User login
AWARD-7: Dulaglutide benefits patients with diabetic renal disease
LISBON – Patients with type 2 diabetes mellitus who also have moderate-to-severe chronic kidney disease (CKD) may be as effectively treated with the glucagonlike peptide–1 receptor agonist dulaglutide (Trulicity) as insulin glargine, the results of an international study showed.
Although comparable effects on glycemic control were seen, patients who received dulaglutide rather than insulin glargine in conjunction with prandial insulin lispro (Humalog) exhibited greater weight loss, had fewer episodes of hypoglycemia, and experienced beneficial effects on two important renal parameters.
The adverse event profile of dulaglutide was typical of that seen with GLP-1 receptor antagonism, noted Dr. Tuttle, who is the executive director of Providence Medical Research Center, Providence Sacred Heart Medical Center in Spokane, Washington, and clinical professor of medicine in the nephrology division at the University of Washington in Seattle.
In Europe, the use of dulaglutide in patients with severely reduced kidney function is not currently recommended, and monitoring is required in the United States in those with gastrointestinal side effects.
AWARD-7 was a randomized, open-label parallel-arm study comparing once-weekly dulaglutide (0.75 mg or 1.5 mg) with insulin glargine plus prandial insulin lispro in 576 subjects who had T2DM and stage 3-4 chronic kidney disease. The aim of the trial was to show noninferiority of the dulaglutide regimen to the insulin glargine regimen.
The trial was open label because the dose of insulin glargine had to be regulated, Dr. Tuttle explained, but the dose of dulaglutide given was blinded. The dose of insulin glargine was targeted to fasting plasma glucose to achieve a value between 5.6 mmol/L and 8.3 mmol/L. The dose of insulin lispro was also adjusted to target preprandial plasma glucose between 6.7 mmol/L and 10.0 mmol/L.
Patients were included if they had a glycated hemoglobin (HbA1c) level of at least 7.5% but less than or equal to 10.5% (at least 57 but less than or equal to 91 mmol/mol) and an eGFR less than 60 but greater than or equal to 15 mL/min per 1.73 m2 at screening.
Approximately 45% of dulaglutide- and 52% of glargine-treated subjects were women; the average age of participants was 65 years, with an average duration of diabetes of around 18 years. The mean HbA1c level at study entry was 8.6% (70.5 mmol/mol), with around half of participants having a HbA1c above 8.5% (69.4 mmol/mol) at entry.
The majority of patients included had an eGFR of less than 45 mL/min per 1.73 m2, and about 30% of patients had stage 4 CKD (eGFR at least 15 but less than 30 mL/min per 1.73 m2), about 45% had macroalbuminuria, and a third or more had microalbuminuria.
The primary endpoint was change in HbA1c from baseline to week 26, and this was comparable for both dulaglutide (at around –1.1% to –1.2%) and insulin glargine (around –1.1%). The effects were maintained at 52 weeks, Dr. Tuttle said, adding that similar percentages (approximately 70% or more) of patients in the groups achieved a target HbA1c of less than 8.0 (64 mmol/mol) at 26 and at 52 weeks. Similar results were seen when the more conventional target of less than 7% (less than 52 mmol/mol) was used, with around 30% of patients achieving this target at 26 and at 52 weeks.
As for weight change, the insulin-treated patients gained about 1 kg in weight over the full course of the study while a dose-dependent decrease in weight of about 2-3 kg was seen with dulaglutide treatment.
“Rates of hypoglycemia were consistently lower in the dulaglutide groups [than in the glargine group],” Dr. Tuttle said, noting “the lowest rates of hypoglycemia were actually seen with the highest dose of dulaglutide.”
The rate of total hypoglycemia (less than or equal to 3.9 mmol/mol) in the 1.5-mg and 0.75-mg dulaglutide groups was 50% and 59.8% of patients, respectively, versus almost 75% of the glargine-treated patients. Rates for documented symptomatic (40.5%, 48.1%, 63.4%), nocturnal (20.5%, 23.8%, 47.9%), and severe (0%, 2.6%, 6.7%) hypoglycemia followed a similar pattern.
“Albuminuria was reduced in all study groups, but there were greater reductions in the patients receiving dulaglutide at 26 weeks,” Dr. Tuttle said. The mean change in UACR from baseline to week 26 was –27.7 for the 1.5-mg dose of dulaglutide, –26.7 for the 0.75-mg dose, and –16.4 for insulin glargine.
The expected rate of eGFR decline at week 26 was also lower with dulaglutide 1.5 mg and 0.75 mg than with glargine, at a respective –0.8%, –3.3%, and –7.7% or –0.1, –0.4, and –1.9 mL/min per 1.73 m2.
“In patients at this stage of CKD, we expect about a 4- to 5-mL per minute loss, so they are right on target or as expected in the insulin group, but this was essentially extinguished in the dulaglutide groups, where there was no significant loss in eGFR during the 26-week time period,” said Dr. Tuttle.
The only difference in side effect profiles between the dulaglutide groups and the glargine group was a higher rate of gastrointestinal side effects. Nausea was seen in 19.8%, 14.2%, and 4.6% of patients given the dulaglutide 1.5 mg, dulaglutide 0.75 mg, and glargine, respectively, with vomiting reported by 13.5%, 8.4%, and 4.6%.
Eli Lilly funded the study. Dr. Tuttle disclosed acting as a consultant on therapies for diabetic kidney disease for Eli Lilly, Boehringer Ingelheim, Gilead, and AstraZeneca.
This article was updated September 28, 2017.
LISBON – Patients with type 2 diabetes mellitus who also have moderate-to-severe chronic kidney disease (CKD) may be as effectively treated with the glucagonlike peptide–1 receptor agonist dulaglutide (Trulicity) as insulin glargine, the results of an international study showed.
Although comparable effects on glycemic control were seen, patients who received dulaglutide rather than insulin glargine in conjunction with prandial insulin lispro (Humalog) exhibited greater weight loss, had fewer episodes of hypoglycemia, and experienced beneficial effects on two important renal parameters.
The adverse event profile of dulaglutide was typical of that seen with GLP-1 receptor antagonism, noted Dr. Tuttle, who is the executive director of Providence Medical Research Center, Providence Sacred Heart Medical Center in Spokane, Washington, and clinical professor of medicine in the nephrology division at the University of Washington in Seattle.
In Europe, the use of dulaglutide in patients with severely reduced kidney function is not currently recommended, and monitoring is required in the United States in those with gastrointestinal side effects.
AWARD-7 was a randomized, open-label parallel-arm study comparing once-weekly dulaglutide (0.75 mg or 1.5 mg) with insulin glargine plus prandial insulin lispro in 576 subjects who had T2DM and stage 3-4 chronic kidney disease. The aim of the trial was to show noninferiority of the dulaglutide regimen to the insulin glargine regimen.
The trial was open label because the dose of insulin glargine had to be regulated, Dr. Tuttle explained, but the dose of dulaglutide given was blinded. The dose of insulin glargine was targeted to fasting plasma glucose to achieve a value between 5.6 mmol/L and 8.3 mmol/L. The dose of insulin lispro was also adjusted to target preprandial plasma glucose between 6.7 mmol/L and 10.0 mmol/L.
Patients were included if they had a glycated hemoglobin (HbA1c) level of at least 7.5% but less than or equal to 10.5% (at least 57 but less than or equal to 91 mmol/mol) and an eGFR less than 60 but greater than or equal to 15 mL/min per 1.73 m2 at screening.
Approximately 45% of dulaglutide- and 52% of glargine-treated subjects were women; the average age of participants was 65 years, with an average duration of diabetes of around 18 years. The mean HbA1c level at study entry was 8.6% (70.5 mmol/mol), with around half of participants having a HbA1c above 8.5% (69.4 mmol/mol) at entry.
The majority of patients included had an eGFR of less than 45 mL/min per 1.73 m2, and about 30% of patients had stage 4 CKD (eGFR at least 15 but less than 30 mL/min per 1.73 m2), about 45% had macroalbuminuria, and a third or more had microalbuminuria.
The primary endpoint was change in HbA1c from baseline to week 26, and this was comparable for both dulaglutide (at around –1.1% to –1.2%) and insulin glargine (around –1.1%). The effects were maintained at 52 weeks, Dr. Tuttle said, adding that similar percentages (approximately 70% or more) of patients in the groups achieved a target HbA1c of less than 8.0 (64 mmol/mol) at 26 and at 52 weeks. Similar results were seen when the more conventional target of less than 7% (less than 52 mmol/mol) was used, with around 30% of patients achieving this target at 26 and at 52 weeks.
As for weight change, the insulin-treated patients gained about 1 kg in weight over the full course of the study while a dose-dependent decrease in weight of about 2-3 kg was seen with dulaglutide treatment.
“Rates of hypoglycemia were consistently lower in the dulaglutide groups [than in the glargine group],” Dr. Tuttle said, noting “the lowest rates of hypoglycemia were actually seen with the highest dose of dulaglutide.”
The rate of total hypoglycemia (less than or equal to 3.9 mmol/mol) in the 1.5-mg and 0.75-mg dulaglutide groups was 50% and 59.8% of patients, respectively, versus almost 75% of the glargine-treated patients. Rates for documented symptomatic (40.5%, 48.1%, 63.4%), nocturnal (20.5%, 23.8%, 47.9%), and severe (0%, 2.6%, 6.7%) hypoglycemia followed a similar pattern.
“Albuminuria was reduced in all study groups, but there were greater reductions in the patients receiving dulaglutide at 26 weeks,” Dr. Tuttle said. The mean change in UACR from baseline to week 26 was –27.7 for the 1.5-mg dose of dulaglutide, –26.7 for the 0.75-mg dose, and –16.4 for insulin glargine.
The expected rate of eGFR decline at week 26 was also lower with dulaglutide 1.5 mg and 0.75 mg than with glargine, at a respective –0.8%, –3.3%, and –7.7% or –0.1, –0.4, and –1.9 mL/min per 1.73 m2.
“In patients at this stage of CKD, we expect about a 4- to 5-mL per minute loss, so they are right on target or as expected in the insulin group, but this was essentially extinguished in the dulaglutide groups, where there was no significant loss in eGFR during the 26-week time period,” said Dr. Tuttle.
The only difference in side effect profiles between the dulaglutide groups and the glargine group was a higher rate of gastrointestinal side effects. Nausea was seen in 19.8%, 14.2%, and 4.6% of patients given the dulaglutide 1.5 mg, dulaglutide 0.75 mg, and glargine, respectively, with vomiting reported by 13.5%, 8.4%, and 4.6%.
Eli Lilly funded the study. Dr. Tuttle disclosed acting as a consultant on therapies for diabetic kidney disease for Eli Lilly, Boehringer Ingelheim, Gilead, and AstraZeneca.
This article was updated September 28, 2017.
LISBON – Patients with type 2 diabetes mellitus who also have moderate-to-severe chronic kidney disease (CKD) may be as effectively treated with the glucagonlike peptide–1 receptor agonist dulaglutide (Trulicity) as insulin glargine, the results of an international study showed.
Although comparable effects on glycemic control were seen, patients who received dulaglutide rather than insulin glargine in conjunction with prandial insulin lispro (Humalog) exhibited greater weight loss, had fewer episodes of hypoglycemia, and experienced beneficial effects on two important renal parameters.
The adverse event profile of dulaglutide was typical of that seen with GLP-1 receptor antagonism, noted Dr. Tuttle, who is the executive director of Providence Medical Research Center, Providence Sacred Heart Medical Center in Spokane, Washington, and clinical professor of medicine in the nephrology division at the University of Washington in Seattle.
In Europe, the use of dulaglutide in patients with severely reduced kidney function is not currently recommended, and monitoring is required in the United States in those with gastrointestinal side effects.
AWARD-7 was a randomized, open-label parallel-arm study comparing once-weekly dulaglutide (0.75 mg or 1.5 mg) with insulin glargine plus prandial insulin lispro in 576 subjects who had T2DM and stage 3-4 chronic kidney disease. The aim of the trial was to show noninferiority of the dulaglutide regimen to the insulin glargine regimen.
The trial was open label because the dose of insulin glargine had to be regulated, Dr. Tuttle explained, but the dose of dulaglutide given was blinded. The dose of insulin glargine was targeted to fasting plasma glucose to achieve a value between 5.6 mmol/L and 8.3 mmol/L. The dose of insulin lispro was also adjusted to target preprandial plasma glucose between 6.7 mmol/L and 10.0 mmol/L.
Patients were included if they had a glycated hemoglobin (HbA1c) level of at least 7.5% but less than or equal to 10.5% (at least 57 but less than or equal to 91 mmol/mol) and an eGFR less than 60 but greater than or equal to 15 mL/min per 1.73 m2 at screening.
Approximately 45% of dulaglutide- and 52% of glargine-treated subjects were women; the average age of participants was 65 years, with an average duration of diabetes of around 18 years. The mean HbA1c level at study entry was 8.6% (70.5 mmol/mol), with around half of participants having a HbA1c above 8.5% (69.4 mmol/mol) at entry.
The majority of patients included had an eGFR of less than 45 mL/min per 1.73 m2, and about 30% of patients had stage 4 CKD (eGFR at least 15 but less than 30 mL/min per 1.73 m2), about 45% had macroalbuminuria, and a third or more had microalbuminuria.
The primary endpoint was change in HbA1c from baseline to week 26, and this was comparable for both dulaglutide (at around –1.1% to –1.2%) and insulin glargine (around –1.1%). The effects were maintained at 52 weeks, Dr. Tuttle said, adding that similar percentages (approximately 70% or more) of patients in the groups achieved a target HbA1c of less than 8.0 (64 mmol/mol) at 26 and at 52 weeks. Similar results were seen when the more conventional target of less than 7% (less than 52 mmol/mol) was used, with around 30% of patients achieving this target at 26 and at 52 weeks.
As for weight change, the insulin-treated patients gained about 1 kg in weight over the full course of the study while a dose-dependent decrease in weight of about 2-3 kg was seen with dulaglutide treatment.
“Rates of hypoglycemia were consistently lower in the dulaglutide groups [than in the glargine group],” Dr. Tuttle said, noting “the lowest rates of hypoglycemia were actually seen with the highest dose of dulaglutide.”
The rate of total hypoglycemia (less than or equal to 3.9 mmol/mol) in the 1.5-mg and 0.75-mg dulaglutide groups was 50% and 59.8% of patients, respectively, versus almost 75% of the glargine-treated patients. Rates for documented symptomatic (40.5%, 48.1%, 63.4%), nocturnal (20.5%, 23.8%, 47.9%), and severe (0%, 2.6%, 6.7%) hypoglycemia followed a similar pattern.
“Albuminuria was reduced in all study groups, but there were greater reductions in the patients receiving dulaglutide at 26 weeks,” Dr. Tuttle said. The mean change in UACR from baseline to week 26 was –27.7 for the 1.5-mg dose of dulaglutide, –26.7 for the 0.75-mg dose, and –16.4 for insulin glargine.
The expected rate of eGFR decline at week 26 was also lower with dulaglutide 1.5 mg and 0.75 mg than with glargine, at a respective –0.8%, –3.3%, and –7.7% or –0.1, –0.4, and –1.9 mL/min per 1.73 m2.
“In patients at this stage of CKD, we expect about a 4- to 5-mL per minute loss, so they are right on target or as expected in the insulin group, but this was essentially extinguished in the dulaglutide groups, where there was no significant loss in eGFR during the 26-week time period,” said Dr. Tuttle.
The only difference in side effect profiles between the dulaglutide groups and the glargine group was a higher rate of gastrointestinal side effects. Nausea was seen in 19.8%, 14.2%, and 4.6% of patients given the dulaglutide 1.5 mg, dulaglutide 0.75 mg, and glargine, respectively, with vomiting reported by 13.5%, 8.4%, and 4.6%.
Eli Lilly funded the study. Dr. Tuttle disclosed acting as a consultant on therapies for diabetic kidney disease for Eli Lilly, Boehringer Ingelheim, Gilead, and AstraZeneca.
This article was updated September 28, 2017.
AT EASD 2017
Key clinical point: Dulaglutide had more beneficial effects on renal parameters than insulin glargine in patients with type 2 diabetes and moderate-to-severe chronic kidney disease.
Major finding: The primary endpoint of change in HbA1c level from baseline to week 26 was comparable for both dulaglutide and insulin glargine.
Data source: A randomized, open-label parallel-arm study comparing once-weekly dulaglutide (0.75 or 1.5 mg) or insulin glargine plus prandial insulin lispro in 576 subjects with type 2 diabetes mellitus and stage 3–4 CKD.
Disclosures: Eli Lilly funded the study. The presenting author has been a consultant on therapies for diabetic kidney disease for Eli Lilly, Boehringer Ingelheim, Gilead, and AstraZeneca.
Letter: Working together to empower our next generation of leaders
Editor:
Dr. Nasim Afsar’s article of June 2, 2017 (“A case for building our leadership skills”) calls for the integration of leadership skills into medical training, and we at the University of Colorado wholeheartedly agree. There are several institutions around the country that are already addressing this problem head on, and we write this letter to highlight a few educational programs we’ve created that demonstrate the power of arming our trainees with this skill set. Furthermore, we wish to encourage collaboration between educators and institutions that are engaged in similar work in the hopes of moving this field forward.
Here at the University of Colorado, a team of Hospital Medicine faculty has created a number of programs to address the leadership education gap in learners at the undergraduate medical education,1 graduate medical education,2 and fellowship levels – creating a pipeline for developing leaders in hospital medicine. These programs include an immersive medical student elective, a dedicated leadership track in the Internal Medicine Residency Program, and a fellowship program in Hospital Medicine focused on Quality Improvement and Health Systems Leadership. Our goal in each of these programs to equip trainees across the spectrum of medical education with the knowledge, attitudes, and skills needed to lead high-functioning teams.
In our 5-year experience with our leadership training pipeline, we’ve learned a few important lessons. First, medical trainees are rarely exposed to the leadership skill set elsewhere in medical training, and are eager to learn new approaches to common problems that they encounter on a daily basis: How do I negotiate with a colleague? How can I motivate team members to change behavior to accomplish a goal? How can I use data to support requests for resources?
Secondly, trainees who are exposed to leadership concepts and who are given the opportunity to practice them through challenging project work in the live system routinely make meaningful changes to the health system. Our trainees have revamped our process of managing interhospital transfers, have decreased rates of inappropriate antibiotic usage, and have enhanced the patient experience in our stroke units. Further, our recent graduates have positioned themselves as leaders in health systems. Our graduates are leading a QI program at a major academic center, being promoted to educational leadership roles such as assistant program director within a residency training program, directing process improvement in a developing country, and leading the operations unit of a large physician group.
As Dr. Afsar highlights, there is much work to be done to better equip trainees with the skill set to lead. We strongly encourage other training programs to develop strategies to teach leadership and create forums for trainees to practice their burgeoning skill set. In addition to responding to Dr. Afsar’s call to develop programs, we should form collaborative working groups through our regional and national organizations to develop comprehensive leadership programs for medical trainees at all levels. Collaborating to empower the next generation of providers is critical to our future as hospitalists as we continue to take the lead in improving and shaping our health care systems.
Tyler Anstett, DO
Manuel Diaz, MD
Emily Gottenborg, MD
University of Colorado School of Medicine, Anschutz Medical Campus, Aurora, Colo.
References
1. Sweigart JR, Tad-Y D, Kneeland P, Williams MV, Glasheen JJ. Hospital Medicine Resident Training Tracks: Developing the Hospital Medicine Pipeline. J Hosp Med. 2017 Mar;12(3):173-176. doi: 10.12788/jhm.2703.
2. Tad-y D, Price L, Cumbler E, Levin D, Wald H, Glasheen J. An experiential quality improvement curriculum for the inpatient setting – part 1: design phase of a QI project. MedEdPORTAL Publications. 2014;10:9841. http://doi.org/10.15766/mep_2374-8265.9841.
Editor:
Dr. Nasim Afsar’s article of June 2, 2017 (“A case for building our leadership skills”) calls for the integration of leadership skills into medical training, and we at the University of Colorado wholeheartedly agree. There are several institutions around the country that are already addressing this problem head on, and we write this letter to highlight a few educational programs we’ve created that demonstrate the power of arming our trainees with this skill set. Furthermore, we wish to encourage collaboration between educators and institutions that are engaged in similar work in the hopes of moving this field forward.
Here at the University of Colorado, a team of Hospital Medicine faculty has created a number of programs to address the leadership education gap in learners at the undergraduate medical education,1 graduate medical education,2 and fellowship levels – creating a pipeline for developing leaders in hospital medicine. These programs include an immersive medical student elective, a dedicated leadership track in the Internal Medicine Residency Program, and a fellowship program in Hospital Medicine focused on Quality Improvement and Health Systems Leadership. Our goal in each of these programs to equip trainees across the spectrum of medical education with the knowledge, attitudes, and skills needed to lead high-functioning teams.
In our 5-year experience with our leadership training pipeline, we’ve learned a few important lessons. First, medical trainees are rarely exposed to the leadership skill set elsewhere in medical training, and are eager to learn new approaches to common problems that they encounter on a daily basis: How do I negotiate with a colleague? How can I motivate team members to change behavior to accomplish a goal? How can I use data to support requests for resources?
Secondly, trainees who are exposed to leadership concepts and who are given the opportunity to practice them through challenging project work in the live system routinely make meaningful changes to the health system. Our trainees have revamped our process of managing interhospital transfers, have decreased rates of inappropriate antibiotic usage, and have enhanced the patient experience in our stroke units. Further, our recent graduates have positioned themselves as leaders in health systems. Our graduates are leading a QI program at a major academic center, being promoted to educational leadership roles such as assistant program director within a residency training program, directing process improvement in a developing country, and leading the operations unit of a large physician group.
As Dr. Afsar highlights, there is much work to be done to better equip trainees with the skill set to lead. We strongly encourage other training programs to develop strategies to teach leadership and create forums for trainees to practice their burgeoning skill set. In addition to responding to Dr. Afsar’s call to develop programs, we should form collaborative working groups through our regional and national organizations to develop comprehensive leadership programs for medical trainees at all levels. Collaborating to empower the next generation of providers is critical to our future as hospitalists as we continue to take the lead in improving and shaping our health care systems.
Tyler Anstett, DO
Manuel Diaz, MD
Emily Gottenborg, MD
University of Colorado School of Medicine, Anschutz Medical Campus, Aurora, Colo.
References
1. Sweigart JR, Tad-Y D, Kneeland P, Williams MV, Glasheen JJ. Hospital Medicine Resident Training Tracks: Developing the Hospital Medicine Pipeline. J Hosp Med. 2017 Mar;12(3):173-176. doi: 10.12788/jhm.2703.
2. Tad-y D, Price L, Cumbler E, Levin D, Wald H, Glasheen J. An experiential quality improvement curriculum for the inpatient setting – part 1: design phase of a QI project. MedEdPORTAL Publications. 2014;10:9841. http://doi.org/10.15766/mep_2374-8265.9841.
Editor:
Dr. Nasim Afsar’s article of June 2, 2017 (“A case for building our leadership skills”) calls for the integration of leadership skills into medical training, and we at the University of Colorado wholeheartedly agree. There are several institutions around the country that are already addressing this problem head on, and we write this letter to highlight a few educational programs we’ve created that demonstrate the power of arming our trainees with this skill set. Furthermore, we wish to encourage collaboration between educators and institutions that are engaged in similar work in the hopes of moving this field forward.
Here at the University of Colorado, a team of Hospital Medicine faculty has created a number of programs to address the leadership education gap in learners at the undergraduate medical education,1 graduate medical education,2 and fellowship levels – creating a pipeline for developing leaders in hospital medicine. These programs include an immersive medical student elective, a dedicated leadership track in the Internal Medicine Residency Program, and a fellowship program in Hospital Medicine focused on Quality Improvement and Health Systems Leadership. Our goal in each of these programs to equip trainees across the spectrum of medical education with the knowledge, attitudes, and skills needed to lead high-functioning teams.
In our 5-year experience with our leadership training pipeline, we’ve learned a few important lessons. First, medical trainees are rarely exposed to the leadership skill set elsewhere in medical training, and are eager to learn new approaches to common problems that they encounter on a daily basis: How do I negotiate with a colleague? How can I motivate team members to change behavior to accomplish a goal? How can I use data to support requests for resources?
Secondly, trainees who are exposed to leadership concepts and who are given the opportunity to practice them through challenging project work in the live system routinely make meaningful changes to the health system. Our trainees have revamped our process of managing interhospital transfers, have decreased rates of inappropriate antibiotic usage, and have enhanced the patient experience in our stroke units. Further, our recent graduates have positioned themselves as leaders in health systems. Our graduates are leading a QI program at a major academic center, being promoted to educational leadership roles such as assistant program director within a residency training program, directing process improvement in a developing country, and leading the operations unit of a large physician group.
As Dr. Afsar highlights, there is much work to be done to better equip trainees with the skill set to lead. We strongly encourage other training programs to develop strategies to teach leadership and create forums for trainees to practice their burgeoning skill set. In addition to responding to Dr. Afsar’s call to develop programs, we should form collaborative working groups through our regional and national organizations to develop comprehensive leadership programs for medical trainees at all levels. Collaborating to empower the next generation of providers is critical to our future as hospitalists as we continue to take the lead in improving and shaping our health care systems.
Tyler Anstett, DO
Manuel Diaz, MD
Emily Gottenborg, MD
University of Colorado School of Medicine, Anschutz Medical Campus, Aurora, Colo.
References
1. Sweigart JR, Tad-Y D, Kneeland P, Williams MV, Glasheen JJ. Hospital Medicine Resident Training Tracks: Developing the Hospital Medicine Pipeline. J Hosp Med. 2017 Mar;12(3):173-176. doi: 10.12788/jhm.2703.
2. Tad-y D, Price L, Cumbler E, Levin D, Wald H, Glasheen J. An experiential quality improvement curriculum for the inpatient setting – part 1: design phase of a QI project. MedEdPORTAL Publications. 2014;10:9841. http://doi.org/10.15766/mep_2374-8265.9841.
ICD-10-CM code changes: What's new for 2018
The list of new and revised International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) codes has been published, with changes becoming effective on October 1, 2017. This year, you can look forward to minimal code changes for gynecologic conditions. The biggest change in this category is the addition of codes that describe a lump in the breast according to which breast and the location on the breast, as well as the addition of a code for prophylactic removal of the fallopian tubes. The codes related to obstetrics will have more extensive changes. You will find revisions to the codes for ectopic pregnancy, a new set of codes for addressing an abnormal fetal heart rate during the antepartum period, and, most welcome of all, an expansion of the single code for antenatal testing to 17 very specific codes.
Gynecologic code changes
The single code N63, Unspecified lump in breast, has been expanded to include codes for both the right and the left breast. Code N63 therefore will be considered invalid after October 1, 2018. Expanded codes include:
- N63.0, Unspecified lump in unspecified breast
- N63.1, Unspecified lump in the right breast
- N63.10, Unspecified lump in the right breast, unspecified quadrant
- N63.11, Unspecified lump in the right breast, upper outer quadrant
- N63.12, Unspecified lump in the right breast, upper inner quadrant
- N63.13, Unspecified lump in the right breast, lower outer quadrant
- N63.14, Unspecified lump in the right breast, lower inner quadrant
- N63.2, Unspecified lump in the left breast
- N63.20, Unspecified lump in the left breast, unspecified quadrant
- N63.21, Unspecified lump in the left breast, upper outer quadrant
- N63.22, Unspecified lump in the left breast, upper inner quadrant
- N63.23, Unspecified lump in the left breast, lower outer quadrant
- N63.24, Unspecified lump in the left breast, lower inner quadrant
- N63.3, Unspecified lump in axillary tail
- N63.31, Unspecified lump in axillary tail of the right breast
- N63.32, Unspecified lump in axillary tail of the left breast
- N63.4, Unspecified lump in breast, subareolar
- N63.41, Unspecified lump in right breast, subareolar
- N63.42, Unspecified lump in left breast, subareolar
Other changes to gynecologic codes
There has been a minor change to the description for code Z31.5, Encounter for genetic counseling. It now is described as "Encounter for procreative genetic counseling."
The code Z40.02, Encounter for prophylactic removal of ovary(s), now refers to one or more ovaries without distinction of right or left, and a new code has been added for removal of the fallopian tube(s), Z40.03, Encounter for prophylactic removal of fallopian tube(s).
The inclusion term "endometriosis of the thorax" has been added to code N80.8, Other endometriosis.
The inclusion term "premenstrual dysphoric disorder" has been deleted from code N94.3, Premenstrual tension syndrome. If the patient has been diagnosed with this condition, the code F32.81, Premenstrual dysphoric disorder, should be reported, as this is considered a mental health issue.
The "excludes 1" note under code Z87.41, Personal history of dysplasia of the female genital tract, has been revised. The codes for personal history of intraepithelial neoplasia III that may not be reported with this code are Z86.001 and Z86.008.
Obstetric code changes
The ectopic pregnancy codes have been revised to include references to the right or left structure affected, which means the codes change from 5 digits to 6 digits in length, and the codes O00.10, O00.11, O00.20, and O00.21 will no longer be valid.
- O00.1, Tubal pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.101, Right tubal pregnancy without intrauterine pregnancy
- O00.102, Left tubal pregnancy without intrauterine pregnancy
- O00.109, Unspecified tubal pregnancy without intrauterine pregnancy
- O00.11, Tubal pregnancy with intrauterine pregnancy
- O00.111, Right tubal pregnancy with intrauterine pregnancy
- O00.112, Left tubal pregnancy with intrauterine pregnancy
- O00.119, Unspecified tubal pregnancy with intrauterine pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.2, Ovarian pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
- O00.201, Right ovarian pregnancy without intrauterine pregnancy
- O00.202, Left ovarian pregnancy without intrauterine pregnancy
- O00.209, Unspecified ovarian pregnancy without intrauterine pregnancy
- O00.21, Ovarian pregnancy with intrauterine pregnancy
- O00.211, Right ovarian pregnancy with intrauterine pregnancy
- O00.212, Left ovarian pregnancy with intrauterine pregnancy
- O00.219, Unspecified ovarian pregnancy with intrauterine pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
New codes for fetal heart rate abnormalities
New codes have been added to report a fetal heart rate or rhythm abnormality during the antepartum period. Until now, there only has been a code that addresses this issue during labor and delivery, O76, Abnormality in fetal heart rate and rhythm complicating labor and delivery.
- O36.83, Maternal care for abnormalities of the fetal heart rate or rhythm
- O36.831, Maternal care for abnormalities of the fetal heart rate or rhythm, first trimester
- O36.832, Maternal care for abnormalities of the fetal heart rate or rhythm, second trimester
- O36.833, Maternal care for abnormalities of the fetal heart rate or rhythm, third trimester
- O36.839, Maternal care for abnormalities of the fetal heart rate or rhythm, unspecified trimester
Several codes redefined
ICD-10 has corrected an "excludes" note error for the code O99.1, Other diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism complicating pregnancy, childbirth, and the puerperium. In 2017, any hemorrhage with coagulation defects defined in code category O45.- or codes O46.0-, O67.0, or O72.3 could be reported with O99.1. This set of codes has now been redefined as an "excludes 1" note, which means that they may not be reported with O99.1 since they are considered inclusive.
More specific codes added for antenatal screening
Great news for those awaiting a more specific code for antenatal screening: The code Z36 has been expanded to more closely match the codes that were available in ICD-9-CM, but it goes beyond the basic list in that codes have been added for things like nonvisualization of anatomic structures on a previous scan and screening for cervical length and fetal lung maturity. Be sure to pay attention to the excludes notes and other inclusive terms.
- Z36, Encounter for antenatal screening of mother (Screening is the testing for disease or disease precursors in asymptomatic individuals so that early detection and treatment can be provided for those who test positive for the disease.)
Includes: Encounter for placental sample (taken vaginally)
Excludes 2: O28.-, Abnormal findings on antenatal screening of mother
- Z36.5, Encounter for antenatal screening for isoimmunization
- Z36.4, Encounter for antenatal screening for fetal growth retardation
Intrauterine growth restriction (IUGR)/small-for-dates - Z36.3, Encounter for antenatal screening for malformations
Screening for a suspected anomaly - Z36.2, Encounter for other antenatal screening follow-up
Nonvisualized anatomy on a previous scan - Z36.1, Encounter for antenatal screening for raised alpha-fetoprotein level
Encounter for antenatal screening for elevated maternal serum alpha-fetoprotein level - Z36.0, Encounter for antenatal screening for chromosomal anomalies
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.8A, Encounter for antenatal screening for other genetic defects
- Z36.89, Encounter for other specified antenatal screening
- Z36.88, Encounter for antenatal screening for fetal macrosomia
Screening for large-for-dates - Z36.87, Encounter for antenatal screening for uncertain dates
- Z36.86, Encounter for antenatal screening for cervical length
Screening for risk of preterm labor - Z36.85, Encounter for antenatal screening for Streptococcus B
- Z36.84, Encounter for antenatal screening for fetal lung maturity
- Z36.83, Encounter for fetal screening for congenital cardiac abnormalities
- Z36.82, Encounter for antenatal screening for nuchal translucency
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.9, Encounter for antenatal screening, unspecified
Code changes for abortion and complications
The code range for use with Z3A, weeks of gestation, has changed from O00-O9A to O09-O9A to reflect the guideline change last year to remove the requirement to use this code with any code that describes pregnancy with an abortive outcome (codes O00-O08).
In addition, if a patient has retained products of conception (POC) after either a spontaneous or elective abortion, report the "without complication" code for the retained POC (O03.4, Incomplete spontaneous abortion without complication, or O07.4, Failed attempted termination of pregnancy without complication). If any other complication occurred in addition to the retained POC, use the code for that particular complication and not O03.4 or O07.4.
Share your thoughts! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
The list of new and revised International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) codes has been published, with changes becoming effective on October 1, 2017. This year, you can look forward to minimal code changes for gynecologic conditions. The biggest change in this category is the addition of codes that describe a lump in the breast according to which breast and the location on the breast, as well as the addition of a code for prophylactic removal of the fallopian tubes. The codes related to obstetrics will have more extensive changes. You will find revisions to the codes for ectopic pregnancy, a new set of codes for addressing an abnormal fetal heart rate during the antepartum period, and, most welcome of all, an expansion of the single code for antenatal testing to 17 very specific codes.
Gynecologic code changes
The single code N63, Unspecified lump in breast, has been expanded to include codes for both the right and the left breast. Code N63 therefore will be considered invalid after October 1, 2018. Expanded codes include:
- N63.0, Unspecified lump in unspecified breast
- N63.1, Unspecified lump in the right breast
- N63.10, Unspecified lump in the right breast, unspecified quadrant
- N63.11, Unspecified lump in the right breast, upper outer quadrant
- N63.12, Unspecified lump in the right breast, upper inner quadrant
- N63.13, Unspecified lump in the right breast, lower outer quadrant
- N63.14, Unspecified lump in the right breast, lower inner quadrant
- N63.2, Unspecified lump in the left breast
- N63.20, Unspecified lump in the left breast, unspecified quadrant
- N63.21, Unspecified lump in the left breast, upper outer quadrant
- N63.22, Unspecified lump in the left breast, upper inner quadrant
- N63.23, Unspecified lump in the left breast, lower outer quadrant
- N63.24, Unspecified lump in the left breast, lower inner quadrant
- N63.3, Unspecified lump in axillary tail
- N63.31, Unspecified lump in axillary tail of the right breast
- N63.32, Unspecified lump in axillary tail of the left breast
- N63.4, Unspecified lump in breast, subareolar
- N63.41, Unspecified lump in right breast, subareolar
- N63.42, Unspecified lump in left breast, subareolar
Other changes to gynecologic codes
There has been a minor change to the description for code Z31.5, Encounter for genetic counseling. It now is described as "Encounter for procreative genetic counseling."
The code Z40.02, Encounter for prophylactic removal of ovary(s), now refers to one or more ovaries without distinction of right or left, and a new code has been added for removal of the fallopian tube(s), Z40.03, Encounter for prophylactic removal of fallopian tube(s).
The inclusion term "endometriosis of the thorax" has been added to code N80.8, Other endometriosis.
The inclusion term "premenstrual dysphoric disorder" has been deleted from code N94.3, Premenstrual tension syndrome. If the patient has been diagnosed with this condition, the code F32.81, Premenstrual dysphoric disorder, should be reported, as this is considered a mental health issue.
The "excludes 1" note under code Z87.41, Personal history of dysplasia of the female genital tract, has been revised. The codes for personal history of intraepithelial neoplasia III that may not be reported with this code are Z86.001 and Z86.008.
Obstetric code changes
The ectopic pregnancy codes have been revised to include references to the right or left structure affected, which means the codes change from 5 digits to 6 digits in length, and the codes O00.10, O00.11, O00.20, and O00.21 will no longer be valid.
- O00.1, Tubal pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.101, Right tubal pregnancy without intrauterine pregnancy
- O00.102, Left tubal pregnancy without intrauterine pregnancy
- O00.109, Unspecified tubal pregnancy without intrauterine pregnancy
- O00.11, Tubal pregnancy with intrauterine pregnancy
- O00.111, Right tubal pregnancy with intrauterine pregnancy
- O00.112, Left tubal pregnancy with intrauterine pregnancy
- O00.119, Unspecified tubal pregnancy with intrauterine pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.2, Ovarian pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
- O00.201, Right ovarian pregnancy without intrauterine pregnancy
- O00.202, Left ovarian pregnancy without intrauterine pregnancy
- O00.209, Unspecified ovarian pregnancy without intrauterine pregnancy
- O00.21, Ovarian pregnancy with intrauterine pregnancy
- O00.211, Right ovarian pregnancy with intrauterine pregnancy
- O00.212, Left ovarian pregnancy with intrauterine pregnancy
- O00.219, Unspecified ovarian pregnancy with intrauterine pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
New codes for fetal heart rate abnormalities
New codes have been added to report a fetal heart rate or rhythm abnormality during the antepartum period. Until now, there only has been a code that addresses this issue during labor and delivery, O76, Abnormality in fetal heart rate and rhythm complicating labor and delivery.
- O36.83, Maternal care for abnormalities of the fetal heart rate or rhythm
- O36.831, Maternal care for abnormalities of the fetal heart rate or rhythm, first trimester
- O36.832, Maternal care for abnormalities of the fetal heart rate or rhythm, second trimester
- O36.833, Maternal care for abnormalities of the fetal heart rate or rhythm, third trimester
- O36.839, Maternal care for abnormalities of the fetal heart rate or rhythm, unspecified trimester
Several codes redefined
ICD-10 has corrected an "excludes" note error for the code O99.1, Other diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism complicating pregnancy, childbirth, and the puerperium. In 2017, any hemorrhage with coagulation defects defined in code category O45.- or codes O46.0-, O67.0, or O72.3 could be reported with O99.1. This set of codes has now been redefined as an "excludes 1" note, which means that they may not be reported with O99.1 since they are considered inclusive.
More specific codes added for antenatal screening
Great news for those awaiting a more specific code for antenatal screening: The code Z36 has been expanded to more closely match the codes that were available in ICD-9-CM, but it goes beyond the basic list in that codes have been added for things like nonvisualization of anatomic structures on a previous scan and screening for cervical length and fetal lung maturity. Be sure to pay attention to the excludes notes and other inclusive terms.
- Z36, Encounter for antenatal screening of mother (Screening is the testing for disease or disease precursors in asymptomatic individuals so that early detection and treatment can be provided for those who test positive for the disease.)
Includes: Encounter for placental sample (taken vaginally)
Excludes 2: O28.-, Abnormal findings on antenatal screening of mother
- Z36.5, Encounter for antenatal screening for isoimmunization
- Z36.4, Encounter for antenatal screening for fetal growth retardation
Intrauterine growth restriction (IUGR)/small-for-dates - Z36.3, Encounter for antenatal screening for malformations
Screening for a suspected anomaly - Z36.2, Encounter for other antenatal screening follow-up
Nonvisualized anatomy on a previous scan - Z36.1, Encounter for antenatal screening for raised alpha-fetoprotein level
Encounter for antenatal screening for elevated maternal serum alpha-fetoprotein level - Z36.0, Encounter for antenatal screening for chromosomal anomalies
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.8A, Encounter for antenatal screening for other genetic defects
- Z36.89, Encounter for other specified antenatal screening
- Z36.88, Encounter for antenatal screening for fetal macrosomia
Screening for large-for-dates - Z36.87, Encounter for antenatal screening for uncertain dates
- Z36.86, Encounter for antenatal screening for cervical length
Screening for risk of preterm labor - Z36.85, Encounter for antenatal screening for Streptococcus B
- Z36.84, Encounter for antenatal screening for fetal lung maturity
- Z36.83, Encounter for fetal screening for congenital cardiac abnormalities
- Z36.82, Encounter for antenatal screening for nuchal translucency
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.9, Encounter for antenatal screening, unspecified
Code changes for abortion and complications
The code range for use with Z3A, weeks of gestation, has changed from O00-O9A to O09-O9A to reflect the guideline change last year to remove the requirement to use this code with any code that describes pregnancy with an abortive outcome (codes O00-O08).
In addition, if a patient has retained products of conception (POC) after either a spontaneous or elective abortion, report the "without complication" code for the retained POC (O03.4, Incomplete spontaneous abortion without complication, or O07.4, Failed attempted termination of pregnancy without complication). If any other complication occurred in addition to the retained POC, use the code for that particular complication and not O03.4 or O07.4.
Share your thoughts! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
The list of new and revised International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) codes has been published, with changes becoming effective on October 1, 2017. This year, you can look forward to minimal code changes for gynecologic conditions. The biggest change in this category is the addition of codes that describe a lump in the breast according to which breast and the location on the breast, as well as the addition of a code for prophylactic removal of the fallopian tubes. The codes related to obstetrics will have more extensive changes. You will find revisions to the codes for ectopic pregnancy, a new set of codes for addressing an abnormal fetal heart rate during the antepartum period, and, most welcome of all, an expansion of the single code for antenatal testing to 17 very specific codes.
Gynecologic code changes
The single code N63, Unspecified lump in breast, has been expanded to include codes for both the right and the left breast. Code N63 therefore will be considered invalid after October 1, 2018. Expanded codes include:
- N63.0, Unspecified lump in unspecified breast
- N63.1, Unspecified lump in the right breast
- N63.10, Unspecified lump in the right breast, unspecified quadrant
- N63.11, Unspecified lump in the right breast, upper outer quadrant
- N63.12, Unspecified lump in the right breast, upper inner quadrant
- N63.13, Unspecified lump in the right breast, lower outer quadrant
- N63.14, Unspecified lump in the right breast, lower inner quadrant
- N63.2, Unspecified lump in the left breast
- N63.20, Unspecified lump in the left breast, unspecified quadrant
- N63.21, Unspecified lump in the left breast, upper outer quadrant
- N63.22, Unspecified lump in the left breast, upper inner quadrant
- N63.23, Unspecified lump in the left breast, lower outer quadrant
- N63.24, Unspecified lump in the left breast, lower inner quadrant
- N63.3, Unspecified lump in axillary tail
- N63.31, Unspecified lump in axillary tail of the right breast
- N63.32, Unspecified lump in axillary tail of the left breast
- N63.4, Unspecified lump in breast, subareolar
- N63.41, Unspecified lump in right breast, subareolar
- N63.42, Unspecified lump in left breast, subareolar
Other changes to gynecologic codes
There has been a minor change to the description for code Z31.5, Encounter for genetic counseling. It now is described as "Encounter for procreative genetic counseling."
The code Z40.02, Encounter for prophylactic removal of ovary(s), now refers to one or more ovaries without distinction of right or left, and a new code has been added for removal of the fallopian tube(s), Z40.03, Encounter for prophylactic removal of fallopian tube(s).
The inclusion term "endometriosis of the thorax" has been added to code N80.8, Other endometriosis.
The inclusion term "premenstrual dysphoric disorder" has been deleted from code N94.3, Premenstrual tension syndrome. If the patient has been diagnosed with this condition, the code F32.81, Premenstrual dysphoric disorder, should be reported, as this is considered a mental health issue.
The "excludes 1" note under code Z87.41, Personal history of dysplasia of the female genital tract, has been revised. The codes for personal history of intraepithelial neoplasia III that may not be reported with this code are Z86.001 and Z86.008.
Obstetric code changes
The ectopic pregnancy codes have been revised to include references to the right or left structure affected, which means the codes change from 5 digits to 6 digits in length, and the codes O00.10, O00.11, O00.20, and O00.21 will no longer be valid.
- O00.1, Tubal pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.101, Right tubal pregnancy without intrauterine pregnancy
- O00.102, Left tubal pregnancy without intrauterine pregnancy
- O00.109, Unspecified tubal pregnancy without intrauterine pregnancy
- O00.11, Tubal pregnancy with intrauterine pregnancy
- O00.111, Right tubal pregnancy with intrauterine pregnancy
- O00.112, Left tubal pregnancy with intrauterine pregnancy
- O00.119, Unspecified tubal pregnancy with intrauterine pregnancy
- O00.10, Tubal pregnancy without intrauterine pregnancy
- O00.2, Ovarian pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
- O00.201, Right ovarian pregnancy without intrauterine pregnancy
- O00.202, Left ovarian pregnancy without intrauterine pregnancy
- O00.209, Unspecified ovarian pregnancy without intrauterine pregnancy
- O00.21, Ovarian pregnancy with intrauterine pregnancy
- O00.211, Right ovarian pregnancy with intrauterine pregnancy
- O00.212, Left ovarian pregnancy with intrauterine pregnancy
- O00.219, Unspecified ovarian pregnancy with intrauterine pregnancy
- O00.20, Ovarian pregnancy without intrauterine pregnancy
New codes for fetal heart rate abnormalities
New codes have been added to report a fetal heart rate or rhythm abnormality during the antepartum period. Until now, there only has been a code that addresses this issue during labor and delivery, O76, Abnormality in fetal heart rate and rhythm complicating labor and delivery.
- O36.83, Maternal care for abnormalities of the fetal heart rate or rhythm
- O36.831, Maternal care for abnormalities of the fetal heart rate or rhythm, first trimester
- O36.832, Maternal care for abnormalities of the fetal heart rate or rhythm, second trimester
- O36.833, Maternal care for abnormalities of the fetal heart rate or rhythm, third trimester
- O36.839, Maternal care for abnormalities of the fetal heart rate or rhythm, unspecified trimester
Several codes redefined
ICD-10 has corrected an "excludes" note error for the code O99.1, Other diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism complicating pregnancy, childbirth, and the puerperium. In 2017, any hemorrhage with coagulation defects defined in code category O45.- or codes O46.0-, O67.0, or O72.3 could be reported with O99.1. This set of codes has now been redefined as an "excludes 1" note, which means that they may not be reported with O99.1 since they are considered inclusive.
More specific codes added for antenatal screening
Great news for those awaiting a more specific code for antenatal screening: The code Z36 has been expanded to more closely match the codes that were available in ICD-9-CM, but it goes beyond the basic list in that codes have been added for things like nonvisualization of anatomic structures on a previous scan and screening for cervical length and fetal lung maturity. Be sure to pay attention to the excludes notes and other inclusive terms.
- Z36, Encounter for antenatal screening of mother (Screening is the testing for disease or disease precursors in asymptomatic individuals so that early detection and treatment can be provided for those who test positive for the disease.)
Includes: Encounter for placental sample (taken vaginally)
Excludes 2: O28.-, Abnormal findings on antenatal screening of mother
- Z36.5, Encounter for antenatal screening for isoimmunization
- Z36.4, Encounter for antenatal screening for fetal growth retardation
Intrauterine growth restriction (IUGR)/small-for-dates - Z36.3, Encounter for antenatal screening for malformations
Screening for a suspected anomaly - Z36.2, Encounter for other antenatal screening follow-up
Nonvisualized anatomy on a previous scan - Z36.1, Encounter for antenatal screening for raised alpha-fetoprotein level
Encounter for antenatal screening for elevated maternal serum alpha-fetoprotein level - Z36.0, Encounter for antenatal screening for chromosomal anomalies
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.8A, Encounter for antenatal screening for other genetic defects
- Z36.89, Encounter for other specified antenatal screening
- Z36.88, Encounter for antenatal screening for fetal macrosomia
Screening for large-for-dates - Z36.87, Encounter for antenatal screening for uncertain dates
- Z36.86, Encounter for antenatal screening for cervical length
Screening for risk of preterm labor - Z36.85, Encounter for antenatal screening for Streptococcus B
- Z36.84, Encounter for antenatal screening for fetal lung maturity
- Z36.83, Encounter for fetal screening for congenital cardiac abnormalities
- Z36.82, Encounter for antenatal screening for nuchal translucency
- Z36.81, Encounter for antenatal screening for hydrops fetalis
- Z36.9, Encounter for antenatal screening, unspecified
Code changes for abortion and complications
The code range for use with Z3A, weeks of gestation, has changed from O00-O9A to O09-O9A to reflect the guideline change last year to remove the requirement to use this code with any code that describes pregnancy with an abortive outcome (codes O00-O08).
In addition, if a patient has retained products of conception (POC) after either a spontaneous or elective abortion, report the "without complication" code for the retained POC (O03.4, Incomplete spontaneous abortion without complication, or O07.4, Failed attempted termination of pregnancy without complication). If any other complication occurred in addition to the retained POC, use the code for that particular complication and not O03.4 or O07.4.
Share your thoughts! Send your Letter to the Editor to [email protected]. Please include your name and the city and state in which you practice.
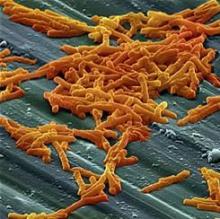
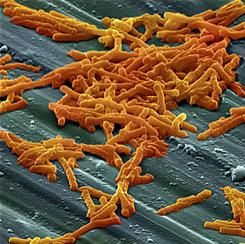
Bezlotoxumab may lower risk of C. difficile readmissions
Clostridium difficile infection (CDI) patients treated with bezlotoxumab were less likely to be readmitted for recurring symptoms within 30 days of discharge, according to a phase 3 trial funded by Merck.
Recurrent CDI is a burden on both patients and providers, increasing health risks with each recurrence and eating through hospital resources, according to Vimalanand S. Prabhu, PhD, associate principal scientist for Merck.
In a randomized, double-blind, placebo-controlled, study of 1,050 CDI patients, a total of 27 (5%) of 530 of those given bezlotoxumab were re-hospitalized 30 days after discharge, compared with 58 (11%) of 520 patients in the placebo group (Clin Infect Dis. 2017 Aug 11. doi. 10.1093/cid/cix523).
Patients were gathered from 322 sites across 30 countries between November 2011 and May 2015.
When measuring CDI-related readmissions, the investigators found use of bezlotoxumab reduced rCDI hospitalizations by 6%, and by approximately 8% in high-risk patients, such as those over 65 years old or with severe CDI.
Bezlotoxumab works by binding to CDI toxin B, a primary cause of CDI symptoms, according to Dr. Prabhu and fellow investigators. The researchers suggested that bezlotoxumab could be a prevailing factor in fighting the rate of CDI infections, which accounted for 29,000 deaths in 2011 (N Engl J Med. 2015 Jun 11;372[24]:2368-9).
Investigators acknowledged that patients admitted for the study may be healthier than the real-world CDI population.
All investigators reported some financial involvement, whether being a full-time employee or acting as a consultant, for Merck, which funded the study. Individually, investigators reported financial ties to similar medical companies, such as Pfizer and AstraZeneca.
AGA offers patient education materials on C. diff that can help your patients better understand the infection. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
[email protected]
On Twitter @eaztweets
Clostridium difficile infection (CDI) patients treated with bezlotoxumab were less likely to be readmitted for recurring symptoms within 30 days of discharge, according to a phase 3 trial funded by Merck.
Recurrent CDI is a burden on both patients and providers, increasing health risks with each recurrence and eating through hospital resources, according to Vimalanand S. Prabhu, PhD, associate principal scientist for Merck.
In a randomized, double-blind, placebo-controlled, study of 1,050 CDI patients, a total of 27 (5%) of 530 of those given bezlotoxumab were re-hospitalized 30 days after discharge, compared with 58 (11%) of 520 patients in the placebo group (Clin Infect Dis. 2017 Aug 11. doi. 10.1093/cid/cix523).
Patients were gathered from 322 sites across 30 countries between November 2011 and May 2015.
When measuring CDI-related readmissions, the investigators found use of bezlotoxumab reduced rCDI hospitalizations by 6%, and by approximately 8% in high-risk patients, such as those over 65 years old or with severe CDI.
Bezlotoxumab works by binding to CDI toxin B, a primary cause of CDI symptoms, according to Dr. Prabhu and fellow investigators. The researchers suggested that bezlotoxumab could be a prevailing factor in fighting the rate of CDI infections, which accounted for 29,000 deaths in 2011 (N Engl J Med. 2015 Jun 11;372[24]:2368-9).
Investigators acknowledged that patients admitted for the study may be healthier than the real-world CDI population.
All investigators reported some financial involvement, whether being a full-time employee or acting as a consultant, for Merck, which funded the study. Individually, investigators reported financial ties to similar medical companies, such as Pfizer and AstraZeneca.
AGA offers patient education materials on C. diff that can help your patients better understand the infection. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
[email protected]
On Twitter @eaztweets
Clostridium difficile infection (CDI) patients treated with bezlotoxumab were less likely to be readmitted for recurring symptoms within 30 days of discharge, according to a phase 3 trial funded by Merck.
Recurrent CDI is a burden on both patients and providers, increasing health risks with each recurrence and eating through hospital resources, according to Vimalanand S. Prabhu, PhD, associate principal scientist for Merck.
In a randomized, double-blind, placebo-controlled, study of 1,050 CDI patients, a total of 27 (5%) of 530 of those given bezlotoxumab were re-hospitalized 30 days after discharge, compared with 58 (11%) of 520 patients in the placebo group (Clin Infect Dis. 2017 Aug 11. doi. 10.1093/cid/cix523).
Patients were gathered from 322 sites across 30 countries between November 2011 and May 2015.
When measuring CDI-related readmissions, the investigators found use of bezlotoxumab reduced rCDI hospitalizations by 6%, and by approximately 8% in high-risk patients, such as those over 65 years old or with severe CDI.
Bezlotoxumab works by binding to CDI toxin B, a primary cause of CDI symptoms, according to Dr. Prabhu and fellow investigators. The researchers suggested that bezlotoxumab could be a prevailing factor in fighting the rate of CDI infections, which accounted for 29,000 deaths in 2011 (N Engl J Med. 2015 Jun 11;372[24]:2368-9).
Investigators acknowledged that patients admitted for the study may be healthier than the real-world CDI population.
All investigators reported some financial involvement, whether being a full-time employee or acting as a consultant, for Merck, which funded the study. Individually, investigators reported financial ties to similar medical companies, such as Pfizer and AstraZeneca.
AGA offers patient education materials on C. diff that can help your patients better understand the infection. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
[email protected]
On Twitter @eaztweets
FROM CLINICAL INFECTIOUS DISEASES
Diabetes infusion sets under voluntary recall
Medtronic announced Sept. 11 that it has started to inform patients worldwide of a voluntary recall of specific lots of infusion sets used with all models of Medtronic insulin pumps.
The recall is for a certain discontinued component in these infusion sets and does not include insulin pumps or glucose sensors. According to recent reports from patients and root-cause analysis, the vent membrane in the recalled infusion sets may be susceptible to being blocked by fluid during the process of priming/fill-tubing. This can lead to potential over-delivery of insulin shortly after an infusion set change and may cause hypoglycemia.
Current manufactured infusion sets include a design update of this component that Medtronic believes reduces the risk of insulin over-delivery after an infusion set change. Medtronic said they are working with patients on recalled infusion sets with the discontinued component to replace the recalled sets with new infusion sets containing the updated component at no cost.
“Our priority is to work with our patients to mitigate risk to patient safety. While we have shipped a significant number of the new and enhanced sets since April, we are committed to replacing recalled infusion sets for all patients,” said Francine Kaufman, MD, chief medical officer of the Diabetes Group at Medtronic in a press release. “Our Medtronic Diabetes team will work as quickly as possible to complete all exchanges to the new and enhanced set and fully support our customers throughout this process.”
Read the full press release on the Food and Drug Administration’s website.
Medtronic announced Sept. 11 that it has started to inform patients worldwide of a voluntary recall of specific lots of infusion sets used with all models of Medtronic insulin pumps.
The recall is for a certain discontinued component in these infusion sets and does not include insulin pumps or glucose sensors. According to recent reports from patients and root-cause analysis, the vent membrane in the recalled infusion sets may be susceptible to being blocked by fluid during the process of priming/fill-tubing. This can lead to potential over-delivery of insulin shortly after an infusion set change and may cause hypoglycemia.
Current manufactured infusion sets include a design update of this component that Medtronic believes reduces the risk of insulin over-delivery after an infusion set change. Medtronic said they are working with patients on recalled infusion sets with the discontinued component to replace the recalled sets with new infusion sets containing the updated component at no cost.
“Our priority is to work with our patients to mitigate risk to patient safety. While we have shipped a significant number of the new and enhanced sets since April, we are committed to replacing recalled infusion sets for all patients,” said Francine Kaufman, MD, chief medical officer of the Diabetes Group at Medtronic in a press release. “Our Medtronic Diabetes team will work as quickly as possible to complete all exchanges to the new and enhanced set and fully support our customers throughout this process.”
Read the full press release on the Food and Drug Administration’s website.
Medtronic announced Sept. 11 that it has started to inform patients worldwide of a voluntary recall of specific lots of infusion sets used with all models of Medtronic insulin pumps.
The recall is for a certain discontinued component in these infusion sets and does not include insulin pumps or glucose sensors. According to recent reports from patients and root-cause analysis, the vent membrane in the recalled infusion sets may be susceptible to being blocked by fluid during the process of priming/fill-tubing. This can lead to potential over-delivery of insulin shortly after an infusion set change and may cause hypoglycemia.
Current manufactured infusion sets include a design update of this component that Medtronic believes reduces the risk of insulin over-delivery after an infusion set change. Medtronic said they are working with patients on recalled infusion sets with the discontinued component to replace the recalled sets with new infusion sets containing the updated component at no cost.
“Our priority is to work with our patients to mitigate risk to patient safety. While we have shipped a significant number of the new and enhanced sets since April, we are committed to replacing recalled infusion sets for all patients,” said Francine Kaufman, MD, chief medical officer of the Diabetes Group at Medtronic in a press release. “Our Medtronic Diabetes team will work as quickly as possible to complete all exchanges to the new and enhanced set and fully support our customers throughout this process.”
Read the full press release on the Food and Drug Administration’s website.
The Importance of Cord Blood and Cord Tissue Stem Cells: Today vs Tomorrow
Click Here to Read Supplement.
Topics include:
- Applications of cord blood stem cells
- Ongoing research with cord blood and cord tissue
- ASCT in autism spectrum disorder
- Patient education and counseling
- Banking options
- Science and education
Faculty/Faculty Disclosure:
Joel Weinthal, MD
Director of Pediatric Stem Cell Transplantation and Attending Physician
Texas Oncology Pediatrics
Medical Director, Apheresis and Stem Cell Laboratory
Medical City Dallas Hospital
Dallas, Texas
Dr. Weinthal reports that he is on the speakers’ bureau and advisory board, and a consultant, for CBR®, Cord Blood Registry®.
Click Here to Read the Supplement.
Click Here to Read Supplement.
Topics include:
- Applications of cord blood stem cells
- Ongoing research with cord blood and cord tissue
- ASCT in autism spectrum disorder
- Patient education and counseling
- Banking options
- Science and education
Faculty/Faculty Disclosure:
Joel Weinthal, MD
Director of Pediatric Stem Cell Transplantation and Attending Physician
Texas Oncology Pediatrics
Medical Director, Apheresis and Stem Cell Laboratory
Medical City Dallas Hospital
Dallas, Texas
Dr. Weinthal reports that he is on the speakers’ bureau and advisory board, and a consultant, for CBR®, Cord Blood Registry®.
Click Here to Read the Supplement.
Click Here to Read Supplement.
Topics include:
- Applications of cord blood stem cells
- Ongoing research with cord blood and cord tissue
- ASCT in autism spectrum disorder
- Patient education and counseling
- Banking options
- Science and education
Faculty/Faculty Disclosure:
Joel Weinthal, MD
Director of Pediatric Stem Cell Transplantation and Attending Physician
Texas Oncology Pediatrics
Medical Director, Apheresis and Stem Cell Laboratory
Medical City Dallas Hospital
Dallas, Texas
Dr. Weinthal reports that he is on the speakers’ bureau and advisory board, and a consultant, for CBR®, Cord Blood Registry®.
Click Here to Read the Supplement.
Targeted therapy may be possible for pityriasis rubra pilaris
CHICAGO – If you’ve ever found that making a diagnosis of pityriasis rubra pilaris is difficult, you’re not alone.
In a recent case series of 100 patients with a median age of 61 years, only 50 patients had an undeniable diagnosis of pityriasis rubra pilaris (PRP). Of those patients, only 26% were diagnosed at initial presentation. The mean delay to diagnosis was 29 months, and 54% required two or more biopsies (JAMA Derm. 2016 Jun 1;152[6]:670-5).
“This is one of those conditions that sometimes you’re going to follow patients and not know what it is right away,” Patricia M. Witman, MD, said at the World Congress of Pediatric Dermatology. Although eczema and contact dermatitis are common diseases where the diagnosis is missed, it’s easy to mistake pityriasis rubra pilaris for psoriasis.
“On the flip side, follicular psoriasis is easy to mistake for PRP,” said Dr. Witman, chief of the division of dermatology at Nationwide Children’s Hospital, Columbus, Ohio. “It’s an uncommon variant that occurs in only about 2.1% of all pediatric psoriasis. These patients can have keratoderma, but they have classic psoriasis on biopsy. Pediatric patients with this subtype do not typically have classic psoriasis plaques.”
PRP is an anti-inflammatory papulosquamous disease with an incidence that ranges between 1:3,500 and 1:400,000. It occurs equally in men and women and has a bimodal onset, with 52%-60% of cases occurring in the 6th or 7th decade of life, and 6%-12% occurring in the 1st or 2nd decade of life, with a mean age of 7 years. Characteristic clinical features include cephalocaudal spread, keratotic follicular papules, well-demarcated orange/red plaques, fine scale, islands of sparing, erythroderma, and palmoplantar keratoderma.
“Even though it’s characteristic, there is a wide spread in the type of disease manifestations,” Dr. Witman said. “There are six different types based on how old you are and on the presentation.”
She limited her presentation to a discussion of three types:
- Classic juvenile type. This type usually presents between ages 5 and 10 and resembles the type I, or classic adult, type, with cephalocaudal spread, follicular keratotic erythematous papules coalescing into plaques, islands of sparing, and typically keratoderma. The scalp dermatitis it causes “often has a little finer scale than the thick micaceous scale we see in psoriasis,” she noted. “Patients can have a photoaggravated presentation with relative sparing of areas protected from the sun.”
- Circumscribed juvenile type. This is the most common pediatric variant. It usually presents between the ages of 3 and 10, with a mean age of 6. It is characterized by sharply demarcated plaques on extensor elbows and knees, as well as follicular hyperkeratosis. About 70% will also have keratoderma. “The Achilles tendon involvement is considered to be fairly pathognomonic for this condition and helps differentiate it from psoriasis, as well as an orange to yellow color of the keratoderma,” Dr. Witman said.
- The atypical juvenile type, or type V. This the familial variant of PRP. It’s also the rarest, occurring in just 6.5% of cases. “It’s autosomal dominant and has incomplete penetrance and variable expression,” she said. “It typically presents in infancy or in the first few years of life. Patients with this form also tend to have a more sclerodermoid palmoplantar keratoderma and ichthyosiform features. It is typically a lifelong condition, but there have been occasional case reports of self-resolution.”
The clinical features of PRP often overlap with psoriasis.
“Although there are some things that are more pathognomonic for PRP, like the Achilles tendon involvement and the keratoderma, for psoriasis we have nail pitting, which we don’t usually see in PRP,” Dr. Witman said. “Sometimes, it’s the skin biopsy that helps us distinguish those defining features, and it may take more than one biopsy to make the diagnosis.”
Dermoscopy can also be helpful. One analysis found that dermoscopy features of PRP include multiple keratotic papules with peripheral rings of erythema that coalesce into a yellow-orange plaque, linear vessels at the periphery of papules, and papules centered on hair (J Am Acad Dermatol. 2015 Jan;72[1]:S58-9).
“Even when you have that definite diagnosis of PRP, you have to remember that PRP can be seen within the context of other disease,” Dr. Witman cautioned. “Malignancy is usually limited to our adult patients with PRP, but infection can certainly trigger PRP in our pediatric patients, most commonly streptococcus. Medication reactions, especially to the biologics, have also been reported to cause PRP-like reactions, as well as autoimmune disease.”
One such entity is referred to as “Wong-like” dermatomyositis, in which patients present with a rash that looks identical to PRP (Ped Dermatol. 2007;24[2]:155-6). “It can occur in both the juvenile and adult populations,” she said. “It has clinical and histopathologic features of PRP, yet it may precede or occur concurrently with a diagnosis of dermatomyositis.”
In 2012, a group of researchers discovered that a gain of function mutation in CARD14 leads to atypical juvenile-type PRP (Am J Hum Genet. 2012 Jul 13;91:163-70). CARD14 is a member of a protein family known as caspase recruitment domain, family member 14, which also is mutated in a variant of familial psoriasis.
“It’s a protein that’s predominantly expressed in the skin, and it’s a known activator of transcription factor nuclear factor kappa light chain enhancer in activated B cells [NFkB], which is responsible for inflammation in the epidermis,” Dr. Witman explained. “What we know is that if you have a gain of function mutation in CARD14, we think that this activates the NFkB pathway and leads to increased inflammation of the skin. The same process would be expected in cases of familial psoriasis.”
Current treatment of PRP is challenging, he said. A recent survey of patients found that 76% found emollients most effective, followed by topical steroids (50%) and salicylic acid (45%) (JAMA Derm. 2016 Jun 1;152[6]:670-5). When it came to systemic therapies, 59% found retinoids most effective, followed by methotrexate (42%) and tumor necrosis factor inhibitors (40%). Only 8% found phototherapy helpful.
Dr. Witman noted that the discovery of the CARD14 mutation as the cause of the familial variant “brings us closer to an understanding of juvenile PRP,” and to the potential for targeted therapy.
“This really raises the question: Do ustekinumab and similar drugs have a future role in the treatment of PRP?” she asked. “We do see anecdotal evidence of clearance in adults using ustekinumab, both those with and without type V PRP and a CARD14 mutation. It has been tried in adult patients, predominantly in those who have failed multiple therapies. But this is anecdotal evidence with isolated case reports. These patients did respond to dosing that is typical for psoriasis.
“At this point, it is not approved for PRP, nor is it approved in children – but it’s something to think about once we have more information,” Dr. Witman noted. “The newer biologics targeting IL[interleukin]-23 and IL-17 may hold promise for PRP, based on what we have learned in psoriasis. But at this point, the safest and most effective therapy for the different variants of PRP in our pediatric patients remains to be seen.”
Dr. Witman reported having no relevant financial disclosures.
CHICAGO – If you’ve ever found that making a diagnosis of pityriasis rubra pilaris is difficult, you’re not alone.
In a recent case series of 100 patients with a median age of 61 years, only 50 patients had an undeniable diagnosis of pityriasis rubra pilaris (PRP). Of those patients, only 26% were diagnosed at initial presentation. The mean delay to diagnosis was 29 months, and 54% required two or more biopsies (JAMA Derm. 2016 Jun 1;152[6]:670-5).
“This is one of those conditions that sometimes you’re going to follow patients and not know what it is right away,” Patricia M. Witman, MD, said at the World Congress of Pediatric Dermatology. Although eczema and contact dermatitis are common diseases where the diagnosis is missed, it’s easy to mistake pityriasis rubra pilaris for psoriasis.
“On the flip side, follicular psoriasis is easy to mistake for PRP,” said Dr. Witman, chief of the division of dermatology at Nationwide Children’s Hospital, Columbus, Ohio. “It’s an uncommon variant that occurs in only about 2.1% of all pediatric psoriasis. These patients can have keratoderma, but they have classic psoriasis on biopsy. Pediatric patients with this subtype do not typically have classic psoriasis plaques.”
PRP is an anti-inflammatory papulosquamous disease with an incidence that ranges between 1:3,500 and 1:400,000. It occurs equally in men and women and has a bimodal onset, with 52%-60% of cases occurring in the 6th or 7th decade of life, and 6%-12% occurring in the 1st or 2nd decade of life, with a mean age of 7 years. Characteristic clinical features include cephalocaudal spread, keratotic follicular papules, well-demarcated orange/red plaques, fine scale, islands of sparing, erythroderma, and palmoplantar keratoderma.
“Even though it’s characteristic, there is a wide spread in the type of disease manifestations,” Dr. Witman said. “There are six different types based on how old you are and on the presentation.”
She limited her presentation to a discussion of three types:
- Classic juvenile type. This type usually presents between ages 5 and 10 and resembles the type I, or classic adult, type, with cephalocaudal spread, follicular keratotic erythematous papules coalescing into plaques, islands of sparing, and typically keratoderma. The scalp dermatitis it causes “often has a little finer scale than the thick micaceous scale we see in psoriasis,” she noted. “Patients can have a photoaggravated presentation with relative sparing of areas protected from the sun.”
- Circumscribed juvenile type. This is the most common pediatric variant. It usually presents between the ages of 3 and 10, with a mean age of 6. It is characterized by sharply demarcated plaques on extensor elbows and knees, as well as follicular hyperkeratosis. About 70% will also have keratoderma. “The Achilles tendon involvement is considered to be fairly pathognomonic for this condition and helps differentiate it from psoriasis, as well as an orange to yellow color of the keratoderma,” Dr. Witman said.
- The atypical juvenile type, or type V. This the familial variant of PRP. It’s also the rarest, occurring in just 6.5% of cases. “It’s autosomal dominant and has incomplete penetrance and variable expression,” she said. “It typically presents in infancy or in the first few years of life. Patients with this form also tend to have a more sclerodermoid palmoplantar keratoderma and ichthyosiform features. It is typically a lifelong condition, but there have been occasional case reports of self-resolution.”
The clinical features of PRP often overlap with psoriasis.
“Although there are some things that are more pathognomonic for PRP, like the Achilles tendon involvement and the keratoderma, for psoriasis we have nail pitting, which we don’t usually see in PRP,” Dr. Witman said. “Sometimes, it’s the skin biopsy that helps us distinguish those defining features, and it may take more than one biopsy to make the diagnosis.”
Dermoscopy can also be helpful. One analysis found that dermoscopy features of PRP include multiple keratotic papules with peripheral rings of erythema that coalesce into a yellow-orange plaque, linear vessels at the periphery of papules, and papules centered on hair (J Am Acad Dermatol. 2015 Jan;72[1]:S58-9).
“Even when you have that definite diagnosis of PRP, you have to remember that PRP can be seen within the context of other disease,” Dr. Witman cautioned. “Malignancy is usually limited to our adult patients with PRP, but infection can certainly trigger PRP in our pediatric patients, most commonly streptococcus. Medication reactions, especially to the biologics, have also been reported to cause PRP-like reactions, as well as autoimmune disease.”
One such entity is referred to as “Wong-like” dermatomyositis, in which patients present with a rash that looks identical to PRP (Ped Dermatol. 2007;24[2]:155-6). “It can occur in both the juvenile and adult populations,” she said. “It has clinical and histopathologic features of PRP, yet it may precede or occur concurrently with a diagnosis of dermatomyositis.”
In 2012, a group of researchers discovered that a gain of function mutation in CARD14 leads to atypical juvenile-type PRP (Am J Hum Genet. 2012 Jul 13;91:163-70). CARD14 is a member of a protein family known as caspase recruitment domain, family member 14, which also is mutated in a variant of familial psoriasis.
“It’s a protein that’s predominantly expressed in the skin, and it’s a known activator of transcription factor nuclear factor kappa light chain enhancer in activated B cells [NFkB], which is responsible for inflammation in the epidermis,” Dr. Witman explained. “What we know is that if you have a gain of function mutation in CARD14, we think that this activates the NFkB pathway and leads to increased inflammation of the skin. The same process would be expected in cases of familial psoriasis.”
Current treatment of PRP is challenging, he said. A recent survey of patients found that 76% found emollients most effective, followed by topical steroids (50%) and salicylic acid (45%) (JAMA Derm. 2016 Jun 1;152[6]:670-5). When it came to systemic therapies, 59% found retinoids most effective, followed by methotrexate (42%) and tumor necrosis factor inhibitors (40%). Only 8% found phototherapy helpful.
Dr. Witman noted that the discovery of the CARD14 mutation as the cause of the familial variant “brings us closer to an understanding of juvenile PRP,” and to the potential for targeted therapy.
“This really raises the question: Do ustekinumab and similar drugs have a future role in the treatment of PRP?” she asked. “We do see anecdotal evidence of clearance in adults using ustekinumab, both those with and without type V PRP and a CARD14 mutation. It has been tried in adult patients, predominantly in those who have failed multiple therapies. But this is anecdotal evidence with isolated case reports. These patients did respond to dosing that is typical for psoriasis.
“At this point, it is not approved for PRP, nor is it approved in children – but it’s something to think about once we have more information,” Dr. Witman noted. “The newer biologics targeting IL[interleukin]-23 and IL-17 may hold promise for PRP, based on what we have learned in psoriasis. But at this point, the safest and most effective therapy for the different variants of PRP in our pediatric patients remains to be seen.”
Dr. Witman reported having no relevant financial disclosures.
CHICAGO – If you’ve ever found that making a diagnosis of pityriasis rubra pilaris is difficult, you’re not alone.
In a recent case series of 100 patients with a median age of 61 years, only 50 patients had an undeniable diagnosis of pityriasis rubra pilaris (PRP). Of those patients, only 26% were diagnosed at initial presentation. The mean delay to diagnosis was 29 months, and 54% required two or more biopsies (JAMA Derm. 2016 Jun 1;152[6]:670-5).
“This is one of those conditions that sometimes you’re going to follow patients and not know what it is right away,” Patricia M. Witman, MD, said at the World Congress of Pediatric Dermatology. Although eczema and contact dermatitis are common diseases where the diagnosis is missed, it’s easy to mistake pityriasis rubra pilaris for psoriasis.
“On the flip side, follicular psoriasis is easy to mistake for PRP,” said Dr. Witman, chief of the division of dermatology at Nationwide Children’s Hospital, Columbus, Ohio. “It’s an uncommon variant that occurs in only about 2.1% of all pediatric psoriasis. These patients can have keratoderma, but they have classic psoriasis on biopsy. Pediatric patients with this subtype do not typically have classic psoriasis plaques.”
PRP is an anti-inflammatory papulosquamous disease with an incidence that ranges between 1:3,500 and 1:400,000. It occurs equally in men and women and has a bimodal onset, with 52%-60% of cases occurring in the 6th or 7th decade of life, and 6%-12% occurring in the 1st or 2nd decade of life, with a mean age of 7 years. Characteristic clinical features include cephalocaudal spread, keratotic follicular papules, well-demarcated orange/red plaques, fine scale, islands of sparing, erythroderma, and palmoplantar keratoderma.
“Even though it’s characteristic, there is a wide spread in the type of disease manifestations,” Dr. Witman said. “There are six different types based on how old you are and on the presentation.”
She limited her presentation to a discussion of three types:
- Classic juvenile type. This type usually presents between ages 5 and 10 and resembles the type I, or classic adult, type, with cephalocaudal spread, follicular keratotic erythematous papules coalescing into plaques, islands of sparing, and typically keratoderma. The scalp dermatitis it causes “often has a little finer scale than the thick micaceous scale we see in psoriasis,” she noted. “Patients can have a photoaggravated presentation with relative sparing of areas protected from the sun.”
- Circumscribed juvenile type. This is the most common pediatric variant. It usually presents between the ages of 3 and 10, with a mean age of 6. It is characterized by sharply demarcated plaques on extensor elbows and knees, as well as follicular hyperkeratosis. About 70% will also have keratoderma. “The Achilles tendon involvement is considered to be fairly pathognomonic for this condition and helps differentiate it from psoriasis, as well as an orange to yellow color of the keratoderma,” Dr. Witman said.
- The atypical juvenile type, or type V. This the familial variant of PRP. It’s also the rarest, occurring in just 6.5% of cases. “It’s autosomal dominant and has incomplete penetrance and variable expression,” she said. “It typically presents in infancy or in the first few years of life. Patients with this form also tend to have a more sclerodermoid palmoplantar keratoderma and ichthyosiform features. It is typically a lifelong condition, but there have been occasional case reports of self-resolution.”
The clinical features of PRP often overlap with psoriasis.
“Although there are some things that are more pathognomonic for PRP, like the Achilles tendon involvement and the keratoderma, for psoriasis we have nail pitting, which we don’t usually see in PRP,” Dr. Witman said. “Sometimes, it’s the skin biopsy that helps us distinguish those defining features, and it may take more than one biopsy to make the diagnosis.”
Dermoscopy can also be helpful. One analysis found that dermoscopy features of PRP include multiple keratotic papules with peripheral rings of erythema that coalesce into a yellow-orange plaque, linear vessels at the periphery of papules, and papules centered on hair (J Am Acad Dermatol. 2015 Jan;72[1]:S58-9).
“Even when you have that definite diagnosis of PRP, you have to remember that PRP can be seen within the context of other disease,” Dr. Witman cautioned. “Malignancy is usually limited to our adult patients with PRP, but infection can certainly trigger PRP in our pediatric patients, most commonly streptococcus. Medication reactions, especially to the biologics, have also been reported to cause PRP-like reactions, as well as autoimmune disease.”
One such entity is referred to as “Wong-like” dermatomyositis, in which patients present with a rash that looks identical to PRP (Ped Dermatol. 2007;24[2]:155-6). “It can occur in both the juvenile and adult populations,” she said. “It has clinical and histopathologic features of PRP, yet it may precede or occur concurrently with a diagnosis of dermatomyositis.”
In 2012, a group of researchers discovered that a gain of function mutation in CARD14 leads to atypical juvenile-type PRP (Am J Hum Genet. 2012 Jul 13;91:163-70). CARD14 is a member of a protein family known as caspase recruitment domain, family member 14, which also is mutated in a variant of familial psoriasis.
“It’s a protein that’s predominantly expressed in the skin, and it’s a known activator of transcription factor nuclear factor kappa light chain enhancer in activated B cells [NFkB], which is responsible for inflammation in the epidermis,” Dr. Witman explained. “What we know is that if you have a gain of function mutation in CARD14, we think that this activates the NFkB pathway and leads to increased inflammation of the skin. The same process would be expected in cases of familial psoriasis.”
Current treatment of PRP is challenging, he said. A recent survey of patients found that 76% found emollients most effective, followed by topical steroids (50%) and salicylic acid (45%) (JAMA Derm. 2016 Jun 1;152[6]:670-5). When it came to systemic therapies, 59% found retinoids most effective, followed by methotrexate (42%) and tumor necrosis factor inhibitors (40%). Only 8% found phototherapy helpful.
Dr. Witman noted that the discovery of the CARD14 mutation as the cause of the familial variant “brings us closer to an understanding of juvenile PRP,” and to the potential for targeted therapy.
“This really raises the question: Do ustekinumab and similar drugs have a future role in the treatment of PRP?” she asked. “We do see anecdotal evidence of clearance in adults using ustekinumab, both those with and without type V PRP and a CARD14 mutation. It has been tried in adult patients, predominantly in those who have failed multiple therapies. But this is anecdotal evidence with isolated case reports. These patients did respond to dosing that is typical for psoriasis.
“At this point, it is not approved for PRP, nor is it approved in children – but it’s something to think about once we have more information,” Dr. Witman noted. “The newer biologics targeting IL[interleukin]-23 and IL-17 may hold promise for PRP, based on what we have learned in psoriasis. But at this point, the safest and most effective therapy for the different variants of PRP in our pediatric patients remains to be seen.”
Dr. Witman reported having no relevant financial disclosures.
AT WCPD 2017
Bedside imaging allowed for individualized PEEP adjustments
A noninvasive bedside imaging technique can individually calibrate positive end-expiratory pressure settings in patients on extracorporeal membrane oxygenation (ECMO) for severe acute respiratory distress syndrome (ARDS), a study showed.
The step-down PEEP (positive end-expiratory pressure) trial could not identify a single PEEP setting that optimally balanced lung overdistension and lung collapse for all 15 patients. But, electrical impedance tomography (EIT) allowed investigators to individually titrate PEEP settings for each patient, Guillaume Franchineau, MD, wrote (Am J Respir Crit Care Med. 2017;196[4]:447-57 doi: 10.1164/rccm.201605-1055OC).
The 4-month study involved 15 patients (aged, 18-79 years) who were in acute respiratory distress syndrome for a variety of reasons, including influenza (7 patients), pneumonia (3), leukemia (2), and 1 case each of Pneumocystis, antisynthetase syndrome, and trauma. All patients were receiving ECMO with a constant driving pressure of 14 cm H2O. After verifying that the inspiratory flow was 0 at the end of inspiration, PEEP was increased to 20 cm H2O (PEEP 20) with a peak inspiratory pressure of 34 cm H2O. PEEP 20 was held for 20 minutes and then lowered by 5 cm H2O decrements with the potential of reaching PEEP 0.
The EIT device, consisting of a silicone belt with 16 surface electrodes, was placed around the thorax aligning with the sixth intercostal parasternal space and connected to a monitor. By measuring conductivity and impeditivity in the underlying tissues, the device generates a low-resolution, two-dimensional image. The image was sufficient to show lung distension and collapse as the PEEP settings changed. Investigators looked for the best compromise between overdistension and collapsed zones, which they defined as the lowest pressure able to limit EIT-assessed collapse to no more than 15% with the least overdistension.
There was no one-size-fits-all PEEP setting, the authors found. The setting that minimized both overdistension and collapse was PEEP 15 in seven patients, PEEP 10 in six patients, and PEEP 5 in two patients.
At each patient’s optimal PEEP setting, the median tidal volume was similar: 3.8 mL/kg ideal body weight for PEEP 15, 3.9 mL/kg ideal body weight for PEEP 10, and 4.3 mL/kg ideal body weight for PEEP 5.
Respiratory system compliance was also similar among the groups, at 20 mL/cm H2O, 18 mL/cm H2O, and 21 mL/cm H2O, respectively. However, arterial partial pressure of oxygen decreased as the PEEP setting decreased, dropping from 148 mm Hg to 128 mm Hg to 100 mm Hg, respectively. Conversely, arterial partial pressure of CO2 increased (32-41 mm Hg).
EIT also allowed clinicians to pinpoint areas of distension or collapse. As PEEP decreased, there was steady ventilation loss in the medial-dorsal and dorsal regions, which shifted to the medial-ventral and ventral regions.
“Most end-expiratory lung impedances were located in medial-dorsal and medial-ventral regions, whereas the dorsal region constantly contributed less than 10% of total end-expiratory lung impedance,” the authors noted.
“The broad variability of EIT-based best compromise PEEPs in these patients with severe ARDS reinforces the need to provide ventilation settings individually tailored to the regional ARDS-lesion distribution,” they concluded. “To achieve that goal, EIT seems to be an interesting bedside noninvasive tool to provide real-time monitoring of the PEEP effect and ventilation distribution on ECMO.”
Dr. Franchineau reported receiving speakers fees from Mapquet.
[email protected]
On Twitter @Alz_Gal
This first study to examine electrical impedance tomography (EIT) in patients under extracorporeal membrane oxygenation shows important clinical potential, but also raises important questions, Claude Guerin, MD, wrote in an accompanying editorial. (Am J Respir Crit Care Med. doi: 10.1164/rccm.201701-0167ed).
The ability to titrate PEEP settings to a patient’s individual needs could substantially reduce the risk of lung derecruitment or damage by overdistension.
The current study, however, has limitations that must be addressed in the next phase of research, before this technique can be adopted into clinical practice, Dr. Guerin said: The 5-cm H20 PEEP steps may be too large to detect relevant changes.
In several other studies, PEEP was reduced more gradually in 2- to 3-cm H2O increments. “Surprisingly, PEEP was reduced to 0 cm H2O in this study, with this step maintained for 20 minutes, raising the risk of derecruitment and further stretching once higher PEEP levels were resumed.”
The investigators did not perform any recruitment maneuvers before proceeding with PEEP adjustment. This is contrary to what has been done in prior animal and human studies.
The computation of driving pressure was done without taking total PEEP into account. “As total PEEP is frequently greater than PEEP in patients with [acute respiratory distress syndrome], driving pressure can be overestimated with the common computation.”
The optimal PEEP that the investigators aimed for was determined retrospectively from an offline analysis of the data; this technique would not be suitable for bedside management. “When ‘optimal’ PEEP was defined from [EIT criteria], from a higher PaO2 [arterial partial pressure of oxygen] or from a higher compliance of the respiratory system during the decremental PEEP trial, these three criteria were observed together in only four patients with [acute respiratory distress syndrome].”
The study was done only once and cannot comply with the need for regular PEEP-level assessments over time, as could be done with some other strategies.
“Further studies should also consider taking into account the role of chest wall mechanics,” Dr. Guerin said.
Nevertheless, he concluded, EIT-based PEEP titration for each individual patient represents a prospective tool for assisting with the treatment of acute respiratory distress syndrome, and should be fully investigated in a large, prospective trial.
Dr. Guerin is a pulmonologist at the Hospital de la Croix Rousse, Lyon, France. He had no relevant financial disclosures.
This first study to examine electrical impedance tomography (EIT) in patients under extracorporeal membrane oxygenation shows important clinical potential, but also raises important questions, Claude Guerin, MD, wrote in an accompanying editorial. (Am J Respir Crit Care Med. doi: 10.1164/rccm.201701-0167ed).
The ability to titrate PEEP settings to a patient’s individual needs could substantially reduce the risk of lung derecruitment or damage by overdistension.
The current study, however, has limitations that must be addressed in the next phase of research, before this technique can be adopted into clinical practice, Dr. Guerin said: The 5-cm H20 PEEP steps may be too large to detect relevant changes.
In several other studies, PEEP was reduced more gradually in 2- to 3-cm H2O increments. “Surprisingly, PEEP was reduced to 0 cm H2O in this study, with this step maintained for 20 minutes, raising the risk of derecruitment and further stretching once higher PEEP levels were resumed.”
The investigators did not perform any recruitment maneuvers before proceeding with PEEP adjustment. This is contrary to what has been done in prior animal and human studies.
The computation of driving pressure was done without taking total PEEP into account. “As total PEEP is frequently greater than PEEP in patients with [acute respiratory distress syndrome], driving pressure can be overestimated with the common computation.”
The optimal PEEP that the investigators aimed for was determined retrospectively from an offline analysis of the data; this technique would not be suitable for bedside management. “When ‘optimal’ PEEP was defined from [EIT criteria], from a higher PaO2 [arterial partial pressure of oxygen] or from a higher compliance of the respiratory system during the decremental PEEP trial, these three criteria were observed together in only four patients with [acute respiratory distress syndrome].”
The study was done only once and cannot comply with the need for regular PEEP-level assessments over time, as could be done with some other strategies.
“Further studies should also consider taking into account the role of chest wall mechanics,” Dr. Guerin said.
Nevertheless, he concluded, EIT-based PEEP titration for each individual patient represents a prospective tool for assisting with the treatment of acute respiratory distress syndrome, and should be fully investigated in a large, prospective trial.
Dr. Guerin is a pulmonologist at the Hospital de la Croix Rousse, Lyon, France. He had no relevant financial disclosures.
This first study to examine electrical impedance tomography (EIT) in patients under extracorporeal membrane oxygenation shows important clinical potential, but also raises important questions, Claude Guerin, MD, wrote in an accompanying editorial. (Am J Respir Crit Care Med. doi: 10.1164/rccm.201701-0167ed).
The ability to titrate PEEP settings to a patient’s individual needs could substantially reduce the risk of lung derecruitment or damage by overdistension.
The current study, however, has limitations that must be addressed in the next phase of research, before this technique can be adopted into clinical practice, Dr. Guerin said: The 5-cm H20 PEEP steps may be too large to detect relevant changes.
In several other studies, PEEP was reduced more gradually in 2- to 3-cm H2O increments. “Surprisingly, PEEP was reduced to 0 cm H2O in this study, with this step maintained for 20 minutes, raising the risk of derecruitment and further stretching once higher PEEP levels were resumed.”
The investigators did not perform any recruitment maneuvers before proceeding with PEEP adjustment. This is contrary to what has been done in prior animal and human studies.
The computation of driving pressure was done without taking total PEEP into account. “As total PEEP is frequently greater than PEEP in patients with [acute respiratory distress syndrome], driving pressure can be overestimated with the common computation.”
The optimal PEEP that the investigators aimed for was determined retrospectively from an offline analysis of the data; this technique would not be suitable for bedside management. “When ‘optimal’ PEEP was defined from [EIT criteria], from a higher PaO2 [arterial partial pressure of oxygen] or from a higher compliance of the respiratory system during the decremental PEEP trial, these three criteria were observed together in only four patients with [acute respiratory distress syndrome].”
The study was done only once and cannot comply with the need for regular PEEP-level assessments over time, as could be done with some other strategies.
“Further studies should also consider taking into account the role of chest wall mechanics,” Dr. Guerin said.
Nevertheless, he concluded, EIT-based PEEP titration for each individual patient represents a prospective tool for assisting with the treatment of acute respiratory distress syndrome, and should be fully investigated in a large, prospective trial.
Dr. Guerin is a pulmonologist at the Hospital de la Croix Rousse, Lyon, France. He had no relevant financial disclosures.
A noninvasive bedside imaging technique can individually calibrate positive end-expiratory pressure settings in patients on extracorporeal membrane oxygenation (ECMO) for severe acute respiratory distress syndrome (ARDS), a study showed.
The step-down PEEP (positive end-expiratory pressure) trial could not identify a single PEEP setting that optimally balanced lung overdistension and lung collapse for all 15 patients. But, electrical impedance tomography (EIT) allowed investigators to individually titrate PEEP settings for each patient, Guillaume Franchineau, MD, wrote (Am J Respir Crit Care Med. 2017;196[4]:447-57 doi: 10.1164/rccm.201605-1055OC).
The 4-month study involved 15 patients (aged, 18-79 years) who were in acute respiratory distress syndrome for a variety of reasons, including influenza (7 patients), pneumonia (3), leukemia (2), and 1 case each of Pneumocystis, antisynthetase syndrome, and trauma. All patients were receiving ECMO with a constant driving pressure of 14 cm H2O. After verifying that the inspiratory flow was 0 at the end of inspiration, PEEP was increased to 20 cm H2O (PEEP 20) with a peak inspiratory pressure of 34 cm H2O. PEEP 20 was held for 20 minutes and then lowered by 5 cm H2O decrements with the potential of reaching PEEP 0.
The EIT device, consisting of a silicone belt with 16 surface electrodes, was placed around the thorax aligning with the sixth intercostal parasternal space and connected to a monitor. By measuring conductivity and impeditivity in the underlying tissues, the device generates a low-resolution, two-dimensional image. The image was sufficient to show lung distension and collapse as the PEEP settings changed. Investigators looked for the best compromise between overdistension and collapsed zones, which they defined as the lowest pressure able to limit EIT-assessed collapse to no more than 15% with the least overdistension.
There was no one-size-fits-all PEEP setting, the authors found. The setting that minimized both overdistension and collapse was PEEP 15 in seven patients, PEEP 10 in six patients, and PEEP 5 in two patients.
At each patient’s optimal PEEP setting, the median tidal volume was similar: 3.8 mL/kg ideal body weight for PEEP 15, 3.9 mL/kg ideal body weight for PEEP 10, and 4.3 mL/kg ideal body weight for PEEP 5.
Respiratory system compliance was also similar among the groups, at 20 mL/cm H2O, 18 mL/cm H2O, and 21 mL/cm H2O, respectively. However, arterial partial pressure of oxygen decreased as the PEEP setting decreased, dropping from 148 mm Hg to 128 mm Hg to 100 mm Hg, respectively. Conversely, arterial partial pressure of CO2 increased (32-41 mm Hg).
EIT also allowed clinicians to pinpoint areas of distension or collapse. As PEEP decreased, there was steady ventilation loss in the medial-dorsal and dorsal regions, which shifted to the medial-ventral and ventral regions.
“Most end-expiratory lung impedances were located in medial-dorsal and medial-ventral regions, whereas the dorsal region constantly contributed less than 10% of total end-expiratory lung impedance,” the authors noted.
“The broad variability of EIT-based best compromise PEEPs in these patients with severe ARDS reinforces the need to provide ventilation settings individually tailored to the regional ARDS-lesion distribution,” they concluded. “To achieve that goal, EIT seems to be an interesting bedside noninvasive tool to provide real-time monitoring of the PEEP effect and ventilation distribution on ECMO.”
Dr. Franchineau reported receiving speakers fees from Mapquet.
[email protected]
On Twitter @Alz_Gal
A noninvasive bedside imaging technique can individually calibrate positive end-expiratory pressure settings in patients on extracorporeal membrane oxygenation (ECMO) for severe acute respiratory distress syndrome (ARDS), a study showed.
The step-down PEEP (positive end-expiratory pressure) trial could not identify a single PEEP setting that optimally balanced lung overdistension and lung collapse for all 15 patients. But, electrical impedance tomography (EIT) allowed investigators to individually titrate PEEP settings for each patient, Guillaume Franchineau, MD, wrote (Am J Respir Crit Care Med. 2017;196[4]:447-57 doi: 10.1164/rccm.201605-1055OC).
The 4-month study involved 15 patients (aged, 18-79 years) who were in acute respiratory distress syndrome for a variety of reasons, including influenza (7 patients), pneumonia (3), leukemia (2), and 1 case each of Pneumocystis, antisynthetase syndrome, and trauma. All patients were receiving ECMO with a constant driving pressure of 14 cm H2O. After verifying that the inspiratory flow was 0 at the end of inspiration, PEEP was increased to 20 cm H2O (PEEP 20) with a peak inspiratory pressure of 34 cm H2O. PEEP 20 was held for 20 minutes and then lowered by 5 cm H2O decrements with the potential of reaching PEEP 0.
The EIT device, consisting of a silicone belt with 16 surface electrodes, was placed around the thorax aligning with the sixth intercostal parasternal space and connected to a monitor. By measuring conductivity and impeditivity in the underlying tissues, the device generates a low-resolution, two-dimensional image. The image was sufficient to show lung distension and collapse as the PEEP settings changed. Investigators looked for the best compromise between overdistension and collapsed zones, which they defined as the lowest pressure able to limit EIT-assessed collapse to no more than 15% with the least overdistension.
There was no one-size-fits-all PEEP setting, the authors found. The setting that minimized both overdistension and collapse was PEEP 15 in seven patients, PEEP 10 in six patients, and PEEP 5 in two patients.
At each patient’s optimal PEEP setting, the median tidal volume was similar: 3.8 mL/kg ideal body weight for PEEP 15, 3.9 mL/kg ideal body weight for PEEP 10, and 4.3 mL/kg ideal body weight for PEEP 5.
Respiratory system compliance was also similar among the groups, at 20 mL/cm H2O, 18 mL/cm H2O, and 21 mL/cm H2O, respectively. However, arterial partial pressure of oxygen decreased as the PEEP setting decreased, dropping from 148 mm Hg to 128 mm Hg to 100 mm Hg, respectively. Conversely, arterial partial pressure of CO2 increased (32-41 mm Hg).
EIT also allowed clinicians to pinpoint areas of distension or collapse. As PEEP decreased, there was steady ventilation loss in the medial-dorsal and dorsal regions, which shifted to the medial-ventral and ventral regions.
“Most end-expiratory lung impedances were located in medial-dorsal and medial-ventral regions, whereas the dorsal region constantly contributed less than 10% of total end-expiratory lung impedance,” the authors noted.
“The broad variability of EIT-based best compromise PEEPs in these patients with severe ARDS reinforces the need to provide ventilation settings individually tailored to the regional ARDS-lesion distribution,” they concluded. “To achieve that goal, EIT seems to be an interesting bedside noninvasive tool to provide real-time monitoring of the PEEP effect and ventilation distribution on ECMO.”
Dr. Franchineau reported receiving speakers fees from Mapquet.
[email protected]
On Twitter @Alz_Gal
FROM THE AMERICAN JOURNAL OF RESPIRATORY AND CRITICAL CARE MEDICINE
Key clinical point:
Major finding: The PEEP settings that minimized both overdistension and collapse were PEEP 15 in seven patients, PEEP 10 in six patients, and PEEP 5 in two patients.
Data source: A prospective study of 15 patients.
Disclosures: Dr. Franchineau reported receiving speakers fees from Mapquet. Dr. Guerin had no relevant financial disclosures.
Pediatric News editorial advisory board welcomes Dr. Tim Joos
Pediatric News welcomes Tim Joos, MD, MPH, to its editorial advisory board.
Dr. Joos is a practicing clinician in combined internal medicine/pediatrics in Seattle. For the last decade, he has worked at a federally qualified community health center in Seattle serving a largely low-income and immigrant population.
Pediatric News welcomes Tim Joos, MD, MPH, to its editorial advisory board.
Dr. Joos is a practicing clinician in combined internal medicine/pediatrics in Seattle. For the last decade, he has worked at a federally qualified community health center in Seattle serving a largely low-income and immigrant population.
Pediatric News welcomes Tim Joos, MD, MPH, to its editorial advisory board.
Dr. Joos is a practicing clinician in combined internal medicine/pediatrics in Seattle. For the last decade, he has worked at a federally qualified community health center in Seattle serving a largely low-income and immigrant population.
Older men benefit from vascular screening
BARCELONA – Population screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension targeted to men aged 65-74 years saved lives in a highly cost-effective way in a Danish randomized study of more than 50,000 men.
During a median follow-up of 4.4 years, total mortality was 7% lower among men invited for this triple-screening panel, compared with uninvited controls – a statistically significant difference achieved without causing any identified serious adverse effects. The cost ran 2,148 euro (about $2,600) per quality adjusted year, making it very “cost attractive,” Jes S. Lindholt, DMSci, said at the annual congress of the European Society of Cardiology.
Dr. Lindholt also said that ongoing studies are assessing the clinical- and cost- effectiveness of screening for AAA and PAD in women in a targeted age range. But for the time being, “we believe the greatest benefit is in men.”
The Viborg Vascular (VIVA) screening trial (ClinicalTrials.gov NCT00662480) randomized all 50,156 men aged 65-74 years living in the central region of Denmark to either receive an invitation to triple disease screening or to receive no invitation and form the control group. Three-quarters of those invited for screening came to screening clinics at 14 regional centers. The examinations identified an AAA in 3%, PAD in 11%, and hypertension in 10%. About a third of people identified with AAA or PAD started treatment with aspirin, a statin, or both, and a small number of those with an AAA underwent surgical repair during the following 5 years. About a third of those newly diagnosed with hypertension began treatment with antihypertensive drugs.
The results showed that for every 169 men invited for screening the program saved one life during follow-up, compared with men in the control arm. “To our knowledge, no prior population-based screening program has shown an impact on overall mortality,” Dr. Lindholt said. Concurrently with his report, the results appeared online (Lancet. 2017 Aug 28. doi: 10.1016/S0140-6736(17)32250-X).
VIVA received no commercial funding. Dr. Lindholt had no disclosures.
[email protected]
On Twitter @mitchelzoler
Triple screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension is a good idea, and the new results from the VIVA trial serve as a call for broader screening initiatives.
Although the patients identified with one or more of the conditions screened received a relatively low rate of interventions, the program nonetheless produced a net benefit. The cost effectiveness of screening was very acceptable, and could potentially further improve if people identified with disease receive treatment sooner. The data showed a modest impact on quality of life, but the findings provided assurance that the screening program produced no excess adverse effects and no decrement in quality of life.

The study was also large and had a median follow-up of more than 4 years. The results also showed the risk for overdiagnosis was no worse than is seen with breast cancer screening.
Andrew M. Kates, MD , is a cardiologist and professor of medicine at Washington University in St. Louis. He had no disclosures. He made these comments as designated discussant for the VIVA trial.
Triple screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension is a good idea, and the new results from the VIVA trial serve as a call for broader screening initiatives.
Although the patients identified with one or more of the conditions screened received a relatively low rate of interventions, the program nonetheless produced a net benefit. The cost effectiveness of screening was very acceptable, and could potentially further improve if people identified with disease receive treatment sooner. The data showed a modest impact on quality of life, but the findings provided assurance that the screening program produced no excess adverse effects and no decrement in quality of life.

The study was also large and had a median follow-up of more than 4 years. The results also showed the risk for overdiagnosis was no worse than is seen with breast cancer screening.
Andrew M. Kates, MD , is a cardiologist and professor of medicine at Washington University in St. Louis. He had no disclosures. He made these comments as designated discussant for the VIVA trial.
Triple screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension is a good idea, and the new results from the VIVA trial serve as a call for broader screening initiatives.
Although the patients identified with one or more of the conditions screened received a relatively low rate of interventions, the program nonetheless produced a net benefit. The cost effectiveness of screening was very acceptable, and could potentially further improve if people identified with disease receive treatment sooner. The data showed a modest impact on quality of life, but the findings provided assurance that the screening program produced no excess adverse effects and no decrement in quality of life.

The study was also large and had a median follow-up of more than 4 years. The results also showed the risk for overdiagnosis was no worse than is seen with breast cancer screening.
Andrew M. Kates, MD , is a cardiologist and professor of medicine at Washington University in St. Louis. He had no disclosures. He made these comments as designated discussant for the VIVA trial.
BARCELONA – Population screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension targeted to men aged 65-74 years saved lives in a highly cost-effective way in a Danish randomized study of more than 50,000 men.
During a median follow-up of 4.4 years, total mortality was 7% lower among men invited for this triple-screening panel, compared with uninvited controls – a statistically significant difference achieved without causing any identified serious adverse effects. The cost ran 2,148 euro (about $2,600) per quality adjusted year, making it very “cost attractive,” Jes S. Lindholt, DMSci, said at the annual congress of the European Society of Cardiology.
Dr. Lindholt also said that ongoing studies are assessing the clinical- and cost- effectiveness of screening for AAA and PAD in women in a targeted age range. But for the time being, “we believe the greatest benefit is in men.”
The Viborg Vascular (VIVA) screening trial (ClinicalTrials.gov NCT00662480) randomized all 50,156 men aged 65-74 years living in the central region of Denmark to either receive an invitation to triple disease screening or to receive no invitation and form the control group. Three-quarters of those invited for screening came to screening clinics at 14 regional centers. The examinations identified an AAA in 3%, PAD in 11%, and hypertension in 10%. About a third of people identified with AAA or PAD started treatment with aspirin, a statin, or both, and a small number of those with an AAA underwent surgical repair during the following 5 years. About a third of those newly diagnosed with hypertension began treatment with antihypertensive drugs.
The results showed that for every 169 men invited for screening the program saved one life during follow-up, compared with men in the control arm. “To our knowledge, no prior population-based screening program has shown an impact on overall mortality,” Dr. Lindholt said. Concurrently with his report, the results appeared online (Lancet. 2017 Aug 28. doi: 10.1016/S0140-6736(17)32250-X).
VIVA received no commercial funding. Dr. Lindholt had no disclosures.
[email protected]
On Twitter @mitchelzoler
BARCELONA – Population screening for abdominal aortic aneurysms, peripheral arterial disease, and hypertension targeted to men aged 65-74 years saved lives in a highly cost-effective way in a Danish randomized study of more than 50,000 men.
During a median follow-up of 4.4 years, total mortality was 7% lower among men invited for this triple-screening panel, compared with uninvited controls – a statistically significant difference achieved without causing any identified serious adverse effects. The cost ran 2,148 euro (about $2,600) per quality adjusted year, making it very “cost attractive,” Jes S. Lindholt, DMSci, said at the annual congress of the European Society of Cardiology.
Dr. Lindholt also said that ongoing studies are assessing the clinical- and cost- effectiveness of screening for AAA and PAD in women in a targeted age range. But for the time being, “we believe the greatest benefit is in men.”
The Viborg Vascular (VIVA) screening trial (ClinicalTrials.gov NCT00662480) randomized all 50,156 men aged 65-74 years living in the central region of Denmark to either receive an invitation to triple disease screening or to receive no invitation and form the control group. Three-quarters of those invited for screening came to screening clinics at 14 regional centers. The examinations identified an AAA in 3%, PAD in 11%, and hypertension in 10%. About a third of people identified with AAA or PAD started treatment with aspirin, a statin, or both, and a small number of those with an AAA underwent surgical repair during the following 5 years. About a third of those newly diagnosed with hypertension began treatment with antihypertensive drugs.
The results showed that for every 169 men invited for screening the program saved one life during follow-up, compared with men in the control arm. “To our knowledge, no prior population-based screening program has shown an impact on overall mortality,” Dr. Lindholt said. Concurrently with his report, the results appeared online (Lancet. 2017 Aug 28. doi: 10.1016/S0140-6736(17)32250-X).
VIVA received no commercial funding. Dr. Lindholt had no disclosures.
[email protected]
On Twitter @mitchelzoler
AT THE ESC CONGRESS 2017
Key clinical point:
Major finding: Overall mortality during median follow-up of 4 years was 7% lower among men invited to screening, compared with unscreened controls.
Data source: VIVA, a randomized, multicenter trial of 50,156 Danish men.
Disclosures: VIVA received no commercial funding. Dr. Lindholt had no disclosures.