User login
Opioid antagonists in pregnancy: Naltrexone or not?
With the increasing concern about rising rates of opioid abuse in the general population, including women of reproductive age and pregnant and breastfeeding women, clear guidelines regarding treatment in pregnancy and lactation are needed.
The Committee on Obstetric Practice of the American College of Obstetricians and Gynecologists and the American Society of Addiction Medicine addressed this issue comprehensively in the ACOG Committee Opinion issued in August 2017.1 In this document, universal screening and medication-assisted treatment for opioid use disorder were recommended. Opioid agonists including methadone and buprenorphine were considered the treatments with the most evidence of benefit, and limited concern about adverse fetal effects, other than predictable and treatable neonatal abstinence syndrome.
Two types of scenarios make this topic relevant. In the first, a woman who has been successful in avoiding relapse by naltrexone treatment, although advised not to become pregnant, could inadvertently conceive. She would then be at risk of relapse if treatment were discontinued. In the second, a woman who overdoses with an opioid in pregnancy might require rapid detoxification with naltrexone in order to survive. In either case, there are quite limited data on potential fetal consequences.
In a 2001 report, Hulse et al. described a series of fetal outcomes following prenatal naltrexone exposure. In one set of cases accumulated from three countries, rapid opiate detoxification with naltrexone was performed for 18 pregnant women. One woman received two detoxification treatments. Two treatments occurred in the first trimester, 11 in the second, and 6 in the third. Maternal and fetal outcomes were said to be unremarkable, except for two cases of low birth weight infants (less than 2,500 g). In another set of cases, seven opioid-dependent women in Australia who had been maintained on 50 mg naltrexone per day became pregnant. In six of the seven cases, naltrexone was discontinued at 7 weeks’ gestation because of the unknown risks of teratogenicity. Of these, three restarted naltrexone maintenance therapy in the second trimester. One mother continued naltrexone throughout pregnancy. One of the seven women delivered at 36 weeks by induction for high blood pressure, and the infant was less than 2,500 g. One other term infant was small at 2,625 g. Otherwise, outcomes were considered normal.3
In two subsequent reports by some of the same authors, pregnancy outcomes in 9 and 17 heroin users with naltrexone implants were unremarkable and comparable to those of women on methadone maintenance therapy.4,5
While the very limited data on naltrexone safety in pregnancy have not suggested substantial increased risks, the numbers are too small to provide strong reassurance, and the animal data remain concerning. Long-term behavioral outcome studies are also lacking. More research in this area is needed to weigh the safety of naltrexone for the fetus against the risk of relapse with discontinuation of this drug.
Dr. Chambers is a professor of pediatrics and director of clinical research at Rady Children’s Hospital and associate director of the Clinical and Translational Research Institute at the University of California, San Diego. She is also director of MotherToBaby California, a past president of the Organization of Teratology Information Specialists, and past president of the Teratology Society. She has no relevant financial disclosures.
References
1. Obstet Gynecol. 2017 Aug;130(2):e81-e94.
2. Curr Neuropharmacol. 2008 Jun;6(2):125–50.
3. Aust N Z J Obstet Gynaecol. 2001 Nov;41(4):424-8.
4. Aust N Z J Obstet Gynaecol. 2002 Feb;42(1):104-5.
5. Int J Gynaecol Obstet. 2004 May;85(2):170-1.
6. Drugs. 2017 Jul;77(11):1211-9.
With the increasing concern about rising rates of opioid abuse in the general population, including women of reproductive age and pregnant and breastfeeding women, clear guidelines regarding treatment in pregnancy and lactation are needed.
The Committee on Obstetric Practice of the American College of Obstetricians and Gynecologists and the American Society of Addiction Medicine addressed this issue comprehensively in the ACOG Committee Opinion issued in August 2017.1 In this document, universal screening and medication-assisted treatment for opioid use disorder were recommended. Opioid agonists including methadone and buprenorphine were considered the treatments with the most evidence of benefit, and limited concern about adverse fetal effects, other than predictable and treatable neonatal abstinence syndrome.
Two types of scenarios make this topic relevant. In the first, a woman who has been successful in avoiding relapse by naltrexone treatment, although advised not to become pregnant, could inadvertently conceive. She would then be at risk of relapse if treatment were discontinued. In the second, a woman who overdoses with an opioid in pregnancy might require rapid detoxification with naltrexone in order to survive. In either case, there are quite limited data on potential fetal consequences.
In a 2001 report, Hulse et al. described a series of fetal outcomes following prenatal naltrexone exposure. In one set of cases accumulated from three countries, rapid opiate detoxification with naltrexone was performed for 18 pregnant women. One woman received two detoxification treatments. Two treatments occurred in the first trimester, 11 in the second, and 6 in the third. Maternal and fetal outcomes were said to be unremarkable, except for two cases of low birth weight infants (less than 2,500 g). In another set of cases, seven opioid-dependent women in Australia who had been maintained on 50 mg naltrexone per day became pregnant. In six of the seven cases, naltrexone was discontinued at 7 weeks’ gestation because of the unknown risks of teratogenicity. Of these, three restarted naltrexone maintenance therapy in the second trimester. One mother continued naltrexone throughout pregnancy. One of the seven women delivered at 36 weeks by induction for high blood pressure, and the infant was less than 2,500 g. One other term infant was small at 2,625 g. Otherwise, outcomes were considered normal.3
In two subsequent reports by some of the same authors, pregnancy outcomes in 9 and 17 heroin users with naltrexone implants were unremarkable and comparable to those of women on methadone maintenance therapy.4,5
While the very limited data on naltrexone safety in pregnancy have not suggested substantial increased risks, the numbers are too small to provide strong reassurance, and the animal data remain concerning. Long-term behavioral outcome studies are also lacking. More research in this area is needed to weigh the safety of naltrexone for the fetus against the risk of relapse with discontinuation of this drug.
Dr. Chambers is a professor of pediatrics and director of clinical research at Rady Children’s Hospital and associate director of the Clinical and Translational Research Institute at the University of California, San Diego. She is also director of MotherToBaby California, a past president of the Organization of Teratology Information Specialists, and past president of the Teratology Society. She has no relevant financial disclosures.
References
1. Obstet Gynecol. 2017 Aug;130(2):e81-e94.
2. Curr Neuropharmacol. 2008 Jun;6(2):125–50.
3. Aust N Z J Obstet Gynaecol. 2001 Nov;41(4):424-8.
4. Aust N Z J Obstet Gynaecol. 2002 Feb;42(1):104-5.
5. Int J Gynaecol Obstet. 2004 May;85(2):170-1.
6. Drugs. 2017 Jul;77(11):1211-9.
With the increasing concern about rising rates of opioid abuse in the general population, including women of reproductive age and pregnant and breastfeeding women, clear guidelines regarding treatment in pregnancy and lactation are needed.
The Committee on Obstetric Practice of the American College of Obstetricians and Gynecologists and the American Society of Addiction Medicine addressed this issue comprehensively in the ACOG Committee Opinion issued in August 2017.1 In this document, universal screening and medication-assisted treatment for opioid use disorder were recommended. Opioid agonists including methadone and buprenorphine were considered the treatments with the most evidence of benefit, and limited concern about adverse fetal effects, other than predictable and treatable neonatal abstinence syndrome.
Two types of scenarios make this topic relevant. In the first, a woman who has been successful in avoiding relapse by naltrexone treatment, although advised not to become pregnant, could inadvertently conceive. She would then be at risk of relapse if treatment were discontinued. In the second, a woman who overdoses with an opioid in pregnancy might require rapid detoxification with naltrexone in order to survive. In either case, there are quite limited data on potential fetal consequences.
In a 2001 report, Hulse et al. described a series of fetal outcomes following prenatal naltrexone exposure. In one set of cases accumulated from three countries, rapid opiate detoxification with naltrexone was performed for 18 pregnant women. One woman received two detoxification treatments. Two treatments occurred in the first trimester, 11 in the second, and 6 in the third. Maternal and fetal outcomes were said to be unremarkable, except for two cases of low birth weight infants (less than 2,500 g). In another set of cases, seven opioid-dependent women in Australia who had been maintained on 50 mg naltrexone per day became pregnant. In six of the seven cases, naltrexone was discontinued at 7 weeks’ gestation because of the unknown risks of teratogenicity. Of these, three restarted naltrexone maintenance therapy in the second trimester. One mother continued naltrexone throughout pregnancy. One of the seven women delivered at 36 weeks by induction for high blood pressure, and the infant was less than 2,500 g. One other term infant was small at 2,625 g. Otherwise, outcomes were considered normal.3
In two subsequent reports by some of the same authors, pregnancy outcomes in 9 and 17 heroin users with naltrexone implants were unremarkable and comparable to those of women on methadone maintenance therapy.4,5
While the very limited data on naltrexone safety in pregnancy have not suggested substantial increased risks, the numbers are too small to provide strong reassurance, and the animal data remain concerning. Long-term behavioral outcome studies are also lacking. More research in this area is needed to weigh the safety of naltrexone for the fetus against the risk of relapse with discontinuation of this drug.
Dr. Chambers is a professor of pediatrics and director of clinical research at Rady Children’s Hospital and associate director of the Clinical and Translational Research Institute at the University of California, San Diego. She is also director of MotherToBaby California, a past president of the Organization of Teratology Information Specialists, and past president of the Teratology Society. She has no relevant financial disclosures.
References
1. Obstet Gynecol. 2017 Aug;130(2):e81-e94.
2. Curr Neuropharmacol. 2008 Jun;6(2):125–50.
3. Aust N Z J Obstet Gynaecol. 2001 Nov;41(4):424-8.
4. Aust N Z J Obstet Gynaecol. 2002 Feb;42(1):104-5.
5. Int J Gynaecol Obstet. 2004 May;85(2):170-1.
6. Drugs. 2017 Jul;77(11):1211-9.
50 years of pediatric dermatology
The world in pediatric dermatology has changed in incredible ways since 1967. In fact, pediatric dermatology was not an organized specialty until years later! This article will look back at some of the history of pediatric dermatology, exploring how different the field was 50 years ago, and how it has evolved into the vibrant field that it is. By looking at some disease states, and differences in practice in relation to the care of dermatologic conditions in children both by pediatricians and dermatologists, we can see the tremendous evolution in our understanding and management of pediatric skin conditions, and perhaps gain insight into the future.
Pediatric dermatology was fairly “neonatal” 50 years ago, with only a few practitioners in the field. Recognizing that up to 30% of pediatric primary care visits include a skin-related problem, and that there was limited training about skin diseases among primary care practitioners and inconsistent training amongst dermatologists, there was a clinical need for establishing the subspecialty of pediatric dermatology. The first international symposium was held in Mexico City in October 1972, and with this meeting the International Society of Pediatric Dermatology was founded. The Society for Pediatric Dermatology (SPD) began in 1973, with Alvin Jacobs, MD, Samuel Weinberg, MD, Nancy Esterly, MD, Sidney Hurwitz, MD, William Weston, MD, and Coleman Jacobson, MD, as some of the initial “founding mothers and fathers.” The journal Pediatric Dermatology released its first issue in 1982 (35 years ago), and the American Academy of Pediatrics did not have a section of dermatology until 1986.
Pediatrics and dermatology: The interface
Many of the first generation of pediatric dermatologists trained as pediatricians prior to pursuing their dermatology work, with some being “assigned” dermatology as pediatric experts, while others did formal residencies in dermatology. This history is important, as pediatric dermatology was, and remains, integrated with pediatrics, even while training in dermatology residencies became standard practice. An important part of the development of the field has been the education of pediatricians and dermatologists by pediatric dermatologists, with a strong sensibility that improved training for both generalists and specialists about pediatric skin disease would yield better care for patients and families.
Initially, there were very few pediatric or dermatology programs in the United States that had pediatric dermatologists. Over the succeeding decades, this is now less common, although even now there are still dermatology and pediatric residency programs that do not have a pediatric dermatologist for either training or to serve their patients. The founding leaders of the SPD set a tone of collaboration nationally and internationally, reaching out to pediatric colleagues and dermatology associates from around the world, and establishing superb educational programs for the exchange of ideas, presentation of challenging cases, and promoting state of the art knowledge of the field. Through annual meetings of the SPD, conferences immediately preceding the American Academy of Dermatology annual meetings, the World Congress of Pediatric Dermatology, and other regional and international meetings, the field developed as the number of practitioners grew, and as the specialized published literature reflected new knowledge in diagnosis and therapy.
Building upon the history of collaboration and reflecting the maturation of the field with a desire to influence the breadth and quantity of research in pediatric dermatology, the Pediatric Dermatology Research Alliance (PeDRA) was formed in 2012. This organization was formed to promote and facilitate high quality collaborative clinical, translational, educational, and basic science research in pediatric dermatology with a vision to create sustainable, collaborative networks to better understand, prevent, treat, and cure dermatologic diseases in children. This network is now composed of over 230 members representing over 68 institutions from the United States and Canada, but including involvement globally from Mexico, Europe, and the Middle East.
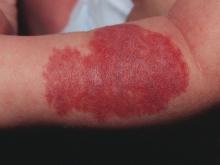
Examples of changing perspectives: hemangiomas
A good way to look at evolution of the field is take a look at some of the similarities and differences in clinical practice in relation to common and uncommon disease states.
A great example is hemangiomas. Some of the first natural history studies on hemangiomas were done in the early 1960s, establishing that many lesions had a typical clinical course of fairly rapid growth, plateau, and involution over time. Of course, the identification of hemangiomas of infancy (or “HOI” in the trade), was confused with vascular malformations, and no one had recognized variant tumors that were distinct, such as rapidly involuting and noninvoluting congenital hemangiomas (RICHs or NICHs), tufted angiomas, and hemangioendotheliomas. PHACE syndrome (posterior fossa brain malformations) had yet to be described (that was done in 1996 by Ilona Frieden and her colleagues). For a time period, hemangiomas were treated with X-rays, before the negative impact of such radiation was acknowledged. For many years after that, even deforming and functionally significant lesions were “followed clinically” for natural involution, presumably a backlash from the radiation therapy interventions.
This story also reflects how organized research efforts helped with the evolution of knowledge and clinical care. The Hemangioma of Infancy Group was formed to take a collaborative approach to characterize and study hemangiomas and related tumors. Beginning with energetic, insightful pediatric dermatologists, and little funding, they changed our knowledge base of how hemangiomas present, the risk factors for their development and the characteristics and multiple organ findings associated with PHACE and other syndromic hemangiomas.
Procedural pediatric dermatology: Tremendous revolution in surgery and laser
The first generation of pediatric dermatologists were considered medical dermatologist specialists. And how important this specialty work was! Acne, atopic dermatitis, psoriasis, diaper and seborrheic dermatitis, and rare genetic syndromes, these conditions were a major part of the work of early pediatric dermatologists (and remain so now). What was not common was for pediatric dermatologists to have procedural or surgical practices, while this now is routinely part of the work of specialists in the field. How did this shift occur?
