User login
Enhancing Opportunities for Physical Activity Among Long-Term Care Residents: A Narrative Review
From the Geriatric Education and Research in Aging Sciences (GERAS) Centre for Aging Research, McMaster University, Hamilton, ON.
Abstract
- Objective. To summarize the literature on improving opportunities for physical activity for residents in long-term care (LTC).
- Method. Narrative review of the literature.
- Results. Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, such as poor mood and increased risk of death, and to improve physical function. This review identifies several strategies for promoting physical activity for LTC residents: incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovative solutions such as robots or interactive technology.
- Conclusion. While the quality of evidence to date is limited, preliminary work suggests that the strategies identified in this article could be included as part of a multifactorial approach to increasing physical activity in LTC.
Keywords: long-term care; nursing homes; physical activity; sedentary; mobility.
The United Nations estimates that between 2013 and 2050 the population aged 60 years or older will double.1 Furthermore, the fastest growth rate will be seen in older adults over the age of 80 years.1 With this demographic shift, a growing number of older adults will require supportive housing, such as long-term care (LTC). Indeed, it is projected that the number of older adults requiring LTC will double by 2036.2
Residents in LTC are often medically complex and experience multimorbidity, cognitive impairment, and functional decline,3 making it difficult for them to engage in physical activity. LTC residents spend approximately 75% of their waking time in sedentary activities (eg, sitting, lying down, watching TV), which amounts to more than 12 hours per day.4-6 Residents with cognitive impairment are even more sedentary, spending as little as 1 minute per day in moderate physical activity and approximately 87% of their time in sedentary activities.7 Additionally, a high prevalence of use of psychotropic drugs and physical restraints contributes to high levels of physical inactivity for residents in LTC.8 Increased time spent in sedentary activities has been associated with adverse health outcomes, such as incidence of cardiovascular disease and type 2 diabetes, and mortality.9-11 Moreover, bed and chair rest are associated with muscle disuse, which can lead to functional impairment.12,13
Given the large amount of time LTC residents spend in sedentary activities and the negative consequences this has on their health, it is essential to find opportunities to engage residents in physical activity throughout the day. This article summarizes evidence about increasing opportunities for physical activity for LTC residents. Physical activity is defined as “any bodily movement produced by skeletal muscles that results in energy expenditure,” while exercise, which is a subset of physical activity, is purposefully planned, structured, and repetitive and has a goal of maintaining or improving physical fitness.14 Previous work has described exercise among LTC residents in detail,8,15,16 and thus exercise is not addressed here. Also, as a narrative review, this article provides an overview of available interventions to improve physical activity for LTC residents and does not provide comments on efficacy or an exhaustive list of potential interventions. Rather, it provides a starting point for LTC homes to consider when providing opportunities to improve physical activity for their residents.
Guidelines for Increasing Physical Activity
There are currently no published evidence-based guidelines for increasing physical activity and reducing sedentary time for residents of LTC homes. However, an international task force of experts in geriatrics, exercise, and LTC research convened in 2015 and made recommendations on this matter.8 They emphasize the importance of considering the needs of residents, family members, health care professionals, LTC staff, and policy-makers when designing strategies to promote movement in LTC.8 This will ensure that the strategies to promote movement will be realistic and sustainable. Additionally, the task force identified motivation and pleasure as key to engaging residents in physical activities, and recommended that interests and preferences should be used to guide the selection of activities.8 The following sections describe example strategies to improve physical activity for residents in LTC that LTC homes can use to help facilitate movement for their residents.
Strategies for Promoting Physical Activity
Leveraging Daily Activities
One approach to promoting physical activity in LTC homes is to systematically use simple strategies embedded within routine care to engage residents in movement.8 Function-focused, or restorative care,17 is a philosophy of care that promotes increasing physical activity and maintaining functional abilities based on the resident’s abilities. Examples include walking with residents to the dining room rather than pushing them in a wheelchair where appropriate, inviting residents to events that require them to leave their room, improving independent wheelchair propulsion for residents who cannot walk, and increasing opportunities for sit-to-stand activities where possible. These activities are scaled to the resident’s underlying physical and cognitive capabilities. A systematic review of function-focused care revealed that it can help maintain functional skills for residents in LTC, and there is no significant risk associated with implementation.18 In a study by Slaughter et al19 that examined the effectiveness of techniques to encourage mobility by residents’ usual caregivers, health care aides prompted residents to perform the sit-to-stand activity 4 times per day, with the number of repetitions individualized based on resident ability, fatigue, and motivation. Residents who completed the sit-to-stand activity had smaller declines in mobility and functional outcomes (ie, less decline on the Functional Independence Measure).19 This study included residents with Alzheimer’s disease and dementia who could transfer independently or with the assistance of one person,20 indicating that this type of intervention is feasible and appropriate for residents with cognitive impairment.
Group Activities
Group activities in LTC homes are another way of engaging residents in physical activity in a motivating and pleasant setting that also encourages social engagement among residents and LTC staff. Group exercise classes can be effective for improving mood and functional outcomes. For example, a systematic review of dance classes in LTC homes revealed an improvement in problematic behaviors, mood, cognition, communication, and socialization.21 Most studies included participants with dementia, and no adverse events were reported, supporting the feasibility and safety of implementing group dance activities for residents with cognitive impairment. Group exercise is the most common delivery method for exercise within LTC homes22 and has been demonstrated to have small positive effects on activities of daily living (ADL; ie, improvement in ADL independence equivalent to 1.3 points on the Barthel Index).23 Other group activities, such as music therapy, have demonstrated improvements in depressive symptoms, emotional well-being, and anxiety for LTC residents with dementia.24 Group activities also provide the opportunity for movement as residents leave their rooms, walk to a new location (if able), and return to their rooms when the activity is complete.
Barriers to Physical Activity and Strategies to Overcome Them
Caregiver-related Factors
LTC staff have limited time to spend promoting physical activity since residents often have complex health care needs and staffing levels are often constrained.25 Indeed, having lower staffing levels has been associated with lower levels of physical activity for residents.26,27 LTC staff have identified a lack of time to walk with residents28,29 and having other tasks to do (eg, clean) as barriers to promoting movement.28,29 However, asking residents to help staff with small household chores, such as folding laundry or clearing dishes, was a facilitator to promoting movement.30 Activating residents by helping them transfer to a wheelchair for independent mobilization around the home or by assisting them to walk where appropriate were also facilitators.30,31 Leveraging facilitators will help staff who have limited time to help residents engage in more physical activity.
Motivation of LTC staff can also be a barrier to encouraging physical activity for residents in LTC. Fear that increasing physical activity will cause adverse events like falls, illness, or exacerbation of symptoms often decreases motivation for staff to facilitate physical activity.32,33 Another potential barrier is the conceptualization of the role of nursing in LTC as protecting residents from harm by encouraging them to engage in “risk-free” activities like staying in bed.34-39 Strategies to increase staff motivation to engage LTC residents in physical activity that have been shown to be effective are verbal prompts, modelling behaviors, goal setting, and home champions to promote function-focused care.17,33,40-43
The Physical Environment
Aspects of the physical environment of LTC homes may facilitate or limit residents’ ability to be physically active. A 2017 systematic review examined elements of the physical environment that acted as barriers and facilitators to physical activity for older adults living in LTC.30 The authors found that the person-environment fit, security, accessibility, and comfort were key components of the physical environment that were associated with residents’ physical activity levels.30 First, an appropriate fit between the residents’ abilities and the demands of the environment was related to improved activity as measured by actigraphy.44 For example, having long hallways between residents’ rooms and common spaces discourages residents who can only walk short distances from walking to these locations. However, residents were more active in larger-scaled LTC homes with shorter distances between different areas (eg, resident rooms and dining rooms).45 Clearly, there must be enough space to encourage walking between areas, but not so much space that walking is not feasible. Residents participating in a focus group identified accessibility and comfort features as being facilitators for walking in the corridor, such as wide corridors, sturdy handrails, carpet, chairs placed at short intervals for seated breaks, windows to look out, plants, and accessible activity rooms and restrooms.45,46 On the other hand, limited things to see and do indoors and outdoors, along with restricted walking areas, were identified as barriers to corridor walking by residents.46
One method for optimizing LTC home architecture to promote movement is to provide therapeutic outdoor spaces, such as gardens. Indeed, therapeutic gardens have been studied as a nonpharmacological method of engaging LTC residents with dementia and have been shown to benefit mood, pain, and fall prevention.47 Secure therapeutic gardens or outdoor spaces provide opportunities for various activities to increase movement, including gardening, animal care, and walking.48 However, there is a higher propensity for residents who use walkers or wheelchairs to slide off paths or become stuck in mud or mulch.49 Residents with physical limitations may require additional supervision in garden spaces, and as such spaces should be designed with improved safety in mind (eg, barriers between paths and places where mud could accumulate). The number of available indoor (eg, a physical therapy gym) and outdoor (eg, gardens) spaces was also found to be positively related to residents’ physical activity levels.50 However, these relationships were mediated by the number of activity programs available in the LTC homes.50 Therefore, having staff available to facilitate activities is also important for promoting physical activity.
Chemical and Physical Restraints
Physical and chemical restraints (eg, antipsychotics and sedatives) are sometimes used to manage the behavioral and psychological symptoms of dementia,51,52 which many residents in LTC experience.3 Though there has been an emphasis in North America to decrease their use, physical and chemical restraints are still used in LTC.53 Physical restraint use is associated with a higher risk of functional and cognitive decline.53,54 Residents who are both physically and chemically restrained through antipsychotic use are at even higher risk for these declines.54 Thus, to improve opportunities for movement in LTC, physical restraint use should be minimized. The risks and benefits of using psychotropic medications that often decrease residents’ physical activity levels must be evaluated individually, and other nonpharmacological strategies should be used to manage the behavioral and psychological symptoms of dementia. These could include functional analysis-based interventions (ie, individualized interventions aimed at identifying unmet needs, causes, antecedents, and consequences of the behavior),55 music therapy,55 or other interventions described above.
Emerging Innovative Interventions
Robots are an emerging nonpharmacological intervention for improving the behavioral and psychological symptoms of dementia and facilitating physical activity in LTC. Robotic animal interventions, where LTC residents interact with robotic animals in an individual or group setting, have been shown to reduce negative behaviors and increase positive mood.56 Additionally, robots are being used in rehabilitation to provide exercise post-stroke57 and could easily be transitioned to do similar tasks in LTC. Robotic interventions are attractive for the LTC sector as they could help relieve the workload demands on an often overloaded sector, and, in the case of pet therapy, surmount regulations for bringing live animals into a LTC home. Though studies examining the use of robots in LTC have mainly focused on the effect of pet therapy on reducing behavioral symptoms, the use of robots to promote physical activity and exercise in LTC is a natural progression for the work that has been done in inpatient rehabilitation.57 On a similar note, an interactive technology (similar to a Kinect system) used to promote 30-minute, twice-weekly physical activity sessions has demonstrated improvements in physical function (Short Physical Performance Battery [SPPB]) for pre-disabled (SPPB of 6 to 9) residents in LTC without dementia.58 The role of technology to promote physical activity in LTC is an emerging area of interest, and future innovations in this area will continue to help facilitate movement.
Quality of Evidence
Most studies aimed at improving physical activity for LTC residents to date are small, have nonrandomized designs, and have limited generalizability and evidence to support the efficacy of the interventions. For example, most studies included in systematic reviews for function-focused care, dance, group exercise, and music therapy are small, observational, or quasi-experimental studies with methodological issues resulting in bias.18,21,23,24 Likewise, the evidence surrounding nonpharmacological interventions for reducing behavioral and psychological symptoms of dementia is of very low to moderate quality.55 Innovative interventions, such as robotics and interactive technology, to promote physical activity in LTC are in their infancy. There are no data syntheses available to date to summarize the available literature on this topic, and conclusions rely on small, nonrandomized designs or extrapolations of results from similar sectors (eg, inpatient rehabilitation). Thus, the studies described in this review can be used as preliminary evidence to support the implementation of interventions to improve physical activity, but discretion should be used when interpreting the efficacy of these interventions.
Discussion
This review identifies several strategies for promoting physical activity for LTC residents, including incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovation solutions like robots or interactive technology. While the quality of evidence to date is limited, preliminary work suggests that strategies identified in this paper could be included as part of a multifactorial approach to increasing physical activity in LTC.
The current evidence does not suggest that any one strategy is more effective at improving physical activity, and it is likely that LTC homes will need to employ a combination of strategies to help residents move more. Additionally, residents’ preferences, goals, and capabilities should always be considered when designing an individualized physical activity plan. For example, if a resident does not like to be outdoors or gardening but enjoys dancing and music, then their physical activity plan should include group dance class and music therapy rather than gardening. LTC homes will need to have a menu of opportunities for movement that residents can choose from so that activities are pleasant and motivating, and therefore more likely to be completed.
Many of the interventions described in this review are safe and feasible to implement with residents who have physical or cognitive impairments. Function-focused care is scaled to the residents’ capabilities and did not increase the risk of falling, though LTC staff require the skills to scale physical activities appropriately.18 Likewise, group dance activities and music therapy were tested with residents with dementia, with no adverse events reported.21,24 However, more work is needed to determine the feasibility of implementing emerging methods, such as robotics and interactive technology, for increasing physical activity for residents with physical and cognitive impairments. Most studies to date have included mobile residents or those with minimal cognitive impairment. Similarly, outdoor garden spaces may be less safe for residents who use walkers or wheelchairs if there is an opportunity for them to slip off paths or get stuck in mud or mulch. LTC homes implementing any of these interventions should evaluate the benefits and risks of each intervention, the resources available within the home to support them (eg, trained staff), and the target residents’ physical and cognitive capabilities.
While increasing physical activity is important, structured exercise is needed to see gains in components of physical fitness such as strength, aerobic capacity, and balance. Indeed, one major consideration highlighted by the aforementioned task force is that every resident who does not have contraindications must also have a personalized multicomponent exercise program as part of their care plan.8 The task force recommends moderate- to high-intensity strength, aerobic, and balance exercises 2 times per week for 35 to 45 minutes per session.8 There is an interrelationship between physical activity and structured exercise: structured exercise programs can certainly be part of a physical activity plan, but physical activity can include more than structured exercise. Physical activity also includes any activity that involves movement, such as walking in gardens or between home areas, or physically participating more in personal care activities (eg, assisting with bathing or dressing).14 Both structured exercise and physical activity are important for LTC residents. Structured exercise provides an opportunity to improve strength and cardiovascular fitness, which aim to decrease the negative effects of sarcopenia and cardiovascular disease, such as disability and death.59,60 However, structured exercise should not be done daily for the same muscle groups.8 Rather, it is recommended for LTC residents to engage in structured exercise 2 times per week.8 Increasing physical activity is a daily goal, as daily physical activity decreases sedentary time, which has negative consequences such as decreased mood61 and increased mortality.62 LTC homes should incorporate strategies to both increase daily physical activity and promote individualized, structured exercise programs.
Conclusion
Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, like poor mood and increased risk of death, and to improve physical function. This review describes several strategies to promote physical activity within LTC homes, such as leveraging daily activities and the physical environment, providing group activities, reducing physical and chemical restraint use, and using innovative technology such as robots. LTC homes can use the information in this review to plan strategies to promote physical activity.
Corresponding author: Caitlin McArthur, MScPT, PhD, Hamilton Health Sciences, St. Peter’s Hospital, 88 Maplewood Avenue, Hamilton, ON L8M 1W9; [email protected].
Financial disclosures: None.
1. United Nations Department of Economic and Social Affairs Population Division. World Population Ageing 2013. New York, NY: United Nations; 2013.
2. Pickard L, Comas-Herrera A, Costa-Font J, et al. Modelling an entitlement to long-term care services for older people in Europe: projections for long-term care expenditure to 2050. J Eur Soc Policy. 2007;17:33-48.
3. Hirdes JP, Mitchell L, Maxwell CJ, White N. Beyond the “iron lungs of gerontology”: Using evidence to shape the future of nursing homes in Canada. Can J Aging. 2011;30:371-390.
4. Chin A Paw MJM, van Poppel MNM, van Mechelen W. Effects of resistance and functional-skills training on habitual activity and constipation among older adults living in long-term care facilities: a randomized controlled trial. BMC Geriatr. 2006;6:9.
5. Ikezoe T, Asakawa Y, Shima H, Kishibuchi K, Ichihashi N. Daytime physical activity patterns and physical fitness in institutionalized elderly women: an exploratory study. Arch Gerontol Geriatr. 2013;57:221-225.
6. Keogh JW, Senior H, Beller EM, Henwood T. Prevalence and risk factors for low habitual walking speed in nursing home residents: an observational study. Arch Phys Med Rehabil. 2015;96:1993-1999.
7. Marmeleira J, Ferreira S, Raimundo A. Physical activity and physical fitness of nursing home residents with cognitive impairment: A pilot study. Exp Gerontol. 2017;100:63-69.
8. de Souto Barreto P, Morley JE, Chodzko-Zajko W, et al. Recommendations on physical activity and exercise for older adults living in long-term care facilities: a taskforce report. J Am Med Dir Assoc. 2016;17:381-392.
9. van der Ploeg HP, Chey T, Korda RJ, et al. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch Intern Med. 2012;172:494-500.
10. Chau JY, Grunseit AC, Chey T, et al. Daily sitting time and all-cause mortality: a meta-analysis. PLoS One. 2013;8:e80000.
11. Grøntved A, Hu FB. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: a meta-analysis. JAMA. 2011;305:2448-2455.
12. Senior HE, Henwood TR, Beller EM, et al. Prevalence and risk factors of sarcopenia among adults living in nursing homes. Maturitas. 2015;82:418-423.
13. Wall BT, Dirks ML, van Loon LJC. Skeletal muscle atrophy during short-term disuse: implications for age-related sarcopenia. Ageing Res Rev. 2013;12:898-906.
14. Caspersen CJ, Powell KE, Christenson GM. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep. 1985;100:126-131.
15. McArthur C, Giangregorio LM. Improving strength and balance for long-term care residents at risk for falling: Suggestions for practice. J Clin Outcomes Manag. 2018;25:28-38.
16. Crocker T, Forster A, Young J, et al. Physical rehabilitation for older people in long-term care. Cochrane Database Syst Rev. 2013;2:CD004294.
17. Resnick B, Galik E, Boltz M, Pretzer-Aboff IE. Implementing Restorative Care Nursing in All Settings. 2nd ed. New York, NY: Spring Publishing Company; 2011.
18. Resnick B, Galik E, Boltz M. Function focused care approaches: literature review of progress and future possibilities. J Am Med Dir Assoc. 2013;14:313-318.
19. Slaughter SE, Estabrooks CA, Jones CA, Wagg AS. Mobility of Vulnerable Elders (MOVE): study protocol to evaluate the implementation and outcomes of a mobility intervention in long-term care facilities. BMC Geriatr. 2011;11:84.
20. Slaughter SE, Wagg AS, Jones CA, et al. Mobility of Vulnerable Elders study: effect of the sit-to-stand activity on mobility, function, and quality of life. J Am Med Dir Assoc. 2015;16(2):138-143.
21. Guzmán-García A, Hughes JC, James IA, Rochester L. Dancing as a psychosocial intervention in care homes: a systematic review of the literature. Int J Geriatr Psychiatry. 2013;28:914-924.
22. McArthur C, Gibbs JC, Patel R, et al. A scoping review of physical rehabilitation in long-term care: interventions, outcomes, tools. Can J Aging/La Rev Can du Vieil. 2017;36:435-452.
23. Crocker T, Young J, Forster A, et al. The effect of physical rehabilitation on activities of daily living in older residents of long-term care facilities: Systematic review with meta-analysis. Age Ageing. 2013;42:682-688.
24. van der Steen JT, Smaling HJ, van der Wouden JC, et al. Music-based therapeutic interventions for people with dementia. Cochrane Database Syst Rev. 2018;7:CD003477.
25. Froggatt K, Davies S, Meyer J. Understanding Care Homes, A Research and Development Perspective. London: Jessica Kingsley Publishers; 2009.
26. Shore BA, Lerman DC, Smith RG, et al. Direct assessment of quality of care in a geriatric nursing home. J Appl Behav Anal. 1995;28:435-448.
27. Bates-Jensen BM, Schnelle JF, Alessi CA, et al. The effects of staffing on in-bed times of nursing home residents. J Am Geriatr Soc. 2004;52:931-938.
28. Ericson-Lidman E, Renström A-S, Åhlin J, Strandberg G. Relatives’ perceptions of residents’ life in a municipal care facility for older people with a focus on quality of life and care environment. Int J Older People Nurs. 2015;10:160-169.
29. Häggström E, Kihlgren A, Kihlgren M, Sörlie V. Relatives’ struggle for an improved and more just care for older people in community care. J Clin Nurs. 2007;16:1749-1757.
30. Douma JG, Volkers KM, Engels G, et al. Setting-related influences on physical inactivity of older adults in residential care settings: a review. BMC Geriatr. 2017;17:97.
31. Zegelin A. ’Tied down’- the process of becoming bedridden through gradual local confinement. J Clin Nurs. 2008;17:2294-2301.
32. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Falls and fall-related injuries associated with function-focused care. Clin Nurs Res. 2012;21:43-63.
33. Pretzer-Aboff I, Galik E. Feasibility and impact of a function focused care intervention for Parkinson’s disease in the community. Nursing Res. 2011;60:276-283.
34. Leditschke IA, Green M, Irvine J, et al. What are the barriers to mobilizing intensive care patients? Cardiopulm Phys Ther J. 2012;23:26-29.
35. Mittmann N, Seung SJ, Pisterzi LF, et al. Nursing workload associated with hospital patient care. Dis Manag Heal Outcomes. 2008;16:53-61.
36. Dykes PC, Carroll DL, Hurley AC, et al. Why do patients in acute care hospitals fall? Can falls be prevented? J Nurs Adm. 2009;39:299-304.
37. Brownie S, Nancarrow S. Effects of person-centered care on residents and staff in aged-care facilities: a systematic review. Clin Interv Aging. 2013;8:1-10.
38. Wakefield BJ, Holman JE. Functional trajectories associated with hospitalization in older adults. West J Nurs Res. 2007;29:161-177.
39. Boltz M, Resnick B, Capezuti E, Shuluk J. Activity restriction vs. self-direction: hospitalised older adults’ response to fear of falling. Int J Older People Nurs. 2014;9:44-53.
40. Resnick B, Galik E, Gruber-Baldini A, Zimmerman S. Testing the effect of function-focused care in assisted living. J Am Geriatr Soc. 2011;59:2233-2240.
41. Galik EM, Resnick B, Gruber-Baldini A, et al. Pilot testing of the restorative care intervention for the cognitively impaired. J Am Med Dir Assoc. 2008;9:516-522.
42. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Implementing a restorative care philosophy of care in assisted living: pilot testing of Res-Care-AL. J Am Acad Nurse Pract. 2009;21:123-133.
43. Resnick B, Gruber-Baldini AL, Zimmerman S, et al. Nursing home resident outcomes from the Res-Care intervention. J Am Geriatr Soc. 2009;57:1156-1165.
44. Pomeroy SH, Scherer Y, Runkawatt V, et al. Person-environment fit and functioning among older adults in a long-term care setting. Geriatr Nurs. 2011;32:368-378.
45. Moos RH, David TG, Lemke S, Postle E. Coping with an intra-institutional relocation: changes in resident and staff behavior patterns. Gerontologist. 1984;24:495-502.
46. Lu Z, Rodiek SD, Shepley MM, Duffy M. Influences of physical environment on corridor walking among assisted living residents. J Appl Gerontol. 2011;30:463-484.
47. Detweiler MB, Sharma T, Detweiler JG, et al. What is the evidence to support the use of therapeutic gardens for the elderly? Psychiatry Investig. 2012;9:100.
48. Blake M, Mitchell G. Horticultural therapy in dementia care: a literature review. Nurs Stand. 2016;30:41-47.
49. Detweiler MB, Murphy PF, Myers LC, Kim KY. Does a wander garden influence inappropriate behaviors in dementia residents? Am J Alzheimers Dis Other Demen. 2008;23:31-45.
50. Joseph A, Zimring C, Harris-Kojetin L, Kiefer K. Presence and visibility of outdoor and indoor physical activity features and participation in physical activity among older adults in retirement communities. J Hous Elderly. 2006;19:141-165.
51. Feng Z, Hirdes JP, Smith TF, et al. Use of physical restraints and antipsychotic medications in nursing homes: a cross-national study. Int J Geriatr Psychiatry. 2009;24:1110-1118.
52. Herrmann N. Recommendations for the management of behavioral and psychological symptoms of dementia. Can J Neurol Sci. 2001;28 Suppl 1:S96-107.
53. Freeman S, Spirgiene L, Martin-Khan M, Hirdes JP. Relationship between restraint use, engagement in social activity, and decline in cognitive status among residents newly admitted to long-term care facilities. Geriatr Gerontol Int. 2017;17:246-255.
54. Foebel AD, Onder G, Finne-Soveri H, et al. Physical restraint and antipsychotic medication use among nursing home residents with dementia. J Am Med Dir Assoc. 2016;17:184.e9-184.e14.
55. Dyer SM, Harrison SL, Laver K, Whitehead C, Crotty M. An overview of systematic reviews of pharmacological and non-pharmacological interventions for the treatment of behavioral and psychological symptoms of dementia. Int Psychogeriatr. 2018;30:295-309.
56. Robinson H, MacDonald B, Kerse N, Broadbent E. The psychosocial effects of a companion robot: a randomized controlled trial. J Am Med Dir Assoc. 2013;14:661-667.
57. Lo K, Stephenson M, Lockwood C. Effectiveness of robotic assisted rehabilitation for mobility and functional ability in adult stroke patients. JBI Database System Rev Implement Rep. 2017;15:3049-3091.
58. Valiani V, Lauzé M, Martel D, et al. A new adaptive home-based exercise technology among older adults living in nursing home: a pilot study on feasibility, acceptability and physical performance. J Nutr Health Aging. 2017;21:819-824.
59. Locquet M, Beaudart C, Hajaoui M, et al. Three-year adverse health consequences of sarcopenia in community-dwelling older adults according to 5 diagnosis definitions. J Am Med Dir Assoc. 2019;20:43-46.e2.
60. Chodzko-Zajko WJ, Proctor DN, Fiatarone Singh MA, et al. Exercise and physical activity for older adults. Med Sci Sports Exerc. 2009;41:1510-1530.
61. Park S-Y, Lee K, Um YJ, Paek S, Ryou IS. Association between physical activity and depressive mood among Korean adults with chronic diseases. Korean J Fam Med. 2018;39:185-190.
62. Loprinzi PD. Light-intensity physical activity and all-cause mortality. Am J Health Promot. 2017;31:340-342.
From the Geriatric Education and Research in Aging Sciences (GERAS) Centre for Aging Research, McMaster University, Hamilton, ON.
Abstract
- Objective. To summarize the literature on improving opportunities for physical activity for residents in long-term care (LTC).
- Method. Narrative review of the literature.
- Results. Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, such as poor mood and increased risk of death, and to improve physical function. This review identifies several strategies for promoting physical activity for LTC residents: incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovative solutions such as robots or interactive technology.
- Conclusion. While the quality of evidence to date is limited, preliminary work suggests that the strategies identified in this article could be included as part of a multifactorial approach to increasing physical activity in LTC.
Keywords: long-term care; nursing homes; physical activity; sedentary; mobility.
The United Nations estimates that between 2013 and 2050 the population aged 60 years or older will double.1 Furthermore, the fastest growth rate will be seen in older adults over the age of 80 years.1 With this demographic shift, a growing number of older adults will require supportive housing, such as long-term care (LTC). Indeed, it is projected that the number of older adults requiring LTC will double by 2036.2
Residents in LTC are often medically complex and experience multimorbidity, cognitive impairment, and functional decline,3 making it difficult for them to engage in physical activity. LTC residents spend approximately 75% of their waking time in sedentary activities (eg, sitting, lying down, watching TV), which amounts to more than 12 hours per day.4-6 Residents with cognitive impairment are even more sedentary, spending as little as 1 minute per day in moderate physical activity and approximately 87% of their time in sedentary activities.7 Additionally, a high prevalence of use of psychotropic drugs and physical restraints contributes to high levels of physical inactivity for residents in LTC.8 Increased time spent in sedentary activities has been associated with adverse health outcomes, such as incidence of cardiovascular disease and type 2 diabetes, and mortality.9-11 Moreover, bed and chair rest are associated with muscle disuse, which can lead to functional impairment.12,13
Given the large amount of time LTC residents spend in sedentary activities and the negative consequences this has on their health, it is essential to find opportunities to engage residents in physical activity throughout the day. This article summarizes evidence about increasing opportunities for physical activity for LTC residents. Physical activity is defined as “any bodily movement produced by skeletal muscles that results in energy expenditure,” while exercise, which is a subset of physical activity, is purposefully planned, structured, and repetitive and has a goal of maintaining or improving physical fitness.14 Previous work has described exercise among LTC residents in detail,8,15,16 and thus exercise is not addressed here. Also, as a narrative review, this article provides an overview of available interventions to improve physical activity for LTC residents and does not provide comments on efficacy or an exhaustive list of potential interventions. Rather, it provides a starting point for LTC homes to consider when providing opportunities to improve physical activity for their residents.
Guidelines for Increasing Physical Activity
There are currently no published evidence-based guidelines for increasing physical activity and reducing sedentary time for residents of LTC homes. However, an international task force of experts in geriatrics, exercise, and LTC research convened in 2015 and made recommendations on this matter.8 They emphasize the importance of considering the needs of residents, family members, health care professionals, LTC staff, and policy-makers when designing strategies to promote movement in LTC.8 This will ensure that the strategies to promote movement will be realistic and sustainable. Additionally, the task force identified motivation and pleasure as key to engaging residents in physical activities, and recommended that interests and preferences should be used to guide the selection of activities.8 The following sections describe example strategies to improve physical activity for residents in LTC that LTC homes can use to help facilitate movement for their residents.
Strategies for Promoting Physical Activity
Leveraging Daily Activities
One approach to promoting physical activity in LTC homes is to systematically use simple strategies embedded within routine care to engage residents in movement.8 Function-focused, or restorative care,17 is a philosophy of care that promotes increasing physical activity and maintaining functional abilities based on the resident’s abilities. Examples include walking with residents to the dining room rather than pushing them in a wheelchair where appropriate, inviting residents to events that require them to leave their room, improving independent wheelchair propulsion for residents who cannot walk, and increasing opportunities for sit-to-stand activities where possible. These activities are scaled to the resident’s underlying physical and cognitive capabilities. A systematic review of function-focused care revealed that it can help maintain functional skills for residents in LTC, and there is no significant risk associated with implementation.18 In a study by Slaughter et al19 that examined the effectiveness of techniques to encourage mobility by residents’ usual caregivers, health care aides prompted residents to perform the sit-to-stand activity 4 times per day, with the number of repetitions individualized based on resident ability, fatigue, and motivation. Residents who completed the sit-to-stand activity had smaller declines in mobility and functional outcomes (ie, less decline on the Functional Independence Measure).19 This study included residents with Alzheimer’s disease and dementia who could transfer independently or with the assistance of one person,20 indicating that this type of intervention is feasible and appropriate for residents with cognitive impairment.
Group Activities
Group activities in LTC homes are another way of engaging residents in physical activity in a motivating and pleasant setting that also encourages social engagement among residents and LTC staff. Group exercise classes can be effective for improving mood and functional outcomes. For example, a systematic review of dance classes in LTC homes revealed an improvement in problematic behaviors, mood, cognition, communication, and socialization.21 Most studies included participants with dementia, and no adverse events were reported, supporting the feasibility and safety of implementing group dance activities for residents with cognitive impairment. Group exercise is the most common delivery method for exercise within LTC homes22 and has been demonstrated to have small positive effects on activities of daily living (ADL; ie, improvement in ADL independence equivalent to 1.3 points on the Barthel Index).23 Other group activities, such as music therapy, have demonstrated improvements in depressive symptoms, emotional well-being, and anxiety for LTC residents with dementia.24 Group activities also provide the opportunity for movement as residents leave their rooms, walk to a new location (if able), and return to their rooms when the activity is complete.
Barriers to Physical Activity and Strategies to Overcome Them
Caregiver-related Factors
LTC staff have limited time to spend promoting physical activity since residents often have complex health care needs and staffing levels are often constrained.25 Indeed, having lower staffing levels has been associated with lower levels of physical activity for residents.26,27 LTC staff have identified a lack of time to walk with residents28,29 and having other tasks to do (eg, clean) as barriers to promoting movement.28,29 However, asking residents to help staff with small household chores, such as folding laundry or clearing dishes, was a facilitator to promoting movement.30 Activating residents by helping them transfer to a wheelchair for independent mobilization around the home or by assisting them to walk where appropriate were also facilitators.30,31 Leveraging facilitators will help staff who have limited time to help residents engage in more physical activity.
Motivation of LTC staff can also be a barrier to encouraging physical activity for residents in LTC. Fear that increasing physical activity will cause adverse events like falls, illness, or exacerbation of symptoms often decreases motivation for staff to facilitate physical activity.32,33 Another potential barrier is the conceptualization of the role of nursing in LTC as protecting residents from harm by encouraging them to engage in “risk-free” activities like staying in bed.34-39 Strategies to increase staff motivation to engage LTC residents in physical activity that have been shown to be effective are verbal prompts, modelling behaviors, goal setting, and home champions to promote function-focused care.17,33,40-43
The Physical Environment
Aspects of the physical environment of LTC homes may facilitate or limit residents’ ability to be physically active. A 2017 systematic review examined elements of the physical environment that acted as barriers and facilitators to physical activity for older adults living in LTC.30 The authors found that the person-environment fit, security, accessibility, and comfort were key components of the physical environment that were associated with residents’ physical activity levels.30 First, an appropriate fit between the residents’ abilities and the demands of the environment was related to improved activity as measured by actigraphy.44 For example, having long hallways between residents’ rooms and common spaces discourages residents who can only walk short distances from walking to these locations. However, residents were more active in larger-scaled LTC homes with shorter distances between different areas (eg, resident rooms and dining rooms).45 Clearly, there must be enough space to encourage walking between areas, but not so much space that walking is not feasible. Residents participating in a focus group identified accessibility and comfort features as being facilitators for walking in the corridor, such as wide corridors, sturdy handrails, carpet, chairs placed at short intervals for seated breaks, windows to look out, plants, and accessible activity rooms and restrooms.45,46 On the other hand, limited things to see and do indoors and outdoors, along with restricted walking areas, were identified as barriers to corridor walking by residents.46
One method for optimizing LTC home architecture to promote movement is to provide therapeutic outdoor spaces, such as gardens. Indeed, therapeutic gardens have been studied as a nonpharmacological method of engaging LTC residents with dementia and have been shown to benefit mood, pain, and fall prevention.47 Secure therapeutic gardens or outdoor spaces provide opportunities for various activities to increase movement, including gardening, animal care, and walking.48 However, there is a higher propensity for residents who use walkers or wheelchairs to slide off paths or become stuck in mud or mulch.49 Residents with physical limitations may require additional supervision in garden spaces, and as such spaces should be designed with improved safety in mind (eg, barriers between paths and places where mud could accumulate). The number of available indoor (eg, a physical therapy gym) and outdoor (eg, gardens) spaces was also found to be positively related to residents’ physical activity levels.50 However, these relationships were mediated by the number of activity programs available in the LTC homes.50 Therefore, having staff available to facilitate activities is also important for promoting physical activity.
Chemical and Physical Restraints
Physical and chemical restraints (eg, antipsychotics and sedatives) are sometimes used to manage the behavioral and psychological symptoms of dementia,51,52 which many residents in LTC experience.3 Though there has been an emphasis in North America to decrease their use, physical and chemical restraints are still used in LTC.53 Physical restraint use is associated with a higher risk of functional and cognitive decline.53,54 Residents who are both physically and chemically restrained through antipsychotic use are at even higher risk for these declines.54 Thus, to improve opportunities for movement in LTC, physical restraint use should be minimized. The risks and benefits of using psychotropic medications that often decrease residents’ physical activity levels must be evaluated individually, and other nonpharmacological strategies should be used to manage the behavioral and psychological symptoms of dementia. These could include functional analysis-based interventions (ie, individualized interventions aimed at identifying unmet needs, causes, antecedents, and consequences of the behavior),55 music therapy,55 or other interventions described above.
Emerging Innovative Interventions
Robots are an emerging nonpharmacological intervention for improving the behavioral and psychological symptoms of dementia and facilitating physical activity in LTC. Robotic animal interventions, where LTC residents interact with robotic animals in an individual or group setting, have been shown to reduce negative behaviors and increase positive mood.56 Additionally, robots are being used in rehabilitation to provide exercise post-stroke57 and could easily be transitioned to do similar tasks in LTC. Robotic interventions are attractive for the LTC sector as they could help relieve the workload demands on an often overloaded sector, and, in the case of pet therapy, surmount regulations for bringing live animals into a LTC home. Though studies examining the use of robots in LTC have mainly focused on the effect of pet therapy on reducing behavioral symptoms, the use of robots to promote physical activity and exercise in LTC is a natural progression for the work that has been done in inpatient rehabilitation.57 On a similar note, an interactive technology (similar to a Kinect system) used to promote 30-minute, twice-weekly physical activity sessions has demonstrated improvements in physical function (Short Physical Performance Battery [SPPB]) for pre-disabled (SPPB of 6 to 9) residents in LTC without dementia.58 The role of technology to promote physical activity in LTC is an emerging area of interest, and future innovations in this area will continue to help facilitate movement.
Quality of Evidence
Most studies aimed at improving physical activity for LTC residents to date are small, have nonrandomized designs, and have limited generalizability and evidence to support the efficacy of the interventions. For example, most studies included in systematic reviews for function-focused care, dance, group exercise, and music therapy are small, observational, or quasi-experimental studies with methodological issues resulting in bias.18,21,23,24 Likewise, the evidence surrounding nonpharmacological interventions for reducing behavioral and psychological symptoms of dementia is of very low to moderate quality.55 Innovative interventions, such as robotics and interactive technology, to promote physical activity in LTC are in their infancy. There are no data syntheses available to date to summarize the available literature on this topic, and conclusions rely on small, nonrandomized designs or extrapolations of results from similar sectors (eg, inpatient rehabilitation). Thus, the studies described in this review can be used as preliminary evidence to support the implementation of interventions to improve physical activity, but discretion should be used when interpreting the efficacy of these interventions.
Discussion
This review identifies several strategies for promoting physical activity for LTC residents, including incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovation solutions like robots or interactive technology. While the quality of evidence to date is limited, preliminary work suggests that strategies identified in this paper could be included as part of a multifactorial approach to increasing physical activity in LTC.
The current evidence does not suggest that any one strategy is more effective at improving physical activity, and it is likely that LTC homes will need to employ a combination of strategies to help residents move more. Additionally, residents’ preferences, goals, and capabilities should always be considered when designing an individualized physical activity plan. For example, if a resident does not like to be outdoors or gardening but enjoys dancing and music, then their physical activity plan should include group dance class and music therapy rather than gardening. LTC homes will need to have a menu of opportunities for movement that residents can choose from so that activities are pleasant and motivating, and therefore more likely to be completed.
Many of the interventions described in this review are safe and feasible to implement with residents who have physical or cognitive impairments. Function-focused care is scaled to the residents’ capabilities and did not increase the risk of falling, though LTC staff require the skills to scale physical activities appropriately.18 Likewise, group dance activities and music therapy were tested with residents with dementia, with no adverse events reported.21,24 However, more work is needed to determine the feasibility of implementing emerging methods, such as robotics and interactive technology, for increasing physical activity for residents with physical and cognitive impairments. Most studies to date have included mobile residents or those with minimal cognitive impairment. Similarly, outdoor garden spaces may be less safe for residents who use walkers or wheelchairs if there is an opportunity for them to slip off paths or get stuck in mud or mulch. LTC homes implementing any of these interventions should evaluate the benefits and risks of each intervention, the resources available within the home to support them (eg, trained staff), and the target residents’ physical and cognitive capabilities.
While increasing physical activity is important, structured exercise is needed to see gains in components of physical fitness such as strength, aerobic capacity, and balance. Indeed, one major consideration highlighted by the aforementioned task force is that every resident who does not have contraindications must also have a personalized multicomponent exercise program as part of their care plan.8 The task force recommends moderate- to high-intensity strength, aerobic, and balance exercises 2 times per week for 35 to 45 minutes per session.8 There is an interrelationship between physical activity and structured exercise: structured exercise programs can certainly be part of a physical activity plan, but physical activity can include more than structured exercise. Physical activity also includes any activity that involves movement, such as walking in gardens or between home areas, or physically participating more in personal care activities (eg, assisting with bathing or dressing).14 Both structured exercise and physical activity are important for LTC residents. Structured exercise provides an opportunity to improve strength and cardiovascular fitness, which aim to decrease the negative effects of sarcopenia and cardiovascular disease, such as disability and death.59,60 However, structured exercise should not be done daily for the same muscle groups.8 Rather, it is recommended for LTC residents to engage in structured exercise 2 times per week.8 Increasing physical activity is a daily goal, as daily physical activity decreases sedentary time, which has negative consequences such as decreased mood61 and increased mortality.62 LTC homes should incorporate strategies to both increase daily physical activity and promote individualized, structured exercise programs.
Conclusion
Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, like poor mood and increased risk of death, and to improve physical function. This review describes several strategies to promote physical activity within LTC homes, such as leveraging daily activities and the physical environment, providing group activities, reducing physical and chemical restraint use, and using innovative technology such as robots. LTC homes can use the information in this review to plan strategies to promote physical activity.
Corresponding author: Caitlin McArthur, MScPT, PhD, Hamilton Health Sciences, St. Peter’s Hospital, 88 Maplewood Avenue, Hamilton, ON L8M 1W9; [email protected].
Financial disclosures: None.
From the Geriatric Education and Research in Aging Sciences (GERAS) Centre for Aging Research, McMaster University, Hamilton, ON.
Abstract
- Objective. To summarize the literature on improving opportunities for physical activity for residents in long-term care (LTC).
- Method. Narrative review of the literature.
- Results. Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, such as poor mood and increased risk of death, and to improve physical function. This review identifies several strategies for promoting physical activity for LTC residents: incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovative solutions such as robots or interactive technology.
- Conclusion. While the quality of evidence to date is limited, preliminary work suggests that the strategies identified in this article could be included as part of a multifactorial approach to increasing physical activity in LTC.
Keywords: long-term care; nursing homes; physical activity; sedentary; mobility.
The United Nations estimates that between 2013 and 2050 the population aged 60 years or older will double.1 Furthermore, the fastest growth rate will be seen in older adults over the age of 80 years.1 With this demographic shift, a growing number of older adults will require supportive housing, such as long-term care (LTC). Indeed, it is projected that the number of older adults requiring LTC will double by 2036.2
Residents in LTC are often medically complex and experience multimorbidity, cognitive impairment, and functional decline,3 making it difficult for them to engage in physical activity. LTC residents spend approximately 75% of their waking time in sedentary activities (eg, sitting, lying down, watching TV), which amounts to more than 12 hours per day.4-6 Residents with cognitive impairment are even more sedentary, spending as little as 1 minute per day in moderate physical activity and approximately 87% of their time in sedentary activities.7 Additionally, a high prevalence of use of psychotropic drugs and physical restraints contributes to high levels of physical inactivity for residents in LTC.8 Increased time spent in sedentary activities has been associated with adverse health outcomes, such as incidence of cardiovascular disease and type 2 diabetes, and mortality.9-11 Moreover, bed and chair rest are associated with muscle disuse, which can lead to functional impairment.12,13
Given the large amount of time LTC residents spend in sedentary activities and the negative consequences this has on their health, it is essential to find opportunities to engage residents in physical activity throughout the day. This article summarizes evidence about increasing opportunities for physical activity for LTC residents. Physical activity is defined as “any bodily movement produced by skeletal muscles that results in energy expenditure,” while exercise, which is a subset of physical activity, is purposefully planned, structured, and repetitive and has a goal of maintaining or improving physical fitness.14 Previous work has described exercise among LTC residents in detail,8,15,16 and thus exercise is not addressed here. Also, as a narrative review, this article provides an overview of available interventions to improve physical activity for LTC residents and does not provide comments on efficacy or an exhaustive list of potential interventions. Rather, it provides a starting point for LTC homes to consider when providing opportunities to improve physical activity for their residents.
Guidelines for Increasing Physical Activity
There are currently no published evidence-based guidelines for increasing physical activity and reducing sedentary time for residents of LTC homes. However, an international task force of experts in geriatrics, exercise, and LTC research convened in 2015 and made recommendations on this matter.8 They emphasize the importance of considering the needs of residents, family members, health care professionals, LTC staff, and policy-makers when designing strategies to promote movement in LTC.8 This will ensure that the strategies to promote movement will be realistic and sustainable. Additionally, the task force identified motivation and pleasure as key to engaging residents in physical activities, and recommended that interests and preferences should be used to guide the selection of activities.8 The following sections describe example strategies to improve physical activity for residents in LTC that LTC homes can use to help facilitate movement for their residents.
Strategies for Promoting Physical Activity
Leveraging Daily Activities
One approach to promoting physical activity in LTC homes is to systematically use simple strategies embedded within routine care to engage residents in movement.8 Function-focused, or restorative care,17 is a philosophy of care that promotes increasing physical activity and maintaining functional abilities based on the resident’s abilities. Examples include walking with residents to the dining room rather than pushing them in a wheelchair where appropriate, inviting residents to events that require them to leave their room, improving independent wheelchair propulsion for residents who cannot walk, and increasing opportunities for sit-to-stand activities where possible. These activities are scaled to the resident’s underlying physical and cognitive capabilities. A systematic review of function-focused care revealed that it can help maintain functional skills for residents in LTC, and there is no significant risk associated with implementation.18 In a study by Slaughter et al19 that examined the effectiveness of techniques to encourage mobility by residents’ usual caregivers, health care aides prompted residents to perform the sit-to-stand activity 4 times per day, with the number of repetitions individualized based on resident ability, fatigue, and motivation. Residents who completed the sit-to-stand activity had smaller declines in mobility and functional outcomes (ie, less decline on the Functional Independence Measure).19 This study included residents with Alzheimer’s disease and dementia who could transfer independently or with the assistance of one person,20 indicating that this type of intervention is feasible and appropriate for residents with cognitive impairment.
Group Activities
Group activities in LTC homes are another way of engaging residents in physical activity in a motivating and pleasant setting that also encourages social engagement among residents and LTC staff. Group exercise classes can be effective for improving mood and functional outcomes. For example, a systematic review of dance classes in LTC homes revealed an improvement in problematic behaviors, mood, cognition, communication, and socialization.21 Most studies included participants with dementia, and no adverse events were reported, supporting the feasibility and safety of implementing group dance activities for residents with cognitive impairment. Group exercise is the most common delivery method for exercise within LTC homes22 and has been demonstrated to have small positive effects on activities of daily living (ADL; ie, improvement in ADL independence equivalent to 1.3 points on the Barthel Index).23 Other group activities, such as music therapy, have demonstrated improvements in depressive symptoms, emotional well-being, and anxiety for LTC residents with dementia.24 Group activities also provide the opportunity for movement as residents leave their rooms, walk to a new location (if able), and return to their rooms when the activity is complete.
Barriers to Physical Activity and Strategies to Overcome Them
Caregiver-related Factors
LTC staff have limited time to spend promoting physical activity since residents often have complex health care needs and staffing levels are often constrained.25 Indeed, having lower staffing levels has been associated with lower levels of physical activity for residents.26,27 LTC staff have identified a lack of time to walk with residents28,29 and having other tasks to do (eg, clean) as barriers to promoting movement.28,29 However, asking residents to help staff with small household chores, such as folding laundry or clearing dishes, was a facilitator to promoting movement.30 Activating residents by helping them transfer to a wheelchair for independent mobilization around the home or by assisting them to walk where appropriate were also facilitators.30,31 Leveraging facilitators will help staff who have limited time to help residents engage in more physical activity.
Motivation of LTC staff can also be a barrier to encouraging physical activity for residents in LTC. Fear that increasing physical activity will cause adverse events like falls, illness, or exacerbation of symptoms often decreases motivation for staff to facilitate physical activity.32,33 Another potential barrier is the conceptualization of the role of nursing in LTC as protecting residents from harm by encouraging them to engage in “risk-free” activities like staying in bed.34-39 Strategies to increase staff motivation to engage LTC residents in physical activity that have been shown to be effective are verbal prompts, modelling behaviors, goal setting, and home champions to promote function-focused care.17,33,40-43
The Physical Environment
Aspects of the physical environment of LTC homes may facilitate or limit residents’ ability to be physically active. A 2017 systematic review examined elements of the physical environment that acted as barriers and facilitators to physical activity for older adults living in LTC.30 The authors found that the person-environment fit, security, accessibility, and comfort were key components of the physical environment that were associated with residents’ physical activity levels.30 First, an appropriate fit between the residents’ abilities and the demands of the environment was related to improved activity as measured by actigraphy.44 For example, having long hallways between residents’ rooms and common spaces discourages residents who can only walk short distances from walking to these locations. However, residents were more active in larger-scaled LTC homes with shorter distances between different areas (eg, resident rooms and dining rooms).45 Clearly, there must be enough space to encourage walking between areas, but not so much space that walking is not feasible. Residents participating in a focus group identified accessibility and comfort features as being facilitators for walking in the corridor, such as wide corridors, sturdy handrails, carpet, chairs placed at short intervals for seated breaks, windows to look out, plants, and accessible activity rooms and restrooms.45,46 On the other hand, limited things to see and do indoors and outdoors, along with restricted walking areas, were identified as barriers to corridor walking by residents.46
One method for optimizing LTC home architecture to promote movement is to provide therapeutic outdoor spaces, such as gardens. Indeed, therapeutic gardens have been studied as a nonpharmacological method of engaging LTC residents with dementia and have been shown to benefit mood, pain, and fall prevention.47 Secure therapeutic gardens or outdoor spaces provide opportunities for various activities to increase movement, including gardening, animal care, and walking.48 However, there is a higher propensity for residents who use walkers or wheelchairs to slide off paths or become stuck in mud or mulch.49 Residents with physical limitations may require additional supervision in garden spaces, and as such spaces should be designed with improved safety in mind (eg, barriers between paths and places where mud could accumulate). The number of available indoor (eg, a physical therapy gym) and outdoor (eg, gardens) spaces was also found to be positively related to residents’ physical activity levels.50 However, these relationships were mediated by the number of activity programs available in the LTC homes.50 Therefore, having staff available to facilitate activities is also important for promoting physical activity.
Chemical and Physical Restraints
Physical and chemical restraints (eg, antipsychotics and sedatives) are sometimes used to manage the behavioral and psychological symptoms of dementia,51,52 which many residents in LTC experience.3 Though there has been an emphasis in North America to decrease their use, physical and chemical restraints are still used in LTC.53 Physical restraint use is associated with a higher risk of functional and cognitive decline.53,54 Residents who are both physically and chemically restrained through antipsychotic use are at even higher risk for these declines.54 Thus, to improve opportunities for movement in LTC, physical restraint use should be minimized. The risks and benefits of using psychotropic medications that often decrease residents’ physical activity levels must be evaluated individually, and other nonpharmacological strategies should be used to manage the behavioral and psychological symptoms of dementia. These could include functional analysis-based interventions (ie, individualized interventions aimed at identifying unmet needs, causes, antecedents, and consequences of the behavior),55 music therapy,55 or other interventions described above.
Emerging Innovative Interventions
Robots are an emerging nonpharmacological intervention for improving the behavioral and psychological symptoms of dementia and facilitating physical activity in LTC. Robotic animal interventions, where LTC residents interact with robotic animals in an individual or group setting, have been shown to reduce negative behaviors and increase positive mood.56 Additionally, robots are being used in rehabilitation to provide exercise post-stroke57 and could easily be transitioned to do similar tasks in LTC. Robotic interventions are attractive for the LTC sector as they could help relieve the workload demands on an often overloaded sector, and, in the case of pet therapy, surmount regulations for bringing live animals into a LTC home. Though studies examining the use of robots in LTC have mainly focused on the effect of pet therapy on reducing behavioral symptoms, the use of robots to promote physical activity and exercise in LTC is a natural progression for the work that has been done in inpatient rehabilitation.57 On a similar note, an interactive technology (similar to a Kinect system) used to promote 30-minute, twice-weekly physical activity sessions has demonstrated improvements in physical function (Short Physical Performance Battery [SPPB]) for pre-disabled (SPPB of 6 to 9) residents in LTC without dementia.58 The role of technology to promote physical activity in LTC is an emerging area of interest, and future innovations in this area will continue to help facilitate movement.
Quality of Evidence
Most studies aimed at improving physical activity for LTC residents to date are small, have nonrandomized designs, and have limited generalizability and evidence to support the efficacy of the interventions. For example, most studies included in systematic reviews for function-focused care, dance, group exercise, and music therapy are small, observational, or quasi-experimental studies with methodological issues resulting in bias.18,21,23,24 Likewise, the evidence surrounding nonpharmacological interventions for reducing behavioral and psychological symptoms of dementia is of very low to moderate quality.55 Innovative interventions, such as robotics and interactive technology, to promote physical activity in LTC are in their infancy. There are no data syntheses available to date to summarize the available literature on this topic, and conclusions rely on small, nonrandomized designs or extrapolations of results from similar sectors (eg, inpatient rehabilitation). Thus, the studies described in this review can be used as preliminary evidence to support the implementation of interventions to improve physical activity, but discretion should be used when interpreting the efficacy of these interventions.
Discussion
This review identifies several strategies for promoting physical activity for LTC residents, including incorporating simple strategies into daily activities, participating in group activities (eg, exercise, dance, or music therapy), using motivational strategies to encourage staff to promote activity, leveraging the physical environment, reducing physical and chemical restraints, and using innovation solutions like robots or interactive technology. While the quality of evidence to date is limited, preliminary work suggests that strategies identified in this paper could be included as part of a multifactorial approach to increasing physical activity in LTC.
The current evidence does not suggest that any one strategy is more effective at improving physical activity, and it is likely that LTC homes will need to employ a combination of strategies to help residents move more. Additionally, residents’ preferences, goals, and capabilities should always be considered when designing an individualized physical activity plan. For example, if a resident does not like to be outdoors or gardening but enjoys dancing and music, then their physical activity plan should include group dance class and music therapy rather than gardening. LTC homes will need to have a menu of opportunities for movement that residents can choose from so that activities are pleasant and motivating, and therefore more likely to be completed.
Many of the interventions described in this review are safe and feasible to implement with residents who have physical or cognitive impairments. Function-focused care is scaled to the residents’ capabilities and did not increase the risk of falling, though LTC staff require the skills to scale physical activities appropriately.18 Likewise, group dance activities and music therapy were tested with residents with dementia, with no adverse events reported.21,24 However, more work is needed to determine the feasibility of implementing emerging methods, such as robotics and interactive technology, for increasing physical activity for residents with physical and cognitive impairments. Most studies to date have included mobile residents or those with minimal cognitive impairment. Similarly, outdoor garden spaces may be less safe for residents who use walkers or wheelchairs if there is an opportunity for them to slip off paths or get stuck in mud or mulch. LTC homes implementing any of these interventions should evaluate the benefits and risks of each intervention, the resources available within the home to support them (eg, trained staff), and the target residents’ physical and cognitive capabilities.
While increasing physical activity is important, structured exercise is needed to see gains in components of physical fitness such as strength, aerobic capacity, and balance. Indeed, one major consideration highlighted by the aforementioned task force is that every resident who does not have contraindications must also have a personalized multicomponent exercise program as part of their care plan.8 The task force recommends moderate- to high-intensity strength, aerobic, and balance exercises 2 times per week for 35 to 45 minutes per session.8 There is an interrelationship between physical activity and structured exercise: structured exercise programs can certainly be part of a physical activity plan, but physical activity can include more than structured exercise. Physical activity also includes any activity that involves movement, such as walking in gardens or between home areas, or physically participating more in personal care activities (eg, assisting with bathing or dressing).14 Both structured exercise and physical activity are important for LTC residents. Structured exercise provides an opportunity to improve strength and cardiovascular fitness, which aim to decrease the negative effects of sarcopenia and cardiovascular disease, such as disability and death.59,60 However, structured exercise should not be done daily for the same muscle groups.8 Rather, it is recommended for LTC residents to engage in structured exercise 2 times per week.8 Increasing physical activity is a daily goal, as daily physical activity decreases sedentary time, which has negative consequences such as decreased mood61 and increased mortality.62 LTC homes should incorporate strategies to both increase daily physical activity and promote individualized, structured exercise programs.
Conclusion
Residents in LTC spend much of their time in sedentary activities such as sitting or lying in bed. Physical activity is important to help decrease the negative effects of sedentary time, like poor mood and increased risk of death, and to improve physical function. This review describes several strategies to promote physical activity within LTC homes, such as leveraging daily activities and the physical environment, providing group activities, reducing physical and chemical restraint use, and using innovative technology such as robots. LTC homes can use the information in this review to plan strategies to promote physical activity.
Corresponding author: Caitlin McArthur, MScPT, PhD, Hamilton Health Sciences, St. Peter’s Hospital, 88 Maplewood Avenue, Hamilton, ON L8M 1W9; [email protected].
Financial disclosures: None.
1. United Nations Department of Economic and Social Affairs Population Division. World Population Ageing 2013. New York, NY: United Nations; 2013.
2. Pickard L, Comas-Herrera A, Costa-Font J, et al. Modelling an entitlement to long-term care services for older people in Europe: projections for long-term care expenditure to 2050. J Eur Soc Policy. 2007;17:33-48.
3. Hirdes JP, Mitchell L, Maxwell CJ, White N. Beyond the “iron lungs of gerontology”: Using evidence to shape the future of nursing homes in Canada. Can J Aging. 2011;30:371-390.
4. Chin A Paw MJM, van Poppel MNM, van Mechelen W. Effects of resistance and functional-skills training on habitual activity and constipation among older adults living in long-term care facilities: a randomized controlled trial. BMC Geriatr. 2006;6:9.
5. Ikezoe T, Asakawa Y, Shima H, Kishibuchi K, Ichihashi N. Daytime physical activity patterns and physical fitness in institutionalized elderly women: an exploratory study. Arch Gerontol Geriatr. 2013;57:221-225.
6. Keogh JW, Senior H, Beller EM, Henwood T. Prevalence and risk factors for low habitual walking speed in nursing home residents: an observational study. Arch Phys Med Rehabil. 2015;96:1993-1999.
7. Marmeleira J, Ferreira S, Raimundo A. Physical activity and physical fitness of nursing home residents with cognitive impairment: A pilot study. Exp Gerontol. 2017;100:63-69.
8. de Souto Barreto P, Morley JE, Chodzko-Zajko W, et al. Recommendations on physical activity and exercise for older adults living in long-term care facilities: a taskforce report. J Am Med Dir Assoc. 2016;17:381-392.
9. van der Ploeg HP, Chey T, Korda RJ, et al. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch Intern Med. 2012;172:494-500.
10. Chau JY, Grunseit AC, Chey T, et al. Daily sitting time and all-cause mortality: a meta-analysis. PLoS One. 2013;8:e80000.
11. Grøntved A, Hu FB. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: a meta-analysis. JAMA. 2011;305:2448-2455.
12. Senior HE, Henwood TR, Beller EM, et al. Prevalence and risk factors of sarcopenia among adults living in nursing homes. Maturitas. 2015;82:418-423.
13. Wall BT, Dirks ML, van Loon LJC. Skeletal muscle atrophy during short-term disuse: implications for age-related sarcopenia. Ageing Res Rev. 2013;12:898-906.
14. Caspersen CJ, Powell KE, Christenson GM. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep. 1985;100:126-131.
15. McArthur C, Giangregorio LM. Improving strength and balance for long-term care residents at risk for falling: Suggestions for practice. J Clin Outcomes Manag. 2018;25:28-38.
16. Crocker T, Forster A, Young J, et al. Physical rehabilitation for older people in long-term care. Cochrane Database Syst Rev. 2013;2:CD004294.
17. Resnick B, Galik E, Boltz M, Pretzer-Aboff IE. Implementing Restorative Care Nursing in All Settings. 2nd ed. New York, NY: Spring Publishing Company; 2011.
18. Resnick B, Galik E, Boltz M. Function focused care approaches: literature review of progress and future possibilities. J Am Med Dir Assoc. 2013;14:313-318.
19. Slaughter SE, Estabrooks CA, Jones CA, Wagg AS. Mobility of Vulnerable Elders (MOVE): study protocol to evaluate the implementation and outcomes of a mobility intervention in long-term care facilities. BMC Geriatr. 2011;11:84.
20. Slaughter SE, Wagg AS, Jones CA, et al. Mobility of Vulnerable Elders study: effect of the sit-to-stand activity on mobility, function, and quality of life. J Am Med Dir Assoc. 2015;16(2):138-143.
21. Guzmán-García A, Hughes JC, James IA, Rochester L. Dancing as a psychosocial intervention in care homes: a systematic review of the literature. Int J Geriatr Psychiatry. 2013;28:914-924.
22. McArthur C, Gibbs JC, Patel R, et al. A scoping review of physical rehabilitation in long-term care: interventions, outcomes, tools. Can J Aging/La Rev Can du Vieil. 2017;36:435-452.
23. Crocker T, Young J, Forster A, et al. The effect of physical rehabilitation on activities of daily living in older residents of long-term care facilities: Systematic review with meta-analysis. Age Ageing. 2013;42:682-688.
24. van der Steen JT, Smaling HJ, van der Wouden JC, et al. Music-based therapeutic interventions for people with dementia. Cochrane Database Syst Rev. 2018;7:CD003477.
25. Froggatt K, Davies S, Meyer J. Understanding Care Homes, A Research and Development Perspective. London: Jessica Kingsley Publishers; 2009.
26. Shore BA, Lerman DC, Smith RG, et al. Direct assessment of quality of care in a geriatric nursing home. J Appl Behav Anal. 1995;28:435-448.
27. Bates-Jensen BM, Schnelle JF, Alessi CA, et al. The effects of staffing on in-bed times of nursing home residents. J Am Geriatr Soc. 2004;52:931-938.
28. Ericson-Lidman E, Renström A-S, Åhlin J, Strandberg G. Relatives’ perceptions of residents’ life in a municipal care facility for older people with a focus on quality of life and care environment. Int J Older People Nurs. 2015;10:160-169.
29. Häggström E, Kihlgren A, Kihlgren M, Sörlie V. Relatives’ struggle for an improved and more just care for older people in community care. J Clin Nurs. 2007;16:1749-1757.
30. Douma JG, Volkers KM, Engels G, et al. Setting-related influences on physical inactivity of older adults in residential care settings: a review. BMC Geriatr. 2017;17:97.
31. Zegelin A. ’Tied down’- the process of becoming bedridden through gradual local confinement. J Clin Nurs. 2008;17:2294-2301.
32. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Falls and fall-related injuries associated with function-focused care. Clin Nurs Res. 2012;21:43-63.
33. Pretzer-Aboff I, Galik E. Feasibility and impact of a function focused care intervention for Parkinson’s disease in the community. Nursing Res. 2011;60:276-283.
34. Leditschke IA, Green M, Irvine J, et al. What are the barriers to mobilizing intensive care patients? Cardiopulm Phys Ther J. 2012;23:26-29.
35. Mittmann N, Seung SJ, Pisterzi LF, et al. Nursing workload associated with hospital patient care. Dis Manag Heal Outcomes. 2008;16:53-61.
36. Dykes PC, Carroll DL, Hurley AC, et al. Why do patients in acute care hospitals fall? Can falls be prevented? J Nurs Adm. 2009;39:299-304.
37. Brownie S, Nancarrow S. Effects of person-centered care on residents and staff in aged-care facilities: a systematic review. Clin Interv Aging. 2013;8:1-10.
38. Wakefield BJ, Holman JE. Functional trajectories associated with hospitalization in older adults. West J Nurs Res. 2007;29:161-177.
39. Boltz M, Resnick B, Capezuti E, Shuluk J. Activity restriction vs. self-direction: hospitalised older adults’ response to fear of falling. Int J Older People Nurs. 2014;9:44-53.
40. Resnick B, Galik E, Gruber-Baldini A, Zimmerman S. Testing the effect of function-focused care in assisted living. J Am Geriatr Soc. 2011;59:2233-2240.
41. Galik EM, Resnick B, Gruber-Baldini A, et al. Pilot testing of the restorative care intervention for the cognitively impaired. J Am Med Dir Assoc. 2008;9:516-522.
42. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Implementing a restorative care philosophy of care in assisted living: pilot testing of Res-Care-AL. J Am Acad Nurse Pract. 2009;21:123-133.
43. Resnick B, Gruber-Baldini AL, Zimmerman S, et al. Nursing home resident outcomes from the Res-Care intervention. J Am Geriatr Soc. 2009;57:1156-1165.
44. Pomeroy SH, Scherer Y, Runkawatt V, et al. Person-environment fit and functioning among older adults in a long-term care setting. Geriatr Nurs. 2011;32:368-378.
45. Moos RH, David TG, Lemke S, Postle E. Coping with an intra-institutional relocation: changes in resident and staff behavior patterns. Gerontologist. 1984;24:495-502.
46. Lu Z, Rodiek SD, Shepley MM, Duffy M. Influences of physical environment on corridor walking among assisted living residents. J Appl Gerontol. 2011;30:463-484.
47. Detweiler MB, Sharma T, Detweiler JG, et al. What is the evidence to support the use of therapeutic gardens for the elderly? Psychiatry Investig. 2012;9:100.
48. Blake M, Mitchell G. Horticultural therapy in dementia care: a literature review. Nurs Stand. 2016;30:41-47.
49. Detweiler MB, Murphy PF, Myers LC, Kim KY. Does a wander garden influence inappropriate behaviors in dementia residents? Am J Alzheimers Dis Other Demen. 2008;23:31-45.
50. Joseph A, Zimring C, Harris-Kojetin L, Kiefer K. Presence and visibility of outdoor and indoor physical activity features and participation in physical activity among older adults in retirement communities. J Hous Elderly. 2006;19:141-165.
51. Feng Z, Hirdes JP, Smith TF, et al. Use of physical restraints and antipsychotic medications in nursing homes: a cross-national study. Int J Geriatr Psychiatry. 2009;24:1110-1118.
52. Herrmann N. Recommendations for the management of behavioral and psychological symptoms of dementia. Can J Neurol Sci. 2001;28 Suppl 1:S96-107.
53. Freeman S, Spirgiene L, Martin-Khan M, Hirdes JP. Relationship between restraint use, engagement in social activity, and decline in cognitive status among residents newly admitted to long-term care facilities. Geriatr Gerontol Int. 2017;17:246-255.
54. Foebel AD, Onder G, Finne-Soveri H, et al. Physical restraint and antipsychotic medication use among nursing home residents with dementia. J Am Med Dir Assoc. 2016;17:184.e9-184.e14.
55. Dyer SM, Harrison SL, Laver K, Whitehead C, Crotty M. An overview of systematic reviews of pharmacological and non-pharmacological interventions for the treatment of behavioral and psychological symptoms of dementia. Int Psychogeriatr. 2018;30:295-309.
56. Robinson H, MacDonald B, Kerse N, Broadbent E. The psychosocial effects of a companion robot: a randomized controlled trial. J Am Med Dir Assoc. 2013;14:661-667.
57. Lo K, Stephenson M, Lockwood C. Effectiveness of robotic assisted rehabilitation for mobility and functional ability in adult stroke patients. JBI Database System Rev Implement Rep. 2017;15:3049-3091.
58. Valiani V, Lauzé M, Martel D, et al. A new adaptive home-based exercise technology among older adults living in nursing home: a pilot study on feasibility, acceptability and physical performance. J Nutr Health Aging. 2017;21:819-824.
59. Locquet M, Beaudart C, Hajaoui M, et al. Three-year adverse health consequences of sarcopenia in community-dwelling older adults according to 5 diagnosis definitions. J Am Med Dir Assoc. 2019;20:43-46.e2.
60. Chodzko-Zajko WJ, Proctor DN, Fiatarone Singh MA, et al. Exercise and physical activity for older adults. Med Sci Sports Exerc. 2009;41:1510-1530.
61. Park S-Y, Lee K, Um YJ, Paek S, Ryou IS. Association between physical activity and depressive mood among Korean adults with chronic diseases. Korean J Fam Med. 2018;39:185-190.
62. Loprinzi PD. Light-intensity physical activity and all-cause mortality. Am J Health Promot. 2017;31:340-342.
1. United Nations Department of Economic and Social Affairs Population Division. World Population Ageing 2013. New York, NY: United Nations; 2013.
2. Pickard L, Comas-Herrera A, Costa-Font J, et al. Modelling an entitlement to long-term care services for older people in Europe: projections for long-term care expenditure to 2050. J Eur Soc Policy. 2007;17:33-48.
3. Hirdes JP, Mitchell L, Maxwell CJ, White N. Beyond the “iron lungs of gerontology”: Using evidence to shape the future of nursing homes in Canada. Can J Aging. 2011;30:371-390.
4. Chin A Paw MJM, van Poppel MNM, van Mechelen W. Effects of resistance and functional-skills training on habitual activity and constipation among older adults living in long-term care facilities: a randomized controlled trial. BMC Geriatr. 2006;6:9.
5. Ikezoe T, Asakawa Y, Shima H, Kishibuchi K, Ichihashi N. Daytime physical activity patterns and physical fitness in institutionalized elderly women: an exploratory study. Arch Gerontol Geriatr. 2013;57:221-225.
6. Keogh JW, Senior H, Beller EM, Henwood T. Prevalence and risk factors for low habitual walking speed in nursing home residents: an observational study. Arch Phys Med Rehabil. 2015;96:1993-1999.
7. Marmeleira J, Ferreira S, Raimundo A. Physical activity and physical fitness of nursing home residents with cognitive impairment: A pilot study. Exp Gerontol. 2017;100:63-69.
8. de Souto Barreto P, Morley JE, Chodzko-Zajko W, et al. Recommendations on physical activity and exercise for older adults living in long-term care facilities: a taskforce report. J Am Med Dir Assoc. 2016;17:381-392.
9. van der Ploeg HP, Chey T, Korda RJ, et al. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch Intern Med. 2012;172:494-500.
10. Chau JY, Grunseit AC, Chey T, et al. Daily sitting time and all-cause mortality: a meta-analysis. PLoS One. 2013;8:e80000.
11. Grøntved A, Hu FB. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: a meta-analysis. JAMA. 2011;305:2448-2455.
12. Senior HE, Henwood TR, Beller EM, et al. Prevalence and risk factors of sarcopenia among adults living in nursing homes. Maturitas. 2015;82:418-423.
13. Wall BT, Dirks ML, van Loon LJC. Skeletal muscle atrophy during short-term disuse: implications for age-related sarcopenia. Ageing Res Rev. 2013;12:898-906.
14. Caspersen CJ, Powell KE, Christenson GM. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep. 1985;100:126-131.
15. McArthur C, Giangregorio LM. Improving strength and balance for long-term care residents at risk for falling: Suggestions for practice. J Clin Outcomes Manag. 2018;25:28-38.
16. Crocker T, Forster A, Young J, et al. Physical rehabilitation for older people in long-term care. Cochrane Database Syst Rev. 2013;2:CD004294.
17. Resnick B, Galik E, Boltz M, Pretzer-Aboff IE. Implementing Restorative Care Nursing in All Settings. 2nd ed. New York, NY: Spring Publishing Company; 2011.
18. Resnick B, Galik E, Boltz M. Function focused care approaches: literature review of progress and future possibilities. J Am Med Dir Assoc. 2013;14:313-318.
19. Slaughter SE, Estabrooks CA, Jones CA, Wagg AS. Mobility of Vulnerable Elders (MOVE): study protocol to evaluate the implementation and outcomes of a mobility intervention in long-term care facilities. BMC Geriatr. 2011;11:84.
20. Slaughter SE, Wagg AS, Jones CA, et al. Mobility of Vulnerable Elders study: effect of the sit-to-stand activity on mobility, function, and quality of life. J Am Med Dir Assoc. 2015;16(2):138-143.
21. Guzmán-García A, Hughes JC, James IA, Rochester L. Dancing as a psychosocial intervention in care homes: a systematic review of the literature. Int J Geriatr Psychiatry. 2013;28:914-924.
22. McArthur C, Gibbs JC, Patel R, et al. A scoping review of physical rehabilitation in long-term care: interventions, outcomes, tools. Can J Aging/La Rev Can du Vieil. 2017;36:435-452.
23. Crocker T, Young J, Forster A, et al. The effect of physical rehabilitation on activities of daily living in older residents of long-term care facilities: Systematic review with meta-analysis. Age Ageing. 2013;42:682-688.
24. van der Steen JT, Smaling HJ, van der Wouden JC, et al. Music-based therapeutic interventions for people with dementia. Cochrane Database Syst Rev. 2018;7:CD003477.
25. Froggatt K, Davies S, Meyer J. Understanding Care Homes, A Research and Development Perspective. London: Jessica Kingsley Publishers; 2009.
26. Shore BA, Lerman DC, Smith RG, et al. Direct assessment of quality of care in a geriatric nursing home. J Appl Behav Anal. 1995;28:435-448.
27. Bates-Jensen BM, Schnelle JF, Alessi CA, et al. The effects of staffing on in-bed times of nursing home residents. J Am Geriatr Soc. 2004;52:931-938.
28. Ericson-Lidman E, Renström A-S, Åhlin J, Strandberg G. Relatives’ perceptions of residents’ life in a municipal care facility for older people with a focus on quality of life and care environment. Int J Older People Nurs. 2015;10:160-169.
29. Häggström E, Kihlgren A, Kihlgren M, Sörlie V. Relatives’ struggle for an improved and more just care for older people in community care. J Clin Nurs. 2007;16:1749-1757.
30. Douma JG, Volkers KM, Engels G, et al. Setting-related influences on physical inactivity of older adults in residential care settings: a review. BMC Geriatr. 2017;17:97.
31. Zegelin A. ’Tied down’- the process of becoming bedridden through gradual local confinement. J Clin Nurs. 2008;17:2294-2301.
32. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Falls and fall-related injuries associated with function-focused care. Clin Nurs Res. 2012;21:43-63.
33. Pretzer-Aboff I, Galik E. Feasibility and impact of a function focused care intervention for Parkinson’s disease in the community. Nursing Res. 2011;60:276-283.
34. Leditschke IA, Green M, Irvine J, et al. What are the barriers to mobilizing intensive care patients? Cardiopulm Phys Ther J. 2012;23:26-29.
35. Mittmann N, Seung SJ, Pisterzi LF, et al. Nursing workload associated with hospital patient care. Dis Manag Heal Outcomes. 2008;16:53-61.
36. Dykes PC, Carroll DL, Hurley AC, et al. Why do patients in acute care hospitals fall? Can falls be prevented? J Nurs Adm. 2009;39:299-304.
37. Brownie S, Nancarrow S. Effects of person-centered care on residents and staff in aged-care facilities: a systematic review. Clin Interv Aging. 2013;8:1-10.
38. Wakefield BJ, Holman JE. Functional trajectories associated with hospitalization in older adults. West J Nurs Res. 2007;29:161-177.
39. Boltz M, Resnick B, Capezuti E, Shuluk J. Activity restriction vs. self-direction: hospitalised older adults’ response to fear of falling. Int J Older People Nurs. 2014;9:44-53.
40. Resnick B, Galik E, Gruber-Baldini A, Zimmerman S. Testing the effect of function-focused care in assisted living. J Am Geriatr Soc. 2011;59:2233-2240.
41. Galik EM, Resnick B, Gruber-Baldini A, et al. Pilot testing of the restorative care intervention for the cognitively impaired. J Am Med Dir Assoc. 2008;9:516-522.
42. Resnick B, Galik E, Gruber-Baldini AL, Zimmerman S. Implementing a restorative care philosophy of care in assisted living: pilot testing of Res-Care-AL. J Am Acad Nurse Pract. 2009;21:123-133.
43. Resnick B, Gruber-Baldini AL, Zimmerman S, et al. Nursing home resident outcomes from the Res-Care intervention. J Am Geriatr Soc. 2009;57:1156-1165.
44. Pomeroy SH, Scherer Y, Runkawatt V, et al. Person-environment fit and functioning among older adults in a long-term care setting. Geriatr Nurs. 2011;32:368-378.
45. Moos RH, David TG, Lemke S, Postle E. Coping with an intra-institutional relocation: changes in resident and staff behavior patterns. Gerontologist. 1984;24:495-502.
46. Lu Z, Rodiek SD, Shepley MM, Duffy M. Influences of physical environment on corridor walking among assisted living residents. J Appl Gerontol. 2011;30:463-484.
47. Detweiler MB, Sharma T, Detweiler JG, et al. What is the evidence to support the use of therapeutic gardens for the elderly? Psychiatry Investig. 2012;9:100.
48. Blake M, Mitchell G. Horticultural therapy in dementia care: a literature review. Nurs Stand. 2016;30:41-47.
49. Detweiler MB, Murphy PF, Myers LC, Kim KY. Does a wander garden influence inappropriate behaviors in dementia residents? Am J Alzheimers Dis Other Demen. 2008;23:31-45.
50. Joseph A, Zimring C, Harris-Kojetin L, Kiefer K. Presence and visibility of outdoor and indoor physical activity features and participation in physical activity among older adults in retirement communities. J Hous Elderly. 2006;19:141-165.
51. Feng Z, Hirdes JP, Smith TF, et al. Use of physical restraints and antipsychotic medications in nursing homes: a cross-national study. Int J Geriatr Psychiatry. 2009;24:1110-1118.
52. Herrmann N. Recommendations for the management of behavioral and psychological symptoms of dementia. Can J Neurol Sci. 2001;28 Suppl 1:S96-107.
53. Freeman S, Spirgiene L, Martin-Khan M, Hirdes JP. Relationship between restraint use, engagement in social activity, and decline in cognitive status among residents newly admitted to long-term care facilities. Geriatr Gerontol Int. 2017;17:246-255.
54. Foebel AD, Onder G, Finne-Soveri H, et al. Physical restraint and antipsychotic medication use among nursing home residents with dementia. J Am Med Dir Assoc. 2016;17:184.e9-184.e14.
55. Dyer SM, Harrison SL, Laver K, Whitehead C, Crotty M. An overview of systematic reviews of pharmacological and non-pharmacological interventions for the treatment of behavioral and psychological symptoms of dementia. Int Psychogeriatr. 2018;30:295-309.
56. Robinson H, MacDonald B, Kerse N, Broadbent E. The psychosocial effects of a companion robot: a randomized controlled trial. J Am Med Dir Assoc. 2013;14:661-667.
57. Lo K, Stephenson M, Lockwood C. Effectiveness of robotic assisted rehabilitation for mobility and functional ability in adult stroke patients. JBI Database System Rev Implement Rep. 2017;15:3049-3091.
58. Valiani V, Lauzé M, Martel D, et al. A new adaptive home-based exercise technology among older adults living in nursing home: a pilot study on feasibility, acceptability and physical performance. J Nutr Health Aging. 2017;21:819-824.
59. Locquet M, Beaudart C, Hajaoui M, et al. Three-year adverse health consequences of sarcopenia in community-dwelling older adults according to 5 diagnosis definitions. J Am Med Dir Assoc. 2019;20:43-46.e2.
60. Chodzko-Zajko WJ, Proctor DN, Fiatarone Singh MA, et al. Exercise and physical activity for older adults. Med Sci Sports Exerc. 2009;41:1510-1530.
61. Park S-Y, Lee K, Um YJ, Paek S, Ryou IS. Association between physical activity and depressive mood among Korean adults with chronic diseases. Korean J Fam Med. 2018;39:185-190.
62. Loprinzi PD. Light-intensity physical activity and all-cause mortality. Am J Health Promot. 2017;31:340-342.
Management of Cardiovascular Disease Risk in Rheumatoid Arthritis
From the Division of Rh
Abstract
- Objective: To review the management of traditional and nontraditional CVD cardiovascular disease risk factors in rheumatoid arthritis (RA).
- Methods: Literature review of the management of CVD risk in RA.
- Results: Because of the increased risk of CVD events and CVD mortality among RA patients, aggressive management of CVD risk is essential. Providers should follow national guidelines for the management of traditional CVD risk factors, including dyslipidemia, hypertension, and diabetes mellitus. Similar efforts are needed in counseling on lifestyle modifications, including smoking cessation, regular exercise, and maintaining a healthy body weight. Because higher RA disease activity is also linked with CVD risk, aggressive treatment of RA to a target of low disease activity or remission is critical. Furthermore, the selection of potentially “cardioprotective” agents such as methotrexate and tumor necrosis factor inhibitors, while limiting use of nonsteroidal anti-inflammatory drugs and glucocorticoids, are strategies that could be employed by rheumatologists to help mitigate CVD risk in their patients with RA.
- Conclusion: Routine assessment of CVD risk, management of traditional CVD risk factors, counseling on healthy lifestyle habits, and aggressive treatment of RA are essential to minimize CVD risk in this population.
Keywords: rheumatoid arthritis; cardiovascular disease; cardiovascular risk assessment; cardiovascular risk management.
Editor’s note: This article is part 2 of a 2-part article. “Assessment of Cardiovascular Disease Risk in Rheumatoid Arthritis” was published in the January/February 2019 issue.
Rheumatoid arthritis (RA) is a systemic autoimmune condition that contributes to an increased risk for cardiovascular disease (CVD) among affected patients. In persons with RA, the risk of incident CVD and CVD mortality are increased by approximately 50% compared with the general population.1,2 To minimize CVD risk in this population, providers must routinely assess for CVD risk factors3 and aggressively manage both traditional and nontraditional CVD risk factors.
Managing Traditional Risk Factors
As in the general population, identification and management of traditional CVD risk factors are crucial to minimize CVD risk in the RA population. A prospective study of 201 RA patients demonstrated that traditional CVD risk factors were in fact more predictive of endothelial dysfunction and carotid atherosclerosis than were disease-related inflammatory markers in RA.4 Management of traditional risk factors is detailed in the following sections, and recommendations for managing all traditional CVD risk factors are summarized in the Table.
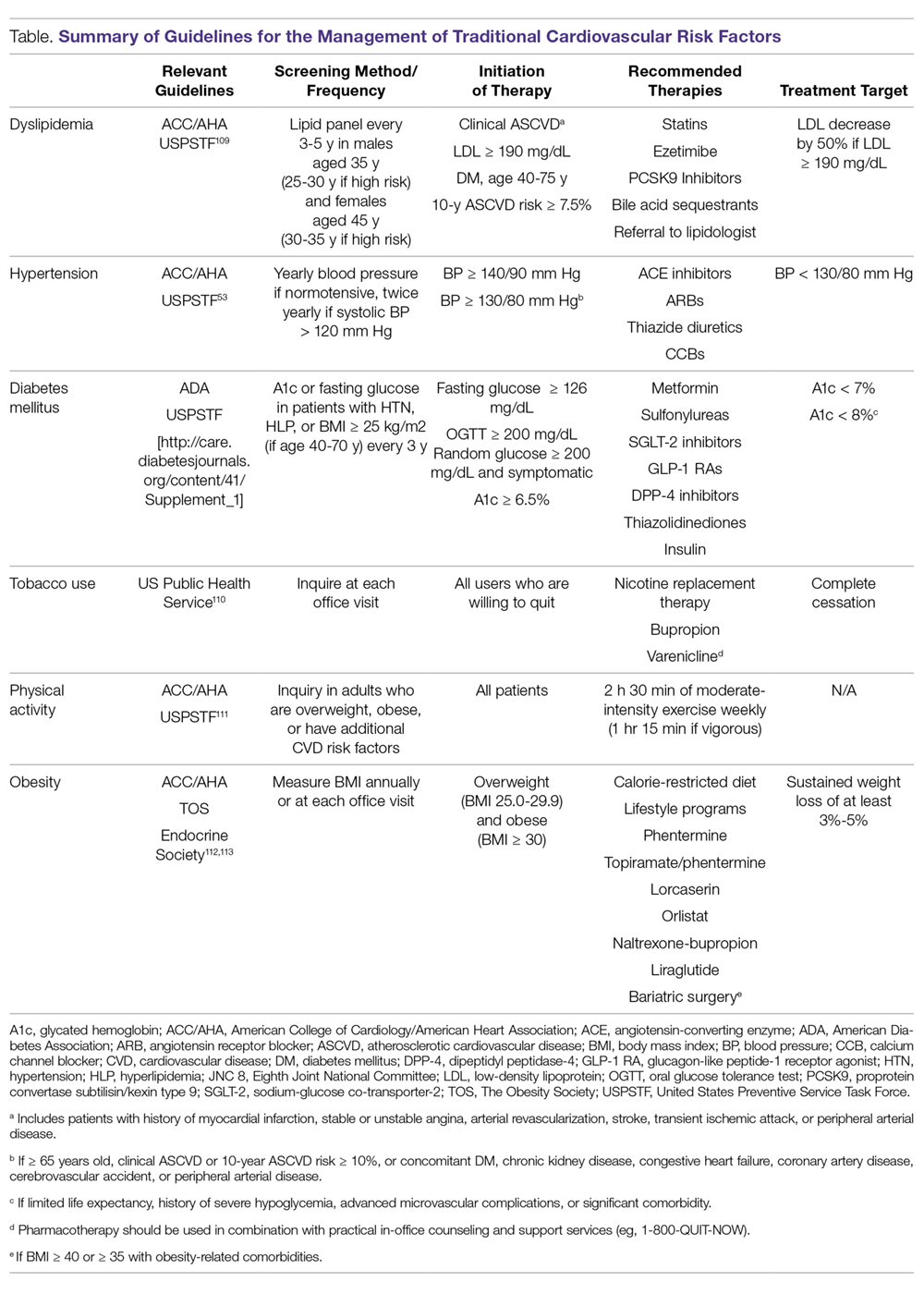
Dyslipidemia
The role of dyslipidemia in atherogenesis is well established, and as a result, lipid levels are nearly universally included in CVD risk stratification tools. However, the interpretation of lipid levels in the context of RA is challenging because of the effects of systemic inflammation on their absolute values. Compared to the general population, patients with RA have lower total cholesterol (TC) and low-density lipoprotein (LDL) levels independent of lipid-lowering therapy.5,6 Despite this, RA patients are at increased risk for CVD. There is even some evidence to suggest a “lipid paradox” in RA, whereby lower TC (< 4 mmol/L) and LDL levels suggest an increased risk of CVD.7,8 In contrast to LDL, higher levels of high-density lipoprotein (HDL) are typically associated with reduced CVD risk, as in the general population.8,9 Interestingly, in a cohort of 16,085 RA patients and 48,499 age- and sex-matched controls, there was no significant difference in the relationship between LDL and CVD risk, suggesting that quantitative lipid levels alone may not entirely explain the CVD mortality gap in RA.9 As such, there is substantial interest in lipoprotein function within the context of CVD risk in RA. Recent investigations have identified impaired HDL function, with reduced cholesterol efflux capacity and antioxidant properties, as well as increased scavenger receptor expression and foam cell formation, in patients with RA.10,11 More research is needed to elucidate how these alterations affect CVD morbidity and mortality and how their measurement could be integrated into improved CVD risk assessment.
Meta-analyses of randomized controlled trials have estimated that lipid-lowering therapy with HMG-CoA reductase inhibitors (statins) reduces the risk of CVD by 25% to 30%; as such, statin therapy has become the standard of care for reduction of CVD risk in the general population.12 Benefits for primary prevention of CVD in RA have also been observed; statin therapy was associated with a reduced risk of CVD events (hazard ratio [HR], 0.45; 95% confidence interval [CI], 0.20-0.98) and all-cause mortality (HR, 0.43; 95% CI, 0.20-0.92) in a population-based cohort study.13 Statins appear to have similar lipid-lowering effects and result in similar CVD risk reduction when used for primary or secondary prevention in RA patients compared to non-RA controls.14-16 Additionally, anti-inflammatory properties of statins may act in synergy with disease-modifying antirheumatic drugs (DMARDs) to improve RA disease activity. In a small study of RA patients, statin therapy improved subjective and objective markers of RA disease activity in conjunction with methotrexate.17
While statins provide robust reduction in CVD risk, some individuals cannot tolerate statin therapy or do not achieve goal LDL levels with statin therapy. Select non-statin LDL-cholesterol-lowering agents have shown promise for reducing CVD events in the general population.18 Ezetimibe, which inhibits cholesterol absorption in the small intestine, very modestly reduced CVD events when added to atorvastatin (relative risk [RR], 0.94; 95% CI, 0.89-0.99) in a double-blind randomized controlled trial.19 Novel monoclonal antibodies to proprotein convertase subtilisin/kexin type 9 (PCSK-9) inhibit the internalization of surface LDL receptors, promoting LDL clearance. Two PCSK-9 inhibitors, alirocumab and evolocumab, were approved by the US Food and Drug Administration (FDA) after randomized controlled trials demonstrated their efficacy in lowering LDL by approximately 60% and reducing CVD events by approximately 15% in patients on maximum-tolerated statin therapy.20-22 To date, non-statin LDL-cholesterol-lowering agents have been subject to limited study in RA.23
Identification and management of dyslipidemia offers an opportunity for substantial CVD risk reduction at the RA population level. Unfortunately, current rates of lipid screening are inadequate in this high-risk group. In a study of 3298 Medicare patients with RA, less than half of RA patients with an indication underwent appropriate lipid screening.24 Additionally, statins are often underutilized for both primary and secondary prevention in RA patients. Only 27% of RA patients meeting National Cholesterol Education Program Adult Treatment Panel III criteria were initiated on statin therapy in a population-based cohort study.25 Among patients discharged after a first myocardial infarction (MI), the odds of receiving lipid-lowering therapy were 31% lower for RA patients (odds ratio [OR], 0.69; 95% CI, 0.58-0.82).26 Similar to the general population, adherence to statins in RA patients appears to be poor.27-30 This raises particular concern considering that a population-based cohort study of RA patients demonstrated a 67% increased risk of MI associated with statin discontinuation, regardless of prior MI status.27 Providers—rheumatologists, primary care providers, and cardiologists alike—need to remain vigilant in efforts to assess CVD risk to identify patients who will benefit from lipid-lowering therapy and to emphasize the importance to patients of statin adherence. Novel models of health-care delivery, health technologies, and patient engagement in care may prove useful for improving lipid screening and management in RA.
Tobacco Use
Cigarette smoking is a shared risk factor for both CVD and RA. Large cohort studies have identified a dose-dependent increased risk of incident RA, particularly seropositive RA, among smokers.31-34 Tobacco smoking has also been associated with increased levels of inflammation and RA disease activity.35 The consequences of tobacco use in the general population are staggering. Among individuals over the age of 30 years, tobacco use is responsible for 12% of all deaths and 10% of all CVD deaths.36 Similar findings are observed in RA; a recent meta-analysis estimated there is a 50% increased risk of CVD events in RA related to smoking tobacco.37 In the general population, smoking cessation markedly lowers CVD risk, and over time CVD risk may approach that of nonsmokers.38,39 Thus, regular counseling and interventions to facilitate smoking cessation are critical to reducing CVD risk in RA patients. RA-specific smoking cessation programs have been proposed, but have yet to outperform standard smoking cessation programs.40
Diabetes Mellitus
It is estimated that almost 10% of the US population has diabetes mellitus (DM), which in isolation portends substantial CVD risk.41 There is an increased prevalence of DM in RA, perhaps owing to factors such as physical inactivity and chronic glucocorticoid use, though a higher level of RA disease activity itself has been associated with increased insulin resistance.42-45 In a cohort of 100 RA patients who were neither obese nor diabetic, RA patients had significantly higher fasting blood glucose and insulin levels than age- and sex-matched controls. These findings were even more pronounced in RA patients with higher levels of disease activity.44 Similar to the general population, DM is associated with poor CVD outcomes in RA.37 Therefore, both appropriate management of diabetes and control of RA disease activity are vitally important to minimize CVD risk related to DM.
Hypertension
Though not a universal finding, there may be an increased prevalence of hypertension in RA patients.31,46 Nonsteroidal anti-inflammatory drug (NSAID) and glucocorticoid use may play a role in the development of hypertension, while DMARDs appear to exert a less substantial effect on blood pressure.47,48 At least one study found that DMARD initiation (particularly for methotrexate and hydroxychloroquine) was associated with significant, albeit small, declines in both systolic and diastolic blood pressure over the first 6 months of treatment.49
Despite its potentially higher prevalence in this population, hypertension is both underdiagnosed and undertreated in RA patients.24,50-52 This is an important deficiency to target because, as in the general population, hypertension is associated with an increased risk of MI (RR, 1.84; 95% CI, 1.38-2.46) and composite CVD outcomes (RR, 2.24; 95% CI, 1.42-3.06) in RA.37 Thresholds for initiation and escalation of antihypertensive therapy are not specific to the RA population; thus, diagnosis and management of hypertension should be informed by the American College of Cardiology/American Heart Association guidelines, treating those with in-office blood pressures exceeding 140/90 mm Hg (> 130/80 mm Hg if aged > 65 years or with concomitant CVD, DM, chronic kidney disease, or 10-year atherosclerotic cardiovascular disease risk > 10%), typically with angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, calcium channel blockers, or thiazide diuretics as comorbidities may dictate or allow.53 Also, the use of NSAIDs and glucocorticoids should be minimized, particularly in those with concomitant hypertension.
Physical Activity
Likely due to factors such as articular pain and stiffness, as well as physical limitations, RA patients are more sedentary than the general population.54,55 In a study of objectively assessed sedentary behavior in RA patients, greater average sedentary time per day and greater number of sedentary bouts (> 20 min) were associated with increased 10-year risk of CVD as assessed by the QRISK2.56 Conversely, the beneficial effects of exercise are well documented. Light to moderate physical activity has been associated with improved cardiovascular outcomes, greater physical function, higher levels of HDL, as well as reduced systemic inflammation and disease activity, and improved endothelial function in RA patients.57-61 While there has been concern that physical activity may result in accelerated joint damage, even high-intensity exercise was shown to be safe without causing significant progression of joint damage.58
Obesity, Weight Loss, and Diet
While obesity is clearly associated with CVD risk in the general population, this relationship is much more complex in RA, as underweight RA patients are also at higher risk for CVD and CVD-related mortality.62-64 One potential explanation for this finding is that pathological weight loss resulting in an underweight body mass index (BMI) is an independent predictor of CVD. In a study of US Veterans with RA, higher rates of weight loss (> 3 kg/m2/year) were associated with increased CVD mortality (HR, 2.27; 95% CI, 1.61-3.19) independent of BMI.65 Systemic inflammation in RA can lead to “rheumatoid cachexia,” characterized by decreased muscle mass, increased adiposity, and increased CVD risk despite a normal or potentially decreased BMI.66 Practitioners should be mindful of not only current body weight, but also patients’ weight trajectories when counseling on lifestyle practices such as healthy diet and regular exercise in RA patients. For obese individuals with RA, healthy weight loss should be encouraged. Interestingly, bariatric surgery in RA patients may improve RA disease activity in addition to its known effects on body weight and DM.67
Counseling on healthy diet with a focus on limiting foods high in saturated- and trans-fatty acids and high glycemic index foods, and increasing consumption of fruits, vegetables, and mono-unsaturated fatty acids is a well-accepted and common practice to help minimize CVD risk in the general population.68 No studies to date have investigated the effect of specific diets on CVD risk in RA patients, and thus we recommend adherence to general population recommendations.
Managing RA-related CVD Risk Factors
Disease Activity
In addition to traditional risk factors, several studies have identified associations between the level of RA disease activity and risk of CVD. In a cohort of US Veterans with RA, CVD-related mortality increased in a dose-dependent manner with higher disease activity categories. In stark contrast, the CVD mortality rates of those in remission paralleled the rates from the general population (standardized mortality ratio [SMR], 0.68; 95% CI, 0.37-1.27).69 In a separate cohort of 1157 RA patients without prior CVD, achieving low disease activity was associated with a lower risk of incident CVD events (HR, 0.65; 95% CI, 0.43-0.99).70 Additionally, high disease activity has been associated with surrogate markers of CVD and other CVD risk factors including NT-proBNP and systolic blood pressure.71,72 While no randomized controlled trial data is available to inform this recommendation, observational data suggest RA should be aggressively treated (ideally to achieve and maintain remission or low disease activity) to minimize CVD risk. While keeping this treatment goal in mind, the differential effects of specific RA therapies on CVD must also be considered.
Glucocorticoids and NSAIDs
With the expanding repertoire of DMARDs available and more aggressive treatment approaches, the role of glucocorticoids and NSAIDs in RA treatment is decreasing over time. While their efficacy for improving pain and stiffness is well established, concern regarding their contribution to CVD risk in RA patients is warranted.
Glucocorticoids are known to have detrimental effects on traditional CVD risk factors such as hypertension, insulin resistance, and dyslipidemia in the general population, as well as in RA patients.73,74 In a meta-analysis of predominantly observational studies of RA patients, glucocorticoid use was associated with an increased risk of CVD events (RR, 1.47; 95% CI, 1.34-1.60), including MI, congestive heart failure (CHF), and cerebrovascular accident (CVA).75 Evidence is conflicting in regards to a clear dose threshold that leads to increased CVD risk with glucocorticoids, though higher doses are associated with greater risk.76-81 As RA patients requiring glucocorticoids typically have higher disease activity, confounding by indication remains a complicating factor in assessing the relative contributions of glucocorticoid use and RA disease activity to elevated CVD risk in many analyses.
The increased CVD risk with NSAID use is not specific to RA and has been well established in the general population.82-84 In the previously mentioned meta-analysis, an increased overall risk of CVD events was observed with NSAID use in RA (RR, 1.18; 95% CI, 1.01-1.38). It should be noted that cyclo-oxygenase 2 (COX-2) inhibitors, in particular rofecoxib (now removed from the market), appeared to drive the majority of this risk (RR, 1.36; 95% CI, 1.10-1.67 in COX-2 inhibitors and RR 1.08, 95% CI, 0.94-1.24 in nonselective NSAIDs), suggesting a potential differential risk among NSAIDs.75 While naproxen has been thought to carry the lowest risk of CVD based on initial studies, this has not been universally observed, including in a recent randomized controlled trial of more than 24,000 RA and osteoarthritis patients.82,85,86
Providers should use the lowest possible dose and duration of glucocorticoids and NSAIDs to achieve symptom relief, with continual efforts to taper or discontinue. Candidates for glucocorticoid and NSAID therapy should be selected carefully, and use of these therapies should be avoided in those with prior CVD or at high risk for CVD based on traditional CVD risk factors. Most importantly, providers should focus on utilizing DMARDs for the management of RA, which more effectively treat RA as well as reduce CVD risk.
Methotrexate
Methotrexate (MTX), a mainstay in the treatment of RA, is a conventional DMARD observed to improve overall survival and mitigate CVD risk in multiple RA cohorts.75,87,88 In a recent meta-analysis comprised of 236,525 RA patients and 5410 CVD events, MTX use was associated with a 28% reduction in overall CVD events across 8 studies (RR, 0.72; 95% CI, 0.57-0.91), substantiating similar findings in a prior meta-analysis.75,88 MTX use was specifically associated with a decreased risk of MI (RR, 0.81; 95% CI, 0.68-0.96). Case-control and cohort studies have cited a 20% to 50% reduced risk of CHF with MTX use.89,90 The potential cardioprotective effect of MTX appears to be both multifactorial and complex, likely mediated through both direct and indirect mechanisms. MTX directly promotes anti-atherogenic lipoprotein function, improves endothelial function, and scavenges free radicals.91,92 Indirectly, MTX likely reduces CVD risk by effectively reducing RA disease activity. Based on these and other data, MTX remains the cornerstone of DMARD therapy in RA patients when targeting CVD risk reduction.
Hydroxychloroquine
Emerging evidence suggests that hydroxychloroquine (HCQ), an antimalarial most often utilized in combination with alternative DMARDs in RA, prevents DM and has beneficial effects on lipid profiles. A recent meta-analysis compiled 3 homogenous observational studies that investigated the effect of HCQ on incident DM. RA patients ever exposed to HCQ had a 40% lower incidence of DM (HR, 0.59; 95% CI, 0.49-0.70).93 Increased duration of HCQ use was shown to further reduce risk of incident DM.94 The aforementioned meta-analysis also pooled 5 studies investigating the effect of HCQ on lipid profiles, with favorable mean differences in TC (–9.82 mg/dL), LDL (–10.61 mg/dL), HDL (4.13 mg/dL), and triglycerides (–19.15 mg/dL) in HCQ users compared to non-users.93 Given these favorable changes to traditional CVD risk factors, it is not surprising that in a retrospective study of 1266 RA patients without prior CVD, HCQ was associated with significantly lower risk of incident CVD. While external validation of these findings is needed, HCQ is an attractive conventional DMARD to be used in RA for CVD risk reduction. Moreover, its combination with MTX and sulfasalazine also shows promise for CVD risk reduction.95,96
TNF Inhibitors
Tumor necrosis factor (TNF) inhibitors are often the initial biologic DMARD therapy used in RA patients not responding to conventional DMARDs. In the previously described meta-analysis, TNF inhibitors were associated with similar reductions in CVD events as MTX (RR, 0.70; 95% CI, 0.54-0.90).75 Of note, there was a trend toward reduced risk of CHF (RR, 0.75; 95% CI, 0.49-1.15) in this same meta-analysis, an area of concern with TNF inhibitor use due to a prior randomized controlled trial demonstrating worsening clinical status in patients with existing moderate-to-severe CHF treated with high-dose infliximab.97 Current RA treatment guidelines recommend avoiding TNF inhibitor use in individuals with CHF.98
Aside from the risk of CHF exacerbation, TNF inhibitors appear to be cardioprotective. Similar to MTX, the mechanism by which TNF inhibition reduces cardiovascular risk is complex and likely due to both direct and indirect mechanisms. Substantial research has been conducted on the effect of TNF inhibition on lipids, with a recent meta-analysis demonstrating increases in HDL and TC, with stable LDL and atherogenic index over treatment follow-up.99 A subsequent meta-analysis not limited to RA patients yielded similar results.100 In addition to quantitative lipid changes, alteration of lipoprotein function, improvement in myocardial function, reduced aortic stiffness, improved blood pressure, and reduced RA disease activity may also be responsible for cardioprotective benefits of these agents.101,102
Non-TNF Biologic and Traditional Synthetic DMARDs
Tocilizumab, an IL-6 inhibitor, can potently increase LDL levels, but it does not appear to increase the risk of CVD events and may actually promote more favorable anti-atherogenic lipoprotein function.103-106 Although these quantitative lipid changes received significant attention in the wake of early reports detailing this effect, similar lipid changes appear to accompany other DMARDs including TNF inhibitors and tofacitinib.107 There have been few studies evaluating the risk of CVD with other non-TNF inhibitor biologic DMARDs and traditional synthetic DMARDs, warranting future study.
Conclusion
To mitigate the increased risk of CVD in RA, primary care and subspecialty providers alike must be aware of this heightened risk in RA, perform frequent assessments of CVD risk,3 and aggressively manage both traditional and nontraditional CVD risk factors. The differential roles in this effort may not be clear; thus, we have proposed a co-management strategy detailed in the Figure. Clear communication between providers is of the utmost importance to ensure effective management of CVD risk.
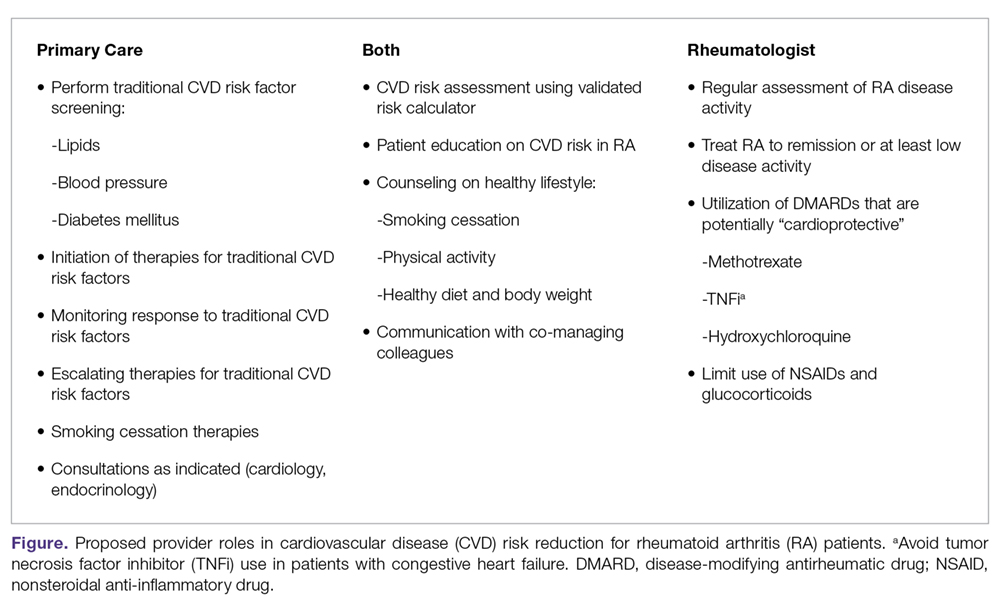
Given limited evidence for RA-specific CVD risk assessments and traditional risk factor treatment targets, management should follow pertinent national guidelines. The importance of lifestyle counseling should not be overlooked, with a focus on smoking cessation, healthy diet and body weight, and regular aerobic exercise. Finally, rheumatologists should aggressively manage RA using a treat-to-target approach, minimize the use of glucocorticoids and NSAIDs, and preferentially select DMARDs that have been associated with lower CVD risk. Through this comprehensive approach, recent trends of improved CVD outcomes in RA will hopefully become more widespread.108
Corresponding author: Bryant R. England, MD; 986270 Nebraska Medical Center, Omaha, NE 68198-6270; [email protected].
Financial disclosures: Dr. England is supported by UNMC Internal Medicine Scientist Development Award, UNMC Physician-Scientist Training Program, the UNMC Mentored Scholars Program, and the Rheumatology Research Foundation Scientist Development Award. Dr. Mikuls is supported by a VA Merit Award (CX000896) and grants from the National Institutes of Health: National Institute of General Medical Sciences (U54GM115458), National Institute on Alcohol Abuse and Alcoholism (R25AA020818), and National Institute of Arthritis and Musculoskeletal and Skin Diseases (2P50AR60772).
1. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
2. Avina-Zubieta JA, Thomas J, Sadatsafavi M, et al. Risk of incident cardiovascular events in patients with rheumatoid arthritis: A meta-analysis of observational studies. Ann Rheum Dis. 2012;71:1524-1529.
3. Johnson TM, Mikuls TR, England BR. Assessment of cardiovascular risk in rheumatoid arthritis. J Clin Outcomes Manage. 2019;26:41-47.
4. Sandoo A, Chanchlani N, Hodson J, et al. Classical cardiovascular disease risk factors associate with vascular function and morphology in rheumatoid arthritis: A six-year prospective study. Arthritis Res Ther. 2013;15:R203.
5. Myasoedova E, Crowson CS, Kremers HM, et al. Total cholesterol and LDL levels decrease before rheumatoid arthritis. Ann Rheum Dis. 2010;69:1310-1314.
6. Liao KP, Cai T, Gainer VS, et al. Lipid and lipoprotein levels and trend in rheumatoid arthritis compared to the general population. Arthritis Care Res (Hoboken). 2013;65:2046-2050.
7. Myasoedova E, Crowson CS, Kremers HM, et al. Lipid paradox in rheumatoid arthritis: The impact of serum lipid measures and systemic inflammation on the risk of cardiovascular disease. Ann Rheum Dis. 2011;70:482-487.
8. Zhang J, Chen L, Delzell E, et al. Republished: The association between inflammatory markers, serum lipids and the risk of cardiovascular events in patients with rheumatoid arthritis. Postgrad Med J. 2014;90:722-729.
9. Liao KP, Liu J, Lu B, et al. Association between lipid levels and major adverse cardiovascular events in rheumatoid arthritis compared to non-rheumatoid arthritis patients. Arthritis Rheumatol. 2015;67:2004-2010.
10. Charles-Schoeman C, Lee YY, Grijalva V, et al. Cholesterol efflux by high density lipoproteins is impaired in patients with active rheumatoid arthritis. Ann Rheum Dis. 2012;71:1157-1162.
11. Voloshyna I, Modayil S, Littlefield MJ, et al. Plasma from rheumatoid arthritis patients promotes pro-atherogenic cholesterol transport gene expression in THP-1 human macrophages. Exp Biol Med (Maywood). 2013 238:1192-1197.
12. Taylor F, Huffman MD, Macedo AF, et al. Statins for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2013;(1):CD004816.
13. Sheng X, Murphy MJ, Macdonald TM, Wei L. Effectiveness of statins on total cholesterol and cardiovascular disease and all-cause mortality in osteoarthritis and rheumatoid arthritis. J Rheumatol. 2012;39:32-40.
14. An J, Alemao E, Reynolds K, et al. Cardiovascular outcomes associated with lowering low-density lipoprotein cholesterol in rheumatoid arthritis and matched nonrheumatoid arthritis. J Rheumatol. 2016;43:1989-1996.
15. Semb AG, Holme I, Kvien TK, Pedersen TR. Intensive lipid lowering in patients with rheumatoid arthritis and previous myocardial infarction: An explorative analysis from the incremental decrease in endpoints through aggressive lipid lowering (IDEAL) trial. Rheumatology (Oxford). 2011;50:324-329.
16. Semb AG, Kvien TK, DeMicco DA, et al. Effect of intensive lipid-lowering therapy on cardiovascular outcome in patients with and those without inflammatory joint disease. Arthritis Rheum. 2012;64:2836-2846.
17. El-Barbary AM, Hussein MS, Rageh EM, et al. Effect of atorvastatin on inflammation and modification of vascular risk factors in rheumatoid arthritis. J Rheumatol. 2011;38:229-235.
18. Writing Committee, Lloyd-Jones DM, Morris PB, et al. 2016 ACC expert consensus decision pathway on the role of non-statin therapies for LDL-cholesterol lowering in the management of atherosclerotic cardiovascular disease risk: A report of the American college of cardiology task force on clinical expert consensus documents. J Am Coll Cardiol. 2016;68:92-125.
19. Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372:2387-2397.
20. Sabatine MS, Giugliano RP, Wiviott SD, et al. Efficacy and safety of evolocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1500-1509.
21. Robinson JG, Farnier M, Krempf M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1489-1499.
22. Sabatine MS, Giugliano RP, Keech AC, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med. 2017;376:1713-1722.
23. Maki-Petaja KM, Booth AD, Hall FC, et al. Ezetimibe and simvastatin reduce inflammation, disease activity, and aortic stiffness and improve endothelial function in rheumatoid arthritis. J Am Coll Cardiol. 2007;50:852-858.
24. Bartels CM, Kind AJ, Everett C, et al. Low frequency of primary lipid screening among medicare patients with rheumatoid arthritis. Arthritis Rheum. 2011;63:1221-1230.
25. Akkara Veetil BM, Myasoedova E, Matteson EL, et al. Use of lipid-lowering agents in rheumatoid arthritis: A population-based cohort study. J Rheumatol. 2013;40:1082-1088.
26. Lindhardsen J, Ahlehoff O, Gislason GH, et al. Initiation and adherence to secondary prevention pharmacotherapy after myocardial infarction in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2012;71:1496-1501.
27. De Vera MA, Choi H, Abrahamowicz M, et al. Statin discontinuation and risk of acute myocardial infarction in patients with rheumatoid arthritis: A population-based cohort study. Ann Rheum Dis. 2011;70:1020-1024.
28. Zhang H, Plutzky J, Skentzos S, et al. Discontinuation of statins in routine care settings: A cohort study. Ann Intern Med. 2013;158:526-534.
29. Zhang H, Plutzky J, Shubina M, Turchin A. Continued statin prescriptions after adverse reactions and patient outcomes: A cohort study. Ann Intern Med. 2017;167:221-227.
30. Lemstra M, Blackburn D, Crawley A, Fung R. Proportion and risk indicators of nonadherence to statin therapy: A meta-analysis. Can J Cardiol. 2012;28:574-580.
31. Boyer JF, Gourraud PA, Cantagrel A, et al. Traditional cardiovascular risk factors in rheumatoid arthritis: A meta-analysis. Joint Bone Spine. 2011;78:179-183.
32. Bergstrom U, Jacobsson LT, Nilsson JA, et al. Pulmonary dysfunction, smoking, socioeconomic status and the risk of developing rheumatoid arthritis. Rheumatology (Oxford). 2011;50:2005-2013.
33. Costenbader KH, Feskanich D, Mandl LA, Karlson EW. Smoking intensity, duration, and cessation, and the risk of rheumatoid arthritis in women. Am J Med. 2006;119:503.e1,503.e9.
34. Klareskog L, Stolt P, Lundberg K, et al. A new model for an etiology of rheumatoid arthritis: Smoking may trigger HLA-DR (shared epitope)-restricted immune reactions to autoantigens modified by citrullination. Arthritis Rheum. 2006;54:38-46.
35. Sokolove J, Wagner CA, Lahey LJ, et al. Increased inflammation and disease activity among current cigarette smokers with rheumatoid arthritis: A cross-sectional analysis of US veterans. Rheumatology (Oxford). 2016;55:1969-1977.
36. World Health Organization. WHO Global Report: Mortality Attributable to Tobacco. Geneva, World Health Organization, 2012.
37. Baghdadi LR, Woodman RJ, Shanahan EM, Mangoni AA. The impact of traditional cardiovascular risk factors on cardiovascular outcomes in patients with rheumatoid arthritis: A systematic review and meta-analysis. PLoS One. 2015;10:e0117952.
38. Centers for Disease Control and Prevention; National Center for Chronic Disease Prevention and Health Promotion. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease: A Report of the Surgeon General. Atlanta (GA): Centers for Disease Control and Prevention; 2010. 6, Cardiovascular Diseases. Available from: https://ncbi.nlm.nih.gov/books/NBK53012/
39. Mons U, Muezzinler A, Gellert C, et al. Impact of smoking and smoking cessation on cardiovascular events and mortality among older adults: Meta-analysis of individual participant data from prospective cohort studies of the CHANCES consortium. BMJ. 2015;350:h1551.
40. Aimer P, Treharne GJ, Stebbings S, Frampton C, Cameron V, Kirby S, et al. Efficacy of a rheumatoid arthritis-specific smoking cessation program: A randomized controlled pilot trial. Arthritis Care Res (Hoboken). 2017;69:28-37.
41. Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2017.
42. Jiang P, Li H, Li X. Diabetes mellitus risk factors in rheumatoid arthritis: A systematic review and meta-analysis. Clin Exp Rheumatol. 2015;33:115-121.
43. Shahin D, Eltoraby E, Mesbah A, Houssen M. Insulin resistance in early untreated rheumatoid arthritis patients. Clin Biochem. 2010;43:661-335.
44. Arias de la Rosa I, Escudero-Contreras A, Rodriguez-Cuenca S, et al. Defective glucose and lipid metabolism in rheumatoid arthritis is determined by chronic inflammation in metabolic tissues. J Intern Med. 2018;84(1):61-77.
45. Wilson JC, Sarsour K, Gale S, et al. Incidence and risk of glucocorticoid-associated adverse effects in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018 Jun 1. doi: 10.1002/acr.23611.
46. Chung CP, Giles JT, Petri M, et al. Prevalence of traditional modifiable cardiovascular risk factors in patients with rheumatoid arthritis: Comparison with control subjects from the multi-ethnic study of atherosclerosis. Semin Arthritis Rheum. 2012;41:535-544.
47. Goodwin JE, Geller DS. Glucocorticoid-induced hypertension. Pediatr Nephrol. 2012;27:1059-1066.
48. Snowden S, Nelson R. The effects of nonsteroidal anti-inflammatory drugs on blood pressure in hypertensive patients. Cardiol Rev. 2011;19:184-191.
49. Baker JF, Sauer B, Teng CC, et al. Initiation of disease-modifying therapies in rheumatoid arthritis is associated with changes in blood pressure. J Clin Rheumatol. 2018;24:203-209.
50. Panoulas VF, Douglas KM, Milionis HJ, et al. Prevalence and associations of hypertension and its control in patients with rheumatoid arthritis. Rheumatology (Oxford). 2007;46:1477-1482.
51. Protogerou AD, Panagiotakos DB, Zampeli E, et al. Arterial hypertension assessed “out-of-office” in a contemporary cohort of rheumatoid arthritis patients free of cardiovascular disease is characterized by high prevalence, low awareness, poor control and increased vascular damage-associated “white coat” phenomenon. Arthritis Res Ther. 2013;15:R142.
52. van Breukelen-van der Stoep DF, van Zeben D, Klop B, et al. Marked underdiagnosis and undertreatment of hypertension and hypercholesterolaemia in rheumatoid arthritis. Rheumatology (Oxford). 2016;55:1210-1216.
53. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American college of cardiology/American heart association task force on clinical practice guidelines. J Am Coll Cardiol. 2018;71:e127-248.
54. Lee J, Dunlop D, Ehrlich-Jones L, et al. Public health impact of risk factors for physical inactivity in adults with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:488-493.
55. Sokka T, Hakkinen A, Kautiainen H, et al. Physical inactivity in patients with rheumatoid arthritis: Data from twenty-one countries in a cross-sectional, international study. Arthritis Rheum. 2008;59:42-50.
56. Fenton SAM, Veldhuijzen van Zanten JJCS, Kitas GD, et al. Sedentary behaviour is associated with increased long-term cardiovascular risk in patients with rheumatoid arthritis independently of moderate-to-vigorous physical activity. BMC Musculoskelet Disord. 2017;18:131,017-1473-9.
57. Byram KW, Oeser AM, Linton MF, et al. Exercise is associated with increased small HDL particle concentration and decreased vascular stiffness in rheumatoid arthritis. J Clin Rheumatol. 2018 May 25. 9.
58. de Jong Z, Munneke M, Zwinderman AH, et al. Is a long-term high-intensity exercise program effective and safe in patients with rheumatoid arthritis? results of a randomized controlled trial. Arthritis Rheum. 2003;48:2415-2424.
59. Stavropoulos-Kalinoglou A, Metsios GS, Veldhuijzen van Zanten JJ, et al. Individualised aerobic and resistance exercise training improves cardiorespiratory fitness and reduces cardiovascular risk in patients with rheumatoid arthritis. Ann Rheum Dis. 2013;72:1819-1825.
60. Khoja SS, Almeida GJ, Chester Wasko M, et al. Association of light-intensity physical activity with lower cardiovascular disease risk burden in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:424-431.
61. Metsios GS, Koutedakis Y, Veldhuijzen van Zanten JJ, et al. Cardiorespiratory fitness levels and their association with cardiovascular profile in patients with rheumatoid arthritis: A cross-sectional study. Rheumatology (Oxford). 2015;54:2215-2220.
62. Escalante A, Haas RW, del Rincon I. Paradoxical effect of body mass index on survival in rheumatoid arthritis: Role of comorbidity and systemic inflammation. Arch Intern Med. 2005;165:1624-1629.
63. Kremers HM, Nicola PJ, Crowson CS, et al. Prognostic importance of low body mass index in relation to cardiovascular mortality in rheumatoid arthritis. Arthritis Rheum. 2004;50:3450-3457.
64. Wolfe F, Michaud K. Effect of body mass index on mortality and clinical status in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:1471-1479.
65. England BR, Baker JF, Sayles H, et al. Body mass index, weight loss, and cause-specific mortality in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018;70:11-18.
66. Dessein PH, Solomon A, Hollan I. Metabolic abnormalities in patients with inflammatory rheumatic diseases. Best Pract Res Clin Rheumatol. 2016;30:901-915.
67. Sparks JA, Halperin F, Karlson JC, et al. Impact of bariatric surgery on patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2015;67:1619-1626.
68. Mente A, de Koning L, Shannon HS, Anand SS. A systematic review of the evidence supporting a causal link between dietary factors and coronary heart disease. Arch Intern Med. 2009;169:659-669.
69. England BR, Sayles H, Michaud K, et al. Cause-specific mortality in male US veterans with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:36-45.
70. Arts EE, Fransen J, Den Broeder AA, et al. Low disease activity (DAS28≤3.2) reduces the risk of first cardiovascular event in rheumatoid arthritis: a time-dependent Cox regression analysis in a large cohort study. Ann Rheum Dis. 2017;76(10):1693-1699.
71. Provan SA, Semb AG, Hisdal J, et al. Remission is the goal for cardiovascular risk management in patients with rheumatoid arthritis: A cross-sectional comparative study. Ann Rheum Dis. 2011;70:812-817.
72. Klarenbeek NB, van der Kooij SM, Huizinga TJ, et al. Blood pressure changes in patients with recent-onset rheumatoid arthritis treated with four different treatment strategies: A post hoc analysis from the BeSt trial. Ann Rheum Dis. 2010;69:1342-1345.
73. Hafstrom I, Rohani M, Deneberg S, et al. Effects of low-dose prednisolone on endothelial function, atherosclerosis, and traditional risk factors for atherosclerosis in patients with rheumatoid arthritis—a randomized study. J Rheumatol. 2007;34:1810-1816.
74. Hoes JN, van der Goes MC, van Raalte DH, et al. Glucose tolerance, insulin sensitivity and beta-cell function in patients with rheumatoid arthritis treated with or without low-to-medium dose glucocorticoids. Ann Rheum Dis. 2011;70:1887-1894.
75. Roubille C. The effects of tumour necrosis factor inhibitors, methotrexate, non-steroidal anti-inflammatory drugs and corticosteroids on cardiovascular events in rheumatoid arthritis, psoriasis and psoriatic arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2003;74:480-489.
76. Ajeganova S, Svensson B, Hafstrom I, BARFOT Study Group. Low-dose prednisolone treatment of early rheumatoid arthritis and late cardiovascular outcome and survival: 10-year follow-up of a 2-year randomised trial. BMJ Open. 2014;4:e004259,2013-004259.
77. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
78. del Rincon I, Battafarano DF, Restrepo JF, et al. Glucocorticoid dose thresholds associated with all-cause and cardiovascular mortality in rheumatoid arthritis. Arthritis Rheumatol. 2014;66:264-272.
79. Davis JM,3rd, Maradit Kremers H, Crowson CS, et al. Glucocorticoids and cardiovascular events in rheumatoid arthritis: A population-based cohort study. Arthritis Rheum. 2007;56:820-830.
80. Zhang J, Xie F, Yun H, et al. Comparative effects of biologics on cardiovascular risk among older patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1813-1818.
81. Greenberg JD, Kremer JM, Curtis JR, et al. Tumour necrosis factor antagonist use and associated risk reduction of cardiovascular events among patients with rheumatoid arthritis. Ann Rheum Dis. 2011;70:576-582.
82. Lindhardsen J, Gislason GH, Jacobsen S, et al. Non-steroidal anti-inflammatory drugs and risk of cardiovascular disease in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2014;73:1515-1521.
83. Schjerning Olsen AM, Fosbol EL, Lindhardsen J, et al. Duration of treatment with nonsteroidal anti-inflammatory drugs and impact on risk of death and recurrent myocardial infarction in patients with prior myocardial infarction: A nationwide cohort study. Circulation. 2011;123:2226-2235.
84. Gislason GH, Rasmussen JN, Abildstrom SZ, et al. Increased mortality and cardiovascular morbidity associated with use of nonsteroidal anti-inflammatory drugs in chronic heart failure. Arch Intern Med. 2009;169:141-149.
85. Trelle S, Reichenbach S, Wandel S, et al. Cardiovascular safety of non-steroidal anti-inflammatory drugs: Network meta-analysis. BMJ. 2011;342:c7086.
86. Nissen SE, Yeomans ND, Solomon DH, et al. Cardiovascular safety of celecoxib, naproxen, or ibuprofen for arthritis. N Engl J Med. 2016;375:2519-2529.
87. Wasko MC, Dasgupta A, Hubert Het al. Propensity-adjusted association of methotrexate with overall survival in rheumatoid arthritis. Arthritis Rheum. 2013;65:334-342.
88. Micha R, Imamura F, Wyler von Ballmoos M, et al. Systematic review and meta-analysis of methotrexate use and risk of cardiovascular disease. Am J Cardiol. 2011;108:1362-1370.
89. Bernatsky S, Hudson M, Suissa S. Anti-rheumatic drug use and risk of hospitalization for congestive heart failure in rheumatoid arthritis. Rheumatology (Oxford). 2005;44:677-680.
90. Myasoedova E, Crowson CS, Nicola PJ, et al. The influence of rheumatoid arthritis disease characteristics on heart failure. J Rheumatol. 2011;38:1601-1606.
91. Ronda N, Greco D, Adorni MP, et al. Newly identified antiatherosclerotic activity of methotrexate and adalimumab: Complementary effects on lipoprotein function and macrophage cholesterol metabolism. Arthritis Rheumatol. 2015;67:1155-1164.
92. Zimmerman MC, Clemens DL, Duryee MJ, et al. Direct antioxidant properties of methotrexate: Inhibition of malondialdehyde-acetaldehyde-protein adduct formation and superoxide scavenging. Redox Biol. 2017;13:588-593.
93. Rempenault C, Combe B, Barnetche T, et al. Metabolic and cardiovascular benefits of hydroxychloroquine in patients with rheumatoid arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2018;77:98-103.
94. Wasko MC, Hubert HB, Lingala VB, et al. Hydroxychloroquine and risk of diabetes in patients with rheumatoid arthritis. JAMA. 2007;298:187-193.
95. Charles-Schoeman C, Wang X, Lee YY, et al. Association of triple therapy with improvement in cholesterol profiles over two-year followup in the treatment of early aggressive rheumatoid arthritis trial. Arthritis Rheumatol. 2016;68:577-586.
96. Charles-Schoeman C, Yin Lee Y, Shahbazian A, et al. Improvement of high-density lipoprotein function in patients with early rheumatoid arthritis treated with methotrexate monotherapy or combination therapies in a randomized controlled trial. Arthritis Rheumatol. 2017;69:46-57.
97. Chung ES, Packer M, Lo KH, , Anti-TNF Therapy Against Congestive Heart Failure Investigators. Randomized, double-blind, placebo-controlled, pilot trial of infliximab, a chimeric monoclonal antibody to tumor necrosis factor-alpha, in patients with moderate-to-severe heart failure: Results of the anti-TNF therapy against congestive heart failure (ATTACH) trial. Circulation. 2003;107:3133-3140.
98. Singh JA, Saag KG, Bridges SL, Jr, et al. 2015 American college of rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68:1-26.
99. Daien CI, Duny Y, Barnetche Tet al. Effect of TNF inhibitors on lipid profile in rheumatoid arthritis: A systematic review with meta-analysis. Ann Rheum Dis. 2012;71:862-868.
100. Di Minno MN, Ambrosino P, Peluso R, et al. Lipid profile changes in patients with rheumatic diseases receiving a treatment with TNF-alpha blockers: A meta-analysis of prospective studies. Ann Med. 2014;46:73-83.
101. Popa C, van Tits LJ, Barrera P, et al. Anti-inflammatory therapy with tumour necrosis factor alpha inhibitors improves high-density lipoprotein cholesterol antioxidative capacity in rheumatoid arthritis patients. Ann Rheum Dis. 2009;68:868-872.
102. O’Neill F, Charakida M, Topham E, et al. Anti-inflammatory treatment improves high-density lipoprotein function in rheumatoid arthritis. Heart. 2017;103:766-773.
103. Nishimoto N, Ito K, Takagi N. Safety and efficacy profiles of tocilizumab monotherapy in Japanese patients with rheumatoid arthritis: Meta-analysis of six initial trials and five long-term extensions. Mod Rheumatol. 2010;20:222-232.
104. Rao VU, Pavlov A, Klearman M, et al. An evaluation of risk factors for major adverse cardiovascular events during tocilizumab therapy. Arthritis Rheumatol. 2015;67:372-380.
105. Gabay C, McInnes IB, Kavanaugh A, et al. Comparison of lipid and lipid-associated cardiovascular risk marker changes after treatment with tocilizumab or adalimumab in patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1806-1812.
106. McInnes IB, Thompson L, Giles JT, et al. Effect of interleukin-6 receptor blockade on surrogates of vascular risk in rheumatoid arthritis: MEASURE, a randomised, placebo-controlled study. Ann Rheum Dis. 2015;74:694-702.
107. Souto A, Salgado E, Maneiro JR, et al. Lipid profile changes in patients with chronic inflammatory arthritis treated with biologic agents and tofacitinib in randomized clinical trials: A systematic review and meta-analysis. Arthritis Rheumatol. 2015;67:117-127.
108. Myasoedova E, Gabriel SE, Matteson EL, et al. Decreased cardiovascular mortality in patients with incident rheumatoid arthritis (RA) in recent years: Dawn of a new era in cardiovascular disease in RA? J Rheumatol. 2017;44:732-739.
109. Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2889-2934.
110. Clinical Practice Guideline Treating Tobacco Use and Dependence 2008 Update Panel, Liaisons, and Staff. A clinical practice guideline for treating tobacco use and dependence: 2008 update. A U.S. public health service report. Am J Prev Med. 2008;35:158-176.
111. Eckel RH, Jakicic JM, Ard JD, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: A report of the American college of cardiology/American heart association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2960-2984.
112. Apovian CM, Aronne LJ, Bessesen DH, et al. Pharmacological management of obesity: An endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2015;100:342-362.
113. Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: A report of the American college of cardiology/American heart association task force on practice guidelines and the obesity society. J Am Coll Cardiol. 2014;63:2985-3023.
From the Division of Rh
Abstract
- Objective: To review the management of traditional and nontraditional CVD cardiovascular disease risk factors in rheumatoid arthritis (RA).
- Methods: Literature review of the management of CVD risk in RA.
- Results: Because of the increased risk of CVD events and CVD mortality among RA patients, aggressive management of CVD risk is essential. Providers should follow national guidelines for the management of traditional CVD risk factors, including dyslipidemia, hypertension, and diabetes mellitus. Similar efforts are needed in counseling on lifestyle modifications, including smoking cessation, regular exercise, and maintaining a healthy body weight. Because higher RA disease activity is also linked with CVD risk, aggressive treatment of RA to a target of low disease activity or remission is critical. Furthermore, the selection of potentially “cardioprotective” agents such as methotrexate and tumor necrosis factor inhibitors, while limiting use of nonsteroidal anti-inflammatory drugs and glucocorticoids, are strategies that could be employed by rheumatologists to help mitigate CVD risk in their patients with RA.
- Conclusion: Routine assessment of CVD risk, management of traditional CVD risk factors, counseling on healthy lifestyle habits, and aggressive treatment of RA are essential to minimize CVD risk in this population.
Keywords: rheumatoid arthritis; cardiovascular disease; cardiovascular risk assessment; cardiovascular risk management.
Editor’s note: This article is part 2 of a 2-part article. “Assessment of Cardiovascular Disease Risk in Rheumatoid Arthritis” was published in the January/February 2019 issue.
Rheumatoid arthritis (RA) is a systemic autoimmune condition that contributes to an increased risk for cardiovascular disease (CVD) among affected patients. In persons with RA, the risk of incident CVD and CVD mortality are increased by approximately 50% compared with the general population.1,2 To minimize CVD risk in this population, providers must routinely assess for CVD risk factors3 and aggressively manage both traditional and nontraditional CVD risk factors.
Managing Traditional Risk Factors
As in the general population, identification and management of traditional CVD risk factors are crucial to minimize CVD risk in the RA population. A prospective study of 201 RA patients demonstrated that traditional CVD risk factors were in fact more predictive of endothelial dysfunction and carotid atherosclerosis than were disease-related inflammatory markers in RA.4 Management of traditional risk factors is detailed in the following sections, and recommendations for managing all traditional CVD risk factors are summarized in the Table.

