User login
Erratic sleep, lack of activity tied to worsening schizophrenia symptoms
The findings also showed that people with schizophrenia spectrum disorders (SSDs) who lived in residential facilities experienced rigid routines, which correlated with a higher degree of negative symptoms.
The rigid routines were problematic for the patients living in residential settings, lead investigator Fabio Ferrarelli, MD, PhD, told this news organization. Dr. Ferrarelli is an associate professor of psychiatry at the University of Pittsburgh.
“Engaging in different activities at different times in activities associated with motivation and social interaction – this helps to ameliorate difficult-to-treat negative symptoms,” he said.
The findings were published online in Molecular Psychiatry.
Need to increase activity levels
While there is no shortage of research on sleep disturbances among people with schizophrenia, research focusing specifically on rest-activity rhythm disturbances and their relationships to symptoms of schizophrenia has been limited by small sample sizes or the lack of a control group, the investigators note.
To address this research gap, the investigators recruited 230 patients with SSD from participating residential facilities and communities throughout Italy. The participants included 108 healthy control participants, 54 community-dwelling patients with SSD who were receiving outpatient services, and 68 patients with SSD who were living in residential facilities.
All participants wore an actigraph for 7 consecutive days so that investigators could monitor sleep-wake patterns.
Compared with healthy control participants, both SSD groups had more total sleep time and spent more time resting or being passive (P < .001). In contrast, healthy control participants were much more active.
Part of the explanation for this may be that most of the control participants had jobs or attended school. In addition, the investigators note that many medications used to treat SSD can be highly sedating, causing some patients to sleep up to 15 hours per day.
Among residential participants with SSD, there was a higher level of inter-daily stability and higher daily rest-activity-rest fragmentation than occurred among healthy control participants or community-dwelling patients with SSD (P < .001). There was also a higher level of negative symptoms among residential participants with SSD than among the community-dwelling group with SSD.
When the findings were taken together, Dr. Ferrarelli and his team interpreted them to mean that inter-daily stability could reflect premature aging or neurodegenerative processes in patients with more severe forms of schizophrenia.
Another explanation could be that the rigid routine of the residential facility was making negative symptoms worse, Dr. Ferrarelli said. It is important to add variety into the mix – getting people to engage in different activities at different times of day would likely help residential SSD patients overcome negative symptoms of the disorder.
Although participants were recruited in Italy, Dr. Ferrarelli said he believes the findings are generalizable.
Bidirectional relationship?
Commenting on the findings, Matcheri Keshavan, MD, professor of psychiatry at Harvard Medical School in Boston, said the results are consistent with “well-known clinical observations that SSD patients tend to spend more time in bed and have more dysregulated sleep.
“Negative symptoms are also common, especially in residential patients. However, it is difficult to determine causality, as we do not know whether excessive sleepiness and decreased physical activity cause negative symptoms, or vice versa, or whether this is a bidirectional relationship,” Dr. Keshavan said.
He emphasized that physical exercise is known to increase sleep quality for people with mental illness and may also improve negative symptoms. “A useful approach in clinical practice is to increase activity levels, especially physical activities like walking and gardening.”
Dr. Keshavan said he would like to see future research that focuses on whether an intervention such as aerobic exercise would improve sleep quality as well as negative symptoms.
He also said that future research should ideally examine the characteristics of sleep alterations in schizophrenia.
“For example, while sleep duration is increased in schizophrenia, studies suggest that time spent in deep sleep is reduced; sleep spindles, which are important for consolidating memory during sleep, are also reduced. Correcting these deficits may improve negative symptoms and cognitive deficits,” he added.
The study was funded by the Italian Ministry of Health and the National Institute of Mental Health. There were no conflicts of interest.
A version of this article first appeared on Medscape.com.
The findings also showed that people with schizophrenia spectrum disorders (SSDs) who lived in residential facilities experienced rigid routines, which correlated with a higher degree of negative symptoms.
The rigid routines were problematic for the patients living in residential settings, lead investigator Fabio Ferrarelli, MD, PhD, told this news organization. Dr. Ferrarelli is an associate professor of psychiatry at the University of Pittsburgh.
“Engaging in different activities at different times in activities associated with motivation and social interaction – this helps to ameliorate difficult-to-treat negative symptoms,” he said.
The findings were published online in Molecular Psychiatry.
Need to increase activity levels
While there is no shortage of research on sleep disturbances among people with schizophrenia, research focusing specifically on rest-activity rhythm disturbances and their relationships to symptoms of schizophrenia has been limited by small sample sizes or the lack of a control group, the investigators note.
To address this research gap, the investigators recruited 230 patients with SSD from participating residential facilities and communities throughout Italy. The participants included 108 healthy control participants, 54 community-dwelling patients with SSD who were receiving outpatient services, and 68 patients with SSD who were living in residential facilities.
All participants wore an actigraph for 7 consecutive days so that investigators could monitor sleep-wake patterns.
Compared with healthy control participants, both SSD groups had more total sleep time and spent more time resting or being passive (P < .001). In contrast, healthy control participants were much more active.
Part of the explanation for this may be that most of the control participants had jobs or attended school. In addition, the investigators note that many medications used to treat SSD can be highly sedating, causing some patients to sleep up to 15 hours per day.
Among residential participants with SSD, there was a higher level of inter-daily stability and higher daily rest-activity-rest fragmentation than occurred among healthy control participants or community-dwelling patients with SSD (P < .001). There was also a higher level of negative symptoms among residential participants with SSD than among the community-dwelling group with SSD.
When the findings were taken together, Dr. Ferrarelli and his team interpreted them to mean that inter-daily stability could reflect premature aging or neurodegenerative processes in patients with more severe forms of schizophrenia.
Another explanation could be that the rigid routine of the residential facility was making negative symptoms worse, Dr. Ferrarelli said. It is important to add variety into the mix – getting people to engage in different activities at different times of day would likely help residential SSD patients overcome negative symptoms of the disorder.
Although participants were recruited in Italy, Dr. Ferrarelli said he believes the findings are generalizable.
Bidirectional relationship?
Commenting on the findings, Matcheri Keshavan, MD, professor of psychiatry at Harvard Medical School in Boston, said the results are consistent with “well-known clinical observations that SSD patients tend to spend more time in bed and have more dysregulated sleep.
“Negative symptoms are also common, especially in residential patients. However, it is difficult to determine causality, as we do not know whether excessive sleepiness and decreased physical activity cause negative symptoms, or vice versa, or whether this is a bidirectional relationship,” Dr. Keshavan said.
He emphasized that physical exercise is known to increase sleep quality for people with mental illness and may also improve negative symptoms. “A useful approach in clinical practice is to increase activity levels, especially physical activities like walking and gardening.”
Dr. Keshavan said he would like to see future research that focuses on whether an intervention such as aerobic exercise would improve sleep quality as well as negative symptoms.
He also said that future research should ideally examine the characteristics of sleep alterations in schizophrenia.
“For example, while sleep duration is increased in schizophrenia, studies suggest that time spent in deep sleep is reduced; sleep spindles, which are important for consolidating memory during sleep, are also reduced. Correcting these deficits may improve negative symptoms and cognitive deficits,” he added.
The study was funded by the Italian Ministry of Health and the National Institute of Mental Health. There were no conflicts of interest.
A version of this article first appeared on Medscape.com.
The findings also showed that people with schizophrenia spectrum disorders (SSDs) who lived in residential facilities experienced rigid routines, which correlated with a higher degree of negative symptoms.
The rigid routines were problematic for the patients living in residential settings, lead investigator Fabio Ferrarelli, MD, PhD, told this news organization. Dr. Ferrarelli is an associate professor of psychiatry at the University of Pittsburgh.
“Engaging in different activities at different times in activities associated with motivation and social interaction – this helps to ameliorate difficult-to-treat negative symptoms,” he said.
The findings were published online in Molecular Psychiatry.
Need to increase activity levels
While there is no shortage of research on sleep disturbances among people with schizophrenia, research focusing specifically on rest-activity rhythm disturbances and their relationships to symptoms of schizophrenia has been limited by small sample sizes or the lack of a control group, the investigators note.
To address this research gap, the investigators recruited 230 patients with SSD from participating residential facilities and communities throughout Italy. The participants included 108 healthy control participants, 54 community-dwelling patients with SSD who were receiving outpatient services, and 68 patients with SSD who were living in residential facilities.
All participants wore an actigraph for 7 consecutive days so that investigators could monitor sleep-wake patterns.
Compared with healthy control participants, both SSD groups had more total sleep time and spent more time resting or being passive (P < .001). In contrast, healthy control participants were much more active.
Part of the explanation for this may be that most of the control participants had jobs or attended school. In addition, the investigators note that many medications used to treat SSD can be highly sedating, causing some patients to sleep up to 15 hours per day.
Among residential participants with SSD, there was a higher level of inter-daily stability and higher daily rest-activity-rest fragmentation than occurred among healthy control participants or community-dwelling patients with SSD (P < .001). There was also a higher level of negative symptoms among residential participants with SSD than among the community-dwelling group with SSD.
When the findings were taken together, Dr. Ferrarelli and his team interpreted them to mean that inter-daily stability could reflect premature aging or neurodegenerative processes in patients with more severe forms of schizophrenia.
Another explanation could be that the rigid routine of the residential facility was making negative symptoms worse, Dr. Ferrarelli said. It is important to add variety into the mix – getting people to engage in different activities at different times of day would likely help residential SSD patients overcome negative symptoms of the disorder.
Although participants were recruited in Italy, Dr. Ferrarelli said he believes the findings are generalizable.
Bidirectional relationship?
Commenting on the findings, Matcheri Keshavan, MD, professor of psychiatry at Harvard Medical School in Boston, said the results are consistent with “well-known clinical observations that SSD patients tend to spend more time in bed and have more dysregulated sleep.
“Negative symptoms are also common, especially in residential patients. However, it is difficult to determine causality, as we do not know whether excessive sleepiness and decreased physical activity cause negative symptoms, or vice versa, or whether this is a bidirectional relationship,” Dr. Keshavan said.
He emphasized that physical exercise is known to increase sleep quality for people with mental illness and may also improve negative symptoms. “A useful approach in clinical practice is to increase activity levels, especially physical activities like walking and gardening.”
Dr. Keshavan said he would like to see future research that focuses on whether an intervention such as aerobic exercise would improve sleep quality as well as negative symptoms.
He also said that future research should ideally examine the characteristics of sleep alterations in schizophrenia.
“For example, while sleep duration is increased in schizophrenia, studies suggest that time spent in deep sleep is reduced; sleep spindles, which are important for consolidating memory during sleep, are also reduced. Correcting these deficits may improve negative symptoms and cognitive deficits,” he added.
The study was funded by the Italian Ministry of Health and the National Institute of Mental Health. There were no conflicts of interest.
A version of this article first appeared on Medscape.com.
FROM MOLECULAR PSYCHIATRY
Harnessing ChatGPT to improve liver disease outcomes
ChatGPT, an artificial intelligence (AI) chatbot, may be helpful for patients with cirrhosis or hepatocellular carcinoma (HCC) and their clinicians by generating easy-to-understand information about the disease, a new study suggests.
; however, the majority of the correct responses were labeled by clinician specialists as “correct but inadequate,” according to the study findings.
The AI tool can also provide empathetic and practical advice to patients and caregivers but falls short in its ability to provide tailored recommendations, the researchers said.
“Patients with cirrhosis and/or liver cancer and their caregivers often have unmet needs and insufficient knowledge about managing and preventing complications of their disease. We found ChatGPT – while it has limitations – can help empower patients and improve health literacy for different populations,” study investigator Brennan Spiegel, MD, director of health services research at Cedars-Sinai, Los Angeles, said in a news release.
The study was published online in Clinical and Molecular Hepatology.
Adjunctive health literacy tool
ChatGPT (Chat Generative Pre-Trained Transformer), developed by OpenAI, is a natural language processing tool that allows users to have personalized conversations with an AI bot capable of providing detailed responses to any question posed.
It has already seen several potential applications in the medical field, but the Cedars-Sinai study is one of the first to examine the chatbot’s ability to answer clinically oriented, disease-specific questions correctly and compare its performance to that of physicians.
The investigators asked ChatGPT 164 questions relevant to patients with cirrhosis and/or HCC across five categories – basic knowledge, diagnosis, treatment, lifestyle, and preventive medicine. The chatbot’s answers were graded independently by two liver transplant specialists.
Overall, ChatGPT answered about 77% of the questions correctly, generating high levels of accuracy in 91 questions across the categories, the researchers reported.
ChatGPT regurgitated extensive knowledge of cirrhosis (79% correct) and HCC (74% correct), but only small proportions were deemed by specialists to be comprehensive (47% in cirrhosis, 41% in HCC).
The chatbot performed better in basic knowledge, lifestyle, and treatment than in the domains of diagnosis and preventive medicine.
The specialists grading ChatGPT felt that 75% of its answers for questions on basic knowledge, treatment, and lifestyle were comprehensive or correct but inadequate. The corresponding percentages for diagnosis and preventive medicine were lower (67% and 50%, respectively). No responses from ChatGPT were graded as completely incorrect.
Responses deemed by the specialists to be “mixed with correct and incorrect/outdated data” were 22% for basic knowledge, 33% for diagnosis, 25% for treatment, 18% for lifestyle, and 50% for preventive medicine.
No substitute for specialists
The investigators also tested ChatGPT on cirrhosis quality measures recommended by the American Association for the Study of Liver Diseases and contained in two published questionnaires. ChatGPT answered 77% of the relevant questions correctly but failed to specify decision-making cutoffs and treatment durations.
ChatGPT also lacked knowledge of variations in regional guidelines, such as HCC screening criteria, but it did offer “practical and multifaceted” advice to patients and caregivers about next steps and adjusting to a new diagnosis.
“We believe ChatGPT to be a very useful adjunctive tool for physicians – not a replacement – but adjunctive tool that provides access to reliable and accurate health information that is easy for many to understand,” Dr. Spiegel said in the news release. “We hope that this can help physicians to empower patients and improve health literacy for patients facing challenging conditions such as cirrhosis and liver cancer.”
ChatGPT could enhance clinician workflow by helping to draft a framework for each tailored question asked by patients and caregivers, the researchers wrote.
“Given the high proportion of either comprehensive or correct but inadequate responses and expected continued improvement over time, we foresee that physicians would only need to revise ChatGPT’s responses to best answer patient queries,” they wrote. “This may not only improve the efficiency of physicians but also decrease the overall cost and burden on the healthcare system.”
In addition, ChatGPT could empower patients to be better informed about their care, the researchers noted.
“This allows for patient-led care and facilitates efficient shared decision-making by providing patients with an additional source of information,” they added.
The study had no specific funding. The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
ChatGPT, an artificial intelligence (AI) chatbot, may be helpful for patients with cirrhosis or hepatocellular carcinoma (HCC) and their clinicians by generating easy-to-understand information about the disease, a new study suggests.
; however, the majority of the correct responses were labeled by clinician specialists as “correct but inadequate,” according to the study findings.
The AI tool can also provide empathetic and practical advice to patients and caregivers but falls short in its ability to provide tailored recommendations, the researchers said.
“Patients with cirrhosis and/or liver cancer and their caregivers often have unmet needs and insufficient knowledge about managing and preventing complications of their disease. We found ChatGPT – while it has limitations – can help empower patients and improve health literacy for different populations,” study investigator Brennan Spiegel, MD, director of health services research at Cedars-Sinai, Los Angeles, said in a news release.
The study was published online in Clinical and Molecular Hepatology.
Adjunctive health literacy tool
ChatGPT (Chat Generative Pre-Trained Transformer), developed by OpenAI, is a natural language processing tool that allows users to have personalized conversations with an AI bot capable of providing detailed responses to any question posed.
It has already seen several potential applications in the medical field, but the Cedars-Sinai study is one of the first to examine the chatbot’s ability to answer clinically oriented, disease-specific questions correctly and compare its performance to that of physicians.
The investigators asked ChatGPT 164 questions relevant to patients with cirrhosis and/or HCC across five categories – basic knowledge, diagnosis, treatment, lifestyle, and preventive medicine. The chatbot’s answers were graded independently by two liver transplant specialists.
Overall, ChatGPT answered about 77% of the questions correctly, generating high levels of accuracy in 91 questions across the categories, the researchers reported.
ChatGPT regurgitated extensive knowledge of cirrhosis (79% correct) and HCC (74% correct), but only small proportions were deemed by specialists to be comprehensive (47% in cirrhosis, 41% in HCC).
The chatbot performed better in basic knowledge, lifestyle, and treatment than in the domains of diagnosis and preventive medicine.
The specialists grading ChatGPT felt that 75% of its answers for questions on basic knowledge, treatment, and lifestyle were comprehensive or correct but inadequate. The corresponding percentages for diagnosis and preventive medicine were lower (67% and 50%, respectively). No responses from ChatGPT were graded as completely incorrect.
Responses deemed by the specialists to be “mixed with correct and incorrect/outdated data” were 22% for basic knowledge, 33% for diagnosis, 25% for treatment, 18% for lifestyle, and 50% for preventive medicine.
No substitute for specialists
The investigators also tested ChatGPT on cirrhosis quality measures recommended by the American Association for the Study of Liver Diseases and contained in two published questionnaires. ChatGPT answered 77% of the relevant questions correctly but failed to specify decision-making cutoffs and treatment durations.
ChatGPT also lacked knowledge of variations in regional guidelines, such as HCC screening criteria, but it did offer “practical and multifaceted” advice to patients and caregivers about next steps and adjusting to a new diagnosis.
“We believe ChatGPT to be a very useful adjunctive tool for physicians – not a replacement – but adjunctive tool that provides access to reliable and accurate health information that is easy for many to understand,” Dr. Spiegel said in the news release. “We hope that this can help physicians to empower patients and improve health literacy for patients facing challenging conditions such as cirrhosis and liver cancer.”
ChatGPT could enhance clinician workflow by helping to draft a framework for each tailored question asked by patients and caregivers, the researchers wrote.
“Given the high proportion of either comprehensive or correct but inadequate responses and expected continued improvement over time, we foresee that physicians would only need to revise ChatGPT’s responses to best answer patient queries,” they wrote. “This may not only improve the efficiency of physicians but also decrease the overall cost and burden on the healthcare system.”
In addition, ChatGPT could empower patients to be better informed about their care, the researchers noted.
“This allows for patient-led care and facilitates efficient shared decision-making by providing patients with an additional source of information,” they added.
The study had no specific funding. The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
ChatGPT, an artificial intelligence (AI) chatbot, may be helpful for patients with cirrhosis or hepatocellular carcinoma (HCC) and their clinicians by generating easy-to-understand information about the disease, a new study suggests.
; however, the majority of the correct responses were labeled by clinician specialists as “correct but inadequate,” according to the study findings.
The AI tool can also provide empathetic and practical advice to patients and caregivers but falls short in its ability to provide tailored recommendations, the researchers said.
“Patients with cirrhosis and/or liver cancer and their caregivers often have unmet needs and insufficient knowledge about managing and preventing complications of their disease. We found ChatGPT – while it has limitations – can help empower patients and improve health literacy for different populations,” study investigator Brennan Spiegel, MD, director of health services research at Cedars-Sinai, Los Angeles, said in a news release.
The study was published online in Clinical and Molecular Hepatology.
Adjunctive health literacy tool
ChatGPT (Chat Generative Pre-Trained Transformer), developed by OpenAI, is a natural language processing tool that allows users to have personalized conversations with an AI bot capable of providing detailed responses to any question posed.
It has already seen several potential applications in the medical field, but the Cedars-Sinai study is one of the first to examine the chatbot’s ability to answer clinically oriented, disease-specific questions correctly and compare its performance to that of physicians.
The investigators asked ChatGPT 164 questions relevant to patients with cirrhosis and/or HCC across five categories – basic knowledge, diagnosis, treatment, lifestyle, and preventive medicine. The chatbot’s answers were graded independently by two liver transplant specialists.
Overall, ChatGPT answered about 77% of the questions correctly, generating high levels of accuracy in 91 questions across the categories, the researchers reported.
ChatGPT regurgitated extensive knowledge of cirrhosis (79% correct) and HCC (74% correct), but only small proportions were deemed by specialists to be comprehensive (47% in cirrhosis, 41% in HCC).
The chatbot performed better in basic knowledge, lifestyle, and treatment than in the domains of diagnosis and preventive medicine.
The specialists grading ChatGPT felt that 75% of its answers for questions on basic knowledge, treatment, and lifestyle were comprehensive or correct but inadequate. The corresponding percentages for diagnosis and preventive medicine were lower (67% and 50%, respectively). No responses from ChatGPT were graded as completely incorrect.
Responses deemed by the specialists to be “mixed with correct and incorrect/outdated data” were 22% for basic knowledge, 33% for diagnosis, 25% for treatment, 18% for lifestyle, and 50% for preventive medicine.
No substitute for specialists
The investigators also tested ChatGPT on cirrhosis quality measures recommended by the American Association for the Study of Liver Diseases and contained in two published questionnaires. ChatGPT answered 77% of the relevant questions correctly but failed to specify decision-making cutoffs and treatment durations.
ChatGPT also lacked knowledge of variations in regional guidelines, such as HCC screening criteria, but it did offer “practical and multifaceted” advice to patients and caregivers about next steps and adjusting to a new diagnosis.
“We believe ChatGPT to be a very useful adjunctive tool for physicians – not a replacement – but adjunctive tool that provides access to reliable and accurate health information that is easy for many to understand,” Dr. Spiegel said in the news release. “We hope that this can help physicians to empower patients and improve health literacy for patients facing challenging conditions such as cirrhosis and liver cancer.”
ChatGPT could enhance clinician workflow by helping to draft a framework for each tailored question asked by patients and caregivers, the researchers wrote.
“Given the high proportion of either comprehensive or correct but inadequate responses and expected continued improvement over time, we foresee that physicians would only need to revise ChatGPT’s responses to best answer patient queries,” they wrote. “This may not only improve the efficiency of physicians but also decrease the overall cost and burden on the healthcare system.”
In addition, ChatGPT could empower patients to be better informed about their care, the researchers noted.
“This allows for patient-led care and facilitates efficient shared decision-making by providing patients with an additional source of information,” they added.
The study had no specific funding. The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM CLINICAL AND MOLECULAR HEPATOLOGY
Unawareness of memory slips could indicate risk for Alzheimer’s
Everyone’s memory fades to some extent as we age, but not everyone will develop Alzheimer’s disease. Screening the most likely people to develop Alzheimer’s remains an ongoing challenge, as some people present only unambiguous symptoms once their disease is advanced.
A new study in JAMA Network Open suggests that one early clue is found in people’s own self-perception of their memory skills. People who are more aware of their own declining memory capacity are less likely to develop Alzheimer’s, the study suggests.
“Some people are very aware of changes in their memory, but many people are unaware,” said study author Patrizia Vannini, PhD, a neurologist at Brigham and Women’s Hospital in Boston. There are gradations of unawareness of memory loss, Dr. Vannini said, from complete unawareness that anything is wrong, to a partial unawareness that memory is declining.
The study compared the records of 436 participants in the Alzheimer’s Disease Neuroimaging Initiative, an Alzheimer’s research institute housed at the University of Southern California. More than 90% of the participants were White, and generally had a college education. Their average age was 75 years, and 53% of participants were women.
Dr. Vannini and colleagues tracked people whose cognitive function was normal at the beginning of the study, based on the Clinical Dementia Rating. Throughout the course of the study, which included data from 2010 to 2021, 91 of the 436 participants experienced a sustained decline in their Clinical Dementia Rating scores, indicating a risk for eventual Alzheimer’s, whereas the other participants held steady.
The people who declined in cognitive function were less aware of slips in their memory, as assessed by discrepancies between people’s self-reports of their own memory skills and the perceptions of someone in their lives. For this part of the study, Dr. Vannini and colleagues used the Everyday Cognition Questionnaire, which evaluates memory tasks such as shopping without a grocery list or recalling conversations from a few days ago. Both the participant and the study partner rated their performance on such tasks compared to 10 years earlier. Those who were less aware of their memory slips were more likely to experience declines in the Clinical Dementia Rating, compared with people with a heightened concern about memory loss (as measured by being more concerned about memory decline than their study partners).
“Partial or complete unawareness is often related to delayed diagnosis of Alzheimer’s, because the patient is unaware they are having problems,” Dr. Vannini said, adding that this is associated with a poorer prognosis as well.
Implications for clinicians
Soo Borson, MD, professor of clinical family medicine at the University of Southern California and coleader of a CDC-funded early dementia detection center at New York University, pointed out that sometimes people are genuinely unaware that their memory is declining, while at other times they know it all too well but say everything is fine when a doctor asks about their current memory status. That may be because people fear the label of “Alzheimer’s,” Dr. Borson suggested, or simply because they don’t want to start a protracted diagnostic pathway that could involve lots of tests and time.
