User login
Copy and paste at your own risk: The dangers of electronic ‘plagiarism’
Between "Hangovers," Bradley Cooper starred in a largely forgettable melodrama called "The Words." The main character was an aspiring writer whose career first skyrockets and then implodes when he plagiarizes an entire novel from a dusty manuscript found buried in an old briefcase bought at an antique store. As art, "The Words" is destined for the on-demand scrap heap, but it may yet be redeemed as a cautionary tale for anyone who creates electronic health records.
While EHRs have many advantages that can improve health care delivery, including easy access and portability, the same technology that affords these advantages can also promote careless practices that may call into question the accuracy of the entire record and make it difficult, if not impossible, for health care providers to defend themselves in court. Among the most troublesome EHR misuses we see in litigation is the inappropriate use of copy and paste functions, whereby a health care provider "plagiarizes" his/her own or a colleague’s prior documentation.
In medical negligence claims, the accuracy of the patient’s medical record and the credibility of the health care providers are often both at issue, and many times the two go hand in hand. Lawyers representing injured patients love to point out errors in the medical record, whether or not the error caused any patient harm, because – the argument goes – if the medical provider was careless in record-keeping, then chances are he/she was also careless in the treatment at issue. So too, if the jury is provided with facts that differ from the medical record, suspicion arises. Thus, an innocent but preoccupied provider is accused of lying or of trying to cover up a treatment error. To avoid these insinuations, clinicians must put time and effort, as well as original thought, into medical record documentation.
Our experience in reviewing medical records for litigation suggests that a surprising number of practitioners routinely copy and paste information from a prior entry in the EHR. The excuses we have heard for this run the gamut from unfamiliarity with the electronic system to lack of time and, ironically, the need to ensure accurate documentation. Similarly, in "The Words," when Bradley Cooper’s character starts copying another author’s manuscript – word for word – onto his laptop, he tells himself that he is doing it simply for inspiration. Excuses aside, this kind of rote replication is seductively easy but fraught with danger, particularly if the EHR later comes under scrutiny.
When data from a prior note in the EHR are copied, little thought or focus is given to context or clarity, and the cobbled-together entry is frequently disorganized and unclear. Worse yet, such copying can result in entering outdated or inaccurate information into the patient’s chart. Even simple errors of this kind can be very damaging. Imagine trying to convince a jury that you are a careful and caring practitioner when it has been pointed out to them that, in your records, your patient’s blood pressure was exactly the same every time she was in your office over the last 5 years. Or that despite the fact that she was experiencing a precipitous, unexplained weight loss, you continued to describe her as morbidly obese. Or that even though her husband died 3 years ago, your records show her "accompanied by spouse" at every visit.
Sometimes EHR plagiarism goes right to the heart of the negligence claim. Where the claim is inappropriate discharge of a patient who died a few days after leaving the hospital, the defense must show that the patient’s condition improved and that troubling symptoms seen on admission responded appropriately to treatment. This effort is hampered by documentation prepared many days or weeks into a hospitalization that copies symptoms and physical findings that are no longer present. Inaccurate information in the EHR can also confuse other medical providers, and the time necessary to reconcile inconsistent information may delay treatment. Likewise, if inaccurate information is relied on for treatment decisions, the results can be disastrous.
It is often argued in litigation that if something doesn’t appear in the medical record it didn’t happen. A corollary to this dubious "rule" is that once bad information is documented in a medical record, it will be redocumented over and over and over again. Predictably, the more times the erroneous data are repeated in the EHR, the more "reliable" it becomes. This problem has been around a long time, but EHR plagiarism has made it worse.
The medical record is the most important evidence in any medical negligence case. While it is true that only a small fraction of medical records will ever see the inside of a courtroom, you should always document assuming the chart in front of you could end up there. This requires time, original thought, accuracy, and completeness. Copying and pasting the electronic medical record, while superficially efficient, is the enemy of these goals, and could leave you – like Bradley Cooper in "The Words" – wondering what happened to your promising career.
Ms. Kane and Mr. Balaguer are in private practice in Wilmington, Del. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University, Philadelphia. He is also editor-in-chief of Redi-Reference Inc., a software company that creates mobile apps.
Between "Hangovers," Bradley Cooper starred in a largely forgettable melodrama called "The Words." The main character was an aspiring writer whose career first skyrockets and then implodes when he plagiarizes an entire novel from a dusty manuscript found buried in an old briefcase bought at an antique store. As art, "The Words" is destined for the on-demand scrap heap, but it may yet be redeemed as a cautionary tale for anyone who creates electronic health records.
While EHRs have many advantages that can improve health care delivery, including easy access and portability, the same technology that affords these advantages can also promote careless practices that may call into question the accuracy of the entire record and make it difficult, if not impossible, for health care providers to defend themselves in court. Among the most troublesome EHR misuses we see in litigation is the inappropriate use of copy and paste functions, whereby a health care provider "plagiarizes" his/her own or a colleague’s prior documentation.
In medical negligence claims, the accuracy of the patient’s medical record and the credibility of the health care providers are often both at issue, and many times the two go hand in hand. Lawyers representing injured patients love to point out errors in the medical record, whether or not the error caused any patient harm, because – the argument goes – if the medical provider was careless in record-keeping, then chances are he/she was also careless in the treatment at issue. So too, if the jury is provided with facts that differ from the medical record, suspicion arises. Thus, an innocent but preoccupied provider is accused of lying or of trying to cover up a treatment error. To avoid these insinuations, clinicians must put time and effort, as well as original thought, into medical record documentation.
Our experience in reviewing medical records for litigation suggests that a surprising number of practitioners routinely copy and paste information from a prior entry in the EHR. The excuses we have heard for this run the gamut from unfamiliarity with the electronic system to lack of time and, ironically, the need to ensure accurate documentation. Similarly, in "The Words," when Bradley Cooper’s character starts copying another author’s manuscript – word for word – onto his laptop, he tells himself that he is doing it simply for inspiration. Excuses aside, this kind of rote replication is seductively easy but fraught with danger, particularly if the EHR later comes under scrutiny.
When data from a prior note in the EHR are copied, little thought or focus is given to context or clarity, and the cobbled-together entry is frequently disorganized and unclear. Worse yet, such copying can result in entering outdated or inaccurate information into the patient’s chart. Even simple errors of this kind can be very damaging. Imagine trying to convince a jury that you are a careful and caring practitioner when it has been pointed out to them that, in your records, your patient’s blood pressure was exactly the same every time she was in your office over the last 5 years. Or that despite the fact that she was experiencing a precipitous, unexplained weight loss, you continued to describe her as morbidly obese. Or that even though her husband died 3 years ago, your records show her "accompanied by spouse" at every visit.
Sometimes EHR plagiarism goes right to the heart of the negligence claim. Where the claim is inappropriate discharge of a patient who died a few days after leaving the hospital, the defense must show that the patient’s condition improved and that troubling symptoms seen on admission responded appropriately to treatment. This effort is hampered by documentation prepared many days or weeks into a hospitalization that copies symptoms and physical findings that are no longer present. Inaccurate information in the EHR can also confuse other medical providers, and the time necessary to reconcile inconsistent information may delay treatment. Likewise, if inaccurate information is relied on for treatment decisions, the results can be disastrous.
It is often argued in litigation that if something doesn’t appear in the medical record it didn’t happen. A corollary to this dubious "rule" is that once bad information is documented in a medical record, it will be redocumented over and over and over again. Predictably, the more times the erroneous data are repeated in the EHR, the more "reliable" it becomes. This problem has been around a long time, but EHR plagiarism has made it worse.
The medical record is the most important evidence in any medical negligence case. While it is true that only a small fraction of medical records will ever see the inside of a courtroom, you should always document assuming the chart in front of you could end up there. This requires time, original thought, accuracy, and completeness. Copying and pasting the electronic medical record, while superficially efficient, is the enemy of these goals, and could leave you – like Bradley Cooper in "The Words" – wondering what happened to your promising career.
Ms. Kane and Mr. Balaguer are in private practice in Wilmington, Del. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University, Philadelphia. He is also editor-in-chief of Redi-Reference Inc., a software company that creates mobile apps.
Between "Hangovers," Bradley Cooper starred in a largely forgettable melodrama called "The Words." The main character was an aspiring writer whose career first skyrockets and then implodes when he plagiarizes an entire novel from a dusty manuscript found buried in an old briefcase bought at an antique store. As art, "The Words" is destined for the on-demand scrap heap, but it may yet be redeemed as a cautionary tale for anyone who creates electronic health records.
While EHRs have many advantages that can improve health care delivery, including easy access and portability, the same technology that affords these advantages can also promote careless practices that may call into question the accuracy of the entire record and make it difficult, if not impossible, for health care providers to defend themselves in court. Among the most troublesome EHR misuses we see in litigation is the inappropriate use of copy and paste functions, whereby a health care provider "plagiarizes" his/her own or a colleague’s prior documentation.