Dyslipidemia
The role of dyslipidemia in atherogenesis is well established, and as a result, lipid levels are nearly universally included in CVD risk stratification tools. However, the interpretation of lipid levels in the context of RA is challenging because of the effects of systemic inflammation on their absolute values. Compared to the general population, patients with RA have lower total cholesterol (TC) and low-density lipoprotein (LDL) levels independent of lipid-lowering therapy.5,6 Despite this, RA patients are at increased risk for CVD. There is even some evidence to suggest a “lipid paradox” in RA, whereby lower TC (< 4 mmol/L) and LDL levels suggest an increased risk of CVD.7,8 In contrast to LDL, higher levels of high-density lipoprotein (HDL) are typically associated with reduced CVD risk, as in the general population.8,9 Interestingly, in a cohort of 16,085 RA patients and 48,499 age- and sex-matched controls, there was no significant difference in the relationship between LDL and CVD risk, suggesting that quantitative lipid levels alone may not entirely explain the CVD mortality gap in RA.9 As such, there is substantial interest in lipoprotein function within the context of CVD risk in RA. Recent investigations have identified impaired HDL function, with reduced cholesterol efflux capacity and antioxidant properties, as well as increased scavenger receptor expression and foam cell formation, in patients with RA.10,11 More research is needed to elucidate how these alterations affect CVD morbidity and mortality and how their measurement could be integrated into improved CVD risk assessment.
Meta-analyses of randomized controlled trials have estimated that lipid-lowering therapy with HMG-CoA reductase inhibitors (statins) reduces the risk of CVD by 25% to 30%; as such, statin therapy has become the standard of care for reduction of CVD risk in the general population.12 Benefits for primary prevention of CVD in RA have also been observed; statin therapy was associated with a reduced risk of CVD events (hazard ratio [HR], 0.45; 95% confidence interval [CI], 0.20-0.98) and all-cause mortality (HR, 0.43; 95% CI, 0.20-0.92) in a population-based cohort study.13 Statins appear to have similar lipid-lowering effects and result in similar CVD risk reduction when used for primary or secondary prevention in RA patients compared to non-RA controls.14-16 Additionally, anti-inflammatory properties of statins may act in synergy with disease-modifying antirheumatic drugs (DMARDs) to improve RA disease activity. In a small study of RA patients, statin therapy improved subjective and objective markers of RA disease activity in conjunction with methotrexate.17
While statins provide robust reduction in CVD risk, some individuals cannot tolerate statin therapy or do not achieve goal LDL levels with statin therapy. Select non-statin LDL-cholesterol-lowering agents have shown promise for reducing CVD events in the general population.18 Ezetimibe, which inhibits cholesterol absorption in the small intestine, very modestly reduced CVD events when added to atorvastatin (relative risk [RR], 0.94; 95% CI, 0.89-0.99) in a double-blind randomized controlled trial.19 Novel monoclonal antibodies to proprotein convertase subtilisin/kexin type 9 (PCSK-9) inhibit the internalization of surface LDL receptors, promoting LDL clearance. Two PCSK-9 inhibitors, alirocumab and evolocumab, were approved by the US Food and Drug Administration (FDA) after randomized controlled trials demonstrated their efficacy in lowering LDL by approximately 60% and reducing CVD events by approximately 15% in patients on maximum-tolerated statin therapy.20-22 To date, non-statin LDL-cholesterol-lowering agents have been subject to limited study in RA.23
Identification and management of dyslipidemia offers an opportunity for substantial CVD risk reduction at the RA population level. Unfortunately, current rates of lipid screening are inadequate in this high-risk group. In a study of 3298 Medicare patients with RA, less than half of RA patients with an indication underwent appropriate lipid screening.24 Additionally, statins are often underutilized for both primary and secondary prevention in RA patients. Only 27% of RA patients meeting National Cholesterol Education Program Adult Treatment Panel III criteria were initiated on statin therapy in a population-based cohort study.25 Among patients discharged after a first myocardial infarction (MI), the odds of receiving lipid-lowering therapy were 31% lower for RA patients (odds ratio [OR], 0.69; 95% CI, 0.58-0.82).26 Similar to the general population, adherence to statins in RA patients appears to be poor.27-30 This raises particular concern considering that a population-based cohort study of RA patients demonstrated a 67% increased risk of MI associated with statin discontinuation, regardless of prior MI status.27 Providers—rheumatologists, primary care providers, and cardiologists alike—need to remain vigilant in efforts to assess CVD risk to identify patients who will benefit from lipid-lowering therapy and to emphasize the importance to patients of statin adherence. Novel models of health-care delivery, health technologies, and patient engagement in care may prove useful for improving lipid screening and management in RA.
Tobacco Use
Cigarette smoking is a shared risk factor for both CVD and RA. Large cohort studies have identified a dose-dependent increased risk of incident RA, particularly seropositive RA, among smokers.31-34 Tobacco smoking has also been associated with increased levels of inflammation and RA disease activity.35 The consequences of tobacco use in the general population are staggering. Among individuals over the age of 30 years, tobacco use is responsible for 12% of all deaths and 10% of all CVD deaths.36 Similar findings are observed in RA; a recent meta-analysis estimated there is a 50% increased risk of CVD events in RA related to smoking tobacco.37 In the general population, smoking cessation markedly lowers CVD risk, and over time CVD risk may approach that of nonsmokers.38,39 Thus, regular counseling and interventions to facilitate smoking cessation are critical to reducing CVD risk in RA patients. RA-specific smoking cessation programs have been proposed, but have yet to outperform standard smoking cessation programs.40
Diabetes Mellitus
It is estimated that almost 10% of the US population has diabetes mellitus (DM), which in isolation portends substantial CVD risk.41 There is an increased prevalence of DM in RA, perhaps owing to factors such as physical inactivity and chronic glucocorticoid use, though a higher level of RA disease activity itself has been associated with increased insulin resistance.42-45 In a cohort of 100 RA patients who were neither obese nor diabetic, RA patients had significantly higher fasting blood glucose and insulin levels than age- and sex-matched controls. These findings were even more pronounced in RA patients with higher levels of disease activity.44 Similar to the general population, DM is associated with poor CVD outcomes in RA.37 Therefore, both appropriate management of diabetes and control of RA disease activity are vitally important to minimize CVD risk related to DM.
Hypertension
Though not a universal finding, there may be an increased prevalence of hypertension in RA patients.31,46 Nonsteroidal anti-inflammatory drug (NSAID) and glucocorticoid use may play a role in the development of hypertension, while DMARDs appear to exert a less substantial effect on blood pressure.47,48 At least one study found that DMARD initiation (particularly for methotrexate and hydroxychloroquine) was associated with significant, albeit small, declines in both systolic and diastolic blood pressure over the first 6 months of treatment.49
Despite its potentially higher prevalence in this population, hypertension is both underdiagnosed and undertreated in RA patients.24,50-52 This is an important deficiency to target because, as in the general population, hypertension is associated with an increased risk of MI (RR, 1.84; 95% CI, 1.38-2.46) and composite CVD outcomes (RR, 2.24; 95% CI, 1.42-3.06) in RA.37 Thresholds for initiation and escalation of antihypertensive therapy are not specific to the RA population; thus, diagnosis and management of hypertension should be informed by the American College of Cardiology/American Heart Association guidelines, treating those with in-office blood pressures exceeding 140/90 mm Hg (> 130/80 mm Hg if aged > 65 years or with concomitant CVD, DM, chronic kidney disease, or 10-year atherosclerotic cardiovascular disease risk > 10%), typically with angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, calcium channel blockers, or thiazide diuretics as comorbidities may dictate or allow.53 Also, the use of NSAIDs and glucocorticoids should be minimized, particularly in those with concomitant hypertension.
Physical Activity
Likely due to factors such as articular pain and stiffness, as well as physical limitations, RA patients are more sedentary than the general population.54,55 In a study of objectively assessed sedentary behavior in RA patients, greater average sedentary time per day and greater number of sedentary bouts (> 20 min) were associated with increased 10-year risk of CVD as assessed by the QRISK2.56 Conversely, the beneficial effects of exercise are well documented. Light to moderate physical activity has been associated with improved cardiovascular outcomes, greater physical function, higher levels of HDL, as well as reduced systemic inflammation and disease activity, and improved endothelial function in RA patients.57-61 While there has been concern that physical activity may result in accelerated joint damage, even high-intensity exercise was shown to be safe without causing significant progression of joint damage.58
Obesity, Weight Loss, and Diet
While obesity is clearly associated with CVD risk in the general population, this relationship is much more complex in RA, as underweight RA patients are also at higher risk for CVD and CVD-related mortality.62-64 One potential explanation for this finding is that pathological weight loss resulting in an underweight body mass index (BMI) is an independent predictor of CVD. In a study of US Veterans with RA, higher rates of weight loss (> 3 kg/m2/year) were associated with increased CVD mortality (HR, 2.27; 95% CI, 1.61-3.19) independent of BMI.65 Systemic inflammation in RA can lead to “rheumatoid cachexia,” characterized by decreased muscle mass, increased adiposity, and increased CVD risk despite a normal or potentially decreased BMI.66 Practitioners should be mindful of not only current body weight, but also patients’ weight trajectories when counseling on lifestyle practices such as healthy diet and regular exercise in RA patients. For obese individuals with RA, healthy weight loss should be encouraged. Interestingly, bariatric surgery in RA patients may improve RA disease activity in addition to its known effects on body weight and DM.67
Counseling on healthy diet with a focus on limiting foods high in saturated- and trans-fatty acids and high glycemic index foods, and increasing consumption of fruits, vegetables, and mono-unsaturated fatty acids is a well-accepted and common practice to help minimize CVD risk in the general population.68 No studies to date have investigated the effect of specific diets on CVD risk in RA patients, and thus we recommend adherence to general population recommendations.
Managing RA-related CVD Risk Factors
Disease Activity
In addition to traditional risk factors, several studies have identified associations between the level of RA disease activity and risk of CVD. In a cohort of US Veterans with RA, CVD-related mortality increased in a dose-dependent manner with higher disease activity categories. In stark contrast, the CVD mortality rates of those in remission paralleled the rates from the general population (standardized mortality ratio [SMR], 0.68; 95% CI, 0.37-1.27).69 In a separate cohort of 1157 RA patients without prior CVD, achieving low disease activity was associated with a lower risk of incident CVD events (HR, 0.65; 95% CI, 0.43-0.99).70 Additionally, high disease activity has been associated with surrogate markers of CVD and other CVD risk factors including NT-proBNP and systolic blood pressure.71,72 While no randomized controlled trial data is available to inform this recommendation, observational data suggest RA should be aggressively treated (ideally to achieve and maintain remission or low disease activity) to minimize CVD risk. While keeping this treatment goal in mind, the differential effects of specific RA therapies on CVD must also be considered.
Glucocorticoids and NSAIDs
With the expanding repertoire of DMARDs available and more aggressive treatment approaches, the role of glucocorticoids and NSAIDs in RA treatment is decreasing over time. While their efficacy for improving pain and stiffness is well established, concern regarding their contribution to CVD risk in RA patients is warranted.
Glucocorticoids are known to have detrimental effects on traditional CVD risk factors such as hypertension, insulin resistance, and dyslipidemia in the general population, as well as in RA patients.73,74 In a meta-analysis of predominantly observational studies of RA patients, glucocorticoid use was associated with an increased risk of CVD events (RR, 1.47; 95% CI, 1.34-1.60), including MI, congestive heart failure (CHF), and cerebrovascular accident (CVA).75 Evidence is conflicting in regards to a clear dose threshold that leads to increased CVD risk with glucocorticoids, though higher doses are associated with greater risk.76-81 As RA patients requiring glucocorticoids typically have higher disease activity, confounding by indication remains a complicating factor in assessing the relative contributions of glucocorticoid use and RA disease activity to elevated CVD risk in many analyses.
The increased CVD risk with NSAID use is not specific to RA and has been well established in the general population.82-84 In the previously mentioned meta-analysis, an increased overall risk of CVD events was observed with NSAID use in RA (RR, 1.18; 95% CI, 1.01-1.38). It should be noted that cyclo-oxygenase 2 (COX-2) inhibitors, in particular rofecoxib (now removed from the market), appeared to drive the majority of this risk (RR, 1.36; 95% CI, 1.10-1.67 in COX-2 inhibitors and RR 1.08, 95% CI, 0.94-1.24 in nonselective NSAIDs), suggesting a potential differential risk among NSAIDs.75 While naproxen has been thought to carry the lowest risk of CVD based on initial studies, this has not been universally observed, including in a recent randomized controlled trial of more than 24,000 RA and osteoarthritis patients.82,85,86
Providers should use the lowest possible dose and duration of glucocorticoids and NSAIDs to achieve symptom relief, with continual efforts to taper or discontinue. Candidates for glucocorticoid and NSAID therapy should be selected carefully, and use of these therapies should be avoided in those with prior CVD or at high risk for CVD based on traditional CVD risk factors. Most importantly, providers should focus on utilizing DMARDs for the management of RA, which more effectively treat RA as well as reduce CVD risk.
Methotrexate
Methotrexate (MTX), a mainstay in the treatment of RA, is a conventional DMARD observed to improve overall survival and mitigate CVD risk in multiple RA cohorts.75,87,88 In a recent meta-analysis comprised of 236,525 RA patients and 5410 CVD events, MTX use was associated with a 28% reduction in overall CVD events across 8 studies (RR, 0.72; 95% CI, 0.57-0.91), substantiating similar findings in a prior meta-analysis.75,88 MTX use was specifically associated with a decreased risk of MI (RR, 0.81; 95% CI, 0.68-0.96). Case-control and cohort studies have cited a 20% to 50% reduced risk of CHF with MTX use.89,90 The potential cardioprotective effect of MTX appears to be both multifactorial and complex, likely mediated through both direct and indirect mechanisms. MTX directly promotes anti-atherogenic lipoprotein function, improves endothelial function, and scavenges free radicals.91,92 Indirectly, MTX likely reduces CVD risk by effectively reducing RA disease activity. Based on these and other data, MTX remains the cornerstone of DMARD therapy in RA patients when targeting CVD risk reduction.
Hydroxychloroquine
Emerging evidence suggests that hydroxychloroquine (HCQ), an antimalarial most often utilized in combination with alternative DMARDs in RA, prevents DM and has beneficial effects on lipid profiles. A recent meta-analysis compiled 3 homogenous observational studies that investigated the effect of HCQ on incident DM. RA patients ever exposed to HCQ had a 40% lower incidence of DM (HR, 0.59; 95% CI, 0.49-0.70).93 Increased duration of HCQ use was shown to further reduce risk of incident DM.94 The aforementioned meta-analysis also pooled 5 studies investigating the effect of HCQ on lipid profiles, with favorable mean differences in TC (–9.82 mg/dL), LDL (–10.61 mg/dL), HDL (4.13 mg/dL), and triglycerides (–19.15 mg/dL) in HCQ users compared to non-users.93 Given these favorable changes to traditional CVD risk factors, it is not surprising that in a retrospective study of 1266 RA patients without prior CVD, HCQ was associated with significantly lower risk of incident CVD. While external validation of these findings is needed, HCQ is an attractive conventional DMARD to be used in RA for CVD risk reduction. Moreover, its combination with MTX and sulfasalazine also shows promise for CVD risk reduction.95,96
TNF Inhibitors
Tumor necrosis factor (TNF) inhibitors are often the initial biologic DMARD therapy used in RA patients not responding to conventional DMARDs. In the previously described meta-analysis, TNF inhibitors were associated with similar reductions in CVD events as MTX (RR, 0.70; 95% CI, 0.54-0.90).75 Of note, there was a trend toward reduced risk of CHF (RR, 0.75; 95% CI, 0.49-1.15) in this same meta-analysis, an area of concern with TNF inhibitor use due to a prior randomized controlled trial demonstrating worsening clinical status in patients with existing moderate-to-severe CHF treated with high-dose infliximab.97 Current RA treatment guidelines recommend avoiding TNF inhibitor use in individuals with CHF.98
Aside from the risk of CHF exacerbation, TNF inhibitors appear to be cardioprotective. Similar to MTX, the mechanism by which TNF inhibition reduces cardiovascular risk is complex and likely due to both direct and indirect mechanisms. Substantial research has been conducted on the effect of TNF inhibition on lipids, with a recent meta-analysis demonstrating increases in HDL and TC, with stable LDL and atherogenic index over treatment follow-up.99 A subsequent meta-analysis not limited to RA patients yielded similar results.100 In addition to quantitative lipid changes, alteration of lipoprotein function, improvement in myocardial function, reduced aortic stiffness, improved blood pressure, and reduced RA disease activity may also be responsible for cardioprotective benefits of these agents.101,102
Non-TNF Biologic and Traditional Synthetic DMARDs
Tocilizumab, an IL-6 inhibitor, can potently increase LDL levels, but it does not appear to increase the risk of CVD events and may actually promote more favorable anti-atherogenic lipoprotein function.103-106 Although these quantitative lipid changes received significant attention in the wake of early reports detailing this effect, similar lipid changes appear to accompany other DMARDs including TNF inhibitors and tofacitinib.107 There have been few studies evaluating the risk of CVD with other non-TNF inhibitor biologic DMARDs and traditional synthetic DMARDs, warranting future study.
Conclusion
To mitigate the increased risk of CVD in RA, primary care and subspecialty providers alike must be aware of this heightened risk in RA, perform frequent assessments of CVD risk,3 and aggressively manage both traditional and nontraditional CVD risk factors. The differential roles in this effort may not be clear; thus, we have proposed a co-management strategy detailed in the Figure. Clear communication between providers is of the utmost importance to ensure effective management of CVD risk.

