User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
Successful Treatment of Severe Dystrophic Nail Psoriasis With Deucravacitinib
Successful Treatment of Severe Dystrophic Nail Psoriasis With Deucravacitinib
To the Editor:
Psoriasis is a chronic inflammatory skin condition that commonly affects the nail matrix and/or nail bed.1 Nail involvement is present in up to 50% of patients with cutaneous psoriasis and 80% of patients with psoriatic arthritis.1 Approximately 5% to 10% of patients with psoriasis demonstrate isolated nail involvement with no skin or joint manifestations.1 Nail psoriasis can cause severe pain and psychological distress, and extreme cases may cause considerable morbidity and functional impairment.2,3 Treatment often requires a long duration and may not result in complete recovery due to the slow rate of nail growth. Patients can progress to permanent nail loss if not treated properly, making early recognition and treatment crucial.1,2 Despite the availability of various treatment options, many cases remain refractory to standard interventions, which underscores the need for novel therapeutic approaches. Herein, we present a severe case of refractory isolated nail psoriasis that was successfully treated with deucravacitinib, an oral tyrosine kinase 2 (TYK2) inhibitor.
A 59-year-old woman presented with a progressive, yellow, hyperkeratotic lesion on the left thumbnail of 2 years’ duration. The patient noted initial discoloration and peeling at the distal end of the nail. Over time, the discoloration progressed to encompass the entire nail. Previous treatments performed by outside physicians including topical corticosteroids, calcineurin inhibitors, and 2 surgeries to remove the nail plate and nail bed all were unsuccessful. The patient also reported severe left thumbnail pain and pruritus that considerably impaired her ability to work. The rest of the nails were unaffected, and she had no personal or family history of psoriasis. Her medical history was notable for hypertension, gastroesophageal reflux disease, and osteomyelitis of the right thumb without nail involvement. Drug allergies included penicillin G benzathine, sulfonamides, amoxicillin, and ciprofloxacin.
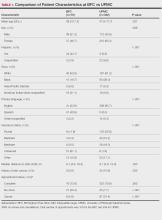
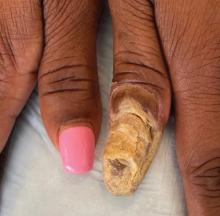
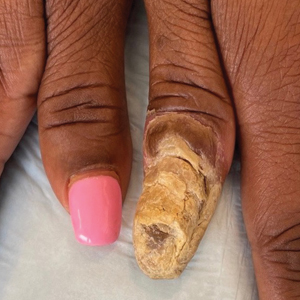
Physical examination of the left thumbnail revealed severe yellow, hyperkeratotic, dystrophic changes with a large, yellow, crumbling hyperkeratotic plaque that extended from approximately 1 cm beyond the nail plate to the proximal end of the distal interphalangeal joint, to and along the lateral nail folds, with extensive distal onycholysis. The proximal and lateral nail folds demonstrated erythema as well as maceration that was extremely tender to minimal palpation (Figure 1). No cutaneous lesions were noted elsewhere on the body. The patient had no tenderness, swelling, or stiffness in any of the joints. The differential diagnosis at the time included squamous cell carcinoma of the nail bed and acrodermatitis continua of Hallopeau.
Radiography of the left thumb revealed irregular swelling and nonspecific soft tissue enlargement at the tip of the digit. A nail clipping from the left thumbnail and 3-mm punch biopsies of the lateral and proximal nail folds as well as the horn of the proximal nail fold (Figure 2) were negative for fungus and confirmed psoriasiform dermatitis of the nail.
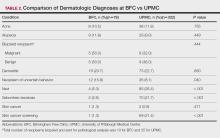
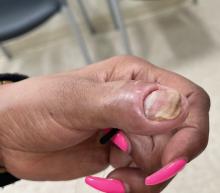
The patient was started on vinegar soaks (1:1 ratio of vinegar to water) every other day as well as urea cream 10%, ammonium lactate 15%, and petrolatum twice daily for 2 months without considerable improvement. Due to lack of improvement during this 2-month period, the patient subsequently was started on oral deucravacitinib 6 mg/d along with continued use of petrolatum twice daily and vinegar soaks every other day. We selected a trial of deucravacitinib for our patient because of its convenient daily oral dosing and promising clinical evidence.4,5 After 2 months of treatment with deucravacitinib, the patient reported substantial improvement and satisfaction with the treatment results. Physical examination of the left thumbnail after 2 months of deucravacitinib treatment revealed mildly hyperkeratotic, yellow, dystrophic changes of the nail with notable improvement of the yellow hyperkeratotic plaque on the distal thumbnail. Normal-appearing nail growth was noted at the proximal nail fold, demonstrating considerable improvement from the initial presentation (Figure 3). However, the patient had developed multiple oral ulcers, generalized pruritus, and an annular urticarial plaque on the left arm. As such, deucravacitinib was discontinued after 2 months of treatment. These symptoms resolved within a week of discontinuing deucravacitinib.
While the etiology of nail psoriasis remains unclear, it is believed to be due to a combination of immunologic, genetic, and environmental factors.3 Classical clinical features include nail pitting, leukonychia, onycholysis, nail bed hyperkeratosis, and splinter hemorrhages.1,3 Our patient exhibited a severe form of nail psoriasis, encompassing the entire nail matrix and bed and extending to the distal interphalangeal joint and lateral nail folds. Previous surgical interventions may have triggered the Koebner phenomenon—which commonly is associated with psoriasis—and resulted in new skin lesions as a secondary response to the surgical trauma.6 The severity of the condition profoundly impacted her quality of life and considerably hindered her ability to work.
Treatment for nail psoriasis includes topical or systemic therapies such as corticosteroids, vitamin D analogs, tacrolimus, and tumor necrosis factor α inhibitors.1,3 Topical treatment is challenging because it is difficult to deliver medication effectively to the nail bed and nail matrix, and patient adherence may be poor.2 Although it has been shown to be effective, intralesional triamcinolone can be associated with pain as the most common adverse effect.7 Systemic medications such as oral methotrexate also may be effective but are contraindicated in pregnant patients and are associated with potential adverse events (AEs), including hepatotoxicity and acute kidney injury.8 The use of biologics may be challenging due to potential AEs and patient reluctance toward injection-based treatments.9
Deucravacitinib is a TYK2 inhibitor approved for treatment of plaque psoriasis.10 Tyrosine kinase 2 is an intracellular kinase that mediates the signaling of IL-23 and other cytokines involved in psoriasis pathogenesis.10 Deucravacitinib selectively binds to the regulatory domain of TYK2, leading to targeted allosteric inhibition of TYK2-mediated IL-23 and type I interferon signaling.4,5,10 Compared with biologics, deucravacitinib is advantageous because it can be administered as a daily oral pill, encouraging high patient compliance.
In the POETYK PSO-1 and PSO-2 phase 3 randomized controlled trials, 20.9% (n=332) and 20.3% (n=510) of deucravacitinib-treated patients with moderate to severe nail involvement achieved a Physician’s Global Assessment of Fingernail score of 0/1 compared with 8.8% (n=165) and 7.9% (n=254) of patients in the placebo group, respectively. All patients in these trials had a diagnosis of plaque psoriasis with at least 10% body surface area involvement; none of the patients had isolated nail psoriasis.4,5
The phase 3 POETYK PSO-1 and PSO-2 trials demonstrated deucravacitinib to be safe and well tolerated with minimal AEs.4,5 However, the development of AEs in our patient, including oral ulcers and generalized pruritus, underscores the need for close monitoring and consideration of potential risks of treatment. Common AEs associated with deucravacitinib include upper respiratory infections (19.2% [n=840]), increased blood creatine phosphokinase levels (2.7% [n=840]), herpes simplex virus (2.0% [n=840]), and mouth ulcers (1.9% [n=840]).11
Patient education also is a crucial component in the treatment of nail psoriasis. Physicians should emphasize the slow growth of nails and need for prolonged treatment. Clear communication and realistic expectations are essential for ensuring patient adherence to treatment.
Our case highlights the potential efficacy and safety of deucravacitinib for treatment of nail psoriasis, potentially laying the groundwork for future clinical studies. Our patient had a severe case of nail psoriasis that involved the entire nail bed and nail plate, resulting in extreme pain, pruritus, and functional impairment. Her case was unique because involvement was isolated to the nail without any accompanying skin or joint manifestations. She showed a favorable response to deucravacitinib within only 2 months of treatment and exhibited considerable improvement of nail psoriasis, with a reported high level of satisfaction with the treatment. We plan to continue to monitor the patient for long-term results. Future randomized clinical trials with longer follow-up periods are crucial to further establish the efficacy and safety of deucravacitinib for treatment of nail psoriasis.
- Hwang JK, Grover C, Iorizzo M, et al. Nail psoriasis and nail lichen planus: updates on diagnosis and management. J Am Acad Dermatol. 2024;90:585-596. doi:10.1016/j.jaad.2023.11.024
- Ji C, Wang H, Bao C, et al. Challenge of nail psoriasis: an update review. Clin Rev Allergy Immunol. 2021;61:377-402. doi:10.1007/s12016-021-08896-9
- Muneer H, Sathe NC, Masood S. Nail psoriasis. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated March 1, 2024. Accessed October 24, 2024. https://www.ncbi.nlm.nih.gov/books/NBK559260/
- Armstrong AW, Gooderham M, Warren RB, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, placebo-controlled phase 3 POETYK PSO-1 trial. J Am Acad Dermatol. 2023;88:29-39. doi:10.1016/j.jaad.2022.07.002
- Strober B, Thaçi D, Sofen H, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, phase 3 Program fOr Evaluation of TYK2 inhibitor psoriasis second trial. J Am Acad Dermatol. 2023;88:40-51. doi:10.1016/j.jaad.2022.08.061
- Sanchez DP, Sonthalia S. Koebner phenomenon. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated November 14, 2022. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK553108/
- Grover C, Kharghoria G, Bansal S. Triamcinolone acetonide injections in nail psoriasis: a pragmatic analysis. Skin Appendage Disord. 2024;10:50-59. doi:10.1159/000534699
- Hanoodi M, Mittal M. Methotrexate. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated August 16, 2023. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK556114/
- Singh JA, Wells GA, Christensen R, et al. Adverse effects of biologics: a network meta-analysis and Cochrane overview. Cochrane Database Syst Rev. 2011;2011:Cd008794. doi:10.1002/14651858.CD008794.pub2
- Thaçi D, Strober B, Gordon KB, et al. Deucravacitinib in moderate to severe psoriasis: clinical and quality-of-life outcomes in a phase 2 trial. Dermatol Ther (Heidelb). 2022;12:495-510. doi:10.1007/s13555-021-00649-y
- Week 0-16: demonstrated safety profile. Bristol-Myers Squibb. 2024. Accessed October 24, 2024. https://www.sotyktuhcp.com/safety-profile?cid=sem_2465603&gclid=CjwKCAiA9ourBhAVEiwA3L5RFnyYqmxbqkz1_zBNPz3dcyHKCSFf1XQ-7acznV0XbR5DDJHYkZcKJxoCWN0QAvD_BwE&gclsrc=aw.ds
To the Editor:
Psoriasis is a chronic inflammatory skin condition that commonly affects the nail matrix and/or nail bed.1 Nail involvement is present in up to 50% of patients with cutaneous psoriasis and 80% of patients with psoriatic arthritis.1 Approximately 5% to 10% of patients with psoriasis demonstrate isolated nail involvement with no skin or joint manifestations.1 Nail psoriasis can cause severe pain and psychological distress, and extreme cases may cause considerable morbidity and functional impairment.2,3 Treatment often requires a long duration and may not result in complete recovery due to the slow rate of nail growth. Patients can progress to permanent nail loss if not treated properly, making early recognition and treatment crucial.1,2 Despite the availability of various treatment options, many cases remain refractory to standard interventions, which underscores the need for novel therapeutic approaches. Herein, we present a severe case of refractory isolated nail psoriasis that was successfully treated with deucravacitinib, an oral tyrosine kinase 2 (TYK2) inhibitor.
A 59-year-old woman presented with a progressive, yellow, hyperkeratotic lesion on the left thumbnail of 2 years’ duration. The patient noted initial discoloration and peeling at the distal end of the nail. Over time, the discoloration progressed to encompass the entire nail. Previous treatments performed by outside physicians including topical corticosteroids, calcineurin inhibitors, and 2 surgeries to remove the nail plate and nail bed all were unsuccessful. The patient also reported severe left thumbnail pain and pruritus that considerably impaired her ability to work. The rest of the nails were unaffected, and she had no personal or family history of psoriasis. Her medical history was notable for hypertension, gastroesophageal reflux disease, and osteomyelitis of the right thumb without nail involvement. Drug allergies included penicillin G benzathine, sulfonamides, amoxicillin, and ciprofloxacin.
Physical examination of the left thumbnail revealed severe yellow, hyperkeratotic, dystrophic changes with a large, yellow, crumbling hyperkeratotic plaque that extended from approximately 1 cm beyond the nail plate to the proximal end of the distal interphalangeal joint, to and along the lateral nail folds, with extensive distal onycholysis. The proximal and lateral nail folds demonstrated erythema as well as maceration that was extremely tender to minimal palpation (Figure 1). No cutaneous lesions were noted elsewhere on the body. The patient had no tenderness, swelling, or stiffness in any of the joints. The differential diagnosis at the time included squamous cell carcinoma of the nail bed and acrodermatitis continua of Hallopeau.
Radiography of the left thumb revealed irregular swelling and nonspecific soft tissue enlargement at the tip of the digit. A nail clipping from the left thumbnail and 3-mm punch biopsies of the lateral and proximal nail folds as well as the horn of the proximal nail fold (Figure 2) were negative for fungus and confirmed psoriasiform dermatitis of the nail.
The patient was started on vinegar soaks (1:1 ratio of vinegar to water) every other day as well as urea cream 10%, ammonium lactate 15%, and petrolatum twice daily for 2 months without considerable improvement. Due to lack of improvement during this 2-month period, the patient subsequently was started on oral deucravacitinib 6 mg/d along with continued use of petrolatum twice daily and vinegar soaks every other day. We selected a trial of deucravacitinib for our patient because of its convenient daily oral dosing and promising clinical evidence.4,5 After 2 months of treatment with deucravacitinib, the patient reported substantial improvement and satisfaction with the treatment results. Physical examination of the left thumbnail after 2 months of deucravacitinib treatment revealed mildly hyperkeratotic, yellow, dystrophic changes of the nail with notable improvement of the yellow hyperkeratotic plaque on the distal thumbnail. Normal-appearing nail growth was noted at the proximal nail fold, demonstrating considerable improvement from the initial presentation (Figure 3). However, the patient had developed multiple oral ulcers, generalized pruritus, and an annular urticarial plaque on the left arm. As such, deucravacitinib was discontinued after 2 months of treatment. These symptoms resolved within a week of discontinuing deucravacitinib.
While the etiology of nail psoriasis remains unclear, it is believed to be due to a combination of immunologic, genetic, and environmental factors.3 Classical clinical features include nail pitting, leukonychia, onycholysis, nail bed hyperkeratosis, and splinter hemorrhages.1,3 Our patient exhibited a severe form of nail psoriasis, encompassing the entire nail matrix and bed and extending to the distal interphalangeal joint and lateral nail folds. Previous surgical interventions may have triggered the Koebner phenomenon—which commonly is associated with psoriasis—and resulted in new skin lesions as a secondary response to the surgical trauma.6 The severity of the condition profoundly impacted her quality of life and considerably hindered her ability to work.
Treatment for nail psoriasis includes topical or systemic therapies such as corticosteroids, vitamin D analogs, tacrolimus, and tumor necrosis factor α inhibitors.1,3 Topical treatment is challenging because it is difficult to deliver medication effectively to the nail bed and nail matrix, and patient adherence may be poor.2 Although it has been shown to be effective, intralesional triamcinolone can be associated with pain as the most common adverse effect.7 Systemic medications such as oral methotrexate also may be effective but are contraindicated in pregnant patients and are associated with potential adverse events (AEs), including hepatotoxicity and acute kidney injury.8 The use of biologics may be challenging due to potential AEs and patient reluctance toward injection-based treatments.9
Deucravacitinib is a TYK2 inhibitor approved for treatment of plaque psoriasis.10 Tyrosine kinase 2 is an intracellular kinase that mediates the signaling of IL-23 and other cytokines involved in psoriasis pathogenesis.10 Deucravacitinib selectively binds to the regulatory domain of TYK2, leading to targeted allosteric inhibition of TYK2-mediated IL-23 and type I interferon signaling.4,5,10 Compared with biologics, deucravacitinib is advantageous because it can be administered as a daily oral pill, encouraging high patient compliance.
In the POETYK PSO-1 and PSO-2 phase 3 randomized controlled trials, 20.9% (n=332) and 20.3% (n=510) of deucravacitinib-treated patients with moderate to severe nail involvement achieved a Physician’s Global Assessment of Fingernail score of 0/1 compared with 8.8% (n=165) and 7.9% (n=254) of patients in the placebo group, respectively. All patients in these trials had a diagnosis of plaque psoriasis with at least 10% body surface area involvement; none of the patients had isolated nail psoriasis.4,5
The phase 3 POETYK PSO-1 and PSO-2 trials demonstrated deucravacitinib to be safe and well tolerated with minimal AEs.4,5 However, the development of AEs in our patient, including oral ulcers and generalized pruritus, underscores the need for close monitoring and consideration of potential risks of treatment. Common AEs associated with deucravacitinib include upper respiratory infections (19.2% [n=840]), increased blood creatine phosphokinase levels (2.7% [n=840]), herpes simplex virus (2.0% [n=840]), and mouth ulcers (1.9% [n=840]).11
Patient education also is a crucial component in the treatment of nail psoriasis. Physicians should emphasize the slow growth of nails and need for prolonged treatment. Clear communication and realistic expectations are essential for ensuring patient adherence to treatment.
Our case highlights the potential efficacy and safety of deucravacitinib for treatment of nail psoriasis, potentially laying the groundwork for future clinical studies. Our patient had a severe case of nail psoriasis that involved the entire nail bed and nail plate, resulting in extreme pain, pruritus, and functional impairment. Her case was unique because involvement was isolated to the nail without any accompanying skin or joint manifestations. She showed a favorable response to deucravacitinib within only 2 months of treatment and exhibited considerable improvement of nail psoriasis, with a reported high level of satisfaction with the treatment. We plan to continue to monitor the patient for long-term results. Future randomized clinical trials with longer follow-up periods are crucial to further establish the efficacy and safety of deucravacitinib for treatment of nail psoriasis.
To the Editor:
Psoriasis is a chronic inflammatory skin condition that commonly affects the nail matrix and/or nail bed.1 Nail involvement is present in up to 50% of patients with cutaneous psoriasis and 80% of patients with psoriatic arthritis.1 Approximately 5% to 10% of patients with psoriasis demonstrate isolated nail involvement with no skin or joint manifestations.1 Nail psoriasis can cause severe pain and psychological distress, and extreme cases may cause considerable morbidity and functional impairment.2,3 Treatment often requires a long duration and may not result in complete recovery due to the slow rate of nail growth. Patients can progress to permanent nail loss if not treated properly, making early recognition and treatment crucial.1,2 Despite the availability of various treatment options, many cases remain refractory to standard interventions, which underscores the need for novel therapeutic approaches. Herein, we present a severe case of refractory isolated nail psoriasis that was successfully treated with deucravacitinib, an oral tyrosine kinase 2 (TYK2) inhibitor.
A 59-year-old woman presented with a progressive, yellow, hyperkeratotic lesion on the left thumbnail of 2 years’ duration. The patient noted initial discoloration and peeling at the distal end of the nail. Over time, the discoloration progressed to encompass the entire nail. Previous treatments performed by outside physicians including topical corticosteroids, calcineurin inhibitors, and 2 surgeries to remove the nail plate and nail bed all were unsuccessful. The patient also reported severe left thumbnail pain and pruritus that considerably impaired her ability to work. The rest of the nails were unaffected, and she had no personal or family history of psoriasis. Her medical history was notable for hypertension, gastroesophageal reflux disease, and osteomyelitis of the right thumb without nail involvement. Drug allergies included penicillin G benzathine, sulfonamides, amoxicillin, and ciprofloxacin.
Physical examination of the left thumbnail revealed severe yellow, hyperkeratotic, dystrophic changes with a large, yellow, crumbling hyperkeratotic plaque that extended from approximately 1 cm beyond the nail plate to the proximal end of the distal interphalangeal joint, to and along the lateral nail folds, with extensive distal onycholysis. The proximal and lateral nail folds demonstrated erythema as well as maceration that was extremely tender to minimal palpation (Figure 1). No cutaneous lesions were noted elsewhere on the body. The patient had no tenderness, swelling, or stiffness in any of the joints. The differential diagnosis at the time included squamous cell carcinoma of the nail bed and acrodermatitis continua of Hallopeau.
Radiography of the left thumb revealed irregular swelling and nonspecific soft tissue enlargement at the tip of the digit. A nail clipping from the left thumbnail and 3-mm punch biopsies of the lateral and proximal nail folds as well as the horn of the proximal nail fold (Figure 2) were negative for fungus and confirmed psoriasiform dermatitis of the nail.
The patient was started on vinegar soaks (1:1 ratio of vinegar to water) every other day as well as urea cream 10%, ammonium lactate 15%, and petrolatum twice daily for 2 months without considerable improvement. Due to lack of improvement during this 2-month period, the patient subsequently was started on oral deucravacitinib 6 mg/d along with continued use of petrolatum twice daily and vinegar soaks every other day. We selected a trial of deucravacitinib for our patient because of its convenient daily oral dosing and promising clinical evidence.4,5 After 2 months of treatment with deucravacitinib, the patient reported substantial improvement and satisfaction with the treatment results. Physical examination of the left thumbnail after 2 months of deucravacitinib treatment revealed mildly hyperkeratotic, yellow, dystrophic changes of the nail with notable improvement of the yellow hyperkeratotic plaque on the distal thumbnail. Normal-appearing nail growth was noted at the proximal nail fold, demonstrating considerable improvement from the initial presentation (Figure 3). However, the patient had developed multiple oral ulcers, generalized pruritus, and an annular urticarial plaque on the left arm. As such, deucravacitinib was discontinued after 2 months of treatment. These symptoms resolved within a week of discontinuing deucravacitinib.
While the etiology of nail psoriasis remains unclear, it is believed to be due to a combination of immunologic, genetic, and environmental factors.3 Classical clinical features include nail pitting, leukonychia, onycholysis, nail bed hyperkeratosis, and splinter hemorrhages.1,3 Our patient exhibited a severe form of nail psoriasis, encompassing the entire nail matrix and bed and extending to the distal interphalangeal joint and lateral nail folds. Previous surgical interventions may have triggered the Koebner phenomenon—which commonly is associated with psoriasis—and resulted in new skin lesions as a secondary response to the surgical trauma.6 The severity of the condition profoundly impacted her quality of life and considerably hindered her ability to work.
Treatment for nail psoriasis includes topical or systemic therapies such as corticosteroids, vitamin D analogs, tacrolimus, and tumor necrosis factor α inhibitors.1,3 Topical treatment is challenging because it is difficult to deliver medication effectively to the nail bed and nail matrix, and patient adherence may be poor.2 Although it has been shown to be effective, intralesional triamcinolone can be associated with pain as the most common adverse effect.7 Systemic medications such as oral methotrexate also may be effective but are contraindicated in pregnant patients and are associated with potential adverse events (AEs), including hepatotoxicity and acute kidney injury.8 The use of biologics may be challenging due to potential AEs and patient reluctance toward injection-based treatments.9
Deucravacitinib is a TYK2 inhibitor approved for treatment of plaque psoriasis.10 Tyrosine kinase 2 is an intracellular kinase that mediates the signaling of IL-23 and other cytokines involved in psoriasis pathogenesis.10 Deucravacitinib selectively binds to the regulatory domain of TYK2, leading to targeted allosteric inhibition of TYK2-mediated IL-23 and type I interferon signaling.4,5,10 Compared with biologics, deucravacitinib is advantageous because it can be administered as a daily oral pill, encouraging high patient compliance.