In medical negligence claims, the accuracy of the patient’s medical record and the credibility of the health care providers are often both at issue, and many times the two go hand in hand. Lawyers representing injured patients love to point out errors in the medical record, whether or not the error caused any patient harm, because – the argument goes – if the medical provider was careless in record-keeping, then chances are he/she was also careless in the treatment at issue. So too, if the jury is provided with facts that differ from the medical record, suspicion arises. Thus, an innocent but preoccupied provider is accused of lying or of trying to cover up a treatment error. To avoid these insinuations, clinicians must put time and effort, as well as original thought, into medical record documentation.
Our experience in reviewing medical records for litigation suggests that a surprising number of practitioners routinely copy and paste information from a prior entry in the EHR. The excuses we have heard for this run the gamut from unfamiliarity with the electronic system to lack of time and, ironically, the need to ensure accurate documentation. Similarly, in "The Words," when Bradley Cooper’s character starts copying another author’s manuscript – word for word – onto his laptop, he tells himself that he is doing it simply for inspiration. Excuses aside, this kind of rote replication is seductively easy but fraught with danger, particularly if the EHR later comes under scrutiny.
When data from a prior note in the EHR are copied, little thought or focus is given to context or clarity, and the cobbled-together entry is frequently disorganized and unclear. Worse yet, such copying can result in entering outdated or inaccurate information into the patient’s chart. Even simple errors of this kind can be very damaging. Imagine trying to convince a jury that you are a careful and caring practitioner when it has been pointed out to them that, in your records, your patient’s blood pressure was exactly the same every time she was in your office over the last 5 years. Or that despite the fact that she was experiencing a precipitous, unexplained weight loss, you continued to describe her as morbidly obese. Or that even though her husband died 3 years ago, your records show her "accompanied by spouse" at every visit.
Sometimes EHR plagiarism goes right to the heart of the negligence claim. Where the claim is inappropriate discharge of a patient who died a few days after leaving the hospital, the defense must show that the patient’s condition improved and that troubling symptoms seen on admission responded appropriately to treatment. This effort is hampered by documentation prepared many days or weeks into a hospitalization that copies symptoms and physical findings that are no longer present. Inaccurate information in the EHR can also confuse other medical providers, and the time necessary to reconcile inconsistent information may delay treatment. Likewise, if inaccurate information is relied on for treatment decisions, the results can be disastrous.
It is often argued in litigation that if something doesn’t appear in the medical record it didn’t happen. A corollary to this dubious "rule" is that once bad information is documented in a medical record, it will be redocumented over and over and over again. Predictably, the more times the erroneous data are repeated in the EHR, the more "reliable" it becomes. This problem has been around a long time, but EHR plagiarism has made it worse.
The medical record is the most important evidence in any medical negligence case. While it is true that only a small fraction of medical records will ever see the inside of a courtroom, you should always document assuming the chart in front of you could end up there. This requires time, original thought, accuracy, and completeness. Copying and pasting the electronic medical record, while superficially efficient, is the enemy of these goals, and could leave you – like Bradley Cooper in "The Words" – wondering what happened to your promising career.
Ms. Kane and Mr. Balaguer are in private practice in Wilmington, Del. Dr. Skolnik is associate director of the family medicine residency program at Abington Memorial Hospital and professor of family and community medicine at Temple University, Philadelphia. He is also editor-in-chief of Redi-Reference Inc., a software company that creates mobile apps.
Physician, heal thyself: my private medicine stash
I’m a pill person. I admit it.
I hate being sick and dealing with the aches and pains of everyday life. I’m the first person to hit the medicine cabinet. When I’m dealing with patients, I don’t want my own body to distract me from theirs.
So in my office, I have this drawer. My secretary calls it "the pharmacy."
As you can see, I have pretty much everything covered: Sudafed, Zyrtec, NSAIDs, an expired Celebrex packet (it’s been a few years since they detailed neurologists), and generics for Tylenol, Excedrin, and Zantac. I even have a nail clipper, ChapStick, an old albuterol metered-dose inhaler, cough drops, Q-tips, and zinc lozenges. An old hemostat that somehow ended up in there; I use it to remove tough staples. (There used to be caffeine pills, but my staff threatened to kill me if I didn’t give them up.)
Does this make me less of a doctor? I hope not. If I don’t feel good, I can’t concentrate as well on the task at hand, and in my case that’s patient care. I don’t pop pills every day, but if I need to, I do.
My staff also occasionally comes in with the seasonal viral crud, or headaches from dealing with headaches, or back pain from carrying 45 pounds of aging x-ray films back to my office. It always helps if I can keep them in shape to handle these days. They know it’s back here if they need anything.
I’m not pushing this philosophy on patients. I always mention, in any medication discussion, that I can’t make them take anything they don’t want to. (I’m also not offering them anything from the drawer – that’s my stash.) But I do emphasize that medications are, in large part, what I have to offer.
But as for me? Physician, heal thyself.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
I’m a pill person. I admit it.
I hate being sick and dealing with the aches and pains of everyday life. I’m the first person to hit the medicine cabinet. When I’m dealing with patients, I don’t want my own body to distract me from theirs.
So in my office, I have this drawer. My secretary calls it "the pharmacy."
As you can see, I have pretty much everything covered: Sudafed, Zyrtec, NSAIDs, an expired Celebrex packet (it’s been a few years since they detailed neurologists), and generics for Tylenol, Excedrin, and Zantac. I even have a nail clipper, ChapStick, an old albuterol metered-dose inhaler, cough drops, Q-tips, and zinc lozenges. An old hemostat that somehow ended up in there; I use it to remove tough staples. (There used to be caffeine pills, but my staff threatened to kill me if I didn’t give them up.)
Does this make me less of a doctor? I hope not. If I don’t feel good, I can’t concentrate as well on the task at hand, and in my case that’s patient care. I don’t pop pills every day, but if I need to, I do.
My staff also occasionally comes in with the seasonal viral crud, or headaches from dealing with headaches, or back pain from carrying 45 pounds of aging x-ray films back to my office. It always helps if I can keep them in shape to handle these days. They know it’s back here if they need anything.
I’m not pushing this philosophy on patients. I always mention, in any medication discussion, that I can’t make them take anything they don’t want to. (I’m also not offering them anything from the drawer – that’s my stash.) But I do emphasize that medications are, in large part, what I have to offer.
But as for me? Physician, heal thyself.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
I’m a pill person. I admit it.
I hate being sick and dealing with the aches and pains of everyday life. I’m the first person to hit the medicine cabinet. When I’m dealing with patients, I don’t want my own body to distract me from theirs.
So in my office, I have this drawer. My secretary calls it "the pharmacy."
As you can see, I have pretty much everything covered: Sudafed, Zyrtec, NSAIDs, an expired Celebrex packet (it’s been a few years since they detailed neurologists), and generics for Tylenol, Excedrin, and Zantac. I even have a nail clipper, ChapStick, an old albuterol metered-dose inhaler, cough drops, Q-tips, and zinc lozenges. An old hemostat that somehow ended up in there; I use it to remove tough staples. (There used to be caffeine pills, but my staff threatened to kill me if I didn’t give them up.)
Does this make me less of a doctor? I hope not. If I don’t feel good, I can’t concentrate as well on the task at hand, and in my case that’s patient care. I don’t pop pills every day, but if I need to, I do.
My staff also occasionally comes in with the seasonal viral crud, or headaches from dealing with headaches, or back pain from carrying 45 pounds of aging x-ray films back to my office. It always helps if I can keep them in shape to handle these days. They know it’s back here if they need anything.
I’m not pushing this philosophy on patients. I always mention, in any medication discussion, that I can’t make them take anything they don’t want to. (I’m also not offering them anything from the drawer – that’s my stash.) But I do emphasize that medications are, in large part, what I have to offer.
But as for me? Physician, heal thyself.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Symple is as simple does
After the surprising, top-line result from the SYMPLICITY HTN-3 trial came out in a press release from Medtronic last January, the question remained of what went wrong: Why did renal denervation fail to outperform a sham procedure in reducing blood pressure?
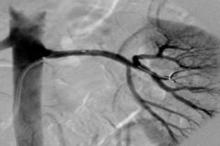
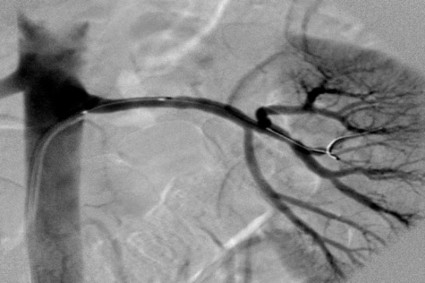
The apparent answer emerged in late March when the full results finally went public in a report at the annual meeting of the American College of Cardiology and in an article in the New England Journal of Medicine. Many of the 364 patients who underwent active denervation – which involves zapping the efferent nerves that run along the outer wall of the renal arteries with a few brief pulses of radiofrequency energy – probably failed to receive adequate treatment, so their renal innervation remained mostly intact. There’s no proof that’s what happened, but it seems plausible given that all the U.S. operators in the trial had no prior experience performing the procedure, as well as the observation several years ago that denervation can produce highly variable results and is very operator dependent.
This variability in success had been documented back in the 2000s by one of the pioneers of renal denervation, Dr. Murray Esler of Melbourne, yet the people who designed SYMPLICITY HTN-3 didn’t pay attention. Their failure to apply what earlier findings had taught about the variability of denervation proved especially egregious, as the interventionalists also couldn’t gauge their procedural success because no easy way exists right now to do this.
But these details didn’t slow the first controlled clinical trial. The concept was so ... simple: Insert catheter into renal artery, throw switch and zap, remove catheter. Easy peasy.
I first heard about renal denervation more than 2 years ago, and marveled at the unmitigated hubris to name the first catheter developed for denervation Symplicity, as well as giving that moniker to a series of uncontrolled and controlled studies that tested the technique. The Symplicity crowd seemed very sure of themselves, of this catheter, and of this procedure.
Fast forward a couple of years and the name morphs into the ironic butt of an expensive, failed trial.
If there is anything I’ve learned during more than 3 decades of covering medicine, it’s that the discipline is hardly ever simple. Think of signaling-pathway diagrams, the ones with all the arrows, boxes, and small fonts. The most reliable reaction when confronted in medicine by something that appears simple is to ask: What am I missing here? Hopefully, when this still-promising technology resurrects, its developers will have learned that lesson.
On Twitter @mitchelzoler
After the surprising, top-line result from the SYMPLICITY HTN-3 trial came out in a press release from Medtronic last January, the question remained of what went wrong: Why did renal denervation fail to outperform a sham procedure in reducing blood pressure?
The apparent answer emerged in late March when the full results finally went public in a report at the annual meeting of the American College of Cardiology and in an article in the New England Journal of Medicine. Many of the 364 patients who underwent active denervation – which involves zapping the efferent nerves that run along the outer wall of the renal arteries with a few brief pulses of radiofrequency energy – probably failed to receive adequate treatment, so their renal innervation remained mostly intact. There’s no proof that’s what happened, but it seems plausible given that all the U.S. operators in the trial had no prior experience performing the procedure, as well as the observation several years ago that denervation can produce highly variable results and is very operator dependent.
This variability in success had been documented back in the 2000s by one of the pioneers of renal denervation, Dr. Murray Esler of Melbourne, yet the people who designed SYMPLICITY HTN-3 didn’t pay attention. Their failure to apply what earlier findings had taught about the variability of denervation proved especially egregious, as the interventionalists also couldn’t gauge their procedural success because no easy way exists right now to do this.
But these details didn’t slow the first controlled clinical trial. The concept was so ... simple: Insert catheter into renal artery, throw switch and zap, remove catheter. Easy peasy.
I first heard about renal denervation more than 2 years ago, and marveled at the unmitigated hubris to name the first catheter developed for denervation Symplicity, as well as giving that moniker to a series of uncontrolled and controlled studies that tested the technique. The Symplicity crowd seemed very sure of themselves, of this catheter, and of this procedure.
Fast forward a couple of years and the name morphs into the ironic butt of an expensive, failed trial.
If there is anything I’ve learned during more than 3 decades of covering medicine, it’s that the discipline is hardly ever simple. Think of signaling-pathway diagrams, the ones with all the arrows, boxes, and small fonts. The most reliable reaction when confronted in medicine by something that appears simple is to ask: What am I missing here? Hopefully, when this still-promising technology resurrects, its developers will have learned that lesson.
On Twitter @mitchelzoler
After the surprising, top-line result from the SYMPLICITY HTN-3 trial came out in a press release from Medtronic last January, the question remained of what went wrong: Why did renal denervation fail to outperform a sham procedure in reducing blood pressure?
The apparent answer emerged in late March when the full results finally went public in a report at the annual meeting of the American College of Cardiology and in an article in the New England Journal of Medicine. Many of the 364 patients who underwent active denervation – which involves zapping the efferent nerves that run along the outer wall of the renal arteries with a few brief pulses of radiofrequency energy – probably failed to receive adequate treatment, so their renal innervation remained mostly intact. There’s no proof that’s what happened, but it seems plausible given that all the U.S. operators in the trial had no prior experience performing the procedure, as well as the observation several years ago that denervation can produce highly variable results and is very operator dependent.
This variability in success had been documented back in the 2000s by one of the pioneers of renal denervation, Dr. Murray Esler of Melbourne, yet the people who designed SYMPLICITY HTN-3 didn’t pay attention. Their failure to apply what earlier findings had taught about the variability of denervation proved especially egregious, as the interventionalists also couldn’t gauge their procedural success because no easy way exists right now to do this.
But these details didn’t slow the first controlled clinical trial. The concept was so ... simple: Insert catheter into renal artery, throw switch and zap, remove catheter. Easy peasy.
I first heard about renal denervation more than 2 years ago, and marveled at the unmitigated hubris to name the first catheter developed for denervation Symplicity, as well as giving that moniker to a series of uncontrolled and controlled studies that tested the technique. The Symplicity crowd seemed very sure of themselves, of this catheter, and of this procedure.
Fast forward a couple of years and the name morphs into the ironic butt of an expensive, failed trial.
If there is anything I’ve learned during more than 3 decades of covering medicine, it’s that the discipline is hardly ever simple. Think of signaling-pathway diagrams, the ones with all the arrows, boxes, and small fonts. The most reliable reaction when confronted in medicine by something that appears simple is to ask: What am I missing here? Hopefully, when this still-promising technology resurrects, its developers will have learned that lesson.
On Twitter @mitchelzoler
Ethical quagmires in preventing and managing concussion
Proper medical surveillance is one of the best tools for preventing and managing concussion. As neurologists, we play a key role in this aspect of concussion prevention and recovery, with the ultimate responsibility of protecting the health and safety of athletes.
That said, there are several instances in which neurologists and sports doctors could face ethical quagmires as they strive toward this goal. One of them is determining when athletes can return to play, if at all, as repetitive injuries are more likely to cause serious brain injury. Those players who have had previous concussions are also at a higher risk for sustaining another one, with football players having a four to six times higher risk than do others with prior concussions. Additionally, those who go back to play too soon are vulnerable to sustaining a second concussion, typically within 10 days of the prior one.
Therefore, much care and consideration must be taken into account when assessing a concussed athlete’s condition. And not all neurologists will be qualified to perform the necessary evaluations, treatment recommendations, and postconcussion follow-up. It is the ethical responsibility of the licensed health care professional to ensure that whoever is treating the concussed athlete is experienced and knowledgeable about treating this type of trauma, including sending the athlete to a different neurologist if necessary.
There’s also a 2013 study that began to take a look at two particular genetic polymorphisms, an amino acid switch in exon 6 of the MAPT (microtubule-associated protein tau) gene and in the promoter region of the APOE (apolipoprotein E) gene, and their relation to postconcussion neurocognitive function/reaction time and outcome in a group of college athletes comprising men’s football and men’s and women’s soccer players. The goal of the study is to determine whether an athlete’s genetic makeup determines the severity of postconcussive brain function. The outcome of the study could potentially add another wrinkle to the question of whether to let players go back to the game or not.
A similar ethical question arises when considering whether to let athletes with certain genetic dispositions play at all. Evidence has been found that boxers with the APOE epsilon-4 allele were more likely to suffer from the effects of chronic traumatic brain injury as their careers went on than did those who did not have the genotype (JAMA 1997;278:136-140). This genotype has also been linked with Alzheimer’s disease (Arch. Neurol. 1995;52:1074-9).
Knowledge of an athlete’s genetic vulnerability to brain injury creates an ethical grey area because the misuse of the information could harm his or her career. Like other HIPAA-protected information, this type of information should be kept confidential. However, sports doctor always needs to keep the athlete’s safety in mind, and if confronted with an athlete who has a genetic predisposition to concussion or poor recovery from concussion, they need to advise the athletes to get regular brain scans to ensure there’s no damage but not necessarily to stop them from playing.
There are other factors at play beyond genetic disposition, and more studies need to be done to get a better understanding of this public health risk. Until then, neurologists need to make careful judgments when dealing with concussions.
Dr. Jordan is the director of the brain injury program and the memory evaluation treatment service at Burke Rehabilitation Hospital in White Plains, N.Y. He also serves as the assistant medical director there. He currently serves as the chief medical officer of the New York State Athletic Commission, as a team physician for USA Boxing, and as a member of the NFL Players Association Mackey-White Traumatic Brain Injury Committee and the NFL Neuro-Cognitive Disability Committee.
Proper medical surveillance is one of the best tools for preventing and managing concussion. As neurologists, we play a key role in this aspect of concussion prevention and recovery, with the ultimate responsibility of protecting the health and safety of athletes.
That said, there are several instances in which neurologists and sports doctors could face ethical quagmires as they strive toward this goal. One of them is determining when athletes can return to play, if at all, as repetitive injuries are more likely to cause serious brain injury. Those players who have had previous concussions are also at a higher risk for sustaining another one, with football players having a four to six times higher risk than do others with prior concussions. Additionally, those who go back to play too soon are vulnerable to sustaining a second concussion, typically within 10 days of the prior one.
Therefore, much care and consideration must be taken into account when assessing a concussed athlete’s condition. And not all neurologists will be qualified to perform the necessary evaluations, treatment recommendations, and postconcussion follow-up. It is the ethical responsibility of the licensed health care professional to ensure that whoever is treating the concussed athlete is experienced and knowledgeable about treating this type of trauma, including sending the athlete to a different neurologist if necessary.
There’s also a 2013 study that began to take a look at two particular genetic polymorphisms, an amino acid switch in exon 6 of the MAPT (microtubule-associated protein tau) gene and in the promoter region of the APOE (apolipoprotein E) gene, and their relation to postconcussion neurocognitive function/reaction time and outcome in a group of college athletes comprising men’s football and men’s and women’s soccer players. The goal of the study is to determine whether an athlete’s genetic makeup determines the severity of postconcussive brain function. The outcome of the study could potentially add another wrinkle to the question of whether to let players go back to the game or not.
A similar ethical question arises when considering whether to let athletes with certain genetic dispositions play at all. Evidence has been found that boxers with the APOE epsilon-4 allele were more likely to suffer from the effects of chronic traumatic brain injury as their careers went on than did those who did not have the genotype (JAMA 1997;278:136-140). This genotype has also been linked with Alzheimer’s disease (Arch. Neurol. 1995;52:1074-9).
Knowledge of an athlete’s genetic vulnerability to brain injury creates an ethical grey area because the misuse of the information could harm his or her career. Like other HIPAA-protected information, this type of information should be kept confidential. However, sports doctor always needs to keep the athlete’s safety in mind, and if confronted with an athlete who has a genetic predisposition to concussion or poor recovery from concussion, they need to advise the athletes to get regular brain scans to ensure there’s no damage but not necessarily to stop them from playing.
There are other factors at play beyond genetic disposition, and more studies need to be done to get a better understanding of this public health risk. Until then, neurologists need to make careful judgments when dealing with concussions.
Dr. Jordan is the director of the brain injury program and the memory evaluation treatment service at Burke Rehabilitation Hospital in White Plains, N.Y. He also serves as the assistant medical director there. He currently serves as the chief medical officer of the New York State Athletic Commission, as a team physician for USA Boxing, and as a member of the NFL Players Association Mackey-White Traumatic Brain Injury Committee and the NFL Neuro-Cognitive Disability Committee.
Proper medical surveillance is one of the best tools for preventing and managing concussion. As neurologists, we play a key role in this aspect of concussion prevention and recovery, with the ultimate responsibility of protecting the health and safety of athletes.
That said, there are several instances in which neurologists and sports doctors could face ethical quagmires as they strive toward this goal. One of them is determining when athletes can return to play, if at all, as repetitive injuries are more likely to cause serious brain injury. Those players who have had previous concussions are also at a higher risk for sustaining another one, with football players having a four to six times higher risk than do others with prior concussions. Additionally, those who go back to play too soon are vulnerable to sustaining a second concussion, typically within 10 days of the prior one.
Therefore, much care and consideration must be taken into account when assessing a concussed athlete’s condition. And not all neurologists will be qualified to perform the necessary evaluations, treatment recommendations, and postconcussion follow-up. It is the ethical responsibility of the licensed health care professional to ensure that whoever is treating the concussed athlete is experienced and knowledgeable about treating this type of trauma, including sending the athlete to a different neurologist if necessary.
There’s also a 2013 study that began to take a look at two particular genetic polymorphisms, an amino acid switch in exon 6 of the MAPT (microtubule-associated protein tau) gene and in the promoter region of the APOE (apolipoprotein E) gene, and their relation to postconcussion neurocognitive function/reaction time and outcome in a group of college athletes comprising men’s football and men’s and women’s soccer players. The goal of the study is to determine whether an athlete’s genetic makeup determines the severity of postconcussive brain function. The outcome of the study could potentially add another wrinkle to the question of whether to let players go back to the game or not.
A similar ethical question arises when considering whether to let athletes with certain genetic dispositions play at all. Evidence has been found that boxers with the APOE epsilon-4 allele were more likely to suffer from the effects of chronic traumatic brain injury as their careers went on than did those who did not have the genotype (JAMA 1997;278:136-140). This genotype has also been linked with Alzheimer’s disease (Arch. Neurol. 1995;52:1074-9).
Knowledge of an athlete’s genetic vulnerability to brain injury creates an ethical grey area because the misuse of the information could harm his or her career. Like other HIPAA-protected information, this type of information should be kept confidential. However, sports doctor always needs to keep the athlete’s safety in mind, and if confronted with an athlete who has a genetic predisposition to concussion or poor recovery from concussion, they need to advise the athletes to get regular brain scans to ensure there’s no damage but not necessarily to stop them from playing.
There are other factors at play beyond genetic disposition, and more studies need to be done to get a better understanding of this public health risk. Until then, neurologists need to make careful judgments when dealing with concussions.
Dr. Jordan is the director of the brain injury program and the memory evaluation treatment service at Burke Rehabilitation Hospital in White Plains, N.Y. He also serves as the assistant medical director there. He currently serves as the chief medical officer of the New York State Athletic Commission, as a team physician for USA Boxing, and as a member of the NFL Players Association Mackey-White Traumatic Brain Injury Committee and the NFL Neuro-Cognitive Disability Committee.
We already tried that ... Refining your behavior management plans
It is the rare family of a child with behavior problems that has not already tried a plan from a book or advice from friends or relatives. They may even have done what their parents did to them, whether it worked or not! The first message you hear in the visit may be "We already tried the star chart thing."
Can you really provide any better advice for changing behavior than what they have already heard?
Unlike casual sources, you know the family well and are a trusted counselor. You may guess meanings the behavior has such as avoiding upset for their "delicate" preemie by not enforcing limits.
But the main way you can provide more effective advice is by knowing the scientific basis for behavior change methods. First, understand the W’s – What is the specific current behavior and What is the desired behavior?; Who is present, When and Where is the behavior most often happening? What does the presence of this behavior mean to the child and family?
You need a thorough understanding of the behavior to advise ways to prevent it by avoiding or reducing demands that the child cannot meet. Reframe the issue as the child lacking skills needed to act appropriately and suggest ways to build them.
The use of rewards or consequences can then be targeted to encouraging skill building or reducing established behavior patterns. In general, positive reinforcement or rewards are more effective than consequences. Why reward? Changing behavior is hard work for the child (and parent), and positive reinforcement helps both initiate and maintain a behavior.
The most effective positive reinforcers are things that are valued by the child, are available infrequently otherwise, are novel, are given contingent on the desired behavior, are related to the desired action, are dosed appropriately; can be delivered immediately and consistently after the desired behavior occurs, and are acceptable to the parent.
Bigger rewards may be needed to start new behaviors (a Barbie got our shy daughter onto the soccer field the first time), but smaller rewards have advantages. Parents will more cheerfully and consistently deliver a 25-cent Pokemon card every time the child cooperates with homework than a $25 video game. Smaller reinforcers also mean less is needed to maintain the behavior. Children are smart – if it takes the promise of Disneyland to sleep in their own bed then it must be pretty bad! Larger rewards also result in less self-satisfaction; the child justifies going along with the plan to get the reward rather than because it was a good idea.
With the ultimate goal of behaving for their own sake, rewards (and later even praise) should be used sparingly and phased out quickly. As children mature, they can be encouraged to self-evaluate, such as asking, "How do you think you handled that?"
Food rewards should be avoided as they can promote emotional attachment to unhealthy snacks, although for children with autism or intellectual disabilities it may be the only effective reinforcement.
All new behaviors are learned better when the reason for change is explained; the child participates in choosing the new behavior and its reward; the desired behavior is named, modeled, and then practiced; and the reinforcement is accompanied by verbal praise. So-called "differential reinforcement" works best when incompatible behavior is rewarded, for example spitting toothpaste in the sink is incompatible with spitting on a sibling.
All inadvertent positive reinforcement for the undesired behavior must be avoided. The subterfuge may be subtle, for example biting may be reinforced if one adult rushes to the child, giving special attention even to scold. Even seemingly aversive things may be positive reinforcers if they result in increasing rather than decreasing a behavior.
Of course, for most children no reward is needed to gain cooperation – just ask! For tougher situations, the optimal frequency of reward comes from a "schedule of reinforcement." At first, reinforcement is likely needed every time and for little pieces of the ultimately desired action ("shaping"). For example, cleaning up toys has to start with the parent picking up 99 and the child 1 (with praise!).
Once the child is doing the new behavior fairly consistently with reinforcement, start "fading" the prompts and rewards. This increases "acting well" spontaneously and helps generalization. You hardly need to teach a parent to fade rewards as they naturally tend to forget, delay, or give fewer prompts. Rewards also can be decreased in amount, delayed, or reserved for increasingly elaborated positive behaviors – all helping solidify the new behavior.
Consequences are mainly needed for younger children and as back up to reinforcement. Similar principles apply to consequences. Consequences are most effective when used infrequently but consistently for the same behavior, unwanted by the child, done immediately after the unwanted behavior, related to the nature of the misbehavior and dosed appropriately (smaller is better!), and acceptable to the parents. The child should have a "clean slate" after the consequence to help restore the relationship. Painful, harsh, scary, or injurious consequences are neither acceptable nor effective.
Two methods of behavior modification I find easy to teach and implement are marks and points.
Marks make reinforcing behavior easy and fun for children 2-7 years old. The adult marks with a pen on the child’s hand along with verbal praise for each behavior "just a little bit better than usual," such as tantrums lasting 1 minute instead of 2, aiming for 6-10 marks per hour. High frequency helps adults notice more and smaller "okay" behaviors, often a deficit. At the end of the marking period each day, give a small reward (such as extra play time, grab bag prize, pennies) for having a "bunch" to confer value to the marks. Give bonus marks for outstanding or spontaneous behaviors (Hey, they’re free!). Marks are faded out when behavior has improved and parents are noticing and praising good behavior. While removal of marks for inappropriate behavior can be used, I do not recommend it as parents are often in a punitive cycle in that case and need to refocus on the positive.
For older children, a "token economy" (star chart) using points, stars, or poker chips is an evidence-based method for behavior change when done correctly. Optimal implementation includes outlining the plan with parent and child together so that the desired behaviors, rewards, and costs are clear and relevant. Together they set the "price" for behaviors (such as 5 earned for 30 minutes of TV without fighting or 10 lost for a squabble). While token economies work for chore compliance, the focus here is for behavior. A key component motivating participation is charging for things taken for granted such as TV, computer, outside play time. Give "bonus points" for initiating, extra acts of kindness, etc. "Purchases" for basics or privileges are deducted from the total kept on a card or a subset of freedoms can be allowed based on a minimum total "in the bank."
Dr. Howard is assistant professor of pediatrics at the Johns Hopkins University School of Medicine, Baltimore, and creator of CHADIS. She has no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to Frontline Medical Communications. E-mail her at [email protected].
It is the rare family of a child with behavior problems that has not already tried a plan from a book or advice from friends or relatives. They may even have done what their parents did to them, whether it worked or not! The first message you hear in the visit may be "We already tried the star chart thing."
Can you really provide any better advice for changing behavior than what they have already heard?
Unlike casual sources, you know the family well and are a trusted counselor. You may guess meanings the behavior has such as avoiding upset for their "delicate" preemie by not enforcing limits.
But the main way you can provide more effective advice is by knowing the scientific basis for behavior change methods. First, understand the W’s – What is the specific current behavior and What is the desired behavior?; Who is present, When and Where is the behavior most often happening? What does the presence of this behavior mean to the child and family?
You need a thorough understanding of the behavior to advise ways to prevent it by avoiding or reducing demands that the child cannot meet. Reframe the issue as the child lacking skills needed to act appropriately and suggest ways to build them.
The use of rewards or consequences can then be targeted to encouraging skill building or reducing established behavior patterns. In general, positive reinforcement or rewards are more effective than consequences. Why reward? Changing behavior is hard work for the child (and parent), and positive reinforcement helps both initiate and maintain a behavior.
The most effective positive reinforcers are things that are valued by the child, are available infrequently otherwise, are novel, are given contingent on the desired behavior, are related to the desired action, are dosed appropriately; can be delivered immediately and consistently after the desired behavior occurs, and are acceptable to the parent.
Bigger rewards may be needed to start new behaviors (a Barbie got our shy daughter onto the soccer field the first time), but smaller rewards have advantages. Parents will more cheerfully and consistently deliver a 25-cent Pokemon card every time the child cooperates with homework than a $25 video game. Smaller reinforcers also mean less is needed to maintain the behavior. Children are smart – if it takes the promise of Disneyland to sleep in their own bed then it must be pretty bad! Larger rewards also result in less self-satisfaction; the child justifies going along with the plan to get the reward rather than because it was a good idea.
With the ultimate goal of behaving for their own sake, rewards (and later even praise) should be used sparingly and phased out quickly. As children mature, they can be encouraged to self-evaluate, such as asking, "How do you think you handled that?"
Food rewards should be avoided as they can promote emotional attachment to unhealthy snacks, although for children with autism or intellectual disabilities it may be the only effective reinforcement.
All new behaviors are learned better when the reason for change is explained; the child participates in choosing the new behavior and its reward; the desired behavior is named, modeled, and then practiced; and the reinforcement is accompanied by verbal praise. So-called "differential reinforcement" works best when incompatible behavior is rewarded, for example spitting toothpaste in the sink is incompatible with spitting on a sibling.
All inadvertent positive reinforcement for the undesired behavior must be avoided. The subterfuge may be subtle, for example biting may be reinforced if one adult rushes to the child, giving special attention even to scold. Even seemingly aversive things may be positive reinforcers if they result in increasing rather than decreasing a behavior.
Of course, for most children no reward is needed to gain cooperation – just ask! For tougher situations, the optimal frequency of reward comes from a "schedule of reinforcement." At first, reinforcement is likely needed every time and for little pieces of the ultimately desired action ("shaping"). For example, cleaning up toys has to start with the parent picking up 99 and the child 1 (with praise!).
Once the child is doing the new behavior fairly consistently with reinforcement, start "fading" the prompts and rewards. This increases "acting well" spontaneously and helps generalization. You hardly need to teach a parent to fade rewards as they naturally tend to forget, delay, or give fewer prompts. Rewards also can be decreased in amount, delayed, or reserved for increasingly elaborated positive behaviors – all helping solidify the new behavior.
Consequences are mainly needed for younger children and as back up to reinforcement. Similar principles apply to consequences. Consequences are most effective when used infrequently but consistently for the same behavior, unwanted by the child, done immediately after the unwanted behavior, related to the nature of the misbehavior and dosed appropriately (smaller is better!), and acceptable to the parents. The child should have a "clean slate" after the consequence to help restore the relationship. Painful, harsh, scary, or injurious consequences are neither acceptable nor effective.
Two methods of behavior modification I find easy to teach and implement are marks and points.
Marks make reinforcing behavior easy and fun for children 2-7 years old. The adult marks with a pen on the child’s hand along with verbal praise for each behavior "just a little bit better than usual," such as tantrums lasting 1 minute instead of 2, aiming for 6-10 marks per hour. High frequency helps adults notice more and smaller "okay" behaviors, often a deficit. At the end of the marking period each day, give a small reward (such as extra play time, grab bag prize, pennies) for having a "bunch" to confer value to the marks. Give bonus marks for outstanding or spontaneous behaviors (Hey, they’re free!). Marks are faded out when behavior has improved and parents are noticing and praising good behavior. While removal of marks for inappropriate behavior can be used, I do not recommend it as parents are often in a punitive cycle in that case and need to refocus on the positive.
For older children, a "token economy" (star chart) using points, stars, or poker chips is an evidence-based method for behavior change when done correctly. Optimal implementation includes outlining the plan with parent and child together so that the desired behaviors, rewards, and costs are clear and relevant. Together they set the "price" for behaviors (such as 5 earned for 30 minutes of TV without fighting or 10 lost for a squabble). While token economies work for chore compliance, the focus here is for behavior. A key component motivating participation is charging for things taken for granted such as TV, computer, outside play time. Give "bonus points" for initiating, extra acts of kindness, etc. "Purchases" for basics or privileges are deducted from the total kept on a card or a subset of freedoms can be allowed based on a minimum total "in the bank."
Dr. Howard is assistant professor of pediatrics at the Johns Hopkins University School of Medicine, Baltimore, and creator of CHADIS. She has no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to Frontline Medical Communications. E-mail her at [email protected].
It is the rare family of a child with behavior problems that has not already tried a plan from a book or advice from friends or relatives. They may even have done what their parents did to them, whether it worked or not! The first message you hear in the visit may be "We already tried the star chart thing."
Can you really provide any better advice for changing behavior than what they have already heard?
Unlike casual sources, you know the family well and are a trusted counselor. You may guess meanings the behavior has such as avoiding upset for their "delicate" preemie by not enforcing limits.
But the main way you can provide more effective advice is by knowing the scientific basis for behavior change methods. First, understand the W’s – What is the specific current behavior and What is the desired behavior?; Who is present, When and Where is the behavior most often happening? What does the presence of this behavior mean to the child and family?
You need a thorough understanding of the behavior to advise ways to prevent it by avoiding or reducing demands that the child cannot meet. Reframe the issue as the child lacking skills needed to act appropriately and suggest ways to build them.
The use of rewards or consequences can then be targeted to encouraging skill building or reducing established behavior patterns. In general, positive reinforcement or rewards are more effective than consequences. Why reward? Changing behavior is hard work for the child (and parent), and positive reinforcement helps both initiate and maintain a behavior.
The most effective positive reinforcers are things that are valued by the child, are available infrequently otherwise, are novel, are given contingent on the desired behavior, are related to the desired action, are dosed appropriately; can be delivered immediately and consistently after the desired behavior occurs, and are acceptable to the parent.
Bigger rewards may be needed to start new behaviors (a Barbie got our shy daughter onto the soccer field the first time), but smaller rewards have advantages. Parents will more cheerfully and consistently deliver a 25-cent Pokemon card every time the child cooperates with homework than a $25 video game. Smaller reinforcers also mean less is needed to maintain the behavior. Children are smart – if it takes the promise of Disneyland to sleep in their own bed then it must be pretty bad! Larger rewards also result in less self-satisfaction; the child justifies going along with the plan to get the reward rather than because it was a good idea.
With the ultimate goal of behaving for their own sake, rewards (and later even praise) should be used sparingly and phased out quickly. As children mature, they can be encouraged to self-evaluate, such as asking, "How do you think you handled that?"
Food rewards should be avoided as they can promote emotional attachment to unhealthy snacks, although for children with autism or intellectual disabilities it may be the only effective reinforcement.
All new behaviors are learned better when the reason for change is explained; the child participates in choosing the new behavior and its reward; the desired behavior is named, modeled, and then practiced; and the reinforcement is accompanied by verbal praise. So-called "differential reinforcement" works best when incompatible behavior is rewarded, for example spitting toothpaste in the sink is incompatible with spitting on a sibling.
All inadvertent positive reinforcement for the undesired behavior must be avoided. The subterfuge may be subtle, for example biting may be reinforced if one adult rushes to the child, giving special attention even to scold. Even seemingly aversive things may be positive reinforcers if they result in increasing rather than decreasing a behavior.
Of course, for most children no reward is needed to gain cooperation – just ask! For tougher situations, the optimal frequency of reward comes from a "schedule of reinforcement." At first, reinforcement is likely needed every time and for little pieces of the ultimately desired action ("shaping"). For example, cleaning up toys has to start with the parent picking up 99 and the child 1 (with praise!).
Once the child is doing the new behavior fairly consistently with reinforcement, start "fading" the prompts and rewards. This increases "acting well" spontaneously and helps generalization. You hardly need to teach a parent to fade rewards as they naturally tend to forget, delay, or give fewer prompts. Rewards also can be decreased in amount, delayed, or reserved for increasingly elaborated positive behaviors – all helping solidify the new behavior.
Consequences are mainly needed for younger children and as back up to reinforcement. Similar principles apply to consequences. Consequences are most effective when used infrequently but consistently for the same behavior, unwanted by the child, done immediately after the unwanted behavior, related to the nature of the misbehavior and dosed appropriately (smaller is better!), and acceptable to the parents. The child should have a "clean slate" after the consequence to help restore the relationship. Painful, harsh, scary, or injurious consequences are neither acceptable nor effective.
Two methods of behavior modification I find easy to teach and implement are marks and points.
Marks make reinforcing behavior easy and fun for children 2-7 years old. The adult marks with a pen on the child’s hand along with verbal praise for each behavior "just a little bit better than usual," such as tantrums lasting 1 minute instead of 2, aiming for 6-10 marks per hour. High frequency helps adults notice more and smaller "okay" behaviors, often a deficit. At the end of the marking period each day, give a small reward (such as extra play time, grab bag prize, pennies) for having a "bunch" to confer value to the marks. Give bonus marks for outstanding or spontaneous behaviors (Hey, they’re free!). Marks are faded out when behavior has improved and parents are noticing and praising good behavior. While removal of marks for inappropriate behavior can be used, I do not recommend it as parents are often in a punitive cycle in that case and need to refocus on the positive.
For older children, a "token economy" (star chart) using points, stars, or poker chips is an evidence-based method for behavior change when done correctly. Optimal implementation includes outlining the plan with parent and child together so that the desired behaviors, rewards, and costs are clear and relevant. Together they set the "price" for behaviors (such as 5 earned for 30 minutes of TV without fighting or 10 lost for a squabble). While token economies work for chore compliance, the focus here is for behavior. A key component motivating participation is charging for things taken for granted such as TV, computer, outside play time. Give "bonus points" for initiating, extra acts of kindness, etc. "Purchases" for basics or privileges are deducted from the total kept on a card or a subset of freedoms can be allowed based on a minimum total "in the bank."
Dr. Howard is assistant professor of pediatrics at the Johns Hopkins University School of Medicine, Baltimore, and creator of CHADIS. She has no other relevant disclosures. Dr. Howard’s contribution to this publication was as a paid expert to Frontline Medical Communications. E-mail her at [email protected].
Healthy teeth, healthy kids
Oral health has deservedly attracted increased attention over recent years. Cavities are the No. 1 chronic disease affecting young children, yet pediatric dentist availability is inadequate, and most pediatricians receive little education on oral health during their training. Additionally, recommendations for good oral health may be hard for parents to implement when their infant is crying for a bottle in the middle of the night or their toddler is fighting all efforts at good tooth brushing.
In my own practice, I feel very lucky to have a close partnership with an excellent pediatric dentistry department from whom I have learned a great deal. I have discovered a lot of facts, but also many practical tips that I have been able to use clinically and pass on to families. The first and most important thing I have learned from my dentistry colleagues is how important it is for pediatric primary care providers to ask about oral health at every visit. There are different ways to incorporate this into your history taking, but I typically ask when I am doing my ear, nose, and throat exam. I find this is most efficient, but also the best time to elicit parents’ questions and concerns about oral health (and also a time for me to provide positive feedback).
The second extremely helpful tip I have learned is how to get a good exam. Older patients are, of course, much more likely to be cooperative, and the very young infants also are fairly easy to examine. A mad 18-month-old, on the other hand, can be a real challenge! Again, as I was taught by my dental colleagues, I ask the parent to sit in a chair and put the child in their lap, facing them and with the child’s legs on either side of the parent’s hips. I also sit in a chair, facing the parent (at which point the child’s back is toward me). The parent then lays the child back along their legs, so that the child’s head is in front of me, and I am looking down their nose into their mouth. This is a perfect angle to be able to control the child’s mouth and get a direct look in – so I can be quick and thorough. For parents whose children really fight tooth brushing, I teach them this technique as well if there are two adults in the house available to help with the dental hygiene routine. In my experience, I find that in addition to providing control and a good angle for an exam, as long as you move them into the position slowly, young children find this a comforting position in which to have their mouth examined. They are somewhat cocooned by the parent’s legs and arms, which seems to help them feel protected and a little calmer.
Finally (and this is perhaps most based on my own experience as a parent), I talk with parents about how important it is to develop a regular routine of twice-daily brushing, even when your toddler fights it. Not every brushing will be perfect. Every parent has had those times where their child clamps down their lips, and you just don’t have the heart to really pry their mouths open to brush all corners of every last tooth. However, if a child learns that this is the routine, the fighting will become less and less with time. I tell parents it is better to get a mediocre tooth brushing in than no brushing at all. I also assure them that, particularly for younger children, they do not have to brush their teeth in the bathroom in front of the sink. As long as you are using an appropriately small amount of toothpaste, you can brush while sitting on the bed reading books or in the rocking chair. Some children do better with the routine of being in the bathroom, while others do better in a safer, feeling more comfortable environment.
Overall, as pediatric providers, we can be important partners with our dental colleagues in making sure that children – and their teeth – are healthy.
Dr. Beers is an assistant professor of pediatrics at Children’s National Medical Center and the George Washington University Medical Center, Washington. She is chair of the American Academy of Pediatrics Committee on Residency Scholarships and president of the District of Columbia chapter of the American Academy of Pediatrics. E-mail Dr. Beers at pdnews@ frontlinemedcom.com.
Oral health has deservedly attracted increased attention over recent years. Cavities are the No. 1 chronic disease affecting young children, yet pediatric dentist availability is inadequate, and most pediatricians receive little education on oral health during their training. Additionally, recommendations for good oral health may be hard for parents to implement when their infant is crying for a bottle in the middle of the night or their toddler is fighting all efforts at good tooth brushing.
In my own practice, I feel very lucky to have a close partnership with an excellent pediatric dentistry department from whom I have learned a great deal. I have discovered a lot of facts, but also many practical tips that I have been able to use clinically and pass on to families. The first and most important thing I have learned from my dentistry colleagues is how important it is for pediatric primary care providers to ask about oral health at every visit. There are different ways to incorporate this into your history taking, but I typically ask when I am doing my ear, nose, and throat exam. I find this is most efficient, but also the best time to elicit parents’ questions and concerns about oral health (and also a time for me to provide positive feedback).
The second extremely helpful tip I have learned is how to get a good exam. Older patients are, of course, much more likely to be cooperative, and the very young infants also are fairly easy to examine. A mad 18-month-old, on the other hand, can be a real challenge! Again, as I was taught by my dental colleagues, I ask the parent to sit in a chair and put the child in their lap, facing them and with the child’s legs on either side of the parent’s hips. I also sit in a chair, facing the parent (at which point the child’s back is toward me). The parent then lays the child back along their legs, so that the child’s head is in front of me, and I am looking down their nose into their mouth. This is a perfect angle to be able to control the child’s mouth and get a direct look in – so I can be quick and thorough. For parents whose children really fight tooth brushing, I teach them this technique as well if there are two adults in the house available to help with the dental hygiene routine. In my experience, I find that in addition to providing control and a good angle for an exam, as long as you move them into the position slowly, young children find this a comforting position in which to have their mouth examined. They are somewhat cocooned by the parent’s legs and arms, which seems to help them feel protected and a little calmer.
Finally (and this is perhaps most based on my own experience as a parent), I talk with parents about how important it is to develop a regular routine of twice-daily brushing, even when your toddler fights it. Not every brushing will be perfect. Every parent has had those times where their child clamps down their lips, and you just don’t have the heart to really pry their mouths open to brush all corners of every last tooth. However, if a child learns that this is the routine, the fighting will become less and less with time. I tell parents it is better to get a mediocre tooth brushing in than no brushing at all. I also assure them that, particularly for younger children, they do not have to brush their teeth in the bathroom in front of the sink. As long as you are using an appropriately small amount of toothpaste, you can brush while sitting on the bed reading books or in the rocking chair. Some children do better with the routine of being in the bathroom, while others do better in a safer, feeling more comfortable environment.
Overall, as pediatric providers, we can be important partners with our dental colleagues in making sure that children – and their teeth – are healthy.
Dr. Beers is an assistant professor of pediatrics at Children’s National Medical Center and the George Washington University Medical Center, Washington. She is chair of the American Academy of Pediatrics Committee on Residency Scholarships and president of the District of Columbia chapter of the American Academy of Pediatrics. E-mail Dr. Beers at pdnews@ frontlinemedcom.com.
Oral health has deservedly attracted increased attention over recent years. Cavities are the No. 1 chronic disease affecting young children, yet pediatric dentist availability is inadequate, and most pediatricians receive little education on oral health during their training. Additionally, recommendations for good oral health may be hard for parents to implement when their infant is crying for a bottle in the middle of the night or their toddler is fighting all efforts at good tooth brushing.
In my own practice, I feel very lucky to have a close partnership with an excellent pediatric dentistry department from whom I have learned a great deal. I have discovered a lot of facts, but also many practical tips that I have been able to use clinically and pass on to families. The first and most important thing I have learned from my dentistry colleagues is how important it is for pediatric primary care providers to ask about oral health at every visit. There are different ways to incorporate this into your history taking, but I typically ask when I am doing my ear, nose, and throat exam. I find this is most efficient, but also the best time to elicit parents’ questions and concerns about oral health (and also a time for me to provide positive feedback).
The second extremely helpful tip I have learned is how to get a good exam. Older patients are, of course, much more likely to be cooperative, and the very young infants also are fairly easy to examine. A mad 18-month-old, on the other hand, can be a real challenge! Again, as I was taught by my dental colleagues, I ask the parent to sit in a chair and put the child in their lap, facing them and with the child’s legs on either side of the parent’s hips. I also sit in a chair, facing the parent (at which point the child’s back is toward me). The parent then lays the child back along their legs, so that the child’s head is in front of me, and I am looking down their nose into their mouth. This is a perfect angle to be able to control the child’s mouth and get a direct look in – so I can be quick and thorough. For parents whose children really fight tooth brushing, I teach them this technique as well if there are two adults in the house available to help with the dental hygiene routine. In my experience, I find that in addition to providing control and a good angle for an exam, as long as you move them into the position slowly, young children find this a comforting position in which to have their mouth examined. They are somewhat cocooned by the parent’s legs and arms, which seems to help them feel protected and a little calmer.
Finally (and this is perhaps most based on my own experience as a parent), I talk with parents about how important it is to develop a regular routine of twice-daily brushing, even when your toddler fights it. Not every brushing will be perfect. Every parent has had those times where their child clamps down their lips, and you just don’t have the heart to really pry their mouths open to brush all corners of every last tooth. However, if a child learns that this is the routine, the fighting will become less and less with time. I tell parents it is better to get a mediocre tooth brushing in than no brushing at all. I also assure them that, particularly for younger children, they do not have to brush their teeth in the bathroom in front of the sink. As long as you are using an appropriately small amount of toothpaste, you can brush while sitting on the bed reading books or in the rocking chair. Some children do better with the routine of being in the bathroom, while others do better in a safer, feeling more comfortable environment.
Overall, as pediatric providers, we can be important partners with our dental colleagues in making sure that children – and their teeth – are healthy.
Dr. Beers is an assistant professor of pediatrics at Children’s National Medical Center and the George Washington University Medical Center, Washington. She is chair of the American Academy of Pediatrics Committee on Residency Scholarships and president of the District of Columbia chapter of the American Academy of Pediatrics. E-mail Dr. Beers at pdnews@ frontlinemedcom.com.
How to spend 2 days as a cognitive cardiologist
WASHINGTON – Another annual meeting of the American College of Cardiology has drawn to a close, and aside from the seemingly endless rain (and brief snow flurries), a lot of interesting discourse took place.
In the heart failure discipline, we have to a large degree become incrementalists: Although there were no blockbusters, important data on renal denervation were released, and corridor discussions about serelaxin and ivabradine were animated. At a time of ICD-10 rollouts, electronic health record (EHR) struggles, board recertification challenges, accreditation, precertification, compliance mandates, and more, it was a delight to be a cognitive cardiologist again. For a few precious moments, we could own our profession again.
We saw no hospital administrators; we did not receive any missives about the (lack of) timeliness of closing encounters in EHRs; we engaged in real peer-to-peer interactions with real peers, unlike the shadow variant we deal with during an appeal of an insurance coverage decision.
And then it was over, ironically with the sun shining. It’s now back to work, but perhaps with renewed purpose. Let’s find ways to reestablish facts on the ground: Our patients and the decisions we make about our patients come first. Research and teaching do, too. Hospital administrators? Send them to a very long annual meeting. And hope that they forget to pack umbrellas.
Dr. Hauptman is professor of internal medicine and assistant dean of clinical-translational research at Saint Louis University and director of heart failure at Saint Louis University Hospital.
WASHINGTON – Another annual meeting of the American College of Cardiology has drawn to a close, and aside from the seemingly endless rain (and brief snow flurries), a lot of interesting discourse took place.
In the heart failure discipline, we have to a large degree become incrementalists: Although there were no blockbusters, important data on renal denervation were released, and corridor discussions about serelaxin and ivabradine were animated. At a time of ICD-10 rollouts, electronic health record (EHR) struggles, board recertification challenges, accreditation, precertification, compliance mandates, and more, it was a delight to be a cognitive cardiologist again. For a few precious moments, we could own our profession again.
We saw no hospital administrators; we did not receive any missives about the (lack of) timeliness of closing encounters in EHRs; we engaged in real peer-to-peer interactions with real peers, unlike the shadow variant we deal with during an appeal of an insurance coverage decision.
And then it was over, ironically with the sun shining. It’s now back to work, but perhaps with renewed purpose. Let’s find ways to reestablish facts on the ground: Our patients and the decisions we make about our patients come first. Research and teaching do, too. Hospital administrators? Send them to a very long annual meeting. And hope that they forget to pack umbrellas.
Dr. Hauptman is professor of internal medicine and assistant dean of clinical-translational research at Saint Louis University and director of heart failure at Saint Louis University Hospital.
WASHINGTON – Another annual meeting of the American College of Cardiology has drawn to a close, and aside from the seemingly endless rain (and brief snow flurries), a lot of interesting discourse took place.
In the heart failure discipline, we have to a large degree become incrementalists: Although there were no blockbusters, important data on renal denervation were released, and corridor discussions about serelaxin and ivabradine were animated. At a time of ICD-10 rollouts, electronic health record (EHR) struggles, board recertification challenges, accreditation, precertification, compliance mandates, and more, it was a delight to be a cognitive cardiologist again. For a few precious moments, we could own our profession again.
We saw no hospital administrators; we did not receive any missives about the (lack of) timeliness of closing encounters in EHRs; we engaged in real peer-to-peer interactions with real peers, unlike the shadow variant we deal with during an appeal of an insurance coverage decision.
And then it was over, ironically with the sun shining. It’s now back to work, but perhaps with renewed purpose. Let’s find ways to reestablish facts on the ground: Our patients and the decisions we make about our patients come first. Research and teaching do, too. Hospital administrators? Send them to a very long annual meeting. And hope that they forget to pack umbrellas.
Dr. Hauptman is professor of internal medicine and assistant dean of clinical-translational research at Saint Louis University and director of heart failure at Saint Louis University Hospital.
Field Therapy in the Treatment of Actinic Keratosis
Human brain mapping project begins to reveal roots of developmental abnormalities
Understanding the neurophysiologic and molecular bases of mental illness, autism, and related conditions remains one of the most challenging frontiers of medicine and neuroscience because despite very prominent symptoms, there is little that clinical diagnostic techniques reveal. The recent report of the BrainSpan Atlas represents a major collaborative attempt to map the human brain from its gestational developmental stages to its adult form (Nature 2014 April 2 [doi:10.1038/nature13185]). Previous work has examined the histology and transcriptomic profiles of 900 neuroanatomical subdivisions (Nature 2012;489:391-9) of two adult human brains that characterized the transcriptomic relationships between different cell types and different cell regions.
Now, based upon four prenatal brains, the atlas displays the gene expression profiles of the developing brain and reveals that many neuropsychiatric disorders, including autism and schizophrenia, have identifiable developmental abnormalities. To what degree these brains are representative of healthy preterm humans is not entirely clear, but the insights gained are remarkable and will certainly contribute importantly to our understanding of these most enigmatic conditions.
Dr. Caselli is a professor of neurology and associate director and clinical core director of the Alzheimer’s Disease Center at the Mayo Clinic in Scottsdale, Ariz. He has no relevant financial disclosures.
Understanding the neurophysiologic and molecular bases of mental illness, autism, and related conditions remains one of the most challenging frontiers of medicine and neuroscience because despite very prominent symptoms, there is little that clinical diagnostic techniques reveal. The recent report of the BrainSpan Atlas represents a major collaborative attempt to map the human brain from its gestational developmental stages to its adult form (Nature 2014 April 2 [doi:10.1038/nature13185]). Previous work has examined the histology and transcriptomic profiles of 900 neuroanatomical subdivisions (Nature 2012;489:391-9) of two adult human brains that characterized the transcriptomic relationships between different cell types and different cell regions.
Now, based upon four prenatal brains, the atlas displays the gene expression profiles of the developing brain and reveals that many neuropsychiatric disorders, including autism and schizophrenia, have identifiable developmental abnormalities. To what degree these brains are representative of healthy preterm humans is not entirely clear, but the insights gained are remarkable and will certainly contribute importantly to our understanding of these most enigmatic conditions.
Dr. Caselli is a professor of neurology and associate director and clinical core director of the Alzheimer’s Disease Center at the Mayo Clinic in Scottsdale, Ariz. He has no relevant financial disclosures.
Understanding the neurophysiologic and molecular bases of mental illness, autism, and related conditions remains one of the most challenging frontiers of medicine and neuroscience because despite very prominent symptoms, there is little that clinical diagnostic techniques reveal. The recent report of the BrainSpan Atlas represents a major collaborative attempt to map the human brain from its gestational developmental stages to its adult form (Nature 2014 April 2 [doi:10.1038/nature13185]). Previous work has examined the histology and transcriptomic profiles of 900 neuroanatomical subdivisions (Nature 2012;489:391-9) of two adult human brains that characterized the transcriptomic relationships between different cell types and different cell regions.
Now, based upon four prenatal brains, the atlas displays the gene expression profiles of the developing brain and reveals that many neuropsychiatric disorders, including autism and schizophrenia, have identifiable developmental abnormalities. To what degree these brains are representative of healthy preterm humans is not entirely clear, but the insights gained are remarkable and will certainly contribute importantly to our understanding of these most enigmatic conditions.
Dr. Caselli is a professor of neurology and associate director and clinical core director of the Alzheimer’s Disease Center at the Mayo Clinic in Scottsdale, Ariz. He has no relevant financial disclosures.
Homeless youths where?
Imagine a place where thousand of teens were homeless, many sleeping on park benches, hungry, and vulnerable. No, this is not a far-away land or third-world country; it’s here in the United States: 1.6 million children will be homeless for some period right here in America, according to the Substance Abuse and Mental Health Services Administration Office of Applied Studies
It’s hard to believe that in one of the richest nations that we would actually have teens walking the streets with no place to go. You might think that these are the wayward teen or the nonconformist, or oppositional defiant teens. But, statistics show that most teens run away to escape abuse they experience at home. Almost 20%-40% of homeless youths identify themselves as LGBT (lesbian, gay, bisexual, or transgender), according to a 2006 report by the National Coalition for the Homeless. Regardless of the reason, the number of homeless children is growing, and the hardship that teens face on the street is even greater than that faced by adults.
Finding shelter as a teen is particularly challenging because many shelters have only a few "youth" beds allotted. There is already a shortage of shelters so the availability is even less for teens. Teens also are particularly vulnerable to sexual predators and human traffickers. Many start by trading sex for food, which puts them at risk of HIV, physical abuse, and likely drug abuse.
Although many of us assume that this is a problem relegated to the inner city, the reality is that these children come from all areas, all cities, and all states. The majority of homeless teens are white (57%), black or African American comprises (27%), then American Indian and Alaskan (3%), according to the SAMHSA Office of Applied Studies (2004). As medical professionals, our critical role is to identify the at-risk teens.
Once we recognize that a teen is in dispute with his or her family because of sexual orientation, drug use, or as a victim of sexual abuse, we have taken the first step to identify a patient at risk.
The second step is to know what resources are available to assist teens that are homeless. The National Runaway Safeline – by phone, at 1-800-RUNAWAY (1-800-786-2929) or at their website, 1800runaway.org – is the national hotline designed to help keep America’s runaway, homeless, and at-risk youth safe and off the streets and to provides access to local shelters.
Homelessness is a growing crisis that affects our youth. If we understand that many of these teens are escaping abuse, it may help to explain why they end up in these situations and to define the support that they need. Remember that shelters are always in need of donations and volunteers.
Dr. Pearce is a pediatrician in Frankfort, Ill. E-mail her at [email protected].
Imagine a place where thousand of teens were homeless, many sleeping on park benches, hungry, and vulnerable. No, this is not a far-away land or third-world country; it’s here in the United States: 1.6 million children will be homeless for some period right here in America, according to the Substance Abuse and Mental Health Services Administration Office of Applied Studies
It’s hard to believe that in one of the richest nations that we would actually have teens walking the streets with no place to go. You might think that these are the wayward teen or the nonconformist, or oppositional defiant teens. But, statistics show that most teens run away to escape abuse they experience at home. Almost 20%-40% of homeless youths identify themselves as LGBT (lesbian, gay, bisexual, or transgender), according to a 2006 report by the National Coalition for the Homeless. Regardless of the reason, the number of homeless children is growing, and the hardship that teens face on the street is even greater than that faced by adults.
Finding shelter as a teen is particularly challenging because many shelters have only a few "youth" beds allotted. There is already a shortage of shelters so the availability is even less for teens. Teens also are particularly vulnerable to sexual predators and human traffickers. Many start by trading sex for food, which puts them at risk of HIV, physical abuse, and likely drug abuse.
Although many of us assume that this is a problem relegated to the inner city, the reality is that these children come from all areas, all cities, and all states. The majority of homeless teens are white (57%), black or African American comprises (27%), then American Indian and Alaskan (3%), according to the SAMHSA Office of Applied Studies (2004). As medical professionals, our critical role is to identify the at-risk teens.
Once we recognize that a teen is in dispute with his or her family because of sexual orientation, drug use, or as a victim of sexual abuse, we have taken the first step to identify a patient at risk.
The second step is to know what resources are available to assist teens that are homeless. The National Runaway Safeline – by phone, at 1-800-RUNAWAY (1-800-786-2929) or at their website, 1800runaway.org – is the national hotline designed to help keep America’s runaway, homeless, and at-risk youth safe and off the streets and to provides access to local shelters.
Homelessness is a growing crisis that affects our youth. If we understand that many of these teens are escaping abuse, it may help to explain why they end up in these situations and to define the support that they need. Remember that shelters are always in need of donations and volunteers.
Dr. Pearce is a pediatrician in Frankfort, Ill. E-mail her at [email protected].
Imagine a place where thousand of teens were homeless, many sleeping on park benches, hungry, and vulnerable. No, this is not a far-away land or third-world country; it’s here in the United States: 1.6 million children will be homeless for some period right here in America, according to the Substance Abuse and Mental Health Services Administration Office of Applied Studies
It’s hard to believe that in one of the richest nations that we would actually have teens walking the streets with no place to go. You might think that these are the wayward teen or the nonconformist, or oppositional defiant teens. But, statistics show that most teens run away to escape abuse they experience at home. Almost 20%-40% of homeless youths identify themselves as LGBT (lesbian, gay, bisexual, or transgender), according to a 2006 report by the National Coalition for the Homeless. Regardless of the reason, the number of homeless children is growing, and the hardship that teens face on the street is even greater than that faced by adults.
Finding shelter as a teen is particularly challenging because many shelters have only a few "youth" beds allotted. There is already a shortage of shelters so the availability is even less for teens. Teens also are particularly vulnerable to sexual predators and human traffickers. Many start by trading sex for food, which puts them at risk of HIV, physical abuse, and likely drug abuse.
Although many of us assume that this is a problem relegated to the inner city, the reality is that these children come from all areas, all cities, and all states. The majority of homeless teens are white (57%), black or African American comprises (27%), then American Indian and Alaskan (3%), according to the SAMHSA Office of Applied Studies (2004). As medical professionals, our critical role is to identify the at-risk teens.
Once we recognize that a teen is in dispute with his or her family because of sexual orientation, drug use, or as a victim of sexual abuse, we have taken the first step to identify a patient at risk.
The second step is to know what resources are available to assist teens that are homeless. The National Runaway Safeline – by phone, at 1-800-RUNAWAY (1-800-786-2929) or at their website, 1800runaway.org – is the national hotline designed to help keep America’s runaway, homeless, and at-risk youth safe and off the streets and to provides access to local shelters.
Homelessness is a growing crisis that affects our youth. If we understand that many of these teens are escaping abuse, it may help to explain why they end up in these situations and to define the support that they need. Remember that shelters are always in need of donations and volunteers.
Dr. Pearce is a pediatrician in Frankfort, Ill. E-mail her at [email protected].