User login
For MD-IQ use only
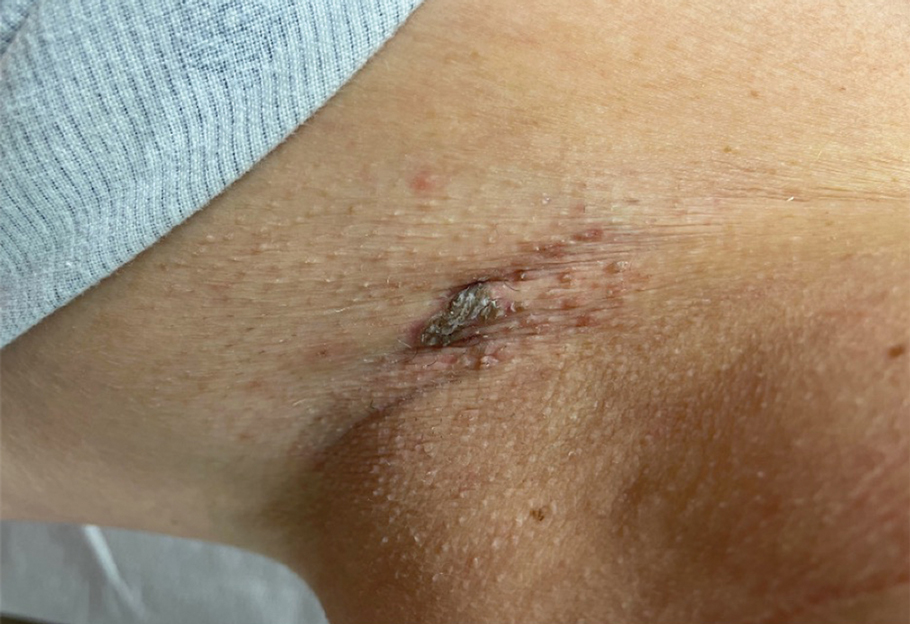
Brown Plaque in the Axilla Following Immobilization of the Arm
The Diagnosis: Granular Parakeratosis
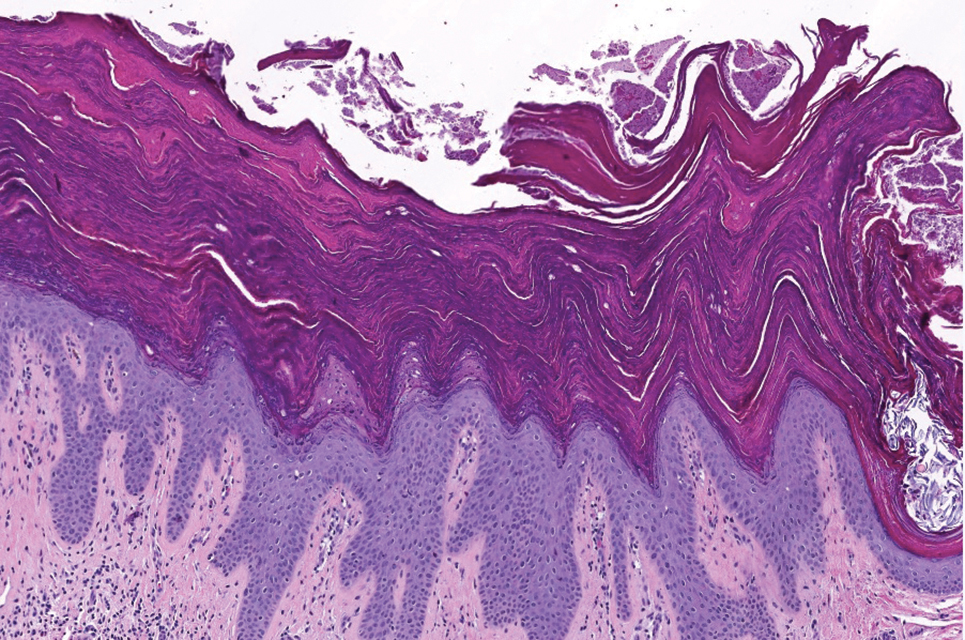
Histopathology demonstrated diffuse parakeratosis with retention of keratohyalin granules throughout the stratum corneum consistent with a diagnosis of granular parakeratosis (Figure), a rare benign cutaneous condition that is thought to occur due to a defect in epidermal differentiation. The lesion resolved without additional treatment.
The pathogenesis of granular parakeratosis is unclear, but a reactive process in which locoregional irritation or occlusion prompts increased cell turnover and prevention of profilaggrin breakdown has been proposed.1,2 The diagnosis is linked to various precipitating agents, most commonly topical products (eg, zinc oxide, antiperspirants) and products with benzalkonium chloride (eg, laundry rinses). These agents are thought to cause retention of keratohyalin granules in the stratum corneum during epidermal differentiation.1,2
Most affected patients are middle-aged women (mean age at diagnosis, 37.8 years).2 Patients present with eruptions of erythematous, brown, hyperkeratotic patches and papules that coalesce into plaques.1,2 These lesions can be pruritic and painful or asymptomatic. They often manifest bilaterally in intertriginous sites, most commonly the axillae, groin, or inguinal folds.1,2
Treatment involves identification and removal of potential triggers including changing antiperspirants, limiting use of irritating agents (eg, topical products with strong fragrances), and reducing heat and moisture in the affected areas. If the lesion persists, stepwise treatment can be initiated with topical agents (eg, corticosteroids, vitamin D analogues, retinoids, keratolytics, calcineurin inhibitors) followed by systemic medications (eg, antibiotics, isotretinoin, antifungals, dexamethasone) and procedures (eg, botulinum toxin injections, surgery, laser, cryotherapy).1,2
Unilateral granular parakeratosis, as seen in our patient, is an uncommon manifestation. Our case supports the theory that occlusion is a precipitating factor for this condition, given persistent axillary exposure to heat, sweat, and friction in the setting of limb immobilization.3
Granular parakeratosis is a challenge to diagnose due to clinical overlap with several other cutaneous conditions; histopathologic confirmation is required. Fox- Fordyce disease is a rare condition that is thought to result from keratin buildup or occlusion of apocrine or apoeccrine sweat ducts leading to duct rupture and surrounding inflammation.4 Common triggers include laser hair removal, hormonal changes, and living conditions that promote hot and humid environments.5 It can manifest similarly to granular parakeratosis, with eruptions of multiple red-violet papules that appear bilaterally in aprocine gland–rich areas, including the axillae and less commonly the genital, periareolar, thoracic, abdominal, and facial areas.4,5 However, most patients with Fox-Fordyce disease tend to be younger females (aged 13–35 years) with severely pruritic lesions,4,5 unlike our patient. In addition, histopathology shows hyperkeratosis, hair follicle plugging, and sweat gland and duct dilation.4
Seborrheic keratoses are common benign epidermal tumors caused by an overproliferation of immature keratinocytes.6,7 Similar to granular parakeratosis, they commonly manifest in older adults as hyperpigmented, well-demarcated, verrucous plaques with a hyperkeratotic surface.6 However, they are more common on the face, neck, trunk, and extremities, and they tend to be asymptomatic, differentiating them from granular parakerosis.6 Histopathology demonstrates a papillomatous epidermal surface, large capillaries in the dermal papillae, and intraepidermal and pseudohorn epidermal cysts.7
Inverse lichen planus, a variant of lichen planus, is a rare inflammatory condition that involves the lysis of basal keratinocytes by CD8+ lymphocytes.8 Similar to granular parakeratosis, lichen planus commonly affects middle-aged women (aged 30–60 years), and this particular variant manifests with asymptomatic or mildly pruritic, hyperpigmented patches and plaques in intertriginous areas. Although it also shows hyperkeratosis on histopathology, it can be differentiated from granular parakeratosis by the additional findings of epidermal hypergranulosis, sawtooth acanthosis of rete ridges, apoptotic keratinocytes in the dermoepidermal junction, and lymphocytic infiltrate in the upper dermis.8
Hailey-Hailey disease (also known as familial benign pemphigus) is a rare condition caused by an autosomaldominant mutation affecting intracellular calcium signaling that impairs keratinocyte adhesion.9 Similar to granular parakeratosis, it is most common in middle-aged adults (aged 30–40 years) and manifests as pruritic and burning lesions in symmetric intertriginous areas that also can be triggered by heat and sweating. However, patients present with recurrent blistering and vesicular lesions that may lead to erosions and secondary infections, which reduced clinical suspicion for this diagnosis in our patient. Histopathology shows suprabasilar and intraepidermal clefts, full-thickness acantholysis, protruding dermal papillae, and a perivascular lymphocytic infiltrate in the superficial dermis.9
- Ding CY, Liu H, Khachemoune A. Granular parakeratosis: a comprehensive review and a critical reappraisal. Am J Clin Dermatol. 2015;16:495-500. doi:10.1007/s40257-015-0148-2
- Ip KH, Li A. Clinical features, histology, and treatment outcomes of granular parakeratosis: a systematic review. Int J Dermatol. 2022;61:973-978. doi:10.1111/ijd.16107
- Mehregan DA, Thomas JE, Mehregan DR. Intertriginous granular parakeratosis. J Am Acad Dermatol. 1998;39:495-496. doi:10.1016/s0190-9622(98)70333-0
- Kamada A, Saga K, Jimbow K. Apoeccrine sweat duct obstruction as a cause for Fox-Fordyce disease. J Am Acad Dermatol. 2003;48:453-455. doi:10.1067/mjd.2003.93
- Salloum A, Bouferraa Y, Bazzi N, et al. Pathophysiology, clinical findings, and management of Fox-Fordyce disease: a systematic review. J Cosmet Dermatol. 2022;21:482-500. doi:10.1111/jocd.14135
- Sun MD, Halpern AC. Advances in the etiology, detection, and clinical management of seborrheic keratoses. Dermatology. 2022;238:205-217. doi:10.1159/000517070
- Minagawa A. Dermoscopy-pathology relationship in seborrheic keratosis. J Dermatol. 2017;44:518-524. doi:10.1111/1346-8138.13657
- Weston G, Payette M. Update on lichen planus and its clinical variants [published online September 16, 2015]. Int J Womens Dermatol. 2015;1:140-149. doi:10.1016/j.ijwd.2015.04.001
- Ben Lagha I, Ashack K, Khachemoune A. Hailey-Hailey disease: an update review with a focus on treatment data. Am J Clin Dermatol. 2020;21:49-68. doi:10.1007/s40257-019-00477-z
The Diagnosis: Granular Parakeratosis
Histopathology demonstrated diffuse parakeratosis with retention of keratohyalin granules throughout the stratum corneum consistent with a diagnosis of granular parakeratosis (Figure), a rare benign cutaneous condition that is thought to occur due to a defect in epidermal differentiation. The lesion resolved without additional treatment.

The pathogenesis of granular parakeratosis is unclear, but a reactive process in which locoregional irritation or occlusion prompts increased cell turnover and prevention of profilaggrin breakdown has been proposed.1,2 The diagnosis is linked to various precipitating agents, most commonly topical products (eg, zinc oxide, antiperspirants) and products with benzalkonium chloride (eg, laundry rinses). These agents are thought to cause retention of keratohyalin granules in the stratum corneum during epidermal differentiation.1,2
Most affected patients are middle-aged women (mean age at diagnosis, 37.8 years).2 Patients present with eruptions of erythematous, brown, hyperkeratotic patches and papules that coalesce into plaques.1,2 These lesions can be pruritic and painful or asymptomatic. They often manifest bilaterally in intertriginous sites, most commonly the axillae, groin, or inguinal folds.1,2
Treatment involves identification and removal of potential triggers including changing antiperspirants, limiting use of irritating agents (eg, topical products with strong fragrances), and reducing heat and moisture in the affected areas. If the lesion persists, stepwise treatment can be initiated with topical agents (eg, corticosteroids, vitamin D analogues, retinoids, keratolytics, calcineurin inhibitors) followed by systemic medications (eg, antibiotics, isotretinoin, antifungals, dexamethasone) and procedures (eg, botulinum toxin injections, surgery, laser, cryotherapy).1,2
Unilateral granular parakeratosis, as seen in our patient, is an uncommon manifestation. Our case supports the theory that occlusion is a precipitating factor for this condition, given persistent axillary exposure to heat, sweat, and friction in the setting of limb immobilization.3
Granular parakeratosis is a challenge to diagnose due to clinical overlap with several other cutaneous conditions; histopathologic confirmation is required. Fox- Fordyce disease is a rare condition that is thought to result from keratin buildup or occlusion of apocrine or apoeccrine sweat ducts leading to duct rupture and surrounding inflammation.4 Common triggers include laser hair removal, hormonal changes, and living conditions that promote hot and humid environments.5 It can manifest similarly to granular parakeratosis, with eruptions of multiple red-violet papules that appear bilaterally in aprocine gland–rich areas, including the axillae and less commonly the genital, periareolar, thoracic, abdominal, and facial areas.4,5 However, most patients with Fox-Fordyce disease tend to be younger females (aged 13–35 years) with severely pruritic lesions,4,5 unlike our patient. In addition, histopathology shows hyperkeratosis, hair follicle plugging, and sweat gland and duct dilation.4
Seborrheic keratoses are common benign epidermal tumors caused by an overproliferation of immature keratinocytes.6,7 Similar to granular parakeratosis, they commonly manifest in older adults as hyperpigmented, well-demarcated, verrucous plaques with a hyperkeratotic surface.6 However, they are more common on the face, neck, trunk, and extremities, and they tend to be asymptomatic, differentiating them from granular parakerosis.6 Histopathology demonstrates a papillomatous epidermal surface, large capillaries in the dermal papillae, and intraepidermal and pseudohorn epidermal cysts.7
Inverse lichen planus, a variant of lichen planus, is a rare inflammatory condition that involves the lysis of basal keratinocytes by CD8+ lymphocytes.8 Similar to granular parakeratosis, lichen planus commonly affects middle-aged women (aged 30–60 years), and this particular variant manifests with asymptomatic or mildly pruritic, hyperpigmented patches and plaques in intertriginous areas. Although it also shows hyperkeratosis on histopathology, it can be differentiated from granular parakeratosis by the additional findings of epidermal hypergranulosis, sawtooth acanthosis of rete ridges, apoptotic keratinocytes in the dermoepidermal junction, and lymphocytic infiltrate in the upper dermis.8
Hailey-Hailey disease (also known as familial benign pemphigus) is a rare condition caused by an autosomaldominant mutation affecting intracellular calcium signaling that impairs keratinocyte adhesion.9 Similar to granular parakeratosis, it is most common in middle-aged adults (aged 30–40 years) and manifests as pruritic and burning lesions in symmetric intertriginous areas that also can be triggered by heat and sweating. However, patients present with recurrent blistering and vesicular lesions that may lead to erosions and secondary infections, which reduced clinical suspicion for this diagnosis in our patient. Histopathology shows suprabasilar and intraepidermal clefts, full-thickness acantholysis, protruding dermal papillae, and a perivascular lymphocytic infiltrate in the superficial dermis.9
The Diagnosis: Granular Parakeratosis
Histopathology demonstrated diffuse parakeratosis with retention of keratohyalin granules throughout the stratum corneum consistent with a diagnosis of granular parakeratosis (Figure), a rare benign cutaneous condition that is thought to occur due to a defect in epidermal differentiation. The lesion resolved without additional treatment.

The pathogenesis of granular parakeratosis is unclear, but a reactive process in which locoregional irritation or occlusion prompts increased cell turnover and prevention of profilaggrin breakdown has been proposed.1,2 The diagnosis is linked to various precipitating agents, most commonly topical products (eg, zinc oxide, antiperspirants) and products with benzalkonium chloride (eg, laundry rinses). These agents are thought to cause retention of keratohyalin granules in the stratum corneum during epidermal differentiation.1,2
Most affected patients are middle-aged women (mean age at diagnosis, 37.8 years).2 Patients present with eruptions of erythematous, brown, hyperkeratotic patches and papules that coalesce into plaques.1,2 These lesions can be pruritic and painful or asymptomatic. They often manifest bilaterally in intertriginous sites, most commonly the axillae, groin, or inguinal folds.1,2
Treatment involves identification and removal of potential triggers including changing antiperspirants, limiting use of irritating agents (eg, topical products with strong fragrances), and reducing heat and moisture in the affected areas. If the lesion persists, stepwise treatment can be initiated with topical agents (eg, corticosteroids, vitamin D analogues, retinoids, keratolytics, calcineurin inhibitors) followed by systemic medications (eg, antibiotics, isotretinoin, antifungals, dexamethasone) and procedures (eg, botulinum toxin injections, surgery, laser, cryotherapy).1,2
Unilateral granular parakeratosis, as seen in our patient, is an uncommon manifestation. Our case supports the theory that occlusion is a precipitating factor for this condition, given persistent axillary exposure to heat, sweat, and friction in the setting of limb immobilization.3
Granular parakeratosis is a challenge to diagnose due to clinical overlap with several other cutaneous conditions; histopathologic confirmation is required. Fox- Fordyce disease is a rare condition that is thought to result from keratin buildup or occlusion of apocrine or apoeccrine sweat ducts leading to duct rupture and surrounding inflammation.4 Common triggers include laser hair removal, hormonal changes, and living conditions that promote hot and humid environments.5 It can manifest similarly to granular parakeratosis, with eruptions of multiple red-violet papules that appear bilaterally in aprocine gland–rich areas, including the axillae and less commonly the genital, periareolar, thoracic, abdominal, and facial areas.4,5 However, most patients with Fox-Fordyce disease tend to be younger females (aged 13–35 years) with severely pruritic lesions,4,5 unlike our patient. In addition, histopathology shows hyperkeratosis, hair follicle plugging, and sweat gland and duct dilation.4
Seborrheic keratoses are common benign epidermal tumors caused by an overproliferation of immature keratinocytes.6,7 Similar to granular parakeratosis, they commonly manifest in older adults as hyperpigmented, well-demarcated, verrucous plaques with a hyperkeratotic surface.6 However, they are more common on the face, neck, trunk, and extremities, and they tend to be asymptomatic, differentiating them from granular parakerosis.6 Histopathology demonstrates a papillomatous epidermal surface, large capillaries in the dermal papillae, and intraepidermal and pseudohorn epidermal cysts.7
Inverse lichen planus, a variant of lichen planus, is a rare inflammatory condition that involves the lysis of basal keratinocytes by CD8+ lymphocytes.8 Similar to granular parakeratosis, lichen planus commonly affects middle-aged women (aged 30–60 years), and this particular variant manifests with asymptomatic or mildly pruritic, hyperpigmented patches and plaques in intertriginous areas. Although it also shows hyperkeratosis on histopathology, it can be differentiated from granular parakeratosis by the additional findings of epidermal hypergranulosis, sawtooth acanthosis of rete ridges, apoptotic keratinocytes in the dermoepidermal junction, and lymphocytic infiltrate in the upper dermis.8
Hailey-Hailey disease (also known as familial benign pemphigus) is a rare condition caused by an autosomaldominant mutation affecting intracellular calcium signaling that impairs keratinocyte adhesion.9 Similar to granular parakeratosis, it is most common in middle-aged adults (aged 30–40 years) and manifests as pruritic and burning lesions in symmetric intertriginous areas that also can be triggered by heat and sweating. However, patients present with recurrent blistering and vesicular lesions that may lead to erosions and secondary infections, which reduced clinical suspicion for this diagnosis in our patient. Histopathology shows suprabasilar and intraepidermal clefts, full-thickness acantholysis, protruding dermal papillae, and a perivascular lymphocytic infiltrate in the superficial dermis.9
- Ding CY, Liu H, Khachemoune A. Granular parakeratosis: a comprehensive review and a critical reappraisal. Am J Clin Dermatol. 2015;16:495-500. doi:10.1007/s40257-015-0148-2
- Ip KH, Li A. Clinical features, histology, and treatment outcomes of granular parakeratosis: a systematic review. Int J Dermatol. 2022;61:973-978. doi:10.1111/ijd.16107
- Mehregan DA, Thomas JE, Mehregan DR. Intertriginous granular parakeratosis. J Am Acad Dermatol. 1998;39:495-496. doi:10.1016/s0190-9622(98)70333-0
- Kamada A, Saga K, Jimbow K. Apoeccrine sweat duct obstruction as a cause for Fox-Fordyce disease. J Am Acad Dermatol. 2003;48:453-455. doi:10.1067/mjd.2003.93
- Salloum A, Bouferraa Y, Bazzi N, et al. Pathophysiology, clinical findings, and management of Fox-Fordyce disease: a systematic review. J Cosmet Dermatol. 2022;21:482-500. doi:10.1111/jocd.14135
- Sun MD, Halpern AC. Advances in the etiology, detection, and clinical management of seborrheic keratoses. Dermatology. 2022;238:205-217. doi:10.1159/000517070
- Minagawa A. Dermoscopy-pathology relationship in seborrheic keratosis. J Dermatol. 2017;44:518-524. doi:10.1111/1346-8138.13657
- Weston G, Payette M. Update on lichen planus and its clinical variants [published online September 16, 2015]. Int J Womens Dermatol. 2015;1:140-149. doi:10.1016/j.ijwd.2015.04.001
- Ben Lagha I, Ashack K, Khachemoune A. Hailey-Hailey disease: an update review with a focus on treatment data. Am J Clin Dermatol. 2020;21:49-68. doi:10.1007/s40257-019-00477-z
- Ding CY, Liu H, Khachemoune A. Granular parakeratosis: a comprehensive review and a critical reappraisal. Am J Clin Dermatol. 2015;16:495-500. doi:10.1007/s40257-015-0148-2
- Ip KH, Li A. Clinical features, histology, and treatment outcomes of granular parakeratosis: a systematic review. Int J Dermatol. 2022;61:973-978. doi:10.1111/ijd.16107
- Mehregan DA, Thomas JE, Mehregan DR. Intertriginous granular parakeratosis. J Am Acad Dermatol. 1998;39:495-496. doi:10.1016/s0190-9622(98)70333-0
- Kamada A, Saga K, Jimbow K. Apoeccrine sweat duct obstruction as a cause for Fox-Fordyce disease. J Am Acad Dermatol. 2003;48:453-455. doi:10.1067/mjd.2003.93
- Salloum A, Bouferraa Y, Bazzi N, et al. Pathophysiology, clinical findings, and management of Fox-Fordyce disease: a systematic review. J Cosmet Dermatol. 2022;21:482-500. doi:10.1111/jocd.14135
- Sun MD, Halpern AC. Advances in the etiology, detection, and clinical management of seborrheic keratoses. Dermatology. 2022;238:205-217. doi:10.1159/000517070
- Minagawa A. Dermoscopy-pathology relationship in seborrheic keratosis. J Dermatol. 2017;44:518-524. doi:10.1111/1346-8138.13657
- Weston G, Payette M. Update on lichen planus and its clinical variants [published online September 16, 2015]. Int J Womens Dermatol. 2015;1:140-149. doi:10.1016/j.ijwd.2015.04.001
- Ben Lagha I, Ashack K, Khachemoune A. Hailey-Hailey disease: an update review with a focus on treatment data. Am J Clin Dermatol. 2020;21:49-68. doi:10.1007/s40257-019-00477-z
A 62-year-old woman presented to our clinic for evaluation of a brown plaque in the left axilla of 2 weeks’ duration. She had a history of a rotator cuff injury and adhesive capsulitis several months prior that required immobilization of the left arm in a shoulder orthosis for several months. After the sling was removed, she noticed the lesion and reported mild cutaneous pain. Physical examination revealed a 1.5-cm, verrucous, red-brown plaque in the left axillary vault. A shave biopsy of the plaque was performed.
A Pharmacist-Led Process to Monitor Discrepant Urine Drug Screen Results
Urine drug screen (UDS) monitoring is a common risk-mitigation strategy tool for prescribing controlled substances.1-3 Not only is UDS monitoring highlighted by clinical practice guidelines for opioid prescribing for chronic pain,1,2 it has also been suggested as best practice for benzodiazepines3 and a consideration for other controlled substances. Monitoring UDSs helps confirm adherence to the prescribed treatment regimen while also screening for substance use that may increase patient risk.
UDS results can be complex and have profound implications for the patient’s treatment plan. Drug metabolites for opioids are particularly complicated; for example, synthetic and semisynthetic opioids are not detected on routine opiate immunoassays.4 This may lead a clinician to falsely assume the patient is not taking their fentanyl or tramadol medication as directed—or potentially even diverting—in the face of a negative opiate result.5 Routine UDSs are also subject to the pitfall of false-positive results due to coprescribed medications; for example, bupropion can lead to a false-positive amphetamine result, whereas sertraline can lead to a false-positive benzodiazepine result.6 Retrospective reviews of clinician behavior surrounding UDS interpretation have demonstrated knowledge gaps and inconsistent communication practices with patients.7,8
Given the complexity of UDS interpretation and its close relationship with medications, pharmacists are positioned to play an important role in the process. Pharmacists are embedded in pain-management teams and involved in prescription drug monitoring programs (PDMPs) for many health systems. The Veterans Health Administration (VHA) has supported the hiring of pain management, opioid safety, and PDMP coordinators (PMOP) at its facilities to provide clinical pain-management guidance, support national initiatives, and uphold legislative requirements.9 In many facilities, a pharmacist is hired specifically for these positions.
Clinical dashboards have been used by pharmacists in a variety of settings.10-13 They allow clinicians at a broad level to target interventions needed across a patient population, then produce a list of actionable patients to facilitate delivery of that intervention on an individual level.13 Between 2021 and 2022, a clinical dashboard to review potentially discrepant UDS results was made available for use at US Department of Veterans Affairs (VA) medical centers. Evidence exists in primary and specialty care settings that implementation of an opioid-prescribing clinical dashboard improves completion rates of risk-mitigation strategies such as UDS and opioid treatment agreements.14,15 To our knowledge there is no published research on the use and outcomes of a clinical dashboard that allows users to efficiently review discrepant UDS results when compared to a list of currently prescribed medications.
Given the availability of the UDS dashboard at the VA Black Hills Health Care System (VABHHCS) in South Dakota and the hiring of a PMOP coordinator pharmacist, the aim of this quality improvement project was 2-fold: to implement a pharmacist-led process to monitor the UDS dashboard for potentially discrepant results and to describe the quantity and types of interventions made by the clinical pharmacist leading this process.
Quality Improvement Project
A clinical UDS dashboard was created by the VA Northwest Health Network and made available for use at VHA sites between 2021 and 2022. The UDS dashboard is housed on a secure, Power BI Report Server (Microsoft), with access restricted to only those with patient health data privileges. The dashboard identifies all local patients with a UDS that returned with a potential discrepancy, defined as an unexpected positive result (eg, a detected substance not recently prescribed or documented on the patient’s medication list) and/or an unexpected negative result (eg, a prescribed substance not detected). The UDS dashboard identifies these discrepancies by comparing the patient’s current medication list (both VHA and non-VHA) to their UDS results.
