User login
Experts debate infection control merits of ‘bare beneath the elbows’
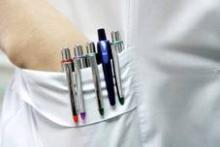
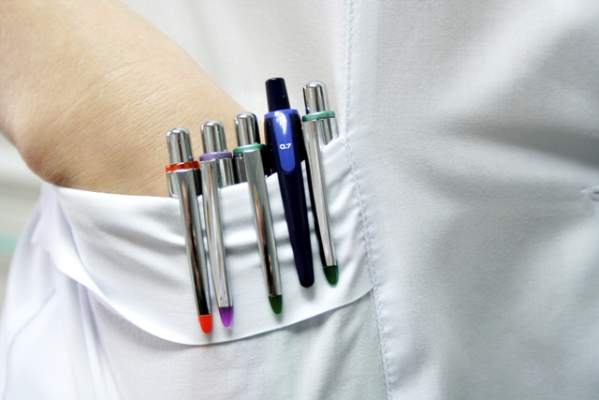
SAN DIEGO – Going tieless and “bare beneath the elbows” has been touted for infection control. But while some clinicians endorse the practice, others call it inconvenient, unprofessional, and distracting. At an annual conference on infectious diseases, two specialists in the field debated going “BBE” and its evidence base.
Widespread practice of BBE dates to at least 2008, when the National Health Service in the United Kingdom mandated it as part of a set of measures to decrease nosocomial transmission of methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile. Clinicians at NHS were directed to leave jewelry, neckties, and wrist watches at home, hang up their lab coats, and wear short sleeves. The policy aims not only to reduce points of physical contact between providers and patients, but also to improve hand and wrist washing, said Dr. Michael Edmond, who is at the University of Iowa Hospitals and Clinics in Iowa City.
Some evidence supports going BBE, said Dr. Edmond. Pathogenic gram-negative rods have been cultured from neckties, scrubs, uniforms, and white coats in multiple studies, he added. Inadequate laundering is part of the problem – clinical faculty in one study reported washing their coats about once every 2 weeks, even less often than medical students did.
“So when is biological plausibility enough to support a change in practice?” Dr. Edmond asked. “There is a potential for benefit in going BBE. There is no risk for harm. And there is minimal cost. On the basis of the same evidence and assumptions, we are willing to wrap ourselves in plastic and confine patients to their hospital rooms – that is, to use contact precautions. And yet, we are not willing to eliminate white coats and ties.”
Patient perception is not at issue, Dr. Edmond argued. Only about half of patients at one British hospital said they wanted physicians to wear traditional white coats, and that proportion dropped to 22% after patients received educational materials on clothing contamination, he noted. In another study, patients ranked their physician’s appearance behind knowledge, compassion, and politeness when asked which characteristics they valued most.
“Without strong evidence for benefit, we should recommend – not mandate – this new practice,” Dr. Edmond concluded.
But Dr. Neil O. Fishman disagreed, calling BBE “an evidence-free zone.” Dr. Fishman, who is at the University of Pennsylvania in Philadelphia, noted a total lack of randomized, controlled trials or well-performed observational studies supporting BBE. “No clinical studies have demonstrated cross-transmission of health care–associated pathogens from a health care provider to a patient,” he said.
Moreover, BBE does not prevent contamination, Dr. Fishman said. Bacterial cultures of the hands of BBE clinicians and controls revealed no differences in total bacteria counts or numbers of clinically significant pathogens, he said. Cultures of white coats and the undersides of wrists also were similar in terms of total bacteria and MRSA counts, he added.
Despite the lack of evidence, BBE has been implemented at NHS “mainly as a political gesture and has had unintended consequences,” Dr. Fishman said. Informal attire has promoted a less-robust view of infection control, junior doctors have adopted scruffy attire and “slovenly” personal hygiene, and all the focus on clothing has distracted from hand washing, he added.
Furthermore, less than 12% of clinicians have complied with BBE, according to Dr. Fishman. Abstainers report feeling cold and not knowing what time it is. Women, in particular, say they have no pockets to carry work essentials. “This is a gender equity issue,” Dr. Fishman said. “Can we afford to promote practices based on limited evidence, a theoretical rationale, or individual opinions? This is a lack of focus on what really matters.”
Dr. Edmond and Dr. Fishman reported no disclosures.
SAN DIEGO – Going tieless and “bare beneath the elbows” has been touted for infection control. But while some clinicians endorse the practice, others call it inconvenient, unprofessional, and distracting. At an annual conference on infectious diseases, two specialists in the field debated going “BBE” and its evidence base.
Widespread practice of BBE dates to at least 2008, when the National Health Service in the United Kingdom mandated it as part of a set of measures to decrease nosocomial transmission of methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile. Clinicians at NHS were directed to leave jewelry, neckties, and wrist watches at home, hang up their lab coats, and wear short sleeves. The policy aims not only to reduce points of physical contact between providers and patients, but also to improve hand and wrist washing, said Dr. Michael Edmond, who is at the University of Iowa Hospitals and Clinics in Iowa City.
Some evidence supports going BBE, said Dr. Edmond. Pathogenic gram-negative rods have been cultured from neckties, scrubs, uniforms, and white coats in multiple studies, he added. Inadequate laundering is part of the problem – clinical faculty in one study reported washing their coats about once every 2 weeks, even less often than medical students did.
“So when is biological plausibility enough to support a change in practice?” Dr. Edmond asked. “There is a potential for benefit in going BBE. There is no risk for harm. And there is minimal cost. On the basis of the same evidence and assumptions, we are willing to wrap ourselves in plastic and confine patients to their hospital rooms – that is, to use contact precautions. And yet, we are not willing to eliminate white coats and ties.”
Patient perception is not at issue, Dr. Edmond argued. Only about half of patients at one British hospital said they wanted physicians to wear traditional white coats, and that proportion dropped to 22% after patients received educational materials on clothing contamination, he noted. In another study, patients ranked their physician’s appearance behind knowledge, compassion, and politeness when asked which characteristics they valued most.
“Without strong evidence for benefit, we should recommend – not mandate – this new practice,” Dr. Edmond concluded.
But Dr. Neil O. Fishman disagreed, calling BBE “an evidence-free zone.” Dr. Fishman, who is at the University of Pennsylvania in Philadelphia, noted a total lack of randomized, controlled trials or well-performed observational studies supporting BBE. “No clinical studies have demonstrated cross-transmission of health care–associated pathogens from a health care provider to a patient,” he said.
Moreover, BBE does not prevent contamination, Dr. Fishman said. Bacterial cultures of the hands of BBE clinicians and controls revealed no differences in total bacteria counts or numbers of clinically significant pathogens, he said. Cultures of white coats and the undersides of wrists also were similar in terms of total bacteria and MRSA counts, he added.
Despite the lack of evidence, BBE has been implemented at NHS “mainly as a political gesture and has had unintended consequences,” Dr. Fishman said. Informal attire has promoted a less-robust view of infection control, junior doctors have adopted scruffy attire and “slovenly” personal hygiene, and all the focus on clothing has distracted from hand washing, he added.
Furthermore, less than 12% of clinicians have complied with BBE, according to Dr. Fishman. Abstainers report feeling cold and not knowing what time it is. Women, in particular, say they have no pockets to carry work essentials. “This is a gender equity issue,” Dr. Fishman said. “Can we afford to promote practices based on limited evidence, a theoretical rationale, or individual opinions? This is a lack of focus on what really matters.”
Dr. Edmond and Dr. Fishman reported no disclosures.
SAN DIEGO – Going tieless and “bare beneath the elbows” has been touted for infection control. But while some clinicians endorse the practice, others call it inconvenient, unprofessional, and distracting. At an annual conference on infectious diseases, two specialists in the field debated going “BBE” and its evidence base.
Widespread practice of BBE dates to at least 2008, when the National Health Service in the United Kingdom mandated it as part of a set of measures to decrease nosocomial transmission of methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile. Clinicians at NHS were directed to leave jewelry, neckties, and wrist watches at home, hang up their lab coats, and wear short sleeves. The policy aims not only to reduce points of physical contact between providers and patients, but also to improve hand and wrist washing, said Dr. Michael Edmond, who is at the University of Iowa Hospitals and Clinics in Iowa City.
Some evidence supports going BBE, said Dr. Edmond. Pathogenic gram-negative rods have been cultured from neckties, scrubs, uniforms, and white coats in multiple studies, he added. Inadequate laundering is part of the problem – clinical faculty in one study reported washing their coats about once every 2 weeks, even less often than medical students did.
“So when is biological plausibility enough to support a change in practice?” Dr. Edmond asked. “There is a potential for benefit in going BBE. There is no risk for harm. And there is minimal cost. On the basis of the same evidence and assumptions, we are willing to wrap ourselves in plastic and confine patients to their hospital rooms – that is, to use contact precautions. And yet, we are not willing to eliminate white coats and ties.”
Patient perception is not at issue, Dr. Edmond argued. Only about half of patients at one British hospital said they wanted physicians to wear traditional white coats, and that proportion dropped to 22% after patients received educational materials on clothing contamination, he noted. In another study, patients ranked their physician’s appearance behind knowledge, compassion, and politeness when asked which characteristics they valued most.
“Without strong evidence for benefit, we should recommend – not mandate – this new practice,” Dr. Edmond concluded.
But Dr. Neil O. Fishman disagreed, calling BBE “an evidence-free zone.” Dr. Fishman, who is at the University of Pennsylvania in Philadelphia, noted a total lack of randomized, controlled trials or well-performed observational studies supporting BBE. “No clinical studies have demonstrated cross-transmission of health care–associated pathogens from a health care provider to a patient,” he said.
Moreover, BBE does not prevent contamination, Dr. Fishman said. Bacterial cultures of the hands of BBE clinicians and controls revealed no differences in total bacteria counts or numbers of clinically significant pathogens, he said. Cultures of white coats and the undersides of wrists also were similar in terms of total bacteria and MRSA counts, he added.
Despite the lack of evidence, BBE has been implemented at NHS “mainly as a political gesture and has had unintended consequences,” Dr. Fishman said. Informal attire has promoted a less-robust view of infection control, junior doctors have adopted scruffy attire and “slovenly” personal hygiene, and all the focus on clothing has distracted from hand washing, he added.
Furthermore, less than 12% of clinicians have complied with BBE, according to Dr. Fishman. Abstainers report feeling cold and not knowing what time it is. Women, in particular, say they have no pockets to carry work essentials. “This is a gender equity issue,” Dr. Fishman said. “Can we afford to promote practices based on limited evidence, a theoretical rationale, or individual opinions? This is a lack of focus on what really matters.”
Dr. Edmond and Dr. Fishman reported no disclosures.
EXPERT ANALYSIS AT IDWEEK 2015
DenseBreast-info.org: What this resource can offer you, and your patients
Read the article Get smart about dense breasts by Wendie Berg, MD, PhD, JoAnn Pushkin, and Cindy Henke-Sarmento (October 2015)
Read the article Get smart about dense breasts by Wendie Berg, MD, PhD, JoAnn Pushkin, and Cindy Henke-Sarmento (October 2015)
Read the article Get smart about dense breasts by Wendie Berg, MD, PhD, JoAnn Pushkin, and Cindy Henke-Sarmento (October 2015)
Access DenseBreast-info.org
VIDEO: Take steps now to keep gram-negative resistance at bay
CHICAGO – Gram-negative bacteria are the new frontier of antimicrobial resistance.
Resistant Escherichia coli, Klebsiella, and other organisms are increasingly common in Asia, South America, and southern Europe, but haven’t quite established themselves yet in the United States.
In an interview at the annual clinical congress of the American College of Surgeons, Dr. John Mazuski, a professor of surgery at Washington University in St. Louis, explained what’s known so far, and the steps to take now to keep the organisms in check.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
CHICAGO – Gram-negative bacteria are the new frontier of antimicrobial resistance.
Resistant Escherichia coli, Klebsiella, and other organisms are increasingly common in Asia, South America, and southern Europe, but haven’t quite established themselves yet in the United States.
In an interview at the annual clinical congress of the American College of Surgeons, Dr. John Mazuski, a professor of surgery at Washington University in St. Louis, explained what’s known so far, and the steps to take now to keep the organisms in check.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
CHICAGO – Gram-negative bacteria are the new frontier of antimicrobial resistance.
Resistant Escherichia coli, Klebsiella, and other organisms are increasingly common in Asia, South America, and southern Europe, but haven’t quite established themselves yet in the United States.
In an interview at the annual clinical congress of the American College of Surgeons, Dr. John Mazuski, a professor of surgery at Washington University in St. Louis, explained what’s known so far, and the steps to take now to keep the organisms in check.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM THE ACS CLINICAL CONGRESS
Managing menopausal symptoms in women with a BRCA mutation
This audiocast was recorded at the North American Menopause Society Annual Meeting held September 30 to October 3, 2015, in Las Vegas, Nevada
For more on this topic, read Dr. Kaunitz's August 2015 Cases in Menopause article, Is menopausal hormone therapy safe when your patient carries a BRCA mutation?
This audiocast was recorded at the North American Menopause Society Annual Meeting held September 30 to October 3, 2015, in Las Vegas, Nevada
For more on this topic, read Dr. Kaunitz's August 2015 Cases in Menopause article, Is menopausal hormone therapy safe when your patient carries a BRCA mutation?
This audiocast was recorded at the North American Menopause Society Annual Meeting held September 30 to October 3, 2015, in Las Vegas, Nevada
For more on this topic, read Dr. Kaunitz's August 2015 Cases in Menopause article, Is menopausal hormone therapy safe when your patient carries a BRCA mutation?
Hospital Groups Might Do Better Without Daytime Admission Shifts, Morning Meetings
You shouldn’t maintain things that do not deliver the value you anticipated when you first put them in place. For example, I thought Netflix streaming would be terrific, but I have used it so infrequently that it probably costs me $50 per movie or show watched. I should probably dump it.
Your hospitalist group might have some operational practices that are not as valuable as they seem and could be replaced with something better. For many groups, this might include doing away with a separate daytime admitter shift and a morning meeting to distribute the overnight admissions.
Daytime Admission Shift
My experience is that hospitalist groups with more than about five daytime doctors almost always have a day-shift person dedicated to seeing new admissions. In most cases, this procedure is implemented with the idea of reducing the stress of other day-shift doctors, who don’t have to interrupt rounds to admit a new patient. Some see a dedicated admitter as a tool to improve ED throughput, because this doctor isn’t tied up with rounds and can immediately start seeing a new admission.
I think an admitter shift does deliver both of these benefits, but its costs make it suboptimal in most settings. For example, a single admitter will impede ED throughput any time more than one new admission is waiting to be seen, and for most groups that will be much of the day. In fact, improved ED throughput is best achieved by having many hospitalists available for admissions, not just a single admitter. (There are many other factors influencing ED throughput, such as whether ED doctors simply send patients to their “floor” bed prior to being seen by a hospitalist. But for this article, I’m just considering the influence of a dedicated admitter.)
I think “silo-ing” work into different roles, such as separating rounding and admitting, makes it more difficult to ensure that each is always working productively. There are likely to be times when the admitter has little or nothing to do, even though the rounders are very busy. Or perhaps the rounders aren’t very busy, but the admitter has just been asked to admit four ED patients at the same time.
While protecting rounders from the stress of admissions is valuable, it comes at the cost of a net increase in hospitalist work, because a new doctor must get to know the patient on the day following admission. And this admitter-to-rounder handoff serves as another opportunity for errors—and probably lowers patient satisfaction.
I think most groups should consider moving the admitter shift into an additional rounder position, dividing admissions across all of the doctors working during the daytime. For example, a group that has six rounders and a separate admitter would change to seven rounders, each available to admit every seventh daytime admission. Each would bear the meaningful stress of having rounds interrupted to admit a new patient, but accepting every seventh daytime admission shouldn’t be too difficult on most days.
Don’t forget that eliminating the admitter means that the list of new patients you take on each morning will be shorter. Mornings may be a little less stressful.
A.M. Distribution
The daytime doctors at many hospitalist groups meet each morning to discuss how the new admissions from the prior night (or even the last 24 hours) will be distributed. Or perhaps one person, sometimes a nurse or clerical staff, arrives very early each day to do this.
Although it might take some careful planning, I think most groups that use this sort of morning distribution should abandon it for a better system. Consider a group in which all six daytime doctors spend an average of 20 minutes distributing patients each morning. Twenty minutes (0.33 hours) times six doctors times 365 days comes to 730 hours annually.
Assuming these doctors are compensated at typical rates, the practice is spending more than $100,000 annually just so the doctors can distribute patients each morning. On top of this, nurses and others at the hospital are usually delayed in learning which daytime hospitalist is caring for each patient. These costs seem unreasonably high.
An alternative is to develop a system by which any admitter, such as a night doctor, who will not be providing subsequent care to a patient can identify by name the doctor who will be providing that care. During the admission encounter, the admitter can tell patient/family, “Dr. Boswell will be taking over your care starting tomorrow. He’s a great guy and has been named one of Portland’s best doctors.” This seems so much better than saying, “One of my partners will be taking over tomorrow. I don’t know which of my partners it will be, but they’re all good doctors.” And Dr. Boswell’s name can be entered into the attending physician field of the EHR so that all hospital staff will know without delay.
MedAptus has recently launched software they call “Assign” that may be able to replace the morning meeting and automate assigning new admissions to each hospitalist. I haven’t seen it in operation, so I can’t speak for its effectiveness, but it might be worthwhile for some groups.
Practical Considerations
The changes I’ve described above might not be optimal for every group, and they may take meaningful work to implement. But I don’t think the difficulty of these things is the biggest barrier. The biggest barrier is probably just inertia in most cases, the same reason I’m still a Netflix streaming subscriber even though I almost never watch it. I did, however, really enjoy the Nexflix original series Lilyhammer.

You shouldn’t maintain things that do not deliver the value you anticipated when you first put them in place. For example, I thought Netflix streaming would be terrific, but I have used it so infrequently that it probably costs me $50 per movie or show watched. I should probably dump it.
Your hospitalist group might have some operational practices that are not as valuable as they seem and could be replaced with something better. For many groups, this might include doing away with a separate daytime admitter shift and a morning meeting to distribute the overnight admissions.
Daytime Admission Shift
My experience is that hospitalist groups with more than about five daytime doctors almost always have a day-shift person dedicated to seeing new admissions. In most cases, this procedure is implemented with the idea of reducing the stress of other day-shift doctors, who don’t have to interrupt rounds to admit a new patient. Some see a dedicated admitter as a tool to improve ED throughput, because this doctor isn’t tied up with rounds and can immediately start seeing a new admission.
I think an admitter shift does deliver both of these benefits, but its costs make it suboptimal in most settings. For example, a single admitter will impede ED throughput any time more than one new admission is waiting to be seen, and for most groups that will be much of the day. In fact, improved ED throughput is best achieved by having many hospitalists available for admissions, not just a single admitter. (There are many other factors influencing ED throughput, such as whether ED doctors simply send patients to their “floor” bed prior to being seen by a hospitalist. But for this article, I’m just considering the influence of a dedicated admitter.)
I think “silo-ing” work into different roles, such as separating rounding and admitting, makes it more difficult to ensure that each is always working productively. There are likely to be times when the admitter has little or nothing to do, even though the rounders are very busy. Or perhaps the rounders aren’t very busy, but the admitter has just been asked to admit four ED patients at the same time.
While protecting rounders from the stress of admissions is valuable, it comes at the cost of a net increase in hospitalist work, because a new doctor must get to know the patient on the day following admission. And this admitter-to-rounder handoff serves as another opportunity for errors—and probably lowers patient satisfaction.
I think most groups should consider moving the admitter shift into an additional rounder position, dividing admissions across all of the doctors working during the daytime. For example, a group that has six rounders and a separate admitter would change to seven rounders, each available to admit every seventh daytime admission. Each would bear the meaningful stress of having rounds interrupted to admit a new patient, but accepting every seventh daytime admission shouldn’t be too difficult on most days.
Don’t forget that eliminating the admitter means that the list of new patients you take on each morning will be shorter. Mornings may be a little less stressful.
A.M. Distribution
The daytime doctors at many hospitalist groups meet each morning to discuss how the new admissions from the prior night (or even the last 24 hours) will be distributed. Or perhaps one person, sometimes a nurse or clerical staff, arrives very early each day to do this.
Although it might take some careful planning, I think most groups that use this sort of morning distribution should abandon it for a better system. Consider a group in which all six daytime doctors spend an average of 20 minutes distributing patients each morning. Twenty minutes (0.33 hours) times six doctors times 365 days comes to 730 hours annually.
Assuming these doctors are compensated at typical rates, the practice is spending more than $100,000 annually just so the doctors can distribute patients each morning. On top of this, nurses and others at the hospital are usually delayed in learning which daytime hospitalist is caring for each patient. These costs seem unreasonably high.
An alternative is to develop a system by which any admitter, such as a night doctor, who will not be providing subsequent care to a patient can identify by name the doctor who will be providing that care. During the admission encounter, the admitter can tell patient/family, “Dr. Boswell will be taking over your care starting tomorrow. He’s a great guy and has been named one of Portland’s best doctors.” This seems so much better than saying, “One of my partners will be taking over tomorrow. I don’t know which of my partners it will be, but they’re all good doctors.” And Dr. Boswell’s name can be entered into the attending physician field of the EHR so that all hospital staff will know without delay.
MedAptus has recently launched software they call “Assign” that may be able to replace the morning meeting and automate assigning new admissions to each hospitalist. I haven’t seen it in operation, so I can’t speak for its effectiveness, but it might be worthwhile for some groups.
Practical Considerations
The changes I’ve described above might not be optimal for every group, and they may take meaningful work to implement. But I don’t think the difficulty of these things is the biggest barrier. The biggest barrier is probably just inertia in most cases, the same reason I’m still a Netflix streaming subscriber even though I almost never watch it. I did, however, really enjoy the Nexflix original series Lilyhammer.

You shouldn’t maintain things that do not deliver the value you anticipated when you first put them in place. For example, I thought Netflix streaming would be terrific, but I have used it so infrequently that it probably costs me $50 per movie or show watched. I should probably dump it.
Your hospitalist group might have some operational practices that are not as valuable as they seem and could be replaced with something better. For many groups, this might include doing away with a separate daytime admitter shift and a morning meeting to distribute the overnight admissions.
Daytime Admission Shift
My experience is that hospitalist groups with more than about five daytime doctors almost always have a day-shift person dedicated to seeing new admissions. In most cases, this procedure is implemented with the idea of reducing the stress of other day-shift doctors, who don’t have to interrupt rounds to admit a new patient. Some see a dedicated admitter as a tool to improve ED throughput, because this doctor isn’t tied up with rounds and can immediately start seeing a new admission.
I think an admitter shift does deliver both of these benefits, but its costs make it suboptimal in most settings. For example, a single admitter will impede ED throughput any time more than one new admission is waiting to be seen, and for most groups that will be much of the day. In fact, improved ED throughput is best achieved by having many hospitalists available for admissions, not just a single admitter. (There are many other factors influencing ED throughput, such as whether ED doctors simply send patients to their “floor” bed prior to being seen by a hospitalist. But for this article, I’m just considering the influence of a dedicated admitter.)
I think “silo-ing” work into different roles, such as separating rounding and admitting, makes it more difficult to ensure that each is always working productively. There are likely to be times when the admitter has little or nothing to do, even though the rounders are very busy. Or perhaps the rounders aren’t very busy, but the admitter has just been asked to admit four ED patients at the same time.
While protecting rounders from the stress of admissions is valuable, it comes at the cost of a net increase in hospitalist work, because a new doctor must get to know the patient on the day following admission. And this admitter-to-rounder handoff serves as another opportunity for errors—and probably lowers patient satisfaction.
I think most groups should consider moving the admitter shift into an additional rounder position, dividing admissions across all of the doctors working during the daytime. For example, a group that has six rounders and a separate admitter would change to seven rounders, each available to admit every seventh daytime admission. Each would bear the meaningful stress of having rounds interrupted to admit a new patient, but accepting every seventh daytime admission shouldn’t be too difficult on most days.
Don’t forget that eliminating the admitter means that the list of new patients you take on each morning will be shorter. Mornings may be a little less stressful.
A.M. Distribution
The daytime doctors at many hospitalist groups meet each morning to discuss how the new admissions from the prior night (or even the last 24 hours) will be distributed. Or perhaps one person, sometimes a nurse or clerical staff, arrives very early each day to do this.
Although it might take some careful planning, I think most groups that use this sort of morning distribution should abandon it for a better system. Consider a group in which all six daytime doctors spend an average of 20 minutes distributing patients each morning. Twenty minutes (0.33 hours) times six doctors times 365 days comes to 730 hours annually.
Assuming these doctors are compensated at typical rates, the practice is spending more than $100,000 annually just so the doctors can distribute patients each morning. On top of this, nurses and others at the hospital are usually delayed in learning which daytime hospitalist is caring for each patient. These costs seem unreasonably high.
An alternative is to develop a system by which any admitter, such as a night doctor, who will not be providing subsequent care to a patient can identify by name the doctor who will be providing that care. During the admission encounter, the admitter can tell patient/family, “Dr. Boswell will be taking over your care starting tomorrow. He’s a great guy and has been named one of Portland’s best doctors.” This seems so much better than saying, “One of my partners will be taking over tomorrow. I don’t know which of my partners it will be, but they’re all good doctors.” And Dr. Boswell’s name can be entered into the attending physician field of the EHR so that all hospital staff will know without delay.
MedAptus has recently launched software they call “Assign” that may be able to replace the morning meeting and automate assigning new admissions to each hospitalist. I haven’t seen it in operation, so I can’t speak for its effectiveness, but it might be worthwhile for some groups.
Practical Considerations
The changes I’ve described above might not be optimal for every group, and they may take meaningful work to implement. But I don’t think the difficulty of these things is the biggest barrier. The biggest barrier is probably just inertia in most cases, the same reason I’m still a Netflix streaming subscriber even though I almost never watch it. I did, however, really enjoy the Nexflix original series Lilyhammer.

Does episiotomy at vacuum delivery increase maternal morbidity?
Episiotomy refers to an incision into the perineal body made during the second stage of labor to expedite delivery. It comes in 2 main flavors (midline and mediolateral), and neither one is particularly palatable. Routine use of episiotomy is strongly discouraged, for several reasons:
- There is little evidence of benefit
- It is associated with an increased risk of short- and long-term complications to both the mother and neonate, including postpartum hemorrhage, severe perineal injury, and pelvic floor dysfunction.1,2
Whether to perform an episiotomy at the time of operative vaginal delivery (forceps or vacuum), however, remains controversial.
Sagi-Dain and Sagi performed a meta- analysis of the existing literature in an effort to answer a single clinically relevant question: Should an episiotomy be performed at the time of vacuum delivery?
Details of the study
The primary endpoint was obstetric anal sphincter injuries (OASIS), which are more commonly referred to in the United States as severe perineal injury (3rd- and 4th-degree perineal laceration). Secondary endpoints were, among others, neonatal outcomes (including Apgar scores, neonatal trauma, shoulder dystocia, neonatal resuscitation, and admission to the neonatal intensive care unit) and maternal complications (including postpartum hemorrhage, perineal infection, urinary retention, urinary/fecal incontinence, prolonged hospital stay, and analgesia use).
Of 812 original research reports initially identified that examined the effect of episiotomy at vacuum delivery on any measure of maternal or neonatal outcome, 15 articles encompassing 350,764 deliveries were included in the final analysis. Of these, 14 were observational cohort studies (13 retrospective and 1 prospective) plus 1 case-control analysis; no randomized trials were identified.
Overall, episiotomy was performed in 64.3% (SD, 18.8%; range, 28.7%-86.0%) of vacuum deliveries and was more common in nulliparous (58.7%; SD, 17.8%) than in multiparous women (34.2%; SD, 14.6%; P = .035). The investigators found that US and Canadian studies reported using mainly median episiotomy, whereas European, Scandinavian, and Australian studies used mainly mediolateral episiotomy.
Overall, OASIS occurred in 8.5% (SD, 10.6%; range 1.0%-23.6%) of vacuum deliveries, with a higher rate occurring in nulliparous compared with multiparous women (9.6%; [SD, 6.2%] vs 1.7% [SD, 1.3%], respectively; P = .031).
Median (midline) episiotomy at the time of vacuum delivery was associated with a significant increase in OASIS in both nulliparous (odds ratio [OR], 5.11; 95% confidence interval [CI], 3.23-8.08) and multip- arous women (OR, 89.4; 95% CI, 11.8-677.1). A similar increase in OASIS was seen when a mediolateral episiotomy was performed at vacuum delivery in multiparous women (OR, 1.27; 95% CI, 1.05-1.53), although no statistically significant relationship was evident between mediolateral episiotomy at vacuum delivery and OASIS in nulliparous women (OR, 0.68; 95% CI, 0.43-1.07). Mediolateral episiotomy also was linked to increased rates of postpartum hemorrhage (OR, 1.82; 95% CI, 1.16-2.86) and analgesia use (OR, 2.10; 95% CI, 1.39-3.17).
Strengths and limitations
Meta-analysis (systematic review) is not synonymous with a review of the literature. It has a very specific methodology and should be treated as original research, albeit in silico. Meta-analyses use precise statistical methods to combine and contrast results from a number of independent original research reports. The current study is an exemplary illustration of just how such an analysis should be conducted. As prescribed by the Meta-analysis Of Observational Studies in Epidemiology (MOOSE) guidelines,3 it included all study designs, both published and unpublished data, and was not limited to English language reports.
In addition, if results were unclear or data were missing, the investigators contacted the authors directly to verify the information. Prior published statistical analyses were disregarded, and the investigators conducted an independent evaluation of the pooled data using each patient as a separate data point. Data classification and coding were clearly described; the analysis was performed independently by 2 separate investigators; and a detailed assessment of data quality, heterogeneity, and sensitivity testing was included.
What this evidence means for practice
Episiotomy at the time of vacuum delivery does not appear to be of benefit, and it more likely than not increases maternal morbidity. This is especially true of median episiotomy (the type used most commonly in the United States), which increases the risk of OASIS at the time of vacuum delivery 5-fold in nulliparous and 89-fold in multiparous women.
Confidence in these conclusions is guarded. Based on the small number of reports, the lack of randomized trials, and the significant heterogeneity between the studies, the authors rated the overall quality of evidence as “low” to “very low” using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) working group criteria. Additional large prospective clinical trials are needed to definitively answer the question of whether episiotomy at vacuum delivery increases maternal morbidity.
Until such studies are available, however, it would be best if obstetric care providers avoid episiotomy at the time of vacuum delivery. On a personal note, I look forward to the day when a medical student turns to an attending and asks: “What is an episiotomy?” And the attending responds: “I don’t know. I’ve never seen one.” Only then will I be ready to retire.
>> Errol R. Norwitz, MD, PhD
1. Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev. 2009;(1):CD000081.
2. Ali U, Norwitz ER. Vacuum-assisted vaginal delivery. Rev Obstet Gynecol. 2009;2(1):5-17.
3. Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008-2012.
Episiotomy refers to an incision into the perineal body made during the second stage of labor to expedite delivery. It comes in 2 main flavors (midline and mediolateral), and neither one is particularly palatable. Routine use of episiotomy is strongly discouraged, for several reasons:
- There is little evidence of benefit
- It is associated with an increased risk of short- and long-term complications to both the mother and neonate, including postpartum hemorrhage, severe perineal injury, and pelvic floor dysfunction.1,2
Whether to perform an episiotomy at the time of operative vaginal delivery (forceps or vacuum), however, remains controversial.
Sagi-Dain and Sagi performed a meta- analysis of the existing literature in an effort to answer a single clinically relevant question: Should an episiotomy be performed at the time of vacuum delivery?
Details of the study
The primary endpoint was obstetric anal sphincter injuries (OASIS), which are more commonly referred to in the United States as severe perineal injury (3rd- and 4th-degree perineal laceration). Secondary endpoints were, among others, neonatal outcomes (including Apgar scores, neonatal trauma, shoulder dystocia, neonatal resuscitation, and admission to the neonatal intensive care unit) and maternal complications (including postpartum hemorrhage, perineal infection, urinary retention, urinary/fecal incontinence, prolonged hospital stay, and analgesia use).
Of 812 original research reports initially identified that examined the effect of episiotomy at vacuum delivery on any measure of maternal or neonatal outcome, 15 articles encompassing 350,764 deliveries were included in the final analysis. Of these, 14 were observational cohort studies (13 retrospective and 1 prospective) plus 1 case-control analysis; no randomized trials were identified.
Overall, episiotomy was performed in 64.3% (SD, 18.8%; range, 28.7%-86.0%) of vacuum deliveries and was more common in nulliparous (58.7%; SD, 17.8%) than in multiparous women (34.2%; SD, 14.6%; P = .035). The investigators found that US and Canadian studies reported using mainly median episiotomy, whereas European, Scandinavian, and Australian studies used mainly mediolateral episiotomy.
Overall, OASIS occurred in 8.5% (SD, 10.6%; range 1.0%-23.6%) of vacuum deliveries, with a higher rate occurring in nulliparous compared with multiparous women (9.6%; [SD, 6.2%] vs 1.7% [SD, 1.3%], respectively; P = .031).
Median (midline) episiotomy at the time of vacuum delivery was associated with a significant increase in OASIS in both nulliparous (odds ratio [OR], 5.11; 95% confidence interval [CI], 3.23-8.08) and multip- arous women (OR, 89.4; 95% CI, 11.8-677.1). A similar increase in OASIS was seen when a mediolateral episiotomy was performed at vacuum delivery in multiparous women (OR, 1.27; 95% CI, 1.05-1.53), although no statistically significant relationship was evident between mediolateral episiotomy at vacuum delivery and OASIS in nulliparous women (OR, 0.68; 95% CI, 0.43-1.07). Mediolateral episiotomy also was linked to increased rates of postpartum hemorrhage (OR, 1.82; 95% CI, 1.16-2.86) and analgesia use (OR, 2.10; 95% CI, 1.39-3.17).
Strengths and limitations
Meta-analysis (systematic review) is not synonymous with a review of the literature. It has a very specific methodology and should be treated as original research, albeit in silico. Meta-analyses use precise statistical methods to combine and contrast results from a number of independent original research reports. The current study is an exemplary illustration of just how such an analysis should be conducted. As prescribed by the Meta-analysis Of Observational Studies in Epidemiology (MOOSE) guidelines,3 it included all study designs, both published and unpublished data, and was not limited to English language reports.
In addition, if results were unclear or data were missing, the investigators contacted the authors directly to verify the information. Prior published statistical analyses were disregarded, and the investigators conducted an independent evaluation of the pooled data using each patient as a separate data point. Data classification and coding were clearly described; the analysis was performed independently by 2 separate investigators; and a detailed assessment of data quality, heterogeneity, and sensitivity testing was included.
What this evidence means for practice
Episiotomy at the time of vacuum delivery does not appear to be of benefit, and it more likely than not increases maternal morbidity. This is especially true of median episiotomy (the type used most commonly in the United States), which increases the risk of OASIS at the time of vacuum delivery 5-fold in nulliparous and 89-fold in multiparous women.
Confidence in these conclusions is guarded. Based on the small number of reports, the lack of randomized trials, and the significant heterogeneity between the studies, the authors rated the overall quality of evidence as “low” to “very low” using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) working group criteria. Additional large prospective clinical trials are needed to definitively answer the question of whether episiotomy at vacuum delivery increases maternal morbidity.
Until such studies are available, however, it would be best if obstetric care providers avoid episiotomy at the time of vacuum delivery. On a personal note, I look forward to the day when a medical student turns to an attending and asks: “What is an episiotomy?” And the attending responds: “I don’t know. I’ve never seen one.” Only then will I be ready to retire.
>> Errol R. Norwitz, MD, PhD
Episiotomy refers to an incision into the perineal body made during the second stage of labor to expedite delivery. It comes in 2 main flavors (midline and mediolateral), and neither one is particularly palatable. Routine use of episiotomy is strongly discouraged, for several reasons:
- There is little evidence of benefit
- It is associated with an increased risk of short- and long-term complications to both the mother and neonate, including postpartum hemorrhage, severe perineal injury, and pelvic floor dysfunction.1,2
Whether to perform an episiotomy at the time of operative vaginal delivery (forceps or vacuum), however, remains controversial.
Sagi-Dain and Sagi performed a meta- analysis of the existing literature in an effort to answer a single clinically relevant question: Should an episiotomy be performed at the time of vacuum delivery?
Details of the study
The primary endpoint was obstetric anal sphincter injuries (OASIS), which are more commonly referred to in the United States as severe perineal injury (3rd- and 4th-degree perineal laceration). Secondary endpoints were, among others, neonatal outcomes (including Apgar scores, neonatal trauma, shoulder dystocia, neonatal resuscitation, and admission to the neonatal intensive care unit) and maternal complications (including postpartum hemorrhage, perineal infection, urinary retention, urinary/fecal incontinence, prolonged hospital stay, and analgesia use).
Of 812 original research reports initially identified that examined the effect of episiotomy at vacuum delivery on any measure of maternal or neonatal outcome, 15 articles encompassing 350,764 deliveries were included in the final analysis. Of these, 14 were observational cohort studies (13 retrospective and 1 prospective) plus 1 case-control analysis; no randomized trials were identified.
Overall, episiotomy was performed in 64.3% (SD, 18.8%; range, 28.7%-86.0%) of vacuum deliveries and was more common in nulliparous (58.7%; SD, 17.8%) than in multiparous women (34.2%; SD, 14.6%; P = .035). The investigators found that US and Canadian studies reported using mainly median episiotomy, whereas European, Scandinavian, and Australian studies used mainly mediolateral episiotomy.
Overall, OASIS occurred in 8.5% (SD, 10.6%; range 1.0%-23.6%) of vacuum deliveries, with a higher rate occurring in nulliparous compared with multiparous women (9.6%; [SD, 6.2%] vs 1.7% [SD, 1.3%], respectively; P = .031).
Median (midline) episiotomy at the time of vacuum delivery was associated with a significant increase in OASIS in both nulliparous (odds ratio [OR], 5.11; 95% confidence interval [CI], 3.23-8.08) and multip- arous women (OR, 89.4; 95% CI, 11.8-677.1). A similar increase in OASIS was seen when a mediolateral episiotomy was performed at vacuum delivery in multiparous women (OR, 1.27; 95% CI, 1.05-1.53), although no statistically significant relationship was evident between mediolateral episiotomy at vacuum delivery and OASIS in nulliparous women (OR, 0.68; 95% CI, 0.43-1.07). Mediolateral episiotomy also was linked to increased rates of postpartum hemorrhage (OR, 1.82; 95% CI, 1.16-2.86) and analgesia use (OR, 2.10; 95% CI, 1.39-3.17).
Strengths and limitations
Meta-analysis (systematic review) is not synonymous with a review of the literature. It has a very specific methodology and should be treated as original research, albeit in silico. Meta-analyses use precise statistical methods to combine and contrast results from a number of independent original research reports. The current study is an exemplary illustration of just how such an analysis should be conducted. As prescribed by the Meta-analysis Of Observational Studies in Epidemiology (MOOSE) guidelines,3 it included all study designs, both published and unpublished data, and was not limited to English language reports.
In addition, if results were unclear or data were missing, the investigators contacted the authors directly to verify the information. Prior published statistical analyses were disregarded, and the investigators conducted an independent evaluation of the pooled data using each patient as a separate data point. Data classification and coding were clearly described; the analysis was performed independently by 2 separate investigators; and a detailed assessment of data quality, heterogeneity, and sensitivity testing was included.
What this evidence means for practice
Episiotomy at the time of vacuum delivery does not appear to be of benefit, and it more likely than not increases maternal morbidity. This is especially true of median episiotomy (the type used most commonly in the United States), which increases the risk of OASIS at the time of vacuum delivery 5-fold in nulliparous and 89-fold in multiparous women.
Confidence in these conclusions is guarded. Based on the small number of reports, the lack of randomized trials, and the significant heterogeneity between the studies, the authors rated the overall quality of evidence as “low” to “very low” using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) working group criteria. Additional large prospective clinical trials are needed to definitively answer the question of whether episiotomy at vacuum delivery increases maternal morbidity.
Until such studies are available, however, it would be best if obstetric care providers avoid episiotomy at the time of vacuum delivery. On a personal note, I look forward to the day when a medical student turns to an attending and asks: “What is an episiotomy?” And the attending responds: “I don’t know. I’ve never seen one.” Only then will I be ready to retire.
>> Errol R. Norwitz, MD, PhD
1. Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev. 2009;(1):CD000081.
2. Ali U, Norwitz ER. Vacuum-assisted vaginal delivery. Rev Obstet Gynecol. 2009;2(1):5-17.
3. Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008-2012.
1. Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev. 2009;(1):CD000081.
2. Ali U, Norwitz ER. Vacuum-assisted vaginal delivery. Rev Obstet Gynecol. 2009;2(1):5-17.
3. Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008-2012.
Which is the more effective treatment for uncomplicated skin infections—clindamycin or trimethoprim-sulfamethoxazole?
Miller and colleagues conducted their study in adults as well as children. Patients were included if they had either a discrete skin abscess or cellulitis, or both. They were excluded if they had one of the following:
- impetigo
- perirectal, genital, or hand infection
- a human or animal bite at the site of infection
- temperature of 38.5° C or higher
- immunocompromise
- morbid obesity
- prosthetic device at the site of infection.
The remaining patients then were stratified into one of 2 groups:
- those with a larger abscess (>5 cm in maximum diameter in adults, proportionally smaller in children) and/or cellulitis
- those who had a smaller abscess.
This study by Miller and colleagues focuses only on the patients in the former group.
Details of the trial
All discrete abscesses were incised and drained, and patients were randomly assigned to either:
- clindamycin, 300 mg 3 times daily for 10 days
- trimethoprim-sulfamethoxazole, 2 single-strength tablets orally twice daily for 10 days.
The primary endpoint was clinical cure at 7 to 10 days after completion of antibiotic therapy.
The study enrolled 524 patients—264 in the clindamycin group and 260 in the trimethoprim-sulfamethoxazole group. Approximately 30% of the patients were children. One hundred sixty patients (30.5%) had a discrete abscess, 280 (53.4%) had cellulitis, and 82 (15.6%) had both an abscess and cellulitis. An incision and drainage procedure was performed in 44.5% of patients. Slightly more than 50% of patients had a microbiological culture.
The most common organism isolated was S aureus (217 of 524 patients, or 41.4%), of which 167 (77%) were methicillin-resistant S aureus (MRSA). Of the 217 isolates identified as S aureus, 27 (12.4%) were resistant to clindamycin, and only one (0.5%) was resistant to trimethoprim-sulfamethoxazole.
Of the 466 patients who were fully evaluable, the rate of cure was 89.5% in the clindamycin group (95% confidence interval [CI], 85.2–93.7) and 88.2% in the trimethoprim-sulfamethoxazole group (95% CI, 83.7–92.7). The difference in the observed rate of clinical cure was not statistically significant.
Eleven of 15 patients in the clindamycin group who had clindamycin-resistant isolates were cured, compared with 77 of 84 patients with susceptible isolates (73.3% vs 91.7%; P = .06). At 1 month after treatment, cure rates remained similar. The overall rates of adverse effects in the 2 groups were similar, at 19%. No patient developed Clostridium difficile-associated diarrhea.
Skin infections can be life-threatening
Skin and skin-structure infections are common—and can influence the decision of when to perform a cesarean delivery, how to prepare the skin before surgery, and where to place the surgical incision. In some patients, these infections can be quite debilitating, even life-threatening. When a discrete abscess (furuncle, carbuncle) is present, the most likely organism is S aureus, and the majority of strains are MRSA. When cellulitis is present, S aureus is less likely, and the dominant organisms are usually streptococci, particularly Streptococcus pyogenes.
Abscesses of any size need incision and drainage and, in most cases, systemic antibiotic therapy. When cellulitis without a discrete abscess is present, the key to treatment is antibiotic therapy.
WHAT THIS EVIDENCE MEANS FOR PRACTICE
For uncomplicated skin and skin-structure infections in immunocompetent women, oral clindamycin and oral trimethoprim-sulfamethoxazole are equally effective; both achieve cures in approximately 90% of patients.
Given that more strains of S aureus were resistant to clindamycin, trimethoprim-sulfamethoxazole may be the preferred agent. It also is less expensive and, in theory at least, less likely to cause drug-induced diarrhea.
Affected patients need to be followed closely because recurrences are common and, in isolated instances, serious complications such as sepsis can develop.
—Patrick Duff, MD
Share your thoughts on this article! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
Miller and colleagues conducted their study in adults as well as children. Patients were included if they had either a discrete skin abscess or cellulitis, or both. They were excluded if they had one of the following:
- impetigo
- perirectal, genital, or hand infection
- a human or animal bite at the site of infection
- temperature of 38.5° C or higher
- immunocompromise
- morbid obesity
- prosthetic device at the site of infection.
The remaining patients then were stratified into one of 2 groups:
- those with a larger abscess (>5 cm in maximum diameter in adults, proportionally smaller in children) and/or cellulitis
- those who had a smaller abscess.
This study by Miller and colleagues focuses only on the patients in the former group.
Details of the trial
All discrete abscesses were incised and drained, and patients were randomly assigned to either:
- clindamycin, 300 mg 3 times daily for 10 days
- trimethoprim-sulfamethoxazole, 2 single-strength tablets orally twice daily for 10 days.
The primary endpoint was clinical cure at 7 to 10 days after completion of antibiotic therapy.
The study enrolled 524 patients—264 in the clindamycin group and 260 in the trimethoprim-sulfamethoxazole group. Approximately 30% of the patients were children. One hundred sixty patients (30.5%) had a discrete abscess, 280 (53.4%) had cellulitis, and 82 (15.6%) had both an abscess and cellulitis. An incision and drainage procedure was performed in 44.5% of patients. Slightly more than 50% of patients had a microbiological culture.
The most common organism isolated was S aureus (217 of 524 patients, or 41.4%), of which 167 (77%) were methicillin-resistant S aureus (MRSA). Of the 217 isolates identified as S aureus, 27 (12.4%) were resistant to clindamycin, and only one (0.5%) was resistant to trimethoprim-sulfamethoxazole.
Of the 466 patients who were fully evaluable, the rate of cure was 89.5% in the clindamycin group (95% confidence interval [CI], 85.2–93.7) and 88.2% in the trimethoprim-sulfamethoxazole group (95% CI, 83.7–92.7). The difference in the observed rate of clinical cure was not statistically significant.
Eleven of 15 patients in the clindamycin group who had clindamycin-resistant isolates were cured, compared with 77 of 84 patients with susceptible isolates (73.3% vs 91.7%; P = .06). At 1 month after treatment, cure rates remained similar. The overall rates of adverse effects in the 2 groups were similar, at 19%. No patient developed Clostridium difficile-associated diarrhea.
Skin infections can be life-threatening
Skin and skin-structure infections are common—and can influence the decision of when to perform a cesarean delivery, how to prepare the skin before surgery, and where to place the surgical incision. In some patients, these infections can be quite debilitating, even life-threatening. When a discrete abscess (furuncle, carbuncle) is present, the most likely organism is S aureus, and the majority of strains are MRSA. When cellulitis is present, S aureus is less likely, and the dominant organisms are usually streptococci, particularly Streptococcus pyogenes.
Abscesses of any size need incision and drainage and, in most cases, systemic antibiotic therapy. When cellulitis without a discrete abscess is present, the key to treatment is antibiotic therapy.
WHAT THIS EVIDENCE MEANS FOR PRACTICE
For uncomplicated skin and skin-structure infections in immunocompetent women, oral clindamycin and oral trimethoprim-sulfamethoxazole are equally effective; both achieve cures in approximately 90% of patients.
Given that more strains of S aureus were resistant to clindamycin, trimethoprim-sulfamethoxazole may be the preferred agent. It also is less expensive and, in theory at least, less likely to cause drug-induced diarrhea.
Affected patients need to be followed closely because recurrences are common and, in isolated instances, serious complications such as sepsis can develop.
—Patrick Duff, MD
Share your thoughts on this article! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
Miller and colleagues conducted their study in adults as well as children. Patients were included if they had either a discrete skin abscess or cellulitis, or both. They were excluded if they had one of the following:
- impetigo
- perirectal, genital, or hand infection
- a human or animal bite at the site of infection
- temperature of 38.5° C or higher
- immunocompromise
- morbid obesity
- prosthetic device at the site of infection.
The remaining patients then were stratified into one of 2 groups:
- those with a larger abscess (>5 cm in maximum diameter in adults, proportionally smaller in children) and/or cellulitis
- those who had a smaller abscess.
This study by Miller and colleagues focuses only on the patients in the former group.
Details of the trial
All discrete abscesses were incised and drained, and patients were randomly assigned to either:
- clindamycin, 300 mg 3 times daily for 10 days
- trimethoprim-sulfamethoxazole, 2 single-strength tablets orally twice daily for 10 days.
The primary endpoint was clinical cure at 7 to 10 days after completion of antibiotic therapy.
The study enrolled 524 patients—264 in the clindamycin group and 260 in the trimethoprim-sulfamethoxazole group. Approximately 30% of the patients were children. One hundred sixty patients (30.5%) had a discrete abscess, 280 (53.4%) had cellulitis, and 82 (15.6%) had both an abscess and cellulitis. An incision and drainage procedure was performed in 44.5% of patients. Slightly more than 50% of patients had a microbiological culture.
The most common organism isolated was S aureus (217 of 524 patients, or 41.4%), of which 167 (77%) were methicillin-resistant S aureus (MRSA). Of the 217 isolates identified as S aureus, 27 (12.4%) were resistant to clindamycin, and only one (0.5%) was resistant to trimethoprim-sulfamethoxazole.
Of the 466 patients who were fully evaluable, the rate of cure was 89.5% in the clindamycin group (95% confidence interval [CI], 85.2–93.7) and 88.2% in the trimethoprim-sulfamethoxazole group (95% CI, 83.7–92.7). The difference in the observed rate of clinical cure was not statistically significant.
Eleven of 15 patients in the clindamycin group who had clindamycin-resistant isolates were cured, compared with 77 of 84 patients with susceptible isolates (73.3% vs 91.7%; P = .06). At 1 month after treatment, cure rates remained similar. The overall rates of adverse effects in the 2 groups were similar, at 19%. No patient developed Clostridium difficile-associated diarrhea.
Skin infections can be life-threatening
Skin and skin-structure infections are common—and can influence the decision of when to perform a cesarean delivery, how to prepare the skin before surgery, and where to place the surgical incision. In some patients, these infections can be quite debilitating, even life-threatening. When a discrete abscess (furuncle, carbuncle) is present, the most likely organism is S aureus, and the majority of strains are MRSA. When cellulitis is present, S aureus is less likely, and the dominant organisms are usually streptococci, particularly Streptococcus pyogenes.
Abscesses of any size need incision and drainage and, in most cases, systemic antibiotic therapy. When cellulitis without a discrete abscess is present, the key to treatment is antibiotic therapy.
WHAT THIS EVIDENCE MEANS FOR PRACTICE
For uncomplicated skin and skin-structure infections in immunocompetent women, oral clindamycin and oral trimethoprim-sulfamethoxazole are equally effective; both achieve cures in approximately 90% of patients.
Given that more strains of S aureus were resistant to clindamycin, trimethoprim-sulfamethoxazole may be the preferred agent. It also is less expensive and, in theory at least, less likely to cause drug-induced diarrhea.
Affected patients need to be followed closely because recurrences are common and, in isolated instances, serious complications such as sepsis can develop.
—Patrick Duff, MD
Share your thoughts on this article! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
VIDEO: Use fiduciary duty to set pain medication boundaries
ORLANDO – Physicians should use the concept of fiduciary duty to set appropriate boundaries with patients taking pain medications, explained Dr. Louis Kuritzky.
Often, patients want treatments that are not in their best interests, noted Dr. Kuritzky of the department of community health and family medicine at the University of Florida, Gainesville.
In an interview at a meeting held by the American Pain Society and Global Academy for Medical Education, Dr. Kuritzky outlined how physicians can take a fiduciary duty approach to set boundaries with patients in a dispassionate manner.
Global Academy and this news organization are owned by the same company. Dr. Kuritzky reported a financial relationship with Lilly.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ORLANDO – Physicians should use the concept of fiduciary duty to set appropriate boundaries with patients taking pain medications, explained Dr. Louis Kuritzky.
Often, patients want treatments that are not in their best interests, noted Dr. Kuritzky of the department of community health and family medicine at the University of Florida, Gainesville.
In an interview at a meeting held by the American Pain Society and Global Academy for Medical Education, Dr. Kuritzky outlined how physicians can take a fiduciary duty approach to set boundaries with patients in a dispassionate manner.
Global Academy and this news organization are owned by the same company. Dr. Kuritzky reported a financial relationship with Lilly.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ORLANDO – Physicians should use the concept of fiduciary duty to set appropriate boundaries with patients taking pain medications, explained Dr. Louis Kuritzky.
Often, patients want treatments that are not in their best interests, noted Dr. Kuritzky of the department of community health and family medicine at the University of Florida, Gainesville.
In an interview at a meeting held by the American Pain Society and Global Academy for Medical Education, Dr. Kuritzky outlined how physicians can take a fiduciary duty approach to set boundaries with patients in a dispassionate manner.
Global Academy and this news organization are owned by the same company. Dr. Kuritzky reported a financial relationship with Lilly.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM PAIN CARE FOR PRIMARY CARE
Why Hospitalist Morale is Declining and Ways to Improve It
Using quotes to ensure that the results were only those that include the two words adjacent to one another, rather than separated, I entered the following phrases into my Google search engine:
- “hospitalist burnout” = 1,580 results
- “hospitalist morale” = 208 results
- “hospitalist well-being” = 0 results
I think the number of results suggests the level of interest in each topic and, if that is the case, clearly thinking about how hospitalists are doing in their careers is more commonly done through the paradigm of burnout than the other two terms. (Of course, there may be other terms that I didn’t consider.) In fact, there have been a handful of published studies of hospitalist burnout and job satisfaction.1,2
Those studies generally have shown both reasonably high levels of job satisfaction and troubling levels of burnout.
But I’ve been thinking about hospitalist morale for a while. I think morale is reasonably distinct from both burnout and job satisfaction.
Causes of a National Decline in Hospitalist Morale
I think hospitalist morale has declined some over the past two or three years across the country. This observation is meaningful because it comes from my experience working with a lot of hospitalist groups coast to coast. But I’m the first to admit it is just anecdotal and is subject to my own biases.
I can think of several things contributing to a decline in morale.
EHR adoption. Near the top of the list is the adoption of EHRs in many hospitals, which typically leads doctors in other specialties to seek hospitalist assistance with EHR-related tasks (e.g. medicine reconciliation and order writing) even in cases where there is little or no clinical reason for hospitalist involvement. Lots of hospitalists complain about this. To be clear, in many hospitals the hospitalists are reasonably content with using the EHR, but they experience ongoing frustration and low morale resulting from nonclinical work other doctors pressure them to take over.
Observation status. Many hospitals began classifying a larger portion of patients as observation status over the last few years; at the same time, patients and families have become more aware of how much of a disadvantage this is. In many cases, it is the hospitalist who takes the brunt of patient and family frustration. This can get awfully stressful and frustrating, and I think it is a contributor to allegations of malpractice.
Budgetary stress. Ever since SHM began collecting survey data in the late 1990s, the financial support hospitals have been providing to hospitalists has increased dramatically. The most recent State of Hospital Medicine report, published in 2104, showed median support provided by hospitals of $156,063 per FTE hospitalist, per year. Some hospitals have begun to resist providing more support, and this translates into stress and lower morale for hospitalists. This is far from a universal issue, but it does lead to lower morale for hospitalists who face it.
Many other factors may be contributing to a national decline in morale, but I think these are some of the most important.
What Can Be Done?
Some hospitalist groups have great morale now and don’t need to do much of anything right now, but some groups should think about a deliberate strategy to improve it.
Sadly, there isn’t a prescription that is sure to work. But there are some things you can try.
Self-care. The field of palliative care has thought a lot about caring for caregivers, and hospitalist groups might want to adopt some of their practices. Search the Internet on “self-care” + “palliative care,” and you’ll find a lot of interesting things. The group I’m part of launched a deliberate program of professionally led and facilitated hospitalist self-care, with high hopes that included mindful meditation, among other things. As soon as we had designed our program, the Mayo Clinic published their favorable experience with a program that was very similar to what we had planned, and I thought we would see similar benefits.3
But, while all who attended the sessions thought they were valuable, attendance was so poor that we ended up cancelling the program. The hospitalists were interested in attending but were either on service and busy seeing patients, or were off and didn’t want to drive in to work solely for the purpose of reducing work stress.
I’m convinced a self-care program is valuable but very tricky to schedule effectively. Maybe others have come up with effective ways of overcoming this problem.
Social connections. Some hospitalist groups seem to have little social and personal connection to other physicians and hospital leaders. I think this results in lower hospitalist morale and tends to be self-reinforcing. If you’re in such a group, you and your hospitalist colleagues should deliberately seek better relationships with other doctors and hospital administrative leaders. Ensure that you visit with others at lunch, talk with them at committee meetings, ask about their vacation and personal activities, and pursue activities with them outside of work.
When these sorts of social connections are strong, work is far more satisfying and you’re much more likely to be treated as a peer by other doctors. I think this is really important and shouldn’t be overlooked if your group is suffering from low morale.
Adaptive work. Lastly, you might want to approach changes to your work and morale as “adaptive work,” rather than “technical work.” Space doesn’t permit a description of these, but it is worth reading about how they differ. Many groups will find value in reframing their approach to aspects of work they don’t like as adaptive work.

References
- Hinami K, Whelan CT, Wolosin RJ, Miller JA, Wetterneck TB. Worklife and satisfaction of hospitalists: toward flourishing careers. J Gen Intern Med. 2012;27(1):28-36.
- Hoff TH, Whitcomb WF, Williams K, Nelson JR, Cheesman RA. Characteristics and work experiences of hospitalists in the United States. Arch Intern Med. 2001;161(6):851-858.
- West CP, Dyrbye LN, Rabatin JT, et al. Intervention to promote physician well-being, job satisfaction, and professionalism: a randomized clinical trial. JAMA Intern Med. 2014;174(4):527-533.
Using quotes to ensure that the results were only those that include the two words adjacent to one another, rather than separated, I entered the following phrases into my Google search engine:
- “hospitalist burnout” = 1,580 results
- “hospitalist morale” = 208 results
- “hospitalist well-being” = 0 results
I think the number of results suggests the level of interest in each topic and, if that is the case, clearly thinking about how hospitalists are doing in their careers is more commonly done through the paradigm of burnout than the other two terms. (Of course, there may be other terms that I didn’t consider.) In fact, there have been a handful of published studies of hospitalist burnout and job satisfaction.1,2
Those studies generally have shown both reasonably high levels of job satisfaction and troubling levels of burnout.
But I’ve been thinking about hospitalist morale for a while. I think morale is reasonably distinct from both burnout and job satisfaction.
Causes of a National Decline in Hospitalist Morale
I think hospitalist morale has declined some over the past two or three years across the country. This observation is meaningful because it comes from my experience working with a lot of hospitalist groups coast to coast. But I’m the first to admit it is just anecdotal and is subject to my own biases.
I can think of several things contributing to a decline in morale.
EHR adoption. Near the top of the list is the adoption of EHRs in many hospitals, which typically leads doctors in other specialties to seek hospitalist assistance with EHR-related tasks (e.g. medicine reconciliation and order writing) even in cases where there is little or no clinical reason for hospitalist involvement. Lots of hospitalists complain about this. To be clear, in many hospitals the hospitalists are reasonably content with using the EHR, but they experience ongoing frustration and low morale resulting from nonclinical work other doctors pressure them to take over.
Observation status. Many hospitals began classifying a larger portion of patients as observation status over the last few years; at the same time, patients and families have become more aware of how much of a disadvantage this is. In many cases, it is the hospitalist who takes the brunt of patient and family frustration. This can get awfully stressful and frustrating, and I think it is a contributor to allegations of malpractice.
Budgetary stress. Ever since SHM began collecting survey data in the late 1990s, the financial support hospitals have been providing to hospitalists has increased dramatically. The most recent State of Hospital Medicine report, published in 2104, showed median support provided by hospitals of $156,063 per FTE hospitalist, per year. Some hospitals have begun to resist providing more support, and this translates into stress and lower morale for hospitalists. This is far from a universal issue, but it does lead to lower morale for hospitalists who face it.
Many other factors may be contributing to a national decline in morale, but I think these are some of the most important.
What Can Be Done?
Some hospitalist groups have great morale now and don’t need to do much of anything right now, but some groups should think about a deliberate strategy to improve it.
Sadly, there isn’t a prescription that is sure to work. But there are some things you can try.
Self-care. The field of palliative care has thought a lot about caring for caregivers, and hospitalist groups might want to adopt some of their practices. Search the Internet on “self-care” + “palliative care,” and you’ll find a lot of interesting things. The group I’m part of launched a deliberate program of professionally led and facilitated hospitalist self-care, with high hopes that included mindful meditation, among other things. As soon as we had designed our program, the Mayo Clinic published their favorable experience with a program that was very similar to what we had planned, and I thought we would see similar benefits.3
But, while all who attended the sessions thought they were valuable, attendance was so poor that we ended up cancelling the program. The hospitalists were interested in attending but were either on service and busy seeing patients, or were off and didn’t want to drive in to work solely for the purpose of reducing work stress.
I’m convinced a self-care program is valuable but very tricky to schedule effectively. Maybe others have come up with effective ways of overcoming this problem.
Social connections. Some hospitalist groups seem to have little social and personal connection to other physicians and hospital leaders. I think this results in lower hospitalist morale and tends to be self-reinforcing. If you’re in such a group, you and your hospitalist colleagues should deliberately seek better relationships with other doctors and hospital administrative leaders. Ensure that you visit with others at lunch, talk with them at committee meetings, ask about their vacation and personal activities, and pursue activities with them outside of work.
When these sorts of social connections are strong, work is far more satisfying and you’re much more likely to be treated as a peer by other doctors. I think this is really important and shouldn’t be overlooked if your group is suffering from low morale.
Adaptive work. Lastly, you might want to approach changes to your work and morale as “adaptive work,” rather than “technical work.” Space doesn’t permit a description of these, but it is worth reading about how they differ. Many groups will find value in reframing their approach to aspects of work they don’t like as adaptive work.

References
- Hinami K, Whelan CT, Wolosin RJ, Miller JA, Wetterneck TB. Worklife and satisfaction of hospitalists: toward flourishing careers. J Gen Intern Med. 2012;27(1):28-36.
- Hoff TH, Whitcomb WF, Williams K, Nelson JR, Cheesman RA. Characteristics and work experiences of hospitalists in the United States. Arch Intern Med. 2001;161(6):851-858.
- West CP, Dyrbye LN, Rabatin JT, et al. Intervention to promote physician well-being, job satisfaction, and professionalism: a randomized clinical trial. JAMA Intern Med. 2014;174(4):527-533.
Using quotes to ensure that the results were only those that include the two words adjacent to one another, rather than separated, I entered the following phrases into my Google search engine:
- “hospitalist burnout” = 1,580 results
- “hospitalist morale” = 208 results
- “hospitalist well-being” = 0 results
I think the number of results suggests the level of interest in each topic and, if that is the case, clearly thinking about how hospitalists are doing in their careers is more commonly done through the paradigm of burnout than the other two terms. (Of course, there may be other terms that I didn’t consider.) In fact, there have been a handful of published studies of hospitalist burnout and job satisfaction.1,2
Those studies generally have shown both reasonably high levels of job satisfaction and troubling levels of burnout.
But I’ve been thinking about hospitalist morale for a while. I think morale is reasonably distinct from both burnout and job satisfaction.
Causes of a National Decline in Hospitalist Morale
I think hospitalist morale has declined some over the past two or three years across the country. This observation is meaningful because it comes from my experience working with a lot of hospitalist groups coast to coast. But I’m the first to admit it is just anecdotal and is subject to my own biases.
I can think of several things contributing to a decline in morale.
EHR adoption. Near the top of the list is the adoption of EHRs in many hospitals, which typically leads doctors in other specialties to seek hospitalist assistance with EHR-related tasks (e.g. medicine reconciliation and order writing) even in cases where there is little or no clinical reason for hospitalist involvement. Lots of hospitalists complain about this. To be clear, in many hospitals the hospitalists are reasonably content with using the EHR, but they experience ongoing frustration and low morale resulting from nonclinical work other doctors pressure them to take over.
Observation status. Many hospitals began classifying a larger portion of patients as observation status over the last few years; at the same time, patients and families have become more aware of how much of a disadvantage this is. In many cases, it is the hospitalist who takes the brunt of patient and family frustration. This can get awfully stressful and frustrating, and I think it is a contributor to allegations of malpractice.
Budgetary stress. Ever since SHM began collecting survey data in the late 1990s, the financial support hospitals have been providing to hospitalists has increased dramatically. The most recent State of Hospital Medicine report, published in 2104, showed median support provided by hospitals of $156,063 per FTE hospitalist, per year. Some hospitals have begun to resist providing more support, and this translates into stress and lower morale for hospitalists. This is far from a universal issue, but it does lead to lower morale for hospitalists who face it.
Many other factors may be contributing to a national decline in morale, but I think these are some of the most important.
What Can Be Done?
Some hospitalist groups have great morale now and don’t need to do much of anything right now, but some groups should think about a deliberate strategy to improve it.
Sadly, there isn’t a prescription that is sure to work. But there are some things you can try.
Self-care. The field of palliative care has thought a lot about caring for caregivers, and hospitalist groups might want to adopt some of their practices. Search the Internet on “self-care” + “palliative care,” and you’ll find a lot of interesting things. The group I’m part of launched a deliberate program of professionally led and facilitated hospitalist self-care, with high hopes that included mindful meditation, among other things. As soon as we had designed our program, the Mayo Clinic published their favorable experience with a program that was very similar to what we had planned, and I thought we would see similar benefits.3
But, while all who attended the sessions thought they were valuable, attendance was so poor that we ended up cancelling the program. The hospitalists were interested in attending but were either on service and busy seeing patients, or were off and didn’t want to drive in to work solely for the purpose of reducing work stress.
I’m convinced a self-care program is valuable but very tricky to schedule effectively. Maybe others have come up with effective ways of overcoming this problem.
Social connections. Some hospitalist groups seem to have little social and personal connection to other physicians and hospital leaders. I think this results in lower hospitalist morale and tends to be self-reinforcing. If you’re in such a group, you and your hospitalist colleagues should deliberately seek better relationships with other doctors and hospital administrative leaders. Ensure that you visit with others at lunch, talk with them at committee meetings, ask about their vacation and personal activities, and pursue activities with them outside of work.
When these sorts of social connections are strong, work is far more satisfying and you’re much more likely to be treated as a peer by other doctors. I think this is really important and shouldn’t be overlooked if your group is suffering from low morale.
Adaptive work. Lastly, you might want to approach changes to your work and morale as “adaptive work,” rather than “technical work.” Space doesn’t permit a description of these, but it is worth reading about how they differ. Many groups will find value in reframing their approach to aspects of work they don’t like as adaptive work.

References
- Hinami K, Whelan CT, Wolosin RJ, Miller JA, Wetterneck TB. Worklife and satisfaction of hospitalists: toward flourishing careers. J Gen Intern Med. 2012;27(1):28-36.
- Hoff TH, Whitcomb WF, Williams K, Nelson JR, Cheesman RA. Characteristics and work experiences of hospitalists in the United States. Arch Intern Med. 2001;161(6):851-858.
- West CP, Dyrbye LN, Rabatin JT, et al. Intervention to promote physician well-being, job satisfaction, and professionalism: a randomized clinical trial. JAMA Intern Med. 2014;174(4):527-533.
Understanding of Mycoplasma-induced mucositis improving
PARK CITY, UTAH – According to emerging evidence in the medical literature, Mycoplasma pneumoniae–induced rash and mucositis is a distinct clinical entity with a distinct etiology and a good prognosis.
At the annual meeting of the Pacific Dermatologic Association, Dr. Erin Mathes shared tips on how to distinguish potentially life-threatening causes of rash and mucositis in children. “You want to think about their age, demographics, and history of medication exposures,” said Dr. Mathes, a pediatric dermatologist at the University of California, San Francisco. “Kids are exposed to viruses and bacteria all the time when they’re in day care. Also think about fever, whether or not they’re sick or well appearing, and the morphology.”
According to a retrospective study of 55 children with Stevens-Johnson Syndrome/toxic epidermal necrolysis (SJS/TEN) at the Hospital for Sick Children, Toronto, and Boston Children’s Hospital between 2000 and 2007, the top three causes of these rare conditions were antiepileptic drugs (29%), followed by M. pneumoniae infection (25%) and antibiotics (20%) (Pediatrics 2011;128[4]:723-8).
Dr. Mathes said that she learned from her mentor, Dr. Ilona Frieden, director of pediatric dermatology at UCSF Benioff Children’s Hospital, that in cases of M. pneumoniae-induced rash and mucositis (MIRM), 90% of the disease burden is the mucositis, and the remaining 10% is cutaneous findings. “So when you see mucositis far out of proportion to rash, think Mycoplasma,” Dr. Mathes said.
She and her associates at UCSF conducted a systematic review of all published cases on Mycoplasma-induced rash and mucositis and included 202 cases from 95 reports in the medical literature (J Am Acad Dermatol. 2015;72:239-45). The mean age of patients was 12 years, 66% were male, and most had a mucosal morphology (oral in 94% of cases, ocular in 82%, and genitourinary findings in 63%). “About one-third of patients had mucosal involvement alone, which is important to remember,” she said.
The patients’ skin involvement was generally mild; 46% was considered to be sparse or scattered, and 19% had moderate involvement. Extensive skin involvement “is rare, but it can happen,” Dr. Mathes said. Outcomes for the 202 patients were “generally good,” with 81% having no sequelae. The rates of recurrence and mucosal complications such as scarring around the mouth were both 8%, the rate of pigmentary alterations was 6%, and the rate of mortality was 3%, “but those cases were prior to the introduction of antibiotics in the 1940s,” she emphasized. “Children, in general, are not dying of Mycoplasma-associated rash and mucositis.”
A study published on July 25, 2015 in Pediatrics (doi:10.1542/peds.2015-0278) described an outbreak of eight Mycoplasma-associated SJS cases at Children’s Hospital Colorado, Aurora, that occurred over a 2-month period. In a case-control analysis comparing hospitalized SJS cases with and without evidence of M. pneumoniae infection, the researchers found that cases of Mycoplasma-associated SJS were significantly more likely to have pneumonia (odds ratio, 10), preceding respiratory symptoms (OR, 30), an erythrocyte sedimentation rate of greater than 35 mg/dL (OR, 22.8), and fewer than three affected skin sites (OR, 4.5).
Dr. Mathes was part of a research team that published diagnostic criteria for MIRM. These include less than 10% body surface area affected, involvement of two or more mucosal sites, the presence of few vesiculobullous lesions/scattered atypical targets with or without targetoid lesions, and clinical and laboratory evidence of atypical pneumonia (J Am Acad Dermatol. 2015;72:239-45).
“Rare cases can have more body surface area detachment, or no rash at all,” she said.
Existing tests for Mycoplasma infection are “not that great,” she continued. “It depends on the manufacturer and what is used as the gold standard.” IgM and IgG have specificity ranges from 25% to 100% and sensitivity ranges from 52% to 100%, she said, while polymerase chain reaction is rapidly becoming the gold standard. “That is usually from a nasal wash or bronchoalveolar lavage. It is very sensitive, but is almost too sensitive, because you can actually shed bacteria in your nasal pharynx for 4 months after an infection. That can lead to false positives.”
At UCSF, Dr. Mathes and her colleagues tend to treat MIRM cases with azithromycin followed by supportive care. “We occasionally use steroids but rarely use IVIG [intravenous immunoglobulin],” she said.
Dr. Mathes reported having no financial disclosures.
PARK CITY, UTAH – According to emerging evidence in the medical literature, Mycoplasma pneumoniae–induced rash and mucositis is a distinct clinical entity with a distinct etiology and a good prognosis.
At the annual meeting of the Pacific Dermatologic Association, Dr. Erin Mathes shared tips on how to distinguish potentially life-threatening causes of rash and mucositis in children. “You want to think about their age, demographics, and history of medication exposures,” said Dr. Mathes, a pediatric dermatologist at the University of California, San Francisco. “Kids are exposed to viruses and bacteria all the time when they’re in day care. Also think about fever, whether or not they’re sick or well appearing, and the morphology.”
According to a retrospective study of 55 children with Stevens-Johnson Syndrome/toxic epidermal necrolysis (SJS/TEN) at the Hospital for Sick Children, Toronto, and Boston Children’s Hospital between 2000 and 2007, the top three causes of these rare conditions were antiepileptic drugs (29%), followed by M. pneumoniae infection (25%) and antibiotics (20%) (Pediatrics 2011;128[4]:723-8).
Dr. Mathes said that she learned from her mentor, Dr. Ilona Frieden, director of pediatric dermatology at UCSF Benioff Children’s Hospital, that in cases of M. pneumoniae-induced rash and mucositis (MIRM), 90% of the disease burden is the mucositis, and the remaining 10% is cutaneous findings. “So when you see mucositis far out of proportion to rash, think Mycoplasma,” Dr. Mathes said.
She and her associates at UCSF conducted a systematic review of all published cases on Mycoplasma-induced rash and mucositis and included 202 cases from 95 reports in the medical literature (J Am Acad Dermatol. 2015;72:239-45). The mean age of patients was 12 years, 66% were male, and most had a mucosal morphology (oral in 94% of cases, ocular in 82%, and genitourinary findings in 63%). “About one-third of patients had mucosal involvement alone, which is important to remember,” she said.
The patients’ skin involvement was generally mild; 46% was considered to be sparse or scattered, and 19% had moderate involvement. Extensive skin involvement “is rare, but it can happen,” Dr. Mathes said. Outcomes for the 202 patients were “generally good,” with 81% having no sequelae. The rates of recurrence and mucosal complications such as scarring around the mouth were both 8%, the rate of pigmentary alterations was 6%, and the rate of mortality was 3%, “but those cases were prior to the introduction of antibiotics in the 1940s,” she emphasized. “Children, in general, are not dying of Mycoplasma-associated rash and mucositis.”
A study published on July 25, 2015 in Pediatrics (doi:10.1542/peds.2015-0278) described an outbreak of eight Mycoplasma-associated SJS cases at Children’s Hospital Colorado, Aurora, that occurred over a 2-month period. In a case-control analysis comparing hospitalized SJS cases with and without evidence of M. pneumoniae infection, the researchers found that cases of Mycoplasma-associated SJS were significantly more likely to have pneumonia (odds ratio, 10), preceding respiratory symptoms (OR, 30), an erythrocyte sedimentation rate of greater than 35 mg/dL (OR, 22.8), and fewer than three affected skin sites (OR, 4.5).
Dr. Mathes was part of a research team that published diagnostic criteria for MIRM. These include less than 10% body surface area affected, involvement of two or more mucosal sites, the presence of few vesiculobullous lesions/scattered atypical targets with or without targetoid lesions, and clinical and laboratory evidence of atypical pneumonia (J Am Acad Dermatol. 2015;72:239-45).
“Rare cases can have more body surface area detachment, or no rash at all,” she said.
Existing tests for Mycoplasma infection are “not that great,” she continued. “It depends on the manufacturer and what is used as the gold standard.” IgM and IgG have specificity ranges from 25% to 100% and sensitivity ranges from 52% to 100%, she said, while polymerase chain reaction is rapidly becoming the gold standard. “That is usually from a nasal wash or bronchoalveolar lavage. It is very sensitive, but is almost too sensitive, because you can actually shed bacteria in your nasal pharynx for 4 months after an infection. That can lead to false positives.”
At UCSF, Dr. Mathes and her colleagues tend to treat MIRM cases with azithromycin followed by supportive care. “We occasionally use steroids but rarely use IVIG [intravenous immunoglobulin],” she said.
Dr. Mathes reported having no financial disclosures.
PARK CITY, UTAH – According to emerging evidence in the medical literature, Mycoplasma pneumoniae–induced rash and mucositis is a distinct clinical entity with a distinct etiology and a good prognosis.
At the annual meeting of the Pacific Dermatologic Association, Dr. Erin Mathes shared tips on how to distinguish potentially life-threatening causes of rash and mucositis in children. “You want to think about their age, demographics, and history of medication exposures,” said Dr. Mathes, a pediatric dermatologist at the University of California, San Francisco. “Kids are exposed to viruses and bacteria all the time when they’re in day care. Also think about fever, whether or not they’re sick or well appearing, and the morphology.”
According to a retrospective study of 55 children with Stevens-Johnson Syndrome/toxic epidermal necrolysis (SJS/TEN) at the Hospital for Sick Children, Toronto, and Boston Children’s Hospital between 2000 and 2007, the top three causes of these rare conditions were antiepileptic drugs (29%), followed by M. pneumoniae infection (25%) and antibiotics (20%) (Pediatrics 2011;128[4]:723-8).
Dr. Mathes said that she learned from her mentor, Dr. Ilona Frieden, director of pediatric dermatology at UCSF Benioff Children’s Hospital, that in cases of M. pneumoniae-induced rash and mucositis (MIRM), 90% of the disease burden is the mucositis, and the remaining 10% is cutaneous findings. “So when you see mucositis far out of proportion to rash, think Mycoplasma,” Dr. Mathes said.
She and her associates at UCSF conducted a systematic review of all published cases on Mycoplasma-induced rash and mucositis and included 202 cases from 95 reports in the medical literature (J Am Acad Dermatol. 2015;72:239-45). The mean age of patients was 12 years, 66% were male, and most had a mucosal morphology (oral in 94% of cases, ocular in 82%, and genitourinary findings in 63%). “About one-third of patients had mucosal involvement alone, which is important to remember,” she said.
The patients’ skin involvement was generally mild; 46% was considered to be sparse or scattered, and 19% had moderate involvement. Extensive skin involvement “is rare, but it can happen,” Dr. Mathes said. Outcomes for the 202 patients were “generally good,” with 81% having no sequelae. The rates of recurrence and mucosal complications such as scarring around the mouth were both 8%, the rate of pigmentary alterations was 6%, and the rate of mortality was 3%, “but those cases were prior to the introduction of antibiotics in the 1940s,” she emphasized. “Children, in general, are not dying of Mycoplasma-associated rash and mucositis.”
A study published on July 25, 2015 in Pediatrics (doi:10.1542/peds.2015-0278) described an outbreak of eight Mycoplasma-associated SJS cases at Children’s Hospital Colorado, Aurora, that occurred over a 2-month period. In a case-control analysis comparing hospitalized SJS cases with and without evidence of M. pneumoniae infection, the researchers found that cases of Mycoplasma-associated SJS were significantly more likely to have pneumonia (odds ratio, 10), preceding respiratory symptoms (OR, 30), an erythrocyte sedimentation rate of greater than 35 mg/dL (OR, 22.8), and fewer than three affected skin sites (OR, 4.5).
Dr. Mathes was part of a research team that published diagnostic criteria for MIRM. These include less than 10% body surface area affected, involvement of two or more mucosal sites, the presence of few vesiculobullous lesions/scattered atypical targets with or without targetoid lesions, and clinical and laboratory evidence of atypical pneumonia (J Am Acad Dermatol. 2015;72:239-45).
“Rare cases can have more body surface area detachment, or no rash at all,” she said.
Existing tests for Mycoplasma infection are “not that great,” she continued. “It depends on the manufacturer and what is used as the gold standard.” IgM and IgG have specificity ranges from 25% to 100% and sensitivity ranges from 52% to 100%, she said, while polymerase chain reaction is rapidly becoming the gold standard. “That is usually from a nasal wash or bronchoalveolar lavage. It is very sensitive, but is almost too sensitive, because you can actually shed bacteria in your nasal pharynx for 4 months after an infection. That can lead to false positives.”
At UCSF, Dr. Mathes and her colleagues tend to treat MIRM cases with azithromycin followed by supportive care. “We occasionally use steroids but rarely use IVIG [intravenous immunoglobulin],” she said.
Dr. Mathes reported having no financial disclosures.
EXPERT ANALYSIS AT PDA 2015