In the POETYK PSO-1 and PSO-2 phase 3 randomized controlled trials, 20.9% (n=332) and 20.3% (n=510) of deucravacitinib-treated patients with moderate to severe nail involvement achieved a Physician’s Global Assessment of Fingernail score of 0/1 compared with 8.8% (n=165) and 7.9% (n=254) of patients in the placebo group, respectively. All patients in these trials had a diagnosis of plaque psoriasis with at least 10% body surface area involvement; none of the patients had isolated nail psoriasis.4,5
The phase 3 POETYK PSO-1 and PSO-2 trials demonstrated deucravacitinib to be safe and well tolerated with minimal AEs.4,5 However, the development of AEs in our patient, including oral ulcers and generalized pruritus, underscores the need for close monitoring and consideration of potential risks of treatment. Common AEs associated with deucravacitinib include upper respiratory infections (19.2% [n=840]), increased blood creatine phosphokinase levels (2.7% [n=840]), herpes simplex virus (2.0% [n=840]), and mouth ulcers (1.9% [n=840]).11
Patient education also is a crucial component in the treatment of nail psoriasis. Physicians should emphasize the slow growth of nails and need for prolonged treatment. Clear communication and realistic expectations are essential for ensuring patient adherence to treatment.
Our case highlights the potential efficacy and safety of deucravacitinib for treatment of nail psoriasis, potentially laying the groundwork for future clinical studies. Our patient had a severe case of nail psoriasis that involved the entire nail bed and nail plate, resulting in extreme pain, pruritus, and functional impairment. Her case was unique because involvement was isolated to the nail without any accompanying skin or joint manifestations. She showed a favorable response to deucravacitinib within only 2 months of treatment and exhibited considerable improvement of nail psoriasis, with a reported high level of satisfaction with the treatment. We plan to continue to monitor the patient for long-term results. Future randomized clinical trials with longer follow-up periods are crucial to further establish the efficacy and safety of deucravacitinib for treatment of nail psoriasis.
- Hwang JK, Grover C, Iorizzo M, et al. Nail psoriasis and nail lichen planus: updates on diagnosis and management. J Am Acad Dermatol. 2024;90:585-596. doi:10.1016/j.jaad.2023.11.024
- Ji C, Wang H, Bao C, et al. Challenge of nail psoriasis: an update review. Clin Rev Allergy Immunol. 2021;61:377-402. doi:10.1007/s12016-021-08896-9
- Muneer H, Sathe NC, Masood S. Nail psoriasis. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated March 1, 2024. Accessed October 24, 2024. https://www.ncbi.nlm.nih.gov/books/NBK559260/
- Armstrong AW, Gooderham M, Warren RB, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, placebo-controlled phase 3 POETYK PSO-1 trial. J Am Acad Dermatol. 2023;88:29-39. doi:10.1016/j.jaad.2022.07.002
- Strober B, Thaçi D, Sofen H, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, phase 3 Program fOr Evaluation of TYK2 inhibitor psoriasis second trial. J Am Acad Dermatol. 2023;88:40-51. doi:10.1016/j.jaad.2022.08.061
- Sanchez DP, Sonthalia S. Koebner phenomenon. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated November 14, 2022. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK553108/
- Grover C, Kharghoria G, Bansal S. Triamcinolone acetonide injections in nail psoriasis: a pragmatic analysis. Skin Appendage Disord. 2024;10:50-59. doi:10.1159/000534699
- Hanoodi M, Mittal M. Methotrexate. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated August 16, 2023. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK556114/
- Singh JA, Wells GA, Christensen R, et al. Adverse effects of biologics: a network meta-analysis and Cochrane overview. Cochrane Database Syst Rev. 2011;2011:Cd008794. doi:10.1002/14651858.CD008794.pub2
- Thaçi D, Strober B, Gordon KB, et al. Deucravacitinib in moderate to severe psoriasis: clinical and quality-of-life outcomes in a phase 2 trial. Dermatol Ther (Heidelb). 2022;12:495-510. doi:10.1007/s13555-021-00649-y
- Week 0-16: demonstrated safety profile. Bristol-Myers Squibb. 2024. Accessed October 24, 2024. https://www.sotyktuhcp.com/safety-profile?cid=sem_2465603&gclid=CjwKCAiA9ourBhAVEiwA3L5RFnyYqmxbqkz1_zBNPz3dcyHKCSFf1XQ-7acznV0XbR5DDJHYkZcKJxoCWN0QAvD_BwE&gclsrc=aw.ds
- Hwang JK, Grover C, Iorizzo M, et al. Nail psoriasis and nail lichen planus: updates on diagnosis and management. J Am Acad Dermatol. 2024;90:585-596. doi:10.1016/j.jaad.2023.11.024
- Ji C, Wang H, Bao C, et al. Challenge of nail psoriasis: an update review. Clin Rev Allergy Immunol. 2021;61:377-402. doi:10.1007/s12016-021-08896-9
- Muneer H, Sathe NC, Masood S. Nail psoriasis. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated March 1, 2024. Accessed October 24, 2024. https://www.ncbi.nlm.nih.gov/books/NBK559260/
- Armstrong AW, Gooderham M, Warren RB, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, placebo-controlled phase 3 POETYK PSO-1 trial. J Am Acad Dermatol. 2023;88:29-39. doi:10.1016/j.jaad.2022.07.002
- Strober B, Thaçi D, Sofen H, et al. Deucravacitinib versus placebo and apremilast in moderate to severe plaque psoriasis: efficacy and safety results from the 52-week, randomized, double-blinded, phase 3 Program fOr Evaluation of TYK2 inhibitor psoriasis second trial. J Am Acad Dermatol. 2023;88:40-51. doi:10.1016/j.jaad.2022.08.061
- Sanchez DP, Sonthalia S. Koebner phenomenon. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated November 14, 2022. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK553108/
- Grover C, Kharghoria G, Bansal S. Triamcinolone acetonide injections in nail psoriasis: a pragmatic analysis. Skin Appendage Disord. 2024;10:50-59. doi:10.1159/000534699
- Hanoodi M, Mittal M. Methotrexate. StatPearls [Internet]. StatPearls Publishing; 2024 Jan-. Updated August 16, 2023. Accessed April 11, 2024. https://www.ncbi.nlm.nih.gov/books/NBK556114/
- Singh JA, Wells GA, Christensen R, et al. Adverse effects of biologics: a network meta-analysis and Cochrane overview. Cochrane Database Syst Rev. 2011;2011:Cd008794. doi:10.1002/14651858.CD008794.pub2
- Thaçi D, Strober B, Gordon KB, et al. Deucravacitinib in moderate to severe psoriasis: clinical and quality-of-life outcomes in a phase 2 trial. Dermatol Ther (Heidelb). 2022;12:495-510. doi:10.1007/s13555-021-00649-y
- Week 0-16: demonstrated safety profile. Bristol-Myers Squibb. 2024. Accessed October 24, 2024. https://www.sotyktuhcp.com/safety-profile?cid=sem_2465603&gclid=CjwKCAiA9ourBhAVEiwA3L5RFnyYqmxbqkz1_zBNPz3dcyHKCSFf1XQ-7acznV0XbR5DDJHYkZcKJxoCWN0QAvD_BwE&gclsrc=aw.ds
Successful Treatment of Severe Dystrophic Nail Psoriasis With Deucravacitinib
Successful Treatment of Severe Dystrophic Nail Psoriasis With Deucravacitinib
PRACTICE POINTS
- Nail psoriasis can masquerade as other dermatologic conditions, including squamous cell carcinoma of the nail bed and acrodermatitis continua of Hallopeau.
- Nail psoriasis can progress to permanent nail loss if not treated properly, making early recognition and treatment crucial.
- Deucravacitinib, an oral tyrosine kinase 2 inhibitor approved for the treatment of plaque psoriasis, has shown promise as an effective treatment for nail psoriasis in cases that are refractory to standard therapies.
25TH Annual Las Vegas Dermatology Seminar Abstract Compendium; Las Vegas, Nevada; September 19-21, 2024
US Study Pinpoints Merkel Cell Risk Factors
TOPLINE:
in the United States.
METHODOLOGY:
- Researchers evaluated 38,020 MCC cases (38% women; 93% non-Hispanic White, 4% Hispanic, 1% non-Hispanic Black) diagnosed in the United States from 2001 to 2019 to estimate the contribution of potentially modifiable risk factors to the burden of MCC.
- Population-based cancer registries and linkages with HIV and transplant registries were utilized to identify MCC cases in patients with HIV, solid organ transplant recipients, and patients with chronic lymphocytic leukemia (CLL).
- Data on cloud-adjusted daily ambient UVR irradiance were merged with cancer registry information on the county of residence at diagnosis to assess UVR exposure. Studies reporting the prevalence of MCPyV in MCC specimens collected in the United States were combined via a meta-analysis.
- The study assessed population attributable fractions of MCC cases that were attributable to major immunosuppressive conditions (HIV, solid organ transplant, and chronic CLL), ambient UVR exposure, and MCPyV.
TAKEAWAY:
- The incidence of MCC was higher in people with HIV (standardized incidence ratio [SIR], 2.78), organ transplant recipients (SIR, 13.1), and patients with CLL (SIR, 5.75) than in the general US population. However, only 2.5% of MCC cases were attributable to these immunosuppressive conditions.
- Non-Hispanic White individuals showed elevated MCC incidence at both lower and higher ambient UVR exposure levels, with incidence rate ratios of 4.05 and 4.91, respectively, for MCC on the head and neck.
- A meta-analysis of 19 case series revealed that 63.8% of MCC cases were attributable to MCPyV, with a similar prevalence observed between immunocompromised and immunocompetent patients.
- Overall, 65.1% of MCC cases were attributable to ambient UVR exposure, with higher attribution for cases diagnosed on the head and neck than those diagnosed on other sites (72.1% vs 60.2%).
IN PRACTICE:
“The results of this study suggest that most MCC cases in the US are attributable to MCPyV and/or ambient UVR [UV radiation] exposure, with a smaller fraction attributable to three major immunosuppressive conditions,” the authors wrote. “Future studies should investigate UVR mutational signature, TMB [tumor mutational burden], and MCPyV prevalence according to race and ethnicity and patient immune status to help clarify the overlap between MCC risk factors.”
SOURCE:
The study was led by Jacob T. Tribble, BA, Division of Cancer Epidemiology and Genetics, National Cancer Institute (NCI), Rockville, Maryland. It was published online on November 27, 2024, in JAMA Dermatology.
LIMITATIONS:
Incidences of MCC may have been inflated because of increased medical surveillance in immunosuppressed populations. The analysis assumed that only cases among non-Hispanic White individuals were associated with UVR. Additionally, the meta-analysis of MCPyV prevalence primarily included studies from large academic institutions, which may not be representative of the entire US population.
DISCLOSURES:
This study was supported in part by the Intramural Research Program of the NCI and the National Institutes of Health Medical Research Scholars Program. Additional funding was provided through a public-private partnership with contributions from the American Association for Dental Research and the Colgate-Palmolive Company to the Foundation for the National Institutes of Health. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including artificial intelligence, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
TOPLINE:
in the United States.
METHODOLOGY:
- Researchers evaluated 38,020 MCC cases (38% women; 93% non-Hispanic White, 4% Hispanic, 1% non-Hispanic Black) diagnosed in the United States from 2001 to 2019 to estimate the contribution of potentially modifiable risk factors to the burden of MCC.
- Population-based cancer registries and linkages with HIV and transplant registries were utilized to identify MCC cases in patients with HIV, solid organ transplant recipients, and patients with chronic lymphocytic leukemia (CLL).
- Data on cloud-adjusted daily ambient UVR irradiance were merged with cancer registry information on the county of residence at diagnosis to assess UVR exposure. Studies reporting the prevalence of MCPyV in MCC specimens collected in the United States were combined via a meta-analysis.
- The study assessed population attributable fractions of MCC cases that were attributable to major immunosuppressive conditions (HIV, solid organ transplant, and chronic CLL), ambient UVR exposure, and MCPyV.
TAKEAWAY:
- The incidence of MCC was higher in people with HIV (standardized incidence ratio [SIR], 2.78), organ transplant recipients (SIR, 13.1), and patients with CLL (SIR, 5.75) than in the general US population. However, only 2.5% of MCC cases were attributable to these immunosuppressive conditions.
- Non-Hispanic White individuals showed elevated MCC incidence at both lower and higher ambient UVR exposure levels, with incidence rate ratios of 4.05 and 4.91, respectively, for MCC on the head and neck.
- A meta-analysis of 19 case series revealed that 63.8% of MCC cases were attributable to MCPyV, with a similar prevalence observed between immunocompromised and immunocompetent patients.
- Overall, 65.1% of MCC cases were attributable to ambient UVR exposure, with higher attribution for cases diagnosed on the head and neck than those diagnosed on other sites (72.1% vs 60.2%).
IN PRACTICE:
“The results of this study suggest that most MCC cases in the US are attributable to MCPyV and/or ambient UVR [UV radiation] exposure, with a smaller fraction attributable to three major immunosuppressive conditions,” the authors wrote. “Future studies should investigate UVR mutational signature, TMB [tumor mutational burden], and MCPyV prevalence according to race and ethnicity and patient immune status to help clarify the overlap between MCC risk factors.”
SOURCE:
The study was led by Jacob T. Tribble, BA, Division of Cancer Epidemiology and Genetics, National Cancer Institute (NCI), Rockville, Maryland. It was published online on November 27, 2024, in JAMA Dermatology.
LIMITATIONS:
Incidences of MCC may have been inflated because of increased medical surveillance in immunosuppressed populations. The analysis assumed that only cases among non-Hispanic White individuals were associated with UVR. Additionally, the meta-analysis of MCPyV prevalence primarily included studies from large academic institutions, which may not be representative of the entire US population.
DISCLOSURES:
This study was supported in part by the Intramural Research Program of the NCI and the National Institutes of Health Medical Research Scholars Program. Additional funding was provided through a public-private partnership with contributions from the American Association for Dental Research and the Colgate-Palmolive Company to the Foundation for the National Institutes of Health. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including artificial intelligence, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
TOPLINE:
in the United States.
METHODOLOGY:
- Researchers evaluated 38,020 MCC cases (38% women; 93% non-Hispanic White, 4% Hispanic, 1% non-Hispanic Black) diagnosed in the United States from 2001 to 2019 to estimate the contribution of potentially modifiable risk factors to the burden of MCC.
- Population-based cancer registries and linkages with HIV and transplant registries were utilized to identify MCC cases in patients with HIV, solid organ transplant recipients, and patients with chronic lymphocytic leukemia (CLL).
- Data on cloud-adjusted daily ambient UVR irradiance were merged with cancer registry information on the county of residence at diagnosis to assess UVR exposure. Studies reporting the prevalence of MCPyV in MCC specimens collected in the United States were combined via a meta-analysis.
- The study assessed population attributable fractions of MCC cases that were attributable to major immunosuppressive conditions (HIV, solid organ transplant, and chronic CLL), ambient UVR exposure, and MCPyV.
TAKEAWAY:
- The incidence of MCC was higher in people with HIV (standardized incidence ratio [SIR], 2.78), organ transplant recipients (SIR, 13.1), and patients with CLL (SIR, 5.75) than in the general US population. However, only 2.5% of MCC cases were attributable to these immunosuppressive conditions.
- Non-Hispanic White individuals showed elevated MCC incidence at both lower and higher ambient UVR exposure levels, with incidence rate ratios of 4.05 and 4.91, respectively, for MCC on the head and neck.
- A meta-analysis of 19 case series revealed that 63.8% of MCC cases were attributable to MCPyV, with a similar prevalence observed between immunocompromised and immunocompetent patients.
- Overall, 65.1% of MCC cases were attributable to ambient UVR exposure, with higher attribution for cases diagnosed on the head and neck than those diagnosed on other sites (72.1% vs 60.2%).
IN PRACTICE:
“The results of this study suggest that most MCC cases in the US are attributable to MCPyV and/or ambient UVR [UV radiation] exposure, with a smaller fraction attributable to three major immunosuppressive conditions,” the authors wrote. “Future studies should investigate UVR mutational signature, TMB [tumor mutational burden], and MCPyV prevalence according to race and ethnicity and patient immune status to help clarify the overlap between MCC risk factors.”
SOURCE:
The study was led by Jacob T. Tribble, BA, Division of Cancer Epidemiology and Genetics, National Cancer Institute (NCI), Rockville, Maryland. It was published online on November 27, 2024, in JAMA Dermatology.
LIMITATIONS:
Incidences of MCC may have been inflated because of increased medical surveillance in immunosuppressed populations. The analysis assumed that only cases among non-Hispanic White individuals were associated with UVR. Additionally, the meta-analysis of MCPyV prevalence primarily included studies from large academic institutions, which may not be representative of the entire US population.
DISCLOSURES:
This study was supported in part by the Intramural Research Program of the NCI and the National Institutes of Health Medical Research Scholars Program. Additional funding was provided through a public-private partnership with contributions from the American Association for Dental Research and the Colgate-Palmolive Company to the Foundation for the National Institutes of Health. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including artificial intelligence, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
A 58-year-old White male presented with lesions on his index and middle finger for 3 months
Syphilis
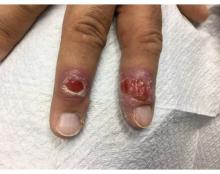
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
Syphilis
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
Syphilis
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
A 58-year-old White male with no significant past medical history presented with lesions on his right index and middle fingers, which had been present for 3 months. The lesions were painless. The patient has a history of hand dermatitis. Upon questioning, the patient said he had not fished or cleaned fish tanks. He did garden occasionally (no roses). He has been using Neosporin on the lesions. He denied any fever or systemic symptoms and had no lymphadenopathy.
What's your diagnosis?
What’s Eating You? Hookworm and Cutaneous Larva Migrans
What’s Eating You? Hookworm and
Cutaneous Larva Migrans
It is estimated that the prevalence of human hookworm infection is approximately 450 million individuals worldwide, representing a substantial global disease burden.1 The annual global public health burden ranges from approximately 2 million to 4 million disability-adjusted life-years and $10 billion to $140 billion in hookwormrelated costs.2 In this article, we discuss the lifecycle, transmission, and disease burden of cutaneous larva migrans (CLM) as well as prevention and treatment strategies.
Background
The Ancylostomatidae nematode family comprises at least 68 known species of hookworm that infect more than 110 different species of mammals.3 Many of these parasites are able to infect more than 1 primary host species, but from a disease perspective they can be classified as either anthropophilic, with humans as the intended host, or zoonotic, with humans as an incidental host. It is important to make this distinction because, though the lifecycles and biology of hookworm species generally are similar, the manifestations of incidental human infection from zoonotic hookworms are different from those of anthropophilic hookworms. Of the anthropophilic species, Necator americanus and Ancylostoma duodenale predominate. In the instance of zoonotic hookworm, dog-infecting A caninum and cat- and doginfecting A braziliense and Uncinaria stenocephala are common causes of incidental human disease.3
The life cycle of Ancylostomatidae organisms is astounding. Through millions of years of co-evolution with mammals,4 these parasitic worms have developed perhaps one of the most circuitous paths to propagate themselves in the natural world. Hookworms start their arduous journey as eggs deposited in soil, sand, and ground vegetation from the feces of infected animals.5 Approximately 1 day after the eggs are deposited, they hatch and begin the larval stage, during which they become infective 1 to 5 weeks later. At this point, the larvae become sensitive to their environment, responding to rising temperatures, increasing carbon dioxide levels, and vibrations in the soil—all of which suggest the presence of a potential host and contribute to a concordant increase in undulatory movement of the larvae.5,6 Here, the most vulnerable tissues include the uncovered soles, palms, and buttocks of host mammals that come into contact with contaminated soil. In an undulating fashion and guided by temperature cues, the larvae locate the skin of the host and utilize a mixture of enzymes including hyaluronidases, metalloprotease, and other proteases to penetrate the epidermis.7 Anthropophilic hookworms such as N americanus and A duodenale will enter the circulatory system; from there, the hookworms migrate through the right-sided cardiopulmonary circuit and eventually ascend into the pulmonary vasculature.8 They then penetrate the lung capillary beds and parenchyma to reach the alveoli, ascend the respiratory tree, and, with the help of the mucociliary escalator, reach the esophagus, where they are swallowed by the host. In the gastrointestinal tract, adult hookworms consume host blood, mate, and lay eggs over a period of approximately 1 to 3 years if left untreated.9 Eggs are laid into the lower gastrointestinal tract, and the journey begins again in feces contacting ground or soil.
Geographic Distribution
Hookworms are found in almost all regions of the world, with species-specific distributions that highlight tropical and subtropical regions. Necator americanus and A duodenale are the most common hookworm species, with the former found predominantly in Southeast Asia and Latin America and the latter in Asia-Pacific regions.10 The highest prevalence of hookworms is in Southeast Asia followed by Sub-Saharan Africa, and the unique climate and soil composition of a region help determine the best environments for specific species of hookworm to thrive.11 In addition, socioeconomics and social determinants of health play a big role in the spread of hookworms, as hygiene practices (eg, wearing clean shoes and clothing, bathing), infrastructure (eg, clean water and streets), and anthelmintic campaigns help reduce transmission.12 Soil-transmitted helminths were once endemic to the southeastern United States, with some reports of approximately 40% of individuals infected in the south in the early 1900s.13 Anthelmintic campaigns such as water, sanitation, and hygiene programs as well as deworming of humans and livestock have proven effective in reducing the prevalence of helminth disease in industrialized nations.13,14 However, zoonotic infections remain a problem in these regions, and in some parts of the United States more than 40% of sampled cats and dogs harbored species such as A braziliense.15
Clinical Manifestation
Initial hookworm infection often goes unnoticed because symptoms can range in severity, but it is characterized by transient ground itch—a local pruritic, erythematous, and papular eruption that develops in response to epidermal penetration.16 Because the larvae must traverse the host from skin to target organs for reproduction over several weeks, iron-deficiency anemia will manifest much later than signs of the initial penetration. In the case of incidental infection from zoonotic Ancylostomatidae organisms, the misguided larvae result in CLM, an often intensely pruritic skin condition that will self-resolve in 2 to 8 weeks with eventual death of the larvae.5
Diagnosis and Pathology of Disease
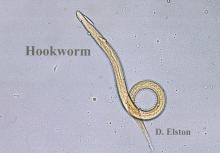
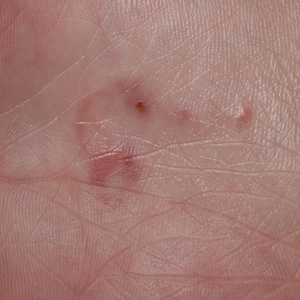
Zoonotic Hookworm—The major presenting sign of zoonotic hookworm infection is CLM. The diagnosis of CLM usually is made clinically, as the larvae themselves are 0.5 mm thick to 10 mm long (Figure 1) and usually extend several centimeters beyond the dermal lesion, with dermoscopy having limited utility.17 Patients may begin to experience itching as little as 1 hour after hookworm penetration of the skin.18 Once in contact with the skin, the hookworms’ hyaluronidases and proteases are capable of breaking through the epidermis, but zoonotic hookworms typically are unable to penetrate the basal layer of the human epidermis and remain entombed between the stratum granulosum and stratum corneum. With the exception of rare cases of direct or indirect pulmonary involvement resulting in Löffler syndrome,19 the larvae will die within weeks to months, and symptoms will subsequently resolve.
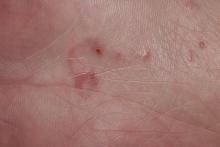
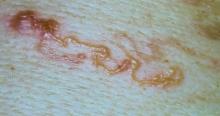
Although the infection generally is self-limiting, the dermatologic manifestations of CLM can be severe and warrant intervention. The lesions start as small reddish papules at the site of penetration (Figure 2), then the hallmark elevated, migrating, serpiginous, urticarial rash develops (Figure 3). Cutaneous larva migrans generally manifests unilaterally and is both erythematous and intensely pruritic. As the larvae migrate, they leave behind 1- to 5-cm tunneled creeping eruptions in their wake. The lesions, which can manifest with pain or be painless, may develop eczematous, bullous, follicular, or impetiginized appearances.20 Atypical manifestations include folliculitis and urticarial plaques.17
cutaneous larval migrans on the palm.
Anthropophilic Hookworm—The lifecycles of N americanus and A duodenale are completed in human infection. Dermatologic manifestations are transient with the development of ground itch at the site of epidermal penetration. The hookworms employ collagenases that allow penetration of the basal layer of the skin, and eosinophilia develops as the parasites travel from the skin to the small intestine. Once attached to the gastrointestinal lumen, blood meals and proteolytic enzymes result in iron-deficiency anemia in the host and may lead to weakness, fatigue, and low birth weights in pregnant patients. With prolonged infection or heavy parasitic burden, patients can develop hypoproteinemia, anasarca, and yellowing of the skin known as chlorosis.11 A clinical diagnosis can be made by examining patient stool samples for eggs, and definitive characterization can be made using molecular tools such as polymerase chain reaction.21,22
Common to hookworm infections is the immune reaction, which promotes inflammation with localized eosinophilia and mastocytosis.11 In a clinical biopsy specimen of gut—usually obtained through esophagogastroduodenoscopy— T-helper (Th) 2–type immune (IL-4, IL-5, IL-9 and IL-13), regulatory Th10 (IL-10 and transcription growth factor β), and some evidence of Th1 (interferon gamma and IL-2) cytokines are present, but little evidence of Th17-type immune response was found.23 It is believed that in zoonotic infections, antiparasitic IgE from basophils are somewhat successful at trapping the helminths in the epidermis, but in the anthropophilic species, IgE and Th2 responses are ineffective at clearing the parasite from the gut, and the defeated immune system transitions to a host-tolerance approach of limiting infection.11 It is now believed that this natural armistice can be manipulated into a potential therapy against autoimmune and inflammatory conditions. Intentional infection with zoonotic whipworm or hookworm has been proposed as a mechanism of switching Th1 and Th2 responses to host-tolerant mechanisms in conditions such as Crohn disease and celiac disease,24 and it has even been hypothesized that prior hookworm infection may reduce the chance of developing allergic conditions such as eczema.25
Treatment and Prevention
The World Health Organization and Centers for Disease Control and Prevention recommend a single oral dose of 400 mg albendazole for adults or 10 to 15 mg/kg in children for CLM. A single dose of ivermectin at 12 mg in adults or 150 μg/kg in children can be used as an alternative where albendazole is not available.11 Topical applications of thiabendazole 10% to 15% under occlusion or 3 times daily for 15 days without occlusion also can manage CLM, and pruritus can be treated with topical corticosteroids for symptomatic relief. Oral albendazole 400 mg twice daily or mebendazole 100 mg twice daily for 3 days or a single 500-mg dose, as well as 11 mg/kg (up to a maximum of 1 g) oral pyrantel pamoate once daily for 3 days can be used to treat intestinal hookworm infection, though it should be avoided in pregnancy. Iron deficiency should be managed with supplementation.11
Prevention of hookworm infection is focused around 2 broad public health efforts: mass drug administration programs and the water, sanitation, and hygiene program. In mass drug administration, treatments such as benzimidazoles are given in mass to communities affected by endemic hookworm as a single dose to reduce the burden of disease. Together, these strategies effectively eliminated hookworms in many developed nations, but areas of resurgence are beginning to surface worldwide. With changes in climate, emerging drug resistance, and socioeconomic disparities, particularly affecting the southeast, a resurgence of hookworm has occurred in the United States.26 One recent study demonstrated that almost one-third (19/55) of children sampled in an impoverished area of rural Alabama had hookworm eggs in their stool.27 Furthermore, pets serve not only as zoonotic reservoirs for CLM recurrence but also as vehicles for the evolution of drug-resistant strains, leading some to call for a ban of animals from beaches and playgrounds as well as tightly controlled veterinary programs.5,28 Ubiquitous benzimidazole use in livestock has led to bendazole-resistant strains, and it is likely that with continued and poorly adherent drug use, more zoonotic and anthropophilic drug-resistant strains of hookworm will emerge.29,30
Conclusion
The burden of hookworm infection and CLM is substantial in parts of the United States. Dermatologists play a critical role in the recognition and management of hookworm infection for both treatment of affected patients and the subsequent prevention of its spread. As drug-resistant strains evolve, clinicians, public health officials, and scientists need to continue to work together to prevent and treat hookworm infection.
- Vos T, Abajobir AA, Abate KH, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1211-1259.
- Bartsch SM, Hotez PJ, Asti L, et al. The global economic and health burden of human hookworm infection. PLoS Negl Trop Dis. 2016;10:E0004922.
- Seguel M, Gottdenker N. The diversity and impact of hookworm infections in wildlife. Int J Parasitol Parasites Wildl. 2017;6:177-194.
- Adams BJ, Peat SM, Dillman AR. Phylogeny and evolution. In: Entomopathogenic Nematodes: Systematics, Phylogeny and Bacterial Symbionts. Brill; 2010:693-733.
- Heukelbach J, Feldmeier H. Epidemiological and clinical characteristics of hookworm-related cutaneous larva migrans. Lancet Infect Dis. 2008;8:302-309.
- Haas W, Haberl B, Idris I, et al. Infective larvae of the human hookworms Necator americanus and Ancylostoma duodenale differ in their orientation behaviour when crawling on surfaces. Parasitol Res. 2005;95:25-29.
- Hotez P, Narasimhan S, Haggerty J, et al. Hyaluronidase from infective Ancylostoma hookworm larvae and its possible function as a virulence factor in tissue invasion and in cutaneous larva migrans. Infect Immun. 1992;60:1018-1023.
- Brooker S, Bethony J, Hotez PJ. Human hookworm infection in the 21st century. Adv Parasitol. 2004;58:197-288.
- Hoagland K, Schad G. Necator americanus and Ancylostoma duodenale: life history parameters and epidemiological implications of two sympatric hookworms of humans. Exp Parasitol. 1978;44:36-49.
- Clements ACA, Alene KA. Global distribution of human hookworm species and differences in their morbidity effects: a systematic review. Lancet Microbe. 2022;3:E72-E79.
- Loukas A, Hotez PJ, Diemert D, et al. Hookworm infection. Nat Rev Dis Primers. 2016;2:1-18.
- Gazzinelli A, Correa-Oliveira R, Yang GJ, et al. A research agenda for helminth diseases of humans: social ecology, environmental determinants, and health systems. PLoS Negl Trop Dis. 2012;6:E1603.
- Starr MC, Montgomery SP. Soil-transmitted helminthiasis in the United States: a systematic review—1940-2010. Am J Trop Med Hyg. 2011;85:680-684.
- Strunz EC, Addiss DG, Stocks ME, et al. Water, sanitation, hygiene, and soil-transmitted helminth infection: a systematic review and metaanalysis. PLoS Med. 2014;11:E1001620.
- Liotta JL, Youn H, Aksel S, et al. Prevalence of Ancylostoma braziliense in dogs from Alachua and Marion Counties, Florida, United States. J Parasitol. 2012;98:1039-1040.
- Hotez PJ, Brooker S, Bethony JM, et al. Hookworm infection. N Engl J Med. 2004;351:799-807.
- Prickett KA, Ferringer TC. What’s eating you? cutaneous larva migrans. Cutis. 2015;95:126-128.
- Feldmeier H, Schuster A. Mini review: hookworm-related cutaneous larva migrans. Eur J Clin Microbiol Infect Dis. 2012;31:915-918.
- Tan SK, Liu TT. Cutaneous larva migrans complicated by Löffler syndrome. Arch Dermatol. 2010;146:210-212.
- Eksomtramage T, Aiempanakit K. Bullous and pustular cutaneous larva migrans: two case reports and a literature review. IDCases. 2018;12:130-132.
- Utzinger J, Rinaldi L, Lohourignon LK, et al. FLOTAC: a new sensitive technique for the diagnosis of hookworm infections in humans. Trans R Soc Trop Med Hyg. 2008;102:84-90.
- Chidambaram M, Parija SC, Toi PC, et al. Evaluation of the utility of conventional polymerase chain reaction for detection and species differentiation in human hookworm infections. Trop Parasitol. 2017;7:111-116.
- Gaze S, McSorley HJ, Daveson J, et al. Characterising the mucosal and systemic immune responses to experimental human hookworm infection. PLoS Pathog. 2012;8:E1002520.
- Croese J, O’Neil J, Masson J, et al. A proof of concept study establishing Necator americanus in Crohn’s patients and reservoir donors. Gut. 2006;55:136-137.
- Mpairwe H, Amoah AS. Parasites and allergy: observations from Africa. Parasite Immunol. 2019;41:E12589.
- Albonico M, Savioli L. Hookworm: a neglected resurgent infection. Editorial. BMJ. 2017;359:j4813.
- McKenna ML, McAtee S, Bryan PE, et al. Human intestinal parasite burden and poor sanitation in rural Alabama. Am J Trop Med Hyg. 2017;97:1623-1628.
- Traversa D. Pet roundworms and hookworms: a continuing need for global worming. Parasit Vectors. 2012;5:1-19.
- Geerts S, Gryseels B. Drug resistance in human helminths: current situation and lessons from livestock. Clin Microbiol Rev. 2000;13:207-222.
- Jimenez Castro PD, Howell SB, Schaefer JJ, et al. Multiple drug resistance in the canine hookworm Ancylostoma caninum: an emerging threat? Parasit Vectors. 2019;12:1-15.
It is estimated that the prevalence of human hookworm infection is approximately 450 million individuals worldwide, representing a substantial global disease burden.1 The annual global public health burden ranges from approximately 2 million to 4 million disability-adjusted life-years and $10 billion to $140 billion in hookwormrelated costs.2 In this article, we discuss the lifecycle, transmission, and disease burden of cutaneous larva migrans (CLM) as well as prevention and treatment strategies.
Background
The Ancylostomatidae nematode family comprises at least 68 known species of hookworm that infect more than 110 different species of mammals.3 Many of these parasites are able to infect more than 1 primary host species, but from a disease perspective they can be classified as either anthropophilic, with humans as the intended host, or zoonotic, with humans as an incidental host. It is important to make this distinction because, though the lifecycles and biology of hookworm species generally are similar, the manifestations of incidental human infection from zoonotic hookworms are different from those of anthropophilic hookworms. Of the anthropophilic species, Necator americanus and Ancylostoma duodenale predominate. In the instance of zoonotic hookworm, dog-infecting A caninum and cat- and doginfecting A braziliense and Uncinaria stenocephala are common causes of incidental human disease.3
The life cycle of Ancylostomatidae organisms is astounding. Through millions of years of co-evolution with mammals,4 these parasitic worms have developed perhaps one of the most circuitous paths to propagate themselves in the natural world. Hookworms start their arduous journey as eggs deposited in soil, sand, and ground vegetation from the feces of infected animals.5 Approximately 1 day after the eggs are deposited, they hatch and begin the larval stage, during which they become infective 1 to 5 weeks later. At this point, the larvae become sensitive to their environment, responding to rising temperatures, increasing carbon dioxide levels, and vibrations in the soil—all of which suggest the presence of a potential host and contribute to a concordant increase in undulatory movement of the larvae.5,6 Here, the most vulnerable tissues include the uncovered soles, palms, and buttocks of host mammals that come into contact with contaminated soil. In an undulating fashion and guided by temperature cues, the larvae locate the skin of the host and utilize a mixture of enzymes including hyaluronidases, metalloprotease, and other proteases to penetrate the epidermis.7 Anthropophilic hookworms such as N americanus and A duodenale will enter the circulatory system; from there, the hookworms migrate through the right-sided cardiopulmonary circuit and eventually ascend into the pulmonary vasculature.8 They then penetrate the lung capillary beds and parenchyma to reach the alveoli, ascend the respiratory tree, and, with the help of the mucociliary escalator, reach the esophagus, where they are swallowed by the host. In the gastrointestinal tract, adult hookworms consume host blood, mate, and lay eggs over a period of approximately 1 to 3 years if left untreated.9 Eggs are laid into the lower gastrointestinal tract, and the journey begins again in feces contacting ground or soil.
Geographic Distribution
Hookworms are found in almost all regions of the world, with species-specific distributions that highlight tropical and subtropical regions. Necator americanus and A duodenale are the most common hookworm species, with the former found predominantly in Southeast Asia and Latin America and the latter in Asia-Pacific regions.10 The highest prevalence of hookworms is in Southeast Asia followed by Sub-Saharan Africa, and the unique climate and soil composition of a region help determine the best environments for specific species of hookworm to thrive.11 In addition, socioeconomics and social determinants of health play a big role in the spread of hookworms, as hygiene practices (eg, wearing clean shoes and clothing, bathing), infrastructure (eg, clean water and streets), and anthelmintic campaigns help reduce transmission.12 Soil-transmitted helminths were once endemic to the southeastern United States, with some reports of approximately 40% of individuals infected in the south in the early 1900s.13 Anthelmintic campaigns such as water, sanitation, and hygiene programs as well as deworming of humans and livestock have proven effective in reducing the prevalence of helminth disease in industrialized nations.13,14 However, zoonotic infections remain a problem in these regions, and in some parts of the United States more than 40% of sampled cats and dogs harbored species such as A braziliense.15
Clinical Manifestation
Initial hookworm infection often goes unnoticed because symptoms can range in severity, but it is characterized by transient ground itch—a local pruritic, erythematous, and papular eruption that develops in response to epidermal penetration.16 Because the larvae must traverse the host from skin to target organs for reproduction over several weeks, iron-deficiency anemia will manifest much later than signs of the initial penetration. In the case of incidental infection from zoonotic Ancylostomatidae organisms, the misguided larvae result in CLM, an often intensely pruritic skin condition that will self-resolve in 2 to 8 weeks with eventual death of the larvae.5
Diagnosis and Pathology of Disease
Zoonotic Hookworm—The major presenting sign of zoonotic hookworm infection is CLM. The diagnosis of CLM usually is made clinically, as the larvae themselves are 0.5 mm thick to 10 mm long (Figure 1) and usually extend several centimeters beyond the dermal lesion, with dermoscopy having limited utility.17 Patients may begin to experience itching as little as 1 hour after hookworm penetration of the skin.18 Once in contact with the skin, the hookworms’ hyaluronidases and proteases are capable of breaking through the epidermis, but zoonotic hookworms typically are unable to penetrate the basal layer of the human epidermis and remain entombed between the stratum granulosum and stratum corneum. With the exception of rare cases of direct or indirect pulmonary involvement resulting in Löffler syndrome,19 the larvae will die within weeks to months, and symptoms will subsequently resolve.
Although the infection generally is self-limiting, the dermatologic manifestations of CLM can be severe and warrant intervention. The lesions start as small reddish papules at the site of penetration (Figure 2), then the hallmark elevated, migrating, serpiginous, urticarial rash develops (Figure 3). Cutaneous larva migrans generally manifests unilaterally and is both erythematous and intensely pruritic. As the larvae migrate, they leave behind 1- to 5-cm tunneled creeping eruptions in their wake. The lesions, which can manifest with pain or be painless, may develop eczematous, bullous, follicular, or impetiginized appearances.20 Atypical manifestations include folliculitis and urticarial plaques.17
cutaneous larval migrans on the palm.
Anthropophilic Hookworm—The lifecycles of N americanus and A duodenale are completed in human infection. Dermatologic manifestations are transient with the development of ground itch at the site of epidermal penetration. The hookworms employ collagenases that allow penetration of the basal layer of the skin, and eosinophilia develops as the parasites travel from the skin to the small intestine. Once attached to the gastrointestinal lumen, blood meals and proteolytic enzymes result in iron-deficiency anemia in the host and may lead to weakness, fatigue, and low birth weights in pregnant patients. With prolonged infection or heavy parasitic burden, patients can develop hypoproteinemia, anasarca, and yellowing of the skin known as chlorosis.11 A clinical diagnosis can be made by examining patient stool samples for eggs, and definitive characterization can be made using molecular tools such as polymerase chain reaction.21,22
Common to hookworm infections is the immune reaction, which promotes inflammation with localized eosinophilia and mastocytosis.11 In a clinical biopsy specimen of gut—usually obtained through esophagogastroduodenoscopy— T-helper (Th) 2–type immune (IL-4, IL-5, IL-9 and IL-13), regulatory Th10 (IL-10 and transcription growth factor β), and some evidence of Th1 (interferon gamma and IL-2) cytokines are present, but little evidence of Th17-type immune response was found.23 It is believed that in zoonotic infections, antiparasitic IgE from basophils are somewhat successful at trapping the helminths in the epidermis, but in the anthropophilic species, IgE and Th2 responses are ineffective at clearing the parasite from the gut, and the defeated immune system transitions to a host-tolerance approach of limiting infection.11 It is now believed that this natural armistice can be manipulated into a potential therapy against autoimmune and inflammatory conditions. Intentional infection with zoonotic whipworm or hookworm has been proposed as a mechanism of switching Th1 and Th2 responses to host-tolerant mechanisms in conditions such as Crohn disease and celiac disease,24 and it has even been hypothesized that prior hookworm infection may reduce the chance of developing allergic conditions such as eczema.25
Treatment and Prevention
The World Health Organization and Centers for Disease Control and Prevention recommend a single oral dose of 400 mg albendazole for adults or 10 to 15 mg/kg in children for CLM. A single dose of ivermectin at 12 mg in adults or 150 μg/kg in children can be used as an alternative where albendazole is not available.11 Topical applications of thiabendazole 10% to 15% under occlusion or 3 times daily for 15 days without occlusion also can manage CLM, and pruritus can be treated with topical corticosteroids for symptomatic relief. Oral albendazole 400 mg twice daily or mebendazole 100 mg twice daily for 3 days or a single 500-mg dose, as well as 11 mg/kg (up to a maximum of 1 g) oral pyrantel pamoate once daily for 3 days can be used to treat intestinal hookworm infection, though it should be avoided in pregnancy. Iron deficiency should be managed with supplementation.11
Prevention of hookworm infection is focused around 2 broad public health efforts: mass drug administration programs and the water, sanitation, and hygiene program. In mass drug administration, treatments such as benzimidazoles are given in mass to communities affected by endemic hookworm as a single dose to reduce the burden of disease. Together, these strategies effectively eliminated hookworms in many developed nations, but areas of resurgence are beginning to surface worldwide. With changes in climate, emerging drug resistance, and socioeconomic disparities, particularly affecting the southeast, a resurgence of hookworm has occurred in the United States.26 One recent study demonstrated that almost one-third (19/55) of children sampled in an impoverished area of rural Alabama had hookworm eggs in their stool.27 Furthermore, pets serve not only as zoonotic reservoirs for CLM recurrence but also as vehicles for the evolution of drug-resistant strains, leading some to call for a ban of animals from beaches and playgrounds as well as tightly controlled veterinary programs.5,28 Ubiquitous benzimidazole use in livestock has led to bendazole-resistant strains, and it is likely that with continued and poorly adherent drug use, more zoonotic and anthropophilic drug-resistant strains of hookworm will emerge.29,30
Conclusion
The burden of hookworm infection and CLM is substantial in parts of the United States. Dermatologists play a critical role in the recognition and management of hookworm infection for both treatment of affected patients and the subsequent prevention of its spread. As drug-resistant strains evolve, clinicians, public health officials, and scientists need to continue to work together to prevent and treat hookworm infection.
It is estimated that the prevalence of human hookworm infection is approximately 450 million individuals worldwide, representing a substantial global disease burden.1 The annual global public health burden ranges from approximately 2 million to 4 million disability-adjusted life-years and $10 billion to $140 billion in hookwormrelated costs.2 In this article, we discuss the lifecycle, transmission, and disease burden of cutaneous larva migrans (CLM) as well as prevention and treatment strategies.
Background
The Ancylostomatidae nematode family comprises at least 68 known species of hookworm that infect more than 110 different species of mammals.3 Many of these parasites are able to infect more than 1 primary host species, but from a disease perspective they can be classified as either anthropophilic, with humans as the intended host, or zoonotic, with humans as an incidental host. It is important to make this distinction because, though the lifecycles and biology of hookworm species generally are similar, the manifestations of incidental human infection from zoonotic hookworms are different from those of anthropophilic hookworms. Of the anthropophilic species, Necator americanus and Ancylostoma duodenale predominate. In the instance of zoonotic hookworm, dog-infecting A caninum and cat- and doginfecting A braziliense and Uncinaria stenocephala are common causes of incidental human disease.3
The life cycle of Ancylostomatidae organisms is astounding. Through millions of years of co-evolution with mammals,4 these parasitic worms have developed perhaps one of the most circuitous paths to propagate themselves in the natural world. Hookworms start their arduous journey as eggs deposited in soil, sand, and ground vegetation from the feces of infected animals.5 Approximately 1 day after the eggs are deposited, they hatch and begin the larval stage, during which they become infective 1 to 5 weeks later. At this point, the larvae become sensitive to their environment, responding to rising temperatures, increasing carbon dioxide levels, and vibrations in the soil—all of which suggest the presence of a potential host and contribute to a concordant increase in undulatory movement of the larvae.5,6 Here, the most vulnerable tissues include the uncovered soles, palms, and buttocks of host mammals that come into contact with contaminated soil. In an undulating fashion and guided by temperature cues, the larvae locate the skin of the host and utilize a mixture of enzymes including hyaluronidases, metalloprotease, and other proteases to penetrate the epidermis.7 Anthropophilic hookworms such as N americanus and A duodenale will enter the circulatory system; from there, the hookworms migrate through the right-sided cardiopulmonary circuit and eventually ascend into the pulmonary vasculature.8 They then penetrate the lung capillary beds and parenchyma to reach the alveoli, ascend the respiratory tree, and, with the help of the mucociliary escalator, reach the esophagus, where they are swallowed by the host. In the gastrointestinal tract, adult hookworms consume host blood, mate, and lay eggs over a period of approximately 1 to 3 years if left untreated.9 Eggs are laid into the lower gastrointestinal tract, and the journey begins again in feces contacting ground or soil.
Geographic Distribution
Hookworms are found in almost all regions of the world, with species-specific distributions that highlight tropical and subtropical regions. Necator americanus and A duodenale are the most common hookworm species, with the former found predominantly in Southeast Asia and Latin America and the latter in Asia-Pacific regions.10 The highest prevalence of hookworms is in Southeast Asia followed by Sub-Saharan Africa, and the unique climate and soil composition of a region help determine the best environments for specific species of hookworm to thrive.11 In addition, socioeconomics and social determinants of health play a big role in the spread of hookworms, as hygiene practices (eg, wearing clean shoes and clothing, bathing), infrastructure (eg, clean water and streets), and anthelmintic campaigns help reduce transmission.12 Soil-transmitted helminths were once endemic to the southeastern United States, with some reports of approximately 40% of individuals infected in the south in the early 1900s.13 Anthelmintic campaigns such as water, sanitation, and hygiene programs as well as deworming of humans and livestock have proven effective in reducing the prevalence of helminth disease in industrialized nations.13,14 However, zoonotic infections remain a problem in these regions, and in some parts of the United States more than 40% of sampled cats and dogs harbored species such as A braziliense.15
Clinical Manifestation
Initial hookworm infection often goes unnoticed because symptoms can range in severity, but it is characterized by transient ground itch—a local pruritic, erythematous, and papular eruption that develops in response to epidermal penetration.16 Because the larvae must traverse the host from skin to target organs for reproduction over several weeks, iron-deficiency anemia will manifest much later than signs of the initial penetration. In the case of incidental infection from zoonotic Ancylostomatidae organisms, the misguided larvae result in CLM, an often intensely pruritic skin condition that will self-resolve in 2 to 8 weeks with eventual death of the larvae.5
Diagnosis and Pathology of Disease
Zoonotic Hookworm—The major presenting sign of zoonotic hookworm infection is CLM. The diagnosis of CLM usually is made clinically, as the larvae themselves are 0.5 mm thick to 10 mm long (Figure 1) and usually extend several centimeters beyond the dermal lesion, with dermoscopy having limited utility.17 Patients may begin to experience itching as little as 1 hour after hookworm penetration of the skin.18 Once in contact with the skin, the hookworms’ hyaluronidases and proteases are capable of breaking through the epidermis, but zoonotic hookworms typically are unable to penetrate the basal layer of the human epidermis and remain entombed between the stratum granulosum and stratum corneum. With the exception of rare cases of direct or indirect pulmonary involvement resulting in Löffler syndrome,19 the larvae will die within weeks to months, and symptoms will subsequently resolve.
Although the infection generally is self-limiting, the dermatologic manifestations of CLM can be severe and warrant intervention. The lesions start as small reddish papules at the site of penetration (Figure 2), then the hallmark elevated, migrating, serpiginous, urticarial rash develops (Figure 3). Cutaneous larva migrans generally manifests unilaterally and is both erythematous and intensely pruritic. As the larvae migrate, they leave behind 1- to 5-cm tunneled creeping eruptions in their wake. The lesions, which can manifest with pain or be painless, may develop eczematous, bullous, follicular, or impetiginized appearances.20 Atypical manifestations include folliculitis and urticarial plaques.17
cutaneous larval migrans on the palm.
