User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
Online support tool improves AD self-management
MONTREAL – for up to 1 year, according to two randomized controlled trials presented at the annual meeting of the International Society of Atopic Dermatitis.
The intervention, directed either at parents of children with AD or young adults with AD, “is very low cost, evidence based, easily accessible, and free from possible commercial bias,” said investigator Kim Thomas, MD, professor of applied dermatology research and codirector of the Centre of Evidence Based Dermatology, faculty of medicine & health sciences, University of Nottingham (England).
The main focus of the intervention, along with general education, is “getting control” of the condition with flare-control creams and “keeping control” with regular emollient use.
Efficacy of the intervention, available free online, was compared with “usual eczema care” in 340 parents of children with AD up to age 12 and 337 young patients with AD aged 13-25. Participants were randomized to the intervention plus usual care or usual care alone. The primary outcome was the Patient-Oriented Eczema Measure(POEM) at 24 weeks, with a further measurement at 52 weeks.
In the parent group, about half were women and 83% were White, and the median age of their children was 4 years. About 50% of parents had a university degree, making them “possibly better educated than we might want our target audience for this type of intervention,” Dr. Thomas commented. Most of the children had moderate AD.
In the young patient group, the mean age was 19 years, more than three-quarters were female, 83% were White, and most had moderate AD.
At 24 weeks, both intervention groups had improved POEM scores, compared with controls, with a mean difference of 1.5 points in the parent group (P = .002) and 1.7 points in the young patient group (P = .04). “A small difference, but statistically significant and sustained,” Dr. Thomas said, adding that this difference was sustained up to 52 weeks.
In terms of mechanism of action, a secondary outcome looked at the concept of enablement, “which again, seemed to be improved in the intervention group, which suggests it’s something to do with being able to understand and cope with their disease better,” she said. The tool is targeted to “people who wouldn’t normally get to a dermatologist and certainly wouldn’t get access to group interventions.”
An additional aim of the intervention was “to provide a single, consistent message received from every point of contact that people might engage with ... [from] community doctors, pharmacists, dermatologists, and importantly, eczema charities all signposting [the intervention] and sharing a consistent message.”
While the intervention is free and available to patients anywhere, Dr. Thomas emphasized that it is tailored to the U.K. health care system. “If people would like to get in touch and help work with us to maybe adapt it slightly to make it more suitable for your own health care systems, that’s something we’d be very happy to look at with you.”
Asked for comment, Natalie Cunningham, MD, panel moderator, was lukewarm about the tool. “It can be a supplement, but you can never replace the one-on-one patient–health care provider interaction,” she told this news organization. “That could be provided by a nondermatologist and supplemented by an online component,” said Dr. Cunningham, from the Izaak Walton Killam Hospital for Children in Halifax, N.S.
“First-line treatment for eczema, no matter what kind of eczema, is topical steroids, and that is something that requires a lot of education – and something you want to do one on one in person because everyone comes to it with a different experience, baggage, or understanding,” she said. “We need to figure out what the barrier is so that you can do the right education.”
In addition, with systemic AD therapies currently approved for children, parents and young patients need to be able to advocate for specialist care to access these medications, she noted.
Dr. Thomas and Dr. Cunningham reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
MONTREAL – for up to 1 year, according to two randomized controlled trials presented at the annual meeting of the International Society of Atopic Dermatitis.
The intervention, directed either at parents of children with AD or young adults with AD, “is very low cost, evidence based, easily accessible, and free from possible commercial bias,” said investigator Kim Thomas, MD, professor of applied dermatology research and codirector of the Centre of Evidence Based Dermatology, faculty of medicine & health sciences, University of Nottingham (England).
The main focus of the intervention, along with general education, is “getting control” of the condition with flare-control creams and “keeping control” with regular emollient use.
Efficacy of the intervention, available free online, was compared with “usual eczema care” in 340 parents of children with AD up to age 12 and 337 young patients with AD aged 13-25. Participants were randomized to the intervention plus usual care or usual care alone. The primary outcome was the Patient-Oriented Eczema Measure(POEM) at 24 weeks, with a further measurement at 52 weeks.
In the parent group, about half were women and 83% were White, and the median age of their children was 4 years. About 50% of parents had a university degree, making them “possibly better educated than we might want our target audience for this type of intervention,” Dr. Thomas commented. Most of the children had moderate AD.
In the young patient group, the mean age was 19 years, more than three-quarters were female, 83% were White, and most had moderate AD.
At 24 weeks, both intervention groups had improved POEM scores, compared with controls, with a mean difference of 1.5 points in the parent group (P = .002) and 1.7 points in the young patient group (P = .04). “A small difference, but statistically significant and sustained,” Dr. Thomas said, adding that this difference was sustained up to 52 weeks.
In terms of mechanism of action, a secondary outcome looked at the concept of enablement, “which again, seemed to be improved in the intervention group, which suggests it’s something to do with being able to understand and cope with their disease better,” she said. The tool is targeted to “people who wouldn’t normally get to a dermatologist and certainly wouldn’t get access to group interventions.”
An additional aim of the intervention was “to provide a single, consistent message received from every point of contact that people might engage with ... [from] community doctors, pharmacists, dermatologists, and importantly, eczema charities all signposting [the intervention] and sharing a consistent message.”
While the intervention is free and available to patients anywhere, Dr. Thomas emphasized that it is tailored to the U.K. health care system. “If people would like to get in touch and help work with us to maybe adapt it slightly to make it more suitable for your own health care systems, that’s something we’d be very happy to look at with you.”
Asked for comment, Natalie Cunningham, MD, panel moderator, was lukewarm about the tool. “It can be a supplement, but you can never replace the one-on-one patient–health care provider interaction,” she told this news organization. “That could be provided by a nondermatologist and supplemented by an online component,” said Dr. Cunningham, from the Izaak Walton Killam Hospital for Children in Halifax, N.S.
“First-line treatment for eczema, no matter what kind of eczema, is topical steroids, and that is something that requires a lot of education – and something you want to do one on one in person because everyone comes to it with a different experience, baggage, or understanding,” she said. “We need to figure out what the barrier is so that you can do the right education.”
In addition, with systemic AD therapies currently approved for children, parents and young patients need to be able to advocate for specialist care to access these medications, she noted.
Dr. Thomas and Dr. Cunningham reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
MONTREAL – for up to 1 year, according to two randomized controlled trials presented at the annual meeting of the International Society of Atopic Dermatitis.
The intervention, directed either at parents of children with AD or young adults with AD, “is very low cost, evidence based, easily accessible, and free from possible commercial bias,” said investigator Kim Thomas, MD, professor of applied dermatology research and codirector of the Centre of Evidence Based Dermatology, faculty of medicine & health sciences, University of Nottingham (England).
The main focus of the intervention, along with general education, is “getting control” of the condition with flare-control creams and “keeping control” with regular emollient use.
Efficacy of the intervention, available free online, was compared with “usual eczema care” in 340 parents of children with AD up to age 12 and 337 young patients with AD aged 13-25. Participants were randomized to the intervention plus usual care or usual care alone. The primary outcome was the Patient-Oriented Eczema Measure(POEM) at 24 weeks, with a further measurement at 52 weeks.
In the parent group, about half were women and 83% were White, and the median age of their children was 4 years. About 50% of parents had a university degree, making them “possibly better educated than we might want our target audience for this type of intervention,” Dr. Thomas commented. Most of the children had moderate AD.
In the young patient group, the mean age was 19 years, more than three-quarters were female, 83% were White, and most had moderate AD.
At 24 weeks, both intervention groups had improved POEM scores, compared with controls, with a mean difference of 1.5 points in the parent group (P = .002) and 1.7 points in the young patient group (P = .04). “A small difference, but statistically significant and sustained,” Dr. Thomas said, adding that this difference was sustained up to 52 weeks.
In terms of mechanism of action, a secondary outcome looked at the concept of enablement, “which again, seemed to be improved in the intervention group, which suggests it’s something to do with being able to understand and cope with their disease better,” she said. The tool is targeted to “people who wouldn’t normally get to a dermatologist and certainly wouldn’t get access to group interventions.”
An additional aim of the intervention was “to provide a single, consistent message received from every point of contact that people might engage with ... [from] community doctors, pharmacists, dermatologists, and importantly, eczema charities all signposting [the intervention] and sharing a consistent message.”
While the intervention is free and available to patients anywhere, Dr. Thomas emphasized that it is tailored to the U.K. health care system. “If people would like to get in touch and help work with us to maybe adapt it slightly to make it more suitable for your own health care systems, that’s something we’d be very happy to look at with you.”
Asked for comment, Natalie Cunningham, MD, panel moderator, was lukewarm about the tool. “It can be a supplement, but you can never replace the one-on-one patient–health care provider interaction,” she told this news organization. “That could be provided by a nondermatologist and supplemented by an online component,” said Dr. Cunningham, from the Izaak Walton Killam Hospital for Children in Halifax, N.S.
“First-line treatment for eczema, no matter what kind of eczema, is topical steroids, and that is something that requires a lot of education – and something you want to do one on one in person because everyone comes to it with a different experience, baggage, or understanding,” she said. “We need to figure out what the barrier is so that you can do the right education.”
In addition, with systemic AD therapies currently approved for children, parents and young patients need to be able to advocate for specialist care to access these medications, she noted.
Dr. Thomas and Dr. Cunningham reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
AT ISAD 2022
Metabolites may distinguish severe subtypes of PAH
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
FROM CHEST
Itchy Red-Brown Spots on a Child
The Diagnosis: Maculopapular Cutaneous Mastocytosis (Urticaria Pigmentosa)
A stroke test revealed urtication at the exact traumatized site (Figure). A skin biopsy performed 2 years prior by another physician in the same hospital had revealed mast cell infiltration of virtually the entire dermis. The diagnosis was then firmly established as maculopapular cutaneous mastocytosis (CM)(also known as urticaria pigmentosa) with both the pathology results and a confirmative stroke test, and no additional biopsy was attempted. Serum IgE and tryptase levels were within the reference range. General recommendations about the avoidance of trigger factors were given to the family, and a new-generation H1 blocker antihistaminic syrup was prescribed for flushing, itching, and urtication.
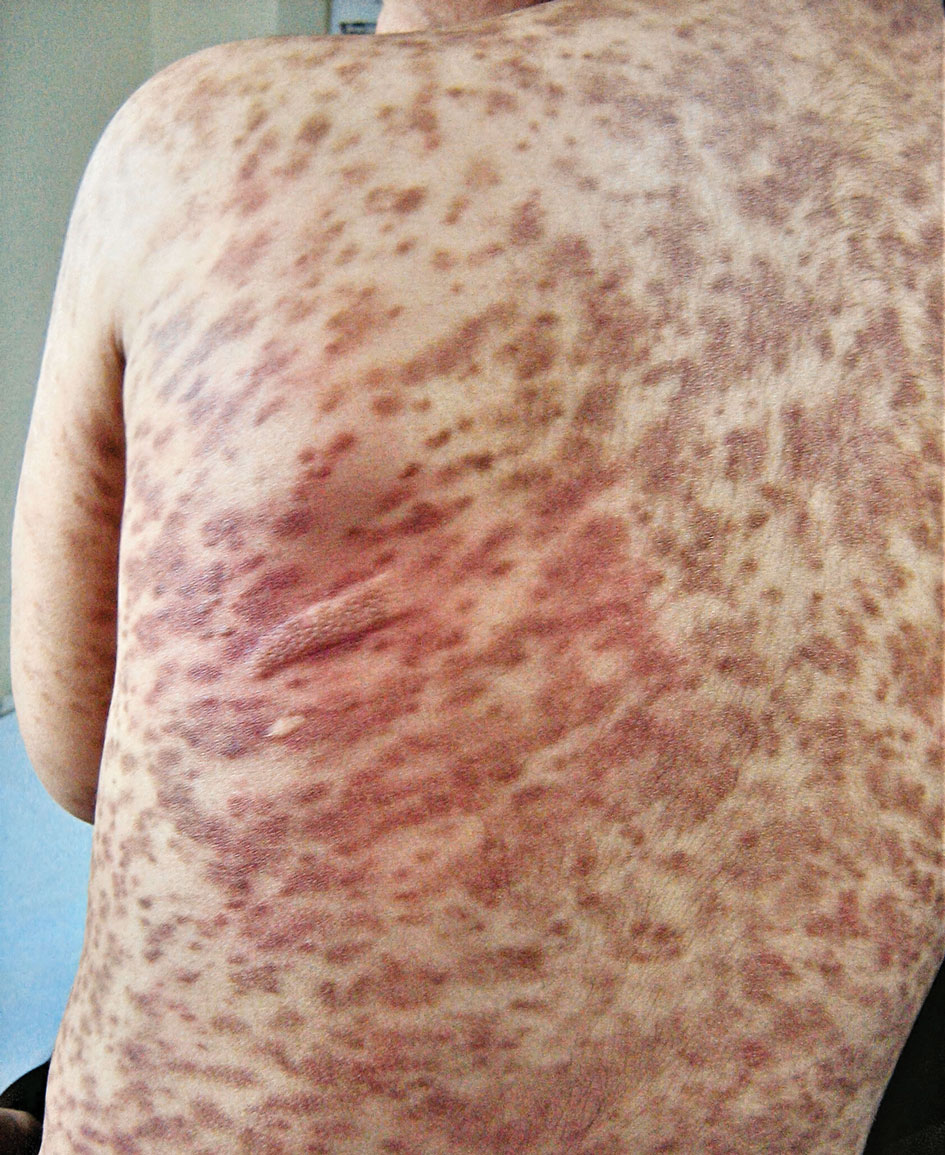
Mastocytosis is a canopy term for a heterogeneous group of disorders caused by clonal proliferation and accumulation of abnormal mast cells within the skin and visceral organs (ie, bone marrow, liver, spleen, lymph nodes, gastrointestinal tract). Cutaneous mastocytosis, the skin-restricted variant, is by far the most common form of childhood mastocytosis (90% of mastocytosis cases in children)1 and generally appears within the first 2 years of life.1-7 Pediatric CM usually is a benign and transient disease with an excellent prognosis and a negligible risk for systemic involvement.2,3,5
The pathogenesis of CM in children is obscure1; however, somatic or germline gain-of-function mutations of the c-KIT proto-oncogene, which encodes KIT (ie, a tyrosine kinase membrane receptor for stem cell factor), may account for most pediatric CM phenotypes.1,3,6 Activating c-KIT mutations leads to constitutive activation of the KIT receptor (expressed on the surface membrane of mast cells) and instigates autonomous (stem cell factor– independent) clonal proliferation, enhanced survival, and accumulation of mast cells.2
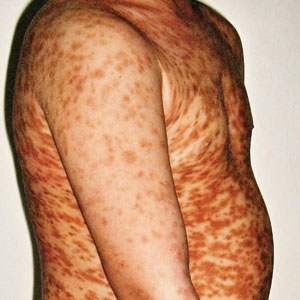
Maculopapular CM is the most common clinical form of CM.2,4,5 In children, maculopapular CM usually presents with polymorphous red-brown lesions of varying sizes and types—macule, papule, plaque, or nodule—on the torso and extremities.1-5 The distribution may be widespread and rarely is almost universal, as in our patient.2 Darier sign typically is positive, with a wheal and flare developing upon stroking or rubbing 1 or several lesions.1-6 The lesions gradually involute and often spontaneously regress at the time of puberty.1-3,5-7
The clinical signs and symptoms of mastocytosis are not only related to mast cell infiltration but also to mast cell activation within the tissues. The release of intracellular mediators from activated mast cells may have local and/or systemic consequences.4,7 Erythema, edema, flushing, pruritus, urticaria, blistering, and dermatographism are among the local cutaneous symptoms of mast cell activation.2-4,7 Systemic symptoms are rare in childhood CM and consist of wheezing, shortness of breath, nausea, vomiting, reflux, abdominal cramping, diarrhea, tachycardia, hypotension, syncope, anaphylaxis, and cyanotic spells.1-7 An elevated serum tryptase level is an indicator of both mast cell burden and risk for mast cell activation in the skin.4,7
Treatment of pediatric CM is conservative and symptomatic.3 Prevention of mediator release may be accomplished through avoidance of trigger factors.1 Alleviation of mediator-related symptoms might be attained using H1 and H2 histamine receptor blockers, oral cromolyn sodium, leukotriene antagonists, and epinephrine autoinjectors.1-3,5 Short-term topical or oral corticosteroids; calcineurin inhibitors (eg, pimecrolimus, tacrolimus); phototherapy; psoralen plus UVA; omalizumab; and innovative agents such as topical miltefosine, nemolizumab (an IL-31 antagonist), kinase inhibitors such as midostaurin, and tyrosine kinase inhibitors such as imatinib and masitinib may be tried in refractory or extensive pediatric CM.1,2,5,6
Although several disorders in childhood may present with red-brown macules and papules, Darier sign is unique to cutaneous mastocytosis. A biopsy also will be helpful in establishing the definitive diagnosis.
Histiocytosis X (also referred to as Langerhans cell histiocytosis) is the most common proliferative histiocytic disorder. Cutaneous lesions are polymorphic and consist of seborrheic involvement of the scalp with yellow, scaly or crusted papules; eroded patches; pustules; vesicles; petechiae; purpura; or red to purplish papules on the groin, abdomen, back, or chest.8
LEOPARD syndrome (also known as Noonan syndrome with multiple lentigines) is an acronym denoting lentigines (multiple), electrocardiographic conduction abnormalities, ocular hypertelorism, pulmonary stenosis, abnormalities of the genitalia, retarded growth, and deafness (sensorineural). The disorder is caused by a genetic mutation involving the PTPN11 gene and currently is categorized under the canopy of RASopathies. Cutaneous findings consist of lentiginous and café-au-lait macules and patches.9
Neurofibromatosis is a genetic disorder with a plethora of cutaneous and systemic manifestations. The type 1 variant that constitutes more than 95% of cases is caused by mutations in the neurofibromin gene. The main cutaneous findings include café-au-lait macules, freckling in axillary and inguinal locations (Crowe sign), and neurofibromas. These lesions may present as macules, patches, papules, or nodules.10
Xanthoma disseminatum is a rare sporadic proliferative histiocyte disorder involving the skin and mucosa. The disorder may be a harbinger of diabetes insipidus. Cutaneous lesions consist of asymptomatic, symmetrical, discrete, erythematous to yellow-brown papules and nodules.11
- Sandru F, Petca RC, Costescu M, et al. Cutaneous mastocytosis in childhood: update from the literature. J Clin Med. 2021;10:1474. doi:10.3390/jcm10071474
- Lange M, Hartmann K, Carter MC, et al. Molecular background, clinical features and management of pediatric mastocytosis: status 2021. Int J Mol Sci. 2021;22:2586. doi:10.3390/ijms22052586
- Castells M, Metcalfe DD, Escribano L. Diagnosis and treatment of cutaneous mastocytosis in children: practical recommendations. Am J Clin Dermatol. 2011;12:259-270. doi:10.2165/11588890-000000000-00000
- Nedoszytko B, Arock M, Lyons JJ, et al. Clinical impact of inherited and acquired genetic variants in mastocytosis. Int J Mol Sci. 2021;22:411. doi:10.3390/ijms22010411
- Nemat K, Abraham S. Cutaneous mastocytosis in childhood. Allergol Select. 2022;6:1-10. doi:10.5414/ALX02304E
- Giona F. Pediatric mastocytosis: an update. Mediterr J Hematol Infect Dis. 2021;13:E2021069. doi:10.4084/MJHID.2021.069
- Brockow K, Plata-Nazar K, Lange M, et al. Mediator-related symptoms and anaphylaxis in children with mastocytosis. Int J Mol Sci. 2021;22:2684. doi:10.3390/ijms22052684
- Grana N. Langerhans cell histiocytosis. Cancer Control. 2014;21: 328-334.
- García-Gil MF, Álvarez-Salafranca M, Valero-Torres A, et al. Melanoma in Noonan syndrome with multiple lentigines (LEOPARD syndrome): a new case. Actas Dermosifiliogr (Engl Ed). 2020;111:619-621.
- Ozarslan B, Russo T, Argenziano G, et al. Cutaneous findings in neurofibromatosis type 1. Cancers (Basel). 2021;13:463.
- Behra A, Sa DK, Naik R, et al. A rare case of persistent xanthoma disseminatum without any systemic involvement. Indian J Dermatol. 2020;65:239-241.
The Diagnosis: Maculopapular Cutaneous Mastocytosis (Urticaria Pigmentosa)
A stroke test revealed urtication at the exact traumatized site (Figure). A skin biopsy performed 2 years prior by another physician in the same hospital had revealed mast cell infiltration of virtually the entire dermis. The diagnosis was then firmly established as maculopapular cutaneous mastocytosis (CM)(also known as urticaria pigmentosa) with both the pathology results and a confirmative stroke test, and no additional biopsy was attempted. Serum IgE and tryptase levels were within the reference range. General recommendations about the avoidance of trigger factors were given to the family, and a new-generation H1 blocker antihistaminic syrup was prescribed for flushing, itching, and urtication.

Mastocytosis is a canopy term for a heterogeneous group of disorders caused by clonal proliferation and accumulation of abnormal mast cells within the skin and visceral organs (ie, bone marrow, liver, spleen, lymph nodes, gastrointestinal tract). Cutaneous mastocytosis, the skin-restricted variant, is by far the most common form of childhood mastocytosis (90% of mastocytosis cases in children)1 and generally appears within the first 2 years of life.1-7 Pediatric CM usually is a benign and transient disease with an excellent prognosis and a negligible risk for systemic involvement.2,3,5
The pathogenesis of CM in children is obscure1; however, somatic or germline gain-of-function mutations of the c-KIT proto-oncogene, which encodes KIT (ie, a tyrosine kinase membrane receptor for stem cell factor), may account for most pediatric CM phenotypes.1,3,6 Activating c-KIT mutations leads to constitutive activation of the KIT receptor (expressed on the surface membrane of mast cells) and instigates autonomous (stem cell factor– independent) clonal proliferation, enhanced survival, and accumulation of mast cells.2
Maculopapular CM is the most common clinical form of CM.2,4,5 In children, maculopapular CM usually presents with polymorphous red-brown lesions of varying sizes and types—macule, papule, plaque, or nodule—on the torso and extremities.1-5 The distribution may be widespread and rarely is almost universal, as in our patient.2 Darier sign typically is positive, with a wheal and flare developing upon stroking or rubbing 1 or several lesions.1-6 The lesions gradually involute and often spontaneously regress at the time of puberty.1-3,5-7
The clinical signs and symptoms of mastocytosis are not only related to mast cell infiltration but also to mast cell activation within the tissues. The release of intracellular mediators from activated mast cells may have local and/or systemic consequences.4,7 Erythema, edema, flushing, pruritus, urticaria, blistering, and dermatographism are among the local cutaneous symptoms of mast cell activation.2-4,7 Systemic symptoms are rare in childhood CM and consist of wheezing, shortness of breath, nausea, vomiting, reflux, abdominal cramping, diarrhea, tachycardia, hypotension, syncope, anaphylaxis, and cyanotic spells.1-7 An elevated serum tryptase level is an indicator of both mast cell burden and risk for mast cell activation in the skin.4,7
Treatment of pediatric CM is conservative and symptomatic.3 Prevention of mediator release may be accomplished through avoidance of trigger factors.1 Alleviation of mediator-related symptoms might be attained using H1 and H2 histamine receptor blockers, oral cromolyn sodium, leukotriene antagonists, and epinephrine autoinjectors.1-3,5 Short-term topical or oral corticosteroids; calcineurin inhibitors (eg, pimecrolimus, tacrolimus); phototherapy; psoralen plus UVA; omalizumab; and innovative agents such as topical miltefosine, nemolizumab (an IL-31 antagonist), kinase inhibitors such as midostaurin, and tyrosine kinase inhibitors such as imatinib and masitinib may be tried in refractory or extensive pediatric CM.1,2,5,6
Although several disorders in childhood may present with red-brown macules and papules, Darier sign is unique to cutaneous mastocytosis. A biopsy also will be helpful in establishing the definitive diagnosis.
Histiocytosis X (also referred to as Langerhans cell histiocytosis) is the most common proliferative histiocytic disorder. Cutaneous lesions are polymorphic and consist of seborrheic involvement of the scalp with yellow, scaly or crusted papules; eroded patches; pustules; vesicles; petechiae; purpura; or red to purplish papules on the groin, abdomen, back, or chest.8
LEOPARD syndrome (also known as Noonan syndrome with multiple lentigines) is an acronym denoting lentigines (multiple), electrocardiographic conduction abnormalities, ocular hypertelorism, pulmonary stenosis, abnormalities of the genitalia, retarded growth, and deafness (sensorineural). The disorder is caused by a genetic mutation involving the PTPN11 gene and currently is categorized under the canopy of RASopathies. Cutaneous findings consist of lentiginous and café-au-lait macules and patches.9
Neurofibromatosis is a genetic disorder with a plethora of cutaneous and systemic manifestations. The type 1 variant that constitutes more than 95% of cases is caused by mutations in the neurofibromin gene. The main cutaneous findings include café-au-lait macules, freckling in axillary and inguinal locations (Crowe sign), and neurofibromas. These lesions may present as macules, patches, papules, or nodules.10
Xanthoma disseminatum is a rare sporadic proliferative histiocyte disorder involving the skin and mucosa. The disorder may be a harbinger of diabetes insipidus. Cutaneous lesions consist of asymptomatic, symmetrical, discrete, erythematous to yellow-brown papules and nodules.11
The Diagnosis: Maculopapular Cutaneous Mastocytosis (Urticaria Pigmentosa)
A stroke test revealed urtication at the exact traumatized site (Figure). A skin biopsy performed 2 years prior by another physician in the same hospital had revealed mast cell infiltration of virtually the entire dermis. The diagnosis was then firmly established as maculopapular cutaneous mastocytosis (CM)(also known as urticaria pigmentosa) with both the pathology results and a confirmative stroke test, and no additional biopsy was attempted. Serum IgE and tryptase levels were within the reference range. General recommendations about the avoidance of trigger factors were given to the family, and a new-generation H1 blocker antihistaminic syrup was prescribed for flushing, itching, and urtication.

Mastocytosis is a canopy term for a heterogeneous group of disorders caused by clonal proliferation and accumulation of abnormal mast cells within the skin and visceral organs (ie, bone marrow, liver, spleen, lymph nodes, gastrointestinal tract). Cutaneous mastocytosis, the skin-restricted variant, is by far the most common form of childhood mastocytosis (90% of mastocytosis cases in children)1 and generally appears within the first 2 years of life.1-7 Pediatric CM usually is a benign and transient disease with an excellent prognosis and a negligible risk for systemic involvement.2,3,5
The pathogenesis of CM in children is obscure1; however, somatic or germline gain-of-function mutations of the c-KIT proto-oncogene, which encodes KIT (ie, a tyrosine kinase membrane receptor for stem cell factor), may account for most pediatric CM phenotypes.1,3,6 Activating c-KIT mutations leads to constitutive activation of the KIT receptor (expressed on the surface membrane of mast cells) and instigates autonomous (stem cell factor– independent) clonal proliferation, enhanced survival, and accumulation of mast cells.2
Maculopapular CM is the most common clinical form of CM.2,4,5 In children, maculopapular CM usually presents with polymorphous red-brown lesions of varying sizes and types—macule, papule, plaque, or nodule—on the torso and extremities.1-5 The distribution may be widespread and rarely is almost universal, as in our patient.2 Darier sign typically is positive, with a wheal and flare developing upon stroking or rubbing 1 or several lesions.1-6 The lesions gradually involute and often spontaneously regress at the time of puberty.1-3,5-7
The clinical signs and symptoms of mastocytosis are not only related to mast cell infiltration but also to mast cell activation within the tissues. The release of intracellular mediators from activated mast cells may have local and/or systemic consequences.4,7 Erythema, edema, flushing, pruritus, urticaria, blistering, and dermatographism are among the local cutaneous symptoms of mast cell activation.2-4,7 Systemic symptoms are rare in childhood CM and consist of wheezing, shortness of breath, nausea, vomiting, reflux, abdominal cramping, diarrhea, tachycardia, hypotension, syncope, anaphylaxis, and cyanotic spells.1-7 An elevated serum tryptase level is an indicator of both mast cell burden and risk for mast cell activation in the skin.4,7
Treatment of pediatric CM is conservative and symptomatic.3 Prevention of mediator release may be accomplished through avoidance of trigger factors.1 Alleviation of mediator-related symptoms might be attained using H1 and H2 histamine receptor blockers, oral cromolyn sodium, leukotriene antagonists, and epinephrine autoinjectors.1-3,5 Short-term topical or oral corticosteroids; calcineurin inhibitors (eg, pimecrolimus, tacrolimus); phototherapy; psoralen plus UVA; omalizumab; and innovative agents such as topical miltefosine, nemolizumab (an IL-31 antagonist), kinase inhibitors such as midostaurin, and tyrosine kinase inhibitors such as imatinib and masitinib may be tried in refractory or extensive pediatric CM.1,2,5,6
Although several disorders in childhood may present with red-brown macules and papules, Darier sign is unique to cutaneous mastocytosis. A biopsy also will be helpful in establishing the definitive diagnosis.
Histiocytosis X (also referred to as Langerhans cell histiocytosis) is the most common proliferative histiocytic disorder. Cutaneous lesions are polymorphic and consist of seborrheic involvement of the scalp with yellow, scaly or crusted papules; eroded patches; pustules; vesicles; petechiae; purpura; or red to purplish papules on the groin, abdomen, back, or chest.8
LEOPARD syndrome (also known as Noonan syndrome with multiple lentigines) is an acronym denoting lentigines (multiple), electrocardiographic conduction abnormalities, ocular hypertelorism, pulmonary stenosis, abnormalities of the genitalia, retarded growth, and deafness (sensorineural). The disorder is caused by a genetic mutation involving the PTPN11 gene and currently is categorized under the canopy of RASopathies. Cutaneous findings consist of lentiginous and café-au-lait macules and patches.9
Neurofibromatosis is a genetic disorder with a plethora of cutaneous and systemic manifestations. The type 1 variant that constitutes more than 95% of cases is caused by mutations in the neurofibromin gene. The main cutaneous findings include café-au-lait macules, freckling in axillary and inguinal locations (Crowe sign), and neurofibromas. These lesions may present as macules, patches, papules, or nodules.10
Xanthoma disseminatum is a rare sporadic proliferative histiocyte disorder involving the skin and mucosa. The disorder may be a harbinger of diabetes insipidus. Cutaneous lesions consist of asymptomatic, symmetrical, discrete, erythematous to yellow-brown papules and nodules.11
- Sandru F, Petca RC, Costescu M, et al. Cutaneous mastocytosis in childhood: update from the literature. J Clin Med. 2021;10:1474. doi:10.3390/jcm10071474
- Lange M, Hartmann K, Carter MC, et al. Molecular background, clinical features and management of pediatric mastocytosis: status 2021. Int J Mol Sci. 2021;22:2586. doi:10.3390/ijms22052586
- Castells M, Metcalfe DD, Escribano L. Diagnosis and treatment of cutaneous mastocytosis in children: practical recommendations. Am J Clin Dermatol. 2011;12:259-270. doi:10.2165/11588890-000000000-00000
- Nedoszytko B, Arock M, Lyons JJ, et al. Clinical impact of inherited and acquired genetic variants in mastocytosis. Int J Mol Sci. 2021;22:411. doi:10.3390/ijms22010411
- Nemat K, Abraham S. Cutaneous mastocytosis in childhood. Allergol Select. 2022;6:1-10. doi:10.5414/ALX02304E
- Giona F. Pediatric mastocytosis: an update. Mediterr J Hematol Infect Dis. 2021;13:E2021069. doi:10.4084/MJHID.2021.069
- Brockow K, Plata-Nazar K, Lange M, et al. Mediator-related symptoms and anaphylaxis in children with mastocytosis. Int J Mol Sci. 2021;22:2684. doi:10.3390/ijms22052684
- Grana N. Langerhans cell histiocytosis. Cancer Control. 2014;21: 328-334.
- García-Gil MF, Álvarez-Salafranca M, Valero-Torres A, et al. Melanoma in Noonan syndrome with multiple lentigines (LEOPARD syndrome): a new case. Actas Dermosifiliogr (Engl Ed). 2020;111:619-621.
- Ozarslan B, Russo T, Argenziano G, et al. Cutaneous findings in neurofibromatosis type 1. Cancers (Basel). 2021;13:463.
- Behra A, Sa DK, Naik R, et al. A rare case of persistent xanthoma disseminatum without any systemic involvement. Indian J Dermatol. 2020;65:239-241.
- Sandru F, Petca RC, Costescu M, et al. Cutaneous mastocytosis in childhood: update from the literature. J Clin Med. 2021;10:1474. doi:10.3390/jcm10071474
- Lange M, Hartmann K, Carter MC, et al. Molecular background, clinical features and management of pediatric mastocytosis: status 2021. Int J Mol Sci. 2021;22:2586. doi:10.3390/ijms22052586
- Castells M, Metcalfe DD, Escribano L. Diagnosis and treatment of cutaneous mastocytosis in children: practical recommendations. Am J Clin Dermatol. 2011;12:259-270. doi:10.2165/11588890-000000000-00000
- Nedoszytko B, Arock M, Lyons JJ, et al. Clinical impact of inherited and acquired genetic variants in mastocytosis. Int J Mol Sci. 2021;22:411. doi:10.3390/ijms22010411
- Nemat K, Abraham S. Cutaneous mastocytosis in childhood. Allergol Select. 2022;6:1-10. doi:10.5414/ALX02304E
- Giona F. Pediatric mastocytosis: an update. Mediterr J Hematol Infect Dis. 2021;13:E2021069. doi:10.4084/MJHID.2021.069
- Brockow K, Plata-Nazar K, Lange M, et al. Mediator-related symptoms and anaphylaxis in children with mastocytosis. Int J Mol Sci. 2021;22:2684. doi:10.3390/ijms22052684
- Grana N. Langerhans cell histiocytosis. Cancer Control. 2014;21: 328-334.
- García-Gil MF, Álvarez-Salafranca M, Valero-Torres A, et al. Melanoma in Noonan syndrome with multiple lentigines (LEOPARD syndrome): a new case. Actas Dermosifiliogr (Engl Ed). 2020;111:619-621.
- Ozarslan B, Russo T, Argenziano G, et al. Cutaneous findings in neurofibromatosis type 1. Cancers (Basel). 2021;13:463.
- Behra A, Sa DK, Naik R, et al. A rare case of persistent xanthoma disseminatum without any systemic involvement. Indian J Dermatol. 2020;65:239-241.
A 5-year-old boy presented with red-brown spots diffusely spread over the body that were present since birth. There were no subjective symptoms, except for rare instances of flushing, itching, and urtication following hot baths and abrasive scrubs. Dermatologic examination revealed widespread brown polymorphic macules and papules of varying sizes on the forehead, neck, torso, and extremities. Physical examination was otherwise normal.
How do patients perceive aesthetic providers on social media?
DENVER – However, in a recent survey, when asked if an aesthetic medical provider’s social media presence positively affects their desire to see that provider, 48% of patients were neutral or had no opinion, while 41% indicated yes.
Those are key findings from the survey, which aimed to evaluate the social media preferences and perceptions of patients who undergo aesthetic procedures.
“Aesthetic providers have firmly established a presence on social media,” Morgan Murphrey, MD, said at the annual meeting of the American Society for Dermatologic Surgery, where she presented the results. “According to the dermatology literature, somewhere between 25% and 50% of patients are looking up aesthetic providers on social media before they even see them in the clinic. This raises the question: How do patients perceive aesthetic providers that are on social media, and what do they want to see on their professional accounts?”
To find out, Dr. Murphrey, chief dermatology resident at the University of California, Davis, and Sabrina Fabi, MD, a San Diego–based cosmetic dermatologist, used Survey Monkey to randomly survey 2,063 individuals in the United States. They used descriptive statistics to analyze characteristics and responses of the study participants.
Of the 2,063 respondents, 651 (32%) indicated that they undergo medical aesthetic treatments including Botox injections, fillers, or laser procedures. More than half (56%) were women, 25% were 18-30 years old, 64% were 31-60 years old, and 11% were 61 years or older.
The three most common social media platforms they used were Facebook (70%), Instagram (65%), and YouTube (63%), followed by TikTok (45%) and Snapchat (29%). When the researchers stratified respondents by income level, individuals making $200,000 or more per year were statistically more likely to be on Instagram while those making less than $200,000 were more likely to be on Facebook and YouTube.
When asked if their aesthetic medical provider’s social media presence positively impacts their desire to see them as a patient, 48% of respondent were neutral or had no opinion, while 41% answered yes. “Only 2% felt strongly about this if the provider was on a specific social media platform, while 9% of respondents preferred that their provider not be on social media,” Dr. Murphrey added.
When asked if the number of social media followers influences their perception of an aesthetic provider as an expert, 43% of respondents answered no while 57% answered yes. “Once you get to about 20,000 followers, there seems to be somewhat of a law of diminishing returns in the number of followers,” she said. However, 55% indicated that they prefer to see a provider with a social media account that is verified with a blue check mark.
As for content published, 70% of respondents found it very important (36%) or important (34%) that a provider show before-and-after photos on their social media pages, while 67% said that they favor viewing personal content such as posts about the provider’s family and hobbies.
“This study summarizes to us that there is really low risk to creating a social media account; it’s something to think about,” Dr. Murphrey said. “Only 9% of respondents really didn’t want aesthetic providers to be on social media, but when we stratified our results, those individuals were less likely to be on social media themselves.”
Patricia Richey, MD, who practices Mohs surgery and cosmetic dermatology in Washington, D.C., and was asked to comment on the results, characterized the findings as important, “as the role of social media (especially visually based platforms like Instagram) will only continue to grow in our dermatologic and aesthetic practices.” Several studies have displayed a trend of plastic surgeons and other subspecialities outnumbering dermatologists within the aesthetic realm of social media, she noted. “As our patients increasingly seek out health care information and advice through these platforms, studies like Dr. Murphrey’s and Dr. Fabi’s are helpful in allowing us to better understand patient preferences and perspectives, in that we, as dermatologists, may be able to better aid their medical decisions in the future,” she added.
Neither the researchers nor Dr. Richey reported having relevant financial disclosures.
DENVER – However, in a recent survey, when asked if an aesthetic medical provider’s social media presence positively affects their desire to see that provider, 48% of patients were neutral or had no opinion, while 41% indicated yes.
Those are key findings from the survey, which aimed to evaluate the social media preferences and perceptions of patients who undergo aesthetic procedures.
“Aesthetic providers have firmly established a presence on social media,” Morgan Murphrey, MD, said at the annual meeting of the American Society for Dermatologic Surgery, where she presented the results. “According to the dermatology literature, somewhere between 25% and 50% of patients are looking up aesthetic providers on social media before they even see them in the clinic. This raises the question: How do patients perceive aesthetic providers that are on social media, and what do they want to see on their professional accounts?”
To find out, Dr. Murphrey, chief dermatology resident at the University of California, Davis, and Sabrina Fabi, MD, a San Diego–based cosmetic dermatologist, used Survey Monkey to randomly survey 2,063 individuals in the United States. They used descriptive statistics to analyze characteristics and responses of the study participants.
Of the 2,063 respondents, 651 (32%) indicated that they undergo medical aesthetic treatments including Botox injections, fillers, or laser procedures. More than half (56%) were women, 25% were 18-30 years old, 64% were 31-60 years old, and 11% were 61 years or older.
The three most common social media platforms they used were Facebook (70%), Instagram (65%), and YouTube (63%), followed by TikTok (45%) and Snapchat (29%). When the researchers stratified respondents by income level, individuals making $200,000 or more per year were statistically more likely to be on Instagram while those making less than $200,000 were more likely to be on Facebook and YouTube.
When asked if their aesthetic medical provider’s social media presence positively impacts their desire to see them as a patient, 48% of respondent were neutral or had no opinion, while 41% answered yes. “Only 2% felt strongly about this if the provider was on a specific social media platform, while 9% of respondents preferred that their provider not be on social media,” Dr. Murphrey added.
When asked if the number of social media followers influences their perception of an aesthetic provider as an expert, 43% of respondents answered no while 57% answered yes. “Once you get to about 20,000 followers, there seems to be somewhat of a law of diminishing returns in the number of followers,” she said. However, 55% indicated that they prefer to see a provider with a social media account that is verified with a blue check mark.
As for content published, 70% of respondents found it very important (36%) or important (34%) that a provider show before-and-after photos on their social media pages, while 67% said that they favor viewing personal content such as posts about the provider’s family and hobbies.
“This study summarizes to us that there is really low risk to creating a social media account; it’s something to think about,” Dr. Murphrey said. “Only 9% of respondents really didn’t want aesthetic providers to be on social media, but when we stratified our results, those individuals were less likely to be on social media themselves.”
Patricia Richey, MD, who practices Mohs surgery and cosmetic dermatology in Washington, D.C., and was asked to comment on the results, characterized the findings as important, “as the role of social media (especially visually based platforms like Instagram) will only continue to grow in our dermatologic and aesthetic practices.” Several studies have displayed a trend of plastic surgeons and other subspecialities outnumbering dermatologists within the aesthetic realm of social media, she noted. “As our patients increasingly seek out health care information and advice through these platforms, studies like Dr. Murphrey’s and Dr. Fabi’s are helpful in allowing us to better understand patient preferences and perspectives, in that we, as dermatologists, may be able to better aid their medical decisions in the future,” she added.
Neither the researchers nor Dr. Richey reported having relevant financial disclosures.
DENVER – However, in a recent survey, when asked if an aesthetic medical provider’s social media presence positively affects their desire to see that provider, 48% of patients were neutral or had no opinion, while 41% indicated yes.
Those are key findings from the survey, which aimed to evaluate the social media preferences and perceptions of patients who undergo aesthetic procedures.
“Aesthetic providers have firmly established a presence on social media,” Morgan Murphrey, MD, said at the annual meeting of the American Society for Dermatologic Surgery, where she presented the results. “According to the dermatology literature, somewhere between 25% and 50% of patients are looking up aesthetic providers on social media before they even see them in the clinic. This raises the question: How do patients perceive aesthetic providers that are on social media, and what do they want to see on their professional accounts?”
To find out, Dr. Murphrey, chief dermatology resident at the University of California, Davis, and Sabrina Fabi, MD, a San Diego–based cosmetic dermatologist, used Survey Monkey to randomly survey 2,063 individuals in the United States. They used descriptive statistics to analyze characteristics and responses of the study participants.
Of the 2,063 respondents, 651 (32%) indicated that they undergo medical aesthetic treatments including Botox injections, fillers, or laser procedures. More than half (56%) were women, 25% were 18-30 years old, 64% were 31-60 years old, and 11% were 61 years or older.
The three most common social media platforms they used were Facebook (70%), Instagram (65%), and YouTube (63%), followed by TikTok (45%) and Snapchat (29%). When the researchers stratified respondents by income level, individuals making $200,000 or more per year were statistically more likely to be on Instagram while those making less than $200,000 were more likely to be on Facebook and YouTube.
When asked if their aesthetic medical provider’s social media presence positively impacts their desire to see them as a patient, 48% of respondent were neutral or had no opinion, while 41% answered yes. “Only 2% felt strongly about this if the provider was on a specific social media platform, while 9% of respondents preferred that their provider not be on social media,” Dr. Murphrey added.
When asked if the number of social media followers influences their perception of an aesthetic provider as an expert, 43% of respondents answered no while 57% answered yes. “Once you get to about 20,000 followers, there seems to be somewhat of a law of diminishing returns in the number of followers,” she said. However, 55% indicated that they prefer to see a provider with a social media account that is verified with a blue check mark.
As for content published, 70% of respondents found it very important (36%) or important (34%) that a provider show before-and-after photos on their social media pages, while 67% said that they favor viewing personal content such as posts about the provider’s family and hobbies.
“This study summarizes to us that there is really low risk to creating a social media account; it’s something to think about,” Dr. Murphrey said. “Only 9% of respondents really didn’t want aesthetic providers to be on social media, but when we stratified our results, those individuals were less likely to be on social media themselves.”
Patricia Richey, MD, who practices Mohs surgery and cosmetic dermatology in Washington, D.C., and was asked to comment on the results, characterized the findings as important, “as the role of social media (especially visually based platforms like Instagram) will only continue to grow in our dermatologic and aesthetic practices.” Several studies have displayed a trend of plastic surgeons and other subspecialities outnumbering dermatologists within the aesthetic realm of social media, she noted. “As our patients increasingly seek out health care information and advice through these platforms, studies like Dr. Murphrey’s and Dr. Fabi’s are helpful in allowing us to better understand patient preferences and perspectives, in that we, as dermatologists, may be able to better aid their medical decisions in the future,” she added.
Neither the researchers nor Dr. Richey reported having relevant financial disclosures.
AT ASDS 2022
An integrative approach to atopic dermatitis features a long list of options
to probiotics and acupressure – that he encourages patients to try as they use the big guns, or as they attempt to wean off of them or avoid their use altogether.
During a presentation at the annual Integrative Dermatology Symposium, Dr. Lio said that he uses “5 pillars” to guide his integrative treatment plans: The skin barrier, the psyche, the microbiome, inflammation, and itch. “I try to flag approaches that predominantly address the categories that I think need the most help,” he said. “And I tell patients [which pillar or pillars] each treatment is addressing.”
Most commonly, the greatest challenge with AD – and the “single biggest weakness of conventional Western medicine” – lies not with getting patients clear in the first place, but in keeping them clear safely, he said. “I don’t think that using immunosuppressive [medications] is okay for the long-term unless there is no other choice,” said Dr. Lio, who cofounded the Chicago Integrative Eczema Center about 6 years ago and is clinical assistant professor of dermatology and pediatrics at Northwestern University, Chicago. Oftentimes, he said, complementary approaches, including dietary changes, can also serve as supportive adjunctive therapy to biologics and JAK inhibitors.
He has three main criteria, or “filters,” for evaluating these treatments before recommending them to patients: At least some clinical evidence for efficacy (preferably randomized trials but not necessarily), safety, and practicality. The “only way we’re going to move things forward [for AD and other conditions] is to try out less tested treatments ... to open up to them,” Dr. Lio said in an interview after the meeting. And in doing so, he said, dermatologists “can connect with a lot of patients whom naysayers can’t connect with.”
An integrative menu
Dr. Lio individualizes plans, suggesting treatments after “listening to patients’ stories” and considering their age, history, symptoms and skin presentation, and other factors. He said he “goes little by little,” telling a patient, for instance, “I’d love for us to try adding a little hemp oil to your diet.”
If patients aren’t pleased with or are tired of treatments, he said in the interview, “we move on and try something else.”
At the meeting, he described some of the treatments on his menu and the supporting evidence for those treatments:
Oral hempseed oil. A randomized crossover study of 20 adult patients with AD found that daily consumption of 2 tablespoons of hempseed oil decreased skin dryness, itchiness, and use of topical medications compared with consumption of olive oil. “It was statistically significant and seemed clinically meaningful,” likely resulting from the high concentration of polyunsaturated fatty acids in the oil, Dr. Lio said.
Topical vitamin B12. In a phase 3 randomized controlled trial of topical B12 applied twice a day for 8 weeks, patients experienced significant improvements in the extent and severity of AD compared with placebo. Another study in children with AD aged 6 months to 18 years found significant improvement in as early as 2 weeks of use. “It really does help, and is very gentle in babies,” Dr. Lio said.
Black tea compresses. “It’s absolutely my favorite kind of compress,” he said. “It was studied on the face and eyelids but I use it all over the body for adults and kids.” A German study of 22 patients with AD or contact facial dermatitis showed significant improvements in facial dermatitis within the first 3 days of treatment with application of black tea dressings plus an emollient cream, with significant reductions in four disease activity scores (the Facial Eczema Area and Severity Index, visual analog scale for pruritus, Investigator’s Global Assessment score, and Patient’s Self-Assessment Score) that continued through day 6.
Oolong tea. In a 2001 study, after 1 month of drinking oolong tea after each meal, 64% of patients with recalcitrant AD who continued with their regular treatment showed marked to moderate improvements in AD, with a beneficial effect first noticed after 1-2 weeks. At 6 months, 54% still had a good response to treatment. “It’s super cheap and accessible,” Dr. Lio said.
Coconut oil. One of the greatest benefits of coconut oil is on the microbiome and the dysbiosis that can result from a disrupted, or “leaky,” skin barrier – especially overgrowth of Staphylococcus aureus, which “drives AD,” Dr. Lio said. In a study of adults with AD from the Philippines, topically applied coconut oil decreased S. aureus colonization by 95% when applied twice daily for 4 weeks, compared with a 50% decrease in an olive oil control group. Other research has shown coconut oil to be superior to mineral oil as a moisturizer, he said at the meeting.
Acupressure. After a pilot study conducted by Dr. Lio and colleagues showed greater decreases in itch (per the visual analogue scale) in adults with AD who applied an acupressure bead at the LI11 point (near the elbow) for 3 minutes three times a week for 4 weeks, than among those who did not use the acupressure tool, Dr. Lio began trying it with some of his patients. “Now I use it broadly,” he added in the interview. “Kids over 10 can figure out how to use it and teenagers love it [to relief itch]. Some don’t use the beads anymore, they just use their fingertips.”
Advice on diet, vitamin D, and probiotics
AD severity is “powerfully” correlated with IgE food allergy, but Dr. Lio said at the meeting that he currently takes a cautious approach toward strict elimination diets.
There is a growing school of thought among allergists, he said, that positive IgE tests without evidence of acute reactions may not indicate true allergy, but rather sensitivity – and may not warrant food eliminations. And as has been shown with peanuts, there can be a serious downside to elimination, as food avoidance can lead to serious allergy later on, he said.
“More and more people are thinking that if you can tolerate [a food], continue it,” he added in the interview. In the absence of clear reactions, the only way to really know if a food is making eczema worse is to do a double-blind, placebo-controlled food challenge test, he noted.
Patients often come to see him believing that food is the “root cause” of their eczema and feeling frustrated, even anxious, about strict dietary restrictions they’ve implemented. But for many of these patients, the right question “would be to ask, why is my eczema causing my food allergy?” he said at the meeting, referring to the epithelial barrier hypothesis, which posits that skin barrier dysfunction can lead to asthma, allergic rhinitis, and food allergy.
Dr. Lio often recommends the Autoimmune Protocol (AIP) diet, a “close cousin” of the paleo diet for patients with AD, as general guidance to be followed “holistically” and often without the strict eliminations it prescribes. Minimizing processed foods and dairy and grains, which “can be inflammatory in some people,” and focusing on whole, nutrient-rich foods – all in keeping with the AIP principles – should have positive effects on the microbiome, overall health, and likely AD as well, he said.
Across the board, Dr. Lio recommends vitamin D (at nationally recommended dosages) and probiotics. Vitamin D has been shown to significantly help a small percentage of patients with eczema, he said, so he advises patients that it’s worth a trial. “I tell patients that I don’t know how to pick that small group out, so let’s try for a few months and see,” he said. “Inevitably, a percentage of patients come back and say it makes a huge difference.”
Dr. Lio’s understanding and use of probiotics has been “dynamic” over the years. “The “best, most reliable evidence” that probiotics can improve AD symptoms comes with the use of multiple probiotic strains together, he said. Based on limited but growing literature, he ensures that recommended formulations for babies include Lactobacillus rhamnosus, and that formulations for adults include Lactobacillus salivarius.
Dr. Lio works closely with dietitians, hypnotherapists, and psychologists – and will occasionally refer interested patients with AD to a Chinese medicine practitioner who personalizes the use of herbal formulations.
He reported no relevant disclosures.
to probiotics and acupressure – that he encourages patients to try as they use the big guns, or as they attempt to wean off of them or avoid their use altogether.
During a presentation at the annual Integrative Dermatology Symposium, Dr. Lio said that he uses “5 pillars” to guide his integrative treatment plans: The skin barrier, the psyche, the microbiome, inflammation, and itch. “I try to flag approaches that predominantly address the categories that I think need the most help,” he said. “And I tell patients [which pillar or pillars] each treatment is addressing.”
Most commonly, the greatest challenge with AD – and the “single biggest weakness of conventional Western medicine” – lies not with getting patients clear in the first place, but in keeping them clear safely, he said. “I don’t think that using immunosuppressive [medications] is okay for the long-term unless there is no other choice,” said Dr. Lio, who cofounded the Chicago Integrative Eczema Center about 6 years ago and is clinical assistant professor of dermatology and pediatrics at Northwestern University, Chicago. Oftentimes, he said, complementary approaches, including dietary changes, can also serve as supportive adjunctive therapy to biologics and JAK inhibitors.
He has three main criteria, or “filters,” for evaluating these treatments before recommending them to patients: At least some clinical evidence for efficacy (preferably randomized trials but not necessarily), safety, and practicality. The “only way we’re going to move things forward [for AD and other conditions] is to try out less tested treatments ... to open up to them,” Dr. Lio said in an interview after the meeting. And in doing so, he said, dermatologists “can connect with a lot of patients whom naysayers can’t connect with.”
An integrative menu
Dr. Lio individualizes plans, suggesting treatments after “listening to patients’ stories” and considering their age, history, symptoms and skin presentation, and other factors. He said he “goes little by little,” telling a patient, for instance, “I’d love for us to try adding a little hemp oil to your diet.”
If patients aren’t pleased with or are tired of treatments, he said in the interview, “we move on and try something else.”
At the meeting, he described some of the treatments on his menu and the supporting evidence for those treatments:
Oral hempseed oil. A randomized crossover study of 20 adult patients with AD found that daily consumption of 2 tablespoons of hempseed oil decreased skin dryness, itchiness, and use of topical medications compared with consumption of olive oil. “It was statistically significant and seemed clinically meaningful,” likely resulting from the high concentration of polyunsaturated fatty acids in the oil, Dr. Lio said.
Topical vitamin B12. In a phase 3 randomized controlled trial of topical B12 applied twice a day for 8 weeks, patients experienced significant improvements in the extent and severity of AD compared with placebo. Another study in children with AD aged 6 months to 18 years found significant improvement in as early as 2 weeks of use. “It really does help, and is very gentle in babies,” Dr. Lio said.
Black tea compresses. “It’s absolutely my favorite kind of compress,” he said. “It was studied on the face and eyelids but I use it all over the body for adults and kids.” A German study of 22 patients with AD or contact facial dermatitis showed significant improvements in facial dermatitis within the first 3 days of treatment with application of black tea dressings plus an emollient cream, with significant reductions in four disease activity scores (the Facial Eczema Area and Severity Index, visual analog scale for pruritus, Investigator’s Global Assessment score, and Patient’s Self-Assessment Score) that continued through day 6.
Oolong tea. In a 2001 study, after 1 month of drinking oolong tea after each meal, 64% of patients with recalcitrant AD who continued with their regular treatment showed marked to moderate improvements in AD, with a beneficial effect first noticed after 1-2 weeks. At 6 months, 54% still had a good response to treatment. “It’s super cheap and accessible,” Dr. Lio said.
Coconut oil. One of the greatest benefits of coconut oil is on the microbiome and the dysbiosis that can result from a disrupted, or “leaky,” skin barrier – especially overgrowth of Staphylococcus aureus, which “drives AD,” Dr. Lio said. In a study of adults with AD from the Philippines, topically applied coconut oil decreased S. aureus colonization by 95% when applied twice daily for 4 weeks, compared with a 50% decrease in an olive oil control group. Other research has shown coconut oil to be superior to mineral oil as a moisturizer, he said at the meeting.
Acupressure. After a pilot study conducted by Dr. Lio and colleagues showed greater decreases in itch (per the visual analogue scale) in adults with AD who applied an acupressure bead at the LI11 point (near the elbow) for 3 minutes three times a week for 4 weeks, than among those who did not use the acupressure tool, Dr. Lio began trying it with some of his patients. “Now I use it broadly,” he added in the interview. “Kids over 10 can figure out how to use it and teenagers love it [to relief itch]. Some don’t use the beads anymore, they just use their fingertips.”
Advice on diet, vitamin D, and probiotics
AD severity is “powerfully” correlated with IgE food allergy, but Dr. Lio said at the meeting that he currently takes a cautious approach toward strict elimination diets.
There is a growing school of thought among allergists, he said, that positive IgE tests without evidence of acute reactions may not indicate true allergy, but rather sensitivity – and may not warrant food eliminations. And as has been shown with peanuts, there can be a serious downside to elimination, as food avoidance can lead to serious allergy later on, he said.
“More and more people are thinking that if you can tolerate [a food], continue it,” he added in the interview. In the absence of clear reactions, the only way to really know if a food is making eczema worse is to do a double-blind, placebo-controlled food challenge test, he noted.
Patients often come to see him believing that food is the “root cause” of their eczema and feeling frustrated, even anxious, about strict dietary restrictions they’ve implemented. But for many of these patients, the right question “would be to ask, why is my eczema causing my food allergy?” he said at the meeting, referring to the epithelial barrier hypothesis, which posits that skin barrier dysfunction can lead to asthma, allergic rhinitis, and food allergy.
Dr. Lio often recommends the Autoimmune Protocol (AIP) diet, a “close cousin” of the paleo diet for patients with AD, as general guidance to be followed “holistically” and often without the strict eliminations it prescribes. Minimizing processed foods and dairy and grains, which “can be inflammatory in some people,” and focusing on whole, nutrient-rich foods – all in keeping with the AIP principles – should have positive effects on the microbiome, overall health, and likely AD as well, he said.
Across the board, Dr. Lio recommends vitamin D (at nationally recommended dosages) and probiotics. Vitamin D has been shown to significantly help a small percentage of patients with eczema, he said, so he advises patients that it’s worth a trial. “I tell patients that I don’t know how to pick that small group out, so let’s try for a few months and see,” he said. “Inevitably, a percentage of patients come back and say it makes a huge difference.”
Dr. Lio’s understanding and use of probiotics has been “dynamic” over the years. “The “best, most reliable evidence” that probiotics can improve AD symptoms comes with the use of multiple probiotic strains together, he said. Based on limited but growing literature, he ensures that recommended formulations for babies include Lactobacillus rhamnosus, and that formulations for adults include Lactobacillus salivarius.
Dr. Lio works closely with dietitians, hypnotherapists, and psychologists – and will occasionally refer interested patients with AD to a Chinese medicine practitioner who personalizes the use of herbal formulations.
He reported no relevant disclosures.
to probiotics and acupressure – that he encourages patients to try as they use the big guns, or as they attempt to wean off of them or avoid their use altogether.
During a presentation at the annual Integrative Dermatology Symposium, Dr. Lio said that he uses “5 pillars” to guide his integrative treatment plans: The skin barrier, the psyche, the microbiome, inflammation, and itch. “I try to flag approaches that predominantly address the categories that I think need the most help,” he said. “And I tell patients [which pillar or pillars] each treatment is addressing.”
Most commonly, the greatest challenge with AD – and the “single biggest weakness of conventional Western medicine” – lies not with getting patients clear in the first place, but in keeping them clear safely, he said. “I don’t think that using immunosuppressive [medications] is okay for the long-term unless there is no other choice,” said Dr. Lio, who cofounded the Chicago Integrative Eczema Center about 6 years ago and is clinical assistant professor of dermatology and pediatrics at Northwestern University, Chicago. Oftentimes, he said, complementary approaches, including dietary changes, can also serve as supportive adjunctive therapy to biologics and JAK inhibitors.
He has three main criteria, or “filters,” for evaluating these treatments before recommending them to patients: At least some clinical evidence for efficacy (preferably randomized trials but not necessarily), safety, and practicality. The “only way we’re going to move things forward [for AD and other conditions] is to try out less tested treatments ... to open up to them,” Dr. Lio said in an interview after the meeting. And in doing so, he said, dermatologists “can connect with a lot of patients whom naysayers can’t connect with.”
An integrative menu
Dr. Lio individualizes plans, suggesting treatments after “listening to patients’ stories” and considering their age, history, symptoms and skin presentation, and other factors. He said he “goes little by little,” telling a patient, for instance, “I’d love for us to try adding a little hemp oil to your diet.”
If patients aren’t pleased with or are tired of treatments, he said in the interview, “we move on and try something else.”
At the meeting, he described some of the treatments on his menu and the supporting evidence for those treatments:
Oral hempseed oil. A randomized crossover study of 20 adult patients with AD found that daily consumption of 2 tablespoons of hempseed oil decreased skin dryness, itchiness, and use of topical medications compared with consumption of olive oil. “It was statistically significant and seemed clinically meaningful,” likely resulting from the high concentration of polyunsaturated fatty acids in the oil, Dr. Lio said.
Topical vitamin B12. In a phase 3 randomized controlled trial of topical B12 applied twice a day for 8 weeks, patients experienced significant improvements in the extent and severity of AD compared with placebo. Another study in children with AD aged 6 months to 18 years found significant improvement in as early as 2 weeks of use. “It really does help, and is very gentle in babies,” Dr. Lio said.
Black tea compresses. “It’s absolutely my favorite kind of compress,” he said. “It was studied on the face and eyelids but I use it all over the body for adults and kids.” A German study of 22 patients with AD or contact facial dermatitis showed significant improvements in facial dermatitis within the first 3 days of treatment with application of black tea dressings plus an emollient cream, with significant reductions in four disease activity scores (the Facial Eczema Area and Severity Index, visual analog scale for pruritus, Investigator’s Global Assessment score, and Patient’s Self-Assessment Score) that continued through day 6.
Oolong tea. In a 2001 study, after 1 month of drinking oolong tea after each meal, 64% of patients with recalcitrant AD who continued with their regular treatment showed marked to moderate improvements in AD, with a beneficial effect first noticed after 1-2 weeks. At 6 months, 54% still had a good response to treatment. “It’s super cheap and accessible,” Dr. Lio said.
Coconut oil. One of the greatest benefits of coconut oil is on the microbiome and the dysbiosis that can result from a disrupted, or “leaky,” skin barrier – especially overgrowth of Staphylococcus aureus, which “drives AD,” Dr. Lio said. In a study of adults with AD from the Philippines, topically applied coconut oil decreased S. aureus colonization by 95% when applied twice daily for 4 weeks, compared with a 50% decrease in an olive oil control group. Other research has shown coconut oil to be superior to mineral oil as a moisturizer, he said at the meeting.
Acupressure. After a pilot study conducted by Dr. Lio and colleagues showed greater decreases in itch (per the visual analogue scale) in adults with AD who applied an acupressure bead at the LI11 point (near the elbow) for 3 minutes three times a week for 4 weeks, than among those who did not use the acupressure tool, Dr. Lio began trying it with some of his patients. “Now I use it broadly,” he added in the interview. “Kids over 10 can figure out how to use it and teenagers love it [to relief itch]. Some don’t use the beads anymore, they just use their fingertips.”
Advice on diet, vitamin D, and probiotics
AD severity is “powerfully” correlated with IgE food allergy, but Dr. Lio said at the meeting that he currently takes a cautious approach toward strict elimination diets.
There is a growing school of thought among allergists, he said, that positive IgE tests without evidence of acute reactions may not indicate true allergy, but rather sensitivity – and may not warrant food eliminations. And as has been shown with peanuts, there can be a serious downside to elimination, as food avoidance can lead to serious allergy later on, he said.
“More and more people are thinking that if you can tolerate [a food], continue it,” he added in the interview. In the absence of clear reactions, the only way to really know if a food is making eczema worse is to do a double-blind, placebo-controlled food challenge test, he noted.
Patients often come to see him believing that food is the “root cause” of their eczema and feeling frustrated, even anxious, about strict dietary restrictions they’ve implemented. But for many of these patients, the right question “would be to ask, why is my eczema causing my food allergy?” he said at the meeting, referring to the epithelial barrier hypothesis, which posits that skin barrier dysfunction can lead to asthma, allergic rhinitis, and food allergy.
Dr. Lio often recommends the Autoimmune Protocol (AIP) diet, a “close cousin” of the paleo diet for patients with AD, as general guidance to be followed “holistically” and often without the strict eliminations it prescribes. Minimizing processed foods and dairy and grains, which “can be inflammatory in some people,” and focusing on whole, nutrient-rich foods – all in keeping with the AIP principles – should have positive effects on the microbiome, overall health, and likely AD as well, he said.
Across the board, Dr. Lio recommends vitamin D (at nationally recommended dosages) and probiotics. Vitamin D has been shown to significantly help a small percentage of patients with eczema, he said, so he advises patients that it’s worth a trial. “I tell patients that I don’t know how to pick that small group out, so let’s try for a few months and see,” he said. “Inevitably, a percentage of patients come back and say it makes a huge difference.”
Dr. Lio’s understanding and use of probiotics has been “dynamic” over the years. “The “best, most reliable evidence” that probiotics can improve AD symptoms comes with the use of multiple probiotic strains together, he said. Based on limited but growing literature, he ensures that recommended formulations for babies include Lactobacillus rhamnosus, and that formulations for adults include Lactobacillus salivarius.
Dr. Lio works closely with dietitians, hypnotherapists, and psychologists – and will occasionally refer interested patients with AD to a Chinese medicine practitioner who personalizes the use of herbal formulations.
He reported no relevant disclosures.
FROM IDS 2022
Commentary: Complementary treatments for AD, November 2022
Still, some patients seek alternative or adjunctive treatment approaches, owing to a desire to identify the root cause of disease, their aversion toward Western medicine, or fear of adverse events. Yepes-Nuñez and colleagues performed a systematic review and meta-analysis including 23 studies of benefits and harms of allergen immunotherapy for AD. I had the privilege of participating in this study and can testify to the astronomical amount of work that went into comprehensively identifying all of the relevant studies and synthesizing the data. We found that adjunctive subcutaneous or sublingual allergen immunotherapy, particularly for house dust mites, led to modest but generally delayed improvements of AD severity, itch, and quality of life, and less definitive effects on sleep disturbance and AD flares. Overall, both were well tolerated, though subcutaneous immunotherapy was associated with more adverse events than sublingual immunotherapy. Allergen immunotherapy requires a significant investment of time by patients and was only modestly effective. Nevertheless, it may be a reasonable approach to consider in select patients with AD.
Benjamin Franklin famously stated that "an ounce of prevention is worth a pound of cure." Likewise, while successful treatment of AD is great, how can we advise patients and caregivers of children who are at high risk for AD? To answer this question, Voigt and Lele performed a systematic review and meta-analysis of 11 randomized controlled trials examining the efficacy of Lactobacillus rhamnosus at preventing AD in children when taken by mothers during pregnancy. They found that L. rhamnosus significantly reduced the risk of developing AD within 2 years, marginally significantly reduced risk at 4-5 years, and significantly reduced risk at 6-7 years, but no significant risk differences were observed at 10-11 years. The authors concluded that use of L. rhamnosus with or without other probiotics during pregnancy reduces the incidence of childhood AD at least up to age 7 years.
Wang and colleagues conducted an observational study of the relationship of home environment exposures with atopic disease, including AD, in 17,881 offspring from Iceland, Norway, Sweden, Denmark, and Estonia who had undergone two follow-up investigations every 10 years. They found that AD was associated with parent-reported visible mold and dampness/mold at home, living in an apartment, and living in newer buildings. Avoidance of these environmental exposures could possibly decrease the risk of developing AD, although future confirmatory studies are needed.
For each of these treatment/prevention approaches, the magnitude of benefit is not very large. Thus, these approaches do not replace our armamentarium of treatments and avoidance strategies for AD. Rather, they can be used complementarily as low-risk add-on interventions with a potential upside.
Still, some patients seek alternative or adjunctive treatment approaches, owing to a desire to identify the root cause of disease, their aversion toward Western medicine, or fear of adverse events. Yepes-Nuñez and colleagues performed a systematic review and meta-analysis including 23 studies of benefits and harms of allergen immunotherapy for AD. I had the privilege of participating in this study and can testify to the astronomical amount of work that went into comprehensively identifying all of the relevant studies and synthesizing the data. We found that adjunctive subcutaneous or sublingual allergen immunotherapy, particularly for house dust mites, led to modest but generally delayed improvements of AD severity, itch, and quality of life, and less definitive effects on sleep disturbance and AD flares. Overall, both were well tolerated, though subcutaneous immunotherapy was associated with more adverse events than sublingual immunotherapy. Allergen immunotherapy requires a significant investment of time by patients and was only modestly effective. Nevertheless, it may be a reasonable approach to consider in select patients with AD.
Benjamin Franklin famously stated that "an ounce of prevention is worth a pound of cure." Likewise, while successful treatment of AD is great, how can we advise patients and caregivers of children who are at high risk for AD? To answer this question, Voigt and Lele performed a systematic review and meta-analysis of 11 randomized controlled trials examining the efficacy of Lactobacillus rhamnosus at preventing AD in children when taken by mothers during pregnancy. They found that L. rhamnosus significantly reduced the risk of developing AD within 2 years, marginally significantly reduced risk at 4-5 years, and significantly reduced risk at 6-7 years, but no significant risk differences were observed at 10-11 years. The authors concluded that use of L. rhamnosus with or without other probiotics during pregnancy reduces the incidence of childhood AD at least up to age 7 years.
Wang and colleagues conducted an observational study of the relationship of home environment exposures with atopic disease, including AD, in 17,881 offspring from Iceland, Norway, Sweden, Denmark, and Estonia who had undergone two follow-up investigations every 10 years. They found that AD was associated with parent-reported visible mold and dampness/mold at home, living in an apartment, and living in newer buildings. Avoidance of these environmental exposures could possibly decrease the risk of developing AD, although future confirmatory studies are needed.
For each of these treatment/prevention approaches, the magnitude of benefit is not very large. Thus, these approaches do not replace our armamentarium of treatments and avoidance strategies for AD. Rather, they can be used complementarily as low-risk add-on interventions with a potential upside.
Still, some patients seek alternative or adjunctive treatment approaches, owing to a desire to identify the root cause of disease, their aversion toward Western medicine, or fear of adverse events. Yepes-Nuñez and colleagues performed a systematic review and meta-analysis including 23 studies of benefits and harms of allergen immunotherapy for AD. I had the privilege of participating in this study and can testify to the astronomical amount of work that went into comprehensively identifying all of the relevant studies and synthesizing the data. We found that adjunctive subcutaneous or sublingual allergen immunotherapy, particularly for house dust mites, led to modest but generally delayed improvements of AD severity, itch, and quality of life, and less definitive effects on sleep disturbance and AD flares. Overall, both were well tolerated, though subcutaneous immunotherapy was associated with more adverse events than sublingual immunotherapy. Allergen immunotherapy requires a significant investment of time by patients and was only modestly effective. Nevertheless, it may be a reasonable approach to consider in select patients with AD.
Benjamin Franklin famously stated that "an ounce of prevention is worth a pound of cure." Likewise, while successful treatment of AD is great, how can we advise patients and caregivers of children who are at high risk for AD? To answer this question, Voigt and Lele performed a systematic review and meta-analysis of 11 randomized controlled trials examining the efficacy of Lactobacillus rhamnosus at preventing AD in children when taken by mothers during pregnancy. They found that L. rhamnosus significantly reduced the risk of developing AD within 2 years, marginally significantly reduced risk at 4-5 years, and significantly reduced risk at 6-7 years, but no significant risk differences were observed at 10-11 years. The authors concluded that use of L. rhamnosus with or without other probiotics during pregnancy reduces the incidence of childhood AD at least up to age 7 years.
Wang and colleagues conducted an observational study of the relationship of home environment exposures with atopic disease, including AD, in 17,881 offspring from Iceland, Norway, Sweden, Denmark, and Estonia who had undergone two follow-up investigations every 10 years. They found that AD was associated with parent-reported visible mold and dampness/mold at home, living in an apartment, and living in newer buildings. Avoidance of these environmental exposures could possibly decrease the risk of developing AD, although future confirmatory studies are needed.
For each of these treatment/prevention approaches, the magnitude of benefit is not very large. Thus, these approaches do not replace our armamentarium of treatments and avoidance strategies for AD. Rather, they can be used complementarily as low-risk add-on interventions with a potential upside.
Younger doctors call for more attention to patients with disabilities
As an undergraduate student at Northeastern University in Boston, Meghan Chin spent her summers working for a day program in Rhode Island. Her charges were adults with various forms of intellectual and developmental disabilities (IDD).
“I was very much a caretaker,” Ms. Chin, now 29, said. “It was everything from helping them get dressed in the morning to getting them to medical appointments.”
During one such visit Ms. Chin got a lesson about how health care looks from the viewpoint of someone with an IDD.
The patient was a woman in her 60s and she was having gastrointestinal issues; symptoms she could have articulated, if asked. “She was perfectly capable of telling a clinician where it hurt, how long she had experienced the problem, and what she had done or not done to alleviate it,” Ms. Chin said.
And of comprehending a response. But she was not given the opportunity.
“She would explain what was going on to the clinician,” Ms. Chin recalled. “And the clinician would turn to me and answer. It was this weird three-way conversation – as if she wasn’t even there in the room with us.”
Ms. Chin was incensed at the rude and disrespectful way the patient had been treated. But her charge didn’t seem upset or surprised. Just resigned. “Sadly, she had become used to this,” Ms. Chin said.
For the young aide, however, the experience was searing. “It didn’t seem right to me,” Ms. Chin said. “That’s why, when I went to medical school, I knew I wanted to do better for this population.”
Serendipity led her to Georgetown University, Washington, where she met Kim Bullock, MD, one of the country’s leading advocates for improved health care delivery to those with IDDs.
Dr. Bullock, an associate professor of family medicine, seeks to create better training and educational opportunities for medical students who will likely encounter patients with these disabilities in their practices.
When Dr. Bullock heard Ms. Chin’s story about the patient being ignored, she was not surprised.
“This is not an unusual or unique situation,” said Dr. Bullock, who is also director of Georgetown’s community health division and a faculty member of the university’s Center for Excellence for Developmental Disabilities. “In fact, it’s quite common and is part of what spurred my own interest in educating pre-med and medical students about effective communication techniques, particularly when addressing neurodiverse patients.”
More than 13% of Americans, or roughly 44 million people, have some form of disability, according to the National Institute on Disability at the University of New Hampshire, a figure that does not include those who are institutionalized. The Centers for Disease Control and Prevention estimates that 17% of children aged 3-17 years have a developmental disability.
Even so, many physicians feel ill-prepared to care for disabled patients. A survey of physicians, published in the journal Health Affairs, found that some lacked the resources and training to properly care for patients with disabilities, or that they struggled to coordinate care for such individuals. Some said they did not know which types of accessible equipment, like adjustable tables and chair scales, were needed or how to use them. And some said they actively try to avoid treating patients with disabilities.
Don’t assume
The first step at correcting the problem, Dr. Bullock said, is to not assume that all IDD patients are incapable of communicating. By talking not to the patient but to their caregiver or spouse or child, as the clinician did with Ms. Chin years ago, “we are taking away their agency, their autonomy to speak for and about themselves.”
Change involves altering physicians’ attitudes and assumptions toward this population, through education. But how?
“The medical school curriculum is tight as it is,” Dr. Bullock acknowledged. “There’s a lot of things students have to learn. People wonder: where we will add this?”
Her suggestion: Incorporate IDD all along the way, through programs or experiences that will enable medical students to see such patients “not as something separate, but as people that have special needs just as other populations have.”
Case in point: Operation House Call, a program in Massachusetts designed to support young health care professionals, by building “confidence, interest, and sensitivity” toward individuals with IDD.
Eight medical and allied health schools, including those at Harvard Medical School and Yale School of Nursing, participate in the program, the centerpiece of which is time spent by teams of medical students in the homes of families with neurodiverse members. “It’s transformational,” said Susan Feeney, DNP, NP-C, director of adult gerontology and family nurse practitioner programs at the graduate school of nursing at the University of Massachusetts, Worcester. “They spend a few hours at the homes of these families, have this interaction with them, and journal about their experiences.”
Dr. Feeney described as “transformational” the experience of the students after getting to know these families. “They all come back profoundly changed,” she told this news organization. “As a medical or health care professional, you meet people in an artificial environment of the clinic and hospital. Here, they become human, like you. It takes the stigma away.”
One area of medicine in which this is an exception is pediatrics, where interaction with children with IDD and their families is common – and close. “They’re going to be much more attuned to this,” Dr. Feeney said. “The problem is primary care or internal medicine. Once these children get into their mid and later 20s, and they need a practitioner to talk to about adult concerns.”
And with adulthood come other medical needs, as the physical demands of age fall no less heavily on individuals with IDDs than those without. For example: “Neurodiverse people get pregnant,” Dr. Bullock said. They also can get heart disease as they age; or require the care of a rheumatologist, a neurologist, an orthopedic surgeon, or any other medical specialty.
Generation gap
Fortunately, the next generation of physicians may be more open to this more inclusionary approach toward a widely misunderstood population.
Like Ms. Chin, Sarah Bdeir had experience with this population prior to beginning her training in medicine. She had volunteered at a school for people with IDD.
“It was one of the best experiences I’ve ever had,” Ms. Bdeir, now 23 and a first-year medical student at Wayne State University, Detroit, said. She found that the neurodiverse individuals she worked with had as many abilities as disabilities. “They are capable of learning, but they do it differently,” she said. “You have to adjust to the way they learn. And you have to step out of your own box.”
Ms. Bdeir also heard about Dr. Bullock’s work and is assisting her in a research project on how to better improve nutritional education for people with IDDs. And although she said it may take time for curriculum boards at medical schools to integrate this kind of training into their programs, she believes they will, in part because the rising cohort of medical students today have an eagerness to engage with and learn more about IDD patients.
As does Ms. Chin.
“When I talk to my peers about this, they’re very receptive,” Ms. Chin said. “They want to learn how to better support the IDD population. And they will learn. I believe in my generation of future doctors.”
A version of this article first appeared on Medscape.com.
As an undergraduate student at Northeastern University in Boston, Meghan Chin spent her summers working for a day program in Rhode Island. Her charges were adults with various forms of intellectual and developmental disabilities (IDD).
“I was very much a caretaker,” Ms. Chin, now 29, said. “It was everything from helping them get dressed in the morning to getting them to medical appointments.”
During one such visit Ms. Chin got a lesson about how health care looks from the viewpoint of someone with an IDD.
The patient was a woman in her 60s and she was having gastrointestinal issues; symptoms she could have articulated, if asked. “She was perfectly capable of telling a clinician where it hurt, how long she had experienced the problem, and what she had done or not done to alleviate it,” Ms. Chin said.
And of comprehending a response. But she was not given the opportunity.
“She would explain what was going on to the clinician,” Ms. Chin recalled. “And the clinician would turn to me and answer. It was this weird three-way conversation – as if she wasn’t even there in the room with us.”
Ms. Chin was incensed at the rude and disrespectful way the patient had been treated. But her charge didn’t seem upset or surprised. Just resigned. “Sadly, she had become used to this,” Ms. Chin said.
For the young aide, however, the experience was searing. “It didn’t seem right to me,” Ms. Chin said. “That’s why, when I went to medical school, I knew I wanted to do better for this population.”
Serendipity led her to Georgetown University, Washington, where she met Kim Bullock, MD, one of the country’s leading advocates for improved health care delivery to those with IDDs.
Dr. Bullock, an associate professor of family medicine, seeks to create better training and educational opportunities for medical students who will likely encounter patients with these disabilities in their practices.
When Dr. Bullock heard Ms. Chin’s story about the patient being ignored, she was not surprised.
“This is not an unusual or unique situation,” said Dr. Bullock, who is also director of Georgetown’s community health division and a faculty member of the university’s Center for Excellence for Developmental Disabilities. “In fact, it’s quite common and is part of what spurred my own interest in educating pre-med and medical students about effective communication techniques, particularly when addressing neurodiverse patients.”
More than 13% of Americans, or roughly 44 million people, have some form of disability, according to the National Institute on Disability at the University of New Hampshire, a figure that does not include those who are institutionalized. The Centers for Disease Control and Prevention estimates that 17% of children aged 3-17 years have a developmental disability.
Even so, many physicians feel ill-prepared to care for disabled patients. A survey of physicians, published in the journal Health Affairs, found that some lacked the resources and training to properly care for patients with disabilities, or that they struggled to coordinate care for such individuals. Some said they did not know which types of accessible equipment, like adjustable tables and chair scales, were needed or how to use them. And some said they actively try to avoid treating patients with disabilities.
Don’t assume
The first step at correcting the problem, Dr. Bullock said, is to not assume that all IDD patients are incapable of communicating. By talking not to the patient but to their caregiver or spouse or child, as the clinician did with Ms. Chin years ago, “we are taking away their agency, their autonomy to speak for and about themselves.”
Change involves altering physicians’ attitudes and assumptions toward this population, through education. But how?
“The medical school curriculum is tight as it is,” Dr. Bullock acknowledged. “There’s a lot of things students have to learn. People wonder: where we will add this?”
Her suggestion: Incorporate IDD all along the way, through programs or experiences that will enable medical students to see such patients “not as something separate, but as people that have special needs just as other populations have.”
Case in point: Operation House Call, a program in Massachusetts designed to support young health care professionals, by building “confidence, interest, and sensitivity” toward individuals with IDD.
Eight medical and allied health schools, including those at Harvard Medical School and Yale School of Nursing, participate in the program, the centerpiece of which is time spent by teams of medical students in the homes of families with neurodiverse members. “It’s transformational,” said Susan Feeney, DNP, NP-C, director of adult gerontology and family nurse practitioner programs at the graduate school of nursing at the University of Massachusetts, Worcester. “They spend a few hours at the homes of these families, have this interaction with them, and journal about their experiences.”
Dr. Feeney described as “transformational” the experience of the students after getting to know these families. “They all come back profoundly changed,” she told this news organization. “As a medical or health care professional, you meet people in an artificial environment of the clinic and hospital. Here, they become human, like you. It takes the stigma away.”
One area of medicine in which this is an exception is pediatrics, where interaction with children with IDD and their families is common – and close. “They’re going to be much more attuned to this,” Dr. Feeney said. “The problem is primary care or internal medicine. Once these children get into their mid and later 20s, and they need a practitioner to talk to about adult concerns.”
And with adulthood come other medical needs, as the physical demands of age fall no less heavily on individuals with IDDs than those without. For example: “Neurodiverse people get pregnant,” Dr. Bullock said. They also can get heart disease as they age; or require the care of a rheumatologist, a neurologist, an orthopedic surgeon, or any other medical specialty.
Generation gap
Fortunately, the next generation of physicians may be more open to this more inclusionary approach toward a widely misunderstood population.
Like Ms. Chin, Sarah Bdeir had experience with this population prior to beginning her training in medicine. She had volunteered at a school for people with IDD.
“It was one of the best experiences I’ve ever had,” Ms. Bdeir, now 23 and a first-year medical student at Wayne State University, Detroit, said. She found that the neurodiverse individuals she worked with had as many abilities as disabilities. “They are capable of learning, but they do it differently,” she said. “You have to adjust to the way they learn. And you have to step out of your own box.”
Ms. Bdeir also heard about Dr. Bullock’s work and is assisting her in a research project on how to better improve nutritional education for people with IDDs. And although she said it may take time for curriculum boards at medical schools to integrate this kind of training into their programs, she believes they will, in part because the rising cohort of medical students today have an eagerness to engage with and learn more about IDD patients.
As does Ms. Chin.
“When I talk to my peers about this, they’re very receptive,” Ms. Chin said. “They want to learn how to better support the IDD population. And they will learn. I believe in my generation of future doctors.”
A version of this article first appeared on Medscape.com.
As an undergraduate student at Northeastern University in Boston, Meghan Chin spent her summers working for a day program in Rhode Island. Her charges were adults with various forms of intellectual and developmental disabilities (IDD).
“I was very much a caretaker,” Ms. Chin, now 29, said. “It was everything from helping them get dressed in the morning to getting them to medical appointments.”
During one such visit Ms. Chin got a lesson about how health care looks from the viewpoint of someone with an IDD.
The patient was a woman in her 60s and she was having gastrointestinal issues; symptoms she could have articulated, if asked. “She was perfectly capable of telling a clinician where it hurt, how long she had experienced the problem, and what she had done or not done to alleviate it,” Ms. Chin said.
And of comprehending a response. But she was not given the opportunity.
“She would explain what was going on to the clinician,” Ms. Chin recalled. “And the clinician would turn to me and answer. It was this weird three-way conversation – as if she wasn’t even there in the room with us.”
Ms. Chin was incensed at the rude and disrespectful way the patient had been treated. But her charge didn’t seem upset or surprised. Just resigned. “Sadly, she had become used to this,” Ms. Chin said.
For the young aide, however, the experience was searing. “It didn’t seem right to me,” Ms. Chin said. “That’s why, when I went to medical school, I knew I wanted to do better for this population.”
Serendipity led her to Georgetown University, Washington, where she met Kim Bullock, MD, one of the country’s leading advocates for improved health care delivery to those with IDDs.
Dr. Bullock, an associate professor of family medicine, seeks to create better training and educational opportunities for medical students who will likely encounter patients with these disabilities in their practices.
When Dr. Bullock heard Ms. Chin’s story about the patient being ignored, she was not surprised.
“This is not an unusual or unique situation,” said Dr. Bullock, who is also director of Georgetown’s community health division and a faculty member of the university’s Center for Excellence for Developmental Disabilities. “In fact, it’s quite common and is part of what spurred my own interest in educating pre-med and medical students about effective communication techniques, particularly when addressing neurodiverse patients.”
More than 13% of Americans, or roughly 44 million people, have some form of disability, according to the National Institute on Disability at the University of New Hampshire, a figure that does not include those who are institutionalized. The Centers for Disease Control and Prevention estimates that 17% of children aged 3-17 years have a developmental disability.
Even so, many physicians feel ill-prepared to care for disabled patients. A survey of physicians, published in the journal Health Affairs, found that some lacked the resources and training to properly care for patients with disabilities, or that they struggled to coordinate care for such individuals. Some said they did not know which types of accessible equipment, like adjustable tables and chair scales, were needed or how to use them. And some said they actively try to avoid treating patients with disabilities.
Don’t assume
The first step at correcting the problem, Dr. Bullock said, is to not assume that all IDD patients are incapable of communicating. By talking not to the patient but to their caregiver or spouse or child, as the clinician did with Ms. Chin years ago, “we are taking away their agency, their autonomy to speak for and about themselves.”
Change involves altering physicians’ attitudes and assumptions toward this population, through education. But how?
“The medical school curriculum is tight as it is,” Dr. Bullock acknowledged. “There’s a lot of things students have to learn. People wonder: where we will add this?”
Her suggestion: Incorporate IDD all along the way, through programs or experiences that will enable medical students to see such patients “not as something separate, but as people that have special needs just as other populations have.”
Case in point: Operation House Call, a program in Massachusetts designed to support young health care professionals, by building “confidence, interest, and sensitivity” toward individuals with IDD.
Eight medical and allied health schools, including those at Harvard Medical School and Yale School of Nursing, participate in the program, the centerpiece of which is time spent by teams of medical students in the homes of families with neurodiverse members. “It’s transformational,” said Susan Feeney, DNP, NP-C, director of adult gerontology and family nurse practitioner programs at the graduate school of nursing at the University of Massachusetts, Worcester. “They spend a few hours at the homes of these families, have this interaction with them, and journal about their experiences.”
Dr. Feeney described as “transformational” the experience of the students after getting to know these families. “They all come back profoundly changed,” she told this news organization. “As a medical or health care professional, you meet people in an artificial environment of the clinic and hospital. Here, they become human, like you. It takes the stigma away.”
One area of medicine in which this is an exception is pediatrics, where interaction with children with IDD and their families is common – and close. “They’re going to be much more attuned to this,” Dr. Feeney said. “The problem is primary care or internal medicine. Once these children get into their mid and later 20s, and they need a practitioner to talk to about adult concerns.”
And with adulthood come other medical needs, as the physical demands of age fall no less heavily on individuals with IDDs than those without. For example: “Neurodiverse people get pregnant,” Dr. Bullock said. They also can get heart disease as they age; or require the care of a rheumatologist, a neurologist, an orthopedic surgeon, or any other medical specialty.
Generation gap
Fortunately, the next generation of physicians may be more open to this more inclusionary approach toward a widely misunderstood population.
Like Ms. Chin, Sarah Bdeir had experience with this population prior to beginning her training in medicine. She had volunteered at a school for people with IDD.
“It was one of the best experiences I’ve ever had,” Ms. Bdeir, now 23 and a first-year medical student at Wayne State University, Detroit, said. She found that the neurodiverse individuals she worked with had as many abilities as disabilities. “They are capable of learning, but they do it differently,” she said. “You have to adjust to the way they learn. And you have to step out of your own box.”
Ms. Bdeir also heard about Dr. Bullock’s work and is assisting her in a research project on how to better improve nutritional education for people with IDDs. And although she said it may take time for curriculum boards at medical schools to integrate this kind of training into their programs, she believes they will, in part because the rising cohort of medical students today have an eagerness to engage with and learn more about IDD patients.
As does Ms. Chin.
“When I talk to my peers about this, they’re very receptive,” Ms. Chin said. “They want to learn how to better support the IDD population. And they will learn. I believe in my generation of future doctors.”
A version of this article first appeared on Medscape.com.
Understanding of capillary malformation characteristics continue to evolve
INDIANAPOLIS – The way Maria C. Garzon, MD, sees it,
“The challenge is, we also use that term to describe a diagnosis,” Dr. Garzon, professor of dermatology and pediatrics at Columbia University, New York, said at the annual meeting of the Society for Pediatric Dermatology. “We have imperfect terminology. We use many different terms like capillary nevi and vascular stain. Instead of port wine stain, we now use the term port wine birthmark, and old terms like nevus flammeus are still used. This leads to diagnostic confusion, and it’s a barrier to developing care guidelines.”
Some capillary malformations, she noted, are benign and fade away while others can cause disfigurement or herald significant medical issues.
Histologically, she continued, not all capillary malformations are composed of capillaries. “Some are composed of postcapillary venules,” she said. “There are also mixed type capillary malformations that include lymphatic tissue, and the capillary malformation of capillary malformation-arteriovenous malformation (CM-AVM) syndrome shares histologic features of evolving AVMs as opposed to classic port wine birthmarks.”
The most recent International Society for the Study of Vascular Anomalies Classification of Vascular Anomalies was published in 2018 and is currently being updated. Other proposed clinical classifications have been published, including one that is diagnosis-specific and includes 20 different types of capillary malformations (J Eur Acad Dermatol Venereol. 2015 29[12]:2295-305, Pediatr Dermatol. 2016;33[6]:570-84).
“There are also syndromic classifications. Another question relates to the role of genomics: Are we ready for a classification that’s based purely on genetic variants, or do we need to incorporate it into existing classifications?” Dr. Garzon said. “Novel testing technologies using cell-free DNA and digital droplet PCR may be used in the future to establish diagnoses.” Genetic variants are found within capillary malformations, and they tend to be associated with three major pathways: the RAS-MAPK/ERK pathway, the PI3K/Akt/mTOR pathway, and the G protein pathway.
The type of capillary malformation that dermatologists and pediatricians most commonly see is nevus simplex, which occurs in 20%-82% of neonates. Other terms used include angel’s kiss, stork bite, salmon patch, nevus flammeus simplex, fading vascular stain, medial telangiectatic nevus, and butterfly mark. “It’s important to differentiate this from a port wine birthmark,” Dr. Garzon said. “This can be challenging when the birthmark is a darker red color. I have cared for patients who were initially thought to have nevus simplex and later found to have Sturge-Weber syndrome.”
Typical locations of nevus simplex include the central forehead/glabella, eyelids, the nape of the neck, scalp (parietal and occipital), nose, lip area (including philtrum), and the back (lumbosacral area and upper back). Most lesions fade/disappear without treatment (J Am Acad Dermatol. 2020;63[5]:805-14). Rare genetic syndromes associated with exaggerated nevus simplex complex include macrocephaly-capillary malformation syndrome and Beckwith-Wiedemann syndrome, “which tells us that this is a heterogeneous group of patients,” she said.
Dr. Garzon added that it’s “incredibly common” to see an eczema flare occurring within a nevus simplex on the nape of the neck. These patients will have a patch of atopic dermatitis that doesn’t get better. “Beneath it is their nevus simplex,” she said. “Remind parents that even after treating the eczema, the pink patch is not going to go away” (Pediatr Rep. 2021;13[1]:131-4).
Meanwhile, the classic port wine birthmark is usually congenital, uniform, and darker red in color. It darkens with maturity and the pattern will correlate with embryonic vasculature. “I am very wary of acquired port wine lesions,” she added. “It’s been described with trauma-related lesions, but early morphea can also mimic a port wine birthmark. You will see this if you’re practicing pediatric dermatology.”
Nearly a decade ago researchers established a link between port wine birthmarks and genetic variants in the GNAQ gene. “We see this in GNA11 as well,” Dr. Garzon said. “These changes are found in isolated port wine stains, and in Sturge-Weber syndrome. We now know that GNAQ drives the formation of large blood vessels through angiopoietin-2,” she noted (Arterioscler Throm Vasc Biol. 2022;42[1]:e27-43).
In general, studies that have examined genotype-phenotype correlations have demonstrated that the classic port wine birthmark is associated with GNAQ while GNA11 variants can be associated with a more reticulated pattern. “But this is not as clearcut as it seems,” she said. Investigators of a recent study showed an association between hypertension and renal anomalies in patients with skin capillary malformations and mosaic GNAQ or GNA11 variants. “This is a new finding,” she said. “Investigators are working to understand this association.”
Port wine birthmarks with the highest risk of Sturge-Weber syndrome include those that involve the forehead, upper eyelid, the midline frontonasal area, the hemifacial area, and median sites. “Patients who have this should be evaluated at birth,” Dr. Garzon said. “You should not delay for 2 months. They should be evaluated by ophthalmology and neurology early.”
The other morphologies commonly seen are “geographic” well-demarcated capillary malformations, which are dark in color. These lesions can be seen in conditions that are associated with genetic variants in PIK3CA (PROS) and include classic Klippel-Trenaunay syndrome, CLOVES (congenital lipomatous overgrowth, vascular malformations, epidermal nevi, scoliosis/skeletal and spinal) syndrome, and CLAPO (capillary malformation of the lower lip, lymphatic malformation of the face and neck, asymmetry of the face and limbs, and partial or generalized overgrowth) syndrome.
“Reticulated stains are much more heterogeneous,” Dr. Garzon said. “They can be localized or widespread. When you see a patient with a widespread reticulated capillary malformation, think about diffuse capillary malformation with overgrowth (DCMO). This condition is clinically and genetically heterogenous with the affected tissue of some patients showing variants in GNA11 while others have variants in PIK3CA. Therefore, a thorough examination at presentation and long-term follow-up is very important.”
Dr. Garzon disclosed that she is a member of the executive board for the International Society for the Study of Vascular Anomalies.
INDIANAPOLIS – The way Maria C. Garzon, MD, sees it,
“The challenge is, we also use that term to describe a diagnosis,” Dr. Garzon, professor of dermatology and pediatrics at Columbia University, New York, said at the annual meeting of the Society for Pediatric Dermatology. “We have imperfect terminology. We use many different terms like capillary nevi and vascular stain. Instead of port wine stain, we now use the term port wine birthmark, and old terms like nevus flammeus are still used. This leads to diagnostic confusion, and it’s a barrier to developing care guidelines.”
Some capillary malformations, she noted, are benign and fade away while others can cause disfigurement or herald significant medical issues.
Histologically, she continued, not all capillary malformations are composed of capillaries. “Some are composed of postcapillary venules,” she said. “There are also mixed type capillary malformations that include lymphatic tissue, and the capillary malformation of capillary malformation-arteriovenous malformation (CM-AVM) syndrome shares histologic features of evolving AVMs as opposed to classic port wine birthmarks.”
The most recent International Society for the Study of Vascular Anomalies Classification of Vascular Anomalies was published in 2018 and is currently being updated. Other proposed clinical classifications have been published, including one that is diagnosis-specific and includes 20 different types of capillary malformations (J Eur Acad Dermatol Venereol. 2015 29[12]:2295-305, Pediatr Dermatol. 2016;33[6]:570-84).
“There are also syndromic classifications. Another question relates to the role of genomics: Are we ready for a classification that’s based purely on genetic variants, or do we need to incorporate it into existing classifications?” Dr. Garzon said. “Novel testing technologies using cell-free DNA and digital droplet PCR may be used in the future to establish diagnoses.” Genetic variants are found within capillary malformations, and they tend to be associated with three major pathways: the RAS-MAPK/ERK pathway, the PI3K/Akt/mTOR pathway, and the G protein pathway.
The type of capillary malformation that dermatologists and pediatricians most commonly see is nevus simplex, which occurs in 20%-82% of neonates. Other terms used include angel’s kiss, stork bite, salmon patch, nevus flammeus simplex, fading vascular stain, medial telangiectatic nevus, and butterfly mark. “It’s important to differentiate this from a port wine birthmark,” Dr. Garzon said. “This can be challenging when the birthmark is a darker red color. I have cared for patients who were initially thought to have nevus simplex and later found to have Sturge-Weber syndrome.”
Typical locations of nevus simplex include the central forehead/glabella, eyelids, the nape of the neck, scalp (parietal and occipital), nose, lip area (including philtrum), and the back (lumbosacral area and upper back). Most lesions fade/disappear without treatment (J Am Acad Dermatol. 2020;63[5]:805-14). Rare genetic syndromes associated with exaggerated nevus simplex complex include macrocephaly-capillary malformation syndrome and Beckwith-Wiedemann syndrome, “which tells us that this is a heterogeneous group of patients,” she said.
Dr. Garzon added that it’s “incredibly common” to see an eczema flare occurring within a nevus simplex on the nape of the neck. These patients will have a patch of atopic dermatitis that doesn’t get better. “Beneath it is their nevus simplex,” she said. “Remind parents that even after treating the eczema, the pink patch is not going to go away” (Pediatr Rep. 2021;13[1]:131-4).
Meanwhile, the classic port wine birthmark is usually congenital, uniform, and darker red in color. It darkens with maturity and the pattern will correlate with embryonic vasculature. “I am very wary of acquired port wine lesions,” she added. “It’s been described with trauma-related lesions, but early morphea can also mimic a port wine birthmark. You will see this if you’re practicing pediatric dermatology.”
Nearly a decade ago researchers established a link between port wine birthmarks and genetic variants in the GNAQ gene. “We see this in GNA11 as well,” Dr. Garzon said. “These changes are found in isolated port wine stains, and in Sturge-Weber syndrome. We now know that GNAQ drives the formation of large blood vessels through angiopoietin-2,” she noted (Arterioscler Throm Vasc Biol. 2022;42[1]:e27-43).
In general, studies that have examined genotype-phenotype correlations have demonstrated that the classic port wine birthmark is associated with GNAQ while GNA11 variants can be associated with a more reticulated pattern. “But this is not as clearcut as it seems,” she said. Investigators of a recent study showed an association between hypertension and renal anomalies in patients with skin capillary malformations and mosaic GNAQ or GNA11 variants. “This is a new finding,” she said. “Investigators are working to understand this association.”
Port wine birthmarks with the highest risk of Sturge-Weber syndrome include those that involve the forehead, upper eyelid, the midline frontonasal area, the hemifacial area, and median sites. “Patients who have this should be evaluated at birth,” Dr. Garzon said. “You should not delay for 2 months. They should be evaluated by ophthalmology and neurology early.”
The other morphologies commonly seen are “geographic” well-demarcated capillary malformations, which are dark in color. These lesions can be seen in conditions that are associated with genetic variants in PIK3CA (PROS) and include classic Klippel-Trenaunay syndrome, CLOVES (congenital lipomatous overgrowth, vascular malformations, epidermal nevi, scoliosis/skeletal and spinal) syndrome, and CLAPO (capillary malformation of the lower lip, lymphatic malformation of the face and neck, asymmetry of the face and limbs, and partial or generalized overgrowth) syndrome.
“Reticulated stains are much more heterogeneous,” Dr. Garzon said. “They can be localized or widespread. When you see a patient with a widespread reticulated capillary malformation, think about diffuse capillary malformation with overgrowth (DCMO). This condition is clinically and genetically heterogenous with the affected tissue of some patients showing variants in GNA11 while others have variants in PIK3CA. Therefore, a thorough examination at presentation and long-term follow-up is very important.”
Dr. Garzon disclosed that she is a member of the executive board for the International Society for the Study of Vascular Anomalies.
INDIANAPOLIS – The way Maria C. Garzon, MD, sees it,
“The challenge is, we also use that term to describe a diagnosis,” Dr. Garzon, professor of dermatology and pediatrics at Columbia University, New York, said at the annual meeting of the Society for Pediatric Dermatology. “We have imperfect terminology. We use many different terms like capillary nevi and vascular stain. Instead of port wine stain, we now use the term port wine birthmark, and old terms like nevus flammeus are still used. This leads to diagnostic confusion, and it’s a barrier to developing care guidelines.”
Some capillary malformations, she noted, are benign and fade away while others can cause disfigurement or herald significant medical issues.
Histologically, she continued, not all capillary malformations are composed of capillaries. “Some are composed of postcapillary venules,” she said. “There are also mixed type capillary malformations that include lymphatic tissue, and the capillary malformation of capillary malformation-arteriovenous malformation (CM-AVM) syndrome shares histologic features of evolving AVMs as opposed to classic port wine birthmarks.”
The most recent International Society for the Study of Vascular Anomalies Classification of Vascular Anomalies was published in 2018 and is currently being updated. Other proposed clinical classifications have been published, including one that is diagnosis-specific and includes 20 different types of capillary malformations (J Eur Acad Dermatol Venereol. 2015 29[12]:2295-305, Pediatr Dermatol. 2016;33[6]:570-84).
“There are also syndromic classifications. Another question relates to the role of genomics: Are we ready for a classification that’s based purely on genetic variants, or do we need to incorporate it into existing classifications?” Dr. Garzon said. “Novel testing technologies using cell-free DNA and digital droplet PCR may be used in the future to establish diagnoses.” Genetic variants are found within capillary malformations, and they tend to be associated with three major pathways: the RAS-MAPK/ERK pathway, the PI3K/Akt/mTOR pathway, and the G protein pathway.
The type of capillary malformation that dermatologists and pediatricians most commonly see is nevus simplex, which occurs in 20%-82% of neonates. Other terms used include angel’s kiss, stork bite, salmon patch, nevus flammeus simplex, fading vascular stain, medial telangiectatic nevus, and butterfly mark. “It’s important to differentiate this from a port wine birthmark,” Dr. Garzon said. “This can be challenging when the birthmark is a darker red color. I have cared for patients who were initially thought to have nevus simplex and later found to have Sturge-Weber syndrome.”
Typical locations of nevus simplex include the central forehead/glabella, eyelids, the nape of the neck, scalp (parietal and occipital), nose, lip area (including philtrum), and the back (lumbosacral area and upper back). Most lesions fade/disappear without treatment (J Am Acad Dermatol. 2020;63[5]:805-14). Rare genetic syndromes associated with exaggerated nevus simplex complex include macrocephaly-capillary malformation syndrome and Beckwith-Wiedemann syndrome, “which tells us that this is a heterogeneous group of patients,” she said.
Dr. Garzon added that it’s “incredibly common” to see an eczema flare occurring within a nevus simplex on the nape of the neck. These patients will have a patch of atopic dermatitis that doesn’t get better. “Beneath it is their nevus simplex,” she said. “Remind parents that even after treating the eczema, the pink patch is not going to go away” (Pediatr Rep. 2021;13[1]:131-4).
Meanwhile, the classic port wine birthmark is usually congenital, uniform, and darker red in color. It darkens with maturity and the pattern will correlate with embryonic vasculature. “I am very wary of acquired port wine lesions,” she added. “It’s been described with trauma-related lesions, but early morphea can also mimic a port wine birthmark. You will see this if you’re practicing pediatric dermatology.”
Nearly a decade ago researchers established a link between port wine birthmarks and genetic variants in the GNAQ gene. “We see this in GNA11 as well,” Dr. Garzon said. “These changes are found in isolated port wine stains, and in Sturge-Weber syndrome. We now know that GNAQ drives the formation of large blood vessels through angiopoietin-2,” she noted (Arterioscler Throm Vasc Biol. 2022;42[1]:e27-43).
In general, studies that have examined genotype-phenotype correlations have demonstrated that the classic port wine birthmark is associated with GNAQ while GNA11 variants can be associated with a more reticulated pattern. “But this is not as clearcut as it seems,” she said. Investigators of a recent study showed an association between hypertension and renal anomalies in patients with skin capillary malformations and mosaic GNAQ or GNA11 variants. “This is a new finding,” she said. “Investigators are working to understand this association.”
Port wine birthmarks with the highest risk of Sturge-Weber syndrome include those that involve the forehead, upper eyelid, the midline frontonasal area, the hemifacial area, and median sites. “Patients who have this should be evaluated at birth,” Dr. Garzon said. “You should not delay for 2 months. They should be evaluated by ophthalmology and neurology early.”
The other morphologies commonly seen are “geographic” well-demarcated capillary malformations, which are dark in color. These lesions can be seen in conditions that are associated with genetic variants in PIK3CA (PROS) and include classic Klippel-Trenaunay syndrome, CLOVES (congenital lipomatous overgrowth, vascular malformations, epidermal nevi, scoliosis/skeletal and spinal) syndrome, and CLAPO (capillary malformation of the lower lip, lymphatic malformation of the face and neck, asymmetry of the face and limbs, and partial or generalized overgrowth) syndrome.
“Reticulated stains are much more heterogeneous,” Dr. Garzon said. “They can be localized or widespread. When you see a patient with a widespread reticulated capillary malformation, think about diffuse capillary malformation with overgrowth (DCMO). This condition is clinically and genetically heterogenous with the affected tissue of some patients showing variants in GNA11 while others have variants in PIK3CA. Therefore, a thorough examination at presentation and long-term follow-up is very important.”
Dr. Garzon disclosed that she is a member of the executive board for the International Society for the Study of Vascular Anomalies.
AT SPD 2022
I’m a physician battling long COVID. I can assure you it’s real
One in 5. It almost seems unimaginable that this is the real number of people who are struggling with long COVID, especially considering how many people in the United States have had COVID-19 at this point (more than 96 million).
Even more unimaginable at this time is that it’s happening to me. I’ve experienced not only the disabling effects of long COVID, but I’ve also seen, firsthand, the frustration of navigating diagnosis and treatment. It’s given me a taste of what millions of other patients are going through.
Vaxxed, masked, and (too) relaxed
I caught COVID-19 (probably Omicron BA.5) that presented as sniffles, making me think it was probably just allergies. However, my resting heart rate was up on my Garmin watch, so of course I got tested and was positive.
With my symptoms virtually nonexistent, it seemed, at the time, merely an inconvenience, because I was forced to isolate away from family and friends, who all stayed negative.
But 2 weeks later, I began to have urticaria – hives – after physical exertion. Did that mean my mast cells were angry? There’s some evidence these immune cells become overactivated in some patients with COVID. Next, I began to experience lightheadedness and the rapid heartbeat of tachycardia. The tachycardia was especially bad any time I physically exerted myself, including on a walk. Imagine me – a lover of all bargain shopping – cutting short a trip to the outlet mall on a particularly bad day when my heart rate was 140 after taking just a few steps. This was orthostatic intolerance.
Then came the severe worsening of my migraines – which are often vestibular, making me nauseated and dizzy on top of the throbbing.
I was of course familiar with these symptoms, as professor and chair of the department of rehabilitation medicine at the Joe R. and Teresa Lozano Long School of Medicine at University of Texas Health Science Center, San Antonio. I developed a post-COVID recovery clinic to help patients.
So I knew about postexertional malaise (PEM) and postexertional symptom exacerbation (PESE), but I was now experiencing these distressing symptoms firsthand.
Clinicians really need to look for this cardinal sign of long COVID as well as evidence of myalgic encephalomyelitis or chronic fatigue syndrome (ME/CFS). ME/CFS is marked by exacerbation of fatigue or symptoms after an activity that could previously be done without these aftereffects. In my case, as an All-American Masters miler with several marathons under my belt, running 5 miles is a walk in the park. But now, I pay for those 5 miles for the rest of the day on the couch or with palpitations, dizziness, and fatigue the following day. Busy clinic day full of procedures? I would have to be sitting by the end of it. Bed by 9 PM was not always early enough.
Becoming a statistic
Here I am, one of the leading experts in the country on caring for people with long COVID, featured in the national news and having testified in front of Congress, and now I am part of that lived experience. Me – a healthy athlete, with no comorbidities, a normal BMI, vaccinated and boosted, and after an almost asymptomatic bout of COVID-19, a victim to long COVID.
You just never know how your body is going to react. Neuroinflammation occurred in studies with mice with mild respiratory COVID and could be happening to me. I did not want a chronic immune-mediated vasculopathy.
So, I did what any other hyperaware physician-researcher would do. I enrolled in the RECOVER trial – a study my own institution is taking part in and one that I recommend to my own patients.
I also decided that I need to access care and not just ignore my symptoms or try to treat them myself.
That’s when things got difficult. There was a wait of at least a month to see my primary care provider – but I was able to use my privileged position as a physician to get in sooner.
My provider said that she had limited knowledge of long COVID, and she hesitated to order some of the tests and treatments that I recommended because they were not yet considered standard of care. I can understand the hesitation. It is engrained in medical education to follow evidence based on the highest-quality research studies. We are slowly learning more about long COVID, but acknowledging the learning curve offers little to patients who need help now.
This has made me realize that we cannot wait on an evidence-based approach – which can take decades to develop – while people are suffering. And it’s important that everyone on the front line learn about some of the manifestations and disease management of long COVID.
I left this first physician visit feeling more defeated than anything and decided to try to push through. That, I quickly realized, was not the right thing to do.
So again, after a couple of significant crashes and days of severe migraines, I phoned a friend: Ratna Bhavaraju-Sanka, MD, the amazing neurologist who treats patients with long COVID alongside me. She squeezed me in on a non-clinic day. Again, I had the privilege to see a specialist most people wait half a year to see. I was diagnosed with both autonomic dysfunction and intractable migraine.
She ordered some intravenous fluids and IV magnesium that would probably help both. But then another obstacle arose. My institution’s infusion center is focused on patients with cancer, and I was unable to schedule treatments there.
Luckily, I knew about the concierge mobile IV hydration therapy companies that come to your house – mostly offering a hangover treatment service. And I am thankful that I had the health literacy and financial ability to pay for some fluids at home.
On another particularly bad day, I phoned other friends – higher-ups at the hospital – who expedited a slot at the hospital infusion center and approval for the IV magnesium.
Thanks to my access, knowledge, and other privileges, I got fairly quick if imperfect care, enrolled in a research trial, and received medications. I knew to pace myself. The vast majority of others with long COVID lack these advantages.
The patient with long COVID
Things I have learned that others can learn, too:
- Acknowledge and recognize that long COVID is a disease that is affecting 1 in 5 Americans who catch COVID. Many look completely “normal on the outside.” Please listen to your patients.
- Autonomic dysfunction is a common manifestation of long COVID. A 10-minute stand test goes a long way in diagnosing this condition, from the American Academy of Physical Medicine and Rehabilitation. It is not just anxiety.
- “That’s only in research” is dismissive and harmful. Think outside the box. Follow guidelines. Consider encouraging patients to sign up for trials.
- Screen for PEM/PESE and teach your patients to pace themselves, because pushing through it or doing graded exercises will be harmful.
- We need to train more physicians to treat postacute sequelae of SARS-CoV-2 infection () and other postinfectious conditions, such as ME/CFS.
If long COVID is hard for physicians to understand and deal with, imagine how difficult it is for patients with no expertise in this area.
It is exponentially harder for those with fewer resources, time, and health literacy. My lived experience with long COVID has shown me that being a patient is never easy. You put your body and fate into the hands of trusted professionals and expect validation and assistance, not gaslighting or gatekeeping.
Along with millions of others, I am tired of waiting.
Dr. Gutierrez is Professor and Distinguished Chair, department of rehabilitation medicine, University of Texas Health Science Center at San Antonio. She reported receiving honoraria for lecturing on long COVID and receiving a research grant from Co-PI for the NIH RECOVER trial.
A version of this article first appeared on Medscape.com.
One in 5. It almost seems unimaginable that this is the real number of people who are struggling with long COVID, especially considering how many people in the United States have had COVID-19 at this point (more than 96 million).
Even more unimaginable at this time is that it’s happening to me. I’ve experienced not only the disabling effects of long COVID, but I’ve also seen, firsthand, the frustration of navigating diagnosis and treatment. It’s given me a taste of what millions of other patients are going through.
Vaxxed, masked, and (too) relaxed
I caught COVID-19 (probably Omicron BA.5) that presented as sniffles, making me think it was probably just allergies. However, my resting heart rate was up on my Garmin watch, so of course I got tested and was positive.
With my symptoms virtually nonexistent, it seemed, at the time, merely an inconvenience, because I was forced to isolate away from family and friends, who all stayed negative.
But 2 weeks later, I began to have urticaria – hives – after physical exertion. Did that mean my mast cells were angry? There’s some evidence these immune cells become overactivated in some patients with COVID. Next, I began to experience lightheadedness and the rapid heartbeat of tachycardia. The tachycardia was especially bad any time I physically exerted myself, including on a walk. Imagine me – a lover of all bargain shopping – cutting short a trip to the outlet mall on a particularly bad day when my heart rate was 140 after taking just a few steps. This was orthostatic intolerance.
Then came the severe worsening of my migraines – which are often vestibular, making me nauseated and dizzy on top of the throbbing.
I was of course familiar with these symptoms, as professor and chair of the department of rehabilitation medicine at the Joe R. and Teresa Lozano Long School of Medicine at University of Texas Health Science Center, San Antonio. I developed a post-COVID recovery clinic to help patients.
So I knew about postexertional malaise (PEM) and postexertional symptom exacerbation (PESE), but I was now experiencing these distressing symptoms firsthand.
Clinicians really need to look for this cardinal sign of long COVID as well as evidence of myalgic encephalomyelitis or chronic fatigue syndrome (ME/CFS). ME/CFS is marked by exacerbation of fatigue or symptoms after an activity that could previously be done without these aftereffects. In my case, as an All-American Masters miler with several marathons under my belt, running 5 miles is a walk in the park. But now, I pay for those 5 miles for the rest of the day on the couch or with palpitations, dizziness, and fatigue the following day. Busy clinic day full of procedures? I would have to be sitting by the end of it. Bed by 9 PM was not always early enough.
Becoming a statistic
Here I am, one of the leading experts in the country on caring for people with long COVID, featured in the national news and having testified in front of Congress, and now I am part of that lived experience. Me – a healthy athlete, with no comorbidities, a normal BMI, vaccinated and boosted, and after an almost asymptomatic bout of COVID-19, a victim to long COVID.
You just never know how your body is going to react. Neuroinflammation occurred in studies with mice with mild respiratory COVID and could be happening to me. I did not want a chronic immune-mediated vasculopathy.
So, I did what any other hyperaware physician-researcher would do. I enrolled in the RECOVER trial – a study my own institution is taking part in and one that I recommend to my own patients.
I also decided that I need to access care and not just ignore my symptoms or try to treat them myself.
That’s when things got difficult. There was a wait of at least a month to see my primary care provider – but I was able to use my privileged position as a physician to get in sooner.
My provider said that she had limited knowledge of long COVID, and she hesitated to order some of the tests and treatments that I recommended because they were not yet considered standard of care. I can understand the hesitation. It is engrained in medical education to follow evidence based on the highest-quality research studies. We are slowly learning more about long COVID, but acknowledging the learning curve offers little to patients who need help now.
This has made me realize that we cannot wait on an evidence-based approach – which can take decades to develop – while people are suffering. And it’s important that everyone on the front line learn about some of the manifestations and disease management of long COVID.
I left this first physician visit feeling more defeated than anything and decided to try to push through. That, I quickly realized, was not the right thing to do.
So again, after a couple of significant crashes and days of severe migraines, I phoned a friend: Ratna Bhavaraju-Sanka, MD, the amazing neurologist who treats patients with long COVID alongside me. She squeezed me in on a non-clinic day. Again, I had the privilege to see a specialist most people wait half a year to see. I was diagnosed with both autonomic dysfunction and intractable migraine.
She ordered some intravenous fluids and IV magnesium that would probably help both. But then another obstacle arose. My institution’s infusion center is focused on patients with cancer, and I was unable to schedule treatments there.
Luckily, I knew about the concierge mobile IV hydration therapy companies that come to your house – mostly offering a hangover treatment service. And I am thankful that I had the health literacy and financial ability to pay for some fluids at home.
On another particularly bad day, I phoned other friends – higher-ups at the hospital – who expedited a slot at the hospital infusion center and approval for the IV magnesium.
Thanks to my access, knowledge, and other privileges, I got fairly quick if imperfect care, enrolled in a research trial, and received medications. I knew to pace myself. The vast majority of others with long COVID lack these advantages.
The patient with long COVID
Things I have learned that others can learn, too:
- Acknowledge and recognize that long COVID is a disease that is affecting 1 in 5 Americans who catch COVID. Many look completely “normal on the outside.” Please listen to your patients.
- Autonomic dysfunction is a common manifestation of long COVID. A 10-minute stand test goes a long way in diagnosing this condition, from the American Academy of Physical Medicine and Rehabilitation. It is not just anxiety.
- “That’s only in research” is dismissive and harmful. Think outside the box. Follow guidelines. Consider encouraging patients to sign up for trials.
- Screen for PEM/PESE and teach your patients to pace themselves, because pushing through it or doing graded exercises will be harmful.
- We need to train more physicians to treat postacute sequelae of SARS-CoV-2 infection () and other postinfectious conditions, such as ME/CFS.
If long COVID is hard for physicians to understand and deal with, imagine how difficult it is for patients with no expertise in this area.
It is exponentially harder for those with fewer resources, time, and health literacy. My lived experience with long COVID has shown me that being a patient is never easy. You put your body and fate into the hands of trusted professionals and expect validation and assistance, not gaslighting or gatekeeping.
Along with millions of others, I am tired of waiting.
Dr. Gutierrez is Professor and Distinguished Chair, department of rehabilitation medicine, University of Texas Health Science Center at San Antonio. She reported receiving honoraria for lecturing on long COVID and receiving a research grant from Co-PI for the NIH RECOVER trial.
A version of this article first appeared on Medscape.com.
One in 5. It almost seems unimaginable that this is the real number of people who are struggling with long COVID, especially considering how many people in the United States have had COVID-19 at this point (more than 96 million).
Even more unimaginable at this time is that it’s happening to me. I’ve experienced not only the disabling effects of long COVID, but I’ve also seen, firsthand, the frustration of navigating diagnosis and treatment. It’s given me a taste of what millions of other patients are going through.
Vaxxed, masked, and (too) relaxed
I caught COVID-19 (probably Omicron BA.5) that presented as sniffles, making me think it was probably just allergies. However, my resting heart rate was up on my Garmin watch, so of course I got tested and was positive.
With my symptoms virtually nonexistent, it seemed, at the time, merely an inconvenience, because I was forced to isolate away from family and friends, who all stayed negative.
But 2 weeks later, I began to have urticaria – hives – after physical exertion. Did that mean my mast cells were angry? There’s some evidence these immune cells become overactivated in some patients with COVID. Next, I began to experience lightheadedness and the rapid heartbeat of tachycardia. The tachycardia was especially bad any time I physically exerted myself, including on a walk. Imagine me – a lover of all bargain shopping – cutting short a trip to the outlet mall on a particularly bad day when my heart rate was 140 after taking just a few steps. This was orthostatic intolerance.
Then came the severe worsening of my migraines – which are often vestibular, making me nauseated and dizzy on top of the throbbing.
I was of course familiar with these symptoms, as professor and chair of the department of rehabilitation medicine at the Joe R. and Teresa Lozano Long School of Medicine at University of Texas Health Science Center, San Antonio. I developed a post-COVID recovery clinic to help patients.
So I knew about postexertional malaise (PEM) and postexertional symptom exacerbation (PESE), but I was now experiencing these distressing symptoms firsthand.
Clinicians really need to look for this cardinal sign of long COVID as well as evidence of myalgic encephalomyelitis or chronic fatigue syndrome (ME/CFS). ME/CFS is marked by exacerbation of fatigue or symptoms after an activity that could previously be done without these aftereffects. In my case, as an All-American Masters miler with several marathons under my belt, running 5 miles is a walk in the park. But now, I pay for those 5 miles for the rest of the day on the couch or with palpitations, dizziness, and fatigue the following day. Busy clinic day full of procedures? I would have to be sitting by the end of it. Bed by 9 PM was not always early enough.
Becoming a statistic
Here I am, one of the leading experts in the country on caring for people with long COVID, featured in the national news and having testified in front of Congress, and now I am part of that lived experience. Me – a healthy athlete, with no comorbidities, a normal BMI, vaccinated and boosted, and after an almost asymptomatic bout of COVID-19, a victim to long COVID.
You just never know how your body is going to react. Neuroinflammation occurred in studies with mice with mild respiratory COVID and could be happening to me. I did not want a chronic immune-mediated vasculopathy.
So, I did what any other hyperaware physician-researcher would do. I enrolled in the RECOVER trial – a study my own institution is taking part in and one that I recommend to my own patients.
I also decided that I need to access care and not just ignore my symptoms or try to treat them myself.
That’s when things got difficult. There was a wait of at least a month to see my primary care provider – but I was able to use my privileged position as a physician to get in sooner.
My provider said that she had limited knowledge of long COVID, and she hesitated to order some of the tests and treatments that I recommended because they were not yet considered standard of care. I can understand the hesitation. It is engrained in medical education to follow evidence based on the highest-quality research studies. We are slowly learning more about long COVID, but acknowledging the learning curve offers little to patients who need help now.
This has made me realize that we cannot wait on an evidence-based approach – which can take decades to develop – while people are suffering. And it’s important that everyone on the front line learn about some of the manifestations and disease management of long COVID.
I left this first physician visit feeling more defeated than anything and decided to try to push through. That, I quickly realized, was not the right thing to do.
So again, after a couple of significant crashes and days of severe migraines, I phoned a friend: Ratna Bhavaraju-Sanka, MD, the amazing neurologist who treats patients with long COVID alongside me. She squeezed me in on a non-clinic day. Again, I had the privilege to see a specialist most people wait half a year to see. I was diagnosed with both autonomic dysfunction and intractable migraine.
She ordered some intravenous fluids and IV magnesium that would probably help both. But then another obstacle arose. My institution’s infusion center is focused on patients with cancer, and I was unable to schedule treatments there.
Luckily, I knew about the concierge mobile IV hydration therapy companies that come to your house – mostly offering a hangover treatment service. And I am thankful that I had the health literacy and financial ability to pay for some fluids at home.
On another particularly bad day, I phoned other friends – higher-ups at the hospital – who expedited a slot at the hospital infusion center and approval for the IV magnesium.
Thanks to my access, knowledge, and other privileges, I got fairly quick if imperfect care, enrolled in a research trial, and received medications. I knew to pace myself. The vast majority of others with long COVID lack these advantages.
The patient with long COVID
Things I have learned that others can learn, too:
- Acknowledge and recognize that long COVID is a disease that is affecting 1 in 5 Americans who catch COVID. Many look completely “normal on the outside.” Please listen to your patients.
- Autonomic dysfunction is a common manifestation of long COVID. A 10-minute stand test goes a long way in diagnosing this condition, from the American Academy of Physical Medicine and Rehabilitation. It is not just anxiety.
- “That’s only in research” is dismissive and harmful. Think outside the box. Follow guidelines. Consider encouraging patients to sign up for trials.
- Screen for PEM/PESE and teach your patients to pace themselves, because pushing through it or doing graded exercises will be harmful.
- We need to train more physicians to treat postacute sequelae of SARS-CoV-2 infection () and other postinfectious conditions, such as ME/CFS.
If long COVID is hard for physicians to understand and deal with, imagine how difficult it is for patients with no expertise in this area.
It is exponentially harder for those with fewer resources, time, and health literacy. My lived experience with long COVID has shown me that being a patient is never easy. You put your body and fate into the hands of trusted professionals and expect validation and assistance, not gaslighting or gatekeeping.
Along with millions of others, I am tired of waiting.
Dr. Gutierrez is Professor and Distinguished Chair, department of rehabilitation medicine, University of Texas Health Science Center at San Antonio. She reported receiving honoraria for lecturing on long COVID and receiving a research grant from Co-PI for the NIH RECOVER trial.
A version of this article first appeared on Medscape.com.
Combining treatment options for scar revision often a useful approach
DENVER –
“It’s important to manage expectations,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual meeting of the American Society for Dermatologic Surgery. “I tell them I can improve their scar and make it look less noticeable, but I can’t make it look like normal skin. It’s going to require multiple treatments. It’s not a one-time thing; it’s going to take several months to see the full benefit. And, it’s an investment of time and money.”
Nonablative, ablative, and fractional resurfacing stimulates dermal fibroblasts to replace lost collagen and elastin. Traditional lasers offer impressive clinical results for scars but are associated with significant preprocedural discomfort, prolonged recovery, and a significant risk of side effects, Dr. Ortiz said, while nonablative lasers are more tolerable with shorter recovery times.
Multiple sessions are required, and results are often less clinically impressive. “It’s often difficult for patients to have a lot of downtime with each treatment so often I prefer to use the nonablative laser, especially for acne scarring,” she said.
Mounting evidence suggests that the sooner scars are treated after they are formed, the better. That may not be feasible for patients with a long history of acne scars, but for surgical scars, Dr. Ortiz prefers to start treatment on the day of suture removal. “Whenever I do that, I always get better results,” she said.
Outcomes may also improve by combining different treatment options, but the type of scar drives the type of modality to consider. There are red scars from postinflammatory erythema, hyperpigmented scars, hypopigmented scars, atrophic scars, hypertrophic scars, spread scars, pin cushion scars, and keloid scars, “which are the most difficult to treat,” she said. “When I’m using a combination approach, I start with the redness component of the scar, because you don’t want to exacerbate nonspecific erythema, or it’ll be difficult to see where the redness is. So, I always use vascular laser first, then a pigment-specific laser, followed by resurfacing, and augmentation with filler if needed.”
Red scars generally fade with time, but that can take several months to more than a year. “If you use a laser, that can speed up the recovery,” said Dr. Ortiz, who is the vice president of the American Society for Laser Medicine and Surgery. “A vascular laser will work, such as KTP, or intense pulsed light. Studies favor a low fluence and a short pulse duration. Pulsed dye laser (PDL) penetrates deeper than KTP, so theoretically you get a bit of collagen remodeling because it can increase TGF-beta [transforming growth factor–beta], so theoretically, PDL is a little bit better than KTP for red scars, but both will work.”
In a comparative study, researchers used purpuric and nonpurpuric parameters to treat surgical scars but found no significant differences between the two treatment settings. “I tend to stick to short pulse duration and low fluence settings,” said Dr. Ortiz, who was not affiliated with the study.
A separate, single-blinded, split scar study, which compared the efficacy of KTP to 595 nm PDL in reduction of erythema in surgical scars, found no significant difference between the two approaches. A review of available therapeutic lasers for acne scarring found that the thermal energy delivered by KTP extends only to the papillary dermis, making it useful for postinflammatory erythema without significant effects on collagen remodeling.
Hyperpigmentation
Use of concomitant bleaching cream can also help as a preventive strategy for hyperpigmentation. But one study of 100 patients found that pretreatment with a bleaching regimen prior to undergoing CO2 laser resurfacing made no significant difference in hyperpigmentation compared with those who received no pretreatment regimen.
When Dr. Ortiz is concerned about hyperpigmentation after laser treatment, she prescribes post-treatment tranexamic acid 325 mg twice daily for 6 months or longer. “I don’t do any kind of workup or labs, but I do not prescribe it if a patient has increased risk of clotting,” she said. Those at increased risk include smokers, those on birth control pills, those on hormonal supplementation, those with a current malignancy, and those with a history of a cerebrovascular accident or deep vein thrombosis.
Hypopigmented, atrophic scars
In Dr. Ortiz’s clinical experience, hypopigmented scars respond well to treatment with the 1550 nonablative laser. “The idea is that you’re removing some of the scarred collagen and it allows the melanocytes to migrate in and repigment,” she said. Following laser treatment, consider applying topical bimatoprost 0.03% twice daily for at least 3 months to optimize results, she added.
For atrophic scars, options include subcision, laser treatment, radiofrequency microneedling, fillers, or biostimulators. “I caution against using permanent fillers because there is a higher risk of granuloma formation,” Dr. Ortiz said. “I tend to use hyaluronic acid fillers, which have a low G prime. I inject superficially.”
She shared a technique she learned from Mathew Avram, MD, JD, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston. It entails spreading the skin with one’s fingers for a scar, especially an acne scar. “If it improves when you spread the skin, then you know it’s amenable to laser treatment,” Dr. Ortiz said. “But if it doesn’t improve when you spread the skin, it probably needs a little subcision. Insert an 18- or 20-gauge tribeveled hypodermic needle or an 18-gauge Nokor under the scar to sever the fibrous components that anchor the scar. This can take more than one treatment. I’ll often do this immediately before resurfacing.”
For hypertrophic scars, consider laser-assisted drug delivery, which creates vertical channels that assist the delivery of topically applied drugs into the skin. “You never want to use something that isn’t meant to be injected into the skin because you can get a granulomatous reaction,” she warned. “I often use topical triamcinolone acetonide, 5-FU, or poly-l-lactic acid.”
Dr. Ortiz noted that botulinum toxin type A may be helpful for scars, despite the paucity of evidence regarding specific mechanisms of action. “There is some thought that it can modulate TGF-beta,” she said. “It also may modulate collagen deposition. Currently we’re looking into Botox alone for keloid scars. The initial results look just okay.”
Dr. Ortiz disclosed that she has received consulting fees from Alastin, Cutera, and Sciton, and honoraria from BTL and Procter & Gamble. She is also a member of the advisory board for Aerolase, Allergan, Bausch Health, Endo, Galderma, Rodan + Fields, and Sciton, and has received equipment from BTL, Sciton, and SmartGraft.
DENVER –
“It’s important to manage expectations,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual meeting of the American Society for Dermatologic Surgery. “I tell them I can improve their scar and make it look less noticeable, but I can’t make it look like normal skin. It’s going to require multiple treatments. It’s not a one-time thing; it’s going to take several months to see the full benefit. And, it’s an investment of time and money.”
Nonablative, ablative, and fractional resurfacing stimulates dermal fibroblasts to replace lost collagen and elastin. Traditional lasers offer impressive clinical results for scars but are associated with significant preprocedural discomfort, prolonged recovery, and a significant risk of side effects, Dr. Ortiz said, while nonablative lasers are more tolerable with shorter recovery times.
Multiple sessions are required, and results are often less clinically impressive. “It’s often difficult for patients to have a lot of downtime with each treatment so often I prefer to use the nonablative laser, especially for acne scarring,” she said.
Mounting evidence suggests that the sooner scars are treated after they are formed, the better. That may not be feasible for patients with a long history of acne scars, but for surgical scars, Dr. Ortiz prefers to start treatment on the day of suture removal. “Whenever I do that, I always get better results,” she said.
Outcomes may also improve by combining different treatment options, but the type of scar drives the type of modality to consider. There are red scars from postinflammatory erythema, hyperpigmented scars, hypopigmented scars, atrophic scars, hypertrophic scars, spread scars, pin cushion scars, and keloid scars, “which are the most difficult to treat,” she said. “When I’m using a combination approach, I start with the redness component of the scar, because you don’t want to exacerbate nonspecific erythema, or it’ll be difficult to see where the redness is. So, I always use vascular laser first, then a pigment-specific laser, followed by resurfacing, and augmentation with filler if needed.”
Red scars generally fade with time, but that can take several months to more than a year. “If you use a laser, that can speed up the recovery,” said Dr. Ortiz, who is the vice president of the American Society for Laser Medicine and Surgery. “A vascular laser will work, such as KTP, or intense pulsed light. Studies favor a low fluence and a short pulse duration. Pulsed dye laser (PDL) penetrates deeper than KTP, so theoretically you get a bit of collagen remodeling because it can increase TGF-beta [transforming growth factor–beta], so theoretically, PDL is a little bit better than KTP for red scars, but both will work.”
In a comparative study, researchers used purpuric and nonpurpuric parameters to treat surgical scars but found no significant differences between the two treatment settings. “I tend to stick to short pulse duration and low fluence settings,” said Dr. Ortiz, who was not affiliated with the study.
A separate, single-blinded, split scar study, which compared the efficacy of KTP to 595 nm PDL in reduction of erythema in surgical scars, found no significant difference between the two approaches. A review of available therapeutic lasers for acne scarring found that the thermal energy delivered by KTP extends only to the papillary dermis, making it useful for postinflammatory erythema without significant effects on collagen remodeling.
Hyperpigmentation
Use of concomitant bleaching cream can also help as a preventive strategy for hyperpigmentation. But one study of 100 patients found that pretreatment with a bleaching regimen prior to undergoing CO2 laser resurfacing made no significant difference in hyperpigmentation compared with those who received no pretreatment regimen.
When Dr. Ortiz is concerned about hyperpigmentation after laser treatment, she prescribes post-treatment tranexamic acid 325 mg twice daily for 6 months or longer. “I don’t do any kind of workup or labs, but I do not prescribe it if a patient has increased risk of clotting,” she said. Those at increased risk include smokers, those on birth control pills, those on hormonal supplementation, those with a current malignancy, and those with a history of a cerebrovascular accident or deep vein thrombosis.
Hypopigmented, atrophic scars
In Dr. Ortiz’s clinical experience, hypopigmented scars respond well to treatment with the 1550 nonablative laser. “The idea is that you’re removing some of the scarred collagen and it allows the melanocytes to migrate in and repigment,” she said. Following laser treatment, consider applying topical bimatoprost 0.03% twice daily for at least 3 months to optimize results, she added.
For atrophic scars, options include subcision, laser treatment, radiofrequency microneedling, fillers, or biostimulators. “I caution against using permanent fillers because there is a higher risk of granuloma formation,” Dr. Ortiz said. “I tend to use hyaluronic acid fillers, which have a low G prime. I inject superficially.”
She shared a technique she learned from Mathew Avram, MD, JD, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston. It entails spreading the skin with one’s fingers for a scar, especially an acne scar. “If it improves when you spread the skin, then you know it’s amenable to laser treatment,” Dr. Ortiz said. “But if it doesn’t improve when you spread the skin, it probably needs a little subcision. Insert an 18- or 20-gauge tribeveled hypodermic needle or an 18-gauge Nokor under the scar to sever the fibrous components that anchor the scar. This can take more than one treatment. I’ll often do this immediately before resurfacing.”
For hypertrophic scars, consider laser-assisted drug delivery, which creates vertical channels that assist the delivery of topically applied drugs into the skin. “You never want to use something that isn’t meant to be injected into the skin because you can get a granulomatous reaction,” she warned. “I often use topical triamcinolone acetonide, 5-FU, or poly-l-lactic acid.”
Dr. Ortiz noted that botulinum toxin type A may be helpful for scars, despite the paucity of evidence regarding specific mechanisms of action. “There is some thought that it can modulate TGF-beta,” she said. “It also may modulate collagen deposition. Currently we’re looking into Botox alone for keloid scars. The initial results look just okay.”
Dr. Ortiz disclosed that she has received consulting fees from Alastin, Cutera, and Sciton, and honoraria from BTL and Procter & Gamble. She is also a member of the advisory board for Aerolase, Allergan, Bausch Health, Endo, Galderma, Rodan + Fields, and Sciton, and has received equipment from BTL, Sciton, and SmartGraft.
DENVER –
“It’s important to manage expectations,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual meeting of the American Society for Dermatologic Surgery. “I tell them I can improve their scar and make it look less noticeable, but I can’t make it look like normal skin. It’s going to require multiple treatments. It’s not a one-time thing; it’s going to take several months to see the full benefit. And, it’s an investment of time and money.”
Nonablative, ablative, and fractional resurfacing stimulates dermal fibroblasts to replace lost collagen and elastin. Traditional lasers offer impressive clinical results for scars but are associated with significant preprocedural discomfort, prolonged recovery, and a significant risk of side effects, Dr. Ortiz said, while nonablative lasers are more tolerable with shorter recovery times.
Multiple sessions are required, and results are often less clinically impressive. “It’s often difficult for patients to have a lot of downtime with each treatment so often I prefer to use the nonablative laser, especially for acne scarring,” she said.
Mounting evidence suggests that the sooner scars are treated after they are formed, the better. That may not be feasible for patients with a long history of acne scars, but for surgical scars, Dr. Ortiz prefers to start treatment on the day of suture removal. “Whenever I do that, I always get better results,” she said.
Outcomes may also improve by combining different treatment options, but the type of scar drives the type of modality to consider. There are red scars from postinflammatory erythema, hyperpigmented scars, hypopigmented scars, atrophic scars, hypertrophic scars, spread scars, pin cushion scars, and keloid scars, “which are the most difficult to treat,” she said. “When I’m using a combination approach, I start with the redness component of the scar, because you don’t want to exacerbate nonspecific erythema, or it’ll be difficult to see where the redness is. So, I always use vascular laser first, then a pigment-specific laser, followed by resurfacing, and augmentation with filler if needed.”
Red scars generally fade with time, but that can take several months to more than a year. “If you use a laser, that can speed up the recovery,” said Dr. Ortiz, who is the vice president of the American Society for Laser Medicine and Surgery. “A vascular laser will work, such as KTP, or intense pulsed light. Studies favor a low fluence and a short pulse duration. Pulsed dye laser (PDL) penetrates deeper than KTP, so theoretically you get a bit of collagen remodeling because it can increase TGF-beta [transforming growth factor–beta], so theoretically, PDL is a little bit better than KTP for red scars, but both will work.”
In a comparative study, researchers used purpuric and nonpurpuric parameters to treat surgical scars but found no significant differences between the two treatment settings. “I tend to stick to short pulse duration and low fluence settings,” said Dr. Ortiz, who was not affiliated with the study.
A separate, single-blinded, split scar study, which compared the efficacy of KTP to 595 nm PDL in reduction of erythema in surgical scars, found no significant difference between the two approaches. A review of available therapeutic lasers for acne scarring found that the thermal energy delivered by KTP extends only to the papillary dermis, making it useful for postinflammatory erythema without significant effects on collagen remodeling.
Hyperpigmentation
Use of concomitant bleaching cream can also help as a preventive strategy for hyperpigmentation. But one study of 100 patients found that pretreatment with a bleaching regimen prior to undergoing CO2 laser resurfacing made no significant difference in hyperpigmentation compared with those who received no pretreatment regimen.
When Dr. Ortiz is concerned about hyperpigmentation after laser treatment, she prescribes post-treatment tranexamic acid 325 mg twice daily for 6 months or longer. “I don’t do any kind of workup or labs, but I do not prescribe it if a patient has increased risk of clotting,” she said. Those at increased risk include smokers, those on birth control pills, those on hormonal supplementation, those with a current malignancy, and those with a history of a cerebrovascular accident or deep vein thrombosis.
Hypopigmented, atrophic scars
In Dr. Ortiz’s clinical experience, hypopigmented scars respond well to treatment with the 1550 nonablative laser. “The idea is that you’re removing some of the scarred collagen and it allows the melanocytes to migrate in and repigment,” she said. Following laser treatment, consider applying topical bimatoprost 0.03% twice daily for at least 3 months to optimize results, she added.
For atrophic scars, options include subcision, laser treatment, radiofrequency microneedling, fillers, or biostimulators. “I caution against using permanent fillers because there is a higher risk of granuloma formation,” Dr. Ortiz said. “I tend to use hyaluronic acid fillers, which have a low G prime. I inject superficially.”
She shared a technique she learned from Mathew Avram, MD, JD, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston. It entails spreading the skin with one’s fingers for a scar, especially an acne scar. “If it improves when you spread the skin, then you know it’s amenable to laser treatment,” Dr. Ortiz said. “But if it doesn’t improve when you spread the skin, it probably needs a little subcision. Insert an 18- or 20-gauge tribeveled hypodermic needle or an 18-gauge Nokor under the scar to sever the fibrous components that anchor the scar. This can take more than one treatment. I’ll often do this immediately before resurfacing.”
For hypertrophic scars, consider laser-assisted drug delivery, which creates vertical channels that assist the delivery of topically applied drugs into the skin. “You never want to use something that isn’t meant to be injected into the skin because you can get a granulomatous reaction,” she warned. “I often use topical triamcinolone acetonide, 5-FU, or poly-l-lactic acid.”
Dr. Ortiz noted that botulinum toxin type A may be helpful for scars, despite the paucity of evidence regarding specific mechanisms of action. “There is some thought that it can modulate TGF-beta,” she said. “It also may modulate collagen deposition. Currently we’re looking into Botox alone for keloid scars. The initial results look just okay.”
Dr. Ortiz disclosed that she has received consulting fees from Alastin, Cutera, and Sciton, and honoraria from BTL and Procter & Gamble. She is also a member of the advisory board for Aerolase, Allergan, Bausch Health, Endo, Galderma, Rodan + Fields, and Sciton, and has received equipment from BTL, Sciton, and SmartGraft.
AT ASDS 2022