User login
Analysis spotlights economic burden of vitiligo in the U.S.
TOPLINE:
METHODOLOGY:
- No published studies have quantified the medical costs and health care resource utilization (HCRU) among patients with vitiligo in the United States, compared with the general population.
- Drawing from the Merative MarketScan Commercial Claims and Encounters database, researchers reviewed the records of 49,512 patients diagnosed with vitiligo between Jan. 1, 2008, and Dec. 31, 2020, and those of 99,024 matched control persons who did not have vitiligo.
- Costs were in 2021 dollars during a 1-year postindex period. The student t test and chi square analysis were used to determine P values.
TAKEAWAY:
- In both cohorts, the median age of patients was 43 years, 79.2% were female, and most (39%) were from the southern region of the United States.
- All-cause total health care costs for patients with vitiligo were significantly higher than those of matched controls ($15,551 vs. $7,735; P < .0001).
- Similarly, medical costs for patients with vitiligo were significantly higher than those of control persons ($11,953 vs. $5,722), as were pharmacy costs ($3,598 vs. $2,014; P < .001 for both associations).
- A significantly greater proportion of patients with vitiligo had higher all-cause HCRU, compared with matched control persons. That included at least one ED visit (17.5% vs 13.4%), at least one inpatient visit (12.9% vs 6.8%), and at least one outpatient visit (99.8% vs. 88.3%; P < .0001 for all associations).
IN PRACTICE:
“These findings reveal an unmet need for cost-effective treatments and highlight the importance of fully identifying the drivers of economic burden for patients with vitiligo,” the authors concluded.
SOURCE:
Khaled Ezzedine, MD, PhD, of the department of dermatology at the Henri Mondor University Hospital, Créteil, France, led the study, which was published in the Journal of Investigative Dermatology.
LIMITATIONS:
The investigators did not evaluate indirect medical costs of vitiligo, such as work productivity, early retirement, and lost opportunities. Also, the results may not be generalizable to populations outside of the United States.
DISCLOSURES:
Dr. Ezzedine has received honoraria as a consultant for AbbVie, Incyte, La Roche–Posay, Pfizer, Pierre Fabre, Sanofi, and Viela Bio. One author is an investigator for Incyte and is a consultant for several pharmaceutical companies. Three authors are AbbVie employees.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- No published studies have quantified the medical costs and health care resource utilization (HCRU) among patients with vitiligo in the United States, compared with the general population.
- Drawing from the Merative MarketScan Commercial Claims and Encounters database, researchers reviewed the records of 49,512 patients diagnosed with vitiligo between Jan. 1, 2008, and Dec. 31, 2020, and those of 99,024 matched control persons who did not have vitiligo.
- Costs were in 2021 dollars during a 1-year postindex period. The student t test and chi square analysis were used to determine P values.
TAKEAWAY:
- In both cohorts, the median age of patients was 43 years, 79.2% were female, and most (39%) were from the southern region of the United States.
- All-cause total health care costs for patients with vitiligo were significantly higher than those of matched controls ($15,551 vs. $7,735; P < .0001).
- Similarly, medical costs for patients with vitiligo were significantly higher than those of control persons ($11,953 vs. $5,722), as were pharmacy costs ($3,598 vs. $2,014; P < .001 for both associations).
- A significantly greater proportion of patients with vitiligo had higher all-cause HCRU, compared with matched control persons. That included at least one ED visit (17.5% vs 13.4%), at least one inpatient visit (12.9% vs 6.8%), and at least one outpatient visit (99.8% vs. 88.3%; P < .0001 for all associations).
IN PRACTICE:
“These findings reveal an unmet need for cost-effective treatments and highlight the importance of fully identifying the drivers of economic burden for patients with vitiligo,” the authors concluded.
SOURCE:
Khaled Ezzedine, MD, PhD, of the department of dermatology at the Henri Mondor University Hospital, Créteil, France, led the study, which was published in the Journal of Investigative Dermatology.
LIMITATIONS:
The investigators did not evaluate indirect medical costs of vitiligo, such as work productivity, early retirement, and lost opportunities. Also, the results may not be generalizable to populations outside of the United States.
DISCLOSURES:
Dr. Ezzedine has received honoraria as a consultant for AbbVie, Incyte, La Roche–Posay, Pfizer, Pierre Fabre, Sanofi, and Viela Bio. One author is an investigator for Incyte and is a consultant for several pharmaceutical companies. Three authors are AbbVie employees.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- No published studies have quantified the medical costs and health care resource utilization (HCRU) among patients with vitiligo in the United States, compared with the general population.
- Drawing from the Merative MarketScan Commercial Claims and Encounters database, researchers reviewed the records of 49,512 patients diagnosed with vitiligo between Jan. 1, 2008, and Dec. 31, 2020, and those of 99,024 matched control persons who did not have vitiligo.
- Costs were in 2021 dollars during a 1-year postindex period. The student t test and chi square analysis were used to determine P values.
TAKEAWAY:
- In both cohorts, the median age of patients was 43 years, 79.2% were female, and most (39%) were from the southern region of the United States.
- All-cause total health care costs for patients with vitiligo were significantly higher than those of matched controls ($15,551 vs. $7,735; P < .0001).
- Similarly, medical costs for patients with vitiligo were significantly higher than those of control persons ($11,953 vs. $5,722), as were pharmacy costs ($3,598 vs. $2,014; P < .001 for both associations).
- A significantly greater proportion of patients with vitiligo had higher all-cause HCRU, compared with matched control persons. That included at least one ED visit (17.5% vs 13.4%), at least one inpatient visit (12.9% vs 6.8%), and at least one outpatient visit (99.8% vs. 88.3%; P < .0001 for all associations).
IN PRACTICE:
“These findings reveal an unmet need for cost-effective treatments and highlight the importance of fully identifying the drivers of economic burden for patients with vitiligo,” the authors concluded.
SOURCE:
Khaled Ezzedine, MD, PhD, of the department of dermatology at the Henri Mondor University Hospital, Créteil, France, led the study, which was published in the Journal of Investigative Dermatology.
LIMITATIONS:
The investigators did not evaluate indirect medical costs of vitiligo, such as work productivity, early retirement, and lost opportunities. Also, the results may not be generalizable to populations outside of the United States.
DISCLOSURES:
Dr. Ezzedine has received honoraria as a consultant for AbbVie, Incyte, La Roche–Posay, Pfizer, Pierre Fabre, Sanofi, and Viela Bio. One author is an investigator for Incyte and is a consultant for several pharmaceutical companies. Three authors are AbbVie employees.
A version of this article first appeared on Medscape.com.
Pediatric psoriasis: Black children, males more likely to have palmoplantar subtype, study finds
TOPLINE:
.
METHODOLOGY:
- Researchers reviewed data on 330 children and youths aged 0-18 years who had received a primary psoriasis diagnosis and who were seen at an academic pediatric dermatology clinic from 2012 to 2022. Among these patients, 50 cases of palmoplantar psoriasis (PP) were identified by pediatric dermatologists.
- The study population was stratified by race/ethnicity on the basis of self-identification. The cohort included White, Black, and Hispanic/Latino patients, as well as patients who identified as other; 71.5% were White persons, 59.1% were female patients.
- The researchers used a regression analysis to investigate the association between race/ethnicity and PP after controlling for multiple confounding variables, including age and gender.
TAKEAWAY:
- Black children were significantly more likely to have PP than White children (adjusted odds ratio, 6.386; P < .0001). PP was diagnosed in 41.9%, 11.5%, and 8.9% of Black, Hispanic/Latino, and White children, respectively.
- Male gender was also identified as an independent risk factor for PP (aOR, 2.241).
- Nail involvement occurred in significantly more Black and Hispanic/Latino patients than in White patients (53.2%, 50.0%, and 33.9%, respectively).
- Black patients had significantly more palm and sole involvement, compared with the other groups (P < .0001 for both); however, White children had significantly more scalp involvement, compared with the other groups (P = .04).
IN PRACTICE:
“Further research is warranted to better understand the degree to which these associations are affected by racial disparities and environmental factors,” as well as potential genetic associations, the researchers noted.
SOURCE:
The corresponding author on the study was Amy Theos, MD, of the department of dermatology at the University of Alabama, Birmingham. The study was published online in Pediatric Dermatology.
LIMITATIONS:
The findings were limited by the small sample size and incomplete data for some patients.
DISCLOSURES:
The study received no outside funding. The researchers had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
TOPLINE:
.
METHODOLOGY:
- Researchers reviewed data on 330 children and youths aged 0-18 years who had received a primary psoriasis diagnosis and who were seen at an academic pediatric dermatology clinic from 2012 to 2022. Among these patients, 50 cases of palmoplantar psoriasis (PP) were identified by pediatric dermatologists.
- The study population was stratified by race/ethnicity on the basis of self-identification. The cohort included White, Black, and Hispanic/Latino patients, as well as patients who identified as other; 71.5% were White persons, 59.1% were female patients.
- The researchers used a regression analysis to investigate the association between race/ethnicity and PP after controlling for multiple confounding variables, including age and gender.
TAKEAWAY:
- Black children were significantly more likely to have PP than White children (adjusted odds ratio, 6.386; P < .0001). PP was diagnosed in 41.9%, 11.5%, and 8.9% of Black, Hispanic/Latino, and White children, respectively.
- Male gender was also identified as an independent risk factor for PP (aOR, 2.241).
- Nail involvement occurred in significantly more Black and Hispanic/Latino patients than in White patients (53.2%, 50.0%, and 33.9%, respectively).
- Black patients had significantly more palm and sole involvement, compared with the other groups (P < .0001 for both); however, White children had significantly more scalp involvement, compared with the other groups (P = .04).
IN PRACTICE:
“Further research is warranted to better understand the degree to which these associations are affected by racial disparities and environmental factors,” as well as potential genetic associations, the researchers noted.
SOURCE:
The corresponding author on the study was Amy Theos, MD, of the department of dermatology at the University of Alabama, Birmingham. The study was published online in Pediatric Dermatology.
LIMITATIONS:
The findings were limited by the small sample size and incomplete data for some patients.
DISCLOSURES:
The study received no outside funding. The researchers had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
TOPLINE:
.
METHODOLOGY:
- Researchers reviewed data on 330 children and youths aged 0-18 years who had received a primary psoriasis diagnosis and who were seen at an academic pediatric dermatology clinic from 2012 to 2022. Among these patients, 50 cases of palmoplantar psoriasis (PP) were identified by pediatric dermatologists.
- The study population was stratified by race/ethnicity on the basis of self-identification. The cohort included White, Black, and Hispanic/Latino patients, as well as patients who identified as other; 71.5% were White persons, 59.1% were female patients.
- The researchers used a regression analysis to investigate the association between race/ethnicity and PP after controlling for multiple confounding variables, including age and gender.
TAKEAWAY:
- Black children were significantly more likely to have PP than White children (adjusted odds ratio, 6.386; P < .0001). PP was diagnosed in 41.9%, 11.5%, and 8.9% of Black, Hispanic/Latino, and White children, respectively.
- Male gender was also identified as an independent risk factor for PP (aOR, 2.241).
- Nail involvement occurred in significantly more Black and Hispanic/Latino patients than in White patients (53.2%, 50.0%, and 33.9%, respectively).
- Black patients had significantly more palm and sole involvement, compared with the other groups (P < .0001 for both); however, White children had significantly more scalp involvement, compared with the other groups (P = .04).
IN PRACTICE:
“Further research is warranted to better understand the degree to which these associations are affected by racial disparities and environmental factors,” as well as potential genetic associations, the researchers noted.
SOURCE:
The corresponding author on the study was Amy Theos, MD, of the department of dermatology at the University of Alabama, Birmingham. The study was published online in Pediatric Dermatology.
LIMITATIONS:
The findings were limited by the small sample size and incomplete data for some patients.
DISCLOSURES:
The study received no outside funding. The researchers had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
The influence of social media on adolescents seeking autism diagnoses
A 16-year-old female presents for a self-identified concern around the possibility that she is experiencing an autism spectrum disorder. She relays to the developmental pediatrician that she has been learning a lot about autism on TikTok and through other social media sites, and has become strongly convinced that she meets medical criteria for this disorder.
A careful developmental history via a detailed interview with the mother reveals normal acquisition of early developmental milestones in addition to long-standing well-modulated eye contact felt to be paired fluidly with directed affect and gestures. The teen is described as having been an engaging toddler and preschooler, without restricted interests or repetitive behaviors, and having had no major challenges in grade school with behaviors, friendships, or academics.
During the pandemic, however, the teen became quite isolated. She developed anxiety with depression, and then started having some new repetitive arm movements within the last 12-18 months. In clinic, the teen makes robustly effortful arm-waving movements, which are noted to wane when she becomes more animated and excited during conversation, and to increase when she is less distracted by conversation and more focused on the movements.
She directs affect nicely toward her mother, while avoiding looking in the direction of the examiner until later in the evaluation when she becomes more relaxed. Prosody of speech and intonation are typical, and she describes having a close group of friends with whom she spends quite a bit of time.
The Autism Diagnostic Observation Schedule (ADOS-2 module 3) is used to gather structured observations, and these social presses yield flowing social engagement with the examiner, good understanding of humor, and overall excellent verbal and nonverbal communication skills. The teen describes hypervigilance around the emotions of others, a natural ease in understanding the perspectives of others, and a quick ability to read the energy of a room. She does have some interest in some more obscure online game forums, but her friends do as well, and she otherwise does not have a history of intrusive fixations. A social history reveals past significant verbal abuse in the home by means of her father during her first 11 years of life, which is described as quite traumatic.
After careful and thoughtful consideration (recognizing the known statistics around girls assigned female at birth, as well as nonbinary individuals and minoritized groups being underdiagnosed with autism), the history and observations are not felt to be consistent with autism, but with anxiety within the context of a trauma and stressor-related disorder. Even when accounting for the possibility of “masking,” the teen still does not meet criteria for autism based on history and presentation. The habit movements are not typical of usual stereotypies or of tics (which tend to increase with excitement and tend to have a more effortless quality), and are felt to possibly be functional in origin. Upon gently sharing these conclusions with the teen, she bursts into tears, stating her friends may now accuse her of lying, as she has already been claiming to have autism online and in person at school.
Countering social media diagnoses
This type of scenario is becoming increasingly common, with teens turning online primarily to social media accounts to gain knowledge around various neurologic and mental health conditions. Greater normalization of neurodiversity and greater access to high-quality information about neurodevelopmental differences is certainly progress, though unfortunately some online depictions of these conditions are simply not accurate. Many adolescents are keenly searching for both their personal identity and also a community through which they might feel wholly accepted, after experiencing some level of isolation during the pandemic followed by increased social discomfort in attempting to reintegrate into school life and society. Connecting the teen with a good-fit therapist and working to replace excessive screen time with exercise, outdoor activities, and in-person engagement with friends and family are also crucial interventions, though they can be incredibly difficult for families to achieve given various patient-specific and societal barriers. The overlap in symptomatology among anxiety, attention-deficit/hyperactivity disorder, and autism spectrum disorders is expansive, making it understandable that young people might misjudge their personal experience of life for a neurodevelopmental disorder for which they do not truly meet criteria. Increasing access to therapists well versed in trauma-informed care is a frequently referenced need, highlighted in this case.
Another case
In contrast to the case scenario above is that of a 19-year-old female presenting for a formal autism evaluation at the urging of her father, who has had concerns around her severe “shyness” throughout her life. He is concerned that she was not able to obtain a high school diploma despite appearing to have adequate cognitive skills, is currently quite isolated, and does not appear equipped to hold a job at this time. He describes her as having been a very quiet and self-directed young child who greatly benefited from the communication and social scaffolding provided by her slightly older and neurotypical sister. She has generally not had true friends, though she had no behavioral or academic difficulties in school other than seeming aloof and unusually quiet. Atypical social approaches have become more apparent over time, as relationship navigation has become more complex with age. She is noted to have frequent stereotyped hand-to-face movements throughout the evaluation, as well as a flat affect and unusual voice quality. She speaks slowly and softly, and while she does make eye contact, it is less well modulated than would be expected. She is very focused on her cat and online interests during conversation, and tends to give stilted answers to open-ended questions. During the interview portion of the ADOS, she demonstrates little insight into friendships and reports feeling very content on her own, though is open to the idea of relationships in the future and would like to learn how to achieve connections with others. Her father reports she tends to be generally quite blunt and has difficulty understanding humor and others’ perspectives. An autism diagnosis is made with the recommendation of application to Developmental Disability Services, given impaired adaptive skills, as a means of utilizing community-based supports to facilitate eventually obtaining a high school equivalency credential, a job, healthier living habits, and comfortable social outlets.
Discussion
It is crucial for providers to be aware of nuanced presentations of autism spectrum disorders that may have been missed in early childhood when social demands are less complicated, particularly in persons identified as female at birth, nonbinary individuals, and those belonging to minority groups. It is also important to address the widely acknowledged trend of adolescents turning to social media influencers for information around neurodevelopmental conditions, at a time in their lives when social anxiety and self-awareness are generally heightened. For an adolescent, a young social media influencer may feel like a more salient and reliable source of information than an adult with various letters after their name. A respectful relationship between a teen and a thoughtful primary care provider can help gain trust to foster open conversations around their concerns, which can further help determine if a referral to a psychologist or developmental pediatrician for a formal autism assessment is truly warranted, highlighting the need for increased diagnostic capacity for such. While it is certainly important for providers to keep an open mind and to have continued awareness around the concept of late autism diagnoses, it is wise to also be aware of this recent trend among adolescents as providers seek to guide youth toward appropriate therapies and services.
Dr. Roth is a developmental and behavioral pediatrician in Eugene, Ore. She has no conflicts of interest.
A 16-year-old female presents for a self-identified concern around the possibility that she is experiencing an autism spectrum disorder. She relays to the developmental pediatrician that she has been learning a lot about autism on TikTok and through other social media sites, and has become strongly convinced that she meets medical criteria for this disorder.
A careful developmental history via a detailed interview with the mother reveals normal acquisition of early developmental milestones in addition to long-standing well-modulated eye contact felt to be paired fluidly with directed affect and gestures. The teen is described as having been an engaging toddler and preschooler, without restricted interests or repetitive behaviors, and having had no major challenges in grade school with behaviors, friendships, or academics.
During the pandemic, however, the teen became quite isolated. She developed anxiety with depression, and then started having some new repetitive arm movements within the last 12-18 months. In clinic, the teen makes robustly effortful arm-waving movements, which are noted to wane when she becomes more animated and excited during conversation, and to increase when she is less distracted by conversation and more focused on the movements.
She directs affect nicely toward her mother, while avoiding looking in the direction of the examiner until later in the evaluation when she becomes more relaxed. Prosody of speech and intonation are typical, and she describes having a close group of friends with whom she spends quite a bit of time.
The Autism Diagnostic Observation Schedule (ADOS-2 module 3) is used to gather structured observations, and these social presses yield flowing social engagement with the examiner, good understanding of humor, and overall excellent verbal and nonverbal communication skills. The teen describes hypervigilance around the emotions of others, a natural ease in understanding the perspectives of others, and a quick ability to read the energy of a room. She does have some interest in some more obscure online game forums, but her friends do as well, and she otherwise does not have a history of intrusive fixations. A social history reveals past significant verbal abuse in the home by means of her father during her first 11 years of life, which is described as quite traumatic.
After careful and thoughtful consideration (recognizing the known statistics around girls assigned female at birth, as well as nonbinary individuals and minoritized groups being underdiagnosed with autism), the history and observations are not felt to be consistent with autism, but with anxiety within the context of a trauma and stressor-related disorder. Even when accounting for the possibility of “masking,” the teen still does not meet criteria for autism based on history and presentation. The habit movements are not typical of usual stereotypies or of tics (which tend to increase with excitement and tend to have a more effortless quality), and are felt to possibly be functional in origin. Upon gently sharing these conclusions with the teen, she bursts into tears, stating her friends may now accuse her of lying, as she has already been claiming to have autism online and in person at school.
Countering social media diagnoses
This type of scenario is becoming increasingly common, with teens turning online primarily to social media accounts to gain knowledge around various neurologic and mental health conditions. Greater normalization of neurodiversity and greater access to high-quality information about neurodevelopmental differences is certainly progress, though unfortunately some online depictions of these conditions are simply not accurate. Many adolescents are keenly searching for both their personal identity and also a community through which they might feel wholly accepted, after experiencing some level of isolation during the pandemic followed by increased social discomfort in attempting to reintegrate into school life and society. Connecting the teen with a good-fit therapist and working to replace excessive screen time with exercise, outdoor activities, and in-person engagement with friends and family are also crucial interventions, though they can be incredibly difficult for families to achieve given various patient-specific and societal barriers. The overlap in symptomatology among anxiety, attention-deficit/hyperactivity disorder, and autism spectrum disorders is expansive, making it understandable that young people might misjudge their personal experience of life for a neurodevelopmental disorder for which they do not truly meet criteria. Increasing access to therapists well versed in trauma-informed care is a frequently referenced need, highlighted in this case.
Another case
In contrast to the case scenario above is that of a 19-year-old female presenting for a formal autism evaluation at the urging of her father, who has had concerns around her severe “shyness” throughout her life. He is concerned that she was not able to obtain a high school diploma despite appearing to have adequate cognitive skills, is currently quite isolated, and does not appear equipped to hold a job at this time. He describes her as having been a very quiet and self-directed young child who greatly benefited from the communication and social scaffolding provided by her slightly older and neurotypical sister. She has generally not had true friends, though she had no behavioral or academic difficulties in school other than seeming aloof and unusually quiet. Atypical social approaches have become more apparent over time, as relationship navigation has become more complex with age. She is noted to have frequent stereotyped hand-to-face movements throughout the evaluation, as well as a flat affect and unusual voice quality. She speaks slowly and softly, and while she does make eye contact, it is less well modulated than would be expected. She is very focused on her cat and online interests during conversation, and tends to give stilted answers to open-ended questions. During the interview portion of the ADOS, she demonstrates little insight into friendships and reports feeling very content on her own, though is open to the idea of relationships in the future and would like to learn how to achieve connections with others. Her father reports she tends to be generally quite blunt and has difficulty understanding humor and others’ perspectives. An autism diagnosis is made with the recommendation of application to Developmental Disability Services, given impaired adaptive skills, as a means of utilizing community-based supports to facilitate eventually obtaining a high school equivalency credential, a job, healthier living habits, and comfortable social outlets.
Discussion
It is crucial for providers to be aware of nuanced presentations of autism spectrum disorders that may have been missed in early childhood when social demands are less complicated, particularly in persons identified as female at birth, nonbinary individuals, and those belonging to minority groups. It is also important to address the widely acknowledged trend of adolescents turning to social media influencers for information around neurodevelopmental conditions, at a time in their lives when social anxiety and self-awareness are generally heightened. For an adolescent, a young social media influencer may feel like a more salient and reliable source of information than an adult with various letters after their name. A respectful relationship between a teen and a thoughtful primary care provider can help gain trust to foster open conversations around their concerns, which can further help determine if a referral to a psychologist or developmental pediatrician for a formal autism assessment is truly warranted, highlighting the need for increased diagnostic capacity for such. While it is certainly important for providers to keep an open mind and to have continued awareness around the concept of late autism diagnoses, it is wise to also be aware of this recent trend among adolescents as providers seek to guide youth toward appropriate therapies and services.
Dr. Roth is a developmental and behavioral pediatrician in Eugene, Ore. She has no conflicts of interest.
A 16-year-old female presents for a self-identified concern around the possibility that she is experiencing an autism spectrum disorder. She relays to the developmental pediatrician that she has been learning a lot about autism on TikTok and through other social media sites, and has become strongly convinced that she meets medical criteria for this disorder.
A careful developmental history via a detailed interview with the mother reveals normal acquisition of early developmental milestones in addition to long-standing well-modulated eye contact felt to be paired fluidly with directed affect and gestures. The teen is described as having been an engaging toddler and preschooler, without restricted interests or repetitive behaviors, and having had no major challenges in grade school with behaviors, friendships, or academics.
During the pandemic, however, the teen became quite isolated. She developed anxiety with depression, and then started having some new repetitive arm movements within the last 12-18 months. In clinic, the teen makes robustly effortful arm-waving movements, which are noted to wane when she becomes more animated and excited during conversation, and to increase when she is less distracted by conversation and more focused on the movements.
She directs affect nicely toward her mother, while avoiding looking in the direction of the examiner until later in the evaluation when she becomes more relaxed. Prosody of speech and intonation are typical, and she describes having a close group of friends with whom she spends quite a bit of time.
The Autism Diagnostic Observation Schedule (ADOS-2 module 3) is used to gather structured observations, and these social presses yield flowing social engagement with the examiner, good understanding of humor, and overall excellent verbal and nonverbal communication skills. The teen describes hypervigilance around the emotions of others, a natural ease in understanding the perspectives of others, and a quick ability to read the energy of a room. She does have some interest in some more obscure online game forums, but her friends do as well, and she otherwise does not have a history of intrusive fixations. A social history reveals past significant verbal abuse in the home by means of her father during her first 11 years of life, which is described as quite traumatic.
After careful and thoughtful consideration (recognizing the known statistics around girls assigned female at birth, as well as nonbinary individuals and minoritized groups being underdiagnosed with autism), the history and observations are not felt to be consistent with autism, but with anxiety within the context of a trauma and stressor-related disorder. Even when accounting for the possibility of “masking,” the teen still does not meet criteria for autism based on history and presentation. The habit movements are not typical of usual stereotypies or of tics (which tend to increase with excitement and tend to have a more effortless quality), and are felt to possibly be functional in origin. Upon gently sharing these conclusions with the teen, she bursts into tears, stating her friends may now accuse her of lying, as she has already been claiming to have autism online and in person at school.
Countering social media diagnoses
This type of scenario is becoming increasingly common, with teens turning online primarily to social media accounts to gain knowledge around various neurologic and mental health conditions. Greater normalization of neurodiversity and greater access to high-quality information about neurodevelopmental differences is certainly progress, though unfortunately some online depictions of these conditions are simply not accurate. Many adolescents are keenly searching for both their personal identity and also a community through which they might feel wholly accepted, after experiencing some level of isolation during the pandemic followed by increased social discomfort in attempting to reintegrate into school life and society. Connecting the teen with a good-fit therapist and working to replace excessive screen time with exercise, outdoor activities, and in-person engagement with friends and family are also crucial interventions, though they can be incredibly difficult for families to achieve given various patient-specific and societal barriers. The overlap in symptomatology among anxiety, attention-deficit/hyperactivity disorder, and autism spectrum disorders is expansive, making it understandable that young people might misjudge their personal experience of life for a neurodevelopmental disorder for which they do not truly meet criteria. Increasing access to therapists well versed in trauma-informed care is a frequently referenced need, highlighted in this case.
Another case
In contrast to the case scenario above is that of a 19-year-old female presenting for a formal autism evaluation at the urging of her father, who has had concerns around her severe “shyness” throughout her life. He is concerned that she was not able to obtain a high school diploma despite appearing to have adequate cognitive skills, is currently quite isolated, and does not appear equipped to hold a job at this time. He describes her as having been a very quiet and self-directed young child who greatly benefited from the communication and social scaffolding provided by her slightly older and neurotypical sister. She has generally not had true friends, though she had no behavioral or academic difficulties in school other than seeming aloof and unusually quiet. Atypical social approaches have become more apparent over time, as relationship navigation has become more complex with age. She is noted to have frequent stereotyped hand-to-face movements throughout the evaluation, as well as a flat affect and unusual voice quality. She speaks slowly and softly, and while she does make eye contact, it is less well modulated than would be expected. She is very focused on her cat and online interests during conversation, and tends to give stilted answers to open-ended questions. During the interview portion of the ADOS, she demonstrates little insight into friendships and reports feeling very content on her own, though is open to the idea of relationships in the future and would like to learn how to achieve connections with others. Her father reports she tends to be generally quite blunt and has difficulty understanding humor and others’ perspectives. An autism diagnosis is made with the recommendation of application to Developmental Disability Services, given impaired adaptive skills, as a means of utilizing community-based supports to facilitate eventually obtaining a high school equivalency credential, a job, healthier living habits, and comfortable social outlets.
Discussion
It is crucial for providers to be aware of nuanced presentations of autism spectrum disorders that may have been missed in early childhood when social demands are less complicated, particularly in persons identified as female at birth, nonbinary individuals, and those belonging to minority groups. It is also important to address the widely acknowledged trend of adolescents turning to social media influencers for information around neurodevelopmental conditions, at a time in their lives when social anxiety and self-awareness are generally heightened. For an adolescent, a young social media influencer may feel like a more salient and reliable source of information than an adult with various letters after their name. A respectful relationship between a teen and a thoughtful primary care provider can help gain trust to foster open conversations around their concerns, which can further help determine if a referral to a psychologist or developmental pediatrician for a formal autism assessment is truly warranted, highlighting the need for increased diagnostic capacity for such. While it is certainly important for providers to keep an open mind and to have continued awareness around the concept of late autism diagnoses, it is wise to also be aware of this recent trend among adolescents as providers seek to guide youth toward appropriate therapies and services.
Dr. Roth is a developmental and behavioral pediatrician in Eugene, Ore. She has no conflicts of interest.
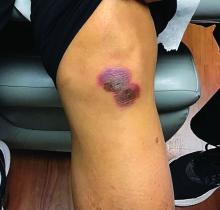
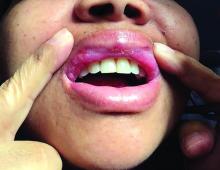
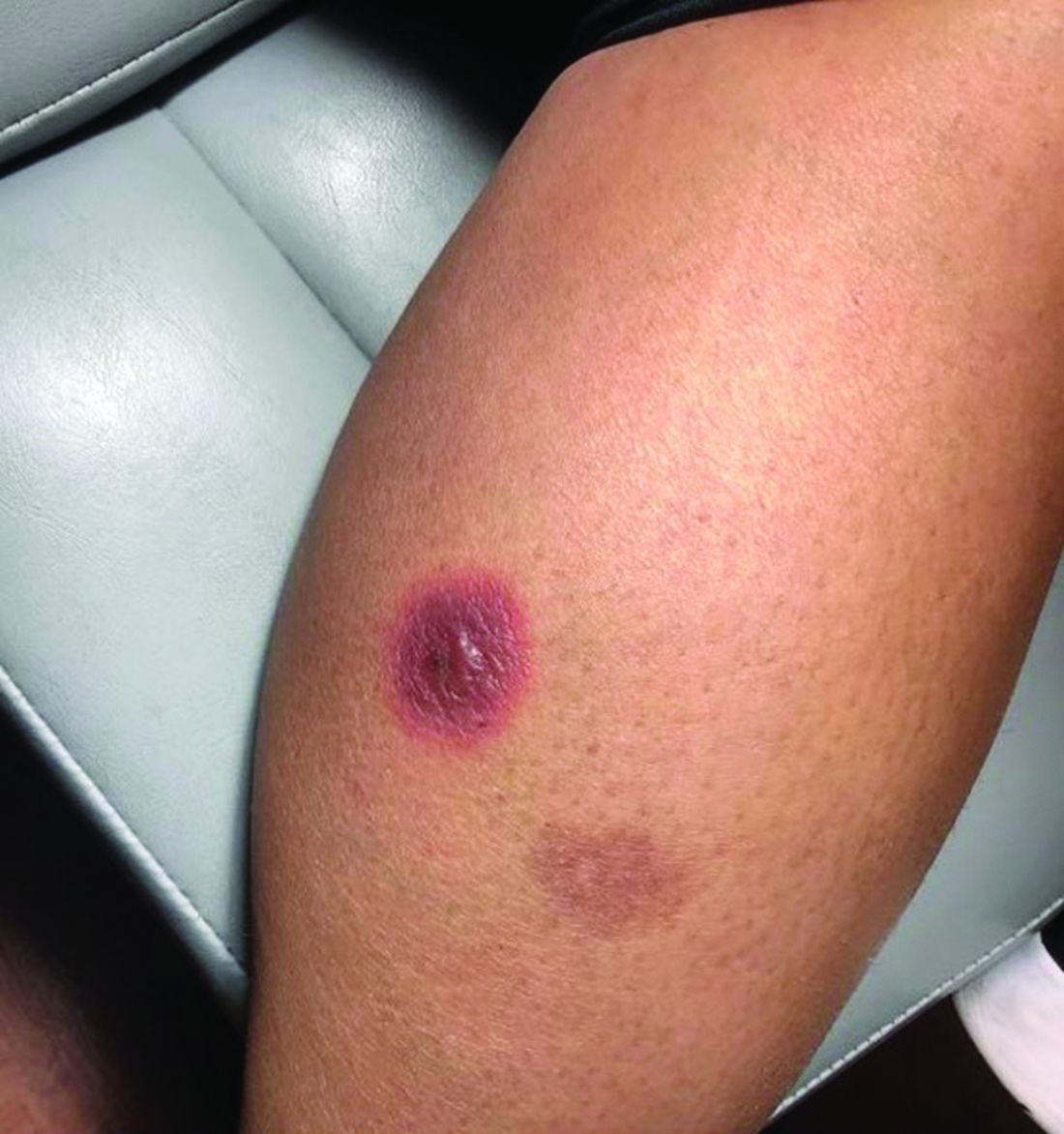
A 42-year-old woman presented with a few days of erosions on her buccal mucosa, tongue, and soft palate
in which lesions present in the same location upon repeated intake of the offending drug. The lesions typically present within 30 minutes to 8 hours of administration of the drug. These reactions can be considered allergic or pseudo-allergic, in which case, there is no notable adaptive immune response. CD8+ T cells appear to play a role in the epidermal injury via release of interferons and interactions with other inflammatory cells.
There are numerous drugs that can precipitate these findings. NSAIDs; antibiotics, such as tetracyclines, sulfonamides; and phenytoin are common offenders. In the case of our patient, naproxen was the offending medication.
The classic presentation of FDE features annular, erythematous to violaceous macules on the skin or mucosa that can be asymptomatic or can produce burning, pain, or pruritus. The most common locations include the trunk and extremities, but the palms, soles, face, scalp, and mucosa can also be impacted. The oral mucosa seems to be the most common mucosal location. Intravenous administration of a drug is associated with more severe symptoms. Systemic symptoms are typically absent, and the eruption may initially be in one location, but may appear elsewhere upon repeated exposure to the offending medication.
The differential diagnosis includes arthropod bite reactions, urticaria, and erythema multiforme. Although FDEs are typically a clinical diagnosis, the histopathology will commonly show a vacuolar interface dermatitis. Furthermore, a variety of immune cells can be found, including neutrophilic, eosinophilic, and lymphocytic infiltrate. A combination of two or more histological patterns often favors the diagnosis of FDE.
Steroid creams can be prescribed to decrease the inflammatory reaction and improve symptoms; however, the definitive treatment of this condition is cessation of the offending agent. Postinflammatory hyperpigmentation is a common symptom after resolution of the condition, and it may take months to fade away. Further darkening can be prevented by practicing sun safety measures such as wearing sunblock, covering the affected areas, and avoiding prolonged sun exposure.
This case and the photos were submitted by Lucas Shapiro, BS, of Nova Southeastern University College of Osteopathic Medicine, Fort Lauderdale, Fla., and Igor Chaplik, DO, Aesthetix Dermatology, Fort Lauderdale. The column was edited by Donna Bilu Martin, MD.
Dr. Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Fla. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Shaker G et al. Cureus. 2022 Aug 23;14(8):e28299.
Srivastava R et al. Indian J Dent. 2015 Apr-Jun;6(2):103-6.
Weyers W, Metze D. Dermatol Pract Concept. 2011 Jan 31;1(1):33-47.
in which lesions present in the same location upon repeated intake of the offending drug. The lesions typically present within 30 minutes to 8 hours of administration of the drug. These reactions can be considered allergic or pseudo-allergic, in which case, there is no notable adaptive immune response. CD8+ T cells appear to play a role in the epidermal injury via release of interferons and interactions with other inflammatory cells.
There are numerous drugs that can precipitate these findings. NSAIDs; antibiotics, such as tetracyclines, sulfonamides; and phenytoin are common offenders. In the case of our patient, naproxen was the offending medication.
The classic presentation of FDE features annular, erythematous to violaceous macules on the skin or mucosa that can be asymptomatic or can produce burning, pain, or pruritus. The most common locations include the trunk and extremities, but the palms, soles, face, scalp, and mucosa can also be impacted. The oral mucosa seems to be the most common mucosal location. Intravenous administration of a drug is associated with more severe symptoms. Systemic symptoms are typically absent, and the eruption may initially be in one location, but may appear elsewhere upon repeated exposure to the offending medication.
The differential diagnosis includes arthropod bite reactions, urticaria, and erythema multiforme. Although FDEs are typically a clinical diagnosis, the histopathology will commonly show a vacuolar interface dermatitis. Furthermore, a variety of immune cells can be found, including neutrophilic, eosinophilic, and lymphocytic infiltrate. A combination of two or more histological patterns often favors the diagnosis of FDE.
Steroid creams can be prescribed to decrease the inflammatory reaction and improve symptoms; however, the definitive treatment of this condition is cessation of the offending agent. Postinflammatory hyperpigmentation is a common symptom after resolution of the condition, and it may take months to fade away. Further darkening can be prevented by practicing sun safety measures such as wearing sunblock, covering the affected areas, and avoiding prolonged sun exposure.
This case and the photos were submitted by Lucas Shapiro, BS, of Nova Southeastern University College of Osteopathic Medicine, Fort Lauderdale, Fla., and Igor Chaplik, DO, Aesthetix Dermatology, Fort Lauderdale. The column was edited by Donna Bilu Martin, MD.
Dr. Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Fla. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Shaker G et al. Cureus. 2022 Aug 23;14(8):e28299.
Srivastava R et al. Indian J Dent. 2015 Apr-Jun;6(2):103-6.
Weyers W, Metze D. Dermatol Pract Concept. 2011 Jan 31;1(1):33-47.
in which lesions present in the same location upon repeated intake of the offending drug. The lesions typically present within 30 minutes to 8 hours of administration of the drug. These reactions can be considered allergic or pseudo-allergic, in which case, there is no notable adaptive immune response. CD8+ T cells appear to play a role in the epidermal injury via release of interferons and interactions with other inflammatory cells.
There are numerous drugs that can precipitate these findings. NSAIDs; antibiotics, such as tetracyclines, sulfonamides; and phenytoin are common offenders. In the case of our patient, naproxen was the offending medication.
The classic presentation of FDE features annular, erythematous to violaceous macules on the skin or mucosa that can be asymptomatic or can produce burning, pain, or pruritus. The most common locations include the trunk and extremities, but the palms, soles, face, scalp, and mucosa can also be impacted. The oral mucosa seems to be the most common mucosal location. Intravenous administration of a drug is associated with more severe symptoms. Systemic symptoms are typically absent, and the eruption may initially be in one location, but may appear elsewhere upon repeated exposure to the offending medication.
The differential diagnosis includes arthropod bite reactions, urticaria, and erythema multiforme. Although FDEs are typically a clinical diagnosis, the histopathology will commonly show a vacuolar interface dermatitis. Furthermore, a variety of immune cells can be found, including neutrophilic, eosinophilic, and lymphocytic infiltrate. A combination of two or more histological patterns often favors the diagnosis of FDE.
Steroid creams can be prescribed to decrease the inflammatory reaction and improve symptoms; however, the definitive treatment of this condition is cessation of the offending agent. Postinflammatory hyperpigmentation is a common symptom after resolution of the condition, and it may take months to fade away. Further darkening can be prevented by practicing sun safety measures such as wearing sunblock, covering the affected areas, and avoiding prolonged sun exposure.
This case and the photos were submitted by Lucas Shapiro, BS, of Nova Southeastern University College of Osteopathic Medicine, Fort Lauderdale, Fla., and Igor Chaplik, DO, Aesthetix Dermatology, Fort Lauderdale. The column was edited by Donna Bilu Martin, MD.
Dr. Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Fla. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to [email protected].
References
Shaker G et al. Cureus. 2022 Aug 23;14(8):e28299.
Srivastava R et al. Indian J Dent. 2015 Apr-Jun;6(2):103-6.
Weyers W, Metze D. Dermatol Pract Concept. 2011 Jan 31;1(1):33-47.
Alert! A decade of type 2 diabetes shortens life by 3.5 years
researchers estimate on the basis of data from studies conducted in 19 high-income countries.
They estimated that, among 50-year-olds, life expectancy of those diagnosed with type 2 diabetes at age 30 is 14 years shorter than that of their peers without diabetes. Among those diagnosed at age 50, life expectancy is 6 years shorter.
The study was recently published in The Lancet – Diabetes and Endocrinology.
The team analyzed data from the Emerging Risk Factors Collaboration and the UK Biobank. The data were from 97 long-term, prospective cohorts and involved 1.5 million participants who were followed for 23.1 million person-years.
“The strongest associations with earlier age at diagnosis of diabetes were for vascular (for example, myocardial infarction and stroke) and other causes of death – mainly respiratory, neurological, and infectious diseases and external causes,” they reported.
Their findings are consistent with previous studies that suggested that younger individuals who develop type 2 diabetes might have higher body mass index (BMI), blood pressure, and lipid levels and that they might experience faster deterioration in glycemic control than individuals who develop diabetes later, potentially leading to premature mortality.
Asked to comment, Anne Peters, MD, director of clinical diabetes programs at the University of Southern California, Los Angeles, who was not involved with this study, said: “We’ve long known that diabetes reduces life expectancy, and the younger you get it the more years you lose. However, this study was from a broader and larger population base than prior studies.
“In this study, the major reason for death was vascular disease, and undertreatment of cardiovascular risk factors may have occurred in the younger individuals. We also don’t know about glucose control.
“I personally think the findings show that we should treat cardiovascular risk factors more aggressively in people diagnosed with [type 2] diabetes in their 30s and 40s,” urged Dr. Peters.
High priority should be given to prevention globally
“Type 2 diabetes used to be seen as a disease that affected older adults, but we’re increasingly seeing people diagnosed earlier in life,” senior author Emanuele Di Angelantonio, MD, PhD, from the University of Cambridge (England), explained in a press release. “As we’ve shown, this means they are at risk of a much shorter life expectancy than they would otherwise have.”
The findings suggest that “high priority should be given to developing and implementing interventions that prevent or delay the onset of [type 2 diabetes], especially as its prevalence among younger age groups is increasing globally,” the study authors wrote.
The results “support the idea that the younger an individual is when they develop type 2 diabetes, the more damage their body accumulates from its impaired metabolism,” added co–senior author Naveed Sattar, MD, PhD, of the University of Glasgow,
Dr. Peters agreed: “People who develop type 2 diabetes at a younger age might have a different, potentially more aggressive type of type 2 diabetes and perhaps need treatment targets that are lower than people who develop type 2 diabetes when they are older.”
“The findings ... suggest that early detection of diabetes by screening followed by intensive glucose management could help prevent long-term complications from the condition,” Dr. Sattar said.
Dr. Peters added: “An issue for some is pregnancy. ... Many of the medications taken for management of CVD [cardiovascular disease] risk factors are contraindicated in pregnancy (as are many of the medications [for treating type 2 diabetes]).
“We need to be careful to risk reduce but take care of the ‘whole person,’ and if of childbearing age, consider the safest approaches to healthy management,” she emphasized.
Study results: Type 2 diabetes diagnosed at age 30, 40, and 50
Previous studies estimated that adults with type 2 diabetes die 6 years earlier on average in comparison with their counterparts who do not have diabetes, but it was not known how diabetes duration affects life span.
To investigate this, the team analyzed individual records from the Emerging Risk Factors Collaboration and the UK Biobank. The primary outcome was all-cause mortality. Other outcomes were deaths from CVD, cancer, and other causes.
Over a median follow-up of 12.5 years, there were 246,670 deaths: 84,443 from cardiovascular causes, 150, 972 from noncardiovascular causes, and 11,255 from unknown/ill-defined causes.
Compared with participants who did not have a history of type 2 diabetes, the hazard ratios for all-cause mortality, adjusted for age and sex, were 2.69 for participants diagnosed at age 30-39, 2.26 for those diagnosed aged 40-49, 1.84 aged 50-59, 1.57 for those aged 60-69, and 1.39 for those diagnosed 70 and older.
These hazard ratios were similar after adjusting for BMI, systolic blood pressure, and total cholesterol, but they were substantially attenuated after further adjusting for fasting glucose or hemoglobin A1c level.
Similar patterns were observed for cause-specific mortality.
“Every decade of earlier diagnosis of diabetes was associated with about 3-4 years of lower life expectancy, highlighting the need to develop and implement interventions that prevent or delay the onset of diabetes and to intensify the treatment of risk factors among young adults diagnosed with diabetes,” the researchers wrote.
The study was funded the British Heart Foundation, the Medical Research Council, the National Institute for Health and Care Research, and Health Data Research UK. Dr. Peters is on advisory boards for Vertex, Eli Lilly, and Medscape, receives research funding from Abbott Diabetes Care and Insulet, and has stock options for Omada Health.
A version of this article first appeared on Medscape.com.
researchers estimate on the basis of data from studies conducted in 19 high-income countries.
They estimated that, among 50-year-olds, life expectancy of those diagnosed with type 2 diabetes at age 30 is 14 years shorter than that of their peers without diabetes. Among those diagnosed at age 50, life expectancy is 6 years shorter.
The study was recently published in The Lancet – Diabetes and Endocrinology.
The team analyzed data from the Emerging Risk Factors Collaboration and the UK Biobank. The data were from 97 long-term, prospective cohorts and involved 1.5 million participants who were followed for 23.1 million person-years.
“The strongest associations with earlier age at diagnosis of diabetes were for vascular (for example, myocardial infarction and stroke) and other causes of death – mainly respiratory, neurological, and infectious diseases and external causes,” they reported.
Their findings are consistent with previous studies that suggested that younger individuals who develop type 2 diabetes might have higher body mass index (BMI), blood pressure, and lipid levels and that they might experience faster deterioration in glycemic control than individuals who develop diabetes later, potentially leading to premature mortality.
Asked to comment, Anne Peters, MD, director of clinical diabetes programs at the University of Southern California, Los Angeles, who was not involved with this study, said: “We’ve long known that diabetes reduces life expectancy, and the younger you get it the more years you lose. However, this study was from a broader and larger population base than prior studies.
“In this study, the major reason for death was vascular disease, and undertreatment of cardiovascular risk factors may have occurred in the younger individuals. We also don’t know about glucose control.
“I personally think the findings show that we should treat cardiovascular risk factors more aggressively in people diagnosed with [type 2] diabetes in their 30s and 40s,” urged Dr. Peters.
High priority should be given to prevention globally
“Type 2 diabetes used to be seen as a disease that affected older adults, but we’re increasingly seeing people diagnosed earlier in life,” senior author Emanuele Di Angelantonio, MD, PhD, from the University of Cambridge (England), explained in a press release. “As we’ve shown, this means they are at risk of a much shorter life expectancy than they would otherwise have.”
The findings suggest that “high priority should be given to developing and implementing interventions that prevent or delay the onset of [type 2 diabetes], especially as its prevalence among younger age groups is increasing globally,” the study authors wrote.
The results “support the idea that the younger an individual is when they develop type 2 diabetes, the more damage their body accumulates from its impaired metabolism,” added co–senior author Naveed Sattar, MD, PhD, of the University of Glasgow,
Dr. Peters agreed: “People who develop type 2 diabetes at a younger age might have a different, potentially more aggressive type of type 2 diabetes and perhaps need treatment targets that are lower than people who develop type 2 diabetes when they are older.”
“The findings ... suggest that early detection of diabetes by screening followed by intensive glucose management could help prevent long-term complications from the condition,” Dr. Sattar said.
Dr. Peters added: “An issue for some is pregnancy. ... Many of the medications taken for management of CVD [cardiovascular disease] risk factors are contraindicated in pregnancy (as are many of the medications [for treating type 2 diabetes]).
“We need to be careful to risk reduce but take care of the ‘whole person,’ and if of childbearing age, consider the safest approaches to healthy management,” she emphasized.
Study results: Type 2 diabetes diagnosed at age 30, 40, and 50
Previous studies estimated that adults with type 2 diabetes die 6 years earlier on average in comparison with their counterparts who do not have diabetes, but it was not known how diabetes duration affects life span.
To investigate this, the team analyzed individual records from the Emerging Risk Factors Collaboration and the UK Biobank. The primary outcome was all-cause mortality. Other outcomes were deaths from CVD, cancer, and other causes.
Over a median follow-up of 12.5 years, there were 246,670 deaths: 84,443 from cardiovascular causes, 150, 972 from noncardiovascular causes, and 11,255 from unknown/ill-defined causes.
Compared with participants who did not have a history of type 2 diabetes, the hazard ratios for all-cause mortality, adjusted for age and sex, were 2.69 for participants diagnosed at age 30-39, 2.26 for those diagnosed aged 40-49, 1.84 aged 50-59, 1.57 for those aged 60-69, and 1.39 for those diagnosed 70 and older.
These hazard ratios were similar after adjusting for BMI, systolic blood pressure, and total cholesterol, but they were substantially attenuated after further adjusting for fasting glucose or hemoglobin A1c level.
Similar patterns were observed for cause-specific mortality.
“Every decade of earlier diagnosis of diabetes was associated with about 3-4 years of lower life expectancy, highlighting the need to develop and implement interventions that prevent or delay the onset of diabetes and to intensify the treatment of risk factors among young adults diagnosed with diabetes,” the researchers wrote.
The study was funded the British Heart Foundation, the Medical Research Council, the National Institute for Health and Care Research, and Health Data Research UK. Dr. Peters is on advisory boards for Vertex, Eli Lilly, and Medscape, receives research funding from Abbott Diabetes Care and Insulet, and has stock options for Omada Health.
A version of this article first appeared on Medscape.com.
researchers estimate on the basis of data from studies conducted in 19 high-income countries.
They estimated that, among 50-year-olds, life expectancy of those diagnosed with type 2 diabetes at age 30 is 14 years shorter than that of their peers without diabetes. Among those diagnosed at age 50, life expectancy is 6 years shorter.
The study was recently published in The Lancet – Diabetes and Endocrinology.
The team analyzed data from the Emerging Risk Factors Collaboration and the UK Biobank. The data were from 97 long-term, prospective cohorts and involved 1.5 million participants who were followed for 23.1 million person-years.
“The strongest associations with earlier age at diagnosis of diabetes were for vascular (for example, myocardial infarction and stroke) and other causes of death – mainly respiratory, neurological, and infectious diseases and external causes,” they reported.
Their findings are consistent with previous studies that suggested that younger individuals who develop type 2 diabetes might have higher body mass index (BMI), blood pressure, and lipid levels and that they might experience faster deterioration in glycemic control than individuals who develop diabetes later, potentially leading to premature mortality.
Asked to comment, Anne Peters, MD, director of clinical diabetes programs at the University of Southern California, Los Angeles, who was not involved with this study, said: “We’ve long known that diabetes reduces life expectancy, and the younger you get it the more years you lose. However, this study was from a broader and larger population base than prior studies.
“In this study, the major reason for death was vascular disease, and undertreatment of cardiovascular risk factors may have occurred in the younger individuals. We also don’t know about glucose control.
“I personally think the findings show that we should treat cardiovascular risk factors more aggressively in people diagnosed with [type 2] diabetes in their 30s and 40s,” urged Dr. Peters.
High priority should be given to prevention globally
“Type 2 diabetes used to be seen as a disease that affected older adults, but we’re increasingly seeing people diagnosed earlier in life,” senior author Emanuele Di Angelantonio, MD, PhD, from the University of Cambridge (England), explained in a press release. “As we’ve shown, this means they are at risk of a much shorter life expectancy than they would otherwise have.”
The findings suggest that “high priority should be given to developing and implementing interventions that prevent or delay the onset of [type 2 diabetes], especially as its prevalence among younger age groups is increasing globally,” the study authors wrote.
The results “support the idea that the younger an individual is when they develop type 2 diabetes, the more damage their body accumulates from its impaired metabolism,” added co–senior author Naveed Sattar, MD, PhD, of the University of Glasgow,
Dr. Peters agreed: “People who develop type 2 diabetes at a younger age might have a different, potentially more aggressive type of type 2 diabetes and perhaps need treatment targets that are lower than people who develop type 2 diabetes when they are older.”
“The findings ... suggest that early detection of diabetes by screening followed by intensive glucose management could help prevent long-term complications from the condition,” Dr. Sattar said.
Dr. Peters added: “An issue for some is pregnancy. ... Many of the medications taken for management of CVD [cardiovascular disease] risk factors are contraindicated in pregnancy (as are many of the medications [for treating type 2 diabetes]).
“We need to be careful to risk reduce but take care of the ‘whole person,’ and if of childbearing age, consider the safest approaches to healthy management,” she emphasized.
Study results: Type 2 diabetes diagnosed at age 30, 40, and 50
Previous studies estimated that adults with type 2 diabetes die 6 years earlier on average in comparison with their counterparts who do not have diabetes, but it was not known how diabetes duration affects life span.
To investigate this, the team analyzed individual records from the Emerging Risk Factors Collaboration and the UK Biobank. The primary outcome was all-cause mortality. Other outcomes were deaths from CVD, cancer, and other causes.
Over a median follow-up of 12.5 years, there were 246,670 deaths: 84,443 from cardiovascular causes, 150, 972 from noncardiovascular causes, and 11,255 from unknown/ill-defined causes.
Compared with participants who did not have a history of type 2 diabetes, the hazard ratios for all-cause mortality, adjusted for age and sex, were 2.69 for participants diagnosed at age 30-39, 2.26 for those diagnosed aged 40-49, 1.84 aged 50-59, 1.57 for those aged 60-69, and 1.39 for those diagnosed 70 and older.
These hazard ratios were similar after adjusting for BMI, systolic blood pressure, and total cholesterol, but they were substantially attenuated after further adjusting for fasting glucose or hemoglobin A1c level.
Similar patterns were observed for cause-specific mortality.
“Every decade of earlier diagnosis of diabetes was associated with about 3-4 years of lower life expectancy, highlighting the need to develop and implement interventions that prevent or delay the onset of diabetes and to intensify the treatment of risk factors among young adults diagnosed with diabetes,” the researchers wrote.
The study was funded the British Heart Foundation, the Medical Research Council, the National Institute for Health and Care Research, and Health Data Research UK. Dr. Peters is on advisory boards for Vertex, Eli Lilly, and Medscape, receives research funding from Abbott Diabetes Care and Insulet, and has stock options for Omada Health.
A version of this article first appeared on Medscape.com.
FROM THE LANCET – DIABETES AND ENDOCRINOLOGY
RVUs: A fair measure of your productivity?
This transcript has been edited for clarity.
The other day, I received a flowery, elaborate email from none other than a physician recruiter: “Beautiful parks, hiking, great schools, blah blah blah, worked RVU production bonus on top of base pay.”
That last part – RVUs. I’m lost. I hear mixed reviews from physicians who work in RVU-based systems. The entire thing seems overly complex and confusing, so let’s clear it up. I did my research, and I’m going to explain RVUs.
Types of RVUs
RVUs, or relative value units, are a standard set by Medicare, used to measure physician productivity and ultimately determine compensation. There are three types:
- Work RVUs (basically everything that happens during a patient encounter).
- Practice expense RVUs.
- Professional liability insurance RVUs.
Now, envision this equation. All three of those RVUs are each multiplied by a geographic practice cost index to come up with a total number, and then that is multiplied by the Medicare conversion factor, which right now is around $33 to $34, to come up with a total dollar amount.
Work RVUs make up the bulk of total RVUs and they get their value from CPT codes. That value is determined by CMS. The AMA’s Relative Value Scale Update Committee, or RUC, which is made up of 32 people from various medical and surgical subspecialties, regularly meets and makes recommendations on the value of various CPT codes.
Is specialty representation fair and balanced?
CMS historically has accepted a high percentage of RUC’s recommendations, so this is a very influential committee. This is also why RUC has led to some controversy, with some stating that there is a lack of primary care representation, and perhaps this is why CPT codes related to procedures tend to reimburse higher.
How does one weigh the value of an hour-long palliative conversation against the quick removal of a benign skin lesion? That’s a loaded question.
This is especially important if your salary, or at least part of it, is determined by total RVUs. You want to have a sense of the pros and cons of working in an RVU system and how this relates to your specialty, your practice, and your schedule.
An RVU-based system provides an objective measure on complex patient encounters, volume, and procedures, and it’s a somewhat unified measure. The cons are pretty clear because these models favor you seeing many patients and billing a lot, and often this favors employers over physicians.
Dr. Patel is a clinical instructor, department of pediatrics, at Columbia University, New York, and a pediatric hospitalist at Morgan Stanley Children’s Hospital of New York–Presbyterian. He reported a conflict of interest with Medumo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
The other day, I received a flowery, elaborate email from none other than a physician recruiter: “Beautiful parks, hiking, great schools, blah blah blah, worked RVU production bonus on top of base pay.”
That last part – RVUs. I’m lost. I hear mixed reviews from physicians who work in RVU-based systems. The entire thing seems overly complex and confusing, so let’s clear it up. I did my research, and I’m going to explain RVUs.
Types of RVUs
RVUs, or relative value units, are a standard set by Medicare, used to measure physician productivity and ultimately determine compensation. There are three types:
- Work RVUs (basically everything that happens during a patient encounter).
- Practice expense RVUs.
- Professional liability insurance RVUs.
Now, envision this equation. All three of those RVUs are each multiplied by a geographic practice cost index to come up with a total number, and then that is multiplied by the Medicare conversion factor, which right now is around $33 to $34, to come up with a total dollar amount.
Work RVUs make up the bulk of total RVUs and they get their value from CPT codes. That value is determined by CMS. The AMA’s Relative Value Scale Update Committee, or RUC, which is made up of 32 people from various medical and surgical subspecialties, regularly meets and makes recommendations on the value of various CPT codes.
Is specialty representation fair and balanced?
CMS historically has accepted a high percentage of RUC’s recommendations, so this is a very influential committee. This is also why RUC has led to some controversy, with some stating that there is a lack of primary care representation, and perhaps this is why CPT codes related to procedures tend to reimburse higher.
How does one weigh the value of an hour-long palliative conversation against the quick removal of a benign skin lesion? That’s a loaded question.
This is especially important if your salary, or at least part of it, is determined by total RVUs. You want to have a sense of the pros and cons of working in an RVU system and how this relates to your specialty, your practice, and your schedule.
An RVU-based system provides an objective measure on complex patient encounters, volume, and procedures, and it’s a somewhat unified measure. The cons are pretty clear because these models favor you seeing many patients and billing a lot, and often this favors employers over physicians.
Dr. Patel is a clinical instructor, department of pediatrics, at Columbia University, New York, and a pediatric hospitalist at Morgan Stanley Children’s Hospital of New York–Presbyterian. He reported a conflict of interest with Medumo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
The other day, I received a flowery, elaborate email from none other than a physician recruiter: “Beautiful parks, hiking, great schools, blah blah blah, worked RVU production bonus on top of base pay.”
That last part – RVUs. I’m lost. I hear mixed reviews from physicians who work in RVU-based systems. The entire thing seems overly complex and confusing, so let’s clear it up. I did my research, and I’m going to explain RVUs.
Types of RVUs
RVUs, or relative value units, are a standard set by Medicare, used to measure physician productivity and ultimately determine compensation. There are three types:
- Work RVUs (basically everything that happens during a patient encounter).
- Practice expense RVUs.
- Professional liability insurance RVUs.
Now, envision this equation. All three of those RVUs are each multiplied by a geographic practice cost index to come up with a total number, and then that is multiplied by the Medicare conversion factor, which right now is around $33 to $34, to come up with a total dollar amount.
Work RVUs make up the bulk of total RVUs and they get their value from CPT codes. That value is determined by CMS. The AMA’s Relative Value Scale Update Committee, or RUC, which is made up of 32 people from various medical and surgical subspecialties, regularly meets and makes recommendations on the value of various CPT codes.
Is specialty representation fair and balanced?
CMS historically has accepted a high percentage of RUC’s recommendations, so this is a very influential committee. This is also why RUC has led to some controversy, with some stating that there is a lack of primary care representation, and perhaps this is why CPT codes related to procedures tend to reimburse higher.
How does one weigh the value of an hour-long palliative conversation against the quick removal of a benign skin lesion? That’s a loaded question.
This is especially important if your salary, or at least part of it, is determined by total RVUs. You want to have a sense of the pros and cons of working in an RVU system and how this relates to your specialty, your practice, and your schedule.
An RVU-based system provides an objective measure on complex patient encounters, volume, and procedures, and it’s a somewhat unified measure. The cons are pretty clear because these models favor you seeing many patients and billing a lot, and often this favors employers over physicians.
Dr. Patel is a clinical instructor, department of pediatrics, at Columbia University, New York, and a pediatric hospitalist at Morgan Stanley Children’s Hospital of New York–Presbyterian. He reported a conflict of interest with Medumo.
A version of this article first appeared on Medscape.com.
Confirmed: Intermittent use of benzodiazepines is the safest option
BARCELONA – results of a large-scale study show.
Investigators matched more than 57,000 chronic benzodiazepine users with nearly 114,000 intermittent users and found that, at 1 year, chronic users had an 8% increased risk for emergency department visits and/or hospitalizations for falls.
Chronic users also had a 25% increased risk for hip fracture, a 4% raised risk for ED visits and/or hospitalizations for any reason, and a 23% increased risk for death.
Study investigator Simon J.C. Davies, MD, PhD, MSc, Centre for Addiction & Mental Health, Toronto, said that the research shows that, where possible, patients older than 65 years with anxiety or insomnia who are taking benzodiazepines should not stay on these medications continuously.
However, he acknowledged that, “in practical terms, there will be some who can’t change or do not want to change” their treatment.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology.
Wide range of adverse outcomes
The authors noted that benzodiazepines are used to treat anxiety and insomnia but are associated with a range of adverse outcomes, including falls, fractures, cognitive impairment, and mortality as well as tolerance and dose escalation.
“These risks are especially relevant in older adults,” they added, noting that some guidelines recommend avoiding the drugs in this population, whereas other suggest short-term benzodiazepine use for a maximum of 4 weeks.
Despite this, “benzodiazepines are widely prescribed in older adults.” One study showed that almost 15% of adults aged 65 years or older received at least one benzodiazepine prescription.
Moreover, chronic use is more common in older versus younger patients.
Benzodiazepine use among older adults “used to be higher,” Dr. Davies said in an interview, at around 20%, but the “numbers have come down,” partly because of the introduction of benzodiazepine-like sleep medications but also because of educational efforts.
“There are certainly campaigns in Ontario to educate physicians,” Dr. Davies said, “but I think more broadly people are aware of the activity of these drugs, and the tolerance and other issues.”
To compare the risk associated with chronic versus intermittent use of benzodiazepines in older adults, the team performed a population-based cohort study using linked health care databases in Ontario.
They focused on adults aged 65 years or older with a first benzodiazepine prescription after at least 1 year without taking the drugs.
Chronic benzodiazepine use was defined as 120 days of prescriptions over the first 180 days after the index prescription. Patients who met these criteria were matched with intermittent users in a 2:1 ratio by age and sex.
Patients were then propensity matched using 24 variables, including health system use in the year prior to the index prescription, clinical diagnoses, prior psychiatric health system use, falls, and income level.
The team identified 57,072 chronic benzodiazepine users and 312,468 intermittent users, of whom, 57,041 and 113,839, respectively, were propensity matched.
As expected, chronic users were prescribed benzodiazepines for more days than were the intermittent users over both the initial 180-day exposure period, at 141 days versus 33 days, and again during a further 180-day follow-up period, at 181 days versus 19 days.
Over the follow-up period, the daily lorazepam dose-equivalents of chronic users four times that of intermittent users.
Hospitalizations and/or ED visits for falls were higher among patients in the chronic benzodiazepine group, at 4.6% versus 3.2% in those who took the drugs intermittently.
After adjusting for benzodiazepine dose, the team found that chronic benzodiazepine use was associated with a significant increase in the risk for falls leading to hospital presentation over the 360-day study period, compared with intermittent use (hazard ratio, 1.08; P = .0124).
Sex differences
In addition, chronic use was linked to a significantly increased risk for hip fracture (HR, 1.25; P = .0095), and long-term care admission (HR, 1.32; P < .0001).
There was also a significant increase in ED visits and/or hospitalizations for any reason with chronic benzodiazepine use versus intermittent use (HR, 1.04; P = .0007), and an increase in the risk for death (HR, 1.23; P < .0001).
A nonsignificant increased risk for wrist fracture was also associated with chronic use of benzodiazepines (HR, 1.02; P = .8683).
Further analysis revealed some sex differences. For instance, men had a marked increase in the risk for hip fracture with chronic use (HR, 1.50; P = .0154), whereas the risk was not significant in women (HR, 1.16; P = .1332). In addition, mortality risk associated with chronic use was higher in men than in women (HR, 1.39; P < .0001 vs. HR, 1.10; P = .2245).
The decision to discontinue chronic benzodiazepine use can be challenging, said Dr. Davies. “If you’re advising people to stop, what happens to the treatment of their anxiety?”
He said that there are many other treatment options for anxiety that don’t come with tolerance or risk for addiction.
“My position would be that intermittent use is perfectly acceptable while you bide your time to explore other treatments. They may be pharmacological; they may, of course, be lifestyle changes, psychotherapies, and so on,” said Dr. Davies.
If, however, patients feel that chronic benzodiazepine use is their only option, this research informs that decision by quantifying the risks.
“We’ve always known that there was a problem, but there haven’t been high-quality epidemiological studies like this that allowed us to say what the numbers are,” said Dr. Davies.
Confirmatory research
In a comment, Christoph U. Correll, MD, professor of psychiatry at Hofstra University, Hempstead, N.Y., noted that the risk associated with benzodiazepine use, especially in older people, has been demonstrated repeatedly.
“In that context, it is not surprising that less continuous exposure to an established risk factor attenuates the risk for these adverse outcomes,” he said.
Dr. Correll, who was not involved in the study pointed out there is nevertheless a “risk of residual confounding by indication.”
In other words, “people with intermittent benzodiazepine use may have less severe underlying illness and better healthy lifestyle behaviors than those requiring chronic benzodiazepine administration.”
Also commenting on the research, Christian Vinkers, MD, PhD, psychiatrist and professor of stress and resilience, Amsterdam University Medical Centre, said that it confirms “once again that long-term benzodiazepine use should not be encouraged.”
“The risk of falls, as well as cognitive side effects and impaired driving skills, with the risk of road accidents, make chronic overuse of benzodiazepines a public health issue. Of course, there is a small group of patients who should have access to long-term use, but it is reasonable to assume that this group is currently too large,” he added.
The study was funded through a grant from the University of Toronto Department of Psychiatry Excellence Funds. No relevant financial relationships were declared.
A version of this article first appeared on Medscape.com.
BARCELONA – results of a large-scale study show.
Investigators matched more than 57,000 chronic benzodiazepine users with nearly 114,000 intermittent users and found that, at 1 year, chronic users had an 8% increased risk for emergency department visits and/or hospitalizations for falls.
Chronic users also had a 25% increased risk for hip fracture, a 4% raised risk for ED visits and/or hospitalizations for any reason, and a 23% increased risk for death.
Study investigator Simon J.C. Davies, MD, PhD, MSc, Centre for Addiction & Mental Health, Toronto, said that the research shows that, where possible, patients older than 65 years with anxiety or insomnia who are taking benzodiazepines should not stay on these medications continuously.
However, he acknowledged that, “in practical terms, there will be some who can’t change or do not want to change” their treatment.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology.
Wide range of adverse outcomes
The authors noted that benzodiazepines are used to treat anxiety and insomnia but are associated with a range of adverse outcomes, including falls, fractures, cognitive impairment, and mortality as well as tolerance and dose escalation.
“These risks are especially relevant in older adults,” they added, noting that some guidelines recommend avoiding the drugs in this population, whereas other suggest short-term benzodiazepine use for a maximum of 4 weeks.
Despite this, “benzodiazepines are widely prescribed in older adults.” One study showed that almost 15% of adults aged 65 years or older received at least one benzodiazepine prescription.
Moreover, chronic use is more common in older versus younger patients.
Benzodiazepine use among older adults “used to be higher,” Dr. Davies said in an interview, at around 20%, but the “numbers have come down,” partly because of the introduction of benzodiazepine-like sleep medications but also because of educational efforts.
“There are certainly campaigns in Ontario to educate physicians,” Dr. Davies said, “but I think more broadly people are aware of the activity of these drugs, and the tolerance and other issues.”
To compare the risk associated with chronic versus intermittent use of benzodiazepines in older adults, the team performed a population-based cohort study using linked health care databases in Ontario.
They focused on adults aged 65 years or older with a first benzodiazepine prescription after at least 1 year without taking the drugs.
Chronic benzodiazepine use was defined as 120 days of prescriptions over the first 180 days after the index prescription. Patients who met these criteria were matched with intermittent users in a 2:1 ratio by age and sex.
Patients were then propensity matched using 24 variables, including health system use in the year prior to the index prescription, clinical diagnoses, prior psychiatric health system use, falls, and income level.
The team identified 57,072 chronic benzodiazepine users and 312,468 intermittent users, of whom, 57,041 and 113,839, respectively, were propensity matched.
As expected, chronic users were prescribed benzodiazepines for more days than were the intermittent users over both the initial 180-day exposure period, at 141 days versus 33 days, and again during a further 180-day follow-up period, at 181 days versus 19 days.
Over the follow-up period, the daily lorazepam dose-equivalents of chronic users four times that of intermittent users.
Hospitalizations and/or ED visits for falls were higher among patients in the chronic benzodiazepine group, at 4.6% versus 3.2% in those who took the drugs intermittently.
After adjusting for benzodiazepine dose, the team found that chronic benzodiazepine use was associated with a significant increase in the risk for falls leading to hospital presentation over the 360-day study period, compared with intermittent use (hazard ratio, 1.08; P = .0124).
Sex differences
In addition, chronic use was linked to a significantly increased risk for hip fracture (HR, 1.25; P = .0095), and long-term care admission (HR, 1.32; P < .0001).
There was also a significant increase in ED visits and/or hospitalizations for any reason with chronic benzodiazepine use versus intermittent use (HR, 1.04; P = .0007), and an increase in the risk for death (HR, 1.23; P < .0001).
A nonsignificant increased risk for wrist fracture was also associated with chronic use of benzodiazepines (HR, 1.02; P = .8683).
Further analysis revealed some sex differences. For instance, men had a marked increase in the risk for hip fracture with chronic use (HR, 1.50; P = .0154), whereas the risk was not significant in women (HR, 1.16; P = .1332). In addition, mortality risk associated with chronic use was higher in men than in women (HR, 1.39; P < .0001 vs. HR, 1.10; P = .2245).
The decision to discontinue chronic benzodiazepine use can be challenging, said Dr. Davies. “If you’re advising people to stop, what happens to the treatment of their anxiety?”
He said that there are many other treatment options for anxiety that don’t come with tolerance or risk for addiction.
“My position would be that intermittent use is perfectly acceptable while you bide your time to explore other treatments. They may be pharmacological; they may, of course, be lifestyle changes, psychotherapies, and so on,” said Dr. Davies.
If, however, patients feel that chronic benzodiazepine use is their only option, this research informs that decision by quantifying the risks.
“We’ve always known that there was a problem, but there haven’t been high-quality epidemiological studies like this that allowed us to say what the numbers are,” said Dr. Davies.
Confirmatory research
In a comment, Christoph U. Correll, MD, professor of psychiatry at Hofstra University, Hempstead, N.Y., noted that the risk associated with benzodiazepine use, especially in older people, has been demonstrated repeatedly.
“In that context, it is not surprising that less continuous exposure to an established risk factor attenuates the risk for these adverse outcomes,” he said.
Dr. Correll, who was not involved in the study pointed out there is nevertheless a “risk of residual confounding by indication.”
In other words, “people with intermittent benzodiazepine use may have less severe underlying illness and better healthy lifestyle behaviors than those requiring chronic benzodiazepine administration.”
Also commenting on the research, Christian Vinkers, MD, PhD, psychiatrist and professor of stress and resilience, Amsterdam University Medical Centre, said that it confirms “once again that long-term benzodiazepine use should not be encouraged.”
“The risk of falls, as well as cognitive side effects and impaired driving skills, with the risk of road accidents, make chronic overuse of benzodiazepines a public health issue. Of course, there is a small group of patients who should have access to long-term use, but it is reasonable to assume that this group is currently too large,” he added.
The study was funded through a grant from the University of Toronto Department of Psychiatry Excellence Funds. No relevant financial relationships were declared.
A version of this article first appeared on Medscape.com.
BARCELONA – results of a large-scale study show.
Investigators matched more than 57,000 chronic benzodiazepine users with nearly 114,000 intermittent users and found that, at 1 year, chronic users had an 8% increased risk for emergency department visits and/or hospitalizations for falls.
Chronic users also had a 25% increased risk for hip fracture, a 4% raised risk for ED visits and/or hospitalizations for any reason, and a 23% increased risk for death.
Study investigator Simon J.C. Davies, MD, PhD, MSc, Centre for Addiction & Mental Health, Toronto, said that the research shows that, where possible, patients older than 65 years with anxiety or insomnia who are taking benzodiazepines should not stay on these medications continuously.
However, he acknowledged that, “in practical terms, there will be some who can’t change or do not want to change” their treatment.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology.
Wide range of adverse outcomes
The authors noted that benzodiazepines are used to treat anxiety and insomnia but are associated with a range of adverse outcomes, including falls, fractures, cognitive impairment, and mortality as well as tolerance and dose escalation.
“These risks are especially relevant in older adults,” they added, noting that some guidelines recommend avoiding the drugs in this population, whereas other suggest short-term benzodiazepine use for a maximum of 4 weeks.
Despite this, “benzodiazepines are widely prescribed in older adults.” One study showed that almost 15% of adults aged 65 years or older received at least one benzodiazepine prescription.
Moreover, chronic use is more common in older versus younger patients.
Benzodiazepine use among older adults “used to be higher,” Dr. Davies said in an interview, at around 20%, but the “numbers have come down,” partly because of the introduction of benzodiazepine-like sleep medications but also because of educational efforts.
“There are certainly campaigns in Ontario to educate physicians,” Dr. Davies said, “but I think more broadly people are aware of the activity of these drugs, and the tolerance and other issues.”
To compare the risk associated with chronic versus intermittent use of benzodiazepines in older adults, the team performed a population-based cohort study using linked health care databases in Ontario.
They focused on adults aged 65 years or older with a first benzodiazepine prescription after at least 1 year without taking the drugs.
Chronic benzodiazepine use was defined as 120 days of prescriptions over the first 180 days after the index prescription. Patients who met these criteria were matched with intermittent users in a 2:1 ratio by age and sex.
Patients were then propensity matched using 24 variables, including health system use in the year prior to the index prescription, clinical diagnoses, prior psychiatric health system use, falls, and income level.
The team identified 57,072 chronic benzodiazepine users and 312,468 intermittent users, of whom, 57,041 and 113,839, respectively, were propensity matched.
As expected, chronic users were prescribed benzodiazepines for more days than were the intermittent users over both the initial 180-day exposure period, at 141 days versus 33 days, and again during a further 180-day follow-up period, at 181 days versus 19 days.
Over the follow-up period, the daily lorazepam dose-equivalents of chronic users four times that of intermittent users.
Hospitalizations and/or ED visits for falls were higher among patients in the chronic benzodiazepine group, at 4.6% versus 3.2% in those who took the drugs intermittently.
After adjusting for benzodiazepine dose, the team found that chronic benzodiazepine use was associated with a significant increase in the risk for falls leading to hospital presentation over the 360-day study period, compared with intermittent use (hazard ratio, 1.08; P = .0124).
Sex differences
In addition, chronic use was linked to a significantly increased risk for hip fracture (HR, 1.25; P = .0095), and long-term care admission (HR, 1.32; P < .0001).
There was also a significant increase in ED visits and/or hospitalizations for any reason with chronic benzodiazepine use versus intermittent use (HR, 1.04; P = .0007), and an increase in the risk for death (HR, 1.23; P < .0001).
A nonsignificant increased risk for wrist fracture was also associated with chronic use of benzodiazepines (HR, 1.02; P = .8683).
Further analysis revealed some sex differences. For instance, men had a marked increase in the risk for hip fracture with chronic use (HR, 1.50; P = .0154), whereas the risk was not significant in women (HR, 1.16; P = .1332). In addition, mortality risk associated with chronic use was higher in men than in women (HR, 1.39; P < .0001 vs. HR, 1.10; P = .2245).
The decision to discontinue chronic benzodiazepine use can be challenging, said Dr. Davies. “If you’re advising people to stop, what happens to the treatment of their anxiety?”
He said that there are many other treatment options for anxiety that don’t come with tolerance or risk for addiction.
“My position would be that intermittent use is perfectly acceptable while you bide your time to explore other treatments. They may be pharmacological; they may, of course, be lifestyle changes, psychotherapies, and so on,” said Dr. Davies.
If, however, patients feel that chronic benzodiazepine use is their only option, this research informs that decision by quantifying the risks.
“We’ve always known that there was a problem, but there haven’t been high-quality epidemiological studies like this that allowed us to say what the numbers are,” said Dr. Davies.
Confirmatory research
In a comment, Christoph U. Correll, MD, professor of psychiatry at Hofstra University, Hempstead, N.Y., noted that the risk associated with benzodiazepine use, especially in older people, has been demonstrated repeatedly.
“In that context, it is not surprising that less continuous exposure to an established risk factor attenuates the risk for these adverse outcomes,” he said.
Dr. Correll, who was not involved in the study pointed out there is nevertheless a “risk of residual confounding by indication.”
In other words, “people with intermittent benzodiazepine use may have less severe underlying illness and better healthy lifestyle behaviors than those requiring chronic benzodiazepine administration.”
Also commenting on the research, Christian Vinkers, MD, PhD, psychiatrist and professor of stress and resilience, Amsterdam University Medical Centre, said that it confirms “once again that long-term benzodiazepine use should not be encouraged.”
“The risk of falls, as well as cognitive side effects and impaired driving skills, with the risk of road accidents, make chronic overuse of benzodiazepines a public health issue. Of course, there is a small group of patients who should have access to long-term use, but it is reasonable to assume that this group is currently too large,” he added.
The study was funded through a grant from the University of Toronto Department of Psychiatry Excellence Funds. No relevant financial relationships were declared.
A version of this article first appeared on Medscape.com.
AT ECNP 2023
Esketamine bests quetiapine for severe depression in head-to-head trial
BARCELONA – (TRD), results of a large, multicenter, head-to-head phase 3 trial show.
Results from the ESCAPE-TRD study, which included 675 participants with TRD, show that esketamine was associated with significantly increased rates of both depression and functional remission, compared with quetiapine.
More than 675 patients were randomly assigned to receive one of the two drugs along with ongoing treatment with an SSRI or a serotonin-norepinephrine reuptake inhibitor (SNRI).
Esketamine increased remission rates at 2 and 8 months over quetiapine by 72% and raised functional remission rates at 8 months by 88% while decreasing adverse event rates.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology and were published online in the New England Journal of Medicine.
New hope
The results provide “some hope for our patients suffering from TRD, which, given the data, is somewhat of a misnomer,” said study investigator Andreas Reif, MD, professor of psychiatry, psychosomatic medicine, and psychotherapy, University Hospital Frankfurt–Goethe University, Frankfurt am Main, Germany, and president-elect of the ECNP.
“These patients are not resistant, they just have resistance to monoaminergic drugs,” he added. Esketamine, he said, is a “new weapon in our armamentarium.”
Dr. Reif said TRD is a serious condition that affects approximately 20%-30% of those with major depressive disorder and has “substantial impact” on patients’ lives, including quality of life and level of functioning.
“We know that esketamine nasal spray is effective in TRD. However, up to now, there were only placebo-controlled trials in addition to ongoing antidepressant treatment,” Dr. Reif noted. Consequently, he added, a head-to-head comparison with an active agent with proven efficacy was “urgently needed.”
For the trial, patients from 171 sites in 24 countries with TRD, defined as a less than 25% improvement in symptoms with two or more consecutive treatments of adequate dosage and duration, were randomly assigned to receive esketamine nasal spray (n = 336) or quetiapine (n = 340) extended release together with ongoing SSRI or SNRI therapy.
Both esketamine and quetiapine were flexibly dosed. The primary endpoint was rates of remission at week 8 on the Montgomery-Åsberg Depression Rating Scale (MADRS). After week 8, patients entered a maintenance phase that lasted to week 32.
Dr. Reif said the study population was representative of a typical TRD population.
The average duration of the current depression episode was more than 5 years, and the average MADRS score was above 30.
Key findings
Results showed that those who received esketamine in combination with an SSRI or SNRI experienced a significantly higher rate of remission at week 8, compared with those treated with quetiapine (27.1% vs. 17.6%; P = .003). This equated to an adjusted odds ratio for remission of 1.74 (P = .003).
Use of esketamine was also associated with a higher rate of remission at week 8, and patients remained relapse free at week 32 (21.7% vs. 14.1% with quetiapine; odds ratio, 1.72; P = .008).
At every time point through the study, the proportion of patients experiencing remission was significantly greater with esketamine than with quetiapine. The absolute rate of remission at week 32 was 55.0%, versus 37.0% (P < .001).
Dr. Reif noted that the definition of remission used in the study was a MADRS score of less than or equal to 10, but if the “more lenient” definition of less than or equal to 12, which has been used previously, were to be applied, the absolute remission rates would rise to 65.1%, versus 46.7%.
Dr. Reif also presented results on functional remission rates beyond 32 weeks – data that were not included in the study as published in NEJM.
While remission rates increased over time in both study arms, the functional remission rate at week 32 was, again, significantly higher with esketamine than with quetiapine (38.1% vs. 25.0%; OR, 1.88; P < .001).
The safety data revealed no new signals, Dr. Reif said. Use of esketamine was associated with a lower rate of treatment-emergent adverse events that led to treatment discontinuation, at 4.2% vs. 11.0% with quetiapine.
Among patients given the ketamine-derived drug, there were lower rates of nervous system disorders, and there were no incidences of weight gain, fatigue, or hangover.
Dr. Reif said the results show that esketamine nasal spray was superior to quetiapine in achieving remission over time and that it “greatly improves patients’ functional impairment” while achieving “generally lower” adverse event rates.
He added that they are currently running a significant number of secondary analyses “to give us a better grasp of which patient benefits most” from esketamine therapy over quetiapine. The results may potentially be used to guide patient selection.
‘Tremendous advance’
Session co-chair Mark Weiser, MD, chairman at the department of psychiatry, Tel Aviv (Israel) University, said in an interview that the results are “very exciting” and offer “further proof of a tremendous advance in our field.”
Dr. Weiser, who was not involved in the study, added that demonstrating functional improvement with esketamine was key.
“It’s great to improve symptoms,” he said, “but to have patients show an improvement in their functionality is really the bottom line of this. Not only do you feel better, but you function better, and that’s of extreme importance and makes us feel very optimistic about the future.”
Josep Antoni Ramos-Quiroga, MD, PhD, head of psychiatry, Vall Hebron University Hospital and Autonomous University of Barcelona, welcomed the findings.
“The results of this study show the superior response and safety of esketamine nasal spray when compared with quetiapine,” he said in a release. “This gives people with treatment-resistant depression more safe treatment options.”
The study was funded by Janssen EMEA. Dr. Reif has relationships with Boehringer Ingelheim, COMPASS, Janssen Pharmaceuticals, LivaNova USA, Medice, Saga Therapeutics, and Shire. Other authors have disclosed numerous relationships with industry.
A version of this article first appeared on Medscape.com.
BARCELONA – (TRD), results of a large, multicenter, head-to-head phase 3 trial show.
Results from the ESCAPE-TRD study, which included 675 participants with TRD, show that esketamine was associated with significantly increased rates of both depression and functional remission, compared with quetiapine.
More than 675 patients were randomly assigned to receive one of the two drugs along with ongoing treatment with an SSRI or a serotonin-norepinephrine reuptake inhibitor (SNRI).
Esketamine increased remission rates at 2 and 8 months over quetiapine by 72% and raised functional remission rates at 8 months by 88% while decreasing adverse event rates.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology and were published online in the New England Journal of Medicine.
New hope
The results provide “some hope for our patients suffering from TRD, which, given the data, is somewhat of a misnomer,” said study investigator Andreas Reif, MD, professor of psychiatry, psychosomatic medicine, and psychotherapy, University Hospital Frankfurt–Goethe University, Frankfurt am Main, Germany, and president-elect of the ECNP.
“These patients are not resistant, they just have resistance to monoaminergic drugs,” he added. Esketamine, he said, is a “new weapon in our armamentarium.”
Dr. Reif said TRD is a serious condition that affects approximately 20%-30% of those with major depressive disorder and has “substantial impact” on patients’ lives, including quality of life and level of functioning.
“We know that esketamine nasal spray is effective in TRD. However, up to now, there were only placebo-controlled trials in addition to ongoing antidepressant treatment,” Dr. Reif noted. Consequently, he added, a head-to-head comparison with an active agent with proven efficacy was “urgently needed.”
For the trial, patients from 171 sites in 24 countries with TRD, defined as a less than 25% improvement in symptoms with two or more consecutive treatments of adequate dosage and duration, were randomly assigned to receive esketamine nasal spray (n = 336) or quetiapine (n = 340) extended release together with ongoing SSRI or SNRI therapy.
Both esketamine and quetiapine were flexibly dosed. The primary endpoint was rates of remission at week 8 on the Montgomery-Åsberg Depression Rating Scale (MADRS). After week 8, patients entered a maintenance phase that lasted to week 32.
Dr. Reif said the study population was representative of a typical TRD population.
The average duration of the current depression episode was more than 5 years, and the average MADRS score was above 30.
Key findings
Results showed that those who received esketamine in combination with an SSRI or SNRI experienced a significantly higher rate of remission at week 8, compared with those treated with quetiapine (27.1% vs. 17.6%; P = .003). This equated to an adjusted odds ratio for remission of 1.74 (P = .003).
Use of esketamine was also associated with a higher rate of remission at week 8, and patients remained relapse free at week 32 (21.7% vs. 14.1% with quetiapine; odds ratio, 1.72; P = .008).
At every time point through the study, the proportion of patients experiencing remission was significantly greater with esketamine than with quetiapine. The absolute rate of remission at week 32 was 55.0%, versus 37.0% (P < .001).
Dr. Reif noted that the definition of remission used in the study was a MADRS score of less than or equal to 10, but if the “more lenient” definition of less than or equal to 12, which has been used previously, were to be applied, the absolute remission rates would rise to 65.1%, versus 46.7%.
Dr. Reif also presented results on functional remission rates beyond 32 weeks – data that were not included in the study as published in NEJM.
While remission rates increased over time in both study arms, the functional remission rate at week 32 was, again, significantly higher with esketamine than with quetiapine (38.1% vs. 25.0%; OR, 1.88; P < .001).
The safety data revealed no new signals, Dr. Reif said. Use of esketamine was associated with a lower rate of treatment-emergent adverse events that led to treatment discontinuation, at 4.2% vs. 11.0% with quetiapine.
Among patients given the ketamine-derived drug, there were lower rates of nervous system disorders, and there were no incidences of weight gain, fatigue, or hangover.
Dr. Reif said the results show that esketamine nasal spray was superior to quetiapine in achieving remission over time and that it “greatly improves patients’ functional impairment” while achieving “generally lower” adverse event rates.
He added that they are currently running a significant number of secondary analyses “to give us a better grasp of which patient benefits most” from esketamine therapy over quetiapine. The results may potentially be used to guide patient selection.
‘Tremendous advance’
Session co-chair Mark Weiser, MD, chairman at the department of psychiatry, Tel Aviv (Israel) University, said in an interview that the results are “very exciting” and offer “further proof of a tremendous advance in our field.”
Dr. Weiser, who was not involved in the study, added that demonstrating functional improvement with esketamine was key.
“It’s great to improve symptoms,” he said, “but to have patients show an improvement in their functionality is really the bottom line of this. Not only do you feel better, but you function better, and that’s of extreme importance and makes us feel very optimistic about the future.”
Josep Antoni Ramos-Quiroga, MD, PhD, head of psychiatry, Vall Hebron University Hospital and Autonomous University of Barcelona, welcomed the findings.
“The results of this study show the superior response and safety of esketamine nasal spray when compared with quetiapine,” he said in a release. “This gives people with treatment-resistant depression more safe treatment options.”
The study was funded by Janssen EMEA. Dr. Reif has relationships with Boehringer Ingelheim, COMPASS, Janssen Pharmaceuticals, LivaNova USA, Medice, Saga Therapeutics, and Shire. Other authors have disclosed numerous relationships with industry.
A version of this article first appeared on Medscape.com.
BARCELONA – (TRD), results of a large, multicenter, head-to-head phase 3 trial show.
Results from the ESCAPE-TRD study, which included 675 participants with TRD, show that esketamine was associated with significantly increased rates of both depression and functional remission, compared with quetiapine.
More than 675 patients were randomly assigned to receive one of the two drugs along with ongoing treatment with an SSRI or a serotonin-norepinephrine reuptake inhibitor (SNRI).
Esketamine increased remission rates at 2 and 8 months over quetiapine by 72% and raised functional remission rates at 8 months by 88% while decreasing adverse event rates.
The findings were presented at the annual meeting of the European College of Neuropsychopharmacology and were published online in the New England Journal of Medicine.
New hope
The results provide “some hope for our patients suffering from TRD, which, given the data, is somewhat of a misnomer,” said study investigator Andreas Reif, MD, professor of psychiatry, psychosomatic medicine, and psychotherapy, University Hospital Frankfurt–Goethe University, Frankfurt am Main, Germany, and president-elect of the ECNP.
“These patients are not resistant, they just have resistance to monoaminergic drugs,” he added. Esketamine, he said, is a “new weapon in our armamentarium.”
Dr. Reif said TRD is a serious condition that affects approximately 20%-30% of those with major depressive disorder and has “substantial impact” on patients’ lives, including quality of life and level of functioning.
“We know that esketamine nasal spray is effective in TRD. However, up to now, there were only placebo-controlled trials in addition to ongoing antidepressant treatment,” Dr. Reif noted. Consequently, he added, a head-to-head comparison with an active agent with proven efficacy was “urgently needed.”
For the trial, patients from 171 sites in 24 countries with TRD, defined as a less than 25% improvement in symptoms with two or more consecutive treatments of adequate dosage and duration, were randomly assigned to receive esketamine nasal spray (n = 336) or quetiapine (n = 340) extended release together with ongoing SSRI or SNRI therapy.
Both esketamine and quetiapine were flexibly dosed. The primary endpoint was rates of remission at week 8 on the Montgomery-Åsberg Depression Rating Scale (MADRS). After week 8, patients entered a maintenance phase that lasted to week 32.
Dr. Reif said the study population was representative of a typical TRD population.
The average duration of the current depression episode was more than 5 years, and the average MADRS score was above 30.
Key findings
Results showed that those who received esketamine in combination with an SSRI or SNRI experienced a significantly higher rate of remission at week 8, compared with those treated with quetiapine (27.1% vs. 17.6%; P = .003). This equated to an adjusted odds ratio for remission of 1.74 (P = .003).
Use of esketamine was also associated with a higher rate of remission at week 8, and patients remained relapse free at week 32 (21.7% vs. 14.1% with quetiapine; odds ratio, 1.72; P = .008).
At every time point through the study, the proportion of patients experiencing remission was significantly greater with esketamine than with quetiapine. The absolute rate of remission at week 32 was 55.0%, versus 37.0% (P < .001).
Dr. Reif noted that the definition of remission used in the study was a MADRS score of less than or equal to 10, but if the “more lenient” definition of less than or equal to 12, which has been used previously, were to be applied, the absolute remission rates would rise to 65.1%, versus 46.7%.
Dr. Reif also presented results on functional remission rates beyond 32 weeks – data that were not included in the study as published in NEJM.
While remission rates increased over time in both study arms, the functional remission rate at week 32 was, again, significantly higher with esketamine than with quetiapine (38.1% vs. 25.0%; OR, 1.88; P < .001).
The safety data revealed no new signals, Dr. Reif said. Use of esketamine was associated with a lower rate of treatment-emergent adverse events that led to treatment discontinuation, at 4.2% vs. 11.0% with quetiapine.
Among patients given the ketamine-derived drug, there were lower rates of nervous system disorders, and there were no incidences of weight gain, fatigue, or hangover.
Dr. Reif said the results show that esketamine nasal spray was superior to quetiapine in achieving remission over time and that it “greatly improves patients’ functional impairment” while achieving “generally lower” adverse event rates.
He added that they are currently running a significant number of secondary analyses “to give us a better grasp of which patient benefits most” from esketamine therapy over quetiapine. The results may potentially be used to guide patient selection.
‘Tremendous advance’
Session co-chair Mark Weiser, MD, chairman at the department of psychiatry, Tel Aviv (Israel) University, said in an interview that the results are “very exciting” and offer “further proof of a tremendous advance in our field.”
Dr. Weiser, who was not involved in the study, added that demonstrating functional improvement with esketamine was key.
“It’s great to improve symptoms,” he said, “but to have patients show an improvement in their functionality is really the bottom line of this. Not only do you feel better, but you function better, and that’s of extreme importance and makes us feel very optimistic about the future.”
Josep Antoni Ramos-Quiroga, MD, PhD, head of psychiatry, Vall Hebron University Hospital and Autonomous University of Barcelona, welcomed the findings.
“The results of this study show the superior response and safety of esketamine nasal spray when compared with quetiapine,” he said in a release. “This gives people with treatment-resistant depression more safe treatment options.”
The study was funded by Janssen EMEA. Dr. Reif has relationships with Boehringer Ingelheim, COMPASS, Janssen Pharmaceuticals, LivaNova USA, Medice, Saga Therapeutics, and Shire. Other authors have disclosed numerous relationships with industry.
A version of this article first appeared on Medscape.com.
AT ECNP 2023
Are they ‘antiobesity medications’ or ‘weight-loss drugs’?
A simple Google search for the terms “weight-loss pens,” “weight-loss drugs,” and “weight-loss medications” displays seven times more results than a search for terms like “antiobesity medications,” “antiobesity drugs,” or “drugs (or medications) to treat obesity.” The same search applied to academic databases yields the opposite results: fewer than 500 results for “weight-loss drugs/agents/medications” and 19,000 results for “antiobesity agents,” for example.
To highlight the importance of the language used to talk about obesity treatment, researchers affiliated with the Brazilian Society of Endocrinology and Metabolism (SBEM) and the Brazilian Association for the Study of Obesity and Metabolic Syndrome (ABESO) released a statement on the subject at the Brazilian Congress of Update in Endocrinology and Metabolism 2023. On the basis of the study by the ABESO and the SBEM, the statement proposes abandoning the use of the term “weight-loss medications” in scientific publications and, most importantly, in the media.
“Put together, we believe that the common use of the term ‘weight-loss medications’ by media and the public, as well as by doctors and the scientific community, contributes to stigma, and certainly that language matters,” study author Paulo Augusto Carvalho Miranda, MD, PhD, chair of SBEM, said in an interview.
“When we refer to these medications as ‘weight-loss drugs,’ we are using derogatory terms to refer to medications that were extensively studied before their launch onto the market and approved by a regulatory authority to treat a disease called obesity,” said study author Márcio Mancini, MD, PhD, deputy chair of the SBEM’s Obesity Department.
Beyond semantics
Another article published by this news organization presents the initiative of a global task force comprising 60 leaders in the clinical management of obesity, who proposed a new name for the disease. According to the leader of the project, Francesco Rubino, MD, “The word is so stigmatized, with so much misunderstanding and misperception, that some might say the only solution is to change the name.” Following this same logic, the authors of the Brazilian study believe that changing how we refer to medications may improve perceptions of health care professionals and patients toward prevention and treatment strategies for obesity.
According to Dr. Miranda, the first step is “remembering that how we refer to people, diseases, and treatments makes all the difference, especially in situations like obesity, a stigmatized disease loaded with misconceptions. It is not merely an issue of semantics, but also an issue of reducing the stigma surrounding the subject.”
According to Dr. Miranda, the primary purpose of the statement is to highlight the uniqueness of the situation and the importance of encouraging the use of the expressions “antiobesity medications” and “medications to treat obesity” to help reduce the stigma and improve adherence and persistence in obesity treatment.
Impact in practice
The statement also emphasizes that obesity pharmacotherapy is widely underused in patients with obesity and that, in the United States, it is prescribed only for approximately 3% of adults with the disease. Weight management programs for this patient population stress implementing lifestyle changes, and only 1.1% of participants are prescribed medications.
According to the statement, the term “weight-loss medications” contributes to the concept that their use has an aesthetic goal and can be consumed by anyone who desires to lose weight.
In addition to ensuring the correct use of language, Dr. Mancini adds that it is essential for doctors to seek and present pharmacologic treatment for obesity as something that will improve patient health. This means stressing that obesity can be controlled with a 10% loss in body weight, just as other chronic diseases, such as diabetes, can be controlled. Moreover, it is important to point out that medications also have a crucial role in optimizing weight maintenance in the long term.
Another issue Dr. Mancini raised is the prejudice that many doctors have against people with obesity. Health professionals should recognize they are also subject to weight bias and that the way they communicate with patients could have a profound effect on health-related outcomes.
“The stigma surrounding obesity can lead to bullying, even in the patient’s home by their relatives; this is very common. Weight stigma is so strong that it hinders patient health and decreases the likelihood of the patient seeking specialized care,” Dr. Mancini warned.
According to the authors, it is of utmost importance to understand that an individual should not be defined by his or disease (as by the use of the terms “obese” or “diabetic”) but rather understood to live with this disease (“individual with obesity” or “with diabetes”). Dr. Mancini suggests the following strategies that health care professionals can adopt while caring for patients with obesity:
- Speak to patients with empathy and respect, avoiding the use of judgmental words.
- Ask if they would like to discuss the “weight issue,” “BMI issue,” terms that are better received by the public, instead of saying “excess fat” or “excess weight.”
- If the patient agrees to talk about the subject, reinforce that this is a chronic health problem that requires longterm treatment and give him or her short, medium, and longterm options.
Lastly, the authors highlighted the importance of differentiating between regulatory agency–approved medications and over-the-counter drugs and supplements that are often sold as “weight-loss agents” and are responsible for an unacceptably high rate of emergency visits.
This article was translated from the Medscape Portuguese Edition. A version appeared on Medscape.com.
A simple Google search for the terms “weight-loss pens,” “weight-loss drugs,” and “weight-loss medications” displays seven times more results than a search for terms like “antiobesity medications,” “antiobesity drugs,” or “drugs (or medications) to treat obesity.” The same search applied to academic databases yields the opposite results: fewer than 500 results for “weight-loss drugs/agents/medications” and 19,000 results for “antiobesity agents,” for example.
To highlight the importance of the language used to talk about obesity treatment, researchers affiliated with the Brazilian Society of Endocrinology and Metabolism (SBEM) and the Brazilian Association for the Study of Obesity and Metabolic Syndrome (ABESO) released a statement on the subject at the Brazilian Congress of Update in Endocrinology and Metabolism 2023. On the basis of the study by the ABESO and the SBEM, the statement proposes abandoning the use of the term “weight-loss medications” in scientific publications and, most importantly, in the media.
“Put together, we believe that the common use of the term ‘weight-loss medications’ by media and the public, as well as by doctors and the scientific community, contributes to stigma, and certainly that language matters,” study author Paulo Augusto Carvalho Miranda, MD, PhD, chair of SBEM, said in an interview.
“When we refer to these medications as ‘weight-loss drugs,’ we are using derogatory terms to refer to medications that were extensively studied before their launch onto the market and approved by a regulatory authority to treat a disease called obesity,” said study author Márcio Mancini, MD, PhD, deputy chair of the SBEM’s Obesity Department.
Beyond semantics
Another article published by this news organization presents the initiative of a global task force comprising 60 leaders in the clinical management of obesity, who proposed a new name for the disease. According to the leader of the project, Francesco Rubino, MD, “The word is so stigmatized, with so much misunderstanding and misperception, that some might say the only solution is to change the name.” Following this same logic, the authors of the Brazilian study believe that changing how we refer to medications may improve perceptions of health care professionals and patients toward prevention and treatment strategies for obesity.
According to Dr. Miranda, the first step is “remembering that how we refer to people, diseases, and treatments makes all the difference, especially in situations like obesity, a stigmatized disease loaded with misconceptions. It is not merely an issue of semantics, but also an issue of reducing the stigma surrounding the subject.”
According to Dr. Miranda, the primary purpose of the statement is to highlight the uniqueness of the situation and the importance of encouraging the use of the expressions “antiobesity medications” and “medications to treat obesity” to help reduce the stigma and improve adherence and persistence in obesity treatment.
Impact in practice
The statement also emphasizes that obesity pharmacotherapy is widely underused in patients with obesity and that, in the United States, it is prescribed only for approximately 3% of adults with the disease. Weight management programs for this patient population stress implementing lifestyle changes, and only 1.1% of participants are prescribed medications.
According to the statement, the term “weight-loss medications” contributes to the concept that their use has an aesthetic goal and can be consumed by anyone who desires to lose weight.
In addition to ensuring the correct use of language, Dr. Mancini adds that it is essential for doctors to seek and present pharmacologic treatment for obesity as something that will improve patient health. This means stressing that obesity can be controlled with a 10% loss in body weight, just as other chronic diseases, such as diabetes, can be controlled. Moreover, it is important to point out that medications also have a crucial role in optimizing weight maintenance in the long term.
Another issue Dr. Mancini raised is the prejudice that many doctors have against people with obesity. Health professionals should recognize they are also subject to weight bias and that the way they communicate with patients could have a profound effect on health-related outcomes.
“The stigma surrounding obesity can lead to bullying, even in the patient’s home by their relatives; this is very common. Weight stigma is so strong that it hinders patient health and decreases the likelihood of the patient seeking specialized care,” Dr. Mancini warned.
According to the authors, it is of utmost importance to understand that an individual should not be defined by his or disease (as by the use of the terms “obese” or “diabetic”) but rather understood to live with this disease (“individual with obesity” or “with diabetes”). Dr. Mancini suggests the following strategies that health care professionals can adopt while caring for patients with obesity:
- Speak to patients with empathy and respect, avoiding the use of judgmental words.
- Ask if they would like to discuss the “weight issue,” “BMI issue,” terms that are better received by the public, instead of saying “excess fat” or “excess weight.”
- If the patient agrees to talk about the subject, reinforce that this is a chronic health problem that requires longterm treatment and give him or her short, medium, and longterm options.
Lastly, the authors highlighted the importance of differentiating between regulatory agency–approved medications and over-the-counter drugs and supplements that are often sold as “weight-loss agents” and are responsible for an unacceptably high rate of emergency visits.
This article was translated from the Medscape Portuguese Edition. A version appeared on Medscape.com.
A simple Google search for the terms “weight-loss pens,” “weight-loss drugs,” and “weight-loss medications” displays seven times more results than a search for terms like “antiobesity medications,” “antiobesity drugs,” or “drugs (or medications) to treat obesity.” The same search applied to academic databases yields the opposite results: fewer than 500 results for “weight-loss drugs/agents/medications” and 19,000 results for “antiobesity agents,” for example.
To highlight the importance of the language used to talk about obesity treatment, researchers affiliated with the Brazilian Society of Endocrinology and Metabolism (SBEM) and the Brazilian Association for the Study of Obesity and Metabolic Syndrome (ABESO) released a statement on the subject at the Brazilian Congress of Update in Endocrinology and Metabolism 2023. On the basis of the study by the ABESO and the SBEM, the statement proposes abandoning the use of the term “weight-loss medications” in scientific publications and, most importantly, in the media.
“Put together, we believe that the common use of the term ‘weight-loss medications’ by media and the public, as well as by doctors and the scientific community, contributes to stigma, and certainly that language matters,” study author Paulo Augusto Carvalho Miranda, MD, PhD, chair of SBEM, said in an interview.
“When we refer to these medications as ‘weight-loss drugs,’ we are using derogatory terms to refer to medications that were extensively studied before their launch onto the market and approved by a regulatory authority to treat a disease called obesity,” said study author Márcio Mancini, MD, PhD, deputy chair of the SBEM’s Obesity Department.
Beyond semantics
Another article published by this news organization presents the initiative of a global task force comprising 60 leaders in the clinical management of obesity, who proposed a new name for the disease. According to the leader of the project, Francesco Rubino, MD, “The word is so stigmatized, with so much misunderstanding and misperception, that some might say the only solution is to change the name.” Following this same logic, the authors of the Brazilian study believe that changing how we refer to medications may improve perceptions of health care professionals and patients toward prevention and treatment strategies for obesity.
According to Dr. Miranda, the first step is “remembering that how we refer to people, diseases, and treatments makes all the difference, especially in situations like obesity, a stigmatized disease loaded with misconceptions. It is not merely an issue of semantics, but also an issue of reducing the stigma surrounding the subject.”
According to Dr. Miranda, the primary purpose of the statement is to highlight the uniqueness of the situation and the importance of encouraging the use of the expressions “antiobesity medications” and “medications to treat obesity” to help reduce the stigma and improve adherence and persistence in obesity treatment.
Impact in practice
The statement also emphasizes that obesity pharmacotherapy is widely underused in patients with obesity and that, in the United States, it is prescribed only for approximately 3% of adults with the disease. Weight management programs for this patient population stress implementing lifestyle changes, and only 1.1% of participants are prescribed medications.
According to the statement, the term “weight-loss medications” contributes to the concept that their use has an aesthetic goal and can be consumed by anyone who desires to lose weight.
In addition to ensuring the correct use of language, Dr. Mancini adds that it is essential for doctors to seek and present pharmacologic treatment for obesity as something that will improve patient health. This means stressing that obesity can be controlled with a 10% loss in body weight, just as other chronic diseases, such as diabetes, can be controlled. Moreover, it is important to point out that medications also have a crucial role in optimizing weight maintenance in the long term.
Another issue Dr. Mancini raised is the prejudice that many doctors have against people with obesity. Health professionals should recognize they are also subject to weight bias and that the way they communicate with patients could have a profound effect on health-related outcomes.
“The stigma surrounding obesity can lead to bullying, even in the patient’s home by their relatives; this is very common. Weight stigma is so strong that it hinders patient health and decreases the likelihood of the patient seeking specialized care,” Dr. Mancini warned.
According to the authors, it is of utmost importance to understand that an individual should not be defined by his or disease (as by the use of the terms “obese” or “diabetic”) but rather understood to live with this disease (“individual with obesity” or “with diabetes”). Dr. Mancini suggests the following strategies that health care professionals can adopt while caring for patients with obesity:
- Speak to patients with empathy and respect, avoiding the use of judgmental words.
- Ask if they would like to discuss the “weight issue,” “BMI issue,” terms that are better received by the public, instead of saying “excess fat” or “excess weight.”
- If the patient agrees to talk about the subject, reinforce that this is a chronic health problem that requires longterm treatment and give him or her short, medium, and longterm options.
Lastly, the authors highlighted the importance of differentiating between regulatory agency–approved medications and over-the-counter drugs and supplements that are often sold as “weight-loss agents” and are responsible for an unacceptably high rate of emergency visits.
This article was translated from the Medscape Portuguese Edition. A version appeared on Medscape.com.
‘Vaginal dryness’ can be fatal. No, really.
This transcript has been edited for clarity.
What do you mean, Dr. Rubin? How is vaginal dryness killing women? We minimize the term vaginal dryness. When women come to our offices and complain of a little vaginal dryness – or they don’t even come to our office to complain of it because the doctor can’t be bothered with a little vaginal dryness — what they don’t understand is that this “little vaginal dryness” is really something called genitourinary syndrome of menopause (GSM). They don’t know that because they’ve never heard of it, and you may have never heard of it either. In 2014, we changed the terms vaginal dryness and vulvovaginal atrophy or atrophic vaginitis to GSM to make it short and simple.
GSM – what does it mean? It’s not just a little vaginal dryness. It turns out that all of the genital and urinary symptoms from menopause just get worse over time. The bladder, the urethra, and the vagina have lots of hormone receptors, including estrogen and testosterone. When the body no longer makes those hormones, the system doesn’t work very well, and genital and urinary symptoms occur that just get worse over time without treatment. Unlike hot flashes, which tend to go away, GSM does not.
What are the symptoms of GSM? Some are sexual: a little vaginal dryness, pain with sex, and worsening orgasm. But there are also genital and urinary symptoms that get worse: itching, burning irritation, rawness, an awareness of their genitals that the patient has never had before. And as a urologist, we see frequency, urgency, and leakage.
The thing that kills women is recurrent urinary tract infections (UTIs). Did you know that UTIs account for 7 million visits and hospitalizations annually and 25% of all infections in older people? In fact, apparently one-third of the total Medicare expenditure is around UTIs. Not preventing UTIs is costing our health care system an enormous amount of money and resources.
Did you know we’ve had safe and effective treatment options for GSM since the 1970s? Vaginal hormones have existed since the 1970s, but we’re using them only for pain with sex and not for GSM. In fact, data show that by using vaginal hormones, we can prevent UTIs by more than 50%. We can save lives using safe, effective, local, low-dose vaginal hormone strategies. And they are safe and effective for all of our patients in pre- and post menopause.
There are five different treatment options: vaginal estrogen inserts, vaginal estrogen creams, vaginal dehydroepiandrosterone (DHEA), low-dose vaginal estrogen rings, and an oral pill option called ospemifene (Osphena). All are used to treat GSM and will only work if your patient actually uses them and continues to use them.
These treatments are safe. They are effective. They do not increase the level of systemic hormones in the bloodstream. I have many patients with breast cancer who use these products as well. The only patients you may want to talk to your oncology colleagues about is women on active aromatase inhibitors.
We have to understand that UTIs kill people and having GSM is debilitating, often requiring pain medication because it can hurt to sit or to wear pads and our patients’ quality of life is severely affected. So please consider learning how to treat GSM. It turns out you don’t have to do exams. You don’t have to do follow-up. You can give these therapies, and women can use them for life.
Now, if your patient has vaginal bleeding, of course they need to see their gynecologist. But this is something every primary care doctor can and should do. As a urologist, we prescribe a lot of tamsulosin (Flomax) for our male patients to help with urination. Vaginal estrogen or DHEA is basically like Flomax for women, but it prevents UTIs and actually works like sildenafil (Viagra) because it can help orgasm and reduce pain with sex.
You have access to affordable, safe, effective treatment options to treat GSM. So check them out and hopefully change the world.
Dr. Rubin is an assistant clinical professor in the department of urology at Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GlaxoSmithKline, and Endo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
What do you mean, Dr. Rubin? How is vaginal dryness killing women? We minimize the term vaginal dryness. When women come to our offices and complain of a little vaginal dryness – or they don’t even come to our office to complain of it because the doctor can’t be bothered with a little vaginal dryness — what they don’t understand is that this “little vaginal dryness” is really something called genitourinary syndrome of menopause (GSM). They don’t know that because they’ve never heard of it, and you may have never heard of it either. In 2014, we changed the terms vaginal dryness and vulvovaginal atrophy or atrophic vaginitis to GSM to make it short and simple.
GSM – what does it mean? It’s not just a little vaginal dryness. It turns out that all of the genital and urinary symptoms from menopause just get worse over time. The bladder, the urethra, and the vagina have lots of hormone receptors, including estrogen and testosterone. When the body no longer makes those hormones, the system doesn’t work very well, and genital and urinary symptoms occur that just get worse over time without treatment. Unlike hot flashes, which tend to go away, GSM does not.
What are the symptoms of GSM? Some are sexual: a little vaginal dryness, pain with sex, and worsening orgasm. But there are also genital and urinary symptoms that get worse: itching, burning irritation, rawness, an awareness of their genitals that the patient has never had before. And as a urologist, we see frequency, urgency, and leakage.
The thing that kills women is recurrent urinary tract infections (UTIs). Did you know that UTIs account for 7 million visits and hospitalizations annually and 25% of all infections in older people? In fact, apparently one-third of the total Medicare expenditure is around UTIs. Not preventing UTIs is costing our health care system an enormous amount of money and resources.
Did you know we’ve had safe and effective treatment options for GSM since the 1970s? Vaginal hormones have existed since the 1970s, but we’re using them only for pain with sex and not for GSM. In fact, data show that by using vaginal hormones, we can prevent UTIs by more than 50%. We can save lives using safe, effective, local, low-dose vaginal hormone strategies. And they are safe and effective for all of our patients in pre- and post menopause.
There are five different treatment options: vaginal estrogen inserts, vaginal estrogen creams, vaginal dehydroepiandrosterone (DHEA), low-dose vaginal estrogen rings, and an oral pill option called ospemifene (Osphena). All are used to treat GSM and will only work if your patient actually uses them and continues to use them.
These treatments are safe. They are effective. They do not increase the level of systemic hormones in the bloodstream. I have many patients with breast cancer who use these products as well. The only patients you may want to talk to your oncology colleagues about is women on active aromatase inhibitors.
We have to understand that UTIs kill people and having GSM is debilitating, often requiring pain medication because it can hurt to sit or to wear pads and our patients’ quality of life is severely affected. So please consider learning how to treat GSM. It turns out you don’t have to do exams. You don’t have to do follow-up. You can give these therapies, and women can use them for life.
Now, if your patient has vaginal bleeding, of course they need to see their gynecologist. But this is something every primary care doctor can and should do. As a urologist, we prescribe a lot of tamsulosin (Flomax) for our male patients to help with urination. Vaginal estrogen or DHEA is basically like Flomax for women, but it prevents UTIs and actually works like sildenafil (Viagra) because it can help orgasm and reduce pain with sex.
You have access to affordable, safe, effective treatment options to treat GSM. So check them out and hopefully change the world.
Dr. Rubin is an assistant clinical professor in the department of urology at Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GlaxoSmithKline, and Endo.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
What do you mean, Dr. Rubin? How is vaginal dryness killing women? We minimize the term vaginal dryness. When women come to our offices and complain of a little vaginal dryness – or they don’t even come to our office to complain of it because the doctor can’t be bothered with a little vaginal dryness — what they don’t understand is that this “little vaginal dryness” is really something called genitourinary syndrome of menopause (GSM). They don’t know that because they’ve never heard of it, and you may have never heard of it either. In 2014, we changed the terms vaginal dryness and vulvovaginal atrophy or atrophic vaginitis to GSM to make it short and simple.
GSM – what does it mean? It’s not just a little vaginal dryness. It turns out that all of the genital and urinary symptoms from menopause just get worse over time. The bladder, the urethra, and the vagina have lots of hormone receptors, including estrogen and testosterone. When the body no longer makes those hormones, the system doesn’t work very well, and genital and urinary symptoms occur that just get worse over time without treatment. Unlike hot flashes, which tend to go away, GSM does not.
What are the symptoms of GSM? Some are sexual: a little vaginal dryness, pain with sex, and worsening orgasm. But there are also genital and urinary symptoms that get worse: itching, burning irritation, rawness, an awareness of their genitals that the patient has never had before. And as a urologist, we see frequency, urgency, and leakage.
The thing that kills women is recurrent urinary tract infections (UTIs). Did you know that UTIs account for 7 million visits and hospitalizations annually and 25% of all infections in older people? In fact, apparently one-third of the total Medicare expenditure is around UTIs. Not preventing UTIs is costing our health care system an enormous amount of money and resources.
Did you know we’ve had safe and effective treatment options for GSM since the 1970s? Vaginal hormones have existed since the 1970s, but we’re using them only for pain with sex and not for GSM. In fact, data show that by using vaginal hormones, we can prevent UTIs by more than 50%. We can save lives using safe, effective, local, low-dose vaginal hormone strategies. And they are safe and effective for all of our patients in pre- and post menopause.
There are five different treatment options: vaginal estrogen inserts, vaginal estrogen creams, vaginal dehydroepiandrosterone (DHEA), low-dose vaginal estrogen rings, and an oral pill option called ospemifene (Osphena). All are used to treat GSM and will only work if your patient actually uses them and continues to use them.
These treatments are safe. They are effective. They do not increase the level of systemic hormones in the bloodstream. I have many patients with breast cancer who use these products as well. The only patients you may want to talk to your oncology colleagues about is women on active aromatase inhibitors.
We have to understand that UTIs kill people and having GSM is debilitating, often requiring pain medication because it can hurt to sit or to wear pads and our patients’ quality of life is severely affected. So please consider learning how to treat GSM. It turns out you don’t have to do exams. You don’t have to do follow-up. You can give these therapies, and women can use them for life.
Now, if your patient has vaginal bleeding, of course they need to see their gynecologist. But this is something every primary care doctor can and should do. As a urologist, we prescribe a lot of tamsulosin (Flomax) for our male patients to help with urination. Vaginal estrogen or DHEA is basically like Flomax for women, but it prevents UTIs and actually works like sildenafil (Viagra) because it can help orgasm and reduce pain with sex.
You have access to affordable, safe, effective treatment options to treat GSM. So check them out and hopefully change the world.
Dr. Rubin is an assistant clinical professor in the department of urology at Georgetown University, Washington. She reported conflicts of interest with Sprout, Maternal Medical, Absorption Pharmaceuticals, GlaxoSmithKline, and Endo.
A version of this article first appeared on Medscape.com.