User login
Diagnosing Adrenal Insufficiency: The ‘Quick and Dirty’ Method
Matthew F. Watto, MD: Welcome back to The Curbsiders. I’m Dr. Matthew Watto, here with America’s primary care physician, Dr. Paul Nelson Williams. Paul, are you ready to talk about some adrenal insufficiency? We had a great conversation with Dr. Atil Kargi, and I’d like you to start us off.
Paul N. Williams, MD: How about thinking about it? It’s a good place to start.
That’s one of the ways this episode changed my approach a little bit. I never really thought about the fact that . It’s such a protean sort of nonspecific presentation. But if you have someone with chronic malaise and poor appetite and maybe unexplained weight loss, and your GI workup is not really leading you anywhere, it’s probably worth thinking about adrenal insufficiency. Even though primary adrenal insufficiency is pretty rare — we’re talking cases per millions — secondary adrenal insufficiency is actually fairly common. It’s probably worth thinking about and testing for more often than I have in the past. So for me, it’s having a lower threshold to start looking for it.
Dr. Watto: When it’s adrenal crisis, you probably think about it, but then it’s too late. Ideally, you would think about it before that happens. But the symptoms can be quite vague. The mineralocorticoid symptoms, like salt cravings, dizziness, near syncope, muscle cramps, might make me think of it because they sound more like something endocrine is going on. But if it’s just a little weight loss, a little fatigue, or a little nausea, that’s everybody.
Dr. Williams: Right. If a patient came to me saying, “I’m craving salt,” that might hasten the workup a little bit, but that’s not the typical presentation.
Dr. Watto: If you are going to check a cortisol level, you should really check it in the morning, between 7 AM and 9 AM. If you check it too early, it might not have peaked yet, so you might get a level that looks low. But if you had checked an hour or 2 later, it might have been above a threshold, and then you would know you could rule out the diagnosis. The cutoffs depend on your source: < 3-5 µg/dL that early in the morning is pretty much diagnostic of adrenal insufficiency. If it’s > 15 µg/dL, that’s a pretty robust cortisol and the patient probably doesn’t have adrenal insufficiency. But if the level is between 5 µg/dL and 15 µg/dL, you’re in a gray zone, and that’s where you might think about doing a stimulation (stim) test.
Dr. Kargi gave us a quick and dirty version of the stim test. Paul, have you had a chance to try this yet?
Dr. Williams: I have not. Have you? I’m sure you’ve been just waiting for the chance.
Dr. Watto: I would love to do this. I don›t know whether I›m set up to do it in the office right now. But this is an aspirational goal for my practice, and I›m sure some physicians are set up in their office already to do it. You can give either intramuscular or subcutaneous cosyntropin 250 µg. You don›t even have to get a baseline cortisol level right before the injection. Let›s say the patient›s previous cortisol level was between 5 µg/dL and 15 µg/dL, so you weren›t sure about the diagnosis. You bring them back to the office one day, give them a shot of cosyntropin, and then 30-60 minutes later, have a random cortisol drawn. If it›s > 19 µg/dL, you›ve ruled out adrenal insufficiency. If it›s anything else, send them to an endocrinologist to sort it out. You might be able to make the diagnosis yourself doing that.
Any treatment pearls to leave the audience with?
Dr. Williams: I hope endocrinologists don›t take issue with this. I say this with respect and admiration, but it feels kind of vibe-based to me. Without a lab value to guide treatment, you are dependent on the patient telling you how they feel much of the time. You have to let their symptoms guide you. It is probably worth noting that because hydrocortisone has a relatively short half-life, within hours, in fact, you typically have to do twice-daily dosing, sometimes even three times daily dosing to get patients to where they feel okay. It sounds like there›s a fair amount of trial and error and some adjustments that you have to make depending on what›s going on with the patient at any given time. You land somewhere between a dose of 15-30 mg per day, but there will be some variability, even within an individual patient, depending on what›s going on with them from a physiologic standpoint.
Dr. Watto: They are going to take one dose in the morning and then a second dose in the afternoon, but they don’t want them to take it too late in the evening because it could cause insomnia, and you want to try to mimic physiologic levels as much as you can. Two thirds of the daily dose is given early in the morning and then another third of the daily dose later in the day if you are prescribing two times daily dosing.
And Dr. Kargi had a low threshold for doubling the dose. If the patient has a cold, double the dose for 2 or 3 days. With a high fever, triple the dose for a few days. If they are going for surgery, they are probably going to be getting some intravenous hydrocortisone while they’re in the hospital.
We really turned over like every stone we could possibly think of on this podcast. There were so many great pearls that we don’t have time to go through them all here. But we talked about steroid tapers and a lot more. You can check it out here.
Dr. Watto has disclosed no relevant financial relationships.
Dr. Williams has disclosed the following relevant financial relationships:Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: The CurbsidersReceived income in an amount equal to or greater than $250 from: The Curbsiders.
A version of this article appeared on Medscape.com.
Matthew F. Watto, MD: Welcome back to The Curbsiders. I’m Dr. Matthew Watto, here with America’s primary care physician, Dr. Paul Nelson Williams. Paul, are you ready to talk about some adrenal insufficiency? We had a great conversation with Dr. Atil Kargi, and I’d like you to start us off.
Paul N. Williams, MD: How about thinking about it? It’s a good place to start.
That’s one of the ways this episode changed my approach a little bit. I never really thought about the fact that . It’s such a protean sort of nonspecific presentation. But if you have someone with chronic malaise and poor appetite and maybe unexplained weight loss, and your GI workup is not really leading you anywhere, it’s probably worth thinking about adrenal insufficiency. Even though primary adrenal insufficiency is pretty rare — we’re talking cases per millions — secondary adrenal insufficiency is actually fairly common. It’s probably worth thinking about and testing for more often than I have in the past. So for me, it’s having a lower threshold to start looking for it.
Dr. Watto: When it’s adrenal crisis, you probably think about it, but then it’s too late. Ideally, you would think about it before that happens. But the symptoms can be quite vague. The mineralocorticoid symptoms, like salt cravings, dizziness, near syncope, muscle cramps, might make me think of it because they sound more like something endocrine is going on. But if it’s just a little weight loss, a little fatigue, or a little nausea, that’s everybody.
Dr. Williams: Right. If a patient came to me saying, “I’m craving salt,” that might hasten the workup a little bit, but that’s not the typical presentation.
Dr. Watto: If you are going to check a cortisol level, you should really check it in the morning, between 7 AM and 9 AM. If you check it too early, it might not have peaked yet, so you might get a level that looks low. But if you had checked an hour or 2 later, it might have been above a threshold, and then you would know you could rule out the diagnosis. The cutoffs depend on your source: < 3-5 µg/dL that early in the morning is pretty much diagnostic of adrenal insufficiency. If it’s > 15 µg/dL, that’s a pretty robust cortisol and the patient probably doesn’t have adrenal insufficiency. But if the level is between 5 µg/dL and 15 µg/dL, you’re in a gray zone, and that’s where you might think about doing a stimulation (stim) test.
Dr. Kargi gave us a quick and dirty version of the stim test. Paul, have you had a chance to try this yet?
Dr. Williams: I have not. Have you? I’m sure you’ve been just waiting for the chance.
Dr. Watto: I would love to do this. I don›t know whether I›m set up to do it in the office right now. But this is an aspirational goal for my practice, and I›m sure some physicians are set up in their office already to do it. You can give either intramuscular or subcutaneous cosyntropin 250 µg. You don›t even have to get a baseline cortisol level right before the injection. Let›s say the patient›s previous cortisol level was between 5 µg/dL and 15 µg/dL, so you weren›t sure about the diagnosis. You bring them back to the office one day, give them a shot of cosyntropin, and then 30-60 minutes later, have a random cortisol drawn. If it›s > 19 µg/dL, you›ve ruled out adrenal insufficiency. If it›s anything else, send them to an endocrinologist to sort it out. You might be able to make the diagnosis yourself doing that.
Any treatment pearls to leave the audience with?
Dr. Williams: I hope endocrinologists don›t take issue with this. I say this with respect and admiration, but it feels kind of vibe-based to me. Without a lab value to guide treatment, you are dependent on the patient telling you how they feel much of the time. You have to let their symptoms guide you. It is probably worth noting that because hydrocortisone has a relatively short half-life, within hours, in fact, you typically have to do twice-daily dosing, sometimes even three times daily dosing to get patients to where they feel okay. It sounds like there›s a fair amount of trial and error and some adjustments that you have to make depending on what›s going on with the patient at any given time. You land somewhere between a dose of 15-30 mg per day, but there will be some variability, even within an individual patient, depending on what›s going on with them from a physiologic standpoint.
Dr. Watto: They are going to take one dose in the morning and then a second dose in the afternoon, but they don’t want them to take it too late in the evening because it could cause insomnia, and you want to try to mimic physiologic levels as much as you can. Two thirds of the daily dose is given early in the morning and then another third of the daily dose later in the day if you are prescribing two times daily dosing.
And Dr. Kargi had a low threshold for doubling the dose. If the patient has a cold, double the dose for 2 or 3 days. With a high fever, triple the dose for a few days. If they are going for surgery, they are probably going to be getting some intravenous hydrocortisone while they’re in the hospital.
We really turned over like every stone we could possibly think of on this podcast. There were so many great pearls that we don’t have time to go through them all here. But we talked about steroid tapers and a lot more. You can check it out here.
Dr. Watto has disclosed no relevant financial relationships.
Dr. Williams has disclosed the following relevant financial relationships:Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: The CurbsidersReceived income in an amount equal to or greater than $250 from: The Curbsiders.
A version of this article appeared on Medscape.com.
Matthew F. Watto, MD: Welcome back to The Curbsiders. I’m Dr. Matthew Watto, here with America’s primary care physician, Dr. Paul Nelson Williams. Paul, are you ready to talk about some adrenal insufficiency? We had a great conversation with Dr. Atil Kargi, and I’d like you to start us off.
Paul N. Williams, MD: How about thinking about it? It’s a good place to start.
That’s one of the ways this episode changed my approach a little bit. I never really thought about the fact that . It’s such a protean sort of nonspecific presentation. But if you have someone with chronic malaise and poor appetite and maybe unexplained weight loss, and your GI workup is not really leading you anywhere, it’s probably worth thinking about adrenal insufficiency. Even though primary adrenal insufficiency is pretty rare — we’re talking cases per millions — secondary adrenal insufficiency is actually fairly common. It’s probably worth thinking about and testing for more often than I have in the past. So for me, it’s having a lower threshold to start looking for it.
Dr. Watto: When it’s adrenal crisis, you probably think about it, but then it’s too late. Ideally, you would think about it before that happens. But the symptoms can be quite vague. The mineralocorticoid symptoms, like salt cravings, dizziness, near syncope, muscle cramps, might make me think of it because they sound more like something endocrine is going on. But if it’s just a little weight loss, a little fatigue, or a little nausea, that’s everybody.
Dr. Williams: Right. If a patient came to me saying, “I’m craving salt,” that might hasten the workup a little bit, but that’s not the typical presentation.
Dr. Watto: If you are going to check a cortisol level, you should really check it in the morning, between 7 AM and 9 AM. If you check it too early, it might not have peaked yet, so you might get a level that looks low. But if you had checked an hour or 2 later, it might have been above a threshold, and then you would know you could rule out the diagnosis. The cutoffs depend on your source: < 3-5 µg/dL that early in the morning is pretty much diagnostic of adrenal insufficiency. If it’s > 15 µg/dL, that’s a pretty robust cortisol and the patient probably doesn’t have adrenal insufficiency. But if the level is between 5 µg/dL and 15 µg/dL, you’re in a gray zone, and that’s where you might think about doing a stimulation (stim) test.
Dr. Kargi gave us a quick and dirty version of the stim test. Paul, have you had a chance to try this yet?
Dr. Williams: I have not. Have you? I’m sure you’ve been just waiting for the chance.
Dr. Watto: I would love to do this. I don›t know whether I›m set up to do it in the office right now. But this is an aspirational goal for my practice, and I›m sure some physicians are set up in their office already to do it. You can give either intramuscular or subcutaneous cosyntropin 250 µg. You don›t even have to get a baseline cortisol level right before the injection. Let›s say the patient›s previous cortisol level was between 5 µg/dL and 15 µg/dL, so you weren›t sure about the diagnosis. You bring them back to the office one day, give them a shot of cosyntropin, and then 30-60 minutes later, have a random cortisol drawn. If it›s > 19 µg/dL, you›ve ruled out adrenal insufficiency. If it›s anything else, send them to an endocrinologist to sort it out. You might be able to make the diagnosis yourself doing that.
Any treatment pearls to leave the audience with?
Dr. Williams: I hope endocrinologists don›t take issue with this. I say this with respect and admiration, but it feels kind of vibe-based to me. Without a lab value to guide treatment, you are dependent on the patient telling you how they feel much of the time. You have to let their symptoms guide you. It is probably worth noting that because hydrocortisone has a relatively short half-life, within hours, in fact, you typically have to do twice-daily dosing, sometimes even three times daily dosing to get patients to where they feel okay. It sounds like there›s a fair amount of trial and error and some adjustments that you have to make depending on what›s going on with the patient at any given time. You land somewhere between a dose of 15-30 mg per day, but there will be some variability, even within an individual patient, depending on what›s going on with them from a physiologic standpoint.
Dr. Watto: They are going to take one dose in the morning and then a second dose in the afternoon, but they don’t want them to take it too late in the evening because it could cause insomnia, and you want to try to mimic physiologic levels as much as you can. Two thirds of the daily dose is given early in the morning and then another third of the daily dose later in the day if you are prescribing two times daily dosing.
And Dr. Kargi had a low threshold for doubling the dose. If the patient has a cold, double the dose for 2 or 3 days. With a high fever, triple the dose for a few days. If they are going for surgery, they are probably going to be getting some intravenous hydrocortisone while they’re in the hospital.
We really turned over like every stone we could possibly think of on this podcast. There were so many great pearls that we don’t have time to go through them all here. But we talked about steroid tapers and a lot more. You can check it out here.
Dr. Watto has disclosed no relevant financial relationships.
Dr. Williams has disclosed the following relevant financial relationships:Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: The CurbsidersReceived income in an amount equal to or greater than $250 from: The Curbsiders.
A version of this article appeared on Medscape.com.
Artificial Sweeteners Alter the Duodenal Microbiome
TOPLINE:
and composition and levels of circulating inflammatory markers.
METHODOLOGY:
- Researchers analyzed samples from the REIMAGINE (Revealing the Entire Intestinal Microbiota and its Associations with the Genetic, Immunologic, and Neuroendocrine Ecosystem) study to assess the potential effects of NSS consumption on the duodenal luminal microbiome.
- They analyzed subjects consuming non-aspartame nonsugar sweeteners (NANS; n = 35) and aspartame only (ASP; n = 9), who were compared with 55 control participants matched for age, sex, and body mass index.
- A subset of 40 participants provided stool samples for additional analysis.
TAKEAWAY:
- Duodenal alpha diversity was lower in NANS consumers vs controls.
- Duodenal relative abundance (RA) of Escherichia, Klebsiella, and Salmonella was lower in both NANS and ASP vs controls, whereas stool RA of these phylum Proteobacteria was increased in both NANS and ASP.
- Compared with controls, NANS and ASP differed in how they altered predicted duodenal microbial metabolic pathways, with NANS impacting polysaccharides biosynthesis and D-galactose degradation and ASP significantly enriching biosynthesis of cylindrospermopsin, a potential cancer-causing agent known to adversely impact the liver and nervous system.
- Circulating levels of interleukin (IL)-1b, a pro-inflammatory cytokine that plays a key role in the immune response, were significantly decreased in NANS vs controls, whereas IL-6 and IL-10, two cytokines with protective properties, were decreased in the ASP group vs controls.
IN PRACTICE:
“Given the crucial role played by small intestinal microbes in digestion, nutrient absorption, immune regulation, and endocrine functions, coupled with the substantial prevalence of NSS consumption among US adults (estimated at 41.4%), our findings have potential implications for metabolic and gastrointestinal health in a considerable proportion of the American adult population.”
SOURCE:
The study, conducted by Ava Hosseini, MPH, and colleagues at Cedars-Sinai, Los Angeles, was published online on November 22, 2023, in iScience.
LIMITATIONS:
The study population may not be representative of healthy individuals as they underwent upper endoscopy for various reasons (eg, evaluation of intestinal complaints). After exclusions, the duodenal sample size for the aspartame group was small. Samples were collected at a single timepoint, limiting the ability to establish causal relationships.
DISCLOSURES:
This research was supported by Frank Lee, the Monica Lester Charitable Trust, and the Elias, Genevieve, and Georgianna Atol Charitable Trust through their support of the Medically Associated Science and Technology Program, Cedars-Sinai, Los Angeles. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
and composition and levels of circulating inflammatory markers.
METHODOLOGY:
- Researchers analyzed samples from the REIMAGINE (Revealing the Entire Intestinal Microbiota and its Associations with the Genetic, Immunologic, and Neuroendocrine Ecosystem) study to assess the potential effects of NSS consumption on the duodenal luminal microbiome.
- They analyzed subjects consuming non-aspartame nonsugar sweeteners (NANS; n = 35) and aspartame only (ASP; n = 9), who were compared with 55 control participants matched for age, sex, and body mass index.
- A subset of 40 participants provided stool samples for additional analysis.
TAKEAWAY:
- Duodenal alpha diversity was lower in NANS consumers vs controls.
- Duodenal relative abundance (RA) of Escherichia, Klebsiella, and Salmonella was lower in both NANS and ASP vs controls, whereas stool RA of these phylum Proteobacteria was increased in both NANS and ASP.
- Compared with controls, NANS and ASP differed in how they altered predicted duodenal microbial metabolic pathways, with NANS impacting polysaccharides biosynthesis and D-galactose degradation and ASP significantly enriching biosynthesis of cylindrospermopsin, a potential cancer-causing agent known to adversely impact the liver and nervous system.
- Circulating levels of interleukin (IL)-1b, a pro-inflammatory cytokine that plays a key role in the immune response, were significantly decreased in NANS vs controls, whereas IL-6 and IL-10, two cytokines with protective properties, were decreased in the ASP group vs controls.
