User login
Distance learning may cause convergence insufficiency
NEW ORLEANS – The increased use of digital screens for school during the COVID-19 pandemic may be causing convergence insufficiency in children, researchers say.
Although the long-term implications for current schoolchildren are not clear, convergence insufficiency sometimes persists for a lifetime, said Kammi Gunton, MD, interim chief of pediatric ophthalmology and strabismus at Wills Eye Hospital, Philadelphia.
“It’s important, if we use digital technology for education, that we are aware that it might contribute to increased eye symptoms in children,” Dr. Gunton told this news organization.
Dr. Gunton’s colleague, Jordan Hamburger, an MD candidate at Sidney Kimmel Medical College, Philadelphia, presented the finding at the American Academy of Ophthalmology 2021 Annual Meeting.
Convergence insufficiency is an impairment of binocularity. Symptoms include headaches while reading, words that seem to move around the page, blurriness, diplopia, and eye fatigue. It can be treated with exercise, prism glasses, or, rarely, surgery.
“We have some kids who improve with either time or maturity, then we have other patients who suffer from it for their entire lives,” Dr. Gunton said.
Previous research has linked the use of digital screens to convergence insufficiency, so when many schools shifted to distance learning for the pandemic, Dr. Gunton and her colleagues wanted to see whether it would have this effect on the students’ eyes.
They surveyed 110 healthy schoolchildren and adolescent students regarding eye symptoms before and after a day of virtual school. The mean age of the participants was 14 years (range, 10-17 years). The participants spent an average of 6.96 hours per day in virtual school. Forty-one percent also attended school in person part time. These students filled out the survey on days when they were in virtual school.
The participants answered questions on the Convergence Insufficiency Symptom Survey (CISS). The survey consists of 15 questions about eye complaints. On each question, the students rated symptoms from 0 to 4, with 4 indicating a severe symptom.
The average sum of the CISS scores rose from 5.17 before school to 9.82 after school, a statistically significant change (P < .001). Sixty-one percent of the participants reported an increase in convergence insufficiency symptoms.
Seventeen percent scored a total of at least 16, which is the threshold score considered suggestive of convergence insufficiency.
The researchers also found that, on average, the more hours each student spent in virtual school, the higher their CISS scores.
This makes sense, because reading requires convergence, Dr. Gunton said. The same problem might occur in traditional school if the students were looking at books all day instead of focusing on objects at various distances in their classrooms, such as the teacher or the whiteboard. “So, in the past, if you read a book, maybe you wouldn’t read for several hours, but now we’re asking children during virtual learning to stay on a device with the camera on,” she said.
Previous research has shown that people blink less when reading or using electronic devices, probably because of their increased concentration. This might explain symptoms such as burning and itching. Fifty-three percent of the students reported an increase in asthenopia symptoms.
The researchers would have liked to have compared the students in virtual school to a matched group of students in traditional school. However, almost all students were enrolled in virtual school when the study was conducted, making such a control difficult.
Although previous research has related virtual learning to myopia, as reported by this news organization, this study did not investigate myopia, and the researchers do not believe that convergence insufficiency causes myopia or vice versa.
Parents can help prevent convergence insufficiency during school by reminding their children to take breaks, Dr. Gunton said. She recommends the 20/20/20 rule: After 20 minutes of work that involves looking at objects nearby, students should take a 20-second break and look at something 20 feet away.
“I also think the take-home message is for parents to ask students if they’re having symptoms,” she said, “and if they hear complaints while kids are on the computers, to have them see an eye doctor and have an evaluation.”
Stephen Lipsky, MD, who wasn’t involved in the study, said he is seeing more cases of eye strain at Children’s Healthcare of Atlanta, where he is a consulting ophthalmologist.
“The study is very valuable in that it shines a light on the fact that these children do have symptoms, such as asthenopia or convergence insufficiency,” he told this news organization. “But I’m optimistic that with a return to more traditional learning, we will return the more traditional incidence of these problems.”
Dr. Gunton and Dr. Lipsky have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
NEW ORLEANS – The increased use of digital screens for school during the COVID-19 pandemic may be causing convergence insufficiency in children, researchers say.
Although the long-term implications for current schoolchildren are not clear, convergence insufficiency sometimes persists for a lifetime, said Kammi Gunton, MD, interim chief of pediatric ophthalmology and strabismus at Wills Eye Hospital, Philadelphia.
“It’s important, if we use digital technology for education, that we are aware that it might contribute to increased eye symptoms in children,” Dr. Gunton told this news organization.
Dr. Gunton’s colleague, Jordan Hamburger, an MD candidate at Sidney Kimmel Medical College, Philadelphia, presented the finding at the American Academy of Ophthalmology 2021 Annual Meeting.
Convergence insufficiency is an impairment of binocularity. Symptoms include headaches while reading, words that seem to move around the page, blurriness, diplopia, and eye fatigue. It can be treated with exercise, prism glasses, or, rarely, surgery.
“We have some kids who improve with either time or maturity, then we have other patients who suffer from it for their entire lives,” Dr. Gunton said.
Previous research has linked the use of digital screens to convergence insufficiency, so when many schools shifted to distance learning for the pandemic, Dr. Gunton and her colleagues wanted to see whether it would have this effect on the students’ eyes.
They surveyed 110 healthy schoolchildren and adolescent students regarding eye symptoms before and after a day of virtual school. The mean age of the participants was 14 years (range, 10-17 years). The participants spent an average of 6.96 hours per day in virtual school. Forty-one percent also attended school in person part time. These students filled out the survey on days when they were in virtual school.
The participants answered questions on the Convergence Insufficiency Symptom Survey (CISS). The survey consists of 15 questions about eye complaints. On each question, the students rated symptoms from 0 to 4, with 4 indicating a severe symptom.
The average sum of the CISS scores rose from 5.17 before school to 9.82 after school, a statistically significant change (P < .001). Sixty-one percent of the participants reported an increase in convergence insufficiency symptoms.
Seventeen percent scored a total of at least 16, which is the threshold score considered suggestive of convergence insufficiency.
The researchers also found that, on average, the more hours each student spent in virtual school, the higher their CISS scores.
This makes sense, because reading requires convergence, Dr. Gunton said. The same problem might occur in traditional school if the students were looking at books all day instead of focusing on objects at various distances in their classrooms, such as the teacher or the whiteboard. “So, in the past, if you read a book, maybe you wouldn’t read for several hours, but now we’re asking children during virtual learning to stay on a device with the camera on,” she said.
Previous research has shown that people blink less when reading or using electronic devices, probably because of their increased concentration. This might explain symptoms such as burning and itching. Fifty-three percent of the students reported an increase in asthenopia symptoms.
The researchers would have liked to have compared the students in virtual school to a matched group of students in traditional school. However, almost all students were enrolled in virtual school when the study was conducted, making such a control difficult.
Although previous research has related virtual learning to myopia, as reported by this news organization, this study did not investigate myopia, and the researchers do not believe that convergence insufficiency causes myopia or vice versa.
Parents can help prevent convergence insufficiency during school by reminding their children to take breaks, Dr. Gunton said. She recommends the 20/20/20 rule: After 20 minutes of work that involves looking at objects nearby, students should take a 20-second break and look at something 20 feet away.
“I also think the take-home message is for parents to ask students if they’re having symptoms,” she said, “and if they hear complaints while kids are on the computers, to have them see an eye doctor and have an evaluation.”
Stephen Lipsky, MD, who wasn’t involved in the study, said he is seeing more cases of eye strain at Children’s Healthcare of Atlanta, where he is a consulting ophthalmologist.
“The study is very valuable in that it shines a light on the fact that these children do have symptoms, such as asthenopia or convergence insufficiency,” he told this news organization. “But I’m optimistic that with a return to more traditional learning, we will return the more traditional incidence of these problems.”
Dr. Gunton and Dr. Lipsky have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
NEW ORLEANS – The increased use of digital screens for school during the COVID-19 pandemic may be causing convergence insufficiency in children, researchers say.
Although the long-term implications for current schoolchildren are not clear, convergence insufficiency sometimes persists for a lifetime, said Kammi Gunton, MD, interim chief of pediatric ophthalmology and strabismus at Wills Eye Hospital, Philadelphia.
“It’s important, if we use digital technology for education, that we are aware that it might contribute to increased eye symptoms in children,” Dr. Gunton told this news organization.
Dr. Gunton’s colleague, Jordan Hamburger, an MD candidate at Sidney Kimmel Medical College, Philadelphia, presented the finding at the American Academy of Ophthalmology 2021 Annual Meeting.
Convergence insufficiency is an impairment of binocularity. Symptoms include headaches while reading, words that seem to move around the page, blurriness, diplopia, and eye fatigue. It can be treated with exercise, prism glasses, or, rarely, surgery.
“We have some kids who improve with either time or maturity, then we have other patients who suffer from it for their entire lives,” Dr. Gunton said.
Previous research has linked the use of digital screens to convergence insufficiency, so when many schools shifted to distance learning for the pandemic, Dr. Gunton and her colleagues wanted to see whether it would have this effect on the students’ eyes.
They surveyed 110 healthy schoolchildren and adolescent students regarding eye symptoms before and after a day of virtual school. The mean age of the participants was 14 years (range, 10-17 years). The participants spent an average of 6.96 hours per day in virtual school. Forty-one percent also attended school in person part time. These students filled out the survey on days when they were in virtual school.
The participants answered questions on the Convergence Insufficiency Symptom Survey (CISS). The survey consists of 15 questions about eye complaints. On each question, the students rated symptoms from 0 to 4, with 4 indicating a severe symptom.
The average sum of the CISS scores rose from 5.17 before school to 9.82 after school, a statistically significant change (P < .001). Sixty-one percent of the participants reported an increase in convergence insufficiency symptoms.
Seventeen percent scored a total of at least 16, which is the threshold score considered suggestive of convergence insufficiency.
The researchers also found that, on average, the more hours each student spent in virtual school, the higher their CISS scores.
This makes sense, because reading requires convergence, Dr. Gunton said. The same problem might occur in traditional school if the students were looking at books all day instead of focusing on objects at various distances in their classrooms, such as the teacher or the whiteboard. “So, in the past, if you read a book, maybe you wouldn’t read for several hours, but now we’re asking children during virtual learning to stay on a device with the camera on,” she said.
Previous research has shown that people blink less when reading or using electronic devices, probably because of their increased concentration. This might explain symptoms such as burning and itching. Fifty-three percent of the students reported an increase in asthenopia symptoms.
The researchers would have liked to have compared the students in virtual school to a matched group of students in traditional school. However, almost all students were enrolled in virtual school when the study was conducted, making such a control difficult.
Although previous research has related virtual learning to myopia, as reported by this news organization, this study did not investigate myopia, and the researchers do not believe that convergence insufficiency causes myopia or vice versa.
Parents can help prevent convergence insufficiency during school by reminding their children to take breaks, Dr. Gunton said. She recommends the 20/20/20 rule: After 20 minutes of work that involves looking at objects nearby, students should take a 20-second break and look at something 20 feet away.
“I also think the take-home message is for parents to ask students if they’re having symptoms,” she said, “and if they hear complaints while kids are on the computers, to have them see an eye doctor and have an evaluation.”
Stephen Lipsky, MD, who wasn’t involved in the study, said he is seeing more cases of eye strain at Children’s Healthcare of Atlanta, where he is a consulting ophthalmologist.
“The study is very valuable in that it shines a light on the fact that these children do have symptoms, such as asthenopia or convergence insufficiency,” he told this news organization. “But I’m optimistic that with a return to more traditional learning, we will return the more traditional incidence of these problems.”
Dr. Gunton and Dr. Lipsky have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM AAO 2021
Moms’ cannabis use in pregnancy tied to anxiety and hyperactivity in offspring
Mothers who use cannabis during pregnancy risk disrupting immune gene networks in the placenta and potentially increasing the risk of anxiety and hyperactivity in their children.
These findings emerged from a study led by Yasmin Hurd, PhD, a professor of psychiatry and director of the Addiction Institute at the Icahn School of Medicine at Mount Sinai, New York, and Yoko Nomura, PhD, a professor of behavioral neuroscience at Queen’s College, City University of New York, that was published online in Proceedings of the National Academy of Sciences.
The analysis assessed the effects of gestational maternal cannabis use on psychosocial and physiological measures in young children as well as its potentially immunomodulatory effect on the in utero environment as reflected in the placental transcriptome.
Participants were drawn from a larger cohort in a study launched in 2012; the investigators evaluated offspring aged 3-6 years for hair hormone levels, neurobehavioral traits on the Behavioral Assessment System for Children survey, and heart rate variability (HRV) at rest and during auditory startle.
The cohort consisted of 322 mother-child dyads and children with prenatal exposure to cannabis were compared with those having no exposure. The cohort consisted of 251 non–cannabis-using mothers and 71 cannabis-using mothers, with mean maternal ages in the two groups of 28.46 years and 25.91 years, respectively, The mothers gave birth at Mount Sinai and they and their children were assessed annually at affiliated medical centers in Mount Sinai’s catchment area.
For a subset of children with behavioral assessments, placental specimens collected at birth were processed for RNA sequencing.
Among the findings:
- Maternal cannabis use was associated with reduced maternal and paternal age, more single-mother pregnancies, state anxiety, trait anxiety, depression, cigarette smoking, and African American race.
- Hair hormone analysis revealed increased cortisol levels in the children of cannabis-using mothers, and was associated with greater anxiety, aggression, and hyperactivity.
- Affected children showed a reduction in the high-frequency component of HRV at baseline, reflecting reduced vagal tone.
- In the placenta, there was reduced expression of many genes involved in immune system function. These included genes for type I interferon, neutrophil, and cytokine-signaling pathways.
Several of these genes organized into coexpression networks that correlated with child anxiety and hyperactivity.
The principal active component of cannabis, tetrahydrocannabinol (THC), targets the endocannabinoid system in placental tissue and the developing brain, the authors noted. Exposure during pregnancy is associated with a range of adverse outcomes from fetal growth restriction to low birth weight and preterm birth.
“There are cannabinoid receptors on immune cells, and it is known that cannabinoids can alter immune function, which is important for maintaining maternal tolerance and protecting the fetus,” Dr. Hurd said. “It’s not surprising that something that affects the immune cells can have an impact on the developing fetus.”
“Overall, our findings reveal a relationship between [maternal cannabis use] and immune response gene networks in the placenta as a potential mediator of risk for anxiety-related problems in early childhood,” Dr. Hurd and colleagues wrote, adding that the results have significant implications for defining mental health issues in the children gestated by cannabis-smoking mothers.
Their results align with previous research indicating a greater risk for psychiatric illness in children with prenatal cannabis exposure from maternal use.
“While data are pretty limited in this realm, there are other studies that demonstrate a relationship between early child developmental and behavioral measures and cannabis use during pregnancy,” Camille Hoffman, MD, MSc, a high-risk obstetrics specialist and an associate professor at the University of Colorado at Denver, Aurora, said in an interview. “Our research group found children exposed to cannabis in utero at 10 weeks’ gestation and beyond were less interactive and more withdrawn than children who were not exposed.”
And THC remains in maternal breast milk even 6 weeks after usage stops.
The long-term effects of prenatal cannabis exposure remain to be determined and it is unknown whether the effects of gestational THC might attenuate as a child grows older. “We use early childhood measures in research as a proxy for the later development of diagnosed mental health conditions or behavioral problems,” Dr. Hoffman explained. “We know when we do this that not every child with an abnormal score early will go on to develop an actual condition. Fortunately, or unfortunately, other factors and exposures during childhood can change the trajectory for the better or worse.”
According to Dr. Hurd, child development is a dynamic process and epigenetic events in utero need not be deterministic. “The important thing is to identify children at risk early and to be able to go in and try to improve the environment they’re being raised in – not in terms of impoverishment but in terms of positive nurturing and giving the mother and family support.”
At the prenatal level, what’s the best advice for cannabis-using mothers-to-be? “If a woman doesn’t know she’s pregnant and has been using cannabis, taking extra choline for the remainder of the pregnancy can help buffer the potential negative impact of the cannabis exposure,” Dr. Hoffman said. The Food and Drug Administration and the American Medical Association recommend a dose of 550 mg daily. “The same is true for alcohol, which we know is also very bad for fetal brain development. This is not to say go ahead and use these substances and just take choline. The choline is more to try and salvage damage to the fetal brain that may have already occurred.”
This study was supported by the National Institute of Mental Health and the National Institute on Drug Abuse. The authors declared no competing interests. Dr. Hoffman disclosed no conflicts of interest with respect to her comments.
Mothers who use cannabis during pregnancy risk disrupting immune gene networks in the placenta and potentially increasing the risk of anxiety and hyperactivity in their children.
These findings emerged from a study led by Yasmin Hurd, PhD, a professor of psychiatry and director of the Addiction Institute at the Icahn School of Medicine at Mount Sinai, New York, and Yoko Nomura, PhD, a professor of behavioral neuroscience at Queen’s College, City University of New York, that was published online in Proceedings of the National Academy of Sciences.
The analysis assessed the effects of gestational maternal cannabis use on psychosocial and physiological measures in young children as well as its potentially immunomodulatory effect on the in utero environment as reflected in the placental transcriptome.
Participants were drawn from a larger cohort in a study launched in 2012; the investigators evaluated offspring aged 3-6 years for hair hormone levels, neurobehavioral traits on the Behavioral Assessment System for Children survey, and heart rate variability (HRV) at rest and during auditory startle.
The cohort consisted of 322 mother-child dyads and children with prenatal exposure to cannabis were compared with those having no exposure. The cohort consisted of 251 non–cannabis-using mothers and 71 cannabis-using mothers, with mean maternal ages in the two groups of 28.46 years and 25.91 years, respectively, The mothers gave birth at Mount Sinai and they and their children were assessed annually at affiliated medical centers in Mount Sinai’s catchment area.
For a subset of children with behavioral assessments, placental specimens collected at birth were processed for RNA sequencing.
Among the findings:
- Maternal cannabis use was associated with reduced maternal and paternal age, more single-mother pregnancies, state anxiety, trait anxiety, depression, cigarette smoking, and African American race.
- Hair hormone analysis revealed increased cortisol levels in the children of cannabis-using mothers, and was associated with greater anxiety, aggression, and hyperactivity.
- Affected children showed a reduction in the high-frequency component of HRV at baseline, reflecting reduced vagal tone.
- In the placenta, there was reduced expression of many genes involved in immune system function. These included genes for type I interferon, neutrophil, and cytokine-signaling pathways.
Several of these genes organized into coexpression networks that correlated with child anxiety and hyperactivity.
The principal active component of cannabis, tetrahydrocannabinol (THC), targets the endocannabinoid system in placental tissue and the developing brain, the authors noted. Exposure during pregnancy is associated with a range of adverse outcomes from fetal growth restriction to low birth weight and preterm birth.
“There are cannabinoid receptors on immune cells, and it is known that cannabinoids can alter immune function, which is important for maintaining maternal tolerance and protecting the fetus,” Dr. Hurd said. “It’s not surprising that something that affects the immune cells can have an impact on the developing fetus.”
“Overall, our findings reveal a relationship between [maternal cannabis use] and immune response gene networks in the placenta as a potential mediator of risk for anxiety-related problems in early childhood,” Dr. Hurd and colleagues wrote, adding that the results have significant implications for defining mental health issues in the children gestated by cannabis-smoking mothers.
Their results align with previous research indicating a greater risk for psychiatric illness in children with prenatal cannabis exposure from maternal use.
“While data are pretty limited in this realm, there are other studies that demonstrate a relationship between early child developmental and behavioral measures and cannabis use during pregnancy,” Camille Hoffman, MD, MSc, a high-risk obstetrics specialist and an associate professor at the University of Colorado at Denver, Aurora, said in an interview. “Our research group found children exposed to cannabis in utero at 10 weeks’ gestation and beyond were less interactive and more withdrawn than children who were not exposed.”
And THC remains in maternal breast milk even 6 weeks after usage stops.
The long-term effects of prenatal cannabis exposure remain to be determined and it is unknown whether the effects of gestational THC might attenuate as a child grows older. “We use early childhood measures in research as a proxy for the later development of diagnosed mental health conditions or behavioral problems,” Dr. Hoffman explained. “We know when we do this that not every child with an abnormal score early will go on to develop an actual condition. Fortunately, or unfortunately, other factors and exposures during childhood can change the trajectory for the better or worse.”
According to Dr. Hurd, child development is a dynamic process and epigenetic events in utero need not be deterministic. “The important thing is to identify children at risk early and to be able to go in and try to improve the environment they’re being raised in – not in terms of impoverishment but in terms of positive nurturing and giving the mother and family support.”
At the prenatal level, what’s the best advice for cannabis-using mothers-to-be? “If a woman doesn’t know she’s pregnant and has been using cannabis, taking extra choline for the remainder of the pregnancy can help buffer the potential negative impact of the cannabis exposure,” Dr. Hoffman said. The Food and Drug Administration and the American Medical Association recommend a dose of 550 mg daily. “The same is true for alcohol, which we know is also very bad for fetal brain development. This is not to say go ahead and use these substances and just take choline. The choline is more to try and salvage damage to the fetal brain that may have already occurred.”
This study was supported by the National Institute of Mental Health and the National Institute on Drug Abuse. The authors declared no competing interests. Dr. Hoffman disclosed no conflicts of interest with respect to her comments.
Mothers who use cannabis during pregnancy risk disrupting immune gene networks in the placenta and potentially increasing the risk of anxiety and hyperactivity in their children.
These findings emerged from a study led by Yasmin Hurd, PhD, a professor of psychiatry and director of the Addiction Institute at the Icahn School of Medicine at Mount Sinai, New York, and Yoko Nomura, PhD, a professor of behavioral neuroscience at Queen’s College, City University of New York, that was published online in Proceedings of the National Academy of Sciences.
The analysis assessed the effects of gestational maternal cannabis use on psychosocial and physiological measures in young children as well as its potentially immunomodulatory effect on the in utero environment as reflected in the placental transcriptome.
Participants were drawn from a larger cohort in a study launched in 2012; the investigators evaluated offspring aged 3-6 years for hair hormone levels, neurobehavioral traits on the Behavioral Assessment System for Children survey, and heart rate variability (HRV) at rest and during auditory startle.
The cohort consisted of 322 mother-child dyads and children with prenatal exposure to cannabis were compared with those having no exposure. The cohort consisted of 251 non–cannabis-using mothers and 71 cannabis-using mothers, with mean maternal ages in the two groups of 28.46 years and 25.91 years, respectively, The mothers gave birth at Mount Sinai and they and their children were assessed annually at affiliated medical centers in Mount Sinai’s catchment area.