Given limited evidence for RA-specific CVD risk assessments and traditional risk factor treatment targets, management should follow pertinent national guidelines. The importance of lifestyle counseling should not be overlooked, with a focus on smoking cessation, healthy diet and body weight, and regular aerobic exercise. Finally, rheumatologists should aggressively manage RA using a treat-to-target approach, minimize the use of glucocorticoids and NSAIDs, and preferentially select DMARDs that have been associated with lower CVD risk. Through this comprehensive approach, recent trends of improved CVD outcomes in RA will hopefully become more widespread.108
Corresponding author: Bryant R. England, MD; 986270 Nebraska Medical Center, Omaha, NE 68198-6270; [email protected].
Financial disclosures: Dr. England is supported by UNMC Internal Medicine Scientist Development Award, UNMC Physician-Scientist Training Program, the UNMC Mentored Scholars Program, and the Rheumatology Research Foundation Scientist Development Award. Dr. Mikuls is supported by a VA Merit Award (CX000896) and grants from the National Institutes of Health: National Institute of General Medical Sciences (U54GM115458), National Institute on Alcohol Abuse and Alcoholism (R25AA020818), and National Institute of Arthritis and Musculoskeletal and Skin Diseases (2P50AR60772).
From the Division of Rh
Abstract
- Objective: To review the management of traditional and nontraditional CVD cardiovascular disease risk factors in rheumatoid arthritis (RA).
- Methods: Literature review of the management of CVD risk in RA.
- Results: Because of the increased risk of CVD events and CVD mortality among RA patients, aggressive management of CVD risk is essential. Providers should follow national guidelines for the management of traditional CVD risk factors, including dyslipidemia, hypertension, and diabetes mellitus. Similar efforts are needed in counseling on lifestyle modifications, including smoking cessation, regular exercise, and maintaining a healthy body weight. Because higher RA disease activity is also linked with CVD risk, aggressive treatment of RA to a target of low disease activity or remission is critical. Furthermore, the selection of potentially “cardioprotective” agents such as methotrexate and tumor necrosis factor inhibitors, while limiting use of nonsteroidal anti-inflammatory drugs and glucocorticoids, are strategies that could be employed by rheumatologists to help mitigate CVD risk in their patients with RA.
- Conclusion: Routine assessment of CVD risk, management of traditional CVD risk factors, counseling on healthy lifestyle habits, and aggressive treatment of RA are essential to minimize CVD risk in this population.
Keywords: rheumatoid arthritis; cardiovascular disease; cardiovascular risk assessment; cardiovascular risk management.
Editor’s note: This article is part 2 of a 2-part article. “Assessment of Cardiovascular Disease Risk in Rheumatoid Arthritis” was published in the January/February 2019 issue.
Rheumatoid arthritis (RA) is a systemic autoimmune condition that contributes to an increased risk for cardiovascular disease (CVD) among affected patients. In persons with RA, the risk of incident CVD and CVD mortality are increased by approximately 50% compared with the general population.1,2 To minimize CVD risk in this population, providers must routinely assess for CVD risk factors3 and aggressively manage both traditional and nontraditional CVD risk factors.
Managing Traditional Risk Factors
As in the general population, identification and management of traditional CVD risk factors are crucial to minimize CVD risk in the RA population. A prospective study of 201 RA patients demonstrated that traditional CVD risk factors were in fact more predictive of endothelial dysfunction and carotid atherosclerosis than were disease-related inflammatory markers in RA.4 Management of traditional risk factors is detailed in the following sections, and recommendations for managing all traditional CVD risk factors are summarized in the Table.