IN PRACTICE:
“Given the crucial role played by small intestinal microbes in digestion, nutrient absorption, immune regulation, and endocrine functions, coupled with the substantial prevalence of NSS consumption among US adults (estimated at 41.4%), our findings have potential implications for metabolic and gastrointestinal health in a considerable proportion of the American adult population.”
SOURCE:
The study, conducted by Ava Hosseini, MPH, and colleagues at Cedars-Sinai, Los Angeles, was published online on November 22, 2023, in iScience.
LIMITATIONS:
The study population may not be representative of healthy individuals as they underwent upper endoscopy for various reasons (eg, evaluation of intestinal complaints). After exclusions, the duodenal sample size for the aspartame group was small. Samples were collected at a single timepoint, limiting the ability to establish causal relationships.
DISCLOSURES:
This research was supported by Frank Lee, the Monica Lester Charitable Trust, and the Elias, Genevieve, and Georgianna Atol Charitable Trust through their support of the Medically Associated Science and Technology Program, Cedars-Sinai, Los Angeles. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
and composition and levels of circulating inflammatory markers.
METHODOLOGY:
- Researchers analyzed samples from the REIMAGINE (Revealing the Entire Intestinal Microbiota and its Associations with the Genetic, Immunologic, and Neuroendocrine Ecosystem) study to assess the potential effects of NSS consumption on the duodenal luminal microbiome.
- They analyzed subjects consuming non-aspartame nonsugar sweeteners (NANS; n = 35) and aspartame only (ASP; n = 9), who were compared with 55 control participants matched for age, sex, and body mass index.
- A subset of 40 participants provided stool samples for additional analysis.
TAKEAWAY:
- Duodenal alpha diversity was lower in NANS consumers vs controls.
- Duodenal relative abundance (RA) of Escherichia, Klebsiella, and Salmonella was lower in both NANS and ASP vs controls, whereas stool RA of these phylum Proteobacteria was increased in both NANS and ASP.
- Compared with controls, NANS and ASP differed in how they altered predicted duodenal microbial metabolic pathways, with NANS impacting polysaccharides biosynthesis and D-galactose degradation and ASP significantly enriching biosynthesis of cylindrospermopsin, a potential cancer-causing agent known to adversely impact the liver and nervous system.
- Circulating levels of interleukin (IL)-1b, a pro-inflammatory cytokine that plays a key role in the immune response, were significantly decreased in NANS vs controls, whereas IL-6 and IL-10, two cytokines with protective properties, were decreased in the ASP group vs controls.
IN PRACTICE:
“Given the crucial role played by small intestinal microbes in digestion, nutrient absorption, immune regulation, and endocrine functions, coupled with the substantial prevalence of NSS consumption among US adults (estimated at 41.4%), our findings have potential implications for metabolic and gastrointestinal health in a considerable proportion of the American adult population.”
SOURCE:
The study, conducted by Ava Hosseini, MPH, and colleagues at Cedars-Sinai, Los Angeles, was published online on November 22, 2023, in iScience.
LIMITATIONS:
The study population may not be representative of healthy individuals as they underwent upper endoscopy for various reasons (eg, evaluation of intestinal complaints). After exclusions, the duodenal sample size for the aspartame group was small. Samples were collected at a single timepoint, limiting the ability to establish causal relationships.
DISCLOSURES:
This research was supported by Frank Lee, the Monica Lester Charitable Trust, and the Elias, Genevieve, and Georgianna Atol Charitable Trust through their support of the Medically Associated Science and Technology Program, Cedars-Sinai, Los Angeles. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
Ascending Thoracic Aortic Aneurysms: A ‘Silver Lining’?
Often known as a “silent killer,” ascending thoracic aortic aneurysms (ATAAs) may grow asymptomatically until they rupture, at which point, mortality is over 90%.
But and by extension, for those who have one, a significantly reduced risk for coronary artery disease and myocardial infarction (MI).
“We noticed in the operating room that many patients we worked on who had an ATAA had pristine arteries, like a teenager’s,” said John Elefteriades, MD, William W.L. Glenn Professor of Cardiothoracic Surgery and former chief of cardiothoracic surgery at Yale University and Yale New Haven Hospital, New Haven, Connecticut. “The same was true of the femoral artery, which we use to hook up to the heart-lung machine.”
Elefteriades and colleagues have been investigating the implications of this association for more than two decades. Many of their studies are highlighted in a recent review of the evidence supporting the protective relationship between ATAAs and the development of atherosclerosis and the possible mechanisms driving the relationship.
“We see four different layers of protection,” said Sandip Mukherjee, MD, medical director of the Aortic Institute at Yale New Haven Hospital and a senior editor of the journal AORTA. Mukherjee collaborated with Elefteriades on many of the studies.
The first layer of protection is lower intima-media thickness, specifically, 0.131 mm lower than in individuals without an ATAA. “It may not seem like very much, but one point can actually translate into a 13%-15% decline in the rate of myocardial infarction or stroke,” Dr. Mukherjee said.
The second layer is lower levels of low-density lipoprotein (LDL) cholesterol. Lower LDL cholesterol levels (75 mg/dL) were associated with increased odds of ATAAs (odds ratio [OR], 1.21), whereas elevated levels (150 mg/dL and 200 mg/dL) were associated with decreased odds of ATAAs (OR, 0.62 and 0.29, respectively).
Lower calcification scores for the coronary arteries are the third layer of protection (6.73 vs 9.36 in one study).
The fourth protective layer is a significantly reduced prevalence of coronary artery disease. A study of individuals with ATAA compared to controls found 61 of those with ATAA had coronary artery disease vs 140 of controls, and 11 vs 83 had experienced an MI. Of note, patients with ATAAs were protected despite having higher body mass indices than controls.
Other MI risk factors such as age increased the risk even among those with an ATAA but, again, much less so than among controls; a multivariable binary logistic regression of data in the team’s review showed that patients with ATAAs were 298, 250, and 232 times less likely to have an MI than if they had a family history of MI, dyslipidemia, or hypertension, respectively.
Why the Protection?
The ligamentum arteriosum separates the ascending from the descending (thoracoabdominal) aorta. ATAAs, located above the ligamentum, tend to be pro-aneurysmal but anti-atherosclerotic. In the descending aorta, below the ligamentum, atherosclerotic aneurysms develop.
The differences between the two sections of the aorta originate in the germ layer in the embryo, Dr. Elefteriades said. “The fundamental difference in tissue of origin translates into marked differences in the character of aneurysms in the different aortic segments.”
What specifically underlies the reduced cardiovascular risk? “We don’t really know, but we think that there may be two possible etiologies,” Dr. Mukherjee said. One hypothesis involves transforming growth factor–beta (TGF-beta), which is overexpressed in patients with ATAA and seems to increase their vulnerability to aneurysms while also conferring protection from coronary disease risk.
Some studies have shown differences in cellular responses to TGF-beta between the thoracic and abdominal aorta, including collagen production and contractility. Others have shown that some patients who have had an MI have polymorphisms that decrease their levels of TGF-beta.
Furthermore, TGF-beta plays a key role in the development of the intimal layer, which could underpin the lack of intimal thickening in patients with ATAA.
But overall, studies have been mixed and challenging to interpret, Dr. Elefteriades and Dr. Mukherjee agreed. TGF-beta has multiple remodeling roles in the body, and it is difficult at this point to isolate its exact role in aortic disease.
Another hypothesis involves matrix metalloproteinases (MMPs), which are dysregulated in patients with ATAA and may confer some protection, Mukherjee said. Several studies have shown higher plasma levels of certain MMPs in patients with ATAAs. MMPs also were found to be elevated in the thoracic aortic walls of patients with ATAA who had an aortic dissection, as well as in the aortic smooth muscle cells in the intima and media.
In addition, some studies have shown increased levels of MMP-2 in the aortas of patients with ATAAs compared with patients with coronary artery disease.
Adding to the mix of possibilities, “We recently found a gene that’s dysregulated in our aneurysm patients that is very intimately related to atherosclerosis,” Dr. Elefteriades said. “But the work is too preliminary to say anything more at this point.”
“It would be fabulous to prove what it is causing this protection,” Dr. Mukherjee added. “But the truth is we don’t know. These are hypotheses.”
“The most important message from our work is that most clinicians need to dissociate an ATAA from the concept of atherosclerosis,” Dr. Elefteriades said. “The ascending aorta is not an atherosclerotic phenomenon.”
How to Manage Patients With ATAA
What does the distinct character of ATAAs mean for patient management? “Finding a drug to treat ATAAs — to prevent growth, rupture, or dissection — has been like a search for the Holy Grail,” Dr. Elefteriades said. “Statins are not necessary, as this is a non-atherosclerotic process. Although sporadic studies have reported beneficial effects from beta-blockers or angiotensin II receptor blockers (ARBs), this has often been based on ‘soft’ evidence, requiring a combination of outcome measures to achieve significance.”
That said, he noted, “The mainstay, common sense treatment is to keep blood pressure controlled. This is usually achieved by a beta-blocker and an ARB, even if the benefit is not via a direct biologic effect on the aneurysmal degenerative process, but via simple hemodynamics — discouraging rupture by keeping pressure in the aorta low.”
Dr. Mukherjee suggested that these patients should be referred to a specialty aneurysm center where their genes will be evaluated, and then the aneurysm will be followed very closely.
“If the aneurysm is larger than 4.5 cm, we screen the patient every single year, and if they have chest pain, we treat them the same way as we treat other aneurysms,” he said. “As a rule of thumb, if the aneurysm reaches 5 cm, it should come out, although the size at which this should happen may differ between 4.5 cm and 5.5 cm, depending on the patient’s body size.”
As for lifestyle management, Dr. Elefteriades said, “Protection from atherosclerosis and MI won’t go away after the aneurysm is removed. We think it’s in the body’s chemistry. But even though it’s very hard for those patients to have a heart attack, we don’t recommend they eat roast beef every night — although I do think they’d be protected from such lifestyle aberrations.”
For now, he added, “Our team is on a hunt to find a drug to treat ascending disease directly and effectively. We have ongoing laboratory experiments with two drugs undergoing investigation at some level. We hope to embark soon on clinical trials.”
‘A Milestone’
James Hamilton Black III, MD, vice chair of the writing committee for the 2022 American College of Cardiology/American Heart Association Aortic Disease Guideline and chief of Division of Vascular Surgery and Endovascular Therapy at Johns Hopkins Medicine, Baltimore, commented on the review and the concept of ATAA’s atherosclerotic protection.
“The association of ascending aortic aneurysms with a lower risk for MI is an interesting one, but it’s probably influenced, at least in part, by the patient population.” That population is at least partially curated since people are coming to an academic center. In addition, Dr. Black noted, “the patients with ATAAs are younger, and so age may be a confounding factor in the analyses. We wouldn’t expect them to have the same burden of atherosclerosis” as older patients.
Nevertheless, he said, “the findings speak to an emerging body of literature suggesting that although the aorta is a single organ, there are certainly different areas, and these would respond quite differently to environmental or genetic or heritable stressors. This isn’t surprising, and there probably are a lot of factors involved.”
Overall, he said, the findings underscore “the precision medicine approaches we need to take with patients with aortic diseases.”
In a commentary on the team’s review article, published in 2022, John G.T. Augoustides, MD, professor of anesthesiology and critical care at the Perelman School of Medicine in Philadelphia, Pennsylvania, suggested that ATAA’s “silver lining” could advance the understanding of thoracic aortic aneurysm (TAA) management, be integrated with the expanding horizons in hereditary thoracic aortic disease, and might be explored in the context of bicuspid aortic valve disease.
Highlighting the “relative absence” of atherosclerosis in ascending aortic aneurysms and its importance is a “milestone in our understanding,” he concluded. “It is likely that future advances in TAAs will be significantly influenced by this observation.”
Dr. Elefteriades, Dr. Mukherjee, and Dr. Black have no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
Often known as a “silent killer,” ascending thoracic aortic aneurysms (ATAAs) may grow asymptomatically until they rupture, at which point, mortality is over 90%.
But and by extension, for those who have one, a significantly reduced risk for coronary artery disease and myocardial infarction (MI).
“We noticed in the operating room that many patients we worked on who had an ATAA had pristine arteries, like a teenager’s,” said John Elefteriades, MD, William W.L. Glenn Professor of Cardiothoracic Surgery and former chief of cardiothoracic surgery at Yale University and Yale New Haven Hospital, New Haven, Connecticut. “The same was true of the femoral artery, which we use to hook up to the heart-lung machine.”
Elefteriades and colleagues have been investigating the implications of this association for more than two decades. Many of their studies are highlighted in a recent review of the evidence supporting the protective relationship between ATAAs and the development of atherosclerosis and the possible mechanisms driving the relationship.
“We see four different layers of protection,” said Sandip Mukherjee, MD, medical director of the Aortic Institute at Yale New Haven Hospital and a senior editor of the journal AORTA. Mukherjee collaborated with Elefteriades on many of the studies.
The first layer of protection is lower intima-media thickness, specifically, 0.131 mm lower than in individuals without an ATAA. “It may not seem like very much, but one point can actually translate into a 13%-15% decline in the rate of myocardial infarction or stroke,” Dr. Mukherjee said.
The second layer is lower levels of low-density lipoprotein (LDL) cholesterol. Lower LDL cholesterol levels (75 mg/dL) were associated with increased odds of ATAAs (odds ratio [OR], 1.21), whereas elevated levels (150 mg/dL and 200 mg/dL) were associated with decreased odds of ATAAs (OR, 0.62 and 0.29, respectively).
Lower calcification scores for the coronary arteries are the third layer of protection (6.73 vs 9.36 in one study).
The fourth protective layer is a significantly reduced prevalence of coronary artery disease. A study of individuals with ATAA compared to controls found 61 of those with ATAA had coronary artery disease vs 140 of controls, and 11 vs 83 had experienced an MI. Of note, patients with ATAAs were protected despite having higher body mass indices than controls.
Other MI risk factors such as age increased the risk even among those with an ATAA but, again, much less so than among controls; a multivariable binary logistic regression of data in the team’s review showed that patients with ATAAs were 298, 250, and 232 times less likely to have an MI than if they had a family history of MI, dyslipidemia, or hypertension, respectively.
Why the Protection?
The ligamentum arteriosum separates the ascending from the descending (thoracoabdominal) aorta. ATAAs, located above the ligamentum, tend to be pro-aneurysmal but anti-atherosclerotic. In the descending aorta, below the ligamentum, atherosclerotic aneurysms develop.
The differences between the two sections of the aorta originate in the germ layer in the embryo, Dr. Elefteriades said. “The fundamental difference in tissue of origin translates into marked differences in the character of aneurysms in the different aortic segments.”
What specifically underlies the reduced cardiovascular risk? “We don’t really know, but we think that there may be two possible etiologies,” Dr. Mukherjee said. One hypothesis involves transforming growth factor–beta (TGF-beta), which is overexpressed in patients with ATAA and seems to increase their vulnerability to aneurysms while also conferring protection from coronary disease risk.
Some studies have shown differences in cellular responses to TGF-beta between the thoracic and abdominal aorta, including collagen production and contractility. Others have shown that some patients who have had an MI have polymorphisms that decrease their levels of TGF-beta.
Furthermore, TGF-beta plays a key role in the development of the intimal layer, which could underpin the lack of intimal thickening in patients with ATAA.
But overall, studies have been mixed and challenging to interpret, Dr. Elefteriades and Dr. Mukherjee agreed. TGF-beta has multiple remodeling roles in the body, and it is difficult at this point to isolate its exact role in aortic disease.
Another hypothesis involves matrix metalloproteinases (MMPs), which are dysregulated in patients with ATAA and may confer some protection, Mukherjee said. Several studies have shown higher plasma levels of certain MMPs in patients with ATAAs. MMPs also were found to be elevated in the thoracic aortic walls of patients with ATAA who had an aortic dissection, as well as in the aortic smooth muscle cells in the intima and media.
In addition, some studies have shown increased levels of MMP-2 in the aortas of patients with ATAAs compared with patients with coronary artery disease.
Adding to the mix of possibilities, “We recently found a gene that’s dysregulated in our aneurysm patients that is very intimately related to atherosclerosis,” Dr. Elefteriades said. “But the work is too preliminary to say anything more at this point.”
“It would be fabulous to prove what it is causing this protection,” Dr. Mukherjee added. “But the truth is we don’t know. These are hypotheses.”
“The most important message from our work is that most clinicians need to dissociate an ATAA from the concept of atherosclerosis,” Dr. Elefteriades said. “The ascending aorta is not an atherosclerotic phenomenon.”
How to Manage Patients With ATAA
What does the distinct character of ATAAs mean for patient management? “Finding a drug to treat ATAAs — to prevent growth, rupture, or dissection — has been like a search for the Holy Grail,” Dr. Elefteriades said. “Statins are not necessary, as this is a non-atherosclerotic process. Although sporadic studies have reported beneficial effects from beta-blockers or angiotensin II receptor blockers (ARBs), this has often been based on ‘soft’ evidence, requiring a combination of outcome measures to achieve significance.”
That said, he noted, “The mainstay, common sense treatment is to keep blood pressure controlled. This is usually achieved by a beta-blocker and an ARB, even if the benefit is not via a direct biologic effect on the aneurysmal degenerative process, but via simple hemodynamics — discouraging rupture by keeping pressure in the aorta low.”
Dr. Mukherjee suggested that these patients should be referred to a specialty aneurysm center where their genes will be evaluated, and then the aneurysm will be followed very closely.
“If the aneurysm is larger than 4.5 cm, we screen the patient every single year, and if they have chest pain, we treat them the same way as we treat other aneurysms,” he said. “As a rule of thumb, if the aneurysm reaches 5 cm, it should come out, although the size at which this should happen may differ between 4.5 cm and 5.5 cm, depending on the patient’s body size.”
As for lifestyle management, Dr. Elefteriades said, “Protection from atherosclerosis and MI won’t go away after the aneurysm is removed. We think it’s in the body’s chemistry. But even though it’s very hard for those patients to have a heart attack, we don’t recommend they eat roast beef every night — although I do think they’d be protected from such lifestyle aberrations.”
For now, he added, “Our team is on a hunt to find a drug to treat ascending disease directly and effectively. We have ongoing laboratory experiments with two drugs undergoing investigation at some level. We hope to embark soon on clinical trials.”