The fundamental shift began to occur with the introduction of the pulsed dye laser in 1989 and the publication of a seminal article in the New England Journal of Medicine (1989 Feb 16;320[7]:416-21) on its utility in treating port-wine stains in children with minimal scarring. Vascular lesions including port-wine stains were common, and pediatric dermatologists managed these patients for both diagnosis and medical management. Also, dermatology residencies at this time offered training in cutaneous surgery, excisions (including Mohs surgery) and repairs, and trainees in pediatric dermatology were “trained up” to high levels of expertise. As lasers were incorporated into dermatology residency work and practices, pediatric dermatologists had the exposure and skill to do this work. An added advantage was having the pediatric knowledge of how to handle children and adolescents in an age appropriate manner, and consideration of methods to minimize the pain and anxiety of procedures. Within a few years, pediatric dermatologists were at the forefront of the use of topical anesthetics (EMLA and liposomal lidocaine) and had general anesthesia privileges for laser and excisional surgery.
So while pediatric dermatologists still do “small procedures” every hour in most practices (cryotherapy for warts, cantharidin for molluscum, shave and punch biopsies), a subset now have extensive procedural practices, which in recent years has extended to pigment lesion lasers (to treat nevus of Ota), hair lasers (to treat perineal areas to prevent pilonidal cyst recurrence or to treat hirsutism), and combinations of lasers to treat hypertrophic, constrictive, and/or deforming scars).
Inflammatory skin disorders: Bread and butter ... and peanut butter?
The care of pediatric inflammatory skin disorders has evolved, but more slowly for some diseases than others. Acne vulgaris now is recognized as much more common under age 12 years than previously, presumably reflecting earlier pubertal changes in our preteens. Over the past 30 years, therapy has evolved with the use of topical retinoids (still underused by pediatricians, considered a “practice gap”), hormonal therapy with combined oral contraceptives, and oral isotretinoin, a powerful but highly effective systemic agent for severe and refractory acne. Specific pediatric guidelines came much later. Pediatric acne expert recommendations were formulated by the American Acne and Rosacea Society and endorsed by the American Academy of Pediatrics in 2013 (Pediatrics. 2013;131:S163-86). Over the past few years, there is a push by experts for more judicious use of antibiotics for acne (oral and topical) to minimize the emergence of bacterial resistance.
Psoriasis has been a condition that has been “behind the revolution,” in that no biologic agent was approved for pediatric psoriasis in the United States until several months ago, lagging behind Europe and elsewhere in the world by almost a decade. Adult psoriasis has been recognized to be associated with a broad set of comorbidities, including obesity and early heart disease, and there is now research on how children are at risk as well, and new recommendations on how to screen children with psoriasis. Moderate to severe psoriasis in adults is now tremendously controllable with biologic agents targeting TNF-alpha, IL 12/23, and IL-17. Etanercept has been approved for children with psoriasis aged 4 years and older, and other biologic agents are under study.
Atopic dermatitis now is ready for its revolution! AD has increased in prevalence from around 5% of the pediatric population 30-plus years ago to 10%-15%. Treatment of most individuals has remained the same over the decades: Good skin care, frequent moisturizers, topical corticosteroids for flares, management of infection if noted. The topical calcineurin inhibitors (TCIs) broadened the therapeutic approach when introduced in 2000 and 2001, but the boxed warning resulted in some practitioners minimizing their utilization of these useful agents.

It has been recognized for years that children with AD have higher risk of developing food allergies than children without AD. A changing understanding of how early food exposure may induce tolerance is changing the world of allergy and influencing the care of children with AD. This is where the peanut butter (or other processed peanut, such as “Bamba”) may be life saving. New guidelines have come from the National Institute of Allergy and Infectious Diseases recommending that infants with severe eczema (or egg allergy, or both) have introduction of age-appropriate peanut-containing food as early as 4-6 months of age to reduce the risk of development of peanut allergy. It is recommended that these infants undergo early evaluation for possible sensitization to peanut protein, with referral to allergists for skin prick tests or serum IgE screens (though if positive, referral to allergists is appropriate), and assess the safety of going ahead with early feeding. It is hoped that following these new guidelines can minimize the development of peanut allergy.
The future
Where will pediatric skin disease, or more importantly, skin health over a lifetime be in 50 years? Can we cure or prevent the consequences of our lethal and life altering genetic diseases such as epidermolysis bullosa or our neurocutaneous disorders? Will our new insights into birthmarks (they are mostly somatic mutations) allow us to form specific, personalized therapies to minimize their impact? Will we be using computers equipped with imaging devices and algorithms to assess our patients’ moles, papules, and nodules? Will our vaccines have wiped out warts, molluscum, and perhaps, acne? Will we have cured our inflammatory skin disorders, or perhaps prevented them by interventions in the neonatal period? No predictions will be offered here, other than that we can look forward to incredible changes for our future generations of health care practitioners, patients, and families.
Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield has served as a consultant for Anacor/Pfizer and Regeneron/Sanofi. Email him at [email protected].
The world in pediatric dermatology has changed in incredible ways since 1967. In fact, pediatric dermatology was not an organized specialty until years later! This article will look back at some of the history of pediatric dermatology, exploring how different the field was 50 years ago, and how it has evolved into the vibrant field that it is. By looking at some disease states, and differences in practice in relation to the care of dermatologic conditions in children both by pediatricians and dermatologists, we can see the tremendous evolution in our understanding and management of pediatric skin conditions, and perhaps gain insight into the future.
Pediatric dermatology was fairly “neonatal” 50 years ago, with only a few practitioners in the field. Recognizing that up to 30% of pediatric primary care visits include a skin-related problem, and that there was limited training about skin diseases among primary care practitioners and inconsistent training amongst dermatologists, there was a clinical need for establishing the subspecialty of pediatric dermatology. The first international symposium was held in Mexico City in October 1972, and with this meeting the International Society of Pediatric Dermatology was founded. The Society for Pediatric Dermatology (SPD) began in 1973, with Alvin Jacobs, MD, Samuel Weinberg, MD, Nancy Esterly, MD, Sidney Hurwitz, MD, William Weston, MD, and Coleman Jacobson, MD, as some of the initial “founding mothers and fathers.” The journal Pediatric Dermatology released its first issue in 1982 (35 years ago), and the American Academy of Pediatrics did not have a section of dermatology until 1986.
Pediatrics and dermatology: The interface
Many of the first generation of pediatric dermatologists trained as pediatricians prior to pursuing their dermatology work, with some being “assigned” dermatology as pediatric experts, while others did formal residencies in dermatology. This history is important, as pediatric dermatology was, and remains, integrated with pediatrics, even while training in dermatology residencies became standard practice. An important part of the development of the field has been the education of pediatricians and dermatologists by pediatric dermatologists, with a strong sensibility that improved training for both generalists and specialists about pediatric skin disease would yield better care for patients and families.
Initially, there were very few pediatric or dermatology programs in the United States that had pediatric dermatologists. Over the succeeding decades, this is now less common, although even now there are still dermatology and pediatric residency programs that do not have a pediatric dermatologist for either training or to serve their patients. The founding leaders of the SPD set a tone of collaboration nationally and internationally, reaching out to pediatric colleagues and dermatology associates from around the world, and establishing superb educational programs for the exchange of ideas, presentation of challenging cases, and promoting state of the art knowledge of the field. Through annual meetings of the SPD, conferences immediately preceding the American Academy of Dermatology annual meetings, the World Congress of Pediatric Dermatology, and other regional and international meetings, the field developed as the number of practitioners grew, and as the specialized published literature reflected new knowledge in diagnosis and therapy.
Building upon the history of collaboration and reflecting the maturation of the field with a desire to influence the breadth and quantity of research in pediatric dermatology, the Pediatric Dermatology Research Alliance (PeDRA) was formed in 2012. This organization was formed to promote and facilitate high quality collaborative clinical, translational, educational, and basic science research in pediatric dermatology with a vision to create sustainable, collaborative networks to better understand, prevent, treat, and cure dermatologic diseases in children. This network is now composed of over 230 members representing over 68 institutions from the United States and Canada, but including involvement globally from Mexico, Europe, and the Middle East.
Examples of changing perspectives: hemangiomas
A good way to look at evolution of the field is take a look at some of the similarities and differences in clinical practice in relation to common and uncommon disease states.
A great example is hemangiomas. Some of the first natural history studies on hemangiomas were done in the early 1960s, establishing that many lesions had a typical clinical course of fairly rapid growth, plateau, and involution over time. Of course, the identification of hemangiomas of infancy (or “HOI” in the trade), was confused with vascular malformations, and no one had recognized variant tumors that were distinct, such as rapidly involuting and noninvoluting congenital hemangiomas (RICHs or NICHs), tufted angiomas, and hemangioendotheliomas. PHACE syndrome (posterior fossa brain malformations) had yet to be described (that was done in 1996 by Ilona Frieden and her colleagues). For a time period, hemangiomas were treated with X-rays, before the negative impact of such radiation was acknowledged. For many years after that, even deforming and functionally significant lesions were “followed clinically” for natural involution, presumably a backlash from the radiation therapy interventions.
This story also reflects how organized research efforts helped with the evolution of knowledge and clinical care. The Hemangioma of Infancy Group was formed to take a collaborative approach to characterize and study hemangiomas and related tumors. Beginning with energetic, insightful pediatric dermatologists, and little funding, they changed our knowledge base of how hemangiomas present, the risk factors for their development and the characteristics and multiple organ findings associated with PHACE and other syndromic hemangiomas.
Procedural pediatric dermatology: Tremendous revolution in surgery and laser
The first generation of pediatric dermatologists were considered medical dermatologist specialists. And how important this specialty work was! Acne, atopic dermatitis, psoriasis, diaper and seborrheic dermatitis, and rare genetic syndromes, these conditions were a major part of the work of early pediatric dermatologists (and remain so now). What was not common was for pediatric dermatologists to have procedural or surgical practices, while this now is routinely part of the work of specialists in the field. How did this shift occur?
The fundamental shift began to occur with the introduction of the pulsed dye laser in 1989 and the publication of a seminal article in the New England Journal of Medicine (1989 Feb 16;320[7]:416-21) on its utility in treating port-wine stains in children with minimal scarring. Vascular lesions including port-wine stains were common, and pediatric dermatologists managed these patients for both diagnosis and medical management. Also, dermatology residencies at this time offered training in cutaneous surgery, excisions (including Mohs surgery) and repairs, and trainees in pediatric dermatology were “trained up” to high levels of expertise. As lasers were incorporated into dermatology residency work and practices, pediatric dermatologists had the exposure and skill to do this work. An added advantage was having the pediatric knowledge of how to handle children and adolescents in an age appropriate manner, and consideration of methods to minimize the pain and anxiety of procedures. Within a few years, pediatric dermatologists were at the forefront of the use of topical anesthetics (EMLA and liposomal lidocaine) and had general anesthesia privileges for laser and excisional surgery.
So while pediatric dermatologists still do “small procedures” every hour in most practices (cryotherapy for warts, cantharidin for molluscum, shave and punch biopsies), a subset now have extensive procedural practices, which in recent years has extended to pigment lesion lasers (to treat nevus of Ota), hair lasers (to treat perineal areas to prevent pilonidal cyst recurrence or to treat hirsutism), and combinations of lasers to treat hypertrophic, constrictive, and/or deforming scars).
Inflammatory skin disorders: Bread and butter ... and peanut butter?
The care of pediatric inflammatory skin disorders has evolved, but more slowly for some diseases than others. Acne vulgaris now is recognized as much more common under age 12 years than previously, presumably reflecting earlier pubertal changes in our preteens. Over the past 30 years, therapy has evolved with the use of topical retinoids (still underused by pediatricians, considered a “practice gap”), hormonal therapy with combined oral contraceptives, and oral isotretinoin, a powerful but highly effective systemic agent for severe and refractory acne. Specific pediatric guidelines came much later. Pediatric acne expert recommendations were formulated by the American Acne and Rosacea Society and endorsed by the American Academy of Pediatrics in 2013 (Pediatrics. 2013;131:S163-86). Over the past few years, there is a push by experts for more judicious use of antibiotics for acne (oral and topical) to minimize the emergence of bacterial resistance.
Psoriasis has been a condition that has been “behind the revolution,” in that no biologic agent was approved for pediatric psoriasis in the United States until several months ago, lagging behind Europe and elsewhere in the world by almost a decade. Adult psoriasis has been recognized to be associated with a broad set of comorbidities, including obesity and early heart disease, and there is now research on how children are at risk as well, and new recommendations on how to screen children with psoriasis. Moderate to severe psoriasis in adults is now tremendously controllable with biologic agents targeting TNF-alpha, IL 12/23, and IL-17. Etanercept has been approved for children with psoriasis aged 4 years and older, and other biologic agents are under study.
Atopic dermatitis now is ready for its revolution! AD has increased in prevalence from around 5% of the pediatric population 30-plus years ago to 10%-15%. Treatment of most individuals has remained the same over the decades: Good skin care, frequent moisturizers, topical corticosteroids for flares, management of infection if noted. The topical calcineurin inhibitors (TCIs) broadened the therapeutic approach when introduced in 2000 and 2001, but the boxed warning resulted in some practitioners minimizing their utilization of these useful agents.

It has been recognized for years that children with AD have higher risk of developing food allergies than children without AD. A changing understanding of how early food exposure may induce tolerance is changing the world of allergy and influencing the care of children with AD. This is where the peanut butter (or other processed peanut, such as “Bamba”) may be life saving. New guidelines have come from the National Institute of Allergy and Infectious Diseases recommending that infants with severe eczema (or egg allergy, or both) have introduction of age-appropriate peanut-containing food as early as 4-6 months of age to reduce the risk of development of peanut allergy. It is recommended that these infants undergo early evaluation for possible sensitization to peanut protein, with referral to allergists for skin prick tests or serum IgE screens (though if positive, referral to allergists is appropriate), and assess the safety of going ahead with early feeding. It is hoped that following these new guidelines can minimize the development of peanut allergy.
The future
Where will pediatric skin disease, or more importantly, skin health over a lifetime be in 50 years? Can we cure or prevent the consequences of our lethal and life altering genetic diseases such as epidermolysis bullosa or our neurocutaneous disorders? Will our new insights into birthmarks (they are mostly somatic mutations) allow us to form specific, personalized therapies to minimize their impact? Will we be using computers equipped with imaging devices and algorithms to assess our patients’ moles, papules, and nodules? Will our vaccines have wiped out warts, molluscum, and perhaps, acne? Will we have cured our inflammatory skin disorders, or perhaps prevented them by interventions in the neonatal period? No predictions will be offered here, other than that we can look forward to incredible changes for our future generations of health care practitioners, patients, and families.
Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield has served as a consultant for Anacor/Pfizer and Regeneron/Sanofi. Email him at [email protected].
The world in pediatric dermatology has changed in incredible ways since 1967. In fact, pediatric dermatology was not an organized specialty until years later! This article will look back at some of the history of pediatric dermatology, exploring how different the field was 50 years ago, and how it has evolved into the vibrant field that it is. By looking at some disease states, and differences in practice in relation to the care of dermatologic conditions in children both by pediatricians and dermatologists, we can see the tremendous evolution in our understanding and management of pediatric skin conditions, and perhaps gain insight into the future.
Pediatric dermatology was fairly “neonatal” 50 years ago, with only a few practitioners in the field. Recognizing that up to 30% of pediatric primary care visits include a skin-related problem, and that there was limited training about skin diseases among primary care practitioners and inconsistent training amongst dermatologists, there was a clinical need for establishing the subspecialty of pediatric dermatology. The first international symposium was held in Mexico City in October 1972, and with this meeting the International Society of Pediatric Dermatology was founded. The Society for Pediatric Dermatology (SPD) began in 1973, with Alvin Jacobs, MD, Samuel Weinberg, MD, Nancy Esterly, MD, Sidney Hurwitz, MD, William Weston, MD, and Coleman Jacobson, MD, as some of the initial “founding mothers and fathers.” The journal Pediatric Dermatology released its first issue in 1982 (35 years ago), and the American Academy of Pediatrics did not have a section of dermatology until 1986.
Pediatrics and dermatology: The interface
Many of the first generation of pediatric dermatologists trained as pediatricians prior to pursuing their dermatology work, with some being “assigned” dermatology as pediatric experts, while others did formal residencies in dermatology. This history is important, as pediatric dermatology was, and remains, integrated with pediatrics, even while training in dermatology residencies became standard practice. An important part of the development of the field has been the education of pediatricians and dermatologists by pediatric dermatologists, with a strong sensibility that improved training for both generalists and specialists about pediatric skin disease would yield better care for patients and families.
Initially, there were very few pediatric or dermatology programs in the United States that had pediatric dermatologists. Over the succeeding decades, this is now less common, although even now there are still dermatology and pediatric residency programs that do not have a pediatric dermatologist for either training or to serve their patients. The founding leaders of the SPD set a tone of collaboration nationally and internationally, reaching out to pediatric colleagues and dermatology associates from around the world, and establishing superb educational programs for the exchange of ideas, presentation of challenging cases, and promoting state of the art knowledge of the field. Through annual meetings of the SPD, conferences immediately preceding the American Academy of Dermatology annual meetings, the World Congress of Pediatric Dermatology, and other regional and international meetings, the field developed as the number of practitioners grew, and as the specialized published literature reflected new knowledge in diagnosis and therapy.
Building upon the history of collaboration and reflecting the maturation of the field with a desire to influence the breadth and quantity of research in pediatric dermatology, the Pediatric Dermatology Research Alliance (PeDRA) was formed in 2012. This organization was formed to promote and facilitate high quality collaborative clinical, translational, educational, and basic science research in pediatric dermatology with a vision to create sustainable, collaborative networks to better understand, prevent, treat, and cure dermatologic diseases in children. This network is now composed of over 230 members representing over 68 institutions from the United States and Canada, but including involvement globally from Mexico, Europe, and the Middle East.
Examples of changing perspectives: hemangiomas
A good way to look at evolution of the field is take a look at some of the similarities and differences in clinical practice in relation to common and uncommon disease states.
A great example is hemangiomas. Some of the first natural history studies on hemangiomas were done in the early 1960s, establishing that many lesions had a typical clinical course of fairly rapid growth, plateau, and involution over time. Of course, the identification of hemangiomas of infancy (or “HOI” in the trade), was confused with vascular malformations, and no one had recognized variant tumors that were distinct, such as rapidly involuting and noninvoluting congenital hemangiomas (RICHs or NICHs), tufted angiomas, and hemangioendotheliomas. PHACE syndrome (posterior fossa brain malformations) had yet to be described (that was done in 1996 by Ilona Frieden and her colleagues). For a time period, hemangiomas were treated with X-rays, before the negative impact of such radiation was acknowledged. For many years after that, even deforming and functionally significant lesions were “followed clinically” for natural involution, presumably a backlash from the radiation therapy interventions.
This story also reflects how organized research efforts helped with the evolution of knowledge and clinical care. The Hemangioma of Infancy Group was formed to take a collaborative approach to characterize and study hemangiomas and related tumors. Beginning with energetic, insightful pediatric dermatologists, and little funding, they changed our knowledge base of how hemangiomas present, the risk factors for their development and the characteristics and multiple organ findings associated with PHACE and other syndromic hemangiomas.
Procedural pediatric dermatology: Tremendous revolution in surgery and laser
The first generation of pediatric dermatologists were considered medical dermatologist specialists. And how important this specialty work was! Acne, atopic dermatitis, psoriasis, diaper and seborrheic dermatitis, and rare genetic syndromes, these conditions were a major part of the work of early pediatric dermatologists (and remain so now). What was not common was for pediatric dermatologists to have procedural or surgical practices, while this now is routinely part of the work of specialists in the field. How did this shift occur?
The fundamental shift began to occur with the introduction of the pulsed dye laser in 1989 and the publication of a seminal article in the New England Journal of Medicine (1989 Feb 16;320[7]:416-21) on its utility in treating port-wine stains in children with minimal scarring. Vascular lesions including port-wine stains were common, and pediatric dermatologists managed these patients for both diagnosis and medical management. Also, dermatology residencies at this time offered training in cutaneous surgery, excisions (including Mohs surgery) and repairs, and trainees in pediatric dermatology were “trained up” to high levels of expertise. As lasers were incorporated into dermatology residency work and practices, pediatric dermatologists had the exposure and skill to do this work. An added advantage was having the pediatric knowledge of how to handle children and adolescents in an age appropriate manner, and consideration of methods to minimize the pain and anxiety of procedures. Within a few years, pediatric dermatologists were at the forefront of the use of topical anesthetics (EMLA and liposomal lidocaine) and had general anesthesia privileges for laser and excisional surgery.
So while pediatric dermatologists still do “small procedures” every hour in most practices (cryotherapy for warts, cantharidin for molluscum, shave and punch biopsies), a subset now have extensive procedural practices, which in recent years has extended to pigment lesion lasers (to treat nevus of Ota), hair lasers (to treat perineal areas to prevent pilonidal cyst recurrence or to treat hirsutism), and combinations of lasers to treat hypertrophic, constrictive, and/or deforming scars).
Inflammatory skin disorders: Bread and butter ... and peanut butter?
The care of pediatric inflammatory skin disorders has evolved, but more slowly for some diseases than others. Acne vulgaris now is recognized as much more common under age 12 years than previously, presumably reflecting earlier pubertal changes in our preteens. Over the past 30 years, therapy has evolved with the use of topical retinoids (still underused by pediatricians, considered a “practice gap”), hormonal therapy with combined oral contraceptives, and oral isotretinoin, a powerful but highly effective systemic agent for severe and refractory acne. Specific pediatric guidelines came much later. Pediatric acne expert recommendations were formulated by the American Acne and Rosacea Society and endorsed by the American Academy of Pediatrics in 2013 (Pediatrics. 2013;131:S163-86). Over the past few years, there is a push by experts for more judicious use of antibiotics for acne (oral and topical) to minimize the emergence of bacterial resistance.
Psoriasis has been a condition that has been “behind the revolution,” in that no biologic agent was approved for pediatric psoriasis in the United States until several months ago, lagging behind Europe and elsewhere in the world by almost a decade. Adult psoriasis has been recognized to be associated with a broad set of comorbidities, including obesity and early heart disease, and there is now research on how children are at risk as well, and new recommendations on how to screen children with psoriasis. Moderate to severe psoriasis in adults is now tremendously controllable with biologic agents targeting TNF-alpha, IL 12/23, and IL-17. Etanercept has been approved for children with psoriasis aged 4 years and older, and other biologic agents are under study.
Atopic dermatitis now is ready for its revolution! AD has increased in prevalence from around 5% of the pediatric population 30-plus years ago to 10%-15%. Treatment of most individuals has remained the same over the decades: Good skin care, frequent moisturizers, topical corticosteroids for flares, management of infection if noted. The topical calcineurin inhibitors (TCIs) broadened the therapeutic approach when introduced in 2000 and 2001, but the boxed warning resulted in some practitioners minimizing their utilization of these useful agents.

It has been recognized for years that children with AD have higher risk of developing food allergies than children without AD. A changing understanding of how early food exposure may induce tolerance is changing the world of allergy and influencing the care of children with AD. This is where the peanut butter (or other processed peanut, such as “Bamba”) may be life saving. New guidelines have come from the National Institute of Allergy and Infectious Diseases recommending that infants with severe eczema (or egg allergy, or both) have introduction of age-appropriate peanut-containing food as early as 4-6 months of age to reduce the risk of development of peanut allergy. It is recommended that these infants undergo early evaluation for possible sensitization to peanut protein, with referral to allergists for skin prick tests or serum IgE screens (though if positive, referral to allergists is appropriate), and assess the safety of going ahead with early feeding. It is hoped that following these new guidelines can minimize the development of peanut allergy.
The future
Where will pediatric skin disease, or more importantly, skin health over a lifetime be in 50 years? Can we cure or prevent the consequences of our lethal and life altering genetic diseases such as epidermolysis bullosa or our neurocutaneous disorders? Will our new insights into birthmarks (they are mostly somatic mutations) allow us to form specific, personalized therapies to minimize their impact? Will we be using computers equipped with imaging devices and algorithms to assess our patients’ moles, papules, and nodules? Will our vaccines have wiped out warts, molluscum, and perhaps, acne? Will we have cured our inflammatory skin disorders, or perhaps prevented them by interventions in the neonatal period? No predictions will be offered here, other than that we can look forward to incredible changes for our future generations of health care practitioners, patients, and families.
Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield has served as a consultant for Anacor/Pfizer and Regeneron/Sanofi. Email him at [email protected].
Missed opportunities: Opioid overdoses and suicide
The current opioid epidemic in the United States has been universally recognized as one of the most important public health issues to date. This crisis has cost nearly $80 billion in lost productivity, treatment (including emergency, medical, psychiatric, and addiction-specific care), and criminal justice involvement.1 Opioid overdoses have increased by 200% since 2000, with more than 33,000 individuals dying from opioid overdoses in 2015 alone.2,3
Currently, overdoses are considered accidental in origin until proved otherwise, and that assumption has become an acceptable hypothesis for the many parties involved: This hypothesis permits the patient to receive the much-needed overdose treatment, the physicians to discharge the patient from the emergency department after resuscitation and medical stabilization, the hospital to collect reimbursement, the pharmaceutical companies to continue to raise prices – and the health system to ignore recidivism and/or long-term outcomes.
However, while well accepted, the accidental overdose hypothesis might not tell the entire story. A recent, competing etiological hypothesis is that many opioid overdoses may, in fact, be misdiagnosed suicide attempts.7 National suicide prevalence has been increasing since 1999, and both all-cause mortality generally and suicides specifically have been increasing in white, male, and middle-aged patients, which encompass the same demographic groups affected by the opioid epidemic.8,9
Also, more than 50% of patients with opioid use disorder have histories of major depressive disorder,which, when untreated, may further drive suicidal thoughts and behavior.10,11Maria A. Oquendo, MD, PHD, immediate past president of the American Psychiatric Association, wrote in a guest post on the blog of Nora D. Volkow, MD, director of the National Institute on Drug Abuse, about the strong link between opioid use disorders and suicidal thoughts and behavior Furthermore, a 2004 literature review on substance use disorders and suicide found that individuals with opioid use disorders had a 13 times greater risk of completed suicide, compared with the general population.12
Additional associations
A recent study of nearly 5 million veterans enrolled in the Veterans Health Administration demonstrated that, even when adjusted for age and comorbid psychiatric diagnoses, opioid use disorder was associated with an increased risk for suicide; particularly striking was that this risk was doubled in women.13
A survey of 40,000 subjects from the 2014 National Survey on Drug Use and Health demonstrated that prescription opioid misuse was associated with an increased risk of suicidal ideation, and weekly misuse was associated with increased suicide planning and attempts.
The data regarding the prevalence of suicidal ideation in patients who have overdosed are limited, although recent evidence from the National Vital Statistics System on adolescent (aged 15-19 years) drug overdose is concerning, with 772 drug overdoses occurring in this age demographic in 2015 alone. Opioids were involved in the vast majority of fatal drug overdoses among this group, and the prevalence of death from opioid overdoses increased during 1999-2007 (0.8/100,000 to 2.7/100,000), stabilized during 2007-2011, declined during 2012-2014 (down to 2.0/100,000) then increased in 2015 (up to 2.4/100,000). While 80.4% of all drug overdoses in this group (including opioids) were considered unintentional, 13.5% were most likely completed suicides.14
These results suggest that, at the very least, some proportion of opioid overdoses are suicide attempts, and the actual prevalence may be much larger. All of this is difficult to discern as these data come from an epidemiological survey with data input as International Classification of Diseases, 10th revision, codes. Thus, the real-life and real-time quality of the psychiatric and postmortem evaluation that led to the determination of a suicide attempt is unknown. More explicitly, because a thorough evaluation and collateral history may have been lacking, this study may have underestimated the prevalence of overdoses that were actual suicide attempts.
Lessons for physicians
Given the epidemiological evidence linking suicidal thoughts and behavior with opioid use disorders, the frequency of overdoses, demographic factors, and recidivism with naloxone rescue, we should be very concerned that many overdoses are unrecognized suicide attempts. Many physicians can recount giving naloxone to a patient – reversing his or her overdose and simultaneously saving his or her life – only to be confronted with anger and combativeness on the part of the patient. When this response occurs, many physicians may attribute the behavioral dysregulation to the patient’s lack of experience with or tolerance to the drug (especially among naive users) or may disregard the emotional response altogether. The danger in physicians’ reacting like this to such behavior is that substantial ambiguity regarding the patient’s motives still remains: Did the patient intentionally use intravenously thinking he or she would die? Was the patient ambivalent about death? Did the patient wish he or she would die – or not wake up? Or was the patient just was playing a version of “Russian roulette” with needles and lethal quantities of opioids?
When considering logical next steps after naloxone reversal to ensure appropriate diagnosis of and treatment for the patient, a psychiatric consultation and thorough evaluation may be indispensable. This is particularly important given that those who attempt suicide or have active suicidal ideation often are evasive about their behavior and current state of mind.15 Thus, these individuals may be unwilling to disclose active suicidal ideation, intent, and/or plans when interviewed. A psychiatrist, however, has the skill set to evaluate risk and protective factors, assess for other psychiatric comorbidities carefully, and make recommendations for safe disposition and comprehensive treatment. Just as a comprehensive cardiovascular evaluation, formulation of a differential diagnosis, and treatment of chronic cardiovascular disease is the standard of care after a cardiac emergency intervention, we suggest quite similar practice standards for an opioid overdose intervention.
Dr. Srivastava is a fourth-year psychiatry resident at Washington University in St. Louis. Dr. Gold is the 17th Distinguished Alumni Professor at the University of Florida, Gainesville, and professor of psychiatry (adjunct) at Washington University. He also serves as chairman of the scientific advisory boards for RiverMend Health.
References
1. Med Care. 2016 Oct;54:901-6.
2. MMWR Morb Mortal Wkly Rep. 2016 Dec 30;65(5051):1445-52.
3. MMWR Morb Mortal Wkly Rep. 2016 Jan 1;64(50-51):1378-82.
4. N Engl J Med. 2016 Dec 8;375(23):2213-15.
5. Drug Alcohol Depend. 2017 Sep 1;178:176-87.
6. BMJ. 2013 Jan 30;346:f174.
7. Nora’s Blog. 2017 Apr 20. https://www.drugabuse.gov/about-nida/noras-blog/2017/04/opioid-use-disorders-suicide-hidden-tragedy-guest-blog
8. NCHS Data Brief. 2016 Apr;(241):1-8.
9. Proc Natl Acad Sci U S A. 2015 Dec 8;112(49):15078-83.
10. Addict Behav. 2009 Jun-Jul;34(6-7):498-504.
11. J Affect Disord. 2013 May;147(1-3):17-28.
12. Drug Alcohol Depend. 2004 Dec 7;76 Suppl:S11-9.
13. Addiction. 2017 Jul;112(7):1193-1201.
14. NCHS Data Brief. 2017 Aug;282:1-7.
15. Am J Psychiatry. 2003 Nov;160(11 Suppl):1-60.
The current opioid epidemic in the United States has been universally recognized as one of the most important public health issues to date. This crisis has cost nearly $80 billion in lost productivity, treatment (including emergency, medical, psychiatric, and addiction-specific care), and criminal justice involvement.1 Opioid overdoses have increased by 200% since 2000, with more than 33,000 individuals dying from opioid overdoses in 2015 alone.2,3
Currently, overdoses are considered accidental in origin until proved otherwise, and that assumption has become an acceptable hypothesis for the many parties involved: This hypothesis permits the patient to receive the much-needed overdose treatment, the physicians to discharge the patient from the emergency department after resuscitation and medical stabilization, the hospital to collect reimbursement, the pharmaceutical companies to continue to raise prices – and the health system to ignore recidivism and/or long-term outcomes.
However, while well accepted, the accidental overdose hypothesis might not tell the entire story. A recent, competing etiological hypothesis is that many opioid overdoses may, in fact, be misdiagnosed suicide attempts.7 National suicide prevalence has been increasing since 1999, and both all-cause mortality generally and suicides specifically have been increasing in white, male, and middle-aged patients, which encompass the same demographic groups affected by the opioid epidemic.8,9
Also, more than 50% of patients with opioid use disorder have histories of major depressive disorder,which, when untreated, may further drive suicidal thoughts and behavior.10,11Maria A. Oquendo, MD, PHD, immediate past president of the American Psychiatric Association, wrote in a guest post on the blog of Nora D. Volkow, MD, director of the National Institute on Drug Abuse, about the strong link between opioid use disorders and suicidal thoughts and behavior Furthermore, a 2004 literature review on substance use disorders and suicide found that individuals with opioid use disorders had a 13 times greater risk of completed suicide, compared with the general population.12
Additional associations
A recent study of nearly 5 million veterans enrolled in the Veterans Health Administration demonstrated that, even when adjusted for age and comorbid psychiatric diagnoses, opioid use disorder was associated with an increased risk for suicide; particularly striking was that this risk was doubled in women.13
A survey of 40,000 subjects from the 2014 National Survey on Drug Use and Health demonstrated that prescription opioid misuse was associated with an increased risk of suicidal ideation, and weekly misuse was associated with increased suicide planning and attempts.
The data regarding the prevalence of suicidal ideation in patients who have overdosed are limited, although recent evidence from the National Vital Statistics System on adolescent (aged 15-19 years) drug overdose is concerning, with 772 drug overdoses occurring in this age demographic in 2015 alone. Opioids were involved in the vast majority of fatal drug overdoses among this group, and the prevalence of death from opioid overdoses increased during 1999-2007 (0.8/100,000 to 2.7/100,000), stabilized during 2007-2011, declined during 2012-2014 (down to 2.0/100,000) then increased in 2015 (up to 2.4/100,000). While 80.4% of all drug overdoses in this group (including opioids) were considered unintentional, 13.5% were most likely completed suicides.14
These results suggest that, at the very least, some proportion of opioid overdoses are suicide attempts, and the actual prevalence may be much larger. All of this is difficult to discern as these data come from an epidemiological survey with data input as International Classification of Diseases, 10th revision, codes. Thus, the real-life and real-time quality of the psychiatric and postmortem evaluation that led to the determination of a suicide attempt is unknown. More explicitly, because a thorough evaluation and collateral history may have been lacking, this study may have underestimated the prevalence of overdoses that were actual suicide attempts.
Lessons for physicians
Given the epidemiological evidence linking suicidal thoughts and behavior with opioid use disorders, the frequency of overdoses, demographic factors, and recidivism with naloxone rescue, we should be very concerned that many overdoses are unrecognized suicide attempts. Many physicians can recount giving naloxone to a patient – reversing his or her overdose and simultaneously saving his or her life – only to be confronted with anger and combativeness on the part of the patient. When this response occurs, many physicians may attribute the behavioral dysregulation to the patient’s lack of experience with or tolerance to the drug (especially among naive users) or may disregard the emotional response altogether. The danger in physicians’ reacting like this to such behavior is that substantial ambiguity regarding the patient’s motives still remains: Did the patient intentionally use intravenously thinking he or she would die? Was the patient ambivalent about death? Did the patient wish he or she would die – or not wake up? Or was the patient just was playing a version of “Russian roulette” with needles and lethal quantities of opioids?
When considering logical next steps after naloxone reversal to ensure appropriate diagnosis of and treatment for the patient, a psychiatric consultation and thorough evaluation may be indispensable. This is particularly important given that those who attempt suicide or have active suicidal ideation often are evasive about their behavior and current state of mind.15 Thus, these individuals may be unwilling to disclose active suicidal ideation, intent, and/or plans when interviewed. A psychiatrist, however, has the skill set to evaluate risk and protective factors, assess for other psychiatric comorbidities carefully, and make recommendations for safe disposition and comprehensive treatment. Just as a comprehensive cardiovascular evaluation, formulation of a differential diagnosis, and treatment of chronic cardiovascular disease is the standard of care after a cardiac emergency intervention, we suggest quite similar practice standards for an opioid overdose intervention.
Dr. Srivastava is a fourth-year psychiatry resident at Washington University in St. Louis. Dr. Gold is the 17th Distinguished Alumni Professor at the University of Florida, Gainesville, and professor of psychiatry (adjunct) at Washington University. He also serves as chairman of the scientific advisory boards for RiverMend Health.
References
1. Med Care. 2016 Oct;54:901-6.
2. MMWR Morb Mortal Wkly Rep. 2016 Dec 30;65(5051):1445-52.
3. MMWR Morb Mortal Wkly Rep. 2016 Jan 1;64(50-51):1378-82.
4. N Engl J Med. 2016 Dec 8;375(23):2213-15.
5. Drug Alcohol Depend. 2017 Sep 1;178:176-87.
6. BMJ. 2013 Jan 30;346:f174.
7. Nora’s Blog. 2017 Apr 20. https://www.drugabuse.gov/about-nida/noras-blog/2017/04/opioid-use-disorders-suicide-hidden-tragedy-guest-blog
8. NCHS Data Brief. 2016 Apr;(241):1-8.
9. Proc Natl Acad Sci U S A. 2015 Dec 8;112(49):15078-83.
10. Addict Behav. 2009 Jun-Jul;34(6-7):498-504.
11. J Affect Disord. 2013 May;147(1-3):17-28.
12. Drug Alcohol Depend. 2004 Dec 7;76 Suppl:S11-9.
13. Addiction. 2017 Jul;112(7):1193-1201.
14. NCHS Data Brief. 2017 Aug;282:1-7.
15. Am J Psychiatry. 2003 Nov;160(11 Suppl):1-60.
The current opioid epidemic in the United States has been universally recognized as one of the most important public health issues to date. This crisis has cost nearly $80 billion in lost productivity, treatment (including emergency, medical, psychiatric, and addiction-specific care), and criminal justice involvement.1 Opioid overdoses have increased by 200% since 2000, with more than 33,000 individuals dying from opioid overdoses in 2015 alone.2,3
Currently, overdoses are considered accidental in origin until proved otherwise, and that assumption has become an acceptable hypothesis for the many parties involved: This hypothesis permits the patient to receive the much-needed overdose treatment, the physicians to discharge the patient from the emergency department after resuscitation and medical stabilization, the hospital to collect reimbursement, the pharmaceutical companies to continue to raise prices – and the health system to ignore recidivism and/or long-term outcomes.
However, while well accepted, the accidental overdose hypothesis might not tell the entire story. A recent, competing etiological hypothesis is that many opioid overdoses may, in fact, be misdiagnosed suicide attempts.7 National suicide prevalence has been increasing since 1999, and both all-cause mortality generally and suicides specifically have been increasing in white, male, and middle-aged patients, which encompass the same demographic groups affected by the opioid epidemic.8,9
Also, more than 50% of patients with opioid use disorder have histories of major depressive disorder,which, when untreated, may further drive suicidal thoughts and behavior.10,11Maria A. Oquendo, MD, PHD, immediate past president of the American Psychiatric Association, wrote in a guest post on the blog of Nora D. Volkow, MD, director of the National Institute on Drug Abuse, about the strong link between opioid use disorders and suicidal thoughts and behavior Furthermore, a 2004 literature review on substance use disorders and suicide found that individuals with opioid use disorders had a 13 times greater risk of completed suicide, compared with the general population.12
Additional associations
A recent study of nearly 5 million veterans enrolled in the Veterans Health Administration demonstrated that, even when adjusted for age and comorbid psychiatric diagnoses, opioid use disorder was associated with an increased risk for suicide; particularly striking was that this risk was doubled in women.13
A survey of 40,000 subjects from the 2014 National Survey on Drug Use and Health demonstrated that prescription opioid misuse was associated with an increased risk of suicidal ideation, and weekly misuse was associated with increased suicide planning and attempts.
The data regarding the prevalence of suicidal ideation in patients who have overdosed are limited, although recent evidence from the National Vital Statistics System on adolescent (aged 15-19 years) drug overdose is concerning, with 772 drug overdoses occurring in this age demographic in 2015 alone. Opioids were involved in the vast majority of fatal drug overdoses among this group, and the prevalence of death from opioid overdoses increased during 1999-2007 (0.8/100,000 to 2.7/100,000), stabilized during 2007-2011, declined during 2012-2014 (down to 2.0/100,000) then increased in 2015 (up to 2.4/100,000). While 80.4% of all drug overdoses in this group (including opioids) were considered unintentional, 13.5% were most likely completed suicides.14
These results suggest that, at the very least, some proportion of opioid overdoses are suicide attempts, and the actual prevalence may be much larger. All of this is difficult to discern as these data come from an epidemiological survey with data input as International Classification of Diseases, 10th revision, codes. Thus, the real-life and real-time quality of the psychiatric and postmortem evaluation that led to the determination of a suicide attempt is unknown. More explicitly, because a thorough evaluation and collateral history may have been lacking, this study may have underestimated the prevalence of overdoses that were actual suicide attempts.
Lessons for physicians
Given the epidemiological evidence linking suicidal thoughts and behavior with opioid use disorders, the frequency of overdoses, demographic factors, and recidivism with naloxone rescue, we should be very concerned that many overdoses are unrecognized suicide attempts. Many physicians can recount giving naloxone to a patient – reversing his or her overdose and simultaneously saving his or her life – only to be confronted with anger and combativeness on the part of the patient. When this response occurs, many physicians may attribute the behavioral dysregulation to the patient’s lack of experience with or tolerance to the drug (especially among naive users) or may disregard the emotional response altogether. The danger in physicians’ reacting like this to such behavior is that substantial ambiguity regarding the patient’s motives still remains: Did the patient intentionally use intravenously thinking he or she would die? Was the patient ambivalent about death? Did the patient wish he or she would die – or not wake up? Or was the patient just was playing a version of “Russian roulette” with needles and lethal quantities of opioids?
When considering logical next steps after naloxone reversal to ensure appropriate diagnosis of and treatment for the patient, a psychiatric consultation and thorough evaluation may be indispensable. This is particularly important given that those who attempt suicide or have active suicidal ideation often are evasive about their behavior and current state of mind.15 Thus, these individuals may be unwilling to disclose active suicidal ideation, intent, and/or plans when interviewed. A psychiatrist, however, has the skill set to evaluate risk and protective factors, assess for other psychiatric comorbidities carefully, and make recommendations for safe disposition and comprehensive treatment. Just as a comprehensive cardiovascular evaluation, formulation of a differential diagnosis, and treatment of chronic cardiovascular disease is the standard of care after a cardiac emergency intervention, we suggest quite similar practice standards for an opioid overdose intervention.
Dr. Srivastava is a fourth-year psychiatry resident at Washington University in St. Louis. Dr. Gold is the 17th Distinguished Alumni Professor at the University of Florida, Gainesville, and professor of psychiatry (adjunct) at Washington University. He also serves as chairman of the scientific advisory boards for RiverMend Health.
References
1. Med Care. 2016 Oct;54:901-6.
2. MMWR Morb Mortal Wkly Rep. 2016 Dec 30;65(5051):1445-52.
3. MMWR Morb Mortal Wkly Rep. 2016 Jan 1;64(50-51):1378-82.
4. N Engl J Med. 2016 Dec 8;375(23):2213-15.
5. Drug Alcohol Depend. 2017 Sep 1;178:176-87.
6. BMJ. 2013 Jan 30;346:f174.
7. Nora’s Blog. 2017 Apr 20. https://www.drugabuse.gov/about-nida/noras-blog/2017/04/opioid-use-disorders-suicide-hidden-tragedy-guest-blog
8. NCHS Data Brief. 2016 Apr;(241):1-8.
9. Proc Natl Acad Sci U S A. 2015 Dec 8;112(49):15078-83.
10. Addict Behav. 2009 Jun-Jul;34(6-7):498-504.
11. J Affect Disord. 2013 May;147(1-3):17-28.
12. Drug Alcohol Depend. 2004 Dec 7;76 Suppl:S11-9.
13. Addiction. 2017 Jul;112(7):1193-1201.
14. NCHS Data Brief. 2017 Aug;282:1-7.
15. Am J Psychiatry. 2003 Nov;160(11 Suppl):1-60.
Test everyone with diagnosed HIV for drug resistance as they enter care
Antiretroviral therapy (ART) for HIV is critical for achieving viral suppression, which improves the health and longevity of people living with infection and dramatically reduces the risk of transmitting HIV to others. Despite these clear benefits, not everyone prescribed ART adheres to their medications, which can result in drug resistance – and transmission of drug-resistant HIV to others.
A Centers for Disease Control and Prevention analysis of eight U.S. cities found that more than 18 percent of 13,393 people with a recent HIV diagnosis had infections that were resistant to at least one form of treatment. Since 2007, the U.S. Department of Health & Human Services has recommended that everyone with diagnosed HIV infection be tested for drug resistance when HIV care begins; however, it’s not known how closely HIV care providers in the United States follow the guidelines.
To learn more, the CDC recently analyzed HIV surveillance data to examine testing patterns among people living with diagnosed HIV who had entered HIV medical care. The results of the study, published in AIDS Care (2017 May. doi: 10.1080/09540121.2017.1316356), indicated that, of the people with HIV diagnosed in 2013 who had entered medical care, only 66% had been tested for resistance. Of those tested, 68% received testing at the beginning of care.
The findings also show that resistance testing is performed less often among certain groups, including males who inject drugs. In recent reports, about a third of people who inject drugs in selected U.S. cities indicated they did not have health insurance, and nearly 80% lived at or below the federal poverty level. Lack of health care access and low socioeconomic status may be potential barriers to receiving medical care and laboratory testing. Additionally, this population might not be aware of available resources that support these services, including those provided through the Ryan White HIV/AIDS Program and federally qualified health centers.
Previous research has also shown that non-HIV specialists are less likely than HIV specialists to order resistance testing for their patients. With potentially more injection drug use and fewer specialist health care services available in less-populated communities, there is an urgent need both to improve HIV testing and increase resistance testing in rural communities. This is important given the growing potential for HIV outbreaks among people who inject drugs, as well as the substantial rise in the number of deaths attributed to opioid use in many communities throughout the nation.
The study findings also indicate that resistance testing is less common among people with higher CD4 counts in some states, including Michigan, New York, and Texas. CD4 cells are a type of white blood cell that helps in protecting the body from infections, but they are also targeted by HIV. CD4 cell counts can be used to determine the stage of HIV infection in a person. As HIV stays in the body longer, CD4 cells decrease. Even if treatment is delayed for a medical reason, such as coinfection with tuberculosis, resistance testing should still be conducted at a person’s entry to care to help ensure treatment success later.
These results have strong implications for clinical practice and management of people with newly diagnosed HIV. More research is needed to identify the factors influencing lacking or delayed resistance testing so that we can address differences in the development of resistance, as well as other clinical outcomes, over time.
Antiretroviral therapy (ART) for HIV is critical for achieving viral suppression, which improves the health and longevity of people living with infection and dramatically reduces the risk of transmitting HIV to others. Despite these clear benefits, not everyone prescribed ART adheres to their medications, which can result in drug resistance – and transmission of drug-resistant HIV to others.
A Centers for Disease Control and Prevention analysis of eight U.S. cities found that more than 18 percent of 13,393 people with a recent HIV diagnosis had infections that were resistant to at least one form of treatment. Since 2007, the U.S. Department of Health & Human Services has recommended that everyone with diagnosed HIV infection be tested for drug resistance when HIV care begins; however, it’s not known how closely HIV care providers in the United States follow the guidelines.
To learn more, the CDC recently analyzed HIV surveillance data to examine testing patterns among people living with diagnosed HIV who had entered HIV medical care. The results of the study, published in AIDS Care (2017 May. doi: 10.1080/09540121.2017.1316356), indicated that, of the people with HIV diagnosed in 2013 who had entered medical care, only 66% had been tested for resistance. Of those tested, 68% received testing at the beginning of care.
The findings also show that resistance testing is performed less often among certain groups, including males who inject drugs. In recent reports, about a third of people who inject drugs in selected U.S. cities indicated they did not have health insurance, and nearly 80% lived at or below the federal poverty level. Lack of health care access and low socioeconomic status may be potential barriers to receiving medical care and laboratory testing. Additionally, this population might not be aware of available resources that support these services, including those provided through the Ryan White HIV/AIDS Program and federally qualified health centers.
Previous research has also shown that non-HIV specialists are less likely than HIV specialists to order resistance testing for their patients. With potentially more injection drug use and fewer specialist health care services available in less-populated communities, there is an urgent need both to improve HIV testing and increase resistance testing in rural communities. This is important given the growing potential for HIV outbreaks among people who inject drugs, as well as the substantial rise in the number of deaths attributed to opioid use in many communities throughout the nation.
The study findings also indicate that resistance testing is less common among people with higher CD4 counts in some states, including Michigan, New York, and Texas. CD4 cells are a type of white blood cell that helps in protecting the body from infections, but they are also targeted by HIV. CD4 cell counts can be used to determine the stage of HIV infection in a person. As HIV stays in the body longer, CD4 cells decrease. Even if treatment is delayed for a medical reason, such as coinfection with tuberculosis, resistance testing should still be conducted at a person’s entry to care to help ensure treatment success later.
These results have strong implications for clinical practice and management of people with newly diagnosed HIV. More research is needed to identify the factors influencing lacking or delayed resistance testing so that we can address differences in the development of resistance, as well as other clinical outcomes, over time.
Antiretroviral therapy (ART) for HIV is critical for achieving viral suppression, which improves the health and longevity of people living with infection and dramatically reduces the risk of transmitting HIV to others. Despite these clear benefits, not everyone prescribed ART adheres to their medications, which can result in drug resistance – and transmission of drug-resistant HIV to others.
A Centers for Disease Control and Prevention analysis of eight U.S. cities found that more than 18 percent of 13,393 people with a recent HIV diagnosis had infections that were resistant to at least one form of treatment. Since 2007, the U.S. Department of Health & Human Services has recommended that everyone with diagnosed HIV infection be tested for drug resistance when HIV care begins; however, it’s not known how closely HIV care providers in the United States follow the guidelines.
To learn more, the CDC recently analyzed HIV surveillance data to examine testing patterns among people living with diagnosed HIV who had entered HIV medical care. The results of the study, published in AIDS Care (2017 May. doi: 10.1080/09540121.2017.1316356), indicated that, of the people with HIV diagnosed in 2013 who had entered medical care, only 66% had been tested for resistance. Of those tested, 68% received testing at the beginning of care.
The findings also show that resistance testing is performed less often among certain groups, including males who inject drugs. In recent reports, about a third of people who inject drugs in selected U.S. cities indicated they did not have health insurance, and nearly 80% lived at or below the federal poverty level. Lack of health care access and low socioeconomic status may be potential barriers to receiving medical care and laboratory testing. Additionally, this population might not be aware of available resources that support these services, including those provided through the Ryan White HIV/AIDS Program and federally qualified health centers.
Previous research has also shown that non-HIV specialists are less likely than HIV specialists to order resistance testing for their patients. With potentially more injection drug use and fewer specialist health care services available in less-populated communities, there is an urgent need both to improve HIV testing and increase resistance testing in rural communities. This is important given the growing potential for HIV outbreaks among people who inject drugs, as well as the substantial rise in the number of deaths attributed to opioid use in many communities throughout the nation.
The study findings also indicate that resistance testing is less common among people with higher CD4 counts in some states, including Michigan, New York, and Texas. CD4 cells are a type of white blood cell that helps in protecting the body from infections, but they are also targeted by HIV. CD4 cell counts can be used to determine the stage of HIV infection in a person. As HIV stays in the body longer, CD4 cells decrease. Even if treatment is delayed for a medical reason, such as coinfection with tuberculosis, resistance testing should still be conducted at a person’s entry to care to help ensure treatment success later.
These results have strong implications for clinical practice and management of people with newly diagnosed HIV. More research is needed to identify the factors influencing lacking or delayed resistance testing so that we can address differences in the development of resistance, as well as other clinical outcomes, over time.
More data show value of CBT for PTSD, anxiety, depression
So often in clinical practice, guidelines and directives about psychiatric treatments lag behind the results we see every day in our offices. Such is the case with cognitive-behavioral therapy.
Earlier this summer, the departments of Veterans Affairs and Defense deemed trauma-focused psychotherapies, such as CBT, as first-line treatments for posttraumatic stress disorder over medication management. Was I surprised by these findings? Absolutely not. Likewise, last year, the American College of Physicians released a guideline recommending CBT as first-line treatment for chronic insomnia disorder in adults. Surprising? Again, not in the least.
Pierre Janet, PhD, MD, the French psychiatrist, psychologist, and neurologist, more than a hundred years ago in his L’Automatisme Psychologique, advanced the idea that thoughts can be challenged and that perceptions leading to mental problems can be reversed. Dr. Janet completed his pioneering work, including an exploration of the power of hypnosis, even though the psychoanalytic movement was in full force and many parallel ideas about treating mental disorders were barely recognized.
By the middle of the 20th century, Albert Ellis, PhD, developed rational emotive behavior therapy, which focused on thoughtfully restructuring irrational beliefs into rational ones that led to improved skills and behaviors. A decade later, the great Aaron T. Beck, MD, developed a true form of CBT. Over the years, Dr. Beck went on to develop controlled clinical trials showing CBT to be more effective in treating a variety of psychiatric disorders, including depression, panic attacks, anxiety disorders, obsessive-compulsive disorders, various phobic disorders, and PTSD.
Yet, despite the effectiveness of CBT, too few young psychiatrists and mental health professionals learn how to use it, and fewer appear to practice it. Traditional psychiatric training, by and large, continues to rely on more psychodynamic approaches, which do have value but take longer to get results than does CBT.
Clearly, partnering with patients and helping them learn new constructs can lead to positive results. More and more research shows that CBT is efficacious for patients across many age and demographic groups.
In one randomized, controlled study of 96 Latino patients with depression, for example, researchers at the University of California, Berkeley, found that group CBT administered in a primary care setting led to a significant decrease in depressive symptoms as measured by the Spanish-language version of the Patient Health Questionnaire (PHQ-9) (Cog Behav Prac. 2017 Apr 17; doi: 10.1016/j.cbpra.2017.03.02). Of the 96 patients, 92 completed the PHQ-9 at least once, and 76 completed a baseline measure of the questionnaire on day 1 of group therapy, the researchers reported. At baseline, the average PHQ-9 score was 13.88, which points to the high end of moderate depression, moving toward moderately severe depression. For every week the patients were enrolled in the therapy, PHQ-9 scores fell by 0.15 points.
The spin on CBT that I created – which I call the learning, philosophizing, and action (LPA) technique – helps patients think through problematic issues and come away with new narratives. I developed and used the LPA technique as part of a smoking-cessation program I ran for many years at the New York University Langone Medical Center. In turn, that program developed into a short-term psychotherapy program with a focus on CBT and hypnosis/relaxation techniques.
We need better codification and organization on what kinds of therapies are and are not suited for specific diagnosable problems. It is hoped that a clearer understanding of genetics, laboratory testing, and imaging, as emphasized by the National Institute of Mental Health’s Research Domain Criteria, will better equip us to decide what works best. Again, for now, helping patients learn and relearn new ways of thinking and behaving, as developed through CBT, is among the best treatments available for many mental health problems.
Dr. London, a psychiatrist who practices in New York, developed and ran a short-term psychotherapy program for 20 years at NYU Langone Medical Center and has been writing columns for 35 years. His new book about helping people feel better fast is expected to be published in fall 2017. He has no disclosures.
So often in clinical practice, guidelines and directives about psychiatric treatments lag behind the results we see every day in our offices. Such is the case with cognitive-behavioral therapy.
Earlier this summer, the departments of Veterans Affairs and Defense deemed trauma-focused psychotherapies, such as CBT, as first-line treatments for posttraumatic stress disorder over medication management. Was I surprised by these findings? Absolutely not. Likewise, last year, the American College of Physicians released a guideline recommending CBT as first-line treatment for chronic insomnia disorder in adults. Surprising? Again, not in the least.
Pierre Janet, PhD, MD, the French psychiatrist, psychologist, and neurologist, more than a hundred years ago in his L’Automatisme Psychologique, advanced the idea that thoughts can be challenged and that perceptions leading to mental problems can be reversed. Dr. Janet completed his pioneering work, including an exploration of the power of hypnosis, even though the psychoanalytic movement was in full force and many parallel ideas about treating mental disorders were barely recognized.
By the middle of the 20th century, Albert Ellis, PhD, developed rational emotive behavior therapy, which focused on thoughtfully restructuring irrational beliefs into rational ones that led to improved skills and behaviors. A decade later, the great Aaron T. Beck, MD, developed a true form of CBT. Over the years, Dr. Beck went on to develop controlled clinical trials showing CBT to be more effective in treating a variety of psychiatric disorders, including depression, panic attacks, anxiety disorders, obsessive-compulsive disorders, various phobic disorders, and PTSD.
Yet, despite the effectiveness of CBT, too few young psychiatrists and mental health professionals learn how to use it, and fewer appear to practice it. Traditional psychiatric training, by and large, continues to rely on more psychodynamic approaches, which do have value but take longer to get results than does CBT.
Clearly, partnering with patients and helping them learn new constructs can lead to positive results. More and more research shows that CBT is efficacious for patients across many age and demographic groups.
In one randomized, controlled study of 96 Latino patients with depression, for example, researchers at the University of California, Berkeley, found that group CBT administered in a primary care setting led to a significant decrease in depressive symptoms as measured by the Spanish-language version of the Patient Health Questionnaire (PHQ-9) (Cog Behav Prac. 2017 Apr 17; doi: 10.1016/j.cbpra.2017.03.02). Of the 96 patients, 92 completed the PHQ-9 at least once, and 76 completed a baseline measure of the questionnaire on day 1 of group therapy, the researchers reported. At baseline, the average PHQ-9 score was 13.88, which points to the high end of moderate depression, moving toward moderately severe depression. For every week the patients were enrolled in the therapy, PHQ-9 scores fell by 0.15 points.
The spin on CBT that I created – which I call the learning, philosophizing, and action (LPA) technique – helps patients think through problematic issues and come away with new narratives. I developed and used the LPA technique as part of a smoking-cessation program I ran for many years at the New York University Langone Medical Center. In turn, that program developed into a short-term psychotherapy program with a focus on CBT and hypnosis/relaxation techniques.
We need better codification and organization on what kinds of therapies are and are not suited for specific diagnosable problems. It is hoped that a clearer understanding of genetics, laboratory testing, and imaging, as emphasized by the National Institute of Mental Health’s Research Domain Criteria, will better equip us to decide what works best. Again, for now, helping patients learn and relearn new ways of thinking and behaving, as developed through CBT, is among the best treatments available for many mental health problems.
Dr. London, a psychiatrist who practices in New York, developed and ran a short-term psychotherapy program for 20 years at NYU Langone Medical Center and has been writing columns for 35 years. His new book about helping people feel better fast is expected to be published in fall 2017. He has no disclosures.
So often in clinical practice, guidelines and directives about psychiatric treatments lag behind the results we see every day in our offices. Such is the case with cognitive-behavioral therapy.
Earlier this summer, the departments of Veterans Affairs and Defense deemed trauma-focused psychotherapies, such as CBT, as first-line treatments for posttraumatic stress disorder over medication management. Was I surprised by these findings? Absolutely not. Likewise, last year, the American College of Physicians released a guideline recommending CBT as first-line treatment for chronic insomnia disorder in adults. Surprising? Again, not in the least.
Pierre Janet, PhD, MD, the French psychiatrist, psychologist, and neurologist, more than a hundred years ago in his L’Automatisme Psychologique, advanced the idea that thoughts can be challenged and that perceptions leading to mental problems can be reversed. Dr. Janet completed his pioneering work, including an exploration of the power of hypnosis, even though the psychoanalytic movement was in full force and many parallel ideas about treating mental disorders were barely recognized.
By the middle of the 20th century, Albert Ellis, PhD, developed rational emotive behavior therapy, which focused on thoughtfully restructuring irrational beliefs into rational ones that led to improved skills and behaviors. A decade later, the great Aaron T. Beck, MD, developed a true form of CBT. Over the years, Dr. Beck went on to develop controlled clinical trials showing CBT to be more effective in treating a variety of psychiatric disorders, including depression, panic attacks, anxiety disorders, obsessive-compulsive disorders, various phobic disorders, and PTSD.
Yet, despite the effectiveness of CBT, too few young psychiatrists and mental health professionals learn how to use it, and fewer appear to practice it. Traditional psychiatric training, by and large, continues to rely on more psychodynamic approaches, which do have value but take longer to get results than does CBT.
Clearly, partnering with patients and helping them learn new constructs can lead to positive results. More and more research shows that CBT is efficacious for patients across many age and demographic groups.
In one randomized, controlled study of 96 Latino patients with depression, for example, researchers at the University of California, Berkeley, found that group CBT administered in a primary care setting led to a significant decrease in depressive symptoms as measured by the Spanish-language version of the Patient Health Questionnaire (PHQ-9) (Cog Behav Prac. 2017 Apr 17; doi: 10.1016/j.cbpra.2017.03.02). Of the 96 patients, 92 completed the PHQ-9 at least once, and 76 completed a baseline measure of the questionnaire on day 1 of group therapy, the researchers reported. At baseline, the average PHQ-9 score was 13.88, which points to the high end of moderate depression, moving toward moderately severe depression. For every week the patients were enrolled in the therapy, PHQ-9 scores fell by 0.15 points.
The spin on CBT that I created – which I call the learning, philosophizing, and action (LPA) technique – helps patients think through problematic issues and come away with new narratives. I developed and used the LPA technique as part of a smoking-cessation program I ran for many years at the New York University Langone Medical Center. In turn, that program developed into a short-term psychotherapy program with a focus on CBT and hypnosis/relaxation techniques.
We need better codification and organization on what kinds of therapies are and are not suited for specific diagnosable problems. It is hoped that a clearer understanding of genetics, laboratory testing, and imaging, as emphasized by the National Institute of Mental Health’s Research Domain Criteria, will better equip us to decide what works best. Again, for now, helping patients learn and relearn new ways of thinking and behaving, as developed through CBT, is among the best treatments available for many mental health problems.
Dr. London, a psychiatrist who practices in New York, developed and ran a short-term psychotherapy program for 20 years at NYU Langone Medical Center and has been writing columns for 35 years. His new book about helping people feel better fast is expected to be published in fall 2017. He has no disclosures.
Fixing the ACA: 11 practical solutions
The Affordable Care Act – Obamacare – is not a disaster. It is not a long-term solution, but it is fixable. Now that repeal and/or replace efforts have failed, Congress should intelligently debate which solutions make the most sense and move forward with legislation to fix the health care system.
Before that can happen, Democrats and Republicans need to make certain acknowledgments.
Democrats should acknowledge that the ACA is flawed. Whereas many experts believe a single-payer system is ultimately going to be the best long-term answer, for our country, we’re just not there yet.
On the other side of the political aisle, Republicans should acknowledge that the ACA is not “a total disaster,” as purported by the president. That’s just not true. The ACA has dramatically reduced the U.S. uninsured population – from 49.9 million in 2010 to 29 million in 2015 (the latest figures), according to the Census Bureau. It cost much less than initially forecast after providing subsidies, assembling accountable care organizations, and providing copayment-free access to a core list of preventive services called the essential health benefits.
Nevertheless, Democrats should acknowledge that the ACA is not affordable. The cost of premiums, copayments, prescription drugs, medical procedures, and subspecialty visits are out of control. Furthermore, Democrats should admit that powerful lobbyists for plaintiffs’ lawyer associations are unwisely influencing their party’s position on tort reform.
So, how can the ACA be fixed? Earlier this year, Republican lawmakers proposed multiple versions of the Better Care Reconciliation Act (BCRA). Unlike the ACA, it really was “a total disaster.” Only 17% of Americans supported the BCRA, according to one poll from NPR/PBS NewsHour/Marist. Further, nearly every major medical organization adamantly opposed it, according to a report from NBC News.
Republicans who despise the ACA often fail to acknowledge what drove up premiums in the first place. Less competition led to higher costs. Republicans shot down the law’s original concept of a “public option.” Nineteen red states refused to expand Medicaid. All these decisions decreased competition in marketplaces.
Now Congress needs to take a deep breath, let go of their hyperpartisan expectations, and listen to these 11 suggestions. How about let’s:
1. Incentivize or persuade more states to expand Medicaid.
2. Create a public option or “public fallback plan” in every state that would compete alongside private plans in the marketplaces.
3. Possibly implement a Cadillac tax on high-cost private plans as recommended by economists.
4. Provide vigorous outreach to the millions of uninsured Americans who are eligible for but not enrolled in Medicaid or the Children’s Health Insurance Program.
5. Invest generously in parent-centered, equitable, high-quality early interventions such as Individuals with Disabilities and Education Act (IDEA) Part C, early childhood special education such as IDEA Part B, and early learning/preschool for young children. High-quality birth-to-5 programs yield $13 for every $1 invested and substantially lower health risks down the road of life.
6. Consider implementing a nationwide sugar tax. Evidence exists that taxing sugary drinks could improve the overall health of the U.S. population which could help to reduce the federal deficit over time.
7. Implement a six-point plan (as originally recommended by Sen. Bernie Sanders [I-Vt.]) to lower prescription drug prices. “Americans pay, by far, the highest prices for prescription drugs in the entire world,” Sen. Sanders notes on his website. He calls for negotiating better deals with drug manufacturers, reimporting prescriptions from Canada, restoring discounts for low-income seniors, prohibiting deals that block generic medications from entering the market, enacting stronger penalties for fraud, and requiring pricing and cost transparency.
8. Expand the role of nurses to filter out which patients need to be seen urgently, and which patients do not need an expensive trip to doctor’s office, urgent care, or emergency department. With appropriate training, nurses can manage behavior change and medication adjustment for chronic conditions; can lead care management teams for patients who are high utilizers of care; and manage transitions of care between the medical home, specialist outpatient, and hospital settings, according to primary care and nursing faculty leaders at the University of California, San Francisco.
9. Bring better accountability to health care by using bundled payments, global payments, and accountable care organizations, while simultaneously improving access and care coordination efforts for people with chronic conditions like mental health disorders and substance abuse, as recommended by the Commonwealth Fund.
10. Expand palliative care programs so far fewer people needlessly suffer and then die in very expensive intensive care units.
11. Enact common-sense tort reform. The overuse of tests and procedures because of fear of malpractice litigation, known as defensive medicine, is indirectly estimated to cost the United States $46 billion annually. According to a 2014 JAMA article, 28% of orders and 13% of costs were judged to be at least partially defensive, and 2.9% of total costs were completely defensive. Most costs were from potentially unnecessary hospitalizations. Survey studies show that greater than 90% of doctors practice defensive medicine, but what separates this perception from careful practice or patient expectations/demands remains controversial.
The main point is this – the Affordable Care Act is indeed fixable. We should not “let Obamacare implode, then deal” as the President tweeted. Whether politicians and other Americans can overcome their hyperpartisan beliefs and expectations remains to be seen.
Kevin P. Marks, MD, is a pediatrician in Eugene, Ore., and a clinical assistant professor at the Oregon Health and Science University, Portland.
The Affordable Care Act – Obamacare – is not a disaster. It is not a long-term solution, but it is fixable. Now that repeal and/or replace efforts have failed, Congress should intelligently debate which solutions make the most sense and move forward with legislation to fix the health care system.
Before that can happen, Democrats and Republicans need to make certain acknowledgments.
Democrats should acknowledge that the ACA is flawed. Whereas many experts believe a single-payer system is ultimately going to be the best long-term answer, for our country, we’re just not there yet.
On the other side of the political aisle, Republicans should acknowledge that the ACA is not “a total disaster,” as purported by the president. That’s just not true. The ACA has dramatically reduced the U.S. uninsured population – from 49.9 million in 2010 to 29 million in 2015 (the latest figures), according to the Census Bureau. It cost much less than initially forecast after providing subsidies, assembling accountable care organizations, and providing copayment-free access to a core list of preventive services called the essential health benefits.
Nevertheless, Democrats should acknowledge that the ACA is not affordable. The cost of premiums, copayments, prescription drugs, medical procedures, and subspecialty visits are out of control. Furthermore, Democrats should admit that powerful lobbyists for plaintiffs’ lawyer associations are unwisely influencing their party’s position on tort reform.
So, how can the ACA be fixed? Earlier this year, Republican lawmakers proposed multiple versions of the Better Care Reconciliation Act (BCRA). Unlike the ACA, it really was “a total disaster.” Only 17% of Americans supported the BCRA, according to one poll from NPR/PBS NewsHour/Marist. Further, nearly every major medical organization adamantly opposed it, according to a report from NBC News.
Republicans who despise the ACA often fail to acknowledge what drove up premiums in the first place. Less competition led to higher costs. Republicans shot down the law’s original concept of a “public option.” Nineteen red states refused to expand Medicaid. All these decisions decreased competition in marketplaces.
Now Congress needs to take a deep breath, let go of their hyperpartisan expectations, and listen to these 11 suggestions. How about let’s:
1. Incentivize or persuade more states to expand Medicaid.
2. Create a public option or “public fallback plan” in every state that would compete alongside private plans in the marketplaces.
3. Possibly implement a Cadillac tax on high-cost private plans as recommended by economists.
4. Provide vigorous outreach to the millions of uninsured Americans who are eligible for but not enrolled in Medicaid or the Children’s Health Insurance Program.
5. Invest generously in parent-centered, equitable, high-quality early interventions such as Individuals with Disabilities and Education Act (IDEA) Part C, early childhood special education such as IDEA Part B, and early learning/preschool for young children. High-quality birth-to-5 programs yield $13 for every $1 invested and substantially lower health risks down the road of life.
6. Consider implementing a nationwide sugar tax. Evidence exists that taxing sugary drinks could improve the overall health of the U.S. population which could help to reduce the federal deficit over time.
7. Implement a six-point plan (as originally recommended by Sen. Bernie Sanders [I-Vt.]) to lower prescription drug prices. “Americans pay, by far, the highest prices for prescription drugs in the entire world,” Sen. Sanders notes on his website. He calls for negotiating better deals with drug manufacturers, reimporting prescriptions from Canada, restoring discounts for low-income seniors, prohibiting deals that block generic medications from entering the market, enacting stronger penalties for fraud, and requiring pricing and cost transparency.
8. Expand the role of nurses to filter out which patients need to be seen urgently, and which patients do not need an expensive trip to doctor’s office, urgent care, or emergency department. With appropriate training, nurses can manage behavior change and medication adjustment for chronic conditions; can lead care management teams for patients who are high utilizers of care; and manage transitions of care between the medical home, specialist outpatient, and hospital settings, according to primary care and nursing faculty leaders at the University of California, San Francisco.
9. Bring better accountability to health care by using bundled payments, global payments, and accountable care organizations, while simultaneously improving access and care coordination efforts for people with chronic conditions like mental health disorders and substance abuse, as recommended by the Commonwealth Fund.
10. Expand palliative care programs so far fewer people needlessly suffer and then die in very expensive intensive care units.
11. Enact common-sense tort reform. The overuse of tests and procedures because of fear of malpractice litigation, known as defensive medicine, is indirectly estimated to cost the United States $46 billion annually. According to a 2014 JAMA article, 28% of orders and 13% of costs were judged to be at least partially defensive, and 2.9% of total costs were completely defensive. Most costs were from potentially unnecessary hospitalizations. Survey studies show that greater than 90% of doctors practice defensive medicine, but what separates this perception from careful practice or patient expectations/demands remains controversial.
The main point is this – the Affordable Care Act is indeed fixable. We should not “let Obamacare implode, then deal” as the President tweeted. Whether politicians and other Americans can overcome their hyperpartisan beliefs and expectations remains to be seen.
Kevin P. Marks, MD, is a pediatrician in Eugene, Ore., and a clinical assistant professor at the Oregon Health and Science University, Portland.
The Affordable Care Act – Obamacare – is not a disaster. It is not a long-term solution, but it is fixable. Now that repeal and/or replace efforts have failed, Congress should intelligently debate which solutions make the most sense and move forward with legislation to fix the health care system.
Before that can happen, Democrats and Republicans need to make certain acknowledgments.
Democrats should acknowledge that the ACA is flawed. Whereas many experts believe a single-payer system is ultimately going to be the best long-term answer, for our country, we’re just not there yet.
On the other side of the political aisle, Republicans should acknowledge that the ACA is not “a total disaster,” as purported by the president. That’s just not true. The ACA has dramatically reduced the U.S. uninsured population – from 49.9 million in 2010 to 29 million in 2015 (the latest figures), according to the Census Bureau. It cost much less than initially forecast after providing subsidies, assembling accountable care organizations, and providing copayment-free access to a core list of preventive services called the essential health benefits.
Nevertheless, Democrats should acknowledge that the ACA is not affordable. The cost of premiums, copayments, prescription drugs, medical procedures, and subspecialty visits are out of control. Furthermore, Democrats should admit that powerful lobbyists for plaintiffs’ lawyer associations are unwisely influencing their party’s position on tort reform.
So, how can the ACA be fixed? Earlier this year, Republican lawmakers proposed multiple versions of the Better Care Reconciliation Act (BCRA). Unlike the ACA, it really was “a total disaster.” Only 17% of Americans supported the BCRA, according to one poll from NPR/PBS NewsHour/Marist. Further, nearly every major medical organization adamantly opposed it, according to a report from NBC News.
Republicans who despise the ACA often fail to acknowledge what drove up premiums in the first place. Less competition led to higher costs. Republicans shot down the law’s original concept of a “public option.” Nineteen red states refused to expand Medicaid. All these decisions decreased competition in marketplaces.
Now Congress needs to take a deep breath, let go of their hyperpartisan expectations, and listen to these 11 suggestions. How about let’s:
1. Incentivize or persuade more states to expand Medicaid.
2. Create a public option or “public fallback plan” in every state that would compete alongside private plans in the marketplaces.
3. Possibly implement a Cadillac tax on high-cost private plans as recommended by economists.
4. Provide vigorous outreach to the millions of uninsured Americans who are eligible for but not enrolled in Medicaid or the Children’s Health Insurance Program.
5. Invest generously in parent-centered, equitable, high-quality early interventions such as Individuals with Disabilities and Education Act (IDEA) Part C, early childhood special education such as IDEA Part B, and early learning/preschool for young children. High-quality birth-to-5 programs yield $13 for every $1 invested and substantially lower health risks down the road of life.
6. Consider implementing a nationwide sugar tax. Evidence exists that taxing sugary drinks could improve the overall health of the U.S. population which could help to reduce the federal deficit over time.
7. Implement a six-point plan (as originally recommended by Sen. Bernie Sanders [I-Vt.]) to lower prescription drug prices. “Americans pay, by far, the highest prices for prescription drugs in the entire world,” Sen. Sanders notes on his website. He calls for negotiating better deals with drug manufacturers, reimporting prescriptions from Canada, restoring discounts for low-income seniors, prohibiting deals that block generic medications from entering the market, enacting stronger penalties for fraud, and requiring pricing and cost transparency.
8. Expand the role of nurses to filter out which patients need to be seen urgently, and which patients do not need an expensive trip to doctor’s office, urgent care, or emergency department. With appropriate training, nurses can manage behavior change and medication adjustment for chronic conditions; can lead care management teams for patients who are high utilizers of care; and manage transitions of care between the medical home, specialist outpatient, and hospital settings, according to primary care and nursing faculty leaders at the University of California, San Francisco.
9. Bring better accountability to health care by using bundled payments, global payments, and accountable care organizations, while simultaneously improving access and care coordination efforts for people with chronic conditions like mental health disorders and substance abuse, as recommended by the Commonwealth Fund.
10. Expand palliative care programs so far fewer people needlessly suffer and then die in very expensive intensive care units.
11. Enact common-sense tort reform. The overuse of tests and procedures because of fear of malpractice litigation, known as defensive medicine, is indirectly estimated to cost the United States $46 billion annually. According to a 2014 JAMA article, 28% of orders and 13% of costs were judged to be at least partially defensive, and 2.9% of total costs were completely defensive. Most costs were from potentially unnecessary hospitalizations. Survey studies show that greater than 90% of doctors practice defensive medicine, but what separates this perception from careful practice or patient expectations/demands remains controversial.
The main point is this – the Affordable Care Act is indeed fixable. We should not “let Obamacare implode, then deal” as the President tweeted. Whether politicians and other Americans can overcome their hyperpartisan beliefs and expectations remains to be seen.
Kevin P. Marks, MD, is a pediatrician in Eugene, Ore., and a clinical assistant professor at the Oregon Health and Science University, Portland.
Mental health courts: Is recidivism what counts?
In 2004, the federal government authorized $50 million for state initiatives to coordinate crime control efforts between the criminal justice and mental health systems. Some of that money was dedicated toward expansion of state mental health courts in an attempt to reduce the number of people with serious mental illness in jails and prisons.
Unlike traditional criminal courts, a mental health court is a nonadversarial problem-solving program that brings together all the stakeholders involved in a defendant’s criminal case and mental health care. A criminal defendant who agrees to participate in mental health court must participate in regular status hearings during which a judge reviews the defendant’s adherence to a court-imposed treatment plan and monitors his progress while on probation. The judge considers input from the prosecutor and the defense attorney, and also from the court’s social worker or case manager. A defendant who agrees to mental health court involvement is often placed on probation rather than sentenced to incarceration and is usually incarcerated for a shorter time pending trial.
Although mental health courts have been in existence for 20 years, data about program efficacy have been mixed. Outcome studies have been hampered by lack of truly blind subject assignment, inadequate controls, and selection bias because many mental health courts exclude defendants charged with serious violent crimes or sex offenses. Also, mental health courts are voluntary programs with significant dropout rates. Nevertheless, proponents of mental health courts believe that they prevent crime, reduce violent offending, and serve to stabilize people with serious mental illness in the community.
In a study published recently in Psychiatric Services (2017 Aug 15. doi: 10.1176/appi.ps.201700107), researchers from North Carolina University, Raleigh, addressed the effect of mental health court involvement on criminal recidivism. Lowder et al. looked at 17 outcome studies of mental health court participants published between 2004 and 2015. These studies included 16,129 participants followed for a minimum of 1 year.
Most of the included studies defined recidivism as a new arrest. For the purpose of the meta-analysis, researchers also included any incarceration, conviction, or new charge. Each study also included a comparison group of defendants processed through usual criminal procedures. Included studies generally looked at reoffending in the year after entry into the program or in the year following exit from the program.
The meta-analysis found a small but significant reduction in criminal recidivism, although the degree of this effect varied considerably between studies, and the effect disappeared completely when only moderate and high-quality studies were considered.
These results should not surprise anyone. Crime is a complex human behavior mediated by more than just psychiatric issues. Poverty, stressful life events, and substance abuse all play a role. And as an outcome variable, an arrest is not a sensitive measure because many crimes go unreported. Defendants with lower rates of reoffending may simply have more forgiving victims; for people with mental illness, that victim is often a family member.
Fortunately, crime prevention is not the sole justification for mental health programs. There are also the intangible social benefits that aren’t measured in these studies – benefits like improved quality of life, restored relationships, and the ability to participate more fully in all the joys that life has to offer. For people with serious mental illness who graduate from mental health court, that’s the outcome that counts.
Dr. Hanson is a forensic psychiatrist and coauthor of “Committed: The Battle over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). The opinions expressed are those of the author only and do not represent those of any of Dr. Hanson’s employers or consultees, including the Maryland Department of Health and Mental Hygiene and the Maryland Division of Correction.
In 2004, the federal government authorized $50 million for state initiatives to coordinate crime control efforts between the criminal justice and mental health systems. Some of that money was dedicated toward expansion of state mental health courts in an attempt to reduce the number of people with serious mental illness in jails and prisons.
Unlike traditional criminal courts, a mental health court is a nonadversarial problem-solving program that brings together all the stakeholders involved in a defendant’s criminal case and mental health care. A criminal defendant who agrees to participate in mental health court must participate in regular status hearings during which a judge reviews the defendant’s adherence to a court-imposed treatment plan and monitors his progress while on probation. The judge considers input from the prosecutor and the defense attorney, and also from the court’s social worker or case manager. A defendant who agrees to mental health court involvement is often placed on probation rather than sentenced to incarceration and is usually incarcerated for a shorter time pending trial.
Although mental health courts have been in existence for 20 years, data about program efficacy have been mixed. Outcome studies have been hampered by lack of truly blind subject assignment, inadequate controls, and selection bias because many mental health courts exclude defendants charged with serious violent crimes or sex offenses. Also, mental health courts are voluntary programs with significant dropout rates. Nevertheless, proponents of mental health courts believe that they prevent crime, reduce violent offending, and serve to stabilize people with serious mental illness in the community.
In a study published recently in Psychiatric Services (2017 Aug 15. doi: 10.1176/appi.ps.201700107), researchers from North Carolina University, Raleigh, addressed the effect of mental health court involvement on criminal recidivism. Lowder et al. looked at 17 outcome studies of mental health court participants published between 2004 and 2015. These studies included 16,129 participants followed for a minimum of 1 year.
Most of the included studies defined recidivism as a new arrest. For the purpose of the meta-analysis, researchers also included any incarceration, conviction, or new charge. Each study also included a comparison group of defendants processed through usual criminal procedures. Included studies generally looked at reoffending in the year after entry into the program or in the year following exit from the program.
The meta-analysis found a small but significant reduction in criminal recidivism, although the degree of this effect varied considerably between studies, and the effect disappeared completely when only moderate and high-quality studies were considered.
These results should not surprise anyone. Crime is a complex human behavior mediated by more than just psychiatric issues. Poverty, stressful life events, and substance abuse all play a role. And as an outcome variable, an arrest is not a sensitive measure because many crimes go unreported. Defendants with lower rates of reoffending may simply have more forgiving victims; for people with mental illness, that victim is often a family member.
Fortunately, crime prevention is not the sole justification for mental health programs. There are also the intangible social benefits that aren’t measured in these studies – benefits like improved quality of life, restored relationships, and the ability to participate more fully in all the joys that life has to offer. For people with serious mental illness who graduate from mental health court, that’s the outcome that counts.
Dr. Hanson is a forensic psychiatrist and coauthor of “Committed: The Battle over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). The opinions expressed are those of the author only and do not represent those of any of Dr. Hanson’s employers or consultees, including the Maryland Department of Health and Mental Hygiene and the Maryland Division of Correction.
In 2004, the federal government authorized $50 million for state initiatives to coordinate crime control efforts between the criminal justice and mental health systems. Some of that money was dedicated toward expansion of state mental health courts in an attempt to reduce the number of people with serious mental illness in jails and prisons.
Unlike traditional criminal courts, a mental health court is a nonadversarial problem-solving program that brings together all the stakeholders involved in a defendant’s criminal case and mental health care. A criminal defendant who agrees to participate in mental health court must participate in regular status hearings during which a judge reviews the defendant’s adherence to a court-imposed treatment plan and monitors his progress while on probation. The judge considers input from the prosecutor and the defense attorney, and also from the court’s social worker or case manager. A defendant who agrees to mental health court involvement is often placed on probation rather than sentenced to incarceration and is usually incarcerated for a shorter time pending trial.
Although mental health courts have been in existence for 20 years, data about program efficacy have been mixed. Outcome studies have been hampered by lack of truly blind subject assignment, inadequate controls, and selection bias because many mental health courts exclude defendants charged with serious violent crimes or sex offenses. Also, mental health courts are voluntary programs with significant dropout rates. Nevertheless, proponents of mental health courts believe that they prevent crime, reduce violent offending, and serve to stabilize people with serious mental illness in the community.
In a study published recently in Psychiatric Services (2017 Aug 15. doi: 10.1176/appi.ps.201700107), researchers from North Carolina University, Raleigh, addressed the effect of mental health court involvement on criminal recidivism. Lowder et al. looked at 17 outcome studies of mental health court participants published between 2004 and 2015. These studies included 16,129 participants followed for a minimum of 1 year.
Most of the included studies defined recidivism as a new arrest. For the purpose of the meta-analysis, researchers also included any incarceration, conviction, or new charge. Each study also included a comparison group of defendants processed through usual criminal procedures. Included studies generally looked at reoffending in the year after entry into the program or in the year following exit from the program.
The meta-analysis found a small but significant reduction in criminal recidivism, although the degree of this effect varied considerably between studies, and the effect disappeared completely when only moderate and high-quality studies were considered.
These results should not surprise anyone. Crime is a complex human behavior mediated by more than just psychiatric issues. Poverty, stressful life events, and substance abuse all play a role. And as an outcome variable, an arrest is not a sensitive measure because many crimes go unreported. Defendants with lower rates of reoffending may simply have more forgiving victims; for people with mental illness, that victim is often a family member.
Fortunately, crime prevention is not the sole justification for mental health programs. There are also the intangible social benefits that aren’t measured in these studies – benefits like improved quality of life, restored relationships, and the ability to participate more fully in all the joys that life has to offer. For people with serious mental illness who graduate from mental health court, that’s the outcome that counts.
Dr. Hanson is a forensic psychiatrist and coauthor of “Committed: The Battle over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). The opinions expressed are those of the author only and do not represent those of any of Dr. Hanson’s employers or consultees, including the Maryland Department of Health and Mental Hygiene and the Maryland Division of Correction.
Consulting for the dead
As the years roll on, it’s nice to be open to new experiences. Till now, for instance, every patient I’ve examined has been alive.
My local hospital called 2 weeks ago. Although I’m on staff, I haven’t consulted on an inpatient there in 20 years.
I ran their skin clinic years ago. Medical residents came to my office for an elective.
“Did you see the glucagonoma on Sefton 6?” a resident would ask.
“No, they didn’t call me for that. They called me for the seborrheic dermatitis on Sefton 4.”
I no longer visit hospitals; nowadays, the main function of my hospital affiliations is to be able to see patients insured on their referral circles. This year, my hospital made a new rule: All dermatologists must cover consults to stay on staff. I drew 3 weeks in June. For 2½ weeks, nobody called. And then, late one morning …
“Hello, doctor. I’m a nurse in the medical ICU. We need your help.”
“Yes?”
“A 25-year-old man died of a drug overdose. We need to harvest his organs. He has skin changes on his back and a blister in his groin, and we need to know that these pose no bar to transplants.”
“I’m stuck in the office,“ I said. “I could come tonight.”
“Can someone else come?” he asked. “Time is critical.”
I told him I would try.
My morning session ended on time. Patient callbacks and lunch could wait. I dashed over to the hospital, phoning the nurse en route. “On my way,” I said, “but I don’t know where the ICU is, and I don’t know your protocols – what forms to fill out and so on.”
He gave me the name of the building and told me to go to the fourth floor. “We’ll have the paperwork ready,” he said.
The parking garage had a free space near the entrance. Asking directions in the lobby, I blundered my way over to the ICU building, newly built and unfamiliar, where the nurse greeted me.
“We appreciate your coming,” he said. “I’ll ask the family at the bedside to leave.”
He introduced a resident, who told me dermatologists dropped by the ICU from time to time to assess issues of graft-versus-host rashes, that sort of thing.
The nurse gave me a yellow paper gown. The patient had his own room. Back in my day, ICUs had no quiet, private spaces.
A middle-aged woman stood by the bed rail – the stepmother of the deceased. What do you say to a newly bereaved family member in this circumstance? “I am your deceased stepson’s dermatology consultant. Pleased to meet you”?
Instead, I said I was sorry for her loss, which seemed pallid but apt. She withdrew.
In bed, was a young man attached to life support. “No track marks,” the nurse observed. “He must have snorted something.”
The nurse and the resident rolled the body over, and I noted the red marks on his back. “Those are from acne,” I said. “No infection.”
Laying him down, they showed me a 1-mm scab at the base of his scrotum. “Appears to be trauma,” I said, “perhaps a scratch. Not herpes or anything infectious.”
Finding nothing else on his integument, I turned to leave. His stepmother was sitting on a chair near the door, her head in her hands. As I passed, she looked up.
In most life settings, including doctors’ offices, there are protocols of behavior, guidelines for how to act, what to say: “We’re all done.” “This should take care of it.” “I will write up a report.” “Nice to have met you.” “Take care.”
I looked down at her tortured face and said, “There is nothing to say.”
At this, I lost my composure, and left.
“I’m not sure what we were concerned about,” said the nurse, “but we appreciate your coming over.” He handed me a sheet of blank paper. I scribbled my nonfindings. Now the transplant wheels could begin to turn.
I left the ICU to its normal goings-on and returned to my office, where the paths of clinical engagement are well worn – and the patients are still alive.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
As the years roll on, it’s nice to be open to new experiences. Till now, for instance, every patient I’ve examined has been alive.
My local hospital called 2 weeks ago. Although I’m on staff, I haven’t consulted on an inpatient there in 20 years.
I ran their skin clinic years ago. Medical residents came to my office for an elective.
“Did you see the glucagonoma on Sefton 6?” a resident would ask.
“No, they didn’t call me for that. They called me for the seborrheic dermatitis on Sefton 4.”
I no longer visit hospitals; nowadays, the main function of my hospital affiliations is to be able to see patients insured on their referral circles. This year, my hospital made a new rule: All dermatologists must cover consults to stay on staff. I drew 3 weeks in June. For 2½ weeks, nobody called. And then, late one morning …
“Hello, doctor. I’m a nurse in the medical ICU. We need your help.”
“Yes?”
“A 25-year-old man died of a drug overdose. We need to harvest his organs. He has skin changes on his back and a blister in his groin, and we need to know that these pose no bar to transplants.”
“I’m stuck in the office,“ I said. “I could come tonight.”
“Can someone else come?” he asked. “Time is critical.”
I told him I would try.
My morning session ended on time. Patient callbacks and lunch could wait. I dashed over to the hospital, phoning the nurse en route. “On my way,” I said, “but I don’t know where the ICU is, and I don’t know your protocols – what forms to fill out and so on.”
He gave me the name of the building and told me to go to the fourth floor. “We’ll have the paperwork ready,” he said.
The parking garage had a free space near the entrance. Asking directions in the lobby, I blundered my way over to the ICU building, newly built and unfamiliar, where the nurse greeted me.
“We appreciate your coming,” he said. “I’ll ask the family at the bedside to leave.”
He introduced a resident, who told me dermatologists dropped by the ICU from time to time to assess issues of graft-versus-host rashes, that sort of thing.
The nurse gave me a yellow paper gown. The patient had his own room. Back in my day, ICUs had no quiet, private spaces.
A middle-aged woman stood by the bed rail – the stepmother of the deceased. What do you say to a newly bereaved family member in this circumstance? “I am your deceased stepson’s dermatology consultant. Pleased to meet you”?
Instead, I said I was sorry for her loss, which seemed pallid but apt. She withdrew.
In bed, was a young man attached to life support. “No track marks,” the nurse observed. “He must have snorted something.”
The nurse and the resident rolled the body over, and I noted the red marks on his back. “Those are from acne,” I said. “No infection.”
Laying him down, they showed me a 1-mm scab at the base of his scrotum. “Appears to be trauma,” I said, “perhaps a scratch. Not herpes or anything infectious.”
Finding nothing else on his integument, I turned to leave. His stepmother was sitting on a chair near the door, her head in her hands. As I passed, she looked up.
In most life settings, including doctors’ offices, there are protocols of behavior, guidelines for how to act, what to say: “We’re all done.” “This should take care of it.” “I will write up a report.” “Nice to have met you.” “Take care.”
I looked down at her tortured face and said, “There is nothing to say.”
At this, I lost my composure, and left.
“I’m not sure what we were concerned about,” said the nurse, “but we appreciate your coming over.” He handed me a sheet of blank paper. I scribbled my nonfindings. Now the transplant wheels could begin to turn.
I left the ICU to its normal goings-on and returned to my office, where the paths of clinical engagement are well worn – and the patients are still alive.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
As the years roll on, it’s nice to be open to new experiences. Till now, for instance, every patient I’ve examined has been alive.
My local hospital called 2 weeks ago. Although I’m on staff, I haven’t consulted on an inpatient there in 20 years.
I ran their skin clinic years ago. Medical residents came to my office for an elective.
“Did you see the glucagonoma on Sefton 6?” a resident would ask.
“No, they didn’t call me for that. They called me for the seborrheic dermatitis on Sefton 4.”
I no longer visit hospitals; nowadays, the main function of my hospital affiliations is to be able to see patients insured on their referral circles. This year, my hospital made a new rule: All dermatologists must cover consults to stay on staff. I drew 3 weeks in June. For 2½ weeks, nobody called. And then, late one morning …
“Hello, doctor. I’m a nurse in the medical ICU. We need your help.”
“Yes?”
“A 25-year-old man died of a drug overdose. We need to harvest his organs. He has skin changes on his back and a blister in his groin, and we need to know that these pose no bar to transplants.”
“I’m stuck in the office,“ I said. “I could come tonight.”
“Can someone else come?” he asked. “Time is critical.”
I told him I would try.
My morning session ended on time. Patient callbacks and lunch could wait. I dashed over to the hospital, phoning the nurse en route. “On my way,” I said, “but I don’t know where the ICU is, and I don’t know your protocols – what forms to fill out and so on.”
He gave me the name of the building and told me to go to the fourth floor. “We’ll have the paperwork ready,” he said.
The parking garage had a free space near the entrance. Asking directions in the lobby, I blundered my way over to the ICU building, newly built and unfamiliar, where the nurse greeted me.
“We appreciate your coming,” he said. “I’ll ask the family at the bedside to leave.”
He introduced a resident, who told me dermatologists dropped by the ICU from time to time to assess issues of graft-versus-host rashes, that sort of thing.
The nurse gave me a yellow paper gown. The patient had his own room. Back in my day, ICUs had no quiet, private spaces.
A middle-aged woman stood by the bed rail – the stepmother of the deceased. What do you say to a newly bereaved family member in this circumstance? “I am your deceased stepson’s dermatology consultant. Pleased to meet you”?
Instead, I said I was sorry for her loss, which seemed pallid but apt. She withdrew.
In bed, was a young man attached to life support. “No track marks,” the nurse observed. “He must have snorted something.”
The nurse and the resident rolled the body over, and I noted the red marks on his back. “Those are from acne,” I said. “No infection.”
Laying him down, they showed me a 1-mm scab at the base of his scrotum. “Appears to be trauma,” I said, “perhaps a scratch. Not herpes or anything infectious.”
Finding nothing else on his integument, I turned to leave. His stepmother was sitting on a chair near the door, her head in her hands. As I passed, she looked up.
In most life settings, including doctors’ offices, there are protocols of behavior, guidelines for how to act, what to say: “We’re all done.” “This should take care of it.” “I will write up a report.” “Nice to have met you.” “Take care.”
I looked down at her tortured face and said, “There is nothing to say.”
At this, I lost my composure, and left.
“I’m not sure what we were concerned about,” said the nurse, “but we appreciate your coming over.” He handed me a sheet of blank paper. I scribbled my nonfindings. Now the transplant wheels could begin to turn.
I left the ICU to its normal goings-on and returned to my office, where the paths of clinical engagement are well worn – and the patients are still alive.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
The cost of experimental medicine
It has been a remarkable summer of milestones and crises for high-technology medicine.
An FDA panel has unanimously approved a gene therapy: The patient’s own immune cells are taken from his or her body, genetically modified, and reinfused to attack cancer. While the treatment has some dangers, it can be worth trying when conventional therapy has failed, and it appears to be curative when it works. Final FDA approval is expected in September.
While those breakthroughs were occurring, the parents of Charlie Gard, an infant in England with a very rare and devastating mitochondrial disease, were seeking experimental therapy for their child. The medical staff disagreed with the parents: They recommended that the best thing for Charlie would be to stop the ventilator and allow him to die, rather than let him to continue to suffer. Three British courts reviewed Charlie’s case and concurred with the medical staff; on appeal, the European Court of Human Rights also denied the parents’ wishes.
End of life cases similar to Charlie’s are not rare. In modern medicine, parents sometimes must make the heart-wrenching decision to stop aggressive therapies and accept that death is imminent and unavoidable. Many factors go into making that decision. Both the courts and medical staff presume that parents are the best decision makers. Generally, medical staff provide emotional and spiritual support to the parents, along with a tincture of time. In the vast majority of cases, parents and physicians come to agree on the course of care, but sometimes, there are irreconcilable disagreements.
It is rare for courts to overrule parents. The government typically intervenes only when the harm from a parent’s choice exceeds some threshold. For instance, it is not in a child’s best interest to be put in a car during a blizzard and driven to the store to get cigarettes. But neither is it wise to have an intrusive government reviewing every choice a parent makes. The potential harm must be large enough, likely enough, and imminent enough before most judges will intervene. The law will insist the child be in a car seat at least.
In Charlie’s case, the medical staff and the judges all explicitly said that the cost of therapy did not factor into their decision making; they looked solely at what was best for Charlie. The focus was on whether the unproven potential benefits of experimental therapy outweighed the risk of suffering caused by the therapy and continued intensive medical care.
Even when a bedside decision ignores the financial impact, money often structures which therapeutic choices are available. There are also issues of equitable access to be raised and weighed. Expenditures impact other social choices.
Money influenced the actions of Martin Shkreli, who is best known as the pharmacy company executive who markedly increased the price of a drug. Mr. Shkreli was recently convicted on three of eight charges for securities fraud, and sentencing is pending; the convictions were not related to the price increase.
The United States has created some amazing technologies to save individual, identifiable lives, but they come at a high price that often costs lives in ways more subtle than the incident in India. At some point, the government and the public are responsible for either financing or rationing care, but that doesn’t absolve the scientists completely. The Russell-Einstein (Pugwash) Manifesto established that scientists have a moral accountability for the negative consequences of creating new technology, and that includes the financial aspects.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected]
It has been a remarkable summer of milestones and crises for high-technology medicine.
An FDA panel has unanimously approved a gene therapy: The patient’s own immune cells are taken from his or her body, genetically modified, and reinfused to attack cancer. While the treatment has some dangers, it can be worth trying when conventional therapy has failed, and it appears to be curative when it works. Final FDA approval is expected in September.
While those breakthroughs were occurring, the parents of Charlie Gard, an infant in England with a very rare and devastating mitochondrial disease, were seeking experimental therapy for their child. The medical staff disagreed with the parents: They recommended that the best thing for Charlie would be to stop the ventilator and allow him to die, rather than let him to continue to suffer. Three British courts reviewed Charlie’s case and concurred with the medical staff; on appeal, the European Court of Human Rights also denied the parents’ wishes.
End of life cases similar to Charlie’s are not rare. In modern medicine, parents sometimes must make the heart-wrenching decision to stop aggressive therapies and accept that death is imminent and unavoidable. Many factors go into making that decision. Both the courts and medical staff presume that parents are the best decision makers. Generally, medical staff provide emotional and spiritual support to the parents, along with a tincture of time. In the vast majority of cases, parents and physicians come to agree on the course of care, but sometimes, there are irreconcilable disagreements.
It is rare for courts to overrule parents. The government typically intervenes only when the harm from a parent’s choice exceeds some threshold. For instance, it is not in a child’s best interest to be put in a car during a blizzard and driven to the store to get cigarettes. But neither is it wise to have an intrusive government reviewing every choice a parent makes. The potential harm must be large enough, likely enough, and imminent enough before most judges will intervene. The law will insist the child be in a car seat at least.
In Charlie’s case, the medical staff and the judges all explicitly said that the cost of therapy did not factor into their decision making; they looked solely at what was best for Charlie. The focus was on whether the unproven potential benefits of experimental therapy outweighed the risk of suffering caused by the therapy and continued intensive medical care.
Even when a bedside decision ignores the financial impact, money often structures which therapeutic choices are available. There are also issues of equitable access to be raised and weighed. Expenditures impact other social choices.
Money influenced the actions of Martin Shkreli, who is best known as the pharmacy company executive who markedly increased the price of a drug. Mr. Shkreli was recently convicted on three of eight charges for securities fraud, and sentencing is pending; the convictions were not related to the price increase.
The United States has created some amazing technologies to save individual, identifiable lives, but they come at a high price that often costs lives in ways more subtle than the incident in India. At some point, the government and the public are responsible for either financing or rationing care, but that doesn’t absolve the scientists completely. The Russell-Einstein (Pugwash) Manifesto established that scientists have a moral accountability for the negative consequences of creating new technology, and that includes the financial aspects.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected]
It has been a remarkable summer of milestones and crises for high-technology medicine.
An FDA panel has unanimously approved a gene therapy: The patient’s own immune cells are taken from his or her body, genetically modified, and reinfused to attack cancer. While the treatment has some dangers, it can be worth trying when conventional therapy has failed, and it appears to be curative when it works. Final FDA approval is expected in September.
While those breakthroughs were occurring, the parents of Charlie Gard, an infant in England with a very rare and devastating mitochondrial disease, were seeking experimental therapy for their child. The medical staff disagreed with the parents: They recommended that the best thing for Charlie would be to stop the ventilator and allow him to die, rather than let him to continue to suffer. Three British courts reviewed Charlie’s case and concurred with the medical staff; on appeal, the European Court of Human Rights also denied the parents’ wishes.
End of life cases similar to Charlie’s are not rare. In modern medicine, parents sometimes must make the heart-wrenching decision to stop aggressive therapies and accept that death is imminent and unavoidable. Many factors go into making that decision. Both the courts and medical staff presume that parents are the best decision makers. Generally, medical staff provide emotional and spiritual support to the parents, along with a tincture of time. In the vast majority of cases, parents and physicians come to agree on the course of care, but sometimes, there are irreconcilable disagreements.
It is rare for courts to overrule parents. The government typically intervenes only when the harm from a parent’s choice exceeds some threshold. For instance, it is not in a child’s best interest to be put in a car during a blizzard and driven to the store to get cigarettes. But neither is it wise to have an intrusive government reviewing every choice a parent makes. The potential harm must be large enough, likely enough, and imminent enough before most judges will intervene. The law will insist the child be in a car seat at least.
In Charlie’s case, the medical staff and the judges all explicitly said that the cost of therapy did not factor into their decision making; they looked solely at what was best for Charlie. The focus was on whether the unproven potential benefits of experimental therapy outweighed the risk of suffering caused by the therapy and continued intensive medical care.
Even when a bedside decision ignores the financial impact, money often structures which therapeutic choices are available. There are also issues of equitable access to be raised and weighed. Expenditures impact other social choices.
Money influenced the actions of Martin Shkreli, who is best known as the pharmacy company executive who markedly increased the price of a drug. Mr. Shkreli was recently convicted on three of eight charges for securities fraud, and sentencing is pending; the convictions were not related to the price increase.
The United States has created some amazing technologies to save individual, identifiable lives, but they come at a high price that often costs lives in ways more subtle than the incident in India. At some point, the government and the public are responsible for either financing or rationing care, but that doesn’t absolve the scientists completely. The Russell-Einstein (Pugwash) Manifesto established that scientists have a moral accountability for the negative consequences of creating new technology, and that includes the financial aspects.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected]