User login
Feds look to retrofit factories to increase COVID vaccine production
The Biden administration is exploring whether factories can be retrofitted to produce more of the Pfizer/BioNTech and Moderna COVID-19 mRNA vaccines to speed up vaccination of the vast majority of Americans.
The announcement comes as the nation is on track to see 479,000-514,000 deaths by the end of February, said Rochelle Walensky, MD, the director of the Centers for Disease Control and Prevention.
Dr. Walensky, speaking to reporters Wednesday in the first briefing from the White House COVID-19 Response Team, said that 1.6 million COVID-19 shots had been administered each day over the past week and that 3.4 million Americans have been fully vaccinated with two doses.
More than 500 million doses will be needed to vaccinate every American older than 16 years, Andy Slavitt, the senior advisor to the COVID-19 response team, told reporters. Pfizer and Moderna are due to deliver an additional 200 million doses near the end of March, and President Biden is seeking to purchase another 200 million doses from the companies, said Mr. Slavitt.
But it may not be enough. Whether companies can retrofit factories to produce vaccines is “something that’s under active exploration,” Mr. Slavitt said.
“This is a national emergency,” said Jeff Zients, the White House COVID-19 response coordinator. “Everything is on the table across the whole supply chain,” he said. He noted that the administration was also buying low-dead-space syringes to help extract an additional sixth dose from every Pfizer vial.
Mr. Slavitt said the team had identified 12 areas in which Mr. Biden was authorized to use the Defense Production Act to spur the manufacture of items such as masks and COVID-19 diagnostics.
More sequencing needed
As new variants emerge, vaccine makers and the CDC are racing to stay a step ahead. “RNA viruses mutate all the time – that’s what they do, that’s their business,” said Anthony Fauci, MD, director of the National Institute of Allergy and Infectious Diseases and Mr. Biden’s chief medical adviser, in the briefing.
Three concerning variants have emerged: the B117, which is circulating widely in the United Kingdom; the B1.351 in South Africa; and the P.1 in Brazil. As of Jan. 26, no cases involving the B1.351 variant have been detected in the United States; one person with the P.1 variant was identified in Minnesota. The CDC has identified 308 cases of the U.K. variant in 26 states, said Dr. Walensky.
The United States is dismally behind in surveillance and sequencing of variants, said Zients. “We are 43rd in the world at genomic sequencing,” which he said was “totally unacceptable.”
Dr. Walensky said the CDC is working on improving data collection and sequencing, but she said more money is needed to “do the amount of sequencing and surveillance that we need in order to be able to detect these when they first start to emerge.”
Both she and Mr. Zients called on Congress to pass Mr. Biden’s proposed American Rescue package, which includes more money for sequencing.
Dr. Fauci said the National Institutes of Health was collaborating with the CDC to determine whether other newly emerging variants pose any threat – such as increased transmissibility or lethality or some other functional characteristic. Scientists will also monitor “in real-time” whether current vaccines continue to make neutralizing antibodies against these mutants.
“With the U.K. variant, what we’re seeing is a very slight, if at all, impact on vaccine-induced antibodies and very little impact on anything else,” he said. With the South African variant, there is “a multifold diminution in the in vitro neutralization by vaccine-induced antibodies,” but “it still is well within the cushion of protection” for the current vaccines.
But, he added, “we have to be concerned looking forward of what the further evolution of this might be.” The anti-COVID monoclonal antibodies – bamlanivimab and the combination of casirivimab and imdevimab – are “more seriously inhibited by this South African strain,” which is spurring development of new monoclonals.
Dr. Fauci also noted that the Johnson & Johnson/Janssen vaccine that is in development – for which phase 3 data may be released within days – was tested in South Africa and Brazil in addition to the United States. The comparative data could help researchers and clinicians make better-informed decisions about what vaccine to use if the South African variant “seeds itself in the U.S.”
A version of this article first appeared on Medscape.com.
The Biden administration is exploring whether factories can be retrofitted to produce more of the Pfizer/BioNTech and Moderna COVID-19 mRNA vaccines to speed up vaccination of the vast majority of Americans.
The announcement comes as the nation is on track to see 479,000-514,000 deaths by the end of February, said Rochelle Walensky, MD, the director of the Centers for Disease Control and Prevention.
Dr. Walensky, speaking to reporters Wednesday in the first briefing from the White House COVID-19 Response Team, said that 1.6 million COVID-19 shots had been administered each day over the past week and that 3.4 million Americans have been fully vaccinated with two doses.
More than 500 million doses will be needed to vaccinate every American older than 16 years, Andy Slavitt, the senior advisor to the COVID-19 response team, told reporters. Pfizer and Moderna are due to deliver an additional 200 million doses near the end of March, and President Biden is seeking to purchase another 200 million doses from the companies, said Mr. Slavitt.
But it may not be enough. Whether companies can retrofit factories to produce vaccines is “something that’s under active exploration,” Mr. Slavitt said.
“This is a national emergency,” said Jeff Zients, the White House COVID-19 response coordinator. “Everything is on the table across the whole supply chain,” he said. He noted that the administration was also buying low-dead-space syringes to help extract an additional sixth dose from every Pfizer vial.
Mr. Slavitt said the team had identified 12 areas in which Mr. Biden was authorized to use the Defense Production Act to spur the manufacture of items such as masks and COVID-19 diagnostics.
More sequencing needed
As new variants emerge, vaccine makers and the CDC are racing to stay a step ahead. “RNA viruses mutate all the time – that’s what they do, that’s their business,” said Anthony Fauci, MD, director of the National Institute of Allergy and Infectious Diseases and Mr. Biden’s chief medical adviser, in the briefing.
Three concerning variants have emerged: the B117, which is circulating widely in the United Kingdom; the B1.351 in South Africa; and the P.1 in Brazil. As of Jan. 26, no cases involving the B1.351 variant have been detected in the United States; one person with the P.1 variant was identified in Minnesota. The CDC has identified 308 cases of the U.K. variant in 26 states, said Dr. Walensky.
The United States is dismally behind in surveillance and sequencing of variants, said Zients. “We are 43rd in the world at genomic sequencing,” which he said was “totally unacceptable.”
Dr. Walensky said the CDC is working on improving data collection and sequencing, but she said more money is needed to “do the amount of sequencing and surveillance that we need in order to be able to detect these when they first start to emerge.”
Both she and Mr. Zients called on Congress to pass Mr. Biden’s proposed American Rescue package, which includes more money for sequencing.
Dr. Fauci said the National Institutes of Health was collaborating with the CDC to determine whether other newly emerging variants pose any threat – such as increased transmissibility or lethality or some other functional characteristic. Scientists will also monitor “in real-time” whether current vaccines continue to make neutralizing antibodies against these mutants.
“With the U.K. variant, what we’re seeing is a very slight, if at all, impact on vaccine-induced antibodies and very little impact on anything else,” he said. With the South African variant, there is “a multifold diminution in the in vitro neutralization by vaccine-induced antibodies,” but “it still is well within the cushion of protection” for the current vaccines.
But, he added, “we have to be concerned looking forward of what the further evolution of this might be.” The anti-COVID monoclonal antibodies – bamlanivimab and the combination of casirivimab and imdevimab – are “more seriously inhibited by this South African strain,” which is spurring development of new monoclonals.
Dr. Fauci also noted that the Johnson & Johnson/Janssen vaccine that is in development – for which phase 3 data may be released within days – was tested in South Africa and Brazil in addition to the United States. The comparative data could help researchers and clinicians make better-informed decisions about what vaccine to use if the South African variant “seeds itself in the U.S.”
A version of this article first appeared on Medscape.com.
The Biden administration is exploring whether factories can be retrofitted to produce more of the Pfizer/BioNTech and Moderna COVID-19 mRNA vaccines to speed up vaccination of the vast majority of Americans.
The announcement comes as the nation is on track to see 479,000-514,000 deaths by the end of February, said Rochelle Walensky, MD, the director of the Centers for Disease Control and Prevention.
Dr. Walensky, speaking to reporters Wednesday in the first briefing from the White House COVID-19 Response Team, said that 1.6 million COVID-19 shots had been administered each day over the past week and that 3.4 million Americans have been fully vaccinated with two doses.
More than 500 million doses will be needed to vaccinate every American older than 16 years, Andy Slavitt, the senior advisor to the COVID-19 response team, told reporters. Pfizer and Moderna are due to deliver an additional 200 million doses near the end of March, and President Biden is seeking to purchase another 200 million doses from the companies, said Mr. Slavitt.
But it may not be enough. Whether companies can retrofit factories to produce vaccines is “something that’s under active exploration,” Mr. Slavitt said.
“This is a national emergency,” said Jeff Zients, the White House COVID-19 response coordinator. “Everything is on the table across the whole supply chain,” he said. He noted that the administration was also buying low-dead-space syringes to help extract an additional sixth dose from every Pfizer vial.
Mr. Slavitt said the team had identified 12 areas in which Mr. Biden was authorized to use the Defense Production Act to spur the manufacture of items such as masks and COVID-19 diagnostics.
More sequencing needed
As new variants emerge, vaccine makers and the CDC are racing to stay a step ahead. “RNA viruses mutate all the time – that’s what they do, that’s their business,” said Anthony Fauci, MD, director of the National Institute of Allergy and Infectious Diseases and Mr. Biden’s chief medical adviser, in the briefing.
Three concerning variants have emerged: the B117, which is circulating widely in the United Kingdom; the B1.351 in South Africa; and the P.1 in Brazil. As of Jan. 26, no cases involving the B1.351 variant have been detected in the United States; one person with the P.1 variant was identified in Minnesota. The CDC has identified 308 cases of the U.K. variant in 26 states, said Dr. Walensky.
The United States is dismally behind in surveillance and sequencing of variants, said Zients. “We are 43rd in the world at genomic sequencing,” which he said was “totally unacceptable.”
Dr. Walensky said the CDC is working on improving data collection and sequencing, but she said more money is needed to “do the amount of sequencing and surveillance that we need in order to be able to detect these when they first start to emerge.”
Both she and Mr. Zients called on Congress to pass Mr. Biden’s proposed American Rescue package, which includes more money for sequencing.
Dr. Fauci said the National Institutes of Health was collaborating with the CDC to determine whether other newly emerging variants pose any threat – such as increased transmissibility or lethality or some other functional characteristic. Scientists will also monitor “in real-time” whether current vaccines continue to make neutralizing antibodies against these mutants.
“With the U.K. variant, what we’re seeing is a very slight, if at all, impact on vaccine-induced antibodies and very little impact on anything else,” he said. With the South African variant, there is “a multifold diminution in the in vitro neutralization by vaccine-induced antibodies,” but “it still is well within the cushion of protection” for the current vaccines.
But, he added, “we have to be concerned looking forward of what the further evolution of this might be.” The anti-COVID monoclonal antibodies – bamlanivimab and the combination of casirivimab and imdevimab – are “more seriously inhibited by this South African strain,” which is spurring development of new monoclonals.
Dr. Fauci also noted that the Johnson & Johnson/Janssen vaccine that is in development – for which phase 3 data may be released within days – was tested in South Africa and Brazil in addition to the United States. The comparative data could help researchers and clinicians make better-informed decisions about what vaccine to use if the South African variant “seeds itself in the U.S.”
A version of this article first appeared on Medscape.com.
Combo testing improves CRC screening participation, but not advanced disease detection
Offering a combination of colonoscopy and fecal immunochemical testing (FIT), either in sequence or by choice, may significantly increase participation in colorectal cancer (CRC) screening, according to a prospective study involving more than 12,000 individuals in Poland.
Still, greater participation did not lead to significantly higher rates of advanced disease detection, reported lead author Nastazja Dagny Pilonis, MD, of the Maria Sklodowska-Curie National Research Institute of Oncology, Warsaw, and colleagues in Gastroenterology.
According to the investigators, screening programs that offer colonoscopy and FIT are more effective than those that offer colonoscopy alone, but an optimal combination protocol has yet to be established, and some parts of the world still rely upon a single diagnostic method.
“In Europe, CRC screening programs often implement only one screening modality: colonoscopy, sigmoidoscopy, or stool testing, depending on the health care provider,” the investigators wrote in Gastroenterology. They noted, however, that national guidelines in the United States recommend strategies that include more than one screening method. “‘One-size-fits-all’ approaches to CRC screening do not result in satisfactory participation” because of behavioral, cultural, and socioeconomic variation among individuals.
To improve understanding of the best ways to improve participation, the investigators conducted a prospective randomized trial, PICCOLINO, via the Polish Colonoscopy Screening Program. In total, 12,485 eligible individuals aged between 55 and 64 years received postal invitations to participate in CRC screening. Individuals were randomized in a 1:1:1 ratio into one of three mailing protocols, each of which involved an initial invitation, and, if needed, a second invitation that offered the following:
- Control group: colonoscopy, with nonresponders receiving the same invitation again
- Sequential group: colonoscopy, with nonresponders or refusers receiving a second invitation that offered FIT
- Choice group: choice between colonoscopy or FIT, with nonresponders receiving the same invitation again
The primary outcome was participation in screening within 18 weeks of enrollment. The secondary outcome was diagnostic yield for either advanced adenoma or CRC.
Out of the three groups, the control group had the lowest participation rate, at 17.5%, compared with 25.8% for the sequential group and 26.5% for the choice group. Multivariable logistic regression showed that individuals in the sequential and choice groups had 64% and 70% higher rates of participation, respectively. Across all groups, age of 60 years or older predicted 12% higher likelihood of participation; in contrast, location more than 40 kilometers from a testing center was associated with an 18% decrease in participation, compared with individuals who lived less than 20 kilometers away.