Anthropophilic Hookworm—The lifecycles of N americanus and A duodenale are completed in human infection. Dermatologic manifestations are transient with the development of ground itch at the site of epidermal penetration. The hookworms employ collagenases that allow penetration of the basal layer of the skin, and eosinophilia develops as the parasites travel from the skin to the small intestine. Once attached to the gastrointestinal lumen, blood meals and proteolytic enzymes result in iron-deficiency anemia in the host and may lead to weakness, fatigue, and low birth weights in pregnant patients. With prolonged infection or heavy parasitic burden, patients can develop hypoproteinemia, anasarca, and yellowing of the skin known as chlorosis.11 A clinical diagnosis can be made by examining patient stool samples for eggs, and definitive characterization can be made using molecular tools such as polymerase chain reaction.21,22
Common to hookworm infections is the immune reaction, which promotes inflammation with localized eosinophilia and mastocytosis.11 In a clinical biopsy specimen of gut—usually obtained through esophagogastroduodenoscopy— T-helper (Th) 2–type immune (IL-4, IL-5, IL-9 and IL-13), regulatory Th10 (IL-10 and transcription growth factor β), and some evidence of Th1 (interferon gamma and IL-2) cytokines are present, but little evidence of Th17-type immune response was found.23 It is believed that in zoonotic infections, antiparasitic IgE from basophils are somewhat successful at trapping the helminths in the epidermis, but in the anthropophilic species, IgE and Th2 responses are ineffective at clearing the parasite from the gut, and the defeated immune system transitions to a host-tolerance approach of limiting infection.11 It is now believed that this natural armistice can be manipulated into a potential therapy against autoimmune and inflammatory conditions. Intentional infection with zoonotic whipworm or hookworm has been proposed as a mechanism of switching Th1 and Th2 responses to host-tolerant mechanisms in conditions such as Crohn disease and celiac disease,24 and it has even been hypothesized that prior hookworm infection may reduce the chance of developing allergic conditions such as eczema.25
Treatment and Prevention
The World Health Organization and Centers for Disease Control and Prevention recommend a single oral dose of 400 mg albendazole for adults or 10 to 15 mg/kg in children for CLM. A single dose of ivermectin at 12 mg in adults or 150 μg/kg in children can be used as an alternative where albendazole is not available.11 Topical applications of thiabendazole 10% to 15% under occlusion or 3 times daily for 15 days without occlusion also can manage CLM, and pruritus can be treated with topical corticosteroids for symptomatic relief. Oral albendazole 400 mg twice daily or mebendazole 100 mg twice daily for 3 days or a single 500-mg dose, as well as 11 mg/kg (up to a maximum of 1 g) oral pyrantel pamoate once daily for 3 days can be used to treat intestinal hookworm infection, though it should be avoided in pregnancy. Iron deficiency should be managed with supplementation.11
Prevention of hookworm infection is focused around 2 broad public health efforts: mass drug administration programs and the water, sanitation, and hygiene program. In mass drug administration, treatments such as benzimidazoles are given in mass to communities affected by endemic hookworm as a single dose to reduce the burden of disease. Together, these strategies effectively eliminated hookworms in many developed nations, but areas of resurgence are beginning to surface worldwide. With changes in climate, emerging drug resistance, and socioeconomic disparities, particularly affecting the southeast, a resurgence of hookworm has occurred in the United States.26 One recent study demonstrated that almost one-third (19/55) of children sampled in an impoverished area of rural Alabama had hookworm eggs in their stool.27 Furthermore, pets serve not only as zoonotic reservoirs for CLM recurrence but also as vehicles for the evolution of drug-resistant strains, leading some to call for a ban of animals from beaches and playgrounds as well as tightly controlled veterinary programs.5,28 Ubiquitous benzimidazole use in livestock has led to bendazole-resistant strains, and it is likely that with continued and poorly adherent drug use, more zoonotic and anthropophilic drug-resistant strains of hookworm will emerge.29,30
Conclusion
The burden of hookworm infection and CLM is substantial in parts of the United States. Dermatologists play a critical role in the recognition and management of hookworm infection for both treatment of affected patients and the subsequent prevention of its spread. As drug-resistant strains evolve, clinicians, public health officials, and scientists need to continue to work together to prevent and treat hookworm infection.
- Vos T, Abajobir AA, Abate KH, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1211-1259.
- Bartsch SM, Hotez PJ, Asti L, et al. The global economic and health burden of human hookworm infection. PLoS Negl Trop Dis. 2016;10:E0004922.
- Seguel M, Gottdenker N. The diversity and impact of hookworm infections in wildlife. Int J Parasitol Parasites Wildl. 2017;6:177-194.
- Adams BJ, Peat SM, Dillman AR. Phylogeny and evolution. In: Entomopathogenic Nematodes: Systematics, Phylogeny and Bacterial Symbionts. Brill; 2010:693-733.
- Heukelbach J, Feldmeier H. Epidemiological and clinical characteristics of hookworm-related cutaneous larva migrans. Lancet Infect Dis. 2008;8:302-309.
- Haas W, Haberl B, Idris I, et al. Infective larvae of the human hookworms Necator americanus and Ancylostoma duodenale differ in their orientation behaviour when crawling on surfaces. Parasitol Res. 2005;95:25-29.
- Hotez P, Narasimhan S, Haggerty J, et al. Hyaluronidase from infective Ancylostoma hookworm larvae and its possible function as a virulence factor in tissue invasion and in cutaneous larva migrans. Infect Immun. 1992;60:1018-1023.
- Brooker S, Bethony J, Hotez PJ. Human hookworm infection in the 21st century. Adv Parasitol. 2004;58:197-288.
- Hoagland K, Schad G. Necator americanus and Ancylostoma duodenale: life history parameters and epidemiological implications of two sympatric hookworms of humans. Exp Parasitol. 1978;44:36-49.
- Clements ACA, Alene KA. Global distribution of human hookworm species and differences in their morbidity effects: a systematic review. Lancet Microbe. 2022;3:E72-E79.
- Loukas A, Hotez PJ, Diemert D, et al. Hookworm infection. Nat Rev Dis Primers. 2016;2:1-18.
- Gazzinelli A, Correa-Oliveira R, Yang GJ, et al. A research agenda for helminth diseases of humans: social ecology, environmental determinants, and health systems. PLoS Negl Trop Dis. 2012;6:E1603.
- Starr MC, Montgomery SP. Soil-transmitted helminthiasis in the United States: a systematic review—1940-2010. Am J Trop Med Hyg. 2011;85:680-684.
- Strunz EC, Addiss DG, Stocks ME, et al. Water, sanitation, hygiene, and soil-transmitted helminth infection: a systematic review and metaanalysis. PLoS Med. 2014;11:E1001620.
- Liotta JL, Youn H, Aksel S, et al. Prevalence of Ancylostoma braziliense in dogs from Alachua and Marion Counties, Florida, United States. J Parasitol. 2012;98:1039-1040.
- Hotez PJ, Brooker S, Bethony JM, et al. Hookworm infection. N Engl J Med. 2004;351:799-807.
- Prickett KA, Ferringer TC. What’s eating you? cutaneous larva migrans. Cutis. 2015;95:126-128.
- Feldmeier H, Schuster A. Mini review: hookworm-related cutaneous larva migrans. Eur J Clin Microbiol Infect Dis. 2012;31:915-918.
- Tan SK, Liu TT. Cutaneous larva migrans complicated by Löffler syndrome. Arch Dermatol. 2010;146:210-212.
- Eksomtramage T, Aiempanakit K. Bullous and pustular cutaneous larva migrans: two case reports and a literature review. IDCases. 2018;12:130-132.
- Utzinger J, Rinaldi L, Lohourignon LK, et al. FLOTAC: a new sensitive technique for the diagnosis of hookworm infections in humans. Trans R Soc Trop Med Hyg. 2008;102:84-90.
- Chidambaram M, Parija SC, Toi PC, et al. Evaluation of the utility of conventional polymerase chain reaction for detection and species differentiation in human hookworm infections. Trop Parasitol. 2017;7:111-116.
- Gaze S, McSorley HJ, Daveson J, et al. Characterising the mucosal and systemic immune responses to experimental human hookworm infection. PLoS Pathog. 2012;8:E1002520.
- Croese J, O’Neil J, Masson J, et al. A proof of concept study establishing Necator americanus in Crohn’s patients and reservoir donors. Gut. 2006;55:136-137.
- Mpairwe H, Amoah AS. Parasites and allergy: observations from Africa. Parasite Immunol. 2019;41:E12589.
- Albonico M, Savioli L. Hookworm: a neglected resurgent infection. Editorial. BMJ. 2017;359:j4813.
- McKenna ML, McAtee S, Bryan PE, et al. Human intestinal parasite burden and poor sanitation in rural Alabama. Am J Trop Med Hyg. 2017;97:1623-1628.
- Traversa D. Pet roundworms and hookworms: a continuing need for global worming. Parasit Vectors. 2012;5:1-19.
- Geerts S, Gryseels B. Drug resistance in human helminths: current situation and lessons from livestock. Clin Microbiol Rev. 2000;13:207-222.
- Jimenez Castro PD, Howell SB, Schaefer JJ, et al. Multiple drug resistance in the canine hookworm Ancylostoma caninum: an emerging threat? Parasit Vectors. 2019;12:1-15.
- Vos T, Abajobir AA, Abate KH, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1211-1259.
- Bartsch SM, Hotez PJ, Asti L, et al. The global economic and health burden of human hookworm infection. PLoS Negl Trop Dis. 2016;10:E0004922.
- Seguel M, Gottdenker N. The diversity and impact of hookworm infections in wildlife. Int J Parasitol Parasites Wildl. 2017;6:177-194.
- Adams BJ, Peat SM, Dillman AR. Phylogeny and evolution. In: Entomopathogenic Nematodes: Systematics, Phylogeny and Bacterial Symbionts. Brill; 2010:693-733.
- Heukelbach J, Feldmeier H. Epidemiological and clinical characteristics of hookworm-related cutaneous larva migrans. Lancet Infect Dis. 2008;8:302-309.
- Haas W, Haberl B, Idris I, et al. Infective larvae of the human hookworms Necator americanus and Ancylostoma duodenale differ in their orientation behaviour when crawling on surfaces. Parasitol Res. 2005;95:25-29.
- Hotez P, Narasimhan S, Haggerty J, et al. Hyaluronidase from infective Ancylostoma hookworm larvae and its possible function as a virulence factor in tissue invasion and in cutaneous larva migrans. Infect Immun. 1992;60:1018-1023.
- Brooker S, Bethony J, Hotez PJ. Human hookworm infection in the 21st century. Adv Parasitol. 2004;58:197-288.
- Hoagland K, Schad G. Necator americanus and Ancylostoma duodenale: life history parameters and epidemiological implications of two sympatric hookworms of humans. Exp Parasitol. 1978;44:36-49.
- Clements ACA, Alene KA. Global distribution of human hookworm species and differences in their morbidity effects: a systematic review. Lancet Microbe. 2022;3:E72-E79.
- Loukas A, Hotez PJ, Diemert D, et al. Hookworm infection. Nat Rev Dis Primers. 2016;2:1-18.
- Gazzinelli A, Correa-Oliveira R, Yang GJ, et al. A research agenda for helminth diseases of humans: social ecology, environmental determinants, and health systems. PLoS Negl Trop Dis. 2012;6:E1603.
- Starr MC, Montgomery SP. Soil-transmitted helminthiasis in the United States: a systematic review—1940-2010. Am J Trop Med Hyg. 2011;85:680-684.
- Strunz EC, Addiss DG, Stocks ME, et al. Water, sanitation, hygiene, and soil-transmitted helminth infection: a systematic review and metaanalysis. PLoS Med. 2014;11:E1001620.
- Liotta JL, Youn H, Aksel S, et al. Prevalence of Ancylostoma braziliense in dogs from Alachua and Marion Counties, Florida, United States. J Parasitol. 2012;98:1039-1040.
- Hotez PJ, Brooker S, Bethony JM, et al. Hookworm infection. N Engl J Med. 2004;351:799-807.
- Prickett KA, Ferringer TC. What’s eating you? cutaneous larva migrans. Cutis. 2015;95:126-128.
- Feldmeier H, Schuster A. Mini review: hookworm-related cutaneous larva migrans. Eur J Clin Microbiol Infect Dis. 2012;31:915-918.
- Tan SK, Liu TT. Cutaneous larva migrans complicated by Löffler syndrome. Arch Dermatol. 2010;146:210-212.
- Eksomtramage T, Aiempanakit K. Bullous and pustular cutaneous larva migrans: two case reports and a literature review. IDCases. 2018;12:130-132.
- Utzinger J, Rinaldi L, Lohourignon LK, et al. FLOTAC: a new sensitive technique for the diagnosis of hookworm infections in humans. Trans R Soc Trop Med Hyg. 2008;102:84-90.
- Chidambaram M, Parija SC, Toi PC, et al. Evaluation of the utility of conventional polymerase chain reaction for detection and species differentiation in human hookworm infections. Trop Parasitol. 2017;7:111-116.
- Gaze S, McSorley HJ, Daveson J, et al. Characterising the mucosal and systemic immune responses to experimental human hookworm infection. PLoS Pathog. 2012;8:E1002520.
- Croese J, O’Neil J, Masson J, et al. A proof of concept study establishing Necator americanus in Crohn’s patients and reservoir donors. Gut. 2006;55:136-137.
- Mpairwe H, Amoah AS. Parasites and allergy: observations from Africa. Parasite Immunol. 2019;41:E12589.
- Albonico M, Savioli L. Hookworm: a neglected resurgent infection. Editorial. BMJ. 2017;359:j4813.
- McKenna ML, McAtee S, Bryan PE, et al. Human intestinal parasite burden and poor sanitation in rural Alabama. Am J Trop Med Hyg. 2017;97:1623-1628.
- Traversa D. Pet roundworms and hookworms: a continuing need for global worming. Parasit Vectors. 2012;5:1-19.
- Geerts S, Gryseels B. Drug resistance in human helminths: current situation and lessons from livestock. Clin Microbiol Rev. 2000;13:207-222.
- Jimenez Castro PD, Howell SB, Schaefer JJ, et al. Multiple drug resistance in the canine hookworm Ancylostoma caninum: an emerging threat? Parasit Vectors. 2019;12:1-15.
What’s Eating You? Hookworm and
Cutaneous Larva Migrans
What’s Eating You? Hookworm and
Cutaneous Larva Migrans
PRACTICE POINTS
- Anthropophilic hookworm infection should be considered with evidence of either transient ground itch or iron-deficient anemia in individuals who go barefoot, permitting ground-to-skin transmission.
- Zoonotic hookworm infection manifests as cutaneous larva migrans, an elevated serpiginous rash that, while usually self-resolving, can be intensely pruritic and should be treated accordingly.
- Considered a neglected tropical disease, hookworm infection still represents an enormous global disease burden. In addition to ongoing afflicted regions, hookworms are making a resurgence in developed nations, and drug-resistant strains have evolved.
Comparing Patient Care Models at a Local Free Clinic vs an Insurance- Based University Medical Center
Comparing Patient Care Models at a Local Free Clinic vs an Insurance- Based University Medical Center
Approximately 25% of Americans have at least one skin condition, and 20% are estimated to develop skin cancer during their lifetime.1,2 However, 40% of the US population lives in areas underserved by dermatologists. 3 The severity and mortality of skin cancers such as melanoma and mycosis fungoides have been positively associated with minoritized race, lack of health insurance, and unstable housing status.4-6 Patients who receive health care at free clinics often are of a racial or ethnic minoritized social group, are uninsured, and/or lack stable housing; this underserved group also includes recent immigrants to the United States who have limited English proficiency (LEP).7 Only 25% of free clinics offer specialty care services such as dermatology.7,8
Of the 42 free clinics and Federally Qualified Health Centers in Pittsburgh, Pennsylvania, the Birmingham Free Clinic (BFC) is one of the few that offers specialty care services including dermatology.9 Founded in 1994, the BFC serves as a safety net for Pittsburgh’s medically underserved population, offering primary and acute care, medication access, and social services. From January 2020 to May 2022, the BFC offered 27 dermatology clinics that provided approximately 100 people with comprehensive care including full-body skin examinations, dermatologic diagnoses and treatments, minor procedures, and dermatopathology services.
In this study, we compared the BFC dermatology patient care model with that of the dermatology department at the University of Pittsburgh Medical Center (UPMC), an insurance-based tertiary referral health care system in western Pennsylvania. By analyzing the demographics, dermatologic diagnoses, and management strategies of both the BFC and UPMC, we gained an understanding of how these patient care models differ and how they can be improved to care for diverse patient populations.
Methods
A retrospective chart review of dermatology patients seen in person at the BFC and UPMC during the period from January 2020 to May 2022 was performed. The UPMC group included patients seen by 3 general dermatologists (including A.J.J.) at matched time points. Data were collected from patients’ first in-person visit during the study period. Variables of interest included patient age, sex, race, ethnicity, primary language, zip code, health insurance status, distance to clinic (estimated using Google Maps to calculate the shortest driving distance from the patient’s zip code to the clinic), history of skin cancer, dermatologic diagnoses, and management strategies. These variables were not collected for patients who cancelled or noshowed their first in-person appointments. All patient charts and notes corresponding to the date and visit of interest were accessed through the electronic medical record (EMR). Patient data were de-identified and stored in a password-protected spreadsheet. Comparisons between the BFC and UPMC patient populations were performed using X2 tests of independence, Fisher exact tests, and Mann-Whitney U tests via SPSS software (IBM). Statistical significance was set at P<.05.
Results
Patient Characteristics—Our analysis included 76 initial appointments at the BFC and 322 at UPMC (Table 1). The mean age for patients at the BFC and UPMC was 39.6 years and 47.8 years, respectively (P=.001). Males accounted for 39 (51.3%) and 112 (34.8%) of BFC and UPMC patients, respectively (P=.008); 2 (0.6%) patients from UPMC were transgender. Of the BFC and UPMC patients, 44.7% (34/76) and 0.9% (3/322) were Hispanic, respectively (P<.001). With regard to race, 52.6% (40/76) of BFC patients were White, 19.7% (15/76) were Black, 6.6% (5/76) were Asian/Pacific Islander (Chinese, 1.3% [1/76]; other Asian, 5.3% [4/76]), and 21.1% (16/76) were American Indian/other/unspecified (American Indian, 1.3% [1/76]; other, 13.2% [10/76]; unspecified, 6.6% [5/76]). At UPMC, 61.2% (197/322) of patients were White, 28.0% (90/322) were Black, 5.3% (17/322) were Asian/Pacific Islander (Chinese, 1.2% [4/322]; Indian [Asian], 1.9% [6/322]; Japanese, 0.3% [1/322]; other Asian, 1.6% [5/322]; other Asian/American Indian, 0.3% [1/322]), and 5.6% (18/322) were American Indian/other/ unspecified (American Indian, 0.3% [1/322]; other, 0.3% [1/322]; unspecified, 5.0% [16/322]). Overall, the BFC patient population was more ethnically and racially diverse than that of UPMC (P<.001).
Forty-six percent (35/76) of BFC patients and 4.3% (14/322) of UPMC patients had LEP (P<.001). Primary languages among BFC patients were 53.9% (41/76) English, 40.8% (31/76) Spanish, and 5.2% (4/76) other/ unspecified (Chinese, 1.3% [1/76]; Indonesian, 2.6% [2/76]; unspecified, 1.3% [1/76]). Primary languages among UPMC patients were 95.7% (308/322) English and 4.3% (14/322) other/unspecified (Chinese, 0.6% [2/322]; Nepali, 0.6% [2/322]; Pali, 0.3% [1/322]; Russian, 0.3% [1/322]; unspecified, 2.5% [8/322]). There were notable differences in insurance status at the BFC vs UPMC (P<.001), with more UPMC patients having private insurance (52.8% [170/322] vs 11.8% [9/76]) and more BFC patients being uninsured (52.8% [51/76] vs 1.9% [6/322]). There was no significant difference in distance to clinic between the 2 groups (P=.183). More UPMC patients had a history of skin cancer (P=.003). More patients at the BFC were no-shows for their appointments (P<.001), and UPMC patients more frequently canceled their appointments (P<.001).
Dermatologic Diagnoses—The most commonly diagnosed dermatologic conditions at the BFC were dermatitis (23.7% [18/76]), neoplasm of uncertain behavior (15.8% [12/76]), alopecia (11.8% [9/76]), and acne (10.5% [8/76]) (Table 2). The most commonly diagnosed conditions at UPMC were nevi (26.4% [85/322]), dermatitis (22.7% [73/322]), seborrheic keratosis (21.7% [70/322]), and skin cancer screening (21.4% [70/322]). Neoplasm of uncertain behavior was more common in BFC vs UPMC patients (P=.040), while UPMC patients were more frequently diagnosed with nevi (P<.001), seborrheic keratosis (P<.001), and skin cancer screening (P<.001). There was no significant difference between the incidence of skin cancer diagnoses in the BFC (1.3% [1/76]) and UPMC (0.6% [2/76]) patient populations (P=.471). Among the biopsied neoplasms, there was also no significant difference in malignant (BFC, 50.0% [5/10]; UPMC, 32.0% [8/25]) and benign (BFC, 50.0% [5/10]; UPMC, 36.0% [9/25]) neoplasms diagnosed at each clinic (P=.444).
Management Strategies—Systemic antibiotics were more frequently prescribed (P<.001) and laboratory testing/ imaging were more frequently ordered (P=.005) at the BFC vs UPMC (Table 3). Patients at the BFC also more frequently required emergency insurance (P=.036). Patients at UPMC were more frequently recommended sunscreen (P=.003) and received education about skin cancer signs by review of the ABCDEs of melanoma (P<.001), sun-protective behaviors (P=.001), and skin examination frequency (P<.001). Notes in the EMR for UPMC patients more frequently specified patient followup instructions (P<.001).
Comment
As of 2020, the city of Pittsburgh had an estimated population of nearly 303,000 based on US Census data.10 Its population is predominantly White (62.7%) followed by Black/African American (22.8%) and Asian (6.5%); 5.9% identify as 2 or more races. Approximately 3.8% identify as Hispanic or Latino. More than 11% of the Pittsburgh population aged 5 years and older speaks a language other than English as their primary language, including Spanish (2.3%), other Indo-European languages (3.9%), and Asian and Pacific Island languages (3.5%).11 More than 5% of the Pittsburgh population does not have health insurance.12
The BFC is located in Pittsburgh’s South Side area, while one of UPMC’s primary dermatology clinics is located in the Oakland district; however, most patients who seek care at these clinics live outside these areas. Our study results indicated that the BFC and UPMC serve distinct groups of people within the Pittsburgh population. The BFC patient population was younger with a higher percentage of patients who were male, Hispanic, racially diverse, and with LEP compared with the UPMC patient population. In this clinical setting, the BFC health care team engages with people from diverse backgrounds and requires greater interpreter and medical support services.
The BFC largely is supported by volunteers, UPMC, grants, and philanthropy. Dermatology clinics are staffed by paid and volunteer team members. Paid team members include 1 nurse and 1 access lead who operates the front desk and registration. Volunteer team members include 1 board-certified dermatologist from UPMC (A.J.J.), or an affiliate clinic and 1 or 2 of each of the following: UPMC dermatology residents, medical or undergraduate students from the University of Pittsburgh, AmeriCorps national service members, and student or community medical interpreters. The onsite pharmacy is run by volunteer faculty, resident, and student pharmacists from the University of Pittsburgh. Dermatology clinics are half-day clinics that occur monthly. Volunteers for each clinic are recruited approximately 1 month in advance.
Dermatology patients at the BFC are referred from the BFC general medicine clinic and nearby Federally Qualified Health Center s for simple to complex medical and surgical dermatologic skin conditions. Each BFC dermatology clinic schedules an average of 7 patients per clinic and places other patients on a wait-list unless more urgent triage is needed. Patients are notified when they are scheduled via phone or text message, and they receive a reminder call or text 1 or 2 days prior to their appointment that also asks them to confirm attendance. Patients with LEP are called with an interpreter and also may receive text reminders that can be translated using Google Translate. Patients are instructed to notify the BFC if they need to cancel or reschedule their appointment. At the end of each visit, patients are given an after-visit summary that lists follow-up instructions, medications prescribed during the visit, and upcoming appointments. The BFC offers bus tickets to help patients get to their appointments. In rare cases, the BFC may pay for a car service to drive patients to and from the clinic.
Dermatology clinics at UPMC use scheduling and self-scheduling systems through which patients can make appointments at a location of their choice with any available board-certified dermatologist or physician assistant. Patients receive a reminder phone call 3 days prior to their appointment instructing them to call the office if they are unable to keep their appointment. Patients signed up for the online portal also receive a reminder message and an option to confirm or cancel their appointment. Patients with cell phone numbers in the UPMC system receive a text message approximately 2 days prior to their appointment that allows them to preregister and pay their copayment in advance. They receive another text 20 minutes prior to their appointment with an option for contactless check-in. At the conclusion of their visit, patients can schedule a follow-up appointment and receive a printed copy of their after-visit summary that provides information about follow-up instructions, prescribed medications, and upcoming visits. They may alternatively access this summary via the online patient portal. Patients are not provided transportation to UPMC clinics, but they are offered parking validation.
