User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
Weight Loss in Later-Life Women: More Than Diet, Exercise
Unwanted weight gain is a common problem for women after menopause. Primary care clinicians have likely heard from patients that attempts at shedding extra pounds are not working.
Aging does: Women gain about 1.5 pounds per year on average starting almost a decade prior to menopause to a decade after their final menstrual cycle, according to research.
“A lot of women are in tears because they have gained 10 or 15 pounds,” said Stephanie Faubion, MD, medical director of The Menopause Society and director of the Mayo Clinic Center for Women’s Health in Jacksonville, Florida.
A shortage of obesity and menopause specialists means primary care clinicians must understand the intersection of weight management and how the body functions after menopause.
“The importance of weight management in midlife cannot be overemphasized,” Dr. Faubion said. “Excess weight around the middle increases the risk of diabetes and heart disease and that is directly related to the loss of estrogen.”
The loss of estrogen due to menopause also causes the redistribution of fat from the thighs, hips, and buttocks to the midsection, which can be more difficult to trim. And women naturally lose muscle mass as they age, in part because the hormone is important to muscle functioning, according to Maria Daniela Hurtado Andrade, MD, PhD, assistant professor of medicine at Mayo Clinic Alix School of Medicine in Jacksonville, Florida.
“Menopause compounds the changes associated with aging: It makes them worse,” Dr. Hurtado Andrade said.
Mounting evidence has linked obesity-related systemic inflammation with an increased risk for cardiovascular disease, including heart attacks and vascular damage.
Michael Knight, MD, clinical associate professor of medicine and a weight loss specialist at the George Washington University in Washington, DC, estimated that more than half of his patients are postmenopausal women.
He recommended clinicians look for adipose tissue dysfunction, which can cause localized insulin resistance and affect metabolic health. Research suggests clinicians can perform a basic metabolic panel, in addition to testing for triglyceride, low-density lipoprotein, and renal function levels. Several other recent studies have pointed to using waist circumference, insulin resistance, or presence of metabolic syndrome to diagnose adipose tissue dysfunction.
Beyond Diet and Exercise
Physicians should ask their patients about physical activity, the type of foods they are eating, and changes in day-to-day movement, Dr. Knight advised.
Pharmacotherapy or surgical options should be considered for some patients, according to Karen Adams, MD, clinical professor of obstetrics and gynecology and a lifestyle medicine specialist at Stanford Medicine in Palo Alto, California. Postmenopausal women who want to lose more than 5%-10% of their body weight likely will need another modality in addition to diet and exercise.
“What’s important is transitioning the patient from feeling like they’ve failed to a mindset of seeking help or seeking care for this condition,” she said. Dr. Adams, a certified menopause specialist, uses the idea of “good enough” with her patients and suggests they think of weight loss as a journey, which may require different tools at various points.
Glucagon-like peptide 1 receptor agonists like semaglutide or tirzepatide are some of the most effective drugs for obesity, according to Dr. Knight.
In addition to these drugs, hormone replacement therapy in combination with the weight loss drug semaglutide may improve weight loss and reduce cardiometabolic risk in postmenopausal women compared with semaglutide alone, as reported in a study Dr. Hurtado Andrade and Dr. Faubion recently coauthored. Improving vasomotor symptoms improved sleep, physical activity, and quality of life, which all can affect efforts to lose weight.
Most patients who struggle to lose weight using diet and exercise methods alone usually do not maintain a healthy weight long term, according to Knight. Physicians need a comprehensive strategy to introduce options like medications or surgery when indicated for long-term, weight management solutions.
Tips for primary care clinicians in helping postmenopausal women lose weight:
- Develop an effective solution that works for your patient’s lifestyle. If you don’t have one, make a referral to a weight loss specialist.
- Educate patients about obesity and postmenopausal weight loss challenges, to help destigmatize the condition. Explain that obesity is a chronic disease, like hypertension or diabetes.
- Exercise suggestions should consider issues like walkable neighborhoods, access and affordability of gym membership, and home broadband access.
- Strength training should be recommended to counter loss of muscle mass that comes with aging.
- Consider a patient’s culture when discussing healthier alternatives to their usual diet.
- Suggest simple changes to start, like eliminating simple carbohydrates — white bread, pasta, and white rice — as a good place to start.
Body mass index was not designed to be a clinical tool and does not fully assess weight in many populations. Risk for chronic diseases and obesity varies depending on whether a person carries weight centrally or on the hips and thighs.
But well before menopause, clinicians can educate their female patients on what body changes to expect and be more mindful about which medications to not prescribe.
People in menopause or perimenopause are frequently prescribed weight-promoting drugs like antidepressants for mood swings or gabapentin for hot flashes. Clinicians should conduct a medication review and look for alternatives to drugs that are associated with weight gain.
The best approach is to try to avoid weight gain in the first place, which can be easier than trying to lose later, Dr. Faubion said. “You can’t just exercise your way out of it,” she said.
Dr. Adams, Dr. Faubion, and Dr. Hurtado Andrade reported no disclosures. Dr. Knight is a former consultant with Novo Nordisk.
A version of this article appeared on Medscape.com.
Unwanted weight gain is a common problem for women after menopause. Primary care clinicians have likely heard from patients that attempts at shedding extra pounds are not working.
Aging does: Women gain about 1.5 pounds per year on average starting almost a decade prior to menopause to a decade after their final menstrual cycle, according to research.
“A lot of women are in tears because they have gained 10 or 15 pounds,” said Stephanie Faubion, MD, medical director of The Menopause Society and director of the Mayo Clinic Center for Women’s Health in Jacksonville, Florida.
A shortage of obesity and menopause specialists means primary care clinicians must understand the intersection of weight management and how the body functions after menopause.
“The importance of weight management in midlife cannot be overemphasized,” Dr. Faubion said. “Excess weight around the middle increases the risk of diabetes and heart disease and that is directly related to the loss of estrogen.”
The loss of estrogen due to menopause also causes the redistribution of fat from the thighs, hips, and buttocks to the midsection, which can be more difficult to trim. And women naturally lose muscle mass as they age, in part because the hormone is important to muscle functioning, according to Maria Daniela Hurtado Andrade, MD, PhD, assistant professor of medicine at Mayo Clinic Alix School of Medicine in Jacksonville, Florida.
“Menopause compounds the changes associated with aging: It makes them worse,” Dr. Hurtado Andrade said.
Mounting evidence has linked obesity-related systemic inflammation with an increased risk for cardiovascular disease, including heart attacks and vascular damage.
Michael Knight, MD, clinical associate professor of medicine and a weight loss specialist at the George Washington University in Washington, DC, estimated that more than half of his patients are postmenopausal women.
He recommended clinicians look for adipose tissue dysfunction, which can cause localized insulin resistance and affect metabolic health. Research suggests clinicians can perform a basic metabolic panel, in addition to testing for triglyceride, low-density lipoprotein, and renal function levels. Several other recent studies have pointed to using waist circumference, insulin resistance, or presence of metabolic syndrome to diagnose adipose tissue dysfunction.
Beyond Diet and Exercise
Physicians should ask their patients about physical activity, the type of foods they are eating, and changes in day-to-day movement, Dr. Knight advised.
Pharmacotherapy or surgical options should be considered for some patients, according to Karen Adams, MD, clinical professor of obstetrics and gynecology and a lifestyle medicine specialist at Stanford Medicine in Palo Alto, California. Postmenopausal women who want to lose more than 5%-10% of their body weight likely will need another modality in addition to diet and exercise.
“What’s important is transitioning the patient from feeling like they’ve failed to a mindset of seeking help or seeking care for this condition,” she said. Dr. Adams, a certified menopause specialist, uses the idea of “good enough” with her patients and suggests they think of weight loss as a journey, which may require different tools at various points.
Glucagon-like peptide 1 receptor agonists like semaglutide or tirzepatide are some of the most effective drugs for obesity, according to Dr. Knight.
In addition to these drugs, hormone replacement therapy in combination with the weight loss drug semaglutide may improve weight loss and reduce cardiometabolic risk in postmenopausal women compared with semaglutide alone, as reported in a study Dr. Hurtado Andrade and Dr. Faubion recently coauthored. Improving vasomotor symptoms improved sleep, physical activity, and quality of life, which all can affect efforts to lose weight.
Most patients who struggle to lose weight using diet and exercise methods alone usually do not maintain a healthy weight long term, according to Knight. Physicians need a comprehensive strategy to introduce options like medications or surgery when indicated for long-term, weight management solutions.
Tips for primary care clinicians in helping postmenopausal women lose weight:
- Develop an effective solution that works for your patient’s lifestyle. If you don’t have one, make a referral to a weight loss specialist.
- Educate patients about obesity and postmenopausal weight loss challenges, to help destigmatize the condition. Explain that obesity is a chronic disease, like hypertension or diabetes.
- Exercise suggestions should consider issues like walkable neighborhoods, access and affordability of gym membership, and home broadband access.
- Strength training should be recommended to counter loss of muscle mass that comes with aging.
- Consider a patient’s culture when discussing healthier alternatives to their usual diet.
- Suggest simple changes to start, like eliminating simple carbohydrates — white bread, pasta, and white rice — as a good place to start.
Body mass index was not designed to be a clinical tool and does not fully assess weight in many populations. Risk for chronic diseases and obesity varies depending on whether a person carries weight centrally or on the hips and thighs.
But well before menopause, clinicians can educate their female patients on what body changes to expect and be more mindful about which medications to not prescribe.
People in menopause or perimenopause are frequently prescribed weight-promoting drugs like antidepressants for mood swings or gabapentin for hot flashes. Clinicians should conduct a medication review and look for alternatives to drugs that are associated with weight gain.
The best approach is to try to avoid weight gain in the first place, which can be easier than trying to lose later, Dr. Faubion said. “You can’t just exercise your way out of it,” she said.
Dr. Adams, Dr. Faubion, and Dr. Hurtado Andrade reported no disclosures. Dr. Knight is a former consultant with Novo Nordisk.
A version of this article appeared on Medscape.com.
Unwanted weight gain is a common problem for women after menopause. Primary care clinicians have likely heard from patients that attempts at shedding extra pounds are not working.
Aging does: Women gain about 1.5 pounds per year on average starting almost a decade prior to menopause to a decade after their final menstrual cycle, according to research.
“A lot of women are in tears because they have gained 10 or 15 pounds,” said Stephanie Faubion, MD, medical director of The Menopause Society and director of the Mayo Clinic Center for Women’s Health in Jacksonville, Florida.
A shortage of obesity and menopause specialists means primary care clinicians must understand the intersection of weight management and how the body functions after menopause.
“The importance of weight management in midlife cannot be overemphasized,” Dr. Faubion said. “Excess weight around the middle increases the risk of diabetes and heart disease and that is directly related to the loss of estrogen.”
The loss of estrogen due to menopause also causes the redistribution of fat from the thighs, hips, and buttocks to the midsection, which can be more difficult to trim. And women naturally lose muscle mass as they age, in part because the hormone is important to muscle functioning, according to Maria Daniela Hurtado Andrade, MD, PhD, assistant professor of medicine at Mayo Clinic Alix School of Medicine in Jacksonville, Florida.
“Menopause compounds the changes associated with aging: It makes them worse,” Dr. Hurtado Andrade said.
Mounting evidence has linked obesity-related systemic inflammation with an increased risk for cardiovascular disease, including heart attacks and vascular damage.
Michael Knight, MD, clinical associate professor of medicine and a weight loss specialist at the George Washington University in Washington, DC, estimated that more than half of his patients are postmenopausal women.
He recommended clinicians look for adipose tissue dysfunction, which can cause localized insulin resistance and affect metabolic health. Research suggests clinicians can perform a basic metabolic panel, in addition to testing for triglyceride, low-density lipoprotein, and renal function levels. Several other recent studies have pointed to using waist circumference, insulin resistance, or presence of metabolic syndrome to diagnose adipose tissue dysfunction.
Beyond Diet and Exercise
Physicians should ask their patients about physical activity, the type of foods they are eating, and changes in day-to-day movement, Dr. Knight advised.
Pharmacotherapy or surgical options should be considered for some patients, according to Karen Adams, MD, clinical professor of obstetrics and gynecology and a lifestyle medicine specialist at Stanford Medicine in Palo Alto, California. Postmenopausal women who want to lose more than 5%-10% of their body weight likely will need another modality in addition to diet and exercise.
“What’s important is transitioning the patient from feeling like they’ve failed to a mindset of seeking help or seeking care for this condition,” she said. Dr. Adams, a certified menopause specialist, uses the idea of “good enough” with her patients and suggests they think of weight loss as a journey, which may require different tools at various points.
Glucagon-like peptide 1 receptor agonists like semaglutide or tirzepatide are some of the most effective drugs for obesity, according to Dr. Knight.
In addition to these drugs, hormone replacement therapy in combination with the weight loss drug semaglutide may improve weight loss and reduce cardiometabolic risk in postmenopausal women compared with semaglutide alone, as reported in a study Dr. Hurtado Andrade and Dr. Faubion recently coauthored. Improving vasomotor symptoms improved sleep, physical activity, and quality of life, which all can affect efforts to lose weight.
Most patients who struggle to lose weight using diet and exercise methods alone usually do not maintain a healthy weight long term, according to Knight. Physicians need a comprehensive strategy to introduce options like medications or surgery when indicated for long-term, weight management solutions.
Tips for primary care clinicians in helping postmenopausal women lose weight:
- Develop an effective solution that works for your patient’s lifestyle. If you don’t have one, make a referral to a weight loss specialist.
- Educate patients about obesity and postmenopausal weight loss challenges, to help destigmatize the condition. Explain that obesity is a chronic disease, like hypertension or diabetes.
- Exercise suggestions should consider issues like walkable neighborhoods, access and affordability of gym membership, and home broadband access.
- Strength training should be recommended to counter loss of muscle mass that comes with aging.
- Consider a patient’s culture when discussing healthier alternatives to their usual diet.
- Suggest simple changes to start, like eliminating simple carbohydrates — white bread, pasta, and white rice — as a good place to start.
Body mass index was not designed to be a clinical tool and does not fully assess weight in many populations. Risk for chronic diseases and obesity varies depending on whether a person carries weight centrally or on the hips and thighs.
But well before menopause, clinicians can educate their female patients on what body changes to expect and be more mindful about which medications to not prescribe.
People in menopause or perimenopause are frequently prescribed weight-promoting drugs like antidepressants for mood swings or gabapentin for hot flashes. Clinicians should conduct a medication review and look for alternatives to drugs that are associated with weight gain.
The best approach is to try to avoid weight gain in the first place, which can be easier than trying to lose later, Dr. Faubion said. “You can’t just exercise your way out of it,” she said.
Dr. Adams, Dr. Faubion, and Dr. Hurtado Andrade reported no disclosures. Dr. Knight is a former consultant with Novo Nordisk.
A version of this article appeared on Medscape.com.
Extraordinary Patients Inspired Father of Cancer Immunotherapy
His pioneering research established interleukin-2 (IL-2) as the first U.S. Food and Drug Administration–approved cancer immunotherapy in 1992.
To recognize his trailblazing work and other achievements, the American Association for Cancer Research (AACR) will award Dr. Rosenberg with the 2024 AACR Award for Lifetime Achievement in Cancer Research at its annual meeting in April.
Dr. Rosenberg, a senior investigator for the Center for Cancer Research at the National Cancer Institute (NCI), and chief of the NCI Surgery Branch, shared the history behind his novel research and the patient stories that inspired his discoveries, during an interview.
Tell us a little about yourself and where you grew up.
Dr. Rosenberg: I grew up in the Bronx. My parents both immigrated to the United States from Poland as teenagers.
As a young boy, did you always want to become a doctor?
Dr. Rosenberg: I think some defining moments on why I decided to go into medicine occurred when I was 6 or 7 years old. The second world war was over, and many of the horrors of the Holocaust became apparent to me. I was brought up as an Orthodox Jew. My parents were quite religious, and I remember postcards coming in one after another about relatives that had died in the death camps. That had a profound influence on me.
How did that experience impact your aspirations?
Dr. Rosenberg: It was an example to me of how evil certain people and groups can be toward one another. I decided at that point, that I wanted to do something good for people, and medicine seemed the most likely way to do that. But also, I was developing a broad scientific interest. I ended up at the Bronx High School of Science and knew that I not only wanted to practice the medicine of today, but I wanted to play a role in helping develop the medicine.
What led to your interest in cancer treatment?
Dr. Rosenberg: Well, as a medical student and resident, it became clear that the field of cancer needed major improvement. We had three major ways to treat cancer: surgery, radiation therapy, and chemotherapy. That could cure about half of the people [who] had cancer. But despite the best application of those three specialties, there were over 600,000 deaths from cancer each year in the United States alone. It was clear to me that new approaches were needed, and I became very interested in taking advantage of the body’s immune system as a source of information to try to make progress.
Were there patients who inspired your research?
Dr. Rosenberg: There were two patients that I saw early in my career that impressed me a great deal. One was a patient that I saw when working in the emergency ward as a resident. A patient came in with right upper quadrant pain that looked like a gallbladder attack. That’s what it was. But when I went through his chart, I saw that he had been at that hospital 12 years earlier with a metastatic gastric cancer. The surgeons had operated. They saw tumor had spread to the liver and could not be removed. They closed the belly, not expecting him to survive. Yet he kept showing up for follow-up visits.
Here he was 12 years later. When I helped operate to take out his gallbladder, there was no evidence of any cancer. The cancer had disappeared in the absence of any external treatment. One of the rarest events in medicine, the spontaneous regression of a cancer. Somehow his body had learned how to destroy the tumor.
Was the second patient’s case as impressive?
Dr. Rosenberg: This patient had received a kidney transplant from a gentleman who died in an auto accident. [The donor’s] kidney contained a cancer deposit, a kidney cancer, unbeknownst to the transplant surgeons. [When the kidney was transplanted], the recipient developed widespread metastatic kidney cancer.
[The recipient] was on immunosuppressive drugs, and so the drugs had to be stopped. [When the immunosuppressive drugs were stopped], the patient’s body rejected the kidney and his cancer disappeared.
That showed me that, in fact, if you could stimulate a strong enough immune reaction, in this case, an [allogeneic] reaction, against foreign tissues from a different individual, that you could make large vascularized, invasive cancers disappear based on immune reactivities. Those were clues that led me toward studying the immune system’s impact on cancer.
From there, how did your work evolve?
Dr. Rosenberg: As chief of the surgery branch at NIH, I began doing research. It was very difficult to manipulate immune cells in the laboratory. They wouldn’t stay alive. But I tried to study immune reactions in patients with cancer to see if there was such a thing as an immune reaction against the cancer. There was no such thing known at the time. There were no cancer antigens and no known immune reactions against the disease in the human.
Around this time, investigators were publishing studies about interleukin-2 (IL-2), or white blood cells known as leukocytes. How did interleukin-2 further your research?
Dr. Rosenberg: The advent of interleukin-2 enabled scientists to grow lymphocytes outside the body. [This] enabled us to grow t-lymphocytes, which are some of the major warriors of the immune system against foreign tissue. After [studying] 66 patients in which we studied interleukin-2 and cells that would develop from it, we finally saw a disappearance of melanoma in a patient that received interleukin-2. And we went on to treat hundreds of patients with that hormone, interleukin-2. In fact, interleukin-2 became the first immunotherapy ever approved by the Food and Drug Administration for the treatment of cancer in humans.
How did this finding impact your future discoveries?
Dr. Rosenberg: [It] led to studies of the mechanism of action of interleukin-2 and to do that, we identified a kind of cell called a tumor infiltrating lymphocyte. What better place, intuitively to look for cells doing battle against the cancer than within the cancer itself?
In 1988, we demonstrated for the first time that transfer of lymphocytes with antitumor activity could cause the regression of melanoma. This was a living drug obtained from melanoma deposits that could be grown outside the body and then readministered to the patient under suitable conditions. Interestingly, [in February the FDA approved that drug as treatment for patients with melanoma]. A company developed it to the point where in multi-institutional studies, they reproduced our results.
And we’ve now emphasized the value of using T cell therapy, t cell transfer, for the treatment of patients with the common solid cancers, the cancers that start anywhere from the colon up through the intestine, the stomach, the pancreas, and the esophagus. Solid tumors such as ovarian cancer, uterine cancer and so on, are also potentially susceptible to this T cell therapy.
We’ve published several papers showing in isolated patients that you could cause major regressions, if not complete regressions, of these solid cancers in the liver, in the breast, the cervix, the colon. That’s a major aspect of what we’re doing now.
I think immunotherapy has come to be recognized as a major fourth arm that can be used to attack cancers, adding to surgery, radiation, and chemotherapy.
What guidance would you have for other physician-investigators or young doctors who want to follow in your path?
Dr. Rosenberg: You have to have a broad base of knowledge. You have to be willing to immerse yourself in a problem so that your mind is working on it when you’re doing things where you can only think. [When] you’re taking a shower, [or] waiting at a red light, your mind is working on this problem because you’re immersed in trying to understand it.
You need to have a laser focus on the goals that you have and not get sidetracked by issues that may be interesting but not directly related to the goals that you’re attempting to achieve.
His pioneering research established interleukin-2 (IL-2) as the first U.S. Food and Drug Administration–approved cancer immunotherapy in 1992.
To recognize his trailblazing work and other achievements, the American Association for Cancer Research (AACR) will award Dr. Rosenberg with the 2024 AACR Award for Lifetime Achievement in Cancer Research at its annual meeting in April.
Dr. Rosenberg, a senior investigator for the Center for Cancer Research at the National Cancer Institute (NCI), and chief of the NCI Surgery Branch, shared the history behind his novel research and the patient stories that inspired his discoveries, during an interview.
Tell us a little about yourself and where you grew up.
Dr. Rosenberg: I grew up in the Bronx. My parents both immigrated to the United States from Poland as teenagers.
As a young boy, did you always want to become a doctor?
Dr. Rosenberg: I think some defining moments on why I decided to go into medicine occurred when I was 6 or 7 years old. The second world war was over, and many of the horrors of the Holocaust became apparent to me. I was brought up as an Orthodox Jew. My parents were quite religious, and I remember postcards coming in one after another about relatives that had died in the death camps. That had a profound influence on me.
How did that experience impact your aspirations?
Dr. Rosenberg: It was an example to me of how evil certain people and groups can be toward one another. I decided at that point, that I wanted to do something good for people, and medicine seemed the most likely way to do that. But also, I was developing a broad scientific interest. I ended up at the Bronx High School of Science and knew that I not only wanted to practice the medicine of today, but I wanted to play a role in helping develop the medicine.
What led to your interest in cancer treatment?
Dr. Rosenberg: Well, as a medical student and resident, it became clear that the field of cancer needed major improvement. We had three major ways to treat cancer: surgery, radiation therapy, and chemotherapy. That could cure about half of the people [who] had cancer. But despite the best application of those three specialties, there were over 600,000 deaths from cancer each year in the United States alone. It was clear to me that new approaches were needed, and I became very interested in taking advantage of the body’s immune system as a source of information to try to make progress.
Were there patients who inspired your research?
Dr. Rosenberg: There were two patients that I saw early in my career that impressed me a great deal. One was a patient that I saw when working in the emergency ward as a resident. A patient came in with right upper quadrant pain that looked like a gallbladder attack. That’s what it was. But when I went through his chart, I saw that he had been at that hospital 12 years earlier with a metastatic gastric cancer. The surgeons had operated. They saw tumor had spread to the liver and could not be removed. They closed the belly, not expecting him to survive. Yet he kept showing up for follow-up visits.
Here he was 12 years later. When I helped operate to take out his gallbladder, there was no evidence of any cancer. The cancer had disappeared in the absence of any external treatment. One of the rarest events in medicine, the spontaneous regression of a cancer. Somehow his body had learned how to destroy the tumor.
Was the second patient’s case as impressive?
Dr. Rosenberg: This patient had received a kidney transplant from a gentleman who died in an auto accident. [The donor’s] kidney contained a cancer deposit, a kidney cancer, unbeknownst to the transplant surgeons. [When the kidney was transplanted], the recipient developed widespread metastatic kidney cancer.
[The recipient] was on immunosuppressive drugs, and so the drugs had to be stopped. [When the immunosuppressive drugs were stopped], the patient’s body rejected the kidney and his cancer disappeared.
That showed me that, in fact, if you could stimulate a strong enough immune reaction, in this case, an [allogeneic] reaction, against foreign tissues from a different individual, that you could make large vascularized, invasive cancers disappear based on immune reactivities. Those were clues that led me toward studying the immune system’s impact on cancer.
From there, how did your work evolve?
Dr. Rosenberg: As chief of the surgery branch at NIH, I began doing research. It was very difficult to manipulate immune cells in the laboratory. They wouldn’t stay alive. But I tried to study immune reactions in patients with cancer to see if there was such a thing as an immune reaction against the cancer. There was no such thing known at the time. There were no cancer antigens and no known immune reactions against the disease in the human.
Around this time, investigators were publishing studies about interleukin-2 (IL-2), or white blood cells known as leukocytes. How did interleukin-2 further your research?
Dr. Rosenberg: The advent of interleukin-2 enabled scientists to grow lymphocytes outside the body. [This] enabled us to grow t-lymphocytes, which are some of the major warriors of the immune system against foreign tissue. After [studying] 66 patients in which we studied interleukin-2 and cells that would develop from it, we finally saw a disappearance of melanoma in a patient that received interleukin-2. And we went on to treat hundreds of patients with that hormone, interleukin-2. In fact, interleukin-2 became the first immunotherapy ever approved by the Food and Drug Administration for the treatment of cancer in humans.
How did this finding impact your future discoveries?
Dr. Rosenberg: [It] led to studies of the mechanism of action of interleukin-2 and to do that, we identified a kind of cell called a tumor infiltrating lymphocyte. What better place, intuitively to look for cells doing battle against the cancer than within the cancer itself?
In 1988, we demonstrated for the first time that transfer of lymphocytes with antitumor activity could cause the regression of melanoma. This was a living drug obtained from melanoma deposits that could be grown outside the body and then readministered to the patient under suitable conditions. Interestingly, [in February the FDA approved that drug as treatment for patients with melanoma]. A company developed it to the point where in multi-institutional studies, they reproduced our results.
And we’ve now emphasized the value of using T cell therapy, t cell transfer, for the treatment of patients with the common solid cancers, the cancers that start anywhere from the colon up through the intestine, the stomach, the pancreas, and the esophagus. Solid tumors such as ovarian cancer, uterine cancer and so on, are also potentially susceptible to this T cell therapy.
We’ve published several papers showing in isolated patients that you could cause major regressions, if not complete regressions, of these solid cancers in the liver, in the breast, the cervix, the colon. That’s a major aspect of what we’re doing now.
I think immunotherapy has come to be recognized as a major fourth arm that can be used to attack cancers, adding to surgery, radiation, and chemotherapy.
What guidance would you have for other physician-investigators or young doctors who want to follow in your path?
Dr. Rosenberg: You have to have a broad base of knowledge. You have to be willing to immerse yourself in a problem so that your mind is working on it when you’re doing things where you can only think. [When] you’re taking a shower, [or] waiting at a red light, your mind is working on this problem because you’re immersed in trying to understand it.
You need to have a laser focus on the goals that you have and not get sidetracked by issues that may be interesting but not directly related to the goals that you’re attempting to achieve.
His pioneering research established interleukin-2 (IL-2) as the first U.S. Food and Drug Administration–approved cancer immunotherapy in 1992.
To recognize his trailblazing work and other achievements, the American Association for Cancer Research (AACR) will award Dr. Rosenberg with the 2024 AACR Award for Lifetime Achievement in Cancer Research at its annual meeting in April.
Dr. Rosenberg, a senior investigator for the Center for Cancer Research at the National Cancer Institute (NCI), and chief of the NCI Surgery Branch, shared the history behind his novel research and the patient stories that inspired his discoveries, during an interview.
Tell us a little about yourself and where you grew up.
Dr. Rosenberg: I grew up in the Bronx. My parents both immigrated to the United States from Poland as teenagers.
As a young boy, did you always want to become a doctor?
Dr. Rosenberg: I think some defining moments on why I decided to go into medicine occurred when I was 6 or 7 years old. The second world war was over, and many of the horrors of the Holocaust became apparent to me. I was brought up as an Orthodox Jew. My parents were quite religious, and I remember postcards coming in one after another about relatives that had died in the death camps. That had a profound influence on me.
How did that experience impact your aspirations?
Dr. Rosenberg: It was an example to me of how evil certain people and groups can be toward one another. I decided at that point, that I wanted to do something good for people, and medicine seemed the most likely way to do that. But also, I was developing a broad scientific interest. I ended up at the Bronx High School of Science and knew that I not only wanted to practice the medicine of today, but I wanted to play a role in helping develop the medicine.
What led to your interest in cancer treatment?
Dr. Rosenberg: Well, as a medical student and resident, it became clear that the field of cancer needed major improvement. We had three major ways to treat cancer: surgery, radiation therapy, and chemotherapy. That could cure about half of the people [who] had cancer. But despite the best application of those three specialties, there were over 600,000 deaths from cancer each year in the United States alone. It was clear to me that new approaches were needed, and I became very interested in taking advantage of the body’s immune system as a source of information to try to make progress.
Were there patients who inspired your research?
Dr. Rosenberg: There were two patients that I saw early in my career that impressed me a great deal. One was a patient that I saw when working in the emergency ward as a resident. A patient came in with right upper quadrant pain that looked like a gallbladder attack. That’s what it was. But when I went through his chart, I saw that he had been at that hospital 12 years earlier with a metastatic gastric cancer. The surgeons had operated. They saw tumor had spread to the liver and could not be removed. They closed the belly, not expecting him to survive. Yet he kept showing up for follow-up visits.
Here he was 12 years later. When I helped operate to take out his gallbladder, there was no evidence of any cancer. The cancer had disappeared in the absence of any external treatment. One of the rarest events in medicine, the spontaneous regression of a cancer. Somehow his body had learned how to destroy the tumor.
Was the second patient’s case as impressive?
Dr. Rosenberg: This patient had received a kidney transplant from a gentleman who died in an auto accident. [The donor’s] kidney contained a cancer deposit, a kidney cancer, unbeknownst to the transplant surgeons. [When the kidney was transplanted], the recipient developed widespread metastatic kidney cancer.
[The recipient] was on immunosuppressive drugs, and so the drugs had to be stopped. [When the immunosuppressive drugs were stopped], the patient’s body rejected the kidney and his cancer disappeared.
That showed me that, in fact, if you could stimulate a strong enough immune reaction, in this case, an [allogeneic] reaction, against foreign tissues from a different individual, that you could make large vascularized, invasive cancers disappear based on immune reactivities. Those were clues that led me toward studying the immune system’s impact on cancer.
From there, how did your work evolve?
Dr. Rosenberg: As chief of the surgery branch at NIH, I began doing research. It was very difficult to manipulate immune cells in the laboratory. They wouldn’t stay alive. But I tried to study immune reactions in patients with cancer to see if there was such a thing as an immune reaction against the cancer. There was no such thing known at the time. There were no cancer antigens and no known immune reactions against the disease in the human.
Around this time, investigators were publishing studies about interleukin-2 (IL-2), or white blood cells known as leukocytes. How did interleukin-2 further your research?
Dr. Rosenberg: The advent of interleukin-2 enabled scientists to grow lymphocytes outside the body. [This] enabled us to grow t-lymphocytes, which are some of the major warriors of the immune system against foreign tissue. After [studying] 66 patients in which we studied interleukin-2 and cells that would develop from it, we finally saw a disappearance of melanoma in a patient that received interleukin-2. And we went on to treat hundreds of patients with that hormone, interleukin-2. In fact, interleukin-2 became the first immunotherapy ever approved by the Food and Drug Administration for the treatment of cancer in humans.
How did this finding impact your future discoveries?
Dr. Rosenberg: [It] led to studies of the mechanism of action of interleukin-2 and to do that, we identified a kind of cell called a tumor infiltrating lymphocyte. What better place, intuitively to look for cells doing battle against the cancer than within the cancer itself?
In 1988, we demonstrated for the first time that transfer of lymphocytes with antitumor activity could cause the regression of melanoma. This was a living drug obtained from melanoma deposits that could be grown outside the body and then readministered to the patient under suitable conditions. Interestingly, [in February the FDA approved that drug as treatment for patients with melanoma]. A company developed it to the point where in multi-institutional studies, they reproduced our results.
And we’ve now emphasized the value of using T cell therapy, t cell transfer, for the treatment of patients with the common solid cancers, the cancers that start anywhere from the colon up through the intestine, the stomach, the pancreas, and the esophagus. Solid tumors such as ovarian cancer, uterine cancer and so on, are also potentially susceptible to this T cell therapy.
We’ve published several papers showing in isolated patients that you could cause major regressions, if not complete regressions, of these solid cancers in the liver, in the breast, the cervix, the colon. That’s a major aspect of what we’re doing now.
I think immunotherapy has come to be recognized as a major fourth arm that can be used to attack cancers, adding to surgery, radiation, and chemotherapy.
What guidance would you have for other physician-investigators or young doctors who want to follow in your path?
Dr. Rosenberg: You have to have a broad base of knowledge. You have to be willing to immerse yourself in a problem so that your mind is working on it when you’re doing things where you can only think. [When] you’re taking a shower, [or] waiting at a red light, your mind is working on this problem because you’re immersed in trying to understand it.
You need to have a laser focus on the goals that you have and not get sidetracked by issues that may be interesting but not directly related to the goals that you’re attempting to achieve.
Paid Parental Leave: Impact on Maternal Mental Health and Child Wellbeing
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
New Research Dissects Transgenerational Obesity and Diabetes
FAIRFAX, VIRGINIA — Nearly 30 years ago, in a 1995 paper, the British physician-epidemiologist David Barker, MD, PhD, wrote about his fetal origins hypothesis — the idea that programs to address fetal undernutrition and low birth weight produced later coronary heart disease (BMJ 1995;311:171-4).
His hypothesis and subsequent research led to the concept of adult diseases of fetal origins, which today extends beyond low birth weight and implicates the in utero environment as a significant determinant of risk for adverse childhood and adult metabolic outcomes and for major chronic diseases, including diabetes and obesity. Studies have shown that the offspring of pregnant mothers with diabetes have a higher risk of developing obesity and diabetes themselves.
“It’s a whole discipline [of research],” E. Albert Reece, MD, PhD, MBA, of the University of Maryland School of Medicine (UMSOM), said in an interview. “But what we’ve never quite understood is the ‘how’ and ‘why’? What are the mechanisms driving the fetal origins of such adverse outcomes in offspring?
At the biennial meeting of the Diabetes in Pregnancy Study Group of North America (DPSG), investigators described studies underway that are digging deeper into the associations between the intrauterine milieu and longer-term offspring health — and that are searching for biological and molecular processes that may be involved.
The studies are like “branches of the Barker hypothesis,” said Dr. Reece, former dean of UMSOM and current director of the UMSOM Center for Advanced Research Training and Innovation, who co-organized the DPSG meeting. “They’re taking the hypothesis and dissecting it by asking, for instance, it is possible that transgenerational obesity may align with the Barker hypothesis? Is it possible that it involves epigenetics regulation? Could we find biomarkers?”
The need for a better understanding of the fetal origins framework — and its subsequent transgenerational impact — is urgent. From 2000 to 2018, the prevalence of childhood obesity increased from 14.7% to 19.2% (a 31% increase) and the prevalence of severe childhood obesity rose from 3.9% to 6.1% (a 56% increase), according to data from the U.S. National Health and Nutrition Examination Survey (Obes Facts. 2022;15[4]:560-9).
Children aged 2-5 years have had an especially sharp increase in obesity (Pediatrics 2018;141[3]:e20173459), Christine Wey Hockett, PhD, of the University of South Dakota School of Medicine, said at the DPSG meeting (Figure 1).
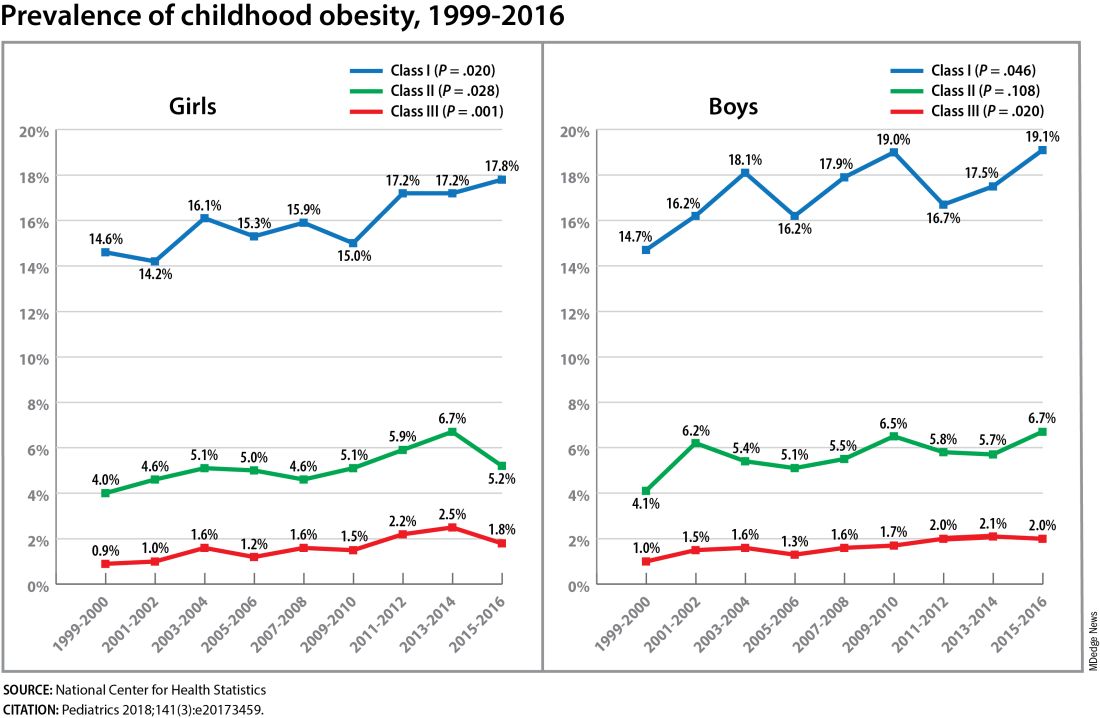
Also notable, she said, is that one-quarter of today’s pediatric diabetes cases are type 2 diabetes, which “is significant as there is a higher prevalence of early complications and comorbidities in youth with type 2 diabetes compared to type 1 diabetes.”
Moreover, recent projections estimate that 57% of today’s children will be obese at 35 years of age (N Engl J Med. 2017;377[22]:2145-53) and that 45% will have diabetes or prediabetes by 2030 (Popul Health Manag. 2017;20[1]:6-12), said Dr. Hockett, assistant professor in the university’s department of pediatrics. An investigator of the Exploring Perinatal Outcomes Among Children (EPOCH) study, which looked at gestational diabetes (GDM) and offspring cardiometabolic risks, she said more chronic disease “at increasingly younger ages [points toward] prebirth influences.”
She noted that there are critical periods postnatally — such as infancy and puberty — that can “impact or further shift the trajectory of chronic disease.” The developmental origins theory posits that life events and biological and environmental processes during the lifespan can modify the effects of intrauterine exposures.
The transgenerational implications “are clear,” she said. “As the number of reproductive-aged individuals with chronic diseases rises, the number of exposed offspring also rises ... It leads to a vicious cycle.”
Deeper Dives Into Associations, Potential Mechanisms
The EPOCH prospective cohort study with which Dr. Hockett was involved gave her a front-seat view of the transgenerational adverse effects of in utero exposure to hyperglycemia. The study recruited ethnically diverse maternal/child dyads from the Kaiser Permanente of Colorado perinatal database from 1992 to 2002 and assessed 418 offspring at two points — a mean age of 10.5 years and 16.5 years — for fasting blood glucose, adiposity, and diet and physical activity. The second visit also involved an oral glucose tolerance test.
The 77 offspring who had been exposed in utero to GDM had a homeostatic model assessment of insulin resistance (HOMA-IR) that was 18% higher, a 19% lower Matsuda index, and a 9% greater HOMA of β-cell function (HOMA-β) than the 341 offspring whose mothers did not have diabetes. Each 5-kg/m2 increase in prepregnancy body mass index predicted increased insulin resistance, but there was no combined effect of both maternal obesity and diabetes in utero.
Exposed offspring had a higher BMI and increased adiposity, but when BMI was controlled for in the analysis of metabolic outcomes, maternal diabetes was still associated with 12% higher HOMA-IR and a 17% lower Matsuda index. “So [the metabolic outcomes] are a direct effect of maternal diabetes,” Dr. Hockett said at the DPSG meeting, noting the fetal overnutrition hypothesis in which maternal glucose, but not maternal insulin, freely passes through the placenta, promoting growth and adiposity in the fetus.
[The EPOCH results on metabolic outcomes and offspring adiposity were published in 2017 and 2019, respectively (Diabet Med. 2017;34:1392-9; Diabetologia. 2019;62:2017-24). In 2020, EPOCH researchers reported sex-specific effects on cardiovascular outcomes, with GDM exposure associated with higher total and LDL cholesterol in girls and higher systolic blood pressure in boys (Pediatr Obes. 2020;15[5]:e12611).]
Now, a new longitudinal cohort study underway in Phoenix, is taking a deeper dive, trying to pinpoint what exactly influences childhood obesity and metabolic risk by following Hispanic and American Indian maternal/child dyads from pregnancy until 18 years postpartum. Researchers are looking not only at associations between maternal risk factors (pregnancy BMI, gestational weight gain, and diabetes in pregnancy) and offspring BMI, adiposity, and growth patterns, but also how various factors during pregnancy — clinical, genetic, lifestyle, biochemical — ”may mediate the associations,” said lead investigator Madhumita Sinha, MD.
“We need a better understanding at the molecular level of the biological processes that lead to obesity in children and that cause metabolic dysfunction,” said Dr. Sinha, who heads the Diabetes Epidemiology and Clinical Research Section of the of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) branch in Phoenix.
The populations being enrolled in the ETCHED study (for Early Tracking of Childhood Health Determinants) are at especially high risk of childhood obesity and metabolic dysfunction. Research conducted decades ago by the NIDDK in Phoenix showed that approximately 50% of Pima Indian children from diabetic pregnancies develop type 2 diabetes by age 25 (N Engl J Med. 1983;308:242-5). Years later, to tease out possible genetic factors, researchers compared siblings born before and after their mother was found to have type 2 diabetes, and found significantly higher rates of diabetes in those born after the mother’s diagnosis, affirming the role of in utero toxicity (Diabetes 2000;49:2208-11).
In the new study, the researchers will look at adipokines and inflammatory biomarkers in the mothers and offspring in addition to traditional anthropometric and glycemic measures. They’ll analyze placental tissue, breast milk, and the gut microbiome longitudinally, and they’ll lean heavily on genomics/epigenomics, proteomics, and metabolomics. “There’s potential,” Dr. Sinha said, “to develop a more accurate predictive and prognostic model of childhood obesity.”
The researchers also will study the role of family, socioeconomics, and environmental factors in influencing child growth patterns and they’ll look at neurodevelopment in infancy and childhood. As of October 2023, almost 80 pregnant women, most with obesity and almost one-third with type 2 diabetes, had enrolled in the study. Over the next several years, the study aims to enroll 750 dyads.
The Timing of In Utero Exposure
Shelley Ehrlich, MD, ScD, MPH, of the University of Cincinnati and Cincinnati Children’s Hospital Medical Center, is aiming, meanwhile, to learn how the timing of in utero exposure to hyperglycemia predicts specific metabolic and cardiovascular morbidities in the adult offspring of diabetic mothers.
“While we know that exposure to maternal diabetes, regardless of type, increases the risk of obesity, insulin resistance, diabetes, renal compromise, and cardiovascular disease in the offspring, there is little known about the level and timing of hyperglycemic exposure during fetal development that triggers these adverse outcomes,” said Dr. Ehrlich. A goal, she said, is to identify gestational profiles that predict phenotypes of offspring at risk for morbidity in later life.
She and other investigators with the TEAM (Transgenerational Effect on Adult Morbidity) study have recruited over 170 offspring of mothers who participated in the Diabetes in Pregnancy Program Project Grant (PPG) at the University of Cincinnati Medical Center from 1978 to 1995 — a landmark study that demonstrated the effect of strict glucose control in reducing major congenital malformations.
The women in the PPG study had frequent glucose monitoring (up to 6-8 times a day) throughout their pregnancies, and now, their recruited offspring, who are up to 43 years of age, are being assessed for obesity, diabetes/metabolic health, cardiovascular disease/cardiac and peripheral vascular structure and function, and other outcomes including those that may be amenable to secondary prevention (J Diabetes Res. Nov 1;2021:6590431).
Preliminary findings from over 170 offspring recruited between 2017 and 2022 suggest that in utero exposure to dysglycemia (as measured by standard deviations of glycohemoglobin) in the third trimester appears to increase the risk of morbid obesity in adulthood, while exposure to dysglycemia in the first trimester increases the risk of impaired glucose tolerance. The risk of B-cell dysfunction, meanwhile, appears to be linked to dysglycemia in the first and third trimesters — particularly the first — Dr. Ehrlich reported.
Cognitive outcomes in offspring have also been assessed and here it appears that dysglycemia in the third trimester is linked to worse scores on the Wechsler Abbreviated Scale of Intelligence (WASI-II), said Katherine Bowers, PhD, MPH, a TEAM study coinvestigator, also of Cincinnati Children’s Hospital Medical Center.
“We’ve already observed [an association between] diabetes in pregnancy and cognition in early childhood and through adolescence, but [the question has been] does this association persist into adulthood?” she said.
Preliminary analyses of 104 offspring show no statistically significant associations between maternal dysglycemia in the first or second trimesters and offspring cognition, but “consistent inverse associations between maternal glycohemoglobin in the third trimester across two [WASI-II] subscales and composite measures of cognition,” Dr. Bowers said.
Their analysis adjusted for a variety of factors, including maternal age, prepregnancy and first trimester BMI, race, family history of diabetes, and diabetes severity/macrovascular complications.
Back In The Laboratory
At the other end of the research spectrum, basic research scientists are also investigating the mechanisms and sequelae of in utero hyperglycemia and other injuries, including congenital malformations, placental adaptive responses and fetal programming. Researchers are asking, for instance, what does placental metabolic reprogramming entail? What role do placental extracellular vesicles play in GDM? Can we alter the in utero environment and thus improve the short and long-term fetal/infant outcomes?
Animal research done at the UMSOM Center for Birth Defects Research, led by Dr. Reece and Peixin Yang, PhD, suggests that “a good portion of in utero injury is due to epigenetics,” Dr. Reece said in the interview. “We’ve shown that under conditions of hyperglycemia, for example, genetic regulation and genetic function can be altered.”
Through in vivo research, they have also shown that antioxidants or membrane stabilizers such as arachidonic acid or myo-inositol, or experimental inhibitors to certain pro-apoptotic intermediates, can individually or collectively result in reduced malformations. “It is highly likely that understanding the biological impact of various altered in utero environments, and then modifying or reversing those environments, will result in short and long-term outcome improvements similar to those shown with congenital malformations,” Dr. Reece said.
FAIRFAX, VIRGINIA — Nearly 30 years ago, in a 1995 paper, the British physician-epidemiologist David Barker, MD, PhD, wrote about his fetal origins hypothesis — the idea that programs to address fetal undernutrition and low birth weight produced later coronary heart disease (BMJ 1995;311:171-4).
His hypothesis and subsequent research led to the concept of adult diseases of fetal origins, which today extends beyond low birth weight and implicates the in utero environment as a significant determinant of risk for adverse childhood and adult metabolic outcomes and for major chronic diseases, including diabetes and obesity. Studies have shown that the offspring of pregnant mothers with diabetes have a higher risk of developing obesity and diabetes themselves.
“It’s a whole discipline [of research],” E. Albert Reece, MD, PhD, MBA, of the University of Maryland School of Medicine (UMSOM), said in an interview. “But what we’ve never quite understood is the ‘how’ and ‘why’? What are the mechanisms driving the fetal origins of such adverse outcomes in offspring?
At the biennial meeting of the Diabetes in Pregnancy Study Group of North America (DPSG), investigators described studies underway that are digging deeper into the associations between the intrauterine milieu and longer-term offspring health — and that are searching for biological and molecular processes that may be involved.
The studies are like “branches of the Barker hypothesis,” said Dr. Reece, former dean of UMSOM and current director of the UMSOM Center for Advanced Research Training and Innovation, who co-organized the DPSG meeting. “They’re taking the hypothesis and dissecting it by asking, for instance, it is possible that transgenerational obesity may align with the Barker hypothesis? Is it possible that it involves epigenetics regulation? Could we find biomarkers?”
The need for a better understanding of the fetal origins framework — and its subsequent transgenerational impact — is urgent. From 2000 to 2018, the prevalence of childhood obesity increased from 14.7% to 19.2% (a 31% increase) and the prevalence of severe childhood obesity rose from 3.9% to 6.1% (a 56% increase), according to data from the U.S. National Health and Nutrition Examination Survey (Obes Facts. 2022;15[4]:560-9).
Children aged 2-5 years have had an especially sharp increase in obesity (Pediatrics 2018;141[3]:e20173459), Christine Wey Hockett, PhD, of the University of South Dakota School of Medicine, said at the DPSG meeting (Figure 1).

Also notable, she said, is that one-quarter of today’s pediatric diabetes cases are type 2 diabetes, which “is significant as there is a higher prevalence of early complications and comorbidities in youth with type 2 diabetes compared to type 1 diabetes.”
Moreover, recent projections estimate that 57% of today’s children will be obese at 35 years of age (N Engl J Med. 2017;377[22]:2145-53) and that 45% will have diabetes or prediabetes by 2030 (Popul Health Manag. 2017;20[1]:6-12), said Dr. Hockett, assistant professor in the university’s department of pediatrics. An investigator of the Exploring Perinatal Outcomes Among Children (EPOCH) study, which looked at gestational diabetes (GDM) and offspring cardiometabolic risks, she said more chronic disease “at increasingly younger ages [points toward] prebirth influences.”
She noted that there are critical periods postnatally — such as infancy and puberty — that can “impact or further shift the trajectory of chronic disease.” The developmental origins theory posits that life events and biological and environmental processes during the lifespan can modify the effects of intrauterine exposures.
The transgenerational implications “are clear,” she said. “As the number of reproductive-aged individuals with chronic diseases rises, the number of exposed offspring also rises ... It leads to a vicious cycle.”
Deeper Dives Into Associations, Potential Mechanisms
The EPOCH prospective cohort study with which Dr. Hockett was involved gave her a front-seat view of the transgenerational adverse effects of in utero exposure to hyperglycemia. The study recruited ethnically diverse maternal/child dyads from the Kaiser Permanente of Colorado perinatal database from 1992 to 2002 and assessed 418 offspring at two points — a mean age of 10.5 years and 16.5 years — for fasting blood glucose, adiposity, and diet and physical activity. The second visit also involved an oral glucose tolerance test.
The 77 offspring who had been exposed in utero to GDM had a homeostatic model assessment of insulin resistance (HOMA-IR) that was 18% higher, a 19% lower Matsuda index, and a 9% greater HOMA of β-cell function (HOMA-β) than the 341 offspring whose mothers did not have diabetes. Each 5-kg/m2 increase in prepregnancy body mass index predicted increased insulin resistance, but there was no combined effect of both maternal obesity and diabetes in utero.
Exposed offspring had a higher BMI and increased adiposity, but when BMI was controlled for in the analysis of metabolic outcomes, maternal diabetes was still associated with 12% higher HOMA-IR and a 17% lower Matsuda index. “So [the metabolic outcomes] are a direct effect of maternal diabetes,” Dr. Hockett said at the DPSG meeting, noting the fetal overnutrition hypothesis in which maternal glucose, but not maternal insulin, freely passes through the placenta, promoting growth and adiposity in the fetus.
[The EPOCH results on metabolic outcomes and offspring adiposity were published in 2017 and 2019, respectively (Diabet Med. 2017;34:1392-9; Diabetologia. 2019;62:2017-24). In 2020, EPOCH researchers reported sex-specific effects on cardiovascular outcomes, with GDM exposure associated with higher total and LDL cholesterol in girls and higher systolic blood pressure in boys (Pediatr Obes. 2020;15[5]:e12611).]
Now, a new longitudinal cohort study underway in Phoenix, is taking a deeper dive, trying to pinpoint what exactly influences childhood obesity and metabolic risk by following Hispanic and American Indian maternal/child dyads from pregnancy until 18 years postpartum. Researchers are looking not only at associations between maternal risk factors (pregnancy BMI, gestational weight gain, and diabetes in pregnancy) and offspring BMI, adiposity, and growth patterns, but also how various factors during pregnancy — clinical, genetic, lifestyle, biochemical — ”may mediate the associations,” said lead investigator Madhumita Sinha, MD.
“We need a better understanding at the molecular level of the biological processes that lead to obesity in children and that cause metabolic dysfunction,” said Dr. Sinha, who heads the Diabetes Epidemiology and Clinical Research Section of the of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) branch in Phoenix.
The populations being enrolled in the ETCHED study (for Early Tracking of Childhood Health Determinants) are at especially high risk of childhood obesity and metabolic dysfunction. Research conducted decades ago by the NIDDK in Phoenix showed that approximately 50% of Pima Indian children from diabetic pregnancies develop type 2 diabetes by age 25 (N Engl J Med. 1983;308:242-5). Years later, to tease out possible genetic factors, researchers compared siblings born before and after their mother was found to have type 2 diabetes, and found significantly higher rates of diabetes in those born after the mother’s diagnosis, affirming the role of in utero toxicity (Diabetes 2000;49:2208-11).
In the new study, the researchers will look at adipokines and inflammatory biomarkers in the mothers and offspring in addition to traditional anthropometric and glycemic measures. They’ll analyze placental tissue, breast milk, and the gut microbiome longitudinally, and they’ll lean heavily on genomics/epigenomics, proteomics, and metabolomics. “There’s potential,” Dr. Sinha said, “to develop a more accurate predictive and prognostic model of childhood obesity.”
The researchers also will study the role of family, socioeconomics, and environmental factors in influencing child growth patterns and they’ll look at neurodevelopment in infancy and childhood. As of October 2023, almost 80 pregnant women, most with obesity and almost one-third with type 2 diabetes, had enrolled in the study. Over the next several years, the study aims to enroll 750 dyads.
The Timing of In Utero Exposure
Shelley Ehrlich, MD, ScD, MPH, of the University of Cincinnati and Cincinnati Children’s Hospital Medical Center, is aiming, meanwhile, to learn how the timing of in utero exposure to hyperglycemia predicts specific metabolic and cardiovascular morbidities in the adult offspring of diabetic mothers.
“While we know that exposure to maternal diabetes, regardless of type, increases the risk of obesity, insulin resistance, diabetes, renal compromise, and cardiovascular disease in the offspring, there is little known about the level and timing of hyperglycemic exposure during fetal development that triggers these adverse outcomes,” said Dr. Ehrlich. A goal, she said, is to identify gestational profiles that predict phenotypes of offspring at risk for morbidity in later life.
She and other investigators with the TEAM (Transgenerational Effect on Adult Morbidity) study have recruited over 170 offspring of mothers who participated in the Diabetes in Pregnancy Program Project Grant (PPG) at the University of Cincinnati Medical Center from 1978 to 1995 — a landmark study that demonstrated the effect of strict glucose control in reducing major congenital malformations.
The women in the PPG study had frequent glucose monitoring (up to 6-8 times a day) throughout their pregnancies, and now, their recruited offspring, who are up to 43 years of age, are being assessed for obesity, diabetes/metabolic health, cardiovascular disease/cardiac and peripheral vascular structure and function, and other outcomes including those that may be amenable to secondary prevention (J Diabetes Res. Nov 1;2021:6590431).
Preliminary findings from over 170 offspring recruited between 2017 and 2022 suggest that in utero exposure to dysglycemia (as measured by standard deviations of glycohemoglobin) in the third trimester appears to increase the risk of morbid obesity in adulthood, while exposure to dysglycemia in the first trimester increases the risk of impaired glucose tolerance. The risk of B-cell dysfunction, meanwhile, appears to be linked to dysglycemia in the first and third trimesters — particularly the first — Dr. Ehrlich reported.
Cognitive outcomes in offspring have also been assessed and here it appears that dysglycemia in the third trimester is linked to worse scores on the Wechsler Abbreviated Scale of Intelligence (WASI-II), said Katherine Bowers, PhD, MPH, a TEAM study coinvestigator, also of Cincinnati Children’s Hospital Medical Center.
“We’ve already observed [an association between] diabetes in pregnancy and cognition in early childhood and through adolescence, but [the question has been] does this association persist into adulthood?” she said.
Preliminary analyses of 104 offspring show no statistically significant associations between maternal dysglycemia in the first or second trimesters and offspring cognition, but “consistent inverse associations between maternal glycohemoglobin in the third trimester across two [WASI-II] subscales and composite measures of cognition,” Dr. Bowers said.
Their analysis adjusted for a variety of factors, including maternal age, prepregnancy and first trimester BMI, race, family history of diabetes, and diabetes severity/macrovascular complications.
Back In The Laboratory
At the other end of the research spectrum, basic research scientists are also investigating the mechanisms and sequelae of in utero hyperglycemia and other injuries, including congenital malformations, placental adaptive responses and fetal programming. Researchers are asking, for instance, what does placental metabolic reprogramming entail? What role do placental extracellular vesicles play in GDM? Can we alter the in utero environment and thus improve the short and long-term fetal/infant outcomes?
Animal research done at the UMSOM Center for Birth Defects Research, led by Dr. Reece and Peixin Yang, PhD, suggests that “a good portion of in utero injury is due to epigenetics,” Dr. Reece said in the interview. “We’ve shown that under conditions of hyperglycemia, for example, genetic regulation and genetic function can be altered.”
Through in vivo research, they have also shown that antioxidants or membrane stabilizers such as arachidonic acid or myo-inositol, or experimental inhibitors to certain pro-apoptotic intermediates, can individually or collectively result in reduced malformations. “It is highly likely that understanding the biological impact of various altered in utero environments, and then modifying or reversing those environments, will result in short and long-term outcome improvements similar to those shown with congenital malformations,” Dr. Reece said.
FAIRFAX, VIRGINIA — Nearly 30 years ago, in a 1995 paper, the British physician-epidemiologist David Barker, MD, PhD, wrote about his fetal origins hypothesis — the idea that programs to address fetal undernutrition and low birth weight produced later coronary heart disease (BMJ 1995;311:171-4).
His hypothesis and subsequent research led to the concept of adult diseases of fetal origins, which today extends beyond low birth weight and implicates the in utero environment as a significant determinant of risk for adverse childhood and adult metabolic outcomes and for major chronic diseases, including diabetes and obesity. Studies have shown that the offspring of pregnant mothers with diabetes have a higher risk of developing obesity and diabetes themselves.
“It’s a whole discipline [of research],” E. Albert Reece, MD, PhD, MBA, of the University of Maryland School of Medicine (UMSOM), said in an interview. “But what we’ve never quite understood is the ‘how’ and ‘why’? What are the mechanisms driving the fetal origins of such adverse outcomes in offspring?
At the biennial meeting of the Diabetes in Pregnancy Study Group of North America (DPSG), investigators described studies underway that are digging deeper into the associations between the intrauterine milieu and longer-term offspring health — and that are searching for biological and molecular processes that may be involved.
The studies are like “branches of the Barker hypothesis,” said Dr. Reece, former dean of UMSOM and current director of the UMSOM Center for Advanced Research Training and Innovation, who co-organized the DPSG meeting. “They’re taking the hypothesis and dissecting it by asking, for instance, it is possible that transgenerational obesity may align with the Barker hypothesis? Is it possible that it involves epigenetics regulation? Could we find biomarkers?”
The need for a better understanding of the fetal origins framework — and its subsequent transgenerational impact — is urgent. From 2000 to 2018, the prevalence of childhood obesity increased from 14.7% to 19.2% (a 31% increase) and the prevalence of severe childhood obesity rose from 3.9% to 6.1% (a 56% increase), according to data from the U.S. National Health and Nutrition Examination Survey (Obes Facts. 2022;15[4]:560-9).
Children aged 2-5 years have had an especially sharp increase in obesity (Pediatrics 2018;141[3]:e20173459), Christine Wey Hockett, PhD, of the University of South Dakota School of Medicine, said at the DPSG meeting (Figure 1).

Also notable, she said, is that one-quarter of today’s pediatric diabetes cases are type 2 diabetes, which “is significant as there is a higher prevalence of early complications and comorbidities in youth with type 2 diabetes compared to type 1 diabetes.”
Moreover, recent projections estimate that 57% of today’s children will be obese at 35 years of age (N Engl J Med. 2017;377[22]:2145-53) and that 45% will have diabetes or prediabetes by 2030 (Popul Health Manag. 2017;20[1]:6-12), said Dr. Hockett, assistant professor in the university’s department of pediatrics. An investigator of the Exploring Perinatal Outcomes Among Children (EPOCH) study, which looked at gestational diabetes (GDM) and offspring cardiometabolic risks, she said more chronic disease “at increasingly younger ages [points toward] prebirth influences.”
She noted that there are critical periods postnatally — such as infancy and puberty — that can “impact or further shift the trajectory of chronic disease.” The developmental origins theory posits that life events and biological and environmental processes during the lifespan can modify the effects of intrauterine exposures.
The transgenerational implications “are clear,” she said. “As the number of reproductive-aged individuals with chronic diseases rises, the number of exposed offspring also rises ... It leads to a vicious cycle.”
Deeper Dives Into Associations, Potential Mechanisms
The EPOCH prospective cohort study with which Dr. Hockett was involved gave her a front-seat view of the transgenerational adverse effects of in utero exposure to hyperglycemia. The study recruited ethnically diverse maternal/child dyads from the Kaiser Permanente of Colorado perinatal database from 1992 to 2002 and assessed 418 offspring at two points — a mean age of 10.5 years and 16.5 years — for fasting blood glucose, adiposity, and diet and physical activity. The second visit also involved an oral glucose tolerance test.
The 77 offspring who had been exposed in utero to GDM had a homeostatic model assessment of insulin resistance (HOMA-IR) that was 18% higher, a 19% lower Matsuda index, and a 9% greater HOMA of β-cell function (HOMA-β) than the 341 offspring whose mothers did not have diabetes. Each 5-kg/m2 increase in prepregnancy body mass index predicted increased insulin resistance, but there was no combined effect of both maternal obesity and diabetes in utero.
Exposed offspring had a higher BMI and increased adiposity, but when BMI was controlled for in the analysis of metabolic outcomes, maternal diabetes was still associated with 12% higher HOMA-IR and a 17% lower Matsuda index. “So [the metabolic outcomes] are a direct effect of maternal diabetes,” Dr. Hockett said at the DPSG meeting, noting the fetal overnutrition hypothesis in which maternal glucose, but not maternal insulin, freely passes through the placenta, promoting growth and adiposity in the fetus.
[The EPOCH results on metabolic outcomes and offspring adiposity were published in 2017 and 2019, respectively (Diabet Med. 2017;34:1392-9; Diabetologia. 2019;62:2017-24). In 2020, EPOCH researchers reported sex-specific effects on cardiovascular outcomes, with GDM exposure associated with higher total and LDL cholesterol in girls and higher systolic blood pressure in boys (Pediatr Obes. 2020;15[5]:e12611).]
Now, a new longitudinal cohort study underway in Phoenix, is taking a deeper dive, trying to pinpoint what exactly influences childhood obesity and metabolic risk by following Hispanic and American Indian maternal/child dyads from pregnancy until 18 years postpartum. Researchers are looking not only at associations between maternal risk factors (pregnancy BMI, gestational weight gain, and diabetes in pregnancy) and offspring BMI, adiposity, and growth patterns, but also how various factors during pregnancy — clinical, genetic, lifestyle, biochemical — ”may mediate the associations,” said lead investigator Madhumita Sinha, MD.
“We need a better understanding at the molecular level of the biological processes that lead to obesity in children and that cause metabolic dysfunction,” said Dr. Sinha, who heads the Diabetes Epidemiology and Clinical Research Section of the of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) branch in Phoenix.
The populations being enrolled in the ETCHED study (for Early Tracking of Childhood Health Determinants) are at especially high risk of childhood obesity and metabolic dysfunction. Research conducted decades ago by the NIDDK in Phoenix showed that approximately 50% of Pima Indian children from diabetic pregnancies develop type 2 diabetes by age 25 (N Engl J Med. 1983;308:242-5). Years later, to tease out possible genetic factors, researchers compared siblings born before and after their mother was found to have type 2 diabetes, and found significantly higher rates of diabetes in those born after the mother’s diagnosis, affirming the role of in utero toxicity (Diabetes 2000;49:2208-11).
In the new study, the researchers will look at adipokines and inflammatory biomarkers in the mothers and offspring in addition to traditional anthropometric and glycemic measures. They’ll analyze placental tissue, breast milk, and the gut microbiome longitudinally, and they’ll lean heavily on genomics/epigenomics, proteomics, and metabolomics. “There’s potential,” Dr. Sinha said, “to develop a more accurate predictive and prognostic model of childhood obesity.”
The researchers also will study the role of family, socioeconomics, and environmental factors in influencing child growth patterns and they’ll look at neurodevelopment in infancy and childhood. As of October 2023, almost 80 pregnant women, most with obesity and almost one-third with type 2 diabetes, had enrolled in the study. Over the next several years, the study aims to enroll 750 dyads.
The Timing of In Utero Exposure
Shelley Ehrlich, MD, ScD, MPH, of the University of Cincinnati and Cincinnati Children’s Hospital Medical Center, is aiming, meanwhile, to learn how the timing of in utero exposure to hyperglycemia predicts specific metabolic and cardiovascular morbidities in the adult offspring of diabetic mothers.
“While we know that exposure to maternal diabetes, regardless of type, increases the risk of obesity, insulin resistance, diabetes, renal compromise, and cardiovascular disease in the offspring, there is little known about the level and timing of hyperglycemic exposure during fetal development that triggers these adverse outcomes,” said Dr. Ehrlich. A goal, she said, is to identify gestational profiles that predict phenotypes of offspring at risk for morbidity in later life.
She and other investigators with the TEAM (Transgenerational Effect on Adult Morbidity) study have recruited over 170 offspring of mothers who participated in the Diabetes in Pregnancy Program Project Grant (PPG) at the University of Cincinnati Medical Center from 1978 to 1995 — a landmark study that demonstrated the effect of strict glucose control in reducing major congenital malformations.
The women in the PPG study had frequent glucose monitoring (up to 6-8 times a day) throughout their pregnancies, and now, their recruited offspring, who are up to 43 years of age, are being assessed for obesity, diabetes/metabolic health, cardiovascular disease/cardiac and peripheral vascular structure and function, and other outcomes including those that may be amenable to secondary prevention (J Diabetes Res. Nov 1;2021:6590431).
Preliminary findings from over 170 offspring recruited between 2017 and 2022 suggest that in utero exposure to dysglycemia (as measured by standard deviations of glycohemoglobin) in the third trimester appears to increase the risk of morbid obesity in adulthood, while exposure to dysglycemia in the first trimester increases the risk of impaired glucose tolerance. The risk of B-cell dysfunction, meanwhile, appears to be linked to dysglycemia in the first and third trimesters — particularly the first — Dr. Ehrlich reported.
Cognitive outcomes in offspring have also been assessed and here it appears that dysglycemia in the third trimester is linked to worse scores on the Wechsler Abbreviated Scale of Intelligence (WASI-II), said Katherine Bowers, PhD, MPH, a TEAM study coinvestigator, also of Cincinnati Children’s Hospital Medical Center.
“We’ve already observed [an association between] diabetes in pregnancy and cognition in early childhood and through adolescence, but [the question has been] does this association persist into adulthood?” she said.
Preliminary analyses of 104 offspring show no statistically significant associations between maternal dysglycemia in the first or second trimesters and offspring cognition, but “consistent inverse associations between maternal glycohemoglobin in the third trimester across two [WASI-II] subscales and composite measures of cognition,” Dr. Bowers said.
Their analysis adjusted for a variety of factors, including maternal age, prepregnancy and first trimester BMI, race, family history of diabetes, and diabetes severity/macrovascular complications.
Back In The Laboratory
At the other end of the research spectrum, basic research scientists are also investigating the mechanisms and sequelae of in utero hyperglycemia and other injuries, including congenital malformations, placental adaptive responses and fetal programming. Researchers are asking, for instance, what does placental metabolic reprogramming entail? What role do placental extracellular vesicles play in GDM? Can we alter the in utero environment and thus improve the short and long-term fetal/infant outcomes?
Animal research done at the UMSOM Center for Birth Defects Research, led by Dr. Reece and Peixin Yang, PhD, suggests that “a good portion of in utero injury is due to epigenetics,” Dr. Reece said in the interview. “We’ve shown that under conditions of hyperglycemia, for example, genetic regulation and genetic function can be altered.”
Through in vivo research, they have also shown that antioxidants or membrane stabilizers such as arachidonic acid or myo-inositol, or experimental inhibitors to certain pro-apoptotic intermediates, can individually or collectively result in reduced malformations. “It is highly likely that understanding the biological impact of various altered in utero environments, and then modifying or reversing those environments, will result in short and long-term outcome improvements similar to those shown with congenital malformations,” Dr. Reece said.
FROM DPSG-NA 2023
Web-Based Aid Educates Women on Tubal Sterilization
Although tubal sterilization is common, especially among those with lower income and education levels, misunderstandings persist about the reversibility of the procedure, and previous studies suggest that many pregnant individuals are not making well-informed decisions, wrote Sonya Borrero, MD, of the University of Pittsburgh, and colleagues.
In a study published in JAMA Network Open, the researchers randomized 350 pregnant individuals with Medicaid insurance to usual care or usual care plus a web-based decision aid in English or Spanish called MyDecision/MiDecisión that included written, audio, and video information about tubal sterilization. The tool also included an interactive table comparing tubal sterilization to other contraceptive options, exercises to clarify patients’ values, knowledge checks, and a final summary report.
The two primary outcomes were knowledge of tubal sterilization based on a 10-question true/false test and decisional conflict about contraceptive choices using the low-literacy Decision Conflict Scale. The participants ranged in age from 21 to 45 years, with a mean age of 29.7 years. Participants were randomized prior to 24 weeks’ gestation, and those in the intervention group completed the intervention immediately using a personal device or a university device in the clinical setting. Further assessments occurred by phone during the third trimester and at 3 months postpartum.
Participants in the decision aid group showed significantly greater knowledge of tubal sterilization compared with controls, with a mean of 76.5% correct responses to the knowledge questions, vs. 55.6% in the control group (P < .001). Decisional conflict scores also were significantly lower in the intervention group compared with controls (mean 12.7 vs. 18.7, P = .002).
The most dramatic knowledge gap related to permanence of tubal sterilization; 90.1% of participants in the intervention group answered correctly that the procedure is not easily reversible, compared to 39.3% of the controls. Similarly, 86.6% of the intervention group responded correctly that the tubes do not “come untied” spontaneously, vs. 33.7% of controls (P < .001 for both).
The findings were limited by several factors including the focus only on pregnant Medicaid patients, the presentation of the decision tool only at a point early in pregnancy, which may have been too soon for some participants to consider tubal sterilization, and a lack of data on long-term satisfaction or regret about tubal sterilization decisions, the researchers noted.
However, the knowledge differences between the intervention and control groups remained significant at the third trimester assessment, they said.
More research is needed in other populations and using other time points, but the current study results suggest that use of the MyDecision/MiDecisión tool in a real-world clinical setting at the actual time of decision-making could improve knowledge and inform patients’ choices, the researchers concluded. Improved patient education also could inform policy decisions about the potential elimination of the 30-day waiting period for sterilization procedures, they said.
The study was supported by the National Institute on Minority Health and Health Disparities. The researchers had no financial conflicts to disclose.
Although tubal sterilization is common, especially among those with lower income and education levels, misunderstandings persist about the reversibility of the procedure, and previous studies suggest that many pregnant individuals are not making well-informed decisions, wrote Sonya Borrero, MD, of the University of Pittsburgh, and colleagues.
In a study published in JAMA Network Open, the researchers randomized 350 pregnant individuals with Medicaid insurance to usual care or usual care plus a web-based decision aid in English or Spanish called MyDecision/MiDecisión that included written, audio, and video information about tubal sterilization. The tool also included an interactive table comparing tubal sterilization to other contraceptive options, exercises to clarify patients’ values, knowledge checks, and a final summary report.
The two primary outcomes were knowledge of tubal sterilization based on a 10-question true/false test and decisional conflict about contraceptive choices using the low-literacy Decision Conflict Scale. The participants ranged in age from 21 to 45 years, with a mean age of 29.7 years. Participants were randomized prior to 24 weeks’ gestation, and those in the intervention group completed the intervention immediately using a personal device or a university device in the clinical setting. Further assessments occurred by phone during the third trimester and at 3 months postpartum.
Participants in the decision aid group showed significantly greater knowledge of tubal sterilization compared with controls, with a mean of 76.5% correct responses to the knowledge questions, vs. 55.6% in the control group (P < .001). Decisional conflict scores also were significantly lower in the intervention group compared with controls (mean 12.7 vs. 18.7, P = .002).
The most dramatic knowledge gap related to permanence of tubal sterilization; 90.1% of participants in the intervention group answered correctly that the procedure is not easily reversible, compared to 39.3% of the controls. Similarly, 86.6% of the intervention group responded correctly that the tubes do not “come untied” spontaneously, vs. 33.7% of controls (P < .001 for both).
The findings were limited by several factors including the focus only on pregnant Medicaid patients, the presentation of the decision tool only at a point early in pregnancy, which may have been too soon for some participants to consider tubal sterilization, and a lack of data on long-term satisfaction or regret about tubal sterilization decisions, the researchers noted.
However, the knowledge differences between the intervention and control groups remained significant at the third trimester assessment, they said.
More research is needed in other populations and using other time points, but the current study results suggest that use of the MyDecision/MiDecisión tool in a real-world clinical setting at the actual time of decision-making could improve knowledge and inform patients’ choices, the researchers concluded. Improved patient education also could inform policy decisions about the potential elimination of the 30-day waiting period for sterilization procedures, they said.
The study was supported by the National Institute on Minority Health and Health Disparities. The researchers had no financial conflicts to disclose.
Although tubal sterilization is common, especially among those with lower income and education levels, misunderstandings persist about the reversibility of the procedure, and previous studies suggest that many pregnant individuals are not making well-informed decisions, wrote Sonya Borrero, MD, of the University of Pittsburgh, and colleagues.
In a study published in JAMA Network Open, the researchers randomized 350 pregnant individuals with Medicaid insurance to usual care or usual care plus a web-based decision aid in English or Spanish called MyDecision/MiDecisión that included written, audio, and video information about tubal sterilization. The tool also included an interactive table comparing tubal sterilization to other contraceptive options, exercises to clarify patients’ values, knowledge checks, and a final summary report.
The two primary outcomes were knowledge of tubal sterilization based on a 10-question true/false test and decisional conflict about contraceptive choices using the low-literacy Decision Conflict Scale. The participants ranged in age from 21 to 45 years, with a mean age of 29.7 years. Participants were randomized prior to 24 weeks’ gestation, and those in the intervention group completed the intervention immediately using a personal device or a university device in the clinical setting. Further assessments occurred by phone during the third trimester and at 3 months postpartum.
Participants in the decision aid group showed significantly greater knowledge of tubal sterilization compared with controls, with a mean of 76.5% correct responses to the knowledge questions, vs. 55.6% in the control group (P < .001). Decisional conflict scores also were significantly lower in the intervention group compared with controls (mean 12.7 vs. 18.7, P = .002).
The most dramatic knowledge gap related to permanence of tubal sterilization; 90.1% of participants in the intervention group answered correctly that the procedure is not easily reversible, compared to 39.3% of the controls. Similarly, 86.6% of the intervention group responded correctly that the tubes do not “come untied” spontaneously, vs. 33.7% of controls (P < .001 for both).
The findings were limited by several factors including the focus only on pregnant Medicaid patients, the presentation of the decision tool only at a point early in pregnancy, which may have been too soon for some participants to consider tubal sterilization, and a lack of data on long-term satisfaction or regret about tubal sterilization decisions, the researchers noted.
However, the knowledge differences between the intervention and control groups remained significant at the third trimester assessment, they said.
More research is needed in other populations and using other time points, but the current study results suggest that use of the MyDecision/MiDecisión tool in a real-world clinical setting at the actual time of decision-making could improve knowledge and inform patients’ choices, the researchers concluded. Improved patient education also could inform policy decisions about the potential elimination of the 30-day waiting period for sterilization procedures, they said.
The study was supported by the National Institute on Minority Health and Health Disparities. The researchers had no financial conflicts to disclose.
FROM JAMA NETWORK OPEN
QOL Not Harmed With Add-On Pembrolizumab in Cervical Cancer
according to patient-reported outcome analyses from the KEYNOTE-A18 trial.
Progression-free survival data from the trial, reported at the 2023 meeting of the European Society for Medical Oncology, showed a 30% reduction in the risk for progression (P =.002) with the addition of pembrolizumab vs placebo, as well as favorable overall survival trends, reported Leslie Randall, MD, with VCU Health in Richmond, Virginia. Now the new analyses bring the “voices of the patients from this large phase 3 study.”
“I think the data can put us at ease and give patients a measure of comfort because there was no detriment in the quality of life,” said Dr. Randall, who presented the data on March 17 at the Society of Gynecologic Oncology (SGO) 2024 conference.
The phase 3 KEYNOTE-A18 trial enrolled 1060 patients new to treatment who had either stage 1B2-2B disease with lymph node involvement or stage 3-4A disease. They were randomly allocated to receive pembrolizumab or placebo plus concurrent chemoradiotherapy.
Patient-reported outcome instruments used in the study were the European Organization for Research and Treatment of Cancer (EORTC) 30-item quality-of-life (QOL) core questionnaire (QLQ-C30), the EORTC cervical cancer–specific module (QLQ-CX24), and the EuroQol EQ-5D-5L visual analog scale (VAS).
Prespecified secondary study endpoints were changes from baseline to week 36 in QLQ-C30 global health status/QOL (GHS/QOL) and physical functioning, and the QLQ-CX24 symptom-experience scale.
At baseline, patient-reported outcome scores were similar between treatment groups. Patients in both treatment groups had an initial decrease in QLQ-C30 GHS/QOL and physical functioning subscale and EQ-5D-5L VAS scores at weeks 3 and 6, but these improved relative to baseline at week 12 and subsequent weeks.
A similar number of patients in the pembrolizumab and placebo groups had improved or stable scores for QLQ-C30 GHS/QOL (76% vs 75%), QLQ-C30 physical functioning (77% vs 77%), QLQ-CX24 symptom experience (85% vs 85%) and EQ-5D-5L VAS (73% vs 76%).
Across all QOL instruments evaluated, there were no meaningful differences in patient-reported outcomes among patients who received pembrolizumab compared with those who received placebo, said Dr. Randall.
The improvement in progression-free survival, coupled with the patient-reported outcomes showing no additional harms to quality of life, support pembrolizumab plus concurrent chemoradiotherapy as a “new standard of care” for patients with high-risk locally advanced cervical cancer, she told attendees.
“We have had stunning success in cervical cancer treatments over the past 10-15 years, and now we see that the addition of pembrolizumab to standard chemotherapy not only improves outcome but very importantly does not significantly impact the quality of life in our patients,” said study discussant R. Wendel Naumann, MD, Atrium Health Levine Cancer Institute, Charlotte, North Carolina.
Funding for KEYNOTE-A18 was provided by Merck. Dr. Randall has disclosed relationships with Seagen/Genmab, Merck, GSK, ImmunoGen, AstraZeneca, and On Target Laboratories. Dr. Naumann has no relevant disclosures.
A version of this article appeared on Medscape.com.
according to patient-reported outcome analyses from the KEYNOTE-A18 trial.
Progression-free survival data from the trial, reported at the 2023 meeting of the European Society for Medical Oncology, showed a 30% reduction in the risk for progression (P =.002) with the addition of pembrolizumab vs placebo, as well as favorable overall survival trends, reported Leslie Randall, MD, with VCU Health in Richmond, Virginia. Now the new analyses bring the “voices of the patients from this large phase 3 study.”
“I think the data can put us at ease and give patients a measure of comfort because there was no detriment in the quality of life,” said Dr. Randall, who presented the data on March 17 at the Society of Gynecologic Oncology (SGO) 2024 conference.
The phase 3 KEYNOTE-A18 trial enrolled 1060 patients new to treatment who had either stage 1B2-2B disease with lymph node involvement or stage 3-4A disease. They were randomly allocated to receive pembrolizumab or placebo plus concurrent chemoradiotherapy.
Patient-reported outcome instruments used in the study were the European Organization for Research and Treatment of Cancer (EORTC) 30-item quality-of-life (QOL) core questionnaire (QLQ-C30), the EORTC cervical cancer–specific module (QLQ-CX24), and the EuroQol EQ-5D-5L visual analog scale (VAS).
Prespecified secondary study endpoints were changes from baseline to week 36 in QLQ-C30 global health status/QOL (GHS/QOL) and physical functioning, and the QLQ-CX24 symptom-experience scale.
At baseline, patient-reported outcome scores were similar between treatment groups. Patients in both treatment groups had an initial decrease in QLQ-C30 GHS/QOL and physical functioning subscale and EQ-5D-5L VAS scores at weeks 3 and 6, but these improved relative to baseline at week 12 and subsequent weeks.
A similar number of patients in the pembrolizumab and placebo groups had improved or stable scores for QLQ-C30 GHS/QOL (76% vs 75%), QLQ-C30 physical functioning (77% vs 77%), QLQ-CX24 symptom experience (85% vs 85%) and EQ-5D-5L VAS (73% vs 76%).
Across all QOL instruments evaluated, there were no meaningful differences in patient-reported outcomes among patients who received pembrolizumab compared with those who received placebo, said Dr. Randall.
The improvement in progression-free survival, coupled with the patient-reported outcomes showing no additional harms to quality of life, support pembrolizumab plus concurrent chemoradiotherapy as a “new standard of care” for patients with high-risk locally advanced cervical cancer, she told attendees.
“We have had stunning success in cervical cancer treatments over the past 10-15 years, and now we see that the addition of pembrolizumab to standard chemotherapy not only improves outcome but very importantly does not significantly impact the quality of life in our patients,” said study discussant R. Wendel Naumann, MD, Atrium Health Levine Cancer Institute, Charlotte, North Carolina.
Funding for KEYNOTE-A18 was provided by Merck. Dr. Randall has disclosed relationships with Seagen/Genmab, Merck, GSK, ImmunoGen, AstraZeneca, and On Target Laboratories. Dr. Naumann has no relevant disclosures.
A version of this article appeared on Medscape.com.
according to patient-reported outcome analyses from the KEYNOTE-A18 trial.
Progression-free survival data from the trial, reported at the 2023 meeting of the European Society for Medical Oncology, showed a 30% reduction in the risk for progression (P =.002) with the addition of pembrolizumab vs placebo, as well as favorable overall survival trends, reported Leslie Randall, MD, with VCU Health in Richmond, Virginia. Now the new analyses bring the “voices of the patients from this large phase 3 study.”
“I think the data can put us at ease and give patients a measure of comfort because there was no detriment in the quality of life,” said Dr. Randall, who presented the data on March 17 at the Society of Gynecologic Oncology (SGO) 2024 conference.
The phase 3 KEYNOTE-A18 trial enrolled 1060 patients new to treatment who had either stage 1B2-2B disease with lymph node involvement or stage 3-4A disease. They were randomly allocated to receive pembrolizumab or placebo plus concurrent chemoradiotherapy.
Patient-reported outcome instruments used in the study were the European Organization for Research and Treatment of Cancer (EORTC) 30-item quality-of-life (QOL) core questionnaire (QLQ-C30), the EORTC cervical cancer–specific module (QLQ-CX24), and the EuroQol EQ-5D-5L visual analog scale (VAS).
Prespecified secondary study endpoints were changes from baseline to week 36 in QLQ-C30 global health status/QOL (GHS/QOL) and physical functioning, and the QLQ-CX24 symptom-experience scale.
At baseline, patient-reported outcome scores were similar between treatment groups. Patients in both treatment groups had an initial decrease in QLQ-C30 GHS/QOL and physical functioning subscale and EQ-5D-5L VAS scores at weeks 3 and 6, but these improved relative to baseline at week 12 and subsequent weeks.
A similar number of patients in the pembrolizumab and placebo groups had improved or stable scores for QLQ-C30 GHS/QOL (76% vs 75%), QLQ-C30 physical functioning (77% vs 77%), QLQ-CX24 symptom experience (85% vs 85%) and EQ-5D-5L VAS (73% vs 76%).
Across all QOL instruments evaluated, there were no meaningful differences in patient-reported outcomes among patients who received pembrolizumab compared with those who received placebo, said Dr. Randall.
The improvement in progression-free survival, coupled with the patient-reported outcomes showing no additional harms to quality of life, support pembrolizumab plus concurrent chemoradiotherapy as a “new standard of care” for patients with high-risk locally advanced cervical cancer, she told attendees.
“We have had stunning success in cervical cancer treatments over the past 10-15 years, and now we see that the addition of pembrolizumab to standard chemotherapy not only improves outcome but very importantly does not significantly impact the quality of life in our patients,” said study discussant R. Wendel Naumann, MD, Atrium Health Levine Cancer Institute, Charlotte, North Carolina.
Funding for KEYNOTE-A18 was provided by Merck. Dr. Randall has disclosed relationships with Seagen/Genmab, Merck, GSK, ImmunoGen, AstraZeneca, and On Target Laboratories. Dr. Naumann has no relevant disclosures.
A version of this article appeared on Medscape.com.
OTC Birth Control Pill Headed to US Pharmacies: What Your Patients Should Know
Primary care clinicians have largely welcomed the arrival of Opill, the first over-the-counter (OTC) birth control pill from Perrigo, which will reach US pharmacy shelves this month. Although the medicine has a long-track record of safe use, physicians and nurse practitioners may want to ready themselves to answer questions from patients about shifting to the option.
The switch to OTC status for the norgestrel-only contraceptive has the support of many physician groups, including the American Medical Association, the American Academy of Family Physicians, and the American College of Obstetricians and Gynecologists (ACOG).
The end of the prescription-requirement removes a barrier to access for many women, especially those who lack insurance. But it also will take away a chief reason many women in their childbearing years make appointments with doctors, as they will no longer need prescriptions for birth control pills.
Anne-Marie Amies Oelschlager, MD, professor of obstetrics and gynecology at University of Washington School of Medicine, in Seattle, Washington, said she is also worried that the availability of an OTC pill will lead to missed opportunities to help patients avoid sexually transmitted diseases. For example, patients can get counseling about the need for testing for sexually transmitted diseases at the start of new relationships during a visit made to obtain a prescription for the pill.
“My hope is that they still follow our recommendations, which is to get tested with every partner,” said Dr. Oelschlager, who cares for many patients in their teens. “Adolescents are at a particularly high risk of infection compared to older ones.”
When clinicians do see patients, they may want to raise the issue of the OTC option and proper use. Patients will need to closely read materials provided for Opill, a step they might skip due to the ready access, according to Diana Zuckerman, PhD, president of the nonprofit National Center for Health Research, which scrutinizes the safety of medical products.
“When something is sold over the counter, it’s perceived by individuals as being safe,” Dr. Zuckerman told this news organization. “There’s less concern and a little less interest in reading the instructions and reading the warnings.”
Considerations for Safety
The US Food and Drug Administration (FDA) in July approved the sales of a daily 0.075 mg norgestrel tablet without prescription. Perrigo told this news organization that it spent the intervening months ensuring retailers and consumers will receive education on the drug.
One of the biggest challenges for people using Opill may be sticking with the dosing schedule, according to Dr. Oelschlager.
“There are going to be people that have a harder time remembering to take a pill every day,” at the same time, said Dr. Oelschlager, who is chair of ACOG’s Clinical Consensus Gynecology Committee. “We need to watch and see what happens as it becomes more widely available, and people start using it.”
Unexpected vaginal bleeding is the most common adverse event linked to this form of birth control, with over one fifth of participants from one study of the OTC drug reporting this side effect, according to an FDA memo.
“It is more likely to be a tolerability issue rather than a safety issue,” the FDA wrote.
Many prescription of birth control options contain estrogen, which is associated with venous thromboembolism (VTE). But Opill contains only norgestrel, a form of progestin, which is not associated with thrombosis. Patients may be more likely to overestimate their potential risks for VTE than to underestimate them, according to Kwuan Paruchabutr, DNP, president of National Association of Nurse Practitioners in Women’s Health and an assistant professor at Georgetown University in Washington, DC.
“This is a progesterone-only pill: The risk is relatively low” of VTE, Dr. Paruchabutr said.
Clinicians should also take special care with patients who are prescribed drugs for seizures, tuberculosis, HIV/AIDS, and pulmonary hypertension or who are taking supplements containing St John’s wort.
Patients in their childbearing years who take isotretinoin are already expected to use some form of birth control.
“All patients on isotretinoin must be registered in the iPLEDGE program, which mandates monthly contraception counseling and monthly pregnancy tests for persons of childbearing potential,” Terrence A. Cronin, Jr, MD, president of the American Academy of Dermatology, told news organization through email.
Dr. Oelschlager noted that many patients who take isotretinoin may benefit from taking a birth control pill containing estrogen, for which they will need a prescription. At least three pills have an FDA-approved indication for treating moderate acne, including Ortho Tri-Cyclen, Estrostep, and Yaz.
The FDA has posted consumer-friendly information about the OTC pill that clinicians can refer their patients to. For clinicians who want more information, ACOG released a practice advisory about the switch in status for this progestin-only pill.
The Cost
While federal laws mandate employer-based and Medicaid plans cover prescription birth control pills for free, the OTC version will carry a cost, according to A. Mark Fendrick, MD, director of the University of Michigan Center for Value-Based Insurance Design in Ann Arbor, Michigan.
Seven states, including New Mexico and New York, already have laws in effect that require health plans to cover certain OTC contraceptives without a prescription, according to a tally kept by the nonprofit research organization KFF.
Dr. Fendrick said it would be helpful for health plans to offer coverage for the OTC pill without copays even if they are not required to do so.
Priced at about $20 a month, Opill “is likely out of reach for many of the individuals who would most benefit from an OTC option,” Dr. Fendrick told this news organization in an email.
The new pill may be utilized most by those who do not have health insurance or have low incomes and cannot afford to see a doctor for a prescription, according to Sally Rafie, PharmD, a pharmacist specialist at University of California San Diego Health and founder of the Birth Control Pharmacist.
The manufacturer’s suggested retail prices will be $19.99 for a 1-month supply and $49.99 for a 3-month supply. Dublin-based Perrigo said it plans to offer a cost-assistance program for the drug in the coming weeks for people who have low incomes and lack insurance.
A version of this article appeared on Medscape.com.
Primary care clinicians have largely welcomed the arrival of Opill, the first over-the-counter (OTC) birth control pill from Perrigo, which will reach US pharmacy shelves this month. Although the medicine has a long-track record of safe use, physicians and nurse practitioners may want to ready themselves to answer questions from patients about shifting to the option.
The switch to OTC status for the norgestrel-only contraceptive has the support of many physician groups, including the American Medical Association, the American Academy of Family Physicians, and the American College of Obstetricians and Gynecologists (ACOG).
The end of the prescription-requirement removes a barrier to access for many women, especially those who lack insurance. But it also will take away a chief reason many women in their childbearing years make appointments with doctors, as they will no longer need prescriptions for birth control pills.
Anne-Marie Amies Oelschlager, MD, professor of obstetrics and gynecology at University of Washington School of Medicine, in Seattle, Washington, said she is also worried that the availability of an OTC pill will lead to missed opportunities to help patients avoid sexually transmitted diseases. For example, patients can get counseling about the need for testing for sexually transmitted diseases at the start of new relationships during a visit made to obtain a prescription for the pill.
“My hope is that they still follow our recommendations, which is to get tested with every partner,” said Dr. Oelschlager, who cares for many patients in their teens. “Adolescents are at a particularly high risk of infection compared to older ones.”
When clinicians do see patients, they may want to raise the issue of the OTC option and proper use. Patients will need to closely read materials provided for Opill, a step they might skip due to the ready access, according to Diana Zuckerman, PhD, president of the nonprofit National Center for Health Research, which scrutinizes the safety of medical products.
“When something is sold over the counter, it’s perceived by individuals as being safe,” Dr. Zuckerman told this news organization. “There’s less concern and a little less interest in reading the instructions and reading the warnings.”
Considerations for Safety
The US Food and Drug Administration (FDA) in July approved the sales of a daily 0.075 mg norgestrel tablet without prescription. Perrigo told this news organization that it spent the intervening months ensuring retailers and consumers will receive education on the drug.
One of the biggest challenges for people using Opill may be sticking with the dosing schedule, according to Dr. Oelschlager.
“There are going to be people that have a harder time remembering to take a pill every day,” at the same time, said Dr. Oelschlager, who is chair of ACOG’s Clinical Consensus Gynecology Committee. “We need to watch and see what happens as it becomes more widely available, and people start using it.”
Unexpected vaginal bleeding is the most common adverse event linked to this form of birth control, with over one fifth of participants from one study of the OTC drug reporting this side effect, according to an FDA memo.
“It is more likely to be a tolerability issue rather than a safety issue,” the FDA wrote.
Many prescription of birth control options contain estrogen, which is associated with venous thromboembolism (VTE). But Opill contains only norgestrel, a form of progestin, which is not associated with thrombosis. Patients may be more likely to overestimate their potential risks for VTE than to underestimate them, according to Kwuan Paruchabutr, DNP, president of National Association of Nurse Practitioners in Women’s Health and an assistant professor at Georgetown University in Washington, DC.
“This is a progesterone-only pill: The risk is relatively low” of VTE, Dr. Paruchabutr said.
Clinicians should also take special care with patients who are prescribed drugs for seizures, tuberculosis, HIV/AIDS, and pulmonary hypertension or who are taking supplements containing St John’s wort.
Patients in their childbearing years who take isotretinoin are already expected to use some form of birth control.
“All patients on isotretinoin must be registered in the iPLEDGE program, which mandates monthly contraception counseling and monthly pregnancy tests for persons of childbearing potential,” Terrence A. Cronin, Jr, MD, president of the American Academy of Dermatology, told news organization through email.
Dr. Oelschlager noted that many patients who take isotretinoin may benefit from taking a birth control pill containing estrogen, for which they will need a prescription. At least three pills have an FDA-approved indication for treating moderate acne, including Ortho Tri-Cyclen, Estrostep, and Yaz.
The FDA has posted consumer-friendly information about the OTC pill that clinicians can refer their patients to. For clinicians who want more information, ACOG released a practice advisory about the switch in status for this progestin-only pill.
The Cost
While federal laws mandate employer-based and Medicaid plans cover prescription birth control pills for free, the OTC version will carry a cost, according to A. Mark Fendrick, MD, director of the University of Michigan Center for Value-Based Insurance Design in Ann Arbor, Michigan.
Seven states, including New Mexico and New York, already have laws in effect that require health plans to cover certain OTC contraceptives without a prescription, according to a tally kept by the nonprofit research organization KFF.
Dr. Fendrick said it would be helpful for health plans to offer coverage for the OTC pill without copays even if they are not required to do so.
Priced at about $20 a month, Opill “is likely out of reach for many of the individuals who would most benefit from an OTC option,” Dr. Fendrick told this news organization in an email.
The new pill may be utilized most by those who do not have health insurance or have low incomes and cannot afford to see a doctor for a prescription, according to Sally Rafie, PharmD, a pharmacist specialist at University of California San Diego Health and founder of the Birth Control Pharmacist.
The manufacturer’s suggested retail prices will be $19.99 for a 1-month supply and $49.99 for a 3-month supply. Dublin-based Perrigo said it plans to offer a cost-assistance program for the drug in the coming weeks for people who have low incomes and lack insurance.
A version of this article appeared on Medscape.com.
Primary care clinicians have largely welcomed the arrival of Opill, the first over-the-counter (OTC) birth control pill from Perrigo, which will reach US pharmacy shelves this month. Although the medicine has a long-track record of safe use, physicians and nurse practitioners may want to ready themselves to answer questions from patients about shifting to the option.
The switch to OTC status for the norgestrel-only contraceptive has the support of many physician groups, including the American Medical Association, the American Academy of Family Physicians, and the American College of Obstetricians and Gynecologists (ACOG).
The end of the prescription-requirement removes a barrier to access for many women, especially those who lack insurance. But it also will take away a chief reason many women in their childbearing years make appointments with doctors, as they will no longer need prescriptions for birth control pills.
Anne-Marie Amies Oelschlager, MD, professor of obstetrics and gynecology at University of Washington School of Medicine, in Seattle, Washington, said she is also worried that the availability of an OTC pill will lead to missed opportunities to help patients avoid sexually transmitted diseases. For example, patients can get counseling about the need for testing for sexually transmitted diseases at the start of new relationships during a visit made to obtain a prescription for the pill.
“My hope is that they still follow our recommendations, which is to get tested with every partner,” said Dr. Oelschlager, who cares for many patients in their teens. “Adolescents are at a particularly high risk of infection compared to older ones.”
When clinicians do see patients, they may want to raise the issue of the OTC option and proper use. Patients will need to closely read materials provided for Opill, a step they might skip due to the ready access, according to Diana Zuckerman, PhD, president of the nonprofit National Center for Health Research, which scrutinizes the safety of medical products.
“When something is sold over the counter, it’s perceived by individuals as being safe,” Dr. Zuckerman told this news organization. “There’s less concern and a little less interest in reading the instructions and reading the warnings.”
Considerations for Safety
The US Food and Drug Administration (FDA) in July approved the sales of a daily 0.075 mg norgestrel tablet without prescription. Perrigo told this news organization that it spent the intervening months ensuring retailers and consumers will receive education on the drug.
One of the biggest challenges for people using Opill may be sticking with the dosing schedule, according to Dr. Oelschlager.
“There are going to be people that have a harder time remembering to take a pill every day,” at the same time, said Dr. Oelschlager, who is chair of ACOG’s Clinical Consensus Gynecology Committee. “We need to watch and see what happens as it becomes more widely available, and people start using it.”
Unexpected vaginal bleeding is the most common adverse event linked to this form of birth control, with over one fifth of participants from one study of the OTC drug reporting this side effect, according to an FDA memo.
“It is more likely to be a tolerability issue rather than a safety issue,” the FDA wrote.
Many prescription of birth control options contain estrogen, which is associated with venous thromboembolism (VTE). But Opill contains only norgestrel, a form of progestin, which is not associated with thrombosis. Patients may be more likely to overestimate their potential risks for VTE than to underestimate them, according to Kwuan Paruchabutr, DNP, president of National Association of Nurse Practitioners in Women’s Health and an assistant professor at Georgetown University in Washington, DC.
“This is a progesterone-only pill: The risk is relatively low” of VTE, Dr. Paruchabutr said.
Clinicians should also take special care with patients who are prescribed drugs for seizures, tuberculosis, HIV/AIDS, and pulmonary hypertension or who are taking supplements containing St John’s wort.
Patients in their childbearing years who take isotretinoin are already expected to use some form of birth control.
“All patients on isotretinoin must be registered in the iPLEDGE program, which mandates monthly contraception counseling and monthly pregnancy tests for persons of childbearing potential,” Terrence A. Cronin, Jr, MD, president of the American Academy of Dermatology, told news organization through email.
Dr. Oelschlager noted that many patients who take isotretinoin may benefit from taking a birth control pill containing estrogen, for which they will need a prescription. At least three pills have an FDA-approved indication for treating moderate acne, including Ortho Tri-Cyclen, Estrostep, and Yaz.
The FDA has posted consumer-friendly information about the OTC pill that clinicians can refer their patients to. For clinicians who want more information, ACOG released a practice advisory about the switch in status for this progestin-only pill.
The Cost
While federal laws mandate employer-based and Medicaid plans cover prescription birth control pills for free, the OTC version will carry a cost, according to A. Mark Fendrick, MD, director of the University of Michigan Center for Value-Based Insurance Design in Ann Arbor, Michigan.
Seven states, including New Mexico and New York, already have laws in effect that require health plans to cover certain OTC contraceptives without a prescription, according to a tally kept by the nonprofit research organization KFF.
Dr. Fendrick said it would be helpful for health plans to offer coverage for the OTC pill without copays even if they are not required to do so.
Priced at about $20 a month, Opill “is likely out of reach for many of the individuals who would most benefit from an OTC option,” Dr. Fendrick told this news organization in an email.
The new pill may be utilized most by those who do not have health insurance or have low incomes and cannot afford to see a doctor for a prescription, according to Sally Rafie, PharmD, a pharmacist specialist at University of California San Diego Health and founder of the Birth Control Pharmacist.
The manufacturer’s suggested retail prices will be $19.99 for a 1-month supply and $49.99 for a 3-month supply. Dublin-based Perrigo said it plans to offer a cost-assistance program for the drug in the coming weeks for people who have low incomes and lack insurance.
A version of this article appeared on Medscape.com.
RUBY: ‘A Huge Win’ for Patients With Advanced or Recurrent Endometrial Cancer
The benefit of the combination of the programmed death protein 1 (PD-1) inhibitor dostarlimab (Jemperli) and chemotherapy was even more pronounced among patients with DNA mismatch repair deficient/microsatellite instability high (dMMR/MSI-H) tumors.
These results, from the second interim analysis of the phase 3 ENGOT-EN6-NSGO/GOG-3031/RUBY trial, were cheered by audience members when they were reported at the Society of Gynecologic Oncology (SGO)’s Annual Meeting on Women’s Cancer, held in San Diego, California.
“Overall survival benefit to the addition of PD-1 inhibitor to chemotherapy upfront for patients with advanced and recurrent MSI-high endometrial cancer: SOLD!” said invited discussant Gini Fleming, medical director of gynecologic oncology at the University of Chicago.
“I think this is a huge win for our patients. It’s something that none of us have seen before over many years of working with endometrial cancer and should be incorporated into everybody’s practice as of yesterday,” she said.
Continued Improvement
Results from the first interim analysis of the trial showed that dostarlimab and chemotherapy significantly improved progression-free survival (PFS) in the dMMR/MSI-H population, and there was an early trend toward improved overall survival, compared with chemotherapy plus placebo.
As Matthew A. Powell, MD from Washington University School of Medicine in Saint Louis, Missouri reported at SGO 2024, that early trend has become an undeniable survival advantage.
At a median follow-up of 37.2 months, the median overall survival was 44.6 months for patients randomized to the combination, compared with 28.2 months for those assigned to chemotherapy plus placebo.
The respective 3-year overall survival (OS) rates were 54.9% and 42.9%, translating into a hazard ratio (HR) for death with dostarlimab/chemotherapy of 0.69 (P = .002).
Among the subset of patients with dMMR/MSI-H tumors the survival benefit conferred by the combination was even greater, with median OS not reached in the dostarlimab group vs 31.4 months in the chemotherapy-alone arm, with respective 3-year OS rates of 78% and 46%. This difference translated into a HR for death with the combination of 0.32 (P = .0002) for patients with deficient mismatch-repair cancers.
“Dostarlimab plus carboplatin-paclitaxel chemotherapy demonstrated statistically significant and clinically meaningful overall survival improvements in the overall population, a substantial unprecedented overall survival benefit in patients with defective mismatch-repair tumors, and a clinically meaningful; 7-month improvement in the OS difference in patients with proficient mismatch-repair tumors,” Dr. Powell said.
RUBY Details
The trial was conducted in 494 patients with primary advanced stage III or IV or first recurrent endometrial cancer who received first-line treatment with standard chemotherapy with carboplatin (area under the concentration–time curve, 5 mg/mL per minute) and paclitaxel (175 mg/m2 of body surface area), every 3 weeks (six cycles). They were also randomized to receive either dostarlimab (1000 mg) or dostarlimab placebo every 6 weeks for up to 3 years.
Within the cohort, 118 patients (23.9%) had dMMR/MSI-H tumors.
At the time of the first interim analysis the estimated progression-free survival at 24 months in the dMMR–MSI-H subgroup was 61.4% in the dostarlimab group vs 15.7 in the placebo group (HR for progression or death, 0.28; P < .001). For the entire cohort, progression-free survival at 24 months was 36.1% vs 18.1% (HR, 0.64; P < .001).
A prespecified exploratory analysis of progression-free survival in proficient MMR, microsatellite stable (MSS) patients was also done, and a clinically relevant benefit was observed.
Overall survival at that time also favored dostarlimab, although it was only mature for 33% of the population. But at 24 months, OS rates were 71.3% vs 56.0% among placebo recipients; this difference approached but did not reach statistical significance.
The overall response rate in the dMMR–MSI-H population vs the placebo group was 77.6% vs 69%, respectively, and 68.1% and 63.4% in the pMMR/MSS population.
The most common adverse events observed were nausea, alopecia, and fatigue. Grade 3 and higher adverse events at the most recent follow-up were more frequent in the dostarlimab group than in the placebo group (72.2% vs 60.2%).
“Importantly, safety was maintained” at the second interim analysis, Dr. Powell said.
“No new safety signals were noted, no new deaths related to therapy were noted with the subsequent 1-year additional analysis time,” he said.
What’s Next?
Dr. Fleming reviewed potential strategies for further improving care of patients with advanced or recurrent endometrial cancer during her discussion.
“What are the next directions for patients with MSI-high disease? Well, obviously could we use immune checkpoint inhibitors without chemotherapy and not compromise results? There are two ongoing trials or trials that we’re awaiting results of that have compared single-agent immune checkpoint inhibitor to just chemotherapy in mismatch repair-deficient advanced disease, and hopefully we can extrapolate from these trials to determine if this might be a more patient-friendly and equally effective strategy, but we don’t yet know,” she said.
Dr. Fleming also noted that ongoing or planned clinical trials will address questions about potential options for patients with MSI-H tumors whose disease progresses on frontline chemotherapy and immunotherapy. Other trials are assessing whether combining radiotherapy with checkpoint inhibitors will be effective in treating patients with earlier-stage tumors, or whether the addition of a PARP inhibitor might offer additional benefit for these patients.
“Immune checkpoint inhibitor should be given first line to patients with advanced/recurrent microsatellite [instability] endometrial cancer, and they should be considered as front line in patients with microsatellite stable disease. At this point, unfortunately, we have no reasonable predictive factors to know which of those patients with microsatellite stable disease will truly benefit. Multiple other agents are being tested in this setting, and will hopefully prove useful in subgroups,” she said.
The study is funded by GlaxoSmithKline. Dr. Powell reports grants/research support from GSK and honoraria/consultation fees from AstraZeneca, Clovis Oncology, Eisai, GSK, Immunogen, and Merck. Dr. Fleming reports serving as an institutional principal investigator for trials sponsored by multiple companies, not including GSK.
The benefit of the combination of the programmed death protein 1 (PD-1) inhibitor dostarlimab (Jemperli) and chemotherapy was even more pronounced among patients with DNA mismatch repair deficient/microsatellite instability high (dMMR/MSI-H) tumors.
These results, from the second interim analysis of the phase 3 ENGOT-EN6-NSGO/GOG-3031/RUBY trial, were cheered by audience members when they were reported at the Society of Gynecologic Oncology (SGO)’s Annual Meeting on Women’s Cancer, held in San Diego, California.
“Overall survival benefit to the addition of PD-1 inhibitor to chemotherapy upfront for patients with advanced and recurrent MSI-high endometrial cancer: SOLD!” said invited discussant Gini Fleming, medical director of gynecologic oncology at the University of Chicago.
“I think this is a huge win for our patients. It’s something that none of us have seen before over many years of working with endometrial cancer and should be incorporated into everybody’s practice as of yesterday,” she said.
Continued Improvement
Results from the first interim analysis of the trial showed that dostarlimab and chemotherapy significantly improved progression-free survival (PFS) in the dMMR/MSI-H population, and there was an early trend toward improved overall survival, compared with chemotherapy plus placebo.
As Matthew A. Powell, MD from Washington University School of Medicine in Saint Louis, Missouri reported at SGO 2024, that early trend has become an undeniable survival advantage.
At a median follow-up of 37.2 months, the median overall survival was 44.6 months for patients randomized to the combination, compared with 28.2 months for those assigned to chemotherapy plus placebo.
The respective 3-year overall survival (OS) rates were 54.9% and 42.9%, translating into a hazard ratio (HR) for death with dostarlimab/chemotherapy of 0.69 (P = .002).
Among the subset of patients with dMMR/MSI-H tumors the survival benefit conferred by the combination was even greater, with median OS not reached in the dostarlimab group vs 31.4 months in the chemotherapy-alone arm, with respective 3-year OS rates of 78% and 46%. This difference translated into a HR for death with the combination of 0.32 (P = .0002) for patients with deficient mismatch-repair cancers.
“Dostarlimab plus carboplatin-paclitaxel chemotherapy demonstrated statistically significant and clinically meaningful overall survival improvements in the overall population, a substantial unprecedented overall survival benefit in patients with defective mismatch-repair tumors, and a clinically meaningful; 7-month improvement in the OS difference in patients with proficient mismatch-repair tumors,” Dr. Powell said.
RUBY Details
The trial was conducted in 494 patients with primary advanced stage III or IV or first recurrent endometrial cancer who received first-line treatment with standard chemotherapy with carboplatin (area under the concentration–time curve, 5 mg/mL per minute) and paclitaxel (175 mg/m2 of body surface area), every 3 weeks (six cycles). They were also randomized to receive either dostarlimab (1000 mg) or dostarlimab placebo every 6 weeks for up to 3 years.
Within the cohort, 118 patients (23.9%) had dMMR/MSI-H tumors.
At the time of the first interim analysis the estimated progression-free survival at 24 months in the dMMR–MSI-H subgroup was 61.4% in the dostarlimab group vs 15.7 in the placebo group (HR for progression or death, 0.28; P < .001). For the entire cohort, progression-free survival at 24 months was 36.1% vs 18.1% (HR, 0.64; P < .001).
A prespecified exploratory analysis of progression-free survival in proficient MMR, microsatellite stable (MSS) patients was also done, and a clinically relevant benefit was observed.
Overall survival at that time also favored dostarlimab, although it was only mature for 33% of the population. But at 24 months, OS rates were 71.3% vs 56.0% among placebo recipients; this difference approached but did not reach statistical significance.
The overall response rate in the dMMR–MSI-H population vs the placebo group was 77.6% vs 69%, respectively, and 68.1% and 63.4% in the pMMR/MSS population.
The most common adverse events observed were nausea, alopecia, and fatigue. Grade 3 and higher adverse events at the most recent follow-up were more frequent in the dostarlimab group than in the placebo group (72.2% vs 60.2%).
“Importantly, safety was maintained” at the second interim analysis, Dr. Powell said.
“No new safety signals were noted, no new deaths related to therapy were noted with the subsequent 1-year additional analysis time,” he said.
What’s Next?
Dr. Fleming reviewed potential strategies for further improving care of patients with advanced or recurrent endometrial cancer during her discussion.
“What are the next directions for patients with MSI-high disease? Well, obviously could we use immune checkpoint inhibitors without chemotherapy and not compromise results? There are two ongoing trials or trials that we’re awaiting results of that have compared single-agent immune checkpoint inhibitor to just chemotherapy in mismatch repair-deficient advanced disease, and hopefully we can extrapolate from these trials to determine if this might be a more patient-friendly and equally effective strategy, but we don’t yet know,” she said.
Dr. Fleming also noted that ongoing or planned clinical trials will address questions about potential options for patients with MSI-H tumors whose disease progresses on frontline chemotherapy and immunotherapy. Other trials are assessing whether combining radiotherapy with checkpoint inhibitors will be effective in treating patients with earlier-stage tumors, or whether the addition of a PARP inhibitor might offer additional benefit for these patients.
“Immune checkpoint inhibitor should be given first line to patients with advanced/recurrent microsatellite [instability] endometrial cancer, and they should be considered as front line in patients with microsatellite stable disease. At this point, unfortunately, we have no reasonable predictive factors to know which of those patients with microsatellite stable disease will truly benefit. Multiple other agents are being tested in this setting, and will hopefully prove useful in subgroups,” she said.
The study is funded by GlaxoSmithKline. Dr. Powell reports grants/research support from GSK and honoraria/consultation fees from AstraZeneca, Clovis Oncology, Eisai, GSK, Immunogen, and Merck. Dr. Fleming reports serving as an institutional principal investigator for trials sponsored by multiple companies, not including GSK.
The benefit of the combination of the programmed death protein 1 (PD-1) inhibitor dostarlimab (Jemperli) and chemotherapy was even more pronounced among patients with DNA mismatch repair deficient/microsatellite instability high (dMMR/MSI-H) tumors.
These results, from the second interim analysis of the phase 3 ENGOT-EN6-NSGO/GOG-3031/RUBY trial, were cheered by audience members when they were reported at the Society of Gynecologic Oncology (SGO)’s Annual Meeting on Women’s Cancer, held in San Diego, California.
“Overall survival benefit to the addition of PD-1 inhibitor to chemotherapy upfront for patients with advanced and recurrent MSI-high endometrial cancer: SOLD!” said invited discussant Gini Fleming, medical director of gynecologic oncology at the University of Chicago.
“I think this is a huge win for our patients. It’s something that none of us have seen before over many years of working with endometrial cancer and should be incorporated into everybody’s practice as of yesterday,” she said.
Continued Improvement
Results from the first interim analysis of the trial showed that dostarlimab and chemotherapy significantly improved progression-free survival (PFS) in the dMMR/MSI-H population, and there was an early trend toward improved overall survival, compared with chemotherapy plus placebo.
As Matthew A. Powell, MD from Washington University School of Medicine in Saint Louis, Missouri reported at SGO 2024, that early trend has become an undeniable survival advantage.
At a median follow-up of 37.2 months, the median overall survival was 44.6 months for patients randomized to the combination, compared with 28.2 months for those assigned to chemotherapy plus placebo.
The respective 3-year overall survival (OS) rates were 54.9% and 42.9%, translating into a hazard ratio (HR) for death with dostarlimab/chemotherapy of 0.69 (P = .002).
Among the subset of patients with dMMR/MSI-H tumors the survival benefit conferred by the combination was even greater, with median OS not reached in the dostarlimab group vs 31.4 months in the chemotherapy-alone arm, with respective 3-year OS rates of 78% and 46%. This difference translated into a HR for death with the combination of 0.32 (P = .0002) for patients with deficient mismatch-repair cancers.
“Dostarlimab plus carboplatin-paclitaxel chemotherapy demonstrated statistically significant and clinically meaningful overall survival improvements in the overall population, a substantial unprecedented overall survival benefit in patients with defective mismatch-repair tumors, and a clinically meaningful; 7-month improvement in the OS difference in patients with proficient mismatch-repair tumors,” Dr. Powell said.
RUBY Details
The trial was conducted in 494 patients with primary advanced stage III or IV or first recurrent endometrial cancer who received first-line treatment with standard chemotherapy with carboplatin (area under the concentration–time curve, 5 mg/mL per minute) and paclitaxel (175 mg/m2 of body surface area), every 3 weeks (six cycles). They were also randomized to receive either dostarlimab (1000 mg) or dostarlimab placebo every 6 weeks for up to 3 years.
Within the cohort, 118 patients (23.9%) had dMMR/MSI-H tumors.
At the time of the first interim analysis the estimated progression-free survival at 24 months in the dMMR–MSI-H subgroup was 61.4% in the dostarlimab group vs 15.7 in the placebo group (HR for progression or death, 0.28; P < .001). For the entire cohort, progression-free survival at 24 months was 36.1% vs 18.1% (HR, 0.64; P < .001).
A prespecified exploratory analysis of progression-free survival in proficient MMR, microsatellite stable (MSS) patients was also done, and a clinically relevant benefit was observed.
Overall survival at that time also favored dostarlimab, although it was only mature for 33% of the population. But at 24 months, OS rates were 71.3% vs 56.0% among placebo recipients; this difference approached but did not reach statistical significance.
The overall response rate in the dMMR–MSI-H population vs the placebo group was 77.6% vs 69%, respectively, and 68.1% and 63.4% in the pMMR/MSS population.
The most common adverse events observed were nausea, alopecia, and fatigue. Grade 3 and higher adverse events at the most recent follow-up were more frequent in the dostarlimab group than in the placebo group (72.2% vs 60.2%).
“Importantly, safety was maintained” at the second interim analysis, Dr. Powell said.
“No new safety signals were noted, no new deaths related to therapy were noted with the subsequent 1-year additional analysis time,” he said.
What’s Next?
Dr. Fleming reviewed potential strategies for further improving care of patients with advanced or recurrent endometrial cancer during her discussion.
“What are the next directions for patients with MSI-high disease? Well, obviously could we use immune checkpoint inhibitors without chemotherapy and not compromise results? There are two ongoing trials or trials that we’re awaiting results of that have compared single-agent immune checkpoint inhibitor to just chemotherapy in mismatch repair-deficient advanced disease, and hopefully we can extrapolate from these trials to determine if this might be a more patient-friendly and equally effective strategy, but we don’t yet know,” she said.
Dr. Fleming also noted that ongoing or planned clinical trials will address questions about potential options for patients with MSI-H tumors whose disease progresses on frontline chemotherapy and immunotherapy. Other trials are assessing whether combining radiotherapy with checkpoint inhibitors will be effective in treating patients with earlier-stage tumors, or whether the addition of a PARP inhibitor might offer additional benefit for these patients.
“Immune checkpoint inhibitor should be given first line to patients with advanced/recurrent microsatellite [instability] endometrial cancer, and they should be considered as front line in patients with microsatellite stable disease. At this point, unfortunately, we have no reasonable predictive factors to know which of those patients with microsatellite stable disease will truly benefit. Multiple other agents are being tested in this setting, and will hopefully prove useful in subgroups,” she said.
The study is funded by GlaxoSmithKline. Dr. Powell reports grants/research support from GSK and honoraria/consultation fees from AstraZeneca, Clovis Oncology, Eisai, GSK, Immunogen, and Merck. Dr. Fleming reports serving as an institutional principal investigator for trials sponsored by multiple companies, not including GSK.
FROM SGO 2024
Combining Targeted Drugs and Radiation in Breast Cancer: What’s Safe?
One reason is studies of new drugs typically exclude concurrent radiotherapy, said Kathy Miller, MD, a contributor to this news organization and professor of oncology and medicine at the Indiana University School of Medicine, Indianapolis, Indiana.
If trials evaluating new targeted therapies included concurrent radiotherapy, it would be challenging to identify whether toxicities came from the drug itself, the radiation, or the combination, Dr. Miller explained.
Given the limited evidence, “we tend to be cautious and conservative” and not combine therapies that “we don’t know are safe or appropriate for patients,” said Chirag Shah, MD, director of breast radiology at the Cleveland Clinic, Cleveland, Ohio.
Below is a guide to what we do and don’t know about combining radiotherapy and systemic treatments in breast cancer.
1. Immunotherapy plus radiotherapy likely safe but evidence is limited
Safety data on combining immune checkpoint inhibitors and radiotherapy in breast cancer are limited because concurrent radiotherapy has typically been excluded in pivotal trials.
The 2020 KEYNOTE-522 trial did provide a rare look at concurrent radiotherapy and immunotherapy in early triple-negative breast cancer. The analysis found “no safety concerns” with concurrent radiotherapy and pembrolizumab, lead investigator Peter Schmid, MD, of Queen Mary University of London, England, told this news organization.
Research on other solid tumor types also suggests that radiotherapy “can be considered safe” alongside immunotherapy, the authors of a recent ESTRO consensus said.
Despite evidence indicating radiotherapy alongside immunotherapy can be safe in patients with breast cancer, “certain aspects, such as patient selection, total dose, and dose per fraction, remain open for debate to achieve the best therapeutic outcomes,” the ESTRO experts cautioned.
2. CDK4/6 inhibitors may be offered with radiotherapy in some settings, not others
CDK4/6 inhibitors are now standard of care for first- or second-line treatment in patients with advanced or metastatic hormone receptor–positive, human epidermal growth factor receptor 2 (HER2)–negative breast cancer.
“Unfortunately, we found no information regarding concurrent radiotherapy in the adjuvant setting” in pivotal trials for palbociclib, abemaciclib, and ribociclib, the ESTRO authors said. In the pivotal trials for palbociclib and abemaciclib, patients had to discontinue immunotherapy before initiating radiotherapy, and in the trial for ribociclib, palliative radiotherapy was allowed for relieving bone pain only.
However, in 2023, a team of experts from 12 countries attempted to piece together the available evidence, publishing a meta-analysis of 11 retrospective studies on the safety of CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic disease.
Although most of these studies had small patient populations, the analysis revealed that CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic breast cancer led to a similar side-effect profile to that observed in trials of the inhibitors given sequentially with adjuvant radiotherapy.
“These findings suggest that the simultaneous administration of CDK4/6 inhibitors and radiotherapy is generally well tolerated,” the ESTRO authors concluded but added that CDK4/6 inhibitors and concomitant radiotherapy should be investigated more in the adjuvant locoregional, whole brain, and intracranial stereotactic radiotherapy settings.
The expert panel did note, however, that CDK4/6 inhibitors and concomitant radiotherapy “could be offered” during palliative and ablative extracranial radiotherapy.
3. Only offer poly (ADP-ribose) polymerase (PARP) inhibitors plus radiotherapy in clinical trial setting
PARP inhibitors olaparib (Lynparza) and talazoprib (Talzenna) are standard of care in patients with metastatic breast cancer who have BRCA1/2 gene mutations. Olaparib is also indicated for high-risk early breast cancer following neoadjuvant or adjuvant chemotherapy.
But data on combining PARP inhibitors with radiotherapy in breast cancer also remain limited.
One ongoing phase 2 trial, comparing olaparib plus radiotherapy to radiotherapy alone in 300 people with inflammatory breast cancer, is aiming to tease out the safety of the combination and whether it improves local control in patients with aggressive disease.
“The desire is to explore the exciting possibility that low doses of PARP inhibition may radiosensitize tumor cells more than normal tissues,” Reshma Jagsi, MD, chair of the Department of Radiation Oncology at Emory University School of Medicine in Atlanta, Georgia, who is leading the study.
Because of potential good or bad interactions between new systemic therapies and radiotherapy, “intentional trial design” is important, Dr. Jagsi said, so we “know the best way to combine treatments in practice to optimize outcomes.”
But given the evidence to date, the ESTRO experts advised waiting until “further research provides more comprehensive safety and efficacy data” in the primary, adjuvant, and metastatic settings. The experts also advised not offering PARP inhibitors and concomitant radiotherapy to treat advanced breast cancer outside of clinical trials.
4. Phosphoinositide 3-kinase inhibitors (PI3K) inhibitors, mammalian target of rapamycin (mTOR) inhibitors, and newer targeted agents should not be offered concurrently with radiotherapy
Clinical trial data on the safety of combining PI3K and mTOR inhibitors with radiation are thin, especially in advanced breast cancer. Typically, radiotherapy within 4 weeks before randomization, or 2 weeks for palliative radiation, was excluded in pivotal trials.
For this reason, the ESTRO team recommended that concurrent radiation with either PI3K inhibitors or mTOR inhibitors “should not be offered.”
ESTRO also cautioned against providing radiation concurrently with newer anti-HER2 tyrosine-kinase drugs, such as neratinib or tucatinib, or newer antibody-drug conjugates such as trastuzumab deruxtecan, until more data emerge on the safety of these combinations.
5. Combining older HER2-targeted drugs and radiotherapy generally safe
The ESTRO authors agreed that older anti-HER2 drugs trastuzumab (Herceptin), pertuzumab (Perjeta), and lapatinib (Tykerb) can be safely used concurrently with locoregional radiotherapy as well.
One of the biggest concerns in the field is how to combine radiation with systemic therapies in the setting of brain metastases, and the data on these older anti-HER2 drugs are relatively clear that it’s safe, Dr. Miller said.
For instance, in a 2019 study of 84 patients with 487 brain metastases, stereotactic radiosurgery given alongside lapatinib led to significantly higher rates of complete responses than stereotactic radiosurgery alone (35% vs 11%) with no increased risk for radiation necrosis.
The ESTRO team agreed, noting that the latest evidence supports the use of trastuzumab, pertuzumab, or lapatinib alongside radiotherapy for whole brain and ablative intracranial stereotactic radiotherapy.
As for older antibody-drug conjugates, trastuzumab emtansine (T-DM1) plus radiotherapy “might be considered” during adjuvant locoregional radiotherapy for breast cancer but should not be offered for whole brain and ablative intracranial stereotactic radiotherapy, the ESTRO team said.
Dr. Jagsi declared the following conflicts in a recent 2024 publication: Stock options for advisory board role in Equity Quotient; grants or contracts from Genentech; and expert witness for Kleinbard, LLC, and Hawks Quindel Law. In the Keynote-522 trial publication Dr. Schmid declared relationships with AstraZeneca, Bayer, Boehringer Ingelheim, Celgene, Eisai, Hoffmann-La Roche, Genetech, Merck, Novartis, and Pfizer. Dr. Shah reported consulting for Impedimed, Videra Surgical, and PreludeDX.
A version of this article appeared on Medscape.com.
One reason is studies of new drugs typically exclude concurrent radiotherapy, said Kathy Miller, MD, a contributor to this news organization and professor of oncology and medicine at the Indiana University School of Medicine, Indianapolis, Indiana.
If trials evaluating new targeted therapies included concurrent radiotherapy, it would be challenging to identify whether toxicities came from the drug itself, the radiation, or the combination, Dr. Miller explained.
Given the limited evidence, “we tend to be cautious and conservative” and not combine therapies that “we don’t know are safe or appropriate for patients,” said Chirag Shah, MD, director of breast radiology at the Cleveland Clinic, Cleveland, Ohio.
Below is a guide to what we do and don’t know about combining radiotherapy and systemic treatments in breast cancer.
1. Immunotherapy plus radiotherapy likely safe but evidence is limited
Safety data on combining immune checkpoint inhibitors and radiotherapy in breast cancer are limited because concurrent radiotherapy has typically been excluded in pivotal trials.
The 2020 KEYNOTE-522 trial did provide a rare look at concurrent radiotherapy and immunotherapy in early triple-negative breast cancer. The analysis found “no safety concerns” with concurrent radiotherapy and pembrolizumab, lead investigator Peter Schmid, MD, of Queen Mary University of London, England, told this news organization.
Research on other solid tumor types also suggests that radiotherapy “can be considered safe” alongside immunotherapy, the authors of a recent ESTRO consensus said.
Despite evidence indicating radiotherapy alongside immunotherapy can be safe in patients with breast cancer, “certain aspects, such as patient selection, total dose, and dose per fraction, remain open for debate to achieve the best therapeutic outcomes,” the ESTRO experts cautioned.
2. CDK4/6 inhibitors may be offered with radiotherapy in some settings, not others
CDK4/6 inhibitors are now standard of care for first- or second-line treatment in patients with advanced or metastatic hormone receptor–positive, human epidermal growth factor receptor 2 (HER2)–negative breast cancer.
“Unfortunately, we found no information regarding concurrent radiotherapy in the adjuvant setting” in pivotal trials for palbociclib, abemaciclib, and ribociclib, the ESTRO authors said. In the pivotal trials for palbociclib and abemaciclib, patients had to discontinue immunotherapy before initiating radiotherapy, and in the trial for ribociclib, palliative radiotherapy was allowed for relieving bone pain only.
However, in 2023, a team of experts from 12 countries attempted to piece together the available evidence, publishing a meta-analysis of 11 retrospective studies on the safety of CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic disease.
Although most of these studies had small patient populations, the analysis revealed that CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic breast cancer led to a similar side-effect profile to that observed in trials of the inhibitors given sequentially with adjuvant radiotherapy.
“These findings suggest that the simultaneous administration of CDK4/6 inhibitors and radiotherapy is generally well tolerated,” the ESTRO authors concluded but added that CDK4/6 inhibitors and concomitant radiotherapy should be investigated more in the adjuvant locoregional, whole brain, and intracranial stereotactic radiotherapy settings.
The expert panel did note, however, that CDK4/6 inhibitors and concomitant radiotherapy “could be offered” during palliative and ablative extracranial radiotherapy.
3. Only offer poly (ADP-ribose) polymerase (PARP) inhibitors plus radiotherapy in clinical trial setting
PARP inhibitors olaparib (Lynparza) and talazoprib (Talzenna) are standard of care in patients with metastatic breast cancer who have BRCA1/2 gene mutations. Olaparib is also indicated for high-risk early breast cancer following neoadjuvant or adjuvant chemotherapy.
But data on combining PARP inhibitors with radiotherapy in breast cancer also remain limited.
One ongoing phase 2 trial, comparing olaparib plus radiotherapy to radiotherapy alone in 300 people with inflammatory breast cancer, is aiming to tease out the safety of the combination and whether it improves local control in patients with aggressive disease.
“The desire is to explore the exciting possibility that low doses of PARP inhibition may radiosensitize tumor cells more than normal tissues,” Reshma Jagsi, MD, chair of the Department of Radiation Oncology at Emory University School of Medicine in Atlanta, Georgia, who is leading the study.
Because of potential good or bad interactions between new systemic therapies and radiotherapy, “intentional trial design” is important, Dr. Jagsi said, so we “know the best way to combine treatments in practice to optimize outcomes.”
But given the evidence to date, the ESTRO experts advised waiting until “further research provides more comprehensive safety and efficacy data” in the primary, adjuvant, and metastatic settings. The experts also advised not offering PARP inhibitors and concomitant radiotherapy to treat advanced breast cancer outside of clinical trials.
4. Phosphoinositide 3-kinase inhibitors (PI3K) inhibitors, mammalian target of rapamycin (mTOR) inhibitors, and newer targeted agents should not be offered concurrently with radiotherapy
Clinical trial data on the safety of combining PI3K and mTOR inhibitors with radiation are thin, especially in advanced breast cancer. Typically, radiotherapy within 4 weeks before randomization, or 2 weeks for palliative radiation, was excluded in pivotal trials.
For this reason, the ESTRO team recommended that concurrent radiation with either PI3K inhibitors or mTOR inhibitors “should not be offered.”
ESTRO also cautioned against providing radiation concurrently with newer anti-HER2 tyrosine-kinase drugs, such as neratinib or tucatinib, or newer antibody-drug conjugates such as trastuzumab deruxtecan, until more data emerge on the safety of these combinations.
5. Combining older HER2-targeted drugs and radiotherapy generally safe
The ESTRO authors agreed that older anti-HER2 drugs trastuzumab (Herceptin), pertuzumab (Perjeta), and lapatinib (Tykerb) can be safely used concurrently with locoregional radiotherapy as well.
One of the biggest concerns in the field is how to combine radiation with systemic therapies in the setting of brain metastases, and the data on these older anti-HER2 drugs are relatively clear that it’s safe, Dr. Miller said.
For instance, in a 2019 study of 84 patients with 487 brain metastases, stereotactic radiosurgery given alongside lapatinib led to significantly higher rates of complete responses than stereotactic radiosurgery alone (35% vs 11%) with no increased risk for radiation necrosis.
The ESTRO team agreed, noting that the latest evidence supports the use of trastuzumab, pertuzumab, or lapatinib alongside radiotherapy for whole brain and ablative intracranial stereotactic radiotherapy.
As for older antibody-drug conjugates, trastuzumab emtansine (T-DM1) plus radiotherapy “might be considered” during adjuvant locoregional radiotherapy for breast cancer but should not be offered for whole brain and ablative intracranial stereotactic radiotherapy, the ESTRO team said.
Dr. Jagsi declared the following conflicts in a recent 2024 publication: Stock options for advisory board role in Equity Quotient; grants or contracts from Genentech; and expert witness for Kleinbard, LLC, and Hawks Quindel Law. In the Keynote-522 trial publication Dr. Schmid declared relationships with AstraZeneca, Bayer, Boehringer Ingelheim, Celgene, Eisai, Hoffmann-La Roche, Genetech, Merck, Novartis, and Pfizer. Dr. Shah reported consulting for Impedimed, Videra Surgical, and PreludeDX.
A version of this article appeared on Medscape.com.
One reason is studies of new drugs typically exclude concurrent radiotherapy, said Kathy Miller, MD, a contributor to this news organization and professor of oncology and medicine at the Indiana University School of Medicine, Indianapolis, Indiana.
If trials evaluating new targeted therapies included concurrent radiotherapy, it would be challenging to identify whether toxicities came from the drug itself, the radiation, or the combination, Dr. Miller explained.
Given the limited evidence, “we tend to be cautious and conservative” and not combine therapies that “we don’t know are safe or appropriate for patients,” said Chirag Shah, MD, director of breast radiology at the Cleveland Clinic, Cleveland, Ohio.
Below is a guide to what we do and don’t know about combining radiotherapy and systemic treatments in breast cancer.
1. Immunotherapy plus radiotherapy likely safe but evidence is limited
Safety data on combining immune checkpoint inhibitors and radiotherapy in breast cancer are limited because concurrent radiotherapy has typically been excluded in pivotal trials.
The 2020 KEYNOTE-522 trial did provide a rare look at concurrent radiotherapy and immunotherapy in early triple-negative breast cancer. The analysis found “no safety concerns” with concurrent radiotherapy and pembrolizumab, lead investigator Peter Schmid, MD, of Queen Mary University of London, England, told this news organization.
Research on other solid tumor types also suggests that radiotherapy “can be considered safe” alongside immunotherapy, the authors of a recent ESTRO consensus said.
Despite evidence indicating radiotherapy alongside immunotherapy can be safe in patients with breast cancer, “certain aspects, such as patient selection, total dose, and dose per fraction, remain open for debate to achieve the best therapeutic outcomes,” the ESTRO experts cautioned.
2. CDK4/6 inhibitors may be offered with radiotherapy in some settings, not others
CDK4/6 inhibitors are now standard of care for first- or second-line treatment in patients with advanced or metastatic hormone receptor–positive, human epidermal growth factor receptor 2 (HER2)–negative breast cancer.
“Unfortunately, we found no information regarding concurrent radiotherapy in the adjuvant setting” in pivotal trials for palbociclib, abemaciclib, and ribociclib, the ESTRO authors said. In the pivotal trials for palbociclib and abemaciclib, patients had to discontinue immunotherapy before initiating radiotherapy, and in the trial for ribociclib, palliative radiotherapy was allowed for relieving bone pain only.
However, in 2023, a team of experts from 12 countries attempted to piece together the available evidence, publishing a meta-analysis of 11 retrospective studies on the safety of CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic disease.
Although most of these studies had small patient populations, the analysis revealed that CDK4/6 inhibitors given concurrently with radiotherapy in patients with metastatic breast cancer led to a similar side-effect profile to that observed in trials of the inhibitors given sequentially with adjuvant radiotherapy.
“These findings suggest that the simultaneous administration of CDK4/6 inhibitors and radiotherapy is generally well tolerated,” the ESTRO authors concluded but added that CDK4/6 inhibitors and concomitant radiotherapy should be investigated more in the adjuvant locoregional, whole brain, and intracranial stereotactic radiotherapy settings.
The expert panel did note, however, that CDK4/6 inhibitors and concomitant radiotherapy “could be offered” during palliative and ablative extracranial radiotherapy.
3. Only offer poly (ADP-ribose) polymerase (PARP) inhibitors plus radiotherapy in clinical trial setting
PARP inhibitors olaparib (Lynparza) and talazoprib (Talzenna) are standard of care in patients with metastatic breast cancer who have BRCA1/2 gene mutations. Olaparib is also indicated for high-risk early breast cancer following neoadjuvant or adjuvant chemotherapy.
But data on combining PARP inhibitors with radiotherapy in breast cancer also remain limited.
One ongoing phase 2 trial, comparing olaparib plus radiotherapy to radiotherapy alone in 300 people with inflammatory breast cancer, is aiming to tease out the safety of the combination and whether it improves local control in patients with aggressive disease.
“The desire is to explore the exciting possibility that low doses of PARP inhibition may radiosensitize tumor cells more than normal tissues,” Reshma Jagsi, MD, chair of the Department of Radiation Oncology at Emory University School of Medicine in Atlanta, Georgia, who is leading the study.
Because of potential good or bad interactions between new systemic therapies and radiotherapy, “intentional trial design” is important, Dr. Jagsi said, so we “know the best way to combine treatments in practice to optimize outcomes.”
But given the evidence to date, the ESTRO experts advised waiting until “further research provides more comprehensive safety and efficacy data” in the primary, adjuvant, and metastatic settings. The experts also advised not offering PARP inhibitors and concomitant radiotherapy to treat advanced breast cancer outside of clinical trials.
4. Phosphoinositide 3-kinase inhibitors (PI3K) inhibitors, mammalian target of rapamycin (mTOR) inhibitors, and newer targeted agents should not be offered concurrently with radiotherapy
Clinical trial data on the safety of combining PI3K and mTOR inhibitors with radiation are thin, especially in advanced breast cancer. Typically, radiotherapy within 4 weeks before randomization, or 2 weeks for palliative radiation, was excluded in pivotal trials.
For this reason, the ESTRO team recommended that concurrent radiation with either PI3K inhibitors or mTOR inhibitors “should not be offered.”
ESTRO also cautioned against providing radiation concurrently with newer anti-HER2 tyrosine-kinase drugs, such as neratinib or tucatinib, or newer antibody-drug conjugates such as trastuzumab deruxtecan, until more data emerge on the safety of these combinations.
5. Combining older HER2-targeted drugs and radiotherapy generally safe
The ESTRO authors agreed that older anti-HER2 drugs trastuzumab (Herceptin), pertuzumab (Perjeta), and lapatinib (Tykerb) can be safely used concurrently with locoregional radiotherapy as well.
One of the biggest concerns in the field is how to combine radiation with systemic therapies in the setting of brain metastases, and the data on these older anti-HER2 drugs are relatively clear that it’s safe, Dr. Miller said.
For instance, in a 2019 study of 84 patients with 487 brain metastases, stereotactic radiosurgery given alongside lapatinib led to significantly higher rates of complete responses than stereotactic radiosurgery alone (35% vs 11%) with no increased risk for radiation necrosis.
The ESTRO team agreed, noting that the latest evidence supports the use of trastuzumab, pertuzumab, or lapatinib alongside radiotherapy for whole brain and ablative intracranial stereotactic radiotherapy.
As for older antibody-drug conjugates, trastuzumab emtansine (T-DM1) plus radiotherapy “might be considered” during adjuvant locoregional radiotherapy for breast cancer but should not be offered for whole brain and ablative intracranial stereotactic radiotherapy, the ESTRO team said.
Dr. Jagsi declared the following conflicts in a recent 2024 publication: Stock options for advisory board role in Equity Quotient; grants or contracts from Genentech; and expert witness for Kleinbard, LLC, and Hawks Quindel Law. In the Keynote-522 trial publication Dr. Schmid declared relationships with AstraZeneca, Bayer, Boehringer Ingelheim, Celgene, Eisai, Hoffmann-La Roche, Genetech, Merck, Novartis, and Pfizer. Dr. Shah reported consulting for Impedimed, Videra Surgical, and PreludeDX.
A version of this article appeared on Medscape.com.
Pediatrics Takes a Hit, Whereas Emergency Medicine Recovers on Match Day
As US medical school graduates learned Friday, March 15, where they would spend their residencies, new Match Day 2024 data showed a loss of interest in pediatrics, whereas emergency medicine regained popularity after concern over last year’s unfilled positions.
Hospitals and medical groups offered 41,503 residency positions in 2024, a 3% increase from last year, according to the data released by the National Resident Matching Program.
But though the number of pediatric residency slots increased slightly from last year, 8% of available positions remained unfilled in 2024 compared with about 3% last year.
Physician leaders and policymakers alike pay keen attention to Match Day results because they can signal future shortages in certain specialties, including primary care. Unfilled slots also can raise concerns over too many residency programs in a specialty.
Medical students’ interest in pediatrics continues to decline in part because it pays less than other specialties, Bryan Carmody, MD, MPH, a pediatric nephrologist known for his medical school commentaries, told this news organization. The number of pediatric applicants from US medical schools peaked in 2015 and has fallen since, he said.
“There’s been a lot of soul searching ... this week, with people speculating about lots of (reasons),” Dr. Carmody said. “I don’t think it’s even debt. You can look at the number of unfilled positions, and it correlates with the expected earning potential of those specialties.”
Family medicine, for example, filled about 88% of its positions this year.
Ob.gyn. residencies retained their popularity despite concerns over abortion and reproductive health rights in many states. The specialty filled 99.6% of its positions, a very slight improvement over last year’s 99% rate.
Though ob.gyn. applicants might prefer programs in states where there are more liberal policies around reproductive health, many won’t be in a position where they can choose that because of the limited number of ob.gyn. slots, Dr. Carmody said.
Unfilled residency slots likely will be filled through the Supplemental Offer and Acceptance Program (SOAP). Applicants who did not match in the first round participate in SOAP for one of the 2562 positions in 787 programs that went unfilled after the matching algorithm was processed. A total of 2575 positions were placed in SOAP, including positions in programs that did not participate in the algorithm phase of the process. There were 83 fewer positions in SOAP in 2024, a decrease of 3.1% compared with last year’s Match. More detailed data on SOAP results will be released later this year.
A version of this article appeared on Medscape.com.
As US medical school graduates learned Friday, March 15, where they would spend their residencies, new Match Day 2024 data showed a loss of interest in pediatrics, whereas emergency medicine regained popularity after concern over last year’s unfilled positions.
Hospitals and medical groups offered 41,503 residency positions in 2024, a 3% increase from last year, according to the data released by the National Resident Matching Program.
But though the number of pediatric residency slots increased slightly from last year, 8% of available positions remained unfilled in 2024 compared with about 3% last year.
Physician leaders and policymakers alike pay keen attention to Match Day results because they can signal future shortages in certain specialties, including primary care. Unfilled slots also can raise concerns over too many residency programs in a specialty.
Medical students’ interest in pediatrics continues to decline in part because it pays less than other specialties, Bryan Carmody, MD, MPH, a pediatric nephrologist known for his medical school commentaries, told this news organization. The number of pediatric applicants from US medical schools peaked in 2015 and has fallen since, he said.
“There’s been a lot of soul searching ... this week, with people speculating about lots of (reasons),” Dr. Carmody said. “I don’t think it’s even debt. You can look at the number of unfilled positions, and it correlates with the expected earning potential of those specialties.”
Family medicine, for example, filled about 88% of its positions this year.
Ob.gyn. residencies retained their popularity despite concerns over abortion and reproductive health rights in many states. The specialty filled 99.6% of its positions, a very slight improvement over last year’s 99% rate.
Though ob.gyn. applicants might prefer programs in states where there are more liberal policies around reproductive health, many won’t be in a position where they can choose that because of the limited number of ob.gyn. slots, Dr. Carmody said.
Unfilled residency slots likely will be filled through the Supplemental Offer and Acceptance Program (SOAP). Applicants who did not match in the first round participate in SOAP for one of the 2562 positions in 787 programs that went unfilled after the matching algorithm was processed. A total of 2575 positions were placed in SOAP, including positions in programs that did not participate in the algorithm phase of the process. There were 83 fewer positions in SOAP in 2024, a decrease of 3.1% compared with last year’s Match. More detailed data on SOAP results will be released later this year.
A version of this article appeared on Medscape.com.
As US medical school graduates learned Friday, March 15, where they would spend their residencies, new Match Day 2024 data showed a loss of interest in pediatrics, whereas emergency medicine regained popularity after concern over last year’s unfilled positions.
Hospitals and medical groups offered 41,503 residency positions in 2024, a 3% increase from last year, according to the data released by the National Resident Matching Program.
But though the number of pediatric residency slots increased slightly from last year, 8% of available positions remained unfilled in 2024 compared with about 3% last year.
Physician leaders and policymakers alike pay keen attention to Match Day results because they can signal future shortages in certain specialties, including primary care. Unfilled slots also can raise concerns over too many residency programs in a specialty.
Medical students’ interest in pediatrics continues to decline in part because it pays less than other specialties, Bryan Carmody, MD, MPH, a pediatric nephrologist known for his medical school commentaries, told this news organization. The number of pediatric applicants from US medical schools peaked in 2015 and has fallen since, he said.
“There’s been a lot of soul searching ... this week, with people speculating about lots of (reasons),” Dr. Carmody said. “I don’t think it’s even debt. You can look at the number of unfilled positions, and it correlates with the expected earning potential of those specialties.”
Family medicine, for example, filled about 88% of its positions this year.
Ob.gyn. residencies retained their popularity despite concerns over abortion and reproductive health rights in many states. The specialty filled 99.6% of its positions, a very slight improvement over last year’s 99% rate.
Though ob.gyn. applicants might prefer programs in states where there are more liberal policies around reproductive health, many won’t be in a position where they can choose that because of the limited number of ob.gyn. slots, Dr. Carmody said.
Unfilled residency slots likely will be filled through the Supplemental Offer and Acceptance Program (SOAP). Applicants who did not match in the first round participate in SOAP for one of the 2562 positions in 787 programs that went unfilled after the matching algorithm was processed. A total of 2575 positions were placed in SOAP, including positions in programs that did not participate in the algorithm phase of the process. There were 83 fewer positions in SOAP in 2024, a decrease of 3.1% compared with last year’s Match. More detailed data on SOAP results will be released later this year.
A version of this article appeared on Medscape.com.




