User login
Autism spectrum disorders
According to the CDC, the prevalence of autism spectrum disorders (ASD) has gone from roughly 1 in 68 children in 2010 to 1 in 36 children in 2020.1 This is nearly a 50% increase over that 10-year period. Over the last several years, there has been evidence suggesting that increasing numbers of young people with ASD or other neurodivergent conditions identify as transgender or gender diverse.2 Experts agree more careful attention must be paid to these patients.
This includes things such as difficulty with communication, possible concrete thinking, and obsessive interests. While earlier research has shown a higher incidence of ASD in those referred to specialized gender medical clinics, it is important to realize that not all of these youth are seeking medical care. They may be brought to the attention of a primary care pediatrician (PCP) if the child has discussed their gender identity at home. It is important that PCPs approach these young people with an open mind and address any coexisting mental health conditions. PCPs must be careful not to dismiss any gender identity concerns as another of the patient’s “obsessions”; rather, they should ensure the patient receives the appropriate mental health care that they need to explore these concerns. One challenge for PCPs is that there is a dearth of mental health professionals who have experience in working with young people who have both gender dysphoria and a neurodivergent condition.
For those clinicians who provide gender-affirming medical care to these young people, it is imperative that they have a thorough understanding of the patient’s gender identity and medical goals before starting any treatment. This may require extensive collaboration with the patient’s mental health provider. The clinician providing medical care may also choose to proceed slower with the introduction of hormones and their subsequent dosing to allow the young person time to continue discussing their effects with their mental health provider. To help clinicians, Dr. John Strang and a multidisciplinary group of collaborators developed a set of guidelines for co-occurring ASD and gender dysphoria in adolescents.3 More recently, Dr. Strang and other collaborators have also developed a questionnaire that can be used by clinicians in the care of these patients.4 The goal of this questionnaire is to allow the young people to “communicate their experiences and needs in a report format attuned to common autistic thinking and communication styles.”
In summary, pediatricians and those who care for children and adolescents need to be aware of the increased association between those with ASD or other neurodivergent conditions and gender dysphoria. To ensure that these young people receive optimal care, it is important to connect them to experts (if possible) in coexisting ASD and gender dysphoria. If such experts are not readily available, the National LGBTQIA+ Health Education Center has developed a resource for providing an affirmative approach to care for these young people.5 While more research is needed to better understand young people with coexisting ASD (or other neurodivergent conditions), taking an individualized approach to their care can help ensure optimal outcomes.
Dr. Cooper is assistant professor of pediatrics at University of Texas Southwestern, Dallas, and an adolescent medicine specialist at Children’s Medical Center Dallas.
References
1. Data & Statistics on Autism Spectrum Disorder. https://www.cdc.gov/ncbddd/autism/data.html.
2. Glidden D et al. Gender dysphoria and autism spectrum disorder: A systematic review of the literature. Sex Med Rev. 2016;4(1):3-14. doi:10.1016/j.sxmr.2015.10.003.
3. Strang JF et al. Initial clinical guidelines for co-occurring autism spectrum disorder and gender dysphoria or incongruence in adolescents. J Clin Child Adolesc Psychol. 2018;47(1):105-15. doi:10.1080/15374416.2016.1228462.
4. Strang JF et. al. The Gender-Diversity and Autism Questionnaire: A Community-Developed Clinical, Research, and Self-Advocacy Tool for Autistic Transgender and Gender-Diverse Young Adults. Autism Adulthood. 2023 Jun 1;5(2):175-90. doi: 10.1089/aut.2023.0002.
5. National LGBT Health Education Center. Neurodiversity & gender-diverse youth: An affirming approach to care 2020. https://www.lgbtqiahealtheducation.org/publication/neurodiversity-gender-diverse-youth-an-affirming-approach-to-care-2020/download
According to the CDC, the prevalence of autism spectrum disorders (ASD) has gone from roughly 1 in 68 children in 2010 to 1 in 36 children in 2020.1 This is nearly a 50% increase over that 10-year period. Over the last several years, there has been evidence suggesting that increasing numbers of young people with ASD or other neurodivergent conditions identify as transgender or gender diverse.2 Experts agree more careful attention must be paid to these patients.
This includes things such as difficulty with communication, possible concrete thinking, and obsessive interests. While earlier research has shown a higher incidence of ASD in those referred to specialized gender medical clinics, it is important to realize that not all of these youth are seeking medical care. They may be brought to the attention of a primary care pediatrician (PCP) if the child has discussed their gender identity at home. It is important that PCPs approach these young people with an open mind and address any coexisting mental health conditions. PCPs must be careful not to dismiss any gender identity concerns as another of the patient’s “obsessions”; rather, they should ensure the patient receives the appropriate mental health care that they need to explore these concerns. One challenge for PCPs is that there is a dearth of mental health professionals who have experience in working with young people who have both gender dysphoria and a neurodivergent condition.
For those clinicians who provide gender-affirming medical care to these young people, it is imperative that they have a thorough understanding of the patient’s gender identity and medical goals before starting any treatment. This may require extensive collaboration with the patient’s mental health provider. The clinician providing medical care may also choose to proceed slower with the introduction of hormones and their subsequent dosing to allow the young person time to continue discussing their effects with their mental health provider. To help clinicians, Dr. John Strang and a multidisciplinary group of collaborators developed a set of guidelines for co-occurring ASD and gender dysphoria in adolescents.3 More recently, Dr. Strang and other collaborators have also developed a questionnaire that can be used by clinicians in the care of these patients.4 The goal of this questionnaire is to allow the young people to “communicate their experiences and needs in a report format attuned to common autistic thinking and communication styles.”
In summary, pediatricians and those who care for children and adolescents need to be aware of the increased association between those with ASD or other neurodivergent conditions and gender dysphoria. To ensure that these young people receive optimal care, it is important to connect them to experts (if possible) in coexisting ASD and gender dysphoria. If such experts are not readily available, the National LGBTQIA+ Health Education Center has developed a resource for providing an affirmative approach to care for these young people.5 While more research is needed to better understand young people with coexisting ASD (or other neurodivergent conditions), taking an individualized approach to their care can help ensure optimal outcomes.
Dr. Cooper is assistant professor of pediatrics at University of Texas Southwestern, Dallas, and an adolescent medicine specialist at Children’s Medical Center Dallas.
References
1. Data & Statistics on Autism Spectrum Disorder. https://www.cdc.gov/ncbddd/autism/data.html.
2. Glidden D et al. Gender dysphoria and autism spectrum disorder: A systematic review of the literature. Sex Med Rev. 2016;4(1):3-14. doi:10.1016/j.sxmr.2015.10.003.
3. Strang JF et al. Initial clinical guidelines for co-occurring autism spectrum disorder and gender dysphoria or incongruence in adolescents. J Clin Child Adolesc Psychol. 2018;47(1):105-15. doi:10.1080/15374416.2016.1228462.
4. Strang JF et. al. The Gender-Diversity and Autism Questionnaire: A Community-Developed Clinical, Research, and Self-Advocacy Tool for Autistic Transgender and Gender-Diverse Young Adults. Autism Adulthood. 2023 Jun 1;5(2):175-90. doi: 10.1089/aut.2023.0002.
5. National LGBT Health Education Center. Neurodiversity & gender-diverse youth: An affirming approach to care 2020. https://www.lgbtqiahealtheducation.org/publication/neurodiversity-gender-diverse-youth-an-affirming-approach-to-care-2020/download
According to the CDC, the prevalence of autism spectrum disorders (ASD) has gone from roughly 1 in 68 children in 2010 to 1 in 36 children in 2020.1 This is nearly a 50% increase over that 10-year period. Over the last several years, there has been evidence suggesting that increasing numbers of young people with ASD or other neurodivergent conditions identify as transgender or gender diverse.2 Experts agree more careful attention must be paid to these patients.
This includes things such as difficulty with communication, possible concrete thinking, and obsessive interests. While earlier research has shown a higher incidence of ASD in those referred to specialized gender medical clinics, it is important to realize that not all of these youth are seeking medical care. They may be brought to the attention of a primary care pediatrician (PCP) if the child has discussed their gender identity at home. It is important that PCPs approach these young people with an open mind and address any coexisting mental health conditions. PCPs must be careful not to dismiss any gender identity concerns as another of the patient’s “obsessions”; rather, they should ensure the patient receives the appropriate mental health care that they need to explore these concerns. One challenge for PCPs is that there is a dearth of mental health professionals who have experience in working with young people who have both gender dysphoria and a neurodivergent condition.
For those clinicians who provide gender-affirming medical care to these young people, it is imperative that they have a thorough understanding of the patient’s gender identity and medical goals before starting any treatment. This may require extensive collaboration with the patient’s mental health provider. The clinician providing medical care may also choose to proceed slower with the introduction of hormones and their subsequent dosing to allow the young person time to continue discussing their effects with their mental health provider. To help clinicians, Dr. John Strang and a multidisciplinary group of collaborators developed a set of guidelines for co-occurring ASD and gender dysphoria in adolescents.3 More recently, Dr. Strang and other collaborators have also developed a questionnaire that can be used by clinicians in the care of these patients.4 The goal of this questionnaire is to allow the young people to “communicate their experiences and needs in a report format attuned to common autistic thinking and communication styles.”
In summary, pediatricians and those who care for children and adolescents need to be aware of the increased association between those with ASD or other neurodivergent conditions and gender dysphoria. To ensure that these young people receive optimal care, it is important to connect them to experts (if possible) in coexisting ASD and gender dysphoria. If such experts are not readily available, the National LGBTQIA+ Health Education Center has developed a resource for providing an affirmative approach to care for these young people.5 While more research is needed to better understand young people with coexisting ASD (or other neurodivergent conditions), taking an individualized approach to their care can help ensure optimal outcomes.
Dr. Cooper is assistant professor of pediatrics at University of Texas Southwestern, Dallas, and an adolescent medicine specialist at Children’s Medical Center Dallas.
References
1. Data & Statistics on Autism Spectrum Disorder. https://www.cdc.gov/ncbddd/autism/data.html.
2. Glidden D et al. Gender dysphoria and autism spectrum disorder: A systematic review of the literature. Sex Med Rev. 2016;4(1):3-14. doi:10.1016/j.sxmr.2015.10.003.
3. Strang JF et al. Initial clinical guidelines for co-occurring autism spectrum disorder and gender dysphoria or incongruence in adolescents. J Clin Child Adolesc Psychol. 2018;47(1):105-15. doi:10.1080/15374416.2016.1228462.
4. Strang JF et. al. The Gender-Diversity and Autism Questionnaire: A Community-Developed Clinical, Research, and Self-Advocacy Tool for Autistic Transgender and Gender-Diverse Young Adults. Autism Adulthood. 2023 Jun 1;5(2):175-90. doi: 10.1089/aut.2023.0002.
5. National LGBT Health Education Center. Neurodiversity & gender-diverse youth: An affirming approach to care 2020. https://www.lgbtqiahealtheducation.org/publication/neurodiversity-gender-diverse-youth-an-affirming-approach-to-care-2020/download
New tool to guide transcatheter aortic valve replacement
TOPLINE:
, results of a new study suggest.
Researchers developed TJ-ICE–guided TAVR to facilitate implanting a heart valve at an optimal depth, guided by direct visualization of the membranous septum (MS) during the procedure.
METHODOLOGY:
- The single-center study included 163 patients with severe aortic stenosis (AS) from an ongoing registry, mean age 85 years, 71% women, and median Society of Thoracic Surgeons score of 6.3%, who underwent TAVR.
- The primary endpoint was the incidence at 30 days of PPMI; secondary endpoints included the feasibility of TJ-ICE–guided TAVR and safety, including complications related to TJ-ICE.
TAKEAWAY:
- Although all patients underwent valve placement in the proper anatomical location, moderate paravalvular leakage (PVL) occurred in four patients, and a second valve was required in two patients, resulting in a device success of 96.3%.
- New PPMI within 30 days was required in 11 patients (6.7%), all because of complete atrioventricular block; patients with baseline right bundle branch block (RBBB) had a higher incidence of new PPMI than did those without RBBB (23.8% vs. 4.2%; P < .001).
- Patients whose device was implanted inside the MS had a significantly lower incidence of new PPMI (overall 2.1% vs. 13.4%; P = .005); this finding was consistent in patients with baseline RBBB (6.7% vs. 66.7%; P = .004) or without RBBB (1.2% vs. 8.2%; P = .041).
- By 30 days, there was one death, which occurred as a result of bleeding in a patient with liver cirrhosis after a successful TAVR procedure; four patients experienced disabling strokes, and vascular complications developed in 16 patients.
IN PRACTICE:
The study demonstrated the “notable feasibility and safety” of TJ-ICE–guided TAVR, the authors write. They point to the “strong association of TAV position with new PPMI rate, which was clearly visualized by ICE during the procedure.”
In an accompanying editorial, Thomas Bartel, MD, PHD, Flexdoc Inc., Düsseldorf, Germany, noted that the study is the first to report a clinical benefit using a TJ-ICE approach, although barriers such as cost and lack of expertise could prevent interventional cardiologists from taking full advantage of ICE monitoring during TAVR, and further research is warranted.
Randomized and prospective trials comparing the accuracy, reproducibility, and outcomes of ICE guidance vs. guidance by transesophageal echocardiography, and pure fluoroscopy and angiography, “need to be performed before ICE imaging is adopted as the primary nonradiographic imaging modality for TAVR.”
SOURCE:
The study was carried out by Tsutomu Murakami, MD, department of cardiology, Tokai University, Isehara, Japan, and colleagues. It was published online in JACC: Asia.
LIMITATIONS:
The retrospective nonrandomized design has inherent limitations. The choice of intraprocedural imaging modality was decided based on heart team discussion, which may have introduced selection bias. Operators’ implantation skills could have influenced the results although most cases involved highly experienced board-certified operators. The limited number of subjects and the relatively low event rates preclude definitive conclusions.
DISCLOSURES:
Dr. Murakami has no relevant conflicts of interest; see paper for disclosures of other study authors. Dr. Bartel has no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
TOPLINE:
, results of a new study suggest.
Researchers developed TJ-ICE–guided TAVR to facilitate implanting a heart valve at an optimal depth, guided by direct visualization of the membranous septum (MS) during the procedure.
METHODOLOGY:
- The single-center study included 163 patients with severe aortic stenosis (AS) from an ongoing registry, mean age 85 years, 71% women, and median Society of Thoracic Surgeons score of 6.3%, who underwent TAVR.
- The primary endpoint was the incidence at 30 days of PPMI; secondary endpoints included the feasibility of TJ-ICE–guided TAVR and safety, including complications related to TJ-ICE.
TAKEAWAY:
- Although all patients underwent valve placement in the proper anatomical location, moderate paravalvular leakage (PVL) occurred in four patients, and a second valve was required in two patients, resulting in a device success of 96.3%.
- New PPMI within 30 days was required in 11 patients (6.7%), all because of complete atrioventricular block; patients with baseline right bundle branch block (RBBB) had a higher incidence of new PPMI than did those without RBBB (23.8% vs. 4.2%; P < .001).
- Patients whose device was implanted inside the MS had a significantly lower incidence of new PPMI (overall 2.1% vs. 13.4%; P = .005); this finding was consistent in patients with baseline RBBB (6.7% vs. 66.7%; P = .004) or without RBBB (1.2% vs. 8.2%; P = .041).
- By 30 days, there was one death, which occurred as a result of bleeding in a patient with liver cirrhosis after a successful TAVR procedure; four patients experienced disabling strokes, and vascular complications developed in 16 patients.
IN PRACTICE:
The study demonstrated the “notable feasibility and safety” of TJ-ICE–guided TAVR, the authors write. They point to the “strong association of TAV position with new PPMI rate, which was clearly visualized by ICE during the procedure.”
In an accompanying editorial, Thomas Bartel, MD, PHD, Flexdoc Inc., Düsseldorf, Germany, noted that the study is the first to report a clinical benefit using a TJ-ICE approach, although barriers such as cost and lack of expertise could prevent interventional cardiologists from taking full advantage of ICE monitoring during TAVR, and further research is warranted.
Randomized and prospective trials comparing the accuracy, reproducibility, and outcomes of ICE guidance vs. guidance by transesophageal echocardiography, and pure fluoroscopy and angiography, “need to be performed before ICE imaging is adopted as the primary nonradiographic imaging modality for TAVR.”
SOURCE:
The study was carried out by Tsutomu Murakami, MD, department of cardiology, Tokai University, Isehara, Japan, and colleagues. It was published online in JACC: Asia.
LIMITATIONS:
The retrospective nonrandomized design has inherent limitations. The choice of intraprocedural imaging modality was decided based on heart team discussion, which may have introduced selection bias. Operators’ implantation skills could have influenced the results although most cases involved highly experienced board-certified operators. The limited number of subjects and the relatively low event rates preclude definitive conclusions.
DISCLOSURES:
Dr. Murakami has no relevant conflicts of interest; see paper for disclosures of other study authors. Dr. Bartel has no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
TOPLINE:
, results of a new study suggest.
Researchers developed TJ-ICE–guided TAVR to facilitate implanting a heart valve at an optimal depth, guided by direct visualization of the membranous septum (MS) during the procedure.
METHODOLOGY:
- The single-center study included 163 patients with severe aortic stenosis (AS) from an ongoing registry, mean age 85 years, 71% women, and median Society of Thoracic Surgeons score of 6.3%, who underwent TAVR.
- The primary endpoint was the incidence at 30 days of PPMI; secondary endpoints included the feasibility of TJ-ICE–guided TAVR and safety, including complications related to TJ-ICE.
TAKEAWAY:
- Although all patients underwent valve placement in the proper anatomical location, moderate paravalvular leakage (PVL) occurred in four patients, and a second valve was required in two patients, resulting in a device success of 96.3%.
- New PPMI within 30 days was required in 11 patients (6.7%), all because of complete atrioventricular block; patients with baseline right bundle branch block (RBBB) had a higher incidence of new PPMI than did those without RBBB (23.8% vs. 4.2%; P < .001).
- Patients whose device was implanted inside the MS had a significantly lower incidence of new PPMI (overall 2.1% vs. 13.4%; P = .005); this finding was consistent in patients with baseline RBBB (6.7% vs. 66.7%; P = .004) or without RBBB (1.2% vs. 8.2%; P = .041).
- By 30 days, there was one death, which occurred as a result of bleeding in a patient with liver cirrhosis after a successful TAVR procedure; four patients experienced disabling strokes, and vascular complications developed in 16 patients.
IN PRACTICE:
The study demonstrated the “notable feasibility and safety” of TJ-ICE–guided TAVR, the authors write. They point to the “strong association of TAV position with new PPMI rate, which was clearly visualized by ICE during the procedure.”
In an accompanying editorial, Thomas Bartel, MD, PHD, Flexdoc Inc., Düsseldorf, Germany, noted that the study is the first to report a clinical benefit using a TJ-ICE approach, although barriers such as cost and lack of expertise could prevent interventional cardiologists from taking full advantage of ICE monitoring during TAVR, and further research is warranted.
Randomized and prospective trials comparing the accuracy, reproducibility, and outcomes of ICE guidance vs. guidance by transesophageal echocardiography, and pure fluoroscopy and angiography, “need to be performed before ICE imaging is adopted as the primary nonradiographic imaging modality for TAVR.”
SOURCE:
The study was carried out by Tsutomu Murakami, MD, department of cardiology, Tokai University, Isehara, Japan, and colleagues. It was published online in JACC: Asia.
LIMITATIONS:
The retrospective nonrandomized design has inherent limitations. The choice of intraprocedural imaging modality was decided based on heart team discussion, which may have introduced selection bias. Operators’ implantation skills could have influenced the results although most cases involved highly experienced board-certified operators. The limited number of subjects and the relatively low event rates preclude definitive conclusions.
DISCLOSURES:
Dr. Murakami has no relevant conflicts of interest; see paper for disclosures of other study authors. Dr. Bartel has no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
Novel triple-threat approach to acne beats placebo
TOPLINE:
A topical fixed-dose combination of three approved acne treatments significantly improves moderate to severe acne with a strong safety profile.
METHODOLOGY:
- The two multicenter studies included 363 individuals aged 9 years and older with moderate to severe acne from 30 centers, including 15 in North America.
- Moderate to severe acne was defined as having 30-100 inflammatory lesions (papules, pustules, or nodules), 35-150 noninflammatory lesions (open or closed comedones), and at least two nodules.
- Participants were randomly assigned to receive treatment with a combination gel containing phosphate 1.2%, 0.15%, and 3.1% (known as IDP-126) or a vehicle gel for once-daily application for 12 weeks.
- Treatment success was defined as a reduction of at least two grades from baseline on the Evaluator’s Global Severity Score (EGSS) and lesion counts of clear (0) or almost clear (1) at weeks 2, 4, 8, and 12.
TAKEAWAY:
- Treatment success occurred in 49.6% of the IDP-126 group, vs 24.9% of the vehicle group in study 1, and in 50.5% of the IDP-126 group, vs 20.5% of the vehicle group in study 2. Overall treatment compliance was 93.7% and 91.3% for studies 1 and 2, respectively (P < .01 for both).
- Patients in the IDP-126 groups for both studies 1 and 2 had significantly greater absolute mean reductions in both inflammatory and noninflammatory lesions from baseline to week 12 compared to the vehicle patients (P ≤ .001 for all).
- Significantly more patients in the IDP-126 group achieved a grade reduction of 2 or more in EGSS compared with those who received the vehicle, with treatment differences of approximately 32% in both studies. Changes in lesion reductions between the treatment and the vehicle groups were significantly greater as early as week 4.
- The most common treatment-related adverse events among patients treated with IDP-126 were erythema, application-site pain, dryness, irritation, and exfoliation. Discontinuation of the study drug as a result of adverse events occurred in 2.5% and 3.3% of these patients in studies 1 and 2, respectively.
IN PRACTICE:
“With its simple treatment regimen containing 3 recommended acne treatments (benzoyl peroxide, a topical retinoid, and a topical antibiotic), IDP-126 is a potential new treatment option for acne,” the researchers concluded.
SOURCE:
The study was led by Linda Stein Gold, MD, of Henry Ford Hospital, Detroit. The study was published online in the Journal of the American Academy of Dermatology.
LIMITATIONS:
In both studies, treatment duration was short, and the studies may not reflect patients’ real-world experiences. The results may be affected by interobserver bias or variation in assessment of acne severity.
DISCLOSURES:
Gold has served as investigator/consultant or speaker for Ortho Dermatologics, LEO Pharma, Dermavant, Incyte, Novartis, AbbVie, Pfizer, Sun Pharma, UCB, Arcutis, and Lilly. Other study coauthors have relationships with multiple companies, including Ortho Dermatologics, which provided medical writing support for the study.
A version of this article first appeared on Medscape.com.
TOPLINE:
A topical fixed-dose combination of three approved acne treatments significantly improves moderate to severe acne with a strong safety profile.
METHODOLOGY:
- The two multicenter studies included 363 individuals aged 9 years and older with moderate to severe acne from 30 centers, including 15 in North America.
- Moderate to severe acne was defined as having 30-100 inflammatory lesions (papules, pustules, or nodules), 35-150 noninflammatory lesions (open or closed comedones), and at least two nodules.
- Participants were randomly assigned to receive treatment with a combination gel containing phosphate 1.2%, 0.15%, and 3.1% (known as IDP-126) or a vehicle gel for once-daily application for 12 weeks.
- Treatment success was defined as a reduction of at least two grades from baseline on the Evaluator’s Global Severity Score (EGSS) and lesion counts of clear (0) or almost clear (1) at weeks 2, 4, 8, and 12.
TAKEAWAY:
- Treatment success occurred in 49.6% of the IDP-126 group, vs 24.9% of the vehicle group in study 1, and in 50.5% of the IDP-126 group, vs 20.5% of the vehicle group in study 2. Overall treatment compliance was 93.7% and 91.3% for studies 1 and 2, respectively (P < .01 for both).
- Patients in the IDP-126 groups for both studies 1 and 2 had significantly greater absolute mean reductions in both inflammatory and noninflammatory lesions from baseline to week 12 compared to the vehicle patients (P ≤ .001 for all).
- Significantly more patients in the IDP-126 group achieved a grade reduction of 2 or more in EGSS compared with those who received the vehicle, with treatment differences of approximately 32% in both studies. Changes in lesion reductions between the treatment and the vehicle groups were significantly greater as early as week 4.
- The most common treatment-related adverse events among patients treated with IDP-126 were erythema, application-site pain, dryness, irritation, and exfoliation. Discontinuation of the study drug as a result of adverse events occurred in 2.5% and 3.3% of these patients in studies 1 and 2, respectively.
IN PRACTICE:
“With its simple treatment regimen containing 3 recommended acne treatments (benzoyl peroxide, a topical retinoid, and a topical antibiotic), IDP-126 is a potential new treatment option for acne,” the researchers concluded.
SOURCE:
The study was led by Linda Stein Gold, MD, of Henry Ford Hospital, Detroit. The study was published online in the Journal of the American Academy of Dermatology.
LIMITATIONS:
In both studies, treatment duration was short, and the studies may not reflect patients’ real-world experiences. The results may be affected by interobserver bias or variation in assessment of acne severity.
DISCLOSURES:
Gold has served as investigator/consultant or speaker for Ortho Dermatologics, LEO Pharma, Dermavant, Incyte, Novartis, AbbVie, Pfizer, Sun Pharma, UCB, Arcutis, and Lilly. Other study coauthors have relationships with multiple companies, including Ortho Dermatologics, which provided medical writing support for the study.
A version of this article first appeared on Medscape.com.
TOPLINE:
A topical fixed-dose combination of three approved acne treatments significantly improves moderate to severe acne with a strong safety profile.
METHODOLOGY:
- The two multicenter studies included 363 individuals aged 9 years and older with moderate to severe acne from 30 centers, including 15 in North America.
- Moderate to severe acne was defined as having 30-100 inflammatory lesions (papules, pustules, or nodules), 35-150 noninflammatory lesions (open or closed comedones), and at least two nodules.
- Participants were randomly assigned to receive treatment with a combination gel containing phosphate 1.2%, 0.15%, and 3.1% (known as IDP-126) or a vehicle gel for once-daily application for 12 weeks.
- Treatment success was defined as a reduction of at least two grades from baseline on the Evaluator’s Global Severity Score (EGSS) and lesion counts of clear (0) or almost clear (1) at weeks 2, 4, 8, and 12.
TAKEAWAY:
- Treatment success occurred in 49.6% of the IDP-126 group, vs 24.9% of the vehicle group in study 1, and in 50.5% of the IDP-126 group, vs 20.5% of the vehicle group in study 2. Overall treatment compliance was 93.7% and 91.3% for studies 1 and 2, respectively (P < .01 for both).
- Patients in the IDP-126 groups for both studies 1 and 2 had significantly greater absolute mean reductions in both inflammatory and noninflammatory lesions from baseline to week 12 compared to the vehicle patients (P ≤ .001 for all).
- Significantly more patients in the IDP-126 group achieved a grade reduction of 2 or more in EGSS compared with those who received the vehicle, with treatment differences of approximately 32% in both studies. Changes in lesion reductions between the treatment and the vehicle groups were significantly greater as early as week 4.
- The most common treatment-related adverse events among patients treated with IDP-126 were erythema, application-site pain, dryness, irritation, and exfoliation. Discontinuation of the study drug as a result of adverse events occurred in 2.5% and 3.3% of these patients in studies 1 and 2, respectively.
IN PRACTICE:
“With its simple treatment regimen containing 3 recommended acne treatments (benzoyl peroxide, a topical retinoid, and a topical antibiotic), IDP-126 is a potential new treatment option for acne,” the researchers concluded.
SOURCE:
The study was led by Linda Stein Gold, MD, of Henry Ford Hospital, Detroit. The study was published online in the Journal of the American Academy of Dermatology.
LIMITATIONS:
In both studies, treatment duration was short, and the studies may not reflect patients’ real-world experiences. The results may be affected by interobserver bias or variation in assessment of acne severity.
DISCLOSURES:
Gold has served as investigator/consultant or speaker for Ortho Dermatologics, LEO Pharma, Dermavant, Incyte, Novartis, AbbVie, Pfizer, Sun Pharma, UCB, Arcutis, and Lilly. Other study coauthors have relationships with multiple companies, including Ortho Dermatologics, which provided medical writing support for the study.
A version of this article first appeared on Medscape.com.
Antibiotics ‘like gold’ for some, driving inappropriate use
Personal beliefs and health care system barriers contribute to inappropriate antibiotic use by patients, report researchers presenting results at an annual scientific meeting on infectious diseases.
Nonprescription antibiotic use includes accessing medication left over from a prior prescribed course, obtained from social networks, and purchased over-the-counter in other countries or illegally in stores and markets in the United States.
Overuse and misuse of antibiotics contributes to a growing threat of antimicrobial resistance, and it is tough to say how common it is, Lindsey A. Laytner, PhD, MPH, with Baylor College of Medicine, Houston, pointed out in her presentation.
“This is an understudied area. We don’t routinely collect these data, so we don’t actually know what the true prevalence is. The factors that contribute to this unsafe practice in the U.S. are also underexplored,” Dr. Laytner said.
To investigate, the researchers conducted in-depth interviews with 86 adults (median age, 49 years; 62% women) to identify patients’ motivations to use antibiotics without a prescription. All of them answered “yes” when asked in a previous survey whether they would use antibiotics without contacting a doctor, nurse, dentist, or clinic.
Dr. Laytner said several prominent themes emerged.
Nearly all interviewees reported nonprescription antibiotic use for symptoms that mostly do not warrant antibiotics. These included symptoms of COVID-19, influenza, and the common cold, as well as for pain management, allergies, and even wounds.
Ineffectively treating symptoms
Many felt they “knew their body, knew what they had, and knew how to treat themselves” without a health care provider, Dr. Laytner said.
They also felt the over-the-counter medicines “don’t always work and that antibiotics are like gold or this cure-all and because they are difficult to get a prescription for, they should be kept on hand,” she explained.
A variety of health care system barriers also contribute to inappropriate antibiotic use, including long wait times to schedule appointments and to see the doctor while at their appointments; high costs for clinic visits and prescriptions; and transportation issues.
Many patients opted to use nonprescription antibiotics out of “convenience,” Laytner added.
She explains that the findings could help inform community-level education efforts on inappropriate use of antibiotics and help shape policies to promote antibiotic stewardship.
Access to care, education
Commenting on the study, Emily Sydnor Spivak, MD, associate professor of medicine at University of Utah, Salt Lake City, said she “wasn’t totally surprised by the results, but found it very interesting how there was a theme of autonomy, or ‘I know my body,’ that seemed to drive patients to get antibiotics for relief of symptoms.”
said Dr. Spivak, who is also medical director of antimicrobial stewardship programs at University of Utah Health and VA Salt Lake City Health Care System.
“Given the lack of access to health care as a reason some patients use nonprescription antibiotics, we need to think about access to the health care system and process changes and policy changes to allow better access. Without better access or interaction with the health care system, we can’t educate patients,” Dr. Spivak said.
The study had no commercial funding. Dr. Laytner and Dr. Spivak report no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Personal beliefs and health care system barriers contribute to inappropriate antibiotic use by patients, report researchers presenting results at an annual scientific meeting on infectious diseases.
Nonprescription antibiotic use includes accessing medication left over from a prior prescribed course, obtained from social networks, and purchased over-the-counter in other countries or illegally in stores and markets in the United States.
Overuse and misuse of antibiotics contributes to a growing threat of antimicrobial resistance, and it is tough to say how common it is, Lindsey A. Laytner, PhD, MPH, with Baylor College of Medicine, Houston, pointed out in her presentation.
“This is an understudied area. We don’t routinely collect these data, so we don’t actually know what the true prevalence is. The factors that contribute to this unsafe practice in the U.S. are also underexplored,” Dr. Laytner said.
To investigate, the researchers conducted in-depth interviews with 86 adults (median age, 49 years; 62% women) to identify patients’ motivations to use antibiotics without a prescription. All of them answered “yes” when asked in a previous survey whether they would use antibiotics without contacting a doctor, nurse, dentist, or clinic.
Dr. Laytner said several prominent themes emerged.
Nearly all interviewees reported nonprescription antibiotic use for symptoms that mostly do not warrant antibiotics. These included symptoms of COVID-19, influenza, and the common cold, as well as for pain management, allergies, and even wounds.
Ineffectively treating symptoms
Many felt they “knew their body, knew what they had, and knew how to treat themselves” without a health care provider, Dr. Laytner said.
They also felt the over-the-counter medicines “don’t always work and that antibiotics are like gold or this cure-all and because they are difficult to get a prescription for, they should be kept on hand,” she explained.
A variety of health care system barriers also contribute to inappropriate antibiotic use, including long wait times to schedule appointments and to see the doctor while at their appointments; high costs for clinic visits and prescriptions; and transportation issues.
Many patients opted to use nonprescription antibiotics out of “convenience,” Laytner added.
She explains that the findings could help inform community-level education efforts on inappropriate use of antibiotics and help shape policies to promote antibiotic stewardship.
Access to care, education
Commenting on the study, Emily Sydnor Spivak, MD, associate professor of medicine at University of Utah, Salt Lake City, said she “wasn’t totally surprised by the results, but found it very interesting how there was a theme of autonomy, or ‘I know my body,’ that seemed to drive patients to get antibiotics for relief of symptoms.”
said Dr. Spivak, who is also medical director of antimicrobial stewardship programs at University of Utah Health and VA Salt Lake City Health Care System.
“Given the lack of access to health care as a reason some patients use nonprescription antibiotics, we need to think about access to the health care system and process changes and policy changes to allow better access. Without better access or interaction with the health care system, we can’t educate patients,” Dr. Spivak said.
The study had no commercial funding. Dr. Laytner and Dr. Spivak report no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Personal beliefs and health care system barriers contribute to inappropriate antibiotic use by patients, report researchers presenting results at an annual scientific meeting on infectious diseases.
Nonprescription antibiotic use includes accessing medication left over from a prior prescribed course, obtained from social networks, and purchased over-the-counter in other countries or illegally in stores and markets in the United States.
Overuse and misuse of antibiotics contributes to a growing threat of antimicrobial resistance, and it is tough to say how common it is, Lindsey A. Laytner, PhD, MPH, with Baylor College of Medicine, Houston, pointed out in her presentation.
“This is an understudied area. We don’t routinely collect these data, so we don’t actually know what the true prevalence is. The factors that contribute to this unsafe practice in the U.S. are also underexplored,” Dr. Laytner said.
To investigate, the researchers conducted in-depth interviews with 86 adults (median age, 49 years; 62% women) to identify patients’ motivations to use antibiotics without a prescription. All of them answered “yes” when asked in a previous survey whether they would use antibiotics without contacting a doctor, nurse, dentist, or clinic.
Dr. Laytner said several prominent themes emerged.
Nearly all interviewees reported nonprescription antibiotic use for symptoms that mostly do not warrant antibiotics. These included symptoms of COVID-19, influenza, and the common cold, as well as for pain management, allergies, and even wounds.
Ineffectively treating symptoms
Many felt they “knew their body, knew what they had, and knew how to treat themselves” without a health care provider, Dr. Laytner said.
They also felt the over-the-counter medicines “don’t always work and that antibiotics are like gold or this cure-all and because they are difficult to get a prescription for, they should be kept on hand,” she explained.
A variety of health care system barriers also contribute to inappropriate antibiotic use, including long wait times to schedule appointments and to see the doctor while at their appointments; high costs for clinic visits and prescriptions; and transportation issues.
Many patients opted to use nonprescription antibiotics out of “convenience,” Laytner added.
She explains that the findings could help inform community-level education efforts on inappropriate use of antibiotics and help shape policies to promote antibiotic stewardship.
Access to care, education
Commenting on the study, Emily Sydnor Spivak, MD, associate professor of medicine at University of Utah, Salt Lake City, said she “wasn’t totally surprised by the results, but found it very interesting how there was a theme of autonomy, or ‘I know my body,’ that seemed to drive patients to get antibiotics for relief of symptoms.”
said Dr. Spivak, who is also medical director of antimicrobial stewardship programs at University of Utah Health and VA Salt Lake City Health Care System.
“Given the lack of access to health care as a reason some patients use nonprescription antibiotics, we need to think about access to the health care system and process changes and policy changes to allow better access. Without better access or interaction with the health care system, we can’t educate patients,” Dr. Spivak said.
The study had no commercial funding. Dr. Laytner and Dr. Spivak report no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
IDWEEK 2023
Trading one’s eggs for a service discount raises tough issues, says ethicist
This transcript has been edited for clarity.
I had a case come to me of a 32-year-old resident who works in a hospital near where I am and was very interested in freezing her eggs. She wasn’t married and was getting worried that maybe she wouldn’t have a partner soon. She was also getting worried that the potential ability of her eggs to be fertilized would begin to decline, which is a phenomenon that does occur with age. She thought, I’m 32; maybe I should freeze my eggs now, as it’s better than to try freezing them when I’m 35 or 37. The potency may be far less.
There are many programs out there now. There have been academic programs for a long time that have been doing egg freezing, and there are many children who have been born successfully. However, it’s also true that people freeze their eggs when they’re 40 years old, and the likelihood of their “working,” if you will, is far less. I wouldn’t say it’s impossible, but age matters. This medical resident knew that and she decided to look into egg freezing.
Well, it turned out that egg freezing is not something that her student insurance plan – or most insurance plans in general – covers. The opportunity to do this is probably going to cost her about $10,000. There are many new egg-freezing infertility programs that have stared up that aren’t part of hospitals. There are clinics that are run for profit. They sometimes encourage women to freeze their eggs.
The student resident quickly found out that there were companies near her who would do egg freezing but would cut a deal if she agreed to take drugs to super-ovulate, make a large number of eggs, and they would be procured if she agreed to give half of them to other women who needed eggs for their infertility treatment. She could keep half and she could get very discounted treatment of egg freezing.
That may be a deal that she’s going to accept. She doesn’t have a path forward. She’s worried about freezing her eggs right now. But there are many ethical considerations that really have to be thought through here.
First and foremost, she’s giving eggs to others. They’re going to use them to try to make children. They can’t make their own eggs, for some reason. She’s going to have some biologically related kids out there. It used to be that you could say to someone who donated sperm or eggs that this will be anonymous.
But in today’s day and age with 23andMe, Ancestry, and better genetic testing, there’s a pretty good likelihood that somebody is going to find out that the person they thought was their biological mom isn’t, and they have someone out there who was the person who, in this case, donated an egg.
Is she willing to risk having that connection, that contact, to have someone enter her life in the future? It’s a situation where she’s donating the eggs, but I’ll tell you that the clinic is going to make far more money using the donated eggs, probably getting $10,000 or $15,000 a cycle with people who are trying to have a child. They’ll make much more money than she’s going to get by donating.
She may get a $5,000 discount, if you will, but the clinic has a business interest. The more they get women involved in bartering their eggs, the more they’re going to profit. In a sense, she’s being coerced, perhaps – I’m going to put it glibly – to sell cheaply. She probably is getting undervalue, even though she needs a path to do this egg freezing.
The other big issue is that we don’t know that egg freezing is going to work for her until someone tries to use those eggs. She may have her own infertility problem not due to age but to other things. Approximately 8%-9% of couples do have infertility problems, sometimes related to gametes. She may never get a partner. Maybe she doesn’t want to use these eggs on her own as a single mom. All of these issues have to be talked through.
What really troubles me here is not so much that someone would choose to barter their eggs, but that they don’t get counseling. They don’t get independent advice about thinking this all through. It’s turning into a business. A business has a commodity – her eggs – that they want. She’s getting more and more desperate, willing to cut a deal to get where she needs to be, but perhaps is not really thinking through all of the ethical dimensions that bartering or trading one’s eggs in order to gain access to freezing entails.
We have to set up a system where there’s independent advice and independent counseling; otherwise, I think we’re closer to exploitation.
A version of this article first appeared on Medscape.com.
Dr. Caplan is director, division of medical ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use.
This transcript has been edited for clarity.
I had a case come to me of a 32-year-old resident who works in a hospital near where I am and was very interested in freezing her eggs. She wasn’t married and was getting worried that maybe she wouldn’t have a partner soon. She was also getting worried that the potential ability of her eggs to be fertilized would begin to decline, which is a phenomenon that does occur with age. She thought, I’m 32; maybe I should freeze my eggs now, as it’s better than to try freezing them when I’m 35 or 37. The potency may be far less.
There are many programs out there now. There have been academic programs for a long time that have been doing egg freezing, and there are many children who have been born successfully. However, it’s also true that people freeze their eggs when they’re 40 years old, and the likelihood of their “working,” if you will, is far less. I wouldn’t say it’s impossible, but age matters. This medical resident knew that and she decided to look into egg freezing.
Well, it turned out that egg freezing is not something that her student insurance plan – or most insurance plans in general – covers. The opportunity to do this is probably going to cost her about $10,000. There are many new egg-freezing infertility programs that have stared up that aren’t part of hospitals. There are clinics that are run for profit. They sometimes encourage women to freeze their eggs.
The student resident quickly found out that there were companies near her who would do egg freezing but would cut a deal if she agreed to take drugs to super-ovulate, make a large number of eggs, and they would be procured if she agreed to give half of them to other women who needed eggs for their infertility treatment. She could keep half and she could get very discounted treatment of egg freezing.
That may be a deal that she’s going to accept. She doesn’t have a path forward. She’s worried about freezing her eggs right now. But there are many ethical considerations that really have to be thought through here.
First and foremost, she’s giving eggs to others. They’re going to use them to try to make children. They can’t make their own eggs, for some reason. She’s going to have some biologically related kids out there. It used to be that you could say to someone who donated sperm or eggs that this will be anonymous.
But in today’s day and age with 23andMe, Ancestry, and better genetic testing, there’s a pretty good likelihood that somebody is going to find out that the person they thought was their biological mom isn’t, and they have someone out there who was the person who, in this case, donated an egg.
Is she willing to risk having that connection, that contact, to have someone enter her life in the future? It’s a situation where she’s donating the eggs, but I’ll tell you that the clinic is going to make far more money using the donated eggs, probably getting $10,000 or $15,000 a cycle with people who are trying to have a child. They’ll make much more money than she’s going to get by donating.
She may get a $5,000 discount, if you will, but the clinic has a business interest. The more they get women involved in bartering their eggs, the more they’re going to profit. In a sense, she’s being coerced, perhaps – I’m going to put it glibly – to sell cheaply. She probably is getting undervalue, even though she needs a path to do this egg freezing.
The other big issue is that we don’t know that egg freezing is going to work for her until someone tries to use those eggs. She may have her own infertility problem not due to age but to other things. Approximately 8%-9% of couples do have infertility problems, sometimes related to gametes. She may never get a partner. Maybe she doesn’t want to use these eggs on her own as a single mom. All of these issues have to be talked through.
What really troubles me here is not so much that someone would choose to barter their eggs, but that they don’t get counseling. They don’t get independent advice about thinking this all through. It’s turning into a business. A business has a commodity – her eggs – that they want. She’s getting more and more desperate, willing to cut a deal to get where she needs to be, but perhaps is not really thinking through all of the ethical dimensions that bartering or trading one’s eggs in order to gain access to freezing entails.
We have to set up a system where there’s independent advice and independent counseling; otherwise, I think we’re closer to exploitation.
A version of this article first appeared on Medscape.com.
Dr. Caplan is director, division of medical ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use.
This transcript has been edited for clarity.
I had a case come to me of a 32-year-old resident who works in a hospital near where I am and was very interested in freezing her eggs. She wasn’t married and was getting worried that maybe she wouldn’t have a partner soon. She was also getting worried that the potential ability of her eggs to be fertilized would begin to decline, which is a phenomenon that does occur with age. She thought, I’m 32; maybe I should freeze my eggs now, as it’s better than to try freezing them when I’m 35 or 37. The potency may be far less.
There are many programs out there now. There have been academic programs for a long time that have been doing egg freezing, and there are many children who have been born successfully. However, it’s also true that people freeze their eggs when they’re 40 years old, and the likelihood of their “working,” if you will, is far less. I wouldn’t say it’s impossible, but age matters. This medical resident knew that and she decided to look into egg freezing.
Well, it turned out that egg freezing is not something that her student insurance plan – or most insurance plans in general – covers. The opportunity to do this is probably going to cost her about $10,000. There are many new egg-freezing infertility programs that have stared up that aren’t part of hospitals. There are clinics that are run for profit. They sometimes encourage women to freeze their eggs.
The student resident quickly found out that there were companies near her who would do egg freezing but would cut a deal if she agreed to take drugs to super-ovulate, make a large number of eggs, and they would be procured if she agreed to give half of them to other women who needed eggs for their infertility treatment. She could keep half and she could get very discounted treatment of egg freezing.
That may be a deal that she’s going to accept. She doesn’t have a path forward. She’s worried about freezing her eggs right now. But there are many ethical considerations that really have to be thought through here.
First and foremost, she’s giving eggs to others. They’re going to use them to try to make children. They can’t make their own eggs, for some reason. She’s going to have some biologically related kids out there. It used to be that you could say to someone who donated sperm or eggs that this will be anonymous.
But in today’s day and age with 23andMe, Ancestry, and better genetic testing, there’s a pretty good likelihood that somebody is going to find out that the person they thought was their biological mom isn’t, and they have someone out there who was the person who, in this case, donated an egg.
Is she willing to risk having that connection, that contact, to have someone enter her life in the future? It’s a situation where she’s donating the eggs, but I’ll tell you that the clinic is going to make far more money using the donated eggs, probably getting $10,000 or $15,000 a cycle with people who are trying to have a child. They’ll make much more money than she’s going to get by donating.
She may get a $5,000 discount, if you will, but the clinic has a business interest. The more they get women involved in bartering their eggs, the more they’re going to profit. In a sense, she’s being coerced, perhaps – I’m going to put it glibly – to sell cheaply. She probably is getting undervalue, even though she needs a path to do this egg freezing.
The other big issue is that we don’t know that egg freezing is going to work for her until someone tries to use those eggs. She may have her own infertility problem not due to age but to other things. Approximately 8%-9% of couples do have infertility problems, sometimes related to gametes. She may never get a partner. Maybe she doesn’t want to use these eggs on her own as a single mom. All of these issues have to be talked through.
What really troubles me here is not so much that someone would choose to barter their eggs, but that they don’t get counseling. They don’t get independent advice about thinking this all through. It’s turning into a business. A business has a commodity – her eggs – that they want. She’s getting more and more desperate, willing to cut a deal to get where she needs to be, but perhaps is not really thinking through all of the ethical dimensions that bartering or trading one’s eggs in order to gain access to freezing entails.
We have to set up a system where there’s independent advice and independent counseling; otherwise, I think we’re closer to exploitation.
A version of this article first appeared on Medscape.com.
Dr. Caplan is director, division of medical ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use.
Should women of childbearing age eat a plant-based diet?
The prospective cohort study followed 11,459 women older than 18 years and evaluated their diet from the beginning using a validated questionnaire about the frequency and quality of plant-based foods. The participants had taken part in the Nurses’ Health Study II (1991-2009). From responses on the questionnaire, the investigators calculated the plant-based diet index (PDI) even among participants with an omnivorous diet. A higher score indicated greater adherence to the PDI.
“We wanted to know how one’s diet leading up to pregnancy influences the pregnancy, so we monitored women for virtually their entire reproductive life – almost 20 years – and gained an awareness of their typical diet before pregnancy,” study author Jorge E. Chavarro, MD, ScD, told this news organization. Dr. Chavarro is a professor of nutrition, epidemiology, and medicine at Harvard Medical School, Boston, and Harvard University’s School of Public Health in Cambridge, Mass. He researches how nutrition and lifestyle influence reproductive health and overall lifelong health in women.
Analysis of the data from the Nurses’ Health Study II revealed that as the proportion of animal products in diets decreased and the proportion of plant-based products increased, the risk of women experiencing hypertensive disorders of pregnancy decreased as well. Women in the highest PDI quintile had a significantly lower risk of hypertensive disorders of pregnancy, in comparison with those in the lowest quintile (relative risk, 0.76). This association was slightly stronger for pregnancy-related hypertension (RR, 0.77) than for preeclampsia (RR, 0.80).
Women in the highest PDI quintile had a 24% lower risk of hypertensive disorders of pregnancy than those in the lowest quintile; the risk of pregnancy-related hypertension decreased in a linear fashion as PDI increased, while the relationship of PDI to preeclampsia was restricted to women in the quintile with the highest adherence.
“It was clearer for pregnancy-related hypertension than for preeclampsia, but a diet made up primarily of plant-based foods seemed to be protective for both,” said Dr. Chavarro. He added that in addition to the problems these conditions cause during pregnancy, both increase the risk of subsequently developing other chronic diseases. “Could it be that modifiable lifestyle factors before and during pregnancy may not only help reduce problems during gestation but also prevent women’s health problems years later? That was the general motivation for this study.”
Mercedes Sotos-Prieto, PhD, a researcher at the Autonomous University of Madrid and an associate professor at Harvard University’s School of Public Health, told this news organization that the study’s methodology was very robust and that the investigators utilized appropriate statistical techniques for the analysis. She highlighted the fact that they used a validated food frequency questionnaire. She believes the study is also important because of the population group it focused on. “There has always been greater resistance when it comes to the diet of pregnant women, and the same is true for older adults. But we have seen that this type of diet, if it’s a quality diet, may be associated with health benefits.” She did not participate in the study.
Dr. Sotos-Prieto has a doctorate in nutritional epidemiology and public health. She works with large epidemiologic cohorts, such as the cohort of American nurses on which this study was based, and ENRICA, a cohort that is representative of the Spanish population and the population of older adults. She is the author of other studies that, like this one, found an association between a plant-based diet and a lower risk of frailty, both in the study involving American nurses and in a study involving a cohort of individuals aged 60 years or older in Spain (ENRICA-1).
Dr. Sotos-Prieto is also principal investigator on a project assessing the risk of cardiovascular disease based on modifiable lifestyles. For this project, the researchers created a tool, the healthy heart test, that can be used to evaluate diet quality “in 5 minutes, because we all know that doctors don’t have any time.” She thinks this test could be implemented in clinical practice to identify lifestyle behaviors that can be improved, such as by replacing refined cereals with whole grains or increasing legume consumption.
Tomatoes and French fries
The greatest benefit of a plant-based diet comes from the diet overall, not from any single food item. That said, these studies use a scoring system to reflect which items are healthy and which are not.
Diet was assessed every 4 years, starting in 1991, using a semiquantitative food frequency questionnaire that recorded the consumption of 131 foods and drinks during the previous year. The researchers determined the average frequency with which participants consumed each food. Eighteen food groups were sorted into three categories: healthy plant-based foods (whole grains, fruits, vegetables, nuts, legumes, vegetable oils, tea, and coffee), unhealthy plant-based foods (fruit juices, refined grains, potatoes, sugary drinks, sweets, and desserts), and animal-based foods (dairy, eggs, fish or shellfish, meat, and various foods of animal origin).
Healthy plant-based foods were given positive scores, while less healthy plant-based foods and the animal-based food groups were given negative scores. The consumption of each food group was classified into PDI using quintiles.
Women in the highest PDI quintile had a significantly lower risk for hypertensive disorders of pregnancy, compared with women in the lowest quintile. There was a negative dose-response relationship between PDI and risk of the disease. “A vegetarian diet isn’t necessarily healthier than a nonvegetarian diet if it’s made up of superfluous foods like French fries and soft drinks,” said Dr. Sotos-Prieto. “The difference lies in the quality of the plant-based foods. That’s what makes the difference between a healthy and an unhealthy diet.”
Give up meat?
Dr. Chavarro said that removing meat from his dinner menu 22 years ago was one of the hardest things he ever did. “Now, it’s no problem,” he said. But he understands that there are people for whom changing the diet by replacing animal products with nonanimal products is difficult. But meat need not be entirely abandoned.
“The women in the highest quintile aren’t necessarily vegetarian or vegan, but they consume much fewer animal-based foods than the others,” he noted. He added that vegetarian or vegan diets are not incompatible with a healthy pregnancy. “All vegans know how to get vitamin B12 from supplements.”
Diet or weight loss?
Much of the benefit observed in the study appears to be related to better weight control. The body mass index between dietary assessment and pregnancy accounted for 39% of the relationship between PDI and hypertensive disorders of pregnancy and 48% of the relationship between PDI and pregnancy-related hypertension.
“Part of the association seems to be explained by better weight control over long periods,” explained Dr. Chavarro. Women who adopted diets with more plant-based foods gained weight more slowly than those who consumed more animal-based foods. “They are different in terms of their weight trajectory over many years. So, part of the association that we observe is related to better long-term weight control. But the other half of the association is attributable to the diet itself and not necessarily to weight.” The authors suggest mechanisms of action such as endothelial dysfunction, inflammation, or blood pressure before pregnancy to explain the association.
Dr. Sotos-Prieto believes that this point is “extremely relevant.” In her opinion, it reveals that controlling weight at the start of pregnancy is important for pregnant women. Weight control may also improve other factors, like gestational diabetes. “I think preventive measures should focus on that. These results show that interventions are needed to increase the likelihood of going into pregnancy with an appropriate weight. And this includes modifying diet.”
Generalizable results?
More than 90% of the participants in the Nurses’ Health Study were White, not Hispanic. Can the results be extrapolated to other populations? “The answer: The study needs to be repeated in other populations,” said Dr. Chavarro, “and that’s going to take time. But even without that information, I think we can use this study to inform other populations, regardless of ethnicity.”
Dr. Sotos-Prieto admitted that this hypothesis has not yet been tested in the Spanish population, but she is the author of a similar study that followed nearly 12,000 Spanish adults for a decade using the same PDI. In this study, every 10-point increase in PDI was associated with a 14% lower risk of mortality from any cause (hazard ratio, 0.86) and a 37% lower risk of death from cardiovascular disease (HR, 0.63). She also believes that the recommendations derived from the study could be generalized to other populations “as long as each country’s culture is taken into account, to see how it can be culturally adapted. If it’s a population that consumes a lot of refined cereals, for example, make small changes to whole grains.”
Weighing the evidence
The study has strengths and limitations, owing to its methodology, and Dr. Chavarro himself recognizes that “in terms of hypertensive disorders of pregnancy specifically, this won’t be the last word.” But there is a pressing need to find answers.
The American College of Obstetricians and Gynecologists and the World Health Organization encourage women to follow healthy diets before and during pregnancy. But they provide little guidance on what constitutes a healthy diet when it comes to minimizing the risks of adverse pregnancy outcomes. “They are quite ambiguous and vague,” said Dr. Chavarro.
These new findings suggest that plant-based diets may be one such strategy, particularly because some evidence was found that these diets may be beneficial for women older than 35 years, who are considered a high-risk group.
“There are certainly many ways to eat healthily, but if we think about these pregnancy complications that can have serious consequences for the mother and the fetus, we might consider this as a healthy diet option,” Dr. Chavarro noted.
But is the evidence robust enough to recommend that patients make changes? “Ideally, there will be more studies,” stated Dr. Chavarro. “There are two ways to understand the problem. One is not making recommendations until you have three controlled clinical trials, which, even with the willingness and funding to do so, will take 15-20 years. But if we have to provide the best available information to those who need it today, I think these are solid results for guiding behavior.
“It’s always better if we can make decisions based on solid, incontrovertible information. But it’s not always available, and you must learn to live in both worlds and make decisions with uncertainties,” he concluded.
Dr. Sotos-Prieto and Dr. Chavarro have disclosed no relevant financial relationships.
This article was translated from the Medscape Spanish Edition. A version of this article first appeared on Medscape.com.
The prospective cohort study followed 11,459 women older than 18 years and evaluated their diet from the beginning using a validated questionnaire about the frequency and quality of plant-based foods. The participants had taken part in the Nurses’ Health Study II (1991-2009). From responses on the questionnaire, the investigators calculated the plant-based diet index (PDI) even among participants with an omnivorous diet. A higher score indicated greater adherence to the PDI.
“We wanted to know how one’s diet leading up to pregnancy influences the pregnancy, so we monitored women for virtually their entire reproductive life – almost 20 years – and gained an awareness of their typical diet before pregnancy,” study author Jorge E. Chavarro, MD, ScD, told this news organization. Dr. Chavarro is a professor of nutrition, epidemiology, and medicine at Harvard Medical School, Boston, and Harvard University’s School of Public Health in Cambridge, Mass. He researches how nutrition and lifestyle influence reproductive health and overall lifelong health in women.
Analysis of the data from the Nurses’ Health Study II revealed that as the proportion of animal products in diets decreased and the proportion of plant-based products increased, the risk of women experiencing hypertensive disorders of pregnancy decreased as well. Women in the highest PDI quintile had a significantly lower risk of hypertensive disorders of pregnancy, in comparison with those in the lowest quintile (relative risk, 0.76). This association was slightly stronger for pregnancy-related hypertension (RR, 0.77) than for preeclampsia (RR, 0.80).
Women in the highest PDI quintile had a 24% lower risk of hypertensive disorders of pregnancy than those in the lowest quintile; the risk of pregnancy-related hypertension decreased in a linear fashion as PDI increased, while the relationship of PDI to preeclampsia was restricted to women in the quintile with the highest adherence.
“It was clearer for pregnancy-related hypertension than for preeclampsia, but a diet made up primarily of plant-based foods seemed to be protective for both,” said Dr. Chavarro. He added that in addition to the problems these conditions cause during pregnancy, both increase the risk of subsequently developing other chronic diseases. “Could it be that modifiable lifestyle factors before and during pregnancy may not only help reduce problems during gestation but also prevent women’s health problems years later? That was the general motivation for this study.”
Mercedes Sotos-Prieto, PhD, a researcher at the Autonomous University of Madrid and an associate professor at Harvard University’s School of Public Health, told this news organization that the study’s methodology was very robust and that the investigators utilized appropriate statistical techniques for the analysis. She highlighted the fact that they used a validated food frequency questionnaire. She believes the study is also important because of the population group it focused on. “There has always been greater resistance when it comes to the diet of pregnant women, and the same is true for older adults. But we have seen that this type of diet, if it’s a quality diet, may be associated with health benefits.” She did not participate in the study.
Dr. Sotos-Prieto has a doctorate in nutritional epidemiology and public health. She works with large epidemiologic cohorts, such as the cohort of American nurses on which this study was based, and ENRICA, a cohort that is representative of the Spanish population and the population of older adults. She is the author of other studies that, like this one, found an association between a plant-based diet and a lower risk of frailty, both in the study involving American nurses and in a study involving a cohort of individuals aged 60 years or older in Spain (ENRICA-1).
Dr. Sotos-Prieto is also principal investigator on a project assessing the risk of cardiovascular disease based on modifiable lifestyles. For this project, the researchers created a tool, the healthy heart test, that can be used to evaluate diet quality “in 5 minutes, because we all know that doctors don’t have any time.” She thinks this test could be implemented in clinical practice to identify lifestyle behaviors that can be improved, such as by replacing refined cereals with whole grains or increasing legume consumption.
Tomatoes and French fries
The greatest benefit of a plant-based diet comes from the diet overall, not from any single food item. That said, these studies use a scoring system to reflect which items are healthy and which are not.
Diet was assessed every 4 years, starting in 1991, using a semiquantitative food frequency questionnaire that recorded the consumption of 131 foods and drinks during the previous year. The researchers determined the average frequency with which participants consumed each food. Eighteen food groups were sorted into three categories: healthy plant-based foods (whole grains, fruits, vegetables, nuts, legumes, vegetable oils, tea, and coffee), unhealthy plant-based foods (fruit juices, refined grains, potatoes, sugary drinks, sweets, and desserts), and animal-based foods (dairy, eggs, fish or shellfish, meat, and various foods of animal origin).
Healthy plant-based foods were given positive scores, while less healthy plant-based foods and the animal-based food groups were given negative scores. The consumption of each food group was classified into PDI using quintiles.
Women in the highest PDI quintile had a significantly lower risk for hypertensive disorders of pregnancy, compared with women in the lowest quintile. There was a negative dose-response relationship between PDI and risk of the disease. “A vegetarian diet isn’t necessarily healthier than a nonvegetarian diet if it’s made up of superfluous foods like French fries and soft drinks,” said Dr. Sotos-Prieto. “The difference lies in the quality of the plant-based foods. That’s what makes the difference between a healthy and an unhealthy diet.”
Give up meat?
Dr. Chavarro said that removing meat from his dinner menu 22 years ago was one of the hardest things he ever did. “Now, it’s no problem,” he said. But he understands that there are people for whom changing the diet by replacing animal products with nonanimal products is difficult. But meat need not be entirely abandoned.
“The women in the highest quintile aren’t necessarily vegetarian or vegan, but they consume much fewer animal-based foods than the others,” he noted. He added that vegetarian or vegan diets are not incompatible with a healthy pregnancy. “All vegans know how to get vitamin B12 from supplements.”
Diet or weight loss?
Much of the benefit observed in the study appears to be related to better weight control. The body mass index between dietary assessment and pregnancy accounted for 39% of the relationship between PDI and hypertensive disorders of pregnancy and 48% of the relationship between PDI and pregnancy-related hypertension.
“Part of the association seems to be explained by better weight control over long periods,” explained Dr. Chavarro. Women who adopted diets with more plant-based foods gained weight more slowly than those who consumed more animal-based foods. “They are different in terms of their weight trajectory over many years. So, part of the association that we observe is related to better long-term weight control. But the other half of the association is attributable to the diet itself and not necessarily to weight.” The authors suggest mechanisms of action such as endothelial dysfunction, inflammation, or blood pressure before pregnancy to explain the association.
Dr. Sotos-Prieto believes that this point is “extremely relevant.” In her opinion, it reveals that controlling weight at the start of pregnancy is important for pregnant women. Weight control may also improve other factors, like gestational diabetes. “I think preventive measures should focus on that. These results show that interventions are needed to increase the likelihood of going into pregnancy with an appropriate weight. And this includes modifying diet.”
Generalizable results?
More than 90% of the participants in the Nurses’ Health Study were White, not Hispanic. Can the results be extrapolated to other populations? “The answer: The study needs to be repeated in other populations,” said Dr. Chavarro, “and that’s going to take time. But even without that information, I think we can use this study to inform other populations, regardless of ethnicity.”
Dr. Sotos-Prieto admitted that this hypothesis has not yet been tested in the Spanish population, but she is the author of a similar study that followed nearly 12,000 Spanish adults for a decade using the same PDI. In this study, every 10-point increase in PDI was associated with a 14% lower risk of mortality from any cause (hazard ratio, 0.86) and a 37% lower risk of death from cardiovascular disease (HR, 0.63). She also believes that the recommendations derived from the study could be generalized to other populations “as long as each country’s culture is taken into account, to see how it can be culturally adapted. If it’s a population that consumes a lot of refined cereals, for example, make small changes to whole grains.”
Weighing the evidence
The study has strengths and limitations, owing to its methodology, and Dr. Chavarro himself recognizes that “in terms of hypertensive disorders of pregnancy specifically, this won’t be the last word.” But there is a pressing need to find answers.
The American College of Obstetricians and Gynecologists and the World Health Organization encourage women to follow healthy diets before and during pregnancy. But they provide little guidance on what constitutes a healthy diet when it comes to minimizing the risks of adverse pregnancy outcomes. “They are quite ambiguous and vague,” said Dr. Chavarro.
These new findings suggest that plant-based diets may be one such strategy, particularly because some evidence was found that these diets may be beneficial for women older than 35 years, who are considered a high-risk group.
“There are certainly many ways to eat healthily, but if we think about these pregnancy complications that can have serious consequences for the mother and the fetus, we might consider this as a healthy diet option,” Dr. Chavarro noted.
But is the evidence robust enough to recommend that patients make changes? “Ideally, there will be more studies,” stated Dr. Chavarro. “There are two ways to understand the problem. One is not making recommendations until you have three controlled clinical trials, which, even with the willingness and funding to do so, will take 15-20 years. But if we have to provide the best available information to those who need it today, I think these are solid results for guiding behavior.
“It’s always better if we can make decisions based on solid, incontrovertible information. But it’s not always available, and you must learn to live in both worlds and make decisions with uncertainties,” he concluded.
Dr. Sotos-Prieto and Dr. Chavarro have disclosed no relevant financial relationships.
This article was translated from the Medscape Spanish Edition. A version of this article first appeared on Medscape.com.
The prospective cohort study followed 11,459 women older than 18 years and evaluated their diet from the beginning using a validated questionnaire about the frequency and quality of plant-based foods. The participants had taken part in the Nurses’ Health Study II (1991-2009). From responses on the questionnaire, the investigators calculated the plant-based diet index (PDI) even among participants with an omnivorous diet. A higher score indicated greater adherence to the PDI.
“We wanted to know how one’s diet leading up to pregnancy influences the pregnancy, so we monitored women for virtually their entire reproductive life – almost 20 years – and gained an awareness of their typical diet before pregnancy,” study author Jorge E. Chavarro, MD, ScD, told this news organization. Dr. Chavarro is a professor of nutrition, epidemiology, and medicine at Harvard Medical School, Boston, and Harvard University’s School of Public Health in Cambridge, Mass. He researches how nutrition and lifestyle influence reproductive health and overall lifelong health in women.
Analysis of the data from the Nurses’ Health Study II revealed that as the proportion of animal products in diets decreased and the proportion of plant-based products increased, the risk of women experiencing hypertensive disorders of pregnancy decreased as well. Women in the highest PDI quintile had a significantly lower risk of hypertensive disorders of pregnancy, in comparison with those in the lowest quintile (relative risk, 0.76). This association was slightly stronger for pregnancy-related hypertension (RR, 0.77) than for preeclampsia (RR, 0.80).
Women in the highest PDI quintile had a 24% lower risk of hypertensive disorders of pregnancy than those in the lowest quintile; the risk of pregnancy-related hypertension decreased in a linear fashion as PDI increased, while the relationship of PDI to preeclampsia was restricted to women in the quintile with the highest adherence.
“It was clearer for pregnancy-related hypertension than for preeclampsia, but a diet made up primarily of plant-based foods seemed to be protective for both,” said Dr. Chavarro. He added that in addition to the problems these conditions cause during pregnancy, both increase the risk of subsequently developing other chronic diseases. “Could it be that modifiable lifestyle factors before and during pregnancy may not only help reduce problems during gestation but also prevent women’s health problems years later? That was the general motivation for this study.”
Mercedes Sotos-Prieto, PhD, a researcher at the Autonomous University of Madrid and an associate professor at Harvard University’s School of Public Health, told this news organization that the study’s methodology was very robust and that the investigators utilized appropriate statistical techniques for the analysis. She highlighted the fact that they used a validated food frequency questionnaire. She believes the study is also important because of the population group it focused on. “There has always been greater resistance when it comes to the diet of pregnant women, and the same is true for older adults. But we have seen that this type of diet, if it’s a quality diet, may be associated with health benefits.” She did not participate in the study.
Dr. Sotos-Prieto has a doctorate in nutritional epidemiology and public health. She works with large epidemiologic cohorts, such as the cohort of American nurses on which this study was based, and ENRICA, a cohort that is representative of the Spanish population and the population of older adults. She is the author of other studies that, like this one, found an association between a plant-based diet and a lower risk of frailty, both in the study involving American nurses and in a study involving a cohort of individuals aged 60 years or older in Spain (ENRICA-1).
Dr. Sotos-Prieto is also principal investigator on a project assessing the risk of cardiovascular disease based on modifiable lifestyles. For this project, the researchers created a tool, the healthy heart test, that can be used to evaluate diet quality “in 5 minutes, because we all know that doctors don’t have any time.” She thinks this test could be implemented in clinical practice to identify lifestyle behaviors that can be improved, such as by replacing refined cereals with whole grains or increasing legume consumption.
Tomatoes and French fries
The greatest benefit of a plant-based diet comes from the diet overall, not from any single food item. That said, these studies use a scoring system to reflect which items are healthy and which are not.
Diet was assessed every 4 years, starting in 1991, using a semiquantitative food frequency questionnaire that recorded the consumption of 131 foods and drinks during the previous year. The researchers determined the average frequency with which participants consumed each food. Eighteen food groups were sorted into three categories: healthy plant-based foods (whole grains, fruits, vegetables, nuts, legumes, vegetable oils, tea, and coffee), unhealthy plant-based foods (fruit juices, refined grains, potatoes, sugary drinks, sweets, and desserts), and animal-based foods (dairy, eggs, fish or shellfish, meat, and various foods of animal origin).
Healthy plant-based foods were given positive scores, while less healthy plant-based foods and the animal-based food groups were given negative scores. The consumption of each food group was classified into PDI using quintiles.
Women in the highest PDI quintile had a significantly lower risk for hypertensive disorders of pregnancy, compared with women in the lowest quintile. There was a negative dose-response relationship between PDI and risk of the disease. “A vegetarian diet isn’t necessarily healthier than a nonvegetarian diet if it’s made up of superfluous foods like French fries and soft drinks,” said Dr. Sotos-Prieto. “The difference lies in the quality of the plant-based foods. That’s what makes the difference between a healthy and an unhealthy diet.”
Give up meat?
Dr. Chavarro said that removing meat from his dinner menu 22 years ago was one of the hardest things he ever did. “Now, it’s no problem,” he said. But he understands that there are people for whom changing the diet by replacing animal products with nonanimal products is difficult. But meat need not be entirely abandoned.
“The women in the highest quintile aren’t necessarily vegetarian or vegan, but they consume much fewer animal-based foods than the others,” he noted. He added that vegetarian or vegan diets are not incompatible with a healthy pregnancy. “All vegans know how to get vitamin B12 from supplements.”
Diet or weight loss?
Much of the benefit observed in the study appears to be related to better weight control. The body mass index between dietary assessment and pregnancy accounted for 39% of the relationship between PDI and hypertensive disorders of pregnancy and 48% of the relationship between PDI and pregnancy-related hypertension.
“Part of the association seems to be explained by better weight control over long periods,” explained Dr. Chavarro. Women who adopted diets with more plant-based foods gained weight more slowly than those who consumed more animal-based foods. “They are different in terms of their weight trajectory over many years. So, part of the association that we observe is related to better long-term weight control. But the other half of the association is attributable to the diet itself and not necessarily to weight.” The authors suggest mechanisms of action such as endothelial dysfunction, inflammation, or blood pressure before pregnancy to explain the association.
Dr. Sotos-Prieto believes that this point is “extremely relevant.” In her opinion, it reveals that controlling weight at the start of pregnancy is important for pregnant women. Weight control may also improve other factors, like gestational diabetes. “I think preventive measures should focus on that. These results show that interventions are needed to increase the likelihood of going into pregnancy with an appropriate weight. And this includes modifying diet.”
Generalizable results?
More than 90% of the participants in the Nurses’ Health Study were White, not Hispanic. Can the results be extrapolated to other populations? “The answer: The study needs to be repeated in other populations,” said Dr. Chavarro, “and that’s going to take time. But even without that information, I think we can use this study to inform other populations, regardless of ethnicity.”
Dr. Sotos-Prieto admitted that this hypothesis has not yet been tested in the Spanish population, but she is the author of a similar study that followed nearly 12,000 Spanish adults for a decade using the same PDI. In this study, every 10-point increase in PDI was associated with a 14% lower risk of mortality from any cause (hazard ratio, 0.86) and a 37% lower risk of death from cardiovascular disease (HR, 0.63). She also believes that the recommendations derived from the study could be generalized to other populations “as long as each country’s culture is taken into account, to see how it can be culturally adapted. If it’s a population that consumes a lot of refined cereals, for example, make small changes to whole grains.”
Weighing the evidence
The study has strengths and limitations, owing to its methodology, and Dr. Chavarro himself recognizes that “in terms of hypertensive disorders of pregnancy specifically, this won’t be the last word.” But there is a pressing need to find answers.
The American College of Obstetricians and Gynecologists and the World Health Organization encourage women to follow healthy diets before and during pregnancy. But they provide little guidance on what constitutes a healthy diet when it comes to minimizing the risks of adverse pregnancy outcomes. “They are quite ambiguous and vague,” said Dr. Chavarro.
These new findings suggest that plant-based diets may be one such strategy, particularly because some evidence was found that these diets may be beneficial for women older than 35 years, who are considered a high-risk group.
“There are certainly many ways to eat healthily, but if we think about these pregnancy complications that can have serious consequences for the mother and the fetus, we might consider this as a healthy diet option,” Dr. Chavarro noted.
But is the evidence robust enough to recommend that patients make changes? “Ideally, there will be more studies,” stated Dr. Chavarro. “There are two ways to understand the problem. One is not making recommendations until you have three controlled clinical trials, which, even with the willingness and funding to do so, will take 15-20 years. But if we have to provide the best available information to those who need it today, I think these are solid results for guiding behavior.
“It’s always better if we can make decisions based on solid, incontrovertible information. But it’s not always available, and you must learn to live in both worlds and make decisions with uncertainties,” he concluded.
Dr. Sotos-Prieto and Dr. Chavarro have disclosed no relevant financial relationships.
This article was translated from the Medscape Spanish Edition. A version of this article first appeared on Medscape.com.
FROM AMERICAN JOURNAL OF OBSTETRICS AND GYNECOLOGY
How PCPs are penalized for positive outcomes from lifestyle change
The Centers for Medicare & Medicaid Services 2022 National Quality Strategy is described as an “ambitious long-term initiative that aims to promote the highest quality outcomes and safest care for all individuals.” It is a commendable goal for an overburdened U.S. health care system that spends more than other high-income counties yet experiences poorer outcomes. But whole-person, person-centered care cannot be achieved under current misaligned quality measures that fail to measure what we purport to value: the quintuple aim of improved health outcomes, cost savings, patient satisfaction, clinician well-being, and health equity.
Lifestyle first
Clinical practice guidelines for many chronic diseases recommend lifestyle intervention as the first and optimal treatment. A growing body of evidence supports lifestyle behavior interventions to treat and, when used intensively, even reverse common chronic conditions such as cardiovascular disease, obesity, and type 2 diabetes, while also providing effective prevention for those conditions. However, no current quality measures consider lifestyle interventions. In fact, some quality measures unintentionally penalize physicians for successfully treating or reversing disease through lifestyle behavior interventions while rewarding clinicians for meeting process measures – usually adherence to medication – regardless of whether health outcomes improved.
Rewarding medication adherence for the treatment of diseases in which lifestyle is a primary therapy (such as hypertension), combined with other health care constraints (lack of lifestyle education, time to spend with patients, and infrastructure support) incentivizes physicians to skip the conversation about lifestyle changes and go straight to medication prescription. Meanwhile, the clinician who takes the extra time to guide a patient toward lifestyle interventions that could treat their current disease and prevent future diseases – without side effects – is penalized.
Misaligned quality measures like these can stifle clinical judgment and risk reducing the practice of medicine to mindless box-checking. In many cases, patients are not even informed that lifestyle behavior change may be a treatment option (much less the first recommended option) for their conditions. This delivery of care is not person-centered and, in fact, may raise questions about the adequacy of informed treatment consent.
Reimbursement barriers
Lifestyle medicine is a growing medical specialty that uses therapeutic lifestyle interventions as a primary modality to treat chronic conditions. Since certification began in 2017, almost 2500 US physicians and 1000 nonphysician health professionals have earned certification. Health systems, including the U.S. military, are increasingly integrating lifestyle medicine. There have been advancements since one survey found that more than half of lifestyle medicine clinicians reported receiving no reimbursement for lifestyle behavior interventions. However, barriers, especially in fee-for-service systems, still inhibit many patients from receiving insurance coverage for comprehensive, interdisciplinary, and whole-person treatments called intensive therapeutic lifestyle change (ITLC) programs.
Existing comprehensive lifestyle programs that patients are eligible for (ie, the Diabetes Prevention Program and intensive behavioral therapy) are often so poorly reimbursed that clinicians and health systems decline to offer them. An example of a well-reimbursed ITLC program is intensive cardiac rehabilitation (ICR), which remains underutilized and limited to a narrow segment of patients, despite ICR›s proven benefits for managing comorbid risk factors such as hemoglobin A1c and weight. Even when lifestyle intervention programs are available and patients are eligible to participate (often through shared medical appointments), patient copays for the frequent visits required to achieve and sustain behavior change – or the lack of reimbursement for interdisciplinary team members – discourage engagement.
Penalizing successful outcomes
Despite the fact that lifestyle behaviors are top contributors to health and, conversely, contribute to up to 80% of chronic diseases, few quality measures focus on screening for lifestyle factors or treating diseases with lifestyle interventions. An example of an existing quality measure is screening or treatment for harmful substance use.
Specific quality measures that penalize lifestyle medicine approaches include pharmacotherapy for type 2 diabetes, dyslipidemia, osteoporosis, and gout as well as approaches to rheumatoid arthritis.
Statins offer a useful example of the conundrum faced by clinicians who want to offer lifestyle interventions. A lifestyle medicine primary care physician had a patient covered by Medicare Advantage who was diagnosed with hyperlipidemia. The patient had total cholesterol of 226 and a triglycerides level of 132. Instead of prescribing the routine statin, the physician prescribed lifestyle behavior modifications. Within 3 weeks, the patient›s total cholesterol improved to 171 and triglycerides to 75. This was a great success for the delighted patient. However, the CMS 5-Star Rating System assigned the primary care physician a grade of C rather than A, which put the physician›s 5-star rating at risk. Why? Because the system bases its score largely on medication compliance. The physician was penalized despite achieving the optimal health outcome, and at a lower cost than with medication. This misalignment does not incentivize patient-centered care because it disregards patient preference, shared decision-making, and evidence-based practice.
Risk adjustment
Rather than automatically managing disease with ever-increasing quantities of costly medications and procedures, lifestyle medicine clinicians first pursue a goal of health restoration when appropriate. But Medicare risk adjustment incentivizes physicians to manage rather than reverse disease. How much Medicare pays health plans is determined in part by how sick the patients are; the sicker the patient, the more Medicare pays, because those patients› costs are expected to be higher. This ensures that health plans are not penalized for enrolling sicker patients. But a physician utilizing diet alone to achieve remission in a patient with type 2 diabetes is penalized financially because, when the risk is adjusted, diabetes is no longer listed among the patient›s conditions. So, Medicare pays the physician less money. That misalignment incentivizes clinicians to manage the symptoms of type 2 diabetes rather than achieve remission, despite remission being the ideal clinical outcome.
Realigning quality measures
Quality measures were developed to quantify health care processes and outcomes, and to ensure the delivery of safe care to all patients. However, over time the number of quality measures has swelled to 2500, evolving into a confusing, time-consuming, and even soul-crushing responsibility for the physician.
Instead of relying heavily on process measures, we must incentivize outcome measures that honor patient autonomy and allow clinicians to offer lifestyle intervention as the first line of treatment. Risk-score calculations should be adjusted so that we stop incentivizing disease management and penalizing disease reversal.
CMS’s proposed development of “a universal foundation” of quality measures is an opportunity to begin the realignment of quality measures and values. This foundation is intended to establish more consistent and meaningful measures, reduce clinician burnout by streamlining the reporting process, and advance health equity. For this change to be successful, it is vital that lifestyle behavior interventions – optimal nutrition, physical activity, restorative sleep, social connections, stress management, and avoidance of harmful substances – become the foundation of universal quality measures. This will ensure that every clinician is incentivized to discuss lifestyle behaviors with patients and pursue the first clinical step recommended by clinical practice guidelines for most chronic diseases. Only then can we truly deliver high-value, whole-person, person-centered care and achieve the quintuple aim.
Dr. Patel is president-elect, American College of Lifestyle Medicine; Lifestyle Medicine Medical Director, Wellvana Health, Midland, Tex. She has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The Centers for Medicare & Medicaid Services 2022 National Quality Strategy is described as an “ambitious long-term initiative that aims to promote the highest quality outcomes and safest care for all individuals.” It is a commendable goal for an overburdened U.S. health care system that spends more than other high-income counties yet experiences poorer outcomes. But whole-person, person-centered care cannot be achieved under current misaligned quality measures that fail to measure what we purport to value: the quintuple aim of improved health outcomes, cost savings, patient satisfaction, clinician well-being, and health equity.
Lifestyle first
Clinical practice guidelines for many chronic diseases recommend lifestyle intervention as the first and optimal treatment. A growing body of evidence supports lifestyle behavior interventions to treat and, when used intensively, even reverse common chronic conditions such as cardiovascular disease, obesity, and type 2 diabetes, while also providing effective prevention for those conditions. However, no current quality measures consider lifestyle interventions. In fact, some quality measures unintentionally penalize physicians for successfully treating or reversing disease through lifestyle behavior interventions while rewarding clinicians for meeting process measures – usually adherence to medication – regardless of whether health outcomes improved.
Rewarding medication adherence for the treatment of diseases in which lifestyle is a primary therapy (such as hypertension), combined with other health care constraints (lack of lifestyle education, time to spend with patients, and infrastructure support) incentivizes physicians to skip the conversation about lifestyle changes and go straight to medication prescription. Meanwhile, the clinician who takes the extra time to guide a patient toward lifestyle interventions that could treat their current disease and prevent future diseases – without side effects – is penalized.
Misaligned quality measures like these can stifle clinical judgment and risk reducing the practice of medicine to mindless box-checking. In many cases, patients are not even informed that lifestyle behavior change may be a treatment option (much less the first recommended option) for their conditions. This delivery of care is not person-centered and, in fact, may raise questions about the adequacy of informed treatment consent.
Reimbursement barriers
Lifestyle medicine is a growing medical specialty that uses therapeutic lifestyle interventions as a primary modality to treat chronic conditions. Since certification began in 2017, almost 2500 US physicians and 1000 nonphysician health professionals have earned certification. Health systems, including the U.S. military, are increasingly integrating lifestyle medicine. There have been advancements since one survey found that more than half of lifestyle medicine clinicians reported receiving no reimbursement for lifestyle behavior interventions. However, barriers, especially in fee-for-service systems, still inhibit many patients from receiving insurance coverage for comprehensive, interdisciplinary, and whole-person treatments called intensive therapeutic lifestyle change (ITLC) programs.
Existing comprehensive lifestyle programs that patients are eligible for (ie, the Diabetes Prevention Program and intensive behavioral therapy) are often so poorly reimbursed that clinicians and health systems decline to offer them. An example of a well-reimbursed ITLC program is intensive cardiac rehabilitation (ICR), which remains underutilized and limited to a narrow segment of patients, despite ICR›s proven benefits for managing comorbid risk factors such as hemoglobin A1c and weight. Even when lifestyle intervention programs are available and patients are eligible to participate (often through shared medical appointments), patient copays for the frequent visits required to achieve and sustain behavior change – or the lack of reimbursement for interdisciplinary team members – discourage engagement.
Penalizing successful outcomes
Despite the fact that lifestyle behaviors are top contributors to health and, conversely, contribute to up to 80% of chronic diseases, few quality measures focus on screening for lifestyle factors or treating diseases with lifestyle interventions. An example of an existing quality measure is screening or treatment for harmful substance use.
Specific quality measures that penalize lifestyle medicine approaches include pharmacotherapy for type 2 diabetes, dyslipidemia, osteoporosis, and gout as well as approaches to rheumatoid arthritis.
Statins offer a useful example of the conundrum faced by clinicians who want to offer lifestyle interventions. A lifestyle medicine primary care physician had a patient covered by Medicare Advantage who was diagnosed with hyperlipidemia. The patient had total cholesterol of 226 and a triglycerides level of 132. Instead of prescribing the routine statin, the physician prescribed lifestyle behavior modifications. Within 3 weeks, the patient›s total cholesterol improved to 171 and triglycerides to 75. This was a great success for the delighted patient. However, the CMS 5-Star Rating System assigned the primary care physician a grade of C rather than A, which put the physician›s 5-star rating at risk. Why? Because the system bases its score largely on medication compliance. The physician was penalized despite achieving the optimal health outcome, and at a lower cost than with medication. This misalignment does not incentivize patient-centered care because it disregards patient preference, shared decision-making, and evidence-based practice.
Risk adjustment
Rather than automatically managing disease with ever-increasing quantities of costly medications and procedures, lifestyle medicine clinicians first pursue a goal of health restoration when appropriate. But Medicare risk adjustment incentivizes physicians to manage rather than reverse disease. How much Medicare pays health plans is determined in part by how sick the patients are; the sicker the patient, the more Medicare pays, because those patients› costs are expected to be higher. This ensures that health plans are not penalized for enrolling sicker patients. But a physician utilizing diet alone to achieve remission in a patient with type 2 diabetes is penalized financially because, when the risk is adjusted, diabetes is no longer listed among the patient›s conditions. So, Medicare pays the physician less money. That misalignment incentivizes clinicians to manage the symptoms of type 2 diabetes rather than achieve remission, despite remission being the ideal clinical outcome.
Realigning quality measures
Quality measures were developed to quantify health care processes and outcomes, and to ensure the delivery of safe care to all patients. However, over time the number of quality measures has swelled to 2500, evolving into a confusing, time-consuming, and even soul-crushing responsibility for the physician.
Instead of relying heavily on process measures, we must incentivize outcome measures that honor patient autonomy and allow clinicians to offer lifestyle intervention as the first line of treatment. Risk-score calculations should be adjusted so that we stop incentivizing disease management and penalizing disease reversal.
CMS’s proposed development of “a universal foundation” of quality measures is an opportunity to begin the realignment of quality measures and values. This foundation is intended to establish more consistent and meaningful measures, reduce clinician burnout by streamlining the reporting process, and advance health equity. For this change to be successful, it is vital that lifestyle behavior interventions – optimal nutrition, physical activity, restorative sleep, social connections, stress management, and avoidance of harmful substances – become the foundation of universal quality measures. This will ensure that every clinician is incentivized to discuss lifestyle behaviors with patients and pursue the first clinical step recommended by clinical practice guidelines for most chronic diseases. Only then can we truly deliver high-value, whole-person, person-centered care and achieve the quintuple aim.
Dr. Patel is president-elect, American College of Lifestyle Medicine; Lifestyle Medicine Medical Director, Wellvana Health, Midland, Tex. She has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The Centers for Medicare & Medicaid Services 2022 National Quality Strategy is described as an “ambitious long-term initiative that aims to promote the highest quality outcomes and safest care for all individuals.” It is a commendable goal for an overburdened U.S. health care system that spends more than other high-income counties yet experiences poorer outcomes. But whole-person, person-centered care cannot be achieved under current misaligned quality measures that fail to measure what we purport to value: the quintuple aim of improved health outcomes, cost savings, patient satisfaction, clinician well-being, and health equity.
Lifestyle first
Clinical practice guidelines for many chronic diseases recommend lifestyle intervention as the first and optimal treatment. A growing body of evidence supports lifestyle behavior interventions to treat and, when used intensively, even reverse common chronic conditions such as cardiovascular disease, obesity, and type 2 diabetes, while also providing effective prevention for those conditions. However, no current quality measures consider lifestyle interventions. In fact, some quality measures unintentionally penalize physicians for successfully treating or reversing disease through lifestyle behavior interventions while rewarding clinicians for meeting process measures – usually adherence to medication – regardless of whether health outcomes improved.
Rewarding medication adherence for the treatment of diseases in which lifestyle is a primary therapy (such as hypertension), combined with other health care constraints (lack of lifestyle education, time to spend with patients, and infrastructure support) incentivizes physicians to skip the conversation about lifestyle changes and go straight to medication prescription. Meanwhile, the clinician who takes the extra time to guide a patient toward lifestyle interventions that could treat their current disease and prevent future diseases – without side effects – is penalized.
Misaligned quality measures like these can stifle clinical judgment and risk reducing the practice of medicine to mindless box-checking. In many cases, patients are not even informed that lifestyle behavior change may be a treatment option (much less the first recommended option) for their conditions. This delivery of care is not person-centered and, in fact, may raise questions about the adequacy of informed treatment consent.
Reimbursement barriers
Lifestyle medicine is a growing medical specialty that uses therapeutic lifestyle interventions as a primary modality to treat chronic conditions. Since certification began in 2017, almost 2500 US physicians and 1000 nonphysician health professionals have earned certification. Health systems, including the U.S. military, are increasingly integrating lifestyle medicine. There have been advancements since one survey found that more than half of lifestyle medicine clinicians reported receiving no reimbursement for lifestyle behavior interventions. However, barriers, especially in fee-for-service systems, still inhibit many patients from receiving insurance coverage for comprehensive, interdisciplinary, and whole-person treatments called intensive therapeutic lifestyle change (ITLC) programs.
Existing comprehensive lifestyle programs that patients are eligible for (ie, the Diabetes Prevention Program and intensive behavioral therapy) are often so poorly reimbursed that clinicians and health systems decline to offer them. An example of a well-reimbursed ITLC program is intensive cardiac rehabilitation (ICR), which remains underutilized and limited to a narrow segment of patients, despite ICR›s proven benefits for managing comorbid risk factors such as hemoglobin A1c and weight. Even when lifestyle intervention programs are available and patients are eligible to participate (often through shared medical appointments), patient copays for the frequent visits required to achieve and sustain behavior change – or the lack of reimbursement for interdisciplinary team members – discourage engagement.
Penalizing successful outcomes
Despite the fact that lifestyle behaviors are top contributors to health and, conversely, contribute to up to 80% of chronic diseases, few quality measures focus on screening for lifestyle factors or treating diseases with lifestyle interventions. An example of an existing quality measure is screening or treatment for harmful substance use.
Specific quality measures that penalize lifestyle medicine approaches include pharmacotherapy for type 2 diabetes, dyslipidemia, osteoporosis, and gout as well as approaches to rheumatoid arthritis.
Statins offer a useful example of the conundrum faced by clinicians who want to offer lifestyle interventions. A lifestyle medicine primary care physician had a patient covered by Medicare Advantage who was diagnosed with hyperlipidemia. The patient had total cholesterol of 226 and a triglycerides level of 132. Instead of prescribing the routine statin, the physician prescribed lifestyle behavior modifications. Within 3 weeks, the patient›s total cholesterol improved to 171 and triglycerides to 75. This was a great success for the delighted patient. However, the CMS 5-Star Rating System assigned the primary care physician a grade of C rather than A, which put the physician›s 5-star rating at risk. Why? Because the system bases its score largely on medication compliance. The physician was penalized despite achieving the optimal health outcome, and at a lower cost than with medication. This misalignment does not incentivize patient-centered care because it disregards patient preference, shared decision-making, and evidence-based practice.
Risk adjustment
Rather than automatically managing disease with ever-increasing quantities of costly medications and procedures, lifestyle medicine clinicians first pursue a goal of health restoration when appropriate. But Medicare risk adjustment incentivizes physicians to manage rather than reverse disease. How much Medicare pays health plans is determined in part by how sick the patients are; the sicker the patient, the more Medicare pays, because those patients› costs are expected to be higher. This ensures that health plans are not penalized for enrolling sicker patients. But a physician utilizing diet alone to achieve remission in a patient with type 2 diabetes is penalized financially because, when the risk is adjusted, diabetes is no longer listed among the patient›s conditions. So, Medicare pays the physician less money. That misalignment incentivizes clinicians to manage the symptoms of type 2 diabetes rather than achieve remission, despite remission being the ideal clinical outcome.
Realigning quality measures
Quality measures were developed to quantify health care processes and outcomes, and to ensure the delivery of safe care to all patients. However, over time the number of quality measures has swelled to 2500, evolving into a confusing, time-consuming, and even soul-crushing responsibility for the physician.
Instead of relying heavily on process measures, we must incentivize outcome measures that honor patient autonomy and allow clinicians to offer lifestyle intervention as the first line of treatment. Risk-score calculations should be adjusted so that we stop incentivizing disease management and penalizing disease reversal.
CMS’s proposed development of “a universal foundation” of quality measures is an opportunity to begin the realignment of quality measures and values. This foundation is intended to establish more consistent and meaningful measures, reduce clinician burnout by streamlining the reporting process, and advance health equity. For this change to be successful, it is vital that lifestyle behavior interventions – optimal nutrition, physical activity, restorative sleep, social connections, stress management, and avoidance of harmful substances – become the foundation of universal quality measures. This will ensure that every clinician is incentivized to discuss lifestyle behaviors with patients and pursue the first clinical step recommended by clinical practice guidelines for most chronic diseases. Only then can we truly deliver high-value, whole-person, person-centered care and achieve the quintuple aim.
Dr. Patel is president-elect, American College of Lifestyle Medicine; Lifestyle Medicine Medical Director, Wellvana Health, Midland, Tex. She has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
‘We’re halfway home’: UCSF’s Dr. Stephen Hauser sketches MS future
MILAN – University of California, San Francisco, neurology professor Stephen Hauser, MD, told colleagues in a highlighted lecture at the 9th Joint ECTRIMS-ACTRIMS meeting.
Going forward, the MS field should emphasize identifying early biomarkers of MS, Dr. Hauser said.
He noted that many experts had anticipated “that, if we could intervene early in the relapsing phase of the disease, we would stabilize neurodegeneration and patient disability. But one of the big surprises was that that was not the case. Instead, the observed course was that by silencing relapses and focal inflammation, a clinically silent, slow, insidious progression continues during the relapsing phase of disease in patients who are not having ongoing relapses.”
Even as focal activity detected via MRI is silenced, “progression continues” he said. “This remains the great unsolved challenge.”
Dr. Hauser asked colleagues to consider a three-stage model of MS that begins with benign autoimmunity followed by pathogenic autoimmunity with subclinical tissue damage. The third stage is clinical autoimmunity.
How can you determine who’s at risk? Genetics can only fill in part of the picture because they can’t pinpoint exactly who’s likely to develop the disease. “In other autoimmune diseases, serologic autoantibodies have been by far the most effective biomarkers,” he said. “There is real-world support – not only in mice – for the concept that autoimmunity begins as a highly focused immune response that then spreads over time.”
In systemic lupus erythematosus, the cascade toward disease begins about 9 years before clinical presentation, he said. It’s 7 months in type 1 diabetes, and 20 years in rheumatoid arthritis. “These have been enormously powerful in designing both observational and therapeutic studies to try to interrupt autoimmunity at the earliest possible stage.”
What can be done if a MS biomarker is developed and shows that a person is at risk? Dr. Hauser highlighted how the anti-CD3 antibody teplizumab has been developed – and Food and Drug Administration approved – to greatly reduce the risk of type 1 diabetes in high-risk patients. Per a 2021 study, a single-14-day course of the drug was linked to lowering the risk of disease over a median 923 days by more than 50% (hazard ratio, 0.457; P < 0.01). Half of those who received the drug were free of diabetes versus just 22% of those treated by placebo.
“We’ve not yet had those serologic biomarkers in MS. But I’d like to show you that maybe we are getting close to having them,” Dr. Hauser said. He pointed to new research into a U.S. Department of Defense serum repository that’s turned up “a pretty rock-solid prediagnostic biomarker specific to MS.”
Moving on to therapy, Dr. Hauser said it’s clear that “the earlier that we treat, the more likely we are to have a large response. Highly effective therapies delivered as first-line therapies have better long-term outcomes for disability then does a graded approach that doesn’t begin with high-efficacy therapy.”
What constitutes a cure?
What else needs to be done going forward? Dr. Hauser called for the MS field to develop a definition of cure. “We should take the lead from cancer therapeutics, where they define what a cure means.” In B-cell leukemia, for example, patients are considered cured “if they remain completely disease-free in terms of clinical symptoms and biomarkers of clonal proliferation for 4 years. They have less than a 1% lifetime risk of relapse. They’re essentially cured. Our equivalent could also be developed for MS.”
He highlighted the IMPACT MS phase 4 trial, a small single-center study of ocrelizumab, which just finished enrollment and will examine the effect of the drug on treatment-naive patients at the moment of their first-ever attack. The primary endpoint is oligoclonal bands in 3 years. “I think more of these studies will probably follow,” Dr. Hauser said.
Is intervention possible at the presymptomatic stage? Targets could be members of families with multiple affected relatives who test positive for the predictive antibody signature and who have a high genetic score, he said. “We could do perhaps an Epstein-Barr virus intervention trial in this population. Then, if we have the courage and are more confident in our biomarkers, perhaps even a therapeutic trial, as has been done in these other diseases.”
As for next-generation therapies, “we’ll need to neutralize multiple cell types, especially in later disease,” he said. Bruton tyrosine kinase inhibitors “seem to be a class of drugs that was designed for the MS patient because they not only hit B cells, but also the plasmablasts that CD20s don’t hit and are the main component of the humoral pathology in chronic MS lesions.”
Dr. Hauser discloses scientific board (Accure, Alector, Annexon), board of directors (Neurona), consulting (BD, Moderna, NGM Bio), and travel reimbursement/writing support (Roche and Novartis).
MILAN – University of California, San Francisco, neurology professor Stephen Hauser, MD, told colleagues in a highlighted lecture at the 9th Joint ECTRIMS-ACTRIMS meeting.
Going forward, the MS field should emphasize identifying early biomarkers of MS, Dr. Hauser said.
He noted that many experts had anticipated “that, if we could intervene early in the relapsing phase of the disease, we would stabilize neurodegeneration and patient disability. But one of the big surprises was that that was not the case. Instead, the observed course was that by silencing relapses and focal inflammation, a clinically silent, slow, insidious progression continues during the relapsing phase of disease in patients who are not having ongoing relapses.”
Even as focal activity detected via MRI is silenced, “progression continues” he said. “This remains the great unsolved challenge.”
Dr. Hauser asked colleagues to consider a three-stage model of MS that begins with benign autoimmunity followed by pathogenic autoimmunity with subclinical tissue damage. The third stage is clinical autoimmunity.
How can you determine who’s at risk? Genetics can only fill in part of the picture because they can’t pinpoint exactly who’s likely to develop the disease. “In other autoimmune diseases, serologic autoantibodies have been by far the most effective biomarkers,” he said. “There is real-world support – not only in mice – for the concept that autoimmunity begins as a highly focused immune response that then spreads over time.”
In systemic lupus erythematosus, the cascade toward disease begins about 9 years before clinical presentation, he said. It’s 7 months in type 1 diabetes, and 20 years in rheumatoid arthritis. “These have been enormously powerful in designing both observational and therapeutic studies to try to interrupt autoimmunity at the earliest possible stage.”
What can be done if a MS biomarker is developed and shows that a person is at risk? Dr. Hauser highlighted how the anti-CD3 antibody teplizumab has been developed – and Food and Drug Administration approved – to greatly reduce the risk of type 1 diabetes in high-risk patients. Per a 2021 study, a single-14-day course of the drug was linked to lowering the risk of disease over a median 923 days by more than 50% (hazard ratio, 0.457; P < 0.01). Half of those who received the drug were free of diabetes versus just 22% of those treated by placebo.
“We’ve not yet had those serologic biomarkers in MS. But I’d like to show you that maybe we are getting close to having them,” Dr. Hauser said. He pointed to new research into a U.S. Department of Defense serum repository that’s turned up “a pretty rock-solid prediagnostic biomarker specific to MS.”
Moving on to therapy, Dr. Hauser said it’s clear that “the earlier that we treat, the more likely we are to have a large response. Highly effective therapies delivered as first-line therapies have better long-term outcomes for disability then does a graded approach that doesn’t begin with high-efficacy therapy.”
What constitutes a cure?
What else needs to be done going forward? Dr. Hauser called for the MS field to develop a definition of cure. “We should take the lead from cancer therapeutics, where they define what a cure means.” In B-cell leukemia, for example, patients are considered cured “if they remain completely disease-free in terms of clinical symptoms and biomarkers of clonal proliferation for 4 years. They have less than a 1% lifetime risk of relapse. They’re essentially cured. Our equivalent could also be developed for MS.”
He highlighted the IMPACT MS phase 4 trial, a small single-center study of ocrelizumab, which just finished enrollment and will examine the effect of the drug on treatment-naive patients at the moment of their first-ever attack. The primary endpoint is oligoclonal bands in 3 years. “I think more of these studies will probably follow,” Dr. Hauser said.
Is intervention possible at the presymptomatic stage? Targets could be members of families with multiple affected relatives who test positive for the predictive antibody signature and who have a high genetic score, he said. “We could do perhaps an Epstein-Barr virus intervention trial in this population. Then, if we have the courage and are more confident in our biomarkers, perhaps even a therapeutic trial, as has been done in these other diseases.”
As for next-generation therapies, “we’ll need to neutralize multiple cell types, especially in later disease,” he said. Bruton tyrosine kinase inhibitors “seem to be a class of drugs that was designed for the MS patient because they not only hit B cells, but also the plasmablasts that CD20s don’t hit and are the main component of the humoral pathology in chronic MS lesions.”
Dr. Hauser discloses scientific board (Accure, Alector, Annexon), board of directors (Neurona), consulting (BD, Moderna, NGM Bio), and travel reimbursement/writing support (Roche and Novartis).
MILAN – University of California, San Francisco, neurology professor Stephen Hauser, MD, told colleagues in a highlighted lecture at the 9th Joint ECTRIMS-ACTRIMS meeting.
Going forward, the MS field should emphasize identifying early biomarkers of MS, Dr. Hauser said.
He noted that many experts had anticipated “that, if we could intervene early in the relapsing phase of the disease, we would stabilize neurodegeneration and patient disability. But one of the big surprises was that that was not the case. Instead, the observed course was that by silencing relapses and focal inflammation, a clinically silent, slow, insidious progression continues during the relapsing phase of disease in patients who are not having ongoing relapses.”
Even as focal activity detected via MRI is silenced, “progression continues” he said. “This remains the great unsolved challenge.”
Dr. Hauser asked colleagues to consider a three-stage model of MS that begins with benign autoimmunity followed by pathogenic autoimmunity with subclinical tissue damage. The third stage is clinical autoimmunity.
How can you determine who’s at risk? Genetics can only fill in part of the picture because they can’t pinpoint exactly who’s likely to develop the disease. “In other autoimmune diseases, serologic autoantibodies have been by far the most effective biomarkers,” he said. “There is real-world support – not only in mice – for the concept that autoimmunity begins as a highly focused immune response that then spreads over time.”
In systemic lupus erythematosus, the cascade toward disease begins about 9 years before clinical presentation, he said. It’s 7 months in type 1 diabetes, and 20 years in rheumatoid arthritis. “These have been enormously powerful in designing both observational and therapeutic studies to try to interrupt autoimmunity at the earliest possible stage.”
What can be done if a MS biomarker is developed and shows that a person is at risk? Dr. Hauser highlighted how the anti-CD3 antibody teplizumab has been developed – and Food and Drug Administration approved – to greatly reduce the risk of type 1 diabetes in high-risk patients. Per a 2021 study, a single-14-day course of the drug was linked to lowering the risk of disease over a median 923 days by more than 50% (hazard ratio, 0.457; P < 0.01). Half of those who received the drug were free of diabetes versus just 22% of those treated by placebo.
“We’ve not yet had those serologic biomarkers in MS. But I’d like to show you that maybe we are getting close to having them,” Dr. Hauser said. He pointed to new research into a U.S. Department of Defense serum repository that’s turned up “a pretty rock-solid prediagnostic biomarker specific to MS.”
Moving on to therapy, Dr. Hauser said it’s clear that “the earlier that we treat, the more likely we are to have a large response. Highly effective therapies delivered as first-line therapies have better long-term outcomes for disability then does a graded approach that doesn’t begin with high-efficacy therapy.”
What constitutes a cure?
What else needs to be done going forward? Dr. Hauser called for the MS field to develop a definition of cure. “We should take the lead from cancer therapeutics, where they define what a cure means.” In B-cell leukemia, for example, patients are considered cured “if they remain completely disease-free in terms of clinical symptoms and biomarkers of clonal proliferation for 4 years. They have less than a 1% lifetime risk of relapse. They’re essentially cured. Our equivalent could also be developed for MS.”
He highlighted the IMPACT MS phase 4 trial, a small single-center study of ocrelizumab, which just finished enrollment and will examine the effect of the drug on treatment-naive patients at the moment of their first-ever attack. The primary endpoint is oligoclonal bands in 3 years. “I think more of these studies will probably follow,” Dr. Hauser said.
Is intervention possible at the presymptomatic stage? Targets could be members of families with multiple affected relatives who test positive for the predictive antibody signature and who have a high genetic score, he said. “We could do perhaps an Epstein-Barr virus intervention trial in this population. Then, if we have the courage and are more confident in our biomarkers, perhaps even a therapeutic trial, as has been done in these other diseases.”
As for next-generation therapies, “we’ll need to neutralize multiple cell types, especially in later disease,” he said. Bruton tyrosine kinase inhibitors “seem to be a class of drugs that was designed for the MS patient because they not only hit B cells, but also the plasmablasts that CD20s don’t hit and are the main component of the humoral pathology in chronic MS lesions.”
Dr. Hauser discloses scientific board (Accure, Alector, Annexon), board of directors (Neurona), consulting (BD, Moderna, NGM Bio), and travel reimbursement/writing support (Roche and Novartis).
AT ECTRIMS 2023
Implementing shared decision making in labor and delivery: TeamBirth is a model for person-centered birthing care
CASE The TeamBirth experience: Making a difference
“At a community hospital in Washington where we had implemented TeamBirth (a labor and delivery shared decision making model), a patient, her partner, a labor and delivery nurse, and myself (an ObGyn) were making a plan for the patient’s induction of labor admission. I asked the patient, a 29-year-old (G2P1001), how we could improve her care in relation to her first birth. Her answer was simple: I want to be treated with respect. Her partner went on to describe their past experience in which the provider was inappropriately texting while in between the patient’s knees during delivery. Our team had the opportunity to undo some of the trauma from her first birth. That’s what I like about TeamBirth. It gives every patient the opportunity, regardless of their background, to define safety and participate in their care experience.”
–Angela Chien, MD, Obstetrician and Quality Improvement leader, Washington
Unfortunately, disrespect and mistreatment are far from an anomaly in the obstetrics setting. In a systematic review of respectful maternity care, the World Health Organization delineated 7 dimensions of maternal mistreatment: physical abuse, sexual abuse, verbal abuse, stigma and discrimination, failure to meet professional standards of care, poor rapport between women and providers, and poor conditions and constraints presented by the health system.1 In 2019, the Giving Voice to Mothers study showed that 17% of birthing people in the United States reported experiencing 1 or more types of maternal mistreatment.2 Rates of mistreatment were disproportionately greater in populations of color, hospital-based births, and among those with social, economic, or health challenges.2 It is well known that Black and African American and American Indian and Alaska Native populations experience the rare events of severe maternal morbidity and mortality more frequently than their White counterparts; the disproportionate burden of mistreatment is lesser known and far more common.
Overlooking the longitudinal harm of a negative birth experience has cascading impact. While an empowering perinatal experience can foster preventive screening and management of chronic disease, a poor experience conversely can seed mistrust at an individual, generational, and community level.
The patient quality enterprise is beginning to shift attention toward maternal experience with the development of PREMs (patient-reported experience measures), PROMs (patient-reported outcome measures), and novel validated scales that assess autonomy and trust.3 Development of a maternal Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey on childbirth is forthcoming.4 Of course, continuing to prioritize physical safety through initiatives on blood pressure monitoring and severe maternal morbidity and mortality remains paramount. Yet emotional and psychological safety also must be recognized as essential pillars of patient safety. Transgressions related to autonomy and dignity, as well as racism, sexism, classicism, and ableism, should be treated as “adverse and never events.”5
How the TeamBirth model works
Shared decision making (SDM) is cited in medical pedagogy as the solution to respectfullyrecognizing social context, integrating subjective experience, and honoring patient autonomy.6 The onus has always been on individual clinicians to exercise SDM. A new practice model, TeamBirth, embeds SDM into the culture and workflow. It offers a behavioral framework to mitigate implicit bias and operationalizes SDM tools, such that every patient is an empowered participant in their care.
TeamBirth was created through Ariadne Labs’ Delivery Decisions Initiative, a research and social impact program that designs, tests, and scales transformative, systems-level solutions that promote quality, equity, and dignity in childbirth. By the end of 2023, TeamBirth will be implemented in more than 100 hospitals across the United States, cumulatively touching over 200,000 lives. (For more information on the TeamBirth model, view the “Why TeamBirth” video at: https://www.youtube.com/watch?v=EoVrSaGk7gc.)
The tenets of TeamBirth are enacted through a patient-facing, shared whiteboard or dry-erase planning board in the labor room (FIGURE 1). Research has demonstrated how dry-erase boards in clinical settings can support safety and dignity in care, especially to improve patient-provider communication, teamwork, and patient satisfaction.7,8 The planning board is initially filled out by a clinical team member and is updated during team “huddles” throughout labor.

Huddles are care plan discussions with the full care team (the patient, nurse, doula and/or other support person(s), delivering provider, and interpreter or social worker as needed). At a minimum, huddles occur on admission, with changes to the clinical course and care plan, and at the request of any team member. Huddles can transpire through in-person, virtual, or phone communication.9 The concept builds on interdisciplinary and patient-centered rounding and establishes a communication system that is suited to the dynamic environment and amplified patient autonomy unique to labor and delivery. Dr. Bob Barbieri, a steadfast leader and champion of TeamBirth implementation at Brigham and Women’s Hospital in Boston (and the Editor in Chief of OBG M
Continue to: Patient response to TeamBirth is positive...
Patient response to TeamBirth is positive
Patients and providers alike have endorsed TeamBirth. In initial pilot testing across 4 sites, 99% of all patients surveyed “definitely” or “somewhat” had the role they wanted in making decisions about their labor.9
In partnership with the Oklahoma Perinatal Quality Improvement Collaborative (OPQIC), the impact of TeamBirth was assessed in a statewide patient cohort (n = 3,121) using the validated Mothers Autonomy in Decision Making (MADM) scale created by the Birth Place Lab at the University of British Columbia. The percentage of patients who scored in the highest MADM quartile was 31.3% higher for patients who indicated participation in a huddle during labor compared with those who did not participate in a huddle. This trend held across all racial and ethnic groups: For example, 93% of non-Hispanic Black/African American patients who had a TeamBirth huddle reported high autonomy, a nearly 20 percentage point increase from those without a huddle (FIGURE 2). Similarly, a higher percentage of agreement was observed across all 7 items in the MADM scale for patients who reported a TeamBirth huddle (FIGURE 3). TeamBirth’s effect has been observed across surveys and multiple validated metrics.
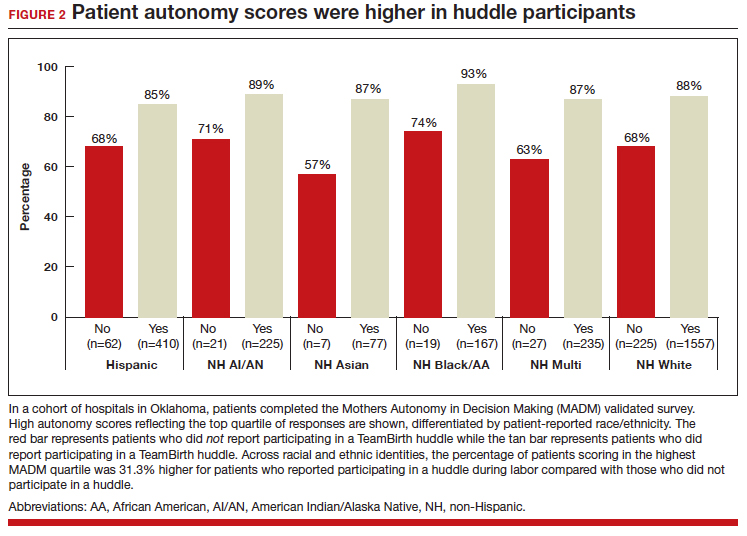
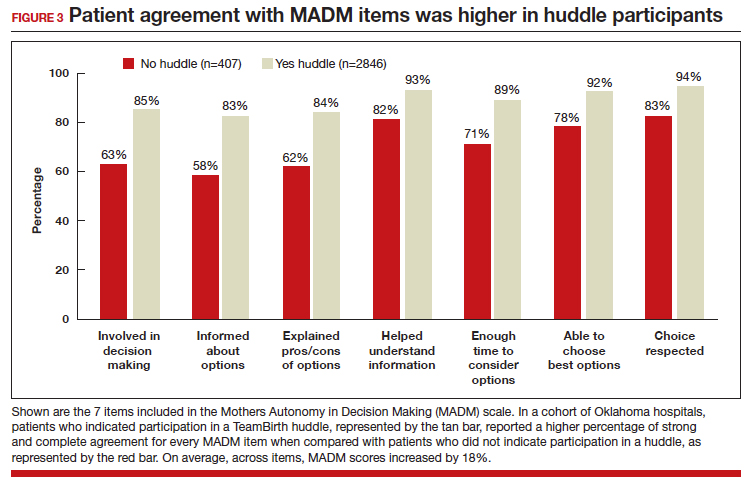
Data collection related to TeamBirth continues to be ongoing, with reported values retrieved on July 14, 2023. Rigorous review of patient-reported outcomes is forthcoming, and assessing impact on clinical outcomes, such as NTSV (nulliparous, term, singleton vertex) cesarean delivery rates and severe maternal morbidity, is on the horizon.
Qualitative survey responses reinforce how patients value TeamBirth and appreciate huddles and whiteboards.
Continue to: Patient testimonials...
Patient testimonials
The following testimonials were obtained from a TeamBirth survey that patients in participating Massachusetts hospitals completed in the postpartum unit prior to discharge.
According to one patient, “TeamBirth is great, feels like all obstacles are covered by multiple people with many talents, expertise. Feels like mom is part of the process, much different than my delivery 2 years ago when I felt like things were decided for me/I was ‘told’ what we were doing and questioned if I felt uneasy about it…. We felt safe and like all things were covered no matter what may happen.”
Another patient, also at a Massachusetts hospital, offered these comments about TeamBirth: “The entire staff was very genuine and my experience the best it could be. They deserve updated whiteboards in every room. I found them to be very useful.”
The clinician perspective
To be certain, clinician workflow must be a consideration for any practice change. The feasibility, acceptability, and safety of the TeamBirth model to clinicians was validated through a study at 4 community hospitals across the United States in which TeamBirth had been implemented in the 8 months prior.9
The clinician response rate was an impressive 78%. Ninety percent of clinicians, including physicians, midwives, and nurses, indicated that they would “definitely” (68%) or “probably” (22%) recommend TeamBirth for use in other labor and delivery units. None of the clinicians surveyed (n = 375) reported that TeamBirth negatively impacted care delivery.9
Obstetricians also provided qualitative commentary, noting that, while at times huddling infringed on efficiency, it also enhanced staff fulfillment. An obstetrician at a Massachusetts hospital observed, “Overall I think [TeamBirth is] helpful in slowing us down a little bit to really make sure that we’re providing the human part of the care, like the communication, and not just the medical care. And I think most providers value the human part and the communication. You know, we all think most providers value good communication with the patients, but when you’re in the middle of running around doing a bunch of stuff, you don’t always remember to prioritize it. And I think that at the end of the day…when you know you’ve communicated well with your patients, you end up feeling better about what you’re doing.”
As with most cross-sectional survey studies, selection bias remains an important caveat; patients and providers may decide to complete or not complete voluntary surveys based on particularly positive or negative experiences.
Metrics aside, obstetricians have an ethical duty to provide dignified and safe care, both physically and psychologically. Collectively, as a specialty, we share the responsibility to mitigate maternal mistreatment. As individuals, we can prevent perpetuation of birth trauma and foster healing and empowerment, one patient at a time, by employing tenets of TeamBirth.
To connect with Delivery Decisions Initiative, visit our website: https://www.ariadnelabs.org/deliverydecisions-initiative/ or contact: deliverydecisions@ ariadnelabs.org
Steps for implementing the TeamBirth model
To incorporate TeamBirth into your practice:
- Make patients the “team captain” and center them as the primary decision maker.
- Elicit patient preferences and subjective experiences to develop a collaborative plan on admission and when changes occur in clinical status.
- Round with and utilize the expertise of the full care team—nurse and midwife or obstetrician, as well as support person(s) and/or doula, learners, interpreter, and social worker as applicable.
- Ensure that the patient knows the names and roles of the care team members and provide updates at shift change.
- If your birthing rooms have a whiteboard, use it to keep the patient and team informed of the plan.
- Delineate status updates by maternal condition, fetal condition, and labor progress.
- Provide explicit permission for patients to call for a team huddle at any time and encourage support from their support people and/or doula. ●
This project is supported by:
- The Oklahoma Department of Health as part of the State Maternal Health Innovation Program Grant, Maternal and Child Health Bureau, Health Resources and Services Administration, Department of Health and Human Services.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award to the Oklahoma State Department of Health. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant T76MC00001 and entitled Training Grant in Maternal and Child Health.
- Point32 Health’s Clinical Innovation Fund.
Data included in this article was collected and analyzed in partnership with the Oklahoma Perinatal Quality Improvement Collaborative, Department of OB/GYN, University of Oklahoma Health Sciences Center, Oklahoma City.
- Bohren MA, Vogel JP, Hunter EC, et al. The mistreatment of women during childbirth in health facilities globally: a mixedmethods systematic review. PLoS Med. 2015;12:e100184. doi:10.1371/journal.pmed.1001847
- Vedam S, Stoll K, Taiwo TK, et al. The Giving Voice to Mothers study: inequity and mistreatment during pregnancy and childbirth in the United States. Reprod Health. 2019;16. doi:10.1186/s12978-019-0729-2
- Kemmerer A, Alteras T. Evolving the maternal health quality measurement enterprise to support the communitybased maternity model. Maternal Health Hub. April 25, 2023. Accessed September 13, 2023. https:/www .maternalhealthhub.org
- Potential CAHPS survey to assess patients’ prenatal and childbirth care experiences. Agency for Healthcare Research and Quality. March 2023. Accessed September 13, 2023. https://www.ahrq.gov/news/cahps-comments-sought.html
- Lyndon A, Davis DA, Sharma AE, et al. Emotional safety is patient safety. BMJ Qual Saf. 2023;32:369-372. doi:10.1136 /bmjqs-2022-015573
- American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 819. Informed consent and shared decision making in obstetrics and gynecology. Obstet Gynecol. 2021;137:e34-e41. Accessed September 13, 2023. https://www.acog.org/clinical/clinical-guidance /committee-opinion/articles/2021/02/informed -consent-and-shared-decision-making-in-obstetrics-and -gynecology
- Goyal AA, Tur K, Mann J, et al. Do bedside visual tools improve patient and caregiver satisfaction? A systematic review of the literature. J Hosp Med. 2017;12:930-936. doi:10.12788 /jhm.2871
- Sehgal NL, Green A, Vidyarthi AR, et al. Patient whiteboards as a communication tool in the hospital setting: a survey of practices and recommendations. J Hosp Med. 2010;5:234-239. doi:10.1002/jhm.638
- Weiseth A, Plough A, Aggarwal R, et al. Improving communication and teamwork during labor: a feasibility, acceptability, and safety study. Birth. 2022:49:637-647. doi:10.1111/birt.12630
CASE The TeamBirth experience: Making a difference
“At a community hospital in Washington where we had implemented TeamBirth (a labor and delivery shared decision making model), a patient, her partner, a labor and delivery nurse, and myself (an ObGyn) were making a plan for the patient’s induction of labor admission. I asked the patient, a 29-year-old (G2P1001), how we could improve her care in relation to her first birth. Her answer was simple: I want to be treated with respect. Her partner went on to describe their past experience in which the provider was inappropriately texting while in between the patient’s knees during delivery. Our team had the opportunity to undo some of the trauma from her first birth. That’s what I like about TeamBirth. It gives every patient the opportunity, regardless of their background, to define safety and participate in their care experience.”
–Angela Chien, MD, Obstetrician and Quality Improvement leader, Washington
Unfortunately, disrespect and mistreatment are far from an anomaly in the obstetrics setting. In a systematic review of respectful maternity care, the World Health Organization delineated 7 dimensions of maternal mistreatment: physical abuse, sexual abuse, verbal abuse, stigma and discrimination, failure to meet professional standards of care, poor rapport between women and providers, and poor conditions and constraints presented by the health system.1 In 2019, the Giving Voice to Mothers study showed that 17% of birthing people in the United States reported experiencing 1 or more types of maternal mistreatment.2 Rates of mistreatment were disproportionately greater in populations of color, hospital-based births, and among those with social, economic, or health challenges.2 It is well known that Black and African American and American Indian and Alaska Native populations experience the rare events of severe maternal morbidity and mortality more frequently than their White counterparts; the disproportionate burden of mistreatment is lesser known and far more common.
Overlooking the longitudinal harm of a negative birth experience has cascading impact. While an empowering perinatal experience can foster preventive screening and management of chronic disease, a poor experience conversely can seed mistrust at an individual, generational, and community level.
The patient quality enterprise is beginning to shift attention toward maternal experience with the development of PREMs (patient-reported experience measures), PROMs (patient-reported outcome measures), and novel validated scales that assess autonomy and trust.3 Development of a maternal Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey on childbirth is forthcoming.4 Of course, continuing to prioritize physical safety through initiatives on blood pressure monitoring and severe maternal morbidity and mortality remains paramount. Yet emotional and psychological safety also must be recognized as essential pillars of patient safety. Transgressions related to autonomy and dignity, as well as racism, sexism, classicism, and ableism, should be treated as “adverse and never events.”5
How the TeamBirth model works
Shared decision making (SDM) is cited in medical pedagogy as the solution to respectfullyrecognizing social context, integrating subjective experience, and honoring patient autonomy.6 The onus has always been on individual clinicians to exercise SDM. A new practice model, TeamBirth, embeds SDM into the culture and workflow. It offers a behavioral framework to mitigate implicit bias and operationalizes SDM tools, such that every patient is an empowered participant in their care.
TeamBirth was created through Ariadne Labs’ Delivery Decisions Initiative, a research and social impact program that designs, tests, and scales transformative, systems-level solutions that promote quality, equity, and dignity in childbirth. By the end of 2023, TeamBirth will be implemented in more than 100 hospitals across the United States, cumulatively touching over 200,000 lives. (For more information on the TeamBirth model, view the “Why TeamBirth” video at: https://www.youtube.com/watch?v=EoVrSaGk7gc.)
The tenets of TeamBirth are enacted through a patient-facing, shared whiteboard or dry-erase planning board in the labor room (FIGURE 1). Research has demonstrated how dry-erase boards in clinical settings can support safety and dignity in care, especially to improve patient-provider communication, teamwork, and patient satisfaction.7,8 The planning board is initially filled out by a clinical team member and is updated during team “huddles” throughout labor.

Huddles are care plan discussions with the full care team (the patient, nurse, doula and/or other support person(s), delivering provider, and interpreter or social worker as needed). At a minimum, huddles occur on admission, with changes to the clinical course and care plan, and at the request of any team member. Huddles can transpire through in-person, virtual, or phone communication.9 The concept builds on interdisciplinary and patient-centered rounding and establishes a communication system that is suited to the dynamic environment and amplified patient autonomy unique to labor and delivery. Dr. Bob Barbieri, a steadfast leader and champion of TeamBirth implementation at Brigham and Women’s Hospital in Boston (and the Editor in Chief of OBG M
Continue to: Patient response to TeamBirth is positive...
Patient response to TeamBirth is positive
Patients and providers alike have endorsed TeamBirth. In initial pilot testing across 4 sites, 99% of all patients surveyed “definitely” or “somewhat” had the role they wanted in making decisions about their labor.9
In partnership with the Oklahoma Perinatal Quality Improvement Collaborative (OPQIC), the impact of TeamBirth was assessed in a statewide patient cohort (n = 3,121) using the validated Mothers Autonomy in Decision Making (MADM) scale created by the Birth Place Lab at the University of British Columbia. The percentage of patients who scored in the highest MADM quartile was 31.3% higher for patients who indicated participation in a huddle during labor compared with those who did not participate in a huddle. This trend held across all racial and ethnic groups: For example, 93% of non-Hispanic Black/African American patients who had a TeamBirth huddle reported high autonomy, a nearly 20 percentage point increase from those without a huddle (FIGURE 2). Similarly, a higher percentage of agreement was observed across all 7 items in the MADM scale for patients who reported a TeamBirth huddle (FIGURE 3). TeamBirth’s effect has been observed across surveys and multiple validated metrics.


Data collection related to TeamBirth continues to be ongoing, with reported values retrieved on July 14, 2023. Rigorous review of patient-reported outcomes is forthcoming, and assessing impact on clinical outcomes, such as NTSV (nulliparous, term, singleton vertex) cesarean delivery rates and severe maternal morbidity, is on the horizon.
Qualitative survey responses reinforce how patients value TeamBirth and appreciate huddles and whiteboards.
Continue to: Patient testimonials...
Patient testimonials
The following testimonials were obtained from a TeamBirth survey that patients in participating Massachusetts hospitals completed in the postpartum unit prior to discharge.
According to one patient, “TeamBirth is great, feels like all obstacles are covered by multiple people with many talents, expertise. Feels like mom is part of the process, much different than my delivery 2 years ago when I felt like things were decided for me/I was ‘told’ what we were doing and questioned if I felt uneasy about it…. We felt safe and like all things were covered no matter what may happen.”
Another patient, also at a Massachusetts hospital, offered these comments about TeamBirth: “The entire staff was very genuine and my experience the best it could be. They deserve updated whiteboards in every room. I found them to be very useful.”
The clinician perspective
To be certain, clinician workflow must be a consideration for any practice change. The feasibility, acceptability, and safety of the TeamBirth model to clinicians was validated through a study at 4 community hospitals across the United States in which TeamBirth had been implemented in the 8 months prior.9
The clinician response rate was an impressive 78%. Ninety percent of clinicians, including physicians, midwives, and nurses, indicated that they would “definitely” (68%) or “probably” (22%) recommend TeamBirth for use in other labor and delivery units. None of the clinicians surveyed (n = 375) reported that TeamBirth negatively impacted care delivery.9
Obstetricians also provided qualitative commentary, noting that, while at times huddling infringed on efficiency, it also enhanced staff fulfillment. An obstetrician at a Massachusetts hospital observed, “Overall I think [TeamBirth is] helpful in slowing us down a little bit to really make sure that we’re providing the human part of the care, like the communication, and not just the medical care. And I think most providers value the human part and the communication. You know, we all think most providers value good communication with the patients, but when you’re in the middle of running around doing a bunch of stuff, you don’t always remember to prioritize it. And I think that at the end of the day…when you know you’ve communicated well with your patients, you end up feeling better about what you’re doing.”
As with most cross-sectional survey studies, selection bias remains an important caveat; patients and providers may decide to complete or not complete voluntary surveys based on particularly positive or negative experiences.
Metrics aside, obstetricians have an ethical duty to provide dignified and safe care, both physically and psychologically. Collectively, as a specialty, we share the responsibility to mitigate maternal mistreatment. As individuals, we can prevent perpetuation of birth trauma and foster healing and empowerment, one patient at a time, by employing tenets of TeamBirth.
To connect with Delivery Decisions Initiative, visit our website: https://www.ariadnelabs.org/deliverydecisions-initiative/ or contact: deliverydecisions@ ariadnelabs.org
Steps for implementing the TeamBirth model
To incorporate TeamBirth into your practice:
- Make patients the “team captain” and center them as the primary decision maker.
- Elicit patient preferences and subjective experiences to develop a collaborative plan on admission and when changes occur in clinical status.
- Round with and utilize the expertise of the full care team—nurse and midwife or obstetrician, as well as support person(s) and/or doula, learners, interpreter, and social worker as applicable.
- Ensure that the patient knows the names and roles of the care team members and provide updates at shift change.
- If your birthing rooms have a whiteboard, use it to keep the patient and team informed of the plan.
- Delineate status updates by maternal condition, fetal condition, and labor progress.
- Provide explicit permission for patients to call for a team huddle at any time and encourage support from their support people and/or doula. ●
This project is supported by:
- The Oklahoma Department of Health as part of the State Maternal Health Innovation Program Grant, Maternal and Child Health Bureau, Health Resources and Services Administration, Department of Health and Human Services.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award to the Oklahoma State Department of Health. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant T76MC00001 and entitled Training Grant in Maternal and Child Health.
- Point32 Health’s Clinical Innovation Fund.
Data included in this article was collected and analyzed in partnership with the Oklahoma Perinatal Quality Improvement Collaborative, Department of OB/GYN, University of Oklahoma Health Sciences Center, Oklahoma City.
CASE The TeamBirth experience: Making a difference
“At a community hospital in Washington where we had implemented TeamBirth (a labor and delivery shared decision making model), a patient, her partner, a labor and delivery nurse, and myself (an ObGyn) were making a plan for the patient’s induction of labor admission. I asked the patient, a 29-year-old (G2P1001), how we could improve her care in relation to her first birth. Her answer was simple: I want to be treated with respect. Her partner went on to describe their past experience in which the provider was inappropriately texting while in between the patient’s knees during delivery. Our team had the opportunity to undo some of the trauma from her first birth. That’s what I like about TeamBirth. It gives every patient the opportunity, regardless of their background, to define safety and participate in their care experience.”
–Angela Chien, MD, Obstetrician and Quality Improvement leader, Washington
Unfortunately, disrespect and mistreatment are far from an anomaly in the obstetrics setting. In a systematic review of respectful maternity care, the World Health Organization delineated 7 dimensions of maternal mistreatment: physical abuse, sexual abuse, verbal abuse, stigma and discrimination, failure to meet professional standards of care, poor rapport between women and providers, and poor conditions and constraints presented by the health system.1 In 2019, the Giving Voice to Mothers study showed that 17% of birthing people in the United States reported experiencing 1 or more types of maternal mistreatment.2 Rates of mistreatment were disproportionately greater in populations of color, hospital-based births, and among those with social, economic, or health challenges.2 It is well known that Black and African American and American Indian and Alaska Native populations experience the rare events of severe maternal morbidity and mortality more frequently than their White counterparts; the disproportionate burden of mistreatment is lesser known and far more common.
Overlooking the longitudinal harm of a negative birth experience has cascading impact. While an empowering perinatal experience can foster preventive screening and management of chronic disease, a poor experience conversely can seed mistrust at an individual, generational, and community level.
The patient quality enterprise is beginning to shift attention toward maternal experience with the development of PREMs (patient-reported experience measures), PROMs (patient-reported outcome measures), and novel validated scales that assess autonomy and trust.3 Development of a maternal Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey on childbirth is forthcoming.4 Of course, continuing to prioritize physical safety through initiatives on blood pressure monitoring and severe maternal morbidity and mortality remains paramount. Yet emotional and psychological safety also must be recognized as essential pillars of patient safety. Transgressions related to autonomy and dignity, as well as racism, sexism, classicism, and ableism, should be treated as “adverse and never events.”5
How the TeamBirth model works
Shared decision making (SDM) is cited in medical pedagogy as the solution to respectfullyrecognizing social context, integrating subjective experience, and honoring patient autonomy.6 The onus has always been on individual clinicians to exercise SDM. A new practice model, TeamBirth, embeds SDM into the culture and workflow. It offers a behavioral framework to mitigate implicit bias and operationalizes SDM tools, such that every patient is an empowered participant in their care.
TeamBirth was created through Ariadne Labs’ Delivery Decisions Initiative, a research and social impact program that designs, tests, and scales transformative, systems-level solutions that promote quality, equity, and dignity in childbirth. By the end of 2023, TeamBirth will be implemented in more than 100 hospitals across the United States, cumulatively touching over 200,000 lives. (For more information on the TeamBirth model, view the “Why TeamBirth” video at: https://www.youtube.com/watch?v=EoVrSaGk7gc.)
The tenets of TeamBirth are enacted through a patient-facing, shared whiteboard or dry-erase planning board in the labor room (FIGURE 1). Research has demonstrated how dry-erase boards in clinical settings can support safety and dignity in care, especially to improve patient-provider communication, teamwork, and patient satisfaction.7,8 The planning board is initially filled out by a clinical team member and is updated during team “huddles” throughout labor.

Huddles are care plan discussions with the full care team (the patient, nurse, doula and/or other support person(s), delivering provider, and interpreter or social worker as needed). At a minimum, huddles occur on admission, with changes to the clinical course and care plan, and at the request of any team member. Huddles can transpire through in-person, virtual, or phone communication.9 The concept builds on interdisciplinary and patient-centered rounding and establishes a communication system that is suited to the dynamic environment and amplified patient autonomy unique to labor and delivery. Dr. Bob Barbieri, a steadfast leader and champion of TeamBirth implementation at Brigham and Women’s Hospital in Boston (and the Editor in Chief of OBG M
Continue to: Patient response to TeamBirth is positive...
Patient response to TeamBirth is positive
Patients and providers alike have endorsed TeamBirth. In initial pilot testing across 4 sites, 99% of all patients surveyed “definitely” or “somewhat” had the role they wanted in making decisions about their labor.9
In partnership with the Oklahoma Perinatal Quality Improvement Collaborative (OPQIC), the impact of TeamBirth was assessed in a statewide patient cohort (n = 3,121) using the validated Mothers Autonomy in Decision Making (MADM) scale created by the Birth Place Lab at the University of British Columbia. The percentage of patients who scored in the highest MADM quartile was 31.3% higher for patients who indicated participation in a huddle during labor compared with those who did not participate in a huddle. This trend held across all racial and ethnic groups: For example, 93% of non-Hispanic Black/African American patients who had a TeamBirth huddle reported high autonomy, a nearly 20 percentage point increase from those without a huddle (FIGURE 2). Similarly, a higher percentage of agreement was observed across all 7 items in the MADM scale for patients who reported a TeamBirth huddle (FIGURE 3). TeamBirth’s effect has been observed across surveys and multiple validated metrics.


Data collection related to TeamBirth continues to be ongoing, with reported values retrieved on July 14, 2023. Rigorous review of patient-reported outcomes is forthcoming, and assessing impact on clinical outcomes, such as NTSV (nulliparous, term, singleton vertex) cesarean delivery rates and severe maternal morbidity, is on the horizon.
Qualitative survey responses reinforce how patients value TeamBirth and appreciate huddles and whiteboards.
Continue to: Patient testimonials...
Patient testimonials
The following testimonials were obtained from a TeamBirth survey that patients in participating Massachusetts hospitals completed in the postpartum unit prior to discharge.
According to one patient, “TeamBirth is great, feels like all obstacles are covered by multiple people with many talents, expertise. Feels like mom is part of the process, much different than my delivery 2 years ago when I felt like things were decided for me/I was ‘told’ what we were doing and questioned if I felt uneasy about it…. We felt safe and like all things were covered no matter what may happen.”
Another patient, also at a Massachusetts hospital, offered these comments about TeamBirth: “The entire staff was very genuine and my experience the best it could be. They deserve updated whiteboards in every room. I found them to be very useful.”
The clinician perspective
To be certain, clinician workflow must be a consideration for any practice change. The feasibility, acceptability, and safety of the TeamBirth model to clinicians was validated through a study at 4 community hospitals across the United States in which TeamBirth had been implemented in the 8 months prior.9
The clinician response rate was an impressive 78%. Ninety percent of clinicians, including physicians, midwives, and nurses, indicated that they would “definitely” (68%) or “probably” (22%) recommend TeamBirth for use in other labor and delivery units. None of the clinicians surveyed (n = 375) reported that TeamBirth negatively impacted care delivery.9
Obstetricians also provided qualitative commentary, noting that, while at times huddling infringed on efficiency, it also enhanced staff fulfillment. An obstetrician at a Massachusetts hospital observed, “Overall I think [TeamBirth is] helpful in slowing us down a little bit to really make sure that we’re providing the human part of the care, like the communication, and not just the medical care. And I think most providers value the human part and the communication. You know, we all think most providers value good communication with the patients, but when you’re in the middle of running around doing a bunch of stuff, you don’t always remember to prioritize it. And I think that at the end of the day…when you know you’ve communicated well with your patients, you end up feeling better about what you’re doing.”
As with most cross-sectional survey studies, selection bias remains an important caveat; patients and providers may decide to complete or not complete voluntary surveys based on particularly positive or negative experiences.
Metrics aside, obstetricians have an ethical duty to provide dignified and safe care, both physically and psychologically. Collectively, as a specialty, we share the responsibility to mitigate maternal mistreatment. As individuals, we can prevent perpetuation of birth trauma and foster healing and empowerment, one patient at a time, by employing tenets of TeamBirth.
To connect with Delivery Decisions Initiative, visit our website: https://www.ariadnelabs.org/deliverydecisions-initiative/ or contact: deliverydecisions@ ariadnelabs.org
Steps for implementing the TeamBirth model
To incorporate TeamBirth into your practice:
- Make patients the “team captain” and center them as the primary decision maker.
- Elicit patient preferences and subjective experiences to develop a collaborative plan on admission and when changes occur in clinical status.
- Round with and utilize the expertise of the full care team—nurse and midwife or obstetrician, as well as support person(s) and/or doula, learners, interpreter, and social worker as applicable.
- Ensure that the patient knows the names and roles of the care team members and provide updates at shift change.
- If your birthing rooms have a whiteboard, use it to keep the patient and team informed of the plan.
- Delineate status updates by maternal condition, fetal condition, and labor progress.
- Provide explicit permission for patients to call for a team huddle at any time and encourage support from their support people and/or doula. ●
This project is supported by:
- The Oklahoma Department of Health as part of the State Maternal Health Innovation Program Grant, Maternal and Child Health Bureau, Health Resources and Services Administration, Department of Health and Human Services.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award to the Oklahoma State Department of Health. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov.
- The Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under grant T76MC00001 and entitled Training Grant in Maternal and Child Health.
- Point32 Health’s Clinical Innovation Fund.
Data included in this article was collected and analyzed in partnership with the Oklahoma Perinatal Quality Improvement Collaborative, Department of OB/GYN, University of Oklahoma Health Sciences Center, Oklahoma City.
- Bohren MA, Vogel JP, Hunter EC, et al. The mistreatment of women during childbirth in health facilities globally: a mixedmethods systematic review. PLoS Med. 2015;12:e100184. doi:10.1371/journal.pmed.1001847
- Vedam S, Stoll K, Taiwo TK, et al. The Giving Voice to Mothers study: inequity and mistreatment during pregnancy and childbirth in the United States. Reprod Health. 2019;16. doi:10.1186/s12978-019-0729-2
- Kemmerer A, Alteras T. Evolving the maternal health quality measurement enterprise to support the communitybased maternity model. Maternal Health Hub. April 25, 2023. Accessed September 13, 2023. https:/www .maternalhealthhub.org
- Potential CAHPS survey to assess patients’ prenatal and childbirth care experiences. Agency for Healthcare Research and Quality. March 2023. Accessed September 13, 2023. https://www.ahrq.gov/news/cahps-comments-sought.html
- Lyndon A, Davis DA, Sharma AE, et al. Emotional safety is patient safety. BMJ Qual Saf. 2023;32:369-372. doi:10.1136 /bmjqs-2022-015573
- American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 819. Informed consent and shared decision making in obstetrics and gynecology. Obstet Gynecol. 2021;137:e34-e41. Accessed September 13, 2023. https://www.acog.org/clinical/clinical-guidance /committee-opinion/articles/2021/02/informed -consent-and-shared-decision-making-in-obstetrics-and -gynecology
- Goyal AA, Tur K, Mann J, et al. Do bedside visual tools improve patient and caregiver satisfaction? A systematic review of the literature. J Hosp Med. 2017;12:930-936. doi:10.12788 /jhm.2871
- Sehgal NL, Green A, Vidyarthi AR, et al. Patient whiteboards as a communication tool in the hospital setting: a survey of practices and recommendations. J Hosp Med. 2010;5:234-239. doi:10.1002/jhm.638
- Weiseth A, Plough A, Aggarwal R, et al. Improving communication and teamwork during labor: a feasibility, acceptability, and safety study. Birth. 2022:49:637-647. doi:10.1111/birt.12630
- Bohren MA, Vogel JP, Hunter EC, et al. The mistreatment of women during childbirth in health facilities globally: a mixedmethods systematic review. PLoS Med. 2015;12:e100184. doi:10.1371/journal.pmed.1001847
- Vedam S, Stoll K, Taiwo TK, et al. The Giving Voice to Mothers study: inequity and mistreatment during pregnancy and childbirth in the United States. Reprod Health. 2019;16. doi:10.1186/s12978-019-0729-2
- Kemmerer A, Alteras T. Evolving the maternal health quality measurement enterprise to support the communitybased maternity model. Maternal Health Hub. April 25, 2023. Accessed September 13, 2023. https:/www .maternalhealthhub.org
- Potential CAHPS survey to assess patients’ prenatal and childbirth care experiences. Agency for Healthcare Research and Quality. March 2023. Accessed September 13, 2023. https://www.ahrq.gov/news/cahps-comments-sought.html
- Lyndon A, Davis DA, Sharma AE, et al. Emotional safety is patient safety. BMJ Qual Saf. 2023;32:369-372. doi:10.1136 /bmjqs-2022-015573
- American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 819. Informed consent and shared decision making in obstetrics and gynecology. Obstet Gynecol. 2021;137:e34-e41. Accessed September 13, 2023. https://www.acog.org/clinical/clinical-guidance /committee-opinion/articles/2021/02/informed -consent-and-shared-decision-making-in-obstetrics-and -gynecology
- Goyal AA, Tur K, Mann J, et al. Do bedside visual tools improve patient and caregiver satisfaction? A systematic review of the literature. J Hosp Med. 2017;12:930-936. doi:10.12788 /jhm.2871
- Sehgal NL, Green A, Vidyarthi AR, et al. Patient whiteboards as a communication tool in the hospital setting: a survey of practices and recommendations. J Hosp Med. 2010;5:234-239. doi:10.1002/jhm.638
- Weiseth A, Plough A, Aggarwal R, et al. Improving communication and teamwork during labor: a feasibility, acceptability, and safety study. Birth. 2022:49:637-647. doi:10.1111/birt.12630