Among the most common dermatologic diagnoses for each group, BFC patients presented for treatment of more acute dermatologic conditions, while UPMC patients presented for more benign and preventive-care conditions. This difference may be attributable to the BFC’s referral and triage system, wherein patients with more urgent problems are given scheduling priority. This patient care model contrasts with UPMC’s scheduling process in which no known formal triage system is utilized. Interestingly, there was no difference in skin cancer incidence despite a higher percentage of preventive skin cancer screenings at UPMC.
Patients at the BFC more often required emergency insurance for surgical interventions, which is consistent with the higher percentage of uninsured individuals in this population. Patients at UPMC more frequently were recommended sunscreen and were educated about skin cancer, sun protection, and skin examination, in part due to this group’s more extensive history of skin cancer and frequent presentation for skin cancer screenings. At the same time, educational materials for skin care at both the BFC and UPMC are populated into the EMR in English, whereas materials in other languages are less readily available.
Our retrospective study had several limitations. Demographic information that relied on clinic-dependent intake questionnaires may be limited due to variable intake processes and patients opting out of self-reporting. By comparing patient populations between 2 clinics, confounding variables such as location and hours of operation may impact the patient demographics recorded at the BFC vs UPMC. Resources and staff availability may affect the management strategies and follow-up care offered by each clinic. Our study period also was unique in that COVID-19 may have affected resources, staffing, scheduling, and logistics at both clinics.
Based on the aforementioned differences between the BFC and UPMC patient characteristics, care models should be strategically designed to support the needs of diverse populations. The BFC patient care model appropriately focuses on communication skills with patients with LEP by using interpreter services. Providing more skin care education and follow-up instructions in patients’ primary languages will help them develop a better understanding of their skin conditions. Another key asset of the BFC patient care model is its provision of social services such as transportation and insurance assistance.
To improve the UPMC patient care model, providing patients with bus tickets and car services may potentially reduce appointment cancellations. Using interpreter services to call and text appointment reminders, as well as interpreter resources to facilitate patient visits and patient instructions, also can mitigate language barriers for patients with LEP. Implementing a triage system into the UPMC scheduling system may help patients with more urgent skin conditions to be seen in a timely manner.
Other investigators have analyzed costs of care and proven the value of dermatologic services at free clinics to guide allocation of supplies and resources, demonstrating an area for future investigation at the BFC.13 A cost analysis of care provided at the BFC compared to UPMC could inform us about the value of the BFC’s services.
Conclusion
The dermatology clinics at the BFC and UPMC have distinct demographics, diagnoses, and management strategies to provide an inclusive patient care model. The services provided by both clinics are necessary to ensure that people in Pittsburgh have access to dermatologic care regardless of social barriers (eg, lack of health insurance, LEP). To achieve greater accessibility and health equity, dermatologic care at the BFC and UPMC can be improved by strengthening communication with people with LEP, providing skin care education, and offering social and scheduling services.
- Lim HW, Collins SAB, Resneck JS, et al. The burden of skin disease in the United States. J Am Acad Dermatol. 2017;76:958-972.e2. doi:10.1016/j.jaad.2016.12.043
- American Academy of Dermatology. Skin cancer. Accessed October 7, 2024. https://www.aad.org/media/stats-skin-cancer
- Suneja T, Smith ED, Chen GJ, et al. Waiting times to see a dermatologist are perceived as too long by dermatologists: implications for the dermatology workforce. Arch Dermatol. 2001;137:1303-1307. doi:10.1001/archderm.137.10.1303
- Grossberg AL, Carranza D, Lamp K, et al. Dermatologic care in the homeless and underserved populations: observations from the Venice Family Clinic. Cutis. 2012;89:25-32.
- Amini A, Rusthoven CG, Waxweiler TV, et al. Association of health insurance with outcomes in adults ages 18 to 64 years with melanoma in the United States. J Am Acad Dermatol. 2016;74:309-316. doi:10.1016/j.jaad.2015.09.054
- Su C, Nguyen KA, Bai HX, et al. Racial disparity in mycosis fungoides: an analysis of 4495 cases from the US National Cancer Database. J Am Acad Dermatol. 2017;77:497-502.e2. doi:10.1016/j.jaad .2017.04.1137
- Darnell JS. Free clinics in the United States: a nationwide survey. Arch Intern Med. 2010;170:946-953. doi:10.1001/archinternmed .2010.107
- Madray V, Ginjupalli S, Hashmi O, et al. Access to dermatology services at free medical clinics: a nationwide cross-sectional survey. J Am Acad Dermatol. 2019;81:245-246. doi:10.1016/j.jaad.2018.12.011
- Pennsylvania free and income-based clinics. Accessed October 7, 2024. https://www.freeclinics.com/sta/pennsylvania
- United States Census Bureau. Decennial census. P1: race. Accessed October 7, 2024. https://data.census.gov/table/DECENNIALPL2020.P1?g=160XX00US4261000
- United States Census Bureau. American community survey. S1601: language spoken at home. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020S1601?g=160XX00US4261000
- United States Census Bureau. S2701: selected characteristics of health insurance coverage in the United States. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020.S2701?g=160XX00US4261000
- Lin CP, Loy S, Boothe WD, et al. Value of Dermatology Nights at a student-run free clinic. Proc (Bayl Univ Med Cent). 2020;34:260-261. doi:10.1080/08998280.2020.1834771
Approximately 25% of Americans have at least one skin condition, and 20% are estimated to develop skin cancer during their lifetime.1,2 However, 40% of the US population lives in areas underserved by dermatologists. 3 The severity and mortality of skin cancers such as melanoma and mycosis fungoides have been positively associated with minoritized race, lack of health insurance, and unstable housing status.4-6 Patients who receive health care at free clinics often are of a racial or ethnic minoritized social group, are uninsured, and/or lack stable housing; this underserved group also includes recent immigrants to the United States who have limited English proficiency (LEP).7 Only 25% of free clinics offer specialty care services such as dermatology.7,8
Of the 42 free clinics and Federally Qualified Health Centers in Pittsburgh, Pennsylvania, the Birmingham Free Clinic (BFC) is one of the few that offers specialty care services including dermatology.9 Founded in 1994, the BFC serves as a safety net for Pittsburgh’s medically underserved population, offering primary and acute care, medication access, and social services. From January 2020 to May 2022, the BFC offered 27 dermatology clinics that provided approximately 100 people with comprehensive care including full-body skin examinations, dermatologic diagnoses and treatments, minor procedures, and dermatopathology services.
In this study, we compared the BFC dermatology patient care model with that of the dermatology department at the University of Pittsburgh Medical Center (UPMC), an insurance-based tertiary referral health care system in western Pennsylvania. By analyzing the demographics, dermatologic diagnoses, and management strategies of both the BFC and UPMC, we gained an understanding of how these patient care models differ and how they can be improved to care for diverse patient populations.
Methods
A retrospective chart review of dermatology patients seen in person at the BFC and UPMC during the period from January 2020 to May 2022 was performed. The UPMC group included patients seen by 3 general dermatologists (including A.J.J.) at matched time points. Data were collected from patients’ first in-person visit during the study period. Variables of interest included patient age, sex, race, ethnicity, primary language, zip code, health insurance status, distance to clinic (estimated using Google Maps to calculate the shortest driving distance from the patient’s zip code to the clinic), history of skin cancer, dermatologic diagnoses, and management strategies. These variables were not collected for patients who cancelled or noshowed their first in-person appointments. All patient charts and notes corresponding to the date and visit of interest were accessed through the electronic medical record (EMR). Patient data were de-identified and stored in a password-protected spreadsheet. Comparisons between the BFC and UPMC patient populations were performed using X2 tests of independence, Fisher exact tests, and Mann-Whitney U tests via SPSS software (IBM). Statistical significance was set at P<.05.
Results
Patient Characteristics—Our analysis included 76 initial appointments at the BFC and 322 at UPMC (Table 1). The mean age for patients at the BFC and UPMC was 39.6 years and 47.8 years, respectively (P=.001). Males accounted for 39 (51.3%) and 112 (34.8%) of BFC and UPMC patients, respectively (P=.008); 2 (0.6%) patients from UPMC were transgender. Of the BFC and UPMC patients, 44.7% (34/76) and 0.9% (3/322) were Hispanic, respectively (P<.001). With regard to race, 52.6% (40/76) of BFC patients were White, 19.7% (15/76) were Black, 6.6% (5/76) were Asian/Pacific Islander (Chinese, 1.3% [1/76]; other Asian, 5.3% [4/76]), and 21.1% (16/76) were American Indian/other/unspecified (American Indian, 1.3% [1/76]; other, 13.2% [10/76]; unspecified, 6.6% [5/76]). At UPMC, 61.2% (197/322) of patients were White, 28.0% (90/322) were Black, 5.3% (17/322) were Asian/Pacific Islander (Chinese, 1.2% [4/322]; Indian [Asian], 1.9% [6/322]; Japanese, 0.3% [1/322]; other Asian, 1.6% [5/322]; other Asian/American Indian, 0.3% [1/322]), and 5.6% (18/322) were American Indian/other/ unspecified (American Indian, 0.3% [1/322]; other, 0.3% [1/322]; unspecified, 5.0% [16/322]). Overall, the BFC patient population was more ethnically and racially diverse than that of UPMC (P<.001).
Forty-six percent (35/76) of BFC patients and 4.3% (14/322) of UPMC patients had LEP (P<.001). Primary languages among BFC patients were 53.9% (41/76) English, 40.8% (31/76) Spanish, and 5.2% (4/76) other/ unspecified (Chinese, 1.3% [1/76]; Indonesian, 2.6% [2/76]; unspecified, 1.3% [1/76]). Primary languages among UPMC patients were 95.7% (308/322) English and 4.3% (14/322) other/unspecified (Chinese, 0.6% [2/322]; Nepali, 0.6% [2/322]; Pali, 0.3% [1/322]; Russian, 0.3% [1/322]; unspecified, 2.5% [8/322]). There were notable differences in insurance status at the BFC vs UPMC (P<.001), with more UPMC patients having private insurance (52.8% [170/322] vs 11.8% [9/76]) and more BFC patients being uninsured (52.8% [51/76] vs 1.9% [6/322]). There was no significant difference in distance to clinic between the 2 groups (P=.183). More UPMC patients had a history of skin cancer (P=.003). More patients at the BFC were no-shows for their appointments (P<.001), and UPMC patients more frequently canceled their appointments (P<.001).
Dermatologic Diagnoses—The most commonly diagnosed dermatologic conditions at the BFC were dermatitis (23.7% [18/76]), neoplasm of uncertain behavior (15.8% [12/76]), alopecia (11.8% [9/76]), and acne (10.5% [8/76]) (Table 2). The most commonly diagnosed conditions at UPMC were nevi (26.4% [85/322]), dermatitis (22.7% [73/322]), seborrheic keratosis (21.7% [70/322]), and skin cancer screening (21.4% [70/322]). Neoplasm of uncertain behavior was more common in BFC vs UPMC patients (P=.040), while UPMC patients were more frequently diagnosed with nevi (P<.001), seborrheic keratosis (P<.001), and skin cancer screening (P<.001). There was no significant difference between the incidence of skin cancer diagnoses in the BFC (1.3% [1/76]) and UPMC (0.6% [2/76]) patient populations (P=.471). Among the biopsied neoplasms, there was also no significant difference in malignant (BFC, 50.0% [5/10]; UPMC, 32.0% [8/25]) and benign (BFC, 50.0% [5/10]; UPMC, 36.0% [9/25]) neoplasms diagnosed at each clinic (P=.444).
Management Strategies—Systemic antibiotics were more frequently prescribed (P<.001) and laboratory testing/ imaging were more frequently ordered (P=.005) at the BFC vs UPMC (Table 3). Patients at the BFC also more frequently required emergency insurance (P=.036). Patients at UPMC were more frequently recommended sunscreen (P=.003) and received education about skin cancer signs by review of the ABCDEs of melanoma (P<.001), sun-protective behaviors (P=.001), and skin examination frequency (P<.001). Notes in the EMR for UPMC patients more frequently specified patient followup instructions (P<.001).
Comment
As of 2020, the city of Pittsburgh had an estimated population of nearly 303,000 based on US Census data.10 Its population is predominantly White (62.7%) followed by Black/African American (22.8%) and Asian (6.5%); 5.9% identify as 2 or more races. Approximately 3.8% identify as Hispanic or Latino. More than 11% of the Pittsburgh population aged 5 years and older speaks a language other than English as their primary language, including Spanish (2.3%), other Indo-European languages (3.9%), and Asian and Pacific Island languages (3.5%).11 More than 5% of the Pittsburgh population does not have health insurance.12
The BFC is located in Pittsburgh’s South Side area, while one of UPMC’s primary dermatology clinics is located in the Oakland district; however, most patients who seek care at these clinics live outside these areas. Our study results indicated that the BFC and UPMC serve distinct groups of people within the Pittsburgh population. The BFC patient population was younger with a higher percentage of patients who were male, Hispanic, racially diverse, and with LEP compared with the UPMC patient population. In this clinical setting, the BFC health care team engages with people from diverse backgrounds and requires greater interpreter and medical support services.
The BFC largely is supported by volunteers, UPMC, grants, and philanthropy. Dermatology clinics are staffed by paid and volunteer team members. Paid team members include 1 nurse and 1 access lead who operates the front desk and registration. Volunteer team members include 1 board-certified dermatologist from UPMC (A.J.J.), or an affiliate clinic and 1 or 2 of each of the following: UPMC dermatology residents, medical or undergraduate students from the University of Pittsburgh, AmeriCorps national service members, and student or community medical interpreters. The onsite pharmacy is run by volunteer faculty, resident, and student pharmacists from the University of Pittsburgh. Dermatology clinics are half-day clinics that occur monthly. Volunteers for each clinic are recruited approximately 1 month in advance.
Dermatology patients at the BFC are referred from the BFC general medicine clinic and nearby Federally Qualified Health Center s for simple to complex medical and surgical dermatologic skin conditions. Each BFC dermatology clinic schedules an average of 7 patients per clinic and places other patients on a wait-list unless more urgent triage is needed. Patients are notified when they are scheduled via phone or text message, and they receive a reminder call or text 1 or 2 days prior to their appointment that also asks them to confirm attendance. Patients with LEP are called with an interpreter and also may receive text reminders that can be translated using Google Translate. Patients are instructed to notify the BFC if they need to cancel or reschedule their appointment. At the end of each visit, patients are given an after-visit summary that lists follow-up instructions, medications prescribed during the visit, and upcoming appointments. The BFC offers bus tickets to help patients get to their appointments. In rare cases, the BFC may pay for a car service to drive patients to and from the clinic.
Dermatology clinics at UPMC use scheduling and self-scheduling systems through which patients can make appointments at a location of their choice with any available board-certified dermatologist or physician assistant. Patients receive a reminder phone call 3 days prior to their appointment instructing them to call the office if they are unable to keep their appointment. Patients signed up for the online portal also receive a reminder message and an option to confirm or cancel their appointment. Patients with cell phone numbers in the UPMC system receive a text message approximately 2 days prior to their appointment that allows them to preregister and pay their copayment in advance. They receive another text 20 minutes prior to their appointment with an option for contactless check-in. At the conclusion of their visit, patients can schedule a follow-up appointment and receive a printed copy of their after-visit summary that provides information about follow-up instructions, prescribed medications, and upcoming visits. They may alternatively access this summary via the online patient portal. Patients are not provided transportation to UPMC clinics, but they are offered parking validation.
Among the most common dermatologic diagnoses for each group, BFC patients presented for treatment of more acute dermatologic conditions, while UPMC patients presented for more benign and preventive-care conditions. This difference may be attributable to the BFC’s referral and triage system, wherein patients with more urgent problems are given scheduling priority. This patient care model contrasts with UPMC’s scheduling process in which no known formal triage system is utilized. Interestingly, there was no difference in skin cancer incidence despite a higher percentage of preventive skin cancer screenings at UPMC.
Patients at the BFC more often required emergency insurance for surgical interventions, which is consistent with the higher percentage of uninsured individuals in this population. Patients at UPMC more frequently were recommended sunscreen and were educated about skin cancer, sun protection, and skin examination, in part due to this group’s more extensive history of skin cancer and frequent presentation for skin cancer screenings. At the same time, educational materials for skin care at both the BFC and UPMC are populated into the EMR in English, whereas materials in other languages are less readily available.
Our retrospective study had several limitations. Demographic information that relied on clinic-dependent intake questionnaires may be limited due to variable intake processes and patients opting out of self-reporting. By comparing patient populations between 2 clinics, confounding variables such as location and hours of operation may impact the patient demographics recorded at the BFC vs UPMC. Resources and staff availability may affect the management strategies and follow-up care offered by each clinic. Our study period also was unique in that COVID-19 may have affected resources, staffing, scheduling, and logistics at both clinics.
Based on the aforementioned differences between the BFC and UPMC patient characteristics, care models should be strategically designed to support the needs of diverse populations. The BFC patient care model appropriately focuses on communication skills with patients with LEP by using interpreter services. Providing more skin care education and follow-up instructions in patients’ primary languages will help them develop a better understanding of their skin conditions. Another key asset of the BFC patient care model is its provision of social services such as transportation and insurance assistance.
To improve the UPMC patient care model, providing patients with bus tickets and car services may potentially reduce appointment cancellations. Using interpreter services to call and text appointment reminders, as well as interpreter resources to facilitate patient visits and patient instructions, also can mitigate language barriers for patients with LEP. Implementing a triage system into the UPMC scheduling system may help patients with more urgent skin conditions to be seen in a timely manner.
Other investigators have analyzed costs of care and proven the value of dermatologic services at free clinics to guide allocation of supplies and resources, demonstrating an area for future investigation at the BFC.13 A cost analysis of care provided at the BFC compared to UPMC could inform us about the value of the BFC’s services.
Conclusion
The dermatology clinics at the BFC and UPMC have distinct demographics, diagnoses, and management strategies to provide an inclusive patient care model. The services provided by both clinics are necessary to ensure that people in Pittsburgh have access to dermatologic care regardless of social barriers (eg, lack of health insurance, LEP). To achieve greater accessibility and health equity, dermatologic care at the BFC and UPMC can be improved by strengthening communication with people with LEP, providing skin care education, and offering social and scheduling services.
Approximately 25% of Americans have at least one skin condition, and 20% are estimated to develop skin cancer during their lifetime.1,2 However, 40% of the US population lives in areas underserved by dermatologists. 3 The severity and mortality of skin cancers such as melanoma and mycosis fungoides have been positively associated with minoritized race, lack of health insurance, and unstable housing status.4-6 Patients who receive health care at free clinics often are of a racial or ethnic minoritized social group, are uninsured, and/or lack stable housing; this underserved group also includes recent immigrants to the United States who have limited English proficiency (LEP).7 Only 25% of free clinics offer specialty care services such as dermatology.7,8
Of the 42 free clinics and Federally Qualified Health Centers in Pittsburgh, Pennsylvania, the Birmingham Free Clinic (BFC) is one of the few that offers specialty care services including dermatology.9 Founded in 1994, the BFC serves as a safety net for Pittsburgh’s medically underserved population, offering primary and acute care, medication access, and social services. From January 2020 to May 2022, the BFC offered 27 dermatology clinics that provided approximately 100 people with comprehensive care including full-body skin examinations, dermatologic diagnoses and treatments, minor procedures, and dermatopathology services.
In this study, we compared the BFC dermatology patient care model with that of the dermatology department at the University of Pittsburgh Medical Center (UPMC), an insurance-based tertiary referral health care system in western Pennsylvania. By analyzing the demographics, dermatologic diagnoses, and management strategies of both the BFC and UPMC, we gained an understanding of how these patient care models differ and how they can be improved to care for diverse patient populations.
Methods
A retrospective chart review of dermatology patients seen in person at the BFC and UPMC during the period from January 2020 to May 2022 was performed. The UPMC group included patients seen by 3 general dermatologists (including A.J.J.) at matched time points. Data were collected from patients’ first in-person visit during the study period. Variables of interest included patient age, sex, race, ethnicity, primary language, zip code, health insurance status, distance to clinic (estimated using Google Maps to calculate the shortest driving distance from the patient’s zip code to the clinic), history of skin cancer, dermatologic diagnoses, and management strategies. These variables were not collected for patients who cancelled or noshowed their first in-person appointments. All patient charts and notes corresponding to the date and visit of interest were accessed through the electronic medical record (EMR). Patient data were de-identified and stored in a password-protected spreadsheet. Comparisons between the BFC and UPMC patient populations were performed using X2 tests of independence, Fisher exact tests, and Mann-Whitney U tests via SPSS software (IBM). Statistical significance was set at P<.05.
Results
Patient Characteristics—Our analysis included 76 initial appointments at the BFC and 322 at UPMC (Table 1). The mean age for patients at the BFC and UPMC was 39.6 years and 47.8 years, respectively (P=.001). Males accounted for 39 (51.3%) and 112 (34.8%) of BFC and UPMC patients, respectively (P=.008); 2 (0.6%) patients from UPMC were transgender. Of the BFC and UPMC patients, 44.7% (34/76) and 0.9% (3/322) were Hispanic, respectively (P<.001). With regard to race, 52.6% (40/76) of BFC patients were White, 19.7% (15/76) were Black, 6.6% (5/76) were Asian/Pacific Islander (Chinese, 1.3% [1/76]; other Asian, 5.3% [4/76]), and 21.1% (16/76) were American Indian/other/unspecified (American Indian, 1.3% [1/76]; other, 13.2% [10/76]; unspecified, 6.6% [5/76]). At UPMC, 61.2% (197/322) of patients were White, 28.0% (90/322) were Black, 5.3% (17/322) were Asian/Pacific Islander (Chinese, 1.2% [4/322]; Indian [Asian], 1.9% [6/322]; Japanese, 0.3% [1/322]; other Asian, 1.6% [5/322]; other Asian/American Indian, 0.3% [1/322]), and 5.6% (18/322) were American Indian/other/ unspecified (American Indian, 0.3% [1/322]; other, 0.3% [1/322]; unspecified, 5.0% [16/322]). Overall, the BFC patient population was more ethnically and racially diverse than that of UPMC (P<.001).
Forty-six percent (35/76) of BFC patients and 4.3% (14/322) of UPMC patients had LEP (P<.001). Primary languages among BFC patients were 53.9% (41/76) English, 40.8% (31/76) Spanish, and 5.2% (4/76) other/ unspecified (Chinese, 1.3% [1/76]; Indonesian, 2.6% [2/76]; unspecified, 1.3% [1/76]). Primary languages among UPMC patients were 95.7% (308/322) English and 4.3% (14/322) other/unspecified (Chinese, 0.6% [2/322]; Nepali, 0.6% [2/322]; Pali, 0.3% [1/322]; Russian, 0.3% [1/322]; unspecified, 2.5% [8/322]). There were notable differences in insurance status at the BFC vs UPMC (P<.001), with more UPMC patients having private insurance (52.8% [170/322] vs 11.8% [9/76]) and more BFC patients being uninsured (52.8% [51/76] vs 1.9% [6/322]). There was no significant difference in distance to clinic between the 2 groups (P=.183). More UPMC patients had a history of skin cancer (P=.003). More patients at the BFC were no-shows for their appointments (P<.001), and UPMC patients more frequently canceled their appointments (P<.001).
Dermatologic Diagnoses—The most commonly diagnosed dermatologic conditions at the BFC were dermatitis (23.7% [18/76]), neoplasm of uncertain behavior (15.8% [12/76]), alopecia (11.8% [9/76]), and acne (10.5% [8/76]) (Table 2). The most commonly diagnosed conditions at UPMC were nevi (26.4% [85/322]), dermatitis (22.7% [73/322]), seborrheic keratosis (21.7% [70/322]), and skin cancer screening (21.4% [70/322]). Neoplasm of uncertain behavior was more common in BFC vs UPMC patients (P=.040), while UPMC patients were more frequently diagnosed with nevi (P<.001), seborrheic keratosis (P<.001), and skin cancer screening (P<.001). There was no significant difference between the incidence of skin cancer diagnoses in the BFC (1.3% [1/76]) and UPMC (0.6% [2/76]) patient populations (P=.471). Among the biopsied neoplasms, there was also no significant difference in malignant (BFC, 50.0% [5/10]; UPMC, 32.0% [8/25]) and benign (BFC, 50.0% [5/10]; UPMC, 36.0% [9/25]) neoplasms diagnosed at each clinic (P=.444).
Management Strategies—Systemic antibiotics were more frequently prescribed (P<.001) and laboratory testing/ imaging were more frequently ordered (P=.005) at the BFC vs UPMC (Table 3). Patients at the BFC also more frequently required emergency insurance (P=.036). Patients at UPMC were more frequently recommended sunscreen (P=.003) and received education about skin cancer signs by review of the ABCDEs of melanoma (P<.001), sun-protective behaviors (P=.001), and skin examination frequency (P<.001). Notes in the EMR for UPMC patients more frequently specified patient followup instructions (P<.001).
Comment
As of 2020, the city of Pittsburgh had an estimated population of nearly 303,000 based on US Census data.10 Its population is predominantly White (62.7%) followed by Black/African American (22.8%) and Asian (6.5%); 5.9% identify as 2 or more races. Approximately 3.8% identify as Hispanic or Latino. More than 11% of the Pittsburgh population aged 5 years and older speaks a language other than English as their primary language, including Spanish (2.3%), other Indo-European languages (3.9%), and Asian and Pacific Island languages (3.5%).11 More than 5% of the Pittsburgh population does not have health insurance.12
The BFC is located in Pittsburgh’s South Side area, while one of UPMC’s primary dermatology clinics is located in the Oakland district; however, most patients who seek care at these clinics live outside these areas. Our study results indicated that the BFC and UPMC serve distinct groups of people within the Pittsburgh population. The BFC patient population was younger with a higher percentage of patients who were male, Hispanic, racially diverse, and with LEP compared with the UPMC patient population. In this clinical setting, the BFC health care team engages with people from diverse backgrounds and requires greater interpreter and medical support services.
The BFC largely is supported by volunteers, UPMC, grants, and philanthropy. Dermatology clinics are staffed by paid and volunteer team members. Paid team members include 1 nurse and 1 access lead who operates the front desk and registration. Volunteer team members include 1 board-certified dermatologist from UPMC (A.J.J.), or an affiliate clinic and 1 or 2 of each of the following: UPMC dermatology residents, medical or undergraduate students from the University of Pittsburgh, AmeriCorps national service members, and student or community medical interpreters. The onsite pharmacy is run by volunteer faculty, resident, and student pharmacists from the University of Pittsburgh. Dermatology clinics are half-day clinics that occur monthly. Volunteers for each clinic are recruited approximately 1 month in advance.
Dermatology patients at the BFC are referred from the BFC general medicine clinic and nearby Federally Qualified Health Center s for simple to complex medical and surgical dermatologic skin conditions. Each BFC dermatology clinic schedules an average of 7 patients per clinic and places other patients on a wait-list unless more urgent triage is needed. Patients are notified when they are scheduled via phone or text message, and they receive a reminder call or text 1 or 2 days prior to their appointment that also asks them to confirm attendance. Patients with LEP are called with an interpreter and also may receive text reminders that can be translated using Google Translate. Patients are instructed to notify the BFC if they need to cancel or reschedule their appointment. At the end of each visit, patients are given an after-visit summary that lists follow-up instructions, medications prescribed during the visit, and upcoming appointments. The BFC offers bus tickets to help patients get to their appointments. In rare cases, the BFC may pay for a car service to drive patients to and from the clinic.
Dermatology clinics at UPMC use scheduling and self-scheduling systems through which patients can make appointments at a location of their choice with any available board-certified dermatologist or physician assistant. Patients receive a reminder phone call 3 days prior to their appointment instructing them to call the office if they are unable to keep their appointment. Patients signed up for the online portal also receive a reminder message and an option to confirm or cancel their appointment. Patients with cell phone numbers in the UPMC system receive a text message approximately 2 days prior to their appointment that allows them to preregister and pay their copayment in advance. They receive another text 20 minutes prior to their appointment with an option for contactless check-in. At the conclusion of their visit, patients can schedule a follow-up appointment and receive a printed copy of their after-visit summary that provides information about follow-up instructions, prescribed medications, and upcoming visits. They may alternatively access this summary via the online patient portal. Patients are not provided transportation to UPMC clinics, but they are offered parking validation.
Among the most common dermatologic diagnoses for each group, BFC patients presented for treatment of more acute dermatologic conditions, while UPMC patients presented for more benign and preventive-care conditions. This difference may be attributable to the BFC’s referral and triage system, wherein patients with more urgent problems are given scheduling priority. This patient care model contrasts with UPMC’s scheduling process in which no known formal triage system is utilized. Interestingly, there was no difference in skin cancer incidence despite a higher percentage of preventive skin cancer screenings at UPMC.
Patients at the BFC more often required emergency insurance for surgical interventions, which is consistent with the higher percentage of uninsured individuals in this population. Patients at UPMC more frequently were recommended sunscreen and were educated about skin cancer, sun protection, and skin examination, in part due to this group’s more extensive history of skin cancer and frequent presentation for skin cancer screenings. At the same time, educational materials for skin care at both the BFC and UPMC are populated into the EMR in English, whereas materials in other languages are less readily available.
Our retrospective study had several limitations. Demographic information that relied on clinic-dependent intake questionnaires may be limited due to variable intake processes and patients opting out of self-reporting. By comparing patient populations between 2 clinics, confounding variables such as location and hours of operation may impact the patient demographics recorded at the BFC vs UPMC. Resources and staff availability may affect the management strategies and follow-up care offered by each clinic. Our study period also was unique in that COVID-19 may have affected resources, staffing, scheduling, and logistics at both clinics.
Based on the aforementioned differences between the BFC and UPMC patient characteristics, care models should be strategically designed to support the needs of diverse populations. The BFC patient care model appropriately focuses on communication skills with patients with LEP by using interpreter services. Providing more skin care education and follow-up instructions in patients’ primary languages will help them develop a better understanding of their skin conditions. Another key asset of the BFC patient care model is its provision of social services such as transportation and insurance assistance.
To improve the UPMC patient care model, providing patients with bus tickets and car services may potentially reduce appointment cancellations. Using interpreter services to call and text appointment reminders, as well as interpreter resources to facilitate patient visits and patient instructions, also can mitigate language barriers for patients with LEP. Implementing a triage system into the UPMC scheduling system may help patients with more urgent skin conditions to be seen in a timely manner.
Other investigators have analyzed costs of care and proven the value of dermatologic services at free clinics to guide allocation of supplies and resources, demonstrating an area for future investigation at the BFC.13 A cost analysis of care provided at the BFC compared to UPMC could inform us about the value of the BFC’s services.
Conclusion
The dermatology clinics at the BFC and UPMC have distinct demographics, diagnoses, and management strategies to provide an inclusive patient care model. The services provided by both clinics are necessary to ensure that people in Pittsburgh have access to dermatologic care regardless of social barriers (eg, lack of health insurance, LEP). To achieve greater accessibility and health equity, dermatologic care at the BFC and UPMC can be improved by strengthening communication with people with LEP, providing skin care education, and offering social and scheduling services.
- Lim HW, Collins SAB, Resneck JS, et al. The burden of skin disease in the United States. J Am Acad Dermatol. 2017;76:958-972.e2. doi:10.1016/j.jaad.2016.12.043
- American Academy of Dermatology. Skin cancer. Accessed October 7, 2024. https://www.aad.org/media/stats-skin-cancer
- Suneja T, Smith ED, Chen GJ, et al. Waiting times to see a dermatologist are perceived as too long by dermatologists: implications for the dermatology workforce. Arch Dermatol. 2001;137:1303-1307. doi:10.1001/archderm.137.10.1303
- Grossberg AL, Carranza D, Lamp K, et al. Dermatologic care in the homeless and underserved populations: observations from the Venice Family Clinic. Cutis. 2012;89:25-32.
- Amini A, Rusthoven CG, Waxweiler TV, et al. Association of health insurance with outcomes in adults ages 18 to 64 years with melanoma in the United States. J Am Acad Dermatol. 2016;74:309-316. doi:10.1016/j.jaad.2015.09.054
- Su C, Nguyen KA, Bai HX, et al. Racial disparity in mycosis fungoides: an analysis of 4495 cases from the US National Cancer Database. J Am Acad Dermatol. 2017;77:497-502.e2. doi:10.1016/j.jaad .2017.04.1137
- Darnell JS. Free clinics in the United States: a nationwide survey. Arch Intern Med. 2010;170:946-953. doi:10.1001/archinternmed .2010.107
- Madray V, Ginjupalli S, Hashmi O, et al. Access to dermatology services at free medical clinics: a nationwide cross-sectional survey. J Am Acad Dermatol. 2019;81:245-246. doi:10.1016/j.jaad.2018.12.011
- Pennsylvania free and income-based clinics. Accessed October 7, 2024. https://www.freeclinics.com/sta/pennsylvania
- United States Census Bureau. Decennial census. P1: race. Accessed October 7, 2024. https://data.census.gov/table/DECENNIALPL2020.P1?g=160XX00US4261000
- United States Census Bureau. American community survey. S1601: language spoken at home. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020S1601?g=160XX00US4261000
- United States Census Bureau. S2701: selected characteristics of health insurance coverage in the United States. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020.S2701?g=160XX00US4261000
- Lin CP, Loy S, Boothe WD, et al. Value of Dermatology Nights at a student-run free clinic. Proc (Bayl Univ Med Cent). 2020;34:260-261. doi:10.1080/08998280.2020.1834771
- Lim HW, Collins SAB, Resneck JS, et al. The burden of skin disease in the United States. J Am Acad Dermatol. 2017;76:958-972.e2. doi:10.1016/j.jaad.2016.12.043
- American Academy of Dermatology. Skin cancer. Accessed October 7, 2024. https://www.aad.org/media/stats-skin-cancer
- Suneja T, Smith ED, Chen GJ, et al. Waiting times to see a dermatologist are perceived as too long by dermatologists: implications for the dermatology workforce. Arch Dermatol. 2001;137:1303-1307. doi:10.1001/archderm.137.10.1303
- Grossberg AL, Carranza D, Lamp K, et al. Dermatologic care in the homeless and underserved populations: observations from the Venice Family Clinic. Cutis. 2012;89:25-32.
- Amini A, Rusthoven CG, Waxweiler TV, et al. Association of health insurance with outcomes in adults ages 18 to 64 years with melanoma in the United States. J Am Acad Dermatol. 2016;74:309-316. doi:10.1016/j.jaad.2015.09.054
- Su C, Nguyen KA, Bai HX, et al. Racial disparity in mycosis fungoides: an analysis of 4495 cases from the US National Cancer Database. J Am Acad Dermatol. 2017;77:497-502.e2. doi:10.1016/j.jaad .2017.04.1137
- Darnell JS. Free clinics in the United States: a nationwide survey. Arch Intern Med. 2010;170:946-953. doi:10.1001/archinternmed .2010.107
- Madray V, Ginjupalli S, Hashmi O, et al. Access to dermatology services at free medical clinics: a nationwide cross-sectional survey. J Am Acad Dermatol. 2019;81:245-246. doi:10.1016/j.jaad.2018.12.011
- Pennsylvania free and income-based clinics. Accessed October 7, 2024. https://www.freeclinics.com/sta/pennsylvania
- United States Census Bureau. Decennial census. P1: race. Accessed October 7, 2024. https://data.census.gov/table/DECENNIALPL2020.P1?g=160XX00US4261000
- United States Census Bureau. American community survey. S1601: language spoken at home. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020S1601?g=160XX00US4261000
- United States Census Bureau. S2701: selected characteristics of health insurance coverage in the United States. Accessed October 7, 2024. https://data.census.gov/table/ACSST5Y2020.S2701?g=160XX00US4261000
- Lin CP, Loy S, Boothe WD, et al. Value of Dermatology Nights at a student-run free clinic. Proc (Bayl Univ Med Cent). 2020;34:260-261. doi:10.1080/08998280.2020.1834771
Comparing Patient Care Models at a Local Free Clinic vs an Insurance- Based University Medical Center
Comparing Patient Care Models at a Local Free Clinic vs an Insurance- Based University Medical Center
PRACTICE POINTS
- Both free clinics and insurance-based health care systems serve dermatology patients with diverse characteristics, necessitating inclusive health care models.
- Dermatologic care can be improved at both free and insurance-based clinics by strengthening communication with individuals with limited English proficiency, providing skin care education, and offering social and scheduling services such as transportation, insurance assistance, and triage.
Building an AI Army of Digital Twins to Fight Cancer
A patient has cancer. It’s decision time.
Clinician and patient alike face, really, the ultimate challenge when making those decisions. They have to consider the patient’s individual circumstances, available treatment options, potential side effects, relevant clinical data such as the patient’s genetic profile and cancer specifics, and more.
“That’s a lot of information to hold,” said Uzma Asghar, PhD, MRCP, a British consultant medical oncologist at The Royal Marsden Hospital and a chief scientific officer at Concr LTD.
What if there were a way to test — quickly and accurately — all the potential paths forward?
That’s the goal of digital twins.
“What the [digital twin] model can do for the clinician is to hold all that information and process it really quickly, within a couple of minutes,” Asghar noted.
A digital twin is more than just a computer model or simulation because it copies a real-world person and relies on real-world data. Some digital twin programs also integrate new information as it becomes available. This technology holds promise for personalized medicine, drug discovery, developing screening strategies, and better understanding diseases.
How to Deliver a Twin
To create a digital twin, experts develop a computer model with data to hone its expertise in an area of medicine, such as cancer types and treatments. Then “you train the model on information it’s seen, and then introduce a patient and patient’s information,” said Asghar.
Asghar is currently working with colleagues to develop digital twins that could eventually help solve the aforementioned cancer scenario — a doctor and patient decide the best course of cancer treatment. But their applications are manifold, particularly in clinical research.
Digital twins often include a machine learning component, which would fall under the umbrella term of AI, said Asghar, but it’s not like ChatGPT or other generative AI modules many people are now familiar with.
“The difference here is the model is not there to replace the clinician or to replace clinical trials,” Asghar noted. Instead, digital twins help make decisions faster in a way that can be more affordable.
Digital Twins to Predict Cancer Outcomes
Asghar is currently involved in UK clinical trials enrolling patients with cancer to test the accuracy of digital twin programs.
At this point, these studies do not yet use digital twins to guide the course of treatment, which is something they hope to do eventually. For now, they are still at the validation phase — the digital twin program makes predictions about the treatments and then the researchers later evaluate how accurate the predictions turned out to be based on real information from the enrolled patients.
Their current model gives predictions for RECIST (response evaluation criteria in solid tumor), treatment response, and survival. In addition to collecting data from ongoing clinical trials, they’ve used retrospective data, such as from the Cancer Tumor Atlas, to test the model.
“We’ve clinically validated it now in over 9000 patients,” said Asghar, who noted that they are constantly testing it on new patients. Their data include 30 chemotherapies and 23 cancer types, but they are focusing on four: Triple-negative breast cancer, cancer of unknown primary, pancreatic cancer, and colorectal cancer.
“The reason for choosing those four cancer types is that they are aggressive, their response to chemotherapy isn’t as great, and the outcome for those patient populations, there’s significant room for improvement,” Asghar explained.
Currently, Asghar said, the model is around 80%-90% correct in predicting what the actual clinical outcomes turn out to be.
The final stage of their work, before it becomes widely available to clinicians, will be to integrate it into a clinical trial in which some clinicians use the model to make decisions about treatment vs some who don’t use the model. By studying patient outcomes in both groups, they will be able to determine the value of the digital twin program they created.
What Else Can a Twin Do? A Lot
While a model that helps clinicians make decisions about cancer treatments may be among the first digital twin programs that become widely available, there are many other kinds of digital twins in the works.
For example, a digital twin could be used as a benchmark for a patient to determine how their cancer might have progressed without treatment. Say a patient’s tumor grew during treatment, it might seem like the treatment failed, but a digital twin might show that if left untreated, the tumor would have grown five times as fast, said Paul Macklin, PhD, professor in the Department of Intelligent Systems Engineering at Indiana University Bloomington.
Alternatively, if the virtual patient’s tumor is around the same size as the real patient’s tumor, “that means that treatment has lost its efficacy. It’s time to do something new,” said Macklin. And a digital twin could help with not only choosing a therapy but also choosing a dosing schedule, he noted.
The models can also be updated as new treatments come out, which could help clinicians virtually explore how they might affect a patient before having that patient switch treatments.
Digital twins could also assist in decision-making based on a patient’s priorities and real-life circumstances. “Maybe your priority is not necessarily to shrink this [tumor] at all costs ... maybe your priority is some mix of that and also quality of life,” Macklin said, referring to potential side effects. Or if someone lives 3 hours from the nearest cancer center, a digital twin could help determine whether less frequent treatments could still be effective.
And while much of the activity around digital twins in biomedical research has been focused on cancer, Asghar said the technology has the potential to be applied to other diseases as well. A digital twin for cardiovascular disease could help doctors choose the best treatment. It could also integrate new information from a smartwatch or glucose monitor to make better predictions and help doctors adjust the treatment plan.
Faster, More Effective Research With Twins
Because digital twin programs can quickly analyze large datasets, they can also make real-world studies more effective and efficient.
Though digital twins would not fully replace real clinical trials, they could help run through preliminary scenarios before starting a full clinical trial, which would “save everybody some money, time and pain and risk,” said Macklin.
It’s also possible to use digital twins to design better screening strategies for early cancer detection and monitoring, said Ioannis Zervantonakis, PhD, a bioengineering professor at the University of Pittsburgh.
Zervantonakis is tapping digital twin technology for research that homes in on understanding tumors. In this case, the digital twin is a virtual representation of a real tumor, complete with its complex network of cells and the surrounding tissue.
Zervantonakis’ lab is using the technology to study cell-cell interactions in the tumor microenvironment, with a focus on human epidermal growth factor receptor 2–targeted therapy resistance in breast cancer. The digital twin they developed will simulate tumor growth, predict drug response, analyze cellular interactions, and optimize treatment strategies.
The Long Push Forward
One big hurdle to making digital twins more widely available is that regulation for the technology is still in progress.
“We’re developing the technology, and what’s also happening is the regulatory framework is being developed in parallel. So we’re almost developing things blindly on the basis that we think this is what the regulators would want,” explained Asghar.
“It’s really important that these technologies are regulated properly, just like drugs, and that’s what we’re pushing and advocating for,” said Asghar, noting that people need to know that like drugs, a digital twin has strengths and limitations.
And while a digital twin can be a cost-saving approach in the long run, it does require funding to get a program built, and finding funds can be difficult because not everyone knows about the technology. More funding means more trials.
With more data, Asghar is hopeful that within a few years, a digital twin model could be available for clinicians to use to help inform treatment decisions. This could lead to more effective treatments and, ultimately, better patient outcomes.
A version of this article appeared on Medscape.com.
A patient has cancer. It’s decision time.
Clinician and patient alike face, really, the ultimate challenge when making those decisions. They have to consider the patient’s individual circumstances, available treatment options, potential side effects, relevant clinical data such as the patient’s genetic profile and cancer specifics, and more.
“That’s a lot of information to hold,” said Uzma Asghar, PhD, MRCP, a British consultant medical oncologist at The Royal Marsden Hospital and a chief scientific officer at Concr LTD.
What if there were a way to test — quickly and accurately — all the potential paths forward?
That’s the goal of digital twins.
“What the [digital twin] model can do for the clinician is to hold all that information and process it really quickly, within a couple of minutes,” Asghar noted.
A digital twin is more than just a computer model or simulation because it copies a real-world person and relies on real-world data. Some digital twin programs also integrate new information as it becomes available. This technology holds promise for personalized medicine, drug discovery, developing screening strategies, and better understanding diseases.
How to Deliver a Twin
To create a digital twin, experts develop a computer model with data to hone its expertise in an area of medicine, such as cancer types and treatments. Then “you train the model on information it’s seen, and then introduce a patient and patient’s information,” said Asghar.
Asghar is currently working with colleagues to develop digital twins that could eventually help solve the aforementioned cancer scenario — a doctor and patient decide the best course of cancer treatment. But their applications are manifold, particularly in clinical research.
Digital twins often include a machine learning component, which would fall under the umbrella term of AI, said Asghar, but it’s not like ChatGPT or other generative AI modules many people are now familiar with.
“The difference here is the model is not there to replace the clinician or to replace clinical trials,” Asghar noted. Instead, digital twins help make decisions faster in a way that can be more affordable.
Digital Twins to Predict Cancer Outcomes
Asghar is currently involved in UK clinical trials enrolling patients with cancer to test the accuracy of digital twin programs.
At this point, these studies do not yet use digital twins to guide the course of treatment, which is something they hope to do eventually. For now, they are still at the validation phase — the digital twin program makes predictions about the treatments and then the researchers later evaluate how accurate the predictions turned out to be based on real information from the enrolled patients.
Their current model gives predictions for RECIST (response evaluation criteria in solid tumor), treatment response, and survival. In addition to collecting data from ongoing clinical trials, they’ve used retrospective data, such as from the Cancer Tumor Atlas, to test the model.
“We’ve clinically validated it now in over 9000 patients,” said Asghar, who noted that they are constantly testing it on new patients. Their data include 30 chemotherapies and 23 cancer types, but they are focusing on four: Triple-negative breast cancer, cancer of unknown primary, pancreatic cancer, and colorectal cancer.
“The reason for choosing those four cancer types is that they are aggressive, their response to chemotherapy isn’t as great, and the outcome for those patient populations, there’s significant room for improvement,” Asghar explained.
Currently, Asghar said, the model is around 80%-90% correct in predicting what the actual clinical outcomes turn out to be.
The final stage of their work, before it becomes widely available to clinicians, will be to integrate it into a clinical trial in which some clinicians use the model to make decisions about treatment vs some who don’t use the model. By studying patient outcomes in both groups, they will be able to determine the value of the digital twin program they created.
What Else Can a Twin Do? A Lot
While a model that helps clinicians make decisions about cancer treatments may be among the first digital twin programs that become widely available, there are many other kinds of digital twins in the works.
For example, a digital twin could be used as a benchmark for a patient to determine how their cancer might have progressed without treatment. Say a patient’s tumor grew during treatment, it might seem like the treatment failed, but a digital twin might show that if left untreated, the tumor would have grown five times as fast, said Paul Macklin, PhD, professor in the Department of Intelligent Systems Engineering at Indiana University Bloomington.
Alternatively, if the virtual patient’s tumor is around the same size as the real patient’s tumor, “that means that treatment has lost its efficacy. It’s time to do something new,” said Macklin. And a digital twin could help with not only choosing a therapy but also choosing a dosing schedule, he noted.
The models can also be updated as new treatments come out, which could help clinicians virtually explore how they might affect a patient before having that patient switch treatments.
Digital twins could also assist in decision-making based on a patient’s priorities and real-life circumstances. “Maybe your priority is not necessarily to shrink this [tumor] at all costs ... maybe your priority is some mix of that and also quality of life,” Macklin said, referring to potential side effects. Or if someone lives 3 hours from the nearest cancer center, a digital twin could help determine whether less frequent treatments could still be effective.
And while much of the activity around digital twins in biomedical research has been focused on cancer, Asghar said the technology has the potential to be applied to other diseases as well. A digital twin for cardiovascular disease could help doctors choose the best treatment. It could also integrate new information from a smartwatch or glucose monitor to make better predictions and help doctors adjust the treatment plan.
Faster, More Effective Research With Twins
Because digital twin programs can quickly analyze large datasets, they can also make real-world studies more effective and efficient.
Though digital twins would not fully replace real clinical trials, they could help run through preliminary scenarios before starting a full clinical trial, which would “save everybody some money, time and pain and risk,” said Macklin.
It’s also possible to use digital twins to design better screening strategies for early cancer detection and monitoring, said Ioannis Zervantonakis, PhD, a bioengineering professor at the University of Pittsburgh.
Zervantonakis is tapping digital twin technology for research that homes in on understanding tumors. In this case, the digital twin is a virtual representation of a real tumor, complete with its complex network of cells and the surrounding tissue.
Zervantonakis’ lab is using the technology to study cell-cell interactions in the tumor microenvironment, with a focus on human epidermal growth factor receptor 2–targeted therapy resistance in breast cancer. The digital twin they developed will simulate tumor growth, predict drug response, analyze cellular interactions, and optimize treatment strategies.
The Long Push Forward
One big hurdle to making digital twins more widely available is that regulation for the technology is still in progress.
“We’re developing the technology, and what’s also happening is the regulatory framework is being developed in parallel. So we’re almost developing things blindly on the basis that we think this is what the regulators would want,” explained Asghar.
