User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
Asymptomatic Umbilical Nodule
The Diagnosis: Sister Mary Joseph Nodule
Histopathologic analysis of the biopsy specimen revealed a dense infiltrate of large, hyperchromatic, mucin-producing cells exhibiting varying degrees of nuclear pleomorphism (Figure 1). Immunohistochemical (IHC) staining was negative for cytokeratin (CK) 20; however, CK7 was found positive (Figure 2), which confirmed the presence of a metastatic adenocarcinoma, consistent with the clinical diagnosis of a Sister Mary Joseph nodule (SMJN). Subsequent IHC workup to determine the site of origin revealed densely positive expression of both cancer antigen 125 and paired homeobox gene 8 (PAX-8)(Figure 3), consistent with primary ovarian disease. Furthermore, expression of estrogen receptor and p53 both were positive within the nuclei, illustrating an aberrant expression pattern. On the other hand, cancer antigen 19-9, caudal-type homeobox 2, gross cystic disease fluid protein 15, and mammaglobin were all determined negative, thus leading to the pathologic diagnosis of a metastatic ovarian adenocarcinoma. Additional workup with computed tomography of the abdomen and pelvis highlighted a large left ovarian mass with multiple omental nodules as well as enlarged retroperitoneal and pelvic lymph nodes.

The SMJN is a rare presentation of internal malignancy that appears as a nodule that metastasizes to the umbilicus. It may be ulcerated or necrotic and is seen in up to 10% of patients with cutaneous metastases from internal malignancy.1 These nodules are named after Sister Mary Joseph, the surgical assistant of Dr. William Mayo who first described the relationship between umbilical nodules seen in patients with gastrointestinal and genitourinary cancer. The most common underlying malignancies include primary gastrointestinal and gynecologic adenocarcinomas. In a retrospective study of 34 patients by Chalya et al,2 the stomach was found to be the most common primary site (41.1%). The presence of an SMJN affords a poor prognosis, with a mean overall survival of 11 months from the time of diagnosis.3 The mechanism of disease dissemination remains unknown but is thought to occur through lymphovascular invasion of tumor cells and spread via the umbilical ligament.1,4
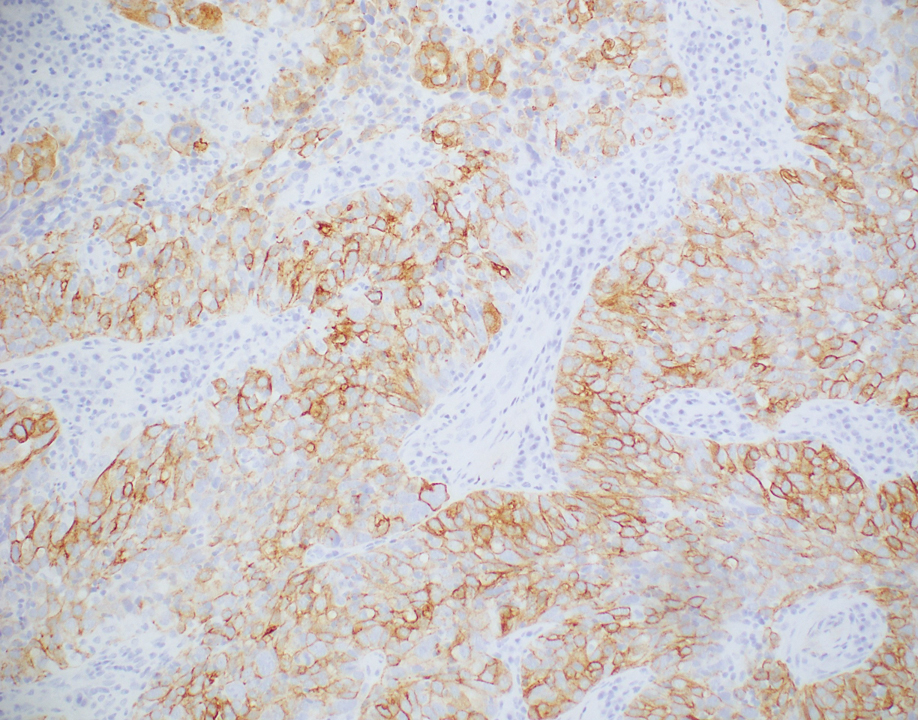
Merkel cell carcinoma is a cutaneous neuroendocrine tumor that most commonly presents in elderly patients as red-violet nodules or plaques. Although Merkel cell carcinoma most frequently is encountered on sun-exposed skin, they also can arise on the trunk and abdomen. Positive IHC staining for CK20 would be expected; however, it was negative in our case.5
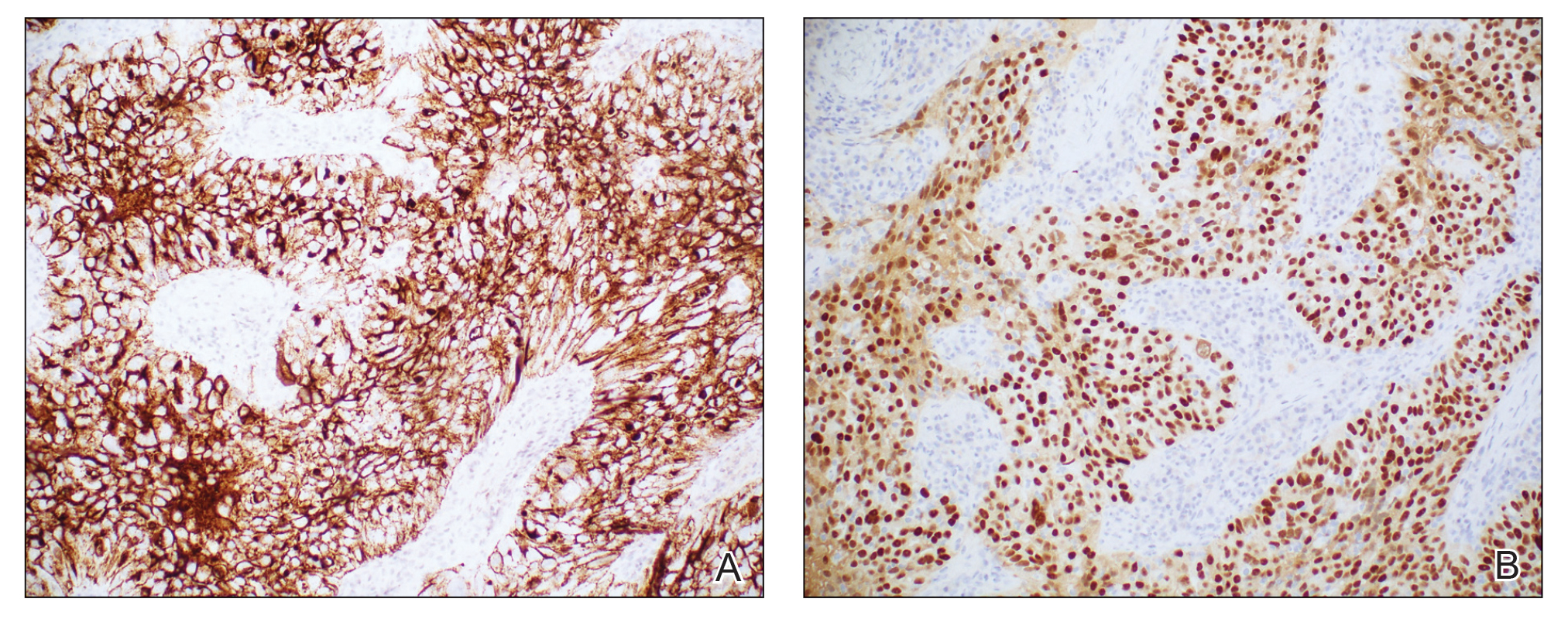
Cutaneous endometriosis is a rare disease presentation and most commonly occurs as a secondary process due to surgical inoculation of the abdominal wall. Primary cutaneous endometriosis in which there is no history of abdominal surgery less frequently is encountered. Patients typically will report pain and cyclical bleeding with menses. Pathology demonstrates ectopic endometrial tissue with glands and uterine myxoid stroma.6
Amelanotic melanoma is an uncommon subtype of malignant melanoma that presents as nonpigmented nodules that have a propensity to ulcerate and bleed. Furthermore, the umbilicus is an exceedingly rare location for primary melanoma. However, one report does exist, and amelanotic melanoma should be considered in the differential for patients with umbilical nodules.7
Dermoid cysts are benign congenital lesions that typically present as a painless, slow-growing, and wellcircumscribed nodule, as similarly experienced by our patient. They most commonly are found on the testicles and ovaries but also are known to arise in embryologic fusion planes, and reports of umbilical lesions exist.8 Dermoid cysts are diagnosed based on histopathology, supporting the need for a biopsy to distinguish a malignant process from benign lesions.9
- Gabriele R, Conte M, Egidi F, et al. Umbilical metastases: current viewpoint. World J Surg Oncol. 2005;3:13.
- Chalya PL, Mabula JB, Rambau PF, et al. Sister Mary Joseph’s nodule at a university teaching hospital in northwestern Tanzania: a retrospective review of 34 cases. World J Surg Oncol. 2013;11:151.
- Leyrat B, Bernadach M, Ginzac A, et al. Sister Mary Joseph nodules: a case report about a rare location of skin metastasis. Case Rep Oncol. 2021;14:664-670.
- Yendluri V, Centeno B, Springett GM. Pancreatic cancer presenting as a Sister Mary Joseph’s nodule: case report and update of the literature. Pancreas. 2007;34:161-164.
- Uchi H. Merkel cell carcinoma: an update and immunotherapy. Front Oncol. 2018;8:48.
- Bittar PG, Hryneewycz KT, Bryant EA. Primary cutaneous endometriosis presenting as an umbilical nodule. JAMA Dermatol. 2021;157:1227.
- Kovitwanichkanont T, Joseph S, Yip L. Hidden in plain sight: umbilical melanoma [published online January 28, 2020]. Med J Aust. 2020;212:154-155.e1.
- Prior A, Anania P, Pacetti M, et al. Dermoid and epidermoid cysts of scalp: case series of 234 consecutive patients. World Neurosurg. 2018;120:119-124.
- Akinci O, Turker C, Erturk MS, et al. Umbilical dermoid cyst: a rare case. Cerrahpasa Med J. 2020;44:51-53.
The Diagnosis: Sister Mary Joseph Nodule
Histopathologic analysis of the biopsy specimen revealed a dense infiltrate of large, hyperchromatic, mucin-producing cells exhibiting varying degrees of nuclear pleomorphism (Figure 1). Immunohistochemical (IHC) staining was negative for cytokeratin (CK) 20; however, CK7 was found positive (Figure 2), which confirmed the presence of a metastatic adenocarcinoma, consistent with the clinical diagnosis of a Sister Mary Joseph nodule (SMJN). Subsequent IHC workup to determine the site of origin revealed densely positive expression of both cancer antigen 125 and paired homeobox gene 8 (PAX-8)(Figure 3), consistent with primary ovarian disease. Furthermore, expression of estrogen receptor and p53 both were positive within the nuclei, illustrating an aberrant expression pattern. On the other hand, cancer antigen 19-9, caudal-type homeobox 2, gross cystic disease fluid protein 15, and mammaglobin were all determined negative, thus leading to the pathologic diagnosis of a metastatic ovarian adenocarcinoma. Additional workup with computed tomography of the abdomen and pelvis highlighted a large left ovarian mass with multiple omental nodules as well as enlarged retroperitoneal and pelvic lymph nodes.

The SMJN is a rare presentation of internal malignancy that appears as a nodule that metastasizes to the umbilicus. It may be ulcerated or necrotic and is seen in up to 10% of patients with cutaneous metastases from internal malignancy.1 These nodules are named after Sister Mary Joseph, the surgical assistant of Dr. William Mayo who first described the relationship between umbilical nodules seen in patients with gastrointestinal and genitourinary cancer. The most common underlying malignancies include primary gastrointestinal and gynecologic adenocarcinomas. In a retrospective study of 34 patients by Chalya et al,2 the stomach was found to be the most common primary site (41.1%). The presence of an SMJN affords a poor prognosis, with a mean overall survival of 11 months from the time of diagnosis.3 The mechanism of disease dissemination remains unknown but is thought to occur through lymphovascular invasion of tumor cells and spread via the umbilical ligament.1,4

Merkel cell carcinoma is a cutaneous neuroendocrine tumor that most commonly presents in elderly patients as red-violet nodules or plaques. Although Merkel cell carcinoma most frequently is encountered on sun-exposed skin, they also can arise on the trunk and abdomen. Positive IHC staining for CK20 would be expected; however, it was negative in our case.5

Cutaneous endometriosis is a rare disease presentation and most commonly occurs as a secondary process due to surgical inoculation of the abdominal wall. Primary cutaneous endometriosis in which there is no history of abdominal surgery less frequently is encountered. Patients typically will report pain and cyclical bleeding with menses. Pathology demonstrates ectopic endometrial tissue with glands and uterine myxoid stroma.6
Amelanotic melanoma is an uncommon subtype of malignant melanoma that presents as nonpigmented nodules that have a propensity to ulcerate and bleed. Furthermore, the umbilicus is an exceedingly rare location for primary melanoma. However, one report does exist, and amelanotic melanoma should be considered in the differential for patients with umbilical nodules.7
Dermoid cysts are benign congenital lesions that typically present as a painless, slow-growing, and wellcircumscribed nodule, as similarly experienced by our patient. They most commonly are found on the testicles and ovaries but also are known to arise in embryologic fusion planes, and reports of umbilical lesions exist.8 Dermoid cysts are diagnosed based on histopathology, supporting the need for a biopsy to distinguish a malignant process from benign lesions.9
The Diagnosis: Sister Mary Joseph Nodule
Histopathologic analysis of the biopsy specimen revealed a dense infiltrate of large, hyperchromatic, mucin-producing cells exhibiting varying degrees of nuclear pleomorphism (Figure 1). Immunohistochemical (IHC) staining was negative for cytokeratin (CK) 20; however, CK7 was found positive (Figure 2), which confirmed the presence of a metastatic adenocarcinoma, consistent with the clinical diagnosis of a Sister Mary Joseph nodule (SMJN). Subsequent IHC workup to determine the site of origin revealed densely positive expression of both cancer antigen 125 and paired homeobox gene 8 (PAX-8)(Figure 3), consistent with primary ovarian disease. Furthermore, expression of estrogen receptor and p53 both were positive within the nuclei, illustrating an aberrant expression pattern. On the other hand, cancer antigen 19-9, caudal-type homeobox 2, gross cystic disease fluid protein 15, and mammaglobin were all determined negative, thus leading to the pathologic diagnosis of a metastatic ovarian adenocarcinoma. Additional workup with computed tomography of the abdomen and pelvis highlighted a large left ovarian mass with multiple omental nodules as well as enlarged retroperitoneal and pelvic lymph nodes.

The SMJN is a rare presentation of internal malignancy that appears as a nodule that metastasizes to the umbilicus. It may be ulcerated or necrotic and is seen in up to 10% of patients with cutaneous metastases from internal malignancy.1 These nodules are named after Sister Mary Joseph, the surgical assistant of Dr. William Mayo who first described the relationship between umbilical nodules seen in patients with gastrointestinal and genitourinary cancer. The most common underlying malignancies include primary gastrointestinal and gynecologic adenocarcinomas. In a retrospective study of 34 patients by Chalya et al,2 the stomach was found to be the most common primary site (41.1%). The presence of an SMJN affords a poor prognosis, with a mean overall survival of 11 months from the time of diagnosis.3 The mechanism of disease dissemination remains unknown but is thought to occur through lymphovascular invasion of tumor cells and spread via the umbilical ligament.1,4

Merkel cell carcinoma is a cutaneous neuroendocrine tumor that most commonly presents in elderly patients as red-violet nodules or plaques. Although Merkel cell carcinoma most frequently is encountered on sun-exposed skin, they also can arise on the trunk and abdomen. Positive IHC staining for CK20 would be expected; however, it was negative in our case.5

Cutaneous endometriosis is a rare disease presentation and most commonly occurs as a secondary process due to surgical inoculation of the abdominal wall. Primary cutaneous endometriosis in which there is no history of abdominal surgery less frequently is encountered. Patients typically will report pain and cyclical bleeding with menses. Pathology demonstrates ectopic endometrial tissue with glands and uterine myxoid stroma.6
Amelanotic melanoma is an uncommon subtype of malignant melanoma that presents as nonpigmented nodules that have a propensity to ulcerate and bleed. Furthermore, the umbilicus is an exceedingly rare location for primary melanoma. However, one report does exist, and amelanotic melanoma should be considered in the differential for patients with umbilical nodules.7
Dermoid cysts are benign congenital lesions that typically present as a painless, slow-growing, and wellcircumscribed nodule, as similarly experienced by our patient. They most commonly are found on the testicles and ovaries but also are known to arise in embryologic fusion planes, and reports of umbilical lesions exist.8 Dermoid cysts are diagnosed based on histopathology, supporting the need for a biopsy to distinguish a malignant process from benign lesions.9
- Gabriele R, Conte M, Egidi F, et al. Umbilical metastases: current viewpoint. World J Surg Oncol. 2005;3:13.
- Chalya PL, Mabula JB, Rambau PF, et al. Sister Mary Joseph’s nodule at a university teaching hospital in northwestern Tanzania: a retrospective review of 34 cases. World J Surg Oncol. 2013;11:151.
- Leyrat B, Bernadach M, Ginzac A, et al. Sister Mary Joseph nodules: a case report about a rare location of skin metastasis. Case Rep Oncol. 2021;14:664-670.
- Yendluri V, Centeno B, Springett GM. Pancreatic cancer presenting as a Sister Mary Joseph’s nodule: case report and update of the literature. Pancreas. 2007;34:161-164.
- Uchi H. Merkel cell carcinoma: an update and immunotherapy. Front Oncol. 2018;8:48.
- Bittar PG, Hryneewycz KT, Bryant EA. Primary cutaneous endometriosis presenting as an umbilical nodule. JAMA Dermatol. 2021;157:1227.
- Kovitwanichkanont T, Joseph S, Yip L. Hidden in plain sight: umbilical melanoma [published online January 28, 2020]. Med J Aust. 2020;212:154-155.e1.
- Prior A, Anania P, Pacetti M, et al. Dermoid and epidermoid cysts of scalp: case series of 234 consecutive patients. World Neurosurg. 2018;120:119-124.
- Akinci O, Turker C, Erturk MS, et al. Umbilical dermoid cyst: a rare case. Cerrahpasa Med J. 2020;44:51-53.
- Gabriele R, Conte M, Egidi F, et al. Umbilical metastases: current viewpoint. World J Surg Oncol. 2005;3:13.
- Chalya PL, Mabula JB, Rambau PF, et al. Sister Mary Joseph’s nodule at a university teaching hospital in northwestern Tanzania: a retrospective review of 34 cases. World J Surg Oncol. 2013;11:151.
- Leyrat B, Bernadach M, Ginzac A, et al. Sister Mary Joseph nodules: a case report about a rare location of skin metastasis. Case Rep Oncol. 2021;14:664-670.
- Yendluri V, Centeno B, Springett GM. Pancreatic cancer presenting as a Sister Mary Joseph’s nodule: case report and update of the literature. Pancreas. 2007;34:161-164.
- Uchi H. Merkel cell carcinoma: an update and immunotherapy. Front Oncol. 2018;8:48.
- Bittar PG, Hryneewycz KT, Bryant EA. Primary cutaneous endometriosis presenting as an umbilical nodule. JAMA Dermatol. 2021;157:1227.
- Kovitwanichkanont T, Joseph S, Yip L. Hidden in plain sight: umbilical melanoma [published online January 28, 2020]. Med J Aust. 2020;212:154-155.e1.
- Prior A, Anania P, Pacetti M, et al. Dermoid and epidermoid cysts of scalp: case series of 234 consecutive patients. World Neurosurg. 2018;120:119-124.
- Akinci O, Turker C, Erturk MS, et al. Umbilical dermoid cyst: a rare case. Cerrahpasa Med J. 2020;44:51-53.
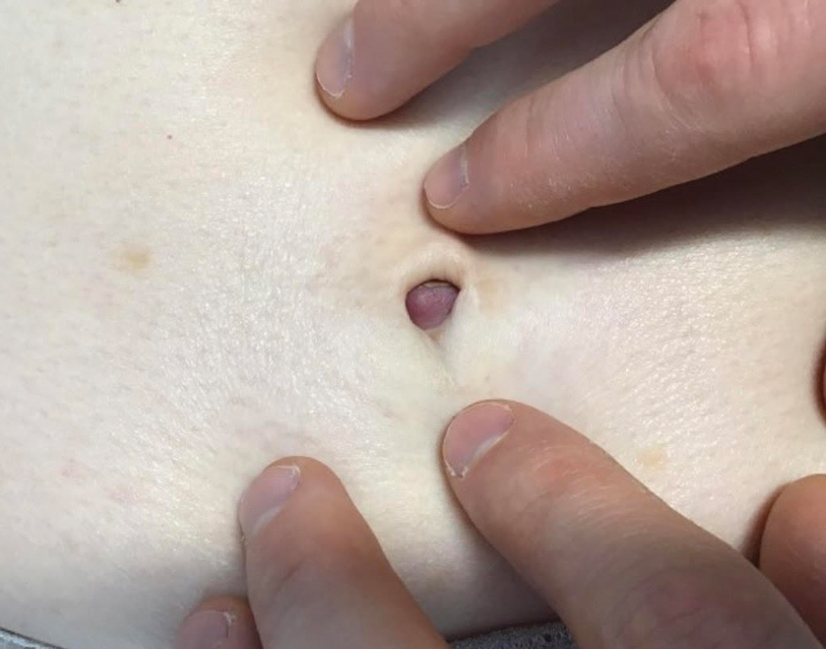
A 64-year-old woman with no notable medical history was referred to our dermatology clinic with an intermittent eczematous rash around the eyelids of 3 months’ duration. While performing a total-body skin examination, a firm pink nodule with a smooth surface incidentally was discovered on the umbilicus. The patient was uncertain when the lesion first appeared and denied any associated symptoms including pain and bleeding. Additionally, a lymph node examination revealed right inguinal lymphadenopathy. Upon further questioning, she reported worsening muscle weakness, fatigue, night sweats, and an unintentional weight loss of 10 pounds. A 6-mm punch biopsy of the umbilical lesion was obtained for routine histopathology.
Dupilumab-associated ocular surface disease in patients with AD: Unraveling the link
MONTREAL – , according to a study presented at the annual meeting of the International Society of Atopic Dermatitis.
In a prospective trial of 69 patients with AD starting dupilumab (Dupixent), baseline OSD was found in 91.3%, with about half of these patients reporting no symptoms, said investigator Roselie Achten, MD, from the National Expertise Center for Atopic Dermatitis at University Medical Center Utrecht, the Netherlands. Among these patients, ophthalmologic assessment revealed no OSD in 6 patients and mild OSD in 37 patients, but moderate and severe disease in 20 and 6 patients, respectively, she said, adding that 71% of the group also reported allergic conjunctivitis at baseline.
The patients enrolled in the study who started dupilumab were aged 36-38 years, with Eczema Area and Severity Index (EASI) scores of 14.7-16.5. Baseline ocular surface health was assessed with the Utrecht Ophthalmic Inflammatory and Allergic disease (UTOPIA) score. Tear fluid was collected to analyze biomarkers and dupilumab levels, and impression cytology was performed to collect conjunctival tissue cells for analysis of goblet cells. These measurements were repeated at 4 and 28 weeks after the start of therapy.
Over 28 weeks of treatment, 14.5% of patients experienced worsening of OSD, with worsening disease associated with a decline in the number of goblet cells. In addition, dupilumab treatment was associated with a significant decline in the production of Mucin5AC, suggesting a decline in function of the goblet cells. “Our hypothesis that the blocking effect of dupilumab on [interleukin-] IL-13 might lead to less goblet cells and less mucin production,” she explained.
In a subset of 48 patients, the researchers also detected significantly higher tear fluid dupilumab levels among those patients with more severe OSD, with comparable serum levels.
OSD has been reported in up to 34% of dupilumab-treated patients with AD and is the most frequently reported side-effect of this treatment, noted Dr. Achten. This side effect is not reported by other patients treated with dupilumab for other indications, she added, “suggesting that AD patients may have a predisposition to develop OSD during dupilumab treatment.”
Indeed, as recently noted by Vivian Shi, MD, from the department of dermatology, University of Arkansas for Medical Sciences, Little Rock, and colleagues, “for reasons not well understood, the incidence of conjunctivitis in dupilumab patients with asthma (0%-2.3%), chronic rhinosinusitis with nasal polyps (1.6%), or eosinophilic esophagitis (0%) is low to none; thus, patients with AD may be particularly susceptible.”
Dr. Achten said that dupilumab-treated patients with AD at her center are prescribed topical tacrolimus and ketotifen eye drops if they develop OSD.
Asked for comment, Melinda Gooderham, MD, who moderated the session, was impressed with the study. “I’d heard about the goblet cells, there were little bits of data here and there, but the tear analysis is something I hadn’t seen before. It was a nice series of experiments that pulled everything together,” she told this news organization. Dr. Gooderham, who is assistant professor at Queens University, in Kingston, Ontario, medical director at the SKiN Centre for Dermatology in Peterborough, Ontario, and consultant physician at Peterborough Regional Health Centre, said that she first began noticing dupilumab-related OSD as an early trial investigator for the drug. “When you put some patients on the drug it’s almost like tipping the balance – that little bit of mucin they’re dependent on is now reduced and it makes them more symptomatic,” she said.
Though she prescribes lubricating eye drops as prophylaxis for all her dupilumab-treated patients with AD, she recommends referring any patients who develop OSD to an ophthalmologist who is familiar with this specific side effect. “If they just see a random ophthalmologist who doesn’t know dupilumab, and doesn’t know the story around it, they could get any sort of diagnosis, or even be told to stop the medication altogether.”
The study was sponsored by Sanofi. Dr. Achten disclosed no other conflicts of interest. Dr. Gooderham is an investigator with Sanofi Genzyme for dupilumab.
A version of this article first appeared on Medscape.com.
MONTREAL – , according to a study presented at the annual meeting of the International Society of Atopic Dermatitis.
In a prospective trial of 69 patients with AD starting dupilumab (Dupixent), baseline OSD was found in 91.3%, with about half of these patients reporting no symptoms, said investigator Roselie Achten, MD, from the National Expertise Center for Atopic Dermatitis at University Medical Center Utrecht, the Netherlands. Among these patients, ophthalmologic assessment revealed no OSD in 6 patients and mild OSD in 37 patients, but moderate and severe disease in 20 and 6 patients, respectively, she said, adding that 71% of the group also reported allergic conjunctivitis at baseline.
The patients enrolled in the study who started dupilumab were aged 36-38 years, with Eczema Area and Severity Index (EASI) scores of 14.7-16.5. Baseline ocular surface health was assessed with the Utrecht Ophthalmic Inflammatory and Allergic disease (UTOPIA) score. Tear fluid was collected to analyze biomarkers and dupilumab levels, and impression cytology was performed to collect conjunctival tissue cells for analysis of goblet cells. These measurements were repeated at 4 and 28 weeks after the start of therapy.
Over 28 weeks of treatment, 14.5% of patients experienced worsening of OSD, with worsening disease associated with a decline in the number of goblet cells. In addition, dupilumab treatment was associated with a significant decline in the production of Mucin5AC, suggesting a decline in function of the goblet cells. “Our hypothesis that the blocking effect of dupilumab on [interleukin-] IL-13 might lead to less goblet cells and less mucin production,” she explained.
In a subset of 48 patients, the researchers also detected significantly higher tear fluid dupilumab levels among those patients with more severe OSD, with comparable serum levels.
OSD has been reported in up to 34% of dupilumab-treated patients with AD and is the most frequently reported side-effect of this treatment, noted Dr. Achten. This side effect is not reported by other patients treated with dupilumab for other indications, she added, “suggesting that AD patients may have a predisposition to develop OSD during dupilumab treatment.”
Indeed, as recently noted by Vivian Shi, MD, from the department of dermatology, University of Arkansas for Medical Sciences, Little Rock, and colleagues, “for reasons not well understood, the incidence of conjunctivitis in dupilumab patients with asthma (0%-2.3%), chronic rhinosinusitis with nasal polyps (1.6%), or eosinophilic esophagitis (0%) is low to none; thus, patients with AD may be particularly susceptible.”
Dr. Achten said that dupilumab-treated patients with AD at her center are prescribed topical tacrolimus and ketotifen eye drops if they develop OSD.
Asked for comment, Melinda Gooderham, MD, who moderated the session, was impressed with the study. “I’d heard about the goblet cells, there were little bits of data here and there, but the tear analysis is something I hadn’t seen before. It was a nice series of experiments that pulled everything together,” she told this news organization. Dr. Gooderham, who is assistant professor at Queens University, in Kingston, Ontario, medical director at the SKiN Centre for Dermatology in Peterborough, Ontario, and consultant physician at Peterborough Regional Health Centre, said that she first began noticing dupilumab-related OSD as an early trial investigator for the drug. “When you put some patients on the drug it’s almost like tipping the balance – that little bit of mucin they’re dependent on is now reduced and it makes them more symptomatic,” she said.
Though she prescribes lubricating eye drops as prophylaxis for all her dupilumab-treated patients with AD, she recommends referring any patients who develop OSD to an ophthalmologist who is familiar with this specific side effect. “If they just see a random ophthalmologist who doesn’t know dupilumab, and doesn’t know the story around it, they could get any sort of diagnosis, or even be told to stop the medication altogether.”
The study was sponsored by Sanofi. Dr. Achten disclosed no other conflicts of interest. Dr. Gooderham is an investigator with Sanofi Genzyme for dupilumab.
A version of this article first appeared on Medscape.com.
MONTREAL – , according to a study presented at the annual meeting of the International Society of Atopic Dermatitis.
In a prospective trial of 69 patients with AD starting dupilumab (Dupixent), baseline OSD was found in 91.3%, with about half of these patients reporting no symptoms, said investigator Roselie Achten, MD, from the National Expertise Center for Atopic Dermatitis at University Medical Center Utrecht, the Netherlands. Among these patients, ophthalmologic assessment revealed no OSD in 6 patients and mild OSD in 37 patients, but moderate and severe disease in 20 and 6 patients, respectively, she said, adding that 71% of the group also reported allergic conjunctivitis at baseline.
The patients enrolled in the study who started dupilumab were aged 36-38 years, with Eczema Area and Severity Index (EASI) scores of 14.7-16.5. Baseline ocular surface health was assessed with the Utrecht Ophthalmic Inflammatory and Allergic disease (UTOPIA) score. Tear fluid was collected to analyze biomarkers and dupilumab levels, and impression cytology was performed to collect conjunctival tissue cells for analysis of goblet cells. These measurements were repeated at 4 and 28 weeks after the start of therapy.
Over 28 weeks of treatment, 14.5% of patients experienced worsening of OSD, with worsening disease associated with a decline in the number of goblet cells. In addition, dupilumab treatment was associated with a significant decline in the production of Mucin5AC, suggesting a decline in function of the goblet cells. “Our hypothesis that the blocking effect of dupilumab on [interleukin-] IL-13 might lead to less goblet cells and less mucin production,” she explained.
In a subset of 48 patients, the researchers also detected significantly higher tear fluid dupilumab levels among those patients with more severe OSD, with comparable serum levels.
OSD has been reported in up to 34% of dupilumab-treated patients with AD and is the most frequently reported side-effect of this treatment, noted Dr. Achten. This side effect is not reported by other patients treated with dupilumab for other indications, she added, “suggesting that AD patients may have a predisposition to develop OSD during dupilumab treatment.”
Indeed, as recently noted by Vivian Shi, MD, from the department of dermatology, University of Arkansas for Medical Sciences, Little Rock, and colleagues, “for reasons not well understood, the incidence of conjunctivitis in dupilumab patients with asthma (0%-2.3%), chronic rhinosinusitis with nasal polyps (1.6%), or eosinophilic esophagitis (0%) is low to none; thus, patients with AD may be particularly susceptible.”
Dr. Achten said that dupilumab-treated patients with AD at her center are prescribed topical tacrolimus and ketotifen eye drops if they develop OSD.
Asked for comment, Melinda Gooderham, MD, who moderated the session, was impressed with the study. “I’d heard about the goblet cells, there were little bits of data here and there, but the tear analysis is something I hadn’t seen before. It was a nice series of experiments that pulled everything together,” she told this news organization. Dr. Gooderham, who is assistant professor at Queens University, in Kingston, Ontario, medical director at the SKiN Centre for Dermatology in Peterborough, Ontario, and consultant physician at Peterborough Regional Health Centre, said that she first began noticing dupilumab-related OSD as an early trial investigator for the drug. “When you put some patients on the drug it’s almost like tipping the balance – that little bit of mucin they’re dependent on is now reduced and it makes them more symptomatic,” she said.
Though she prescribes lubricating eye drops as prophylaxis for all her dupilumab-treated patients with AD, she recommends referring any patients who develop OSD to an ophthalmologist who is familiar with this specific side effect. “If they just see a random ophthalmologist who doesn’t know dupilumab, and doesn’t know the story around it, they could get any sort of diagnosis, or even be told to stop the medication altogether.”
The study was sponsored by Sanofi. Dr. Achten disclosed no other conflicts of interest. Dr. Gooderham is an investigator with Sanofi Genzyme for dupilumab.
A version of this article first appeared on Medscape.com.
FROM ISAD 2022
Achieving diversity, equity and inclusion: Invite everyone and build a team
What you really don’t want to do, if you want to improve diversity, equity, and inclusion (DEI) at your academic institution, is to recruit diverse people to your program and then have them come and feel not included, said Vivian Asare, MD. “That can work against your efforts,” she stated in an oral presentation at the annual meeting of the American College of Chest Physicians (CHEST). Dr. Asare is assistant professor and vice chief of DEI for Yale Pulmonary, Critical Care, and Sleep Medicine, and associate medical director of Yale Centers for Sleep Medicine, New Haven, Conn.
In offering a path to successful DEI, Dr. Asare said: “The first step is to build a team and discuss your mission. Invite everyone to participate and include your leadership because they’re the ones who set the stage, ensure sustainability, and can be a liaison with faculty.” Then a DEI leader should be elected, she added.
The next and very important step is to survey the current institutional climate. That entails speaking directly with the stakeholders (faculty, staff, trainees) and identifying their specific concerns and what they think is lacking. Retreats, serious group discussions, and self-reflecting (asking “what initiatives would be good for us?”), and meeting one-on-one with individuals for a truly personalized approach are among potentially productive strategies for identifying the priorities and DEI-related topics specific to a particular academic sleep program.
Dr. Asare offered up a sample DEI survey (Am J Obstet Gynecol. 2020 Nov;223[5]:715.e1-715.e7), that made direct statements inviting the respondent to check off one of the following responses: Yes, No, Somewhat, Do not know, and Not applicable. Among sample statements:
- Our department is actively committed to issues of diversity, equity, and inclusion.
- Faculty searches in the department regularly attract a diverse pool of highly qualified candidates and/or attract a pool that represents the availability of MDs in this field.
- Our outreach and recruitment processes employ targeted practices for attracting diverse populations.
Dr. Asare said that a survey can be a simple approach for garnering information that can be useful for prioritizing DEI topics of concern and igniting interest in them. Engagement requires regular DEI committee meetings with minutes or a newsletter and with updates and topics brought to faculty meetings.
Key DEI areas of focus
Dr. Asare listed several key DEI areas: Recruitment/retention, mentorship, scholarship, and inclusion and community engagement. Under scholarship, for example, she cited topics for potential inclusion in a DEI curriculum: Unconscious bias and anti-racism training, racism, discrimination and microaggression education (bystander/deescalation training), cultural competency and awareness, workplace civility, and health disparities. “We all know that implicit bias in providers is a reality, unfortunately,” Dr. Asare said. Being aware of these implicit biases is a start, but instruction on how to actively overcome them has to be provided. Tools may include perspective-taking, exploring common identity, and self-reflection.
To create an inclusive environment for all faculty, trainees, and staff may involve establishing a “welcome committee” for new faculty, perhaps with designating a “peer buddy,” creating social events and other opportunities for all opinions and ideas to be heard and valued. Particularly for underserved and disadvantaged patient populations, patient advocacy and community service need to be fostered through support groups and provision of resources.
Summarizing, Dr. Asare reiterated several key elements for a successful DEI program: Build a team and discuss the mission, survey the current climate allowing open communication and dialogue, plan and engage, organize, and form areas of DEI focus. Find out where you are and where you want to be with respect to DEI, she concluded.
Dr. Asare declared that she had no conflicts of interest.
What you really don’t want to do, if you want to improve diversity, equity, and inclusion (DEI) at your academic institution, is to recruit diverse people to your program and then have them come and feel not included, said Vivian Asare, MD. “That can work against your efforts,” she stated in an oral presentation at the annual meeting of the American College of Chest Physicians (CHEST). Dr. Asare is assistant professor and vice chief of DEI for Yale Pulmonary, Critical Care, and Sleep Medicine, and associate medical director of Yale Centers for Sleep Medicine, New Haven, Conn.
In offering a path to successful DEI, Dr. Asare said: “The first step is to build a team and discuss your mission. Invite everyone to participate and include your leadership because they’re the ones who set the stage, ensure sustainability, and can be a liaison with faculty.” Then a DEI leader should be elected, she added.
The next and very important step is to survey the current institutional climate. That entails speaking directly with the stakeholders (faculty, staff, trainees) and identifying their specific concerns and what they think is lacking. Retreats, serious group discussions, and self-reflecting (asking “what initiatives would be good for us?”), and meeting one-on-one with individuals for a truly personalized approach are among potentially productive strategies for identifying the priorities and DEI-related topics specific to a particular academic sleep program.
Dr. Asare offered up a sample DEI survey (Am J Obstet Gynecol. 2020 Nov;223[5]:715.e1-715.e7), that made direct statements inviting the respondent to check off one of the following responses: Yes, No, Somewhat, Do not know, and Not applicable. Among sample statements:
- Our department is actively committed to issues of diversity, equity, and inclusion.
- Faculty searches in the department regularly attract a diverse pool of highly qualified candidates and/or attract a pool that represents the availability of MDs in this field.
- Our outreach and recruitment processes employ targeted practices for attracting diverse populations.
Dr. Asare said that a survey can be a simple approach for garnering information that can be useful for prioritizing DEI topics of concern and igniting interest in them. Engagement requires regular DEI committee meetings with minutes or a newsletter and with updates and topics brought to faculty meetings.
Key DEI areas of focus
Dr. Asare listed several key DEI areas: Recruitment/retention, mentorship, scholarship, and inclusion and community engagement. Under scholarship, for example, she cited topics for potential inclusion in a DEI curriculum: Unconscious bias and anti-racism training, racism, discrimination and microaggression education (bystander/deescalation training), cultural competency and awareness, workplace civility, and health disparities. “We all know that implicit bias in providers is a reality, unfortunately,” Dr. Asare said. Being aware of these implicit biases is a start, but instruction on how to actively overcome them has to be provided. Tools may include perspective-taking, exploring common identity, and self-reflection.
To create an inclusive environment for all faculty, trainees, and staff may involve establishing a “welcome committee” for new faculty, perhaps with designating a “peer buddy,” creating social events and other opportunities for all opinions and ideas to be heard and valued. Particularly for underserved and disadvantaged patient populations, patient advocacy and community service need to be fostered through support groups and provision of resources.
Summarizing, Dr. Asare reiterated several key elements for a successful DEI program: Build a team and discuss the mission, survey the current climate allowing open communication and dialogue, plan and engage, organize, and form areas of DEI focus. Find out where you are and where you want to be with respect to DEI, she concluded.
Dr. Asare declared that she had no conflicts of interest.
What you really don’t want to do, if you want to improve diversity, equity, and inclusion (DEI) at your academic institution, is to recruit diverse people to your program and then have them come and feel not included, said Vivian Asare, MD. “That can work against your efforts,” she stated in an oral presentation at the annual meeting of the American College of Chest Physicians (CHEST). Dr. Asare is assistant professor and vice chief of DEI for Yale Pulmonary, Critical Care, and Sleep Medicine, and associate medical director of Yale Centers for Sleep Medicine, New Haven, Conn.
In offering a path to successful DEI, Dr. Asare said: “The first step is to build a team and discuss your mission. Invite everyone to participate and include your leadership because they’re the ones who set the stage, ensure sustainability, and can be a liaison with faculty.” Then a DEI leader should be elected, she added.
The next and very important step is to survey the current institutional climate. That entails speaking directly with the stakeholders (faculty, staff, trainees) and identifying their specific concerns and what they think is lacking. Retreats, serious group discussions, and self-reflecting (asking “what initiatives would be good for us?”), and meeting one-on-one with individuals for a truly personalized approach are among potentially productive strategies for identifying the priorities and DEI-related topics specific to a particular academic sleep program.
Dr. Asare offered up a sample DEI survey (Am J Obstet Gynecol. 2020 Nov;223[5]:715.e1-715.e7), that made direct statements inviting the respondent to check off one of the following responses: Yes, No, Somewhat, Do not know, and Not applicable. Among sample statements:
- Our department is actively committed to issues of diversity, equity, and inclusion.
- Faculty searches in the department regularly attract a diverse pool of highly qualified candidates and/or attract a pool that represents the availability of MDs in this field.
- Our outreach and recruitment processes employ targeted practices for attracting diverse populations.
Dr. Asare said that a survey can be a simple approach for garnering information that can be useful for prioritizing DEI topics of concern and igniting interest in them. Engagement requires regular DEI committee meetings with minutes or a newsletter and with updates and topics brought to faculty meetings.
Key DEI areas of focus
Dr. Asare listed several key DEI areas: Recruitment/retention, mentorship, scholarship, and inclusion and community engagement. Under scholarship, for example, she cited topics for potential inclusion in a DEI curriculum: Unconscious bias and anti-racism training, racism, discrimination and microaggression education (bystander/deescalation training), cultural competency and awareness, workplace civility, and health disparities. “We all know that implicit bias in providers is a reality, unfortunately,” Dr. Asare said. Being aware of these implicit biases is a start, but instruction on how to actively overcome them has to be provided. Tools may include perspective-taking, exploring common identity, and self-reflection.
To create an inclusive environment for all faculty, trainees, and staff may involve establishing a “welcome committee” for new faculty, perhaps with designating a “peer buddy,” creating social events and other opportunities for all opinions and ideas to be heard and valued. Particularly for underserved and disadvantaged patient populations, patient advocacy and community service need to be fostered through support groups and provision of resources.
Summarizing, Dr. Asare reiterated several key elements for a successful DEI program: Build a team and discuss the mission, survey the current climate allowing open communication and dialogue, plan and engage, organize, and form areas of DEI focus. Find out where you are and where you want to be with respect to DEI, she concluded.
Dr. Asare declared that she had no conflicts of interest.
FROM CHEST 2022
Ready or not, hands-free devices are coming
Denver – When Anne Chapas, MD, was asked to help conduct a clinical trial of a wearable, hands-free device for remodeling of the face and submental area, she responded with a healthy dose of skepticism.
“My first thought was, ‘this is crazy. It looks like a Storm Trooper helmet,’ ” Dr. Chapas, founder and medical director of UnionDerm, New York, said at the annual meeting of the American Society for Dermatologic Surgery. “But it’s the first FDA-cleared device that uses bipolar radiofrequency to target the lower third of the face and the submental area of the face. We wanted to see how it works.”
Its bipolar radiofrequency (RF) component reaches 4 mm in depth and travels from central to outer electrodes. The device features real-time temperature monitoring and the ability to delivery energy at lower temps for longer periods of time compared with hands-on approaches. No cooling is required.
“It is able to treat a large surface area simultaneously to achieve maximal tissue contraction,” Dr. Chapas said. “What we’ve learned in decades of RF technology is that it’s not just about heat. It has to be the right amount of heat for the right amount of time. That’s what’s difficult when we’re doing our own individual treatments. How many pulses do we need? How is that heat dissipating? Are we getting the amount of heat we need? Is the patient in pain? We need to take that data from the individual provider and come up with an automated system. That’s what this device is trying to accomplish.”
In a prospective trial, she and her colleagues enrolled 40 patients between the ages of 36 and 75 years with visible signs of facial aging who were seeking skin tightening treatments at one of three centers in the United States. They underwent three biweekly treatments with the Evoke device to the lower face and submental area where a target temperature of 42°-43° C was maintained for 41 minutes, or about 20 minutes for each site.
For the primary safety endpoint, investigators and blinded evaluators used a 4-point Likert scale before treatment, and 1, 3, and 6 months post-treatment. Follow-up visit satisfaction metrics were the patient’s skin appearance evaluation and overall satisfaction, and the investigator improvement rating based on an analysis of volumetric data from 3D imaging software. Chin and cheek discomfort metrics were assessed at all treatments. The subject satisfaction metrics were measured on an 11-point scale where 0 is most comfortable and 10 is most uncomfortable.
In terms of safety, patients tolerated the treatments well and rated their average discomfort from 0.643 to 1.45 on the 11-point Likert scale. “The subject satisfaction rate was about 80%, which is in line with other devices, such as microfocused ultrasound,” said Dr. Chapas, who is also a clinical instructor of dermatology at the Mount Sinai Medical Center, New York.
“The physicians were a little tougher on their assessments. We felt there was about a 65%-70% success rate after the three treatment timepoints.” One possible reason for the disparity between the patient and physician assessments is that patients “may be more accepting of meager results from a hands-free treatment.”
Expect to see more hands-free devices hit the dermatology market in the coming months and years ahead, Dr. Chapas said. Before clinicians incorporate such systems into their practices, she advises them to review existing evidence for the technology, including published data and asking for demonstrations. “If it’s not efficacious, you’ve just wasted everybody’s time,” she said. “Also, is it practical for your office? Do you have the space for it? What staff training is involved? Is it truly automated?”
She added, “If you have a device that’s hands-free but someone must stay in the room with the patient for an hour, does that really help the flow of your practice? And finally, what do your patients want? Do they want to come back multiple times, or do they prefer one-and-done treatments?”
Other questions to consider, she said, include, who benefits from these treatments. Does it fill an unmet need for patients, and for clinicians? Does it help with operator fatigue? How are more consistent treatments achieved? Can the technology be applied to broad body areas?
“The hands-free revolution has been building,” Dr. Chapas commented. “The next generation of lasers and energy devices are going to be coming into our offices, so we should think carefully about how to incorporate them.”
Dr. Chapas disclosed that she is an investigator for InMode (the manufacturer of Evoke), Cutera, and Galderma, and a speaker for Allergan.
Denver – When Anne Chapas, MD, was asked to help conduct a clinical trial of a wearable, hands-free device for remodeling of the face and submental area, she responded with a healthy dose of skepticism.
“My first thought was, ‘this is crazy. It looks like a Storm Trooper helmet,’ ” Dr. Chapas, founder and medical director of UnionDerm, New York, said at the annual meeting of the American Society for Dermatologic Surgery. “But it’s the first FDA-cleared device that uses bipolar radiofrequency to target the lower third of the face and the submental area of the face. We wanted to see how it works.”
Its bipolar radiofrequency (RF) component reaches 4 mm in depth and travels from central to outer electrodes. The device features real-time temperature monitoring and the ability to delivery energy at lower temps for longer periods of time compared with hands-on approaches. No cooling is required.
“It is able to treat a large surface area simultaneously to achieve maximal tissue contraction,” Dr. Chapas said. “What we’ve learned in decades of RF technology is that it’s not just about heat. It has to be the right amount of heat for the right amount of time. That’s what’s difficult when we’re doing our own individual treatments. How many pulses do we need? How is that heat dissipating? Are we getting the amount of heat we need? Is the patient in pain? We need to take that data from the individual provider and come up with an automated system. That’s what this device is trying to accomplish.”
In a prospective trial, she and her colleagues enrolled 40 patients between the ages of 36 and 75 years with visible signs of facial aging who were seeking skin tightening treatments at one of three centers in the United States. They underwent three biweekly treatments with the Evoke device to the lower face and submental area where a target temperature of 42°-43° C was maintained for 41 minutes, or about 20 minutes for each site.
For the primary safety endpoint, investigators and blinded evaluators used a 4-point Likert scale before treatment, and 1, 3, and 6 months post-treatment. Follow-up visit satisfaction metrics were the patient’s skin appearance evaluation and overall satisfaction, and the investigator improvement rating based on an analysis of volumetric data from 3D imaging software. Chin and cheek discomfort metrics were assessed at all treatments. The subject satisfaction metrics were measured on an 11-point scale where 0 is most comfortable and 10 is most uncomfortable.
In terms of safety, patients tolerated the treatments well and rated their average discomfort from 0.643 to 1.45 on the 11-point Likert scale. “The subject satisfaction rate was about 80%, which is in line with other devices, such as microfocused ultrasound,” said Dr. Chapas, who is also a clinical instructor of dermatology at the Mount Sinai Medical Center, New York.
“The physicians were a little tougher on their assessments. We felt there was about a 65%-70% success rate after the three treatment timepoints.” One possible reason for the disparity between the patient and physician assessments is that patients “may be more accepting of meager results from a hands-free treatment.”
Expect to see more hands-free devices hit the dermatology market in the coming months and years ahead, Dr. Chapas said. Before clinicians incorporate such systems into their practices, she advises them to review existing evidence for the technology, including published data and asking for demonstrations. “If it’s not efficacious, you’ve just wasted everybody’s time,” she said. “Also, is it practical for your office? Do you have the space for it? What staff training is involved? Is it truly automated?”
She added, “If you have a device that’s hands-free but someone must stay in the room with the patient for an hour, does that really help the flow of your practice? And finally, what do your patients want? Do they want to come back multiple times, or do they prefer one-and-done treatments?”
Other questions to consider, she said, include, who benefits from these treatments. Does it fill an unmet need for patients, and for clinicians? Does it help with operator fatigue? How are more consistent treatments achieved? Can the technology be applied to broad body areas?
“The hands-free revolution has been building,” Dr. Chapas commented. “The next generation of lasers and energy devices are going to be coming into our offices, so we should think carefully about how to incorporate them.”
Dr. Chapas disclosed that she is an investigator for InMode (the manufacturer of Evoke), Cutera, and Galderma, and a speaker for Allergan.
Denver – When Anne Chapas, MD, was asked to help conduct a clinical trial of a wearable, hands-free device for remodeling of the face and submental area, she responded with a healthy dose of skepticism.
“My first thought was, ‘this is crazy. It looks like a Storm Trooper helmet,’ ” Dr. Chapas, founder and medical director of UnionDerm, New York, said at the annual meeting of the American Society for Dermatologic Surgery. “But it’s the first FDA-cleared device that uses bipolar radiofrequency to target the lower third of the face and the submental area of the face. We wanted to see how it works.”
Its bipolar radiofrequency (RF) component reaches 4 mm in depth and travels from central to outer electrodes. The device features real-time temperature monitoring and the ability to delivery energy at lower temps for longer periods of time compared with hands-on approaches. No cooling is required.
“It is able to treat a large surface area simultaneously to achieve maximal tissue contraction,” Dr. Chapas said. “What we’ve learned in decades of RF technology is that it’s not just about heat. It has to be the right amount of heat for the right amount of time. That’s what’s difficult when we’re doing our own individual treatments. How many pulses do we need? How is that heat dissipating? Are we getting the amount of heat we need? Is the patient in pain? We need to take that data from the individual provider and come up with an automated system. That’s what this device is trying to accomplish.”
In a prospective trial, she and her colleagues enrolled 40 patients between the ages of 36 and 75 years with visible signs of facial aging who were seeking skin tightening treatments at one of three centers in the United States. They underwent three biweekly treatments with the Evoke device to the lower face and submental area where a target temperature of 42°-43° C was maintained for 41 minutes, or about 20 minutes for each site.
For the primary safety endpoint, investigators and blinded evaluators used a 4-point Likert scale before treatment, and 1, 3, and 6 months post-treatment. Follow-up visit satisfaction metrics were the patient’s skin appearance evaluation and overall satisfaction, and the investigator improvement rating based on an analysis of volumetric data from 3D imaging software. Chin and cheek discomfort metrics were assessed at all treatments. The subject satisfaction metrics were measured on an 11-point scale where 0 is most comfortable and 10 is most uncomfortable.
In terms of safety, patients tolerated the treatments well and rated their average discomfort from 0.643 to 1.45 on the 11-point Likert scale. “The subject satisfaction rate was about 80%, which is in line with other devices, such as microfocused ultrasound,” said Dr. Chapas, who is also a clinical instructor of dermatology at the Mount Sinai Medical Center, New York.
“The physicians were a little tougher on their assessments. We felt there was about a 65%-70% success rate after the three treatment timepoints.” One possible reason for the disparity between the patient and physician assessments is that patients “may be more accepting of meager results from a hands-free treatment.”
Expect to see more hands-free devices hit the dermatology market in the coming months and years ahead, Dr. Chapas said. Before clinicians incorporate such systems into their practices, she advises them to review existing evidence for the technology, including published data and asking for demonstrations. “If it’s not efficacious, you’ve just wasted everybody’s time,” she said. “Also, is it practical for your office? Do you have the space for it? What staff training is involved? Is it truly automated?”
She added, “If you have a device that’s hands-free but someone must stay in the room with the patient for an hour, does that really help the flow of your practice? And finally, what do your patients want? Do they want to come back multiple times, or do they prefer one-and-done treatments?”
Other questions to consider, she said, include, who benefits from these treatments. Does it fill an unmet need for patients, and for clinicians? Does it help with operator fatigue? How are more consistent treatments achieved? Can the technology be applied to broad body areas?
“The hands-free revolution has been building,” Dr. Chapas commented. “The next generation of lasers and energy devices are going to be coming into our offices, so we should think carefully about how to incorporate them.”
Dr. Chapas disclosed that she is an investigator for InMode (the manufacturer of Evoke), Cutera, and Galderma, and a speaker for Allergan.
AT ASDS 2022
Alcohol use disorder and atopic dermatitis: Is there a link?
Key clinical point: Patients with atopic dermatitis (AD) have a 50% higher chance of developing alcohol use disorder (AUD) than people without AD and should be screened when appropriate.
Major finding: Patients with AD had a significantly higher chance of developing AUD (odds ratio 1.50; P < .001) than controls without AD.
Study details: Findings are from the All of Us cohort including 11,752 patients with AD and 47,008 matched controls.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Fan R et al. Alcohol use disorder among adults with atopic dermatitis: A case-control study in the All of Us research program. J Am Acad Dermatol. 2022 (Sep 20). Doi: 10.1016/j.jaad.2022.09.015
Key clinical point: Patients with atopic dermatitis (AD) have a 50% higher chance of developing alcohol use disorder (AUD) than people without AD and should be screened when appropriate.
Major finding: Patients with AD had a significantly higher chance of developing AUD (odds ratio 1.50; P < .001) than controls without AD.
Study details: Findings are from the All of Us cohort including 11,752 patients with AD and 47,008 matched controls.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Fan R et al. Alcohol use disorder among adults with atopic dermatitis: A case-control study in the All of Us research program. J Am Acad Dermatol. 2022 (Sep 20). Doi: 10.1016/j.jaad.2022.09.015
Key clinical point: Patients with atopic dermatitis (AD) have a 50% higher chance of developing alcohol use disorder (AUD) than people without AD and should be screened when appropriate.
Major finding: Patients with AD had a significantly higher chance of developing AUD (odds ratio 1.50; P < .001) than controls without AD.
Study details: Findings are from the All of Us cohort including 11,752 patients with AD and 47,008 matched controls.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Fan R et al. Alcohol use disorder among adults with atopic dermatitis: A case-control study in the All of Us research program. J Am Acad Dermatol. 2022 (Sep 20). Doi: 10.1016/j.jaad.2022.09.015
Dampness and mold increase risk for atopic dermatitis
Key clinical point: The presence of dampness and mold at home affected offspring health outcomes negatively by increasing the prevalence of atopic dermatitis (AD).
Major finding: AD was associated with visible mold (odds ratio [OR] 1.35; P = .001) and dampness/mold at home between the first and second follow-up (OR 1.18; P = .008) and during both follow-up periods (OR 1.38; P < .001).
Study details: Findings are from the Respiratory Health in Northern Europe study including 17,881 offspring aged ≤30 years who had undergone two follow-up investigations every 10 years. Of these, 17.3% had developed AD.
Disclosures: This study was supported by the Icelandic Research Council and other sources. The authors declared no conflicts of interest.
Source: Wang J et al. Asthma, allergic rhinitis and atopic dermatitis in association with home environment—The RHINE study. Sci Total Environ. 2022;853:158609 (Sep 8). Doi: 10.1016/j.scitotenv.2022.158609
Key clinical point: The presence of dampness and mold at home affected offspring health outcomes negatively by increasing the prevalence of atopic dermatitis (AD).
Major finding: AD was associated with visible mold (odds ratio [OR] 1.35; P = .001) and dampness/mold at home between the first and second follow-up (OR 1.18; P = .008) and during both follow-up periods (OR 1.38; P < .001).
Study details: Findings are from the Respiratory Health in Northern Europe study including 17,881 offspring aged ≤30 years who had undergone two follow-up investigations every 10 years. Of these, 17.3% had developed AD.
Disclosures: This study was supported by the Icelandic Research Council and other sources. The authors declared no conflicts of interest.
Source: Wang J et al. Asthma, allergic rhinitis and atopic dermatitis in association with home environment—The RHINE study. Sci Total Environ. 2022;853:158609 (Sep 8). Doi: 10.1016/j.scitotenv.2022.158609
Key clinical point: The presence of dampness and mold at home affected offspring health outcomes negatively by increasing the prevalence of atopic dermatitis (AD).
Major finding: AD was associated with visible mold (odds ratio [OR] 1.35; P = .001) and dampness/mold at home between the first and second follow-up (OR 1.18; P = .008) and during both follow-up periods (OR 1.38; P < .001).
Study details: Findings are from the Respiratory Health in Northern Europe study including 17,881 offspring aged ≤30 years who had undergone two follow-up investigations every 10 years. Of these, 17.3% had developed AD.
Disclosures: This study was supported by the Icelandic Research Council and other sources. The authors declared no conflicts of interest.
Source: Wang J et al. Asthma, allergic rhinitis and atopic dermatitis in association with home environment—The RHINE study. Sci Total Environ. 2022;853:158609 (Sep 8). Doi: 10.1016/j.scitotenv.2022.158609
Meta-analysis demonstrates long-term atopic dermatitis prevention with L. rhamnosus probiotic
Key clinical point: Lactobacillus rhamnosus, with or without other probiotics, reduced the incidence risk for atopic dermatitis (AD) in children when administered to mothers and infants in the perinatal period.
Major finding: The risk of developing AD was significantly reduced at 2 years (risk ratio [RR] 0.60; P < .00001) and 6-7 years (RR 0.62; P < .00001) with L. rhamnosus or L. rhamnosus + other probiotic strains.
Study details: Findings are from a meta-analysis of 11 randomized controlled trials that reported the incidence of AD after oral administration of L. rhamnosus or L. rhamnasos + other probiotics during pregnancy and post-pregnancy in mothers and infants.
Disclosures: J Voigt received partial funding. The authors declared serving as an evidence assessment expert or an executive for Lil Mixins, a manufacturer of probiotic supplements.
Source: Voigt J and Lele M. Lactobacillus rhamnosus used in the perinatal period for the prevention of atopic dermatitis in infants: A systematic review and meta-analysis of randomized trials. Am J Clin Dermatol. 2022;23:801–811 (Sep 26). Doi: 10.1007/s40257-022-00723-x
Key clinical point: Lactobacillus rhamnosus, with or without other probiotics, reduced the incidence risk for atopic dermatitis (AD) in children when administered to mothers and infants in the perinatal period.
Major finding: The risk of developing AD was significantly reduced at 2 years (risk ratio [RR] 0.60; P < .00001) and 6-7 years (RR 0.62; P < .00001) with L. rhamnosus or L. rhamnosus + other probiotic strains.
Study details: Findings are from a meta-analysis of 11 randomized controlled trials that reported the incidence of AD after oral administration of L. rhamnosus or L. rhamnasos + other probiotics during pregnancy and post-pregnancy in mothers and infants.
Disclosures: J Voigt received partial funding. The authors declared serving as an evidence assessment expert or an executive for Lil Mixins, a manufacturer of probiotic supplements.
Source: Voigt J and Lele M. Lactobacillus rhamnosus used in the perinatal period for the prevention of atopic dermatitis in infants: A systematic review and meta-analysis of randomized trials. Am J Clin Dermatol. 2022;23:801–811 (Sep 26). Doi: 10.1007/s40257-022-00723-x
Key clinical point: Lactobacillus rhamnosus, with or without other probiotics, reduced the incidence risk for atopic dermatitis (AD) in children when administered to mothers and infants in the perinatal period.
Major finding: The risk of developing AD was significantly reduced at 2 years (risk ratio [RR] 0.60; P < .00001) and 6-7 years (RR 0.62; P < .00001) with L. rhamnosus or L. rhamnosus + other probiotic strains.
Study details: Findings are from a meta-analysis of 11 randomized controlled trials that reported the incidence of AD after oral administration of L. rhamnosus or L. rhamnasos + other probiotics during pregnancy and post-pregnancy in mothers and infants.
Disclosures: J Voigt received partial funding. The authors declared serving as an evidence assessment expert or an executive for Lil Mixins, a manufacturer of probiotic supplements.
Source: Voigt J and Lele M. Lactobacillus rhamnosus used in the perinatal period for the prevention of atopic dermatitis in infants: A systematic review and meta-analysis of randomized trials. Am J Clin Dermatol. 2022;23:801–811 (Sep 26). Doi: 10.1007/s40257-022-00723-x
Atopic dermatitis: Meta-analysis demonstrates efficacy of allergen immunotherapy
Key clinical point: Patients with atopic dermatitis (AD) who received adjunctive allergen immunotherapy (AIT) reported improvements in disease severity and quality of life despite an increase in the rate of adverse events (AE).
Major finding: AIT vs no AIT improved disease severity (risk ratio [RR] 1.53; 95% CI 1.31-1.78) and the Dermatology Life Quality Index by at least 4 points (RR 1.44; 95% CI 1.03-2.01). The rates of local (RR 1.65; 95% CI 1.48-1.64) and systemic (RR 1.37; 95% CI 1.15-1.64) AE were higher with AIT vs placebo.
Study details: Findings are from a meta-analysis of 23 randomized controlled trials including 1957 adult and pediatric patients with moderate-to-severe AD who were randomly assigned to adjunctive AIT (subcutaneous or sublingual immunotherapy) or no AIT (placebo or standard care).
Disclosures: This study was supported by the American Academy of Allergy, Asthma, & Immunology and other sources. The authors declared no conflicts of interest.
Source: Yepes-Nuñez JJ et al. Allergen immunotherapy for atopic dermatitis: A systematic review and meta-analysis of benefits and harms. J Allergy Clin Immunol. 2022 (Sep 30). Doi: 10.1016/j.jaci.2022.09.020
Key clinical point: Patients with atopic dermatitis (AD) who received adjunctive allergen immunotherapy (AIT) reported improvements in disease severity and quality of life despite an increase in the rate of adverse events (AE).
Major finding: AIT vs no AIT improved disease severity (risk ratio [RR] 1.53; 95% CI 1.31-1.78) and the Dermatology Life Quality Index by at least 4 points (RR 1.44; 95% CI 1.03-2.01). The rates of local (RR 1.65; 95% CI 1.48-1.64) and systemic (RR 1.37; 95% CI 1.15-1.64) AE were higher with AIT vs placebo.
Study details: Findings are from a meta-analysis of 23 randomized controlled trials including 1957 adult and pediatric patients with moderate-to-severe AD who were randomly assigned to adjunctive AIT (subcutaneous or sublingual immunotherapy) or no AIT (placebo or standard care).
Disclosures: This study was supported by the American Academy of Allergy, Asthma, & Immunology and other sources. The authors declared no conflicts of interest.
Source: Yepes-Nuñez JJ et al. Allergen immunotherapy for atopic dermatitis: A systematic review and meta-analysis of benefits and harms. J Allergy Clin Immunol. 2022 (Sep 30). Doi: 10.1016/j.jaci.2022.09.020
Key clinical point: Patients with atopic dermatitis (AD) who received adjunctive allergen immunotherapy (AIT) reported improvements in disease severity and quality of life despite an increase in the rate of adverse events (AE).
Major finding: AIT vs no AIT improved disease severity (risk ratio [RR] 1.53; 95% CI 1.31-1.78) and the Dermatology Life Quality Index by at least 4 points (RR 1.44; 95% CI 1.03-2.01). The rates of local (RR 1.65; 95% CI 1.48-1.64) and systemic (RR 1.37; 95% CI 1.15-1.64) AE were higher with AIT vs placebo.
Study details: Findings are from a meta-analysis of 23 randomized controlled trials including 1957 adult and pediatric patients with moderate-to-severe AD who were randomly assigned to adjunctive AIT (subcutaneous or sublingual immunotherapy) or no AIT (placebo or standard care).
Disclosures: This study was supported by the American Academy of Allergy, Asthma, & Immunology and other sources. The authors declared no conflicts of interest.
Source: Yepes-Nuñez JJ et al. Allergen immunotherapy for atopic dermatitis: A systematic review and meta-analysis of benefits and harms. J Allergy Clin Immunol. 2022 (Sep 30). Doi: 10.1016/j.jaci.2022.09.020
Some immunomodulatory treatments increase risk for COVID-19 complications in atopic dermatitis
Key clinical point: Rate of COVID-19 hospitalizations varied by treatment modalities in patients with atopic dermatitis (AD) who received immunomodulatory drugs.
Major finding: Rate of COVID-19 hospitalizations was higher among patients who received topical treatment vs dupilumab (adjusted odds ratio [aOR] 4.99; 95% CI 1.4-20.84) or combination therapy with systemic corticosteroids vs monotherapy with nonsteroidal immunosuppressants (aOR 45.75; 95% CI 4.54-616.22).
Study details: Findings are from the SECURE-AD registry including 442 patients with AD and a diagnosis of COVID-19 who received immunomodulatory treatments.
Disclosures: This study is funded by the University of Amsterdam and other sources. Some authors declared serving as employees or receiving grants, consulting fees, honoraria, or travel support from several sources.
Source: Musters AH et al. The effects of systemic immunomodulatory treatments on COVID-19 outcomes in patients with atopic dermatitis: Results from the global SECURE-AD registry. J Eur Acad Dermatol Venereol. 2022 (Sep 28). Doi: 10.1111/jdv.18613
Key clinical point: Rate of COVID-19 hospitalizations varied by treatment modalities in patients with atopic dermatitis (AD) who received immunomodulatory drugs.
Major finding: Rate of COVID-19 hospitalizations was higher among patients who received topical treatment vs dupilumab (adjusted odds ratio [aOR] 4.99; 95% CI 1.4-20.84) or combination therapy with systemic corticosteroids vs monotherapy with nonsteroidal immunosuppressants (aOR 45.75; 95% CI 4.54-616.22).
Study details: Findings are from the SECURE-AD registry including 442 patients with AD and a diagnosis of COVID-19 who received immunomodulatory treatments.
Disclosures: This study is funded by the University of Amsterdam and other sources. Some authors declared serving as employees or receiving grants, consulting fees, honoraria, or travel support from several sources.
Source: Musters AH et al. The effects of systemic immunomodulatory treatments on COVID-19 outcomes in patients with atopic dermatitis: Results from the global SECURE-AD registry. J Eur Acad Dermatol Venereol. 2022 (Sep 28). Doi: 10.1111/jdv.18613
Key clinical point: Rate of COVID-19 hospitalizations varied by treatment modalities in patients with atopic dermatitis (AD) who received immunomodulatory drugs.
Major finding: Rate of COVID-19 hospitalizations was higher among patients who received topical treatment vs dupilumab (adjusted odds ratio [aOR] 4.99; 95% CI 1.4-20.84) or combination therapy with systemic corticosteroids vs monotherapy with nonsteroidal immunosuppressants (aOR 45.75; 95% CI 4.54-616.22).
Study details: Findings are from the SECURE-AD registry including 442 patients with AD and a diagnosis of COVID-19 who received immunomodulatory treatments.
Disclosures: This study is funded by the University of Amsterdam and other sources. Some authors declared serving as employees or receiving grants, consulting fees, honoraria, or travel support from several sources.
Source: Musters AH et al. The effects of systemic immunomodulatory treatments on COVID-19 outcomes in patients with atopic dermatitis: Results from the global SECURE-AD registry. J Eur Acad Dermatol Venereol. 2022 (Sep 28). Doi: 10.1111/jdv.18613
Moderate-to-severe atopic dermatitis: Tralokinumab with or without TCS effective and safe in North American population
Key clinical point: Tralokinumab, with or without topical corticosteroids (TCS), demonstrated significant efficacy in reducing disease severity and was well-tolerated in North American patients with moderate-to-severe atopic dermatitis (AD).
Major finding: At week 16, a significantly higher proportion of patients receiving tralokinumab vs placebo achieved ≥75% improvement in the Eczema Area and Severity Index in ECZTRA 1/2 (40.1% vs 19.4%; P < .001) and ECZTRA 3 (58.1% vs 37.0%; P = .012) studies. Tralokinumab with or without TCS was also well-tolerated in the North American population.
Study details: Findings are from a post hoc analysis of three tralokinumab trials including patients with moderate-to-severe AD who were randomly assigned to receive tralokinumab or placebo, both with TCS as needed (ECZTRA 3; n = 160) or without TCS (ECZTRA 1 and 2; n = 559).
Disclosures: The ECZTRA trials were sponsored by LEO Pharma A/S. Three authors declared being current or former employees of LEO Pharma. The other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Tralokinumab efficacy and safety, with or without topical corticosteroids, in North American adults with moderate-to-severe atopic dermatitis: A subanalysis of phase 3 trials ECZTRA 1, 2, and 3. Dermatol Ther (Heidelb). 2022 (Sep 24). Doi: 10.1007/s13555-022-00805-y
Key clinical point: Tralokinumab, with or without topical corticosteroids (TCS), demonstrated significant efficacy in reducing disease severity and was well-tolerated in North American patients with moderate-to-severe atopic dermatitis (AD).
Major finding: At week 16, a significantly higher proportion of patients receiving tralokinumab vs placebo achieved ≥75% improvement in the Eczema Area and Severity Index in ECZTRA 1/2 (40.1% vs 19.4%; P < .001) and ECZTRA 3 (58.1% vs 37.0%; P = .012) studies. Tralokinumab with or without TCS was also well-tolerated in the North American population.
Study details: Findings are from a post hoc analysis of three tralokinumab trials including patients with moderate-to-severe AD who were randomly assigned to receive tralokinumab or placebo, both with TCS as needed (ECZTRA 3; n = 160) or without TCS (ECZTRA 1 and 2; n = 559).
Disclosures: The ECZTRA trials were sponsored by LEO Pharma A/S. Three authors declared being current or former employees of LEO Pharma. The other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Tralokinumab efficacy and safety, with or without topical corticosteroids, in North American adults with moderate-to-severe atopic dermatitis: A subanalysis of phase 3 trials ECZTRA 1, 2, and 3. Dermatol Ther (Heidelb). 2022 (Sep 24). Doi: 10.1007/s13555-022-00805-y
Key clinical point: Tralokinumab, with or without topical corticosteroids (TCS), demonstrated significant efficacy in reducing disease severity and was well-tolerated in North American patients with moderate-to-severe atopic dermatitis (AD).
Major finding: At week 16, a significantly higher proportion of patients receiving tralokinumab vs placebo achieved ≥75% improvement in the Eczema Area and Severity Index in ECZTRA 1/2 (40.1% vs 19.4%; P < .001) and ECZTRA 3 (58.1% vs 37.0%; P = .012) studies. Tralokinumab with or without TCS was also well-tolerated in the North American population.
Study details: Findings are from a post hoc analysis of three tralokinumab trials including patients with moderate-to-severe AD who were randomly assigned to receive tralokinumab or placebo, both with TCS as needed (ECZTRA 3; n = 160) or without TCS (ECZTRA 1 and 2; n = 559).
Disclosures: The ECZTRA trials were sponsored by LEO Pharma A/S. Three authors declared being current or former employees of LEO Pharma. The other authors reported ties with several sources, including LEO Pharma.
Source: Blauvelt A et al. Tralokinumab efficacy and safety, with or without topical corticosteroids, in North American adults with moderate-to-severe atopic dermatitis: A subanalysis of phase 3 trials ECZTRA 1, 2, and 3. Dermatol Ther (Heidelb). 2022 (Sep 24). Doi: 10.1007/s13555-022-00805-y