User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
Poor Oral Health Tied to Worse Brain Health
In a large observational study of middle-aged adults without stroke or dementia, poor oral health was strongly associated with multiple neuroimaging markers of white matter injury.
“Because the neuroimaging markers evaluated in this study precede and are established risk factors of stroke and dementia, our results suggest that oral health, an easily modifiable process, may be a promising target for very early interventions focused on improving brain health,” wrote the authors, led by Cyprien A. Rivier, MD, MS, with the Department of Neurology, Yale University School of Medicine, New Haven, Connecticut.
The study was published online on December 20, 2023, in Neurology.
Research data came from 40,175 adults (mean age, 55 years; 53% women) with no history of stroke or dementia who enrolled in the UK Biobank from 2006 to 2010 and had brain MRI between 2014 and 2016.
Altogether, 5470 (14%) participants had poor oral health, defined as the presence of dentures or loose teeth. Those with poor (vs optimal) oral health were older, more likely to be male, and had higher prevalence of hypertension, hypercholesterolemia, diabetes, overweight/obesity, and current or past smoking history.
In a multivariable model, poor oral health was associated with a 9% increase in white matter hyperintensity (WMH) volume (P < .001), a well-established marker of clinically silent cerebrovascular disease.
Poor oral health was also associated with a 10% change in aggregate fractional anisotropy (FA) score (P < .001) and a 5% change in aggregate mean diffusivity (MD) score (P < .001), two diffusion tensor imaging metrics that accurately represent white matter disintegrity.
Genetic analyses using Mendelian randomization confirmed these associations. Individuals who were genetically prone to poor oral health had a 30% increase in WMH volume (P < .001), 43% change in aggregate FA score (P < .001), and 10% change in aggregate MD score (P < .01), the researchers reported.
These findings, they noted, add to prior epidemiologic evidence for an association between poor oral health and a higher risk for clinical outcomes related to brain health, including cognitive decline.
‘Huge Dividends’
The authors of an accompanying editorial praised the authors for looking at the consequences of poor oral health in a “new and powerful way by using as their outcome MRI-defined white matter injury, which is associated with, but antedates by many years, cognitive decline and stroke.”
“The fact that these imaging changes are seen in asymptomatic persons offers the hope that if the association is causal, interventions to improve oral health could pay huge dividends in subsequent brain health,” wrote Steven J. Kittner, MD, MPH, and Breana L. Taylor, MD, with the Department of Neurology, University of Maryland School of Medicine in Baltimore.
“The mechanisms mediating the relationship between the oral health genetic risk score and white matter injury are likely to be complex, but the authors have taken an important step forward in addressing a hypothesis of immense public health importance,” they added.
Data from the World Health Organization suggested that oral diseases, which are largely preventable, affect nearly 3.5 billion people globally, with three out of four people affected in middle-income countries.
Funding for the study was provided in part by grants from the National Institutes of Health, the American Heart Association, and the Neurocritical Care Society Research Fellowship. The authors and editorialists disclosed no relevant conflicts of interest.
Megan Brooks has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
In a large observational study of middle-aged adults without stroke or dementia, poor oral health was strongly associated with multiple neuroimaging markers of white matter injury.
“Because the neuroimaging markers evaluated in this study precede and are established risk factors of stroke and dementia, our results suggest that oral health, an easily modifiable process, may be a promising target for very early interventions focused on improving brain health,” wrote the authors, led by Cyprien A. Rivier, MD, MS, with the Department of Neurology, Yale University School of Medicine, New Haven, Connecticut.
The study was published online on December 20, 2023, in Neurology.
Research data came from 40,175 adults (mean age, 55 years; 53% women) with no history of stroke or dementia who enrolled in the UK Biobank from 2006 to 2010 and had brain MRI between 2014 and 2016.
Altogether, 5470 (14%) participants had poor oral health, defined as the presence of dentures or loose teeth. Those with poor (vs optimal) oral health were older, more likely to be male, and had higher prevalence of hypertension, hypercholesterolemia, diabetes, overweight/obesity, and current or past smoking history.
In a multivariable model, poor oral health was associated with a 9% increase in white matter hyperintensity (WMH) volume (P < .001), a well-established marker of clinically silent cerebrovascular disease.
Poor oral health was also associated with a 10% change in aggregate fractional anisotropy (FA) score (P < .001) and a 5% change in aggregate mean diffusivity (MD) score (P < .001), two diffusion tensor imaging metrics that accurately represent white matter disintegrity.
Genetic analyses using Mendelian randomization confirmed these associations. Individuals who were genetically prone to poor oral health had a 30% increase in WMH volume (P < .001), 43% change in aggregate FA score (P < .001), and 10% change in aggregate MD score (P < .01), the researchers reported.
These findings, they noted, add to prior epidemiologic evidence for an association between poor oral health and a higher risk for clinical outcomes related to brain health, including cognitive decline.
‘Huge Dividends’
The authors of an accompanying editorial praised the authors for looking at the consequences of poor oral health in a “new and powerful way by using as their outcome MRI-defined white matter injury, which is associated with, but antedates by many years, cognitive decline and stroke.”
“The fact that these imaging changes are seen in asymptomatic persons offers the hope that if the association is causal, interventions to improve oral health could pay huge dividends in subsequent brain health,” wrote Steven J. Kittner, MD, MPH, and Breana L. Taylor, MD, with the Department of Neurology, University of Maryland School of Medicine in Baltimore.
“The mechanisms mediating the relationship between the oral health genetic risk score and white matter injury are likely to be complex, but the authors have taken an important step forward in addressing a hypothesis of immense public health importance,” they added.
Data from the World Health Organization suggested that oral diseases, which are largely preventable, affect nearly 3.5 billion people globally, with three out of four people affected in middle-income countries.
Funding for the study was provided in part by grants from the National Institutes of Health, the American Heart Association, and the Neurocritical Care Society Research Fellowship. The authors and editorialists disclosed no relevant conflicts of interest.
Megan Brooks has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
In a large observational study of middle-aged adults without stroke or dementia, poor oral health was strongly associated with multiple neuroimaging markers of white matter injury.
“Because the neuroimaging markers evaluated in this study precede and are established risk factors of stroke and dementia, our results suggest that oral health, an easily modifiable process, may be a promising target for very early interventions focused on improving brain health,” wrote the authors, led by Cyprien A. Rivier, MD, MS, with the Department of Neurology, Yale University School of Medicine, New Haven, Connecticut.
The study was published online on December 20, 2023, in Neurology.
Research data came from 40,175 adults (mean age, 55 years; 53% women) with no history of stroke or dementia who enrolled in the UK Biobank from 2006 to 2010 and had brain MRI between 2014 and 2016.
Altogether, 5470 (14%) participants had poor oral health, defined as the presence of dentures or loose teeth. Those with poor (vs optimal) oral health were older, more likely to be male, and had higher prevalence of hypertension, hypercholesterolemia, diabetes, overweight/obesity, and current or past smoking history.
In a multivariable model, poor oral health was associated with a 9% increase in white matter hyperintensity (WMH) volume (P < .001), a well-established marker of clinically silent cerebrovascular disease.
Poor oral health was also associated with a 10% change in aggregate fractional anisotropy (FA) score (P < .001) and a 5% change in aggregate mean diffusivity (MD) score (P < .001), two diffusion tensor imaging metrics that accurately represent white matter disintegrity.
Genetic analyses using Mendelian randomization confirmed these associations. Individuals who were genetically prone to poor oral health had a 30% increase in WMH volume (P < .001), 43% change in aggregate FA score (P < .001), and 10% change in aggregate MD score (P < .01), the researchers reported.
These findings, they noted, add to prior epidemiologic evidence for an association between poor oral health and a higher risk for clinical outcomes related to brain health, including cognitive decline.
‘Huge Dividends’
The authors of an accompanying editorial praised the authors for looking at the consequences of poor oral health in a “new and powerful way by using as their outcome MRI-defined white matter injury, which is associated with, but antedates by many years, cognitive decline and stroke.”
“The fact that these imaging changes are seen in asymptomatic persons offers the hope that if the association is causal, interventions to improve oral health could pay huge dividends in subsequent brain health,” wrote Steven J. Kittner, MD, MPH, and Breana L. Taylor, MD, with the Department of Neurology, University of Maryland School of Medicine in Baltimore.
“The mechanisms mediating the relationship between the oral health genetic risk score and white matter injury are likely to be complex, but the authors have taken an important step forward in addressing a hypothesis of immense public health importance,” they added.
Data from the World Health Organization suggested that oral diseases, which are largely preventable, affect nearly 3.5 billion people globally, with three out of four people affected in middle-income countries.
Funding for the study was provided in part by grants from the National Institutes of Health, the American Heart Association, and the Neurocritical Care Society Research Fellowship. The authors and editorialists disclosed no relevant conflicts of interest.
Megan Brooks has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Intermittent Energy Restriction Tied to Gut, Brain Changes
TOPLINE:
In people with obesity, weight loss by intermittent energy restriction (IER) has multiple, dynamic effects on the brain-gut-microbiome (BGM) axis, including reduced activity in brain regions affecting eating behavior and increased microbial diversity in the gut, over the short term, new research suggested.
METHODOLOGY:
- Researchers studied 25 individuals with obesity in China who successfully lost weight during a three-phase IER intervention. In the first phase, participants were on a normal diet without restriction for 4 days. In the second, they were on a tightly controlled diet of clinically formulated IER meals every other day that decreased stepwise in caloric value to one quarter of their basic energy intake over 32 days. The last phase was a 30-day low-controlled fasting period.
- Blood and stool samples were collected at baseline, at the midpoint and endpoint of the tightly controlled fasting phase, and at the endpoint of the low-controlled fasting phase.
- A functional MRI was used to determine the activity of specific brain regions, and metagenomic sequencing was performed to identify differentially abundant gut microbes and pathways from stool samples.
TAKEAWAY:
- Patients lost weight (7.6 kg on average) and showed sustained, significant reductions on several measures, including body mass index, body fat, systolic blood pressure, and serum levels of glycosylated hemoglobin during the IER. Diastolic blood pressure, serum levels of fasting plasma glucose, total cholesterol, various lipids, and levels of several key liver enzymes were significantly decreased at at least one timepoint during the IER.
- IER reduced the activity of obesity-related brain regions (ie, the inferior frontal orbital gyrus in the cognitive control circuit, the putamen in the emotion and learning circuit, and the anterior cingulate cortex in the sensory circuit) at different timepoints during the intervention. No significant changes were observed in brain activity in the reward circuit.
- Gut microbial diversity increased during the tightly controlled fasting phase. The abundance of the probiotic Faecalibacterium prausnitzii, Parabacteroides distasonis, and Bacterokles uniformis was elevated during this phase. The abundance of pathogenic Escherichia coli was reduced across multiple timepoints. A correlation analysis revealed longitudinal correlations between gut bacteria abundance alterations and brain activity changes.
- Overall, there was a dynamical alteration of the BGM axis during weight loss using IER, although whether changes in the gut microbiome drive changes in the brain, or vice versa, is still unknown.
IN PRACTICE:
“IER induced constant, significant reductions in the activity of eating behavior-related brain regions…[and] significant, dynamic changes in the abundance of some gut bacteria. Importantly, gut microbiota alterations correlated with brain activity changes across different timepoints in IER intervention. These data suggest that the dynamic interplay between the brain and gut microbiota plays an important role in weight loss,” the authors wrote.
SOURCE:
Jing Zhou, Henan Provincial People’s Hospital, Zhengzhou University People’s Hospital, Henan University People’s Hospital, Zhengzhou, China, led the study, which was published online on December 30, 2023, in Frontiers in Cellular and Infection Microbiology.
LIMITATIONS:
The study examines BGM axis changes during weight loss only in the short term and does not establish causation. Longer follow-up is needed to establish the BGM axis changes that may influence long-term weight loss.
DISCLOSURES:
This work was supported by the National Natural Science Foundation of China, the National Key R&D Program of China, Young and Middle-Aged Health Science and Technology Innovative Talent Cultivation Project of Henan Provincial Leading Talents, and the Medical Science and Technology Research Program of Henan Province. One coauthor was employed by a supplement company and another by a biotech company. No other disclosures were reported.
A version of this article appeared on Medscape.com.
TOPLINE:
In people with obesity, weight loss by intermittent energy restriction (IER) has multiple, dynamic effects on the brain-gut-microbiome (BGM) axis, including reduced activity in brain regions affecting eating behavior and increased microbial diversity in the gut, over the short term, new research suggested.
METHODOLOGY:
- Researchers studied 25 individuals with obesity in China who successfully lost weight during a three-phase IER intervention. In the first phase, participants were on a normal diet without restriction for 4 days. In the second, they were on a tightly controlled diet of clinically formulated IER meals every other day that decreased stepwise in caloric value to one quarter of their basic energy intake over 32 days. The last phase was a 30-day low-controlled fasting period.
- Blood and stool samples were collected at baseline, at the midpoint and endpoint of the tightly controlled fasting phase, and at the endpoint of the low-controlled fasting phase.
- A functional MRI was used to determine the activity of specific brain regions, and metagenomic sequencing was performed to identify differentially abundant gut microbes and pathways from stool samples.
TAKEAWAY:
- Patients lost weight (7.6 kg on average) and showed sustained, significant reductions on several measures, including body mass index, body fat, systolic blood pressure, and serum levels of glycosylated hemoglobin during the IER. Diastolic blood pressure, serum levels of fasting plasma glucose, total cholesterol, various lipids, and levels of several key liver enzymes were significantly decreased at at least one timepoint during the IER.
- IER reduced the activity of obesity-related brain regions (ie, the inferior frontal orbital gyrus in the cognitive control circuit, the putamen in the emotion and learning circuit, and the anterior cingulate cortex in the sensory circuit) at different timepoints during the intervention. No significant changes were observed in brain activity in the reward circuit.
- Gut microbial diversity increased during the tightly controlled fasting phase. The abundance of the probiotic Faecalibacterium prausnitzii, Parabacteroides distasonis, and Bacterokles uniformis was elevated during this phase. The abundance of pathogenic Escherichia coli was reduced across multiple timepoints. A correlation analysis revealed longitudinal correlations between gut bacteria abundance alterations and brain activity changes.
- Overall, there was a dynamical alteration of the BGM axis during weight loss using IER, although whether changes in the gut microbiome drive changes in the brain, or vice versa, is still unknown.
IN PRACTICE:
“IER induced constant, significant reductions in the activity of eating behavior-related brain regions…[and] significant, dynamic changes in the abundance of some gut bacteria. Importantly, gut microbiota alterations correlated with brain activity changes across different timepoints in IER intervention. These data suggest that the dynamic interplay between the brain and gut microbiota plays an important role in weight loss,” the authors wrote.
SOURCE:
Jing Zhou, Henan Provincial People’s Hospital, Zhengzhou University People’s Hospital, Henan University People’s Hospital, Zhengzhou, China, led the study, which was published online on December 30, 2023, in Frontiers in Cellular and Infection Microbiology.
LIMITATIONS:
The study examines BGM axis changes during weight loss only in the short term and does not establish causation. Longer follow-up is needed to establish the BGM axis changes that may influence long-term weight loss.
DISCLOSURES:
This work was supported by the National Natural Science Foundation of China, the National Key R&D Program of China, Young and Middle-Aged Health Science and Technology Innovative Talent Cultivation Project of Henan Provincial Leading Talents, and the Medical Science and Technology Research Program of Henan Province. One coauthor was employed by a supplement company and another by a biotech company. No other disclosures were reported.
A version of this article appeared on Medscape.com.
TOPLINE:
In people with obesity, weight loss by intermittent energy restriction (IER) has multiple, dynamic effects on the brain-gut-microbiome (BGM) axis, including reduced activity in brain regions affecting eating behavior and increased microbial diversity in the gut, over the short term, new research suggested.
METHODOLOGY:
- Researchers studied 25 individuals with obesity in China who successfully lost weight during a three-phase IER intervention. In the first phase, participants were on a normal diet without restriction for 4 days. In the second, they were on a tightly controlled diet of clinically formulated IER meals every other day that decreased stepwise in caloric value to one quarter of their basic energy intake over 32 days. The last phase was a 30-day low-controlled fasting period.
- Blood and stool samples were collected at baseline, at the midpoint and endpoint of the tightly controlled fasting phase, and at the endpoint of the low-controlled fasting phase.
- A functional MRI was used to determine the activity of specific brain regions, and metagenomic sequencing was performed to identify differentially abundant gut microbes and pathways from stool samples.
TAKEAWAY:
- Patients lost weight (7.6 kg on average) and showed sustained, significant reductions on several measures, including body mass index, body fat, systolic blood pressure, and serum levels of glycosylated hemoglobin during the IER. Diastolic blood pressure, serum levels of fasting plasma glucose, total cholesterol, various lipids, and levels of several key liver enzymes were significantly decreased at at least one timepoint during the IER.
- IER reduced the activity of obesity-related brain regions (ie, the inferior frontal orbital gyrus in the cognitive control circuit, the putamen in the emotion and learning circuit, and the anterior cingulate cortex in the sensory circuit) at different timepoints during the intervention. No significant changes were observed in brain activity in the reward circuit.
- Gut microbial diversity increased during the tightly controlled fasting phase. The abundance of the probiotic Faecalibacterium prausnitzii, Parabacteroides distasonis, and Bacterokles uniformis was elevated during this phase. The abundance of pathogenic Escherichia coli was reduced across multiple timepoints. A correlation analysis revealed longitudinal correlations between gut bacteria abundance alterations and brain activity changes.
- Overall, there was a dynamical alteration of the BGM axis during weight loss using IER, although whether changes in the gut microbiome drive changes in the brain, or vice versa, is still unknown.
IN PRACTICE:
“IER induced constant, significant reductions in the activity of eating behavior-related brain regions…[and] significant, dynamic changes in the abundance of some gut bacteria. Importantly, gut microbiota alterations correlated with brain activity changes across different timepoints in IER intervention. These data suggest that the dynamic interplay between the brain and gut microbiota plays an important role in weight loss,” the authors wrote.
SOURCE:
Jing Zhou, Henan Provincial People’s Hospital, Zhengzhou University People’s Hospital, Henan University People’s Hospital, Zhengzhou, China, led the study, which was published online on December 30, 2023, in Frontiers in Cellular and Infection Microbiology.
LIMITATIONS:
The study examines BGM axis changes during weight loss only in the short term and does not establish causation. Longer follow-up is needed to establish the BGM axis changes that may influence long-term weight loss.
DISCLOSURES:
This work was supported by the National Natural Science Foundation of China, the National Key R&D Program of China, Young and Middle-Aged Health Science and Technology Innovative Talent Cultivation Project of Henan Provincial Leading Talents, and the Medical Science and Technology Research Program of Henan Province. One coauthor was employed by a supplement company and another by a biotech company. No other disclosures were reported.
A version of this article appeared on Medscape.com.
Dieting and Gout: Intensive Weight Loss Not Especially Helpful for Symptoms
TOPLINE:
An intensive weight loss program is safe for individuals with gout and obesity but does not ease gout symptoms compared with a “control diet” with basic nutritional counseling.
METHODOLOGY:
- Weight loss is recommended as a gout management strategy, despite little clinical evidence.
- Researchers recruited 61 patients with gout and obesity to participate in a 16-week, randomized, nonblinded, parallel-group trial in Denmark.
- A total of 29 participants were assigned to an intensive, low-calorie diet with provided meal replacements.
- Another 32 participants were assigned to the “control diet” with basic nutritional counseling.
TAKEAWAY:
- Patients in the intensive group lost more weight (−15.4 kg/34 lbs) than those the control group (−7.7 kg/17 lbs).
- There were no differences in pain, fatigue, or gout flares between the two groups.
- Weight loss was associated with reduction in serum urate (SU).
- Patients in the intervention group had a numerically larger mean SU change (−0.6 mg/dL) than the control group (−0.3 mg/dL), but this difference was not statistically significant.
IN PRACTICE:
Weight loss can lower SU levels, but this did not translate to improved gout symptoms.
SOURCE:
Robin Christensen, PhD, and Kristian Zobbe, MD, PhD, of the Parker Institute at Bispebjerg and Frederiksberg Hospital in Copenhagen, Denmark, were co-first authors of the study, published on January 2, 2024, in Arthritis & Rheumatology.
LIMITATIONS:
The study had a relatively small sample size and short-term intervention period, which may have made it difficult to detect differences between the intervention and control groups. Patients in the control group lost a significant amount of weight, which also affected comparisons between the two groups.
DISCLOSURES:
Several of the authors disclosed financial relationships with pharmaceutical companies. The Parker Institute, which funded the study, is supported by grants from the Oak Foundation and the Danish Rheumatism Association.
A version of this article appeared on Medscape.com.
TOPLINE:
An intensive weight loss program is safe for individuals with gout and obesity but does not ease gout symptoms compared with a “control diet” with basic nutritional counseling.
METHODOLOGY:
- Weight loss is recommended as a gout management strategy, despite little clinical evidence.
- Researchers recruited 61 patients with gout and obesity to participate in a 16-week, randomized, nonblinded, parallel-group trial in Denmark.
- A total of 29 participants were assigned to an intensive, low-calorie diet with provided meal replacements.
- Another 32 participants were assigned to the “control diet” with basic nutritional counseling.
TAKEAWAY:
- Patients in the intensive group lost more weight (−15.4 kg/34 lbs) than those the control group (−7.7 kg/17 lbs).
- There were no differences in pain, fatigue, or gout flares between the two groups.
- Weight loss was associated with reduction in serum urate (SU).
- Patients in the intervention group had a numerically larger mean SU change (−0.6 mg/dL) than the control group (−0.3 mg/dL), but this difference was not statistically significant.
IN PRACTICE:
Weight loss can lower SU levels, but this did not translate to improved gout symptoms.
SOURCE:
Robin Christensen, PhD, and Kristian Zobbe, MD, PhD, of the Parker Institute at Bispebjerg and Frederiksberg Hospital in Copenhagen, Denmark, were co-first authors of the study, published on January 2, 2024, in Arthritis & Rheumatology.
LIMITATIONS:
The study had a relatively small sample size and short-term intervention period, which may have made it difficult to detect differences between the intervention and control groups. Patients in the control group lost a significant amount of weight, which also affected comparisons between the two groups.
DISCLOSURES:
Several of the authors disclosed financial relationships with pharmaceutical companies. The Parker Institute, which funded the study, is supported by grants from the Oak Foundation and the Danish Rheumatism Association.
A version of this article appeared on Medscape.com.
TOPLINE:
An intensive weight loss program is safe for individuals with gout and obesity but does not ease gout symptoms compared with a “control diet” with basic nutritional counseling.
METHODOLOGY:
- Weight loss is recommended as a gout management strategy, despite little clinical evidence.
- Researchers recruited 61 patients with gout and obesity to participate in a 16-week, randomized, nonblinded, parallel-group trial in Denmark.
- A total of 29 participants were assigned to an intensive, low-calorie diet with provided meal replacements.
- Another 32 participants were assigned to the “control diet” with basic nutritional counseling.
TAKEAWAY:
- Patients in the intensive group lost more weight (−15.4 kg/34 lbs) than those the control group (−7.7 kg/17 lbs).
- There were no differences in pain, fatigue, or gout flares between the two groups.
- Weight loss was associated with reduction in serum urate (SU).
- Patients in the intervention group had a numerically larger mean SU change (−0.6 mg/dL) than the control group (−0.3 mg/dL), but this difference was not statistically significant.
IN PRACTICE:
Weight loss can lower SU levels, but this did not translate to improved gout symptoms.
SOURCE:
Robin Christensen, PhD, and Kristian Zobbe, MD, PhD, of the Parker Institute at Bispebjerg and Frederiksberg Hospital in Copenhagen, Denmark, were co-first authors of the study, published on January 2, 2024, in Arthritis & Rheumatology.
LIMITATIONS:
The study had a relatively small sample size and short-term intervention period, which may have made it difficult to detect differences between the intervention and control groups. Patients in the control group lost a significant amount of weight, which also affected comparisons between the two groups.
DISCLOSURES:
Several of the authors disclosed financial relationships with pharmaceutical companies. The Parker Institute, which funded the study, is supported by grants from the Oak Foundation and the Danish Rheumatism Association.
A version of this article appeared on Medscape.com.
Eli Lilly Offers Obesity Drug Directly to Consumers
Eli Lilly, maker of the anti-obesity drug Zepbound, announced this week the launch of LillyDirect, a direct-to-patient portal, allowing some patients to obtain its drug for as little as $25 a month.
The move is seen as a major shift in the way these popular medications can reach patients.
For many of the 42 million Americans with obesity, weight loss medications such as Wegovy, Saxenda, and the brand-new Zepbound can be a godsend, helping them lose the excess pounds they’ve struggled with for decades or a lifetime.
But getting these medications has been a struggle for many who are eligible. Shortages of the drugs have been one barrier, and costs of up to $1,300 monthly — the price tag without insurance coverage — are another hurdle.
But 2024 may be a much brighter year, thanks to Lilly’s new portal as well as other developments:
Insurance coverage on private health plans, while still spotty, may be improving. Federal legislators are fighting a 2003 law that forbids Medicare from paying for the medications when prescribed for obesity.
New research found that semaglutide (Wegovy) can reduce the risk of recurrent strokes and heart attacks as well as deaths from cardiovascular events in those with obesity and preexisting cardiovascular disease (or diseases of the heart and blood vessels), a finding experts said should get the attention of health insurers.
The medications, also referred to as GLP-1 agonists, work by activating the receptors of hormones (called glucagon-like peptide 1 and others) that are naturally released after eating. That, in turn, makes you feel more full, leading to weight loss of up to 22% for some. The medications are approved for those with a body mass index (BMI) of 30 or a BMI of 27 with at least one other weight-related health condition such as high blood pressure or high cholesterol. The medicines, injected weekly or more often, are prescribed along with advice about a reduced-calorie diet and increased physical activity.
LillyDirect
Patients can access the obesity medicines through the telehealth platform FORM. Patients reach independent telehealth providers, according to Lilly, who can complement a patient’s current doctor or be an alternative to in-patient care in some cases.
Eli Lilly officials did not respond to requests for comment.
Some obesity experts welcomed the new service. “Any program that improves availability and affordability of these ground-breaking medications is welcome news for our long-suffering patients,” said Louis Aronne, MD, director of the Comprehensive Weight Control Center at Weill Cornell Medicine in New York City, a long-time obesity researcher.
“It’s a great move for Lilly to do,” agreed Caroline Apovian, MD, a professor of medicine at Harvard Medical School and co-director of the Center for Weight Management and Wellness at Brigham & Women’s Hospital in Boston, who is also a veteran obesity specialist. “It is trying to help the accessibility issue and do it responsibly.”
“The bottom line is, there is an overwhelming amount of consumer need and desire for these medications and not enough channels [to provide them],” said Zeev Neuwirth, MD, a former executive at Atrium Health who writes about health care trends. “Eli Lilly is responding to a market need that is out there and quite honestly continuing to grow.”
There are still concerns and questions, Dr. Neuwirth said, “especially since this is to my knowledge the first of its kind in terms of a pharmaceutical manufacturer directly dispensing medication in this nontraditional way.”
He called for transparency between telehealth providers and the pharmaceutical company to rule out any conflicts of interest.
The American College of Physicians, an organization of internal medicine doctors and others, issued a statement expressing concern. Omar T. Atiq, MD, group’s president, said his organization is “concerned by the development of websites that enable patients to order prescription medications directly from the drugmakers. While information on in-person care is available, this direct-to-consumer approach is primarily oriented around the use of telehealth services to prescribe a drug maker’s products.”
The group urged that an established patient-doctor relationship be present, or that care should happen in consultation with a doctor who does have an established relationship (the latter an option offered by Lilly). “These direct-to-consumer services have the potential to leave patients confused and misinformed about medications.”
Heart Attack, Stroke Reduction Benefits
Previous research has found that the GLP-1 medicines such as Ozempic (semaglutide), which the FDA approved to treat diabetes, also reduce the risk of cardiovascular issues such as strokes and heart attacks. Now, new research finds that semaglutide at the Wegovy dose (usually slightly higher than the Ozempic dose for diabetes) also has those benefits in those who don›t have a diabetes diagnosis but do have obesity and cardiovascular disease.
In a clinical trial sponsored by Novo Nordisk, the maker of Wegovy, half of more than 17,000 people with obesity were given semaglutide (Wegovy); the other half got a placebo. Compared to those on the placebo, those who took the Wegovy had a 20% reduction in strokes, heart attacks, and deaths from cardiovascular causes over a 33-month period.
The study results are a “big deal,” Dr. Aronne said. The results make it clear that those with obesity but not diabetes will get the cardiovascular benefits from the treatment as well. While more analysis is necessary, he said the important point is that the study showed that reducing body weight is linked to improvement in critical health outcomes.
As the research evolves, he said, it’s going to be difficult for insurers to deny medications in the face of those findings, which promise reductions in long-term health care costs.
Insurance Coverage
In November, the American Medical Association voted to adopt a policy to urge insurance coverage for evidence-based treatment for obesity, including the new obesity medications.
“No single organization is going to be able to convince insurers and employers to cover this,” Dr. Aronne said. “But I think a prominent organization like the AMA adding their voice to the rising chorus is going to help.”
Coverage of GLP-1 medications could nearly double in 2024, according to a survey of 500 human resources decision-makers released in October by Accolade, a personalized health care advocacy and delivery company. While 25% of respondents said they currently offered coverage when the survey was done in August and September, 43% said they intend to offer coverage in 2024.
In an email, David Allen, a spokesperson for America’s Health Insurance Plans, a health care industry association, said: “Every American deserves affordable coverage and high-quality care, and that includes coverage and care for evidence-based obesity treatments and therapies.”
He said “clinical leaders and other experts at health insurance providers routinely review the evidence for all types of treatments, including treatments for obesity, and offer multiple options to patients — ranging from lifestyle changes and nutrition counseling, to surgical interventions, to prescription drugs.”
Mr. Allen said the evidence that obesity drugs help with weight loss “is still evolving.”
“And some patients are experiencing bad effects related to these drugs such as vomiting and nausea, for example, and the likelihood of gaining the weight back when discontinuing the drugs,” he said.
Others are fighting for Medicare coverage, while some experts contend the costs of that coverage would be overwhelming. A bipartisan bill, the Treat and Reduce Obesity Act of 2023, would allow coverage under Medicare›s prescription drug benefit for drugs used for the treatment of obesity or for weigh loss management for people who are overweight. Some say it›s an uphill climb, citing a Vanderbilt University analysis that found giving just 10% of Medicare-eligible patients the drugs would cost $13.6 billion to more than $26 billion.
However, a white paper from the University of Southern California concluded that the value to society of covering the drugs for Medicare recipients would equal nearly $1 trillion over 10 years, citing savings in hospitalizations and other health care costs.
Comprehensive insurance coverage is needed, Dr. Apovian said. Private insurance plans, Medicare, and Medicaid must all realize the importance of covering what has been now shown to be life-saving drugs, she said.
Broader coverage might also reduce the number of patients getting obesity drugs from unreliable sources, in an effort to save money, and having adverse effects. The FDA warned against counterfeit semaglutide in December.
Long-Term Picture
Research suggests the obesity medications must be taken continuously, at least for most people, to maintain the weight loss. In a study of patients on Zepbound, Dr. Aronne and colleagues found that withdrawing the medication led people to regain weight, while continuing it led to maintaining and even increasing the initial weight loss. While some may be able to use the medications only from time to time, “the majority will have to take these on a chronic basis,” Dr. Aronne said.
Obesity, like high blood pressure and other chronic conditions, needs continuous treatment, Dr. Apovian said. No one would suggest withdrawing blood pressure medications that stabilize blood pressure; the same should be true for the obesity drugs, she said.
Dr. Apovian consults for FORM, the telehealth platform Lilly uses for LillyDirect, and consults for Novo Nordisk, which makes Saxenda and Wegovy. Dr. Aronne is a consultant and investigator for Novo Nordisk, Eli Lilly, and other companies.
A version of this article appeared on WebMD.com.
Eli Lilly, maker of the anti-obesity drug Zepbound, announced this week the launch of LillyDirect, a direct-to-patient portal, allowing some patients to obtain its drug for as little as $25 a month.
The move is seen as a major shift in the way these popular medications can reach patients.
For many of the 42 million Americans with obesity, weight loss medications such as Wegovy, Saxenda, and the brand-new Zepbound can be a godsend, helping them lose the excess pounds they’ve struggled with for decades or a lifetime.
But getting these medications has been a struggle for many who are eligible. Shortages of the drugs have been one barrier, and costs of up to $1,300 monthly — the price tag without insurance coverage — are another hurdle.
But 2024 may be a much brighter year, thanks to Lilly’s new portal as well as other developments:
Insurance coverage on private health plans, while still spotty, may be improving. Federal legislators are fighting a 2003 law that forbids Medicare from paying for the medications when prescribed for obesity.
New research found that semaglutide (Wegovy) can reduce the risk of recurrent strokes and heart attacks as well as deaths from cardiovascular events in those with obesity and preexisting cardiovascular disease (or diseases of the heart and blood vessels), a finding experts said should get the attention of health insurers.
The medications, also referred to as GLP-1 agonists, work by activating the receptors of hormones (called glucagon-like peptide 1 and others) that are naturally released after eating. That, in turn, makes you feel more full, leading to weight loss of up to 22% for some. The medications are approved for those with a body mass index (BMI) of 30 or a BMI of 27 with at least one other weight-related health condition such as high blood pressure or high cholesterol. The medicines, injected weekly or more often, are prescribed along with advice about a reduced-calorie diet and increased physical activity.
LillyDirect
Patients can access the obesity medicines through the telehealth platform FORM. Patients reach independent telehealth providers, according to Lilly, who can complement a patient’s current doctor or be an alternative to in-patient care in some cases.
Eli Lilly officials did not respond to requests for comment.
Some obesity experts welcomed the new service. “Any program that improves availability and affordability of these ground-breaking medications is welcome news for our long-suffering patients,” said Louis Aronne, MD, director of the Comprehensive Weight Control Center at Weill Cornell Medicine in New York City, a long-time obesity researcher.
“It’s a great move for Lilly to do,” agreed Caroline Apovian, MD, a professor of medicine at Harvard Medical School and co-director of the Center for Weight Management and Wellness at Brigham & Women’s Hospital in Boston, who is also a veteran obesity specialist. “It is trying to help the accessibility issue and do it responsibly.”
“The bottom line is, there is an overwhelming amount of consumer need and desire for these medications and not enough channels [to provide them],” said Zeev Neuwirth, MD, a former executive at Atrium Health who writes about health care trends. “Eli Lilly is responding to a market need that is out there and quite honestly continuing to grow.”
There are still concerns and questions, Dr. Neuwirth said, “especially since this is to my knowledge the first of its kind in terms of a pharmaceutical manufacturer directly dispensing medication in this nontraditional way.”
He called for transparency between telehealth providers and the pharmaceutical company to rule out any conflicts of interest.
The American College of Physicians, an organization of internal medicine doctors and others, issued a statement expressing concern. Omar T. Atiq, MD, group’s president, said his organization is “concerned by the development of websites that enable patients to order prescription medications directly from the drugmakers. While information on in-person care is available, this direct-to-consumer approach is primarily oriented around the use of telehealth services to prescribe a drug maker’s products.”
The group urged that an established patient-doctor relationship be present, or that care should happen in consultation with a doctor who does have an established relationship (the latter an option offered by Lilly). “These direct-to-consumer services have the potential to leave patients confused and misinformed about medications.”
Heart Attack, Stroke Reduction Benefits
Previous research has found that the GLP-1 medicines such as Ozempic (semaglutide), which the FDA approved to treat diabetes, also reduce the risk of cardiovascular issues such as strokes and heart attacks. Now, new research finds that semaglutide at the Wegovy dose (usually slightly higher than the Ozempic dose for diabetes) also has those benefits in those who don›t have a diabetes diagnosis but do have obesity and cardiovascular disease.
In a clinical trial sponsored by Novo Nordisk, the maker of Wegovy, half of more than 17,000 people with obesity were given semaglutide (Wegovy); the other half got a placebo. Compared to those on the placebo, those who took the Wegovy had a 20% reduction in strokes, heart attacks, and deaths from cardiovascular causes over a 33-month period.
The study results are a “big deal,” Dr. Aronne said. The results make it clear that those with obesity but not diabetes will get the cardiovascular benefits from the treatment as well. While more analysis is necessary, he said the important point is that the study showed that reducing body weight is linked to improvement in critical health outcomes.
As the research evolves, he said, it’s going to be difficult for insurers to deny medications in the face of those findings, which promise reductions in long-term health care costs.
Insurance Coverage
In November, the American Medical Association voted to adopt a policy to urge insurance coverage for evidence-based treatment for obesity, including the new obesity medications.
“No single organization is going to be able to convince insurers and employers to cover this,” Dr. Aronne said. “But I think a prominent organization like the AMA adding their voice to the rising chorus is going to help.”
Coverage of GLP-1 medications could nearly double in 2024, according to a survey of 500 human resources decision-makers released in October by Accolade, a personalized health care advocacy and delivery company. While 25% of respondents said they currently offered coverage when the survey was done in August and September, 43% said they intend to offer coverage in 2024.
In an email, David Allen, a spokesperson for America’s Health Insurance Plans, a health care industry association, said: “Every American deserves affordable coverage and high-quality care, and that includes coverage and care for evidence-based obesity treatments and therapies.”
He said “clinical leaders and other experts at health insurance providers routinely review the evidence for all types of treatments, including treatments for obesity, and offer multiple options to patients — ranging from lifestyle changes and nutrition counseling, to surgical interventions, to prescription drugs.”
Mr. Allen said the evidence that obesity drugs help with weight loss “is still evolving.”
“And some patients are experiencing bad effects related to these drugs such as vomiting and nausea, for example, and the likelihood of gaining the weight back when discontinuing the drugs,” he said.
Others are fighting for Medicare coverage, while some experts contend the costs of that coverage would be overwhelming. A bipartisan bill, the Treat and Reduce Obesity Act of 2023, would allow coverage under Medicare›s prescription drug benefit for drugs used for the treatment of obesity or for weigh loss management for people who are overweight. Some say it›s an uphill climb, citing a Vanderbilt University analysis that found giving just 10% of Medicare-eligible patients the drugs would cost $13.6 billion to more than $26 billion.
However, a white paper from the University of Southern California concluded that the value to society of covering the drugs for Medicare recipients would equal nearly $1 trillion over 10 years, citing savings in hospitalizations and other health care costs.
Comprehensive insurance coverage is needed, Dr. Apovian said. Private insurance plans, Medicare, and Medicaid must all realize the importance of covering what has been now shown to be life-saving drugs, she said.
Broader coverage might also reduce the number of patients getting obesity drugs from unreliable sources, in an effort to save money, and having adverse effects. The FDA warned against counterfeit semaglutide in December.
Long-Term Picture
Research suggests the obesity medications must be taken continuously, at least for most people, to maintain the weight loss. In a study of patients on Zepbound, Dr. Aronne and colleagues found that withdrawing the medication led people to regain weight, while continuing it led to maintaining and even increasing the initial weight loss. While some may be able to use the medications only from time to time, “the majority will have to take these on a chronic basis,” Dr. Aronne said.
Obesity, like high blood pressure and other chronic conditions, needs continuous treatment, Dr. Apovian said. No one would suggest withdrawing blood pressure medications that stabilize blood pressure; the same should be true for the obesity drugs, she said.
Dr. Apovian consults for FORM, the telehealth platform Lilly uses for LillyDirect, and consults for Novo Nordisk, which makes Saxenda and Wegovy. Dr. Aronne is a consultant and investigator for Novo Nordisk, Eli Lilly, and other companies.
A version of this article appeared on WebMD.com.
Eli Lilly, maker of the anti-obesity drug Zepbound, announced this week the launch of LillyDirect, a direct-to-patient portal, allowing some patients to obtain its drug for as little as $25 a month.
The move is seen as a major shift in the way these popular medications can reach patients.
For many of the 42 million Americans with obesity, weight loss medications such as Wegovy, Saxenda, and the brand-new Zepbound can be a godsend, helping them lose the excess pounds they’ve struggled with for decades or a lifetime.
But getting these medications has been a struggle for many who are eligible. Shortages of the drugs have been one barrier, and costs of up to $1,300 monthly — the price tag without insurance coverage — are another hurdle.
But 2024 may be a much brighter year, thanks to Lilly’s new portal as well as other developments:
Insurance coverage on private health plans, while still spotty, may be improving. Federal legislators are fighting a 2003 law that forbids Medicare from paying for the medications when prescribed for obesity.
New research found that semaglutide (Wegovy) can reduce the risk of recurrent strokes and heart attacks as well as deaths from cardiovascular events in those with obesity and preexisting cardiovascular disease (or diseases of the heart and blood vessels), a finding experts said should get the attention of health insurers.
The medications, also referred to as GLP-1 agonists, work by activating the receptors of hormones (called glucagon-like peptide 1 and others) that are naturally released after eating. That, in turn, makes you feel more full, leading to weight loss of up to 22% for some. The medications are approved for those with a body mass index (BMI) of 30 or a BMI of 27 with at least one other weight-related health condition such as high blood pressure or high cholesterol. The medicines, injected weekly or more often, are prescribed along with advice about a reduced-calorie diet and increased physical activity.
LillyDirect
Patients can access the obesity medicines through the telehealth platform FORM. Patients reach independent telehealth providers, according to Lilly, who can complement a patient’s current doctor or be an alternative to in-patient care in some cases.
Eli Lilly officials did not respond to requests for comment.
Some obesity experts welcomed the new service. “Any program that improves availability and affordability of these ground-breaking medications is welcome news for our long-suffering patients,” said Louis Aronne, MD, director of the Comprehensive Weight Control Center at Weill Cornell Medicine in New York City, a long-time obesity researcher.
“It’s a great move for Lilly to do,” agreed Caroline Apovian, MD, a professor of medicine at Harvard Medical School and co-director of the Center for Weight Management and Wellness at Brigham & Women’s Hospital in Boston, who is also a veteran obesity specialist. “It is trying to help the accessibility issue and do it responsibly.”
“The bottom line is, there is an overwhelming amount of consumer need and desire for these medications and not enough channels [to provide them],” said Zeev Neuwirth, MD, a former executive at Atrium Health who writes about health care trends. “Eli Lilly is responding to a market need that is out there and quite honestly continuing to grow.”
There are still concerns and questions, Dr. Neuwirth said, “especially since this is to my knowledge the first of its kind in terms of a pharmaceutical manufacturer directly dispensing medication in this nontraditional way.”
He called for transparency between telehealth providers and the pharmaceutical company to rule out any conflicts of interest.
The American College of Physicians, an organization of internal medicine doctors and others, issued a statement expressing concern. Omar T. Atiq, MD, group’s president, said his organization is “concerned by the development of websites that enable patients to order prescription medications directly from the drugmakers. While information on in-person care is available, this direct-to-consumer approach is primarily oriented around the use of telehealth services to prescribe a drug maker’s products.”
The group urged that an established patient-doctor relationship be present, or that care should happen in consultation with a doctor who does have an established relationship (the latter an option offered by Lilly). “These direct-to-consumer services have the potential to leave patients confused and misinformed about medications.”
Heart Attack, Stroke Reduction Benefits
Previous research has found that the GLP-1 medicines such as Ozempic (semaglutide), which the FDA approved to treat diabetes, also reduce the risk of cardiovascular issues such as strokes and heart attacks. Now, new research finds that semaglutide at the Wegovy dose (usually slightly higher than the Ozempic dose for diabetes) also has those benefits in those who don›t have a diabetes diagnosis but do have obesity and cardiovascular disease.
In a clinical trial sponsored by Novo Nordisk, the maker of Wegovy, half of more than 17,000 people with obesity were given semaglutide (Wegovy); the other half got a placebo. Compared to those on the placebo, those who took the Wegovy had a 20% reduction in strokes, heart attacks, and deaths from cardiovascular causes over a 33-month period.
The study results are a “big deal,” Dr. Aronne said. The results make it clear that those with obesity but not diabetes will get the cardiovascular benefits from the treatment as well. While more analysis is necessary, he said the important point is that the study showed that reducing body weight is linked to improvement in critical health outcomes.
As the research evolves, he said, it’s going to be difficult for insurers to deny medications in the face of those findings, which promise reductions in long-term health care costs.
Insurance Coverage
In November, the American Medical Association voted to adopt a policy to urge insurance coverage for evidence-based treatment for obesity, including the new obesity medications.
“No single organization is going to be able to convince insurers and employers to cover this,” Dr. Aronne said. “But I think a prominent organization like the AMA adding their voice to the rising chorus is going to help.”
Coverage of GLP-1 medications could nearly double in 2024, according to a survey of 500 human resources decision-makers released in October by Accolade, a personalized health care advocacy and delivery company. While 25% of respondents said they currently offered coverage when the survey was done in August and September, 43% said they intend to offer coverage in 2024.
In an email, David Allen, a spokesperson for America’s Health Insurance Plans, a health care industry association, said: “Every American deserves affordable coverage and high-quality care, and that includes coverage and care for evidence-based obesity treatments and therapies.”
He said “clinical leaders and other experts at health insurance providers routinely review the evidence for all types of treatments, including treatments for obesity, and offer multiple options to patients — ranging from lifestyle changes and nutrition counseling, to surgical interventions, to prescription drugs.”
Mr. Allen said the evidence that obesity drugs help with weight loss “is still evolving.”
“And some patients are experiencing bad effects related to these drugs such as vomiting and nausea, for example, and the likelihood of gaining the weight back when discontinuing the drugs,” he said.
Others are fighting for Medicare coverage, while some experts contend the costs of that coverage would be overwhelming. A bipartisan bill, the Treat and Reduce Obesity Act of 2023, would allow coverage under Medicare›s prescription drug benefit for drugs used for the treatment of obesity or for weigh loss management for people who are overweight. Some say it›s an uphill climb, citing a Vanderbilt University analysis that found giving just 10% of Medicare-eligible patients the drugs would cost $13.6 billion to more than $26 billion.
However, a white paper from the University of Southern California concluded that the value to society of covering the drugs for Medicare recipients would equal nearly $1 trillion over 10 years, citing savings in hospitalizations and other health care costs.
Comprehensive insurance coverage is needed, Dr. Apovian said. Private insurance plans, Medicare, and Medicaid must all realize the importance of covering what has been now shown to be life-saving drugs, she said.
Broader coverage might also reduce the number of patients getting obesity drugs from unreliable sources, in an effort to save money, and having adverse effects. The FDA warned against counterfeit semaglutide in December.
Long-Term Picture
Research suggests the obesity medications must be taken continuously, at least for most people, to maintain the weight loss. In a study of patients on Zepbound, Dr. Aronne and colleagues found that withdrawing the medication led people to regain weight, while continuing it led to maintaining and even increasing the initial weight loss. While some may be able to use the medications only from time to time, “the majority will have to take these on a chronic basis,” Dr. Aronne said.
Obesity, like high blood pressure and other chronic conditions, needs continuous treatment, Dr. Apovian said. No one would suggest withdrawing blood pressure medications that stabilize blood pressure; the same should be true for the obesity drugs, she said.
Dr. Apovian consults for FORM, the telehealth platform Lilly uses for LillyDirect, and consults for Novo Nordisk, which makes Saxenda and Wegovy. Dr. Aronne is a consultant and investigator for Novo Nordisk, Eli Lilly, and other companies.
A version of this article appeared on WebMD.com.
A Counterintuitive Approach to Lowering Cholesterol in Children
With the flip of the calendar a few short weeks ago, gyms and fitness centers began ramping up their advertising campaigns in hopes of attracting the horde of resolution makers searching for a place where they can inject some exercise into their sedentary lives. A recent survey by C.S. Mott’s Children’s Hospital found that even young people are setting health-related goals with more than half of the parents of 11- to 18-year-olds reporting their children were setting personal goals for themselves. More than 40% of the young people listed more exercise as a target.
However, our personal and professional experiences have taught us that achieving goals, particularly when it comes to exercise, is far more difficult than setting the target. Finding an exercise buddy can be an important motivator on the days when just lacing up one’s sneakers is a stumbling block. Investing in a gym membership and sweating with a peer group can help. However, it is an investment that rarely pays a dividend. Exercise isn’t fun for everyone. For adults, showing up at a gym may be just one more reminder of how they have already lost their competitive edge over their leaner and fitter peers. If they aren’t lucky enough to find a sport or activity that they enjoy, the loneliness of the long-distance runner has little appeal.
A recent study on children in the United Kingdom suggests that at least when it comes to teens and young adults we as physicians may actually have been making things worse for our obese patients by urging them to accept unrealistic activity goals. While it is already known that sedentary time is responsible for 70% of the total increase in cholesterol as children advance to young adulthood an unqualified recommendation for more exercise may not be the best advice.
In an interview with the study author, Andre O. Agbaje MD, MPH, said that in his large study population “light physical activity outperforms moderate to vigorous physical activity by five to eight times in lowering lipids”. While we may be surprised by this counterintuitive finding, Dr. Agbaje points out that an increase in sedentariness from 6 to 9 hours per day translates into a loss of 3 hours of light physical activity. In other words if you’re not sedentary you must be standing at attention or engaged in some light activity.
In my experience, and I suspect yours, it is difficult to get adults to do something, particularly if that something involves exerting energy, even a small amount of energy. The general admonishment of “be more active” is often met with a blank stare and the sometimes unspoken question “Like what?”
You could fall into a bottomless trap with them by suggesting a long list of activities, many of which are probably ones you do or would enjoy but don’t happen to fit with any of their interests or capabilities. Your chances of hitting on a perfect activity that the patient will attempt, let alone adopt, is very slim. Those of you with more patience than I have may choose to persist with this strategy. You could argue that even if the patient only dabbles briefly in one of your recommended activities, this is a minor victory worth celebrating. Who knows? The brief jolt of energy they received from this activity may prompt them to seek and find something else that works.
My interpretation of Dr. Agbaje’s findings is this: If we are going to suggest more activity, aim low. Don’t even mention the heavily weighted words “sport” or “exercise,” which are likely to dredge up bad memories. For adults, “Go shopping” or “Visit a friend” may be sufficient to at least get the person off the couch and on their feet and moving, even if very briefly.
The second message from this study applies more to children and adolescents and is one of those unusual instances in which a negative intervention may be more effective than a positive approach. Acknowledging that we are likely to have difficulty finding even a light activity that the child enjoys, why not pivot to the other side of the equation? Make a list of the child’s primary sedentary “activities.” Then suggest the parents put the child on a couch potato diet by immediately cutting in half the time he or she spends being sedentary. By definition, this will automatically increase his or her light physical activity by 50%. According to Dr. Agbaje’s data, this should be more effective in lowering lipids than in the unlikely event of finding a moderate activity the child accepts.
You can argue that the child will hound his or her parents unmercifully asking to be entertained. This may be true and this persistent complaining will be more likely to come from the older the child and the longer that the child has been allowed to be sedentary. Although the child may appear to have lost the ability to self amuse, I contend this isn’t a permanent loss and, This is another example of how saying “No!” in the right circumstances is often the most effective remedy for an unhealthy situation. I would never claim saying “No” is easy and helping parents to learn how to say “No” is one of our most difficult challenges. But, nothing else seems to be working.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
With the flip of the calendar a few short weeks ago, gyms and fitness centers began ramping up their advertising campaigns in hopes of attracting the horde of resolution makers searching for a place where they can inject some exercise into their sedentary lives. A recent survey by C.S. Mott’s Children’s Hospital found that even young people are setting health-related goals with more than half of the parents of 11- to 18-year-olds reporting their children were setting personal goals for themselves. More than 40% of the young people listed more exercise as a target.
However, our personal and professional experiences have taught us that achieving goals, particularly when it comes to exercise, is far more difficult than setting the target. Finding an exercise buddy can be an important motivator on the days when just lacing up one’s sneakers is a stumbling block. Investing in a gym membership and sweating with a peer group can help. However, it is an investment that rarely pays a dividend. Exercise isn’t fun for everyone. For adults, showing up at a gym may be just one more reminder of how they have already lost their competitive edge over their leaner and fitter peers. If they aren’t lucky enough to find a sport or activity that they enjoy, the loneliness of the long-distance runner has little appeal.
A recent study on children in the United Kingdom suggests that at least when it comes to teens and young adults we as physicians may actually have been making things worse for our obese patients by urging them to accept unrealistic activity goals. While it is already known that sedentary time is responsible for 70% of the total increase in cholesterol as children advance to young adulthood an unqualified recommendation for more exercise may not be the best advice.
In an interview with the study author, Andre O. Agbaje MD, MPH, said that in his large study population “light physical activity outperforms moderate to vigorous physical activity by five to eight times in lowering lipids”. While we may be surprised by this counterintuitive finding, Dr. Agbaje points out that an increase in sedentariness from 6 to 9 hours per day translates into a loss of 3 hours of light physical activity. In other words if you’re not sedentary you must be standing at attention or engaged in some light activity.
In my experience, and I suspect yours, it is difficult to get adults to do something, particularly if that something involves exerting energy, even a small amount of energy. The general admonishment of “be more active” is often met with a blank stare and the sometimes unspoken question “Like what?”
You could fall into a bottomless trap with them by suggesting a long list of activities, many of which are probably ones you do or would enjoy but don’t happen to fit with any of their interests or capabilities. Your chances of hitting on a perfect activity that the patient will attempt, let alone adopt, is very slim. Those of you with more patience than I have may choose to persist with this strategy. You could argue that even if the patient only dabbles briefly in one of your recommended activities, this is a minor victory worth celebrating. Who knows? The brief jolt of energy they received from this activity may prompt them to seek and find something else that works.
My interpretation of Dr. Agbaje’s findings is this: If we are going to suggest more activity, aim low. Don’t even mention the heavily weighted words “sport” or “exercise,” which are likely to dredge up bad memories. For adults, “Go shopping” or “Visit a friend” may be sufficient to at least get the person off the couch and on their feet and moving, even if very briefly.
The second message from this study applies more to children and adolescents and is one of those unusual instances in which a negative intervention may be more effective than a positive approach. Acknowledging that we are likely to have difficulty finding even a light activity that the child enjoys, why not pivot to the other side of the equation? Make a list of the child’s primary sedentary “activities.” Then suggest the parents put the child on a couch potato diet by immediately cutting in half the time he or she spends being sedentary. By definition, this will automatically increase his or her light physical activity by 50%. According to Dr. Agbaje’s data, this should be more effective in lowering lipids than in the unlikely event of finding a moderate activity the child accepts.
You can argue that the child will hound his or her parents unmercifully asking to be entertained. This may be true and this persistent complaining will be more likely to come from the older the child and the longer that the child has been allowed to be sedentary. Although the child may appear to have lost the ability to self amuse, I contend this isn’t a permanent loss and, This is another example of how saying “No!” in the right circumstances is often the most effective remedy for an unhealthy situation. I would never claim saying “No” is easy and helping parents to learn how to say “No” is one of our most difficult challenges. But, nothing else seems to be working.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
With the flip of the calendar a few short weeks ago, gyms and fitness centers began ramping up their advertising campaigns in hopes of attracting the horde of resolution makers searching for a place where they can inject some exercise into their sedentary lives. A recent survey by C.S. Mott’s Children’s Hospital found that even young people are setting health-related goals with more than half of the parents of 11- to 18-year-olds reporting their children were setting personal goals for themselves. More than 40% of the young people listed more exercise as a target.
However, our personal and professional experiences have taught us that achieving goals, particularly when it comes to exercise, is far more difficult than setting the target. Finding an exercise buddy can be an important motivator on the days when just lacing up one’s sneakers is a stumbling block. Investing in a gym membership and sweating with a peer group can help. However, it is an investment that rarely pays a dividend. Exercise isn’t fun for everyone. For adults, showing up at a gym may be just one more reminder of how they have already lost their competitive edge over their leaner and fitter peers. If they aren’t lucky enough to find a sport or activity that they enjoy, the loneliness of the long-distance runner has little appeal.
A recent study on children in the United Kingdom suggests that at least when it comes to teens and young adults we as physicians may actually have been making things worse for our obese patients by urging them to accept unrealistic activity goals. While it is already known that sedentary time is responsible for 70% of the total increase in cholesterol as children advance to young adulthood an unqualified recommendation for more exercise may not be the best advice.
In an interview with the study author, Andre O. Agbaje MD, MPH, said that in his large study population “light physical activity outperforms moderate to vigorous physical activity by five to eight times in lowering lipids”. While we may be surprised by this counterintuitive finding, Dr. Agbaje points out that an increase in sedentariness from 6 to 9 hours per day translates into a loss of 3 hours of light physical activity. In other words if you’re not sedentary you must be standing at attention or engaged in some light activity.
In my experience, and I suspect yours, it is difficult to get adults to do something, particularly if that something involves exerting energy, even a small amount of energy. The general admonishment of “be more active” is often met with a blank stare and the sometimes unspoken question “Like what?”
You could fall into a bottomless trap with them by suggesting a long list of activities, many of which are probably ones you do or would enjoy but don’t happen to fit with any of their interests or capabilities. Your chances of hitting on a perfect activity that the patient will attempt, let alone adopt, is very slim. Those of you with more patience than I have may choose to persist with this strategy. You could argue that even if the patient only dabbles briefly in one of your recommended activities, this is a minor victory worth celebrating. Who knows? The brief jolt of energy they received from this activity may prompt them to seek and find something else that works.
My interpretation of Dr. Agbaje’s findings is this: If we are going to suggest more activity, aim low. Don’t even mention the heavily weighted words “sport” or “exercise,” which are likely to dredge up bad memories. For adults, “Go shopping” or “Visit a friend” may be sufficient to at least get the person off the couch and on their feet and moving, even if very briefly.
The second message from this study applies more to children and adolescents and is one of those unusual instances in which a negative intervention may be more effective than a positive approach. Acknowledging that we are likely to have difficulty finding even a light activity that the child enjoys, why not pivot to the other side of the equation? Make a list of the child’s primary sedentary “activities.” Then suggest the parents put the child on a couch potato diet by immediately cutting in half the time he or she spends being sedentary. By definition, this will automatically increase his or her light physical activity by 50%. According to Dr. Agbaje’s data, this should be more effective in lowering lipids than in the unlikely event of finding a moderate activity the child accepts.
You can argue that the child will hound his or her parents unmercifully asking to be entertained. This may be true and this persistent complaining will be more likely to come from the older the child and the longer that the child has been allowed to be sedentary. Although the child may appear to have lost the ability to self amuse, I contend this isn’t a permanent loss and, This is another example of how saying “No!” in the right circumstances is often the most effective remedy for an unhealthy situation. I would never claim saying “No” is easy and helping parents to learn how to say “No” is one of our most difficult challenges. But, nothing else seems to be working.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
Healthcare Violence: Doctors and Nurses Are Bearing the Brunt of Business Pressures
This transcript has been edited for clarity.
This month, I want to tackle the difficult subject of violence toward healthcare workers. There’s a reason this is top of mind for me in my practice, but I want to start by acknowledging that this has been a much larger issue for our profession and one that has been growing for a number of years now.
They also estimate that that rate doubled between 2011 and 2018. I think that range is important because it proves this was a problem, and a crescendoing problem, even before COVID.
Another thing I think is relevant is to look at where in the healthcare system are these attacks most likely. In the emergency room, ER staff have seen hostility toward them rise by at least 25% over the past several years. Some of the seeds of mistrust that were sown between the general public and the scientific and medical communities around the pandemic. I think there’s some explanation there for why that might be a particular crucible.
Perhaps most disturbingly of all, 60% of the victims of healthcare workplace violence are bedside nurses. There is something about the intensity of the inpatient setting that makes nerves particularly frayed and unfortunately makes patients and family members more likely to lash out. I think it’s actually the heightened sense of mortality.
I’m not excusing any of these behaviors, but maybe it’s akin to road rage. On the road, behind the wheel, tiny gestures can actually be, on some level, perceived as threats to our survival. Another driver swerving into your lane activates a fight-or-flight response, you feel threatened, and you might respond in the moment very rashly. I wonder if we’re not seeing that, quite unfairly, play out against bedside staff in our hospitals.
Here’s the thing. Those of us who practice in the outpatient setting — 95% of my work, for instance, happens in clinic — are not immune to this either. There are some very harrowing recent examples of physicians being killed, typically at gunpoint, often by patients, sometimes by aggrieved family members, in their offices. An orthopedist in Tennessee, a back surgeon in Tulsa, along with three of their colleagues. In the latter case, the assailant specifically blamed the surgeon for their pain.
This is where I think things get even more scary. We have to be the bearers of bad news in our profession. This has long been the task of the oncologist, in particular, to convey things that people don’t want to hear.
I think what brought this to my mind in terms of my reading was an incredible article in The ASCO Post and also in the Journal of Clinical Oncology by Dr. Noelle LoConte, who’s a medical oncologist in Wisconsin. The article is called, “I Want to Kill You,” and it recounts her telling a previously stage III colon cancer patient, with whom she thought she had good rapport, that the disease had recurred. The patient’s immediate reaction in the heat of that moment was to say, Dr LoConte, I want to kill you. I want to blow your face off.
Already, there’s clearly tension when we are telling people what they don’t want to hear. I think the final piece of the puzzle goes back to the intrusion of the business of healthcare on the practice of medicine. This is what I witnessed very recently. One of the things that’s interesting to think about is how what we do is now framed as customer service. I know there’s deriding of this model, but if perception is reality, we have a system where patients are set up to view themselves as consumers.
Let’s say, for instance, you’re in the unfortunate circumstance of being diagnosed with cancer and your insurer gives you the option to go to multiple oncologists. If you’re online browsing for oncologists, how do you differentiate me from some of my colleagues? The answer on these rating websites often has to do with domains that are about the overall experience — not just the patient-doctor interaction but also things like wait time, friendliness of staff, and promptness of care delivery.
That, I think, is the final piece of the puzzle, because what I really risk when I sit down with a patient and lay out a treatment plan is overpromising and underdelivering. I am long used to citing median overall survival for expectation of outcome. Of course, every patient wants to be an exceptional responder. Most patients want to be on the latter half of median survival. No one wants to be on the disappointingly shorter half.
My point is that I’ve long been able to mitigate that uncertainty for patients. What is getting harder and harder to explain away is the delay incurred between someone’s diagnosis, my meeting them and laying out a treatment plan, and their actual initiation of that therapy.
This finally brings me to my recent personal encounter. I have long taken care of a patient, much like Dr LoConte’s, with an extremely calm demeanor. I thought we had a great therapeutic alliance. I had to tell the patient that the disease had recurred, and then I laid out a treatment plan. It took weeks and then months for the insurer to approve this plan despite my providing my note in a timely fashion with a mountain of evidence behind the regimen that I’d selected.
This is where I think insurers — when they deny, deflect, and delay — are not taking adequate responsibility for the impact that has on the therapeutic alliance between a patient and their doctor. These people are trusting us with their lives. As an oncologist, I’ve already told them something they didn’t want to hear, and now I’m compounding that with the uncertainty of when we can actually begin treatment.
This gentleman — who, again, is normally extremely kind and affable — showed up at my office and was incredibly hostile toward me and my staff because of the delay that he was encountering. We literally couldn’t tell him when his insurer was going to approve his treatment, which would have been financially disastrous if he had tried to pay for it himself out of pocket. He needed his insurer’s approval before we could start, but we didn’t know when he could start. That uncertainty and not knowing was gnawing away at him until he was at the end of his rope.
What I’m here to say is that this has been a difficult couple of years in healthcare. I’m well aware that our ER staff are on the front lines, as are our bedside and inpatient teams. Even in the outpatient setting, I think we’re seeing this crucible and we’re seeing the pressure just grow, and grow, and grow. It’s like fracking. The more you increase the pressure, the more eventually you’re going to find out where the cracks are.
These patients are the ultimate stakeholders. It’s their lives on the line, and we should be concerned, but perhaps ultimately not surprised, that they’re lashing out to be heard. Given no other resort, they are taking out their frustration and their aggression on us. It›s not fair, but I am newly aware of it because, in a patient with whom I thought we had a superb rapport, I saw that vanish. As soon as he thought that his life was at risk, his fight-or-flight response kicked in. I was not dealing with the same man I knew. I was dealing with someone who was desperate and who just wanted to know when he could get the treatment.
I think this has taken the likelihood of workplace hostility to a whole other level for those of us in healthcare.
For any patients listening, I beg of you, please don’t shoot the messenger. We are here to serve you the best we can, but there are many external factors at play. We are doing our best to mitigate those for you so we can deliver the care that we promised in as timely a fashion as we can.
I hope everyone out there can stay safe. Thank you.
Dr. Lewis is director of gastrointestinal oncology at Intermountain Healthcare in Salt Lake City, Utah. He has an interest in neuroendocrine tumors, hereditary cancer syndromes, and patient-physician communication. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
This transcript has been edited for clarity.
This month, I want to tackle the difficult subject of violence toward healthcare workers. There’s a reason this is top of mind for me in my practice, but I want to start by acknowledging that this has been a much larger issue for our profession and one that has been growing for a number of years now.
They also estimate that that rate doubled between 2011 and 2018. I think that range is important because it proves this was a problem, and a crescendoing problem, even before COVID.
Another thing I think is relevant is to look at where in the healthcare system are these attacks most likely. In the emergency room, ER staff have seen hostility toward them rise by at least 25% over the past several years. Some of the seeds of mistrust that were sown between the general public and the scientific and medical communities around the pandemic. I think there’s some explanation there for why that might be a particular crucible.
Perhaps most disturbingly of all, 60% of the victims of healthcare workplace violence are bedside nurses. There is something about the intensity of the inpatient setting that makes nerves particularly frayed and unfortunately makes patients and family members more likely to lash out. I think it’s actually the heightened sense of mortality.
I’m not excusing any of these behaviors, but maybe it’s akin to road rage. On the road, behind the wheel, tiny gestures can actually be, on some level, perceived as threats to our survival. Another driver swerving into your lane activates a fight-or-flight response, you feel threatened, and you might respond in the moment very rashly. I wonder if we’re not seeing that, quite unfairly, play out against bedside staff in our hospitals.
Here’s the thing. Those of us who practice in the outpatient setting — 95% of my work, for instance, happens in clinic — are not immune to this either. There are some very harrowing recent examples of physicians being killed, typically at gunpoint, often by patients, sometimes by aggrieved family members, in their offices. An orthopedist in Tennessee, a back surgeon in Tulsa, along with three of their colleagues. In the latter case, the assailant specifically blamed the surgeon for their pain.
This is where I think things get even more scary. We have to be the bearers of bad news in our profession. This has long been the task of the oncologist, in particular, to convey things that people don’t want to hear.
I think what brought this to my mind in terms of my reading was an incredible article in The ASCO Post and also in the Journal of Clinical Oncology by Dr. Noelle LoConte, who’s a medical oncologist in Wisconsin. The article is called, “I Want to Kill You,” and it recounts her telling a previously stage III colon cancer patient, with whom she thought she had good rapport, that the disease had recurred. The patient’s immediate reaction in the heat of that moment was to say, Dr LoConte, I want to kill you. I want to blow your face off.
Already, there’s clearly tension when we are telling people what they don’t want to hear. I think the final piece of the puzzle goes back to the intrusion of the business of healthcare on the practice of medicine. This is what I witnessed very recently. One of the things that’s interesting to think about is how what we do is now framed as customer service. I know there’s deriding of this model, but if perception is reality, we have a system where patients are set up to view themselves as consumers.
Let’s say, for instance, you’re in the unfortunate circumstance of being diagnosed with cancer and your insurer gives you the option to go to multiple oncologists. If you’re online browsing for oncologists, how do you differentiate me from some of my colleagues? The answer on these rating websites often has to do with domains that are about the overall experience — not just the patient-doctor interaction but also things like wait time, friendliness of staff, and promptness of care delivery.
That, I think, is the final piece of the puzzle, because what I really risk when I sit down with a patient and lay out a treatment plan is overpromising and underdelivering. I am long used to citing median overall survival for expectation of outcome. Of course, every patient wants to be an exceptional responder. Most patients want to be on the latter half of median survival. No one wants to be on the disappointingly shorter half.
My point is that I’ve long been able to mitigate that uncertainty for patients. What is getting harder and harder to explain away is the delay incurred between someone’s diagnosis, my meeting them and laying out a treatment plan, and their actual initiation of that therapy.
This finally brings me to my recent personal encounter. I have long taken care of a patient, much like Dr LoConte’s, with an extremely calm demeanor. I thought we had a great therapeutic alliance. I had to tell the patient that the disease had recurred, and then I laid out a treatment plan. It took weeks and then months for the insurer to approve this plan despite my providing my note in a timely fashion with a mountain of evidence behind the regimen that I’d selected.
This is where I think insurers — when they deny, deflect, and delay — are not taking adequate responsibility for the impact that has on the therapeutic alliance between a patient and their doctor. These people are trusting us with their lives. As an oncologist, I’ve already told them something they didn’t want to hear, and now I’m compounding that with the uncertainty of when we can actually begin treatment.
This gentleman — who, again, is normally extremely kind and affable — showed up at my office and was incredibly hostile toward me and my staff because of the delay that he was encountering. We literally couldn’t tell him when his insurer was going to approve his treatment, which would have been financially disastrous if he had tried to pay for it himself out of pocket. He needed his insurer’s approval before we could start, but we didn’t know when he could start. That uncertainty and not knowing was gnawing away at him until he was at the end of his rope.
What I’m here to say is that this has been a difficult couple of years in healthcare. I’m well aware that our ER staff are on the front lines, as are our bedside and inpatient teams. Even in the outpatient setting, I think we’re seeing this crucible and we’re seeing the pressure just grow, and grow, and grow. It’s like fracking. The more you increase the pressure, the more eventually you’re going to find out where the cracks are.
These patients are the ultimate stakeholders. It’s their lives on the line, and we should be concerned, but perhaps ultimately not surprised, that they’re lashing out to be heard. Given no other resort, they are taking out their frustration and their aggression on us. It›s not fair, but I am newly aware of it because, in a patient with whom I thought we had a superb rapport, I saw that vanish. As soon as he thought that his life was at risk, his fight-or-flight response kicked in. I was not dealing with the same man I knew. I was dealing with someone who was desperate and who just wanted to know when he could get the treatment.
I think this has taken the likelihood of workplace hostility to a whole other level for those of us in healthcare.
For any patients listening, I beg of you, please don’t shoot the messenger. We are here to serve you the best we can, but there are many external factors at play. We are doing our best to mitigate those for you so we can deliver the care that we promised in as timely a fashion as we can.
I hope everyone out there can stay safe. Thank you.
Dr. Lewis is director of gastrointestinal oncology at Intermountain Healthcare in Salt Lake City, Utah. He has an interest in neuroendocrine tumors, hereditary cancer syndromes, and patient-physician communication. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
This transcript has been edited for clarity.
This month, I want to tackle the difficult subject of violence toward healthcare workers. There’s a reason this is top of mind for me in my practice, but I want to start by acknowledging that this has been a much larger issue for our profession and one that has been growing for a number of years now.
They also estimate that that rate doubled between 2011 and 2018. I think that range is important because it proves this was a problem, and a crescendoing problem, even before COVID.
Another thing I think is relevant is to look at where in the healthcare system are these attacks most likely. In the emergency room, ER staff have seen hostility toward them rise by at least 25% over the past several years. Some of the seeds of mistrust that were sown between the general public and the scientific and medical communities around the pandemic. I think there’s some explanation there for why that might be a particular crucible.
Perhaps most disturbingly of all, 60% of the victims of healthcare workplace violence are bedside nurses. There is something about the intensity of the inpatient setting that makes nerves particularly frayed and unfortunately makes patients and family members more likely to lash out. I think it’s actually the heightened sense of mortality.
I’m not excusing any of these behaviors, but maybe it’s akin to road rage. On the road, behind the wheel, tiny gestures can actually be, on some level, perceived as threats to our survival. Another driver swerving into your lane activates a fight-or-flight response, you feel threatened, and you might respond in the moment very rashly. I wonder if we’re not seeing that, quite unfairly, play out against bedside staff in our hospitals.
Here’s the thing. Those of us who practice in the outpatient setting — 95% of my work, for instance, happens in clinic — are not immune to this either. There are some very harrowing recent examples of physicians being killed, typically at gunpoint, often by patients, sometimes by aggrieved family members, in their offices. An orthopedist in Tennessee, a back surgeon in Tulsa, along with three of their colleagues. In the latter case, the assailant specifically blamed the surgeon for their pain.
This is where I think things get even more scary. We have to be the bearers of bad news in our profession. This has long been the task of the oncologist, in particular, to convey things that people don’t want to hear.
I think what brought this to my mind in terms of my reading was an incredible article in The ASCO Post and also in the Journal of Clinical Oncology by Dr. Noelle LoConte, who’s a medical oncologist in Wisconsin. The article is called, “I Want to Kill You,” and it recounts her telling a previously stage III colon cancer patient, with whom she thought she had good rapport, that the disease had recurred. The patient’s immediate reaction in the heat of that moment was to say, Dr LoConte, I want to kill you. I want to blow your face off.
Already, there’s clearly tension when we are telling people what they don’t want to hear. I think the final piece of the puzzle goes back to the intrusion of the business of healthcare on the practice of medicine. This is what I witnessed very recently. One of the things that’s interesting to think about is how what we do is now framed as customer service. I know there’s deriding of this model, but if perception is reality, we have a system where patients are set up to view themselves as consumers.
Let’s say, for instance, you’re in the unfortunate circumstance of being diagnosed with cancer and your insurer gives you the option to go to multiple oncologists. If you’re online browsing for oncologists, how do you differentiate me from some of my colleagues? The answer on these rating websites often has to do with domains that are about the overall experience — not just the patient-doctor interaction but also things like wait time, friendliness of staff, and promptness of care delivery.
That, I think, is the final piece of the puzzle, because what I really risk when I sit down with a patient and lay out a treatment plan is overpromising and underdelivering. I am long used to citing median overall survival for expectation of outcome. Of course, every patient wants to be an exceptional responder. Most patients want to be on the latter half of median survival. No one wants to be on the disappointingly shorter half.
My point is that I’ve long been able to mitigate that uncertainty for patients. What is getting harder and harder to explain away is the delay incurred between someone’s diagnosis, my meeting them and laying out a treatment plan, and their actual initiation of that therapy.
This finally brings me to my recent personal encounter. I have long taken care of a patient, much like Dr LoConte’s, with an extremely calm demeanor. I thought we had a great therapeutic alliance. I had to tell the patient that the disease had recurred, and then I laid out a treatment plan. It took weeks and then months for the insurer to approve this plan despite my providing my note in a timely fashion with a mountain of evidence behind the regimen that I’d selected.
This is where I think insurers — when they deny, deflect, and delay — are not taking adequate responsibility for the impact that has on the therapeutic alliance between a patient and their doctor. These people are trusting us with their lives. As an oncologist, I’ve already told them something they didn’t want to hear, and now I’m compounding that with the uncertainty of when we can actually begin treatment.
This gentleman — who, again, is normally extremely kind and affable — showed up at my office and was incredibly hostile toward me and my staff because of the delay that he was encountering. We literally couldn’t tell him when his insurer was going to approve his treatment, which would have been financially disastrous if he had tried to pay for it himself out of pocket. He needed his insurer’s approval before we could start, but we didn’t know when he could start. That uncertainty and not knowing was gnawing away at him until he was at the end of his rope.
What I’m here to say is that this has been a difficult couple of years in healthcare. I’m well aware that our ER staff are on the front lines, as are our bedside and inpatient teams. Even in the outpatient setting, I think we’re seeing this crucible and we’re seeing the pressure just grow, and grow, and grow. It’s like fracking. The more you increase the pressure, the more eventually you’re going to find out where the cracks are.
These patients are the ultimate stakeholders. It’s their lives on the line, and we should be concerned, but perhaps ultimately not surprised, that they’re lashing out to be heard. Given no other resort, they are taking out their frustration and their aggression on us. It›s not fair, but I am newly aware of it because, in a patient with whom I thought we had a superb rapport, I saw that vanish. As soon as he thought that his life was at risk, his fight-or-flight response kicked in. I was not dealing with the same man I knew. I was dealing with someone who was desperate and who just wanted to know when he could get the treatment.
I think this has taken the likelihood of workplace hostility to a whole other level for those of us in healthcare.
For any patients listening, I beg of you, please don’t shoot the messenger. We are here to serve you the best we can, but there are many external factors at play. We are doing our best to mitigate those for you so we can deliver the care that we promised in as timely a fashion as we can.
I hope everyone out there can stay safe. Thank you.
Dr. Lewis is director of gastrointestinal oncology at Intermountain Healthcare in Salt Lake City, Utah. He has an interest in neuroendocrine tumors, hereditary cancer syndromes, and patient-physician communication. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Are Post-Meal Insulin Surges Beneficial?
Rapid surges in insulin following a meal are associated with favorable long-term cardiometabolic benefits, including improvements in beta cell function and a lower risk for the development of prediabetes or diabetes, contrary to some concerns of the surges being indicative of more negative effects.
“There are practitioners who subscribe to this notion of higher insulin levels being a bad thing, and sometimes are making recommendations to patients to limit their insulin fluctuations after the meal,” said first author Ravi Retnakaran, MD, an endocrinologist and Boehringer Ingelheim Chair in Beta-cell Preservation, Function and Regeneration at the Leadership Sinai Centre for Diabetes at Mount Sinai Hospital, Toronto, Ontario, in a press statement.
“But it’s not that simple,” he said. “We observed that a robust post-challenge insulin secretory response, once adjusted for glucose levels, is only associated with beneficial metabolic effects.”
The findings were published on December 13, 2023, in eClinicalMedicine, part of The Lancet Discovery Science.
Insulin levels increase after food consumption in the normal management of blood glucose; however, some research has suggested that more rapid spikes in insulin, especially after a high-carbohydrate meal, are linked to an anabolic state contributing to weight gain and insulin resistance.
As public awareness of those reports has grown, “patients are coming in concerned about the possibility of their insulin levels being high, and there is confusion about the physiology of these effects,” Dr. Retnakaran told this news organization.
However, other studies have shown that the effects of insulin surges are important relative to baseline factors, including ambient glycemia and, specifically, baseline glucose levels prior to a meal.
Therefore, a more appropriate assessment is to use a corrected insulin response, measuring insulin secretion at 30 minutes after an oral glucose challenge, in relation to baseline glucose levels, research has suggested.
To investigate the issue in a longitudinal context, Dr. Retnakaran and colleagues conducted a prospective cohort study of 306 pregnant women representing a full range of glucose tolerance, who were enrolled at a hospital in Toronto between October 2003 and March 2014.
The women received comprehensive cardiometabolic testing, including oral glucose tolerance tests at 1-year, 3-year, and 5-year postpartum, and their baseline post-challenge insulinemia was established using corrected insulin response at 1 year.
Over 4 years of follow-up, a progressive worsening of cardiometabolic factors was associated with higher tertiles of corrected insulin responses at baseline, including waist circumference (P = .016), high-density lipoprotein (P = .018), C-reactive protein (CRP; P = .006), and insulin sensitivity (P < .001).
However, those trends were also associated with progressively improved beta cell function (P < .001).
After adjustment in the longitudinal analysis for the clinical risk factors for diabetes, including age, ethnicity, family history of diabetes, and body mass index (BMI) at 1 year, a higher corrected insulin response tertile at baseline was independently associated with improved Insulin Secretion-Sensitivity Index-2 and insulinogenic index/insulin resistance index (IGI/HOMA-IR), as well as lower glycemia, as observed on fasting and 2-hour glucose at 3 years and 5 years (all P < .001).
The insulin response was meanwhile not associated with BMI, waist, lipids, CRP, or insulin sensitivity or resistance.
Importantly, the highest corrected insulin response tertile at 1-year postpartum was also significantly associated with a lower risk for prediabetes or diabetes than the lowest tertile at 3 years (adjusted OR [aOR], 0.19) as well as 5 years (aOR, 0.18).
“The real question in my mind was whether we had the statistical power to be able to demonstrate a longitudinal beneficial effect on glucose regulation, but we did,” Dr. Retnakaran told this news organization. “The results show lower prediabetes and diabetes among people who had the most robust postprandial insulin excursion at 1-year postpartum.”
While the unadjusted analyses at baseline showed adverse as well as favorable outcomes, “adjusted longitudinal analyses revealed consistent independent associations of higher complete insulin response with better beta cell function, lower glycemia, and lower risk of prediabetes or diabetes in the years thereafter,” the authors reported.
“This evidence should help push back concern around the postprandial insulin spike,” Dr. Retnakaran said.
Commenting on the study, James D. Johnson, PhD, a professor of cellular and physiological sciences and director of the Life Sciences Institute at the University of British Columbia, Canada, noted that “it is already well-known that the loss of postprandial first phase insulin secretion can be a key and early defect in the transition to prediabetes and type 2 diabetes. That is not new, but the confirmatory data are welcome,” he told this news organization.
However, with other data linking high insulin with adiposity and insulin resistance, “the nuance and subtleties are critical for us to understand the directions of the causality,” he said.
“It is quite possible that both of these models are true at different life stages and/or in different people. There may be more than one pathway to diabetes. This is the nature of science and progress.”
A key caveat is that with a specific cohort of pregnant women, the question remains of the generalizability to men and to those younger or older than childbearing age.
Nevertheless, “I think this is an interesting and important study,” Dr. Johnson said. “More data on this topic is always welcome, but I am not sure this will be the final say in this debate.”
The authors and Dr. Johnson had no disclosures to report.
A version of this article appeared on Medscape.com.
Rapid surges in insulin following a meal are associated with favorable long-term cardiometabolic benefits, including improvements in beta cell function and a lower risk for the development of prediabetes or diabetes, contrary to some concerns of the surges being indicative of more negative effects.
“There are practitioners who subscribe to this notion of higher insulin levels being a bad thing, and sometimes are making recommendations to patients to limit their insulin fluctuations after the meal,” said first author Ravi Retnakaran, MD, an endocrinologist and Boehringer Ingelheim Chair in Beta-cell Preservation, Function and Regeneration at the Leadership Sinai Centre for Diabetes at Mount Sinai Hospital, Toronto, Ontario, in a press statement.
“But it’s not that simple,” he said. “We observed that a robust post-challenge insulin secretory response, once adjusted for glucose levels, is only associated with beneficial metabolic effects.”
The findings were published on December 13, 2023, in eClinicalMedicine, part of The Lancet Discovery Science.
Insulin levels increase after food consumption in the normal management of blood glucose; however, some research has suggested that more rapid spikes in insulin, especially after a high-carbohydrate meal, are linked to an anabolic state contributing to weight gain and insulin resistance.
As public awareness of those reports has grown, “patients are coming in concerned about the possibility of their insulin levels being high, and there is confusion about the physiology of these effects,” Dr. Retnakaran told this news organization.
However, other studies have shown that the effects of insulin surges are important relative to baseline factors, including ambient glycemia and, specifically, baseline glucose levels prior to a meal.
Therefore, a more appropriate assessment is to use a corrected insulin response, measuring insulin secretion at 30 minutes after an oral glucose challenge, in relation to baseline glucose levels, research has suggested.
To investigate the issue in a longitudinal context, Dr. Retnakaran and colleagues conducted a prospective cohort study of 306 pregnant women representing a full range of glucose tolerance, who were enrolled at a hospital in Toronto between October 2003 and March 2014.
The women received comprehensive cardiometabolic testing, including oral glucose tolerance tests at 1-year, 3-year, and 5-year postpartum, and their baseline post-challenge insulinemia was established using corrected insulin response at 1 year.
Over 4 years of follow-up, a progressive worsening of cardiometabolic factors was associated with higher tertiles of corrected insulin responses at baseline, including waist circumference (P = .016), high-density lipoprotein (P = .018), C-reactive protein (CRP; P = .006), and insulin sensitivity (P < .001).
However, those trends were also associated with progressively improved beta cell function (P < .001).
After adjustment in the longitudinal analysis for the clinical risk factors for diabetes, including age, ethnicity, family history of diabetes, and body mass index (BMI) at 1 year, a higher corrected insulin response tertile at baseline was independently associated with improved Insulin Secretion-Sensitivity Index-2 and insulinogenic index/insulin resistance index (IGI/HOMA-IR), as well as lower glycemia, as observed on fasting and 2-hour glucose at 3 years and 5 years (all P < .001).
The insulin response was meanwhile not associated with BMI, waist, lipids, CRP, or insulin sensitivity or resistance.
Importantly, the highest corrected insulin response tertile at 1-year postpartum was also significantly associated with a lower risk for prediabetes or diabetes than the lowest tertile at 3 years (adjusted OR [aOR], 0.19) as well as 5 years (aOR, 0.18).
“The real question in my mind was whether we had the statistical power to be able to demonstrate a longitudinal beneficial effect on glucose regulation, but we did,” Dr. Retnakaran told this news organization. “The results show lower prediabetes and diabetes among people who had the most robust postprandial insulin excursion at 1-year postpartum.”
While the unadjusted analyses at baseline showed adverse as well as favorable outcomes, “adjusted longitudinal analyses revealed consistent independent associations of higher complete insulin response with better beta cell function, lower glycemia, and lower risk of prediabetes or diabetes in the years thereafter,” the authors reported.
“This evidence should help push back concern around the postprandial insulin spike,” Dr. Retnakaran said.
Commenting on the study, James D. Johnson, PhD, a professor of cellular and physiological sciences and director of the Life Sciences Institute at the University of British Columbia, Canada, noted that “it is already well-known that the loss of postprandial first phase insulin secretion can be a key and early defect in the transition to prediabetes and type 2 diabetes. That is not new, but the confirmatory data are welcome,” he told this news organization.
However, with other data linking high insulin with adiposity and insulin resistance, “the nuance and subtleties are critical for us to understand the directions of the causality,” he said.
“It is quite possible that both of these models are true at different life stages and/or in different people. There may be more than one pathway to diabetes. This is the nature of science and progress.”
A key caveat is that with a specific cohort of pregnant women, the question remains of the generalizability to men and to those younger or older than childbearing age.
Nevertheless, “I think this is an interesting and important study,” Dr. Johnson said. “More data on this topic is always welcome, but I am not sure this will be the final say in this debate.”
The authors and Dr. Johnson had no disclosures to report.
A version of this article appeared on Medscape.com.
Rapid surges in insulin following a meal are associated with favorable long-term cardiometabolic benefits, including improvements in beta cell function and a lower risk for the development of prediabetes or diabetes, contrary to some concerns of the surges being indicative of more negative effects.
“There are practitioners who subscribe to this notion of higher insulin levels being a bad thing, and sometimes are making recommendations to patients to limit their insulin fluctuations after the meal,” said first author Ravi Retnakaran, MD, an endocrinologist and Boehringer Ingelheim Chair in Beta-cell Preservation, Function and Regeneration at the Leadership Sinai Centre for Diabetes at Mount Sinai Hospital, Toronto, Ontario, in a press statement.
“But it’s not that simple,” he said. “We observed that a robust post-challenge insulin secretory response, once adjusted for glucose levels, is only associated with beneficial metabolic effects.”
The findings were published on December 13, 2023, in eClinicalMedicine, part of The Lancet Discovery Science.
Insulin levels increase after food consumption in the normal management of blood glucose; however, some research has suggested that more rapid spikes in insulin, especially after a high-carbohydrate meal, are linked to an anabolic state contributing to weight gain and insulin resistance.
As public awareness of those reports has grown, “patients are coming in concerned about the possibility of their insulin levels being high, and there is confusion about the physiology of these effects,” Dr. Retnakaran told this news organization.
However, other studies have shown that the effects of insulin surges are important relative to baseline factors, including ambient glycemia and, specifically, baseline glucose levels prior to a meal.
Therefore, a more appropriate assessment is to use a corrected insulin response, measuring insulin secretion at 30 minutes after an oral glucose challenge, in relation to baseline glucose levels, research has suggested.
To investigate the issue in a longitudinal context, Dr. Retnakaran and colleagues conducted a prospective cohort study of 306 pregnant women representing a full range of glucose tolerance, who were enrolled at a hospital in Toronto between October 2003 and March 2014.
The women received comprehensive cardiometabolic testing, including oral glucose tolerance tests at 1-year, 3-year, and 5-year postpartum, and their baseline post-challenge insulinemia was established using corrected insulin response at 1 year.
Over 4 years of follow-up, a progressive worsening of cardiometabolic factors was associated with higher tertiles of corrected insulin responses at baseline, including waist circumference (P = .016), high-density lipoprotein (P = .018), C-reactive protein (CRP; P = .006), and insulin sensitivity (P < .001).
However, those trends were also associated with progressively improved beta cell function (P < .001).
After adjustment in the longitudinal analysis for the clinical risk factors for diabetes, including age, ethnicity, family history of diabetes, and body mass index (BMI) at 1 year, a higher corrected insulin response tertile at baseline was independently associated with improved Insulin Secretion-Sensitivity Index-2 and insulinogenic index/insulin resistance index (IGI/HOMA-IR), as well as lower glycemia, as observed on fasting and 2-hour glucose at 3 years and 5 years (all P < .001).
The insulin response was meanwhile not associated with BMI, waist, lipids, CRP, or insulin sensitivity or resistance.
Importantly, the highest corrected insulin response tertile at 1-year postpartum was also significantly associated with a lower risk for prediabetes or diabetes than the lowest tertile at 3 years (adjusted OR [aOR], 0.19) as well as 5 years (aOR, 0.18).
“The real question in my mind was whether we had the statistical power to be able to demonstrate a longitudinal beneficial effect on glucose regulation, but we did,” Dr. Retnakaran told this news organization. “The results show lower prediabetes and diabetes among people who had the most robust postprandial insulin excursion at 1-year postpartum.”
While the unadjusted analyses at baseline showed adverse as well as favorable outcomes, “adjusted longitudinal analyses revealed consistent independent associations of higher complete insulin response with better beta cell function, lower glycemia, and lower risk of prediabetes or diabetes in the years thereafter,” the authors reported.
“This evidence should help push back concern around the postprandial insulin spike,” Dr. Retnakaran said.
Commenting on the study, James D. Johnson, PhD, a professor of cellular and physiological sciences and director of the Life Sciences Institute at the University of British Columbia, Canada, noted that “it is already well-known that the loss of postprandial first phase insulin secretion can be a key and early defect in the transition to prediabetes and type 2 diabetes. That is not new, but the confirmatory data are welcome,” he told this news organization.
However, with other data linking high insulin with adiposity and insulin resistance, “the nuance and subtleties are critical for us to understand the directions of the causality,” he said.
“It is quite possible that both of these models are true at different life stages and/or in different people. There may be more than one pathway to diabetes. This is the nature of science and progress.”
A key caveat is that with a specific cohort of pregnant women, the question remains of the generalizability to men and to those younger or older than childbearing age.
Nevertheless, “I think this is an interesting and important study,” Dr. Johnson said. “More data on this topic is always welcome, but I am not sure this will be the final say in this debate.”
The authors and Dr. Johnson had no disclosures to report.
A version of this article appeared on Medscape.com.
Evidence Grows for SGLT2 Inhibitors in Rheumatology
Over just a decade, sodium-glucose cotransporter-2 (SGLT2) inhibitors have revolutionized the second-line treatment of type 2 diabetes by improving the control of blood sugar, and they’re also being used to treat heart failure and chronic kidney disease. Now, there’s growing evidence that the medications have the potential to play a role in the treatment of a variety of rheumatologic diseases — gout, systemic lupus erythematosus (SLE), and lupus nephritis.
“I suspect that SGLT2 inhibitors may have a role in multiple rheumatic diseases,” said rheumatologist April Jorge, MD, of Harvard Medical School and Massachusetts General Hospital, Boston.
In gout, for example, “SGLT2 inhibitors hold great promise as a multipurpose treatment option,” said rheumatologist Chio Yokose, MD, MSc, also of Harvard Medical School and Massachusetts General Hospital. Both Dr. Jorge and Dr. Yokose spoke at recent medical conferences and in interviews about the potential value of the drugs in rheumatology.
There’s a big caveat. For the moment, SGLT2 inhibitors aren’t cleared for use in the treatment of rheumatologic conditions, and neither physician is ready to recommend prescribing them off-label outside of their FDA-approved indications.
But studies could pave the way toward more approved uses in rheumatology. And there’s good news for now: Many rheumatology patients may already be eligible to take the drugs because of other medical conditions. In gout, for example, “sizable proportions of patients have comorbidities for which they are already indicated,” Dr. Yokose said.
Research Hints at Gout-Busting Potential
The first SGLT2 inhibitor canagliflozin (Invokana), received FDA approval in 2013, followed by dapagliflozin (Farxiga), empagliflozin (Jardiance), ertugliflozin (Steglatro), and bexagliflozin (Brenzavvy). The drugs “lower blood sugar by causing the kidneys to remove sugar from the body through urine,” reports the National Kidney Foundation, and they “help to protect the kidneys and heart in people with CKD [chronic kidney disease].”
As Dr. Yokose noted in a presentation at the 2023 Gout Hyperuricemia and Crystal Associated Disease Network research symposium, SGLT2 inhibitors “have really become blockbuster drugs, and they’ve now been integrated into multiple professional society guidelines and recommendations.”
These drugs should not be confused with the wildly popular medications known as glucagon-like peptide-1 (GLP1) agonists, which include medications such as semaglutide (Ozempic and Wegovy). These drugs are generally administered via injection — unlike the oral SGLT2 inhibitors — and they’re variously indicated for type 2 diabetes and obesity.
Dr. Yokose highlighted research findings about the drugs in gout. A 2020 study, for example, tracked 295,907 US adults with type 2 diabetes who received a new prescription for an SGLT2 inhibitor or GLP1 agonist during 2013-2017. Those in the SGLT2 inhibitor group had a 36% lower risk of newly diagnosed gout (hazard ratio [HR], 0.64; 95% CI, 0.57-0.72), the researchers reported.
A similar study, a 2021 report from Taiwan, also linked SGLT2 inhibitors to improvement in gout incidence vs. dipeptidyl peptidase 4 (DPP4) inhibitors, diabetes drugs that are not linked to lower serum urate levels. In an adjusted analysis, the risk of gout was 11% lower in the SGLT2 inhibitor group (adjusted HR, 0.86; 95% CI, 0.78-0.95).
What about recurrent gout? In a 2023 study, Dr. Yokose and colleagues tracked patients with type 2 diabetes who began SGLT2 inhibitors or DPP4 inhibitors. Over the period from 2013 to 2017, those who took SGLT2 inhibitors were less likely to have gout flares (rate ratio [RR], 0.66; 95% CI, 0.57-0.75) and gout-primary emergency department visits/hospitalizations (RR, 0.52; 95% CI, 0.32-0.84).
“This finding requires further replication in other populations and compared to other drugs,” Dr. Yokose cautioned.
Another 2023 study analyzed UK data and reached similar results regarding risk of recurrent gout.
Lower Urate Levels and Less Inflammation Could Be Key
How might SGLT2 inhibitors reduce the risk of gout? Multiple studies have linked the drugs to lower serum urate levels, Dr. Yokose said, but researchers often excluded patients with gout.
For a small new study presented at the 2023 annual meeting of the American College of Rheumatology but not yet published, Dr. Yokose and colleagues reported that patients with gout who began SGLT2 inhibitors had lower urate levels than those who began a sulfonylurea, another second-line agent for type 2 diabetes. During the study period, up to 3 months before and after initiation, 43.5% of patients in the SGLT2 inhibitor group reached a target serum urate of < 6 mg/dL vs. 4.2% of sulfonylurea initiators.
“The magnitude of this reduction, while not as large as what can be achieved with appropriately titrated urate-lowering therapy such as allopurinol or febuxostat, is also not negligible. It’s believed to be between 1.5-2.0 mg/dL among patients with gout,” Dr. Yokose said. “Also, SGLT2 inhibitors are purported to have some anti-inflammatory effects that may target the same pathways responsible for the profound inflammation associated with acute gout flares. However, both the exact mechanisms underlying the serum urate-lowering and anti-inflammatory effects of SGLT2 [inhibitors] require further research and clarification.”
Moving forward, she said, “I would love to see some prospective studies of SGLT2 inhibitor use among patients with gout, looking at serum urate and clinical gout endpoints, as well as biomarkers to understand better the beneficial effects of SGLT2 inhibitors as it pertains to patients with gout.”
In Lupus, Findings Are More Mixed
Studies of SGLT2 inhibitors have excluded patients with lupus, limiting insight into their benefits in that specific population, said Dr. Jorge of Massachusetts General Hospital and Harvard Medical School. However, “one small phase I/II trial showed an acceptable safety profile of dapagliflozin add-on therapy in adult patients with SLE,” she said.
Her team is working to expand understanding about the drugs in people with lupus. At the 2023 ACR annual meeting, she presented the findings of a study that tracked patients with SLE who took SGLT2 inhibitors (n = 426, including 154 with lupus nephritis) or DPP4 inhibitors (n = 865, including 270 with lupus nephritis). Patients who took SGLT2 inhibitors had lower risks of major adverse cardiac events (HR, 0.69; 95% CI, 0.48-0.99) and renal progression (HR, 0.71; 95% CI, 0.51-0.98).
“Our results are promising, but the majority of patient with lupus who had received SGLT2 inhibitors also had the comorbidity of type 2 diabetes as a separate indication for SGLT2 inhibitor use,” Dr. Jorge said. “We still need to study the impact of SGLT2 inhibitors in patients with SLE and lupus nephritis who do not have a separate indication for the medication.”
Dr. Jorge added that “we do not yet know the ideal time to initiate SGLT2 inhibitors in the treatment of lupus nephritis. Specifically, it is not yet known whether these medications should be used in patients with persistent proteinuria due to damage from lupus nephritis or whether there is also a role to start these medications in patients with active lupus nephritis who are undergoing induction immunosuppression regimens.”
However, another study released at the 2023 ACR annual meeting suggested that SGLT2 inhibitors may not have a beneficial effect in lupus nephritis: “We observed a reduction in decline in eGFR [estimated glomerular filtration rate] after starting SGLT2 inhibitors; however, this reduction was not statistically significant … early experience suggested marginal benefit of SGLT2 inhibitors in SLE,” researchers from Johns Hopkins University, and the University of Maryland, Baltimore, reported.
“My cohort is not showing miracles from SGLT2 inhibitors,” study lead author Michelle Petri, MD, MPH, of Johns Hopkins, said in an interview.
Still, new European Alliance of Associations for Rheumatology recommendations for SLE now advise to consider the use of the drugs in patients with lupus nephritis who have reduced eGFR. Meanwhile, “the American College of Rheumatology is currently developing new treatment guidelines for SLE and for lupus nephritis, and SGLT2 inhibitors will likely be a topic of consideration,” Dr. Jorge added.
As for mechanism, Dr. Jorge said it’s not clear how the drugs may affect lupus. “It’s proposed that they have benefits in hemodynamic effects as well as potentially anti-inflammatory effects. The hemodynamic effects, including reducing intraglomerular hyperfiltration and reducing blood pressure, likely have similar benefits in patients with chronic kidney disease due to diabetic nephropathy or due to lupus nephritis with damage/scarring and persistent proteinuria. Patients with SLE and other chronic, systemic rheumatic diseases such as ANCA [antineutrophilic cytoplasmic antibody]-associated vasculitis also develop kidney disease and cardiovascular events mediated by inflammatory processes.”
Side Effects and Cost: Where Do They Fit In?
According to Dr. Yokose, SGLT2 inhibitors “are generally quite well-tolerated, and very serious adverse effects are rare.” Side effects include disrupted urination, increased thirst, genital infections, flu-like symptoms, and swelling.
Urinary-related problems are understandable “because these drugs cause the kidneys to pass more glucose into the urine,” University of Hong Kong cardiac specialist Bernard Cheung, MBBCh, PhD, who has studied SGLT2 inhibitors, said in an interview.
In Dr. Yokose’s 2023 study of SGLT2 inhibitors in recurrent gout, patients who took the drugs were 2.15 times more likely than the comparison group to have genital infections (hazard ratio, 2.15; 95% CI, 1.39-3.30). This finding “was what we’d expect,” she said.
She added that genital infection rates were higher among patients with diabetes, women, and uncircumcised men. “Fortunately, most experienced just a single mild episode that can readily be treated with topical therapy. There does not appear to be an increased risk of urinary tract infections.”
Dr. Cheung added that “doctors should be aware of a rare adverse effect called euglycemic ketoacidosis, in which the patient has increased ketones in the blood causing it to be more acidic than normal, but the blood glucose remains within the normal range.”
As for cost, goodrx.com reports that several SGLT2 inhibitors run about $550-$683 per month, making them expensive but still cheaper than GLP-1 agonists, which can cost $1,000 or more per month. Unlike the most popular GLP-1 agonists such as Ozempic, none of the SGLT2 inhibitors are in short supply, according to the American Society of Health-System Pharmacists.
“If someone with gout already has a cardiovascular-kidney-metabolic indication for SGLT2 inhibitors and also stands to benefit in terms of lowering serum urate and risk of recurrent gout flares, there is potential for high benefit relative to cost,” Dr. Yokose said.
She added: “It is well-documented that current gout care is suboptimal, and many patients end up in the emergency room or hospitalized for gout, which in and of itself is quite costly both for the patient and the health care system. Therefore, streamlining or integrating gout and comorbidity care with SGLT2 inhibitors could potentially be quite beneficial for patients with gout.”
In regard to lupus, “many patients with lupus undergo multiple hospitalizations related to their disease, which is a source of high health care costs,” Dr. Jorge said. “Additionally, chronic kidney disease and cardiovascular disease are major causes of disability and premature mortality. Further studies will be needed to better understand whether benefits of SGLT2 inhibitors may outweigh the costs of treatment.”
As for prescribing the drugs in lupus now, Dr. Jorge said they can be an option in lupus nephritis. “There is not a clear consensus of the ideal timing to initiate SGLT2 inhibitors — e.g., degree of proteinuria or eGFR range,” she said. “However, it is less controversial that SGLT2 inhibitors should be considered in particular for patients with lupus nephritis with ongoing proteinuria despite adequate treatment with conventional therapies.”
As for gout, Dr. Yokose isn’t ready to prescribe the drugs to patients who don’t have comorbidities that can be treated by the medications. However, she noted that those patients are rare.
“If I see a patient with gout with one or more of these comorbidities, and I see that they are not already on an SGLT2 inhibitor, I definitely take the time to talk to the patient about this exciting class of drugs and will consult with their other physicians about getting them started on an SGLT2 inhibitor.”
Dr. Yokose, Dr. Petri, and Dr. Cheung have no relevant disclosures. Dr. Jorge disclosed serving as a site investigator for SLE clinical trials funded by Bristol-Myers Squibb and Cabaletta Bio; the trials are not related to SGLT2 inhibitors.
Over just a decade, sodium-glucose cotransporter-2 (SGLT2) inhibitors have revolutionized the second-line treatment of type 2 diabetes by improving the control of blood sugar, and they’re also being used to treat heart failure and chronic kidney disease. Now, there’s growing evidence that the medications have the potential to play a role in the treatment of a variety of rheumatologic diseases — gout, systemic lupus erythematosus (SLE), and lupus nephritis.
“I suspect that SGLT2 inhibitors may have a role in multiple rheumatic diseases,” said rheumatologist April Jorge, MD, of Harvard Medical School and Massachusetts General Hospital, Boston.
In gout, for example, “SGLT2 inhibitors hold great promise as a multipurpose treatment option,” said rheumatologist Chio Yokose, MD, MSc, also of Harvard Medical School and Massachusetts General Hospital. Both Dr. Jorge and Dr. Yokose spoke at recent medical conferences and in interviews about the potential value of the drugs in rheumatology.
There’s a big caveat. For the moment, SGLT2 inhibitors aren’t cleared for use in the treatment of rheumatologic conditions, and neither physician is ready to recommend prescribing them off-label outside of their FDA-approved indications.
But studies could pave the way toward more approved uses in rheumatology. And there’s good news for now: Many rheumatology patients may already be eligible to take the drugs because of other medical conditions. In gout, for example, “sizable proportions of patients have comorbidities for which they are already indicated,” Dr. Yokose said.
Research Hints at Gout-Busting Potential
The first SGLT2 inhibitor canagliflozin (Invokana), received FDA approval in 2013, followed by dapagliflozin (Farxiga), empagliflozin (Jardiance), ertugliflozin (Steglatro), and bexagliflozin (Brenzavvy). The drugs “lower blood sugar by causing the kidneys to remove sugar from the body through urine,” reports the National Kidney Foundation, and they “help to protect the kidneys and heart in people with CKD [chronic kidney disease].”
As Dr. Yokose noted in a presentation at the 2023 Gout Hyperuricemia and Crystal Associated Disease Network research symposium, SGLT2 inhibitors “have really become blockbuster drugs, and they’ve now been integrated into multiple professional society guidelines and recommendations.”
These drugs should not be confused with the wildly popular medications known as glucagon-like peptide-1 (GLP1) agonists, which include medications such as semaglutide (Ozempic and Wegovy). These drugs are generally administered via injection — unlike the oral SGLT2 inhibitors — and they’re variously indicated for type 2 diabetes and obesity.
Dr. Yokose highlighted research findings about the drugs in gout. A 2020 study, for example, tracked 295,907 US adults with type 2 diabetes who received a new prescription for an SGLT2 inhibitor or GLP1 agonist during 2013-2017. Those in the SGLT2 inhibitor group had a 36% lower risk of newly diagnosed gout (hazard ratio [HR], 0.64; 95% CI, 0.57-0.72), the researchers reported.
A similar study, a 2021 report from Taiwan, also linked SGLT2 inhibitors to improvement in gout incidence vs. dipeptidyl peptidase 4 (DPP4) inhibitors, diabetes drugs that are not linked to lower serum urate levels. In an adjusted analysis, the risk of gout was 11% lower in the SGLT2 inhibitor group (adjusted HR, 0.86; 95% CI, 0.78-0.95).
What about recurrent gout? In a 2023 study, Dr. Yokose and colleagues tracked patients with type 2 diabetes who began SGLT2 inhibitors or DPP4 inhibitors. Over the period from 2013 to 2017, those who took SGLT2 inhibitors were less likely to have gout flares (rate ratio [RR], 0.66; 95% CI, 0.57-0.75) and gout-primary emergency department visits/hospitalizations (RR, 0.52; 95% CI, 0.32-0.84).
“This finding requires further replication in other populations and compared to other drugs,” Dr. Yokose cautioned.
Another 2023 study analyzed UK data and reached similar results regarding risk of recurrent gout.
Lower Urate Levels and Less Inflammation Could Be Key
How might SGLT2 inhibitors reduce the risk of gout? Multiple studies have linked the drugs to lower serum urate levels, Dr. Yokose said, but researchers often excluded patients with gout.
For a small new study presented at the 2023 annual meeting of the American College of Rheumatology but not yet published, Dr. Yokose and colleagues reported that patients with gout who began SGLT2 inhibitors had lower urate levels than those who began a sulfonylurea, another second-line agent for type 2 diabetes. During the study period, up to 3 months before and after initiation, 43.5% of patients in the SGLT2 inhibitor group reached a target serum urate of < 6 mg/dL vs. 4.2% of sulfonylurea initiators.
“The magnitude of this reduction, while not as large as what can be achieved with appropriately titrated urate-lowering therapy such as allopurinol or febuxostat, is also not negligible. It’s believed to be between 1.5-2.0 mg/dL among patients with gout,” Dr. Yokose said. “Also, SGLT2 inhibitors are purported to have some anti-inflammatory effects that may target the same pathways responsible for the profound inflammation associated with acute gout flares. However, both the exact mechanisms underlying the serum urate-lowering and anti-inflammatory effects of SGLT2 [inhibitors] require further research and clarification.”
Moving forward, she said, “I would love to see some prospective studies of SGLT2 inhibitor use among patients with gout, looking at serum urate and clinical gout endpoints, as well as biomarkers to understand better the beneficial effects of SGLT2 inhibitors as it pertains to patients with gout.”
In Lupus, Findings Are More Mixed
Studies of SGLT2 inhibitors have excluded patients with lupus, limiting insight into their benefits in that specific population, said Dr. Jorge of Massachusetts General Hospital and Harvard Medical School. However, “one small phase I/II trial showed an acceptable safety profile of dapagliflozin add-on therapy in adult patients with SLE,” she said.
Her team is working to expand understanding about the drugs in people with lupus. At the 2023 ACR annual meeting, she presented the findings of a study that tracked patients with SLE who took SGLT2 inhibitors (n = 426, including 154 with lupus nephritis) or DPP4 inhibitors (n = 865, including 270 with lupus nephritis). Patients who took SGLT2 inhibitors had lower risks of major adverse cardiac events (HR, 0.69; 95% CI, 0.48-0.99) and renal progression (HR, 0.71; 95% CI, 0.51-0.98).
“Our results are promising, but the majority of patient with lupus who had received SGLT2 inhibitors also had the comorbidity of type 2 diabetes as a separate indication for SGLT2 inhibitor use,” Dr. Jorge said. “We still need to study the impact of SGLT2 inhibitors in patients with SLE and lupus nephritis who do not have a separate indication for the medication.”
Dr. Jorge added that “we do not yet know the ideal time to initiate SGLT2 inhibitors in the treatment of lupus nephritis. Specifically, it is not yet known whether these medications should be used in patients with persistent proteinuria due to damage from lupus nephritis or whether there is also a role to start these medications in patients with active lupus nephritis who are undergoing induction immunosuppression regimens.”
However, another study released at the 2023 ACR annual meeting suggested that SGLT2 inhibitors may not have a beneficial effect in lupus nephritis: “We observed a reduction in decline in eGFR [estimated glomerular filtration rate] after starting SGLT2 inhibitors; however, this reduction was not statistically significant … early experience suggested marginal benefit of SGLT2 inhibitors in SLE,” researchers from Johns Hopkins University, and the University of Maryland, Baltimore, reported.
“My cohort is not showing miracles from SGLT2 inhibitors,” study lead author Michelle Petri, MD, MPH, of Johns Hopkins, said in an interview.
Still, new European Alliance of Associations for Rheumatology recommendations for SLE now advise to consider the use of the drugs in patients with lupus nephritis who have reduced eGFR. Meanwhile, “the American College of Rheumatology is currently developing new treatment guidelines for SLE and for lupus nephritis, and SGLT2 inhibitors will likely be a topic of consideration,” Dr. Jorge added.
As for mechanism, Dr. Jorge said it’s not clear how the drugs may affect lupus. “It’s proposed that they have benefits in hemodynamic effects as well as potentially anti-inflammatory effects. The hemodynamic effects, including reducing intraglomerular hyperfiltration and reducing blood pressure, likely have similar benefits in patients with chronic kidney disease due to diabetic nephropathy or due to lupus nephritis with damage/scarring and persistent proteinuria. Patients with SLE and other chronic, systemic rheumatic diseases such as ANCA [antineutrophilic cytoplasmic antibody]-associated vasculitis also develop kidney disease and cardiovascular events mediated by inflammatory processes.”
Side Effects and Cost: Where Do They Fit In?
According to Dr. Yokose, SGLT2 inhibitors “are generally quite well-tolerated, and very serious adverse effects are rare.” Side effects include disrupted urination, increased thirst, genital infections, flu-like symptoms, and swelling.
Urinary-related problems are understandable “because these drugs cause the kidneys to pass more glucose into the urine,” University of Hong Kong cardiac specialist Bernard Cheung, MBBCh, PhD, who has studied SGLT2 inhibitors, said in an interview.
In Dr. Yokose’s 2023 study of SGLT2 inhibitors in recurrent gout, patients who took the drugs were 2.15 times more likely than the comparison group to have genital infections (hazard ratio, 2.15; 95% CI, 1.39-3.30). This finding “was what we’d expect,” she said.
She added that genital infection rates were higher among patients with diabetes, women, and uncircumcised men. “Fortunately, most experienced just a single mild episode that can readily be treated with topical therapy. There does not appear to be an increased risk of urinary tract infections.”
Dr. Cheung added that “doctors should be aware of a rare adverse effect called euglycemic ketoacidosis, in which the patient has increased ketones in the blood causing it to be more acidic than normal, but the blood glucose remains within the normal range.”
As for cost, goodrx.com reports that several SGLT2 inhibitors run about $550-$683 per month, making them expensive but still cheaper than GLP-1 agonists, which can cost $1,000 or more per month. Unlike the most popular GLP-1 agonists such as Ozempic, none of the SGLT2 inhibitors are in short supply, according to the American Society of Health-System Pharmacists.
“If someone with gout already has a cardiovascular-kidney-metabolic indication for SGLT2 inhibitors and also stands to benefit in terms of lowering serum urate and risk of recurrent gout flares, there is potential for high benefit relative to cost,” Dr. Yokose said.
She added: “It is well-documented that current gout care is suboptimal, and many patients end up in the emergency room or hospitalized for gout, which in and of itself is quite costly both for the patient and the health care system. Therefore, streamlining or integrating gout and comorbidity care with SGLT2 inhibitors could potentially be quite beneficial for patients with gout.”
In regard to lupus, “many patients with lupus undergo multiple hospitalizations related to their disease, which is a source of high health care costs,” Dr. Jorge said. “Additionally, chronic kidney disease and cardiovascular disease are major causes of disability and premature mortality. Further studies will be needed to better understand whether benefits of SGLT2 inhibitors may outweigh the costs of treatment.”
As for prescribing the drugs in lupus now, Dr. Jorge said they can be an option in lupus nephritis. “There is not a clear consensus of the ideal timing to initiate SGLT2 inhibitors — e.g., degree of proteinuria or eGFR range,” she said. “However, it is less controversial that SGLT2 inhibitors should be considered in particular for patients with lupus nephritis with ongoing proteinuria despite adequate treatment with conventional therapies.”
As for gout, Dr. Yokose isn’t ready to prescribe the drugs to patients who don’t have comorbidities that can be treated by the medications. However, she noted that those patients are rare.
“If I see a patient with gout with one or more of these comorbidities, and I see that they are not already on an SGLT2 inhibitor, I definitely take the time to talk to the patient about this exciting class of drugs and will consult with their other physicians about getting them started on an SGLT2 inhibitor.”
Dr. Yokose, Dr. Petri, and Dr. Cheung have no relevant disclosures. Dr. Jorge disclosed serving as a site investigator for SLE clinical trials funded by Bristol-Myers Squibb and Cabaletta Bio; the trials are not related to SGLT2 inhibitors.
Over just a decade, sodium-glucose cotransporter-2 (SGLT2) inhibitors have revolutionized the second-line treatment of type 2 diabetes by improving the control of blood sugar, and they’re also being used to treat heart failure and chronic kidney disease. Now, there’s growing evidence that the medications have the potential to play a role in the treatment of a variety of rheumatologic diseases — gout, systemic lupus erythematosus (SLE), and lupus nephritis.
“I suspect that SGLT2 inhibitors may have a role in multiple rheumatic diseases,” said rheumatologist April Jorge, MD, of Harvard Medical School and Massachusetts General Hospital, Boston.
In gout, for example, “SGLT2 inhibitors hold great promise as a multipurpose treatment option,” said rheumatologist Chio Yokose, MD, MSc, also of Harvard Medical School and Massachusetts General Hospital. Both Dr. Jorge and Dr. Yokose spoke at recent medical conferences and in interviews about the potential value of the drugs in rheumatology.
There’s a big caveat. For the moment, SGLT2 inhibitors aren’t cleared for use in the treatment of rheumatologic conditions, and neither physician is ready to recommend prescribing them off-label outside of their FDA-approved indications.
But studies could pave the way toward more approved uses in rheumatology. And there’s good news for now: Many rheumatology patients may already be eligible to take the drugs because of other medical conditions. In gout, for example, “sizable proportions of patients have comorbidities for which they are already indicated,” Dr. Yokose said.
Research Hints at Gout-Busting Potential
The first SGLT2 inhibitor canagliflozin (Invokana), received FDA approval in 2013, followed by dapagliflozin (Farxiga), empagliflozin (Jardiance), ertugliflozin (Steglatro), and bexagliflozin (Brenzavvy). The drugs “lower blood sugar by causing the kidneys to remove sugar from the body through urine,” reports the National Kidney Foundation, and they “help to protect the kidneys and heart in people with CKD [chronic kidney disease].”
As Dr. Yokose noted in a presentation at the 2023 Gout Hyperuricemia and Crystal Associated Disease Network research symposium, SGLT2 inhibitors “have really become blockbuster drugs, and they’ve now been integrated into multiple professional society guidelines and recommendations.”
These drugs should not be confused with the wildly popular medications known as glucagon-like peptide-1 (GLP1) agonists, which include medications such as semaglutide (Ozempic and Wegovy). These drugs are generally administered via injection — unlike the oral SGLT2 inhibitors — and they’re variously indicated for type 2 diabetes and obesity.
Dr. Yokose highlighted research findings about the drugs in gout. A 2020 study, for example, tracked 295,907 US adults with type 2 diabetes who received a new prescription for an SGLT2 inhibitor or GLP1 agonist during 2013-2017. Those in the SGLT2 inhibitor group had a 36% lower risk of newly diagnosed gout (hazard ratio [HR], 0.64; 95% CI, 0.57-0.72), the researchers reported.
A similar study, a 2021 report from Taiwan, also linked SGLT2 inhibitors to improvement in gout incidence vs. dipeptidyl peptidase 4 (DPP4) inhibitors, diabetes drugs that are not linked to lower serum urate levels. In an adjusted analysis, the risk of gout was 11% lower in the SGLT2 inhibitor group (adjusted HR, 0.86; 95% CI, 0.78-0.95).
What about recurrent gout? In a 2023 study, Dr. Yokose and colleagues tracked patients with type 2 diabetes who began SGLT2 inhibitors or DPP4 inhibitors. Over the period from 2013 to 2017, those who took SGLT2 inhibitors were less likely to have gout flares (rate ratio [RR], 0.66; 95% CI, 0.57-0.75) and gout-primary emergency department visits/hospitalizations (RR, 0.52; 95% CI, 0.32-0.84).
“This finding requires further replication in other populations and compared to other drugs,” Dr. Yokose cautioned.
Another 2023 study analyzed UK data and reached similar results regarding risk of recurrent gout.
Lower Urate Levels and Less Inflammation Could Be Key
How might SGLT2 inhibitors reduce the risk of gout? Multiple studies have linked the drugs to lower serum urate levels, Dr. Yokose said, but researchers often excluded patients with gout.
For a small new study presented at the 2023 annual meeting of the American College of Rheumatology but not yet published, Dr. Yokose and colleagues reported that patients with gout who began SGLT2 inhibitors had lower urate levels than those who began a sulfonylurea, another second-line agent for type 2 diabetes. During the study period, up to 3 months before and after initiation, 43.5% of patients in the SGLT2 inhibitor group reached a target serum urate of < 6 mg/dL vs. 4.2% of sulfonylurea initiators.
“The magnitude of this reduction, while not as large as what can be achieved with appropriately titrated urate-lowering therapy such as allopurinol or febuxostat, is also not negligible. It’s believed to be between 1.5-2.0 mg/dL among patients with gout,” Dr. Yokose said. “Also, SGLT2 inhibitors are purported to have some anti-inflammatory effects that may target the same pathways responsible for the profound inflammation associated with acute gout flares. However, both the exact mechanisms underlying the serum urate-lowering and anti-inflammatory effects of SGLT2 [inhibitors] require further research and clarification.”
Moving forward, she said, “I would love to see some prospective studies of SGLT2 inhibitor use among patients with gout, looking at serum urate and clinical gout endpoints, as well as biomarkers to understand better the beneficial effects of SGLT2 inhibitors as it pertains to patients with gout.”
In Lupus, Findings Are More Mixed
Studies of SGLT2 inhibitors have excluded patients with lupus, limiting insight into their benefits in that specific population, said Dr. Jorge of Massachusetts General Hospital and Harvard Medical School. However, “one small phase I/II trial showed an acceptable safety profile of dapagliflozin add-on therapy in adult patients with SLE,” she said.
Her team is working to expand understanding about the drugs in people with lupus. At the 2023 ACR annual meeting, she presented the findings of a study that tracked patients with SLE who took SGLT2 inhibitors (n = 426, including 154 with lupus nephritis) or DPP4 inhibitors (n = 865, including 270 with lupus nephritis). Patients who took SGLT2 inhibitors had lower risks of major adverse cardiac events (HR, 0.69; 95% CI, 0.48-0.99) and renal progression (HR, 0.71; 95% CI, 0.51-0.98).
“Our results are promising, but the majority of patient with lupus who had received SGLT2 inhibitors also had the comorbidity of type 2 diabetes as a separate indication for SGLT2 inhibitor use,” Dr. Jorge said. “We still need to study the impact of SGLT2 inhibitors in patients with SLE and lupus nephritis who do not have a separate indication for the medication.”
Dr. Jorge added that “we do not yet know the ideal time to initiate SGLT2 inhibitors in the treatment of lupus nephritis. Specifically, it is not yet known whether these medications should be used in patients with persistent proteinuria due to damage from lupus nephritis or whether there is also a role to start these medications in patients with active lupus nephritis who are undergoing induction immunosuppression regimens.”
However, another study released at the 2023 ACR annual meeting suggested that SGLT2 inhibitors may not have a beneficial effect in lupus nephritis: “We observed a reduction in decline in eGFR [estimated glomerular filtration rate] after starting SGLT2 inhibitors; however, this reduction was not statistically significant … early experience suggested marginal benefit of SGLT2 inhibitors in SLE,” researchers from Johns Hopkins University, and the University of Maryland, Baltimore, reported.
“My cohort is not showing miracles from SGLT2 inhibitors,” study lead author Michelle Petri, MD, MPH, of Johns Hopkins, said in an interview.
Still, new European Alliance of Associations for Rheumatology recommendations for SLE now advise to consider the use of the drugs in patients with lupus nephritis who have reduced eGFR. Meanwhile, “the American College of Rheumatology is currently developing new treatment guidelines for SLE and for lupus nephritis, and SGLT2 inhibitors will likely be a topic of consideration,” Dr. Jorge added.
As for mechanism, Dr. Jorge said it’s not clear how the drugs may affect lupus. “It’s proposed that they have benefits in hemodynamic effects as well as potentially anti-inflammatory effects. The hemodynamic effects, including reducing intraglomerular hyperfiltration and reducing blood pressure, likely have similar benefits in patients with chronic kidney disease due to diabetic nephropathy or due to lupus nephritis with damage/scarring and persistent proteinuria. Patients with SLE and other chronic, systemic rheumatic diseases such as ANCA [antineutrophilic cytoplasmic antibody]-associated vasculitis also develop kidney disease and cardiovascular events mediated by inflammatory processes.”
Side Effects and Cost: Where Do They Fit In?
According to Dr. Yokose, SGLT2 inhibitors “are generally quite well-tolerated, and very serious adverse effects are rare.” Side effects include disrupted urination, increased thirst, genital infections, flu-like symptoms, and swelling.
Urinary-related problems are understandable “because these drugs cause the kidneys to pass more glucose into the urine,” University of Hong Kong cardiac specialist Bernard Cheung, MBBCh, PhD, who has studied SGLT2 inhibitors, said in an interview.
In Dr. Yokose’s 2023 study of SGLT2 inhibitors in recurrent gout, patients who took the drugs were 2.15 times more likely than the comparison group to have genital infections (hazard ratio, 2.15; 95% CI, 1.39-3.30). This finding “was what we’d expect,” she said.
She added that genital infection rates were higher among patients with diabetes, women, and uncircumcised men. “Fortunately, most experienced just a single mild episode that can readily be treated with topical therapy. There does not appear to be an increased risk of urinary tract infections.”
Dr. Cheung added that “doctors should be aware of a rare adverse effect called euglycemic ketoacidosis, in which the patient has increased ketones in the blood causing it to be more acidic than normal, but the blood glucose remains within the normal range.”
As for cost, goodrx.com reports that several SGLT2 inhibitors run about $550-$683 per month, making them expensive but still cheaper than GLP-1 agonists, which can cost $1,000 or more per month. Unlike the most popular GLP-1 agonists such as Ozempic, none of the SGLT2 inhibitors are in short supply, according to the American Society of Health-System Pharmacists.
“If someone with gout already has a cardiovascular-kidney-metabolic indication for SGLT2 inhibitors and also stands to benefit in terms of lowering serum urate and risk of recurrent gout flares, there is potential for high benefit relative to cost,” Dr. Yokose said.
She added: “It is well-documented that current gout care is suboptimal, and many patients end up in the emergency room or hospitalized for gout, which in and of itself is quite costly both for the patient and the health care system. Therefore, streamlining or integrating gout and comorbidity care with SGLT2 inhibitors could potentially be quite beneficial for patients with gout.”
In regard to lupus, “many patients with lupus undergo multiple hospitalizations related to their disease, which is a source of high health care costs,” Dr. Jorge said. “Additionally, chronic kidney disease and cardiovascular disease are major causes of disability and premature mortality. Further studies will be needed to better understand whether benefits of SGLT2 inhibitors may outweigh the costs of treatment.”
As for prescribing the drugs in lupus now, Dr. Jorge said they can be an option in lupus nephritis. “There is not a clear consensus of the ideal timing to initiate SGLT2 inhibitors — e.g., degree of proteinuria or eGFR range,” she said. “However, it is less controversial that SGLT2 inhibitors should be considered in particular for patients with lupus nephritis with ongoing proteinuria despite adequate treatment with conventional therapies.”
As for gout, Dr. Yokose isn’t ready to prescribe the drugs to patients who don’t have comorbidities that can be treated by the medications. However, she noted that those patients are rare.
“If I see a patient with gout with one or more of these comorbidities, and I see that they are not already on an SGLT2 inhibitor, I definitely take the time to talk to the patient about this exciting class of drugs and will consult with their other physicians about getting them started on an SGLT2 inhibitor.”
Dr. Yokose, Dr. Petri, and Dr. Cheung have no relevant disclosures. Dr. Jorge disclosed serving as a site investigator for SLE clinical trials funded by Bristol-Myers Squibb and Cabaletta Bio; the trials are not related to SGLT2 inhibitors.
Asymptomatic Violaceous Plaques on the Face and Back
The Diagnosis: Cutaneous Sarcoidosis
A biopsy of a plaque on the back confirmed cutaneous sarcoidosis (CS). A chest radiograph demonstrated hilar nodes, and a referral was placed for comanagement with a pulmonologist. Histopathology was critical in making the diagnosis, with well-circumscribed noncaseating granulomas present in the dermis. The granulomas in CS often are described as naked, as there are minimal lymphocytes present and plasma cells normally are absent.1 Because the lungs are the most common site of involvement, a chest radiograph is necessary to examine for systemic sarcoidosis. Laboratory workup is used to evaluate for lymphopenia, hypercalcemia, elevated blood sedimentation rate, and elevated angiotensin- converting enzyme levels, which are common in systemic sarcoidosis.1
Sarcoidosis is a multisystemic granulomatous disorder with an unknown etiology. It is believed to develop in genetically predisposed individuals as a reaction to unidentified antigens in the environment.1 Helper T cells (TH1) respond to these environmental antigens in those who are susceptible, which leads to the disease process, but paradoxically, even with the elevation of cellular immune activity at the sites of the granulomatous inflammation, the peripheral immune response in these patients is suppressed as shown by lymphopenia.2
Cutaneous sarcoidosis is found in approximately one-third of patients with systemic sarcoidosis but can occur without systemic involvement.1,2 Sarcoidosis is reported worldwide and affects patients of all races and ethnicities, ages, and sexes but does have a higher prevalence among Black individuals in the United States, patients younger than 40 years (peak incidence, 20–29 years of age), and females.2 In 80% of patients, CS occurs before systemic sarcoidosis develops, or they may develop simultaneously.1
Cutaneous sarcoidosis has a wide range of clinical presentations that are classified as specific and nonspecific. Specific lesions in CS contain noncaseating granulomas while nonspecific lesions in CS appear as reactive processes.2 The most common specific presentation of CS includes papules that are brown in pigmentation in lighter skin tones and red to violaceous in darker skin tones (Figure). The most common nonspecific skin manifestation is erythema nodosum, which represents a hypersensitivity reaction. Cutaneous sarcoidosis can appear as hypopigmented or hyperpigmented patches or plaques.1
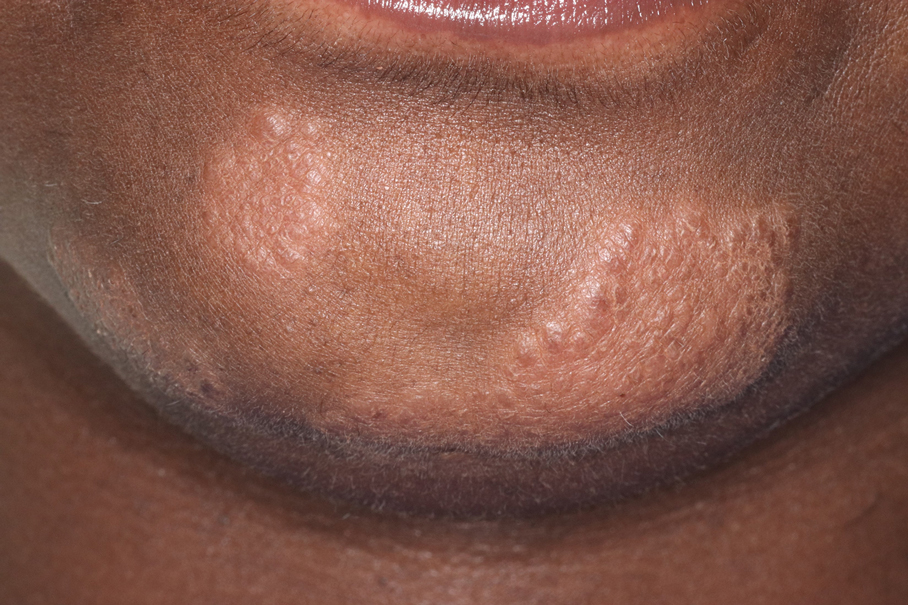
Treatments for CS vary based on the individual.1 For milder and more localized cases, topical or intralesional steroids may be used. If systemic sarcoidosis is suspected or if there is diffuse involvement of the skin, systemic steroids, antimalarials (eg, hydroxychloroquine), low-dose methotrexate, minocycline, allopurinol, azathioprine, isotretinoin, tumor necrosis factor α inhibitors, or psoralen plus long-wave UVA radiation may be used. If systemic sarcoidosis is present, referral to a pulmonologist is recommended for co-management.1
Cutaneous sarcoidosis is known as the “great imitator,” and there are multiple diseases to consider in the differential that are distinguished by the physical findings.1 In our case of a middle-aged Black woman with indurated plaques, a few diagnoses to consider were psoriasis, discoid lupus erythematosus (DLE), mycosis fungoides (MF), and tinea infection.
Psoriasis is a common disease, and 90% of patients have chronic plaquelike disease with well-demarcated erythematous plaques that have a silver-gray scale and a positive Auspitz sign (also known as pinpoint bleeding).3 Plaques often are distributed on the trunk, limb extensors, and scalp, along with nail changes. Some patients also have joint pain, indicating psoriatic arthritis. The etiology of psoriasis is unknown, but it develops due to unrestrained keratinocyte proliferation and defective differentiation, which leads to histopathology showing regular acanthosis and papillary dermal ectasia with rouleaux. Mild cases typically are treated with topical steroids or vitamin D, while more severe cases are treated with methotrexate, cyclosporine, retinoids, or biologics.3
Discoid lupus erythematosus occurs 4 times more often in Black patients than in White patients. Clinically, DLE begins as well-defined, erythematous, scaly patches that expand with hyperpigmentation at the periphery and leave an atrophic, scarred, hypopigmented center.4 It typically is localized to the head and neck, but in cases where it disseminates elsewhere on the body, the risk for systemic lupus erythematosus increases from 1.2% to 28%.5 Histopathology of DLE shows vacuolar degeneration of the basal cell layer in the epidermis along with patchy lymphocytic infiltrate in the dermis. Treatments range from topical steroids for mild cases to antimalarial agents, retinoids, anti-inflammatory drugs, and calcineurin inhibitors for more severe cases.4
Although there are multiple types of cutaneous T-cell lymphoma, the most common is MF, which traditionally is nonaggressive. The typical patient with MF is older than 60 years and presents with indolent, ongoing, flat to minimally indurated patches or plaques that have cigarette paper scale. As MF progresses, some plaques grow into tumors and can become more aggressive. Histologically, MF changes based on its clinical stage, with the initial phase showing epidermotropic atypical lymphocytes and later phases showing less epitheliotropic, larger, atypical lymphocytes. The treatment algorithm varies depending on cutaneous T-cell lymphoma staging.6
Tinea infections are caused by dermatophytes. In prepubertal children, they predominantly appear as tinea corporis (on the body) or tinea capitis (on the scalp), but in adults they appear as tinea cruris (on the groin), tinea pedis (on the feet), or tinea unguium (on the nails).7 Tinea infections classically are known to appear as an annular patch with an active erythematous scaling border and central clearing. The patches can be pruritic. Potassium hydroxide preparation of a skin scraping is a quick test to use in the office; if the results are inconclusive, a culture may be required. Treatment depends on the location of the infection but typically involves either topical or oral antifungal agents.7
- Tchernev G, Cardoso JC, Chokoeva AA, et al. The “mystery” of cutaneous sarcoidosis: facts and controversies. Int J Immunopathol Pharmacol. 2014;27:321-330. doi:10.1177/039463201402700302
- Ali MM, Atwan AA, Gonzalez ML. Cutaneous sarcoidosis: updates in the pathogenesis. J Eur Acad Dermatol Venereol. 2010;24:747-755. doi:10.1111/j.1468-3083.2009.03517.x
- Rendon A, Schäkel K. Psoriasis pathogenesis and treatment [published online March 23, 2019]. Int J Mol Sci. 2019;20:1475. doi:10.3390/ijms20061475
- McDaniel B, Sukumaran S, Koritala T, et al. Discoid lupus erythematosus. StatPearls [Internet]. StatPearls Publishing; 2023. Accessed December 11, 2023. https://www.ncbi.nlm.nih.gov/books/NBK493145/
- Bhat MR, Hulmani M, Dandakeri S, et al. Disseminated discoid lupus erythematosus leading to squamous cell carcinoma. Indian J Dermatol. 2012;57:158-161. doi:10.4103/0019-5154.94298
- Pulitzer M. Cutaneous T-cell Lymphoma. Clin Lab Med. 2017; 37:527-546. doi:10.1016/j.cll.2017.06.006
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014;90:702-710.
The Diagnosis: Cutaneous Sarcoidosis
A biopsy of a plaque on the back confirmed cutaneous sarcoidosis (CS). A chest radiograph demonstrated hilar nodes, and a referral was placed for comanagement with a pulmonologist. Histopathology was critical in making the diagnosis, with well-circumscribed noncaseating granulomas present in the dermis. The granulomas in CS often are described as naked, as there are minimal lymphocytes present and plasma cells normally are absent.1 Because the lungs are the most common site of involvement, a chest radiograph is necessary to examine for systemic sarcoidosis. Laboratory workup is used to evaluate for lymphopenia, hypercalcemia, elevated blood sedimentation rate, and elevated angiotensin- converting enzyme levels, which are common in systemic sarcoidosis.1
Sarcoidosis is a multisystemic granulomatous disorder with an unknown etiology. It is believed to develop in genetically predisposed individuals as a reaction to unidentified antigens in the environment.1 Helper T cells (TH1) respond to these environmental antigens in those who are susceptible, which leads to the disease process, but paradoxically, even with the elevation of cellular immune activity at the sites of the granulomatous inflammation, the peripheral immune response in these patients is suppressed as shown by lymphopenia.2
Cutaneous sarcoidosis is found in approximately one-third of patients with systemic sarcoidosis but can occur without systemic involvement.1,2 Sarcoidosis is reported worldwide and affects patients of all races and ethnicities, ages, and sexes but does have a higher prevalence among Black individuals in the United States, patients younger than 40 years (peak incidence, 20–29 years of age), and females.2 In 80% of patients, CS occurs before systemic sarcoidosis develops, or they may develop simultaneously.1
Cutaneous sarcoidosis has a wide range of clinical presentations that are classified as specific and nonspecific. Specific lesions in CS contain noncaseating granulomas while nonspecific lesions in CS appear as reactive processes.2 The most common specific presentation of CS includes papules that are brown in pigmentation in lighter skin tones and red to violaceous in darker skin tones (Figure). The most common nonspecific skin manifestation is erythema nodosum, which represents a hypersensitivity reaction. Cutaneous sarcoidosis can appear as hypopigmented or hyperpigmented patches or plaques.1

Treatments for CS vary based on the individual.1 For milder and more localized cases, topical or intralesional steroids may be used. If systemic sarcoidosis is suspected or if there is diffuse involvement of the skin, systemic steroids, antimalarials (eg, hydroxychloroquine), low-dose methotrexate, minocycline, allopurinol, azathioprine, isotretinoin, tumor necrosis factor α inhibitors, or psoralen plus long-wave UVA radiation may be used. If systemic sarcoidosis is present, referral to a pulmonologist is recommended for co-management.1
Cutaneous sarcoidosis is known as the “great imitator,” and there are multiple diseases to consider in the differential that are distinguished by the physical findings.1 In our case of a middle-aged Black woman with indurated plaques, a few diagnoses to consider were psoriasis, discoid lupus erythematosus (DLE), mycosis fungoides (MF), and tinea infection.
Psoriasis is a common disease, and 90% of patients have chronic plaquelike disease with well-demarcated erythematous plaques that have a silver-gray scale and a positive Auspitz sign (also known as pinpoint bleeding).3 Plaques often are distributed on the trunk, limb extensors, and scalp, along with nail changes. Some patients also have joint pain, indicating psoriatic arthritis. The etiology of psoriasis is unknown, but it develops due to unrestrained keratinocyte proliferation and defective differentiation, which leads to histopathology showing regular acanthosis and papillary dermal ectasia with rouleaux. Mild cases typically are treated with topical steroids or vitamin D, while more severe cases are treated with methotrexate, cyclosporine, retinoids, or biologics.3
Discoid lupus erythematosus occurs 4 times more often in Black patients than in White patients. Clinically, DLE begins as well-defined, erythematous, scaly patches that expand with hyperpigmentation at the periphery and leave an atrophic, scarred, hypopigmented center.4 It typically is localized to the head and neck, but in cases where it disseminates elsewhere on the body, the risk for systemic lupus erythematosus increases from 1.2% to 28%.5 Histopathology of DLE shows vacuolar degeneration of the basal cell layer in the epidermis along with patchy lymphocytic infiltrate in the dermis. Treatments range from topical steroids for mild cases to antimalarial agents, retinoids, anti-inflammatory drugs, and calcineurin inhibitors for more severe cases.4
Although there are multiple types of cutaneous T-cell lymphoma, the most common is MF, which traditionally is nonaggressive. The typical patient with MF is older than 60 years and presents with indolent, ongoing, flat to minimally indurated patches or plaques that have cigarette paper scale. As MF progresses, some plaques grow into tumors and can become more aggressive. Histologically, MF changes based on its clinical stage, with the initial phase showing epidermotropic atypical lymphocytes and later phases showing less epitheliotropic, larger, atypical lymphocytes. The treatment algorithm varies depending on cutaneous T-cell lymphoma staging.6
Tinea infections are caused by dermatophytes. In prepubertal children, they predominantly appear as tinea corporis (on the body) or tinea capitis (on the scalp), but in adults they appear as tinea cruris (on the groin), tinea pedis (on the feet), or tinea unguium (on the nails).7 Tinea infections classically are known to appear as an annular patch with an active erythematous scaling border and central clearing. The patches can be pruritic. Potassium hydroxide preparation of a skin scraping is a quick test to use in the office; if the results are inconclusive, a culture may be required. Treatment depends on the location of the infection but typically involves either topical or oral antifungal agents.7
The Diagnosis: Cutaneous Sarcoidosis
A biopsy of a plaque on the back confirmed cutaneous sarcoidosis (CS). A chest radiograph demonstrated hilar nodes, and a referral was placed for comanagement with a pulmonologist. Histopathology was critical in making the diagnosis, with well-circumscribed noncaseating granulomas present in the dermis. The granulomas in CS often are described as naked, as there are minimal lymphocytes present and plasma cells normally are absent.1 Because the lungs are the most common site of involvement, a chest radiograph is necessary to examine for systemic sarcoidosis. Laboratory workup is used to evaluate for lymphopenia, hypercalcemia, elevated blood sedimentation rate, and elevated angiotensin- converting enzyme levels, which are common in systemic sarcoidosis.1
Sarcoidosis is a multisystemic granulomatous disorder with an unknown etiology. It is believed to develop in genetically predisposed individuals as a reaction to unidentified antigens in the environment.1 Helper T cells (TH1) respond to these environmental antigens in those who are susceptible, which leads to the disease process, but paradoxically, even with the elevation of cellular immune activity at the sites of the granulomatous inflammation, the peripheral immune response in these patients is suppressed as shown by lymphopenia.2
Cutaneous sarcoidosis is found in approximately one-third of patients with systemic sarcoidosis but can occur without systemic involvement.1,2 Sarcoidosis is reported worldwide and affects patients of all races and ethnicities, ages, and sexes but does have a higher prevalence among Black individuals in the United States, patients younger than 40 years (peak incidence, 20–29 years of age), and females.2 In 80% of patients, CS occurs before systemic sarcoidosis develops, or they may develop simultaneously.1
Cutaneous sarcoidosis has a wide range of clinical presentations that are classified as specific and nonspecific. Specific lesions in CS contain noncaseating granulomas while nonspecific lesions in CS appear as reactive processes.2 The most common specific presentation of CS includes papules that are brown in pigmentation in lighter skin tones and red to violaceous in darker skin tones (Figure). The most common nonspecific skin manifestation is erythema nodosum, which represents a hypersensitivity reaction. Cutaneous sarcoidosis can appear as hypopigmented or hyperpigmented patches or plaques.1

Treatments for CS vary based on the individual.1 For milder and more localized cases, topical or intralesional steroids may be used. If systemic sarcoidosis is suspected or if there is diffuse involvement of the skin, systemic steroids, antimalarials (eg, hydroxychloroquine), low-dose methotrexate, minocycline, allopurinol, azathioprine, isotretinoin, tumor necrosis factor α inhibitors, or psoralen plus long-wave UVA radiation may be used. If systemic sarcoidosis is present, referral to a pulmonologist is recommended for co-management.1
Cutaneous sarcoidosis is known as the “great imitator,” and there are multiple diseases to consider in the differential that are distinguished by the physical findings.1 In our case of a middle-aged Black woman with indurated plaques, a few diagnoses to consider were psoriasis, discoid lupus erythematosus (DLE), mycosis fungoides (MF), and tinea infection.
Psoriasis is a common disease, and 90% of patients have chronic plaquelike disease with well-demarcated erythematous plaques that have a silver-gray scale and a positive Auspitz sign (also known as pinpoint bleeding).3 Plaques often are distributed on the trunk, limb extensors, and scalp, along with nail changes. Some patients also have joint pain, indicating psoriatic arthritis. The etiology of psoriasis is unknown, but it develops due to unrestrained keratinocyte proliferation and defective differentiation, which leads to histopathology showing regular acanthosis and papillary dermal ectasia with rouleaux. Mild cases typically are treated with topical steroids or vitamin D, while more severe cases are treated with methotrexate, cyclosporine, retinoids, or biologics.3
Discoid lupus erythematosus occurs 4 times more often in Black patients than in White patients. Clinically, DLE begins as well-defined, erythematous, scaly patches that expand with hyperpigmentation at the periphery and leave an atrophic, scarred, hypopigmented center.4 It typically is localized to the head and neck, but in cases where it disseminates elsewhere on the body, the risk for systemic lupus erythematosus increases from 1.2% to 28%.5 Histopathology of DLE shows vacuolar degeneration of the basal cell layer in the epidermis along with patchy lymphocytic infiltrate in the dermis. Treatments range from topical steroids for mild cases to antimalarial agents, retinoids, anti-inflammatory drugs, and calcineurin inhibitors for more severe cases.4
Although there are multiple types of cutaneous T-cell lymphoma, the most common is MF, which traditionally is nonaggressive. The typical patient with MF is older than 60 years and presents with indolent, ongoing, flat to minimally indurated patches or plaques that have cigarette paper scale. As MF progresses, some plaques grow into tumors and can become more aggressive. Histologically, MF changes based on its clinical stage, with the initial phase showing epidermotropic atypical lymphocytes and later phases showing less epitheliotropic, larger, atypical lymphocytes. The treatment algorithm varies depending on cutaneous T-cell lymphoma staging.6
Tinea infections are caused by dermatophytes. In prepubertal children, they predominantly appear as tinea corporis (on the body) or tinea capitis (on the scalp), but in adults they appear as tinea cruris (on the groin), tinea pedis (on the feet), or tinea unguium (on the nails).7 Tinea infections classically are known to appear as an annular patch with an active erythematous scaling border and central clearing. The patches can be pruritic. Potassium hydroxide preparation of a skin scraping is a quick test to use in the office; if the results are inconclusive, a culture may be required. Treatment depends on the location of the infection but typically involves either topical or oral antifungal agents.7
- Tchernev G, Cardoso JC, Chokoeva AA, et al. The “mystery” of cutaneous sarcoidosis: facts and controversies. Int J Immunopathol Pharmacol. 2014;27:321-330. doi:10.1177/039463201402700302
- Ali MM, Atwan AA, Gonzalez ML. Cutaneous sarcoidosis: updates in the pathogenesis. J Eur Acad Dermatol Venereol. 2010;24:747-755. doi:10.1111/j.1468-3083.2009.03517.x
- Rendon A, Schäkel K. Psoriasis pathogenesis and treatment [published online March 23, 2019]. Int J Mol Sci. 2019;20:1475. doi:10.3390/ijms20061475
- McDaniel B, Sukumaran S, Koritala T, et al. Discoid lupus erythematosus. StatPearls [Internet]. StatPearls Publishing; 2023. Accessed December 11, 2023. https://www.ncbi.nlm.nih.gov/books/NBK493145/
- Bhat MR, Hulmani M, Dandakeri S, et al. Disseminated discoid lupus erythematosus leading to squamous cell carcinoma. Indian J Dermatol. 2012;57:158-161. doi:10.4103/0019-5154.94298
- Pulitzer M. Cutaneous T-cell Lymphoma. Clin Lab Med. 2017; 37:527-546. doi:10.1016/j.cll.2017.06.006
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014;90:702-710.
- Tchernev G, Cardoso JC, Chokoeva AA, et al. The “mystery” of cutaneous sarcoidosis: facts and controversies. Int J Immunopathol Pharmacol. 2014;27:321-330. doi:10.1177/039463201402700302
- Ali MM, Atwan AA, Gonzalez ML. Cutaneous sarcoidosis: updates in the pathogenesis. J Eur Acad Dermatol Venereol. 2010;24:747-755. doi:10.1111/j.1468-3083.2009.03517.x
- Rendon A, Schäkel K. Psoriasis pathogenesis and treatment [published online March 23, 2019]. Int J Mol Sci. 2019;20:1475. doi:10.3390/ijms20061475
- McDaniel B, Sukumaran S, Koritala T, et al. Discoid lupus erythematosus. StatPearls [Internet]. StatPearls Publishing; 2023. Accessed December 11, 2023. https://www.ncbi.nlm.nih.gov/books/NBK493145/
- Bhat MR, Hulmani M, Dandakeri S, et al. Disseminated discoid lupus erythematosus leading to squamous cell carcinoma. Indian J Dermatol. 2012;57:158-161. doi:10.4103/0019-5154.94298
- Pulitzer M. Cutaneous T-cell Lymphoma. Clin Lab Med. 2017; 37:527-546. doi:10.1016/j.cll.2017.06.006
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014;90:702-710.
A 35-year-old Black woman presented to dermatology as a new patient for evaluation of an asymptomatic rash that had enlarged and spread to involve both the face and back over the last 4 months. She had not tried any treatments. She had no notable medical history and was uncertain of her family history. Physical examination showed indurated, flesh-colored to violaceous plaques around the alar-facial groove (top), nasal tip, chin, and back (bottom). The mucosae and nails were not involved.
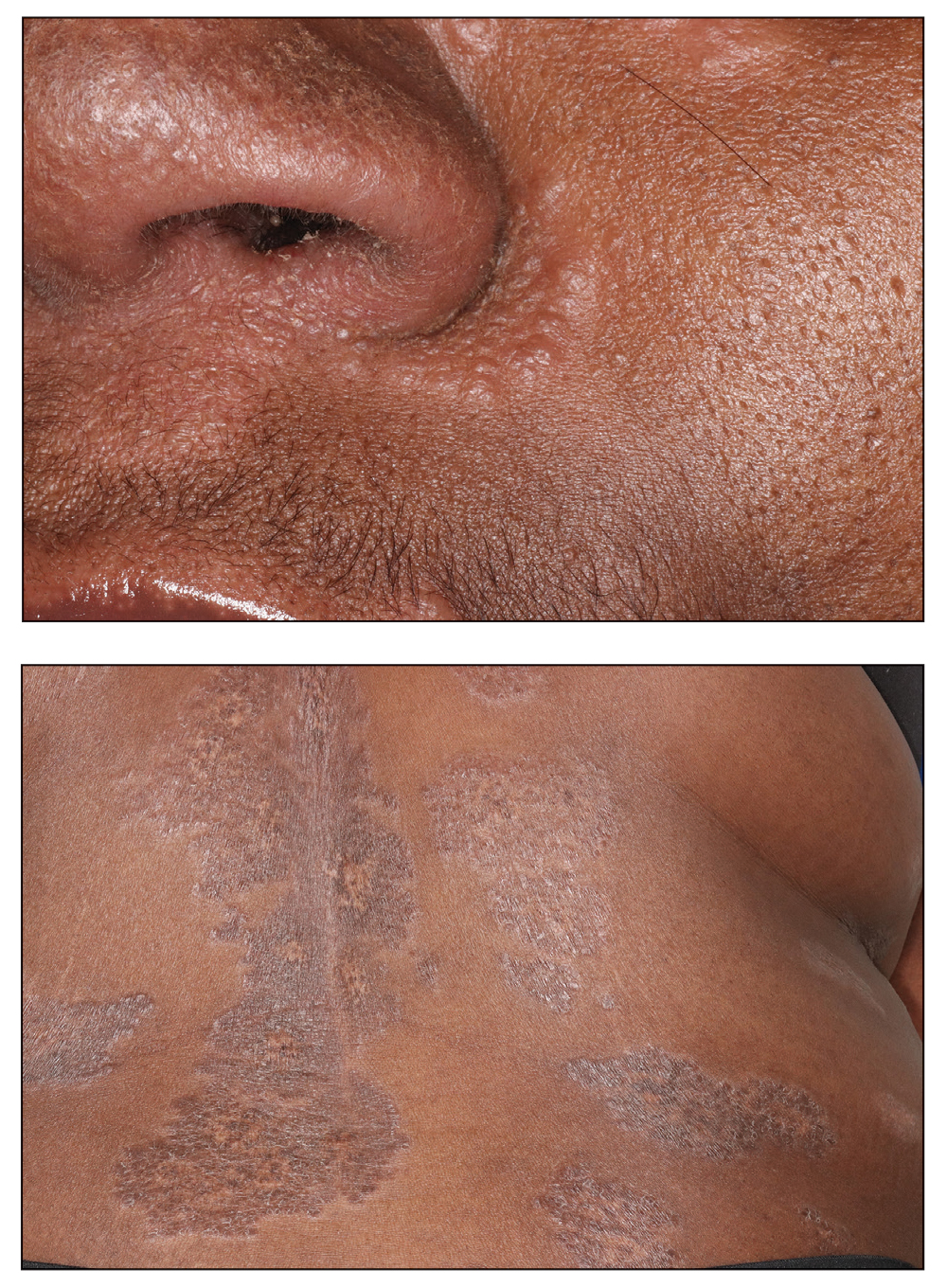
US Dermatologic Drug Approvals Rose Between 2012 and 2022
TOPLINE:
METHODOLOGY:
- Only five new drugs for diseases treated mostly by dermatologists were approved by the FDA between 1999 and 2009.
- In a cross-sectional analysis to characterize the frequency and degree of innovation of dermatologic drugs approved more recently, researchers identified new and supplemental dermatologic drugs approved between January 1, 2012, and December 31, 2022, from FDA lists, Centers for Medicare & Medicaid Services CenterWatch, and peer-reviewed articles.
- They used five proxy measures to estimate each drug’s degree of innovation: FDA designation (first in class, advance in class, or addition to class), independent clinical usefulness ratings, and benefit ratings by health technology assessment organizations.
TAKEAWAY:
- The study authors identified 52 new drug applications and 26 supplemental new indications approved by the FDA for dermatologic indications between 2012 and 2022.
- Of the 52 new drugs, the researchers categorized 11 (21%) as first in class and 13 (25%) as first in indication.
- An analysis of benefit ratings available for 38 of the drugs showed that 15 (39%) were rated as being clinically useful or having high added therapeutic benefit.
- Of the 10 supplemental new indications with ratings by any organization, 3 (30%) were rated as clinically useful or having high added therapeutic benefit.
IN PRACTICE:
While innovative drug development in dermatology may have increased, “these findings also highlight opportunities to develop more truly innovative dermatologic agents, particularly for diseases with unmet therapeutic need,” the authors wrote.
SOURCE:
First author Samir Kamat, MD, of the Medical Education Department at Icahn School of Medicine at Mount Sinai, New York City, and corresponding author Ravi Gupta, MD, MSHP, of the Internal Medicine Division at Johns Hopkins University, Baltimore, Maryland, led the research. The study was published online as a research letter on December 20, 2023, in JAMA Dermatology.
LIMITATIONS:
They include the use of individual indications to assess clinical usefulness and benefit ratings. Many drugs, particularly supplemental indications, lacked such ratings. Reformulations of already marketed drugs or indications were not included.
DISCLOSURES:
Dr. Kamat and Dr. Gupta had no relevant disclosures. Three coauthors reported having received financial support outside of the submitted work.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Only five new drugs for diseases treated mostly by dermatologists were approved by the FDA between 1999 and 2009.
- In a cross-sectional analysis to characterize the frequency and degree of innovation of dermatologic drugs approved more recently, researchers identified new and supplemental dermatologic drugs approved between January 1, 2012, and December 31, 2022, from FDA lists, Centers for Medicare & Medicaid Services CenterWatch, and peer-reviewed articles.
- They used five proxy measures to estimate each drug’s degree of innovation: FDA designation (first in class, advance in class, or addition to class), independent clinical usefulness ratings, and benefit ratings by health technology assessment organizations.
TAKEAWAY:
- The study authors identified 52 new drug applications and 26 supplemental new indications approved by the FDA for dermatologic indications between 2012 and 2022.
- Of the 52 new drugs, the researchers categorized 11 (21%) as first in class and 13 (25%) as first in indication.
- An analysis of benefit ratings available for 38 of the drugs showed that 15 (39%) were rated as being clinically useful or having high added therapeutic benefit.
- Of the 10 supplemental new indications with ratings by any organization, 3 (30%) were rated as clinically useful or having high added therapeutic benefit.
IN PRACTICE:
While innovative drug development in dermatology may have increased, “these findings also highlight opportunities to develop more truly innovative dermatologic agents, particularly for diseases with unmet therapeutic need,” the authors wrote.
SOURCE:
First author Samir Kamat, MD, of the Medical Education Department at Icahn School of Medicine at Mount Sinai, New York City, and corresponding author Ravi Gupta, MD, MSHP, of the Internal Medicine Division at Johns Hopkins University, Baltimore, Maryland, led the research. The study was published online as a research letter on December 20, 2023, in JAMA Dermatology.
LIMITATIONS:
They include the use of individual indications to assess clinical usefulness and benefit ratings. Many drugs, particularly supplemental indications, lacked such ratings. Reformulations of already marketed drugs or indications were not included.
DISCLOSURES:
Dr. Kamat and Dr. Gupta had no relevant disclosures. Three coauthors reported having received financial support outside of the submitted work.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Only five new drugs for diseases treated mostly by dermatologists were approved by the FDA between 1999 and 2009.
- In a cross-sectional analysis to characterize the frequency and degree of innovation of dermatologic drugs approved more recently, researchers identified new and supplemental dermatologic drugs approved between January 1, 2012, and December 31, 2022, from FDA lists, Centers for Medicare & Medicaid Services CenterWatch, and peer-reviewed articles.
- They used five proxy measures to estimate each drug’s degree of innovation: FDA designation (first in class, advance in class, or addition to class), independent clinical usefulness ratings, and benefit ratings by health technology assessment organizations.
TAKEAWAY:
- The study authors identified 52 new drug applications and 26 supplemental new indications approved by the FDA for dermatologic indications between 2012 and 2022.
- Of the 52 new drugs, the researchers categorized 11 (21%) as first in class and 13 (25%) as first in indication.
- An analysis of benefit ratings available for 38 of the drugs showed that 15 (39%) were rated as being clinically useful or having high added therapeutic benefit.
- Of the 10 supplemental new indications with ratings by any organization, 3 (30%) were rated as clinically useful or having high added therapeutic benefit.
IN PRACTICE:
While innovative drug development in dermatology may have increased, “these findings also highlight opportunities to develop more truly innovative dermatologic agents, particularly for diseases with unmet therapeutic need,” the authors wrote.
SOURCE:
First author Samir Kamat, MD, of the Medical Education Department at Icahn School of Medicine at Mount Sinai, New York City, and corresponding author Ravi Gupta, MD, MSHP, of the Internal Medicine Division at Johns Hopkins University, Baltimore, Maryland, led the research. The study was published online as a research letter on December 20, 2023, in JAMA Dermatology.
LIMITATIONS:
They include the use of individual indications to assess clinical usefulness and benefit ratings. Many drugs, particularly supplemental indications, lacked such ratings. Reformulations of already marketed drugs or indications were not included.
DISCLOSURES:
Dr. Kamat and Dr. Gupta had no relevant disclosures. Three coauthors reported having received financial support outside of the submitted work.
A version of this article appeared on Medscape.com.