“It’s really important that these technologies are regulated properly, just like drugs, and that’s what we’re pushing and advocating for,” said Asghar, noting that people need to know that like drugs, a digital twin has strengths and limitations.
And while a digital twin can be a cost-saving approach in the long run, it does require funding to get a program built, and finding funds can be difficult because not everyone knows about the technology. More funding means more trials.
With more data, Asghar is hopeful that within a few years, a digital twin model could be available for clinicians to use to help inform treatment decisions. This could lead to more effective treatments and, ultimately, better patient outcomes.
A version of this article appeared on Medscape.com.
A patient has cancer. It’s decision time.
Clinician and patient alike face, really, the ultimate challenge when making those decisions. They have to consider the patient’s individual circumstances, available treatment options, potential side effects, relevant clinical data such as the patient’s genetic profile and cancer specifics, and more.
“That’s a lot of information to hold,” said Uzma Asghar, PhD, MRCP, a British consultant medical oncologist at The Royal Marsden Hospital and a chief scientific officer at Concr LTD.
What if there were a way to test — quickly and accurately — all the potential paths forward?
That’s the goal of digital twins.
“What the [digital twin] model can do for the clinician is to hold all that information and process it really quickly, within a couple of minutes,” Asghar noted.
A digital twin is more than just a computer model or simulation because it copies a real-world person and relies on real-world data. Some digital twin programs also integrate new information as it becomes available. This technology holds promise for personalized medicine, drug discovery, developing screening strategies, and better understanding diseases.
How to Deliver a Twin
To create a digital twin, experts develop a computer model with data to hone its expertise in an area of medicine, such as cancer types and treatments. Then “you train the model on information it’s seen, and then introduce a patient and patient’s information,” said Asghar.
Asghar is currently working with colleagues to develop digital twins that could eventually help solve the aforementioned cancer scenario — a doctor and patient decide the best course of cancer treatment. But their applications are manifold, particularly in clinical research.
Digital twins often include a machine learning component, which would fall under the umbrella term of AI, said Asghar, but it’s not like ChatGPT or other generative AI modules many people are now familiar with.
“The difference here is the model is not there to replace the clinician or to replace clinical trials,” Asghar noted. Instead, digital twins help make decisions faster in a way that can be more affordable.
Digital Twins to Predict Cancer Outcomes
Asghar is currently involved in UK clinical trials enrolling patients with cancer to test the accuracy of digital twin programs.
At this point, these studies do not yet use digital twins to guide the course of treatment, which is something they hope to do eventually. For now, they are still at the validation phase — the digital twin program makes predictions about the treatments and then the researchers later evaluate how accurate the predictions turned out to be based on real information from the enrolled patients.
Their current model gives predictions for RECIST (response evaluation criteria in solid tumor), treatment response, and survival. In addition to collecting data from ongoing clinical trials, they’ve used retrospective data, such as from the Cancer Tumor Atlas, to test the model.
“We’ve clinically validated it now in over 9000 patients,” said Asghar, who noted that they are constantly testing it on new patients. Their data include 30 chemotherapies and 23 cancer types, but they are focusing on four: Triple-negative breast cancer, cancer of unknown primary, pancreatic cancer, and colorectal cancer.
“The reason for choosing those four cancer types is that they are aggressive, their response to chemotherapy isn’t as great, and the outcome for those patient populations, there’s significant room for improvement,” Asghar explained.
Currently, Asghar said, the model is around 80%-90% correct in predicting what the actual clinical outcomes turn out to be.
The final stage of their work, before it becomes widely available to clinicians, will be to integrate it into a clinical trial in which some clinicians use the model to make decisions about treatment vs some who don’t use the model. By studying patient outcomes in both groups, they will be able to determine the value of the digital twin program they created.
What Else Can a Twin Do? A Lot
While a model that helps clinicians make decisions about cancer treatments may be among the first digital twin programs that become widely available, there are many other kinds of digital twins in the works.
For example, a digital twin could be used as a benchmark for a patient to determine how their cancer might have progressed without treatment. Say a patient’s tumor grew during treatment, it might seem like the treatment failed, but a digital twin might show that if left untreated, the tumor would have grown five times as fast, said Paul Macklin, PhD, professor in the Department of Intelligent Systems Engineering at Indiana University Bloomington.
Alternatively, if the virtual patient’s tumor is around the same size as the real patient’s tumor, “that means that treatment has lost its efficacy. It’s time to do something new,” said Macklin. And a digital twin could help with not only choosing a therapy but also choosing a dosing schedule, he noted.
The models can also be updated as new treatments come out, which could help clinicians virtually explore how they might affect a patient before having that patient switch treatments.
Digital twins could also assist in decision-making based on a patient’s priorities and real-life circumstances. “Maybe your priority is not necessarily to shrink this [tumor] at all costs ... maybe your priority is some mix of that and also quality of life,” Macklin said, referring to potential side effects. Or if someone lives 3 hours from the nearest cancer center, a digital twin could help determine whether less frequent treatments could still be effective.
And while much of the activity around digital twins in biomedical research has been focused on cancer, Asghar said the technology has the potential to be applied to other diseases as well. A digital twin for cardiovascular disease could help doctors choose the best treatment. It could also integrate new information from a smartwatch or glucose monitor to make better predictions and help doctors adjust the treatment plan.
Faster, More Effective Research With Twins
Because digital twin programs can quickly analyze large datasets, they can also make real-world studies more effective and efficient.
Though digital twins would not fully replace real clinical trials, they could help run through preliminary scenarios before starting a full clinical trial, which would “save everybody some money, time and pain and risk,” said Macklin.
It’s also possible to use digital twins to design better screening strategies for early cancer detection and monitoring, said Ioannis Zervantonakis, PhD, a bioengineering professor at the University of Pittsburgh.
Zervantonakis is tapping digital twin technology for research that homes in on understanding tumors. In this case, the digital twin is a virtual representation of a real tumor, complete with its complex network of cells and the surrounding tissue.
Zervantonakis’ lab is using the technology to study cell-cell interactions in the tumor microenvironment, with a focus on human epidermal growth factor receptor 2–targeted therapy resistance in breast cancer. The digital twin they developed will simulate tumor growth, predict drug response, analyze cellular interactions, and optimize treatment strategies.
The Long Push Forward
One big hurdle to making digital twins more widely available is that regulation for the technology is still in progress.
“We’re developing the technology, and what’s also happening is the regulatory framework is being developed in parallel. So we’re almost developing things blindly on the basis that we think this is what the regulators would want,” explained Asghar.
“It’s really important that these technologies are regulated properly, just like drugs, and that’s what we’re pushing and advocating for,” said Asghar, noting that people need to know that like drugs, a digital twin has strengths and limitations.
And while a digital twin can be a cost-saving approach in the long run, it does require funding to get a program built, and finding funds can be difficult because not everyone knows about the technology. More funding means more trials.
With more data, Asghar is hopeful that within a few years, a digital twin model could be available for clinicians to use to help inform treatment decisions. This could lead to more effective treatments and, ultimately, better patient outcomes.
A version of this article appeared on Medscape.com.
Study Finds No Significant Effect of Low-Dose Oral Minoxidil on BP
TOPLINE:
but is associated with a slight increase in heart rate and a 5% incidence of hypotensive symptoms.
METHODOLOGY:
- Researchers conducted a systematic review and meta-analysis of 16 studies, which involved 2387 patients with alopecia (60.7% women) who received minoxidil, a vasodilator originally developed as an antihypertensive, at doses of 5 mg or less per day.
- Outcomes included changes in mean arterial pressure, systolic BP, diastolic BP, and heart rate.
- Mean differences were calculated between pretreatment and posttreatment values.
TAKEAWAY:
- Hypotensive symptoms were reported in 5% patients, with no significant hypotensive episodes. About 1.8% patients experienced lightheadedness or syncope, 1.2% experienced dizziness, 0.9% had tachycardia, and 0.8% had palpitations.
- LDOM did not significantly alter systolic BP (mean difference, –0.13; 95% CI, –2.67 to 2.41), diastolic BP (mean difference, –1.25; 95% CI, –3.21 to 0.71), and mean arterial pressure (mean difference, –1.92; 95% CI, –4.00 to 0.17).
- LDOM led to a significant increase in heart rate (mean difference, 2.67 beats/min; 95% CI, 0.34-5.01), a difference the authors wrote would “likely not be clinically significant for most patients.”
- Hypertrichosis was the most common side effect (59.6%) and reason for stopping treatment (accounting for nearly 35% of discontinuations).
IN PRACTICE:
“LDOM appears to be a safe treatment for alopecia with no significant impact on blood pressure,” the authors wrote, noting that the study “addresses gaps in clinical knowledge involving LDOM.” Based on their results, they recommended that BP and heart rate “do not need to be closely monitored in patients without prior cardiovascular risk history.”
SOURCE:
The study was led by Matthew Chen, BS, Stony Brook Dermatology in New York. It was published online in The Journal of the American Academy of Dermatology.
LIMITATIONS:
The studies included had small sample sizes and retrospective designs, which may limit the reliability of the findings. Additional limitations include the absence of control groups, a potential recall bias in adverse effect reporting, and variability in dosing regimens and BP monitoring.
DISCLOSURES:
The authors reported no external funding or conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
but is associated with a slight increase in heart rate and a 5% incidence of hypotensive symptoms.
METHODOLOGY:
- Researchers conducted a systematic review and meta-analysis of 16 studies, which involved 2387 patients with alopecia (60.7% women) who received minoxidil, a vasodilator originally developed as an antihypertensive, at doses of 5 mg or less per day.
- Outcomes included changes in mean arterial pressure, systolic BP, diastolic BP, and heart rate.
- Mean differences were calculated between pretreatment and posttreatment values.
TAKEAWAY:
- Hypotensive symptoms were reported in 5% patients, with no significant hypotensive episodes. About 1.8% patients experienced lightheadedness or syncope, 1.2% experienced dizziness, 0.9% had tachycardia, and 0.8% had palpitations.
- LDOM did not significantly alter systolic BP (mean difference, –0.13; 95% CI, –2.67 to 2.41), diastolic BP (mean difference, –1.25; 95% CI, –3.21 to 0.71), and mean arterial pressure (mean difference, –1.92; 95% CI, –4.00 to 0.17).
- LDOM led to a significant increase in heart rate (mean difference, 2.67 beats/min; 95% CI, 0.34-5.01), a difference the authors wrote would “likely not be clinically significant for most patients.”
- Hypertrichosis was the most common side effect (59.6%) and reason for stopping treatment (accounting for nearly 35% of discontinuations).
IN PRACTICE:
“LDOM appears to be a safe treatment for alopecia with no significant impact on blood pressure,” the authors wrote, noting that the study “addresses gaps in clinical knowledge involving LDOM.” Based on their results, they recommended that BP and heart rate “do not need to be closely monitored in patients without prior cardiovascular risk history.”
SOURCE:
The study was led by Matthew Chen, BS, Stony Brook Dermatology in New York. It was published online in The Journal of the American Academy of Dermatology.
LIMITATIONS:
The studies included had small sample sizes and retrospective designs, which may limit the reliability of the findings. Additional limitations include the absence of control groups, a potential recall bias in adverse effect reporting, and variability in dosing regimens and BP monitoring.
DISCLOSURES:
The authors reported no external funding or conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
but is associated with a slight increase in heart rate and a 5% incidence of hypotensive symptoms.
METHODOLOGY:
- Researchers conducted a systematic review and meta-analysis of 16 studies, which involved 2387 patients with alopecia (60.7% women) who received minoxidil, a vasodilator originally developed as an antihypertensive, at doses of 5 mg or less per day.
- Outcomes included changes in mean arterial pressure, systolic BP, diastolic BP, and heart rate.
- Mean differences were calculated between pretreatment and posttreatment values.
TAKEAWAY:
- Hypotensive symptoms were reported in 5% patients, with no significant hypotensive episodes. About 1.8% patients experienced lightheadedness or syncope, 1.2% experienced dizziness, 0.9% had tachycardia, and 0.8% had palpitations.
- LDOM did not significantly alter systolic BP (mean difference, –0.13; 95% CI, –2.67 to 2.41), diastolic BP (mean difference, –1.25; 95% CI, –3.21 to 0.71), and mean arterial pressure (mean difference, –1.92; 95% CI, –4.00 to 0.17).
- LDOM led to a significant increase in heart rate (mean difference, 2.67 beats/min; 95% CI, 0.34-5.01), a difference the authors wrote would “likely not be clinically significant for most patients.”
- Hypertrichosis was the most common side effect (59.6%) and reason for stopping treatment (accounting for nearly 35% of discontinuations).
IN PRACTICE:
“LDOM appears to be a safe treatment for alopecia with no significant impact on blood pressure,” the authors wrote, noting that the study “addresses gaps in clinical knowledge involving LDOM.” Based on their results, they recommended that BP and heart rate “do not need to be closely monitored in patients without prior cardiovascular risk history.”
SOURCE:
The study was led by Matthew Chen, BS, Stony Brook Dermatology in New York. It was published online in The Journal of the American Academy of Dermatology.
LIMITATIONS:
The studies included had small sample sizes and retrospective designs, which may limit the reliability of the findings. Additional limitations include the absence of control groups, a potential recall bias in adverse effect reporting, and variability in dosing regimens and BP monitoring.
DISCLOSURES:
The authors reported no external funding or conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Barzolvolimab Effective for CSU in Phase 2 Study
of an ongoing phase 2 study.
Moreover, in the study, barzolvolimab, an anti-KIT monoclonal antibody that inhibits the activation of and depletes mast cells, induced comparable responses in a subset of patients who had taken omalizumab, an anti–immunoglobulin E monoclonal antibody approved by the Food and Drug Administration for treating CSU.
The findings were presented at the annual European Academy of Dermatology and Venereology (EADV) 2024 Congress. Barzolvolimab is being developed by Celldex Therapeutics.
“Barzolvolimab treatment resulted in rapid, profound, and durable improvement in UAS7 [weekly Urticaria Activity Score 7],” said presenter Martin Metz, MD, professor of dermatology, Institute of Allergology, Charité – Universitätsmedizin Berlin in Germany, “with a deepening of response over 52 weeks in patients with antihistamine-refractory CSU.”
“Similar robust improvement was seen in patients previously treated with omalizumab, including refractory patients,” he added.
Because barzolvolimab was well tolerated over the course of the follow-up period, Metz said, it “has the potential to be an important new treatment option,” noting that patients are now being enrolled in global phase 3 studies of barzolvolimab.
Sustained Symptom Relief
Ana M. Giménez-Arnau, MD, PhD, associate professor of dermatology, Autonomous University and Pompeu Fabra University, Barcelona, Spain, told Medscape Medical News that the results are important, as they showed people who switched from placebo to the active drug also saw a long-term benefit.
What is “remarkable” about barzolvolimab, continued Giménez-Arnau, who was not involved in the study, is that it is the first drug to target the KIT receptor on mast cells and interfere with stimulating growth factors, thus making the cells that drive the development of CSU “disappear.”
The study included three different barzolvolimab regimens, with the 150-mg dose every 4 weeks and the 300-mg dose every 8 weeks achieving similar results, noted Giménez-Arnau.
For her, there are important questions to answer around the pharmacokinetic and pharmacodynamic profiles of the two regimens that remain, but she underlined that for the patient, the choice of regimen could have an impact on their quality of life.
“If we give 300 mg every 8 weeks,” she said, it appears “you can achieve disease control” while halving the frequency of subcutaneous injections.
She said that it would be “interesting to know” if 300 mg every 8 weeks is given as two 150-mg injections every 2 months or one 300-mg injection. If it is the former, Giménez Arnau said, “This is potentially an important benefit for the patient.”
Sustained Benefits at 1 Year
The study enrolled 208 patients with antihistamine-refractory CSU at sites in 10 countries, randomizing them to one of four arms: Subcutaneous injections of barzolvolimab 75 mg or 150 mg every 4 weeks, 300 mg every 8 weeks, or placebo every 4 weeks.
The mean age in each arm was between 42 and 47 years, and around 75% were women. Across the arms, 64%-76% had severe disease, as measured on the UAS7, at a mean score of 30.0-31.3. Around 20% had previously been treated with omalizumab.
Patients were treated for 16 weeks, during which time they completed daily and weekly diaries and attended six clinic visits at weeks 0, 2, 4, 8, 12, and 16. Results from the trial published earlier this year demonstrated that both the regimens (150 mg every 4 weeks and 300 mg every 8 weeks) achieved clinically meaningful and statistically significant improvement in UAS7, the primary endpoint, vs placebo at 12 weeks.
Participants in the barzolvolimab 75 mg and placebo arms were then randomized to receive barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, and those who had been in the 150-mg and 300-mg treatment arms continued with that treatment for a further 36 weeks. (The remaining patients have been continued on a further 24-week follow-up, but the data are not yet available.)
By the 52-week follow-up, 25% of patients who started in each of the barzolvolimab arms had discontinued treatment, as well as 16% first randomized to the placebo arm.
Metz reported that the improvements in UAS7 scores, observed as early as week 1, were sustained through week 52 in patients in both the ongoing 150-mg and 300-mg arms. Patients who initially started in the placebo and the barzolvolimab 75-mg groups caught up with those who had started on the higher doses, so that by week 52, there were no significant differences in urticaria activity, hives, or itch scores between the arms.
By week 52, the proportion of patients achieving well-controlled disease, defined as a UAS7 score ≤ 6, was 73.7% in the barzolvolimab 150 mg every 4-week arm and 68.2% in the 300 mg barzolvolimab every 8-week arm.
Notably, just 12.8% of patients in the placebo arm had achieved well-controlled CSU by week 16, but after switching to barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, 63% reached that target at week 52.
“Maybe even more striking and very interesting to look at,” said Metz, was the complete control of symptoms, meaning “not one single wheal and no itch.” By week 52, 52% of those on 300 mg every 8 weeks and 71.1% of those on 150 mg every 4 weeks had a complete response, with no itch/hives (UAS7 of 0).
Importantly, complete responses with barzolvolimab were observed early and were sustained or improved to week 52, Metz said, with, again, placebo and former barzolvolimab 75 mg patients catching up with those who started on 150 mg every 4 weeks and 300 mg every 8 weeks once they switched at week 16.
“This is the best data for chronic spontaneous urticaria that we have so far seen,” he said, adding that the responses were seen regardless of prior experience with omalizumab.
Changes in Hair Color, Skin Pigmentation
As for safety, during the first 16 weeks, 66% of those on active treatment and 39% on placebo experienced at least one adverse event. There were no treatment-related serious adverse events, compared with two among those who received treatment for the full 52 weeks.
The most common adverse events with active treatment were hair color changes (14% in the first 16 weeks and 26% among those treated for the full 52 weeks), neutropenia/reduced neutrophil count (9% in the first 16 weeks and 17% among those treated for the full 52 weeks), and skin hypopigmentation (1% in the first 16 weeks, 13% among those treated for the full 52 weeks, and 19% among those who switched from placebo to active treatment at 36 weeks). Urticaria was reported by 10% among patients on active treatment and 10% among those on placebo in the first 16 weeks, and by 15% of those treated for the full 52 weeks.
In the post-presentation discussion, Metz explained that the hypopigmentation appears to start around the hair follicle and is diffuse, so tends to look like vitiligo.
He suggested that the melanocytes around the hair follicle “seem to be the ones that are more stressed, maybe because of the hair follicle cycling,” adding that the effect is reversible and does not appear to be dose dependent.
The study was funded by Celldex Therapeutics. Metz declared relationships with AbbVie, ALK-Abelló, Almirall, Amgen, argenx, AstraZeneca, Astria, Attovia Therapeutics, Celldex, Celltrion, Escient Pharmaceuticals, Galen, Galderma, GSK, Incyte, Jasper, Lilly, Novartis, Pfizer, Pharvaris, Regeneron, Sanofi, Teva, Third Harmonic Bio, and Vifor.
A version of this article first appeared on Medscape.com.
of an ongoing phase 2 study.
Moreover, in the study, barzolvolimab, an anti-KIT monoclonal antibody that inhibits the activation of and depletes mast cells, induced comparable responses in a subset of patients who had taken omalizumab, an anti–immunoglobulin E monoclonal antibody approved by the Food and Drug Administration for treating CSU.
The findings were presented at the annual European Academy of Dermatology and Venereology (EADV) 2024 Congress. Barzolvolimab is being developed by Celldex Therapeutics.
“Barzolvolimab treatment resulted in rapid, profound, and durable improvement in UAS7 [weekly Urticaria Activity Score 7],” said presenter Martin Metz, MD, professor of dermatology, Institute of Allergology, Charité – Universitätsmedizin Berlin in Germany, “with a deepening of response over 52 weeks in patients with antihistamine-refractory CSU.”
“Similar robust improvement was seen in patients previously treated with omalizumab, including refractory patients,” he added.
Because barzolvolimab was well tolerated over the course of the follow-up period, Metz said, it “has the potential to be an important new treatment option,” noting that patients are now being enrolled in global phase 3 studies of barzolvolimab.
Sustained Symptom Relief
Ana M. Giménez-Arnau, MD, PhD, associate professor of dermatology, Autonomous University and Pompeu Fabra University, Barcelona, Spain, told Medscape Medical News that the results are important, as they showed people who switched from placebo to the active drug also saw a long-term benefit.
What is “remarkable” about barzolvolimab, continued Giménez-Arnau, who was not involved in the study, is that it is the first drug to target the KIT receptor on mast cells and interfere with stimulating growth factors, thus making the cells that drive the development of CSU “disappear.”
The study included three different barzolvolimab regimens, with the 150-mg dose every 4 weeks and the 300-mg dose every 8 weeks achieving similar results, noted Giménez-Arnau.
For her, there are important questions to answer around the pharmacokinetic and pharmacodynamic profiles of the two regimens that remain, but she underlined that for the patient, the choice of regimen could have an impact on their quality of life.
“If we give 300 mg every 8 weeks,” she said, it appears “you can achieve disease control” while halving the frequency of subcutaneous injections.
She said that it would be “interesting to know” if 300 mg every 8 weeks is given as two 150-mg injections every 2 months or one 300-mg injection. If it is the former, Giménez Arnau said, “This is potentially an important benefit for the patient.”
Sustained Benefits at 1 Year
The study enrolled 208 patients with antihistamine-refractory CSU at sites in 10 countries, randomizing them to one of four arms: Subcutaneous injections of barzolvolimab 75 mg or 150 mg every 4 weeks, 300 mg every 8 weeks, or placebo every 4 weeks.
The mean age in each arm was between 42 and 47 years, and around 75% were women. Across the arms, 64%-76% had severe disease, as measured on the UAS7, at a mean score of 30.0-31.3. Around 20% had previously been treated with omalizumab.
Patients were treated for 16 weeks, during which time they completed daily and weekly diaries and attended six clinic visits at weeks 0, 2, 4, 8, 12, and 16. Results from the trial published earlier this year demonstrated that both the regimens (150 mg every 4 weeks and 300 mg every 8 weeks) achieved clinically meaningful and statistically significant improvement in UAS7, the primary endpoint, vs placebo at 12 weeks.
Participants in the barzolvolimab 75 mg and placebo arms were then randomized to receive barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, and those who had been in the 150-mg and 300-mg treatment arms continued with that treatment for a further 36 weeks. (The remaining patients have been continued on a further 24-week follow-up, but the data are not yet available.)
By the 52-week follow-up, 25% of patients who started in each of the barzolvolimab arms had discontinued treatment, as well as 16% first randomized to the placebo arm.
Metz reported that the improvements in UAS7 scores, observed as early as week 1, were sustained through week 52 in patients in both the ongoing 150-mg and 300-mg arms. Patients who initially started in the placebo and the barzolvolimab 75-mg groups caught up with those who had started on the higher doses, so that by week 52, there were no significant differences in urticaria activity, hives, or itch scores between the arms.
By week 52, the proportion of patients achieving well-controlled disease, defined as a UAS7 score ≤ 6, was 73.7% in the barzolvolimab 150 mg every 4-week arm and 68.2% in the 300 mg barzolvolimab every 8-week arm.
Notably, just 12.8% of patients in the placebo arm had achieved well-controlled CSU by week 16, but after switching to barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, 63% reached that target at week 52.
“Maybe even more striking and very interesting to look at,” said Metz, was the complete control of symptoms, meaning “not one single wheal and no itch.” By week 52, 52% of those on 300 mg every 8 weeks and 71.1% of those on 150 mg every 4 weeks had a complete response, with no itch/hives (UAS7 of 0).
Importantly, complete responses with barzolvolimab were observed early and were sustained or improved to week 52, Metz said, with, again, placebo and former barzolvolimab 75 mg patients catching up with those who started on 150 mg every 4 weeks and 300 mg every 8 weeks once they switched at week 16.