While the control and sequential groups had similar rates of colonoscopy participation, at 17.5% and 15.9%, respectively (P = .788), this rate was significantly lower, at 8.5%, in the choice group (P = .001). Conversely, the sequential group had a significantly lower rate of FITs than the choice group, at 9.9% versus 17.9%, respectively (P = .001). Among participants with a positive FIT, diagnostic work-up colonoscopies were performed in 70.0% of those in the sequential group and 73.3% in the choice group, “despite active call-recall efforts.”
Across all invited individuals, advanced disease detection rates were similar across groups, at 1.1% for both the control and the sequential group and 1.2% for the choice group. Among those who were actually screened, the control group had a slightly higher diagnostic yield for advanced neoplasia, at 6.5%, compared with 4.2% in the sequential group and 4.4% in the choice group; however, these differences were not statistically significant. In contrast, significantly more adenomas of any kind were detected in the control and sequential groups (5.6% for both) than the choice group (3.9%) (P < .001).
“Although the strategies which included FIT showed higher participation rates than the strategy of offering colonoscopy alone, these strategies did not result in increased detection rates of advanced neoplasia in the intention to screen analysis,” the investigators wrote. “An absolute increase in participation rates of 8%-10% seems insufficient to translate into higher advanced neoplasia detection at the population level.”
Dr. Pilonis and colleagues also suggested that the relatively low rate of diagnostic colonoscopy after positive FIT contributed to the suboptimal diagnostic yield.
“These rates are unsatisfactory taking into account significant call-recall efforts, but are within the range reported in other studies,” they wrote.
They also wrote that their study compared participation and detection between one-time colonoscopy and one-time screening strategies combining colonoscopy and FIT. In acknowledging this, they noted that these approaches have different screening intervals and uptake over time: “FIT has been shown to achieve higher participation rates than colonoscopy for one time screening, but its uptake over several rounds may not be superior to one time colonoscopy.” Furthermore, detection rates of the sequential or choice strategies for advanced disease may rise over time with further implementation, so the one-time screening may not be sufficient to reveal what could become significant differences.
The study was funded by the Polish Ministry of Health, the Polish Foundation of Gastroenterology, and the Centre of Postgraduate Medical Education in Warsaw. FITs, materials, and reagents were provided by Eiken Chemical. The investigators disclosed relationships with Boston Scientific, AbbVie, Olympus, and others.
Offering a combination of colonoscopy and fecal immunochemical testing (FIT), either in sequence or by choice, may significantly increase participation in colorectal cancer (CRC) screening, according to a prospective study involving more than 12,000 individuals in Poland.
Still, greater participation did not lead to significantly higher rates of advanced disease detection, reported lead author Nastazja Dagny Pilonis, MD, of the Maria Sklodowska-Curie National Research Institute of Oncology, Warsaw, and colleagues in Gastroenterology.
According to the investigators, screening programs that offer colonoscopy and FIT are more effective than those that offer colonoscopy alone, but an optimal combination protocol has yet to be established, and some parts of the world still rely upon a single diagnostic method.
“In Europe, CRC screening programs often implement only one screening modality: colonoscopy, sigmoidoscopy, or stool testing, depending on the health care provider,” the investigators wrote in Gastroenterology. They noted, however, that national guidelines in the United States recommend strategies that include more than one screening method. “‘One-size-fits-all’ approaches to CRC screening do not result in satisfactory participation” because of behavioral, cultural, and socioeconomic variation among individuals.
To improve understanding of the best ways to improve participation, the investigators conducted a prospective randomized trial, PICCOLINO, via the Polish Colonoscopy Screening Program. In total, 12,485 eligible individuals aged between 55 and 64 years received postal invitations to participate in CRC screening. Individuals were randomized in a 1:1:1 ratio into one of three mailing protocols, each of which involved an initial invitation, and, if needed, a second invitation that offered the following:
- Control group: colonoscopy, with nonresponders receiving the same invitation again
- Sequential group: colonoscopy, with nonresponders or refusers receiving a second invitation that offered FIT
- Choice group: choice between colonoscopy or FIT, with nonresponders receiving the same invitation again
The primary outcome was participation in screening within 18 weeks of enrollment. The secondary outcome was diagnostic yield for either advanced adenoma or CRC.
Out of the three groups, the control group had the lowest participation rate, at 17.5%, compared with 25.8% for the sequential group and 26.5% for the choice group. Multivariable logistic regression showed that individuals in the sequential and choice groups had 64% and 70% higher rates of participation, respectively. Across all groups, age of 60 years or older predicted 12% higher likelihood of participation; in contrast, location more than 40 kilometers from a testing center was associated with an 18% decrease in participation, compared with individuals who lived less than 20 kilometers away.
While the control and sequential groups had similar rates of colonoscopy participation, at 17.5% and 15.9%, respectively (P = .788), this rate was significantly lower, at 8.5%, in the choice group (P = .001). Conversely, the sequential group had a significantly lower rate of FITs than the choice group, at 9.9% versus 17.9%, respectively (P = .001). Among participants with a positive FIT, diagnostic work-up colonoscopies were performed in 70.0% of those in the sequential group and 73.3% in the choice group, “despite active call-recall efforts.”
Across all invited individuals, advanced disease detection rates were similar across groups, at 1.1% for both the control and the sequential group and 1.2% for the choice group. Among those who were actually screened, the control group had a slightly higher diagnostic yield for advanced neoplasia, at 6.5%, compared with 4.2% in the sequential group and 4.4% in the choice group; however, these differences were not statistically significant. In contrast, significantly more adenomas of any kind were detected in the control and sequential groups (5.6% for both) than the choice group (3.9%) (P < .001).
“Although the strategies which included FIT showed higher participation rates than the strategy of offering colonoscopy alone, these strategies did not result in increased detection rates of advanced neoplasia in the intention to screen analysis,” the investigators wrote. “An absolute increase in participation rates of 8%-10% seems insufficient to translate into higher advanced neoplasia detection at the population level.”
Dr. Pilonis and colleagues also suggested that the relatively low rate of diagnostic colonoscopy after positive FIT contributed to the suboptimal diagnostic yield.
“These rates are unsatisfactory taking into account significant call-recall efforts, but are within the range reported in other studies,” they wrote.
They also wrote that their study compared participation and detection between one-time colonoscopy and one-time screening strategies combining colonoscopy and FIT. In acknowledging this, they noted that these approaches have different screening intervals and uptake over time: “FIT has been shown to achieve higher participation rates than colonoscopy for one time screening, but its uptake over several rounds may not be superior to one time colonoscopy.” Furthermore, detection rates of the sequential or choice strategies for advanced disease may rise over time with further implementation, so the one-time screening may not be sufficient to reveal what could become significant differences.
The study was funded by the Polish Ministry of Health, the Polish Foundation of Gastroenterology, and the Centre of Postgraduate Medical Education in Warsaw. FITs, materials, and reagents were provided by Eiken Chemical. The investigators disclosed relationships with Boston Scientific, AbbVie, Olympus, and others.
Offering a combination of colonoscopy and fecal immunochemical testing (FIT), either in sequence or by choice, may significantly increase participation in colorectal cancer (CRC) screening, according to a prospective study involving more than 12,000 individuals in Poland.
Still, greater participation did not lead to significantly higher rates of advanced disease detection, reported lead author Nastazja Dagny Pilonis, MD, of the Maria Sklodowska-Curie National Research Institute of Oncology, Warsaw, and colleagues in Gastroenterology.
According to the investigators, screening programs that offer colonoscopy and FIT are more effective than those that offer colonoscopy alone, but an optimal combination protocol has yet to be established, and some parts of the world still rely upon a single diagnostic method.
“In Europe, CRC screening programs often implement only one screening modality: colonoscopy, sigmoidoscopy, or stool testing, depending on the health care provider,” the investigators wrote in Gastroenterology. They noted, however, that national guidelines in the United States recommend strategies that include more than one screening method. “‘One-size-fits-all’ approaches to CRC screening do not result in satisfactory participation” because of behavioral, cultural, and socioeconomic variation among individuals.
To improve understanding of the best ways to improve participation, the investigators conducted a prospective randomized trial, PICCOLINO, via the Polish Colonoscopy Screening Program. In total, 12,485 eligible individuals aged between 55 and 64 years received postal invitations to participate in CRC screening. Individuals were randomized in a 1:1:1 ratio into one of three mailing protocols, each of which involved an initial invitation, and, if needed, a second invitation that offered the following:
- Control group: colonoscopy, with nonresponders receiving the same invitation again
- Sequential group: colonoscopy, with nonresponders or refusers receiving a second invitation that offered FIT
- Choice group: choice between colonoscopy or FIT, with nonresponders receiving the same invitation again
The primary outcome was participation in screening within 18 weeks of enrollment. The secondary outcome was diagnostic yield for either advanced adenoma or CRC.
Out of the three groups, the control group had the lowest participation rate, at 17.5%, compared with 25.8% for the sequential group and 26.5% for the choice group. Multivariable logistic regression showed that individuals in the sequential and choice groups had 64% and 70% higher rates of participation, respectively. Across all groups, age of 60 years or older predicted 12% higher likelihood of participation; in contrast, location more than 40 kilometers from a testing center was associated with an 18% decrease in participation, compared with individuals who lived less than 20 kilometers away.
While the control and sequential groups had similar rates of colonoscopy participation, at 17.5% and 15.9%, respectively (P = .788), this rate was significantly lower, at 8.5%, in the choice group (P = .001). Conversely, the sequential group had a significantly lower rate of FITs than the choice group, at 9.9% versus 17.9%, respectively (P = .001). Among participants with a positive FIT, diagnostic work-up colonoscopies were performed in 70.0% of those in the sequential group and 73.3% in the choice group, “despite active call-recall efforts.”
Across all invited individuals, advanced disease detection rates were similar across groups, at 1.1% for both the control and the sequential group and 1.2% for the choice group. Among those who were actually screened, the control group had a slightly higher diagnostic yield for advanced neoplasia, at 6.5%, compared with 4.2% in the sequential group and 4.4% in the choice group; however, these differences were not statistically significant. In contrast, significantly more adenomas of any kind were detected in the control and sequential groups (5.6% for both) than the choice group (3.9%) (P < .001).
“Although the strategies which included FIT showed higher participation rates than the strategy of offering colonoscopy alone, these strategies did not result in increased detection rates of advanced neoplasia in the intention to screen analysis,” the investigators wrote. “An absolute increase in participation rates of 8%-10% seems insufficient to translate into higher advanced neoplasia detection at the population level.”
Dr. Pilonis and colleagues also suggested that the relatively low rate of diagnostic colonoscopy after positive FIT contributed to the suboptimal diagnostic yield.
“These rates are unsatisfactory taking into account significant call-recall efforts, but are within the range reported in other studies,” they wrote.
They also wrote that their study compared participation and detection between one-time colonoscopy and one-time screening strategies combining colonoscopy and FIT. In acknowledging this, they noted that these approaches have different screening intervals and uptake over time: “FIT has been shown to achieve higher participation rates than colonoscopy for one time screening, but its uptake over several rounds may not be superior to one time colonoscopy.” Furthermore, detection rates of the sequential or choice strategies for advanced disease may rise over time with further implementation, so the one-time screening may not be sufficient to reveal what could become significant differences.
The study was funded by the Polish Ministry of Health, the Polish Foundation of Gastroenterology, and the Centre of Postgraduate Medical Education in Warsaw. FITs, materials, and reagents were provided by Eiken Chemical. The investigators disclosed relationships with Boston Scientific, AbbVie, Olympus, and others.
FROM GASTROENTEROLOGY
Chart review for cosmetic procedures: 2019 was a good year
Cosmetic procedures continued to increase in popularity in 2019, and body sculpting and laser/light/energy-based procedures led the way, according to a survey by the American Society of Dermatologic Surgery.

the largest proportional rise among the major categories of cosmetic procedures, the ASDS reported in its annual member survey.
Use of laser/light/energy-based devices was up by a much lower 18%, but the increase in the actual number of procedures – nearly 637,000 more than 2018 – was larger than any other category, the ASDS said.
Procedures categorized as “other rejuvenation” – microneedling, platelet-rich plasma, hair rejuvenation, and thread lifts – were another bright spot in the cosmetic lineup in 2019, rising 38% over their 2018 volume. Injectable neuromodulator treatments, which were second in overall volume with almost 2.4 million procedures, were up by 12.5% in 2019, compared with 2018, the ASDS said.
The injectable soft-tissue fillers, however, did not produce any noteworthy gain in the volume of procedures for the second consecutive year. Meanwhile, the number of chemical peel procedures dropped by almost 16% in 2019 after rising for the last 2 years, the ASDS reported.
A closer look at the body-sculpting sector also shows some declines in 2019, despite the overall success: Cryolipolysis procedures were down by 10.3% and deoxycholic acid procedures slipped 13.7%. The biggest addition – over 157,000 procedures – came from muscle-toning devices, which were new to the survey last year, the ASDS noted.
The survey was conducted among the society’s members from May 7 to July 31, 2020, and the 514 responses were generalized to the entire ASDS membership of over 6,400 physicians.
Cosmetic procedures continued to increase in popularity in 2019, and body sculpting and laser/light/energy-based procedures led the way, according to a survey by the American Society of Dermatologic Surgery.

the largest proportional rise among the major categories of cosmetic procedures, the ASDS reported in its annual member survey.
Use of laser/light/energy-based devices was up by a much lower 18%, but the increase in the actual number of procedures – nearly 637,000 more than 2018 – was larger than any other category, the ASDS said.
Procedures categorized as “other rejuvenation” – microneedling, platelet-rich plasma, hair rejuvenation, and thread lifts – were another bright spot in the cosmetic lineup in 2019, rising 38% over their 2018 volume. Injectable neuromodulator treatments, which were second in overall volume with almost 2.4 million procedures, were up by 12.5% in 2019, compared with 2018, the ASDS said.
The injectable soft-tissue fillers, however, did not produce any noteworthy gain in the volume of procedures for the second consecutive year. Meanwhile, the number of chemical peel procedures dropped by almost 16% in 2019 after rising for the last 2 years, the ASDS reported.
A closer look at the body-sculpting sector also shows some declines in 2019, despite the overall success: Cryolipolysis procedures were down by 10.3% and deoxycholic acid procedures slipped 13.7%. The biggest addition – over 157,000 procedures – came from muscle-toning devices, which were new to the survey last year, the ASDS noted.
The survey was conducted among the society’s members from May 7 to July 31, 2020, and the 514 responses were generalized to the entire ASDS membership of over 6,400 physicians.
Cosmetic procedures continued to increase in popularity in 2019, and body sculpting and laser/light/energy-based procedures led the way, according to a survey by the American Society of Dermatologic Surgery.

the largest proportional rise among the major categories of cosmetic procedures, the ASDS reported in its annual member survey.
Use of laser/light/energy-based devices was up by a much lower 18%, but the increase in the actual number of procedures – nearly 637,000 more than 2018 – was larger than any other category, the ASDS said.
Procedures categorized as “other rejuvenation” – microneedling, platelet-rich plasma, hair rejuvenation, and thread lifts – were another bright spot in the cosmetic lineup in 2019, rising 38% over their 2018 volume. Injectable neuromodulator treatments, which were second in overall volume with almost 2.4 million procedures, were up by 12.5% in 2019, compared with 2018, the ASDS said.
The injectable soft-tissue fillers, however, did not produce any noteworthy gain in the volume of procedures for the second consecutive year. Meanwhile, the number of chemical peel procedures dropped by almost 16% in 2019 after rising for the last 2 years, the ASDS reported.
A closer look at the body-sculpting sector also shows some declines in 2019, despite the overall success: Cryolipolysis procedures were down by 10.3% and deoxycholic acid procedures slipped 13.7%. The biggest addition – over 157,000 procedures – came from muscle-toning devices, which were new to the survey last year, the ASDS noted.
The survey was conducted among the society’s members from May 7 to July 31, 2020, and the 514 responses were generalized to the entire ASDS membership of over 6,400 physicians.
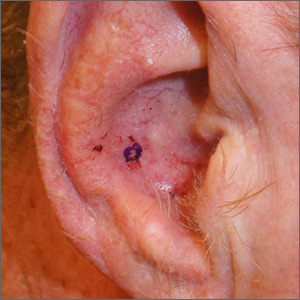
Are there COVID-19–related ‘long-haul’ skin issues?
– as a result of infection with or exposure to the SARS-CoV-2 virus, but some dermatologists question if the skin signs and symptoms are truly related.
In their commentary in the Lancet Infectious Diseases, Esther P. Freeman, MD, PhD, and colleagues who lead and participate in the American Academy of Dermatology’s international registry said their analysis “revealed a previously unreported subset of patients who experience long-haul symptoms in dermatology-dominant COVID-19.”
Some of the data was presented at the 29th European Academy of Dermatology and Venereology in late October 2020, but has since been updated with more cases.
Dermatologists who spoke with this news organization said it has not been settled that some skin manifestations – such as pernio/chilblains rashes, seen primarily in nonhospitalized patients, and described in the registry – are definitively caused by COVID. They also noted that in some cases, patients who initially test negative for COVID-19 by polymerase chain reaction (PCR) sometimes do not ever develop antibodies, which could mean they were never actually exposed to SARS-CoV-2.
“I still question whether the perniosis is directly related to infection with SARS-CoV-2 or not,” said Anthony Fernandez, MD, PhD, director of medical and inpatient dermatology and assistant professor of dermatopathology at the Cleveland Clinic. His uncertainty is driven by the lack of seroconversion and that few cases were seen over the summer in the United States – suggesting that it may still be a result of cold temperatures.
“I’m not sure there is a definitive correct answer, definitely not that everyone would agree on,” said Christine Ko, MD, professor of dermatology and pathology at Yale University, New Haven, Conn.
Dr. Freeman, however, believed that pernio and especially persistent lesions are caused by an immune response to COVID.
In an interview, she noted the multiple cases of patients in the registry who did seroconvert and that, while a registry is not a perfect means of getting an answer, it is good for generating questions. Taken collectively, the cases in the registry can “tell a story for further hypotheses,” said Dr. Freeman, who is director of global health dermatology at Massachusetts General Hospital and assistant professor of dermatology at Harvard University, both in Boston.
“We were noticing this signal across the world” that patients “developed these toe lesions and they never got better,” said Dr. Freeman. Generally, people who experience pernio, also described as COVID toes or “COVID fingers,” recover in 4-8 weeks. But in the registry, “we did have this subset of patients who really were experiencing these very longstanding symptoms,” she added.
Two patients with lab-confirmed COVID have had long-lasting pernio of 133 days and 150 days. “I’m caring for a cohort in Boston who have had long COVID of the skin and symptoms for over 10 months,” Dr. Freeman said.
Pernio dominates
The registry – a collaboration between the AAD and the International League of Dermatological Societies – was launched in April 2020. Any medical professional can enter case information. From April to October, 1,030 total cases and 331 laboratory-confirmed or suspected COVID-19 cases with dermatological manifestations were entered from 41 countries.
Most of the cases were just recorded at a single time point, which is an acknowledged limitation of the study.
Dr. Freeman and colleagues reached out to registry participants in June and August to get updates on COVID lab test results and sign and symptom duration. Overall, 234 total and 96 lab-confirmed COVID infections had more lengthy data about sign and symptom duration.
Pernio lasted a median of 15 days in patients with suspected disease and 12 days for those with lab-confirmed COVID, compared with a median of 7 days for morbilliform eruptions, 4 days for urticarial eruptions, and 20 days for papulosquamous eruptions – all in patients with lab-confirmed disease.
Of the 103 cases of pernio, 7 had symptoms lasting more than 60 days. Only two of those seven patients had lab-confirmed COVID. Initially, the one patient tested negative with nasopharyngeal PCR, and serum IgM and IgG. Six weeks after pernio onset, the patient – still experiencing fatigue and pernio – seroconverted to anti–SARS-CoV-2 IgM positivity.
The other long-haul patient, after a negative PCR, tested positive for SARS-CoV-2 serum IgG 1 month after pernio onset.
Robust immune response?
Dr. Freeman said these patients might have a very high interferon response initially to the virus, which makes for a mild to nonexistent disease, but could create inflammation elsewhere. “I almost view the toes as an innocent bystander of a robust immune response to SARS-CoV-2.”
Although he has not seen extended pernio or other skin manifestations in his patients, Dr. Fernandez said the interferon hypothesis is “fair,” and “the best that’s out there.” Dr. Fernandez is currently studying cutaneous manifestations of COVID-19 as a principal investigator of a trial sponsored by the Clinical and Translational Science Collaborative of Cleveland.
Dr. Ko said in an interview that she has not observed long-haul skin issues in her patients, but Yale colleagues have.
In a study, she and Yale colleagues published in September, SARS-CoV-2 spike protein was detected in perniotic lesions, but not nuclear protein or viral RNA. The test they used – immunohistochemistry – can be nonspecific, which muddied results.
She does not think there is replicating virus in the skin or the lesions. Instead, said Dr. Ko, “either there is viral spike protein that has somehow become disassociated from actively replicating virus that somehow got deposited in endothelial cells,” or the staining “was spurious,” or some other protein is cross-reacting. “And the people who are unlucky enough to have that protein in their endothelial cells can manifest this COVID-toe, COVID-finger phenomenon.”
To her, it’s an unsolved mystery. “The weird thing is, we’ve never before had this much perniosis,” Dr. Ko said.
Dr. Fernandez is not convinced yet, noting that, in Cleveland, more pernio cases were observed in March and April than in the summer. “If it is a manifestation of the infection then you also need the right environment, the cold weather for this manifestation to present,” he said. “Or, it really isn’t a direct manifestation of COVID-19 but may be more related to other factors,” such as lifestyle changes related to limitations implemented to help mitigate the spread of the disease.
“To me the jury is still out whether or not the perniotic lesions really can tell us something about a patient’s exposure and infection with SARS-CoV-2,” he said.
Dr. Freeman reported receiving a grant from the International League of Dermatological Societies and nonfinancial support from the AAD for the study. Dr. Ko reported no conflicts. Dr. Fernadnez had no disclosures.
– as a result of infection with or exposure to the SARS-CoV-2 virus, but some dermatologists question if the skin signs and symptoms are truly related.
In their commentary in the Lancet Infectious Diseases, Esther P. Freeman, MD, PhD, and colleagues who lead and participate in the American Academy of Dermatology’s international registry said their analysis “revealed a previously unreported subset of patients who experience long-haul symptoms in dermatology-dominant COVID-19.”
Some of the data was presented at the 29th European Academy of Dermatology and Venereology in late October 2020, but has since been updated with more cases.
Dermatologists who spoke with this news organization said it has not been settled that some skin manifestations – such as pernio/chilblains rashes, seen primarily in nonhospitalized patients, and described in the registry – are definitively caused by COVID. They also noted that in some cases, patients who initially test negative for COVID-19 by polymerase chain reaction (PCR) sometimes do not ever develop antibodies, which could mean they were never actually exposed to SARS-CoV-2.
“I still question whether the perniosis is directly related to infection with SARS-CoV-2 or not,” said Anthony Fernandez, MD, PhD, director of medical and inpatient dermatology and assistant professor of dermatopathology at the Cleveland Clinic. His uncertainty is driven by the lack of seroconversion and that few cases were seen over the summer in the United States – suggesting that it may still be a result of cold temperatures.
“I’m not sure there is a definitive correct answer, definitely not that everyone would agree on,” said Christine Ko, MD, professor of dermatology and pathology at Yale University, New Haven, Conn.
Dr. Freeman, however, believed that pernio and especially persistent lesions are caused by an immune response to COVID.
In an interview, she noted the multiple cases of patients in the registry who did seroconvert and that, while a registry is not a perfect means of getting an answer, it is good for generating questions. Taken collectively, the cases in the registry can “tell a story for further hypotheses,” said Dr. Freeman, who is director of global health dermatology at Massachusetts General Hospital and assistant professor of dermatology at Harvard University, both in Boston.
“We were noticing this signal across the world” that patients “developed these toe lesions and they never got better,” said Dr. Freeman. Generally, people who experience pernio, also described as COVID toes or “COVID fingers,” recover in 4-8 weeks. But in the registry, “we did have this subset of patients who really were experiencing these very longstanding symptoms,” she added.
Two patients with lab-confirmed COVID have had long-lasting pernio of 133 days and 150 days. “I’m caring for a cohort in Boston who have had long COVID of the skin and symptoms for over 10 months,” Dr. Freeman said.
Pernio dominates
The registry – a collaboration between the AAD and the International League of Dermatological Societies – was launched in April 2020. Any medical professional can enter case information. From April to October, 1,030 total cases and 331 laboratory-confirmed or suspected COVID-19 cases with dermatological manifestations were entered from 41 countries.
Most of the cases were just recorded at a single time point, which is an acknowledged limitation of the study.
Dr. Freeman and colleagues reached out to registry participants in June and August to get updates on COVID lab test results and sign and symptom duration. Overall, 234 total and 96 lab-confirmed COVID infections had more lengthy data about sign and symptom duration.
Pernio lasted a median of 15 days in patients with suspected disease and 12 days for those with lab-confirmed COVID, compared with a median of 7 days for morbilliform eruptions, 4 days for urticarial eruptions, and 20 days for papulosquamous eruptions – all in patients with lab-confirmed disease.
Of the 103 cases of pernio, 7 had symptoms lasting more than 60 days. Only two of those seven patients had lab-confirmed COVID. Initially, the one patient tested negative with nasopharyngeal PCR, and serum IgM and IgG. Six weeks after pernio onset, the patient – still experiencing fatigue and pernio – seroconverted to anti–SARS-CoV-2 IgM positivity.
The other long-haul patient, after a negative PCR, tested positive for SARS-CoV-2 serum IgG 1 month after pernio onset.
Robust immune response?
Dr. Freeman said these patients might have a very high interferon response initially to the virus, which makes for a mild to nonexistent disease, but could create inflammation elsewhere. “I almost view the toes as an innocent bystander of a robust immune response to SARS-CoV-2.”
Although he has not seen extended pernio or other skin manifestations in his patients, Dr. Fernandez said the interferon hypothesis is “fair,” and “the best that’s out there.” Dr. Fernandez is currently studying cutaneous manifestations of COVID-19 as a principal investigator of a trial sponsored by the Clinical and Translational Science Collaborative of Cleveland.
Dr. Ko said in an interview that she has not observed long-haul skin issues in her patients, but Yale colleagues have.
In a study, she and Yale colleagues published in September, SARS-CoV-2 spike protein was detected in perniotic lesions, but not nuclear protein or viral RNA. The test they used – immunohistochemistry – can be nonspecific, which muddied results.
She does not think there is replicating virus in the skin or the lesions. Instead, said Dr. Ko, “either there is viral spike protein that has somehow become disassociated from actively replicating virus that somehow got deposited in endothelial cells,” or the staining “was spurious,” or some other protein is cross-reacting. “And the people who are unlucky enough to have that protein in their endothelial cells can manifest this COVID-toe, COVID-finger phenomenon.”
To her, it’s an unsolved mystery. “The weird thing is, we’ve never before had this much perniosis,” Dr. Ko said.
Dr. Fernandez is not convinced yet, noting that, in Cleveland, more pernio cases were observed in March and April than in the summer. “If it is a manifestation of the infection then you also need the right environment, the cold weather for this manifestation to present,” he said. “Or, it really isn’t a direct manifestation of COVID-19 but may be more related to other factors,” such as lifestyle changes related to limitations implemented to help mitigate the spread of the disease.
“To me the jury is still out whether or not the perniotic lesions really can tell us something about a patient’s exposure and infection with SARS-CoV-2,” he said.
Dr. Freeman reported receiving a grant from the International League of Dermatological Societies and nonfinancial support from the AAD for the study. Dr. Ko reported no conflicts. Dr. Fernadnez had no disclosures.
– as a result of infection with or exposure to the SARS-CoV-2 virus, but some dermatologists question if the skin signs and symptoms are truly related.
In their commentary in the Lancet Infectious Diseases, Esther P. Freeman, MD, PhD, and colleagues who lead and participate in the American Academy of Dermatology’s international registry said their analysis “revealed a previously unreported subset of patients who experience long-haul symptoms in dermatology-dominant COVID-19.”
Some of the data was presented at the 29th European Academy of Dermatology and Venereology in late October 2020, but has since been updated with more cases.
Dermatologists who spoke with this news organization said it has not been settled that some skin manifestations – such as pernio/chilblains rashes, seen primarily in nonhospitalized patients, and described in the registry – are definitively caused by COVID. They also noted that in some cases, patients who initially test negative for COVID-19 by polymerase chain reaction (PCR) sometimes do not ever develop antibodies, which could mean they were never actually exposed to SARS-CoV-2.
“I still question whether the perniosis is directly related to infection with SARS-CoV-2 or not,” said Anthony Fernandez, MD, PhD, director of medical and inpatient dermatology and assistant professor of dermatopathology at the Cleveland Clinic. His uncertainty is driven by the lack of seroconversion and that few cases were seen over the summer in the United States – suggesting that it may still be a result of cold temperatures.
“I’m not sure there is a definitive correct answer, definitely not that everyone would agree on,” said Christine Ko, MD, professor of dermatology and pathology at Yale University, New Haven, Conn.
Dr. Freeman, however, believed that pernio and especially persistent lesions are caused by an immune response to COVID.
In an interview, she noted the multiple cases of patients in the registry who did seroconvert and that, while a registry is not a perfect means of getting an answer, it is good for generating questions. Taken collectively, the cases in the registry can “tell a story for further hypotheses,” said Dr. Freeman, who is director of global health dermatology at Massachusetts General Hospital and assistant professor of dermatology at Harvard University, both in Boston.
“We were noticing this signal across the world” that patients “developed these toe lesions and they never got better,” said Dr. Freeman. Generally, people who experience pernio, also described as COVID toes or “COVID fingers,” recover in 4-8 weeks. But in the registry, “we did have this subset of patients who really were experiencing these very longstanding symptoms,” she added.
Two patients with lab-confirmed COVID have had long-lasting pernio of 133 days and 150 days. “I’m caring for a cohort in Boston who have had long COVID of the skin and symptoms for over 10 months,” Dr. Freeman said.
Pernio dominates
The registry – a collaboration between the AAD and the International League of Dermatological Societies – was launched in April 2020. Any medical professional can enter case information. From April to October, 1,030 total cases and 331 laboratory-confirmed or suspected COVID-19 cases with dermatological manifestations were entered from 41 countries.
Most of the cases were just recorded at a single time point, which is an acknowledged limitation of the study.
Dr. Freeman and colleagues reached out to registry participants in June and August to get updates on COVID lab test results and sign and symptom duration. Overall, 234 total and 96 lab-confirmed COVID infections had more lengthy data about sign and symptom duration.
Pernio lasted a median of 15 days in patients with suspected disease and 12 days for those with lab-confirmed COVID, compared with a median of 7 days for morbilliform eruptions, 4 days for urticarial eruptions, and 20 days for papulosquamous eruptions – all in patients with lab-confirmed disease.
Of the 103 cases of pernio, 7 had symptoms lasting more than 60 days. Only two of those seven patients had lab-confirmed COVID. Initially, the one patient tested negative with nasopharyngeal PCR, and serum IgM and IgG. Six weeks after pernio onset, the patient – still experiencing fatigue and pernio – seroconverted to anti–SARS-CoV-2 IgM positivity.
The other long-haul patient, after a negative PCR, tested positive for SARS-CoV-2 serum IgG 1 month after pernio onset.
Robust immune response?
Dr. Freeman said these patients might have a very high interferon response initially to the virus, which makes for a mild to nonexistent disease, but could create inflammation elsewhere. “I almost view the toes as an innocent bystander of a robust immune response to SARS-CoV-2.”
Although he has not seen extended pernio or other skin manifestations in his patients, Dr. Fernandez said the interferon hypothesis is “fair,” and “the best that’s out there.” Dr. Fernandez is currently studying cutaneous manifestations of COVID-19 as a principal investigator of a trial sponsored by the Clinical and Translational Science Collaborative of Cleveland.
Dr. Ko said in an interview that she has not observed long-haul skin issues in her patients, but Yale colleagues have.
In a study, she and Yale colleagues published in September, SARS-CoV-2 spike protein was detected in perniotic lesions, but not nuclear protein or viral RNA. The test they used – immunohistochemistry – can be nonspecific, which muddied results.
She does not think there is replicating virus in the skin or the lesions. Instead, said Dr. Ko, “either there is viral spike protein that has somehow become disassociated from actively replicating virus that somehow got deposited in endothelial cells,” or the staining “was spurious,” or some other protein is cross-reacting. “And the people who are unlucky enough to have that protein in their endothelial cells can manifest this COVID-toe, COVID-finger phenomenon.”
To her, it’s an unsolved mystery. “The weird thing is, we’ve never before had this much perniosis,” Dr. Ko said.
Dr. Fernandez is not convinced yet, noting that, in Cleveland, more pernio cases were observed in March and April than in the summer. “If it is a manifestation of the infection then you also need the right environment, the cold weather for this manifestation to present,” he said. “Or, it really isn’t a direct manifestation of COVID-19 but may be more related to other factors,” such as lifestyle changes related to limitations implemented to help mitigate the spread of the disease.
“To me the jury is still out whether or not the perniotic lesions really can tell us something about a patient’s exposure and infection with SARS-CoV-2,” he said.
Dr. Freeman reported receiving a grant from the International League of Dermatological Societies and nonfinancial support from the AAD for the study. Dr. Ko reported no conflicts. Dr. Fernadnez had no disclosures.
FROM THE LANCET INFECTIOUS DISEASES
Naltrexone cuts hospitalization, deaths in alcohol use disorder
Naltrexone reduces the risk for hospitalization for alcohol use disorder (AUD), regardless of whether it is used alone or in conjunction with disulfiram or acamprosate, research suggests.
Investigators analyzed 10-year data on more than 125,000 Swedish residents with AUD and found that naltrexone, used as monotherapy or combined with acamprosate or disulfiram, was associated with significantly lower risk for AUD hospitalization or all-cause hospitalization in comparison with patients who did not use AUD medication. The patients ranged in age from 16 to 64 years.
By contrast, benzodiazepines and acamprosate monotherapy were associated with increased risk for AUD hospitalization.
“The take-home message for practicing clinicians would be that especially naltrexone use is associated with favorable treatment outcomes and should be utilized as part of the treatment protocol for AUD,” study investigator Milja Heikkinen, MD, specialist in forensic psychiatry and addiction medicine, University of Eastern Finland, Kuopio, told this news organization.
On the other hand, “benzodiazepines should be avoided and should not be administered other than for alcohol withdrawal symptoms,” she said.
The study was published online Jan. 4 in Addiction.
Real-world data
Previous research has shown that disulfiram, acamprosate, naltrexone, and nalmefene are efficacious in treating AUD, but most studies have been randomized controlled trials or meta-analyses, the authors write.
“Very little is known about overall health outcomes (such as risks of hospitalization and mortality) associated with specific treatments in real-world circumstances,” they write.
“The study was motivated by the fact that, although AUD is a significant public health concern, very little is known, especially about the comparative effectiveness of medications indicated in AUD,” said Dr. Heikkinen.
who had been diagnosed with AUD (62.5% men; mean [standard deviation] age, 38.1 [15.9] years). They followed the cohort over a median of 4.6 years (interquartile range, 2.1-.2 years).
During the follow-up period, roughly one-fourth of patients (25.6) underwent treatment with one or more drugs.

The main outcome measure was AUD-related hospitalization. Secondary outcomes were hospitalization for any cause and for alcohol-related somatic causes; all-cause mortality; and work disability.
Two types of analyses were conducted. The within-individual analyses, designed to eliminate selection bias, compared the use of a medication to periods during which the same individual was not using the medication.
Between-individual analyses (adjusted for sex, age, educational level, number of previous AUD-related hospitalizations, time since first AUD diagnosis, comorbidities, and use of other medications) utilized a “traditional” multivariate-adjusted Cox hazards regression model.
AUD pharmacotherapy ‘underutilized’
Close to one-fourth of patients (23.9%) experienced the main outcome event (AUD-related hospitalization) during the follow-up period.
The within-individual analysis showed that naltrexone – whether used as monotherapy or adjunctively with disulfiram or acamprosate – “was associated with a significantly lower risk of AUD-related hospitalization, compared to those time periods in which the same individual did not use any AUD medication,” the authors report.
By contrast, they state, acamprosate monotherapy and benzodiazepines were associated with a significantly higher risk for AUD-related hospitalization.
Similar results were obtained in the between-individual analysis. Longer duration of naltrexone use was associated with lower risk for AUD-related hospitalization.
The pattern was also found when the outcome was hospitalization for any cause. However, unlike the findings of the within-individual model, the second model found that acamprosate monotherapy was not associated with a higher risk for any-cause hospitalization.
Polytherapy, including combinations of the four AUD medications, as well as disulfiram monotherapy were similarly associated with lower risk for hospitalization for alcohol-related somatic causes.
Of the overall cohort, 6.2% died during the follow-up period. No association was found between disulfiram, acamprosate, nalmefene, and naltrexone use and all-cause mortality. By contrast, benzodiazepine use was associated with a significantly higher mortality rate (hazard ratio, 1.11; 95% confidence interval, 1.04-1.19).
“AUD drugs are underutilized, despite AUD being a significant public health concern,” Dr. Heikkinen noted. On the other hand, benzodiazepine use is “very common.”
‘Ravages’ of benzodiazepines
Commenting on the study in an interview, John Krystal, MD, professor and chair of psychiatry and director of the Center for the Translational Neuroscience of Alcoholism, Yale University, New Haven, Conn., said, “The main message from the study for practicing clinicians is that treatment works.”
Dr. Krystal, who was not involved with the study, noted that “many practicing clinicians are discouraged by the course of their patients with AUD, and this study highlights that naltrexone, perhaps in combination with other medications, may be effective in preventing hospitalization and, presumably, other hospitalization-related complications of AUD.”
Also commenting on the study, Raymond Anton, MD, professor, department of psychiatry and behavioral sciences, Medical University of South Carolina, Charleston, suggested that the “clinical knowledge of the harm of benzodiazepines in those with AUD is reinforced by these findings.”
In fact, the harm of benzodiazepines might be the study’s “most important message ... [a message that was] recently highlighted by the Netflix series “The Queen’s Gambit”, which shows the ravages of using both together, or how one leads to potential addiction with the other,” said Dr. Anton, who was not involved with the study.
The other “big take-home message is that naltrexone should be used more frequently,” said Dr. Anton, distinguished professor of psychiatry at the university and scientific director of the Charleston Alcohol Research Center. He noted that there are “recent data suggesting some clinical and genetic indicators that predict responsiveness to these medications, improving efficacy.”
The study was funded by the Finnish Ministry of Social Affairs and Health. Dr. Heikkinen reports no relevant financial relationships. The other authors’ disclosures are listed on the original article. Dr. Krystal consults for companies currently developing other treatments for AUDs and receives medications to test from AstraZeneca and Novartis for NIAAA-funded research programs. Dr. Anton has consulted for Alkermes, Lipha, and Lundbeck in the past. He is also chair of the Alcohol Clinical Trials Initiative, which is a public-private partnership partially sponsored by several companies and has received grant funding from the National Institutes of Health/National Institute on Alcohol Abuse and Alcoholism to study pharmacotherapies, including naltrexone, nalmefene, and acamprosate.
A version of this article first appeared on Medscape.com.
Naltrexone reduces the risk for hospitalization for alcohol use disorder (AUD), regardless of whether it is used alone or in conjunction with disulfiram or acamprosate, research suggests.
Investigators analyzed 10-year data on more than 125,000 Swedish residents with AUD and found that naltrexone, used as monotherapy or combined with acamprosate or disulfiram, was associated with significantly lower risk for AUD hospitalization or all-cause hospitalization in comparison with patients who did not use AUD medication. The patients ranged in age from 16 to 64 years.
By contrast, benzodiazepines and acamprosate monotherapy were associated with increased risk for AUD hospitalization.
“The take-home message for practicing clinicians would be that especially naltrexone use is associated with favorable treatment outcomes and should be utilized as part of the treatment protocol for AUD,” study investigator Milja Heikkinen, MD, specialist in forensic psychiatry and addiction medicine, University of Eastern Finland, Kuopio, told this news organization.
On the other hand, “benzodiazepines should be avoided and should not be administered other than for alcohol withdrawal symptoms,” she said.
The study was published online Jan. 4 in Addiction.
Real-world data
Previous research has shown that disulfiram, acamprosate, naltrexone, and nalmefene are efficacious in treating AUD, but most studies have been randomized controlled trials or meta-analyses, the authors write.
“Very little is known about overall health outcomes (such as risks of hospitalization and mortality) associated with specific treatments in real-world circumstances,” they write.
“The study was motivated by the fact that, although AUD is a significant public health concern, very little is known, especially about the comparative effectiveness of medications indicated in AUD,” said Dr. Heikkinen.
who had been diagnosed with AUD (62.5% men; mean [standard deviation] age, 38.1 [15.9] years). They followed the cohort over a median of 4.6 years (interquartile range, 2.1-.2 years).
During the follow-up period, roughly one-fourth of patients (25.6) underwent treatment with one or more drugs.

The main outcome measure was AUD-related hospitalization. Secondary outcomes were hospitalization for any cause and for alcohol-related somatic causes; all-cause mortality; and work disability.
Two types of analyses were conducted. The within-individual analyses, designed to eliminate selection bias, compared the use of a medication to periods during which the same individual was not using the medication.
Between-individual analyses (adjusted for sex, age, educational level, number of previous AUD-related hospitalizations, time since first AUD diagnosis, comorbidities, and use of other medications) utilized a “traditional” multivariate-adjusted Cox hazards regression model.
AUD pharmacotherapy ‘underutilized’
Close to one-fourth of patients (23.9%) experienced the main outcome event (AUD-related hospitalization) during the follow-up period.
The within-individual analysis showed that naltrexone – whether used as monotherapy or adjunctively with disulfiram or acamprosate – “was associated with a significantly lower risk of AUD-related hospitalization, compared to those time periods in which the same individual did not use any AUD medication,” the authors report.
By contrast, they state, acamprosate monotherapy and benzodiazepines were associated with a significantly higher risk for AUD-related hospitalization.
Similar results were obtained in the between-individual analysis. Longer duration of naltrexone use was associated with lower risk for AUD-related hospitalization.
The pattern was also found when the outcome was hospitalization for any cause. However, unlike the findings of the within-individual model, the second model found that acamprosate monotherapy was not associated with a higher risk for any-cause hospitalization.
Polytherapy, including combinations of the four AUD medications, as well as disulfiram monotherapy were similarly associated with lower risk for hospitalization for alcohol-related somatic causes.
Of the overall cohort, 6.2% died during the follow-up period. No association was found between disulfiram, acamprosate, nalmefene, and naltrexone use and all-cause mortality. By contrast, benzodiazepine use was associated with a significantly higher mortality rate (hazard ratio, 1.11; 95% confidence interval, 1.04-1.19).
“AUD drugs are underutilized, despite AUD being a significant public health concern,” Dr. Heikkinen noted. On the other hand, benzodiazepine use is “very common.”
‘Ravages’ of benzodiazepines
Commenting on the study in an interview, John Krystal, MD, professor and chair of psychiatry and director of the Center for the Translational Neuroscience of Alcoholism, Yale University, New Haven, Conn., said, “The main message from the study for practicing clinicians is that treatment works.”
Dr. Krystal, who was not involved with the study, noted that “many practicing clinicians are discouraged by the course of their patients with AUD, and this study highlights that naltrexone, perhaps in combination with other medications, may be effective in preventing hospitalization and, presumably, other hospitalization-related complications of AUD.”
Also commenting on the study, Raymond Anton, MD, professor, department of psychiatry and behavioral sciences, Medical University of South Carolina, Charleston, suggested that the “clinical knowledge of the harm of benzodiazepines in those with AUD is reinforced by these findings.”
In fact, the harm of benzodiazepines might be the study’s “most important message ... [a message that was] recently highlighted by the Netflix series “The Queen’s Gambit”, which shows the ravages of using both together, or how one leads to potential addiction with the other,” said Dr. Anton, who was not involved with the study.
The other “big take-home message is that naltrexone should be used more frequently,” said Dr. Anton, distinguished professor of psychiatry at the university and scientific director of the Charleston Alcohol Research Center. He noted that there are “recent data suggesting some clinical and genetic indicators that predict responsiveness to these medications, improving efficacy.”
The study was funded by the Finnish Ministry of Social Affairs and Health. Dr. Heikkinen reports no relevant financial relationships. The other authors’ disclosures are listed on the original article. Dr. Krystal consults for companies currently developing other treatments for AUDs and receives medications to test from AstraZeneca and Novartis for NIAAA-funded research programs. Dr. Anton has consulted for Alkermes, Lipha, and Lundbeck in the past. He is also chair of the Alcohol Clinical Trials Initiative, which is a public-private partnership partially sponsored by several companies and has received grant funding from the National Institutes of Health/National Institute on Alcohol Abuse and Alcoholism to study pharmacotherapies, including naltrexone, nalmefene, and acamprosate.
A version of this article first appeared on Medscape.com.
Naltrexone reduces the risk for hospitalization for alcohol use disorder (AUD), regardless of whether it is used alone or in conjunction with disulfiram or acamprosate, research suggests.
Investigators analyzed 10-year data on more than 125,000 Swedish residents with AUD and found that naltrexone, used as monotherapy or combined with acamprosate or disulfiram, was associated with significantly lower risk for AUD hospitalization or all-cause hospitalization in comparison with patients who did not use AUD medication. The patients ranged in age from 16 to 64 years.
By contrast, benzodiazepines and acamprosate monotherapy were associated with increased risk for AUD hospitalization.
“The take-home message for practicing clinicians would be that especially naltrexone use is associated with favorable treatment outcomes and should be utilized as part of the treatment protocol for AUD,” study investigator Milja Heikkinen, MD, specialist in forensic psychiatry and addiction medicine, University of Eastern Finland, Kuopio, told this news organization.
On the other hand, “benzodiazepines should be avoided and should not be administered other than for alcohol withdrawal symptoms,” she said.
The study was published online Jan. 4 in Addiction.
Real-world data
Previous research has shown that disulfiram, acamprosate, naltrexone, and nalmefene are efficacious in treating AUD, but most studies have been randomized controlled trials or meta-analyses, the authors write.
“Very little is known about overall health outcomes (such as risks of hospitalization and mortality) associated with specific treatments in real-world circumstances,” they write.
“The study was motivated by the fact that, although AUD is a significant public health concern, very little is known, especially about the comparative effectiveness of medications indicated in AUD,” said Dr. Heikkinen.
who had been diagnosed with AUD (62.5% men; mean [standard deviation] age, 38.1 [15.9] years). They followed the cohort over a median of 4.6 years (interquartile range, 2.1-.2 years).
During the follow-up period, roughly one-fourth of patients (25.6) underwent treatment with one or more drugs.

The main outcome measure was AUD-related hospitalization. Secondary outcomes were hospitalization for any cause and for alcohol-related somatic causes; all-cause mortality; and work disability.
Two types of analyses were conducted. The within-individual analyses, designed to eliminate selection bias, compared the use of a medication to periods during which the same individual was not using the medication.
Between-individual analyses (adjusted for sex, age, educational level, number of previous AUD-related hospitalizations, time since first AUD diagnosis, comorbidities, and use of other medications) utilized a “traditional” multivariate-adjusted Cox hazards regression model.
AUD pharmacotherapy ‘underutilized’
Close to one-fourth of patients (23.9%) experienced the main outcome event (AUD-related hospitalization) during the follow-up period.
The within-individual analysis showed that naltrexone – whether used as monotherapy or adjunctively with disulfiram or acamprosate – “was associated with a significantly lower risk of AUD-related hospitalization, compared to those time periods in which the same individual did not use any AUD medication,” the authors report.
By contrast, they state, acamprosate monotherapy and benzodiazepines were associated with a significantly higher risk for AUD-related hospitalization.
Similar results were obtained in the between-individual analysis. Longer duration of naltrexone use was associated with lower risk for AUD-related hospitalization.
The pattern was also found when the outcome was hospitalization for any cause. However, unlike the findings of the within-individual model, the second model found that acamprosate monotherapy was not associated with a higher risk for any-cause hospitalization.
Polytherapy, including combinations of the four AUD medications, as well as disulfiram monotherapy were similarly associated with lower risk for hospitalization for alcohol-related somatic causes.
Of the overall cohort, 6.2% died during the follow-up period. No association was found between disulfiram, acamprosate, nalmefene, and naltrexone use and all-cause mortality. By contrast, benzodiazepine use was associated with a significantly higher mortality rate (hazard ratio, 1.11; 95% confidence interval, 1.04-1.19).
“AUD drugs are underutilized, despite AUD being a significant public health concern,” Dr. Heikkinen noted. On the other hand, benzodiazepine use is “very common.”
‘Ravages’ of benzodiazepines
Commenting on the study in an interview, John Krystal, MD, professor and chair of psychiatry and director of the Center for the Translational Neuroscience of Alcoholism, Yale University, New Haven, Conn., said, “The main message from the study for practicing clinicians is that treatment works.”
Dr. Krystal, who was not involved with the study, noted that “many practicing clinicians are discouraged by the course of their patients with AUD, and this study highlights that naltrexone, perhaps in combination with other medications, may be effective in preventing hospitalization and, presumably, other hospitalization-related complications of AUD.”
Also commenting on the study, Raymond Anton, MD, professor, department of psychiatry and behavioral sciences, Medical University of South Carolina, Charleston, suggested that the “clinical knowledge of the harm of benzodiazepines in those with AUD is reinforced by these findings.”
In fact, the harm of benzodiazepines might be the study’s “most important message ... [a message that was] recently highlighted by the Netflix series “The Queen’s Gambit”, which shows the ravages of using both together, or how one leads to potential addiction with the other,” said Dr. Anton, who was not involved with the study.
The other “big take-home message is that naltrexone should be used more frequently,” said Dr. Anton, distinguished professor of psychiatry at the university and scientific director of the Charleston Alcohol Research Center. He noted that there are “recent data suggesting some clinical and genetic indicators that predict responsiveness to these medications, improving efficacy.”
The study was funded by the Finnish Ministry of Social Affairs and Health. Dr. Heikkinen reports no relevant financial relationships. The other authors’ disclosures are listed on the original article. Dr. Krystal consults for companies currently developing other treatments for AUDs and receives medications to test from AstraZeneca and Novartis for NIAAA-funded research programs. Dr. Anton has consulted for Alkermes, Lipha, and Lundbeck in the past. He is also chair of the Alcohol Clinical Trials Initiative, which is a public-private partnership partially sponsored by several companies and has received grant funding from the National Institutes of Health/National Institute on Alcohol Abuse and Alcoholism to study pharmacotherapies, including naltrexone, nalmefene, and acamprosate.
A version of this article first appeared on Medscape.com.
A hard-to-reach bleeding lesion
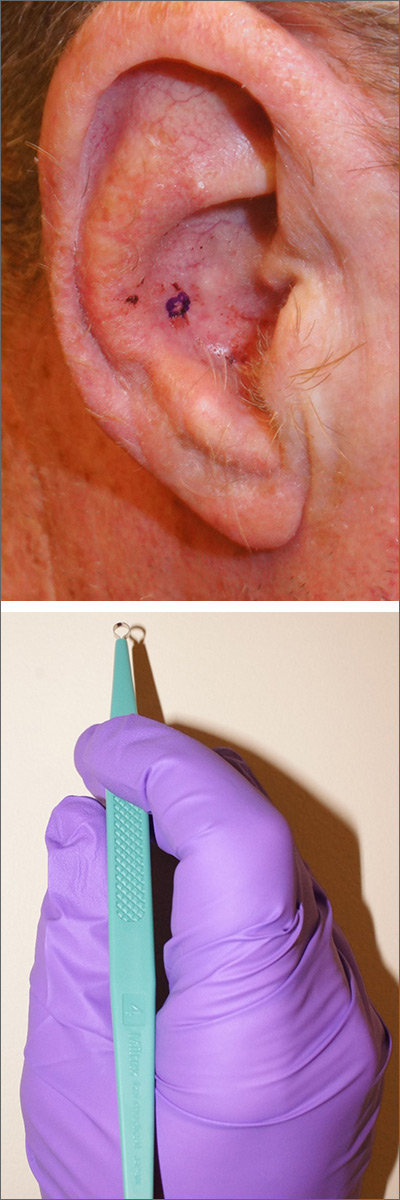
The history and exam were all suspicious for basal cell carcinoma (BCC), the most common of all cancers in the United States. (In African Americans, the most common skin cancer is squamous cell carcinoma). The suspicious lesion in this case was in a crevice, making it difficult to obtain a shave or punch biopsy.
As a result, a 4-mm disposable sterile curette was used (Figure). After informed consent was obtained, the lesion was cleansed with alcohol and marked with a surgical marker. Then, buffered lidocaine 1% with epinephrine was injected with a small syringe. Using a firm scraping motion with gentle rotation, a 4-mm sample of the lesion was quickly obtained and placed in standard formalin. Hemostasis was immediately obtained with firm application of 70% aluminum chloride in water using a cotton-tipped applicator. Heavy petrolatum was applied as a dressing.
The patient was confirmed to have a BCC and underwent Mohs surgery with clear margins after 1 stage. This case demonstrates the utility of a curette as a biopsy instrument for patients presenting with suspicious lesions in hard-to-reach places.
Text and photos courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. (Photo copyright retained.)
Yang YW, DiCaudo DJ. Effects of curettage after shave biopsy of unexpected melanoma: a retrospective review. J Am Acad Dermatol. 2018;78:1000-1002.

The history and exam were all suspicious for basal cell carcinoma (BCC), the most common of all cancers in the United States. (In African Americans, the most common skin cancer is squamous cell carcinoma). The suspicious lesion in this case was in a crevice, making it difficult to obtain a shave or punch biopsy.
As a result, a 4-mm disposable sterile curette was used (Figure). After informed consent was obtained, the lesion was cleansed with alcohol and marked with a surgical marker. Then, buffered lidocaine 1% with epinephrine was injected with a small syringe. Using a firm scraping motion with gentle rotation, a 4-mm sample of the lesion was quickly obtained and placed in standard formalin. Hemostasis was immediately obtained with firm application of 70% aluminum chloride in water using a cotton-tipped applicator. Heavy petrolatum was applied as a dressing.
The patient was confirmed to have a BCC and underwent Mohs surgery with clear margins after 1 stage. This case demonstrates the utility of a curette as a biopsy instrument for patients presenting with suspicious lesions in hard-to-reach places.
Text and photos courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. (Photo copyright retained.)

The history and exam were all suspicious for basal cell carcinoma (BCC), the most common of all cancers in the United States. (In African Americans, the most common skin cancer is squamous cell carcinoma). The suspicious lesion in this case was in a crevice, making it difficult to obtain a shave or punch biopsy.
As a result, a 4-mm disposable sterile curette was used (Figure). After informed consent was obtained, the lesion was cleansed with alcohol and marked with a surgical marker. Then, buffered lidocaine 1% with epinephrine was injected with a small syringe. Using a firm scraping motion with gentle rotation, a 4-mm sample of the lesion was quickly obtained and placed in standard formalin. Hemostasis was immediately obtained with firm application of 70% aluminum chloride in water using a cotton-tipped applicator. Heavy petrolatum was applied as a dressing.
The patient was confirmed to have a BCC and underwent Mohs surgery with clear margins after 1 stage. This case demonstrates the utility of a curette as a biopsy instrument for patients presenting with suspicious lesions in hard-to-reach places.
Text and photos courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. (Photo copyright retained.)
Yang YW, DiCaudo DJ. Effects of curettage after shave biopsy of unexpected melanoma: a retrospective review. J Am Acad Dermatol. 2018;78:1000-1002.
Yang YW, DiCaudo DJ. Effects of curettage after shave biopsy of unexpected melanoma: a retrospective review. J Am Acad Dermatol. 2018;78:1000-1002.
NAFLD linked to worse outcomes in IBD
Nonalcoholic fatty liver disease (NAFLD) in patients with inflammatory bowel disease (IBD) is associated with worse outcomes, and that relationship may be influenced by nonmetabolic factors. That is the conclusion of a new nationwide database analysis. NAFLD is common in IBD, with an estimated prevalence of 27%-32%.
Previous, smaller studies showed possible links between NAFLD and a history of IBD surgery, IBD disease activity, and metabolic factors, “but none of the studies looked at it on the scale that we did, and our study was more focused on outcomes than simply examining factors associated with both NAFLD and IBD,” Shaya Noorian, MD, of UCLA Medical Center in Los Angeles, said in an interview. Dr. Noorian presented the research at the annual congress of the Crohn’s & Colitis Foundation and the American Gastroenterological Association.
Dr. Noorian and colleagues found higher rates of hospital readmission, longer hospitalization, and higher costs, but not higher rates of death among patients with both Crohn’s disease or ulcerative colitis and NAFLD. The researchers analyzed data from patients in the Nationwide Readmissions Database (2016-2017), using ICD-10 codes to identify patients with IBD and NAFLD, along with propensity-matched controls. The study included 3,655 with Crohn’s disease and NAFLD and 7,482 without, and there were 2,026 with ulcerative colitis and NAFLD 4,094 without.
IBD hospital readmission rates were higher with comorbid NAFLD in Crohn’s disease (hazard ratio, 1.98; 95% confidence interval, 1.8-2.17; P < .001) and ulcerative colitis (HR, 1.97; 95% CI, 1.67-2.32; P < .001). Comorbid NAFLD was associated with additional length of stay Crohn’s disease (0.74 days; 95% CI, 0.29-1.18; P < .01) and ulcerative colitis (0.84 days; 0.32-1.35, respectively; P < .01), and there was additional cost of care with both Crohn’s disease ($7,766; 95% CI, $2,693-$12,839; P < .01) and ulcerative colitis ($11,496; 95% CI, $4,361-$18,631; P < .01).
Kaplan Meier curves for IBD readmission-free survival versus days since discharge showed clear separation in both Crohn’s disease and ulcerative colitis among patients with versus those without NAFLD.
Although evidence points to nonmetabolic factors being involved, metabolic factors such as obesity and diabetes are likely important as well. “We still do recognize that it’s very likely that these metabolic factors play a role in developing NAFLD in IBD. I think the fact that there are worse outcomes in patients with NAFLD supports the fact that we should do our best to control the metabolic factors like diabetes, obesity, et cetera. We don’t want to minimize that aspect of it. But I think the fact that there were still worse outcomes after adjusting for metabolic factors emphasizes the importance of researching these factors further to see which ones are the main contributors. If we can find the main contributor, whether that’s medication, IBD disease burden, or history of surgery, perhaps we can use that information to prevent development or progression of NAFLD,” said Dr. Noorian.
“Historical reports have examined the relationship between Crohn’s disease and NAFLD. The currently study included both Crohn’s and ulcerative colitis, thus impressively demonstrating the importance of this interaction across IBD,” said Matthew Ciorba, MD, director of the IBD Center at Washington University in St. Louis, who attended the session.
“This is the largest study to date, and the signal is very clear. It really does underscore the need [to study not just how] medications and other factors influence the clinical syndrome, but how it happens mechanistically. There are a multitude of metabolic interactions going on between the gut and liver. We need to understand this better – not just at the systemic level, but at the enterohepatic circulation level,” said Dr. Ciorba.
Possible mechanisms include liver toxicity due to medication, IBD-associated inflammation, or changes to gut bacteria, according to Dr. Noorian.
The study also brings to light something that could become an emerging problem. “In the past, Crohn’s patients were oftentimes thin because their Crohn’s disease wasn’t well treated. They were taking steroids all the time, so they had fat redistribution, including to the liver. Now we see IBD patients who are obese, and most are not underweight. It has become a compounding problem at this point with both conditions contributing to morbidity,” said Dr. Ciorba.
The study had no source of funding. Dr. Noorian and Dr. Ciorba have no relevant financial disclosures.
Nonalcoholic fatty liver disease (NAFLD) in patients with inflammatory bowel disease (IBD) is associated with worse outcomes, and that relationship may be influenced by nonmetabolic factors. That is the conclusion of a new nationwide database analysis. NAFLD is common in IBD, with an estimated prevalence of 27%-32%.
Previous, smaller studies showed possible links between NAFLD and a history of IBD surgery, IBD disease activity, and metabolic factors, “but none of the studies looked at it on the scale that we did, and our study was more focused on outcomes than simply examining factors associated with both NAFLD and IBD,” Shaya Noorian, MD, of UCLA Medical Center in Los Angeles, said in an interview. Dr. Noorian presented the research at the annual congress of the Crohn’s & Colitis Foundation and the American Gastroenterological Association.
Dr. Noorian and colleagues found higher rates of hospital readmission, longer hospitalization, and higher costs, but not higher rates of death among patients with both Crohn’s disease or ulcerative colitis and NAFLD. The researchers analyzed data from patients in the Nationwide Readmissions Database (2016-2017), using ICD-10 codes to identify patients with IBD and NAFLD, along with propensity-matched controls. The study included 3,655 with Crohn’s disease and NAFLD and 7,482 without, and there were 2,026 with ulcerative colitis and NAFLD 4,094 without.
IBD hospital readmission rates were higher with comorbid NAFLD in Crohn’s disease (hazard ratio, 1.98; 95% confidence interval, 1.8-2.17; P < .001) and ulcerative colitis (HR, 1.97; 95% CI, 1.67-2.32; P < .001). Comorbid NAFLD was associated with additional length of stay Crohn’s disease (0.74 days; 95% CI, 0.29-1.18; P < .01) and ulcerative colitis (0.84 days; 0.32-1.35, respectively; P < .01), and there was additional cost of care with both Crohn’s disease ($7,766; 95% CI, $2,693-$12,839; P < .01) and ulcerative colitis ($11,496; 95% CI, $4,361-$18,631; P < .01).
Kaplan Meier curves for IBD readmission-free survival versus days since discharge showed clear separation in both Crohn’s disease and ulcerative colitis among patients with versus those without NAFLD.
Although evidence points to nonmetabolic factors being involved, metabolic factors such as obesity and diabetes are likely important as well. “We still do recognize that it’s very likely that these metabolic factors play a role in developing NAFLD in IBD. I think the fact that there are worse outcomes in patients with NAFLD supports the fact that we should do our best to control the metabolic factors like diabetes, obesity, et cetera. We don’t want to minimize that aspect of it. But I think the fact that there were still worse outcomes after adjusting for metabolic factors emphasizes the importance of researching these factors further to see which ones are the main contributors. If we can find the main contributor, whether that’s medication, IBD disease burden, or history of surgery, perhaps we can use that information to prevent development or progression of NAFLD,” said Dr. Noorian.
“Historical reports have examined the relationship between Crohn’s disease and NAFLD. The currently study included both Crohn’s and ulcerative colitis, thus impressively demonstrating the importance of this interaction across IBD,” said Matthew Ciorba, MD, director of the IBD Center at Washington University in St. Louis, who attended the session.
“This is the largest study to date, and the signal is very clear. It really does underscore the need [to study not just how] medications and other factors influence the clinical syndrome, but how it happens mechanistically. There are a multitude of metabolic interactions going on between the gut and liver. We need to understand this better – not just at the systemic level, but at the enterohepatic circulation level,” said Dr. Ciorba.
Possible mechanisms include liver toxicity due to medication, IBD-associated inflammation, or changes to gut bacteria, according to Dr. Noorian.
The study also brings to light something that could become an emerging problem. “In the past, Crohn’s patients were oftentimes thin because their Crohn’s disease wasn’t well treated. They were taking steroids all the time, so they had fat redistribution, including to the liver. Now we see IBD patients who are obese, and most are not underweight. It has become a compounding problem at this point with both conditions contributing to morbidity,” said Dr. Ciorba.
The study had no source of funding. Dr. Noorian and Dr. Ciorba have no relevant financial disclosures.
Nonalcoholic fatty liver disease (NAFLD) in patients with inflammatory bowel disease (IBD) is associated with worse outcomes, and that relationship may be influenced by nonmetabolic factors. That is the conclusion of a new nationwide database analysis. NAFLD is common in IBD, with an estimated prevalence of 27%-32%.
Previous, smaller studies showed possible links between NAFLD and a history of IBD surgery, IBD disease activity, and metabolic factors, “but none of the studies looked at it on the scale that we did, and our study was more focused on outcomes than simply examining factors associated with both NAFLD and IBD,” Shaya Noorian, MD, of UCLA Medical Center in Los Angeles, said in an interview. Dr. Noorian presented the research at the annual congress of the Crohn’s & Colitis Foundation and the American Gastroenterological Association.
Dr. Noorian and colleagues found higher rates of hospital readmission, longer hospitalization, and higher costs, but not higher rates of death among patients with both Crohn’s disease or ulcerative colitis and NAFLD. The researchers analyzed data from patients in the Nationwide Readmissions Database (2016-2017), using ICD-10 codes to identify patients with IBD and NAFLD, along with propensity-matched controls. The study included 3,655 with Crohn’s disease and NAFLD and 7,482 without, and there were 2,026 with ulcerative colitis and NAFLD 4,094 without.
IBD hospital readmission rates were higher with comorbid NAFLD in Crohn’s disease (hazard ratio, 1.98; 95% confidence interval, 1.8-2.17; P < .001) and ulcerative colitis (HR, 1.97; 95% CI, 1.67-2.32; P < .001). Comorbid NAFLD was associated with additional length of stay Crohn’s disease (0.74 days; 95% CI, 0.29-1.18; P < .01) and ulcerative colitis (0.84 days; 0.32-1.35, respectively; P < .01), and there was additional cost of care with both Crohn’s disease ($7,766; 95% CI, $2,693-$12,839; P < .01) and ulcerative colitis ($11,496; 95% CI, $4,361-$18,631; P < .01).
Kaplan Meier curves for IBD readmission-free survival versus days since discharge showed clear separation in both Crohn’s disease and ulcerative colitis among patients with versus those without NAFLD.
Although evidence points to nonmetabolic factors being involved, metabolic factors such as obesity and diabetes are likely important as well. “We still do recognize that it’s very likely that these metabolic factors play a role in developing NAFLD in IBD. I think the fact that there are worse outcomes in patients with NAFLD supports the fact that we should do our best to control the metabolic factors like diabetes, obesity, et cetera. We don’t want to minimize that aspect of it. But I think the fact that there were still worse outcomes after adjusting for metabolic factors emphasizes the importance of researching these factors further to see which ones are the main contributors. If we can find the main contributor, whether that’s medication, IBD disease burden, or history of surgery, perhaps we can use that information to prevent development or progression of NAFLD,” said Dr. Noorian.
“Historical reports have examined the relationship between Crohn’s disease and NAFLD. The currently study included both Crohn’s and ulcerative colitis, thus impressively demonstrating the importance of this interaction across IBD,” said Matthew Ciorba, MD, director of the IBD Center at Washington University in St. Louis, who attended the session.
“This is the largest study to date, and the signal is very clear. It really does underscore the need [to study not just how] medications and other factors influence the clinical syndrome, but how it happens mechanistically. There are a multitude of metabolic interactions going on between the gut and liver. We need to understand this better – not just at the systemic level, but at the enterohepatic circulation level,” said Dr. Ciorba.
Possible mechanisms include liver toxicity due to medication, IBD-associated inflammation, or changes to gut bacteria, according to Dr. Noorian.
The study also brings to light something that could become an emerging problem. “In the past, Crohn’s patients were oftentimes thin because their Crohn’s disease wasn’t well treated. They were taking steroids all the time, so they had fat redistribution, including to the liver. Now we see IBD patients who are obese, and most are not underweight. It has become a compounding problem at this point with both conditions contributing to morbidity,” said Dr. Ciorba.
The study had no source of funding. Dr. Noorian and Dr. Ciorba have no relevant financial disclosures.
FROM THE CROHN’S & COLITIS CONGRESS
Can ‘big’ be healthy? Yes – and no
While many people were committing to their New Year’s resolutions to lose weight, in January 2020 Cosmopolitan UK magazine released covers portraying 11 women of different shapes and sizes, with the headline, “This is healthy!” Each version of the cover features one or more of the 11 women wearing athletic gear and makeup, some of whom are caught mid-action – boxing, doing yoga, or simply rejoicing in being who they are. Seeing these, I was reminded of a patient I cared for as an intern.
Janet Spears (not her real name) was thin. Standing barely 5 feet 3 inches, she weighed 110 pounds. For those out there who think of size in terms of body mass index (BMI), it was about 20 kg/m2, solidly in the “normal” category. At the age of 62, despite this healthy BMI, she had so much plaque in her arteries that she needed surgery to improve blood flow to her foot.
Admittedly, whenever I had read about people with high cholesterol, type 2 diabetes, or atherosclerosis, I pictured bigger people. But when I met Ms. Spears, I realized that one’s health cannot necessarily be inferred from physical appearance.
As a bariatric surgeon board certified in obesity medicine, I’ve probably spent more time thinking and learning about obesity than most people – and yet I still didn’t know what to make of the Cosmopolitan covers.
I saw the reaction on Twitter before I saw the magazines themselves, and I quickly observed a number of people decrying the covers, suggesting that they promote obesity:
Multiple people suggested that this was inappropriate, especially in the context of the COVID-19 pandemic and the fact that people with obesity are at risk for worse outcomes, compared with those without obesity. (As an aside, these comments suggest that people did not read the associated article, which is about fitness and body image more than it is about obesity.)
Does size reflect health?
Putting the pandemic aside for a moment, the question the magazine covers raise is whether physical appearance reflects health. That’s what got me thinking about Ms. Spears, who, though appearing healthy, was sick enough that she needed to have major surgery. This whole conversation hinges, of course, on one’s definition of health.
A common knee-jerk response, especially from physicians, would be to say that obesity is by definition unhealthy. Some researchers have suggested though that a segment of people with obesity fall into a category called metabolically healthy obesity, which is typically characterized by a limited set of data such as cholesterol, blood sugar, and blood pressure. Indeed, some people with obesity have normal values in those categories.
Being metabolically healthy, however, does not preclude other medical problems associated with obesity, including joint pain, cancer, and mood disorders, among other issues. So even those who have metabolically healthy obesity are not necessarily immune to the many other obesity-related conditions.
What about body positivity?
As I delved further into the conversation about these covers, I saw people embracing the idea of promoting different-sized bodies. With almost two thirds of the U.S. population having overweight or obesity, one might argue that it’s high time magazine covers and the media reflect the reality in our hometowns. Unrealistic images in the media are associated with negative self-image and disordered eating, so perhaps embracing the shapes of real people may help us all have healthier attitudes toward our bodies.
That said, this idea can be taken too far. The Health at Every Size movement, which some might consider to be the ultimate body-positivity movement, espouses the idea that size and health are completely unrelated. That crosses a line between what we know to be true – that, at a population level, higher weight is associated with more medical problems – and fake news.
Another idea to consider is fitness, as opposed to health. Fitness can be defined multiple ways, but if we consider it to be measured exercise capacity, those who are more fit have a longer life expectancy than those with lower fitness levels at a given BMI. While some feel that the Cosmopolitan covers promote obesity and are therefore irresponsible, it’s at least as likely that highlighting people with obesity being active may inspire others with obesity to do the same.
Now let’s bring the pandemic back into the picture. As much as we all wish that it was over, with uncontrolled spread in every state and record numbers of people dying, COVID-19 is still very much a part of our reality. Having obesity increases the risk of having a severe case of COVID-19 if infected. Patients with obesity are also more likely than those without obesity to be hospitalized, require intensive care, and die with COVID-19.
Guiding the conversation
Pandemic or not, the truth is that obesity is related to multiple medical problems. That does not mean that every person with obesity has medical problems. The musician Lizzo, for example, is someone with obesity who considers herself to be healthy. She posts images and videos of working out and shares her personal fitness routine with her millions of fans. As a physician, I worry about the medical conditions – metabolic or otherwise – that someone like her may develop. But I love how she embraces who she is while striving to be healthier.
Most of the critical comments I have seen about the Cosmopolitan covers have, at best, bordered on fat shaming; others are solidly in that category. And the vitriol aimed at the larger models is despicable. It seems that conversations about obesity often vacillate from one extreme (fat shaming) to the other (extreme body positivity).
Although it may not sell magazines, I would love to see more nuanced, fact-based discussions, both in the media and in our clinics. We can start by acknowledging the fact that people of different sizes can be healthy. The truth is that we can’t tell very much about a person’s health from their outward appearance, and we should probably stop trying to make such inferences.
Assessment of health is most accurately judged by each person with their medical team, not by observers who use media images as part of their own propaganda machine, pushing one extreme view or another. As physicians, we have the opportunity and the responsibility to support our patients in the pursuit of health, without shame or judgment. Maybe that’s a New Year’s resolution worth committing to.
Arghavan Salles, MD, PhD, is a bariatric surgeon.
A version of this article first appeared on Medscape.com.
While many people were committing to their New Year’s resolutions to lose weight, in January 2020 Cosmopolitan UK magazine released covers portraying 11 women of different shapes and sizes, with the headline, “This is healthy!” Each version of the cover features one or more of the 11 women wearing athletic gear and makeup, some of whom are caught mid-action – boxing, doing yoga, or simply rejoicing in being who they are. Seeing these, I was reminded of a patient I cared for as an intern.
Janet Spears (not her real name) was thin. Standing barely 5 feet 3 inches, she weighed 110 pounds. For those out there who think of size in terms of body mass index (BMI), it was about 20 kg/m2, solidly in the “normal” category. At the age of 62, despite this healthy BMI, she had so much plaque in her arteries that she needed surgery to improve blood flow to her foot.
Admittedly, whenever I had read about people with high cholesterol, type 2 diabetes, or atherosclerosis, I pictured bigger people. But when I met Ms. Spears, I realized that one’s health cannot necessarily be inferred from physical appearance.
As a bariatric surgeon board certified in obesity medicine, I’ve probably spent more time thinking and learning about obesity than most people – and yet I still didn’t know what to make of the Cosmopolitan covers.
I saw the reaction on Twitter before I saw the magazines themselves, and I quickly observed a number of people decrying the covers, suggesting that they promote obesity:
Multiple people suggested that this was inappropriate, especially in the context of the COVID-19 pandemic and the fact that people with obesity are at risk for worse outcomes, compared with those without obesity. (As an aside, these comments suggest that people did not read the associated article, which is about fitness and body image more than it is about obesity.)
Does size reflect health?
Putting the pandemic aside for a moment, the question the magazine covers raise is whether physical appearance reflects health. That’s what got me thinking about Ms. Spears, who, though appearing healthy, was sick enough that she needed to have major surgery. This whole conversation hinges, of course, on one’s definition of health.
A common knee-jerk response, especially from physicians, would be to say that obesity is by definition unhealthy. Some researchers have suggested though that a segment of people with obesity fall into a category called metabolically healthy obesity, which is typically characterized by a limited set of data such as cholesterol, blood sugar, and blood pressure. Indeed, some people with obesity have normal values in those categories.
Being metabolically healthy, however, does not preclude other medical problems associated with obesity, including joint pain, cancer, and mood disorders, among other issues. So even those who have metabolically healthy obesity are not necessarily immune to the many other obesity-related conditions.
What about body positivity?
As I delved further into the conversation about these covers, I saw people embracing the idea of promoting different-sized bodies. With almost two thirds of the U.S. population having overweight or obesity, one might argue that it’s high time magazine covers and the media reflect the reality in our hometowns. Unrealistic images in the media are associated with negative self-image and disordered eating, so perhaps embracing the shapes of real people may help us all have healthier attitudes toward our bodies.
That said, this idea can be taken too far. The Health at Every Size movement, which some might consider to be the ultimate body-positivity movement, espouses the idea that size and health are completely unrelated. That crosses a line between what we know to be true – that, at a population level, higher weight is associated with more medical problems – and fake news.
Another idea to consider is fitness, as opposed to health. Fitness can be defined multiple ways, but if we consider it to be measured exercise capacity, those who are more fit have a longer life expectancy than those with lower fitness levels at a given BMI. While some feel that the Cosmopolitan covers promote obesity and are therefore irresponsible, it’s at least as likely that highlighting people with obesity being active may inspire others with obesity to do the same.
Now let’s bring the pandemic back into the picture. As much as we all wish that it was over, with uncontrolled spread in every state and record numbers of people dying, COVID-19 is still very much a part of our reality. Having obesity increases the risk of having a severe case of COVID-19 if infected. Patients with obesity are also more likely than those without obesity to be hospitalized, require intensive care, and die with COVID-19.
Guiding the conversation
Pandemic or not, the truth is that obesity is related to multiple medical problems. That does not mean that every person with obesity has medical problems. The musician Lizzo, for example, is someone with obesity who considers herself to be healthy. She posts images and videos of working out and shares her personal fitness routine with her millions of fans. As a physician, I worry about the medical conditions – metabolic or otherwise – that someone like her may develop. But I love how she embraces who she is while striving to be healthier.
Most of the critical comments I have seen about the Cosmopolitan covers have, at best, bordered on fat shaming; others are solidly in that category. And the vitriol aimed at the larger models is despicable. It seems that conversations about obesity often vacillate from one extreme (fat shaming) to the other (extreme body positivity).
Although it may not sell magazines, I would love to see more nuanced, fact-based discussions, both in the media and in our clinics. We can start by acknowledging the fact that people of different sizes can be healthy. The truth is that we can’t tell very much about a person’s health from their outward appearance, and we should probably stop trying to make such inferences.
Assessment of health is most accurately judged by each person with their medical team, not by observers who use media images as part of their own propaganda machine, pushing one extreme view or another. As physicians, we have the opportunity and the responsibility to support our patients in the pursuit of health, without shame or judgment. Maybe that’s a New Year’s resolution worth committing to.
Arghavan Salles, MD, PhD, is a bariatric surgeon.
A version of this article first appeared on Medscape.com.
While many people were committing to their New Year’s resolutions to lose weight, in January 2020 Cosmopolitan UK magazine released covers portraying 11 women of different shapes and sizes, with the headline, “This is healthy!” Each version of the cover features one or more of the 11 women wearing athletic gear and makeup, some of whom are caught mid-action – boxing, doing yoga, or simply rejoicing in being who they are. Seeing these, I was reminded of a patient I cared for as an intern.
Janet Spears (not her real name) was thin. Standing barely 5 feet 3 inches, she weighed 110 pounds. For those out there who think of size in terms of body mass index (BMI), it was about 20 kg/m2, solidly in the “normal” category. At the age of 62, despite this healthy BMI, she had so much plaque in her arteries that she needed surgery to improve blood flow to her foot.
Admittedly, whenever I had read about people with high cholesterol, type 2 diabetes, or atherosclerosis, I pictured bigger people. But when I met Ms. Spears, I realized that one’s health cannot necessarily be inferred from physical appearance.
As a bariatric surgeon board certified in obesity medicine, I’ve probably spent more time thinking and learning about obesity than most people – and yet I still didn’t know what to make of the Cosmopolitan covers.
I saw the reaction on Twitter before I saw the magazines themselves, and I quickly observed a number of people decrying the covers, suggesting that they promote obesity:
Multiple people suggested that this was inappropriate, especially in the context of the COVID-19 pandemic and the fact that people with obesity are at risk for worse outcomes, compared with those without obesity. (As an aside, these comments suggest that people did not read the associated article, which is about fitness and body image more than it is about obesity.)
Does size reflect health?
Putting the pandemic aside for a moment, the question the magazine covers raise is whether physical appearance reflects health. That’s what got me thinking about Ms. Spears, who, though appearing healthy, was sick enough that she needed to have major surgery. This whole conversation hinges, of course, on one’s definition of health.
A common knee-jerk response, especially from physicians, would be to say that obesity is by definition unhealthy. Some researchers have suggested though that a segment of people with obesity fall into a category called metabolically healthy obesity, which is typically characterized by a limited set of data such as cholesterol, blood sugar, and blood pressure. Indeed, some people with obesity have normal values in those categories.
Being metabolically healthy, however, does not preclude other medical problems associated with obesity, including joint pain, cancer, and mood disorders, among other issues. So even those who have metabolically healthy obesity are not necessarily immune to the many other obesity-related conditions.
What about body positivity?
As I delved further into the conversation about these covers, I saw people embracing the idea of promoting different-sized bodies. With almost two thirds of the U.S. population having overweight or obesity, one might argue that it’s high time magazine covers and the media reflect the reality in our hometowns. Unrealistic images in the media are associated with negative self-image and disordered eating, so perhaps embracing the shapes of real people may help us all have healthier attitudes toward our bodies.
That said, this idea can be taken too far. The Health at Every Size movement, which some might consider to be the ultimate body-positivity movement, espouses the idea that size and health are completely unrelated. That crosses a line between what we know to be true – that, at a population level, higher weight is associated with more medical problems – and fake news.
Another idea to consider is fitness, as opposed to health. Fitness can be defined multiple ways, but if we consider it to be measured exercise capacity, those who are more fit have a longer life expectancy than those with lower fitness levels at a given BMI. While some feel that the Cosmopolitan covers promote obesity and are therefore irresponsible, it’s at least as likely that highlighting people with obesity being active may inspire others with obesity to do the same.
Now let’s bring the pandemic back into the picture. As much as we all wish that it was over, with uncontrolled spread in every state and record numbers of people dying, COVID-19 is still very much a part of our reality. Having obesity increases the risk of having a severe case of COVID-19 if infected. Patients with obesity are also more likely than those without obesity to be hospitalized, require intensive care, and die with COVID-19.
Guiding the conversation
Pandemic or not, the truth is that obesity is related to multiple medical problems. That does not mean that every person with obesity has medical problems. The musician Lizzo, for example, is someone with obesity who considers herself to be healthy. She posts images and videos of working out and shares her personal fitness routine with her millions of fans. As a physician, I worry about the medical conditions – metabolic or otherwise – that someone like her may develop. But I love how she embraces who she is while striving to be healthier.
Most of the critical comments I have seen about the Cosmopolitan covers have, at best, bordered on fat shaming; others are solidly in that category. And the vitriol aimed at the larger models is despicable. It seems that conversations about obesity often vacillate from one extreme (fat shaming) to the other (extreme body positivity).
Although it may not sell magazines, I would love to see more nuanced, fact-based discussions, both in the media and in our clinics. We can start by acknowledging the fact that people of different sizes can be healthy. The truth is that we can’t tell very much about a person’s health from their outward appearance, and we should probably stop trying to make such inferences.
Assessment of health is most accurately judged by each person with their medical team, not by observers who use media images as part of their own propaganda machine, pushing one extreme view or another. As physicians, we have the opportunity and the responsibility to support our patients in the pursuit of health, without shame or judgment. Maybe that’s a New Year’s resolution worth committing to.
Arghavan Salles, MD, PhD, is a bariatric surgeon.
A version of this article first appeared on Medscape.com.
Menopause, not aging, may influence brain volume
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
Postmenopausal women not only have larger brain volume than women who are premenopausal, but they also experience larger reductions in brain volume over time, reported Ananthan Ambikairajah of the Centre for Research on Ageing, Health and Wellbeing, Australian National University, Canberra, and associates. Their report was published in Menopause.
In this large population-based cohort of 5,072 women aged 37-73 years, the goal of the study was to look at links between brain volume and measures of menstruation history, such as menopausal status, age at menopause, age at menarche, and the duration of a woman’s reproductive stage, but to do so within the context of how it relates to dementia prevalence. Citing a study in The Lancet Neurology, the authors noted that the age-standardized prevalence for dementia is 17% higher in women than in men, and they speculated that it may be important to look beyond age for answers.
What about menstrual history and Alzheimer’s disease?
According to the Framingham Study in Neurology, the remaining lifetime risk of Alzheimer’s disease (AD) is nearly double for a 65-year-old woman (12%) compared with a 65-year-old man (6.3%), leading Mr. Ambikairajah and associates to conclude that “menstruation history may also be particularly relevant, given that it is unique to female aging.” They further speculated, citing several related studies, that because AD pathology is initiated decades prior to the onset of clinical signs, menstruation history and its effects on brain health may, in fact, be reflected in brain volume.
Postmenopausal women had 0.82% and 1.33% larger total brain and hippocampal volume, respectively, compared with premenopausal women. Postmenopausal women had a 23% greater decrease in total brain volume but not in hippocampal volume over time, compared with premenopausal women.
As Braak and Braak illustrated in Acta Neuropathologica, chronic inflammation has been linked to brain shrinkage “consistent with the pattern of results in the present study,” Mr. Ambikairajah and colleagues noted, adding that longitudinal neuroimaging/biomarker studies are needed to explore this further.
What made this study unique was its ability to match pre- and postmenopausal women for age, a critically important attribute “given that aging and menopause both progress concurrently, which can make it difficult to determine the individual contribution of each for measures of brain health,” the authors explained.
In an interview, Constance Bohon, MD, an ob.gyn. in private practice and assistant clinical professor, George Washington University, Washington, observed: “The conclusion [in this study] is that an early age of menarche, delayed age of menopause and increased duration of the reproductive stage is negatively associated with brain volume.”
What of the neuroprotective effects of endogenous estrogen?
“Their findings are not consistent with a neuroprotective effect of endogenous estrogen exposure on brain volume,” she noted, adding that the study “did not assess the effect of exogenous estrogen on brain volume. Neither was the effect of exogenous or endogenous estrogen on cerebral blood flow assessed. In a study published in Obstetrics & Gynecology, the conclusion was that oophorectomy before the age of natural menopause is associated with a decrease in cognitive impairment and dementia. There was no assessment of brain volume or cerebral blood flow. Likewise in a report published in Neurobiology of Aging, Maki P and Resnick S M. concluded that estrogen helps maintain hippocampal and prefrontal function as women age,” observed Dr. Bohon, noting that the study did not assess brain volume.
“It is unclear whether the most predictive assessment for worsening cognition and dementia is the finding of decreased total brain volume, decreased hippocampal volume, or decreased cerebral blood flow. The effect of both endogenous and exogenous estrogen on the risk for dementia needs further evaluation,” she cautioned.
Mr. Ambikairajah cited one financial disclosure; the remaining contributors had no relevant disclosures.
FROM MENOPAUSE
New COPD mortality risk model includes imaging-derived variables
All-cause mortality in patients with COPD over 10 years of follow-up was accurately predicted by a newly developed model based on a point system incorporating imaging-derived variables.
Identifying risk factors is important to develop treatments and preventive strategies, but the role of imaging variables in COPD mortality among smokers has not been well studied, wrote investigator Matthew Strand, PhD, of National Jewish Health in Denver, and colleagues.
An established risk model is the body mass index–airflow Obstruction-Dyspnea-Exercise capacity (BODE) index, developed to predict mortality in COPD patients over a 4-year period. The investigators noted that while models such as BODE provide useful information about predictors of mortality in COPD, they were developed using participants in the Global initiative for obstructive Lung Disease (GOLD) spirometry grades 1-4, and have been largely constructed without quantitative computed tomography (CT) imaging variables until recently.
“The BODE index was created as a simple point scoring system to predict risk of all-cause mortality within 4 years, and is based on FEV1 [forced expiratory volume at 1 second], [6-minute walk test], dyspnea and BMI, a subset of predictors we considered in our model,” the investigators noted. The new model includes data from pulmonary function tests and volumetric CT scans.
In a study published in Chronic Obstructive Pulmonary Diseases, the researchers identified 9,074 current and past smokers in the COPD Genetic Epidemiology study (COPDGene) for whom complete data were available. They developed a point system to determine mortality risk in current and former smokers after controlling for multiple risk factors. The average age of the study population was 60 years. All participants were current or former smokers with a smoking history of at least 10 pack-years.
Assessments of the study participants included a medical history, pre- and post-bronchodilator spirometry, a 6-minute walk distance test, and inspiratory and expiratory CT scans. The researchers analyzed mortality risk in the context of Global Initiative for Obstructive Lung Disease (GOLD) classifications of patients in the sample.
Overall, the average 10-year mortality risk was 18% for women and 25% for men. Performance on the 6-minute walk test (distances less than 500 feet), FEV1 (less than 20), and older age (80 years and older) were the strongest predictors of mortality.
The model showed strong predictive accuracy, with an area under the receiver operating characteristic curve averaging 0.797 that was validated in an external cohort, the researchers said.
The study findings were limited by the observational design that does not allow for estimating the causal effects of such modifiable factors as smoking cessation, that might impact the walking test and FEV1 values, the researchers noted. In addition, the model did not allow for testing the effects of smoking vs. not smoking.
However, the model developed in the study “will allow physicians and patients to better understand factors affecting risk of an adverse event, some of which may be modifiable,” the researchers said. “The risk estimates can be used to target groups of individuals for future clinical trials, including those not currently classified as having COPD based on GOLD criteria,” they said.
The study was supported by the National Heart, Lung, and Blood Institute and by the COPD Foundation through contributions to an industry advisory committee including AstraZeneca, Boehringer-Ingelheim, Genentech, GlaxoSmithKline, Novartis, Pfizer, Siemens, and Sunovion.
All-cause mortality in patients with COPD over 10 years of follow-up was accurately predicted by a newly developed model based on a point system incorporating imaging-derived variables.
Identifying risk factors is important to develop treatments and preventive strategies, but the role of imaging variables in COPD mortality among smokers has not been well studied, wrote investigator Matthew Strand, PhD, of National Jewish Health in Denver, and colleagues.
An established risk model is the body mass index–airflow Obstruction-Dyspnea-Exercise capacity (BODE) index, developed to predict mortality in COPD patients over a 4-year period. The investigators noted that while models such as BODE provide useful information about predictors of mortality in COPD, they were developed using participants in the Global initiative for obstructive Lung Disease (GOLD) spirometry grades 1-4, and have been largely constructed without quantitative computed tomography (CT) imaging variables until recently.
“The BODE index was created as a simple point scoring system to predict risk of all-cause mortality within 4 years, and is based on FEV1 [forced expiratory volume at 1 second], [6-minute walk test], dyspnea and BMI, a subset of predictors we considered in our model,” the investigators noted. The new model includes data from pulmonary function tests and volumetric CT scans.
In a study published in Chronic Obstructive Pulmonary Diseases, the researchers identified 9,074 current and past smokers in the COPD Genetic Epidemiology study (COPDGene) for whom complete data were available. They developed a point system to determine mortality risk in current and former smokers after controlling for multiple risk factors. The average age of the study population was 60 years. All participants were current or former smokers with a smoking history of at least 10 pack-years.
Assessments of the study participants included a medical history, pre- and post-bronchodilator spirometry, a 6-minute walk distance test, and inspiratory and expiratory CT scans. The researchers analyzed mortality risk in the context of Global Initiative for Obstructive Lung Disease (GOLD) classifications of patients in the sample.
Overall, the average 10-year mortality risk was 18% for women and 25% for men. Performance on the 6-minute walk test (distances less than 500 feet), FEV1 (less than 20), and older age (80 years and older) were the strongest predictors of mortality.
The model showed strong predictive accuracy, with an area under the receiver operating characteristic curve averaging 0.797 that was validated in an external cohort, the researchers said.
The study findings were limited by the observational design that does not allow for estimating the causal effects of such modifiable factors as smoking cessation, that might impact the walking test and FEV1 values, the researchers noted. In addition, the model did not allow for testing the effects of smoking vs. not smoking.
However, the model developed in the study “will allow physicians and patients to better understand factors affecting risk of an adverse event, some of which may be modifiable,” the researchers said. “The risk estimates can be used to target groups of individuals for future clinical trials, including those not currently classified as having COPD based on GOLD criteria,” they said.
The study was supported by the National Heart, Lung, and Blood Institute and by the COPD Foundation through contributions to an industry advisory committee including AstraZeneca, Boehringer-Ingelheim, Genentech, GlaxoSmithKline, Novartis, Pfizer, Siemens, and Sunovion.
All-cause mortality in patients with COPD over 10 years of follow-up was accurately predicted by a newly developed model based on a point system incorporating imaging-derived variables.
Identifying risk factors is important to develop treatments and preventive strategies, but the role of imaging variables in COPD mortality among smokers has not been well studied, wrote investigator Matthew Strand, PhD, of National Jewish Health in Denver, and colleagues.
An established risk model is the body mass index–airflow Obstruction-Dyspnea-Exercise capacity (BODE) index, developed to predict mortality in COPD patients over a 4-year period. The investigators noted that while models such as BODE provide useful information about predictors of mortality in COPD, they were developed using participants in the Global initiative for obstructive Lung Disease (GOLD) spirometry grades 1-4, and have been largely constructed without quantitative computed tomography (CT) imaging variables until recently.
“The BODE index was created as a simple point scoring system to predict risk of all-cause mortality within 4 years, and is based on FEV1 [forced expiratory volume at 1 second], [6-minute walk test], dyspnea and BMI, a subset of predictors we considered in our model,” the investigators noted. The new model includes data from pulmonary function tests and volumetric CT scans.
In a study published in Chronic Obstructive Pulmonary Diseases, the researchers identified 9,074 current and past smokers in the COPD Genetic Epidemiology study (COPDGene) for whom complete data were available. They developed a point system to determine mortality risk in current and former smokers after controlling for multiple risk factors. The average age of the study population was 60 years. All participants were current or former smokers with a smoking history of at least 10 pack-years.
Assessments of the study participants included a medical history, pre- and post-bronchodilator spirometry, a 6-minute walk distance test, and inspiratory and expiratory CT scans. The researchers analyzed mortality risk in the context of Global Initiative for Obstructive Lung Disease (GOLD) classifications of patients in the sample.
Overall, the average 10-year mortality risk was 18% for women and 25% for men. Performance on the 6-minute walk test (distances less than 500 feet), FEV1 (less than 20), and older age (80 years and older) were the strongest predictors of mortality.
The model showed strong predictive accuracy, with an area under the receiver operating characteristic curve averaging 0.797 that was validated in an external cohort, the researchers said.
The study findings were limited by the observational design that does not allow for estimating the causal effects of such modifiable factors as smoking cessation, that might impact the walking test and FEV1 values, the researchers noted. In addition, the model did not allow for testing the effects of smoking vs. not smoking.
However, the model developed in the study “will allow physicians and patients to better understand factors affecting risk of an adverse event, some of which may be modifiable,” the researchers said. “The risk estimates can be used to target groups of individuals for future clinical trials, including those not currently classified as having COPD based on GOLD criteria,” they said.
The study was supported by the National Heart, Lung, and Blood Institute and by the COPD Foundation through contributions to an industry advisory committee including AstraZeneca, Boehringer-Ingelheim, Genentech, GlaxoSmithKline, Novartis, Pfizer, Siemens, and Sunovion.
FROM CHRONIC OBSTRUCTIVE PULMONARY DISEASES