For a subset of children with behavioral assessments, placental specimens collected at birth were processed for RNA sequencing.
Among the findings:
- Maternal cannabis use was associated with reduced maternal and paternal age, more single-mother pregnancies, state anxiety, trait anxiety, depression, cigarette smoking, and African American race.
- Hair hormone analysis revealed increased cortisol levels in the children of cannabis-using mothers, and was associated with greater anxiety, aggression, and hyperactivity.
- Affected children showed a reduction in the high-frequency component of HRV at baseline, reflecting reduced vagal tone.
- In the placenta, there was reduced expression of many genes involved in immune system function. These included genes for type I interferon, neutrophil, and cytokine-signaling pathways.
Several of these genes organized into coexpression networks that correlated with child anxiety and hyperactivity.
The principal active component of cannabis, tetrahydrocannabinol (THC), targets the endocannabinoid system in placental tissue and the developing brain, the authors noted. Exposure during pregnancy is associated with a range of adverse outcomes from fetal growth restriction to low birth weight and preterm birth.
“There are cannabinoid receptors on immune cells, and it is known that cannabinoids can alter immune function, which is important for maintaining maternal tolerance and protecting the fetus,” Dr. Hurd said. “It’s not surprising that something that affects the immune cells can have an impact on the developing fetus.”
“Overall, our findings reveal a relationship between [maternal cannabis use] and immune response gene networks in the placenta as a potential mediator of risk for anxiety-related problems in early childhood,” Dr. Hurd and colleagues wrote, adding that the results have significant implications for defining mental health issues in the children gestated by cannabis-smoking mothers.
Their results align with previous research indicating a greater risk for psychiatric illness in children with prenatal cannabis exposure from maternal use.
“While data are pretty limited in this realm, there are other studies that demonstrate a relationship between early child developmental and behavioral measures and cannabis use during pregnancy,” Camille Hoffman, MD, MSc, a high-risk obstetrics specialist and an associate professor at the University of Colorado at Denver, Aurora, said in an interview. “Our research group found children exposed to cannabis in utero at 10 weeks’ gestation and beyond were less interactive and more withdrawn than children who were not exposed.”
And THC remains in maternal breast milk even 6 weeks after usage stops.
The long-term effects of prenatal cannabis exposure remain to be determined and it is unknown whether the effects of gestational THC might attenuate as a child grows older. “We use early childhood measures in research as a proxy for the later development of diagnosed mental health conditions or behavioral problems,” Dr. Hoffman explained. “We know when we do this that not every child with an abnormal score early will go on to develop an actual condition. Fortunately, or unfortunately, other factors and exposures during childhood can change the trajectory for the better or worse.”
According to Dr. Hurd, child development is a dynamic process and epigenetic events in utero need not be deterministic. “The important thing is to identify children at risk early and to be able to go in and try to improve the environment they’re being raised in – not in terms of impoverishment but in terms of positive nurturing and giving the mother and family support.”
At the prenatal level, what’s the best advice for cannabis-using mothers-to-be? “If a woman doesn’t know she’s pregnant and has been using cannabis, taking extra choline for the remainder of the pregnancy can help buffer the potential negative impact of the cannabis exposure,” Dr. Hoffman said. The Food and Drug Administration and the American Medical Association recommend a dose of 550 mg daily. “The same is true for alcohol, which we know is also very bad for fetal brain development. This is not to say go ahead and use these substances and just take choline. The choline is more to try and salvage damage to the fetal brain that may have already occurred.”
This study was supported by the National Institute of Mental Health and the National Institute on Drug Abuse. The authors declared no competing interests. Dr. Hoffman disclosed no conflicts of interest with respect to her comments.
FROM PROCEEDINGS OF THE NATIONAL ACADEMY OF SCIENCES
More tools for the COVID toolbox
I was recently asked to see a 16-year-old, unvaccinated (against COVID-19) adolescent with hypothyroidism and obesity (body mass index 37 kg/m2) seen in the pediatric emergency department with tachycardia, O2 saturation 96%, urinary tract infection, poor appetite, and nausea. Her chest x-ray had low lung volumes but no infiltrates. She was noted to be dehydrated. Testing for COVID-19 was PCR positive.1
She was observed overnight, tolerated oral rehydration, and was being readied for discharge. Pediatric Infectious Diseases was called about prescribing remdesivir.
Remdesivir was not indicated as its current use is limited to inpatients with oxygen desaturations less than 94%. Infectious Diseases Society of America guidelines do recommend the use of monoclonal antibodies against the SARS-CoV-2 spike protein for prevention of COVID disease progression in high-risk individuals. Specifically, the IDSA guidelines say, “Among ambulatory patients with mild to moderate COVID-19 at high risk for progression to severe disease, bamlanivimab/etesevimab, casirivimab/imdevimab, or sotrovimab rather than no neutralizing antibody treatment.”
The Food and Drug Administration’s Emergency Use Authorization (EUA) allowed use of specific monoclonal antibodies (casirivimab/imdevimab in combination, bamlanivimab/etesevimab in combination, and sotrovimab alone) for individuals 12 years and above with a minimum weight of 40 kg with high-risk conditions, describing the evidence as moderate certainty.2
Several questions have arisen regarding their use. Which children qualify under the EUA? Are the available monoclonal antibodies effective for SARS-CoV-2 variants? What adverse events were observed? Are there implementation hurdles?
Unlike the EUA for prophylactic use, which targeted unvaccinated individuals and those unlikely to have a good antibody response to vaccine, use of monoclonal antibody for prevention of progression does not have such restrictions. Effectiveness may vary by local variant susceptibility and should be considered in the choice of the most appropriate monoclonal antibody therapy. Reductions in hospitalization and progression to critical disease status were reported from phase 3 studies; reductions were also observed in mortality in some, but not all, studies. Enhanced viral clearance on day 7 was observed with few subjects having persistent high viral load.
Which children qualify under the EUA? Adolescents 12 years and older and over 40 kg are eligible if a high risk condition is present. High-risk conditions include body mass index at the 85th percentile or higher, immunosuppressive disease, or receipt of immunosuppressive therapies, or baseline (pre-COVID infection) medical-related technological dependence such as tracheostomy or positive pressure ventilation. Additional high-risk conditions are neurodevelopmental disorders, sickle cell disease, congenital or acquired heart disease, asthma, or reactive airway or other chronic respiratory disease that requires daily medication for control, diabetes, chronic kidney disease, or pregnancy.3
Are the available monoclonal antibodies effective for SARS-CoV-2 variants? Of course, this is a critical question and relies on knowledge of the dominant variant in a specific geographic location. The CDC data on which variants are susceptible to which monoclonal therapies were updated as of Oct. 21 online (see Table 1). Local departments of public health often will have current data on the dominant variant in the community. Currently, the dominant variant in the United States is Delta and it is anticipated to be susceptible to the three monoclonal treatments authorized under the EUA based on in vitro neutralizing assays.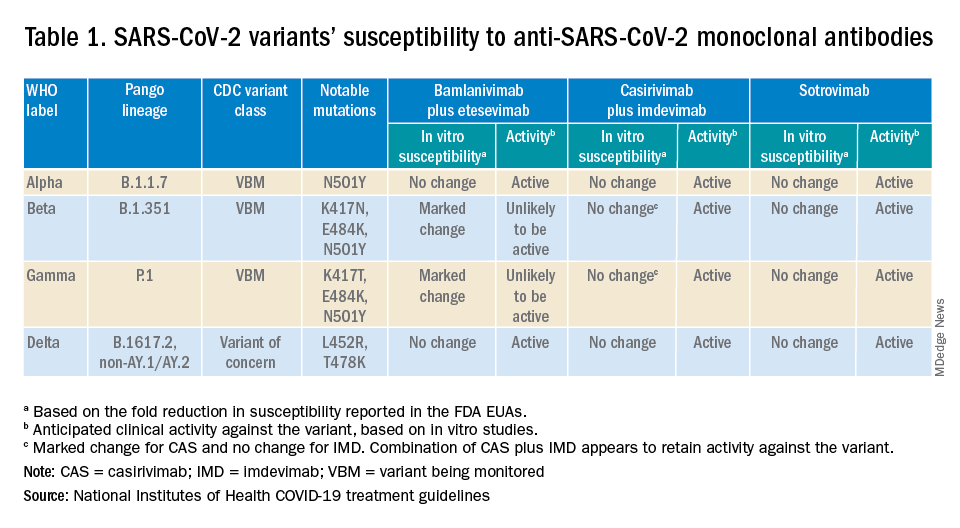
What adverse events were observed? Monoclonal antibody infusions are in general safe but anaphylaxis has been reported. Other infusion-related adverse events include urticaria, pruritis, flushing, pyrexia, shortness of breath, chest tightness, nausea, vomiting, and rash. Nearly all events were grade 1, mild, or grade 2, moderate. For nonsevere infusion-related reactions, consider slowing the infusion; if necessary, the infusion should be stopped.
Implementation challenges
The first challenge is finding a location to infuse the monoclonal antibodies. Although they can be given subcutaneously, the dose is large and little, if any, time is saved as the recommendation is for observation post administration for 1 hour. The challenge we and other centers may face is that the patients are COVID PCR+ and therefore our usual infusion program, which often is occupied by individuals already compromised and at high risk for severe COVID, is an undesirable location. We are planning to use the emergency department to accommodate such patients currently, but even that solution creates challenges for a busy, urban medical center.

Summary
Anti–SARS-CoV-2 monoclonal antibodies are an important part of the therapeutic approach to minimizing disease severity. Clinicians should review high-risk conditions in adolescents who are PCR+ for SARS-CoV-2 and have mild to moderate symptoms. Medical care systems should implement programs to make monoclonal infusions available for such high-risk adolescents.4 Obesity and asthma reactive airways or requiring daily medication for control are the two most common conditions that place adolescents with COVID-19 at risk for progression to hospitalization and severe disease in addition to the more traditional immune-compromising conditions and medical fragility.
Dr. Pelton is professor of pediatrics and epidemiology at Boston University schools of medicine and public health and senior attending physician in pediatric infectious diseases, Boston Medical Center. Email him at [email protected].
References
1. Federal Response to COVID-19: Monoclonal Antibody Clinical Implementation Guide. U.S. Department of Health and Human Services. 2021 Sep 2.
2. Bhimraj A et al. IDSA Guidelines on the Treatment and Management of Patients with COVID-19. Last updated 2021 Nov 9.
3. Anti-SARS-CoV-2 Monoclonal Antibodies. National Institutes of Health’s COVID 19 Treatment Guidelines. Last updated 2021 Oct 19.
4. Spreading the Word on the Benefits of Monoclonal Antibodies for COVID-19, by Hannah R. Buchdahl. CDC Foundation, 2021 Jul 2.
I was recently asked to see a 16-year-old, unvaccinated (against COVID-19) adolescent with hypothyroidism and obesity (body mass index 37 kg/m2) seen in the pediatric emergency department with tachycardia, O2 saturation 96%, urinary tract infection, poor appetite, and nausea. Her chest x-ray had low lung volumes but no infiltrates. She was noted to be dehydrated. Testing for COVID-19 was PCR positive.1
She was observed overnight, tolerated oral rehydration, and was being readied for discharge. Pediatric Infectious Diseases was called about prescribing remdesivir.
Remdesivir was not indicated as its current use is limited to inpatients with oxygen desaturations less than 94%. Infectious Diseases Society of America guidelines do recommend the use of monoclonal antibodies against the SARS-CoV-2 spike protein for prevention of COVID disease progression in high-risk individuals. Specifically, the IDSA guidelines say, “Among ambulatory patients with mild to moderate COVID-19 at high risk for progression to severe disease, bamlanivimab/etesevimab, casirivimab/imdevimab, or sotrovimab rather than no neutralizing antibody treatment.”
The Food and Drug Administration’s Emergency Use Authorization (EUA) allowed use of specific monoclonal antibodies (casirivimab/imdevimab in combination, bamlanivimab/etesevimab in combination, and sotrovimab alone) for individuals 12 years and above with a minimum weight of 40 kg with high-risk conditions, describing the evidence as moderate certainty.2
Several questions have arisen regarding their use. Which children qualify under the EUA? Are the available monoclonal antibodies effective for SARS-CoV-2 variants? What adverse events were observed? Are there implementation hurdles?
Unlike the EUA for prophylactic use, which targeted unvaccinated individuals and those unlikely to have a good antibody response to vaccine, use of monoclonal antibody for prevention of progression does not have such restrictions. Effectiveness may vary by local variant susceptibility and should be considered in the choice of the most appropriate monoclonal antibody therapy. Reductions in hospitalization and progression to critical disease status were reported from phase 3 studies; reductions were also observed in mortality in some, but not all, studies. Enhanced viral clearance on day 7 was observed with few subjects having persistent high viral load.
Which children qualify under the EUA? Adolescents 12 years and older and over 40 kg are eligible if a high risk condition is present. High-risk conditions include body mass index at the 85th percentile or higher, immunosuppressive disease, or receipt of immunosuppressive therapies, or baseline (pre-COVID infection) medical-related technological dependence such as tracheostomy or positive pressure ventilation. Additional high-risk conditions are neurodevelopmental disorders, sickle cell disease, congenital or acquired heart disease, asthma, or reactive airway or other chronic respiratory disease that requires daily medication for control, diabetes, chronic kidney disease, or pregnancy.3
Are the available monoclonal antibodies effective for SARS-CoV-2 variants? Of course, this is a critical question and relies on knowledge of the dominant variant in a specific geographic location. The CDC data on which variants are susceptible to which monoclonal therapies were updated as of Oct. 21 online (see Table 1). Local departments of public health often will have current data on the dominant variant in the community. Currently, the dominant variant in the United States is Delta and it is anticipated to be susceptible to the three monoclonal treatments authorized under the EUA based on in vitro neutralizing assays.
What adverse events were observed? Monoclonal antibody infusions are in general safe but anaphylaxis has been reported. Other infusion-related adverse events include urticaria, pruritis, flushing, pyrexia, shortness of breath, chest tightness, nausea, vomiting, and rash. Nearly all events were grade 1, mild, or grade 2, moderate. For nonsevere infusion-related reactions, consider slowing the infusion; if necessary, the infusion should be stopped.
Implementation challenges
The first challenge is finding a location to infuse the monoclonal antibodies. Although they can be given subcutaneously, the dose is large and little, if any, time is saved as the recommendation is for observation post administration for 1 hour. The challenge we and other centers may face is that the patients are COVID PCR+ and therefore our usual infusion program, which often is occupied by individuals already compromised and at high risk for severe COVID, is an undesirable location. We are planning to use the emergency department to accommodate such patients currently, but even that solution creates challenges for a busy, urban medical center.

Summary
Anti–SARS-CoV-2 monoclonal antibodies are an important part of the therapeutic approach to minimizing disease severity. Clinicians should review high-risk conditions in adolescents who are PCR+ for SARS-CoV-2 and have mild to moderate symptoms. Medical care systems should implement programs to make monoclonal infusions available for such high-risk adolescents.4 Obesity and asthma reactive airways or requiring daily medication for control are the two most common conditions that place adolescents with COVID-19 at risk for progression to hospitalization and severe disease in addition to the more traditional immune-compromising conditions and medical fragility.
Dr. Pelton is professor of pediatrics and epidemiology at Boston University schools of medicine and public health and senior attending physician in pediatric infectious diseases, Boston Medical Center. Email him at [email protected].
References
1. Federal Response to COVID-19: Monoclonal Antibody Clinical Implementation Guide. U.S. Department of Health and Human Services. 2021 Sep 2.
2. Bhimraj A et al. IDSA Guidelines on the Treatment and Management of Patients with COVID-19. Last updated 2021 Nov 9.
3. Anti-SARS-CoV-2 Monoclonal Antibodies. National Institutes of Health’s COVID 19 Treatment Guidelines. Last updated 2021 Oct 19.
4. Spreading the Word on the Benefits of Monoclonal Antibodies for COVID-19, by Hannah R. Buchdahl. CDC Foundation, 2021 Jul 2.
I was recently asked to see a 16-year-old, unvaccinated (against COVID-19) adolescent with hypothyroidism and obesity (body mass index 37 kg/m2) seen in the pediatric emergency department with tachycardia, O2 saturation 96%, urinary tract infection, poor appetite, and nausea. Her chest x-ray had low lung volumes but no infiltrates. She was noted to be dehydrated. Testing for COVID-19 was PCR positive.1
She was observed overnight, tolerated oral rehydration, and was being readied for discharge. Pediatric Infectious Diseases was called about prescribing remdesivir.
Remdesivir was not indicated as its current use is limited to inpatients with oxygen desaturations less than 94%. Infectious Diseases Society of America guidelines do recommend the use of monoclonal antibodies against the SARS-CoV-2 spike protein for prevention of COVID disease progression in high-risk individuals. Specifically, the IDSA guidelines say, “Among ambulatory patients with mild to moderate COVID-19 at high risk for progression to severe disease, bamlanivimab/etesevimab, casirivimab/imdevimab, or sotrovimab rather than no neutralizing antibody treatment.”
The Food and Drug Administration’s Emergency Use Authorization (EUA) allowed use of specific monoclonal antibodies (casirivimab/imdevimab in combination, bamlanivimab/etesevimab in combination, and sotrovimab alone) for individuals 12 years and above with a minimum weight of 40 kg with high-risk conditions, describing the evidence as moderate certainty.2
Several questions have arisen regarding their use. Which children qualify under the EUA? Are the available monoclonal antibodies effective for SARS-CoV-2 variants? What adverse events were observed? Are there implementation hurdles?
Unlike the EUA for prophylactic use, which targeted unvaccinated individuals and those unlikely to have a good antibody response to vaccine, use of monoclonal antibody for prevention of progression does not have such restrictions. Effectiveness may vary by local variant susceptibility and should be considered in the choice of the most appropriate monoclonal antibody therapy. Reductions in hospitalization and progression to critical disease status were reported from phase 3 studies; reductions were also observed in mortality in some, but not all, studies. Enhanced viral clearance on day 7 was observed with few subjects having persistent high viral load.
Which children qualify under the EUA? Adolescents 12 years and older and over 40 kg are eligible if a high risk condition is present. High-risk conditions include body mass index at the 85th percentile or higher, immunosuppressive disease, or receipt of immunosuppressive therapies, or baseline (pre-COVID infection) medical-related technological dependence such as tracheostomy or positive pressure ventilation. Additional high-risk conditions are neurodevelopmental disorders, sickle cell disease, congenital or acquired heart disease, asthma, or reactive airway or other chronic respiratory disease that requires daily medication for control, diabetes, chronic kidney disease, or pregnancy.3
Are the available monoclonal antibodies effective for SARS-CoV-2 variants? Of course, this is a critical question and relies on knowledge of the dominant variant in a specific geographic location. The CDC data on which variants are susceptible to which monoclonal therapies were updated as of Oct. 21 online (see Table 1). Local departments of public health often will have current data on the dominant variant in the community. Currently, the dominant variant in the United States is Delta and it is anticipated to be susceptible to the three monoclonal treatments authorized under the EUA based on in vitro neutralizing assays.
What adverse events were observed? Monoclonal antibody infusions are in general safe but anaphylaxis has been reported. Other infusion-related adverse events include urticaria, pruritis, flushing, pyrexia, shortness of breath, chest tightness, nausea, vomiting, and rash. Nearly all events were grade 1, mild, or grade 2, moderate. For nonsevere infusion-related reactions, consider slowing the infusion; if necessary, the infusion should be stopped.
Implementation challenges
The first challenge is finding a location to infuse the monoclonal antibodies. Although they can be given subcutaneously, the dose is large and little, if any, time is saved as the recommendation is for observation post administration for 1 hour. The challenge we and other centers may face is that the patients are COVID PCR+ and therefore our usual infusion program, which often is occupied by individuals already compromised and at high risk for severe COVID, is an undesirable location. We are planning to use the emergency department to accommodate such patients currently, but even that solution creates challenges for a busy, urban medical center.

Summary
Anti–SARS-CoV-2 monoclonal antibodies are an important part of the therapeutic approach to minimizing disease severity. Clinicians should review high-risk conditions in adolescents who are PCR+ for SARS-CoV-2 and have mild to moderate symptoms. Medical care systems should implement programs to make monoclonal infusions available for such high-risk adolescents.4 Obesity and asthma reactive airways or requiring daily medication for control are the two most common conditions that place adolescents with COVID-19 at risk for progression to hospitalization and severe disease in addition to the more traditional immune-compromising conditions and medical fragility.
Dr. Pelton is professor of pediatrics and epidemiology at Boston University schools of medicine and public health and senior attending physician in pediatric infectious diseases, Boston Medical Center. Email him at [email protected].
References
1. Federal Response to COVID-19: Monoclonal Antibody Clinical Implementation Guide. U.S. Department of Health and Human Services. 2021 Sep 2.
2. Bhimraj A et al. IDSA Guidelines on the Treatment and Management of Patients with COVID-19. Last updated 2021 Nov 9.
3. Anti-SARS-CoV-2 Monoclonal Antibodies. National Institutes of Health’s COVID 19 Treatment Guidelines. Last updated 2021 Oct 19.
4. Spreading the Word on the Benefits of Monoclonal Antibodies for COVID-19, by Hannah R. Buchdahl. CDC Foundation, 2021 Jul 2.
Perinatal research and the Tooth Fairy
How much did you get per tooth from the Tooth Fairy? How much do your children or grandchildren receive each time they lose a baby tooth? In my family the Tooth Fairy seems to be more than keeping with inflation. Has she ever been caught in the act of swapping cash for enamel in your home? Has she every slipped up one night but managed to resurrect her credibility the following night by doubling the reward? And, by the way, what does the Tooth Fairy do with all those teeth, and who’s funding her nocturnal switcheroos?
A recent study from the Center for Genomic Medicine at the Massachusetts General Hospital in Boston may provide an answer to at least one of those questions. It turns out some researchers have been collecting baby teeth in hopes of assessing prenatal and perinatal stress in infants.
Not surprisingly, teeth are like trees, preserving a history of the environment in their growth rings. The Boston researchers hypothesized that the thickness of one particular growth line referred to as the neonatal line (NNL) might reflect prenatal and immediate postnatal environmental stress. Using data and naturally shed teeth collected in an English longitudinal study, the authors discovered that the teeth of children whose mothers had a long history of severe depression or other psychiatric problems and children of mothers who at 32 weeks’ gestation experienced anxiety and/or depression were more likely to have thicker NNLs. On the other hand, the teeth of children whose mothers had received “significant social support” in the immediate postnatal period exhibited thinner NNLs.
