient coughs up pink frothy sputum during a Mohs surgical procedure. Another pops two ibuprofen 20 minutes before a biopsy and goes into anaphylaxis once the procedure is underway.
These aren’t scenarios concocted for an emergency training film, but real-life events that transpired in the private practice of Dr. Alexander Miller, a Mohs surgeon in private practice in Yorba Linda, Calif.
"Stuff happens," he said during the meeting sponsored by the American Society for Mohs Surgery. "You’ve got to be prepared."
Preparedness begins with a preoperative consultation, said Dr. Edward H. Yob, a Mohs surgeon in private practice in Tulsa, Okla., who noted that it’s an "odd week" when he doesn’t find at least one prospective patient with a systolic blood pressure well over 200 mm Hg.
Mohs surgeons who meet their patients for the first time during the surgical appointment might never realize that the patient in his 50s with nitroglycerine on his medication list actually requires the medication 1-2 times a day. Dr. Yob sent this patient for a cardiac consultation, eventually deciding to schedule his procedure in a hospital operating room.
"You have to decide how far you’re going to take this, whether you’re going to monitor patients. In our office, we don’t monitor. We take blood pressure, pulse oximetry, and pulse. [Beyond that], we have our cutoff and say, ‘We won’t operate on this patient in the office,’ " he said.
However, an occasional medical emergency is bound to strike, regardless of how thorough the preoperative workup might be, both surgeons agreed.
For that, planning is the key.
"Designate a 911 caller," suggested Dr. Miller. "[While the staff is] sort of scared and wide-eyed and gaga, [someone needs] to actually call 911."
Likewise, he said, "Train yourself to maintain composure and calmness, and do the steps that are required."
Maintain CPR certification and proficiency, and have the right equipment on hand, he recommended.
Dr. Yob said the extent of equipment required will depend not only on the complexity level of patients accepted for Mohs surgery, but also the practice’s proximity to the hospital.
"How long does it take for an ambulance to get there?" he asked.
At a minimum, an office performing Mohs surgery should have available oxygen, Benadryl, atropine, epinephrine, intravenous supplies, and oral and intravenous dextrose.
An automated external defibrillator is an element of state-of-the-art care, said Dr. Yob.
A review of internet sites found that such units are available for about $2,400 and up, and come with simple instructions designed to be easily followed even in the pressure of an emergency.
Dr. Yob and Dr. Miller reported no disclosures pertaining to their talks.
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY
Point/Counterpoint: What is the first-line treatment of choice for metastatic BRAF-mutant melanoma?
Consider immunotherapy as first-line treatment.
Application of immunotherapy is becoming increasingly more sophisticated as we learn to control the many signals that activate and deactivate T cells. We now have two approved immunotherapies for metastatic melanoma – high-dose interleukin-2 (Proleukin) and ipilimumab (Yervoy) – and at least two investigational ones – adoptive T-cell therapy and a novel antibody to PD-1 (MDX-1106; ASCO 2010 annual meeting. Abstract 2506) – that are especially promising.
There is no question that if you give only a single agent and compare agents head to head, ipilimumab will lose to vemurafenib (Zelboraf), a targeted BRAF inhibitor, in terms of response rate, progression-free survival, and probably median survival. But our goal is the best overall outcome in this population, and in that regard, the sequencing of agents comes into play, and there may be advantages to giving immunotherapy first.
The first of several factors to consider when selecting initial therapy is that immunotherapy can produce long-term durable remissions; for example, about 5% of patients given high-dose interleukin-2 have a remission lasting more than 2 years, in some cases more than 10 years, often without maintenance therapy (Clin. Cancer Res. 2006;12:2353s-8s). In contrast, virtually all patients given targeted agents will require some sort of second therapy when they have progression.
Second, the actual treatment duration of immunotherapy is quite limited, and patients having a response may never need a second therapy. But for targeted therapy, as far as we can tell, patients will have to remain on that therapy forever.
A third factor is the speed of response. Reponses to immunotherapy are slow, in some cases taking at least 12 weeks, whereas responses to targeted agents often occur within days. So it may be difficult to give immunotherapy if you wait until a patient has progression on the targeted agent, whereas the targeted agent works so quickly that it may still be an option after failure of immunotherapy.
It is also noteworthy that targeted therapy can be associated with fulminant relapse. Our limited experience has been that a subset of patients has incredibly rapid progression when this therapy begins to fail and the targeted agent is discontinued, so there’s no opportunity to give immunotherapy at that point.
To be sure, patients with high tumor burden and very rapid tumor progression at initial metastatic presentation are generally not good candidates for receiving immunotherapy first. So you really have to look at the overall patient and consider potential predictive markers like low baseline lymphocyte count (which would disfavor immunotherapy) and preexisting autoimmune disease (which would exclude patients from some immunotherapies and favor targeted therapy).
Fourth, it has been proposed that giving immunotherapy first and targeted therapy second may be synergistic. Admittedly, this is purely theoretical. But the idea is that ipilimumab, for instance, remains in the body for up to 3 months, so if a patient starts to develop progression on this agent and a targeted agent is given at that time, you are essentially giving combination therapy.
Also, antitumor immunity may play an important role in the efficacy of targeted therapy. Very interesting preclinical data suggest that some of the activity of targeted agents requires existing immune responses (Cancer Cell. 2010;18:485-98), so inducing or expanding an immune response first may produce a better overall effect from the targeted agent. Clinically, evidence was presented that vemurafenib induces T-cell infiltrates in the tumor.
In conclusion, there are compelling reasons to consider immunotherapy as first-line therapy for melanoma. At present, we sometimes have to make difficult choices between initial therapies based on the individual patient, existing data, and our clinical judgment. But future treatment will likely entail use of these therapies in combination to optimize outcomes. Those trials are being planned. There are all sorts of possible combinations coming down the road that will likely improve outcomes.
Dr. Sznol is professor of medical oncology and codirector of the melanoma program at Yale Cancer Center, New Haven, Conn. He disclosed that he is a consultant to Bristol-Myers Squibb (manufacturer of ipilimumab) and Genesis Biopharma (a developer of adoptive cell therapies).
BRAF-targeted therapy has better overall survival.
About half of melanomas have a mutation of BRAF, providing a target for therapy that at the present time has demonstrated great promise. Vemurafenib achieves rapid, often dramatic responses in most patients. In BRIM-2, a phase II trial among patients who had had a failure of a prior therapy, nearly all had regression of disease on vemurafenib and more than 50% achieved a confirmed RECIST (Response Evaluation Criteria in Solid Tumors) clinical response (N. Engl. J. Med., in press). In BRIM-3, a phase III trial among patients with untreated disease, vemurafenib provided a dramatic improvement in both progression-free survival and overall survival over dacarbazine with hazard ratios of 0.26 and 0.37, respectively (N. Engl. J. Med. 2011;364:2507-16).