Dr. Borson, who was not involved in the study, noted that the population was predominantly White and well-educated, and by definition included people who were concerned enough about potential memory loss to become part of an Alzheimer’s research network. This limits the generalizability of this study’s results to other populations, Dr. Borson said.
Despite that limitation, in Dr. Borson’s view the study points to the continued importance of clinicians (ideally a primary care doctor who knows the patient well) engaging with patients about their brain health once they reach midlife. A doctor could ask if patients have noticed a decline in their thinking or memory over the last year, for example, or a more open-ended question about any memory concerns.
Although some patients may choose to withhold concerns about their memory, Dr. Borson acknowledged, the overall thrust of these questions is to provide a safe space for patients to air their concerns if they so choose. In some cases it would be appropriate to do a simple memory test on the spot, and then proceed accordingly – either for further tests if something of concern emerges, or to reassure the patient if the test doesn’t yield anything of note. In the latter case some patients will still want further tests for additional reassurance, and Dr. Borson thinks doctors should facilitate that request even if in their own judgment nothing is wrong.
“This is not like testing for impaired kidney function by doing a serum creatinine test,” Dr. Borson said. While the orientation of the health care system is toward quick and easy answers for everything, detecting possible dementia eludes such an approach.
Dr. Vannini reports funding from the National Institutes of Health National Institute on Aging. Dr. Borson reported no disclosures.
Everyone’s memory fades to some extent as we age, but not everyone will develop Alzheimer’s disease. Screening the most likely people to develop Alzheimer’s remains an ongoing challenge, as some people present only unambiguous symptoms once their disease is advanced.
A new study in JAMA Network Open suggests that one early clue is found in people’s own self-perception of their memory skills. People who are more aware of their own declining memory capacity are less likely to develop Alzheimer’s, the study suggests.
“Some people are very aware of changes in their memory, but many people are unaware,” said study author Patrizia Vannini, PhD, a neurologist at Brigham and Women’s Hospital in Boston. There are gradations of unawareness of memory loss, Dr. Vannini said, from complete unawareness that anything is wrong, to a partial unawareness that memory is declining.
The study compared the records of 436 participants in the Alzheimer’s Disease Neuroimaging Initiative, an Alzheimer’s research institute housed at the University of Southern California. More than 90% of the participants were White, and generally had a college education. Their average age was 75 years, and 53% of participants were women.
Dr. Vannini and colleagues tracked people whose cognitive function was normal at the beginning of the study, based on the Clinical Dementia Rating. Throughout the course of the study, which included data from 2010 to 2021, 91 of the 436 participants experienced a sustained decline in their Clinical Dementia Rating scores, indicating a risk for eventual Alzheimer’s, whereas the other participants held steady.
The people who declined in cognitive function were less aware of slips in their memory, as assessed by discrepancies between people’s self-reports of their own memory skills and the perceptions of someone in their lives. For this part of the study, Dr. Vannini and colleagues used the Everyday Cognition Questionnaire, which evaluates memory tasks such as shopping without a grocery list or recalling conversations from a few days ago. Both the participant and the study partner rated their performance on such tasks compared to 10 years earlier. Those who were less aware of their memory slips were more likely to experience declines in the Clinical Dementia Rating, compared with people with a heightened concern about memory loss (as measured by being more concerned about memory decline than their study partners).
“Partial or complete unawareness is often related to delayed diagnosis of Alzheimer’s, because the patient is unaware they are having problems,” Dr. Vannini said, adding that this is associated with a poorer prognosis as well.
Implications for clinicians
Soo Borson, MD, professor of clinical family medicine at the University of Southern California and coleader of a CDC-funded early dementia detection center at New York University, pointed out that sometimes people are genuinely unaware that their memory is declining, while at other times they know it all too well but say everything is fine when a doctor asks about their current memory status. That may be because people fear the label of “Alzheimer’s,” Dr. Borson suggested, or simply because they don’t want to start a protracted diagnostic pathway that could involve lots of tests and time.
Dr. Borson, who was not involved in the study, noted that the population was predominantly White and well-educated, and by definition included people who were concerned enough about potential memory loss to become part of an Alzheimer’s research network. This limits the generalizability of this study’s results to other populations, Dr. Borson said.
Despite that limitation, in Dr. Borson’s view the study points to the continued importance of clinicians (ideally a primary care doctor who knows the patient well) engaging with patients about their brain health once they reach midlife. A doctor could ask if patients have noticed a decline in their thinking or memory over the last year, for example, or a more open-ended question about any memory concerns.
Although some patients may choose to withhold concerns about their memory, Dr. Borson acknowledged, the overall thrust of these questions is to provide a safe space for patients to air their concerns if they so choose. In some cases it would be appropriate to do a simple memory test on the spot, and then proceed accordingly – either for further tests if something of concern emerges, or to reassure the patient if the test doesn’t yield anything of note. In the latter case some patients will still want further tests for additional reassurance, and Dr. Borson thinks doctors should facilitate that request even if in their own judgment nothing is wrong.
“This is not like testing for impaired kidney function by doing a serum creatinine test,” Dr. Borson said. While the orientation of the health care system is toward quick and easy answers for everything, detecting possible dementia eludes such an approach.
Dr. Vannini reports funding from the National Institutes of Health National Institute on Aging. Dr. Borson reported no disclosures.
Everyone’s memory fades to some extent as we age, but not everyone will develop Alzheimer’s disease. Screening the most likely people to develop Alzheimer’s remains an ongoing challenge, as some people present only unambiguous symptoms once their disease is advanced.
A new study in JAMA Network Open suggests that one early clue is found in people’s own self-perception of their memory skills. People who are more aware of their own declining memory capacity are less likely to develop Alzheimer’s, the study suggests.
“Some people are very aware of changes in their memory, but many people are unaware,” said study author Patrizia Vannini, PhD, a neurologist at Brigham and Women’s Hospital in Boston. There are gradations of unawareness of memory loss, Dr. Vannini said, from complete unawareness that anything is wrong, to a partial unawareness that memory is declining.
The study compared the records of 436 participants in the Alzheimer’s Disease Neuroimaging Initiative, an Alzheimer’s research institute housed at the University of Southern California. More than 90% of the participants were White, and generally had a college education. Their average age was 75 years, and 53% of participants were women.
Dr. Vannini and colleagues tracked people whose cognitive function was normal at the beginning of the study, based on the Clinical Dementia Rating. Throughout the course of the study, which included data from 2010 to 2021, 91 of the 436 participants experienced a sustained decline in their Clinical Dementia Rating scores, indicating a risk for eventual Alzheimer’s, whereas the other participants held steady.
The people who declined in cognitive function were less aware of slips in their memory, as assessed by discrepancies between people’s self-reports of their own memory skills and the perceptions of someone in their lives. For this part of the study, Dr. Vannini and colleagues used the Everyday Cognition Questionnaire, which evaluates memory tasks such as shopping without a grocery list or recalling conversations from a few days ago. Both the participant and the study partner rated their performance on such tasks compared to 10 years earlier. Those who were less aware of their memory slips were more likely to experience declines in the Clinical Dementia Rating, compared with people with a heightened concern about memory loss (as measured by being more concerned about memory decline than their study partners).
“Partial or complete unawareness is often related to delayed diagnosis of Alzheimer’s, because the patient is unaware they are having problems,” Dr. Vannini said, adding that this is associated with a poorer prognosis as well.
Implications for clinicians
Soo Borson, MD, professor of clinical family medicine at the University of Southern California and coleader of a CDC-funded early dementia detection center at New York University, pointed out that sometimes people are genuinely unaware that their memory is declining, while at other times they know it all too well but say everything is fine when a doctor asks about their current memory status. That may be because people fear the label of “Alzheimer’s,” Dr. Borson suggested, or simply because they don’t want to start a protracted diagnostic pathway that could involve lots of tests and time.
Dr. Borson, who was not involved in the study, noted that the population was predominantly White and well-educated, and by definition included people who were concerned enough about potential memory loss to become part of an Alzheimer’s research network. This limits the generalizability of this study’s results to other populations, Dr. Borson said.
Despite that limitation, in Dr. Borson’s view the study points to the continued importance of clinicians (ideally a primary care doctor who knows the patient well) engaging with patients about their brain health once they reach midlife. A doctor could ask if patients have noticed a decline in their thinking or memory over the last year, for example, or a more open-ended question about any memory concerns.
Although some patients may choose to withhold concerns about their memory, Dr. Borson acknowledged, the overall thrust of these questions is to provide a safe space for patients to air their concerns if they so choose. In some cases it would be appropriate to do a simple memory test on the spot, and then proceed accordingly – either for further tests if something of concern emerges, or to reassure the patient if the test doesn’t yield anything of note. In the latter case some patients will still want further tests for additional reassurance, and Dr. Borson thinks doctors should facilitate that request even if in their own judgment nothing is wrong.
“This is not like testing for impaired kidney function by doing a serum creatinine test,” Dr. Borson said. While the orientation of the health care system is toward quick and easy answers for everything, detecting possible dementia eludes such an approach.
Dr. Vannini reports funding from the National Institutes of Health National Institute on Aging. Dr. Borson reported no disclosures.
FROM JAMA NETWORK OPEN
Drug combo improves recurrence-free survival after HCC resection
ORLANDO – Patients with hepatocellular carcinoma (HCC) who undergo surgery or thermal ablation with curative intent are at high risk for recurrence, but currently, no adjuvant therapy standard of care exists for these patients.
New findings signal a promising option for these patients. The combination of the immune checkpoint inhibitor atezolizumab (Tecentriq) and the angiogenesis inhibitor bevacizumab (Avastin) was associated with a significant improvement in recurrence-free survival, compared with active surveillance, and represents the first option to show efficacy in the adjuvant setting following surgical resection of HCCs for patients at high risk for recurrence.
among patients who received the combination therapy in comparison with active surveillance. However, the overall survival data remain immature.
The data come from an interim analysis of the IMbrave050 trial, which was presented at the annual meeting of the American Association for Cancer Research.
“Atezolizumab plus bevacizumab may be a practice-changing adjuvant treatment options for patients with high-risk HCC,” said lead investigator Pierce Chow, MBBS, PhD, codirector of the National Cancer Centre Singapore Comprehensive Liver Cancer Clinic. He presented the results in an oral abstract session at the meeting. The combination “may also change clinical indications for surgical resection” because clinicians may be more likely to consider resection for patients at extremely high risk for recurrence if the risk of recurrence can be reduced with this combination.
In the previous IMbrave150 trial, the combination of atezolizumab and bevacizumab significantly improved outcomes for patients with high-risk and non–high-risk unresectable HCC, compared with the standard of care sorafenib (Nexavar).
In that trial, the median overall survival in the intention-to-treat population was 19.2 months for patients who received atezolizumab-bevacizumab versus 13.4 months for patients who received sorafenib (P = .0009).
The combination was also associated with improvements in progression-free survival and objective response rates, compared with sorafenib.
On the basis of these results, the IMbrave050 investigators explored whether the same benefits would occur for patients with resectable disease considered to be at high risk for recurrence owing to tumor size, vascular invasion, or poor tumor differentiation. The trial compared the combination for 334 patients with active surveillance, also for 334 patients, in the adjuvant setting.
Patients were considered good candidates for thermal ablation if they had a single tumor greater than 2 cm, but not larger than 5 cm in its longest dimension, or if they had four or fewer tumors, all of which were no larger than 5 cm. For all other patients, surgical resection was recommended.
The median age of the patients was 60. For about half of patients in each arm, the expression level of programmed death–ligand-1 (PD-L1) was 1% or higher.
After a median follow-up of 17.4 months, the 12-month recurrence-free survival rate, as assessed by independent review, was 78% for patients in the treatment arm, compared with 65% for patients who were assigned to active surveillance (hazard ratio, 0.72; P = .012). This finding was generally consistent across clinical subgroups, including groups based on age, sex, race/ethnicity, performance status, PD-L1 expression, number of high-risk features, Barcelona Clinic Liver Cancer stage, cancer etiology, procedure type, microvascular invasion, or tumor numbers and size.
Of 133 patients on active surveillance who experienced a protocol-defined recurrence event, 81 (61%) crossed over to the atezolizumab/bevacizumab arm.
The overall survival benefit of the combination therapy was less clear. Dr. Chow called the overall survival data “highly immature” at the time of data cutoff.
Overall, 47 patients died – 7 more in the combination arm (27 vs. 20). More specifically, 17 patients in the combination arm and 16 on active surveillance died from progressive disease; 6 patients in the treatment arm versus 1 on surveillance died from adverse events. The remaining deaths were attributed to other causes. Two deaths in the combination arm were considered treatment related, one from esophageal varices hemorrhage, and the other from ischemic stroke.
Dr. Chow said a number of deaths attributed to HCC recurrence was similar between the groups. There were three COVID-19–related deaths within 1 year of randomization, all in the combination arm.
As for adverse events, the safety of the combination was largely consistent with that reported in the IMbrave150 trial. Nearly all patients experienced at least one adverse event. Treatment-related grade 3 or 4 adverse events occurred in 34.9% of patients in the combination group, and serious treatment-related events occurred in 13.3%.
The most common adverse events of any grade were proteinuria, hypertension, decreased platelet count, increases in liver enzyme level, hypothyroidism, arthralgia, pruritus, rash, increase in serum bilirubin level, and fever.
Invited discussant Stephen L. Chan, MD, from the Chinese University of Hong Kong, said the study was “definitely” relevant to clinicians and addresses “a very important unmet need.”
Dr. Chan noted that he thinks this combination will “likely” be practice changing, given the improvement in recurrence-free survival, but “certainly we need more data to guide us in patient selection.”
The study was funded by F. Hoffman–La Roche. Dr. Chow has consulting for and has received honoraria and grant/research support from Roche and others. Dr. Chan has received honoraria from Roche and consulting fees and grant/research support from others.
A version of this article first appeared on Medscape.com.
ORLANDO – Patients with hepatocellular carcinoma (HCC) who undergo surgery or thermal ablation with curative intent are at high risk for recurrence, but currently, no adjuvant therapy standard of care exists for these patients.
New findings signal a promising option for these patients. The combination of the immune checkpoint inhibitor atezolizumab (Tecentriq) and the angiogenesis inhibitor bevacizumab (Avastin) was associated with a significant improvement in recurrence-free survival, compared with active surveillance, and represents the first option to show efficacy in the adjuvant setting following surgical resection of HCCs for patients at high risk for recurrence.
among patients who received the combination therapy in comparison with active surveillance. However, the overall survival data remain immature.
The data come from an interim analysis of the IMbrave050 trial, which was presented at the annual meeting of the American Association for Cancer Research.
“Atezolizumab plus bevacizumab may be a practice-changing adjuvant treatment options for patients with high-risk HCC,” said lead investigator Pierce Chow, MBBS, PhD, codirector of the National Cancer Centre Singapore Comprehensive Liver Cancer Clinic. He presented the results in an oral abstract session at the meeting. The combination “may also change clinical indications for surgical resection” because clinicians may be more likely to consider resection for patients at extremely high risk for recurrence if the risk of recurrence can be reduced with this combination.
In the previous IMbrave150 trial, the combination of atezolizumab and bevacizumab significantly improved outcomes for patients with high-risk and non–high-risk unresectable HCC, compared with the standard of care sorafenib (Nexavar).
In that trial, the median overall survival in the intention-to-treat population was 19.2 months for patients who received atezolizumab-bevacizumab versus 13.4 months for patients who received sorafenib (P = .0009).
The combination was also associated with improvements in progression-free survival and objective response rates, compared with sorafenib.
On the basis of these results, the IMbrave050 investigators explored whether the same benefits would occur for patients with resectable disease considered to be at high risk for recurrence owing to tumor size, vascular invasion, or poor tumor differentiation. The trial compared the combination for 334 patients with active surveillance, also for 334 patients, in the adjuvant setting.
Patients were considered good candidates for thermal ablation if they had a single tumor greater than 2 cm, but not larger than 5 cm in its longest dimension, or if they had four or fewer tumors, all of which were no larger than 5 cm. For all other patients, surgical resection was recommended.
The median age of the patients was 60. For about half of patients in each arm, the expression level of programmed death–ligand-1 (PD-L1) was 1% or higher.
After a median follow-up of 17.4 months, the 12-month recurrence-free survival rate, as assessed by independent review, was 78% for patients in the treatment arm, compared with 65% for patients who were assigned to active surveillance (hazard ratio, 0.72; P = .012). This finding was generally consistent across clinical subgroups, including groups based on age, sex, race/ethnicity, performance status, PD-L1 expression, number of high-risk features, Barcelona Clinic Liver Cancer stage, cancer etiology, procedure type, microvascular invasion, or tumor numbers and size.
Of 133 patients on active surveillance who experienced a protocol-defined recurrence event, 81 (61%) crossed over to the atezolizumab/bevacizumab arm.
The overall survival benefit of the combination therapy was less clear. Dr. Chow called the overall survival data “highly immature” at the time of data cutoff.
Overall, 47 patients died – 7 more in the combination arm (27 vs. 20). More specifically, 17 patients in the combination arm and 16 on active surveillance died from progressive disease; 6 patients in the treatment arm versus 1 on surveillance died from adverse events. The remaining deaths were attributed to other causes. Two deaths in the combination arm were considered treatment related, one from esophageal varices hemorrhage, and the other from ischemic stroke.
Dr. Chow said a number of deaths attributed to HCC recurrence was similar between the groups. There were three COVID-19–related deaths within 1 year of randomization, all in the combination arm.
As for adverse events, the safety of the combination was largely consistent with that reported in the IMbrave150 trial. Nearly all patients experienced at least one adverse event. Treatment-related grade 3 or 4 adverse events occurred in 34.9% of patients in the combination group, and serious treatment-related events occurred in 13.3%.
The most common adverse events of any grade were proteinuria, hypertension, decreased platelet count, increases in liver enzyme level, hypothyroidism, arthralgia, pruritus, rash, increase in serum bilirubin level, and fever.
Invited discussant Stephen L. Chan, MD, from the Chinese University of Hong Kong, said the study was “definitely” relevant to clinicians and addresses “a very important unmet need.”
Dr. Chan noted that he thinks this combination will “likely” be practice changing, given the improvement in recurrence-free survival, but “certainly we need more data to guide us in patient selection.”
The study was funded by F. Hoffman–La Roche. Dr. Chow has consulting for and has received honoraria and grant/research support from Roche and others. Dr. Chan has received honoraria from Roche and consulting fees and grant/research support from others.
A version of this article first appeared on Medscape.com.
ORLANDO – Patients with hepatocellular carcinoma (HCC) who undergo surgery or thermal ablation with curative intent are at high risk for recurrence, but currently, no adjuvant therapy standard of care exists for these patients.
New findings signal a promising option for these patients. The combination of the immune checkpoint inhibitor atezolizumab (Tecentriq) and the angiogenesis inhibitor bevacizumab (Avastin) was associated with a significant improvement in recurrence-free survival, compared with active surveillance, and represents the first option to show efficacy in the adjuvant setting following surgical resection of HCCs for patients at high risk for recurrence.
among patients who received the combination therapy in comparison with active surveillance. However, the overall survival data remain immature.
The data come from an interim analysis of the IMbrave050 trial, which was presented at the annual meeting of the American Association for Cancer Research.
“Atezolizumab plus bevacizumab may be a practice-changing adjuvant treatment options for patients with high-risk HCC,” said lead investigator Pierce Chow, MBBS, PhD, codirector of the National Cancer Centre Singapore Comprehensive Liver Cancer Clinic. He presented the results in an oral abstract session at the meeting. The combination “may also change clinical indications for surgical resection” because clinicians may be more likely to consider resection for patients at extremely high risk for recurrence if the risk of recurrence can be reduced with this combination.
In the previous IMbrave150 trial, the combination of atezolizumab and bevacizumab significantly improved outcomes for patients with high-risk and non–high-risk unresectable HCC, compared with the standard of care sorafenib (Nexavar).
In that trial, the median overall survival in the intention-to-treat population was 19.2 months for patients who received atezolizumab-bevacizumab versus 13.4 months for patients who received sorafenib (P = .0009).
The combination was also associated with improvements in progression-free survival and objective response rates, compared with sorafenib.
On the basis of these results, the IMbrave050 investigators explored whether the same benefits would occur for patients with resectable disease considered to be at high risk for recurrence owing to tumor size, vascular invasion, or poor tumor differentiation. The trial compared the combination for 334 patients with active surveillance, also for 334 patients, in the adjuvant setting.
Patients were considered good candidates for thermal ablation if they had a single tumor greater than 2 cm, but not larger than 5 cm in its longest dimension, or if they had four or fewer tumors, all of which were no larger than 5 cm. For all other patients, surgical resection was recommended.
The median age of the patients was 60. For about half of patients in each arm, the expression level of programmed death–ligand-1 (PD-L1) was 1% or higher.
After a median follow-up of 17.4 months, the 12-month recurrence-free survival rate, as assessed by independent review, was 78% for patients in the treatment arm, compared with 65% for patients who were assigned to active surveillance (hazard ratio, 0.72; P = .012). This finding was generally consistent across clinical subgroups, including groups based on age, sex, race/ethnicity, performance status, PD-L1 expression, number of high-risk features, Barcelona Clinic Liver Cancer stage, cancer etiology, procedure type, microvascular invasion, or tumor numbers and size.
Of 133 patients on active surveillance who experienced a protocol-defined recurrence event, 81 (61%) crossed over to the atezolizumab/bevacizumab arm.
The overall survival benefit of the combination therapy was less clear. Dr. Chow called the overall survival data “highly immature” at the time of data cutoff.
Overall, 47 patients died – 7 more in the combination arm (27 vs. 20). More specifically, 17 patients in the combination arm and 16 on active surveillance died from progressive disease; 6 patients in the treatment arm versus 1 on surveillance died from adverse events. The remaining deaths were attributed to other causes. Two deaths in the combination arm were considered treatment related, one from esophageal varices hemorrhage, and the other from ischemic stroke.
Dr. Chow said a number of deaths attributed to HCC recurrence was similar between the groups. There were three COVID-19–related deaths within 1 year of randomization, all in the combination arm.
As for adverse events, the safety of the combination was largely consistent with that reported in the IMbrave150 trial. Nearly all patients experienced at least one adverse event. Treatment-related grade 3 or 4 adverse events occurred in 34.9% of patients in the combination group, and serious treatment-related events occurred in 13.3%.
The most common adverse events of any grade were proteinuria, hypertension, decreased platelet count, increases in liver enzyme level, hypothyroidism, arthralgia, pruritus, rash, increase in serum bilirubin level, and fever.
Invited discussant Stephen L. Chan, MD, from the Chinese University of Hong Kong, said the study was “definitely” relevant to clinicians and addresses “a very important unmet need.”
Dr. Chan noted that he thinks this combination will “likely” be practice changing, given the improvement in recurrence-free survival, but “certainly we need more data to guide us in patient selection.”
The study was funded by F. Hoffman–La Roche. Dr. Chow has consulting for and has received honoraria and grant/research support from Roche and others. Dr. Chan has received honoraria from Roche and consulting fees and grant/research support from others.
A version of this article first appeared on Medscape.com.
AT AACR 2023
Tirzepatide scores win in second obesity trial, SURMOUNT-2
The “twincretin” tirzepatide (Mounjaro) has proven successful in SURMOUNT-2, the second pivotal trial for the drug as an antiobesity agent, according to top-line results reported April 27 by tirzepatide’s manufacturer, Lilly, in a press release. The company reveals that tirzepatide achieved both of its primary endpoints in the trial, as well as all its key secondary endpoints.
The findings pave the way for tirzepatide to likely receive Food and Drug Administration approval as a treatment for obesity, perhaps before the end of 2023.
Tirzepatide received FDA approval in May 2022 for the treatment of type 2 diabetes in adults, under the brand name Mounjaro, and some people have already been using it off-label to treat obesity.
Tirzepatide is a dual glucagonlike peptide–1 (GLP-1) agonist and glucose-dependent insulinotropic polypeptide agonist. Several GLP-1 receptor agonists are already approved in the United States, including semaglutide, a once-weekly injection, which is approved as Wegovy for patients with obesity and as Ozempic for treatment of type 2 diabetes.
These agents have been incredibly popular among celebrity influencers, and with use of the #Ozempic hashtag and others on social media, this has led to unprecedented use of these products for weight loss, often among those who do not even have obesity or type 2 diabetes. Subsequently, patients with type 2 diabetes and obesity who need them have often struggled to obtain them, owing to shortages following this phenomenon.
SURMOUNT-2: Weight loss around 15%, less than seen in SURMOUNT-1
SURMOUNT-2 enrolled 938 adults with overweight or obesity and type 2 diabetes and had dual primary endpoints that both focused on weight loss, compared with placebo.
The first completed pivotal trial of tirzepatide for weight loss, SURMOUNT-1, enrolled people with overweight or obesity but no diabetes and had its main results reported in 2022. At the time, the weight loss achieved with tirzepatide, was described as “unprecedented,” with those given the highest dose in that trial (15 mg subcutaneously per week) losing an average of 20%-22% of body weight over 72 weeks, depending on the specific statistical analysis used.