The UDS dashboard displays a summary of UDSs performed, unexpected negative results, unexpected positive results, and potential discrepancies. The user may also specify the laboratory type and time frame of interest to limit displayed results. The user can then view patient-specific data for any category. Among the data are the patient’s UDS results and the completion date, detected (or nondetected) substance(s), ordering clinician, associated medication(s) with last fill date and days’ supply, and whether a confirmatory test has been performed in the past year.
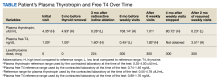
VABHHCS uses an extended UDS immunoassay (PROFILE-V, MEDTOX Diagnostics) that reports on 11 substances: opiates, oxycodone, buprenorphine, methadone, amphetamines, methamphetamine, barbiturates, benzodiazepines, cocaine metabolites, cannabinoids (tetrahydrocannabinol [THC]), and phencyclidine. These substances appear on the UDS dashboard. The project protocol initially included monitoring for tramadol but that was later removed because it was not available with this UDS immunoassay.
Pharmacist Process
Either the PMOP coordinator or pharmacy resident monitored the UDS dashboard weekly. Any patients identified as having a potential discrepancy were reviewed. If the discrepancy was determined to be significant, the PMOP coordinator or pharmacy resident would review the patient electronic health record. If warranted, the patient was contacted and asked about newly prescribed medications, missed and recent medication doses, and illicit substance use. Potential interventions during in-depth review included: (1) discussing future actions with the primary care clinician and/or prescriber of the controlled substance; (2) ordering a confirmatory test on the original urine sample; (3) evaluating for sources of potential false-positive results; (4) completing an updated PDMP if not performed within the past year; (5) referring patients for substance use disorder treatment or counseling; or (6) consulting the local narcotics review committee. A progress note was entered into the electronic health record with the findings and any actions taken, and an alert for the primary care clinician and/or prescriber of the controlled substance.
Implementation and Analysis
This quality improvement project spanned 16 weeks from June 2022 through September 2022. Any patient with a UDS that returned with a significant discrepancy was reviewed. The primary outcome was interventions made by the PMOP coordinator or pharmacy resident, as well as time taken to perform the in-depth review of each patient. Patient demographics were also collected. The protocol for this project was approved by the VABHHCS pharmacy and therapeutics committee and was determined to meet guidelines for a nonresearch quality improvement project.
Results
From June 2022 through September 2022, 700 UDSs were performed at VABHHCS with 278 (39.7%) patients identified as having a potential discrepancy based on UDS results. Sixty patients (8.6%) had significant discrepancies that warranted in-depth review. The most common reasons for determining whether a potential discrepancy was not significant included unexpected negatives due to documented non-VA medications no longer being prescribed, unexpected positives due to recent expiration of a controlled substance prescription the patient was still taking, or unexpected positives due to the detection of a substance for which the clinician was already aware. During the 16-week study period, the mean number of patients warranting in-depth review was 4 per week.
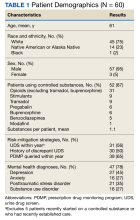
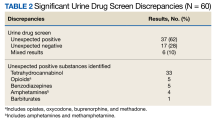
The patients were predominantly male with a mean age of 61 years, and most (87%) were prescribed at least 1 controlled substance (mean, 1.1), primarily opioids for pain management (Table 1). Most patients had recent substance risk mitigation with UDS (56%) and PDMP (65%) checks within the past year. Of the 60 patients reviewed with significant UDS discrepancies, 50% had a history of discrepant UDS results. Of the 60 UDS discrepancies, there were 37 unexpected positive results (62%), 17 unexpected negative results (28%), and 10 patients with both positive and negative results (17%). THC was the most frequently detected substance, followed by opiates, benzodiazepines, and amphetamines (Table 2).
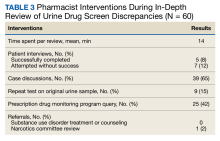
Each in-depth review with interventions by the PMOP coordinator or pharmacy resident lasted a mean of 14 minutes (Table 3). Five patients were successfully contacted for an interview and 7 patients could not be contacted. The ordering clinician of the UDS sometimes had contacted these patients prior to the PMOP coordinator or pharmacy resident reviewing the UDS dashboard, eliminating the need for additional follow-up.
The most common pharmacist intervention was discussing future actions with the primary care clinician and/or prescriber of the controlled substance (n = 39; 65%). These conversations resulted in actions such as ordering a repeat UDS with confirmatory testing at a future date or agreeing that the clinician would discuss the results and subsequent actions with the patient at an upcoming visit. Pharmacist interventions also included 25 PDMP queries (42%) and 9 orders of confirmatory UDS on the original urine sample (15%). Only 1 patient was evaluated by the narcotics review committee, which resulted in a controlled substance flag being placed on their profile. No patients were referred to substance use disorder treatment or counseling. It was offered to and declined by 1 patient, and 3 patients were already engaged in these services.
Medication therapies that could contribute to false-positive results were also evaluated. Fourteen patients who tested positive for THC had a prescription for a nonsteroidal anti-inflammatory drug or proton-pump inhibitor, which could have created a false-positive result.6 One patient who tested positive for amphetamines had a prescription for phentermine.16 No other potential false-positive results were identified.
Discussion
Findings of this project illustrate that the use of a clinical pharmacist to monitor a dashboard of discrepant UDS results created opportunities for collaboration with clinicians and impacted confirmatory testing and PDMP monitoring practices.
At the local level, the process had numerous benefits. First, it was a reasonable amount of workload to generate pharmacist interventions: the PMOP coordinator conducted an average of 4 in-depth reviews weekly, each lasting about 14 minutes. Thus, the UDS dashboard allowed the PMOP coordinator to actively surveil all incoming UDS results for potential discrepancies in about 1 hour each week. Pairing the automation of the UDS dashboard with the clinical judgment of the PMOP coordinator seemed to maximize efficiency. VABHHCS provides primary and secondary medical and surgical care to a rural population of approximately 20,000 patients across 5 states; the time required at facilities that serve a higher volume of patients may be greater.
Second, the project served as an opportunity for the PMOP coordinator to provide case-specific clinician education on UDS monitoring. As medication experts, pharmacists can apply their medication-related knowledge to UDS interpretation. This includes understanding drug metabolism and classification and how they apply to UDS results, as well as recognizing medication therapies that could contribute to false-positive UDS results. Research suggests that clinicians may have gaps in their knowledge and may welcome pharmacist assistance in interpreting UDS results.7,8
Third, the project helped improve rates of confirmatory testing for those with unexpected positive UDS results. Confirmatory testing should be strongly considered if positive results would have significant implications on the future course of treatment.4 The PMOP coordinator ordered a confirmatory test on 9 patients using the same urine sample used to conduct the initial UDS, minimizing the burden on the patient and laboratory staff. Confirmatory testing was limited by the laboratory’s sample retention period; if the need for confirmatory testing was not recognized soon enough, the sample would no longer be available for retesting. Health systems may consider the use of reflexive confirmatory testing with UDS as an alternative approach, although this may come at an additional cost and may not be warranted in many cases (eg, only 39.7% of all potential discrepancies were deemed as significant within our project).
There were notable incidental findings in our quality improvement project. Among patients with a significant discrepancy on UDS, 50% had a history of ≥ 1 discrepant UDS result. This further emphasizes the importance of appropriate use and interpretation of UDS monitoring for all clinicians, as this may prevent prolonged and potentially inappropriate treatment regimens. Secondly, rates of mental health diagnoses among those with a significant UDS discrepancy seemed relatively high compared to population-level data. For example, among veterans, the overall lifetime prevalence of posttraumatic stress disorder is estimated to be 8.0%; in our project, 35% of patients with a significant UDS discrepancy had a posttraumatic stress disorder diagnosis.17 This relationship may be an area of further study.
Lastly, it was surprising that the overall rates of UDS and PDMP checks within the past year were 56% and 65%, respectively. VABHHCS requires veterans on controlled substances to have these risk-mitigation strategies performed annually, so our suspicion is that many were falling out due to having been most recently evaluated 12 to 16 months prior. This may represent a limitation of our data-collection method, which reviewed only the previous 12 months.
Limitations
This project was carried out over a period of only 4 months. As a result, only 60 patients received an in-depth review from the PMOP coordinator. Second, the timeliness of the intervention seemed crucial, as delayed in-depth reviews resulted in fewer opportunities to order confirmatory tests or collaborate with clinicians prior to devising an updated plan. Additionally, our process called for UDS dashboard monitoring once a week. Given that the laboratory held samples for only 48 hours, twice- or thrice-weekly review of the UDS dashboard would have allowed for more confirmatory testing, along with more immediate clinician collaboration. Most importantly, the outcomes of this project are only presented via descriptive statistics and without the results of any comparison group, making it impossible to draw firm conclusions about this approach compared to standard-care processes.
Conclusions
This quality improvement project has proven to be valuable at VABHHCS and we intend to continue this pharmacist-led process to monitor the UDS dashboard. VABHHCS leadership are also discussing UDS practices more broadly to further enhance patient management. Within the VA, the PMOP coordinator—charged with being the local coordinator of appropriate pain management and opioid safety practices—is well positioned to assume these responsibilities. Outside of the VA, a pain-management clinical pharmacist or any pharmacist embedded within primary care could similarly perform these duties. Previous literature regarding the implementation of clinical dashboards suggests that with the appropriate software engineering teams and infrastructure, this tool could also be feasibly developed and implemented at other health systems relatively quickly.14
Overall, a pharmacist-led process to efficiently monitor a dashboard of discrepant UDS results led to opportunities for collaboration with clinicians and positively impacted confirmatory testing and PDMP monitoring at a rural VA health system.
Acknowledgments
The authors express their gratitude to Patrick Spoutz, PharmD, BCPS, VISN 20 Pharmacist Executive, for introducing and sharing the UDS dashboard with our team.
1. Dowell D, Ragan KR, Jones CM, Baldwin GT, Chou R. CDC Clinical Practice Guideline for Prescribing Opioids for Pain - United States, 2022. MMWR Recomm Rep. 2022;71(3):1-95. doi:10.15585/mmwr.rr7103a1
2. US Department of Defense, US Department of Veterans Affairs. VA/DoD clinical practice guidelines for the use of opioids in the management of chronic pain. Version 4.0. Published 2002. Accessed January 22, 2024. https://www.healthquality.va.gov/guidelines/Pain/cot/VADoDOpioidsCPG.pdf
3. Champion C, Kameg BN. Best practices in benzodiazepine prescribing and management in primary care. Nurse Pract. 2021;46(3):30-36.doi:10.1097/01.NPR.0000733684.24949.19
4. Kale N. Urine drug tests: ordering and interpretation. Am Fam Physician. 2019;99(1):33-39.
5. Gillespie E, Cunningham JM, Indovina KA. Interpretation of the urine drug screen. The Hospitalist. May 2, 2022. Accessed January 19, 2024. https://www.the-hospitalist.org/hospitalist/article/32085/interpreting-diagnostic-tests/interpretation-of-the-urine-drug-screen/
6. Schwebach A, Ball J. Urine drug screening: minimizing false-positives and false-negatives to optimize patient care. US Pharm. 2016;41(8):26-30.
7. Starrels JL, Fox AD, Kunins HV, Cunningham CO. They don’t know what they don’t know: internal medicine residents’ knowledge and confidence in urine drug test interpretation for patients with chronic pain. J Gen Intern Med. 2012;27(11):1521-1527. doi:10.1007/s11606-012-2165-7
8. Chua I, Petrides AK, Schiff GD, et al. Provider misinterpretation, documentation, and follow-up of definitive urine drug testing results. J Gen Intern Med. 2020;35(1):283-290. doi:10.1007/s11606-019-05514-5
9. US Department of Veterans Affairs, Veterans Health Administration. VHA Pain Management, Opioid Safety, and Prescription Drug Monitoring Program (PMOP) National Program Field Roles and Responsibilities Manual. October 2021 (V1).[Source not verified]
10. Dorsch MP, Chen CS, Allen AL, et al. Nationwide implementation of a population management dashboard for monitoring direct oral anticoagulants: insights from the Veterans Affairs Health System. Circ Cardiovasc Qual Outcomes. 2023;16(2):e009256. doi:10.1161/CIRCOUTCOMES.122.009256
11. Hu AM, Pepin MJ, Hashem MG, et al. Development of a specialty medication clinical dashboard to improve tumor necrosis factor-α inhibitor safety and adherence monitoring. Am J Health Syst Pharm. 2022;79(8):683-688. doi:10.1093/ajhp/zxab454
12. Homsted FAE, Magee CE, Nesin N. Population health management in a small health system: impact of controlled substance stewardship in a patient-centered medical home. Am J Health Syst Pharm. 2017;74(18):1468-1475. doi:10.2146/ajhp161032
13. US Department of Veterans Affairs, Veterans Health Administration, Pharmacy Benefits (PBM) Services, Clinical Pharmacy Practice Office. Fact Sheet: CPS Role in Population Health Management. 2019. [Source not verified]
14. Anderson D, Zlateva I, Khatri K, Ciaburri N. Using health information technology to improve adherence to opioid prescribing guidelines in primary care. Clin J Pain. 2015;31(6):573-579. doi:10.1097/AJP.0000000000000177
15. Wang EJ, Helgesen R, Johr CR, Lacko HS, Ashburn MA, Merkel PA. Targeted program in an academic rheumatology practice to improve compliance with opioid prescribing guidelines for the treatment of chronic pain. Arthritis Care Res (Hoboken). 2021;73(10):1425-1429. doi:10.1002/acr.24354
16. Moeller KE, Kissack JC, Atayee RS, Lee KC. Clinical interpretation of urine drug tests: what clinicians need to know about urine drug screens. Mayo Clin Proc. 2017;92(5):774-796. doi:10.1016/j.mayocp.2016.12.007
17. Wisco BE, Marx BP, Wolf EJ, Miller MW, Southwick SM, Pietrzak RH. Posttraumatic stress disorder in the US veteran population: results from the National Health and Resilience in Veterans Study. J Clin Psychiatry. 2014;75(12):1338-46. doi:10.4088/JCP.14m09328
Urine drug screen (UDS) monitoring is a common risk-mitigation strategy tool for prescribing controlled substances.1-3 Not only is UDS monitoring highlighted by clinical practice guidelines for opioid prescribing for chronic pain,1,2 it has also been suggested as best practice for benzodiazepines3 and a consideration for other controlled substances. Monitoring UDSs helps confirm adherence to the prescribed treatment regimen while also screening for substance use that may increase patient risk.
UDS results can be complex and have profound implications for the patient’s treatment plan. Drug metabolites for opioids are particularly complicated; for example, synthetic and semisynthetic opioids are not detected on routine opiate immunoassays.4 This may lead a clinician to falsely assume the patient is not taking their fentanyl or tramadol medication as directed—or potentially even diverting—in the face of a negative opiate result.5 Routine UDSs are also subject to the pitfall of false-positive results due to coprescribed medications; for example, bupropion can lead to a false-positive amphetamine result, whereas sertraline can lead to a false-positive benzodiazepine result.6 Retrospective reviews of clinician behavior surrounding UDS interpretation have demonstrated knowledge gaps and inconsistent communication practices with patients.7,8
Given the complexity of UDS interpretation and its close relationship with medications, pharmacists are positioned to play an important role in the process. Pharmacists are embedded in pain-management teams and involved in prescription drug monitoring programs (PDMPs) for many health systems. The Veterans Health Administration (VHA) has supported the hiring of pain management, opioid safety, and PDMP coordinators (PMOP) at its facilities to provide clinical pain-management guidance, support national initiatives, and uphold legislative requirements.9 In many facilities, a pharmacist is hired specifically for these positions.
Clinical dashboards have been used by pharmacists in a variety of settings.10-13 They allow clinicians at a broad level to target interventions needed across a patient population, then produce a list of actionable patients to facilitate delivery of that intervention on an individual level.13 Between 2021 and 2022, a clinical dashboard to review potentially discrepant UDS results was made available for use at US Department of Veterans Affairs (VA) medical centers. Evidence exists in primary and specialty care settings that implementation of an opioid-prescribing clinical dashboard improves completion rates of risk-mitigation strategies such as UDS and opioid treatment agreements.14,15 To our knowledge there is no published research on the use and outcomes of a clinical dashboard that allows users to efficiently review discrepant UDS results when compared to a list of currently prescribed medications.
Given the availability of the UDS dashboard at the VA Black Hills Health Care System (VABHHCS) in South Dakota and the hiring of a PMOP coordinator pharmacist, the aim of this quality improvement project was 2-fold: to implement a pharmacist-led process to monitor the UDS dashboard for potentially discrepant results and to describe the quantity and types of interventions made by the clinical pharmacist leading this process.
Quality Improvement Project
A clinical UDS dashboard was created by the VA Northwest Health Network and made available for use at VHA sites between 2021 and 2022. The UDS dashboard is housed on a secure, Power BI Report Server (Microsoft), with access restricted to only those with patient health data privileges. The dashboard identifies all local patients with a UDS that returned with a potential discrepancy, defined as an unexpected positive result (eg, a detected substance not recently prescribed or documented on the patient’s medication list) and/or an unexpected negative result (eg, a prescribed substance not detected). The UDS dashboard identifies these discrepancies by comparing the patient’s current medication list (both VHA and non-VHA) to their UDS results.
The UDS dashboard displays a summary of UDSs performed, unexpected negative results, unexpected positive results, and potential discrepancies. The user may also specify the laboratory type and time frame of interest to limit displayed results. The user can then view patient-specific data for any category. Among the data are the patient’s UDS results and the completion date, detected (or nondetected) substance(s), ordering clinician, associated medication(s) with last fill date and days’ supply, and whether a confirmatory test has been performed in the past year.
VABHHCS uses an extended UDS immunoassay (PROFILE-V, MEDTOX Diagnostics) that reports on 11 substances: opiates, oxycodone, buprenorphine, methadone, amphetamines, methamphetamine, barbiturates, benzodiazepines, cocaine metabolites, cannabinoids (tetrahydrocannabinol [THC]), and phencyclidine. These substances appear on the UDS dashboard. The project protocol initially included monitoring for tramadol but that was later removed because it was not available with this UDS immunoassay.
Pharmacist Process
Either the PMOP coordinator or pharmacy resident monitored the UDS dashboard weekly. Any patients identified as having a potential discrepancy were reviewed. If the discrepancy was determined to be significant, the PMOP coordinator or pharmacy resident would review the patient electronic health record. If warranted, the patient was contacted and asked about newly prescribed medications, missed and recent medication doses, and illicit substance use. Potential interventions during in-depth review included: (1) discussing future actions with the primary care clinician and/or prescriber of the controlled substance; (2) ordering a confirmatory test on the original urine sample; (3) evaluating for sources of potential false-positive results; (4) completing an updated PDMP if not performed within the past year; (5) referring patients for substance use disorder treatment or counseling; or (6) consulting the local narcotics review committee. A progress note was entered into the electronic health record with the findings and any actions taken, and an alert for the primary care clinician and/or prescriber of the controlled substance.
Implementation and Analysis
This quality improvement project spanned 16 weeks from June 2022 through September 2022. Any patient with a UDS that returned with a significant discrepancy was reviewed. The primary outcome was interventions made by the PMOP coordinator or pharmacy resident, as well as time taken to perform the in-depth review of each patient. Patient demographics were also collected. The protocol for this project was approved by the VABHHCS pharmacy and therapeutics committee and was determined to meet guidelines for a nonresearch quality improvement project.
Results
From June 2022 through September 2022, 700 UDSs were performed at VABHHCS with 278 (39.7%) patients identified as having a potential discrepancy based on UDS results. Sixty patients (8.6%) had significant discrepancies that warranted in-depth review. The most common reasons for determining whether a potential discrepancy was not significant included unexpected negatives due to documented non-VA medications no longer being prescribed, unexpected positives due to recent expiration of a controlled substance prescription the patient was still taking, or unexpected positives due to the detection of a substance for which the clinician was already aware. During the 16-week study period, the mean number of patients warranting in-depth review was 4 per week.
The patients were predominantly male with a mean age of 61 years, and most (87%) were prescribed at least 1 controlled substance (mean, 1.1), primarily opioids for pain management (Table 1). Most patients had recent substance risk mitigation with UDS (56%) and PDMP (65%) checks within the past year. Of the 60 patients reviewed with significant UDS discrepancies, 50% had a history of discrepant UDS results. Of the 60 UDS discrepancies, there were 37 unexpected positive results (62%), 17 unexpected negative results (28%), and 10 patients with both positive and negative results (17%). THC was the most frequently detected substance, followed by opiates, benzodiazepines, and amphetamines (Table 2).
Each in-depth review with interventions by the PMOP coordinator or pharmacy resident lasted a mean of 14 minutes (Table 3). Five patients were successfully contacted for an interview and 7 patients could not be contacted. The ordering clinician of the UDS sometimes had contacted these patients prior to the PMOP coordinator or pharmacy resident reviewing the UDS dashboard, eliminating the need for additional follow-up.
The most common pharmacist intervention was discussing future actions with the primary care clinician and/or prescriber of the controlled substance (n = 39; 65%). These conversations resulted in actions such as ordering a repeat UDS with confirmatory testing at a future date or agreeing that the clinician would discuss the results and subsequent actions with the patient at an upcoming visit. Pharmacist interventions also included 25 PDMP queries (42%) and 9 orders of confirmatory UDS on the original urine sample (15%). Only 1 patient was evaluated by the narcotics review committee, which resulted in a controlled substance flag being placed on their profile. No patients were referred to substance use disorder treatment or counseling. It was offered to and declined by 1 patient, and 3 patients were already engaged in these services.
Medication therapies that could contribute to false-positive results were also evaluated. Fourteen patients who tested positive for THC had a prescription for a nonsteroidal anti-inflammatory drug or proton-pump inhibitor, which could have created a false-positive result.6 One patient who tested positive for amphetamines had a prescription for phentermine.16 No other potential false-positive results were identified.
Discussion
Findings of this project illustrate that the use of a clinical pharmacist to monitor a dashboard of discrepant UDS results created opportunities for collaboration with clinicians and impacted confirmatory testing and PDMP monitoring practices.
At the local level, the process had numerous benefits. First, it was a reasonable amount of workload to generate pharmacist interventions: the PMOP coordinator conducted an average of 4 in-depth reviews weekly, each lasting about 14 minutes. Thus, the UDS dashboard allowed the PMOP coordinator to actively surveil all incoming UDS results for potential discrepancies in about 1 hour each week. Pairing the automation of the UDS dashboard with the clinical judgment of the PMOP coordinator seemed to maximize efficiency. VABHHCS provides primary and secondary medical and surgical care to a rural population of approximately 20,000 patients across 5 states; the time required at facilities that serve a higher volume of patients may be greater.
Second, the project served as an opportunity for the PMOP coordinator to provide case-specific clinician education on UDS monitoring. As medication experts, pharmacists can apply their medication-related knowledge to UDS interpretation. This includes understanding drug metabolism and classification and how they apply to UDS results, as well as recognizing medication therapies that could contribute to false-positive UDS results. Research suggests that clinicians may have gaps in their knowledge and may welcome pharmacist assistance in interpreting UDS results.7,8
Third, the project helped improve rates of confirmatory testing for those with unexpected positive UDS results. Confirmatory testing should be strongly considered if positive results would have significant implications on the future course of treatment.4 The PMOP coordinator ordered a confirmatory test on 9 patients using the same urine sample used to conduct the initial UDS, minimizing the burden on the patient and laboratory staff. Confirmatory testing was limited by the laboratory’s sample retention period; if the need for confirmatory testing was not recognized soon enough, the sample would no longer be available for retesting. Health systems may consider the use of reflexive confirmatory testing with UDS as an alternative approach, although this may come at an additional cost and may not be warranted in many cases (eg, only 39.7% of all potential discrepancies were deemed as significant within our project).
There were notable incidental findings in our quality improvement project. Among patients with a significant discrepancy on UDS, 50% had a history of ≥ 1 discrepant UDS result. This further emphasizes the importance of appropriate use and interpretation of UDS monitoring for all clinicians, as this may prevent prolonged and potentially inappropriate treatment regimens. Secondly, rates of mental health diagnoses among those with a significant UDS discrepancy seemed relatively high compared to population-level data. For example, among veterans, the overall lifetime prevalence of posttraumatic stress disorder is estimated to be 8.0%; in our project, 35% of patients with a significant UDS discrepancy had a posttraumatic stress disorder diagnosis.17 This relationship may be an area of further study.
Lastly, it was surprising that the overall rates of UDS and PDMP checks within the past year were 56% and 65%, respectively. VABHHCS requires veterans on controlled substances to have these risk-mitigation strategies performed annually, so our suspicion is that many were falling out due to having been most recently evaluated 12 to 16 months prior. This may represent a limitation of our data-collection method, which reviewed only the previous 12 months.
Limitations
This project was carried out over a period of only 4 months. As a result, only 60 patients received an in-depth review from the PMOP coordinator. Second, the timeliness of the intervention seemed crucial, as delayed in-depth reviews resulted in fewer opportunities to order confirmatory tests or collaborate with clinicians prior to devising an updated plan. Additionally, our process called for UDS dashboard monitoring once a week. Given that the laboratory held samples for only 48 hours, twice- or thrice-weekly review of the UDS dashboard would have allowed for more confirmatory testing, along with more immediate clinician collaboration. Most importantly, the outcomes of this project are only presented via descriptive statistics and without the results of any comparison group, making it impossible to draw firm conclusions about this approach compared to standard-care processes.
Conclusions
This quality improvement project has proven to be valuable at VABHHCS and we intend to continue this pharmacist-led process to monitor the UDS dashboard. VABHHCS leadership are also discussing UDS practices more broadly to further enhance patient management. Within the VA, the PMOP coordinator—charged with being the local coordinator of appropriate pain management and opioid safety practices—is well positioned to assume these responsibilities. Outside of the VA, a pain-management clinical pharmacist or any pharmacist embedded within primary care could similarly perform these duties. Previous literature regarding the implementation of clinical dashboards suggests that with the appropriate software engineering teams and infrastructure, this tool could also be feasibly developed and implemented at other health systems relatively quickly.14
Overall, a pharmacist-led process to efficiently monitor a dashboard of discrepant UDS results led to opportunities for collaboration with clinicians and positively impacted confirmatory testing and PDMP monitoring at a rural VA health system.
Acknowledgments
The authors express their gratitude to Patrick Spoutz, PharmD, BCPS, VISN 20 Pharmacist Executive, for introducing and sharing the UDS dashboard with our team.
Urine drug screen (UDS) monitoring is a common risk-mitigation strategy tool for prescribing controlled substances.1-3 Not only is UDS monitoring highlighted by clinical practice guidelines for opioid prescribing for chronic pain,1,2 it has also been suggested as best practice for benzodiazepines3 and a consideration for other controlled substances. Monitoring UDSs helps confirm adherence to the prescribed treatment regimen while also screening for substance use that may increase patient risk.
UDS results can be complex and have profound implications for the patient’s treatment plan. Drug metabolites for opioids are particularly complicated; for example, synthetic and semisynthetic opioids are not detected on routine opiate immunoassays.4 This may lead a clinician to falsely assume the patient is not taking their fentanyl or tramadol medication as directed—or potentially even diverting—in the face of a negative opiate result.5 Routine UDSs are also subject to the pitfall of false-positive results due to coprescribed medications; for example, bupropion can lead to a false-positive amphetamine result, whereas sertraline can lead to a false-positive benzodiazepine result.6 Retrospective reviews of clinician behavior surrounding UDS interpretation have demonstrated knowledge gaps and inconsistent communication practices with patients.7,8
Given the complexity of UDS interpretation and its close relationship with medications, pharmacists are positioned to play an important role in the process. Pharmacists are embedded in pain-management teams and involved in prescription drug monitoring programs (PDMPs) for many health systems. The Veterans Health Administration (VHA) has supported the hiring of pain management, opioid safety, and PDMP coordinators (PMOP) at its facilities to provide clinical pain-management guidance, support national initiatives, and uphold legislative requirements.9 In many facilities, a pharmacist is hired specifically for these positions.
Clinical dashboards have been used by pharmacists in a variety of settings.10-13 They allow clinicians at a broad level to target interventions needed across a patient population, then produce a list of actionable patients to facilitate delivery of that intervention on an individual level.13 Between 2021 and 2022, a clinical dashboard to review potentially discrepant UDS results was made available for use at US Department of Veterans Affairs (VA) medical centers. Evidence exists in primary and specialty care settings that implementation of an opioid-prescribing clinical dashboard improves completion rates of risk-mitigation strategies such as UDS and opioid treatment agreements.14,15 To our knowledge there is no published research on the use and outcomes of a clinical dashboard that allows users to efficiently review discrepant UDS results when compared to a list of currently prescribed medications.
Given the availability of the UDS dashboard at the VA Black Hills Health Care System (VABHHCS) in South Dakota and the hiring of a PMOP coordinator pharmacist, the aim of this quality improvement project was 2-fold: to implement a pharmacist-led process to monitor the UDS dashboard for potentially discrepant results and to describe the quantity and types of interventions made by the clinical pharmacist leading this process.
Quality Improvement Project
A clinical UDS dashboard was created by the VA Northwest Health Network and made available for use at VHA sites between 2021 and 2022. The UDS dashboard is housed on a secure, Power BI Report Server (Microsoft), with access restricted to only those with patient health data privileges. The dashboard identifies all local patients with a UDS that returned with a potential discrepancy, defined as an unexpected positive result (eg, a detected substance not recently prescribed or documented on the patient’s medication list) and/or an unexpected negative result (eg, a prescribed substance not detected). The UDS dashboard identifies these discrepancies by comparing the patient’s current medication list (both VHA and non-VHA) to their UDS results.
The UDS dashboard displays a summary of UDSs performed, unexpected negative results, unexpected positive results, and potential discrepancies. The user may also specify the laboratory type and time frame of interest to limit displayed results. The user can then view patient-specific data for any category. Among the data are the patient’s UDS results and the completion date, detected (or nondetected) substance(s), ordering clinician, associated medication(s) with last fill date and days’ supply, and whether a confirmatory test has been performed in the past year.
VABHHCS uses an extended UDS immunoassay (PROFILE-V, MEDTOX Diagnostics) that reports on 11 substances: opiates, oxycodone, buprenorphine, methadone, amphetamines, methamphetamine, barbiturates, benzodiazepines, cocaine metabolites, cannabinoids (tetrahydrocannabinol [THC]), and phencyclidine. These substances appear on the UDS dashboard. The project protocol initially included monitoring for tramadol but that was later removed because it was not available with this UDS immunoassay.
Pharmacist Process
Either the PMOP coordinator or pharmacy resident monitored the UDS dashboard weekly. Any patients identified as having a potential discrepancy were reviewed. If the discrepancy was determined to be significant, the PMOP coordinator or pharmacy resident would review the patient electronic health record. If warranted, the patient was contacted and asked about newly prescribed medications, missed and recent medication doses, and illicit substance use. Potential interventions during in-depth review included: (1) discussing future actions with the primary care clinician and/or prescriber of the controlled substance; (2) ordering a confirmatory test on the original urine sample; (3) evaluating for sources of potential false-positive results; (4) completing an updated PDMP if not performed within the past year; (5) referring patients for substance use disorder treatment or counseling; or (6) consulting the local narcotics review committee. A progress note was entered into the electronic health record with the findings and any actions taken, and an alert for the primary care clinician and/or prescriber of the controlled substance.
Implementation and Analysis
This quality improvement project spanned 16 weeks from June 2022 through September 2022. Any patient with a UDS that returned with a significant discrepancy was reviewed. The primary outcome was interventions made by the PMOP coordinator or pharmacy resident, as well as time taken to perform the in-depth review of each patient. Patient demographics were also collected. The protocol for this project was approved by the VABHHCS pharmacy and therapeutics committee and was determined to meet guidelines for a nonresearch quality improvement project.
Results
From June 2022 through September 2022, 700 UDSs were performed at VABHHCS with 278 (39.7%) patients identified as having a potential discrepancy based on UDS results. Sixty patients (8.6%) had significant discrepancies that warranted in-depth review. The most common reasons for determining whether a potential discrepancy was not significant included unexpected negatives due to documented non-VA medications no longer being prescribed, unexpected positives due to recent expiration of a controlled substance prescription the patient was still taking, or unexpected positives due to the detection of a substance for which the clinician was already aware. During the 16-week study period, the mean number of patients warranting in-depth review was 4 per week.
The patients were predominantly male with a mean age of 61 years, and most (87%) were prescribed at least 1 controlled substance (mean, 1.1), primarily opioids for pain management (Table 1). Most patients had recent substance risk mitigation with UDS (56%) and PDMP (65%) checks within the past year. Of the 60 patients reviewed with significant UDS discrepancies, 50% had a history of discrepant UDS results. Of the 60 UDS discrepancies, there were 37 unexpected positive results (62%), 17 unexpected negative results (28%), and 10 patients with both positive and negative results (17%). THC was the most frequently detected substance, followed by opiates, benzodiazepines, and amphetamines (Table 2).
Each in-depth review with interventions by the PMOP coordinator or pharmacy resident lasted a mean of 14 minutes (Table 3). Five patients were successfully contacted for an interview and 7 patients could not be contacted. The ordering clinician of the UDS sometimes had contacted these patients prior to the PMOP coordinator or pharmacy resident reviewing the UDS dashboard, eliminating the need for additional follow-up.
The most common pharmacist intervention was discussing future actions with the primary care clinician and/or prescriber of the controlled substance (n = 39; 65%). These conversations resulted in actions such as ordering a repeat UDS with confirmatory testing at a future date or agreeing that the clinician would discuss the results and subsequent actions with the patient at an upcoming visit. Pharmacist interventions also included 25 PDMP queries (42%) and 9 orders of confirmatory UDS on the original urine sample (15%). Only 1 patient was evaluated by the narcotics review committee, which resulted in a controlled substance flag being placed on their profile. No patients were referred to substance use disorder treatment or counseling. It was offered to and declined by 1 patient, and 3 patients were already engaged in these services.
Medication therapies that could contribute to false-positive results were also evaluated. Fourteen patients who tested positive for THC had a prescription for a nonsteroidal anti-inflammatory drug or proton-pump inhibitor, which could have created a false-positive result.6 One patient who tested positive for amphetamines had a prescription for phentermine.16 No other potential false-positive results were identified.
Discussion
Findings of this project illustrate that the use of a clinical pharmacist to monitor a dashboard of discrepant UDS results created opportunities for collaboration with clinicians and impacted confirmatory testing and PDMP monitoring practices.
At the local level, the process had numerous benefits. First, it was a reasonable amount of workload to generate pharmacist interventions: the PMOP coordinator conducted an average of 4 in-depth reviews weekly, each lasting about 14 minutes. Thus, the UDS dashboard allowed the PMOP coordinator to actively surveil all incoming UDS results for potential discrepancies in about 1 hour each week. Pairing the automation of the UDS dashboard with the clinical judgment of the PMOP coordinator seemed to maximize efficiency. VABHHCS provides primary and secondary medical and surgical care to a rural population of approximately 20,000 patients across 5 states; the time required at facilities that serve a higher volume of patients may be greater.
Second, the project served as an opportunity for the PMOP coordinator to provide case-specific clinician education on UDS monitoring. As medication experts, pharmacists can apply their medication-related knowledge to UDS interpretation. This includes understanding drug metabolism and classification and how they apply to UDS results, as well as recognizing medication therapies that could contribute to false-positive UDS results. Research suggests that clinicians may have gaps in their knowledge and may welcome pharmacist assistance in interpreting UDS results.7,8
Third, the project helped improve rates of confirmatory testing for those with unexpected positive UDS results. Confirmatory testing should be strongly considered if positive results would have significant implications on the future course of treatment.4 The PMOP coordinator ordered a confirmatory test on 9 patients using the same urine sample used to conduct the initial UDS, minimizing the burden on the patient and laboratory staff. Confirmatory testing was limited by the laboratory’s sample retention period; if the need for confirmatory testing was not recognized soon enough, the sample would no longer be available for retesting. Health systems may consider the use of reflexive confirmatory testing with UDS as an alternative approach, although this may come at an additional cost and may not be warranted in many cases (eg, only 39.7% of all potential discrepancies were deemed as significant within our project).
There were notable incidental findings in our quality improvement project. Among patients with a significant discrepancy on UDS, 50% had a history of ≥ 1 discrepant UDS result. This further emphasizes the importance of appropriate use and interpretation of UDS monitoring for all clinicians, as this may prevent prolonged and potentially inappropriate treatment regimens. Secondly, rates of mental health diagnoses among those with a significant UDS discrepancy seemed relatively high compared to population-level data. For example, among veterans, the overall lifetime prevalence of posttraumatic stress disorder is estimated to be 8.0%; in our project, 35% of patients with a significant UDS discrepancy had a posttraumatic stress disorder diagnosis.17 This relationship may be an area of further study.
Lastly, it was surprising that the overall rates of UDS and PDMP checks within the past year were 56% and 65%, respectively. VABHHCS requires veterans on controlled substances to have these risk-mitigation strategies performed annually, so our suspicion is that many were falling out due to having been most recently evaluated 12 to 16 months prior. This may represent a limitation of our data-collection method, which reviewed only the previous 12 months.
Limitations
This project was carried out over a period of only 4 months. As a result, only 60 patients received an in-depth review from the PMOP coordinator. Second, the timeliness of the intervention seemed crucial, as delayed in-depth reviews resulted in fewer opportunities to order confirmatory tests or collaborate with clinicians prior to devising an updated plan. Additionally, our process called for UDS dashboard monitoring once a week. Given that the laboratory held samples for only 48 hours, twice- or thrice-weekly review of the UDS dashboard would have allowed for more confirmatory testing, along with more immediate clinician collaboration. Most importantly, the outcomes of this project are only presented via descriptive statistics and without the results of any comparison group, making it impossible to draw firm conclusions about this approach compared to standard-care processes.
Conclusions
This quality improvement project has proven to be valuable at VABHHCS and we intend to continue this pharmacist-led process to monitor the UDS dashboard. VABHHCS leadership are also discussing UDS practices more broadly to further enhance patient management. Within the VA, the PMOP coordinator—charged with being the local coordinator of appropriate pain management and opioid safety practices—is well positioned to assume these responsibilities. Outside of the VA, a pain-management clinical pharmacist or any pharmacist embedded within primary care could similarly perform these duties. Previous literature regarding the implementation of clinical dashboards suggests that with the appropriate software engineering teams and infrastructure, this tool could also be feasibly developed and implemented at other health systems relatively quickly.14
Overall, a pharmacist-led process to efficiently monitor a dashboard of discrepant UDS results led to opportunities for collaboration with clinicians and positively impacted confirmatory testing and PDMP monitoring at a rural VA health system.
Acknowledgments
The authors express their gratitude to Patrick Spoutz, PharmD, BCPS, VISN 20 Pharmacist Executive, for introducing and sharing the UDS dashboard with our team.
1. Dowell D, Ragan KR, Jones CM, Baldwin GT, Chou R. CDC Clinical Practice Guideline for Prescribing Opioids for Pain - United States, 2022. MMWR Recomm Rep. 2022;71(3):1-95. doi:10.15585/mmwr.rr7103a1
2. US Department of Defense, US Department of Veterans Affairs. VA/DoD clinical practice guidelines for the use of opioids in the management of chronic pain. Version 4.0. Published 2002. Accessed January 22, 2024. https://www.healthquality.va.gov/guidelines/Pain/cot/VADoDOpioidsCPG.pdf
3. Champion C, Kameg BN. Best practices in benzodiazepine prescribing and management in primary care. Nurse Pract. 2021;46(3):30-36.doi:10.1097/01.NPR.0000733684.24949.19
4. Kale N. Urine drug tests: ordering and interpretation. Am Fam Physician. 2019;99(1):33-39.
5. Gillespie E, Cunningham JM, Indovina KA. Interpretation of the urine drug screen. The Hospitalist. May 2, 2022. Accessed January 19, 2024. https://www.the-hospitalist.org/hospitalist/article/32085/interpreting-diagnostic-tests/interpretation-of-the-urine-drug-screen/
6. Schwebach A, Ball J. Urine drug screening: minimizing false-positives and false-negatives to optimize patient care. US Pharm. 2016;41(8):26-30.
7. Starrels JL, Fox AD, Kunins HV, Cunningham CO. They don’t know what they don’t know: internal medicine residents’ knowledge and confidence in urine drug test interpretation for patients with chronic pain. J Gen Intern Med. 2012;27(11):1521-1527. doi:10.1007/s11606-012-2165-7
8. Chua I, Petrides AK, Schiff GD, et al. Provider misinterpretation, documentation, and follow-up of definitive urine drug testing results. J Gen Intern Med. 2020;35(1):283-290. doi:10.1007/s11606-019-05514-5
9. US Department of Veterans Affairs, Veterans Health Administration. VHA Pain Management, Opioid Safety, and Prescription Drug Monitoring Program (PMOP) National Program Field Roles and Responsibilities Manual. October 2021 (V1).[Source not verified]
10. Dorsch MP, Chen CS, Allen AL, et al. Nationwide implementation of a population management dashboard for monitoring direct oral anticoagulants: insights from the Veterans Affairs Health System. Circ Cardiovasc Qual Outcomes. 2023;16(2):e009256. doi:10.1161/CIRCOUTCOMES.122.009256
11. Hu AM, Pepin MJ, Hashem MG, et al. Development of a specialty medication clinical dashboard to improve tumor necrosis factor-α inhibitor safety and adherence monitoring. Am J Health Syst Pharm. 2022;79(8):683-688. doi:10.1093/ajhp/zxab454
12. Homsted FAE, Magee CE, Nesin N. Population health management in a small health system: impact of controlled substance stewardship in a patient-centered medical home. Am J Health Syst Pharm. 2017;74(18):1468-1475. doi:10.2146/ajhp161032
13. US Department of Veterans Affairs, Veterans Health Administration, Pharmacy Benefits (PBM) Services, Clinical Pharmacy Practice Office. Fact Sheet: CPS Role in Population Health Management. 2019. [Source not verified]
14. Anderson D, Zlateva I, Khatri K, Ciaburri N. Using health information technology to improve adherence to opioid prescribing guidelines in primary care. Clin J Pain. 2015;31(6):573-579. doi:10.1097/AJP.0000000000000177
15. Wang EJ, Helgesen R, Johr CR, Lacko HS, Ashburn MA, Merkel PA. Targeted program in an academic rheumatology practice to improve compliance with opioid prescribing guidelines for the treatment of chronic pain. Arthritis Care Res (Hoboken). 2021;73(10):1425-1429. doi:10.1002/acr.24354
16. Moeller KE, Kissack JC, Atayee RS, Lee KC. Clinical interpretation of urine drug tests: what clinicians need to know about urine drug screens. Mayo Clin Proc. 2017;92(5):774-796. doi:10.1016/j.mayocp.2016.12.007
17. Wisco BE, Marx BP, Wolf EJ, Miller MW, Southwick SM, Pietrzak RH. Posttraumatic stress disorder in the US veteran population: results from the National Health and Resilience in Veterans Study. J Clin Psychiatry. 2014;75(12):1338-46. doi:10.4088/JCP.14m09328
1. Dowell D, Ragan KR, Jones CM, Baldwin GT, Chou R. CDC Clinical Practice Guideline for Prescribing Opioids for Pain - United States, 2022. MMWR Recomm Rep. 2022;71(3):1-95. doi:10.15585/mmwr.rr7103a1
2. US Department of Defense, US Department of Veterans Affairs. VA/DoD clinical practice guidelines for the use of opioids in the management of chronic pain. Version 4.0. Published 2002. Accessed January 22, 2024. https://www.healthquality.va.gov/guidelines/Pain/cot/VADoDOpioidsCPG.pdf
3. Champion C, Kameg BN. Best practices in benzodiazepine prescribing and management in primary care. Nurse Pract. 2021;46(3):30-36.doi:10.1097/01.NPR.0000733684.24949.19
4. Kale N. Urine drug tests: ordering and interpretation. Am Fam Physician. 2019;99(1):33-39.
5. Gillespie E, Cunningham JM, Indovina KA. Interpretation of the urine drug screen. The Hospitalist. May 2, 2022. Accessed January 19, 2024. https://www.the-hospitalist.org/hospitalist/article/32085/interpreting-diagnostic-tests/interpretation-of-the-urine-drug-screen/
6. Schwebach A, Ball J. Urine drug screening: minimizing false-positives and false-negatives to optimize patient care. US Pharm. 2016;41(8):26-30.
7. Starrels JL, Fox AD, Kunins HV, Cunningham CO. They don’t know what they don’t know: internal medicine residents’ knowledge and confidence in urine drug test interpretation for patients with chronic pain. J Gen Intern Med. 2012;27(11):1521-1527. doi:10.1007/s11606-012-2165-7
8. Chua I, Petrides AK, Schiff GD, et al. Provider misinterpretation, documentation, and follow-up of definitive urine drug testing results. J Gen Intern Med. 2020;35(1):283-290. doi:10.1007/s11606-019-05514-5
9. US Department of Veterans Affairs, Veterans Health Administration. VHA Pain Management, Opioid Safety, and Prescription Drug Monitoring Program (PMOP) National Program Field Roles and Responsibilities Manual. October 2021 (V1).[Source not verified]
10. Dorsch MP, Chen CS, Allen AL, et al. Nationwide implementation of a population management dashboard for monitoring direct oral anticoagulants: insights from the Veterans Affairs Health System. Circ Cardiovasc Qual Outcomes. 2023;16(2):e009256. doi:10.1161/CIRCOUTCOMES.122.009256
11. Hu AM, Pepin MJ, Hashem MG, et al. Development of a specialty medication clinical dashboard to improve tumor necrosis factor-α inhibitor safety and adherence monitoring. Am J Health Syst Pharm. 2022;79(8):683-688. doi:10.1093/ajhp/zxab454
12. Homsted FAE, Magee CE, Nesin N. Population health management in a small health system: impact of controlled substance stewardship in a patient-centered medical home. Am J Health Syst Pharm. 2017;74(18):1468-1475. doi:10.2146/ajhp161032
13. US Department of Veterans Affairs, Veterans Health Administration, Pharmacy Benefits (PBM) Services, Clinical Pharmacy Practice Office. Fact Sheet: CPS Role in Population Health Management. 2019. [Source not verified]
14. Anderson D, Zlateva I, Khatri K, Ciaburri N. Using health information technology to improve adherence to opioid prescribing guidelines in primary care. Clin J Pain. 2015;31(6):573-579. doi:10.1097/AJP.0000000000000177
15. Wang EJ, Helgesen R, Johr CR, Lacko HS, Ashburn MA, Merkel PA. Targeted program in an academic rheumatology practice to improve compliance with opioid prescribing guidelines for the treatment of chronic pain. Arthritis Care Res (Hoboken). 2021;73(10):1425-1429. doi:10.1002/acr.24354
16. Moeller KE, Kissack JC, Atayee RS, Lee KC. Clinical interpretation of urine drug tests: what clinicians need to know about urine drug screens. Mayo Clin Proc. 2017;92(5):774-796. doi:10.1016/j.mayocp.2016.12.007
17. Wisco BE, Marx BP, Wolf EJ, Miller MW, Southwick SM, Pietrzak RH. Posttraumatic stress disorder in the US veteran population: results from the National Health and Resilience in Veterans Study. J Clin Psychiatry. 2014;75(12):1338-46. doi:10.4088/JCP.14m09328
Medication-Nonadherent Hypothyroidism Requiring Frequent Primary Care Visits to Achieve Euthyroidism
Nonadherence to medications is an issue across health care. In endocrinology, hypothyroidism, a deficiency of thyroid hormones, is most often treated with levothyroxine and if left untreated can lead to myxedema coma, which can lead to death due to multiorgan dysfunction.1 Therefore, adherence to levothyroxine is very important in preventing fatal complications.
We present the case of a patient with persistent primary hypothyroidism who was suspected to be nonadherent to levothyroxine, although the patient consistently claimed adherence. The patient’s plasma thyrotropin (TSH) level improved to reference range after 6 weeks of weekly primary care clinic visits. After stopping the visits, his plasma TSH level increased again, so 9 more weeks of visits resumed, which again helped bring down his plasma TSH levels.
Case Presentation
A male patient aged 67 years presented to the Dayton Veterans Affairs Medical Center (VAMC) endocrinology clinic for evaluation of thyroid nodules. The patient reported no history of neck irradiation and a physical examination was unremarkable. At that time, laboratory results showed a slightly elevated plasma TSH level of 4.35 uIU/mL (reference range, 0.35-4.00 uIU/mL) and normal free thyroxine (T4) of 1.00 ng/dL (reference range, 0.74-1.46 ng/dL). Later that year, the patient underwent a total thyroidectomy at the Cincinnati VAMC for Hurthle cell variant papillary thyroid carcinoma that was noted on biopsy at the Dayton VAMC. After surgical pathology results were available, the patient started levothyroxine 200 mcg daily, although 224 mcg would have been more appropriate based on his 142 kg weight. Due to a history of arrhythmia, the goal plasma TSH level was 0.10 to 0.50 uIU/mL. The patient subsequently underwent radioactive iodine ablation. After levothyroxine dose adjustments, the patient’s plasma TSH level was noted to be within his target range at 0.28 uIU/mL 3 months postablation.
Over the next 5 years the patient had regular laboratory tests during which his plasma TSH level rose and were typically high despite adjusting levothyroxine doses between 200 mcg and 325 mcg. The patient received counseling on taking the medication in the morning on an empty stomach and waiting at least 1 hour before consuming anything, and he went to many follow-up visits at the Dayton VAMC endocrinology clinic. He reported no vomiting or diarrhea but endorsed weight gain once. The patient also had high free T4 at times and did not take extra levothyroxine before undergoing laboratory tests.
Nonadherence to levothyroxine was suspected, but the patient insisted he was adherent. He received the medication in the mail regularly, generally had 90-day refills unless a dose change was made, used a pill box, and had social support from his son, but he did not use a phone alarm to remind him to take it. A home care nurse made weekly visits to make sure the remaining levothyroxine pill counts were correct; however, the patient continued to have difficulty maintaining daily adherence at home as indicated by the nurse’s pill counts not aligning with the number of pills which should have been left if the patient was talking the pills daily.
The patient was asked to visit a local community-based outpatient clinic (CBOC) weekly (to avoid patient travel time to Dayton VAMC > 1 hour) to check pill counts and assess adherence. The patient went to the CBOC clinic for these visits, during which pill counts indicated much better but not 100% adherence. After 6 weeks of clinic visits, his plasma TSH decreased to 1.01 uIU/mL, which was within the reference range, and the patient stopped coming to the weekly clinic visits (Table). Four months later, the patient's plasma TSH levels increased to 80.72 uIU/mL. Nonadherence to levothyroxine was suspected again. He was asked to resume weekly clinic visits, and the life-threatening effects of hypothyroidism and not taking levothyroxine were discussed with the patient and his son. The patient made CBOC clinic visits for 9 weeks, after which his plasma TSH level was low at 0.23 uIU/mL.
Discussion
There are multiple important causes to consider in patients with persistent hypothyroidism. One is medication nonadherence, which was most likely seen in the patient in this case. Missing even 1 day of levothyroxine can affect TSH and thyroid hormone levels for several days due to the long half-life of the medication.2 Hepp and colleagues found that patients with hypothyroidism were significantly more likely to be nonadherent to levothyroxine if they had comorbid conditions such as type 2 diabetes or were obese.3 Another study of levothyroxine adherence found that the most common reason for missing doses was forgetfulness.4 However, memory and cognition impairments can also be symptoms of hypothyroidism itself; Haskard-Zolnierek and colleagues found a significant association between nonadherence to levothyroxine and self-reported brain fog in patients with hypothyroidism.5
Another cause of persistent hypothyroidism is malabsorption. Absorption of levothyroxine can be affected by intestinal malabsorption due to inflammatory bowel disease, lactose intolerance, or gastrointestinal infection, as well as several foods, drinks (eg, coffee), medications, vitamins, and supplements (eg, proton-pump inhibitors and calcium).2,6 Levothyroxine is absorbed mainly at the jejunum and upper ileum, so any pathologies or ingested items that would directly or indirectly affect absorption at those sites can affect levothyroxine absorption.2
A liquid levothyroxine formulation can help with malabsorption.2 Alternatively, weight gain may lead to a need for increasing the dosage of levothyroxine.2,6 Other factors that can affect TSH levels include Addison disease, dysregulation of the hypothalamic-pituitary-thyroid axis, and TSH heterophile antibodies.2
Research describes methods that have effectively treated hypothyroidism in patients struggling with levothyroxine adherence. Two case reports describe weekly visits for levothyroxine administration successfully treating uncontrolled hypothyroidism.7,8 A meta-analysis found that while weekly levothyroxine tablets led to a higher mean TSH level than daily use, weekly use still led to reference-range TSH levels, suggesting that weekly levothyroxine may be a helpful alternative for nonadherent patients.9 Alternatively, patients taking levothyroxine tablets have been shown to forget to take their medication more frequently compared to those taking the liquid formulation.10,11 Additionally, a study by El Helou and colleagues found that adherence to levothyroxine was significantly improved when patients had endocrinology visits once a month and when the endocrinologist provided information about hypothyroidism.12
Another method that may improve adherence to levothyroxine is telehealth visits. This would be especially helpful for patients who live far from the clinic or do not have the time, transportation, or financial means to visit the clinic for weekly visits to assess medication adherence. Additionally, patients may be afraid of admitting to a health care professional that they are nonadherent. Clinicians must be tactful when asking about adherence to make the patient feel comfortable with admitting to nonadherence if their cognition is not impaired. Then, a patient-led conversation can occur regarding realistic ways the patient feels they can work toward adherence.
To our knowledge, the patient in this case report had no symptoms of intestinal malabsorption, and weight gain was not thought to be the issue, as levothyroxine dosage was adjusted multiple times. His plasma TSH levels returned to reference range after weekly pill count visits for 6 weeks and after weekly pill count visits for 9 weeks. Therefore, nonadherence to levothyroxine was suspected to be the cause of frequently elevated plasma TSH levels despite the patient’s insistence on adherence. While the patient did not report memory issues, cognitive impairments due to hypothyroidism may have been contributing to his probable nonadherence. Additionally, he had comorbidities, such as type 2 diabetes mellitus and obesity, which may have made adherence more difficult.
Levothyroxine was also only prescribed in daily tablet form, so the frequency and formulation may have also contributed to nonadherence. While the home nurse was originally sent to assess the patient’s adherence, the care team could have had the nurse start giving the patient weekly levothyroxine once nonadherence was determined to be a likely issue. The patient’s adherence only improved when he went to the clinic for pill counts but not when the home nurse came to his house weekly; this could be because the patient knew he had to invest the time to physically go to clinic visits for pill checks, motivating him to increase adherence.
Conclusions
This case reports a patient with frequently high plasma TSH levels achieving normalization of plasma TSH levels after weekly medication adherence checks at a primary care clinic. Weekly visits to a clinic seem impractical compared to weekly dosing with a visiting nurse; however, after review of the literature, this may be an approach to consider in the future. This strategy may especially help in cases of persistent abnormal plasma TSH levels in which no etiology can be found other than suspected medication nonadherence. Knowing their medication use will be checked at weekly clinic visits may motivate patients to be adherent.
1. Chaker L, Bianco AC, Jonklaas J, Peeters RP. Hypothyroidism. Lancet. 2017;390(10101):1550-1562. doi:10.1016/S0140-6736(17)30703-1
2. Centanni M, Benvenga S, Sachmechi I. Diagnosis and management of treatment-refractory hypothyroidism: an expert consensus report. J Endocrinol Invest. 2017;40(12):1289-1301. doi:10.1007/s40618-017-0706-y
3. Hepp Z, Lage MJ, Espaillat R, Gossain VV. The association between adherence to levothyroxine and economic and clinical outcomes in patients with hypothyroidism in the US. J Med Econ. 2018;21(9):912-919. doi:10.1080/13696998.2018.1484749
4. Shakya Shrestha S, Risal K, Shrestha R, Bhatta RD. Medication Adherence to Levothyroxine Therapy among Hypothyroid Patients and their Clinical Outcomes with Special Reference to Thyroid Function Parameters. Kathmandu Univ Med J (KUMJ). 2018;16(62):129-137.
5. Haskard-Zolnierek K, Wilson C, Pruin J, Deason R, Howard K. The Relationship Between Brain Fog and Medication Adherence for Individuals With Hypothyroidism. Clin Nurs Res. 2022;31(3):445-452. doi:10.1177/10547738211038127
6. McNally LJ, Ofiaeli CI, Oyibo SO. Treatment-refractory hypothyroidism. BMJ. 2019;364:l579. Published 2019 Feb 25. doi:10.1136/bmj.l579
7. Nakano Y, Hashimoto K, Ohkiba N, et al. A Case of Refractory Hypothyroidism due to Poor Compliance Treated with the Weekly Intravenous and Oral Levothyroxine Administration. Case Rep Endocrinol. 2019;2019:5986014. Published 2019 Feb 5. doi:10.1155/2019/5986014
8. Kiran Z, Shaikh KS, Fatima N, Tariq N, Baloch AA. Levothyroxine absorption test followed by directly observed treatment on an outpatient basis to address long-term high TSH levels in a hypothyroid patient: a case report. J Med Case Rep. 2023;17(1):24. Published 2023 Jan 25. doi:10.1186/s13256-023-03760-0
9. Chiu HH, Larrazabal R Jr, Uy AB, Jimeno C. Weekly Versus Daily Levothyroxine Tablet Replacement in Adults with Hypothyroidism: A Meta-Analysis. J ASEAN Fed Endocr Soc. 2021;36(2):156-160. doi:10.15605/jafes.036.02.07
10. Cappelli C, Castello R, Marini F, et al. Adherence to Levothyroxine Treatment Among Patients With Hypothyroidism: A Northeastern Italian Survey. Front Endocrinol (Lausanne). 2018;9:699. Published 2018 Nov 23. doi:10.3389/fendo.2018.00699
11. Bocale R, Desideri G, Barini A, et al. Long-Term Adherence to Levothyroxine Replacement Therapy in Thyroidectomized Patients. J Clin Med. 2022;11(15):4296. Published 2022 Jul 24. doi:10.3390/jcm11154296
12. El Helou S, Hallit S, Awada S, et al. Adherence to levothyroxine among patients with hypothyroidism in Lebanon. East Mediterr Health J. 2019;25(3):149-159. Published 2019 Apr 25. doi:10.26719/emhj.18.022
Nonadherence to medications is an issue across health care. In endocrinology, hypothyroidism, a deficiency of thyroid hormones, is most often treated with levothyroxine and if left untreated can lead to myxedema coma, which can lead to death due to multiorgan dysfunction.1 Therefore, adherence to levothyroxine is very important in preventing fatal complications.
We present the case of a patient with persistent primary hypothyroidism who was suspected to be nonadherent to levothyroxine, although the patient consistently claimed adherence. The patient’s plasma thyrotropin (TSH) level improved to reference range after 6 weeks of weekly primary care clinic visits. After stopping the visits, his plasma TSH level increased again, so 9 more weeks of visits resumed, which again helped bring down his plasma TSH levels.
Case Presentation
A male patient aged 67 years presented to the Dayton Veterans Affairs Medical Center (VAMC) endocrinology clinic for evaluation of thyroid nodules. The patient reported no history of neck irradiation and a physical examination was unremarkable. At that time, laboratory results showed a slightly elevated plasma TSH level of 4.35 uIU/mL (reference range, 0.35-4.00 uIU/mL) and normal free thyroxine (T4) of 1.00 ng/dL (reference range, 0.74-1.46 ng/dL). Later that year, the patient underwent a total thyroidectomy at the Cincinnati VAMC for Hurthle cell variant papillary thyroid carcinoma that was noted on biopsy at the Dayton VAMC. After surgical pathology results were available, the patient started levothyroxine 200 mcg daily, although 224 mcg would have been more appropriate based on his 142 kg weight. Due to a history of arrhythmia, the goal plasma TSH level was 0.10 to 0.50 uIU/mL. The patient subsequently underwent radioactive iodine ablation. After levothyroxine dose adjustments, the patient’s plasma TSH level was noted to be within his target range at 0.28 uIU/mL 3 months postablation.
Over the next 5 years the patient had regular laboratory tests during which his plasma TSH level rose and were typically high despite adjusting levothyroxine doses between 200 mcg and 325 mcg. The patient received counseling on taking the medication in the morning on an empty stomach and waiting at least 1 hour before consuming anything, and he went to many follow-up visits at the Dayton VAMC endocrinology clinic. He reported no vomiting or diarrhea but endorsed weight gain once. The patient also had high free T4 at times and did not take extra levothyroxine before undergoing laboratory tests.
Nonadherence to levothyroxine was suspected, but the patient insisted he was adherent. He received the medication in the mail regularly, generally had 90-day refills unless a dose change was made, used a pill box, and had social support from his son, but he did not use a phone alarm to remind him to take it. A home care nurse made weekly visits to make sure the remaining levothyroxine pill counts were correct; however, the patient continued to have difficulty maintaining daily adherence at home as indicated by the nurse’s pill counts not aligning with the number of pills which should have been left if the patient was talking the pills daily.
The patient was asked to visit a local community-based outpatient clinic (CBOC) weekly (to avoid patient travel time to Dayton VAMC > 1 hour) to check pill counts and assess adherence. The patient went to the CBOC clinic for these visits, during which pill counts indicated much better but not 100% adherence. After 6 weeks of clinic visits, his plasma TSH decreased to 1.01 uIU/mL, which was within the reference range, and the patient stopped coming to the weekly clinic visits (Table). Four months later, the patient's plasma TSH levels increased to 80.72 uIU/mL. Nonadherence to levothyroxine was suspected again. He was asked to resume weekly clinic visits, and the life-threatening effects of hypothyroidism and not taking levothyroxine were discussed with the patient and his son. The patient made CBOC clinic visits for 9 weeks, after which his plasma TSH level was low at 0.23 uIU/mL.
Discussion
There are multiple important causes to consider in patients with persistent hypothyroidism. One is medication nonadherence, which was most likely seen in the patient in this case. Missing even 1 day of levothyroxine can affect TSH and thyroid hormone levels for several days due to the long half-life of the medication.2 Hepp and colleagues found that patients with hypothyroidism were significantly more likely to be nonadherent to levothyroxine if they had comorbid conditions such as type 2 diabetes or were obese.3 Another study of levothyroxine adherence found that the most common reason for missing doses was forgetfulness.4 However, memory and cognition impairments can also be symptoms of hypothyroidism itself; Haskard-Zolnierek and colleagues found a significant association between nonadherence to levothyroxine and self-reported brain fog in patients with hypothyroidism.5
Another cause of persistent hypothyroidism is malabsorption. Absorption of levothyroxine can be affected by intestinal malabsorption due to inflammatory bowel disease, lactose intolerance, or gastrointestinal infection, as well as several foods, drinks (eg, coffee), medications, vitamins, and supplements (eg, proton-pump inhibitors and calcium).2,6 Levothyroxine is absorbed mainly at the jejunum and upper ileum, so any pathologies or ingested items that would directly or indirectly affect absorption at those sites can affect levothyroxine absorption.2
A liquid levothyroxine formulation can help with malabsorption.2 Alternatively, weight gain may lead to a need for increasing the dosage of levothyroxine.2,6 Other factors that can affect TSH levels include Addison disease, dysregulation of the hypothalamic-pituitary-thyroid axis, and TSH heterophile antibodies.2
Research describes methods that have effectively treated hypothyroidism in patients struggling with levothyroxine adherence. Two case reports describe weekly visits for levothyroxine administration successfully treating uncontrolled hypothyroidism.7,8 A meta-analysis found that while weekly levothyroxine tablets led to a higher mean TSH level than daily use, weekly use still led to reference-range TSH levels, suggesting that weekly levothyroxine may be a helpful alternative for nonadherent patients.9 Alternatively, patients taking levothyroxine tablets have been shown to forget to take their medication more frequently compared to those taking the liquid formulation.10,11 Additionally, a study by El Helou and colleagues found that adherence to levothyroxine was significantly improved when patients had endocrinology visits once a month and when the endocrinologist provided information about hypothyroidism.12
Another method that may improve adherence to levothyroxine is telehealth visits. This would be especially helpful for patients who live far from the clinic or do not have the time, transportation, or financial means to visit the clinic for weekly visits to assess medication adherence. Additionally, patients may be afraid of admitting to a health care professional that they are nonadherent. Clinicians must be tactful when asking about adherence to make the patient feel comfortable with admitting to nonadherence if their cognition is not impaired. Then, a patient-led conversation can occur regarding realistic ways the patient feels they can work toward adherence.
To our knowledge, the patient in this case report had no symptoms of intestinal malabsorption, and weight gain was not thought to be the issue, as levothyroxine dosage was adjusted multiple times. His plasma TSH levels returned to reference range after weekly pill count visits for 6 weeks and after weekly pill count visits for 9 weeks. Therefore, nonadherence to levothyroxine was suspected to be the cause of frequently elevated plasma TSH levels despite the patient’s insistence on adherence. While the patient did not report memory issues, cognitive impairments due to hypothyroidism may have been contributing to his probable nonadherence. Additionally, he had comorbidities, such as type 2 diabetes mellitus and obesity, which may have made adherence more difficult.
Levothyroxine was also only prescribed in daily tablet form, so the frequency and formulation may have also contributed to nonadherence. While the home nurse was originally sent to assess the patient’s adherence, the care team could have had the nurse start giving the patient weekly levothyroxine once nonadherence was determined to be a likely issue. The patient’s adherence only improved when he went to the clinic for pill counts but not when the home nurse came to his house weekly; this could be because the patient knew he had to invest the time to physically go to clinic visits for pill checks, motivating him to increase adherence.
Conclusions
This case reports a patient with frequently high plasma TSH levels achieving normalization of plasma TSH levels after weekly medication adherence checks at a primary care clinic. Weekly visits to a clinic seem impractical compared to weekly dosing with a visiting nurse; however, after review of the literature, this may be an approach to consider in the future. This strategy may especially help in cases of persistent abnormal plasma TSH levels in which no etiology can be found other than suspected medication nonadherence. Knowing their medication use will be checked at weekly clinic visits may motivate patients to be adherent.
Nonadherence to medications is an issue across health care. In endocrinology, hypothyroidism, a deficiency of thyroid hormones, is most often treated with levothyroxine and if left untreated can lead to myxedema coma, which can lead to death due to multiorgan dysfunction.1 Therefore, adherence to levothyroxine is very important in preventing fatal complications.
We present the case of a patient with persistent primary hypothyroidism who was suspected to be nonadherent to levothyroxine, although the patient consistently claimed adherence. The patient’s plasma thyrotropin (TSH) level improved to reference range after 6 weeks of weekly primary care clinic visits. After stopping the visits, his plasma TSH level increased again, so 9 more weeks of visits resumed, which again helped bring down his plasma TSH levels.
Case Presentation
A male patient aged 67 years presented to the Dayton Veterans Affairs Medical Center (VAMC) endocrinology clinic for evaluation of thyroid nodules. The patient reported no history of neck irradiation and a physical examination was unremarkable. At that time, laboratory results showed a slightly elevated plasma TSH level of 4.35 uIU/mL (reference range, 0.35-4.00 uIU/mL) and normal free thyroxine (T4) of 1.00 ng/dL (reference range, 0.74-1.46 ng/dL). Later that year, the patient underwent a total thyroidectomy at the Cincinnati VAMC for Hurthle cell variant papillary thyroid carcinoma that was noted on biopsy at the Dayton VAMC. After surgical pathology results were available, the patient started levothyroxine 200 mcg daily, although 224 mcg would have been more appropriate based on his 142 kg weight. Due to a history of arrhythmia, the goal plasma TSH level was 0.10 to 0.50 uIU/mL. The patient subsequently underwent radioactive iodine ablation. After levothyroxine dose adjustments, the patient’s plasma TSH level was noted to be within his target range at 0.28 uIU/mL 3 months postablation.
Over the next 5 years the patient had regular laboratory tests during which his plasma TSH level rose and were typically high despite adjusting levothyroxine doses between 200 mcg and 325 mcg. The patient received counseling on taking the medication in the morning on an empty stomach and waiting at least 1 hour before consuming anything, and he went to many follow-up visits at the Dayton VAMC endocrinology clinic. He reported no vomiting or diarrhea but endorsed weight gain once. The patient also had high free T4 at times and did not take extra levothyroxine before undergoing laboratory tests.
Nonadherence to levothyroxine was suspected, but the patient insisted he was adherent. He received the medication in the mail regularly, generally had 90-day refills unless a dose change was made, used a pill box, and had social support from his son, but he did not use a phone alarm to remind him to take it. A home care nurse made weekly visits to make sure the remaining levothyroxine pill counts were correct; however, the patient continued to have difficulty maintaining daily adherence at home as indicated by the nurse’s pill counts not aligning with the number of pills which should have been left if the patient was talking the pills daily.
The patient was asked to visit a local community-based outpatient clinic (CBOC) weekly (to avoid patient travel time to Dayton VAMC > 1 hour) to check pill counts and assess adherence. The patient went to the CBOC clinic for these visits, during which pill counts indicated much better but not 100% adherence. After 6 weeks of clinic visits, his plasma TSH decreased to 1.01 uIU/mL, which was within the reference range, and the patient stopped coming to the weekly clinic visits (Table). Four months later, the patient's plasma TSH levels increased to 80.72 uIU/mL. Nonadherence to levothyroxine was suspected again. He was asked to resume weekly clinic visits, and the life-threatening effects of hypothyroidism and not taking levothyroxine were discussed with the patient and his son. The patient made CBOC clinic visits for 9 weeks, after which his plasma TSH level was low at 0.23 uIU/mL.
Discussion
There are multiple important causes to consider in patients with persistent hypothyroidism. One is medication nonadherence, which was most likely seen in the patient in this case. Missing even 1 day of levothyroxine can affect TSH and thyroid hormone levels for several days due to the long half-life of the medication.2 Hepp and colleagues found that patients with hypothyroidism were significantly more likely to be nonadherent to levothyroxine if they had comorbid conditions such as type 2 diabetes or were obese.3 Another study of levothyroxine adherence found that the most common reason for missing doses was forgetfulness.4 However, memory and cognition impairments can also be symptoms of hypothyroidism itself; Haskard-Zolnierek and colleagues found a significant association between nonadherence to levothyroxine and self-reported brain fog in patients with hypothyroidism.5
Another cause of persistent hypothyroidism is malabsorption. Absorption of levothyroxine can be affected by intestinal malabsorption due to inflammatory bowel disease, lactose intolerance, or gastrointestinal infection, as well as several foods, drinks (eg, coffee), medications, vitamins, and supplements (eg, proton-pump inhibitors and calcium).2,6 Levothyroxine is absorbed mainly at the jejunum and upper ileum, so any pathologies or ingested items that would directly or indirectly affect absorption at those sites can affect levothyroxine absorption.2
A liquid levothyroxine formulation can help with malabsorption.2 Alternatively, weight gain may lead to a need for increasing the dosage of levothyroxine.2,6 Other factors that can affect TSH levels include Addison disease, dysregulation of the hypothalamic-pituitary-thyroid axis, and TSH heterophile antibodies.2
Research describes methods that have effectively treated hypothyroidism in patients struggling with levothyroxine adherence. Two case reports describe weekly visits for levothyroxine administration successfully treating uncontrolled hypothyroidism.7,8 A meta-analysis found that while weekly levothyroxine tablets led to a higher mean TSH level than daily use, weekly use still led to reference-range TSH levels, suggesting that weekly levothyroxine may be a helpful alternative for nonadherent patients.9 Alternatively, patients taking levothyroxine tablets have been shown to forget to take their medication more frequently compared to those taking the liquid formulation.10,11 Additionally, a study by El Helou and colleagues found that adherence to levothyroxine was significantly improved when patients had endocrinology visits once a month and when the endocrinologist provided information about hypothyroidism.12
Another method that may improve adherence to levothyroxine is telehealth visits. This would be especially helpful for patients who live far from the clinic or do not have the time, transportation, or financial means to visit the clinic for weekly visits to assess medication adherence. Additionally, patients may be afraid of admitting to a health care professional that they are nonadherent. Clinicians must be tactful when asking about adherence to make the patient feel comfortable with admitting to nonadherence if their cognition is not impaired. Then, a patient-led conversation can occur regarding realistic ways the patient feels they can work toward adherence.
To our knowledge, the patient in this case report had no symptoms of intestinal malabsorption, and weight gain was not thought to be the issue, as levothyroxine dosage was adjusted multiple times. His plasma TSH levels returned to reference range after weekly pill count visits for 6 weeks and after weekly pill count visits for 9 weeks. Therefore, nonadherence to levothyroxine was suspected to be the cause of frequently elevated plasma TSH levels despite the patient’s insistence on adherence. While the patient did not report memory issues, cognitive impairments due to hypothyroidism may have been contributing to his probable nonadherence. Additionally, he had comorbidities, such as type 2 diabetes mellitus and obesity, which may have made adherence more difficult.
Levothyroxine was also only prescribed in daily tablet form, so the frequency and formulation may have also contributed to nonadherence. While the home nurse was originally sent to assess the patient’s adherence, the care team could have had the nurse start giving the patient weekly levothyroxine once nonadherence was determined to be a likely issue. The patient’s adherence only improved when he went to the clinic for pill counts but not when the home nurse came to his house weekly; this could be because the patient knew he had to invest the time to physically go to clinic visits for pill checks, motivating him to increase adherence.
Conclusions
This case reports a patient with frequently high plasma TSH levels achieving normalization of plasma TSH levels after weekly medication adherence checks at a primary care clinic. Weekly visits to a clinic seem impractical compared to weekly dosing with a visiting nurse; however, after review of the literature, this may be an approach to consider in the future. This strategy may especially help in cases of persistent abnormal plasma TSH levels in which no etiology can be found other than suspected medication nonadherence. Knowing their medication use will be checked at weekly clinic visits may motivate patients to be adherent.
1. Chaker L, Bianco AC, Jonklaas J, Peeters RP. Hypothyroidism. Lancet. 2017;390(10101):1550-1562. doi:10.1016/S0140-6736(17)30703-1
2. Centanni M, Benvenga S, Sachmechi I. Diagnosis and management of treatment-refractory hypothyroidism: an expert consensus report. J Endocrinol Invest. 2017;40(12):1289-1301. doi:10.1007/s40618-017-0706-y
3. Hepp Z, Lage MJ, Espaillat R, Gossain VV. The association between adherence to levothyroxine and economic and clinical outcomes in patients with hypothyroidism in the US. J Med Econ. 2018;21(9):912-919. doi:10.1080/13696998.2018.1484749
4. Shakya Shrestha S, Risal K, Shrestha R, Bhatta RD. Medication Adherence to Levothyroxine Therapy among Hypothyroid Patients and their Clinical Outcomes with Special Reference to Thyroid Function Parameters. Kathmandu Univ Med J (KUMJ). 2018;16(62):129-137.
5. Haskard-Zolnierek K, Wilson C, Pruin J, Deason R, Howard K. The Relationship Between Brain Fog and Medication Adherence for Individuals With Hypothyroidism. Clin Nurs Res. 2022;31(3):445-452. doi:10.1177/10547738211038127
6. McNally LJ, Ofiaeli CI, Oyibo SO. Treatment-refractory hypothyroidism. BMJ. 2019;364:l579. Published 2019 Feb 25. doi:10.1136/bmj.l579
7. Nakano Y, Hashimoto K, Ohkiba N, et al. A Case of Refractory Hypothyroidism due to Poor Compliance Treated with the Weekly Intravenous and Oral Levothyroxine Administration. Case Rep Endocrinol. 2019;2019:5986014. Published 2019 Feb 5. doi:10.1155/2019/5986014
8. Kiran Z, Shaikh KS, Fatima N, Tariq N, Baloch AA. Levothyroxine absorption test followed by directly observed treatment on an outpatient basis to address long-term high TSH levels in a hypothyroid patient: a case report. J Med Case Rep. 2023;17(1):24. Published 2023 Jan 25. doi:10.1186/s13256-023-03760-0
9. Chiu HH, Larrazabal R Jr, Uy AB, Jimeno C. Weekly Versus Daily Levothyroxine Tablet Replacement in Adults with Hypothyroidism: A Meta-Analysis. J ASEAN Fed Endocr Soc. 2021;36(2):156-160. doi:10.15605/jafes.036.02.07
10. Cappelli C, Castello R, Marini F, et al. Adherence to Levothyroxine Treatment Among Patients With Hypothyroidism: A Northeastern Italian Survey. Front Endocrinol (Lausanne). 2018;9:699. Published 2018 Nov 23. doi:10.3389/fendo.2018.00699
11. Bocale R, Desideri G, Barini A, et al. Long-Term Adherence to Levothyroxine Replacement Therapy in Thyroidectomized Patients. J Clin Med. 2022;11(15):4296. Published 2022 Jul 24. doi:10.3390/jcm11154296
12. El Helou S, Hallit S, Awada S, et al. Adherence to levothyroxine among patients with hypothyroidism in Lebanon. East Mediterr Health J. 2019;25(3):149-159. Published 2019 Apr 25. doi:10.26719/emhj.18.022
1. Chaker L, Bianco AC, Jonklaas J, Peeters RP. Hypothyroidism. Lancet. 2017;390(10101):1550-1562. doi:10.1016/S0140-6736(17)30703-1
2. Centanni M, Benvenga S, Sachmechi I. Diagnosis and management of treatment-refractory hypothyroidism: an expert consensus report. J Endocrinol Invest. 2017;40(12):1289-1301. doi:10.1007/s40618-017-0706-y
3. Hepp Z, Lage MJ, Espaillat R, Gossain VV. The association between adherence to levothyroxine and economic and clinical outcomes in patients with hypothyroidism in the US. J Med Econ. 2018;21(9):912-919. doi:10.1080/13696998.2018.1484749
4. Shakya Shrestha S, Risal K, Shrestha R, Bhatta RD. Medication Adherence to Levothyroxine Therapy among Hypothyroid Patients and their Clinical Outcomes with Special Reference to Thyroid Function Parameters. Kathmandu Univ Med J (KUMJ). 2018;16(62):129-137.
5. Haskard-Zolnierek K, Wilson C, Pruin J, Deason R, Howard K. The Relationship Between Brain Fog and Medication Adherence for Individuals With Hypothyroidism. Clin Nurs Res. 2022;31(3):445-452. doi:10.1177/10547738211038127
6. McNally LJ, Ofiaeli CI, Oyibo SO. Treatment-refractory hypothyroidism. BMJ. 2019;364:l579. Published 2019 Feb 25. doi:10.1136/bmj.l579
7. Nakano Y, Hashimoto K, Ohkiba N, et al. A Case of Refractory Hypothyroidism due to Poor Compliance Treated with the Weekly Intravenous and Oral Levothyroxine Administration. Case Rep Endocrinol. 2019;2019:5986014. Published 2019 Feb 5. doi:10.1155/2019/5986014
8. Kiran Z, Shaikh KS, Fatima N, Tariq N, Baloch AA. Levothyroxine absorption test followed by directly observed treatment on an outpatient basis to address long-term high TSH levels in a hypothyroid patient: a case report. J Med Case Rep. 2023;17(1):24. Published 2023 Jan 25. doi:10.1186/s13256-023-03760-0
9. Chiu HH, Larrazabal R Jr, Uy AB, Jimeno C. Weekly Versus Daily Levothyroxine Tablet Replacement in Adults with Hypothyroidism: A Meta-Analysis. J ASEAN Fed Endocr Soc. 2021;36(2):156-160. doi:10.15605/jafes.036.02.07
10. Cappelli C, Castello R, Marini F, et al. Adherence to Levothyroxine Treatment Among Patients With Hypothyroidism: A Northeastern Italian Survey. Front Endocrinol (Lausanne). 2018;9:699. Published 2018 Nov 23. doi:10.3389/fendo.2018.00699
11. Bocale R, Desideri G, Barini A, et al. Long-Term Adherence to Levothyroxine Replacement Therapy in Thyroidectomized Patients. J Clin Med. 2022;11(15):4296. Published 2022 Jul 24. doi:10.3390/jcm11154296
12. El Helou S, Hallit S, Awada S, et al. Adherence to levothyroxine among patients with hypothyroidism in Lebanon. East Mediterr Health J. 2019;25(3):149-159. Published 2019 Apr 25. doi:10.26719/emhj.18.022
Patient-Reported Outcomes Predict Mortality in Cutaneous Chronic GVHD
. Independent of potential confounders, these PROs moreover predicted non-relapse mortality for all three disease subtypes, making PROs potentially useful adjuncts for risk stratification and treatment decisions, the study authors said.
“These two findings highlight the importance of patient-reported outcomes in measuring this disease,” lead author Emily Baumrin, MD, MSCE, assistant professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, told this news organization. The study was published online February 28 in JAMA Dermatology.
Symptoms and QOL
The investigators monitored 436 patients from the Chronic GVHD Consortium until December 2020. The Lee Symptom Scale (LSS) skin subscale was used to evaluate symptom burden and the Functional Assessment of Cancer Therapy–Bone Marrow Transplantation (FACT-BMT) was used to measure quality of life.
Patients with sclerotic GVHD and combination disease at diagnosis had significantly worse median LSS scores than did those with epidermal disease (25, 35, and 20 points, respectively; P = .01). Patients with sclerotic disease had worse median FACT-BMT scores versus those with epidermal involvement (104 versus 109 points, respectively; P = .08).
Although these scores improved with all skin subtypes, LSS skin subscale and FACT-BMT scores remained significantly worse (by 9.0 points and 6.1 points, respectively) for patients with combination and sclerotic disease versus those with epidermal disease after adjusting for potential confounders.
Regarding mortality, every 7-point worsening (clinically meaningful difference) in FACT-BMT score at diagnosis of skin chronic GVHD conferred 9.1% increases in odds of both all-cause mortality and non-relapse mortality, after adjustment for factors such as age and sex. Likewise, for every 11 points worsening (clinically meaningful difference) in LSS skin subscale scores at diagnosis, researchers observed odds increases of 10% in all-cause mortality and 16.4% in non-relapse mortality.
Because patients with combination disease had only slightly more epidermal body surface area (BSA) involvement but significantly higher symptom burden than the other subtypes, the authors added, combination disease may represent a distinct phenotype. “Since we’ve also shown that the severity of patient-reported outcomes is associated with mortality,” Dr. Baumrin said in the interview, “perhaps these patients are at the highest risk of mortality as well.”
A growing population
Although many might think of chronic GVHD as rare, she noted, the number of allogeneic hematopoietic cell transplant (HCT) survivors living in the United States is growing. In a modeling study published in October of 2013 in Biology of Blood and Marrow Transplantation, authors predicted that by 2030, this figure will reach 502,000 — about half of whom will develop chronic GVHD, she said.
With more HCTs being performed each year and ongoing improvements in supportive care, patients are living longer post transplant. “Therefore, many transplant survivors are being taken care of in the community outside of transplant centers.”
Accordingly, Dr. Baumrin said, study findings are relevant to dermatologists in academic and transplant centers and the community who provide skin cancer screenings or other dermatologic care for transplant recipients. “Upon diagnosis of chronic GVHD, the evaluation of disease burden by patient-reported outcome measures may assist in assessing disease severity and response to treatments over time — and to stratify patients at higher risk for mortality and communicate that back to transplant physicians.”
Incorporating PROs into clinical practice might prove especially helpful for patients with sclerotic chronic cutaneous GVHD. Currently, clinicians assess cutaneous GVHD clinically, using parameters including skin thickness. The National Institutes of Health (NIH) Skin Score, used in clinical trials, also measures BSA.
“The issue with sclerosis is, it’s hard to determine clinical severity based on physical examination alone,” Dr. Baumrin said. It can be difficult to quantify skin thickness and changes over time. “So it’s hard to detect improvements, which are often slow. Patient-reported outcome measures may be a more sensitive way to detect response to treatment than our clinical assessments, which are often crude for sclerotic disease.”
In a secondary analysis of the phase 2 clinical trial of belumosudil, a treatment for chronic GVHD, published in October 2022 in Transplantation and Cellular Therapy, response rate was around 30% measured by NIH Skin Score and 77% by PROs. “Our clinical examination in sclerotic type disease falls short in terms of determining therapeutic benefit. PROs might complement those clinical measures,” she said.
Future research will involve determining and validating which PROs matter most clinically and to patients, added Dr. Baumrin. Although widely used in evaluating transplant patients, LSS skin subscale and FACT-BMT scores may not represent patients’ experience of living with cutaneous chronic GVHD as effectively as might other tools such as the Dermatology Life Quality Index (DLQI) or Patient-Reported Outcomes Measurement Information System (PROMIS) measures, she explained.
Study strengths included authors’ use of well-validated PROs rather than novel unvalidated measures, Sandra A. Mitchell, PhD, CRNP, of the National Cancer Institute, Rockville, Maryland, and Edward W. Cowen, MD, MHSc, of the Dermatology Branch at the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), Bethesda, Maryland, wrote in an accompanying editorial in JAMA Dermatology. However, they added, incorporating causes of death might have revealed that the excess mortality associated with sclerotic disease stemmed at least partly from adverse effects of prolonged immunosuppression, particularly infection.
If future studies establish this to be the case, said Dr. Baumrin, reducing immunosuppression might be warranted for these patients. “And if death is primarily due to chronic GVHD itself, maybe we should treat more aggressively. PROs can help guide this decision.”
The study was supported by the NIH/NIAMS and the University of Pennsylvania. Dr. Baumrin and three coauthors report no relevant financial relationships; other authors had disclosures related to several pharmaceutical companies. Dr. Mitchell and Dr. Cowen had no disclosures.
. Independent of potential confounders, these PROs moreover predicted non-relapse mortality for all three disease subtypes, making PROs potentially useful adjuncts for risk stratification and treatment decisions, the study authors said.
“These two findings highlight the importance of patient-reported outcomes in measuring this disease,” lead author Emily Baumrin, MD, MSCE, assistant professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, told this news organization. The study was published online February 28 in JAMA Dermatology.
Symptoms and QOL
The investigators monitored 436 patients from the Chronic GVHD Consortium until December 2020. The Lee Symptom Scale (LSS) skin subscale was used to evaluate symptom burden and the Functional Assessment of Cancer Therapy–Bone Marrow Transplantation (FACT-BMT) was used to measure quality of life.
Patients with sclerotic GVHD and combination disease at diagnosis had significantly worse median LSS scores than did those with epidermal disease (25, 35, and 20 points, respectively; P = .01). Patients with sclerotic disease had worse median FACT-BMT scores versus those with epidermal involvement (104 versus 109 points, respectively; P = .08).
Although these scores improved with all skin subtypes, LSS skin subscale and FACT-BMT scores remained significantly worse (by 9.0 points and 6.1 points, respectively) for patients with combination and sclerotic disease versus those with epidermal disease after adjusting for potential confounders.
Regarding mortality, every 7-point worsening (clinically meaningful difference) in FACT-BMT score at diagnosis of skin chronic GVHD conferred 9.1% increases in odds of both all-cause mortality and non-relapse mortality, after adjustment for factors such as age and sex. Likewise, for every 11 points worsening (clinically meaningful difference) in LSS skin subscale scores at diagnosis, researchers observed odds increases of 10% in all-cause mortality and 16.4% in non-relapse mortality.
Because patients with combination disease had only slightly more epidermal body surface area (BSA) involvement but significantly higher symptom burden than the other subtypes, the authors added, combination disease may represent a distinct phenotype. “Since we’ve also shown that the severity of patient-reported outcomes is associated with mortality,” Dr. Baumrin said in the interview, “perhaps these patients are at the highest risk of mortality as well.”
A growing population
Although many might think of chronic GVHD as rare, she noted, the number of allogeneic hematopoietic cell transplant (HCT) survivors living in the United States is growing. In a modeling study published in October of 2013 in Biology of Blood and Marrow Transplantation, authors predicted that by 2030, this figure will reach 502,000 — about half of whom will develop chronic GVHD, she said.
With more HCTs being performed each year and ongoing improvements in supportive care, patients are living longer post transplant. “Therefore, many transplant survivors are being taken care of in the community outside of transplant centers.”
Accordingly, Dr. Baumrin said, study findings are relevant to dermatologists in academic and transplant centers and the community who provide skin cancer screenings or other dermatologic care for transplant recipients. “Upon diagnosis of chronic GVHD, the evaluation of disease burden by patient-reported outcome measures may assist in assessing disease severity and response to treatments over time — and to stratify patients at higher risk for mortality and communicate that back to transplant physicians.”
Incorporating PROs into clinical practice might prove especially helpful for patients with sclerotic chronic cutaneous GVHD. Currently, clinicians assess cutaneous GVHD clinically, using parameters including skin thickness. The National Institutes of Health (NIH) Skin Score, used in clinical trials, also measures BSA.
“The issue with sclerosis is, it’s hard to determine clinical severity based on physical examination alone,” Dr. Baumrin said. It can be difficult to quantify skin thickness and changes over time. “So it’s hard to detect improvements, which are often slow. Patient-reported outcome measures may be a more sensitive way to detect response to treatment than our clinical assessments, which are often crude for sclerotic disease.”
In a secondary analysis of the phase 2 clinical trial of belumosudil, a treatment for chronic GVHD, published in October 2022 in Transplantation and Cellular Therapy, response rate was around 30% measured by NIH Skin Score and 77% by PROs. “Our clinical examination in sclerotic type disease falls short in terms of determining therapeutic benefit. PROs might complement those clinical measures,” she said.
Future research will involve determining and validating which PROs matter most clinically and to patients, added Dr. Baumrin. Although widely used in evaluating transplant patients, LSS skin subscale and FACT-BMT scores may not represent patients’ experience of living with cutaneous chronic GVHD as effectively as might other tools such as the Dermatology Life Quality Index (DLQI) or Patient-Reported Outcomes Measurement Information System (PROMIS) measures, she explained.
Study strengths included authors’ use of well-validated PROs rather than novel unvalidated measures, Sandra A. Mitchell, PhD, CRNP, of the National Cancer Institute, Rockville, Maryland, and Edward W. Cowen, MD, MHSc, of the Dermatology Branch at the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), Bethesda, Maryland, wrote in an accompanying editorial in JAMA Dermatology. However, they added, incorporating causes of death might have revealed that the excess mortality associated with sclerotic disease stemmed at least partly from adverse effects of prolonged immunosuppression, particularly infection.
If future studies establish this to be the case, said Dr. Baumrin, reducing immunosuppression might be warranted for these patients. “And if death is primarily due to chronic GVHD itself, maybe we should treat more aggressively. PROs can help guide this decision.”
The study was supported by the NIH/NIAMS and the University of Pennsylvania. Dr. Baumrin and three coauthors report no relevant financial relationships; other authors had disclosures related to several pharmaceutical companies. Dr. Mitchell and Dr. Cowen had no disclosures.
. Independent of potential confounders, these PROs moreover predicted non-relapse mortality for all three disease subtypes, making PROs potentially useful adjuncts for risk stratification and treatment decisions, the study authors said.
“These two findings highlight the importance of patient-reported outcomes in measuring this disease,” lead author Emily Baumrin, MD, MSCE, assistant professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, told this news organization. The study was published online February 28 in JAMA Dermatology.
Symptoms and QOL
The investigators monitored 436 patients from the Chronic GVHD Consortium until December 2020. The Lee Symptom Scale (LSS) skin subscale was used to evaluate symptom burden and the Functional Assessment of Cancer Therapy–Bone Marrow Transplantation (FACT-BMT) was used to measure quality of life.
Patients with sclerotic GVHD and combination disease at diagnosis had significantly worse median LSS scores than did those with epidermal disease (25, 35, and 20 points, respectively; P = .01). Patients with sclerotic disease had worse median FACT-BMT scores versus those with epidermal involvement (104 versus 109 points, respectively; P = .08).
Although these scores improved with all skin subtypes, LSS skin subscale and FACT-BMT scores remained significantly worse (by 9.0 points and 6.1 points, respectively) for patients with combination and sclerotic disease versus those with epidermal disease after adjusting for potential confounders.
Regarding mortality, every 7-point worsening (clinically meaningful difference) in FACT-BMT score at diagnosis of skin chronic GVHD conferred 9.1% increases in odds of both all-cause mortality and non-relapse mortality, after adjustment for factors such as age and sex. Likewise, for every 11 points worsening (clinically meaningful difference) in LSS skin subscale scores at diagnosis, researchers observed odds increases of 10% in all-cause mortality and 16.4% in non-relapse mortality.
Because patients with combination disease had only slightly more epidermal body surface area (BSA) involvement but significantly higher symptom burden than the other subtypes, the authors added, combination disease may represent a distinct phenotype. “Since we’ve also shown that the severity of patient-reported outcomes is associated with mortality,” Dr. Baumrin said in the interview, “perhaps these patients are at the highest risk of mortality as well.”
A growing population
Although many might think of chronic GVHD as rare, she noted, the number of allogeneic hematopoietic cell transplant (HCT) survivors living in the United States is growing. In a modeling study published in October of 2013 in Biology of Blood and Marrow Transplantation, authors predicted that by 2030, this figure will reach 502,000 — about half of whom will develop chronic GVHD, she said.
With more HCTs being performed each year and ongoing improvements in supportive care, patients are living longer post transplant. “Therefore, many transplant survivors are being taken care of in the community outside of transplant centers.”
Accordingly, Dr. Baumrin said, study findings are relevant to dermatologists in academic and transplant centers and the community who provide skin cancer screenings or other dermatologic care for transplant recipients. “Upon diagnosis of chronic GVHD, the evaluation of disease burden by patient-reported outcome measures may assist in assessing disease severity and response to treatments over time — and to stratify patients at higher risk for mortality and communicate that back to transplant physicians.”
Incorporating PROs into clinical practice might prove especially helpful for patients with sclerotic chronic cutaneous GVHD. Currently, clinicians assess cutaneous GVHD clinically, using parameters including skin thickness. The National Institutes of Health (NIH) Skin Score, used in clinical trials, also measures BSA.
“The issue with sclerosis is, it’s hard to determine clinical severity based on physical examination alone,” Dr. Baumrin said. It can be difficult to quantify skin thickness and changes over time. “So it’s hard to detect improvements, which are often slow. Patient-reported outcome measures may be a more sensitive way to detect response to treatment than our clinical assessments, which are often crude for sclerotic disease.”
In a secondary analysis of the phase 2 clinical trial of belumosudil, a treatment for chronic GVHD, published in October 2022 in Transplantation and Cellular Therapy, response rate was around 30% measured by NIH Skin Score and 77% by PROs. “Our clinical examination in sclerotic type disease falls short in terms of determining therapeutic benefit. PROs might complement those clinical measures,” she said.
Future research will involve determining and validating which PROs matter most clinically and to patients, added Dr. Baumrin. Although widely used in evaluating transplant patients, LSS skin subscale and FACT-BMT scores may not represent patients’ experience of living with cutaneous chronic GVHD as effectively as might other tools such as the Dermatology Life Quality Index (DLQI) or Patient-Reported Outcomes Measurement Information System (PROMIS) measures, she explained.
Study strengths included authors’ use of well-validated PROs rather than novel unvalidated measures, Sandra A. Mitchell, PhD, CRNP, of the National Cancer Institute, Rockville, Maryland, and Edward W. Cowen, MD, MHSc, of the Dermatology Branch at the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), Bethesda, Maryland, wrote in an accompanying editorial in JAMA Dermatology. However, they added, incorporating causes of death might have revealed that the excess mortality associated with sclerotic disease stemmed at least partly from adverse effects of prolonged immunosuppression, particularly infection.
If future studies establish this to be the case, said Dr. Baumrin, reducing immunosuppression might be warranted for these patients. “And if death is primarily due to chronic GVHD itself, maybe we should treat more aggressively. PROs can help guide this decision.”
The study was supported by the NIH/NIAMS and the University of Pennsylvania. Dr. Baumrin and three coauthors report no relevant financial relationships; other authors had disclosures related to several pharmaceutical companies. Dr. Mitchell and Dr. Cowen had no disclosures.
FROM JAMA DERMATOLOGY
Bigfoot, Bermuda Triangle, ‘No Lido With Epi’?
“Fingers, toes, ears, and nose are places where epinephrine never goes,” Thomas Ehlers, DPM, wrote in Podiatry Today. “That is an adage I heard during podiatry school, my clerkships, and from various attendings throughout my training.”
But as Dr. Ehlers added, epinephrine gets a bad rap. The catchy admonition “has been proven a myth time and time again.”
So Although medical trainees across multiple disciplines are taught to fear the practice, citing the potential for gangrene, its reputation for harm is not supported by the evidence.
Lack of Feeling Doesn’t Care About Your Facts
The debate surfaced anew in response to a recent column by Kenny Lin, MD, MPH, family physician and associate director of the Lancaster General Hospital Family Medicine Residency, in Lancaster, Pennsylvania, about the rather pedestrian topic of why he no longer performs surgery to correct ingrown toenails. Dr. Lin’s admission that he used to do the procedure with a combination of epinephrine and lidocaine turned into a major focus of the comments — many of them harshly critical of the practice:
“Epinephrine is not an appropriate drug to use for podiatry or use in any peripheral area. Gangrene?” one commenter posted.
“Leave epi out of lidocaine to fingers, toes, nose, and ear lobes,” another wrote.
“No lido with epi, whether or not it is contraindicated, because: If there’s any adverse outcome, a lawyer will find plenty of references saying it was contraindicated,” a reader chimed in.
Other commenters disagreed, with one saying, “Please, folks, don’t show that you trained 50 years ago and haven’t changed practice since…”
For Dr. Lin, the response was surprising given what he believes to be the lack of evidence supporting the purported dangers.
“When I think about this, it’s something that was taught to me during residency — that they should not be used on certain areas,” Dr. Lin said. “But since then, studies have been published looking at thousands of cases of people using epinephrine with lidocaine and haven’t found any cases of necrosis.”
Many doctors, like Dr. Lin, say they were cautioned against this in their training. Others don’t remember exactly where they’ve heard it but recognize the idea has a nebulous hold on practice.
Combining epinephrine with lidocaine helps make the numbing last longer, stops bleeding, and reduces the use of lidocaine required, all of which improve the chances of an effective and comfortable intervention for the patient, Dr. Lin said. The approach also reduces the use of tourniquets, which come with their own risks including nerve injury.
However, in areas with limited circulation, this vasoconstrictive effect may be more pronounced, potentially leading to complications for patients with complicating factors.
Clinicians who regularly use the combination of epinephrine and lidocaine for surgery do concede that it can pose certain hazards and considerations in areas without robust blood flow.
But the literature largely points to its safety.
In 2001, California-based plastic and reconstructive surgeon Keith Denkler, MD, published a deep dive on the topic starting in the 19th century, including a review of Index Medicus from 1880 to 1966, a computer review of the National Library of Medicine database from 1966 to 2000, and major textbooks from 1900 to 2000.
He found a total of 48 cases of digital gangrene — but most involved the use of cocaine or procaine. Of the 48 cases, 21 involved the use of epinephrine, and 17 used an unknown concentration based on manual dilution.
“Multiple other concurrent conditions (hot soaks, tight tourniquets, and infection) existed in these case reports, making it difficult to determine the exact cause of the tissue insult,” Dr. Denkler wrote.
In a 2010 retrospective review in the Journal of the American Society of Plastic Surgeons, authors examined 1111 cases involving digital and hand surgery. Of the 611 patients who received injections of 1% lidocaine with epinephrine, none experienced digital necrosis.
Another review from 2003 touted the combination’s safety, in hopes to “help dispel the myth that epinephrine has no place in podiatric anesthesia.” But authors noted limitations of use, including “known sensitivity, thyrotoxicosis, and use of either tricyclic antidepressants or monoamine oxidase inhibitors.”
James Christina, DPM, executive director and CEO of the American Podiatric Medical Association, echoed that sentiment. He said he regularly used the combination to correct bunions, hammer toes, and ingrown toenails over his 20 years of practicing but acknowledged the technique is not appropriate for all such patients.
“There’s always been caution when using epinephrine with local anesthetic,” Dr. Christina told this news organization. “You need a healthy patient with normal circulation and no other complications; someone without vascular compromise.”
Marie Hanna, MD, MEHP, chief of regional anesthesia and acute pain management at Johns Hopkins University, Baltimore, counts herself among the cautious. Citing Principles of Office Anesthesia: Part I. Infiltrative Anesthesia, Dr. Hanna said epinephrine should never be used in digital and penile blocks or in skin flaps with marginal viability.
“It is perfectly fine in certain areas, like the wrist or the arm,” Dr. Hanna said. “But specifically for use in end organs like nose, fingers, ears, toes — all of these with tenuous blood supply — it is not good practice.”
The divide among doctors comes down to theoretical concern, rather than empirical basis, said Rebecca Johnson, MD, chair of the American Society of Anesthesiologists committee on Regional Anesthesia and Acute Pain Medicine and a faculty member at Mayo Clinic, in Rochester, Minnesota.
“It’s just one of those myths we have in practice,” she said.
And legally, Dr. Johnson noted, the mere existence of a myth can be enough of a deterrent for medical practitioners: “Like anything, when you’re trying to do the right thing, if a complication would occur for another reason, you’d want to make sure a jury of your peers didn’t bring up that myth.”
The sources in this story reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
“Fingers, toes, ears, and nose are places where epinephrine never goes,” Thomas Ehlers, DPM, wrote in Podiatry Today. “That is an adage I heard during podiatry school, my clerkships, and from various attendings throughout my training.”
But as Dr. Ehlers added, epinephrine gets a bad rap. The catchy admonition “has been proven a myth time and time again.”
So Although medical trainees across multiple disciplines are taught to fear the practice, citing the potential for gangrene, its reputation for harm is not supported by the evidence.
Lack of Feeling Doesn’t Care About Your Facts
The debate surfaced anew in response to a recent column by Kenny Lin, MD, MPH, family physician and associate director of the Lancaster General Hospital Family Medicine Residency, in Lancaster, Pennsylvania, about the rather pedestrian topic of why he no longer performs surgery to correct ingrown toenails. Dr. Lin’s admission that he used to do the procedure with a combination of epinephrine and lidocaine turned into a major focus of the comments — many of them harshly critical of the practice:
“Epinephrine is not an appropriate drug to use for podiatry or use in any peripheral area. Gangrene?” one commenter posted.
“Leave epi out of lidocaine to fingers, toes, nose, and ear lobes,” another wrote.
“No lido with epi, whether or not it is contraindicated, because: If there’s any adverse outcome, a lawyer will find plenty of references saying it was contraindicated,” a reader chimed in.
Other commenters disagreed, with one saying, “Please, folks, don’t show that you trained 50 years ago and haven’t changed practice since…”
For Dr. Lin, the response was surprising given what he believes to be the lack of evidence supporting the purported dangers.
“When I think about this, it’s something that was taught to me during residency — that they should not be used on certain areas,” Dr. Lin said. “But since then, studies have been published looking at thousands of cases of people using epinephrine with lidocaine and haven’t found any cases of necrosis.”
Many doctors, like Dr. Lin, say they were cautioned against this in their training. Others don’t remember exactly where they’ve heard it but recognize the idea has a nebulous hold on practice.
Combining epinephrine with lidocaine helps make the numbing last longer, stops bleeding, and reduces the use of lidocaine required, all of which improve the chances of an effective and comfortable intervention for the patient, Dr. Lin said. The approach also reduces the use of tourniquets, which come with their own risks including nerve injury.
However, in areas with limited circulation, this vasoconstrictive effect may be more pronounced, potentially leading to complications for patients with complicating factors.
Clinicians who regularly use the combination of epinephrine and lidocaine for surgery do concede that it can pose certain hazards and considerations in areas without robust blood flow.
But the literature largely points to its safety.
In 2001, California-based plastic and reconstructive surgeon Keith Denkler, MD, published a deep dive on the topic starting in the 19th century, including a review of Index Medicus from 1880 to 1966, a computer review of the National Library of Medicine database from 1966 to 2000, and major textbooks from 1900 to 2000.
He found a total of 48 cases of digital gangrene — but most involved the use of cocaine or procaine. Of the 48 cases, 21 involved the use of epinephrine, and 17 used an unknown concentration based on manual dilution.
“Multiple other concurrent conditions (hot soaks, tight tourniquets, and infection) existed in these case reports, making it difficult to determine the exact cause of the tissue insult,” Dr. Denkler wrote.
In a 2010 retrospective review in the Journal of the American Society of Plastic Surgeons, authors examined 1111 cases involving digital and hand surgery. Of the 611 patients who received injections of 1% lidocaine with epinephrine, none experienced digital necrosis.
Another review from 2003 touted the combination’s safety, in hopes to “help dispel the myth that epinephrine has no place in podiatric anesthesia.” But authors noted limitations of use, including “known sensitivity, thyrotoxicosis, and use of either tricyclic antidepressants or monoamine oxidase inhibitors.”
James Christina, DPM, executive director and CEO of the American Podiatric Medical Association, echoed that sentiment. He said he regularly used the combination to correct bunions, hammer toes, and ingrown toenails over his 20 years of practicing but acknowledged the technique is not appropriate for all such patients.
“There’s always been caution when using epinephrine with local anesthetic,” Dr. Christina told this news organization. “You need a healthy patient with normal circulation and no other complications; someone without vascular compromise.”
Marie Hanna, MD, MEHP, chief of regional anesthesia and acute pain management at Johns Hopkins University, Baltimore, counts herself among the cautious. Citing Principles of Office Anesthesia: Part I. Infiltrative Anesthesia, Dr. Hanna said epinephrine should never be used in digital and penile blocks or in skin flaps with marginal viability.
“It is perfectly fine in certain areas, like the wrist or the arm,” Dr. Hanna said. “But specifically for use in end organs like nose, fingers, ears, toes — all of these with tenuous blood supply — it is not good practice.”
The divide among doctors comes down to theoretical concern, rather than empirical basis, said Rebecca Johnson, MD, chair of the American Society of Anesthesiologists committee on Regional Anesthesia and Acute Pain Medicine and a faculty member at Mayo Clinic, in Rochester, Minnesota.
“It’s just one of those myths we have in practice,” she said.
And legally, Dr. Johnson noted, the mere existence of a myth can be enough of a deterrent for medical practitioners: “Like anything, when you’re trying to do the right thing, if a complication would occur for another reason, you’d want to make sure a jury of your peers didn’t bring up that myth.”
The sources in this story reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
“Fingers, toes, ears, and nose are places where epinephrine never goes,” Thomas Ehlers, DPM, wrote in Podiatry Today. “That is an adage I heard during podiatry school, my clerkships, and from various attendings throughout my training.”
But as Dr. Ehlers added, epinephrine gets a bad rap. The catchy admonition “has been proven a myth time and time again.”
So Although medical trainees across multiple disciplines are taught to fear the practice, citing the potential for gangrene, its reputation for harm is not supported by the evidence.
Lack of Feeling Doesn’t Care About Your Facts
The debate surfaced anew in response to a recent column by Kenny Lin, MD, MPH, family physician and associate director of the Lancaster General Hospital Family Medicine Residency, in Lancaster, Pennsylvania, about the rather pedestrian topic of why he no longer performs surgery to correct ingrown toenails. Dr. Lin’s admission that he used to do the procedure with a combination of epinephrine and lidocaine turned into a major focus of the comments — many of them harshly critical of the practice:
“Epinephrine is not an appropriate drug to use for podiatry or use in any peripheral area. Gangrene?” one commenter posted.
“Leave epi out of lidocaine to fingers, toes, nose, and ear lobes,” another wrote.
“No lido with epi, whether or not it is contraindicated, because: If there’s any adverse outcome, a lawyer will find plenty of references saying it was contraindicated,” a reader chimed in.
Other commenters disagreed, with one saying, “Please, folks, don’t show that you trained 50 years ago and haven’t changed practice since…”
For Dr. Lin, the response was surprising given what he believes to be the lack of evidence supporting the purported dangers.
“When I think about this, it’s something that was taught to me during residency — that they should not be used on certain areas,” Dr. Lin said. “But since then, studies have been published looking at thousands of cases of people using epinephrine with lidocaine and haven’t found any cases of necrosis.”
Many doctors, like Dr. Lin, say they were cautioned against this in their training. Others don’t remember exactly where they’ve heard it but recognize the idea has a nebulous hold on practice.
Combining epinephrine with lidocaine helps make the numbing last longer, stops bleeding, and reduces the use of lidocaine required, all of which improve the chances of an effective and comfortable intervention for the patient, Dr. Lin said. The approach also reduces the use of tourniquets, which come with their own risks including nerve injury.
However, in areas with limited circulation, this vasoconstrictive effect may be more pronounced, potentially leading to complications for patients with complicating factors.
Clinicians who regularly use the combination of epinephrine and lidocaine for surgery do concede that it can pose certain hazards and considerations in areas without robust blood flow.
But the literature largely points to its safety.
In 2001, California-based plastic and reconstructive surgeon Keith Denkler, MD, published a deep dive on the topic starting in the 19th century, including a review of Index Medicus from 1880 to 1966, a computer review of the National Library of Medicine database from 1966 to 2000, and major textbooks from 1900 to 2000.
He found a total of 48 cases of digital gangrene — but most involved the use of cocaine or procaine. Of the 48 cases, 21 involved the use of epinephrine, and 17 used an unknown concentration based on manual dilution.
“Multiple other concurrent conditions (hot soaks, tight tourniquets, and infection) existed in these case reports, making it difficult to determine the exact cause of the tissue insult,” Dr. Denkler wrote.
In a 2010 retrospective review in the Journal of the American Society of Plastic Surgeons, authors examined 1111 cases involving digital and hand surgery. Of the 611 patients who received injections of 1% lidocaine with epinephrine, none experienced digital necrosis.
Another review from 2003 touted the combination’s safety, in hopes to “help dispel the myth that epinephrine has no place in podiatric anesthesia.” But authors noted limitations of use, including “known sensitivity, thyrotoxicosis, and use of either tricyclic antidepressants or monoamine oxidase inhibitors.”
James Christina, DPM, executive director and CEO of the American Podiatric Medical Association, echoed that sentiment. He said he regularly used the combination to correct bunions, hammer toes, and ingrown toenails over his 20 years of practicing but acknowledged the technique is not appropriate for all such patients.
“There’s always been caution when using epinephrine with local anesthetic,” Dr. Christina told this news organization. “You need a healthy patient with normal circulation and no other complications; someone without vascular compromise.”
Marie Hanna, MD, MEHP, chief of regional anesthesia and acute pain management at Johns Hopkins University, Baltimore, counts herself among the cautious. Citing Principles of Office Anesthesia: Part I. Infiltrative Anesthesia, Dr. Hanna said epinephrine should never be used in digital and penile blocks or in skin flaps with marginal viability.
“It is perfectly fine in certain areas, like the wrist or the arm,” Dr. Hanna said. “But specifically for use in end organs like nose, fingers, ears, toes — all of these with tenuous blood supply — it is not good practice.”
The divide among doctors comes down to theoretical concern, rather than empirical basis, said Rebecca Johnson, MD, chair of the American Society of Anesthesiologists committee on Regional Anesthesia and Acute Pain Medicine and a faculty member at Mayo Clinic, in Rochester, Minnesota.
“It’s just one of those myths we have in practice,” she said.
And legally, Dr. Johnson noted, the mere existence of a myth can be enough of a deterrent for medical practitioners: “Like anything, when you’re trying to do the right thing, if a complication would occur for another reason, you’d want to make sure a jury of your peers didn’t bring up that myth.”
The sources in this story reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
Oral Herpes Tied to Double Dementia Risk in Older Adults
TOPLINE:
A history of herpes simplex virus (HSV) is associated with a more than doubling of the risk for dementia in older people, results of a prospective epidemiological study showed.
METHODOLOGY:
- The study included 1002 dementia-free 70-year-olds from the Prospective Investigation of Vasculature in Uppsala Seniors cohort who were assessed at baseline and at age 75 and 80 years and followed through medical records at age 85 years.
- Researchers collected and analyzed blood samples to detect anti-HSV and anti-HSV-1 immunoglobulin (Ig) G, anti-cytomegalovirus (CMV) IgG, anti-HSV IgM, and anti-HSV and anti-CMV IgG levels and apolipoprotein epsilon 4 (APOE 4) status of participants.
- Investigators collected information on anti-herpesvirus drug treatment and reviewed dementia diagnoses obtained from medical records to classify as established or probable dementia or Alzheimer’s disease (AD).
TAKEAWAY:
- 82% of participants were anti-HSV IgG carriers, of which 6% had received drug treatment for herpes virus, and 7% of participants developed all-cause dementia and 4% AD during the median 15-year follow up.
- In HSV and HSV-1 subsamples, treatment for herpes virus was not significantly associated with lower risks for AD (HR, 1.46, P = .532 and HR, 1.64; P = .419, respectively) or dementia (HR 1.70; P = .222 and HR, 1.60; P = .320, respectively).
- There was no significant interaction between anti-HSV IgG seroprevalence and APOE 4 with regard to dementia risk, likely due to underpowering, and there were no associations between anti-CMV IgG positivity or anti-HSV IgM positivity and AD or dementia.
IN PRACTICE:
“What’s special about this particular study is that the participants are roughly the same age, which makes the results even more reliable since age differences, which are otherwise linked to the development of dementia, cannot confuse the results,” lead author Erika Vestin, a medical student in the Department of Public Health and Caring Sciences, Clinical Geriatrics, Uppsala University, Sweden, said in a press release. Findings may drive dementia research further towards treating the illness at an early stage using common anti-herpes virus drugs, Ms. Vestin added.
SOURCE:
The study, with Ms. Vestin as lead author, was published online on February 14, 2024, in the Journal of Alzheimer’s Disease.
LIMITATIONS:
The study underrepresented people with diabetes, heart failure, and stroke and lacked information on treatment compliance, dosage, and length and number of prescriptions, which prevented analysis of dose dependency. Since dementia data collection relied on medical records, dementia cases may be underreported. Some cases of AD could have been misclassified as vascular dementia or other dementia.
DISCLOSURES:
The study was supported by the Gun and Bertil Stohne’s Foundation, Swedish Dementia Association, Swedish Society of Medicine, Märta Lundqvist Foundation, Thureus Foundation, Region Uppsala, Gamla Tjänarinnor Foundation, and Swedish Brain Foundation. The authors had no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
A history of herpes simplex virus (HSV) is associated with a more than doubling of the risk for dementia in older people, results of a prospective epidemiological study showed.
METHODOLOGY:
- The study included 1002 dementia-free 70-year-olds from the Prospective Investigation of Vasculature in Uppsala Seniors cohort who were assessed at baseline and at age 75 and 80 years and followed through medical records at age 85 years.
- Researchers collected and analyzed blood samples to detect anti-HSV and anti-HSV-1 immunoglobulin (Ig) G, anti-cytomegalovirus (CMV) IgG, anti-HSV IgM, and anti-HSV and anti-CMV IgG levels and apolipoprotein epsilon 4 (APOE 4) status of participants.
- Investigators collected information on anti-herpesvirus drug treatment and reviewed dementia diagnoses obtained from medical records to classify as established or probable dementia or Alzheimer’s disease (AD).
TAKEAWAY:
- 82% of participants were anti-HSV IgG carriers, of which 6% had received drug treatment for herpes virus, and 7% of participants developed all-cause dementia and 4% AD during the median 15-year follow up.
- In HSV and HSV-1 subsamples, treatment for herpes virus was not significantly associated with lower risks for AD (HR, 1.46, P = .532 and HR, 1.64; P = .419, respectively) or dementia (HR 1.70; P = .222 and HR, 1.60; P = .320, respectively).
- There was no significant interaction between anti-HSV IgG seroprevalence and APOE 4 with regard to dementia risk, likely due to underpowering, and there were no associations between anti-CMV IgG positivity or anti-HSV IgM positivity and AD or dementia.
IN PRACTICE:
“What’s special about this particular study is that the participants are roughly the same age, which makes the results even more reliable since age differences, which are otherwise linked to the development of dementia, cannot confuse the results,” lead author Erika Vestin, a medical student in the Department of Public Health and Caring Sciences, Clinical Geriatrics, Uppsala University, Sweden, said in a press release. Findings may drive dementia research further towards treating the illness at an early stage using common anti-herpes virus drugs, Ms. Vestin added.
SOURCE:
The study, with Ms. Vestin as lead author, was published online on February 14, 2024, in the Journal of Alzheimer’s Disease.
LIMITATIONS:
The study underrepresented people with diabetes, heart failure, and stroke and lacked information on treatment compliance, dosage, and length and number of prescriptions, which prevented analysis of dose dependency. Since dementia data collection relied on medical records, dementia cases may be underreported. Some cases of AD could have been misclassified as vascular dementia or other dementia.
DISCLOSURES:
The study was supported by the Gun and Bertil Stohne’s Foundation, Swedish Dementia Association, Swedish Society of Medicine, Märta Lundqvist Foundation, Thureus Foundation, Region Uppsala, Gamla Tjänarinnor Foundation, and Swedish Brain Foundation. The authors had no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
A history of herpes simplex virus (HSV) is associated with a more than doubling of the risk for dementia in older people, results of a prospective epidemiological study showed.
METHODOLOGY:
- The study included 1002 dementia-free 70-year-olds from the Prospective Investigation of Vasculature in Uppsala Seniors cohort who were assessed at baseline and at age 75 and 80 years and followed through medical records at age 85 years.
- Researchers collected and analyzed blood samples to detect anti-HSV and anti-HSV-1 immunoglobulin (Ig) G, anti-cytomegalovirus (CMV) IgG, anti-HSV IgM, and anti-HSV and anti-CMV IgG levels and apolipoprotein epsilon 4 (APOE 4) status of participants.
- Investigators collected information on anti-herpesvirus drug treatment and reviewed dementia diagnoses obtained from medical records to classify as established or probable dementia or Alzheimer’s disease (AD).
TAKEAWAY:
- 82% of participants were anti-HSV IgG carriers, of which 6% had received drug treatment for herpes virus, and 7% of participants developed all-cause dementia and 4% AD during the median 15-year follow up.
- In HSV and HSV-1 subsamples, treatment for herpes virus was not significantly associated with lower risks for AD (HR, 1.46, P = .532 and HR, 1.64; P = .419, respectively) or dementia (HR 1.70; P = .222 and HR, 1.60; P = .320, respectively).
- There was no significant interaction between anti-HSV IgG seroprevalence and APOE 4 with regard to dementia risk, likely due to underpowering, and there were no associations between anti-CMV IgG positivity or anti-HSV IgM positivity and AD or dementia.
IN PRACTICE:
“What’s special about this particular study is that the participants are roughly the same age, which makes the results even more reliable since age differences, which are otherwise linked to the development of dementia, cannot confuse the results,” lead author Erika Vestin, a medical student in the Department of Public Health and Caring Sciences, Clinical Geriatrics, Uppsala University, Sweden, said in a press release. Findings may drive dementia research further towards treating the illness at an early stage using common anti-herpes virus drugs, Ms. Vestin added.
SOURCE:
The study, with Ms. Vestin as lead author, was published online on February 14, 2024, in the Journal of Alzheimer’s Disease.
LIMITATIONS:
The study underrepresented people with diabetes, heart failure, and stroke and lacked information on treatment compliance, dosage, and length and number of prescriptions, which prevented analysis of dose dependency. Since dementia data collection relied on medical records, dementia cases may be underreported. Some cases of AD could have been misclassified as vascular dementia or other dementia.
DISCLOSURES:
The study was supported by the Gun and Bertil Stohne’s Foundation, Swedish Dementia Association, Swedish Society of Medicine, Märta Lundqvist Foundation, Thureus Foundation, Region Uppsala, Gamla Tjänarinnor Foundation, and Swedish Brain Foundation. The authors had no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
FDA Removes Harmful Chemicals From Food Packaging
Issued on February 28, 2024, “this means the major source of dietary exposure to PFAS from food packaging like fast-food wrappers, microwave popcorn bags, take-out paperboard containers, and pet food bags is being eliminated,” the FDA said in a statement.
In 2020, the FDA had secured commitments from manufacturers to stop selling products containing PFAS used in the food packaging for grease-proofing. “Today’s announcement marks the fulfillment of these voluntary commitments,” according to the agency.
PFAS, a class of thousands of chemicals also called “forever chemicals” are widely used in consumer and industrial products. People may be exposed via contaminated food packaging (although perhaps no longer in the United States) or occupationally. Studies have found that some PFAS disrupt hormones including estrogen and testosterone, whereas others may impair thyroid function.
Endocrine Society Report Sounds the Alarm About PFAS and Others
The FDA’s announcement came just 2 days after the Endocrine Society issued a new alarm about the human health dangers from environmental EDCs including PFAS in a report covering the latest science.
“Endocrine disrupting chemicals” are individual substances or mixtures that can interfere with natural hormonal function, leading to disease or even death. Many are ubiquitous in the modern environment and contribute to a wide range of human diseases.
The new report Endocrine Disrupting Chemicals: Threats to Human Health was issued jointly with the International Pollutants Elimination Network (IPEN), a global advocacy organization. It’s an update to the Endocrine Society’s 2015 report, providing new data on the endocrine-disrupting substances previously covered and adding four EDCs not discussed in that document: Pesticides, plastics, PFAS, and children’s products containing arsenic.
At a briefing held during the United Nations Environment Assembly meeting in Nairobi, Kenya, last week, the new report’s lead author Andrea C. Gore, PhD, of the University of Texas at Austin, noted, “A well-established body of scientific research indicates that endocrine-disrupting chemicals that are part of our daily lives are making us more susceptible to reproductive disorders, cancer, diabetes, obesity, heart disease, and other serious health conditions.”
Added Dr. Gore, who is also a member of the Endocrine Society’s Board of Directors, “These chemicals pose particularly serious risks to pregnant women and children. Now is the time for the UN Environment Assembly and other global policymakers to take action to address this threat to public health.”
While the science has been emerging rapidly, global and national chemical control policies haven’t kept up, the authors said. Of particular concern is that EDCs behave differently from other chemicals in many ways, including that even very low-dose exposures can pose health threats, but policies thus far haven’t dealt with that aspect.
Moreover, “the effects of low doses cannot be predicted by the effects observed at high doses. This means there may be no safe dose for exposure to EDCs,” according to the report.
Exposures can come from household products, including furniture, toys, and food packages, as well as electronics building materials and cosmetics. These chemicals are also in the outdoor environment, via pesticides, air pollution, and industrial waste.
“IPEN and the Endocrine Society call for chemical regulations based on the most modern scientific understanding of how hormones act and how EDCs can perturb these actions. We work to educate policy makers in global, regional, and national government assemblies and help ensure that regulations correlate with current scientific understanding,” they said in the report.
New Data on Four Classes of EDCs
Chapters of the report summarized the latest information about the science of EDCs and their links to endocrine disease and real-world exposure. It included a special section about “EDCs throughout the plastics life cycle” and a summary of the links between EDCs and climate change.
The report reviewed three pesticides, including the world’s most heavily applied herbicide, glycophosphate. Exposures can occur directly from the air, water, dust, and food residues. Recent data linked glycophosphate to adverse reproductive health outcomes.
Two toxic plastic chemicals, phthalates and bisphenols, are present in personal care products, among others. Emerging evidence links them with impaired neurodevelopment, leading to impaired cognitive function, learning, attention, and impulsivity.
Arsenic has long been linked to human health conditions including cancer, but more recent evidence finds it can disrupt multiple endocrine systems and lead to metabolic conditions including diabetes, reproductive dysfunction, and cardiovascular and neurocognitive conditions.
The special section about plastics noted that they are made from fossil fuels and chemicals, including many toxic substances that are known or suspected EDCs. People who live near plastic production facilities or waste dumps may be at greatest risk, but anyone can be exposed using any plastic product. Plastic waste disposal is increasingly problematic and often foisted on lower- and middle-income countries.
‘Additional Education and Awareness-Raising Among Stakeholders Remain Necessary’
Policies aimed at reducing human health risks from EDCs have included the 2022 Plastics Treaty, a resolution adopted by 175 countries at the United Nations Environmental Assembly that “may be a significant step toward global control of plastics and elimination of threats from exposures to EDCs in plastics,” the report said.
The authors added, “While significant progress has been made in recent years connecting scientific advances on EDCs with health-protective policies, additional education and awareness-raising among stakeholders remain necessary to achieve a safer and more sustainable environment that minimizes exposure to these harmful chemicals.”
The document was produced with financial contributions from the Government of Sweden, the Tides Foundation, Passport Foundation, and other donors.
A version of this article appeared on Medscape.com.
Issued on February 28, 2024, “this means the major source of dietary exposure to PFAS from food packaging like fast-food wrappers, microwave popcorn bags, take-out paperboard containers, and pet food bags is being eliminated,” the FDA said in a statement.
In 2020, the FDA had secured commitments from manufacturers to stop selling products containing PFAS used in the food packaging for grease-proofing. “Today’s announcement marks the fulfillment of these voluntary commitments,” according to the agency.
PFAS, a class of thousands of chemicals also called “forever chemicals” are widely used in consumer and industrial products. People may be exposed via contaminated food packaging (although perhaps no longer in the United States) or occupationally. Studies have found that some PFAS disrupt hormones including estrogen and testosterone, whereas others may impair thyroid function.
Endocrine Society Report Sounds the Alarm About PFAS and Others
The FDA’s announcement came just 2 days after the Endocrine Society issued a new alarm about the human health dangers from environmental EDCs including PFAS in a report covering the latest science.
“Endocrine disrupting chemicals” are individual substances or mixtures that can interfere with natural hormonal function, leading to disease or even death. Many are ubiquitous in the modern environment and contribute to a wide range of human diseases.
The new report Endocrine Disrupting Chemicals: Threats to Human Health was issued jointly with the International Pollutants Elimination Network (IPEN), a global advocacy organization. It’s an update to the Endocrine Society’s 2015 report, providing new data on the endocrine-disrupting substances previously covered and adding four EDCs not discussed in that document: Pesticides, plastics, PFAS, and children’s products containing arsenic.
At a briefing held during the United Nations Environment Assembly meeting in Nairobi, Kenya, last week, the new report’s lead author Andrea C. Gore, PhD, of the University of Texas at Austin, noted, “A well-established body of scientific research indicates that endocrine-disrupting chemicals that are part of our daily lives are making us more susceptible to reproductive disorders, cancer, diabetes, obesity, heart disease, and other serious health conditions.”
Added Dr. Gore, who is also a member of the Endocrine Society’s Board of Directors, “These chemicals pose particularly serious risks to pregnant women and children. Now is the time for the UN Environment Assembly and other global policymakers to take action to address this threat to public health.”
While the science has been emerging rapidly, global and national chemical control policies haven’t kept up, the authors said. Of particular concern is that EDCs behave differently from other chemicals in many ways, including that even very low-dose exposures can pose health threats, but policies thus far haven’t dealt with that aspect.
Moreover, “the effects of low doses cannot be predicted by the effects observed at high doses. This means there may be no safe dose for exposure to EDCs,” according to the report.
Exposures can come from household products, including furniture, toys, and food packages, as well as electronics building materials and cosmetics. These chemicals are also in the outdoor environment, via pesticides, air pollution, and industrial waste.
“IPEN and the Endocrine Society call for chemical regulations based on the most modern scientific understanding of how hormones act and how EDCs can perturb these actions. We work to educate policy makers in global, regional, and national government assemblies and help ensure that regulations correlate with current scientific understanding,” they said in the report.
New Data on Four Classes of EDCs
Chapters of the report summarized the latest information about the science of EDCs and their links to endocrine disease and real-world exposure. It included a special section about “EDCs throughout the plastics life cycle” and a summary of the links between EDCs and climate change.
The report reviewed three pesticides, including the world’s most heavily applied herbicide, glycophosphate. Exposures can occur directly from the air, water, dust, and food residues. Recent data linked glycophosphate to adverse reproductive health outcomes.
Two toxic plastic chemicals, phthalates and bisphenols, are present in personal care products, among others. Emerging evidence links them with impaired neurodevelopment, leading to impaired cognitive function, learning, attention, and impulsivity.
Arsenic has long been linked to human health conditions including cancer, but more recent evidence finds it can disrupt multiple endocrine systems and lead to metabolic conditions including diabetes, reproductive dysfunction, and cardiovascular and neurocognitive conditions.
The special section about plastics noted that they are made from fossil fuels and chemicals, including many toxic substances that are known or suspected EDCs. People who live near plastic production facilities or waste dumps may be at greatest risk, but anyone can be exposed using any plastic product. Plastic waste disposal is increasingly problematic and often foisted on lower- and middle-income countries.
‘Additional Education and Awareness-Raising Among Stakeholders Remain Necessary’
Policies aimed at reducing human health risks from EDCs have included the 2022 Plastics Treaty, a resolution adopted by 175 countries at the United Nations Environmental Assembly that “may be a significant step toward global control of plastics and elimination of threats from exposures to EDCs in plastics,” the report said.
The authors added, “While significant progress has been made in recent years connecting scientific advances on EDCs with health-protective policies, additional education and awareness-raising among stakeholders remain necessary to achieve a safer and more sustainable environment that minimizes exposure to these harmful chemicals.”
The document was produced with financial contributions from the Government of Sweden, the Tides Foundation, Passport Foundation, and other donors.
A version of this article appeared on Medscape.com.
Issued on February 28, 2024, “this means the major source of dietary exposure to PFAS from food packaging like fast-food wrappers, microwave popcorn bags, take-out paperboard containers, and pet food bags is being eliminated,” the FDA said in a statement.
In 2020, the FDA had secured commitments from manufacturers to stop selling products containing PFAS used in the food packaging for grease-proofing. “Today’s announcement marks the fulfillment of these voluntary commitments,” according to the agency.
PFAS, a class of thousands of chemicals also called “forever chemicals” are widely used in consumer and industrial products. People may be exposed via contaminated food packaging (although perhaps no longer in the United States) or occupationally. Studies have found that some PFAS disrupt hormones including estrogen and testosterone, whereas others may impair thyroid function.
Endocrine Society Report Sounds the Alarm About PFAS and Others
The FDA’s announcement came just 2 days after the Endocrine Society issued a new alarm about the human health dangers from environmental EDCs including PFAS in a report covering the latest science.
“Endocrine disrupting chemicals” are individual substances or mixtures that can interfere with natural hormonal function, leading to disease or even death. Many are ubiquitous in the modern environment and contribute to a wide range of human diseases.
The new report Endocrine Disrupting Chemicals: Threats to Human Health was issued jointly with the International Pollutants Elimination Network (IPEN), a global advocacy organization. It’s an update to the Endocrine Society’s 2015 report, providing new data on the endocrine-disrupting substances previously covered and adding four EDCs not discussed in that document: Pesticides, plastics, PFAS, and children’s products containing arsenic.
At a briefing held during the United Nations Environment Assembly meeting in Nairobi, Kenya, last week, the new report’s lead author Andrea C. Gore, PhD, of the University of Texas at Austin, noted, “A well-established body of scientific research indicates that endocrine-disrupting chemicals that are part of our daily lives are making us more susceptible to reproductive disorders, cancer, diabetes, obesity, heart disease, and other serious health conditions.”
Added Dr. Gore, who is also a member of the Endocrine Society’s Board of Directors, “These chemicals pose particularly serious risks to pregnant women and children. Now is the time for the UN Environment Assembly and other global policymakers to take action to address this threat to public health.”
While the science has been emerging rapidly, global and national chemical control policies haven’t kept up, the authors said. Of particular concern is that EDCs behave differently from other chemicals in many ways, including that even very low-dose exposures can pose health threats, but policies thus far haven’t dealt with that aspect.
Moreover, “the effects of low doses cannot be predicted by the effects observed at high doses. This means there may be no safe dose for exposure to EDCs,” according to the report.
Exposures can come from household products, including furniture, toys, and food packages, as well as electronics building materials and cosmetics. These chemicals are also in the outdoor environment, via pesticides, air pollution, and industrial waste.
“IPEN and the Endocrine Society call for chemical regulations based on the most modern scientific understanding of how hormones act and how EDCs can perturb these actions. We work to educate policy makers in global, regional, and national government assemblies and help ensure that regulations correlate with current scientific understanding,” they said in the report.
New Data on Four Classes of EDCs
Chapters of the report summarized the latest information about the science of EDCs and their links to endocrine disease and real-world exposure. It included a special section about “EDCs throughout the plastics life cycle” and a summary of the links between EDCs and climate change.
The report reviewed three pesticides, including the world’s most heavily applied herbicide, glycophosphate. Exposures can occur directly from the air, water, dust, and food residues. Recent data linked glycophosphate to adverse reproductive health outcomes.
Two toxic plastic chemicals, phthalates and bisphenols, are present in personal care products, among others. Emerging evidence links them with impaired neurodevelopment, leading to impaired cognitive function, learning, attention, and impulsivity.
Arsenic has long been linked to human health conditions including cancer, but more recent evidence finds it can disrupt multiple endocrine systems and lead to metabolic conditions including diabetes, reproductive dysfunction, and cardiovascular and neurocognitive conditions.
The special section about plastics noted that they are made from fossil fuels and chemicals, including many toxic substances that are known or suspected EDCs. People who live near plastic production facilities or waste dumps may be at greatest risk, but anyone can be exposed using any plastic product. Plastic waste disposal is increasingly problematic and often foisted on lower- and middle-income countries.
‘Additional Education and Awareness-Raising Among Stakeholders Remain Necessary’
Policies aimed at reducing human health risks from EDCs have included the 2022 Plastics Treaty, a resolution adopted by 175 countries at the United Nations Environmental Assembly that “may be a significant step toward global control of plastics and elimination of threats from exposures to EDCs in plastics,” the report said.
The authors added, “While significant progress has been made in recent years connecting scientific advances on EDCs with health-protective policies, additional education and awareness-raising among stakeholders remain necessary to achieve a safer and more sustainable environment that minimizes exposure to these harmful chemicals.”
The document was produced with financial contributions from the Government of Sweden, the Tides Foundation, Passport Foundation, and other donors.
A version of this article appeared on Medscape.com.
Shining a Light on Colorectal Cancer
For more than two decades, March has been designated Colorectal Cancer Awareness Month. This annual observance serves as a reminder to spread the word in our local and national communities regarding the value of colorectal cancer screening and prevention. CRC prevention through screening and surveillance is a core part of our practice as gastroenterologists and plays a critical role in improving outcomes and reducing mortality from the second leading cause of cancer deaths in the US.
While we have made great strides in increasing awareness among patients of the need for screening, overall screening rates remain well below our national target of 80% and significant disparities in screening persist. By disseminating key information about risk factors, promoting early detection through evidence-based screening, continuing to improve access to care by reducing financial and other barriers, and educating patients about available screening options that best fit their needs and preferences, we can continue to move the needle in improving overall screening rates and optimizing outcomes.
In this month’s issue of GIHN, we feature an excellent narrative review by Dr. Samir Gupta and colleagues describing the phenomenon of “birth cohort CRC,” which is thought to explain recent changes in CRC epidemiology, including rising incidence of early-onset colorectal cancer. We also highlight a timely study out of Kaiser Permanente investigating how best to communicate with patients with prior low-risk adenomas regarding updated colonoscopy intervals given recent guideline changes extending surveillance intervals from 5 to 7-10 years. This question is particularly relevant to resource-constrained healthcare settings, where proactive de-implementation of outdated surveillance intervals could improve access for other patients with more immediate need.
In our March Member Spotlight, we feature Dr. Andy Tau of Austin Gastroenterology, who shares important insights regarding his career as a GI hospitalist, a growing area of GI practice. Finally, in this month’s Perspectives column, Drs. Michael Weinstein of Capital Digestive Care and Paul Berggreen of GI Alliance provide powerful contrasting perspectives highlighting the pros and cons of private equity in GI and how to evaluate if it’s right for your practice. I found it to be a particularly fascinating read!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
For more than two decades, March has been designated Colorectal Cancer Awareness Month. This annual observance serves as a reminder to spread the word in our local and national communities regarding the value of colorectal cancer screening and prevention. CRC prevention through screening and surveillance is a core part of our practice as gastroenterologists and plays a critical role in improving outcomes and reducing mortality from the second leading cause of cancer deaths in the US.
While we have made great strides in increasing awareness among patients of the need for screening, overall screening rates remain well below our national target of 80% and significant disparities in screening persist. By disseminating key information about risk factors, promoting early detection through evidence-based screening, continuing to improve access to care by reducing financial and other barriers, and educating patients about available screening options that best fit their needs and preferences, we can continue to move the needle in improving overall screening rates and optimizing outcomes.
In this month’s issue of GIHN, we feature an excellent narrative review by Dr. Samir Gupta and colleagues describing the phenomenon of “birth cohort CRC,” which is thought to explain recent changes in CRC epidemiology, including rising incidence of early-onset colorectal cancer. We also highlight a timely study out of Kaiser Permanente investigating how best to communicate with patients with prior low-risk adenomas regarding updated colonoscopy intervals given recent guideline changes extending surveillance intervals from 5 to 7-10 years. This question is particularly relevant to resource-constrained healthcare settings, where proactive de-implementation of outdated surveillance intervals could improve access for other patients with more immediate need.
In our March Member Spotlight, we feature Dr. Andy Tau of Austin Gastroenterology, who shares important insights regarding his career as a GI hospitalist, a growing area of GI practice. Finally, in this month’s Perspectives column, Drs. Michael Weinstein of Capital Digestive Care and Paul Berggreen of GI Alliance provide powerful contrasting perspectives highlighting the pros and cons of private equity in GI and how to evaluate if it’s right for your practice. I found it to be a particularly fascinating read!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
For more than two decades, March has been designated Colorectal Cancer Awareness Month. This annual observance serves as a reminder to spread the word in our local and national communities regarding the value of colorectal cancer screening and prevention. CRC prevention through screening and surveillance is a core part of our practice as gastroenterologists and plays a critical role in improving outcomes and reducing mortality from the second leading cause of cancer deaths in the US.
While we have made great strides in increasing awareness among patients of the need for screening, overall screening rates remain well below our national target of 80% and significant disparities in screening persist. By disseminating key information about risk factors, promoting early detection through evidence-based screening, continuing to improve access to care by reducing financial and other barriers, and educating patients about available screening options that best fit their needs and preferences, we can continue to move the needle in improving overall screening rates and optimizing outcomes.
In this month’s issue of GIHN, we feature an excellent narrative review by Dr. Samir Gupta and colleagues describing the phenomenon of “birth cohort CRC,” which is thought to explain recent changes in CRC epidemiology, including rising incidence of early-onset colorectal cancer. We also highlight a timely study out of Kaiser Permanente investigating how best to communicate with patients with prior low-risk adenomas regarding updated colonoscopy intervals given recent guideline changes extending surveillance intervals from 5 to 7-10 years. This question is particularly relevant to resource-constrained healthcare settings, where proactive de-implementation of outdated surveillance intervals could improve access for other patients with more immediate need.
In our March Member Spotlight, we feature Dr. Andy Tau of Austin Gastroenterology, who shares important insights regarding his career as a GI hospitalist, a growing area of GI practice. Finally, in this month’s Perspectives column, Drs. Michael Weinstein of Capital Digestive Care and Paul Berggreen of GI Alliance provide powerful contrasting perspectives highlighting the pros and cons of private equity in GI and how to evaluate if it’s right for your practice. I found it to be a particularly fascinating read!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
‘There’s Nothing Left to Try’: Oncologists on Managing Grief
Dr. Lewis was well acquainted with cancer grief long before he became an oncologist. Dr. Lewis’ father died of a rare, hereditary cancer syndrome when he was only 14. The condition, which causes tumors to grow in the endocrine glands, can be hard to identify and, if found late, deadly.
In some ways, Dr. Lewis’ career caring for patients with advanced cancers was born out of that first loss. He centered his practice around helping patients diagnosed at late stages, like his father.
But that comes at a cost. Many patients will die.
Dr. Lewis’ encounter with his colleague led him to inventory his practice. He found that well over half of his patients died within 2 years following their advanced cancer diagnosis.
To stave off the grief of so many losses, Dr. Lewis became an eternal optimist in the clinic, in search of the Hail Mary chemotherapy, any way to eke out a few more months only to be ambushed by grief when a patient did finally pass.
At funerals — which he made every effort to attend — Dr. Lewis couldn’t help but think, “If I had done my job better, none of us with be here.” His grief started to mingle with this sense of guilt.
It became a cycle: Denial shrouded in optimism, grief, then a toxic guilt. The pattern became untenable for his colleagues. And his partner finally called him out.
Few medical specialties draw physicians as close to their patients as oncology. The long courses of treatment-spanning years can foster an intimacy that is comforting for patients and fulfilling for physicians. But that closeness can also set doctors up for an acute grief when the end of life comes.
Experts agree that no amount of training in medical school prepares an oncologist to navigate the grief that comes with losing patients. Five oncologists spoke with this news organization about the boundaries they rely on to sustain their careers.
Don’t Go to Funerals
Don Dizon, MD, who specializes in women’s cancers, established an essential boundary 20 years ago: Never go to funerals. In his early days at Memorial Sloan Kettering Cancer Center, the death of each patient dealt him a crushing blow. He’d go to the funerals in search of closure, but that only added to the weight of his grief.
“When I started in oncology, I just remember the most tragic cases were the ones I was taking care of,” recalled Dr. Dizon, now director of the Pelvic Malignancies Program at Lifespan Cancer Institute in Lincoln, Rhode Island.
Dr. Dizon recalled one young mother who was diagnosed with ovarian cancer. She responded to treatment, but it was short-lived, and her cancer progressed, he said. Multiple treatments followed, but none were effective. Eventually, Dr. Dizon had to tell her that “there’s nothing left to try.”
At her funeral, watching her grieving husband with their daughter who had just started to walk, Dr. Dizon was overwhelmed with despair.
“When you have to do this multiple times a year,” the grief becomes untenable, he said. Sensing the difficulty I was having as a new attending, “my boss stopped sending me patients because he knew I was in trouble emotionally.”
That’s when Dr. Dizon started looking for other ways to get closure.
Today, he tries to say his goodbyes before a patient dies. After the final treatment or before hospice, Dr. Dizon has a parting conversation with his patients to express the privilege of caring for them and all he learned from them. These talks help him and his patient connect in their last moments together.
The Price of Wildly Happy Days
Molly Taylor, MD, MS, a pediatric oncologist in Seattle, sees the deeply sad days as the price an oncologist pays to be witness to the “wildly happy ones.”
Dr. Taylor has gone to patients’ funerals, has even been asked to speak at them, but she has also attended patients’ weddings.
To some degree, doctors get good at compartmentalizing, and they become accustomed to tragedy, she said. But there are some patients who stick with you, “and that is a whole other level of grief,” Dr. Taylor said.
Several years into her practice, one of Dr. Taylor’s patients, someone who reminded her of her own child, died. The death came as a surprise, and the finality of it took her breath away, she said. The sadness only deepened as days went by. “I felt that mother’s grief and still do,” she said.
The patient’s funeral was one of the most difficult moments in her career as an oncologist. Even weeks later, she caught herself picturing the family huddled together that day.
Taking long walks, commiserating with colleagues who get it, and watching the occasional cat video can help take the immediate sting away. But the pain of losing a patient can be long lasting and processing that grief can be a lonely endeavor.
“We need space to recognize grief for all providers, all the people that touch these patients’ lives — the nurses, the translators, the cleaning staff,” Dr. Taylor said. Otherwise, you start to believe you’re the only one feeling the weight of the loss.
While it doesn’t make the losses any less poignant, Dr. Taylor finds solace in the good moments: Patient graduations and weddings, survivors who now volunteer at the hospital, and a patient who had a baby of her own this past year. If facing grief daily has taught Dr. Taylor anything, it is to not let the good moments pass unnoticed.
Towing the Line
Ten years ago, Tina Rizack, MD, walked into the ICU to see a young mother holding her 6-year-old daughter. The mother had necrotizing fasciitis that had gone undiagnosed.
As Dr. Rizack stood in the doorway watching the embrace, she saw a grim future: A child without her mother. This realization hit too close to home, she said. “I still think about that case.”
In her training, Dr. Rizack, now medical director of hematology/oncology at St. Anne’s in Fall River, Massachusetts, worked with a social worker who taught her how to deal with these tough cases — most importantly, how to not take them home with her.
Over the years, Dr. Rizack learned how to build and sustain a firm barrier between work and outside work.
She doesn’t go to funerals or give out her cell phone number. If charts need to be done, she prefers to stay late at the clinic instead of bringing them home.
And she invests in the simple moments that help her detach from the day-to-day in the clinic — rooting for her kids at their games, carving out time for family meals most days, and having relaxed movie nights on the couch.
“It’s hard sometimes,” she said. But “I really do need the line.” Because without it, she can’t show up for her patients the way she wants and needs to.
Establishing the work-life boundary means that when at work, Dr. Rizack can be all in for her patients. Even after her patients’ treatment ends, she makes sure to check on them at home or in hospice. For her, sticking with patients over the long term offers some closure.
“I want to love work, and if I’m there all the time, I’m not going to love it,” she said.
Trading Funerals for the Bedside
Like many other oncologists, Charles Blanke, MD, finds that going to patients’ funerals makes the loss seem more profound. Being at the bedside when they die is not as painful, he said. In fact, being there when his patients die offers him some comfort. He rarely misses a patient’s death because now Dr. Blanke’s patients can schedule their departure.
An oncologist at the Knight Cancer Institute in Portland, Oregon, Dr. Blanke specializes in end-of-life care with an emphasis on death with dignity, also known as medical aid in dying. He admits it’s not a role every physician is comfortable with.
“If you’re paralyzed by grief, you can’t do this for a living,” he said. But he’s able to do the work because he genuinely feels he’s helping patients get “the relief they so strongly desire” in their last moments.
When cancer care can’t give them the life they wanted, he can give them control over when and how they die. And the ability to honor their last wishes offers him some closure as well.
“You know what kind of end they have. You know it was peaceful. You see them achieve the thing that was the most important to them,” he said.
Despite this process, he still encounters some circumstances utterly heart-wrenching — the very young patients who have advanced disease. Some of these patients choose to die because they can’t afford to continue treatment. Others don’t have a support system. In these instances, Dr. Blanke is often the only one in the room.
Believe it or not, he said, the paperwork — and there’s a lot of it in his line of work — helps remind Dr. Blanke that patients’ last wishes are being honored.
Making Changes
After Dr. Lewis was confronted by his partner, he began to face the shortcomings of his own coping strategies. His practice hired a social worker to help staff process difficult experiences. After the loss of every patient, the practice comes together to share and process the loss.
For him, funerals remain helpful, providing a sort of solace, so he continues to go when he can. But how to grieve is something each doctor has to figure out, he said.
Deaths still hit hard, especially the ones he doesn’t see coming. The patients who remind him of his dad can also be hard. They restart a cycle of grief from his teenage years.
The difference now is he has space to voice those concerns and someone objective to help his process.
“It’s a privilege to prepare [patients for death] and help them build their legacy,” he said. But it’s also an unrelenting challenge to navigate that grief, he said.
Still, the grief lets Dr. Lewis know he’s still engaged.
“The day I don’t feel something is probably the day I need to take a break or walk away.”
A version of this article appeared on Medscape.com.
Dr. Lewis was well acquainted with cancer grief long before he became an oncologist. Dr. Lewis’ father died of a rare, hereditary cancer syndrome when he was only 14. The condition, which causes tumors to grow in the endocrine glands, can be hard to identify and, if found late, deadly.
In some ways, Dr. Lewis’ career caring for patients with advanced cancers was born out of that first loss. He centered his practice around helping patients diagnosed at late stages, like his father.
But that comes at a cost. Many patients will die.
Dr. Lewis’ encounter with his colleague led him to inventory his practice. He found that well over half of his patients died within 2 years following their advanced cancer diagnosis.
To stave off the grief of so many losses, Dr. Lewis became an eternal optimist in the clinic, in search of the Hail Mary chemotherapy, any way to eke out a few more months only to be ambushed by grief when a patient did finally pass.
At funerals — which he made every effort to attend — Dr. Lewis couldn’t help but think, “If I had done my job better, none of us with be here.” His grief started to mingle with this sense of guilt.
It became a cycle: Denial shrouded in optimism, grief, then a toxic guilt. The pattern became untenable for his colleagues. And his partner finally called him out.
Few medical specialties draw physicians as close to their patients as oncology. The long courses of treatment-spanning years can foster an intimacy that is comforting for patients and fulfilling for physicians. But that closeness can also set doctors up for an acute grief when the end of life comes.
Experts agree that no amount of training in medical school prepares an oncologist to navigate the grief that comes with losing patients. Five oncologists spoke with this news organization about the boundaries they rely on to sustain their careers.
Don’t Go to Funerals
Don Dizon, MD, who specializes in women’s cancers, established an essential boundary 20 years ago: Never go to funerals. In his early days at Memorial Sloan Kettering Cancer Center, the death of each patient dealt him a crushing blow. He’d go to the funerals in search of closure, but that only added to the weight of his grief.
“When I started in oncology, I just remember the most tragic cases were the ones I was taking care of,” recalled Dr. Dizon, now director of the Pelvic Malignancies Program at Lifespan Cancer Institute in Lincoln, Rhode Island.
Dr. Dizon recalled one young mother who was diagnosed with ovarian cancer. She responded to treatment, but it was short-lived, and her cancer progressed, he said. Multiple treatments followed, but none were effective. Eventually, Dr. Dizon had to tell her that “there’s nothing left to try.”
At her funeral, watching her grieving husband with their daughter who had just started to walk, Dr. Dizon was overwhelmed with despair.
“When you have to do this multiple times a year,” the grief becomes untenable, he said. Sensing the difficulty I was having as a new attending, “my boss stopped sending me patients because he knew I was in trouble emotionally.”
That’s when Dr. Dizon started looking for other ways to get closure.
Today, he tries to say his goodbyes before a patient dies. After the final treatment or before hospice, Dr. Dizon has a parting conversation with his patients to express the privilege of caring for them and all he learned from them. These talks help him and his patient connect in their last moments together.
The Price of Wildly Happy Days
Molly Taylor, MD, MS, a pediatric oncologist in Seattle, sees the deeply sad days as the price an oncologist pays to be witness to the “wildly happy ones.”
Dr. Taylor has gone to patients’ funerals, has even been asked to speak at them, but she has also attended patients’ weddings.
To some degree, doctors get good at compartmentalizing, and they become accustomed to tragedy, she said. But there are some patients who stick with you, “and that is a whole other level of grief,” Dr. Taylor said.
Several years into her practice, one of Dr. Taylor’s patients, someone who reminded her of her own child, died. The death came as a surprise, and the finality of it took her breath away, she said. The sadness only deepened as days went by. “I felt that mother’s grief and still do,” she said.
The patient’s funeral was one of the most difficult moments in her career as an oncologist. Even weeks later, she caught herself picturing the family huddled together that day.
Taking long walks, commiserating with colleagues who get it, and watching the occasional cat video can help take the immediate sting away. But the pain of losing a patient can be long lasting and processing that grief can be a lonely endeavor.
“We need space to recognize grief for all providers, all the people that touch these patients’ lives — the nurses, the translators, the cleaning staff,” Dr. Taylor said. Otherwise, you start to believe you’re the only one feeling the weight of the loss.
While it doesn’t make the losses any less poignant, Dr. Taylor finds solace in the good moments: Patient graduations and weddings, survivors who now volunteer at the hospital, and a patient who had a baby of her own this past year. If facing grief daily has taught Dr. Taylor anything, it is to not let the good moments pass unnoticed.
Towing the Line
Ten years ago, Tina Rizack, MD, walked into the ICU to see a young mother holding her 6-year-old daughter. The mother had necrotizing fasciitis that had gone undiagnosed.
As Dr. Rizack stood in the doorway watching the embrace, she saw a grim future: A child without her mother. This realization hit too close to home, she said. “I still think about that case.”
In her training, Dr. Rizack, now medical director of hematology/oncology at St. Anne’s in Fall River, Massachusetts, worked with a social worker who taught her how to deal with these tough cases — most importantly, how to not take them home with her.
Over the years, Dr. Rizack learned how to build and sustain a firm barrier between work and outside work.
She doesn’t go to funerals or give out her cell phone number. If charts need to be done, she prefers to stay late at the clinic instead of bringing them home.
And she invests in the simple moments that help her detach from the day-to-day in the clinic — rooting for her kids at their games, carving out time for family meals most days, and having relaxed movie nights on the couch.
“It’s hard sometimes,” she said. But “I really do need the line.” Because without it, she can’t show up for her patients the way she wants and needs to.
Establishing the work-life boundary means that when at work, Dr. Rizack can be all in for her patients. Even after her patients’ treatment ends, she makes sure to check on them at home or in hospice. For her, sticking with patients over the long term offers some closure.
“I want to love work, and if I’m there all the time, I’m not going to love it,” she said.
Trading Funerals for the Bedside
Like many other oncologists, Charles Blanke, MD, finds that going to patients’ funerals makes the loss seem more profound. Being at the bedside when they die is not as painful, he said. In fact, being there when his patients die offers him some comfort. He rarely misses a patient’s death because now Dr. Blanke’s patients can schedule their departure.
An oncologist at the Knight Cancer Institute in Portland, Oregon, Dr. Blanke specializes in end-of-life care with an emphasis on death with dignity, also known as medical aid in dying. He admits it’s not a role every physician is comfortable with.
“If you’re paralyzed by grief, you can’t do this for a living,” he said. But he’s able to do the work because he genuinely feels he’s helping patients get “the relief they so strongly desire” in their last moments.
When cancer care can’t give them the life they wanted, he can give them control over when and how they die. And the ability to honor their last wishes offers him some closure as well.
“You know what kind of end they have. You know it was peaceful. You see them achieve the thing that was the most important to them,” he said.
Despite this process, he still encounters some circumstances utterly heart-wrenching — the very young patients who have advanced disease. Some of these patients choose to die because they can’t afford to continue treatment. Others don’t have a support system. In these instances, Dr. Blanke is often the only one in the room.
Believe it or not, he said, the paperwork — and there’s a lot of it in his line of work — helps remind Dr. Blanke that patients’ last wishes are being honored.
Making Changes
After Dr. Lewis was confronted by his partner, he began to face the shortcomings of his own coping strategies. His practice hired a social worker to help staff process difficult experiences. After the loss of every patient, the practice comes together to share and process the loss.
For him, funerals remain helpful, providing a sort of solace, so he continues to go when he can. But how to grieve is something each doctor has to figure out, he said.
Deaths still hit hard, especially the ones he doesn’t see coming. The patients who remind him of his dad can also be hard. They restart a cycle of grief from his teenage years.
The difference now is he has space to voice those concerns and someone objective to help his process.
“It’s a privilege to prepare [patients for death] and help them build their legacy,” he said. But it’s also an unrelenting challenge to navigate that grief, he said.
Still, the grief lets Dr. Lewis know he’s still engaged.
“The day I don’t feel something is probably the day I need to take a break or walk away.”
A version of this article appeared on Medscape.com.
Dr. Lewis was well acquainted with cancer grief long before he became an oncologist. Dr. Lewis’ father died of a rare, hereditary cancer syndrome when he was only 14. The condition, which causes tumors to grow in the endocrine glands, can be hard to identify and, if found late, deadly.
In some ways, Dr. Lewis’ career caring for patients with advanced cancers was born out of that first loss. He centered his practice around helping patients diagnosed at late stages, like his father.
But that comes at a cost. Many patients will die.
Dr. Lewis’ encounter with his colleague led him to inventory his practice. He found that well over half of his patients died within 2 years following their advanced cancer diagnosis.
To stave off the grief of so many losses, Dr. Lewis became an eternal optimist in the clinic, in search of the Hail Mary chemotherapy, any way to eke out a few more months only to be ambushed by grief when a patient did finally pass.
At funerals — which he made every effort to attend — Dr. Lewis couldn’t help but think, “If I had done my job better, none of us with be here.” His grief started to mingle with this sense of guilt.
It became a cycle: Denial shrouded in optimism, grief, then a toxic guilt. The pattern became untenable for his colleagues. And his partner finally called him out.
Few medical specialties draw physicians as close to their patients as oncology. The long courses of treatment-spanning years can foster an intimacy that is comforting for patients and fulfilling for physicians. But that closeness can also set doctors up for an acute grief when the end of life comes.
Experts agree that no amount of training in medical school prepares an oncologist to navigate the grief that comes with losing patients. Five oncologists spoke with this news organization about the boundaries they rely on to sustain their careers.
Don’t Go to Funerals
Don Dizon, MD, who specializes in women’s cancers, established an essential boundary 20 years ago: Never go to funerals. In his early days at Memorial Sloan Kettering Cancer Center, the death of each patient dealt him a crushing blow. He’d go to the funerals in search of closure, but that only added to the weight of his grief.
“When I started in oncology, I just remember the most tragic cases were the ones I was taking care of,” recalled Dr. Dizon, now director of the Pelvic Malignancies Program at Lifespan Cancer Institute in Lincoln, Rhode Island.
Dr. Dizon recalled one young mother who was diagnosed with ovarian cancer. She responded to treatment, but it was short-lived, and her cancer progressed, he said. Multiple treatments followed, but none were effective. Eventually, Dr. Dizon had to tell her that “there’s nothing left to try.”
At her funeral, watching her grieving husband with their daughter who had just started to walk, Dr. Dizon was overwhelmed with despair.
“When you have to do this multiple times a year,” the grief becomes untenable, he said. Sensing the difficulty I was having as a new attending, “my boss stopped sending me patients because he knew I was in trouble emotionally.”
That’s when Dr. Dizon started looking for other ways to get closure.
Today, he tries to say his goodbyes before a patient dies. After the final treatment or before hospice, Dr. Dizon has a parting conversation with his patients to express the privilege of caring for them and all he learned from them. These talks help him and his patient connect in their last moments together.
The Price of Wildly Happy Days
Molly Taylor, MD, MS, a pediatric oncologist in Seattle, sees the deeply sad days as the price an oncologist pays to be witness to the “wildly happy ones.”
Dr. Taylor has gone to patients’ funerals, has even been asked to speak at them, but she has also attended patients’ weddings.
To some degree, doctors get good at compartmentalizing, and they become accustomed to tragedy, she said. But there are some patients who stick with you, “and that is a whole other level of grief,” Dr. Taylor said.
Several years into her practice, one of Dr. Taylor’s patients, someone who reminded her of her own child, died. The death came as a surprise, and the finality of it took her breath away, she said. The sadness only deepened as days went by. “I felt that mother’s grief and still do,” she said.
The patient’s funeral was one of the most difficult moments in her career as an oncologist. Even weeks later, she caught herself picturing the family huddled together that day.
Taking long walks, commiserating with colleagues who get it, and watching the occasional cat video can help take the immediate sting away. But the pain of losing a patient can be long lasting and processing that grief can be a lonely endeavor.
“We need space to recognize grief for all providers, all the people that touch these patients’ lives — the nurses, the translators, the cleaning staff,” Dr. Taylor said. Otherwise, you start to believe you’re the only one feeling the weight of the loss.
While it doesn’t make the losses any less poignant, Dr. Taylor finds solace in the good moments: Patient graduations and weddings, survivors who now volunteer at the hospital, and a patient who had a baby of her own this past year. If facing grief daily has taught Dr. Taylor anything, it is to not let the good moments pass unnoticed.
Towing the Line
Ten years ago, Tina Rizack, MD, walked into the ICU to see a young mother holding her 6-year-old daughter. The mother had necrotizing fasciitis that had gone undiagnosed.
As Dr. Rizack stood in the doorway watching the embrace, she saw a grim future: A child without her mother. This realization hit too close to home, she said. “I still think about that case.”
In her training, Dr. Rizack, now medical director of hematology/oncology at St. Anne’s in Fall River, Massachusetts, worked with a social worker who taught her how to deal with these tough cases — most importantly, how to not take them home with her.
Over the years, Dr. Rizack learned how to build and sustain a firm barrier between work and outside work.
She doesn’t go to funerals or give out her cell phone number. If charts need to be done, she prefers to stay late at the clinic instead of bringing them home.
And she invests in the simple moments that help her detach from the day-to-day in the clinic — rooting for her kids at their games, carving out time for family meals most days, and having relaxed movie nights on the couch.
“It’s hard sometimes,” she said. But “I really do need the line.” Because without it, she can’t show up for her patients the way she wants and needs to.
Establishing the work-life boundary means that when at work, Dr. Rizack can be all in for her patients. Even after her patients’ treatment ends, she makes sure to check on them at home or in hospice. For her, sticking with patients over the long term offers some closure.
“I want to love work, and if I’m there all the time, I’m not going to love it,” she said.
Trading Funerals for the Bedside
Like many other oncologists, Charles Blanke, MD, finds that going to patients’ funerals makes the loss seem more profound. Being at the bedside when they die is not as painful, he said. In fact, being there when his patients die offers him some comfort. He rarely misses a patient’s death because now Dr. Blanke’s patients can schedule their departure.
An oncologist at the Knight Cancer Institute in Portland, Oregon, Dr. Blanke specializes in end-of-life care with an emphasis on death with dignity, also known as medical aid in dying. He admits it’s not a role every physician is comfortable with.
“If you’re paralyzed by grief, you can’t do this for a living,” he said. But he’s able to do the work because he genuinely feels he’s helping patients get “the relief they so strongly desire” in their last moments.
When cancer care can’t give them the life they wanted, he can give them control over when and how they die. And the ability to honor their last wishes offers him some closure as well.
“You know what kind of end they have. You know it was peaceful. You see them achieve the thing that was the most important to them,” he said.
Despite this process, he still encounters some circumstances utterly heart-wrenching — the very young patients who have advanced disease. Some of these patients choose to die because they can’t afford to continue treatment. Others don’t have a support system. In these instances, Dr. Blanke is often the only one in the room.
Believe it or not, he said, the paperwork — and there’s a lot of it in his line of work — helps remind Dr. Blanke that patients’ last wishes are being honored.
Making Changes
After Dr. Lewis was confronted by his partner, he began to face the shortcomings of his own coping strategies. His practice hired a social worker to help staff process difficult experiences. After the loss of every patient, the practice comes together to share and process the loss.
For him, funerals remain helpful, providing a sort of solace, so he continues to go when he can. But how to grieve is something each doctor has to figure out, he said.
Deaths still hit hard, especially the ones he doesn’t see coming. The patients who remind him of his dad can also be hard. They restart a cycle of grief from his teenage years.
The difference now is he has space to voice those concerns and someone objective to help his process.
“It’s a privilege to prepare [patients for death] and help them build their legacy,” he said. But it’s also an unrelenting challenge to navigate that grief, he said.
Still, the grief lets Dr. Lewis know he’s still engaged.
“The day I don’t feel something is probably the day I need to take a break or walk away.”
A version of this article appeared on Medscape.com.
Will 2024 Be Easier on the Eyes?
The burdens that monthly or every-other-month injections in the eye impose on patients with retinal diseases are well-known to be barriers to care for many people with these conditions. Making treatment less onerous has driven research into new treatments since the US Food and Drug Administration (FDA) approved ranibizumab (Lucentis) in 2006 as the first anti–vascular endothelial growth factor (VEGF) for the treatment of age-related macular degeneration (AMD) and other retinal diseases.
Those Several of those investigational therapies are poised to hit meaningful milestones in 2024.
Regular Eye Injections: How We Got Here
Ranibizumab originally received approval as a monthly injection. Since then, protocols have evolved to space those injections out to every other month in some, but not all, patients.
New drugs have emerged that require less frequent injections. In 2022, the anti-VEGF and angiopoietin-2 inhibitor faricimab (Vabysmo) was approved for dosing up to every 4 months. Last year, the FDA approved a high-dose formulation of the anti-VEGF treatment aflibercept 8 mg (Eylea HD) to be given every 2-4 months, as well.
But even these treatments require patients going to the office at least three or four times a year for injections, Reginald Sanders, MD, president of the American Society of Retina Specialist, Chicago, and a retina specialist in Washington, DC, told this news organization. “Now with injections, you have the anxiety of getting the injections, you have the inconvenience of coming in on a regular basis to get the injections, and you have mild discomfort — but you don’t go blind,” Dr. Sanders said.
Studies have shown patients with AMD or diabetic macular edema are better off getting more frequent injections, but still drug developers are seeking the holy grail of fewer injections. “How do we make these treatments last longer?” Dr. Sanders said. “Durability has become the catchword in our field. Instead of lasting a month or 2, can it last 3 months? Can it last 6 months? Or even a year? Can you get one injection and be done with it?”
Or, no injection at all?
“We’re looking for incremental improvements and longer-acting drugs, trying to lengthen the time between injections for wet AMD patients,” said David Boyer, MD, a retina specialist in Los Angeles.
Two Drugs May Be Better Than One
One combination treatment, sozinibercept, targets VEGF-C and D. The therapy is in two phase 3 trials: One in combination with aflibercept 2 mg (Eylea), which targets VEGF-A and B along with placental growth factor, and the other in combination with ranibizumab, which targets VEGF-A only. Data from one of those trials are expected this year, Dr. Boyer said.
A phase 2 trial last year reported that patients on combination sozinibercept-ranibizumab had significantly better visual acuity improvement than patients on ranibizumab only. The phase 3 trials ShORe with ranibizumab and COAST with aflibercept are evaluating improvements in visual acuity and retinal anatomy.
Two other combination therapies are in phase 2 trials, both with aflibercept: UBX1325 or foselutoclax, a small-molecule inhibitor of B-cell lymphoma extra-large, and umedaptanib pegol, an anti-fibroblast growth factor-2 aptamer. In the foselutoclax-aflibercept trial, 40% of patients didn’t need a supplemental anti-VEGF injection through 48 weeks, and 64% went treatment-free for more than 24 weeks.
Phase 2 trials of intravitreal umedaptanib pegol-aflibercept combination therapy in nAMD last year showed no superiority in vision and anatomical improvements over aflibercept alone but did find the combination halted disease progression, with “striking improvement” in previously untreated patients.
Novel Drug Delivery Systems
A host of novel drug delivery systems that could stretch out intervals between injections are in human trials. In 2021, the FDA approved one such system, the refillable port delivery system (PDS) implant with ranibizumab (Susvimo). PDS is a small cylinder implanted into the eye and filled with 100 mg/mL of ranibizumab, to be released for 6 months or so, then refilled in the physician’s office when it’s empty.
But new implants of PDS were halted in 2022 after the manufacturer, Genentech, received reports the device leaked. Genentech said it has fixed those problems and confirmed the device should again become available for implants this year.
The most advanced novel drug delivery system in clinical trials is EYP-1901, a depot that contains the tyrosine kinase inhibitor (TKI) vorolanib. The depot is inserted under the ocular surface, where it biodegrades over 6 months as it releases the drug. A phase 3 trial is due to start enrollment at midyear.
An intravitreal implant with the TKI axitinib (Axpaxli) is in a phase 3 trial in nAMD and is due to start a phase 3 trial in diabetic retinopathy this year. At least four other implants, some of which biodegrade as they release the active ingredient, are in phase 1 or 2 trials.
TKIs themselves are a drug class worth watching in retina, said Jennifer I. Lim, MD, director of the retina service at the University of Illinois Chicago and president of the Retina Society.
“With TKIs, which activate intracellularly, in combination with anti-VEGFs will result in enhanced durability and possibly more efficacy for AMD,” Dr. Lim said. “TKIs in the phase 2 studies showed a marked reduction in the need for anti-VEGF injections in previously difficult-to-treat, high-need patient.”
Potential for Orals and Topicals
Topical eye drops are commonly used for anti-glaucoma drugs and antibiotics and corticosteroids for eye infections and inflammation, but using them for retinal disease has been a challenge. By the time the drug reaches the back of the eye, it has lost much of its pharmacokinetic activity. Three drops are in clinical trials for diabetic eye disease, with one, OCS-01, a preservative-free formulation of the corticosteroid dexamethasone, scheduled this year to enter a phase 3 trial.
At least four oral tablets are in early-stage human trials for diabetic eye disease. Four others are in clinical trials to treat geographic atrophy or early-stage dry AMD. They include tinlarebant, which is in phase 3 trials for geographic atrophy and Stargardt disease, an inherited retinal disorder.
Two other oral tablets are in human trials for inherited retinal disease. Like tinlarebant, emixustat has been in a phase 3 trial for Stargardt disease but showed no clinically significant improvement in macular atrophy. An early readout of an ongoing phase 2 trial of glideuretinol, a modified form of vitamin A, demonstrated slowed growth of macular atrophy in Stargardt.
These new and emerging treatments may potentially enable retina specialists to manage a rapidly growing aging population more efficiently, Dr. Sanders said.
“We have to figure out, on one hand, how do we catch the disease earlier? Like in other fields of medicine, the earlier you treat someone, the better,” Dr. Sanders said. “And also, how do we efficiently see these patients earlier to get therapy? Using implants or more durable drugs may be able to help us to treat more people more efficiently.”
Dr. Lim disclosed financial relationships with AbbVie/Allergan, Adverum Biotechnologies, Alimera Sciences, Bausch + Lomb, Chengdu Kanghong Biotechnology, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Novartis, Regeneron Pharmaceuticals, RegenxBio, Santen, SparingVision, Stealth BioTherapeutics, Unity Biotechnology, and Viridian.
Dr. Boyer disclosed financial relationships with 4D Molecular Therapeutics, AbbVie/Allergan, Adverum Biotechnologies, Aldeyra Therapeutics, Alimera Sciences, Alkahest, Allegro, Amgen, Annexon Biosciences, Apellis Pharmaceuticals, AsclepiX Therapeutics, Aviceda Therapeutics, Bausch + Lomb, Bayer, Belite Bio, Clearside Biomedical, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Nano scope Therapeutics, Novartis, Ocugen, Oculist, Ocuphire Pharma, Opthea, Pfizer, Regeneron Pharmaceuticals, RegenxBio, Sanofi, Stilbite Zhuhai, Stealth BioTherapeutics, Thea Laboratories, and Unity Biotechnology. Dr. Sanders had no relevant disclosures.
A version of this article appeared on Medscape.com.
The burdens that monthly or every-other-month injections in the eye impose on patients with retinal diseases are well-known to be barriers to care for many people with these conditions. Making treatment less onerous has driven research into new treatments since the US Food and Drug Administration (FDA) approved ranibizumab (Lucentis) in 2006 as the first anti–vascular endothelial growth factor (VEGF) for the treatment of age-related macular degeneration (AMD) and other retinal diseases.
Those Several of those investigational therapies are poised to hit meaningful milestones in 2024.
Regular Eye Injections: How We Got Here
Ranibizumab originally received approval as a monthly injection. Since then, protocols have evolved to space those injections out to every other month in some, but not all, patients.
New drugs have emerged that require less frequent injections. In 2022, the anti-VEGF and angiopoietin-2 inhibitor faricimab (Vabysmo) was approved for dosing up to every 4 months. Last year, the FDA approved a high-dose formulation of the anti-VEGF treatment aflibercept 8 mg (Eylea HD) to be given every 2-4 months, as well.
But even these treatments require patients going to the office at least three or four times a year for injections, Reginald Sanders, MD, president of the American Society of Retina Specialist, Chicago, and a retina specialist in Washington, DC, told this news organization. “Now with injections, you have the anxiety of getting the injections, you have the inconvenience of coming in on a regular basis to get the injections, and you have mild discomfort — but you don’t go blind,” Dr. Sanders said.
Studies have shown patients with AMD or diabetic macular edema are better off getting more frequent injections, but still drug developers are seeking the holy grail of fewer injections. “How do we make these treatments last longer?” Dr. Sanders said. “Durability has become the catchword in our field. Instead of lasting a month or 2, can it last 3 months? Can it last 6 months? Or even a year? Can you get one injection and be done with it?”
Or, no injection at all?
“We’re looking for incremental improvements and longer-acting drugs, trying to lengthen the time between injections for wet AMD patients,” said David Boyer, MD, a retina specialist in Los Angeles.
Two Drugs May Be Better Than One
One combination treatment, sozinibercept, targets VEGF-C and D. The therapy is in two phase 3 trials: One in combination with aflibercept 2 mg (Eylea), which targets VEGF-A and B along with placental growth factor, and the other in combination with ranibizumab, which targets VEGF-A only. Data from one of those trials are expected this year, Dr. Boyer said.
A phase 2 trial last year reported that patients on combination sozinibercept-ranibizumab had significantly better visual acuity improvement than patients on ranibizumab only. The phase 3 trials ShORe with ranibizumab and COAST with aflibercept are evaluating improvements in visual acuity and retinal anatomy.
Two other combination therapies are in phase 2 trials, both with aflibercept: UBX1325 or foselutoclax, a small-molecule inhibitor of B-cell lymphoma extra-large, and umedaptanib pegol, an anti-fibroblast growth factor-2 aptamer. In the foselutoclax-aflibercept trial, 40% of patients didn’t need a supplemental anti-VEGF injection through 48 weeks, and 64% went treatment-free for more than 24 weeks.
Phase 2 trials of intravitreal umedaptanib pegol-aflibercept combination therapy in nAMD last year showed no superiority in vision and anatomical improvements over aflibercept alone but did find the combination halted disease progression, with “striking improvement” in previously untreated patients.
Novel Drug Delivery Systems
A host of novel drug delivery systems that could stretch out intervals between injections are in human trials. In 2021, the FDA approved one such system, the refillable port delivery system (PDS) implant with ranibizumab (Susvimo). PDS is a small cylinder implanted into the eye and filled with 100 mg/mL of ranibizumab, to be released for 6 months or so, then refilled in the physician’s office when it’s empty.
But new implants of PDS were halted in 2022 after the manufacturer, Genentech, received reports the device leaked. Genentech said it has fixed those problems and confirmed the device should again become available for implants this year.
The most advanced novel drug delivery system in clinical trials is EYP-1901, a depot that contains the tyrosine kinase inhibitor (TKI) vorolanib. The depot is inserted under the ocular surface, where it biodegrades over 6 months as it releases the drug. A phase 3 trial is due to start enrollment at midyear.
An intravitreal implant with the TKI axitinib (Axpaxli) is in a phase 3 trial in nAMD and is due to start a phase 3 trial in diabetic retinopathy this year. At least four other implants, some of which biodegrade as they release the active ingredient, are in phase 1 or 2 trials.
TKIs themselves are a drug class worth watching in retina, said Jennifer I. Lim, MD, director of the retina service at the University of Illinois Chicago and president of the Retina Society.
“With TKIs, which activate intracellularly, in combination with anti-VEGFs will result in enhanced durability and possibly more efficacy for AMD,” Dr. Lim said. “TKIs in the phase 2 studies showed a marked reduction in the need for anti-VEGF injections in previously difficult-to-treat, high-need patient.”
Potential for Orals and Topicals
Topical eye drops are commonly used for anti-glaucoma drugs and antibiotics and corticosteroids for eye infections and inflammation, but using them for retinal disease has been a challenge. By the time the drug reaches the back of the eye, it has lost much of its pharmacokinetic activity. Three drops are in clinical trials for diabetic eye disease, with one, OCS-01, a preservative-free formulation of the corticosteroid dexamethasone, scheduled this year to enter a phase 3 trial.
At least four oral tablets are in early-stage human trials for diabetic eye disease. Four others are in clinical trials to treat geographic atrophy or early-stage dry AMD. They include tinlarebant, which is in phase 3 trials for geographic atrophy and Stargardt disease, an inherited retinal disorder.
Two other oral tablets are in human trials for inherited retinal disease. Like tinlarebant, emixustat has been in a phase 3 trial for Stargardt disease but showed no clinically significant improvement in macular atrophy. An early readout of an ongoing phase 2 trial of glideuretinol, a modified form of vitamin A, demonstrated slowed growth of macular atrophy in Stargardt.
These new and emerging treatments may potentially enable retina specialists to manage a rapidly growing aging population more efficiently, Dr. Sanders said.
“We have to figure out, on one hand, how do we catch the disease earlier? Like in other fields of medicine, the earlier you treat someone, the better,” Dr. Sanders said. “And also, how do we efficiently see these patients earlier to get therapy? Using implants or more durable drugs may be able to help us to treat more people more efficiently.”
Dr. Lim disclosed financial relationships with AbbVie/Allergan, Adverum Biotechnologies, Alimera Sciences, Bausch + Lomb, Chengdu Kanghong Biotechnology, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Novartis, Regeneron Pharmaceuticals, RegenxBio, Santen, SparingVision, Stealth BioTherapeutics, Unity Biotechnology, and Viridian.
Dr. Boyer disclosed financial relationships with 4D Molecular Therapeutics, AbbVie/Allergan, Adverum Biotechnologies, Aldeyra Therapeutics, Alimera Sciences, Alkahest, Allegro, Amgen, Annexon Biosciences, Apellis Pharmaceuticals, AsclepiX Therapeutics, Aviceda Therapeutics, Bausch + Lomb, Bayer, Belite Bio, Clearside Biomedical, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Nano scope Therapeutics, Novartis, Ocugen, Oculist, Ocuphire Pharma, Opthea, Pfizer, Regeneron Pharmaceuticals, RegenxBio, Sanofi, Stilbite Zhuhai, Stealth BioTherapeutics, Thea Laboratories, and Unity Biotechnology. Dr. Sanders had no relevant disclosures.
A version of this article appeared on Medscape.com.
The burdens that monthly or every-other-month injections in the eye impose on patients with retinal diseases are well-known to be barriers to care for many people with these conditions. Making treatment less onerous has driven research into new treatments since the US Food and Drug Administration (FDA) approved ranibizumab (Lucentis) in 2006 as the first anti–vascular endothelial growth factor (VEGF) for the treatment of age-related macular degeneration (AMD) and other retinal diseases.
Those Several of those investigational therapies are poised to hit meaningful milestones in 2024.
Regular Eye Injections: How We Got Here
Ranibizumab originally received approval as a monthly injection. Since then, protocols have evolved to space those injections out to every other month in some, but not all, patients.
New drugs have emerged that require less frequent injections. In 2022, the anti-VEGF and angiopoietin-2 inhibitor faricimab (Vabysmo) was approved for dosing up to every 4 months. Last year, the FDA approved a high-dose formulation of the anti-VEGF treatment aflibercept 8 mg (Eylea HD) to be given every 2-4 months, as well.
But even these treatments require patients going to the office at least three or four times a year for injections, Reginald Sanders, MD, president of the American Society of Retina Specialist, Chicago, and a retina specialist in Washington, DC, told this news organization. “Now with injections, you have the anxiety of getting the injections, you have the inconvenience of coming in on a regular basis to get the injections, and you have mild discomfort — but you don’t go blind,” Dr. Sanders said.
Studies have shown patients with AMD or diabetic macular edema are better off getting more frequent injections, but still drug developers are seeking the holy grail of fewer injections. “How do we make these treatments last longer?” Dr. Sanders said. “Durability has become the catchword in our field. Instead of lasting a month or 2, can it last 3 months? Can it last 6 months? Or even a year? Can you get one injection and be done with it?”
Or, no injection at all?
“We’re looking for incremental improvements and longer-acting drugs, trying to lengthen the time between injections for wet AMD patients,” said David Boyer, MD, a retina specialist in Los Angeles.
Two Drugs May Be Better Than One
One combination treatment, sozinibercept, targets VEGF-C and D. The therapy is in two phase 3 trials: One in combination with aflibercept 2 mg (Eylea), which targets VEGF-A and B along with placental growth factor, and the other in combination with ranibizumab, which targets VEGF-A only. Data from one of those trials are expected this year, Dr. Boyer said.
A phase 2 trial last year reported that patients on combination sozinibercept-ranibizumab had significantly better visual acuity improvement than patients on ranibizumab only. The phase 3 trials ShORe with ranibizumab and COAST with aflibercept are evaluating improvements in visual acuity and retinal anatomy.
Two other combination therapies are in phase 2 trials, both with aflibercept: UBX1325 or foselutoclax, a small-molecule inhibitor of B-cell lymphoma extra-large, and umedaptanib pegol, an anti-fibroblast growth factor-2 aptamer. In the foselutoclax-aflibercept trial, 40% of patients didn’t need a supplemental anti-VEGF injection through 48 weeks, and 64% went treatment-free for more than 24 weeks.
Phase 2 trials of intravitreal umedaptanib pegol-aflibercept combination therapy in nAMD last year showed no superiority in vision and anatomical improvements over aflibercept alone but did find the combination halted disease progression, with “striking improvement” in previously untreated patients.
Novel Drug Delivery Systems
A host of novel drug delivery systems that could stretch out intervals between injections are in human trials. In 2021, the FDA approved one such system, the refillable port delivery system (PDS) implant with ranibizumab (Susvimo). PDS is a small cylinder implanted into the eye and filled with 100 mg/mL of ranibizumab, to be released for 6 months or so, then refilled in the physician’s office when it’s empty.
But new implants of PDS were halted in 2022 after the manufacturer, Genentech, received reports the device leaked. Genentech said it has fixed those problems and confirmed the device should again become available for implants this year.
The most advanced novel drug delivery system in clinical trials is EYP-1901, a depot that contains the tyrosine kinase inhibitor (TKI) vorolanib. The depot is inserted under the ocular surface, where it biodegrades over 6 months as it releases the drug. A phase 3 trial is due to start enrollment at midyear.
An intravitreal implant with the TKI axitinib (Axpaxli) is in a phase 3 trial in nAMD and is due to start a phase 3 trial in diabetic retinopathy this year. At least four other implants, some of which biodegrade as they release the active ingredient, are in phase 1 or 2 trials.
TKIs themselves are a drug class worth watching in retina, said Jennifer I. Lim, MD, director of the retina service at the University of Illinois Chicago and president of the Retina Society.
“With TKIs, which activate intracellularly, in combination with anti-VEGFs will result in enhanced durability and possibly more efficacy for AMD,” Dr. Lim said. “TKIs in the phase 2 studies showed a marked reduction in the need for anti-VEGF injections in previously difficult-to-treat, high-need patient.”
Potential for Orals and Topicals
Topical eye drops are commonly used for anti-glaucoma drugs and antibiotics and corticosteroids for eye infections and inflammation, but using them for retinal disease has been a challenge. By the time the drug reaches the back of the eye, it has lost much of its pharmacokinetic activity. Three drops are in clinical trials for diabetic eye disease, with one, OCS-01, a preservative-free formulation of the corticosteroid dexamethasone, scheduled this year to enter a phase 3 trial.
At least four oral tablets are in early-stage human trials for diabetic eye disease. Four others are in clinical trials to treat geographic atrophy or early-stage dry AMD. They include tinlarebant, which is in phase 3 trials for geographic atrophy and Stargardt disease, an inherited retinal disorder.
Two other oral tablets are in human trials for inherited retinal disease. Like tinlarebant, emixustat has been in a phase 3 trial for Stargardt disease but showed no clinically significant improvement in macular atrophy. An early readout of an ongoing phase 2 trial of glideuretinol, a modified form of vitamin A, demonstrated slowed growth of macular atrophy in Stargardt.
These new and emerging treatments may potentially enable retina specialists to manage a rapidly growing aging population more efficiently, Dr. Sanders said.
“We have to figure out, on one hand, how do we catch the disease earlier? Like in other fields of medicine, the earlier you treat someone, the better,” Dr. Sanders said. “And also, how do we efficiently see these patients earlier to get therapy? Using implants or more durable drugs may be able to help us to treat more people more efficiently.”
Dr. Lim disclosed financial relationships with AbbVie/Allergan, Adverum Biotechnologies, Alimera Sciences, Bausch + Lomb, Chengdu Kanghong Biotechnology, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Novartis, Regeneron Pharmaceuticals, RegenxBio, Santen, SparingVision, Stealth BioTherapeutics, Unity Biotechnology, and Viridian.
Dr. Boyer disclosed financial relationships with 4D Molecular Therapeutics, AbbVie/Allergan, Adverum Biotechnologies, Aldeyra Therapeutics, Alimera Sciences, Alkahest, Allegro, Amgen, Annexon Biosciences, Apellis Pharmaceuticals, AsclepiX Therapeutics, Aviceda Therapeutics, Bausch + Lomb, Bayer, Belite Bio, Clearside Biomedical, Eyepoint Pharmaceuticals, Genentech/ Roche, Graybug Vision, Iveric Bio, Janssen Pharmaceuticals, Nano scope Therapeutics, Novartis, Ocugen, Oculist, Ocuphire Pharma, Opthea, Pfizer, Regeneron Pharmaceuticals, RegenxBio, Sanofi, Stilbite Zhuhai, Stealth BioTherapeutics, Thea Laboratories, and Unity Biotechnology. Dr. Sanders had no relevant disclosures.
A version of this article appeared on Medscape.com.