User login
Plastic IUD placement instruments prevent uterine perforations
Key clinical point: In a biomechanical ex vivo analysis, metal uterine sounds caused uterine perforation, but the manufacturer’s plastic intrauterine device placement rod did not.
Major finding: The lowest mean maximum force generated for IUD placement was 12.3 Newtons with the levonorgestrel intrauterine system placement instrument, followed by 14.1 Newtons with the copper T380A intrauterine device placement instrument 14.1 Newtons; the highest mean maximum force of 17.9 N occurred with the metal sound (P < 0.01).
Study details: The data come from 16 premenopausal women with benign conditions who provided hysterectomy sections at a single center.
Disclosures: The study was funded indirectly through grants to the University of Utah from Bayer, Bioceptive, Sebela, Medicines 360, Merck, and Cooper Surgical. Lead author Dr. Duncan had no financial conflicts to disclose.
Source: Duncan J et al. BMC Womens Health. 2021 Apr 7. doi: 10.1186/s12905-021-01285-6.
Key clinical point: In a biomechanical ex vivo analysis, metal uterine sounds caused uterine perforation, but the manufacturer’s plastic intrauterine device placement rod did not.
Major finding: The lowest mean maximum force generated for IUD placement was 12.3 Newtons with the levonorgestrel intrauterine system placement instrument, followed by 14.1 Newtons with the copper T380A intrauterine device placement instrument 14.1 Newtons; the highest mean maximum force of 17.9 N occurred with the metal sound (P < 0.01).
Study details: The data come from 16 premenopausal women with benign conditions who provided hysterectomy sections at a single center.
Disclosures: The study was funded indirectly through grants to the University of Utah from Bayer, Bioceptive, Sebela, Medicines 360, Merck, and Cooper Surgical. Lead author Dr. Duncan had no financial conflicts to disclose.
Source: Duncan J et al. BMC Womens Health. 2021 Apr 7. doi: 10.1186/s12905-021-01285-6.
Key clinical point: In a biomechanical ex vivo analysis, metal uterine sounds caused uterine perforation, but the manufacturer’s plastic intrauterine device placement rod did not.
Major finding: The lowest mean maximum force generated for IUD placement was 12.3 Newtons with the levonorgestrel intrauterine system placement instrument, followed by 14.1 Newtons with the copper T380A intrauterine device placement instrument 14.1 Newtons; the highest mean maximum force of 17.9 N occurred with the metal sound (P < 0.01).
Study details: The data come from 16 premenopausal women with benign conditions who provided hysterectomy sections at a single center.
Disclosures: The study was funded indirectly through grants to the University of Utah from Bayer, Bioceptive, Sebela, Medicines 360, Merck, and Cooper Surgical. Lead author Dr. Duncan had no financial conflicts to disclose.
Source: Duncan J et al. BMC Womens Health. 2021 Apr 7. doi: 10.1186/s12905-021-01285-6.
Oral contraceptive use shows no impact on later heart failure risk
Key clinical point: Use of oral contraceptives by women of reproductive age was not associated with increased risk of heart failure later in life, but the potential impact of different formulations and dosages deserves further research.
Major finding: Over an average of 12 years’ follow-up, the researchers identified 138 incident cases of heart failure. The incidence of heart failure was not significantly associated with heart failure in multivariate analysis (hazard ratio 0.96); however, any OC use was positively associated with left ventricular end-diastolic mass (P = 0.006) and stroke volume (P = 0.01 and P = 0.005 for left and right ventricles, respectively).
Study details: The data come from a retrospective study of 3,594 women with an average age of 62 years who were enrolled in the Multi‐Ethnic Study of Atherosclerosis and could provide data on oral contraceptive use.
Disclosures: The study was supported by the Guangdong Peak Project, the Science and Technology Planning Project of Guangdong Province, Natural Science Foundation of Guangdong Province, and the National Key Research and Development Program of China. The researchers had no financial conflicts to disclose.
Source: Luo D et al. ESC Heart Fail. 2021 Apr 9. doi: 10.1002/ehf2.13328.
Key clinical point: Use of oral contraceptives by women of reproductive age was not associated with increased risk of heart failure later in life, but the potential impact of different formulations and dosages deserves further research.
Major finding: Over an average of 12 years’ follow-up, the researchers identified 138 incident cases of heart failure. The incidence of heart failure was not significantly associated with heart failure in multivariate analysis (hazard ratio 0.96); however, any OC use was positively associated with left ventricular end-diastolic mass (P = 0.006) and stroke volume (P = 0.01 and P = 0.005 for left and right ventricles, respectively).
Study details: The data come from a retrospective study of 3,594 women with an average age of 62 years who were enrolled in the Multi‐Ethnic Study of Atherosclerosis and could provide data on oral contraceptive use.
Disclosures: The study was supported by the Guangdong Peak Project, the Science and Technology Planning Project of Guangdong Province, Natural Science Foundation of Guangdong Province, and the National Key Research and Development Program of China. The researchers had no financial conflicts to disclose.
Source: Luo D et al. ESC Heart Fail. 2021 Apr 9. doi: 10.1002/ehf2.13328.
Key clinical point: Use of oral contraceptives by women of reproductive age was not associated with increased risk of heart failure later in life, but the potential impact of different formulations and dosages deserves further research.
Major finding: Over an average of 12 years’ follow-up, the researchers identified 138 incident cases of heart failure. The incidence of heart failure was not significantly associated with heart failure in multivariate analysis (hazard ratio 0.96); however, any OC use was positively associated with left ventricular end-diastolic mass (P = 0.006) and stroke volume (P = 0.01 and P = 0.005 for left and right ventricles, respectively).
Study details: The data come from a retrospective study of 3,594 women with an average age of 62 years who were enrolled in the Multi‐Ethnic Study of Atherosclerosis and could provide data on oral contraceptive use.
Disclosures: The study was supported by the Guangdong Peak Project, the Science and Technology Planning Project of Guangdong Province, Natural Science Foundation of Guangdong Province, and the National Key Research and Development Program of China. The researchers had no financial conflicts to disclose.
Source: Luo D et al. ESC Heart Fail. 2021 Apr 9. doi: 10.1002/ehf2.13328.
More signs COVID shots are safe for pregnant women
As the U.S. races to vaccinate millions of people against the coronavirus, pregnant women face the extra challenge of not knowing whether the vaccines are safe for them or their unborn babies.
None of the recent COVID-19 vaccine trials, including those for Pfizer, Moderna, and Johnson & Johnson, enrolled pregnant or breastfeeding women because they consider them a high-risk group.
That was despite the Society for Maternal-Fetal Medicine and the American College of Obstetricians and Gynecologists asking that pregnant and breastfeeding women be included in trials. The Food and Drug Administration even included pregnant women in the COVID-19 vaccine emergency use authorization (EUA) because of their higher risk of having a more severe disease.
Despite that lack of clinical trial data, more and more smaller studies are suggesting that the vaccines are safe for both mother and child.
Pfizer is now studying its two-dose vaccine in 4,000 pregnant and breastfeeding women to see how safe, tolerated, and robust their immune response is. Researchers will also look at how safe the vaccine is for infants and whether mothers pass along antibodies to children. But the preliminary results won’t be available until the end of the year, a Pfizer spokesperson says.
Without that information, pregnant women are less likely to get vaccinated, according to a large international survey. Less than 45% of pregnant women in the United States said they intended to get vaccinated even when they were told the vaccine was safe and 90% effective. That figure rises to 52% of pregnant women in 16 countries, including the United States, compared with 74% of nonpregnant women willing to be vaccinated. The findings were published online March 1, 2021, in the European Journal of Epidemiology.
The vaccine-hesitant pregnant women in the international study were most concerned that the COVID-19 vaccine could harm their developing fetuses, a worry related to the lack of clinical evidence in pregnant women, said lead researcher Julia Wu, ScD, an epidemiologist at the Harvard School of Public Health’s Human Immunomics Initiative in Boston.
The information vacuum also increases the chances that “people will fall victim to misinformation campaigns like the one on social media that claims that the COVID-19 vaccine causes infertility,” Dr. Wu said. This unfounded claim has deterred some women of childbearing age from getting the vaccine.
Deciding to get vaccinated
Frontline health care professionals were in the first group eligible to receive the vaccine in December 2020. “All of us who were pregnant ... had to decide whether to wait for the data, because we don’t know what the risks are, or go ahead and get it [the vaccine]. We had been dealing with the pandemic for months and were afraid of being exposed to the virus and infecting family members,” said Jacqueline Parchem, MD, a maternal-fetal medicine specialist at the University of Texas Health Science Center, Houston.
Given the lack of safety data, the CDC guidance to pregnant women has been to consult with their doctors and that it’s a personal choice. The Center for Disease Control and Prevention’s latest vaccine guidance said that “there is no evidence that antibodies formed from COVID-19 vaccination cause any problem with pregnancy, including the development of the placenta.”
The CDC is monitoring vaccinated people through its v-safe program and reported on April 12 that more than 86,000 v-safe participants said they were pregnant when they were vaccinated.
Health care workers who were nursing their infants when they were eligible for the vaccine faced a similar dilemma as pregnant women – they lacked the data on them to make a truly informed decision.
“I was nervous about the vaccine side effects for myself and whether my son Bennett, who was about a year old, would experience any of these himself,” said Christa Carrig, a labor and delivery nurse at Massachusetts General Hospital in Boston, who was breastfeeding at the time.
She and Dr. Parchem know that pregnant women with COVID-19 are more likely to have severe illness and complications such as high blood pressure and preterm delivery. “Pregnancy takes a toll on the body. When a woman gets COVID-19 and that insult is added, women who were otherwise young and healthy get much sicker than you would expect,” said Ms. Carrig.
“As a high-risk pregnancy specialist, I know that, with COVID, that babies don’t do well when moms are sick,” said Dr. Parchem.
Pregnant women accounted for more than 84,629 cases of COVID-19 and 95 deaths in the United States between Jan. 22 last year and April 12 this year, according to the CDC COVID data tracker.
Dr. Parchem and Ms. Carrig decided to get vaccinated because of their high risk of exposure to COVID-19 at work. After the second dose, Ms. Carrig reported chills but Bennett had no side effects from breastfeeding. Dr. Parchem, who delivered a healthy baby boy in February, reported no side effects other than a sore arm.
“There’s also a psychological benefit to returning to some sense of normalcy,” said Dr. Parchem. “My mother was finally able to visit us to see the new baby after we were all vaccinated. This was the first visit in more than a year.”
New study results
Ms. Carrig was one of 131 vaccinated hospital workers in the Boston area who took part in the first study to profile the immune response in pregnant and breastfeeding women and compare it with both nonpregnant and pregnant women who had COVID-19.
The study was not designed to evaluate the safety of the vaccines or whether they prevent COVID-19 illness and hospitalizations. That is the role of the large vaccine trials, the authors said.
The participants were aged 18-45 years and received both doses of either Pfizer or Moderna vaccines during one of their trimesters. They provided blood and/or breast milk samples after each vaccine dose, 2-6 weeks after the last dose, and at delivery for the 10 who gave birth during the study.
The vaccines produced a similar strong antibody response among the pregnant/breastfeeding women and nonpregnant women. Their antibody levels were much higher than those found in the pregnant women who had COVID-19, the researchers reported on March 25, 2021, in the American Journal of Obstetrics and Gynecology.
“This is important because a lot of people tend to think once they’ve had COVID-19, they are protected from the virus. This finding suggests that the vaccines produce a stronger antibody response than the infection itself, and this might be important for long-lasting protection against COVID-19,” said Dr. Parchem.
The study also addressed whether newborns benefit from the antibodies produced by their mothers. “In the 10 women who delivered, we detected antibodies in their umbilical cords and breast milk,” says Andrea Edlow, MD, lead researcher and a maternal-fetal medicine specialist at Massachusetts General Hospital.
Newborns are particularly vulnerable to respiratory infections because they have small airways and their immune systems are underdeveloped. These infections can be lethal early in life.
“The public health strategy is to vaccinate mothers against respiratory viruses, bacteria, and parasites that neonates up to 6 months are exposed to. Influenza and pertussis (whooping cough) are two examples of vaccines that we give mothers that we know transfer [antibodies] across the umbilical cord,” said Dr. Edlow.
But this “passive transfer immunity” is different from active immunity, when the body produces its own antibody immune response, she explains.
A different study, also published in March, confirmed that antibodies were transferred from 27 vaccinated pregnant mothers to their infants when they delivered. A new finding was that the women who were vaccinated with both doses and earlier in their third semester passed on more antibodies than the women who were vaccinated later or with only one dose.
Impact of the studies
The Society for Maternal-Fetal Medicine updated its guidance on counseling pregnant and lactating patients about the COVID-19 vaccines to include Dr. Edlow’s study.
“We were struck by how much pregnant and breastfeeding women want to participate in research and to help others in the same situation make decisions. I hope this will be an example to drug companies doing research on new vaccines in the future – that they should not be left behind and can make decisions themselves whether to participate after weighing the risks and benefits,” said Dr. Edlow.
She continues to enroll more vaccinated women in her study in the Boston area, including non–health care workers who have asked to take part.
“It was worth getting vaccinated and participating in the study. I know that I have antibodies and it worked and that I passed them on to Bennett. Also, I know that all the information is available for other women who are questioning whether to get vaccinated or not,” said Ms. Carrig.
Dr. Parchem is also taking part in the CDC’s v-safe pregnancy registry, which is collecting health and safety data on vaccinated pregnant women.
Before she was vaccinated, Dr. Parchem said, “my advice was very measured because we lacked data either saying that it definitely works or showing that it was unsafe. Now that we have this data supporting the benefits, I feel more confident in recommending the vaccines.”
A version of this article first appeared on Medscape.com.
As the U.S. races to vaccinate millions of people against the coronavirus, pregnant women face the extra challenge of not knowing whether the vaccines are safe for them or their unborn babies.
None of the recent COVID-19 vaccine trials, including those for Pfizer, Moderna, and Johnson & Johnson, enrolled pregnant or breastfeeding women because they consider them a high-risk group.
That was despite the Society for Maternal-Fetal Medicine and the American College of Obstetricians and Gynecologists asking that pregnant and breastfeeding women be included in trials. The Food and Drug Administration even included pregnant women in the COVID-19 vaccine emergency use authorization (EUA) because of their higher risk of having a more severe disease.
Despite that lack of clinical trial data, more and more smaller studies are suggesting that the vaccines are safe for both mother and child.
Pfizer is now studying its two-dose vaccine in 4,000 pregnant and breastfeeding women to see how safe, tolerated, and robust their immune response is. Researchers will also look at how safe the vaccine is for infants and whether mothers pass along antibodies to children. But the preliminary results won’t be available until the end of the year, a Pfizer spokesperson says.
Without that information, pregnant women are less likely to get vaccinated, according to a large international survey. Less than 45% of pregnant women in the United States said they intended to get vaccinated even when they were told the vaccine was safe and 90% effective. That figure rises to 52% of pregnant women in 16 countries, including the United States, compared with 74% of nonpregnant women willing to be vaccinated. The findings were published online March 1, 2021, in the European Journal of Epidemiology.
The vaccine-hesitant pregnant women in the international study were most concerned that the COVID-19 vaccine could harm their developing fetuses, a worry related to the lack of clinical evidence in pregnant women, said lead researcher Julia Wu, ScD, an epidemiologist at the Harvard School of Public Health’s Human Immunomics Initiative in Boston.
The information vacuum also increases the chances that “people will fall victim to misinformation campaigns like the one on social media that claims that the COVID-19 vaccine causes infertility,” Dr. Wu said. This unfounded claim has deterred some women of childbearing age from getting the vaccine.
Deciding to get vaccinated
Frontline health care professionals were in the first group eligible to receive the vaccine in December 2020. “All of us who were pregnant ... had to decide whether to wait for the data, because we don’t know what the risks are, or go ahead and get it [the vaccine]. We had been dealing with the pandemic for months and were afraid of being exposed to the virus and infecting family members,” said Jacqueline Parchem, MD, a maternal-fetal medicine specialist at the University of Texas Health Science Center, Houston.
Given the lack of safety data, the CDC guidance to pregnant women has been to consult with their doctors and that it’s a personal choice. The Center for Disease Control and Prevention’s latest vaccine guidance said that “there is no evidence that antibodies formed from COVID-19 vaccination cause any problem with pregnancy, including the development of the placenta.”
The CDC is monitoring vaccinated people through its v-safe program and reported on April 12 that more than 86,000 v-safe participants said they were pregnant when they were vaccinated.
Health care workers who were nursing their infants when they were eligible for the vaccine faced a similar dilemma as pregnant women – they lacked the data on them to make a truly informed decision.
“I was nervous about the vaccine side effects for myself and whether my son Bennett, who was about a year old, would experience any of these himself,” said Christa Carrig, a labor and delivery nurse at Massachusetts General Hospital in Boston, who was breastfeeding at the time.
She and Dr. Parchem know that pregnant women with COVID-19 are more likely to have severe illness and complications such as high blood pressure and preterm delivery. “Pregnancy takes a toll on the body. When a woman gets COVID-19 and that insult is added, women who were otherwise young and healthy get much sicker than you would expect,” said Ms. Carrig.
“As a high-risk pregnancy specialist, I know that, with COVID, that babies don’t do well when moms are sick,” said Dr. Parchem.
Pregnant women accounted for more than 84,629 cases of COVID-19 and 95 deaths in the United States between Jan. 22 last year and April 12 this year, according to the CDC COVID data tracker.
Dr. Parchem and Ms. Carrig decided to get vaccinated because of their high risk of exposure to COVID-19 at work. After the second dose, Ms. Carrig reported chills but Bennett had no side effects from breastfeeding. Dr. Parchem, who delivered a healthy baby boy in February, reported no side effects other than a sore arm.
“There’s also a psychological benefit to returning to some sense of normalcy,” said Dr. Parchem. “My mother was finally able to visit us to see the new baby after we were all vaccinated. This was the first visit in more than a year.”
New study results
Ms. Carrig was one of 131 vaccinated hospital workers in the Boston area who took part in the first study to profile the immune response in pregnant and breastfeeding women and compare it with both nonpregnant and pregnant women who had COVID-19.
The study was not designed to evaluate the safety of the vaccines or whether they prevent COVID-19 illness and hospitalizations. That is the role of the large vaccine trials, the authors said.
The participants were aged 18-45 years and received both doses of either Pfizer or Moderna vaccines during one of their trimesters. They provided blood and/or breast milk samples after each vaccine dose, 2-6 weeks after the last dose, and at delivery for the 10 who gave birth during the study.
The vaccines produced a similar strong antibody response among the pregnant/breastfeeding women and nonpregnant women. Their antibody levels were much higher than those found in the pregnant women who had COVID-19, the researchers reported on March 25, 2021, in the American Journal of Obstetrics and Gynecology.
“This is important because a lot of people tend to think once they’ve had COVID-19, they are protected from the virus. This finding suggests that the vaccines produce a stronger antibody response than the infection itself, and this might be important for long-lasting protection against COVID-19,” said Dr. Parchem.
The study also addressed whether newborns benefit from the antibodies produced by their mothers. “In the 10 women who delivered, we detected antibodies in their umbilical cords and breast milk,” says Andrea Edlow, MD, lead researcher and a maternal-fetal medicine specialist at Massachusetts General Hospital.
Newborns are particularly vulnerable to respiratory infections because they have small airways and their immune systems are underdeveloped. These infections can be lethal early in life.
“The public health strategy is to vaccinate mothers against respiratory viruses, bacteria, and parasites that neonates up to 6 months are exposed to. Influenza and pertussis (whooping cough) are two examples of vaccines that we give mothers that we know transfer [antibodies] across the umbilical cord,” said Dr. Edlow.
But this “passive transfer immunity” is different from active immunity, when the body produces its own antibody immune response, she explains.
A different study, also published in March, confirmed that antibodies were transferred from 27 vaccinated pregnant mothers to their infants when they delivered. A new finding was that the women who were vaccinated with both doses and earlier in their third semester passed on more antibodies than the women who were vaccinated later or with only one dose.
Impact of the studies
The Society for Maternal-Fetal Medicine updated its guidance on counseling pregnant and lactating patients about the COVID-19 vaccines to include Dr. Edlow’s study.
“We were struck by how much pregnant and breastfeeding women want to participate in research and to help others in the same situation make decisions. I hope this will be an example to drug companies doing research on new vaccines in the future – that they should not be left behind and can make decisions themselves whether to participate after weighing the risks and benefits,” said Dr. Edlow.
She continues to enroll more vaccinated women in her study in the Boston area, including non–health care workers who have asked to take part.
“It was worth getting vaccinated and participating in the study. I know that I have antibodies and it worked and that I passed them on to Bennett. Also, I know that all the information is available for other women who are questioning whether to get vaccinated or not,” said Ms. Carrig.
Dr. Parchem is also taking part in the CDC’s v-safe pregnancy registry, which is collecting health and safety data on vaccinated pregnant women.
Before she was vaccinated, Dr. Parchem said, “my advice was very measured because we lacked data either saying that it definitely works or showing that it was unsafe. Now that we have this data supporting the benefits, I feel more confident in recommending the vaccines.”
A version of this article first appeared on Medscape.com.
As the U.S. races to vaccinate millions of people against the coronavirus, pregnant women face the extra challenge of not knowing whether the vaccines are safe for them or their unborn babies.
None of the recent COVID-19 vaccine trials, including those for Pfizer, Moderna, and Johnson & Johnson, enrolled pregnant or breastfeeding women because they consider them a high-risk group.
That was despite the Society for Maternal-Fetal Medicine and the American College of Obstetricians and Gynecologists asking that pregnant and breastfeeding women be included in trials. The Food and Drug Administration even included pregnant women in the COVID-19 vaccine emergency use authorization (EUA) because of their higher risk of having a more severe disease.
Despite that lack of clinical trial data, more and more smaller studies are suggesting that the vaccines are safe for both mother and child.
Pfizer is now studying its two-dose vaccine in 4,000 pregnant and breastfeeding women to see how safe, tolerated, and robust their immune response is. Researchers will also look at how safe the vaccine is for infants and whether mothers pass along antibodies to children. But the preliminary results won’t be available until the end of the year, a Pfizer spokesperson says.
Without that information, pregnant women are less likely to get vaccinated, according to a large international survey. Less than 45% of pregnant women in the United States said they intended to get vaccinated even when they were told the vaccine was safe and 90% effective. That figure rises to 52% of pregnant women in 16 countries, including the United States, compared with 74% of nonpregnant women willing to be vaccinated. The findings were published online March 1, 2021, in the European Journal of Epidemiology.
The vaccine-hesitant pregnant women in the international study were most concerned that the COVID-19 vaccine could harm their developing fetuses, a worry related to the lack of clinical evidence in pregnant women, said lead researcher Julia Wu, ScD, an epidemiologist at the Harvard School of Public Health’s Human Immunomics Initiative in Boston.
The information vacuum also increases the chances that “people will fall victim to misinformation campaigns like the one on social media that claims that the COVID-19 vaccine causes infertility,” Dr. Wu said. This unfounded claim has deterred some women of childbearing age from getting the vaccine.
Deciding to get vaccinated
Frontline health care professionals were in the first group eligible to receive the vaccine in December 2020. “All of us who were pregnant ... had to decide whether to wait for the data, because we don’t know what the risks are, or go ahead and get it [the vaccine]. We had been dealing with the pandemic for months and were afraid of being exposed to the virus and infecting family members,” said Jacqueline Parchem, MD, a maternal-fetal medicine specialist at the University of Texas Health Science Center, Houston.
Given the lack of safety data, the CDC guidance to pregnant women has been to consult with their doctors and that it’s a personal choice. The Center for Disease Control and Prevention’s latest vaccine guidance said that “there is no evidence that antibodies formed from COVID-19 vaccination cause any problem with pregnancy, including the development of the placenta.”
The CDC is monitoring vaccinated people through its v-safe program and reported on April 12 that more than 86,000 v-safe participants said they were pregnant when they were vaccinated.
Health care workers who were nursing their infants when they were eligible for the vaccine faced a similar dilemma as pregnant women – they lacked the data on them to make a truly informed decision.
“I was nervous about the vaccine side effects for myself and whether my son Bennett, who was about a year old, would experience any of these himself,” said Christa Carrig, a labor and delivery nurse at Massachusetts General Hospital in Boston, who was breastfeeding at the time.
She and Dr. Parchem know that pregnant women with COVID-19 are more likely to have severe illness and complications such as high blood pressure and preterm delivery. “Pregnancy takes a toll on the body. When a woman gets COVID-19 and that insult is added, women who were otherwise young and healthy get much sicker than you would expect,” said Ms. Carrig.
“As a high-risk pregnancy specialist, I know that, with COVID, that babies don’t do well when moms are sick,” said Dr. Parchem.
Pregnant women accounted for more than 84,629 cases of COVID-19 and 95 deaths in the United States between Jan. 22 last year and April 12 this year, according to the CDC COVID data tracker.
Dr. Parchem and Ms. Carrig decided to get vaccinated because of their high risk of exposure to COVID-19 at work. After the second dose, Ms. Carrig reported chills but Bennett had no side effects from breastfeeding. Dr. Parchem, who delivered a healthy baby boy in February, reported no side effects other than a sore arm.
“There’s also a psychological benefit to returning to some sense of normalcy,” said Dr. Parchem. “My mother was finally able to visit us to see the new baby after we were all vaccinated. This was the first visit in more than a year.”
New study results
Ms. Carrig was one of 131 vaccinated hospital workers in the Boston area who took part in the first study to profile the immune response in pregnant and breastfeeding women and compare it with both nonpregnant and pregnant women who had COVID-19.
The study was not designed to evaluate the safety of the vaccines or whether they prevent COVID-19 illness and hospitalizations. That is the role of the large vaccine trials, the authors said.
The participants were aged 18-45 years and received both doses of either Pfizer or Moderna vaccines during one of their trimesters. They provided blood and/or breast milk samples after each vaccine dose, 2-6 weeks after the last dose, and at delivery for the 10 who gave birth during the study.
The vaccines produced a similar strong antibody response among the pregnant/breastfeeding women and nonpregnant women. Their antibody levels were much higher than those found in the pregnant women who had COVID-19, the researchers reported on March 25, 2021, in the American Journal of Obstetrics and Gynecology.
“This is important because a lot of people tend to think once they’ve had COVID-19, they are protected from the virus. This finding suggests that the vaccines produce a stronger antibody response than the infection itself, and this might be important for long-lasting protection against COVID-19,” said Dr. Parchem.
The study also addressed whether newborns benefit from the antibodies produced by their mothers. “In the 10 women who delivered, we detected antibodies in their umbilical cords and breast milk,” says Andrea Edlow, MD, lead researcher and a maternal-fetal medicine specialist at Massachusetts General Hospital.
Newborns are particularly vulnerable to respiratory infections because they have small airways and their immune systems are underdeveloped. These infections can be lethal early in life.
“The public health strategy is to vaccinate mothers against respiratory viruses, bacteria, and parasites that neonates up to 6 months are exposed to. Influenza and pertussis (whooping cough) are two examples of vaccines that we give mothers that we know transfer [antibodies] across the umbilical cord,” said Dr. Edlow.
But this “passive transfer immunity” is different from active immunity, when the body produces its own antibody immune response, she explains.
A different study, also published in March, confirmed that antibodies were transferred from 27 vaccinated pregnant mothers to their infants when they delivered. A new finding was that the women who were vaccinated with both doses and earlier in their third semester passed on more antibodies than the women who were vaccinated later or with only one dose.
Impact of the studies
The Society for Maternal-Fetal Medicine updated its guidance on counseling pregnant and lactating patients about the COVID-19 vaccines to include Dr. Edlow’s study.
“We were struck by how much pregnant and breastfeeding women want to participate in research and to help others in the same situation make decisions. I hope this will be an example to drug companies doing research on new vaccines in the future – that they should not be left behind and can make decisions themselves whether to participate after weighing the risks and benefits,” said Dr. Edlow.
She continues to enroll more vaccinated women in her study in the Boston area, including non–health care workers who have asked to take part.
“It was worth getting vaccinated and participating in the study. I know that I have antibodies and it worked and that I passed them on to Bennett. Also, I know that all the information is available for other women who are questioning whether to get vaccinated or not,” said Ms. Carrig.
Dr. Parchem is also taking part in the CDC’s v-safe pregnancy registry, which is collecting health and safety data on vaccinated pregnant women.
Before she was vaccinated, Dr. Parchem said, “my advice was very measured because we lacked data either saying that it definitely works or showing that it was unsafe. Now that we have this data supporting the benefits, I feel more confident in recommending the vaccines.”
A version of this article first appeared on Medscape.com.
Cannabis for migraine strongly linked to rebound headache
, preliminary research suggests, although the direction of the relationship is unclear. Researchers at Stanford (Calif.) University found a significant increase in the likelihood of medication overuse headache (rebound headache) in chronic migraine patients who use cannabis.
“This study shows that there is some kind of association between cannabis use and medication overuse headache in people with chronic migraine,” said lead investigator Niushen Zhang, MD, a clinical assistant professor at Stanford.
“But it is unclear at this time whether patients are using cannabis to treat medication overuse headache or if cannabis is contributing to the development medication overuse headache, or both,” she said.
The findings were presented at the American Academy of Neurology’s 2021 annual meeting.
Sixfold increase
“Medication overuse occurs in about 1% to 3% of the general population. It affects nearly one-third of the patients (mostly patients with chronic migraine) seen at tertiary care centers such as the Stanford Headache Center,” Dr. Zhang said.
From clinical observations, patients with chronic migraine and medication overuse headache appear to be concomitantly using cannabis products, yet there is currently very little research on this topic, she added.
To investigate, the researchers reviewed the records of 368 adults who experienced chronic migraine (15 or more migraine days per month) for at least 1 year. Of the 368 patients, 150 were using cannabis, and 218 were not. In addition, 212 had medication overuse headache, and 156 did not.
Results showed that patients who used cannabis were nearly six times more likely to have medication overuse headache than those who did not use cannabis (odds ratio, 5.99; 95% confidence interval, 3.45-10.43; P < .0001).
There were significant bidirectional relationships between current cannabis use, opioid use, and medication overuse headache.
Jury out on cannabis for migraine
Commenting on the findings, Teshamae Monteith, MD, of the University of Miami, noted, “With increased legalization, greater access, and less stigmatization, there are more individuals using cannabis for migraine, but there is no solid evidence to suggest that cannabis is effective for acute or preventive treatment of migraine.”
The study is “interesting,” Dr. Monteith said, but, owing to methodologic limitations, it is not clear that cannabis contributes to medication overuse headache. “Patients with medication overuse headaches may have more comorbidities, such as anxiety, depression, and sleep disorders, that are driving the cannabis use. The patients on cannabis also had higher rates of opiate use, which itself is a stronger contributor to medication overuse headache and may indicate the presence of other pain disorders,” Dr. Monteith said.
“It is not clear if these patients were appropriately treated with migraine prevention; patients that use cannabis sometimes report that they prefer to avoid pharmaceutical treatments, such as antidepressants, etc., used for migraine,” Dr. Monteith noted.
She said that at this point, she would advise clinicians to ask about cannabis use “and let patients know that we do not know enough about the long-term effects of cannabis on the migraine brain.”
Most importantly, Dr. Monteith said, she would “encourage clinicians to be sensitive to the high prevalence of migraine, chronic migraine, and medication overuse. If we can treat more effectively and prevent migraine progression, which includes addressing comorbidities, there would be a lot less medication overuse headache.”
Also weighing in on the study, Jessica Ailani, MD, director, Medstar Georgetown Headache Center, Washington, D.C., noted that there is no conclusive evidence that cannabis is an effective acute or preventive treatment for migraine. “There is a suggestion that cannabis can help treat a migraine attack, but there is uncertainty about concentration of cannabidiol (CBD) to tetrahydrocannabinol (THC) needed to achieve pain freedom,” Dr. Ailani said.
“There has also been some concern about interactions between CBD and other medications used to treat migraine and that CBD can cause a condition known as reversible cerebral vasoconstrictive syndrome. These are reasons to be cautious with CBD,” Dr. Ailani added.
“At this time there is limited advice we can give our patients except that more studies need to be done. If cannabis is used, it should be reported, and medications that may interact with cannabis should be avoided. A headache calendar should be kept to ensure frequency of migraine and headache attacks do not go up,” said Dr. Ailani.
The study had no specific funding. Dr. Zhang, Dr. Monteith, and Dr. Ailani have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
, preliminary research suggests, although the direction of the relationship is unclear. Researchers at Stanford (Calif.) University found a significant increase in the likelihood of medication overuse headache (rebound headache) in chronic migraine patients who use cannabis.
“This study shows that there is some kind of association between cannabis use and medication overuse headache in people with chronic migraine,” said lead investigator Niushen Zhang, MD, a clinical assistant professor at Stanford.
“But it is unclear at this time whether patients are using cannabis to treat medication overuse headache or if cannabis is contributing to the development medication overuse headache, or both,” she said.
The findings were presented at the American Academy of Neurology’s 2021 annual meeting.
Sixfold increase
“Medication overuse occurs in about 1% to 3% of the general population. It affects nearly one-third of the patients (mostly patients with chronic migraine) seen at tertiary care centers such as the Stanford Headache Center,” Dr. Zhang said.
From clinical observations, patients with chronic migraine and medication overuse headache appear to be concomitantly using cannabis products, yet there is currently very little research on this topic, she added.
To investigate, the researchers reviewed the records of 368 adults who experienced chronic migraine (15 or more migraine days per month) for at least 1 year. Of the 368 patients, 150 were using cannabis, and 218 were not. In addition, 212 had medication overuse headache, and 156 did not.
Results showed that patients who used cannabis were nearly six times more likely to have medication overuse headache than those who did not use cannabis (odds ratio, 5.99; 95% confidence interval, 3.45-10.43; P < .0001).
There were significant bidirectional relationships between current cannabis use, opioid use, and medication overuse headache.
Jury out on cannabis for migraine
Commenting on the findings, Teshamae Monteith, MD, of the University of Miami, noted, “With increased legalization, greater access, and less stigmatization, there are more individuals using cannabis for migraine, but there is no solid evidence to suggest that cannabis is effective for acute or preventive treatment of migraine.”
The study is “interesting,” Dr. Monteith said, but, owing to methodologic limitations, it is not clear that cannabis contributes to medication overuse headache. “Patients with medication overuse headaches may have more comorbidities, such as anxiety, depression, and sleep disorders, that are driving the cannabis use. The patients on cannabis also had higher rates of opiate use, which itself is a stronger contributor to medication overuse headache and may indicate the presence of other pain disorders,” Dr. Monteith said.
“It is not clear if these patients were appropriately treated with migraine prevention; patients that use cannabis sometimes report that they prefer to avoid pharmaceutical treatments, such as antidepressants, etc., used for migraine,” Dr. Monteith noted.
She said that at this point, she would advise clinicians to ask about cannabis use “and let patients know that we do not know enough about the long-term effects of cannabis on the migraine brain.”
Most importantly, Dr. Monteith said, she would “encourage clinicians to be sensitive to the high prevalence of migraine, chronic migraine, and medication overuse. If we can treat more effectively and prevent migraine progression, which includes addressing comorbidities, there would be a lot less medication overuse headache.”
Also weighing in on the study, Jessica Ailani, MD, director, Medstar Georgetown Headache Center, Washington, D.C., noted that there is no conclusive evidence that cannabis is an effective acute or preventive treatment for migraine. “There is a suggestion that cannabis can help treat a migraine attack, but there is uncertainty about concentration of cannabidiol (CBD) to tetrahydrocannabinol (THC) needed to achieve pain freedom,” Dr. Ailani said.
“There has also been some concern about interactions between CBD and other medications used to treat migraine and that CBD can cause a condition known as reversible cerebral vasoconstrictive syndrome. These are reasons to be cautious with CBD,” Dr. Ailani added.
“At this time there is limited advice we can give our patients except that more studies need to be done. If cannabis is used, it should be reported, and medications that may interact with cannabis should be avoided. A headache calendar should be kept to ensure frequency of migraine and headache attacks do not go up,” said Dr. Ailani.
The study had no specific funding. Dr. Zhang, Dr. Monteith, and Dr. Ailani have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
, preliminary research suggests, although the direction of the relationship is unclear. Researchers at Stanford (Calif.) University found a significant increase in the likelihood of medication overuse headache (rebound headache) in chronic migraine patients who use cannabis.
“This study shows that there is some kind of association between cannabis use and medication overuse headache in people with chronic migraine,” said lead investigator Niushen Zhang, MD, a clinical assistant professor at Stanford.
“But it is unclear at this time whether patients are using cannabis to treat medication overuse headache or if cannabis is contributing to the development medication overuse headache, or both,” she said.
The findings were presented at the American Academy of Neurology’s 2021 annual meeting.
Sixfold increase
“Medication overuse occurs in about 1% to 3% of the general population. It affects nearly one-third of the patients (mostly patients with chronic migraine) seen at tertiary care centers such as the Stanford Headache Center,” Dr. Zhang said.
From clinical observations, patients with chronic migraine and medication overuse headache appear to be concomitantly using cannabis products, yet there is currently very little research on this topic, she added.
To investigate, the researchers reviewed the records of 368 adults who experienced chronic migraine (15 or more migraine days per month) for at least 1 year. Of the 368 patients, 150 were using cannabis, and 218 were not. In addition, 212 had medication overuse headache, and 156 did not.
Results showed that patients who used cannabis were nearly six times more likely to have medication overuse headache than those who did not use cannabis (odds ratio, 5.99; 95% confidence interval, 3.45-10.43; P < .0001).
There were significant bidirectional relationships between current cannabis use, opioid use, and medication overuse headache.
Jury out on cannabis for migraine
Commenting on the findings, Teshamae Monteith, MD, of the University of Miami, noted, “With increased legalization, greater access, and less stigmatization, there are more individuals using cannabis for migraine, but there is no solid evidence to suggest that cannabis is effective for acute or preventive treatment of migraine.”
The study is “interesting,” Dr. Monteith said, but, owing to methodologic limitations, it is not clear that cannabis contributes to medication overuse headache. “Patients with medication overuse headaches may have more comorbidities, such as anxiety, depression, and sleep disorders, that are driving the cannabis use. The patients on cannabis also had higher rates of opiate use, which itself is a stronger contributor to medication overuse headache and may indicate the presence of other pain disorders,” Dr. Monteith said.
“It is not clear if these patients were appropriately treated with migraine prevention; patients that use cannabis sometimes report that they prefer to avoid pharmaceutical treatments, such as antidepressants, etc., used for migraine,” Dr. Monteith noted.
She said that at this point, she would advise clinicians to ask about cannabis use “and let patients know that we do not know enough about the long-term effects of cannabis on the migraine brain.”
Most importantly, Dr. Monteith said, she would “encourage clinicians to be sensitive to the high prevalence of migraine, chronic migraine, and medication overuse. If we can treat more effectively and prevent migraine progression, which includes addressing comorbidities, there would be a lot less medication overuse headache.”
Also weighing in on the study, Jessica Ailani, MD, director, Medstar Georgetown Headache Center, Washington, D.C., noted that there is no conclusive evidence that cannabis is an effective acute or preventive treatment for migraine. “There is a suggestion that cannabis can help treat a migraine attack, but there is uncertainty about concentration of cannabidiol (CBD) to tetrahydrocannabinol (THC) needed to achieve pain freedom,” Dr. Ailani said.
“There has also been some concern about interactions between CBD and other medications used to treat migraine and that CBD can cause a condition known as reversible cerebral vasoconstrictive syndrome. These are reasons to be cautious with CBD,” Dr. Ailani added.
“At this time there is limited advice we can give our patients except that more studies need to be done. If cannabis is used, it should be reported, and medications that may interact with cannabis should be avoided. A headache calendar should be kept to ensure frequency of migraine and headache attacks do not go up,” said Dr. Ailani.
The study had no specific funding. Dr. Zhang, Dr. Monteith, and Dr. Ailani have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
From AAN 2021
Nondopamine antipsychotic shows clinical signal in Parkinson’s disease psychosis
according to results of a proof-of-principle study presented at the 2021 annual meeting of the American Academy of Neurology.
In presenting study results, Stuart H. Isaacson, MD, of the Parkinson’s Disease and Movement Disorders Center in Boca Raton, Fla., noted the one potential advantage of SEP-363856 is that it does not require blood monitoring, unlike clozapine, often used as an alternative to pimavanserin, the only Food and Drug Administration–approved treatment for Parkinson’s disease psychosis.* Quetiapine has also been used off label for Parkinson’s disease psychosis, but Dr. Isaacson said this lacks the evidence supporting the other two options and has side effects including sedation and orthostatic hypotension.
“Other non–FDA-approved treatment options are limited due to their lack of efficacy, safety concerns, and exacerbation of motor symptoms,” he said.
The study involved 38 patients, 24 of whom received SEP-363856 and the rest placebo, and evaluated total scores for the novel Scale for the Assessment of Positive Symptoms for Parkinson’s Disease Psychosis (SAPS-PD) after 6 weeks of treatment. The treatment group was given one of three doses: 25 mg (n = 11), 50 mg (n = 9), and 75 mg (n = 10).
Dr. Isaacson described SEP-363856 as a novel molecule that has agonist activity at TARR1, which regulates dopamine, norepinephrine, and serotonin, as well as serotonin receptor 5-HT1A, but has no activity at the dopamine receptor D2.
“There did appear to be improvement with this medication in patients’ psychosis symptoms, using the SAPS-PD subscale to identify the frequency and severity of hallucinations and delusions, but there was also improvement in the placebo group in this small study,” Dr. Isaacson said. “That did not demonstrate significance.” The improvement was maintained through the study period.
But the gap between the treatment and placebo groups widened as the degree of response increased. The rates were identical for the 30% or above response and the 50% or above response subgroups: 27.3% and 37.5% for placebo and treatment groups, respectively. However, 25% of patients taking SEP-363856 had a 100% response in terms of SAPS-PD score versus 0% in the placebo group, Dr. Isaacson said.
The study also found Mini-Mental State Examination (MMSE) scores improved more in the treatment group, with the gap wider in those with baseline MMSE scores below 24 versus scores above 24: –5.2 (standard deviation, 2.81) versus –2.1 (SD, 3.00; P = .460).
“The scope of daytime and nighttime sleep both showed improvement, with the score for daytime sleep being significant,” Dr. Isaacson said of the treatment group. “Importantly, UPDRS [Unified Parkinson’s Disease Rating Scale] Part III motor scores showed no difference from placebo. Indeed, there was a trend toward improvement, but this again was not significant.” That’s noteworthy, he said, because other antipsychotics, with the exception of clozapine – which requires blood monitoring – are contraindicated in PDP because of their effect on motor function.
During question-and-answer, Dr. Isaacson noted that the complete response rate of 25% with SEP-363856 compared favorably with the 14% complete response rate reported with pimavanserin in the pivotal trial.
“Hopefully greater-powered studies will be performed to further identify and determine the safety and efficacy and tolerably of SEP-363856 in Parkinson’s psychosis, aiming to minimize the placebo effect and to try to hopefully identify its efficacy in relationship to other treatments,” Dr. Isaacson said.
“Right now with only one approved treatment, one that has efficacy but requires blood monitoring, and another treatment that may be fraught sometimes with sleepiness and other side effects, we need other alternatives for our patients as many of them resort to lowering and lowering their dopaminergic therapies with the consequence [of] worsening motor activity,” Dr. Isaacson said.
“This study further supports the concept that Parkinson’s disease psychosis involves much more than simply dopamine,” said Daniel E. Kremens, MD, codirector of the Parkinson’s disease and movement disorders division at Thomas Jefferson University, Philadelphia. “Targeting nondopaminergic targets allows us to treat the psychosis without worsening motor symptoms. By targeting TAAR-1 along with 5HT1A, SEP-363856 is a novel compound that appears to be well tolerated and may treat PDP without worsening motor symptoms,”
Sunovion Pharmaceuticals provided funding for the study. Dr. Isaacson has no financial relationships to disclose. Three study coauthors are employees of Sunovion. Dr. Kremens reported serving as a consultant to Sunovion.
*Correction, 5/17/21: An earlier version of this article misstated the blood monitoring requirements for pimavanserin.
according to results of a proof-of-principle study presented at the 2021 annual meeting of the American Academy of Neurology.
In presenting study results, Stuart H. Isaacson, MD, of the Parkinson’s Disease and Movement Disorders Center in Boca Raton, Fla., noted the one potential advantage of SEP-363856 is that it does not require blood monitoring, unlike clozapine, often used as an alternative to pimavanserin, the only Food and Drug Administration–approved treatment for Parkinson’s disease psychosis.* Quetiapine has also been used off label for Parkinson’s disease psychosis, but Dr. Isaacson said this lacks the evidence supporting the other two options and has side effects including sedation and orthostatic hypotension.
“Other non–FDA-approved treatment options are limited due to their lack of efficacy, safety concerns, and exacerbation of motor symptoms,” he said.
The study involved 38 patients, 24 of whom received SEP-363856 and the rest placebo, and evaluated total scores for the novel Scale for the Assessment of Positive Symptoms for Parkinson’s Disease Psychosis (SAPS-PD) after 6 weeks of treatment. The treatment group was given one of three doses: 25 mg (n = 11), 50 mg (n = 9), and 75 mg (n = 10).
Dr. Isaacson described SEP-363856 as a novel molecule that has agonist activity at TARR1, which regulates dopamine, norepinephrine, and serotonin, as well as serotonin receptor 5-HT1A, but has no activity at the dopamine receptor D2.
“There did appear to be improvement with this medication in patients’ psychosis symptoms, using the SAPS-PD subscale to identify the frequency and severity of hallucinations and delusions, but there was also improvement in the placebo group in this small study,” Dr. Isaacson said. “That did not demonstrate significance.” The improvement was maintained through the study period.
But the gap between the treatment and placebo groups widened as the degree of response increased. The rates were identical for the 30% or above response and the 50% or above response subgroups: 27.3% and 37.5% for placebo and treatment groups, respectively. However, 25% of patients taking SEP-363856 had a 100% response in terms of SAPS-PD score versus 0% in the placebo group, Dr. Isaacson said.
The study also found Mini-Mental State Examination (MMSE) scores improved more in the treatment group, with the gap wider in those with baseline MMSE scores below 24 versus scores above 24: –5.2 (standard deviation, 2.81) versus –2.1 (SD, 3.00; P = .460).
“The scope of daytime and nighttime sleep both showed improvement, with the score for daytime sleep being significant,” Dr. Isaacson said of the treatment group. “Importantly, UPDRS [Unified Parkinson’s Disease Rating Scale] Part III motor scores showed no difference from placebo. Indeed, there was a trend toward improvement, but this again was not significant.” That’s noteworthy, he said, because other antipsychotics, with the exception of clozapine – which requires blood monitoring – are contraindicated in PDP because of their effect on motor function.
During question-and-answer, Dr. Isaacson noted that the complete response rate of 25% with SEP-363856 compared favorably with the 14% complete response rate reported with pimavanserin in the pivotal trial.
“Hopefully greater-powered studies will be performed to further identify and determine the safety and efficacy and tolerably of SEP-363856 in Parkinson’s psychosis, aiming to minimize the placebo effect and to try to hopefully identify its efficacy in relationship to other treatments,” Dr. Isaacson said.
“Right now with only one approved treatment, one that has efficacy but requires blood monitoring, and another treatment that may be fraught sometimes with sleepiness and other side effects, we need other alternatives for our patients as many of them resort to lowering and lowering their dopaminergic therapies with the consequence [of] worsening motor activity,” Dr. Isaacson said.
“This study further supports the concept that Parkinson’s disease psychosis involves much more than simply dopamine,” said Daniel E. Kremens, MD, codirector of the Parkinson’s disease and movement disorders division at Thomas Jefferson University, Philadelphia. “Targeting nondopaminergic targets allows us to treat the psychosis without worsening motor symptoms. By targeting TAAR-1 along with 5HT1A, SEP-363856 is a novel compound that appears to be well tolerated and may treat PDP without worsening motor symptoms,”
Sunovion Pharmaceuticals provided funding for the study. Dr. Isaacson has no financial relationships to disclose. Three study coauthors are employees of Sunovion. Dr. Kremens reported serving as a consultant to Sunovion.
*Correction, 5/17/21: An earlier version of this article misstated the blood monitoring requirements for pimavanserin.
according to results of a proof-of-principle study presented at the 2021 annual meeting of the American Academy of Neurology.
In presenting study results, Stuart H. Isaacson, MD, of the Parkinson’s Disease and Movement Disorders Center in Boca Raton, Fla., noted the one potential advantage of SEP-363856 is that it does not require blood monitoring, unlike clozapine, often used as an alternative to pimavanserin, the only Food and Drug Administration–approved treatment for Parkinson’s disease psychosis.* Quetiapine has also been used off label for Parkinson’s disease psychosis, but Dr. Isaacson said this lacks the evidence supporting the other two options and has side effects including sedation and orthostatic hypotension.
“Other non–FDA-approved treatment options are limited due to their lack of efficacy, safety concerns, and exacerbation of motor symptoms,” he said.
The study involved 38 patients, 24 of whom received SEP-363856 and the rest placebo, and evaluated total scores for the novel Scale for the Assessment of Positive Symptoms for Parkinson’s Disease Psychosis (SAPS-PD) after 6 weeks of treatment. The treatment group was given one of three doses: 25 mg (n = 11), 50 mg (n = 9), and 75 mg (n = 10).
Dr. Isaacson described SEP-363856 as a novel molecule that has agonist activity at TARR1, which regulates dopamine, norepinephrine, and serotonin, as well as serotonin receptor 5-HT1A, but has no activity at the dopamine receptor D2.
“There did appear to be improvement with this medication in patients’ psychosis symptoms, using the SAPS-PD subscale to identify the frequency and severity of hallucinations and delusions, but there was also improvement in the placebo group in this small study,” Dr. Isaacson said. “That did not demonstrate significance.” The improvement was maintained through the study period.
But the gap between the treatment and placebo groups widened as the degree of response increased. The rates were identical for the 30% or above response and the 50% or above response subgroups: 27.3% and 37.5% for placebo and treatment groups, respectively. However, 25% of patients taking SEP-363856 had a 100% response in terms of SAPS-PD score versus 0% in the placebo group, Dr. Isaacson said.
The study also found Mini-Mental State Examination (MMSE) scores improved more in the treatment group, with the gap wider in those with baseline MMSE scores below 24 versus scores above 24: –5.2 (standard deviation, 2.81) versus –2.1 (SD, 3.00; P = .460).
“The scope of daytime and nighttime sleep both showed improvement, with the score for daytime sleep being significant,” Dr. Isaacson said of the treatment group. “Importantly, UPDRS [Unified Parkinson’s Disease Rating Scale] Part III motor scores showed no difference from placebo. Indeed, there was a trend toward improvement, but this again was not significant.” That’s noteworthy, he said, because other antipsychotics, with the exception of clozapine – which requires blood monitoring – are contraindicated in PDP because of their effect on motor function.
During question-and-answer, Dr. Isaacson noted that the complete response rate of 25% with SEP-363856 compared favorably with the 14% complete response rate reported with pimavanserin in the pivotal trial.
“Hopefully greater-powered studies will be performed to further identify and determine the safety and efficacy and tolerably of SEP-363856 in Parkinson’s psychosis, aiming to minimize the placebo effect and to try to hopefully identify its efficacy in relationship to other treatments,” Dr. Isaacson said.
“Right now with only one approved treatment, one that has efficacy but requires blood monitoring, and another treatment that may be fraught sometimes with sleepiness and other side effects, we need other alternatives for our patients as many of them resort to lowering and lowering their dopaminergic therapies with the consequence [of] worsening motor activity,” Dr. Isaacson said.
“This study further supports the concept that Parkinson’s disease psychosis involves much more than simply dopamine,” said Daniel E. Kremens, MD, codirector of the Parkinson’s disease and movement disorders division at Thomas Jefferson University, Philadelphia. “Targeting nondopaminergic targets allows us to treat the psychosis without worsening motor symptoms. By targeting TAAR-1 along with 5HT1A, SEP-363856 is a novel compound that appears to be well tolerated and may treat PDP without worsening motor symptoms,”
Sunovion Pharmaceuticals provided funding for the study. Dr. Isaacson has no financial relationships to disclose. Three study coauthors are employees of Sunovion. Dr. Kremens reported serving as a consultant to Sunovion.
*Correction, 5/17/21: An earlier version of this article misstated the blood monitoring requirements for pimavanserin.
FROM AAN 2021
Helpful giant rodents and our old friend, the hookworm
Rat-ting out coronavirus
Did you know there is a possibility that giant rodents could rat out coronavirus? Not many people are keen on the presence of a 3-foot-long African giant pouched rat, but they have already been trained to sniff out diseases that are dangerous to humans, such as brucellosis and tuberculosis, according to researchers at the University of Glasgow.
Professor Dan Haydon and his associates believe there is a good possibility that the rats can be trained to sniff out COVID-19. Dogs have been helpful in sniffing for COVID-19 at airports and are being trained to detect it through armpit sweat, making detection of the virus easier for travelers and staff. Even robots have gotten into the COVID-19 detecting act.
Since African giant pouched rats can grow to be the size of a small dog and “are easily tamed as companion animals,” it seems likely that they have the potential to do the same. That is, sniffing for COVID-19, not appearing at your local airport. That’s still gross.
Stay healthy, get a parasite bestie
The key to health could actually be swimming around in your gut. Researchers from University College London have found that a parasitic worm could be the answer to longevity and avoidance of chronic diseases.
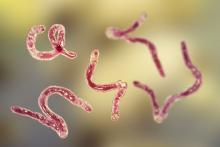
The seeming immunity from inflammatory diseases such as arthritis, diabetes, and multiple sclerosis may come from helminth parasites, or hookworms – parasites that have been coexisting harmlessly with the human body for thousands of years. The investigators went so far as to call them “old friends,” but the kind that you rarely see at reunions or call up for a favor.
As a result of modern sanitation and improved hygiene, humans and hookworms are seeing much less of each other, which may be a factor in the rise of “aging-associated inflammation” such as COVID-19 symptoms, they suggested. So is there a way to get these old friends back?
“Restorative hookworm treatments” could help with heart disease or dementia, according to the investigators, but maybe you’re not totally on board with getting an actual parasite in your system. We get it. There are helminth-derived proteins that have already been tested to get the job done.
Maybe old friends really do make the best friends.
I love the smell of microbe-infected aerosols in the morning
Have you gone into a public restroom and just stood around for a while appreciating the fine aromas? No? You haven’t? You do your business and get out? Well, it’s a good thing you act like a normal person, because the aerosols released when toilets flush can contain all sorts of nasty bacteria and viruses.
The authors of a new study published in Physics of Fluids came to this groundbreaking conclusion by going to a public bathroom, sticking particle counters above a urinal and a toilet, and letting them sit for a while. After 3 hours and 100 flushes, the ambient level of particles 0.3-3 mcm in diameter had increased dramatically, with particles sized 0.5-1 mcm particularly prone to lingering. For those particles, the level from baseline increased by over 200%.
This is a major concern, the researchers said, because the sort of microbes that are expelled through feces, urine, and vomit can include some pretty nasty things. Ebola, noroviruses that can cause food poisoning, and even good old SARS-CoV-2 can be expelled from the body but remain viable for a time in these aerosols. The researchers recommended improving the ventilation systems in restrooms so that aerosols don’t hang around for hours at a time. Plus, it might make the place not smell like a, uh, public restroom.
Not to question the research and the people behind it, but we’re not sure how necessary it was to give people another reason not to hang out in a place where hundreds, if not thousands, of people come to relieve themselves. There’s a reason we’re supposed to “stop and smell the roses” and not “stop and smell the public bathroom.”
World ends not with a bang but with a cheeseburger
Speaking of old sayings, one of our favorites, “You are what you eat,” may offer a culinary explanation for those who do enjoy the ambiance of a fine, aerosol-infested public restroom.
That explanation involves the high-calorie, high-fat smorgasbord known as the Western diet and some mice who were forced to consume it. Those mice, it turns out, were more anxious and less cognitively advanced than their counterparts who were not eating “highly palatable, energy dense foods (e.g., high saturated fat, high sugar) that are commonly consumed by humans,” according to the authors of a recent literature review.
“Consumption of a Western diet is related to poorer cognitive performance across the lifespan,” the investigators said, adding that consumption of a Western diet “during critical early life stages of development has negative consequences on various cognitive abilities later in adulthood.”
To show their appreciation for the sacrifices these brave test subjects had made in the name of science, the scientists released the Western diet–addled rodents from captivity. Not only did they survive and thrive in the wilds of darkest suburbia, but within 6 months almost half of them were running for Congress.
Rat-ting out coronavirus
Did you know there is a possibility that giant rodents could rat out coronavirus? Not many people are keen on the presence of a 3-foot-long African giant pouched rat, but they have already been trained to sniff out diseases that are dangerous to humans, such as brucellosis and tuberculosis, according to researchers at the University of Glasgow.
Professor Dan Haydon and his associates believe there is a good possibility that the rats can be trained to sniff out COVID-19. Dogs have been helpful in sniffing for COVID-19 at airports and are being trained to detect it through armpit sweat, making detection of the virus easier for travelers and staff. Even robots have gotten into the COVID-19 detecting act.
Since African giant pouched rats can grow to be the size of a small dog and “are easily tamed as companion animals,” it seems likely that they have the potential to do the same. That is, sniffing for COVID-19, not appearing at your local airport. That’s still gross.
Stay healthy, get a parasite bestie
The key to health could actually be swimming around in your gut. Researchers from University College London have found that a parasitic worm could be the answer to longevity and avoidance of chronic diseases.
The seeming immunity from inflammatory diseases such as arthritis, diabetes, and multiple sclerosis may come from helminth parasites, or hookworms – parasites that have been coexisting harmlessly with the human body for thousands of years. The investigators went so far as to call them “old friends,” but the kind that you rarely see at reunions or call up for a favor.
As a result of modern sanitation and improved hygiene, humans and hookworms are seeing much less of each other, which may be a factor in the rise of “aging-associated inflammation” such as COVID-19 symptoms, they suggested. So is there a way to get these old friends back?
“Restorative hookworm treatments” could help with heart disease or dementia, according to the investigators, but maybe you’re not totally on board with getting an actual parasite in your system. We get it. There are helminth-derived proteins that have already been tested to get the job done.
Maybe old friends really do make the best friends.
I love the smell of microbe-infected aerosols in the morning
Have you gone into a public restroom and just stood around for a while appreciating the fine aromas? No? You haven’t? You do your business and get out? Well, it’s a good thing you act like a normal person, because the aerosols released when toilets flush can contain all sorts of nasty bacteria and viruses.
The authors of a new study published in Physics of Fluids came to this groundbreaking conclusion by going to a public bathroom, sticking particle counters above a urinal and a toilet, and letting them sit for a while. After 3 hours and 100 flushes, the ambient level of particles 0.3-3 mcm in diameter had increased dramatically, with particles sized 0.5-1 mcm particularly prone to lingering. For those particles, the level from baseline increased by over 200%.
This is a major concern, the researchers said, because the sort of microbes that are expelled through feces, urine, and vomit can include some pretty nasty things. Ebola, noroviruses that can cause food poisoning, and even good old SARS-CoV-2 can be expelled from the body but remain viable for a time in these aerosols. The researchers recommended improving the ventilation systems in restrooms so that aerosols don’t hang around for hours at a time. Plus, it might make the place not smell like a, uh, public restroom.
Not to question the research and the people behind it, but we’re not sure how necessary it was to give people another reason not to hang out in a place where hundreds, if not thousands, of people come to relieve themselves. There’s a reason we’re supposed to “stop and smell the roses” and not “stop and smell the public bathroom.”
World ends not with a bang but with a cheeseburger
Speaking of old sayings, one of our favorites, “You are what you eat,” may offer a culinary explanation for those who do enjoy the ambiance of a fine, aerosol-infested public restroom.
That explanation involves the high-calorie, high-fat smorgasbord known as the Western diet and some mice who were forced to consume it. Those mice, it turns out, were more anxious and less cognitively advanced than their counterparts who were not eating “highly palatable, energy dense foods (e.g., high saturated fat, high sugar) that are commonly consumed by humans,” according to the authors of a recent literature review.
“Consumption of a Western diet is related to poorer cognitive performance across the lifespan,” the investigators said, adding that consumption of a Western diet “during critical early life stages of development has negative consequences on various cognitive abilities later in adulthood.”
To show their appreciation for the sacrifices these brave test subjects had made in the name of science, the scientists released the Western diet–addled rodents from captivity. Not only did they survive and thrive in the wilds of darkest suburbia, but within 6 months almost half of them were running for Congress.
Rat-ting out coronavirus
Did you know there is a possibility that giant rodents could rat out coronavirus? Not many people are keen on the presence of a 3-foot-long African giant pouched rat, but they have already been trained to sniff out diseases that are dangerous to humans, such as brucellosis and tuberculosis, according to researchers at the University of Glasgow.
Professor Dan Haydon and his associates believe there is a good possibility that the rats can be trained to sniff out COVID-19. Dogs have been helpful in sniffing for COVID-19 at airports and are being trained to detect it through armpit sweat, making detection of the virus easier for travelers and staff. Even robots have gotten into the COVID-19 detecting act.
Since African giant pouched rats can grow to be the size of a small dog and “are easily tamed as companion animals,” it seems likely that they have the potential to do the same. That is, sniffing for COVID-19, not appearing at your local airport. That’s still gross.
Stay healthy, get a parasite bestie
The key to health could actually be swimming around in your gut. Researchers from University College London have found that a parasitic worm could be the answer to longevity and avoidance of chronic diseases.
The seeming immunity from inflammatory diseases such as arthritis, diabetes, and multiple sclerosis may come from helminth parasites, or hookworms – parasites that have been coexisting harmlessly with the human body for thousands of years. The investigators went so far as to call them “old friends,” but the kind that you rarely see at reunions or call up for a favor.
As a result of modern sanitation and improved hygiene, humans and hookworms are seeing much less of each other, which may be a factor in the rise of “aging-associated inflammation” such as COVID-19 symptoms, they suggested. So is there a way to get these old friends back?
“Restorative hookworm treatments” could help with heart disease or dementia, according to the investigators, but maybe you’re not totally on board with getting an actual parasite in your system. We get it. There are helminth-derived proteins that have already been tested to get the job done.
Maybe old friends really do make the best friends.
I love the smell of microbe-infected aerosols in the morning
Have you gone into a public restroom and just stood around for a while appreciating the fine aromas? No? You haven’t? You do your business and get out? Well, it’s a good thing you act like a normal person, because the aerosols released when toilets flush can contain all sorts of nasty bacteria and viruses.
The authors of a new study published in Physics of Fluids came to this groundbreaking conclusion by going to a public bathroom, sticking particle counters above a urinal and a toilet, and letting them sit for a while. After 3 hours and 100 flushes, the ambient level of particles 0.3-3 mcm in diameter had increased dramatically, with particles sized 0.5-1 mcm particularly prone to lingering. For those particles, the level from baseline increased by over 200%.
This is a major concern, the researchers said, because the sort of microbes that are expelled through feces, urine, and vomit can include some pretty nasty things. Ebola, noroviruses that can cause food poisoning, and even good old SARS-CoV-2 can be expelled from the body but remain viable for a time in these aerosols. The researchers recommended improving the ventilation systems in restrooms so that aerosols don’t hang around for hours at a time. Plus, it might make the place not smell like a, uh, public restroom.
Not to question the research and the people behind it, but we’re not sure how necessary it was to give people another reason not to hang out in a place where hundreds, if not thousands, of people come to relieve themselves. There’s a reason we’re supposed to “stop and smell the roses” and not “stop and smell the public bathroom.”
World ends not with a bang but with a cheeseburger
Speaking of old sayings, one of our favorites, “You are what you eat,” may offer a culinary explanation for those who do enjoy the ambiance of a fine, aerosol-infested public restroom.
That explanation involves the high-calorie, high-fat smorgasbord known as the Western diet and some mice who were forced to consume it. Those mice, it turns out, were more anxious and less cognitively advanced than their counterparts who were not eating “highly palatable, energy dense foods (e.g., high saturated fat, high sugar) that are commonly consumed by humans,” according to the authors of a recent literature review.
“Consumption of a Western diet is related to poorer cognitive performance across the lifespan,” the investigators said, adding that consumption of a Western diet “during critical early life stages of development has negative consequences on various cognitive abilities later in adulthood.”
To show their appreciation for the sacrifices these brave test subjects had made in the name of science, the scientists released the Western diet–addled rodents from captivity. Not only did they survive and thrive in the wilds of darkest suburbia, but within 6 months almost half of them were running for Congress.
Gene therapy shows promise for Sanfilippo syndrome
. Most of the benefit from the treatment came in patients who began treatment at younger age, but comparisons to natural history controls showed profound improvement among many recipients, some of whom attained normal developmental trajectories.
The study was presented at the American Academy of Neurology’s 2021 annual meeting by Kevin Flanigan, MD, an attending neurologist at Nationwide Children’s Hospital in Columbus, Ohio. He highlighted the improved developmental outcomes. “There’s been nothing shown to change the cognitive pathway of the disease. This is the first time it’s been seen as a treatment effect,” Dr. Flanigan said during a follow-up Q&A session.
The therapy was delivered using an adeno-associated virus-9 (AAV-9) vector, which led one questioner to ask about potential safety concerns, since AAV-associated risks date back to the death of Jesse Gelsinger in 1999. “There is concern about AAV therapies related to immune responses to potentially complement-mediated activation and thrombocytopenic syndrome, which has led to clinical holds on some other AAV-9 products related to muscular dystrophies. We’ve not seen signals of anything reminiscent of that, and we’re at AAV-9 dosages that are quite similar to what’s been used elsewhere in the field,” said Dr. Flanigan.
The results have him optimistic about the therapy. “I do think if it continues to be increasing divergent from the natural history, it will be questionable as to whether a subsequent trial will be necessary for this. That’s a decision for the [Food and Drug Administration] and the company to decide. Each observation point that goes by, each patient treated, and each time we get more data, I get more and more confident. It’s really gratifying to watch,” said Dr. Flanigan.
The study confirms the potential of gene replacement therapy autosomal recessive conditions, according to Nicholas Johnson, MD, associate professor of neurology at Virginia Commonwealth University, Richmond, as well as a fellow of the American Academy of Neurology. “Where the genetic problem is loss of gene function, the ability to replace that gene using a viral approach is going to be transformative across the board for many of these different conditions, including Sanfilippo syndrome,” said Dr. Johnson, who attended the session but was not involved in the research.
Toxicity could remain an issue, even in the absence of AAV-based safety concerns. “The rate limiting step in terms of gene replacement therapy development likely relates to the ability to provide those therapies to larger adults, because many approaches are weight based and it’s unclear what the upper limit of toxicity would be for adults,” said Dr. Johnson.
Transpher A study results
Dr. Flanigan presented results from Transpher A, a phase 1/2 clinical trial that has enrolled 20 patients to date in three cohorts: Cohort 1, with 3 patients, received 5 x 1,012 vg/kg, and had a mean follow-up of 58 months; cohort 2, with 3 patients, received 1 x 1,013 vg/kg, and had a mean follow-up of 49 months; and cohort 3, with 14 patients, received 3 x 1,013 vg/kg, with a mean follow-up of 24 months. Included patients ranged from birth to age 2, or older than age 2 with a development quotient of 60 or higher on the Bayley Scale.
Dr. Flanigan showed a plot of developmental progress compared with natural history controls, which showed that patients treated before age 2 or with a developmental quotient of 60 or higher had improved outcomes compared to other patients in the high dose cohort. They continued to show normal developmental progression at 30-36 months post treatment, at a time when the natural history data suggested they would suffer cognitive decline. Two years after administration, this group had cerebral spinal fluid levels of heparan sulfate that fell below the lower limit of detection. Patients in the high-dose cohort had normalized CSF levels of GM2 and GM3 gangliosides, and there were reductions in plasma heparan sulfate and urinary glycosaminoglycans. There was also a sustained decrease in liver volume.
The highest dose group was originally given to older patients, and most were similar to the natural history cohort, though some did stabilize. “More compellingly, patients (in the high-dose group) who were treated younger actually showed continued increase in development. One individual follows the normal development quotient line, and we would say that these are really quite distinct from what we typically see in patients,” said Dr. Flanigan.
The treatment was well tolerated. There were no deaths or treatment-related serious adverse events, and no clinically-significant adverse events within the first 5 years of follow-up.
The study was funded by Abeona Therapeutics. Dr. Flanigan has been on advisory boards for Apic Bio and 4D Molecular Therapeutics, consulted for Encoded Therapeutics, and has received royalties from Audentes Therapeutics. Dr. Flanigan has received funding from and been a consultant for Avidity.
. Most of the benefit from the treatment came in patients who began treatment at younger age, but comparisons to natural history controls showed profound improvement among many recipients, some of whom attained normal developmental trajectories.
The study was presented at the American Academy of Neurology’s 2021 annual meeting by Kevin Flanigan, MD, an attending neurologist at Nationwide Children’s Hospital in Columbus, Ohio. He highlighted the improved developmental outcomes. “There’s been nothing shown to change the cognitive pathway of the disease. This is the first time it’s been seen as a treatment effect,” Dr. Flanigan said during a follow-up Q&A session.
The therapy was delivered using an adeno-associated virus-9 (AAV-9) vector, which led one questioner to ask about potential safety concerns, since AAV-associated risks date back to the death of Jesse Gelsinger in 1999. “There is concern about AAV therapies related to immune responses to potentially complement-mediated activation and thrombocytopenic syndrome, which has led to clinical holds on some other AAV-9 products related to muscular dystrophies. We’ve not seen signals of anything reminiscent of that, and we’re at AAV-9 dosages that are quite similar to what’s been used elsewhere in the field,” said Dr. Flanigan.
The results have him optimistic about the therapy. “I do think if it continues to be increasing divergent from the natural history, it will be questionable as to whether a subsequent trial will be necessary for this. That’s a decision for the [Food and Drug Administration] and the company to decide. Each observation point that goes by, each patient treated, and each time we get more data, I get more and more confident. It’s really gratifying to watch,” said Dr. Flanigan.
The study confirms the potential of gene replacement therapy autosomal recessive conditions, according to Nicholas Johnson, MD, associate professor of neurology at Virginia Commonwealth University, Richmond, as well as a fellow of the American Academy of Neurology. “Where the genetic problem is loss of gene function, the ability to replace that gene using a viral approach is going to be transformative across the board for many of these different conditions, including Sanfilippo syndrome,” said Dr. Johnson, who attended the session but was not involved in the research.
Toxicity could remain an issue, even in the absence of AAV-based safety concerns. “The rate limiting step in terms of gene replacement therapy development likely relates to the ability to provide those therapies to larger adults, because many approaches are weight based and it’s unclear what the upper limit of toxicity would be for adults,” said Dr. Johnson.
Transpher A study results
Dr. Flanigan presented results from Transpher A, a phase 1/2 clinical trial that has enrolled 20 patients to date in three cohorts: Cohort 1, with 3 patients, received 5 x 1,012 vg/kg, and had a mean follow-up of 58 months; cohort 2, with 3 patients, received 1 x 1,013 vg/kg, and had a mean follow-up of 49 months; and cohort 3, with 14 patients, received 3 x 1,013 vg/kg, with a mean follow-up of 24 months. Included patients ranged from birth to age 2, or older than age 2 with a development quotient of 60 or higher on the Bayley Scale.
Dr. Flanigan showed a plot of developmental progress compared with natural history controls, which showed that patients treated before age 2 or with a developmental quotient of 60 or higher had improved outcomes compared to other patients in the high dose cohort. They continued to show normal developmental progression at 30-36 months post treatment, at a time when the natural history data suggested they would suffer cognitive decline. Two years after administration, this group had cerebral spinal fluid levels of heparan sulfate that fell below the lower limit of detection. Patients in the high-dose cohort had normalized CSF levels of GM2 and GM3 gangliosides, and there were reductions in plasma heparan sulfate and urinary glycosaminoglycans. There was also a sustained decrease in liver volume.
The highest dose group was originally given to older patients, and most were similar to the natural history cohort, though some did stabilize. “More compellingly, patients (in the high-dose group) who were treated younger actually showed continued increase in development. One individual follows the normal development quotient line, and we would say that these are really quite distinct from what we typically see in patients,” said Dr. Flanigan.
The treatment was well tolerated. There were no deaths or treatment-related serious adverse events, and no clinically-significant adverse events within the first 5 years of follow-up.
The study was funded by Abeona Therapeutics. Dr. Flanigan has been on advisory boards for Apic Bio and 4D Molecular Therapeutics, consulted for Encoded Therapeutics, and has received royalties from Audentes Therapeutics. Dr. Flanigan has received funding from and been a consultant for Avidity.
. Most of the benefit from the treatment came in patients who began treatment at younger age, but comparisons to natural history controls showed profound improvement among many recipients, some of whom attained normal developmental trajectories.
The study was presented at the American Academy of Neurology’s 2021 annual meeting by Kevin Flanigan, MD, an attending neurologist at Nationwide Children’s Hospital in Columbus, Ohio. He highlighted the improved developmental outcomes. “There’s been nothing shown to change the cognitive pathway of the disease. This is the first time it’s been seen as a treatment effect,” Dr. Flanigan said during a follow-up Q&A session.
The therapy was delivered using an adeno-associated virus-9 (AAV-9) vector, which led one questioner to ask about potential safety concerns, since AAV-associated risks date back to the death of Jesse Gelsinger in 1999. “There is concern about AAV therapies related to immune responses to potentially complement-mediated activation and thrombocytopenic syndrome, which has led to clinical holds on some other AAV-9 products related to muscular dystrophies. We’ve not seen signals of anything reminiscent of that, and we’re at AAV-9 dosages that are quite similar to what’s been used elsewhere in the field,” said Dr. Flanigan.
The results have him optimistic about the therapy. “I do think if it continues to be increasing divergent from the natural history, it will be questionable as to whether a subsequent trial will be necessary for this. That’s a decision for the [Food and Drug Administration] and the company to decide. Each observation point that goes by, each patient treated, and each time we get more data, I get more and more confident. It’s really gratifying to watch,” said Dr. Flanigan.
The study confirms the potential of gene replacement therapy autosomal recessive conditions, according to Nicholas Johnson, MD, associate professor of neurology at Virginia Commonwealth University, Richmond, as well as a fellow of the American Academy of Neurology. “Where the genetic problem is loss of gene function, the ability to replace that gene using a viral approach is going to be transformative across the board for many of these different conditions, including Sanfilippo syndrome,” said Dr. Johnson, who attended the session but was not involved in the research.
Toxicity could remain an issue, even in the absence of AAV-based safety concerns. “The rate limiting step in terms of gene replacement therapy development likely relates to the ability to provide those therapies to larger adults, because many approaches are weight based and it’s unclear what the upper limit of toxicity would be for adults,” said Dr. Johnson.
Transpher A study results
Dr. Flanigan presented results from Transpher A, a phase 1/2 clinical trial that has enrolled 20 patients to date in three cohorts: Cohort 1, with 3 patients, received 5 x 1,012 vg/kg, and had a mean follow-up of 58 months; cohort 2, with 3 patients, received 1 x 1,013 vg/kg, and had a mean follow-up of 49 months; and cohort 3, with 14 patients, received 3 x 1,013 vg/kg, with a mean follow-up of 24 months. Included patients ranged from birth to age 2, or older than age 2 with a development quotient of 60 or higher on the Bayley Scale.
Dr. Flanigan showed a plot of developmental progress compared with natural history controls, which showed that patients treated before age 2 or with a developmental quotient of 60 or higher had improved outcomes compared to other patients in the high dose cohort. They continued to show normal developmental progression at 30-36 months post treatment, at a time when the natural history data suggested they would suffer cognitive decline. Two years after administration, this group had cerebral spinal fluid levels of heparan sulfate that fell below the lower limit of detection. Patients in the high-dose cohort had normalized CSF levels of GM2 and GM3 gangliosides, and there were reductions in plasma heparan sulfate and urinary glycosaminoglycans. There was also a sustained decrease in liver volume.
The highest dose group was originally given to older patients, and most were similar to the natural history cohort, though some did stabilize. “More compellingly, patients (in the high-dose group) who were treated younger actually showed continued increase in development. One individual follows the normal development quotient line, and we would say that these are really quite distinct from what we typically see in patients,” said Dr. Flanigan.
The treatment was well tolerated. There were no deaths or treatment-related serious adverse events, and no clinically-significant adverse events within the first 5 years of follow-up.
The study was funded by Abeona Therapeutics. Dr. Flanigan has been on advisory boards for Apic Bio and 4D Molecular Therapeutics, consulted for Encoded Therapeutics, and has received royalties from Audentes Therapeutics. Dr. Flanigan has received funding from and been a consultant for Avidity.
FROM AAN 2021
Investigative gepant liver profile comparable with standard of care
according to results of a multicenter, open-label trial presented at the 2021 annual meeting of the American Academy of Neurology.
The trial included 739 patients, 543 of whom were randomized to daily oral atogepant with the remainder assigned to the existing standard of care oral migraine prevention medication, said Messoud Ashina, MD, PhD, of the Danish Headache Center at the University of Copenhagen. Initially, 67% (n = 364) of the atogepant patients reported treatment-emergent adverse events (TEAEs). However, he noted, the rate of TEAEs related to treatment was actually 18% (n = 98), and the rate of serious AEs was 4.4% (n = 24); 31 patients (5.7%) discontinued therapy because of TEAEs.
Those rates compared favorably with the standard of care group, Dr. Ashina said. In that group, the rate of TEAEs was 78.6% (154/196), and the rate of treatment-related TEAEs was 36.2% (n = 71).
In the atogepant group, the most common TEAEs were upper respiratory tract infection (10.3%, n = 56), constipation (7.2%, n = 39) and nausea (6.3%, n = 34). “With constipation in particular most cases were mild to moderate,” Dr. Ashina said. “Only one case was considered severe and it resolved before the end of the trial.” One patient discontinued treatment because of constipation.
Most significantly, said Dr. Ashina, “No hepatic safety issues were identified.” In the atogepant group, 2.4% of patients (n = 13) had ALT/AST levels at three times the upper limit of normal versus 3.2% (n = 6) in the standard of care group.
During question-and-answer, Dr. Ashina was pressed on the rate or urinary tract infections in the atogepant patients – 5.2% (n = 28), a measure not reported in the standard of care group – but he said there was no indication the UTIs resulted from atogepant itself. “I assume if there was some problems with urinary tract infections because of the kidneys then you would expect to see the lab data showing that,” he added in an interview. “There were no differences in lab abnormalities between the two groups.”
While Dr. Ashina said “I don’t think it’s something of concern” with regard to the UTI risk, he added: “It doesn’t mean that we don’t have to be careful. As physicians, we have to exhibit pharmacovigilance all the time, especially with the new drugs coming out over the next 5 years. But don’t panic.”
Stephen D. Silberstein, MD, director of the headache center at Thomas Jefferson University, Philadelphia, agreed that the hepatic values reported in the open-label trial are important. “What’s really nice about this study is the fact that we now know that this particular gepant when given on a regular basis for 1 year has no problem with liver or kidney function,” he said in an interview.
Dr. Ashina said once-daily oral atogepant could potentially be a desirable alternative migraine preventive treatment to monoclonal antibodies and their quarterly injections and a second-line therapy when other treatments don’t work. However, Dr. Silverstein noted that patients typically aren’t as compliant with self-administered oral medications as they are with periodic injections.
Allergan/AbbVie sponsored the trial. Dr. Ashina reported financial relationships with Allergan/AbbVie, Amgen, Eli Lilly, Lundbeck, Novartis, and Teva. Dr. Silberstein is a trial investigator.
according to results of a multicenter, open-label trial presented at the 2021 annual meeting of the American Academy of Neurology.
The trial included 739 patients, 543 of whom were randomized to daily oral atogepant with the remainder assigned to the existing standard of care oral migraine prevention medication, said Messoud Ashina, MD, PhD, of the Danish Headache Center at the University of Copenhagen. Initially, 67% (n = 364) of the atogepant patients reported treatment-emergent adverse events (TEAEs). However, he noted, the rate of TEAEs related to treatment was actually 18% (n = 98), and the rate of serious AEs was 4.4% (n = 24); 31 patients (5.7%) discontinued therapy because of TEAEs.
Those rates compared favorably with the standard of care group, Dr. Ashina said. In that group, the rate of TEAEs was 78.6% (154/196), and the rate of treatment-related TEAEs was 36.2% (n = 71).
In the atogepant group, the most common TEAEs were upper respiratory tract infection (10.3%, n = 56), constipation (7.2%, n = 39) and nausea (6.3%, n = 34). “With constipation in particular most cases were mild to moderate,” Dr. Ashina said. “Only one case was considered severe and it resolved before the end of the trial.” One patient discontinued treatment because of constipation.
Most significantly, said Dr. Ashina, “No hepatic safety issues were identified.” In the atogepant group, 2.4% of patients (n = 13) had ALT/AST levels at three times the upper limit of normal versus 3.2% (n = 6) in the standard of care group.
During question-and-answer, Dr. Ashina was pressed on the rate or urinary tract infections in the atogepant patients – 5.2% (n = 28), a measure not reported in the standard of care group – but he said there was no indication the UTIs resulted from atogepant itself. “I assume if there was some problems with urinary tract infections because of the kidneys then you would expect to see the lab data showing that,” he added in an interview. “There were no differences in lab abnormalities between the two groups.”
While Dr. Ashina said “I don’t think it’s something of concern” with regard to the UTI risk, he added: “It doesn’t mean that we don’t have to be careful. As physicians, we have to exhibit pharmacovigilance all the time, especially with the new drugs coming out over the next 5 years. But don’t panic.”
Stephen D. Silberstein, MD, director of the headache center at Thomas Jefferson University, Philadelphia, agreed that the hepatic values reported in the open-label trial are important. “What’s really nice about this study is the fact that we now know that this particular gepant when given on a regular basis for 1 year has no problem with liver or kidney function,” he said in an interview.
Dr. Ashina said once-daily oral atogepant could potentially be a desirable alternative migraine preventive treatment to monoclonal antibodies and their quarterly injections and a second-line therapy when other treatments don’t work. However, Dr. Silverstein noted that patients typically aren’t as compliant with self-administered oral medications as they are with periodic injections.
Allergan/AbbVie sponsored the trial. Dr. Ashina reported financial relationships with Allergan/AbbVie, Amgen, Eli Lilly, Lundbeck, Novartis, and Teva. Dr. Silberstein is a trial investigator.
according to results of a multicenter, open-label trial presented at the 2021 annual meeting of the American Academy of Neurology.
The trial included 739 patients, 543 of whom were randomized to daily oral atogepant with the remainder assigned to the existing standard of care oral migraine prevention medication, said Messoud Ashina, MD, PhD, of the Danish Headache Center at the University of Copenhagen. Initially, 67% (n = 364) of the atogepant patients reported treatment-emergent adverse events (TEAEs). However, he noted, the rate of TEAEs related to treatment was actually 18% (n = 98), and the rate of serious AEs was 4.4% (n = 24); 31 patients (5.7%) discontinued therapy because of TEAEs.
Those rates compared favorably with the standard of care group, Dr. Ashina said. In that group, the rate of TEAEs was 78.6% (154/196), and the rate of treatment-related TEAEs was 36.2% (n = 71).
In the atogepant group, the most common TEAEs were upper respiratory tract infection (10.3%, n = 56), constipation (7.2%, n = 39) and nausea (6.3%, n = 34). “With constipation in particular most cases were mild to moderate,” Dr. Ashina said. “Only one case was considered severe and it resolved before the end of the trial.” One patient discontinued treatment because of constipation.
Most significantly, said Dr. Ashina, “No hepatic safety issues were identified.” In the atogepant group, 2.4% of patients (n = 13) had ALT/AST levels at three times the upper limit of normal versus 3.2% (n = 6) in the standard of care group.
During question-and-answer, Dr. Ashina was pressed on the rate or urinary tract infections in the atogepant patients – 5.2% (n = 28), a measure not reported in the standard of care group – but he said there was no indication the UTIs resulted from atogepant itself. “I assume if there was some problems with urinary tract infections because of the kidneys then you would expect to see the lab data showing that,” he added in an interview. “There were no differences in lab abnormalities between the two groups.”
While Dr. Ashina said “I don’t think it’s something of concern” with regard to the UTI risk, he added: “It doesn’t mean that we don’t have to be careful. As physicians, we have to exhibit pharmacovigilance all the time, especially with the new drugs coming out over the next 5 years. But don’t panic.”
Stephen D. Silberstein, MD, director of the headache center at Thomas Jefferson University, Philadelphia, agreed that the hepatic values reported in the open-label trial are important. “What’s really nice about this study is the fact that we now know that this particular gepant when given on a regular basis for 1 year has no problem with liver or kidney function,” he said in an interview.
Dr. Ashina said once-daily oral atogepant could potentially be a desirable alternative migraine preventive treatment to monoclonal antibodies and their quarterly injections and a second-line therapy when other treatments don’t work. However, Dr. Silverstein noted that patients typically aren’t as compliant with self-administered oral medications as they are with periodic injections.
Allergan/AbbVie sponsored the trial. Dr. Ashina reported financial relationships with Allergan/AbbVie, Amgen, Eli Lilly, Lundbeck, Novartis, and Teva. Dr. Silberstein is a trial investigator.
FROM AAN 2021
The neurology of long-haul COVID-19
Long-haul neurologic symptoms of COVID-19 seem to be distinct from neurologic conditions found in acute disease. Much work remains to be done to understand the biological mechanisms behind these problems, but inflammation and autoimmune responses may play a role in some cases.
Those were some of the takeaways from a talk by Serena Spudich, MD, who presented her research at the 2021 annual meeting of the American Academy of Neurology. Dr. Spudich is the division chief of neurologic infections and global neurology and codirector of the Center for Neuroepidemiology and Clinical Neurological Research at Yale University, New Haven, Conn.
Examining the nervous system’s involvement in COVID-19
Even early on in the pandemic, it became clear that there were lingering complaints of neuromuscular problems, cognitive dysfunction, and mood and psychiatric issues. Breathing and heart rate problems also can arise. “There seems to be a preponderance of syndromes that reflect involvement of the nervous system,” said Dr. Spudich.
To try to understand the etiology of these persistent problems, Dr. Spudich said it’s important to examine the nervous system’s involvement in acute COVID-19. She has been involved in these efforts since early in the pandemic, when she ran an inpatient consult service at Yale dedicated to neurologic effects of acute COVID-19. She witnessed complications including stroke, encephalopathy, and seizures, among others.
Stroke during acute COVID-19 seemed to be associated with inflammation and endothelial activation or endotheliopathy. SARS-CoV-2 has been undetectable in the cerebrospinal fluid (CSF) of patients with acute COVID-19 and neurologic symptoms, but inflammatory cytokines can be present along with increased frequency of B cells. Anti–SARS-CoV-2 antibodies have also been found in CSF, some of which were auto reactive to brain tissue. The immune response was altered, compared with healthy controls, and in the CNS, compared with in the blood, “raising the question of whether inflammation and autoimmunity may be underlying causes of these syndromes,” said Dr. Spudich.
She also pointed to an MRI study of autopsied brain tissue of patients with COVID-19 and neurologic complications, which showed indications of both hemorrhagic and ischemic microvascular injury. “It’s just a reminder that, during acute COVID-19, there may be inflammation in the brain, there may be autoimmune reactions, and there may be vascular changes that underlie some of the neurologic syndromes that are seen,” said Dr. Spudich.
A panoply of different syndromes
In October, Yale set up a post-COVID neurologic clinic that brought together pulmonary, cardiology, and psychiatric specialists, many of whom saw the same patients, about 60% of whom had cognitive impairment, more than 40% had neuromuscular problems, and over 30% headache. “There’s not a single entity of a post-COVID neurologic syndrome. There’s a panoply of different syndromes that may have similar or distinct etiologies,” said Dr. Spudich.
Most patients were in their 30s, 40s, or 50s. That doesn’t necessarily mean this is the most common age range for these issues, though. There could be some bias if these individuals are seeking specialty care because they expected to recover from COVID-19 quickly. But it could be that there is something biologically unique among this age group that predisposes them to complications. Regardless, two out of three patients were never hospitalized, “suggesting that even mild COVID-19 can lead to some long-term sequelae,” said Dr. Spudich.
One potential explanation for long-term neurologic syndromes is that they are an extension of the inflammation, autoimmunity, and immune perturbation occurring during acute disease. One study looked at 18 cancer patients who had neurologic complications with COVID-19. Two months after onset, they had elevated markers of neuroinflammation and neuronal injury in the cerebral spinal fluid compared to cancer patients with no history of COVID-19.
Looking for biologic markers
An Italian study looked at patients who were evaluated during acute hospitalization and again 3 months later, and found that some markers of inflation in the blood were associated with later cognitive impairment. The patients were more severely ill, so it’s not clear what the findings mean for patients who present with neurologic symptoms after milder illness.
A PET scan study of 35 patients with persistent neurologic symptoms found patterns of reduced fluorodeoxyglucose uptake in some regions of the brain that are believed to be associated with some symptoms. Lower values were associated with greater severity for symptoms like memory dysfunction, and anosmia. “Why there might be hypometabolism in these regions I think needs to be assessed and used as a biomarker to associate hypometabolism with other kinds of processes in blood and spinal fluid,” said Dr. Spudich.
Along with colleagues at Yale, Dr. Spudich is conducting the MIND study, which is using PET and MRI imaging along with blood and CSF biomarkers to track the progress of patients after COVID-19. There are few results to discuss since only 20 patients have been recruited so far, except that brain imaging and blood values are generally normal despite neurologic complaints. Most were not hospitalized for COVID-19. Dr. Spudich highlighted one man in his 30s who developed new-onset psychosis, despite no previous history. Although clinical tests were all negative, a novel autoantibody detection method revealed a previously unknown autoreactive antibody in his spinal fluid. “This may suggest that there is autoantibody production in some individuals with post–COVID-19 psychosis, and potentially other syndromes,” said Dr. Spudich.
The research task ahead
The case illustrates the task ahead for neurology. “There’s a real research mandate to understand the biological substrates of these diverse disorders, not only to address the emergent public health concern and reduce the stigma in our patients, but to develop targeted therapeutic interventions,” said Dr. Spudich.
Anna Cervantes-Arslanian, MD, an associate professor of neurology at Boston University who also treats and studies patients with post-COVID neurologic symptoms, agreed with that assessment. “It’s not like every patient that has muscle aches and fatigue also has brain fog. It’s really hard to parse them out into specific phenotypes that are pretty classic. Some people will have all of those things, some will have very few of them,” said Dr. Cervantes-Arslanian. “We need to be able to identify them sand see if there is clustering of symptoms so we can better look into what the biological underpinnings are. That’s the first step to thinking about a therapeutic target.”
Dr. Spudich and Dr. Cervantes-Arslanian had no relevant financial disclosures.
Long-haul neurologic symptoms of COVID-19 seem to be distinct from neurologic conditions found in acute disease. Much work remains to be done to understand the biological mechanisms behind these problems, but inflammation and autoimmune responses may play a role in some cases.
Those were some of the takeaways from a talk by Serena Spudich, MD, who presented her research at the 2021 annual meeting of the American Academy of Neurology. Dr. Spudich is the division chief of neurologic infections and global neurology and codirector of the Center for Neuroepidemiology and Clinical Neurological Research at Yale University, New Haven, Conn.
Examining the nervous system’s involvement in COVID-19
Even early on in the pandemic, it became clear that there were lingering complaints of neuromuscular problems, cognitive dysfunction, and mood and psychiatric issues. Breathing and heart rate problems also can arise. “There seems to be a preponderance of syndromes that reflect involvement of the nervous system,” said Dr. Spudich.
To try to understand the etiology of these persistent problems, Dr. Spudich said it’s important to examine the nervous system’s involvement in acute COVID-19. She has been involved in these efforts since early in the pandemic, when she ran an inpatient consult service at Yale dedicated to neurologic effects of acute COVID-19. She witnessed complications including stroke, encephalopathy, and seizures, among others.
Stroke during acute COVID-19 seemed to be associated with inflammation and endothelial activation or endotheliopathy. SARS-CoV-2 has been undetectable in the cerebrospinal fluid (CSF) of patients with acute COVID-19 and neurologic symptoms, but inflammatory cytokines can be present along with increased frequency of B cells. Anti–SARS-CoV-2 antibodies have also been found in CSF, some of which were auto reactive to brain tissue. The immune response was altered, compared with healthy controls, and in the CNS, compared with in the blood, “raising the question of whether inflammation and autoimmunity may be underlying causes of these syndromes,” said Dr. Spudich.
She also pointed to an MRI study of autopsied brain tissue of patients with COVID-19 and neurologic complications, which showed indications of both hemorrhagic and ischemic microvascular injury. “It’s just a reminder that, during acute COVID-19, there may be inflammation in the brain, there may be autoimmune reactions, and there may be vascular changes that underlie some of the neurologic syndromes that are seen,” said Dr. Spudich.
A panoply of different syndromes
In October, Yale set up a post-COVID neurologic clinic that brought together pulmonary, cardiology, and psychiatric specialists, many of whom saw the same patients, about 60% of whom had cognitive impairment, more than 40% had neuromuscular problems, and over 30% headache. “There’s not a single entity of a post-COVID neurologic syndrome. There’s a panoply of different syndromes that may have similar or distinct etiologies,” said Dr. Spudich.
Most patients were in their 30s, 40s, or 50s. That doesn’t necessarily mean this is the most common age range for these issues, though. There could be some bias if these individuals are seeking specialty care because they expected to recover from COVID-19 quickly. But it could be that there is something biologically unique among this age group that predisposes them to complications. Regardless, two out of three patients were never hospitalized, “suggesting that even mild COVID-19 can lead to some long-term sequelae,” said Dr. Spudich.
One potential explanation for long-term neurologic syndromes is that they are an extension of the inflammation, autoimmunity, and immune perturbation occurring during acute disease. One study looked at 18 cancer patients who had neurologic complications with COVID-19. Two months after onset, they had elevated markers of neuroinflammation and neuronal injury in the cerebral spinal fluid compared to cancer patients with no history of COVID-19.
Looking for biologic markers
An Italian study looked at patients who were evaluated during acute hospitalization and again 3 months later, and found that some markers of inflation in the blood were associated with later cognitive impairment. The patients were more severely ill, so it’s not clear what the findings mean for patients who present with neurologic symptoms after milder illness.
A PET scan study of 35 patients with persistent neurologic symptoms found patterns of reduced fluorodeoxyglucose uptake in some regions of the brain that are believed to be associated with some symptoms. Lower values were associated with greater severity for symptoms like memory dysfunction, and anosmia. “Why there might be hypometabolism in these regions I think needs to be assessed and used as a biomarker to associate hypometabolism with other kinds of processes in blood and spinal fluid,” said Dr. Spudich.
Along with colleagues at Yale, Dr. Spudich is conducting the MIND study, which is using PET and MRI imaging along with blood and CSF biomarkers to track the progress of patients after COVID-19. There are few results to discuss since only 20 patients have been recruited so far, except that brain imaging and blood values are generally normal despite neurologic complaints. Most were not hospitalized for COVID-19. Dr. Spudich highlighted one man in his 30s who developed new-onset psychosis, despite no previous history. Although clinical tests were all negative, a novel autoantibody detection method revealed a previously unknown autoreactive antibody in his spinal fluid. “This may suggest that there is autoantibody production in some individuals with post–COVID-19 psychosis, and potentially other syndromes,” said Dr. Spudich.
The research task ahead
The case illustrates the task ahead for neurology. “There’s a real research mandate to understand the biological substrates of these diverse disorders, not only to address the emergent public health concern and reduce the stigma in our patients, but to develop targeted therapeutic interventions,” said Dr. Spudich.
Anna Cervantes-Arslanian, MD, an associate professor of neurology at Boston University who also treats and studies patients with post-COVID neurologic symptoms, agreed with that assessment. “It’s not like every patient that has muscle aches and fatigue also has brain fog. It’s really hard to parse them out into specific phenotypes that are pretty classic. Some people will have all of those things, some will have very few of them,” said Dr. Cervantes-Arslanian. “We need to be able to identify them sand see if there is clustering of symptoms so we can better look into what the biological underpinnings are. That’s the first step to thinking about a therapeutic target.”
Dr. Spudich and Dr. Cervantes-Arslanian had no relevant financial disclosures.
Long-haul neurologic symptoms of COVID-19 seem to be distinct from neurologic conditions found in acute disease. Much work remains to be done to understand the biological mechanisms behind these problems, but inflammation and autoimmune responses may play a role in some cases.
Those were some of the takeaways from a talk by Serena Spudich, MD, who presented her research at the 2021 annual meeting of the American Academy of Neurology. Dr. Spudich is the division chief of neurologic infections and global neurology and codirector of the Center for Neuroepidemiology and Clinical Neurological Research at Yale University, New Haven, Conn.
Examining the nervous system’s involvement in COVID-19
Even early on in the pandemic, it became clear that there were lingering complaints of neuromuscular problems, cognitive dysfunction, and mood and psychiatric issues. Breathing and heart rate problems also can arise. “There seems to be a preponderance of syndromes that reflect involvement of the nervous system,” said Dr. Spudich.
To try to understand the etiology of these persistent problems, Dr. Spudich said it’s important to examine the nervous system’s involvement in acute COVID-19. She has been involved in these efforts since early in the pandemic, when she ran an inpatient consult service at Yale dedicated to neurologic effects of acute COVID-19. She witnessed complications including stroke, encephalopathy, and seizures, among others.
Stroke during acute COVID-19 seemed to be associated with inflammation and endothelial activation or endotheliopathy. SARS-CoV-2 has been undetectable in the cerebrospinal fluid (CSF) of patients with acute COVID-19 and neurologic symptoms, but inflammatory cytokines can be present along with increased frequency of B cells. Anti–SARS-CoV-2 antibodies have also been found in CSF, some of which were auto reactive to brain tissue. The immune response was altered, compared with healthy controls, and in the CNS, compared with in the blood, “raising the question of whether inflammation and autoimmunity may be underlying causes of these syndromes,” said Dr. Spudich.
She also pointed to an MRI study of autopsied brain tissue of patients with COVID-19 and neurologic complications, which showed indications of both hemorrhagic and ischemic microvascular injury. “It’s just a reminder that, during acute COVID-19, there may be inflammation in the brain, there may be autoimmune reactions, and there may be vascular changes that underlie some of the neurologic syndromes that are seen,” said Dr. Spudich.
A panoply of different syndromes
In October, Yale set up a post-COVID neurologic clinic that brought together pulmonary, cardiology, and psychiatric specialists, many of whom saw the same patients, about 60% of whom had cognitive impairment, more than 40% had neuromuscular problems, and over 30% headache. “There’s not a single entity of a post-COVID neurologic syndrome. There’s a panoply of different syndromes that may have similar or distinct etiologies,” said Dr. Spudich.
Most patients were in their 30s, 40s, or 50s. That doesn’t necessarily mean this is the most common age range for these issues, though. There could be some bias if these individuals are seeking specialty care because they expected to recover from COVID-19 quickly. But it could be that there is something biologically unique among this age group that predisposes them to complications. Regardless, two out of three patients were never hospitalized, “suggesting that even mild COVID-19 can lead to some long-term sequelae,” said Dr. Spudich.
One potential explanation for long-term neurologic syndromes is that they are an extension of the inflammation, autoimmunity, and immune perturbation occurring during acute disease. One study looked at 18 cancer patients who had neurologic complications with COVID-19. Two months after onset, they had elevated markers of neuroinflammation and neuronal injury in the cerebral spinal fluid compared to cancer patients with no history of COVID-19.
Looking for biologic markers
An Italian study looked at patients who were evaluated during acute hospitalization and again 3 months later, and found that some markers of inflation in the blood were associated with later cognitive impairment. The patients were more severely ill, so it’s not clear what the findings mean for patients who present with neurologic symptoms after milder illness.
A PET scan study of 35 patients with persistent neurologic symptoms found patterns of reduced fluorodeoxyglucose uptake in some regions of the brain that are believed to be associated with some symptoms. Lower values were associated with greater severity for symptoms like memory dysfunction, and anosmia. “Why there might be hypometabolism in these regions I think needs to be assessed and used as a biomarker to associate hypometabolism with other kinds of processes in blood and spinal fluid,” said Dr. Spudich.
Along with colleagues at Yale, Dr. Spudich is conducting the MIND study, which is using PET and MRI imaging along with blood and CSF biomarkers to track the progress of patients after COVID-19. There are few results to discuss since only 20 patients have been recruited so far, except that brain imaging and blood values are generally normal despite neurologic complaints. Most were not hospitalized for COVID-19. Dr. Spudich highlighted one man in his 30s who developed new-onset psychosis, despite no previous history. Although clinical tests were all negative, a novel autoantibody detection method revealed a previously unknown autoreactive antibody in his spinal fluid. “This may suggest that there is autoantibody production in some individuals with post–COVID-19 psychosis, and potentially other syndromes,” said Dr. Spudich.
The research task ahead
The case illustrates the task ahead for neurology. “There’s a real research mandate to understand the biological substrates of these diverse disorders, not only to address the emergent public health concern and reduce the stigma in our patients, but to develop targeted therapeutic interventions,” said Dr. Spudich.
Anna Cervantes-Arslanian, MD, an associate professor of neurology at Boston University who also treats and studies patients with post-COVID neurologic symptoms, agreed with that assessment. “It’s not like every patient that has muscle aches and fatigue also has brain fog. It’s really hard to parse them out into specific phenotypes that are pretty classic. Some people will have all of those things, some will have very few of them,” said Dr. Cervantes-Arslanian. “We need to be able to identify them sand see if there is clustering of symptoms so we can better look into what the biological underpinnings are. That’s the first step to thinking about a therapeutic target.”
Dr. Spudich and Dr. Cervantes-Arslanian had no relevant financial disclosures.
FROM AAN 2021
AHA statement on obesity emphasizes abdominal fat, AFib
An updated American Heart Association scientific statement on the role of obesity in cardiovascular disease provides the first new guidance in 15 years, drawing on evidence that’s emerged in that time to clarify the potential of newer drug therapies and interventions like bariatric surgery and lifestyle modifications to curtail cardiovascular disease risks.
“The timing of this information is important because the obesity epidemic contributes significantly to the global burden of cardiovascular disease and numerous chronic health conditions that also impact heart disease,” said Tiffany Powell-Wiley, MD, MPH, chair of the volunteer statement writing group.
“One of the big takeaways that I hope people get from the statement is really making it clear that obesity is a complex disease, and that it is multifactorial,” Dr. Powell-Wiley said in an interview. “There are not just biological reasons why individuals have obesity, but there are environmental, psychosocial, and really multilevel factors that contribute to the development and course of obesity.”
Most significantly, Dr. Powell-Wiley said, “we want to emphasize that we really want to have cardiologists think about and focus on abdominal obesity in particular.”
A metric for cardiovascular risk that seems to gain credibility in the statement is the relationship of waist circumference to height regardless of overall weight. “That is a very important finding that we can now really think of waist circumference as an important measure in our clinical practice,” said Dr. Powell-Wiley, chief of the Social Determinants of Obesity and Cardiovascular Risk Laboratory in the division of intramural research at the National Heart, Lung, and Blood Institute. “We want to get across to providers that this is something that should be measured and should be followed over time, based on data from the last 15 years that waist circumference and abdominal obesity are associated with higher cardiovascular risk regardless of body mass index.”
The statement provides potentially groundbreaking advice on atrial fibrillation as a consequence of weight, noted Dr. Powell-Wiley. “Up until recently, we haven’t really thought about weight management as a part of managing Afib [atrial fibrillation],” she said. “This statement highlights the need to think about weight management in addition to anticoagulation as part of the pieces for managing Afib.”
Evidence on interventions
The statement, published in Circulation, also dives into the evidence surrounding the varied interventions for managing weight.
“The biggest area where there’s much more data is bariatric surgery,” said Dr. Powell-Wiley. “There’s clear evidence that bariatric surgery lowers cardio mortality and all-cause mortality for patients, but we’ve also seen data around lifestyle interventions, with the Look AHEAD trial, which showed that while there were improvements in CV [cardiovascular] risk factors, we didn’t see the reduction in CV mortality that we wanted to see.”
The statement noted that the Look AHEAD trial (for Action for Health in Diabetes) of people with type 2 diabetes failed to show a significant reduction in major adverse cardiac events or CV mortality after almost 10 years of an intensive weight-loss intervention. Dr. Powell-Wiley added that the result seemed to be related more to the lack of weight loss with lifestyle interventions when compared with bariatric surgery.
The statement also addressed the effectiveness of drug treatments for weight control in managing CV risk, and while the evidence supporting pharmacotherapy specifically for weight loss has been mixed, emerging treatments have shown promise, Dr. Powell-Wiley said. “I think we now have some bright spots with new therapies that have been developed for diabetes and heart failure, such as the SGLT2 inhibitors as well as the GLP-1 agonists, and how they can also appear to improve weight and likely will improve CV mortality in patients with obesity.”
The “obesity paradox,” which Dr. Powell-Wiley noted is “definitely a controversial topic,” is also addressed in the statement. “We try to explain what it is and what we know about it right now,” she said. “We know for instance that patients with obesity, particularly those who have class 1 obesity or patients who are overweight, seem to do better in the short term in relation to coronary artery disease and heart failure, but the reasons for that are not necessarily clear.”
The statement also provides evidence-based insights on the use of diagnostic tools, including stress echocardiography and cardiac MRI as well as coronary angiography, and the clinical significance of specific echocardiographic changes in obese patients.
The writing committee also identified areas that need future research. “It’s really important to emphasize what we learned about the complexity of obesity over this time period,” Dr. Powell-Wiley said. “But again, we don’t have all the answers; there’s a lot more work to be done to understand what type of lifestyle intervention might be most beneficial, especially with addressing abdominal obesity, and how these new therapeutics around heart failure and diabetes may be useful in patients with obesity.
Obesity in adolescents is another area that needs further research, Dr. Powell-Wiley said. “How do we prevent obesity in those populations when we know they’re at risk for so much as they get older? Once you have obesity it’s hard to change that trajectory.”
The scientific statement was prepared by the volunteer writing group on behalf of the AHA’s Council on Lifestyle and Cardiometabolic Health, the Council on Cardiovascular and Stroke Nursing, the Council on Clinical Cardiology, the Council on Epidemiology and Prevention, and the Stroke Council. Committee vice chair Paul Poirier, MD, PhD, reported financial relationships with Abbott, Amgen, AstraZeneca, Bausch Health, Bayer, Boehringer Ingelheim, Eli Lilly, Janssen, Novartis, Novo Nordisk, Sanofi, Servier, and HLS Therapeutics. One committee member disclosed a financial relationship with AstraZeneca. Dr. Powell-Wiley and the other committee members have no relationships to disclose.
An updated American Heart Association scientific statement on the role of obesity in cardiovascular disease provides the first new guidance in 15 years, drawing on evidence that’s emerged in that time to clarify the potential of newer drug therapies and interventions like bariatric surgery and lifestyle modifications to curtail cardiovascular disease risks.
“The timing of this information is important because the obesity epidemic contributes significantly to the global burden of cardiovascular disease and numerous chronic health conditions that also impact heart disease,” said Tiffany Powell-Wiley, MD, MPH, chair of the volunteer statement writing group.
“One of the big takeaways that I hope people get from the statement is really making it clear that obesity is a complex disease, and that it is multifactorial,” Dr. Powell-Wiley said in an interview. “There are not just biological reasons why individuals have obesity, but there are environmental, psychosocial, and really multilevel factors that contribute to the development and course of obesity.”
Most significantly, Dr. Powell-Wiley said, “we want to emphasize that we really want to have cardiologists think about and focus on abdominal obesity in particular.”
A metric for cardiovascular risk that seems to gain credibility in the statement is the relationship of waist circumference to height regardless of overall weight. “That is a very important finding that we can now really think of waist circumference as an important measure in our clinical practice,” said Dr. Powell-Wiley, chief of the Social Determinants of Obesity and Cardiovascular Risk Laboratory in the division of intramural research at the National Heart, Lung, and Blood Institute. “We want to get across to providers that this is something that should be measured and should be followed over time, based on data from the last 15 years that waist circumference and abdominal obesity are associated with higher cardiovascular risk regardless of body mass index.”
The statement provides potentially groundbreaking advice on atrial fibrillation as a consequence of weight, noted Dr. Powell-Wiley. “Up until recently, we haven’t really thought about weight management as a part of managing Afib [atrial fibrillation],” she said. “This statement highlights the need to think about weight management in addition to anticoagulation as part of the pieces for managing Afib.”
Evidence on interventions
The statement, published in Circulation, also dives into the evidence surrounding the varied interventions for managing weight.
“The biggest area where there’s much more data is bariatric surgery,” said Dr. Powell-Wiley. “There’s clear evidence that bariatric surgery lowers cardio mortality and all-cause mortality for patients, but we’ve also seen data around lifestyle interventions, with the Look AHEAD trial, which showed that while there were improvements in CV [cardiovascular] risk factors, we didn’t see the reduction in CV mortality that we wanted to see.”
The statement noted that the Look AHEAD trial (for Action for Health in Diabetes) of people with type 2 diabetes failed to show a significant reduction in major adverse cardiac events or CV mortality after almost 10 years of an intensive weight-loss intervention. Dr. Powell-Wiley added that the result seemed to be related more to the lack of weight loss with lifestyle interventions when compared with bariatric surgery.
The statement also addressed the effectiveness of drug treatments for weight control in managing CV risk, and while the evidence supporting pharmacotherapy specifically for weight loss has been mixed, emerging treatments have shown promise, Dr. Powell-Wiley said. “I think we now have some bright spots with new therapies that have been developed for diabetes and heart failure, such as the SGLT2 inhibitors as well as the GLP-1 agonists, and how they can also appear to improve weight and likely will improve CV mortality in patients with obesity.”
The “obesity paradox,” which Dr. Powell-Wiley noted is “definitely a controversial topic,” is also addressed in the statement. “We try to explain what it is and what we know about it right now,” she said. “We know for instance that patients with obesity, particularly those who have class 1 obesity or patients who are overweight, seem to do better in the short term in relation to coronary artery disease and heart failure, but the reasons for that are not necessarily clear.”
The statement also provides evidence-based insights on the use of diagnostic tools, including stress echocardiography and cardiac MRI as well as coronary angiography, and the clinical significance of specific echocardiographic changes in obese patients.
The writing committee also identified areas that need future research. “It’s really important to emphasize what we learned about the complexity of obesity over this time period,” Dr. Powell-Wiley said. “But again, we don’t have all the answers; there’s a lot more work to be done to understand what type of lifestyle intervention might be most beneficial, especially with addressing abdominal obesity, and how these new therapeutics around heart failure and diabetes may be useful in patients with obesity.
Obesity in adolescents is another area that needs further research, Dr. Powell-Wiley said. “How do we prevent obesity in those populations when we know they’re at risk for so much as they get older? Once you have obesity it’s hard to change that trajectory.”
The scientific statement was prepared by the volunteer writing group on behalf of the AHA’s Council on Lifestyle and Cardiometabolic Health, the Council on Cardiovascular and Stroke Nursing, the Council on Clinical Cardiology, the Council on Epidemiology and Prevention, and the Stroke Council. Committee vice chair Paul Poirier, MD, PhD, reported financial relationships with Abbott, Amgen, AstraZeneca, Bausch Health, Bayer, Boehringer Ingelheim, Eli Lilly, Janssen, Novartis, Novo Nordisk, Sanofi, Servier, and HLS Therapeutics. One committee member disclosed a financial relationship with AstraZeneca. Dr. Powell-Wiley and the other committee members have no relationships to disclose.
An updated American Heart Association scientific statement on the role of obesity in cardiovascular disease provides the first new guidance in 15 years, drawing on evidence that’s emerged in that time to clarify the potential of newer drug therapies and interventions like bariatric surgery and lifestyle modifications to curtail cardiovascular disease risks.
“The timing of this information is important because the obesity epidemic contributes significantly to the global burden of cardiovascular disease and numerous chronic health conditions that also impact heart disease,” said Tiffany Powell-Wiley, MD, MPH, chair of the volunteer statement writing group.
“One of the big takeaways that I hope people get from the statement is really making it clear that obesity is a complex disease, and that it is multifactorial,” Dr. Powell-Wiley said in an interview. “There are not just biological reasons why individuals have obesity, but there are environmental, psychosocial, and really multilevel factors that contribute to the development and course of obesity.”
Most significantly, Dr. Powell-Wiley said, “we want to emphasize that we really want to have cardiologists think about and focus on abdominal obesity in particular.”
A metric for cardiovascular risk that seems to gain credibility in the statement is the relationship of waist circumference to height regardless of overall weight. “That is a very important finding that we can now really think of waist circumference as an important measure in our clinical practice,” said Dr. Powell-Wiley, chief of the Social Determinants of Obesity and Cardiovascular Risk Laboratory in the division of intramural research at the National Heart, Lung, and Blood Institute. “We want to get across to providers that this is something that should be measured and should be followed over time, based on data from the last 15 years that waist circumference and abdominal obesity are associated with higher cardiovascular risk regardless of body mass index.”
The statement provides potentially groundbreaking advice on atrial fibrillation as a consequence of weight, noted Dr. Powell-Wiley. “Up until recently, we haven’t really thought about weight management as a part of managing Afib [atrial fibrillation],” she said. “This statement highlights the need to think about weight management in addition to anticoagulation as part of the pieces for managing Afib.”
Evidence on interventions
The statement, published in Circulation, also dives into the evidence surrounding the varied interventions for managing weight.
“The biggest area where there’s much more data is bariatric surgery,” said Dr. Powell-Wiley. “There’s clear evidence that bariatric surgery lowers cardio mortality and all-cause mortality for patients, but we’ve also seen data around lifestyle interventions, with the Look AHEAD trial, which showed that while there were improvements in CV [cardiovascular] risk factors, we didn’t see the reduction in CV mortality that we wanted to see.”
The statement noted that the Look AHEAD trial (for Action for Health in Diabetes) of people with type 2 diabetes failed to show a significant reduction in major adverse cardiac events or CV mortality after almost 10 years of an intensive weight-loss intervention. Dr. Powell-Wiley added that the result seemed to be related more to the lack of weight loss with lifestyle interventions when compared with bariatric surgery.
The statement also addressed the effectiveness of drug treatments for weight control in managing CV risk, and while the evidence supporting pharmacotherapy specifically for weight loss has been mixed, emerging treatments have shown promise, Dr. Powell-Wiley said. “I think we now have some bright spots with new therapies that have been developed for diabetes and heart failure, such as the SGLT2 inhibitors as well as the GLP-1 agonists, and how they can also appear to improve weight and likely will improve CV mortality in patients with obesity.”
The “obesity paradox,” which Dr. Powell-Wiley noted is “definitely a controversial topic,” is also addressed in the statement. “We try to explain what it is and what we know about it right now,” she said. “We know for instance that patients with obesity, particularly those who have class 1 obesity or patients who are overweight, seem to do better in the short term in relation to coronary artery disease and heart failure, but the reasons for that are not necessarily clear.”
The statement also provides evidence-based insights on the use of diagnostic tools, including stress echocardiography and cardiac MRI as well as coronary angiography, and the clinical significance of specific echocardiographic changes in obese patients.
The writing committee also identified areas that need future research. “It’s really important to emphasize what we learned about the complexity of obesity over this time period,” Dr. Powell-Wiley said. “But again, we don’t have all the answers; there’s a lot more work to be done to understand what type of lifestyle intervention might be most beneficial, especially with addressing abdominal obesity, and how these new therapeutics around heart failure and diabetes may be useful in patients with obesity.
Obesity in adolescents is another area that needs further research, Dr. Powell-Wiley said. “How do we prevent obesity in those populations when we know they’re at risk for so much as they get older? Once you have obesity it’s hard to change that trajectory.”
The scientific statement was prepared by the volunteer writing group on behalf of the AHA’s Council on Lifestyle and Cardiometabolic Health, the Council on Cardiovascular and Stroke Nursing, the Council on Clinical Cardiology, the Council on Epidemiology and Prevention, and the Stroke Council. Committee vice chair Paul Poirier, MD, PhD, reported financial relationships with Abbott, Amgen, AstraZeneca, Bausch Health, Bayer, Boehringer Ingelheim, Eli Lilly, Janssen, Novartis, Novo Nordisk, Sanofi, Servier, and HLS Therapeutics. One committee member disclosed a financial relationship with AstraZeneca. Dr. Powell-Wiley and the other committee members have no relationships to disclose.
FROM CIRCULATION