For SURMOUNT-2’s first primary endpoint, 72 weeks of weekly subcutaneous injections with tirzepatide at dosages of 10 mg or 15 mg led to an average weight loss from baseline of 13.4% and 15.7%, respectively, compared with an average loss of 3.3% from baseline in the placebo-treated control arm.
For the second primary endpoint, 81.6% of people on the 10-mg dose and 86.4% on the 15-mg dose achieved at least 5% weight loss from baseline, compared with 30.5% of controls who had at least 5% weight loss from baseline.
In one key secondary endpoint, tirzepatide at dosages of 10 mg or 15 mg weekly produced at least a 15% cut in weight from baseline in 41.4% and 51.8% of participants, respectively, compared with a 2.6% rate of this endpoint in the placebo controls.
So the extent of weight loss seen in in SURMOUNT-2 was somewhat less than was reported in SURMOUNT-1, a finding consistent with many prior studies of incretin-based weight-loss agents, which seem to pack a more potent weight-loss punch in people without type 2 diabetes.
Lilly did not specifically report the treatment effect of tirzepatide on hemoglobin A1c in SURMOUNT-2, only saying that the effect was similar to what had been seen in the series of five SURPASS trials that led to the approval of tirzepatide for type 2 diabetes.
Lilly also reported that the safety profile of tirzepatide in SURMOUNT-2 generally matched what was seen in SURMOUNT-1 as well as in the SURPASS trials. The most common adverse events in SURMOUNT-2 involved gastrointestinal symptoms, such as nausea, diarrhea, and vomiting; these were generally mild to moderate in severity and clustered during the dose-escalation phase at the start of treatment. Treatment discontinuations caused by adverse effects were 3.8% on the 10-mg dosage, 7.4% on the 15-mg dosage, and 3.8% on placebo.
SURMOUNT-2 enrolled patients in the United States, Puerto Rico, and five other countries. All participants also received interventions designed to reduce their calorie intake and increase their physical activity.
More SURMOUNT-2 results at ADA in June
Lilly also announced that researchers would report more complete results from SURMOUNT-2 at the 2023 scientific sessions of the American Diabetes Association, being held in San Diego in late June, and publish the findings in a major medical journal.
Results from two additional phase 3 trials of tirzepatide in people with overweight or obesity, SURMOUNT-3 and SURMOUNT-4, are expected later in 2023.
Lilly started an application to the FDA for an indication for weight loss in October 2022 under a fast track designation by the agency, and the data collected in SURMOUNT-2 are expected to complete this application, which would then be subject to an FDA decision within about 6 months. Lilly said in its April 27 press release that it anticipates an FDA decision on this application may occur before the end of 2023.
SURMOUNT-2 and all of the other tirzepatide trials were sponsored by Lilly.
A version of this article first appeared on Medscape.com.
The “twincretin” tirzepatide (Mounjaro) has proven successful in SURMOUNT-2, the second pivotal trial for the drug as an antiobesity agent, according to top-line results reported April 27 by tirzepatide’s manufacturer, Lilly, in a press release. The company reveals that tirzepatide achieved both of its primary endpoints in the trial, as well as all its key secondary endpoints.
The findings pave the way for tirzepatide to likely receive Food and Drug Administration approval as a treatment for obesity, perhaps before the end of 2023.
Tirzepatide received FDA approval in May 2022 for the treatment of type 2 diabetes in adults, under the brand name Mounjaro, and some people have already been using it off-label to treat obesity.
Tirzepatide is a dual glucagonlike peptide–1 (GLP-1) agonist and glucose-dependent insulinotropic polypeptide agonist. Several GLP-1 receptor agonists are already approved in the United States, including semaglutide, a once-weekly injection, which is approved as Wegovy for patients with obesity and as Ozempic for treatment of type 2 diabetes.
These agents have been incredibly popular among celebrity influencers, and with use of the #Ozempic hashtag and others on social media, this has led to unprecedented use of these products for weight loss, often among those who do not even have obesity or type 2 diabetes. Subsequently, patients with type 2 diabetes and obesity who need them have often struggled to obtain them, owing to shortages following this phenomenon.
SURMOUNT-2: Weight loss around 15%, less than seen in SURMOUNT-1
SURMOUNT-2 enrolled 938 adults with overweight or obesity and type 2 diabetes and had dual primary endpoints that both focused on weight loss, compared with placebo.
The first completed pivotal trial of tirzepatide for weight loss, SURMOUNT-1, enrolled people with overweight or obesity but no diabetes and had its main results reported in 2022. At the time, the weight loss achieved with tirzepatide, was described as “unprecedented,” with those given the highest dose in that trial (15 mg subcutaneously per week) losing an average of 20%-22% of body weight over 72 weeks, depending on the specific statistical analysis used.
For SURMOUNT-2’s first primary endpoint, 72 weeks of weekly subcutaneous injections with tirzepatide at dosages of 10 mg or 15 mg led to an average weight loss from baseline of 13.4% and 15.7%, respectively, compared with an average loss of 3.3% from baseline in the placebo-treated control arm.
For the second primary endpoint, 81.6% of people on the 10-mg dose and 86.4% on the 15-mg dose achieved at least 5% weight loss from baseline, compared with 30.5% of controls who had at least 5% weight loss from baseline.
In one key secondary endpoint, tirzepatide at dosages of 10 mg or 15 mg weekly produced at least a 15% cut in weight from baseline in 41.4% and 51.8% of participants, respectively, compared with a 2.6% rate of this endpoint in the placebo controls.
So the extent of weight loss seen in in SURMOUNT-2 was somewhat less than was reported in SURMOUNT-1, a finding consistent with many prior studies of incretin-based weight-loss agents, which seem to pack a more potent weight-loss punch in people without type 2 diabetes.
Lilly did not specifically report the treatment effect of tirzepatide on hemoglobin A1c in SURMOUNT-2, only saying that the effect was similar to what had been seen in the series of five SURPASS trials that led to the approval of tirzepatide for type 2 diabetes.
Lilly also reported that the safety profile of tirzepatide in SURMOUNT-2 generally matched what was seen in SURMOUNT-1 as well as in the SURPASS trials. The most common adverse events in SURMOUNT-2 involved gastrointestinal symptoms, such as nausea, diarrhea, and vomiting; these were generally mild to moderate in severity and clustered during the dose-escalation phase at the start of treatment. Treatment discontinuations caused by adverse effects were 3.8% on the 10-mg dosage, 7.4% on the 15-mg dosage, and 3.8% on placebo.
SURMOUNT-2 enrolled patients in the United States, Puerto Rico, and five other countries. All participants also received interventions designed to reduce their calorie intake and increase their physical activity.
More SURMOUNT-2 results at ADA in June
Lilly also announced that researchers would report more complete results from SURMOUNT-2 at the 2023 scientific sessions of the American Diabetes Association, being held in San Diego in late June, and publish the findings in a major medical journal.
Results from two additional phase 3 trials of tirzepatide in people with overweight or obesity, SURMOUNT-3 and SURMOUNT-4, are expected later in 2023.
Lilly started an application to the FDA for an indication for weight loss in October 2022 under a fast track designation by the agency, and the data collected in SURMOUNT-2 are expected to complete this application, which would then be subject to an FDA decision within about 6 months. Lilly said in its April 27 press release that it anticipates an FDA decision on this application may occur before the end of 2023.
SURMOUNT-2 and all of the other tirzepatide trials were sponsored by Lilly.
A version of this article first appeared on Medscape.com.
The “twincretin” tirzepatide (Mounjaro) has proven successful in SURMOUNT-2, the second pivotal trial for the drug as an antiobesity agent, according to top-line results reported April 27 by tirzepatide’s manufacturer, Lilly, in a press release. The company reveals that tirzepatide achieved both of its primary endpoints in the trial, as well as all its key secondary endpoints.
The findings pave the way for tirzepatide to likely receive Food and Drug Administration approval as a treatment for obesity, perhaps before the end of 2023.
Tirzepatide received FDA approval in May 2022 for the treatment of type 2 diabetes in adults, under the brand name Mounjaro, and some people have already been using it off-label to treat obesity.
Tirzepatide is a dual glucagonlike peptide–1 (GLP-1) agonist and glucose-dependent insulinotropic polypeptide agonist. Several GLP-1 receptor agonists are already approved in the United States, including semaglutide, a once-weekly injection, which is approved as Wegovy for patients with obesity and as Ozempic for treatment of type 2 diabetes.
These agents have been incredibly popular among celebrity influencers, and with use of the #Ozempic hashtag and others on social media, this has led to unprecedented use of these products for weight loss, often among those who do not even have obesity or type 2 diabetes. Subsequently, patients with type 2 diabetes and obesity who need them have often struggled to obtain them, owing to shortages following this phenomenon.
SURMOUNT-2: Weight loss around 15%, less than seen in SURMOUNT-1
SURMOUNT-2 enrolled 938 adults with overweight or obesity and type 2 diabetes and had dual primary endpoints that both focused on weight loss, compared with placebo.
The first completed pivotal trial of tirzepatide for weight loss, SURMOUNT-1, enrolled people with overweight or obesity but no diabetes and had its main results reported in 2022. At the time, the weight loss achieved with tirzepatide, was described as “unprecedented,” with those given the highest dose in that trial (15 mg subcutaneously per week) losing an average of 20%-22% of body weight over 72 weeks, depending on the specific statistical analysis used.
For SURMOUNT-2’s first primary endpoint, 72 weeks of weekly subcutaneous injections with tirzepatide at dosages of 10 mg or 15 mg led to an average weight loss from baseline of 13.4% and 15.7%, respectively, compared with an average loss of 3.3% from baseline in the placebo-treated control arm.
For the second primary endpoint, 81.6% of people on the 10-mg dose and 86.4% on the 15-mg dose achieved at least 5% weight loss from baseline, compared with 30.5% of controls who had at least 5% weight loss from baseline.
In one key secondary endpoint, tirzepatide at dosages of 10 mg or 15 mg weekly produced at least a 15% cut in weight from baseline in 41.4% and 51.8% of participants, respectively, compared with a 2.6% rate of this endpoint in the placebo controls.
So the extent of weight loss seen in in SURMOUNT-2 was somewhat less than was reported in SURMOUNT-1, a finding consistent with many prior studies of incretin-based weight-loss agents, which seem to pack a more potent weight-loss punch in people without type 2 diabetes.
Lilly did not specifically report the treatment effect of tirzepatide on hemoglobin A1c in SURMOUNT-2, only saying that the effect was similar to what had been seen in the series of five SURPASS trials that led to the approval of tirzepatide for type 2 diabetes.
Lilly also reported that the safety profile of tirzepatide in SURMOUNT-2 generally matched what was seen in SURMOUNT-1 as well as in the SURPASS trials. The most common adverse events in SURMOUNT-2 involved gastrointestinal symptoms, such as nausea, diarrhea, and vomiting; these were generally mild to moderate in severity and clustered during the dose-escalation phase at the start of treatment. Treatment discontinuations caused by adverse effects were 3.8% on the 10-mg dosage, 7.4% on the 15-mg dosage, and 3.8% on placebo.
SURMOUNT-2 enrolled patients in the United States, Puerto Rico, and five other countries. All participants also received interventions designed to reduce their calorie intake and increase their physical activity.
More SURMOUNT-2 results at ADA in June
Lilly also announced that researchers would report more complete results from SURMOUNT-2 at the 2023 scientific sessions of the American Diabetes Association, being held in San Diego in late June, and publish the findings in a major medical journal.
Results from two additional phase 3 trials of tirzepatide in people with overweight or obesity, SURMOUNT-3 and SURMOUNT-4, are expected later in 2023.
Lilly started an application to the FDA for an indication for weight loss in October 2022 under a fast track designation by the agency, and the data collected in SURMOUNT-2 are expected to complete this application, which would then be subject to an FDA decision within about 6 months. Lilly said in its April 27 press release that it anticipates an FDA decision on this application may occur before the end of 2023.
SURMOUNT-2 and all of the other tirzepatide trials were sponsored by Lilly.
A version of this article first appeared on Medscape.com.
Erythema Ab Igne: A Clinical Review
Erythema ab igne (EAI)(also known as toasted skin syndrome) was first described in the British Journal of Dermatology in the 20th century, 1 though it was known by physicians long before. Reticular netlike skin changes were seen in association with patients who spent extended time directly next to a heat source. This association led to the name of this condition, which literally means “redness by fire.” Indeed, EAI induced by chronic heat exposure has been described across the world for centuries. For example, in the cold regions of northern China, people used to sleep on beds of hot bricks called kang to stay warm at night. The people of India’s Kashmir district carried pots of hot coals called kangri next to the skin under large woven shawls to stay warm. In the past, Irish women often spent much time by a turf- or peat-burning fire. Chronic heat exposure in these cases can lead not only to EAI but also to aggressive types of cancer, often with a latency of 30 years or more. 2
More recently, the invention of home central heating led to a stark decrease in the number of cases associated with combustion-based heat, with a transition to etiologies such as use of hot water bottles, electric blankets, and electric space heaters. Over time, technological advances led to ever-increasing potential causes for EAI, such as laptops or cell phones, car heaters and heated seats, heated blankets,3,4 infrared lamps for food, and even medical devices such as ultrasound-based heating products and convective temperature management systems for hospitalized patients. As technology evolves, so do the potential causes of EAI, requiring clinicians to diagnose and deduce the cause through a thorough social and medical history as well as a workup on the present illness with considerations for the anatomical location.5-7 Herein, we describe the etiology of EAI, diagnosis, and treatment options.
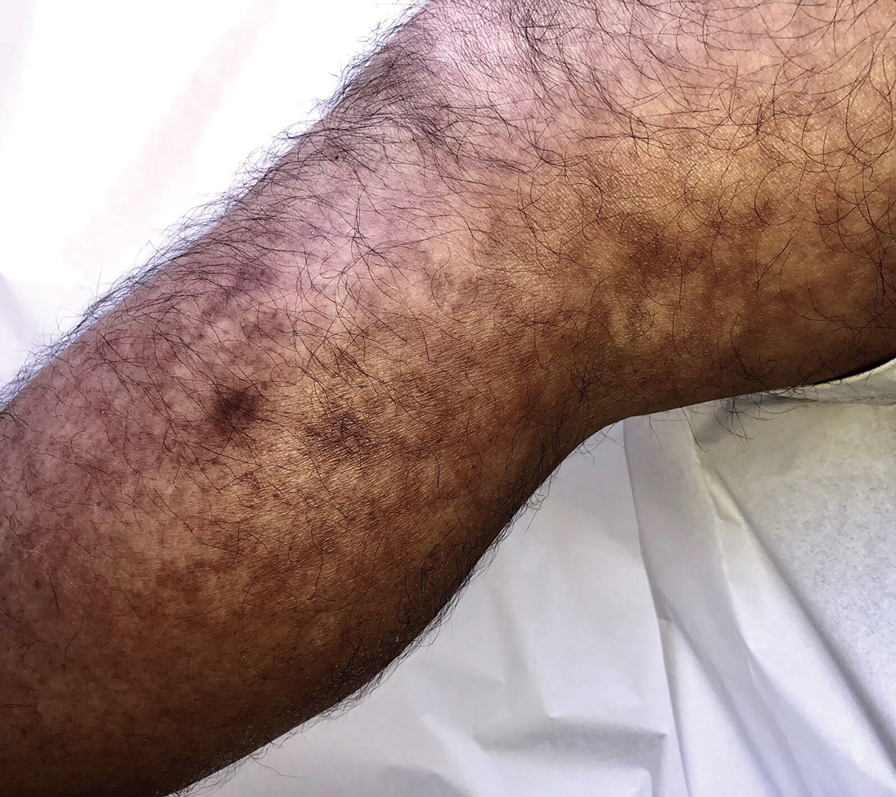
Clinical Characteristics
Erythema ab igne begins as mild, transient, and erythematous macules and patches in a reticular pattern that resolve minutes to hours after removal of the heat source. With weeks to months of continued or repeated application of the heat source, the affected area eventually becomes hyperpigmented where there once was erythema (Figures 1 and 2). Sometimes papules, bullae, telangiectasia, and hyperkeratosis also form. The rash usually is asymptomatic, though pain, pruritus, and dysesthesia have been reported.7 Dermoscopy of EAI in the hyperpigmented stage can reveal diffuse superficial dark pigmentation, telangiectasia, and mild whitish scaling.8 Although the pathogenesis has remained elusive over the years, lesions do seem to be mostly associated with cumulative exposure to heat rather than length of exposure.7
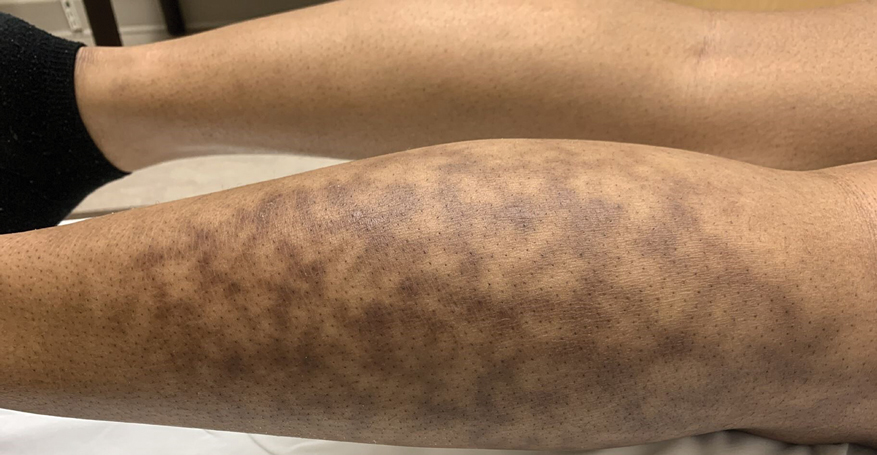
Etiology of EAI
Anatomic Location—The affected site depends on the source of heat (Table). Classic examples of this condition include a patient with EAI presenting on the anterior thighs after working in front of a hot oven or a patient with chronic back pain presenting with lower-back EAI secondary to frequent use of a hot water bottle or heating pad.7 With evolving technology over the last few decades, new etiologies have become more common—teenagers are presenting with anterior thigh EAI secondary to frequent laptop use2-29; patients are holding warm cell phones in their pant pockets, leading to unilateral geometric EAI on the anterior thigh (front pocket) or buttock (back pocket)30; plug-in radiators under computer desks are causing EAI on the lower legs31-34; and automobile seat heaters have been shown to cause EAI on the posterior legs.5,35-37 Clinicians should consider anatomic location a critical clue for etiology.
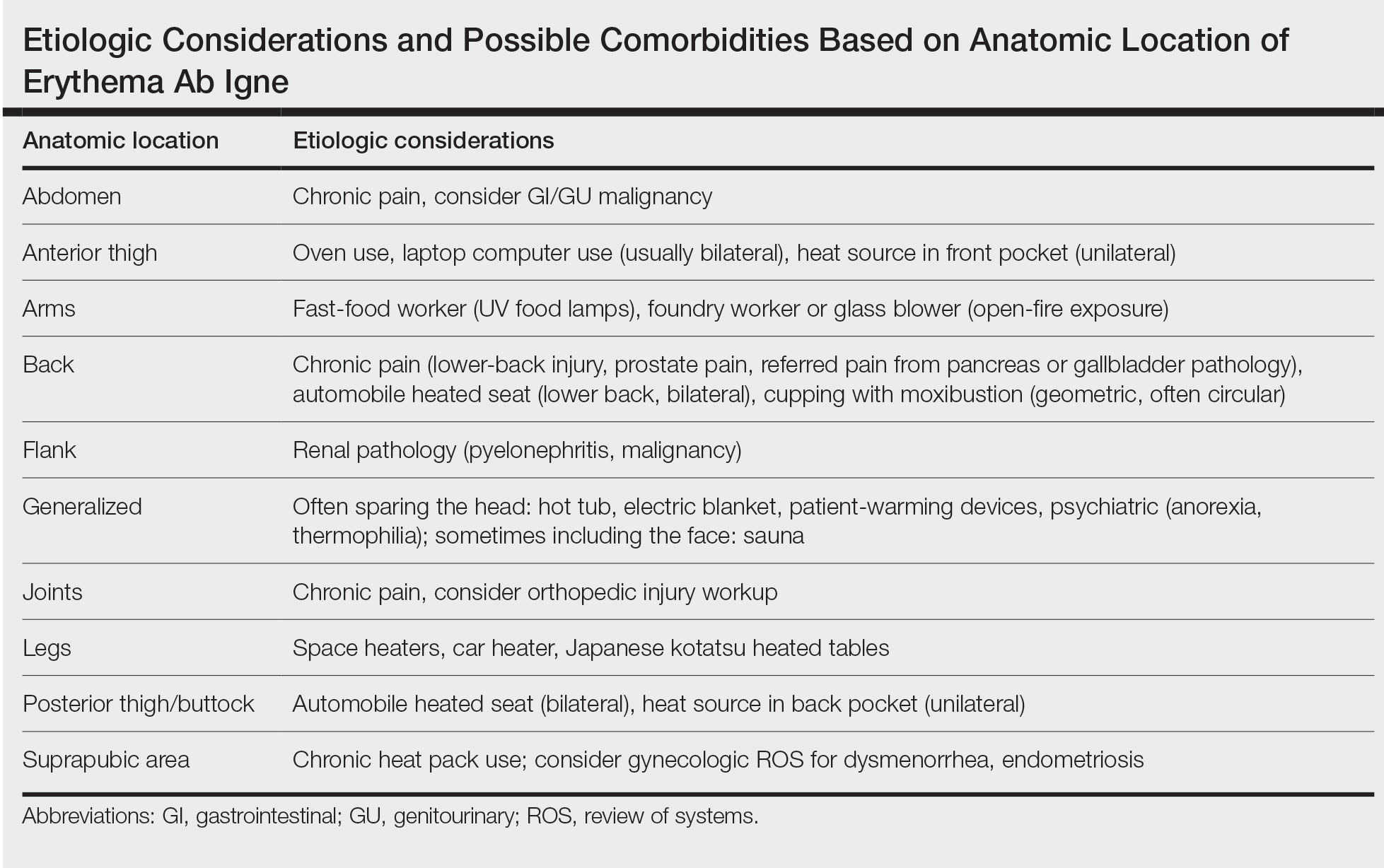
Social History—There are rarer and more highly specific causes of EAI than simple heat exposure that can be parsed from a patient’s social history. Occupational exposure has been documented, such as bakers with exposure to ovens, foundry workers with exposure to heated metals, or fast-food workers with chronic exposure to infrared food lamps.6,7 There also are cultural practices that can cause EAI. For example, the practice of cupping with moxibustion was shown to create a specific pattern in the shape of the cultural tool used.38 When footbaths with Chinese herbal remedies are performed frequently with high heat, they can lead to EAI on the feet with a linear border at the ankles. There also have been reports of kotatsu (heated tables in Japan) leading to lower-body EAI.39,40 These cultural practices also are more common in patients with darker skin types, which can lead to hyperpigmentation that is difficult to treat, making early diagnosis important.7
Medical History—Case reports have shown EAI caused by patients attempting to use heat-based methods for pain relief of an underlying serious disease such as cancer, bowel pathology (abdominal EAI), spinal disc prolapse (midline back EAI),41 sickle cell anemia, and renal pathology (posterior upper flank EAI).6,7,40-49 Patients with hypothyroidism or anorexia have been noted to have generalized EAI sparing the face secondary to repeated and extended hot baths or showers.50-53 One patient with schizophrenia was shown to have associated thermophilia due to a delusion that led the patient to soak in hot baths for long periods of time, leading to EAI.54 Finally, all physicians should be aware of iatrogenic causes of EAI, such as use of warming devices, ultrasound-based warming techniques, and laser therapy for lipolysis. Inquire about the patient’s surgical history or intensive care unit stays as well as alternative medicine or chiropractic visits. Obtaining a history of medical procedures can be enlightening when an etiology is not immediately clear.7,55,56
Diagnosis
Erythema ab igne is a clinical diagnosis based on recognizable cutaneous findings and a clear history of moderate heat exposure. However, when a clinical diagnosis of EAI is not certain (eg, when unable to obtain a clear history from the patient) or when malignant transformation is suspected, a biopsy can be performed. Pathologically, hematoxylin and eosin staining of EAI classically reveals dilated small vascular channels in the superficial dermis, hence a clinically reticular rash; interface dermatitis clinically manifesting as erythema; and pigment incontinence with melanin-laden macrophages consistent with clinical hyperpigmentation. Finally, for unclear reasons, increased numbers of elastic fibers classically are seen in biopsies of EAI.7
Differential Diagnosis
The differential diagnosis for a reticular patch includes livedo reticularis (Figure 3), which usually manifests as a more generalized rash in patients with chronic disease or coagulopathy such as systemic lupus erythematosus, cryoglobulinemia, or Raynaud phenomenon. When differentiating EAI from livedo reticularis or cutis marmorata, consider that both alternative diagnoses are more vascular appearing and are associated with cold exposure rather than heat exposure. In cases that are less reticular, livedo racemosa can be considered in the differential diagnosis. Finally, poikiloderma of Civatte can be reticular, particularly on dermoscopy, but the distribution on the neck with submental sparing should help to distinguish it from EAI unless a heat source around the neck is identified while taking the patient’s history.7
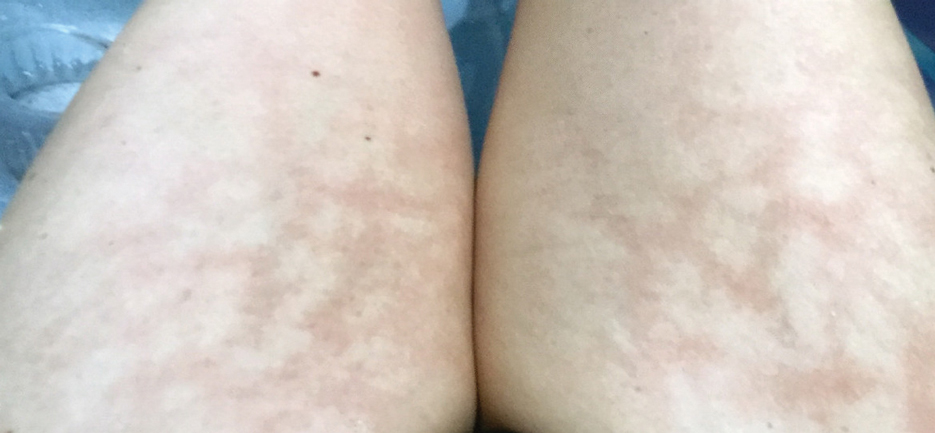
In babies, a reticular generalized rash is most likely to be cutis marmorata (Figure 4), which is a physiologic response to cold exposure that resolves with rewarming of the skin. A more serious condition—cutis marmorata telangiectatica congenita (Figure 5)—usually is present at birth, most frequently involves a single extremity, and notably does not resolve with rewarming. This is an important differential for EAI in children because it can be associated with vascular and neurologic anomalies as well as limb asymmetry. Finally, port-wine stains can sometimes be reticular in appearance and can mimic the early erythematous stages of EAI. However, unlike the erythematous stage of EAI, the port-wine stains will be present at birth.7
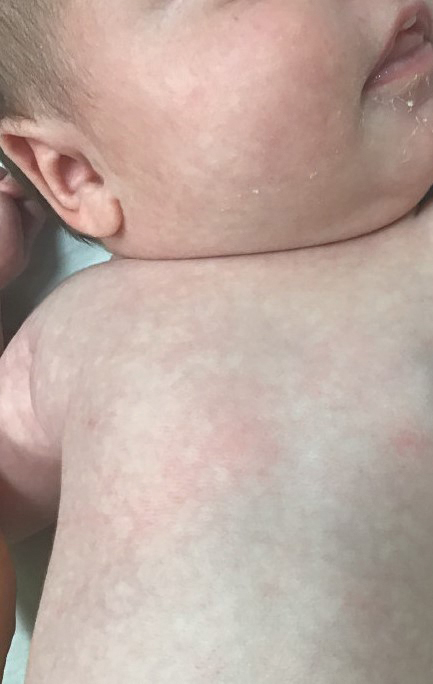
Emerging in 2020, an important differential diagnosis to consider is a cutaneous manifestation of COVID-19 infection. An erythematous, reticular, chilblainlike or transient livedo reticularis–like rash has been described as a cutaneous manifestation of COVID-19. Although the pathophysiology is still being elucidated, it is suspected that this is caused by a major vaso-occlusive crisis secondary to COVID-19–induced thrombotic vasculopathy. Interestingly, the majority of patients with this COVID-related exanthem also displayed symptoms of COVID-19 (eg, fever, cough) at the time of presentation,57-60 but there also have been cases in patients who were asymptomatic or mildly symptomatic.60
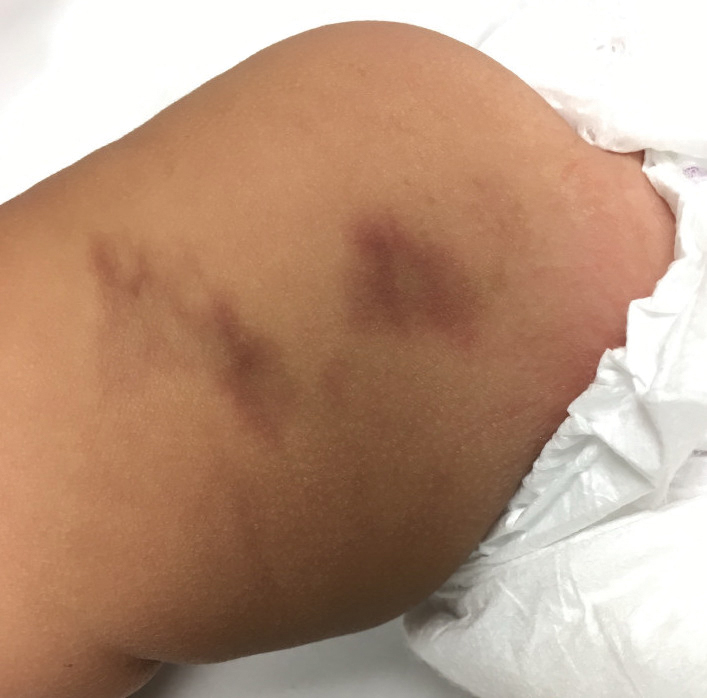
In some cases, EAI is an indication to screen for an underlying disease. For example, uncontrolled pain is an opportunity to improve interventions such as modifying the patient’s pain-control regimen, placing a palliative care pain consultation, or checking if the patient has had age-appropriate screenings for malignancy. New focal pain in a patient with a prior diagnosis of cancer may be a sign of a new metastasis. A thermophilic patient leaves opportunity to assess for underlying medical causes such as thyroid abnormalities or social/psychological issues. Geriatric patients who are diagnosed with EAI may need to be assessed for dementia or home safety issues. Patients with a history of diabetes mellitus can unknowingly develop EAI on the lower extremities, which may signal a need to assess the patient for peripheral neuropathy. Patients with gastroparesis secondary to diabetes also may develop EAI on the abdomen secondary to heating pad use for discomfort. These examples are a reminder to consider possible secondary comorbidities in all diagnoses of EAI.7
Prognosis
Although the prognosis of EAI is excellent if caught early, failure to diagnose this condition can lead to permanent discoloration of the skin and even malignancy.6 A rare sequela includes squamous cell carcinoma, most commonly seen in chronic cases of the lower leg, which is likely related to chronic inflammation of the skin.61-65 Rare cases of poorly differentiated carcinoma,66 cutaneous marginal zone lymphoma,67 and Merkel cell carcinoma68 have been reported. Patients diagnosed with EAI should receive normal periodic surveillance of the skin based on their medical history, though the physician should have an increased suspicion and plan for biopsy of any nodules or ulcerations found on the skin of the affected area.7
Treatments
Once the diagnosis of EAI is made, treatment starts with removal of the heat source causing the rash. Because the rash usually is asymptomatic, further treatment typically is not required. The discoloration can resolve over months or years, but permanent hyperpigmentation is not uncommon. If hyperpigmentation persists despite removal of the heat source and the patient desires further treatment for discoloration, there are few treatment options, none of which are approved by the US Food and Drug Administration for this condition.7 There is some evidence for the use of Nd:YAG lasers to reduce hyperpigmentation in EAI.69 There have been some reports of treatment using topical hydroquinone and topical tretinoin in an attempt to lighten the skin. If associated hyperkeratosis or other epithelial atypia is present, the use of 5-fluorouracil may show some improvement.70 One case report has been published of successful treatment with systemic mesoglycan and topical bioflavonoids.71 It also is conceivable that medications used to treat postinflammatory hyperpigmentation may be helpful in this condition (eg, kojic acid, arbutin, mild topical steroids, azelaic acid). Patients with darker skin may experience permanent discoloration and may not be good candidates for alternative treatments such as laser therapy due to the risk for inducible hyperpigmentation.7
Conclusion
No matter the etiology, EAI usually is a benign skin condition that is treated by removal of the causative heat source. Once a diagnosis is made, the clinician must work with the patient to determine the etiology. Care must be taken to ensure that there are no underlying signs, such as chronic pain or psychiatric illness, that could point to associated conditions. Rarely, sequalae such as cancers have been documented in areas of chronic EAI. Once the heat source is identified and removed, any remaining hyperpigmentation usually will self-resolve over months to years, though this may take longer in patients with darker skin types. If more aggressive treatment is preferred by the patient, laser therapy, topical medications, and oral over-the-counter vitamins have been tried with minimal responses.
- Perry. Case of erythema ab igne. Br J Dermatol. 1900;xxiii:375.
- Bose S, Ortonee JP. Diseases affected by heat. In: Parish LC, Millikan LE, Amer M, et al. Global Dermatology Diagnosis and Management According to Geography, Climate, and Culture. Springer-Varlag; 1994:83-92.
- Leal-Lobato MM, Blasco-Morente G. Electric blanket induced erythema ab igne [in Spanish]. Semergen. 2015;41:456-457. doi:10.1016/j.semerg.2014.12.008
- Huynh N, Sarma D, Huerter C. Erythema ab igne: a case report and review of the literature. Cutis. 2011;88:290-292.
- Kesty K, Feldman SR. Erythema ab igne: evolving technology, evolving presentation. Dermatol Online J. 2014;20. doi:10.5070/D32011024689
- Miller K, Hunt R, Chu J, et al. Erythema ab igne. Dermatol Online J. 2011;17:28.
- Smith ML. Environmental and sports-related skin diseases. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Elsevier; 2018:1569-1594.
- Errichetti E, Stinco G. Dermoscopy in general dermatology: a practical overview. Dermatol Ther (Heidelb). 2016;6:471-507. doi:10.1007/s13555-016-0141-6
- Guarneri C, Tchernev G, Wollina U, et al. Erythema ab igne caused by laptop computer. Open Access Maced J Med Sci. 2017;5:490-492. doi:10.3889/oamjms.2017.137
- Arnold AW, Itin PH. Laptop computer-induced erythema ab igne in a child and review of the literature. Pediatrics. 2010;126:E1227-E1230. doi:10.1542/peds.2010-1390
- Dickman J, Kessler S. Unilateral reticulated patch localized to the anterior thigh. JAAD Case Rep. 2018;4:746-748. doi:10.1016/j.jdcr.2018.06.007
- Boffa MJ. Laptop computer-induced erythema ab igne on the left breast. Cutis. 2011;87:175-176.
- Li K, Barankin B. Cutaneous manifestations of modern technology use. J Cutan Med Surg. 2011;15:347-353. doi:10.2310/7750.2011.10053
- Riahi RR, Cohen PR. Laptop-induced erythema ab igne: report and review of literature. Dermatol Online J. 2012;18:5.
- Andersen F. Laptop-thighs--laptop-induced erythema ab igne [in Danish]. Ugeskr Laeger. 2010;172:635.
- Jagtman BA. Erythema ab igne due to a laptop computer. Contact Dermatitis. 2004;50:105. doi:10.1111/j.0105-1873.2004.0295g.x
- Olechowska M, Kisiel K, Ruszkowska L, et al. Erythema ab igne (EAI) induced by a laptop computer: report of two cases. J Dtsch Dermatol Ges. doi:10.1111/j.1610-0387.2014.12387
- Nayak SUK, Shenoi SD, Prabhu S. Laptop induced erythema ab igne. Indian J Dermatol. 2012;57:131-132. doi:10.4103/0019-5154.94284
- Salvio AG, Nunes AJ, Angarita DPR. Laptop computer induced erythema ab igne: a new presentation of an old disease. An Bras Dermatol. 2016;91:79-80. doi:10.1590/abd1806-4841.20165139
- Schummer C, Tittelbach J, Elsner P. Right-sided laptop dermatitis [in German]. Dtsch Med Wochenschr. 2015;140:1376-1377. doi:10.1055/s-0041-103615
- Manoharan D. Erythema ab igne: usual site, unusual cause. J Pharm Bioallied Sci. 2015;7(suppl 1):S74-S75. doi:10.4103/0975-7406.155811
- Giraldi S, Diettrich F, Abbage KT, et al. Erythema ab igne induced by a laptop computer in an adolescent. An Bras Dermatol. 2011;86:128-130. doi:10.1590/S0365-05962011000100018
- Secher LLS, Vind-Kezunovic D, Zachariae COC. Side-effects to the use of laptop computers: erythema ab igne. Dermatol Reports. 2010;31:E11. doi:10.4081/dr.2010.e11
- Botten D, Langley RGB, Webb A. Academic branding: erythema ab igne and use of laptop computers. CMAJ. 2010;182:E857. doi:10.1503/cmaj.091868
- Bilic M, Adams BB. Erythema ab igne induced by a laptop computer. J Am Acad Dermatol. 2004;50:973-974. doi:10.1016/j.jaad.2003.08.007
- Fu LW, Vender R. Erythema ab igne caused by laptop computer gaming - a case report. Int J Dermatol. 2012;51:716-717. doi:10.1111/j.1365-4632.2011.05033.x
- Levinbook WS, Mallett J, Grant-Kels JM. Laptop computer-associated erythema ab igne. Cutis. 2007;80:319-320.
- Mohr MR, Scott KA, Pariser RM, et al. Laptop computer-induced erythema ab igne: a case report. Cutis. 2007;79:59-60.
- Cantor AS, Bartling SJ. Laptop computer-induced hyperpigmentation. Dermatol Online J. 2018;24:13030/qt6k37r9wm.
- Kaptanog˘lu AF, Mullaaziz D. Erythema ab igne in the palmar area induced by smart phone: case report. Turkiye Klin J Med Sci. 2015;35:284-286. doi:10.5336/medsci.2015-46976
- Redding KS, Watts AN, Lee J, et al. Space heater-induced bullous erythema ab igne. Cutis. 2017;100:E9-E10.
- Goorland J, Edens MA, Baudoin TD. An emergency department presentation of erythema ab igne caused by repeated heater exposure. J La State Med Soc. 2016;168:33-34.
- Kokturk A, Kaya TI, Baz K, et al. Bullous erythema ab igne. Dermatol Online J. 2003;9:18.
- Brzezinski P, Ismail S, Chiriac A. Radiator-induced erythema ab igne in 8-year-old girl. Rev Chil Pediatr. 2014;85:239-240. doi:10.4067/S0370-41062014000200015
- Adams BB. Heated car seat-induced erythema ab igne. Arch Dermatol. 2012;148:265-266. doi:10.1001/archdermatol.2011.2207
- Helm TN, Spigel GT, Helm KF. Erythema ab igne caused by a car heater. Cutis. 1997;59:81-82.
- Gregory JF, Beute TC. Erythema ab igne. J Spec Oper Med. 2013;13:115-119. doi:10.55460/5AVH-NZHY
- Chua S, Chen Q, Lee HY. Erythema ab igne and dermal scarring caused by cupping and moxibustion treatment. J Dtsch Dermatol Ges. 2015;13:337-338. doi:10.1111/ddg.12581
- Chen JF, Liu YC, Chen YF, et al. Erythema ab igne after footbath with Chinese herbal remedies. J Chinese Med Assoc. 2011;74:51-53. doi:10.1016/j.jcma.2011.01.009
- Baltazar D, Brockman R, Simpson E. Kotatsu-induced erythema ab igne. An Bras Dermatol. 2019;94:253-254. doi:10.1590/abd1806-4841.20198792
- Baig M, Byrne F. Erythema ab igne and its relation to spinal pathology. Cureus. 2018;10:e2914. doi:10.7759/cureus.2914
- Aria AB, Chen L, Silapunt S. Erythema ab igne from heating pad use: a report of three clinical cases and a differential diagnosis. Cureus. 2018;10:e2635. doi:10.7759/cureus.2635
- Milchak M, Smucker J, Chung CG, et al. Erythema ab igne due to heating pad use: a case report and review of clinical presentation, prevention, and complications. Case Rep Med. 2016;1862480. doi:10.1155/2016/1862480
- Gmuca S, Yu J, Weiss PF, et al. Erythema ab igne in an adolescent with chronic pain: an alarming cutaneous eruption from heat exposure. Pediatr Emerg Care. 2020;36:e236-e238. doi:10.1097/PEC.0000000000001460
- Dizdarevic A, Karim OA, Bygum A. A reddish brown reticulated hyperpigmented erythema on the abdomen of a girl. Erythema ab igne, also known as toasted skin syndrome, caused by a heating pad onthe abdomen. Acta Derm Venereol. 2014;94:365-367. doi:10.2340/00015555-1722
- Chatterjee S. Erythema ab igne from prolonged use of a heating pad. Mayo Clin Proc. 2005;80:1500. doi:10.4065/80.11.1500
- Waldorf DS, Rast MF, Garofalo VJ. Heating-pad erythematous dermatitis “erythema ab igne.” JAMA. 1971;218:1704. doi:10.1001/jama.1971.03190240056023
- South AM, Crispin MK, Marqueling AL, et al. A hyperpigmented reticular rash in a patient on peritoneal dialysis. Perit Dial Int. 2016;36:677-700. doi:10.3747/pdi.2016.00042
- Ravindran R. Erythema ab igne in an individual with diabetes and gastroparesis. BMJ Case Rep. 2017;2017:bcr2014203856. doi:10.1136/bcr-2014-203856
- Dessinioti C, Katsambas A, Tzavela E, et al. Erythema ab igne in three girls with anorexia nervosa. Pediatr Dermatol. 2016;33:e149-e150. doi:10.1111/pde.12770
- Fischer J, Rein K, Erfurt-Berge C, et al. Three cases of erythema ab igne (EAI) in patients with eating disorders. Neuropsychiatr. 2010;24:141-143.
- Docx MKF, Simons A, Ramet J, et al. Erythema ab igne in an adolescent with anorexia nervosa. Int J Eat Disord. 2013;46:381-383. doi:10.1002/eat.22075
- Turan E, Cimen V, Haytoglu NSK, et al. A case of bullous erythema ab igne accompanied by anemia and subclinical hypothyroidism. Dermatol Online J. 2014;20:223366.
- Pavithran K. Erythema ab igne, schizophrenia and thermophilia. Indian J Dermatol Venereol Leprol. 1987;53:181-182.
- Dellavelle R, Gillum P. Erythema ab igne following heating/cooling blanket use in the intensive care unit. Cutis. 2000;66:136-138.
- Park SY, Kim SM, Yoon TJ. Erythema ab igne caused by weight loss heating pad. Korean J Dermatol. 2007;45:489-491.
- Sachdeva M, Gianotti R, Shah M, et al. Cutaneous manifestations of COVID-19: report of three cases and a review of literature. J Dermatol Sci. 2020;98:75-81. doi:10.1016/j.jdermsci.2020.04.011
- Gisondi P, Plaserico S, Bordin C, et al. Cutaneous manifestations of SARS‐CoV‐2 infection: a clinical update. J Eur Acad Dermatol Venereol. 2020;34:2499-2504. doi:10.1111/jdv.16774
- Manalo IF, Smith MK, Cheeley J, et al. A dermatologic manifestation of COVID-19: transient livedo reticularis. J Am Acad Dermatol. 2020;83:700. doi:10.1016/j.jaad.2020.04.018
- Zhao Q, Fang X, Pang Z, et al. COVID‐19 and cutaneous manifestations: a systematic review. J Eur Acad Dermatol Venereol. 2020;34:2505-2510. doi:10.1111/jdv.16778
- Akasaka T, Kon S. Two cases of squamous cell carcinoma arising from erythema ab igne. Nihon Hifuka Gakkai Zasshi. 1989;99:735-742.
- Arrington JH 3rd, Lockman DS. Thermal keratoses and squamous cell carcinoma in situ associated with erythema ab igne. Arch Dermatol. 1979;115:1226-1228.
- Wharton JB, Sheehan DJ, Lesher JL Jr. Squamous cell carcinoma in situ arising in the setting of erythema ab igne. J Drugs Dermatol. 2008;7:488-489.
- Wollina U, Helm C, Hansel G, et al. Two cases of erythema ab igne, one with a squamous cell carcinoma. G Ital Dermatol Venereol. 2007;142:415-418.
- Rudolph CM, Soyer HP, Wolf P, et al. Squamous cell carcinoma arising in erythema ab igne. Hautarzt. 2000;51:260-263. doi:10.1007/s001050051115
- Sigmon JR, Cantrell J, Teague D, et al. Poorly differentiated carcinoma arising in the setting of erythema ab igne. Am J Dermatopathol. 2013;35:676-678. doi:10.1097/DAD.0b013e3182871648
- Wharton J, Roffwarg D, Miller J, et al. Cutaneous marginal zone lymphoma arising in the setting of erythema ab igne. J Am Acad Dermatol. 2010;62:1080-1081. doi:10.1016/j.jaad.2009.08.005
- Jones CS, Tyring SK, Lee PC, et al. Development of neuroendocrine (Merkel cell) carcinoma mixed with squamous cell carcinoma in erythema ab igne. Arch Dermatol. 1988;124:110-113.
- Kim HW, Kim EJ, Park HC, et al. Erythema ab igne successfully treated with low fluenced 1,064-nm Q-switched neodymium-doped yttrium aluminum garnet laser. J Cosmet Laser Ther. 2014;16:147-148. doi:10.3109/14764172.2013.854623
- Tan S, Bertucci V. Erythema ab igne: an old condition new again. CMAJ. 2000;62:77-78.
- Gianfaldoni S, Gianfaldoni R, Tchernev G, et al. Erythema ab igne successfully treated with mesoglycan and bioflavonoids: a case-report. Open Access Maced J Med Sci. 2017;5:432-435. doi:10.3889/oamjms.2017.123
Erythema ab igne (EAI)(also known as toasted skin syndrome) was first described in the British Journal of Dermatology in the 20th century, 1 though it was known by physicians long before. Reticular netlike skin changes were seen in association with patients who spent extended time directly next to a heat source. This association led to the name of this condition, which literally means “redness by fire.” Indeed, EAI induced by chronic heat exposure has been described across the world for centuries. For example, in the cold regions of northern China, people used to sleep on beds of hot bricks called kang to stay warm at night. The people of India’s Kashmir district carried pots of hot coals called kangri next to the skin under large woven shawls to stay warm. In the past, Irish women often spent much time by a turf- or peat-burning fire. Chronic heat exposure in these cases can lead not only to EAI but also to aggressive types of cancer, often with a latency of 30 years or more. 2
More recently, the invention of home central heating led to a stark decrease in the number of cases associated with combustion-based heat, with a transition to etiologies such as use of hot water bottles, electric blankets, and electric space heaters. Over time, technological advances led to ever-increasing potential causes for EAI, such as laptops or cell phones, car heaters and heated seats, heated blankets,3,4 infrared lamps for food, and even medical devices such as ultrasound-based heating products and convective temperature management systems for hospitalized patients. As technology evolves, so do the potential causes of EAI, requiring clinicians to diagnose and deduce the cause through a thorough social and medical history as well as a workup on the present illness with considerations for the anatomical location.5-7 Herein, we describe the etiology of EAI, diagnosis, and treatment options.

Clinical Characteristics
Erythema ab igne begins as mild, transient, and erythematous macules and patches in a reticular pattern that resolve minutes to hours after removal of the heat source. With weeks to months of continued or repeated application of the heat source, the affected area eventually becomes hyperpigmented where there once was erythema (Figures 1 and 2). Sometimes papules, bullae, telangiectasia, and hyperkeratosis also form. The rash usually is asymptomatic, though pain, pruritus, and dysesthesia have been reported.7 Dermoscopy of EAI in the hyperpigmented stage can reveal diffuse superficial dark pigmentation, telangiectasia, and mild whitish scaling.8 Although the pathogenesis has remained elusive over the years, lesions do seem to be mostly associated with cumulative exposure to heat rather than length of exposure.7

Etiology of EAI
Anatomic Location—The affected site depends on the source of heat (Table). Classic examples of this condition include a patient with EAI presenting on the anterior thighs after working in front of a hot oven or a patient with chronic back pain presenting with lower-back EAI secondary to frequent use of a hot water bottle or heating pad.7 With evolving technology over the last few decades, new etiologies have become more common—teenagers are presenting with anterior thigh EAI secondary to frequent laptop use2-29; patients are holding warm cell phones in their pant pockets, leading to unilateral geometric EAI on the anterior thigh (front pocket) or buttock (back pocket)30; plug-in radiators under computer desks are causing EAI on the lower legs31-34; and automobile seat heaters have been shown to cause EAI on the posterior legs.5,35-37 Clinicians should consider anatomic location a critical clue for etiology.

Social History—There are rarer and more highly specific causes of EAI than simple heat exposure that can be parsed from a patient’s social history. Occupational exposure has been documented, such as bakers with exposure to ovens, foundry workers with exposure to heated metals, or fast-food workers with chronic exposure to infrared food lamps.6,7 There also are cultural practices that can cause EAI. For example, the practice of cupping with moxibustion was shown to create a specific pattern in the shape of the cultural tool used.38 When footbaths with Chinese herbal remedies are performed frequently with high heat, they can lead to EAI on the feet with a linear border at the ankles. There also have been reports of kotatsu (heated tables in Japan) leading to lower-body EAI.39,40 These cultural practices also are more common in patients with darker skin types, which can lead to hyperpigmentation that is difficult to treat, making early diagnosis important.7
Medical History—Case reports have shown EAI caused by patients attempting to use heat-based methods for pain relief of an underlying serious disease such as cancer, bowel pathology (abdominal EAI), spinal disc prolapse (midline back EAI),41 sickle cell anemia, and renal pathology (posterior upper flank EAI).6,7,40-49 Patients with hypothyroidism or anorexia have been noted to have generalized EAI sparing the face secondary to repeated and extended hot baths or showers.50-53 One patient with schizophrenia was shown to have associated thermophilia due to a delusion that led the patient to soak in hot baths for long periods of time, leading to EAI.54 Finally, all physicians should be aware of iatrogenic causes of EAI, such as use of warming devices, ultrasound-based warming techniques, and laser therapy for lipolysis. Inquire about the patient’s surgical history or intensive care unit stays as well as alternative medicine or chiropractic visits. Obtaining a history of medical procedures can be enlightening when an etiology is not immediately clear.7,55,56
Diagnosis
Erythema ab igne is a clinical diagnosis based on recognizable cutaneous findings and a clear history of moderate heat exposure. However, when a clinical diagnosis of EAI is not certain (eg, when unable to obtain a clear history from the patient) or when malignant transformation is suspected, a biopsy can be performed. Pathologically, hematoxylin and eosin staining of EAI classically reveals dilated small vascular channels in the superficial dermis, hence a clinically reticular rash; interface dermatitis clinically manifesting as erythema; and pigment incontinence with melanin-laden macrophages consistent with clinical hyperpigmentation. Finally, for unclear reasons, increased numbers of elastic fibers classically are seen in biopsies of EAI.7
Differential Diagnosis
The differential diagnosis for a reticular patch includes livedo reticularis (Figure 3), which usually manifests as a more generalized rash in patients with chronic disease or coagulopathy such as systemic lupus erythematosus, cryoglobulinemia, or Raynaud phenomenon. When differentiating EAI from livedo reticularis or cutis marmorata, consider that both alternative diagnoses are more vascular appearing and are associated with cold exposure rather than heat exposure. In cases that are less reticular, livedo racemosa can be considered in the differential diagnosis. Finally, poikiloderma of Civatte can be reticular, particularly on dermoscopy, but the distribution on the neck with submental sparing should help to distinguish it from EAI unless a heat source around the neck is identified while taking the patient’s history.7

In babies, a reticular generalized rash is most likely to be cutis marmorata (Figure 4), which is a physiologic response to cold exposure that resolves with rewarming of the skin. A more serious condition—cutis marmorata telangiectatica congenita (Figure 5)—usually is present at birth, most frequently involves a single extremity, and notably does not resolve with rewarming. This is an important differential for EAI in children because it can be associated with vascular and neurologic anomalies as well as limb asymmetry. Finally, port-wine stains can sometimes be reticular in appearance and can mimic the early erythematous stages of EAI. However, unlike the erythematous stage of EAI, the port-wine stains will be present at birth.7

Emerging in 2020, an important differential diagnosis to consider is a cutaneous manifestation of COVID-19 infection. An erythematous, reticular, chilblainlike or transient livedo reticularis–like rash has been described as a cutaneous manifestation of COVID-19. Although the pathophysiology is still being elucidated, it is suspected that this is caused by a major vaso-occlusive crisis secondary to COVID-19–induced thrombotic vasculopathy. Interestingly, the majority of patients with this COVID-related exanthem also displayed symptoms of COVID-19 (eg, fever, cough) at the time of presentation,57-60 but there also have been cases in patients who were asymptomatic or mildly symptomatic.60

In some cases, EAI is an indication to screen for an underlying disease. For example, uncontrolled pain is an opportunity to improve interventions such as modifying the patient’s pain-control regimen, placing a palliative care pain consultation, or checking if the patient has had age-appropriate screenings for malignancy. New focal pain in a patient with a prior diagnosis of cancer may be a sign of a new metastasis. A thermophilic patient leaves opportunity to assess for underlying medical causes such as thyroid abnormalities or social/psychological issues. Geriatric patients who are diagnosed with EAI may need to be assessed for dementia or home safety issues. Patients with a history of diabetes mellitus can unknowingly develop EAI on the lower extremities, which may signal a need to assess the patient for peripheral neuropathy. Patients with gastroparesis secondary to diabetes also may develop EAI on the abdomen secondary to heating pad use for discomfort. These examples are a reminder to consider possible secondary comorbidities in all diagnoses of EAI.7
Prognosis
Although the prognosis of EAI is excellent if caught early, failure to diagnose this condition can lead to permanent discoloration of the skin and even malignancy.6 A rare sequela includes squamous cell carcinoma, most commonly seen in chronic cases of the lower leg, which is likely related to chronic inflammation of the skin.61-65 Rare cases of poorly differentiated carcinoma,66 cutaneous marginal zone lymphoma,67 and Merkel cell carcinoma68 have been reported. Patients diagnosed with EAI should receive normal periodic surveillance of the skin based on their medical history, though the physician should have an increased suspicion and plan for biopsy of any nodules or ulcerations found on the skin of the affected area.7
Treatments
Once the diagnosis of EAI is made, treatment starts with removal of the heat source causing the rash. Because the rash usually is asymptomatic, further treatment typically is not required. The discoloration can resolve over months or years, but permanent hyperpigmentation is not uncommon. If hyperpigmentation persists despite removal of the heat source and the patient desires further treatment for discoloration, there are few treatment options, none of which are approved by the US Food and Drug Administration for this condition.7 There is some evidence for the use of Nd:YAG lasers to reduce hyperpigmentation in EAI.69 There have been some reports of treatment using topical hydroquinone and topical tretinoin in an attempt to lighten the skin. If associated hyperkeratosis or other epithelial atypia is present, the use of 5-fluorouracil may show some improvement.70 One case report has been published of successful treatment with systemic mesoglycan and topical bioflavonoids.71 It also is conceivable that medications used to treat postinflammatory hyperpigmentation may be helpful in this condition (eg, kojic acid, arbutin, mild topical steroids, azelaic acid). Patients with darker skin may experience permanent discoloration and may not be good candidates for alternative treatments such as laser therapy due to the risk for inducible hyperpigmentation.7
Conclusion
No matter the etiology, EAI usually is a benign skin condition that is treated by removal of the causative heat source. Once a diagnosis is made, the clinician must work with the patient to determine the etiology. Care must be taken to ensure that there are no underlying signs, such as chronic pain or psychiatric illness, that could point to associated conditions. Rarely, sequalae such as cancers have been documented in areas of chronic EAI. Once the heat source is identified and removed, any remaining hyperpigmentation usually will self-resolve over months to years, though this may take longer in patients with darker skin types. If more aggressive treatment is preferred by the patient, laser therapy, topical medications, and oral over-the-counter vitamins have been tried with minimal responses.
Erythema ab igne (EAI)(also known as toasted skin syndrome) was first described in the British Journal of Dermatology in the 20th century, 1 though it was known by physicians long before. Reticular netlike skin changes were seen in association with patients who spent extended time directly next to a heat source. This association led to the name of this condition, which literally means “redness by fire.” Indeed, EAI induced by chronic heat exposure has been described across the world for centuries. For example, in the cold regions of northern China, people used to sleep on beds of hot bricks called kang to stay warm at night. The people of India’s Kashmir district carried pots of hot coals called kangri next to the skin under large woven shawls to stay warm. In the past, Irish women often spent much time by a turf- or peat-burning fire. Chronic heat exposure in these cases can lead not only to EAI but also to aggressive types of cancer, often with a latency of 30 years or more. 2
More recently, the invention of home central heating led to a stark decrease in the number of cases associated with combustion-based heat, with a transition to etiologies such as use of hot water bottles, electric blankets, and electric space heaters. Over time, technological advances led to ever-increasing potential causes for EAI, such as laptops or cell phones, car heaters and heated seats, heated blankets,3,4 infrared lamps for food, and even medical devices such as ultrasound-based heating products and convective temperature management systems for hospitalized patients. As technology evolves, so do the potential causes of EAI, requiring clinicians to diagnose and deduce the cause through a thorough social and medical history as well as a workup on the present illness with considerations for the anatomical location.5-7 Herein, we describe the etiology of EAI, diagnosis, and treatment options.

Clinical Characteristics
Erythema ab igne begins as mild, transient, and erythematous macules and patches in a reticular pattern that resolve minutes to hours after removal of the heat source. With weeks to months of continued or repeated application of the heat source, the affected area eventually becomes hyperpigmented where there once was erythema (Figures 1 and 2). Sometimes papules, bullae, telangiectasia, and hyperkeratosis also form. The rash usually is asymptomatic, though pain, pruritus, and dysesthesia have been reported.7 Dermoscopy of EAI in the hyperpigmented stage can reveal diffuse superficial dark pigmentation, telangiectasia, and mild whitish scaling.8 Although the pathogenesis has remained elusive over the years, lesions do seem to be mostly associated with cumulative exposure to heat rather than length of exposure.7

Etiology of EAI
Anatomic Location—The affected site depends on the source of heat (Table). Classic examples of this condition include a patient with EAI presenting on the anterior thighs after working in front of a hot oven or a patient with chronic back pain presenting with lower-back EAI secondary to frequent use of a hot water bottle or heating pad.7 With evolving technology over the last few decades, new etiologies have become more common—teenagers are presenting with anterior thigh EAI secondary to frequent laptop use2-29; patients are holding warm cell phones in their pant pockets, leading to unilateral geometric EAI on the anterior thigh (front pocket) or buttock (back pocket)30; plug-in radiators under computer desks are causing EAI on the lower legs31-34; and automobile seat heaters have been shown to cause EAI on the posterior legs.5,35-37 Clinicians should consider anatomic location a critical clue for etiology.

Social History—There are rarer and more highly specific causes of EAI than simple heat exposure that can be parsed from a patient’s social history. Occupational exposure has been documented, such as bakers with exposure to ovens, foundry workers with exposure to heated metals, or fast-food workers with chronic exposure to infrared food lamps.6,7 There also are cultural practices that can cause EAI. For example, the practice of cupping with moxibustion was shown to create a specific pattern in the shape of the cultural tool used.38 When footbaths with Chinese herbal remedies are performed frequently with high heat, they can lead to EAI on the feet with a linear border at the ankles. There also have been reports of kotatsu (heated tables in Japan) leading to lower-body EAI.39,40 These cultural practices also are more common in patients with darker skin types, which can lead to hyperpigmentation that is difficult to treat, making early diagnosis important.7
Medical History—Case reports have shown EAI caused by patients attempting to use heat-based methods for pain relief of an underlying serious disease such as cancer, bowel pathology (abdominal EAI), spinal disc prolapse (midline back EAI),41 sickle cell anemia, and renal pathology (posterior upper flank EAI).6,7,40-49 Patients with hypothyroidism or anorexia have been noted to have generalized EAI sparing the face secondary to repeated and extended hot baths or showers.50-53 One patient with schizophrenia was shown to have associated thermophilia due to a delusion that led the patient to soak in hot baths for long periods of time, leading to EAI.54 Finally, all physicians should be aware of iatrogenic causes of EAI, such as use of warming devices, ultrasound-based warming techniques, and laser therapy for lipolysis. Inquire about the patient’s surgical history or intensive care unit stays as well as alternative medicine or chiropractic visits. Obtaining a history of medical procedures can be enlightening when an etiology is not immediately clear.7,55,56
Diagnosis
Erythema ab igne is a clinical diagnosis based on recognizable cutaneous findings and a clear history of moderate heat exposure. However, when a clinical diagnosis of EAI is not certain (eg, when unable to obtain a clear history from the patient) or when malignant transformation is suspected, a biopsy can be performed. Pathologically, hematoxylin and eosin staining of EAI classically reveals dilated small vascular channels in the superficial dermis, hence a clinically reticular rash; interface dermatitis clinically manifesting as erythema; and pigment incontinence with melanin-laden macrophages consistent with clinical hyperpigmentation. Finally, for unclear reasons, increased numbers of elastic fibers classically are seen in biopsies of EAI.7
Differential Diagnosis
The differential diagnosis for a reticular patch includes livedo reticularis (Figure 3), which usually manifests as a more generalized rash in patients with chronic disease or coagulopathy such as systemic lupus erythematosus, cryoglobulinemia, or Raynaud phenomenon. When differentiating EAI from livedo reticularis or cutis marmorata, consider that both alternative diagnoses are more vascular appearing and are associated with cold exposure rather than heat exposure. In cases that are less reticular, livedo racemosa can be considered in the differential diagnosis. Finally, poikiloderma of Civatte can be reticular, particularly on dermoscopy, but the distribution on the neck with submental sparing should help to distinguish it from EAI unless a heat source around the neck is identified while taking the patient’s history.7

In babies, a reticular generalized rash is most likely to be cutis marmorata (Figure 4), which is a physiologic response to cold exposure that resolves with rewarming of the skin. A more serious condition—cutis marmorata telangiectatica congenita (Figure 5)—usually is present at birth, most frequently involves a single extremity, and notably does not resolve with rewarming. This is an important differential for EAI in children because it can be associated with vascular and neurologic anomalies as well as limb asymmetry. Finally, port-wine stains can sometimes be reticular in appearance and can mimic the early erythematous stages of EAI. However, unlike the erythematous stage of EAI, the port-wine stains will be present at birth.7

Emerging in 2020, an important differential diagnosis to consider is a cutaneous manifestation of COVID-19 infection. An erythematous, reticular, chilblainlike or transient livedo reticularis–like rash has been described as a cutaneous manifestation of COVID-19. Although the pathophysiology is still being elucidated, it is suspected that this is caused by a major vaso-occlusive crisis secondary to COVID-19–induced thrombotic vasculopathy. Interestingly, the majority of patients with this COVID-related exanthem also displayed symptoms of COVID-19 (eg, fever, cough) at the time of presentation,57-60 but there also have been cases in patients who were asymptomatic or mildly symptomatic.60

In some cases, EAI is an indication to screen for an underlying disease. For example, uncontrolled pain is an opportunity to improve interventions such as modifying the patient’s pain-control regimen, placing a palliative care pain consultation, or checking if the patient has had age-appropriate screenings for malignancy. New focal pain in a patient with a prior diagnosis of cancer may be a sign of a new metastasis. A thermophilic patient leaves opportunity to assess for underlying medical causes such as thyroid abnormalities or social/psychological issues. Geriatric patients who are diagnosed with EAI may need to be assessed for dementia or home safety issues. Patients with a history of diabetes mellitus can unknowingly develop EAI on the lower extremities, which may signal a need to assess the patient for peripheral neuropathy. Patients with gastroparesis secondary to diabetes also may develop EAI on the abdomen secondary to heating pad use for discomfort. These examples are a reminder to consider possible secondary comorbidities in all diagnoses of EAI.7
Prognosis
Although the prognosis of EAI is excellent if caught early, failure to diagnose this condition can lead to permanent discoloration of the skin and even malignancy.6 A rare sequela includes squamous cell carcinoma, most commonly seen in chronic cases of the lower leg, which is likely related to chronic inflammation of the skin.61-65 Rare cases of poorly differentiated carcinoma,66 cutaneous marginal zone lymphoma,67 and Merkel cell carcinoma68 have been reported. Patients diagnosed with EAI should receive normal periodic surveillance of the skin based on their medical history, though the physician should have an increased suspicion and plan for biopsy of any nodules or ulcerations found on the skin of the affected area.7
Treatments
Once the diagnosis of EAI is made, treatment starts with removal of the heat source causing the rash. Because the rash usually is asymptomatic, further treatment typically is not required. The discoloration can resolve over months or years, but permanent hyperpigmentation is not uncommon. If hyperpigmentation persists despite removal of the heat source and the patient desires further treatment for discoloration, there are few treatment options, none of which are approved by the US Food and Drug Administration for this condition.7 There is some evidence for the use of Nd:YAG lasers to reduce hyperpigmentation in EAI.69 There have been some reports of treatment using topical hydroquinone and topical tretinoin in an attempt to lighten the skin. If associated hyperkeratosis or other epithelial atypia is present, the use of 5-fluorouracil may show some improvement.70 One case report has been published of successful treatment with systemic mesoglycan and topical bioflavonoids.71 It also is conceivable that medications used to treat postinflammatory hyperpigmentation may be helpful in this condition (eg, kojic acid, arbutin, mild topical steroids, azelaic acid). Patients with darker skin may experience permanent discoloration and may not be good candidates for alternative treatments such as laser therapy due to the risk for inducible hyperpigmentation.7
Conclusion
No matter the etiology, EAI usually is a benign skin condition that is treated by removal of the causative heat source. Once a diagnosis is made, the clinician must work with the patient to determine the etiology. Care must be taken to ensure that there are no underlying signs, such as chronic pain or psychiatric illness, that could point to associated conditions. Rarely, sequalae such as cancers have been documented in areas of chronic EAI. Once the heat source is identified and removed, any remaining hyperpigmentation usually will self-resolve over months to years, though this may take longer in patients with darker skin types. If more aggressive treatment is preferred by the patient, laser therapy, topical medications, and oral over-the-counter vitamins have been tried with minimal responses.
- Perry. Case of erythema ab igne. Br J Dermatol. 1900;xxiii:375.
- Bose S, Ortonee JP. Diseases affected by heat. In: Parish LC, Millikan LE, Amer M, et al. Global Dermatology Diagnosis and Management According to Geography, Climate, and Culture. Springer-Varlag; 1994:83-92.
- Leal-Lobato MM, Blasco-Morente G. Electric blanket induced erythema ab igne [in Spanish]. Semergen. 2015;41:456-457. doi:10.1016/j.semerg.2014.12.008
- Huynh N, Sarma D, Huerter C. Erythema ab igne: a case report and review of the literature. Cutis. 2011;88:290-292.
- Kesty K, Feldman SR. Erythema ab igne: evolving technology, evolving presentation. Dermatol Online J. 2014;20. doi:10.5070/D32011024689
- Miller K, Hunt R, Chu J, et al. Erythema ab igne. Dermatol Online J. 2011;17:28.
- Smith ML. Environmental and sports-related skin diseases. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Elsevier; 2018:1569-1594.
- Errichetti E, Stinco G. Dermoscopy in general dermatology: a practical overview. Dermatol Ther (Heidelb). 2016;6:471-507. doi:10.1007/s13555-016-0141-6
- Guarneri C, Tchernev G, Wollina U, et al. Erythema ab igne caused by laptop computer. Open Access Maced J Med Sci. 2017;5:490-492. doi:10.3889/oamjms.2017.137
- Arnold AW, Itin PH. Laptop computer-induced erythema ab igne in a child and review of the literature. Pediatrics. 2010;126:E1227-E1230. doi:10.1542/peds.2010-1390
- Dickman J, Kessler S. Unilateral reticulated patch localized to the anterior thigh. JAAD Case Rep. 2018;4:746-748. doi:10.1016/j.jdcr.2018.06.007
- Boffa MJ. Laptop computer-induced erythema ab igne on the left breast. Cutis. 2011;87:175-176.
- Li K, Barankin B. Cutaneous manifestations of modern technology use. J Cutan Med Surg. 2011;15:347-353. doi:10.2310/7750.2011.10053
- Riahi RR, Cohen PR. Laptop-induced erythema ab igne: report and review of literature. Dermatol Online J. 2012;18:5.
- Andersen F. Laptop-thighs--laptop-induced erythema ab igne [in Danish]. Ugeskr Laeger. 2010;172:635.
- Jagtman BA. Erythema ab igne due to a laptop computer. Contact Dermatitis. 2004;50:105. doi:10.1111/j.0105-1873.2004.0295g.x
- Olechowska M, Kisiel K, Ruszkowska L, et al. Erythema ab igne (EAI) induced by a laptop computer: report of two cases. J Dtsch Dermatol Ges. doi:10.1111/j.1610-0387.2014.12387
- Nayak SUK, Shenoi SD, Prabhu S. Laptop induced erythema ab igne. Indian J Dermatol. 2012;57:131-132. doi:10.4103/0019-5154.94284
- Salvio AG, Nunes AJ, Angarita DPR. Laptop computer induced erythema ab igne: a new presentation of an old disease. An Bras Dermatol. 2016;91:79-80. doi:10.1590/abd1806-4841.20165139
- Schummer C, Tittelbach J, Elsner P. Right-sided laptop dermatitis [in German]. Dtsch Med Wochenschr. 2015;140:1376-1377. doi:10.1055/s-0041-103615
- Manoharan D. Erythema ab igne: usual site, unusual cause. J Pharm Bioallied Sci. 2015;7(suppl 1):S74-S75. doi:10.4103/0975-7406.155811
- Giraldi S, Diettrich F, Abbage KT, et al. Erythema ab igne induced by a laptop computer in an adolescent. An Bras Dermatol. 2011;86:128-130. doi:10.1590/S0365-05962011000100018
- Secher LLS, Vind-Kezunovic D, Zachariae COC. Side-effects to the use of laptop computers: erythema ab igne. Dermatol Reports. 2010;31:E11. doi:10.4081/dr.2010.e11
- Botten D, Langley RGB, Webb A. Academic branding: erythema ab igne and use of laptop computers. CMAJ. 2010;182:E857. doi:10.1503/cmaj.091868
- Bilic M, Adams BB. Erythema ab igne induced by a laptop computer. J Am Acad Dermatol. 2004;50:973-974. doi:10.1016/j.jaad.2003.08.007
- Fu LW, Vender R. Erythema ab igne caused by laptop computer gaming - a case report. Int J Dermatol. 2012;51:716-717. doi:10.1111/j.1365-4632.2011.05033.x
- Levinbook WS, Mallett J, Grant-Kels JM. Laptop computer-associated erythema ab igne. Cutis. 2007;80:319-320.
- Mohr MR, Scott KA, Pariser RM, et al. Laptop computer-induced erythema ab igne: a case report. Cutis. 2007;79:59-60.
- Cantor AS, Bartling SJ. Laptop computer-induced hyperpigmentation. Dermatol Online J. 2018;24:13030/qt6k37r9wm.
- Kaptanog˘lu AF, Mullaaziz D. Erythema ab igne in the palmar area induced by smart phone: case report. Turkiye Klin J Med Sci. 2015;35:284-286. doi:10.5336/medsci.2015-46976
- Redding KS, Watts AN, Lee J, et al. Space heater-induced bullous erythema ab igne. Cutis. 2017;100:E9-E10.
- Goorland J, Edens MA, Baudoin TD. An emergency department presentation of erythema ab igne caused by repeated heater exposure. J La State Med Soc. 2016;168:33-34.
- Kokturk A, Kaya TI, Baz K, et al. Bullous erythema ab igne. Dermatol Online J. 2003;9:18.
- Brzezinski P, Ismail S, Chiriac A. Radiator-induced erythema ab igne in 8-year-old girl. Rev Chil Pediatr. 2014;85:239-240. doi:10.4067/S0370-41062014000200015
- Adams BB. Heated car seat-induced erythema ab igne. Arch Dermatol. 2012;148:265-266. doi:10.1001/archdermatol.2011.2207
- Helm TN, Spigel GT, Helm KF. Erythema ab igne caused by a car heater. Cutis. 1997;59:81-82.
