User login
Biosimilars poised to save $54 billion over the next decade
Biosimilars could reduce overall spending on biologic products by $54 billion from 2017 to 2026, according to new research from the Rand Corp.
Given the level of uncertainty surrounding the biosimilars market, however, the range of savings could be as low at $24 billion or as high as $150 billion.
“Because of limited U.S. experience with biosimilars, the key assumptions on market share and biosimilar prices are ‘best guesses’ based on anecdotes or professional opinion,” Andrew Mulcahy, PhD, a health policy researcher at Rand, and his colleagues, wrote in a perspective report.
“Whether actual cost savings end up above or below our baseline estimate hinges in large part on whether manufacturers continue to have a business case to invest in developing and marketing biosimilars,” the authors noted, citing a number of areas, including intellectual property litigation, payment, price competition, nonprice competition from reference biologic manufacturers, naming convention, and interchangeability.
Getting over these hurdles could require legislative or regulatory solutions.
“The pervasive uncertainty in the U.S. biosimilar market – including questions as to whether the market will be sustainable and lead to cost savings, as intended – presents two choices for policymakers,” Dr. Mulcahy and his colleagues wrote. “One strategy is to let the market continue to develop under current policies,” with stability coming from experience.
The alternative could be policy levers to “help steer the U.S. biosimilar market more quickly to a sustainable, competitive state,” they continued. “For example, regulators at the FDA could experiment with new approaches to provide stronger, earlier signals through guidance documents or other mechanisms on expectations surrounding interchangeability and other topics.”
The FDA appears to be moving on the latter. In an Oct. 23 blog post, FDA Commissioner Scott Gottlieb, MD, and Leah Christl, PhD, associate director for therapeutic biologics in the office of new drugs at the FDA’s Center for Drug Evaluation and Research, outlined a number of recent tools to help biosimilar adoption. The resources provide basics such as the basic definition associated with biosimilars (i.e., what is a biosimilar and a reference product, and what it means to be interchangeable), the standards of approval that biosimilars must go through, and easily accessible information on what the FDA is using to review biosimilarity.
“Next, FDA plans to embark on additional research with health care professionals to learn more about the types of information prescribers need to properly communicate with their patients about biosimilars,” Commissioner Gottlieb and Dr. Christl wrote. “An increase in market competition, offered by a growing complement of biosimilars, may lead to meaningfully reduced costs for both patients and our health care system.”
The Centers for Medicare & Medicaid Services also plays a role in developing policy to spur biosimilar adoption, Dr. Mulcahy and his colleagues wrote. They note work being done by the Medicare Payment Advisory Commission on recommendations that could address payment for physician-administered biosimilars under Part B, as well as incentives in the Part D prescription drug program to steer patients and providers toward lower cost biosimilars when appropriate. CMS changed current payment policy for biosimilars for 2018, which may have an effect.
“Beyond FDA regulation, payment, and coverage, both government and industry could play a role in educating patients and providers about the potential cost savings from biosimilars, much like both groups have done for generic drugs,” they stated. “While our study does not address whether policy action is needed now, it is likely that the answer will become clearer over the next 1 to 3 years as the market continues to develop.”
Biosimilars could reduce overall spending on biologic products by $54 billion from 2017 to 2026, according to new research from the Rand Corp.
Given the level of uncertainty surrounding the biosimilars market, however, the range of savings could be as low at $24 billion or as high as $150 billion.
“Because of limited U.S. experience with biosimilars, the key assumptions on market share and biosimilar prices are ‘best guesses’ based on anecdotes or professional opinion,” Andrew Mulcahy, PhD, a health policy researcher at Rand, and his colleagues, wrote in a perspective report.
“Whether actual cost savings end up above or below our baseline estimate hinges in large part on whether manufacturers continue to have a business case to invest in developing and marketing biosimilars,” the authors noted, citing a number of areas, including intellectual property litigation, payment, price competition, nonprice competition from reference biologic manufacturers, naming convention, and interchangeability.
Getting over these hurdles could require legislative or regulatory solutions.
“The pervasive uncertainty in the U.S. biosimilar market – including questions as to whether the market will be sustainable and lead to cost savings, as intended – presents two choices for policymakers,” Dr. Mulcahy and his colleagues wrote. “One strategy is to let the market continue to develop under current policies,” with stability coming from experience.
The alternative could be policy levers to “help steer the U.S. biosimilar market more quickly to a sustainable, competitive state,” they continued. “For example, regulators at the FDA could experiment with new approaches to provide stronger, earlier signals through guidance documents or other mechanisms on expectations surrounding interchangeability and other topics.”
The FDA appears to be moving on the latter. In an Oct. 23 blog post, FDA Commissioner Scott Gottlieb, MD, and Leah Christl, PhD, associate director for therapeutic biologics in the office of new drugs at the FDA’s Center for Drug Evaluation and Research, outlined a number of recent tools to help biosimilar adoption. The resources provide basics such as the basic definition associated with biosimilars (i.e., what is a biosimilar and a reference product, and what it means to be interchangeable), the standards of approval that biosimilars must go through, and easily accessible information on what the FDA is using to review biosimilarity.
“Next, FDA plans to embark on additional research with health care professionals to learn more about the types of information prescribers need to properly communicate with their patients about biosimilars,” Commissioner Gottlieb and Dr. Christl wrote. “An increase in market competition, offered by a growing complement of biosimilars, may lead to meaningfully reduced costs for both patients and our health care system.”
The Centers for Medicare & Medicaid Services also plays a role in developing policy to spur biosimilar adoption, Dr. Mulcahy and his colleagues wrote. They note work being done by the Medicare Payment Advisory Commission on recommendations that could address payment for physician-administered biosimilars under Part B, as well as incentives in the Part D prescription drug program to steer patients and providers toward lower cost biosimilars when appropriate. CMS changed current payment policy for biosimilars for 2018, which may have an effect.
“Beyond FDA regulation, payment, and coverage, both government and industry could play a role in educating patients and providers about the potential cost savings from biosimilars, much like both groups have done for generic drugs,” they stated. “While our study does not address whether policy action is needed now, it is likely that the answer will become clearer over the next 1 to 3 years as the market continues to develop.”
Biosimilars could reduce overall spending on biologic products by $54 billion from 2017 to 2026, according to new research from the Rand Corp.
Given the level of uncertainty surrounding the biosimilars market, however, the range of savings could be as low at $24 billion or as high as $150 billion.
“Because of limited U.S. experience with biosimilars, the key assumptions on market share and biosimilar prices are ‘best guesses’ based on anecdotes or professional opinion,” Andrew Mulcahy, PhD, a health policy researcher at Rand, and his colleagues, wrote in a perspective report.
“Whether actual cost savings end up above or below our baseline estimate hinges in large part on whether manufacturers continue to have a business case to invest in developing and marketing biosimilars,” the authors noted, citing a number of areas, including intellectual property litigation, payment, price competition, nonprice competition from reference biologic manufacturers, naming convention, and interchangeability.
Getting over these hurdles could require legislative or regulatory solutions.
“The pervasive uncertainty in the U.S. biosimilar market – including questions as to whether the market will be sustainable and lead to cost savings, as intended – presents two choices for policymakers,” Dr. Mulcahy and his colleagues wrote. “One strategy is to let the market continue to develop under current policies,” with stability coming from experience.
The alternative could be policy levers to “help steer the U.S. biosimilar market more quickly to a sustainable, competitive state,” they continued. “For example, regulators at the FDA could experiment with new approaches to provide stronger, earlier signals through guidance documents or other mechanisms on expectations surrounding interchangeability and other topics.”
The FDA appears to be moving on the latter. In an Oct. 23 blog post, FDA Commissioner Scott Gottlieb, MD, and Leah Christl, PhD, associate director for therapeutic biologics in the office of new drugs at the FDA’s Center for Drug Evaluation and Research, outlined a number of recent tools to help biosimilar adoption. The resources provide basics such as the basic definition associated with biosimilars (i.e., what is a biosimilar and a reference product, and what it means to be interchangeable), the standards of approval that biosimilars must go through, and easily accessible information on what the FDA is using to review biosimilarity.
“Next, FDA plans to embark on additional research with health care professionals to learn more about the types of information prescribers need to properly communicate with their patients about biosimilars,” Commissioner Gottlieb and Dr. Christl wrote. “An increase in market competition, offered by a growing complement of biosimilars, may lead to meaningfully reduced costs for both patients and our health care system.”
The Centers for Medicare & Medicaid Services also plays a role in developing policy to spur biosimilar adoption, Dr. Mulcahy and his colleagues wrote. They note work being done by the Medicare Payment Advisory Commission on recommendations that could address payment for physician-administered biosimilars under Part B, as well as incentives in the Part D prescription drug program to steer patients and providers toward lower cost biosimilars when appropriate. CMS changed current payment policy for biosimilars for 2018, which may have an effect.
“Beyond FDA regulation, payment, and coverage, both government and industry could play a role in educating patients and providers about the potential cost savings from biosimilars, much like both groups have done for generic drugs,” they stated. “While our study does not address whether policy action is needed now, it is likely that the answer will become clearer over the next 1 to 3 years as the market continues to develop.”
Force Protection in the Spotlight at AMSUS Meeting
From the battlefront to the home front, the face of federal health is changing. Federal Practitioner recently talked with VADM Michael Cowan, MD, executive director of AMSUS, as he prepares for its upcoming 2017 annual meeting. The meeting will focus on the continuation of care from the DoD to VA and PHS.
"When an injury or illness is successfully treated, the responsibility of the health system to that person is not done," VADM Cowan said. "We have seen a revolution in health care, and we are celebrating that revolution. Survival is a wonderful thing, but wouldn't we be cruel if we only saved those people and were done?"
According to VADM Cowan, the meeting will be structured to have frontline and battlefield topics early in the week. Later in the week the focus will turn to providing long-term health care. The meeting will conclude by bringing in patients so that the focus remains patient centered.
In addition to keynote addresses from VA leaders like Secretary David J. Shulkin, MD, and Deputy Under Secretary for Health for Organizational Excellence Carolyn Clancy, MD, the meeting will include presentations on hurricane relief efforts, a keynote address from Surgeon General VADM Jerome M. Adams, MD, MH; and the CDC's new global rapid response team. More information on the conference can be found at amsusmeeting.org.
From the battlefront to the home front, the face of federal health is changing. Federal Practitioner recently talked with VADM Michael Cowan, MD, executive director of AMSUS, as he prepares for its upcoming 2017 annual meeting. The meeting will focus on the continuation of care from the DoD to VA and PHS.
"When an injury or illness is successfully treated, the responsibility of the health system to that person is not done," VADM Cowan said. "We have seen a revolution in health care, and we are celebrating that revolution. Survival is a wonderful thing, but wouldn't we be cruel if we only saved those people and were done?"
According to VADM Cowan, the meeting will be structured to have frontline and battlefield topics early in the week. Later in the week the focus will turn to providing long-term health care. The meeting will conclude by bringing in patients so that the focus remains patient centered.
In addition to keynote addresses from VA leaders like Secretary David J. Shulkin, MD, and Deputy Under Secretary for Health for Organizational Excellence Carolyn Clancy, MD, the meeting will include presentations on hurricane relief efforts, a keynote address from Surgeon General VADM Jerome M. Adams, MD, MH; and the CDC's new global rapid response team. More information on the conference can be found at amsusmeeting.org.
From the battlefront to the home front, the face of federal health is changing. Federal Practitioner recently talked with VADM Michael Cowan, MD, executive director of AMSUS, as he prepares for its upcoming 2017 annual meeting. The meeting will focus on the continuation of care from the DoD to VA and PHS.
"When an injury or illness is successfully treated, the responsibility of the health system to that person is not done," VADM Cowan said. "We have seen a revolution in health care, and we are celebrating that revolution. Survival is a wonderful thing, but wouldn't we be cruel if we only saved those people and were done?"
According to VADM Cowan, the meeting will be structured to have frontline and battlefield topics early in the week. Later in the week the focus will turn to providing long-term health care. The meeting will conclude by bringing in patients so that the focus remains patient centered.
In addition to keynote addresses from VA leaders like Secretary David J. Shulkin, MD, and Deputy Under Secretary for Health for Organizational Excellence Carolyn Clancy, MD, the meeting will include presentations on hurricane relief efforts, a keynote address from Surgeon General VADM Jerome M. Adams, MD, MH; and the CDC's new global rapid response team. More information on the conference can be found at amsusmeeting.org.
VIDEO: How to manage surgical pain in opioid addiction treatment
NEW ORLEANS – How do you manage surgical pain when someone is in treatment for opioid addiction? And how do you manage chronic pain?
It is possible to give patients opioids for post-op pain without increasing the risk of relapse, according to Margaret Chaplin, MD, a staff psychiatrist at Community Mental Health Affiliates in New Britain, Conn.
Dr. Chaplin generally uses buprenorphine and naloxone (Suboxone) for opioid use disorder, and she likes to keep her patients on it for surgery. That often means, however, talking with skeptical surgeons and anesthesiologists beforehand, and reminding them that buprenorphine itself has analgesic effects. Meanwhile, when her patients have chronic pain, sometimes they need help understanding that aspirin and acetaminophen help, even if they don’t give patients a warm, fuzzy feeling.
Dr. Chaplin shared those tips and more about pain management in opioid addiction in an interview at the American Psychiatric Association’s Institute on Psychiatric Services.
NEW ORLEANS – How do you manage surgical pain when someone is in treatment for opioid addiction? And how do you manage chronic pain?
It is possible to give patients opioids for post-op pain without increasing the risk of relapse, according to Margaret Chaplin, MD, a staff psychiatrist at Community Mental Health Affiliates in New Britain, Conn.
Dr. Chaplin generally uses buprenorphine and naloxone (Suboxone) for opioid use disorder, and she likes to keep her patients on it for surgery. That often means, however, talking with skeptical surgeons and anesthesiologists beforehand, and reminding them that buprenorphine itself has analgesic effects. Meanwhile, when her patients have chronic pain, sometimes they need help understanding that aspirin and acetaminophen help, even if they don’t give patients a warm, fuzzy feeling.
Dr. Chaplin shared those tips and more about pain management in opioid addiction in an interview at the American Psychiatric Association’s Institute on Psychiatric Services.
NEW ORLEANS – How do you manage surgical pain when someone is in treatment for opioid addiction? And how do you manage chronic pain?
It is possible to give patients opioids for post-op pain without increasing the risk of relapse, according to Margaret Chaplin, MD, a staff psychiatrist at Community Mental Health Affiliates in New Britain, Conn.
Dr. Chaplin generally uses buprenorphine and naloxone (Suboxone) for opioid use disorder, and she likes to keep her patients on it for surgery. That often means, however, talking with skeptical surgeons and anesthesiologists beforehand, and reminding them that buprenorphine itself has analgesic effects. Meanwhile, when her patients have chronic pain, sometimes they need help understanding that aspirin and acetaminophen help, even if they don’t give patients a warm, fuzzy feeling.
Dr. Chaplin shared those tips and more about pain management in opioid addiction in an interview at the American Psychiatric Association’s Institute on Psychiatric Services.
AT IPS 2017
Multiple Comorbidities: Does Age Matter?
The stereotype of someone with multiple comorbid conditions (MCCs) is an older, often overweight person. But according to an analysis of data from > 200,000 respondents in the 2015 Behavioral Risk Factor Surveillance System (BRFSS), people aged < 65 years are more likely to report MCCs, such as asthma, cognitive impairment, depression, smoking, obesity, disability, and lower quality of life (QOL). In fact, research indicates that most people with MCCs are of working age.
The study compared 2 groups of adults with MCCs: those aged > 65 years with those aged < 65 years. The researchers found significant differences by age group in 18 measures, suggesting that adults aged < 65 years were “worse off” compared with those aged > 65 years. Results were similar regardless of whether diabetes, depression, hypertension, and high cholesterol were included.
Other results from BRFSS data have shown that people with ≥ 3 chronic conditions are more likely to report poor QOL than those with fewer conditions. But that analysis did not compare age groups, the researchers say. In this study, most uninsured adults were aged < 65 years, and the younger adults with MCCs were more likely to report a cost barrier to health care. They also were less likely to report a recent routine check-up. According to the study. these are important findings because managing and treating existing chronic conditions and diagnosing incident ones are key to preventing worse health in the future. The younger cohort had lower levels of well-recognized risk factors—diabetes, hypertension, high cholesterol—than the older, but their levels were still high enough to be concerning.
A “somewhat unexpected” finding was that the younger group had a high rate of cognitive impairment. That could be the result of lack of sleep, side effects of medication, or use of illicit drugs, the researcher notes, and may not be associated with future risk of dementia. Whatever the cause, though, the researcher adds that being cognitively impaired can affect someone’s ability to manage other chronic conditions.
The stereotype of someone with multiple comorbid conditions (MCCs) is an older, often overweight person. But according to an analysis of data from > 200,000 respondents in the 2015 Behavioral Risk Factor Surveillance System (BRFSS), people aged < 65 years are more likely to report MCCs, such as asthma, cognitive impairment, depression, smoking, obesity, disability, and lower quality of life (QOL). In fact, research indicates that most people with MCCs are of working age.
The study compared 2 groups of adults with MCCs: those aged > 65 years with those aged < 65 years. The researchers found significant differences by age group in 18 measures, suggesting that adults aged < 65 years were “worse off” compared with those aged > 65 years. Results were similar regardless of whether diabetes, depression, hypertension, and high cholesterol were included.
Other results from BRFSS data have shown that people with ≥ 3 chronic conditions are more likely to report poor QOL than those with fewer conditions. But that analysis did not compare age groups, the researchers say. In this study, most uninsured adults were aged < 65 years, and the younger adults with MCCs were more likely to report a cost barrier to health care. They also were less likely to report a recent routine check-up. According to the study. these are important findings because managing and treating existing chronic conditions and diagnosing incident ones are key to preventing worse health in the future. The younger cohort had lower levels of well-recognized risk factors—diabetes, hypertension, high cholesterol—than the older, but their levels were still high enough to be concerning.
A “somewhat unexpected” finding was that the younger group had a high rate of cognitive impairment. That could be the result of lack of sleep, side effects of medication, or use of illicit drugs, the researcher notes, and may not be associated with future risk of dementia. Whatever the cause, though, the researcher adds that being cognitively impaired can affect someone’s ability to manage other chronic conditions.
The stereotype of someone with multiple comorbid conditions (MCCs) is an older, often overweight person. But according to an analysis of data from > 200,000 respondents in the 2015 Behavioral Risk Factor Surveillance System (BRFSS), people aged < 65 years are more likely to report MCCs, such as asthma, cognitive impairment, depression, smoking, obesity, disability, and lower quality of life (QOL). In fact, research indicates that most people with MCCs are of working age.
The study compared 2 groups of adults with MCCs: those aged > 65 years with those aged < 65 years. The researchers found significant differences by age group in 18 measures, suggesting that adults aged < 65 years were “worse off” compared with those aged > 65 years. Results were similar regardless of whether diabetes, depression, hypertension, and high cholesterol were included.
Other results from BRFSS data have shown that people with ≥ 3 chronic conditions are more likely to report poor QOL than those with fewer conditions. But that analysis did not compare age groups, the researchers say. In this study, most uninsured adults were aged < 65 years, and the younger adults with MCCs were more likely to report a cost barrier to health care. They also were less likely to report a recent routine check-up. According to the study. these are important findings because managing and treating existing chronic conditions and diagnosing incident ones are key to preventing worse health in the future. The younger cohort had lower levels of well-recognized risk factors—diabetes, hypertension, high cholesterol—than the older, but their levels were still high enough to be concerning.
A “somewhat unexpected” finding was that the younger group had a high rate of cognitive impairment. That could be the result of lack of sleep, side effects of medication, or use of illicit drugs, the researcher notes, and may not be associated with future risk of dementia. Whatever the cause, though, the researcher adds that being cognitively impaired can affect someone’s ability to manage other chronic conditions.
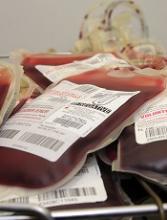
Results support early blood transfusion
Early blood transfusion is associated with improved survival among people with severe trauma sustained during combat, according to research published in JAMA.
Researchers studied medically evacuated US military personnel fighting in Afghanistan and found that patients who received blood products prior to hospitalization or within 15 minutes of medical evacuation were more likely to be alive at 24 hours and 30 days, when compared to patients who had delayed transfusions or did not receive transfusions.
Stacy A. Shackelford, MD, of Ft. Sam Houston in San Antonio, Texas, and her colleagues conducted this study to examine the association of prehospital transfusion and time to initial transfusion with injury survival.
The study included US military combat casualties in Afghanistan between April 1, 2012, and August 7, 2015. Eligible patients were rescued alive by medical evacuation from the point of injury with either:
- A traumatic limb amputation at or above the knee or elbow
- Shock, defined as a systolic blood pressure of less than 90 mm Hg or a heart rate greater than 120 beats per minute.
The study included 502, mostly male (98%), patients with a median age of 25 (range, 22 to 29). There were 55 patients who received prehospital transfusions (of red blood cells and/or plasma) and 447 who did not.
The rate of death within 24 hours of medical evacuation was 5% (3/55) among prehospital transfusion recipients and 19% (85/447) among nonrecipients (P=0.01). The rate of death by day 30 was 11% (6/55) and 23% (102/447), respectively (P=0.04).
The researchers also matched nonrecipients and recipients of prehospital transfusion by mechanism of injury, prehospital shock, severity of limb amputation, head injury, and torso hemorrhage. And the team adjusted their analyses for patient age, injury year, transport team, tourniquet use, and time to medical evacuation.
There were 386 matched patients with complete covariate data. Among these patients, the association of survival with prehospital transfusion remained significant at 24 hours and 30 days.
At 24 hours, the adjusted hazard ratio (aHR) for mortality was 0.26 (P=0.02). There were 3 deaths among the 54 prehospital transfusion recipients and 67 deaths among the 332 matched nonrecipients.
At 30 days, the aHR was 0.39 (P=0.03). There were 6 deaths among the 54 prehospital transfusion recipients and 76 deaths among the 332 matched nonrecipients.
The researchers also found that shorter time to initial transfusion, whether it occurred prior to or during hospitalization, was associated with reduced 24-hour mortality.
Transfusions occurring within 15 minutes of medical evacuation (a median of 36 minutes after injury) were associated with reduced mortality at 24 hours.
The aHR was 0.17 (P=0.02). There were 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation and 68 deaths among the 324 patients who received delayed transfusions or did not receive transfusions.
When the researchers eliminated patients who did not receive transfusions, the aHR was 0.23 (P=0.04). There were 47 deaths among the 303 patients who received delayed transfusions (compared to 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation). ![]()
Early blood transfusion is associated with improved survival among people with severe trauma sustained during combat, according to research published in JAMA.
Researchers studied medically evacuated US military personnel fighting in Afghanistan and found that patients who received blood products prior to hospitalization or within 15 minutes of medical evacuation were more likely to be alive at 24 hours and 30 days, when compared to patients who had delayed transfusions or did not receive transfusions.
Stacy A. Shackelford, MD, of Ft. Sam Houston in San Antonio, Texas, and her colleagues conducted this study to examine the association of prehospital transfusion and time to initial transfusion with injury survival.
The study included US military combat casualties in Afghanistan between April 1, 2012, and August 7, 2015. Eligible patients were rescued alive by medical evacuation from the point of injury with either:
- A traumatic limb amputation at or above the knee or elbow
- Shock, defined as a systolic blood pressure of less than 90 mm Hg or a heart rate greater than 120 beats per minute.
The study included 502, mostly male (98%), patients with a median age of 25 (range, 22 to 29). There were 55 patients who received prehospital transfusions (of red blood cells and/or plasma) and 447 who did not.
The rate of death within 24 hours of medical evacuation was 5% (3/55) among prehospital transfusion recipients and 19% (85/447) among nonrecipients (P=0.01). The rate of death by day 30 was 11% (6/55) and 23% (102/447), respectively (P=0.04).
The researchers also matched nonrecipients and recipients of prehospital transfusion by mechanism of injury, prehospital shock, severity of limb amputation, head injury, and torso hemorrhage. And the team adjusted their analyses for patient age, injury year, transport team, tourniquet use, and time to medical evacuation.
There were 386 matched patients with complete covariate data. Among these patients, the association of survival with prehospital transfusion remained significant at 24 hours and 30 days.
At 24 hours, the adjusted hazard ratio (aHR) for mortality was 0.26 (P=0.02). There were 3 deaths among the 54 prehospital transfusion recipients and 67 deaths among the 332 matched nonrecipients.
At 30 days, the aHR was 0.39 (P=0.03). There were 6 deaths among the 54 prehospital transfusion recipients and 76 deaths among the 332 matched nonrecipients.
The researchers also found that shorter time to initial transfusion, whether it occurred prior to or during hospitalization, was associated with reduced 24-hour mortality.
Transfusions occurring within 15 minutes of medical evacuation (a median of 36 minutes after injury) were associated with reduced mortality at 24 hours.
The aHR was 0.17 (P=0.02). There were 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation and 68 deaths among the 324 patients who received delayed transfusions or did not receive transfusions.
When the researchers eliminated patients who did not receive transfusions, the aHR was 0.23 (P=0.04). There were 47 deaths among the 303 patients who received delayed transfusions (compared to 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation). ![]()
Early blood transfusion is associated with improved survival among people with severe trauma sustained during combat, according to research published in JAMA.
Researchers studied medically evacuated US military personnel fighting in Afghanistan and found that patients who received blood products prior to hospitalization or within 15 minutes of medical evacuation were more likely to be alive at 24 hours and 30 days, when compared to patients who had delayed transfusions or did not receive transfusions.
Stacy A. Shackelford, MD, of Ft. Sam Houston in San Antonio, Texas, and her colleagues conducted this study to examine the association of prehospital transfusion and time to initial transfusion with injury survival.
The study included US military combat casualties in Afghanistan between April 1, 2012, and August 7, 2015. Eligible patients were rescued alive by medical evacuation from the point of injury with either:
- A traumatic limb amputation at or above the knee or elbow
- Shock, defined as a systolic blood pressure of less than 90 mm Hg or a heart rate greater than 120 beats per minute.
The study included 502, mostly male (98%), patients with a median age of 25 (range, 22 to 29). There were 55 patients who received prehospital transfusions (of red blood cells and/or plasma) and 447 who did not.
The rate of death within 24 hours of medical evacuation was 5% (3/55) among prehospital transfusion recipients and 19% (85/447) among nonrecipients (P=0.01). The rate of death by day 30 was 11% (6/55) and 23% (102/447), respectively (P=0.04).
The researchers also matched nonrecipients and recipients of prehospital transfusion by mechanism of injury, prehospital shock, severity of limb amputation, head injury, and torso hemorrhage. And the team adjusted their analyses for patient age, injury year, transport team, tourniquet use, and time to medical evacuation.
There were 386 matched patients with complete covariate data. Among these patients, the association of survival with prehospital transfusion remained significant at 24 hours and 30 days.
At 24 hours, the adjusted hazard ratio (aHR) for mortality was 0.26 (P=0.02). There were 3 deaths among the 54 prehospital transfusion recipients and 67 deaths among the 332 matched nonrecipients.
At 30 days, the aHR was 0.39 (P=0.03). There were 6 deaths among the 54 prehospital transfusion recipients and 76 deaths among the 332 matched nonrecipients.
The researchers also found that shorter time to initial transfusion, whether it occurred prior to or during hospitalization, was associated with reduced 24-hour mortality.
Transfusions occurring within 15 minutes of medical evacuation (a median of 36 minutes after injury) were associated with reduced mortality at 24 hours.
The aHR was 0.17 (P=0.02). There were 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation and 68 deaths among the 324 patients who received delayed transfusions or did not receive transfusions.
When the researchers eliminated patients who did not receive transfusions, the aHR was 0.23 (P=0.04). There were 47 deaths among the 303 patients who received delayed transfusions (compared to 2 deaths among the 62 patients who received a transfusion within 15 minutes of medical evacuation). ![]()
CCSs more likely to stay at jobs to keep health insurance
Survey results suggest childhood cancer survivors (CCSs) in the US are more likely than individuals without a history of cancer to experience “job lock,” or staying at a job to keep work-related health insurance.
CCSs are also more likely than individuals without a history of cancer to report problems paying medical bills and being denied health insurance.
Anne Kirchhoff, PhD, of Huntsman Cancer Institute at the University of Utah in Salt Lake City, and her colleagues reported these findings in JAMA Oncology.
The researchers analyzed 394 CCSs from pediatric oncology institutions across the US, along with 128 of their siblings who had no history of cancer. All study participants worked 35 hours or more per week.
The most common cancer diagnosis among CCSs was leukemia (35.4%), followed by Hodgkin lymphoma (14.9%). Most patients had undergone chemotherapy (77.2%), radiotherapy (63.9%), and surgery (81.1%).
Overall, sociodemographic and clinical characteristics were similar between CCSs and siblings. However, CCSs were more likely than siblings to have severe, disabling, or life-threatening chronic conditions—33.9% and 17.7%, respectively (P<0.001).
Most CCSs (88.0%) and siblings (88.5%) had employer-sponsored health insurance. Three percent of siblings and 5.3% of CCSs had individual insurance; 1.9% and 2.3%, respectively, had public insurance; and 6.7% and 4.4%, respectively, were uninsured.
Results
CCSs were more likely than siblings to report:
- Job lock—23.2% and 16.9%, respectively (P=0.16)
- Problems paying medical bills—20.1% and 12.9%, respectively (P=0.09)
- Denial of health insurance—13.4% and 1.8%, respectively (P<0.001).
In a multivariable analysis, insurance denial remained significantly more common among CCSs than siblings (relative risk [RR]=7.38).
In another multivariable analysis, 38% of CCSs with a previous insurance denial reported job lock, compared with 20% of those who never experienced insurance denial (RR=1.60). And 44% of CCSs who reported problems paying their medical bills also reported job lock, compared to 16% of those who had no problems paying medical bills (RR=2.43).
The researchers also found that female CCSs (RR=1.70) and CCSs with severe, disabling, or life-threatening chronic conditions (RR=1.72) were more likely to report job lock.
“This information gives us a feel for high-risk groups of survivors who may need more information about insurance,” Dr Kirchhoff said. “Many people experience a gap in education and literacy around insurance, and it’s important for people to understand their options—even those who are employed and consistently had access to insurance through work. We want to know what their concerns are so we can help patients and survivors. Getting healthcare should not be a worry for cancer survivors.”
“Survivors have been through a lot when they were younger and understand the importance of making sure they can get healthcare when they need it. I think a lot of them also saw what their parents and families went through in terms of the financial stress and burden of dealing with a health crisis. So they’re just primed to understand the importance of health insurance.”
Dr Kirchhoff noted that this study was conducted as the Affordable Care Act was rolling out. Therefore, she would like to do a follow-up study to see if the insurance exchanges and Medicaid expansion lessened job-related insurance worries. ![]()
Survey results suggest childhood cancer survivors (CCSs) in the US are more likely than individuals without a history of cancer to experience “job lock,” or staying at a job to keep work-related health insurance.
CCSs are also more likely than individuals without a history of cancer to report problems paying medical bills and being denied health insurance.
Anne Kirchhoff, PhD, of Huntsman Cancer Institute at the University of Utah in Salt Lake City, and her colleagues reported these findings in JAMA Oncology.
The researchers analyzed 394 CCSs from pediatric oncology institutions across the US, along with 128 of their siblings who had no history of cancer. All study participants worked 35 hours or more per week.
The most common cancer diagnosis among CCSs was leukemia (35.4%), followed by Hodgkin lymphoma (14.9%). Most patients had undergone chemotherapy (77.2%), radiotherapy (63.9%), and surgery (81.1%).
Overall, sociodemographic and clinical characteristics were similar between CCSs and siblings. However, CCSs were more likely than siblings to have severe, disabling, or life-threatening chronic conditions—33.9% and 17.7%, respectively (P<0.001).
Most CCSs (88.0%) and siblings (88.5%) had employer-sponsored health insurance. Three percent of siblings and 5.3% of CCSs had individual insurance; 1.9% and 2.3%, respectively, had public insurance; and 6.7% and 4.4%, respectively, were uninsured.
Results
CCSs were more likely than siblings to report:
- Job lock—23.2% and 16.9%, respectively (P=0.16)
- Problems paying medical bills—20.1% and 12.9%, respectively (P=0.09)
- Denial of health insurance—13.4% and 1.8%, respectively (P<0.001).
In a multivariable analysis, insurance denial remained significantly more common among CCSs than siblings (relative risk [RR]=7.38).
In another multivariable analysis, 38% of CCSs with a previous insurance denial reported job lock, compared with 20% of those who never experienced insurance denial (RR=1.60). And 44% of CCSs who reported problems paying their medical bills also reported job lock, compared to 16% of those who had no problems paying medical bills (RR=2.43).
The researchers also found that female CCSs (RR=1.70) and CCSs with severe, disabling, or life-threatening chronic conditions (RR=1.72) were more likely to report job lock.
“This information gives us a feel for high-risk groups of survivors who may need more information about insurance,” Dr Kirchhoff said. “Many people experience a gap in education and literacy around insurance, and it’s important for people to understand their options—even those who are employed and consistently had access to insurance through work. We want to know what their concerns are so we can help patients and survivors. Getting healthcare should not be a worry for cancer survivors.”
“Survivors have been through a lot when they were younger and understand the importance of making sure they can get healthcare when they need it. I think a lot of them also saw what their parents and families went through in terms of the financial stress and burden of dealing with a health crisis. So they’re just primed to understand the importance of health insurance.”
Dr Kirchhoff noted that this study was conducted as the Affordable Care Act was rolling out. Therefore, she would like to do a follow-up study to see if the insurance exchanges and Medicaid expansion lessened job-related insurance worries. ![]()
Survey results suggest childhood cancer survivors (CCSs) in the US are more likely than individuals without a history of cancer to experience “job lock,” or staying at a job to keep work-related health insurance.
CCSs are also more likely than individuals without a history of cancer to report problems paying medical bills and being denied health insurance.
Anne Kirchhoff, PhD, of Huntsman Cancer Institute at the University of Utah in Salt Lake City, and her colleagues reported these findings in JAMA Oncology.
The researchers analyzed 394 CCSs from pediatric oncology institutions across the US, along with 128 of their siblings who had no history of cancer. All study participants worked 35 hours or more per week.
The most common cancer diagnosis among CCSs was leukemia (35.4%), followed by Hodgkin lymphoma (14.9%). Most patients had undergone chemotherapy (77.2%), radiotherapy (63.9%), and surgery (81.1%).
Overall, sociodemographic and clinical characteristics were similar between CCSs and siblings. However, CCSs were more likely than siblings to have severe, disabling, or life-threatening chronic conditions—33.9% and 17.7%, respectively (P<0.001).
Most CCSs (88.0%) and siblings (88.5%) had employer-sponsored health insurance. Three percent of siblings and 5.3% of CCSs had individual insurance; 1.9% and 2.3%, respectively, had public insurance; and 6.7% and 4.4%, respectively, were uninsured.
Results
CCSs were more likely than siblings to report:
- Job lock—23.2% and 16.9%, respectively (P=0.16)
- Problems paying medical bills—20.1% and 12.9%, respectively (P=0.09)
- Denial of health insurance—13.4% and 1.8%, respectively (P<0.001).
In a multivariable analysis, insurance denial remained significantly more common among CCSs than siblings (relative risk [RR]=7.38).
In another multivariable analysis, 38% of CCSs with a previous insurance denial reported job lock, compared with 20% of those who never experienced insurance denial (RR=1.60). And 44% of CCSs who reported problems paying their medical bills also reported job lock, compared to 16% of those who had no problems paying medical bills (RR=2.43).
The researchers also found that female CCSs (RR=1.70) and CCSs with severe, disabling, or life-threatening chronic conditions (RR=1.72) were more likely to report job lock.
“This information gives us a feel for high-risk groups of survivors who may need more information about insurance,” Dr Kirchhoff said. “Many people experience a gap in education and literacy around insurance, and it’s important for people to understand their options—even those who are employed and consistently had access to insurance through work. We want to know what their concerns are so we can help patients and survivors. Getting healthcare should not be a worry for cancer survivors.”
“Survivors have been through a lot when they were younger and understand the importance of making sure they can get healthcare when they need it. I think a lot of them also saw what their parents and families went through in terms of the financial stress and burden of dealing with a health crisis. So they’re just primed to understand the importance of health insurance.”
Dr Kirchhoff noted that this study was conducted as the Affordable Care Act was rolling out. Therefore, she would like to do a follow-up study to see if the insurance exchanges and Medicaid expansion lessened job-related insurance worries. ![]()
Drug receives breakthrough designation for DLBCL
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to MOR208, an Fc-enhanced monoclonal antibody directed against CD19.
The designation is for MOR208 to be used in combination with lenalidomide to treat adults with relapsed or refractory diffuse large B-cell lymphoma (DLBCL) who are not eligible for high-dose chemotherapy and autologous stem cell transplant.
The FDA’s breakthrough designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
The designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
The breakthrough designation for MOR208 is based on preliminary data from the ongoing phase 2 L-MIND study (NCT02399085).
In this trial, researchers are evaluating MOR208 in combination with lenalidomide in patients with relapsed/refractory DLBCL who are ineligible for high-dose chemotherapy and autologous stem cell transplant.
Preliminary data from this trial were presented at ASCO 2017.* Of the 44 patients enrolled at the data cut-off, 34 were evaluable for efficacy.
The objective response rate was 56% (19/34), and the complete response rate was 32% (11/34). Sixteen of the 19 responders were still on study at the data cut-off point.
The most frequent adverse events of grade 3 or higher were neutropenia (32%), thrombocytopenia (9%), and leukopenia (9%). As of the data cut-off, 27% of patients required a reduction of the lenalidomide dose due to side effects.
“We expect to report further data from our ongoing phase 2 L-MIND trial with MOR208 plus lenalidomide at this year’s American Society of Hematology conference in December,” said Malte Peters, chief development officer of MorphoSys AG, the company developing MOR208.
“In addition, we are currently evaluating MOR208 in combination with bendamustine in our phase 3 B-MIND trial.”
The B-MIND study is designed to compare MOR208 plus bendamustine to rituximab plus bendamustine in patients with relapsed/refractory DLBCL who are not eligible for high-dose chemotherapy and autologous stem cell transplant. ![]()
*Data in the abstract differ from the data presented at the meeting.
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to MOR208, an Fc-enhanced monoclonal antibody directed against CD19.
The designation is for MOR208 to be used in combination with lenalidomide to treat adults with relapsed or refractory diffuse large B-cell lymphoma (DLBCL) who are not eligible for high-dose chemotherapy and autologous stem cell transplant.
The FDA’s breakthrough designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
The designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
The breakthrough designation for MOR208 is based on preliminary data from the ongoing phase 2 L-MIND study (NCT02399085).
In this trial, researchers are evaluating MOR208 in combination with lenalidomide in patients with relapsed/refractory DLBCL who are ineligible for high-dose chemotherapy and autologous stem cell transplant.
Preliminary data from this trial were presented at ASCO 2017.* Of the 44 patients enrolled at the data cut-off, 34 were evaluable for efficacy.
The objective response rate was 56% (19/34), and the complete response rate was 32% (11/34). Sixteen of the 19 responders were still on study at the data cut-off point.
The most frequent adverse events of grade 3 or higher were neutropenia (32%), thrombocytopenia (9%), and leukopenia (9%). As of the data cut-off, 27% of patients required a reduction of the lenalidomide dose due to side effects.
“We expect to report further data from our ongoing phase 2 L-MIND trial with MOR208 plus lenalidomide at this year’s American Society of Hematology conference in December,” said Malte Peters, chief development officer of MorphoSys AG, the company developing MOR208.
“In addition, we are currently evaluating MOR208 in combination with bendamustine in our phase 3 B-MIND trial.”
The B-MIND study is designed to compare MOR208 plus bendamustine to rituximab plus bendamustine in patients with relapsed/refractory DLBCL who are not eligible for high-dose chemotherapy and autologous stem cell transplant. ![]()
*Data in the abstract differ from the data presented at the meeting.
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to MOR208, an Fc-enhanced monoclonal antibody directed against CD19.
The designation is for MOR208 to be used in combination with lenalidomide to treat adults with relapsed or refractory diffuse large B-cell lymphoma (DLBCL) who are not eligible for high-dose chemotherapy and autologous stem cell transplant.
The FDA’s breakthrough designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
The designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
The breakthrough designation for MOR208 is based on preliminary data from the ongoing phase 2 L-MIND study (NCT02399085).
In this trial, researchers are evaluating MOR208 in combination with lenalidomide in patients with relapsed/refractory DLBCL who are ineligible for high-dose chemotherapy and autologous stem cell transplant.
Preliminary data from this trial were presented at ASCO 2017.* Of the 44 patients enrolled at the data cut-off, 34 were evaluable for efficacy.
The objective response rate was 56% (19/34), and the complete response rate was 32% (11/34). Sixteen of the 19 responders were still on study at the data cut-off point.
The most frequent adverse events of grade 3 or higher were neutropenia (32%), thrombocytopenia (9%), and leukopenia (9%). As of the data cut-off, 27% of patients required a reduction of the lenalidomide dose due to side effects.
“We expect to report further data from our ongoing phase 2 L-MIND trial with MOR208 plus lenalidomide at this year’s American Society of Hematology conference in December,” said Malte Peters, chief development officer of MorphoSys AG, the company developing MOR208.
“In addition, we are currently evaluating MOR208 in combination with bendamustine in our phase 3 B-MIND trial.”
The B-MIND study is designed to compare MOR208 plus bendamustine to rituximab plus bendamustine in patients with relapsed/refractory DLBCL who are not eligible for high-dose chemotherapy and autologous stem cell transplant. ![]()
*Data in the abstract differ from the data presented at the meeting.
Optimizing dose of carfilzomib in rel/ref MM
Top-line results from the phase 3 A.R.R.O.W. trial support a 70 mg/m2 weekly dose of carfilzomib in combination with dexamethasone for patients with relapsed and refractory multiple myeloma (MM).
The data suggest a weekly dose of carfilzomib at 70 mg/m2 is more effective than, and just as safe as, a twice-weekly dose of carfilzomib at 27 mg/m2.
These results were recently announced by Amgen, makers of carfilzomib.
The A.R.R.O.W. trial included 478 patients with relapsed and refractory MM who had received 2 to 3 prior therapies, including bortezomib and an immunomodulatory drug.
Patients were randomized to receive once-weekly carfilzomib (20 mg/m2 on day 1 of cycle 1; 70 mg/m2 on days 8 and 15 of cycle 1; and 70 mg/m2 on days 1, 8 and 15 of subsequent cycles) with dexamethasone (40 mg) or twice-weekly carfilzomib (20 mg/m2 on days 1 and 2 of cycle 1; 27 mg/m2 on days 8, 9, 15 and 16 of cycle 1; and 27 mg/m2 on days 1, 2, 8, 9, 15 and 16 of subsequent cycles) with dexamethasone (40 mg).
The study’s primary endpoint is progression-free survival (PFS).
Patients treated with the once-weekly regimen had significantly better PFS than patients who received carfilzomib twice weekly. The median PFS was 11.2 months and 7.6 months, respectively (hazard ratio=0.69, 95% confidence interval, 0.54–0.88).
The overall safety profile of the once-weekly regimen was comparable to that of the twice-weekly regimen.
The most frequently reported treatment-emergent adverse events (occurring in at least 20% of patients) in either treatment arm were anemia, diarrhea, fatigue, hypertension, insomnia, and pyrexia. ![]()
Top-line results from the phase 3 A.R.R.O.W. trial support a 70 mg/m2 weekly dose of carfilzomib in combination with dexamethasone for patients with relapsed and refractory multiple myeloma (MM).
The data suggest a weekly dose of carfilzomib at 70 mg/m2 is more effective than, and just as safe as, a twice-weekly dose of carfilzomib at 27 mg/m2.
These results were recently announced by Amgen, makers of carfilzomib.
The A.R.R.O.W. trial included 478 patients with relapsed and refractory MM who had received 2 to 3 prior therapies, including bortezomib and an immunomodulatory drug.
Patients were randomized to receive once-weekly carfilzomib (20 mg/m2 on day 1 of cycle 1; 70 mg/m2 on days 8 and 15 of cycle 1; and 70 mg/m2 on days 1, 8 and 15 of subsequent cycles) with dexamethasone (40 mg) or twice-weekly carfilzomib (20 mg/m2 on days 1 and 2 of cycle 1; 27 mg/m2 on days 8, 9, 15 and 16 of cycle 1; and 27 mg/m2 on days 1, 2, 8, 9, 15 and 16 of subsequent cycles) with dexamethasone (40 mg).
The study’s primary endpoint is progression-free survival (PFS).
Patients treated with the once-weekly regimen had significantly better PFS than patients who received carfilzomib twice weekly. The median PFS was 11.2 months and 7.6 months, respectively (hazard ratio=0.69, 95% confidence interval, 0.54–0.88).
The overall safety profile of the once-weekly regimen was comparable to that of the twice-weekly regimen.
The most frequently reported treatment-emergent adverse events (occurring in at least 20% of patients) in either treatment arm were anemia, diarrhea, fatigue, hypertension, insomnia, and pyrexia. ![]()
Top-line results from the phase 3 A.R.R.O.W. trial support a 70 mg/m2 weekly dose of carfilzomib in combination with dexamethasone for patients with relapsed and refractory multiple myeloma (MM).
The data suggest a weekly dose of carfilzomib at 70 mg/m2 is more effective than, and just as safe as, a twice-weekly dose of carfilzomib at 27 mg/m2.
These results were recently announced by Amgen, makers of carfilzomib.
The A.R.R.O.W. trial included 478 patients with relapsed and refractory MM who had received 2 to 3 prior therapies, including bortezomib and an immunomodulatory drug.
Patients were randomized to receive once-weekly carfilzomib (20 mg/m2 on day 1 of cycle 1; 70 mg/m2 on days 8 and 15 of cycle 1; and 70 mg/m2 on days 1, 8 and 15 of subsequent cycles) with dexamethasone (40 mg) or twice-weekly carfilzomib (20 mg/m2 on days 1 and 2 of cycle 1; 27 mg/m2 on days 8, 9, 15 and 16 of cycle 1; and 27 mg/m2 on days 1, 2, 8, 9, 15 and 16 of subsequent cycles) with dexamethasone (40 mg).
The study’s primary endpoint is progression-free survival (PFS).
Patients treated with the once-weekly regimen had significantly better PFS than patients who received carfilzomib twice weekly. The median PFS was 11.2 months and 7.6 months, respectively (hazard ratio=0.69, 95% confidence interval, 0.54–0.88).
The overall safety profile of the once-weekly regimen was comparable to that of the twice-weekly regimen.
The most frequently reported treatment-emergent adverse events (occurring in at least 20% of patients) in either treatment arm were anemia, diarrhea, fatigue, hypertension, insomnia, and pyrexia. ![]()
Hypertension: How Low to Go When Treating Older Adults
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Pediatric Dermatology Consult - November 2017
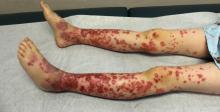
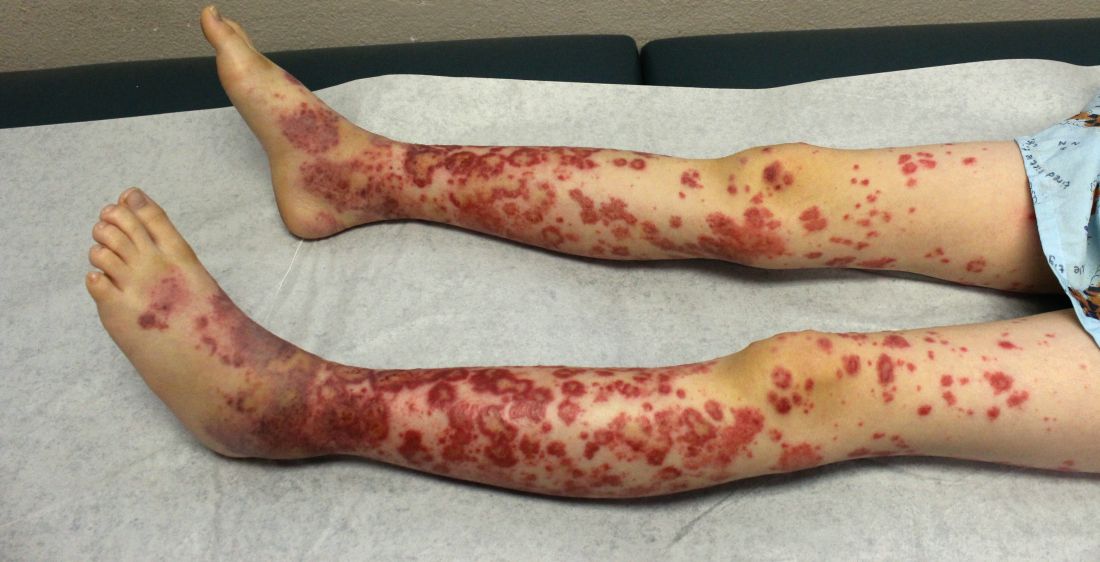
The patient was diagnosed with Henoch-Schönlein purpura (HSP) based on clinical presentation of the lesions and associated symptoms of arthralgia and abdominal pain. Urinalysis was obtained and found to be unremarkable, at presentation and follow-up, and treatment with naproxen 5 mg/kg divided into two doses per day was started for pain relief. A prednisone taper starting at 1 mg/kg per day for 3 weeks also was started due to the presence of severe abdominal pain and bullae on exam. The patient was followed with regular urine studies and blood pressure checks for 2 months, and these also were within normal limits.
HSP, also known as anaphylactoid purpura and immunoglobulin A (IgA) vasculitis, is a small vessel leukocytoclastic vasculitis characterized by the perivascular deposition of IgA1-based immune complexes in the walls of arterioles and postcapillary venules.1 In the vast majority of cases, the condition resolves spontaneously in 4-6 weeks and does not require any specific treatment,2 although NSAIDs and systemic corticosteroids can be used for mild-to-moderate and severe pain, respectively.3
HSP is the most common vasculitis in children, with a peak incidence in boys under the age of 5 years. It occurs worldwide, more commonly among whites and Asians, less commonly among blacks, and recent studies from the Czech Republic,4 Taiwan,5 Spain,6 France,7 South Korea,8 and the United Kingdom9 have shown similar incidence rates of 10-20 per 100,000 children. HSP does occur in adults, but is less common, and is known to carry a worse prognosis – in particular, a higher risk of progression to chronic kidney disease. The disease is more commonly seen in winter months,1 unsurprisingly as upper respiratory tract infections also are more common in these months.10
Pathogenesis
The exact pathogenesis of HSP is the subject of ongoing investigation and continued controversy. Mutations and polymorphisms in mannose-binding lectin, interleukins 1 and 8, vascular endothelial growth factor, and alpha-1-antitrypsin have been associated with HSP.3 Immunoglobulin A (IgA) normally exists in two heavily glycosylated forms – IgA1 and IgA2. Abnormal glycosylation, particularly undergalactosylation, of IgA1, the predominant form of IgA in serum and mucosal secretions, has been linked to HSP.11 HSP has been associated with group A streptococcal infections, Bartonella henselae (cat scratch fever) and numerous drugs,12 although no definitive causal or mechanistic explanation has been identified.
Diagnosis
Two major diagnostic criteria for HSP are widely in use, one developed by the American College of Rheumatology (ACR) in 199013 and the other by the European League Against Rheumatism (EULAR) in 2005.14 Both the ACR and EULAR criteria include acute abdominal pain, purpura, and microscopic evidence of vasculitis. Almost all patients with HSP have cutaneous purpura, and many of these patients have palpable purpura, which is pathognomonic of a leukocytoclastic vasculitis, but palpable purpura is not needed for diagnosis. The ACR criteria additionally include age of 20 years or younger, while the EULAR criteria include arthralgias and the presence of hematuria or proteinuria. Ancillary testing usually is not required to make the diagnosis, but when the diagnosis is not clear histopathologic analysis of a skin sample can identify leukocytoclastic vasculitis. Other laboratory studies that may be needed to rule out other conditions, as well as other organ involvement, include a complete blood count, which can be done to rule out thrombocytopenia as a cause of purpura, a metabolic panel, coagulation studies, occult blood test of stool, abdominal imaging, and urinalysis (UA), which can identify proteinuria or hematuria.
Abdominal pain in HSP is believed to be a result of vasculitis of the gastric, mesenteric, and/or colic vasculature. Bleeding from the inflamed vasculature rarely can lead to gross hematochezia, frank melena, or hematemesis. One serious, potential complication of HSP-related mesenteric vasculitis is intussusception, which is otherwise rare in children older than 2 years. Intussusception should be suspected if features of the classic triad of episodic abdominal pain, sausage-shaped abdominal mass, and currant jelly stool are present. Abdominal ultrasound can help to determine whether intussusception is present.
The purpura in HSP presents in waves or crops, and crops last 5-10 days each. Complete resolution takes 4-6 weeks. If biopsy is desired to confirm the diagnosis, it should be done on a lesion less than 24 hours old. This allows for identification of perivascular IgA on histopathology: beyond 24 hours, IgG and IgM also leak out, contributing to a less specific histopathologic picture.
Accurate diagnosis of HSP is important to guide therapy and anticipate potential complications. Wegener’s granulomatosis (A), also known as granulomatosis with polyangiitis, classically involves the upper and lower respiratory tract and the kidneys, leading to a presentation of epistaxis, cough, and hypertension. It occurs more commonly in adults than children. Finkelstein disease (B), also known as acute hemorrhagic edema of infancy (AHEI), is characterized by the development of petechial, urticarial, or targetoid plaques over 24-48 hours with tender edema and fever in children aged less than 2 years. Unlike HSP, AHEI typically does not involve the gastrointestinal tract, kidneys, or joints. Biopsy of skin lesions of AHEI reveals IgA deposition and leukocytoclastic vasculitis, leading some authors to consider it a closely related entity to HSP. Microscopic polyangiitis (D) is an uncommon pauci-immune vasculitis similar to Wegener’s granulomatosis, but lacking granulomas. It presents typically in the 5th decade of life with fever, fatigue, weight loss, and renal involvement. IgA nephropathy (E), also known as synpharyngitic nephritis and Berger disease, is less likely than HSP to cause a rash, joint pain, or abdominal pain. The nomenclature of HSP (whose alternate name is IgA vasculitis) reflects the multi-organ nature of HSP in comparison to IgA nephropathy, which is more likely to be limited to the kidneys.
Treatment
Aside from intussusception and renal disease, which may result from HSP, treatment is not typically required for HSP as it resolves spontaneously. Patients with significant arthralgias are likely to benefit from NSAIDs such as naproxen 5-20 mg/kg per day, although NSAIDs should be avoided if there is significant renal dysfunction or GI bleeding. Patients with severe abdominal pain or joint pain may be more likely to benefit from oral corticosteroids, particularly prednisone 1-2 mg/kg per day. A meta-analysis showed that corticosteroids significantly reduce the duration of symptoms if given early in the course of disease.15
The prognosis is usually excellent, except for a very small sample of the population (5%) that can develop end-stage renal disease. It is recommended that all children with HSP continue monitoring blood pressure and UA either weekly or biweekly for the first 2 months and then once a month for 6-12 months.16
First described in 1801 by a British physician, HSP is a common and usually self-limited disease for which our understanding has advanced greatly over the past 2 centuries, yet for which many important questions regarding pathophysiology remain unanswered. No diagnostic tests or treatments are needed for the majority of patients. Providers should include HSP in the differential diagnosis for the child with unexplained abdominal pain, renal dysfunction, or nonthrombocytopenic purpura.
Mr. Kusari is a medical student at the University of California, San Diego. Dr. Matiz is a practicing dermatologist at Southern California Permanente Medical Group in La Mesa, California. Dr. Matiz and Mr. Kusari said they had no relevant financial disclosures. Email them at [email protected].
References
1. “Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence”, 5th ed. (New York: Elsevier, 2016).
2. Lancet. 2007;369(9566):976-8.
3. “Dermatology”, 3rd ed. (Philadelphia: Elsevier Saunders, 2012).
4. J Rheumatol. 2004 Nov;31(11):2295-9.
5. Rheumatology (Oxford). 2005 May;44(5):618-22.
6. Medicine (Baltimore). 2014 Mar;93(2):106-13.
7. Rheumatology (Oxford). 2017;56(8):1358-66.
8. J Korean Med Sci. 2014 Feb;29(2):198-203.
9. Lancet. 2002 Oct 19;360(9341):1197-202.
10. Rhinology. 2015 Jun;53(2):99-106.
11. PLoS One. 2016 Nov 21;11(11):e0166700.
12. Pediatr Infect Dis J. 2002 Jan;21(1):28-31.
13. Arthritis Rheum. 1990 Aug;33(8):1114-21.
14. Ann Rheum Dis. 2006 Jul;65(7):936-41.
15. Pediatrics. 2007 Nov;120(5):1079-87.
16. Arch Dis Child. 2010 Nov;95(11):877-82.
The patient was diagnosed with Henoch-Schönlein purpura (HSP) based on clinical presentation of the lesions and associated symptoms of arthralgia and abdominal pain. Urinalysis was obtained and found to be unremarkable, at presentation and follow-up, and treatment with naproxen 5 mg/kg divided into two doses per day was started for pain relief. A prednisone taper starting at 1 mg/kg per day for 3 weeks also was started due to the presence of severe abdominal pain and bullae on exam. The patient was followed with regular urine studies and blood pressure checks for 2 months, and these also were within normal limits.
HSP, also known as anaphylactoid purpura and immunoglobulin A (IgA) vasculitis, is a small vessel leukocytoclastic vasculitis characterized by the perivascular deposition of IgA1-based immune complexes in the walls of arterioles and postcapillary venules.1 In the vast majority of cases, the condition resolves spontaneously in 4-6 weeks and does not require any specific treatment,2 although NSAIDs and systemic corticosteroids can be used for mild-to-moderate and severe pain, respectively.3
HSP is the most common vasculitis in children, with a peak incidence in boys under the age of 5 years. It occurs worldwide, more commonly among whites and Asians, less commonly among blacks, and recent studies from the Czech Republic,4 Taiwan,5 Spain,6 France,7 South Korea,8 and the United Kingdom9 have shown similar incidence rates of 10-20 per 100,000 children. HSP does occur in adults, but is less common, and is known to carry a worse prognosis – in particular, a higher risk of progression to chronic kidney disease. The disease is more commonly seen in winter months,1 unsurprisingly as upper respiratory tract infections also are more common in these months.10
Pathogenesis
The exact pathogenesis of HSP is the subject of ongoing investigation and continued controversy. Mutations and polymorphisms in mannose-binding lectin, interleukins 1 and 8, vascular endothelial growth factor, and alpha-1-antitrypsin have been associated with HSP.3 Immunoglobulin A (IgA) normally exists in two heavily glycosylated forms – IgA1 and IgA2. Abnormal glycosylation, particularly undergalactosylation, of IgA1, the predominant form of IgA in serum and mucosal secretions, has been linked to HSP.11 HSP has been associated with group A streptococcal infections, Bartonella henselae (cat scratch fever) and numerous drugs,12 although no definitive causal or mechanistic explanation has been identified.
Diagnosis
Two major diagnostic criteria for HSP are widely in use, one developed by the American College of Rheumatology (ACR) in 199013 and the other by the European League Against Rheumatism (EULAR) in 2005.14 Both the ACR and EULAR criteria include acute abdominal pain, purpura, and microscopic evidence of vasculitis. Almost all patients with HSP have cutaneous purpura, and many of these patients have palpable purpura, which is pathognomonic of a leukocytoclastic vasculitis, but palpable purpura is not needed for diagnosis. The ACR criteria additionally include age of 20 years or younger, while the EULAR criteria include arthralgias and the presence of hematuria or proteinuria. Ancillary testing usually is not required to make the diagnosis, but when the diagnosis is not clear histopathologic analysis of a skin sample can identify leukocytoclastic vasculitis. Other laboratory studies that may be needed to rule out other conditions, as well as other organ involvement, include a complete blood count, which can be done to rule out thrombocytopenia as a cause of purpura, a metabolic panel, coagulation studies, occult blood test of stool, abdominal imaging, and urinalysis (UA), which can identify proteinuria or hematuria.
Abdominal pain in HSP is believed to be a result of vasculitis of the gastric, mesenteric, and/or colic vasculature. Bleeding from the inflamed vasculature rarely can lead to gross hematochezia, frank melena, or hematemesis. One serious, potential complication of HSP-related mesenteric vasculitis is intussusception, which is otherwise rare in children older than 2 years. Intussusception should be suspected if features of the classic triad of episodic abdominal pain, sausage-shaped abdominal mass, and currant jelly stool are present. Abdominal ultrasound can help to determine whether intussusception is present.
The purpura in HSP presents in waves or crops, and crops last 5-10 days each. Complete resolution takes 4-6 weeks. If biopsy is desired to confirm the diagnosis, it should be done on a lesion less than 24 hours old. This allows for identification of perivascular IgA on histopathology: beyond 24 hours, IgG and IgM also leak out, contributing to a less specific histopathologic picture.
Accurate diagnosis of HSP is important to guide therapy and anticipate potential complications. Wegener’s granulomatosis (A), also known as granulomatosis with polyangiitis, classically involves the upper and lower respiratory tract and the kidneys, leading to a presentation of epistaxis, cough, and hypertension. It occurs more commonly in adults than children. Finkelstein disease (B), also known as acute hemorrhagic edema of infancy (AHEI), is characterized by the development of petechial, urticarial, or targetoid plaques over 24-48 hours with tender edema and fever in children aged less than 2 years. Unlike HSP, AHEI typically does not involve the gastrointestinal tract, kidneys, or joints. Biopsy of skin lesions of AHEI reveals IgA deposition and leukocytoclastic vasculitis, leading some authors to consider it a closely related entity to HSP. Microscopic polyangiitis (D) is an uncommon pauci-immune vasculitis similar to Wegener’s granulomatosis, but lacking granulomas. It presents typically in the 5th decade of life with fever, fatigue, weight loss, and renal involvement. IgA nephropathy (E), also known as synpharyngitic nephritis and Berger disease, is less likely than HSP to cause a rash, joint pain, or abdominal pain. The nomenclature of HSP (whose alternate name is IgA vasculitis) reflects the multi-organ nature of HSP in comparison to IgA nephropathy, which is more likely to be limited to the kidneys.
Treatment
Aside from intussusception and renal disease, which may result from HSP, treatment is not typically required for HSP as it resolves spontaneously. Patients with significant arthralgias are likely to benefit from NSAIDs such as naproxen 5-20 mg/kg per day, although NSAIDs should be avoided if there is significant renal dysfunction or GI bleeding. Patients with severe abdominal pain or joint pain may be more likely to benefit from oral corticosteroids, particularly prednisone 1-2 mg/kg per day. A meta-analysis showed that corticosteroids significantly reduce the duration of symptoms if given early in the course of disease.15
The prognosis is usually excellent, except for a very small sample of the population (5%) that can develop end-stage renal disease. It is recommended that all children with HSP continue monitoring blood pressure and UA either weekly or biweekly for the first 2 months and then once a month for 6-12 months.16
First described in 1801 by a British physician, HSP is a common and usually self-limited disease for which our understanding has advanced greatly over the past 2 centuries, yet for which many important questions regarding pathophysiology remain unanswered. No diagnostic tests or treatments are needed for the majority of patients. Providers should include HSP in the differential diagnosis for the child with unexplained abdominal pain, renal dysfunction, or nonthrombocytopenic purpura.
Mr. Kusari is a medical student at the University of California, San Diego. Dr. Matiz is a practicing dermatologist at Southern California Permanente Medical Group in La Mesa, California. Dr. Matiz and Mr. Kusari said they had no relevant financial disclosures. Email them at [email protected].
References
1. “Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence”, 5th ed. (New York: Elsevier, 2016).
2. Lancet. 2007;369(9566):976-8.
3. “Dermatology”, 3rd ed. (Philadelphia: Elsevier Saunders, 2012).
4. J Rheumatol. 2004 Nov;31(11):2295-9.
5. Rheumatology (Oxford). 2005 May;44(5):618-22.
6. Medicine (Baltimore). 2014 Mar;93(2):106-13.
7. Rheumatology (Oxford). 2017;56(8):1358-66.
8. J Korean Med Sci. 2014 Feb;29(2):198-203.
9. Lancet. 2002 Oct 19;360(9341):1197-202.
10. Rhinology. 2015 Jun;53(2):99-106.
11. PLoS One. 2016 Nov 21;11(11):e0166700.
12. Pediatr Infect Dis J. 2002 Jan;21(1):28-31.
13. Arthritis Rheum. 1990 Aug;33(8):1114-21.
14. Ann Rheum Dis. 2006 Jul;65(7):936-41.
15. Pediatrics. 2007 Nov;120(5):1079-87.
16. Arch Dis Child. 2010 Nov;95(11):877-82.
The patient was diagnosed with Henoch-Schönlein purpura (HSP) based on clinical presentation of the lesions and associated symptoms of arthralgia and abdominal pain. Urinalysis was obtained and found to be unremarkable, at presentation and follow-up, and treatment with naproxen 5 mg/kg divided into two doses per day was started for pain relief. A prednisone taper starting at 1 mg/kg per day for 3 weeks also was started due to the presence of severe abdominal pain and bullae on exam. The patient was followed with regular urine studies and blood pressure checks for 2 months, and these also were within normal limits.
HSP, also known as anaphylactoid purpura and immunoglobulin A (IgA) vasculitis, is a small vessel leukocytoclastic vasculitis characterized by the perivascular deposition of IgA1-based immune complexes in the walls of arterioles and postcapillary venules.1 In the vast majority of cases, the condition resolves spontaneously in 4-6 weeks and does not require any specific treatment,2 although NSAIDs and systemic corticosteroids can be used for mild-to-moderate and severe pain, respectively.3
HSP is the most common vasculitis in children, with a peak incidence in boys under the age of 5 years. It occurs worldwide, more commonly among whites and Asians, less commonly among blacks, and recent studies from the Czech Republic,4 Taiwan,5 Spain,6 France,7 South Korea,8 and the United Kingdom9 have shown similar incidence rates of 10-20 per 100,000 children. HSP does occur in adults, but is less common, and is known to carry a worse prognosis – in particular, a higher risk of progression to chronic kidney disease. The disease is more commonly seen in winter months,1 unsurprisingly as upper respiratory tract infections also are more common in these months.10
Pathogenesis
The exact pathogenesis of HSP is the subject of ongoing investigation and continued controversy. Mutations and polymorphisms in mannose-binding lectin, interleukins 1 and 8, vascular endothelial growth factor, and alpha-1-antitrypsin have been associated with HSP.3 Immunoglobulin A (IgA) normally exists in two heavily glycosylated forms – IgA1 and IgA2. Abnormal glycosylation, particularly undergalactosylation, of IgA1, the predominant form of IgA in serum and mucosal secretions, has been linked to HSP.11 HSP has been associated with group A streptococcal infections, Bartonella henselae (cat scratch fever) and numerous drugs,12 although no definitive causal or mechanistic explanation has been identified.
Diagnosis
Two major diagnostic criteria for HSP are widely in use, one developed by the American College of Rheumatology (ACR) in 199013 and the other by the European League Against Rheumatism (EULAR) in 2005.14 Both the ACR and EULAR criteria include acute abdominal pain, purpura, and microscopic evidence of vasculitis. Almost all patients with HSP have cutaneous purpura, and many of these patients have palpable purpura, which is pathognomonic of a leukocytoclastic vasculitis, but palpable purpura is not needed for diagnosis. The ACR criteria additionally include age of 20 years or younger, while the EULAR criteria include arthralgias and the presence of hematuria or proteinuria. Ancillary testing usually is not required to make the diagnosis, but when the diagnosis is not clear histopathologic analysis of a skin sample can identify leukocytoclastic vasculitis. Other laboratory studies that may be needed to rule out other conditions, as well as other organ involvement, include a complete blood count, which can be done to rule out thrombocytopenia as a cause of purpura, a metabolic panel, coagulation studies, occult blood test of stool, abdominal imaging, and urinalysis (UA), which can identify proteinuria or hematuria.
Abdominal pain in HSP is believed to be a result of vasculitis of the gastric, mesenteric, and/or colic vasculature. Bleeding from the inflamed vasculature rarely can lead to gross hematochezia, frank melena, or hematemesis. One serious, potential complication of HSP-related mesenteric vasculitis is intussusception, which is otherwise rare in children older than 2 years. Intussusception should be suspected if features of the classic triad of episodic abdominal pain, sausage-shaped abdominal mass, and currant jelly stool are present. Abdominal ultrasound can help to determine whether intussusception is present.
The purpura in HSP presents in waves or crops, and crops last 5-10 days each. Complete resolution takes 4-6 weeks. If biopsy is desired to confirm the diagnosis, it should be done on a lesion less than 24 hours old. This allows for identification of perivascular IgA on histopathology: beyond 24 hours, IgG and IgM also leak out, contributing to a less specific histopathologic picture.
Accurate diagnosis of HSP is important to guide therapy and anticipate potential complications. Wegener’s granulomatosis (A), also known as granulomatosis with polyangiitis, classically involves the upper and lower respiratory tract and the kidneys, leading to a presentation of epistaxis, cough, and hypertension. It occurs more commonly in adults than children. Finkelstein disease (B), also known as acute hemorrhagic edema of infancy (AHEI), is characterized by the development of petechial, urticarial, or targetoid plaques over 24-48 hours with tender edema and fever in children aged less than 2 years. Unlike HSP, AHEI typically does not involve the gastrointestinal tract, kidneys, or joints. Biopsy of skin lesions of AHEI reveals IgA deposition and leukocytoclastic vasculitis, leading some authors to consider it a closely related entity to HSP. Microscopic polyangiitis (D) is an uncommon pauci-immune vasculitis similar to Wegener’s granulomatosis, but lacking granulomas. It presents typically in the 5th decade of life with fever, fatigue, weight loss, and renal involvement. IgA nephropathy (E), also known as synpharyngitic nephritis and Berger disease, is less likely than HSP to cause a rash, joint pain, or abdominal pain. The nomenclature of HSP (whose alternate name is IgA vasculitis) reflects the multi-organ nature of HSP in comparison to IgA nephropathy, which is more likely to be limited to the kidneys.
Treatment
Aside from intussusception and renal disease, which may result from HSP, treatment is not typically required for HSP as it resolves spontaneously. Patients with significant arthralgias are likely to benefit from NSAIDs such as naproxen 5-20 mg/kg per day, although NSAIDs should be avoided if there is significant renal dysfunction or GI bleeding. Patients with severe abdominal pain or joint pain may be more likely to benefit from oral corticosteroids, particularly prednisone 1-2 mg/kg per day. A meta-analysis showed that corticosteroids significantly reduce the duration of symptoms if given early in the course of disease.15
The prognosis is usually excellent, except for a very small sample of the population (5%) that can develop end-stage renal disease. It is recommended that all children with HSP continue monitoring blood pressure and UA either weekly or biweekly for the first 2 months and then once a month for 6-12 months.16
First described in 1801 by a British physician, HSP is a common and usually self-limited disease for which our understanding has advanced greatly over the past 2 centuries, yet for which many important questions regarding pathophysiology remain unanswered. No diagnostic tests or treatments are needed for the majority of patients. Providers should include HSP in the differential diagnosis for the child with unexplained abdominal pain, renal dysfunction, or nonthrombocytopenic purpura.
Mr. Kusari is a medical student at the University of California, San Diego. Dr. Matiz is a practicing dermatologist at Southern California Permanente Medical Group in La Mesa, California. Dr. Matiz and Mr. Kusari said they had no relevant financial disclosures. Email them at [email protected].
References
1. “Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence”, 5th ed. (New York: Elsevier, 2016).
2. Lancet. 2007;369(9566):976-8.
3. “Dermatology”, 3rd ed. (Philadelphia: Elsevier Saunders, 2012).
4. J Rheumatol. 2004 Nov;31(11):2295-9.
5. Rheumatology (Oxford). 2005 May;44(5):618-22.
6. Medicine (Baltimore). 2014 Mar;93(2):106-13.
7. Rheumatology (Oxford). 2017;56(8):1358-66.
8. J Korean Med Sci. 2014 Feb;29(2):198-203.
9. Lancet. 2002 Oct 19;360(9341):1197-202.
10. Rhinology. 2015 Jun;53(2):99-106.
11. PLoS One. 2016 Nov 21;11(11):e0166700.
12. Pediatr Infect Dis J. 2002 Jan;21(1):28-31.
13. Arthritis Rheum. 1990 Aug;33(8):1114-21.
14. Ann Rheum Dis. 2006 Jul;65(7):936-41.
15. Pediatrics. 2007 Nov;120(5):1079-87.
16. Arch Dis Child. 2010 Nov;95(11):877-82.
Clinical presentation
A healthy 9-year-old boy presents with 1 week history of a rash that began as “bruises” on both ankles that subsequently ascended over a few days to the proximal lower extremities and upper extremities. The rash has been painful and pruritic at times. The patient’s mother reports regular application of hydrocortisone cream for itch and pain relief, and this has been somewhat successful.
The patient has a history of longstanding constipation and abdominal pain, but over the past week has reported abdominal pain that is different and more severe than his usual abdominal pain. This abdominal pain has limited oral intake over the past 2 days. The patient and family also report bilateral pain of the wrists and elbows, which has limited his daily activities. The patient and mother deny fevers, chills, cough, coryza, and any sick contacts.
His vital signs are stable. On physical examination there is mild conjunctival injection, no intraoral lesions, and no lymphadenopathy or hepatosplenomegaly. The abdomen is not distended but it is tender to deep palpation. Bowel sounds are present. On skin examination, there are multiple purpuric annular plaques with central clearing, some with bullae and petechiae, on the bilateral buttocks and legs. There is bilateral pedal edema. On the arms, there are a few polymorphic pink and red annular to targetoid plaques.