User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
Expert shares her tips for diagnosing, treating onychomycosis
NEW ORLEANS – .
“The PAS [periodic acid-Schiff] stain is very popular because it can identify the presence or absence of fungal elements, but a fungal culture will identify the organism living in the nail,” Dr. Elewski, professor and chair of dermatology at the University of Alabama, Birmingham, said at the annual meeting of the American Academy of Dermatology. “You also could do a PCR to identify the organism, with or without a KOH or PAS stain. It is often helpful to know what organism is causing the infection.”
While waiting for lab results, there are three clinical clues to look for – the first being that an infection likely resides in the toenail. “You almost never see dermatophyte onychomycosis in the fingernails without it being in the toenails, too,” Dr. Elewski said.
The presence of tinea pedis is a second clinical clue. “Sometimes it’s subtle, so I will ask the patient, ‘Have you been treating yourself for athlete’s foot?’ If they say ‘no, I’ve never had it,’ put down on your list that it’s unlikely they have onychomycosis. How is the fungus going to jump from the floor into the nail without taking a little vacation on the bottom of the foot? It just isn’t going to happen.”
The presence of dermatophytoma is the third clinical clue. “These are dermatophyte abscesses encased in a biofilm, and they’re really hard to treat,” she said.
Treatments
Clinicians typically turn to one of three oral drugs for treating onychomycosis: terbinafine, itraconazole, and fluconazole, Dr. Elewski noted. Referring to terbinafine as “the gold standard,” she said that she typically writes a prescription for 90 250-mg pills. “When I give terbinafine, I often do baseline liver profiling, depending on the patient’s age, their state of health, their comorbidities, and other medications they’re taking,” she said. “If they’re 18 years old and otherwise healthy, I probably don’t.” While she generally prescribes 90 pills, she added, “keep in mind that 90 pills are not going to cure everybody. I see the patient 4 months later because the drug should stay in the nail for 30 days or more at therapeutic levels after you take that 90-day course.”
Another option is itraconazole, which can be taken at a dose of 200 mg a day for 12 weeks, or at a pulse dose, where patients take 400 mg every day for 1 week, 1 week a month, for 4 consecutive months. “I’ll often do a baseline liver profile with itraconazole, too,” Dr. Elewski said. “I don’t think you have to, but it makes sense if it’s feasible for you. Decide that based on each patient.”
Itraconazole can’t be given concomitantly with statins because of the potential for rhabdomyolysis. For patients taking statins, she consults with their physicians to make sure it’s safe to stop the statin a couple of days before and after their scheduled pulse dose of itraconazole. “This involves 1 week per month of taking itraconazole without the statin,” she said. “Or they could stop statins for the time you treat, if cleared by their doctor.”
As for fluconazole, Dr. Elewski usually prescribes 200 mg once or twice per week until the nail is normal. She offers patients the mnemonic for “Fungal Fridays” or Toesdays” as a way for them to remember which day to take the fluconazole.
According to data in the package inserts, rates of complete and mycologic cures are 38% and 70% for terbinafine, respectively, 14% and 54% for itraconazole, and 37% to 48% and 47% to 62% for fluconazole. “These cures are not 100% based on the standard course [of the drug],” Dr. Elewski noted. “I don’t use the standard course. I believe in treating to terminate. You want to kill the fungus.”
Resistant dermatophytes ‘are coming’
Halting treatment with an oral drug at a particular time point instead of when the nail is fungal-free likely contributes to resistant strains, she added, noting that she has at least two dozen patients in her practice with dermatophyte resistance documented in labs. “We need to be antifungal stewards, because resistant dermatophytes are coming to us,” she said. “They’re here already, and we don’t want it to be endemic in the U.S.”
In a published study from 2020, researchers from India enrolled 200 patients with relapsing tinea corporis, tinea cruris, and tinea faciei and allocated 50 each to treatment with either fluconazole, griseofulvin, itraconazole, or terbinafine. At week 4, all treatment arms had cure rates of less than 8%. At week 8, the cure rates were 42% for fluconazole, 16% for griseofulvin, 28% for terbinafine, and 66% for itraconazole.
Based in part on these study findings, Dr. Elewski said that she has become more aggressive in her therapeutic approach, including treating some of her patients on terbinafine for a minimum of 6 months. “If that’s not enough, I keep treating,” she said. “But, patients may not respond to terbinafine; we see resistance. So, itraconazole may be our best drug going forward for treating onychomycosis. You just have to watch out for side effects of itraconazole, mainly drug-drug interactions.”
Dr. Elewski reported having no relevant financial disclosures related to her presentation.
NEW ORLEANS – .
“The PAS [periodic acid-Schiff] stain is very popular because it can identify the presence or absence of fungal elements, but a fungal culture will identify the organism living in the nail,” Dr. Elewski, professor and chair of dermatology at the University of Alabama, Birmingham, said at the annual meeting of the American Academy of Dermatology. “You also could do a PCR to identify the organism, with or without a KOH or PAS stain. It is often helpful to know what organism is causing the infection.”
While waiting for lab results, there are three clinical clues to look for – the first being that an infection likely resides in the toenail. “You almost never see dermatophyte onychomycosis in the fingernails without it being in the toenails, too,” Dr. Elewski said.
The presence of tinea pedis is a second clinical clue. “Sometimes it’s subtle, so I will ask the patient, ‘Have you been treating yourself for athlete’s foot?’ If they say ‘no, I’ve never had it,’ put down on your list that it’s unlikely they have onychomycosis. How is the fungus going to jump from the floor into the nail without taking a little vacation on the bottom of the foot? It just isn’t going to happen.”
The presence of dermatophytoma is the third clinical clue. “These are dermatophyte abscesses encased in a biofilm, and they’re really hard to treat,” she said.
Treatments
Clinicians typically turn to one of three oral drugs for treating onychomycosis: terbinafine, itraconazole, and fluconazole, Dr. Elewski noted. Referring to terbinafine as “the gold standard,” she said that she typically writes a prescription for 90 250-mg pills. “When I give terbinafine, I often do baseline liver profiling, depending on the patient’s age, their state of health, their comorbidities, and other medications they’re taking,” she said. “If they’re 18 years old and otherwise healthy, I probably don’t.” While she generally prescribes 90 pills, she added, “keep in mind that 90 pills are not going to cure everybody. I see the patient 4 months later because the drug should stay in the nail for 30 days or more at therapeutic levels after you take that 90-day course.”
Another option is itraconazole, which can be taken at a dose of 200 mg a day for 12 weeks, or at a pulse dose, where patients take 400 mg every day for 1 week, 1 week a month, for 4 consecutive months. “I’ll often do a baseline liver profile with itraconazole, too,” Dr. Elewski said. “I don’t think you have to, but it makes sense if it’s feasible for you. Decide that based on each patient.”
Itraconazole can’t be given concomitantly with statins because of the potential for rhabdomyolysis. For patients taking statins, she consults with their physicians to make sure it’s safe to stop the statin a couple of days before and after their scheduled pulse dose of itraconazole. “This involves 1 week per month of taking itraconazole without the statin,” she said. “Or they could stop statins for the time you treat, if cleared by their doctor.”
As for fluconazole, Dr. Elewski usually prescribes 200 mg once or twice per week until the nail is normal. She offers patients the mnemonic for “Fungal Fridays” or Toesdays” as a way for them to remember which day to take the fluconazole.
According to data in the package inserts, rates of complete and mycologic cures are 38% and 70% for terbinafine, respectively, 14% and 54% for itraconazole, and 37% to 48% and 47% to 62% for fluconazole. “These cures are not 100% based on the standard course [of the drug],” Dr. Elewski noted. “I don’t use the standard course. I believe in treating to terminate. You want to kill the fungus.”
Resistant dermatophytes ‘are coming’
Halting treatment with an oral drug at a particular time point instead of when the nail is fungal-free likely contributes to resistant strains, she added, noting that she has at least two dozen patients in her practice with dermatophyte resistance documented in labs. “We need to be antifungal stewards, because resistant dermatophytes are coming to us,” she said. “They’re here already, and we don’t want it to be endemic in the U.S.”
In a published study from 2020, researchers from India enrolled 200 patients with relapsing tinea corporis, tinea cruris, and tinea faciei and allocated 50 each to treatment with either fluconazole, griseofulvin, itraconazole, or terbinafine. At week 4, all treatment arms had cure rates of less than 8%. At week 8, the cure rates were 42% for fluconazole, 16% for griseofulvin, 28% for terbinafine, and 66% for itraconazole.
Based in part on these study findings, Dr. Elewski said that she has become more aggressive in her therapeutic approach, including treating some of her patients on terbinafine for a minimum of 6 months. “If that’s not enough, I keep treating,” she said. “But, patients may not respond to terbinafine; we see resistance. So, itraconazole may be our best drug going forward for treating onychomycosis. You just have to watch out for side effects of itraconazole, mainly drug-drug interactions.”
Dr. Elewski reported having no relevant financial disclosures related to her presentation.
NEW ORLEANS – .
“The PAS [periodic acid-Schiff] stain is very popular because it can identify the presence or absence of fungal elements, but a fungal culture will identify the organism living in the nail,” Dr. Elewski, professor and chair of dermatology at the University of Alabama, Birmingham, said at the annual meeting of the American Academy of Dermatology. “You also could do a PCR to identify the organism, with or without a KOH or PAS stain. It is often helpful to know what organism is causing the infection.”
While waiting for lab results, there are three clinical clues to look for – the first being that an infection likely resides in the toenail. “You almost never see dermatophyte onychomycosis in the fingernails without it being in the toenails, too,” Dr. Elewski said.
The presence of tinea pedis is a second clinical clue. “Sometimes it’s subtle, so I will ask the patient, ‘Have you been treating yourself for athlete’s foot?’ If they say ‘no, I’ve never had it,’ put down on your list that it’s unlikely they have onychomycosis. How is the fungus going to jump from the floor into the nail without taking a little vacation on the bottom of the foot? It just isn’t going to happen.”
The presence of dermatophytoma is the third clinical clue. “These are dermatophyte abscesses encased in a biofilm, and they’re really hard to treat,” she said.
Treatments
Clinicians typically turn to one of three oral drugs for treating onychomycosis: terbinafine, itraconazole, and fluconazole, Dr. Elewski noted. Referring to terbinafine as “the gold standard,” she said that she typically writes a prescription for 90 250-mg pills. “When I give terbinafine, I often do baseline liver profiling, depending on the patient’s age, their state of health, their comorbidities, and other medications they’re taking,” she said. “If they’re 18 years old and otherwise healthy, I probably don’t.” While she generally prescribes 90 pills, she added, “keep in mind that 90 pills are not going to cure everybody. I see the patient 4 months later because the drug should stay in the nail for 30 days or more at therapeutic levels after you take that 90-day course.”
Another option is itraconazole, which can be taken at a dose of 200 mg a day for 12 weeks, or at a pulse dose, where patients take 400 mg every day for 1 week, 1 week a month, for 4 consecutive months. “I’ll often do a baseline liver profile with itraconazole, too,” Dr. Elewski said. “I don’t think you have to, but it makes sense if it’s feasible for you. Decide that based on each patient.”
Itraconazole can’t be given concomitantly with statins because of the potential for rhabdomyolysis. For patients taking statins, she consults with their physicians to make sure it’s safe to stop the statin a couple of days before and after their scheduled pulse dose of itraconazole. “This involves 1 week per month of taking itraconazole without the statin,” she said. “Or they could stop statins for the time you treat, if cleared by their doctor.”
As for fluconazole, Dr. Elewski usually prescribes 200 mg once or twice per week until the nail is normal. She offers patients the mnemonic for “Fungal Fridays” or Toesdays” as a way for them to remember which day to take the fluconazole.
According to data in the package inserts, rates of complete and mycologic cures are 38% and 70% for terbinafine, respectively, 14% and 54% for itraconazole, and 37% to 48% and 47% to 62% for fluconazole. “These cures are not 100% based on the standard course [of the drug],” Dr. Elewski noted. “I don’t use the standard course. I believe in treating to terminate. You want to kill the fungus.”
Resistant dermatophytes ‘are coming’
Halting treatment with an oral drug at a particular time point instead of when the nail is fungal-free likely contributes to resistant strains, she added, noting that she has at least two dozen patients in her practice with dermatophyte resistance documented in labs. “We need to be antifungal stewards, because resistant dermatophytes are coming to us,” she said. “They’re here already, and we don’t want it to be endemic in the U.S.”
In a published study from 2020, researchers from India enrolled 200 patients with relapsing tinea corporis, tinea cruris, and tinea faciei and allocated 50 each to treatment with either fluconazole, griseofulvin, itraconazole, or terbinafine. At week 4, all treatment arms had cure rates of less than 8%. At week 8, the cure rates were 42% for fluconazole, 16% for griseofulvin, 28% for terbinafine, and 66% for itraconazole.
Based in part on these study findings, Dr. Elewski said that she has become more aggressive in her therapeutic approach, including treating some of her patients on terbinafine for a minimum of 6 months. “If that’s not enough, I keep treating,” she said. “But, patients may not respond to terbinafine; we see resistance. So, itraconazole may be our best drug going forward for treating onychomycosis. You just have to watch out for side effects of itraconazole, mainly drug-drug interactions.”
Dr. Elewski reported having no relevant financial disclosures related to her presentation.
AT AAD 2023
FDA approves new Merkel cell carcinoma treatment
the agency announced.
This marks the first regulatory approval for the PD-1 inhibitor. The FDA granted accelerated approval for the drug on the basis of tumor response rate and duration of response from the POD1UM-201 trial. Drugmaker Incyte said that “continued approval of Zynyz for this indication may be contingent upon verification and description of clinical benefit in confirmatory trials.”
MCC is a rare and aggressive skin cancer with a high rate of metastatic disease and an estimated 5-year overall survival of just 14% among those who present with metastatic disease. Incidence is rapidly increasing in the United States, particularly among adults older than 65 years, Incyte noted.
“More than a third of patients with MCC present with regional or distant metastases, which are associated with high rates of mortality,” principal author Shailender Bhatia, MD, of the University of Washington and Fred Hutchinson Cancer Center, both in Seattle, said in a news release. “The approval of Zynyz offers health care providers another first-line treatment option against MCC that can result in durable responses in patients with metastatic disease.”
POD1UM-201 was an open-label, single-arm, phase 2 study that evaluated the agent in 65 systemic treatment–naive adults with metastatic or recurrent locally advanced MCC.
Overall, 52% of patients had an objective response rate. A complete response was observed in 12 patients (18%), and a partial response was observed in 22 patients (34%).
Duration of response ranged from 1.1 to 24.9 months; 76% of responders experienced responses of 6 months or longer, and 62% experienced responses of 12 months or longer.
Study participants received a 500-mg dose of retifanlimab every 4 weeks for up to 24 weeks or until disease progression or unacceptable toxicity. Serious adverse events occurred in 22% of patients and most often included fatigue, arrhythmia, and pneumonitis; 11% of patients discontinued treatment because of serious adverse events.
Retifanlimab may cause a severe or life-threatening immune response during treatment or after discontinuation. Patients should be advised to immediately report any new or worsening signs or symptoms to their health care provider. Side effects can also be reported to the FDA.
A version of this article first appeared on Medscape.com.
the agency announced.
This marks the first regulatory approval for the PD-1 inhibitor. The FDA granted accelerated approval for the drug on the basis of tumor response rate and duration of response from the POD1UM-201 trial. Drugmaker Incyte said that “continued approval of Zynyz for this indication may be contingent upon verification and description of clinical benefit in confirmatory trials.”
MCC is a rare and aggressive skin cancer with a high rate of metastatic disease and an estimated 5-year overall survival of just 14% among those who present with metastatic disease. Incidence is rapidly increasing in the United States, particularly among adults older than 65 years, Incyte noted.
“More than a third of patients with MCC present with regional or distant metastases, which are associated with high rates of mortality,” principal author Shailender Bhatia, MD, of the University of Washington and Fred Hutchinson Cancer Center, both in Seattle, said in a news release. “The approval of Zynyz offers health care providers another first-line treatment option against MCC that can result in durable responses in patients with metastatic disease.”
POD1UM-201 was an open-label, single-arm, phase 2 study that evaluated the agent in 65 systemic treatment–naive adults with metastatic or recurrent locally advanced MCC.
Overall, 52% of patients had an objective response rate. A complete response was observed in 12 patients (18%), and a partial response was observed in 22 patients (34%).
Duration of response ranged from 1.1 to 24.9 months; 76% of responders experienced responses of 6 months or longer, and 62% experienced responses of 12 months or longer.
Study participants received a 500-mg dose of retifanlimab every 4 weeks for up to 24 weeks or until disease progression or unacceptable toxicity. Serious adverse events occurred in 22% of patients and most often included fatigue, arrhythmia, and pneumonitis; 11% of patients discontinued treatment because of serious adverse events.
Retifanlimab may cause a severe or life-threatening immune response during treatment or after discontinuation. Patients should be advised to immediately report any new or worsening signs or symptoms to their health care provider. Side effects can also be reported to the FDA.
A version of this article first appeared on Medscape.com.
the agency announced.
This marks the first regulatory approval for the PD-1 inhibitor. The FDA granted accelerated approval for the drug on the basis of tumor response rate and duration of response from the POD1UM-201 trial. Drugmaker Incyte said that “continued approval of Zynyz for this indication may be contingent upon verification and description of clinical benefit in confirmatory trials.”
