User login
White House to end COVID vaccine mandate for federal workers
The move means vaccines will no longer be required for workers who are federal employees, federal contractors, Head Start early education employees, workers at Medicare-certified health care facilities, and those who work at U.S. borders. International air travelers will no longer be required to prove their vaccination status. The requirement will be lifted at the end of the day on May 11, which is also when the federal public health emergency declaration ends.
“While vaccination remains one of the most important tools in advancing the health and safety of employees and promoting the efficiency of workplaces, we are now in a different phase of our response when these measures are no longer necessary,” an announcement from the White House stated.
White House officials credited vaccine requirements with saving millions of lives, noting that the rules ensured “the safety of workers in critical workforces including those in the healthcare and education sectors, protecting themselves and the populations they serve, and strengthening their ability to provide services without disruptions to operations.”
More than 100 million people were subject to the vaccine requirement, The Associated Press reported. All but 2% of those covered by the mandate had received at least one dose or had a pending or approved exception on file by January 2022, the Biden administration said, noting that COVID deaths have dropped 95% since January 2021 and hospitalizations are down nearly 91%.
In January, vaccine requirements were lifted for U.S. military members.
On the government-run website Safer Federal Workforce, which helped affected organizations put federal COVID rules into place, agencies were told to “take no action to implement or enforce the COVID-19 vaccination requirement” at this time.
A version of this article first appeared on WebMD.com.
The move means vaccines will no longer be required for workers who are federal employees, federal contractors, Head Start early education employees, workers at Medicare-certified health care facilities, and those who work at U.S. borders. International air travelers will no longer be required to prove their vaccination status. The requirement will be lifted at the end of the day on May 11, which is also when the federal public health emergency declaration ends.
“While vaccination remains one of the most important tools in advancing the health and safety of employees and promoting the efficiency of workplaces, we are now in a different phase of our response when these measures are no longer necessary,” an announcement from the White House stated.
White House officials credited vaccine requirements with saving millions of lives, noting that the rules ensured “the safety of workers in critical workforces including those in the healthcare and education sectors, protecting themselves and the populations they serve, and strengthening their ability to provide services without disruptions to operations.”
More than 100 million people were subject to the vaccine requirement, The Associated Press reported. All but 2% of those covered by the mandate had received at least one dose or had a pending or approved exception on file by January 2022, the Biden administration said, noting that COVID deaths have dropped 95% since January 2021 and hospitalizations are down nearly 91%.
In January, vaccine requirements were lifted for U.S. military members.
On the government-run website Safer Federal Workforce, which helped affected organizations put federal COVID rules into place, agencies were told to “take no action to implement or enforce the COVID-19 vaccination requirement” at this time.
A version of this article first appeared on WebMD.com.
The move means vaccines will no longer be required for workers who are federal employees, federal contractors, Head Start early education employees, workers at Medicare-certified health care facilities, and those who work at U.S. borders. International air travelers will no longer be required to prove their vaccination status. The requirement will be lifted at the end of the day on May 11, which is also when the federal public health emergency declaration ends.
“While vaccination remains one of the most important tools in advancing the health and safety of employees and promoting the efficiency of workplaces, we are now in a different phase of our response when these measures are no longer necessary,” an announcement from the White House stated.
White House officials credited vaccine requirements with saving millions of lives, noting that the rules ensured “the safety of workers in critical workforces including those in the healthcare and education sectors, protecting themselves and the populations they serve, and strengthening their ability to provide services without disruptions to operations.”
More than 100 million people were subject to the vaccine requirement, The Associated Press reported. All but 2% of those covered by the mandate had received at least one dose or had a pending or approved exception on file by January 2022, the Biden administration said, noting that COVID deaths have dropped 95% since January 2021 and hospitalizations are down nearly 91%.
In January, vaccine requirements were lifted for U.S. military members.
On the government-run website Safer Federal Workforce, which helped affected organizations put federal COVID rules into place, agencies were told to “take no action to implement or enforce the COVID-19 vaccination requirement” at this time.
A version of this article first appeared on WebMD.com.
U.S. incidence, prevalence of myasthenia gravis is rising
, an analysis of new claims data shows. Investigators speculate the rise of this rare disorder may be due to “increased diagnosis and more awareness of the disease over time, which has been shown in several studies,” study investigator Ema Rodrigues, DSc, MPH, with Alexion Pharmaceuticals, Boston.
Dr. Rodrigues presented her research at the 2023 annual meeting of the American Academy of Neurology.
Myasthenia gravis is a rare neuromuscular disease characterized by muscle weakness and fatigue caused by the binding of autoantibodies at the neuromuscular junction. It affects the voluntary muscles of the body, especially those that control the eyes, mouth, throat, and limbs.
In Europe, the incidence and prevalence of myasthenia gravis has increased for the past several decades. In the United States, increasing prevalence has also been observed, but recent estimates are lacking, making it tough to gauge the true burden of disease, Dr. Rodrigues explained.
Claims-based analysis
To investigate, Dr. Rodrigues and colleagues analyzed claims data (commercial, Medicare, and Medicaid) and electronic health records representing over 300 million patients in the United States from 2011 to present.
They calculated sex- and age-specific incidence and prevalence of myasthenia gravis for the year 2021 using U.S. Census data.
Prevalent patients were identified as having one or more myasthenia gravis records in 2021 and two or more myasthenia gravis records, at least 30 days apart, from 2016 to 2021. This cohort had 78,225 patients.
Incident patients were identified as those with a myasthenia gravis record in 2021 and no previous myasthenia gravis record from 2019 to 2020. This cohort had 4,214 patients.
For both the prevalent and incident cohort, the distribution of male and female patients was roughly 50/50, with a slightly higher proportion of females in the incident cohort, Dr. Rodrigues reported.
When looking at age groups, there were “very few pediatric patients,” she noted, with less than 1% of the patients under the age of 12. The highest proportion of patients were 65 years or older. The mean age was 67 in the prevalent cohort and 68 in the incident cohort.
In 2021, the overall incidence of myasthenia gravis was 3.2 per 100,000 with similar estimates for males and females (3.2 vs. 3.1 per 100,000, respectively).
Total prevalence was estimated to be 37.0 per 100,000 with sex-specific estimates being comparable at 37.3 and 36.7 per 100,000 for males and females, respectively.
The incidence and prevalence of myasthenia gravis increased with age, ranging from 0.3 and 0.4 per 100,000, respectively, in children younger than age 2 years, to 10.2 and 116.8 per 100,000, respectively, in people 65 and older.
These estimates are “significantly higher” than those from a prior U.S. analysis from 2003, Dr. Rodrigues told attendees, but they are quite similar to the estimates that were reported in Sweden in 2020.
A limitation of the analysis is that patients who do not seek care regularly may have not been identified due to inclusion criteria, potentially leading to underestimates. Also, no information was available on the myasthenia gravis subtype (ocular vs. generalized).
Underestimated burden
Reached for comment, Richard J. Nowak, MD, MS, director of the Yale Myasthenia Gravis Clinic, Yale School of Medicine, New Haven, Conn., noted that the new report, “albeit limited as a claims-based analysis, presents modern data on incidence and prevalence of myasthenia gravis in the United States.”
“It suggests that the current estimates of myasthenia gravis in the United States are too low and that the true impact/burden of myasthenia gravis is greater. While we are unable to verify the accuracy of the diagnosis, the total myasthenia gravis population is likely to be about 100,000, which is higher than prior estimates.”
“This, in fact, might be driven by greater disease awareness and increased diagnosis along with decreased mortality and longer life expectancy,” Dr. Nowak said.
“Anecdotally, we are most certainly seeing patients with new-onset myasthenia gravis in their 70s, 80s, and even 90s in recent years. The EXPLORE-MG registry published data from a tertiary center on age of onset breakdown showing myasthenia gravis can present at any age,” Dr. Nowak added.
Funding for the study was provided by Alexion, AstraZeneca Rare Disease. Dr. Rodrigues receives compensation and owns stock as an employee of Alexion, AstraZeneca Rare Diseases. Dr. Nowak has no relevant disclosures.
A version of this article originally appeared on Medscape.com.
, an analysis of new claims data shows. Investigators speculate the rise of this rare disorder may be due to “increased diagnosis and more awareness of the disease over time, which has been shown in several studies,” study investigator Ema Rodrigues, DSc, MPH, with Alexion Pharmaceuticals, Boston.
Dr. Rodrigues presented her research at the 2023 annual meeting of the American Academy of Neurology.
Myasthenia gravis is a rare neuromuscular disease characterized by muscle weakness and fatigue caused by the binding of autoantibodies at the neuromuscular junction. It affects the voluntary muscles of the body, especially those that control the eyes, mouth, throat, and limbs.
In Europe, the incidence and prevalence of myasthenia gravis has increased for the past several decades. In the United States, increasing prevalence has also been observed, but recent estimates are lacking, making it tough to gauge the true burden of disease, Dr. Rodrigues explained.
Claims-based analysis
To investigate, Dr. Rodrigues and colleagues analyzed claims data (commercial, Medicare, and Medicaid) and electronic health records representing over 300 million patients in the United States from 2011 to present.
They calculated sex- and age-specific incidence and prevalence of myasthenia gravis for the year 2021 using U.S. Census data.
Prevalent patients were identified as having one or more myasthenia gravis records in 2021 and two or more myasthenia gravis records, at least 30 days apart, from 2016 to 2021. This cohort had 78,225 patients.
Incident patients were identified as those with a myasthenia gravis record in 2021 and no previous myasthenia gravis record from 2019 to 2020. This cohort had 4,214 patients.
For both the prevalent and incident cohort, the distribution of male and female patients was roughly 50/50, with a slightly higher proportion of females in the incident cohort, Dr. Rodrigues reported.
When looking at age groups, there were “very few pediatric patients,” she noted, with less than 1% of the patients under the age of 12. The highest proportion of patients were 65 years or older. The mean age was 67 in the prevalent cohort and 68 in the incident cohort.
In 2021, the overall incidence of myasthenia gravis was 3.2 per 100,000 with similar estimates for males and females (3.2 vs. 3.1 per 100,000, respectively).
Total prevalence was estimated to be 37.0 per 100,000 with sex-specific estimates being comparable at 37.3 and 36.7 per 100,000 for males and females, respectively.
The incidence and prevalence of myasthenia gravis increased with age, ranging from 0.3 and 0.4 per 100,000, respectively, in children younger than age 2 years, to 10.2 and 116.8 per 100,000, respectively, in people 65 and older.
These estimates are “significantly higher” than those from a prior U.S. analysis from 2003, Dr. Rodrigues told attendees, but they are quite similar to the estimates that were reported in Sweden in 2020.
A limitation of the analysis is that patients who do not seek care regularly may have not been identified due to inclusion criteria, potentially leading to underestimates. Also, no information was available on the myasthenia gravis subtype (ocular vs. generalized).
Underestimated burden
Reached for comment, Richard J. Nowak, MD, MS, director of the Yale Myasthenia Gravis Clinic, Yale School of Medicine, New Haven, Conn., noted that the new report, “albeit limited as a claims-based analysis, presents modern data on incidence and prevalence of myasthenia gravis in the United States.”
“It suggests that the current estimates of myasthenia gravis in the United States are too low and that the true impact/burden of myasthenia gravis is greater. While we are unable to verify the accuracy of the diagnosis, the total myasthenia gravis population is likely to be about 100,000, which is higher than prior estimates.”
“This, in fact, might be driven by greater disease awareness and increased diagnosis along with decreased mortality and longer life expectancy,” Dr. Nowak said.
“Anecdotally, we are most certainly seeing patients with new-onset myasthenia gravis in their 70s, 80s, and even 90s in recent years. The EXPLORE-MG registry published data from a tertiary center on age of onset breakdown showing myasthenia gravis can present at any age,” Dr. Nowak added.
Funding for the study was provided by Alexion, AstraZeneca Rare Disease. Dr. Rodrigues receives compensation and owns stock as an employee of Alexion, AstraZeneca Rare Diseases. Dr. Nowak has no relevant disclosures.
A version of this article originally appeared on Medscape.com.
, an analysis of new claims data shows. Investigators speculate the rise of this rare disorder may be due to “increased diagnosis and more awareness of the disease over time, which has been shown in several studies,” study investigator Ema Rodrigues, DSc, MPH, with Alexion Pharmaceuticals, Boston.
Dr. Rodrigues presented her research at the 2023 annual meeting of the American Academy of Neurology.
Myasthenia gravis is a rare neuromuscular disease characterized by muscle weakness and fatigue caused by the binding of autoantibodies at the neuromuscular junction. It affects the voluntary muscles of the body, especially those that control the eyes, mouth, throat, and limbs.
In Europe, the incidence and prevalence of myasthenia gravis has increased for the past several decades. In the United States, increasing prevalence has also been observed, but recent estimates are lacking, making it tough to gauge the true burden of disease, Dr. Rodrigues explained.
Claims-based analysis
To investigate, Dr. Rodrigues and colleagues analyzed claims data (commercial, Medicare, and Medicaid) and electronic health records representing over 300 million patients in the United States from 2011 to present.
They calculated sex- and age-specific incidence and prevalence of myasthenia gravis for the year 2021 using U.S. Census data.
Prevalent patients were identified as having one or more myasthenia gravis records in 2021 and two or more myasthenia gravis records, at least 30 days apart, from 2016 to 2021. This cohort had 78,225 patients.
Incident patients were identified as those with a myasthenia gravis record in 2021 and no previous myasthenia gravis record from 2019 to 2020. This cohort had 4,214 patients.
For both the prevalent and incident cohort, the distribution of male and female patients was roughly 50/50, with a slightly higher proportion of females in the incident cohort, Dr. Rodrigues reported.
When looking at age groups, there were “very few pediatric patients,” she noted, with less than 1% of the patients under the age of 12. The highest proportion of patients were 65 years or older. The mean age was 67 in the prevalent cohort and 68 in the incident cohort.
In 2021, the overall incidence of myasthenia gravis was 3.2 per 100,000 with similar estimates for males and females (3.2 vs. 3.1 per 100,000, respectively).
Total prevalence was estimated to be 37.0 per 100,000 with sex-specific estimates being comparable at 37.3 and 36.7 per 100,000 for males and females, respectively.
The incidence and prevalence of myasthenia gravis increased with age, ranging from 0.3 and 0.4 per 100,000, respectively, in children younger than age 2 years, to 10.2 and 116.8 per 100,000, respectively, in people 65 and older.
These estimates are “significantly higher” than those from a prior U.S. analysis from 2003, Dr. Rodrigues told attendees, but they are quite similar to the estimates that were reported in Sweden in 2020.
A limitation of the analysis is that patients who do not seek care regularly may have not been identified due to inclusion criteria, potentially leading to underestimates. Also, no information was available on the myasthenia gravis subtype (ocular vs. generalized).
Underestimated burden
Reached for comment, Richard J. Nowak, MD, MS, director of the Yale Myasthenia Gravis Clinic, Yale School of Medicine, New Haven, Conn., noted that the new report, “albeit limited as a claims-based analysis, presents modern data on incidence and prevalence of myasthenia gravis in the United States.”
“It suggests that the current estimates of myasthenia gravis in the United States are too low and that the true impact/burden of myasthenia gravis is greater. While we are unable to verify the accuracy of the diagnosis, the total myasthenia gravis population is likely to be about 100,000, which is higher than prior estimates.”
“This, in fact, might be driven by greater disease awareness and increased diagnosis along with decreased mortality and longer life expectancy,” Dr. Nowak said.
“Anecdotally, we are most certainly seeing patients with new-onset myasthenia gravis in their 70s, 80s, and even 90s in recent years. The EXPLORE-MG registry published data from a tertiary center on age of onset breakdown showing myasthenia gravis can present at any age,” Dr. Nowak added.
Funding for the study was provided by Alexion, AstraZeneca Rare Disease. Dr. Rodrigues receives compensation and owns stock as an employee of Alexion, AstraZeneca Rare Diseases. Dr. Nowak has no relevant disclosures.
A version of this article originally appeared on Medscape.com.
From AAN 2023
Step count–heart rate link confirmed in children
, according to a study presented at the Pediatric Academic Societies annual meeting.
The new findings provide a new means for pediatricians to measure physical fitness, the researchers said.
“It really changes the way we evaluate kids’ fitness and gives us a new method of judging physical fitness other than body mass index,” said Susan Gasparino, MD, an instructor in pediatrics at the University of Rochester (N.Y.) Medical Center, who led the study.
Using data from the 2005 to 2006 National Health and Nutrition Examination Survey, Dr. Gasparino and her colleagues examined the association between resting heart rate (RHR) and step count among 899 children and 1,640 adolescents aged 6-19 years.
In the adolescent group, the mean RHR was 74.9 among those who walked more than 10,000 steps per day (n = 414) and 79.3 for those whose step counts fell below that cutoff (n = 1,226) (P < .001). For each additional 1,000 steps per day, RHR decreased by an average of 0.7 beats per minute in this group (P < .001).
In the younger age group, mean RHR was 85.3 among children who took more than 10,000 steps per day (n = 447) and 86.3 among those who did not reach that threshold (n = 452) (P = .29). For each additional 1,000 steps per day, RHR decreased by an average of 0.3 bpm in this group (P = .02)
Dr. Gasparino said next steps in research could include controlling for confounders, such as baseline anxiety and medications that could blunt the heart rate.
Broader implications
If similar results bear out in future studies, monitoring RHR could be incorporated into fitness programs for children and adolescents. Doing so could obviate “the need for intensive treadmill assessments using VO2max, time-consuming and emotionally fraught school-based physical fitness tests, and the fear and potential shame of the scale,” the researchers said.
Dr. Gasparino said measuring RHR during a 3-minute step test could help organizations and governments determine whether fitness programs are improving cardiovascular and overall health and could help them direct “funding and resources to the programs that are effective.” Such a test could also be incorporated into pediatrician wellness checks, she noted.
“It’s an exciting development, and [RHR measurement] holds a lot of promise as a clinical tool that can be applicable in a lot of settings,” said Nicholas M. Edwards, MD, MPH, a sports medicine pediatrician and an associate professor of orthopedics at the University of Minnesota in Minneapolis.
Dr. Edwards said that, because measurement of fitness in clinical settings is difficult, finding ways to “assess fitness in the office with the equipment already at hand would be a superb development.”
If use of RHR to measure fitness “is validated in a clinical setting,” Dr. Edwards said, “I think adoption would be a natural next step.”
Dr. Edwards has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
, according to a study presented at the Pediatric Academic Societies annual meeting.
The new findings provide a new means for pediatricians to measure physical fitness, the researchers said.
“It really changes the way we evaluate kids’ fitness and gives us a new method of judging physical fitness other than body mass index,” said Susan Gasparino, MD, an instructor in pediatrics at the University of Rochester (N.Y.) Medical Center, who led the study.
Using data from the 2005 to 2006 National Health and Nutrition Examination Survey, Dr. Gasparino and her colleagues examined the association between resting heart rate (RHR) and step count among 899 children and 1,640 adolescents aged 6-19 years.
In the adolescent group, the mean RHR was 74.9 among those who walked more than 10,000 steps per day (n = 414) and 79.3 for those whose step counts fell below that cutoff (n = 1,226) (P < .001). For each additional 1,000 steps per day, RHR decreased by an average of 0.7 beats per minute in this group (P < .001).
In the younger age group, mean RHR was 85.3 among children who took more than 10,000 steps per day (n = 447) and 86.3 among those who did not reach that threshold (n = 452) (P = .29). For each additional 1,000 steps per day, RHR decreased by an average of 0.3 bpm in this group (P = .02)
Dr. Gasparino said next steps in research could include controlling for confounders, such as baseline anxiety and medications that could blunt the heart rate.
Broader implications
If similar results bear out in future studies, monitoring RHR could be incorporated into fitness programs for children and adolescents. Doing so could obviate “the need for intensive treadmill assessments using VO2max, time-consuming and emotionally fraught school-based physical fitness tests, and the fear and potential shame of the scale,” the researchers said.
Dr. Gasparino said measuring RHR during a 3-minute step test could help organizations and governments determine whether fitness programs are improving cardiovascular and overall health and could help them direct “funding and resources to the programs that are effective.” Such a test could also be incorporated into pediatrician wellness checks, she noted.
“It’s an exciting development, and [RHR measurement] holds a lot of promise as a clinical tool that can be applicable in a lot of settings,” said Nicholas M. Edwards, MD, MPH, a sports medicine pediatrician and an associate professor of orthopedics at the University of Minnesota in Minneapolis.
Dr. Edwards said that, because measurement of fitness in clinical settings is difficult, finding ways to “assess fitness in the office with the equipment already at hand would be a superb development.”
If use of RHR to measure fitness “is validated in a clinical setting,” Dr. Edwards said, “I think adoption would be a natural next step.”
Dr. Edwards has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
, according to a study presented at the Pediatric Academic Societies annual meeting.
The new findings provide a new means for pediatricians to measure physical fitness, the researchers said.
“It really changes the way we evaluate kids’ fitness and gives us a new method of judging physical fitness other than body mass index,” said Susan Gasparino, MD, an instructor in pediatrics at the University of Rochester (N.Y.) Medical Center, who led the study.
Using data from the 2005 to 2006 National Health and Nutrition Examination Survey, Dr. Gasparino and her colleagues examined the association between resting heart rate (RHR) and step count among 899 children and 1,640 adolescents aged 6-19 years.
In the adolescent group, the mean RHR was 74.9 among those who walked more than 10,000 steps per day (n = 414) and 79.3 for those whose step counts fell below that cutoff (n = 1,226) (P < .001). For each additional 1,000 steps per day, RHR decreased by an average of 0.7 beats per minute in this group (P < .001).
In the younger age group, mean RHR was 85.3 among children who took more than 10,000 steps per day (n = 447) and 86.3 among those who did not reach that threshold (n = 452) (P = .29). For each additional 1,000 steps per day, RHR decreased by an average of 0.3 bpm in this group (P = .02)
Dr. Gasparino said next steps in research could include controlling for confounders, such as baseline anxiety and medications that could blunt the heart rate.
Broader implications
If similar results bear out in future studies, monitoring RHR could be incorporated into fitness programs for children and adolescents. Doing so could obviate “the need for intensive treadmill assessments using VO2max, time-consuming and emotionally fraught school-based physical fitness tests, and the fear and potential shame of the scale,” the researchers said.
Dr. Gasparino said measuring RHR during a 3-minute step test could help organizations and governments determine whether fitness programs are improving cardiovascular and overall health and could help them direct “funding and resources to the programs that are effective.” Such a test could also be incorporated into pediatrician wellness checks, she noted.
“It’s an exciting development, and [RHR measurement] holds a lot of promise as a clinical tool that can be applicable in a lot of settings,” said Nicholas M. Edwards, MD, MPH, a sports medicine pediatrician and an associate professor of orthopedics at the University of Minnesota in Minneapolis.
Dr. Edwards said that, because measurement of fitness in clinical settings is difficult, finding ways to “assess fitness in the office with the equipment already at hand would be a superb development.”
If use of RHR to measure fitness “is validated in a clinical setting,” Dr. Edwards said, “I think adoption would be a natural next step.”
Dr. Edwards has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
FROM PAS 2023
Head-to-head comparison of migraine meds reveals top options
BOSTON – , a new real-world analysis of data on more than 3 million migraine attacks shows.
The findings “align with results of clinical trials and recommendations from clinical treatment guidelines” and provide insights to complement clinical practice, said study investigator Chia-Chun Chiang, MD, a neurologist with Mayo Clinic, Rochester, Minn.
The findings were presented at the 2023 annual meeting of the American Academy of Neurology.
The power of big data
Despite a wide variety of acute migraine medications that are available, large-scale, head-to-head comparisons of treatment effectiveness from real-world patient experience reports are lacking, Dr. Chiang explained.
“To the best of our knowledge, this is the first study that simultaneously compared multiple acute migraine medications using a Big Data analysis approach based on real-world patient-provided data,” she said.
The researchers extracted more than 10 million self-reported migraine attack records from a migraine smartphone app called Migraine Buddy, where users can document whether a treatment was helpful, somewhat helpful, unsure, or unhelpful.
They analyzed 25 acute medications among seven classes: acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), triptans, combination analgesics (acetaminophen/aspirin/caffeine), ergots, antiemetics, and opioids. The newer gepants and ditan medication classes of medications were not included because of the relatively lower numbers of usage when data was extracted (2014-2020).
The researchers employed a two-level nested logistic regression model to analyze the odds of treatment effectiveness of each medication by adjusting concurrent medications and the covariance within the same user.
The final analysis included more than 3.1 million migraine attacks among 278,000 users globally.
Using ibuprofen as the reference, triptans, ergots, and antiemetics had the highest efficacy with mean odds ratios of 4.8, 3.02, and 2.67, respectively, followed by opioids (OR, 2.49), NSAIDs (OR, 1.94), combination analgesics (OR, 1.69), others (OR, 1.49), and acetaminophen (OR, 0.83).
Individual medications with the highest patient-reported effectiveness were eletriptan (Relpax; OR, 6.1), zolmitriptan (Zomig; OR, 5.7) and sumatriptan (Zecuity; OR, 5.2).
This migraine medication comparative effectiveness analysis, based on patient-reported outcomes, “supports and complements the treatment recommendations from national headache societies based on randomized controlled trials and meta-analyses and strongly supports the use of triptans,” Dr. Chiang said.
End of trial-and-error?
Commenting on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said “This is a great study of Big Data in that it shows the power of the smartphone to collect real-world data and smart researchers like at Mayo Clinic to analyze them.”
“The study sheds light on how different therapeutics compare with each other. The next iteration of this line of research, I would hope, would be to determine if particular medications are effective for a particular migraine population, and even down to individuals with migraine,” said Dr. Lakhan, who wasn’t involved in the study.
“Once those models are appropriately built, long gone will be the era of trial-and-error medicine,” Dr. Lakhan added.
The study had no specific funding. Dr. Chiang has served as a consultant for Satsuma. Dr. Lakhan reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
BOSTON – , a new real-world analysis of data on more than 3 million migraine attacks shows.
The findings “align with results of clinical trials and recommendations from clinical treatment guidelines” and provide insights to complement clinical practice, said study investigator Chia-Chun Chiang, MD, a neurologist with Mayo Clinic, Rochester, Minn.
The findings were presented at the 2023 annual meeting of the American Academy of Neurology.
The power of big data
Despite a wide variety of acute migraine medications that are available, large-scale, head-to-head comparisons of treatment effectiveness from real-world patient experience reports are lacking, Dr. Chiang explained.
“To the best of our knowledge, this is the first study that simultaneously compared multiple acute migraine medications using a Big Data analysis approach based on real-world patient-provided data,” she said.
The researchers extracted more than 10 million self-reported migraine attack records from a migraine smartphone app called Migraine Buddy, where users can document whether a treatment was helpful, somewhat helpful, unsure, or unhelpful.
They analyzed 25 acute medications among seven classes: acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), triptans, combination analgesics (acetaminophen/aspirin/caffeine), ergots, antiemetics, and opioids. The newer gepants and ditan medication classes of medications were not included because of the relatively lower numbers of usage when data was extracted (2014-2020).
The researchers employed a two-level nested logistic regression model to analyze the odds of treatment effectiveness of each medication by adjusting concurrent medications and the covariance within the same user.
The final analysis included more than 3.1 million migraine attacks among 278,000 users globally.
Using ibuprofen as the reference, triptans, ergots, and antiemetics had the highest efficacy with mean odds ratios of 4.8, 3.02, and 2.67, respectively, followed by opioids (OR, 2.49), NSAIDs (OR, 1.94), combination analgesics (OR, 1.69), others (OR, 1.49), and acetaminophen (OR, 0.83).
Individual medications with the highest patient-reported effectiveness were eletriptan (Relpax; OR, 6.1), zolmitriptan (Zomig; OR, 5.7) and sumatriptan (Zecuity; OR, 5.2).
This migraine medication comparative effectiveness analysis, based on patient-reported outcomes, “supports and complements the treatment recommendations from national headache societies based on randomized controlled trials and meta-analyses and strongly supports the use of triptans,” Dr. Chiang said.
End of trial-and-error?
Commenting on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said “This is a great study of Big Data in that it shows the power of the smartphone to collect real-world data and smart researchers like at Mayo Clinic to analyze them.”
“The study sheds light on how different therapeutics compare with each other. The next iteration of this line of research, I would hope, would be to determine if particular medications are effective for a particular migraine population, and even down to individuals with migraine,” said Dr. Lakhan, who wasn’t involved in the study.
“Once those models are appropriately built, long gone will be the era of trial-and-error medicine,” Dr. Lakhan added.
The study had no specific funding. Dr. Chiang has served as a consultant for Satsuma. Dr. Lakhan reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
BOSTON – , a new real-world analysis of data on more than 3 million migraine attacks shows.
The findings “align with results of clinical trials and recommendations from clinical treatment guidelines” and provide insights to complement clinical practice, said study investigator Chia-Chun Chiang, MD, a neurologist with Mayo Clinic, Rochester, Minn.
The findings were presented at the 2023 annual meeting of the American Academy of Neurology.
The power of big data
Despite a wide variety of acute migraine medications that are available, large-scale, head-to-head comparisons of treatment effectiveness from real-world patient experience reports are lacking, Dr. Chiang explained.
“To the best of our knowledge, this is the first study that simultaneously compared multiple acute migraine medications using a Big Data analysis approach based on real-world patient-provided data,” she said.
The researchers extracted more than 10 million self-reported migraine attack records from a migraine smartphone app called Migraine Buddy, where users can document whether a treatment was helpful, somewhat helpful, unsure, or unhelpful.
They analyzed 25 acute medications among seven classes: acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), triptans, combination analgesics (acetaminophen/aspirin/caffeine), ergots, antiemetics, and opioids. The newer gepants and ditan medication classes of medications were not included because of the relatively lower numbers of usage when data was extracted (2014-2020).
The researchers employed a two-level nested logistic regression model to analyze the odds of treatment effectiveness of each medication by adjusting concurrent medications and the covariance within the same user.
The final analysis included more than 3.1 million migraine attacks among 278,000 users globally.
Using ibuprofen as the reference, triptans, ergots, and antiemetics had the highest efficacy with mean odds ratios of 4.8, 3.02, and 2.67, respectively, followed by opioids (OR, 2.49), NSAIDs (OR, 1.94), combination analgesics (OR, 1.69), others (OR, 1.49), and acetaminophen (OR, 0.83).
Individual medications with the highest patient-reported effectiveness were eletriptan (Relpax; OR, 6.1), zolmitriptan (Zomig; OR, 5.7) and sumatriptan (Zecuity; OR, 5.2).
This migraine medication comparative effectiveness analysis, based on patient-reported outcomes, “supports and complements the treatment recommendations from national headache societies based on randomized controlled trials and meta-analyses and strongly supports the use of triptans,” Dr. Chiang said.
End of trial-and-error?
Commenting on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said “This is a great study of Big Data in that it shows the power of the smartphone to collect real-world data and smart researchers like at Mayo Clinic to analyze them.”
“The study sheds light on how different therapeutics compare with each other. The next iteration of this line of research, I would hope, would be to determine if particular medications are effective for a particular migraine population, and even down to individuals with migraine,” said Dr. Lakhan, who wasn’t involved in the study.
“Once those models are appropriately built, long gone will be the era of trial-and-error medicine,” Dr. Lakhan added.
The study had no specific funding. Dr. Chiang has served as a consultant for Satsuma. Dr. Lakhan reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AT AAN 2023
Oral antiamyloid shows disease-modifying potential Phase 3 trial underway
BOSTON – , represented by positive changes in plasma and imaging biomarkers of Alzheimer’s disease pathology.
Use of the drug, ALZ-801 (Alzheon), led to a significant reduction of plasma phosphorylated–tau 181 (p-tau181) , a marker of amyloid-induced neuronal injury in Alzheimer’s disease, as well as slowing of hippocampal atrophy and stabilization of cognition.
“The 12-month results of our phase 2 trial support the finding that ALZ-801 blocks misfolding of amyloid monomers and subsequent formation of neurotoxic amyloid oligomers, the key initial step in the amyloid aggregation cascade, which leads to a rapid and sustained reduction of brain neurodegeneration as measured by plasma p-tau181,” John Hey, PhD, Alzheon’s chief scientific officer, said in a statement.
“The severalfold greater reduction on the p-tau181 biomarker in plasma compared to plaque-clearing antiamyloid antibodies, combined with preservation of brain hippocampal volume and their positive correlations with cognitive benefits, further validate the disease-modifying effects of ALZ-801 in Alzheimer’s patients,” Dr. Hey added.
The results were presented at the 2023 annual meeting of the American Academy of Neurology.
ALZ-801 is an optimized prodrug of tramiprosate that has been shown to inhibit amyloid-beta 42 aggregation into toxic oligomers.
The ongoing phase 2 study is evaluating the effects of oral ALZ-801 (265 mg twice daily) on biomarkers of Alzheimer’s disease pathology for 84 adults with early Alzheimer’s disease who have either the APOE4/4 or APOE3/4 genotype. These genotypes represent the majority of patients with Alzheimer’s disease.
The mean age of the cohort was 69 years, and 51% are women; 70% had mild cognitive impairment, and 30% had mild Alzheimer’s disease. The mean Mini-Mental State Examination score for the cohort was 26.0. Roughly half were taking a cholinesterase inhibitor.
Significant plasma p-tau181 reduction was observed at 13 weeks. Levels were reduced by 41% by 52 weeks (P = .016). There was also a significant 5% reduction in plasma amyloid-beta 42 and 40 at 52 weeks (P = .002 and P = .005, respectively), Dr. Hey reported.
After 12 months of treatment, hippocampal atrophy was reduced by about 23%, and expansion of ventricular volume was reduced by about 15%, both in comparison with matched controls from the Alzheimer’s Disease Neuroimaging Initiative.
Composite cognitive z-score improved significantly at 13 and 26 weeks and remained above baseline at 52 weeks in comparison with matched ADNI controls. “These are very promising data,” Dr. Hey told conference attendees.
He noted that the safety profile of ALZ-801 remains favorable and consistent with prior safety data. Common adverse events were mild nausea and SARS-CoV-2 infection. There were no drug-related serious events or amyloid-related imaging abnormalities–edema (ARIA-E).
The phase 3 APOLLOE4 study of ALZ-801 is underway. This double-blind, randomized study is comparing oral ALZ-801 with placebo over 78 weeks for roughly 300 adults with early Alzheimer’s disease who have the APOE4/4 genotype. APOLLOE4 is expected to be completed in mid 2024.
The APOLLOE4 study is supported by a $47 million grant from the National Institute on Aging. The U.S. Food and Drug Administration has granted ALZ-801 fast-track designation.
More accessible option?
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, noted that the “biggest difference between this drug and others is that it is taken orally, rather than delivered through an infusion. This is important and valuable for reducing patient and caregiver burden and increasing ease of use and access.”
It’s also noteworthy that ALZ-801 was not associated with ARIA-E, “which has been reported in other antiamyloid trials and can occasionally be serious,” Dr. Griffin said.
Overall, he said the results are “encouraging, but more work is needed. If studies results continue to be positive, this treatment may provide a more accessible option for people who are at higher risk of ARIA,” Dr. Griffin said.
The study was funded by Alzheon. Dr. Hey is an employee of Alzheon and holds stock in the company. Dr. Griffin has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
BOSTON – , represented by positive changes in plasma and imaging biomarkers of Alzheimer’s disease pathology.
Use of the drug, ALZ-801 (Alzheon), led to a significant reduction of plasma phosphorylated–tau 181 (p-tau181) , a marker of amyloid-induced neuronal injury in Alzheimer’s disease, as well as slowing of hippocampal atrophy and stabilization of cognition.
“The 12-month results of our phase 2 trial support the finding that ALZ-801 blocks misfolding of amyloid monomers and subsequent formation of neurotoxic amyloid oligomers, the key initial step in the amyloid aggregation cascade, which leads to a rapid and sustained reduction of brain neurodegeneration as measured by plasma p-tau181,” John Hey, PhD, Alzheon’s chief scientific officer, said in a statement.
“The severalfold greater reduction on the p-tau181 biomarker in plasma compared to plaque-clearing antiamyloid antibodies, combined with preservation of brain hippocampal volume and their positive correlations with cognitive benefits, further validate the disease-modifying effects of ALZ-801 in Alzheimer’s patients,” Dr. Hey added.
The results were presented at the 2023 annual meeting of the American Academy of Neurology.
ALZ-801 is an optimized prodrug of tramiprosate that has been shown to inhibit amyloid-beta 42 aggregation into toxic oligomers.
The ongoing phase 2 study is evaluating the effects of oral ALZ-801 (265 mg twice daily) on biomarkers of Alzheimer’s disease pathology for 84 adults with early Alzheimer’s disease who have either the APOE4/4 or APOE3/4 genotype. These genotypes represent the majority of patients with Alzheimer’s disease.
The mean age of the cohort was 69 years, and 51% are women; 70% had mild cognitive impairment, and 30% had mild Alzheimer’s disease. The mean Mini-Mental State Examination score for the cohort was 26.0. Roughly half were taking a cholinesterase inhibitor.
Significant plasma p-tau181 reduction was observed at 13 weeks. Levels were reduced by 41% by 52 weeks (P = .016). There was also a significant 5% reduction in plasma amyloid-beta 42 and 40 at 52 weeks (P = .002 and P = .005, respectively), Dr. Hey reported.
After 12 months of treatment, hippocampal atrophy was reduced by about 23%, and expansion of ventricular volume was reduced by about 15%, both in comparison with matched controls from the Alzheimer’s Disease Neuroimaging Initiative.
Composite cognitive z-score improved significantly at 13 and 26 weeks and remained above baseline at 52 weeks in comparison with matched ADNI controls. “These are very promising data,” Dr. Hey told conference attendees.
He noted that the safety profile of ALZ-801 remains favorable and consistent with prior safety data. Common adverse events were mild nausea and SARS-CoV-2 infection. There were no drug-related serious events or amyloid-related imaging abnormalities–edema (ARIA-E).
The phase 3 APOLLOE4 study of ALZ-801 is underway. This double-blind, randomized study is comparing oral ALZ-801 with placebo over 78 weeks for roughly 300 adults with early Alzheimer’s disease who have the APOE4/4 genotype. APOLLOE4 is expected to be completed in mid 2024.
The APOLLOE4 study is supported by a $47 million grant from the National Institute on Aging. The U.S. Food and Drug Administration has granted ALZ-801 fast-track designation.
More accessible option?
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, noted that the “biggest difference between this drug and others is that it is taken orally, rather than delivered through an infusion. This is important and valuable for reducing patient and caregiver burden and increasing ease of use and access.”
It’s also noteworthy that ALZ-801 was not associated with ARIA-E, “which has been reported in other antiamyloid trials and can occasionally be serious,” Dr. Griffin said.
Overall, he said the results are “encouraging, but more work is needed. If studies results continue to be positive, this treatment may provide a more accessible option for people who are at higher risk of ARIA,” Dr. Griffin said.
The study was funded by Alzheon. Dr. Hey is an employee of Alzheon and holds stock in the company. Dr. Griffin has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
BOSTON – , represented by positive changes in plasma and imaging biomarkers of Alzheimer’s disease pathology.
Use of the drug, ALZ-801 (Alzheon), led to a significant reduction of plasma phosphorylated–tau 181 (p-tau181) , a marker of amyloid-induced neuronal injury in Alzheimer’s disease, as well as slowing of hippocampal atrophy and stabilization of cognition.
“The 12-month results of our phase 2 trial support the finding that ALZ-801 blocks misfolding of amyloid monomers and subsequent formation of neurotoxic amyloid oligomers, the key initial step in the amyloid aggregation cascade, which leads to a rapid and sustained reduction of brain neurodegeneration as measured by plasma p-tau181,” John Hey, PhD, Alzheon’s chief scientific officer, said in a statement.
“The severalfold greater reduction on the p-tau181 biomarker in plasma compared to plaque-clearing antiamyloid antibodies, combined with preservation of brain hippocampal volume and their positive correlations with cognitive benefits, further validate the disease-modifying effects of ALZ-801 in Alzheimer’s patients,” Dr. Hey added.
The results were presented at the 2023 annual meeting of the American Academy of Neurology.
ALZ-801 is an optimized prodrug of tramiprosate that has been shown to inhibit amyloid-beta 42 aggregation into toxic oligomers.
The ongoing phase 2 study is evaluating the effects of oral ALZ-801 (265 mg twice daily) on biomarkers of Alzheimer’s disease pathology for 84 adults with early Alzheimer’s disease who have either the APOE4/4 or APOE3/4 genotype. These genotypes represent the majority of patients with Alzheimer’s disease.
The mean age of the cohort was 69 years, and 51% are women; 70% had mild cognitive impairment, and 30% had mild Alzheimer’s disease. The mean Mini-Mental State Examination score for the cohort was 26.0. Roughly half were taking a cholinesterase inhibitor.
Significant plasma p-tau181 reduction was observed at 13 weeks. Levels were reduced by 41% by 52 weeks (P = .016). There was also a significant 5% reduction in plasma amyloid-beta 42 and 40 at 52 weeks (P = .002 and P = .005, respectively), Dr. Hey reported.
After 12 months of treatment, hippocampal atrophy was reduced by about 23%, and expansion of ventricular volume was reduced by about 15%, both in comparison with matched controls from the Alzheimer’s Disease Neuroimaging Initiative.
Composite cognitive z-score improved significantly at 13 and 26 weeks and remained above baseline at 52 weeks in comparison with matched ADNI controls. “These are very promising data,” Dr. Hey told conference attendees.
He noted that the safety profile of ALZ-801 remains favorable and consistent with prior safety data. Common adverse events were mild nausea and SARS-CoV-2 infection. There were no drug-related serious events or amyloid-related imaging abnormalities–edema (ARIA-E).
The phase 3 APOLLOE4 study of ALZ-801 is underway. This double-blind, randomized study is comparing oral ALZ-801 with placebo over 78 weeks for roughly 300 adults with early Alzheimer’s disease who have the APOE4/4 genotype. APOLLOE4 is expected to be completed in mid 2024.
The APOLLOE4 study is supported by a $47 million grant from the National Institute on Aging. The U.S. Food and Drug Administration has granted ALZ-801 fast-track designation.
More accessible option?
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, noted that the “biggest difference between this drug and others is that it is taken orally, rather than delivered through an infusion. This is important and valuable for reducing patient and caregiver burden and increasing ease of use and access.”
It’s also noteworthy that ALZ-801 was not associated with ARIA-E, “which has been reported in other antiamyloid trials and can occasionally be serious,” Dr. Griffin said.
Overall, he said the results are “encouraging, but more work is needed. If studies results continue to be positive, this treatment may provide a more accessible option for people who are at higher risk of ARIA,” Dr. Griffin said.
The study was funded by Alzheon. Dr. Hey is an employee of Alzheon and holds stock in the company. Dr. Griffin has disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
FROM AAN 2023
Patients With Newly Diagnosed Mantle Cell Lymphoma and the Relevance of Clinical Trials
What is the significance of the recent TRIANGLE study on mantle cell lymphoma (MCL)?
Dr. LaCasce: The TRIANGLE study is extremely important in previously untreated, transplant-eligible patients with MCL. The cutoff age for transplants varies by center and is between 60 and 75 years. In the absence of a TP53 mutation, we have typically used induction chemotherapy followed by autologous stem-cell transplant (ASCT), followed by 3 years of maintenance rituximab. Obviously, this is a lot of therapy.
The TRIANGLE study was a 3-arm study in which ibrutinib-containing therapy was compared with standard RCHOP/RDHAP followed by ASCT. Maintenance rituximab became standard of care midway through the trial and was added. In the first experimental arm, ibrutinib was combined with RCHOP and then given as maintenance for 2 years following ASCT. The second experimental arm included the same schedule of ibrutinib and omitted the ASCT.
The results are early, but what has been presented thus far, ibrutinib induction and maintenance with ASCT is clearly superior to the standard arm with ASCT. Although the data are not statistically mature, the failure-free survival of the 2 ibrutinib arms was similar, suggesting that transplant may not be necessary. Longer follow-up is necessary to confirm this conclusion and assess overall survival in all 3 arms.
If the results hold, ASCT could become a thing of the past or perhaps used in the second line. With the favorable activity of chimeric antigen receptor (CAR) T-cell therapy, however, it is unclear whether ASCT would be used in second line. Avoiding the sequential use of ASCT and CAR T-cell therapy is appealing given the stem-cell damage that can result. It is appealing to think about not using ASCT upfront, because ASCT increases the risk of myelodysplastic syndrome.
The TRIANGLE data are likely to change the frontline management of MCL. Although ibrutinib was the first Bruton tyrosine kinase (BTK) inhibitor approved in MCL and has obviously changed the field dramatically, it is significantly less well-tolerated than the next generation of drugs—acalabrutinib and zanubrutinib. I suspect these will be substituted for ibrutinib and we will see even more tolerable upfront regimens for patients with newly diagnosed MCL.
Have there been any disparities that you found in patients newly diagnosed with MCL regarding age, sex, or ethnicity?
Dr. LaCasce: MCL typically affects patients in their 60s. It is rare in young patients, and approximately 75% of the cases are male. If you look at the demographics, it is more common in White patients and less common in Hispanic and African American patients. In addition, there is an association with farming, which likely contribute to the demographics of patients with MCL.
What is your recommended approach to managing patients newly diagnosed with MCL in your day-to-day practice?
Dr. LaCasce: Management is a bit tricky right now because the TRIANGLE study is not part of any guidelines thus far. Therefore, most would argue the standard treatment continues to include ASCT upfront. There is an important, large randomized study (NCT03267433) going on in the United States that is assessing the role of ASCT in patients who are in MRD-negative complete remission at the end of induction therapy. These patients are randomized to ASCT plus maintenance rituximab versus maintenance rituximab alone.
We are still enrolling patients to participate in this study, which is addressing a different question than TRIANGLE. I think we will learn a lot from this study. For patients who are not interested in participating in this study, we talk about the risks and benefits of ASCT.
One or 2 years ago, I would have strongly encouraged patients who were appropriate candidates to consider transplant in first remission. With the TRIANGLE data, however, and now that we have CAR T-cell therapy, I think it is more important to tailor the recommendation to the individual patient. If a patient is reluctant about ASCT and the associated risks, I do not push it.
If patients want the most aggressive approach associated with the longest remissions, at this moment, before TRIANGLE findings have been adopted into guidelines, I continue to recommend ASCT. For patients who have TP53 mutation, however, we treat with typically less aggressive therapy, as this patient population does not benefit from ASCT. We look forward to more data incorporating BTK inhibitors upfront, particularly for this group of patients, who tend to have a more adverse prognosis.
Do you feel MCL data and clinical trials are important areas of focus for your colleagues?
Dr. LaCasce: Yes. I think it is a rapidly evolving field, which is really exciting. We are seeing data now from the bispecific antibodies in the relapsed/refractory setting. We also need more data using pirtobrutinib for patients who have had BTK inhibitors and compare pirtobrutinib (a non-covalent BTK inhibitor) with the covalent BTK inhibitors.
I would strongly encourage patients to participate in clinical trials so that we can better answer these important questions. When patients go online and read about MCL, they often see a median survival of 3 to 4 years, which is completely outdated. The overall prognosis of MCL has changed dramatically since I have been in the field. Hopefully, survival will continue to improve, and therapies will become more tolerable, as well.
What is the significance of the recent TRIANGLE study on mantle cell lymphoma (MCL)?
Dr. LaCasce: The TRIANGLE study is extremely important in previously untreated, transplant-eligible patients with MCL. The cutoff age for transplants varies by center and is between 60 and 75 years. In the absence of a TP53 mutation, we have typically used induction chemotherapy followed by autologous stem-cell transplant (ASCT), followed by 3 years of maintenance rituximab. Obviously, this is a lot of therapy.
The TRIANGLE study was a 3-arm study in which ibrutinib-containing therapy was compared with standard RCHOP/RDHAP followed by ASCT. Maintenance rituximab became standard of care midway through the trial and was added. In the first experimental arm, ibrutinib was combined with RCHOP and then given as maintenance for 2 years following ASCT. The second experimental arm included the same schedule of ibrutinib and omitted the ASCT.
The results are early, but what has been presented thus far, ibrutinib induction and maintenance with ASCT is clearly superior to the standard arm with ASCT. Although the data are not statistically mature, the failure-free survival of the 2 ibrutinib arms was similar, suggesting that transplant may not be necessary. Longer follow-up is necessary to confirm this conclusion and assess overall survival in all 3 arms.
If the results hold, ASCT could become a thing of the past or perhaps used in the second line. With the favorable activity of chimeric antigen receptor (CAR) T-cell therapy, however, it is unclear whether ASCT would be used in second line. Avoiding the sequential use of ASCT and CAR T-cell therapy is appealing given the stem-cell damage that can result. It is appealing to think about not using ASCT upfront, because ASCT increases the risk of myelodysplastic syndrome.
The TRIANGLE data are likely to change the frontline management of MCL. Although ibrutinib was the first Bruton tyrosine kinase (BTK) inhibitor approved in MCL and has obviously changed the field dramatically, it is significantly less well-tolerated than the next generation of drugs—acalabrutinib and zanubrutinib. I suspect these will be substituted for ibrutinib and we will see even more tolerable upfront regimens for patients with newly diagnosed MCL.
Have there been any disparities that you found in patients newly diagnosed with MCL regarding age, sex, or ethnicity?
Dr. LaCasce: MCL typically affects patients in their 60s. It is rare in young patients, and approximately 75% of the cases are male. If you look at the demographics, it is more common in White patients and less common in Hispanic and African American patients. In addition, there is an association with farming, which likely contribute to the demographics of patients with MCL.
What is your recommended approach to managing patients newly diagnosed with MCL in your day-to-day practice?
Dr. LaCasce: Management is a bit tricky right now because the TRIANGLE study is not part of any guidelines thus far. Therefore, most would argue the standard treatment continues to include ASCT upfront. There is an important, large randomized study (NCT03267433) going on in the United States that is assessing the role of ASCT in patients who are in MRD-negative complete remission at the end of induction therapy. These patients are randomized to ASCT plus maintenance rituximab versus maintenance rituximab alone.
We are still enrolling patients to participate in this study, which is addressing a different question than TRIANGLE. I think we will learn a lot from this study. For patients who are not interested in participating in this study, we talk about the risks and benefits of ASCT.
One or 2 years ago, I would have strongly encouraged patients who were appropriate candidates to consider transplant in first remission. With the TRIANGLE data, however, and now that we have CAR T-cell therapy, I think it is more important to tailor the recommendation to the individual patient. If a patient is reluctant about ASCT and the associated risks, I do not push it.
If patients want the most aggressive approach associated with the longest remissions, at this moment, before TRIANGLE findings have been adopted into guidelines, I continue to recommend ASCT. For patients who have TP53 mutation, however, we treat with typically less aggressive therapy, as this patient population does not benefit from ASCT. We look forward to more data incorporating BTK inhibitors upfront, particularly for this group of patients, who tend to have a more adverse prognosis.
Do you feel MCL data and clinical trials are important areas of focus for your colleagues?
Dr. LaCasce: Yes. I think it is a rapidly evolving field, which is really exciting. We are seeing data now from the bispecific antibodies in the relapsed/refractory setting. We also need more data using pirtobrutinib for patients who have had BTK inhibitors and compare pirtobrutinib (a non-covalent BTK inhibitor) with the covalent BTK inhibitors.
I would strongly encourage patients to participate in clinical trials so that we can better answer these important questions. When patients go online and read about MCL, they often see a median survival of 3 to 4 years, which is completely outdated. The overall prognosis of MCL has changed dramatically since I have been in the field. Hopefully, survival will continue to improve, and therapies will become more tolerable, as well.
What is the significance of the recent TRIANGLE study on mantle cell lymphoma (MCL)?
Dr. LaCasce: The TRIANGLE study is extremely important in previously untreated, transplant-eligible patients with MCL. The cutoff age for transplants varies by center and is between 60 and 75 years. In the absence of a TP53 mutation, we have typically used induction chemotherapy followed by autologous stem-cell transplant (ASCT), followed by 3 years of maintenance rituximab. Obviously, this is a lot of therapy.
The TRIANGLE study was a 3-arm study in which ibrutinib-containing therapy was compared with standard RCHOP/RDHAP followed by ASCT. Maintenance rituximab became standard of care midway through the trial and was added. In the first experimental arm, ibrutinib was combined with RCHOP and then given as maintenance for 2 years following ASCT. The second experimental arm included the same schedule of ibrutinib and omitted the ASCT.
The results are early, but what has been presented thus far, ibrutinib induction and maintenance with ASCT is clearly superior to the standard arm with ASCT. Although the data are not statistically mature, the failure-free survival of the 2 ibrutinib arms was similar, suggesting that transplant may not be necessary. Longer follow-up is necessary to confirm this conclusion and assess overall survival in all 3 arms.
If the results hold, ASCT could become a thing of the past or perhaps used in the second line. With the favorable activity of chimeric antigen receptor (CAR) T-cell therapy, however, it is unclear whether ASCT would be used in second line. Avoiding the sequential use of ASCT and CAR T-cell therapy is appealing given the stem-cell damage that can result. It is appealing to think about not using ASCT upfront, because ASCT increases the risk of myelodysplastic syndrome.
The TRIANGLE data are likely to change the frontline management of MCL. Although ibrutinib was the first Bruton tyrosine kinase (BTK) inhibitor approved in MCL and has obviously changed the field dramatically, it is significantly less well-tolerated than the next generation of drugs—acalabrutinib and zanubrutinib. I suspect these will be substituted for ibrutinib and we will see even more tolerable upfront regimens for patients with newly diagnosed MCL.
Have there been any disparities that you found in patients newly diagnosed with MCL regarding age, sex, or ethnicity?
Dr. LaCasce: MCL typically affects patients in their 60s. It is rare in young patients, and approximately 75% of the cases are male. If you look at the demographics, it is more common in White patients and less common in Hispanic and African American patients. In addition, there is an association with farming, which likely contribute to the demographics of patients with MCL.
What is your recommended approach to managing patients newly diagnosed with MCL in your day-to-day practice?
Dr. LaCasce: Management is a bit tricky right now because the TRIANGLE study is not part of any guidelines thus far. Therefore, most would argue the standard treatment continues to include ASCT upfront. There is an important, large randomized study (NCT03267433) going on in the United States that is assessing the role of ASCT in patients who are in MRD-negative complete remission at the end of induction therapy. These patients are randomized to ASCT plus maintenance rituximab versus maintenance rituximab alone.
We are still enrolling patients to participate in this study, which is addressing a different question than TRIANGLE. I think we will learn a lot from this study. For patients who are not interested in participating in this study, we talk about the risks and benefits of ASCT.
One or 2 years ago, I would have strongly encouraged patients who were appropriate candidates to consider transplant in first remission. With the TRIANGLE data, however, and now that we have CAR T-cell therapy, I think it is more important to tailor the recommendation to the individual patient. If a patient is reluctant about ASCT and the associated risks, I do not push it.
If patients want the most aggressive approach associated with the longest remissions, at this moment, before TRIANGLE findings have been adopted into guidelines, I continue to recommend ASCT. For patients who have TP53 mutation, however, we treat with typically less aggressive therapy, as this patient population does not benefit from ASCT. We look forward to more data incorporating BTK inhibitors upfront, particularly for this group of patients, who tend to have a more adverse prognosis.
Do you feel MCL data and clinical trials are important areas of focus for your colleagues?
Dr. LaCasce: Yes. I think it is a rapidly evolving field, which is really exciting. We are seeing data now from the bispecific antibodies in the relapsed/refractory setting. We also need more data using pirtobrutinib for patients who have had BTK inhibitors and compare pirtobrutinib (a non-covalent BTK inhibitor) with the covalent BTK inhibitors.
I would strongly encourage patients to participate in clinical trials so that we can better answer these important questions. When patients go online and read about MCL, they often see a median survival of 3 to 4 years, which is completely outdated. The overall prognosis of MCL has changed dramatically since I have been in the field. Hopefully, survival will continue to improve, and therapies will become more tolerable, as well.
Long-COVID rate may be higher with rheumatic diseases
MANCHESTER, England – Data from the COVAD-2 e-survey suggest that people with a rheumatic disease are twice as likely as are those without to experience long-term effects after contracting COVID-19.
The prevalence of post–COVID-19 condition (PCC), the term the World Health Organization advocates for describing the widely popularized term long COVID, was 10.8% among people with autoimmune rheumatic diseases (AIRDs) vs. 5.3% among those with no autoimmune condition (designated as “healthy controls”). The odds ratio was 2.1, with a 95% confidence interval of 1.4-3.2 and a P-value of .002.
The prevalence in people with nonrheumatic autoimmune diseases was also higher than it was in the control participants but still lower, at 7.3%, than in those with AIRDs.
“Our findings highlight the importance of close monitoring for PCC,” Arvind Nune, MBBCh, MSc, said in a virtual poster presentation at the annual meeting of the British Society for Rheumatology.
They also show the need for “appropriate referral for optimized multidisciplinary care for patients with autoimmune rheumatic diseases during the recovery period following COVID-19,” added Dr. Nune, who works for Southport (England) and Ormskirk Hospital NHS Trust.
In an interview, he noted that it was patients who had a severe COVID-19 course or had other coexisting conditions that appeared to experience more long-term effects than did their less-affected counterparts.
Commenting on the study, Jeffrey A. Sparks, MD, MMSc, told this news organization: “This is one of the first studies to find that the prevalence of long COVID is higher among people with systemic rheumatic diseases than those without.”
Dr. Sparks, who is based at Brigham and Women’s Hospital and Harvard Medical School in Boston, added: “Since the symptoms of long COVID and rheumatic diseases can overlap substantially, more work will need to be done to determine whether COVID may have induced flares, new symptoms, or whether the finding is due to the presence of the chronic rheumatic disease.”
The COVAD study
Using an electronic survey platform, the COVAD study has been set up to look at the long-term efficacy and safety of COVID-19 vaccinations in patients with AIRDs. It’s now a large international effort involving more than 150 collaborating clinics in 106 countries.
A huge amount of data has been collected. “We collected demographics, details of autoimmune disease, including treatment, comorbidity, COVID infection, vaccination history and outcomes, date on flares, and validated patient-reported outcomes, including pain, fatigue, physical function, and quality of life,” Dr. Nune said in his presentation.
A total of 12,358 people who were invited to participate responded to the e-survey. Of them, 2,640 were confirmed to have COVID-19. Because the analysis aimed to look at PCC, anyone who had completed the survey less than 3 months after infection was excluded. This left 1,677 eligible respondents, of whom, an overall 8.7% (n = 136) were identified as having PCC.
“The [WHO] definition for PCC was employed, which is persistent signs or symptoms beyond 3 months of COVID-19 infection lasting at least 2 months,” Dr. Nune told this news organization.
“Symptoms could be anything from fatigue to breathlessness to arthralgias,” he added. However, the focus of the present analysis was to look at how many people were experiencing the condition rather than specific symptoms.
A higher risk for PCC was seen in women than in men (OR, 2.9; 95% CI, 1.1-7.7; P = .037) in the entire cohort.
In addition, those with comorbidities were found to have a greater chance of long-term sequelae from COVID-19 than were those without comorbid disease (OR, 2.8; 95% CI, 1.4-5.7; P = .005).
Patients who experienced more severe acute COVID-19, such as those who needed intensive care treatment, oxygen therapy, or advanced treatment for COVID-19 with monoclonal antibodies, were significantly more likely to later have PCC than were those who did not (OR, 3.8; 95% CI, 1.1-13.6; P = .039).
Having PCC was also associated with poorer patient-reported outcomes for physical function, compared with not having PCC. “However, no association with disease flares of underlying rheumatic diseases or immunosuppressive drugs used were noted,” Dr. Nune said.
These new findings from the COVAD study should be published soon. Dr. Nune suggested that the findings might be used to help identify patients early so that they can be referred to the appropriate services in good time.
The COVAD study was independently supported. Dr. Nune reports no relevant financial relationships. Dr. Sparks is supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the R. Bruce and Joan M. Mickey Research Scholar Fund, and the Llura Gund Award for Rheumatoid Arthritis Research and Care. Dr. Sparks has received research support from Bristol-Myers Squibb and performed consultancy for AbbVie, Amgen, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead, Inova Diagnostics, Janssen, Optum, and Pfizer.
MANCHESTER, England – Data from the COVAD-2 e-survey suggest that people with a rheumatic disease are twice as likely as are those without to experience long-term effects after contracting COVID-19.
The prevalence of post–COVID-19 condition (PCC), the term the World Health Organization advocates for describing the widely popularized term long COVID, was 10.8% among people with autoimmune rheumatic diseases (AIRDs) vs. 5.3% among those with no autoimmune condition (designated as “healthy controls”). The odds ratio was 2.1, with a 95% confidence interval of 1.4-3.2 and a P-value of .002.
The prevalence in people with nonrheumatic autoimmune diseases was also higher than it was in the control participants but still lower, at 7.3%, than in those with AIRDs.
“Our findings highlight the importance of close monitoring for PCC,” Arvind Nune, MBBCh, MSc, said in a virtual poster presentation at the annual meeting of the British Society for Rheumatology.
They also show the need for “appropriate referral for optimized multidisciplinary care for patients with autoimmune rheumatic diseases during the recovery period following COVID-19,” added Dr. Nune, who works for Southport (England) and Ormskirk Hospital NHS Trust.
In an interview, he noted that it was patients who had a severe COVID-19 course or had other coexisting conditions that appeared to experience more long-term effects than did their less-affected counterparts.
Commenting on the study, Jeffrey A. Sparks, MD, MMSc, told this news organization: “This is one of the first studies to find that the prevalence of long COVID is higher among people with systemic rheumatic diseases than those without.”
Dr. Sparks, who is based at Brigham and Women’s Hospital and Harvard Medical School in Boston, added: “Since the symptoms of long COVID and rheumatic diseases can overlap substantially, more work will need to be done to determine whether COVID may have induced flares, new symptoms, or whether the finding is due to the presence of the chronic rheumatic disease.”
The COVAD study
Using an electronic survey platform, the COVAD study has been set up to look at the long-term efficacy and safety of COVID-19 vaccinations in patients with AIRDs. It’s now a large international effort involving more than 150 collaborating clinics in 106 countries.
A huge amount of data has been collected. “We collected demographics, details of autoimmune disease, including treatment, comorbidity, COVID infection, vaccination history and outcomes, date on flares, and validated patient-reported outcomes, including pain, fatigue, physical function, and quality of life,” Dr. Nune said in his presentation.
A total of 12,358 people who were invited to participate responded to the e-survey. Of them, 2,640 were confirmed to have COVID-19. Because the analysis aimed to look at PCC, anyone who had completed the survey less than 3 months after infection was excluded. This left 1,677 eligible respondents, of whom, an overall 8.7% (n = 136) were identified as having PCC.
“The [WHO] definition for PCC was employed, which is persistent signs or symptoms beyond 3 months of COVID-19 infection lasting at least 2 months,” Dr. Nune told this news organization.
“Symptoms could be anything from fatigue to breathlessness to arthralgias,” he added. However, the focus of the present analysis was to look at how many people were experiencing the condition rather than specific symptoms.
A higher risk for PCC was seen in women than in men (OR, 2.9; 95% CI, 1.1-7.7; P = .037) in the entire cohort.
In addition, those with comorbidities were found to have a greater chance of long-term sequelae from COVID-19 than were those without comorbid disease (OR, 2.8; 95% CI, 1.4-5.7; P = .005).
Patients who experienced more severe acute COVID-19, such as those who needed intensive care treatment, oxygen therapy, or advanced treatment for COVID-19 with monoclonal antibodies, were significantly more likely to later have PCC than were those who did not (OR, 3.8; 95% CI, 1.1-13.6; P = .039).
Having PCC was also associated with poorer patient-reported outcomes for physical function, compared with not having PCC. “However, no association with disease flares of underlying rheumatic diseases or immunosuppressive drugs used were noted,” Dr. Nune said.
These new findings from the COVAD study should be published soon. Dr. Nune suggested that the findings might be used to help identify patients early so that they can be referred to the appropriate services in good time.
The COVAD study was independently supported. Dr. Nune reports no relevant financial relationships. Dr. Sparks is supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the R. Bruce and Joan M. Mickey Research Scholar Fund, and the Llura Gund Award for Rheumatoid Arthritis Research and Care. Dr. Sparks has received research support from Bristol-Myers Squibb and performed consultancy for AbbVie, Amgen, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead, Inova Diagnostics, Janssen, Optum, and Pfizer.
MANCHESTER, England – Data from the COVAD-2 e-survey suggest that people with a rheumatic disease are twice as likely as are those without to experience long-term effects after contracting COVID-19.
The prevalence of post–COVID-19 condition (PCC), the term the World Health Organization advocates for describing the widely popularized term long COVID, was 10.8% among people with autoimmune rheumatic diseases (AIRDs) vs. 5.3% among those with no autoimmune condition (designated as “healthy controls”). The odds ratio was 2.1, with a 95% confidence interval of 1.4-3.2 and a P-value of .002.
The prevalence in people with nonrheumatic autoimmune diseases was also higher than it was in the control participants but still lower, at 7.3%, than in those with AIRDs.
“Our findings highlight the importance of close monitoring for PCC,” Arvind Nune, MBBCh, MSc, said in a virtual poster presentation at the annual meeting of the British Society for Rheumatology.
They also show the need for “appropriate referral for optimized multidisciplinary care for patients with autoimmune rheumatic diseases during the recovery period following COVID-19,” added Dr. Nune, who works for Southport (England) and Ormskirk Hospital NHS Trust.
In an interview, he noted that it was patients who had a severe COVID-19 course or had other coexisting conditions that appeared to experience more long-term effects than did their less-affected counterparts.
Commenting on the study, Jeffrey A. Sparks, MD, MMSc, told this news organization: “This is one of the first studies to find that the prevalence of long COVID is higher among people with systemic rheumatic diseases than those without.”
Dr. Sparks, who is based at Brigham and Women’s Hospital and Harvard Medical School in Boston, added: “Since the symptoms of long COVID and rheumatic diseases can overlap substantially, more work will need to be done to determine whether COVID may have induced flares, new symptoms, or whether the finding is due to the presence of the chronic rheumatic disease.”
The COVAD study
Using an electronic survey platform, the COVAD study has been set up to look at the long-term efficacy and safety of COVID-19 vaccinations in patients with AIRDs. It’s now a large international effort involving more than 150 collaborating clinics in 106 countries.
A huge amount of data has been collected. “We collected demographics, details of autoimmune disease, including treatment, comorbidity, COVID infection, vaccination history and outcomes, date on flares, and validated patient-reported outcomes, including pain, fatigue, physical function, and quality of life,” Dr. Nune said in his presentation.
A total of 12,358 people who were invited to participate responded to the e-survey. Of them, 2,640 were confirmed to have COVID-19. Because the analysis aimed to look at PCC, anyone who had completed the survey less than 3 months after infection was excluded. This left 1,677 eligible respondents, of whom, an overall 8.7% (n = 136) were identified as having PCC.
“The [WHO] definition for PCC was employed, which is persistent signs or symptoms beyond 3 months of COVID-19 infection lasting at least 2 months,” Dr. Nune told this news organization.
“Symptoms could be anything from fatigue to breathlessness to arthralgias,” he added. However, the focus of the present analysis was to look at how many people were experiencing the condition rather than specific symptoms.
A higher risk for PCC was seen in women than in men (OR, 2.9; 95% CI, 1.1-7.7; P = .037) in the entire cohort.
In addition, those with comorbidities were found to have a greater chance of long-term sequelae from COVID-19 than were those without comorbid disease (OR, 2.8; 95% CI, 1.4-5.7; P = .005).
Patients who experienced more severe acute COVID-19, such as those who needed intensive care treatment, oxygen therapy, or advanced treatment for COVID-19 with monoclonal antibodies, were significantly more likely to later have PCC than were those who did not (OR, 3.8; 95% CI, 1.1-13.6; P = .039).
Having PCC was also associated with poorer patient-reported outcomes for physical function, compared with not having PCC. “However, no association with disease flares of underlying rheumatic diseases or immunosuppressive drugs used were noted,” Dr. Nune said.
These new findings from the COVAD study should be published soon. Dr. Nune suggested that the findings might be used to help identify patients early so that they can be referred to the appropriate services in good time.
The COVAD study was independently supported. Dr. Nune reports no relevant financial relationships. Dr. Sparks is supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the R. Bruce and Joan M. Mickey Research Scholar Fund, and the Llura Gund Award for Rheumatoid Arthritis Research and Care. Dr. Sparks has received research support from Bristol-Myers Squibb and performed consultancy for AbbVie, Amgen, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead, Inova Diagnostics, Janssen, Optum, and Pfizer.
AT BSR 2023
The nation’s health secretary has this obstetrician on call
She’s seen progress, albeit slow, over three decades, yet the number of maternal deaths each year continues to rise.
Luckily, she’s got the ear of President Joe Biden’s health secretary.
Dr. Reyes, 64, is married to Health and Human Services Secretary Xavier Becerra, who is championing the administration’s initiative to require all states to provide Medicaid coverage to mothers for a year after giving birth. In March, the Centers for Disease Control and Prevention released data showing a 40% increase in U.S. maternal deaths from 2020 to 2021. The mortality rate among Black women was 2.6 times that of white women, no matter their economic status.
Over the years, Mr. Becerra has spoken highly of his wife’s expertise, but she downplays her influence, saying her husband of nearly 35 years “had it in him to begin with” to improve health care for women and to demand fewer pregnancy-related deaths. She, too, describes the nation’s high maternal mortality rate as unacceptable and preventable.
Dr. Reyes, a Latina who grew up as one of eight children in California’s agricultural heartland, now practices perinatology at the University of California, Davis. She is a member of a California Department of Public Health panel that reviews cases of maternal deaths and recommends improvements. And she chairs the board of the California Health Care Foundation, a nonprofit that works to increase health care access. (California Healthline is an editorially independent service of the California Health Care Foundation.)
Her work has been a blend of medicine and advocacy, and she worries recent federal court rulings will erode hard-fought victories regarding the safety of pregnant women and their babies. She discussed the nation’s maternal health crisis and health care disparities in an interview, which has been edited for length and clarity.
Question: When did you first realize there are disparities in the health care system?
Answer: When I was in high school in the Fresno Unified School District, we were under a consent decree to desegregate. And I was, at the time, student body president at Roosevelt High School. I was asked to be on this unified school district desegregation task force, where the district had to come up with a plan.
It was a time when I really had incredible exposure to how policies are made at a larger level, societal level, that really determine where people live, where they can seek health care, where they go to school. That experience had a tremendous impact on my life in terms of what I wanted to do in a career and how to give back.
Q: The U.S. has one of the best health care systems in the world, yet the maternal mortality rate is high compared with other developed countries. Why do think that is?
A. What we know by the CDC and maternal mortality review committees is that about 60% of maternal deaths are considered preventable. And that’s really been a lot of what I’ve tried to focus on: What can we do to reduce the severity of disease? Or what can we do within the role that we play in maternal health that can reduce that?
We know that there are societal issues absolutely that increase women’s risks and there are public health issues. But there’s a role that hospitals play in helping reduce that risk. Ten years ago, I was on the maternal mortality review committee for the state of California when we started reviewing cases of women who died within hospital systems to see, “Is there a role that we can play in a hospital system to reduce that risk?”
We recognized that sometimes there were conditions that were not recognized early enough so that there was a delay in the care. Sometimes there was a misdiagnosis. Or in some hospital systems, especially rural systems where there aren’t as many resources, sometimes there was the lack of specialists available. So, we’ve identified these risks and said, “We can do something about them.”
Q: You served on a federal panel 20 years ago that published a groundbreaking report identifying racism in health care. It seems as if we could be much further along.
A. The purpose of that committee was to really answer the question: Do patients receive a different level of care based on race? Looking back, we knew there was something there, but we really didn’t know. And it took months for the committee to come to that agreement, that there was a difference. I mean, that was honestly monumental, because we just didn’t have that level of consensus before. And so just to say “That treatment is unequal and it’s unacceptable” was really profound.
We thought that the 700-page report was going to be a time period where there was going to be tremendous movement, and I think I’ve learned over 20 years that change doesn’t happen quickly, especially when providers and health systems don’t see that they play a role. It’s like … “OK, so maybe it exists, but not for me.”
We all saw George Floyd and how he was treated. And during COVID we saw a tremendous difference in who was dying, right? Underrepresented minorities – certainly much higher. It was that culmination that made us realize the elephant in the room. We can’t ignore that this does exist, that there is a difference in how people are treated, even in our health care system.
Q: When addressing racism in health care, you talk about diversifying not just the health care workforce, but also the boardrooms of hospitals and health systems. Why is that important?
A. At the board level, change is hard. But we all play a role because leadership really helps determine much of what’s carried out. So, to have a leadership that is understanding and representative of the communities they serve, I think it has been demonstrated that we do make a difference.
Q: As a health care provider, do you have a wish list of policies you’d like the government to take up?
A. There was tremendous effort around offering preventive health services as a part of what was covered under the Affordable Care Act. And individuals exhaled, finally thinking this is a tremendous win, especially for women in pregnancy. Because we fought for preventive health services to help them have access so they can prepare for their pregnancy. So, for women, this was huge. But now with the Texas federal court ruling that the U.S. Preventive Services Task Force didn’t have any authority, it is a tremendous step backward.
We have culturally, linguistically appropriate standards in place, but it’s a matter in terms of how they’re carried out by state and by individual hospital systems. My wish list is that we really do listen to our patients, speak to them in a language of their choice, and provide them written materials in the language of their choice. We don’t fully do that.
Q: You mentioned one Texas ruling on the ACA. What’s your take on the ruling by another Texas judge suspending the abortion pill? And the U.S. Supreme Court’s overturning of Roe v. Wade?A. As a maternal-fetal medicine specialist who tries to help women plan for pregnancies, those rulings are a tremendous setback.
Q: And what about women of color? Will they find access to abortion services more difficult?
A. Oh, absolutely. When we speak of underrepresented minorities or those with less resources, they have less resources to then seek the appropriate care. Some women may have the opportunity to go to a different state or seek care elsewhere if their state doesn’t provide it. Many women just don’t have those resources to devote to them and don’t have a choice. So, we will see that disparity widen.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
She’s seen progress, albeit slow, over three decades, yet the number of maternal deaths each year continues to rise.
Luckily, she’s got the ear of President Joe Biden’s health secretary.
Dr. Reyes, 64, is married to Health and Human Services Secretary Xavier Becerra, who is championing the administration’s initiative to require all states to provide Medicaid coverage to mothers for a year after giving birth. In March, the Centers for Disease Control and Prevention released data showing a 40% increase in U.S. maternal deaths from 2020 to 2021. The mortality rate among Black women was 2.6 times that of white women, no matter their economic status.
Over the years, Mr. Becerra has spoken highly of his wife’s expertise, but she downplays her influence, saying her husband of nearly 35 years “had it in him to begin with” to improve health care for women and to demand fewer pregnancy-related deaths. She, too, describes the nation’s high maternal mortality rate as unacceptable and preventable.
Dr. Reyes, a Latina who grew up as one of eight children in California’s agricultural heartland, now practices perinatology at the University of California, Davis. She is a member of a California Department of Public Health panel that reviews cases of maternal deaths and recommends improvements. And she chairs the board of the California Health Care Foundation, a nonprofit that works to increase health care access. (California Healthline is an editorially independent service of the California Health Care Foundation.)
Her work has been a blend of medicine and advocacy, and she worries recent federal court rulings will erode hard-fought victories regarding the safety of pregnant women and their babies. She discussed the nation’s maternal health crisis and health care disparities in an interview, which has been edited for length and clarity.
Question: When did you first realize there are disparities in the health care system?
Answer: When I was in high school in the Fresno Unified School District, we were under a consent decree to desegregate. And I was, at the time, student body president at Roosevelt High School. I was asked to be on this unified school district desegregation task force, where the district had to come up with a plan.
It was a time when I really had incredible exposure to how policies are made at a larger level, societal level, that really determine where people live, where they can seek health care, where they go to school. That experience had a tremendous impact on my life in terms of what I wanted to do in a career and how to give back.
Q: The U.S. has one of the best health care systems in the world, yet the maternal mortality rate is high compared with other developed countries. Why do think that is?
A. What we know by the CDC and maternal mortality review committees is that about 60% of maternal deaths are considered preventable. And that’s really been a lot of what I’ve tried to focus on: What can we do to reduce the severity of disease? Or what can we do within the role that we play in maternal health that can reduce that?
We know that there are societal issues absolutely that increase women’s risks and there are public health issues. But there’s a role that hospitals play in helping reduce that risk. Ten years ago, I was on the maternal mortality review committee for the state of California when we started reviewing cases of women who died within hospital systems to see, “Is there a role that we can play in a hospital system to reduce that risk?”
We recognized that sometimes there were conditions that were not recognized early enough so that there was a delay in the care. Sometimes there was a misdiagnosis. Or in some hospital systems, especially rural systems where there aren’t as many resources, sometimes there was the lack of specialists available. So, we’ve identified these risks and said, “We can do something about them.”
Q: You served on a federal panel 20 years ago that published a groundbreaking report identifying racism in health care. It seems as if we could be much further along.
A. The purpose of that committee was to really answer the question: Do patients receive a different level of care based on race? Looking back, we knew there was something there, but we really didn’t know. And it took months for the committee to come to that agreement, that there was a difference. I mean, that was honestly monumental, because we just didn’t have that level of consensus before. And so just to say “That treatment is unequal and it’s unacceptable” was really profound.
We thought that the 700-page report was going to be a time period where there was going to be tremendous movement, and I think I’ve learned over 20 years that change doesn’t happen quickly, especially when providers and health systems don’t see that they play a role. It’s like … “OK, so maybe it exists, but not for me.”
We all saw George Floyd and how he was treated. And during COVID we saw a tremendous difference in who was dying, right? Underrepresented minorities – certainly much higher. It was that culmination that made us realize the elephant in the room. We can’t ignore that this does exist, that there is a difference in how people are treated, even in our health care system.
Q: When addressing racism in health care, you talk about diversifying not just the health care workforce, but also the boardrooms of hospitals and health systems. Why is that important?
A. At the board level, change is hard. But we all play a role because leadership really helps determine much of what’s carried out. So, to have a leadership that is understanding and representative of the communities they serve, I think it has been demonstrated that we do make a difference.
Q: As a health care provider, do you have a wish list of policies you’d like the government to take up?
A. There was tremendous effort around offering preventive health services as a part of what was covered under the Affordable Care Act. And individuals exhaled, finally thinking this is a tremendous win, especially for women in pregnancy. Because we fought for preventive health services to help them have access so they can prepare for their pregnancy. So, for women, this was huge. But now with the Texas federal court ruling that the U.S. Preventive Services Task Force didn’t have any authority, it is a tremendous step backward.
We have culturally, linguistically appropriate standards in place, but it’s a matter in terms of how they’re carried out by state and by individual hospital systems. My wish list is that we really do listen to our patients, speak to them in a language of their choice, and provide them written materials in the language of their choice. We don’t fully do that.
Q: You mentioned one Texas ruling on the ACA. What’s your take on the ruling by another Texas judge suspending the abortion pill? And the U.S. Supreme Court’s overturning of Roe v. Wade?A. As a maternal-fetal medicine specialist who tries to help women plan for pregnancies, those rulings are a tremendous setback.
Q: And what about women of color? Will they find access to abortion services more difficult?
A. Oh, absolutely. When we speak of underrepresented minorities or those with less resources, they have less resources to then seek the appropriate care. Some women may have the opportunity to go to a different state or seek care elsewhere if their state doesn’t provide it. Many women just don’t have those resources to devote to them and don’t have a choice. So, we will see that disparity widen.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
She’s seen progress, albeit slow, over three decades, yet the number of maternal deaths each year continues to rise.
Luckily, she’s got the ear of President Joe Biden’s health secretary.
Dr. Reyes, 64, is married to Health and Human Services Secretary Xavier Becerra, who is championing the administration’s initiative to require all states to provide Medicaid coverage to mothers for a year after giving birth. In March, the Centers for Disease Control and Prevention released data showing a 40% increase in U.S. maternal deaths from 2020 to 2021. The mortality rate among Black women was 2.6 times that of white women, no matter their economic status.
Over the years, Mr. Becerra has spoken highly of his wife’s expertise, but she downplays her influence, saying her husband of nearly 35 years “had it in him to begin with” to improve health care for women and to demand fewer pregnancy-related deaths. She, too, describes the nation’s high maternal mortality rate as unacceptable and preventable.
Dr. Reyes, a Latina who grew up as one of eight children in California’s agricultural heartland, now practices perinatology at the University of California, Davis. She is a member of a California Department of Public Health panel that reviews cases of maternal deaths and recommends improvements. And she chairs the board of the California Health Care Foundation, a nonprofit that works to increase health care access. (California Healthline is an editorially independent service of the California Health Care Foundation.)
Her work has been a blend of medicine and advocacy, and she worries recent federal court rulings will erode hard-fought victories regarding the safety of pregnant women and their babies. She discussed the nation’s maternal health crisis and health care disparities in an interview, which has been edited for length and clarity.
Question: When did you first realize there are disparities in the health care system?
Answer: When I was in high school in the Fresno Unified School District, we were under a consent decree to desegregate. And I was, at the time, student body president at Roosevelt High School. I was asked to be on this unified school district desegregation task force, where the district had to come up with a plan.
It was a time when I really had incredible exposure to how policies are made at a larger level, societal level, that really determine where people live, where they can seek health care, where they go to school. That experience had a tremendous impact on my life in terms of what I wanted to do in a career and how to give back.
Q: The U.S. has one of the best health care systems in the world, yet the maternal mortality rate is high compared with other developed countries. Why do think that is?
A. What we know by the CDC and maternal mortality review committees is that about 60% of maternal deaths are considered preventable. And that’s really been a lot of what I’ve tried to focus on: What can we do to reduce the severity of disease? Or what can we do within the role that we play in maternal health that can reduce that?
We know that there are societal issues absolutely that increase women’s risks and there are public health issues. But there’s a role that hospitals play in helping reduce that risk. Ten years ago, I was on the maternal mortality review committee for the state of California when we started reviewing cases of women who died within hospital systems to see, “Is there a role that we can play in a hospital system to reduce that risk?”
We recognized that sometimes there were conditions that were not recognized early enough so that there was a delay in the care. Sometimes there was a misdiagnosis. Or in some hospital systems, especially rural systems where there aren’t as many resources, sometimes there was the lack of specialists available. So, we’ve identified these risks and said, “We can do something about them.”
Q: You served on a federal panel 20 years ago that published a groundbreaking report identifying racism in health care. It seems as if we could be much further along.
A. The purpose of that committee was to really answer the question: Do patients receive a different level of care based on race? Looking back, we knew there was something there, but we really didn’t know. And it took months for the committee to come to that agreement, that there was a difference. I mean, that was honestly monumental, because we just didn’t have that level of consensus before. And so just to say “That treatment is unequal and it’s unacceptable” was really profound.
We thought that the 700-page report was going to be a time period where there was going to be tremendous movement, and I think I’ve learned over 20 years that change doesn’t happen quickly, especially when providers and health systems don’t see that they play a role. It’s like … “OK, so maybe it exists, but not for me.”
We all saw George Floyd and how he was treated. And during COVID we saw a tremendous difference in who was dying, right? Underrepresented minorities – certainly much higher. It was that culmination that made us realize the elephant in the room. We can’t ignore that this does exist, that there is a difference in how people are treated, even in our health care system.
Q: When addressing racism in health care, you talk about diversifying not just the health care workforce, but also the boardrooms of hospitals and health systems. Why is that important?
A. At the board level, change is hard. But we all play a role because leadership really helps determine much of what’s carried out. So, to have a leadership that is understanding and representative of the communities they serve, I think it has been demonstrated that we do make a difference.
Q: As a health care provider, do you have a wish list of policies you’d like the government to take up?
A. There was tremendous effort around offering preventive health services as a part of what was covered under the Affordable Care Act. And individuals exhaled, finally thinking this is a tremendous win, especially for women in pregnancy. Because we fought for preventive health services to help them have access so they can prepare for their pregnancy. So, for women, this was huge. But now with the Texas federal court ruling that the U.S. Preventive Services Task Force didn’t have any authority, it is a tremendous step backward.
We have culturally, linguistically appropriate standards in place, but it’s a matter in terms of how they’re carried out by state and by individual hospital systems. My wish list is that we really do listen to our patients, speak to them in a language of their choice, and provide them written materials in the language of their choice. We don’t fully do that.
Q: You mentioned one Texas ruling on the ACA. What’s your take on the ruling by another Texas judge suspending the abortion pill? And the U.S. Supreme Court’s overturning of Roe v. Wade?A. As a maternal-fetal medicine specialist who tries to help women plan for pregnancies, those rulings are a tremendous setback.
Q: And what about women of color? Will they find access to abortion services more difficult?
A. Oh, absolutely. When we speak of underrepresented minorities or those with less resources, they have less resources to then seek the appropriate care. Some women may have the opportunity to go to a different state or seek care elsewhere if their state doesn’t provide it. Many women just don’t have those resources to devote to them and don’t have a choice. So, we will see that disparity widen.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
Pustules on face
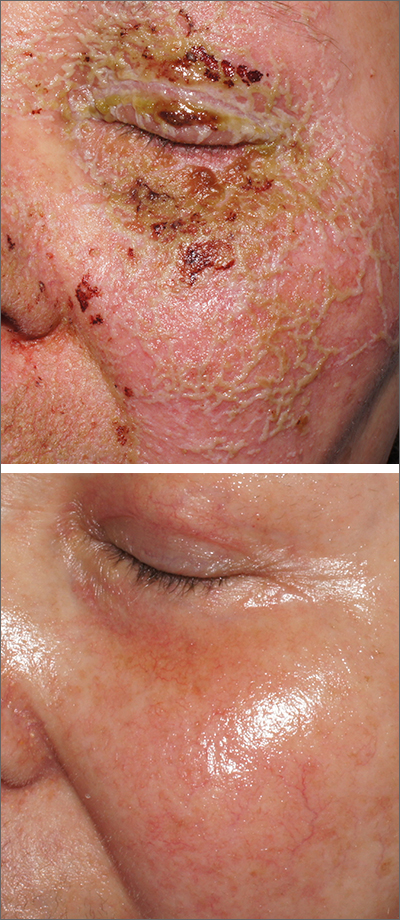
A review of the patient’s chemotherapy medications revealed that 4 weeks earlier, panitumumab had been added to her folinic acid, fluorouracil, and irinotecan (FOLFIRI) regimen. The physician diagnosed this acneiform eruption as an adverse effect of the panitumumab.
Panitumumab is a monoclonal antibody that works to inhibit epidermal growth factor receptor (EGFR) proteins that are overexpressed on some solid tumors and responsible for cancer cell proliferation. EGFR inhibitor–induced acneiform eruptions are common in patients receiving panitumumab.
EGFR proteins have been a target of chemotherapy since the approval of the small molecule erlotinib in 2004. Panitumumab and cetuximab are monoclonal antibodies targeting EGFR and improve long-term survival in patients with metastatic colorectal cancer when added to other standard chemotherapy regimens. EGFR is found throughout the epidermis and all EGFR inhibitors may cause unique skin toxicity not seen with other chemotherapy agents. In 1 study of 229 patients, 59% of patients exhibited skin toxicity at Day 15; the most common examples included widespread acne-like papules and pustules or an eczema-like manifestation.1 Eruptions may be worsened by significant sun exposure while on panitumumab. In this case, the acneiform eruption occurred more intensely along visible facial telangiectasias.
When EGFR inhibitor–induced acneiform eruption occurs, patients commonly develop skin toxicity within the first 2 to 4 weeks of therapy. Pre-therapy doxycycline or minocycline and/or topical steroids may help prevent toxicities from occurring. These same therapies may be used to treat symptoms after they have occurred. More severe cases with systemic symptoms or failure to improve with the above measures may need prednisone or cessation of therapy.
This patient was started on topical hydrocortisone 2.5% ointment twice daily and oral doxycycline 100 mg bid for 6 weeks. She had dramatic improvement within 3 weeks. Doxycycline was subsequently continued at a dose of 100 mg/d and the patient was able to continue with her chemotherapy combination for several more months. Unfortunately, her colon cancer progressed despite therapy and she ultimately died from cancer-related complications.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.
1. Bouché O, Ben Abdelghani M, Labourey JL, et al. Management of skin toxicities during panitumumab treatment in metastatic colorectal cancer. World J Gastroenterol. 2019;25:4007-4018. doi: 10.3748/wjg.v25.i29.4007

A review of the patient’s chemotherapy medications revealed that 4 weeks earlier, panitumumab had been added to her folinic acid, fluorouracil, and irinotecan (FOLFIRI) regimen. The physician diagnosed this acneiform eruption as an adverse effect of the panitumumab.
Panitumumab is a monoclonal antibody that works to inhibit epidermal growth factor receptor (EGFR) proteins that are overexpressed on some solid tumors and responsible for cancer cell proliferation. EGFR inhibitor–induced acneiform eruptions are common in patients receiving panitumumab.
EGFR proteins have been a target of chemotherapy since the approval of the small molecule erlotinib in 2004. Panitumumab and cetuximab are monoclonal antibodies targeting EGFR and improve long-term survival in patients with metastatic colorectal cancer when added to other standard chemotherapy regimens. EGFR is found throughout the epidermis and all EGFR inhibitors may cause unique skin toxicity not seen with other chemotherapy agents. In 1 study of 229 patients, 59% of patients exhibited skin toxicity at Day 15; the most common examples included widespread acne-like papules and pustules or an eczema-like manifestation.1 Eruptions may be worsened by significant sun exposure while on panitumumab. In this case, the acneiform eruption occurred more intensely along visible facial telangiectasias.
When EGFR inhibitor–induced acneiform eruption occurs, patients commonly develop skin toxicity within the first 2 to 4 weeks of therapy. Pre-therapy doxycycline or minocycline and/or topical steroids may help prevent toxicities from occurring. These same therapies may be used to treat symptoms after they have occurred. More severe cases with systemic symptoms or failure to improve with the above measures may need prednisone or cessation of therapy.
This patient was started on topical hydrocortisone 2.5% ointment twice daily and oral doxycycline 100 mg bid for 6 weeks. She had dramatic improvement within 3 weeks. Doxycycline was subsequently continued at a dose of 100 mg/d and the patient was able to continue with her chemotherapy combination for several more months. Unfortunately, her colon cancer progressed despite therapy and she ultimately died from cancer-related complications.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.

A review of the patient’s chemotherapy medications revealed that 4 weeks earlier, panitumumab had been added to her folinic acid, fluorouracil, and irinotecan (FOLFIRI) regimen. The physician diagnosed this acneiform eruption as an adverse effect of the panitumumab.
Panitumumab is a monoclonal antibody that works to inhibit epidermal growth factor receptor (EGFR) proteins that are overexpressed on some solid tumors and responsible for cancer cell proliferation. EGFR inhibitor–induced acneiform eruptions are common in patients receiving panitumumab.
EGFR proteins have been a target of chemotherapy since the approval of the small molecule erlotinib in 2004. Panitumumab and cetuximab are monoclonal antibodies targeting EGFR and improve long-term survival in patients with metastatic colorectal cancer when added to other standard chemotherapy regimens. EGFR is found throughout the epidermis and all EGFR inhibitors may cause unique skin toxicity not seen with other chemotherapy agents. In 1 study of 229 patients, 59% of patients exhibited skin toxicity at Day 15; the most common examples included widespread acne-like papules and pustules or an eczema-like manifestation.1 Eruptions may be worsened by significant sun exposure while on panitumumab. In this case, the acneiform eruption occurred more intensely along visible facial telangiectasias.
When EGFR inhibitor–induced acneiform eruption occurs, patients commonly develop skin toxicity within the first 2 to 4 weeks of therapy. Pre-therapy doxycycline or minocycline and/or topical steroids may help prevent toxicities from occurring. These same therapies may be used to treat symptoms after they have occurred. More severe cases with systemic symptoms or failure to improve with the above measures may need prednisone or cessation of therapy.
This patient was started on topical hydrocortisone 2.5% ointment twice daily and oral doxycycline 100 mg bid for 6 weeks. She had dramatic improvement within 3 weeks. Doxycycline was subsequently continued at a dose of 100 mg/d and the patient was able to continue with her chemotherapy combination for several more months. Unfortunately, her colon cancer progressed despite therapy and she ultimately died from cancer-related complications.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.
1. Bouché O, Ben Abdelghani M, Labourey JL, et al. Management of skin toxicities during panitumumab treatment in metastatic colorectal cancer. World J Gastroenterol. 2019;25:4007-4018. doi: 10.3748/wjg.v25.i29.4007
1. Bouché O, Ben Abdelghani M, Labourey JL, et al. Management of skin toxicities during panitumumab treatment in metastatic colorectal cancer. World J Gastroenterol. 2019;25:4007-4018. doi: 10.3748/wjg.v25.i29.4007