User login
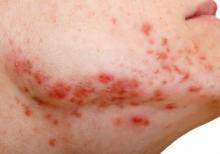
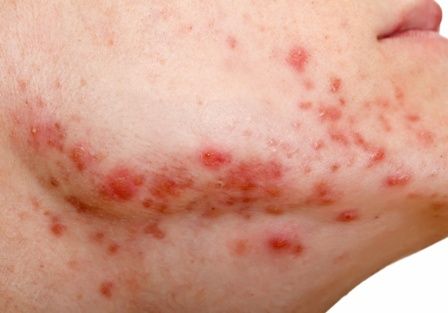
TCA and punch excision are two options for icepick acne scars
WAIKOLOA, HAWAII – Dermatologists can certainly improve icepick acne scars, but they have to be careful not to make them worse, according to dermatologist Nazanin Saedi, MD, director of the Jefferson Laser Surgery and Cosmetic Dermatology Center at Thomas Jefferson University, Philadelphia.
.
After about three to five TCA treatments, most patients will have a better than 50% improvement, Dr. Saedi said, but the treatment isn’t for darker skin types – Fitzpatrick types V or VI – because of the risk of pigmentation changes. Dr. Saedi uses toothpicks to apply a small amount of 80% TCA to the base of the scar, and waits for the “frost” to appear. It’s important not to reapply the TCA. “A lot of people double dip and ... keep dipping into the scar,” which causes more damage.
For patients with darker skin types, or those who don’t want to go through a series of treatments, punch excision is an option, with nonablative laser treatment a week later when sutures are removed. “Some patients heal beautifully,” but some patients may have a spread scar or a small atrophic scar at the punch site, she noted. Options to treat atrophic scarring after treatment are laser treatments and fillers.
She offered her advice in an interview at the Hawaii Dermatology Seminar, provided by the Global Academy for Medical Education/Skin Disease Education Foundation. It’s important to set realistic expectations, Dr. Saedi said.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Dermatologists can certainly improve icepick acne scars, but they have to be careful not to make them worse, according to dermatologist Nazanin Saedi, MD, director of the Jefferson Laser Surgery and Cosmetic Dermatology Center at Thomas Jefferson University, Philadelphia.
.
After about three to five TCA treatments, most patients will have a better than 50% improvement, Dr. Saedi said, but the treatment isn’t for darker skin types – Fitzpatrick types V or VI – because of the risk of pigmentation changes. Dr. Saedi uses toothpicks to apply a small amount of 80% TCA to the base of the scar, and waits for the “frost” to appear. It’s important not to reapply the TCA. “A lot of people double dip and ... keep dipping into the scar,” which causes more damage.
For patients with darker skin types, or those who don’t want to go through a series of treatments, punch excision is an option, with nonablative laser treatment a week later when sutures are removed. “Some patients heal beautifully,” but some patients may have a spread scar or a small atrophic scar at the punch site, she noted. Options to treat atrophic scarring after treatment are laser treatments and fillers.
She offered her advice in an interview at the Hawaii Dermatology Seminar, provided by the Global Academy for Medical Education/Skin Disease Education Foundation. It’s important to set realistic expectations, Dr. Saedi said.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – Dermatologists can certainly improve icepick acne scars, but they have to be careful not to make them worse, according to dermatologist Nazanin Saedi, MD, director of the Jefferson Laser Surgery and Cosmetic Dermatology Center at Thomas Jefferson University, Philadelphia.
.
After about three to five TCA treatments, most patients will have a better than 50% improvement, Dr. Saedi said, but the treatment isn’t for darker skin types – Fitzpatrick types V or VI – because of the risk of pigmentation changes. Dr. Saedi uses toothpicks to apply a small amount of 80% TCA to the base of the scar, and waits for the “frost” to appear. It’s important not to reapply the TCA. “A lot of people double dip and ... keep dipping into the scar,” which causes more damage.
For patients with darker skin types, or those who don’t want to go through a series of treatments, punch excision is an option, with nonablative laser treatment a week later when sutures are removed. “Some patients heal beautifully,” but some patients may have a spread scar or a small atrophic scar at the punch site, she noted. Options to treat atrophic scarring after treatment are laser treatments and fillers.
She offered her advice in an interview at the Hawaii Dermatology Seminar, provided by the Global Academy for Medical Education/Skin Disease Education Foundation. It’s important to set realistic expectations, Dr. Saedi said.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR
Trump bars abortion referrals from family planning program
The U.S. Department of Health & Human Services has finalized sweeping changes to the federal Title X family planning program, pulling back funds from clinics that provide abortion counseling or that refer patients for abortion services, regardless of whether the money is used for other health care services.
Under the final rule, announced Feb. 22 by HHS, women’s health clinics are ineligible for Title X funding if they offer, promote, or support abortion as a method of family planning. Title X grants generally go to health centers that provide reproductive health care – such as STD-testing, cancer screenings, and contraception – to low-income families.
In a fact sheet, HHS stated the final rule will provide for clear financial and physical separation between Title X and non-Title X activities, reduce confusion on the part of Title X clinics and the public about permissible Title X activities, and improve program transparency by requiring more complete reporting by grantees about their partnerships with referral agencies.
“The final rule ensures compliance with statutory program integrity provisions governing the program and, in particular, the statutory prohibition on funding programs where abortion is a method of family planning,” department officials said in a statement. “The final rule amends the Title X regulation, which had not been substantially updated in nearly 2 decades, and makes notable improvements designed to increase the number of patients served and improve the quality of their care.”
Lisa Hollier, MD, president for the American College of Obstetricians and Gynecologists (ACOG) said the final rule threatens the ability of women’s health care providers to deliver medically accurate and comprehensive reproductive health care and poses significant harms to women’s health.
“As the only federal program exclusively dedicated to providing low-income patients with access to family planning and preventive health services and information, [Title X] plays a vital role in the landscape of women’s health care,” Dr. Hollier said during a Feb. 22 press conference. “By weakening the requirements for the scope of contraceptive care provided by grant recipients and restricting the types of care recipients can discuss with patients, the final rule fundamentally harms the scope and purpose of this historic program.”
The American Medical Association also expressed disappointment, referring to the final requirement as a “gag rule” between physicians and patients.
“This rule interferes with and imposes restrictions on the patient-physician relationship,” Barbara L. McAneny, MD, AMA President said in a statement. “For all intents and purposes, it imposes a gag rule on what information physicians can provide to their patients. The patient-physician relationship relies on trust, open conversation and informed decision making and the government should not be telling physicians what they can and cannot say to their patients.”
Under the rule, proposed last year, physicians are prohibited from discussing abortion options with pregnant women, from sharing abortion information, and from making abortion referrals if the clinic receives Title X funds. The regulation permits, but no longer requires, nondirective pregnancy counseling, including nondirective counseling on abortion. In its statement, HHS officials said the new rule ensures “conscience protections” for Title X health providers by eliminating the requirement for providers to counsel on and refer for abortion.
Susan B. Anthony List, an anti-abortion group, praised the final rule as a measure that disentangles taxpayers from the “big abortion industry led by Planned Parenthood.”
“The Protect Life Rule does not cut family planning funding by a single dime, and instead directs tax dollars to entities that provide health care to women but do not perform abortions,” said SBA List President Marjorie Dannenfelser in a statement. “The Title X program was not intended to be a slush fund for abortion businesses like Planned Parenthood, which violently ends the lives of more than 332,000 unborn babies a year and receives almost $60 million a year in Title X taxpayer dollars.”
Emily Stewart, vice president of public policy for the Planned Parenthood Federation of America indicated that the group plans to fight the rule in court.
“Since day one, the Trump-Pence administration has aggressively targeted the health, rights, and bodily autonomy of people of color, people with low incomes, and women,” she said in a statement. “We’re going to fight this rule through every possible avenue.”
The final rule has been submitted to the Federal Register for publication.
The U.S. Department of Health & Human Services has finalized sweeping changes to the federal Title X family planning program, pulling back funds from clinics that provide abortion counseling or that refer patients for abortion services, regardless of whether the money is used for other health care services.
Under the final rule, announced Feb. 22 by HHS, women’s health clinics are ineligible for Title X funding if they offer, promote, or support abortion as a method of family planning. Title X grants generally go to health centers that provide reproductive health care – such as STD-testing, cancer screenings, and contraception – to low-income families.
In a fact sheet, HHS stated the final rule will provide for clear financial and physical separation between Title X and non-Title X activities, reduce confusion on the part of Title X clinics and the public about permissible Title X activities, and improve program transparency by requiring more complete reporting by grantees about their partnerships with referral agencies.
“The final rule ensures compliance with statutory program integrity provisions governing the program and, in particular, the statutory prohibition on funding programs where abortion is a method of family planning,” department officials said in a statement. “The final rule amends the Title X regulation, which had not been substantially updated in nearly 2 decades, and makes notable improvements designed to increase the number of patients served and improve the quality of their care.”
Lisa Hollier, MD, president for the American College of Obstetricians and Gynecologists (ACOG) said the final rule threatens the ability of women’s health care providers to deliver medically accurate and comprehensive reproductive health care and poses significant harms to women’s health.
“As the only federal program exclusively dedicated to providing low-income patients with access to family planning and preventive health services and information, [Title X] plays a vital role in the landscape of women’s health care,” Dr. Hollier said during a Feb. 22 press conference. “By weakening the requirements for the scope of contraceptive care provided by grant recipients and restricting the types of care recipients can discuss with patients, the final rule fundamentally harms the scope and purpose of this historic program.”
The American Medical Association also expressed disappointment, referring to the final requirement as a “gag rule” between physicians and patients.
“This rule interferes with and imposes restrictions on the patient-physician relationship,” Barbara L. McAneny, MD, AMA President said in a statement. “For all intents and purposes, it imposes a gag rule on what information physicians can provide to their patients. The patient-physician relationship relies on trust, open conversation and informed decision making and the government should not be telling physicians what they can and cannot say to their patients.”
Under the rule, proposed last year, physicians are prohibited from discussing abortion options with pregnant women, from sharing abortion information, and from making abortion referrals if the clinic receives Title X funds. The regulation permits, but no longer requires, nondirective pregnancy counseling, including nondirective counseling on abortion. In its statement, HHS officials said the new rule ensures “conscience protections” for Title X health providers by eliminating the requirement for providers to counsel on and refer for abortion.
Susan B. Anthony List, an anti-abortion group, praised the final rule as a measure that disentangles taxpayers from the “big abortion industry led by Planned Parenthood.”
“The Protect Life Rule does not cut family planning funding by a single dime, and instead directs tax dollars to entities that provide health care to women but do not perform abortions,” said SBA List President Marjorie Dannenfelser in a statement. “The Title X program was not intended to be a slush fund for abortion businesses like Planned Parenthood, which violently ends the lives of more than 332,000 unborn babies a year and receives almost $60 million a year in Title X taxpayer dollars.”
Emily Stewart, vice president of public policy for the Planned Parenthood Federation of America indicated that the group plans to fight the rule in court.
“Since day one, the Trump-Pence administration has aggressively targeted the health, rights, and bodily autonomy of people of color, people with low incomes, and women,” she said in a statement. “We’re going to fight this rule through every possible avenue.”
The final rule has been submitted to the Federal Register for publication.
The U.S. Department of Health & Human Services has finalized sweeping changes to the federal Title X family planning program, pulling back funds from clinics that provide abortion counseling or that refer patients for abortion services, regardless of whether the money is used for other health care services.
Under the final rule, announced Feb. 22 by HHS, women’s health clinics are ineligible for Title X funding if they offer, promote, or support abortion as a method of family planning. Title X grants generally go to health centers that provide reproductive health care – such as STD-testing, cancer screenings, and contraception – to low-income families.
In a fact sheet, HHS stated the final rule will provide for clear financial and physical separation between Title X and non-Title X activities, reduce confusion on the part of Title X clinics and the public about permissible Title X activities, and improve program transparency by requiring more complete reporting by grantees about their partnerships with referral agencies.
“The final rule ensures compliance with statutory program integrity provisions governing the program and, in particular, the statutory prohibition on funding programs where abortion is a method of family planning,” department officials said in a statement. “The final rule amends the Title X regulation, which had not been substantially updated in nearly 2 decades, and makes notable improvements designed to increase the number of patients served and improve the quality of their care.”
Lisa Hollier, MD, president for the American College of Obstetricians and Gynecologists (ACOG) said the final rule threatens the ability of women’s health care providers to deliver medically accurate and comprehensive reproductive health care and poses significant harms to women’s health.
“As the only federal program exclusively dedicated to providing low-income patients with access to family planning and preventive health services and information, [Title X] plays a vital role in the landscape of women’s health care,” Dr. Hollier said during a Feb. 22 press conference. “By weakening the requirements for the scope of contraceptive care provided by grant recipients and restricting the types of care recipients can discuss with patients, the final rule fundamentally harms the scope and purpose of this historic program.”
The American Medical Association also expressed disappointment, referring to the final requirement as a “gag rule” between physicians and patients.
“This rule interferes with and imposes restrictions on the patient-physician relationship,” Barbara L. McAneny, MD, AMA President said in a statement. “For all intents and purposes, it imposes a gag rule on what information physicians can provide to their patients. The patient-physician relationship relies on trust, open conversation and informed decision making and the government should not be telling physicians what they can and cannot say to their patients.”
Under the rule, proposed last year, physicians are prohibited from discussing abortion options with pregnant women, from sharing abortion information, and from making abortion referrals if the clinic receives Title X funds. The regulation permits, but no longer requires, nondirective pregnancy counseling, including nondirective counseling on abortion. In its statement, HHS officials said the new rule ensures “conscience protections” for Title X health providers by eliminating the requirement for providers to counsel on and refer for abortion.
Susan B. Anthony List, an anti-abortion group, praised the final rule as a measure that disentangles taxpayers from the “big abortion industry led by Planned Parenthood.”
“The Protect Life Rule does not cut family planning funding by a single dime, and instead directs tax dollars to entities that provide health care to women but do not perform abortions,” said SBA List President Marjorie Dannenfelser in a statement. “The Title X program was not intended to be a slush fund for abortion businesses like Planned Parenthood, which violently ends the lives of more than 332,000 unborn babies a year and receives almost $60 million a year in Title X taxpayer dollars.”
Emily Stewart, vice president of public policy for the Planned Parenthood Federation of America indicated that the group plans to fight the rule in court.
“Since day one, the Trump-Pence administration has aggressively targeted the health, rights, and bodily autonomy of people of color, people with low incomes, and women,” she said in a statement. “We’re going to fight this rule through every possible avenue.”
The final rule has been submitted to the Federal Register for publication.
Debunking Acne Myths: Patients Need Photoprotection, Not a Tan
Myth: Getting a Tan Helps Improve Acne
Acne has a multifaceted impact on patients, and facial acne in particular can impair self-image, psychological well-being, and ability to develop relationships. Patients cope with the clinical presentation of the disease in various ways, such as wearing makeup to cover blemishes, changing their hair color or diet, or getting regular facials. A common misconception is that a tan will help resolve acne.
A 2014 study on the burden of adult female acne (N=208) found that 5.3% of patients go to tanning salons or lay out in the sun to cope with their acne and 17% use self-tanning products to make their acne less visible. Many patients (40%) also believed that sunscreen exacerbates acne. Furthermore, a study of adolescents in Stockholm reported that those with acne, eczema, or psoriasis used sunbeds more than others without skin diseases.
The risk of developing skin cancer from sun exposure or UV light has been well established, and there is no evidence that UV light helps improve acne. A 2015 review of the literature on tanning bed use and phototherapy associated with treatment of conditions such as acne reported that experimental trials have been conducted for various light source therapies (eg, blue light, red-blue light, photodynamic therapy); however, there is no direct evidence for UV light.
In fact, acne patients should be counseled on the importance of photoprotection. Many acne therapies leave patients predisposed to UV damage, and UV damage generates free radical formation, which has been implicated in acne flares.
Expert Commentary
Often I hear from patients they feel tanning helps improve their acne. I tell them there is no evidence this is at all true. Just like cream makeup can camouflage acne, so too can tanning. But, trying to hide your blemishes does not actually help nor treat them. And moreover, tanning is so dangerous for potential skin cancer later in life.
—Lawrence J. Green, MD (Washington, DC)
Boldeman C, Beitner H, Jansson B, et al. Sunbed use in relation to phenotype, erythema, sunscreen use and skin diseases. a questionnaire survey among Swedish adolescents. Br J Dermatol. 1996;135:712-726.
Bowe WP, Kircik LH. The importance of photoprotection and moisturization in treating acne vulgaris. J Drugs Dermatol. 2014;13:S89-S94.
Radack KP, Farhangian ME, Anderson KL, et al. A review of the use of tanning beds as a dermatological treatment. Dermatol Ther (Heidelb). 2015;5:37-51.
Tanghetti EA, Kawata AK, Daniels SR, et al. Understanding the burden of adult female acne. J Clin Aesthet Dermatol. 2014;7:22-30.
Myth: Getting a Tan Helps Improve Acne
Acne has a multifaceted impact on patients, and facial acne in particular can impair self-image, psychological well-being, and ability to develop relationships. Patients cope with the clinical presentation of the disease in various ways, such as wearing makeup to cover blemishes, changing their hair color or diet, or getting regular facials. A common misconception is that a tan will help resolve acne.
A 2014 study on the burden of adult female acne (N=208) found that 5.3% of patients go to tanning salons or lay out in the sun to cope with their acne and 17% use self-tanning products to make their acne less visible. Many patients (40%) also believed that sunscreen exacerbates acne. Furthermore, a study of adolescents in Stockholm reported that those with acne, eczema, or psoriasis used sunbeds more than others without skin diseases.
The risk of developing skin cancer from sun exposure or UV light has been well established, and there is no evidence that UV light helps improve acne. A 2015 review of the literature on tanning bed use and phototherapy associated with treatment of conditions such as acne reported that experimental trials have been conducted for various light source therapies (eg, blue light, red-blue light, photodynamic therapy); however, there is no direct evidence for UV light.
In fact, acne patients should be counseled on the importance of photoprotection. Many acne therapies leave patients predisposed to UV damage, and UV damage generates free radical formation, which has been implicated in acne flares.
Expert Commentary
Often I hear from patients they feel tanning helps improve their acne. I tell them there is no evidence this is at all true. Just like cream makeup can camouflage acne, so too can tanning. But, trying to hide your blemishes does not actually help nor treat them. And moreover, tanning is so dangerous for potential skin cancer later in life.
—Lawrence J. Green, MD (Washington, DC)
Myth: Getting a Tan Helps Improve Acne
Acne has a multifaceted impact on patients, and facial acne in particular can impair self-image, psychological well-being, and ability to develop relationships. Patients cope with the clinical presentation of the disease in various ways, such as wearing makeup to cover blemishes, changing their hair color or diet, or getting regular facials. A common misconception is that a tan will help resolve acne.
A 2014 study on the burden of adult female acne (N=208) found that 5.3% of patients go to tanning salons or lay out in the sun to cope with their acne and 17% use self-tanning products to make their acne less visible. Many patients (40%) also believed that sunscreen exacerbates acne. Furthermore, a study of adolescents in Stockholm reported that those with acne, eczema, or psoriasis used sunbeds more than others without skin diseases.
The risk of developing skin cancer from sun exposure or UV light has been well established, and there is no evidence that UV light helps improve acne. A 2015 review of the literature on tanning bed use and phototherapy associated with treatment of conditions such as acne reported that experimental trials have been conducted for various light source therapies (eg, blue light, red-blue light, photodynamic therapy); however, there is no direct evidence for UV light.
In fact, acne patients should be counseled on the importance of photoprotection. Many acne therapies leave patients predisposed to UV damage, and UV damage generates free radical formation, which has been implicated in acne flares.
Expert Commentary
Often I hear from patients they feel tanning helps improve their acne. I tell them there is no evidence this is at all true. Just like cream makeup can camouflage acne, so too can tanning. But, trying to hide your blemishes does not actually help nor treat them. And moreover, tanning is so dangerous for potential skin cancer later in life.
—Lawrence J. Green, MD (Washington, DC)
Boldeman C, Beitner H, Jansson B, et al. Sunbed use in relation to phenotype, erythema, sunscreen use and skin diseases. a questionnaire survey among Swedish adolescents. Br J Dermatol. 1996;135:712-726.
Bowe WP, Kircik LH. The importance of photoprotection and moisturization in treating acne vulgaris. J Drugs Dermatol. 2014;13:S89-S94.
Radack KP, Farhangian ME, Anderson KL, et al. A review of the use of tanning beds as a dermatological treatment. Dermatol Ther (Heidelb). 2015;5:37-51.
Tanghetti EA, Kawata AK, Daniels SR, et al. Understanding the burden of adult female acne. J Clin Aesthet Dermatol. 2014;7:22-30.
Boldeman C, Beitner H, Jansson B, et al. Sunbed use in relation to phenotype, erythema, sunscreen use and skin diseases. a questionnaire survey among Swedish adolescents. Br J Dermatol. 1996;135:712-726.
Bowe WP, Kircik LH. The importance of photoprotection and moisturization in treating acne vulgaris. J Drugs Dermatol. 2014;13:S89-S94.
Radack KP, Farhangian ME, Anderson KL, et al. A review of the use of tanning beds as a dermatological treatment. Dermatol Ther (Heidelb). 2015;5:37-51.
Tanghetti EA, Kawata AK, Daniels SR, et al. Understanding the burden of adult female acne. J Clin Aesthet Dermatol. 2014;7:22-30.
Don’t fear spironolactone, isotretinoin, OCs for acne
WAIKOLOA, HAWAII – There’s really , of the department of dermatology at the University of Alabama at Birmingham.
There have been concerns with all three in the past, but most of the worries have been recently laid to rest.
The news hasn’t reached everyone, though, so, by and large, they are “tools I think we are not using enough of,” Dr. Harper said in an interview. With isotretinoin, for instance, it really isn’t necessary to do blood work for lipids and liver function every month, a daunting prospect for patients; baseline testing with a repeat at 2 months is sufficient, as long as there’s no dose escalation and results are acceptable, with the exception of a monthly pregnancy test for women, she noted. Meanwhile, there’s no evidence of a link with inflammatory bowel disease, and wound healing isn’t as much of an issue as once thought.
It’s the same story with spironolactone. Hyperkalemia is a long-standing concern, but it turns out that “in healthy young women taking spironolactone for acne, we don’t need to be checking potassium.” As far as breast cancer goes, the potential risk with spironolactone hasn’t panned out in the literature, and there may not be “a link at all,” Dr. Harper said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
There are caveats, of course. Hormonal treatments shouldn’t be used in young women until they’ve established their menstrual cycle. OCs should not be used in smokers, or people who have hypertension or migraines, among other conditions. Also, elevated triglycerides remain a concern with isotretinoin. “The number I would want people to remember is 500 [mg/dL],” the threshold when triglycerides become a problem.
In the interview, Dr. Harper explained the new thinking on these three options, and shared her treatment tips, including what to do if patients’ triglycerides hit the 500 mg/dL mark.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – There’s really , of the department of dermatology at the University of Alabama at Birmingham.
There have been concerns with all three in the past, but most of the worries have been recently laid to rest.
The news hasn’t reached everyone, though, so, by and large, they are “tools I think we are not using enough of,” Dr. Harper said in an interview. With isotretinoin, for instance, it really isn’t necessary to do blood work for lipids and liver function every month, a daunting prospect for patients; baseline testing with a repeat at 2 months is sufficient, as long as there’s no dose escalation and results are acceptable, with the exception of a monthly pregnancy test for women, she noted. Meanwhile, there’s no evidence of a link with inflammatory bowel disease, and wound healing isn’t as much of an issue as once thought.
It’s the same story with spironolactone. Hyperkalemia is a long-standing concern, but it turns out that “in healthy young women taking spironolactone for acne, we don’t need to be checking potassium.” As far as breast cancer goes, the potential risk with spironolactone hasn’t panned out in the literature, and there may not be “a link at all,” Dr. Harper said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
There are caveats, of course. Hormonal treatments shouldn’t be used in young women until they’ve established their menstrual cycle. OCs should not be used in smokers, or people who have hypertension or migraines, among other conditions. Also, elevated triglycerides remain a concern with isotretinoin. “The number I would want people to remember is 500 [mg/dL],” the threshold when triglycerides become a problem.
In the interview, Dr. Harper explained the new thinking on these three options, and shared her treatment tips, including what to do if patients’ triglycerides hit the 500 mg/dL mark.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
WAIKOLOA, HAWAII – There’s really , of the department of dermatology at the University of Alabama at Birmingham.
There have been concerns with all three in the past, but most of the worries have been recently laid to rest.
The news hasn’t reached everyone, though, so, by and large, they are “tools I think we are not using enough of,” Dr. Harper said in an interview. With isotretinoin, for instance, it really isn’t necessary to do blood work for lipids and liver function every month, a daunting prospect for patients; baseline testing with a repeat at 2 months is sufficient, as long as there’s no dose escalation and results are acceptable, with the exception of a monthly pregnancy test for women, she noted. Meanwhile, there’s no evidence of a link with inflammatory bowel disease, and wound healing isn’t as much of an issue as once thought.
It’s the same story with spironolactone. Hyperkalemia is a long-standing concern, but it turns out that “in healthy young women taking spironolactone for acne, we don’t need to be checking potassium.” As far as breast cancer goes, the potential risk with spironolactone hasn’t panned out in the literature, and there may not be “a link at all,” Dr. Harper said at the Hawaii Dermatology Seminar provided by the Global Academy for Medical Education/Skin Disease Education Foundation.
There are caveats, of course. Hormonal treatments shouldn’t be used in young women until they’ve established their menstrual cycle. OCs should not be used in smokers, or people who have hypertension or migraines, among other conditions. Also, elevated triglycerides remain a concern with isotretinoin. “The number I would want people to remember is 500 [mg/dL],” the threshold when triglycerides become a problem.
In the interview, Dr. Harper explained the new thinking on these three options, and shared her treatment tips, including what to do if patients’ triglycerides hit the 500 mg/dL mark.
SDEF/Global Academy for Medical Education and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR
Antibiotic use in dermatology declining, with one exception
Dermatologists are prescribing fewer antibiotics for acne and rosacea, but prescribing after dermatologic surgery has increased in the past decade.
In a study published online Jan. 16 in JAMA Dermatology, researchers report the results of a cross-sectional analysis of antibiotic prescribing by 11,986 dermatologists between 2008 and 2016, using commercial claims data.
The analysis showed that, over this period of time, the overall rate of antibiotic prescribing by dermatologists decreased by 36.6%, from 3.36 courses per 100 dermatologist visits to 2.13 courses. In particular, antibiotic prescribing for acne decreased by 28.1%, from 11.76 courses per 100 visits to 8.45 courses, and for rosacea it decreased by 18.1%, from 10.89 courses per 100 visits to 8.92 courses.
John S. Barbieri, MD, of the department of dermatology, University of Pennsylvania, and his coauthors described the overall decline in antibiotic prescribing as “encouraging,” considering that in 2013 dermatologists were identified as the “most frequent prescribers of oral antibiotics per clinician.” The decline resulted in an estimated 480,000 fewer antibiotic courses a year, they noted.
“Much of the decrease in extended courses of antibiotic therapy is associated with visits for acne and rosacea,” they wrote. “Although recent guidelines suggest limiting the duration of therapy in this patient population, course duration has remained stable over time, suggesting that this decrease may be due to fewer patients being treated with antibiotics rather than patients being treated for a shorter duration.”
However, the rate of oral antibiotic prescriptions associated with surgical visits increased by 69.6%, from 3.92 courses per 100 visits to 6.65. This increase was concerning, given the risk of surgical-site infections was low, the authors pointed out. “In addition, a 2008 advisory statement on antibiotic prophylaxis recommends single-dose perioperative antibiotics for patients at increased risk of surgical-site infection,” they added.
The study also noted a 35.3% increase in antibiotic prescribing for cysts and a 3.2% increase for hidradenitis suppurativa.
Over the entire study period, nearly 1 million courses of oral antibiotics were prescribed. Doxycycline hyclate accounted for around one quarter of prescriptions, as did minocycline, while 19.9% of prescriptions were for cephalexin.
“Given the low rate of infectious complications, even for Mohs surgery, and the lack of evidence to support the use of prolonged rather than single-dose perioperative regimens, the postoperative courses of antibiotics identified in this study may increase risks to patients without substantial benefits,” they added.
The study was partly supported by the National Institute of Arthritis and Musculoskeletal Skin Diseases. No conflicts of interest were declared.
SOURCE: Barbieri J et al. JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4944.
Reducing antibiotic prescribing in dermatology – as in so many other areas of medical practice – is a challenge, but there are a number of strategies that can help.
The first is to take a wait-and-see approach, which has been shown to be effective for childhood otitis media. Communication training for physicians can also help them to manage patient requests for antibiotics by working out the patient’s level of understanding of their condition and treatment options, and their expectations, and getting them to agree to keep antibiotics as a contingency plan. There are clinical decision support tools available to help physicians identify high-risk surgical patients who may require postoperative antibiotics.
It will help to have alternative treatment options for conditions such as acne and rosacea, such as better topical therapies, and an increase in clinical trials for these therapies will hopefully provide more options for patients.
Joslyn S. Kirby, MD, and Jordan S. Lim, MB, are in the department of dermatology, Penn State University, Hershey. These comments are taken from an accompanying editorial (JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4877). They had no disclosures.
Reducing antibiotic prescribing in dermatology – as in so many other areas of medical practice – is a challenge, but there are a number of strategies that can help.
The first is to take a wait-and-see approach, which has been shown to be effective for childhood otitis media. Communication training for physicians can also help them to manage patient requests for antibiotics by working out the patient’s level of understanding of their condition and treatment options, and their expectations, and getting them to agree to keep antibiotics as a contingency plan. There are clinical decision support tools available to help physicians identify high-risk surgical patients who may require postoperative antibiotics.
It will help to have alternative treatment options for conditions such as acne and rosacea, such as better topical therapies, and an increase in clinical trials for these therapies will hopefully provide more options for patients.
Joslyn S. Kirby, MD, and Jordan S. Lim, MB, are in the department of dermatology, Penn State University, Hershey. These comments are taken from an accompanying editorial (JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4877). They had no disclosures.
Reducing antibiotic prescribing in dermatology – as in so many other areas of medical practice – is a challenge, but there are a number of strategies that can help.
The first is to take a wait-and-see approach, which has been shown to be effective for childhood otitis media. Communication training for physicians can also help them to manage patient requests for antibiotics by working out the patient’s level of understanding of their condition and treatment options, and their expectations, and getting them to agree to keep antibiotics as a contingency plan. There are clinical decision support tools available to help physicians identify high-risk surgical patients who may require postoperative antibiotics.
It will help to have alternative treatment options for conditions such as acne and rosacea, such as better topical therapies, and an increase in clinical trials for these therapies will hopefully provide more options for patients.
Joslyn S. Kirby, MD, and Jordan S. Lim, MB, are in the department of dermatology, Penn State University, Hershey. These comments are taken from an accompanying editorial (JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4877). They had no disclosures.
Dermatologists are prescribing fewer antibiotics for acne and rosacea, but prescribing after dermatologic surgery has increased in the past decade.
In a study published online Jan. 16 in JAMA Dermatology, researchers report the results of a cross-sectional analysis of antibiotic prescribing by 11,986 dermatologists between 2008 and 2016, using commercial claims data.
The analysis showed that, over this period of time, the overall rate of antibiotic prescribing by dermatologists decreased by 36.6%, from 3.36 courses per 100 dermatologist visits to 2.13 courses. In particular, antibiotic prescribing for acne decreased by 28.1%, from 11.76 courses per 100 visits to 8.45 courses, and for rosacea it decreased by 18.1%, from 10.89 courses per 100 visits to 8.92 courses.
John S. Barbieri, MD, of the department of dermatology, University of Pennsylvania, and his coauthors described the overall decline in antibiotic prescribing as “encouraging,” considering that in 2013 dermatologists were identified as the “most frequent prescribers of oral antibiotics per clinician.” The decline resulted in an estimated 480,000 fewer antibiotic courses a year, they noted.
“Much of the decrease in extended courses of antibiotic therapy is associated with visits for acne and rosacea,” they wrote. “Although recent guidelines suggest limiting the duration of therapy in this patient population, course duration has remained stable over time, suggesting that this decrease may be due to fewer patients being treated with antibiotics rather than patients being treated for a shorter duration.”
However, the rate of oral antibiotic prescriptions associated with surgical visits increased by 69.6%, from 3.92 courses per 100 visits to 6.65. This increase was concerning, given the risk of surgical-site infections was low, the authors pointed out. “In addition, a 2008 advisory statement on antibiotic prophylaxis recommends single-dose perioperative antibiotics for patients at increased risk of surgical-site infection,” they added.
The study also noted a 35.3% increase in antibiotic prescribing for cysts and a 3.2% increase for hidradenitis suppurativa.
Over the entire study period, nearly 1 million courses of oral antibiotics were prescribed. Doxycycline hyclate accounted for around one quarter of prescriptions, as did minocycline, while 19.9% of prescriptions were for cephalexin.
“Given the low rate of infectious complications, even for Mohs surgery, and the lack of evidence to support the use of prolonged rather than single-dose perioperative regimens, the postoperative courses of antibiotics identified in this study may increase risks to patients without substantial benefits,” they added.
The study was partly supported by the National Institute of Arthritis and Musculoskeletal Skin Diseases. No conflicts of interest were declared.
SOURCE: Barbieri J et al. JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4944.
Dermatologists are prescribing fewer antibiotics for acne and rosacea, but prescribing after dermatologic surgery has increased in the past decade.
In a study published online Jan. 16 in JAMA Dermatology, researchers report the results of a cross-sectional analysis of antibiotic prescribing by 11,986 dermatologists between 2008 and 2016, using commercial claims data.
The analysis showed that, over this period of time, the overall rate of antibiotic prescribing by dermatologists decreased by 36.6%, from 3.36 courses per 100 dermatologist visits to 2.13 courses. In particular, antibiotic prescribing for acne decreased by 28.1%, from 11.76 courses per 100 visits to 8.45 courses, and for rosacea it decreased by 18.1%, from 10.89 courses per 100 visits to 8.92 courses.
John S. Barbieri, MD, of the department of dermatology, University of Pennsylvania, and his coauthors described the overall decline in antibiotic prescribing as “encouraging,” considering that in 2013 dermatologists were identified as the “most frequent prescribers of oral antibiotics per clinician.” The decline resulted in an estimated 480,000 fewer antibiotic courses a year, they noted.
“Much of the decrease in extended courses of antibiotic therapy is associated with visits for acne and rosacea,” they wrote. “Although recent guidelines suggest limiting the duration of therapy in this patient population, course duration has remained stable over time, suggesting that this decrease may be due to fewer patients being treated with antibiotics rather than patients being treated for a shorter duration.”
However, the rate of oral antibiotic prescriptions associated with surgical visits increased by 69.6%, from 3.92 courses per 100 visits to 6.65. This increase was concerning, given the risk of surgical-site infections was low, the authors pointed out. “In addition, a 2008 advisory statement on antibiotic prophylaxis recommends single-dose perioperative antibiotics for patients at increased risk of surgical-site infection,” they added.
The study also noted a 35.3% increase in antibiotic prescribing for cysts and a 3.2% increase for hidradenitis suppurativa.
Over the entire study period, nearly 1 million courses of oral antibiotics were prescribed. Doxycycline hyclate accounted for around one quarter of prescriptions, as did minocycline, while 19.9% of prescriptions were for cephalexin.
“Given the low rate of infectious complications, even for Mohs surgery, and the lack of evidence to support the use of prolonged rather than single-dose perioperative regimens, the postoperative courses of antibiotics identified in this study may increase risks to patients without substantial benefits,” they added.
The study was partly supported by the National Institute of Arthritis and Musculoskeletal Skin Diseases. No conflicts of interest were declared.
SOURCE: Barbieri J et al. JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4944.
FROM JAMA DERMATOLOGY
Key clinical point: Antibiotic prescriptions by dermatologists have decreased since 2008.
Major finding: Between 2008 and 2016, antibiotic prescriptions by dermatologists dropped by 36.6%.
Study details: Cross-sectional analysis of antibiotic prescribing by 11,986 dermatologists from 2008 to 2016.
Disclosures: The study was partly supported by the National Institute of Arthritis and Musculoskeletal Skin Diseases. The authors had no disclosures.
Source: Barbieri J et al. JAMA Dermatology. 2019 Jan 16. doi: 10.1001/jamadermatol.2018.4944.
Isotretinoin treatment reorganizes dermal microbiome in acne patients
GRAND CAYMAN, CAYMAN ISLANDS – Isotretinoin, the go-to guy for severe acne, may not be so much a local cop as a community organizer, Kenneth B. Gordon, MD, said at the meeting provided by Global Academy for Medical Education.
“It now appears that with and that the microbial community is replenished with the types associated with healthy skin,” said Dr. Gordon, professor and chair of dermatology at the Medical College of Wisconsin, Milwaukee. When these new bacteria move in, they push pathogenic species out of the neighborhood “and create a new skin microbial community. Maybe this is the real reason our patients tend to stay better, once we get them better with isotretinoin.”
Dr. Gordon discussed new data published last October in the Journal of Investigative Dermatology (J Invest Dermatol. 2018 Oct 24. doi: 10.1016/j.jid.2018.09.023). In a letter to the editor, William H. McCoy, IV, MD, PhD, of Washington University, St. Louis, and his associates suggest that isotretinoin induces a “sebaceous drought,” which shifts the skin microbiome from pathogenic to normophysiological.
Isotretinoin is the gold standard treatment for severe acne, but its method of action has never been fully elucidated, Dr. Gordon said. It clearly targets the sebaceous gland – decreasing sebocyte proliferation and suppressing sebum production – but an emerging body of research suggests that the drug also markedly affects dermal microbial colonization.
The entire concept of a skin microbiome is nearly as new as this new concept of isotretinoin’s effect upon it. Only in the last few years have researchers begun to characterize the complex microbial film that keeps skin healthy and resistant to infection. Dermal dysbiosis has now been associated with acne, psoriasis and psoriatic arthritis, and atopic dermatitis.
The 2-year pilot study compared the dermal microbiome of isotretinoin-treated acne patients with that of patients with untreated acne and normal skin. Skin samples underwent genomic analysis before isotretinoin treatment, at several periods during treatment, and about 5 months after treatment stopped. Untreated controls were evaluated at baseline and at 2, 5, and 10 months.
Not surprisingly, before treatment the microbiome was similar in both acne groups, but markedly different from that seen in normal skin. As isotretinoin’s “oil drought” dragged on, levels of Cutibacterium acnes (the new appellation for P. acnes) declined. Staphylococcus species initially increased, but then declined as well. Simultaneously, four new taxa (Rothia, Flavobacterium, Enterobacter, and Micrococcus) increased. Most patients had a restructuring of their Propionibacterium community, populated largely by the less-pathogenic strains found on normal skin.
“We suggest that isotretinoin creates a Propionibacterium ‘population bottleneck’ that selects for ‘healthy’ Propionibacterium communities and other sebaceous skin taxa that persist after treatment, resulting in long-term acne remission [i.e., normal skin],” the investigators wrote.
This is a new and very exciting finding, Dr. Gordon commented. “It appears that the reason our isotretinoin patients stay better once they get better is not from targeting the sebaceous gland itself, but by repairing the skin’s microbiome and getting it back to normal.”
Dr. Gordon reported financial relationships with numerous pharmaceutical companies. Global Academy and this news organization are owned by the same parent company.
This article was updated 2/1/19.
GRAND CAYMAN, CAYMAN ISLANDS – Isotretinoin, the go-to guy for severe acne, may not be so much a local cop as a community organizer, Kenneth B. Gordon, MD, said at the meeting provided by Global Academy for Medical Education.
“It now appears that with and that the microbial community is replenished with the types associated with healthy skin,” said Dr. Gordon, professor and chair of dermatology at the Medical College of Wisconsin, Milwaukee. When these new bacteria move in, they push pathogenic species out of the neighborhood “and create a new skin microbial community. Maybe this is the real reason our patients tend to stay better, once we get them better with isotretinoin.”
Dr. Gordon discussed new data published last October in the Journal of Investigative Dermatology (J Invest Dermatol. 2018 Oct 24. doi: 10.1016/j.jid.2018.09.023). In a letter to the editor, William H. McCoy, IV, MD, PhD, of Washington University, St. Louis, and his associates suggest that isotretinoin induces a “sebaceous drought,” which shifts the skin microbiome from pathogenic to normophysiological.
Isotretinoin is the gold standard treatment for severe acne, but its method of action has never been fully elucidated, Dr. Gordon said. It clearly targets the sebaceous gland – decreasing sebocyte proliferation and suppressing sebum production – but an emerging body of research suggests that the drug also markedly affects dermal microbial colonization.
The entire concept of a skin microbiome is nearly as new as this new concept of isotretinoin’s effect upon it. Only in the last few years have researchers begun to characterize the complex microbial film that keeps skin healthy and resistant to infection. Dermal dysbiosis has now been associated with acne, psoriasis and psoriatic arthritis, and atopic dermatitis.
The 2-year pilot study compared the dermal microbiome of isotretinoin-treated acne patients with that of patients with untreated acne and normal skin. Skin samples underwent genomic analysis before isotretinoin treatment, at several periods during treatment, and about 5 months after treatment stopped. Untreated controls were evaluated at baseline and at 2, 5, and 10 months.
Not surprisingly, before treatment the microbiome was similar in both acne groups, but markedly different from that seen in normal skin. As isotretinoin’s “oil drought” dragged on, levels of Cutibacterium acnes (the new appellation for P. acnes) declined. Staphylococcus species initially increased, but then declined as well. Simultaneously, four new taxa (Rothia, Flavobacterium, Enterobacter, and Micrococcus) increased. Most patients had a restructuring of their Propionibacterium community, populated largely by the less-pathogenic strains found on normal skin.
“We suggest that isotretinoin creates a Propionibacterium ‘population bottleneck’ that selects for ‘healthy’ Propionibacterium communities and other sebaceous skin taxa that persist after treatment, resulting in long-term acne remission [i.e., normal skin],” the investigators wrote.
This is a new and very exciting finding, Dr. Gordon commented. “It appears that the reason our isotretinoin patients stay better once they get better is not from targeting the sebaceous gland itself, but by repairing the skin’s microbiome and getting it back to normal.”
Dr. Gordon reported financial relationships with numerous pharmaceutical companies. Global Academy and this news organization are owned by the same parent company.
This article was updated 2/1/19.
GRAND CAYMAN, CAYMAN ISLANDS – Isotretinoin, the go-to guy for severe acne, may not be so much a local cop as a community organizer, Kenneth B. Gordon, MD, said at the meeting provided by Global Academy for Medical Education.
“It now appears that with and that the microbial community is replenished with the types associated with healthy skin,” said Dr. Gordon, professor and chair of dermatology at the Medical College of Wisconsin, Milwaukee. When these new bacteria move in, they push pathogenic species out of the neighborhood “and create a new skin microbial community. Maybe this is the real reason our patients tend to stay better, once we get them better with isotretinoin.”
Dr. Gordon discussed new data published last October in the Journal of Investigative Dermatology (J Invest Dermatol. 2018 Oct 24. doi: 10.1016/j.jid.2018.09.023). In a letter to the editor, William H. McCoy, IV, MD, PhD, of Washington University, St. Louis, and his associates suggest that isotretinoin induces a “sebaceous drought,” which shifts the skin microbiome from pathogenic to normophysiological.
Isotretinoin is the gold standard treatment for severe acne, but its method of action has never been fully elucidated, Dr. Gordon said. It clearly targets the sebaceous gland – decreasing sebocyte proliferation and suppressing sebum production – but an emerging body of research suggests that the drug also markedly affects dermal microbial colonization.
The entire concept of a skin microbiome is nearly as new as this new concept of isotretinoin’s effect upon it. Only in the last few years have researchers begun to characterize the complex microbial film that keeps skin healthy and resistant to infection. Dermal dysbiosis has now been associated with acne, psoriasis and psoriatic arthritis, and atopic dermatitis.
The 2-year pilot study compared the dermal microbiome of isotretinoin-treated acne patients with that of patients with untreated acne and normal skin. Skin samples underwent genomic analysis before isotretinoin treatment, at several periods during treatment, and about 5 months after treatment stopped. Untreated controls were evaluated at baseline and at 2, 5, and 10 months.
Not surprisingly, before treatment the microbiome was similar in both acne groups, but markedly different from that seen in normal skin. As isotretinoin’s “oil drought” dragged on, levels of Cutibacterium acnes (the new appellation for P. acnes) declined. Staphylococcus species initially increased, but then declined as well. Simultaneously, four new taxa (Rothia, Flavobacterium, Enterobacter, and Micrococcus) increased. Most patients had a restructuring of their Propionibacterium community, populated largely by the less-pathogenic strains found on normal skin.
“We suggest that isotretinoin creates a Propionibacterium ‘population bottleneck’ that selects for ‘healthy’ Propionibacterium communities and other sebaceous skin taxa that persist after treatment, resulting in long-term acne remission [i.e., normal skin],” the investigators wrote.
This is a new and very exciting finding, Dr. Gordon commented. “It appears that the reason our isotretinoin patients stay better once they get better is not from targeting the sebaceous gland itself, but by repairing the skin’s microbiome and getting it back to normal.”
Dr. Gordon reported financial relationships with numerous pharmaceutical companies. Global Academy and this news organization are owned by the same parent company.
This article was updated 2/1/19.
REPORTING FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
Review looks at effectiveness of isotretinoin for acne
There is when based on reductions in inflammatory lesion counts, according to a recent Cochrane Review.
“The current recommendation of clinical guidelines that oral isotretinoin should be the first-line treatment for moderate to severe acne unresponsive to previous therapies, being more effective than the use of oral antibiotics plus topical agents, underpins current dermatological practice,” Caroline S. Costa, MD, from the Emergency Medicine and Evidence-Based Medicine department at Universidade Federal de São Paulo and her colleagues wrote in their review. “The recommendation cannot be fully supported with certainty by the finding of this review; however, neither does this review challenge it.”
Dr. Costa and her colleagues identified 31 randomized, controlled trials in the Cochrane Skin Group Specialised Register, CENTRAL, MEDLINE, Embase, PsycINFO, and LILACS databases up to July 2017, which altogether included 3,836 participants with mild to severe acne who were aged 12-55 years. The patients received treatment with oral isotretinoin versus placebo or other treatments, such as antibiotics.
In 3 studies that altogether included 400 participants and compared isotretinoin with oral antibiotics plus topical treatments, there was no significant difference with isotretinoin in decreases in the investigator-assessed inflammatory lesion count in participants with moderate to severe acne after 20-24 weeks (risk ratio, 1.01; 95% confidence interval, 0.96-1.06). One serious side effect – Stevens-Johnson syndrome – was noted in the isotretinoin-treated group (RR, 3.00; 95% CI, 0.12-72.98). These results were based on “very-low-quality evidence,” the authors noted.
Two studies also comparing isotretinoin with oral antibiotics and topical treatments in a total of 351 participants showed a 15% improvement in acne severity (RR, 1.15; 95% CI, 1.00-1.32) as assessed by physician’s global evaluation but with a greater number of adverse events considered less severe (RR, 1.67; 95% CI, 1.42-1.98), such as vomiting, nausea, dry lips and skin, and cheilitis.
With regard to dosing, one study with 154 participants with severe acne showed 0.05 mg/kg per day of isotretinoin reduced inflammatory lesion count by 79% after 20 weeks, while 0.1 mg/kg per day and 0.2 mg/kg per day reduced inflammatory lesion counts by 80% and 84%, respectively, after 20 weeks. A different study of 150 participants with severe acne found a 95% decrease in inflammatory lesion counts for 58% of participants receiving 0.1 mg/kg per day, 80% of participants receiving 0.5 mg/kg per day, and 90% of participants receiving 1 mg/kg per day of oral isotretinoin after 20 weeks.
In a randomized, controlled trial with 40 participants with moderate acne comparing intermittent dosing (0.5-0.7 mg/kg per day for 1 week per month), continuous conventional dosing (0.5-0.7 mg/kg per day), and continuous low dosing (0.25-0.4 mg/kg per day) of oral isotretinoin found greater differences in mean decreased numbers of inflammatory lesions among participants in the continuous low dose (a decrease of 3.72 lesions; 95% CI, 2.13-5.31) and continuous conventional dose (a decrease of 3.87 lesions; 95% CI, 2.31-5.43) groups. The authors noted they were unable to perform a meta-analysis because of study heterogeneity in the three studies examining the primary outcome.
In 14 studies with a total of 906 participants who had moderate and severe acne, the authors noted there were no severe adverse events with different doses and regimens of isotretinoin treatment from 12 weeks to 32 weeks or at follow-up at the end of treatment at up to 48 weeks. There were some adverse events, such as skin dryness, hair loss, and itching in 13 studies with a total of 858 participants.
No birth defects were reported in the studies.
The authors took special note of the low-quality evidence in the review, and said that future studies should include larger sample sizes to observe more rare adverse events, as well as create subgroups with results based on acne severity, longer duration and follow-up, standardization of primary outcomes, and adherence to the 2010 CONSORT statement for reporting parallel-group randomized trials.
“With the aim of providing reliable physician guidelines and a robust evidence-based support for daily clinical practice in acne therapy, future randomized clinical trials on oral isotretinoin for acne should focus on treatment of acne when there is insufficient response to therapy with oral antibiotics plus topical agents,” Dr. Costa and her colleagues wrote.
Dr. Costa reports receiving a grant from the Brazilian government granting agency Coordenação de Aperfeicoamento de Pessoal de Nivel Superior. Another author reported a board membership with Bayer for studies and research and is a paid lecturer for a continuing medical education program on adult female acne. The remaining five authors reported no relevant conflicts of interest.
SOURCE: Costa CS et al. Cochrane Database Syst Rev. 2018. doi: 10.1002/14651858.CD009435.pub2.
I think dermatologists would agree with the assertions of the Cochrane Review that there is limited evidence according to today’s standards of quality evidence. The Cochrane Review process examines available data, ranking it by the quality of the data. The paper by Costa et al. shows where the Cochrane Review process is fatally flawed. It assumes that, where the highest quality data is lacking, the medication in question must be ineffective or that this at least casts doubt on its efficacy.
Isotretinoin was approved for use in acne in the 1980s. If you look at one initial report by Peck et al. examining the efficacy of isotretinoin versus placebo in patients with very severe nodulocystic acne, the isotretinoin group was so effective that half of the patients in the placebo arm broke code because of a 57% worsening of their acne and went to the treatment arm. Overall, there was a 95% improvement in the isotretinoin-treated group at the end of treatment (J Am Acad Dermatol. 1982 Apr;6[4 Pt 2 Suppl]:735-45). This study truly reflects how effective isotretinoin is in the treatment of severe acne, and any dermatologist who uses isotretinoin knows that for a fact. I suspect that, if someone applied the Cochrane Review process to insulin, they also would question its efficacy.
I agree there are questionable data on high versus standard versus low dosing. For most patients, standard dosing of 1.0 mg/kg per day over 20-24 weeks will result in complete and sustained clearance. There are always outliers, however, and alternative dosing may be needed – either higher cumulative dosing to achieve clearance or longer lower dosing to manage side effects.
The authors clearly have limited experience in treating acne, or the aim of the article was simply a review of available data with no consideration of actual clinical usage. However, if patients see this report, it could undermine dermatologists’ efforts to care for their patients with acne. It is rather irresponsible to publish these types of reviews, in which the efficacy of the medication in question was established long ago and is clearly without question, and it really discredits the integrity of the Cochrane Review.
Andrea L. Zaenglein, MD , is professor of dermatology and pediatric dermatology at Pennsylvania State University, Hershey, Penn., and is a cochair of the American Academy of Dermatology’s most recent acne management guidelines ( J Am Acad Dermatol. 2016 May;74[5]:945-73.e33 ). She reports being a consultant for Sun Pharmaceutical Industries.
I think dermatologists would agree with the assertions of the Cochrane Review that there is limited evidence according to today’s standards of quality evidence. The Cochrane Review process examines available data, ranking it by the quality of the data. The paper by Costa et al. shows where the Cochrane Review process is fatally flawed. It assumes that, where the highest quality data is lacking, the medication in question must be ineffective or that this at least casts doubt on its efficacy.
Isotretinoin was approved for use in acne in the 1980s. If you look at one initial report by Peck et al. examining the efficacy of isotretinoin versus placebo in patients with very severe nodulocystic acne, the isotretinoin group was so effective that half of the patients in the placebo arm broke code because of a 57% worsening of their acne and went to the treatment arm. Overall, there was a 95% improvement in the isotretinoin-treated group at the end of treatment (J Am Acad Dermatol. 1982 Apr;6[4 Pt 2 Suppl]:735-45). This study truly reflects how effective isotretinoin is in the treatment of severe acne, and any dermatologist who uses isotretinoin knows that for a fact. I suspect that, if someone applied the Cochrane Review process to insulin, they also would question its efficacy.
I agree there are questionable data on high versus standard versus low dosing. For most patients, standard dosing of 1.0 mg/kg per day over 20-24 weeks will result in complete and sustained clearance. There are always outliers, however, and alternative dosing may be needed – either higher cumulative dosing to achieve clearance or longer lower dosing to manage side effects.
The authors clearly have limited experience in treating acne, or the aim of the article was simply a review of available data with no consideration of actual clinical usage. However, if patients see this report, it could undermine dermatologists’ efforts to care for their patients with acne. It is rather irresponsible to publish these types of reviews, in which the efficacy of the medication in question was established long ago and is clearly without question, and it really discredits the integrity of the Cochrane Review.
Andrea L. Zaenglein, MD , is professor of dermatology and pediatric dermatology at Pennsylvania State University, Hershey, Penn., and is a cochair of the American Academy of Dermatology’s most recent acne management guidelines ( J Am Acad Dermatol. 2016 May;74[5]:945-73.e33 ). She reports being a consultant for Sun Pharmaceutical Industries.
I think dermatologists would agree with the assertions of the Cochrane Review that there is limited evidence according to today’s standards of quality evidence. The Cochrane Review process examines available data, ranking it by the quality of the data. The paper by Costa et al. shows where the Cochrane Review process is fatally flawed. It assumes that, where the highest quality data is lacking, the medication in question must be ineffective or that this at least casts doubt on its efficacy.
Isotretinoin was approved for use in acne in the 1980s. If you look at one initial report by Peck et al. examining the efficacy of isotretinoin versus placebo in patients with very severe nodulocystic acne, the isotretinoin group was so effective that half of the patients in the placebo arm broke code because of a 57% worsening of their acne and went to the treatment arm. Overall, there was a 95% improvement in the isotretinoin-treated group at the end of treatment (J Am Acad Dermatol. 1982 Apr;6[4 Pt 2 Suppl]:735-45). This study truly reflects how effective isotretinoin is in the treatment of severe acne, and any dermatologist who uses isotretinoin knows that for a fact. I suspect that, if someone applied the Cochrane Review process to insulin, they also would question its efficacy.
I agree there are questionable data on high versus standard versus low dosing. For most patients, standard dosing of 1.0 mg/kg per day over 20-24 weeks will result in complete and sustained clearance. There are always outliers, however, and alternative dosing may be needed – either higher cumulative dosing to achieve clearance or longer lower dosing to manage side effects.
The authors clearly have limited experience in treating acne, or the aim of the article was simply a review of available data with no consideration of actual clinical usage. However, if patients see this report, it could undermine dermatologists’ efforts to care for their patients with acne. It is rather irresponsible to publish these types of reviews, in which the efficacy of the medication in question was established long ago and is clearly without question, and it really discredits the integrity of the Cochrane Review.
Andrea L. Zaenglein, MD , is professor of dermatology and pediatric dermatology at Pennsylvania State University, Hershey, Penn., and is a cochair of the American Academy of Dermatology’s most recent acne management guidelines ( J Am Acad Dermatol. 2016 May;74[5]:945-73.e33 ). She reports being a consultant for Sun Pharmaceutical Industries.
There is when based on reductions in inflammatory lesion counts, according to a recent Cochrane Review.
“The current recommendation of clinical guidelines that oral isotretinoin should be the first-line treatment for moderate to severe acne unresponsive to previous therapies, being more effective than the use of oral antibiotics plus topical agents, underpins current dermatological practice,” Caroline S. Costa, MD, from the Emergency Medicine and Evidence-Based Medicine department at Universidade Federal de São Paulo and her colleagues wrote in their review. “The recommendation cannot be fully supported with certainty by the finding of this review; however, neither does this review challenge it.”
Dr. Costa and her colleagues identified 31 randomized, controlled trials in the Cochrane Skin Group Specialised Register, CENTRAL, MEDLINE, Embase, PsycINFO, and LILACS databases up to July 2017, which altogether included 3,836 participants with mild to severe acne who were aged 12-55 years. The patients received treatment with oral isotretinoin versus placebo or other treatments, such as antibiotics.
In 3 studies that altogether included 400 participants and compared isotretinoin with oral antibiotics plus topical treatments, there was no significant difference with isotretinoin in decreases in the investigator-assessed inflammatory lesion count in participants with moderate to severe acne after 20-24 weeks (risk ratio, 1.01; 95% confidence interval, 0.96-1.06). One serious side effect – Stevens-Johnson syndrome – was noted in the isotretinoin-treated group (RR, 3.00; 95% CI, 0.12-72.98). These results were based on “very-low-quality evidence,” the authors noted.
Two studies also comparing isotretinoin with oral antibiotics and topical treatments in a total of 351 participants showed a 15% improvement in acne severity (RR, 1.15; 95% CI, 1.00-1.32) as assessed by physician’s global evaluation but with a greater number of adverse events considered less severe (RR, 1.67; 95% CI, 1.42-1.98), such as vomiting, nausea, dry lips and skin, and cheilitis.
With regard to dosing, one study with 154 participants with severe acne showed 0.05 mg/kg per day of isotretinoin reduced inflammatory lesion count by 79% after 20 weeks, while 0.1 mg/kg per day and 0.2 mg/kg per day reduced inflammatory lesion counts by 80% and 84%, respectively, after 20 weeks. A different study of 150 participants with severe acne found a 95% decrease in inflammatory lesion counts for 58% of participants receiving 0.1 mg/kg per day, 80% of participants receiving 0.5 mg/kg per day, and 90% of participants receiving 1 mg/kg per day of oral isotretinoin after 20 weeks.
In a randomized, controlled trial with 40 participants with moderate acne comparing intermittent dosing (0.5-0.7 mg/kg per day for 1 week per month), continuous conventional dosing (0.5-0.7 mg/kg per day), and continuous low dosing (0.25-0.4 mg/kg per day) of oral isotretinoin found greater differences in mean decreased numbers of inflammatory lesions among participants in the continuous low dose (a decrease of 3.72 lesions; 95% CI, 2.13-5.31) and continuous conventional dose (a decrease of 3.87 lesions; 95% CI, 2.31-5.43) groups. The authors noted they were unable to perform a meta-analysis because of study heterogeneity in the three studies examining the primary outcome.
In 14 studies with a total of 906 participants who had moderate and severe acne, the authors noted there were no severe adverse events with different doses and regimens of isotretinoin treatment from 12 weeks to 32 weeks or at follow-up at the end of treatment at up to 48 weeks. There were some adverse events, such as skin dryness, hair loss, and itching in 13 studies with a total of 858 participants.
No birth defects were reported in the studies.
The authors took special note of the low-quality evidence in the review, and said that future studies should include larger sample sizes to observe more rare adverse events, as well as create subgroups with results based on acne severity, longer duration and follow-up, standardization of primary outcomes, and adherence to the 2010 CONSORT statement for reporting parallel-group randomized trials.
“With the aim of providing reliable physician guidelines and a robust evidence-based support for daily clinical practice in acne therapy, future randomized clinical trials on oral isotretinoin for acne should focus on treatment of acne when there is insufficient response to therapy with oral antibiotics plus topical agents,” Dr. Costa and her colleagues wrote.
Dr. Costa reports receiving a grant from the Brazilian government granting agency Coordenação de Aperfeicoamento de Pessoal de Nivel Superior. Another author reported a board membership with Bayer for studies and research and is a paid lecturer for a continuing medical education program on adult female acne. The remaining five authors reported no relevant conflicts of interest.
SOURCE: Costa CS et al. Cochrane Database Syst Rev. 2018. doi: 10.1002/14651858.CD009435.pub2.
There is when based on reductions in inflammatory lesion counts, according to a recent Cochrane Review.
“The current recommendation of clinical guidelines that oral isotretinoin should be the first-line treatment for moderate to severe acne unresponsive to previous therapies, being more effective than the use of oral antibiotics plus topical agents, underpins current dermatological practice,” Caroline S. Costa, MD, from the Emergency Medicine and Evidence-Based Medicine department at Universidade Federal de São Paulo and her colleagues wrote in their review. “The recommendation cannot be fully supported with certainty by the finding of this review; however, neither does this review challenge it.”
Dr. Costa and her colleagues identified 31 randomized, controlled trials in the Cochrane Skin Group Specialised Register, CENTRAL, MEDLINE, Embase, PsycINFO, and LILACS databases up to July 2017, which altogether included 3,836 participants with mild to severe acne who were aged 12-55 years. The patients received treatment with oral isotretinoin versus placebo or other treatments, such as antibiotics.
In 3 studies that altogether included 400 participants and compared isotretinoin with oral antibiotics plus topical treatments, there was no significant difference with isotretinoin in decreases in the investigator-assessed inflammatory lesion count in participants with moderate to severe acne after 20-24 weeks (risk ratio, 1.01; 95% confidence interval, 0.96-1.06). One serious side effect – Stevens-Johnson syndrome – was noted in the isotretinoin-treated group (RR, 3.00; 95% CI, 0.12-72.98). These results were based on “very-low-quality evidence,” the authors noted.
Two studies also comparing isotretinoin with oral antibiotics and topical treatments in a total of 351 participants showed a 15% improvement in acne severity (RR, 1.15; 95% CI, 1.00-1.32) as assessed by physician’s global evaluation but with a greater number of adverse events considered less severe (RR, 1.67; 95% CI, 1.42-1.98), such as vomiting, nausea, dry lips and skin, and cheilitis.
With regard to dosing, one study with 154 participants with severe acne showed 0.05 mg/kg per day of isotretinoin reduced inflammatory lesion count by 79% after 20 weeks, while 0.1 mg/kg per day and 0.2 mg/kg per day reduced inflammatory lesion counts by 80% and 84%, respectively, after 20 weeks. A different study of 150 participants with severe acne found a 95% decrease in inflammatory lesion counts for 58% of participants receiving 0.1 mg/kg per day, 80% of participants receiving 0.5 mg/kg per day, and 90% of participants receiving 1 mg/kg per day of oral isotretinoin after 20 weeks.
In a randomized, controlled trial with 40 participants with moderate acne comparing intermittent dosing (0.5-0.7 mg/kg per day for 1 week per month), continuous conventional dosing (0.5-0.7 mg/kg per day), and continuous low dosing (0.25-0.4 mg/kg per day) of oral isotretinoin found greater differences in mean decreased numbers of inflammatory lesions among participants in the continuous low dose (a decrease of 3.72 lesions; 95% CI, 2.13-5.31) and continuous conventional dose (a decrease of 3.87 lesions; 95% CI, 2.31-5.43) groups. The authors noted they were unable to perform a meta-analysis because of study heterogeneity in the three studies examining the primary outcome.
In 14 studies with a total of 906 participants who had moderate and severe acne, the authors noted there were no severe adverse events with different doses and regimens of isotretinoin treatment from 12 weeks to 32 weeks or at follow-up at the end of treatment at up to 48 weeks. There were some adverse events, such as skin dryness, hair loss, and itching in 13 studies with a total of 858 participants.
No birth defects were reported in the studies.
The authors took special note of the low-quality evidence in the review, and said that future studies should include larger sample sizes to observe more rare adverse events, as well as create subgroups with results based on acne severity, longer duration and follow-up, standardization of primary outcomes, and adherence to the 2010 CONSORT statement for reporting parallel-group randomized trials.
“With the aim of providing reliable physician guidelines and a robust evidence-based support for daily clinical practice in acne therapy, future randomized clinical trials on oral isotretinoin for acne should focus on treatment of acne when there is insufficient response to therapy with oral antibiotics plus topical agents,” Dr. Costa and her colleagues wrote.
Dr. Costa reports receiving a grant from the Brazilian government granting agency Coordenação de Aperfeicoamento de Pessoal de Nivel Superior. Another author reported a board membership with Bayer for studies and research and is a paid lecturer for a continuing medical education program on adult female acne. The remaining five authors reported no relevant conflicts of interest.
SOURCE: Costa CS et al. Cochrane Database Syst Rev. 2018. doi: 10.1002/14651858.CD009435.pub2.
FROM COCHRANE DATABASE OF SYSTEMATIC REVIEWS
Key clinical point: A Cochrane Review found low quality of evidence surrounding oral isotretinoin’s effectiveness for acne.
Major finding: Isotretinoin did not decrease inflammatory lesion count, compared with (risk ratio, 1.01; 95% confidence interval, 0.96-1.06), in 3 studies, and there was low evidence to suggest daily treatment was more effective than treatment for 1 week per month.
Study details: A Cochrane Review of 31 studies that altogether included 3,836 patients with mild to severe acne who received oral isotretinoin, placebo, or other treatments such as antibiotics.
Disclosures: Dr. Costa reported receiving a grant from the Brazilian government granting agency Coordenação de Aperfeicoamento de Pessoal de Nivel Superior. Dr. Bagatin reported a board membership with Bayer for studies and research and is a paid lecturer for a continuing medical education program on adult female acne. The other authors report no relevant conflicts of interest.
Source: Costa CS et al. Cochrane Database Syst Rev. 2018. doi: 10.1002/14651858.CD009435.pub2.
Innovations in Dermatology: Laboratory Monitoring With Isotretinoin



An iPledge Halloween
It was a dark and stormy night.
OK, it was a warm and sunny afternoon. But Halloween was approaching. Strange things happen. Plus, the patient’s name was Ichabod ...
OK, his name was Jerry. Jerry came to Boston from Chula Taco, Calif., to study at CIT, the famed Boston Chipotle Institute of Technology. He’d finished 4 months of isotretinoin and needed one more.
I asked him to call iPledge to request a transfer to me. He called back later to say that This seemed odd, since his pills had only run out 3 days before.
Having confirmed his name, address, telephone number, and the last four digits of his social security number, I tried enrolling him on iPledge at 5:30 p.m. (Cue: thunder and lightning), expecting to get a request for an override code. Instead the screen just asked for his iPledge number (you have to use the old one, you know). I called iPledge (my favorite pastime), identified myself by the usual means (Full name. iPledge ID number. Date of personal significance. Office telephone. Thank you. How can I help you?).
I explained my dilemma. The representative asked that I verify Jerry’s identity. I gave her his name, date of birth, and the last four of his social.
“We have his name and date of birth,” she said, “but the social security digits don’t match.” She asked for his phone number, but his Boston number didn’t match what she had. “Do you have his address?” she asked. I did not, since he’d given me his Boston address, not his California one.
I left her on hold and called Jerry on my cell. He confirmed that the social security digits he’d given me were correct. He gave me his mother’s cell phone number, but that also turned out not to be what iPledge had on file.
“What other identifying information can I give you?” I asked the iPledge rep. “How about his home address?” she said. Back to my cell: “Jerry, what’s your home address?” “It’s 2470 Chalupa Drive, Chula Taco, California 9090909-090909,” he said.
I repeated that to the iPledge representative. “Please hold a moment,” she said.
She was back. “The street address is correct,” she said, “The ZIP is correct. But the town is wrong.”
The town is wrong? If Jerry didn’t know either the last four of his social or his town, how did he get Amazon deliveries? Was this identity theft by an Accutane seeker? Maybe Jerry was really a Russian spy with dry lips posing as an acne patient! (Cue: screeches, howls, more thunder.)
“Can you tell me which town you have listed for him?” I asked iPledge.
“No,” she said, “because you haven’t identified him properly yet,” (emphasis added).
Back to the cell: “Jerry, are you sure you know what town you live in?” He insisted he did. (But then, so would a spy, wouldn’t he?)
In near despair, I returned to the iPledge rep. “I really want to get this patient his medication, “I said. “And I really want to go home. Can you help either of us?”
“Let me get my supervisor,” she said. “This may take a few minutes.” I hung up on Jerry and, in a blaze of multitasking, filled out three Prior Authorization forms for clindamycin gel.
“I found your patient,” said the rep, returning at last. “Not only that, I was able to reregister him in the iPledge program. Want to know his iPledge number?
Of course!
“Now that he’s registered,” I said, “could you give me the name of the town you have him listed as living in on Chalupa Drive?”
“Sure,” she said, “We have him in Rancho Carmen Miranda. Can help you with anything else today?”
“No, thanks ...”
“Would you be willing to take a 2-minute survey ...?”
“No, but thank you very much!” I said, hanging up in triumph. (Cue: sunshine, violins.)
Back to the cell: “Jerry, you’re in! Here’s your iPledge number.”
“Thanks, Doc.”
“By the way, Jerry, iPledge has you living in the town of Rancho Carmen Miranda. Do you live there?”
“No,” said Jerry. “I don’t.”
“Well, Jerry, for 1 more month, for federal purposes, you do!”
I’m sure there’s a good explanation for all this. I just don’t want to know it. Just pass the candy corn.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
It was a dark and stormy night.
OK, it was a warm and sunny afternoon. But Halloween was approaching. Strange things happen. Plus, the patient’s name was Ichabod ...
OK, his name was Jerry. Jerry came to Boston from Chula Taco, Calif., to study at CIT, the famed Boston Chipotle Institute of Technology. He’d finished 4 months of isotretinoin and needed one more.
I asked him to call iPledge to request a transfer to me. He called back later to say that This seemed odd, since his pills had only run out 3 days before.
Having confirmed his name, address, telephone number, and the last four digits of his social security number, I tried enrolling him on iPledge at 5:30 p.m. (Cue: thunder and lightning), expecting to get a request for an override code. Instead the screen just asked for his iPledge number (you have to use the old one, you know). I called iPledge (my favorite pastime), identified myself by the usual means (Full name. iPledge ID number. Date of personal significance. Office telephone. Thank you. How can I help you?).
I explained my dilemma. The representative asked that I verify Jerry’s identity. I gave her his name, date of birth, and the last four of his social.
“We have his name and date of birth,” she said, “but the social security digits don’t match.” She asked for his phone number, but his Boston number didn’t match what she had. “Do you have his address?” she asked. I did not, since he’d given me his Boston address, not his California one.
I left her on hold and called Jerry on my cell. He confirmed that the social security digits he’d given me were correct. He gave me his mother’s cell phone number, but that also turned out not to be what iPledge had on file.
“What other identifying information can I give you?” I asked the iPledge rep. “How about his home address?” she said. Back to my cell: “Jerry, what’s your home address?” “It’s 2470 Chalupa Drive, Chula Taco, California 9090909-090909,” he said.
I repeated that to the iPledge representative. “Please hold a moment,” she said.
She was back. “The street address is correct,” she said, “The ZIP is correct. But the town is wrong.”
The town is wrong? If Jerry didn’t know either the last four of his social or his town, how did he get Amazon deliveries? Was this identity theft by an Accutane seeker? Maybe Jerry was really a Russian spy with dry lips posing as an acne patient! (Cue: screeches, howls, more thunder.)
“Can you tell me which town you have listed for him?” I asked iPledge.
“No,” she said, “because you haven’t identified him properly yet,” (emphasis added).
Back to the cell: “Jerry, are you sure you know what town you live in?” He insisted he did. (But then, so would a spy, wouldn’t he?)
In near despair, I returned to the iPledge rep. “I really want to get this patient his medication, “I said. “And I really want to go home. Can you help either of us?”
“Let me get my supervisor,” she said. “This may take a few minutes.” I hung up on Jerry and, in a blaze of multitasking, filled out three Prior Authorization forms for clindamycin gel.
“I found your patient,” said the rep, returning at last. “Not only that, I was able to reregister him in the iPledge program. Want to know his iPledge number?
Of course!
“Now that he’s registered,” I said, “could you give me the name of the town you have him listed as living in on Chalupa Drive?”
“Sure,” she said, “We have him in Rancho Carmen Miranda. Can help you with anything else today?”
“No, thanks ...”
“Would you be willing to take a 2-minute survey ...?”
“No, but thank you very much!” I said, hanging up in triumph. (Cue: sunshine, violins.)
Back to the cell: “Jerry, you’re in! Here’s your iPledge number.”
“Thanks, Doc.”
“By the way, Jerry, iPledge has you living in the town of Rancho Carmen Miranda. Do you live there?”
“No,” said Jerry. “I don’t.”
“Well, Jerry, for 1 more month, for federal purposes, you do!”
I’m sure there’s a good explanation for all this. I just don’t want to know it. Just pass the candy corn.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
It was a dark and stormy night.
OK, it was a warm and sunny afternoon. But Halloween was approaching. Strange things happen. Plus, the patient’s name was Ichabod ...
OK, his name was Jerry. Jerry came to Boston from Chula Taco, Calif., to study at CIT, the famed Boston Chipotle Institute of Technology. He’d finished 4 months of isotretinoin and needed one more.
I asked him to call iPledge to request a transfer to me. He called back later to say that This seemed odd, since his pills had only run out 3 days before.
Having confirmed his name, address, telephone number, and the last four digits of his social security number, I tried enrolling him on iPledge at 5:30 p.m. (Cue: thunder and lightning), expecting to get a request for an override code. Instead the screen just asked for his iPledge number (you have to use the old one, you know). I called iPledge (my favorite pastime), identified myself by the usual means (Full name. iPledge ID number. Date of personal significance. Office telephone. Thank you. How can I help you?).
I explained my dilemma. The representative asked that I verify Jerry’s identity. I gave her his name, date of birth, and the last four of his social.
“We have his name and date of birth,” she said, “but the social security digits don’t match.” She asked for his phone number, but his Boston number didn’t match what she had. “Do you have his address?” she asked. I did not, since he’d given me his Boston address, not his California one.
I left her on hold and called Jerry on my cell. He confirmed that the social security digits he’d given me were correct. He gave me his mother’s cell phone number, but that also turned out not to be what iPledge had on file.
“What other identifying information can I give you?” I asked the iPledge rep. “How about his home address?” she said. Back to my cell: “Jerry, what’s your home address?” “It’s 2470 Chalupa Drive, Chula Taco, California 9090909-090909,” he said.
I repeated that to the iPledge representative. “Please hold a moment,” she said.
She was back. “The street address is correct,” she said, “The ZIP is correct. But the town is wrong.”
The town is wrong? If Jerry didn’t know either the last four of his social or his town, how did he get Amazon deliveries? Was this identity theft by an Accutane seeker? Maybe Jerry was really a Russian spy with dry lips posing as an acne patient! (Cue: screeches, howls, more thunder.)
“Can you tell me which town you have listed for him?” I asked iPledge.
“No,” she said, “because you haven’t identified him properly yet,” (emphasis added).
Back to the cell: “Jerry, are you sure you know what town you live in?” He insisted he did. (But then, so would a spy, wouldn’t he?)
In near despair, I returned to the iPledge rep. “I really want to get this patient his medication, “I said. “And I really want to go home. Can you help either of us?”
“Let me get my supervisor,” she said. “This may take a few minutes.” I hung up on Jerry and, in a blaze of multitasking, filled out three Prior Authorization forms for clindamycin gel.
“I found your patient,” said the rep, returning at last. “Not only that, I was able to reregister him in the iPledge program. Want to know his iPledge number?
Of course!
“Now that he’s registered,” I said, “could you give me the name of the town you have him listed as living in on Chalupa Drive?”
“Sure,” she said, “We have him in Rancho Carmen Miranda. Can help you with anything else today?”
“No, thanks ...”
“Would you be willing to take a 2-minute survey ...?”
“No, but thank you very much!” I said, hanging up in triumph. (Cue: sunshine, violins.)
Back to the cell: “Jerry, you’re in! Here’s your iPledge number.”
“Thanks, Doc.”
“By the way, Jerry, iPledge has you living in the town of Rancho Carmen Miranda. Do you live there?”
“No,” said Jerry. “I don’t.”
“Well, Jerry, for 1 more month, for federal purposes, you do!”
I’m sure there’s a good explanation for all this. I just don’t want to know it. Just pass the candy corn.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years. His second book, “Act Like a Doctor, Think Like a Patient,” is available at amazon.com and barnesandnoble.com. Write to him at [email protected].
Topical retinoid found effective as microneedling for acne scars
according to a new study.
In a prospective, randomized, split-face study of adults with postacne scarring, both treatments resulted in similar efficacy after 6 months, reported T.P. Afra, MD, and associates from the department of dermatology, venereology, and leprology at the Postgraduate Institute of Medical Education and Research in Chandigarh, India. While the clinical usefulness of microneedling as a procedure for postacne scarring is well established, research exploring the effectiveness of topical therapies for acne scarring that could be used at home is lacking. “A home-based topical treatment with a comparable efficacy to microneedling and that is well tolerated would be a useful addition in the armamentarium of acne scar management,” they wrote in the study, published in JAMA Facial Plastic Surgery.
The study included 34 patients, aged 18-30 years, with grade 2-4 facial atrophic acne scars at their initial visit to the research team’s skin clinic. One side of each participants face was randomized to receive microneedling treatment for four sessions over 3 months (using a dermaroller with 1.5-mm needles). Topical tazarotene gel 0.1%, a retinoid approved by the Food and Drug Administration as a treatment for mild to moderate facial acne, was applied to the other side of their face once a night during the same time. Almost 81% were skin phototypes IV, the rest were type III or V. Patients followed up every month for 3 months, then at 6 months.
Changes in acne scar severity from baseline, the primary outcome, were assessed using Goodman and Baron quantitative and qualitative scores and a subjective dermatologist score. Patient satisfaction measured with a Patient Global Assessment (PGA) score and adverse events were secondary outcomes.
In 31 patients (91.2%), overall improvements from baseline to the 6-month visit in quantitative acne scar severity scores for both treatments were seen, with significant improvements from baseline to 6 months: A median improvement of 3 on the sides of the face treated with microneedling and a median improvement of 2.5 on the sides of the face treated with tazarotene (between-group comparison, P = .42). The qualitative acne scar severity score did not significantly improve with either treatment, the investigators noted.
The median improvement in the independent dermatologist score was also comparable for both methods at 3 and 6 months.
At 6 months, improvement in the mean PGA score was “slightly but significantly superior” for the microneedling treatment, compared with that for tazarotene (mean of 5.86 vs. 5.76, respectively; P less than .001), with both falling into the “satisfactory” range for the PGA, the investigators wrote. They also noted a positive correlation between previous exposure to oral isotretinoin and patient satisfaction.
“Although collagen accumulation has been considered a drawback of isotretinoin therapy owing to the development of hypertrophic scars, the better atrophic acne scar outcomes observed for both the present treatment groups in patients with a history of isotretinoin treatment indicates that the collagen accumulation in this case may actually be beneficial,” they wrote.
The topical retinoid was well tolerated by participants, with less than a third reporting dryness and scaling, and adverse effects associated with microneedling were described as “minimal.”
“The use of a modality such as tazarotene that prevents acne flares while addressing acne scarring is a practical addition to clinical practice,” the investigators concluded. “Tazarotene gel 0.1% would be a useful alternative to microneedling in the management of atrophic acne scars. Such a home-based medical management option for acne scarring may decrease physician dependence and health care expenditures for patients with postacne scarring.”
The study authors noted that, as collagen remodeling is a continuous process lasting more than 1 year, a limitation of their study was its short-follow-up of 6 months. However, a strength of the study was its use of validated acne scar severity scoring tools as well as patient and physician assessment of scar improvement in the outcome assessments.
The authors had no disclosures to report.
SOURCE: Afra TP et al. JAMA Facial Plast Surg. 2018 Nov 15. doi: 10.1001/jamafacial.2018.1404.
according to a new study.
In a prospective, randomized, split-face study of adults with postacne scarring, both treatments resulted in similar efficacy after 6 months, reported T.P. Afra, MD, and associates from the department of dermatology, venereology, and leprology at the Postgraduate Institute of Medical Education and Research in Chandigarh, India. While the clinical usefulness of microneedling as a procedure for postacne scarring is well established, research exploring the effectiveness of topical therapies for acne scarring that could be used at home is lacking. “A home-based topical treatment with a comparable efficacy to microneedling and that is well tolerated would be a useful addition in the armamentarium of acne scar management,” they wrote in the study, published in JAMA Facial Plastic Surgery.
The study included 34 patients, aged 18-30 years, with grade 2-4 facial atrophic acne scars at their initial visit to the research team’s skin clinic. One side of each participants face was randomized to receive microneedling treatment for four sessions over 3 months (using a dermaroller with 1.5-mm needles). Topical tazarotene gel 0.1%, a retinoid approved by the Food and Drug Administration as a treatment for mild to moderate facial acne, was applied to the other side of their face once a night during the same time. Almost 81% were skin phototypes IV, the rest were type III or V. Patients followed up every month for 3 months, then at 6 months.
Changes in acne scar severity from baseline, the primary outcome, were assessed using Goodman and Baron quantitative and qualitative scores and a subjective dermatologist score. Patient satisfaction measured with a Patient Global Assessment (PGA) score and adverse events were secondary outcomes.
In 31 patients (91.2%), overall improvements from baseline to the 6-month visit in quantitative acne scar severity scores for both treatments were seen, with significant improvements from baseline to 6 months: A median improvement of 3 on the sides of the face treated with microneedling and a median improvement of 2.5 on the sides of the face treated with tazarotene (between-group comparison, P = .42). The qualitative acne scar severity score did not significantly improve with either treatment, the investigators noted.
The median improvement in the independent dermatologist score was also comparable for both methods at 3 and 6 months.
At 6 months, improvement in the mean PGA score was “slightly but significantly superior” for the microneedling treatment, compared with that for tazarotene (mean of 5.86 vs. 5.76, respectively; P less than .001), with both falling into the “satisfactory” range for the PGA, the investigators wrote. They also noted a positive correlation between previous exposure to oral isotretinoin and patient satisfaction.
“Although collagen accumulation has been considered a drawback of isotretinoin therapy owing to the development of hypertrophic scars, the better atrophic acne scar outcomes observed for both the present treatment groups in patients with a history of isotretinoin treatment indicates that the collagen accumulation in this case may actually be beneficial,” they wrote.
The topical retinoid was well tolerated by participants, with less than a third reporting dryness and scaling, and adverse effects associated with microneedling were described as “minimal.”
“The use of a modality such as tazarotene that prevents acne flares while addressing acne scarring is a practical addition to clinical practice,” the investigators concluded. “Tazarotene gel 0.1% would be a useful alternative to microneedling in the management of atrophic acne scars. Such a home-based medical management option for acne scarring may decrease physician dependence and health care expenditures for patients with postacne scarring.”
The study authors noted that, as collagen remodeling is a continuous process lasting more than 1 year, a limitation of their study was its short-follow-up of 6 months. However, a strength of the study was its use of validated acne scar severity scoring tools as well as patient and physician assessment of scar improvement in the outcome assessments.
The authors had no disclosures to report.
SOURCE: Afra TP et al. JAMA Facial Plast Surg. 2018 Nov 15. doi: 10.1001/jamafacial.2018.1404.
according to a new study.
In a prospective, randomized, split-face study of adults with postacne scarring, both treatments resulted in similar efficacy after 6 months, reported T.P. Afra, MD, and associates from the department of dermatology, venereology, and leprology at the Postgraduate Institute of Medical Education and Research in Chandigarh, India. While the clinical usefulness of microneedling as a procedure for postacne scarring is well established, research exploring the effectiveness of topical therapies for acne scarring that could be used at home is lacking. “A home-based topical treatment with a comparable efficacy to microneedling and that is well tolerated would be a useful addition in the armamentarium of acne scar management,” they wrote in the study, published in JAMA Facial Plastic Surgery.
The study included 34 patients, aged 18-30 years, with grade 2-4 facial atrophic acne scars at their initial visit to the research team’s skin clinic. One side of each participants face was randomized to receive microneedling treatment for four sessions over 3 months (using a dermaroller with 1.5-mm needles). Topical tazarotene gel 0.1%, a retinoid approved by the Food and Drug Administration as a treatment for mild to moderate facial acne, was applied to the other side of their face once a night during the same time. Almost 81% were skin phototypes IV, the rest were type III or V. Patients followed up every month for 3 months, then at 6 months.
Changes in acne scar severity from baseline, the primary outcome, were assessed using Goodman and Baron quantitative and qualitative scores and a subjective dermatologist score. Patient satisfaction measured with a Patient Global Assessment (PGA) score and adverse events were secondary outcomes.
In 31 patients (91.2%), overall improvements from baseline to the 6-month visit in quantitative acne scar severity scores for both treatments were seen, with significant improvements from baseline to 6 months: A median improvement of 3 on the sides of the face treated with microneedling and a median improvement of 2.5 on the sides of the face treated with tazarotene (between-group comparison, P = .42). The qualitative acne scar severity score did not significantly improve with either treatment, the investigators noted.
The median improvement in the independent dermatologist score was also comparable for both methods at 3 and 6 months.
At 6 months, improvement in the mean PGA score was “slightly but significantly superior” for the microneedling treatment, compared with that for tazarotene (mean of 5.86 vs. 5.76, respectively; P less than .001), with both falling into the “satisfactory” range for the PGA, the investigators wrote. They also noted a positive correlation between previous exposure to oral isotretinoin and patient satisfaction.
“Although collagen accumulation has been considered a drawback of isotretinoin therapy owing to the development of hypertrophic scars, the better atrophic acne scar outcomes observed for both the present treatment groups in patients with a history of isotretinoin treatment indicates that the collagen accumulation in this case may actually be beneficial,” they wrote.
The topical retinoid was well tolerated by participants, with less than a third reporting dryness and scaling, and adverse effects associated with microneedling were described as “minimal.”
“The use of a modality such as tazarotene that prevents acne flares while addressing acne scarring is a practical addition to clinical practice,” the investigators concluded. “Tazarotene gel 0.1% would be a useful alternative to microneedling in the management of atrophic acne scars. Such a home-based medical management option for acne scarring may decrease physician dependence and health care expenditures for patients with postacne scarring.”
The study authors noted that, as collagen remodeling is a continuous process lasting more than 1 year, a limitation of their study was its short-follow-up of 6 months. However, a strength of the study was its use of validated acne scar severity scoring tools as well as patient and physician assessment of scar improvement in the outcome assessments.
The authors had no disclosures to report.
SOURCE: Afra TP et al. JAMA Facial Plast Surg. 2018 Nov 15. doi: 10.1001/jamafacial.2018.1404.
FROM JAMA FACIAL PLASTIC SURGERY
Key clinical point: The topical retinoid tazarotene could be a home-based option for treating atrophic acne scarring.
Major finding: Improvements in acne scarring were similar with microneedling and nightly applications of tazarotene gel 0.1% after 6 months.
Study details: A prospective, observer-blinded, split-face, randomized, clinical trial involving 34 patients with grade 2-4 facial atrophic postacne scars.
Disclosures: The authors had no disclosures to report.
Source: Afra TP et al. JAMA Facial Plast Surg. 2018 Nov 15. doi: 10.1001/jamafacial.2018.1404.