Based on anecdotal observations, I think most of us already suspected that the children whose mothers had significant psychiatric illness began life with a challenge, but it is nice to know that we may now have a tool to document one small bit of evidence of the structural damage that occurred during this period of stress. Of course, the prior owners of these baby teeth won’t benefit from the findings in this study; however, the evidence that social support during the critical perinatal period can ameliorate the damage might stimulate more robust prenatal programs for mother and infants at risk in the future.
It will be interesting to see if this investigative tool becomes more widely used to determine the degree to which a variety of potential perinatal stressors are manifesting themselves in structural change in newborns. For example, collecting baby teeth from neonatal ICU graduates may answer some questions about how certain environmental conditions such as sound, vibration, bright light, and temperature may result in long-term damage to the infants. Most of us suspect that skin-to-skin contact with mother and kangaroo care are beneficial. A study that includes a survey of NNLs might go a long way toward supporting our suspicions.
I can even imagine that a deep retrospective study of NNLs in baby teeth collected over the last 100 years might demonstrate the effect of phenomena such as wars, natural disasters, forced migration, and pandemics, to name a few.
It may be time to put out a nationwide call to all Tooth Fairies both active and retired to dig deep in their top bureau drawers. Those little bits of long-forgotten enamel may hold the answers to a plethora of unanswered questions about those critical months surrounding the birth of a child.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
How much did you get per tooth from the Tooth Fairy? How much do your children or grandchildren receive each time they lose a baby tooth? In my family the Tooth Fairy seems to be more than keeping with inflation. Has she ever been caught in the act of swapping cash for enamel in your home? Has she every slipped up one night but managed to resurrect her credibility the following night by doubling the reward? And, by the way, what does the Tooth Fairy do with all those teeth, and who’s funding her nocturnal switcheroos?
A recent study from the Center for Genomic Medicine at the Massachusetts General Hospital in Boston may provide an answer to at least one of those questions. It turns out some researchers have been collecting baby teeth in hopes of assessing prenatal and perinatal stress in infants.
Not surprisingly, teeth are like trees, preserving a history of the environment in their growth rings. The Boston researchers hypothesized that the thickness of one particular growth line referred to as the neonatal line (NNL) might reflect prenatal and immediate postnatal environmental stress. Using data and naturally shed teeth collected in an English longitudinal study, the authors discovered that the teeth of children whose mothers had a long history of severe depression or other psychiatric problems and children of mothers who at 32 weeks’ gestation experienced anxiety and/or depression were more likely to have thicker NNLs. On the other hand, the teeth of children whose mothers had received “significant social support” in the immediate postnatal period exhibited thinner NNLs.
Based on anecdotal observations, I think most of us already suspected that the children whose mothers had significant psychiatric illness began life with a challenge, but it is nice to know that we may now have a tool to document one small bit of evidence of the structural damage that occurred during this period of stress. Of course, the prior owners of these baby teeth won’t benefit from the findings in this study; however, the evidence that social support during the critical perinatal period can ameliorate the damage might stimulate more robust prenatal programs for mother and infants at risk in the future.
It will be interesting to see if this investigative tool becomes more widely used to determine the degree to which a variety of potential perinatal stressors are manifesting themselves in structural change in newborns. For example, collecting baby teeth from neonatal ICU graduates may answer some questions about how certain environmental conditions such as sound, vibration, bright light, and temperature may result in long-term damage to the infants. Most of us suspect that skin-to-skin contact with mother and kangaroo care are beneficial. A study that includes a survey of NNLs might go a long way toward supporting our suspicions.
I can even imagine that a deep retrospective study of NNLs in baby teeth collected over the last 100 years might demonstrate the effect of phenomena such as wars, natural disasters, forced migration, and pandemics, to name a few.
It may be time to put out a nationwide call to all Tooth Fairies both active and retired to dig deep in their top bureau drawers. Those little bits of long-forgotten enamel may hold the answers to a plethora of unanswered questions about those critical months surrounding the birth of a child.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
How much did you get per tooth from the Tooth Fairy? How much do your children or grandchildren receive each time they lose a baby tooth? In my family the Tooth Fairy seems to be more than keeping with inflation. Has she ever been caught in the act of swapping cash for enamel in your home? Has she every slipped up one night but managed to resurrect her credibility the following night by doubling the reward? And, by the way, what does the Tooth Fairy do with all those teeth, and who’s funding her nocturnal switcheroos?
A recent study from the Center for Genomic Medicine at the Massachusetts General Hospital in Boston may provide an answer to at least one of those questions. It turns out some researchers have been collecting baby teeth in hopes of assessing prenatal and perinatal stress in infants.
Not surprisingly, teeth are like trees, preserving a history of the environment in their growth rings. The Boston researchers hypothesized that the thickness of one particular growth line referred to as the neonatal line (NNL) might reflect prenatal and immediate postnatal environmental stress. Using data and naturally shed teeth collected in an English longitudinal study, the authors discovered that the teeth of children whose mothers had a long history of severe depression or other psychiatric problems and children of mothers who at 32 weeks’ gestation experienced anxiety and/or depression were more likely to have thicker NNLs. On the other hand, the teeth of children whose mothers had received “significant social support” in the immediate postnatal period exhibited thinner NNLs.
Based on anecdotal observations, I think most of us already suspected that the children whose mothers had significant psychiatric illness began life with a challenge, but it is nice to know that we may now have a tool to document one small bit of evidence of the structural damage that occurred during this period of stress. Of course, the prior owners of these baby teeth won’t benefit from the findings in this study; however, the evidence that social support during the critical perinatal period can ameliorate the damage might stimulate more robust prenatal programs for mother and infants at risk in the future.
It will be interesting to see if this investigative tool becomes more widely used to determine the degree to which a variety of potential perinatal stressors are manifesting themselves in structural change in newborns. For example, collecting baby teeth from neonatal ICU graduates may answer some questions about how certain environmental conditions such as sound, vibration, bright light, and temperature may result in long-term damage to the infants. Most of us suspect that skin-to-skin contact with mother and kangaroo care are beneficial. A study that includes a survey of NNLs might go a long way toward supporting our suspicions.
I can even imagine that a deep retrospective study of NNLs in baby teeth collected over the last 100 years might demonstrate the effect of phenomena such as wars, natural disasters, forced migration, and pandemics, to name a few.
It may be time to put out a nationwide call to all Tooth Fairies both active and retired to dig deep in their top bureau drawers. Those little bits of long-forgotten enamel may hold the answers to a plethora of unanswered questions about those critical months surrounding the birth of a child.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
St. Jude hoards billions while many of its families drain their savings
A series of sharp knocks on his driver’s side window startled Jason Burt awake.
It was the middle of the night on a Saturday in 2016. Burt was sleeping in his pickup truck in the parking lot of St. Jude Children’s Research Hospital in downtown Memphis, Tenn., where his 5-year-old daughter was being treated for brain cancer. He’d driven more than 500 miles from his home in Central Texas to visit her.
A St. Jude security guard peered into the truck and asked Burt what he was doing. Burt explained that his daughter and her mother, his ex-girlfriend, were staying in the hospital’s free patient housing. But St. Jude provides housing for only one parent. Burt, a school bus driver making $20,000 a year, told the guard he couldn’t afford a hotel. The guard let the exhausted father go back to sleep.
St. Jude would do no more to find him a place to stay.
“They were aware of the situation,” Burt said. “I didn’t push anything. I was just grateful she was getting treated and I was doing what I needed to do.”
St. Jude is the largest and most highly regarded health care charity in the country. Each year, the Memphis hospital’s fundraisers send out hundreds of millions of letters, many with heart-wrenching photographs of children left bald from battling cancer. Celebrities like Jennifer Aniston and Sofia Vergara sing the hospital’s praises in televised advertisements. This year, St. Jude’s fundraising reached outer space. The SpaceX Inspiration4 mission in September included a former St. Jude patient as a crew member.
Last year, St. Jude raised a record $2 billion. U.S. News & World Report ranked it the country’s 10th-best children’s cancer hospital, and St. Jude raised roughly as much as the nine hospitals ahead of it put together. It currently has $5.2 billion in reserves, a sum large enough to run the institution at current levels for the next four and a half years without a single additional donation.
St. Jude makes a unique promise as part of its fundraising: “Families never receive a bill from St. Jude for treatment, travel, housing or food – because all a family should worry about is helping their child live.”
But for many families, treatment at St. Jude does not relieve all the financial burdens they incur in getting care for their children, including housing, travel, and food costs that fall outside the hospital’s strict limits, a ProPublica investigation has found.
While families may not receive a bill from St. Jude, the hospital doesn’t cover what’s usually the biggest source of financial stress associated with childhood cancer: The loss of income as parents quit or take leave from jobs to be with their child during treatment. For many families, the consequence is missed payments for cars, utilities, and cellphones. Others face eviction or foreclosure because they can’t keep up with rent and mortgage payments.
Parents at St. Jude have exhausted savings and retirement accounts, borrowed from family and friends, or asked other charities for aid. ProPublica identified more than 100 St. Jude families seeking financial help through the online fundraiser GoFundMe, with half of the campaigns started in the past two years. We counted scores of other events like concerts and yard sales organized to help St. Jude families in need.
One family relied on a mixed martial arts fighter to help raise money for expenses like car repairs and cellphone bills, items that St. Jude would not cover. Another spent $10,000, originally saved to purchase a home, on costs related to treatment at St. Jude.
Only about half of the $7.3 billion St. Jude has received in contributions in the past five fiscal years went to the hospital’s research and caring for patients, according to its financial filings with the Internal Revenue Service. About 30% covered the cost of its fundraising operations, and the remaining 20%, or $1 of every $5 donated, increased its reserve fund.
Further, ProPublica found, a substantial portion of the cost for treatment is paid not by St. Jude but by families’ private insurance or by Medicaid, the government insurance program for low-income families. About 90% of patients are insured, bringing in more than $100 million in reimbursements for treatment a year. If a family shows up at St. Jude without insurance, a company hired by the charity helps them find it. St. Jude does cover copays and deductibles, an unusual benefit.
St. Jude spends about $500 million a year on patient services – a figure that includes all medical care and other assistance. Very little of what St. Jude raises from the public goes to pay for food, travel, and housing for families, the investigation found. Last year, it was 2% of the money raised, or nearly $40 million.
In written responses to ProPublica, lawyers for St. Jude and its fundraising arm, the American Lebanese Syrian Associated Charities, or ALSAC, emphasized that countless families have benefited from the charity provided since the hospital opened its doors in 1962.
“ProPublica should be celebrating St. Jude and ALSAC for their commitment to finding cures, saving children’s lives, and optimizing patient outcomes,” one of their letters said.
It is unquestioned that St. Jude has helped thousands of children and their families over the decades. Patients have offered scores of testimonials about the hospital’s generosity and care.
“This often comes as a huge relief to families who often expect to sell all their belongings just so their children can get the medical care and treatment they need to save their lives,” the hospital’s lawyers wrote. “St. Jude and ALSAC understand that this arrangement cannot cover all financial obligations of all families, nor can St. Jude or ALSAC shield families from all the financial and emotional effects” of a child’s illness.
St. Jude said it discloses the limits of its aid to families on its website and in material provided to those whose children are admitted to the hospital. That includes the rule Burt ran into, that the hospital covers the travel and housing costs of only one caregiver and one patient. For many families, the daily food budget is capped at $50. In some cases, hotel stays en route are provided only if families travel more than 500 miles to get to St. Jude.
St. Jude said its assistance is “based on guidelines to ensure fairness and responsible use of donor funds” and on remaining compliant with a federal anti-kickback statute that makes it a criminal offense to offer something of value to induce a medical referral. St. Jude declined to explain how the law affects the amount or type of financial assistance it provides to families.
“St. Jude has never promised anyone – neither patients nor the public in general – that it can solve all financial problems,” the letter said.
When parents need additional financial help, St. Jude’s social workers often send them to smaller charities or in some cases suggest that they apply for government aid.
They refer many to the Andrew McDonough B+ Foundation, which gives more than $2.5 million a year in grants to thousands of families of pediatric cancer patients at hospitals across the country to help cover rent, utilities, and other urgent expenses.
Joe McDonough, the foundation’s founder and president, said St. Jude families have the same money problems as families of patients at other children’s hospitals, even though he said St. Jude’s marketing creates the public perception that it alleviates these burdens.
“People say to me, ‘Why are you helping St. Jude families?’ ” McDonough said. “Well, what happens when a family lives in Augusta, Georgia, and they’re being treated at St. Jude? They still have to pay the rent on their apartment back in Augusta, Georgia. They still have to make their car payment. And it’s not my position to say whether St. Jude should be paying for all those expenses or not. I’m just explaining that it’s not a totally free ride.”
The help St. Jude provides to families may soon be increasing.
After ProPublica provided St. Jude with the findings of its reporting, the hospital informed families of a dramatic expansion in the assistance it will give to parents and other relatives during their kids’ treatment in Memphis.
Among the most significant changes are increasing travel benefits to two parents instead of one and covering regular trips to Memphis for siblings and other loved ones. St. Jude’s letter to parents said the changes take effect Nov. 15.
That would’ve made a big difference for Burt.
Burt’s daughter, whom ProPublica is not identifying at her mother’s request, was originally diagnosed with cancer in early 2015, when doctors discovered a tumor pressing against her brain stem. She had successful emergency surgery to remove the mass at Dell Children’s Medical Center in Austin, Texas. Medicaid and Dell Children’s covered the bill, but the family was still faced with the cost of her ongoing treatment.
“At that point I’m thinking: ‘What am I going to do? I guess I’m selling my house, whatever it takes,’” Burt recalled. “Honestly, that was probably a big deciding factor for St. Jude.”
St. Jude accepted Burt’s daughter into a clinical trial, and the family moved to the hospital’s patient housing in Memphis for several months. Both parents stopped working for a time, and people in their hometown raised cash to pay their bills.
Her cancer relapsed the following year with several new, inoperable brain tumors. Burt and his daughter’s mom broke up during that round of treatment, and financial problems piled up.
Burt said his credit score dropped so low that utility companies refused to set up service unless he first paid a deposit. One of the family’s cars was repossessed, he said. Burt’s 2005 Chevrolet Colorado pickup has 300,000 miles on it, many of them logged on trips from Texas to Memphis. When Burt’s daughter was at St. Jude for treatment or exams, he’d work all week, then visit on many weekends where he would spend Saturday night sleeping in the hospital parking lot.
He asked hospital officials if he could sleep in St. Jude’s housing, but they turned him down, he said.
Burt said he was happy with the care St. Jude provided. His daughter’s health is stable, he said, and brain scans taken during her September exam confirmed her two remaining tumors haven’t grown. But he’s still trying to recover financially.
“It’s five years now,” Burt said, “and I’m not completely caught up yet.”
A fundraising giant
St. Jude began with a fledgling entertainer praying for a career break.
When Danny Thomas, a comic and actor best known for the TV sitcom “Make Room for Daddy,” was struggling to earn a living in the late 1930s, the devout Roman Catholic went to church and asked for help from the patron saint of desperate cases, St. Jude Thaddeus. If he made it big, Thomas promised to build “a shrine where the poor and the helpless and the hopeless may come for comfort and aid,” according to a history published by ALSAC.
Within five years, Thomas became a star and worked to fulfill his promise by building a children’s hospital named after St. Jude and a fundraising organization to support it. Thomas, whose parents were Lebanese immigrants, recruited others who shared his Middle Eastern roots to help.
He used his fame to raise the hospital’s profile, appearing in ads for St. Jude and hosting fundraising events starring the likes of Elvis Presley and Sammy Davis Jr. Thomas’ daughter Marlo, herself a TV star, succeeded him in championing St. Jude.
Today, St. Jude is a specialty treatment and research center with about 5,700 employees and 73 beds. Other top children’s hospitals have more staff and beds, and they also treat more conditions.
Though St. Jude raises money across the world, most of its patients come from Tennessee and surrounding states. Patients from elsewhere are usually enrolled in clinical trials.
ALSAC, which handles St. Jude’s fundraising and investments, has 2,188 employees in Memphis and in 36 regional offices across the country. More than 400 of the fundraising arm’s employees are paid over $100,000, according to IRS filings. The charity takes in so much money each year that it regularly steers hundreds of millions of dollars in donations to reserve accounts, the filings show.
Overall, St. Jude’s reserve has grown by 58% over the past five fiscal years, during which it has added $1.9 billion to its investment accounts and shifted its portfolio toward financial products designed to generate bigger returns than stocks, bonds, and mutual funds traditionally deliver. The charity stowed more than a third of the new surplus, $688 million, in riskier private equity investments.
IRS rules do not limit the size of a nonprofit’s reserves, and experts on charitable finance differ on best practices.
St. Jude meets Better Business Bureau guidelines, which call for charities to maintain reserves of less than three times total expenses, but other experts expressed alarm that the hospital had accumulated such a large sum of money.
The size of the St. Jude reserve is “staggering,” said Laura Otten, the director of LaSalle University’s master program in nonprofit leadership. She said a typical reserve for a nonprofit the size of St. Jude is one to two years of expenses. Donors generally want to know their dollars are being put to work, she said.
The hospital said it needs a large reserve because its unique operating model relies on donations to fund annual operating costs. “[W]e are highly donor-dependent and subject to the economic driven vagaries of charitable giving,” the hospital said in a written response to ProPublica questions.
But the hospital’s reserve is already more than large enough to buffer against recessions and potential drops in donations, said Ge Bai, a professor of accounting and health policy at Johns Hopkins University. “They should be spending the money as aggressively as they raise it, but they seem to be hoarding,” Bai said.
The hospital said it is also raising billions to fund the construction of new housing and research space, although its plans do not currently include spending any of the reserve on new facilities.
St. Jude’s reserves have ballooned at a time when researchers, oncologists, advocates, and families complain about a dearth of funding for pediatric cancer studies nationally.
Dozens of other children’s hospitals across the country have research divisions devoted to pediatric cancer and enroll their patients in clinical trials for new drugs and procedures. They pay for research staff and studies in part with donations from their local communities, often competing directly against St. Jude. ALSAC has regional offices in several U.S. cities with elite pediatric cancer centers of their own, including Atlanta, Chicago, Denver, and Seattle.
Coury Shadyac, an ALSAC vice president and daughter of the organization’s CEO, Richard Shadyac Jr., oversees a team of 45 fundraisers along the West Coast “raising $300 million annually” for St. Jude, according to her LinkedIn profile. That’s $100 million more in donations than either Children’s Hospital Los Angeles or Seattle Children’s Hospital, two of the nation’s leading pediatric cancer institutions, received in fiscal year 2019, IRS disclosures show. But it’s only a small part of St. Jude’s fundraising haul.
ALSAC’s ubiquitous fundraising has led to concerns that it undercuts other hospitals’ campaigns. Some doctors interviewed by ProPublica said they have encouraged donors to give their money to hospitals closer to home.
David Clark, a pediatrician and former longtime chairperson of pediatrics at Albany Medical Center in New York, said St. Jude raises tens of thousands of dollars in his region that does little to benefit the children with cancer in his area since almost all are treated locally. ALSAC has a fundraising office located a few miles from Albany Medical.
“They think of every way they can to make money and the least amount of ways to spend it,” Clark said. “They deceive people into supporting something that is totally dishonest.”
Nearly all St. Jude solicitations feature the hospital’s patients – the children usually smiling and bald from treatment – along with the familiar promise that it never sends families a bill.
It’s a message that ALSAC has tested and researched to maximize donations. Donors appreciate the promise to never bill families, said Mary Kate Tolan, an ALSAC executive, in a podcast last year. She added that no parent should have to take out a second mortgage or lose their job because their child is being treated at St. Jude.
Alternative messaging to the no-bills promise did not “perform as well,” said Tolan, who develops emerging technologies for ALSAC. Tolan did not return requests for comment.
“Borrowing and begging”
Catherine Rainey thought she would be free of financial worry when her 2-year-old daughter Harlee was admitted to St. Jude last year.
“The first thing my dad said was: ‘Catherine, you have nothing to worry about. They raise billions of dollars. Anytime you have a problem, you tell them and they will take care of it,’ ” she said.
But like many families, the Raineys discovered that St. Jude’s charity came with limits on payments for expenses such as travel that could be bewildering.
Harlee ended up at St. Jude after first going to nearby Niswonger Children’s Hospital in Johnson City, Tenn., in October 2020. The doctors there discovered a cancerous mass attached to her right kidney. The hospital is a St. Jude affiliate, and the doctors recommended the toddler be treated in Memphis.
Rainey, a single mother of two young girls, had to leave her job as a nurse for months to be with Harlee at St. Jude. The loss of income quickly created problems. “My family, we don’t come from money,” she said. “We are not doctors and billionaires. We make it. That is it.”
St. Jude did provide food and housing on campus. But the hospital said it couldn’t help with the items that were causing Rainey to worry, including car payments, insurance, and cellphone bills.
Rainey’s boss set up a GoFundMe account to help make up some of her lost income. A small local charity, Kari’s Heart Foundation, also helped out by paying about $3,000 worth of phone bills and car payments, staving off repossession.
“It was just a bunch of borrowing and begging,” Rainey said of her experience while her daughter was treated in Memphis. “They acted like it was coming out of their own pocket.”
Harlee has checkups at St. Jude every three months that last about four days. The costs of travel to and from St. Jude put an additional strain on Rainey and Harlee. St. Jude is an eight-hour ride, without stops, from Rainey’s home in Appalachia, Va., a town of 1,432 people near the Kentucky border.
Rainey said her daughter generally can make it about two-thirds of the way, with frequent stops, before she has had enough. “When she is done, she is really done,” Rainey said. “She will scream, cry, and kick.”
In July, in advance of an August trip to Memphis, Rainey called the patient services department at St. Jude to see whether they could help pay for a hotel to break up the travel day — an expense Rainey said she could not afford.
To qualify for a hotel reimbursement, Rainey said, St. Jude told her she had to live more than 500 miles from Memphis. The ride from her home to the hospital is 530 miles (a measurement ProPublica confirmed with mapping tools). However, Rainey said, St. Jude told her it measured the trip from city limit to city limit and came up with a distance of 491 miles. Even using that metric, the distance is still more than 500 miles, ProPublica found.
When she challenged the hospital’s stance, Rainey said she was berated by a patient services representative.
“I was feeling pissed off, and I was crying,” Rainey said of the interaction. “You give up your whole life for your child, and they tell you don’t worry about anything, we will cover this and then they tell you to just push through the drive.”
Rainey did what she could to make the trip go smoothly: She configured a small table to extend across her daughter’s car seat, so Harlee could play with the coloring books, markers, and Play-Doh bought for the ride. She packed snacks and a cooler full of drinks. Since Harlee was still potty training, she brought extra towels and clothes for accidents. The final step was handing Harlee her Baby Yoda doll once she settled into her car seat. Rainey had sewed a port in the doll’s chest to mirror the one Harlee has in hers.
About three hours from Memphis, Harlee was crying inconsolably. Rainey pulled off the interstate and stopped at the first hotel she could find. She later learned it had been described in online reviews as “awful,” a “nightmare,” “disgusting,” and “horrible.”
“I didn’t know the area,” she said. “The hotel was garbage. It just made it worse.”
The drive home also required a hotel stop, but this time Rainey was able to find one that was cleaner. A $100 donation from a local charity helped to offset the cost.
Among the changes St. Jude is making is to reimburse families like Rainey’s, who live more than 400 miles from the hospital, for an overnight stay at a hotel when making the trip to Memphis.
Rainey said she was called by a St. Jude representative after ProPublica asked about her situation and was told the hospital would pay for her past hotel stays when traveling back and forth to St. Jude. The representative, Rainey said, also told her the hospital discovered the way it had been measuring mileage was inaccurate.
“I am not the only one,” Rainey said. “There are others. They should reimburse all the families.”
The anxiety of unpaid bills piling up, combined with caring for a child undergoing chemotherapy or radiation, takes a severe toll on parents and guardians, said Christopher Hope, a UPS driver who started a Memphis-based foundation after meeting St. Jude parents who were in financial crisis.
Hope’s small charity spent $12,000 last year to help families. Parents in St. Jude social media groups often refer families in need to it. The charity has helped families cover mortgage and car payments.
“I never knew anything about this until hearing about it from families,” Hope said. “All we hear is about kids and treatment, not the other side of it.”
“It’s not free”
In addition to charities like Hope’s, St. Jude families have repeatedly turned to fundraising sites and networks of their relatives, friends, and neighbors to help cover basic expenses while unable to work during their children’s treatment. Parents’ requests on fundraising sites are sometimes desperate pleas.
In January 2017, one father in North Carolina said he’d had to abandon a business venture to take time for his son to receive care at St. Jude. His income had plummeted. He asked friends to give as little as $10 to “at least make it possible to survive.”
This year, a mother in Memphis whose 1-year-old son receives care at St. Jude for sickle cell disorder ran out of medical leave and couldn’t work her shifts at a clothing distribution center. After the child had a flare-up in July requiring several days of treatment at the hospital, she said she returned home to find her power shut off. Sitting in a dark apartment, unable to pay her utility bills, she set up a GoFundMe campaign. She received less than $20 through the site; her relatives eventually pooled $350 to get her electricity restored.
Even parents with stable jobs and private health insurance often take on debt and need outside help.
When Taylr and Treg Murphy’s 17-year-old son Peyton was diagnosed with cancer and needed monthslong treatment at St. Jude in 2017, the entire family – mom, dad, sister, and brother – went with him, traveling from their home in Lafayette, La., to Memphis. Treg took a leave from his job at an oil mining company and Taylr, who works at her mother’s bakery, did the same.
“We knew that it was going to be a collective team effort,” Treg said. “Without even a discussion, we figured that if Peyton’s got to go for the surgery, we’re all going.”
Peyton had an enormous tumor that had grown out of his right femur and was crowding his knee. Rounds of chemotherapy appeared to have killed osteosarcoma cells elsewhere in his body. But he needed to undergo a procedure called limb-sparing surgery that would require weeks of recovery time at the hospital.
The hospital agreed to allow all five family members to stay for free at St. Jude if they bunked together in a single room. It assigned them a spot in Tri Delta Place, its hotel-like short-term patient residence on the campus. Tri Delta is set up for visits of up to seven days, according to the hospital’s guide for volunteers, but the Murphys were there for almost 50.
Taylr said the unit at Tri Delta had no oven or stove and St. Jude provided no grocery money, instead allotting them a $50-per-day credit at the hospital cafeteria, Kay Kafe – not enough to feed the family of five. As the weeks wore on, the Murphys split grilled cheese sandwiches and paid for food out of pocket.
After ProPublica asked about the hospital’s food allowances, St. Jude said it would increase them as part of the changes scheduled to go into effect this month. The hospital switched from a $50-a-day cap per family to providing $25 a day to each family member. For a family of four, that would double the food benefit. A weekly stipend given to families in long-term housing was increased to $150 from $125.
For the Murphys, it was the loss of their work income, more than out-of-pocket expenses, that put them into a financial hole as Peyton’s treatment went on. Treg’s employer couldn’t pay him during his long absences.
Fearful of being evicted or having their car repossessed, Taylr said she asked a St. Jude social worker for assistance. The social worker helped her apply for grants from other charities. Taylr said the B+ Foundation paid their rent one month, which ensured they’d have a home to return to.
In the years since his initial treatment, Peyton has gone back to St. Jude repeatedly for exams and surgeries to remove malignant growths in his lungs. Taylr and Treg have missed more work to bring Peyton to Memphis, costing them thousands of dollars more in income.
By the start of this year, Taylr and Treg said they were about $20,000 in debt and panicking. Dustin Poirier, a former UFC champion from their hometown, heard from a friend about Peyton and the family’s financial trouble. He donated $10,000 to them from his personal charity and in May hosted a local fundraiser that collected enough to pay off their credit cards.
St. Jude families sometimes commiserate about money problems with each other, Taylr said, but few are aware of the extent of the hospital’s unspent resources. The Murphys said they didn’t know St. Jude has more than $5 billion in reserve or that it continues to raise hundreds of millions of dollars in surplus donations each year.
“That’s just insane,” Taylr said. “That just blows my mind. When we first started getting treated, people would be like, ‘Oh, St. Jude covers everything, that’s awesome.’ That’s not how it works. People don’t understand that. I truly didn’t understand before I got into St. Jude.”
Taylr and Treg said the doctors at St. Jude are “amazing” and they’re grateful for their son’s care. But they bristled at the assumption that it was covered by the hospital’s charity. The family’s insurance paid a substantial part of the bills.
“It’s not free,” Taylr said. “My husband works very hard for the insurance we have – and they are billed.” The Murphys pay $12,000 in health insurance premiums each year.
Their struggle continues. Peyton’s cancer has relapsed, and he’s making regular trips with his mom or dad back to St. Jude for chemotherapy. The family is again applying for help from other charities.
Wiped out savings
The costs associated with care at St. Jude caused at least one family to stop going to Memphis altogether.
Last winter, Kelly Edwards was excitedly searching through Tulsa real estate listings after years of diligently saving $10,000 for a down payment on a house. She craved a permanent home for herself and the two young brothers she had taken in five years earlier at the behest of a family friend. She hoped to adopt the boys, now 13 and 9, who call her mom.
In February, the older boy, DJ, was lethargic and uninterested in his schoolwork. After several doctor visits, he was diagnosed with acute lymphoblastic leukemia at a Tulsa hospital. The cancer, referred to as ALL, is the most common type among children, with survival rates that exceed 90%. A day after his diagnosis, DJ and Edwards were driving six hours to Memphis for treatment at St. Jude, which is affiliated with the Oklahoma hospital.
The pair stayed for free at an independently operated Ronald McDonald House near St. Jude, and a weekly stipend from the hospital helped to pay for meals – aid that Edwards said was a blessing. DJ had health insurance through the Oklahoma Medicaid program.
But as with the Murphys, lost income soon put Edwards’ family into financial jeopardy. She works as a supervisor for a company that delivers packages for Amazon. After she used up two weeks of paid time off, she stopped getting paychecks. The bills, however, kept coming: rent, car payments, utilities. To that was added the $250 a week she paid a friend to stay with DJ’s younger brother and her two dogs in Tulsa.
Within four months, her house savings were wiped out. Edwards said she told her St. Jude social worker about her financial woes but got no additional help.
One of Edwards’ adult daughters started a GoFundMe campaign to help, bringing in just over $3,000. Edwards said she appreciated the aid but believes donations were kept low by the widespread perception that St. Jude families don’t have financial problems.
“Everyone hears that everything is taken care of by St. Jude,” she said. “That is not true, but everyone has that mentality.” She said someone she knew asked her “what is that money going for if St. Jude’s is paying for everything?”
DJ was scheduled to go back to St. Jude for three weeks of treatment in August, but Edwards decided she simply couldn’t afford it. “I don’t have the money to go back and forth,” she said. She worked with DJ’s local doctors and found that the hospital near her home in Tulsa could provide the same treatment he was scheduled to get in Tennessee.
The local treatment allowed her to continue working some shifts and to be at home with both of her boys. DJ is also happier when he is home, Edwards said.
Edwards and the boys are now living in a small house her brother owns just outside Tulsa. Late on a recent weekday afternoon, DJ slowly shuffled into the living room, exhausted from a day of chemotherapy treatment.
He is in the midst of a 20-week regimen where he receives the cancer-killing drugs every other day, just one phase of a nearly three-year treatment plan. He wore an orange knit hat, T-shirt, and shorts. He rubbed his eyes before asking a visitor, “How is your day going?” He smiled at the positive response. When he heard the family was eating steak for dinner, he eagerly jumped up to start helping in the kitchen. After they moved in, Edwards hung family portraits on the walls to make it feel homier. She doesn’t expect they will be moving again any time soon.
The dream of buying a home of their own is gone.
Former ProPublica reporter Marshall Allen contributed reporting. Kirsten Berg contributed research.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
A series of sharp knocks on his driver’s side window startled Jason Burt awake.
It was the middle of the night on a Saturday in 2016. Burt was sleeping in his pickup truck in the parking lot of St. Jude Children’s Research Hospital in downtown Memphis, Tenn., where his 5-year-old daughter was being treated for brain cancer. He’d driven more than 500 miles from his home in Central Texas to visit her.
A St. Jude security guard peered into the truck and asked Burt what he was doing. Burt explained that his daughter and her mother, his ex-girlfriend, were staying in the hospital’s free patient housing. But St. Jude provides housing for only one parent. Burt, a school bus driver making $20,000 a year, told the guard he couldn’t afford a hotel. The guard let the exhausted father go back to sleep.
St. Jude would do no more to find him a place to stay.
“They were aware of the situation,” Burt said. “I didn’t push anything. I was just grateful she was getting treated and I was doing what I needed to do.”
St. Jude is the largest and most highly regarded health care charity in the country. Each year, the Memphis hospital’s fundraisers send out hundreds of millions of letters, many with heart-wrenching photographs of children left bald from battling cancer. Celebrities like Jennifer Aniston and Sofia Vergara sing the hospital’s praises in televised advertisements. This year, St. Jude’s fundraising reached outer space. The SpaceX Inspiration4 mission in September included a former St. Jude patient as a crew member.
Last year, St. Jude raised a record $2 billion. U.S. News & World Report ranked it the country’s 10th-best children’s cancer hospital, and St. Jude raised roughly as much as the nine hospitals ahead of it put together. It currently has $5.2 billion in reserves, a sum large enough to run the institution at current levels for the next four and a half years without a single additional donation.
St. Jude makes a unique promise as part of its fundraising: “Families never receive a bill from St. Jude for treatment, travel, housing or food – because all a family should worry about is helping their child live.”
But for many families, treatment at St. Jude does not relieve all the financial burdens they incur in getting care for their children, including housing, travel, and food costs that fall outside the hospital’s strict limits, a ProPublica investigation has found.
While families may not receive a bill from St. Jude, the hospital doesn’t cover what’s usually the biggest source of financial stress associated with childhood cancer: The loss of income as parents quit or take leave from jobs to be with their child during treatment. For many families, the consequence is missed payments for cars, utilities, and cellphones. Others face eviction or foreclosure because they can’t keep up with rent and mortgage payments.
Parents at St. Jude have exhausted savings and retirement accounts, borrowed from family and friends, or asked other charities for aid. ProPublica identified more than 100 St. Jude families seeking financial help through the online fundraiser GoFundMe, with half of the campaigns started in the past two years. We counted scores of other events like concerts and yard sales organized to help St. Jude families in need.
One family relied on a mixed martial arts fighter to help raise money for expenses like car repairs and cellphone bills, items that St. Jude would not cover. Another spent $10,000, originally saved to purchase a home, on costs related to treatment at St. Jude.
Only about half of the $7.3 billion St. Jude has received in contributions in the past five fiscal years went to the hospital’s research and caring for patients, according to its financial filings with the Internal Revenue Service. About 30% covered the cost of its fundraising operations, and the remaining 20%, or $1 of every $5 donated, increased its reserve fund.
Further, ProPublica found, a substantial portion of the cost for treatment is paid not by St. Jude but by families’ private insurance or by Medicaid, the government insurance program for low-income families. About 90% of patients are insured, bringing in more than $100 million in reimbursements for treatment a year. If a family shows up at St. Jude without insurance, a company hired by the charity helps them find it. St. Jude does cover copays and deductibles, an unusual benefit.
St. Jude spends about $500 million a year on patient services – a figure that includes all medical care and other assistance. Very little of what St. Jude raises from the public goes to pay for food, travel, and housing for families, the investigation found. Last year, it was 2% of the money raised, or nearly $40 million.
In written responses to ProPublica, lawyers for St. Jude and its fundraising arm, the American Lebanese Syrian Associated Charities, or ALSAC, emphasized that countless families have benefited from the charity provided since the hospital opened its doors in 1962.
“ProPublica should be celebrating St. Jude and ALSAC for their commitment to finding cures, saving children’s lives, and optimizing patient outcomes,” one of their letters said.
It is unquestioned that St. Jude has helped thousands of children and their families over the decades. Patients have offered scores of testimonials about the hospital’s generosity and care.
“This often comes as a huge relief to families who often expect to sell all their belongings just so their children can get the medical care and treatment they need to save their lives,” the hospital’s lawyers wrote. “St. Jude and ALSAC understand that this arrangement cannot cover all financial obligations of all families, nor can St. Jude or ALSAC shield families from all the financial and emotional effects” of a child’s illness.
St. Jude said it discloses the limits of its aid to families on its website and in material provided to those whose children are admitted to the hospital. That includes the rule Burt ran into, that the hospital covers the travel and housing costs of only one caregiver and one patient. For many families, the daily food budget is capped at $50. In some cases, hotel stays en route are provided only if families travel more than 500 miles to get to St. Jude.
St. Jude said its assistance is “based on guidelines to ensure fairness and responsible use of donor funds” and on remaining compliant with a federal anti-kickback statute that makes it a criminal offense to offer something of value to induce a medical referral. St. Jude declined to explain how the law affects the amount or type of financial assistance it provides to families.
“St. Jude has never promised anyone – neither patients nor the public in general – that it can solve all financial problems,” the letter said.
When parents need additional financial help, St. Jude’s social workers often send them to smaller charities or in some cases suggest that they apply for government aid.
They refer many to the Andrew McDonough B+ Foundation, which gives more than $2.5 million a year in grants to thousands of families of pediatric cancer patients at hospitals across the country to help cover rent, utilities, and other urgent expenses.
Joe McDonough, the foundation’s founder and president, said St. Jude families have the same money problems as families of patients at other children’s hospitals, even though he said St. Jude’s marketing creates the public perception that it alleviates these burdens.
“People say to me, ‘Why are you helping St. Jude families?’ ” McDonough said. “Well, what happens when a family lives in Augusta, Georgia, and they’re being treated at St. Jude? They still have to pay the rent on their apartment back in Augusta, Georgia. They still have to make their car payment. And it’s not my position to say whether St. Jude should be paying for all those expenses or not. I’m just explaining that it’s not a totally free ride.”
The help St. Jude provides to families may soon be increasing.
After ProPublica provided St. Jude with the findings of its reporting, the hospital informed families of a dramatic expansion in the assistance it will give to parents and other relatives during their kids’ treatment in Memphis.
Among the most significant changes are increasing travel benefits to two parents instead of one and covering regular trips to Memphis for siblings and other loved ones. St. Jude’s letter to parents said the changes take effect Nov. 15.
That would’ve made a big difference for Burt.
Burt’s daughter, whom ProPublica is not identifying at her mother’s request, was originally diagnosed with cancer in early 2015, when doctors discovered a tumor pressing against her brain stem. She had successful emergency surgery to remove the mass at Dell Children’s Medical Center in Austin, Texas. Medicaid and Dell Children’s covered the bill, but the family was still faced with the cost of her ongoing treatment.
“At that point I’m thinking: ‘What am I going to do? I guess I’m selling my house, whatever it takes,’” Burt recalled. “Honestly, that was probably a big deciding factor for St. Jude.”
St. Jude accepted Burt’s daughter into a clinical trial, and the family moved to the hospital’s patient housing in Memphis for several months. Both parents stopped working for a time, and people in their hometown raised cash to pay their bills.
Her cancer relapsed the following year with several new, inoperable brain tumors. Burt and his daughter’s mom broke up during that round of treatment, and financial problems piled up.
Burt said his credit score dropped so low that utility companies refused to set up service unless he first paid a deposit. One of the family’s cars was repossessed, he said. Burt’s 2005 Chevrolet Colorado pickup has 300,000 miles on it, many of them logged on trips from Texas to Memphis. When Burt’s daughter was at St. Jude for treatment or exams, he’d work all week, then visit on many weekends where he would spend Saturday night sleeping in the hospital parking lot.
He asked hospital officials if he could sleep in St. Jude’s housing, but they turned him down, he said.
Burt said he was happy with the care St. Jude provided. His daughter’s health is stable, he said, and brain scans taken during her September exam confirmed her two remaining tumors haven’t grown. But he’s still trying to recover financially.
“It’s five years now,” Burt said, “and I’m not completely caught up yet.”
A fundraising giant
St. Jude began with a fledgling entertainer praying for a career break.
When Danny Thomas, a comic and actor best known for the TV sitcom “Make Room for Daddy,” was struggling to earn a living in the late 1930s, the devout Roman Catholic went to church and asked for help from the patron saint of desperate cases, St. Jude Thaddeus. If he made it big, Thomas promised to build “a shrine where the poor and the helpless and the hopeless may come for comfort and aid,” according to a history published by ALSAC.
Within five years, Thomas became a star and worked to fulfill his promise by building a children’s hospital named after St. Jude and a fundraising organization to support it. Thomas, whose parents were Lebanese immigrants, recruited others who shared his Middle Eastern roots to help.
He used his fame to raise the hospital’s profile, appearing in ads for St. Jude and hosting fundraising events starring the likes of Elvis Presley and Sammy Davis Jr. Thomas’ daughter Marlo, herself a TV star, succeeded him in championing St. Jude.
Today, St. Jude is a specialty treatment and research center with about 5,700 employees and 73 beds. Other top children’s hospitals have more staff and beds, and they also treat more conditions.
Though St. Jude raises money across the world, most of its patients come from Tennessee and surrounding states. Patients from elsewhere are usually enrolled in clinical trials.
ALSAC, which handles St. Jude’s fundraising and investments, has 2,188 employees in Memphis and in 36 regional offices across the country. More than 400 of the fundraising arm’s employees are paid over $100,000, according to IRS filings. The charity takes in so much money each year that it regularly steers hundreds of millions of dollars in donations to reserve accounts, the filings show.
Overall, St. Jude’s reserve has grown by 58% over the past five fiscal years, during which it has added $1.9 billion to its investment accounts and shifted its portfolio toward financial products designed to generate bigger returns than stocks, bonds, and mutual funds traditionally deliver. The charity stowed more than a third of the new surplus, $688 million, in riskier private equity investments.
IRS rules do not limit the size of a nonprofit’s reserves, and experts on charitable finance differ on best practices.
St. Jude meets Better Business Bureau guidelines, which call for charities to maintain reserves of less than three times total expenses, but other experts expressed alarm that the hospital had accumulated such a large sum of money.
The size of the St. Jude reserve is “staggering,” said Laura Otten, the director of LaSalle University’s master program in nonprofit leadership. She said a typical reserve for a nonprofit the size of St. Jude is one to two years of expenses. Donors generally want to know their dollars are being put to work, she said.
The hospital said it needs a large reserve because its unique operating model relies on donations to fund annual operating costs. “[W]e are highly donor-dependent and subject to the economic driven vagaries of charitable giving,” the hospital said in a written response to ProPublica questions.
But the hospital’s reserve is already more than large enough to buffer against recessions and potential drops in donations, said Ge Bai, a professor of accounting and health policy at Johns Hopkins University. “They should be spending the money as aggressively as they raise it, but they seem to be hoarding,” Bai said.
The hospital said it is also raising billions to fund the construction of new housing and research space, although its plans do not currently include spending any of the reserve on new facilities.
St. Jude’s reserves have ballooned at a time when researchers, oncologists, advocates, and families complain about a dearth of funding for pediatric cancer studies nationally.
Dozens of other children’s hospitals across the country have research divisions devoted to pediatric cancer and enroll their patients in clinical trials for new drugs and procedures. They pay for research staff and studies in part with donations from their local communities, often competing directly against St. Jude. ALSAC has regional offices in several U.S. cities with elite pediatric cancer centers of their own, including Atlanta, Chicago, Denver, and Seattle.
Coury Shadyac, an ALSAC vice president and daughter of the organization’s CEO, Richard Shadyac Jr., oversees a team of 45 fundraisers along the West Coast “raising $300 million annually” for St. Jude, according to her LinkedIn profile. That’s $100 million more in donations than either Children’s Hospital Los Angeles or Seattle Children’s Hospital, two of the nation’s leading pediatric cancer institutions, received in fiscal year 2019, IRS disclosures show. But it’s only a small part of St. Jude’s fundraising haul.
ALSAC’s ubiquitous fundraising has led to concerns that it undercuts other hospitals’ campaigns. Some doctors interviewed by ProPublica said they have encouraged donors to give their money to hospitals closer to home.
David Clark, a pediatrician and former longtime chairperson of pediatrics at Albany Medical Center in New York, said St. Jude raises tens of thousands of dollars in his region that does little to benefit the children with cancer in his area since almost all are treated locally. ALSAC has a fundraising office located a few miles from Albany Medical.
“They think of every way they can to make money and the least amount of ways to spend it,” Clark said. “They deceive people into supporting something that is totally dishonest.”
Nearly all St. Jude solicitations feature the hospital’s patients – the children usually smiling and bald from treatment – along with the familiar promise that it never sends families a bill.
It’s a message that ALSAC has tested and researched to maximize donations. Donors appreciate the promise to never bill families, said Mary Kate Tolan, an ALSAC executive, in a podcast last year. She added that no parent should have to take out a second mortgage or lose their job because their child is being treated at St. Jude.
Alternative messaging to the no-bills promise did not “perform as well,” said Tolan, who develops emerging technologies for ALSAC. Tolan did not return requests for comment.
“Borrowing and begging”
Catherine Rainey thought she would be free of financial worry when her 2-year-old daughter Harlee was admitted to St. Jude last year.
“The first thing my dad said was: ‘Catherine, you have nothing to worry about. They raise billions of dollars. Anytime you have a problem, you tell them and they will take care of it,’ ” she said.
But like many families, the Raineys discovered that St. Jude’s charity came with limits on payments for expenses such as travel that could be bewildering.
Harlee ended up at St. Jude after first going to nearby Niswonger Children’s Hospital in Johnson City, Tenn., in October 2020. The doctors there discovered a cancerous mass attached to her right kidney. The hospital is a St. Jude affiliate, and the doctors recommended the toddler be treated in Memphis.
Rainey, a single mother of two young girls, had to leave her job as a nurse for months to be with Harlee at St. Jude. The loss of income quickly created problems. “My family, we don’t come from money,” she said. “We are not doctors and billionaires. We make it. That is it.”
St. Jude did provide food and housing on campus. But the hospital said it couldn’t help with the items that were causing Rainey to worry, including car payments, insurance, and cellphone bills.
Rainey’s boss set up a GoFundMe account to help make up some of her lost income. A small local charity, Kari’s Heart Foundation, also helped out by paying about $3,000 worth of phone bills and car payments, staving off repossession.
“It was just a bunch of borrowing and begging,” Rainey said of her experience while her daughter was treated in Memphis. “They acted like it was coming out of their own pocket.”
Harlee has checkups at St. Jude every three months that last about four days. The costs of travel to and from St. Jude put an additional strain on Rainey and Harlee. St. Jude is an eight-hour ride, without stops, from Rainey’s home in Appalachia, Va., a town of 1,432 people near the Kentucky border.
Rainey said her daughter generally can make it about two-thirds of the way, with frequent stops, before she has had enough. “When she is done, she is really done,” Rainey said. “She will scream, cry, and kick.”
In July, in advance of an August trip to Memphis, Rainey called the patient services department at St. Jude to see whether they could help pay for a hotel to break up the travel day — an expense Rainey said she could not afford.
To qualify for a hotel reimbursement, Rainey said, St. Jude told her she had to live more than 500 miles from Memphis. The ride from her home to the hospital is 530 miles (a measurement ProPublica confirmed with mapping tools). However, Rainey said, St. Jude told her it measured the trip from city limit to city limit and came up with a distance of 491 miles. Even using that metric, the distance is still more than 500 miles, ProPublica found.
When she challenged the hospital’s stance, Rainey said she was berated by a patient services representative.
“I was feeling pissed off, and I was crying,” Rainey said of the interaction. “You give up your whole life for your child, and they tell you don’t worry about anything, we will cover this and then they tell you to just push through the drive.”
Rainey did what she could to make the trip go smoothly: She configured a small table to extend across her daughter’s car seat, so Harlee could play with the coloring books, markers, and Play-Doh bought for the ride. She packed snacks and a cooler full of drinks. Since Harlee was still potty training, she brought extra towels and clothes for accidents. The final step was handing Harlee her Baby Yoda doll once she settled into her car seat. Rainey had sewed a port in the doll’s chest to mirror the one Harlee has in hers.
About three hours from Memphis, Harlee was crying inconsolably. Rainey pulled off the interstate and stopped at the first hotel she could find. She later learned it had been described in online reviews as “awful,” a “nightmare,” “disgusting,” and “horrible.”
“I didn’t know the area,” she said. “The hotel was garbage. It just made it worse.”
The drive home also required a hotel stop, but this time Rainey was able to find one that was cleaner. A $100 donation from a local charity helped to offset the cost.
Among the changes St. Jude is making is to reimburse families like Rainey’s, who live more than 400 miles from the hospital, for an overnight stay at a hotel when making the trip to Memphis.
Rainey said she was called by a St. Jude representative after ProPublica asked about her situation and was told the hospital would pay for her past hotel stays when traveling back and forth to St. Jude. The representative, Rainey said, also told her the hospital discovered the way it had been measuring mileage was inaccurate.
“I am not the only one,” Rainey said. “There are others. They should reimburse all the families.”
The anxiety of unpaid bills piling up, combined with caring for a child undergoing chemotherapy or radiation, takes a severe toll on parents and guardians, said Christopher Hope, a UPS driver who started a Memphis-based foundation after meeting St. Jude parents who were in financial crisis.
Hope’s small charity spent $12,000 last year to help families. Parents in St. Jude social media groups often refer families in need to it. The charity has helped families cover mortgage and car payments.
“I never knew anything about this until hearing about it from families,” Hope said. “All we hear is about kids and treatment, not the other side of it.”
“It’s not free”
In addition to charities like Hope’s, St. Jude families have repeatedly turned to fundraising sites and networks of their relatives, friends, and neighbors to help cover basic expenses while unable to work during their children’s treatment. Parents’ requests on fundraising sites are sometimes desperate pleas.
In January 2017, one father in North Carolina said he’d had to abandon a business venture to take time for his son to receive care at St. Jude. His income had plummeted. He asked friends to give as little as $10 to “at least make it possible to survive.”
This year, a mother in Memphis whose 1-year-old son receives care at St. Jude for sickle cell disorder ran out of medical leave and couldn’t work her shifts at a clothing distribution center. After the child had a flare-up in July requiring several days of treatment at the hospital, she said she returned home to find her power shut off. Sitting in a dark apartment, unable to pay her utility bills, she set up a GoFundMe campaign. She received less than $20 through the site; her relatives eventually pooled $350 to get her electricity restored.
Even parents with stable jobs and private health insurance often take on debt and need outside help.
When Taylr and Treg Murphy’s 17-year-old son Peyton was diagnosed with cancer and needed monthslong treatment at St. Jude in 2017, the entire family – mom, dad, sister, and brother – went with him, traveling from their home in Lafayette, La., to Memphis. Treg took a leave from his job at an oil mining company and Taylr, who works at her mother’s bakery, did the same.
“We knew that it was going to be a collective team effort,” Treg said. “Without even a discussion, we figured that if Peyton’s got to go for the surgery, we’re all going.”
Peyton had an enormous tumor that had grown out of his right femur and was crowding his knee. Rounds of chemotherapy appeared to have killed osteosarcoma cells elsewhere in his body. But he needed to undergo a procedure called limb-sparing surgery that would require weeks of recovery time at the hospital.
The hospital agreed to allow all five family members to stay for free at St. Jude if they bunked together in a single room. It assigned them a spot in Tri Delta Place, its hotel-like short-term patient residence on the campus. Tri Delta is set up for visits of up to seven days, according to the hospital’s guide for volunteers, but the Murphys were there for almost 50.
Taylr said the unit at Tri Delta had no oven or stove and St. Jude provided no grocery money, instead allotting them a $50-per-day credit at the hospital cafeteria, Kay Kafe – not enough to feed the family of five. As the weeks wore on, the Murphys split grilled cheese sandwiches and paid for food out of pocket.
After ProPublica asked about the hospital’s food allowances, St. Jude said it would increase them as part of the changes scheduled to go into effect this month. The hospital switched from a $50-a-day cap per family to providing $25 a day to each family member. For a family of four, that would double the food benefit. A weekly stipend given to families in long-term housing was increased to $150 from $125.
For the Murphys, it was the loss of their work income, more than out-of-pocket expenses, that put them into a financial hole as Peyton’s treatment went on. Treg’s employer couldn’t pay him during his long absences.
Fearful of being evicted or having their car repossessed, Taylr said she asked a St. Jude social worker for assistance. The social worker helped her apply for grants from other charities. Taylr said the B+ Foundation paid their rent one month, which ensured they’d have a home to return to.
In the years since his initial treatment, Peyton has gone back to St. Jude repeatedly for exams and surgeries to remove malignant growths in his lungs. Taylr and Treg have missed more work to bring Peyton to Memphis, costing them thousands of dollars more in income.
By the start of this year, Taylr and Treg said they were about $20,000 in debt and panicking. Dustin Poirier, a former UFC champion from their hometown, heard from a friend about Peyton and the family’s financial trouble. He donated $10,000 to them from his personal charity and in May hosted a local fundraiser that collected enough to pay off their credit cards.
St. Jude families sometimes commiserate about money problems with each other, Taylr said, but few are aware of the extent of the hospital’s unspent resources. The Murphys said they didn’t know St. Jude has more than $5 billion in reserve or that it continues to raise hundreds of millions of dollars in surplus donations each year.
“That’s just insane,” Taylr said. “That just blows my mind. When we first started getting treated, people would be like, ‘Oh, St. Jude covers everything, that’s awesome.’ That’s not how it works. People don’t understand that. I truly didn’t understand before I got into St. Jude.”
Taylr and Treg said the doctors at St. Jude are “amazing” and they’re grateful for their son’s care. But they bristled at the assumption that it was covered by the hospital’s charity. The family’s insurance paid a substantial part of the bills.
“It’s not free,” Taylr said. “My husband works very hard for the insurance we have – and they are billed.” The Murphys pay $12,000 in health insurance premiums each year.
Their struggle continues. Peyton’s cancer has relapsed, and he’s making regular trips with his mom or dad back to St. Jude for chemotherapy. The family is again applying for help from other charities.
Wiped out savings
The costs associated with care at St. Jude caused at least one family to stop going to Memphis altogether.
Last winter, Kelly Edwards was excitedly searching through Tulsa real estate listings after years of diligently saving $10,000 for a down payment on a house. She craved a permanent home for herself and the two young brothers she had taken in five years earlier at the behest of a family friend. She hoped to adopt the boys, now 13 and 9, who call her mom.
In February, the older boy, DJ, was lethargic and uninterested in his schoolwork. After several doctor visits, he was diagnosed with acute lymphoblastic leukemia at a Tulsa hospital. The cancer, referred to as ALL, is the most common type among children, with survival rates that exceed 90%. A day after his diagnosis, DJ and Edwards were driving six hours to Memphis for treatment at St. Jude, which is affiliated with the Oklahoma hospital.
The pair stayed for free at an independently operated Ronald McDonald House near St. Jude, and a weekly stipend from the hospital helped to pay for meals – aid that Edwards said was a blessing. DJ had health insurance through the Oklahoma Medicaid program.
But as with the Murphys, lost income soon put Edwards’ family into financial jeopardy. She works as a supervisor for a company that delivers packages for Amazon. After she used up two weeks of paid time off, she stopped getting paychecks. The bills, however, kept coming: rent, car payments, utilities. To that was added the $250 a week she paid a friend to stay with DJ’s younger brother and her two dogs in Tulsa.
Within four months, her house savings were wiped out. Edwards said she told her St. Jude social worker about her financial woes but got no additional help.
One of Edwards’ adult daughters started a GoFundMe campaign to help, bringing in just over $3,000. Edwards said she appreciated the aid but believes donations were kept low by the widespread perception that St. Jude families don’t have financial problems.
“Everyone hears that everything is taken care of by St. Jude,” she said. “That is not true, but everyone has that mentality.” She said someone she knew asked her “what is that money going for if St. Jude’s is paying for everything?”
DJ was scheduled to go back to St. Jude for three weeks of treatment in August, but Edwards decided she simply couldn’t afford it. “I don’t have the money to go back and forth,” she said. She worked with DJ’s local doctors and found that the hospital near her home in Tulsa could provide the same treatment he was scheduled to get in Tennessee.
The local treatment allowed her to continue working some shifts and to be at home with both of her boys. DJ is also happier when he is home, Edwards said.
Edwards and the boys are now living in a small house her brother owns just outside Tulsa. Late on a recent weekday afternoon, DJ slowly shuffled into the living room, exhausted from a day of chemotherapy treatment.
He is in the midst of a 20-week regimen where he receives the cancer-killing drugs every other day, just one phase of a nearly three-year treatment plan. He wore an orange knit hat, T-shirt, and shorts. He rubbed his eyes before asking a visitor, “How is your day going?” He smiled at the positive response. When he heard the family was eating steak for dinner, he eagerly jumped up to start helping in the kitchen. After they moved in, Edwards hung family portraits on the walls to make it feel homier. She doesn’t expect they will be moving again any time soon.
The dream of buying a home of their own is gone.
Former ProPublica reporter Marshall Allen contributed reporting. Kirsten Berg contributed research.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
A series of sharp knocks on his driver’s side window startled Jason Burt awake.
It was the middle of the night on a Saturday in 2016. Burt was sleeping in his pickup truck in the parking lot of St. Jude Children’s Research Hospital in downtown Memphis, Tenn., where his 5-year-old daughter was being treated for brain cancer. He’d driven more than 500 miles from his home in Central Texas to visit her.
A St. Jude security guard peered into the truck and asked Burt what he was doing. Burt explained that his daughter and her mother, his ex-girlfriend, were staying in the hospital’s free patient housing. But St. Jude provides housing for only one parent. Burt, a school bus driver making $20,000 a year, told the guard he couldn’t afford a hotel. The guard let the exhausted father go back to sleep.
St. Jude would do no more to find him a place to stay.
“They were aware of the situation,” Burt said. “I didn’t push anything. I was just grateful she was getting treated and I was doing what I needed to do.”
St. Jude is the largest and most highly regarded health care charity in the country. Each year, the Memphis hospital’s fundraisers send out hundreds of millions of letters, many with heart-wrenching photographs of children left bald from battling cancer. Celebrities like Jennifer Aniston and Sofia Vergara sing the hospital’s praises in televised advertisements. This year, St. Jude’s fundraising reached outer space. The SpaceX Inspiration4 mission in September included a former St. Jude patient as a crew member.
Last year, St. Jude raised a record $2 billion. U.S. News & World Report ranked it the country’s 10th-best children’s cancer hospital, and St. Jude raised roughly as much as the nine hospitals ahead of it put together. It currently has $5.2 billion in reserves, a sum large enough to run the institution at current levels for the next four and a half years without a single additional donation.
St. Jude makes a unique promise as part of its fundraising: “Families never receive a bill from St. Jude for treatment, travel, housing or food – because all a family should worry about is helping their child live.”
But for many families, treatment at St. Jude does not relieve all the financial burdens they incur in getting care for their children, including housing, travel, and food costs that fall outside the hospital’s strict limits, a ProPublica investigation has found.
While families may not receive a bill from St. Jude, the hospital doesn’t cover what’s usually the biggest source of financial stress associated with childhood cancer: The loss of income as parents quit or take leave from jobs to be with their child during treatment. For many families, the consequence is missed payments for cars, utilities, and cellphones. Others face eviction or foreclosure because they can’t keep up with rent and mortgage payments.
Parents at St. Jude have exhausted savings and retirement accounts, borrowed from family and friends, or asked other charities for aid. ProPublica identified more than 100 St. Jude families seeking financial help through the online fundraiser GoFundMe, with half of the campaigns started in the past two years. We counted scores of other events like concerts and yard sales organized to help St. Jude families in need.
One family relied on a mixed martial arts fighter to help raise money for expenses like car repairs and cellphone bills, items that St. Jude would not cover. Another spent $10,000, originally saved to purchase a home, on costs related to treatment at St. Jude.
Only about half of the $7.3 billion St. Jude has received in contributions in the past five fiscal years went to the hospital’s research and caring for patients, according to its financial filings with the Internal Revenue Service. About 30% covered the cost of its fundraising operations, and the remaining 20%, or $1 of every $5 donated, increased its reserve fund.
Further, ProPublica found, a substantial portion of the cost for treatment is paid not by St. Jude but by families’ private insurance or by Medicaid, the government insurance program for low-income families. About 90% of patients are insured, bringing in more than $100 million in reimbursements for treatment a year. If a family shows up at St. Jude without insurance, a company hired by the charity helps them find it. St. Jude does cover copays and deductibles, an unusual benefit.
St. Jude spends about $500 million a year on patient services – a figure that includes all medical care and other assistance. Very little of what St. Jude raises from the public goes to pay for food, travel, and housing for families, the investigation found. Last year, it was 2% of the money raised, or nearly $40 million.
In written responses to ProPublica, lawyers for St. Jude and its fundraising arm, the American Lebanese Syrian Associated Charities, or ALSAC, emphasized that countless families have benefited from the charity provided since the hospital opened its doors in 1962.
“ProPublica should be celebrating St. Jude and ALSAC for their commitment to finding cures, saving children’s lives, and optimizing patient outcomes,” one of their letters said.
It is unquestioned that St. Jude has helped thousands of children and their families over the decades. Patients have offered scores of testimonials about the hospital’s generosity and care.
“This often comes as a huge relief to families who often expect to sell all their belongings just so their children can get the medical care and treatment they need to save their lives,” the hospital’s lawyers wrote. “St. Jude and ALSAC understand that this arrangement cannot cover all financial obligations of all families, nor can St. Jude or ALSAC shield families from all the financial and emotional effects” of a child’s illness.
St. Jude said it discloses the limits of its aid to families on its website and in material provided to those whose children are admitted to the hospital. That includes the rule Burt ran into, that the hospital covers the travel and housing costs of only one caregiver and one patient. For many families, the daily food budget is capped at $50. In some cases, hotel stays en route are provided only if families travel more than 500 miles to get to St. Jude.
St. Jude said its assistance is “based on guidelines to ensure fairness and responsible use of donor funds” and on remaining compliant with a federal anti-kickback statute that makes it a criminal offense to offer something of value to induce a medical referral. St. Jude declined to explain how the law affects the amount or type of financial assistance it provides to families.
“St. Jude has never promised anyone – neither patients nor the public in general – that it can solve all financial problems,” the letter said.
When parents need additional financial help, St. Jude’s social workers often send them to smaller charities or in some cases suggest that they apply for government aid.
They refer many to the Andrew McDonough B+ Foundation, which gives more than $2.5 million a year in grants to thousands of families of pediatric cancer patients at hospitals across the country to help cover rent, utilities, and other urgent expenses.
Joe McDonough, the foundation’s founder and president, said St. Jude families have the same money problems as families of patients at other children’s hospitals, even though he said St. Jude’s marketing creates the public perception that it alleviates these burdens.
“People say to me, ‘Why are you helping St. Jude families?’ ” McDonough said. “Well, what happens when a family lives in Augusta, Georgia, and they’re being treated at St. Jude? They still have to pay the rent on their apartment back in Augusta, Georgia. They still have to make their car payment. And it’s not my position to say whether St. Jude should be paying for all those expenses or not. I’m just explaining that it’s not a totally free ride.”
The help St. Jude provides to families may soon be increasing.
After ProPublica provided St. Jude with the findings of its reporting, the hospital informed families of a dramatic expansion in the assistance it will give to parents and other relatives during their kids’ treatment in Memphis.
Among the most significant changes are increasing travel benefits to two parents instead of one and covering regular trips to Memphis for siblings and other loved ones. St. Jude’s letter to parents said the changes take effect Nov. 15.
That would’ve made a big difference for Burt.
Burt’s daughter, whom ProPublica is not identifying at her mother’s request, was originally diagnosed with cancer in early 2015, when doctors discovered a tumor pressing against her brain stem. She had successful emergency surgery to remove the mass at Dell Children’s Medical Center in Austin, Texas. Medicaid and Dell Children’s covered the bill, but the family was still faced with the cost of her ongoing treatment.
“At that point I’m thinking: ‘What am I going to do? I guess I’m selling my house, whatever it takes,’” Burt recalled. “Honestly, that was probably a big deciding factor for St. Jude.”
St. Jude accepted Burt’s daughter into a clinical trial, and the family moved to the hospital’s patient housing in Memphis for several months. Both parents stopped working for a time, and people in their hometown raised cash to pay their bills.
Her cancer relapsed the following year with several new, inoperable brain tumors. Burt and his daughter’s mom broke up during that round of treatment, and financial problems piled up.
Burt said his credit score dropped so low that utility companies refused to set up service unless he first paid a deposit. One of the family’s cars was repossessed, he said. Burt’s 2005 Chevrolet Colorado pickup has 300,000 miles on it, many of them logged on trips from Texas to Memphis. When Burt’s daughter was at St. Jude for treatment or exams, he’d work all week, then visit on many weekends where he would spend Saturday night sleeping in the hospital parking lot.
He asked hospital officials if he could sleep in St. Jude’s housing, but they turned him down, he said.
Burt said he was happy with the care St. Jude provided. His daughter’s health is stable, he said, and brain scans taken during her September exam confirmed her two remaining tumors haven’t grown. But he’s still trying to recover financially.
“It’s five years now,” Burt said, “and I’m not completely caught up yet.”
A fundraising giant
St. Jude began with a fledgling entertainer praying for a career break.
When Danny Thomas, a comic and actor best known for the TV sitcom “Make Room for Daddy,” was struggling to earn a living in the late 1930s, the devout Roman Catholic went to church and asked for help from the patron saint of desperate cases, St. Jude Thaddeus. If he made it big, Thomas promised to build “a shrine where the poor and the helpless and the hopeless may come for comfort and aid,” according to a history published by ALSAC.
Within five years, Thomas became a star and worked to fulfill his promise by building a children’s hospital named after St. Jude and a fundraising organization to support it. Thomas, whose parents were Lebanese immigrants, recruited others who shared his Middle Eastern roots to help.
He used his fame to raise the hospital’s profile, appearing in ads for St. Jude and hosting fundraising events starring the likes of Elvis Presley and Sammy Davis Jr. Thomas’ daughter Marlo, herself a TV star, succeeded him in championing St. Jude.
Today, St. Jude is a specialty treatment and research center with about 5,700 employees and 73 beds. Other top children’s hospitals have more staff and beds, and they also treat more conditions.
Though St. Jude raises money across the world, most of its patients come from Tennessee and surrounding states. Patients from elsewhere are usually enrolled in clinical trials.
ALSAC, which handles St. Jude’s fundraising and investments, has 2,188 employees in Memphis and in 36 regional offices across the country. More than 400 of the fundraising arm’s employees are paid over $100,000, according to IRS filings. The charity takes in so much money each year that it regularly steers hundreds of millions of dollars in donations to reserve accounts, the filings show.
Overall, St. Jude’s reserve has grown by 58% over the past five fiscal years, during which it has added $1.9 billion to its investment accounts and shifted its portfolio toward financial products designed to generate bigger returns than stocks, bonds, and mutual funds traditionally deliver. The charity stowed more than a third of the new surplus, $688 million, in riskier private equity investments.
IRS rules do not limit the size of a nonprofit’s reserves, and experts on charitable finance differ on best practices.
St. Jude meets Better Business Bureau guidelines, which call for charities to maintain reserves of less than three times total expenses, but other experts expressed alarm that the hospital had accumulated such a large sum of money.
The size of the St. Jude reserve is “staggering,” said Laura Otten, the director of LaSalle University’s master program in nonprofit leadership. She said a typical reserve for a nonprofit the size of St. Jude is one to two years of expenses. Donors generally want to know their dollars are being put to work, she said.
The hospital said it needs a large reserve because its unique operating model relies on donations to fund annual operating costs. “[W]e are highly donor-dependent and subject to the economic driven vagaries of charitable giving,” the hospital said in a written response to ProPublica questions.
But the hospital’s reserve is already more than large enough to buffer against recessions and potential drops in donations, said Ge Bai, a professor of accounting and health policy at Johns Hopkins University. “They should be spending the money as aggressively as they raise it, but they seem to be hoarding,” Bai said.
The hospital said it is also raising billions to fund the construction of new housing and research space, although its plans do not currently include spending any of the reserve on new facilities.
St. Jude’s reserves have ballooned at a time when researchers, oncologists, advocates, and families complain about a dearth of funding for pediatric cancer studies nationally.
Dozens of other children’s hospitals across the country have research divisions devoted to pediatric cancer and enroll their patients in clinical trials for new drugs and procedures. They pay for research staff and studies in part with donations from their local communities, often competing directly against St. Jude. ALSAC has regional offices in several U.S. cities with elite pediatric cancer centers of their own, including Atlanta, Chicago, Denver, and Seattle.
Coury Shadyac, an ALSAC vice president and daughter of the organization’s CEO, Richard Shadyac Jr., oversees a team of 45 fundraisers along the West Coast “raising $300 million annually” for St. Jude, according to her LinkedIn profile. That’s $100 million more in donations than either Children’s Hospital Los Angeles or Seattle Children’s Hospital, two of the nation’s leading pediatric cancer institutions, received in fiscal year 2019, IRS disclosures show. But it’s only a small part of St. Jude’s fundraising haul.
ALSAC’s ubiquitous fundraising has led to concerns that it undercuts other hospitals’ campaigns. Some doctors interviewed by ProPublica said they have encouraged donors to give their money to hospitals closer to home.
David Clark, a pediatrician and former longtime chairperson of pediatrics at Albany Medical Center in New York, said St. Jude raises tens of thousands of dollars in his region that does little to benefit the children with cancer in his area since almost all are treated locally. ALSAC has a fundraising office located a few miles from Albany Medical.
“They think of every way they can to make money and the least amount of ways to spend it,” Clark said. “They deceive people into supporting something that is totally dishonest.”
Nearly all St. Jude solicitations feature the hospital’s patients – the children usually smiling and bald from treatment – along with the familiar promise that it never sends families a bill.
It’s a message that ALSAC has tested and researched to maximize donations. Donors appreciate the promise to never bill families, said Mary Kate Tolan, an ALSAC executive, in a podcast last year. She added that no parent should have to take out a second mortgage or lose their job because their child is being treated at St. Jude.
Alternative messaging to the no-bills promise did not “perform as well,” said Tolan, who develops emerging technologies for ALSAC. Tolan did not return requests for comment.
“Borrowing and begging”
Catherine Rainey thought she would be free of financial worry when her 2-year-old daughter Harlee was admitted to St. Jude last year.
“The first thing my dad said was: ‘Catherine, you have nothing to worry about. They raise billions of dollars. Anytime you have a problem, you tell them and they will take care of it,’ ” she said.
But like many families, the Raineys discovered that St. Jude’s charity came with limits on payments for expenses such as travel that could be bewildering.
Harlee ended up at St. Jude after first going to nearby Niswonger Children’s Hospital in Johnson City, Tenn., in October 2020. The doctors there discovered a cancerous mass attached to her right kidney. The hospital is a St. Jude affiliate, and the doctors recommended the toddler be treated in Memphis.
Rainey, a single mother of two young girls, had to leave her job as a nurse for months to be with Harlee at St. Jude. The loss of income quickly created problems. “My family, we don’t come from money,” she said. “We are not doctors and billionaires. We make it. That is it.”
St. Jude did provide food and housing on campus. But the hospital said it couldn’t help with the items that were causing Rainey to worry, including car payments, insurance, and cellphone bills.
Rainey’s boss set up a GoFundMe account to help make up some of her lost income. A small local charity, Kari’s Heart Foundation, also helped out by paying about $3,000 worth of phone bills and car payments, staving off repossession.
“It was just a bunch of borrowing and begging,” Rainey said of her experience while her daughter was treated in Memphis. “They acted like it was coming out of their own pocket.”
Harlee has checkups at St. Jude every three months that last about four days. The costs of travel to and from St. Jude put an additional strain on Rainey and Harlee. St. Jude is an eight-hour ride, without stops, from Rainey’s home in Appalachia, Va., a town of 1,432 people near the Kentucky border.
Rainey said her daughter generally can make it about two-thirds of the way, with frequent stops, before she has had enough. “When she is done, she is really done,” Rainey said. “She will scream, cry, and kick.”
In July, in advance of an August trip to Memphis, Rainey called the patient services department at St. Jude to see whether they could help pay for a hotel to break up the travel day — an expense Rainey said she could not afford.
To qualify for a hotel reimbursement, Rainey said, St. Jude told her she had to live more than 500 miles from Memphis. The ride from her home to the hospital is 530 miles (a measurement ProPublica confirmed with mapping tools). However, Rainey said, St. Jude told her it measured the trip from city limit to city limit and came up with a distance of 491 miles. Even using that metric, the distance is still more than 500 miles, ProPublica found.
When she challenged the hospital’s stance, Rainey said she was berated by a patient services representative.
“I was feeling pissed off, and I was crying,” Rainey said of the interaction. “You give up your whole life for your child, and they tell you don’t worry about anything, we will cover this and then they tell you to just push through the drive.”
Rainey did what she could to make the trip go smoothly: She configured a small table to extend across her daughter’s car seat, so Harlee could play with the coloring books, markers, and Play-Doh bought for the ride. She packed snacks and a cooler full of drinks. Since Harlee was still potty training, she brought extra towels and clothes for accidents. The final step was handing Harlee her Baby Yoda doll once she settled into her car seat. Rainey had sewed a port in the doll’s chest to mirror the one Harlee has in hers.
About three hours from Memphis, Harlee was crying inconsolably. Rainey pulled off the interstate and stopped at the first hotel she could find. She later learned it had been described in online reviews as “awful,” a “nightmare,” “disgusting,” and “horrible.”
“I didn’t know the area,” she said. “The hotel was garbage. It just made it worse.”
The drive home also required a hotel stop, but this time Rainey was able to find one that was cleaner. A $100 donation from a local charity helped to offset the cost.
Among the changes St. Jude is making is to reimburse families like Rainey’s, who live more than 400 miles from the hospital, for an overnight stay at a hotel when making the trip to Memphis.
Rainey said she was called by a St. Jude representative after ProPublica asked about her situation and was told the hospital would pay for her past hotel stays when traveling back and forth to St. Jude. The representative, Rainey said, also told her the hospital discovered the way it had been measuring mileage was inaccurate.
“I am not the only one,” Rainey said. “There are others. They should reimburse all the families.”
The anxiety of unpaid bills piling up, combined with caring for a child undergoing chemotherapy or radiation, takes a severe toll on parents and guardians, said Christopher Hope, a UPS driver who started a Memphis-based foundation after meeting St. Jude parents who were in financial crisis.
Hope’s small charity spent $12,000 last year to help families. Parents in St. Jude social media groups often refer families in need to it. The charity has helped families cover mortgage and car payments.
“I never knew anything about this until hearing about it from families,” Hope said. “All we hear is about kids and treatment, not the other side of it.”
“It’s not free”
In addition to charities like Hope’s, St. Jude families have repeatedly turned to fundraising sites and networks of their relatives, friends, and neighbors to help cover basic expenses while unable to work during their children’s treatment. Parents’ requests on fundraising sites are sometimes desperate pleas.
In January 2017, one father in North Carolina said he’d had to abandon a business venture to take time for his son to receive care at St. Jude. His income had plummeted. He asked friends to give as little as $10 to “at least make it possible to survive.”
This year, a mother in Memphis whose 1-year-old son receives care at St. Jude for sickle cell disorder ran out of medical leave and couldn’t work her shifts at a clothing distribution center. After the child had a flare-up in July requiring several days of treatment at the hospital, she said she returned home to find her power shut off. Sitting in a dark apartment, unable to pay her utility bills, she set up a GoFundMe campaign. She received less than $20 through the site; her relatives eventually pooled $350 to get her electricity restored.
Even parents with stable jobs and private health insurance often take on debt and need outside help.
When Taylr and Treg Murphy’s 17-year-old son Peyton was diagnosed with cancer and needed monthslong treatment at St. Jude in 2017, the entire family – mom, dad, sister, and brother – went with him, traveling from their home in Lafayette, La., to Memphis. Treg took a leave from his job at an oil mining company and Taylr, who works at her mother’s bakery, did the same.
“We knew that it was going to be a collective team effort,” Treg said. “Without even a discussion, we figured that if Peyton’s got to go for the surgery, we’re all going.”
Peyton had an enormous tumor that had grown out of his right femur and was crowding his knee. Rounds of chemotherapy appeared to have killed osteosarcoma cells elsewhere in his body. But he needed to undergo a procedure called limb-sparing surgery that would require weeks of recovery time at the hospital.
The hospital agreed to allow all five family members to stay for free at St. Jude if they bunked together in a single room. It assigned them a spot in Tri Delta Place, its hotel-like short-term patient residence on the campus. Tri Delta is set up for visits of up to seven days, according to the hospital’s guide for volunteers, but the Murphys were there for almost 50.
Taylr said the unit at Tri Delta had no oven or stove and St. Jude provided no grocery money, instead allotting them a $50-per-day credit at the hospital cafeteria, Kay Kafe – not enough to feed the family of five. As the weeks wore on, the Murphys split grilled cheese sandwiches and paid for food out of pocket.
After ProPublica asked about the hospital’s food allowances, St. Jude said it would increase them as part of the changes scheduled to go into effect this month. The hospital switched from a $50-a-day cap per family to providing $25 a day to each family member. For a family of four, that would double the food benefit. A weekly stipend given to families in long-term housing was increased to $150 from $125.
For the Murphys, it was the loss of their work income, more than out-of-pocket expenses, that put them into a financial hole as Peyton’s treatment went on. Treg’s employer couldn’t pay him during his long absences.
Fearful of being evicted or having their car repossessed, Taylr said she asked a St. Jude social worker for assistance. The social worker helped her apply for grants from other charities. Taylr said the B+ Foundation paid their rent one month, which ensured they’d have a home to return to.
In the years since his initial treatment, Peyton has gone back to St. Jude repeatedly for exams and surgeries to remove malignant growths in his lungs. Taylr and Treg have missed more work to bring Peyton to Memphis, costing them thousands of dollars more in income.
By the start of this year, Taylr and Treg said they were about $20,000 in debt and panicking. Dustin Poirier, a former UFC champion from their hometown, heard from a friend about Peyton and the family’s financial trouble. He donated $10,000 to them from his personal charity and in May hosted a local fundraiser that collected enough to pay off their credit cards.
St. Jude families sometimes commiserate about money problems with each other, Taylr said, but few are aware of the extent of the hospital’s unspent resources. The Murphys said they didn’t know St. Jude has more than $5 billion in reserve or that it continues to raise hundreds of millions of dollars in surplus donations each year.
“That’s just insane,” Taylr said. “That just blows my mind. When we first started getting treated, people would be like, ‘Oh, St. Jude covers everything, that’s awesome.’ That’s not how it works. People don’t understand that. I truly didn’t understand before I got into St. Jude.”
Taylr and Treg said the doctors at St. Jude are “amazing” and they’re grateful for their son’s care. But they bristled at the assumption that it was covered by the hospital’s charity. The family’s insurance paid a substantial part of the bills.
“It’s not free,” Taylr said. “My husband works very hard for the insurance we have – and they are billed.” The Murphys pay $12,000 in health insurance premiums each year.
Their struggle continues. Peyton’s cancer has relapsed, and he’s making regular trips with his mom or dad back to St. Jude for chemotherapy. The family is again applying for help from other charities.
Wiped out savings
The costs associated with care at St. Jude caused at least one family to stop going to Memphis altogether.
Last winter, Kelly Edwards was excitedly searching through Tulsa real estate listings after years of diligently saving $10,000 for a down payment on a house. She craved a permanent home for herself and the two young brothers she had taken in five years earlier at the behest of a family friend. She hoped to adopt the boys, now 13 and 9, who call her mom.
In February, the older boy, DJ, was lethargic and uninterested in his schoolwork. After several doctor visits, he was diagnosed with acute lymphoblastic leukemia at a Tulsa hospital. The cancer, referred to as ALL, is the most common type among children, with survival rates that exceed 90%. A day after his diagnosis, DJ and Edwards were driving six hours to Memphis for treatment at St. Jude, which is affiliated with the Oklahoma hospital.
The pair stayed for free at an independently operated Ronald McDonald House near St. Jude, and a weekly stipend from the hospital helped to pay for meals – aid that Edwards said was a blessing. DJ had health insurance through the Oklahoma Medicaid program.
But as with the Murphys, lost income soon put Edwards’ family into financial jeopardy. She works as a supervisor for a company that delivers packages for Amazon. After she used up two weeks of paid time off, she stopped getting paychecks. The bills, however, kept coming: rent, car payments, utilities. To that was added the $250 a week she paid a friend to stay with DJ’s younger brother and her two dogs in Tulsa.
Within four months, her house savings were wiped out. Edwards said she told her St. Jude social worker about her financial woes but got no additional help.
One of Edwards’ adult daughters started a GoFundMe campaign to help, bringing in just over $3,000. Edwards said she appreciated the aid but believes donations were kept low by the widespread perception that St. Jude families don’t have financial problems.
“Everyone hears that everything is taken care of by St. Jude,” she said. “That is not true, but everyone has that mentality.” She said someone she knew asked her “what is that money going for if St. Jude’s is paying for everything?”
DJ was scheduled to go back to St. Jude for three weeks of treatment in August, but Edwards decided she simply couldn’t afford it. “I don’t have the money to go back and forth,” she said. She worked with DJ’s local doctors and found that the hospital near her home in Tulsa could provide the same treatment he was scheduled to get in Tennessee.
The local treatment allowed her to continue working some shifts and to be at home with both of her boys. DJ is also happier when he is home, Edwards said.
Edwards and the boys are now living in a small house her brother owns just outside Tulsa. Late on a recent weekday afternoon, DJ slowly shuffled into the living room, exhausted from a day of chemotherapy treatment.
He is in the midst of a 20-week regimen where he receives the cancer-killing drugs every other day, just one phase of a nearly three-year treatment plan. He wore an orange knit hat, T-shirt, and shorts. He rubbed his eyes before asking a visitor, “How is your day going?” He smiled at the positive response. When he heard the family was eating steak for dinner, he eagerly jumped up to start helping in the kitchen. After they moved in, Edwards hung family portraits on the walls to make it feel homier. She doesn’t expect they will be moving again any time soon.
The dream of buying a home of their own is gone.
Former ProPublica reporter Marshall Allen contributed reporting. Kirsten Berg contributed research.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
Children and COVID: Youngest vaccinees off to a slower start

Specific figures for children aged 5-11 years are not yet available, but CDC data show that 1.55 million children under the age of 12 years had received at least one dose of COVID-19 vaccine as of Nov. 15, of whom almost 204,000 already had been vaccinated before Nov. 2. For children aged 12-15, the first 2 weeks after approval on May 12 produced almost 2.1 million vaccine initiations, according to the CDC’s COVID Data Tracker.
That dataset reveals several other noteworthy differences between the two age groups in the 10 days after approval:
- There were over 7,000 vaccine initiations on the first day in the 12-15 group; the younger group had 32.
- The older children reached 100,000 per day in 3 days; the younger children took 8 days.
- The older group topped 200,000 vaccinations per day on six different days; the younger group didn’t get above 175,000.
Children under 12 made up 27.5% of vaccine initiations in all age groups during the 2 weeks from Nov. 2 to Nov. 15, versus 3.4% for 12- to 15-year-olds and 1.2% for 16- and 17-year-olds, the CDC said, while also reporting that 3.6% of children under age 12 had received at least one dose of the COVID vaccine, compared with 57.8% of those aged 12-15 and 64.4% of 16- to 17-year-olds.
Meanwhile, the first full week of November marked the second consecutive increase in the number of weekly child COVID cases, with 122,000 reported for Nov. 5-11. The number of new cases has now surpassed 100,000 for 14 consecutive weeks, the American Academy of Pediatrics and the Children’s Hospital Association said in their weekly COVID report. That report, which covers state health departments, has not included current information from Alabama, Nebraska, and Texas since the summer.
Regionally, the increases over the past 2 weeks were spread out among the East, the Midwest, and the West, while the decline that had been going on for several weeks in the South has largely come to a halt. The states with the highest percent increases over those 2 weeks are all in New England: Maine, New Hampshire, and Vermont, the AAP and CHA noted. In a separate report, the AAP said that Vermont has the second-highest child vaccination rate (81%) in the country, just behind Massachusetts (82%).

Specific figures for children aged 5-11 years are not yet available, but CDC data show that 1.55 million children under the age of 12 years had received at least one dose of COVID-19 vaccine as of Nov. 15, of whom almost 204,000 already had been vaccinated before Nov. 2. For children aged 12-15, the first 2 weeks after approval on May 12 produced almost 2.1 million vaccine initiations, according to the CDC’s COVID Data Tracker.
That dataset reveals several other noteworthy differences between the two age groups in the 10 days after approval:
- There were over 7,000 vaccine initiations on the first day in the 12-15 group; the younger group had 32.
- The older children reached 100,000 per day in 3 days; the younger children took 8 days.
- The older group topped 200,000 vaccinations per day on six different days; the younger group didn’t get above 175,000.
Children under 12 made up 27.5% of vaccine initiations in all age groups during the 2 weeks from Nov. 2 to Nov. 15, versus 3.4% for 12- to 15-year-olds and 1.2% for 16- and 17-year-olds, the CDC said, while also reporting that 3.6% of children under age 12 had received at least one dose of the COVID vaccine, compared with 57.8% of those aged 12-15 and 64.4% of 16- to 17-year-olds.
Meanwhile, the first full week of November marked the second consecutive increase in the number of weekly child COVID cases, with 122,000 reported for Nov. 5-11. The number of new cases has now surpassed 100,000 for 14 consecutive weeks, the American Academy of Pediatrics and the Children’s Hospital Association said in their weekly COVID report. That report, which covers state health departments, has not included current information from Alabama, Nebraska, and Texas since the summer.
Regionally, the increases over the past 2 weeks were spread out among the East, the Midwest, and the West, while the decline that had been going on for several weeks in the South has largely come to a halt. The states with the highest percent increases over those 2 weeks are all in New England: Maine, New Hampshire, and Vermont, the AAP and CHA noted. In a separate report, the AAP said that Vermont has the second-highest child vaccination rate (81%) in the country, just behind Massachusetts (82%).

Specific figures for children aged 5-11 years are not yet available, but CDC data show that 1.55 million children under the age of 12 years had received at least one dose of COVID-19 vaccine as of Nov. 15, of whom almost 204,000 already had been vaccinated before Nov. 2. For children aged 12-15, the first 2 weeks after approval on May 12 produced almost 2.1 million vaccine initiations, according to the CDC’s COVID Data Tracker.
That dataset reveals several other noteworthy differences between the two age groups in the 10 days after approval:
- There were over 7,000 vaccine initiations on the first day in the 12-15 group; the younger group had 32.
- The older children reached 100,000 per day in 3 days; the younger children took 8 days.
- The older group topped 200,000 vaccinations per day on six different days; the younger group didn’t get above 175,000.
Children under 12 made up 27.5% of vaccine initiations in all age groups during the 2 weeks from Nov. 2 to Nov. 15, versus 3.4% for 12- to 15-year-olds and 1.2% for 16- and 17-year-olds, the CDC said, while also reporting that 3.6% of children under age 12 had received at least one dose of the COVID vaccine, compared with 57.8% of those aged 12-15 and 64.4% of 16- to 17-year-olds.
Meanwhile, the first full week of November marked the second consecutive increase in the number of weekly child COVID cases, with 122,000 reported for Nov. 5-11. The number of new cases has now surpassed 100,000 for 14 consecutive weeks, the American Academy of Pediatrics and the Children’s Hospital Association said in their weekly COVID report. That report, which covers state health departments, has not included current information from Alabama, Nebraska, and Texas since the summer.
Regionally, the increases over the past 2 weeks were spread out among the East, the Midwest, and the West, while the decline that had been going on for several weeks in the South has largely come to a halt. The states with the highest percent increases over those 2 weeks are all in New England: Maine, New Hampshire, and Vermont, the AAP and CHA noted. In a separate report, the AAP said that Vermont has the second-highest child vaccination rate (81%) in the country, just behind Massachusetts (82%).
Two-thirds of preschoolers correctly identified emotions of masked adults
Some are concerned about the effects of adults working in preschools wearing face masks on the ability of young children to learn to recognize emotions, study author Juliane Schneider, MD, of University Hospital Lausanne (Switzerland), and colleagues wrote. Previous studies using photographs of faces with digitally added masks have suggested that young children’s emotional recognition was worse with masked faces.
In the study published in JAMA Pediatrics, the researchers tested the impact of masks on the ability of preschool children to identify joy, anger, and sadness. The study included 135 girls and 141 boys aged 36-72 months with a mean age of 52.4 months. The tests were conducted at nine daycare centers.
Children were shown photographs of 15 actors (5 men and 10 women) with and without surgical face masks. The total data set included 90 pictures illustrating joy, anger, and sadness. The children were shown the pictures at random, and they could either name the emotion, point to a card with emoticons showing the three emotions, or respond “I don’t know” or “quit the experiment.” Test sessions lasted approximately 7 minutes per child. Effect sizes were calculated using X2 and Cramer V tests.
Overall, 68.8% of the children correctly identified the emotion portrayed; the correct response rate was 70.6% for faces without face masks and 66.9% for those with face masks. Correct recognition of joy was significantly higher for faces without masks than for those with masks (94.8% vs. 87.3), as was correct recognition of sadness (54.1% vs. 48.9%; P < .001 for both). Recognition of anger was not significantly different for unmasked and masked faces (62.2% vs. 64.6%, P = .10).
No significant differences in correct responses appeared between boys and girls and the rate of correct responses increased significantly with age. The rates of “I don’t know,” and “quit the experiment” responses were 3.1% and 2.2%, respectively. In an analysis of incorrect responses, approximately 25% of the children confused anger and sadness, and 21% misidentified joy for images of anger or sadness.
“Overall, participants in this study, who had been exposed to face masks for nearly a year, recognized emotions on pictures better than has been reported in previous research, even with face masks,” the researchers wrote.
The study findings were limited by several factors including the use of static pictures versus real individuals, which limits generalizability, and the lack of data on children with developmental issues, the researchers noted.
Despite relatively small differences and weak effect size (Cramer V scores of 0.2 or less for all), the results show a stronger recognition of emotion, compared with other studies, and highlight the importance of investigating the impact of face masks on other aspects of child development as the COVID-19 pandemic persists, the researchers concluded.
The study received no outside funding. The researchers had no relevant financial conflicts to disclose.
Some are concerned about the effects of adults working in preschools wearing face masks on the ability of young children to learn to recognize emotions, study author Juliane Schneider, MD, of University Hospital Lausanne (Switzerland), and colleagues wrote. Previous studies using photographs of faces with digitally added masks have suggested that young children’s emotional recognition was worse with masked faces.
In the study published in JAMA Pediatrics, the researchers tested the impact of masks on the ability of preschool children to identify joy, anger, and sadness. The study included 135 girls and 141 boys aged 36-72 months with a mean age of 52.4 months. The tests were conducted at nine daycare centers.
Children were shown photographs of 15 actors (5 men and 10 women) with and without surgical face masks. The total data set included 90 pictures illustrating joy, anger, and sadness. The children were shown the pictures at random, and they could either name the emotion, point to a card with emoticons showing the three emotions, or respond “I don’t know” or “quit the experiment.” Test sessions lasted approximately 7 minutes per child. Effect sizes were calculated using X2 and Cramer V tests.
Overall, 68.8% of the children correctly identified the emotion portrayed; the correct response rate was 70.6% for faces without face masks and 66.9% for those with face masks. Correct recognition of joy was significantly higher for faces without masks than for those with masks (94.8% vs. 87.3), as was correct recognition of sadness (54.1% vs. 48.9%; P < .001 for both). Recognition of anger was not significantly different for unmasked and masked faces (62.2% vs. 64.6%, P = .10).
No significant differences in correct responses appeared between boys and girls and the rate of correct responses increased significantly with age. The rates of “I don’t know,” and “quit the experiment” responses were 3.1% and 2.2%, respectively. In an analysis of incorrect responses, approximately 25% of the children confused anger and sadness, and 21% misidentified joy for images of anger or sadness.
“Overall, participants in this study, who had been exposed to face masks for nearly a year, recognized emotions on pictures better than has been reported in previous research, even with face masks,” the researchers wrote.
The study findings were limited by several factors including the use of static pictures versus real individuals, which limits generalizability, and the lack of data on children with developmental issues, the researchers noted.
Despite relatively small differences and weak effect size (Cramer V scores of 0.2 or less for all), the results show a stronger recognition of emotion, compared with other studies, and highlight the importance of investigating the impact of face masks on other aspects of child development as the COVID-19 pandemic persists, the researchers concluded.
The study received no outside funding. The researchers had no relevant financial conflicts to disclose.
Some are concerned about the effects of adults working in preschools wearing face masks on the ability of young children to learn to recognize emotions, study author Juliane Schneider, MD, of University Hospital Lausanne (Switzerland), and colleagues wrote. Previous studies using photographs of faces with digitally added masks have suggested that young children’s emotional recognition was worse with masked faces.
In the study published in JAMA Pediatrics, the researchers tested the impact of masks on the ability of preschool children to identify joy, anger, and sadness. The study included 135 girls and 141 boys aged 36-72 months with a mean age of 52.4 months. The tests were conducted at nine daycare centers.
Children were shown photographs of 15 actors (5 men and 10 women) with and without surgical face masks. The total data set included 90 pictures illustrating joy, anger, and sadness. The children were shown the pictures at random, and they could either name the emotion, point to a card with emoticons showing the three emotions, or respond “I don’t know” or “quit the experiment.” Test sessions lasted approximately 7 minutes per child. Effect sizes were calculated using X2 and Cramer V tests.
Overall, 68.8% of the children correctly identified the emotion portrayed; the correct response rate was 70.6% for faces without face masks and 66.9% for those with face masks. Correct recognition of joy was significantly higher for faces without masks than for those with masks (94.8% vs. 87.3), as was correct recognition of sadness (54.1% vs. 48.9%; P < .001 for both). Recognition of anger was not significantly different for unmasked and masked faces (62.2% vs. 64.6%, P = .10).
No significant differences in correct responses appeared between boys and girls and the rate of correct responses increased significantly with age. The rates of “I don’t know,” and “quit the experiment” responses were 3.1% and 2.2%, respectively. In an analysis of incorrect responses, approximately 25% of the children confused anger and sadness, and 21% misidentified joy for images of anger or sadness.
“Overall, participants in this study, who had been exposed to face masks for nearly a year, recognized emotions on pictures better than has been reported in previous research, even with face masks,” the researchers wrote.
The study findings were limited by several factors including the use of static pictures versus real individuals, which limits generalizability, and the lack of data on children with developmental issues, the researchers noted.
Despite relatively small differences and weak effect size (Cramer V scores of 0.2 or less for all), the results show a stronger recognition of emotion, compared with other studies, and highlight the importance of investigating the impact of face masks on other aspects of child development as the COVID-19 pandemic persists, the researchers concluded.
The study received no outside funding. The researchers had no relevant financial conflicts to disclose.
FROM JAMA PEDIATRICS
What is the diagnosis?
Numerous morphologies of skin rashes have been described in the setting of COVID-19, including pernio, livedoid rash, exanthem, and vasculitis. This classic constellation of symptoms (palpable purpura on buttocks/legs, abdominal pain, arthralgia, hematuria) is highly consistent with Henoch-Schonlein purpura (HSP). There are now multiple case reports of COVID-19–associated HSP.
HSP is the most common type of childhood systemic vasculitis. It is mediated by immunoglobulin A (IgA) immune complex deposition and has been associated with respiratory tract infections, streptococcal species, parainfluenza virus, and human parvovirus B19, medications, vaccinations, and malignancies. HSP is usually a self-limiting disease, with a course over 4-6 weeks, and can affect multiple organs, including the skin, gastrointestinal tract, joints, and the kidneys. The diagnostic criteria include palpable purpura in the presence of one or more of the following: diffuse abdominal pain, arthritis or arthralgia, any biopsy showing predominant IgA deposition, and renal involvement in the form of hematuria or proteinuria. Renal disease is variable and is the most significant indicator of long-term prognosis. This teenager was treated with oral corticosteroids because of the severe periarticular edema and responded rapidly. His subsequent urine analyses normalized.
What is on the differential?
Multisystem inflammatory syndrome in children (MIS-C) is a rare, potentially fatal, complication of COVID-19 infection that causes inflammation of multiple organs, including the heart, lungs, kidneys, brain, skin, eyes, or the gastrointestinal tract. It commonly affects children around ages 8-9 years. Initial symptoms include fever, rash, red eyes, diarrhea, and vomiting that appear 2-6 weeks post COVID-19 infection. Like HSP, MIS-C can present with edema of the extremities, worsening hand/foot pain, and hematuria; however, the absence of both fever and the pattern of system involvement seen with MIS-C and classic findings in this patient are more consistent with HSP.
Reactive infectious mucocutaneous eruption (RIME) was recently coined to encompass both infection-associated Stevens-Johnson eruptions including Mycoplasma pneumoniae-induced rash and mucositis (MIRM) and mucocutaneous eruptions caused by nonmycoplasma pathogens (including Chlamydia pneumoniae, human parainfluenza virus 2, rhinovirus, adenovirus, enterovirus, human metapneumovirus, influenza B virus, and COVID-19). It is usually seen in male children and adolescents. Prodromal symptoms include cough, fever, and malaise and they precede the prominent feature of mucositis. Our patient’s lack of mucosal involvement is not consistent with RIME.
Perniosis (chilblains) is characterized by localized edematous patches of erythema or cyanosis on exposed extremities, that may be associated with cold exposure. Lesions are usually symmetric and self-limiting, and symptoms can include numbness, tingling, pruritus, burning, or pain. Pernio-like skin lesions have been seen during the COVID-19 pandemic, though many patients have negative testing for infection by PCR and serology. Pernio may also be seen with autoimmune diseases or malignancy.
Meningococcemia is a rare disease caused by infection with gram-negative diplococci bacteria Neisseria meningitidis and spreads through saliva or respiratory secretions. Its clinical presentation can vary widely, from transient fever to fulminant disease. It is characterized by upper respiratory tract infection, fever, and petechial lesions associated with thrombocytopenia and coagulopathy.
Dr. Eichenfield is vice chair of the department of dermatology and professor of dermatology and pediatrics at the University of California, San Diego, and Rady Children’s Hospital, San Diego. Ms. Laborada is a pediatric dermatology research associate in the division of pediatric and adolescent dermatology at the University of California, San Diego, and Rady Children’s Hospital. Dr. Eichenfield and Ms. Laborada have no relevant financial disclosures.
References
AlGhoozi DA, AlKhayyat HM. BMJ Case Reports CP 2021;14:e239910.
Jacobi M et al. Pediatr Infect Dis J. 2021;40(2):e93-4.
Paller A, Mancini AJ. Hurwitz clinical pediatric dermatology: A textbook of skin disorders of childhood and adolescence. 4th ed. Philadelphia (PA): Elsevier Saunders; 2011.
Radia T et al. Paediatr Respir Rev. 2021;38:51-7.
Ramien ML. Clin Exp Dermatol. 2021;46(3):420-9.
Numerous morphologies of skin rashes have been described in the setting of COVID-19, including pernio, livedoid rash, exanthem, and vasculitis. This classic constellation of symptoms (palpable purpura on buttocks/legs, abdominal pain, arthralgia, hematuria) is highly consistent with Henoch-Schonlein purpura (HSP). There are now multiple case reports of COVID-19–associated HSP.
HSP is the most common type of childhood systemic vasculitis. It is mediated by immunoglobulin A (IgA) immune complex deposition and has been associated with respiratory tract infections, streptococcal species, parainfluenza virus, and human parvovirus B19, medications, vaccinations, and malignancies. HSP is usually a self-limiting disease, with a course over 4-6 weeks, and can affect multiple organs, including the skin, gastrointestinal tract, joints, and the kidneys. The diagnostic criteria include palpable purpura in the presence of one or more of the following: diffuse abdominal pain, arthritis or arthralgia, any biopsy showing predominant IgA deposition, and renal involvement in the form of hematuria or proteinuria. Renal disease is variable and is the most significant indicator of long-term prognosis. This teenager was treated with oral corticosteroids because of the severe periarticular edema and responded rapidly. His subsequent urine analyses normalized.
What is on the differential?
Multisystem inflammatory syndrome in children (MIS-C) is a rare, potentially fatal, complication of COVID-19 infection that causes inflammation of multiple organs, including the heart, lungs, kidneys, brain, skin, eyes, or the gastrointestinal tract. It commonly affects children around ages 8-9 years. Initial symptoms include fever, rash, red eyes, diarrhea, and vomiting that appear 2-6 weeks post COVID-19 infection. Like HSP, MIS-C can present with edema of the extremities, worsening hand/foot pain, and hematuria; however, the absence of both fever and the pattern of system involvement seen with MIS-C and classic findings in this patient are more consistent with HSP.
Reactive infectious mucocutaneous eruption (RIME) was recently coined to encompass both infection-associated Stevens-Johnson eruptions including Mycoplasma pneumoniae-induced rash and mucositis (MIRM) and mucocutaneous eruptions caused by nonmycoplasma pathogens (including Chlamydia pneumoniae, human parainfluenza virus 2, rhinovirus, adenovirus, enterovirus, human metapneumovirus, influenza B virus, and COVID-19). It is usually seen in male children and adolescents. Prodromal symptoms include cough, fever, and malaise and they precede the prominent feature of mucositis. Our patient’s lack of mucosal involvement is not consistent with RIME.
Perniosis (chilblains) is characterized by localized edematous patches of erythema or cyanosis on exposed extremities, that may be associated with cold exposure. Lesions are usually symmetric and self-limiting, and symptoms can include numbness, tingling, pruritus, burning, or pain. Pernio-like skin lesions have been seen during the COVID-19 pandemic, though many patients have negative testing for infection by PCR and serology. Pernio may also be seen with autoimmune diseases or malignancy.
Meningococcemia is a rare disease caused by infection with gram-negative diplococci bacteria Neisseria meningitidis and spreads through saliva or respiratory secretions. Its clinical presentation can vary widely, from transient fever to fulminant disease. It is characterized by upper respiratory tract infection, fever, and petechial lesions associated with thrombocytopenia and coagulopathy.
Dr. Eichenfield is vice chair of the department of dermatology and professor of dermatology and pediatrics at the University of California, San Diego, and Rady Children’s Hospital, San Diego. Ms. Laborada is a pediatric dermatology research associate in the division of pediatric and adolescent dermatology at the University of California, San Diego, and Rady Children’s Hospital. Dr. Eichenfield and Ms. Laborada have no relevant financial disclosures.
References
AlGhoozi DA, AlKhayyat HM. BMJ Case Reports CP 2021;14:e239910.
Jacobi M et al. Pediatr Infect Dis J. 2021;40(2):e93-4.
Paller A, Mancini AJ. Hurwitz clinical pediatric dermatology: A textbook of skin disorders of childhood and adolescence. 4th ed. Philadelphia (PA): Elsevier Saunders; 2011.
Radia T et al. Paediatr Respir Rev. 2021;38:51-7.
Ramien ML. Clin Exp Dermatol. 2021;46(3):420-9.
Numerous morphologies of skin rashes have been described in the setting of COVID-19, including pernio, livedoid rash, exanthem, and vasculitis. This classic constellation of symptoms (palpable purpura on buttocks/legs, abdominal pain, arthralgia, hematuria) is highly consistent with Henoch-Schonlein purpura (HSP). There are now multiple case reports of COVID-19–associated HSP.
HSP is the most common type of childhood systemic vasculitis. It is mediated by immunoglobulin A (IgA) immune complex deposition and has been associated with respiratory tract infections, streptococcal species, parainfluenza virus, and human parvovirus B19, medications, vaccinations, and malignancies. HSP is usually a self-limiting disease, with a course over 4-6 weeks, and can affect multiple organs, including the skin, gastrointestinal tract, joints, and the kidneys. The diagnostic criteria include palpable purpura in the presence of one or more of the following: diffuse abdominal pain, arthritis or arthralgia, any biopsy showing predominant IgA deposition, and renal involvement in the form of hematuria or proteinuria. Renal disease is variable and is the most significant indicator of long-term prognosis. This teenager was treated with oral corticosteroids because of the severe periarticular edema and responded rapidly. His subsequent urine analyses normalized.
What is on the differential?
Multisystem inflammatory syndrome in children (MIS-C) is a rare, potentially fatal, complication of COVID-19 infection that causes inflammation of multiple organs, including the heart, lungs, kidneys, brain, skin, eyes, or the gastrointestinal tract. It commonly affects children around ages 8-9 years. Initial symptoms include fever, rash, red eyes, diarrhea, and vomiting that appear 2-6 weeks post COVID-19 infection. Like HSP, MIS-C can present with edema of the extremities, worsening hand/foot pain, and hematuria; however, the absence of both fever and the pattern of system involvement seen with MIS-C and classic findings in this patient are more consistent with HSP.
Reactive infectious mucocutaneous eruption (RIME) was recently coined to encompass both infection-associated Stevens-Johnson eruptions including Mycoplasma pneumoniae-induced rash and mucositis (MIRM) and mucocutaneous eruptions caused by nonmycoplasma pathogens (including Chlamydia pneumoniae, human parainfluenza virus 2, rhinovirus, adenovirus, enterovirus, human metapneumovirus, influenza B virus, and COVID-19). It is usually seen in male children and adolescents. Prodromal symptoms include cough, fever, and malaise and they precede the prominent feature of mucositis. Our patient’s lack of mucosal involvement is not consistent with RIME.
Perniosis (chilblains) is characterized by localized edematous patches of erythema or cyanosis on exposed extremities, that may be associated with cold exposure. Lesions are usually symmetric and self-limiting, and symptoms can include numbness, tingling, pruritus, burning, or pain. Pernio-like skin lesions have been seen during the COVID-19 pandemic, though many patients have negative testing for infection by PCR and serology. Pernio may also be seen with autoimmune diseases or malignancy.
Meningococcemia is a rare disease caused by infection with gram-negative diplococci bacteria Neisseria meningitidis and spreads through saliva or respiratory secretions. Its clinical presentation can vary widely, from transient fever to fulminant disease. It is characterized by upper respiratory tract infection, fever, and petechial lesions associated with thrombocytopenia and coagulopathy.
Dr. Eichenfield is vice chair of the department of dermatology and professor of dermatology and pediatrics at the University of California, San Diego, and Rady Children’s Hospital, San Diego. Ms. Laborada is a pediatric dermatology research associate in the division of pediatric and adolescent dermatology at the University of California, San Diego, and Rady Children’s Hospital. Dr. Eichenfield and Ms. Laborada have no relevant financial disclosures.
References
AlGhoozi DA, AlKhayyat HM. BMJ Case Reports CP 2021;14:e239910.
Jacobi M et al. Pediatr Infect Dis J. 2021;40(2):e93-4.
Paller A, Mancini AJ. Hurwitz clinical pediatric dermatology: A textbook of skin disorders of childhood and adolescence. 4th ed. Philadelphia (PA): Elsevier Saunders; 2011.
Radia T et al. Paediatr Respir Rev. 2021;38:51-7.
Ramien ML. Clin Exp Dermatol. 2021;46(3):420-9.
Step right up, folks, for a public dissection
The greatest autopsy on Earth?
The LOTME staff would like to apologize in advance. The following item contains historical facts.
P.T. Barnum is a rather controversial figure in American history. The greatest show on Earth was certainly popular in its day. However, Barnum got his start in 1835 by leasing a slave named Joyce Heth, an elderly Black woman who told vivid stories of caring for a young George Washington. He toured her around the country, advertising her as a 160-year-old woman who served as George Washington’s nanny. When Ms. Heth died the next year, Barnum sold tickets to the autopsy, charging the equivalent of $30 in today’s money.
When a doctor announced that Ms. Heth was actually 75-80 when she died, it caused great controversy in the press and ruined Barnum’s career. Wait, no, that’s not right. The opposite, actually. He weathered the storm, built his famous circus, and never again committed a hoax.
It’s difficult to quantify how wrong publicly dissecting a person and charging people to see said dissection is, but that was almost 200 years ago. At the very least, we can say that such terrible behavior is firmly in the distant past.
Oh wait.
David Saunders, a 98-year-old veteran of World War II and the Korean War, donated his body to science. His body, however, was purchased by DeathScience.org from a medical lab – with the buyer supposedly misleading the medical lab about its intentions, which was for use at the traveling Oddities and Curiosities Expo. Tickets went for up to $500 each to witness the public autopsy of Mr. Saunders’ body, which took place at a Marriott in Portland, Ore. It promised to be an exciting, all-day event from 9 a.m. to 4 p.m., with a break for lunch, of course. You can’t have an autopsy without a catered lunch.
Another public autopsy event was scheduled in Seattle but canceled after news of the first event broke. Oh, and for that extra little kick, Mr. Saunders died from COVID-19, meaning that all those paying customers were exposed.
P.T. Barnum is probably rolling over in his grave right now. His autopsy tickets were a bargain.
Go ahead, have that soda before math
We should all know by now that sugary drinks are bad, even artificially sweetened ones. It might not always stop us from drinking them, but we know the deal. But what if sugary drinks like soda could be helpful for girls in school?
You read that right. We said girls. A soda before class might have boys bouncing off the walls, but not girls. A recent study showed that not only was girls’ behavior unaffected by having a sugary drink, their math skills even improved.
Researchers analyzed the behavior of 4- to 6-year-old children before and after having a sugary drink. The sugar rush was actually calming for girls and helped them perform better with numerical skills, but the opposite was true for boys. “Our study is the first to provide large-scale experimental evidence on the impact of sugary drinks on preschool children. The results clearly indicate a causal impact of sugary drinks on children’s behavior and test scores,” Fritz Schiltz, PhD, said in a written statement.
This probably isn’t the green light to have as many sugary drinks as you want, but it might be interesting to see how your work is affected after a soda.
Chicken nuggets and the meat paradox
Two young children are fighting over the last chicken nugget when an adult comes in to see what’s going on.
Liam: Vegetable!
Olivia: Meat!
Liam: Chicken nuggets are vegetables!
Olivia: No, dorkface! They’re meat.
Caregiver: Good news, kids. You’re both right.
Olivia: How can we both be right?
At this point, a woman enters the room. She’s wearing a white lab coat, so she must be a scientist.
Dr. Scientist: You can’t both be right, Olivia. You are being fed a serving of the meat paradox. That’s why Liam here doesn’t know that chicken nuggets are made of chicken, which is a form of meat. Sadly, he’s not the only one.
In a recent study, scientists from Furman University in Greenville, S.C., found that 38% of 176 children aged 4-7 years thought that chicken nuggets were vegetables and more than 46% identified French fries as animal based.
Olivia: Did our caregiver lie to us, Dr. Scientist?
Dr. Scientist: Yes, Olivia. The researchers I mentioned explained that “many people experience unease while eating meat. Omnivores eat foods that entail animal suffering and death while at the same time endorsing the compassionate treatment of animals.” That’s the meat paradox.
Liam: What else did they say, Dr. Scientist?
Dr. Scientist: Over 70% of those children said that cows and pigs were not edible and 5% thought that cats and horses were. The investigators wrote “that children and youth should be viewed as agents of environmental change” in the future, but suggested that parents need to bring honesty to the table.
Caregiver: How did you get in here anyway? And how do you know their names?
Dr. Scientist: I’ve been rooting through your garbage for years. All in the name of science, of course.
Bedtimes aren’t just for children
There are multiple ways to prevent heart disease, but what if it could be as easy as switching your bedtime? A recent study in European Heart Journal–Digital Health suggests that there’s a sweet spot when it comes to sleep timing.
Through smartwatch-like devices, researchers measured the sleep-onset and wake-up times for 7 days in 88,026 participants aged 43-79 years. After 5.7 years of follow-up to see if anyone had a heart attack, stroke, or any other cardiovascular event, 3.6% developed some kind of cardiovascular disease.
Those who went to bed between 10 p.m. and 11 p.m. had a lower risk of developing heart disease. The risk was 25% higher for subjects who went to bed at midnight or later, 24% higher for bedtimes before 10 p.m., and 12% higher for bedtimes between 11 p.m. and midnight.
So, why can you go to bed before “The Tonight Show” and lower your cardiovascular risk but not before the nightly news? Well, it has something to do with your body’s natural clock.
“The optimum time to go to sleep is at a specific point in the body’s 24-hour cycle and deviations may be detrimental to health. The riskiest time was after midnight, potentially because it may reduce the likelihood of seeing morning light, which resets the body clock,” said study author Dr. David Plans of the University of Exeter, England.
Although a sleep schedule is preferred, it isn’t realistic all the time for those in certain occupations who might have to resort to other methods to keep their circadian clocks ticking optimally for their health. But if all it takes is prescribing a sleep time to reduce heart disease on a massive scale it would make a great “low-cost public health target.”
So bedtimes aren’t just for children.
The greatest autopsy on Earth?
The LOTME staff would like to apologize in advance. The following item contains historical facts.
P.T. Barnum is a rather controversial figure in American history. The greatest show on Earth was certainly popular in its day. However, Barnum got his start in 1835 by leasing a slave named Joyce Heth, an elderly Black woman who told vivid stories of caring for a young George Washington. He toured her around the country, advertising her as a 160-year-old woman who served as George Washington’s nanny. When Ms. Heth died the next year, Barnum sold tickets to the autopsy, charging the equivalent of $30 in today’s money.
When a doctor announced that Ms. Heth was actually 75-80 when she died, it caused great controversy in the press and ruined Barnum’s career. Wait, no, that’s not right. The opposite, actually. He weathered the storm, built his famous circus, and never again committed a hoax.
It’s difficult to quantify how wrong publicly dissecting a person and charging people to see said dissection is, but that was almost 200 years ago. At the very least, we can say that such terrible behavior is firmly in the distant past.
Oh wait.
David Saunders, a 98-year-old veteran of World War II and the Korean War, donated his body to science. His body, however, was purchased by DeathScience.org from a medical lab – with the buyer supposedly misleading the medical lab about its intentions, which was for use at the traveling Oddities and Curiosities Expo. Tickets went for up to $500 each to witness the public autopsy of Mr. Saunders’ body, which took place at a Marriott in Portland, Ore. It promised to be an exciting, all-day event from 9 a.m. to 4 p.m., with a break for lunch, of course. You can’t have an autopsy without a catered lunch.
Another public autopsy event was scheduled in Seattle but canceled after news of the first event broke. Oh, and for that extra little kick, Mr. Saunders died from COVID-19, meaning that all those paying customers were exposed.
P.T. Barnum is probably rolling over in his grave right now. His autopsy tickets were a bargain.
Go ahead, have that soda before math
We should all know by now that sugary drinks are bad, even artificially sweetened ones. It might not always stop us from drinking them, but we know the deal. But what if sugary drinks like soda could be helpful for girls in school?
You read that right. We said girls. A soda before class might have boys bouncing off the walls, but not girls. A recent study showed that not only was girls’ behavior unaffected by having a sugary drink, their math skills even improved.
Researchers analyzed the behavior of 4- to 6-year-old children before and after having a sugary drink. The sugar rush was actually calming for girls and helped them perform better with numerical skills, but the opposite was true for boys. “Our study is the first to provide large-scale experimental evidence on the impact of sugary drinks on preschool children. The results clearly indicate a causal impact of sugary drinks on children’s behavior and test scores,” Fritz Schiltz, PhD, said in a written statement.
This probably isn’t the green light to have as many sugary drinks as you want, but it might be interesting to see how your work is affected after a soda.
Chicken nuggets and the meat paradox
Two young children are fighting over the last chicken nugget when an adult comes in to see what’s going on.
Liam: Vegetable!
Olivia: Meat!
Liam: Chicken nuggets are vegetables!
Olivia: No, dorkface! They’re meat.
Caregiver: Good news, kids. You’re both right.
Olivia: How can we both be right?
At this point, a woman enters the room. She’s wearing a white lab coat, so she must be a scientist.
Dr. Scientist: You can’t both be right, Olivia. You are being fed a serving of the meat paradox. That’s why Liam here doesn’t know that chicken nuggets are made of chicken, which is a form of meat. Sadly, he’s not the only one.
In a recent study, scientists from Furman University in Greenville, S.C., found that 38% of 176 children aged 4-7 years thought that chicken nuggets were vegetables and more than 46% identified French fries as animal based.
Olivia: Did our caregiver lie to us, Dr. Scientist?
Dr. Scientist: Yes, Olivia. The researchers I mentioned explained that “many people experience unease while eating meat. Omnivores eat foods that entail animal suffering and death while at the same time endorsing the compassionate treatment of animals.” That’s the meat paradox.
Liam: What else did they say, Dr. Scientist?
Dr. Scientist: Over 70% of those children said that cows and pigs were not edible and 5% thought that cats and horses were. The investigators wrote “that children and youth should be viewed as agents of environmental change” in the future, but suggested that parents need to bring honesty to the table.
Caregiver: How did you get in here anyway? And how do you know their names?
Dr. Scientist: I’ve been rooting through your garbage for years. All in the name of science, of course.
Bedtimes aren’t just for children
There are multiple ways to prevent heart disease, but what if it could be as easy as switching your bedtime? A recent study in European Heart Journal–Digital Health suggests that there’s a sweet spot when it comes to sleep timing.
Through smartwatch-like devices, researchers measured the sleep-onset and wake-up times for 7 days in 88,026 participants aged 43-79 years. After 5.7 years of follow-up to see if anyone had a heart attack, stroke, or any other cardiovascular event, 3.6% developed some kind of cardiovascular disease.
Those who went to bed between 10 p.m. and 11 p.m. had a lower risk of developing heart disease. The risk was 25% higher for subjects who went to bed at midnight or later, 24% higher for bedtimes before 10 p.m., and 12% higher for bedtimes between 11 p.m. and midnight.
So, why can you go to bed before “The Tonight Show” and lower your cardiovascular risk but not before the nightly news? Well, it has something to do with your body’s natural clock.
“The optimum time to go to sleep is at a specific point in the body’s 24-hour cycle and deviations may be detrimental to health. The riskiest time was after midnight, potentially because it may reduce the likelihood of seeing morning light, which resets the body clock,” said study author Dr. David Plans of the University of Exeter, England.
Although a sleep schedule is preferred, it isn’t realistic all the time for those in certain occupations who might have to resort to other methods to keep their circadian clocks ticking optimally for their health. But if all it takes is prescribing a sleep time to reduce heart disease on a massive scale it would make a great “low-cost public health target.”
So bedtimes aren’t just for children.
The greatest autopsy on Earth?
The LOTME staff would like to apologize in advance. The following item contains historical facts.
P.T. Barnum is a rather controversial figure in American history. The greatest show on Earth was certainly popular in its day. However, Barnum got his start in 1835 by leasing a slave named Joyce Heth, an elderly Black woman who told vivid stories of caring for a young George Washington. He toured her around the country, advertising her as a 160-year-old woman who served as George Washington’s nanny. When Ms. Heth died the next year, Barnum sold tickets to the autopsy, charging the equivalent of $30 in today’s money.
When a doctor announced that Ms. Heth was actually 75-80 when she died, it caused great controversy in the press and ruined Barnum’s career. Wait, no, that’s not right. The opposite, actually. He weathered the storm, built his famous circus, and never again committed a hoax.
It’s difficult to quantify how wrong publicly dissecting a person and charging people to see said dissection is, but that was almost 200 years ago. At the very least, we can say that such terrible behavior is firmly in the distant past.
Oh wait.
David Saunders, a 98-year-old veteran of World War II and the Korean War, donated his body to science. His body, however, was purchased by DeathScience.org from a medical lab – with the buyer supposedly misleading the medical lab about its intentions, which was for use at the traveling Oddities and Curiosities Expo. Tickets went for up to $500 each to witness the public autopsy of Mr. Saunders’ body, which took place at a Marriott in Portland, Ore. It promised to be an exciting, all-day event from 9 a.m. to 4 p.m., with a break for lunch, of course. You can’t have an autopsy without a catered lunch.
Another public autopsy event was scheduled in Seattle but canceled after news of the first event broke. Oh, and for that extra little kick, Mr. Saunders died from COVID-19, meaning that all those paying customers were exposed.
P.T. Barnum is probably rolling over in his grave right now. His autopsy tickets were a bargain.
Go ahead, have that soda before math
We should all know by now that sugary drinks are bad, even artificially sweetened ones. It might not always stop us from drinking them, but we know the deal. But what if sugary drinks like soda could be helpful for girls in school?
You read that right. We said girls. A soda before class might have boys bouncing off the walls, but not girls. A recent study showed that not only was girls’ behavior unaffected by having a sugary drink, their math skills even improved.
Researchers analyzed the behavior of 4- to 6-year-old children before and after having a sugary drink. The sugar rush was actually calming for girls and helped them perform better with numerical skills, but the opposite was true for boys. “Our study is the first to provide large-scale experimental evidence on the impact of sugary drinks on preschool children. The results clearly indicate a causal impact of sugary drinks on children’s behavior and test scores,” Fritz Schiltz, PhD, said in a written statement.
This probably isn’t the green light to have as many sugary drinks as you want, but it might be interesting to see how your work is affected after a soda.
Chicken nuggets and the meat paradox
Two young children are fighting over the last chicken nugget when an adult comes in to see what’s going on.
Liam: Vegetable!
Olivia: Meat!
Liam: Chicken nuggets are vegetables!
Olivia: No, dorkface! They’re meat.
Caregiver: Good news, kids. You’re both right.
Olivia: How can we both be right?
At this point, a woman enters the room. She’s wearing a white lab coat, so she must be a scientist.
Dr. Scientist: You can’t both be right, Olivia. You are being fed a serving of the meat paradox. That’s why Liam here doesn’t know that chicken nuggets are made of chicken, which is a form of meat. Sadly, he’s not the only one.
In a recent study, scientists from Furman University in Greenville, S.C., found that 38% of 176 children aged 4-7 years thought that chicken nuggets were vegetables and more than 46% identified French fries as animal based.
Olivia: Did our caregiver lie to us, Dr. Scientist?
Dr. Scientist: Yes, Olivia. The researchers I mentioned explained that “many people experience unease while eating meat. Omnivores eat foods that entail animal suffering and death while at the same time endorsing the compassionate treatment of animals.” That’s the meat paradox.
Liam: What else did they say, Dr. Scientist?
Dr. Scientist: Over 70% of those children said that cows and pigs were not edible and 5% thought that cats and horses were. The investigators wrote “that children and youth should be viewed as agents of environmental change” in the future, but suggested that parents need to bring honesty to the table.
Caregiver: How did you get in here anyway? And how do you know their names?
Dr. Scientist: I’ve been rooting through your garbage for years. All in the name of science, of course.
Bedtimes aren’t just for children
There are multiple ways to prevent heart disease, but what if it could be as easy as switching your bedtime? A recent study in European Heart Journal–Digital Health suggests that there’s a sweet spot when it comes to sleep timing.
Through smartwatch-like devices, researchers measured the sleep-onset and wake-up times for 7 days in 88,026 participants aged 43-79 years. After 5.7 years of follow-up to see if anyone had a heart attack, stroke, or any other cardiovascular event, 3.6% developed some kind of cardiovascular disease.
Those who went to bed between 10 p.m. and 11 p.m. had a lower risk of developing heart disease. The risk was 25% higher for subjects who went to bed at midnight or later, 24% higher for bedtimes before 10 p.m., and 12% higher for bedtimes between 11 p.m. and midnight.
So, why can you go to bed before “The Tonight Show” and lower your cardiovascular risk but not before the nightly news? Well, it has something to do with your body’s natural clock.
“The optimum time to go to sleep is at a specific point in the body’s 24-hour cycle and deviations may be detrimental to health. The riskiest time was after midnight, potentially because it may reduce the likelihood of seeing morning light, which resets the body clock,” said study author Dr. David Plans of the University of Exeter, England.
Although a sleep schedule is preferred, it isn’t realistic all the time for those in certain occupations who might have to resort to other methods to keep their circadian clocks ticking optimally for their health. But if all it takes is prescribing a sleep time to reduce heart disease on a massive scale it would make a great “low-cost public health target.”
So bedtimes aren’t just for children.
Enriched infant formula offers no academic benefit later: Study
Infants who are given nutrient- or supplement-enriched formula milk do not later have higher academic scores as adolescents than those fed with standard formula, a study published online in the BMJ suggests.
One goal of modifying infant formula has been to make long-term cognitive outcomes similar to those for breast-fed infants, the authors noted. Rates for breastfeeding beyond 6 weeks are low in many parts of the world and more than 60% of babies worldwide under the age of 6 months are given formula to replace or supplement breast milk, the paper states.
So far, research has been inconclusive on benefits, though enhancements continue to be added and claims have been made as to their benefits on cognition in advertising. Long-term trials are difficult as researchers move on and participants are lost to follow-up.
In a new study, however, researchers led by Maximiliane L. Verfürden, MsC, with the University College of London’s Great Ormond Street Institute of Child Health, linked data from seven dormant, randomized, controlled infant formula trials to participants’ performance later as adolescents in the United Kingdom on mandatory national school math and English exams at ages 11 and 16 and found no difference in scores.
They followed 1,763 adolescents who had been participants in the formula trials, which were conducted between 1993 and 2001, and were able to link 91.2% (1,607) to academic records.
They found “no benefit of the infant formula modifications on cognitive outcomes.”
Three types of formula studied
In this study, the researchers discuss three widely available types of modified infant formulas that have been promoted as benefiting cognitive development: formula enriched with nutrients; formula supplemented with long-chain polyunsaturated fatty acids (LCPUFAs); and follow-on formula fortified with iron.
In one supplement group the academic results were worse than for those given standard formula. At age 11, children who had been given the LCPUFA-enhanced formula scored lower in both English and math.
“Given the potential associations between the source of LCPUFAs and adverse cognitive outcomes, long-term follow-up of trials testing infant formulas from other sources of LCPUFAs is recommended,” the authors wrote.
Nutrients can harm, editorialist says
Charlotte Wright, BM BCH, MSc, a pediatrician and epidemiologist with the Glasgow Royal Hospital for Children in Glasgow, who was not part of the study, coauthored an editorial that accompanied the article in the BMJ.
Dr. Wright and nutritionist Ada L. Gargia, PhD, at the University of Glasgow, wrote that nutrients in some formula enhancements can harm and that infant milk trials often have been poorly conducted.
The editorialists point to a large systematic review of formula milk trials published this year in the BMJ by Helfer et al. that found that most were funded by industry.
“Helfer and colleagues’ review found that 80% of studies were at high risk of bias, mainly because of selective reporting, with 92% of abstracts mentioning positive findings, despite only 42% of trials finding statistically significant differences in a stated primary outcome,” they wrote.
Dr. Wright, who runs a specialist feeding clinic for children, said in an interview that the study is valuable in that it has follow-up “to an age when adult cognition can be robustly assessed.”
She noted that the authors say additives that have been shown to be harmful are still routinely added.
“There is now evidence that adding LCPUFAs results in lower cognition and that giving extra iron to healthy children increases their risk of infection and may even slow their growth,” she said.
But advertisements to the contrary are quickly found in an Internet search, she said, even if no specific claims are made for them.
She gave an example of an advertisement for a commonly used enhanced formula, which reads: “Our formulation contains our highest levels of DHA (Omega 3 LCPs) and is enriched with iron to support normal cognitive development.”
The formula studies were done more than 20 years ago, but Dr. Wright said that does not downplay their relevance.
The basic formulation of the formulas hasn’t changed much, she said, and the additives are still present.
This work was supported by the Economic and Social Research Council UCL, Bloomsbury and East London Doctoral Training Partnership and a Great Ormond Street Hospital Charity Research grant. Full disclosures for all authors are available with the full text of the paper. Dr. Wright and Dr. Garcia declared no relevant financial relationships.
Infants who are given nutrient- or supplement-enriched formula milk do not later have higher academic scores as adolescents than those fed with standard formula, a study published online in the BMJ suggests.
One goal of modifying infant formula has been to make long-term cognitive outcomes similar to those for breast-fed infants, the authors noted. Rates for breastfeeding beyond 6 weeks are low in many parts of the world and more than 60% of babies worldwide under the age of 6 months are given formula to replace or supplement breast milk, the paper states.
So far, research has been inconclusive on benefits, though enhancements continue to be added and claims have been made as to their benefits on cognition in advertising. Long-term trials are difficult as researchers move on and participants are lost to follow-up.
In a new study, however, researchers led by Maximiliane L. Verfürden, MsC, with the University College of London’s Great Ormond Street Institute of Child Health, linked data from seven dormant, randomized, controlled infant formula trials to participants’ performance later as adolescents in the United Kingdom on mandatory national school math and English exams at ages 11 and 16 and found no difference in scores.
They followed 1,763 adolescents who had been participants in the formula trials, which were conducted between 1993 and 2001, and were able to link 91.2% (1,607) to academic records.
They found “no benefit of the infant formula modifications on cognitive outcomes.”
Three types of formula studied
In this study, the researchers discuss three widely available types of modified infant formulas that have been promoted as benefiting cognitive development: formula enriched with nutrients; formula supplemented with long-chain polyunsaturated fatty acids (LCPUFAs); and follow-on formula fortified with iron.
In one supplement group the academic results were worse than for those given standard formula. At age 11, children who had been given the LCPUFA-enhanced formula scored lower in both English and math.
“Given the potential associations between the source of LCPUFAs and adverse cognitive outcomes, long-term follow-up of trials testing infant formulas from other sources of LCPUFAs is recommended,” the authors wrote.
Nutrients can harm, editorialist says
Charlotte Wright, BM BCH, MSc, a pediatrician and epidemiologist with the Glasgow Royal Hospital for Children in Glasgow, who was not part of the study, coauthored an editorial that accompanied the article in the BMJ.
Dr. Wright and nutritionist Ada L. Gargia, PhD, at the University of Glasgow, wrote that nutrients in some formula enhancements can harm and that infant milk trials often have been poorly conducted.
The editorialists point to a large systematic review of formula milk trials published this year in the BMJ by Helfer et al. that found that most were funded by industry.
“Helfer and colleagues’ review found that 80% of studies were at high risk of bias, mainly because of selective reporting, with 92% of abstracts mentioning positive findings, despite only 42% of trials finding statistically significant differences in a stated primary outcome,” they wrote.
Dr. Wright, who runs a specialist feeding clinic for children, said in an interview that the study is valuable in that it has follow-up “to an age when adult cognition can be robustly assessed.”
She noted that the authors say additives that have been shown to be harmful are still routinely added.
“There is now evidence that adding LCPUFAs results in lower cognition and that giving extra iron to healthy children increases their risk of infection and may even slow their growth,” she said.
But advertisements to the contrary are quickly found in an Internet search, she said, even if no specific claims are made for them.
She gave an example of an advertisement for a commonly used enhanced formula, which reads: “Our formulation contains our highest levels of DHA (Omega 3 LCPs) and is enriched with iron to support normal cognitive development.”
The formula studies were done more than 20 years ago, but Dr. Wright said that does not downplay their relevance.
The basic formulation of the formulas hasn’t changed much, she said, and the additives are still present.
This work was supported by the Economic and Social Research Council UCL, Bloomsbury and East London Doctoral Training Partnership and a Great Ormond Street Hospital Charity Research grant. Full disclosures for all authors are available with the full text of the paper. Dr. Wright and Dr. Garcia declared no relevant financial relationships.
Infants who are given nutrient- or supplement-enriched formula milk do not later have higher academic scores as adolescents than those fed with standard formula, a study published online in the BMJ suggests.
One goal of modifying infant formula has been to make long-term cognitive outcomes similar to those for breast-fed infants, the authors noted. Rates for breastfeeding beyond 6 weeks are low in many parts of the world and more than 60% of babies worldwide under the age of 6 months are given formula to replace or supplement breast milk, the paper states.
So far, research has been inconclusive on benefits, though enhancements continue to be added and claims have been made as to their benefits on cognition in advertising. Long-term trials are difficult as researchers move on and participants are lost to follow-up.
In a new study, however, researchers led by Maximiliane L. Verfürden, MsC, with the University College of London’s Great Ormond Street Institute of Child Health, linked data from seven dormant, randomized, controlled infant formula trials to participants’ performance later as adolescents in the United Kingdom on mandatory national school math and English exams at ages 11 and 16 and found no difference in scores.
They followed 1,763 adolescents who had been participants in the formula trials, which were conducted between 1993 and 2001, and were able to link 91.2% (1,607) to academic records.
They found “no benefit of the infant formula modifications on cognitive outcomes.”
Three types of formula studied
In this study, the researchers discuss three widely available types of modified infant formulas that have been promoted as benefiting cognitive development: formula enriched with nutrients; formula supplemented with long-chain polyunsaturated fatty acids (LCPUFAs); and follow-on formula fortified with iron.
In one supplement group the academic results were worse than for those given standard formula. At age 11, children who had been given the LCPUFA-enhanced formula scored lower in both English and math.
“Given the potential associations between the source of LCPUFAs and adverse cognitive outcomes, long-term follow-up of trials testing infant formulas from other sources of LCPUFAs is recommended,” the authors wrote.
Nutrients can harm, editorialist says
Charlotte Wright, BM BCH, MSc, a pediatrician and epidemiologist with the Glasgow Royal Hospital for Children in Glasgow, who was not part of the study, coauthored an editorial that accompanied the article in the BMJ.
Dr. Wright and nutritionist Ada L. Gargia, PhD, at the University of Glasgow, wrote that nutrients in some formula enhancements can harm and that infant milk trials often have been poorly conducted.
The editorialists point to a large systematic review of formula milk trials published this year in the BMJ by Helfer et al. that found that most were funded by industry.
“Helfer and colleagues’ review found that 80% of studies were at high risk of bias, mainly because of selective reporting, with 92% of abstracts mentioning positive findings, despite only 42% of trials finding statistically significant differences in a stated primary outcome,” they wrote.
Dr. Wright, who runs a specialist feeding clinic for children, said in an interview that the study is valuable in that it has follow-up “to an age when adult cognition can be robustly assessed.”
She noted that the authors say additives that have been shown to be harmful are still routinely added.
“There is now evidence that adding LCPUFAs results in lower cognition and that giving extra iron to healthy children increases their risk of infection and may even slow their growth,” she said.
But advertisements to the contrary are quickly found in an Internet search, she said, even if no specific claims are made for them.
She gave an example of an advertisement for a commonly used enhanced formula, which reads: “Our formulation contains our highest levels of DHA (Omega 3 LCPs) and is enriched with iron to support normal cognitive development.”
The formula studies were done more than 20 years ago, but Dr. Wright said that does not downplay their relevance.
The basic formulation of the formulas hasn’t changed much, she said, and the additives are still present.
This work was supported by the Economic and Social Research Council UCL, Bloomsbury and East London Doctoral Training Partnership and a Great Ormond Street Hospital Charity Research grant. Full disclosures for all authors are available with the full text of the paper. Dr. Wright and Dr. Garcia declared no relevant financial relationships.
FROM THE BMJ