MCC is a rare and aggressive skin cancer with a high rate of metastatic disease and an estimated 5-year overall survival of just 14% among those who present with metastatic disease. Incidence is rapidly increasing in the United States, particularly among adults older than 65 years, Incyte noted.
“More than a third of patients with MCC present with regional or distant metastases, which are associated with high rates of mortality,” principal author Shailender Bhatia, MD, of the University of Washington and Fred Hutchinson Cancer Center, both in Seattle, said in a news release. “The approval of Zynyz offers health care providers another first-line treatment option against MCC that can result in durable responses in patients with metastatic disease.”
POD1UM-201 was an open-label, single-arm, phase 2 study that evaluated the agent in 65 systemic treatment–naive adults with metastatic or recurrent locally advanced MCC.
Overall, 52% of patients had an objective response rate. A complete response was observed in 12 patients (18%), and a partial response was observed in 22 patients (34%).
Duration of response ranged from 1.1 to 24.9 months; 76% of responders experienced responses of 6 months or longer, and 62% experienced responses of 12 months or longer.
Study participants received a 500-mg dose of retifanlimab every 4 weeks for up to 24 weeks or until disease progression or unacceptable toxicity. Serious adverse events occurred in 22% of patients and most often included fatigue, arrhythmia, and pneumonitis; 11% of patients discontinued treatment because of serious adverse events.
Retifanlimab may cause a severe or life-threatening immune response during treatment or after discontinuation. Patients should be advised to immediately report any new or worsening signs or symptoms to their health care provider. Side effects can also be reported to the FDA.
A version of this article first appeared on Medscape.com.
Celebrity death finally solved – with locks of hair
This transcript has been edited for clarity.
I’m going to open this week with a case.
A 56-year-old musician presents with diffuse abdominal pain, cramping, and jaundice. His medical history is notable for years of diffuse abdominal complaints, characterized by disabling bouts of diarrhea.
In addition to the jaundice, this acute illness was accompanied by fever as well as diffuse edema and ascites. The patient underwent several abdominal paracenteses to drain excess fluid. One consulting physician administered alcohol to relieve pain, to little avail.
The patient succumbed to his illness. An autopsy showed diffuse liver injury, as well as papillary necrosis of the kidneys. Notably, the nerves of his auditory canal were noted to be thickened, along with the bony part of the skull, consistent with Paget disease of the bone and explaining, potentially, why the talented musician had gone deaf at such a young age.
An interesting note on social history: The patient had apparently developed some feelings for the niece of that doctor who prescribed alcohol. Her name was Therese, perhaps mistranscribed as Elise, and it seems that he may have written this song for her.
We’re talking about this paper in Current Biology, by Tristan Begg and colleagues, which gives us a look into the very genome of what some would argue is the world’s greatest composer.
The ability to extract DNA from older specimens has transformed the fields of anthropology, archaeology, and history, and now, perhaps, musicology as well.
The researchers identified eight locks of hair in private and public collections, all attributed to the maestro.
Four of the samples had an intact chain of custody from the time the hair was cut. DNA sequencing on these four and an additional one of the eight locks came from the same individual, a male of European heritage.
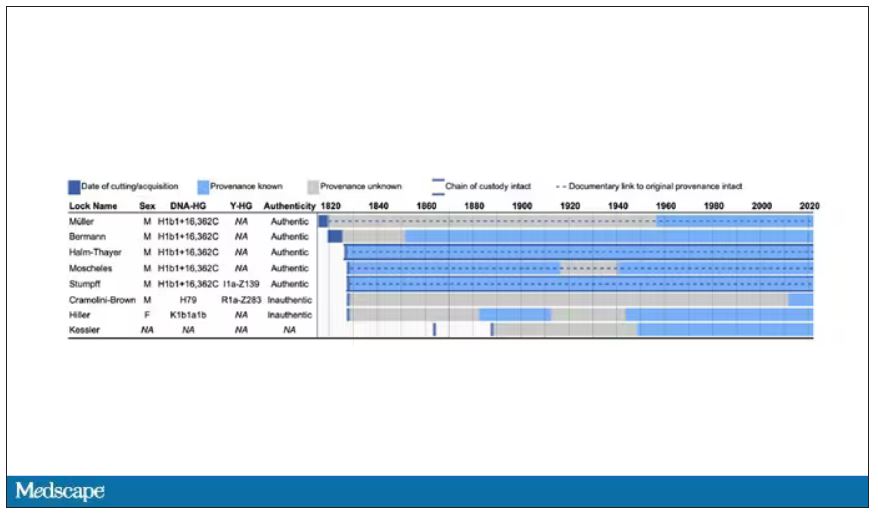
The three locks with less documentation came from three other unrelated individuals. Interestingly, analysis of one of those hair samples – the so-called Hiller Lock – had shown high levels of lead, leading historians to speculate that lead poisoning could account for some of Beethoven’s symptoms.

DNA analysis of that hair reveals it to have come from a woman likely of North African, Middle Eastern, or Jewish ancestry. We can no longer presume that plumbism was involved in Beethoven’s death. Beethoven’s ancestry turns out to be less exotic and maps quite well to ethnic German populations today.
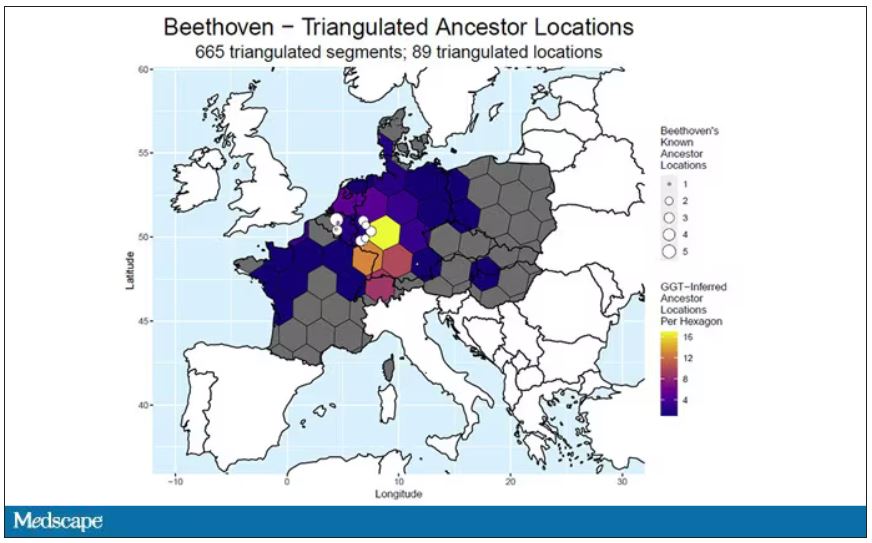
In fact, there are van Beethovens alive as we speak, primarily in Belgium. Genealogic records suggest that these van Beethovens share a common ancestor with the virtuoso composer, a man by the name of Aert van Beethoven.
But the DNA reveals a scandal.
The Y-chromosome that Beethoven inherited was not Aert van Beethoven’s. Questions of Beethoven’s paternity have been raised before, but this evidence strongly suggests an extramarital paternity event, at least in the generations preceding his birth. That’s right – Beethoven may not have been a Beethoven.
With five locks now essentially certain to have come from Beethoven himself, the authors could use DNA analysis to try to explain three significant health problems he experienced throughout his life and death: his hearing loss, his terrible gastrointestinal issues, and his liver failure.
Let’s start with the most disappointing results, explanations for his hearing loss. No genetic cause was forthcoming, though the authors note that they have little to go on in regard to the genetic risk for otosclerosis, to which his hearing loss has often been attributed. Lead poisoning is, of course, possible here, though this report focuses only on genetics – there was no testing for lead – and as I mentioned, the lock that was strongly lead-positive in prior studies is almost certainly inauthentic.
What about his lifelong GI complaints? Some have suggested celiac disease or lactose intolerance as explanations. These can essentially be ruled out by the genetic analysis, which shows no risk alleles for celiac disease and the presence of the lactase-persistence gene which confers the ability to metabolize lactose throughout one’s life. IBS is harder to assess genetically, but for what it’s worth, he scored quite low on a polygenic risk score for the condition, in just the 9th percentile of risk. We should probably be looking elsewhere to explain the GI distress.
The genetic information bore much more fruit in regard to his liver disease. Remember that Beethoven’s autopsy showed cirrhosis. His polygenic risk score for liver cirrhosis puts him in the 96th percentile of risk. He was also heterozygous for two variants that can cause hereditary hemochromatosis. The risk for cirrhosis among those with these variants is increased by the use of alcohol. And historical accounts are quite clear that Beethoven consumed more than his share.
But it wasn’t just Beethoven’s DNA in these hair follicles. Analysis of a follicle from later in his life revealed the unmistakable presence of hepatitis B virus. Endemic in Europe at the time, this was a common cause of liver failure and is likely to have contributed to, if not directly caused, Beethoven’s demise.
It’s hard to read these results and not marvel at the fact that, two centuries after his death, our fascination with Beethoven has led us to probe every corner of his life – his letters, his writings, his medical records, and now his very DNA. What are we actually looking for? Is it relevant to us today what caused his hearing loss? His stomach troubles? Even his death? Will it help any patients in the future? I propose that what we are actually trying to understand is something ineffable: Genius of magnitude that is rarely seen in one or many lifetimes. And our scientific tools, as sharp as they may have become, are still far too blunt to probe the depths of that transcendence.
In any case, friends, no more of these sounds. Let us sing more cheerful songs, more full of joy.
For Medscape, I’m Perry Wilson.
Dr. Wilson is associate professor, department of medicine, and director, Clinical and Translational Research Accelerator, at Yale University, New Haven, Conn. He reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I’m going to open this week with a case.
A 56-year-old musician presents with diffuse abdominal pain, cramping, and jaundice. His medical history is notable for years of diffuse abdominal complaints, characterized by disabling bouts of diarrhea.
In addition to the jaundice, this acute illness was accompanied by fever as well as diffuse edema and ascites. The patient underwent several abdominal paracenteses to drain excess fluid. One consulting physician administered alcohol to relieve pain, to little avail.
The patient succumbed to his illness. An autopsy showed diffuse liver injury, as well as papillary necrosis of the kidneys. Notably, the nerves of his auditory canal were noted to be thickened, along with the bony part of the skull, consistent with Paget disease of the bone and explaining, potentially, why the talented musician had gone deaf at such a young age.
An interesting note on social history: The patient had apparently developed some feelings for the niece of that doctor who prescribed alcohol. Her name was Therese, perhaps mistranscribed as Elise, and it seems that he may have written this song for her.
We’re talking about this paper in Current Biology, by Tristan Begg and colleagues, which gives us a look into the very genome of what some would argue is the world’s greatest composer.
The ability to extract DNA from older specimens has transformed the fields of anthropology, archaeology, and history, and now, perhaps, musicology as well.
The researchers identified eight locks of hair in private and public collections, all attributed to the maestro.
Four of the samples had an intact chain of custody from the time the hair was cut. DNA sequencing on these four and an additional one of the eight locks came from the same individual, a male of European heritage.

The three locks with less documentation came from three other unrelated individuals. Interestingly, analysis of one of those hair samples – the so-called Hiller Lock – had shown high levels of lead, leading historians to speculate that lead poisoning could account for some of Beethoven’s symptoms.

DNA analysis of that hair reveals it to have come from a woman likely of North African, Middle Eastern, or Jewish ancestry. We can no longer presume that plumbism was involved in Beethoven’s death. Beethoven’s ancestry turns out to be less exotic and maps quite well to ethnic German populations today.

In fact, there are van Beethovens alive as we speak, primarily in Belgium. Genealogic records suggest that these van Beethovens share a common ancestor with the virtuoso composer, a man by the name of Aert van Beethoven.
But the DNA reveals a scandal.
The Y-chromosome that Beethoven inherited was not Aert van Beethoven’s. Questions of Beethoven’s paternity have been raised before, but this evidence strongly suggests an extramarital paternity event, at least in the generations preceding his birth. That’s right – Beethoven may not have been a Beethoven.
With five locks now essentially certain to have come from Beethoven himself, the authors could use DNA analysis to try to explain three significant health problems he experienced throughout his life and death: his hearing loss, his terrible gastrointestinal issues, and his liver failure.
Let’s start with the most disappointing results, explanations for his hearing loss. No genetic cause was forthcoming, though the authors note that they have little to go on in regard to the genetic risk for otosclerosis, to which his hearing loss has often been attributed. Lead poisoning is, of course, possible here, though this report focuses only on genetics – there was no testing for lead – and as I mentioned, the lock that was strongly lead-positive in prior studies is almost certainly inauthentic.
What about his lifelong GI complaints? Some have suggested celiac disease or lactose intolerance as explanations. These can essentially be ruled out by the genetic analysis, which shows no risk alleles for celiac disease and the presence of the lactase-persistence gene which confers the ability to metabolize lactose throughout one’s life. IBS is harder to assess genetically, but for what it’s worth, he scored quite low on a polygenic risk score for the condition, in just the 9th percentile of risk. We should probably be looking elsewhere to explain the GI distress.
The genetic information bore much more fruit in regard to his liver disease. Remember that Beethoven’s autopsy showed cirrhosis. His polygenic risk score for liver cirrhosis puts him in the 96th percentile of risk. He was also heterozygous for two variants that can cause hereditary hemochromatosis. The risk for cirrhosis among those with these variants is increased by the use of alcohol. And historical accounts are quite clear that Beethoven consumed more than his share.
But it wasn’t just Beethoven’s DNA in these hair follicles. Analysis of a follicle from later in his life revealed the unmistakable presence of hepatitis B virus. Endemic in Europe at the time, this was a common cause of liver failure and is likely to have contributed to, if not directly caused, Beethoven’s demise.

It’s hard to read these results and not marvel at the fact that, two centuries after his death, our fascination with Beethoven has led us to probe every corner of his life – his letters, his writings, his medical records, and now his very DNA. What are we actually looking for? Is it relevant to us today what caused his hearing loss? His stomach troubles? Even his death? Will it help any patients in the future? I propose that what we are actually trying to understand is something ineffable: Genius of magnitude that is rarely seen in one or many lifetimes. And our scientific tools, as sharp as they may have become, are still far too blunt to probe the depths of that transcendence.
In any case, friends, no more of these sounds. Let us sing more cheerful songs, more full of joy.
For Medscape, I’m Perry Wilson.
Dr. Wilson is associate professor, department of medicine, and director, Clinical and Translational Research Accelerator, at Yale University, New Haven, Conn. He reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I’m going to open this week with a case.
A 56-year-old musician presents with diffuse abdominal pain, cramping, and jaundice. His medical history is notable for years of diffuse abdominal complaints, characterized by disabling bouts of diarrhea.
In addition to the jaundice, this acute illness was accompanied by fever as well as diffuse edema and ascites. The patient underwent several abdominal paracenteses to drain excess fluid. One consulting physician administered alcohol to relieve pain, to little avail.
The patient succumbed to his illness. An autopsy showed diffuse liver injury, as well as papillary necrosis of the kidneys. Notably, the nerves of his auditory canal were noted to be thickened, along with the bony part of the skull, consistent with Paget disease of the bone and explaining, potentially, why the talented musician had gone deaf at such a young age.
An interesting note on social history: The patient had apparently developed some feelings for the niece of that doctor who prescribed alcohol. Her name was Therese, perhaps mistranscribed as Elise, and it seems that he may have written this song for her.
We’re talking about this paper in Current Biology, by Tristan Begg and colleagues, which gives us a look into the very genome of what some would argue is the world’s greatest composer.
The ability to extract DNA from older specimens has transformed the fields of anthropology, archaeology, and history, and now, perhaps, musicology as well.
The researchers identified eight locks of hair in private and public collections, all attributed to the maestro.
Four of the samples had an intact chain of custody from the time the hair was cut. DNA sequencing on these four and an additional one of the eight locks came from the same individual, a male of European heritage.

The three locks with less documentation came from three other unrelated individuals. Interestingly, analysis of one of those hair samples – the so-called Hiller Lock – had shown high levels of lead, leading historians to speculate that lead poisoning could account for some of Beethoven’s symptoms.

DNA analysis of that hair reveals it to have come from a woman likely of North African, Middle Eastern, or Jewish ancestry. We can no longer presume that plumbism was involved in Beethoven’s death. Beethoven’s ancestry turns out to be less exotic and maps quite well to ethnic German populations today.

In fact, there are van Beethovens alive as we speak, primarily in Belgium. Genealogic records suggest that these van Beethovens share a common ancestor with the virtuoso composer, a man by the name of Aert van Beethoven.
But the DNA reveals a scandal.
The Y-chromosome that Beethoven inherited was not Aert van Beethoven’s. Questions of Beethoven’s paternity have been raised before, but this evidence strongly suggests an extramarital paternity event, at least in the generations preceding his birth. That’s right – Beethoven may not have been a Beethoven.
With five locks now essentially certain to have come from Beethoven himself, the authors could use DNA analysis to try to explain three significant health problems he experienced throughout his life and death: his hearing loss, his terrible gastrointestinal issues, and his liver failure.
Let’s start with the most disappointing results, explanations for his hearing loss. No genetic cause was forthcoming, though the authors note that they have little to go on in regard to the genetic risk for otosclerosis, to which his hearing loss has often been attributed. Lead poisoning is, of course, possible here, though this report focuses only on genetics – there was no testing for lead – and as I mentioned, the lock that was strongly lead-positive in prior studies is almost certainly inauthentic.
What about his lifelong GI complaints? Some have suggested celiac disease or lactose intolerance as explanations. These can essentially be ruled out by the genetic analysis, which shows no risk alleles for celiac disease and the presence of the lactase-persistence gene which confers the ability to metabolize lactose throughout one’s life. IBS is harder to assess genetically, but for what it’s worth, he scored quite low on a polygenic risk score for the condition, in just the 9th percentile of risk. We should probably be looking elsewhere to explain the GI distress.
The genetic information bore much more fruit in regard to his liver disease. Remember that Beethoven’s autopsy showed cirrhosis. His polygenic risk score for liver cirrhosis puts him in the 96th percentile of risk. He was also heterozygous for two variants that can cause hereditary hemochromatosis. The risk for cirrhosis among those with these variants is increased by the use of alcohol. And historical accounts are quite clear that Beethoven consumed more than his share.
But it wasn’t just Beethoven’s DNA in these hair follicles. Analysis of a follicle from later in his life revealed the unmistakable presence of hepatitis B virus. Endemic in Europe at the time, this was a common cause of liver failure and is likely to have contributed to, if not directly caused, Beethoven’s demise.

It’s hard to read these results and not marvel at the fact that, two centuries after his death, our fascination with Beethoven has led us to probe every corner of his life – his letters, his writings, his medical records, and now his very DNA. What are we actually looking for? Is it relevant to us today what caused his hearing loss? His stomach troubles? Even his death? Will it help any patients in the future? I propose that what we are actually trying to understand is something ineffable: Genius of magnitude that is rarely seen in one or many lifetimes. And our scientific tools, as sharp as they may have become, are still far too blunt to probe the depths of that transcendence.
In any case, friends, no more of these sounds. Let us sing more cheerful songs, more full of joy.
For Medscape, I’m Perry Wilson.
Dr. Wilson is associate professor, department of medicine, and director, Clinical and Translational Research Accelerator, at Yale University, New Haven, Conn. He reported no conflicts of interest.
A version of this article first appeared on Medscape.com.
Nurse makes millions selling her licensing exam study sheets
Ms. Beggs, 28, sells one-page study sheets or bundles of sheets, sometimes with colorful drawings, conversation bubbles and underlining, that boil down concepts for particular conditions into easy-to-understand language.
The biggest seller on Ms. Beggs’ online marketplace Etsy site, RNExplained, is a bundle of study guides covering eight core nursing classes. The notes range in price from $2 to $150. More than 70,000 customers have bought the $60 bundle, according to the website.
Ms. Beggs’ business developed in a “very unintentional” way when COVID hit with just months left in her nursing program at Mount Saint Mary’s University, Los Angeles, she told this news organization.
Classes had switched to Zoom, and she had no one to study with as she prepared to take her board exams.
“The best way I know how to study is to teach things out loud. But because I had nobody to teach out loud to, I would literally teach them to the wall,” Ms. Beggs said. “I would record myself so I could play it back and teach myself these topics that were hard for me to understand.”
Just for fun, she says, she posted them on TikTok and the responses started flowing in, with followers asking where she was selling the sheets. She now has more than 660,000 TikTok followers and 9 million likes.
Ms. Beggs said that every sheet highlights a condition, and she has made 308 of them.
Traditional classroom lessons typically teach one medical condition in 5-6 pages, Ms. Beggs said. “I go straight to the point.”
One reviewer on Ms. Beggs’ Etsy site appreciated the handwritten notes, calling them “simplified and concise.” Another commented: “Definitely helped me pass my last exam.”
Ms. Beggs says that her notes may seem simple, but each page represents comprehensive research.
“I have to go through not just one source of information to make sure my information is factual,” Ms. Beggs says. “What you teach in California might be a little different than what you teach in Florida. It’s very meticulous. The lab values will be a little different everywhere you go.”
She acknowledges her competition, noting that there are many other study guides for the NCLEX and nursing courses.
Nursing groups weigh in
Dawn Kappel, spokesperson for the National Council of State Boards of Nursing, which oversees NCLEX, said in an interview that “NCSBN has no issue with the current content of Stephanee Beggs’ business venture.”
For many students, the study guides will be helpful, especially for visual learners, said Carole Kenner, PhD, RN, dean and professor in the School of Nursing and Health Sciences at The College of New Jersey.
But for students “who are less confident in their knowledge, I would want to see a lot more in-depth explanation and rationale,” Dr. Kenner said.
“Since the NCLEX is moving to more cased-based scenarios, the next-gen unfolding cases, you really have to understand a lot of the rationale.”
The notes remind Dr. Kenner of traditional flash cards. “I don’t think it will work for all students, but even the fanciest of onsite review courses are useful to everyone,” she said.
‘Not cutting corners’
As an emergency nurse, Ms. Beggs said, “I have the experience as a nurse to show people that what you are learning will be seen in real life.”
“The way I teach my brand is not to take shortcuts. I love to teach to understand rather than teaching to memorize for an exam.”
She said she sees her guides as a supplement to learning, not a replacement.
“It’s not cutting corners,” she says. “I condense a medical condition that could take a very long time to understand and break it into layman’s terms.”
Ms. Beggs said when people hear about the $2 million, they often ask her whether she plans to give up her shifts in the emergency department for the more lucrative venture.
The answer is no, at least not yet.
“Aside from teaching, I genuinely love being at the bedside,” Ms. Beggs said. “I don’t foresee myself leaving that for good for as long as I can handle both.” She acknowledged, though, that her business now takes up most of her time.
“I love everything about both aspects, so it’s hard for me to choose.”
A version of this article first appeared on Medscape.com.
Ms. Beggs, 28, sells one-page study sheets or bundles of sheets, sometimes with colorful drawings, conversation bubbles and underlining, that boil down concepts for particular conditions into easy-to-understand language.
The biggest seller on Ms. Beggs’ online marketplace Etsy site, RNExplained, is a bundle of study guides covering eight core nursing classes. The notes range in price from $2 to $150. More than 70,000 customers have bought the $60 bundle, according to the website.
Ms. Beggs’ business developed in a “very unintentional” way when COVID hit with just months left in her nursing program at Mount Saint Mary’s University, Los Angeles, she told this news organization.
Classes had switched to Zoom, and she had no one to study with as she prepared to take her board exams.
“The best way I know how to study is to teach things out loud. But because I had nobody to teach out loud to, I would literally teach them to the wall,” Ms. Beggs said. “I would record myself so I could play it back and teach myself these topics that were hard for me to understand.”
Just for fun, she says, she posted them on TikTok and the responses started flowing in, with followers asking where she was selling the sheets. She now has more than 660,000 TikTok followers and 9 million likes.
Ms. Beggs said that every sheet highlights a condition, and she has made 308 of them.
Traditional classroom lessons typically teach one medical condition in 5-6 pages, Ms. Beggs said. “I go straight to the point.”
One reviewer on Ms. Beggs’ Etsy site appreciated the handwritten notes, calling them “simplified and concise.” Another commented: “Definitely helped me pass my last exam.”
Ms. Beggs says that her notes may seem simple, but each page represents comprehensive research.
“I have to go through not just one source of information to make sure my information is factual,” Ms. Beggs says. “What you teach in California might be a little different than what you teach in Florida. It’s very meticulous. The lab values will be a little different everywhere you go.”
She acknowledges her competition, noting that there are many other study guides for the NCLEX and nursing courses.
Nursing groups weigh in
Dawn Kappel, spokesperson for the National Council of State Boards of Nursing, which oversees NCLEX, said in an interview that “NCSBN has no issue with the current content of Stephanee Beggs’ business venture.”
For many students, the study guides will be helpful, especially for visual learners, said Carole Kenner, PhD, RN, dean and professor in the School of Nursing and Health Sciences at The College of New Jersey.
But for students “who are less confident in their knowledge, I would want to see a lot more in-depth explanation and rationale,” Dr. Kenner said.
“Since the NCLEX is moving to more cased-based scenarios, the next-gen unfolding cases, you really have to understand a lot of the rationale.”
The notes remind Dr. Kenner of traditional flash cards. “I don’t think it will work for all students, but even the fanciest of onsite review courses are useful to everyone,” she said.
‘Not cutting corners’
As an emergency nurse, Ms. Beggs said, “I have the experience as a nurse to show people that what you are learning will be seen in real life.”
“The way I teach my brand is not to take shortcuts. I love to teach to understand rather than teaching to memorize for an exam.”
She said she sees her guides as a supplement to learning, not a replacement.
“It’s not cutting corners,” she says. “I condense a medical condition that could take a very long time to understand and break it into layman’s terms.”
Ms. Beggs said when people hear about the $2 million, they often ask her whether she plans to give up her shifts in the emergency department for the more lucrative venture.
The answer is no, at least not yet.
“Aside from teaching, I genuinely love being at the bedside,” Ms. Beggs said. “I don’t foresee myself leaving that for good for as long as I can handle both.” She acknowledged, though, that her business now takes up most of her time.
“I love everything about both aspects, so it’s hard for me to choose.”
A version of this article first appeared on Medscape.com.
Ms. Beggs, 28, sells one-page study sheets or bundles of sheets, sometimes with colorful drawings, conversation bubbles and underlining, that boil down concepts for particular conditions into easy-to-understand language.
The biggest seller on Ms. Beggs’ online marketplace Etsy site, RNExplained, is a bundle of study guides covering eight core nursing classes. The notes range in price from $2 to $150. More than 70,000 customers have bought the $60 bundle, according to the website.
Ms. Beggs’ business developed in a “very unintentional” way when COVID hit with just months left in her nursing program at Mount Saint Mary’s University, Los Angeles, she told this news organization.
Classes had switched to Zoom, and she had no one to study with as she prepared to take her board exams.
“The best way I know how to study is to teach things out loud. But because I had nobody to teach out loud to, I would literally teach them to the wall,” Ms. Beggs said. “I would record myself so I could play it back and teach myself these topics that were hard for me to understand.”
Just for fun, she says, she posted them on TikTok and the responses started flowing in, with followers asking where she was selling the sheets. She now has more than 660,000 TikTok followers and 9 million likes.
Ms. Beggs said that every sheet highlights a condition, and she has made 308 of them.
Traditional classroom lessons typically teach one medical condition in 5-6 pages, Ms. Beggs said. “I go straight to the point.”
One reviewer on Ms. Beggs’ Etsy site appreciated the handwritten notes, calling them “simplified and concise.” Another commented: “Definitely helped me pass my last exam.”
Ms. Beggs says that her notes may seem simple, but each page represents comprehensive research.
“I have to go through not just one source of information to make sure my information is factual,” Ms. Beggs says. “What you teach in California might be a little different than what you teach in Florida. It’s very meticulous. The lab values will be a little different everywhere you go.”
She acknowledges her competition, noting that there are many other study guides for the NCLEX and nursing courses.
Nursing groups weigh in
Dawn Kappel, spokesperson for the National Council of State Boards of Nursing, which oversees NCLEX, said in an interview that “NCSBN has no issue with the current content of Stephanee Beggs’ business venture.”
For many students, the study guides will be helpful, especially for visual learners, said Carole Kenner, PhD, RN, dean and professor in the School of Nursing and Health Sciences at The College of New Jersey.
But for students “who are less confident in their knowledge, I would want to see a lot more in-depth explanation and rationale,” Dr. Kenner said.
“Since the NCLEX is moving to more cased-based scenarios, the next-gen unfolding cases, you really have to understand a lot of the rationale.”
The notes remind Dr. Kenner of traditional flash cards. “I don’t think it will work for all students, but even the fanciest of onsite review courses are useful to everyone,” she said.
‘Not cutting corners’
As an emergency nurse, Ms. Beggs said, “I have the experience as a nurse to show people that what you are learning will be seen in real life.”
“The way I teach my brand is not to take shortcuts. I love to teach to understand rather than teaching to memorize for an exam.”
She said she sees her guides as a supplement to learning, not a replacement.
“It’s not cutting corners,” she says. “I condense a medical condition that could take a very long time to understand and break it into layman’s terms.”
Ms. Beggs said when people hear about the $2 million, they often ask her whether she plans to give up her shifts in the emergency department for the more lucrative venture.
The answer is no, at least not yet.
“Aside from teaching, I genuinely love being at the bedside,” Ms. Beggs said. “I don’t foresee myself leaving that for good for as long as I can handle both.” She acknowledged, though, that her business now takes up most of her time.
“I love everything about both aspects, so it’s hard for me to choose.”
A version of this article first appeared on Medscape.com.
Severe atopic dermatitis linked with significant overall morbidity
Key clinical point: Compared with mild atopic dermatitis (AD), severe AD results in an increased risk for overall morbidity.
Major finding: Patients with severe vs mild AD had a significantly increased risk for other dermatitis, extragenital herpes, urticaria, impetigo, cellulitis, varicella zoster virus, abscess, sepsis, conjunctivitis, alopecia areata, asthma, allergic rhinitis and conjunctivitis, stress-related and somatoform diseases, intervertebral disc disorders, osteoporosis, and lymphomas (all P < .001), as well as condylomas, rosacea, certain psychiatric disorders, migraine, sleep apnea, other sleep disorders, hypertension, atherosclerosis, enthesopathies, and drug-induced cataract (all P < .05). However, patients with moderate or severe vs mild AD had a lower risk for prostate cancer (P < .05).
Study details: The data come from a retrospective real-world cohort study including 124,038 patients with mild (n = 53,046), moderate (n = 46,296), or severe (n = 24,696) AD.
Disclosures: This study was sponsored by AbbVie. Some authors reported ties, including employment and stock ownership, with AbbVie and others.
Source: Kiiski V et al. Effect of disease severity on comorbid conditions in atopic dermatitis: Nationwide registry-based investigation in Finnish adults. Acta Derm Venereol. 2023;103:adv00882 (Mar 8). Doi: 10.2340/actadv.v103.4447
Key clinical point: Compared with mild atopic dermatitis (AD), severe AD results in an increased risk for overall morbidity.
Major finding: Patients with severe vs mild AD had a significantly increased risk for other dermatitis, extragenital herpes, urticaria, impetigo, cellulitis, varicella zoster virus, abscess, sepsis, conjunctivitis, alopecia areata, asthma, allergic rhinitis and conjunctivitis, stress-related and somatoform diseases, intervertebral disc disorders, osteoporosis, and lymphomas (all P < .001), as well as condylomas, rosacea, certain psychiatric disorders, migraine, sleep apnea, other sleep disorders, hypertension, atherosclerosis, enthesopathies, and drug-induced cataract (all P < .05). However, patients with moderate or severe vs mild AD had a lower risk for prostate cancer (P < .05).
Study details: The data come from a retrospective real-world cohort study including 124,038 patients with mild (n = 53,046), moderate (n = 46,296), or severe (n = 24,696) AD.
Disclosures: This study was sponsored by AbbVie. Some authors reported ties, including employment and stock ownership, with AbbVie and others.
Source: Kiiski V et al. Effect of disease severity on comorbid conditions in atopic dermatitis: Nationwide registry-based investigation in Finnish adults. Acta Derm Venereol. 2023;103:adv00882 (Mar 8). Doi: 10.2340/actadv.v103.4447
Key clinical point: Compared with mild atopic dermatitis (AD), severe AD results in an increased risk for overall morbidity.
Major finding: Patients with severe vs mild AD had a significantly increased risk for other dermatitis, extragenital herpes, urticaria, impetigo, cellulitis, varicella zoster virus, abscess, sepsis, conjunctivitis, alopecia areata, asthma, allergic rhinitis and conjunctivitis, stress-related and somatoform diseases, intervertebral disc disorders, osteoporosis, and lymphomas (all P < .001), as well as condylomas, rosacea, certain psychiatric disorders, migraine, sleep apnea, other sleep disorders, hypertension, atherosclerosis, enthesopathies, and drug-induced cataract (all P < .05). However, patients with moderate or severe vs mild AD had a lower risk for prostate cancer (P < .05).
Study details: The data come from a retrospective real-world cohort study including 124,038 patients with mild (n = 53,046), moderate (n = 46,296), or severe (n = 24,696) AD.
Disclosures: This study was sponsored by AbbVie. Some authors reported ties, including employment and stock ownership, with AbbVie and others.
Source: Kiiski V et al. Effect of disease severity on comorbid conditions in atopic dermatitis: Nationwide registry-based investigation in Finnish adults. Acta Derm Venereol. 2023;103:adv00882 (Mar 8). Doi: 10.2340/actadv.v103.4447
Skin biomarkers in infants aged 2 months predictive of future atopic dermatitis onset
Key clinical point: Stratum corneum (SC) lipid and cytokine levels in infants aged 2 months can predict the future onset of atopic dermatitis (AD) up to 2 years of age.
Major finding: The SC levels of protein-bound ceramides were decreased (P = .0058), whereas those of unsaturated sphingomyelin (P < .0001), thymic stromal lymphopoietin (P = .0032), and interleukin-13 (IL13; P < .0001) increased in infants with vs without a family history of atopic diseases. A combination of family history and high IL13, high 26:1-sphingomyelin, and low O30:0(C22S)-ceramide levels had a strong predictive power for AD onset by 2 years of age (adjusted odds ratio 54.0; 95% CI 9.2-317.5).
Study details: This observational study included 111 asymptomatic infants with or without a family history of atopic diseases who underwent skin tape strip analysis at 2 months of age.
Disclosures: This study was funded by Edelstein Family Chair of Pediatric Allergy-Immunology at National Jewish Health, Denver, Colorado, and the Korea Environment Industry and Technology Institute (KEITI) through Environmental Health Action Program, funded by Korea Ministry of Environment. Some authors reported ties with various organizations.
Source: Berdyshev E et al. Stratum corneum lipid and cytokine biomarkers at two months of age predict the future onset of atopic dermatitis. J Allergy Clin Immunol. 2023 (Feb 22). Doi: 10.1016/j.jaci.2023.02.013
Key clinical point: Stratum corneum (SC) lipid and cytokine levels in infants aged 2 months can predict the future onset of atopic dermatitis (AD) up to 2 years of age.
Major finding: The SC levels of protein-bound ceramides were decreased (P = .0058), whereas those of unsaturated sphingomyelin (P < .0001), thymic stromal lymphopoietin (P = .0032), and interleukin-13 (IL13; P < .0001) increased in infants with vs without a family history of atopic diseases. A combination of family history and high IL13, high 26:1-sphingomyelin, and low O30:0(C22S)-ceramide levels had a strong predictive power for AD onset by 2 years of age (adjusted odds ratio 54.0; 95% CI 9.2-317.5).
Study details: This observational study included 111 asymptomatic infants with or without a family history of atopic diseases who underwent skin tape strip analysis at 2 months of age.
Disclosures: This study was funded by Edelstein Family Chair of Pediatric Allergy-Immunology at National Jewish Health, Denver, Colorado, and the Korea Environment Industry and Technology Institute (KEITI) through Environmental Health Action Program, funded by Korea Ministry of Environment. Some authors reported ties with various organizations.
Source: Berdyshev E et al. Stratum corneum lipid and cytokine biomarkers at two months of age predict the future onset of atopic dermatitis. J Allergy Clin Immunol. 2023 (Feb 22). Doi: 10.1016/j.jaci.2023.02.013
Key clinical point: Stratum corneum (SC) lipid and cytokine levels in infants aged 2 months can predict the future onset of atopic dermatitis (AD) up to 2 years of age.
Major finding: The SC levels of protein-bound ceramides were decreased (P = .0058), whereas those of unsaturated sphingomyelin (P < .0001), thymic stromal lymphopoietin (P = .0032), and interleukin-13 (IL13; P < .0001) increased in infants with vs without a family history of atopic diseases. A combination of family history and high IL13, high 26:1-sphingomyelin, and low O30:0(C22S)-ceramide levels had a strong predictive power for AD onset by 2 years of age (adjusted odds ratio 54.0; 95% CI 9.2-317.5).
Study details: This observational study included 111 asymptomatic infants with or without a family history of atopic diseases who underwent skin tape strip analysis at 2 months of age.
Disclosures: This study was funded by Edelstein Family Chair of Pediatric Allergy-Immunology at National Jewish Health, Denver, Colorado, and the Korea Environment Industry and Technology Institute (KEITI) through Environmental Health Action Program, funded by Korea Ministry of Environment. Some authors reported ties with various organizations.
Source: Berdyshev E et al. Stratum corneum lipid and cytokine biomarkers at two months of age predict the future onset of atopic dermatitis. J Allergy Clin Immunol. 2023 (Feb 22). Doi: 10.1016/j.jaci.2023.02.013
Crisaborole improves sleep outcomes in pediatric mild-to-moderate atopic dermatitis
Key clinical point: Crisaborole was effective in reducing sleep disturbance in pediatric patients with mild-to-moderate atopic dermatitis (AD).
Major finding: At day 29, a significantly lower proportion of patients reported sleep disturbance in the crisaborole vs vehicle group (48.5% vs 57.7%; P = .001). Crisaborole led to a 32.2% decrease in the proportion of infants with ≥1 night of disturbed sleep.
Study details: This post hoc analysis included infants aged 3 to <24 months (CARE 1; n = 137), patients aged 2 to <16 years (pooled CORE 1/CORE 2; n = 1227), and families of patients aged 2 to <18 years (pooled CORE 1/CORE 2; n = 1313) with mild-to-moderate AD who received crisaborole or vehicle twice daily for 28 days.
Disclosures: This study was sponsored by Pfizer Inc. Some authors declared serving as speakers and consultants for or receiving speaker and consulting fees from various sources, including Pfizer. Six authors declared being employees of and holding stocks in Pfizer Inc.
Source: Fowler J et al. Impact of crisaborole on sleep outcomes in pediatric patients with mild-to-moderate atopic dermatitis. Dermatol Ther (Heidelb). 2023 (Feb 22). Doi: 10.1007/s13555-023-00899-y
Key clinical point: Crisaborole was effective in reducing sleep disturbance in pediatric patients with mild-to-moderate atopic dermatitis (AD).
Major finding: At day 29, a significantly lower proportion of patients reported sleep disturbance in the crisaborole vs vehicle group (48.5% vs 57.7%; P = .001). Crisaborole led to a 32.2% decrease in the proportion of infants with ≥1 night of disturbed sleep.
Study details: This post hoc analysis included infants aged 3 to <24 months (CARE 1; n = 137), patients aged 2 to <16 years (pooled CORE 1/CORE 2; n = 1227), and families of patients aged 2 to <18 years (pooled CORE 1/CORE 2; n = 1313) with mild-to-moderate AD who received crisaborole or vehicle twice daily for 28 days.
Disclosures: This study was sponsored by Pfizer Inc. Some authors declared serving as speakers and consultants for or receiving speaker and consulting fees from various sources, including Pfizer. Six authors declared being employees of and holding stocks in Pfizer Inc.
Source: Fowler J et al. Impact of crisaborole on sleep outcomes in pediatric patients with mild-to-moderate atopic dermatitis. Dermatol Ther (Heidelb). 2023 (Feb 22). Doi: 10.1007/s13555-023-00899-y
Key clinical point: Crisaborole was effective in reducing sleep disturbance in pediatric patients with mild-to-moderate atopic dermatitis (AD).
Major finding: At day 29, a significantly lower proportion of patients reported sleep disturbance in the crisaborole vs vehicle group (48.5% vs 57.7%; P = .001). Crisaborole led to a 32.2% decrease in the proportion of infants with ≥1 night of disturbed sleep.
Study details: This post hoc analysis included infants aged 3 to <24 months (CARE 1; n = 137), patients aged 2 to <16 years (pooled CORE 1/CORE 2; n = 1227), and families of patients aged 2 to <18 years (pooled CORE 1/CORE 2; n = 1313) with mild-to-moderate AD who received crisaborole or vehicle twice daily for 28 days.
Disclosures: This study was sponsored by Pfizer Inc. Some authors declared serving as speakers and consultants for or receiving speaker and consulting fees from various sources, including Pfizer. Six authors declared being employees of and holding stocks in Pfizer Inc.
Source: Fowler J et al. Impact of crisaborole on sleep outcomes in pediatric patients with mild-to-moderate atopic dermatitis. Dermatol Ther (Heidelb). 2023 (Feb 22). Doi: 10.1007/s13555-023-00899-y
Atopic dermatitis is positively linked with the risk for gastroesophageal reflux disease
Key clinical point: Adult patients with atopic dermatitis (AD) are at an increased risk of developing subsequent gastroesophageal reflux disease (GERD).
Major finding: Patients with AD vs matched control individuals had a 15% higher risk for subsequent GERD (adjusted hazard ratio [aHR] 1.15; P = .0013), with the risk being higher in women (aHR 1.17; P = .0120) vs men (aHR 1.15; P = .0343) with AD.
Study details: The data come from a retrospective population-based cohort study including 9164 patients aged ≥20 years with AD and 9164 matched control individuals without AD.
Disclosures: This study was supported by a grant of the National Research Foundation of Korea funded by the Ministry of Education, Science, and Technology. The authors declared no conflicts of interest.
Source: Lee SW et al. Atopic dermatitis and risk of gastroesophageal reflux disease: A nationwide population-based study. PLoS One. 2023;18(2):e0281883 (Feb 17). Doi: 10.1371/journal.pone.0281883
Key clinical point: Adult patients with atopic dermatitis (AD) are at an increased risk of developing subsequent gastroesophageal reflux disease (GERD).
Major finding: Patients with AD vs matched control individuals had a 15% higher risk for subsequent GERD (adjusted hazard ratio [aHR] 1.15; P = .0013), with the risk being higher in women (aHR 1.17; P = .0120) vs men (aHR 1.15; P = .0343) with AD.
Study details: The data come from a retrospective population-based cohort study including 9164 patients aged ≥20 years with AD and 9164 matched control individuals without AD.
Disclosures: This study was supported by a grant of the National Research Foundation of Korea funded by the Ministry of Education, Science, and Technology. The authors declared no conflicts of interest.
Source: Lee SW et al. Atopic dermatitis and risk of gastroesophageal reflux disease: A nationwide population-based study. PLoS One. 2023;18(2):e0281883 (Feb 17). Doi: 10.1371/journal.pone.0281883
Key clinical point: Adult patients with atopic dermatitis (AD) are at an increased risk of developing subsequent gastroesophageal reflux disease (GERD).
Major finding: Patients with AD vs matched control individuals had a 15% higher risk for subsequent GERD (adjusted hazard ratio [aHR] 1.15; P = .0013), with the risk being higher in women (aHR 1.17; P = .0120) vs men (aHR 1.15; P = .0343) with AD.
Study details: The data come from a retrospective population-based cohort study including 9164 patients aged ≥20 years with AD and 9164 matched control individuals without AD.
Disclosures: This study was supported by a grant of the National Research Foundation of Korea funded by the Ministry of Education, Science, and Technology. The authors declared no conflicts of interest.
Source: Lee SW et al. Atopic dermatitis and risk of gastroesophageal reflux disease: A nationwide population-based study. PLoS One. 2023;18(2):e0281883 (Feb 17). Doi: 10.1371/journal.pone.0281883
Season of birth influences the risk for atopic dermatitis in early infancy
Key clinical point: Environmental conditions characterized by the month of birth affect the risk of developing eczema and atopic dermatitis (AD) in infants until 1 year of age.
Major finding: With infants born in spring as a reference, those born in autumn had the highest risk for eczema at 6 months (adjusted odds ratio [aOR] 2.19; 95% CI 2.10-2.30) and 1 year (aOR 1.08; 95% CI 1.02-1.14) of age and for physician-diagnosed AD up to 1 year of age (aOR 1.33; 95% CI 1.20-1.47), whereas those born in summer had the highest risk for eczema at the age of 1 month (aOR 1.19; 95% CI 1.14-1.24).
Study details: This study analyzed the data of 81,615 infants from a prospective birth cohort study, the Japan Environment and Children’s Study (JECS).
Disclosures: The JECS is supported by the Ministry of the Environment, Japan. The authors declared no conflicts of interest.
Source: Tsuchida A et al. Season of birth and atopic dermatitis in early infancy: Results from the Japan Environment and Children’s Study. BMC Pediatr. 2023;23(1):78 (Feb 15). Doi: 10.1186/s12887-023-03878-6
Key clinical point: Environmental conditions characterized by the month of birth affect the risk of developing eczema and atopic dermatitis (AD) in infants until 1 year of age.
Major finding: With infants born in spring as a reference, those born in autumn had the highest risk for eczema at 6 months (adjusted odds ratio [aOR] 2.19; 95% CI 2.10-2.30) and 1 year (aOR 1.08; 95% CI 1.02-1.14) of age and for physician-diagnosed AD up to 1 year of age (aOR 1.33; 95% CI 1.20-1.47), whereas those born in summer had the highest risk for eczema at the age of 1 month (aOR 1.19; 95% CI 1.14-1.24).
Study details: This study analyzed the data of 81,615 infants from a prospective birth cohort study, the Japan Environment and Children’s Study (JECS).
Disclosures: The JECS is supported by the Ministry of the Environment, Japan. The authors declared no conflicts of interest.
Source: Tsuchida A et al. Season of birth and atopic dermatitis in early infancy: Results from the Japan Environment and Children’s Study. BMC Pediatr. 2023;23(1):78 (Feb 15). Doi: 10.1186/s12887-023-03878-6
Key clinical point: Environmental conditions characterized by the month of birth affect the risk of developing eczema and atopic dermatitis (AD) in infants until 1 year of age.
Major finding: With infants born in spring as a reference, those born in autumn had the highest risk for eczema at 6 months (adjusted odds ratio [aOR] 2.19; 95% CI 2.10-2.30) and 1 year (aOR 1.08; 95% CI 1.02-1.14) of age and for physician-diagnosed AD up to 1 year of age (aOR 1.33; 95% CI 1.20-1.47), whereas those born in summer had the highest risk for eczema at the age of 1 month (aOR 1.19; 95% CI 1.14-1.24).
Study details: This study analyzed the data of 81,615 infants from a prospective birth cohort study, the Japan Environment and Children’s Study (JECS).
Disclosures: The JECS is supported by the Ministry of the Environment, Japan. The authors declared no conflicts of interest.
Source: Tsuchida A et al. Season of birth and atopic dermatitis in early infancy: Results from the Japan Environment and Children’s Study. BMC Pediatr. 2023;23(1):78 (Feb 15). Doi: 10.1186/s12887-023-03878-6
Pruritus reduction crucial for improving other inflammatory symptoms in nemolizumab-treated atopic dermatitis
Key clinical point: Patients with atopic dermatitis (AD) who experienced greater pruritus reductions after nemolizumab treatment also showed clinically meaningful improvements in other pruritus and cutaneous symptoms.
Major finding: At week 16, a greater proportion of pruritus Visual Analogy Scale (VAS) responders (≥50% improvement) vs nonresponders achieved a pruritus VAS score of <30 mm (81.6% vs 0%), ≥50% improvement in the Eczema Area and Severity Index score (65.3% vs 44.7%), ≥4-point improvement in pruritus numerical rating scale score (89.6% vs 2.1%), and 5-level itch score of ≤1 (42.9% vs 3.2%).
Study details: This post hoc analysis of the Nemolizumab-JP01 study Part A included 215 patients with inadequately controlled AD who had been randomly assigned to receive subcutaneous 60 mg nemolizumab (n = 143) or placebo (n = 72) every 4 weeks for 16 weeks.
Disclosures: This study was funded by Maruho. Some authors declared receiving grants or personal fees from various organizations, including Maruho. Two authors declared being employees of Maruho.
Source: Kabashima K et al for the Nemolizumab-JP01 Study Group. Clinically meaningful improvements in cutaneous lesions and quality of life measures in patients with atopic dermatitis with greater pruritus reductions after treatment with 60 mg nemolizumab subcutaneously every 4 weeks: Subgroup analysis from a phase 3, randomized, controlled trial. J Dermatolog Treat. 2023;1-13 (Feb 13). Doi: 10.1080/09546634.2023.2177096
Key clinical point: Patients with atopic dermatitis (AD) who experienced greater pruritus reductions after nemolizumab treatment also showed clinically meaningful improvements in other pruritus and cutaneous symptoms.
Major finding: At week 16, a greater proportion of pruritus Visual Analogy Scale (VAS) responders (≥50% improvement) vs nonresponders achieved a pruritus VAS score of <30 mm (81.6% vs 0%), ≥50% improvement in the Eczema Area and Severity Index score (65.3% vs 44.7%), ≥4-point improvement in pruritus numerical rating scale score (89.6% vs 2.1%), and 5-level itch score of ≤1 (42.9% vs 3.2%).
Study details: This post hoc analysis of the Nemolizumab-JP01 study Part A included 215 patients with inadequately controlled AD who had been randomly assigned to receive subcutaneous 60 mg nemolizumab (n = 143) or placebo (n = 72) every 4 weeks for 16 weeks.
Disclosures: This study was funded by Maruho. Some authors declared receiving grants or personal fees from various organizations, including Maruho. Two authors declared being employees of Maruho.
Source: Kabashima K et al for the Nemolizumab-JP01 Study Group. Clinically meaningful improvements in cutaneous lesions and quality of life measures in patients with atopic dermatitis with greater pruritus reductions after treatment with 60 mg nemolizumab subcutaneously every 4 weeks: Subgroup analysis from a phase 3, randomized, controlled trial. J Dermatolog Treat. 2023;1-13 (Feb 13). Doi: 10.1080/09546634.2023.2177096
Key clinical point: Patients with atopic dermatitis (AD) who experienced greater pruritus reductions after nemolizumab treatment also showed clinically meaningful improvements in other pruritus and cutaneous symptoms.
Major finding: At week 16, a greater proportion of pruritus Visual Analogy Scale (VAS) responders (≥50% improvement) vs nonresponders achieved a pruritus VAS score of <30 mm (81.6% vs 0%), ≥50% improvement in the Eczema Area and Severity Index score (65.3% vs 44.7%), ≥4-point improvement in pruritus numerical rating scale score (89.6% vs 2.1%), and 5-level itch score of ≤1 (42.9% vs 3.2%).
Study details: This post hoc analysis of the Nemolizumab-JP01 study Part A included 215 patients with inadequately controlled AD who had been randomly assigned to receive subcutaneous 60 mg nemolizumab (n = 143) or placebo (n = 72) every 4 weeks for 16 weeks.
Disclosures: This study was funded by Maruho. Some authors declared receiving grants or personal fees from various organizations, including Maruho. Two authors declared being employees of Maruho.
Source: Kabashima K et al for the Nemolizumab-JP01 Study Group. Clinically meaningful improvements in cutaneous lesions and quality of life measures in patients with atopic dermatitis with greater pruritus reductions after treatment with 60 mg nemolizumab subcutaneously every 4 weeks: Subgroup analysis from a phase 3, randomized, controlled trial. J Dermatolog Treat. 2023;1-13 (Feb 13). Doi: 10.1080/09546634.2023.2177096