One misconception about vemurafenib therapy is that everybody is going to have a relapse in 6-7 months and die. The progression-free survival has a median of 6.8 months, but we are seeing impressive median overall survival, with a 15.9-month median in BRIM-2, probably the longest in any similar trial. The 63% relative reduction in the risk of death in BRIM-3 with vemurafenib benefited nearly all subgroups but was most impressive in patients having high lactate dehydrogenase (LDH) levels or M1c disease. We are unlikely to get good long-term survival data from this trial because of the early favorable result and allowance of crossover.
Another misconception about vemurafenib therapy is that most patients will have aggressive disease at relapse, and there will not be an opportunity for a second therapy. In fact, many patients have a localized relapse, undergo resection, and can continue on the vemurafenib. My experience has been that the patients having an aggressive relapse are those who enrolled in the trial with aggressive disease, and would not have been appropriate for other treatments. They did have a great improvement in their quality of life, albeit not for as long as hoped.
With all the limitations of comparisons between trials, vemurafenib compared with ipilimumab has been associated with better rates of overall survival at 1 year (54%-58% vs. 46%) and 2 years (33% vs. 24%). And there is a huge improvement in the disease control rate (86% vs. 44%).
Unquestionably, some patients have highly durable remissions with immunotherapy, but a major frustration is our inability to pick out this small subset of patients up front – prior to therapy.
Vemurafenib is probably the only effective therapy we have ever had for symptomatic patients with a high LDH level, who need rapid improvement in their performance status. I honestly had never seen a patient with those characteristics respond to anything until vemurafenib.
Finally, there may be some science suggesting that giving vemurafenib after ipilimumab is better, but there is not one bit of data to show that you are not able to achieve a durable remission to ipilimumab after failure of a BRAF inhibitor. More research on the sequencing of therapies is needed. In BRIM-2, only about 5% of patients had previously received ipilimumab. And although an analysis is being done among the 24% who got ipilimumab after stopping vemurafenib, it is a post hoc analysis, and the goal is simply to ascertain any contribution to the overall survival result.
In conclusion, in this era of targeted agents, it is essential that all melanomas be genotyped. It is my view that patients with symptomatic bulky disease or an increased LDH level should get vemurafenib. Patients with indolent disease, asymptomatic M1a or M1b disease, could get either; I can’t make any passionate argument that they all should get vemurafenib. But if you’re trying to put a patient into remission for as long as you can with a good quality of life, then vemurafenib is much more likely to do that. Ultimately, we need trials evaluating the issues of sequencing and combination therapy.
Dr. Sosman is professor of medicine and director of the melanoma program at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He disclosed that he is a consultant to, and receives research support from, GlaxoSmithKline (manufacturer of investigational targeted therapies for melanoma) and Roche (manufacturer of vemurafenib).
Consider immunotherapy as first-line treatment.
Application of immunotherapy is becoming increasingly more sophisticated as we learn to control the many signals that activate and deactivate T cells. We now have two approved immunotherapies for metastatic melanoma – high-dose interleukin-2 (Proleukin) and ipilimumab (Yervoy) – and at least two investigational ones – adoptive T-cell therapy and a novel antibody to PD-1 (MDX-1106; ASCO 2010 annual meeting. Abstract 2506) – that are especially promising.
There is no question that if you give only a single agent and compare agents head to head, ipilimumab will lose to vemurafenib (Zelboraf), a targeted BRAF inhibitor, in terms of response rate, progression-free survival, and probably median survival. But our goal is the best overall outcome in this population, and in that regard, the sequencing of agents comes into play, and there may be advantages to giving immunotherapy first.
The first of several factors to consider when selecting initial therapy is that immunotherapy can produce long-term durable remissions; for example, about 5% of patients given high-dose interleukin-2 have a remission lasting more than 2 years, in some cases more than 10 years, often without maintenance therapy (Clin. Cancer Res. 2006;12:2353s-8s). In contrast, virtually all patients given targeted agents will require some sort of second therapy when they have progression.
Second, the actual treatment duration of immunotherapy is quite limited, and patients having a response may never need a second therapy. But for targeted therapy, as far as we can tell, patients will have to remain on that therapy forever.
A third factor is the speed of response. Reponses to immunotherapy are slow, in some cases taking at least 12 weeks, whereas responses to targeted agents often occur within days. So it may be difficult to give immunotherapy if you wait until a patient has progression on the targeted agent, whereas the targeted agent works so quickly that it may still be an option after failure of immunotherapy.
It is also noteworthy that targeted therapy can be associated with fulminant relapse. Our limited experience has been that a subset of patients has incredibly rapid progression when this therapy begins to fail and the targeted agent is discontinued, so there’s no opportunity to give immunotherapy at that point.
To be sure, patients with high tumor burden and very rapid tumor progression at initial metastatic presentation are generally not good candidates for receiving immunotherapy first. So you really have to look at the overall patient and consider potential predictive markers like low baseline lymphocyte count (which would disfavor immunotherapy) and preexisting autoimmune disease (which would exclude patients from some immunotherapies and favor targeted therapy).
Fourth, it has been proposed that giving immunotherapy first and targeted therapy second may be synergistic. Admittedly, this is purely theoretical. But the idea is that ipilimumab, for instance, remains in the body for up to 3 months, so if a patient starts to develop progression on this agent and a targeted agent is given at that time, you are essentially giving combination therapy.
Also, antitumor immunity may play an important role in the efficacy of targeted therapy. Very interesting preclinical data suggest that some of the activity of targeted agents requires existing immune responses (Cancer Cell. 2010;18:485-98), so inducing or expanding an immune response first may produce a better overall effect from the targeted agent. Clinically, evidence was presented that vemurafenib induces T-cell infiltrates in the tumor.
In conclusion, there are compelling reasons to consider immunotherapy as first-line therapy for melanoma. At present, we sometimes have to make difficult choices between initial therapies based on the individual patient, existing data, and our clinical judgment. But future treatment will likely entail use of these therapies in combination to optimize outcomes. Those trials are being planned. There are all sorts of possible combinations coming down the road that will likely improve outcomes.
Dr. Sznol is professor of medical oncology and codirector of the melanoma program at Yale Cancer Center, New Haven, Conn. He disclosed that he is a consultant to Bristol-Myers Squibb (manufacturer of ipilimumab) and Genesis Biopharma (a developer of adoptive cell therapies).
BRAF-targeted therapy has better overall survival.
About half of melanomas have a mutation of BRAF, providing a target for therapy that at the present time has demonstrated great promise. Vemurafenib achieves rapid, often dramatic responses in most patients. In BRIM-2, a phase II trial among patients who had had a failure of a prior therapy, nearly all had regression of disease on vemurafenib and more than 50% achieved a confirmed RECIST (Response Evaluation Criteria in Solid Tumors) clinical response (N. Engl. J. Med., in press). In BRIM-3, a phase III trial among patients with untreated disease, vemurafenib provided a dramatic improvement in both progression-free survival and overall survival over dacarbazine with hazard ratios of 0.26 and 0.37, respectively (N. Engl. J. Med. 2011;364:2507-16).
One misconception about vemurafenib therapy is that everybody is going to have a relapse in 6-7 months and die. The progression-free survival has a median of 6.8 months, but we are seeing impressive median overall survival, with a 15.9-month median in BRIM-2, probably the longest in any similar trial. The 63% relative reduction in the risk of death in BRIM-3 with vemurafenib benefited nearly all subgroups but was most impressive in patients having high lactate dehydrogenase (LDH) levels or M1c disease. We are unlikely to get good long-term survival data from this trial because of the early favorable result and allowance of crossover.
Another misconception about vemurafenib therapy is that most patients will have aggressive disease at relapse, and there will not be an opportunity for a second therapy. In fact, many patients have a localized relapse, undergo resection, and can continue on the vemurafenib. My experience has been that the patients having an aggressive relapse are those who enrolled in the trial with aggressive disease, and would not have been appropriate for other treatments. They did have a great improvement in their quality of life, albeit not for as long as hoped.
With all the limitations of comparisons between trials, vemurafenib compared with ipilimumab has been associated with better rates of overall survival at 1 year (54%-58% vs. 46%) and 2 years (33% vs. 24%). And there is a huge improvement in the disease control rate (86% vs. 44%).
Unquestionably, some patients have highly durable remissions with immunotherapy, but a major frustration is our inability to pick out this small subset of patients up front – prior to therapy.
Vemurafenib is probably the only effective therapy we have ever had for symptomatic patients with a high LDH level, who need rapid improvement in their performance status. I honestly had never seen a patient with those characteristics respond to anything until vemurafenib.
Finally, there may be some science suggesting that giving vemurafenib after ipilimumab is better, but there is not one bit of data to show that you are not able to achieve a durable remission to ipilimumab after failure of a BRAF inhibitor. More research on the sequencing of therapies is needed. In BRIM-2, only about 5% of patients had previously received ipilimumab. And although an analysis is being done among the 24% who got ipilimumab after stopping vemurafenib, it is a post hoc analysis, and the goal is simply to ascertain any contribution to the overall survival result.
In conclusion, in this era of targeted agents, it is essential that all melanomas be genotyped. It is my view that patients with symptomatic bulky disease or an increased LDH level should get vemurafenib. Patients with indolent disease, asymptomatic M1a or M1b disease, could get either; I can’t make any passionate argument that they all should get vemurafenib. But if you’re trying to put a patient into remission for as long as you can with a good quality of life, then vemurafenib is much more likely to do that. Ultimately, we need trials evaluating the issues of sequencing and combination therapy.
Dr. Sosman is professor of medicine and director of the melanoma program at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He disclosed that he is a consultant to, and receives research support from, GlaxoSmithKline (manufacturer of investigational targeted therapies for melanoma) and Roche (manufacturer of vemurafenib).
Consider immunotherapy as first-line treatment.
Application of immunotherapy is becoming increasingly more sophisticated as we learn to control the many signals that activate and deactivate T cells. We now have two approved immunotherapies for metastatic melanoma – high-dose interleukin-2 (Proleukin) and ipilimumab (Yervoy) – and at least two investigational ones – adoptive T-cell therapy and a novel antibody to PD-1 (MDX-1106; ASCO 2010 annual meeting. Abstract 2506) – that are especially promising.
There is no question that if you give only a single agent and compare agents head to head, ipilimumab will lose to vemurafenib (Zelboraf), a targeted BRAF inhibitor, in terms of response rate, progression-free survival, and probably median survival. But our goal is the best overall outcome in this population, and in that regard, the sequencing of agents comes into play, and there may be advantages to giving immunotherapy first.
The first of several factors to consider when selecting initial therapy is that immunotherapy can produce long-term durable remissions; for example, about 5% of patients given high-dose interleukin-2 have a remission lasting more than 2 years, in some cases more than 10 years, often without maintenance therapy (Clin. Cancer Res. 2006;12:2353s-8s). In contrast, virtually all patients given targeted agents will require some sort of second therapy when they have progression.
Second, the actual treatment duration of immunotherapy is quite limited, and patients having a response may never need a second therapy. But for targeted therapy, as far as we can tell, patients will have to remain on that therapy forever.
A third factor is the speed of response. Reponses to immunotherapy are slow, in some cases taking at least 12 weeks, whereas responses to targeted agents often occur within days. So it may be difficult to give immunotherapy if you wait until a patient has progression on the targeted agent, whereas the targeted agent works so quickly that it may still be an option after failure of immunotherapy.
It is also noteworthy that targeted therapy can be associated with fulminant relapse. Our limited experience has been that a subset of patients has incredibly rapid progression when this therapy begins to fail and the targeted agent is discontinued, so there’s no opportunity to give immunotherapy at that point.
To be sure, patients with high tumor burden and very rapid tumor progression at initial metastatic presentation are generally not good candidates for receiving immunotherapy first. So you really have to look at the overall patient and consider potential predictive markers like low baseline lymphocyte count (which would disfavor immunotherapy) and preexisting autoimmune disease (which would exclude patients from some immunotherapies and favor targeted therapy).
Fourth, it has been proposed that giving immunotherapy first and targeted therapy second may be synergistic. Admittedly, this is purely theoretical. But the idea is that ipilimumab, for instance, remains in the body for up to 3 months, so if a patient starts to develop progression on this agent and a targeted agent is given at that time, you are essentially giving combination therapy.
Also, antitumor immunity may play an important role in the efficacy of targeted therapy. Very interesting preclinical data suggest that some of the activity of targeted agents requires existing immune responses (Cancer Cell. 2010;18:485-98), so inducing or expanding an immune response first may produce a better overall effect from the targeted agent. Clinically, evidence was presented that vemurafenib induces T-cell infiltrates in the tumor.
In conclusion, there are compelling reasons to consider immunotherapy as first-line therapy for melanoma. At present, we sometimes have to make difficult choices between initial therapies based on the individual patient, existing data, and our clinical judgment. But future treatment will likely entail use of these therapies in combination to optimize outcomes. Those trials are being planned. There are all sorts of possible combinations coming down the road that will likely improve outcomes.
Dr. Sznol is professor of medical oncology and codirector of the melanoma program at Yale Cancer Center, New Haven, Conn. He disclosed that he is a consultant to Bristol-Myers Squibb (manufacturer of ipilimumab) and Genesis Biopharma (a developer of adoptive cell therapies).
BRAF-targeted therapy has better overall survival.
About half of melanomas have a mutation of BRAF, providing a target for therapy that at the present time has demonstrated great promise. Vemurafenib achieves rapid, often dramatic responses in most patients. In BRIM-2, a phase II trial among patients who had had a failure of a prior therapy, nearly all had regression of disease on vemurafenib and more than 50% achieved a confirmed RECIST (Response Evaluation Criteria in Solid Tumors) clinical response (N. Engl. J. Med., in press). In BRIM-3, a phase III trial among patients with untreated disease, vemurafenib provided a dramatic improvement in both progression-free survival and overall survival over dacarbazine with hazard ratios of 0.26 and 0.37, respectively (N. Engl. J. Med. 2011;364:2507-16).
One misconception about vemurafenib therapy is that everybody is going to have a relapse in 6-7 months and die. The progression-free survival has a median of 6.8 months, but we are seeing impressive median overall survival, with a 15.9-month median in BRIM-2, probably the longest in any similar trial. The 63% relative reduction in the risk of death in BRIM-3 with vemurafenib benefited nearly all subgroups but was most impressive in patients having high lactate dehydrogenase (LDH) levels or M1c disease. We are unlikely to get good long-term survival data from this trial because of the early favorable result and allowance of crossover.
Another misconception about vemurafenib therapy is that most patients will have aggressive disease at relapse, and there will not be an opportunity for a second therapy. In fact, many patients have a localized relapse, undergo resection, and can continue on the vemurafenib. My experience has been that the patients having an aggressive relapse are those who enrolled in the trial with aggressive disease, and would not have been appropriate for other treatments. They did have a great improvement in their quality of life, albeit not for as long as hoped.
With all the limitations of comparisons between trials, vemurafenib compared with ipilimumab has been associated with better rates of overall survival at 1 year (54%-58% vs. 46%) and 2 years (33% vs. 24%). And there is a huge improvement in the disease control rate (86% vs. 44%).
Unquestionably, some patients have highly durable remissions with immunotherapy, but a major frustration is our inability to pick out this small subset of patients up front – prior to therapy.
Vemurafenib is probably the only effective therapy we have ever had for symptomatic patients with a high LDH level, who need rapid improvement in their performance status. I honestly had never seen a patient with those characteristics respond to anything until vemurafenib.
Finally, there may be some science suggesting that giving vemurafenib after ipilimumab is better, but there is not one bit of data to show that you are not able to achieve a durable remission to ipilimumab after failure of a BRAF inhibitor. More research on the sequencing of therapies is needed. In BRIM-2, only about 5% of patients had previously received ipilimumab. And although an analysis is being done among the 24% who got ipilimumab after stopping vemurafenib, it is a post hoc analysis, and the goal is simply to ascertain any contribution to the overall survival result.
In conclusion, in this era of targeted agents, it is essential that all melanomas be genotyped. It is my view that patients with symptomatic bulky disease or an increased LDH level should get vemurafenib. Patients with indolent disease, asymptomatic M1a or M1b disease, could get either; I can’t make any passionate argument that they all should get vemurafenib. But if you’re trying to put a patient into remission for as long as you can with a good quality of life, then vemurafenib is much more likely to do that. Ultimately, we need trials evaluating the issues of sequencing and combination therapy.
Dr. Sosman is professor of medicine and director of the melanoma program at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He disclosed that he is a consultant to, and receives research support from, GlaxoSmithKline (manufacturer of investigational targeted therapies for melanoma) and Roche (manufacturer of vemurafenib).
Supplement Captures Snapshot of Melanoma Epidemiology
While the recently published supplement on melanoma in the Journal of the American Academy of Dermatology doesn’t offer evidence of many new trends, it does provide an important estimate of the burden of the disease and suggests new targets for education and surveillance.
"The best way to characterize this nice ensemble of studies is that it literally takes a pulse on the epidemic," Dr. Hensin Tsao said of the collection of studies (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S1-143) in an interview. Dr. Tsao is the clinical director of the Melanoma Center and Pigmented Lesion Center at Massachusetts General Hospital in Boston.
Dr. Randall K. Roenigk, a professor of dermatology at the Mayo Clinic in Rochester, Minn., agreed. "It summarizes some facts that are pretty well known but it solidifies some [others]," he said in an interview.
The supplements were published as a joint effort by the American Academy of Dermatology and the Centers for Disease Control and Prevention. The included studies were largely based on data from the Surveillance, Epidemiology, and End Results (SEER) registry that is maintained by the National Cancer Institute.
"The incidence of melanoma is still increasing, and the mortality has not decreased," said Dr. Tsao. "So the biggest take-home message is that this burden is still growing."
Dr. Roenigk noted that "people interpret that one of two ways. They either say that it’s increasing because we’re doing a better job of surveillance or that people are just getting more cancers. However, he added, "some people say that the death rate should also increase if the incidence rate is increasing; but because it’s flat, some people say that maybe our criteria for diagnosis have changed a little bit ... I don’t know if [the supplement] answers that. It’s a little bit of a controversy. But the positive spin on it would be that while the incidence rate is increasing, we’re able to catch it in time that the death rate is staying about the same."
The take home messages from the supplement include: cancer incidence is increasing in younger individuals, particularly younger women; the greatest melanoma mortality is seen among elderly men; and dermatologists have an important chance to improve surveillance of melanoma by reporting their data to registries, such as the SEER database.
Young Women
The study of melanoma in adolescents and young adults aged 15-39 years (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S38-49) found the incidence of melanoma to be rising in that age group. "There have been a number of studies in this younger age group showing the incidence shooting up, especially among women," said Dr. Tsao. "This study substantiates previously published data."
According to Dr. Roenigk, it has been suggested that "the increased incidence in melanoma could just be due to people living longer ... but obviously with people under the age of 40 it’s not so much living longer, it’s probably behavioral or it’s environmental ... but not necessarily longevity."
Dr. Tsao noted that the increasing melanoma incidence in this age group "has implications for what we can do now on some regulatory level ... and for what we expect to happen in 20 years. Are we going to get a whole cohort of advanced-disease women because there is a lag time in the formation of [melanomas] ... It’s a cautionary tale for the future but it’s certainly a point of intervention now."
Tanning beds continue to be a source of controversy at all levels of government nationwide. The AAD, states, local organizations, and others are working to tackle the issue of access to tanning beds.
Education may prove even harder. "We have a lot of room to improve ... despite pretty heavy messaging ... people are either fatigued with the message or they have competing interests," said Dr. Tsao. "There are even more and more studies out there suggesting that even the long-wave ‘safer tans’ like UVA can cause the same types of genetic damage ... I’m not sure that the words ‘safe tan’ makes any sense. A lot of exposure even to long-wave UVA may lead to the chronic skin cancer environment in the skin."
Older Men
The other newer information asks who is dying from melanoma. "Overall, yes, young women are getting melanoma," but if you’re asking who is dying from melanoma, it is old men. You’ll see this theme throughout many of the articles," said Dr. Tsao. "Elderly men are getting to be the most susceptible group – it appears – for melanoma if you look at the death rates." In this age group the rates of melanoma mortality are much greater in men than in women (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S78-86).
"This is going to have clinical impact down the line," Dr. Tsao noted. "Many of these [older] people have melanomas on the head and neck, which appear to have a worse prognosis." These tumors are thick, often nodular in subtype and with a lot of negative features in the pathology report. "We don’t really understand this phenotype – it may be the tumor, it may be the host, it may be the chronically sun-damaged skin surface."
However, "the question is how you get that group to be potentially screened – and how screening within this group is going to impact mortality," he noted. "We’re still optimistic that with proper screening, we can make a difference in mortality."