- Gregory JF, Beute TC. Erythema ab igne. J Spec Oper Med. 2013;13:115-119. doi:10.55460/5AVH-NZHY
- Chua S, Chen Q, Lee HY. Erythema ab igne and dermal scarring caused by cupping and moxibustion treatment. J Dtsch Dermatol Ges. 2015;13:337-338. doi:10.1111/ddg.12581
- Chen JF, Liu YC, Chen YF, et al. Erythema ab igne after footbath with Chinese herbal remedies. J Chinese Med Assoc. 2011;74:51-53. doi:10.1016/j.jcma.2011.01.009
- Baltazar D, Brockman R, Simpson E. Kotatsu-induced erythema ab igne. An Bras Dermatol. 2019;94:253-254. doi:10.1590/abd1806-4841.20198792
- Baig M, Byrne F. Erythema ab igne and its relation to spinal pathology. Cureus. 2018;10:e2914. doi:10.7759/cureus.2914
- Aria AB, Chen L, Silapunt S. Erythema ab igne from heating pad use: a report of three clinical cases and a differential diagnosis. Cureus. 2018;10:e2635. doi:10.7759/cureus.2635
- Milchak M, Smucker J, Chung CG, et al. Erythema ab igne due to heating pad use: a case report and review of clinical presentation, prevention, and complications. Case Rep Med. 2016;1862480. doi:10.1155/2016/1862480
- Gmuca S, Yu J, Weiss PF, et al. Erythema ab igne in an adolescent with chronic pain: an alarming cutaneous eruption from heat exposure. Pediatr Emerg Care. 2020;36:e236-e238. doi:10.1097/PEC.0000000000001460
- Dizdarevic A, Karim OA, Bygum A. A reddish brown reticulated hyperpigmented erythema on the abdomen of a girl. Erythema ab igne, also known as toasted skin syndrome, caused by a heating pad onthe abdomen. Acta Derm Venereol. 2014;94:365-367. doi:10.2340/00015555-1722
- Chatterjee S. Erythema ab igne from prolonged use of a heating pad. Mayo Clin Proc. 2005;80:1500. doi:10.4065/80.11.1500
- Waldorf DS, Rast MF, Garofalo VJ. Heating-pad erythematous dermatitis “erythema ab igne.” JAMA. 1971;218:1704. doi:10.1001/jama.1971.03190240056023
- South AM, Crispin MK, Marqueling AL, et al. A hyperpigmented reticular rash in a patient on peritoneal dialysis. Perit Dial Int. 2016;36:677-700. doi:10.3747/pdi.2016.00042
- Ravindran R. Erythema ab igne in an individual with diabetes and gastroparesis. BMJ Case Rep. 2017;2017:bcr2014203856. doi:10.1136/bcr-2014-203856
- Dessinioti C, Katsambas A, Tzavela E, et al. Erythema ab igne in three girls with anorexia nervosa. Pediatr Dermatol. 2016;33:e149-e150. doi:10.1111/pde.12770
- Fischer J, Rein K, Erfurt-Berge C, et al. Three cases of erythema ab igne (EAI) in patients with eating disorders. Neuropsychiatr. 2010;24:141-143.
- Docx MKF, Simons A, Ramet J, et al. Erythema ab igne in an adolescent with anorexia nervosa. Int J Eat Disord. 2013;46:381-383. doi:10.1002/eat.22075
- Turan E, Cimen V, Haytoglu NSK, et al. A case of bullous erythema ab igne accompanied by anemia and subclinical hypothyroidism. Dermatol Online J. 2014;20:223366.
- Pavithran K. Erythema ab igne, schizophrenia and thermophilia. Indian J Dermatol Venereol Leprol. 1987;53:181-182.
- Dellavelle R, Gillum P. Erythema ab igne following heating/cooling blanket use in the intensive care unit. Cutis. 2000;66:136-138.
- Park SY, Kim SM, Yoon TJ. Erythema ab igne caused by weight loss heating pad. Korean J Dermatol. 2007;45:489-491.
- Sachdeva M, Gianotti R, Shah M, et al. Cutaneous manifestations of COVID-19: report of three cases and a review of literature. J Dermatol Sci. 2020;98:75-81. doi:10.1016/j.jdermsci.2020.04.011
- Gisondi P, Plaserico S, Bordin C, et al. Cutaneous manifestations of SARS‐CoV‐2 infection: a clinical update. J Eur Acad Dermatol Venereol. 2020;34:2499-2504. doi:10.1111/jdv.16774
- Manalo IF, Smith MK, Cheeley J, et al. A dermatologic manifestation of COVID-19: transient livedo reticularis. J Am Acad Dermatol. 2020;83:700. doi:10.1016/j.jaad.2020.04.018
- Zhao Q, Fang X, Pang Z, et al. COVID‐19 and cutaneous manifestations: a systematic review. J Eur Acad Dermatol Venereol. 2020;34:2505-2510. doi:10.1111/jdv.16778
- Akasaka T, Kon S. Two cases of squamous cell carcinoma arising from erythema ab igne. Nihon Hifuka Gakkai Zasshi. 1989;99:735-742.
- Arrington JH 3rd, Lockman DS. Thermal keratoses and squamous cell carcinoma in situ associated with erythema ab igne. Arch Dermatol. 1979;115:1226-1228.
- Wharton JB, Sheehan DJ, Lesher JL Jr. Squamous cell carcinoma in situ arising in the setting of erythema ab igne. J Drugs Dermatol. 2008;7:488-489.
- Wollina U, Helm C, Hansel G, et al. Two cases of erythema ab igne, one with a squamous cell carcinoma. G Ital Dermatol Venereol. 2007;142:415-418.
- Rudolph CM, Soyer HP, Wolf P, et al. Squamous cell carcinoma arising in erythema ab igne. Hautarzt. 2000;51:260-263. doi:10.1007/s001050051115
- Sigmon JR, Cantrell J, Teague D, et al. Poorly differentiated carcinoma arising in the setting of erythema ab igne. Am J Dermatopathol. 2013;35:676-678. doi:10.1097/DAD.0b013e3182871648
- Wharton J, Roffwarg D, Miller J, et al. Cutaneous marginal zone lymphoma arising in the setting of erythema ab igne. J Am Acad Dermatol. 2010;62:1080-1081. doi:10.1016/j.jaad.2009.08.005
- Jones CS, Tyring SK, Lee PC, et al. Development of neuroendocrine (Merkel cell) carcinoma mixed with squamous cell carcinoma in erythema ab igne. Arch Dermatol. 1988;124:110-113.
- Kim HW, Kim EJ, Park HC, et al. Erythema ab igne successfully treated with low fluenced 1,064-nm Q-switched neodymium-doped yttrium aluminum garnet laser. J Cosmet Laser Ther. 2014;16:147-148. doi:10.3109/14764172.2013.854623
- Tan S, Bertucci V. Erythema ab igne: an old condition new again. CMAJ. 2000;62:77-78.
- Gianfaldoni S, Gianfaldoni R, Tchernev G, et al. Erythema ab igne successfully treated with mesoglycan and bioflavonoids: a case-report. Open Access Maced J Med Sci. 2017;5:432-435. doi:10.3889/oamjms.2017.123
- Perry. Case of erythema ab igne. Br J Dermatol. 1900;xxiii:375.
- Bose S, Ortonee JP. Diseases affected by heat. In: Parish LC, Millikan LE, Amer M, et al. Global Dermatology Diagnosis and Management According to Geography, Climate, and Culture. Springer-Varlag; 1994:83-92.
- Leal-Lobato MM, Blasco-Morente G. Electric blanket induced erythema ab igne [in Spanish]. Semergen. 2015;41:456-457. doi:10.1016/j.semerg.2014.12.008
- Huynh N, Sarma D, Huerter C. Erythema ab igne: a case report and review of the literature. Cutis. 2011;88:290-292.
- Kesty K, Feldman SR. Erythema ab igne: evolving technology, evolving presentation. Dermatol Online J. 2014;20. doi:10.5070/D32011024689
- Miller K, Hunt R, Chu J, et al. Erythema ab igne. Dermatol Online J. 2011;17:28.
- Smith ML. Environmental and sports-related skin diseases. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Elsevier; 2018:1569-1594.
- Errichetti E, Stinco G. Dermoscopy in general dermatology: a practical overview. Dermatol Ther (Heidelb). 2016;6:471-507. doi:10.1007/s13555-016-0141-6
- Guarneri C, Tchernev G, Wollina U, et al. Erythema ab igne caused by laptop computer. Open Access Maced J Med Sci. 2017;5:490-492. doi:10.3889/oamjms.2017.137
- Arnold AW, Itin PH. Laptop computer-induced erythema ab igne in a child and review of the literature. Pediatrics. 2010;126:E1227-E1230. doi:10.1542/peds.2010-1390
- Dickman J, Kessler S. Unilateral reticulated patch localized to the anterior thigh. JAAD Case Rep. 2018;4:746-748. doi:10.1016/j.jdcr.2018.06.007
- Boffa MJ. Laptop computer-induced erythema ab igne on the left breast. Cutis. 2011;87:175-176.
- Li K, Barankin B. Cutaneous manifestations of modern technology use. J Cutan Med Surg. 2011;15:347-353. doi:10.2310/7750.2011.10053
- Riahi RR, Cohen PR. Laptop-induced erythema ab igne: report and review of literature. Dermatol Online J. 2012;18:5.
- Andersen F. Laptop-thighs--laptop-induced erythema ab igne [in Danish]. Ugeskr Laeger. 2010;172:635.
- Jagtman BA. Erythema ab igne due to a laptop computer. Contact Dermatitis. 2004;50:105. doi:10.1111/j.0105-1873.2004.0295g.x
- Olechowska M, Kisiel K, Ruszkowska L, et al. Erythema ab igne (EAI) induced by a laptop computer: report of two cases. J Dtsch Dermatol Ges. doi:10.1111/j.1610-0387.2014.12387
- Nayak SUK, Shenoi SD, Prabhu S. Laptop induced erythema ab igne. Indian J Dermatol. 2012;57:131-132. doi:10.4103/0019-5154.94284
- Salvio AG, Nunes AJ, Angarita DPR. Laptop computer induced erythema ab igne: a new presentation of an old disease. An Bras Dermatol. 2016;91:79-80. doi:10.1590/abd1806-4841.20165139
- Schummer C, Tittelbach J, Elsner P. Right-sided laptop dermatitis [in German]. Dtsch Med Wochenschr. 2015;140:1376-1377. doi:10.1055/s-0041-103615
- Manoharan D. Erythema ab igne: usual site, unusual cause. J Pharm Bioallied Sci. 2015;7(suppl 1):S74-S75. doi:10.4103/0975-7406.155811
- Giraldi S, Diettrich F, Abbage KT, et al. Erythema ab igne induced by a laptop computer in an adolescent. An Bras Dermatol. 2011;86:128-130. doi:10.1590/S0365-05962011000100018
- Secher LLS, Vind-Kezunovic D, Zachariae COC. Side-effects to the use of laptop computers: erythema ab igne. Dermatol Reports. 2010;31:E11. doi:10.4081/dr.2010.e11
- Botten D, Langley RGB, Webb A. Academic branding: erythema ab igne and use of laptop computers. CMAJ. 2010;182:E857. doi:10.1503/cmaj.091868
- Bilic M, Adams BB. Erythema ab igne induced by a laptop computer. J Am Acad Dermatol. 2004;50:973-974. doi:10.1016/j.jaad.2003.08.007
- Fu LW, Vender R. Erythema ab igne caused by laptop computer gaming - a case report. Int J Dermatol. 2012;51:716-717. doi:10.1111/j.1365-4632.2011.05033.x
- Levinbook WS, Mallett J, Grant-Kels JM. Laptop computer-associated erythema ab igne. Cutis. 2007;80:319-320.
- Mohr MR, Scott KA, Pariser RM, et al. Laptop computer-induced erythema ab igne: a case report. Cutis. 2007;79:59-60.
- Cantor AS, Bartling SJ. Laptop computer-induced hyperpigmentation. Dermatol Online J. 2018;24:13030/qt6k37r9wm.
- Kaptanog˘lu AF, Mullaaziz D. Erythema ab igne in the palmar area induced by smart phone: case report. Turkiye Klin J Med Sci. 2015;35:284-286. doi:10.5336/medsci.2015-46976
- Redding KS, Watts AN, Lee J, et al. Space heater-induced bullous erythema ab igne. Cutis. 2017;100:E9-E10.
- Goorland J, Edens MA, Baudoin TD. An emergency department presentation of erythema ab igne caused by repeated heater exposure. J La State Med Soc. 2016;168:33-34.
- Kokturk A, Kaya TI, Baz K, et al. Bullous erythema ab igne. Dermatol Online J. 2003;9:18.
- Brzezinski P, Ismail S, Chiriac A. Radiator-induced erythema ab igne in 8-year-old girl. Rev Chil Pediatr. 2014;85:239-240. doi:10.4067/S0370-41062014000200015
- Adams BB. Heated car seat-induced erythema ab igne. Arch Dermatol. 2012;148:265-266. doi:10.1001/archdermatol.2011.2207
- Helm TN, Spigel GT, Helm KF. Erythema ab igne caused by a car heater. Cutis. 1997;59:81-82.
- Gregory JF, Beute TC. Erythema ab igne. J Spec Oper Med. 2013;13:115-119. doi:10.55460/5AVH-NZHY
- Chua S, Chen Q, Lee HY. Erythema ab igne and dermal scarring caused by cupping and moxibustion treatment. J Dtsch Dermatol Ges. 2015;13:337-338. doi:10.1111/ddg.12581
- Chen JF, Liu YC, Chen YF, et al. Erythema ab igne after footbath with Chinese herbal remedies. J Chinese Med Assoc. 2011;74:51-53. doi:10.1016/j.jcma.2011.01.009
- Baltazar D, Brockman R, Simpson E. Kotatsu-induced erythema ab igne. An Bras Dermatol. 2019;94:253-254. doi:10.1590/abd1806-4841.20198792
- Baig M, Byrne F. Erythema ab igne and its relation to spinal pathology. Cureus. 2018;10:e2914. doi:10.7759/cureus.2914
- Aria AB, Chen L, Silapunt S. Erythema ab igne from heating pad use: a report of three clinical cases and a differential diagnosis. Cureus. 2018;10:e2635. doi:10.7759/cureus.2635
- Milchak M, Smucker J, Chung CG, et al. Erythema ab igne due to heating pad use: a case report and review of clinical presentation, prevention, and complications. Case Rep Med. 2016;1862480. doi:10.1155/2016/1862480
- Gmuca S, Yu J, Weiss PF, et al. Erythema ab igne in an adolescent with chronic pain: an alarming cutaneous eruption from heat exposure. Pediatr Emerg Care. 2020;36:e236-e238. doi:10.1097/PEC.0000000000001460
- Dizdarevic A, Karim OA, Bygum A. A reddish brown reticulated hyperpigmented erythema on the abdomen of a girl. Erythema ab igne, also known as toasted skin syndrome, caused by a heating pad onthe abdomen. Acta Derm Venereol. 2014;94:365-367. doi:10.2340/00015555-1722
- Chatterjee S. Erythema ab igne from prolonged use of a heating pad. Mayo Clin Proc. 2005;80:1500. doi:10.4065/80.11.1500
- Waldorf DS, Rast MF, Garofalo VJ. Heating-pad erythematous dermatitis “erythema ab igne.” JAMA. 1971;218:1704. doi:10.1001/jama.1971.03190240056023
- South AM, Crispin MK, Marqueling AL, et al. A hyperpigmented reticular rash in a patient on peritoneal dialysis. Perit Dial Int. 2016;36:677-700. doi:10.3747/pdi.2016.00042
- Ravindran R. Erythema ab igne in an individual with diabetes and gastroparesis. BMJ Case Rep. 2017;2017:bcr2014203856. doi:10.1136/bcr-2014-203856
- Dessinioti C, Katsambas A, Tzavela E, et al. Erythema ab igne in three girls with anorexia nervosa. Pediatr Dermatol. 2016;33:e149-e150. doi:10.1111/pde.12770
- Fischer J, Rein K, Erfurt-Berge C, et al. Three cases of erythema ab igne (EAI) in patients with eating disorders. Neuropsychiatr. 2010;24:141-143.
- Docx MKF, Simons A, Ramet J, et al. Erythema ab igne in an adolescent with anorexia nervosa. Int J Eat Disord. 2013;46:381-383. doi:10.1002/eat.22075
- Turan E, Cimen V, Haytoglu NSK, et al. A case of bullous erythema ab igne accompanied by anemia and subclinical hypothyroidism. Dermatol Online J. 2014;20:223366.
- Pavithran K. Erythema ab igne, schizophrenia and thermophilia. Indian J Dermatol Venereol Leprol. 1987;53:181-182.
- Dellavelle R, Gillum P. Erythema ab igne following heating/cooling blanket use in the intensive care unit. Cutis. 2000;66:136-138.
- Park SY, Kim SM, Yoon TJ. Erythema ab igne caused by weight loss heating pad. Korean J Dermatol. 2007;45:489-491.
- Sachdeva M, Gianotti R, Shah M, et al. Cutaneous manifestations of COVID-19: report of three cases and a review of literature. J Dermatol Sci. 2020;98:75-81. doi:10.1016/j.jdermsci.2020.04.011
- Gisondi P, Plaserico S, Bordin C, et al. Cutaneous manifestations of SARS‐CoV‐2 infection: a clinical update. J Eur Acad Dermatol Venereol. 2020;34:2499-2504. doi:10.1111/jdv.16774
- Manalo IF, Smith MK, Cheeley J, et al. A dermatologic manifestation of COVID-19: transient livedo reticularis. J Am Acad Dermatol. 2020;83:700. doi:10.1016/j.jaad.2020.04.018
- Zhao Q, Fang X, Pang Z, et al. COVID‐19 and cutaneous manifestations: a systematic review. J Eur Acad Dermatol Venereol. 2020;34:2505-2510. doi:10.1111/jdv.16778
- Akasaka T, Kon S. Two cases of squamous cell carcinoma arising from erythema ab igne. Nihon Hifuka Gakkai Zasshi. 1989;99:735-742.
- Arrington JH 3rd, Lockman DS. Thermal keratoses and squamous cell carcinoma in situ associated with erythema ab igne. Arch Dermatol. 1979;115:1226-1228.
- Wharton JB, Sheehan DJ, Lesher JL Jr. Squamous cell carcinoma in situ arising in the setting of erythema ab igne. J Drugs Dermatol. 2008;7:488-489.
- Wollina U, Helm C, Hansel G, et al. Two cases of erythema ab igne, one with a squamous cell carcinoma. G Ital Dermatol Venereol. 2007;142:415-418.
- Rudolph CM, Soyer HP, Wolf P, et al. Squamous cell carcinoma arising in erythema ab igne. Hautarzt. 2000;51:260-263. doi:10.1007/s001050051115
- Sigmon JR, Cantrell J, Teague D, et al. Poorly differentiated carcinoma arising in the setting of erythema ab igne. Am J Dermatopathol. 2013;35:676-678. doi:10.1097/DAD.0b013e3182871648
- Wharton J, Roffwarg D, Miller J, et al. Cutaneous marginal zone lymphoma arising in the setting of erythema ab igne. J Am Acad Dermatol. 2010;62:1080-1081. doi:10.1016/j.jaad.2009.08.005
- Jones CS, Tyring SK, Lee PC, et al. Development of neuroendocrine (Merkel cell) carcinoma mixed with squamous cell carcinoma in erythema ab igne. Arch Dermatol. 1988;124:110-113.
- Kim HW, Kim EJ, Park HC, et al. Erythema ab igne successfully treated with low fluenced 1,064-nm Q-switched neodymium-doped yttrium aluminum garnet laser. J Cosmet Laser Ther. 2014;16:147-148. doi:10.3109/14764172.2013.854623
- Tan S, Bertucci V. Erythema ab igne: an old condition new again. CMAJ. 2000;62:77-78.
- Gianfaldoni S, Gianfaldoni R, Tchernev G, et al. Erythema ab igne successfully treated with mesoglycan and bioflavonoids: a case-report. Open Access Maced J Med Sci. 2017;5:432-435. doi:10.3889/oamjms.2017.123
Practice Points
- Erythema ab igne (EAI) is a skin condition caused by chronic exposure to heat; removal of the heat source often will result in self-resolution of the rash.
- Erythema ab igne can be a sign of underlying illness in patients self-treating chronic pain with application of heat.
- Recognition and discontinuation of the exposure with close observation are key components in the treatment of EAI.
Could combining topical antioxidants with a nonablative laser prevent acne scars?
PHOENIX – lesions, results from a prospective, single-center study showed.
“Acne vulgaris is the most common inflammatory dermatosis worldwide, often resulting in sequelae such as scarring, PIE, and PIH,” presenting author Jamie Hu, MD, said at the annual conference of the American Society for Laser Medicine and Surgery, where the study results were presented during an abstract session. “This dyschromia can cause greater psychological distress than the original acne lesions, and disproportionately affects skin of color patients.”
Blemish-prone skin is known to have higher levels of sebum and lower levels of antioxidants, leading to lipid peroxidation and oxidative stress, resulting in proliferation of Cutibacterium acnes and an inflammatory cascade that has recently been implicated in postinflammatory dyschromia and the development of PIE and PIH, noted Dr. Hu, a dermatology resident at the University of Miami. “Therefore, the use of antioxidants presents an opportunity to disrupt blemish and dyschromia,” she said.
One such antioxidant is silymarin, which is derived from the milk thistle plant. Recent studies have demonstrated that silymarin reduces proinflammatory mediators, prevents lipid peroxidation, and presents a new way to target the treatment of both acne and postinflammatory dyschromia.
Dr. Hu’s mentor, Jill S. Waibel, MD, owner and medical director of the Miami Dermatology and Laser Institute, hypothesized that nonablative laser therapy followed by topical application of silymarin would improve acne-associated postinflammatory dyschromia. To test her hunch, she conducted a 12-week, prospective trial in which 24 patients with PIE and/or PIH were randomized to one of two treatment arms: laser treatment with topical antioxidants or laser treatment with vehicle control. Patients received three laser treatments, each 1 month apart. The topical antioxidant used was Silymarin CF, a serum that contains 0.5% silymarin, 0.5% salicylic acid, 15% L-ascorbic acid, and 0.5% ferulic acid. (The study was sponsored by SkinCeuticals, the manufacturer of the serum.)
Laser selection was made primarily on the type of dyschromia, with PIE patients receiving treatment with the pulsed dye laser and PIH patients receiving treatment with the 1,927-nm thulium laser. Patients were treated on days 0, 28, and 56 of the 12-week study, followed by immediate application of topical antioxidants or vehicle control. They were also instructed to apply the assigned topical twice daily for the duration of the study. Patients ranged in age from 21 to 61 years, and 20 had skin types III-IV.
To evaluate efficacy, the researchers conducted blinded clinical assessments with the postacne hyperpigmentation index (PAHPI) and the Global Aesthetic Improvement Scale (GAIS), instrumentation with the Mexameter, a device that captures erythema and melanin index values, and visual diagnostics with optical coherence tomography (OCT).
Dr. Hu reported that at week 12, the PAHPI in the silymarin-plus-laser treatment group fell from an average of 3.18 to 1.74 (a decrease of 1.44), which suggested an improvement trend, compared with the laser treatment–only group, whose PAHPI fell from an average of 3.25 to 1.97 (a decrease of 1.28).
As for the GAIS, a one-time score assessed at the end of the trial, the average score for all patients was 3.24, which translated to “much improved/very much improved.” Patients in the silymarin-plus-laser treatment group had higher average scores compared with patients in the laser treatment–only group (3.35 vs. 3.10, respectively), but the differences did not reach statistical significance.
According to results of the Mexameter assessment, paired t-tests showed that the levels of intralesional melanin decreased significantly for patients in the silymarin-plus-laser treatment group, compared with the laser treatment–only group (P < .05). OCT assessments demonstrated an increase in dermal brightness in both groups, corresponding to an increase in dermal collagen, as well as an increase in blood vessel density.
In an interview at the meeting, Dr. Waibel, subsection chief of dermatology at Baptist Hospital of Miami, said that future studies will focus on long-term follow-up to determine if acne scars can be prevented by combining silymarin with lasers to prevent PIH and PIE. “That would be priceless,” she said. “I believe that the PIH is what causes damage to the collagen, and that damage to the collagen is what causes the scarring. So, if we can prevent or treat PIH, we may be able to prevent scarring.”
This approach, she added, “would decrease the pharmaceutical cost because I think there are many dermatologists who are treating PEI and PIH as active acne. You really have to have a keen eye for understanding the differences and you really have to be looking, because PIE and PIH are flat, whereas active acne consists of either comedones or nodules.”
She noted that in skin of color patients, she has seen PIH persist for 9 or 10 months after treatment with isotretinoin. “It’s not the isotretinoin causing the scars, or even the acne, it’s the prolonged inflammation,” she said.
Catherine M. DiGiorgio, MD, a Boston-based laser and cosmetic dermatologist who was asked to comment on the study, said that patients and dermatologists frequently seek alternatives to hydroquinone for unwanted hyperpigmentation.
“This topical contains an active ingredient – silymarin – obtained from the milk thistle plant along with several already well known topicals used for the treatment of acne and PIH,” said Dr. DiGiorgio, program co-chair of the 2023 ASLMS conference. “Further and larger studies are needed to demonstrate and support the effectiveness of this product and silymarin for PIH and/or PIE.”
Also commenting on the results, Ray Jalian, MD, a Los Angeles–based laser and cosmetic dermatologist, told this news organization that the study findings demonstrate the power of combining topical and laser treatment for more effective improvement in acne-related PIH.
“While the study failed to show statistically significant improvement in postinflammatory erythema with concomitant laser and topical therapy versus laser alone, the promising data supporting concurrent use of topicals and fractional lasers for treatment of PIH, particularly in dark skin phototypes, is a clinically impactful contribution to our daily practice,” he said.
Dr. Waibel disclosed that she has conducted clinical trials for many device and pharmaceutical companies including SkinCeuticals. Dr. Hu, Dr. DiGiorgio, and Dr. Jalian were not involved with the study and reported having no relevant disclosures.
