User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
When Should a Pediatrician Suspect a Rare Disease?
A wise medical precept is attributed to Theodore Woodward, MD (1914-2005): “When you hear hoofbeats, think of horses, not zebras.” Primary care pediatricians, however, often find themselves confronting so-called rare or uncommon diseases (“zebras”) in their offices. The pressing challenge is to know when to suspect them. How can one reconcile the need to dispel uncertainty with the use of diagnostic tests that can be costly and invasive? When can the desire to reassure parents mean delaying the detection of a potentially treatable condition?
“It may seem like wordplay, but it’s not uncommon to have a rare disease,” noted Alejandro Fainboim, MD, a specialist in rare diseases and head of the Multivalent Day Hospital at the Ricardo Gutiérrez Children’s Hospital in Buenos Aires, Argentina. “And pediatricians are the first line of defense in detecting these types of pathologies. To make the diagnosis, we have to consider them. And to consider them, we must be knowledgeable. That’s why sometimes, ignorance slows down the diagnosis,” Dr. Fainboim made his remarks during an online seminar organized for the press on the eve of Rare Disease Day, which is commemorated on February 29th.
There are more than 8000 rare diseases, which generally are defined as those affecting fewer than five people per 10,000. But collectively, one in every 13 people has one of these diseases, and one in every two diagnosed patients is a child. Dr. Fainboim emphasized that most of these rare diseases are severe or very severe, hereditary, degenerative, and potentially fatal. And although they are pediatric pathologies, some manifest later in adulthood.
“The major problem we pediatricians face is that we’re handed a model from adults to solve pediatric diseases. So, signs and symptoms are described that we won’t find early on, but we have to anticipate and learn to decode some that are hidden,” he remarked.
Diagnostic delays and repeated consultations with various doctors before identification are common. Dr. Fainboim added that in industrialized countries, the diagnosis of these diseases takes between 5 and 10 years, and in low-income countries, up to 30 years or more. However, “this has improved significantly in recent years,” he said.
Unnoticed Signs
Specialists who treat patients with rare diseases often feel that there were obvious signs that went unnoticed and should have aroused the suspicion of the primary care physician. An example is paroxysmal nocturnal hemoglobinuria, which affects 13-14 people per million inhabitants and can appear at any age, although the incidence is higher in the third decade of life.
“In my 50 years as a doctor, I’ve seen seven or eight patients with paroxysmal nocturnal hemoglobinuria,” said Elsa Nucifora, MD, a hematologist at the Italian Hospital of Buenos Aires, Argentina. But “the diagnosis is so easy” that doctors could make it if they “were to think instead of acting automatically because they’re in a hurry,” she added. The diagnosis should be considered “every time anemia occurs in a young person, with certain characteristics, instead of giving them iron like everyone else and ‘we’ll see later’…the diagnosis is in two or three steps, so it’s not complicated.”
Similar situations occur with more than 1000 neuromuscular diseases involving mutations in more than 600 genes, including spinal muscular atrophy and muscular dystrophies.
“What are the most common manifestations? The hypotonic infant, the child who walks late, who falls frequently, who can’t climb stairs, who later may have difficulty breathing, who loses strength: These are presentations often unrecognized by doctors not in the specialty,” said Alberto Dubrovsky, MD, director of the Department of Neurology and the Neuromuscular Diseases Unit at the Favaloro University Neuroscience Institute in Buenos Aires, Argentina, during the seminar. “And considering that these diseases are diagnosed based on genetic mutations that need to be known to search for and request them, we are faced with a truly complex scenario that requires subspecialization.”
In a study recently published in the Argentine Archives of Pediatrics, Dr. Dubrovsky and colleagues interviewed 112 families of Argentine patients with molecular diagnoses of spinal muscular atrophy types I, II, and III and found that in 75%-85% of cases, the first signs of the disease (such as hypotonia, developmental delay, inability to achieve bipedal standing, or frequent falls) were recognized by parents. For type I, the most severe and early onset, in only 17.5% of cases did a neonatologist or pediatrician first notice something. Of the 72 patients with types II and III, where routine checks are less frequent than in the first months of life, only one doctor detected the first signs of the disease before parents or other relatives.
In the same study, the median time elapsed between the first sign and confirmed molecular diagnosis was 2, 10, and 31.5 months for types I, II, and III, respectively. The delay “is primarily due to the lack of clinical suspicion on the part of the intervening physician, who often dismisses or misinterprets the signs reported by parents, as reflected in the alternative diagnoses invoked,” the authors wrote.
“I don’t even ask for suspicion of a specific rare disease because that requires specialization. What I ask for is a kind of recognition or realization that something is happening and then request a consultation with the specialist to ensure proper care,” said Dr. Dubrovsky.
In another study conducted among 70 Argentine patients under age 13 years who were diagnosed with Duchenne muscular dystrophy (one of the most severe forms of muscular dystrophy), 82% of the pediatricians who were initially consulted for any problem in motor agility that parents, other relatives, or teachers had detected dismissed the observation. “They’re told to wait, that it will mature a little more,” said Dr. Dubrovsky. This explains why the time to diagnosis in Argentina from the first signs is around 2 years. The delays are unfortunate because “today we have treatments capable of interfering with the disease’s progression slope, reducing its progression, or eventually stopping it,” he said.
“Do you mind that primary care pediatricians don’t notice or dismiss signs and symptoms strongly suggestive of one of these rare diseases? Does it frustrate you?” this news organization asked asked Dr. Dubrovsky. “Sometimes it does make me angry, but many times it’s understood that there can’t be highly trained specialists everywhere to realize and request diagnostic tests. One must consider the circumstances in each case, and that’s why we work in education,” he replied.
Rules and Experience
In an interview, Dr. Fainboim highlighted key factors that should prompt a pediatrician’s suspicion. One is common symptoms expressed in a more intense or complicated way or when many symptoms coexist in the same patient, even if each one separately is benign or not so severe.
Dr. Fainboim also recommended establishing a therapeutic alliance with parents. “We shouldn’t undermine what parents say, especially those who have other children and already know what normal child development is like. This is a very important milestone.
“We have to strengthen the suspicion clue, and for that, we rely on standards and our experience, which we keep refining. As Wilde said, experience is the sum of our mistakes. But there’s no universal answer. Not all families are the same. Not all diseases manifest in the same way. And unless there’s an imminent risk to life or function, one can wait and take the time to evaluate it. For example, if I have a child with slowed developmental milestones, what I have to do is teach how to stimulate them or send them for stimulation with another professional. And I observe the response to this initial basic treatment. If I see no response, the alarms start to grow louder,” said Dr. Fainboim.
Pablo Barvosa, MD, the principal physician in the outpatient area of the Juan P. Garrahan Pediatric Hospital in Buenos Aires, Argentina, and a member of the Working Group on Genetics and Rare Diseases of the Argentine Society of Pediatrics, told this news organization about other factors that should be considered for detecting these pathologies. Dr. Barvosa did not participate in the online seminar.
“Patients with rare diseases have common symptoms. What needs to be done is to prioritize those symptoms that behave abnormally, that have an unusual evolution compared with normal situations. For example, children who go into a coma after a fasting episode or after eating a certain food,” he said.
Dr. Barvosa also suggested considering when patients belong to certain communities where there is a lot of endogamy, due to the higher incidence of hereditary diseases. “Attention should be heightened when parents are cousins or relatives,” he pointed out.
“My view is that doctors should think more and better, be rational, sequential. If a disease is treated and resolved, but we find out that the child had 26 previous hospitalizations in the last 2 years, something is wrong. We have to look at the patient’s and family’s life histories. If a mother had 15 miscarriages, that’s a warning sign. We have to find a common thread. Be a sharp-witted pediatrician,” said Dr. Barvosa.
The suspicion and diagnosis of a rare disease can be devastating for families and painful for the professional, but even if there is no specific treatment, “something can always be done for patients,” he added.
And in certain circumstances, identifying a rare disease can reverse the ominous “stamp” of a wrong diagnosis. Dr. Barvosa commented on the case of a 7-year-old boy he attended at the hospital in 2014. The boy presented as quadriplegic, with no mobility in his limbs, and the parents were convinced he had that condition because he had fallen from the roof of the house. Although imaging techniques did not show a spinal injury, it was assumed to be a case of spinal cord injury without radiographic abnormality. But something caught Dr. Barvosa’s attention: The boy had well-developed abdominal muscles, as if he were an athlete. So, he requested an electromyogram, and the muscle was found to be in permanent contraction.
“The patient didn’t have a spinal cord injury: He had Isaacs’ syndrome,” said Dr. Barvosa. The syndrome also is known as acquired neuromyotonia, a rare condition of hyperexcitability of peripheral nerves that activate muscle fibers. “That is treated with anticonvulsants, such as phenytoin. Within a week, he was walking again, and shortly after, he was playing soccer. When I presented the case at a conference, I cried with emotion. That’s why the pediatrician must be insistent, be like the gadfly that stings in the ear” when there are clinical elements that don’t quite fit into a clear diagnosis, he added.
In recent publications, Dr. Dubrovsky has reported receiving fees for consultations or research from PTC, Sarepta, Biogen, Sanofi Genzyme, Takeda Avexis, Novartis, Raffo, and Roche. Dr. Nucifora has received fees from Jansen LATAM. Dr. Fainboim reported receiving fees from Sanofi. Dr. Barvosa has declared no relevant financial conflicts of interest. The webinar was organized by Urban Comunicaciones.
This story was translated from the Medscape Spanish edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
A wise medical precept is attributed to Theodore Woodward, MD (1914-2005): “When you hear hoofbeats, think of horses, not zebras.” Primary care pediatricians, however, often find themselves confronting so-called rare or uncommon diseases (“zebras”) in their offices. The pressing challenge is to know when to suspect them. How can one reconcile the need to dispel uncertainty with the use of diagnostic tests that can be costly and invasive? When can the desire to reassure parents mean delaying the detection of a potentially treatable condition?
“It may seem like wordplay, but it’s not uncommon to have a rare disease,” noted Alejandro Fainboim, MD, a specialist in rare diseases and head of the Multivalent Day Hospital at the Ricardo Gutiérrez Children’s Hospital in Buenos Aires, Argentina. “And pediatricians are the first line of defense in detecting these types of pathologies. To make the diagnosis, we have to consider them. And to consider them, we must be knowledgeable. That’s why sometimes, ignorance slows down the diagnosis,” Dr. Fainboim made his remarks during an online seminar organized for the press on the eve of Rare Disease Day, which is commemorated on February 29th.
There are more than 8000 rare diseases, which generally are defined as those affecting fewer than five people per 10,000. But collectively, one in every 13 people has one of these diseases, and one in every two diagnosed patients is a child. Dr. Fainboim emphasized that most of these rare diseases are severe or very severe, hereditary, degenerative, and potentially fatal. And although they are pediatric pathologies, some manifest later in adulthood.
“The major problem we pediatricians face is that we’re handed a model from adults to solve pediatric diseases. So, signs and symptoms are described that we won’t find early on, but we have to anticipate and learn to decode some that are hidden,” he remarked.
Diagnostic delays and repeated consultations with various doctors before identification are common. Dr. Fainboim added that in industrialized countries, the diagnosis of these diseases takes between 5 and 10 years, and in low-income countries, up to 30 years or more. However, “this has improved significantly in recent years,” he said.
Unnoticed Signs
Specialists who treat patients with rare diseases often feel that there were obvious signs that went unnoticed and should have aroused the suspicion of the primary care physician. An example is paroxysmal nocturnal hemoglobinuria, which affects 13-14 people per million inhabitants and can appear at any age, although the incidence is higher in the third decade of life.
“In my 50 years as a doctor, I’ve seen seven or eight patients with paroxysmal nocturnal hemoglobinuria,” said Elsa Nucifora, MD, a hematologist at the Italian Hospital of Buenos Aires, Argentina. But “the diagnosis is so easy” that doctors could make it if they “were to think instead of acting automatically because they’re in a hurry,” she added. The diagnosis should be considered “every time anemia occurs in a young person, with certain characteristics, instead of giving them iron like everyone else and ‘we’ll see later’…the diagnosis is in two or three steps, so it’s not complicated.”
Similar situations occur with more than 1000 neuromuscular diseases involving mutations in more than 600 genes, including spinal muscular atrophy and muscular dystrophies.
“What are the most common manifestations? The hypotonic infant, the child who walks late, who falls frequently, who can’t climb stairs, who later may have difficulty breathing, who loses strength: These are presentations often unrecognized by doctors not in the specialty,” said Alberto Dubrovsky, MD, director of the Department of Neurology and the Neuromuscular Diseases Unit at the Favaloro University Neuroscience Institute in Buenos Aires, Argentina, during the seminar. “And considering that these diseases are diagnosed based on genetic mutations that need to be known to search for and request them, we are faced with a truly complex scenario that requires subspecialization.”
In a study recently published in the Argentine Archives of Pediatrics, Dr. Dubrovsky and colleagues interviewed 112 families of Argentine patients with molecular diagnoses of spinal muscular atrophy types I, II, and III and found that in 75%-85% of cases, the first signs of the disease (such as hypotonia, developmental delay, inability to achieve bipedal standing, or frequent falls) were recognized by parents. For type I, the most severe and early onset, in only 17.5% of cases did a neonatologist or pediatrician first notice something. Of the 72 patients with types II and III, where routine checks are less frequent than in the first months of life, only one doctor detected the first signs of the disease before parents or other relatives.
In the same study, the median time elapsed between the first sign and confirmed molecular diagnosis was 2, 10, and 31.5 months for types I, II, and III, respectively. The delay “is primarily due to the lack of clinical suspicion on the part of the intervening physician, who often dismisses or misinterprets the signs reported by parents, as reflected in the alternative diagnoses invoked,” the authors wrote.
“I don’t even ask for suspicion of a specific rare disease because that requires specialization. What I ask for is a kind of recognition or realization that something is happening and then request a consultation with the specialist to ensure proper care,” said Dr. Dubrovsky.
In another study conducted among 70 Argentine patients under age 13 years who were diagnosed with Duchenne muscular dystrophy (one of the most severe forms of muscular dystrophy), 82% of the pediatricians who were initially consulted for any problem in motor agility that parents, other relatives, or teachers had detected dismissed the observation. “They’re told to wait, that it will mature a little more,” said Dr. Dubrovsky. This explains why the time to diagnosis in Argentina from the first signs is around 2 years. The delays are unfortunate because “today we have treatments capable of interfering with the disease’s progression slope, reducing its progression, or eventually stopping it,” he said.
“Do you mind that primary care pediatricians don’t notice or dismiss signs and symptoms strongly suggestive of one of these rare diseases? Does it frustrate you?” this news organization asked asked Dr. Dubrovsky. “Sometimes it does make me angry, but many times it’s understood that there can’t be highly trained specialists everywhere to realize and request diagnostic tests. One must consider the circumstances in each case, and that’s why we work in education,” he replied.
Rules and Experience
In an interview, Dr. Fainboim highlighted key factors that should prompt a pediatrician’s suspicion. One is common symptoms expressed in a more intense or complicated way or when many symptoms coexist in the same patient, even if each one separately is benign or not so severe.
Dr. Fainboim also recommended establishing a therapeutic alliance with parents. “We shouldn’t undermine what parents say, especially those who have other children and already know what normal child development is like. This is a very important milestone.
“We have to strengthen the suspicion clue, and for that, we rely on standards and our experience, which we keep refining. As Wilde said, experience is the sum of our mistakes. But there’s no universal answer. Not all families are the same. Not all diseases manifest in the same way. And unless there’s an imminent risk to life or function, one can wait and take the time to evaluate it. For example, if I have a child with slowed developmental milestones, what I have to do is teach how to stimulate them or send them for stimulation with another professional. And I observe the response to this initial basic treatment. If I see no response, the alarms start to grow louder,” said Dr. Fainboim.
Pablo Barvosa, MD, the principal physician in the outpatient area of the Juan P. Garrahan Pediatric Hospital in Buenos Aires, Argentina, and a member of the Working Group on Genetics and Rare Diseases of the Argentine Society of Pediatrics, told this news organization about other factors that should be considered for detecting these pathologies. Dr. Barvosa did not participate in the online seminar.
“Patients with rare diseases have common symptoms. What needs to be done is to prioritize those symptoms that behave abnormally, that have an unusual evolution compared with normal situations. For example, children who go into a coma after a fasting episode or after eating a certain food,” he said.
Dr. Barvosa also suggested considering when patients belong to certain communities where there is a lot of endogamy, due to the higher incidence of hereditary diseases. “Attention should be heightened when parents are cousins or relatives,” he pointed out.
“My view is that doctors should think more and better, be rational, sequential. If a disease is treated and resolved, but we find out that the child had 26 previous hospitalizations in the last 2 years, something is wrong. We have to look at the patient’s and family’s life histories. If a mother had 15 miscarriages, that’s a warning sign. We have to find a common thread. Be a sharp-witted pediatrician,” said Dr. Barvosa.
The suspicion and diagnosis of a rare disease can be devastating for families and painful for the professional, but even if there is no specific treatment, “something can always be done for patients,” he added.
And in certain circumstances, identifying a rare disease can reverse the ominous “stamp” of a wrong diagnosis. Dr. Barvosa commented on the case of a 7-year-old boy he attended at the hospital in 2014. The boy presented as quadriplegic, with no mobility in his limbs, and the parents were convinced he had that condition because he had fallen from the roof of the house. Although imaging techniques did not show a spinal injury, it was assumed to be a case of spinal cord injury without radiographic abnormality. But something caught Dr. Barvosa’s attention: The boy had well-developed abdominal muscles, as if he were an athlete. So, he requested an electromyogram, and the muscle was found to be in permanent contraction.
“The patient didn’t have a spinal cord injury: He had Isaacs’ syndrome,” said Dr. Barvosa. The syndrome also is known as acquired neuromyotonia, a rare condition of hyperexcitability of peripheral nerves that activate muscle fibers. “That is treated with anticonvulsants, such as phenytoin. Within a week, he was walking again, and shortly after, he was playing soccer. When I presented the case at a conference, I cried with emotion. That’s why the pediatrician must be insistent, be like the gadfly that stings in the ear” when there are clinical elements that don’t quite fit into a clear diagnosis, he added.
In recent publications, Dr. Dubrovsky has reported receiving fees for consultations or research from PTC, Sarepta, Biogen, Sanofi Genzyme, Takeda Avexis, Novartis, Raffo, and Roche. Dr. Nucifora has received fees from Jansen LATAM. Dr. Fainboim reported receiving fees from Sanofi. Dr. Barvosa has declared no relevant financial conflicts of interest. The webinar was organized by Urban Comunicaciones.