Dr. Tsao uses the mnemonic MENN (male, elderly, neck/scalp/trunk, nodular type melanoma) to thoroughly check for melanomas in this patient population, regardless of the reason for presentation.
Melanoma Registries
"One of the ways that we can study the burden of a skin disease is by having nationalized records. It doesn’t exist for most other skin diseases," said Dr. Tsao. "Still, most dermatologists in practice don’t think about registering their melanomas, even though this is one of the most codified disorders in all of dermatology ... maybe this is something that we need to work on ... the only way that we can make progress toward documenting the burden of skin disease is that we document the burden of skin disease."
There are likely a large number of melanomas that are diagnosed in the community and the question is whether those are getting recorded in a registry. "In most large hospitals or tertiary care centers, cancers undergo registration. But this may not be the case in private practice," Dr. Tsao said. "If we’re underestimating the burden of melanoma, then in some ways we’re shortchanging ourselves. Given the long-range surveillance, dermatologists are becoming the primary caretakers of melanoma patients in this country in terms of sheer volume ... dermatologists have an opportunity to detect at an early stage and to deflect these patients away from advanced disease."
While the recently published supplement on melanoma in the Journal of the American Academy of Dermatology doesn’t offer evidence of many new trends, it does provide an important estimate of the burden of the disease and suggests new targets for education and surveillance.
"The best way to characterize this nice ensemble of studies is that it literally takes a pulse on the epidemic," Dr. Hensin Tsao said of the collection of studies (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S1-143) in an interview. Dr. Tsao is the clinical director of the Melanoma Center and Pigmented Lesion Center at Massachusetts General Hospital in Boston.
Dr. Randall K. Roenigk, a professor of dermatology at the Mayo Clinic in Rochester, Minn., agreed. "It summarizes some facts that are pretty well known but it solidifies some [others]," he said in an interview.
The supplements were published as a joint effort by the American Academy of Dermatology and the Centers for Disease Control and Prevention. The included studies were largely based on data from the Surveillance, Epidemiology, and End Results (SEER) registry that is maintained by the National Cancer Institute.
"The incidence of melanoma is still increasing, and the mortality has not decreased," said Dr. Tsao. "So the biggest take-home message is that this burden is still growing."
Dr. Roenigk noted that "people interpret that one of two ways. They either say that it’s increasing because we’re doing a better job of surveillance or that people are just getting more cancers. However, he added, "some people say that the death rate should also increase if the incidence rate is increasing; but because it’s flat, some people say that maybe our criteria for diagnosis have changed a little bit ... I don’t know if [the supplement] answers that. It’s a little bit of a controversy. But the positive spin on it would be that while the incidence rate is increasing, we’re able to catch it in time that the death rate is staying about the same."
The take home messages from the supplement include: cancer incidence is increasing in younger individuals, particularly younger women; the greatest melanoma mortality is seen among elderly men; and dermatologists have an important chance to improve surveillance of melanoma by reporting their data to registries, such as the SEER database.
Young Women
The study of melanoma in adolescents and young adults aged 15-39 years (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S38-49) found the incidence of melanoma to be rising in that age group. "There have been a number of studies in this younger age group showing the incidence shooting up, especially among women," said Dr. Tsao. "This study substantiates previously published data."
According to Dr. Roenigk, it has been suggested that "the increased incidence in melanoma could just be due to people living longer ... but obviously with people under the age of 40 it’s not so much living longer, it’s probably behavioral or it’s environmental ... but not necessarily longevity."
Dr. Tsao noted that the increasing melanoma incidence in this age group "has implications for what we can do now on some regulatory level ... and for what we expect to happen in 20 years. Are we going to get a whole cohort of advanced-disease women because there is a lag time in the formation of [melanomas] ... It’s a cautionary tale for the future but it’s certainly a point of intervention now."
Tanning beds continue to be a source of controversy at all levels of government nationwide. The AAD, states, local organizations, and others are working to tackle the issue of access to tanning beds.
Education may prove even harder. "We have a lot of room to improve ... despite pretty heavy messaging ... people are either fatigued with the message or they have competing interests," said Dr. Tsao. "There are even more and more studies out there suggesting that even the long-wave ‘safer tans’ like UVA can cause the same types of genetic damage ... I’m not sure that the words ‘safe tan’ makes any sense. A lot of exposure even to long-wave UVA may lead to the chronic skin cancer environment in the skin."
Older Men
The other newer information asks who is dying from melanoma. "Overall, yes, young women are getting melanoma," but if you’re asking who is dying from melanoma, it is old men. You’ll see this theme throughout many of the articles," said Dr. Tsao. "Elderly men are getting to be the most susceptible group – it appears – for melanoma if you look at the death rates." In this age group the rates of melanoma mortality are much greater in men than in women (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S78-86).
"This is going to have clinical impact down the line," Dr. Tsao noted. "Many of these [older] people have melanomas on the head and neck, which appear to have a worse prognosis." These tumors are thick, often nodular in subtype and with a lot of negative features in the pathology report. "We don’t really understand this phenotype – it may be the tumor, it may be the host, it may be the chronically sun-damaged skin surface."
However, "the question is how you get that group to be potentially screened – and how screening within this group is going to impact mortality," he noted. "We’re still optimistic that with proper screening, we can make a difference in mortality."
Dr. Tsao uses the mnemonic MENN (male, elderly, neck/scalp/trunk, nodular type melanoma) to thoroughly check for melanomas in this patient population, regardless of the reason for presentation.
Melanoma Registries
"One of the ways that we can study the burden of a skin disease is by having nationalized records. It doesn’t exist for most other skin diseases," said Dr. Tsao. "Still, most dermatologists in practice don’t think about registering their melanomas, even though this is one of the most codified disorders in all of dermatology ... maybe this is something that we need to work on ... the only way that we can make progress toward documenting the burden of skin disease is that we document the burden of skin disease."
There are likely a large number of melanomas that are diagnosed in the community and the question is whether those are getting recorded in a registry. "In most large hospitals or tertiary care centers, cancers undergo registration. But this may not be the case in private practice," Dr. Tsao said. "If we’re underestimating the burden of melanoma, then in some ways we’re shortchanging ourselves. Given the long-range surveillance, dermatologists are becoming the primary caretakers of melanoma patients in this country in terms of sheer volume ... dermatologists have an opportunity to detect at an early stage and to deflect these patients away from advanced disease."
While the recently published supplement on melanoma in the Journal of the American Academy of Dermatology doesn’t offer evidence of many new trends, it does provide an important estimate of the burden of the disease and suggests new targets for education and surveillance.
"The best way to characterize this nice ensemble of studies is that it literally takes a pulse on the epidemic," Dr. Hensin Tsao said of the collection of studies (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S1-143) in an interview. Dr. Tsao is the clinical director of the Melanoma Center and Pigmented Lesion Center at Massachusetts General Hospital in Boston.
Dr. Randall K. Roenigk, a professor of dermatology at the Mayo Clinic in Rochester, Minn., agreed. "It summarizes some facts that are pretty well known but it solidifies some [others]," he said in an interview.
The supplements were published as a joint effort by the American Academy of Dermatology and the Centers for Disease Control and Prevention. The included studies were largely based on data from the Surveillance, Epidemiology, and End Results (SEER) registry that is maintained by the National Cancer Institute.
"The incidence of melanoma is still increasing, and the mortality has not decreased," said Dr. Tsao. "So the biggest take-home message is that this burden is still growing."
Dr. Roenigk noted that "people interpret that one of two ways. They either say that it’s increasing because we’re doing a better job of surveillance or that people are just getting more cancers. However, he added, "some people say that the death rate should also increase if the incidence rate is increasing; but because it’s flat, some people say that maybe our criteria for diagnosis have changed a little bit ... I don’t know if [the supplement] answers that. It’s a little bit of a controversy. But the positive spin on it would be that while the incidence rate is increasing, we’re able to catch it in time that the death rate is staying about the same."
The take home messages from the supplement include: cancer incidence is increasing in younger individuals, particularly younger women; the greatest melanoma mortality is seen among elderly men; and dermatologists have an important chance to improve surveillance of melanoma by reporting their data to registries, such as the SEER database.
Young Women
The study of melanoma in adolescents and young adults aged 15-39 years (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S38-49) found the incidence of melanoma to be rising in that age group. "There have been a number of studies in this younger age group showing the incidence shooting up, especially among women," said Dr. Tsao. "This study substantiates previously published data."
According to Dr. Roenigk, it has been suggested that "the increased incidence in melanoma could just be due to people living longer ... but obviously with people under the age of 40 it’s not so much living longer, it’s probably behavioral or it’s environmental ... but not necessarily longevity."
Dr. Tsao noted that the increasing melanoma incidence in this age group "has implications for what we can do now on some regulatory level ... and for what we expect to happen in 20 years. Are we going to get a whole cohort of advanced-disease women because there is a lag time in the formation of [melanomas] ... It’s a cautionary tale for the future but it’s certainly a point of intervention now."
Tanning beds continue to be a source of controversy at all levels of government nationwide. The AAD, states, local organizations, and others are working to tackle the issue of access to tanning beds.
Education may prove even harder. "We have a lot of room to improve ... despite pretty heavy messaging ... people are either fatigued with the message or they have competing interests," said Dr. Tsao. "There are even more and more studies out there suggesting that even the long-wave ‘safer tans’ like UVA can cause the same types of genetic damage ... I’m not sure that the words ‘safe tan’ makes any sense. A lot of exposure even to long-wave UVA may lead to the chronic skin cancer environment in the skin."
Older Men
The other newer information asks who is dying from melanoma. "Overall, yes, young women are getting melanoma," but if you’re asking who is dying from melanoma, it is old men. You’ll see this theme throughout many of the articles," said Dr. Tsao. "Elderly men are getting to be the most susceptible group – it appears – for melanoma if you look at the death rates." In this age group the rates of melanoma mortality are much greater in men than in women (J. Am. Acad. Dermatol 2011;65[suppl. 1]:S78-86).
"This is going to have clinical impact down the line," Dr. Tsao noted. "Many of these [older] people have melanomas on the head and neck, which appear to have a worse prognosis." These tumors are thick, often nodular in subtype and with a lot of negative features in the pathology report. "We don’t really understand this phenotype – it may be the tumor, it may be the host, it may be the chronically sun-damaged skin surface."
However, "the question is how you get that group to be potentially screened – and how screening within this group is going to impact mortality," he noted. "We’re still optimistic that with proper screening, we can make a difference in mortality."
Dr. Tsao uses the mnemonic MENN (male, elderly, neck/scalp/trunk, nodular type melanoma) to thoroughly check for melanomas in this patient population, regardless of the reason for presentation.
Melanoma Registries
"One of the ways that we can study the burden of a skin disease is by having nationalized records. It doesn’t exist for most other skin diseases," said Dr. Tsao. "Still, most dermatologists in practice don’t think about registering their melanomas, even though this is one of the most codified disorders in all of dermatology ... maybe this is something that we need to work on ... the only way that we can make progress toward documenting the burden of skin disease is that we document the burden of skin disease."
There are likely a large number of melanomas that are diagnosed in the community and the question is whether those are getting recorded in a registry. "In most large hospitals or tertiary care centers, cancers undergo registration. But this may not be the case in private practice," Dr. Tsao said. "If we’re underestimating the burden of melanoma, then in some ways we’re shortchanging ourselves. Given the long-range surveillance, dermatologists are becoming the primary caretakers of melanoma patients in this country in terms of sheer volume ... dermatologists have an opportunity to detect at an early stage and to deflect these patients away from advanced disease."
Treatment Costs Low for Nonmelanoma Skin Cancers
The average annual cost of treatment for nonmelanoma skin cancers was $788 per adult in 2005-2008, according to a report from the Agency for Healthcare Research and Quality.
The average for nonmelanoma skin cancers, the most common type of cancer diagnosed in the United States, was lower than the annual costs of other common cancers.
The average number of adults treated for nonmelanoma skin cancers (mainly basal cell and squamous cell) was 3.72 million per year from 2005 to 2008. That compares with 1.46 million per year for breast cancer, 1.2 million for prostate cancer, 570,000 for colon cancer, and 450,000 for lung cancer, according to data from the Medical Expenditure Panel Survey.
Nonmelanoma skin cancers accounted for about $2.9 billion of the $75.7 billion in average annual spending for cancer care among adults in 2005-2008, the report noted.
Note: Based on data from the Medical Expenditure Panel Survey, 2005-2008.
Source: Agency for Healthcare Research and Quality
The average annual cost of treatment for nonmelanoma skin cancers was $788 per adult in 2005-2008, according to a report from the Agency for Healthcare Research and Quality.
The average for nonmelanoma skin cancers, the most common type of cancer diagnosed in the United States, was lower than the annual costs of other common cancers.
The average number of adults treated for nonmelanoma skin cancers (mainly basal cell and squamous cell) was 3.72 million per year from 2005 to 2008. That compares with 1.46 million per year for breast cancer, 1.2 million for prostate cancer, 570,000 for colon cancer, and 450,000 for lung cancer, according to data from the Medical Expenditure Panel Survey.
Nonmelanoma skin cancers accounted for about $2.9 billion of the $75.7 billion in average annual spending for cancer care among adults in 2005-2008, the report noted.
Note: Based on data from the Medical Expenditure Panel Survey, 2005-2008.
Source: Agency for Healthcare Research and Quality
The average annual cost of treatment for nonmelanoma skin cancers was $788 per adult in 2005-2008, according to a report from the Agency for Healthcare Research and Quality.
The average for nonmelanoma skin cancers, the most common type of cancer diagnosed in the United States, was lower than the annual costs of other common cancers.
The average number of adults treated for nonmelanoma skin cancers (mainly basal cell and squamous cell) was 3.72 million per year from 2005 to 2008. That compares with 1.46 million per year for breast cancer, 1.2 million for prostate cancer, 570,000 for colon cancer, and 450,000 for lung cancer, according to data from the Medical Expenditure Panel Survey.
Nonmelanoma skin cancers accounted for about $2.9 billion of the $75.7 billion in average annual spending for cancer care among adults in 2005-2008, the report noted.
Note: Based on data from the Medical Expenditure Panel Survey, 2005-2008.
Source: Agency for Healthcare Research and Quality
USPTF Urges Counseling Against Sun Exposure
The U.S. Preventive Services Task Force has recommended that physicians counsel children, adolescents, and young adults on minimizing their ultraviolet radiation exposure to reduce their risk of skin cancer.
The recommendation was issued in draft form, which means that it is open for comment until Dec. 6. It was based on an evidence review published in February.
The USPTF focused on children and adults aged 10-24 years, grading the evidence supporting its recommendation as a B. Under that rubric, "there is high certainty that the net benefit is moderate or there is moderate certainty that the net benefit is moderate to substantial."
However, the panel concluded that the evidence is "insufficient" to determine the risks and benefits of such counseling for adults.
The American Academy of Dermatology lauded the USPTF for its recommendation but took issue with its conclusion on adults. The AAD "is pleased that the USPSTF has recommended that sun protection counseling is important for children, adolescents, and young adults with fair skin types," said AAD President Ronald L. Moy. "However, the Academy believes sun protection counseling is important for everyone, including the adult population."
When the USPTF last looked at counseling, in 2003, it concluded there was insufficient evidence to support it for either children or adults.
In its update, however, the panel noted there being plenty of data showing that counseling is linked to behavior changes that lead to less sun exposure, at least in children. The USPTF also determined that there were no negative consequences to children being told to stay out of the sun. There was no decrease in outdoor activity or increase in body mass in the studies the panel reviewed. The studies did not assess the impact on vitamin D levels in children or adults.
The committee looked at studies on tanning bed use, also. There was not enough evidence to assess the association between use of tanning beds and the risk of squamous or basal cell carcinoma, reported the panel. A number of studies did, however, show an increased risk of melanoma with tanning beds.
Tanning beds are still an issue for the AAD, though.
"More than 3.5 million skin cancers in more than 2 million people are diagnosed annually, and excessive exposure to ultraviolet radiation from the sun and tanning beds is the most preventable cause of all skin cancers," said Dr. Moy.
The USPTF is funded by the Agency for Healthcare Quality and Research.
The U.S. Preventive Services Task Force has recommended that physicians counsel children, adolescents, and young adults on minimizing their ultraviolet radiation exposure to reduce their risk of skin cancer.
The recommendation was issued in draft form, which means that it is open for comment until Dec. 6. It was based on an evidence review published in February.
The USPTF focused on children and adults aged 10-24 years, grading the evidence supporting its recommendation as a B. Under that rubric, "there is high certainty that the net benefit is moderate or there is moderate certainty that the net benefit is moderate to substantial."
However, the panel concluded that the evidence is "insufficient" to determine the risks and benefits of such counseling for adults.
The American Academy of Dermatology lauded the USPTF for its recommendation but took issue with its conclusion on adults. The AAD "is pleased that the USPSTF has recommended that sun protection counseling is important for children, adolescents, and young adults with fair skin types," said AAD President Ronald L. Moy. "However, the Academy believes sun protection counseling is important for everyone, including the adult population."
When the USPTF last looked at counseling, in 2003, it concluded there was insufficient evidence to support it for either children or adults.
In its update, however, the panel noted there being plenty of data showing that counseling is linked to behavior changes that lead to less sun exposure, at least in children. The USPTF also determined that there were no negative consequences to children being told to stay out of the sun. There was no decrease in outdoor activity or increase in body mass in the studies the panel reviewed. The studies did not assess the impact on vitamin D levels in children or adults.
The committee looked at studies on tanning bed use, also. There was not enough evidence to assess the association between use of tanning beds and the risk of squamous or basal cell carcinoma, reported the panel. A number of studies did, however, show an increased risk of melanoma with tanning beds.
Tanning beds are still an issue for the AAD, though.
"More than 3.5 million skin cancers in more than 2 million people are diagnosed annually, and excessive exposure to ultraviolet radiation from the sun and tanning beds is the most preventable cause of all skin cancers," said Dr. Moy.
The USPTF is funded by the Agency for Healthcare Quality and Research.
The U.S. Preventive Services Task Force has recommended that physicians counsel children, adolescents, and young adults on minimizing their ultraviolet radiation exposure to reduce their risk of skin cancer.
The recommendation was issued in draft form, which means that it is open for comment until Dec. 6. It was based on an evidence review published in February.
The USPTF focused on children and adults aged 10-24 years, grading the evidence supporting its recommendation as a B. Under that rubric, "there is high certainty that the net benefit is moderate or there is moderate certainty that the net benefit is moderate to substantial."
However, the panel concluded that the evidence is "insufficient" to determine the risks and benefits of such counseling for adults.
The American Academy of Dermatology lauded the USPTF for its recommendation but took issue with its conclusion on adults. The AAD "is pleased that the USPSTF has recommended that sun protection counseling is important for children, adolescents, and young adults with fair skin types," said AAD President Ronald L. Moy. "However, the Academy believes sun protection counseling is important for everyone, including the adult population."
When the USPTF last looked at counseling, in 2003, it concluded there was insufficient evidence to support it for either children or adults.
In its update, however, the panel noted there being plenty of data showing that counseling is linked to behavior changes that lead to less sun exposure, at least in children. The USPTF also determined that there were no negative consequences to children being told to stay out of the sun. There was no decrease in outdoor activity or increase in body mass in the studies the panel reviewed. The studies did not assess the impact on vitamin D levels in children or adults.
The committee looked at studies on tanning bed use, also. There was not enough evidence to assess the association between use of tanning beds and the risk of squamous or basal cell carcinoma, reported the panel. A number of studies did, however, show an increased risk of melanoma with tanning beds.
Tanning beds are still an issue for the AAD, though.
"More than 3.5 million skin cancers in more than 2 million people are diagnosed annually, and excessive exposure to ultraviolet radiation from the sun and tanning beds is the most preventable cause of all skin cancers," said Dr. Moy.
The USPTF is funded by the Agency for Healthcare Quality and Research.
NCAA Athletes Not Using Sunscreen
WASHINGTON – Despite high levels of sun exposure, nearly half of collegiate athletes don't use sunscreen, according to a recent survey.
The anonymous survey of 290 athletes from two universities – one on the East Coast and one on the West Coast – found that 96% of respondents believed sunscreen would help protect them from skin cancer. Yet, 43% of the athletes surveyed reported never using sunscreen, 31% reported only using sunscreen 1-3 days per week, 18% reported using sunscreen 4-6 days per week, and 8% reported using sunscreen every day of the week.
On average, the athletes reported spending 4 hours a day outdoors for 10 months a year, said Dr. Ashley Wysong, a resident in the department of dermatology at Stanford (Calif.) University.