“This is the best data for chronic spontaneous urticaria that we have so far seen,” he said, adding that the responses were seen regardless of prior experience with omalizumab.
Changes in Hair Color, Skin Pigmentation
As for safety, during the first 16 weeks, 66% of those on active treatment and 39% on placebo experienced at least one adverse event. There were no treatment-related serious adverse events, compared with two among those who received treatment for the full 52 weeks.
The most common adverse events with active treatment were hair color changes (14% in the first 16 weeks and 26% among those treated for the full 52 weeks), neutropenia/reduced neutrophil count (9% in the first 16 weeks and 17% among those treated for the full 52 weeks), and skin hypopigmentation (1% in the first 16 weeks, 13% among those treated for the full 52 weeks, and 19% among those who switched from placebo to active treatment at 36 weeks). Urticaria was reported by 10% among patients on active treatment and 10% among those on placebo in the first 16 weeks, and by 15% of those treated for the full 52 weeks.
In the post-presentation discussion, Metz explained that the hypopigmentation appears to start around the hair follicle and is diffuse, so tends to look like vitiligo.
He suggested that the melanocytes around the hair follicle “seem to be the ones that are more stressed, maybe because of the hair follicle cycling,” adding that the effect is reversible and does not appear to be dose dependent.
The study was funded by Celldex Therapeutics. Metz declared relationships with AbbVie, ALK-Abelló, Almirall, Amgen, argenx, AstraZeneca, Astria, Attovia Therapeutics, Celldex, Celltrion, Escient Pharmaceuticals, Galen, Galderma, GSK, Incyte, Jasper, Lilly, Novartis, Pfizer, Pharvaris, Regeneron, Sanofi, Teva, Third Harmonic Bio, and Vifor.
A version of this article first appeared on Medscape.com.
of an ongoing phase 2 study.
Moreover, in the study, barzolvolimab, an anti-KIT monoclonal antibody that inhibits the activation of and depletes mast cells, induced comparable responses in a subset of patients who had taken omalizumab, an anti–immunoglobulin E monoclonal antibody approved by the Food and Drug Administration for treating CSU.
The findings were presented at the annual European Academy of Dermatology and Venereology (EADV) 2024 Congress. Barzolvolimab is being developed by Celldex Therapeutics.
“Barzolvolimab treatment resulted in rapid, profound, and durable improvement in UAS7 [weekly Urticaria Activity Score 7],” said presenter Martin Metz, MD, professor of dermatology, Institute of Allergology, Charité – Universitätsmedizin Berlin in Germany, “with a deepening of response over 52 weeks in patients with antihistamine-refractory CSU.”
“Similar robust improvement was seen in patients previously treated with omalizumab, including refractory patients,” he added.
Because barzolvolimab was well tolerated over the course of the follow-up period, Metz said, it “has the potential to be an important new treatment option,” noting that patients are now being enrolled in global phase 3 studies of barzolvolimab.
Sustained Symptom Relief
Ana M. Giménez-Arnau, MD, PhD, associate professor of dermatology, Autonomous University and Pompeu Fabra University, Barcelona, Spain, told Medscape Medical News that the results are important, as they showed people who switched from placebo to the active drug also saw a long-term benefit.
What is “remarkable” about barzolvolimab, continued Giménez-Arnau, who was not involved in the study, is that it is the first drug to target the KIT receptor on mast cells and interfere with stimulating growth factors, thus making the cells that drive the development of CSU “disappear.”
The study included three different barzolvolimab regimens, with the 150-mg dose every 4 weeks and the 300-mg dose every 8 weeks achieving similar results, noted Giménez-Arnau.
For her, there are important questions to answer around the pharmacokinetic and pharmacodynamic profiles of the two regimens that remain, but she underlined that for the patient, the choice of regimen could have an impact on their quality of life.
“If we give 300 mg every 8 weeks,” she said, it appears “you can achieve disease control” while halving the frequency of subcutaneous injections.
She said that it would be “interesting to know” if 300 mg every 8 weeks is given as two 150-mg injections every 2 months or one 300-mg injection. If it is the former, Giménez Arnau said, “This is potentially an important benefit for the patient.”
Sustained Benefits at 1 Year
The study enrolled 208 patients with antihistamine-refractory CSU at sites in 10 countries, randomizing them to one of four arms: Subcutaneous injections of barzolvolimab 75 mg or 150 mg every 4 weeks, 300 mg every 8 weeks, or placebo every 4 weeks.
The mean age in each arm was between 42 and 47 years, and around 75% were women. Across the arms, 64%-76% had severe disease, as measured on the UAS7, at a mean score of 30.0-31.3. Around 20% had previously been treated with omalizumab.
Patients were treated for 16 weeks, during which time they completed daily and weekly diaries and attended six clinic visits at weeks 0, 2, 4, 8, 12, and 16. Results from the trial published earlier this year demonstrated that both the regimens (150 mg every 4 weeks and 300 mg every 8 weeks) achieved clinically meaningful and statistically significant improvement in UAS7, the primary endpoint, vs placebo at 12 weeks.
Participants in the barzolvolimab 75 mg and placebo arms were then randomized to receive barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, and those who had been in the 150-mg and 300-mg treatment arms continued with that treatment for a further 36 weeks. (The remaining patients have been continued on a further 24-week follow-up, but the data are not yet available.)
By the 52-week follow-up, 25% of patients who started in each of the barzolvolimab arms had discontinued treatment, as well as 16% first randomized to the placebo arm.
Metz reported that the improvements in UAS7 scores, observed as early as week 1, were sustained through week 52 in patients in both the ongoing 150-mg and 300-mg arms. Patients who initially started in the placebo and the barzolvolimab 75-mg groups caught up with those who had started on the higher doses, so that by week 52, there were no significant differences in urticaria activity, hives, or itch scores between the arms.
By week 52, the proportion of patients achieving well-controlled disease, defined as a UAS7 score ≤ 6, was 73.7% in the barzolvolimab 150 mg every 4-week arm and 68.2% in the 300 mg barzolvolimab every 8-week arm.
Notably, just 12.8% of patients in the placebo arm had achieved well-controlled CSU by week 16, but after switching to barzolvolimab 150 mg every 4 weeks or 300 mg every 8 weeks, 63% reached that target at week 52.
“Maybe even more striking and very interesting to look at,” said Metz, was the complete control of symptoms, meaning “not one single wheal and no itch.” By week 52, 52% of those on 300 mg every 8 weeks and 71.1% of those on 150 mg every 4 weeks had a complete response, with no itch/hives (UAS7 of 0).
Importantly, complete responses with barzolvolimab were observed early and were sustained or improved to week 52, Metz said, with, again, placebo and former barzolvolimab 75 mg patients catching up with those who started on 150 mg every 4 weeks and 300 mg every 8 weeks once they switched at week 16.
“This is the best data for chronic spontaneous urticaria that we have so far seen,” he said, adding that the responses were seen regardless of prior experience with omalizumab.
Changes in Hair Color, Skin Pigmentation
As for safety, during the first 16 weeks, 66% of those on active treatment and 39% on placebo experienced at least one adverse event. There were no treatment-related serious adverse events, compared with two among those who received treatment for the full 52 weeks.
The most common adverse events with active treatment were hair color changes (14% in the first 16 weeks and 26% among those treated for the full 52 weeks), neutropenia/reduced neutrophil count (9% in the first 16 weeks and 17% among those treated for the full 52 weeks), and skin hypopigmentation (1% in the first 16 weeks, 13% among those treated for the full 52 weeks, and 19% among those who switched from placebo to active treatment at 36 weeks). Urticaria was reported by 10% among patients on active treatment and 10% among those on placebo in the first 16 weeks, and by 15% of those treated for the full 52 weeks.
In the post-presentation discussion, Metz explained that the hypopigmentation appears to start around the hair follicle and is diffuse, so tends to look like vitiligo.
He suggested that the melanocytes around the hair follicle “seem to be the ones that are more stressed, maybe because of the hair follicle cycling,” adding that the effect is reversible and does not appear to be dose dependent.
The study was funded by Celldex Therapeutics. Metz declared relationships with AbbVie, ALK-Abelló, Almirall, Amgen, argenx, AstraZeneca, Astria, Attovia Therapeutics, Celldex, Celltrion, Escient Pharmaceuticals, Galen, Galderma, GSK, Incyte, Jasper, Lilly, Novartis, Pfizer, Pharvaris, Regeneron, Sanofi, Teva, Third Harmonic Bio, and Vifor.
A version of this article first appeared on Medscape.com.
FROM EADV 2024
Children With Severe Atopic Dermatitis Catch Up on Growth With Dupilumab
AMSTERDAM — , revealed a post hoc trial analysis.
The research was presented at the European Academy of Dermatology and Venereology (EADV) 2024 Congress.
The trial included a “rigorously selected … well-characterized, well-studied” population of children aged 6-11 years, said presenter Alan D. Irvine, MD, DSc, professor of dermatology, Trinity College Dublin, Ireland.
It showed that “severe atopic dermatitis does cause restriction of growth, as well as a higher weight, and therefore obviously a higher BMI [body mass index].”
He continued, however, that children at the lower percentiles of height receiving prompt treatment with dupilumab (Dupixent) “were able to rapidly move through the centiles over the 16 weeks of the study, and that may be the window for catch-up growth … when children are growing rapidly.”
Anna Yasmine Kirkorian, MD, chief of dermatology, Children’s National Hospital, Washington, DC, who was not involved in the study, said that she was “surprised” at the degree of growth achieved over the study period, as height is not something that jumps up “overnight.”
“On the other hand, it fits with my experience with children who’ve had the brakes on all of their life due to inflammation, whether it be height, going to school, sleeping — everything is sort of put on pause by this terrible inflammatory process,” she said.
“When you take the brakes off, they get to be who they are going to be,” Kirkorian added. “So I was surprised by the speed of it, but not by the fact that height was acquired.”
Her belief is that in the pre-dupilumab era, severe atopic dermatitis was often insufficiently controlled, so children were “smaller than you would predict from parental height,” and the treatment is “allowing them to reach their genetic potential.”
Post Hoc Analysis
In his presentation, Irvine emphasized that it has been clearly demonstrated that adolescents with moderate and severe atopic dermatitis have a significantly higher likelihood of being below the 25th percentile of height on growth reference charts.
Such children are also at a higher risk of having low bone mineral density and low serum alkaline phosphatase (ALP) levels . While data presented at the EADV 2023 Congress showed that dupilumab significantly increased serum levels of bone ALP compared with placebo, the underlying mechanism remains unclear.
For the current analysis, Irvine and colleagues determined that the proportion of children aged 6-11 years with severe atopic dermatitis and lower stature reach a ≥ 5 centile improvement in height following 16 weeks of dupilumab treatment.
They examined data from the LIBERTY AD PEDS trial, in which patients aged 6-11 years with severe atopic dermatitis were randomized to 300 mg dupilumab every 4 weeks or placebo along with a mild or moderately potent topical corticosteroid. The study found that, overall, dupilumab was associated with significant improvements in signs, symptoms, and quality of life compared with placebo.
Height measures at baseline revealed that “more boys and more girls were below the 50th centile than you would predict for a healthy, normal control population,” Irvine said. “If we look at weight, we see the opposite,” he continued, “with a disproportionate number of boys and girls who are above the 50th centile for weight at baseline.”
Consequently, “we’re seeing these children who are shorter and heavier than the predicted healthy weight range and, as a result, obviously have higher BMI,” Irvine noted, with 67% girls and 62% boys found to have a higher BMI than normal for their age.
After 16 weeks of treatment with dupilumab, there was a much greater gain in height than that seen among those on placebo, with the most pronounced effect seen in children who had the lowest height at baseline. Indeed, among children in the lowest 25% height percentile at baseline, 30.6% on dupilumab vs 11.9% on placebo experienced an increase in height of 5 centiles or more(P < .05).
“This reflects what we see in clinical practice,” Irvine said. “Children often grow dramatically on treatment for atopic dermatitis.”
Among patients with a baseline height below the 30th percentile, 31.9% treated with dupilumab vs 11.1% treated with placebo gained at least 5 centiles in height. The figures for children below the 40th height percentile at baseline were 31.3% vs 15.5% (P < .05 for both).
Although there remained a marked difference in the proportion of children below the 50th height percentile at baseline gaining 5 centiles or more in height, at 29.0% with dupilumab versus 15.7% with placebo, it was no longer significant.
“So the effect of catch-up growth, or growth through the centiles, is most marked in those who are in the 40th centile or below,” Irvine said, indicating that the “more growth restricted kids have much more potential to catch up.”
‘Convincing’ Data
Overall, Kirkorian said in the interview, the data are “convincing” and support her view that severe atopic dermatitis is a “terrible chronic disease that we really underappreciate.” Atopic dermatitis, she added, “should get the respect that any severe chronic illness would have, whether that be arthritis, diabetes, or cardiac disease, because it is a systemic disorder that … profoundly affects quality of life, every minute of every day.”
However, “we don’t get all the referrals we should, until the child has suffered for years and years, and the family has suffered,” as there is a bias that it can be outgrown — although not everybody does — and it “doesn’t look as conspicuous as other chronic skin disorders,” such as psoriasis.
“Now with this study,” Kirkorian said, “it gives us a really compelling point to make to parents, to the community, and to insurers that not only are we affecting the quality of life from the itch standpoint [with dupilumab] but we may have long profound effects on growth and bone health.”
The research was sponsored by Sanofi and Regeneron Pharmaceuticals. Irvine declared relationships with AbbVie, Arena Pharmaceuticals, BenevolentAI, Chugai Pharmaceutical, Dermavant, Eli Lily, Genentech, LEO Pharma, Menlo Therapeutics, Novartis, Pfizer, Regeneron, Sanofi, UCB, DS Biopharma, and Inflazome. Kirkorian declared relationships with Dermavant, Verrica Pharmaceuticals, Pfizer, and Incyte.
A version of this article first appeared on Medscape.com.
AMSTERDAM — , revealed a post hoc trial analysis.
The research was presented at the European Academy of Dermatology and Venereology (EADV) 2024 Congress.
The trial included a “rigorously selected … well-characterized, well-studied” population of children aged 6-11 years, said presenter Alan D. Irvine, MD, DSc, professor of dermatology, Trinity College Dublin, Ireland.
It showed that “severe atopic dermatitis does cause restriction of growth, as well as a higher weight, and therefore obviously a higher BMI [body mass index].”
He continued, however, that children at the lower percentiles of height receiving prompt treatment with dupilumab (Dupixent) “were able to rapidly move through the centiles over the 16 weeks of the study, and that may be the window for catch-up growth … when children are growing rapidly.”
Anna Yasmine Kirkorian, MD, chief of dermatology, Children’s National Hospital, Washington, DC, who was not involved in the study, said that she was “surprised” at the degree of growth achieved over the study period, as height is not something that jumps up “overnight.”
“On the other hand, it fits with my experience with children who’ve had the brakes on all of their life due to inflammation, whether it be height, going to school, sleeping — everything is sort of put on pause by this terrible inflammatory process,” she said.
“When you take the brakes off, they get to be who they are going to be,” Kirkorian added. “So I was surprised by the speed of it, but not by the fact that height was acquired.”
Her belief is that in the pre-dupilumab era, severe atopic dermatitis was often insufficiently controlled, so children were “smaller than you would predict from parental height,” and the treatment is “allowing them to reach their genetic potential.”
Post Hoc Analysis
In his presentation, Irvine emphasized that it has been clearly demonstrated that adolescents with moderate and severe atopic dermatitis have a significantly higher likelihood of being below the 25th percentile of height on growth reference charts.
Such children are also at a higher risk of having low bone mineral density and low serum alkaline phosphatase (ALP) levels . While data presented at the EADV 2023 Congress showed that dupilumab significantly increased serum levels of bone ALP compared with placebo, the underlying mechanism remains unclear.
For the current analysis, Irvine and colleagues determined that the proportion of children aged 6-11 years with severe atopic dermatitis and lower stature reach a ≥ 5 centile improvement in height following 16 weeks of dupilumab treatment.
They examined data from the LIBERTY AD PEDS trial, in which patients aged 6-11 years with severe atopic dermatitis were randomized to 300 mg dupilumab every 4 weeks or placebo along with a mild or moderately potent topical corticosteroid. The study found that, overall, dupilumab was associated with significant improvements in signs, symptoms, and quality of life compared with placebo.
Height measures at baseline revealed that “more boys and more girls were below the 50th centile than you would predict for a healthy, normal control population,” Irvine said. “If we look at weight, we see the opposite,” he continued, “with a disproportionate number of boys and girls who are above the 50th centile for weight at baseline.”
Consequently, “we’re seeing these children who are shorter and heavier than the predicted healthy weight range and, as a result, obviously have higher BMI,” Irvine noted, with 67% girls and 62% boys found to have a higher BMI than normal for their age.
After 16 weeks of treatment with dupilumab, there was a much greater gain in height than that seen among those on placebo, with the most pronounced effect seen in children who had the lowest height at baseline. Indeed, among children in the lowest 25% height percentile at baseline, 30.6% on dupilumab vs 11.9% on placebo experienced an increase in height of 5 centiles or more(P < .05).
“This reflects what we see in clinical practice,” Irvine said. “Children often grow dramatically on treatment for atopic dermatitis.”
Among patients with a baseline height below the 30th percentile, 31.9% treated with dupilumab vs 11.1% treated with placebo gained at least 5 centiles in height. The figures for children below the 40th height percentile at baseline were 31.3% vs 15.5% (P < .05 for both).
Although there remained a marked difference in the proportion of children below the 50th height percentile at baseline gaining 5 centiles or more in height, at 29.0% with dupilumab versus 15.7% with placebo, it was no longer significant.
“So the effect of catch-up growth, or growth through the centiles, is most marked in those who are in the 40th centile or below,” Irvine said, indicating that the “more growth restricted kids have much more potential to catch up.”
‘Convincing’ Data
Overall, Kirkorian said in the interview, the data are “convincing” and support her view that severe atopic dermatitis is a “terrible chronic disease that we really underappreciate.” Atopic dermatitis, she added, “should get the respect that any severe chronic illness would have, whether that be arthritis, diabetes, or cardiac disease, because it is a systemic disorder that … profoundly affects quality of life, every minute of every day.”
However, “we don’t get all the referrals we should, until the child has suffered for years and years, and the family has suffered,” as there is a bias that it can be outgrown — although not everybody does — and it “doesn’t look as conspicuous as other chronic skin disorders,” such as psoriasis.
“Now with this study,” Kirkorian said, “it gives us a really compelling point to make to parents, to the community, and to insurers that not only are we affecting the quality of life from the itch standpoint [with dupilumab] but we may have long profound effects on growth and bone health.”
The research was sponsored by Sanofi and Regeneron Pharmaceuticals. Irvine declared relationships with AbbVie, Arena Pharmaceuticals, BenevolentAI, Chugai Pharmaceutical, Dermavant, Eli Lily, Genentech, LEO Pharma, Menlo Therapeutics, Novartis, Pfizer, Regeneron, Sanofi, UCB, DS Biopharma, and Inflazome. Kirkorian declared relationships with Dermavant, Verrica Pharmaceuticals, Pfizer, and Incyte.
A version of this article first appeared on Medscape.com.
AMSTERDAM — , revealed a post hoc trial analysis.
The research was presented at the European Academy of Dermatology and Venereology (EADV) 2024 Congress.
The trial included a “rigorously selected … well-characterized, well-studied” population of children aged 6-11 years, said presenter Alan D. Irvine, MD, DSc, professor of dermatology, Trinity College Dublin, Ireland.
It showed that “severe atopic dermatitis does cause restriction of growth, as well as a higher weight, and therefore obviously a higher BMI [body mass index].”
He continued, however, that children at the lower percentiles of height receiving prompt treatment with dupilumab (Dupixent) “were able to rapidly move through the centiles over the 16 weeks of the study, and that may be the window for catch-up growth … when children are growing rapidly.”
Anna Yasmine Kirkorian, MD, chief of dermatology, Children’s National Hospital, Washington, DC, who was not involved in the study, said that she was “surprised” at the degree of growth achieved over the study period, as height is not something that jumps up “overnight.”
“On the other hand, it fits with my experience with children who’ve had the brakes on all of their life due to inflammation, whether it be height, going to school, sleeping — everything is sort of put on pause by this terrible inflammatory process,” she said.
“When you take the brakes off, they get to be who they are going to be,” Kirkorian added. “So I was surprised by the speed of it, but not by the fact that height was acquired.”
Her belief is that in the pre-dupilumab era, severe atopic dermatitis was often insufficiently controlled, so children were “smaller than you would predict from parental height,” and the treatment is “allowing them to reach their genetic potential.”
Post Hoc Analysis
In his presentation, Irvine emphasized that it has been clearly demonstrated that adolescents with moderate and severe atopic dermatitis have a significantly higher likelihood of being below the 25th percentile of height on growth reference charts.
Such children are also at a higher risk of having low bone mineral density and low serum alkaline phosphatase (ALP) levels . While data presented at the EADV 2023 Congress showed that dupilumab significantly increased serum levels of bone ALP compared with placebo, the underlying mechanism remains unclear.
For the current analysis, Irvine and colleagues determined that the proportion of children aged 6-11 years with severe atopic dermatitis and lower stature reach a ≥ 5 centile improvement in height following 16 weeks of dupilumab treatment.
They examined data from the LIBERTY AD PEDS trial, in which patients aged 6-11 years with severe atopic dermatitis were randomized to 300 mg dupilumab every 4 weeks or placebo along with a mild or moderately potent topical corticosteroid. The study found that, overall, dupilumab was associated with significant improvements in signs, symptoms, and quality of life compared with placebo.
Height measures at baseline revealed that “more boys and more girls were below the 50th centile than you would predict for a healthy, normal control population,” Irvine said. “If we look at weight, we see the opposite,” he continued, “with a disproportionate number of boys and girls who are above the 50th centile for weight at baseline.”
Consequently, “we’re seeing these children who are shorter and heavier than the predicted healthy weight range and, as a result, obviously have higher BMI,” Irvine noted, with 67% girls and 62% boys found to have a higher BMI than normal for their age.
After 16 weeks of treatment with dupilumab, there was a much greater gain in height than that seen among those on placebo, with the most pronounced effect seen in children who had the lowest height at baseline. Indeed, among children in the lowest 25% height percentile at baseline, 30.6% on dupilumab vs 11.9% on placebo experienced an increase in height of 5 centiles or more(P < .05).
“This reflects what we see in clinical practice,” Irvine said. “Children often grow dramatically on treatment for atopic dermatitis.”
Among patients with a baseline height below the 30th percentile, 31.9% treated with dupilumab vs 11.1% treated with placebo gained at least 5 centiles in height. The figures for children below the 40th height percentile at baseline were 31.3% vs 15.5% (P < .05 for both).
Although there remained a marked difference in the proportion of children below the 50th height percentile at baseline gaining 5 centiles or more in height, at 29.0% with dupilumab versus 15.7% with placebo, it was no longer significant.
“So the effect of catch-up growth, or growth through the centiles, is most marked in those who are in the 40th centile or below,” Irvine said, indicating that the “more growth restricted kids have much more potential to catch up.”
‘Convincing’ Data
Overall, Kirkorian said in the interview, the data are “convincing” and support her view that severe atopic dermatitis is a “terrible chronic disease that we really underappreciate.” Atopic dermatitis, she added, “should get the respect that any severe chronic illness would have, whether that be arthritis, diabetes, or cardiac disease, because it is a systemic disorder that … profoundly affects quality of life, every minute of every day.”
However, “we don’t get all the referrals we should, until the child has suffered for years and years, and the family has suffered,” as there is a bias that it can be outgrown — although not everybody does — and it “doesn’t look as conspicuous as other chronic skin disorders,” such as psoriasis.
“Now with this study,” Kirkorian said, “it gives us a really compelling point to make to parents, to the community, and to insurers that not only are we affecting the quality of life from the itch standpoint [with dupilumab] but we may have long profound effects on growth and bone health.”
The research was sponsored by Sanofi and Regeneron Pharmaceuticals. Irvine declared relationships with AbbVie, Arena Pharmaceuticals, BenevolentAI, Chugai Pharmaceutical, Dermavant, Eli Lily, Genentech, LEO Pharma, Menlo Therapeutics, Novartis, Pfizer, Regeneron, Sanofi, UCB, DS Biopharma, and Inflazome. Kirkorian declared relationships with Dermavant, Verrica Pharmaceuticals, Pfizer, and Incyte.
A version of this article first appeared on Medscape.com.
FROM EADV 2024