PHOENIX – lesions, results from a prospective, single-center study showed.
“Acne vulgaris is the most common inflammatory dermatosis worldwide, often resulting in sequelae such as scarring, PIE, and PIH,” presenting author Jamie Hu, MD, said at the annual conference of the American Society for Laser Medicine and Surgery, where the study results were presented during an abstract session. “This dyschromia can cause greater psychological distress than the original acne lesions, and disproportionately affects skin of color patients.”
Blemish-prone skin is known to have higher levels of sebum and lower levels of antioxidants, leading to lipid peroxidation and oxidative stress, resulting in proliferation of Cutibacterium acnes and an inflammatory cascade that has recently been implicated in postinflammatory dyschromia and the development of PIE and PIH, noted Dr. Hu, a dermatology resident at the University of Miami. “Therefore, the use of antioxidants presents an opportunity to disrupt blemish and dyschromia,” she said.
One such antioxidant is silymarin, which is derived from the milk thistle plant. Recent studies have demonstrated that silymarin reduces proinflammatory mediators, prevents lipid peroxidation, and presents a new way to target the treatment of both acne and postinflammatory dyschromia.
Dr. Hu’s mentor, Jill S. Waibel, MD, owner and medical director of the Miami Dermatology and Laser Institute, hypothesized that nonablative laser therapy followed by topical application of silymarin would improve acne-associated postinflammatory dyschromia. To test her hunch, she conducted a 12-week, prospective trial in which 24 patients with PIE and/or PIH were randomized to one of two treatment arms: laser treatment with topical antioxidants or laser treatment with vehicle control. Patients received three laser treatments, each 1 month apart. The topical antioxidant used was Silymarin CF, a serum that contains 0.5% silymarin, 0.5% salicylic acid, 15% L-ascorbic acid, and 0.5% ferulic acid. (The study was sponsored by SkinCeuticals, the manufacturer of the serum.)
Laser selection was made primarily on the type of dyschromia, with PIE patients receiving treatment with the pulsed dye laser and PIH patients receiving treatment with the 1,927-nm thulium laser. Patients were treated on days 0, 28, and 56 of the 12-week study, followed by immediate application of topical antioxidants or vehicle control. They were also instructed to apply the assigned topical twice daily for the duration of the study. Patients ranged in age from 21 to 61 years, and 20 had skin types III-IV.
To evaluate efficacy, the researchers conducted blinded clinical assessments with the postacne hyperpigmentation index (PAHPI) and the Global Aesthetic Improvement Scale (GAIS), instrumentation with the Mexameter, a device that captures erythema and melanin index values, and visual diagnostics with optical coherence tomography (OCT).
Dr. Hu reported that at week 12, the PAHPI in the silymarin-plus-laser treatment group fell from an average of 3.18 to 1.74 (a decrease of 1.44), which suggested an improvement trend, compared with the laser treatment–only group, whose PAHPI fell from an average of 3.25 to 1.97 (a decrease of 1.28).
As for the GAIS, a one-time score assessed at the end of the trial, the average score for all patients was 3.24, which translated to “much improved/very much improved.” Patients in the silymarin-plus-laser treatment group had higher average scores compared with patients in the laser treatment–only group (3.35 vs. 3.10, respectively), but the differences did not reach statistical significance.
According to results of the Mexameter assessment, paired t-tests showed that the levels of intralesional melanin decreased significantly for patients in the silymarin-plus-laser treatment group, compared with the laser treatment–only group (P < .05). OCT assessments demonstrated an increase in dermal brightness in both groups, corresponding to an increase in dermal collagen, as well as an increase in blood vessel density.
In an interview at the meeting, Dr. Waibel, subsection chief of dermatology at Baptist Hospital of Miami, said that future studies will focus on long-term follow-up to determine if acne scars can be prevented by combining silymarin with lasers to prevent PIH and PIE. “That would be priceless,” she said. “I believe that the PIH is what causes damage to the collagen, and that damage to the collagen is what causes the scarring. So, if we can prevent or treat PIH, we may be able to prevent scarring.”
This approach, she added, “would decrease the pharmaceutical cost because I think there are many dermatologists who are treating PEI and PIH as active acne. You really have to have a keen eye for understanding the differences and you really have to be looking, because PIE and PIH are flat, whereas active acne consists of either comedones or nodules.”
She noted that in skin of color patients, she has seen PIH persist for 9 or 10 months after treatment with isotretinoin. “It’s not the isotretinoin causing the scars, or even the acne, it’s the prolonged inflammation,” she said.
Catherine M. DiGiorgio, MD, a Boston-based laser and cosmetic dermatologist who was asked to comment on the study, said that patients and dermatologists frequently seek alternatives to hydroquinone for unwanted hyperpigmentation.
“This topical contains an active ingredient – silymarin – obtained from the milk thistle plant along with several already well known topicals used for the treatment of acne and PIH,” said Dr. DiGiorgio, program co-chair of the 2023 ASLMS conference. “Further and larger studies are needed to demonstrate and support the effectiveness of this product and silymarin for PIH and/or PIE.”
Also commenting on the results, Ray Jalian, MD, a Los Angeles–based laser and cosmetic dermatologist, told this news organization that the study findings demonstrate the power of combining topical and laser treatment for more effective improvement in acne-related PIH.
“While the study failed to show statistically significant improvement in postinflammatory erythema with concomitant laser and topical therapy versus laser alone, the promising data supporting concurrent use of topicals and fractional lasers for treatment of PIH, particularly in dark skin phototypes, is a clinically impactful contribution to our daily practice,” he said.
Dr. Waibel disclosed that she has conducted clinical trials for many device and pharmaceutical companies including SkinCeuticals. Dr. Hu, Dr. DiGiorgio, and Dr. Jalian were not involved with the study and reported having no relevant disclosures.
PHOENIX – lesions, results from a prospective, single-center study showed.
“Acne vulgaris is the most common inflammatory dermatosis worldwide, often resulting in sequelae such as scarring, PIE, and PIH,” presenting author Jamie Hu, MD, said at the annual conference of the American Society for Laser Medicine and Surgery, where the study results were presented during an abstract session. “This dyschromia can cause greater psychological distress than the original acne lesions, and disproportionately affects skin of color patients.”
Blemish-prone skin is known to have higher levels of sebum and lower levels of antioxidants, leading to lipid peroxidation and oxidative stress, resulting in proliferation of Cutibacterium acnes and an inflammatory cascade that has recently been implicated in postinflammatory dyschromia and the development of PIE and PIH, noted Dr. Hu, a dermatology resident at the University of Miami. “Therefore, the use of antioxidants presents an opportunity to disrupt blemish and dyschromia,” she said.
One such antioxidant is silymarin, which is derived from the milk thistle plant. Recent studies have demonstrated that silymarin reduces proinflammatory mediators, prevents lipid peroxidation, and presents a new way to target the treatment of both acne and postinflammatory dyschromia.
Dr. Hu’s mentor, Jill S. Waibel, MD, owner and medical director of the Miami Dermatology and Laser Institute, hypothesized that nonablative laser therapy followed by topical application of silymarin would improve acne-associated postinflammatory dyschromia. To test her hunch, she conducted a 12-week, prospective trial in which 24 patients with PIE and/or PIH were randomized to one of two treatment arms: laser treatment with topical antioxidants or laser treatment with vehicle control. Patients received three laser treatments, each 1 month apart. The topical antioxidant used was Silymarin CF, a serum that contains 0.5% silymarin, 0.5% salicylic acid, 15% L-ascorbic acid, and 0.5% ferulic acid. (The study was sponsored by SkinCeuticals, the manufacturer of the serum.)
Laser selection was made primarily on the type of dyschromia, with PIE patients receiving treatment with the pulsed dye laser and PIH patients receiving treatment with the 1,927-nm thulium laser. Patients were treated on days 0, 28, and 56 of the 12-week study, followed by immediate application of topical antioxidants or vehicle control. They were also instructed to apply the assigned topical twice daily for the duration of the study. Patients ranged in age from 21 to 61 years, and 20 had skin types III-IV.
To evaluate efficacy, the researchers conducted blinded clinical assessments with the postacne hyperpigmentation index (PAHPI) and the Global Aesthetic Improvement Scale (GAIS), instrumentation with the Mexameter, a device that captures erythema and melanin index values, and visual diagnostics with optical coherence tomography (OCT).
Dr. Hu reported that at week 12, the PAHPI in the silymarin-plus-laser treatment group fell from an average of 3.18 to 1.74 (a decrease of 1.44), which suggested an improvement trend, compared with the laser treatment–only group, whose PAHPI fell from an average of 3.25 to 1.97 (a decrease of 1.28).
As for the GAIS, a one-time score assessed at the end of the trial, the average score for all patients was 3.24, which translated to “much improved/very much improved.” Patients in the silymarin-plus-laser treatment group had higher average scores compared with patients in the laser treatment–only group (3.35 vs. 3.10, respectively), but the differences did not reach statistical significance.
According to results of the Mexameter assessment, paired t-tests showed that the levels of intralesional melanin decreased significantly for patients in the silymarin-plus-laser treatment group, compared with the laser treatment–only group (P < .05). OCT assessments demonstrated an increase in dermal brightness in both groups, corresponding to an increase in dermal collagen, as well as an increase in blood vessel density.
In an interview at the meeting, Dr. Waibel, subsection chief of dermatology at Baptist Hospital of Miami, said that future studies will focus on long-term follow-up to determine if acne scars can be prevented by combining silymarin with lasers to prevent PIH and PIE. “That would be priceless,” she said. “I believe that the PIH is what causes damage to the collagen, and that damage to the collagen is what causes the scarring. So, if we can prevent or treat PIH, we may be able to prevent scarring.”
This approach, she added, “would decrease the pharmaceutical cost because I think there are many dermatologists who are treating PEI and PIH as active acne. You really have to have a keen eye for understanding the differences and you really have to be looking, because PIE and PIH are flat, whereas active acne consists of either comedones or nodules.”
She noted that in skin of color patients, she has seen PIH persist for 9 or 10 months after treatment with isotretinoin. “It’s not the isotretinoin causing the scars, or even the acne, it’s the prolonged inflammation,” she said.
Catherine M. DiGiorgio, MD, a Boston-based laser and cosmetic dermatologist who was asked to comment on the study, said that patients and dermatologists frequently seek alternatives to hydroquinone for unwanted hyperpigmentation.
“This topical contains an active ingredient – silymarin – obtained from the milk thistle plant along with several already well known topicals used for the treatment of acne and PIH,” said Dr. DiGiorgio, program co-chair of the 2023 ASLMS conference. “Further and larger studies are needed to demonstrate and support the effectiveness of this product and silymarin for PIH and/or PIE.”
Also commenting on the results, Ray Jalian, MD, a Los Angeles–based laser and cosmetic dermatologist, told this news organization that the study findings demonstrate the power of combining topical and laser treatment for more effective improvement in acne-related PIH.
“While the study failed to show statistically significant improvement in postinflammatory erythema with concomitant laser and topical therapy versus laser alone, the promising data supporting concurrent use of topicals and fractional lasers for treatment of PIH, particularly in dark skin phototypes, is a clinically impactful contribution to our daily practice,” he said.
Dr. Waibel disclosed that she has conducted clinical trials for many device and pharmaceutical companies including SkinCeuticals. Dr. Hu, Dr. DiGiorgio, and Dr. Jalian were not involved with the study and reported having no relevant disclosures.
AT ASLMS 2023
Liver transplants for CRC metastases: Coming into its own?
Liver transplant is an effective therapy for patients with primary liver cancer, and outcomes after transplantation are often superior to surgical resection. But the pool of potential patients is increasing, as transplantation is now emerging as an attractive option for select patients with nonresectable colorectal cancer (CRC) liver metastases, as well as those with intrahepatic cholangiocarcinoma (CCA).
Transplant is here to stay
To date, the only curative or potentially curative therapy for patients with CRC liver metastases and intrahepatic CCA has been the combination of systemic therapies and R0 resection, said Gonzalo Sapisochin Cantis, MD, associate professor, department of surgery, University of Toronto.
The new idea is that, for patients with unresectable disease, total hepatectomy followed by a liver transplant may be a promising strategy. “This is a very hot topic in transplant oncology,” he said.
Liver transplantation is already established as the best treatment option for patients with primary hepatocellular carcinoma, which has become the main indication for liver transplantation at many centers.
For patients with CRC metastases and intrahepatic CCA, liver transplantation may help cure some patients by extending the conventional margins of surgical oncology, he suggested. “This is basically going to work in patients who have exclusive liver-restricted disease and not in those with metastatic disease. The efficacy is going to be seen by objective and sustained response to some sort of neoadjuvant therapy.”
However, Dr. Sapisochin emphasized liver transplantation is not an option for every patient. “We’re going to have to have clear inclusion and exclusion criteria that need to be defined a priori.”
Intrahepatic CCA has historically been considered a contraindication for liver transplantation. Surgical resection is the preferred first-line treatment and the only one that is potentially curative, he explained. However, most patients are not candidates for surgery, and even if they do have a resection, many of these patients will experience a recurrence, usually in the liver.
There are some studies that support transplantation in this patient population, including one by Dr. Sapisochin and colleagues. That study looked at patients who were transplanted under the assumption that they had hepatocellular carcinoma but were found to actually have intrahepatic CCA. The recurrence rate at 5 years was 18%, and 5-year survival was 65%.
“We were able to show that those patients with small tumors actually can do very well after transplant, with survivals over 70%-80%, which in this population is a very good outcome,” he said.
Transplant for CRC metastases
Unresectable liver metastases from colorectal cancer can also be challenging to treat, he said. Surgical resection is the only potential cure with a combination of systemic chemotherapy, but only a minority of patients are candidates for surgery.
Data supporting transplantation for CRC metastases have been emerging. One trial was conducted by researchers in Norway, who developed the Oslo score for risk stratification. “Those with risk factors had worse outcomes, and obviously, having a large tumor diameter, a high CEA (carcinoembryonic antigen), progressing on chemotherapy, or a short interval between the primary resection and the transplant were risk factors for recurrence,” Dr. Sapisochin said.
The 10-year survival among patients with a low Oslo score was 50%. “We’re talking about patients who had no resection possibility and received a transplant after systemic chemotherapy, and they had a 10-year survival of 50%,” he emphasized.
However, Dr. Sapisochin acknowledged the biggest problem transplant surgeons face is that there are not enough donor organs.
One solution is living donor liver transplantation. “Given that this is an unlimited source, you can utilize this as extended criteria and it adds another graft to the system,” he explained.
“We have a protocol for living donor liver transplantations for patients with colorectal liver metastasis,” Dr. Sapisochin said. “We’ve done seven cases so far with pretty good outcomes. One patient, unfortunately, passed away 39 months after transplant with lung metastases, but the rest are alive with no recurrence.”*
More available organs?
R. Mark Ghobrial, MD, PhD, director of the J.C. Walter Jr. Transplant Center at Houston Methodist Hospital, said that, 5 years ago, he was very cautious about liver transplantation for intrahepatic CCA.
He pointed out that, although transplantation for hepatocellular cancer was being done in the 1990s, the results were so poor that a moratorium was placed on the practice. “But now liver transplantation has become the definitive therapy for hepatocellular cancer, and intrahepatic cholangiocarcinoma is going the same way,” he said.
Dr. Ghobrial reiterated that one of the issues in transplantation for oncology patients is the limited supply of available organs, but he believes the landscape for liver transplantation has changed, resulting in more available organs. One factor is that hepatitis C has become curable with the advent of new therapies, and hence, the need for transplantation for patients with this disease has plummeted.
“I’ve done about maybe 800 transplants in the last 5 years. I’ve only transplanted two patients with hepatitis C,” he said. “Now we are doing more transplants for alcoholic liver disease and cancer.”
Improvements in technology are also allowing for more livers to become useable, he pointed out. One example is normothermic machine perfusion, which has entered the clinical arena in the last decade. The technique has shown promising results in improving the quality of marginal organs and increasing the pool of liver grafts.
Another factor that has increased the number of livers available for transplantation is the move to accept organs from circulatory death donors, as well as donations after brain death. “Our transplantation was about 4% of donors after cardiac death, but today this has gone up to almost 16% or 20% of the livers,” Dr. Ghobrial said. “In some centers this has gone up to about 50%.
“Liver transplantation for intrahepatic cholangiocarcinoma and colorectal cancer metastases has come of age for selected patients,” he said.
More caution needed
However, another expert urged some caution, warning that live donation carries risk. Yuman Fong, MD, a surgical oncologist with City of Hope National Medical Center, Duarte, Calif., said that around “1 in 600 live donors die from donation. That is a healthy person dying. This is not a small issue.”
He pointed out that if the criteria for transplant is greatly liberalized, the 5-year survival will not be as high as demonstrated in clinical trials.
Writing about the issue in a recent editorial, Dr. Fong pointed out that cadaveric livers for transplant remain a finite resource and that more than 1,000 patients still die every year on the waiting list for a transplant.
A more reasonable approach would be to advocate for this type of program in regions of the world where cadaveric livers are more plentiful or centers with established living donor transplant programs.
“For us to develop this resource and safeguard patients, family organ donors, and resources, we need to develop what are the best inclusion criteria,” Dr. Fong said. “We have to optimize use of all cadaveric organs and determine if we are willing to transplant borderline organs.”
Ethics of transplanting
Ethicist Arthur L. Caplan, PhD, the Drs. William F. and Virginia Connolly Mitty Professor of Bioethics at New York University, said this is an interesting development in the field of liver transplantation. “There have been attempts in the past, and many did not end well, such as with Steve Jobs. But transplantation is always pushing to expand eligibility, and there has also been much success with that.”
However, Dr. Caplan emphasized the new data are innovative and experimental, which may control how many centers will be able to perform liver transplants in these cancer patient populations. “It has to be data driven as we are dealing with an exceedingly scarce source,” he said. “We know that people can do well, but it adds more stress to the supply of organs, and some patients may not do as well.”
He also emphasized that live donation is not a panacea. “Liver donation from a live donor is not the same as live donation for a kidney. It is much riskier and not that common. So not quite the same.”
The bottom line is that livers for transplantation are a scarce resource and transplant may work well in some cancer patients but not others, he emphasized. “Morally, we want to save lives, but not by adding in people who may not do well. If programs try to stretch the criteria, some may try transplants with more marginal organs.”
Dr. Sapisochin has disclosed relationships with Bayer, Roche, Novartis, Integra, AstraZeneca, Chiesi, Evidera, and Stryker. Dr. Ghobrial reported no relevant financial relationships. Dr. Fong has reported being a scientific consultant for Medtronic and Johnson & Johnson and receiving royalties from Merck and Imugene. Dr. Caplan writes a regular column on ethics for Medscape.
A version of this article first appeared on Medscape.com.
Correction, 4/28/23 - An earlier version of this article misstated when the patient passed away.
Liver transplant is an effective therapy for patients with primary liver cancer, and outcomes after transplantation are often superior to surgical resection. But the pool of potential patients is increasing, as transplantation is now emerging as an attractive option for select patients with nonresectable colorectal cancer (CRC) liver metastases, as well as those with intrahepatic cholangiocarcinoma (CCA).
Transplant is here to stay
To date, the only curative or potentially curative therapy for patients with CRC liver metastases and intrahepatic CCA has been the combination of systemic therapies and R0 resection, said Gonzalo Sapisochin Cantis, MD, associate professor, department of surgery, University of Toronto.
The new idea is that, for patients with unresectable disease, total hepatectomy followed by a liver transplant may be a promising strategy. “This is a very hot topic in transplant oncology,” he said.
Liver transplantation is already established as the best treatment option for patients with primary hepatocellular carcinoma, which has become the main indication for liver transplantation at many centers.
For patients with CRC metastases and intrahepatic CCA, liver transplantation may help cure some patients by extending the conventional margins of surgical oncology, he suggested. “This is basically going to work in patients who have exclusive liver-restricted disease and not in those with metastatic disease. The efficacy is going to be seen by objective and sustained response to some sort of neoadjuvant therapy.”
However, Dr. Sapisochin emphasized liver transplantation is not an option for every patient. “We’re going to have to have clear inclusion and exclusion criteria that need to be defined a priori.”
Intrahepatic CCA has historically been considered a contraindication for liver transplantation. Surgical resection is the preferred first-line treatment and the only one that is potentially curative, he explained. However, most patients are not candidates for surgery, and even if they do have a resection, many of these patients will experience a recurrence, usually in the liver.
There are some studies that support transplantation in this patient population, including one by Dr. Sapisochin and colleagues. That study looked at patients who were transplanted under the assumption that they had hepatocellular carcinoma but were found to actually have intrahepatic CCA. The recurrence rate at 5 years was 18%, and 5-year survival was 65%.
“We were able to show that those patients with small tumors actually can do very well after transplant, with survivals over 70%-80%, which in this population is a very good outcome,” he said.
Transplant for CRC metastases
Unresectable liver metastases from colorectal cancer can also be challenging to treat, he said. Surgical resection is the only potential cure with a combination of systemic chemotherapy, but only a minority of patients are candidates for surgery.
Data supporting transplantation for CRC metastases have been emerging. One trial was conducted by researchers in Norway, who developed the Oslo score for risk stratification. “Those with risk factors had worse outcomes, and obviously, having a large tumor diameter, a high CEA (carcinoembryonic antigen), progressing on chemotherapy, or a short interval between the primary resection and the transplant were risk factors for recurrence,” Dr. Sapisochin said.
The 10-year survival among patients with a low Oslo score was 50%. “We’re talking about patients who had no resection possibility and received a transplant after systemic chemotherapy, and they had a 10-year survival of 50%,” he emphasized.
However, Dr. Sapisochin acknowledged the biggest problem transplant surgeons face is that there are not enough donor organs.
One solution is living donor liver transplantation. “Given that this is an unlimited source, you can utilize this as extended criteria and it adds another graft to the system,” he explained.
“We have a protocol for living donor liver transplantations for patients with colorectal liver metastasis,” Dr. Sapisochin said. “We’ve done seven cases so far with pretty good outcomes. One patient, unfortunately, passed away 39 months after transplant with lung metastases, but the rest are alive with no recurrence.”*
More available organs?
R. Mark Ghobrial, MD, PhD, director of the J.C. Walter Jr. Transplant Center at Houston Methodist Hospital, said that, 5 years ago, he was very cautious about liver transplantation for intrahepatic CCA.
He pointed out that, although transplantation for hepatocellular cancer was being done in the 1990s, the results were so poor that a moratorium was placed on the practice. “But now liver transplantation has become the definitive therapy for hepatocellular cancer, and intrahepatic cholangiocarcinoma is going the same way,” he said.
Dr. Ghobrial reiterated that one of the issues in transplantation for oncology patients is the limited supply of available organs, but he believes the landscape for liver transplantation has changed, resulting in more available organs. One factor is that hepatitis C has become curable with the advent of new therapies, and hence, the need for transplantation for patients with this disease has plummeted.
“I’ve done about maybe 800 transplants in the last 5 years. I’ve only transplanted two patients with hepatitis C,” he said. “Now we are doing more transplants for alcoholic liver disease and cancer.”
Improvements in technology are also allowing for more livers to become useable, he pointed out. One example is normothermic machine perfusion, which has entered the clinical arena in the last decade. The technique has shown promising results in improving the quality of marginal organs and increasing the pool of liver grafts.
Another factor that has increased the number of livers available for transplantation is the move to accept organs from circulatory death donors, as well as donations after brain death. “Our transplantation was about 4% of donors after cardiac death, but today this has gone up to almost 16% or 20% of the livers,” Dr. Ghobrial said. “In some centers this has gone up to about 50%.
“Liver transplantation for intrahepatic cholangiocarcinoma and colorectal cancer metastases has come of age for selected patients,” he said.
More caution needed
However, another expert urged some caution, warning that live donation carries risk. Yuman Fong, MD, a surgical oncologist with City of Hope National Medical Center, Duarte, Calif., said that around “1 in 600 live donors die from donation. That is a healthy person dying. This is not a small issue.”
He pointed out that if the criteria for transplant is greatly liberalized, the 5-year survival will not be as high as demonstrated in clinical trials.
Writing about the issue in a recent editorial, Dr. Fong pointed out that cadaveric livers for transplant remain a finite resource and that more than 1,000 patients still die every year on the waiting list for a transplant.
A more reasonable approach would be to advocate for this type of program in regions of the world where cadaveric livers are more plentiful or centers with established living donor transplant programs.
“For us to develop this resource and safeguard patients, family organ donors, and resources, we need to develop what are the best inclusion criteria,” Dr. Fong said. “We have to optimize use of all cadaveric organs and determine if we are willing to transplant borderline organs.”
Ethics of transplanting
Ethicist Arthur L. Caplan, PhD, the Drs. William F. and Virginia Connolly Mitty Professor of Bioethics at New York University, said this is an interesting development in the field of liver transplantation. “There have been attempts in the past, and many did not end well, such as with Steve Jobs. But transplantation is always pushing to expand eligibility, and there has also been much success with that.”