With more than 400,000 NCAA collegiate athletes in universities across the nation, "An organized educational campaign by dermatologists, the NCAA, member universities, and individual coaches may be beneficial" in achieving better sun protection among college athletes, said Dr. Wysong, a former six-time NCAA All-American and national champion in middle distance running.
The survey, which included 13 outdoor sports, found that the percentage of athletes who wore sunscreen increased with the frequency of coaches or athletic administrators speaking with them about sun protection.
Survey respondents listed several reasons for not using sunscreen. The most common was forgetting to use it (63%), followed by inconvenience of use (41%), and "I like to be tan" (39%). Other reasons the athletes reported for not using sunscreen included: belief that they don’t burn (35%), the greasy feel of sunscreen (34%), and the time it takes for application (22%).
Not surprisingly, sunburns were common among the participants. Nearly 84% reported experiencing at least one sunburn in the past year, with 28% reporting four or more, and 10% reporting a blistering sunburn.
The majority of respondents were Fitzpatrick Skin Type I and II, but all skin types were represented in the study, the authors reported.
A few factors contributed to sunscreen use: living in the West Coast, female gender, number of sunburns in the past year, belief in the risk of skin cancer, knowing someone with skin cancer, and worry about wrinkles.
A study by researchers at the University of Cincinnati reached a similar conclusion, finding "a need for improved primary prevention of ultraviolet damage" among college athletes. The survey found that 85% of athletes at four universities reported no sunscreen use during the prior week, and only 7% reported using sunscreen at least three times during that time period (J. Am. Acad. Dermatol. 2005;53:237-41).
Dr. Wysong said that sun protective behavior extends beyond just the athletes themselves, because "they are role models for younger kids."
To follow-up their study, the authors are planning to hand out educational literature to freshmen athletes and conduct before and after questionnaires on sunscreen use.
Dr. Wysong reported having no conflicts of interest.
WASHINGTON – Despite high levels of sun exposure, nearly half of collegiate athletes don't use sunscreen, according to a recent survey.
The anonymous survey of 290 athletes from two universities – one on the East Coast and one on the West Coast – found that 96% of respondents believed sunscreen would help protect them from skin cancer. Yet, 43% of the athletes surveyed reported never using sunscreen, 31% reported only using sunscreen 1-3 days per week, 18% reported using sunscreen 4-6 days per week, and 8% reported using sunscreen every day of the week.
On average, the athletes reported spending 4 hours a day outdoors for 10 months a year, said Dr. Ashley Wysong, a resident in the department of dermatology at Stanford (Calif.) University.
With more than 400,000 NCAA collegiate athletes in universities across the nation, "An organized educational campaign by dermatologists, the NCAA, member universities, and individual coaches may be beneficial" in achieving better sun protection among college athletes, said Dr. Wysong, a former six-time NCAA All-American and national champion in middle distance running.
The survey, which included 13 outdoor sports, found that the percentage of athletes who wore sunscreen increased with the frequency of coaches or athletic administrators speaking with them about sun protection.
Survey respondents listed several reasons for not using sunscreen. The most common was forgetting to use it (63%), followed by inconvenience of use (41%), and "I like to be tan" (39%). Other reasons the athletes reported for not using sunscreen included: belief that they don’t burn (35%), the greasy feel of sunscreen (34%), and the time it takes for application (22%).
Not surprisingly, sunburns were common among the participants. Nearly 84% reported experiencing at least one sunburn in the past year, with 28% reporting four or more, and 10% reporting a blistering sunburn.
The majority of respondents were Fitzpatrick Skin Type I and II, but all skin types were represented in the study, the authors reported.
A few factors contributed to sunscreen use: living in the West Coast, female gender, number of sunburns in the past year, belief in the risk of skin cancer, knowing someone with skin cancer, and worry about wrinkles.
A study by researchers at the University of Cincinnati reached a similar conclusion, finding "a need for improved primary prevention of ultraviolet damage" among college athletes. The survey found that 85% of athletes at four universities reported no sunscreen use during the prior week, and only 7% reported using sunscreen at least three times during that time period (J. Am. Acad. Dermatol. 2005;53:237-41).
Dr. Wysong said that sun protective behavior extends beyond just the athletes themselves, because "they are role models for younger kids."
To follow-up their study, the authors are planning to hand out educational literature to freshmen athletes and conduct before and after questionnaires on sunscreen use.
Dr. Wysong reported having no conflicts of interest.
WASHINGTON – Despite high levels of sun exposure, nearly half of collegiate athletes don't use sunscreen, according to a recent survey.
The anonymous survey of 290 athletes from two universities – one on the East Coast and one on the West Coast – found that 96% of respondents believed sunscreen would help protect them from skin cancer. Yet, 43% of the athletes surveyed reported never using sunscreen, 31% reported only using sunscreen 1-3 days per week, 18% reported using sunscreen 4-6 days per week, and 8% reported using sunscreen every day of the week.
On average, the athletes reported spending 4 hours a day outdoors for 10 months a year, said Dr. Ashley Wysong, a resident in the department of dermatology at Stanford (Calif.) University.
With more than 400,000 NCAA collegiate athletes in universities across the nation, "An organized educational campaign by dermatologists, the NCAA, member universities, and individual coaches may be beneficial" in achieving better sun protection among college athletes, said Dr. Wysong, a former six-time NCAA All-American and national champion in middle distance running.
The survey, which included 13 outdoor sports, found that the percentage of athletes who wore sunscreen increased with the frequency of coaches or athletic administrators speaking with them about sun protection.
Survey respondents listed several reasons for not using sunscreen. The most common was forgetting to use it (63%), followed by inconvenience of use (41%), and "I like to be tan" (39%). Other reasons the athletes reported for not using sunscreen included: belief that they don’t burn (35%), the greasy feel of sunscreen (34%), and the time it takes for application (22%).
Not surprisingly, sunburns were common among the participants. Nearly 84% reported experiencing at least one sunburn in the past year, with 28% reporting four or more, and 10% reporting a blistering sunburn.
The majority of respondents were Fitzpatrick Skin Type I and II, but all skin types were represented in the study, the authors reported.
A few factors contributed to sunscreen use: living in the West Coast, female gender, number of sunburns in the past year, belief in the risk of skin cancer, knowing someone with skin cancer, and worry about wrinkles.
A study by researchers at the University of Cincinnati reached a similar conclusion, finding "a need for improved primary prevention of ultraviolet damage" among college athletes. The survey found that 85% of athletes at four universities reported no sunscreen use during the prior week, and only 7% reported using sunscreen at least three times during that time period (J. Am. Acad. Dermatol. 2005;53:237-41).
Dr. Wysong said that sun protective behavior extends beyond just the athletes themselves, because "they are role models for younger kids."
To follow-up their study, the authors are planning to hand out educational literature to freshmen athletes and conduct before and after questionnaires on sunscreen use.
Dr. Wysong reported having no conflicts of interest.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY