User login
It is time to separate the O from the G
Two very different specialties, obstetrics (O) and gynecology (G), were fused into one in 1889. It is difficult to conceive that, with the expansion of both specialties in knowledge, procedures, and subspecialties, they still remain as one after 130 years. The American College of Obstetricians and Gynecologists was founded in 1952, and after 68 years no major changes have been made to accept or incorporate that there is a need to consider O and G as two different specialties.
Obstetrics and gynecology are the only specialties dedicated exclusively to women but with a very different purpose: the O is for reproduction, the G is for prevention and management of genital diseases. The specialties of O and G are so different the only thing in common is the patient.
It is time to separate the O from the G.
Are we training surgically competent residents?
No, we are not. There is an adequate volume for training and practice in O with close to 3.8 million births a year (the number cited by the Centers for Disease Control and Prevention in 2018). Not surprisingly, there is a need for trainees and also for practitioners in rural areas. As a result, the surgical training and practice in G is not optimal. If the number of hysterectomies was even near that of deliveries, there would be an adequate volume for everyone in training and in practice. But this is not the case.
The Accreditation Council for Graduate Medical Education (ACGME) mandates OG residents to graduate with a minimum of 70 minimally invasive hysterectomies (MIH), including laparoscopic (LH), vaginal (VH), and laparoscopic vaginally assisted (LAVH). In 2017, 51% of graduating residents fell below the minimum of 70 MIH.1 Because the learning curve of LH ranges from 30 to 80 cases,2 it is not surprising most residents feel surgically inadequate at graduation to function independently.
Increased procedures and technologies with reduced training hours
Let’s look at hysterectomies. From two techniques, vaginal and abdominal, they have expanded to LH, LAVH, robotic, single-site LH, single-site robotic, and recently single-port robotic. In addition, different and new technologies for hysteroscopy and myomectomy procedures have been developed.
All these operations are supposed to be part of any training program as ACGME demands “OG residents must be able to competently perform all medical, diagnostic, and surgical procedures considered essential for the area of practice.”3 In addition, primary care has been added to OG residency training: “Primary health care management from adolescence through reproductive age to midlife and beyond is integral to any ob.gyn.’s practice” and “Obstetrician-gynecologists are viewed by some entities as being primary care physicians for women, especially as coordinators of care among most reproductive-aged women,” according to ACOG.4
All this with reduced training hours.
The number of training hours a week has been reduced to 80, while it used to be over 100 hours. If you do the math, 20 fewer hours a week for 4 years amounts to 4,240 hours, equivalent to 180 days, equal to 6 months.
Graduating residents must pass a written and an oral exam for certification and with this are approved to enter the operating room and operate on women without a surgical skills test.
A simple test shows that elimination of the O for 1 year improves laparoscopic performance
We compared the time to perform three basic laparoscopic skills by fourth-year OG residents with that of fellows at the end of their first year in a minimally invasive G fellowship.5 The mean time for the residents completing the three tasks within the allotted time was 16 minutes, compared with 3.5 minutes for fellows: a four times faster performance.
Are there enough patients to maintain surgical skills after residency?
No, there are not.
Consider the following reality after residency. Decreasing number of surgeries and increasing numbers of OGs results in what you have already guessed: a lower surgical volume per OG.
Since 1979, the number of G surgeries has decreased by almost half (46%) while the number of OGs has doubled (54%) resulting in an 81% decrease of number of surgeries per OG, from 132 in 1979 to 25 in 2007.6 For hysterectomies, there has been a continuous yearly decline per G from 28 in 1980 to 9.8 in 2007 and to 8.5 in 2010.7,8
Would any mother feel comfortable having an obstetrician for her pregnancy and delivery performing only 8.5 deliveries a year?
Where do we go from here?
Separate the training and practice of O and G, an initiative already started in some residency programs and in some institutions in the United States. The O and the G both include a medical and a surgical practice.
We need to start accepting there is a need for different practices: medical O, medical G, surgical O, and surgical G. It is not new, it is already happening, it is the case in our institution since inception, and it is expanding across the country because it is needed. Graduating residents recognize this need as noticed by the increasing number seeking subspecialty training, from 7% in 2000 to 19.5% in 2012.4
Will this require some patients to drive away from home to obtain the best possible care? Yes. It is not a new concept, and it already is occurring for patients traveling to specialized centers away from home for certain conditions. In some countries, the practice is restricted to only a few centers. In Sweden, for instance, patients diagnosed with gynecologic cancer must travel to one of only seven centers subspecialized in gynecologic malignancies.
Conclusion
We need to start someday. We already are late after 130 years. We need to provide optimal care for women. They are our mothers. They deserve it. Let the O deliver O care, let the G provide G care, and we will reap improved results.
Dr. Magrina is with the department of medical and surgical gynecology at the Mayo Clinic in Phoenix. The author has no conflict of interest or financial involvement with this manuscript.
References
1. Am J Obstet Gynecol. 2019 Nov 22. doi: 10.1016/j.ajog.2019.11.1258.
2. Clin Obstet Gynecol. 2011 Sep;54(3):376-81.
3. Accreditation Council for Graduate Medical Education. Program requirements for GME in Obstetrics and Gynecology 2017.
4. “The obstetrician-gynecologist workforce in the United States: Facts, figures, and implications, 2017” (Washington, D.C.: ACOG, 2017).
5. J Minim Invasive Gynecol. 2008 Jul-Aug;15(4):410-3.
6. J Minim Invasive Gynecol. 2014 Jul-Aug;21(4):501-3.
7. National Health Statistics Report. Hysterectomy in the U.S. and oophorectomy 1979-2007. http://www.cdc.gov/nchs/products/nhsr.htm.
8. The Healthcare Cost and Utilization Project – Nationwide Inpatient Sample: Agency for Health Care Research Quality. 2013.
Two very different specialties, obstetrics (O) and gynecology (G), were fused into one in 1889. It is difficult to conceive that, with the expansion of both specialties in knowledge, procedures, and subspecialties, they still remain as one after 130 years. The American College of Obstetricians and Gynecologists was founded in 1952, and after 68 years no major changes have been made to accept or incorporate that there is a need to consider O and G as two different specialties.
Obstetrics and gynecology are the only specialties dedicated exclusively to women but with a very different purpose: the O is for reproduction, the G is for prevention and management of genital diseases. The specialties of O and G are so different the only thing in common is the patient.
It is time to separate the O from the G.
Are we training surgically competent residents?
No, we are not. There is an adequate volume for training and practice in O with close to 3.8 million births a year (the number cited by the Centers for Disease Control and Prevention in 2018). Not surprisingly, there is a need for trainees and also for practitioners in rural areas. As a result, the surgical training and practice in G is not optimal. If the number of hysterectomies was even near that of deliveries, there would be an adequate volume for everyone in training and in practice. But this is not the case.
The Accreditation Council for Graduate Medical Education (ACGME) mandates OG residents to graduate with a minimum of 70 minimally invasive hysterectomies (MIH), including laparoscopic (LH), vaginal (VH), and laparoscopic vaginally assisted (LAVH). In 2017, 51% of graduating residents fell below the minimum of 70 MIH.1 Because the learning curve of LH ranges from 30 to 80 cases,2 it is not surprising most residents feel surgically inadequate at graduation to function independently.
Increased procedures and technologies with reduced training hours
Let’s look at hysterectomies. From two techniques, vaginal and abdominal, they have expanded to LH, LAVH, robotic, single-site LH, single-site robotic, and recently single-port robotic. In addition, different and new technologies for hysteroscopy and myomectomy procedures have been developed.
All these operations are supposed to be part of any training program as ACGME demands “OG residents must be able to competently perform all medical, diagnostic, and surgical procedures considered essential for the area of practice.”3 In addition, primary care has been added to OG residency training: “Primary health care management from adolescence through reproductive age to midlife and beyond is integral to any ob.gyn.’s practice” and “Obstetrician-gynecologists are viewed by some entities as being primary care physicians for women, especially as coordinators of care among most reproductive-aged women,” according to ACOG.4
All this with reduced training hours.
The number of training hours a week has been reduced to 80, while it used to be over 100 hours. If you do the math, 20 fewer hours a week for 4 years amounts to 4,240 hours, equivalent to 180 days, equal to 6 months.
Graduating residents must pass a written and an oral exam for certification and with this are approved to enter the operating room and operate on women without a surgical skills test.
A simple test shows that elimination of the O for 1 year improves laparoscopic performance
We compared the time to perform three basic laparoscopic skills by fourth-year OG residents with that of fellows at the end of their first year in a minimally invasive G fellowship.5 The mean time for the residents completing the three tasks within the allotted time was 16 minutes, compared with 3.5 minutes for fellows: a four times faster performance.
Are there enough patients to maintain surgical skills after residency?
No, there are not.
Consider the following reality after residency. Decreasing number of surgeries and increasing numbers of OGs results in what you have already guessed: a lower surgical volume per OG.
Since 1979, the number of G surgeries has decreased by almost half (46%) while the number of OGs has doubled (54%) resulting in an 81% decrease of number of surgeries per OG, from 132 in 1979 to 25 in 2007.6 For hysterectomies, there has been a continuous yearly decline per G from 28 in 1980 to 9.8 in 2007 and to 8.5 in 2010.7,8
Would any mother feel comfortable having an obstetrician for her pregnancy and delivery performing only 8.5 deliveries a year?
Where do we go from here?
Separate the training and practice of O and G, an initiative already started in some residency programs and in some institutions in the United States. The O and the G both include a medical and a surgical practice.
We need to start accepting there is a need for different practices: medical O, medical G, surgical O, and surgical G. It is not new, it is already happening, it is the case in our institution since inception, and it is expanding across the country because it is needed. Graduating residents recognize this need as noticed by the increasing number seeking subspecialty training, from 7% in 2000 to 19.5% in 2012.4
Will this require some patients to drive away from home to obtain the best possible care? Yes. It is not a new concept, and it already is occurring for patients traveling to specialized centers away from home for certain conditions. In some countries, the practice is restricted to only a few centers. In Sweden, for instance, patients diagnosed with gynecologic cancer must travel to one of only seven centers subspecialized in gynecologic malignancies.
Conclusion
We need to start someday. We already are late after 130 years. We need to provide optimal care for women. They are our mothers. They deserve it. Let the O deliver O care, let the G provide G care, and we will reap improved results.
Dr. Magrina is with the department of medical and surgical gynecology at the Mayo Clinic in Phoenix. The author has no conflict of interest or financial involvement with this manuscript.
References
1. Am J Obstet Gynecol. 2019 Nov 22. doi: 10.1016/j.ajog.2019.11.1258.
2. Clin Obstet Gynecol. 2011 Sep;54(3):376-81.
3. Accreditation Council for Graduate Medical Education. Program requirements for GME in Obstetrics and Gynecology 2017.
4. “The obstetrician-gynecologist workforce in the United States: Facts, figures, and implications, 2017” (Washington, D.C.: ACOG, 2017).
5. J Minim Invasive Gynecol. 2008 Jul-Aug;15(4):410-3.
6. J Minim Invasive Gynecol. 2014 Jul-Aug;21(4):501-3.
7. National Health Statistics Report. Hysterectomy in the U.S. and oophorectomy 1979-2007. http://www.cdc.gov/nchs/products/nhsr.htm.
8. The Healthcare Cost and Utilization Project – Nationwide Inpatient Sample: Agency for Health Care Research Quality. 2013.
Two very different specialties, obstetrics (O) and gynecology (G), were fused into one in 1889. It is difficult to conceive that, with the expansion of both specialties in knowledge, procedures, and subspecialties, they still remain as one after 130 years. The American College of Obstetricians and Gynecologists was founded in 1952, and after 68 years no major changes have been made to accept or incorporate that there is a need to consider O and G as two different specialties.
Obstetrics and gynecology are the only specialties dedicated exclusively to women but with a very different purpose: the O is for reproduction, the G is for prevention and management of genital diseases. The specialties of O and G are so different the only thing in common is the patient.
It is time to separate the O from the G.
Are we training surgically competent residents?
No, we are not. There is an adequate volume for training and practice in O with close to 3.8 million births a year (the number cited by the Centers for Disease Control and Prevention in 2018). Not surprisingly, there is a need for trainees and also for practitioners in rural areas. As a result, the surgical training and practice in G is not optimal. If the number of hysterectomies was even near that of deliveries, there would be an adequate volume for everyone in training and in practice. But this is not the case.
The Accreditation Council for Graduate Medical Education (ACGME) mandates OG residents to graduate with a minimum of 70 minimally invasive hysterectomies (MIH), including laparoscopic (LH), vaginal (VH), and laparoscopic vaginally assisted (LAVH). In 2017, 51% of graduating residents fell below the minimum of 70 MIH.1 Because the learning curve of LH ranges from 30 to 80 cases,2 it is not surprising most residents feel surgically inadequate at graduation to function independently.
Increased procedures and technologies with reduced training hours
Let’s look at hysterectomies. From two techniques, vaginal and abdominal, they have expanded to LH, LAVH, robotic, single-site LH, single-site robotic, and recently single-port robotic. In addition, different and new technologies for hysteroscopy and myomectomy procedures have been developed.
All these operations are supposed to be part of any training program as ACGME demands “OG residents must be able to competently perform all medical, diagnostic, and surgical procedures considered essential for the area of practice.”3 In addition, primary care has been added to OG residency training: “Primary health care management from adolescence through reproductive age to midlife and beyond is integral to any ob.gyn.’s practice” and “Obstetrician-gynecologists are viewed by some entities as being primary care physicians for women, especially as coordinators of care among most reproductive-aged women,” according to ACOG.4
All this with reduced training hours.
The number of training hours a week has been reduced to 80, while it used to be over 100 hours. If you do the math, 20 fewer hours a week for 4 years amounts to 4,240 hours, equivalent to 180 days, equal to 6 months.
Graduating residents must pass a written and an oral exam for certification and with this are approved to enter the operating room and operate on women without a surgical skills test.
A simple test shows that elimination of the O for 1 year improves laparoscopic performance
We compared the time to perform three basic laparoscopic skills by fourth-year OG residents with that of fellows at the end of their first year in a minimally invasive G fellowship.5 The mean time for the residents completing the three tasks within the allotted time was 16 minutes, compared with 3.5 minutes for fellows: a four times faster performance.
Are there enough patients to maintain surgical skills after residency?
No, there are not.
Consider the following reality after residency. Decreasing number of surgeries and increasing numbers of OGs results in what you have already guessed: a lower surgical volume per OG.
Since 1979, the number of G surgeries has decreased by almost half (46%) while the number of OGs has doubled (54%) resulting in an 81% decrease of number of surgeries per OG, from 132 in 1979 to 25 in 2007.6 For hysterectomies, there has been a continuous yearly decline per G from 28 in 1980 to 9.8 in 2007 and to 8.5 in 2010.7,8
Would any mother feel comfortable having an obstetrician for her pregnancy and delivery performing only 8.5 deliveries a year?
Where do we go from here?
Separate the training and practice of O and G, an initiative already started in some residency programs and in some institutions in the United States. The O and the G both include a medical and a surgical practice.
We need to start accepting there is a need for different practices: medical O, medical G, surgical O, and surgical G. It is not new, it is already happening, it is the case in our institution since inception, and it is expanding across the country because it is needed. Graduating residents recognize this need as noticed by the increasing number seeking subspecialty training, from 7% in 2000 to 19.5% in 2012.4
Will this require some patients to drive away from home to obtain the best possible care? Yes. It is not a new concept, and it already is occurring for patients traveling to specialized centers away from home for certain conditions. In some countries, the practice is restricted to only a few centers. In Sweden, for instance, patients diagnosed with gynecologic cancer must travel to one of only seven centers subspecialized in gynecologic malignancies.
Conclusion
We need to start someday. We already are late after 130 years. We need to provide optimal care for women. They are our mothers. They deserve it. Let the O deliver O care, let the G provide G care, and we will reap improved results.
Dr. Magrina is with the department of medical and surgical gynecology at the Mayo Clinic in Phoenix. The author has no conflict of interest or financial involvement with this manuscript.
References
1. Am J Obstet Gynecol. 2019 Nov 22. doi: 10.1016/j.ajog.2019.11.1258.
2. Clin Obstet Gynecol. 2011 Sep;54(3):376-81.
3. Accreditation Council for Graduate Medical Education. Program requirements for GME in Obstetrics and Gynecology 2017.
4. “The obstetrician-gynecologist workforce in the United States: Facts, figures, and implications, 2017” (Washington, D.C.: ACOG, 2017).
5. J Minim Invasive Gynecol. 2008 Jul-Aug;15(4):410-3.
6. J Minim Invasive Gynecol. 2014 Jul-Aug;21(4):501-3.
7. National Health Statistics Report. Hysterectomy in the U.S. and oophorectomy 1979-2007. http://www.cdc.gov/nchs/products/nhsr.htm.
8. The Healthcare Cost and Utilization Project – Nationwide Inpatient Sample: Agency for Health Care Research Quality. 2013.
Understanding the cervicovaginal microbiome and how it affects preterm birth
Prematurity remains the leading cause of neonatal morbidity and mortality, accounting for $26 billion a year in immediate costs, despite the implementation in obstetrics of a host of risk stratification algorithms and strategies for risk reduction, including the use of some medications.
It now is questionable whether injectable 17-alpha hydroxyprogesterone caproate (Makena) truly is efficacious in women who’ve had a prior spontaneous preterm birth (sPTB) – a Food and Drug Administration advisory committee last year recommended withdrawing it from the market based on results of an FDA confirmatory study. Even if the drug were efficacious, only a small percentage of the women who have an sPTB have had a prior one. The majority of sPTB occurs among women without such a history.
Vaginal progesterone appears to confer some protection in women found to have a short cervix during the second trimester, but this approach also has limited reach: Only 9% of women with sPTB had an antecedent short cervix in a 2017 study.1 Like a history of sPTB, screening for short cervical length is a potentially helpful strategy for risk reduction, but it is not a strategy that will significantly impact the overall rate of prematurity.
We’ve fallen short in our goals to significantly reduce the public health impact of prematurity partly because we still do not understand the exact pathways and mechanisms by which sPTB occurs. The main working paradigm for myself and many other researchers over the past 2 decades has centered on infection in the uterus triggering inflammation, followed by cervical remodeling and ripening. Research in animal models, as well as human clinical trials targeting various infections and inflammation, have led to some insights and discoveries, but no successful interventions.
In the past decade, however, our research framework for understanding sPTB incorporates new questions about immunologic, microbiological, and molecular/cellular events that happen in the cervicovaginal space. We’ve learned more about the cervicovaginal microbiota, and most recently, our research at the University of Pennsylvania has elucidated the role that nonoptimal bacteria play in disrupting the cervical endothelial barrier and initiating the process of cervical remodeling that likely precedes sPTB.
We also know that this association is stronger in black women and may help explain some of the observed racial disparities in sPTB. Although more research is needed to determine specific therapeutic strategies, new doors are open.
Host immune-microbial interactions
This new research paradigm has involved stepping back and asking basic questions, such as, what do we really know about the cervicovaginal space? In actuality, we know very little. We know little about the immune function of the vaginal and cervical epithelial cells in pregnancy, for instance, and there is a large gap in knowledge regarding the biomechanics of the cervix – a remarkable organ that can change shape and function in a matter of minutes. Studies on the biomechanics of the cervix during pregnancy and in labor are still in their infancy.
However, lessons can be drawn from research on inflammatory bowel disease and other disorders involving the gut. In the gastrointestinal tract, epithelial cells have been found to act as sentinels, forming a mucosal barrier against bacterial pathogens and secreting various immune factors. Research in this field also has shown that microbes living in the gut produce metabolites; that these microbial metabolites may be the key messengers from the microbial communities to the epithelial barrier; and that the microbes, microbial metabolites, and immune responses are responsible for triggering inflammatory processes in the tissues underneath.
In 2011, Jacques Ravel, PhD, who was part of the National Institutes of Health’s Human Microbiome Project, characterized the vaginal microbiome of reproductive-age women for the first time.2 His paper classified the vaginal microbial communities of approximately 400 asymptomatic women of various ethnicities into five “community state types” (CSTs) based on the predominant bacteria found in the cervicovaginal space.3
On the heels of his research, Dr. Ravel and I launched an NIH-funded study involving a prospective cohort of 2,000 women with singleton pregnancies – the Motherhood & Microbiome cohort – to look at the cervicovaginal microbiota, the local immune response, and the risk of sPTB.4 Cervicovaginal samples were collected at 16-20 weeks’ gestation and during two subsequent clinical visits. From this cohort, which was composed mostly of African American women (74.5%), we conducted a nested case-controlled study of 103 cases of sPTB and 432 women who delivered at term, matched for race.
We carefully adjudicated the deliveries in our 2,000-person cohort so that we homed in on sPTB as opposed to preterm births that are medically indicated for reasons such as fetal distress or preeclampsia. (Several prior studies looking at the associations between the cervicovaginal microbiome had a heterogeneous phenotyping of PTB that made it hard to draw definitive conclusions.)
Our focus in assessing the microbiome and immunologic profiles was on the samples collected at the earliest time points in pregnancy because we hoped to detect a “signature” that could predict an outcome months later. Indeed, we found that the nonoptimal microbiota, known in microbiological terms as CST IV, was associated with about a 150% increased risk of sPTB. This community comprises a dominant array of anaerobic bacteria and a paucity of Lactobacillus species.
We also found that a larger proportion of African American women, compared with non–African American women, had this nonoptimal microbiota early in pregnancy (40% vs. 15%), which is consistent with previous studies in pregnancy and nonpregnancy showing lower levels of Lactobacillus species in the cervicovaginal microbiome of African American women.
Even more interesting was the finding that, although the rate of sPTB was higher in African American women and the effect of CST IV on sPTB was stronger in these women, the risk of sPTB couldn’t be explained solely by the presence of CST IV. Some women with this nonoptimal microbiome delivered at term, whereas others with more optimal microbiome types had sPTBs. This suggests that other factors contribute to African American women having a nonoptimal microbiota and being especially predisposed to sPTB.
Through the study’s immunologic profiling, we found a significant difference in the cervicovaginal levels of an immune factor, beta-defensin 2, between African American women who delivered at term and those who had a sPTB. Women who had a sPTB, even those who had higher levels of Lactobacillus species, had lower levels of beta-defensin 2. This association was not found in non–African American women.
Beta-defensin 2 is a host-derived antimicrobial peptide that, like other antimicrobial peptides, works at epithelial-mucosal barriers to combat bacteria; we have knowledge of its action from research on the gut, as well as some studies of the vaginal space in nonpregnant women that have focused on sexually transmitted infections.
Most exciting for us was the finding that higher levels of beta-defensin 2 appeared to lower the risk of sPTB in women who had a nonoptimal cervicovaginal microbiota. There’s an interplay between the host and the microbiota, in other words, and it’s one that could be essential to manipulate as we seek to reduce sPTB.
The cervical epithelial barrier
In the laboratory, meanwhile, we are learning how certain microbes are mechanistically involved in the pathogenesis of sPTB. Research over the last decade has suggested that disruption or breakdown of the cervical epithelial barrier drives cervical remodeling processes that precede sPTB. The question now is, do cervicovaginal bacteria associated with sPTB, or a nonoptimal cervicovaginal microbiota, cause disruption of the vaginal and cervical epithelial barrier – and how?
Using an in vitro model system, we found that Mobiluncus curtisii/mulieris, the bacterial taxa with the strongest association with sPTB in our Motherhood & Microbiome cohort and one that has long been associated with bacterial vaginosis, had a plethora of effects. It increased cell permeability and the expression of inflammatory mediators associated with cervical epithelial breakdown, and it altered expression of microRNAs that have been associated with sPTB in human studies.
Our study on Mobiluncus has served as proof of concept to us that, not only is the bacteria associated with sPTB, but that there are multiple mechanisms by which it can disrupt the cervicovaginal barrier and lead to cervical remodeling.5
The findings echo previous in vitro research on Gardnerella vaginalis, another anaerobic bacterium that has been associated with bacterial vaginosis and adverse obstetric outcomes, including sPTB.6 Using similar models, we found that G. vaginalis disrupts the cervical epithelial barrier through diverse mechanisms including the cleavage of certain proteins, the up-regulation of proinflammatory immune mediators, and altered gene expression.
Lactobacillus crispatus, on the other hand, conferred protection to the cervical epithelial barrier in this study by mitigating various G. vaginalis–induced effects.
Learning more about host-microbe interactions and the role of microbial metabolites in these interactions, as well as the role of altered gene expression in cervical function, will help us to more fully understand the biological mechanisms regulating cervicovaginal epithelial cells. At this point, we know that, as in the gut, bacteria commonly found in the cervicovaginal space play a significant role in regulating the function of epithelial cells (in both optimal and nonoptimal microbiota), and that various bacteria associated with sPTB contribute to poor outcomes by breaking down the cervical epithelium.
Therapeutic implications
Our growing knowledge of the cervicovaginal microbiota does not yet support screening or any particular interventions. We don’t know, for instance, that administering probiotics or prebiotics orally or vaginally will have any effect on rates of sPTB.
Ongoing research at all levels holds promise, however, for the development of diagnostics to identify women at risk for sPTB, and for the development of therapeutic strategies that aim to modify the microbiome and/or modify the immune response. We know from other areas of medicine that there are realistic ways to modulate the immune response and/or microbiota in a system to alter risk.
We need to more thoroughly understand the risk of particular microbiota and immune response factors – and how they vary by race and ethnicity – and we need to study the cervicovaginal microbiota of women before and during pregnancy to learn whether there is something about pregnancy or even about intercourse that can change one’s microbiome to a less favorable state.
It may well be possible in the near future to identify high-risk states of nonoptimal microbiota before conception – microbiota that, in and of themselves, may not be pathogenic but that become detrimental during pregnancy – and it should be possible to screen women early in pregnancy for microbial or immune signatures or both.
The question often arises in medicine of the validity of screening without having achieved certainty about treatments. However, in obstetrics, where we have different levels of care and the ability to personalize monitoring and care, identifying those at greatest risk still has value. Ultimately, with enough investment in all levels of research (basic, translational, and clinical), we can develop interventions and therapeutics that address a biologically plausible mechanism of sPTB and, as a result, achieve significant reductions in the rate of prematurity.
Dr. Elovitz is the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia. She disclosed holding a patent on a method to determine risk of preterm birth that relates to the microbiome. Email her at [email protected].
References
1. JAMA. 2017 Mar 14;317(10):1047-56.
2. NIH Human Microbiome Project. https://hmpdacc.org/.
3. PNAS. 2011 Mar 15;108 (Supplement 1):4680-7.
4. Nat Commun. 2019 Mar 21. doi: 10.1038/s41467-019-09285-9.
5. Anaerobe. 2019 Nov 21. doi: 10.1016/j.anaerobe.2019.102127.
6. Front Microbiol. 2018 Oct 8. doi: 10.3389/fmicb.2018.02181.
Prematurity remains the leading cause of neonatal morbidity and mortality, accounting for $26 billion a year in immediate costs, despite the implementation in obstetrics of a host of risk stratification algorithms and strategies for risk reduction, including the use of some medications.
It now is questionable whether injectable 17-alpha hydroxyprogesterone caproate (Makena) truly is efficacious in women who’ve had a prior spontaneous preterm birth (sPTB) – a Food and Drug Administration advisory committee last year recommended withdrawing it from the market based on results of an FDA confirmatory study. Even if the drug were efficacious, only a small percentage of the women who have an sPTB have had a prior one. The majority of sPTB occurs among women without such a history.
Vaginal progesterone appears to confer some protection in women found to have a short cervix during the second trimester, but this approach also has limited reach: Only 9% of women with sPTB had an antecedent short cervix in a 2017 study.1 Like a history of sPTB, screening for short cervical length is a potentially helpful strategy for risk reduction, but it is not a strategy that will significantly impact the overall rate of prematurity.
We’ve fallen short in our goals to significantly reduce the public health impact of prematurity partly because we still do not understand the exact pathways and mechanisms by which sPTB occurs. The main working paradigm for myself and many other researchers over the past 2 decades has centered on infection in the uterus triggering inflammation, followed by cervical remodeling and ripening. Research in animal models, as well as human clinical trials targeting various infections and inflammation, have led to some insights and discoveries, but no successful interventions.
In the past decade, however, our research framework for understanding sPTB incorporates new questions about immunologic, microbiological, and molecular/cellular events that happen in the cervicovaginal space. We’ve learned more about the cervicovaginal microbiota, and most recently, our research at the University of Pennsylvania has elucidated the role that nonoptimal bacteria play in disrupting the cervical endothelial barrier and initiating the process of cervical remodeling that likely precedes sPTB.
We also know that this association is stronger in black women and may help explain some of the observed racial disparities in sPTB. Although more research is needed to determine specific therapeutic strategies, new doors are open.
Host immune-microbial interactions
This new research paradigm has involved stepping back and asking basic questions, such as, what do we really know about the cervicovaginal space? In actuality, we know very little. We know little about the immune function of the vaginal and cervical epithelial cells in pregnancy, for instance, and there is a large gap in knowledge regarding the biomechanics of the cervix – a remarkable organ that can change shape and function in a matter of minutes. Studies on the biomechanics of the cervix during pregnancy and in labor are still in their infancy.
However, lessons can be drawn from research on inflammatory bowel disease and other disorders involving the gut. In the gastrointestinal tract, epithelial cells have been found to act as sentinels, forming a mucosal barrier against bacterial pathogens and secreting various immune factors. Research in this field also has shown that microbes living in the gut produce metabolites; that these microbial metabolites may be the key messengers from the microbial communities to the epithelial barrier; and that the microbes, microbial metabolites, and immune responses are responsible for triggering inflammatory processes in the tissues underneath.
In 2011, Jacques Ravel, PhD, who was part of the National Institutes of Health’s Human Microbiome Project, characterized the vaginal microbiome of reproductive-age women for the first time.2 His paper classified the vaginal microbial communities of approximately 400 asymptomatic women of various ethnicities into five “community state types” (CSTs) based on the predominant bacteria found in the cervicovaginal space.3
On the heels of his research, Dr. Ravel and I launched an NIH-funded study involving a prospective cohort of 2,000 women with singleton pregnancies – the Motherhood & Microbiome cohort – to look at the cervicovaginal microbiota, the local immune response, and the risk of sPTB.4 Cervicovaginal samples were collected at 16-20 weeks’ gestation and during two subsequent clinical visits. From this cohort, which was composed mostly of African American women (74.5%), we conducted a nested case-controlled study of 103 cases of sPTB and 432 women who delivered at term, matched for race.
We carefully adjudicated the deliveries in our 2,000-person cohort so that we homed in on sPTB as opposed to preterm births that are medically indicated for reasons such as fetal distress or preeclampsia. (Several prior studies looking at the associations between the cervicovaginal microbiome had a heterogeneous phenotyping of PTB that made it hard to draw definitive conclusions.)
Our focus in assessing the microbiome and immunologic profiles was on the samples collected at the earliest time points in pregnancy because we hoped to detect a “signature” that could predict an outcome months later. Indeed, we found that the nonoptimal microbiota, known in microbiological terms as CST IV, was associated with about a 150% increased risk of sPTB. This community comprises a dominant array of anaerobic bacteria and a paucity of Lactobacillus species.
We also found that a larger proportion of African American women, compared with non–African American women, had this nonoptimal microbiota early in pregnancy (40% vs. 15%), which is consistent with previous studies in pregnancy and nonpregnancy showing lower levels of Lactobacillus species in the cervicovaginal microbiome of African American women.
Even more interesting was the finding that, although the rate of sPTB was higher in African American women and the effect of CST IV on sPTB was stronger in these women, the risk of sPTB couldn’t be explained solely by the presence of CST IV. Some women with this nonoptimal microbiome delivered at term, whereas others with more optimal microbiome types had sPTBs. This suggests that other factors contribute to African American women having a nonoptimal microbiota and being especially predisposed to sPTB.
Through the study’s immunologic profiling, we found a significant difference in the cervicovaginal levels of an immune factor, beta-defensin 2, between African American women who delivered at term and those who had a sPTB. Women who had a sPTB, even those who had higher levels of Lactobacillus species, had lower levels of beta-defensin 2. This association was not found in non–African American women.
Beta-defensin 2 is a host-derived antimicrobial peptide that, like other antimicrobial peptides, works at epithelial-mucosal barriers to combat bacteria; we have knowledge of its action from research on the gut, as well as some studies of the vaginal space in nonpregnant women that have focused on sexually transmitted infections.
Most exciting for us was the finding that higher levels of beta-defensin 2 appeared to lower the risk of sPTB in women who had a nonoptimal cervicovaginal microbiota. There’s an interplay between the host and the microbiota, in other words, and it’s one that could be essential to manipulate as we seek to reduce sPTB.
The cervical epithelial barrier
In the laboratory, meanwhile, we are learning how certain microbes are mechanistically involved in the pathogenesis of sPTB. Research over the last decade has suggested that disruption or breakdown of the cervical epithelial barrier drives cervical remodeling processes that precede sPTB. The question now is, do cervicovaginal bacteria associated with sPTB, or a nonoptimal cervicovaginal microbiota, cause disruption of the vaginal and cervical epithelial barrier – and how?
Using an in vitro model system, we found that Mobiluncus curtisii/mulieris, the bacterial taxa with the strongest association with sPTB in our Motherhood & Microbiome cohort and one that has long been associated with bacterial vaginosis, had a plethora of effects. It increased cell permeability and the expression of inflammatory mediators associated with cervical epithelial breakdown, and it altered expression of microRNAs that have been associated with sPTB in human studies.
Our study on Mobiluncus has served as proof of concept to us that, not only is the bacteria associated with sPTB, but that there are multiple mechanisms by which it can disrupt the cervicovaginal barrier and lead to cervical remodeling.5
The findings echo previous in vitro research on Gardnerella vaginalis, another anaerobic bacterium that has been associated with bacterial vaginosis and adverse obstetric outcomes, including sPTB.6 Using similar models, we found that G. vaginalis disrupts the cervical epithelial barrier through diverse mechanisms including the cleavage of certain proteins, the up-regulation of proinflammatory immune mediators, and altered gene expression.
Lactobacillus crispatus, on the other hand, conferred protection to the cervical epithelial barrier in this study by mitigating various G. vaginalis–induced effects.
Learning more about host-microbe interactions and the role of microbial metabolites in these interactions, as well as the role of altered gene expression in cervical function, will help us to more fully understand the biological mechanisms regulating cervicovaginal epithelial cells. At this point, we know that, as in the gut, bacteria commonly found in the cervicovaginal space play a significant role in regulating the function of epithelial cells (in both optimal and nonoptimal microbiota), and that various bacteria associated with sPTB contribute to poor outcomes by breaking down the cervical epithelium.
Therapeutic implications
Our growing knowledge of the cervicovaginal microbiota does not yet support screening or any particular interventions. We don’t know, for instance, that administering probiotics or prebiotics orally or vaginally will have any effect on rates of sPTB.
Ongoing research at all levels holds promise, however, for the development of diagnostics to identify women at risk for sPTB, and for the development of therapeutic strategies that aim to modify the microbiome and/or modify the immune response. We know from other areas of medicine that there are realistic ways to modulate the immune response and/or microbiota in a system to alter risk.
We need to more thoroughly understand the risk of particular microbiota and immune response factors – and how they vary by race and ethnicity – and we need to study the cervicovaginal microbiota of women before and during pregnancy to learn whether there is something about pregnancy or even about intercourse that can change one’s microbiome to a less favorable state.
It may well be possible in the near future to identify high-risk states of nonoptimal microbiota before conception – microbiota that, in and of themselves, may not be pathogenic but that become detrimental during pregnancy – and it should be possible to screen women early in pregnancy for microbial or immune signatures or both.
The question often arises in medicine of the validity of screening without having achieved certainty about treatments. However, in obstetrics, where we have different levels of care and the ability to personalize monitoring and care, identifying those at greatest risk still has value. Ultimately, with enough investment in all levels of research (basic, translational, and clinical), we can develop interventions and therapeutics that address a biologically plausible mechanism of sPTB and, as a result, achieve significant reductions in the rate of prematurity.
Dr. Elovitz is the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia. She disclosed holding a patent on a method to determine risk of preterm birth that relates to the microbiome. Email her at [email protected].
References
1. JAMA. 2017 Mar 14;317(10):1047-56.
2. NIH Human Microbiome Project. https://hmpdacc.org/.
3. PNAS. 2011 Mar 15;108 (Supplement 1):4680-7.
4. Nat Commun. 2019 Mar 21. doi: 10.1038/s41467-019-09285-9.
5. Anaerobe. 2019 Nov 21. doi: 10.1016/j.anaerobe.2019.102127.
6. Front Microbiol. 2018 Oct 8. doi: 10.3389/fmicb.2018.02181.
Prematurity remains the leading cause of neonatal morbidity and mortality, accounting for $26 billion a year in immediate costs, despite the implementation in obstetrics of a host of risk stratification algorithms and strategies for risk reduction, including the use of some medications.
It now is questionable whether injectable 17-alpha hydroxyprogesterone caproate (Makena) truly is efficacious in women who’ve had a prior spontaneous preterm birth (sPTB) – a Food and Drug Administration advisory committee last year recommended withdrawing it from the market based on results of an FDA confirmatory study. Even if the drug were efficacious, only a small percentage of the women who have an sPTB have had a prior one. The majority of sPTB occurs among women without such a history.
Vaginal progesterone appears to confer some protection in women found to have a short cervix during the second trimester, but this approach also has limited reach: Only 9% of women with sPTB had an antecedent short cervix in a 2017 study.1 Like a history of sPTB, screening for short cervical length is a potentially helpful strategy for risk reduction, but it is not a strategy that will significantly impact the overall rate of prematurity.
We’ve fallen short in our goals to significantly reduce the public health impact of prematurity partly because we still do not understand the exact pathways and mechanisms by which sPTB occurs. The main working paradigm for myself and many other researchers over the past 2 decades has centered on infection in the uterus triggering inflammation, followed by cervical remodeling and ripening. Research in animal models, as well as human clinical trials targeting various infections and inflammation, have led to some insights and discoveries, but no successful interventions.
In the past decade, however, our research framework for understanding sPTB incorporates new questions about immunologic, microbiological, and molecular/cellular events that happen in the cervicovaginal space. We’ve learned more about the cervicovaginal microbiota, and most recently, our research at the University of Pennsylvania has elucidated the role that nonoptimal bacteria play in disrupting the cervical endothelial barrier and initiating the process of cervical remodeling that likely precedes sPTB.
We also know that this association is stronger in black women and may help explain some of the observed racial disparities in sPTB. Although more research is needed to determine specific therapeutic strategies, new doors are open.
Host immune-microbial interactions
This new research paradigm has involved stepping back and asking basic questions, such as, what do we really know about the cervicovaginal space? In actuality, we know very little. We know little about the immune function of the vaginal and cervical epithelial cells in pregnancy, for instance, and there is a large gap in knowledge regarding the biomechanics of the cervix – a remarkable organ that can change shape and function in a matter of minutes. Studies on the biomechanics of the cervix during pregnancy and in labor are still in their infancy.
However, lessons can be drawn from research on inflammatory bowel disease and other disorders involving the gut. In the gastrointestinal tract, epithelial cells have been found to act as sentinels, forming a mucosal barrier against bacterial pathogens and secreting various immune factors. Research in this field also has shown that microbes living in the gut produce metabolites; that these microbial metabolites may be the key messengers from the microbial communities to the epithelial barrier; and that the microbes, microbial metabolites, and immune responses are responsible for triggering inflammatory processes in the tissues underneath.
In 2011, Jacques Ravel, PhD, who was part of the National Institutes of Health’s Human Microbiome Project, characterized the vaginal microbiome of reproductive-age women for the first time.2 His paper classified the vaginal microbial communities of approximately 400 asymptomatic women of various ethnicities into five “community state types” (CSTs) based on the predominant bacteria found in the cervicovaginal space.3
On the heels of his research, Dr. Ravel and I launched an NIH-funded study involving a prospective cohort of 2,000 women with singleton pregnancies – the Motherhood & Microbiome cohort – to look at the cervicovaginal microbiota, the local immune response, and the risk of sPTB.4 Cervicovaginal samples were collected at 16-20 weeks’ gestation and during two subsequent clinical visits. From this cohort, which was composed mostly of African American women (74.5%), we conducted a nested case-controlled study of 103 cases of sPTB and 432 women who delivered at term, matched for race.
We carefully adjudicated the deliveries in our 2,000-person cohort so that we homed in on sPTB as opposed to preterm births that are medically indicated for reasons such as fetal distress or preeclampsia. (Several prior studies looking at the associations between the cervicovaginal microbiome had a heterogeneous phenotyping of PTB that made it hard to draw definitive conclusions.)
Our focus in assessing the microbiome and immunologic profiles was on the samples collected at the earliest time points in pregnancy because we hoped to detect a “signature” that could predict an outcome months later. Indeed, we found that the nonoptimal microbiota, known in microbiological terms as CST IV, was associated with about a 150% increased risk of sPTB. This community comprises a dominant array of anaerobic bacteria and a paucity of Lactobacillus species.
We also found that a larger proportion of African American women, compared with non–African American women, had this nonoptimal microbiota early in pregnancy (40% vs. 15%), which is consistent with previous studies in pregnancy and nonpregnancy showing lower levels of Lactobacillus species in the cervicovaginal microbiome of African American women.
Even more interesting was the finding that, although the rate of sPTB was higher in African American women and the effect of CST IV on sPTB was stronger in these women, the risk of sPTB couldn’t be explained solely by the presence of CST IV. Some women with this nonoptimal microbiome delivered at term, whereas others with more optimal microbiome types had sPTBs. This suggests that other factors contribute to African American women having a nonoptimal microbiota and being especially predisposed to sPTB.
Through the study’s immunologic profiling, we found a significant difference in the cervicovaginal levels of an immune factor, beta-defensin 2, between African American women who delivered at term and those who had a sPTB. Women who had a sPTB, even those who had higher levels of Lactobacillus species, had lower levels of beta-defensin 2. This association was not found in non–African American women.
Beta-defensin 2 is a host-derived antimicrobial peptide that, like other antimicrobial peptides, works at epithelial-mucosal barriers to combat bacteria; we have knowledge of its action from research on the gut, as well as some studies of the vaginal space in nonpregnant women that have focused on sexually transmitted infections.
Most exciting for us was the finding that higher levels of beta-defensin 2 appeared to lower the risk of sPTB in women who had a nonoptimal cervicovaginal microbiota. There’s an interplay between the host and the microbiota, in other words, and it’s one that could be essential to manipulate as we seek to reduce sPTB.
The cervical epithelial barrier
In the laboratory, meanwhile, we are learning how certain microbes are mechanistically involved in the pathogenesis of sPTB. Research over the last decade has suggested that disruption or breakdown of the cervical epithelial barrier drives cervical remodeling processes that precede sPTB. The question now is, do cervicovaginal bacteria associated with sPTB, or a nonoptimal cervicovaginal microbiota, cause disruption of the vaginal and cervical epithelial barrier – and how?
Using an in vitro model system, we found that Mobiluncus curtisii/mulieris, the bacterial taxa with the strongest association with sPTB in our Motherhood & Microbiome cohort and one that has long been associated with bacterial vaginosis, had a plethora of effects. It increased cell permeability and the expression of inflammatory mediators associated with cervical epithelial breakdown, and it altered expression of microRNAs that have been associated with sPTB in human studies.
Our study on Mobiluncus has served as proof of concept to us that, not only is the bacteria associated with sPTB, but that there are multiple mechanisms by which it can disrupt the cervicovaginal barrier and lead to cervical remodeling.5
The findings echo previous in vitro research on Gardnerella vaginalis, another anaerobic bacterium that has been associated with bacterial vaginosis and adverse obstetric outcomes, including sPTB.6 Using similar models, we found that G. vaginalis disrupts the cervical epithelial barrier through diverse mechanisms including the cleavage of certain proteins, the up-regulation of proinflammatory immune mediators, and altered gene expression.
Lactobacillus crispatus, on the other hand, conferred protection to the cervical epithelial barrier in this study by mitigating various G. vaginalis–induced effects.
Learning more about host-microbe interactions and the role of microbial metabolites in these interactions, as well as the role of altered gene expression in cervical function, will help us to more fully understand the biological mechanisms regulating cervicovaginal epithelial cells. At this point, we know that, as in the gut, bacteria commonly found in the cervicovaginal space play a significant role in regulating the function of epithelial cells (in both optimal and nonoptimal microbiota), and that various bacteria associated with sPTB contribute to poor outcomes by breaking down the cervical epithelium.
Therapeutic implications
Our growing knowledge of the cervicovaginal microbiota does not yet support screening or any particular interventions. We don’t know, for instance, that administering probiotics or prebiotics orally or vaginally will have any effect on rates of sPTB.
Ongoing research at all levels holds promise, however, for the development of diagnostics to identify women at risk for sPTB, and for the development of therapeutic strategies that aim to modify the microbiome and/or modify the immune response. We know from other areas of medicine that there are realistic ways to modulate the immune response and/or microbiota in a system to alter risk.
We need to more thoroughly understand the risk of particular microbiota and immune response factors – and how they vary by race and ethnicity – and we need to study the cervicovaginal microbiota of women before and during pregnancy to learn whether there is something about pregnancy or even about intercourse that can change one’s microbiome to a less favorable state.
It may well be possible in the near future to identify high-risk states of nonoptimal microbiota before conception – microbiota that, in and of themselves, may not be pathogenic but that become detrimental during pregnancy – and it should be possible to screen women early in pregnancy for microbial or immune signatures or both.
The question often arises in medicine of the validity of screening without having achieved certainty about treatments. However, in obstetrics, where we have different levels of care and the ability to personalize monitoring and care, identifying those at greatest risk still has value. Ultimately, with enough investment in all levels of research (basic, translational, and clinical), we can develop interventions and therapeutics that address a biologically plausible mechanism of sPTB and, as a result, achieve significant reductions in the rate of prematurity.
Dr. Elovitz is the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia. She disclosed holding a patent on a method to determine risk of preterm birth that relates to the microbiome. Email her at [email protected].
References
1. JAMA. 2017 Mar 14;317(10):1047-56.
2. NIH Human Microbiome Project. https://hmpdacc.org/.
3. PNAS. 2011 Mar 15;108 (Supplement 1):4680-7.
4. Nat Commun. 2019 Mar 21. doi: 10.1038/s41467-019-09285-9.
5. Anaerobe. 2019 Nov 21. doi: 10.1016/j.anaerobe.2019.102127.
6. Front Microbiol. 2018 Oct 8. doi: 10.3389/fmicb.2018.02181.
Preterm birth: Under the microscope
Preventing infant mortality remains a significant challenge for ob.gyns. Despite the availability of a multitude of preventive and treatment options and some of the best possible medical care offered in the world, the United States lags behind many other developed and developing countries in its rate of infant deaths, which was an estimated 5.8 deaths per 1,000 live births in 2017. We can, and must, do better.
One of the major contributing factors to infant mortality is preterm birth. Defined as birth occurring prior to 37 weeks’ gestation, preterm birth is associated with a myriad of severe neonatal sequelae: low birth weight, bacterial sepsis, neonatal hemorrhage, and respiratory distress syndrome, among others. Therefore, many within the clinical and biomedical research spheres recognize that preventing preterm birth means reducing infant deaths.
However, therein lies the conundrum. We know very little about what causes preterm birth, which renders the current therapeutic strategies – such as use of progesterone supplements or cerclage placement – good for some but not all patients. It is thus vital to continue research to unravel the underlying mechanisms of preterm birth.
A promising area of investigation is the field of microbiome research, which has made great strides in advancing our awareness of the critical role of the millions of organisms living on and within us in maintaining health and fighting disease. For example, we now realize that eradicating all the commensals in our gastrointestinal tract has unintended and very negative consequences and, for patients whose good bacteria have been eliminated, fecal transplant is a therapeutic option. Therefore, it stands to reason that the microbes found in the vagina contribute significantly to women’s overall reproductive health.
The publication of the groundbreaking study characterizing the vaginal microbiome species in reproductive-age women opened new avenues of research into how these organisms contribute to women’s health. Importantly, this work, led initially by Jacques Ravel, PhD, a professor in the department of microbiology & immunology and associate director of the Institute for Genome Sciences at the University of Maryland School of Medicine, has spawned additional investigations into the potential role of the vaginal microbiome in preterm birth.
To provide some insight into the research around how the microorganisms in the vagina may induce or prevent preterm birth is our guest author, Michal A. Elovitz, MD, the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia.
Dr. Reece, who specializes in maternal-fetal medicine, is executive vice president for medical affairs at the University of Maryland School of Medicine as well as the John Z. and Akiko K. Bowers Distinguished Professor and dean of the school of medicine. He is the medical editor of this column. He said he had no relevant financial disclosures. Contact him at [email protected].
Preventing infant mortality remains a significant challenge for ob.gyns. Despite the availability of a multitude of preventive and treatment options and some of the best possible medical care offered in the world, the United States lags behind many other developed and developing countries in its rate of infant deaths, which was an estimated 5.8 deaths per 1,000 live births in 2017. We can, and must, do better.
One of the major contributing factors to infant mortality is preterm birth. Defined as birth occurring prior to 37 weeks’ gestation, preterm birth is associated with a myriad of severe neonatal sequelae: low birth weight, bacterial sepsis, neonatal hemorrhage, and respiratory distress syndrome, among others. Therefore, many within the clinical and biomedical research spheres recognize that preventing preterm birth means reducing infant deaths.
However, therein lies the conundrum. We know very little about what causes preterm birth, which renders the current therapeutic strategies – such as use of progesterone supplements or cerclage placement – good for some but not all patients. It is thus vital to continue research to unravel the underlying mechanisms of preterm birth.
A promising area of investigation is the field of microbiome research, which has made great strides in advancing our awareness of the critical role of the millions of organisms living on and within us in maintaining health and fighting disease. For example, we now realize that eradicating all the commensals in our gastrointestinal tract has unintended and very negative consequences and, for patients whose good bacteria have been eliminated, fecal transplant is a therapeutic option. Therefore, it stands to reason that the microbes found in the vagina contribute significantly to women’s overall reproductive health.
The publication of the groundbreaking study characterizing the vaginal microbiome species in reproductive-age women opened new avenues of research into how these organisms contribute to women’s health. Importantly, this work, led initially by Jacques Ravel, PhD, a professor in the department of microbiology & immunology and associate director of the Institute for Genome Sciences at the University of Maryland School of Medicine, has spawned additional investigations into the potential role of the vaginal microbiome in preterm birth.
To provide some insight into the research around how the microorganisms in the vagina may induce or prevent preterm birth is our guest author, Michal A. Elovitz, MD, the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia.
Dr. Reece, who specializes in maternal-fetal medicine, is executive vice president for medical affairs at the University of Maryland School of Medicine as well as the John Z. and Akiko K. Bowers Distinguished Professor and dean of the school of medicine. He is the medical editor of this column. He said he had no relevant financial disclosures. Contact him at [email protected].
Preventing infant mortality remains a significant challenge for ob.gyns. Despite the availability of a multitude of preventive and treatment options and some of the best possible medical care offered in the world, the United States lags behind many other developed and developing countries in its rate of infant deaths, which was an estimated 5.8 deaths per 1,000 live births in 2017. We can, and must, do better.
One of the major contributing factors to infant mortality is preterm birth. Defined as birth occurring prior to 37 weeks’ gestation, preterm birth is associated with a myriad of severe neonatal sequelae: low birth weight, bacterial sepsis, neonatal hemorrhage, and respiratory distress syndrome, among others. Therefore, many within the clinical and biomedical research spheres recognize that preventing preterm birth means reducing infant deaths.
However, therein lies the conundrum. We know very little about what causes preterm birth, which renders the current therapeutic strategies – such as use of progesterone supplements or cerclage placement – good for some but not all patients. It is thus vital to continue research to unravel the underlying mechanisms of preterm birth.
A promising area of investigation is the field of microbiome research, which has made great strides in advancing our awareness of the critical role of the millions of organisms living on and within us in maintaining health and fighting disease. For example, we now realize that eradicating all the commensals in our gastrointestinal tract has unintended and very negative consequences and, for patients whose good bacteria have been eliminated, fecal transplant is a therapeutic option. Therefore, it stands to reason that the microbes found in the vagina contribute significantly to women’s overall reproductive health.
The publication of the groundbreaking study characterizing the vaginal microbiome species in reproductive-age women opened new avenues of research into how these organisms contribute to women’s health. Importantly, this work, led initially by Jacques Ravel, PhD, a professor in the department of microbiology & immunology and associate director of the Institute for Genome Sciences at the University of Maryland School of Medicine, has spawned additional investigations into the potential role of the vaginal microbiome in preterm birth.
To provide some insight into the research around how the microorganisms in the vagina may induce or prevent preterm birth is our guest author, Michal A. Elovitz, MD, the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health, vice chair of translational research, and director of the Maternal and Child Health Research Center, department of obstetrics and gynecology, at the University of Pennsylvania, Philadelphia.
Dr. Reece, who specializes in maternal-fetal medicine, is executive vice president for medical affairs at the University of Maryland School of Medicine as well as the John Z. and Akiko K. Bowers Distinguished Professor and dean of the school of medicine. He is the medical editor of this column. He said he had no relevant financial disclosures. Contact him at [email protected].
Are patient portals living up to the hype? Ask your mother-in-law!
While preparing to write this technology column, I received a great deal of insight from the unlikeliest of sources: my mother-in-law.
Now don’t get me wrong – she’s a truly lovely, intelligent, and capable woman. I have sought her advice often on many things and have always been impressed by her wisdom and pragmatism, but I’ve just never thought of asking her for her opinion on medicine or technology, as I considered her knowledge of both subjects to be limited.
This occasion changed my opinion. In fact, I believe that, as health care IT becomes more complex, people like my mother-in-law may be exactly who we should be looking to for answers.
A few weeks ago, my mother-in-law and I were discussing her recent trip to the doctor. When she mentioned some lab tests, I suggested that we log in to her patient portal to view the results. This elicited several questions and a declaration of frustration.
“Which portal?” she asked. “I have so many and can’t keep all of the websites and passwords straight! Why can’t all of my doctors use the same portal, and why do they all have different password requirements?”
As she spoke these words, I was immediately struck with an unfortunate reality of EHRs: We have done a brilliant job creating state-of-the-art digital castles and have filled them with the data needed to revolutionize care and improve population health – but we haven’t given our patients the keys to get inside.
We must ask ourselves if, in trying to construct fortresses of information around our patients, we have lost sight of the individuals in the center. I believe that we can answer this question and improve the benefits of patient portals, but we all must agree to a few simple steps to streamline the experience for everyone.
Make it easy
A study recently published in the Journal of General Internal Medicine surveyed several hospitals on their usage of patient portals. After determining whether or not the institutions had such portals, the authors then investigated to find out what, if any, guidance was provided to patients about how to use them.
Their findings are frustrating, though not surprising. While 89% of hospitals had some form of patient portal, only 65% of those “had links that were easily found, defined as links accessible within two clicks from the home page.”
Furthermore, even in cases where portals were easily found, good instructions on how to use them were missing. Those instructions that did exist centered on rules and restrictions and laying out “terms and conditions” and informing patients on “what not to do,” rather than explaining how to make the most of the experience.
According to the authors, “this focus on curtailing behavior, and the hurdles placed on finding and understanding guidance, suggest that some hospitals may be prioritizing reducing liability over improving the patient experience with portals.”
If we want our patients to use them, portals must be easy to access and intuitive to use. They also must provide value.
Make it meaningful
Patient portals have proliferated exponentially over the last 10 years, thanks to government incentive programs. One such program, known as “meaningful use,” is primarily responsible for this, as it made implementation of a patient portal one of its core requirements.
Sadly, in spite of its oft-reviled name, the meaningful use program never defined patient-friendly standards of usability for patient portals. As a result, current portals just aren’t very good. Patients like my mother-in-law find them to be too numerous, too unfriendly to use, and too limited, so they are not being used to their full potential.
In fact, many institutions may choose not to enable all of the available features in order to limit technical issues and reduce the burden on providers. In the study referenced above, only 63% of portals offered the ability for patients to communicate directly with their physicians, and only 43% offered the ability to refill prescriptions.
When enabled, these functions improve patient engagement and efficiency. Without them, patients are less likely to log on, and physicians are forced to rely on less-efficient telephone calls or traditional letters to communicate results to their patients.
Put the patient, not the portal, at the center
History has all but forgotten the attempts by tech giants such as Google and Microsoft to create personal health records. While these initially seemed like a wonderful concept, they sadly proved to be a total flop. Some patients embraced the idea, but security concerns and the lack of buy-in from EHR vendors significantly limited their uptake.
They may simply have been ahead of their time.
A decade later, wearable technology and telemedicine are ushering in a new era of patient-centric care. Individuals have been embracing a greater share of the responsibility for their own personal health information, yet most EHRs lack the ability to easily incorporate data acquired outside physicians’ offices.
It’s time for EHR vendors to go all in and change that. Instead of enslaving patients to the tyranny of fragmented health records, they should prioritize the creation of a robust, standardized, and portable health record that travels with the patient, not the other way around.
Have any other ideas on how to improve patient engagement? We’d love to hear about them and share them in a future column.
If you want to contribute but don’t have any ideas, we have a suggestion: Ask your mother-in-law. You may be surprised at what you learn!
Dr. Notte is a family physician and associate chief medical information officer for Abington (Pa.) Hospital–Jefferson Health. Follow him on twitter (@doctornotte). Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Philadelphia, and associate director of the family medicine residency program at Abington Hospital–Jefferson Health.
Reference
Lee JL et al. J Gen Intern Med. 2019 Nov 12. doi: 10.1007/s11606-019-05528-z.
While preparing to write this technology column, I received a great deal of insight from the unlikeliest of sources: my mother-in-law.
Now don’t get me wrong – she’s a truly lovely, intelligent, and capable woman. I have sought her advice often on many things and have always been impressed by her wisdom and pragmatism, but I’ve just never thought of asking her for her opinion on medicine or technology, as I considered her knowledge of both subjects to be limited.
This occasion changed my opinion. In fact, I believe that, as health care IT becomes more complex, people like my mother-in-law may be exactly who we should be looking to for answers.
A few weeks ago, my mother-in-law and I were discussing her recent trip to the doctor. When she mentioned some lab tests, I suggested that we log in to her patient portal to view the results. This elicited several questions and a declaration of frustration.
“Which portal?” she asked. “I have so many and can’t keep all of the websites and passwords straight! Why can’t all of my doctors use the same portal, and why do they all have different password requirements?”
As she spoke these words, I was immediately struck with an unfortunate reality of EHRs: We have done a brilliant job creating state-of-the-art digital castles and have filled them with the data needed to revolutionize care and improve population health – but we haven’t given our patients the keys to get inside.
We must ask ourselves if, in trying to construct fortresses of information around our patients, we have lost sight of the individuals in the center. I believe that we can answer this question and improve the benefits of patient portals, but we all must agree to a few simple steps to streamline the experience for everyone.
Make it easy
A study recently published in the Journal of General Internal Medicine surveyed several hospitals on their usage of patient portals. After determining whether or not the institutions had such portals, the authors then investigated to find out what, if any, guidance was provided to patients about how to use them.
Their findings are frustrating, though not surprising. While 89% of hospitals had some form of patient portal, only 65% of those “had links that were easily found, defined as links accessible within two clicks from the home page.”
Furthermore, even in cases where portals were easily found, good instructions on how to use them were missing. Those instructions that did exist centered on rules and restrictions and laying out “terms and conditions” and informing patients on “what not to do,” rather than explaining how to make the most of the experience.
According to the authors, “this focus on curtailing behavior, and the hurdles placed on finding and understanding guidance, suggest that some hospitals may be prioritizing reducing liability over improving the patient experience with portals.”
If we want our patients to use them, portals must be easy to access and intuitive to use. They also must provide value.
Make it meaningful
Patient portals have proliferated exponentially over the last 10 years, thanks to government incentive programs. One such program, known as “meaningful use,” is primarily responsible for this, as it made implementation of a patient portal one of its core requirements.
Sadly, in spite of its oft-reviled name, the meaningful use program never defined patient-friendly standards of usability for patient portals. As a result, current portals just aren’t very good. Patients like my mother-in-law find them to be too numerous, too unfriendly to use, and too limited, so they are not being used to their full potential.
In fact, many institutions may choose not to enable all of the available features in order to limit technical issues and reduce the burden on providers. In the study referenced above, only 63% of portals offered the ability for patients to communicate directly with their physicians, and only 43% offered the ability to refill prescriptions.
When enabled, these functions improve patient engagement and efficiency. Without them, patients are less likely to log on, and physicians are forced to rely on less-efficient telephone calls or traditional letters to communicate results to their patients.
Put the patient, not the portal, at the center
History has all but forgotten the attempts by tech giants such as Google and Microsoft to create personal health records. While these initially seemed like a wonderful concept, they sadly proved to be a total flop. Some patients embraced the idea, but security concerns and the lack of buy-in from EHR vendors significantly limited their uptake.
They may simply have been ahead of their time.
A decade later, wearable technology and telemedicine are ushering in a new era of patient-centric care. Individuals have been embracing a greater share of the responsibility for their own personal health information, yet most EHRs lack the ability to easily incorporate data acquired outside physicians’ offices.
It’s time for EHR vendors to go all in and change that. Instead of enslaving patients to the tyranny of fragmented health records, they should prioritize the creation of a robust, standardized, and portable health record that travels with the patient, not the other way around.
Have any other ideas on how to improve patient engagement? We’d love to hear about them and share them in a future column.
If you want to contribute but don’t have any ideas, we have a suggestion: Ask your mother-in-law. You may be surprised at what you learn!
Dr. Notte is a family physician and associate chief medical information officer for Abington (Pa.) Hospital–Jefferson Health. Follow him on twitter (@doctornotte). Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Philadelphia, and associate director of the family medicine residency program at Abington Hospital–Jefferson Health.
Reference
Lee JL et al. J Gen Intern Med. 2019 Nov 12. doi: 10.1007/s11606-019-05528-z.
While preparing to write this technology column, I received a great deal of insight from the unlikeliest of sources: my mother-in-law.
Now don’t get me wrong – she’s a truly lovely, intelligent, and capable woman. I have sought her advice often on many things and have always been impressed by her wisdom and pragmatism, but I’ve just never thought of asking her for her opinion on medicine or technology, as I considered her knowledge of both subjects to be limited.
This occasion changed my opinion. In fact, I believe that, as health care IT becomes more complex, people like my mother-in-law may be exactly who we should be looking to for answers.
A few weeks ago, my mother-in-law and I were discussing her recent trip to the doctor. When she mentioned some lab tests, I suggested that we log in to her patient portal to view the results. This elicited several questions and a declaration of frustration.
“Which portal?” she asked. “I have so many and can’t keep all of the websites and passwords straight! Why can’t all of my doctors use the same portal, and why do they all have different password requirements?”
As she spoke these words, I was immediately struck with an unfortunate reality of EHRs: We have done a brilliant job creating state-of-the-art digital castles and have filled them with the data needed to revolutionize care and improve population health – but we haven’t given our patients the keys to get inside.
We must ask ourselves if, in trying to construct fortresses of information around our patients, we have lost sight of the individuals in the center. I believe that we can answer this question and improve the benefits of patient portals, but we all must agree to a few simple steps to streamline the experience for everyone.
Make it easy
A study recently published in the Journal of General Internal Medicine surveyed several hospitals on their usage of patient portals. After determining whether or not the institutions had such portals, the authors then investigated to find out what, if any, guidance was provided to patients about how to use them.
Their findings are frustrating, though not surprising. While 89% of hospitals had some form of patient portal, only 65% of those “had links that were easily found, defined as links accessible within two clicks from the home page.”
Furthermore, even in cases where portals were easily found, good instructions on how to use them were missing. Those instructions that did exist centered on rules and restrictions and laying out “terms and conditions” and informing patients on “what not to do,” rather than explaining how to make the most of the experience.
According to the authors, “this focus on curtailing behavior, and the hurdles placed on finding and understanding guidance, suggest that some hospitals may be prioritizing reducing liability over improving the patient experience with portals.”
If we want our patients to use them, portals must be easy to access and intuitive to use. They also must provide value.
Make it meaningful
Patient portals have proliferated exponentially over the last 10 years, thanks to government incentive programs. One such program, known as “meaningful use,” is primarily responsible for this, as it made implementation of a patient portal one of its core requirements.
Sadly, in spite of its oft-reviled name, the meaningful use program never defined patient-friendly standards of usability for patient portals. As a result, current portals just aren’t very good. Patients like my mother-in-law find them to be too numerous, too unfriendly to use, and too limited, so they are not being used to their full potential.
In fact, many institutions may choose not to enable all of the available features in order to limit technical issues and reduce the burden on providers. In the study referenced above, only 63% of portals offered the ability for patients to communicate directly with their physicians, and only 43% offered the ability to refill prescriptions.
When enabled, these functions improve patient engagement and efficiency. Without them, patients are less likely to log on, and physicians are forced to rely on less-efficient telephone calls or traditional letters to communicate results to their patients.
Put the patient, not the portal, at the center
History has all but forgotten the attempts by tech giants such as Google and Microsoft to create personal health records. While these initially seemed like a wonderful concept, they sadly proved to be a total flop. Some patients embraced the idea, but security concerns and the lack of buy-in from EHR vendors significantly limited their uptake.
They may simply have been ahead of their time.
A decade later, wearable technology and telemedicine are ushering in a new era of patient-centric care. Individuals have been embracing a greater share of the responsibility for their own personal health information, yet most EHRs lack the ability to easily incorporate data acquired outside physicians’ offices.
It’s time for EHR vendors to go all in and change that. Instead of enslaving patients to the tyranny of fragmented health records, they should prioritize the creation of a robust, standardized, and portable health record that travels with the patient, not the other way around.
Have any other ideas on how to improve patient engagement? We’d love to hear about them and share them in a future column.
If you want to contribute but don’t have any ideas, we have a suggestion: Ask your mother-in-law. You may be surprised at what you learn!
Dr. Notte is a family physician and associate chief medical information officer for Abington (Pa.) Hospital–Jefferson Health. Follow him on twitter (@doctornotte). Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Philadelphia, and associate director of the family medicine residency program at Abington Hospital–Jefferson Health.
Reference
Lee JL et al. J Gen Intern Med. 2019 Nov 12. doi: 10.1007/s11606-019-05528-z.
How to beat bullying in the workplace
Cyberbullying can prove particularly insidious
Bullying happens to our patients and sometimes to the doctors in the medical community. As psychiatrists, we need to share information on how to spot it and deal with it in the workplace.
We can view bullying as the endpoint in a continuum with authority at one end and harassment at the other extreme. Discipline maintains order but those in charge can be misguided or mean spirited.
Bullying is bad and prevalent, but is it inevitable in the workplace? There are three categories: those who get bullied, those who bully, and those who witness bullying. Any one, two, or even all three can apply in a work environment. Some escape the problem, and for them, bullying remains theoretical, a phenomenon to understand.
How do we define bullying? You know it when you see it; bullying interferes with functioning. It includes harsh language, threats, snubbing, screaming, and undermining.
Case is illustrative
Helen, a medical consultant on a surgical unit, was reading a chart when another internist arrived for the same purpose. He introduced himself as a new full-time assistant to the head of medical consultations. Helen greeted him and said: “Since I started with this case, I will continue. There was probably an error in the referral process.” Bill looked concerned. “But he has uncontrolled diabetes.” Taken aback, Helen said: “I think I can handle it. I’ve been on the hospital staff for 25 years.”
Then the bullying began. On occasion, Bill and a resident consulted on patients Helen was treating already, as though her input were nonexistent. When Helen inquired about this, rather than attribute it to an error in communication within a large hospital, Bill diminished the value of her input. She asked, “How many medical consultants does a patient need?” She decided to confront Bill and tell him that he had no reason to treat her with disrespect. After that, Bill’s disparaging remarks intensified and he threatened her saying, “I’m not someone you want to go up against.” Bill sent her an email, “You are demeaning and harsh to the staff; if you want to retain your hospital credentials you must change your behavior.” In her response, Helen agreed to meet with Bill and she emailed, “It is not in my nature to mistreat anyone, staff or patient.” The meeting never happened.
Helen sought me out for psychiatric consultation and psychotherapy because she felt demoralized. Confused by Bill’s assault on her reputation, she needed a strategy and confirmation of her worth. We conceived a plan. Helen decided to get busy and get better. She redoubled her efforts to be cordial, and she remained effective with her patients. I suggested that she confide in a trusted senior attending at the hospital, which she did. She aired her insights to him. Excellence mattered and the threats disappeared. Bill had no power over Helen after all. She was a voluntary attending. She never succumbed to despair; rather she converted her response to the threats into useful energy.
When does authority become harassment?
A pecking order exists in every organization because, from the CEO to the janitor, it is necessary to maintain productivity. But when does this hierarchy become abusive? Discipline gets learned early. Those who are familiar with the comic strip “Calvin and Hobbes” by Bill Watterson may remember the 6-year-old boy asserting his intention to stay home from school – only to be forced to the bus stop by his mother. Call that authority, discipline, or even bullying, but it represents a child’s first encounter with obedience despite protest. When authority interferes rather than enhances effectiveness, question the methods used to attain order.
The vulnerable
If you do your job and you do it well, there should be no bullying. It is hard to know why a target gets chosen for harassment. However, some questions may need answering by the target. Does he or she avoid conflict even when there is bad behavior? Does past trauma immobilize him into passivity? Such issues necessitate self examination. Psychotherapy helps to uncover and clear up these issues.
Is bullying a fact of life?
In “Lord of the Flies,” William Golding portrays a fictional group of unsupervised boys abandoned on an island. An initial hierarchy descends into threats and eventual violence. Consider the animal world. In the wild, a wolf pack isolates a caribou from the herd to kill and devour. On a farm, llamas raised for yarn establish which llama is in charge. Those cases illustrate the hierarchy that exists because there is the need for food or reproductive prowess.
In the workplace, isolation of the target is common when authority extends to bullying. According to Robert Sapolsky, PhD, a neuroscientist and author, there are biological underpinnings for group conformity. This implies that colleagues who stand apart feel distress and get relief when they join the ganging up on a target. Those who watch harassment may hide from confronting it or even from pointing it out to protect themselves.
How do bullies think?
Challenge the bully at your own peril, because expecting a bully to change is futile. Recall Helen’s confrontation with Bill. It provoked him. His power to harass her came from his perceived position. Bullies regard the pleasant person as weak. Bullies can fall into two categories: Sadists who get pleasure from seeing others suffer, and opportunists. The latter focus only on their goals and disregard concerns expressed by others. Outside of the workplace, they may be reasonable. If workplace morale deteriorates along with productivity, the bully gets ousted. Otherwise, companies usually protect high performers at the expense of targets.
Is bullying different in medicine?
It can happen in a training program. The ingredients for bullying exist, including imbalance of power. Often, there are no witnesses, and there can be lack of accountability because of changing authorities. Just as technology can help make harassment possible, it also enables the target to spot and document inappropriate communications by saving emails and texts. Whenever a need for advancement exists along with changing authority, bullying gets tolerated. Who wants to be derailed by reporting? Those in training have the goal of completing a program. If they report bullying, they fear antagonism and retribution, a personal expense that can deter advancement.
Remedies
Let truth and fairness be your guide. That is easy to say and hard to do, but there are helpful personal and legal resources.
Personal capability
Get busy; get better. That became Helen’s method of choice. She focused on her role and productivity, not on her hurt. Helen shunned victimhood. With the help of psychotherapy and by confiding in a mentor, she prevailed. What works is recalling challenges that were mastered and the qualities that made for success. Acquire skills, build a good reputation, be assertive, not defensive.
The group is powerful, and that means it is important to build alliances above and below in the organizational hierarchy; cultivate friendship with trustworthy people. Occasionally, there is unwarranted ganging up on a manager, bullying from below. It is more likely to happen to a newly appointed supervisor. A way to avert that is to communicate with staff throughout the institution and remain accessible.
Legal options
What are legal options to confront bullying? Of note, workplace bullying is not necessarily illegal. According to one employment attorney, “There is no law that prohibits uncivil behavior on the job.” However, under Title VII of the federal law enacted in 1964, there are protected characteristics such as race, color, national origin, sex, age, and disability. The Equal Employment Opportunity Commission enforces Title VII. In cases of assault or stalking, harassment is illegal and criminal.
Some employees report to Human Resources or seek out their company’s employee assistance program. As useful as those options may be, they are part of the company and potentially partial to the administration. There can be incentives to protect those with power against a complainant. For assistance, it is preferable to enlist an outside attorney and a therapist in the community.
Advocacy exists. The Workplace Bullying Institute maintains a website, holds workshops, promotes literature, and offers information. The National Employment Lawyers Association can provide referrals or recommendations that come from other legal sources. Cases rarely reach court because of the expense of a trial; rather, the parties reach a financial settlement. When there is cause, an employment attorney can best pursue justice for the worker.
Conclusion
Get busy; get better is the solution to bullying. Avoid victimhood. That means prepare: Update the resume, seek opportunities, and identify allies. Bullies get beaten; as Abraham Lincoln said, “You can fool some of the people some of the time but you can’t fool all of the people all of the time.”
According to the Workplace Bullying Institute, 7 out of 10 bullied workers either resign or get fired. You should leave only when the leaving is better than the staying. Bullying brings out the worst in the workplace. Those who bully isolate the target. Coworkers often shun the target, fearing for their own position; they may even participate in the harassment. Psychiatrists need to remain sensitive to harassment in their own environment and for their patients. We have tools to address bullying in the workplace and a moral responsibility to combat it.
References
Workplace Bullying Institute (WBI)
National Employment Lawyers Association (NELA)
“Ozymandias” by Percy Bysshe Shelley
BY BEN HINDELL, PSY.D.
Cyberbullying is willful, repeated harm inflicted with the use of computers, cell phones, and other electronic devices. In some cases, a single message may be viewed by multiple people because the text and pictures are posted elsewhere.
Technology makes is possible to harass at any hour. The concept of willful harm is essential. Without interaction between sender and recipient, nuances are lost. Face to face might make a communication benign instead of malevolent or threatening. This has implications for the workplace, where colleagues increasingly communicate by email rather than discuss matters in person or by telephone.
Steps for survivors of cyberbullying
- Do not respond immediately to an inflammatory message, post, or email. Gather your thoughts and avoid responding in anger.
- Keep calm and rational, not emotional.
- Try to respond in person and work to avoid a conflict.
- Remember, your interpretation may differ from what was intended.
- Communicate openly and honestly and not defensively.
- Calmly indicate you were offended and you want the comments to stop.
- Move up the chain of command, if comments don’t cease.
- Save all messages and posts as evidence.
- Report the cyberbullying to your employer. Human resources may get involved.
- Detach from the cyberbully, if it continues. Block social media, cell phone messaging, and emails.
- Find support from friends, family, and a psychotherapist, if needed. As a last resort, it may become necessary to enlist an attorney.
- Take the high road; remain calm and professional at work. The bully may be seeking a reaction from the behavior. Prevent it.
All of the elements of workplace bullying apply to cyberbullying, but the latter can be more insidious. Psychiatrists and psychologists are able to support patients who deal with cyberbullying and help them cope successfully.
Dr. Cohen is in private practice and is a clinical assistant professor of psychiatry at Weill Cornell Medical Center of New York-Presbyterian Hospital, and psychiatric consultant at the Hospital for Special Surgery, also in New York. She made changes to the patient’s story to protect confidentiality.
Dr. Hindell is a psychologist with the Mental Health Service of Colorado College, Colorado Springs. He also practices psychotherapy in Denver. Dr. Hindell is the son of Dr. Cohen.
Cyberbullying can prove particularly insidious
Cyberbullying can prove particularly insidious
Bullying happens to our patients and sometimes to the doctors in the medical community. As psychiatrists, we need to share information on how to spot it and deal with it in the workplace.
We can view bullying as the endpoint in a continuum with authority at one end and harassment at the other extreme. Discipline maintains order but those in charge can be misguided or mean spirited.
Bullying is bad and prevalent, but is it inevitable in the workplace? There are three categories: those who get bullied, those who bully, and those who witness bullying. Any one, two, or even all three can apply in a work environment. Some escape the problem, and for them, bullying remains theoretical, a phenomenon to understand.
How do we define bullying? You know it when you see it; bullying interferes with functioning. It includes harsh language, threats, snubbing, screaming, and undermining.
Case is illustrative
Helen, a medical consultant on a surgical unit, was reading a chart when another internist arrived for the same purpose. He introduced himself as a new full-time assistant to the head of medical consultations. Helen greeted him and said: “Since I started with this case, I will continue. There was probably an error in the referral process.” Bill looked concerned. “But he has uncontrolled diabetes.” Taken aback, Helen said: “I think I can handle it. I’ve been on the hospital staff for 25 years.”
Then the bullying began. On occasion, Bill and a resident consulted on patients Helen was treating already, as though her input were nonexistent. When Helen inquired about this, rather than attribute it to an error in communication within a large hospital, Bill diminished the value of her input. She asked, “How many medical consultants does a patient need?” She decided to confront Bill and tell him that he had no reason to treat her with disrespect. After that, Bill’s disparaging remarks intensified and he threatened her saying, “I’m not someone you want to go up against.” Bill sent her an email, “You are demeaning and harsh to the staff; if you want to retain your hospital credentials you must change your behavior.” In her response, Helen agreed to meet with Bill and she emailed, “It is not in my nature to mistreat anyone, staff or patient.” The meeting never happened.
Helen sought me out for psychiatric consultation and psychotherapy because she felt demoralized. Confused by Bill’s assault on her reputation, she needed a strategy and confirmation of her worth. We conceived a plan. Helen decided to get busy and get better. She redoubled her efforts to be cordial, and she remained effective with her patients. I suggested that she confide in a trusted senior attending at the hospital, which she did. She aired her insights to him. Excellence mattered and the threats disappeared. Bill had no power over Helen after all. She was a voluntary attending. She never succumbed to despair; rather she converted her response to the threats into useful energy.
When does authority become harassment?
A pecking order exists in every organization because, from the CEO to the janitor, it is necessary to maintain productivity. But when does this hierarchy become abusive? Discipline gets learned early. Those who are familiar with the comic strip “Calvin and Hobbes” by Bill Watterson may remember the 6-year-old boy asserting his intention to stay home from school – only to be forced to the bus stop by his mother. Call that authority, discipline, or even bullying, but it represents a child’s first encounter with obedience despite protest. When authority interferes rather than enhances effectiveness, question the methods used to attain order.
The vulnerable
If you do your job and you do it well, there should be no bullying. It is hard to know why a target gets chosen for harassment. However, some questions may need answering by the target. Does he or she avoid conflict even when there is bad behavior? Does past trauma immobilize him into passivity? Such issues necessitate self examination. Psychotherapy helps to uncover and clear up these issues.
Is bullying a fact of life?
In “Lord of the Flies,” William Golding portrays a fictional group of unsupervised boys abandoned on an island. An initial hierarchy descends into threats and eventual violence. Consider the animal world. In the wild, a wolf pack isolates a caribou from the herd to kill and devour. On a farm, llamas raised for yarn establish which llama is in charge. Those cases illustrate the hierarchy that exists because there is the need for food or reproductive prowess.
In the workplace, isolation of the target is common when authority extends to bullying. According to Robert Sapolsky, PhD, a neuroscientist and author, there are biological underpinnings for group conformity. This implies that colleagues who stand apart feel distress and get relief when they join the ganging up on a target. Those who watch harassment may hide from confronting it or even from pointing it out to protect themselves.
How do bullies think?
Challenge the bully at your own peril, because expecting a bully to change is futile. Recall Helen’s confrontation with Bill. It provoked him. His power to harass her came from his perceived position. Bullies regard the pleasant person as weak. Bullies can fall into two categories: Sadists who get pleasure from seeing others suffer, and opportunists. The latter focus only on their goals and disregard concerns expressed by others. Outside of the workplace, they may be reasonable. If workplace morale deteriorates along with productivity, the bully gets ousted. Otherwise, companies usually protect high performers at the expense of targets.
Is bullying different in medicine?
It can happen in a training program. The ingredients for bullying exist, including imbalance of power. Often, there are no witnesses, and there can be lack of accountability because of changing authorities. Just as technology can help make harassment possible, it also enables the target to spot and document inappropriate communications by saving emails and texts. Whenever a need for advancement exists along with changing authority, bullying gets tolerated. Who wants to be derailed by reporting? Those in training have the goal of completing a program. If they report bullying, they fear antagonism and retribution, a personal expense that can deter advancement.
Remedies
Let truth and fairness be your guide. That is easy to say and hard to do, but there are helpful personal and legal resources.
Personal capability
Get busy; get better. That became Helen’s method of choice. She focused on her role and productivity, not on her hurt. Helen shunned victimhood. With the help of psychotherapy and by confiding in a mentor, she prevailed. What works is recalling challenges that were mastered and the qualities that made for success. Acquire skills, build a good reputation, be assertive, not defensive.
The group is powerful, and that means it is important to build alliances above and below in the organizational hierarchy; cultivate friendship with trustworthy people. Occasionally, there is unwarranted ganging up on a manager, bullying from below. It is more likely to happen to a newly appointed supervisor. A way to avert that is to communicate with staff throughout the institution and remain accessible.
Legal options
What are legal options to confront bullying? Of note, workplace bullying is not necessarily illegal. According to one employment attorney, “There is no law that prohibits uncivil behavior on the job.” However, under Title VII of the federal law enacted in 1964, there are protected characteristics such as race, color, national origin, sex, age, and disability. The Equal Employment Opportunity Commission enforces Title VII. In cases of assault or stalking, harassment is illegal and criminal.
Some employees report to Human Resources or seek out their company’s employee assistance program. As useful as those options may be, they are part of the company and potentially partial to the administration. There can be incentives to protect those with power against a complainant. For assistance, it is preferable to enlist an outside attorney and a therapist in the community.
Advocacy exists. The Workplace Bullying Institute maintains a website, holds workshops, promotes literature, and offers information. The National Employment Lawyers Association can provide referrals or recommendations that come from other legal sources. Cases rarely reach court because of the expense of a trial; rather, the parties reach a financial settlement. When there is cause, an employment attorney can best pursue justice for the worker.
Conclusion
Get busy; get better is the solution to bullying. Avoid victimhood. That means prepare: Update the resume, seek opportunities, and identify allies. Bullies get beaten; as Abraham Lincoln said, “You can fool some of the people some of the time but you can’t fool all of the people all of the time.”
According to the Workplace Bullying Institute, 7 out of 10 bullied workers either resign or get fired. You should leave only when the leaving is better than the staying. Bullying brings out the worst in the workplace. Those who bully isolate the target. Coworkers often shun the target, fearing for their own position; they may even participate in the harassment. Psychiatrists need to remain sensitive to harassment in their own environment and for their patients. We have tools to address bullying in the workplace and a moral responsibility to combat it.
References
Workplace Bullying Institute (WBI)
National Employment Lawyers Association (NELA)
“Ozymandias” by Percy Bysshe Shelley
BY BEN HINDELL, PSY.D.
Cyberbullying is willful, repeated harm inflicted with the use of computers, cell phones, and other electronic devices. In some cases, a single message may be viewed by multiple people because the text and pictures are posted elsewhere.
Technology makes is possible to harass at any hour. The concept of willful harm is essential. Without interaction between sender and recipient, nuances are lost. Face to face might make a communication benign instead of malevolent or threatening. This has implications for the workplace, where colleagues increasingly communicate by email rather than discuss matters in person or by telephone.
Steps for survivors of cyberbullying
- Do not respond immediately to an inflammatory message, post, or email. Gather your thoughts and avoid responding in anger.
- Keep calm and rational, not emotional.
- Try to respond in person and work to avoid a conflict.
- Remember, your interpretation may differ from what was intended.
- Communicate openly and honestly and not defensively.
- Calmly indicate you were offended and you want the comments to stop.
- Move up the chain of command, if comments don’t cease.
- Save all messages and posts as evidence.
- Report the cyberbullying to your employer. Human resources may get involved.
- Detach from the cyberbully, if it continues. Block social media, cell phone messaging, and emails.
- Find support from friends, family, and a psychotherapist, if needed. As a last resort, it may become necessary to enlist an attorney.
- Take the high road; remain calm and professional at work. The bully may be seeking a reaction from the behavior. Prevent it.
All of the elements of workplace bullying apply to cyberbullying, but the latter can be more insidious. Psychiatrists and psychologists are able to support patients who deal with cyberbullying and help them cope successfully.
Dr. Cohen is in private practice and is a clinical assistant professor of psychiatry at Weill Cornell Medical Center of New York-Presbyterian Hospital, and psychiatric consultant at the Hospital for Special Surgery, also in New York. She made changes to the patient’s story to protect confidentiality.
Dr. Hindell is a psychologist with the Mental Health Service of Colorado College, Colorado Springs. He also practices psychotherapy in Denver. Dr. Hindell is the son of Dr. Cohen.
Bullying happens to our patients and sometimes to the doctors in the medical community. As psychiatrists, we need to share information on how to spot it and deal with it in the workplace.
We can view bullying as the endpoint in a continuum with authority at one end and harassment at the other extreme. Discipline maintains order but those in charge can be misguided or mean spirited.
Bullying is bad and prevalent, but is it inevitable in the workplace? There are three categories: those who get bullied, those who bully, and those who witness bullying. Any one, two, or even all three can apply in a work environment. Some escape the problem, and for them, bullying remains theoretical, a phenomenon to understand.
How do we define bullying? You know it when you see it; bullying interferes with functioning. It includes harsh language, threats, snubbing, screaming, and undermining.
Case is illustrative
Helen, a medical consultant on a surgical unit, was reading a chart when another internist arrived for the same purpose. He introduced himself as a new full-time assistant to the head of medical consultations. Helen greeted him and said: “Since I started with this case, I will continue. There was probably an error in the referral process.” Bill looked concerned. “But he has uncontrolled diabetes.” Taken aback, Helen said: “I think I can handle it. I’ve been on the hospital staff for 25 years.”
Then the bullying began. On occasion, Bill and a resident consulted on patients Helen was treating already, as though her input were nonexistent. When Helen inquired about this, rather than attribute it to an error in communication within a large hospital, Bill diminished the value of her input. She asked, “How many medical consultants does a patient need?” She decided to confront Bill and tell him that he had no reason to treat her with disrespect. After that, Bill’s disparaging remarks intensified and he threatened her saying, “I’m not someone you want to go up against.” Bill sent her an email, “You are demeaning and harsh to the staff; if you want to retain your hospital credentials you must change your behavior.” In her response, Helen agreed to meet with Bill and she emailed, “It is not in my nature to mistreat anyone, staff or patient.” The meeting never happened.
Helen sought me out for psychiatric consultation and psychotherapy because she felt demoralized. Confused by Bill’s assault on her reputation, she needed a strategy and confirmation of her worth. We conceived a plan. Helen decided to get busy and get better. She redoubled her efforts to be cordial, and she remained effective with her patients. I suggested that she confide in a trusted senior attending at the hospital, which she did. She aired her insights to him. Excellence mattered and the threats disappeared. Bill had no power over Helen after all. She was a voluntary attending. She never succumbed to despair; rather she converted her response to the threats into useful energy.
When does authority become harassment?
A pecking order exists in every organization because, from the CEO to the janitor, it is necessary to maintain productivity. But when does this hierarchy become abusive? Discipline gets learned early. Those who are familiar with the comic strip “Calvin and Hobbes” by Bill Watterson may remember the 6-year-old boy asserting his intention to stay home from school – only to be forced to the bus stop by his mother. Call that authority, discipline, or even bullying, but it represents a child’s first encounter with obedience despite protest. When authority interferes rather than enhances effectiveness, question the methods used to attain order.
The vulnerable
If you do your job and you do it well, there should be no bullying. It is hard to know why a target gets chosen for harassment. However, some questions may need answering by the target. Does he or she avoid conflict even when there is bad behavior? Does past trauma immobilize him into passivity? Such issues necessitate self examination. Psychotherapy helps to uncover and clear up these issues.
Is bullying a fact of life?
In “Lord of the Flies,” William Golding portrays a fictional group of unsupervised boys abandoned on an island. An initial hierarchy descends into threats and eventual violence. Consider the animal world. In the wild, a wolf pack isolates a caribou from the herd to kill and devour. On a farm, llamas raised for yarn establish which llama is in charge. Those cases illustrate the hierarchy that exists because there is the need for food or reproductive prowess.
In the workplace, isolation of the target is common when authority extends to bullying. According to Robert Sapolsky, PhD, a neuroscientist and author, there are biological underpinnings for group conformity. This implies that colleagues who stand apart feel distress and get relief when they join the ganging up on a target. Those who watch harassment may hide from confronting it or even from pointing it out to protect themselves.
How do bullies think?
Challenge the bully at your own peril, because expecting a bully to change is futile. Recall Helen’s confrontation with Bill. It provoked him. His power to harass her came from his perceived position. Bullies regard the pleasant person as weak. Bullies can fall into two categories: Sadists who get pleasure from seeing others suffer, and opportunists. The latter focus only on their goals and disregard concerns expressed by others. Outside of the workplace, they may be reasonable. If workplace morale deteriorates along with productivity, the bully gets ousted. Otherwise, companies usually protect high performers at the expense of targets.
Is bullying different in medicine?
It can happen in a training program. The ingredients for bullying exist, including imbalance of power. Often, there are no witnesses, and there can be lack of accountability because of changing authorities. Just as technology can help make harassment possible, it also enables the target to spot and document inappropriate communications by saving emails and texts. Whenever a need for advancement exists along with changing authority, bullying gets tolerated. Who wants to be derailed by reporting? Those in training have the goal of completing a program. If they report bullying, they fear antagonism and retribution, a personal expense that can deter advancement.
Remedies
Let truth and fairness be your guide. That is easy to say and hard to do, but there are helpful personal and legal resources.
Personal capability
Get busy; get better. That became Helen’s method of choice. She focused on her role and productivity, not on her hurt. Helen shunned victimhood. With the help of psychotherapy and by confiding in a mentor, she prevailed. What works is recalling challenges that were mastered and the qualities that made for success. Acquire skills, build a good reputation, be assertive, not defensive.
The group is powerful, and that means it is important to build alliances above and below in the organizational hierarchy; cultivate friendship with trustworthy people. Occasionally, there is unwarranted ganging up on a manager, bullying from below. It is more likely to happen to a newly appointed supervisor. A way to avert that is to communicate with staff throughout the institution and remain accessible.
Legal options
What are legal options to confront bullying? Of note, workplace bullying is not necessarily illegal. According to one employment attorney, “There is no law that prohibits uncivil behavior on the job.” However, under Title VII of the federal law enacted in 1964, there are protected characteristics such as race, color, national origin, sex, age, and disability. The Equal Employment Opportunity Commission enforces Title VII. In cases of assault or stalking, harassment is illegal and criminal.
Some employees report to Human Resources or seek out their company’s employee assistance program. As useful as those options may be, they are part of the company and potentially partial to the administration. There can be incentives to protect those with power against a complainant. For assistance, it is preferable to enlist an outside attorney and a therapist in the community.
Advocacy exists. The Workplace Bullying Institute maintains a website, holds workshops, promotes literature, and offers information. The National Employment Lawyers Association can provide referrals or recommendations that come from other legal sources. Cases rarely reach court because of the expense of a trial; rather, the parties reach a financial settlement. When there is cause, an employment attorney can best pursue justice for the worker.
Conclusion
Get busy; get better is the solution to bullying. Avoid victimhood. That means prepare: Update the resume, seek opportunities, and identify allies. Bullies get beaten; as Abraham Lincoln said, “You can fool some of the people some of the time but you can’t fool all of the people all of the time.”
According to the Workplace Bullying Institute, 7 out of 10 bullied workers either resign or get fired. You should leave only when the leaving is better than the staying. Bullying brings out the worst in the workplace. Those who bully isolate the target. Coworkers often shun the target, fearing for their own position; they may even participate in the harassment. Psychiatrists need to remain sensitive to harassment in their own environment and for their patients. We have tools to address bullying in the workplace and a moral responsibility to combat it.
References
Workplace Bullying Institute (WBI)
National Employment Lawyers Association (NELA)
“Ozymandias” by Percy Bysshe Shelley
BY BEN HINDELL, PSY.D.
Cyberbullying is willful, repeated harm inflicted with the use of computers, cell phones, and other electronic devices. In some cases, a single message may be viewed by multiple people because the text and pictures are posted elsewhere.
Technology makes is possible to harass at any hour. The concept of willful harm is essential. Without interaction between sender and recipient, nuances are lost. Face to face might make a communication benign instead of malevolent or threatening. This has implications for the workplace, where colleagues increasingly communicate by email rather than discuss matters in person or by telephone.
Steps for survivors of cyberbullying
- Do not respond immediately to an inflammatory message, post, or email. Gather your thoughts and avoid responding in anger.
- Keep calm and rational, not emotional.
- Try to respond in person and work to avoid a conflict.
- Remember, your interpretation may differ from what was intended.
- Communicate openly and honestly and not defensively.
- Calmly indicate you were offended and you want the comments to stop.
- Move up the chain of command, if comments don’t cease.
- Save all messages and posts as evidence.
- Report the cyberbullying to your employer. Human resources may get involved.
- Detach from the cyberbully, if it continues. Block social media, cell phone messaging, and emails.
- Find support from friends, family, and a psychotherapist, if needed. As a last resort, it may become necessary to enlist an attorney.
- Take the high road; remain calm and professional at work. The bully may be seeking a reaction from the behavior. Prevent it.
All of the elements of workplace bullying apply to cyberbullying, but the latter can be more insidious. Psychiatrists and psychologists are able to support patients who deal with cyberbullying and help them cope successfully.
Dr. Cohen is in private practice and is a clinical assistant professor of psychiatry at Weill Cornell Medical Center of New York-Presbyterian Hospital, and psychiatric consultant at the Hospital for Special Surgery, also in New York. She made changes to the patient’s story to protect confidentiality.
Dr. Hindell is a psychologist with the Mental Health Service of Colorado College, Colorado Springs. He also practices psychotherapy in Denver. Dr. Hindell is the son of Dr. Cohen.
ID Blog: SARS-CoV-2 – What’s in a name?
Coming up with a moniker for the new coronavirus shows the perils of naming names.
There is no Baby Book of Names or hurricane alphabet to readily name diseases and their causal entities. Throughout history and even in the modern era, a host of considerations have intruded on the decision as to what to call these blights upon humanity. Names have varied from inflammatory to misleading, from colloquial to scientific. And when it concerns a new epidemiological entity such as the latest coronavirus outbreak originating in China, health organizations, media, politicians, scientific taxonomy commissions, and the public at large all have a stake in the naming.
From “Wuhan virus” to “novel coronavirus-2019” to “COVID-19 virus,” the name of the new coronavirus that first appeared in China has been evolving to its now official designation: SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2). But where did the final name come from, how does such a name become official, and who makes it so?
Virus taxonomy
The Coronavirus Study Group (CSG) of the International Committee on Taxonomy of Viruses (ICTV) named the new coronavirus SARS-CoV-2 based upon its genetic relationship to the original SARS-CoV that caused an outbreak of disease in 2002–2003.
According to the ICTV website, the first internationally organized attempts to introduce order into the bewildering variety of viruses took place at the International Congress of Microbiology held in Moscow in 1966 where a committee was created that later became the ICTV and was given the task of developing a single, universal taxonomic scheme for all the viruses infecting animals, plants, fungi, bacteria, and archaea. The ICTV was created as a committee of the virology division of the International Union of Microbiological Societies and is governed by statutes approved by the virology division. Virus classification and nomenclature are subject to rules set out in an International Code.
These designate that: “The universal virus classification system shall employ the hierarchical levels of realm, subrealm, kingdom, subkingdom, phylum, subphylum, class, subclass, order, suborder, family, subfamily, genus, subgenus and species.”
Many of the topmost areas of classification are based on whether the viruses are DNA or RNA, single or double stranded, and have a simple protein shell or a complex lipoprotein envelope. Other levels of classification include host species, type of replication, and type of diseases they cause, the later exemplified in the SARS designation for this virus.
There are 98 international study groups (SGs) covering all major virus orders, families, and genera that are part of the ICTV, and it was the one dedicated to the single-stranded RNA coronaviruses, the CSG, that came up with the SARS-CoV-2 name and first referenced it in their Feb 11 publication in the Cold Springs Harbor preprint journal bioRxiv.
“Based on phylogeny, taxonomy and established practice, the CSG formally recognizes this virus as a sister to severe acute respiratory syndrome coronaviruses (SARS-CoVs) of the species severe acute respiratory syndrome–related coronavirus and designates it as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2),” they wrote.
According to the National Center for Biotechnology Information Taxonomy Browser, with respect to the original SARS CoV virus, of which this is a relative, the full taxonomic designation is: Viruses, Riboviria, Nidovirales, Cornidovirineae, Coronaviridae, Orthocoronavirinae, Betacoronavirus, Sarbecovirus.
The problem with naming names
The World Health Organization currently is not using the official scientific name of the virus, but rather is merely labeling it with regard to the disease: COVID-19, which simply refers to coronavirus disease 2019.
They are following a modern standard by which disease names avoid inflammatory connotations with people and places. Too often in the past from syphilis as the “French pox,” the 1918 influenza as the “Spanish flu,” AIDS as the “gay plague,” Middle East Respiratory Syndrome (MERS), and the currently named “WuFlu,” which made an appearance early in the new outbreak and which is symbolic of a sudden wave of anti-Asian, and specifically Chinese, prejudice.
Chinatown districts even in the United States are being affected economically through unwarranted fear associated with the virus. And there have been equivalently virulent outbreaks of hate speech against Asian individuals in places untouched by the new virus.
However, although SARS-CoV-2 as a name avoids such problems, different considerations led the WHO to reject it in its discussions, determining that its use ties it to tightly to the much more deadly SARS-CoV-1 virus in the public mind, risking greater fear and panic, especially in Asia, where SARS-CoV-1 had the biggest impact.
Back in 1896, William Sykes, MD, writing in the first flush of the triumph of germ theory in modern medicine, attempted to give some guidance to how medical science should best come up with new names of diseases by merging the demands of common parlance with those of taxonomic legitimacy. His “On the Origin and History of Disease-Names,” published in the Lancet, had clearcut advice: “It is vain to attempt to replace a folk name or one widely adopted by the people by a new one deliberately coined by scholars, and this for the following reasons: first, whatever names may be accepted by medical men must be translated by them into the vernacular of their patients, and by a resulting reaction the vernacular name comes to be the commoner one with themselves; and, secondly, there is no continuity or unchangeableness in the terms invented by savants, which are amended, improved upon, and displaced by the next writer on the subject, or, even more absurdly still, by the very inventors themselves in a subsequent publication.”
This is the reason that virus taxonomy provides names based upon unchangeable scientific descriptors of the actual disease causing entity, as illustrated by the decisions of the ICTV. In addition, the genomic sequences being provided by the scientific community are all being organized under the SARS-CoV-2 name and thus are cementing that moniker as the only acceptable scientific one.
Whether the rest of the world universally adopts SARS-CoV-2 as a name is still in question. If the outbreak spreads significantly beyond its current limits, fear and confusion – and simply the need for a more familiar-sounding label – may lead the general public to adopt more colloquial designations than those that science attempts to impose, as Dr. Sykes suggested back in 1896. That remains to be seen.
[email protected]
Mark Lesney is the managing editor of MDedge.com/IDPractioner. He has a PhD in plant virology and a PhD in the history of science, with a focus on the history of biotechnology and medicine. He has served as an adjunct assistant professor of the department of biochemistry and molecular & cellular biology at Georgetown University, Washington.
Coming up with a moniker for the new coronavirus shows the perils of naming names.
Coming up with a moniker for the new coronavirus shows the perils of naming names.
There is no Baby Book of Names or hurricane alphabet to readily name diseases and their causal entities. Throughout history and even in the modern era, a host of considerations have intruded on the decision as to what to call these blights upon humanity. Names have varied from inflammatory to misleading, from colloquial to scientific. And when it concerns a new epidemiological entity such as the latest coronavirus outbreak originating in China, health organizations, media, politicians, scientific taxonomy commissions, and the public at large all have a stake in the naming.
From “Wuhan virus” to “novel coronavirus-2019” to “COVID-19 virus,” the name of the new coronavirus that first appeared in China has been evolving to its now official designation: SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2). But where did the final name come from, how does such a name become official, and who makes it so?
Virus taxonomy
The Coronavirus Study Group (CSG) of the International Committee on Taxonomy of Viruses (ICTV) named the new coronavirus SARS-CoV-2 based upon its genetic relationship to the original SARS-CoV that caused an outbreak of disease in 2002–2003.
According to the ICTV website, the first internationally organized attempts to introduce order into the bewildering variety of viruses took place at the International Congress of Microbiology held in Moscow in 1966 where a committee was created that later became the ICTV and was given the task of developing a single, universal taxonomic scheme for all the viruses infecting animals, plants, fungi, bacteria, and archaea. The ICTV was created as a committee of the virology division of the International Union of Microbiological Societies and is governed by statutes approved by the virology division. Virus classification and nomenclature are subject to rules set out in an International Code.
These designate that: “The universal virus classification system shall employ the hierarchical levels of realm, subrealm, kingdom, subkingdom, phylum, subphylum, class, subclass, order, suborder, family, subfamily, genus, subgenus and species.”
Many of the topmost areas of classification are based on whether the viruses are DNA or RNA, single or double stranded, and have a simple protein shell or a complex lipoprotein envelope. Other levels of classification include host species, type of replication, and type of diseases they cause, the later exemplified in the SARS designation for this virus.
There are 98 international study groups (SGs) covering all major virus orders, families, and genera that are part of the ICTV, and it was the one dedicated to the single-stranded RNA coronaviruses, the CSG, that came up with the SARS-CoV-2 name and first referenced it in their Feb 11 publication in the Cold Springs Harbor preprint journal bioRxiv.
“Based on phylogeny, taxonomy and established practice, the CSG formally recognizes this virus as a sister to severe acute respiratory syndrome coronaviruses (SARS-CoVs) of the species severe acute respiratory syndrome–related coronavirus and designates it as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2),” they wrote.
According to the National Center for Biotechnology Information Taxonomy Browser, with respect to the original SARS CoV virus, of which this is a relative, the full taxonomic designation is: Viruses, Riboviria, Nidovirales, Cornidovirineae, Coronaviridae, Orthocoronavirinae, Betacoronavirus, Sarbecovirus.
The problem with naming names
The World Health Organization currently is not using the official scientific name of the virus, but rather is merely labeling it with regard to the disease: COVID-19, which simply refers to coronavirus disease 2019.
They are following a modern standard by which disease names avoid inflammatory connotations with people and places. Too often in the past from syphilis as the “French pox,” the 1918 influenza as the “Spanish flu,” AIDS as the “gay plague,” Middle East Respiratory Syndrome (MERS), and the currently named “WuFlu,” which made an appearance early in the new outbreak and which is symbolic of a sudden wave of anti-Asian, and specifically Chinese, prejudice.
Chinatown districts even in the United States are being affected economically through unwarranted fear associated with the virus. And there have been equivalently virulent outbreaks of hate speech against Asian individuals in places untouched by the new virus.
However, although SARS-CoV-2 as a name avoids such problems, different considerations led the WHO to reject it in its discussions, determining that its use ties it to tightly to the much more deadly SARS-CoV-1 virus in the public mind, risking greater fear and panic, especially in Asia, where SARS-CoV-1 had the biggest impact.
Back in 1896, William Sykes, MD, writing in the first flush of the triumph of germ theory in modern medicine, attempted to give some guidance to how medical science should best come up with new names of diseases by merging the demands of common parlance with those of taxonomic legitimacy. His “On the Origin and History of Disease-Names,” published in the Lancet, had clearcut advice: “It is vain to attempt to replace a folk name or one widely adopted by the people by a new one deliberately coined by scholars, and this for the following reasons: first, whatever names may be accepted by medical men must be translated by them into the vernacular of their patients, and by a resulting reaction the vernacular name comes to be the commoner one with themselves; and, secondly, there is no continuity or unchangeableness in the terms invented by savants, which are amended, improved upon, and displaced by the next writer on the subject, or, even more absurdly still, by the very inventors themselves in a subsequent publication.”
This is the reason that virus taxonomy provides names based upon unchangeable scientific descriptors of the actual disease causing entity, as illustrated by the decisions of the ICTV. In addition, the genomic sequences being provided by the scientific community are all being organized under the SARS-CoV-2 name and thus are cementing that moniker as the only acceptable scientific one.
Whether the rest of the world universally adopts SARS-CoV-2 as a name is still in question. If the outbreak spreads significantly beyond its current limits, fear and confusion – and simply the need for a more familiar-sounding label – may lead the general public to adopt more colloquial designations than those that science attempts to impose, as Dr. Sykes suggested back in 1896. That remains to be seen.
[email protected]
Mark Lesney is the managing editor of MDedge.com/IDPractioner. He has a PhD in plant virology and a PhD in the history of science, with a focus on the history of biotechnology and medicine. He has served as an adjunct assistant professor of the department of biochemistry and molecular & cellular biology at Georgetown University, Washington.
There is no Baby Book of Names or hurricane alphabet to readily name diseases and their causal entities. Throughout history and even in the modern era, a host of considerations have intruded on the decision as to what to call these blights upon humanity. Names have varied from inflammatory to misleading, from colloquial to scientific. And when it concerns a new epidemiological entity such as the latest coronavirus outbreak originating in China, health organizations, media, politicians, scientific taxonomy commissions, and the public at large all have a stake in the naming.
From “Wuhan virus” to “novel coronavirus-2019” to “COVID-19 virus,” the name of the new coronavirus that first appeared in China has been evolving to its now official designation: SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2). But where did the final name come from, how does such a name become official, and who makes it so?
Virus taxonomy
The Coronavirus Study Group (CSG) of the International Committee on Taxonomy of Viruses (ICTV) named the new coronavirus SARS-CoV-2 based upon its genetic relationship to the original SARS-CoV that caused an outbreak of disease in 2002–2003.
According to the ICTV website, the first internationally organized attempts to introduce order into the bewildering variety of viruses took place at the International Congress of Microbiology held in Moscow in 1966 where a committee was created that later became the ICTV and was given the task of developing a single, universal taxonomic scheme for all the viruses infecting animals, plants, fungi, bacteria, and archaea. The ICTV was created as a committee of the virology division of the International Union of Microbiological Societies and is governed by statutes approved by the virology division. Virus classification and nomenclature are subject to rules set out in an International Code.
These designate that: “The universal virus classification system shall employ the hierarchical levels of realm, subrealm, kingdom, subkingdom, phylum, subphylum, class, subclass, order, suborder, family, subfamily, genus, subgenus and species.”
Many of the topmost areas of classification are based on whether the viruses are DNA or RNA, single or double stranded, and have a simple protein shell or a complex lipoprotein envelope. Other levels of classification include host species, type of replication, and type of diseases they cause, the later exemplified in the SARS designation for this virus.
There are 98 international study groups (SGs) covering all major virus orders, families, and genera that are part of the ICTV, and it was the one dedicated to the single-stranded RNA coronaviruses, the CSG, that came up with the SARS-CoV-2 name and first referenced it in their Feb 11 publication in the Cold Springs Harbor preprint journal bioRxiv.
“Based on phylogeny, taxonomy and established practice, the CSG formally recognizes this virus as a sister to severe acute respiratory syndrome coronaviruses (SARS-CoVs) of the species severe acute respiratory syndrome–related coronavirus and designates it as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2),” they wrote.
According to the National Center for Biotechnology Information Taxonomy Browser, with respect to the original SARS CoV virus, of which this is a relative, the full taxonomic designation is: Viruses, Riboviria, Nidovirales, Cornidovirineae, Coronaviridae, Orthocoronavirinae, Betacoronavirus, Sarbecovirus.
The problem with naming names
The World Health Organization currently is not using the official scientific name of the virus, but rather is merely labeling it with regard to the disease: COVID-19, which simply refers to coronavirus disease 2019.
They are following a modern standard by which disease names avoid inflammatory connotations with people and places. Too often in the past from syphilis as the “French pox,” the 1918 influenza as the “Spanish flu,” AIDS as the “gay plague,” Middle East Respiratory Syndrome (MERS), and the currently named “WuFlu,” which made an appearance early in the new outbreak and which is symbolic of a sudden wave of anti-Asian, and specifically Chinese, prejudice.
Chinatown districts even in the United States are being affected economically through unwarranted fear associated with the virus. And there have been equivalently virulent outbreaks of hate speech against Asian individuals in places untouched by the new virus.
However, although SARS-CoV-2 as a name avoids such problems, different considerations led the WHO to reject it in its discussions, determining that its use ties it to tightly to the much more deadly SARS-CoV-1 virus in the public mind, risking greater fear and panic, especially in Asia, where SARS-CoV-1 had the biggest impact.
Back in 1896, William Sykes, MD, writing in the first flush of the triumph of germ theory in modern medicine, attempted to give some guidance to how medical science should best come up with new names of diseases by merging the demands of common parlance with those of taxonomic legitimacy. His “On the Origin and History of Disease-Names,” published in the Lancet, had clearcut advice: “It is vain to attempt to replace a folk name or one widely adopted by the people by a new one deliberately coined by scholars, and this for the following reasons: first, whatever names may be accepted by medical men must be translated by them into the vernacular of their patients, and by a resulting reaction the vernacular name comes to be the commoner one with themselves; and, secondly, there is no continuity or unchangeableness in the terms invented by savants, which are amended, improved upon, and displaced by the next writer on the subject, or, even more absurdly still, by the very inventors themselves in a subsequent publication.”
This is the reason that virus taxonomy provides names based upon unchangeable scientific descriptors of the actual disease causing entity, as illustrated by the decisions of the ICTV. In addition, the genomic sequences being provided by the scientific community are all being organized under the SARS-CoV-2 name and thus are cementing that moniker as the only acceptable scientific one.
Whether the rest of the world universally adopts SARS-CoV-2 as a name is still in question. If the outbreak spreads significantly beyond its current limits, fear and confusion – and simply the need for a more familiar-sounding label – may lead the general public to adopt more colloquial designations than those that science attempts to impose, as Dr. Sykes suggested back in 1896. That remains to be seen.
[email protected]
Mark Lesney is the managing editor of MDedge.com/IDPractioner. He has a PhD in plant virology and a PhD in the history of science, with a focus on the history of biotechnology and medicine. He has served as an adjunct assistant professor of the department of biochemistry and molecular & cellular biology at Georgetown University, Washington.
Transporting the high-risk psychiatric patient: Clinical and legal challenges
“I’ve given up, doctor. We gave it our best, but I am at the point where I want to end my life.” You receive this call at 2 a.m., and you’re flooded with a series of emotions and are bewildered – until your training kicks in.
Countless hours of working with patients in emergency department settings while on call as a resident inform your ability to triage the situation. Years of supervision guide your supportive statements as you work collaboratively with your patient to address the emotional and existential distress. As the call proceeds and you realize that your patient will require hospitalization, you are struck by a sobering question: “How am I going to arrange for my patient to go to the nearest hospital in the middle of the night?”
The options for transporting patients with serious mental illness (SMI) typically vary from bad to worse and usually filter down to three possibilities:
1. Get a friend or family member to transport them to the nearest ED.
2. Call emergency medical services (EMS) for transport to the nearest ED.
3. Call the police and request transport to the nearest ED.
Several factors would determine which of those options you would use alone or in combination. Current training paradigms for mental health professionals offer a limited body of literature on evidenced-based strategies for patients with SMI. At best – if not handled properly – these experiences can aggravate patients’ mental health conditions. At worst, they can lead to the loss of our patients. Together, we have more than 40 years’ experience working in complex mental health care systems that run the gamut, from providing direct clinical care to directing mental health care divisions.
Sobering statistics prevail
In 2017, suicide was the 10th leading cause of death in the United States, accounting for more than 47,000 deaths. Suicide was the second-leading cause of death among individuals aged 10-34 and the fourth leading cause of death for individuals aged 35- 54.1 In 2017, more than 70,200 Americans died from a drug overdose, including illicit drugs and prescription opioids.2 Drug overdose deaths nearly quadrupled between 1999 and 2017, from 16,849 deaths to 70,237, respectively.2
The life expectancy of an American with SMI is 14-32 years less than that of the average population.3 Those numbers are on par with many sub-Saharan countries, including Sudan and Ethiopia, and surpass the health disparities for most racial and ethnic groups.
The decrease in life expectancy for people with SMI is rarely the result of suicide but rather the effect of medical comorbidities, including heart disease, stroke, pulmonary disease, diabetes, and cancer.3 Individuals with SMI are much more likely to suffer from chronic illnesses that are associated with co-occurring addictions, side effects of psychotropic medications, and social determinants of mental health, such as poverty.
Major depressive disorder among people with SMI presents acute and chronic medical risks. For example, people with major depressive disorder are at a higher risk for stroke and cardiovascular disease.4 There is a threefold increase in cardiac-related deaths for individuals who experience depression after a heart attack.5 In addition, depression increases the risk of cardiac-related death after a heart attack more than any other risk factor, except for congestive heart failure.6
The transportation challenge
When the complexity of psychiatric conditions is conceptualized to include decreased life expectancy because of medical comorbidities, medical complications that can result from psychotropic medications, and the high incidence of co-occurring substance use disorders (SUDs), it is clear why we are concerned about the type of transport used for patients experiencing a psychiatric emergency.
A common practice for patients presenting for medical treatment for a mental health condition is for them to be transported by law enforcement in handcuffs, or by private vehicle, because of a lack of medical transport options.
One tragic example occurred on Sept. 18, 2018, when two Horry County, S.C., deputies were providing a hospital-to-hospital transport for two mental health patients. The patients, who had no legal charges and were not under arrest, were locked in a transport cage in the back of a law enforcement vehicle for transport during Hurricane Florence. While the driver tried to move through floodwaters, the car stalled and became submerged. The patients were unable to open the locked cage door, and the deputies responsible for the transport did not have a key to unlock the cage.
The two women died as a result of the incident. Both deputies are facing two counts of involuntary manslaughter – with a potential prison sentence of 5 years each.7
The system that promotes the use of law enforcement to transport medical patients who are not in legal custody perpetuates a high risk to patients. Also at risk are law enforcement professionals who often are not adequately trained to evaluate, intervene, and manage patients in need of medical treatment (for acute medical, SUDs, or mental illness).
Recommendations for transporting high-risk patients
The legal and regulatory standards required by the Centers for Medicare & Medicaid Services guidelines8 for behavioral health patients are consistent in saying that law enforcement restraints cannot be used in hospital settings – unless the patient is under law enforcement custody. If the patient is admitted to an inpatient psychiatric unit, law enforcement restraints are never allowed to be used. Despite those guidelines for handling these situations within hospital settings, a similar standard does not exist for interhospital transport of high-risk behavioral health patients.
Patients often are transported between facilities by law enforcement, and at times, with the use of law enforcement restraints. However, use of law enforcement for interhospital transport of patients not in the custody of law enforcement is both detrimental to and clinically dangerous for the patient. Not only does the scenario put the patient at risk, but it also places law enforcement professionals at risk with the potential for legal liability if the patient medically decompensates during the transport.
Also, using law enforcement to intervene and provide transportation for behavioral health patients in crisis might cause further harm to the patient’s psychological condition and deter the patient from presenting for treatment.
The appropriate level of interfacility transport for a behavioral health patient requiring an inpatient level of care is secure transport with trained medical professionals. If necessary, restraint guidelines should follow the same standard as they do in hospital settings. In situations with high risk for violence or agitation, law enforcement should be requested to accompany EMS during the transport. Handling the situation in this way allows for a collaborative approach to provide adequate medical support, and provide for the physical safety and security of the patient – and of EMS personnel.
Across police and sheriffs’ departments nationwide, law enforcement officers are required to transport mental health patients from one location or hospital to another. Hospitals and outpatient locations, often with no alternative, rely on local law enforcement agencies to provide safe transport between acute and mental health facilities. Departmental policies and the widespread belief that mental health patients automatically pose a substantial danger to themselves or others have led to these patients being handcuffed and put in the back of police cruisers. Essentially, they are treated like criminals who are under arrest.
The CMS has strict criteria for ordering, applying, evaluating, reevaluating, and reporting restraint-associated deaths. Likewise, The Joint Commission, during its accreditation survey, rightly scrutinizes a facility’s use of restraints. Both the CMS and The Joint Commission define restraint by the function of the device and not the type of the device.
According to the CMS, a restraint is any manual method, physical or mechanic device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely. Within a police cruiser, handcuffs on a mental health patient who is not under arrest would fall squarely within this definition of restraint.
A patient’s current behavior or clinical needs – not history or diagnosis – should determine whether a restraint is warranted. A patient experiencing a psychiatric crisis who is not under arrest might very well escalate and become destructive and combative when being placed in handcuffs in the back of a police vehicle. What should police do at that point? Should they arrest the individual? We offer the following five recommendations.
Key recommendations
- Patients who require interhospital transport for an acute behavioral health crisis should be transported by medical professionals with the training and expertise to manage mental health and medical conditions.
- Interhospital transport restraint guidelines should be in line with CMS guidelines for hospital restraints. No patient that is not under law enforcement custody should be transported in law enforcement restraints.
- Patients at high risk for violence/agitation (an underlying condition causing violence/agitation may include dementia, traumatic brain injuries, delirium, SUDs, or psychiatric conditions) should be managed in accordance with medically indicated intervention such as medical restraints or medications.
- If required, a request should be made for law enforcement officers to accompany EMS to provide support and to ensure the safety of the patient and EMS professionals during the transport.
- EMS professionals should receive specific training to manage acute psychiatric and SUD conditions, and should be aware of the life-threatening medical complications that can result from SUDs and psychiatric conditions/medications.
We recognize that patients with SMI require clinicians to work collaboratively, perhaps with law enforcement, to safely transport them from one point to another. Only when the rules we have outlined are followed will our patients get transported in such ways that allow them to get the care they need.
Dr. Norris is editor-in-chief of MDedge Psychiatry, and assistant professor of psychiatry and behavioral sciences at George Washington University, Washington. He serves as assistant dean of student affairs at the university, and medical director of psychiatric and behavioral sciences at GWU Hospital. Ms. Palmieri is a managing partner of Healthcare Legal Education & Consulting Network (HLECN), and the chief clinical officer and cofounder of XFERALL. HLECN focuses on clinical education and training, and XFERALL is a company that provides a technology platform aimed at improving access to care for behavioral health and medical patients. Ms. Slater is a managing partner of legal education for HLECN, and a trial attorney at Colley Shroyer & Abraham in Columbus, Ohio. Mr. Whaley is director of the safety and security department at GWU Hospital.
References
1. National Institute of Mental Health: Suicide.
2. National Institute on Drug Abuse. Overdose death rates. Revised January 2019.
3. Post by former NIMH Director Thomas Insel: No health without mental health. Sept. 6, 2011.
4. Dhar AK and Barton DA. Depression and the link with cardiovascular disease. Front Psychiatry. 2016 Mar 21;7:33.
5. Lichtman JH et al. Depression and coronary heart disease. Circulation. 2008;118:1768-75.
6. Hare DL et al. Depression and cardiovascular disease: A clinical review. European Heart J. 2014 Jun;35(21):1365-72.
7. “ ‘How many people have to die?’ SC mental health patients endure nightmare transport.” The News & Observer. 2019 May 29.
8. 42 C.F.R. Part 482. Part IV. Department of Health and Human Services. Medicare & Medicaid programs; Hospital conditions of participation; Patients’ rights; Final rule. 2006 Dec 8.
“I’ve given up, doctor. We gave it our best, but I am at the point where I want to end my life.” You receive this call at 2 a.m., and you’re flooded with a series of emotions and are bewildered – until your training kicks in.
Countless hours of working with patients in emergency department settings while on call as a resident inform your ability to triage the situation. Years of supervision guide your supportive statements as you work collaboratively with your patient to address the emotional and existential distress. As the call proceeds and you realize that your patient will require hospitalization, you are struck by a sobering question: “How am I going to arrange for my patient to go to the nearest hospital in the middle of the night?”
The options for transporting patients with serious mental illness (SMI) typically vary from bad to worse and usually filter down to three possibilities:
1. Get a friend or family member to transport them to the nearest ED.
2. Call emergency medical services (EMS) for transport to the nearest ED.
3. Call the police and request transport to the nearest ED.
Several factors would determine which of those options you would use alone or in combination. Current training paradigms for mental health professionals offer a limited body of literature on evidenced-based strategies for patients with SMI. At best – if not handled properly – these experiences can aggravate patients’ mental health conditions. At worst, they can lead to the loss of our patients. Together, we have more than 40 years’ experience working in complex mental health care systems that run the gamut, from providing direct clinical care to directing mental health care divisions.
Sobering statistics prevail
In 2017, suicide was the 10th leading cause of death in the United States, accounting for more than 47,000 deaths. Suicide was the second-leading cause of death among individuals aged 10-34 and the fourth leading cause of death for individuals aged 35- 54.1 In 2017, more than 70,200 Americans died from a drug overdose, including illicit drugs and prescription opioids.2 Drug overdose deaths nearly quadrupled between 1999 and 2017, from 16,849 deaths to 70,237, respectively.2
The life expectancy of an American with SMI is 14-32 years less than that of the average population.3 Those numbers are on par with many sub-Saharan countries, including Sudan and Ethiopia, and surpass the health disparities for most racial and ethnic groups.
The decrease in life expectancy for people with SMI is rarely the result of suicide but rather the effect of medical comorbidities, including heart disease, stroke, pulmonary disease, diabetes, and cancer.3 Individuals with SMI are much more likely to suffer from chronic illnesses that are associated with co-occurring addictions, side effects of psychotropic medications, and social determinants of mental health, such as poverty.
Major depressive disorder among people with SMI presents acute and chronic medical risks. For example, people with major depressive disorder are at a higher risk for stroke and cardiovascular disease.4 There is a threefold increase in cardiac-related deaths for individuals who experience depression after a heart attack.5 In addition, depression increases the risk of cardiac-related death after a heart attack more than any other risk factor, except for congestive heart failure.6
The transportation challenge
When the complexity of psychiatric conditions is conceptualized to include decreased life expectancy because of medical comorbidities, medical complications that can result from psychotropic medications, and the high incidence of co-occurring substance use disorders (SUDs), it is clear why we are concerned about the type of transport used for patients experiencing a psychiatric emergency.
A common practice for patients presenting for medical treatment for a mental health condition is for them to be transported by law enforcement in handcuffs, or by private vehicle, because of a lack of medical transport options.
One tragic example occurred on Sept. 18, 2018, when two Horry County, S.C., deputies were providing a hospital-to-hospital transport for two mental health patients. The patients, who had no legal charges and were not under arrest, were locked in a transport cage in the back of a law enforcement vehicle for transport during Hurricane Florence. While the driver tried to move through floodwaters, the car stalled and became submerged. The patients were unable to open the locked cage door, and the deputies responsible for the transport did not have a key to unlock the cage.
The two women died as a result of the incident. Both deputies are facing two counts of involuntary manslaughter – with a potential prison sentence of 5 years each.7
The system that promotes the use of law enforcement to transport medical patients who are not in legal custody perpetuates a high risk to patients. Also at risk are law enforcement professionals who often are not adequately trained to evaluate, intervene, and manage patients in need of medical treatment (for acute medical, SUDs, or mental illness).
Recommendations for transporting high-risk patients
The legal and regulatory standards required by the Centers for Medicare & Medicaid Services guidelines8 for behavioral health patients are consistent in saying that law enforcement restraints cannot be used in hospital settings – unless the patient is under law enforcement custody. If the patient is admitted to an inpatient psychiatric unit, law enforcement restraints are never allowed to be used. Despite those guidelines for handling these situations within hospital settings, a similar standard does not exist for interhospital transport of high-risk behavioral health patients.
Patients often are transported between facilities by law enforcement, and at times, with the use of law enforcement restraints. However, use of law enforcement for interhospital transport of patients not in the custody of law enforcement is both detrimental to and clinically dangerous for the patient. Not only does the scenario put the patient at risk, but it also places law enforcement professionals at risk with the potential for legal liability if the patient medically decompensates during the transport.
Also, using law enforcement to intervene and provide transportation for behavioral health patients in crisis might cause further harm to the patient’s psychological condition and deter the patient from presenting for treatment.
The appropriate level of interfacility transport for a behavioral health patient requiring an inpatient level of care is secure transport with trained medical professionals. If necessary, restraint guidelines should follow the same standard as they do in hospital settings. In situations with high risk for violence or agitation, law enforcement should be requested to accompany EMS during the transport. Handling the situation in this way allows for a collaborative approach to provide adequate medical support, and provide for the physical safety and security of the patient – and of EMS personnel.
Across police and sheriffs’ departments nationwide, law enforcement officers are required to transport mental health patients from one location or hospital to another. Hospitals and outpatient locations, often with no alternative, rely on local law enforcement agencies to provide safe transport between acute and mental health facilities. Departmental policies and the widespread belief that mental health patients automatically pose a substantial danger to themselves or others have led to these patients being handcuffed and put in the back of police cruisers. Essentially, they are treated like criminals who are under arrest.
The CMS has strict criteria for ordering, applying, evaluating, reevaluating, and reporting restraint-associated deaths. Likewise, The Joint Commission, during its accreditation survey, rightly scrutinizes a facility’s use of restraints. Both the CMS and The Joint Commission define restraint by the function of the device and not the type of the device.
According to the CMS, a restraint is any manual method, physical or mechanic device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely. Within a police cruiser, handcuffs on a mental health patient who is not under arrest would fall squarely within this definition of restraint.
A patient’s current behavior or clinical needs – not history or diagnosis – should determine whether a restraint is warranted. A patient experiencing a psychiatric crisis who is not under arrest might very well escalate and become destructive and combative when being placed in handcuffs in the back of a police vehicle. What should police do at that point? Should they arrest the individual? We offer the following five recommendations.
Key recommendations
- Patients who require interhospital transport for an acute behavioral health crisis should be transported by medical professionals with the training and expertise to manage mental health and medical conditions.
- Interhospital transport restraint guidelines should be in line with CMS guidelines for hospital restraints. No patient that is not under law enforcement custody should be transported in law enforcement restraints.
- Patients at high risk for violence/agitation (an underlying condition causing violence/agitation may include dementia, traumatic brain injuries, delirium, SUDs, or psychiatric conditions) should be managed in accordance with medically indicated intervention such as medical restraints or medications.
- If required, a request should be made for law enforcement officers to accompany EMS to provide support and to ensure the safety of the patient and EMS professionals during the transport.
- EMS professionals should receive specific training to manage acute psychiatric and SUD conditions, and should be aware of the life-threatening medical complications that can result from SUDs and psychiatric conditions/medications.
We recognize that patients with SMI require clinicians to work collaboratively, perhaps with law enforcement, to safely transport them from one point to another. Only when the rules we have outlined are followed will our patients get transported in such ways that allow them to get the care they need.
Dr. Norris is editor-in-chief of MDedge Psychiatry, and assistant professor of psychiatry and behavioral sciences at George Washington University, Washington. He serves as assistant dean of student affairs at the university, and medical director of psychiatric and behavioral sciences at GWU Hospital. Ms. Palmieri is a managing partner of Healthcare Legal Education & Consulting Network (HLECN), and the chief clinical officer and cofounder of XFERALL. HLECN focuses on clinical education and training, and XFERALL is a company that provides a technology platform aimed at improving access to care for behavioral health and medical patients. Ms. Slater is a managing partner of legal education for HLECN, and a trial attorney at Colley Shroyer & Abraham in Columbus, Ohio. Mr. Whaley is director of the safety and security department at GWU Hospital.
References
1. National Institute of Mental Health: Suicide.
2. National Institute on Drug Abuse. Overdose death rates. Revised January 2019.
3. Post by former NIMH Director Thomas Insel: No health without mental health. Sept. 6, 2011.
4. Dhar AK and Barton DA. Depression and the link with cardiovascular disease. Front Psychiatry. 2016 Mar 21;7:33.
5. Lichtman JH et al. Depression and coronary heart disease. Circulation. 2008;118:1768-75.
6. Hare DL et al. Depression and cardiovascular disease: A clinical review. European Heart J. 2014 Jun;35(21):1365-72.
7. “ ‘How many people have to die?’ SC mental health patients endure nightmare transport.” The News & Observer. 2019 May 29.
8. 42 C.F.R. Part 482. Part IV. Department of Health and Human Services. Medicare & Medicaid programs; Hospital conditions of participation; Patients’ rights; Final rule. 2006 Dec 8.
“I’ve given up, doctor. We gave it our best, but I am at the point where I want to end my life.” You receive this call at 2 a.m., and you’re flooded with a series of emotions and are bewildered – until your training kicks in.
Countless hours of working with patients in emergency department settings while on call as a resident inform your ability to triage the situation. Years of supervision guide your supportive statements as you work collaboratively with your patient to address the emotional and existential distress. As the call proceeds and you realize that your patient will require hospitalization, you are struck by a sobering question: “How am I going to arrange for my patient to go to the nearest hospital in the middle of the night?”
The options for transporting patients with serious mental illness (SMI) typically vary from bad to worse and usually filter down to three possibilities:
1. Get a friend or family member to transport them to the nearest ED.
2. Call emergency medical services (EMS) for transport to the nearest ED.
3. Call the police and request transport to the nearest ED.
Several factors would determine which of those options you would use alone or in combination. Current training paradigms for mental health professionals offer a limited body of literature on evidenced-based strategies for patients with SMI. At best – if not handled properly – these experiences can aggravate patients’ mental health conditions. At worst, they can lead to the loss of our patients. Together, we have more than 40 years’ experience working in complex mental health care systems that run the gamut, from providing direct clinical care to directing mental health care divisions.
Sobering statistics prevail
In 2017, suicide was the 10th leading cause of death in the United States, accounting for more than 47,000 deaths. Suicide was the second-leading cause of death among individuals aged 10-34 and the fourth leading cause of death for individuals aged 35- 54.1 In 2017, more than 70,200 Americans died from a drug overdose, including illicit drugs and prescription opioids.2 Drug overdose deaths nearly quadrupled between 1999 and 2017, from 16,849 deaths to 70,237, respectively.2
The life expectancy of an American with SMI is 14-32 years less than that of the average population.3 Those numbers are on par with many sub-Saharan countries, including Sudan and Ethiopia, and surpass the health disparities for most racial and ethnic groups.
The decrease in life expectancy for people with SMI is rarely the result of suicide but rather the effect of medical comorbidities, including heart disease, stroke, pulmonary disease, diabetes, and cancer.3 Individuals with SMI are much more likely to suffer from chronic illnesses that are associated with co-occurring addictions, side effects of psychotropic medications, and social determinants of mental health, such as poverty.
Major depressive disorder among people with SMI presents acute and chronic medical risks. For example, people with major depressive disorder are at a higher risk for stroke and cardiovascular disease.4 There is a threefold increase in cardiac-related deaths for individuals who experience depression after a heart attack.5 In addition, depression increases the risk of cardiac-related death after a heart attack more than any other risk factor, except for congestive heart failure.6
The transportation challenge
When the complexity of psychiatric conditions is conceptualized to include decreased life expectancy because of medical comorbidities, medical complications that can result from psychotropic medications, and the high incidence of co-occurring substance use disorders (SUDs), it is clear why we are concerned about the type of transport used for patients experiencing a psychiatric emergency.
A common practice for patients presenting for medical treatment for a mental health condition is for them to be transported by law enforcement in handcuffs, or by private vehicle, because of a lack of medical transport options.
One tragic example occurred on Sept. 18, 2018, when two Horry County, S.C., deputies were providing a hospital-to-hospital transport for two mental health patients. The patients, who had no legal charges and were not under arrest, were locked in a transport cage in the back of a law enforcement vehicle for transport during Hurricane Florence. While the driver tried to move through floodwaters, the car stalled and became submerged. The patients were unable to open the locked cage door, and the deputies responsible for the transport did not have a key to unlock the cage.
The two women died as a result of the incident. Both deputies are facing two counts of involuntary manslaughter – with a potential prison sentence of 5 years each.7
The system that promotes the use of law enforcement to transport medical patients who are not in legal custody perpetuates a high risk to patients. Also at risk are law enforcement professionals who often are not adequately trained to evaluate, intervene, and manage patients in need of medical treatment (for acute medical, SUDs, or mental illness).
Recommendations for transporting high-risk patients
The legal and regulatory standards required by the Centers for Medicare & Medicaid Services guidelines8 for behavioral health patients are consistent in saying that law enforcement restraints cannot be used in hospital settings – unless the patient is under law enforcement custody. If the patient is admitted to an inpatient psychiatric unit, law enforcement restraints are never allowed to be used. Despite those guidelines for handling these situations within hospital settings, a similar standard does not exist for interhospital transport of high-risk behavioral health patients.
Patients often are transported between facilities by law enforcement, and at times, with the use of law enforcement restraints. However, use of law enforcement for interhospital transport of patients not in the custody of law enforcement is both detrimental to and clinically dangerous for the patient. Not only does the scenario put the patient at risk, but it also places law enforcement professionals at risk with the potential for legal liability if the patient medically decompensates during the transport.
Also, using law enforcement to intervene and provide transportation for behavioral health patients in crisis might cause further harm to the patient’s psychological condition and deter the patient from presenting for treatment.
The appropriate level of interfacility transport for a behavioral health patient requiring an inpatient level of care is secure transport with trained medical professionals. If necessary, restraint guidelines should follow the same standard as they do in hospital settings. In situations with high risk for violence or agitation, law enforcement should be requested to accompany EMS during the transport. Handling the situation in this way allows for a collaborative approach to provide adequate medical support, and provide for the physical safety and security of the patient – and of EMS personnel.
Across police and sheriffs’ departments nationwide, law enforcement officers are required to transport mental health patients from one location or hospital to another. Hospitals and outpatient locations, often with no alternative, rely on local law enforcement agencies to provide safe transport between acute and mental health facilities. Departmental policies and the widespread belief that mental health patients automatically pose a substantial danger to themselves or others have led to these patients being handcuffed and put in the back of police cruisers. Essentially, they are treated like criminals who are under arrest.
The CMS has strict criteria for ordering, applying, evaluating, reevaluating, and reporting restraint-associated deaths. Likewise, The Joint Commission, during its accreditation survey, rightly scrutinizes a facility’s use of restraints. Both the CMS and The Joint Commission define restraint by the function of the device and not the type of the device.
According to the CMS, a restraint is any manual method, physical or mechanic device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely. Within a police cruiser, handcuffs on a mental health patient who is not under arrest would fall squarely within this definition of restraint.
A patient’s current behavior or clinical needs – not history or diagnosis – should determine whether a restraint is warranted. A patient experiencing a psychiatric crisis who is not under arrest might very well escalate and become destructive and combative when being placed in handcuffs in the back of a police vehicle. What should police do at that point? Should they arrest the individual? We offer the following five recommendations.
Key recommendations
- Patients who require interhospital transport for an acute behavioral health crisis should be transported by medical professionals with the training and expertise to manage mental health and medical conditions.
- Interhospital transport restraint guidelines should be in line with CMS guidelines for hospital restraints. No patient that is not under law enforcement custody should be transported in law enforcement restraints.
- Patients at high risk for violence/agitation (an underlying condition causing violence/agitation may include dementia, traumatic brain injuries, delirium, SUDs, or psychiatric conditions) should be managed in accordance with medically indicated intervention such as medical restraints or medications.
- If required, a request should be made for law enforcement officers to accompany EMS to provide support and to ensure the safety of the patient and EMS professionals during the transport.
- EMS professionals should receive specific training to manage acute psychiatric and SUD conditions, and should be aware of the life-threatening medical complications that can result from SUDs and psychiatric conditions/medications.
We recognize that patients with SMI require clinicians to work collaboratively, perhaps with law enforcement, to safely transport them from one point to another. Only when the rules we have outlined are followed will our patients get transported in such ways that allow them to get the care they need.
Dr. Norris is editor-in-chief of MDedge Psychiatry, and assistant professor of psychiatry and behavioral sciences at George Washington University, Washington. He serves as assistant dean of student affairs at the university, and medical director of psychiatric and behavioral sciences at GWU Hospital. Ms. Palmieri is a managing partner of Healthcare Legal Education & Consulting Network (HLECN), and the chief clinical officer and cofounder of XFERALL. HLECN focuses on clinical education and training, and XFERALL is a company that provides a technology platform aimed at improving access to care for behavioral health and medical patients. Ms. Slater is a managing partner of legal education for HLECN, and a trial attorney at Colley Shroyer & Abraham in Columbus, Ohio. Mr. Whaley is director of the safety and security department at GWU Hospital.
References
1. National Institute of Mental Health: Suicide.
2. National Institute on Drug Abuse. Overdose death rates. Revised January 2019.
3. Post by former NIMH Director Thomas Insel: No health without mental health. Sept. 6, 2011.
4. Dhar AK and Barton DA. Depression and the link with cardiovascular disease. Front Psychiatry. 2016 Mar 21;7:33.
5. Lichtman JH et al. Depression and coronary heart disease. Circulation. 2008;118:1768-75.
6. Hare DL et al. Depression and cardiovascular disease: A clinical review. European Heart J. 2014 Jun;35(21):1365-72.
7. “ ‘How many people have to die?’ SC mental health patients endure nightmare transport.” The News & Observer. 2019 May 29.
8. 42 C.F.R. Part 482. Part IV. Department of Health and Human Services. Medicare & Medicaid programs; Hospital conditions of participation; Patients’ rights; Final rule. 2006 Dec 8.
June Medical Services v. Russo: Understanding this high-stakes abortion case
On March 4, 2020, the Supreme Court of the United States (SCOTUS) will hear opening arguments for June Medical Services v. Russo. (Please note that this case was originally referred to as June Medical Services v. Gee. However, Secretary Rebekah Gee resigned from her position on January 31, 2020, and was replaced by Interim Secretary Stephen Russo.) The case will examine a Louisiana law (Louisiana Act 620, or LA 620), originally passed in 2014, that requires physicians to have hospital admitting privileges within 30 miles of where they provide abortion services.1 When LA 620 was signed into law in 2014, 5 of Louisiana’s 6 abortion clinics would not have met the standards created by this legislation and would have been forced to close, potentially leaving the vast majority of women in Louisiana without access to an abortion provider, and disproportionately impacting poor and rural women. Prior to enactment of this law, physicians at these 5 clinics attempted to obtain admitting privileges, and all were denied. The denials occurred due to two main reasons—because the providers admitted too few patients each year to qualify for hospital privileges or simply because they provided abortion care.2 Shortly after this legislation was signed into law, the Center for Reproductive Rights (CRR) challenged the law, citing the undue burden it created for patients attempting to access abortion care.
Prior case also considered question of hospital privileges for abortion providers
Interestingly, SCOTUS already has ruled on this very question. In 1992, the Court ruled in Planned Parenthood of Southeastern Pennsylvania v. Casey that it is unconstitutional for a state to create an “undue burden” on a woman’s right to abortion prior to fetal viability.3 And in 2016, when considering whether or not requiring abortion providers to obtain hospital privileges creates an undue burden in Whole Women’s Health (WWH) v. Hellerstedt, the Supreme Court’s answer was yes, it does. WWH, with legal aid from CRR, challenged Texas House Bill 2 (H.B. 2), which similar to LA 620, required abortion providers to have local admitting privileges. Based largely on the precedent set in Casey, SCOTUS ruled 5-3 in favor of WWH.
The Louisiana law currently in question was written and challenged in district court simultaneous to the Supreme Court’s review of WWH. The district court declared LA 620 invalid and permanently enjoined its enforcement, finding the law would “drastically burden women’s right to choose abortions.”4 However, the US Court of Appeals for the Fifth Circuit reviewed the case and overturned the district court decision, finding the lower court’s analysis erroneous and stating, “no clinics will likely be forced to close on account of [LA 620].” The Fifth Circuit panel ruled that, despite the precedent of WWH, LA 620 did not create an undue burden because of state-level differences in admitting privileges, demographics, and geography. They also found that only 30% of the 2 million women living in Louisiana would be impacted by the law, predominantly via longer wait times, and argued that this does not represent significant burden. The plaintiffs filed for an emergency stay with SCOTUS, who granted the stay pending a full hearing. On March 4, the Supreme Court will hear arguments to determine if the Fifth Circuit was correct in drawing a distinction between LA 620 and the SCOTUS verdict in WWH.
Targeted restrictions on abortion providers
LA 620 joins a long series of laws meant to enact targeted restrictions on abortion providers, or “TRAP” laws. TRAP laws are written to limit access to abortion under the guise of improving patient safety, despite ample evidence to the contrary, and include such various regulations as admitting privileges, facilities requirements, waiting periods, and parental or partner notification. Many such laws have been enacted in the last decade, and many struck down based on judicial precedent.
How the Supreme Court has ruled in the past
When a case is appealed to the Supreme Court, the court can either decline to hear the case, thereby leaving the lower courts’ ruling in place, or choose to hear the case in full and either affirm or overturn the lower court’s decision. After issuing a ruling in WWH, the 2016-2017 Roberts Court declined to hear challenges from other states with similarly overturned laws, leaving the laws struck down. In electing to hear June Medical Services v. Russo, the court has the opportunity to uphold or overturn the Fifth Circuit Court’s decision. However, today’s Supreme Court differs greatly from the Supreme Court in 2016.
In 2016, the court ruled 5-3 to overturn H.B. 2 in WWH shortly after the death of Justice Antonin Scalia. Scalia was replaced by Justice Neil Gorsuch, a Constitutional originalist who has never directly ruled on an abortion case.5 In 2018, Justice Anthony Kennedy, who authored the court’s majority opinion on Casey and was among the majority on WWH, retired, and was replaced by Justice Brett Kavanaugh. Kavanaugh has ruled once on the right to abortion in Garza v. Hargan in 2017, where he argued that precedent states that the government has “permissible interests in favoring fetal life…and refraining from facilitating abortion,” and that significant delay in care did not constitute undue burden.6 In regard to the 5-4 stay issued by the court in June Medical Services, Kavanaugh joined Gorsuch in voting to deny the application for stay, and was the only justice to issue an opinion alongside the ruling, arguing that because the doctors in question had not applied for and been denied admitting privileges since the WWH ruling, the case hinges on theoretical rather than demonstrable undue burden.7 Appointed by President Donald Trump, both Gorsuch and Kavanaugh are widely considered to be conservative judges, and while neither has a strong judicial record on abortion rights, both are anticipated to side with the conservative majority on the court.
The Supreme Court rarely overturns its own precedent, but concerns are high
The question of precedent will be central in SCOTUS hearing June Medical Services v. Russo so quickly after the WWH decision. Additionally, in hearing this case, the court will have the opportunity to reexamine all relevant precedent, including the Planned Parenthood of Southeastern Pennsylvania v. Casey decision and even Roe v. Wade. With a conservative court and an increasingly charged political environment, reproductive rights advocates fear that the June Medical Services v. Russo ruling may be the first step toward dismantling judicial protection of abortion rights in the United States.
If SCOTUS rules against June Medical Services, stating that admitting privileges do not cause an undue burden for women seeking to access abortion care, other states likely will introduce and enact similar legislation. These TRAP laws have the potential to limit or eliminate access to abortion for 25 million people of reproductive age. Numerous studies have demonstrated that limiting access to abortion care does not decrease the number of abortions but can result in patients using unsafe means to obtain an abortion.8
The medical community recognizes the danger of enacting restrictive legislation. The American College of Obstetricians and Gynecologists (ACOG), along with the American Medical Association, the Society of Maternal-Fetal Medicine, the Association for Sexual and Reproductive Medicine, the American Association of Family Practitioners, and many others, filed an amicus curiae in support of the June Medical Services plaintiffs.9 These brief filings are critical to ensuring the courts hear physician voices in this important legal decision, and ACOG’s briefs have been quoted in several previous Supreme Court opinions, concurrences, and dissents.
Action items
- Although June Medical Services v. Russo’s decision will not be made until early summer 2020, we can continue to use our voices and expertise to speak out against laws designed to limit access to abortion—at the state and federal levels. As women’s health clinicians, we see the impact abortion restrictions have on our patients, especially our low income and rural patients. Sharing these stories with our legislators, testifying for or against legislation, and speaking out in our communities can have a powerful impact. Check with your local ACOG chapter or with ACOG’s state and government affairs office for more information.
- Follow along with this case at SCOTUS Blog.
- Lastly, make sure you are registered to vote. We are in an election year, and using our voices in and out of the ballot box is critical. You can register here.
- HB338. Louisiana State Legislature. 2014. http://www.legis.la.gov/legis/BillInfo.aspx?s=14RS&b=ACT620&sbi=y. Accessed February 19, 2020.
- Nash E, Donovan MK. Admitting priveleges are back at the U.S. Supreme Court with serious implications for abortion access. Guttmacher Institute. Updated December 3, 2019.
- Planned Parenthood of Southeastern Pennsylvania v. Casey. Cornell Law School Legal Information Institute. https://www.law.cornell.edu/supremecourt/text/505/833. Accessed February 20, 2020.
- June Medical Services LLC v Gee. Oyez. www.oyez.org/cases/2019/18-1323. Accessed February 20, 2020.
- Neil Gorsuch. Oyez. https://www.oyez.org/justices/neil_gorsuch. Accessed February 20, 2020.
- Judge Kavanaugh’s Judicial Record on the Right to Abortion. Center for Reproductive Rights. https://www.reproductiverights.org/sites/crr.civicactions.net/files/documents/factsheets/Judge-Kavanaugh-Judicial-Record-on-the-Right-to-Abortion2.pdf. Accessed February 20, 2020.
- Kavanaugh B. (2019, February 7). June Medical Services, L.L.C, v. Gee, 586 U.S. ____ (2019). Supreme Court of the United States. https://www.supremecourt.gov/opinions/18pdf/18a774_3ebh.pdf. Accessed February 20, 2020.
- Cohen SA. Facts and consequences: Legality, incidence and safety of abortion worldwide. November 20, 2009.
- June Medical Services, LLC v. Russo. SCOTUSblog. February 6, 2020. https://www.scotusblog.com/case-files/cases/june-medical-services-llc-v-russo/. Accessed February 20, 2020.
On March 4, 2020, the Supreme Court of the United States (SCOTUS) will hear opening arguments for June Medical Services v. Russo. (Please note that this case was originally referred to as June Medical Services v. Gee. However, Secretary Rebekah Gee resigned from her position on January 31, 2020, and was replaced by Interim Secretary Stephen Russo.) The case will examine a Louisiana law (Louisiana Act 620, or LA 620), originally passed in 2014, that requires physicians to have hospital admitting privileges within 30 miles of where they provide abortion services.1 When LA 620 was signed into law in 2014, 5 of Louisiana’s 6 abortion clinics would not have met the standards created by this legislation and would have been forced to close, potentially leaving the vast majority of women in Louisiana without access to an abortion provider, and disproportionately impacting poor and rural women. Prior to enactment of this law, physicians at these 5 clinics attempted to obtain admitting privileges, and all were denied. The denials occurred due to two main reasons—because the providers admitted too few patients each year to qualify for hospital privileges or simply because they provided abortion care.2 Shortly after this legislation was signed into law, the Center for Reproductive Rights (CRR) challenged the law, citing the undue burden it created for patients attempting to access abortion care.
Prior case also considered question of hospital privileges for abortion providers
Interestingly, SCOTUS already has ruled on this very question. In 1992, the Court ruled in Planned Parenthood of Southeastern Pennsylvania v. Casey that it is unconstitutional for a state to create an “undue burden” on a woman’s right to abortion prior to fetal viability.3 And in 2016, when considering whether or not requiring abortion providers to obtain hospital privileges creates an undue burden in Whole Women’s Health (WWH) v. Hellerstedt, the Supreme Court’s answer was yes, it does. WWH, with legal aid from CRR, challenged Texas House Bill 2 (H.B. 2), which similar to LA 620, required abortion providers to have local admitting privileges. Based largely on the precedent set in Casey, SCOTUS ruled 5-3 in favor of WWH.
The Louisiana law currently in question was written and challenged in district court simultaneous to the Supreme Court’s review of WWH. The district court declared LA 620 invalid and permanently enjoined its enforcement, finding the law would “drastically burden women’s right to choose abortions.”4 However, the US Court of Appeals for the Fifth Circuit reviewed the case and overturned the district court decision, finding the lower court’s analysis erroneous and stating, “no clinics will likely be forced to close on account of [LA 620].” The Fifth Circuit panel ruled that, despite the precedent of WWH, LA 620 did not create an undue burden because of state-level differences in admitting privileges, demographics, and geography. They also found that only 30% of the 2 million women living in Louisiana would be impacted by the law, predominantly via longer wait times, and argued that this does not represent significant burden. The plaintiffs filed for an emergency stay with SCOTUS, who granted the stay pending a full hearing. On March 4, the Supreme Court will hear arguments to determine if the Fifth Circuit was correct in drawing a distinction between LA 620 and the SCOTUS verdict in WWH.
Targeted restrictions on abortion providers
LA 620 joins a long series of laws meant to enact targeted restrictions on abortion providers, or “TRAP” laws. TRAP laws are written to limit access to abortion under the guise of improving patient safety, despite ample evidence to the contrary, and include such various regulations as admitting privileges, facilities requirements, waiting periods, and parental or partner notification. Many such laws have been enacted in the last decade, and many struck down based on judicial precedent.
How the Supreme Court has ruled in the past
When a case is appealed to the Supreme Court, the court can either decline to hear the case, thereby leaving the lower courts’ ruling in place, or choose to hear the case in full and either affirm or overturn the lower court’s decision. After issuing a ruling in WWH, the 2016-2017 Roberts Court declined to hear challenges from other states with similarly overturned laws, leaving the laws struck down. In electing to hear June Medical Services v. Russo, the court has the opportunity to uphold or overturn the Fifth Circuit Court’s decision. However, today’s Supreme Court differs greatly from the Supreme Court in 2016.
In 2016, the court ruled 5-3 to overturn H.B. 2 in WWH shortly after the death of Justice Antonin Scalia. Scalia was replaced by Justice Neil Gorsuch, a Constitutional originalist who has never directly ruled on an abortion case.5 In 2018, Justice Anthony Kennedy, who authored the court’s majority opinion on Casey and was among the majority on WWH, retired, and was replaced by Justice Brett Kavanaugh. Kavanaugh has ruled once on the right to abortion in Garza v. Hargan in 2017, where he argued that precedent states that the government has “permissible interests in favoring fetal life…and refraining from facilitating abortion,” and that significant delay in care did not constitute undue burden.6 In regard to the 5-4 stay issued by the court in June Medical Services, Kavanaugh joined Gorsuch in voting to deny the application for stay, and was the only justice to issue an opinion alongside the ruling, arguing that because the doctors in question had not applied for and been denied admitting privileges since the WWH ruling, the case hinges on theoretical rather than demonstrable undue burden.7 Appointed by President Donald Trump, both Gorsuch and Kavanaugh are widely considered to be conservative judges, and while neither has a strong judicial record on abortion rights, both are anticipated to side with the conservative majority on the court.
The Supreme Court rarely overturns its own precedent, but concerns are high
The question of precedent will be central in SCOTUS hearing June Medical Services v. Russo so quickly after the WWH decision. Additionally, in hearing this case, the court will have the opportunity to reexamine all relevant precedent, including the Planned Parenthood of Southeastern Pennsylvania v. Casey decision and even Roe v. Wade. With a conservative court and an increasingly charged political environment, reproductive rights advocates fear that the June Medical Services v. Russo ruling may be the first step toward dismantling judicial protection of abortion rights in the United States.
If SCOTUS rules against June Medical Services, stating that admitting privileges do not cause an undue burden for women seeking to access abortion care, other states likely will introduce and enact similar legislation. These TRAP laws have the potential to limit or eliminate access to abortion for 25 million people of reproductive age. Numerous studies have demonstrated that limiting access to abortion care does not decrease the number of abortions but can result in patients using unsafe means to obtain an abortion.8
The medical community recognizes the danger of enacting restrictive legislation. The American College of Obstetricians and Gynecologists (ACOG), along with the American Medical Association, the Society of Maternal-Fetal Medicine, the Association for Sexual and Reproductive Medicine, the American Association of Family Practitioners, and many others, filed an amicus curiae in support of the June Medical Services plaintiffs.9 These brief filings are critical to ensuring the courts hear physician voices in this important legal decision, and ACOG’s briefs have been quoted in several previous Supreme Court opinions, concurrences, and dissents.
Action items
- Although June Medical Services v. Russo’s decision will not be made until early summer 2020, we can continue to use our voices and expertise to speak out against laws designed to limit access to abortion—at the state and federal levels. As women’s health clinicians, we see the impact abortion restrictions have on our patients, especially our low income and rural patients. Sharing these stories with our legislators, testifying for or against legislation, and speaking out in our communities can have a powerful impact. Check with your local ACOG chapter or with ACOG’s state and government affairs office for more information.
- Follow along with this case at SCOTUS Blog.
- Lastly, make sure you are registered to vote. We are in an election year, and using our voices in and out of the ballot box is critical. You can register here.
On March 4, 2020, the Supreme Court of the United States (SCOTUS) will hear opening arguments for June Medical Services v. Russo. (Please note that this case was originally referred to as June Medical Services v. Gee. However, Secretary Rebekah Gee resigned from her position on January 31, 2020, and was replaced by Interim Secretary Stephen Russo.) The case will examine a Louisiana law (Louisiana Act 620, or LA 620), originally passed in 2014, that requires physicians to have hospital admitting privileges within 30 miles of where they provide abortion services.1 When LA 620 was signed into law in 2014, 5 of Louisiana’s 6 abortion clinics would not have met the standards created by this legislation and would have been forced to close, potentially leaving the vast majority of women in Louisiana without access to an abortion provider, and disproportionately impacting poor and rural women. Prior to enactment of this law, physicians at these 5 clinics attempted to obtain admitting privileges, and all were denied. The denials occurred due to two main reasons—because the providers admitted too few patients each year to qualify for hospital privileges or simply because they provided abortion care.2 Shortly after this legislation was signed into law, the Center for Reproductive Rights (CRR) challenged the law, citing the undue burden it created for patients attempting to access abortion care.
Prior case also considered question of hospital privileges for abortion providers
Interestingly, SCOTUS already has ruled on this very question. In 1992, the Court ruled in Planned Parenthood of Southeastern Pennsylvania v. Casey that it is unconstitutional for a state to create an “undue burden” on a woman’s right to abortion prior to fetal viability.3 And in 2016, when considering whether or not requiring abortion providers to obtain hospital privileges creates an undue burden in Whole Women’s Health (WWH) v. Hellerstedt, the Supreme Court’s answer was yes, it does. WWH, with legal aid from CRR, challenged Texas House Bill 2 (H.B. 2), which similar to LA 620, required abortion providers to have local admitting privileges. Based largely on the precedent set in Casey, SCOTUS ruled 5-3 in favor of WWH.
The Louisiana law currently in question was written and challenged in district court simultaneous to the Supreme Court’s review of WWH. The district court declared LA 620 invalid and permanently enjoined its enforcement, finding the law would “drastically burden women’s right to choose abortions.”4 However, the US Court of Appeals for the Fifth Circuit reviewed the case and overturned the district court decision, finding the lower court’s analysis erroneous and stating, “no clinics will likely be forced to close on account of [LA 620].” The Fifth Circuit panel ruled that, despite the precedent of WWH, LA 620 did not create an undue burden because of state-level differences in admitting privileges, demographics, and geography. They also found that only 30% of the 2 million women living in Louisiana would be impacted by the law, predominantly via longer wait times, and argued that this does not represent significant burden. The plaintiffs filed for an emergency stay with SCOTUS, who granted the stay pending a full hearing. On March 4, the Supreme Court will hear arguments to determine if the Fifth Circuit was correct in drawing a distinction between LA 620 and the SCOTUS verdict in WWH.
Targeted restrictions on abortion providers
LA 620 joins a long series of laws meant to enact targeted restrictions on abortion providers, or “TRAP” laws. TRAP laws are written to limit access to abortion under the guise of improving patient safety, despite ample evidence to the contrary, and include such various regulations as admitting privileges, facilities requirements, waiting periods, and parental or partner notification. Many such laws have been enacted in the last decade, and many struck down based on judicial precedent.
How the Supreme Court has ruled in the past
When a case is appealed to the Supreme Court, the court can either decline to hear the case, thereby leaving the lower courts’ ruling in place, or choose to hear the case in full and either affirm or overturn the lower court’s decision. After issuing a ruling in WWH, the 2016-2017 Roberts Court declined to hear challenges from other states with similarly overturned laws, leaving the laws struck down. In electing to hear June Medical Services v. Russo, the court has the opportunity to uphold or overturn the Fifth Circuit Court’s decision. However, today’s Supreme Court differs greatly from the Supreme Court in 2016.
In 2016, the court ruled 5-3 to overturn H.B. 2 in WWH shortly after the death of Justice Antonin Scalia. Scalia was replaced by Justice Neil Gorsuch, a Constitutional originalist who has never directly ruled on an abortion case.5 In 2018, Justice Anthony Kennedy, who authored the court’s majority opinion on Casey and was among the majority on WWH, retired, and was replaced by Justice Brett Kavanaugh. Kavanaugh has ruled once on the right to abortion in Garza v. Hargan in 2017, where he argued that precedent states that the government has “permissible interests in favoring fetal life…and refraining from facilitating abortion,” and that significant delay in care did not constitute undue burden.6 In regard to the 5-4 stay issued by the court in June Medical Services, Kavanaugh joined Gorsuch in voting to deny the application for stay, and was the only justice to issue an opinion alongside the ruling, arguing that because the doctors in question had not applied for and been denied admitting privileges since the WWH ruling, the case hinges on theoretical rather than demonstrable undue burden.7 Appointed by President Donald Trump, both Gorsuch and Kavanaugh are widely considered to be conservative judges, and while neither has a strong judicial record on abortion rights, both are anticipated to side with the conservative majority on the court.
The Supreme Court rarely overturns its own precedent, but concerns are high
The question of precedent will be central in SCOTUS hearing June Medical Services v. Russo so quickly after the WWH decision. Additionally, in hearing this case, the court will have the opportunity to reexamine all relevant precedent, including the Planned Parenthood of Southeastern Pennsylvania v. Casey decision and even Roe v. Wade. With a conservative court and an increasingly charged political environment, reproductive rights advocates fear that the June Medical Services v. Russo ruling may be the first step toward dismantling judicial protection of abortion rights in the United States.
If SCOTUS rules against June Medical Services, stating that admitting privileges do not cause an undue burden for women seeking to access abortion care, other states likely will introduce and enact similar legislation. These TRAP laws have the potential to limit or eliminate access to abortion for 25 million people of reproductive age. Numerous studies have demonstrated that limiting access to abortion care does not decrease the number of abortions but can result in patients using unsafe means to obtain an abortion.8
The medical community recognizes the danger of enacting restrictive legislation. The American College of Obstetricians and Gynecologists (ACOG), along with the American Medical Association, the Society of Maternal-Fetal Medicine, the Association for Sexual and Reproductive Medicine, the American Association of Family Practitioners, and many others, filed an amicus curiae in support of the June Medical Services plaintiffs.9 These brief filings are critical to ensuring the courts hear physician voices in this important legal decision, and ACOG’s briefs have been quoted in several previous Supreme Court opinions, concurrences, and dissents.
Action items
- Although June Medical Services v. Russo’s decision will not be made until early summer 2020, we can continue to use our voices and expertise to speak out against laws designed to limit access to abortion—at the state and federal levels. As women’s health clinicians, we see the impact abortion restrictions have on our patients, especially our low income and rural patients. Sharing these stories with our legislators, testifying for or against legislation, and speaking out in our communities can have a powerful impact. Check with your local ACOG chapter or with ACOG’s state and government affairs office for more information.
- Follow along with this case at SCOTUS Blog.
- Lastly, make sure you are registered to vote. We are in an election year, and using our voices in and out of the ballot box is critical. You can register here.
- HB338. Louisiana State Legislature. 2014. http://www.legis.la.gov/legis/BillInfo.aspx?s=14RS&b=ACT620&sbi=y. Accessed February 19, 2020.
- Nash E, Donovan MK. Admitting priveleges are back at the U.S. Supreme Court with serious implications for abortion access. Guttmacher Institute. Updated December 3, 2019.
- Planned Parenthood of Southeastern Pennsylvania v. Casey. Cornell Law School Legal Information Institute. https://www.law.cornell.edu/supremecourt/text/505/833. Accessed February 20, 2020.
- June Medical Services LLC v Gee. Oyez. www.oyez.org/cases/2019/18-1323. Accessed February 20, 2020.
- Neil Gorsuch. Oyez. https://www.oyez.org/justices/neil_gorsuch. Accessed February 20, 2020.
- Judge Kavanaugh’s Judicial Record on the Right to Abortion. Center for Reproductive Rights. https://www.reproductiverights.org/sites/crr.civicactions.net/files/documents/factsheets/Judge-Kavanaugh-Judicial-Record-on-the-Right-to-Abortion2.pdf. Accessed February 20, 2020.
- Kavanaugh B. (2019, February 7). June Medical Services, L.L.C, v. Gee, 586 U.S. ____ (2019). Supreme Court of the United States. https://www.supremecourt.gov/opinions/18pdf/18a774_3ebh.pdf. Accessed February 20, 2020.
- Cohen SA. Facts and consequences: Legality, incidence and safety of abortion worldwide. November 20, 2009.
- June Medical Services, LLC v. Russo. SCOTUSblog. February 6, 2020. https://www.scotusblog.com/case-files/cases/june-medical-services-llc-v-russo/. Accessed February 20, 2020.
- HB338. Louisiana State Legislature. 2014. http://www.legis.la.gov/legis/BillInfo.aspx?s=14RS&b=ACT620&sbi=y. Accessed February 19, 2020.
- Nash E, Donovan MK. Admitting priveleges are back at the U.S. Supreme Court with serious implications for abortion access. Guttmacher Institute. Updated December 3, 2019.
- Planned Parenthood of Southeastern Pennsylvania v. Casey. Cornell Law School Legal Information Institute. https://www.law.cornell.edu/supremecourt/text/505/833. Accessed February 20, 2020.
- June Medical Services LLC v Gee. Oyez. www.oyez.org/cases/2019/18-1323. Accessed February 20, 2020.
- Neil Gorsuch. Oyez. https://www.oyez.org/justices/neil_gorsuch. Accessed February 20, 2020.
- Judge Kavanaugh’s Judicial Record on the Right to Abortion. Center for Reproductive Rights. https://www.reproductiverights.org/sites/crr.civicactions.net/files/documents/factsheets/Judge-Kavanaugh-Judicial-Record-on-the-Right-to-Abortion2.pdf. Accessed February 20, 2020.
- Kavanaugh B. (2019, February 7). June Medical Services, L.L.C, v. Gee, 586 U.S. ____ (2019). Supreme Court of the United States. https://www.supremecourt.gov/opinions/18pdf/18a774_3ebh.pdf. Accessed February 20, 2020.
- Cohen SA. Facts and consequences: Legality, incidence and safety of abortion worldwide. November 20, 2009.
- June Medical Services, LLC v. Russo. SCOTUSblog. February 6, 2020. https://www.scotusblog.com/case-files/cases/june-medical-services-llc-v-russo/. Accessed February 20, 2020.
Nail dystrophy and nail plate thinning
At a follow-up visit, a biopsy of the skin on the fingertips was performed, which showed lichenoid lymphocytic inflammatory infiltrate with associated hyperkeratosis, hypergranulosis, and acanthosis.
No fungal elements were seen. The findings were consistent with lichen planus.
The patient was started on hydroxychloroquine. It was recommended she start a 6-week course of oral prednisone, but the mother was opposed to systemic treatment because of potential side effects.
She continued topical betamethasone without much change. Topical tacrolimus later was recommended to use on off days of betamethasone, which led to no improvement. Narrow-band UVB also was started with minimal improvement. Unfortunately,
Nail lichen planus (NLP) in children is not a common condition.1 In a recent series from Chiheb et al., NLP was reported in 90 patients, of which 40% were children; a quarter of the patients reported having extracutaneous involvement as well.2 In another childhood LP series,14 % of the children presented with nail disease.3 It can be a severe disease that, if not treated aggressively, may lead to destruction of the nail bed. This condition seems to be more prevalent in boys than girls and more prevalent in African American children.3 Unfortunately, in this patient’s case, the mother was hesitant to use systemic therapy and aggressive treatment was delayed.
Possible but not clear associations with autoimmune conditions such as vitiligo, autoimmune thyroiditis, myasthenia gravis, alopecia areata, thymoma, autoimmune polyendocrinopathy, atopic dermatitis, and lichen nitidus have been described in children with LP.
The clinical characteristics of NLP include nail plate thinning with longitudinal ridging and fissuring, with or without pterygium; trachyonychia; and erythema of the lunula when the nail matrix is involved. When the nail bed is affected, the patient can present with onycholysis with or without subungual hyperkeratosis and violaceous hue of the nail bed.4 NLP can have three different clinical presentations described by Tosti et al., which include typical NLP, 20‐nail dystrophy (trachyonychia), and idiopathic nail atrophy. Idiopathic nail atrophy is described solely in children as an acute and rapid progression that leads to destruction of the nail within months, which appears to be the clinical presentation in our patient.
The differential diagnosis of nail dystrophy in children includes infectious processes such as onychomycosis, especially when children present with onycholysis and subungual hyperkeratosis. Because of this, it is recommended to perform a nail culture or submit a sample of nail clippings for microscopic evaluation to confirm the diagnosis of onychomycosis prior to starting systemic therapy in children. Fingernail involvement without toenail involvement is an unusual presentation of onychomycosis.
Twenty-nail dystrophy – also known as trachyonychia – can be caused by several inflammatory skin conditions such as lichen planus, psoriasis, eczema, pemphigus vulgaris, and alopecia areata. Clinically, there is uniformly monomorphic thinning of the nail plate with longitudinal ridging without splitting or pterygium.1 This is a benign condition and should not cause scarring. About 10% of the cases of 20-nail dystrophy are caused by lichen planus.
Nail psoriasis is characterized by nail pitting, oil spots on the nail plate, leukonychia, subungual hyperkeratosis, and onycholysis, as well as nail crumbling, which were not seen in our patient. Although her initial presentation was of 20-nail dystrophy, which also can be a presentation of nail psoriasis, its rapid evolution with associated nail atrophy and pterygium make it unlikely to be psoriasis in this particular patient.
Patients with pachyonychia congenita – which is a genetic disorder or keratinization caused by mutations on several genes encoding keratin such as K6a, K16, K17, K6b, and possibly K6c – present with nail thickening (pachyonychia) and discoloration of the nails, as well as pincer nails. These patients also present with oral leukokeratosis and focal palmoplantar keratoderma.
The main treatment of lichen planus is potent topical corticosteroids.
For nail disease, topical treatment may not be effective and systemic treatment may be necessary. Systemic corticosteroids have been used in several pediatric series varying from a short course given at a dose of 1- 2 mg/kg per day for 2 weeks to a longer 3-month course followed by tapering.3 There are several protocols of intramuscular triamcinolone at a dose of 0.5 mg/kg in children in once a month injections for about 3 months that have been reported successful with minimal side effects.1 Other medications reported useful in patients with NLP include dapsone and acitretin. Other treatment options include narrow-band UVB and PUVA.3
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego. Email her at [email protected].
References
1. Arch Dermatol. 2001 Aug;137(8):1027-32.
2. Ann Dermatol Venereol. 2015 Jan;142(1):21-5.
3. Pediatr Dermatol. 2014 Jan-Feb;31(1):59-67.
4. Dermatological diseases, in “Nails: Diagnosis, Therapy, and Surgery,” 3rd ed. (Oxford: Elsevier Saunders, 2005, p. 105).
At a follow-up visit, a biopsy of the skin on the fingertips was performed, which showed lichenoid lymphocytic inflammatory infiltrate with associated hyperkeratosis, hypergranulosis, and acanthosis.
No fungal elements were seen. The findings were consistent with lichen planus.
The patient was started on hydroxychloroquine. It was recommended she start a 6-week course of oral prednisone, but the mother was opposed to systemic treatment because of potential side effects.
She continued topical betamethasone without much change. Topical tacrolimus later was recommended to use on off days of betamethasone, which led to no improvement. Narrow-band UVB also was started with minimal improvement. Unfortunately,
Nail lichen planus (NLP) in children is not a common condition.1 In a recent series from Chiheb et al., NLP was reported in 90 patients, of which 40% were children; a quarter of the patients reported having extracutaneous involvement as well.2 In another childhood LP series,14 % of the children presented with nail disease.3 It can be a severe disease that, if not treated aggressively, may lead to destruction of the nail bed. This condition seems to be more prevalent in boys than girls and more prevalent in African American children.3 Unfortunately, in this patient’s case, the mother was hesitant to use systemic therapy and aggressive treatment was delayed.
Possible but not clear associations with autoimmune conditions such as vitiligo, autoimmune thyroiditis, myasthenia gravis, alopecia areata, thymoma, autoimmune polyendocrinopathy, atopic dermatitis, and lichen nitidus have been described in children with LP.
The clinical characteristics of NLP include nail plate thinning with longitudinal ridging and fissuring, with or without pterygium; trachyonychia; and erythema of the lunula when the nail matrix is involved. When the nail bed is affected, the patient can present with onycholysis with or without subungual hyperkeratosis and violaceous hue of the nail bed.4 NLP can have three different clinical presentations described by Tosti et al., which include typical NLP, 20‐nail dystrophy (trachyonychia), and idiopathic nail atrophy. Idiopathic nail atrophy is described solely in children as an acute and rapid progression that leads to destruction of the nail within months, which appears to be the clinical presentation in our patient.
The differential diagnosis of nail dystrophy in children includes infectious processes such as onychomycosis, especially when children present with onycholysis and subungual hyperkeratosis. Because of this, it is recommended to perform a nail culture or submit a sample of nail clippings for microscopic evaluation to confirm the diagnosis of onychomycosis prior to starting systemic therapy in children. Fingernail involvement without toenail involvement is an unusual presentation of onychomycosis.
Twenty-nail dystrophy – also known as trachyonychia – can be caused by several inflammatory skin conditions such as lichen planus, psoriasis, eczema, pemphigus vulgaris, and alopecia areata. Clinically, there is uniformly monomorphic thinning of the nail plate with longitudinal ridging without splitting or pterygium.1 This is a benign condition and should not cause scarring. About 10% of the cases of 20-nail dystrophy are caused by lichen planus.
Nail psoriasis is characterized by nail pitting, oil spots on the nail plate, leukonychia, subungual hyperkeratosis, and onycholysis, as well as nail crumbling, which were not seen in our patient. Although her initial presentation was of 20-nail dystrophy, which also can be a presentation of nail psoriasis, its rapid evolution with associated nail atrophy and pterygium make it unlikely to be psoriasis in this particular patient.
Patients with pachyonychia congenita – which is a genetic disorder or keratinization caused by mutations on several genes encoding keratin such as K6a, K16, K17, K6b, and possibly K6c – present with nail thickening (pachyonychia) and discoloration of the nails, as well as pincer nails. These patients also present with oral leukokeratosis and focal palmoplantar keratoderma.
The main treatment of lichen planus is potent topical corticosteroids.
For nail disease, topical treatment may not be effective and systemic treatment may be necessary. Systemic corticosteroids have been used in several pediatric series varying from a short course given at a dose of 1- 2 mg/kg per day for 2 weeks to a longer 3-month course followed by tapering.3 There are several protocols of intramuscular triamcinolone at a dose of 0.5 mg/kg in children in once a month injections for about 3 months that have been reported successful with minimal side effects.1 Other medications reported useful in patients with NLP include dapsone and acitretin. Other treatment options include narrow-band UVB and PUVA.3
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego. Email her at [email protected].
References
1. Arch Dermatol. 2001 Aug;137(8):1027-32.
2. Ann Dermatol Venereol. 2015 Jan;142(1):21-5.
3. Pediatr Dermatol. 2014 Jan-Feb;31(1):59-67.
4. Dermatological diseases, in “Nails: Diagnosis, Therapy, and Surgery,” 3rd ed. (Oxford: Elsevier Saunders, 2005, p. 105).
At a follow-up visit, a biopsy of the skin on the fingertips was performed, which showed lichenoid lymphocytic inflammatory infiltrate with associated hyperkeratosis, hypergranulosis, and acanthosis.
No fungal elements were seen. The findings were consistent with lichen planus.
The patient was started on hydroxychloroquine. It was recommended she start a 6-week course of oral prednisone, but the mother was opposed to systemic treatment because of potential side effects.
She continued topical betamethasone without much change. Topical tacrolimus later was recommended to use on off days of betamethasone, which led to no improvement. Narrow-band UVB also was started with minimal improvement. Unfortunately,
Nail lichen planus (NLP) in children is not a common condition.1 In a recent series from Chiheb et al., NLP was reported in 90 patients, of which 40% were children; a quarter of the patients reported having extracutaneous involvement as well.2 In another childhood LP series,14 % of the children presented with nail disease.3 It can be a severe disease that, if not treated aggressively, may lead to destruction of the nail bed. This condition seems to be more prevalent in boys than girls and more prevalent in African American children.3 Unfortunately, in this patient’s case, the mother was hesitant to use systemic therapy and aggressive treatment was delayed.
Possible but not clear associations with autoimmune conditions such as vitiligo, autoimmune thyroiditis, myasthenia gravis, alopecia areata, thymoma, autoimmune polyendocrinopathy, atopic dermatitis, and lichen nitidus have been described in children with LP.
The clinical characteristics of NLP include nail plate thinning with longitudinal ridging and fissuring, with or without pterygium; trachyonychia; and erythema of the lunula when the nail matrix is involved. When the nail bed is affected, the patient can present with onycholysis with or without subungual hyperkeratosis and violaceous hue of the nail bed.4 NLP can have three different clinical presentations described by Tosti et al., which include typical NLP, 20‐nail dystrophy (trachyonychia), and idiopathic nail atrophy. Idiopathic nail atrophy is described solely in children as an acute and rapid progression that leads to destruction of the nail within months, which appears to be the clinical presentation in our patient.
The differential diagnosis of nail dystrophy in children includes infectious processes such as onychomycosis, especially when children present with onycholysis and subungual hyperkeratosis. Because of this, it is recommended to perform a nail culture or submit a sample of nail clippings for microscopic evaluation to confirm the diagnosis of onychomycosis prior to starting systemic therapy in children. Fingernail involvement without toenail involvement is an unusual presentation of onychomycosis.
Twenty-nail dystrophy – also known as trachyonychia – can be caused by several inflammatory skin conditions such as lichen planus, psoriasis, eczema, pemphigus vulgaris, and alopecia areata. Clinically, there is uniformly monomorphic thinning of the nail plate with longitudinal ridging without splitting or pterygium.1 This is a benign condition and should not cause scarring. About 10% of the cases of 20-nail dystrophy are caused by lichen planus.
Nail psoriasis is characterized by nail pitting, oil spots on the nail plate, leukonychia, subungual hyperkeratosis, and onycholysis, as well as nail crumbling, which were not seen in our patient. Although her initial presentation was of 20-nail dystrophy, which also can be a presentation of nail psoriasis, its rapid evolution with associated nail atrophy and pterygium make it unlikely to be psoriasis in this particular patient.
Patients with pachyonychia congenita – which is a genetic disorder or keratinization caused by mutations on several genes encoding keratin such as K6a, K16, K17, K6b, and possibly K6c – present with nail thickening (pachyonychia) and discoloration of the nails, as well as pincer nails. These patients also present with oral leukokeratosis and focal palmoplantar keratoderma.
The main treatment of lichen planus is potent topical corticosteroids.
For nail disease, topical treatment may not be effective and systemic treatment may be necessary. Systemic corticosteroids have been used in several pediatric series varying from a short course given at a dose of 1- 2 mg/kg per day for 2 weeks to a longer 3-month course followed by tapering.3 There are several protocols of intramuscular triamcinolone at a dose of 0.5 mg/kg in children in once a month injections for about 3 months that have been reported successful with minimal side effects.1 Other medications reported useful in patients with NLP include dapsone and acitretin. Other treatment options include narrow-band UVB and PUVA.3
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego. Email her at [email protected].
References
1. Arch Dermatol. 2001 Aug;137(8):1027-32.
2. Ann Dermatol Venereol. 2015 Jan;142(1):21-5.
3. Pediatr Dermatol. 2014 Jan-Feb;31(1):59-67.
4. Dermatological diseases, in “Nails: Diagnosis, Therapy, and Surgery,” 3rd ed. (Oxford: Elsevier Saunders, 2005, p. 105).
An 8-year-old female child comes to our pediatric dermatology clinic for evaluation of onychomycosis on her fingernails. The mother stated the child started developing funny-looking nails 1 year prior to the visit. It started with only two fingernails affected and now has spread to all her fingernails. Her toenails are not involved.
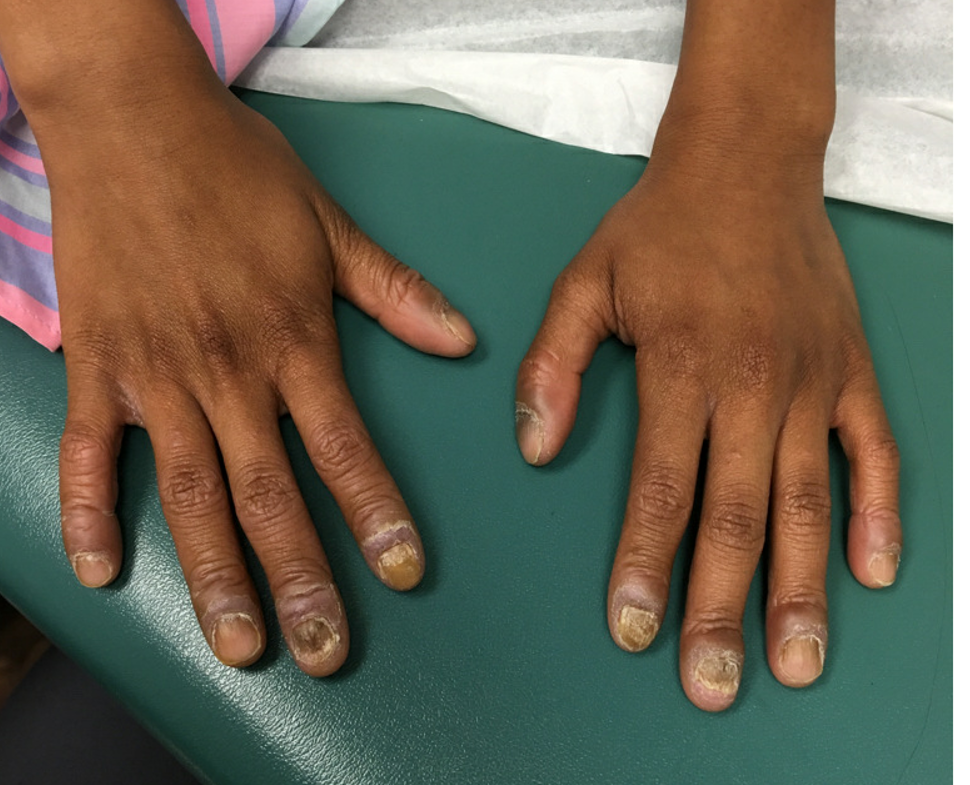
She denied any pain or itching. She initially was treated with topical antifungal medications as well as tea tree oil, apple cider vinegar, and a 6-week course of oral griseofulvin without any improvement. Her nails progressively have gotten much worse. She has no history of atopic dermatitis or any other skin conditions. She denied any joint pain, sun sensitivity, hair loss, or any other symptoms. The mother denied any family history of nail fungus, ringworm, psoriasis, or eczema.
She likes to play basketball and enjoys arts and crafts. She has a cat and a dog; neither of them have any skin problems.
On physical examination, there is nail dystrophy with nail plate thinning and longitudinal fissuring of all fingernails but not of the toenails. She also has hyperpigmented violaceous plaques on the surrounding periungual skin. There are no other skin lesions, and there are no oral or genital lesions. There is no scalp involvement or hair loss. At follow-up several months later, she had complete destruction of the nail plate with scar formation.
A fungal culture was performed, as well as microscopic analysis of the nail with periodic acid fast and giemsa stains, which showed no fungal organisms.
She initially was treated with topical betamethasone twice a day for 6 weeks and then 2 weeks on and 2 weeks off without much change.
Play it as it lies: Handling lying by kids
“Not my son!” your patient’s parent rants. “If he lies to me, he will regret it for a long time.” While your first reaction may be to agree that a child lying to a parent crosses a kind of moral line in the sand, lying is a far more nuanced part of parenting worth a deeper understanding.
In order to lie, a child has to develop cognitive and social understanding. Typically developing children look to see what is interesting to others, called “joint attention,” at around 12-18 months. Failure to do this is one of the early signs of autism reflecting atypical social understanding. At around 3.5 years, children may attempt to deceive if they have broken a rule. The study demonstrating this may sound a lot like home: Children are left alone with a tempting toy but told not to touch it. Although they do touch it while the adult is out of sight, they say rather sweetly (and eventually convincingly) that they did not, even though the toy was clearly moved! While boys generally have more behavior problems, girls and children with better verbal skills achieve deceit at an earlier age, some as young as 2 years. At this stage, children become aware that the adult can’t know exactly what they know. If the parent shows high emotion to what they consider a lie, this can be a topic for testing! Children with ADHD often lack the inhibition needed for early mastery of deception, and children with autism later or not at all. They don’t see the social point to lying nor can they fake a facial expression. They have a case of intractable honesty!
The inability to refrain from telling the truth can result in social rejection, for example when a child rats on a peer for a trivial misdeed in class. Even though he is speaking the truth and “following the (teacher’s) rules,” he did not see that the cost of breaking the (peer) social rules was more important. By age 6 years, children typically figure out that what another person thinks may not be true – their belief may be incorrect or a “false belief.” This understanding is called Theory of Mind, missing or delayed in autism. Only 40% of high-functioning children with autism passed false belief testing at ages 6- to 13-years-old, compared with 95% of typical age-matched peers (Physiol Behav. 2010 Jun 1;100[3]:268-76). The percentage of children on the spectrum understanding false beliefs more closely matched that of preschoolers (39%). At a later age and given extra time to think, some children with autism can do better at this kind of perspective taking, but many continue having difficulty understanding thoughts of others, especially social expectations or motivations (such as flirting, status seeking, and making an excuse) even as adults. This can impair social relationships even when desire to fit in and IQ are otherwise high.
On the other hand, ADHD is a common condition in which “lying” comes from saying the first thing that comes to mind even if the child knows otherwise. A wise parent of one of my patients with ADHD told me about her “30 second rule” where she would give her child that extra time and walk away briefly to “be sure that is what you wanted to say,” with praise rather than give a consequence for changing the story to the truth. This is an important concept we pediatricians need to know: Punishing lying in children tends to result in more, not less, lying and more sneakiness. Instead, parents need to be advised to recall the origins of the word discipline as being “to teach.”
When children lie there are four basic scenarios: They may not know the rules, they may know but have something they want more, they may be impulsive, or they may have developed an attitude of seeking to con the adults whom they feel are mean as a way to have some power in the relationship and get back at them. Clearly, we do not want to push children to this fourth resort by harsh reactions to lying. We have seen particular difficulty with harsh reactions to lying in parents from strong, rule-oriented careers such as police officers, military, and ministers. Asking “How would your parent have handled this?” often will reveal reasons for their tough but backfiring stance.
Lying can work to get what one wants and nearly all children try it. As with other new milestones, children practice this “skill,” much to parents’ dismay. Parents generally can tell if children are lying; they see it on their faces, hear the story from siblings, or see evidence of what happened. Lying provides an important opportunity for the adult to stop, take some breaths, touch the child, and empathize: “It is hard to admit a mistake. I know you did not mean to do it. But you are young, and I know that you are good and honest inside, and will get stronger and braver at telling the truth as you get older. Will you promise to try harder?” In some cases a consequence may be appropriate, for example if something was broken. Usually, simply empathizing and focusing on the expectation for improvement will increase the child’s desire to please the parents rather than get back at them. Actual rewards for honesty improve truth telling by 1.5 times if the reward is big enough.
But it is important to recognize that we all make split second tactical decisions about our actions based on how safe we feel in the situation and our knowledge of social rules and costs. Children over time need to learn that it is safe to tell the truth among family members and that they will not be harshly dealt with. It is a subtle task, but important to learn that deception is a tool that can be important used judiciously when required socially (I have a curfew) or in dangerous situations (I did not see the thug), but can undermine relationships and should not be used with your allies (family and friends).
But parenting involves lying also, which can be a model for the child. Sarcasm is a peculiar form of problematic adult lying. The adults say the opposite or an exaggeration of what they really mean, usually with a smirk or other nonverbal cue to their intent. This is confusing, if not infuriating, to immature children or those who do not understand this twisted communication. It is best to avoid sarcasm with children, or at least be sure to explain it so the children gain understanding over time.
Parents need to “lie” to their children to some extent to reassure and allow for development of confidence. What adult hasn’t said “It’s going to be all right” about a looming storm, car crash, or illness, when actually there is uncertainty. Children count on adults to keep them safe emotionally and physically from things they can’t yet handle. To move forward developmentally, children need adults to be brave leaders, even when the adults don’t feel confident. Some parents think their children must know the “truth” in every instance. Those children are often painfully anxious and overwhelmed.
There is plenty of time for more facts later when the child has the thinking and emotional power to handle the truth.
Dr. Howard is assistant professor of pediatrics at Johns Hopkins University, Baltimore, and creator of CHADIS (www.CHADIS.com). She had no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to MDedge News. E-mail her at [email protected].
“Not my son!” your patient’s parent rants. “If he lies to me, he will regret it for a long time.” While your first reaction may be to agree that a child lying to a parent crosses a kind of moral line in the sand, lying is a far more nuanced part of parenting worth a deeper understanding.
In order to lie, a child has to develop cognitive and social understanding. Typically developing children look to see what is interesting to others, called “joint attention,” at around 12-18 months. Failure to do this is one of the early signs of autism reflecting atypical social understanding. At around 3.5 years, children may attempt to deceive if they have broken a rule. The study demonstrating this may sound a lot like home: Children are left alone with a tempting toy but told not to touch it. Although they do touch it while the adult is out of sight, they say rather sweetly (and eventually convincingly) that they did not, even though the toy was clearly moved! While boys generally have more behavior problems, girls and children with better verbal skills achieve deceit at an earlier age, some as young as 2 years. At this stage, children become aware that the adult can’t know exactly what they know. If the parent shows high emotion to what they consider a lie, this can be a topic for testing! Children with ADHD often lack the inhibition needed for early mastery of deception, and children with autism later or not at all. They don’t see the social point to lying nor can they fake a facial expression. They have a case of intractable honesty!
The inability to refrain from telling the truth can result in social rejection, for example when a child rats on a peer for a trivial misdeed in class. Even though he is speaking the truth and “following the (teacher’s) rules,” he did not see that the cost of breaking the (peer) social rules was more important. By age 6 years, children typically figure out that what another person thinks may not be true – their belief may be incorrect or a “false belief.” This understanding is called Theory of Mind, missing or delayed in autism. Only 40% of high-functioning children with autism passed false belief testing at ages 6- to 13-years-old, compared with 95% of typical age-matched peers (Physiol Behav. 2010 Jun 1;100[3]:268-76). The percentage of children on the spectrum understanding false beliefs more closely matched that of preschoolers (39%). At a later age and given extra time to think, some children with autism can do better at this kind of perspective taking, but many continue having difficulty understanding thoughts of others, especially social expectations or motivations (such as flirting, status seeking, and making an excuse) even as adults. This can impair social relationships even when desire to fit in and IQ are otherwise high.
On the other hand, ADHD is a common condition in which “lying” comes from saying the first thing that comes to mind even if the child knows otherwise. A wise parent of one of my patients with ADHD told me about her “30 second rule” where she would give her child that extra time and walk away briefly to “be sure that is what you wanted to say,” with praise rather than give a consequence for changing the story to the truth. This is an important concept we pediatricians need to know: Punishing lying in children tends to result in more, not less, lying and more sneakiness. Instead, parents need to be advised to recall the origins of the word discipline as being “to teach.”
When children lie there are four basic scenarios: They may not know the rules, they may know but have something they want more, they may be impulsive, or they may have developed an attitude of seeking to con the adults whom they feel are mean as a way to have some power in the relationship and get back at them. Clearly, we do not want to push children to this fourth resort by harsh reactions to lying. We have seen particular difficulty with harsh reactions to lying in parents from strong, rule-oriented careers such as police officers, military, and ministers. Asking “How would your parent have handled this?” often will reveal reasons for their tough but backfiring stance.
Lying can work to get what one wants and nearly all children try it. As with other new milestones, children practice this “skill,” much to parents’ dismay. Parents generally can tell if children are lying; they see it on their faces, hear the story from siblings, or see evidence of what happened. Lying provides an important opportunity for the adult to stop, take some breaths, touch the child, and empathize: “It is hard to admit a mistake. I know you did not mean to do it. But you are young, and I know that you are good and honest inside, and will get stronger and braver at telling the truth as you get older. Will you promise to try harder?” In some cases a consequence may be appropriate, for example if something was broken. Usually, simply empathizing and focusing on the expectation for improvement will increase the child’s desire to please the parents rather than get back at them. Actual rewards for honesty improve truth telling by 1.5 times if the reward is big enough.
But it is important to recognize that we all make split second tactical decisions about our actions based on how safe we feel in the situation and our knowledge of social rules and costs. Children over time need to learn that it is safe to tell the truth among family members and that they will not be harshly dealt with. It is a subtle task, but important to learn that deception is a tool that can be important used judiciously when required socially (I have a curfew) or in dangerous situations (I did not see the thug), but can undermine relationships and should not be used with your allies (family and friends).
But parenting involves lying also, which can be a model for the child. Sarcasm is a peculiar form of problematic adult lying. The adults say the opposite or an exaggeration of what they really mean, usually with a smirk or other nonverbal cue to their intent. This is confusing, if not infuriating, to immature children or those who do not understand this twisted communication. It is best to avoid sarcasm with children, or at least be sure to explain it so the children gain understanding over time.
Parents need to “lie” to their children to some extent to reassure and allow for development of confidence. What adult hasn’t said “It’s going to be all right” about a looming storm, car crash, or illness, when actually there is uncertainty. Children count on adults to keep them safe emotionally and physically from things they can’t yet handle. To move forward developmentally, children need adults to be brave leaders, even when the adults don’t feel confident. Some parents think their children must know the “truth” in every instance. Those children are often painfully anxious and overwhelmed.
There is plenty of time for more facts later when the child has the thinking and emotional power to handle the truth.
Dr. Howard is assistant professor of pediatrics at Johns Hopkins University, Baltimore, and creator of CHADIS (www.CHADIS.com). She had no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to MDedge News. E-mail her at [email protected].
“Not my son!” your patient’s parent rants. “If he lies to me, he will regret it for a long time.” While your first reaction may be to agree that a child lying to a parent crosses a kind of moral line in the sand, lying is a far more nuanced part of parenting worth a deeper understanding.
In order to lie, a child has to develop cognitive and social understanding. Typically developing children look to see what is interesting to others, called “joint attention,” at around 12-18 months. Failure to do this is one of the early signs of autism reflecting atypical social understanding. At around 3.5 years, children may attempt to deceive if they have broken a rule. The study demonstrating this may sound a lot like home: Children are left alone with a tempting toy but told not to touch it. Although they do touch it while the adult is out of sight, they say rather sweetly (and eventually convincingly) that they did not, even though the toy was clearly moved! While boys generally have more behavior problems, girls and children with better verbal skills achieve deceit at an earlier age, some as young as 2 years. At this stage, children become aware that the adult can’t know exactly what they know. If the parent shows high emotion to what they consider a lie, this can be a topic for testing! Children with ADHD often lack the inhibition needed for early mastery of deception, and children with autism later or not at all. They don’t see the social point to lying nor can they fake a facial expression. They have a case of intractable honesty!
The inability to refrain from telling the truth can result in social rejection, for example when a child rats on a peer for a trivial misdeed in class. Even though he is speaking the truth and “following the (teacher’s) rules,” he did not see that the cost of breaking the (peer) social rules was more important. By age 6 years, children typically figure out that what another person thinks may not be true – their belief may be incorrect or a “false belief.” This understanding is called Theory of Mind, missing or delayed in autism. Only 40% of high-functioning children with autism passed false belief testing at ages 6- to 13-years-old, compared with 95% of typical age-matched peers (Physiol Behav. 2010 Jun 1;100[3]:268-76). The percentage of children on the spectrum understanding false beliefs more closely matched that of preschoolers (39%). At a later age and given extra time to think, some children with autism can do better at this kind of perspective taking, but many continue having difficulty understanding thoughts of others, especially social expectations or motivations (such as flirting, status seeking, and making an excuse) even as adults. This can impair social relationships even when desire to fit in and IQ are otherwise high.
On the other hand, ADHD is a common condition in which “lying” comes from saying the first thing that comes to mind even if the child knows otherwise. A wise parent of one of my patients with ADHD told me about her “30 second rule” where she would give her child that extra time and walk away briefly to “be sure that is what you wanted to say,” with praise rather than give a consequence for changing the story to the truth. This is an important concept we pediatricians need to know: Punishing lying in children tends to result in more, not less, lying and more sneakiness. Instead, parents need to be advised to recall the origins of the word discipline as being “to teach.”
When children lie there are four basic scenarios: They may not know the rules, they may know but have something they want more, they may be impulsive, or they may have developed an attitude of seeking to con the adults whom they feel are mean as a way to have some power in the relationship and get back at them. Clearly, we do not want to push children to this fourth resort by harsh reactions to lying. We have seen particular difficulty with harsh reactions to lying in parents from strong, rule-oriented careers such as police officers, military, and ministers. Asking “How would your parent have handled this?” often will reveal reasons for their tough but backfiring stance.
Lying can work to get what one wants and nearly all children try it. As with other new milestones, children practice this “skill,” much to parents’ dismay. Parents generally can tell if children are lying; they see it on their faces, hear the story from siblings, or see evidence of what happened. Lying provides an important opportunity for the adult to stop, take some breaths, touch the child, and empathize: “It is hard to admit a mistake. I know you did not mean to do it. But you are young, and I know that you are good and honest inside, and will get stronger and braver at telling the truth as you get older. Will you promise to try harder?” In some cases a consequence may be appropriate, for example if something was broken. Usually, simply empathizing and focusing on the expectation for improvement will increase the child’s desire to please the parents rather than get back at them. Actual rewards for honesty improve truth telling by 1.5 times if the reward is big enough.
But it is important to recognize that we all make split second tactical decisions about our actions based on how safe we feel in the situation and our knowledge of social rules and costs. Children over time need to learn that it is safe to tell the truth among family members and that they will not be harshly dealt with. It is a subtle task, but important to learn that deception is a tool that can be important used judiciously when required socially (I have a curfew) or in dangerous situations (I did not see the thug), but can undermine relationships and should not be used with your allies (family and friends).
But parenting involves lying also, which can be a model for the child. Sarcasm is a peculiar form of problematic adult lying. The adults say the opposite or an exaggeration of what they really mean, usually with a smirk or other nonverbal cue to their intent. This is confusing, if not infuriating, to immature children or those who do not understand this twisted communication. It is best to avoid sarcasm with children, or at least be sure to explain it so the children gain understanding over time.
Parents need to “lie” to their children to some extent to reassure and allow for development of confidence. What adult hasn’t said “It’s going to be all right” about a looming storm, car crash, or illness, when actually there is uncertainty. Children count on adults to keep them safe emotionally and physically from things they can’t yet handle. To move forward developmentally, children need adults to be brave leaders, even when the adults don’t feel confident. Some parents think their children must know the “truth” in every instance. Those children are often painfully anxious and overwhelmed.
There is plenty of time for more facts later when the child has the thinking and emotional power to handle the truth.
Dr. Howard is assistant professor of pediatrics at Johns Hopkins University, Baltimore, and creator of CHADIS (www.CHADIS.com). She had no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to MDedge News. E-mail her at [email protected].