‘A Milestone’
James Hamilton Black III, MD, vice chair of the writing committee for the 2022 American College of Cardiology/American Heart Association Aortic Disease Guideline and chief of Division of Vascular Surgery and Endovascular Therapy at Johns Hopkins Medicine, Baltimore, commented on the review and the concept of ATAA’s atherosclerotic protection.
“The association of ascending aortic aneurysms with a lower risk for MI is an interesting one, but it’s probably influenced, at least in part, by the patient population.” That population is at least partially curated since people are coming to an academic center. In addition, Dr. Black noted, “the patients with ATAAs are younger, and so age may be a confounding factor in the analyses. We wouldn’t expect them to have the same burden of atherosclerosis” as older patients.
Nevertheless, he said, “the findings speak to an emerging body of literature suggesting that although the aorta is a single organ, there are certainly different areas, and these would respond quite differently to environmental or genetic or heritable stressors. This isn’t surprising, and there probably are a lot of factors involved.”
Overall, he said, the findings underscore “the precision medicine approaches we need to take with patients with aortic diseases.”
In a commentary on the team’s review article, published in 2022, John G.T. Augoustides, MD, professor of anesthesiology and critical care at the Perelman School of Medicine in Philadelphia, Pennsylvania, suggested that ATAA’s “silver lining” could advance the understanding of thoracic aortic aneurysm (TAA) management, be integrated with the expanding horizons in hereditary thoracic aortic disease, and might be explored in the context of bicuspid aortic valve disease.
Highlighting the “relative absence” of atherosclerosis in ascending aortic aneurysms and its importance is a “milestone in our understanding,” he concluded. “It is likely that future advances in TAAs will be significantly influenced by this observation.”
Dr. Elefteriades, Dr. Mukherjee, and Dr. Black have no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
Often known as a “silent killer,” ascending thoracic aortic aneurysms (ATAAs) may grow asymptomatically until they rupture, at which point, mortality is over 90%.
But and by extension, for those who have one, a significantly reduced risk for coronary artery disease and myocardial infarction (MI).
“We noticed in the operating room that many patients we worked on who had an ATAA had pristine arteries, like a teenager’s,” said John Elefteriades, MD, William W.L. Glenn Professor of Cardiothoracic Surgery and former chief of cardiothoracic surgery at Yale University and Yale New Haven Hospital, New Haven, Connecticut. “The same was true of the femoral artery, which we use to hook up to the heart-lung machine.”
Elefteriades and colleagues have been investigating the implications of this association for more than two decades. Many of their studies are highlighted in a recent review of the evidence supporting the protective relationship between ATAAs and the development of atherosclerosis and the possible mechanisms driving the relationship.
“We see four different layers of protection,” said Sandip Mukherjee, MD, medical director of the Aortic Institute at Yale New Haven Hospital and a senior editor of the journal AORTA. Mukherjee collaborated with Elefteriades on many of the studies.
The first layer of protection is lower intima-media thickness, specifically, 0.131 mm lower than in individuals without an ATAA. “It may not seem like very much, but one point can actually translate into a 13%-15% decline in the rate of myocardial infarction or stroke,” Dr. Mukherjee said.
The second layer is lower levels of low-density lipoprotein (LDL) cholesterol. Lower LDL cholesterol levels (75 mg/dL) were associated with increased odds of ATAAs (odds ratio [OR], 1.21), whereas elevated levels (150 mg/dL and 200 mg/dL) were associated with decreased odds of ATAAs (OR, 0.62 and 0.29, respectively).
Lower calcification scores for the coronary arteries are the third layer of protection (6.73 vs 9.36 in one study).
The fourth protective layer is a significantly reduced prevalence of coronary artery disease. A study of individuals with ATAA compared to controls found 61 of those with ATAA had coronary artery disease vs 140 of controls, and 11 vs 83 had experienced an MI. Of note, patients with ATAAs were protected despite having higher body mass indices than controls.
Other MI risk factors such as age increased the risk even among those with an ATAA but, again, much less so than among controls; a multivariable binary logistic regression of data in the team’s review showed that patients with ATAAs were 298, 250, and 232 times less likely to have an MI than if they had a family history of MI, dyslipidemia, or hypertension, respectively.
Why the Protection?
The ligamentum arteriosum separates the ascending from the descending (thoracoabdominal) aorta. ATAAs, located above the ligamentum, tend to be pro-aneurysmal but anti-atherosclerotic. In the descending aorta, below the ligamentum, atherosclerotic aneurysms develop.
The differences between the two sections of the aorta originate in the germ layer in the embryo, Dr. Elefteriades said. “The fundamental difference in tissue of origin translates into marked differences in the character of aneurysms in the different aortic segments.”
What specifically underlies the reduced cardiovascular risk? “We don’t really know, but we think that there may be two possible etiologies,” Dr. Mukherjee said. One hypothesis involves transforming growth factor–beta (TGF-beta), which is overexpressed in patients with ATAA and seems to increase their vulnerability to aneurysms while also conferring protection from coronary disease risk.
Some studies have shown differences in cellular responses to TGF-beta between the thoracic and abdominal aorta, including collagen production and contractility. Others have shown that some patients who have had an MI have polymorphisms that decrease their levels of TGF-beta.
Furthermore, TGF-beta plays a key role in the development of the intimal layer, which could underpin the lack of intimal thickening in patients with ATAA.
But overall, studies have been mixed and challenging to interpret, Dr. Elefteriades and Dr. Mukherjee agreed. TGF-beta has multiple remodeling roles in the body, and it is difficult at this point to isolate its exact role in aortic disease.
Another hypothesis involves matrix metalloproteinases (MMPs), which are dysregulated in patients with ATAA and may confer some protection, Mukherjee said. Several studies have shown higher plasma levels of certain MMPs in patients with ATAAs. MMPs also were found to be elevated in the thoracic aortic walls of patients with ATAA who had an aortic dissection, as well as in the aortic smooth muscle cells in the intima and media.
In addition, some studies have shown increased levels of MMP-2 in the aortas of patients with ATAAs compared with patients with coronary artery disease.
Adding to the mix of possibilities, “We recently found a gene that’s dysregulated in our aneurysm patients that is very intimately related to atherosclerosis,” Dr. Elefteriades said. “But the work is too preliminary to say anything more at this point.”
“It would be fabulous to prove what it is causing this protection,” Dr. Mukherjee added. “But the truth is we don’t know. These are hypotheses.”
“The most important message from our work is that most clinicians need to dissociate an ATAA from the concept of atherosclerosis,” Dr. Elefteriades said. “The ascending aorta is not an atherosclerotic phenomenon.”
How to Manage Patients With ATAA
What does the distinct character of ATAAs mean for patient management? “Finding a drug to treat ATAAs — to prevent growth, rupture, or dissection — has been like a search for the Holy Grail,” Dr. Elefteriades said. “Statins are not necessary, as this is a non-atherosclerotic process. Although sporadic studies have reported beneficial effects from beta-blockers or angiotensin II receptor blockers (ARBs), this has often been based on ‘soft’ evidence, requiring a combination of outcome measures to achieve significance.”
That said, he noted, “The mainstay, common sense treatment is to keep blood pressure controlled. This is usually achieved by a beta-blocker and an ARB, even if the benefit is not via a direct biologic effect on the aneurysmal degenerative process, but via simple hemodynamics — discouraging rupture by keeping pressure in the aorta low.”
Dr. Mukherjee suggested that these patients should be referred to a specialty aneurysm center where their genes will be evaluated, and then the aneurysm will be followed very closely.
“If the aneurysm is larger than 4.5 cm, we screen the patient every single year, and if they have chest pain, we treat them the same way as we treat other aneurysms,” he said. “As a rule of thumb, if the aneurysm reaches 5 cm, it should come out, although the size at which this should happen may differ between 4.5 cm and 5.5 cm, depending on the patient’s body size.”
As for lifestyle management, Dr. Elefteriades said, “Protection from atherosclerosis and MI won’t go away after the aneurysm is removed. We think it’s in the body’s chemistry. But even though it’s very hard for those patients to have a heart attack, we don’t recommend they eat roast beef every night — although I do think they’d be protected from such lifestyle aberrations.”
For now, he added, “Our team is on a hunt to find a drug to treat ascending disease directly and effectively. We have ongoing laboratory experiments with two drugs undergoing investigation at some level. We hope to embark soon on clinical trials.”
‘A Milestone’
James Hamilton Black III, MD, vice chair of the writing committee for the 2022 American College of Cardiology/American Heart Association Aortic Disease Guideline and chief of Division of Vascular Surgery and Endovascular Therapy at Johns Hopkins Medicine, Baltimore, commented on the review and the concept of ATAA’s atherosclerotic protection.
“The association of ascending aortic aneurysms with a lower risk for MI is an interesting one, but it’s probably influenced, at least in part, by the patient population.” That population is at least partially curated since people are coming to an academic center. In addition, Dr. Black noted, “the patients with ATAAs are younger, and so age may be a confounding factor in the analyses. We wouldn’t expect them to have the same burden of atherosclerosis” as older patients.
Nevertheless, he said, “the findings speak to an emerging body of literature suggesting that although the aorta is a single organ, there are certainly different areas, and these would respond quite differently to environmental or genetic or heritable stressors. This isn’t surprising, and there probably are a lot of factors involved.”
Overall, he said, the findings underscore “the precision medicine approaches we need to take with patients with aortic diseases.”
In a commentary on the team’s review article, published in 2022, John G.T. Augoustides, MD, professor of anesthesiology and critical care at the Perelman School of Medicine in Philadelphia, Pennsylvania, suggested that ATAA’s “silver lining” could advance the understanding of thoracic aortic aneurysm (TAA) management, be integrated with the expanding horizons in hereditary thoracic aortic disease, and might be explored in the context of bicuspid aortic valve disease.
Highlighting the “relative absence” of atherosclerosis in ascending aortic aneurysms and its importance is a “milestone in our understanding,” he concluded. “It is likely that future advances in TAAs will be significantly influenced by this observation.”
Dr. Elefteriades, Dr. Mukherjee, and Dr. Black have no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
What Is the Best Way to Manage Axial Spondyloarthritis in Primary Care?
When axial spondyloarthritis (SpA) is suspected, a “prompt referral to a rheumatologist” is in order. But with the referral possibly taking several weeks, if not months in some parts of the world, how can primary care practitioners manage patients with this type of chronic back pain in the meantime? And what is the long-term role of the primary care practitioner in managing someone diagnosed with the condition? This news organization asked rheumatologist Marina Magrey, MD, and general internal medicine physician Debra Leizman, MD, for their expert advice.
Steps to Manage Suspected Axial SpA
“As [primary care practitioners] identify patients who they suspect may have axial spondyloarthritis, the first thing they should do is a prompt referral to a rheumatologist so that there is a timely diagnosis,” said Dr. Magrey, who heads up the division of rheumatology at University Hospitals Cleveland Medical Center and is professor of medicine at Case Western Reserve University School of Medicine in Cleveland, Ohio.
Importantly, the referral should “explicitly say that they’re suspecting axial spondyloarthritis” and not just chronic back pain, Dr. Magrey added, otherwise it may not “hit the radar” that patients need to be seen as soon as possible. Results of lab tests such as C-reactive protein, erythrocyte sedimentation rate, and human leukocyte antigen B27, along with basic pelvic imaging results, are useful to note on the referral. “If the patient comes with that information, it makes it much easier for the rheumatologist,” she said.
Additionally,
First-Line Treatment Options
“The goal is to improve the quality of life for our patients: To reduce pain, fatigue, inflammation,” Dr. Magrey noted. “So, starting a nonsteroidal anti-inflammatory drug [NSAID] with physical therapy is very useful” in primary care, she added. These remain the “cornerstone” of treatment for axial SpA even in secondary care.
Dr. Leizman agreed that her “go to” treatment for suspected axial SpA is physical therapy alongside one of the many NSAIDs available, such as naproxen or celecoxib. She may also use topical treatments such as lidocaine or diclofenac.
“I’m not going to start any biologics; I leave that for my rheumatologist,” said Dr. Leizman, who is a senior attending physician in the division of general internal medicine at University Hospitals Cleveland Medical Center and associate professor of medicine at Case Western Reserve University.
“If I think it’s a possibility that the patient will be going on to a biologic; however, I will try to check their TB status, immunizations, and vaccination titers, making sure that the patient is up to date and as healthy otherwise as possible so that they will be primed and ready, hopefully, to go on to the biologics,” she added.
Dr. Magrey cautioned that disease-modifying antirheumatic drugs, such as methotrexate and sulfasalazine, and systemic steroids such as oral prednisone “do not work in axial spondyloarthritis, so they are not recommended.”
Does the Choice of NSAID Matter?
The choice of NSAID is really down to the personal choice of the physician in agreement with the patient, and of course whether the medical insurance will cover it, Dr. Magrey observed. There appears to be little difference between the available NSAIDs, and it doesn’t appear to matter whether they are long-acting and taken once a day — which may be a convenient option for some patients — or short-acting and taken twice a day. The important point is that patients are taking these drugs continuously and not on demand and that they are being given at full dose.
“Start with one NSAID at the maximum strength, and then you try that for 2-4 weeks. If that doesn’t work, switch to another one,” Dr. Magrey advised.
American College of Rheumatology (ACR) guidelines for axial SpA recommend that a trial of at least two NSAIDs is undertaken before any biologic treatment is considered, but because the presentation of axial SpA is so heterogeneous, the decision to escalate treatment — usually to a tumor necrosis factor inhibitor first — is best left until after the referral and the diagnosis had been confirmed, she suggested.
What Type of Physical Therapy Works?
Physical therapy and nonpharmacologic ways to help people are integral to optimal patient management. But these still need to be prescribed and administered by a qualified physiotherapist, which means another, separate referral that can also take time, as it’s important to match the patient to the right physiotherapist, Dr. Leizman observed.
Patients need to be informed about the benefits of regular exercise, and suggesting low-impact exercises for the back can be helpful, Dr. Magrey noted.
“Supervised physical therapy is preferred over unsupervised back exercises,” Dr. Magrey said, summarizing current ACR recommendations, which also suggest that land-based activities are preferred over water-based exercises and group physical therapy rather than home-based exercises, according to the available evidence, although it is of low-to-moderate quality.
What type of physical therapy to recommend really boils down to what services are available, what facilities the patient has access to, and what they feel they are capable of doing or are willing to do.
Back pain can be frustrating for patients, said Dr. Leizman, because they hurt when they move, and there’s not a simple solution of “do this or that and you’ll get better.”
“If it’s possible for a patient to do aqua therapy, that has been a good option for many of my patients who are unable to get moving on land without pain,” she said, and “I’ve had some great success with some yoga therapists who work with my patients.”
Long-term Role of the Primary Care Practitioner
Once referred, patients with axial SpA will usually be seen by their rheumatologists at least twice a year to monitor their response to treatment. Primary care practitioners will also continue to see these people for other reasons and can help monitor for drug toxicity by performing blood and liver function tests, as well as looking for signs of associated conditions such as uveitis, psoriasis, and inflammatory bowel disease and referring patients on to other specialists as required.
Treating the inflammatory back pain may sometimes help treat the related conditions and vice versa, but not always, noted Dr. Leizman. Communication between professionals is thus very important to ensure that everyone is on the same page, and regular updates help enormously.
Dr. Leizman tries to see all her patients regularly, at least once a year, but it can be once or twice a year, depending on their age, how healthy they are, and what underlying conditions they may have that she is also managing along with the inflammatory back condition. It is a balancing act to prevent too many appointments, she said, but also helps patients manage the multiple recommendations.
At these appointments, she’ll not only check on patients’ progress and ensure that they have had all the tests that they should have, but she’ll also discuss general measures that may help with patients’ general health, such as weight control, their ability to manage disease processes with other daily activities of living, and other creative coping mechanisms.
“The weight discussion is never easy, but it is helpful to address the impact of weight if it may be contributing to their discomfort,” Dr. Leizman said. “I also think that there are diets patients can choose that are less inflammatory and that can be beneficial.”
Ultimately, “I want my patients to be on the least amount of medicine possible,” Dr. Leizman said. “If they need medications, I support my rheumatologists’ recommendations. I help my patients as they try whatever works to make them feel better, both the nonpharmaceutical options and the medications,” she said.
“Importantly, I am there for support as a resource and a partner,” Leizman added. “I’m the main quarterback for my patients.”
Key Takeaways
- Prompt referral to a rheumatologist remains key.
- The treatment goal is to improve patients’ quality of life by reducing symptoms such as pain and fatigue.
- Physical therapy and NSAIDs remain first-line treatment in primary care.
- NSAID treatment should be at the full recommended dose and given continuously, not as needed.
- The choice of NSAID does not matter; try switching the NSAID if no effects are seen.
- Physical therapy such as water-based activities and yoga may be beneficial, but exercise programs should be prescribed by a qualified therapist.
- Remember general health advice regarding diet and nutrition can be helpful.
A version of this article appeared on Medscape.com.
When axial spondyloarthritis (SpA) is suspected, a “prompt referral to a rheumatologist” is in order. But with the referral possibly taking several weeks, if not months in some parts of the world, how can primary care practitioners manage patients with this type of chronic back pain in the meantime? And what is the long-term role of the primary care practitioner in managing someone diagnosed with the condition? This news organization asked rheumatologist Marina Magrey, MD, and general internal medicine physician Debra Leizman, MD, for their expert advice.
Steps to Manage Suspected Axial SpA
“As [primary care practitioners] identify patients who they suspect may have axial spondyloarthritis, the first thing they should do is a prompt referral to a rheumatologist so that there is a timely diagnosis,” said Dr. Magrey, who heads up the division of rheumatology at University Hospitals Cleveland Medical Center and is professor of medicine at Case Western Reserve University School of Medicine in Cleveland, Ohio.
Importantly, the referral should “explicitly say that they’re suspecting axial spondyloarthritis” and not just chronic back pain, Dr. Magrey added, otherwise it may not “hit the radar” that patients need to be seen as soon as possible. Results of lab tests such as C-reactive protein, erythrocyte sedimentation rate, and human leukocyte antigen B27, along with basic pelvic imaging results, are useful to note on the referral. “If the patient comes with that information, it makes it much easier for the rheumatologist,” she said.
Additionally,
First-Line Treatment Options
“The goal is to improve the quality of life for our patients: To reduce pain, fatigue, inflammation,” Dr. Magrey noted. “So, starting a nonsteroidal anti-inflammatory drug [NSAID] with physical therapy is very useful” in primary care, she added. These remain the “cornerstone” of treatment for axial SpA even in secondary care.
Dr. Leizman agreed that her “go to” treatment for suspected axial SpA is physical therapy alongside one of the many NSAIDs available, such as naproxen or celecoxib. She may also use topical treatments such as lidocaine or diclofenac.
“I’m not going to start any biologics; I leave that for my rheumatologist,” said Dr. Leizman, who is a senior attending physician in the division of general internal medicine at University Hospitals Cleveland Medical Center and associate professor of medicine at Case Western Reserve University.
“If I think it’s a possibility that the patient will be going on to a biologic; however, I will try to check their TB status, immunizations, and vaccination titers, making sure that the patient is up to date and as healthy otherwise as possible so that they will be primed and ready, hopefully, to go on to the biologics,” she added.
Dr. Magrey cautioned that disease-modifying antirheumatic drugs, such as methotrexate and sulfasalazine, and systemic steroids such as oral prednisone “do not work in axial spondyloarthritis, so they are not recommended.”
Does the Choice of NSAID Matter?
The choice of NSAID is really down to the personal choice of the physician in agreement with the patient, and of course whether the medical insurance will cover it, Dr. Magrey observed. There appears to be little difference between the available NSAIDs, and it doesn’t appear to matter whether they are long-acting and taken once a day — which may be a convenient option for some patients — or short-acting and taken twice a day. The important point is that patients are taking these drugs continuously and not on demand and that they are being given at full dose.
“Start with one NSAID at the maximum strength, and then you try that for 2-4 weeks. If that doesn’t work, switch to another one,” Dr. Magrey advised.
American College of Rheumatology (ACR) guidelines for axial SpA recommend that a trial of at least two NSAIDs is undertaken before any biologic treatment is considered, but because the presentation of axial SpA is so heterogeneous, the decision to escalate treatment — usually to a tumor necrosis factor inhibitor first — is best left until after the referral and the diagnosis had been confirmed, she suggested.
What Type of Physical Therapy Works?
Physical therapy and nonpharmacologic ways to help people are integral to optimal patient management. But these still need to be prescribed and administered by a qualified physiotherapist, which means another, separate referral that can also take time, as it’s important to match the patient to the right physiotherapist, Dr. Leizman observed.
Patients need to be informed about the benefits of regular exercise, and suggesting low-impact exercises for the back can be helpful, Dr. Magrey noted.
“Supervised physical therapy is preferred over unsupervised back exercises,” Dr. Magrey said, summarizing current ACR recommendations, which also suggest that land-based activities are preferred over water-based exercises and group physical therapy rather than home-based exercises, according to the available evidence, although it is of low-to-moderate quality.
What type of physical therapy to recommend really boils down to what services are available, what facilities the patient has access to, and what they feel they are capable of doing or are willing to do.
Back pain can be frustrating for patients, said Dr. Leizman, because they hurt when they move, and there’s not a simple solution of “do this or that and you’ll get better.”
“If it’s possible for a patient to do aqua therapy, that has been a good option for many of my patients who are unable to get moving on land without pain,” she said, and “I’ve had some great success with some yoga therapists who work with my patients.”
Long-term Role of the Primary Care Practitioner
Once referred, patients with axial SpA will usually be seen by their rheumatologists at least twice a year to monitor their response to treatment. Primary care practitioners will also continue to see these people for other reasons and can help monitor for drug toxicity by performing blood and liver function tests, as well as looking for signs of associated conditions such as uveitis, psoriasis, and inflammatory bowel disease and referring patients on to other specialists as required.
Treating the inflammatory back pain may sometimes help treat the related conditions and vice versa, but not always, noted Dr. Leizman. Communication between professionals is thus very important to ensure that everyone is on the same page, and regular updates help enormously.
Dr. Leizman tries to see all her patients regularly, at least once a year, but it can be once or twice a year, depending on their age, how healthy they are, and what underlying conditions they may have that she is also managing along with the inflammatory back condition. It is a balancing act to prevent too many appointments, she said, but also helps patients manage the multiple recommendations.
At these appointments, she’ll not only check on patients’ progress and ensure that they have had all the tests that they should have, but she’ll also discuss general measures that may help with patients’ general health, such as weight control, their ability to manage disease processes with other daily activities of living, and other creative coping mechanisms.
“The weight discussion is never easy, but it is helpful to address the impact of weight if it may be contributing to their discomfort,” Dr. Leizman said. “I also think that there are diets patients can choose that are less inflammatory and that can be beneficial.”
Ultimately, “I want my patients to be on the least amount of medicine possible,” Dr. Leizman said. “If they need medications, I support my rheumatologists’ recommendations. I help my patients as they try whatever works to make them feel better, both the nonpharmaceutical options and the medications,” she said.
“Importantly, I am there for support as a resource and a partner,” Leizman added. “I’m the main quarterback for my patients.”
Key Takeaways
- Prompt referral to a rheumatologist remains key.
- The treatment goal is to improve patients’ quality of life by reducing symptoms such as pain and fatigue.
- Physical therapy and NSAIDs remain first-line treatment in primary care.
- NSAID treatment should be at the full recommended dose and given continuously, not as needed.
- The choice of NSAID does not matter; try switching the NSAID if no effects are seen.
- Physical therapy such as water-based activities and yoga may be beneficial, but exercise programs should be prescribed by a qualified therapist.
- Remember general health advice regarding diet and nutrition can be helpful.
A version of this article appeared on Medscape.com.
When axial spondyloarthritis (SpA) is suspected, a “prompt referral to a rheumatologist” is in order. But with the referral possibly taking several weeks, if not months in some parts of the world, how can primary care practitioners manage patients with this type of chronic back pain in the meantime? And what is the long-term role of the primary care practitioner in managing someone diagnosed with the condition? This news organization asked rheumatologist Marina Magrey, MD, and general internal medicine physician Debra Leizman, MD, for their expert advice.
Steps to Manage Suspected Axial SpA
“As [primary care practitioners] identify patients who they suspect may have axial spondyloarthritis, the first thing they should do is a prompt referral to a rheumatologist so that there is a timely diagnosis,” said Dr. Magrey, who heads up the division of rheumatology at University Hospitals Cleveland Medical Center and is professor of medicine at Case Western Reserve University School of Medicine in Cleveland, Ohio.
Importantly, the referral should “explicitly say that they’re suspecting axial spondyloarthritis” and not just chronic back pain, Dr. Magrey added, otherwise it may not “hit the radar” that patients need to be seen as soon as possible. Results of lab tests such as C-reactive protein, erythrocyte sedimentation rate, and human leukocyte antigen B27, along with basic pelvic imaging results, are useful to note on the referral. “If the patient comes with that information, it makes it much easier for the rheumatologist,” she said.
Additionally,
First-Line Treatment Options
“The goal is to improve the quality of life for our patients: To reduce pain, fatigue, inflammation,” Dr. Magrey noted. “So, starting a nonsteroidal anti-inflammatory drug [NSAID] with physical therapy is very useful” in primary care, she added. These remain the “cornerstone” of treatment for axial SpA even in secondary care.
Dr. Leizman agreed that her “go to” treatment for suspected axial SpA is physical therapy alongside one of the many NSAIDs available, such as naproxen or celecoxib. She may also use topical treatments such as lidocaine or diclofenac.
“I’m not going to start any biologics; I leave that for my rheumatologist,” said Dr. Leizman, who is a senior attending physician in the division of general internal medicine at University Hospitals Cleveland Medical Center and associate professor of medicine at Case Western Reserve University.
“If I think it’s a possibility that the patient will be going on to a biologic; however, I will try to check their TB status, immunizations, and vaccination titers, making sure that the patient is up to date and as healthy otherwise as possible so that they will be primed and ready, hopefully, to go on to the biologics,” she added.
Dr. Magrey cautioned that disease-modifying antirheumatic drugs, such as methotrexate and sulfasalazine, and systemic steroids such as oral prednisone “do not work in axial spondyloarthritis, so they are not recommended.”
Does the Choice of NSAID Matter?
The choice of NSAID is really down to the personal choice of the physician in agreement with the patient, and of course whether the medical insurance will cover it, Dr. Magrey observed. There appears to be little difference between the available NSAIDs, and it doesn’t appear to matter whether they are long-acting and taken once a day — which may be a convenient option for some patients — or short-acting and taken twice a day. The important point is that patients are taking these drugs continuously and not on demand and that they are being given at full dose.
“Start with one NSAID at the maximum strength, and then you try that for 2-4 weeks. If that doesn’t work, switch to another one,” Dr. Magrey advised.
American College of Rheumatology (ACR) guidelines for axial SpA recommend that a trial of at least two NSAIDs is undertaken before any biologic treatment is considered, but because the presentation of axial SpA is so heterogeneous, the decision to escalate treatment — usually to a tumor necrosis factor inhibitor first — is best left until after the referral and the diagnosis had been confirmed, she suggested.
What Type of Physical Therapy Works?
Physical therapy and nonpharmacologic ways to help people are integral to optimal patient management. But these still need to be prescribed and administered by a qualified physiotherapist, which means another, separate referral that can also take time, as it’s important to match the patient to the right physiotherapist, Dr. Leizman observed.
Patients need to be informed about the benefits of regular exercise, and suggesting low-impact exercises for the back can be helpful, Dr. Magrey noted.
“Supervised physical therapy is preferred over unsupervised back exercises,” Dr. Magrey said, summarizing current ACR recommendations, which also suggest that land-based activities are preferred over water-based exercises and group physical therapy rather than home-based exercises, according to the available evidence, although it is of low-to-moderate quality.
What type of physical therapy to recommend really boils down to what services are available, what facilities the patient has access to, and what they feel they are capable of doing or are willing to do.
Back pain can be frustrating for patients, said Dr. Leizman, because they hurt when they move, and there’s not a simple solution of “do this or that and you’ll get better.”
“If it’s possible for a patient to do aqua therapy, that has been a good option for many of my patients who are unable to get moving on land without pain,” she said, and “I’ve had some great success with some yoga therapists who work with my patients.”
Long-term Role of the Primary Care Practitioner
Once referred, patients with axial SpA will usually be seen by their rheumatologists at least twice a year to monitor their response to treatment. Primary care practitioners will also continue to see these people for other reasons and can help monitor for drug toxicity by performing blood and liver function tests, as well as looking for signs of associated conditions such as uveitis, psoriasis, and inflammatory bowel disease and referring patients on to other specialists as required.
Treating the inflammatory back pain may sometimes help treat the related conditions and vice versa, but not always, noted Dr. Leizman. Communication between professionals is thus very important to ensure that everyone is on the same page, and regular updates help enormously.
Dr. Leizman tries to see all her patients regularly, at least once a year, but it can be once or twice a year, depending on their age, how healthy they are, and what underlying conditions they may have that she is also managing along with the inflammatory back condition. It is a balancing act to prevent too many appointments, she said, but also helps patients manage the multiple recommendations.
At these appointments, she’ll not only check on patients’ progress and ensure that they have had all the tests that they should have, but she’ll also discuss general measures that may help with patients’ general health, such as weight control, their ability to manage disease processes with other daily activities of living, and other creative coping mechanisms.
“The weight discussion is never easy, but it is helpful to address the impact of weight if it may be contributing to their discomfort,” Dr. Leizman said. “I also think that there are diets patients can choose that are less inflammatory and that can be beneficial.”
Ultimately, “I want my patients to be on the least amount of medicine possible,” Dr. Leizman said. “If they need medications, I support my rheumatologists’ recommendations. I help my patients as they try whatever works to make them feel better, both the nonpharmaceutical options and the medications,” she said.
“Importantly, I am there for support as a resource and a partner,” Leizman added. “I’m the main quarterback for my patients.”
Key Takeaways
- Prompt referral to a rheumatologist remains key.
- The treatment goal is to improve patients’ quality of life by reducing symptoms such as pain and fatigue.
- Physical therapy and NSAIDs remain first-line treatment in primary care.
- NSAID treatment should be at the full recommended dose and given continuously, not as needed.
- The choice of NSAID does not matter; try switching the NSAID if no effects are seen.
- Physical therapy such as water-based activities and yoga may be beneficial, but exercise programs should be prescribed by a qualified therapist.
- Remember general health advice regarding diet and nutrition can be helpful.
A version of this article appeared on Medscape.com.
Migratory Nodules in a Traveler
The Diagnosis: Gnathostomiasis
The biopsy demonstrated a dense, eosinophilic, granulomatous infiltrate surrounding sections of a parasite with skeletal muscle bundles and intestines containing a brush border and luminal debris (Figure), which was consistent with a diagnosis of gnathostomiasis. Upon further questioning, he revealed that while in Peru he frequently consumed ceviche, which is a dish typically made from fresh raw fish cured in lemon or lime juice. He subsequently was treated with oral ivermectin 0.2 mg/kg once daily for 2 days with no evidence of recurrence 12 months later.
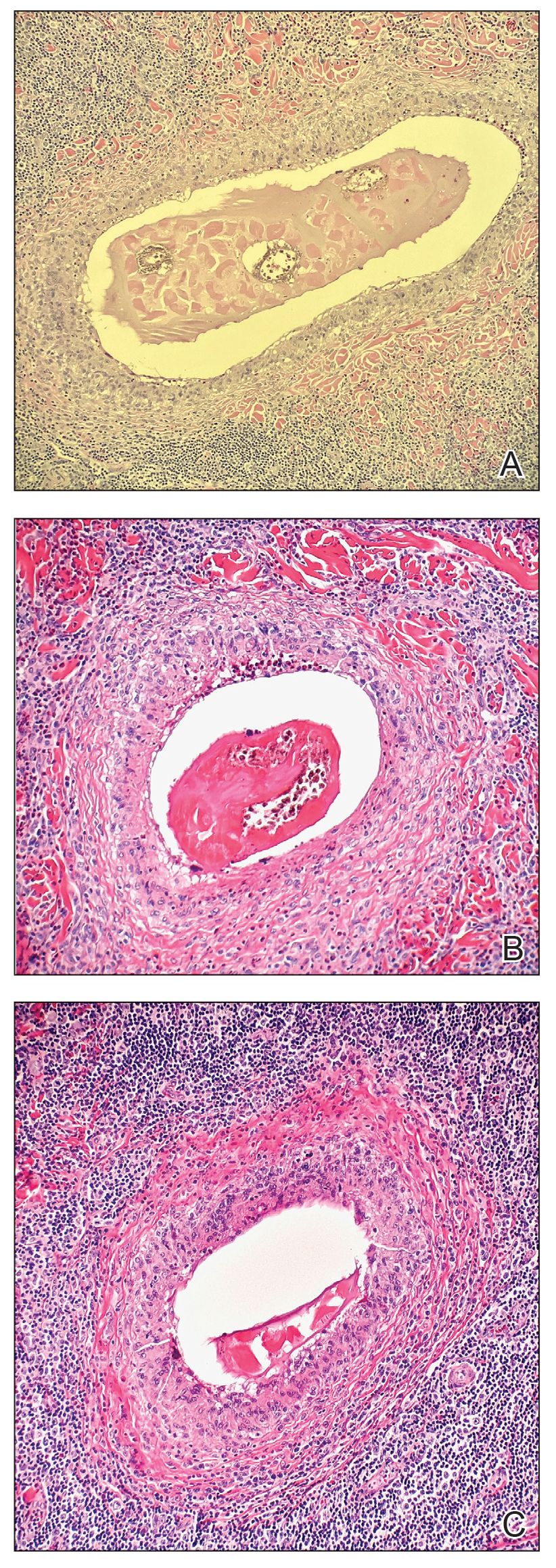
Cutaneous gnathostomiasis is the most common manifestation of infection caused by the third-stage larvae of the genus Gnathostoma. The nematode is endemic to tropical and subtropical regions of Japan and Southeast Asia, particularly Thailand. The disease has been increasingly observed in Central and South America. Humans can become infected through ingestion of undercooked meats, particularly freshwater fish but also poultry, snakes, or frogs. Few cases have been reported in North America and Europe presumably due to more stringent regulations governing the sourcing and storage of fish for consumption.1-3 Restaurants in endemic regions also may use cheaper local freshwater or brackish fish compared to restaurants in the West, which use more expensive saltwater fish that do not harbor Gnathostoma species.1 There is a false belief among restauranteurs and consumers that the larvae can be reliably killed by marinating meat in citrus juice or with concurrent consumption of alcohol or hot spices.2 Adequately cooking or freezing meat to 20 °C for 3 to 5 days are the only effective ways to ensure that the larvae are killed.1-3
The parasite requires its natural definitive hosts—fish-eating mammals such as pigs, cats, and dogs—to complete its life cycle and reproduce. Humans are accidental hosts in whom the parasite fails to reach sexual maturity.1-3 Consequently, symptoms commonly are due to the migration of only 1 larva, but occasionally infection with 2 or more has been observed.1,4
Human infection initially may result in malaise, fever, anorexia, abdominal pain, nausea, vomiting, and diarrhea as the parasite migrates through the stomach, intestines, and liver. After 2 to 4 weeks, larvae may reach the skin where they most commonly create ill-defined, erythematous, indurated, round or oval plaques or nodules described as nodular migratory panniculitis. These lesions tend to develop on the trunk or arms and correspond to the location of the migrating worm.1,3,5 The larvae have been observed to migrate at 1 cm/h.6 Symptoms often wax and wane, with individual nodules lasting approximately 1 to 2 weeks. Uniquely, larval migration can result in a trail of subcutaneous hemorrhage that is considered pathognomonic and helps to differentiate gnathostomiasis from other forms of parasitosis such as strongyloidiasis and sparganosis.1,3 Larvae are highly motile and invasive, and they are capable of producing a wide range of symptoms affecting virtually any part of the body.1,2 Depending on the anatomic location of the migrating worm, infection also may result in neurologic, gastrointestinal, pulmonary, or ocular symptoms.1-3,7 Eosinophilia is common but can subside in the chronic stage, as seen in our patient.1
The classic triad of intermittent migratory nodules, eosinophilia, and a history of travel to Southeast Asia or another endemic region should raise suspicion for gnathostomiasis.1-3,5,7 Unfortunately, confirmatory testing such as Gnathostoma serology is not readily available in the United States, and available serologic tests demonstrate frequent false positives and incomplete crossreactivity.1,2,8 Accordingly, the diagnosis most commonly is solidified by combining cardinal clinical features with histologic findings of a dense eosinophilic inflammatory infiltrate involving the dermis and hypodermis.2,5 In one study, the larva itself was only found in 12 of 66 (18%) skin biopsy specimens from patients with gnathostomiasis.5 If the larva is detected within the sections, it ranges from 2.5 to 12.5 mm in length and 0.4 to 1.2 mm in width and can exhibit cuticular spines, intestinal cells, and characteristic large lateral chords.1,5
The treatment of choice is surgical removal of the worm. Oral albendazole (400–800 mg/d for 21 days) also is considered a first-line treatment and results in clinical cure in approximately 90% of cases. Two doses of oral ivermectin (0.2 mg/kg) spaced 24 to 48 hours apart is an acceptable alternative with comparable efficacy.1-3 Care should be taken if involvement of the central nervous system is suspected, as antihelminthic treatment theoretically could be deleterious due to an inflammatory response to the dying larvae.1,2,9
In the differential diagnosis, loiasis can resemble gnathostomiasis, but the former is endemic to Africa.3 Cutaneous larva migrans most frequently is caused by hookworms from the genus Ancylostoma, which classically leads to superficial serpiginous linear plaques that migrate at a rate of several millimeters per day. However, the larvae are believed to lack the collagenase enzyme required to penetrate the epidermal basement membrane and thus are not capable of producing deep-seated nodules or visceral symptoms.3 Strongyloidiasis (larva currens) generally exhibits a more linear morphology, and infection would result in positive Strongyloides serology.7 Erythema nodosum is a septal panniculitis that can be triggered by infection, pregnancy, medications, connective tissue diseases, inflammatory conditions, and underlying malignancy.10
- Herman JS, Chiodini PL. Gnathostomiasis, another emerging imported disease. Clin Microbiol Rev. 2009;22:484-492.
- Liu GH, Sun MM, Elsheikha HM, et al. Human gnathostomiasis: a neglected food-borne zoonosis. Parasit Vectors. 2020;13:616.
- Tyring SK. Gnathostomiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. 2nd ed. Elsevier; 2017:77-78.
- Rusnak JM, Lucey DR. Clinical gnathostomiasis: case report and review of the English-language literature. Clin Infect Dis. 1993;16:33-50.
- Magaña M, Messina M, Bustamante F, et al. Gnathostomiasis: clinicopathologic study. Am J Dermatopathol. 2004;26:91-95.
- Chandenier J, Husson J, Canaple S, et al. Medullary gnathostomiasis in a white patient: use of immunodiagnosis and magnetic resonance imaging. Clin Infect Dis. 2001;32:E154-E157.
- Hamilton WL, Agranoff D. Imported gnathostomiasis manifesting as cutaneous larva migrans and Löffler’s syndrome. BMJ Case Rep. 2018;2018:bcr2017223132.
- Neumayr A, Ollague J, Bravo F, et al. Cross-reactivity pattern of Asian and American human gnathostomiasis in western blot assays using crude antigens prepared from Gnathostoma spinigerum and Gnathostoma binucleatum third-stage larvae. Am J Trop Med Hyg. 2016;95:413-416.
- Kraivichian K, Nuchprayoon S, Sitichalernchai P, et al. Treatment of cutaneous gnathostomiasis with ivermectin. Am J Trop Med Hyg. 2004;71:623-628.
- Pérez-Garza DM, Chavez-Alvarez S, Ocampo-Candiani J, et al. Erythema nodosum: a practical approach and diagnostic algorithm. Am J Clin Dermatol. 2021;22:367-378.
The Diagnosis: Gnathostomiasis
The biopsy demonstrated a dense, eosinophilic, granulomatous infiltrate surrounding sections of a parasite with skeletal muscle bundles and intestines containing a brush border and luminal debris (Figure), which was consistent with a diagnosis of gnathostomiasis. Upon further questioning, he revealed that while in Peru he frequently consumed ceviche, which is a dish typically made from fresh raw fish cured in lemon or lime juice. He subsequently was treated with oral ivermectin 0.2 mg/kg once daily for 2 days with no evidence of recurrence 12 months later.

Cutaneous gnathostomiasis is the most common manifestation of infection caused by the third-stage larvae of the genus Gnathostoma. The nematode is endemic to tropical and subtropical regions of Japan and Southeast Asia, particularly Thailand. The disease has been increasingly observed in Central and South America. Humans can become infected through ingestion of undercooked meats, particularly freshwater fish but also poultry, snakes, or frogs. Few cases have been reported in North America and Europe presumably due to more stringent regulations governing the sourcing and storage of fish for consumption.1-3 Restaurants in endemic regions also may use cheaper local freshwater or brackish fish compared to restaurants in the West, which use more expensive saltwater fish that do not harbor Gnathostoma species.1 There is a false belief among restauranteurs and consumers that the larvae can be reliably killed by marinating meat in citrus juice or with concurrent consumption of alcohol or hot spices.2 Adequately cooking or freezing meat to 20 °C for 3 to 5 days are the only effective ways to ensure that the larvae are killed.1-3
The parasite requires its natural definitive hosts—fish-eating mammals such as pigs, cats, and dogs—to complete its life cycle and reproduce. Humans are accidental hosts in whom the parasite fails to reach sexual maturity.1-3 Consequently, symptoms commonly are due to the migration of only 1 larva, but occasionally infection with 2 or more has been observed.1,4
Human infection initially may result in malaise, fever, anorexia, abdominal pain, nausea, vomiting, and diarrhea as the parasite migrates through the stomach, intestines, and liver. After 2 to 4 weeks, larvae may reach the skin where they most commonly create ill-defined, erythematous, indurated, round or oval plaques or nodules described as nodular migratory panniculitis. These lesions tend to develop on the trunk or arms and correspond to the location of the migrating worm.1,3,5 The larvae have been observed to migrate at 1 cm/h.6 Symptoms often wax and wane, with individual nodules lasting approximately 1 to 2 weeks. Uniquely, larval migration can result in a trail of subcutaneous hemorrhage that is considered pathognomonic and helps to differentiate gnathostomiasis from other forms of parasitosis such as strongyloidiasis and sparganosis.1,3 Larvae are highly motile and invasive, and they are capable of producing a wide range of symptoms affecting virtually any part of the body.1,2 Depending on the anatomic location of the migrating worm, infection also may result in neurologic, gastrointestinal, pulmonary, or ocular symptoms.1-3,7 Eosinophilia is common but can subside in the chronic stage, as seen in our patient.1
The classic triad of intermittent migratory nodules, eosinophilia, and a history of travel to Southeast Asia or another endemic region should raise suspicion for gnathostomiasis.1-3,5,7 Unfortunately, confirmatory testing such as Gnathostoma serology is not readily available in the United States, and available serologic tests demonstrate frequent false positives and incomplete crossreactivity.1,2,8 Accordingly, the diagnosis most commonly is solidified by combining cardinal clinical features with histologic findings of a dense eosinophilic inflammatory infiltrate involving the dermis and hypodermis.2,5 In one study, the larva itself was only found in 12 of 66 (18%) skin biopsy specimens from patients with gnathostomiasis.5 If the larva is detected within the sections, it ranges from 2.5 to 12.5 mm in length and 0.4 to 1.2 mm in width and can exhibit cuticular spines, intestinal cells, and characteristic large lateral chords.1,5
The treatment of choice is surgical removal of the worm. Oral albendazole (400–800 mg/d for 21 days) also is considered a first-line treatment and results in clinical cure in approximately 90% of cases. Two doses of oral ivermectin (0.2 mg/kg) spaced 24 to 48 hours apart is an acceptable alternative with comparable efficacy.1-3 Care should be taken if involvement of the central nervous system is suspected, as antihelminthic treatment theoretically could be deleterious due to an inflammatory response to the dying larvae.1,2,9
In the differential diagnosis, loiasis can resemble gnathostomiasis, but the former is endemic to Africa.3 Cutaneous larva migrans most frequently is caused by hookworms from the genus Ancylostoma, which classically leads to superficial serpiginous linear plaques that migrate at a rate of several millimeters per day. However, the larvae are believed to lack the collagenase enzyme required to penetrate the epidermal basement membrane and thus are not capable of producing deep-seated nodules or visceral symptoms.3 Strongyloidiasis (larva currens) generally exhibits a more linear morphology, and infection would result in positive Strongyloides serology.7 Erythema nodosum is a septal panniculitis that can be triggered by infection, pregnancy, medications, connective tissue diseases, inflammatory conditions, and underlying malignancy.10
The Diagnosis: Gnathostomiasis
The biopsy demonstrated a dense, eosinophilic, granulomatous infiltrate surrounding sections of a parasite with skeletal muscle bundles and intestines containing a brush border and luminal debris (Figure), which was consistent with a diagnosis of gnathostomiasis. Upon further questioning, he revealed that while in Peru he frequently consumed ceviche, which is a dish typically made from fresh raw fish cured in lemon or lime juice. He subsequently was treated with oral ivermectin 0.2 mg/kg once daily for 2 days with no evidence of recurrence 12 months later.

Cutaneous gnathostomiasis is the most common manifestation of infection caused by the third-stage larvae of the genus Gnathostoma. The nematode is endemic to tropical and subtropical regions of Japan and Southeast Asia, particularly Thailand. The disease has been increasingly observed in Central and South America. Humans can become infected through ingestion of undercooked meats, particularly freshwater fish but also poultry, snakes, or frogs. Few cases have been reported in North America and Europe presumably due to more stringent regulations governing the sourcing and storage of fish for consumption.1-3 Restaurants in endemic regions also may use cheaper local freshwater or brackish fish compared to restaurants in the West, which use more expensive saltwater fish that do not harbor Gnathostoma species.1 There is a false belief among restauranteurs and consumers that the larvae can be reliably killed by marinating meat in citrus juice or with concurrent consumption of alcohol or hot spices.2 Adequately cooking or freezing meat to 20 °C for 3 to 5 days are the only effective ways to ensure that the larvae are killed.1-3
The parasite requires its natural definitive hosts—fish-eating mammals such as pigs, cats, and dogs—to complete its life cycle and reproduce. Humans are accidental hosts in whom the parasite fails to reach sexual maturity.1-3 Consequently, symptoms commonly are due to the migration of only 1 larva, but occasionally infection with 2 or more has been observed.1,4
Human infection initially may result in malaise, fever, anorexia, abdominal pain, nausea, vomiting, and diarrhea as the parasite migrates through the stomach, intestines, and liver. After 2 to 4 weeks, larvae may reach the skin where they most commonly create ill-defined, erythematous, indurated, round or oval plaques or nodules described as nodular migratory panniculitis. These lesions tend to develop on the trunk or arms and correspond to the location of the migrating worm.1,3,5 The larvae have been observed to migrate at 1 cm/h.6 Symptoms often wax and wane, with individual nodules lasting approximately 1 to 2 weeks. Uniquely, larval migration can result in a trail of subcutaneous hemorrhage that is considered pathognomonic and helps to differentiate gnathostomiasis from other forms of parasitosis such as strongyloidiasis and sparganosis.1,3 Larvae are highly motile and invasive, and they are capable of producing a wide range of symptoms affecting virtually any part of the body.1,2 Depending on the anatomic location of the migrating worm, infection also may result in neurologic, gastrointestinal, pulmonary, or ocular symptoms.1-3,7 Eosinophilia is common but can subside in the chronic stage, as seen in our patient.1
The classic triad of intermittent migratory nodules, eosinophilia, and a history of travel to Southeast Asia or another endemic region should raise suspicion for gnathostomiasis.1-3,5,7 Unfortunately, confirmatory testing such as Gnathostoma serology is not readily available in the United States, and available serologic tests demonstrate frequent false positives and incomplete crossreactivity.1,2,8 Accordingly, the diagnosis most commonly is solidified by combining cardinal clinical features with histologic findings of a dense eosinophilic inflammatory infiltrate involving the dermis and hypodermis.2,5 In one study, the larva itself was only found in 12 of 66 (18%) skin biopsy specimens from patients with gnathostomiasis.5 If the larva is detected within the sections, it ranges from 2.5 to 12.5 mm in length and 0.4 to 1.2 mm in width and can exhibit cuticular spines, intestinal cells, and characteristic large lateral chords.1,5
The treatment of choice is surgical removal of the worm. Oral albendazole (400–800 mg/d for 21 days) also is considered a first-line treatment and results in clinical cure in approximately 90% of cases. Two doses of oral ivermectin (0.2 mg/kg) spaced 24 to 48 hours apart is an acceptable alternative with comparable efficacy.1-3 Care should be taken if involvement of the central nervous system is suspected, as antihelminthic treatment theoretically could be deleterious due to an inflammatory response to the dying larvae.1,2,9
In the differential diagnosis, loiasis can resemble gnathostomiasis, but the former is endemic to Africa.3 Cutaneous larva migrans most frequently is caused by hookworms from the genus Ancylostoma, which classically leads to superficial serpiginous linear plaques that migrate at a rate of several millimeters per day. However, the larvae are believed to lack the collagenase enzyme required to penetrate the epidermal basement membrane and thus are not capable of producing deep-seated nodules or visceral symptoms.3 Strongyloidiasis (larva currens) generally exhibits a more linear morphology, and infection would result in positive Strongyloides serology.7 Erythema nodosum is a septal panniculitis that can be triggered by infection, pregnancy, medications, connective tissue diseases, inflammatory conditions, and underlying malignancy.10
- Herman JS, Chiodini PL. Gnathostomiasis, another emerging imported disease. Clin Microbiol Rev. 2009;22:484-492.
- Liu GH, Sun MM, Elsheikha HM, et al. Human gnathostomiasis: a neglected food-borne zoonosis. Parasit Vectors. 2020;13:616.
- Tyring SK. Gnathostomiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. 2nd ed. Elsevier; 2017:77-78.
- Rusnak JM, Lucey DR. Clinical gnathostomiasis: case report and review of the English-language literature. Clin Infect Dis. 1993;16:33-50.
- Magaña M, Messina M, Bustamante F, et al. Gnathostomiasis: clinicopathologic study. Am J Dermatopathol. 2004;26:91-95.
- Chandenier J, Husson J, Canaple S, et al. Medullary gnathostomiasis in a white patient: use of immunodiagnosis and magnetic resonance imaging. Clin Infect Dis. 2001;32:E154-E157.
- Hamilton WL, Agranoff D. Imported gnathostomiasis manifesting as cutaneous larva migrans and Löffler’s syndrome. BMJ Case Rep. 2018;2018:bcr2017223132.
- Neumayr A, Ollague J, Bravo F, et al. Cross-reactivity pattern of Asian and American human gnathostomiasis in western blot assays using crude antigens prepared from Gnathostoma spinigerum and Gnathostoma binucleatum third-stage larvae. Am J Trop Med Hyg. 2016;95:413-416.
- Kraivichian K, Nuchprayoon S, Sitichalernchai P, et al. Treatment of cutaneous gnathostomiasis with ivermectin. Am J Trop Med Hyg. 2004;71:623-628.
- Pérez-Garza DM, Chavez-Alvarez S, Ocampo-Candiani J, et al. Erythema nodosum: a practical approach and diagnostic algorithm. Am J Clin Dermatol. 2021;22:367-378.
- Herman JS, Chiodini PL. Gnathostomiasis, another emerging imported disease. Clin Microbiol Rev. 2009;22:484-492.
- Liu GH, Sun MM, Elsheikha HM, et al. Human gnathostomiasis: a neglected food-borne zoonosis. Parasit Vectors. 2020;13:616.
- Tyring SK. Gnathostomiasis. In: Tyring SK, Lupi O, Hengge UR, eds. Tropical Dermatology. 2nd ed. Elsevier; 2017:77-78.
- Rusnak JM, Lucey DR. Clinical gnathostomiasis: case report and review of the English-language literature. Clin Infect Dis. 1993;16:33-50.
- Magaña M, Messina M, Bustamante F, et al. Gnathostomiasis: clinicopathologic study. Am J Dermatopathol. 2004;26:91-95.
- Chandenier J, Husson J, Canaple S, et al. Medullary gnathostomiasis in a white patient: use of immunodiagnosis and magnetic resonance imaging. Clin Infect Dis. 2001;32:E154-E157.
- Hamilton WL, Agranoff D. Imported gnathostomiasis manifesting as cutaneous larva migrans and Löffler’s syndrome. BMJ Case Rep. 2018;2018:bcr2017223132.
- Neumayr A, Ollague J, Bravo F, et al. Cross-reactivity pattern of Asian and American human gnathostomiasis in western blot assays using crude antigens prepared from Gnathostoma spinigerum and Gnathostoma binucleatum third-stage larvae. Am J Trop Med Hyg. 2016;95:413-416.
- Kraivichian K, Nuchprayoon S, Sitichalernchai P, et al. Treatment of cutaneous gnathostomiasis with ivermectin. Am J Trop Med Hyg. 2004;71:623-628.
- Pérez-Garza DM, Chavez-Alvarez S, Ocampo-Candiani J, et al. Erythema nodosum: a practical approach and diagnostic algorithm. Am J Clin Dermatol. 2021;22:367-378.
A 41-year-old man presented to a dermatology clinic in the United States with a migratory subcutaneous nodule overlying the left upper chest that initially developed 12 months prior and continued to migrate along the trunk and proximal aspect of the arms. The patient had spent the last 3 years residing in Peru. He never observed more than 1 nodule at a time and denied associated fever, headache, visual changes, chest pain, cough, abdominal pain, and diarrhea. Laboratory studies including a blood eosinophil count and serum Strongyloides immunoglobulins were within reference range. An excisional biopsy was performed.
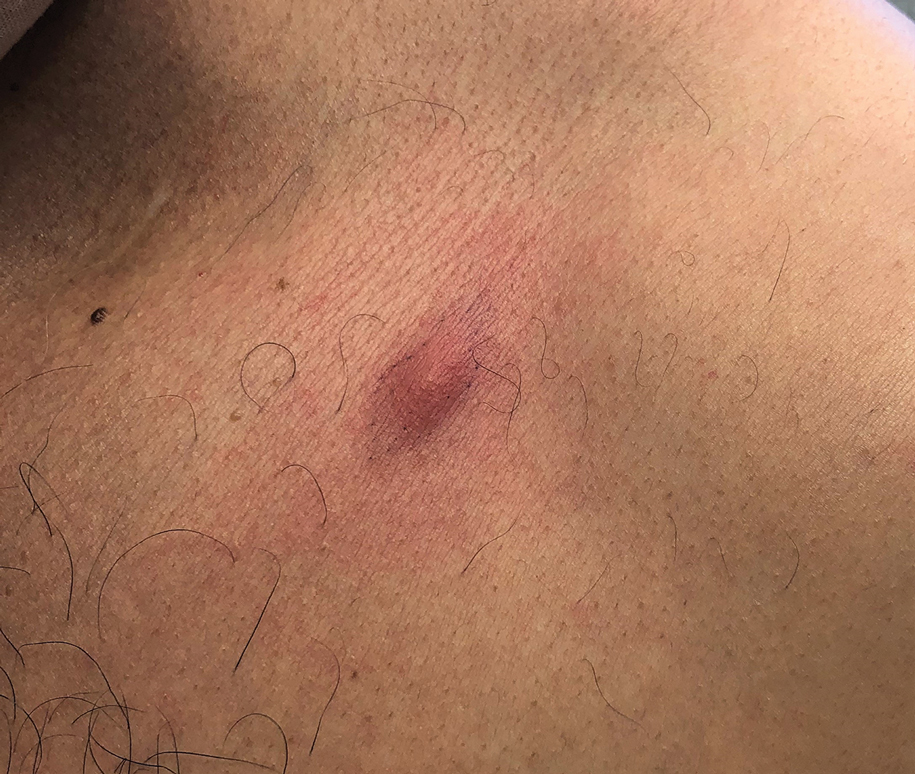
Public Citizen seeks stronger warning for Botox, related products
.
The nonprofit watchdog group successfully petitioned the FDA in 2008 to require a warning for Botox and related products regarding the risk of distant spread of the toxin. In its latest petition to the agency, it says that the injectables need additional warnings about the possibility of iatrogenic botulism with initial and repeated doses and that individuals who contract the condition may need botulinum antitoxin to avert temporary muscle paralysis, hospitalization, and death.
The current warning does not contain any information about the potential need for antitoxin and downplays the need for giving antitoxin in the settings of excessive dosing, accidental injection, and oral ingestion, said Public Citizen.
“Our petition is based on clear postmarketing evidence that refutes industry propaganda claiming that Botox and related drugs are ‘always safe’ and that no ‘definitive’ cases of botulism have occurred with recommended doses,” Azza AbuDagga, PhD, health services researcher at Public Citizen’s Health Research Group, said in a statement.
Public Citizen said that using data from the FDA’s Adverse Event Reporting System (FAERS), it found 5414 reports of serious outcomes from botulinum toxin products from January 1989 through March 2021. Almost 22% involved cosmetic indications and about 78% involved therapeutic indications.
Of the 5414 reports, 121 (2%) specified botulism as an adverse reaction; 89 involved therapeutic uses of a botulinum toxin products, and 32 involved cosmetic uses. Many of those 121 reports involved doses within the recommended range for the indication, according to Public Citizen.
The group is also asking the FDA to remove what it calls misleading promotional statements in the labeling of Botox and Botox Cosmetic and from the medication guides for those products. The labels state that there have been “no definitive serious adverse event reports of distant spread of toxin effect” with either the cosmetic use or for use in treating chronic migraine, severe underarm sweating, blepharospasm, or strabismus. These statements do not appear in similar labeling in other countries, such as Canada and the United Kingdom, said Public Citizen.
“The FDA needs to implement our two requested actions quickly to warn the public in unambiguous terms about the risk of botulism associated with the use of Botox and related drugs,” Dr. AbuDagga said in the Public Citizen statement. “This will allow health care professionals and patients to make more informed decisions about the benefit-risk profile of these widely used drugs.”
The Public Citizen petition would apply to all seven approved botulinum toxin biological products: abobotulinumtoxinA (Dysport), daxibotulinumtoxinA-lanm (Daxxify), incobotulinumtoxinA (Xeomin), onabotulinumtoxinA (Botox, Botox Cosmetic), prabotulinumtoxinA-xvfs (Jeuveau) and rimabotulinumtoxinB (Myobloc).
An FDA spokesperson said the agency is reviewing the citizen petition, and that generally the agency does not comment on pending petitions. “When we respond to the petition, we will respond directly to the petitioner and post the response in the designated agency docket,” the spokesperson told this news organization. At press time, Botox manufacturer AbbVie had not responded to a request for a comment.
Botulinum toxin is the most-used product for nonsurgical cosmetic procedures, according to the International Society of Aesthetic Plastic Surgery (ISAPS). The ISAPS reported that there were more than 7 million botulinum toxin procedures performed by plastic surgeons worldwide in 2021.
The American Society of Plastic Surgery reported that its members performed 4.4 million Botox procedures in 2020, while the American Society of Dermatologic Surgery (ASDS) said its members performed 2.3 million wrinkle-relaxing procedures in 2019, a 60% increase since 2012.
.
The nonprofit watchdog group successfully petitioned the FDA in 2008 to require a warning for Botox and related products regarding the risk of distant spread of the toxin. In its latest petition to the agency, it says that the injectables need additional warnings about the possibility of iatrogenic botulism with initial and repeated doses and that individuals who contract the condition may need botulinum antitoxin to avert temporary muscle paralysis, hospitalization, and death.
The current warning does not contain any information about the potential need for antitoxin and downplays the need for giving antitoxin in the settings of excessive dosing, accidental injection, and oral ingestion, said Public Citizen.
“Our petition is based on clear postmarketing evidence that refutes industry propaganda claiming that Botox and related drugs are ‘always safe’ and that no ‘definitive’ cases of botulism have occurred with recommended doses,” Azza AbuDagga, PhD, health services researcher at Public Citizen’s Health Research Group, said in a statement.
Public Citizen said that using data from the FDA’s Adverse Event Reporting System (FAERS), it found 5414 reports of serious outcomes from botulinum toxin products from January 1989 through March 2021. Almost 22% involved cosmetic indications and about 78% involved therapeutic indications.
Of the 5414 reports, 121 (2%) specified botulism as an adverse reaction; 89 involved therapeutic uses of a botulinum toxin products, and 32 involved cosmetic uses. Many of those 121 reports involved doses within the recommended range for the indication, according to Public Citizen.
The group is also asking the FDA to remove what it calls misleading promotional statements in the labeling of Botox and Botox Cosmetic and from the medication guides for those products. The labels state that there have been “no definitive serious adverse event reports of distant spread of toxin effect” with either the cosmetic use or for use in treating chronic migraine, severe underarm sweating, blepharospasm, or strabismus. These statements do not appear in similar labeling in other countries, such as Canada and the United Kingdom, said Public Citizen.
“The FDA needs to implement our two requested actions quickly to warn the public in unambiguous terms about the risk of botulism associated with the use of Botox and related drugs,” Dr. AbuDagga said in the Public Citizen statement. “This will allow health care professionals and patients to make more informed decisions about the benefit-risk profile of these widely used drugs.”
The Public Citizen petition would apply to all seven approved botulinum toxin biological products: abobotulinumtoxinA (Dysport), daxibotulinumtoxinA-lanm (Daxxify), incobotulinumtoxinA (Xeomin), onabotulinumtoxinA (Botox, Botox Cosmetic), prabotulinumtoxinA-xvfs (Jeuveau) and rimabotulinumtoxinB (Myobloc).
An FDA spokesperson said the agency is reviewing the citizen petition, and that generally the agency does not comment on pending petitions. “When we respond to the petition, we will respond directly to the petitioner and post the response in the designated agency docket,” the spokesperson told this news organization. At press time, Botox manufacturer AbbVie had not responded to a request for a comment.
Botulinum toxin is the most-used product for nonsurgical cosmetic procedures, according to the International Society of Aesthetic Plastic Surgery (ISAPS). The ISAPS reported that there were more than 7 million botulinum toxin procedures performed by plastic surgeons worldwide in 2021.
The American Society of Plastic Surgery reported that its members performed 4.4 million Botox procedures in 2020, while the American Society of Dermatologic Surgery (ASDS) said its members performed 2.3 million wrinkle-relaxing procedures in 2019, a 60% increase since 2012.
.
The nonprofit watchdog group successfully petitioned the FDA in 2008 to require a warning for Botox and related products regarding the risk of distant spread of the toxin. In its latest petition to the agency, it says that the injectables need additional warnings about the possibility of iatrogenic botulism with initial and repeated doses and that individuals who contract the condition may need botulinum antitoxin to avert temporary muscle paralysis, hospitalization, and death.
The current warning does not contain any information about the potential need for antitoxin and downplays the need for giving antitoxin in the settings of excessive dosing, accidental injection, and oral ingestion, said Public Citizen.
“Our petition is based on clear postmarketing evidence that refutes industry propaganda claiming that Botox and related drugs are ‘always safe’ and that no ‘definitive’ cases of botulism have occurred with recommended doses,” Azza AbuDagga, PhD, health services researcher at Public Citizen’s Health Research Group, said in a statement.
Public Citizen said that using data from the FDA’s Adverse Event Reporting System (FAERS), it found 5414 reports of serious outcomes from botulinum toxin products from January 1989 through March 2021. Almost 22% involved cosmetic indications and about 78% involved therapeutic indications.
Of the 5414 reports, 121 (2%) specified botulism as an adverse reaction; 89 involved therapeutic uses of a botulinum toxin products, and 32 involved cosmetic uses. Many of those 121 reports involved doses within the recommended range for the indication, according to Public Citizen.
The group is also asking the FDA to remove what it calls misleading promotional statements in the labeling of Botox and Botox Cosmetic and from the medication guides for those products. The labels state that there have been “no definitive serious adverse event reports of distant spread of toxin effect” with either the cosmetic use or for use in treating chronic migraine, severe underarm sweating, blepharospasm, or strabismus. These statements do not appear in similar labeling in other countries, such as Canada and the United Kingdom, said Public Citizen.
“The FDA needs to implement our two requested actions quickly to warn the public in unambiguous terms about the risk of botulism associated with the use of Botox and related drugs,” Dr. AbuDagga said in the Public Citizen statement. “This will allow health care professionals and patients to make more informed decisions about the benefit-risk profile of these widely used drugs.”
The Public Citizen petition would apply to all seven approved botulinum toxin biological products: abobotulinumtoxinA (Dysport), daxibotulinumtoxinA-lanm (Daxxify), incobotulinumtoxinA (Xeomin), onabotulinumtoxinA (Botox, Botox Cosmetic), prabotulinumtoxinA-xvfs (Jeuveau) and rimabotulinumtoxinB (Myobloc).
An FDA spokesperson said the agency is reviewing the citizen petition, and that generally the agency does not comment on pending petitions. “When we respond to the petition, we will respond directly to the petitioner and post the response in the designated agency docket,” the spokesperson told this news organization. At press time, Botox manufacturer AbbVie had not responded to a request for a comment.
Botulinum toxin is the most-used product for nonsurgical cosmetic procedures, according to the International Society of Aesthetic Plastic Surgery (ISAPS). The ISAPS reported that there were more than 7 million botulinum toxin procedures performed by plastic surgeons worldwide in 2021.
The American Society of Plastic Surgery reported that its members performed 4.4 million Botox procedures in 2020, while the American Society of Dermatologic Surgery (ASDS) said its members performed 2.3 million wrinkle-relaxing procedures in 2019, a 60% increase since 2012.
Clinical Takeaways in Thrombocytopenia From ASH 2023
The clinical takeaways in immune thrombocytopenia (ITP) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition include the relative merits of advanced therapies, efficacy of novel therapies, and infection risk for patients with chronic ITP.
Dr Howard Liebman, of the Keck School of Medicine in Los Angeles, California, opens with a database analysis of patients with primary ITP who were first-time users of advanced therapies, such as rituximab and thrombopoietin (TPO) receptor agonists. The analysis found that despite their relative merits, all the drugs carried a significant risk for adverse events.
Next, he reports on a study examining whether newly diagnosed patients or patients with chronic ITP had better results from the use of avatrombopag, a TPO receptor agonist. Reassuringly, there were no differences in outcomes.
Dr Liebman then discusses the updated results of an ongoing study of rilzabrutinib, a Bruton kinase inhibitor. This analysis showed that the drug achieved rapid, stable, and durable platelet responses.
He next turns to a Danish registry study on infection in patients with chronic ITP, which revealed an ongoing, cumulative risk for infection over 10 years.
Finally, Dr Liebman reports on a study that showed women who develop ITP during pregnancy require more interventions than do women with chronic ITP who become pregnant, and many develop chronic disease after delivery.
--
Howard A. Liebman, MD, Professor of Medicine and Pathology, University of Southern California, Keck School of Medicine; Attending Physician, Department of Medicine, Hematology, Norris Comprehensive Cancer Center, Keck Medicine at University of Southern California, Los Angeles, California
Howard A. Liebman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a consultant for: Novartis; Sanofi; Sobi
Received research grant from: Janssen Pharmaceuticals; Sanofi
The clinical takeaways in immune thrombocytopenia (ITP) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition include the relative merits of advanced therapies, efficacy of novel therapies, and infection risk for patients with chronic ITP.
Dr Howard Liebman, of the Keck School of Medicine in Los Angeles, California, opens with a database analysis of patients with primary ITP who were first-time users of advanced therapies, such as rituximab and thrombopoietin (TPO) receptor agonists. The analysis found that despite their relative merits, all the drugs carried a significant risk for adverse events.
Next, he reports on a study examining whether newly diagnosed patients or patients with chronic ITP had better results from the use of avatrombopag, a TPO receptor agonist. Reassuringly, there were no differences in outcomes.
Dr Liebman then discusses the updated results of an ongoing study of rilzabrutinib, a Bruton kinase inhibitor. This analysis showed that the drug achieved rapid, stable, and durable platelet responses.
He next turns to a Danish registry study on infection in patients with chronic ITP, which revealed an ongoing, cumulative risk for infection over 10 years.
Finally, Dr Liebman reports on a study that showed women who develop ITP during pregnancy require more interventions than do women with chronic ITP who become pregnant, and many develop chronic disease after delivery.
--
Howard A. Liebman, MD, Professor of Medicine and Pathology, University of Southern California, Keck School of Medicine; Attending Physician, Department of Medicine, Hematology, Norris Comprehensive Cancer Center, Keck Medicine at University of Southern California, Los Angeles, California
Howard A. Liebman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a consultant for: Novartis; Sanofi; Sobi
Received research grant from: Janssen Pharmaceuticals; Sanofi
The clinical takeaways in immune thrombocytopenia (ITP) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition include the relative merits of advanced therapies, efficacy of novel therapies, and infection risk for patients with chronic ITP.
Dr Howard Liebman, of the Keck School of Medicine in Los Angeles, California, opens with a database analysis of patients with primary ITP who were first-time users of advanced therapies, such as rituximab and thrombopoietin (TPO) receptor agonists. The analysis found that despite their relative merits, all the drugs carried a significant risk for adverse events.
Next, he reports on a study examining whether newly diagnosed patients or patients with chronic ITP had better results from the use of avatrombopag, a TPO receptor agonist. Reassuringly, there were no differences in outcomes.
Dr Liebman then discusses the updated results of an ongoing study of rilzabrutinib, a Bruton kinase inhibitor. This analysis showed that the drug achieved rapid, stable, and durable platelet responses.
He next turns to a Danish registry study on infection in patients with chronic ITP, which revealed an ongoing, cumulative risk for infection over 10 years.
Finally, Dr Liebman reports on a study that showed women who develop ITP during pregnancy require more interventions than do women with chronic ITP who become pregnant, and many develop chronic disease after delivery.
--
Howard A. Liebman, MD, Professor of Medicine and Pathology, University of Southern California, Keck School of Medicine; Attending Physician, Department of Medicine, Hematology, Norris Comprehensive Cancer Center, Keck Medicine at University of Southern California, Los Angeles, California
Howard A. Liebman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a consultant for: Novartis; Sanofi; Sobi
Received research grant from: Janssen Pharmaceuticals; Sanofi

Diffuse Large B-Cell Lymphoma Highlights From ASH 2023
Highlights in diffuse large B-cell lymphoma (DLBCL) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition that are particularly relevant to Veterans Health Administration (VHA) patients are reported by Dr Nicholas Burwick of Puget Sound VA Health Care System.
Dr Burwick begins with a large VHA study examining racial disparities in DLBCL outcomes among veterans. Importantly, overall survival was not significantly different across racial groups.
He next covers two studies in the DLBCL frontline setting. The first examines the efficacy of standard-dose R-CHOP; reduced-intensity R-CHOP; and an anthracycline alternative regimen among older patients. Standard-dose R-CHOP yielded superior results in patients aged 70- to 79-years but not for those older than 80 years, a group that merits further study.
The second frontline study focused on the chemotherapy-free regimen mosunetuzumab plus the antibody-drug conjugate polatuzumab vedotin (pola) in patients who are older and unfit for chemotherapy. The combination showed good preliminary efficacy.
Turning to relapsed/refractory patients, Dr Burwick discusses a real-world study examining response rates to tafasitamab in White vs Black/African American patients and non-Hispanic vs Hispanic patients. Differences between the two groups proved minimal.
Finally, he discusses a study of the bispecific antibody glofitamab and pola in heavily pretreated patients that showed promising results in this population.
--
Nicholas R. Burwick, MD, Associate Professor, Department of Medicine, Division of Hematology, University of Washington; Staff Physician, Department of Medicine, Division of Hematology, Puget Sound VA Health Care System, Seattle, Washington
Nicholas R. Burwick, MD, has disclosed no relevant financial relationships
Highlights in diffuse large B-cell lymphoma (DLBCL) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition that are particularly relevant to Veterans Health Administration (VHA) patients are reported by Dr Nicholas Burwick of Puget Sound VA Health Care System.
Dr Burwick begins with a large VHA study examining racial disparities in DLBCL outcomes among veterans. Importantly, overall survival was not significantly different across racial groups.
He next covers two studies in the DLBCL frontline setting. The first examines the efficacy of standard-dose R-CHOP; reduced-intensity R-CHOP; and an anthracycline alternative regimen among older patients. Standard-dose R-CHOP yielded superior results in patients aged 70- to 79-years but not for those older than 80 years, a group that merits further study.
The second frontline study focused on the chemotherapy-free regimen mosunetuzumab plus the antibody-drug conjugate polatuzumab vedotin (pola) in patients who are older and unfit for chemotherapy. The combination showed good preliminary efficacy.
Turning to relapsed/refractory patients, Dr Burwick discusses a real-world study examining response rates to tafasitamab in White vs Black/African American patients and non-Hispanic vs Hispanic patients. Differences between the two groups proved minimal.
Finally, he discusses a study of the bispecific antibody glofitamab and pola in heavily pretreated patients that showed promising results in this population.
--
Nicholas R. Burwick, MD, Associate Professor, Department of Medicine, Division of Hematology, University of Washington; Staff Physician, Department of Medicine, Division of Hematology, Puget Sound VA Health Care System, Seattle, Washington
Nicholas R. Burwick, MD, has disclosed no relevant financial relationships
Highlights in diffuse large B-cell lymphoma (DLBCL) from the 2023 American Society of Hematology (ASH) Annual Meeting and Exposition that are particularly relevant to Veterans Health Administration (VHA) patients are reported by Dr Nicholas Burwick of Puget Sound VA Health Care System.
Dr Burwick begins with a large VHA study examining racial disparities in DLBCL outcomes among veterans. Importantly, overall survival was not significantly different across racial groups.
He next covers two studies in the DLBCL frontline setting. The first examines the efficacy of standard-dose R-CHOP; reduced-intensity R-CHOP; and an anthracycline alternative regimen among older patients. Standard-dose R-CHOP yielded superior results in patients aged 70- to 79-years but not for those older than 80 years, a group that merits further study.
The second frontline study focused on the chemotherapy-free regimen mosunetuzumab plus the antibody-drug conjugate polatuzumab vedotin (pola) in patients who are older and unfit for chemotherapy. The combination showed good preliminary efficacy.
Turning to relapsed/refractory patients, Dr Burwick discusses a real-world study examining response rates to tafasitamab in White vs Black/African American patients and non-Hispanic vs Hispanic patients. Differences between the two groups proved minimal.
Finally, he discusses a study of the bispecific antibody glofitamab and pola in heavily pretreated patients that showed promising results in this population.
--
Nicholas R. Burwick, MD, Associate Professor, Department of Medicine, Division of Hematology, University of Washington; Staff Physician, Department of Medicine, Division of Hematology, Puget Sound VA Health Care System, Seattle, Washington
Nicholas R. Burwick, MD, has disclosed no relevant financial relationships

Should Physicians Offer Patients Medical Credit Cards?
With healthcare costs rising and payer reimbursements dwindling, many physicians are focusing even more on collecting outstanding patient balances.
Medical credit cards can be a popular choice to fill this gap because doctors get reimbursed upfront while patients receive special financing offers and the care they seek or need.
But, in recent months, federal officials have questioned whether these arrangements are genuinely win-win or if the cards prey on low-income and vulnerable individuals and warrant tighter regulatory oversight.
In July, the Consumer Financial Protection Bureau (CFPB), the US Department of Health and Human Services, and the US Department of Treasury announced an inquiry into medical credit cards. The agencies sought public comments from patients and providers to determine how much they are used.
Medical credit cards typically offer 0% or low-interest terms ranging from 6 to 24 months. Minimum monthly payments are required, often as low as $30 and not usually enough to pay the balance by the end of the promotional period.
After the introductory rate, card issuers may charge interest rates approaching 30% — not just on the remaining balance but on the original amount financed, adding considerably to total out-of-pocket costs.
Ophthalmologist Michael A. Brusco, MD, FACS, specializes in laser-assisted in situ keratomileuses and vision correction at his practice in the greater Washington, DC, area. He told this news organization that nearly all his patients are self-paying, and just under half utilize one of two medical credit cards he offers through third-party vendors, CareCredit and Alphaeon Credit.
“We are clear with our patients that it is interest-free only if they make all payments on time, and if they don’t, then the penalties and fees skyrocket,” Dr. Brusco said.
Patients pay no interest if they make the minimum monthly payments and pay the entire balance by the end of the term. Brusco said those who qualify and abide by those conditions can benefit from spreading healthcare expenses over several months and reducing the stress and financial strain associated with a larger, one-time payment.
He acknowledged that deferred interest can be problematic if patients are caught unaware but said his staff has received training from both vendors on clearly explaining the plans to patients. If someone doesn’t think they can pay off the balance in the timeframe, he suggests they pursue an alternative payment method.
Community Catalyst, a nonprofit health advocacy organization, has joined 60 other groups urging the Biden Administration to ban deferred interest medical credit cards.
They say that patients don’t understand what they are signing up for due to comments like these:
“Even though I’ve made monthly automatic payments on my account, as long as I have any balance on my account by [the end of the promotion], I’d be charged a 26.99% interest rate on the whole medical bill of [$2700].”
“I had nearly [$700] of interest that had accumulated within 4 months…based on one [$2000] charge. The employees at medical offices are selling a product they know little about without fully disclosing the terms and conditions to their patients.”
Historically, patients who apply for the cards have tended to use them to finance cosmetic or other lifestyle medicine procedures, but the CFPB said patients increasingly rely on them for routine and emergency care, which may contribute to growing medical debts and collections balances.
Federal authorities have expressed concerns that doctors may direct patients toward these financial arrangements instead of properly screening them for assistance programs or pursuing the sometimes arduous claims process to capture reimbursement from payers.
Growth of Medical Credit Card Market
One of the most widely used cards, CareCredit, is owned by Synchrony Bank and accepted at over 260,000 locations. Beyond private practices, the vendor has multiyear deals with over 300 hospitals, including Kaiser Permanente and the Cleveland Clinic.
Despite growing popularity and acceptance within the medical community, the cards may work well for some, but not all, patients.
According to a CFPB report released earlier this year, deferred interest medical credit cards were used to pay nearly $23 billion in healthcare expenses from 2018 to 2020. Individuals unable to stick to the terms paid $1 billion in deferred interest payments during that period. Three quarters of CareCredit consumers pay no interest, the organization reported.
Healthcare costs are likely driving demand for medical credit cards. In a recent survey by the Commonwealth Fund, almost half of respondents said it was very or somewhat difficult to afford care even when having insurance coverage through an employer, individual, or government plan. Consumers in the survey cited the high costs as a reason why they delayed or skipped care and prescription medication in the past year, including 29% of those with employer coverage and 42% with Medicare.
These dynamics can leave doctors between a rock and a hard place, said Alan P. Sager, PhD, a professor of health law, policy, and management at Boston University School of Public Health. He told this news organization that medical credit cards can keep cash flowing for doctors and provide elective and necessary care for patients, but the double-digit interest rates outside of the promotional periods can put patients at risk of bankruptcy. He views them as a short-term solution to a more significant problem.
“What doctors need and deserve is patients who have full coverage so that there are no medical debts and no need for medical credit cards,” said Dr. Sager.
Doctor Groups Weigh In
The Medical Group Management Association (MGMA), representing more than 15,000 medical groups, said in its public comments that Medicare cuts and staffing and inflation challenges have made running a profitable practice challenging, particularly for rural and less-resourced offices.
The organization said medical credit cards with transparent terms and conditions can help patients afford care and keep practice doors open amid rising operational costs. However, MGMA worries that the CFPB’s inquiry could “perpetuate the notion that it is acceptable for payment not to be rendered immediately after clinical services are provided, and it’s ok that payments are often subject to significant delays.”
Meanwhile, the American Society of Plastic Surgeons (ASPS) has endorsed CareCredit for over 20 years. In response to the CFPB’s request for information, the association said it supports medical credit cards that offer promotional low- or no-interest terms.
Steven Williams, MD, ASPS president, told this news organization that patients appreciate multiple payment options and the flexibility to move forward with care on short notice. Still, he said that it requires due diligence on everyone’s part.
“Lenders have a responsibility to educate their customers, and it’s critical that lending products have full disclosure in plain and clear language. And with any substantial purchase, patients need to analyze how much it adds to the bottom line,” he said.
A version of this article appeared on Medscape.com.
With healthcare costs rising and payer reimbursements dwindling, many physicians are focusing even more on collecting outstanding patient balances.
Medical credit cards can be a popular choice to fill this gap because doctors get reimbursed upfront while patients receive special financing offers and the care they seek or need.
But, in recent months, federal officials have questioned whether these arrangements are genuinely win-win or if the cards prey on low-income and vulnerable individuals and warrant tighter regulatory oversight.
In July, the Consumer Financial Protection Bureau (CFPB), the US Department of Health and Human Services, and the US Department of Treasury announced an inquiry into medical credit cards. The agencies sought public comments from patients and providers to determine how much they are used.
Medical credit cards typically offer 0% or low-interest terms ranging from 6 to 24 months. Minimum monthly payments are required, often as low as $30 and not usually enough to pay the balance by the end of the promotional period.
After the introductory rate, card issuers may charge interest rates approaching 30% — not just on the remaining balance but on the original amount financed, adding considerably to total out-of-pocket costs.
Ophthalmologist Michael A. Brusco, MD, FACS, specializes in laser-assisted in situ keratomileuses and vision correction at his practice in the greater Washington, DC, area. He told this news organization that nearly all his patients are self-paying, and just under half utilize one of two medical credit cards he offers through third-party vendors, CareCredit and Alphaeon Credit.
“We are clear with our patients that it is interest-free only if they make all payments on time, and if they don’t, then the penalties and fees skyrocket,” Dr. Brusco said.
Patients pay no interest if they make the minimum monthly payments and pay the entire balance by the end of the term. Brusco said those who qualify and abide by those conditions can benefit from spreading healthcare expenses over several months and reducing the stress and financial strain associated with a larger, one-time payment.
He acknowledged that deferred interest can be problematic if patients are caught unaware but said his staff has received training from both vendors on clearly explaining the plans to patients. If someone doesn’t think they can pay off the balance in the timeframe, he suggests they pursue an alternative payment method.
Community Catalyst, a nonprofit health advocacy organization, has joined 60 other groups urging the Biden Administration to ban deferred interest medical credit cards.
They say that patients don’t understand what they are signing up for due to comments like these:
“Even though I’ve made monthly automatic payments on my account, as long as I have any balance on my account by [the end of the promotion], I’d be charged a 26.99% interest rate on the whole medical bill of [$2700].”
“I had nearly [$700] of interest that had accumulated within 4 months…based on one [$2000] charge. The employees at medical offices are selling a product they know little about without fully disclosing the terms and conditions to their patients.”
Historically, patients who apply for the cards have tended to use them to finance cosmetic or other lifestyle medicine procedures, but the CFPB said patients increasingly rely on them for routine and emergency care, which may contribute to growing medical debts and collections balances.
Federal authorities have expressed concerns that doctors may direct patients toward these financial arrangements instead of properly screening them for assistance programs or pursuing the sometimes arduous claims process to capture reimbursement from payers.
Growth of Medical Credit Card Market
One of the most widely used cards, CareCredit, is owned by Synchrony Bank and accepted at over 260,000 locations. Beyond private practices, the vendor has multiyear deals with over 300 hospitals, including Kaiser Permanente and the Cleveland Clinic.
Despite growing popularity and acceptance within the medical community, the cards may work well for some, but not all, patients.
According to a CFPB report released earlier this year, deferred interest medical credit cards were used to pay nearly $23 billion in healthcare expenses from 2018 to 2020. Individuals unable to stick to the terms paid $1 billion in deferred interest payments during that period. Three quarters of CareCredit consumers pay no interest, the organization reported.
Healthcare costs are likely driving demand for medical credit cards. In a recent survey by the Commonwealth Fund, almost half of respondents said it was very or somewhat difficult to afford care even when having insurance coverage through an employer, individual, or government plan. Consumers in the survey cited the high costs as a reason why they delayed or skipped care and prescription medication in the past year, including 29% of those with employer coverage and 42% with Medicare.
These dynamics can leave doctors between a rock and a hard place, said Alan P. Sager, PhD, a professor of health law, policy, and management at Boston University School of Public Health. He told this news organization that medical credit cards can keep cash flowing for doctors and provide elective and necessary care for patients, but the double-digit interest rates outside of the promotional periods can put patients at risk of bankruptcy. He views them as a short-term solution to a more significant problem.
“What doctors need and deserve is patients who have full coverage so that there are no medical debts and no need for medical credit cards,” said Dr. Sager.
Doctor Groups Weigh In
The Medical Group Management Association (MGMA), representing more than 15,000 medical groups, said in its public comments that Medicare cuts and staffing and inflation challenges have made running a profitable practice challenging, particularly for rural and less-resourced offices.
The organization said medical credit cards with transparent terms and conditions can help patients afford care and keep practice doors open amid rising operational costs. However, MGMA worries that the CFPB’s inquiry could “perpetuate the notion that it is acceptable for payment not to be rendered immediately after clinical services are provided, and it’s ok that payments are often subject to significant delays.”
Meanwhile, the American Society of Plastic Surgeons (ASPS) has endorsed CareCredit for over 20 years. In response to the CFPB’s request for information, the association said it supports medical credit cards that offer promotional low- or no-interest terms.
Steven Williams, MD, ASPS president, told this news organization that patients appreciate multiple payment options and the flexibility to move forward with care on short notice. Still, he said that it requires due diligence on everyone’s part.
“Lenders have a responsibility to educate their customers, and it’s critical that lending products have full disclosure in plain and clear language. And with any substantial purchase, patients need to analyze how much it adds to the bottom line,” he said.
A version of this article appeared on Medscape.com.
With healthcare costs rising and payer reimbursements dwindling, many physicians are focusing even more on collecting outstanding patient balances.
Medical credit cards can be a popular choice to fill this gap because doctors get reimbursed upfront while patients receive special financing offers and the care they seek or need.
But, in recent months, federal officials have questioned whether these arrangements are genuinely win-win or if the cards prey on low-income and vulnerable individuals and warrant tighter regulatory oversight.
In July, the Consumer Financial Protection Bureau (CFPB), the US Department of Health and Human Services, and the US Department of Treasury announced an inquiry into medical credit cards. The agencies sought public comments from patients and providers to determine how much they are used.
Medical credit cards typically offer 0% or low-interest terms ranging from 6 to 24 months. Minimum monthly payments are required, often as low as $30 and not usually enough to pay the balance by the end of the promotional period.
After the introductory rate, card issuers may charge interest rates approaching 30% — not just on the remaining balance but on the original amount financed, adding considerably to total out-of-pocket costs.
Ophthalmologist Michael A. Brusco, MD, FACS, specializes in laser-assisted in situ keratomileuses and vision correction at his practice in the greater Washington, DC, area. He told this news organization that nearly all his patients are self-paying, and just under half utilize one of two medical credit cards he offers through third-party vendors, CareCredit and Alphaeon Credit.
“We are clear with our patients that it is interest-free only if they make all payments on time, and if they don’t, then the penalties and fees skyrocket,” Dr. Brusco said.
Patients pay no interest if they make the minimum monthly payments and pay the entire balance by the end of the term. Brusco said those who qualify and abide by those conditions can benefit from spreading healthcare expenses over several months and reducing the stress and financial strain associated with a larger, one-time payment.
He acknowledged that deferred interest can be problematic if patients are caught unaware but said his staff has received training from both vendors on clearly explaining the plans to patients. If someone doesn’t think they can pay off the balance in the timeframe, he suggests they pursue an alternative payment method.
Community Catalyst, a nonprofit health advocacy organization, has joined 60 other groups urging the Biden Administration to ban deferred interest medical credit cards.
They say that patients don’t understand what they are signing up for due to comments like these:
“Even though I’ve made monthly automatic payments on my account, as long as I have any balance on my account by [the end of the promotion], I’d be charged a 26.99% interest rate on the whole medical bill of [$2700].”
“I had nearly [$700] of interest that had accumulated within 4 months…based on one [$2000] charge. The employees at medical offices are selling a product they know little about without fully disclosing the terms and conditions to their patients.”
Historically, patients who apply for the cards have tended to use them to finance cosmetic or other lifestyle medicine procedures, but the CFPB said patients increasingly rely on them for routine and emergency care, which may contribute to growing medical debts and collections balances.
Federal authorities have expressed concerns that doctors may direct patients toward these financial arrangements instead of properly screening them for assistance programs or pursuing the sometimes arduous claims process to capture reimbursement from payers.
Growth of Medical Credit Card Market
One of the most widely used cards, CareCredit, is owned by Synchrony Bank and accepted at over 260,000 locations. Beyond private practices, the vendor has multiyear deals with over 300 hospitals, including Kaiser Permanente and the Cleveland Clinic.
Despite growing popularity and acceptance within the medical community, the cards may work well for some, but not all, patients.
According to a CFPB report released earlier this year, deferred interest medical credit cards were used to pay nearly $23 billion in healthcare expenses from 2018 to 2020. Individuals unable to stick to the terms paid $1 billion in deferred interest payments during that period. Three quarters of CareCredit consumers pay no interest, the organization reported.
Healthcare costs are likely driving demand for medical credit cards. In a recent survey by the Commonwealth Fund, almost half of respondents said it was very or somewhat difficult to afford care even when having insurance coverage through an employer, individual, or government plan. Consumers in the survey cited the high costs as a reason why they delayed or skipped care and prescription medication in the past year, including 29% of those with employer coverage and 42% with Medicare.
These dynamics can leave doctors between a rock and a hard place, said Alan P. Sager, PhD, a professor of health law, policy, and management at Boston University School of Public Health. He told this news organization that medical credit cards can keep cash flowing for doctors and provide elective and necessary care for patients, but the double-digit interest rates outside of the promotional periods can put patients at risk of bankruptcy. He views them as a short-term solution to a more significant problem.
“What doctors need and deserve is patients who have full coverage so that there are no medical debts and no need for medical credit cards,” said Dr. Sager.
Doctor Groups Weigh In
The Medical Group Management Association (MGMA), representing more than 15,000 medical groups, said in its public comments that Medicare cuts and staffing and inflation challenges have made running a profitable practice challenging, particularly for rural and less-resourced offices.
The organization said medical credit cards with transparent terms and conditions can help patients afford care and keep practice doors open amid rising operational costs. However, MGMA worries that the CFPB’s inquiry could “perpetuate the notion that it is acceptable for payment not to be rendered immediately after clinical services are provided, and it’s ok that payments are often subject to significant delays.”
Meanwhile, the American Society of Plastic Surgeons (ASPS) has endorsed CareCredit for over 20 years. In response to the CFPB’s request for information, the association said it supports medical credit cards that offer promotional low- or no-interest terms.
Steven Williams, MD, ASPS president, told this news organization that patients appreciate multiple payment options and the flexibility to move forward with care on short notice. Still, he said that it requires due diligence on everyone’s part.
“Lenders have a responsibility to educate their customers, and it’s critical that lending products have full disclosure in plain and clear language. And with any substantial purchase, patients need to analyze how much it adds to the bottom line,” he said.
A version of this article appeared on Medscape.com.
JAMA Internal Medicine Editor Recaps 2023’s High-Impact Research
Harvard Medical School’s Sharon K. Inouye, MD, MPH, is editor in chief of JAMA Internal Medicine and a leading voice in American gerontology. We asked her to choose five of the influential journal’s most impactful studies from 2023 and highlight important take-home messages for internists and their colleagues.
Q: One of the studies you chose suggests that the antiviral nirmatrelvir (Paxlovid) can ward off long COVID. Could you recap the findings?
A: Researchers followed a group of more than 280,000 Department of Veterans Affairs patients who were seen in 2022, had a positive COVID test, and had at least one risk factor for severe COVID. They focused on those who survived to 30 days after their COVID infection and compared those who received the drug within the first 5 days of a positive test with an equivalent control group.
They found that 13 long COVID symptoms were all significantly less common (relative risk = 0.74) in those who received nirmatrelvir. This was true no matter whether they’d ever had a COVID vaccination.
Q: How should this research affect clinical practice?
A: You can’t generalize from this to everyone because, of course, not everyone was included in this study. But it is highly suggestive that this drug is very effective for preventing long COVID.
Nirmatrelvir was touted as being able to shorten duration of illness and prevent hospitalization. But if you were low risk or you were already well into your COVID course, it wasn’t like rush, rush, rush to the doctor to get it.
This changes that equation because we know long COVID is such a huge issue. The vast majority of doctors who work with COVID patients and know this are now being more aggressive about prescribing it.
Q: What about patients whom the CDC considers to be at less risk — people with up-to-date vaccinations who are under 50 with mild-to-moderate COVID and no higher-risk medical conditions? Should they take nirmatrelvir?
A: The evidence is not 100% in yet. A study like this one needs to be repeated and include younger people without any risk factors to see if we see the same thing. So it’s a personal choice, and a personal calculus needs to be done. A lot of people are making that choice [to take the drug], and it can be a rational decision.
Q: You also chose a study that links high thyroid hormone levels to higher rates of dementia. What did it reveal?
A: This study looks at patients who had thyrotoxicosis — a thyroid level that’s too high — from hormone produced endogenously, and exogenously. Researchers tracked almost 66,000 patients aged 65 and older and found that thyrotoxicosis from all causes, whether it was endogenous or exogenous, was linked to an increased risk of dementia in a dose-response relationship (adjusted hazard ratio = 1.39).
Q: Is there a clinical take-home message here?
A: When we start patients on thyroid medication, they don’t always get reassessed on a regular basis. Given this finding, a TSH [thyroid-stimulating hormone] level is indicated during the annual wellness check that patients on Medicare can get every year.
Q: Is TSH measured as part of routine blood tests?
A: No it’s not. It has to be ordered. I think that’s why we’re seeing this problem to begin with — because it’s not something we all have awareness about. I wasn’t aware myself that mildly high levels of thyroid could increase the risk of cognitive impairment. Certainly, I’m going to be much more aware in my practice.
Q: You also picked a study about silicosis in workers who are exposed to dust when they make engineered stone countertops, also known as quartz countertops. What were the findings?
A: Silicosis is a very serious lung condition that develops from exposure to crystalline silica. Essentially, sand gets inhaled into the lungs. Workers can be exposed when they’re making engineered stone countertops, the most popular countertops now in the United States.
This study is based on statewide surveys from 2019 to 2022 that the California Department of Public Health does routinely. They gathered cases of silicosis and found 52 — all men with an average age of 45. All but one were Latino immigrants, and most either had no insurance or very poor insurance.
Q: The study found that “diagnosis was delayed in 58%, with 38% presenting with advanced disease (progressive massive fibrosis), and 19% died.” What does that tell you?
A: It’s a very serious condition. Once it gets to the advanced stage, it will just continue to progress, and the person will die. That’s why it’s so important to know that it’s absolutely preventable.
Q: Is there a message here for internists?
A: If you treat a lot of immigrants or work in an area where there are a lot of industrial workers, you’re going to want to have a very high suspicion about it. If you see an atypical pattern on the chest x-ray or via diffusion scoring, have a low threshold for getting a pulmonary function test.
Doctors need to be aware and diagnose this very quickly. When patients present, you can pull them out of that work environment or put mitigation systems into place.
Q: California regulators were expected to put emergency rules into place in late December to protect workers. Did this study play a role in focusing attention on the problem?
A: This article, along with a commentary and podcast that we put out, really helped with advocacy to improve health and safety for workers at stone-cutting and fabrication shops.
Q: You were impressed by another study about airborne dangers, this one linking air pollution to dementia. What did researchers discover?
A: [This analysis] of more than 27,000 people in the Health and Retirement Study, a respected and rich database, found that exposure to air pollution was associated with greater rates of dementia — an increase of about 8% a year. Exposure to agricultural emissions and wildfire smoke were most robustly associated with a greater risk of dementia.
Q: How are these findings important, especially in light of the unhealthy air spawned by recent wildfires in the United States and Canada?
A: Studies like this will make it even more compelling that we are better prepared for air quality issues.
I grew up in Los Angeles, where smog and pollution were very big issues. I was constantly hearing about various mitigation strategies that were going into place. But after I moved to the East Coast, I almost never heard about prevention.
Now, I’m hoping we can keep this topic in the national conversation.
Q: You also highlighted a systematic review of the use of restraints in the emergency department. Why did you choose this research?
A: At JAMA Internal Medicine, we’re really focused on ways we can address health disparities and raise awareness of potential unconscious bias.
This review looked at 10 studies that included more than 2.5 million patient encounters, including 24,000 incidents of physical restraint use. They found that the overall rate of use of restraints was low at below 1%.
But when they are used, Black patients were 1.3 times more likely to be restrained than White patients.
Q: What’s the message here?
A: This is an important start to recognizing these differences and then changing our behavior. Perhaps restraints don’t need to be used as often in light of evidence, for example, of increased rates of misdiagnosis of psychosis in the Black population.
Q: How should physicians change their approach to restraints?
A: Restraints are not to be used to control disruption — wild behavior or verbal outbursts. They’re for when someone is a danger to themselves or others.
Dr. Inouye has no conflicts of interest.
Harvard Medical School’s Sharon K. Inouye, MD, MPH, is editor in chief of JAMA Internal Medicine and a leading voice in American gerontology. We asked her to choose five of the influential journal’s most impactful studies from 2023 and highlight important take-home messages for internists and their colleagues.
Q: One of the studies you chose suggests that the antiviral nirmatrelvir (Paxlovid) can ward off long COVID. Could you recap the findings?
A: Researchers followed a group of more than 280,000 Department of Veterans Affairs patients who were seen in 2022, had a positive COVID test, and had at least one risk factor for severe COVID. They focused on those who survived to 30 days after their COVID infection and compared those who received the drug within the first 5 days of a positive test with an equivalent control group.
They found that 13 long COVID symptoms were all significantly less common (relative risk = 0.74) in those who received nirmatrelvir. This was true no matter whether they’d ever had a COVID vaccination.
Q: How should this research affect clinical practice?
A: You can’t generalize from this to everyone because, of course, not everyone was included in this study. But it is highly suggestive that this drug is very effective for preventing long COVID.
Nirmatrelvir was touted as being able to shorten duration of illness and prevent hospitalization. But if you were low risk or you were already well into your COVID course, it wasn’t like rush, rush, rush to the doctor to get it.
This changes that equation because we know long COVID is such a huge issue. The vast majority of doctors who work with COVID patients and know this are now being more aggressive about prescribing it.
Q: What about patients whom the CDC considers to be at less risk — people with up-to-date vaccinations who are under 50 with mild-to-moderate COVID and no higher-risk medical conditions? Should they take nirmatrelvir?
A: The evidence is not 100% in yet. A study like this one needs to be repeated and include younger people without any risk factors to see if we see the same thing. So it’s a personal choice, and a personal calculus needs to be done. A lot of people are making that choice [to take the drug], and it can be a rational decision.
Q: You also chose a study that links high thyroid hormone levels to higher rates of dementia. What did it reveal?
A: This study looks at patients who had thyrotoxicosis — a thyroid level that’s too high — from hormone produced endogenously, and exogenously. Researchers tracked almost 66,000 patients aged 65 and older and found that thyrotoxicosis from all causes, whether it was endogenous or exogenous, was linked to an increased risk of dementia in a dose-response relationship (adjusted hazard ratio = 1.39).
Q: Is there a clinical take-home message here?
A: When we start patients on thyroid medication, they don’t always get reassessed on a regular basis. Given this finding, a TSH [thyroid-stimulating hormone] level is indicated during the annual wellness check that patients on Medicare can get every year.
Q: Is TSH measured as part of routine blood tests?
A: No it’s not. It has to be ordered. I think that’s why we’re seeing this problem to begin with — because it’s not something we all have awareness about. I wasn’t aware myself that mildly high levels of thyroid could increase the risk of cognitive impairment. Certainly, I’m going to be much more aware in my practice.
Q: You also picked a study about silicosis in workers who are exposed to dust when they make engineered stone countertops, also known as quartz countertops. What were the findings?
A: Silicosis is a very serious lung condition that develops from exposure to crystalline silica. Essentially, sand gets inhaled into the lungs. Workers can be exposed when they’re making engineered stone countertops, the most popular countertops now in the United States.
This study is based on statewide surveys from 2019 to 2022 that the California Department of Public Health does routinely. They gathered cases of silicosis and found 52 — all men with an average age of 45. All but one were Latino immigrants, and most either had no insurance or very poor insurance.
Q: The study found that “diagnosis was delayed in 58%, with 38% presenting with advanced disease (progressive massive fibrosis), and 19% died.” What does that tell you?
A: It’s a very serious condition. Once it gets to the advanced stage, it will just continue to progress, and the person will die. That’s why it’s so important to know that it’s absolutely preventable.
Q: Is there a message here for internists?
A: If you treat a lot of immigrants or work in an area where there are a lot of industrial workers, you’re going to want to have a very high suspicion about it. If you see an atypical pattern on the chest x-ray or via diffusion scoring, have a low threshold for getting a pulmonary function test.
Doctors need to be aware and diagnose this very quickly. When patients present, you can pull them out of that work environment or put mitigation systems into place.
Q: California regulators were expected to put emergency rules into place in late December to protect workers. Did this study play a role in focusing attention on the problem?
A: This article, along with a commentary and podcast that we put out, really helped with advocacy to improve health and safety for workers at stone-cutting and fabrication shops.
Q: You were impressed by another study about airborne dangers, this one linking air pollution to dementia. What did researchers discover?
A: [This analysis] of more than 27,000 people in the Health and Retirement Study, a respected and rich database, found that exposure to air pollution was associated with greater rates of dementia — an increase of about 8% a year. Exposure to agricultural emissions and wildfire smoke were most robustly associated with a greater risk of dementia.
Q: How are these findings important, especially in light of the unhealthy air spawned by recent wildfires in the United States and Canada?
A: Studies like this will make it even more compelling that we are better prepared for air quality issues.
I grew up in Los Angeles, where smog and pollution were very big issues. I was constantly hearing about various mitigation strategies that were going into place. But after I moved to the East Coast, I almost never heard about prevention.
Now, I’m hoping we can keep this topic in the national conversation.
Q: You also highlighted a systematic review of the use of restraints in the emergency department. Why did you choose this research?
A: At JAMA Internal Medicine, we’re really focused on ways we can address health disparities and raise awareness of potential unconscious bias.
This review looked at 10 studies that included more than 2.5 million patient encounters, including 24,000 incidents of physical restraint use. They found that the overall rate of use of restraints was low at below 1%.
But when they are used, Black patients were 1.3 times more likely to be restrained than White patients.
Q: What’s the message here?
A: This is an important start to recognizing these differences and then changing our behavior. Perhaps restraints don’t need to be used as often in light of evidence, for example, of increased rates of misdiagnosis of psychosis in the Black population.
Q: How should physicians change their approach to restraints?
A: Restraints are not to be used to control disruption — wild behavior or verbal outbursts. They’re for when someone is a danger to themselves or others.
Dr. Inouye has no conflicts of interest.
Harvard Medical School’s Sharon K. Inouye, MD, MPH, is editor in chief of JAMA Internal Medicine and a leading voice in American gerontology. We asked her to choose five of the influential journal’s most impactful studies from 2023 and highlight important take-home messages for internists and their colleagues.
Q: One of the studies you chose suggests that the antiviral nirmatrelvir (Paxlovid) can ward off long COVID. Could you recap the findings?
A: Researchers followed a group of more than 280,000 Department of Veterans Affairs patients who were seen in 2022, had a positive COVID test, and had at least one risk factor for severe COVID. They focused on those who survived to 30 days after their COVID infection and compared those who received the drug within the first 5 days of a positive test with an equivalent control group.
They found that 13 long COVID symptoms were all significantly less common (relative risk = 0.74) in those who received nirmatrelvir. This was true no matter whether they’d ever had a COVID vaccination.
Q: How should this research affect clinical practice?
A: You can’t generalize from this to everyone because, of course, not everyone was included in this study. But it is highly suggestive that this drug is very effective for preventing long COVID.
Nirmatrelvir was touted as being able to shorten duration of illness and prevent hospitalization. But if you were low risk or you were already well into your COVID course, it wasn’t like rush, rush, rush to the doctor to get it.
This changes that equation because we know long COVID is such a huge issue. The vast majority of doctors who work with COVID patients and know this are now being more aggressive about prescribing it.
Q: What about patients whom the CDC considers to be at less risk — people with up-to-date vaccinations who are under 50 with mild-to-moderate COVID and no higher-risk medical conditions? Should they take nirmatrelvir?
A: The evidence is not 100% in yet. A study like this one needs to be repeated and include younger people without any risk factors to see if we see the same thing. So it’s a personal choice, and a personal calculus needs to be done. A lot of people are making that choice [to take the drug], and it can be a rational decision.
Q: You also chose a study that links high thyroid hormone levels to higher rates of dementia. What did it reveal?
A: This study looks at patients who had thyrotoxicosis — a thyroid level that’s too high — from hormone produced endogenously, and exogenously. Researchers tracked almost 66,000 patients aged 65 and older and found that thyrotoxicosis from all causes, whether it was endogenous or exogenous, was linked to an increased risk of dementia in a dose-response relationship (adjusted hazard ratio = 1.39).
Q: Is there a clinical take-home message here?
A: When we start patients on thyroid medication, they don’t always get reassessed on a regular basis. Given this finding, a TSH [thyroid-stimulating hormone] level is indicated during the annual wellness check that patients on Medicare can get every year.
Q: Is TSH measured as part of routine blood tests?
A: No it’s not. It has to be ordered. I think that’s why we’re seeing this problem to begin with — because it’s not something we all have awareness about. I wasn’t aware myself that mildly high levels of thyroid could increase the risk of cognitive impairment. Certainly, I’m going to be much more aware in my practice.
Q: You also picked a study about silicosis in workers who are exposed to dust when they make engineered stone countertops, also known as quartz countertops. What were the findings?
A: Silicosis is a very serious lung condition that develops from exposure to crystalline silica. Essentially, sand gets inhaled into the lungs. Workers can be exposed when they’re making engineered stone countertops, the most popular countertops now in the United States.
This study is based on statewide surveys from 2019 to 2022 that the California Department of Public Health does routinely. They gathered cases of silicosis and found 52 — all men with an average age of 45. All but one were Latino immigrants, and most either had no insurance or very poor insurance.
Q: The study found that “diagnosis was delayed in 58%, with 38% presenting with advanced disease (progressive massive fibrosis), and 19% died.” What does that tell you?
A: It’s a very serious condition. Once it gets to the advanced stage, it will just continue to progress, and the person will die. That’s why it’s so important to know that it’s absolutely preventable.
Q: Is there a message here for internists?
A: If you treat a lot of immigrants or work in an area where there are a lot of industrial workers, you’re going to want to have a very high suspicion about it. If you see an atypical pattern on the chest x-ray or via diffusion scoring, have a low threshold for getting a pulmonary function test.
Doctors need to be aware and diagnose this very quickly. When patients present, you can pull them out of that work environment or put mitigation systems into place.
Q: California regulators were expected to put emergency rules into place in late December to protect workers. Did this study play a role in focusing attention on the problem?
A: This article, along with a commentary and podcast that we put out, really helped with advocacy to improve health and safety for workers at stone-cutting and fabrication shops.
Q: You were impressed by another study about airborne dangers, this one linking air pollution to dementia. What did researchers discover?
A: [This analysis] of more than 27,000 people in the Health and Retirement Study, a respected and rich database, found that exposure to air pollution was associated with greater rates of dementia — an increase of about 8% a year. Exposure to agricultural emissions and wildfire smoke were most robustly associated with a greater risk of dementia.
Q: How are these findings important, especially in light of the unhealthy air spawned by recent wildfires in the United States and Canada?
A: Studies like this will make it even more compelling that we are better prepared for air quality issues.
I grew up in Los Angeles, where smog and pollution were very big issues. I was constantly hearing about various mitigation strategies that were going into place. But after I moved to the East Coast, I almost never heard about prevention.
Now, I’m hoping we can keep this topic in the national conversation.
Q: You also highlighted a systematic review of the use of restraints in the emergency department. Why did you choose this research?
A: At JAMA Internal Medicine, we’re really focused on ways we can address health disparities and raise awareness of potential unconscious bias.
This review looked at 10 studies that included more than 2.5 million patient encounters, including 24,000 incidents of physical restraint use. They found that the overall rate of use of restraints was low at below 1%.
But when they are used, Black patients were 1.3 times more likely to be restrained than White patients.
Q: What’s the message here?
A: This is an important start to recognizing these differences and then changing our behavior. Perhaps restraints don’t need to be used as often in light of evidence, for example, of increased rates of misdiagnosis of psychosis in the Black population.
Q: How should physicians change their approach to restraints?
A: Restraints are not to be used to control disruption — wild behavior or verbal outbursts. They’re for when someone is a danger to themselves or others.
Dr. Inouye has no conflicts of interest.