This story was translated from the Medscape Spanish edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
A wise medical precept is attributed to Theodore Woodward, MD (1914-2005): “When you hear hoofbeats, think of horses, not zebras.” Primary care pediatricians, however, often find themselves confronting so-called rare or uncommon diseases (“zebras”) in their offices. The pressing challenge is to know when to suspect them. How can one reconcile the need to dispel uncertainty with the use of diagnostic tests that can be costly and invasive? When can the desire to reassure parents mean delaying the detection of a potentially treatable condition?
“It may seem like wordplay, but it’s not uncommon to have a rare disease,” noted Alejandro Fainboim, MD, a specialist in rare diseases and head of the Multivalent Day Hospital at the Ricardo Gutiérrez Children’s Hospital in Buenos Aires, Argentina. “And pediatricians are the first line of defense in detecting these types of pathologies. To make the diagnosis, we have to consider them. And to consider them, we must be knowledgeable. That’s why sometimes, ignorance slows down the diagnosis,” Dr. Fainboim made his remarks during an online seminar organized for the press on the eve of Rare Disease Day, which is commemorated on February 29th.
There are more than 8000 rare diseases, which generally are defined as those affecting fewer than five people per 10,000. But collectively, one in every 13 people has one of these diseases, and one in every two diagnosed patients is a child. Dr. Fainboim emphasized that most of these rare diseases are severe or very severe, hereditary, degenerative, and potentially fatal. And although they are pediatric pathologies, some manifest later in adulthood.
“The major problem we pediatricians face is that we’re handed a model from adults to solve pediatric diseases. So, signs and symptoms are described that we won’t find early on, but we have to anticipate and learn to decode some that are hidden,” he remarked.
Diagnostic delays and repeated consultations with various doctors before identification are common. Dr. Fainboim added that in industrialized countries, the diagnosis of these diseases takes between 5 and 10 years, and in low-income countries, up to 30 years or more. However, “this has improved significantly in recent years,” he said.
Unnoticed Signs
Specialists who treat patients with rare diseases often feel that there were obvious signs that went unnoticed and should have aroused the suspicion of the primary care physician. An example is paroxysmal nocturnal hemoglobinuria, which affects 13-14 people per million inhabitants and can appear at any age, although the incidence is higher in the third decade of life.
“In my 50 years as a doctor, I’ve seen seven or eight patients with paroxysmal nocturnal hemoglobinuria,” said Elsa Nucifora, MD, a hematologist at the Italian Hospital of Buenos Aires, Argentina. But “the diagnosis is so easy” that doctors could make it if they “were to think instead of acting automatically because they’re in a hurry,” she added. The diagnosis should be considered “every time anemia occurs in a young person, with certain characteristics, instead of giving them iron like everyone else and ‘we’ll see later’…the diagnosis is in two or three steps, so it’s not complicated.”
Similar situations occur with more than 1000 neuromuscular diseases involving mutations in more than 600 genes, including spinal muscular atrophy and muscular dystrophies.
“What are the most common manifestations? The hypotonic infant, the child who walks late, who falls frequently, who can’t climb stairs, who later may have difficulty breathing, who loses strength: These are presentations often unrecognized by doctors not in the specialty,” said Alberto Dubrovsky, MD, director of the Department of Neurology and the Neuromuscular Diseases Unit at the Favaloro University Neuroscience Institute in Buenos Aires, Argentina, during the seminar. “And considering that these diseases are diagnosed based on genetic mutations that need to be known to search for and request them, we are faced with a truly complex scenario that requires subspecialization.”
In a study recently published in the Argentine Archives of Pediatrics, Dr. Dubrovsky and colleagues interviewed 112 families of Argentine patients with molecular diagnoses of spinal muscular atrophy types I, II, and III and found that in 75%-85% of cases, the first signs of the disease (such as hypotonia, developmental delay, inability to achieve bipedal standing, or frequent falls) were recognized by parents. For type I, the most severe and early onset, in only 17.5% of cases did a neonatologist or pediatrician first notice something. Of the 72 patients with types II and III, where routine checks are less frequent than in the first months of life, only one doctor detected the first signs of the disease before parents or other relatives.
In the same study, the median time elapsed between the first sign and confirmed molecular diagnosis was 2, 10, and 31.5 months for types I, II, and III, respectively. The delay “is primarily due to the lack of clinical suspicion on the part of the intervening physician, who often dismisses or misinterprets the signs reported by parents, as reflected in the alternative diagnoses invoked,” the authors wrote.
“I don’t even ask for suspicion of a specific rare disease because that requires specialization. What I ask for is a kind of recognition or realization that something is happening and then request a consultation with the specialist to ensure proper care,” said Dr. Dubrovsky.
In another study conducted among 70 Argentine patients under age 13 years who were diagnosed with Duchenne muscular dystrophy (one of the most severe forms of muscular dystrophy), 82% of the pediatricians who were initially consulted for any problem in motor agility that parents, other relatives, or teachers had detected dismissed the observation. “They’re told to wait, that it will mature a little more,” said Dr. Dubrovsky. This explains why the time to diagnosis in Argentina from the first signs is around 2 years. The delays are unfortunate because “today we have treatments capable of interfering with the disease’s progression slope, reducing its progression, or eventually stopping it,” he said.
“Do you mind that primary care pediatricians don’t notice or dismiss signs and symptoms strongly suggestive of one of these rare diseases? Does it frustrate you?” this news organization asked asked Dr. Dubrovsky. “Sometimes it does make me angry, but many times it’s understood that there can’t be highly trained specialists everywhere to realize and request diagnostic tests. One must consider the circumstances in each case, and that’s why we work in education,” he replied.
Rules and Experience
In an interview, Dr. Fainboim highlighted key factors that should prompt a pediatrician’s suspicion. One is common symptoms expressed in a more intense or complicated way or when many symptoms coexist in the same patient, even if each one separately is benign or not so severe.
Dr. Fainboim also recommended establishing a therapeutic alliance with parents. “We shouldn’t undermine what parents say, especially those who have other children and already know what normal child development is like. This is a very important milestone.
“We have to strengthen the suspicion clue, and for that, we rely on standards and our experience, which we keep refining. As Wilde said, experience is the sum of our mistakes. But there’s no universal answer. Not all families are the same. Not all diseases manifest in the same way. And unless there’s an imminent risk to life or function, one can wait and take the time to evaluate it. For example, if I have a child with slowed developmental milestones, what I have to do is teach how to stimulate them or send them for stimulation with another professional. And I observe the response to this initial basic treatment. If I see no response, the alarms start to grow louder,” said Dr. Fainboim.
Pablo Barvosa, MD, the principal physician in the outpatient area of the Juan P. Garrahan Pediatric Hospital in Buenos Aires, Argentina, and a member of the Working Group on Genetics and Rare Diseases of the Argentine Society of Pediatrics, told this news organization about other factors that should be considered for detecting these pathologies. Dr. Barvosa did not participate in the online seminar.
“Patients with rare diseases have common symptoms. What needs to be done is to prioritize those symptoms that behave abnormally, that have an unusual evolution compared with normal situations. For example, children who go into a coma after a fasting episode or after eating a certain food,” he said.
Dr. Barvosa also suggested considering when patients belong to certain communities where there is a lot of endogamy, due to the higher incidence of hereditary diseases. “Attention should be heightened when parents are cousins or relatives,” he pointed out.
“My view is that doctors should think more and better, be rational, sequential. If a disease is treated and resolved, but we find out that the child had 26 previous hospitalizations in the last 2 years, something is wrong. We have to look at the patient’s and family’s life histories. If a mother had 15 miscarriages, that’s a warning sign. We have to find a common thread. Be a sharp-witted pediatrician,” said Dr. Barvosa.
The suspicion and diagnosis of a rare disease can be devastating for families and painful for the professional, but even if there is no specific treatment, “something can always be done for patients,” he added.
And in certain circumstances, identifying a rare disease can reverse the ominous “stamp” of a wrong diagnosis. Dr. Barvosa commented on the case of a 7-year-old boy he attended at the hospital in 2014. The boy presented as quadriplegic, with no mobility in his limbs, and the parents were convinced he had that condition because he had fallen from the roof of the house. Although imaging techniques did not show a spinal injury, it was assumed to be a case of spinal cord injury without radiographic abnormality. But something caught Dr. Barvosa’s attention: The boy had well-developed abdominal muscles, as if he were an athlete. So, he requested an electromyogram, and the muscle was found to be in permanent contraction.
“The patient didn’t have a spinal cord injury: He had Isaacs’ syndrome,” said Dr. Barvosa. The syndrome also is known as acquired neuromyotonia, a rare condition of hyperexcitability of peripheral nerves that activate muscle fibers. “That is treated with anticonvulsants, such as phenytoin. Within a week, he was walking again, and shortly after, he was playing soccer. When I presented the case at a conference, I cried with emotion. That’s why the pediatrician must be insistent, be like the gadfly that stings in the ear” when there are clinical elements that don’t quite fit into a clear diagnosis, he added.
In recent publications, Dr. Dubrovsky has reported receiving fees for consultations or research from PTC, Sarepta, Biogen, Sanofi Genzyme, Takeda Avexis, Novartis, Raffo, and Roche. Dr. Nucifora has received fees from Jansen LATAM. Dr. Fainboim reported receiving fees from Sanofi. Dr. Barvosa has declared no relevant financial conflicts of interest. The webinar was organized by Urban Comunicaciones.
This story was translated from the Medscape Spanish edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
Vitamin D Supplements May Be a Double-Edged Sword
This transcript has been edited for clarity.
Welcome to Impact Factor, your weekly dose of commentary on a new medical study. I’m Dr F. Perry Wilson of the Yale School of Medicine.
Imagine, if you will, the great Cathedral of Our Lady of Correlation. You walk through the majestic oak doors depicting the link between ice cream sales and shark attacks, past the rose window depicting the cardiovascular benefits of red wine, and down the aisles frescoed in dramatic images showing how Facebook usage is associated with less life satisfaction. And then you reach the altar, the holy of holies where, emblazoned in shimmering pyrite, you see the patron saint of this church: vitamin D.
Yes, if you’ve watched this space, then you know that I have little truck with the wildly popular supplement. In all of clinical research, I believe that there is no molecule with stronger data for correlation and weaker data for causation.
Low serum vitamin D levels have been linked to higher risks for heart disease, cancer, falls, COVID, dementia, C diff, and others. And yet, when we do randomized trials of vitamin D supplementation — the thing that can prove that the low level was causally linked to the outcome of interest — we get negative results.
Trials aren’t perfect, of course, and we’ll talk in a moment about a big one that had some issues. But we are at a point where we need to either be vitamin D apologists, saying, “Forget what those lying RCTs tell you and buy this supplement” — an $800 million-a-year industry, by the way — or conclude that vitamin D levels are a convenient marker of various lifestyle factors that are associated with better outcomes: markers of exercise, getting outside, eating a varied diet.
Or perhaps vitamin D supplements have real effects. It’s just that the beneficial effects are matched by the harmful ones. Stay tuned.
The Women’s Health Initiative remains among the largest randomized trials of vitamin D and calcium supplementation ever conducted — and a major contributor to the negative outcomes of vitamin D trials.
But if you dig into the inclusion and exclusion criteria for this trial, you’ll find that individuals were allowed to continue taking vitamins and supplements while they were in the trial, regardless of their randomization status. In fact, the majority took supplements at baseline, and more took supplements over time.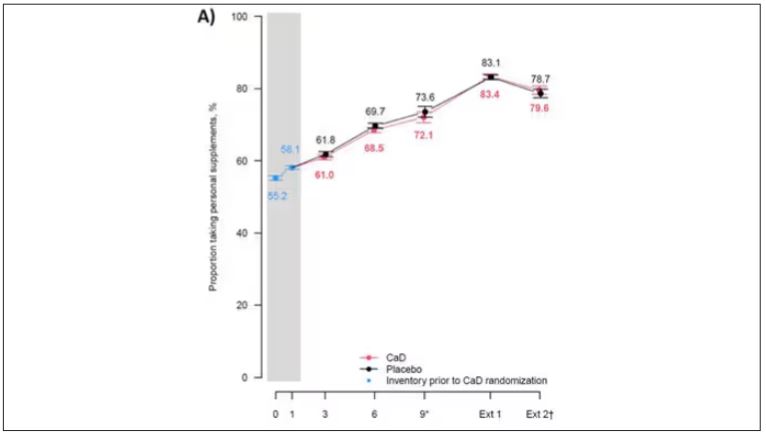
That means, of course, that people in the placebo group, who were getting sugar pills instead of vitamin D and calcium, may have been taking vitamin D and calcium on the side. That would certainly bias the results of the trial toward the null, which is what the primary analyses showed. To wit, the original analysis of the Women’s Health Initiative trial showed no effect of randomization to vitamin D supplementation on improving cancer or cardiovascular outcomes.
But the Women’s Health Initiative trial started 30 years ago. Today, with the benefit of decades of follow-up, we can re-investigate — and perhaps re-litigate — those findings, courtesy of this study, “Long-Term Effect of Randomization to Calcium and Vitamin D Supplementation on Health in Older Women” appearing in Annals of Internal Medicine.
Dr Cynthia Thomson, of the Mel and Enid Zuckerman College of Public Health at the University of Arizona, and colleagues led this updated analysis focused on two findings that had been hinted at, but not statistically confirmed, in other vitamin D studies: a potential for the supplement to reduce the risk for cancer, and a potential for it to increase the risk for heart disease.
The randomized trial itself only lasted 7 years. What we are seeing in this analysis of 36,282 women is outcomes that happened at any time from randomization to the end of 2023 — around 20 years after the randomization to supplementation stopped. But, the researchers would argue, that’s probably okay. Cancer and heart disease take time to develop; we see lung cancer long after people stop smoking. So a history of consistent vitamin D supplementation may indeed be protective — or harmful.
Here are the top-line results. Those randomized to vitamin D and calcium supplementation had a 7% reduction in the rate of death from cancer, driven primarily by a reduction in colorectal cancer. This was statistically significant. Also statistically significant? Those randomized to supplementation had a 6% increase in the rate of death from cardiovascular disease. Put those findings together and what do you get? Stone-cold nothing, in terms of overall mortality.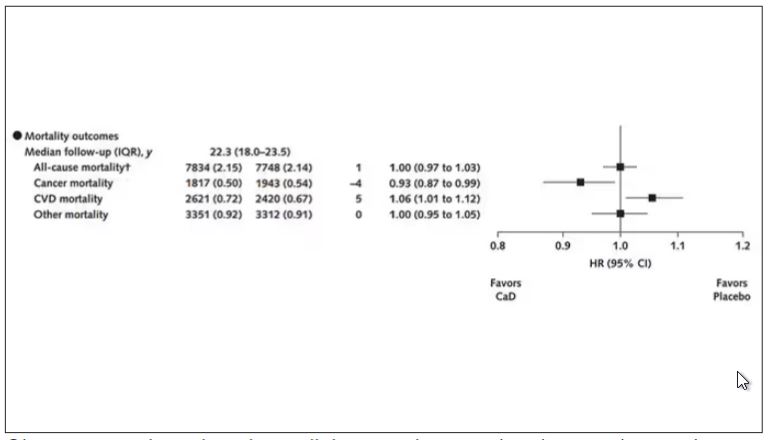
Okay, you say, but what about all that supplementation that was happening outside of the context of the trial, biasing our results toward the null?
The researchers finally clue us in.
First of all, I’ll tell you that, yes, people who were supplementing outside of the trial had higher baseline vitamin D levels — a median of 54.5 nmol/L vs 32.8 nmol/L. This may be because they were supplementing with vitamin D, but it could also be because people who take supplements tend to do other healthy things — another correlation to add to the great cathedral.
To get a better view of the real effects of randomization, the authors restricted the analysis to just those who did not use outside supplements. If vitamin D supplements help, then these are the people they should help. This group had about a 11% reduction in the incidence of cancer — statistically significant — and a 7% reduction in cancer mortality that did not meet the bar for statistical significance.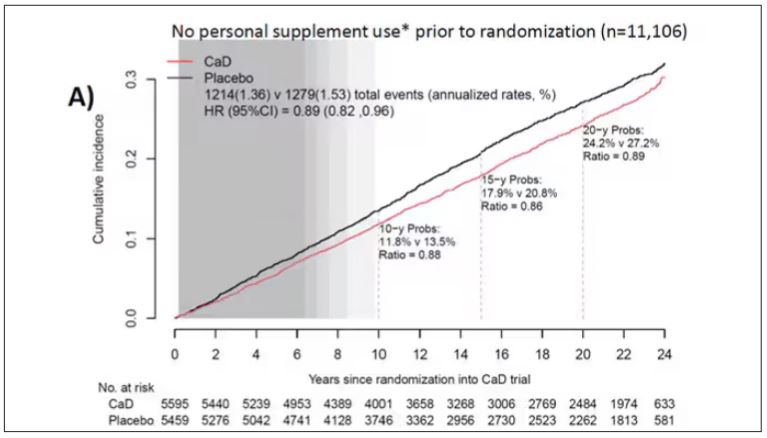
There was no increase in cardiovascular disease among this group. But this small effect on cancer was nowhere near enough to significantly reduce the rate of all-cause mortality.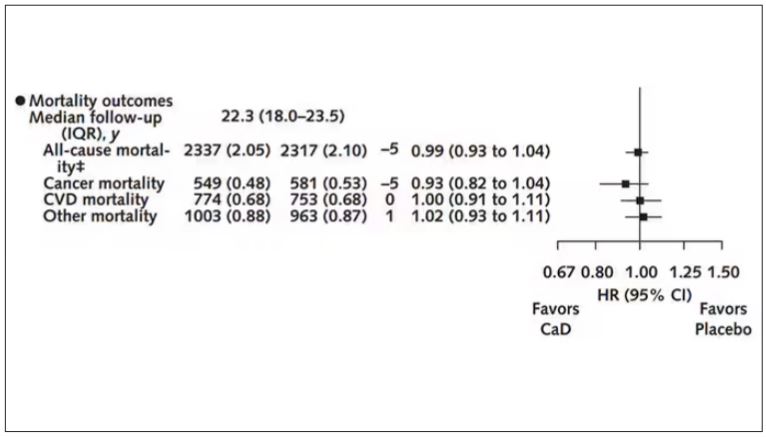
Among those using supplements, vitamin D supplementation didn’t really move the needle on any outcome.
I know what you’re thinking: How many of these women were vitamin D deficient when we got started? These results may simply be telling us that people who have normal vitamin D levels are fine to go without supplementation.
Nearly three fourths of women who were not taking supplements entered the trial with vitamin D levels below the 50 nmol/L cutoff that the authors suggest would qualify for deficiency. Around half of those who used supplements were deficient. And yet, frustratingly, I could not find data on the effect of randomization to supplementation stratified by baseline vitamin D level. I even reached out to Dr Thomson to ask about this. She replied, “We did not stratify on baseline values because the numbers are too small statistically to test this.” Sorry.
In the meantime, I can tell you that for your “average woman,” vitamin D supplementation likely has no effect on mortality. It might modestly reduce the risk for certain cancers while increasing the risk for heart disease (probably through coronary calcification). So, there might be some room for personalization here. Perhaps women with a strong family history of cancer or other risk factors would do better with supplements, and those with a high risk for heart disease would do worse. Seems like a strategy that could be tested in a clinical trial. But maybe we could ask the participants to give up their extracurricular supplement use before they enter the trial. F. Perry Wilson, MD, MSCE, has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
F. Perry Wilson, MD, MSCE, is an associate professor of medicine and public health and director of Yale’s Clinical and Translational Research Accelerator. His science communication work can be found in the Huffington Post, on NPR, and here on Medscape. He tweets @fperrywilson and his book, How Medicine Works and When It Doesn’t, is available now.
This transcript has been edited for clarity.
Welcome to Impact Factor, your weekly dose of commentary on a new medical study. I’m Dr F. Perry Wilson of the Yale School of Medicine.
Imagine, if you will, the great Cathedral of Our Lady of Correlation. You walk through the majestic oak doors depicting the link between ice cream sales and shark attacks, past the rose window depicting the cardiovascular benefits of red wine, and down the aisles frescoed in dramatic images showing how Facebook usage is associated with less life satisfaction. And then you reach the altar, the holy of holies where, emblazoned in shimmering pyrite, you see the patron saint of this church: vitamin D.
Yes, if you’ve watched this space, then you know that I have little truck with the wildly popular supplement. In all of clinical research, I believe that there is no molecule with stronger data for correlation and weaker data for causation.
Low serum vitamin D levels have been linked to higher risks for heart disease, cancer, falls, COVID, dementia, C diff, and others. And yet, when we do randomized trials of vitamin D supplementation — the thing that can prove that the low level was causally linked to the outcome of interest — we get negative results.
Trials aren’t perfect, of course, and we’ll talk in a moment about a big one that had some issues. But we are at a point where we need to either be vitamin D apologists, saying, “Forget what those lying RCTs tell you and buy this supplement” — an $800 million-a-year industry, by the way — or conclude that vitamin D levels are a convenient marker of various lifestyle factors that are associated with better outcomes: markers of exercise, getting outside, eating a varied diet.
Or perhaps vitamin D supplements have real effects. It’s just that the beneficial effects are matched by the harmful ones. Stay tuned.
The Women’s Health Initiative remains among the largest randomized trials of vitamin D and calcium supplementation ever conducted — and a major contributor to the negative outcomes of vitamin D trials.
But if you dig into the inclusion and exclusion criteria for this trial, you’ll find that individuals were allowed to continue taking vitamins and supplements while they were in the trial, regardless of their randomization status. In fact, the majority took supplements at baseline, and more took supplements over time.
That means, of course, that people in the placebo group, who were getting sugar pills instead of vitamin D and calcium, may have been taking vitamin D and calcium on the side. That would certainly bias the results of the trial toward the null, which is what the primary analyses showed. To wit, the original analysis of the Women’s Health Initiative trial showed no effect of randomization to vitamin D supplementation on improving cancer or cardiovascular outcomes.
But the Women’s Health Initiative trial started 30 years ago. Today, with the benefit of decades of follow-up, we can re-investigate — and perhaps re-litigate — those findings, courtesy of this study, “Long-Term Effect of Randomization to Calcium and Vitamin D Supplementation on Health in Older Women” appearing in Annals of Internal Medicine.
Dr Cynthia Thomson, of the Mel and Enid Zuckerman College of Public Health at the University of Arizona, and colleagues led this updated analysis focused on two findings that had been hinted at, but not statistically confirmed, in other vitamin D studies: a potential for the supplement to reduce the risk for cancer, and a potential for it to increase the risk for heart disease.
The randomized trial itself only lasted 7 years. What we are seeing in this analysis of 36,282 women is outcomes that happened at any time from randomization to the end of 2023 — around 20 years after the randomization to supplementation stopped. But, the researchers would argue, that’s probably okay. Cancer and heart disease take time to develop; we see lung cancer long after people stop smoking. So a history of consistent vitamin D supplementation may indeed be protective — or harmful.
Here are the top-line results. Those randomized to vitamin D and calcium supplementation had a 7% reduction in the rate of death from cancer, driven primarily by a reduction in colorectal cancer. This was statistically significant. Also statistically significant? Those randomized to supplementation had a 6% increase in the rate of death from cardiovascular disease. Put those findings together and what do you get? Stone-cold nothing, in terms of overall mortality.
Okay, you say, but what about all that supplementation that was happening outside of the context of the trial, biasing our results toward the null?
The researchers finally clue us in.
First of all, I’ll tell you that, yes, people who were supplementing outside of the trial had higher baseline vitamin D levels — a median of 54.5 nmol/L vs 32.8 nmol/L. This may be because they were supplementing with vitamin D, but it could also be because people who take supplements tend to do other healthy things — another correlation to add to the great cathedral.
To get a better view of the real effects of randomization, the authors restricted the analysis to just those who did not use outside supplements. If vitamin D supplements help, then these are the people they should help. This group had about a 11% reduction in the incidence of cancer — statistically significant — and a 7% reduction in cancer mortality that did not meet the bar for statistical significance.
There was no increase in cardiovascular disease among this group. But this small effect on cancer was nowhere near enough to significantly reduce the rate of all-cause mortality.
Among those using supplements, vitamin D supplementation didn’t really move the needle on any outcome.
I know what you’re thinking: How many of these women were vitamin D deficient when we got started? These results may simply be telling us that people who have normal vitamin D levels are fine to go without supplementation.
Nearly three fourths of women who were not taking supplements entered the trial with vitamin D levels below the 50 nmol/L cutoff that the authors suggest would qualify for deficiency. Around half of those who used supplements were deficient. And yet, frustratingly, I could not find data on the effect of randomization to supplementation stratified by baseline vitamin D level. I even reached out to Dr Thomson to ask about this. She replied, “We did not stratify on baseline values because the numbers are too small statistically to test this.” Sorry.
In the meantime, I can tell you that for your “average woman,” vitamin D supplementation likely has no effect on mortality. It might modestly reduce the risk for certain cancers while increasing the risk for heart disease (probably through coronary calcification). So, there might be some room for personalization here. Perhaps women with a strong family history of cancer or other risk factors would do better with supplements, and those with a high risk for heart disease would do worse. Seems like a strategy that could be tested in a clinical trial. But maybe we could ask the participants to give up their extracurricular supplement use before they enter the trial. F. Perry Wilson, MD, MSCE, has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
F. Perry Wilson, MD, MSCE, is an associate professor of medicine and public health and director of Yale’s Clinical and Translational Research Accelerator. His science communication work can be found in the Huffington Post, on NPR, and here on Medscape. He tweets @fperrywilson and his book, How Medicine Works and When It Doesn’t, is available now.
This transcript has been edited for clarity.
Welcome to Impact Factor, your weekly dose of commentary on a new medical study. I’m Dr F. Perry Wilson of the Yale School of Medicine.
Imagine, if you will, the great Cathedral of Our Lady of Correlation. You walk through the majestic oak doors depicting the link between ice cream sales and shark attacks, past the rose window depicting the cardiovascular benefits of red wine, and down the aisles frescoed in dramatic images showing how Facebook usage is associated with less life satisfaction. And then you reach the altar, the holy of holies where, emblazoned in shimmering pyrite, you see the patron saint of this church: vitamin D.
Yes, if you’ve watched this space, then you know that I have little truck with the wildly popular supplement. In all of clinical research, I believe that there is no molecule with stronger data for correlation and weaker data for causation.
Low serum vitamin D levels have been linked to higher risks for heart disease, cancer, falls, COVID, dementia, C diff, and others. And yet, when we do randomized trials of vitamin D supplementation — the thing that can prove that the low level was causally linked to the outcome of interest — we get negative results.
Trials aren’t perfect, of course, and we’ll talk in a moment about a big one that had some issues. But we are at a point where we need to either be vitamin D apologists, saying, “Forget what those lying RCTs tell you and buy this supplement” — an $800 million-a-year industry, by the way — or conclude that vitamin D levels are a convenient marker of various lifestyle factors that are associated with better outcomes: markers of exercise, getting outside, eating a varied diet.
Or perhaps vitamin D supplements have real effects. It’s just that the beneficial effects are matched by the harmful ones. Stay tuned.
The Women’s Health Initiative remains among the largest randomized trials of vitamin D and calcium supplementation ever conducted — and a major contributor to the negative outcomes of vitamin D trials.
But if you dig into the inclusion and exclusion criteria for this trial, you’ll find that individuals were allowed to continue taking vitamins and supplements while they were in the trial, regardless of their randomization status. In fact, the majority took supplements at baseline, and more took supplements over time.
That means, of course, that people in the placebo group, who were getting sugar pills instead of vitamin D and calcium, may have been taking vitamin D and calcium on the side. That would certainly bias the results of the trial toward the null, which is what the primary analyses showed. To wit, the original analysis of the Women’s Health Initiative trial showed no effect of randomization to vitamin D supplementation on improving cancer or cardiovascular outcomes.
But the Women’s Health Initiative trial started 30 years ago. Today, with the benefit of decades of follow-up, we can re-investigate — and perhaps re-litigate — those findings, courtesy of this study, “Long-Term Effect of Randomization to Calcium and Vitamin D Supplementation on Health in Older Women” appearing in Annals of Internal Medicine.
Dr Cynthia Thomson, of the Mel and Enid Zuckerman College of Public Health at the University of Arizona, and colleagues led this updated analysis focused on two findings that had been hinted at, but not statistically confirmed, in other vitamin D studies: a potential for the supplement to reduce the risk for cancer, and a potential for it to increase the risk for heart disease.
The randomized trial itself only lasted 7 years. What we are seeing in this analysis of 36,282 women is outcomes that happened at any time from randomization to the end of 2023 — around 20 years after the randomization to supplementation stopped. But, the researchers would argue, that’s probably okay. Cancer and heart disease take time to develop; we see lung cancer long after people stop smoking. So a history of consistent vitamin D supplementation may indeed be protective — or harmful.
Here are the top-line results. Those randomized to vitamin D and calcium supplementation had a 7% reduction in the rate of death from cancer, driven primarily by a reduction in colorectal cancer. This was statistically significant. Also statistically significant? Those randomized to supplementation had a 6% increase in the rate of death from cardiovascular disease. Put those findings together and what do you get? Stone-cold nothing, in terms of overall mortality.
Okay, you say, but what about all that supplementation that was happening outside of the context of the trial, biasing our results toward the null?
The researchers finally clue us in.
First of all, I’ll tell you that, yes, people who were supplementing outside of the trial had higher baseline vitamin D levels — a median of 54.5 nmol/L vs 32.8 nmol/L. This may be because they were supplementing with vitamin D, but it could also be because people who take supplements tend to do other healthy things — another correlation to add to the great cathedral.
To get a better view of the real effects of randomization, the authors restricted the analysis to just those who did not use outside supplements. If vitamin D supplements help, then these are the people they should help. This group had about a 11% reduction in the incidence of cancer — statistically significant — and a 7% reduction in cancer mortality that did not meet the bar for statistical significance.
There was no increase in cardiovascular disease among this group. But this small effect on cancer was nowhere near enough to significantly reduce the rate of all-cause mortality.
Among those using supplements, vitamin D supplementation didn’t really move the needle on any outcome.
I know what you’re thinking: How many of these women were vitamin D deficient when we got started? These results may simply be telling us that people who have normal vitamin D levels are fine to go without supplementation.
Nearly three fourths of women who were not taking supplements entered the trial with vitamin D levels below the 50 nmol/L cutoff that the authors suggest would qualify for deficiency. Around half of those who used supplements were deficient. And yet, frustratingly, I could not find data on the effect of randomization to supplementation stratified by baseline vitamin D level. I even reached out to Dr Thomson to ask about this. She replied, “We did not stratify on baseline values because the numbers are too small statistically to test this.” Sorry.
In the meantime, I can tell you that for your “average woman,” vitamin D supplementation likely has no effect on mortality. It might modestly reduce the risk for certain cancers while increasing the risk for heart disease (probably through coronary calcification). So, there might be some room for personalization here. Perhaps women with a strong family history of cancer or other risk factors would do better with supplements, and those with a high risk for heart disease would do worse. Seems like a strategy that could be tested in a clinical trial. But maybe we could ask the participants to give up their extracurricular supplement use before they enter the trial. F. Perry Wilson, MD, MSCE, has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
F. Perry Wilson, MD, MSCE, is an associate professor of medicine and public health and director of Yale’s Clinical and Translational Research Accelerator. His science communication work can be found in the Huffington Post, on NPR, and here on Medscape. He tweets @fperrywilson and his book, How Medicine Works and When It Doesn’t, is available now.
Long-Term Calcium and Vitamin D: Cancer Deaths Down, CVD Deaths Up in Older Women?
Some doctors may be scratching their heads over a new analysis reporting that combined calcium and vitamin D (CaD) supplements appear to be associated with a slight 6% increase in cardiovascular (CVD) mortality, a slight 7% decrease in cancer risk, and no effect on osteoporotic fracture in postmenopausal women.
The study, in Annals of Internal Medicine, found no effect of supplementation on all-cause mortality.
The findings emerged from an analysis of more than 20 years’ follow-up data on a randomized trial in postmenopausal women conducted as part of the Women’s Health Initiative (WHI).
Cynthia A. Thomson, PhD, RD, first author and cancer prevention scientist at the Arizona Cancer Center and a professor of health promotion sciences at the University of Arizona in Tucson said the findings recommend individualized assessment of the need for supplements for older women as they consider them in hopes of preventing fractures.
“Evaluate your patients individually and understand that there are some who may benefit from supplementation, for example, in terms of reducing colorectal cancer mortality,” Dr. Thomson said in an interview. The approach should be nuanced. “If you check the adequacy of vitamin D and calcium in their diets, supplementation may not be needed.” She added that supplementation is best considered in the context of a woman’s overall health profile, including risk factors for fracture, heart disease, and cancer, especially colorectal cancer (CRC).
Study Details
The investigators conducted postintervention follow-up of the WHI’s 7-year multicenter randomized intervention trial of CaD vs placebo.
Since existing evidence of long-term health outcomes was limited, the trial, begun in 1999 and closed in 2005, enrolled 36,282 postmenopausal women (mean age 62) with no history of breast or colorectal cancer. They were randomly assigned 1:1 to supplementation with 1000 mg of calcium carbonate (400 mg elemental calcium) plus 400 IU of vitamin D3 daily or placebo, taken twice daily in half doses.
Study outcomes were incidence of CRC, total and invasive breast cancer; disease-specific and all-cause mortality; total CVD; and hip fracture measured through December 2020, with analyses stratified by personal supplement usage.
Cancer. CaD was associated with reduced incident total cancer, CRC, and invasive breast cancer — notably among participants not taking CaD before randomization. Cancer incidence estimates varied widely, the authors noted, when stratified by supplement use before randomization. Noting that CaD seemed to have more cancer-related impact in those without prior supplementation, the authors suggested supplementation may affect cancer biology primarily by augmenting nutrient insufficiency.
An estimated 7% reduction in cancer mortality was observed after a median cumulative follow-up of 22.3 years: 1817 vs 1943 deaths (hazard ratio, 0.93; 95% CI, 0.87-0.99).
CVD. An estimated 6% increase in CVD mortality was seen in the CaD group: 2621 vs 2420 deaths (HR, 1.06; 95% CI, 1.01-1.12). Pretrial supplement users were found to be at higher CVD risk.
Hip fracture. No effect on hip fracture risk was measured, but the authors cautioned that hip fracture and CVD outcomes were available only for a subset of participants, and the effects of calcium alone vs vitamin D alone vs the combination could not be disentangled.
In a small subgroup analysis, some CaD users were seen to respond in terms of bone mineral density but since only 4 of the study’s 40 sites collected such information, the study was underpowered to examine the effect. ”Many other studies, however, show a response to supplementation in women who already have bone mineral deficits,” Dr. Thomson said.
The Calcification Question
One of the possible mechanisms of harm is that high-dose calcium supplements can increase the rate of blood coagulation and promote vascular calcification, said Emma Laing, PhD, RD, director of dietetics at the University of Georgia in Athens and a spokesperson for the Chicago-based Academy of Nutrition and Dietetics.
“Other factors that should be considered when determining a patient’s CVD risk are race, genetic predisposition, medical and social history, response to stress, and lifestyle behaviors, as well as the length of time supplements have been consumed,” added Dr. Laing, who was not involved in the WHI analysis.
“We asked ourselves if CaD supplements might contribute to calcification of the coronary arteries, since some believe this to be the case, although the literature is mixed,” said Dr. Thomson.
“So we did a shorter ancillary study in a small sample of several hundred [women] to see if there was any increase in calcification” and no difference was seen on imaging across the two arms. “However, women who were already on supplements before entering the study seemed to be at higher CVD risk,” she said.
Added study coauthor JoAnn E. Manson, MD, DrPH, chief of the division of preventive medicine at Brigham and Women’s Hospital and professor of women’s health at Harvard Medical School, both in Boston: “With no increase or decrease in coronary artery calcium at the end of the trial, we don’t believe starting or continuing calcium/vitamin D supplements should require screening for coronary artery disease.”
Some randomized trials and systematic reviews, however, have observed an increased risk of CVD in healthy patients on calcium supplements, with one Korean meta-analysis reporting a 15% increase in CVD risk in healthy postmenopausal women taking calcium supplements. Another meta-analysis found a link between calcium supplements and a greater risk of various cardiovascular outcomes, especially myocardial infarction.
Vitamin D Supplementation
As for vitamin D only supplementation, an updated meta-analysis including more than 83,000 individuals showed that it confers no cardiovascular protection and is therefore not indicated for this purpose.
Practice Considerations
Offering an outsider’s perspective, Sarah G. Candler, MD, MPH, an internist in Houston specializing in primary care for older high-risk adults, said: “Unfortunately, this latest study continues the trend of creating more questions than answers. If the adverse outcome of CVD death is a result of supplementation, it is unclear if this is due to the vitamin D, the calcium, or both. And it is unclear if this is dose dependent, time dependent, or due to concurrent risk factors unique to certain populations.
“It is recommended that patients at risk of osteoporosis based on age, sex, medications, and lifestyle be screened for osteoporosis and treated accordingly, including supplementation with CaD,” Dr. Candler said. “It remains unclear whether supplementation with CaD in the absence of osteoporosis and osteopenia is net beneficial or harmful, and at this time I would not recommend it to my patients.”
Added Dr. Manson: “The very small increase seen in cardiovascular mortality wouldn’t be a reason to discontinue supplementation among women who have been advised by their healthcare providers to take these supplements for bone health or other purposes.
“Among those at usual risk of fracture, we recommend trying to obtain adequate calcium and vitamin D from food sources first and to use supplements only for the purpose of filling gaps in intake,” Dr. Manson continued. Overall, the findings support the national recommended dietary allowances for daily calcium intake of 1200 mg and daily vitamin D intake of 600-800 IU among postmenopausal women for maintenance of bone health, she said.
While a 2022 study found that vitamin D supplementation alone did not prevent fractures in healthy adults, other research has shown that a calcium/vitamin D combination is more likely to protect the skeleton.
“Patients at risk for fractures will probably benefit from calcium and/or vitamin D supplementation if they do not meet dietary intake requirements, have malabsorption syndromes, are taking medications that affect nutrient absorption, or if they are older and not regularly exposed to sunlight,” said Dr. Laing. “A combination of biochemical, imaging, functional, and dietary intake data can help determine if a supplement is warranted.”
She stressed that additional research is needed in more diverse populations before changing practice guidelines. “However, doctors should continue to weigh the risks and benefits of prescribing supplements for each patient.”
The WHI program is funded by the National Heart, Lung, and Blood Institute. Dr. Thomson disclosed no competing interests. Dr. Manson reported a relationship with Mars Edge. Multiple authors reported grant support from government funding agencies. The outside commentators had no relevant competing interests to disclose.
Some doctors may be scratching their heads over a new analysis reporting that combined calcium and vitamin D (CaD) supplements appear to be associated with a slight 6% increase in cardiovascular (CVD) mortality, a slight 7% decrease in cancer risk, and no effect on osteoporotic fracture in postmenopausal women.
The study, in Annals of Internal Medicine, found no effect of supplementation on all-cause mortality.
The findings emerged from an analysis of more than 20 years’ follow-up data on a randomized trial in postmenopausal women conducted as part of the Women’s Health Initiative (WHI).
Cynthia A. Thomson, PhD, RD, first author and cancer prevention scientist at the Arizona Cancer Center and a professor of health promotion sciences at the University of Arizona in Tucson said the findings recommend individualized assessment of the need for supplements for older women as they consider them in hopes of preventing fractures.
“Evaluate your patients individually and understand that there are some who may benefit from supplementation, for example, in terms of reducing colorectal cancer mortality,” Dr. Thomson said in an interview. The approach should be nuanced. “If you check the adequacy of vitamin D and calcium in their diets, supplementation may not be needed.” She added that supplementation is best considered in the context of a woman’s overall health profile, including risk factors for fracture, heart disease, and cancer, especially colorectal cancer (CRC).
Study Details
The investigators conducted postintervention follow-up of the WHI’s 7-year multicenter randomized intervention trial of CaD vs placebo.
Since existing evidence of long-term health outcomes was limited, the trial, begun in 1999 and closed in 2005, enrolled 36,282 postmenopausal women (mean age 62) with no history of breast or colorectal cancer. They were randomly assigned 1:1 to supplementation with 1000 mg of calcium carbonate (400 mg elemental calcium) plus 400 IU of vitamin D3 daily or placebo, taken twice daily in half doses.
Study outcomes were incidence of CRC, total and invasive breast cancer; disease-specific and all-cause mortality; total CVD; and hip fracture measured through December 2020, with analyses stratified by personal supplement usage.
Cancer. CaD was associated with reduced incident total cancer, CRC, and invasive breast cancer — notably among participants not taking CaD before randomization. Cancer incidence estimates varied widely, the authors noted, when stratified by supplement use before randomization. Noting that CaD seemed to have more cancer-related impact in those without prior supplementation, the authors suggested supplementation may affect cancer biology primarily by augmenting nutrient insufficiency.
An estimated 7% reduction in cancer mortality was observed after a median cumulative follow-up of 22.3 years: 1817 vs 1943 deaths (hazard ratio, 0.93; 95% CI, 0.87-0.99).
CVD. An estimated 6% increase in CVD mortality was seen in the CaD group: 2621 vs 2420 deaths (HR, 1.06; 95% CI, 1.01-1.12). Pretrial supplement users were found to be at higher CVD risk.
Hip fracture. No effect on hip fracture risk was measured, but the authors cautioned that hip fracture and CVD outcomes were available only for a subset of participants, and the effects of calcium alone vs vitamin D alone vs the combination could not be disentangled.
In a small subgroup analysis, some CaD users were seen to respond in terms of bone mineral density but since only 4 of the study’s 40 sites collected such information, the study was underpowered to examine the effect. ”Many other studies, however, show a response to supplementation in women who already have bone mineral deficits,” Dr. Thomson said.
The Calcification Question
One of the possible mechanisms of harm is that high-dose calcium supplements can increase the rate of blood coagulation and promote vascular calcification, said Emma Laing, PhD, RD, director of dietetics at the University of Georgia in Athens and a spokesperson for the Chicago-based Academy of Nutrition and Dietetics.
“Other factors that should be considered when determining a patient’s CVD risk are race, genetic predisposition, medical and social history, response to stress, and lifestyle behaviors, as well as the length of time supplements have been consumed,” added Dr. Laing, who was not involved in the WHI analysis.
“We asked ourselves if CaD supplements might contribute to calcification of the coronary arteries, since some believe this to be the case, although the literature is mixed,” said Dr. Thomson.
“So we did a shorter ancillary study in a small sample of several hundred [women] to see if there was any increase in calcification” and no difference was seen on imaging across the two arms. “However, women who were already on supplements before entering the study seemed to be at higher CVD risk,” she said.
Added study coauthor JoAnn E. Manson, MD, DrPH, chief of the division of preventive medicine at Brigham and Women’s Hospital and professor of women’s health at Harvard Medical School, both in Boston: “With no increase or decrease in coronary artery calcium at the end of the trial, we don’t believe starting or continuing calcium/vitamin D supplements should require screening for coronary artery disease.”
Some randomized trials and systematic reviews, however, have observed an increased risk of CVD in healthy patients on calcium supplements, with one Korean meta-analysis reporting a 15% increase in CVD risk in healthy postmenopausal women taking calcium supplements. Another meta-analysis found a link between calcium supplements and a greater risk of various cardiovascular outcomes, especially myocardial infarction.
Vitamin D Supplementation
As for vitamin D only supplementation, an updated meta-analysis including more than 83,000 individuals showed that it confers no cardiovascular protection and is therefore not indicated for this purpose.
Practice Considerations
Offering an outsider’s perspective, Sarah G. Candler, MD, MPH, an internist in Houston specializing in primary care for older high-risk adults, said: “Unfortunately, this latest study continues the trend of creating more questions than answers. If the adverse outcome of CVD death is a result of supplementation, it is unclear if this is due to the vitamin D, the calcium, or both. And it is unclear if this is dose dependent, time dependent, or due to concurrent risk factors unique to certain populations.
“It is recommended that patients at risk of osteoporosis based on age, sex, medications, and lifestyle be screened for osteoporosis and treated accordingly, including supplementation with CaD,” Dr. Candler said. “It remains unclear whether supplementation with CaD in the absence of osteoporosis and osteopenia is net beneficial or harmful, and at this time I would not recommend it to my patients.”
Added Dr. Manson: “The very small increase seen in cardiovascular mortality wouldn’t be a reason to discontinue supplementation among women who have been advised by their healthcare providers to take these supplements for bone health or other purposes.
“Among those at usual risk of fracture, we recommend trying to obtain adequate calcium and vitamin D from food sources first and to use supplements only for the purpose of filling gaps in intake,” Dr. Manson continued. Overall, the findings support the national recommended dietary allowances for daily calcium intake of 1200 mg and daily vitamin D intake of 600-800 IU among postmenopausal women for maintenance of bone health, she said.
While a 2022 study found that vitamin D supplementation alone did not prevent fractures in healthy adults, other research has shown that a calcium/vitamin D combination is more likely to protect the skeleton.
“Patients at risk for fractures will probably benefit from calcium and/or vitamin D supplementation if they do not meet dietary intake requirements, have malabsorption syndromes, are taking medications that affect nutrient absorption, or if they are older and not regularly exposed to sunlight,” said Dr. Laing. “A combination of biochemical, imaging, functional, and dietary intake data can help determine if a supplement is warranted.”
She stressed that additional research is needed in more diverse populations before changing practice guidelines. “However, doctors should continue to weigh the risks and benefits of prescribing supplements for each patient.”
The WHI program is funded by the National Heart, Lung, and Blood Institute. Dr. Thomson disclosed no competing interests. Dr. Manson reported a relationship with Mars Edge. Multiple authors reported grant support from government funding agencies. The outside commentators had no relevant competing interests to disclose.
Some doctors may be scratching their heads over a new analysis reporting that combined calcium and vitamin D (CaD) supplements appear to be associated with a slight 6% increase in cardiovascular (CVD) mortality, a slight 7% decrease in cancer risk, and no effect on osteoporotic fracture in postmenopausal women.
The study, in Annals of Internal Medicine, found no effect of supplementation on all-cause mortality.
The findings emerged from an analysis of more than 20 years’ follow-up data on a randomized trial in postmenopausal women conducted as part of the Women’s Health Initiative (WHI).
Cynthia A. Thomson, PhD, RD, first author and cancer prevention scientist at the Arizona Cancer Center and a professor of health promotion sciences at the University of Arizona in Tucson said the findings recommend individualized assessment of the need for supplements for older women as they consider them in hopes of preventing fractures.
“Evaluate your patients individually and understand that there are some who may benefit from supplementation, for example, in terms of reducing colorectal cancer mortality,” Dr. Thomson said in an interview. The approach should be nuanced. “If you check the adequacy of vitamin D and calcium in their diets, supplementation may not be needed.” She added that supplementation is best considered in the context of a woman’s overall health profile, including risk factors for fracture, heart disease, and cancer, especially colorectal cancer (CRC).
Study Details
The investigators conducted postintervention follow-up of the WHI’s 7-year multicenter randomized intervention trial of CaD vs placebo.
Since existing evidence of long-term health outcomes was limited, the trial, begun in 1999 and closed in 2005, enrolled 36,282 postmenopausal women (mean age 62) with no history of breast or colorectal cancer. They were randomly assigned 1:1 to supplementation with 1000 mg of calcium carbonate (400 mg elemental calcium) plus 400 IU of vitamin D3 daily or placebo, taken twice daily in half doses.
Study outcomes were incidence of CRC, total and invasive breast cancer; disease-specific and all-cause mortality; total CVD; and hip fracture measured through December 2020, with analyses stratified by personal supplement usage.
Cancer. CaD was associated with reduced incident total cancer, CRC, and invasive breast cancer — notably among participants not taking CaD before randomization. Cancer incidence estimates varied widely, the authors noted, when stratified by supplement use before randomization. Noting that CaD seemed to have more cancer-related impact in those without prior supplementation, the authors suggested supplementation may affect cancer biology primarily by augmenting nutrient insufficiency.
An estimated 7% reduction in cancer mortality was observed after a median cumulative follow-up of 22.3 years: 1817 vs 1943 deaths (hazard ratio, 0.93; 95% CI, 0.87-0.99).
CVD. An estimated 6% increase in CVD mortality was seen in the CaD group: 2621 vs 2420 deaths (HR, 1.06; 95% CI, 1.01-1.12). Pretrial supplement users were found to be at higher CVD risk.
Hip fracture. No effect on hip fracture risk was measured, but the authors cautioned that hip fracture and CVD outcomes were available only for a subset of participants, and the effects of calcium alone vs vitamin D alone vs the combination could not be disentangled.
In a small subgroup analysis, some CaD users were seen to respond in terms of bone mineral density but since only 4 of the study’s 40 sites collected such information, the study was underpowered to examine the effect. ”Many other studies, however, show a response to supplementation in women who already have bone mineral deficits,” Dr. Thomson said.
The Calcification Question
One of the possible mechanisms of harm is that high-dose calcium supplements can increase the rate of blood coagulation and promote vascular calcification, said Emma Laing, PhD, RD, director of dietetics at the University of Georgia in Athens and a spokesperson for the Chicago-based Academy of Nutrition and Dietetics.
“Other factors that should be considered when determining a patient’s CVD risk are race, genetic predisposition, medical and social history, response to stress, and lifestyle behaviors, as well as the length of time supplements have been consumed,” added Dr. Laing, who was not involved in the WHI analysis.
“We asked ourselves if CaD supplements might contribute to calcification of the coronary arteries, since some believe this to be the case, although the literature is mixed,” said Dr. Thomson.
“So we did a shorter ancillary study in a small sample of several hundred [women] to see if there was any increase in calcification” and no difference was seen on imaging across the two arms. “However, women who were already on supplements before entering the study seemed to be at higher CVD risk,” she said.
Added study coauthor JoAnn E. Manson, MD, DrPH, chief of the division of preventive medicine at Brigham and Women’s Hospital and professor of women’s health at Harvard Medical School, both in Boston: “With no increase or decrease in coronary artery calcium at the end of the trial, we don’t believe starting or continuing calcium/vitamin D supplements should require screening for coronary artery disease.”
Some randomized trials and systematic reviews, however, have observed an increased risk of CVD in healthy patients on calcium supplements, with one Korean meta-analysis reporting a 15% increase in CVD risk in healthy postmenopausal women taking calcium supplements. Another meta-analysis found a link between calcium supplements and a greater risk of various cardiovascular outcomes, especially myocardial infarction.
Vitamin D Supplementation
As for vitamin D only supplementation, an updated meta-analysis including more than 83,000 individuals showed that it confers no cardiovascular protection and is therefore not indicated for this purpose.
Practice Considerations
Offering an outsider’s perspective, Sarah G. Candler, MD, MPH, an internist in Houston specializing in primary care for older high-risk adults, said: “Unfortunately, this latest study continues the trend of creating more questions than answers. If the adverse outcome of CVD death is a result of supplementation, it is unclear if this is due to the vitamin D, the calcium, or both. And it is unclear if this is dose dependent, time dependent, or due to concurrent risk factors unique to certain populations.
“It is recommended that patients at risk of osteoporosis based on age, sex, medications, and lifestyle be screened for osteoporosis and treated accordingly, including supplementation with CaD,” Dr. Candler said. “It remains unclear whether supplementation with CaD in the absence of osteoporosis and osteopenia is net beneficial or harmful, and at this time I would not recommend it to my patients.”
Added Dr. Manson: “The very small increase seen in cardiovascular mortality wouldn’t be a reason to discontinue supplementation among women who have been advised by their healthcare providers to take these supplements for bone health or other purposes.
“Among those at usual risk of fracture, we recommend trying to obtain adequate calcium and vitamin D from food sources first and to use supplements only for the purpose of filling gaps in intake,” Dr. Manson continued. Overall, the findings support the national recommended dietary allowances for daily calcium intake of 1200 mg and daily vitamin D intake of 600-800 IU among postmenopausal women for maintenance of bone health, she said.
While a 2022 study found that vitamin D supplementation alone did not prevent fractures in healthy adults, other research has shown that a calcium/vitamin D combination is more likely to protect the skeleton.
“Patients at risk for fractures will probably benefit from calcium and/or vitamin D supplementation if they do not meet dietary intake requirements, have malabsorption syndromes, are taking medications that affect nutrient absorption, or if they are older and not regularly exposed to sunlight,” said Dr. Laing. “A combination of biochemical, imaging, functional, and dietary intake data can help determine if a supplement is warranted.”
She stressed that additional research is needed in more diverse populations before changing practice guidelines. “However, doctors should continue to weigh the risks and benefits of prescribing supplements for each patient.”
The WHI program is funded by the National Heart, Lung, and Blood Institute. Dr. Thomson disclosed no competing interests. Dr. Manson reported a relationship with Mars Edge. Multiple authors reported grant support from government funding agencies. The outside commentators had no relevant competing interests to disclose.
FROM ANNALS OF INTERNAL MEDICINE
Look Beyond BMI: Metabolic Factors’ Link to Cancer Explained
The new research finds that adults with persistent metabolic syndrome that worsens over time are at increased risk for any type of cancer.
The conditions that make up metabolic syndrome (high blood pressure, high blood sugar, increased abdominal adiposity, and high cholesterol and triglycerides) have been associated with an increased risk of diseases, including heart disease, stroke, and type 2 diabetes, wrote Li Deng, PhD, of Capital Medical University, Beijing, and colleagues.
However, a single assessment of metabolic syndrome at one point in time is inadequate to show an association with cancer risk over time, they said. In the current study, the researchers used models to examine the association between trajectory patterns of metabolic syndrome over time and the risk of overall and specific cancer types. They also examined the impact of chronic inflammation concurrent with metabolic syndrome.
What We Know About Metabolic Syndrome and Cancer Risk
A systematic review and meta-analysis published in Diabetes Care in 2012 showed an association between the presence of metabolic syndrome and an increased risk of various cancers including liver, bladder, pancreatic, breast, and colorectal.
More recently, a 2020 study published in Diabetes showed evidence of increased risk for certain cancers (pancreatic, kidney, uterine, cervical) but no increased risk for cancer overall.
In addition, a 2022 study by some of the current study researchers of the same Chinese cohort focused on the role of inflammation in combination with metabolic syndrome on colorectal cancer specifically, and found an increased risk for cancer when both metabolic syndrome and inflammation were present.
However, the reasons for this association between metabolic syndrome and cancer remain unclear, and the effect of the fluctuating nature of metabolic syndrome over time on long-term cancer risk has not been explored, the researchers wrote.
“There is emerging evidence that even normal weight individuals who are metabolically unhealthy may be at an elevated cancer risk, and we need better metrics to define the underlying metabolic dysfunction in obesity,” Sheetal Hardikar, MBBS, PhD, MPH, an investigator at the Huntsman Cancer Institute, University of Utah, said in an interview.
Dr. Hardikar, who serves as assistant professor in the department of population health sciences at the University of Utah, was not involved in the current study. She and her colleagues published a research paper on data from the National Health and Nutrition Examination Survey in 2023 that showed an increased risk of obesity-related cancer.
What New Study Adds to Related Research
Previous studies have consistently reported an approximately 30% increased risk of cancer with metabolic syndrome, Dr. Hardikar said. “What is unique about this study is the examination of metabolic syndrome trajectories over four years, and not just the presence of metabolic syndrome at one point in time,” she said.
In the new study, published in Cancer on March 11 (doi: 10.1002/cncr.35235), 44,115 adults in China were separated into four trajectories based on metabolic syndrome scores for the period from 2006 to 2010. The scores were based on clinical evidence of metabolic syndrome, defined using the International Diabetes Federation criteria of central obesity and the presence of at least two other factors including increased triglycerides, decreased HDL cholesterol, high blood pressure (or treatment for previously diagnosed hypertension), and increased fasting plasma glucose (or previous diagnosis of type 2 diabetes).
The average age of the participants was 49 years; the mean body mass index ranged from approximately 22 kg/m2 in the low-stable group to approximately 28 kg/m2 in the elevated-increasing group.
The four trajectories of metabolic syndrome were low-stable (10.56% of participants), moderate-low (40.84%), moderate-high (41.46%), and elevated-increasing (7.14%), based on trends from the individuals’ initial physical exams on entering the study.
Over a median follow-up period of 9.4 years (from 2010 to 2021), 2,271 cancer diagnoses were reported in the study population. Those with an elevated-increasing metabolic syndrome trajectory had 1.3 times the risk of any cancer compared with those in the low-stable group. Risk for breast cancer, endometrial cancer, kidney cancer, colorectal cancer, and liver cancer in the highest trajectory group were 2.1, 3.3, 4.5, 2.5, and 1.6 times higher, respectively, compared to the lowest group. The increased risk in the elevated-trajectory group for all cancer types persisted when the low-stable, moderate-low, and moderate-high trajectory pattern groups were combined.
The researchers also examined the impact of chronic inflammation and found that individuals with persistently high metabolic syndrome scores and concurrent chronic inflammation had the highest risks of breast, endometrial, colon, and liver cancer. However, individuals with persistently high metabolic syndrome scores and no concurrent chronic inflammation had the highest risk of kidney cancer.
What Are the Limitations of This Research?
The researchers of the current study acknowledged the lack of information on other causes of cancer, including dietary habits, hepatitis C infection, and Helicobacter pylori infection. Other limitations include the focus only on individuals from a single community of mainly middle-aged men in China that may not generalize to other populations.
Also, the metabolic syndrome trajectories did not change much over time, which may be related to the short 4-year study period.
Using the International Diabetes Federation criteria was another limitation, because it prevented the assessment of cancer risk in normal weight individuals with metabolic dysfunction, Dr. Hardikar noted.
Does Metabolic Syndrome Cause Cancer?
“This research suggests that proactive and continuous management of metabolic syndrome may serve as an essential strategy in preventing cancer,” senior author Han-Ping Shi, MD, PhD, of Capital Medical University in Beijing, noted in a statement on the study.
More research is needed to assess the impact of these interventions on cancer risk. However, the data from the current study can guide future research that may lead to more targeted treatments and more effective preventive strategies, he continued.
“Current evidence based on this study and many other reports strongly suggests an increased risk for cancer associated with metabolic syndrome,” Dr. Hardikar said in an interview. The data serve as a reminder to clinicians to look beyond BMI as the only measure of obesity, and to consider metabolic factors together to identify individuals at increased risk for cancer, she said.
“We must continue to educate patients about obesity and all the chronic conditions it may lead to, but we cannot ignore this emerging phenotype of being of normal weight but metabolically unhealthy,” Dr. Hardikar emphasized.
What Additional Research is Needed?
Looking ahead, “we need well-designed interventions to test causality for metabolic syndrome and cancer risk, though the evidence from the observational studies is very strong,” Dr. Hardikar said.
In addition, a consensus is needed to better define metabolic dysfunction,and to explore cancer risk in normal weight but metabolically unhealthy individuals, she said.
The study was supported by the National Key Research and Development Program of China. The researchers and Dr. Hardikar had no financial conflicts to disclose.
The new research finds that adults with persistent metabolic syndrome that worsens over time are at increased risk for any type of cancer.
The conditions that make up metabolic syndrome (high blood pressure, high blood sugar, increased abdominal adiposity, and high cholesterol and triglycerides) have been associated with an increased risk of diseases, including heart disease, stroke, and type 2 diabetes, wrote Li Deng, PhD, of Capital Medical University, Beijing, and colleagues.
However, a single assessment of metabolic syndrome at one point in time is inadequate to show an association with cancer risk over time, they said. In the current study, the researchers used models to examine the association between trajectory patterns of metabolic syndrome over time and the risk of overall and specific cancer types. They also examined the impact of chronic inflammation concurrent with metabolic syndrome.
What We Know About Metabolic Syndrome and Cancer Risk
A systematic review and meta-analysis published in Diabetes Care in 2012 showed an association between the presence of metabolic syndrome and an increased risk of various cancers including liver, bladder, pancreatic, breast, and colorectal.
More recently, a 2020 study published in Diabetes showed evidence of increased risk for certain cancers (pancreatic, kidney, uterine, cervical) but no increased risk for cancer overall.
In addition, a 2022 study by some of the current study researchers of the same Chinese cohort focused on the role of inflammation in combination with metabolic syndrome on colorectal cancer specifically, and found an increased risk for cancer when both metabolic syndrome and inflammation were present.
However, the reasons for this association between metabolic syndrome and cancer remain unclear, and the effect of the fluctuating nature of metabolic syndrome over time on long-term cancer risk has not been explored, the researchers wrote.
“There is emerging evidence that even normal weight individuals who are metabolically unhealthy may be at an elevated cancer risk, and we need better metrics to define the underlying metabolic dysfunction in obesity,” Sheetal Hardikar, MBBS, PhD, MPH, an investigator at the Huntsman Cancer Institute, University of Utah, said in an interview.
Dr. Hardikar, who serves as assistant professor in the department of population health sciences at the University of Utah, was not involved in the current study. She and her colleagues published a research paper on data from the National Health and Nutrition Examination Survey in 2023 that showed an increased risk of obesity-related cancer.
What New Study Adds to Related Research
Previous studies have consistently reported an approximately 30% increased risk of cancer with metabolic syndrome, Dr. Hardikar said. “What is unique about this study is the examination of metabolic syndrome trajectories over four years, and not just the presence of metabolic syndrome at one point in time,” she said.
In the new study, published in Cancer on March 11 (doi: 10.1002/cncr.35235), 44,115 adults in China were separated into four trajectories based on metabolic syndrome scores for the period from 2006 to 2010. The scores were based on clinical evidence of metabolic syndrome, defined using the International Diabetes Federation criteria of central obesity and the presence of at least two other factors including increased triglycerides, decreased HDL cholesterol, high blood pressure (or treatment for previously diagnosed hypertension), and increased fasting plasma glucose (or previous diagnosis of type 2 diabetes).
The average age of the participants was 49 years; the mean body mass index ranged from approximately 22 kg/m2 in the low-stable group to approximately 28 kg/m2 in the elevated-increasing group.
The four trajectories of metabolic syndrome were low-stable (10.56% of participants), moderate-low (40.84%), moderate-high (41.46%), and elevated-increasing (7.14%), based on trends from the individuals’ initial physical exams on entering the study.
Over a median follow-up period of 9.4 years (from 2010 to 2021), 2,271 cancer diagnoses were reported in the study population. Those with an elevated-increasing metabolic syndrome trajectory had 1.3 times the risk of any cancer compared with those in the low-stable group. Risk for breast cancer, endometrial cancer, kidney cancer, colorectal cancer, and liver cancer in the highest trajectory group were 2.1, 3.3, 4.5, 2.5, and 1.6 times higher, respectively, compared to the lowest group. The increased risk in the elevated-trajectory group for all cancer types persisted when the low-stable, moderate-low, and moderate-high trajectory pattern groups were combined.
The researchers also examined the impact of chronic inflammation and found that individuals with persistently high metabolic syndrome scores and concurrent chronic inflammation had the highest risks of breast, endometrial, colon, and liver cancer. However, individuals with persistently high metabolic syndrome scores and no concurrent chronic inflammation had the highest risk of kidney cancer.
What Are the Limitations of This Research?
The researchers of the current study acknowledged the lack of information on other causes of cancer, including dietary habits, hepatitis C infection, and Helicobacter pylori infection. Other limitations include the focus only on individuals from a single community of mainly middle-aged men in China that may not generalize to other populations.
Also, the metabolic syndrome trajectories did not change much over time, which may be related to the short 4-year study period.
Using the International Diabetes Federation criteria was another limitation, because it prevented the assessment of cancer risk in normal weight individuals with metabolic dysfunction, Dr. Hardikar noted.
Does Metabolic Syndrome Cause Cancer?
“This research suggests that proactive and continuous management of metabolic syndrome may serve as an essential strategy in preventing cancer,” senior author Han-Ping Shi, MD, PhD, of Capital Medical University in Beijing, noted in a statement on the study.
More research is needed to assess the impact of these interventions on cancer risk. However, the data from the current study can guide future research that may lead to more targeted treatments and more effective preventive strategies, he continued.
“Current evidence based on this study and many other reports strongly suggests an increased risk for cancer associated with metabolic syndrome,” Dr. Hardikar said in an interview. The data serve as a reminder to clinicians to look beyond BMI as the only measure of obesity, and to consider metabolic factors together to identify individuals at increased risk for cancer, she said.
“We must continue to educate patients about obesity and all the chronic conditions it may lead to, but we cannot ignore this emerging phenotype of being of normal weight but metabolically unhealthy,” Dr. Hardikar emphasized.
What Additional Research is Needed?
Looking ahead, “we need well-designed interventions to test causality for metabolic syndrome and cancer risk, though the evidence from the observational studies is very strong,” Dr. Hardikar said.
In addition, a consensus is needed to better define metabolic dysfunction,and to explore cancer risk in normal weight but metabolically unhealthy individuals, she said.
The study was supported by the National Key Research and Development Program of China. The researchers and Dr. Hardikar had no financial conflicts to disclose.
The new research finds that adults with persistent metabolic syndrome that worsens over time are at increased risk for any type of cancer.
The conditions that make up metabolic syndrome (high blood pressure, high blood sugar, increased abdominal adiposity, and high cholesterol and triglycerides) have been associated with an increased risk of diseases, including heart disease, stroke, and type 2 diabetes, wrote Li Deng, PhD, of Capital Medical University, Beijing, and colleagues.
However, a single assessment of metabolic syndrome at one point in time is inadequate to show an association with cancer risk over time, they said. In the current study, the researchers used models to examine the association between trajectory patterns of metabolic syndrome over time and the risk of overall and specific cancer types. They also examined the impact of chronic inflammation concurrent with metabolic syndrome.
What We Know About Metabolic Syndrome and Cancer Risk
A systematic review and meta-analysis published in Diabetes Care in 2012 showed an association between the presence of metabolic syndrome and an increased risk of various cancers including liver, bladder, pancreatic, breast, and colorectal.
More recently, a 2020 study published in Diabetes showed evidence of increased risk for certain cancers (pancreatic, kidney, uterine, cervical) but no increased risk for cancer overall.
In addition, a 2022 study by some of the current study researchers of the same Chinese cohort focused on the role of inflammation in combination with metabolic syndrome on colorectal cancer specifically, and found an increased risk for cancer when both metabolic syndrome and inflammation were present.
However, the reasons for this association between metabolic syndrome and cancer remain unclear, and the effect of the fluctuating nature of metabolic syndrome over time on long-term cancer risk has not been explored, the researchers wrote.
“There is emerging evidence that even normal weight individuals who are metabolically unhealthy may be at an elevated cancer risk, and we need better metrics to define the underlying metabolic dysfunction in obesity,” Sheetal Hardikar, MBBS, PhD, MPH, an investigator at the Huntsman Cancer Institute, University of Utah, said in an interview.
Dr. Hardikar, who serves as assistant professor in the department of population health sciences at the University of Utah, was not involved in the current study. She and her colleagues published a research paper on data from the National Health and Nutrition Examination Survey in 2023 that showed an increased risk of obesity-related cancer.
What New Study Adds to Related Research
Previous studies have consistently reported an approximately 30% increased risk of cancer with metabolic syndrome, Dr. Hardikar said. “What is unique about this study is the examination of metabolic syndrome trajectories over four years, and not just the presence of metabolic syndrome at one point in time,” she said.
In the new study, published in Cancer on March 11 (doi: 10.1002/cncr.35235), 44,115 adults in China were separated into four trajectories based on metabolic syndrome scores for the period from 2006 to 2010. The scores were based on clinical evidence of metabolic syndrome, defined using the International Diabetes Federation criteria of central obesity and the presence of at least two other factors including increased triglycerides, decreased HDL cholesterol, high blood pressure (or treatment for previously diagnosed hypertension), and increased fasting plasma glucose (or previous diagnosis of type 2 diabetes).
The average age of the participants was 49 years; the mean body mass index ranged from approximately 22 kg/m2 in the low-stable group to approximately 28 kg/m2 in the elevated-increasing group.
The four trajectories of metabolic syndrome were low-stable (10.56% of participants), moderate-low (40.84%), moderate-high (41.46%), and elevated-increasing (7.14%), based on trends from the individuals’ initial physical exams on entering the study.
Over a median follow-up period of 9.4 years (from 2010 to 2021), 2,271 cancer diagnoses were reported in the study population. Those with an elevated-increasing metabolic syndrome trajectory had 1.3 times the risk of any cancer compared with those in the low-stable group. Risk for breast cancer, endometrial cancer, kidney cancer, colorectal cancer, and liver cancer in the highest trajectory group were 2.1, 3.3, 4.5, 2.5, and 1.6 times higher, respectively, compared to the lowest group. The increased risk in the elevated-trajectory group for all cancer types persisted when the low-stable, moderate-low, and moderate-high trajectory pattern groups were combined.
The researchers also examined the impact of chronic inflammation and found that individuals with persistently high metabolic syndrome scores and concurrent chronic inflammation had the highest risks of breast, endometrial, colon, and liver cancer. However, individuals with persistently high metabolic syndrome scores and no concurrent chronic inflammation had the highest risk of kidney cancer.
What Are the Limitations of This Research?
The researchers of the current study acknowledged the lack of information on other causes of cancer, including dietary habits, hepatitis C infection, and Helicobacter pylori infection. Other limitations include the focus only on individuals from a single community of mainly middle-aged men in China that may not generalize to other populations.
Also, the metabolic syndrome trajectories did not change much over time, which may be related to the short 4-year study period.
Using the International Diabetes Federation criteria was another limitation, because it prevented the assessment of cancer risk in normal weight individuals with metabolic dysfunction, Dr. Hardikar noted.
Does Metabolic Syndrome Cause Cancer?
“This research suggests that proactive and continuous management of metabolic syndrome may serve as an essential strategy in preventing cancer,” senior author Han-Ping Shi, MD, PhD, of Capital Medical University in Beijing, noted in a statement on the study.
More research is needed to assess the impact of these interventions on cancer risk. However, the data from the current study can guide future research that may lead to more targeted treatments and more effective preventive strategies, he continued.
“Current evidence based on this study and many other reports strongly suggests an increased risk for cancer associated with metabolic syndrome,” Dr. Hardikar said in an interview. The data serve as a reminder to clinicians to look beyond BMI as the only measure of obesity, and to consider metabolic factors together to identify individuals at increased risk for cancer, she said.
“We must continue to educate patients about obesity and all the chronic conditions it may lead to, but we cannot ignore this emerging phenotype of being of normal weight but metabolically unhealthy,” Dr. Hardikar emphasized.
What Additional Research is Needed?
Looking ahead, “we need well-designed interventions to test causality for metabolic syndrome and cancer risk, though the evidence from the observational studies is very strong,” Dr. Hardikar said.
In addition, a consensus is needed to better define metabolic dysfunction,and to explore cancer risk in normal weight but metabolically unhealthy individuals, she said.
The study was supported by the National Key Research and Development Program of China. The researchers and Dr. Hardikar had no financial conflicts to disclose.
FROM CANCER
Semaglutide Curbs MASLD Severity in People Living With HIV
Semaglutide improved metabolic dysfunction–associated steatotic liver disease (MASLD) among people living with HIV, and in some cases resolved it completely, according to results from the SLIM LIVER study presented by the AIDS Clinical Trials Group (ACTG) at this year’s Conference on Retroviruses and Opportunistic Infections (CROI) 2024 Annual Meeting in Denver.
Furthermore, although muscle volume decreased with weight loss, participants did not experience significant changes in muscle quality or physical function.
‘A First’
SLIM LIVER is the first study evaluating semaglutide as a treatment of MASLD among people living with HIV.
The phase 2b, single-arm pilot study enrolled adults living with HIV who were virally suppressed and had central adiposity, insulin resistance or prediabetes, and steatotic liver disease.
Participants self-injected semaglutide weekly at increasing doses until they reached a 1-mg dose at week 4. At 24 weeks, the study team assessed changes in participants’ intra-hepatic triglyceride content using magnetic resonance imaging-proton density fat fraction.
The primary analysis results from SLIM LIVER were reported in an oral presentation, “Semaglutide Reduces Metabolic-Associated Steatotic Liver Disease in People With HIV: The SLIM LIVER Study,” on March 5 by Jordan E. Lake, MD, MSc, of UTHealth Houston.
A subgroup analysis of the study was provided in a poster, “Effects of Semaglutide on Muscle Structure and Function in the SLIM LIVER Study,” presented on March 4 by Grace L. Ditzenberger, PT, DPT, of the University of Colorado Anschutz Medical Campus in Aurora.
In the primary analysis, the median age of the 49 participants was 52 years, 43% were women (cisgender and transgender), the mean body mass index was 35, 39% were Hispanic and 33% were Black/African American, and 82% were taking antiretroviral therapy that included an integrase inhibitor.
Liver fat was reduced by an average of 31%, with 29% of participants experiencing a complete resolution (5% or less liver fat) of MASLD. They also experienced weight loss, reduced fasting blood glucose, and reduced fasting triglycerides, consistent with effects observed in studies of semaglutide in people without HIV.
The sub-analysis of the 46 participants for whom muscle measurements were available showed that muscle volume (measured in the psoas) decreased but with no significant change in physical function.
Semaglutide was generally well tolerated, with an adverse event profile similar to that seen in individuals without HIV.
The most common adverse events were gastrointestinal (ie, nausea, diarrhea, vomiting, and abdominal pain). Two participants experienced more significant adverse events possibly related to semaglutide but were able to continue in the study.
All participants completed the full 24 weeks of therapy at the originally prescribed dose.
Potential Impact
“Even at the low dose of 1 mg every week, most participants lost significant weight, and weight loss was closely associated with improvements in MASLD,” Dr. Lake said. “Additional research will assess the secondary effects of semaglutide on systemic inflammation and metabolism and determine whether semaglutide may have unique risks or benefits for people living with HIV.”
“These findings have the potential to have a significant impact on the health and quality of life of people living with HIV,” added ACTG Chair Judith Currier, MD, MSc, University of California Los Angeles.
The SLIM LIVER study was sponsored by the US National Institute of Allergy and Infectious Diseases (NIAID), with additional funding from UTHealth Houston McGovern School of Medicine. ACTG is a clinical trials network focused on HIV and other infectious diseases, funded by NIAID and collaborating institutes of the US National Institutes of Health.
No conflicts of interest were reported.
A version of this article appeared on Medscape.com.
Semaglutide improved metabolic dysfunction–associated steatotic liver disease (MASLD) among people living with HIV, and in some cases resolved it completely, according to results from the SLIM LIVER study presented by the AIDS Clinical Trials Group (ACTG) at this year’s Conference on Retroviruses and Opportunistic Infections (CROI) 2024 Annual Meeting in Denver.
Furthermore, although muscle volume decreased with weight loss, participants did not experience significant changes in muscle quality or physical function.
‘A First’
SLIM LIVER is the first study evaluating semaglutide as a treatment of MASLD among people living with HIV.
The phase 2b, single-arm pilot study enrolled adults living with HIV who were virally suppressed and had central adiposity, insulin resistance or prediabetes, and steatotic liver disease.
Participants self-injected semaglutide weekly at increasing doses until they reached a 1-mg dose at week 4. At 24 weeks, the study team assessed changes in participants’ intra-hepatic triglyceride content using magnetic resonance imaging-proton density fat fraction.
The primary analysis results from SLIM LIVER were reported in an oral presentation, “Semaglutide Reduces Metabolic-Associated Steatotic Liver Disease in People With HIV: The SLIM LIVER Study,” on March 5 by Jordan E. Lake, MD, MSc, of UTHealth Houston.
A subgroup analysis of the study was provided in a poster, “Effects of Semaglutide on Muscle Structure and Function in the SLIM LIVER Study,” presented on March 4 by Grace L. Ditzenberger, PT, DPT, of the University of Colorado Anschutz Medical Campus in Aurora.
In the primary analysis, the median age of the 49 participants was 52 years, 43% were women (cisgender and transgender), the mean body mass index was 35, 39% were Hispanic and 33% were Black/African American, and 82% were taking antiretroviral therapy that included an integrase inhibitor.
Liver fat was reduced by an average of 31%, with 29% of participants experiencing a complete resolution (5% or less liver fat) of MASLD. They also experienced weight loss, reduced fasting blood glucose, and reduced fasting triglycerides, consistent with effects observed in studies of semaglutide in people without HIV.
The sub-analysis of the 46 participants for whom muscle measurements were available showed that muscle volume (measured in the psoas) decreased but with no significant change in physical function.
Semaglutide was generally well tolerated, with an adverse event profile similar to that seen in individuals without HIV.
The most common adverse events were gastrointestinal (ie, nausea, diarrhea, vomiting, and abdominal pain). Two participants experienced more significant adverse events possibly related to semaglutide but were able to continue in the study.
All participants completed the full 24 weeks of therapy at the originally prescribed dose.
Potential Impact
“Even at the low dose of 1 mg every week, most participants lost significant weight, and weight loss was closely associated with improvements in MASLD,” Dr. Lake said. “Additional research will assess the secondary effects of semaglutide on systemic inflammation and metabolism and determine whether semaglutide may have unique risks or benefits for people living with HIV.”
“These findings have the potential to have a significant impact on the health and quality of life of people living with HIV,” added ACTG Chair Judith Currier, MD, MSc, University of California Los Angeles.
The SLIM LIVER study was sponsored by the US National Institute of Allergy and Infectious Diseases (NIAID), with additional funding from UTHealth Houston McGovern School of Medicine. ACTG is a clinical trials network focused on HIV and other infectious diseases, funded by NIAID and collaborating institutes of the US National Institutes of Health.
No conflicts of interest were reported.
A version of this article appeared on Medscape.com.
Semaglutide improved metabolic dysfunction–associated steatotic liver disease (MASLD) among people living with HIV, and in some cases resolved it completely, according to results from the SLIM LIVER study presented by the AIDS Clinical Trials Group (ACTG) at this year’s Conference on Retroviruses and Opportunistic Infections (CROI) 2024 Annual Meeting in Denver.
Furthermore, although muscle volume decreased with weight loss, participants did not experience significant changes in muscle quality or physical function.
‘A First’
SLIM LIVER is the first study evaluating semaglutide as a treatment of MASLD among people living with HIV.
The phase 2b, single-arm pilot study enrolled adults living with HIV who were virally suppressed and had central adiposity, insulin resistance or prediabetes, and steatotic liver disease.
Participants self-injected semaglutide weekly at increasing doses until they reached a 1-mg dose at week 4. At 24 weeks, the study team assessed changes in participants’ intra-hepatic triglyceride content using magnetic resonance imaging-proton density fat fraction.
The primary analysis results from SLIM LIVER were reported in an oral presentation, “Semaglutide Reduces Metabolic-Associated Steatotic Liver Disease in People With HIV: The SLIM LIVER Study,” on March 5 by Jordan E. Lake, MD, MSc, of UTHealth Houston.
A subgroup analysis of the study was provided in a poster, “Effects of Semaglutide on Muscle Structure and Function in the SLIM LIVER Study,” presented on March 4 by Grace L. Ditzenberger, PT, DPT, of the University of Colorado Anschutz Medical Campus in Aurora.
In the primary analysis, the median age of the 49 participants was 52 years, 43% were women (cisgender and transgender), the mean body mass index was 35, 39% were Hispanic and 33% were Black/African American, and 82% were taking antiretroviral therapy that included an integrase inhibitor.
Liver fat was reduced by an average of 31%, with 29% of participants experiencing a complete resolution (5% or less liver fat) of MASLD. They also experienced weight loss, reduced fasting blood glucose, and reduced fasting triglycerides, consistent with effects observed in studies of semaglutide in people without HIV.
The sub-analysis of the 46 participants for whom muscle measurements were available showed that muscle volume (measured in the psoas) decreased but with no significant change in physical function.
Semaglutide was generally well tolerated, with an adverse event profile similar to that seen in individuals without HIV.
The most common adverse events were gastrointestinal (ie, nausea, diarrhea, vomiting, and abdominal pain). Two participants experienced more significant adverse events possibly related to semaglutide but were able to continue in the study.
All participants completed the full 24 weeks of therapy at the originally prescribed dose.
Potential Impact
“Even at the low dose of 1 mg every week, most participants lost significant weight, and weight loss was closely associated with improvements in MASLD,” Dr. Lake said. “Additional research will assess the secondary effects of semaglutide on systemic inflammation and metabolism and determine whether semaglutide may have unique risks or benefits for people living with HIV.”
“These findings have the potential to have a significant impact on the health and quality of life of people living with HIV,” added ACTG Chair Judith Currier, MD, MSc, University of California Los Angeles.
The SLIM LIVER study was sponsored by the US National Institute of Allergy and Infectious Diseases (NIAID), with additional funding from UTHealth Houston McGovern School of Medicine. ACTG is a clinical trials network focused on HIV and other infectious diseases, funded by NIAID and collaborating institutes of the US National Institutes of Health.
No conflicts of interest were reported.
A version of this article appeared on Medscape.com.
FROM CROI 2024
The Role of Growth Hormone Mediators in Youth-Onset T2D
TOPLINE:
Changes in plasma growth hormone mediators such as growth hormone receptor (GHR) and insulin-like growth factor-binding protein 1 (IGFBP-1) were associated with glycemic failure in youth-onset type 2 diabetes (T2D), an analysis of the TODAY trial showed.
METHODOLOGY:
- In youth, T2D often occurs during or after puberty, hinting at hormonal influences in the development and/or progression of the disease.
- This secondary analysis assessed the role of growth hormone mediators including insulin-like growth factor-1 (IGF-1), GHR, and IGFBP-1 in glycemic failure in a subset of 398 youths, aged 10-17 years, with a T2D duration of less than 2 years (62% girls; 21% White).
- The participants were followed up for a mean of 3.9 years.
- The primary outcomes included glycemic failure, defined as an A1c level of 8% or more for 6 months, or acute metabolic decompensation requiring insulin.
- Other assessments included baseline and 36-month measures of glycemia, insulin sensitivity, high molecular weight adiponectin, and beta cell function.
TAKEAWAY:
- Of 398 participants, 182 (46%) experienced glycemic failure, while 216 (54%) retained glycemic control.
- At 36 months, youths with glycemic failure had lower IGF-1 levels (P < .001) and higher log2 GHR (P = .03) and log2 IGFBP-1 (P = .009) levels than those who maintained glycemic control.
- A greater increase in IGF-1 level at 36 months was associated with lower odds of glycemic failure (odds ratio [OR], 0.995; P < .001).
- Increased levels of log2 GHR and log2 IGFBP-1 were associated with higher odds of glycemic failure (OR, 1.75; P = .04 and OR, 1.37; P = .007, respectively). Results were adjusted for body mass index (BMI), suggesting that associations between GHR level and glycemic outcomes exist independent of BMI.
- Interhormonal correlations suggested an association between glucose metabolism and growth hormone signaling or a shared process leading to changes in both processes.
IN PRACTICE:
“Our study has identified GHR level as a novel biomarker of decrease in glycemic control in youths with T2D,” the study authors wrote. Future research is needed, with an emphasis on assessing alterations in growth hormone mediators which may contribute to diabetes complications in youth.
SOURCE:
The study, published online in JAMA Network Open, was led by Chang Lu, MD, Division of Endocrinology, Boston Children’s Hospital, and Joslin Diabetes Center at Harvard Medical School, Boston, Massachusetts.
LIMITATIONS:
The study did not include a control group (individuals without diabetes). The cohort largely included youth in late puberty or after puberty, affecting subgroup analysis. Moreover, only circulating growth hormone mediators were measured, limiting the identity of the source tissue of the hormone and the target organs.
DISCLOSURES:
Some authors reported receiving grants from the National Institutes of Health and National Institute of Diabetes and Digestive and Kidney Diseases while conducting the study. Also, certain authors reported receiving grants and personal fees from various trusts as well as pharmaceutical, healthcare, and medical technology companies outside the submitted work.
TOPLINE:
Changes in plasma growth hormone mediators such as growth hormone receptor (GHR) and insulin-like growth factor-binding protein 1 (IGFBP-1) were associated with glycemic failure in youth-onset type 2 diabetes (T2D), an analysis of the TODAY trial showed.
METHODOLOGY:
- In youth, T2D often occurs during or after puberty, hinting at hormonal influences in the development and/or progression of the disease.
- This secondary analysis assessed the role of growth hormone mediators including insulin-like growth factor-1 (IGF-1), GHR, and IGFBP-1 in glycemic failure in a subset of 398 youths, aged 10-17 years, with a T2D duration of less than 2 years (62% girls; 21% White).
- The participants were followed up for a mean of 3.9 years.
- The primary outcomes included glycemic failure, defined as an A1c level of 8% or more for 6 months, or acute metabolic decompensation requiring insulin.
- Other assessments included baseline and 36-month measures of glycemia, insulin sensitivity, high molecular weight adiponectin, and beta cell function.
TAKEAWAY:
- Of 398 participants, 182 (46%) experienced glycemic failure, while 216 (54%) retained glycemic control.
- At 36 months, youths with glycemic failure had lower IGF-1 levels (P < .001) and higher log2 GHR (P = .03) and log2 IGFBP-1 (P = .009) levels than those who maintained glycemic control.
- A greater increase in IGF-1 level at 36 months was associated with lower odds of glycemic failure (odds ratio [OR], 0.995; P < .001).
- Increased levels of log2 GHR and log2 IGFBP-1 were associated with higher odds of glycemic failure (OR, 1.75; P = .04 and OR, 1.37; P = .007, respectively). Results were adjusted for body mass index (BMI), suggesting that associations between GHR level and glycemic outcomes exist independent of BMI.
- Interhormonal correlations suggested an association between glucose metabolism and growth hormone signaling or a shared process leading to changes in both processes.
IN PRACTICE:
“Our study has identified GHR level as a novel biomarker of decrease in glycemic control in youths with T2D,” the study authors wrote. Future research is needed, with an emphasis on assessing alterations in growth hormone mediators which may contribute to diabetes complications in youth.
SOURCE:
The study, published online in JAMA Network Open, was led by Chang Lu, MD, Division of Endocrinology, Boston Children’s Hospital, and Joslin Diabetes Center at Harvard Medical School, Boston, Massachusetts.
LIMITATIONS:
The study did not include a control group (individuals without diabetes). The cohort largely included youth in late puberty or after puberty, affecting subgroup analysis. Moreover, only circulating growth hormone mediators were measured, limiting the identity of the source tissue of the hormone and the target organs.
DISCLOSURES:
Some authors reported receiving grants from the National Institutes of Health and National Institute of Diabetes and Digestive and Kidney Diseases while conducting the study. Also, certain authors reported receiving grants and personal fees from various trusts as well as pharmaceutical, healthcare, and medical technology companies outside the submitted work.
TOPLINE:
Changes in plasma growth hormone mediators such as growth hormone receptor (GHR) and insulin-like growth factor-binding protein 1 (IGFBP-1) were associated with glycemic failure in youth-onset type 2 diabetes (T2D), an analysis of the TODAY trial showed.
METHODOLOGY:
- In youth, T2D often occurs during or after puberty, hinting at hormonal influences in the development and/or progression of the disease.
- This secondary analysis assessed the role of growth hormone mediators including insulin-like growth factor-1 (IGF-1), GHR, and IGFBP-1 in glycemic failure in a subset of 398 youths, aged 10-17 years, with a T2D duration of less than 2 years (62% girls; 21% White).
- The participants were followed up for a mean of 3.9 years.
- The primary outcomes included glycemic failure, defined as an A1c level of 8% or more for 6 months, or acute metabolic decompensation requiring insulin.
- Other assessments included baseline and 36-month measures of glycemia, insulin sensitivity, high molecular weight adiponectin, and beta cell function.
TAKEAWAY:
- Of 398 participants, 182 (46%) experienced glycemic failure, while 216 (54%) retained glycemic control.
- At 36 months, youths with glycemic failure had lower IGF-1 levels (P < .001) and higher log2 GHR (P = .03) and log2 IGFBP-1 (P = .009) levels than those who maintained glycemic control.
- A greater increase in IGF-1 level at 36 months was associated with lower odds of glycemic failure (odds ratio [OR], 0.995; P < .001).
- Increased levels of log2 GHR and log2 IGFBP-1 were associated with higher odds of glycemic failure (OR, 1.75; P = .04 and OR, 1.37; P = .007, respectively). Results were adjusted for body mass index (BMI), suggesting that associations between GHR level and glycemic outcomes exist independent of BMI.
- Interhormonal correlations suggested an association between glucose metabolism and growth hormone signaling or a shared process leading to changes in both processes.
IN PRACTICE:
“Our study has identified GHR level as a novel biomarker of decrease in glycemic control in youths with T2D,” the study authors wrote. Future research is needed, with an emphasis on assessing alterations in growth hormone mediators which may contribute to diabetes complications in youth.
SOURCE:
The study, published online in JAMA Network Open, was led by Chang Lu, MD, Division of Endocrinology, Boston Children’s Hospital, and Joslin Diabetes Center at Harvard Medical School, Boston, Massachusetts.
LIMITATIONS:
The study did not include a control group (individuals without diabetes). The cohort largely included youth in late puberty or after puberty, affecting subgroup analysis. Moreover, only circulating growth hormone mediators were measured, limiting the identity of the source tissue of the hormone and the target organs.
DISCLOSURES:
Some authors reported receiving grants from the National Institutes of Health and National Institute of Diabetes and Digestive and Kidney Diseases while conducting the study. Also, certain authors reported receiving grants and personal fees from various trusts as well as pharmaceutical, healthcare, and medical technology companies outside the submitted work.
Vitamin D Supplement Protects Insulin-Producing Cells in T1D
TOPLINE:
The remission period of type 1 diabetes (T1D) can be prolonged with high-dose ergocalciferol (a vitamin D analog), by preserving the function of insulin-producing beta cells in newly diagnosed patients.
METHODOLOGY:
- Beta cells may retain approximately 30%-50% function at the time of T1D diagnosis and continue producing insulin for months or years.
- Researchers conducted a secondary post hoc analysis of a randomized clinical trial looking at residual beta function and vitamin D supplementation in 36 youths (age, 10-21 years; mean age, 13.5 years; 33.3% women) with recently diagnosed T1D.
- Participants were randomly assigned to receive vitamin D (50,000 international units) or placebo every week for 2 months and then biweekly for 10 months.
- Mixed-meal tolerance tests were performed after overnight fasting at 0, 3, 6, 9, and 12 months, and blood draws were obtained 30 minutes and 90 minutes for post-meal C-peptide and glucose estimations.
- The fasting proinsulin to C-peptide ratio (PI:C) and the percentage change in the area under the curve of C-peptide from baseline (%ΔAUC) were calculated to test the effect of vitamin D on beta-cell function.
TAKEAWAY:
- Vitamin D supplementation improved the insulin secretion capacity of beta cells, as observed by the decrease in the mean fasting PI:C ratio compared with placebo (−0.0009 vs 0.0011; P =.01).
- The reduction in %ΔAUC of C-peptide was notably slower with vitamin D than placebo (−2.8% vs −4.7%; P =.03), indicating a longer delay in the loss of C-peptide.
IN PRACTICE:
“It is exciting to know that vitamin D could protect the beta cells of the pancreas and increase the natural production of good and functional insulin in these patients. This, in turn, prolongs the honeymoon phase of type 1 diabetes and leads to reduced long-term complications of this disease,” Benjamin Udoka Nwosu, MD, Northwell Health, Division of Endocrinology, Department of Pediatrics, Cohen Children’s Medical Center, New Hyde Park, New York, the principal author, said in a press release.
SOURCE:
The study was published online in JAMA Network Open.
LIMITATIONS:
It was a single-center study.
DISCLOSURES:
The study was supported by the National Institute of Diabetes and Digestive and Kidney Diseases. The authors did not report any conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
The remission period of type 1 diabetes (T1D) can be prolonged with high-dose ergocalciferol (a vitamin D analog), by preserving the function of insulin-producing beta cells in newly diagnosed patients.
METHODOLOGY:
- Beta cells may retain approximately 30%-50% function at the time of T1D diagnosis and continue producing insulin for months or years.
- Researchers conducted a secondary post hoc analysis of a randomized clinical trial looking at residual beta function and vitamin D supplementation in 36 youths (age, 10-21 years; mean age, 13.5 years; 33.3% women) with recently diagnosed T1D.
- Participants were randomly assigned to receive vitamin D (50,000 international units) or placebo every week for 2 months and then biweekly for 10 months.
- Mixed-meal tolerance tests were performed after overnight fasting at 0, 3, 6, 9, and 12 months, and blood draws were obtained 30 minutes and 90 minutes for post-meal C-peptide and glucose estimations.
- The fasting proinsulin to C-peptide ratio (PI:C) and the percentage change in the area under the curve of C-peptide from baseline (%ΔAUC) were calculated to test the effect of vitamin D on beta-cell function.
TAKEAWAY:
- Vitamin D supplementation improved the insulin secretion capacity of beta cells, as observed by the decrease in the mean fasting PI:C ratio compared with placebo (−0.0009 vs 0.0011; P =.01).
- The reduction in %ΔAUC of C-peptide was notably slower with vitamin D than placebo (−2.8% vs −4.7%; P =.03), indicating a longer delay in the loss of C-peptide.
IN PRACTICE:
“It is exciting to know that vitamin D could protect the beta cells of the pancreas and increase the natural production of good and functional insulin in these patients. This, in turn, prolongs the honeymoon phase of type 1 diabetes and leads to reduced long-term complications of this disease,” Benjamin Udoka Nwosu, MD, Northwell Health, Division of Endocrinology, Department of Pediatrics, Cohen Children’s Medical Center, New Hyde Park, New York, the principal author, said in a press release.
SOURCE:
The study was published online in JAMA Network Open.
LIMITATIONS:
It was a single-center study.
DISCLOSURES:
The study was supported by the National Institute of Diabetes and Digestive and Kidney Diseases. The authors did not report any conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
The remission period of type 1 diabetes (T1D) can be prolonged with high-dose ergocalciferol (a vitamin D analog), by preserving the function of insulin-producing beta cells in newly diagnosed patients.
METHODOLOGY:
- Beta cells may retain approximately 30%-50% function at the time of T1D diagnosis and continue producing insulin for months or years.
- Researchers conducted a secondary post hoc analysis of a randomized clinical trial looking at residual beta function and vitamin D supplementation in 36 youths (age, 10-21 years; mean age, 13.5 years; 33.3% women) with recently diagnosed T1D.
- Participants were randomly assigned to receive vitamin D (50,000 international units) or placebo every week for 2 months and then biweekly for 10 months.
- Mixed-meal tolerance tests were performed after overnight fasting at 0, 3, 6, 9, and 12 months, and blood draws were obtained 30 minutes and 90 minutes for post-meal C-peptide and glucose estimations.
- The fasting proinsulin to C-peptide ratio (PI:C) and the percentage change in the area under the curve of C-peptide from baseline (%ΔAUC) were calculated to test the effect of vitamin D on beta-cell function.
TAKEAWAY:
- Vitamin D supplementation improved the insulin secretion capacity of beta cells, as observed by the decrease in the mean fasting PI:C ratio compared with placebo (−0.0009 vs 0.0011; P =.01).
- The reduction in %ΔAUC of C-peptide was notably slower with vitamin D than placebo (−2.8% vs −4.7%; P =.03), indicating a longer delay in the loss of C-peptide.
IN PRACTICE:
“It is exciting to know that vitamin D could protect the beta cells of the pancreas and increase the natural production of good and functional insulin in these patients. This, in turn, prolongs the honeymoon phase of type 1 diabetes and leads to reduced long-term complications of this disease,” Benjamin Udoka Nwosu, MD, Northwell Health, Division of Endocrinology, Department of Pediatrics, Cohen Children’s Medical Center, New Hyde Park, New York, the principal author, said in a press release.
SOURCE:
The study was published online in JAMA Network Open.
LIMITATIONS:
It was a single-center study.
DISCLOSURES:
The study was supported by the National Institute of Diabetes and Digestive and Kidney Diseases. The authors did not report any conflicts of interest.
A version of this article appeared on Medscape.com.
Higher Dietary Niacin Tied to Lower Mortality Risk in MASLD
TOPLINE:
Higher dietary niacin intake is associated with a lower risk for all-cause mortality among people with metabolic dysfunction-associated steatotic liver disease (MASLD), but there is no connection between niacin consumption and cardiovascular disease (CVD) mortality, a recent study suggested.
METHODOLOGY:
- Researchers analyzed data from the National Health and Nutrition Examination Survey (2003-2018) for 4315 adults with MASLD (mean age, 52.5 years; 55%, men; 67%, non-Hispanic White).
- Dietary niacin intake levels were based on two 24-hour dietary recall interviews to report the types and quantities of foods that participants consumed in the 24 hours prior to the interviews.
- Participants were categorized by tertile of dietary niacin intake: Tertile 1 (n = 1440), < 18.4 mg; tertile 2 (n = 1441), 18.5-26.6 mg; and tertile 3 (n = 1434), > 26.7 mg.
TAKEAWAY:
- During a median follow-up of 8.8 years, 566 deaths occurred, of which 197 were attributed to CVD.
- Compared with participants with a niacin intake of 18.4 mg or lower (the lowest tertile), the multivariable-adjusted hazard ratios (HRs) for participants with a niacin intake of 26.7 mg or higher (the highest tertile) were 0.70 for all-cause mortality and 0.65 for CVD mortality.
- For the subgroup with diabetes compared with the reference group (the first tertile), the HR of all-cause mortality in the third tertile was 0.82.
- When the subgroup without diabetes was compared with the reference group, the HR of all-cause mortality in the third tertile was 0.58, suggesting a significant interaction between niacin and diabetes with the risk of all-cause mortality.
- An inverse association between dietary niacin intake and all-cause mortality was seen in sensitivity analyses, when excluding a participant who died within 2 years of follow-up.
IN PRACTICE:
“Higher dietary niacin intake was associated with a lower risk of all-cause mortality,” but not CVD, among individuals with MASLD, and “the dose-response association…needs to be further investigated to determine optimal intake level,” the authors wrote.
SOURCE:
The study, led by Jie Pan, MD, Sun Yat-sen University, Guangzhou, China, was published online in JAMA Network Open.
LIMITATIONS:
Physical activity data were missing and could not be adjusted for. The National Death Index used by the researchers has only “modest” ability to accurately classify CVD mortality, and the dietary data were subject to recall bias.
DISCLOSURES:
One author was supported by a grant from the National Nature Science Foundation of China. No other conflicts of interest were reported.
A version of this article appeared on Medscape.com.
TOPLINE:
Higher dietary niacin intake is associated with a lower risk for all-cause mortality among people with metabolic dysfunction-associated steatotic liver disease (MASLD), but there is no connection between niacin consumption and cardiovascular disease (CVD) mortality, a recent study suggested.
METHODOLOGY:
- Researchers analyzed data from the National Health and Nutrition Examination Survey (2003-2018) for 4315 adults with MASLD (mean age, 52.5 years; 55%, men; 67%, non-Hispanic White).
- Dietary niacin intake levels were based on two 24-hour dietary recall interviews to report the types and quantities of foods that participants consumed in the 24 hours prior to the interviews.
- Participants were categorized by tertile of dietary niacin intake: Tertile 1 (n = 1440), < 18.4 mg; tertile 2 (n = 1441), 18.5-26.6 mg; and tertile 3 (n = 1434), > 26.7 mg.
TAKEAWAY:
- During a median follow-up of 8.8 years, 566 deaths occurred, of which 197 were attributed to CVD.
- Compared with participants with a niacin intake of 18.4 mg or lower (the lowest tertile), the multivariable-adjusted hazard ratios (HRs) for participants with a niacin intake of 26.7 mg or higher (the highest tertile) were 0.70 for all-cause mortality and 0.65 for CVD mortality.
- For the subgroup with diabetes compared with the reference group (the first tertile), the HR of all-cause mortality in the third tertile was 0.82.
- When the subgroup without diabetes was compared with the reference group, the HR of all-cause mortality in the third tertile was 0.58, suggesting a significant interaction between niacin and diabetes with the risk of all-cause mortality.
- An inverse association between dietary niacin intake and all-cause mortality was seen in sensitivity analyses, when excluding a participant who died within 2 years of follow-up.
IN PRACTICE:
“Higher dietary niacin intake was associated with a lower risk of all-cause mortality,” but not CVD, among individuals with MASLD, and “the dose-response association…needs to be further investigated to determine optimal intake level,” the authors wrote.
SOURCE:
The study, led by Jie Pan, MD, Sun Yat-sen University, Guangzhou, China, was published online in JAMA Network Open.
LIMITATIONS:
Physical activity data were missing and could not be adjusted for. The National Death Index used by the researchers has only “modest” ability to accurately classify CVD mortality, and the dietary data were subject to recall bias.
DISCLOSURES:
One author was supported by a grant from the National Nature Science Foundation of China. No other conflicts of interest were reported.
A version of this article appeared on Medscape.com.
TOPLINE:
Higher dietary niacin intake is associated with a lower risk for all-cause mortality among people with metabolic dysfunction-associated steatotic liver disease (MASLD), but there is no connection between niacin consumption and cardiovascular disease (CVD) mortality, a recent study suggested.
METHODOLOGY:
- Researchers analyzed data from the National Health and Nutrition Examination Survey (2003-2018) for 4315 adults with MASLD (mean age, 52.5 years; 55%, men; 67%, non-Hispanic White).
- Dietary niacin intake levels were based on two 24-hour dietary recall interviews to report the types and quantities of foods that participants consumed in the 24 hours prior to the interviews.
- Participants were categorized by tertile of dietary niacin intake: Tertile 1 (n = 1440), < 18.4 mg; tertile 2 (n = 1441), 18.5-26.6 mg; and tertile 3 (n = 1434), > 26.7 mg.
TAKEAWAY:
- During a median follow-up of 8.8 years, 566 deaths occurred, of which 197 were attributed to CVD.
- Compared with participants with a niacin intake of 18.4 mg or lower (the lowest tertile), the multivariable-adjusted hazard ratios (HRs) for participants with a niacin intake of 26.7 mg or higher (the highest tertile) were 0.70 for all-cause mortality and 0.65 for CVD mortality.
- For the subgroup with diabetes compared with the reference group (the first tertile), the HR of all-cause mortality in the third tertile was 0.82.
- When the subgroup without diabetes was compared with the reference group, the HR of all-cause mortality in the third tertile was 0.58, suggesting a significant interaction between niacin and diabetes with the risk of all-cause mortality.
- An inverse association between dietary niacin intake and all-cause mortality was seen in sensitivity analyses, when excluding a participant who died within 2 years of follow-up.
IN PRACTICE:
“Higher dietary niacin intake was associated with a lower risk of all-cause mortality,” but not CVD, among individuals with MASLD, and “the dose-response association…needs to be further investigated to determine optimal intake level,” the authors wrote.
SOURCE:
The study, led by Jie Pan, MD, Sun Yat-sen University, Guangzhou, China, was published online in JAMA Network Open.
LIMITATIONS:
Physical activity data were missing and could not be adjusted for. The National Death Index used by the researchers has only “modest” ability to accurately classify CVD mortality, and the dietary data were subject to recall bias.
DISCLOSURES:
One author was supported by a grant from the National Nature Science Foundation of China. No other conflicts of interest were reported.
A version of this article appeared on Medscape.com.
Is a 1-Hour Glucose Test Better at Predicting T2D Risk?
A new position statement from the International Diabetes Federation advises using a 1-hour 75-g oral glucose tolerance test (OGTT) to improve identification of people at risk of developing type 2 diabetes.
“There are many, many people who may appear ‘normal’ if you use A1c or fasting glucose, but if you do a glucose tolerance test, they may have an abnormality after a glucose load. …The 1-hour plasma glucose has been found to be a more sensitive biomarker for the earlier identification of these high-risk individuals,” lead author Michael Bergman, MD, professor of medicine and population health at New York University Grossman School of Medicine, New York City, told this news organization in an interview.
Dr. Bergman presented the document, written by a 22-member international expert panel, on March 6, 2024, at the annual Advanced Technologies & Treatments for Diabetes meeting. It was simultaneously published in Diabetes Research and Clinical Practice.
This is the International Diabetes Federation’s (IDF’s) proposed screening algorithm for “intermediate hyperglycemia” and type 2 diabetes:
- At-risk high-risk individuals are first screened with a validated questionnaire such as the FINDRISK or the American Diabetes Association’s (ADA’s) risk screening tool.
- People identified as high risk should undergo laboratory screening with a 1-hour 75-g OGTT (although a 2-hour OGTT, fasting glucose, or A1c, as currently recommended by several organizations, is still considered acceptable).
- People with a 1-hour plasma glucose value at or above 155 mg (8.6 mmol/L) are considered to have intermediate hyperglycemia and should be prescribed lifestyle intervention and referred to a diabetes prevention program.
- Those with a 1-hour value greater than or equal to 209 mg/dL (11.6 mmol/L) are considered to have type 2 diabetes and should have a repeat test to confirm the diagnosis, with referral for further evaluation and treatment.
The new guidance is based on increasing evidence that the 1-hour test is a better predictor than other tests, including the 2-hour OGTT, of progression to type 2 diabetes and its associated complications, in a variety of populations. The document cites data showing that a plasma glucose of 155 mg/dl or greater on the 1-hour post-75-g test can identify people with undiagnosed type 2 diabetes or who are at increased risk but who have “normal” glucose tolerance as defined by an A1c < 5.7% (38.8 mmol/mol), a fasting plasma glucose < 100 mg/dL (5.6 mmol/L), or a 2-hour value below 140 mg/dL (7.8 mmol/L).
However, even though a 1-hour test may be more convenient than the traditional 2-hour test, incorporating OGTT into busy clinical practice may still pose logistical problems and may not improve ultimate outcomes, Elizabeth Selvin, PhD, MPH, of the Johns Hopkins University Bloomberg School of Public Health, Baltimore, Maryland, told this news organization. “I worry that emphasizing a burdensome test is not going to improve diabetes screening or diabetes prevention. Doing more 1-hour glucose screening is not going to get more people into diabetes prevention programs.”
When an audience member raised the logistics concern during the session Q&A, Dr. Bergman replied, “It’s no different than recommending colonoscopy or a mammogram. … I tell patients that we want to learn more about what is going on before we make a firm diagnosis. … I’ve done more than a hundred 1-hour glucose tolerance tests and have not seen one patient who refused because of inconvenience. Everything depends on the way we discuss things with patients.”
Recommendation Based on Emerging Evidence
“Intermediate hyperglycemia” is the World Health Organization’s term to refer to either impaired fasting glucose (IFG) or impaired glucose tolerance (IGT). These conditions are often called “prediabetes,” especially in the United States, but that term has been controversial because not everyone with IFG and IGT will go on to develop type 2 diabetes, said Dr. Bergman, who is also director of the NYU Langone Diabetes Prevention Program.
“With ‘prediabetes’ you’re labeling someone with a disease they may not develop. It’s not normal, but it’s not diabetes, so it’s an intermediate state,” he explained.
The statement provides a detailed summary of the data from 19 studies supporting use of a 1-hour plasma glucose of ≥ 155 mg/dL (8.6 mmol/L) to diagnose intermediate hyperglycemia and type 2 diabetes, including links between that level of glycemia and worsened metabolic and atherogenic profiles, risk for microvascular and macrovascular complications and mortality, and identification of risks for obstructive sleep apnea, cystic fibrosis-related diabetes mellitus, fatty liver disease, and premature mortality.
One major problem with current testing, Dr. Bergman said, is that “there is a huge disconnect between A1c and glucose values. … Only about 30% of individuals with an abnormal A1c will have an abnormal fasting glucose, and the inverse is also true. There’s a big mismatch between the two.”
Current guidelines suggest using both A1c and fasting glucose, but Dr. Bergman said that even then “you’re still missing about 20-30% who have IGT. … Part of the problem is that the criteria we use for defining abnormal fasting and 2-hour levels are too high. … 140 [mg/dL] for the 2-hour is too high and 100 [mg/dL] fasting is too high. … And that’s one of the reasons why many people progress to type 2 diabetes, because we’re using screening thresholds that are nonphysiologic.”
But Dr. Selvin disagrees, pointing to her own work showing that “using a combination of fasting glucose and A1c for screening does an excellent job at identifying high-risk individuals.”
She’s also unconvinced by other data cited in the paper. “I am deeply skeptical about 1-hour glucose being more prognostic than all other glycemic tests. … Associations of glucose tests with incident diabetes are inherently a circular analysis since diabetes is defined by elevations in those same tests. It is helpful to look at progression of diabetes, but these analyses are not simple and doing them well, especially with head-to-head comparisons against different glycemic tests, is hard,” she said.
In her view, “lifestyle interventions and weight loss should be recommended in at-risk individuals, including those with overweight and obesity, hypertension, metabolic syndrome, etc., regardless of 1-hour glucose test results.”
She added, “If we want to prevent diabetes, we need to focus on preventing weight gain and obesity and managing cardiometabolic risk factors. Lifestyle interventions are not effective unless they are intensive and patients are highly adherent. We need to make lifestyle interventions available and affordable for patients. That is the big barrier. I don’t think more screening with 1-hour glucose is going to help.”
Dr. Bergman pointed out that the International Diabetes Federation represents more than 100 countries, including many that are middle- and low-income. “They need a simple, cost-effective tool for screening effectively. A1c is more expensive, and fasting glucose alone will underestimate disease prevalence. So, the IDF felt, after doing a fairly comprehensive due diligence, that the data warranted recommendation of the 1-hour glucose.”
He’s hoping other organizations like the ADA and the World Health Organization will sign on to bring this guidance into the primary care arena. This news organization reached out to ADA for comment, but their representative hadn’t responded by press time.
Dr. Bergman had no disclosures. Dr. Selvin was supported by the National Institutes of Health.
A version of this article appeared on Medscape.com.
A new position statement from the International Diabetes Federation advises using a 1-hour 75-g oral glucose tolerance test (OGTT) to improve identification of people at risk of developing type 2 diabetes.
“There are many, many people who may appear ‘normal’ if you use A1c or fasting glucose, but if you do a glucose tolerance test, they may have an abnormality after a glucose load. …The 1-hour plasma glucose has been found to be a more sensitive biomarker for the earlier identification of these high-risk individuals,” lead author Michael Bergman, MD, professor of medicine and population health at New York University Grossman School of Medicine, New York City, told this news organization in an interview.
Dr. Bergman presented the document, written by a 22-member international expert panel, on March 6, 2024, at the annual Advanced Technologies & Treatments for Diabetes meeting. It was simultaneously published in Diabetes Research and Clinical Practice.
This is the International Diabetes Federation’s (IDF’s) proposed screening algorithm for “intermediate hyperglycemia” and type 2 diabetes:
- At-risk high-risk individuals are first screened with a validated questionnaire such as the FINDRISK or the American Diabetes Association’s (ADA’s) risk screening tool.
- People identified as high risk should undergo laboratory screening with a 1-hour 75-g OGTT (although a 2-hour OGTT, fasting glucose, or A1c, as currently recommended by several organizations, is still considered acceptable).
- People with a 1-hour plasma glucose value at or above 155 mg (8.6 mmol/L) are considered to have intermediate hyperglycemia and should be prescribed lifestyle intervention and referred to a diabetes prevention program.
- Those with a 1-hour value greater than or equal to 209 mg/dL (11.6 mmol/L) are considered to have type 2 diabetes and should have a repeat test to confirm the diagnosis, with referral for further evaluation and treatment.
The new guidance is based on increasing evidence that the 1-hour test is a better predictor than other tests, including the 2-hour OGTT, of progression to type 2 diabetes and its associated complications, in a variety of populations. The document cites data showing that a plasma glucose of 155 mg/dl or greater on the 1-hour post-75-g test can identify people with undiagnosed type 2 diabetes or who are at increased risk but who have “normal” glucose tolerance as defined by an A1c < 5.7% (38.8 mmol/mol), a fasting plasma glucose < 100 mg/dL (5.6 mmol/L), or a 2-hour value below 140 mg/dL (7.8 mmol/L).
However, even though a 1-hour test may be more convenient than the traditional 2-hour test, incorporating OGTT into busy clinical practice may still pose logistical problems and may not improve ultimate outcomes, Elizabeth Selvin, PhD, MPH, of the Johns Hopkins University Bloomberg School of Public Health, Baltimore, Maryland, told this news organization. “I worry that emphasizing a burdensome test is not going to improve diabetes screening or diabetes prevention. Doing more 1-hour glucose screening is not going to get more people into diabetes prevention programs.”
When an audience member raised the logistics concern during the session Q&A, Dr. Bergman replied, “It’s no different than recommending colonoscopy or a mammogram. … I tell patients that we want to learn more about what is going on before we make a firm diagnosis. … I’ve done more than a hundred 1-hour glucose tolerance tests and have not seen one patient who refused because of inconvenience. Everything depends on the way we discuss things with patients.”
Recommendation Based on Emerging Evidence
“Intermediate hyperglycemia” is the World Health Organization’s term to refer to either impaired fasting glucose (IFG) or impaired glucose tolerance (IGT). These conditions are often called “prediabetes,” especially in the United States, but that term has been controversial because not everyone with IFG and IGT will go on to develop type 2 diabetes, said Dr. Bergman, who is also director of the NYU Langone Diabetes Prevention Program.
“With ‘prediabetes’ you’re labeling someone with a disease they may not develop. It’s not normal, but it’s not diabetes, so it’s an intermediate state,” he explained.
The statement provides a detailed summary of the data from 19 studies supporting use of a 1-hour plasma glucose of ≥ 155 mg/dL (8.6 mmol/L) to diagnose intermediate hyperglycemia and type 2 diabetes, including links between that level of glycemia and worsened metabolic and atherogenic profiles, risk for microvascular and macrovascular complications and mortality, and identification of risks for obstructive sleep apnea, cystic fibrosis-related diabetes mellitus, fatty liver disease, and premature mortality.
One major problem with current testing, Dr. Bergman said, is that “there is a huge disconnect between A1c and glucose values. … Only about 30% of individuals with an abnormal A1c will have an abnormal fasting glucose, and the inverse is also true. There’s a big mismatch between the two.”
Current guidelines suggest using both A1c and fasting glucose, but Dr. Bergman said that even then “you’re still missing about 20-30% who have IGT. … Part of the problem is that the criteria we use for defining abnormal fasting and 2-hour levels are too high. … 140 [mg/dL] for the 2-hour is too high and 100 [mg/dL] fasting is too high. … And that’s one of the reasons why many people progress to type 2 diabetes, because we’re using screening thresholds that are nonphysiologic.”
But Dr. Selvin disagrees, pointing to her own work showing that “using a combination of fasting glucose and A1c for screening does an excellent job at identifying high-risk individuals.”
She’s also unconvinced by other data cited in the paper. “I am deeply skeptical about 1-hour glucose being more prognostic than all other glycemic tests. … Associations of glucose tests with incident diabetes are inherently a circular analysis since diabetes is defined by elevations in those same tests. It is helpful to look at progression of diabetes, but these analyses are not simple and doing them well, especially with head-to-head comparisons against different glycemic tests, is hard,” she said.
In her view, “lifestyle interventions and weight loss should be recommended in at-risk individuals, including those with overweight and obesity, hypertension, metabolic syndrome, etc., regardless of 1-hour glucose test results.”
She added, “If we want to prevent diabetes, we need to focus on preventing weight gain and obesity and managing cardiometabolic risk factors. Lifestyle interventions are not effective unless they are intensive and patients are highly adherent. We need to make lifestyle interventions available and affordable for patients. That is the big barrier. I don’t think more screening with 1-hour glucose is going to help.”
Dr. Bergman pointed out that the International Diabetes Federation represents more than 100 countries, including many that are middle- and low-income. “They need a simple, cost-effective tool for screening effectively. A1c is more expensive, and fasting glucose alone will underestimate disease prevalence. So, the IDF felt, after doing a fairly comprehensive due diligence, that the data warranted recommendation of the 1-hour glucose.”
He’s hoping other organizations like the ADA and the World Health Organization will sign on to bring this guidance into the primary care arena. This news organization reached out to ADA for comment, but their representative hadn’t responded by press time.
Dr. Bergman had no disclosures. Dr. Selvin was supported by the National Institutes of Health.
A version of this article appeared on Medscape.com.
A new position statement from the International Diabetes Federation advises using a 1-hour 75-g oral glucose tolerance test (OGTT) to improve identification of people at risk of developing type 2 diabetes.
“There are many, many people who may appear ‘normal’ if you use A1c or fasting glucose, but if you do a glucose tolerance test, they may have an abnormality after a glucose load. …The 1-hour plasma glucose has been found to be a more sensitive biomarker for the earlier identification of these high-risk individuals,” lead author Michael Bergman, MD, professor of medicine and population health at New York University Grossman School of Medicine, New York City, told this news organization in an interview.
Dr. Bergman presented the document, written by a 22-member international expert panel, on March 6, 2024, at the annual Advanced Technologies & Treatments for Diabetes meeting. It was simultaneously published in Diabetes Research and Clinical Practice.
This is the International Diabetes Federation’s (IDF’s) proposed screening algorithm for “intermediate hyperglycemia” and type 2 diabetes:
- At-risk high-risk individuals are first screened with a validated questionnaire such as the FINDRISK or the American Diabetes Association’s (ADA’s) risk screening tool.
- People identified as high risk should undergo laboratory screening with a 1-hour 75-g OGTT (although a 2-hour OGTT, fasting glucose, or A1c, as currently recommended by several organizations, is still considered acceptable).
- People with a 1-hour plasma glucose value at or above 155 mg (8.6 mmol/L) are considered to have intermediate hyperglycemia and should be prescribed lifestyle intervention and referred to a diabetes prevention program.
- Those with a 1-hour value greater than or equal to 209 mg/dL (11.6 mmol/L) are considered to have type 2 diabetes and should have a repeat test to confirm the diagnosis, with referral for further evaluation and treatment.
The new guidance is based on increasing evidence that the 1-hour test is a better predictor than other tests, including the 2-hour OGTT, of progression to type 2 diabetes and its associated complications, in a variety of populations. The document cites data showing that a plasma glucose of 155 mg/dl or greater on the 1-hour post-75-g test can identify people with undiagnosed type 2 diabetes or who are at increased risk but who have “normal” glucose tolerance as defined by an A1c < 5.7% (38.8 mmol/mol), a fasting plasma glucose < 100 mg/dL (5.6 mmol/L), or a 2-hour value below 140 mg/dL (7.8 mmol/L).
However, even though a 1-hour test may be more convenient than the traditional 2-hour test, incorporating OGTT into busy clinical practice may still pose logistical problems and may not improve ultimate outcomes, Elizabeth Selvin, PhD, MPH, of the Johns Hopkins University Bloomberg School of Public Health, Baltimore, Maryland, told this news organization. “I worry that emphasizing a burdensome test is not going to improve diabetes screening or diabetes prevention. Doing more 1-hour glucose screening is not going to get more people into diabetes prevention programs.”
When an audience member raised the logistics concern during the session Q&A, Dr. Bergman replied, “It’s no different than recommending colonoscopy or a mammogram. … I tell patients that we want to learn more about what is going on before we make a firm diagnosis. … I’ve done more than a hundred 1-hour glucose tolerance tests and have not seen one patient who refused because of inconvenience. Everything depends on the way we discuss things with patients.”
Recommendation Based on Emerging Evidence
“Intermediate hyperglycemia” is the World Health Organization’s term to refer to either impaired fasting glucose (IFG) or impaired glucose tolerance (IGT). These conditions are often called “prediabetes,” especially in the United States, but that term has been controversial because not everyone with IFG and IGT will go on to develop type 2 diabetes, said Dr. Bergman, who is also director of the NYU Langone Diabetes Prevention Program.
“With ‘prediabetes’ you’re labeling someone with a disease they may not develop. It’s not normal, but it’s not diabetes, so it’s an intermediate state,” he explained.
The statement provides a detailed summary of the data from 19 studies supporting use of a 1-hour plasma glucose of ≥ 155 mg/dL (8.6 mmol/L) to diagnose intermediate hyperglycemia and type 2 diabetes, including links between that level of glycemia and worsened metabolic and atherogenic profiles, risk for microvascular and macrovascular complications and mortality, and identification of risks for obstructive sleep apnea, cystic fibrosis-related diabetes mellitus, fatty liver disease, and premature mortality.
One major problem with current testing, Dr. Bergman said, is that “there is a huge disconnect between A1c and glucose values. … Only about 30% of individuals with an abnormal A1c will have an abnormal fasting glucose, and the inverse is also true. There’s a big mismatch between the two.”
Current guidelines suggest using both A1c and fasting glucose, but Dr. Bergman said that even then “you’re still missing about 20-30% who have IGT. … Part of the problem is that the criteria we use for defining abnormal fasting and 2-hour levels are too high. … 140 [mg/dL] for the 2-hour is too high and 100 [mg/dL] fasting is too high. … And that’s one of the reasons why many people progress to type 2 diabetes, because we’re using screening thresholds that are nonphysiologic.”
But Dr. Selvin disagrees, pointing to her own work showing that “using a combination of fasting glucose and A1c for screening does an excellent job at identifying high-risk individuals.”
She’s also unconvinced by other data cited in the paper. “I am deeply skeptical about 1-hour glucose being more prognostic than all other glycemic tests. … Associations of glucose tests with incident diabetes are inherently a circular analysis since diabetes is defined by elevations in those same tests. It is helpful to look at progression of diabetes, but these analyses are not simple and doing them well, especially with head-to-head comparisons against different glycemic tests, is hard,” she said.
In her view, “lifestyle interventions and weight loss should be recommended in at-risk individuals, including those with overweight and obesity, hypertension, metabolic syndrome, etc., regardless of 1-hour glucose test results.”
She added, “If we want to prevent diabetes, we need to focus on preventing weight gain and obesity and managing cardiometabolic risk factors. Lifestyle interventions are not effective unless they are intensive and patients are highly adherent. We need to make lifestyle interventions available and affordable for patients. That is the big barrier. I don’t think more screening with 1-hour glucose is going to help.”
Dr. Bergman pointed out that the International Diabetes Federation represents more than 100 countries, including many that are middle- and low-income. “They need a simple, cost-effective tool for screening effectively. A1c is more expensive, and fasting glucose alone will underestimate disease prevalence. So, the IDF felt, after doing a fairly comprehensive due diligence, that the data warranted recommendation of the 1-hour glucose.”
He’s hoping other organizations like the ADA and the World Health Organization will sign on to bring this guidance into the primary care arena. This news organization reached out to ADA for comment, but their representative hadn’t responded by press time.
Dr. Bergman had no disclosures. Dr. Selvin was supported by the National Institutes of Health.
A version of this article appeared on Medscape.com.
Study Sounds Alert About GLP-1 RA Use and Aspiration Risk
TOPLINE:
Patients on weekly glucagon-like peptide-1 receptor agonists (GLP-1 RAs) have high residual gastric content, a major risk factor for aspiration under anesthesia, despite following fasting guidelines before undergoing elective procedures.
METHODOLOGY:
- The increasing use of GLP-1 RAs to manage weight and hyperglycemia has sparked safety concerns because of the drugs’ association with slow gastric emptying, a major risk factor for aspiration under anesthesia.
- This cross-sectional study used gastric ultrasonography to examine the link between GLP-1 RA use and the prevalence of increased residual gastric content.
- All 124 participants (median age, 56 years; 60% women) — half of whom received once-weekly GLP-1 RAs such as semaglutide, dulaglutide, or tirzepatide — adhered to the guideline-recommended fasting duration before undergoing elective procedures under anesthesia.
- The primary outcome focused on identifying increased residual gastric content, defined by the presence of solids, thick liquids, or > 1.5 mL/kg of clear liquids on ultrasound.
- An exploratory analysis examined the association between the duration of GLP-1 RA discontinuation and increased residual gastric content.
TAKEAWAY:
- The adjusted prevalence of increased residual gastric content was 30.5% (95% CI, 9.9%-51.2%) higher in participants who received GLP-1 RA than those who did not.
- Most patients took their last dose of GLP-1 RA within 5 days before their procedure, but elevated residual gastric content persisted even after 7 days of GLP-1 RA discontinuation.
- There was also no significant association between the type of GLP-1 RA used and the prevalence of increased residual gastric content.
IN PRACTICE:
“We expect healthcare professionals will encounter these classes of drugs with increasing frequency in the perioperative period. Perioperative physicians, including anesthesiologists, surgeons, and primary care physicians, should be well-informed about the safety implications of GLP-1 RA drugs,” the authors wrote.
SOURCE:
The study was led by Sudipta Sen, MD, from the Department of Anesthesiology, Critical Care and Pain Medicine, McGovern Medical School, University of Texas Health Center at Houston, Houston, Texas, and published online in JAMA Surgery.
LIMITATIONS:
Residual gastric content, the primary outcome, served as a proxy for aspiration risk and does not have an exact threshold of volume associated with increased risk. The study did not directly evaluate aspiration events. The authors also acknowledged potential bias from unmeasured confounders owing to the observational nature of this study. A small sample size limited the ability to detect a risk difference for each additional day of drug discontinuation before surgery.
DISCLOSURES:
One of the authors reported receiving a grant from the National Institutes of Health. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
Patients on weekly glucagon-like peptide-1 receptor agonists (GLP-1 RAs) have high residual gastric content, a major risk factor for aspiration under anesthesia, despite following fasting guidelines before undergoing elective procedures.
METHODOLOGY:
- The increasing use of GLP-1 RAs to manage weight and hyperglycemia has sparked safety concerns because of the drugs’ association with slow gastric emptying, a major risk factor for aspiration under anesthesia.
- This cross-sectional study used gastric ultrasonography to examine the link between GLP-1 RA use and the prevalence of increased residual gastric content.
- All 124 participants (median age, 56 years; 60% women) — half of whom received once-weekly GLP-1 RAs such as semaglutide, dulaglutide, or tirzepatide — adhered to the guideline-recommended fasting duration before undergoing elective procedures under anesthesia.
- The primary outcome focused on identifying increased residual gastric content, defined by the presence of solids, thick liquids, or > 1.5 mL/kg of clear liquids on ultrasound.
- An exploratory analysis examined the association between the duration of GLP-1 RA discontinuation and increased residual gastric content.
TAKEAWAY:
- The adjusted prevalence of increased residual gastric content was 30.5% (95% CI, 9.9%-51.2%) higher in participants who received GLP-1 RA than those who did not.
- Most patients took their last dose of GLP-1 RA within 5 days before their procedure, but elevated residual gastric content persisted even after 7 days of GLP-1 RA discontinuation.
- There was also no significant association between the type of GLP-1 RA used and the prevalence of increased residual gastric content.
IN PRACTICE:
“We expect healthcare professionals will encounter these classes of drugs with increasing frequency in the perioperative period. Perioperative physicians, including anesthesiologists, surgeons, and primary care physicians, should be well-informed about the safety implications of GLP-1 RA drugs,” the authors wrote.
SOURCE:
The study was led by Sudipta Sen, MD, from the Department of Anesthesiology, Critical Care and Pain Medicine, McGovern Medical School, University of Texas Health Center at Houston, Houston, Texas, and published online in JAMA Surgery.
LIMITATIONS:
Residual gastric content, the primary outcome, served as a proxy for aspiration risk and does not have an exact threshold of volume associated with increased risk. The study did not directly evaluate aspiration events. The authors also acknowledged potential bias from unmeasured confounders owing to the observational nature of this study. A small sample size limited the ability to detect a risk difference for each additional day of drug discontinuation before surgery.
DISCLOSURES:
One of the authors reported receiving a grant from the National Institutes of Health. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
Patients on weekly glucagon-like peptide-1 receptor agonists (GLP-1 RAs) have high residual gastric content, a major risk factor for aspiration under anesthesia, despite following fasting guidelines before undergoing elective procedures.
METHODOLOGY:
- The increasing use of GLP-1 RAs to manage weight and hyperglycemia has sparked safety concerns because of the drugs’ association with slow gastric emptying, a major risk factor for aspiration under anesthesia.
- This cross-sectional study used gastric ultrasonography to examine the link between GLP-1 RA use and the prevalence of increased residual gastric content.
- All 124 participants (median age, 56 years; 60% women) — half of whom received once-weekly GLP-1 RAs such as semaglutide, dulaglutide, or tirzepatide — adhered to the guideline-recommended fasting duration before undergoing elective procedures under anesthesia.
- The primary outcome focused on identifying increased residual gastric content, defined by the presence of solids, thick liquids, or > 1.5 mL/kg of clear liquids on ultrasound.
- An exploratory analysis examined the association between the duration of GLP-1 RA discontinuation and increased residual gastric content.
TAKEAWAY:
- The adjusted prevalence of increased residual gastric content was 30.5% (95% CI, 9.9%-51.2%) higher in participants who received GLP-1 RA than those who did not.
- Most patients took their last dose of GLP-1 RA within 5 days before their procedure, but elevated residual gastric content persisted even after 7 days of GLP-1 RA discontinuation.
- There was also no significant association between the type of GLP-1 RA used and the prevalence of increased residual gastric content.
IN PRACTICE:
“We expect healthcare professionals will encounter these classes of drugs with increasing frequency in the perioperative period. Perioperative physicians, including anesthesiologists, surgeons, and primary care physicians, should be well-informed about the safety implications of GLP-1 RA drugs,” the authors wrote.
SOURCE:
The study was led by Sudipta Sen, MD, from the Department of Anesthesiology, Critical Care and Pain Medicine, McGovern Medical School, University of Texas Health Center at Houston, Houston, Texas, and published online in JAMA Surgery.
LIMITATIONS:
Residual gastric content, the primary outcome, served as a proxy for aspiration risk and does not have an exact threshold of volume associated with increased risk. The study did not directly evaluate aspiration events. The authors also acknowledged potential bias from unmeasured confounders owing to the observational nature of this study. A small sample size limited the ability to detect a risk difference for each additional day of drug discontinuation before surgery.
DISCLOSURES:
One of the authors reported receiving a grant from the National Institutes of Health. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.