Dyslipidemia
The role of dyslipidemia in atherogenesis is well established, and as a result, lipid levels are nearly universally included in CVD risk stratification tools. However, the interpretation of lipid levels in the context of RA is challenging because of the effects of systemic inflammation on their absolute values. Compared to the general population, patients with RA have lower total cholesterol (TC) and low-density lipoprotein (LDL) levels independent of lipid-lowering therapy.5,6 Despite this, RA patients are at increased risk for CVD. There is even some evidence to suggest a “lipid paradox” in RA, whereby lower TC (< 4 mmol/L) and LDL levels suggest an increased risk of CVD.7,8 In contrast to LDL, higher levels of high-density lipoprotein (HDL) are typically associated with reduced CVD risk, as in the general population.8,9 Interestingly, in a cohort of 16,085 RA patients and 48,499 age- and sex-matched controls, there was no significant difference in the relationship between LDL and CVD risk, suggesting that quantitative lipid levels alone may not entirely explain the CVD mortality gap in RA.9 As such, there is substantial interest in lipoprotein function within the context of CVD risk in RA. Recent investigations have identified impaired HDL function, with reduced cholesterol efflux capacity and antioxidant properties, as well as increased scavenger receptor expression and foam cell formation, in patients with RA.10,11 More research is needed to elucidate how these alterations affect CVD morbidity and mortality and how their measurement could be integrated into improved CVD risk assessment.
Meta-analyses of randomized controlled trials have estimated that lipid-lowering therapy with HMG-CoA reductase inhibitors (statins) reduces the risk of CVD by 25% to 30%; as such, statin therapy has become the standard of care for reduction of CVD risk in the general population.12 Benefits for primary prevention of CVD in RA have also been observed; statin therapy was associated with a reduced risk of CVD events (hazard ratio [HR], 0.45; 95% confidence interval [CI], 0.20-0.98) and all-cause mortality (HR, 0.43; 95% CI, 0.20-0.92) in a population-based cohort study.13 Statins appear to have similar lipid-lowering effects and result in similar CVD risk reduction when used for primary or secondary prevention in RA patients compared to non-RA controls.14-16 Additionally, anti-inflammatory properties of statins may act in synergy with disease-modifying antirheumatic drugs (DMARDs) to improve RA disease activity. In a small study of RA patients, statin therapy improved subjective and objective markers of RA disease activity in conjunction with methotrexate.17
While statins provide robust reduction in CVD risk, some individuals cannot tolerate statin therapy or do not achieve goal LDL levels with statin therapy. Select non-statin LDL-cholesterol-lowering agents have shown promise for reducing CVD events in the general population.18 Ezetimibe, which inhibits cholesterol absorption in the small intestine, very modestly reduced CVD events when added to atorvastatin (relative risk [RR], 0.94; 95% CI, 0.89-0.99) in a double-blind randomized controlled trial.19 Novel monoclonal antibodies to proprotein convertase subtilisin/kexin type 9 (PCSK-9) inhibit the internalization of surface LDL receptors, promoting LDL clearance. Two PCSK-9 inhibitors, alirocumab and evolocumab, were approved by the US Food and Drug Administration (FDA) after randomized controlled trials demonstrated their efficacy in lowering LDL by approximately 60% and reducing CVD events by approximately 15% in patients on maximum-tolerated statin therapy.20-22 To date, non-statin LDL-cholesterol-lowering agents have been subject to limited study in RA.23
Identification and management of dyslipidemia offers an opportunity for substantial CVD risk reduction at the RA population level. Unfortunately, current rates of lipid screening are inadequate in this high-risk group. In a study of 3298 Medicare patients with RA, less than half of RA patients with an indication underwent appropriate lipid screening.24 Additionally, statins are often underutilized for both primary and secondary prevention in RA patients. Only 27% of RA patients meeting National Cholesterol Education Program Adult Treatment Panel III criteria were initiated on statin therapy in a population-based cohort study.25 Among patients discharged after a first myocardial infarction (MI), the odds of receiving lipid-lowering therapy were 31% lower for RA patients (odds ratio [OR], 0.69; 95% CI, 0.58-0.82).26 Similar to the general population, adherence to statins in RA patients appears to be poor.27-30 This raises particular concern considering that a population-based cohort study of RA patients demonstrated a 67% increased risk of MI associated with statin discontinuation, regardless of prior MI status.27 Providers—rheumatologists, primary care providers, and cardiologists alike—need to remain vigilant in efforts to assess CVD risk to identify patients who will benefit from lipid-lowering therapy and to emphasize the importance to patients of statin adherence. Novel models of health-care delivery, health technologies, and patient engagement in care may prove useful for improving lipid screening and management in RA.
Tobacco Use
Cigarette smoking is a shared risk factor for both CVD and RA. Large cohort studies have identified a dose-dependent increased risk of incident RA, particularly seropositive RA, among smokers.31-34 Tobacco smoking has also been associated with increased levels of inflammation and RA disease activity.35 The consequences of tobacco use in the general population are staggering. Among individuals over the age of 30 years, tobacco use is responsible for 12% of all deaths and 10% of all CVD deaths.36 Similar findings are observed in RA; a recent meta-analysis estimated there is a 50% increased risk of CVD events in RA related to smoking tobacco.37 In the general population, smoking cessation markedly lowers CVD risk, and over time CVD risk may approach that of nonsmokers.38,39 Thus, regular counseling and interventions to facilitate smoking cessation are critical to reducing CVD risk in RA patients. RA-specific smoking cessation programs have been proposed, but have yet to outperform standard smoking cessation programs.40
Diabetes Mellitus
It is estimated that almost 10% of the US population has diabetes mellitus (DM), which in isolation portends substantial CVD risk.41 There is an increased prevalence of DM in RA, perhaps owing to factors such as physical inactivity and chronic glucocorticoid use, though a higher level of RA disease activity itself has been associated with increased insulin resistance.42-45 In a cohort of 100 RA patients who were neither obese nor diabetic, RA patients had significantly higher fasting blood glucose and insulin levels than age- and sex-matched controls. These findings were even more pronounced in RA patients with higher levels of disease activity.44 Similar to the general population, DM is associated with poor CVD outcomes in RA.37 Therefore, both appropriate management of diabetes and control of RA disease activity are vitally important to minimize CVD risk related to DM.
Hypertension
Though not a universal finding, there may be an increased prevalence of hypertension in RA patients.31,46 Nonsteroidal anti-inflammatory drug (NSAID) and glucocorticoid use may play a role in the development of hypertension, while DMARDs appear to exert a less substantial effect on blood pressure.47,48 At least one study found that DMARD initiation (particularly for methotrexate and hydroxychloroquine) was associated with significant, albeit small, declines in both systolic and diastolic blood pressure over the first 6 months of treatment.49
Despite its potentially higher prevalence in this population, hypertension is both underdiagnosed and undertreated in RA patients.24,50-52 This is an important deficiency to target because, as in the general population, hypertension is associated with an increased risk of MI (RR, 1.84; 95% CI, 1.38-2.46) and composite CVD outcomes (RR, 2.24; 95% CI, 1.42-3.06) in RA.37 Thresholds for initiation and escalation of antihypertensive therapy are not specific to the RA population; thus, diagnosis and management of hypertension should be informed by the American College of Cardiology/American Heart Association guidelines, treating those with in-office blood pressures exceeding 140/90 mm Hg (> 130/80 mm Hg if aged > 65 years or with concomitant CVD, DM, chronic kidney disease, or 10-year atherosclerotic cardiovascular disease risk > 10%), typically with angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, calcium channel blockers, or thiazide diuretics as comorbidities may dictate or allow.53 Also, the use of NSAIDs and glucocorticoids should be minimized, particularly in those with concomitant hypertension.
Physical Activity
Likely due to factors such as articular pain and stiffness, as well as physical limitations, RA patients are more sedentary than the general population.54,55 In a study of objectively assessed sedentary behavior in RA patients, greater average sedentary time per day and greater number of sedentary bouts (> 20 min) were associated with increased 10-year risk of CVD as assessed by the QRISK2.56 Conversely, the beneficial effects of exercise are well documented. Light to moderate physical activity has been associated with improved cardiovascular outcomes, greater physical function, higher levels of HDL, as well as reduced systemic inflammation and disease activity, and improved endothelial function in RA patients.57-61 While there has been concern that physical activity may result in accelerated joint damage, even high-intensity exercise was shown to be safe without causing significant progression of joint damage.58
Obesity, Weight Loss, and Diet
While obesity is clearly associated with CVD risk in the general population, this relationship is much more complex in RA, as underweight RA patients are also at higher risk for CVD and CVD-related mortality.62-64 One potential explanation for this finding is that pathological weight loss resulting in an underweight body mass index (BMI) is an independent predictor of CVD. In a study of US Veterans with RA, higher rates of weight loss (> 3 kg/m2/year) were associated with increased CVD mortality (HR, 2.27; 95% CI, 1.61-3.19) independent of BMI.65 Systemic inflammation in RA can lead to “rheumatoid cachexia,” characterized by decreased muscle mass, increased adiposity, and increased CVD risk despite a normal or potentially decreased BMI.66 Practitioners should be mindful of not only current body weight, but also patients’ weight trajectories when counseling on lifestyle practices such as healthy diet and regular exercise in RA patients. For obese individuals with RA, healthy weight loss should be encouraged. Interestingly, bariatric surgery in RA patients may improve RA disease activity in addition to its known effects on body weight and DM.67
Counseling on healthy diet with a focus on limiting foods high in saturated- and trans-fatty acids and high glycemic index foods, and increasing consumption of fruits, vegetables, and mono-unsaturated fatty acids is a well-accepted and common practice to help minimize CVD risk in the general population.68 No studies to date have investigated the effect of specific diets on CVD risk in RA patients, and thus we recommend adherence to general population recommendations.
Managing RA-related CVD Risk Factors
Disease Activity
In addition to traditional risk factors, several studies have identified associations between the level of RA disease activity and risk of CVD. In a cohort of US Veterans with RA, CVD-related mortality increased in a dose-dependent manner with higher disease activity categories. In stark contrast, the CVD mortality rates of those in remission paralleled the rates from the general population (standardized mortality ratio [SMR], 0.68; 95% CI, 0.37-1.27).69 In a separate cohort of 1157 RA patients without prior CVD, achieving low disease activity was associated with a lower risk of incident CVD events (HR, 0.65; 95% CI, 0.43-0.99).70 Additionally, high disease activity has been associated with surrogate markers of CVD and other CVD risk factors including NT-proBNP and systolic blood pressure.71,72 While no randomized controlled trial data is available to inform this recommendation, observational data suggest RA should be aggressively treated (ideally to achieve and maintain remission or low disease activity) to minimize CVD risk. While keeping this treatment goal in mind, the differential effects of specific RA therapies on CVD must also be considered.
Glucocorticoids and NSAIDs
With the expanding repertoire of DMARDs available and more aggressive treatment approaches, the role of glucocorticoids and NSAIDs in RA treatment is decreasing over time. While their efficacy for improving pain and stiffness is well established, concern regarding their contribution to CVD risk in RA patients is warranted.
Glucocorticoids are known to have detrimental effects on traditional CVD risk factors such as hypertension, insulin resistance, and dyslipidemia in the general population, as well as in RA patients.73,74 In a meta-analysis of predominantly observational studies of RA patients, glucocorticoid use was associated with an increased risk of CVD events (RR, 1.47; 95% CI, 1.34-1.60), including MI, congestive heart failure (CHF), and cerebrovascular accident (CVA).75 Evidence is conflicting in regards to a clear dose threshold that leads to increased CVD risk with glucocorticoids, though higher doses are associated with greater risk.76-81 As RA patients requiring glucocorticoids typically have higher disease activity, confounding by indication remains a complicating factor in assessing the relative contributions of glucocorticoid use and RA disease activity to elevated CVD risk in many analyses.
The increased CVD risk with NSAID use is not specific to RA and has been well established in the general population.82-84 In the previously mentioned meta-analysis, an increased overall risk of CVD events was observed with NSAID use in RA (RR, 1.18; 95% CI, 1.01-1.38). It should be noted that cyclo-oxygenase 2 (COX-2) inhibitors, in particular rofecoxib (now removed from the market), appeared to drive the majority of this risk (RR, 1.36; 95% CI, 1.10-1.67 in COX-2 inhibitors and RR 1.08, 95% CI, 0.94-1.24 in nonselective NSAIDs), suggesting a potential differential risk among NSAIDs.75 While naproxen has been thought to carry the lowest risk of CVD based on initial studies, this has not been universally observed, including in a recent randomized controlled trial of more than 24,000 RA and osteoarthritis patients.82,85,86
Providers should use the lowest possible dose and duration of glucocorticoids and NSAIDs to achieve symptom relief, with continual efforts to taper or discontinue. Candidates for glucocorticoid and NSAID therapy should be selected carefully, and use of these therapies should be avoided in those with prior CVD or at high risk for CVD based on traditional CVD risk factors. Most importantly, providers should focus on utilizing DMARDs for the management of RA, which more effectively treat RA as well as reduce CVD risk.
Methotrexate
Methotrexate (MTX), a mainstay in the treatment of RA, is a conventional DMARD observed to improve overall survival and mitigate CVD risk in multiple RA cohorts.75,87,88 In a recent meta-analysis comprised of 236,525 RA patients and 5410 CVD events, MTX use was associated with a 28% reduction in overall CVD events across 8 studies (RR, 0.72; 95% CI, 0.57-0.91), substantiating similar findings in a prior meta-analysis.75,88 MTX use was specifically associated with a decreased risk of MI (RR, 0.81; 95% CI, 0.68-0.96). Case-control and cohort studies have cited a 20% to 50% reduced risk of CHF with MTX use.89,90 The potential cardioprotective effect of MTX appears to be both multifactorial and complex, likely mediated through both direct and indirect mechanisms. MTX directly promotes anti-atherogenic lipoprotein function, improves endothelial function, and scavenges free radicals.91,92 Indirectly, MTX likely reduces CVD risk by effectively reducing RA disease activity. Based on these and other data, MTX remains the cornerstone of DMARD therapy in RA patients when targeting CVD risk reduction.
Hydroxychloroquine
Emerging evidence suggests that hydroxychloroquine (HCQ), an antimalarial most often utilized in combination with alternative DMARDs in RA, prevents DM and has beneficial effects on lipid profiles. A recent meta-analysis compiled 3 homogenous observational studies that investigated the effect of HCQ on incident DM. RA patients ever exposed to HCQ had a 40% lower incidence of DM (HR, 0.59; 95% CI, 0.49-0.70).93 Increased duration of HCQ use was shown to further reduce risk of incident DM.94 The aforementioned meta-analysis also pooled 5 studies investigating the effect of HCQ on lipid profiles, with favorable mean differences in TC (–9.82 mg/dL), LDL (–10.61 mg/dL), HDL (4.13 mg/dL), and triglycerides (–19.15 mg/dL) in HCQ users compared to non-users.93 Given these favorable changes to traditional CVD risk factors, it is not surprising that in a retrospective study of 1266 RA patients without prior CVD, HCQ was associated with significantly lower risk of incident CVD. While external validation of these findings is needed, HCQ is an attractive conventional DMARD to be used in RA for CVD risk reduction. Moreover, its combination with MTX and sulfasalazine also shows promise for CVD risk reduction.95,96
TNF Inhibitors
Tumor necrosis factor (TNF) inhibitors are often the initial biologic DMARD therapy used in RA patients not responding to conventional DMARDs. In the previously described meta-analysis, TNF inhibitors were associated with similar reductions in CVD events as MTX (RR, 0.70; 95% CI, 0.54-0.90).75 Of note, there was a trend toward reduced risk of CHF (RR, 0.75; 95% CI, 0.49-1.15) in this same meta-analysis, an area of concern with TNF inhibitor use due to a prior randomized controlled trial demonstrating worsening clinical status in patients with existing moderate-to-severe CHF treated with high-dose infliximab.97 Current RA treatment guidelines recommend avoiding TNF inhibitor use in individuals with CHF.98
Aside from the risk of CHF exacerbation, TNF inhibitors appear to be cardioprotective. Similar to MTX, the mechanism by which TNF inhibition reduces cardiovascular risk is complex and likely due to both direct and indirect mechanisms. Substantial research has been conducted on the effect of TNF inhibition on lipids, with a recent meta-analysis demonstrating increases in HDL and TC, with stable LDL and atherogenic index over treatment follow-up.99 A subsequent meta-analysis not limited to RA patients yielded similar results.100 In addition to quantitative lipid changes, alteration of lipoprotein function, improvement in myocardial function, reduced aortic stiffness, improved blood pressure, and reduced RA disease activity may also be responsible for cardioprotective benefits of these agents.101,102
Non-TNF Biologic and Traditional Synthetic DMARDs
Tocilizumab, an IL-6 inhibitor, can potently increase LDL levels, but it does not appear to increase the risk of CVD events and may actually promote more favorable anti-atherogenic lipoprotein function.103-106 Although these quantitative lipid changes received significant attention in the wake of early reports detailing this effect, similar lipid changes appear to accompany other DMARDs including TNF inhibitors and tofacitinib.107 There have been few studies evaluating the risk of CVD with other non-TNF inhibitor biologic DMARDs and traditional synthetic DMARDs, warranting future study.
Conclusion
To mitigate the increased risk of CVD in RA, primary care and subspecialty providers alike must be aware of this heightened risk in RA, perform frequent assessments of CVD risk,3 and aggressively manage both traditional and nontraditional CVD risk factors. The differential roles in this effort may not be clear; thus, we have proposed a co-management strategy detailed in the Figure. Clear communication between providers is of the utmost importance to ensure effective management of CVD risk.

Given limited evidence for RA-specific CVD risk assessments and traditional risk factor treatment targets, management should follow pertinent national guidelines. The importance of lifestyle counseling should not be overlooked, with a focus on smoking cessation, healthy diet and body weight, and regular aerobic exercise. Finally, rheumatologists should aggressively manage RA using a treat-to-target approach, minimize the use of glucocorticoids and NSAIDs, and preferentially select DMARDs that have been associated with lower CVD risk. Through this comprehensive approach, recent trends of improved CVD outcomes in RA will hopefully become more widespread.108
Corresponding author: Bryant R. England, MD; 986270 Nebraska Medical Center, Omaha, NE 68198-6270; [email protected].
Financial disclosures: Dr. England is supported by UNMC Internal Medicine Scientist Development Award, UNMC Physician-Scientist Training Program, the UNMC Mentored Scholars Program, and the Rheumatology Research Foundation Scientist Development Award. Dr. Mikuls is supported by a VA Merit Award (CX000896) and grants from the National Institutes of Health: National Institute of General Medical Sciences (U54GM115458), National Institute on Alcohol Abuse and Alcoholism (R25AA020818), and National Institute of Arthritis and Musculoskeletal and Skin Diseases (2P50AR60772).
1. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
2. Avina-Zubieta JA, Thomas J, Sadatsafavi M, et al. Risk of incident cardiovascular events in patients with rheumatoid arthritis: A meta-analysis of observational studies. Ann Rheum Dis. 2012;71:1524-1529.
3. Johnson TM, Mikuls TR, England BR. Assessment of cardiovascular risk in rheumatoid arthritis. J Clin Outcomes Manage. 2019;26:41-47.
4. Sandoo A, Chanchlani N, Hodson J, et al. Classical cardiovascular disease risk factors associate with vascular function and morphology in rheumatoid arthritis: A six-year prospective study. Arthritis Res Ther. 2013;15:R203.
5. Myasoedova E, Crowson CS, Kremers HM, et al. Total cholesterol and LDL levels decrease before rheumatoid arthritis. Ann Rheum Dis. 2010;69:1310-1314.
6. Liao KP, Cai T, Gainer VS, et al. Lipid and lipoprotein levels and trend in rheumatoid arthritis compared to the general population. Arthritis Care Res (Hoboken). 2013;65:2046-2050.
7. Myasoedova E, Crowson CS, Kremers HM, et al. Lipid paradox in rheumatoid arthritis: The impact of serum lipid measures and systemic inflammation on the risk of cardiovascular disease. Ann Rheum Dis. 2011;70:482-487.
8. Zhang J, Chen L, Delzell E, et al. Republished: The association between inflammatory markers, serum lipids and the risk of cardiovascular events in patients with rheumatoid arthritis. Postgrad Med J. 2014;90:722-729.
9. Liao KP, Liu J, Lu B, et al. Association between lipid levels and major adverse cardiovascular events in rheumatoid arthritis compared to non-rheumatoid arthritis patients. Arthritis Rheumatol. 2015;67:2004-2010.
10. Charles-Schoeman C, Lee YY, Grijalva V, et al. Cholesterol efflux by high density lipoproteins is impaired in patients with active rheumatoid arthritis. Ann Rheum Dis. 2012;71:1157-1162.
11. Voloshyna I, Modayil S, Littlefield MJ, et al. Plasma from rheumatoid arthritis patients promotes pro-atherogenic cholesterol transport gene expression in THP-1 human macrophages. Exp Biol Med (Maywood). 2013 238:1192-1197.
12. Taylor F, Huffman MD, Macedo AF, et al. Statins for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2013;(1):CD004816.
13. Sheng X, Murphy MJ, Macdonald TM, Wei L. Effectiveness of statins on total cholesterol and cardiovascular disease and all-cause mortality in osteoarthritis and rheumatoid arthritis. J Rheumatol. 2012;39:32-40.
14. An J, Alemao E, Reynolds K, et al. Cardiovascular outcomes associated with lowering low-density lipoprotein cholesterol in rheumatoid arthritis and matched nonrheumatoid arthritis. J Rheumatol. 2016;43:1989-1996.
15. Semb AG, Holme I, Kvien TK, Pedersen TR. Intensive lipid lowering in patients with rheumatoid arthritis and previous myocardial infarction: An explorative analysis from the incremental decrease in endpoints through aggressive lipid lowering (IDEAL) trial. Rheumatology (Oxford). 2011;50:324-329.
16. Semb AG, Kvien TK, DeMicco DA, et al. Effect of intensive lipid-lowering therapy on cardiovascular outcome in patients with and those without inflammatory joint disease. Arthritis Rheum. 2012;64:2836-2846.
17. El-Barbary AM, Hussein MS, Rageh EM, et al. Effect of atorvastatin on inflammation and modification of vascular risk factors in rheumatoid arthritis. J Rheumatol. 2011;38:229-235.
18. Writing Committee, Lloyd-Jones DM, Morris PB, et al. 2016 ACC expert consensus decision pathway on the role of non-statin therapies for LDL-cholesterol lowering in the management of atherosclerotic cardiovascular disease risk: A report of the American college of cardiology task force on clinical expert consensus documents. J Am Coll Cardiol. 2016;68:92-125.
19. Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372:2387-2397.
20. Sabatine MS, Giugliano RP, Wiviott SD, et al. Efficacy and safety of evolocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1500-1509.
21. Robinson JG, Farnier M, Krempf M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1489-1499.
22. Sabatine MS, Giugliano RP, Keech AC, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med. 2017;376:1713-1722.
23. Maki-Petaja KM, Booth AD, Hall FC, et al. Ezetimibe and simvastatin reduce inflammation, disease activity, and aortic stiffness and improve endothelial function in rheumatoid arthritis. J Am Coll Cardiol. 2007;50:852-858.
24. Bartels CM, Kind AJ, Everett C, et al. Low frequency of primary lipid screening among medicare patients with rheumatoid arthritis. Arthritis Rheum. 2011;63:1221-1230.
25. Akkara Veetil BM, Myasoedova E, Matteson EL, et al. Use of lipid-lowering agents in rheumatoid arthritis: A population-based cohort study. J Rheumatol. 2013;40:1082-1088.
26. Lindhardsen J, Ahlehoff O, Gislason GH, et al. Initiation and adherence to secondary prevention pharmacotherapy after myocardial infarction in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2012;71:1496-1501.
27. De Vera MA, Choi H, Abrahamowicz M, et al. Statin discontinuation and risk of acute myocardial infarction in patients with rheumatoid arthritis: A population-based cohort study. Ann Rheum Dis. 2011;70:1020-1024.
28. Zhang H, Plutzky J, Skentzos S, et al. Discontinuation of statins in routine care settings: A cohort study. Ann Intern Med. 2013;158:526-534.
29. Zhang H, Plutzky J, Shubina M, Turchin A. Continued statin prescriptions after adverse reactions and patient outcomes: A cohort study. Ann Intern Med. 2017;167:221-227.
30. Lemstra M, Blackburn D, Crawley A, Fung R. Proportion and risk indicators of nonadherence to statin therapy: A meta-analysis. Can J Cardiol. 2012;28:574-580.
31. Boyer JF, Gourraud PA, Cantagrel A, et al. Traditional cardiovascular risk factors in rheumatoid arthritis: A meta-analysis. Joint Bone Spine. 2011;78:179-183.
32. Bergstrom U, Jacobsson LT, Nilsson JA, et al. Pulmonary dysfunction, smoking, socioeconomic status and the risk of developing rheumatoid arthritis. Rheumatology (Oxford). 2011;50:2005-2013.
33. Costenbader KH, Feskanich D, Mandl LA, Karlson EW. Smoking intensity, duration, and cessation, and the risk of rheumatoid arthritis in women. Am J Med. 2006;119:503.e1,503.e9.
34. Klareskog L, Stolt P, Lundberg K, et al. A new model for an etiology of rheumatoid arthritis: Smoking may trigger HLA-DR (shared epitope)-restricted immune reactions to autoantigens modified by citrullination. Arthritis Rheum. 2006;54:38-46.
35. Sokolove J, Wagner CA, Lahey LJ, et al. Increased inflammation and disease activity among current cigarette smokers with rheumatoid arthritis: A cross-sectional analysis of US veterans. Rheumatology (Oxford). 2016;55:1969-1977.
36. World Health Organization. WHO Global Report: Mortality Attributable to Tobacco. Geneva, World Health Organization, 2012.
37. Baghdadi LR, Woodman RJ, Shanahan EM, Mangoni AA. The impact of traditional cardiovascular risk factors on cardiovascular outcomes in patients with rheumatoid arthritis: A systematic review and meta-analysis. PLoS One. 2015;10:e0117952.
38. Centers for Disease Control and Prevention; National Center for Chronic Disease Prevention and Health Promotion. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease: A Report of the Surgeon General. Atlanta (GA): Centers for Disease Control and Prevention; 2010. 6, Cardiovascular Diseases. Available from: https://ncbi.nlm.nih.gov/books/NBK53012/
39. Mons U, Muezzinler A, Gellert C, et al. Impact of smoking and smoking cessation on cardiovascular events and mortality among older adults: Meta-analysis of individual participant data from prospective cohort studies of the CHANCES consortium. BMJ. 2015;350:h1551.
40. Aimer P, Treharne GJ, Stebbings S, Frampton C, Cameron V, Kirby S, et al. Efficacy of a rheumatoid arthritis-specific smoking cessation program: A randomized controlled pilot trial. Arthritis Care Res (Hoboken). 2017;69:28-37.
41. Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2017.
42. Jiang P, Li H, Li X. Diabetes mellitus risk factors in rheumatoid arthritis: A systematic review and meta-analysis. Clin Exp Rheumatol. 2015;33:115-121.
43. Shahin D, Eltoraby E, Mesbah A, Houssen M. Insulin resistance in early untreated rheumatoid arthritis patients. Clin Biochem. 2010;43:661-335.
44. Arias de la Rosa I, Escudero-Contreras A, Rodriguez-Cuenca S, et al. Defective glucose and lipid metabolism in rheumatoid arthritis is determined by chronic inflammation in metabolic tissues. J Intern Med. 2018;84(1):61-77.
45. Wilson JC, Sarsour K, Gale S, et al. Incidence and risk of glucocorticoid-associated adverse effects in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018 Jun 1. doi: 10.1002/acr.23611.
46. Chung CP, Giles JT, Petri M, et al. Prevalence of traditional modifiable cardiovascular risk factors in patients with rheumatoid arthritis: Comparison with control subjects from the multi-ethnic study of atherosclerosis. Semin Arthritis Rheum. 2012;41:535-544.
47. Goodwin JE, Geller DS. Glucocorticoid-induced hypertension. Pediatr Nephrol. 2012;27:1059-1066.
48. Snowden S, Nelson R. The effects of nonsteroidal anti-inflammatory drugs on blood pressure in hypertensive patients. Cardiol Rev. 2011;19:184-191.
49. Baker JF, Sauer B, Teng CC, et al. Initiation of disease-modifying therapies in rheumatoid arthritis is associated with changes in blood pressure. J Clin Rheumatol. 2018;24:203-209.
50. Panoulas VF, Douglas KM, Milionis HJ, et al. Prevalence and associations of hypertension and its control in patients with rheumatoid arthritis. Rheumatology (Oxford). 2007;46:1477-1482.
51. Protogerou AD, Panagiotakos DB, Zampeli E, et al. Arterial hypertension assessed “out-of-office” in a contemporary cohort of rheumatoid arthritis patients free of cardiovascular disease is characterized by high prevalence, low awareness, poor control and increased vascular damage-associated “white coat” phenomenon. Arthritis Res Ther. 2013;15:R142.
52. van Breukelen-van der Stoep DF, van Zeben D, Klop B, et al. Marked underdiagnosis and undertreatment of hypertension and hypercholesterolaemia in rheumatoid arthritis. Rheumatology (Oxford). 2016;55:1210-1216.
53. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American college of cardiology/American heart association task force on clinical practice guidelines. J Am Coll Cardiol. 2018;71:e127-248.
54. Lee J, Dunlop D, Ehrlich-Jones L, et al. Public health impact of risk factors for physical inactivity in adults with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:488-493.
55. Sokka T, Hakkinen A, Kautiainen H, et al. Physical inactivity in patients with rheumatoid arthritis: Data from twenty-one countries in a cross-sectional, international study. Arthritis Rheum. 2008;59:42-50.
56. Fenton SAM, Veldhuijzen van Zanten JJCS, Kitas GD, et al. Sedentary behaviour is associated with increased long-term cardiovascular risk in patients with rheumatoid arthritis independently of moderate-to-vigorous physical activity. BMC Musculoskelet Disord. 2017;18:131,017-1473-9.
57. Byram KW, Oeser AM, Linton MF, et al. Exercise is associated with increased small HDL particle concentration and decreased vascular stiffness in rheumatoid arthritis. J Clin Rheumatol. 2018 May 25. 9.
58. de Jong Z, Munneke M, Zwinderman AH, et al. Is a long-term high-intensity exercise program effective and safe in patients with rheumatoid arthritis? results of a randomized controlled trial. Arthritis Rheum. 2003;48:2415-2424.
59. Stavropoulos-Kalinoglou A, Metsios GS, Veldhuijzen van Zanten JJ, et al. Individualised aerobic and resistance exercise training improves cardiorespiratory fitness and reduces cardiovascular risk in patients with rheumatoid arthritis. Ann Rheum Dis. 2013;72:1819-1825.
60. Khoja SS, Almeida GJ, Chester Wasko M, et al. Association of light-intensity physical activity with lower cardiovascular disease risk burden in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:424-431.
61. Metsios GS, Koutedakis Y, Veldhuijzen van Zanten JJ, et al. Cardiorespiratory fitness levels and their association with cardiovascular profile in patients with rheumatoid arthritis: A cross-sectional study. Rheumatology (Oxford). 2015;54:2215-2220.
62. Escalante A, Haas RW, del Rincon I. Paradoxical effect of body mass index on survival in rheumatoid arthritis: Role of comorbidity and systemic inflammation. Arch Intern Med. 2005;165:1624-1629.
63. Kremers HM, Nicola PJ, Crowson CS, et al. Prognostic importance of low body mass index in relation to cardiovascular mortality in rheumatoid arthritis. Arthritis Rheum. 2004;50:3450-3457.
64. Wolfe F, Michaud K. Effect of body mass index on mortality and clinical status in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:1471-1479.
65. England BR, Baker JF, Sayles H, et al. Body mass index, weight loss, and cause-specific mortality in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018;70:11-18.
66. Dessein PH, Solomon A, Hollan I. Metabolic abnormalities in patients with inflammatory rheumatic diseases. Best Pract Res Clin Rheumatol. 2016;30:901-915.
67. Sparks JA, Halperin F, Karlson JC, et al. Impact of bariatric surgery on patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2015;67:1619-1626.
68. Mente A, de Koning L, Shannon HS, Anand SS. A systematic review of the evidence supporting a causal link between dietary factors and coronary heart disease. Arch Intern Med. 2009;169:659-669.
69. England BR, Sayles H, Michaud K, et al. Cause-specific mortality in male US veterans with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:36-45.
70. Arts EE, Fransen J, Den Broeder AA, et al. Low disease activity (DAS28≤3.2) reduces the risk of first cardiovascular event in rheumatoid arthritis: a time-dependent Cox regression analysis in a large cohort study. Ann Rheum Dis. 2017;76(10):1693-1699.
71. Provan SA, Semb AG, Hisdal J, et al. Remission is the goal for cardiovascular risk management in patients with rheumatoid arthritis: A cross-sectional comparative study. Ann Rheum Dis. 2011;70:812-817.
72. Klarenbeek NB, van der Kooij SM, Huizinga TJ, et al. Blood pressure changes in patients with recent-onset rheumatoid arthritis treated with four different treatment strategies: A post hoc analysis from the BeSt trial. Ann Rheum Dis. 2010;69:1342-1345.
73. Hafstrom I, Rohani M, Deneberg S, et al. Effects of low-dose prednisolone on endothelial function, atherosclerosis, and traditional risk factors for atherosclerosis in patients with rheumatoid arthritis—a randomized study. J Rheumatol. 2007;34:1810-1816.
74. Hoes JN, van der Goes MC, van Raalte DH, et al. Glucose tolerance, insulin sensitivity and beta-cell function in patients with rheumatoid arthritis treated with or without low-to-medium dose glucocorticoids. Ann Rheum Dis. 2011;70:1887-1894.
75. Roubille C. The effects of tumour necrosis factor inhibitors, methotrexate, non-steroidal anti-inflammatory drugs and corticosteroids on cardiovascular events in rheumatoid arthritis, psoriasis and psoriatic arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2003;74:480-489.
76. Ajeganova S, Svensson B, Hafstrom I, BARFOT Study Group. Low-dose prednisolone treatment of early rheumatoid arthritis and late cardiovascular outcome and survival: 10-year follow-up of a 2-year randomised trial. BMJ Open. 2014;4:e004259,2013-004259.
77. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
78. del Rincon I, Battafarano DF, Restrepo JF, et al. Glucocorticoid dose thresholds associated with all-cause and cardiovascular mortality in rheumatoid arthritis. Arthritis Rheumatol. 2014;66:264-272.
79. Davis JM,3rd, Maradit Kremers H, Crowson CS, et al. Glucocorticoids and cardiovascular events in rheumatoid arthritis: A population-based cohort study. Arthritis Rheum. 2007;56:820-830.
80. Zhang J, Xie F, Yun H, et al. Comparative effects of biologics on cardiovascular risk among older patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1813-1818.
81. Greenberg JD, Kremer JM, Curtis JR, et al. Tumour necrosis factor antagonist use and associated risk reduction of cardiovascular events among patients with rheumatoid arthritis. Ann Rheum Dis. 2011;70:576-582.
82. Lindhardsen J, Gislason GH, Jacobsen S, et al. Non-steroidal anti-inflammatory drugs and risk of cardiovascular disease in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2014;73:1515-1521.
83. Schjerning Olsen AM, Fosbol EL, Lindhardsen J, et al. Duration of treatment with nonsteroidal anti-inflammatory drugs and impact on risk of death and recurrent myocardial infarction in patients with prior myocardial infarction: A nationwide cohort study. Circulation. 2011;123:2226-2235.
84. Gislason GH, Rasmussen JN, Abildstrom SZ, et al. Increased mortality and cardiovascular morbidity associated with use of nonsteroidal anti-inflammatory drugs in chronic heart failure. Arch Intern Med. 2009;169:141-149.
85. Trelle S, Reichenbach S, Wandel S, et al. Cardiovascular safety of non-steroidal anti-inflammatory drugs: Network meta-analysis. BMJ. 2011;342:c7086.
86. Nissen SE, Yeomans ND, Solomon DH, et al. Cardiovascular safety of celecoxib, naproxen, or ibuprofen for arthritis. N Engl J Med. 2016;375:2519-2529.
87. Wasko MC, Dasgupta A, Hubert Het al. Propensity-adjusted association of methotrexate with overall survival in rheumatoid arthritis. Arthritis Rheum. 2013;65:334-342.
88. Micha R, Imamura F, Wyler von Ballmoos M, et al. Systematic review and meta-analysis of methotrexate use and risk of cardiovascular disease. Am J Cardiol. 2011;108:1362-1370.
89. Bernatsky S, Hudson M, Suissa S. Anti-rheumatic drug use and risk of hospitalization for congestive heart failure in rheumatoid arthritis. Rheumatology (Oxford). 2005;44:677-680.
90. Myasoedova E, Crowson CS, Nicola PJ, et al. The influence of rheumatoid arthritis disease characteristics on heart failure. J Rheumatol. 2011;38:1601-1606.
91. Ronda N, Greco D, Adorni MP, et al. Newly identified antiatherosclerotic activity of methotrexate and adalimumab: Complementary effects on lipoprotein function and macrophage cholesterol metabolism. Arthritis Rheumatol. 2015;67:1155-1164.
92. Zimmerman MC, Clemens DL, Duryee MJ, et al. Direct antioxidant properties of methotrexate: Inhibition of malondialdehyde-acetaldehyde-protein adduct formation and superoxide scavenging. Redox Biol. 2017;13:588-593.
93. Rempenault C, Combe B, Barnetche T, et al. Metabolic and cardiovascular benefits of hydroxychloroquine in patients with rheumatoid arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2018;77:98-103.
94. Wasko MC, Hubert HB, Lingala VB, et al. Hydroxychloroquine and risk of diabetes in patients with rheumatoid arthritis. JAMA. 2007;298:187-193.
95. Charles-Schoeman C, Wang X, Lee YY, et al. Association of triple therapy with improvement in cholesterol profiles over two-year followup in the treatment of early aggressive rheumatoid arthritis trial. Arthritis Rheumatol. 2016;68:577-586.
96. Charles-Schoeman C, Yin Lee Y, Shahbazian A, et al. Improvement of high-density lipoprotein function in patients with early rheumatoid arthritis treated with methotrexate monotherapy or combination therapies in a randomized controlled trial. Arthritis Rheumatol. 2017;69:46-57.
97. Chung ES, Packer M, Lo KH, , Anti-TNF Therapy Against Congestive Heart Failure Investigators. Randomized, double-blind, placebo-controlled, pilot trial of infliximab, a chimeric monoclonal antibody to tumor necrosis factor-alpha, in patients with moderate-to-severe heart failure: Results of the anti-TNF therapy against congestive heart failure (ATTACH) trial. Circulation. 2003;107:3133-3140.
98. Singh JA, Saag KG, Bridges SL, Jr, et al. 2015 American college of rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68:1-26.
99. Daien CI, Duny Y, Barnetche Tet al. Effect of TNF inhibitors on lipid profile in rheumatoid arthritis: A systematic review with meta-analysis. Ann Rheum Dis. 2012;71:862-868.
100. Di Minno MN, Ambrosino P, Peluso R, et al. Lipid profile changes in patients with rheumatic diseases receiving a treatment with TNF-alpha blockers: A meta-analysis of prospective studies. Ann Med. 2014;46:73-83.
101. Popa C, van Tits LJ, Barrera P, et al. Anti-inflammatory therapy with tumour necrosis factor alpha inhibitors improves high-density lipoprotein cholesterol antioxidative capacity in rheumatoid arthritis patients. Ann Rheum Dis. 2009;68:868-872.
102. O’Neill F, Charakida M, Topham E, et al. Anti-inflammatory treatment improves high-density lipoprotein function in rheumatoid arthritis. Heart. 2017;103:766-773.
103. Nishimoto N, Ito K, Takagi N. Safety and efficacy profiles of tocilizumab monotherapy in Japanese patients with rheumatoid arthritis: Meta-analysis of six initial trials and five long-term extensions. Mod Rheumatol. 2010;20:222-232.
104. Rao VU, Pavlov A, Klearman M, et al. An evaluation of risk factors for major adverse cardiovascular events during tocilizumab therapy. Arthritis Rheumatol. 2015;67:372-380.
105. Gabay C, McInnes IB, Kavanaugh A, et al. Comparison of lipid and lipid-associated cardiovascular risk marker changes after treatment with tocilizumab or adalimumab in patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1806-1812.
106. McInnes IB, Thompson L, Giles JT, et al. Effect of interleukin-6 receptor blockade on surrogates of vascular risk in rheumatoid arthritis: MEASURE, a randomised, placebo-controlled study. Ann Rheum Dis. 2015;74:694-702.
107. Souto A, Salgado E, Maneiro JR, et al. Lipid profile changes in patients with chronic inflammatory arthritis treated with biologic agents and tofacitinib in randomized clinical trials: A systematic review and meta-analysis. Arthritis Rheumatol. 2015;67:117-127.
108. Myasoedova E, Gabriel SE, Matteson EL, et al. Decreased cardiovascular mortality in patients with incident rheumatoid arthritis (RA) in recent years: Dawn of a new era in cardiovascular disease in RA? J Rheumatol. 2017;44:732-739.
109. Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2889-2934.
110. Clinical Practice Guideline Treating Tobacco Use and Dependence 2008 Update Panel, Liaisons, and Staff. A clinical practice guideline for treating tobacco use and dependence: 2008 update. A U.S. public health service report. Am J Prev Med. 2008;35:158-176.
111. Eckel RH, Jakicic JM, Ard JD, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: A report of the American college of cardiology/American heart association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2960-2984.
112. Apovian CM, Aronne LJ, Bessesen DH, et al. Pharmacological management of obesity: An endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2015;100:342-362.
113. Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: A report of the American college of cardiology/American heart association task force on practice guidelines and the obesity society. J Am Coll Cardiol. 2014;63:2985-3023.
1. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
2. Avina-Zubieta JA, Thomas J, Sadatsafavi M, et al. Risk of incident cardiovascular events in patients with rheumatoid arthritis: A meta-analysis of observational studies. Ann Rheum Dis. 2012;71:1524-1529.
3. Johnson TM, Mikuls TR, England BR. Assessment of cardiovascular risk in rheumatoid arthritis. J Clin Outcomes Manage. 2019;26:41-47.
4. Sandoo A, Chanchlani N, Hodson J, et al. Classical cardiovascular disease risk factors associate with vascular function and morphology in rheumatoid arthritis: A six-year prospective study. Arthritis Res Ther. 2013;15:R203.
5. Myasoedova E, Crowson CS, Kremers HM, et al. Total cholesterol and LDL levels decrease before rheumatoid arthritis. Ann Rheum Dis. 2010;69:1310-1314.
6. Liao KP, Cai T, Gainer VS, et al. Lipid and lipoprotein levels and trend in rheumatoid arthritis compared to the general population. Arthritis Care Res (Hoboken). 2013;65:2046-2050.
7. Myasoedova E, Crowson CS, Kremers HM, et al. Lipid paradox in rheumatoid arthritis: The impact of serum lipid measures and systemic inflammation on the risk of cardiovascular disease. Ann Rheum Dis. 2011;70:482-487.
8. Zhang J, Chen L, Delzell E, et al. Republished: The association between inflammatory markers, serum lipids and the risk of cardiovascular events in patients with rheumatoid arthritis. Postgrad Med J. 2014;90:722-729.
9. Liao KP, Liu J, Lu B, et al. Association between lipid levels and major adverse cardiovascular events in rheumatoid arthritis compared to non-rheumatoid arthritis patients. Arthritis Rheumatol. 2015;67:2004-2010.
10. Charles-Schoeman C, Lee YY, Grijalva V, et al. Cholesterol efflux by high density lipoproteins is impaired in patients with active rheumatoid arthritis. Ann Rheum Dis. 2012;71:1157-1162.
11. Voloshyna I, Modayil S, Littlefield MJ, et al. Plasma from rheumatoid arthritis patients promotes pro-atherogenic cholesterol transport gene expression in THP-1 human macrophages. Exp Biol Med (Maywood). 2013 238:1192-1197.
12. Taylor F, Huffman MD, Macedo AF, et al. Statins for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2013;(1):CD004816.
13. Sheng X, Murphy MJ, Macdonald TM, Wei L. Effectiveness of statins on total cholesterol and cardiovascular disease and all-cause mortality in osteoarthritis and rheumatoid arthritis. J Rheumatol. 2012;39:32-40.
14. An J, Alemao E, Reynolds K, et al. Cardiovascular outcomes associated with lowering low-density lipoprotein cholesterol in rheumatoid arthritis and matched nonrheumatoid arthritis. J Rheumatol. 2016;43:1989-1996.
15. Semb AG, Holme I, Kvien TK, Pedersen TR. Intensive lipid lowering in patients with rheumatoid arthritis and previous myocardial infarction: An explorative analysis from the incremental decrease in endpoints through aggressive lipid lowering (IDEAL) trial. Rheumatology (Oxford). 2011;50:324-329.
16. Semb AG, Kvien TK, DeMicco DA, et al. Effect of intensive lipid-lowering therapy on cardiovascular outcome in patients with and those without inflammatory joint disease. Arthritis Rheum. 2012;64:2836-2846.
17. El-Barbary AM, Hussein MS, Rageh EM, et al. Effect of atorvastatin on inflammation and modification of vascular risk factors in rheumatoid arthritis. J Rheumatol. 2011;38:229-235.
18. Writing Committee, Lloyd-Jones DM, Morris PB, et al. 2016 ACC expert consensus decision pathway on the role of non-statin therapies for LDL-cholesterol lowering in the management of atherosclerotic cardiovascular disease risk: A report of the American college of cardiology task force on clinical expert consensus documents. J Am Coll Cardiol. 2016;68:92-125.
19. Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372:2387-2397.
20. Sabatine MS, Giugliano RP, Wiviott SD, et al. Efficacy and safety of evolocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1500-1509.
21. Robinson JG, Farnier M, Krempf M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1489-1499.
22. Sabatine MS, Giugliano RP, Keech AC, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med. 2017;376:1713-1722.
23. Maki-Petaja KM, Booth AD, Hall FC, et al. Ezetimibe and simvastatin reduce inflammation, disease activity, and aortic stiffness and improve endothelial function in rheumatoid arthritis. J Am Coll Cardiol. 2007;50:852-858.
24. Bartels CM, Kind AJ, Everett C, et al. Low frequency of primary lipid screening among medicare patients with rheumatoid arthritis. Arthritis Rheum. 2011;63:1221-1230.
25. Akkara Veetil BM, Myasoedova E, Matteson EL, et al. Use of lipid-lowering agents in rheumatoid arthritis: A population-based cohort study. J Rheumatol. 2013;40:1082-1088.
26. Lindhardsen J, Ahlehoff O, Gislason GH, et al. Initiation and adherence to secondary prevention pharmacotherapy after myocardial infarction in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2012;71:1496-1501.
27. De Vera MA, Choi H, Abrahamowicz M, et al. Statin discontinuation and risk of acute myocardial infarction in patients with rheumatoid arthritis: A population-based cohort study. Ann Rheum Dis. 2011;70:1020-1024.
28. Zhang H, Plutzky J, Skentzos S, et al. Discontinuation of statins in routine care settings: A cohort study. Ann Intern Med. 2013;158:526-534.
29. Zhang H, Plutzky J, Shubina M, Turchin A. Continued statin prescriptions after adverse reactions and patient outcomes: A cohort study. Ann Intern Med. 2017;167:221-227.
30. Lemstra M, Blackburn D, Crawley A, Fung R. Proportion and risk indicators of nonadherence to statin therapy: A meta-analysis. Can J Cardiol. 2012;28:574-580.
31. Boyer JF, Gourraud PA, Cantagrel A, et al. Traditional cardiovascular risk factors in rheumatoid arthritis: A meta-analysis. Joint Bone Spine. 2011;78:179-183.
32. Bergstrom U, Jacobsson LT, Nilsson JA, et al. Pulmonary dysfunction, smoking, socioeconomic status and the risk of developing rheumatoid arthritis. Rheumatology (Oxford). 2011;50:2005-2013.
33. Costenbader KH, Feskanich D, Mandl LA, Karlson EW. Smoking intensity, duration, and cessation, and the risk of rheumatoid arthritis in women. Am J Med. 2006;119:503.e1,503.e9.
34. Klareskog L, Stolt P, Lundberg K, et al. A new model for an etiology of rheumatoid arthritis: Smoking may trigger HLA-DR (shared epitope)-restricted immune reactions to autoantigens modified by citrullination. Arthritis Rheum. 2006;54:38-46.
35. Sokolove J, Wagner CA, Lahey LJ, et al. Increased inflammation and disease activity among current cigarette smokers with rheumatoid arthritis: A cross-sectional analysis of US veterans. Rheumatology (Oxford). 2016;55:1969-1977.
36. World Health Organization. WHO Global Report: Mortality Attributable to Tobacco. Geneva, World Health Organization, 2012.
37. Baghdadi LR, Woodman RJ, Shanahan EM, Mangoni AA. The impact of traditional cardiovascular risk factors on cardiovascular outcomes in patients with rheumatoid arthritis: A systematic review and meta-analysis. PLoS One. 2015;10:e0117952.
38. Centers for Disease Control and Prevention; National Center for Chronic Disease Prevention and Health Promotion. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease: A Report of the Surgeon General. Atlanta (GA): Centers for Disease Control and Prevention; 2010. 6, Cardiovascular Diseases. Available from: https://ncbi.nlm.nih.gov/books/NBK53012/
39. Mons U, Muezzinler A, Gellert C, et al. Impact of smoking and smoking cessation on cardiovascular events and mortality among older adults: Meta-analysis of individual participant data from prospective cohort studies of the CHANCES consortium. BMJ. 2015;350:h1551.
40. Aimer P, Treharne GJ, Stebbings S, Frampton C, Cameron V, Kirby S, et al. Efficacy of a rheumatoid arthritis-specific smoking cessation program: A randomized controlled pilot trial. Arthritis Care Res (Hoboken). 2017;69:28-37.
41. Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2017.
42. Jiang P, Li H, Li X. Diabetes mellitus risk factors in rheumatoid arthritis: A systematic review and meta-analysis. Clin Exp Rheumatol. 2015;33:115-121.
43. Shahin D, Eltoraby E, Mesbah A, Houssen M. Insulin resistance in early untreated rheumatoid arthritis patients. Clin Biochem. 2010;43:661-335.
44. Arias de la Rosa I, Escudero-Contreras A, Rodriguez-Cuenca S, et al. Defective glucose and lipid metabolism in rheumatoid arthritis is determined by chronic inflammation in metabolic tissues. J Intern Med. 2018;84(1):61-77.
45. Wilson JC, Sarsour K, Gale S, et al. Incidence and risk of glucocorticoid-associated adverse effects in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018 Jun 1. doi: 10.1002/acr.23611.
46. Chung CP, Giles JT, Petri M, et al. Prevalence of traditional modifiable cardiovascular risk factors in patients with rheumatoid arthritis: Comparison with control subjects from the multi-ethnic study of atherosclerosis. Semin Arthritis Rheum. 2012;41:535-544.
47. Goodwin JE, Geller DS. Glucocorticoid-induced hypertension. Pediatr Nephrol. 2012;27:1059-1066.
48. Snowden S, Nelson R. The effects of nonsteroidal anti-inflammatory drugs on blood pressure in hypertensive patients. Cardiol Rev. 2011;19:184-191.
49. Baker JF, Sauer B, Teng CC, et al. Initiation of disease-modifying therapies in rheumatoid arthritis is associated with changes in blood pressure. J Clin Rheumatol. 2018;24:203-209.
50. Panoulas VF, Douglas KM, Milionis HJ, et al. Prevalence and associations of hypertension and its control in patients with rheumatoid arthritis. Rheumatology (Oxford). 2007;46:1477-1482.
51. Protogerou AD, Panagiotakos DB, Zampeli E, et al. Arterial hypertension assessed “out-of-office” in a contemporary cohort of rheumatoid arthritis patients free of cardiovascular disease is characterized by high prevalence, low awareness, poor control and increased vascular damage-associated “white coat” phenomenon. Arthritis Res Ther. 2013;15:R142.
52. van Breukelen-van der Stoep DF, van Zeben D, Klop B, et al. Marked underdiagnosis and undertreatment of hypertension and hypercholesterolaemia in rheumatoid arthritis. Rheumatology (Oxford). 2016;55:1210-1216.
53. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American college of cardiology/American heart association task force on clinical practice guidelines. J Am Coll Cardiol. 2018;71:e127-248.
54. Lee J, Dunlop D, Ehrlich-Jones L, et al. Public health impact of risk factors for physical inactivity in adults with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:488-493.
55. Sokka T, Hakkinen A, Kautiainen H, et al. Physical inactivity in patients with rheumatoid arthritis: Data from twenty-one countries in a cross-sectional, international study. Arthritis Rheum. 2008;59:42-50.
56. Fenton SAM, Veldhuijzen van Zanten JJCS, Kitas GD, et al. Sedentary behaviour is associated with increased long-term cardiovascular risk in patients with rheumatoid arthritis independently of moderate-to-vigorous physical activity. BMC Musculoskelet Disord. 2017;18:131,017-1473-9.
57. Byram KW, Oeser AM, Linton MF, et al. Exercise is associated with increased small HDL particle concentration and decreased vascular stiffness in rheumatoid arthritis. J Clin Rheumatol. 2018 May 25. 9.
58. de Jong Z, Munneke M, Zwinderman AH, et al. Is a long-term high-intensity exercise program effective and safe in patients with rheumatoid arthritis? results of a randomized controlled trial. Arthritis Rheum. 2003;48:2415-2424.
59. Stavropoulos-Kalinoglou A, Metsios GS, Veldhuijzen van Zanten JJ, et al. Individualised aerobic and resistance exercise training improves cardiorespiratory fitness and reduces cardiovascular risk in patients with rheumatoid arthritis. Ann Rheum Dis. 2013;72:1819-1825.
60. Khoja SS, Almeida GJ, Chester Wasko M, et al. Association of light-intensity physical activity with lower cardiovascular disease risk burden in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:424-431.
61. Metsios GS, Koutedakis Y, Veldhuijzen van Zanten JJ, et al. Cardiorespiratory fitness levels and their association with cardiovascular profile in patients with rheumatoid arthritis: A cross-sectional study. Rheumatology (Oxford). 2015;54:2215-2220.
62. Escalante A, Haas RW, del Rincon I. Paradoxical effect of body mass index on survival in rheumatoid arthritis: Role of comorbidity and systemic inflammation. Arch Intern Med. 2005;165:1624-1629.
63. Kremers HM, Nicola PJ, Crowson CS, et al. Prognostic importance of low body mass index in relation to cardiovascular mortality in rheumatoid arthritis. Arthritis Rheum. 2004;50:3450-3457.
64. Wolfe F, Michaud K. Effect of body mass index on mortality and clinical status in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012;64:1471-1479.
65. England BR, Baker JF, Sayles H, et al. Body mass index, weight loss, and cause-specific mortality in rheumatoid arthritis. Arthritis Care Res (Hoboken). 2018;70:11-18.
66. Dessein PH, Solomon A, Hollan I. Metabolic abnormalities in patients with inflammatory rheumatic diseases. Best Pract Res Clin Rheumatol. 2016;30:901-915.
67. Sparks JA, Halperin F, Karlson JC, et al. Impact of bariatric surgery on patients with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2015;67:1619-1626.
68. Mente A, de Koning L, Shannon HS, Anand SS. A systematic review of the evidence supporting a causal link between dietary factors and coronary heart disease. Arch Intern Med. 2009;169:659-669.
69. England BR, Sayles H, Michaud K, et al. Cause-specific mortality in male US veterans with rheumatoid arthritis. Arthritis Care Res (Hoboken). 2016;68:36-45.
70. Arts EE, Fransen J, Den Broeder AA, et al. Low disease activity (DAS28≤3.2) reduces the risk of first cardiovascular event in rheumatoid arthritis: a time-dependent Cox regression analysis in a large cohort study. Ann Rheum Dis. 2017;76(10):1693-1699.
71. Provan SA, Semb AG, Hisdal J, et al. Remission is the goal for cardiovascular risk management in patients with rheumatoid arthritis: A cross-sectional comparative study. Ann Rheum Dis. 2011;70:812-817.
72. Klarenbeek NB, van der Kooij SM, Huizinga TJ, et al. Blood pressure changes in patients with recent-onset rheumatoid arthritis treated with four different treatment strategies: A post hoc analysis from the BeSt trial. Ann Rheum Dis. 2010;69:1342-1345.
73. Hafstrom I, Rohani M, Deneberg S, et al. Effects of low-dose prednisolone on endothelial function, atherosclerosis, and traditional risk factors for atherosclerosis in patients with rheumatoid arthritis—a randomized study. J Rheumatol. 2007;34:1810-1816.
74. Hoes JN, van der Goes MC, van Raalte DH, et al. Glucose tolerance, insulin sensitivity and beta-cell function in patients with rheumatoid arthritis treated with or without low-to-medium dose glucocorticoids. Ann Rheum Dis. 2011;70:1887-1894.
75. Roubille C. The effects of tumour necrosis factor inhibitors, methotrexate, non-steroidal anti-inflammatory drugs and corticosteroids on cardiovascular events in rheumatoid arthritis, psoriasis and psoriatic arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2003;74:480-489.
76. Ajeganova S, Svensson B, Hafstrom I, BARFOT Study Group. Low-dose prednisolone treatment of early rheumatoid arthritis and late cardiovascular outcome and survival: 10-year follow-up of a 2-year randomised trial. BMJ Open. 2014;4:e004259,2013-004259.
77. Avina-Zubieta JA, Choi HK, Sadatsafavi M, et al. Risk of cardiovascular mortality in patients with rheumatoid arthritis: A meta-analysis of observational studies. Arthritis Rheum. 2008;59:1690-1697.
78. del Rincon I, Battafarano DF, Restrepo JF, et al. Glucocorticoid dose thresholds associated with all-cause and cardiovascular mortality in rheumatoid arthritis. Arthritis Rheumatol. 2014;66:264-272.
79. Davis JM,3rd, Maradit Kremers H, Crowson CS, et al. Glucocorticoids and cardiovascular events in rheumatoid arthritis: A population-based cohort study. Arthritis Rheum. 2007;56:820-830.
80. Zhang J, Xie F, Yun H, et al. Comparative effects of biologics on cardiovascular risk among older patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1813-1818.
81. Greenberg JD, Kremer JM, Curtis JR, et al. Tumour necrosis factor antagonist use and associated risk reduction of cardiovascular events among patients with rheumatoid arthritis. Ann Rheum Dis. 2011;70:576-582.
82. Lindhardsen J, Gislason GH, Jacobsen S, et al. Non-steroidal anti-inflammatory drugs and risk of cardiovascular disease in patients with rheumatoid arthritis: A nationwide cohort study. Ann Rheum Dis. 2014;73:1515-1521.
83. Schjerning Olsen AM, Fosbol EL, Lindhardsen J, et al. Duration of treatment with nonsteroidal anti-inflammatory drugs and impact on risk of death and recurrent myocardial infarction in patients with prior myocardial infarction: A nationwide cohort study. Circulation. 2011;123:2226-2235.
84. Gislason GH, Rasmussen JN, Abildstrom SZ, et al. Increased mortality and cardiovascular morbidity associated with use of nonsteroidal anti-inflammatory drugs in chronic heart failure. Arch Intern Med. 2009;169:141-149.
85. Trelle S, Reichenbach S, Wandel S, et al. Cardiovascular safety of non-steroidal anti-inflammatory drugs: Network meta-analysis. BMJ. 2011;342:c7086.
86. Nissen SE, Yeomans ND, Solomon DH, et al. Cardiovascular safety of celecoxib, naproxen, or ibuprofen for arthritis. N Engl J Med. 2016;375:2519-2529.
87. Wasko MC, Dasgupta A, Hubert Het al. Propensity-adjusted association of methotrexate with overall survival in rheumatoid arthritis. Arthritis Rheum. 2013;65:334-342.
88. Micha R, Imamura F, Wyler von Ballmoos M, et al. Systematic review and meta-analysis of methotrexate use and risk of cardiovascular disease. Am J Cardiol. 2011;108:1362-1370.
89. Bernatsky S, Hudson M, Suissa S. Anti-rheumatic drug use and risk of hospitalization for congestive heart failure in rheumatoid arthritis. Rheumatology (Oxford). 2005;44:677-680.
90. Myasoedova E, Crowson CS, Nicola PJ, et al. The influence of rheumatoid arthritis disease characteristics on heart failure. J Rheumatol. 2011;38:1601-1606.
91. Ronda N, Greco D, Adorni MP, et al. Newly identified antiatherosclerotic activity of methotrexate and adalimumab: Complementary effects on lipoprotein function and macrophage cholesterol metabolism. Arthritis Rheumatol. 2015;67:1155-1164.
92. Zimmerman MC, Clemens DL, Duryee MJ, et al. Direct antioxidant properties of methotrexate: Inhibition of malondialdehyde-acetaldehyde-protein adduct formation and superoxide scavenging. Redox Biol. 2017;13:588-593.
93. Rempenault C, Combe B, Barnetche T, et al. Metabolic and cardiovascular benefits of hydroxychloroquine in patients with rheumatoid arthritis: A systematic review and meta-analysis. Ann Rheum Dis. 2018;77:98-103.
94. Wasko MC, Hubert HB, Lingala VB, et al. Hydroxychloroquine and risk of diabetes in patients with rheumatoid arthritis. JAMA. 2007;298:187-193.
95. Charles-Schoeman C, Wang X, Lee YY, et al. Association of triple therapy with improvement in cholesterol profiles over two-year followup in the treatment of early aggressive rheumatoid arthritis trial. Arthritis Rheumatol. 2016;68:577-586.
96. Charles-Schoeman C, Yin Lee Y, Shahbazian A, et al. Improvement of high-density lipoprotein function in patients with early rheumatoid arthritis treated with methotrexate monotherapy or combination therapies in a randomized controlled trial. Arthritis Rheumatol. 2017;69:46-57.
97. Chung ES, Packer M, Lo KH, , Anti-TNF Therapy Against Congestive Heart Failure Investigators. Randomized, double-blind, placebo-controlled, pilot trial of infliximab, a chimeric monoclonal antibody to tumor necrosis factor-alpha, in patients with moderate-to-severe heart failure: Results of the anti-TNF therapy against congestive heart failure (ATTACH) trial. Circulation. 2003;107:3133-3140.
98. Singh JA, Saag KG, Bridges SL, Jr, et al. 2015 American college of rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68:1-26.
99. Daien CI, Duny Y, Barnetche Tet al. Effect of TNF inhibitors on lipid profile in rheumatoid arthritis: A systematic review with meta-analysis. Ann Rheum Dis. 2012;71:862-868.
100. Di Minno MN, Ambrosino P, Peluso R, et al. Lipid profile changes in patients with rheumatic diseases receiving a treatment with TNF-alpha blockers: A meta-analysis of prospective studies. Ann Med. 2014;46:73-83.
101. Popa C, van Tits LJ, Barrera P, et al. Anti-inflammatory therapy with tumour necrosis factor alpha inhibitors improves high-density lipoprotein cholesterol antioxidative capacity in rheumatoid arthritis patients. Ann Rheum Dis. 2009;68:868-872.
102. O’Neill F, Charakida M, Topham E, et al. Anti-inflammatory treatment improves high-density lipoprotein function in rheumatoid arthritis. Heart. 2017;103:766-773.
103. Nishimoto N, Ito K, Takagi N. Safety and efficacy profiles of tocilizumab monotherapy in Japanese patients with rheumatoid arthritis: Meta-analysis of six initial trials and five long-term extensions. Mod Rheumatol. 2010;20:222-232.
104. Rao VU, Pavlov A, Klearman M, et al. An evaluation of risk factors for major adverse cardiovascular events during tocilizumab therapy. Arthritis Rheumatol. 2015;67:372-380.
105. Gabay C, McInnes IB, Kavanaugh A, et al. Comparison of lipid and lipid-associated cardiovascular risk marker changes after treatment with tocilizumab or adalimumab in patients with rheumatoid arthritis. Ann Rheum Dis. 2016;75:1806-1812.
106. McInnes IB, Thompson L, Giles JT, et al. Effect of interleukin-6 receptor blockade on surrogates of vascular risk in rheumatoid arthritis: MEASURE, a randomised, placebo-controlled study. Ann Rheum Dis. 2015;74:694-702.
107. Souto A, Salgado E, Maneiro JR, et al. Lipid profile changes in patients with chronic inflammatory arthritis treated with biologic agents and tofacitinib in randomized clinical trials: A systematic review and meta-analysis. Arthritis Rheumatol. 2015;67:117-127.
108. Myasoedova E, Gabriel SE, Matteson EL, et al. Decreased cardiovascular mortality in patients with incident rheumatoid arthritis (RA) in recent years: Dawn of a new era in cardiovascular disease in RA? J Rheumatol. 2017;44:732-739.
109. Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2889-2934.
110. Clinical Practice Guideline Treating Tobacco Use and Dependence 2008 Update Panel, Liaisons, and Staff. A clinical practice guideline for treating tobacco use and dependence: 2008 update. A U.S. public health service report. Am J Prev Med. 2008;35:158-176.
111. Eckel RH, Jakicic JM, Ard JD, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: A report of the American college of cardiology/American heart association task force on practice guidelines. J Am Coll Cardiol. 2014;63:2960-2984.
112. Apovian CM, Aronne LJ, Bessesen DH, et al. Pharmacological management of obesity: An endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2015;100:342-362.
113. Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: A report of the American college of cardiology/American heart association task force on practice guidelines and the obesity society. J Am Coll Cardiol. 2014;63:2985-3023.
Point-of-Care versus Central Laboratory Glucose Testing in Postoperative Cardiac Surgery Patients
From the Maine Medical Center, Portland, ME (Dr. Kramer, Ms. Palmeri, Dr. Robich, Mr. Groom, Dr. Hayes, Ms. Janoushek, Dr. Rappold, Dr. Swarz, and Dr. Quinn), and the Center for Outcomes Research and Evaluation, Maine Medical Center Research Institute, Portland, ME (Dr. Lucas).
Abstract
- Objective. To determine the accuracy of the glucometer currently used for point-of-care testing (POCT) of blood glucose in our cardiothoracic surgery intensive care unit (CTICU).
- Design. Prospective cohort study.
- Setting. Tertiary care community hospital affiliated with a school of medicine.
- Participants. Coronary artery bypass graft (CABG) surgery patients.
- Measurements. Blood glucose levels obtained via POCT with a glucometer using fingerstick and radial artery blood samples were compared with values obtained via central laboratory testing of radial artery blood samples (gold standard) in 106 CABG patients on continuous insulin infusions (CII) upon arrival to the CTICU from the operating room and 102 CABG patients on CII in the CTICU 6 hours later.
- Results. Fingerstick POCT and central lab blood glucose values correlated well (r = 0.83 for admission and 0.86 for 6-hour values), but the mean values were significantly different as determined by paired t-tests. Upon arrival, the fingerstick POCT mean value was 120.9 mg/dL, while the central laboratory value was 127.9 mg/dL (P value = 0.03). At the 6-hour time point, the mean value for fingerstick POCT was 129.7 mg/dL compared to a central laboratory value of 137.3 (P value = 0.02).
- Conclusion. The blood glucose POCT values correlated well with central laboratory values, but the values were statistically significantly different. Nevertheless, accurate clinical decisions were made despite the inaccuracies of POCT glucose testing, as experienced bedside nurses were able to use the glucometer successfully and safely. The device’s results informed them when the blood glucose was out of a prescibed range and the direction of the change, and they were able to adjust the CII accordingly.
Keywords: quality improvement; glucose management; point-of-care testing; critical care.
Achieving glycemic control in patients with and without diabetes during coronary artery bypass graft (CABG) surgery is associated with reduced perioperative morbidity and mortality and improved long-term survival.1 Hyperglycemia has detrimental effects on the cardiovascular system and insulin has beneficial effects on the ischemic myocardium.2 The current recommendations of the Society of Thoracic Surgery regarding blood glucose management include the use of continuous insulin infusions (CII) during and after surgery in the critical care unit,3 keeping blood glucose in a moderate range. Glucometers are commonly used in the critical care perioperative setting for point-of-care testing (POCT) for timely determinations of blood glucose levels for patients on CII.
POCT for glucose monitoring is a valuable tool for managing patients with diabetes in the outpatient setting. Evolving from urinary test strips that depended on a colorimetric model, glucometers now incoroporate digital technology that allows patients to determine their blood glucose using a drop of blood from a fingerstick. The US Food and Drug Administration’s approval for most glucose POCT technology includes home use by diabetic patients and use in the hospital setting, with the exception of critically ill patients, who may be affected by hypoxemia, poor capillary perfusion, tissue edema, severe anemia4 or other pathophysiologic states that could impact the accuracy of the devices. For example, poor peripheral perfusion related to shock or vasoconstrictors and interstitial edema are variables that could contribute to an erroneous reading. Therefore, many glucometers used in the critical care setting are being used off-label. Because much of the current POCT technology for glucose monitoring may provide erroneous results in certain ranges and in some clinical settings, the safety of most glucometers has been called into question.5,6
Given the concern regarding the potential inaccuracies of commonly used glucometers in the critical care setting, we undertook a quality improvement project to analyze the clinical performance of the glucometer currently used in our critically ill postoperative cardiac surgery population. The cardiac surgery division policy at our institution is to place all patients, both diabetic and nondiabetic, on a CII intraoperatively and to continue the infusion for at least 24 to 48 hours postoperatively. The CII start rate is determined utilizing the division’s Insulin Start Chart, and then the CII is adjusted according to the nomogram through the postoperative course. Both the Insulin Start Chart and nomogram have been previously described by Kramer et al.7
Currently, POCT of glucose in all post cardiac surgery patients is done hourly or more frequently in the first 24 to 48 hours after surgery in order to adjust the CII. In patients undergoing the stress of cardiac surgery, the action of insulin is counter-regulated by glucagon, epinephrine, norepinephrine, cortisol, and growth hormone. The resulting varying degrees of insulin resistance in this population of patients requires close monitoring of blood glucose, keeping it in a prescribed range, which in our center is 110 to 150 mg/dL, both in diabetic and nondiabetic patients. Frequent laboratory and POCT determinations of glucose are made. Providers and bedside nurses adjust the CII according to central laboratory values, POCT values, and trends, as previously described.7
Methods
Setting
Maine Medical Center is a 600-bed tertiary care teaching hospital. It is a level 1 trauma center where 1000 cardiac surgical operations are performed annually. POCT glucose monitoring is relied upon to monitor blood glucose and adjust the CII accordingly. This project, which did not require any additional procedures outside of the standard of care for this population of patients, was reviewed by the Institutional Review Board, who determined that this activity does not meet either the definition of research as specified under 45 CFR 46.102 (d) or the definition of clinical investigation as specified in 21 CFR 56.102 (c).
Patients
Using central laboratory glucose values drawn from the radial artery as the gold standard, we created a registry of consecutive postoperative cardiac surgery patients who had undergone CABG surgery and had blood glucose determinations from both POCT (fingerstick and radial artery samples) and central laboratory testing (radial artery sample) during a 7-month period (May 2016 through February 2017). To be included in the registry, patients had to (1) be postoperative following isolated CABG or CABG plus Maze procedure; (2) have been on cardiopulmonary bypass (CPB); (3) have radial arterial lines; and (4) be on a CII. A total of 116 patients qualified according to the inclusion criteria. Patients missing glucose results in 1 or more of the variables were excluded from data analysis.
Measurements and Variables
Using a POCT glucometer (FreeStyle Precision Pro, Abbott Laboratories, Abbott Park, IL), blood glucose conentrations were measured on samples obtained from both fingerstick and radial artery. Concurrently, radial arterial blood was sent to the central laboratory for glucose measurement. Blood glucose values were compared in CABG patients on CII upon arrival to the cardiothoracic surgery intensive care unit (CTICU) from the operating room and CABG patients on CII 6 hours after arrival in the CTICU. During the 6-hour interval, blood glucose levels were tested hourly or more frequently, allowing nurses to identify trends in blood glucose changes in order to keep blood glucose in the prescribed goal range of 110 to 150 mg/dL. At each of these 2 time points, on arrival to CTICU and 6 hours later, blood glucose values obtained with radial artery POCT and fingerstick POCT were compared with values obtained with central laboratory testing of radial artery samples. The amount of blood required was 1 drop each for POCT fingerstick and POCT radial artery and 2 mL for central lab testing.
Patient characteristics were identified from the electronic medical record. The variables recorded were type of operation, time on CPB, time of CTICU arrival, temperature, vasoconstrictor infusions (norepinephrine, vasopressin, phenylephrine), preoperative diagnosis of diabetes mellitus, preoperative HbA1c, and hemoglobin/hematocrit. Hemoglobin/hematocrit was only available at the time of the patient’s arrival to CTICU. The study was completed within the confines of our center’s standard of care protocol for postoperative cardiac surgical patients.
Analysis
We used standard statistical techniques to describe the study population, including proportions for categorical variables and means (standard deviations) for continuous variables. Correlation and regression techniques were used to describe the relationship between POCT and laboratory (gold standard) tests, both measured as continuous variables, and paired t-tests with Bonferroni correction were used to compare the central tendency and range of these comparisons. We calculated the differences between the gold standard measure and the POCT measure as an indication of outliers (ie, cases in which the 2 tests gave markedly different results). We examined plots to ascertain at which levels of the gold standard test these outliers occurred. An interim analysis was done at the halfway point and submitted to the Institutional Review Board, but no correction to the P value was done based on this analysis, which was largely qualitative. We used Bonferroni correction to declare a P value of 0.025 statistically significant with the 2-way comparisons of both fingerstick and radial artery values to central laboratory values. When the data was stratified by a clinical characteristic creating a 4-way comparison, we used Bonferroni correction to declare a P value of 0.0125 to be statistically significant when comparing both fingerstick and radial artery values to central laboratory values.
Results
Glucose POCT evaluations were carried out on 116 consecutive patients who underwent CABG surgery with or without a Maze procedure on CPB with a CII and an arterial line. Due to missing glucose results in 1 or more of the variables, 10 patients were excluded from data analysis for the time point of arrival in the CTICU and 14 patients were excluded from data analysis for the time point of 6 hours post CTICU arrival. This gave a final count of 106 CABG patients for CTICU arrival data analysis and 102 CABG patients for the 6 hours after CTICU arrival data analysis.
Patients ranged in age from 43 to 85 years, with a mean of age of 66 years, 22% were were women, 41% were diabetic, and 18% had peripheral vascular disease (Table 1). The average preoperative HbA1c was 6.4% ± 1.3% (range, 4.6% to 11.1%). Mean time on CBP for the group was 101 ± 31 minutes (range, 43 to 233 minutes). Postoperative mean hematocrit and hemoglobin were 32.5% and 11.4 g/dL, respectively. The average core temperature of patients on arrival was 36.0°C, which rose to an average of 36.6°C 6 hours later. A vasoconstrictor drip was infusing on 52% of patients upon CTICU arrival; 65% had a vasoconstrictor drip infusing 6 hours after arrival to the CTICU. Hemoglobin results were available only upon CTICU arrival as they are not routinely checked at 6 hours; 74 (64%) patients had a hemoglobin < 12 g/dL.
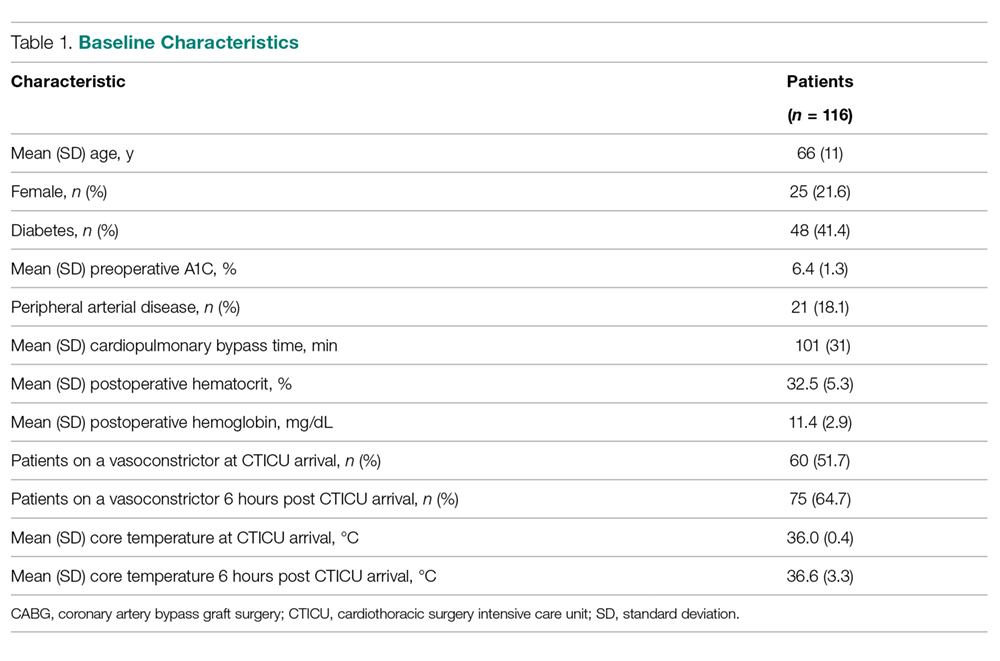
Compared to central laboratory testing, which we are defining as the gold standard, fingerstick POCT performed better on arrival, while radial artery POCT performed better at 6 hours (Table 2). At CTICU arrival, the mean blood glucose value for fingerstick POCT was 121 ± 24.1 mg/dL, 116 ± 27.2 mg/dL for radial artery POCT, and 128 ± 23.5 mg/dL for central lab testing. The difference in mean blood glucose between the fingerstick POCT and central lab testing was not statistically significant (P = 0.032), while the difference in mean blood glucose between radial artery POCT and central lab testing was statistically significant (P = 0.001). At 6 hours post arrival to the CTICU, the mean fingerstick POCT blood glucose value was 130 ± 23.9 mg/dL, compared to the mean central lab testing value of 137 ± 22.4 mg/dL; this difference was statistically significant (P = 0.019), while the radial artery POCT blood glucose value (133 ± 24.6 mg/dL) was not significantly different from the central lab testing value.
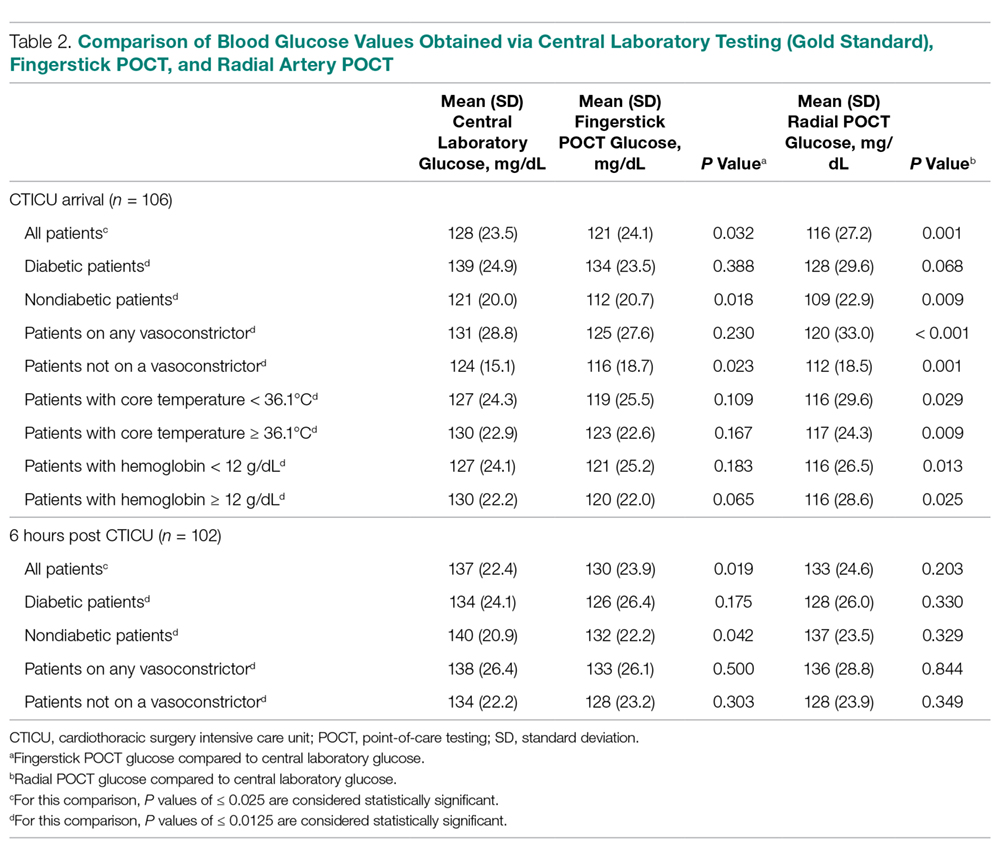
Blood glucose values from fingerstick POCT and central laboratory testing correlated well (r = 0.83 for admission and 0.86 for 6-hour values), as did radial artery POCT and central lab values (r = 0.87 for admission and 0.90 for 6-hour values) (Figures 1, 2, 3, and 4). Comparing individual values for fingerstick POCT and central lab testing, within-person differences between the 2 values ranged from –45 to 25 mg/dL, with 21% of pairs discrepant by 20 mg/dL or more (Figure 1); results were similar at 6 hours (Figure 2), with slightly less discrepancy.
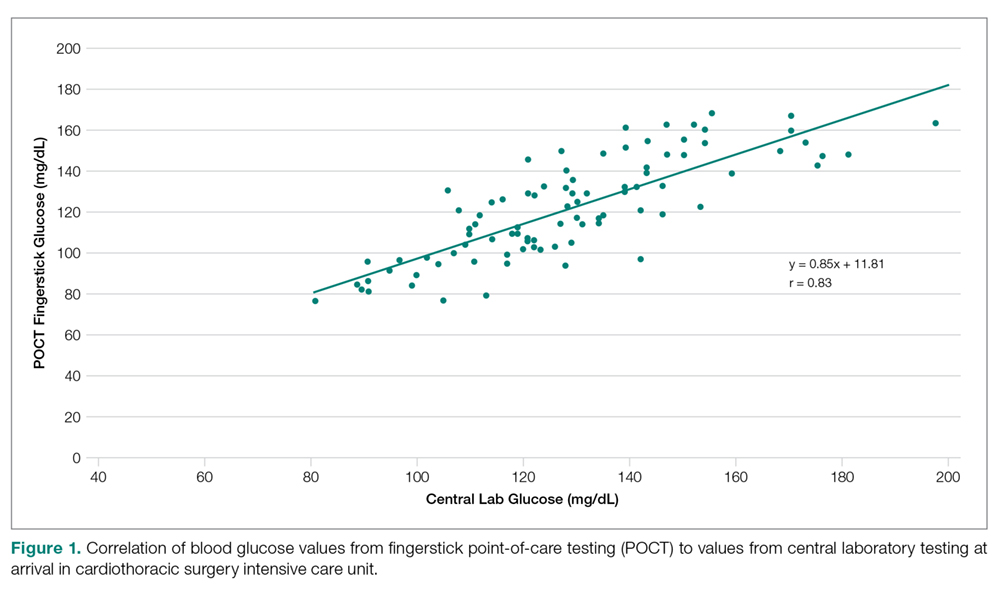
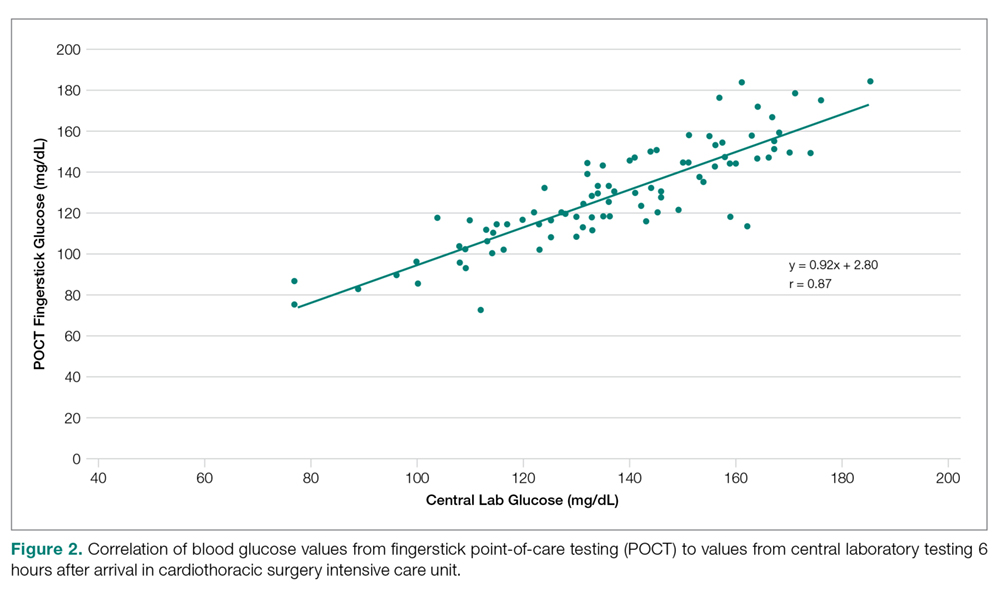
The differences between radial artery POCT and central lab testing values at CTICU arrival ranged from –43 to 80 mg/dL, with 24% of pairs discrepant by 20 mg/dL or more (Figure 3). At 6 hours post CTICU arrival, the difference between radial artery POCT and central lab testing values ranged from –130 to 27 mg/dL, with 11% of pairs discrepant by 20 mg/dL or more (Figure 4). Ninety-two percent of central laboratory values were either close to (± 20) or within the moderate glycemic control target range (110–150 mg/dL).
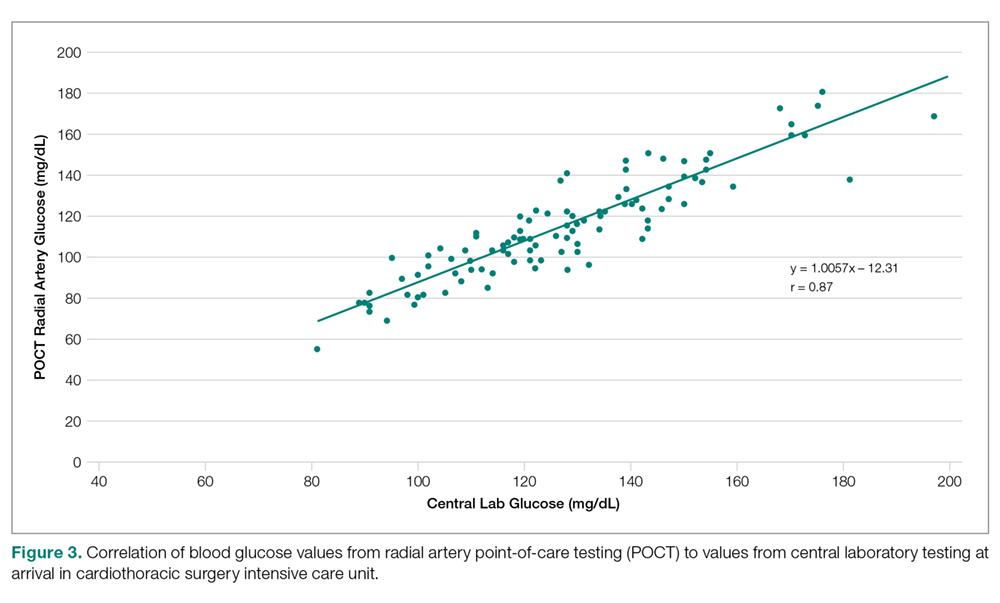
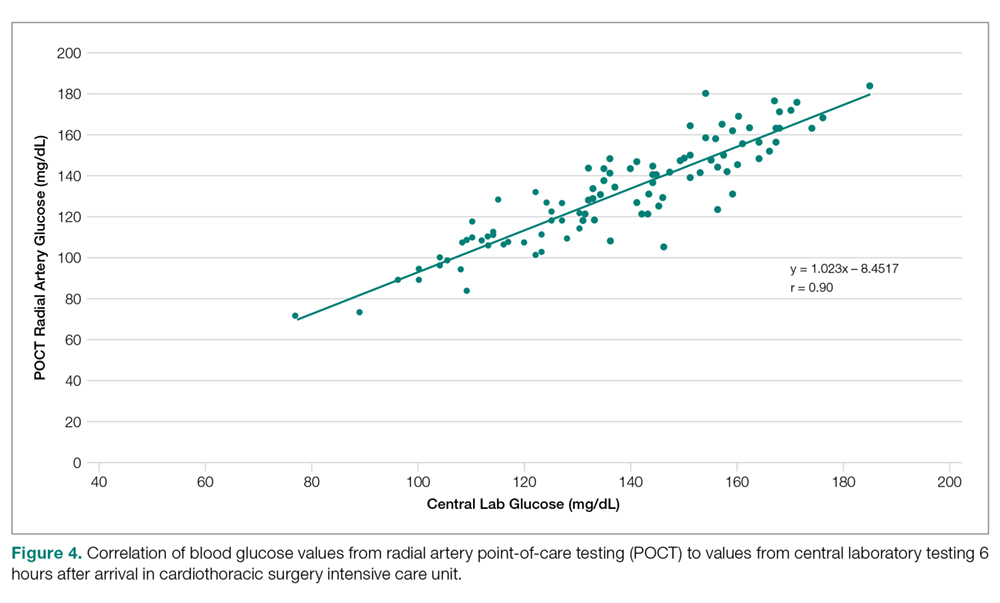
When the patient cohort was stratified by anemia, diabetes, body temperature, and receipt of vasoconstrictor, there were no significant differences between mean fingerstick POCT and central lab testing values for any strata on CTICU arrival, while there were significant differences between radial artery POCT and central lab testing means for both vasoconstrictor strata as well as for patients with core temperature > 36.1°C (Table 2). At 6 hours, there were no statistically significant differences when stratified for receipt of vasoconstrictor or presence of diabetes. Stratification for anemia or core body temperature was not done for patients at the 6-hour post CTICU arrival time because no hemoglobin value was available and all patients except 1 reached a core temperature of 36.1°C.
Although we measured POCT values obtained using 2 different blood sample sources, fingerstick POCT performed better than radial artery POCT testing with regard to the mean values when compared with the central lab. However, radial artery POCT performed better with regard to correlation with the central lab value. In other words, fingerstick POCT values were less significantly different than radial artery POCT values when compared with the central lab, while radial artery POCT values correlated better with values from the central lab. In spite of this unexplained variability in differences and correlation, the blood glucose values stayed in the target goal range (Figures 1-4).
Discussion
The accuracy of glucose POCT in the critical care setting has been called into question.4,5 The clinical demands of glucose management using CII include timely and accurate guidance in postoperaptive cardiac surgery, in this case, CABG. A previous study compared POCT and central laboratory blood glucose values in medical intensive care unit patients,8 but not in patients who have had CABG surgery. Another study has reviewed the difference in glucose values from POCT and central lab analysis in the critically ill population, but not in the post cardiac surgical population.9 We have shown that the POCT blood glucose values correlate well with the clinical lab values, but the values are statistically different. Our study adds an additional observation in that, although the POCT inconsistencies were statistically significant, they were not clinically significant. That is, POCT of blood glucose was inaccurate, but it still helped guide care by providing enough information to keep the blood glucose in range (most of the time) and allowing the bedside nurse to detect trends and make appropriate adjustments to the infusion. However, given these inconsistencies, we recommend a low threshold for sending additional samples to the central lab to double-check the glucose values, especially when they are outside the prescribed range. Our analysis provides some measure of reassurance with regard to current postoperative CABG glucose management by showing that the limitations of the blood glucose meter do not jeopardize the safety of patients. Nonetheless, we look forward to advances in the accuracy of POCT blood glucose technology so that critical care patients can be better managed when blood glucose is outside the prescribed range.
This analysis of 116 CABG patients points out both the inaccuracy and the utility of a representative POCT glucometer (in this case, the FreeStyle Precision Pro) used at the bedside to manage CIIs in postoperative CABG patients, keeping the blood glucose level in the moderate control range (110-150 mg/dL). The correlation plot shows that in this population the bedside nurses were able to keep blood glucose in range most of the time, in spite of the inaccuracy of POCT of blood glucose, given that the error of the test fits in the wide margin of 40 mg/dL. The fact that the 6-hour values were slightly less variable than the admission values indicates that sequential determinations of blood glucose over the 6-hour period to detect trends allowed good clinical management even in the face of such inaccuracy. The correlation allows the inaccurate number (blood glucose value) to indicate direction, and frequent determinations allow the bedside nurse to keep that number in the prescribed range most of the time in this population of patients.
Conclusion
We have found that glucometer blood glucose determinations in our center used on a homogenous population (CABG surgery) utilizing a single type of glucometer correlated well with those of the central lab, but were not always accurate. In spite of the inaccuracies, experienced bedside nurses were able to use the instrument successfully and safely, as it informed them if the blood glucose was in or out of a predetermined range and in which direction it was going.
Acknowledgment: The authors are indebted to the nurses of the Cardiothoracic Surgery Intensive Care Unit at Maine Medical Center for their support and assistance, without which this analysis would not have been possible.
Corresponding author: Robert S. Kramer, MD, Division of Cardiothoracic Surgery, Maine Medical Center Cardiovascular Institute, 22 Bramhall St., Portland ME 04102; [email protected].
Financial disclosures: None.
1. Furnary AP, Gao G, Grunkemeier GL, et al. Continuous insulin infusion reduces mortality in patients with diabetes undergoing coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2003;125:1007-1021.
2. Lazar H. Glycemic control during coronary artery bypass graft surgery. ISRN Cardiol. 2012;2012:292490.
3. Lazar HL, McDonnell M, Chipkin SR, et al; Society of Thoracic Surgeons Blood Glucose Guideline Task Force. The Society of Thoracic Surgeons Practice Guideline Series: blood glucose management during adult cardiac surgery. Ann Thorac Surg. 2009;87:663-669.
4. US Food and Drug Administration. Blood Glucose Monitoring Test Systems for Prescription Point of Care Use. Guidance for Industry and Food and Drug Administration Staff,.www.fda.gov/downloads/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/UCM380325.pdf. Accessed March 8, 2019.
5. Finkielman JD, Oyen LJ, Afess B. Agreement between bedside blood and plasma glucose measurement in the ICU Setting. Chest. 2005;127:1749-1511.
6. Pidcoke HF, Wade CE, Mann EA, et al. Anemia causes hypoglycemia in ICU patients due to error in single-channel glucometers: methods of reducing patient risk. Crit Care Med. 2010;38:471-476.
7. Kramer R, Groom R, Weldner D, et al. Glycemic control reduces deep sternal wound infection: a multidisciplinary approach. Arch Surg. 2008;143:451-456.
8. Peterson JR, Graves DF, Tacker DH, et al. Comparison of POCT and central laboratory blood glucose results using arterial, capillary, and venous samples from MICU patients on a tight glycemic protocol. Clinica Chimica Acta. 2008;396:10-13.
9. Cook A, Laughlin D, Moore M, et al. Differences in glucose values obtained from point-of-care glucose meters and laboratory analysis in critically ill patients. Am J Crit Care. 2009;18:65-72.
From the Maine Medical Center, Portland, ME (Dr. Kramer, Ms. Palmeri, Dr. Robich, Mr. Groom, Dr. Hayes, Ms. Janoushek, Dr. Rappold, Dr. Swarz, and Dr. Quinn), and the Center for Outcomes Research and Evaluation, Maine Medical Center Research Institute, Portland, ME (Dr. Lucas).
Abstract
- Objective. To determine the accuracy of the glucometer currently used for point-of-care testing (POCT) of blood glucose in our cardiothoracic surgery intensive care unit (CTICU).
- Design. Prospective cohort study.
- Setting. Tertiary care community hospital affiliated with a school of medicine.
- Participants. Coronary artery bypass graft (CABG) surgery patients.
- Measurements. Blood glucose levels obtained via POCT with a glucometer using fingerstick and radial artery blood samples were compared with values obtained via central laboratory testing of radial artery blood samples (gold standard) in 106 CABG patients on continuous insulin infusions (CII) upon arrival to the CTICU from the operating room and 102 CABG patients on CII in the CTICU 6 hours later.
- Results. Fingerstick POCT and central lab blood glucose values correlated well (r = 0.83 for admission and 0.86 for 6-hour values), but the mean values were significantly different as determined by paired t-tests. Upon arrival, the fingerstick POCT mean value was 120.9 mg/dL, while the central laboratory value was 127.9 mg/dL (P value = 0.03). At the 6-hour time point, the mean value for fingerstick POCT was 129.7 mg/dL compared to a central laboratory value of 137.3 (P value = 0.02).
- Conclusion. The blood glucose POCT values correlated well with central laboratory values, but the values were statistically significantly different. Nevertheless, accurate clinical decisions were made despite the inaccuracies of POCT glucose testing, as experienced bedside nurses were able to use the glucometer successfully and safely. The device’s results informed them when the blood glucose was out of a prescibed range and the direction of the change, and they were able to adjust the CII accordingly.
Keywords: quality improvement; glucose management; point-of-care testing; critical care.
Achieving glycemic control in patients with and without diabetes during coronary artery bypass graft (CABG) surgery is associated with reduced perioperative morbidity and mortality and improved long-term survival.1 Hyperglycemia has detrimental effects on the cardiovascular system and insulin has beneficial effects on the ischemic myocardium.2 The current recommendations of the Society of Thoracic Surgery regarding blood glucose management include the use of continuous insulin infusions (CII) during and after surgery in the critical care unit,3 keeping blood glucose in a moderate range. Glucometers are commonly used in the critical care perioperative setting for point-of-care testing (POCT) for timely determinations of blood glucose levels for patients on CII.
POCT for glucose monitoring is a valuable tool for managing patients with diabetes in the outpatient setting. Evolving from urinary test strips that depended on a colorimetric model, glucometers now incoroporate digital technology that allows patients to determine their blood glucose using a drop of blood from a fingerstick. The US Food and Drug Administration’s approval for most glucose POCT technology includes home use by diabetic patients and use in the hospital setting, with the exception of critically ill patients, who may be affected by hypoxemia, poor capillary perfusion, tissue edema, severe anemia4 or other pathophysiologic states that could impact the accuracy of the devices. For example, poor peripheral perfusion related to shock or vasoconstrictors and interstitial edema are variables that could contribute to an erroneous reading. Therefore, many glucometers used in the critical care setting are being used off-label. Because much of the current POCT technology for glucose monitoring may provide erroneous results in certain ranges and in some clinical settings, the safety of most glucometers has been called into question.5,6
Given the concern regarding the potential inaccuracies of commonly used glucometers in the critical care setting, we undertook a quality improvement project to analyze the clinical performance of the glucometer currently used in our critically ill postoperative cardiac surgery population. The cardiac surgery division policy at our institution is to place all patients, both diabetic and nondiabetic, on a CII intraoperatively and to continue the infusion for at least 24 to 48 hours postoperatively. The CII start rate is determined utilizing the division’s Insulin Start Chart, and then the CII is adjusted according to the nomogram through the postoperative course. Both the Insulin Start Chart and nomogram have been previously described by Kramer et al.7
Currently, POCT of glucose in all post cardiac surgery patients is done hourly or more frequently in the first 24 to 48 hours after surgery in order to adjust the CII. In patients undergoing the stress of cardiac surgery, the action of insulin is counter-regulated by glucagon, epinephrine, norepinephrine, cortisol, and growth hormone. The resulting varying degrees of insulin resistance in this population of patients requires close monitoring of blood glucose, keeping it in a prescribed range, which in our center is 110 to 150 mg/dL, both in diabetic and nondiabetic patients. Frequent laboratory and POCT determinations of glucose are made. Providers and bedside nurses adjust the CII according to central laboratory values, POCT values, and trends, as previously described.7
Methods
Setting
Maine Medical Center is a 600-bed tertiary care teaching hospital. It is a level 1 trauma center where 1000 cardiac surgical operations are performed annually. POCT glucose monitoring is relied upon to monitor blood glucose and adjust the CII accordingly. This project, which did not require any additional procedures outside of the standard of care for this population of patients, was reviewed by the Institutional Review Board, who determined that this activity does not meet either the definition of research as specified under 45 CFR 46.102 (d) or the definition of clinical investigation as specified in 21 CFR 56.102 (c).
Patients
Using central laboratory glucose values drawn from the radial artery as the gold standard, we created a registry of consecutive postoperative cardiac surgery patients who had undergone CABG surgery and had blood glucose determinations from both POCT (fingerstick and radial artery samples) and central laboratory testing (radial artery sample) during a 7-month period (May 2016 through February 2017). To be included in the registry, patients had to (1) be postoperative following isolated CABG or CABG plus Maze procedure; (2) have been on cardiopulmonary bypass (CPB); (3) have radial arterial lines; and (4) be on a CII. A total of 116 patients qualified according to the inclusion criteria. Patients missing glucose results in 1 or more of the variables were excluded from data analysis.
Measurements and Variables
Using a POCT glucometer (FreeStyle Precision Pro, Abbott Laboratories, Abbott Park, IL), blood glucose conentrations were measured on samples obtained from both fingerstick and radial artery. Concurrently, radial arterial blood was sent to the central laboratory for glucose measurement. Blood glucose values were compared in CABG patients on CII upon arrival to the cardiothoracic surgery intensive care unit (CTICU) from the operating room and CABG patients on CII 6 hours after arrival in the CTICU. During the 6-hour interval, blood glucose levels were tested hourly or more frequently, allowing nurses to identify trends in blood glucose changes in order to keep blood glucose in the prescribed goal range of 110 to 150 mg/dL. At each of these 2 time points, on arrival to CTICU and 6 hours later, blood glucose values obtained with radial artery POCT and fingerstick POCT were compared with values obtained with central laboratory testing of radial artery samples. The amount of blood required was 1 drop each for POCT fingerstick and POCT radial artery and 2 mL for central lab testing.
Patient characteristics were identified from the electronic medical record. The variables recorded were type of operation, time on CPB, time of CTICU arrival, temperature, vasoconstrictor infusions (norepinephrine, vasopressin, phenylephrine), preoperative diagnosis of diabetes mellitus, preoperative HbA1c, and hemoglobin/hematocrit. Hemoglobin/hematocrit was only available at the time of the patient’s arrival to CTICU. The study was completed within the confines of our center’s standard of care protocol for postoperative cardiac surgical patients.
Analysis
We used standard statistical techniques to describe the study population, including proportions for categorical variables and means (standard deviations) for continuous variables. Correlation and regression techniques were used to describe the relationship between POCT and laboratory (gold standard) tests, both measured as continuous variables, and paired t-tests with Bonferroni correction were used to compare the central tendency and range of these comparisons. We calculated the differences between the gold standard measure and the POCT measure as an indication of outliers (ie, cases in which the 2 tests gave markedly different results). We examined plots to ascertain at which levels of the gold standard test these outliers occurred. An interim analysis was done at the halfway point and submitted to the Institutional Review Board, but no correction to the P value was done based on this analysis, which was largely qualitative. We used Bonferroni correction to declare a P value of 0.025 statistically significant with the 2-way comparisons of both fingerstick and radial artery values to central laboratory values. When the data was stratified by a clinical characteristic creating a 4-way comparison, we used Bonferroni correction to declare a P value of 0.0125 to be statistically significant when comparing both fingerstick and radial artery values to central laboratory values.
Results
Glucose POCT evaluations were carried out on 116 consecutive patients who underwent CABG surgery with or without a Maze procedure on CPB with a CII and an arterial line. Due to missing glucose results in 1 or more of the variables, 10 patients were excluded from data analysis for the time point of arrival in the CTICU and 14 patients were excluded from data analysis for the time point of 6 hours post CTICU arrival. This gave a final count of 106 CABG patients for CTICU arrival data analysis and 102 CABG patients for the 6 hours after CTICU arrival data analysis.
Patients ranged in age from 43 to 85 years, with a mean of age of 66 years, 22% were were women, 41% were diabetic, and 18% had peripheral vascular disease (Table 1). The average preoperative HbA1c was 6.4% ± 1.3% (range, 4.6% to 11.1%). Mean time on CBP for the group was 101 ± 31 minutes (range, 43 to 233 minutes). Postoperative mean hematocrit and hemoglobin were 32.5% and 11.4 g/dL, respectively. The average core temperature of patients on arrival was 36.0°C, which rose to an average of 36.6°C 6 hours later. A vasoconstrictor drip was infusing on 52% of patients upon CTICU arrival; 65% had a vasoconstrictor drip infusing 6 hours after arrival to the CTICU. Hemoglobin results were available only upon CTICU arrival as they are not routinely checked at 6 hours; 74 (64%) patients had a hemoglobin < 12 g/dL.

Compared to central laboratory testing, which we are defining as the gold standard, fingerstick POCT performed better on arrival, while radial artery POCT performed better at 6 hours (Table 2). At CTICU arrival, the mean blood glucose value for fingerstick POCT was 121 ± 24.1 mg/dL, 116 ± 27.2 mg/dL for radial artery POCT, and 128 ± 23.5 mg/dL for central lab testing. The difference in mean blood glucose between the fingerstick POCT and central lab testing was not statistically significant (P = 0.032), while the difference in mean blood glucose between radial artery POCT and central lab testing was statistically significant (P = 0.001). At 6 hours post arrival to the CTICU, the mean fingerstick POCT blood glucose value was 130 ± 23.9 mg/dL, compared to the mean central lab testing value of 137 ± 22.4 mg/dL; this difference was statistically significant (P = 0.019), while the radial artery POCT blood glucose value (133 ± 24.6 mg/dL) was not significantly different from the central lab testing value.

Blood glucose values from fingerstick POCT and central laboratory testing correlated well (r = 0.83 for admission and 0.86 for 6-hour values), as did radial artery POCT and central lab values (r = 0.87 for admission and 0.90 for 6-hour values) (Figures 1, 2, 3, and 4). Comparing individual values for fingerstick POCT and central lab testing, within-person differences between the 2 values ranged from –45 to 25 mg/dL, with 21% of pairs discrepant by 20 mg/dL or more (Figure 1); results were similar at 6 hours (Figure 2), with slightly less discrepancy.


The differences between radial artery POCT and central lab testing values at CTICU arrival ranged from –43 to 80 mg/dL, with 24% of pairs discrepant by 20 mg/dL or more (Figure 3). At 6 hours post CTICU arrival, the difference between radial artery POCT and central lab testing values ranged from –130 to 27 mg/dL, with 11% of pairs discrepant by 20 mg/dL or more (Figure 4). Ninety-two percent of central laboratory values were either close to (± 20) or within the moderate glycemic control target range (110–150 mg/dL).


When the patient cohort was stratified by anemia, diabetes, body temperature, and receipt of vasoconstrictor, there were no significant differences between mean fingerstick POCT and central lab testing values for any strata on CTICU arrival, while there were significant differences between radial artery POCT and central lab testing means for both vasoconstrictor strata as well as for patients with core temperature > 36.1°C (Table 2). At 6 hours, there were no statistically significant differences when stratified for receipt of vasoconstrictor or presence of diabetes. Stratification for anemia or core body temperature was not done for patients at the 6-hour post CTICU arrival time because no hemoglobin value was available and all patients except 1 reached a core temperature of 36.1°C.
Although we measured POCT values obtained using 2 different blood sample sources, fingerstick POCT performed better than radial artery POCT testing with regard to the mean values when compared with the central lab. However, radial artery POCT performed better with regard to correlation with the central lab value. In other words, fingerstick POCT values were less significantly different than radial artery POCT values when compared with the central lab, while radial artery POCT values correlated better with values from the central lab. In spite of this unexplained variability in differences and correlation, the blood glucose values stayed in the target goal range (Figures 1-4).
Discussion
The accuracy of glucose POCT in the critical care setting has been called into question.4,5 The clinical demands of glucose management using CII include timely and accurate guidance in postoperaptive cardiac surgery, in this case, CABG. A previous study compared POCT and central laboratory blood glucose values in medical intensive care unit patients,8 but not in patients who have had CABG surgery. Another study has reviewed the difference in glucose values from POCT and central lab analysis in the critically ill population, but not in the post cardiac surgical population.9 We have shown that the POCT blood glucose values correlate well with the clinical lab values, but the values are statistically different. Our study adds an additional observation in that, although the POCT inconsistencies were statistically significant, they were not clinically significant. That is, POCT of blood glucose was inaccurate, but it still helped guide care by providing enough information to keep the blood glucose in range (most of the time) and allowing the bedside nurse to detect trends and make appropriate adjustments to the infusion. However, given these inconsistencies, we recommend a low threshold for sending additional samples to the central lab to double-check the glucose values, especially when they are outside the prescribed range. Our analysis provides some measure of reassurance with regard to current postoperative CABG glucose management by showing that the limitations of the blood glucose meter do not jeopardize the safety of patients. Nonetheless, we look forward to advances in the accuracy of POCT blood glucose technology so that critical care patients can be better managed when blood glucose is outside the prescribed range.
This analysis of 116 CABG patients points out both the inaccuracy and the utility of a representative POCT glucometer (in this case, the FreeStyle Precision Pro) used at the bedside to manage CIIs in postoperative CABG patients, keeping the blood glucose level in the moderate control range (110-150 mg/dL). The correlation plot shows that in this population the bedside nurses were able to keep blood glucose in range most of the time, in spite of the inaccuracy of POCT of blood glucose, given that the error of the test fits in the wide margin of 40 mg/dL. The fact that the 6-hour values were slightly less variable than the admission values indicates that sequential determinations of blood glucose over the 6-hour period to detect trends allowed good clinical management even in the face of such inaccuracy. The correlation allows the inaccurate number (blood glucose value) to indicate direction, and frequent determinations allow the bedside nurse to keep that number in the prescribed range most of the time in this population of patients.
Conclusion
We have found that glucometer blood glucose determinations in our center used on a homogenous population (CABG surgery) utilizing a single type of glucometer correlated well with those of the central lab, but were not always accurate. In spite of the inaccuracies, experienced bedside nurses were able to use the instrument successfully and safely, as it informed them if the blood glucose was in or out of a predetermined range and in which direction it was going.
Acknowledgment: The authors are indebted to the nurses of the Cardiothoracic Surgery Intensive Care Unit at Maine Medical Center for their support and assistance, without which this analysis would not have been possible.
Corresponding author: Robert S. Kramer, MD, Division of Cardiothoracic Surgery, Maine Medical Center Cardiovascular Institute, 22 Bramhall St., Portland ME 04102; [email protected].
Financial disclosures: None.
From the Maine Medical Center, Portland, ME (Dr. Kramer, Ms. Palmeri, Dr. Robich, Mr. Groom, Dr. Hayes, Ms. Janoushek, Dr. Rappold, Dr. Swarz, and Dr. Quinn), and the Center for Outcomes Research and Evaluation, Maine Medical Center Research Institute, Portland, ME (Dr. Lucas).
Abstract
- Objective. To determine the accuracy of the glucometer currently used for point-of-care testing (POCT) of blood glucose in our cardiothoracic surgery intensive care unit (CTICU).
- Design. Prospective cohort study.
- Setting. Tertiary care community hospital affiliated with a school of medicine.
- Participants. Coronary artery bypass graft (CABG) surgery patients.
- Measurements. Blood glucose levels obtained via POCT with a glucometer using fingerstick and radial artery blood samples were compared with values obtained via central laboratory testing of radial artery blood samples (gold standard) in 106 CABG patients on continuous insulin infusions (CII) upon arrival to the CTICU from the operating room and 102 CABG patients on CII in the CTICU 6 hours later.
- Results. Fingerstick POCT and central lab blood glucose values correlated well (r = 0.83 for admission and 0.86 for 6-hour values), but the mean values were significantly different as determined by paired t-tests. Upon arrival, the fingerstick POCT mean value was 120.9 mg/dL, while the central laboratory value was 127.9 mg/dL (P value = 0.03). At the 6-hour time point, the mean value for fingerstick POCT was 129.7 mg/dL compared to a central laboratory value of 137.3 (P value = 0.02).
- Conclusion. The blood glucose POCT values correlated well with central laboratory values, but the values were statistically significantly different. Nevertheless, accurate clinical decisions were made despite the inaccuracies of POCT glucose testing, as experienced bedside nurses were able to use the glucometer successfully and safely. The device’s results informed them when the blood glucose was out of a prescibed range and the direction of the change, and they were able to adjust the CII accordingly.
Keywords: quality improvement; glucose management; point-of-care testing; critical care.
Achieving glycemic control in patients with and without diabetes during coronary artery bypass graft (CABG) surgery is associated with reduced perioperative morbidity and mortality and improved long-term survival.1 Hyperglycemia has detrimental effects on the cardiovascular system and insulin has beneficial effects on the ischemic myocardium.2 The current recommendations of the Society of Thoracic Surgery regarding blood glucose management include the use of continuous insulin infusions (CII) during and after surgery in the critical care unit,3 keeping blood glucose in a moderate range. Glucometers are commonly used in the critical care perioperative setting for point-of-care testing (POCT) for timely determinations of blood glucose levels for patients on CII.
POCT for glucose monitoring is a valuable tool for managing patients with diabetes in the outpatient setting. Evolving from urinary test strips that depended on a colorimetric model, glucometers now incoroporate digital technology that allows patients to determine their blood glucose using a drop of blood from a fingerstick. The US Food and Drug Administration’s approval for most glucose POCT technology includes home use by diabetic patients and use in the hospital setting, with the exception of critically ill patients, who may be affected by hypoxemia, poor capillary perfusion, tissue edema, severe anemia4 or other pathophysiologic states that could impact the accuracy of the devices. For example, poor peripheral perfusion related to shock or vasoconstrictors and interstitial edema are variables that could contribute to an erroneous reading. Therefore, many glucometers used in the critical care setting are being used off-label. Because much of the current POCT technology for glucose monitoring may provide erroneous results in certain ranges and in some clinical settings, the safety of most glucometers has been called into question.5,6
Given the concern regarding the potential inaccuracies of commonly used glucometers in the critical care setting, we undertook a quality improvement project to analyze the clinical performance of the glucometer currently used in our critically ill postoperative cardiac surgery population. The cardiac surgery division policy at our institution is to place all patients, both diabetic and nondiabetic, on a CII intraoperatively and to continue the infusion for at least 24 to 48 hours postoperatively. The CII start rate is determined utilizing the division’s Insulin Start Chart, and then the CII is adjusted according to the nomogram through the postoperative course. Both the Insulin Start Chart and nomogram have been previously described by Kramer et al.7
Currently, POCT of glucose in all post cardiac surgery patients is done hourly or more frequently in the first 24 to 48 hours after surgery in order to adjust the CII. In patients undergoing the stress of cardiac surgery, the action of insulin is counter-regulated by glucagon, epinephrine, norepinephrine, cortisol, and growth hormone. The resulting varying degrees of insulin resistance in this population of patients requires close monitoring of blood glucose, keeping it in a prescribed range, which in our center is 110 to 150 mg/dL, both in diabetic and nondiabetic patients. Frequent laboratory and POCT determinations of glucose are made. Providers and bedside nurses adjust the CII according to central laboratory values, POCT values, and trends, as previously described.7
Methods
Setting
Maine Medical Center is a 600-bed tertiary care teaching hospital. It is a level 1 trauma center where 1000 cardiac surgical operations are performed annually. POCT glucose monitoring is relied upon to monitor blood glucose and adjust the CII accordingly. This project, which did not require any additional procedures outside of the standard of care for this population of patients, was reviewed by the Institutional Review Board, who determined that this activity does not meet either the definition of research as specified under 45 CFR 46.102 (d) or the definition of clinical investigation as specified in 21 CFR 56.102 (c).
Patients
Using central laboratory glucose values drawn from the radial artery as the gold standard, we created a registry of consecutive postoperative cardiac surgery patients who had undergone CABG surgery and had blood glucose determinations from both POCT (fingerstick and radial artery samples) and central laboratory testing (radial artery sample) during a 7-month period (May 2016 through February 2017). To be included in the registry, patients had to (1) be postoperative following isolated CABG or CABG plus Maze procedure; (2) have been on cardiopulmonary bypass (CPB); (3) have radial arterial lines; and (4) be on a CII. A total of 116 patients qualified according to the inclusion criteria. Patients missing glucose results in 1 or more of the variables were excluded from data analysis.
Measurements and Variables
Using a POCT glucometer (FreeStyle Precision Pro, Abbott Laboratories, Abbott Park, IL), blood glucose conentrations were measured on samples obtained from both fingerstick and radial artery. Concurrently, radial arterial blood was sent to the central laboratory for glucose measurement. Blood glucose values were compared in CABG patients on CII upon arrival to the cardiothoracic surgery intensive care unit (CTICU) from the operating room and CABG patients on CII 6 hours after arrival in the CTICU. During the 6-hour interval, blood glucose levels were tested hourly or more frequently, allowing nurses to identify trends in blood glucose changes in order to keep blood glucose in the prescribed goal range of 110 to 150 mg/dL. At each of these 2 time points, on arrival to CTICU and 6 hours later, blood glucose values obtained with radial artery POCT and fingerstick POCT were compared with values obtained with central laboratory testing of radial artery samples. The amount of blood required was 1 drop each for POCT fingerstick and POCT radial artery and 2 mL for central lab testing.
Patient characteristics were identified from the electronic medical record. The variables recorded were type of operation, time on CPB, time of CTICU arrival, temperature, vasoconstrictor infusions (norepinephrine, vasopressin, phenylephrine), preoperative diagnosis of diabetes mellitus, preoperative HbA1c, and hemoglobin/hematocrit. Hemoglobin/hematocrit was only available at the time of the patient’s arrival to CTICU. The study was completed within the confines of our center’s standard of care protocol for postoperative cardiac surgical patients.
Analysis
We used standard statistical techniques to describe the study population, including proportions for categorical variables and means (standard deviations) for continuous variables. Correlation and regression techniques were used to describe the relationship between POCT and laboratory (gold standard) tests, both measured as continuous variables, and paired t-tests with Bonferroni correction were used to compare the central tendency and range of these comparisons. We calculated the differences between the gold standard measure and the POCT measure as an indication of outliers (ie, cases in which the 2 tests gave markedly different results). We examined plots to ascertain at which levels of the gold standard test these outliers occurred. An interim analysis was done at the halfway point and submitted to the Institutional Review Board, but no correction to the P value was done based on this analysis, which was largely qualitative. We used Bonferroni correction to declare a P value of 0.025 statistically significant with the 2-way comparisons of both fingerstick and radial artery values to central laboratory values. When the data was stratified by a clinical characteristic creating a 4-way comparison, we used Bonferroni correction to declare a P value of 0.0125 to be statistically significant when comparing both fingerstick and radial artery values to central laboratory values.
Results
Glucose POCT evaluations were carried out on 116 consecutive patients who underwent CABG surgery with or without a Maze procedure on CPB with a CII and an arterial line. Due to missing glucose results in 1 or more of the variables, 10 patients were excluded from data analysis for the time point of arrival in the CTICU and 14 patients were excluded from data analysis for the time point of 6 hours post CTICU arrival. This gave a final count of 106 CABG patients for CTICU arrival data analysis and 102 CABG patients for the 6 hours after CTICU arrival data analysis.
Patients ranged in age from 43 to 85 years, with a mean of age of 66 years, 22% were were women, 41% were diabetic, and 18% had peripheral vascular disease (Table 1). The average preoperative HbA1c was 6.4% ± 1.3% (range, 4.6% to 11.1%). Mean time on CBP for the group was 101 ± 31 minutes (range, 43 to 233 minutes). Postoperative mean hematocrit and hemoglobin were 32.5% and 11.4 g/dL, respectively. The average core temperature of patients on arrival was 36.0°C, which rose to an average of 36.6°C 6 hours later. A vasoconstrictor drip was infusing on 52% of patients upon CTICU arrival; 65% had a vasoconstrictor drip infusing 6 hours after arrival to the CTICU. Hemoglobin results were available only upon CTICU arrival as they are not routinely checked at 6 hours; 74 (64%) patients had a hemoglobin < 12 g/dL.

Compared to central laboratory testing, which we are defining as the gold standard, fingerstick POCT performed better on arrival, while radial artery POCT performed better at 6 hours (Table 2). At CTICU arrival, the mean blood glucose value for fingerstick POCT was 121 ± 24.1 mg/dL, 116 ± 27.2 mg/dL for radial artery POCT, and 128 ± 23.5 mg/dL for central lab testing. The difference in mean blood glucose between the fingerstick POCT and central lab testing was not statistically significant (P = 0.032), while the difference in mean blood glucose between radial artery POCT and central lab testing was statistically significant (P = 0.001). At 6 hours post arrival to the CTICU, the mean fingerstick POCT blood glucose value was 130 ± 23.9 mg/dL, compared to the mean central lab testing value of 137 ± 22.4 mg/dL; this difference was statistically significant (P = 0.019), while the radial artery POCT blood glucose value (133 ± 24.6 mg/dL) was not significantly different from the central lab testing value.

Blood glucose values from fingerstick POCT and central laboratory testing correlated well (r = 0.83 for admission and 0.86 for 6-hour values), as did radial artery POCT and central lab values (r = 0.87 for admission and 0.90 for 6-hour values) (Figures 1, 2, 3, and 4). Comparing individual values for fingerstick POCT and central lab testing, within-person differences between the 2 values ranged from –45 to 25 mg/dL, with 21% of pairs discrepant by 20 mg/dL or more (Figure 1); results were similar at 6 hours (Figure 2), with slightly less discrepancy.


The differences between radial artery POCT and central lab testing values at CTICU arrival ranged from –43 to 80 mg/dL, with 24% of pairs discrepant by 20 mg/dL or more (Figure 3). At 6 hours post CTICU arrival, the difference between radial artery POCT and central lab testing values ranged from –130 to 27 mg/dL, with 11% of pairs discrepant by 20 mg/dL or more (Figure 4). Ninety-two percent of central laboratory values were either close to (± 20) or within the moderate glycemic control target range (110–150 mg/dL).


When the patient cohort was stratified by anemia, diabetes, body temperature, and receipt of vasoconstrictor, there were no significant differences between mean fingerstick POCT and central lab testing values for any strata on CTICU arrival, while there were significant differences between radial artery POCT and central lab testing means for both vasoconstrictor strata as well as for patients with core temperature > 36.1°C (Table 2). At 6 hours, there were no statistically significant differences when stratified for receipt of vasoconstrictor or presence of diabetes. Stratification for anemia or core body temperature was not done for patients at the 6-hour post CTICU arrival time because no hemoglobin value was available and all patients except 1 reached a core temperature of 36.1°C.
Although we measured POCT values obtained using 2 different blood sample sources, fingerstick POCT performed better than radial artery POCT testing with regard to the mean values when compared with the central lab. However, radial artery POCT performed better with regard to correlation with the central lab value. In other words, fingerstick POCT values were less significantly different than radial artery POCT values when compared with the central lab, while radial artery POCT values correlated better with values from the central lab. In spite of this unexplained variability in differences and correlation, the blood glucose values stayed in the target goal range (Figures 1-4).
Discussion
The accuracy of glucose POCT in the critical care setting has been called into question.4,5 The clinical demands of glucose management using CII include timely and accurate guidance in postoperaptive cardiac surgery, in this case, CABG. A previous study compared POCT and central laboratory blood glucose values in medical intensive care unit patients,8 but not in patients who have had CABG surgery. Another study has reviewed the difference in glucose values from POCT and central lab analysis in the critically ill population, but not in the post cardiac surgical population.9 We have shown that the POCT blood glucose values correlate well with the clinical lab values, but the values are statistically different. Our study adds an additional observation in that, although the POCT inconsistencies were statistically significant, they were not clinically significant. That is, POCT of blood glucose was inaccurate, but it still helped guide care by providing enough information to keep the blood glucose in range (most of the time) and allowing the bedside nurse to detect trends and make appropriate adjustments to the infusion. However, given these inconsistencies, we recommend a low threshold for sending additional samples to the central lab to double-check the glucose values, especially when they are outside the prescribed range. Our analysis provides some measure of reassurance with regard to current postoperative CABG glucose management by showing that the limitations of the blood glucose meter do not jeopardize the safety of patients. Nonetheless, we look forward to advances in the accuracy of POCT blood glucose technology so that critical care patients can be better managed when blood glucose is outside the prescribed range.
This analysis of 116 CABG patients points out both the inaccuracy and the utility of a representative POCT glucometer (in this case, the FreeStyle Precision Pro) used at the bedside to manage CIIs in postoperative CABG patients, keeping the blood glucose level in the moderate control range (110-150 mg/dL). The correlation plot shows that in this population the bedside nurses were able to keep blood glucose in range most of the time, in spite of the inaccuracy of POCT of blood glucose, given that the error of the test fits in the wide margin of 40 mg/dL. The fact that the 6-hour values were slightly less variable than the admission values indicates that sequential determinations of blood glucose over the 6-hour period to detect trends allowed good clinical management even in the face of such inaccuracy. The correlation allows the inaccurate number (blood glucose value) to indicate direction, and frequent determinations allow the bedside nurse to keep that number in the prescribed range most of the time in this population of patients.
Conclusion
We have found that glucometer blood glucose determinations in our center used on a homogenous population (CABG surgery) utilizing a single type of glucometer correlated well with those of the central lab, but were not always accurate. In spite of the inaccuracies, experienced bedside nurses were able to use the instrument successfully and safely, as it informed them if the blood glucose was in or out of a predetermined range and in which direction it was going.
Acknowledgment: The authors are indebted to the nurses of the Cardiothoracic Surgery Intensive Care Unit at Maine Medical Center for their support and assistance, without which this analysis would not have been possible.
Corresponding author: Robert S. Kramer, MD, Division of Cardiothoracic Surgery, Maine Medical Center Cardiovascular Institute, 22 Bramhall St., Portland ME 04102; [email protected].
Financial disclosures: None.
1. Furnary AP, Gao G, Grunkemeier GL, et al. Continuous insulin infusion reduces mortality in patients with diabetes undergoing coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2003;125:1007-1021.
2. Lazar H. Glycemic control during coronary artery bypass graft surgery. ISRN Cardiol. 2012;2012:292490.
3. Lazar HL, McDonnell M, Chipkin SR, et al; Society of Thoracic Surgeons Blood Glucose Guideline Task Force. The Society of Thoracic Surgeons Practice Guideline Series: blood glucose management during adult cardiac surgery. Ann Thorac Surg. 2009;87:663-669.
4. US Food and Drug Administration. Blood Glucose Monitoring Test Systems for Prescription Point of Care Use. Guidance for Industry and Food and Drug Administration Staff,.www.fda.gov/downloads/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/UCM380325.pdf. Accessed March 8, 2019.
5. Finkielman JD, Oyen LJ, Afess B. Agreement between bedside blood and plasma glucose measurement in the ICU Setting. Chest. 2005;127:1749-1511.
6. Pidcoke HF, Wade CE, Mann EA, et al. Anemia causes hypoglycemia in ICU patients due to error in single-channel glucometers: methods of reducing patient risk. Crit Care Med. 2010;38:471-476.
7. Kramer R, Groom R, Weldner D, et al. Glycemic control reduces deep sternal wound infection: a multidisciplinary approach. Arch Surg. 2008;143:451-456.
8. Peterson JR, Graves DF, Tacker DH, et al. Comparison of POCT and central laboratory blood glucose results using arterial, capillary, and venous samples from MICU patients on a tight glycemic protocol. Clinica Chimica Acta. 2008;396:10-13.
9. Cook A, Laughlin D, Moore M, et al. Differences in glucose values obtained from point-of-care glucose meters and laboratory analysis in critically ill patients. Am J Crit Care. 2009;18:65-72.
1. Furnary AP, Gao G, Grunkemeier GL, et al. Continuous insulin infusion reduces mortality in patients with diabetes undergoing coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2003;125:1007-1021.
2. Lazar H. Glycemic control during coronary artery bypass graft surgery. ISRN Cardiol. 2012;2012:292490.
3. Lazar HL, McDonnell M, Chipkin SR, et al; Society of Thoracic Surgeons Blood Glucose Guideline Task Force. The Society of Thoracic Surgeons Practice Guideline Series: blood glucose management during adult cardiac surgery. Ann Thorac Surg. 2009;87:663-669.
4. US Food and Drug Administration. Blood Glucose Monitoring Test Systems for Prescription Point of Care Use. Guidance for Industry and Food and Drug Administration Staff,.www.fda.gov/downloads/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/UCM380325.pdf. Accessed March 8, 2019.
5. Finkielman JD, Oyen LJ, Afess B. Agreement between bedside blood and plasma glucose measurement in the ICU Setting. Chest. 2005;127:1749-1511.
6. Pidcoke HF, Wade CE, Mann EA, et al. Anemia causes hypoglycemia in ICU patients due to error in single-channel glucometers: methods of reducing patient risk. Crit Care Med. 2010;38:471-476.
7. Kramer R, Groom R, Weldner D, et al. Glycemic control reduces deep sternal wound infection: a multidisciplinary approach. Arch Surg. 2008;143:451-456.
8. Peterson JR, Graves DF, Tacker DH, et al. Comparison of POCT and central laboratory blood glucose results using arterial, capillary, and venous samples from MICU patients on a tight glycemic protocol. Clinica Chimica Acta. 2008;396:10-13.
9. Cook A, Laughlin D, Moore M, et al. Differences in glucose values obtained from point-of-care glucose meters and laboratory analysis in critically ill patients. Am J Crit Care. 2009;18:65-72.
Is Patient Satisfaction the Same Immediately After the First Visit Compared to Two Weeks Later?
From the Department of Surgery and Perioperative Care, Dell Medical School, The University of Texas at Austin, Austin, TX (Dr. Kortlever, Ms. Haidar, Dr. Reichel, Dr. Driscoll, Dr. Ring, and Dr. Vagner) and University Medical Center Utrecht, Utrecht, The Netherlands (Dr. Teunis).
Abstract
- Objective: Patient satisfaction is considered a quality measure. Satisfaction is typically measured directly after an in-person visit in research and 2 weeks later in practice surveys. We assessed if there was a difference in immediate and delayed measurement of satisfaction.
- Questions: (1) There is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) and (2) perceived empathy (measured by the Jefferson Scale of Patient Perceptions of Physician Empathy [JSPPPE]) immediately after the initial visit compared to 2 weeks later. (3) Change in disability (measured by the Patient-Reported Outcome Measurement Information System Physical Function-Upper Extremity [PROMIS PF-UE]) is not independently associated with change in satisfaction and (4) empathy after the initial visit compared to 2 weeks later.
- Methods: 150 new patients completed a survey of demographics, satisfaction with the surgeon, rating of the surgeon’s empathy, and upper extremity specific limitations. The satisfaction, empathy, and limitation questionnaires were repeated 2 weeks later.
- Results: We found a slight but significant decrease in satisfaction 2 weeks after the in-person visit (–0.41, P = 0.001). There was no significant change in perceived empathy (–0.71, P = 0.19). Change in limitations did not account for a change in satisfaction (P = 0.79) or perceived empathy (P = 0.93).
- Conclusion: Satisfaction and perceived empathy are relatively stable constructs that can be measured immediately after the visit.
Keywords: satisfaction, empathy, change, upper extremity, disability.
Patient satisfaction is increasingly being used as a performance measure to evaluate quality of care.1-8 Patient satisfaction correlates with adherence with recommended treatment.1,6,8-10 Satisfaction measured on an 11-point ordinal scale immediately after the visit correlates strongly with the perception of clinician empathy.2,3 Indeed, some satisfaction questionnaires such as the Medical Interview Satisfaction Scale (MISS)11,12 have questions very similar to empathy questionnaires. It may be that satisfaction is a construct similar to feeling that your doctor listened and cared about you as an individual (perceived physician empathy).
Higher ratings of satisfaction also seem to be related to a physician’s communication style.1,4,7-10 One study of 13 fertility doctors found that training in effective communication strategies led to improved patient satisfaction.7 A qualitative study of 36 patients, health professionals, and clinical support staff in an orthopaedic outpatient setting held interviews and focus group sessions to identify themes influencing patient satisfaction.4 Communication and expectation were among the 7 themes identified. We have noticed a high ceiling effect (maximum scores) with measures of patient satisfaction and perceived empathy.2,3 Another study also noted a high ceiling effect when using an ordinal scale.5 It may be that people with a positive feeling shortly after a health care encounter give top ratings out of politeness or gratefulness. It is also possible they will feel differently a few weeks after they leave the office. Furthermore, ratings of satisfaction gathered by a practice or health care system for practice assessment/improvement are often obtained several days to weeks after the visit, while research often obtains satisfaction ratings immediately after the visit for practical reasons. There may be differences between immediate and delayed measurement of satisfaction beyond the mentioned social norms.
Therefore, this study tested the primary null hypothesis that there is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) immediately after the initial visit compared to 2 weeks later. Additionally, we assessed the difference in perceived empathy immediately after the initial visit compared to 2 weeks later, and whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
Methods
Study Design
After Institutional Review Board approval of this prospective, longitudinal, observational cohort study, we prospectively enrolled 150 adult patients between November 29, 2017 and January 10, 2018. Patients were seen at 5 orthopaedic clinics in a large urban area. We included all new English-speaking patients aged 18 to 89 years who were visiting 1 of 6 participating orthopaedic surgeons for any upper extremity problem and who were able to provide informed consent. We excluded follow-up visits and patients who were unable to speak and understand English. Four research assistants who were not involved with patient treatment described the study to patients before or after the visit with the surgeon. We were granted a waiver of written informed consent; patients indicated their consent by completing the surveys.
Patients could choose either phone or email as their preferred mode of contact for follow-up in this study. For patients who selected email as the preferred mode of contact, the follow-up survey was sent automatically 2 weeks after completion date, and a maximum of 3 reminder emails with 2-day time intervals between them were sent to those who did not respond to the initial invitation. For patients who selected phone as the preferred mode of contact, the follow-up survey was done by an English-speaking research assistant who was not involved with patient treatment. When a response was not obtained on the initial phone call, 3 additional phone calls were made (1 later that same day and 2 the next day). One patient declined participation because he was not interested in the study and had no time after his visit.
Measurements
Patients were asked to complete a set of questionnaires at the end of their visit:
1. A demographic questionnaire consisting of preferred mode of contact for follow-up (phone or email), age, sex, race/ethnicity, marital status, education status, work status, insurance status, and type of visit (first visit or second opinion);
2. An 11-point ordinal measure of satisfaction with the surgeon, with scores ranging from 0 (Worst Surgeon Possible) to 10 (Best Surgeon Possible);
3. The patient’s rating of the surgeon’s empathy, measured by the Jefferson Scale of Patient Perceptions of Physician Empathy (JSPPPE).13 The JSPPPE is a 5-item questionnaire, measured on a 7-point Likert scale, with scores ranging from 1 (Strongly Disagree) to 7 (Strongly Agree), that assesses agreement with statements about the physician. The total score is the sum of all item scores (5-35), with higher scores representing a higher degree of perceived physician empathy.
4. Upper extremity disability, measured by the Patient-Reported Outcomes Measurement Information System Physical Function-Upper Extremity (PROMIS PF-UE) Computer Adaptive Test (CAT).14-16 This is a measure of physical limitations in the upper extremity. It can be completed with as few as 4 questions while still achieving high precision in scoring and thereby decreasing survey burden. PROMIS presents a continuous T-score with a mean of 50 and standard deviation (SD) of 10, with higher scores reflecting better physical function compared to the average of the US general population.15
After completing the initial questionnaire, the research assistant filled out the office and surgeon name and asked the surgeon to complete the diagnosis. All questionnaires were administered on an encrypted tablet via the secure, HIPAA-compliant electronic platform REDCap (Research Electronic Data Capture), a web-based application for building and managing online surveys and databases.17 The follow-up survey was sent automatically or was done by phone call as previously described. The follow-up survey consisted of (1) the 11-point ordinal measure of satisfaction with the surgeon, (2) the JSPPPE for perceived empathy, and (3) the PROMIS PF-UE for physical limitations in the upper extremity.
Analysis
Continuous variables are presented as mean ± SD and discrete data as proportions. We used Student’s t-tests to assess baseline differences between continuous variables and Fisher’s exact tests for discrete variables. To assess differences in satisfaction and perceived empathy after 2 weeks, we used Student’s paired t-tests. We created 2 multilevel multivariable linear regression models to assess factors associated with (1) change in satisfaction with the surgeon and (2) change in perceived physician empathy. These models account for correlation of patients treated by the same surgeon. We selected variables to be included in the final models by running multilevel models with only 1 independent variable of interest (Appendix 1). Variables with P < 0.10 were included in our final models. We also included change in PROMIS PF-UE in both models because this was our variable of interest. We considered P < 0.05 significant.
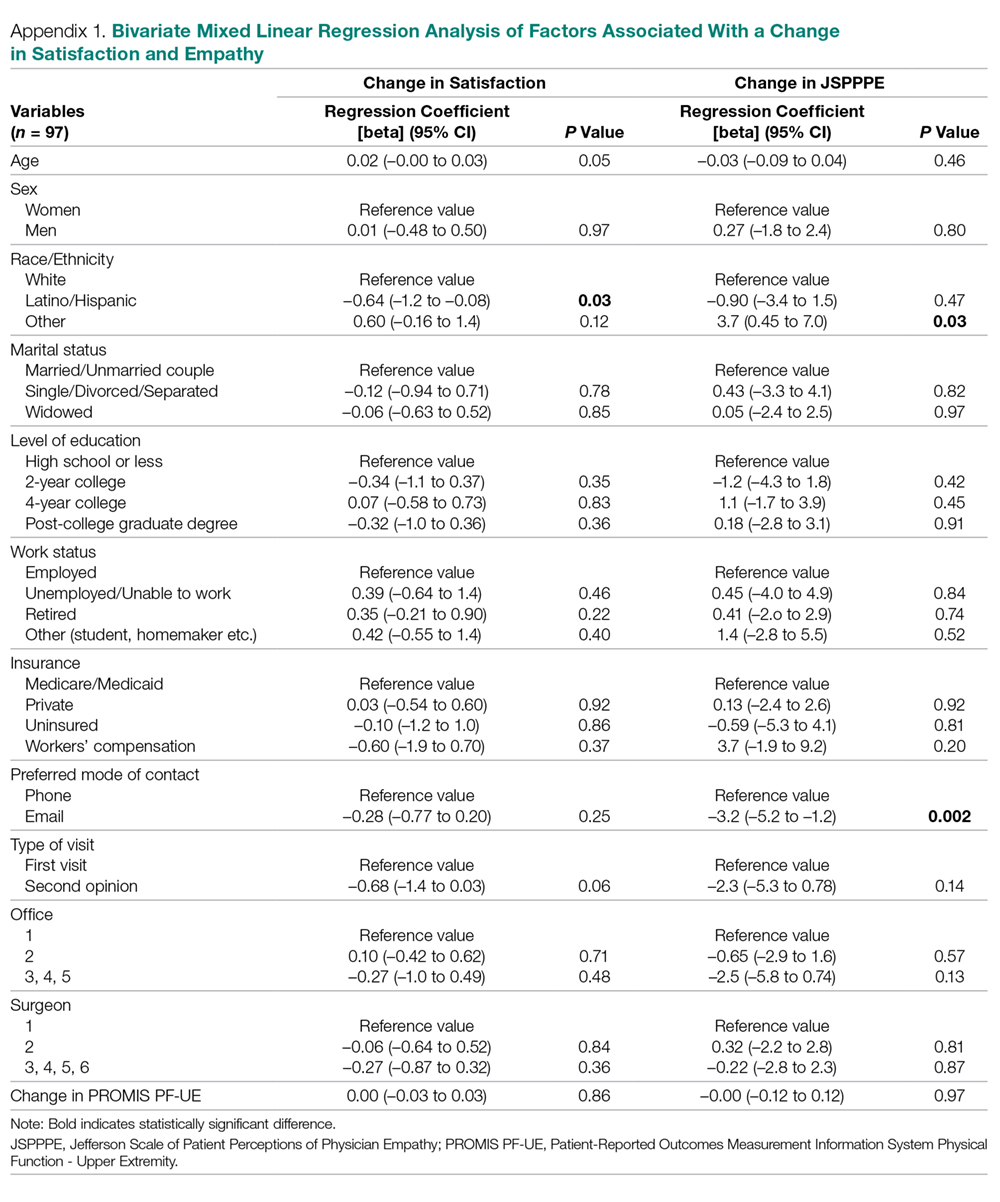
We performed a power analysis for the difference in patient satisfaction immediately after the first visit compared to 2 weeks later. Based on our pilot data where we found an initial mean satisfaction score of 9.4 and mean satisfaction score after 2 weeks of 9.1 (SD of difference 1.0), a priori power analysis showed that we needed a minimum sample size of 90 patients to detect a difference with power set at 0.80 and alpha set at 0.05. In order to account for loss to follow-up as previously noted,18 we enrolled 67% more patients (total of 150).
Results
Respondent Characteristics
None of the 150 patients were excluded from the analysis. The study patients’ mean age was 51 ± 16 years (range, 18-87 years), and 73 (49%) were men (Table 1). Mean scores directly after the visit were 9.4 ± 1.2 (range, 2-10) for satisfaction with the surgeon, 31 ± 5.2 (range, 9-35) for perceived physician empathy, and 40 ± 10 (range 15-56) for upper extremity disability. Most patients (n = 130, 87%) were seen in 2 of 5 offices, and 106 (71%) were seen by 2 out of 6 participating surgeons.
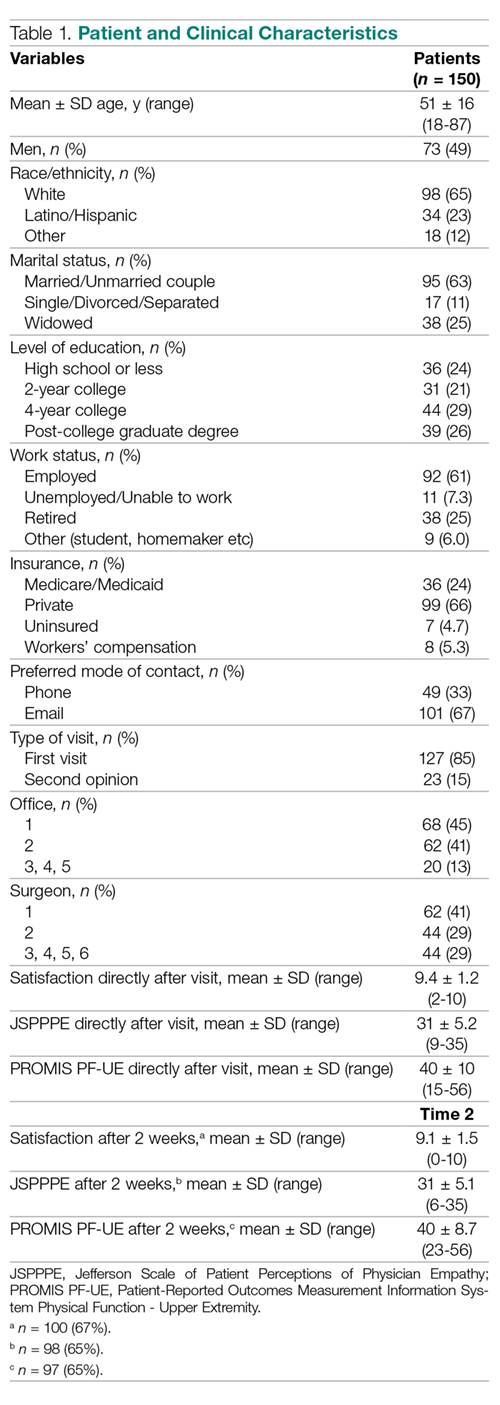
Ninety-seven (65%) patients completed their follow-up assessment 2 weeks after their initial visit, 49 (51%) by phone and 48 (49%) by email. This is a slightly better rate than the 36% rate reported in previous research.18 After 2 weeks, the mean score for satisfaction with the surgeon was 9.1 ± 1.5 (range, 0-10), the mean perceived empathy score was 31 ± 5.1 (range, 6-35), and the mean upper extremity disability score was 40 ± 8.7 (range, 23-56). Responders did not differ from nonresponders based on demographic data (Table 2). However, nonresponders had lower perceived empathy scores directly after their visit (P = 0.03) and none had initially chosen phone as their preferred mode of contact for follow-up (P < 0.001). A list of all diagnoses with frequencies the surgeons stated is listed in Appendix 2.
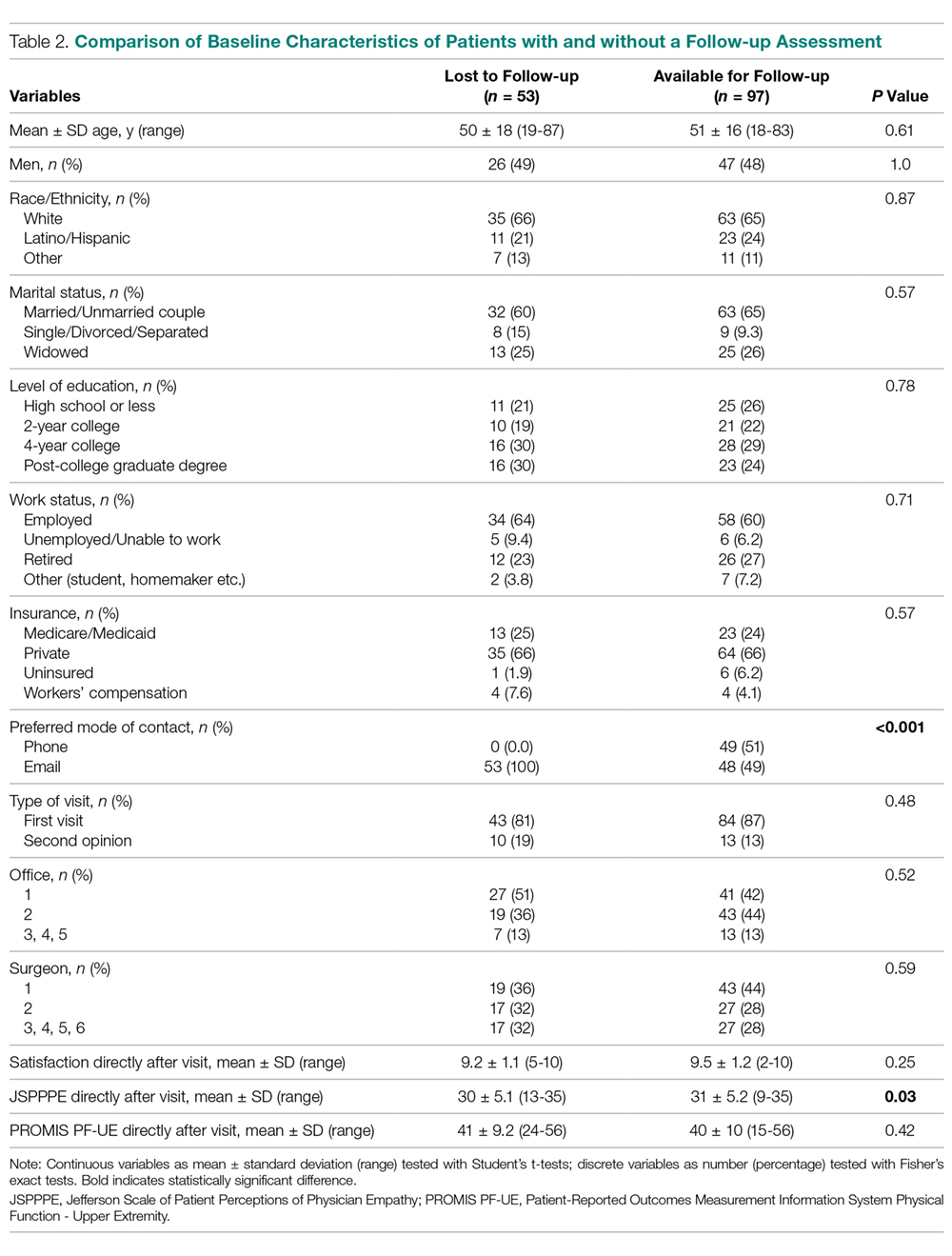
Difference in Satisfaction with the Surgeon
Satisfaction with the surgeon 2 weeks after the in-person visit was slightly, but significantly, lower on bivariate analysis compared to satisfaction with the surgeon immediately after the initial visit (–0.41 ± 1.2, P = 0.001; Table 3).
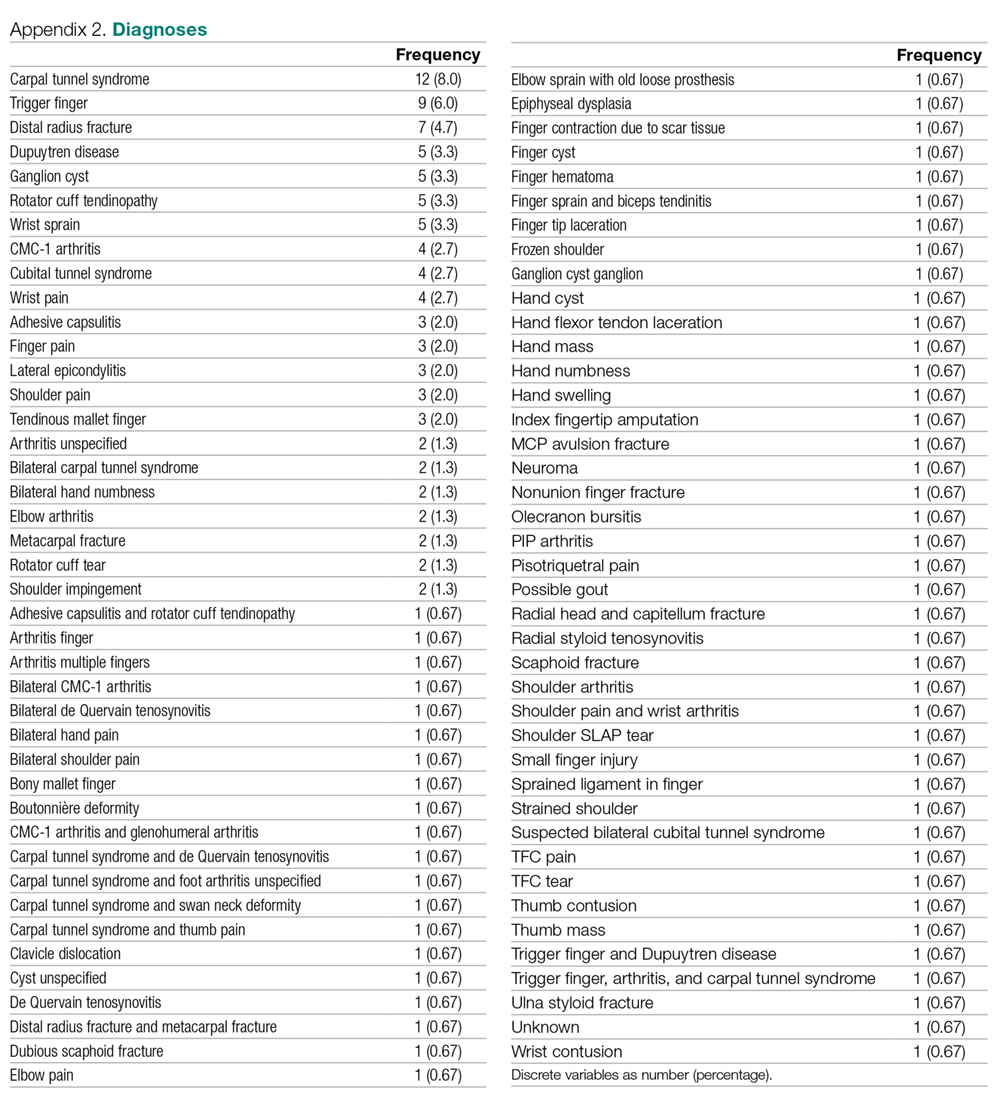
Difference in Perceived Physician Empathy
Perceived physician empathy 2 weeks after the in-person visit was not significantly lower on bivariate analysis compared to perceived physician empathy immediately after the initial visit (–0.71 ± 5.3, P = 0.19; Table 3).
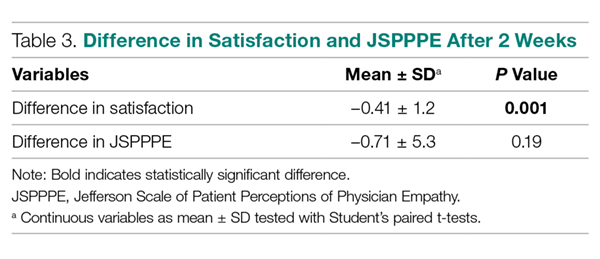
Factors Associated with Change in Satisfaction with the Surgeon
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in satisfaction with the surgeon (regression coefficient [beta], 0.00 [95% confidence interval {CI}, –0.02 to 0.03]; standard error [SE], 0.01; P = 0.79 [Table 4]). Being Latino was independently associated with less change in satisfaction with the surgeon (beta coefficient, –0.57 [95% CI, –1.1 to 0.00]; SE, 0.29; P = 0.049).
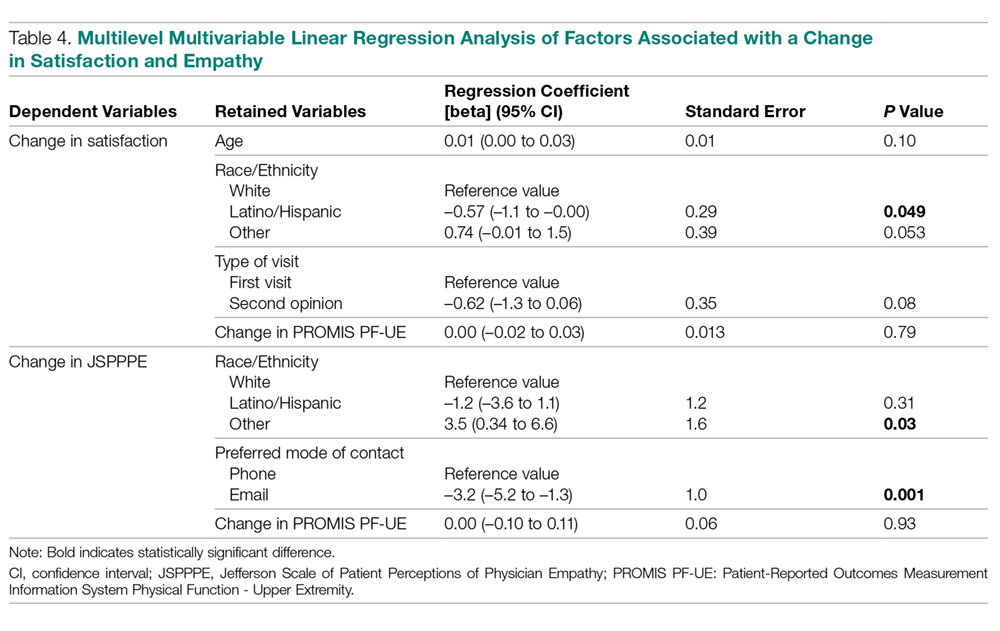
Factors Associated with Change in Perceived Physician Empathy
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in perceived physician empathy (beta coefficient = 0.00 [95% CI, –0.10 to 0.11]; SE, 0.06; P = 0.93 [Table 4]). Race/ethnicity other than white or Latino was independently associated with more change in perceived physician empathy (beta coefficient, 3.5 [95% CI, 0.34 to 6.6]; SE, 1.6; P = 0.030), and preferring email as mode of contact for follow-up was independently associated with less change in perceived physician empathy (beta coefficient, –3.2 [95% CI, –5.2 to –1.3]; SE, 1.0; P = 0.001).
Discussion
Patient satisfaction is considered a quality measure1-8 and is typically measured directly after an in-person visit. This study tested differences in patient satisfaction and perceived empathy immediately after the initial visit compared to 2 weeks later. In addition, we assessed whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
We acknowledge some study limitations. First, we only measured satisfaction based on 1 visit rather than multiple visits over time. It might be that satisfaction ratings differ when the physician-patient relationship is more established. However, we found overall high satisfaction ratings and a well-established relationship might not add to this finding. Second, surgeons were aware of the study and its purpose, which might have resulted in subconsciously altering the behavior to improve satisfaction. The effect of people acting differently as a result of being observed is called the Hawthorne effect.19 Third, we only used 1 simple ordinal measure to assess patient satisfaction with the surgeon. There is a wide variety of satisfaction measures,20 though the focus of this study was not to test the best possible satisfaction measure but to assess changes in satisfaction over time and its predictors. The simple 11-point ordinal satisfaction measure has proved reliable.6 Fourth, 35% of patients did not make a second rating. This is not unusual for phone or email studies. Our response rate was relatively high compared to other studies in our field,18 perhaps because the time to the second assessment was only 2 weeks and all people were available for follow-up by phone. Fifth, we analyzed 4 surgeons as 1 group and 3 offices as 1 group since we did not enroll enough patients per surgeon and office for individual analysis. However, multilevel linear analysis takes surgeon specific factors into account within that group.
The finding that satisfaction with the surgeon after 2 weeks was significantly lower on bivariate analysis compared to immediately after the initial visit is different from a study that found small increases in satisfaction after 2 weeks and 3 months,1 but comparable to another study in our field.21 Although significant, we believe the decrease in satisfaction is probably not clinically relevant. It might also be that satisfaction at follow-up is lower than measured, but that the least satisfied people did not respond on the follow-up survey.
We found no significant change in perceived empathy after 2 weeks. Since empathy is a strong driver of satisfaction,2,4-7 we did not expect to find differing results for empathy and for satisfaction over time. Both satisfaction and empathy seem to be relatively durable measures with current measurement tools.
The finding that change in disability was neither independently associated with change in satisfaction nor change in empathy is consistent with prior research.2,3,21 We cannot adequately study the impact of changes since we did not find an important change in either satisfaction or empathy over time. Jackson et al found higher satisfaction ratings over time in patients who had an increase in physical function and a decrease in symptoms.1 They also found that met expectations was associated with higher satisfaction immediately after the visit, after 2 weeks, and after 3 months.1 We feel that met expectations and fewer symptoms and limitations are likely highly co-linear with satisfaction. We therefore may not be able to learn much about one from the others.
The slight change we found in satisfaction with the surgeon among Latino patients was significantly less than the change among white patients. This suggests Latino patients might have a more stable opinion over time (a cultural phenomenon), or it might be spurious given the small number of Latino patients included in the study. The same can be said for the finding that race/ethnicity other than white or Latino was independently associated with greater change in empathy. Providing email as the preferred mode of contact was found to be independently associated with less change in perceived empathy compared to follow-up by phone. We had a 100% success rate for our follow-ups by phone. Our findings suggest that patients might more easily switch ratings on an 11-point ordinal scale than on a 5-item Likert scale. However, both measures are often rated at the ceiling of the scale.2,21
Conclusion
Satisfaction and perceived empathy are relatively stable constructs, are not clearly associated with other factors, and are strongly correlated with one another. This study supports the research practice of measuring satisfaction immediately after the visit, which is more convenient for both participant and researcher and avoids the loss of more than one third of the patients, and those with a worse experience in particular. To improve the utility and interpretation of patient-reported experience measures such as these, we might direct our efforts to developing scales with less ceiling effect.
Corresponding author: David Ring, MD, PhD, Dell Medical School, The University of Texas at Austin, Health Discovery Building HDB 6.706, 1701 Trinity St., Austin, TX 78705; [email protected].
Financial disclosures: Dr. Ring has or may receive payment or benefits from Skeletal Dynamics, Wright Medical for elbow implants, Deputy Editor for Clinical Orthopaedics and Related Research, Universities and Hospitals, Lawyers outside the submitted work.
Dr. Teunis has or may receive payment or benefits from VCC, PATIENT+, and AO Trauma TK network unrelated to this work and consultant fees from Synthes.
1. Jackson JL, Chamberlin J, Kroenke K. Predictors of patient satisfaction. Soc Sci Med. 2001;52:609-620.
2. Menendez ME, Chen NC, Mudgal CS, et al. Physician empathy as a driver of hand surgery patient satisfaction. J Hand Surg Am. 2015;40(9):1860-1865.
3. Parrish RC 2nd, Menendez ME, Mudgal CS, et al. Patient Satisfaction and its relation to perceived visit duration with a hand surgeon. J Hand Surg Am. 2016;41(2):257-262.
4. Waters S, Edmondston SJ, Yates PJ, Gucciardi DF. Identification of factors influencing patient satisfaction with orthopaedic outpatient clinic consultation: A qualitative study. Man Ther. 2016;25:48-55.
5. Voutilainen A, Pitkaaho T, Kvist T, Vehvilainen-Julkunen K. How to ask about patient satisfaction? The visual analogue scale is less vulnerable to confounding factors and ceiling effect than a symmetric Likert scale. J Adv Nurs. 2016;72:946-957.
6. van Berckel MM, Bosma NH, Hageman MG, et al. The correlation between a numerical rating scale of patient satisfaction with current management of an upper extremity disorder and a general measure of satisfaction with the medical visit. Hand (N Y). 2017;12:202-206.
7. Garcia D, Bautista O, Venereo L, et al. Training in empathic skills improves the patient-physician relationship during the first consultation in a fertility clinic. Fertil Steril. 2013;99:1413-1418.
8. Fitzpatrick RM, Hopkins A. Patients’ satisfaction with communication in neurological outpatient clinics. J Psychosom Res. 1981;25:329-334.
9. Kincey J, Bradshaw P, Ley P. Patients’ satisfaction and reported acceptance of advice in general practice. J R Coll Gen Pract. 1975;25:558-566.
10. Ley P, Whitworth MA, Skilbeck CE, et al. Improving doctor-patient communication in general practice. J R Coll Gen Pract. 1976;26:720-724.
11. Meakin R, Weinman J. The ‘Medical Interview Satisfaction Scale’ (MISS-21) adapted for British general practice. Fam Pract. 2002;19:257-263.
12. Wolf MH, Putnam SM, James SA, Stiles WB. The Medical Interview Satisfaction Scale: development of a scale to measure patient perceptions of physician behavior. J Behav Med. 1978;1:391-401.
13. Kane GC, Gotto JL, Mangione S, et al. Jefferson Scale of Patient’s Perceptions of Physician Empathy: preliminary psychometric data. Croat Med J. 2007;48:81-86.
14. Beckmann JT , Hung M, Voss MW, et al. Evaluation of the patient-reported outcomes measurement information system upper extremity computer adaptive test. J Hand Surg Am. 2016;41:739-744.
15. PROMIS. PROMIS PF Scoring. Available at www.healthmeasures.net/administrator/components/com_instruments/uploads/PROMIS%20Physical%20Function%20Scoring%20Manual.pdf. Accessed March 1, 2019.
16. PROMIS. PROMIS Measures. Available at wwwnihpromisorg. Accessed March 1, 2019.
17. Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377-381.
18. Bot AG, Anderson JA, Neuhaus V, Ring D. Factors associated with survey response in hand surgery research. Clin Orthop Relat Res. 2013;471(10):3237-3242.
19. Sedgwick P, Greenwood N. Understanding the Hawthorne effect. BMJ. 2015;351:h4672.
20. Ross CK, Steward CA, Sinacore JM. A comparative study of seven measures of patient satisfaction. Med Care. 1995;33:392-406.
21. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res. 2015;473:2362-2368.
From the Department of Surgery and Perioperative Care, Dell Medical School, The University of Texas at Austin, Austin, TX (Dr. Kortlever, Ms. Haidar, Dr. Reichel, Dr. Driscoll, Dr. Ring, and Dr. Vagner) and University Medical Center Utrecht, Utrecht, The Netherlands (Dr. Teunis).
Abstract
- Objective: Patient satisfaction is considered a quality measure. Satisfaction is typically measured directly after an in-person visit in research and 2 weeks later in practice surveys. We assessed if there was a difference in immediate and delayed measurement of satisfaction.
- Questions: (1) There is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) and (2) perceived empathy (measured by the Jefferson Scale of Patient Perceptions of Physician Empathy [JSPPPE]) immediately after the initial visit compared to 2 weeks later. (3) Change in disability (measured by the Patient-Reported Outcome Measurement Information System Physical Function-Upper Extremity [PROMIS PF-UE]) is not independently associated with change in satisfaction and (4) empathy after the initial visit compared to 2 weeks later.
- Methods: 150 new patients completed a survey of demographics, satisfaction with the surgeon, rating of the surgeon’s empathy, and upper extremity specific limitations. The satisfaction, empathy, and limitation questionnaires were repeated 2 weeks later.
- Results: We found a slight but significant decrease in satisfaction 2 weeks after the in-person visit (–0.41, P = 0.001). There was no significant change in perceived empathy (–0.71, P = 0.19). Change in limitations did not account for a change in satisfaction (P = 0.79) or perceived empathy (P = 0.93).
- Conclusion: Satisfaction and perceived empathy are relatively stable constructs that can be measured immediately after the visit.
Keywords: satisfaction, empathy, change, upper extremity, disability.
Patient satisfaction is increasingly being used as a performance measure to evaluate quality of care.1-8 Patient satisfaction correlates with adherence with recommended treatment.1,6,8-10 Satisfaction measured on an 11-point ordinal scale immediately after the visit correlates strongly with the perception of clinician empathy.2,3 Indeed, some satisfaction questionnaires such as the Medical Interview Satisfaction Scale (MISS)11,12 have questions very similar to empathy questionnaires. It may be that satisfaction is a construct similar to feeling that your doctor listened and cared about you as an individual (perceived physician empathy).
Higher ratings of satisfaction also seem to be related to a physician’s communication style.1,4,7-10 One study of 13 fertility doctors found that training in effective communication strategies led to improved patient satisfaction.7 A qualitative study of 36 patients, health professionals, and clinical support staff in an orthopaedic outpatient setting held interviews and focus group sessions to identify themes influencing patient satisfaction.4 Communication and expectation were among the 7 themes identified. We have noticed a high ceiling effect (maximum scores) with measures of patient satisfaction and perceived empathy.2,3 Another study also noted a high ceiling effect when using an ordinal scale.5 It may be that people with a positive feeling shortly after a health care encounter give top ratings out of politeness or gratefulness. It is also possible they will feel differently a few weeks after they leave the office. Furthermore, ratings of satisfaction gathered by a practice or health care system for practice assessment/improvement are often obtained several days to weeks after the visit, while research often obtains satisfaction ratings immediately after the visit for practical reasons. There may be differences between immediate and delayed measurement of satisfaction beyond the mentioned social norms.
Therefore, this study tested the primary null hypothesis that there is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) immediately after the initial visit compared to 2 weeks later. Additionally, we assessed the difference in perceived empathy immediately after the initial visit compared to 2 weeks later, and whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
Methods
Study Design
After Institutional Review Board approval of this prospective, longitudinal, observational cohort study, we prospectively enrolled 150 adult patients between November 29, 2017 and January 10, 2018. Patients were seen at 5 orthopaedic clinics in a large urban area. We included all new English-speaking patients aged 18 to 89 years who were visiting 1 of 6 participating orthopaedic surgeons for any upper extremity problem and who were able to provide informed consent. We excluded follow-up visits and patients who were unable to speak and understand English. Four research assistants who were not involved with patient treatment described the study to patients before or after the visit with the surgeon. We were granted a waiver of written informed consent; patients indicated their consent by completing the surveys.
Patients could choose either phone or email as their preferred mode of contact for follow-up in this study. For patients who selected email as the preferred mode of contact, the follow-up survey was sent automatically 2 weeks after completion date, and a maximum of 3 reminder emails with 2-day time intervals between them were sent to those who did not respond to the initial invitation. For patients who selected phone as the preferred mode of contact, the follow-up survey was done by an English-speaking research assistant who was not involved with patient treatment. When a response was not obtained on the initial phone call, 3 additional phone calls were made (1 later that same day and 2 the next day). One patient declined participation because he was not interested in the study and had no time after his visit.
Measurements
Patients were asked to complete a set of questionnaires at the end of their visit:
1. A demographic questionnaire consisting of preferred mode of contact for follow-up (phone or email), age, sex, race/ethnicity, marital status, education status, work status, insurance status, and type of visit (first visit or second opinion);
2. An 11-point ordinal measure of satisfaction with the surgeon, with scores ranging from 0 (Worst Surgeon Possible) to 10 (Best Surgeon Possible);
3. The patient’s rating of the surgeon’s empathy, measured by the Jefferson Scale of Patient Perceptions of Physician Empathy (JSPPPE).13 The JSPPPE is a 5-item questionnaire, measured on a 7-point Likert scale, with scores ranging from 1 (Strongly Disagree) to 7 (Strongly Agree), that assesses agreement with statements about the physician. The total score is the sum of all item scores (5-35), with higher scores representing a higher degree of perceived physician empathy.
4. Upper extremity disability, measured by the Patient-Reported Outcomes Measurement Information System Physical Function-Upper Extremity (PROMIS PF-UE) Computer Adaptive Test (CAT).14-16 This is a measure of physical limitations in the upper extremity. It can be completed with as few as 4 questions while still achieving high precision in scoring and thereby decreasing survey burden. PROMIS presents a continuous T-score with a mean of 50 and standard deviation (SD) of 10, with higher scores reflecting better physical function compared to the average of the US general population.15
After completing the initial questionnaire, the research assistant filled out the office and surgeon name and asked the surgeon to complete the diagnosis. All questionnaires were administered on an encrypted tablet via the secure, HIPAA-compliant electronic platform REDCap (Research Electronic Data Capture), a web-based application for building and managing online surveys and databases.17 The follow-up survey was sent automatically or was done by phone call as previously described. The follow-up survey consisted of (1) the 11-point ordinal measure of satisfaction with the surgeon, (2) the JSPPPE for perceived empathy, and (3) the PROMIS PF-UE for physical limitations in the upper extremity.
Analysis
Continuous variables are presented as mean ± SD and discrete data as proportions. We used Student’s t-tests to assess baseline differences between continuous variables and Fisher’s exact tests for discrete variables. To assess differences in satisfaction and perceived empathy after 2 weeks, we used Student’s paired t-tests. We created 2 multilevel multivariable linear regression models to assess factors associated with (1) change in satisfaction with the surgeon and (2) change in perceived physician empathy. These models account for correlation of patients treated by the same surgeon. We selected variables to be included in the final models by running multilevel models with only 1 independent variable of interest (Appendix 1). Variables with P < 0.10 were included in our final models. We also included change in PROMIS PF-UE in both models because this was our variable of interest. We considered P < 0.05 significant.

We performed a power analysis for the difference in patient satisfaction immediately after the first visit compared to 2 weeks later. Based on our pilot data where we found an initial mean satisfaction score of 9.4 and mean satisfaction score after 2 weeks of 9.1 (SD of difference 1.0), a priori power analysis showed that we needed a minimum sample size of 90 patients to detect a difference with power set at 0.80 and alpha set at 0.05. In order to account for loss to follow-up as previously noted,18 we enrolled 67% more patients (total of 150).
Results
Respondent Characteristics
None of the 150 patients were excluded from the analysis. The study patients’ mean age was 51 ± 16 years (range, 18-87 years), and 73 (49%) were men (Table 1). Mean scores directly after the visit were 9.4 ± 1.2 (range, 2-10) for satisfaction with the surgeon, 31 ± 5.2 (range, 9-35) for perceived physician empathy, and 40 ± 10 (range 15-56) for upper extremity disability. Most patients (n = 130, 87%) were seen in 2 of 5 offices, and 106 (71%) were seen by 2 out of 6 participating surgeons.

Ninety-seven (65%) patients completed their follow-up assessment 2 weeks after their initial visit, 49 (51%) by phone and 48 (49%) by email. This is a slightly better rate than the 36% rate reported in previous research.18 After 2 weeks, the mean score for satisfaction with the surgeon was 9.1 ± 1.5 (range, 0-10), the mean perceived empathy score was 31 ± 5.1 (range, 6-35), and the mean upper extremity disability score was 40 ± 8.7 (range, 23-56). Responders did not differ from nonresponders based on demographic data (Table 2). However, nonresponders had lower perceived empathy scores directly after their visit (P = 0.03) and none had initially chosen phone as their preferred mode of contact for follow-up (P < 0.001). A list of all diagnoses with frequencies the surgeons stated is listed in Appendix 2.

Difference in Satisfaction with the Surgeon
Satisfaction with the surgeon 2 weeks after the in-person visit was slightly, but significantly, lower on bivariate analysis compared to satisfaction with the surgeon immediately after the initial visit (–0.41 ± 1.2, P = 0.001; Table 3).

Difference in Perceived Physician Empathy
Perceived physician empathy 2 weeks after the in-person visit was not significantly lower on bivariate analysis compared to perceived physician empathy immediately after the initial visit (–0.71 ± 5.3, P = 0.19; Table 3).

Factors Associated with Change in Satisfaction with the Surgeon
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in satisfaction with the surgeon (regression coefficient [beta], 0.00 [95% confidence interval {CI}, –0.02 to 0.03]; standard error [SE], 0.01; P = 0.79 [Table 4]). Being Latino was independently associated with less change in satisfaction with the surgeon (beta coefficient, –0.57 [95% CI, –1.1 to 0.00]; SE, 0.29; P = 0.049).

Factors Associated with Change in Perceived Physician Empathy
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in perceived physician empathy (beta coefficient = 0.00 [95% CI, –0.10 to 0.11]; SE, 0.06; P = 0.93 [Table 4]). Race/ethnicity other than white or Latino was independently associated with more change in perceived physician empathy (beta coefficient, 3.5 [95% CI, 0.34 to 6.6]; SE, 1.6; P = 0.030), and preferring email as mode of contact for follow-up was independently associated with less change in perceived physician empathy (beta coefficient, –3.2 [95% CI, –5.2 to –1.3]; SE, 1.0; P = 0.001).
Discussion
Patient satisfaction is considered a quality measure1-8 and is typically measured directly after an in-person visit. This study tested differences in patient satisfaction and perceived empathy immediately after the initial visit compared to 2 weeks later. In addition, we assessed whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
We acknowledge some study limitations. First, we only measured satisfaction based on 1 visit rather than multiple visits over time. It might be that satisfaction ratings differ when the physician-patient relationship is more established. However, we found overall high satisfaction ratings and a well-established relationship might not add to this finding. Second, surgeons were aware of the study and its purpose, which might have resulted in subconsciously altering the behavior to improve satisfaction. The effect of people acting differently as a result of being observed is called the Hawthorne effect.19 Third, we only used 1 simple ordinal measure to assess patient satisfaction with the surgeon. There is a wide variety of satisfaction measures,20 though the focus of this study was not to test the best possible satisfaction measure but to assess changes in satisfaction over time and its predictors. The simple 11-point ordinal satisfaction measure has proved reliable.6 Fourth, 35% of patients did not make a second rating. This is not unusual for phone or email studies. Our response rate was relatively high compared to other studies in our field,18 perhaps because the time to the second assessment was only 2 weeks and all people were available for follow-up by phone. Fifth, we analyzed 4 surgeons as 1 group and 3 offices as 1 group since we did not enroll enough patients per surgeon and office for individual analysis. However, multilevel linear analysis takes surgeon specific factors into account within that group.
The finding that satisfaction with the surgeon after 2 weeks was significantly lower on bivariate analysis compared to immediately after the initial visit is different from a study that found small increases in satisfaction after 2 weeks and 3 months,1 but comparable to another study in our field.21 Although significant, we believe the decrease in satisfaction is probably not clinically relevant. It might also be that satisfaction at follow-up is lower than measured, but that the least satisfied people did not respond on the follow-up survey.
We found no significant change in perceived empathy after 2 weeks. Since empathy is a strong driver of satisfaction,2,4-7 we did not expect to find differing results for empathy and for satisfaction over time. Both satisfaction and empathy seem to be relatively durable measures with current measurement tools.
The finding that change in disability was neither independently associated with change in satisfaction nor change in empathy is consistent with prior research.2,3,21 We cannot adequately study the impact of changes since we did not find an important change in either satisfaction or empathy over time. Jackson et al found higher satisfaction ratings over time in patients who had an increase in physical function and a decrease in symptoms.1 They also found that met expectations was associated with higher satisfaction immediately after the visit, after 2 weeks, and after 3 months.1 We feel that met expectations and fewer symptoms and limitations are likely highly co-linear with satisfaction. We therefore may not be able to learn much about one from the others.
The slight change we found in satisfaction with the surgeon among Latino patients was significantly less than the change among white patients. This suggests Latino patients might have a more stable opinion over time (a cultural phenomenon), or it might be spurious given the small number of Latino patients included in the study. The same can be said for the finding that race/ethnicity other than white or Latino was independently associated with greater change in empathy. Providing email as the preferred mode of contact was found to be independently associated with less change in perceived empathy compared to follow-up by phone. We had a 100% success rate for our follow-ups by phone. Our findings suggest that patients might more easily switch ratings on an 11-point ordinal scale than on a 5-item Likert scale. However, both measures are often rated at the ceiling of the scale.2,21
Conclusion
Satisfaction and perceived empathy are relatively stable constructs, are not clearly associated with other factors, and are strongly correlated with one another. This study supports the research practice of measuring satisfaction immediately after the visit, which is more convenient for both participant and researcher and avoids the loss of more than one third of the patients, and those with a worse experience in particular. To improve the utility and interpretation of patient-reported experience measures such as these, we might direct our efforts to developing scales with less ceiling effect.
Corresponding author: David Ring, MD, PhD, Dell Medical School, The University of Texas at Austin, Health Discovery Building HDB 6.706, 1701 Trinity St., Austin, TX 78705; [email protected].
Financial disclosures: Dr. Ring has or may receive payment or benefits from Skeletal Dynamics, Wright Medical for elbow implants, Deputy Editor for Clinical Orthopaedics and Related Research, Universities and Hospitals, Lawyers outside the submitted work.
Dr. Teunis has or may receive payment or benefits from VCC, PATIENT+, and AO Trauma TK network unrelated to this work and consultant fees from Synthes.
From the Department of Surgery and Perioperative Care, Dell Medical School, The University of Texas at Austin, Austin, TX (Dr. Kortlever, Ms. Haidar, Dr. Reichel, Dr. Driscoll, Dr. Ring, and Dr. Vagner) and University Medical Center Utrecht, Utrecht, The Netherlands (Dr. Teunis).
Abstract
- Objective: Patient satisfaction is considered a quality measure. Satisfaction is typically measured directly after an in-person visit in research and 2 weeks later in practice surveys. We assessed if there was a difference in immediate and delayed measurement of satisfaction.
- Questions: (1) There is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) and (2) perceived empathy (measured by the Jefferson Scale of Patient Perceptions of Physician Empathy [JSPPPE]) immediately after the initial visit compared to 2 weeks later. (3) Change in disability (measured by the Patient-Reported Outcome Measurement Information System Physical Function-Upper Extremity [PROMIS PF-UE]) is not independently associated with change in satisfaction and (4) empathy after the initial visit compared to 2 weeks later.
- Methods: 150 new patients completed a survey of demographics, satisfaction with the surgeon, rating of the surgeon’s empathy, and upper extremity specific limitations. The satisfaction, empathy, and limitation questionnaires were repeated 2 weeks later.
- Results: We found a slight but significant decrease in satisfaction 2 weeks after the in-person visit (–0.41, P = 0.001). There was no significant change in perceived empathy (–0.71, P = 0.19). Change in limitations did not account for a change in satisfaction (P = 0.79) or perceived empathy (P = 0.93).
- Conclusion: Satisfaction and perceived empathy are relatively stable constructs that can be measured immediately after the visit.
Keywords: satisfaction, empathy, change, upper extremity, disability.
Patient satisfaction is increasingly being used as a performance measure to evaluate quality of care.1-8 Patient satisfaction correlates with adherence with recommended treatment.1,6,8-10 Satisfaction measured on an 11-point ordinal scale immediately after the visit correlates strongly with the perception of clinician empathy.2,3 Indeed, some satisfaction questionnaires such as the Medical Interview Satisfaction Scale (MISS)11,12 have questions very similar to empathy questionnaires. It may be that satisfaction is a construct similar to feeling that your doctor listened and cared about you as an individual (perceived physician empathy).
Higher ratings of satisfaction also seem to be related to a physician’s communication style.1,4,7-10 One study of 13 fertility doctors found that training in effective communication strategies led to improved patient satisfaction.7 A qualitative study of 36 patients, health professionals, and clinical support staff in an orthopaedic outpatient setting held interviews and focus group sessions to identify themes influencing patient satisfaction.4 Communication and expectation were among the 7 themes identified. We have noticed a high ceiling effect (maximum scores) with measures of patient satisfaction and perceived empathy.2,3 Another study also noted a high ceiling effect when using an ordinal scale.5 It may be that people with a positive feeling shortly after a health care encounter give top ratings out of politeness or gratefulness. It is also possible they will feel differently a few weeks after they leave the office. Furthermore, ratings of satisfaction gathered by a practice or health care system for practice assessment/improvement are often obtained several days to weeks after the visit, while research often obtains satisfaction ratings immediately after the visit for practical reasons. There may be differences between immediate and delayed measurement of satisfaction beyond the mentioned social norms.
Therefore, this study tested the primary null hypothesis that there is no difference in patient satisfaction (measured by Numerical Rating Scale [NRS]) immediately after the initial visit compared to 2 weeks later. Additionally, we assessed the difference in perceived empathy immediately after the initial visit compared to 2 weeks later, and whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
Methods
Study Design
After Institutional Review Board approval of this prospective, longitudinal, observational cohort study, we prospectively enrolled 150 adult patients between November 29, 2017 and January 10, 2018. Patients were seen at 5 orthopaedic clinics in a large urban area. We included all new English-speaking patients aged 18 to 89 years who were visiting 1 of 6 participating orthopaedic surgeons for any upper extremity problem and who were able to provide informed consent. We excluded follow-up visits and patients who were unable to speak and understand English. Four research assistants who were not involved with patient treatment described the study to patients before or after the visit with the surgeon. We were granted a waiver of written informed consent; patients indicated their consent by completing the surveys.
Patients could choose either phone or email as their preferred mode of contact for follow-up in this study. For patients who selected email as the preferred mode of contact, the follow-up survey was sent automatically 2 weeks after completion date, and a maximum of 3 reminder emails with 2-day time intervals between them were sent to those who did not respond to the initial invitation. For patients who selected phone as the preferred mode of contact, the follow-up survey was done by an English-speaking research assistant who was not involved with patient treatment. When a response was not obtained on the initial phone call, 3 additional phone calls were made (1 later that same day and 2 the next day). One patient declined participation because he was not interested in the study and had no time after his visit.
Measurements
Patients were asked to complete a set of questionnaires at the end of their visit:
1. A demographic questionnaire consisting of preferred mode of contact for follow-up (phone or email), age, sex, race/ethnicity, marital status, education status, work status, insurance status, and type of visit (first visit or second opinion);
2. An 11-point ordinal measure of satisfaction with the surgeon, with scores ranging from 0 (Worst Surgeon Possible) to 10 (Best Surgeon Possible);
3. The patient’s rating of the surgeon’s empathy, measured by the Jefferson Scale of Patient Perceptions of Physician Empathy (JSPPPE).13 The JSPPPE is a 5-item questionnaire, measured on a 7-point Likert scale, with scores ranging from 1 (Strongly Disagree) to 7 (Strongly Agree), that assesses agreement with statements about the physician. The total score is the sum of all item scores (5-35), with higher scores representing a higher degree of perceived physician empathy.
4. Upper extremity disability, measured by the Patient-Reported Outcomes Measurement Information System Physical Function-Upper Extremity (PROMIS PF-UE) Computer Adaptive Test (CAT).14-16 This is a measure of physical limitations in the upper extremity. It can be completed with as few as 4 questions while still achieving high precision in scoring and thereby decreasing survey burden. PROMIS presents a continuous T-score with a mean of 50 and standard deviation (SD) of 10, with higher scores reflecting better physical function compared to the average of the US general population.15
After completing the initial questionnaire, the research assistant filled out the office and surgeon name and asked the surgeon to complete the diagnosis. All questionnaires were administered on an encrypted tablet via the secure, HIPAA-compliant electronic platform REDCap (Research Electronic Data Capture), a web-based application for building and managing online surveys and databases.17 The follow-up survey was sent automatically or was done by phone call as previously described. The follow-up survey consisted of (1) the 11-point ordinal measure of satisfaction with the surgeon, (2) the JSPPPE for perceived empathy, and (3) the PROMIS PF-UE for physical limitations in the upper extremity.
Analysis
Continuous variables are presented as mean ± SD and discrete data as proportions. We used Student’s t-tests to assess baseline differences between continuous variables and Fisher’s exact tests for discrete variables. To assess differences in satisfaction and perceived empathy after 2 weeks, we used Student’s paired t-tests. We created 2 multilevel multivariable linear regression models to assess factors associated with (1) change in satisfaction with the surgeon and (2) change in perceived physician empathy. These models account for correlation of patients treated by the same surgeon. We selected variables to be included in the final models by running multilevel models with only 1 independent variable of interest (Appendix 1). Variables with P < 0.10 were included in our final models. We also included change in PROMIS PF-UE in both models because this was our variable of interest. We considered P < 0.05 significant.

We performed a power analysis for the difference in patient satisfaction immediately after the first visit compared to 2 weeks later. Based on our pilot data where we found an initial mean satisfaction score of 9.4 and mean satisfaction score after 2 weeks of 9.1 (SD of difference 1.0), a priori power analysis showed that we needed a minimum sample size of 90 patients to detect a difference with power set at 0.80 and alpha set at 0.05. In order to account for loss to follow-up as previously noted,18 we enrolled 67% more patients (total of 150).
Results
Respondent Characteristics
None of the 150 patients were excluded from the analysis. The study patients’ mean age was 51 ± 16 years (range, 18-87 years), and 73 (49%) were men (Table 1). Mean scores directly after the visit were 9.4 ± 1.2 (range, 2-10) for satisfaction with the surgeon, 31 ± 5.2 (range, 9-35) for perceived physician empathy, and 40 ± 10 (range 15-56) for upper extremity disability. Most patients (n = 130, 87%) were seen in 2 of 5 offices, and 106 (71%) were seen by 2 out of 6 participating surgeons.

Ninety-seven (65%) patients completed their follow-up assessment 2 weeks after their initial visit, 49 (51%) by phone and 48 (49%) by email. This is a slightly better rate than the 36% rate reported in previous research.18 After 2 weeks, the mean score for satisfaction with the surgeon was 9.1 ± 1.5 (range, 0-10), the mean perceived empathy score was 31 ± 5.1 (range, 6-35), and the mean upper extremity disability score was 40 ± 8.7 (range, 23-56). Responders did not differ from nonresponders based on demographic data (Table 2). However, nonresponders had lower perceived empathy scores directly after their visit (P = 0.03) and none had initially chosen phone as their preferred mode of contact for follow-up (P < 0.001). A list of all diagnoses with frequencies the surgeons stated is listed in Appendix 2.

Difference in Satisfaction with the Surgeon
Satisfaction with the surgeon 2 weeks after the in-person visit was slightly, but significantly, lower on bivariate analysis compared to satisfaction with the surgeon immediately after the initial visit (–0.41 ± 1.2, P = 0.001; Table 3).

Difference in Perceived Physician Empathy
Perceived physician empathy 2 weeks after the in-person visit was not significantly lower on bivariate analysis compared to perceived physician empathy immediately after the initial visit (–0.71 ± 5.3, P = 0.19; Table 3).

Factors Associated with Change in Satisfaction with the Surgeon
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in satisfaction with the surgeon (regression coefficient [beta], 0.00 [95% confidence interval {CI}, –0.02 to 0.03]; standard error [SE], 0.01; P = 0.79 [Table 4]). Being Latino was independently associated with less change in satisfaction with the surgeon (beta coefficient, –0.57 [95% CI, –1.1 to 0.00]; SE, 0.29; P = 0.049).

Factors Associated with Change in Perceived Physician Empathy
Accounting for potential interaction of variables using multilevel multivariable analysis, change in disability of the upper extremity was not associated with change in perceived physician empathy (beta coefficient = 0.00 [95% CI, –0.10 to 0.11]; SE, 0.06; P = 0.93 [Table 4]). Race/ethnicity other than white or Latino was independently associated with more change in perceived physician empathy (beta coefficient, 3.5 [95% CI, 0.34 to 6.6]; SE, 1.6; P = 0.030), and preferring email as mode of contact for follow-up was independently associated with less change in perceived physician empathy (beta coefficient, –3.2 [95% CI, –5.2 to –1.3]; SE, 1.0; P = 0.001).
Discussion
Patient satisfaction is considered a quality measure1-8 and is typically measured directly after an in-person visit. This study tested differences in patient satisfaction and perceived empathy immediately after the initial visit compared to 2 weeks later. In addition, we assessed whether change in disability was independently associated with change in satisfaction and empathy after the initial visit compared to 2 weeks later.
We acknowledge some study limitations. First, we only measured satisfaction based on 1 visit rather than multiple visits over time. It might be that satisfaction ratings differ when the physician-patient relationship is more established. However, we found overall high satisfaction ratings and a well-established relationship might not add to this finding. Second, surgeons were aware of the study and its purpose, which might have resulted in subconsciously altering the behavior to improve satisfaction. The effect of people acting differently as a result of being observed is called the Hawthorne effect.19 Third, we only used 1 simple ordinal measure to assess patient satisfaction with the surgeon. There is a wide variety of satisfaction measures,20 though the focus of this study was not to test the best possible satisfaction measure but to assess changes in satisfaction over time and its predictors. The simple 11-point ordinal satisfaction measure has proved reliable.6 Fourth, 35% of patients did not make a second rating. This is not unusual for phone or email studies. Our response rate was relatively high compared to other studies in our field,18 perhaps because the time to the second assessment was only 2 weeks and all people were available for follow-up by phone. Fifth, we analyzed 4 surgeons as 1 group and 3 offices as 1 group since we did not enroll enough patients per surgeon and office for individual analysis. However, multilevel linear analysis takes surgeon specific factors into account within that group.
The finding that satisfaction with the surgeon after 2 weeks was significantly lower on bivariate analysis compared to immediately after the initial visit is different from a study that found small increases in satisfaction after 2 weeks and 3 months,1 but comparable to another study in our field.21 Although significant, we believe the decrease in satisfaction is probably not clinically relevant. It might also be that satisfaction at follow-up is lower than measured, but that the least satisfied people did not respond on the follow-up survey.
We found no significant change in perceived empathy after 2 weeks. Since empathy is a strong driver of satisfaction,2,4-7 we did not expect to find differing results for empathy and for satisfaction over time. Both satisfaction and empathy seem to be relatively durable measures with current measurement tools.
The finding that change in disability was neither independently associated with change in satisfaction nor change in empathy is consistent with prior research.2,3,21 We cannot adequately study the impact of changes since we did not find an important change in either satisfaction or empathy over time. Jackson et al found higher satisfaction ratings over time in patients who had an increase in physical function and a decrease in symptoms.1 They also found that met expectations was associated with higher satisfaction immediately after the visit, after 2 weeks, and after 3 months.1 We feel that met expectations and fewer symptoms and limitations are likely highly co-linear with satisfaction. We therefore may not be able to learn much about one from the others.
The slight change we found in satisfaction with the surgeon among Latino patients was significantly less than the change among white patients. This suggests Latino patients might have a more stable opinion over time (a cultural phenomenon), or it might be spurious given the small number of Latino patients included in the study. The same can be said for the finding that race/ethnicity other than white or Latino was independently associated with greater change in empathy. Providing email as the preferred mode of contact was found to be independently associated with less change in perceived empathy compared to follow-up by phone. We had a 100% success rate for our follow-ups by phone. Our findings suggest that patients might more easily switch ratings on an 11-point ordinal scale than on a 5-item Likert scale. However, both measures are often rated at the ceiling of the scale.2,21
Conclusion
Satisfaction and perceived empathy are relatively stable constructs, are not clearly associated with other factors, and are strongly correlated with one another. This study supports the research practice of measuring satisfaction immediately after the visit, which is more convenient for both participant and researcher and avoids the loss of more than one third of the patients, and those with a worse experience in particular. To improve the utility and interpretation of patient-reported experience measures such as these, we might direct our efforts to developing scales with less ceiling effect.
Corresponding author: David Ring, MD, PhD, Dell Medical School, The University of Texas at Austin, Health Discovery Building HDB 6.706, 1701 Trinity St., Austin, TX 78705; [email protected].
Financial disclosures: Dr. Ring has or may receive payment or benefits from Skeletal Dynamics, Wright Medical for elbow implants, Deputy Editor for Clinical Orthopaedics and Related Research, Universities and Hospitals, Lawyers outside the submitted work.
Dr. Teunis has or may receive payment or benefits from VCC, PATIENT+, and AO Trauma TK network unrelated to this work and consultant fees from Synthes.
1. Jackson JL, Chamberlin J, Kroenke K. Predictors of patient satisfaction. Soc Sci Med. 2001;52:609-620.
2. Menendez ME, Chen NC, Mudgal CS, et al. Physician empathy as a driver of hand surgery patient satisfaction. J Hand Surg Am. 2015;40(9):1860-1865.
3. Parrish RC 2nd, Menendez ME, Mudgal CS, et al. Patient Satisfaction and its relation to perceived visit duration with a hand surgeon. J Hand Surg Am. 2016;41(2):257-262.
4. Waters S, Edmondston SJ, Yates PJ, Gucciardi DF. Identification of factors influencing patient satisfaction with orthopaedic outpatient clinic consultation: A qualitative study. Man Ther. 2016;25:48-55.
5. Voutilainen A, Pitkaaho T, Kvist T, Vehvilainen-Julkunen K. How to ask about patient satisfaction? The visual analogue scale is less vulnerable to confounding factors and ceiling effect than a symmetric Likert scale. J Adv Nurs. 2016;72:946-957.
6. van Berckel MM, Bosma NH, Hageman MG, et al. The correlation between a numerical rating scale of patient satisfaction with current management of an upper extremity disorder and a general measure of satisfaction with the medical visit. Hand (N Y). 2017;12:202-206.
7. Garcia D, Bautista O, Venereo L, et al. Training in empathic skills improves the patient-physician relationship during the first consultation in a fertility clinic. Fertil Steril. 2013;99:1413-1418.
8. Fitzpatrick RM, Hopkins A. Patients’ satisfaction with communication in neurological outpatient clinics. J Psychosom Res. 1981;25:329-334.
9. Kincey J, Bradshaw P, Ley P. Patients’ satisfaction and reported acceptance of advice in general practice. J R Coll Gen Pract. 1975;25:558-566.
10. Ley P, Whitworth MA, Skilbeck CE, et al. Improving doctor-patient communication in general practice. J R Coll Gen Pract. 1976;26:720-724.
11. Meakin R, Weinman J. The ‘Medical Interview Satisfaction Scale’ (MISS-21) adapted for British general practice. Fam Pract. 2002;19:257-263.
12. Wolf MH, Putnam SM, James SA, Stiles WB. The Medical Interview Satisfaction Scale: development of a scale to measure patient perceptions of physician behavior. J Behav Med. 1978;1:391-401.
13. Kane GC, Gotto JL, Mangione S, et al. Jefferson Scale of Patient’s Perceptions of Physician Empathy: preliminary psychometric data. Croat Med J. 2007;48:81-86.
14. Beckmann JT , Hung M, Voss MW, et al. Evaluation of the patient-reported outcomes measurement information system upper extremity computer adaptive test. J Hand Surg Am. 2016;41:739-744.
15. PROMIS. PROMIS PF Scoring. Available at www.healthmeasures.net/administrator/components/com_instruments/uploads/PROMIS%20Physical%20Function%20Scoring%20Manual.pdf. Accessed March 1, 2019.
16. PROMIS. PROMIS Measures. Available at wwwnihpromisorg. Accessed March 1, 2019.
17. Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377-381.
18. Bot AG, Anderson JA, Neuhaus V, Ring D. Factors associated with survey response in hand surgery research. Clin Orthop Relat Res. 2013;471(10):3237-3242.
19. Sedgwick P, Greenwood N. Understanding the Hawthorne effect. BMJ. 2015;351:h4672.
20. Ross CK, Steward CA, Sinacore JM. A comparative study of seven measures of patient satisfaction. Med Care. 1995;33:392-406.
21. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res. 2015;473:2362-2368.
1. Jackson JL, Chamberlin J, Kroenke K. Predictors of patient satisfaction. Soc Sci Med. 2001;52:609-620.
2. Menendez ME, Chen NC, Mudgal CS, et al. Physician empathy as a driver of hand surgery patient satisfaction. J Hand Surg Am. 2015;40(9):1860-1865.
3. Parrish RC 2nd, Menendez ME, Mudgal CS, et al. Patient Satisfaction and its relation to perceived visit duration with a hand surgeon. J Hand Surg Am. 2016;41(2):257-262.
4. Waters S, Edmondston SJ, Yates PJ, Gucciardi DF. Identification of factors influencing patient satisfaction with orthopaedic outpatient clinic consultation: A qualitative study. Man Ther. 2016;25:48-55.
5. Voutilainen A, Pitkaaho T, Kvist T, Vehvilainen-Julkunen K. How to ask about patient satisfaction? The visual analogue scale is less vulnerable to confounding factors and ceiling effect than a symmetric Likert scale. J Adv Nurs. 2016;72:946-957.
6. van Berckel MM, Bosma NH, Hageman MG, et al. The correlation between a numerical rating scale of patient satisfaction with current management of an upper extremity disorder and a general measure of satisfaction with the medical visit. Hand (N Y). 2017;12:202-206.
7. Garcia D, Bautista O, Venereo L, et al. Training in empathic skills improves the patient-physician relationship during the first consultation in a fertility clinic. Fertil Steril. 2013;99:1413-1418.
8. Fitzpatrick RM, Hopkins A. Patients’ satisfaction with communication in neurological outpatient clinics. J Psychosom Res. 1981;25:329-334.
9. Kincey J, Bradshaw P, Ley P. Patients’ satisfaction and reported acceptance of advice in general practice. J R Coll Gen Pract. 1975;25:558-566.
10. Ley P, Whitworth MA, Skilbeck CE, et al. Improving doctor-patient communication in general practice. J R Coll Gen Pract. 1976;26:720-724.
11. Meakin R, Weinman J. The ‘Medical Interview Satisfaction Scale’ (MISS-21) adapted for British general practice. Fam Pract. 2002;19:257-263.
12. Wolf MH, Putnam SM, James SA, Stiles WB. The Medical Interview Satisfaction Scale: development of a scale to measure patient perceptions of physician behavior. J Behav Med. 1978;1:391-401.
13. Kane GC, Gotto JL, Mangione S, et al. Jefferson Scale of Patient’s Perceptions of Physician Empathy: preliminary psychometric data. Croat Med J. 2007;48:81-86.
14. Beckmann JT , Hung M, Voss MW, et al. Evaluation of the patient-reported outcomes measurement information system upper extremity computer adaptive test. J Hand Surg Am. 2016;41:739-744.
15. PROMIS. PROMIS PF Scoring. Available at www.healthmeasures.net/administrator/components/com_instruments/uploads/PROMIS%20Physical%20Function%20Scoring%20Manual.pdf. Accessed March 1, 2019.
16. PROMIS. PROMIS Measures. Available at wwwnihpromisorg. Accessed March 1, 2019.
17. Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377-381.
18. Bot AG, Anderson JA, Neuhaus V, Ring D. Factors associated with survey response in hand surgery research. Clin Orthop Relat Res. 2013;471(10):3237-3242.
19. Sedgwick P, Greenwood N. Understanding the Hawthorne effect. BMJ. 2015;351:h4672.
20. Ross CK, Steward CA, Sinacore JM. A comparative study of seven measures of patient satisfaction. Med Care. 1995;33:392-406.
21. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res. 2015;473:2362-2368.
Multicomponent Exercise Program Can Reverse Hospitalization-Associated Functional Decline in Elderly Patients
Study Overview
Objective. To assess the effects of an individualized, multicomponent exercise intervention on the functional status of very elderly patients who were acutely hospitalized compared with those who received usual care.
Design. A single-center, single-blind randomized clinical trial comparing elderly (≥ 75 years old) hospitalized patients who received in-hospital exercise (ie, individualized low-intensity resistance, balance, and walking exercises) versus control (ie, usual care that included physical rehabilitation if needed) interventions. The exercise intervention was adapted from the multicomponent physical exercise program Vivifrail and was supervised and conducted by a fitness specialist in 2 daily (1 morning and 1 evening) sessions lasting 20 minutes for 5 to 7 consecutive days. The morning session consisted of supervised and individualized progressive resistance, balance, and walking exercises. The evening session consisted of functional unsupervised exercises including light weights, extension and flexion of knee and hip, and walking.
Setting and participants. The study was conducted in an acute care unit in a tertiary public hospital in Navarra, Spain, between 1 February 2015 and 30 August 2017. A total of 370 elderly patients undergoing acute care hospitalization were enrolled in the study and randomly assigned to receive in-hospital exercise or control intervention. Inclusion criteria were: age ≥ 75 years, Barthel Index score ≥ 60, and ambulatory with or without assistance.
Main outcome measures. The primary outcome was change in functional capacity from baseline (beginning of exercise or control intervention) to hospital discharge as assessed by the Barthel Index of independence and the Short Physical Performance Battery (SPPB). Secondary outcomes were changes in cognitive capacity (Mini-Mental State Examination [MMSE]) and mood status (Yesavage Geriatric Depression Scale [GDS]), quality of life (QoL; EuroQol-5D), handgrip strength (dominant hand), incident delirium (Confusion Assessment Method), length of stay (LOS), falls during hospitalization, transfer after discharge, and readmission rate and mortality at 3 months after discharge. Intention-to-treat analysis was conducted.
Main results. Of the 370 patients included in the study’s analyses, 209 (56.5%) were women, mean age was 87.3 ± 4.9 years (range, 75-101 years; 130 [35.1%] nonagenarians). The median LOS was 8 days in both groups (interquartile range [IQR], 4 and 4 days, respectively). The median duration of the intervention was 5 days (IQR, 0 days), with 5 ± 1 morning and 4 ± 1 evening sessions in the exercise group. Adherence to the exercise intervention was high (95.8% for morning sessions; 83.4% for evening sessions), and no adverse effects were observed with the intervention.
The in-hospital exercise intervention program yielded significant benefits over usual care in functional outcomes in elderly patients. The exercise group had an increased change in measures of functional capacity compared to the usual care group (ie, Barthel Index, 6.9 points; 95% confidence interval [CI], 4.4-9.5; SPPB score, 2.2 points; 95% CI, 1.7-2.6). Furthermore, acute hospitalization led to an impairment in functional capacity from baseline to discharge in the Barthel Index (−5.0 points; 95% CI, −6.8 to −3.2) in the usual care group. In contrast, exercise intervention reversed this decline and improved functional outcomes as assessed by Barthel Index (1.9 points; 95% CI, 0.2-3.7) and SPPB score (2.4 points; 95% CI, 2.1-2.7).
The beneficial effects of the in-hospital exercise intervention extended to secondary end points indicative of cognitive capacity (MMSE, 1.8 points; 95% CI, 1.3-2.3), mood status (GDS, −2.0 points; 95% CI, −2.5 to −1.6), QoL (EuroQol-5D, 13.2 points; 95% CI, 8.2-18.2), and handgrip strength (2.3 kg; 95% CI, 1.8-2.8) compared to those who received usual care. In contrast, no differences were observed between groups that received exercise intervention and usual care in incident delirium, LOS, falls during hospitalization, transfer after discharge, and 3-month hospital readmission rate and mortality.
Conclusion. An individualized, multicomponent physical exercise program that includes low-intensity resistance, balance, and walking exercises performed during the course of hospitalization (average of 5 days) can reverse functional decline associated with acute hospitalization in very elderly patients. Furthermore, this in-hospital exercise intervention is safe and has a high adherence rate, and thus represents an opportunity to improve quality of care in this vulnerable population.
Commentary
Frail elderly patients are highly susceptible to adverse outcomes of acute hospitalization, including functional decline, disability, nursing home placement, rehospitalization, and mortality.1 Mobility limitation, a major hazard of hospitalization, has been associated with poorer functional recovery and increased vulnerability to these major adverse events after hospital discharge.2-4 Interdisciplinary care models delivered during hospitalization (eg, Geriatric Evaluation Unit, Acute Care for Elders) that emphasize functional independence and provide protocols for exercise and rehabilitation have demonstrated reduced hospital LOS, discharge to nursing home, and mortality, and improved functional status in elderly patients.5-7 Despite this evidence, significant gaps in knowledge exist in understanding whether early implementation of an individualized, multicomponent exercise training program can benefit the oldest old patients who are acutely hospitalized.
This study reported by Martinez-Velilla and colleagues provides an important and timely investigation in examining the effects of an individualized, multicomponent (ie, low-intensity resistance, balance, and walking) in-hospital exercise intervention on functional outcomes of hospitalized octogenarians and nonagenarians. The authors reported that such an intervention, administered 2 sessions per day for 5 to 7 consecutive days, can be safely implemented and reverse functional decline (ie, improvement in Barthel Index and SPPB score over course of hospital stay) typically associated with acute hospitalization in these vulnerable individuals. These findings are particularly significant given the paucity of randomized controlled trials evaluating the impact of exercise intervention in preserving functional capacity of geriatric patients in the setting of acute hospitalization. While much more research is needed to facilitate future development of a consensus opinion in this regard, results from this study provide the rationale that implementation of an individualized multicomponent exercise program is feasible and safe and may attenuate functional decline in hospitalized older patients. Finally, the beneficial effects of in-hospital exercise intervention may extend to cognitive capacity, mood status, and QoL—domains that are essential to optimizing patient-centered care in the frailest elderly patients.
The study was well conceived with a number of strengths, including its randomized clinical trial design. In addition, the trial patients were advanced in age (35.1% were nonagenarians), which is particularly important because this is a vulnerable population that is frequently excluded from participation in trials of exercise interventions and because the evidence-base for physical activity guidelines is suboptimal. Moreover, the authors demonstrated that an individualized multicomponent exercise program could be successfully implemented in elderly patients in an acute setting via daily exercise sessions. This test of feasibility is significant in that clinical trials in exercise intervention in geriatrics are commonly performed in nonacute settings in the community, long-term care facilities, or subacute care. The major limitation in this study centers on the generalizability of its findings. It was noted that some patients were not assessed for changes from baseline to discharge on the Barthel Index (6.1%) and SPPB (2.3%) because of their poor condition. The exclusion of the most debilitated patients limits the application of the study’s key findings to the frailest elderly patients, who are most likely to require acute hospital care.
Applications for Clinical Pract
Functional decline is an exceedingly common adverse outcome associated with hospitalization in older patients. While more evidence is needed, early implementation of an individualized, multicomponent exercise regimen during hospitalization may help to prevent functional decline in vulnerable elderly patients.
—Fred Ko, MD, MS
1. Goldwater DS, Dharmarajan K, McEwan BS, Krumholz HM. Is posthospital syndrome a result of hospitalization-induced allostatic overload? J Hosp Med. 2018;13(5).doi:10.12788/jhm.2986.
2. Creditor MC. Hazards of hospitalization of the elderly. Ann Intern Med. 1993;118:219-223.
3. Minnick AF, Mion LC, Johnson ME, et al. Prevalence and variation of physical restraint use in acute care settings in the US. J Nurs Scholarsh. 2007;39:30-37.
4. Zisberg A, Shadmi E, Sinoff G et al. Low mobility during hospitalization and functional decline in older adults. J Am Geriatr Soc. 2011;59:266-273.
5. Rubenstein LZ, et al. Effectiveness of a geriatric evaluation unit. A randomized clinical trial. N Engl J Med. 1984;311:1664-1670.
6. Landefeld CS, Palmer RM, Kresevic DM, et al. A randomized trial of care in a hospital medical unit especially designed to improve the functional outcomes of acutely ill older patients. N Engl J Med. 1995;332:1338-1344.
7. de Morton NA, Keating JL, Jeffs K. Exercise for acutely hospitalised older medical patients. Cochrane Database Syst Rev. 2007;CD005955.
Study Overview
Objective. To assess the effects of an individualized, multicomponent exercise intervention on the functional status of very elderly patients who were acutely hospitalized compared with those who received usual care.
Design. A single-center, single-blind randomized clinical trial comparing elderly (≥ 75 years old) hospitalized patients who received in-hospital exercise (ie, individualized low-intensity resistance, balance, and walking exercises) versus control (ie, usual care that included physical rehabilitation if needed) interventions. The exercise intervention was adapted from the multicomponent physical exercise program Vivifrail and was supervised and conducted by a fitness specialist in 2 daily (1 morning and 1 evening) sessions lasting 20 minutes for 5 to 7 consecutive days. The morning session consisted of supervised and individualized progressive resistance, balance, and walking exercises. The evening session consisted of functional unsupervised exercises including light weights, extension and flexion of knee and hip, and walking.
Setting and participants. The study was conducted in an acute care unit in a tertiary public hospital in Navarra, Spain, between 1 February 2015 and 30 August 2017. A total of 370 elderly patients undergoing acute care hospitalization were enrolled in the study and randomly assigned to receive in-hospital exercise or control intervention. Inclusion criteria were: age ≥ 75 years, Barthel Index score ≥ 60, and ambulatory with or without assistance.
Main outcome measures. The primary outcome was change in functional capacity from baseline (beginning of exercise or control intervention) to hospital discharge as assessed by the Barthel Index of independence and the Short Physical Performance Battery (SPPB). Secondary outcomes were changes in cognitive capacity (Mini-Mental State Examination [MMSE]) and mood status (Yesavage Geriatric Depression Scale [GDS]), quality of life (QoL; EuroQol-5D), handgrip strength (dominant hand), incident delirium (Confusion Assessment Method), length of stay (LOS), falls during hospitalization, transfer after discharge, and readmission rate and mortality at 3 months after discharge. Intention-to-treat analysis was conducted.
Main results. Of the 370 patients included in the study’s analyses, 209 (56.5%) were women, mean age was 87.3 ± 4.9 years (range, 75-101 years; 130 [35.1%] nonagenarians). The median LOS was 8 days in both groups (interquartile range [IQR], 4 and 4 days, respectively). The median duration of the intervention was 5 days (IQR, 0 days), with 5 ± 1 morning and 4 ± 1 evening sessions in the exercise group. Adherence to the exercise intervention was high (95.8% for morning sessions; 83.4% for evening sessions), and no adverse effects were observed with the intervention.
The in-hospital exercise intervention program yielded significant benefits over usual care in functional outcomes in elderly patients. The exercise group had an increased change in measures of functional capacity compared to the usual care group (ie, Barthel Index, 6.9 points; 95% confidence interval [CI], 4.4-9.5; SPPB score, 2.2 points; 95% CI, 1.7-2.6). Furthermore, acute hospitalization led to an impairment in functional capacity from baseline to discharge in the Barthel Index (−5.0 points; 95% CI, −6.8 to −3.2) in the usual care group. In contrast, exercise intervention reversed this decline and improved functional outcomes as assessed by Barthel Index (1.9 points; 95% CI, 0.2-3.7) and SPPB score (2.4 points; 95% CI, 2.1-2.7).
The beneficial effects of the in-hospital exercise intervention extended to secondary end points indicative of cognitive capacity (MMSE, 1.8 points; 95% CI, 1.3-2.3), mood status (GDS, −2.0 points; 95% CI, −2.5 to −1.6), QoL (EuroQol-5D, 13.2 points; 95% CI, 8.2-18.2), and handgrip strength (2.3 kg; 95% CI, 1.8-2.8) compared to those who received usual care. In contrast, no differences were observed between groups that received exercise intervention and usual care in incident delirium, LOS, falls during hospitalization, transfer after discharge, and 3-month hospital readmission rate and mortality.
Conclusion. An individualized, multicomponent physical exercise program that includes low-intensity resistance, balance, and walking exercises performed during the course of hospitalization (average of 5 days) can reverse functional decline associated with acute hospitalization in very elderly patients. Furthermore, this in-hospital exercise intervention is safe and has a high adherence rate, and thus represents an opportunity to improve quality of care in this vulnerable population.
Commentary
Frail elderly patients are highly susceptible to adverse outcomes of acute hospitalization, including functional decline, disability, nursing home placement, rehospitalization, and mortality.1 Mobility limitation, a major hazard of hospitalization, has been associated with poorer functional recovery and increased vulnerability to these major adverse events after hospital discharge.2-4 Interdisciplinary care models delivered during hospitalization (eg, Geriatric Evaluation Unit, Acute Care for Elders) that emphasize functional independence and provide protocols for exercise and rehabilitation have demonstrated reduced hospital LOS, discharge to nursing home, and mortality, and improved functional status in elderly patients.5-7 Despite this evidence, significant gaps in knowledge exist in understanding whether early implementation of an individualized, multicomponent exercise training program can benefit the oldest old patients who are acutely hospitalized.
This study reported by Martinez-Velilla and colleagues provides an important and timely investigation in examining the effects of an individualized, multicomponent (ie, low-intensity resistance, balance, and walking) in-hospital exercise intervention on functional outcomes of hospitalized octogenarians and nonagenarians. The authors reported that such an intervention, administered 2 sessions per day for 5 to 7 consecutive days, can be safely implemented and reverse functional decline (ie, improvement in Barthel Index and SPPB score over course of hospital stay) typically associated with acute hospitalization in these vulnerable individuals. These findings are particularly significant given the paucity of randomized controlled trials evaluating the impact of exercise intervention in preserving functional capacity of geriatric patients in the setting of acute hospitalization. While much more research is needed to facilitate future development of a consensus opinion in this regard, results from this study provide the rationale that implementation of an individualized multicomponent exercise program is feasible and safe and may attenuate functional decline in hospitalized older patients. Finally, the beneficial effects of in-hospital exercise intervention may extend to cognitive capacity, mood status, and QoL—domains that are essential to optimizing patient-centered care in the frailest elderly patients.
The study was well conceived with a number of strengths, including its randomized clinical trial design. In addition, the trial patients were advanced in age (35.1% were nonagenarians), which is particularly important because this is a vulnerable population that is frequently excluded from participation in trials of exercise interventions and because the evidence-base for physical activity guidelines is suboptimal. Moreover, the authors demonstrated that an individualized multicomponent exercise program could be successfully implemented in elderly patients in an acute setting via daily exercise sessions. This test of feasibility is significant in that clinical trials in exercise intervention in geriatrics are commonly performed in nonacute settings in the community, long-term care facilities, or subacute care. The major limitation in this study centers on the generalizability of its findings. It was noted that some patients were not assessed for changes from baseline to discharge on the Barthel Index (6.1%) and SPPB (2.3%) because of their poor condition. The exclusion of the most debilitated patients limits the application of the study’s key findings to the frailest elderly patients, who are most likely to require acute hospital care.
Applications for Clinical Pract
Functional decline is an exceedingly common adverse outcome associated with hospitalization in older patients. While more evidence is needed, early implementation of an individualized, multicomponent exercise regimen during hospitalization may help to prevent functional decline in vulnerable elderly patients.
—Fred Ko, MD, MS
Study Overview
Objective. To assess the effects of an individualized, multicomponent exercise intervention on the functional status of very elderly patients who were acutely hospitalized compared with those who received usual care.
Design. A single-center, single-blind randomized clinical trial comparing elderly (≥ 75 years old) hospitalized patients who received in-hospital exercise (ie, individualized low-intensity resistance, balance, and walking exercises) versus control (ie, usual care that included physical rehabilitation if needed) interventions. The exercise intervention was adapted from the multicomponent physical exercise program Vivifrail and was supervised and conducted by a fitness specialist in 2 daily (1 morning and 1 evening) sessions lasting 20 minutes for 5 to 7 consecutive days. The morning session consisted of supervised and individualized progressive resistance, balance, and walking exercises. The evening session consisted of functional unsupervised exercises including light weights, extension and flexion of knee and hip, and walking.
Setting and participants. The study was conducted in an acute care unit in a tertiary public hospital in Navarra, Spain, between 1 February 2015 and 30 August 2017. A total of 370 elderly patients undergoing acute care hospitalization were enrolled in the study and randomly assigned to receive in-hospital exercise or control intervention. Inclusion criteria were: age ≥ 75 years, Barthel Index score ≥ 60, and ambulatory with or without assistance.
Main outcome measures. The primary outcome was change in functional capacity from baseline (beginning of exercise or control intervention) to hospital discharge as assessed by the Barthel Index of independence and the Short Physical Performance Battery (SPPB). Secondary outcomes were changes in cognitive capacity (Mini-Mental State Examination [MMSE]) and mood status (Yesavage Geriatric Depression Scale [GDS]), quality of life (QoL; EuroQol-5D), handgrip strength (dominant hand), incident delirium (Confusion Assessment Method), length of stay (LOS), falls during hospitalization, transfer after discharge, and readmission rate and mortality at 3 months after discharge. Intention-to-treat analysis was conducted.
Main results. Of the 370 patients included in the study’s analyses, 209 (56.5%) were women, mean age was 87.3 ± 4.9 years (range, 75-101 years; 130 [35.1%] nonagenarians). The median LOS was 8 days in both groups (interquartile range [IQR], 4 and 4 days, respectively). The median duration of the intervention was 5 days (IQR, 0 days), with 5 ± 1 morning and 4 ± 1 evening sessions in the exercise group. Adherence to the exercise intervention was high (95.8% for morning sessions; 83.4% for evening sessions), and no adverse effects were observed with the intervention.
The in-hospital exercise intervention program yielded significant benefits over usual care in functional outcomes in elderly patients. The exercise group had an increased change in measures of functional capacity compared to the usual care group (ie, Barthel Index, 6.9 points; 95% confidence interval [CI], 4.4-9.5; SPPB score, 2.2 points; 95% CI, 1.7-2.6). Furthermore, acute hospitalization led to an impairment in functional capacity from baseline to discharge in the Barthel Index (−5.0 points; 95% CI, −6.8 to −3.2) in the usual care group. In contrast, exercise intervention reversed this decline and improved functional outcomes as assessed by Barthel Index (1.9 points; 95% CI, 0.2-3.7) and SPPB score (2.4 points; 95% CI, 2.1-2.7).
The beneficial effects of the in-hospital exercise intervention extended to secondary end points indicative of cognitive capacity (MMSE, 1.8 points; 95% CI, 1.3-2.3), mood status (GDS, −2.0 points; 95% CI, −2.5 to −1.6), QoL (EuroQol-5D, 13.2 points; 95% CI, 8.2-18.2), and handgrip strength (2.3 kg; 95% CI, 1.8-2.8) compared to those who received usual care. In contrast, no differences were observed between groups that received exercise intervention and usual care in incident delirium, LOS, falls during hospitalization, transfer after discharge, and 3-month hospital readmission rate and mortality.
Conclusion. An individualized, multicomponent physical exercise program that includes low-intensity resistance, balance, and walking exercises performed during the course of hospitalization (average of 5 days) can reverse functional decline associated with acute hospitalization in very elderly patients. Furthermore, this in-hospital exercise intervention is safe and has a high adherence rate, and thus represents an opportunity to improve quality of care in this vulnerable population.
Commentary
Frail elderly patients are highly susceptible to adverse outcomes of acute hospitalization, including functional decline, disability, nursing home placement, rehospitalization, and mortality.1 Mobility limitation, a major hazard of hospitalization, has been associated with poorer functional recovery and increased vulnerability to these major adverse events after hospital discharge.2-4 Interdisciplinary care models delivered during hospitalization (eg, Geriatric Evaluation Unit, Acute Care for Elders) that emphasize functional independence and provide protocols for exercise and rehabilitation have demonstrated reduced hospital LOS, discharge to nursing home, and mortality, and improved functional status in elderly patients.5-7 Despite this evidence, significant gaps in knowledge exist in understanding whether early implementation of an individualized, multicomponent exercise training program can benefit the oldest old patients who are acutely hospitalized.
This study reported by Martinez-Velilla and colleagues provides an important and timely investigation in examining the effects of an individualized, multicomponent (ie, low-intensity resistance, balance, and walking) in-hospital exercise intervention on functional outcomes of hospitalized octogenarians and nonagenarians. The authors reported that such an intervention, administered 2 sessions per day for 5 to 7 consecutive days, can be safely implemented and reverse functional decline (ie, improvement in Barthel Index and SPPB score over course of hospital stay) typically associated with acute hospitalization in these vulnerable individuals. These findings are particularly significant given the paucity of randomized controlled trials evaluating the impact of exercise intervention in preserving functional capacity of geriatric patients in the setting of acute hospitalization. While much more research is needed to facilitate future development of a consensus opinion in this regard, results from this study provide the rationale that implementation of an individualized multicomponent exercise program is feasible and safe and may attenuate functional decline in hospitalized older patients. Finally, the beneficial effects of in-hospital exercise intervention may extend to cognitive capacity, mood status, and QoL—domains that are essential to optimizing patient-centered care in the frailest elderly patients.
The study was well conceived with a number of strengths, including its randomized clinical trial design. In addition, the trial patients were advanced in age (35.1% were nonagenarians), which is particularly important because this is a vulnerable population that is frequently excluded from participation in trials of exercise interventions and because the evidence-base for physical activity guidelines is suboptimal. Moreover, the authors demonstrated that an individualized multicomponent exercise program could be successfully implemented in elderly patients in an acute setting via daily exercise sessions. This test of feasibility is significant in that clinical trials in exercise intervention in geriatrics are commonly performed in nonacute settings in the community, long-term care facilities, or subacute care. The major limitation in this study centers on the generalizability of its findings. It was noted that some patients were not assessed for changes from baseline to discharge on the Barthel Index (6.1%) and SPPB (2.3%) because of their poor condition. The exclusion of the most debilitated patients limits the application of the study’s key findings to the frailest elderly patients, who are most likely to require acute hospital care.
Applications for Clinical Pract
Functional decline is an exceedingly common adverse outcome associated with hospitalization in older patients. While more evidence is needed, early implementation of an individualized, multicomponent exercise regimen during hospitalization may help to prevent functional decline in vulnerable elderly patients.
—Fred Ko, MD, MS
1. Goldwater DS, Dharmarajan K, McEwan BS, Krumholz HM. Is posthospital syndrome a result of hospitalization-induced allostatic overload? J Hosp Med. 2018;13(5).doi:10.12788/jhm.2986.
2. Creditor MC. Hazards of hospitalization of the elderly. Ann Intern Med. 1993;118:219-223.
3. Minnick AF, Mion LC, Johnson ME, et al. Prevalence and variation of physical restraint use in acute care settings in the US. J Nurs Scholarsh. 2007;39:30-37.
4. Zisberg A, Shadmi E, Sinoff G et al. Low mobility during hospitalization and functional decline in older adults. J Am Geriatr Soc. 2011;59:266-273.
5. Rubenstein LZ, et al. Effectiveness of a geriatric evaluation unit. A randomized clinical trial. N Engl J Med. 1984;311:1664-1670.
6. Landefeld CS, Palmer RM, Kresevic DM, et al. A randomized trial of care in a hospital medical unit especially designed to improve the functional outcomes of acutely ill older patients. N Engl J Med. 1995;332:1338-1344.
7. de Morton NA, Keating JL, Jeffs K. Exercise for acutely hospitalised older medical patients. Cochrane Database Syst Rev. 2007;CD005955.
1. Goldwater DS, Dharmarajan K, McEwan BS, Krumholz HM. Is posthospital syndrome a result of hospitalization-induced allostatic overload? J Hosp Med. 2018;13(5).doi:10.12788/jhm.2986.
2. Creditor MC. Hazards of hospitalization of the elderly. Ann Intern Med. 1993;118:219-223.
3. Minnick AF, Mion LC, Johnson ME, et al. Prevalence and variation of physical restraint use in acute care settings in the US. J Nurs Scholarsh. 2007;39:30-37.
4. Zisberg A, Shadmi E, Sinoff G et al. Low mobility during hospitalization and functional decline in older adults. J Am Geriatr Soc. 2011;59:266-273.
5. Rubenstein LZ, et al. Effectiveness of a geriatric evaluation unit. A randomized clinical trial. N Engl J Med. 1984;311:1664-1670.
6. Landefeld CS, Palmer RM, Kresevic DM, et al. A randomized trial of care in a hospital medical unit especially designed to improve the functional outcomes of acutely ill older patients. N Engl J Med. 1995;332:1338-1344.
7. de Morton NA, Keating JL, Jeffs K. Exercise for acutely hospitalised older medical patients. Cochrane Database Syst Rev. 2007;CD005955.
Androgen Deprivation Therapy Combined with Radiation in High-Risk Prostate Cancer . . . How Long Do We Go?
Study Overview
Objective. To compare the outcomes of 18 months versus 36 months of androgen deprivation therapy (ADT) combined with radiation in high-risk prostate cancer (HRPC).
Design. Phase 3 multicenter, randomized superiority trial.
Participants. This study enrolled patients aged ≤ 80 years with HRPC. All patients had no evidence of regional or distant metastasis. High-risk disease was defined as any of the following: clinical stage T3 or T4, prostate-specific antigen (PSA) level > 20 ng/mL, or Gleason score > 7.
Methods. Prior to randomization, all patients received 4 months of ADT with goserelin 10.8 mg and anti-androgen therapy with bicalutamide 50 mg daily for 30 days. Patients were then randomly assigned to 18 (short arm) or 36 (long arm) months of ADT in combination with radiation therapy (RT). The randomization was stratified by stage (T1-2 vs T3-4), Gleason score (< 7 vs > 7) and PSA level (< 20 ng/mL vs > 20 ng/mL). The standard radiation dose was 70 Gy to the prostate and 44 Gy to the pelvis. Computed tomography or magnetic resonance imaging exam of the abdomen and pelvis and a bone scan were performed to rule out regional or distant metastases. PSA level was monitored every 3 months for 18 months, every 6 months up to the third year, and yearly thereafter.
Main outcome measures. The 2 primary outcomes were overall survival (OS) and quality of life (QoL) at 5 years. The secondary end points were biochemical failure (BF)defined as PSA nadir plus 2, disease-free survival (DFS), and site(s) of tumor relapse.
Main results. The 5-year OS was 91% and 86% for the 36- and 18-month groups, respectively (P = 0.07). The 10-year OS was 62% for both groups (P = 0.7), and the global hazard ratio (HR) was 1.02 (P = 0.8). The disease-specific survival (DSS) was similar in both groups at 5 years (98% vs 97%) and at 10 years (91% vs 92%) in the long versus short arm, respectively. The rate of prostate cancer–specific death was 21% versus 23% in the long versus short arm, respectively. In a multivariate analysis for OS, only age and Gleason score > 7 were statistically significant survival predictors. BF rate at 10 years was 25% for 36 months as compared with 31% for 18 months (HR, 0.71, P = 0.02). The 10-year DFS rates were 45% and 39% for 36 and 18 months, respectively (HR, 0.68, P = 0.08). Forty patients in the long arm versus 43 in the short arm developed distant metastasis. Both groups developed similar sites of metastasis, which was predominantly osseous. Some aspects of the EORTC30 and PR25 scales were significant, mostly pertaining to sexual activity, fatigue, and hormone-related symptoms in favor of the 18-month group. The median time to testosterone recovery after completion of ADT was 2.1 years for the short arm versus 4 years in the long arm (P = 0.02). The compliance rate with ADT was 88% in the short arm versus 53% in the long arm. The main reason for nonadherence was side effects in 54% of the patients in the long arm and 31% in the short arm.
Conclusion. The results of the current study suggest that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months in patients with HRPC.
Commentary
The role of ADT for HRPC in combination with RT has been well established by evidence from several trials; however, the comparator arms and patient characteristics between these studies have been quite heterogeneous. For instance, the Radiation Therapy Oncology Group (RTOG) 85-31 trial compared indefinite ADT with RT versus RT alone and showed significantly better 10-year OS in the ADT plus RT arm.1 Similarly, the European Organisation for Research and Treatment of Cancer (EROTC) 22961 trial showed an OS benefit for 36 months versus 6 months of ADT in combination with radiation.2 Additionally, the RTOG 92-02 trial, which compared 4 months versus 24 months of ADT with radiation, also found a significantly improved 10-year OS with a longer course of ADT.3 Taken together these data suggest that 4 to 6 months of ADT is inferior to 24 to 36 months of ADT in HRPC.
Several differences, however, exist in patient characteristics between the present trial and the earlier trials, justifiably reflecting the change of practice in the PSA era. For instance, the present study has a higher percentage of patients with Gleason scores 8-10 (60%) compared to the EROTC and RTOG studies (15%-35%) and a lower percentage of patients with T3 and T4 tumors. Patients with high Gleason scores are believed to have a higher risk of micro-metastasis at the time of diagnosis and higher chances of castration resistance. Therefore, inclusion of a (presumably) larger high-risk patient subgroup in the present study lends further credence to results indicating similar OS with a shorter course of ADT. A post hoc analysis including only patients with Gleason score 8-10 performed for OS, DSS, BF, and DFS showed no significant difference in any of these variables between the arms. Analysis of the interaction between ADT duration in the Gleason 8-10 subgroup versus Gleason 7 for OS, DFS, DSS and BF found no significant differences. This again suggests that 18 months of ADT may be sufficient for this high-risk group; however, it is difficult to draw definitive conclusions from this unplanned subgroup analysis.
Based on the results of the current study, it seems that 18 months of ADT is adequate for many, but not necessarily all, patients. For instance, there was a significantly higher incidence of BF in the 18-month arm. Applying this data to younger patients may require a more nuanced approach, as it is possible that with longer follow-up this higher rate of BF may translate into a difference in OS. Therefore, life expectancy and comorbid conditions always need to be incorporated into clinical decision making with regards to ADT duration. In a study by Rose et al, the risk of prostate cancer–specific mortality significantly decreased by using ADT plus RT for men with HRPC with a low, but not a high, competing mortality score.4 The clinical significance of this finding is that adding ADT to RT might significantly reduce the risk of death from prostate cancer only in the setting of low competing risks.
Another concept to ponder is the optimum duration of ADT in the era of RT dose escalation. Currently, there are emerging techniques for delivering higher radiation doses and combining brachytherapy with external beam radiotherapy for HRPC, and the role of whole pelvic radiation is being investigated. New data suggests that higher radiation doses can lead to improvement in outcomes for HRPC. The DART01/05 study compared 4 versus 24 months of ADT with 76 to 82 Gy of RT and reported improved 5-year OS, DFS, and metastasis-free survival with longer ADT duration.5 Moreover, Kishan et al reported improved prostate cancer–specific mortality when brachytherapy boost was added to radiation compared to radiation alone in patients with Gleason scores 9 and 10.6 Therefore, the optimal duration of ADT in the setting of dose-escalated radiotherapy is not yet known. Also, it is important to note that unlike the prior RTOG and EORTC studies, this study did not include patients with evidence of regional nodal disease, and thus the present data should not be applied to this patient population.
Applications to Clinical Practice
This study’s results suggesting that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months of ADT in patients with HRPC should be interpreted with caution when treating very young patients, since the higher rate of BF in the short arm may impact the OS with longer follow-up. Additionally, patients’ QoL and tolerance to ADT-related adverse effects should be taken into consideration given that compliance with 36 months of ADT was only 53% in this study.
—Jailan Elayoubi, MD, Michigan State University, East Lansing, MI
1. Pilepich MV, Winter K, Lawton CA, et al. Androgen suppression adjuvant to definitive radiotherapy in prostate carcinoma—long-term results of phase III RTOG 85–31. Int J Radiat Oncol Biol Phys. 2005;61:1285-1290.
2. Bolla M, de Reijke TM, Van Tienhoven G, et al. Duration of androgen suppression in the treatment of prostate cancer. N Engl J Med. 2009;360:2516-2527.
3. Horwitz EM, Bae K, Hanks GE, Porter A, et al. Ten-year follow-up of radiation therapy oncology group protocol 92-02: a phase III trial of the duration of elective androgen deprivation in locally advanced prostate cancer. J Clin Oncol. 2008;26:2497–2504.
4. Rose BS, Chen MH, Wu J, et al. Androgen deprivation therapy use in the setting of high-dose radiation therapy and the risk of prostate cancer-specific mortality stratified by the extent of competing mortality. Int J Radiat Oncol Biol Phys. 2016;96:778-784.
5. Zapatero A, Guerrero A, Maldonado X, et al. High-dose radiotherapy with short-term or long-term androgen deprivation in localised prostate cancer (DART01/05 GICOR): a randomised, controlled, phase 3 trial. Lancet Oncol. 2015;16:320-327.
6. Kishan, AU, Cook, RR, Ciezki, JP, et al. Radical prostatectomy, external beam radiotherapy, or external beam radiotherapy with brachytherapy boost and disease progression and mortality in patients with gleason score 9-10 prostate cancer. JAMA. 2018;319:896-905.
Study Overview
Objective. To compare the outcomes of 18 months versus 36 months of androgen deprivation therapy (ADT) combined with radiation in high-risk prostate cancer (HRPC).
Design. Phase 3 multicenter, randomized superiority trial.
Participants. This study enrolled patients aged ≤ 80 years with HRPC. All patients had no evidence of regional or distant metastasis. High-risk disease was defined as any of the following: clinical stage T3 or T4, prostate-specific antigen (PSA) level > 20 ng/mL, or Gleason score > 7.
Methods. Prior to randomization, all patients received 4 months of ADT with goserelin 10.8 mg and anti-androgen therapy with bicalutamide 50 mg daily for 30 days. Patients were then randomly assigned to 18 (short arm) or 36 (long arm) months of ADT in combination with radiation therapy (RT). The randomization was stratified by stage (T1-2 vs T3-4), Gleason score (< 7 vs > 7) and PSA level (< 20 ng/mL vs > 20 ng/mL). The standard radiation dose was 70 Gy to the prostate and 44 Gy to the pelvis. Computed tomography or magnetic resonance imaging exam of the abdomen and pelvis and a bone scan were performed to rule out regional or distant metastases. PSA level was monitored every 3 months for 18 months, every 6 months up to the third year, and yearly thereafter.
Main outcome measures. The 2 primary outcomes were overall survival (OS) and quality of life (QoL) at 5 years. The secondary end points were biochemical failure (BF)defined as PSA nadir plus 2, disease-free survival (DFS), and site(s) of tumor relapse.
Main results. The 5-year OS was 91% and 86% for the 36- and 18-month groups, respectively (P = 0.07). The 10-year OS was 62% for both groups (P = 0.7), and the global hazard ratio (HR) was 1.02 (P = 0.8). The disease-specific survival (DSS) was similar in both groups at 5 years (98% vs 97%) and at 10 years (91% vs 92%) in the long versus short arm, respectively. The rate of prostate cancer–specific death was 21% versus 23% in the long versus short arm, respectively. In a multivariate analysis for OS, only age and Gleason score > 7 were statistically significant survival predictors. BF rate at 10 years was 25% for 36 months as compared with 31% for 18 months (HR, 0.71, P = 0.02). The 10-year DFS rates were 45% and 39% for 36 and 18 months, respectively (HR, 0.68, P = 0.08). Forty patients in the long arm versus 43 in the short arm developed distant metastasis. Both groups developed similar sites of metastasis, which was predominantly osseous. Some aspects of the EORTC30 and PR25 scales were significant, mostly pertaining to sexual activity, fatigue, and hormone-related symptoms in favor of the 18-month group. The median time to testosterone recovery after completion of ADT was 2.1 years for the short arm versus 4 years in the long arm (P = 0.02). The compliance rate with ADT was 88% in the short arm versus 53% in the long arm. The main reason for nonadherence was side effects in 54% of the patients in the long arm and 31% in the short arm.
Conclusion. The results of the current study suggest that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months in patients with HRPC.
Commentary
The role of ADT for HRPC in combination with RT has been well established by evidence from several trials; however, the comparator arms and patient characteristics between these studies have been quite heterogeneous. For instance, the Radiation Therapy Oncology Group (RTOG) 85-31 trial compared indefinite ADT with RT versus RT alone and showed significantly better 10-year OS in the ADT plus RT arm.1 Similarly, the European Organisation for Research and Treatment of Cancer (EROTC) 22961 trial showed an OS benefit for 36 months versus 6 months of ADT in combination with radiation.2 Additionally, the RTOG 92-02 trial, which compared 4 months versus 24 months of ADT with radiation, also found a significantly improved 10-year OS with a longer course of ADT.3 Taken together these data suggest that 4 to 6 months of ADT is inferior to 24 to 36 months of ADT in HRPC.
Several differences, however, exist in patient characteristics between the present trial and the earlier trials, justifiably reflecting the change of practice in the PSA era. For instance, the present study has a higher percentage of patients with Gleason scores 8-10 (60%) compared to the EROTC and RTOG studies (15%-35%) and a lower percentage of patients with T3 and T4 tumors. Patients with high Gleason scores are believed to have a higher risk of micro-metastasis at the time of diagnosis and higher chances of castration resistance. Therefore, inclusion of a (presumably) larger high-risk patient subgroup in the present study lends further credence to results indicating similar OS with a shorter course of ADT. A post hoc analysis including only patients with Gleason score 8-10 performed for OS, DSS, BF, and DFS showed no significant difference in any of these variables between the arms. Analysis of the interaction between ADT duration in the Gleason 8-10 subgroup versus Gleason 7 for OS, DFS, DSS and BF found no significant differences. This again suggests that 18 months of ADT may be sufficient for this high-risk group; however, it is difficult to draw definitive conclusions from this unplanned subgroup analysis.
Based on the results of the current study, it seems that 18 months of ADT is adequate for many, but not necessarily all, patients. For instance, there was a significantly higher incidence of BF in the 18-month arm. Applying this data to younger patients may require a more nuanced approach, as it is possible that with longer follow-up this higher rate of BF may translate into a difference in OS. Therefore, life expectancy and comorbid conditions always need to be incorporated into clinical decision making with regards to ADT duration. In a study by Rose et al, the risk of prostate cancer–specific mortality significantly decreased by using ADT plus RT for men with HRPC with a low, but not a high, competing mortality score.4 The clinical significance of this finding is that adding ADT to RT might significantly reduce the risk of death from prostate cancer only in the setting of low competing risks.
Another concept to ponder is the optimum duration of ADT in the era of RT dose escalation. Currently, there are emerging techniques for delivering higher radiation doses and combining brachytherapy with external beam radiotherapy for HRPC, and the role of whole pelvic radiation is being investigated. New data suggests that higher radiation doses can lead to improvement in outcomes for HRPC. The DART01/05 study compared 4 versus 24 months of ADT with 76 to 82 Gy of RT and reported improved 5-year OS, DFS, and metastasis-free survival with longer ADT duration.5 Moreover, Kishan et al reported improved prostate cancer–specific mortality when brachytherapy boost was added to radiation compared to radiation alone in patients with Gleason scores 9 and 10.6 Therefore, the optimal duration of ADT in the setting of dose-escalated radiotherapy is not yet known. Also, it is important to note that unlike the prior RTOG and EORTC studies, this study did not include patients with evidence of regional nodal disease, and thus the present data should not be applied to this patient population.
Applications to Clinical Practice
This study’s results suggesting that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months of ADT in patients with HRPC should be interpreted with caution when treating very young patients, since the higher rate of BF in the short arm may impact the OS with longer follow-up. Additionally, patients’ QoL and tolerance to ADT-related adverse effects should be taken into consideration given that compliance with 36 months of ADT was only 53% in this study.
—Jailan Elayoubi, MD, Michigan State University, East Lansing, MI
Study Overview
Objective. To compare the outcomes of 18 months versus 36 months of androgen deprivation therapy (ADT) combined with radiation in high-risk prostate cancer (HRPC).
Design. Phase 3 multicenter, randomized superiority trial.
Participants. This study enrolled patients aged ≤ 80 years with HRPC. All patients had no evidence of regional or distant metastasis. High-risk disease was defined as any of the following: clinical stage T3 or T4, prostate-specific antigen (PSA) level > 20 ng/mL, or Gleason score > 7.
Methods. Prior to randomization, all patients received 4 months of ADT with goserelin 10.8 mg and anti-androgen therapy with bicalutamide 50 mg daily for 30 days. Patients were then randomly assigned to 18 (short arm) or 36 (long arm) months of ADT in combination with radiation therapy (RT). The randomization was stratified by stage (T1-2 vs T3-4), Gleason score (< 7 vs > 7) and PSA level (< 20 ng/mL vs > 20 ng/mL). The standard radiation dose was 70 Gy to the prostate and 44 Gy to the pelvis. Computed tomography or magnetic resonance imaging exam of the abdomen and pelvis and a bone scan were performed to rule out regional or distant metastases. PSA level was monitored every 3 months for 18 months, every 6 months up to the third year, and yearly thereafter.
Main outcome measures. The 2 primary outcomes were overall survival (OS) and quality of life (QoL) at 5 years. The secondary end points were biochemical failure (BF)defined as PSA nadir plus 2, disease-free survival (DFS), and site(s) of tumor relapse.
Main results. The 5-year OS was 91% and 86% for the 36- and 18-month groups, respectively (P = 0.07). The 10-year OS was 62% for both groups (P = 0.7), and the global hazard ratio (HR) was 1.02 (P = 0.8). The disease-specific survival (DSS) was similar in both groups at 5 years (98% vs 97%) and at 10 years (91% vs 92%) in the long versus short arm, respectively. The rate of prostate cancer–specific death was 21% versus 23% in the long versus short arm, respectively. In a multivariate analysis for OS, only age and Gleason score > 7 were statistically significant survival predictors. BF rate at 10 years was 25% for 36 months as compared with 31% for 18 months (HR, 0.71, P = 0.02). The 10-year DFS rates were 45% and 39% for 36 and 18 months, respectively (HR, 0.68, P = 0.08). Forty patients in the long arm versus 43 in the short arm developed distant metastasis. Both groups developed similar sites of metastasis, which was predominantly osseous. Some aspects of the EORTC30 and PR25 scales were significant, mostly pertaining to sexual activity, fatigue, and hormone-related symptoms in favor of the 18-month group. The median time to testosterone recovery after completion of ADT was 2.1 years for the short arm versus 4 years in the long arm (P = 0.02). The compliance rate with ADT was 88% in the short arm versus 53% in the long arm. The main reason for nonadherence was side effects in 54% of the patients in the long arm and 31% in the short arm.
Conclusion. The results of the current study suggest that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months in patients with HRPC.
Commentary
The role of ADT for HRPC in combination with RT has been well established by evidence from several trials; however, the comparator arms and patient characteristics between these studies have been quite heterogeneous. For instance, the Radiation Therapy Oncology Group (RTOG) 85-31 trial compared indefinite ADT with RT versus RT alone and showed significantly better 10-year OS in the ADT plus RT arm.1 Similarly, the European Organisation for Research and Treatment of Cancer (EROTC) 22961 trial showed an OS benefit for 36 months versus 6 months of ADT in combination with radiation.2 Additionally, the RTOG 92-02 trial, which compared 4 months versus 24 months of ADT with radiation, also found a significantly improved 10-year OS with a longer course of ADT.3 Taken together these data suggest that 4 to 6 months of ADT is inferior to 24 to 36 months of ADT in HRPC.
Several differences, however, exist in patient characteristics between the present trial and the earlier trials, justifiably reflecting the change of practice in the PSA era. For instance, the present study has a higher percentage of patients with Gleason scores 8-10 (60%) compared to the EROTC and RTOG studies (15%-35%) and a lower percentage of patients with T3 and T4 tumors. Patients with high Gleason scores are believed to have a higher risk of micro-metastasis at the time of diagnosis and higher chances of castration resistance. Therefore, inclusion of a (presumably) larger high-risk patient subgroup in the present study lends further credence to results indicating similar OS with a shorter course of ADT. A post hoc analysis including only patients with Gleason score 8-10 performed for OS, DSS, BF, and DFS showed no significant difference in any of these variables between the arms. Analysis of the interaction between ADT duration in the Gleason 8-10 subgroup versus Gleason 7 for OS, DFS, DSS and BF found no significant differences. This again suggests that 18 months of ADT may be sufficient for this high-risk group; however, it is difficult to draw definitive conclusions from this unplanned subgroup analysis.
Based on the results of the current study, it seems that 18 months of ADT is adequate for many, but not necessarily all, patients. For instance, there was a significantly higher incidence of BF in the 18-month arm. Applying this data to younger patients may require a more nuanced approach, as it is possible that with longer follow-up this higher rate of BF may translate into a difference in OS. Therefore, life expectancy and comorbid conditions always need to be incorporated into clinical decision making with regards to ADT duration. In a study by Rose et al, the risk of prostate cancer–specific mortality significantly decreased by using ADT plus RT for men with HRPC with a low, but not a high, competing mortality score.4 The clinical significance of this finding is that adding ADT to RT might significantly reduce the risk of death from prostate cancer only in the setting of low competing risks.
Another concept to ponder is the optimum duration of ADT in the era of RT dose escalation. Currently, there are emerging techniques for delivering higher radiation doses and combining brachytherapy with external beam radiotherapy for HRPC, and the role of whole pelvic radiation is being investigated. New data suggests that higher radiation doses can lead to improvement in outcomes for HRPC. The DART01/05 study compared 4 versus 24 months of ADT with 76 to 82 Gy of RT and reported improved 5-year OS, DFS, and metastasis-free survival with longer ADT duration.5 Moreover, Kishan et al reported improved prostate cancer–specific mortality when brachytherapy boost was added to radiation compared to radiation alone in patients with Gleason scores 9 and 10.6 Therefore, the optimal duration of ADT in the setting of dose-escalated radiotherapy is not yet known. Also, it is important to note that unlike the prior RTOG and EORTC studies, this study did not include patients with evidence of regional nodal disease, and thus the present data should not be applied to this patient population.
Applications to Clinical Practice
This study’s results suggesting that 18 months of ADT in combination with RT yields similar 10-year OS and improved QoL compared with 36 months of ADT in patients with HRPC should be interpreted with caution when treating very young patients, since the higher rate of BF in the short arm may impact the OS with longer follow-up. Additionally, patients’ QoL and tolerance to ADT-related adverse effects should be taken into consideration given that compliance with 36 months of ADT was only 53% in this study.
—Jailan Elayoubi, MD, Michigan State University, East Lansing, MI
1. Pilepich MV, Winter K, Lawton CA, et al. Androgen suppression adjuvant to definitive radiotherapy in prostate carcinoma—long-term results of phase III RTOG 85–31. Int J Radiat Oncol Biol Phys. 2005;61:1285-1290.
2. Bolla M, de Reijke TM, Van Tienhoven G, et al. Duration of androgen suppression in the treatment of prostate cancer. N Engl J Med. 2009;360:2516-2527.
3. Horwitz EM, Bae K, Hanks GE, Porter A, et al. Ten-year follow-up of radiation therapy oncology group protocol 92-02: a phase III trial of the duration of elective androgen deprivation in locally advanced prostate cancer. J Clin Oncol. 2008;26:2497–2504.
4. Rose BS, Chen MH, Wu J, et al. Androgen deprivation therapy use in the setting of high-dose radiation therapy and the risk of prostate cancer-specific mortality stratified by the extent of competing mortality. Int J Radiat Oncol Biol Phys. 2016;96:778-784.
5. Zapatero A, Guerrero A, Maldonado X, et al. High-dose radiotherapy with short-term or long-term androgen deprivation in localised prostate cancer (DART01/05 GICOR): a randomised, controlled, phase 3 trial. Lancet Oncol. 2015;16:320-327.
6. Kishan, AU, Cook, RR, Ciezki, JP, et al. Radical prostatectomy, external beam radiotherapy, or external beam radiotherapy with brachytherapy boost and disease progression and mortality in patients with gleason score 9-10 prostate cancer. JAMA. 2018;319:896-905.
1. Pilepich MV, Winter K, Lawton CA, et al. Androgen suppression adjuvant to definitive radiotherapy in prostate carcinoma—long-term results of phase III RTOG 85–31. Int J Radiat Oncol Biol Phys. 2005;61:1285-1290.
2. Bolla M, de Reijke TM, Van Tienhoven G, et al. Duration of androgen suppression in the treatment of prostate cancer. N Engl J Med. 2009;360:2516-2527.
3. Horwitz EM, Bae K, Hanks GE, Porter A, et al. Ten-year follow-up of radiation therapy oncology group protocol 92-02: a phase III trial of the duration of elective androgen deprivation in locally advanced prostate cancer. J Clin Oncol. 2008;26:2497–2504.
4. Rose BS, Chen MH, Wu J, et al. Androgen deprivation therapy use in the setting of high-dose radiation therapy and the risk of prostate cancer-specific mortality stratified by the extent of competing mortality. Int J Radiat Oncol Biol Phys. 2016;96:778-784.
5. Zapatero A, Guerrero A, Maldonado X, et al. High-dose radiotherapy with short-term or long-term androgen deprivation in localised prostate cancer (DART01/05 GICOR): a randomised, controlled, phase 3 trial. Lancet Oncol. 2015;16:320-327.
6. Kishan, AU, Cook, RR, Ciezki, JP, et al. Radical prostatectomy, external beam radiotherapy, or external beam radiotherapy with brachytherapy boost and disease progression and mortality in patients with gleason score 9-10 prostate cancer. JAMA. 2018;319:896-905.
A.I. and U 2
In a previous Letter from Maine I wrote about a study performed in China in which more than half a million patients were diagnosed by an artificial intelligence (A.I.) system that was able to extract and analyze information from their electronic medical records. The system was at least as accurate as physicians who had access to the same data (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). I ended my column with the hopeful assumption that despite incredible advances in A.I., the practice of medicine always would include a human element. However, I left unexplained exactly how physicians would fit into the post-A.I. revolution. In the weeks since I submitted that column, I have been searching for roles that might remain for physicians after A.I. has snatched their bread and butter of diagnosis and management.
I easily can envision a system in which the patient enters her chief complaint and current symptoms into her smartphone or tablet. Using its database of the patient’s past, family, and social history, the system generates a list of laboratory and imaging studies, some of which the patient may be able to submit directly from her handheld device. For example, the system may be able to use the patient’s phone to “examine” her. The A.I. system then generates a diagnosis.
If the diagnosed condition and management is simple and straightforward, such as a rash, the information could be communicated to the patient directly, with a short paragraph of explanation and list of persistent symptoms that would indicate that the condition was not improving as expected. A contact dermatitis comes to mind here.
However, suppose the A.I. system determines that the patient has a 90% chance of having stage IV pancreatic cancer, with a life expectancy of 6 months. Is this the kind of information you would like to learn about yourself by clicking “Your Diagnosis” box on your phone while you were having lunch with a friend? Obviously, a diagnosis of this severity should be communicated human to human, even though it was generated by a highly accurate computer system. And this communication would best be done in the form of a dialogue with someone who knows the patient and has some understanding of how she might understand and cope with the information. In the absence of a prior relationship, the dialogue should occur in real time and face to face at a minimum. I guess we have to acknowledge that FaceTime or Skype might be acceptable here.
Fortunately, stage IV cancers are rare, but there are a bazillion other conditions that, while not serious, require a nuanced explanation as part of a successful management plan that takes into account the patient’s level of anxiety and cognitive abilities. A boilerplate paragraph or two spit out by an A.I. system isn’t good health care. Although I know many physicians do rely on printed handouts for conditions they feel is a no-brainer.
The bottom line is that even when a machine may be better than we are at making some diagnoses, there always will be a role for a human to help other humans understand and cope with those diagnoses. At this point, physicians would appear be the obvious choice to fill that role. How we will get reimbursed for our communication skills is unclear.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
In a previous Letter from Maine I wrote about a study performed in China in which more than half a million patients were diagnosed by an artificial intelligence (A.I.) system that was able to extract and analyze information from their electronic medical records. The system was at least as accurate as physicians who had access to the same data (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). I ended my column with the hopeful assumption that despite incredible advances in A.I., the practice of medicine always would include a human element. However, I left unexplained exactly how physicians would fit into the post-A.I. revolution. In the weeks since I submitted that column, I have been searching for roles that might remain for physicians after A.I. has snatched their bread and butter of diagnosis and management.
I easily can envision a system in which the patient enters her chief complaint and current symptoms into her smartphone or tablet. Using its database of the patient’s past, family, and social history, the system generates a list of laboratory and imaging studies, some of which the patient may be able to submit directly from her handheld device. For example, the system may be able to use the patient’s phone to “examine” her. The A.I. system then generates a diagnosis.
If the diagnosed condition and management is simple and straightforward, such as a rash, the information could be communicated to the patient directly, with a short paragraph of explanation and list of persistent symptoms that would indicate that the condition was not improving as expected. A contact dermatitis comes to mind here.
However, suppose the A.I. system determines that the patient has a 90% chance of having stage IV pancreatic cancer, with a life expectancy of 6 months. Is this the kind of information you would like to learn about yourself by clicking “Your Diagnosis” box on your phone while you were having lunch with a friend? Obviously, a diagnosis of this severity should be communicated human to human, even though it was generated by a highly accurate computer system. And this communication would best be done in the form of a dialogue with someone who knows the patient and has some understanding of how she might understand and cope with the information. In the absence of a prior relationship, the dialogue should occur in real time and face to face at a minimum. I guess we have to acknowledge that FaceTime or Skype might be acceptable here.
Fortunately, stage IV cancers are rare, but there are a bazillion other conditions that, while not serious, require a nuanced explanation as part of a successful management plan that takes into account the patient’s level of anxiety and cognitive abilities. A boilerplate paragraph or two spit out by an A.I. system isn’t good health care. Although I know many physicians do rely on printed handouts for conditions they feel is a no-brainer.
The bottom line is that even when a machine may be better than we are at making some diagnoses, there always will be a role for a human to help other humans understand and cope with those diagnoses. At this point, physicians would appear be the obvious choice to fill that role. How we will get reimbursed for our communication skills is unclear.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
In a previous Letter from Maine I wrote about a study performed in China in which more than half a million patients were diagnosed by an artificial intelligence (A.I.) system that was able to extract and analyze information from their electronic medical records. The system was at least as accurate as physicians who had access to the same data (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). I ended my column with the hopeful assumption that despite incredible advances in A.I., the practice of medicine always would include a human element. However, I left unexplained exactly how physicians would fit into the post-A.I. revolution. In the weeks since I submitted that column, I have been searching for roles that might remain for physicians after A.I. has snatched their bread and butter of diagnosis and management.
I easily can envision a system in which the patient enters her chief complaint and current symptoms into her smartphone or tablet. Using its database of the patient’s past, family, and social history, the system generates a list of laboratory and imaging studies, some of which the patient may be able to submit directly from her handheld device. For example, the system may be able to use the patient’s phone to “examine” her. The A.I. system then generates a diagnosis.
If the diagnosed condition and management is simple and straightforward, such as a rash, the information could be communicated to the patient directly, with a short paragraph of explanation and list of persistent symptoms that would indicate that the condition was not improving as expected. A contact dermatitis comes to mind here.
However, suppose the A.I. system determines that the patient has a 90% chance of having stage IV pancreatic cancer, with a life expectancy of 6 months. Is this the kind of information you would like to learn about yourself by clicking “Your Diagnosis” box on your phone while you were having lunch with a friend? Obviously, a diagnosis of this severity should be communicated human to human, even though it was generated by a highly accurate computer system. And this communication would best be done in the form of a dialogue with someone who knows the patient and has some understanding of how she might understand and cope with the information. In the absence of a prior relationship, the dialogue should occur in real time and face to face at a minimum. I guess we have to acknowledge that FaceTime or Skype might be acceptable here.
Fortunately, stage IV cancers are rare, but there are a bazillion other conditions that, while not serious, require a nuanced explanation as part of a successful management plan that takes into account the patient’s level of anxiety and cognitive abilities. A boilerplate paragraph or two spit out by an A.I. system isn’t good health care. Although I know many physicians do rely on printed handouts for conditions they feel is a no-brainer.
The bottom line is that even when a machine may be better than we are at making some diagnoses, there always will be a role for a human to help other humans understand and cope with those diagnoses. At this point, physicians would appear be the obvious choice to fill that role. How we will get reimbursed for our communication skills is unclear.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
Food allergy can be revealed in the epidermis of children with atopic dermatitis
according to a study of children with and without AD and FA.
The researchers included 62 children aged 4-17 years, who were divided into three groups: atopic dermatitis and food allergy (AD FA+, n = 21), atopic dermatitis and no food allergy (AD FA−, n = 19), and nonatopic controls (NA, n = 22).
“In this prospective clinical study with laboratory personnel blinded to minimize bias, we demonstrate that children with AD FA+ represent a unique endotype that can be distinguished from AD FA− or NA,” wrote Donald Y. M. Leung, MD, of National Jewish Health, Denver, and his coauthors. Their work was published online in Science Translational Medicine.
According to three different scoring systems, the two AD groups were measured to have similar skin disease severity. Dr. Leung and colleagues then used skin tape stripping to measure the first layer of skin tissue for transepidermal water loss (TEWL) and stratum corneum (SC) composition, along with other variables that would indicate a difference between AD FA+ and the other groups.
Upon analysis, children in the AD FA+ group were found to have “a constellation of SC attributes,” including increased TEWL and lower levels of filaggrin gene breakdown products (urocanic acid and pyroglutamic acid) at nonlesional layers. In addition, there was an increase of Staphylococcus aureus on the nonlesional skin of AD FA+, compared with NA.
The coauthors shared the study’s limitations, which included transcriptome analysis being successful for only a fraction of the patients and the lack of skin biopsies, which would be useful to confirm “the potential role of changes in the deeper layers of skin.” However, they also noted that using minimally invasive STS led to more patients providing samples, and thus less bias in collection. “Although future studies are needed to validate our findings,” Dr. Leung and his associates wrote, “our current data support the concept that primary and secondary prevention of AD and FA in this subset of AD should focus on improving skin barrier function.”
The study was funded by the National Institute of Health/The National Institute of Allergy and Infectious Diseases’ Atopic Dermatitis Research Network, with partial support from the Edelstein Family Chair for Pediatric Allergy at NIH and a NIH/National Center for Advancing Translational Sciences Colorado Clinical and Translational Science Awards grant. Three of the authors declared being inventors of a patent that covers methods of identifying AD with FA as a unique endotype. No other conflicts of interest were reported.
SOURCE: Leung DYM et al. Sci Transl Med. 2019 Feb 20. doi: 10.1126/scitranslmed.aav2685.
according to a study of children with and without AD and FA.
The researchers included 62 children aged 4-17 years, who were divided into three groups: atopic dermatitis and food allergy (AD FA+, n = 21), atopic dermatitis and no food allergy (AD FA−, n = 19), and nonatopic controls (NA, n = 22).
“In this prospective clinical study with laboratory personnel blinded to minimize bias, we demonstrate that children with AD FA+ represent a unique endotype that can be distinguished from AD FA− or NA,” wrote Donald Y. M. Leung, MD, of National Jewish Health, Denver, and his coauthors. Their work was published online in Science Translational Medicine.
According to three different scoring systems, the two AD groups were measured to have similar skin disease severity. Dr. Leung and colleagues then used skin tape stripping to measure the first layer of skin tissue for transepidermal water loss (TEWL) and stratum corneum (SC) composition, along with other variables that would indicate a difference between AD FA+ and the other groups.
Upon analysis, children in the AD FA+ group were found to have “a constellation of SC attributes,” including increased TEWL and lower levels of filaggrin gene breakdown products (urocanic acid and pyroglutamic acid) at nonlesional layers. In addition, there was an increase of Staphylococcus aureus on the nonlesional skin of AD FA+, compared with NA.
The coauthors shared the study’s limitations, which included transcriptome analysis being successful for only a fraction of the patients and the lack of skin biopsies, which would be useful to confirm “the potential role of changes in the deeper layers of skin.” However, they also noted that using minimally invasive STS led to more patients providing samples, and thus less bias in collection. “Although future studies are needed to validate our findings,” Dr. Leung and his associates wrote, “our current data support the concept that primary and secondary prevention of AD and FA in this subset of AD should focus on improving skin barrier function.”
The study was funded by the National Institute of Health/The National Institute of Allergy and Infectious Diseases’ Atopic Dermatitis Research Network, with partial support from the Edelstein Family Chair for Pediatric Allergy at NIH and a NIH/National Center for Advancing Translational Sciences Colorado Clinical and Translational Science Awards grant. Three of the authors declared being inventors of a patent that covers methods of identifying AD with FA as a unique endotype. No other conflicts of interest were reported.
SOURCE: Leung DYM et al. Sci Transl Med. 2019 Feb 20. doi: 10.1126/scitranslmed.aav2685.
according to a study of children with and without AD and FA.
The researchers included 62 children aged 4-17 years, who were divided into three groups: atopic dermatitis and food allergy (AD FA+, n = 21), atopic dermatitis and no food allergy (AD FA−, n = 19), and nonatopic controls (NA, n = 22).
“In this prospective clinical study with laboratory personnel blinded to minimize bias, we demonstrate that children with AD FA+ represent a unique endotype that can be distinguished from AD FA− or NA,” wrote Donald Y. M. Leung, MD, of National Jewish Health, Denver, and his coauthors. Their work was published online in Science Translational Medicine.
According to three different scoring systems, the two AD groups were measured to have similar skin disease severity. Dr. Leung and colleagues then used skin tape stripping to measure the first layer of skin tissue for transepidermal water loss (TEWL) and stratum corneum (SC) composition, along with other variables that would indicate a difference between AD FA+ and the other groups.
Upon analysis, children in the AD FA+ group were found to have “a constellation of SC attributes,” including increased TEWL and lower levels of filaggrin gene breakdown products (urocanic acid and pyroglutamic acid) at nonlesional layers. In addition, there was an increase of Staphylococcus aureus on the nonlesional skin of AD FA+, compared with NA.
The coauthors shared the study’s limitations, which included transcriptome analysis being successful for only a fraction of the patients and the lack of skin biopsies, which would be useful to confirm “the potential role of changes in the deeper layers of skin.” However, they also noted that using minimally invasive STS led to more patients providing samples, and thus less bias in collection. “Although future studies are needed to validate our findings,” Dr. Leung and his associates wrote, “our current data support the concept that primary and secondary prevention of AD and FA in this subset of AD should focus on improving skin barrier function.”
The study was funded by the National Institute of Health/The National Institute of Allergy and Infectious Diseases’ Atopic Dermatitis Research Network, with partial support from the Edelstein Family Chair for Pediatric Allergy at NIH and a NIH/National Center for Advancing Translational Sciences Colorado Clinical and Translational Science Awards grant. Three of the authors declared being inventors of a patent that covers methods of identifying AD with FA as a unique endotype. No other conflicts of interest were reported.
SOURCE: Leung DYM et al. Sci Transl Med. 2019 Feb 20. doi: 10.1126/scitranslmed.aav2685.
FROM SCIENCE TRANSLATIONAL MEDICINE
Key clinical point: Children with both atopic dermatitis and food allergy can be distinguished from those with just atopic dermatitis via their nonlesional skin surface.
Major finding: Those in the AD FA+ group were found to have “a constellation of stratum corneum attributes,” including increased TEWL and lower levels of filaggrin gene breakdown products.
Study details: A prospective clinical study of 62 children aged 4-17 years who were divided into three groups: atopic dermatitis and food allergy, atopic dermatitis and no food allergy, and nonatopic controls.
Disclosures: The study was funded by the National Institute of Health/The National Institute of Allergy and Infectious Diseases’ Atopic Dermatitis Research Network, with partial support from the Edelstein Family Chair for Pediatric Allergy at NIH and a NIH/National Center for Advancing Translational Sciences Colorado Clinical and Translational Science Awards grant. Three of the authors declared being inventors of a patent that covers methods of identifying AD with FA as a unique endotype. No other conflicts of interest were reported.
Source: Leung DYM et al. Sci Transl Med. 2019 Feb 20. doi: 10.1126/scitranslmed.aav2685.
Sleeping poorly may mean itching more
Study results showing an association between active atopic dermatitis (AD) and poor sleep quality were published in JAMA Pediatrics by a group of dermatologists at the University of California, San Francisco (JAMA Pediatr. 2019 Mar 4. doi: 10.1001/jamapediatrics.2019.0025). The data on the sleep quality and quantity of nearly 14,000 children were collected over span of 11 years. Of these children, slightly fewer than 5,000 met the researchers’ definition of atopic dermatitis.
Although the sleep duration of children with and without AD was not statistically different, the reports of poor sleep quality and sleep disturbances by children with AD were dramatically more frequent – a nearly 50% higher chance of having more sleep-quality disturbances. In addition, children with more severe active disease were even more likely to report poor sleep quality – almost 80%.
I suspect that you’re not surprised by these findings. You have probably heard numerous tales of poor sleep from families who have children with AD. It just makes sense that a child whose skin is dry and itchy will have trouble sleeping. I’m sure you have struggled to help parents be more diligent about applying moisturizing creams and lotions, and have been aggressive with steroid creams during flare-ups. You may have added sleep onset-promoting antihistamines when topical treatments haven’t been as effective as you had hoped.
Has your working assumption always been that if you can get the child’s skin settled down, the itching will improve and the child will have an easier time falling asleep? But have you ever considered flipping the equation over and tried to be more aggressive in managing the child’s sleep problems?
Like many other folks with psoriasis, I have noticed that my itching is worse when I am tired, and particularly worse in that evil interval between crawling into bed and falling asleep. As the grandparent of a child with AD, I have observed a similar phenomenon. While I am not going to claim that sleep deprivation causes psoriasis or AD, I think that we need to consider the association between poor sleep quality and itching as a feedback loop that must be interrupted. This means that in addition to recommending topicals and moisturizing strategies, we must learn more about our patients’ sleep habits and suggest appropriate sleep hygiene practices.
Many parents aren’t aware of the cruel paradox that an overtired child is more likely to have trouble falling asleep. Has the child been allowed to give up his nap prematurely? Is bedtime at an appropriate hour, and does it consist of a limited number of sleep-promoting rituals? Is the bedroom dark enough, cool enough, and free of electronic distractions?
Providing effective counseling on sleep hygiene is time consuming and requires that you have first convinced the parents that the child’s itching is being aggravated by his sleep deprivation and not just the other way around. Successful management may require a close working relationship between the child’s pediatrician and his dermatologist, with both physicians reinforcing each other’s message that atopic dermatitis isn’t just skin deep.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “Is My Child Overtired?: The Sleep Solution for Raising Happier, Healthier Children.” Email him at [email protected].
Study results showing an association between active atopic dermatitis (AD) and poor sleep quality were published in JAMA Pediatrics by a group of dermatologists at the University of California, San Francisco (JAMA Pediatr. 2019 Mar 4. doi: 10.1001/jamapediatrics.2019.0025). The data on the sleep quality and quantity of nearly 14,000 children were collected over span of 11 years. Of these children, slightly fewer than 5,000 met the researchers’ definition of atopic dermatitis.
Although the sleep duration of children with and without AD was not statistically different, the reports of poor sleep quality and sleep disturbances by children with AD were dramatically more frequent – a nearly 50% higher chance of having more sleep-quality disturbances. In addition, children with more severe active disease were even more likely to report poor sleep quality – almost 80%.
I suspect that you’re not surprised by these findings. You have probably heard numerous tales of poor sleep from families who have children with AD. It just makes sense that a child whose skin is dry and itchy will have trouble sleeping. I’m sure you have struggled to help parents be more diligent about applying moisturizing creams and lotions, and have been aggressive with steroid creams during flare-ups. You may have added sleep onset-promoting antihistamines when topical treatments haven’t been as effective as you had hoped.
Has your working assumption always been that if you can get the child’s skin settled down, the itching will improve and the child will have an easier time falling asleep? But have you ever considered flipping the equation over and tried to be more aggressive in managing the child’s sleep problems?
Like many other folks with psoriasis, I have noticed that my itching is worse when I am tired, and particularly worse in that evil interval between crawling into bed and falling asleep. As the grandparent of a child with AD, I have observed a similar phenomenon. While I am not going to claim that sleep deprivation causes psoriasis or AD, I think that we need to consider the association between poor sleep quality and itching as a feedback loop that must be interrupted. This means that in addition to recommending topicals and moisturizing strategies, we must learn more about our patients’ sleep habits and suggest appropriate sleep hygiene practices.
Many parents aren’t aware of the cruel paradox that an overtired child is more likely to have trouble falling asleep. Has the child been allowed to give up his nap prematurely? Is bedtime at an appropriate hour, and does it consist of a limited number of sleep-promoting rituals? Is the bedroom dark enough, cool enough, and free of electronic distractions?
Providing effective counseling on sleep hygiene is time consuming and requires that you have first convinced the parents that the child’s itching is being aggravated by his sleep deprivation and not just the other way around. Successful management may require a close working relationship between the child’s pediatrician and his dermatologist, with both physicians reinforcing each other’s message that atopic dermatitis isn’t just skin deep.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “Is My Child Overtired?: The Sleep Solution for Raising Happier, Healthier Children.” Email him at [email protected].
Study results showing an association between active atopic dermatitis (AD) and poor sleep quality were published in JAMA Pediatrics by a group of dermatologists at the University of California, San Francisco (JAMA Pediatr. 2019 Mar 4. doi: 10.1001/jamapediatrics.2019.0025). The data on the sleep quality and quantity of nearly 14,000 children were collected over span of 11 years. Of these children, slightly fewer than 5,000 met the researchers’ definition of atopic dermatitis.
Although the sleep duration of children with and without AD was not statistically different, the reports of poor sleep quality and sleep disturbances by children with AD were dramatically more frequent – a nearly 50% higher chance of having more sleep-quality disturbances. In addition, children with more severe active disease were even more likely to report poor sleep quality – almost 80%.
I suspect that you’re not surprised by these findings. You have probably heard numerous tales of poor sleep from families who have children with AD. It just makes sense that a child whose skin is dry and itchy will have trouble sleeping. I’m sure you have struggled to help parents be more diligent about applying moisturizing creams and lotions, and have been aggressive with steroid creams during flare-ups. You may have added sleep onset-promoting antihistamines when topical treatments haven’t been as effective as you had hoped.
Has your working assumption always been that if you can get the child’s skin settled down, the itching will improve and the child will have an easier time falling asleep? But have you ever considered flipping the equation over and tried to be more aggressive in managing the child’s sleep problems?
Like many other folks with psoriasis, I have noticed that my itching is worse when I am tired, and particularly worse in that evil interval between crawling into bed and falling asleep. As the grandparent of a child with AD, I have observed a similar phenomenon. While I am not going to claim that sleep deprivation causes psoriasis or AD, I think that we need to consider the association between poor sleep quality and itching as a feedback loop that must be interrupted. This means that in addition to recommending topicals and moisturizing strategies, we must learn more about our patients’ sleep habits and suggest appropriate sleep hygiene practices.
Many parents aren’t aware of the cruel paradox that an overtired child is more likely to have trouble falling asleep. Has the child been allowed to give up his nap prematurely? Is bedtime at an appropriate hour, and does it consist of a limited number of sleep-promoting rituals? Is the bedroom dark enough, cool enough, and free of electronic distractions?
Providing effective counseling on sleep hygiene is time consuming and requires that you have first convinced the parents that the child’s itching is being aggravated by his sleep deprivation and not just the other way around. Successful management may require a close working relationship between the child’s pediatrician and his dermatologist, with both physicians reinforcing each other’s message that atopic dermatitis isn’t just skin deep.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “Is My Child Overtired?: The Sleep Solution for Raising Happier, Healthier Children.” Email him at [email protected].
Scales assessing pediatric OCD possess little symptom overlap
There is considerable heterogeneity among symptoms included in various freely available, self-reported scales assessing obsessive-compulsive disorder in pediatric populations, according to Rachel Visontay and her associates at the University of New South Wales, Sydney.
They reviewed seven scales that exclusively assessed obsessive-compulsive disorder (OCD) and measured both obsessive and compulsive components in their study, published in the Journal of Obsessive-Compulsive and Related Disorders. The scales are:
- Children’s Florida Obsessive Compulsive Inventory.
- Children’s Yale-Brown Obsessive Compulsive Scale Symptom Checklist.
- Leyton Obsessional Inventory–Child Version.
- Children’s Obsessional Compulsive Inventory–Revised–Self Report.
- Obsessive Compulsive Inventory–Child Version.
- OCD Family Functioning Scale.
- Short OCD Screener.
A total of 54 umbrella symptoms were included over all seven scales: 32 obsessions, 21 compulsion, and 1 other symptom (Give poor class presentations despite planning). Half of these symptoms were unique to one scale but were more commonly obsessions (18 of 32) than compulsions (8 of 21). No obsession symptom appeared on more than five of the seven scales, but two compulsion symptoms (cleaning and checking compulsion) did appear on all scales.
The mean overlap between scales after Jaccard analysis was 0.14 for obsessions and 0.39 for compulsions, indicating very weak and weak overlap, respectively. The correlation between number of included symptoms and mean overlap was 0.43 for obsessions, indicating that scale length did play a role in determining overlap, but was –0.09 for compulsions, indicating no relationship between scale length and symptom overlap.
“While youth OCD scales generally measure the same broader construct, they might have different scopes within that construct, or may be more or less comprehensive than one another. As such, low content overlap does not necessarily mean a scale is ‘worse’ than one with higher overlap,” the investigators wrote. “However, researchers and
The study authors reported no conflicts of interest. The study was funded by a University of New South Wales Medicine, Neuroscience, Mental Health and Addiction Theme and SPHERE Mindgardens Clinical Academic Group collaborative research seed funding grant.
There is considerable heterogeneity among symptoms included in various freely available, self-reported scales assessing obsessive-compulsive disorder in pediatric populations, according to Rachel Visontay and her associates at the University of New South Wales, Sydney.
They reviewed seven scales that exclusively assessed obsessive-compulsive disorder (OCD) and measured both obsessive and compulsive components in their study, published in the Journal of Obsessive-Compulsive and Related Disorders. The scales are:
- Children’s Florida Obsessive Compulsive Inventory.
- Children’s Yale-Brown Obsessive Compulsive Scale Symptom Checklist.
- Leyton Obsessional Inventory–Child Version.
- Children’s Obsessional Compulsive Inventory–Revised–Self Report.
- Obsessive Compulsive Inventory–Child Version.
- OCD Family Functioning Scale.
- Short OCD Screener.
A total of 54 umbrella symptoms were included over all seven scales: 32 obsessions, 21 compulsion, and 1 other symptom (Give poor class presentations despite planning). Half of these symptoms were unique to one scale but were more commonly obsessions (18 of 32) than compulsions (8 of 21). No obsession symptom appeared on more than five of the seven scales, but two compulsion symptoms (cleaning and checking compulsion) did appear on all scales.
The mean overlap between scales after Jaccard analysis was 0.14 for obsessions and 0.39 for compulsions, indicating very weak and weak overlap, respectively. The correlation between number of included symptoms and mean overlap was 0.43 for obsessions, indicating that scale length did play a role in determining overlap, but was –0.09 for compulsions, indicating no relationship between scale length and symptom overlap.
“While youth OCD scales generally measure the same broader construct, they might have different scopes within that construct, or may be more or less comprehensive than one another. As such, low content overlap does not necessarily mean a scale is ‘worse’ than one with higher overlap,” the investigators wrote. “However, researchers and
The study authors reported no conflicts of interest. The study was funded by a University of New South Wales Medicine, Neuroscience, Mental Health and Addiction Theme and SPHERE Mindgardens Clinical Academic Group collaborative research seed funding grant.
There is considerable heterogeneity among symptoms included in various freely available, self-reported scales assessing obsessive-compulsive disorder in pediatric populations, according to Rachel Visontay and her associates at the University of New South Wales, Sydney.
They reviewed seven scales that exclusively assessed obsessive-compulsive disorder (OCD) and measured both obsessive and compulsive components in their study, published in the Journal of Obsessive-Compulsive and Related Disorders. The scales are:
- Children’s Florida Obsessive Compulsive Inventory.
- Children’s Yale-Brown Obsessive Compulsive Scale Symptom Checklist.
- Leyton Obsessional Inventory–Child Version.
- Children’s Obsessional Compulsive Inventory–Revised–Self Report.
- Obsessive Compulsive Inventory–Child Version.
- OCD Family Functioning Scale.
- Short OCD Screener.
A total of 54 umbrella symptoms were included over all seven scales: 32 obsessions, 21 compulsion, and 1 other symptom (Give poor class presentations despite planning). Half of these symptoms were unique to one scale but were more commonly obsessions (18 of 32) than compulsions (8 of 21). No obsession symptom appeared on more than five of the seven scales, but two compulsion symptoms (cleaning and checking compulsion) did appear on all scales.
The mean overlap between scales after Jaccard analysis was 0.14 for obsessions and 0.39 for compulsions, indicating very weak and weak overlap, respectively. The correlation between number of included symptoms and mean overlap was 0.43 for obsessions, indicating that scale length did play a role in determining overlap, but was –0.09 for compulsions, indicating no relationship between scale length and symptom overlap.
“While youth OCD scales generally measure the same broader construct, they might have different scopes within that construct, or may be more or less comprehensive than one another. As such, low content overlap does not necessarily mean a scale is ‘worse’ than one with higher overlap,” the investigators wrote. “However, researchers and
The study authors reported no conflicts of interest. The study was funded by a University of New South Wales Medicine, Neuroscience, Mental Health and Addiction Theme and SPHERE Mindgardens Clinical Academic Group collaborative research seed funding grant.
FROM THE JOURNAL OF OBSESSIVE-COMPULSIVE AND RELATED DISORDERS