However, Dr. Caplan emphasized the new data are innovative and experimental, which may control how many centers will be able to perform liver transplants in these cancer patient populations. “It has to be data driven as we are dealing with an exceedingly scarce source,” he said. “We know that people can do well, but it adds more stress to the supply of organs, and some patients may not do as well.”
He also emphasized that live donation is not a panacea. “Liver donation from a live donor is not the same as live donation for a kidney. It is much riskier and not that common. So not quite the same.”
The bottom line is that livers for transplantation are a scarce resource and transplant may work well in some cancer patients but not others, he emphasized. “Morally, we want to save lives, but not by adding in people who may not do well. If programs try to stretch the criteria, some may try transplants with more marginal organs.”
Dr. Sapisochin has disclosed relationships with Bayer, Roche, Novartis, Integra, AstraZeneca, Chiesi, Evidera, and Stryker. Dr. Ghobrial reported no relevant financial relationships. Dr. Fong has reported being a scientific consultant for Medtronic and Johnson & Johnson and receiving royalties from Merck and Imugene. Dr. Caplan writes a regular column on ethics for Medscape.
A version of this article first appeared on Medscape.com.
Correction, 4/28/23 - An earlier version of this article misstated when the patient passed away.
Liver transplant is an effective therapy for patients with primary liver cancer, and outcomes after transplantation are often superior to surgical resection. But the pool of potential patients is increasing, as transplantation is now emerging as an attractive option for select patients with nonresectable colorectal cancer (CRC) liver metastases, as well as those with intrahepatic cholangiocarcinoma (CCA).
Transplant is here to stay
To date, the only curative or potentially curative therapy for patients with CRC liver metastases and intrahepatic CCA has been the combination of systemic therapies and R0 resection, said Gonzalo Sapisochin Cantis, MD, associate professor, department of surgery, University of Toronto.
The new idea is that, for patients with unresectable disease, total hepatectomy followed by a liver transplant may be a promising strategy. “This is a very hot topic in transplant oncology,” he said.
Liver transplantation is already established as the best treatment option for patients with primary hepatocellular carcinoma, which has become the main indication for liver transplantation at many centers.
For patients with CRC metastases and intrahepatic CCA, liver transplantation may help cure some patients by extending the conventional margins of surgical oncology, he suggested. “This is basically going to work in patients who have exclusive liver-restricted disease and not in those with metastatic disease. The efficacy is going to be seen by objective and sustained response to some sort of neoadjuvant therapy.”
However, Dr. Sapisochin emphasized liver transplantation is not an option for every patient. “We’re going to have to have clear inclusion and exclusion criteria that need to be defined a priori.”
Intrahepatic CCA has historically been considered a contraindication for liver transplantation. Surgical resection is the preferred first-line treatment and the only one that is potentially curative, he explained. However, most patients are not candidates for surgery, and even if they do have a resection, many of these patients will experience a recurrence, usually in the liver.
There are some studies that support transplantation in this patient population, including one by Dr. Sapisochin and colleagues. That study looked at patients who were transplanted under the assumption that they had hepatocellular carcinoma but were found to actually have intrahepatic CCA. The recurrence rate at 5 years was 18%, and 5-year survival was 65%.
“We were able to show that those patients with small tumors actually can do very well after transplant, with survivals over 70%-80%, which in this population is a very good outcome,” he said.
Transplant for CRC metastases
Unresectable liver metastases from colorectal cancer can also be challenging to treat, he said. Surgical resection is the only potential cure with a combination of systemic chemotherapy, but only a minority of patients are candidates for surgery.
Data supporting transplantation for CRC metastases have been emerging. One trial was conducted by researchers in Norway, who developed the Oslo score for risk stratification. “Those with risk factors had worse outcomes, and obviously, having a large tumor diameter, a high CEA (carcinoembryonic antigen), progressing on chemotherapy, or a short interval between the primary resection and the transplant were risk factors for recurrence,” Dr. Sapisochin said.
The 10-year survival among patients with a low Oslo score was 50%. “We’re talking about patients who had no resection possibility and received a transplant after systemic chemotherapy, and they had a 10-year survival of 50%,” he emphasized.
However, Dr. Sapisochin acknowledged the biggest problem transplant surgeons face is that there are not enough donor organs.
One solution is living donor liver transplantation. “Given that this is an unlimited source, you can utilize this as extended criteria and it adds another graft to the system,” he explained.
“We have a protocol for living donor liver transplantations for patients with colorectal liver metastasis,” Dr. Sapisochin said. “We’ve done seven cases so far with pretty good outcomes. One patient, unfortunately, passed away 39 months after transplant with lung metastases, but the rest are alive with no recurrence.”*
More available organs?
R. Mark Ghobrial, MD, PhD, director of the J.C. Walter Jr. Transplant Center at Houston Methodist Hospital, said that, 5 years ago, he was very cautious about liver transplantation for intrahepatic CCA.
He pointed out that, although transplantation for hepatocellular cancer was being done in the 1990s, the results were so poor that a moratorium was placed on the practice. “But now liver transplantation has become the definitive therapy for hepatocellular cancer, and intrahepatic cholangiocarcinoma is going the same way,” he said.
Dr. Ghobrial reiterated that one of the issues in transplantation for oncology patients is the limited supply of available organs, but he believes the landscape for liver transplantation has changed, resulting in more available organs. One factor is that hepatitis C has become curable with the advent of new therapies, and hence, the need for transplantation for patients with this disease has plummeted.
“I’ve done about maybe 800 transplants in the last 5 years. I’ve only transplanted two patients with hepatitis C,” he said. “Now we are doing more transplants for alcoholic liver disease and cancer.”
Improvements in technology are also allowing for more livers to become useable, he pointed out. One example is normothermic machine perfusion, which has entered the clinical arena in the last decade. The technique has shown promising results in improving the quality of marginal organs and increasing the pool of liver grafts.
Another factor that has increased the number of livers available for transplantation is the move to accept organs from circulatory death donors, as well as donations after brain death. “Our transplantation was about 4% of donors after cardiac death, but today this has gone up to almost 16% or 20% of the livers,” Dr. Ghobrial said. “In some centers this has gone up to about 50%.
“Liver transplantation for intrahepatic cholangiocarcinoma and colorectal cancer metastases has come of age for selected patients,” he said.
More caution needed
However, another expert urged some caution, warning that live donation carries risk. Yuman Fong, MD, a surgical oncologist with City of Hope National Medical Center, Duarte, Calif., said that around “1 in 600 live donors die from donation. That is a healthy person dying. This is not a small issue.”
He pointed out that if the criteria for transplant is greatly liberalized, the 5-year survival will not be as high as demonstrated in clinical trials.
Writing about the issue in a recent editorial, Dr. Fong pointed out that cadaveric livers for transplant remain a finite resource and that more than 1,000 patients still die every year on the waiting list for a transplant.
A more reasonable approach would be to advocate for this type of program in regions of the world where cadaveric livers are more plentiful or centers with established living donor transplant programs.
“For us to develop this resource and safeguard patients, family organ donors, and resources, we need to develop what are the best inclusion criteria,” Dr. Fong said. “We have to optimize use of all cadaveric organs and determine if we are willing to transplant borderline organs.”
Ethics of transplanting
Ethicist Arthur L. Caplan, PhD, the Drs. William F. and Virginia Connolly Mitty Professor of Bioethics at New York University, said this is an interesting development in the field of liver transplantation. “There have been attempts in the past, and many did not end well, such as with Steve Jobs. But transplantation is always pushing to expand eligibility, and there has also been much success with that.”
However, Dr. Caplan emphasized the new data are innovative and experimental, which may control how many centers will be able to perform liver transplants in these cancer patient populations. “It has to be data driven as we are dealing with an exceedingly scarce source,” he said. “We know that people can do well, but it adds more stress to the supply of organs, and some patients may not do as well.”
He also emphasized that live donation is not a panacea. “Liver donation from a live donor is not the same as live donation for a kidney. It is much riskier and not that common. So not quite the same.”
The bottom line is that livers for transplantation are a scarce resource and transplant may work well in some cancer patients but not others, he emphasized. “Morally, we want to save lives, but not by adding in people who may not do well. If programs try to stretch the criteria, some may try transplants with more marginal organs.”
Dr. Sapisochin has disclosed relationships with Bayer, Roche, Novartis, Integra, AstraZeneca, Chiesi, Evidera, and Stryker. Dr. Ghobrial reported no relevant financial relationships. Dr. Fong has reported being a scientific consultant for Medtronic and Johnson & Johnson and receiving royalties from Merck and Imugene. Dr. Caplan writes a regular column on ethics for Medscape.
A version of this article first appeared on Medscape.com.
Correction, 4/28/23 - An earlier version of this article misstated when the patient passed away.
FROM ASCO GU 2023
Liver disease does not worsen IVF outcomes
Having chronic liver disease does not affect outcomes for women who undergo in vitro fertilization (IVF), new research suggests.
The study, published online in the American Journal of Gastroenterology, compared women with and those without chronic liver disease who had normal ovarian reserve and who underwent assisted reproductive technology (ART) treatment in a high-volume fertility practice from 2002 to 2021.
“IVF treatment and pregnancy outcomes were not significantly different compared to controls,” the researchers wrote.
Women with liver disease may experience impaired fertility. For example, women with chronic liver disease, such as hepatitis C virus infection, may have premature ovarian insufficiency, while women with advanced liver disease, cirrhosis, and hepatic decompensation are known to have abnormally low gonadotropin levels.
leading to “an immediate need for the clinical assessment of reproductive potential in women with chronic liver disease,” the authors wrote.
The literature about ART treatment outcomes for women with liver disease was limited and may not reflect current therapy protocols, researchers found.
“To the best of our knowledge, this study is the largest to date to evaluate IVF efficacy in women with liver disease,” they wrote.
Similar outcomes
Researchers identified 295 women with liver disease (mean age, 37.8 ± 5.2 years) who underwent 1,033 contemporary, standard ART treatment cycles. Six patients (2%) had cirrhosis, eight (2.7%) had undergone liver transplantation, and 281 (95.3%) had chronic liver disease, of which viral hepatitis B and C infections were the most prevalent. The final study population consisted of 115 women who underwent 186 IVF cycles, as well as embryo biopsy for genetic testing.
The control group consisted of all the women at the treatment center without liver disease who received contemporary, standard ART treatment because of male factor infertility, which served as an indication that the women had normal ovarian reserve and were considered fertile. These 624 patients underwent 868 IVF cycles with embryo biopsy.
The mean age of the patients with liver disease was significantly higher than that of the control participants. Mean body mass index was also significantly higher for the patients with liver disease, and there were differences in baseline levels of selected hormones, compared with control participants. In addition, among those with liver disease, the number of oocytes retrieved was significantly lower (12.3 ± 7.6 vs. 16.5 ± 8.2; P < .05), as were the number of mature oocytes (9.1 ± 6.2 vs. 12.6 ± 6.7; P < .05), the number of fertilized embryos (7.0 ± 5.2 vs. 9.9 ± 5.9; P < .05), the number of embryos for which biopsy was performed (3.4 ± 2.2 vs. 5.1 ± 3.5; P < .05), and the number of euploid embryos (1.6 ± 1.4 vs. 2.7 ± 2.4; P < .05), compared with control participants.
Among the two groups, there were no statistically significant differences in mature oocyte rate (an indicator of response to controlled ovarian stimulation), fertilization per mature oocyte rate (an indicator of oocyte quality and ability to be fertilized), or embryo ploidy rate (an indicator of genetically normal embryos), as determined by embryo biopsy, the researchers write.
A subanalysis of women who went on to have a single thawed euploid (chromosomally normal) embryo transfer to achieve pregnancy found no statistically significant differences in rates of clinical pregnancy, clinical pregnancy loss, or live births between the liver disease group and the control group.
“Overall, women with chronic liver disease can be counseled that IVF treatment will not significantly differ in response to controlled ovarian stimulation, embryo fertilization rate, or ploidy outcome compared to women without liver disease,” the researchers wrote.
Data for patient counseling
The results could change the current common thinking among clinicians that IVF should not be conducted until liver disease is under optimal control, first author Jessica Lee, BS, a student at Icahn School of Medicine at Mount Sinai, New York, said.
“There was a knowledge gap for studies in the United States, and we hope this study will not only help patients with liver disease but also providers with counseling,” she said.
The findings suggest that “even if you have chronic liver disease and it’s not fully optimized, that should not interfere with pursuing IVF,” said principal investigator Tatyana Kushner, MD, an associate professor of medicine in liver diseases at the Icahn School.
Women with liver disease whose fertility is impaired should receive counseling about fertility preservation options earlier to help access fertility care, the researchers write.
The study’s findings are “encouraging,” said Monika Sarkar, MD, associate professor of medicine in gastroenterology at the University of California, San Francisco.
“With rising numbers of young adults with liver disease, it is encouraging to see dedicated studies that address a topic of importance to our patients – namely, their reproductive health,” she said. “The current study nicely expands beyond previous data to include a control population without liver disease.”
Differences in oocyte numbers
Although there were no differences in the success rate of embryo transfer, the researchers did see differences in the number of oocytes. Only 37 mature oocytes made it to transfer in the liver disease group, compared with 609 in the control group, noted Dr. Sarkar, who was not involved with the study.
“The challenge of ART is less at the level of embryo transfer, which is very successful once a euploid embryo is achieved, but rather at the earlier step of retrieval of mature oocytes,” Dr. Sarkar said. “Here, the authors found that patients with liver disease had a significantly lower number of oocytes retrieved, number of mature oocytes, and lower number of fertilized embryos.”
The data suggest that fewer eggs are retrieved per cycle from patients with liver disease, “which ultimately will lower the success per cycle,” Dr. Sarkar said.
“This suggests that referring women with chronic liver disease to ART sooner may help to optimize outcomes,” she added. “Larger data evaluating ability to achieve mature oocytes and subsequent fertilization will also be key for determining whether ART success differs by presence, severity, and type of liver disease.”
As more research on ART outcomes in women with liver disease is conducted, subspecialists in gastrointestinal and liver disease may gain confidence in counseling patients, Dr. Sarkar said.
Ms. Lee, Dr. Kushner, and Dr. Sarkar report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Having chronic liver disease does not affect outcomes for women who undergo in vitro fertilization (IVF), new research suggests.
The study, published online in the American Journal of Gastroenterology, compared women with and those without chronic liver disease who had normal ovarian reserve and who underwent assisted reproductive technology (ART) treatment in a high-volume fertility practice from 2002 to 2021.
“IVF treatment and pregnancy outcomes were not significantly different compared to controls,” the researchers wrote.
Women with liver disease may experience impaired fertility. For example, women with chronic liver disease, such as hepatitis C virus infection, may have premature ovarian insufficiency, while women with advanced liver disease, cirrhosis, and hepatic decompensation are known to have abnormally low gonadotropin levels.
leading to “an immediate need for the clinical assessment of reproductive potential in women with chronic liver disease,” the authors wrote.
The literature about ART treatment outcomes for women with liver disease was limited and may not reflect current therapy protocols, researchers found.
“To the best of our knowledge, this study is the largest to date to evaluate IVF efficacy in women with liver disease,” they wrote.
Similar outcomes
Researchers identified 295 women with liver disease (mean age, 37.8 ± 5.2 years) who underwent 1,033 contemporary, standard ART treatment cycles. Six patients (2%) had cirrhosis, eight (2.7%) had undergone liver transplantation, and 281 (95.3%) had chronic liver disease, of which viral hepatitis B and C infections were the most prevalent. The final study population consisted of 115 women who underwent 186 IVF cycles, as well as embryo biopsy for genetic testing.
The control group consisted of all the women at the treatment center without liver disease who received contemporary, standard ART treatment because of male factor infertility, which served as an indication that the women had normal ovarian reserve and were considered fertile. These 624 patients underwent 868 IVF cycles with embryo biopsy.
The mean age of the patients with liver disease was significantly higher than that of the control participants. Mean body mass index was also significantly higher for the patients with liver disease, and there were differences in baseline levels of selected hormones, compared with control participants. In addition, among those with liver disease, the number of oocytes retrieved was significantly lower (12.3 ± 7.6 vs. 16.5 ± 8.2; P < .05), as were the number of mature oocytes (9.1 ± 6.2 vs. 12.6 ± 6.7; P < .05), the number of fertilized embryos (7.0 ± 5.2 vs. 9.9 ± 5.9; P < .05), the number of embryos for which biopsy was performed (3.4 ± 2.2 vs. 5.1 ± 3.5; P < .05), and the number of euploid embryos (1.6 ± 1.4 vs. 2.7 ± 2.4; P < .05), compared with control participants.
Among the two groups, there were no statistically significant differences in mature oocyte rate (an indicator of response to controlled ovarian stimulation), fertilization per mature oocyte rate (an indicator of oocyte quality and ability to be fertilized), or embryo ploidy rate (an indicator of genetically normal embryos), as determined by embryo biopsy, the researchers write.
A subanalysis of women who went on to have a single thawed euploid (chromosomally normal) embryo transfer to achieve pregnancy found no statistically significant differences in rates of clinical pregnancy, clinical pregnancy loss, or live births between the liver disease group and the control group.
“Overall, women with chronic liver disease can be counseled that IVF treatment will not significantly differ in response to controlled ovarian stimulation, embryo fertilization rate, or ploidy outcome compared to women without liver disease,” the researchers wrote.
Data for patient counseling
The results could change the current common thinking among clinicians that IVF should not be conducted until liver disease is under optimal control, first author Jessica Lee, BS, a student at Icahn School of Medicine at Mount Sinai, New York, said.
“There was a knowledge gap for studies in the United States, and we hope this study will not only help patients with liver disease but also providers with counseling,” she said.
The findings suggest that “even if you have chronic liver disease and it’s not fully optimized, that should not interfere with pursuing IVF,” said principal investigator Tatyana Kushner, MD, an associate professor of medicine in liver diseases at the Icahn School.
Women with liver disease whose fertility is impaired should receive counseling about fertility preservation options earlier to help access fertility care, the researchers write.
The study’s findings are “encouraging,” said Monika Sarkar, MD, associate professor of medicine in gastroenterology at the University of California, San Francisco.
“With rising numbers of young adults with liver disease, it is encouraging to see dedicated studies that address a topic of importance to our patients – namely, their reproductive health,” she said. “The current study nicely expands beyond previous data to include a control population without liver disease.”
Differences in oocyte numbers
Although there were no differences in the success rate of embryo transfer, the researchers did see differences in the number of oocytes. Only 37 mature oocytes made it to transfer in the liver disease group, compared with 609 in the control group, noted Dr. Sarkar, who was not involved with the study.
“The challenge of ART is less at the level of embryo transfer, which is very successful once a euploid embryo is achieved, but rather at the earlier step of retrieval of mature oocytes,” Dr. Sarkar said. “Here, the authors found that patients with liver disease had a significantly lower number of oocytes retrieved, number of mature oocytes, and lower number of fertilized embryos.”
The data suggest that fewer eggs are retrieved per cycle from patients with liver disease, “which ultimately will lower the success per cycle,” Dr. Sarkar said.
“This suggests that referring women with chronic liver disease to ART sooner may help to optimize outcomes,” she added. “Larger data evaluating ability to achieve mature oocytes and subsequent fertilization will also be key for determining whether ART success differs by presence, severity, and type of liver disease.”
As more research on ART outcomes in women with liver disease is conducted, subspecialists in gastrointestinal and liver disease may gain confidence in counseling patients, Dr. Sarkar said.
Ms. Lee, Dr. Kushner, and Dr. Sarkar report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Having chronic liver disease does not affect outcomes for women who undergo in vitro fertilization (IVF), new research suggests.
The study, published online in the American Journal of Gastroenterology, compared women with and those without chronic liver disease who had normal ovarian reserve and who underwent assisted reproductive technology (ART) treatment in a high-volume fertility practice from 2002 to 2021.
“IVF treatment and pregnancy outcomes were not significantly different compared to controls,” the researchers wrote.
Women with liver disease may experience impaired fertility. For example, women with chronic liver disease, such as hepatitis C virus infection, may have premature ovarian insufficiency, while women with advanced liver disease, cirrhosis, and hepatic decompensation are known to have abnormally low gonadotropin levels.
leading to “an immediate need for the clinical assessment of reproductive potential in women with chronic liver disease,” the authors wrote.
The literature about ART treatment outcomes for women with liver disease was limited and may not reflect current therapy protocols, researchers found.
“To the best of our knowledge, this study is the largest to date to evaluate IVF efficacy in women with liver disease,” they wrote.
Similar outcomes
Researchers identified 295 women with liver disease (mean age, 37.8 ± 5.2 years) who underwent 1,033 contemporary, standard ART treatment cycles. Six patients (2%) had cirrhosis, eight (2.7%) had undergone liver transplantation, and 281 (95.3%) had chronic liver disease, of which viral hepatitis B and C infections were the most prevalent. The final study population consisted of 115 women who underwent 186 IVF cycles, as well as embryo biopsy for genetic testing.
The control group consisted of all the women at the treatment center without liver disease who received contemporary, standard ART treatment because of male factor infertility, which served as an indication that the women had normal ovarian reserve and were considered fertile. These 624 patients underwent 868 IVF cycles with embryo biopsy.
The mean age of the patients with liver disease was significantly higher than that of the control participants. Mean body mass index was also significantly higher for the patients with liver disease, and there were differences in baseline levels of selected hormones, compared with control participants. In addition, among those with liver disease, the number of oocytes retrieved was significantly lower (12.3 ± 7.6 vs. 16.5 ± 8.2; P < .05), as were the number of mature oocytes (9.1 ± 6.2 vs. 12.6 ± 6.7; P < .05), the number of fertilized embryos (7.0 ± 5.2 vs. 9.9 ± 5.9; P < .05), the number of embryos for which biopsy was performed (3.4 ± 2.2 vs. 5.1 ± 3.5; P < .05), and the number of euploid embryos (1.6 ± 1.4 vs. 2.7 ± 2.4; P < .05), compared with control participants.
Among the two groups, there were no statistically significant differences in mature oocyte rate (an indicator of response to controlled ovarian stimulation), fertilization per mature oocyte rate (an indicator of oocyte quality and ability to be fertilized), or embryo ploidy rate (an indicator of genetically normal embryos), as determined by embryo biopsy, the researchers write.
A subanalysis of women who went on to have a single thawed euploid (chromosomally normal) embryo transfer to achieve pregnancy found no statistically significant differences in rates of clinical pregnancy, clinical pregnancy loss, or live births between the liver disease group and the control group.
“Overall, women with chronic liver disease can be counseled that IVF treatment will not significantly differ in response to controlled ovarian stimulation, embryo fertilization rate, or ploidy outcome compared to women without liver disease,” the researchers wrote.
Data for patient counseling
The results could change the current common thinking among clinicians that IVF should not be conducted until liver disease is under optimal control, first author Jessica Lee, BS, a student at Icahn School of Medicine at Mount Sinai, New York, said.
“There was a knowledge gap for studies in the United States, and we hope this study will not only help patients with liver disease but also providers with counseling,” she said.
The findings suggest that “even if you have chronic liver disease and it’s not fully optimized, that should not interfere with pursuing IVF,” said principal investigator Tatyana Kushner, MD, an associate professor of medicine in liver diseases at the Icahn School.
Women with liver disease whose fertility is impaired should receive counseling about fertility preservation options earlier to help access fertility care, the researchers write.
The study’s findings are “encouraging,” said Monika Sarkar, MD, associate professor of medicine in gastroenterology at the University of California, San Francisco.
“With rising numbers of young adults with liver disease, it is encouraging to see dedicated studies that address a topic of importance to our patients – namely, their reproductive health,” she said. “The current study nicely expands beyond previous data to include a control population without liver disease.”
Differences in oocyte numbers
Although there were no differences in the success rate of embryo transfer, the researchers did see differences in the number of oocytes. Only 37 mature oocytes made it to transfer in the liver disease group, compared with 609 in the control group, noted Dr. Sarkar, who was not involved with the study.
“The challenge of ART is less at the level of embryo transfer, which is very successful once a euploid embryo is achieved, but rather at the earlier step of retrieval of mature oocytes,” Dr. Sarkar said. “Here, the authors found that patients with liver disease had a significantly lower number of oocytes retrieved, number of mature oocytes, and lower number of fertilized embryos.”
The data suggest that fewer eggs are retrieved per cycle from patients with liver disease, “which ultimately will lower the success per cycle,” Dr. Sarkar said.
“This suggests that referring women with chronic liver disease to ART sooner may help to optimize outcomes,” she added. “Larger data evaluating ability to achieve mature oocytes and subsequent fertilization will also be key for determining whether ART success differs by presence, severity, and type of liver disease.”
As more research on ART outcomes in women with liver disease is conducted, subspecialists in gastrointestinal and liver disease may gain confidence in counseling patients, Dr. Sarkar said.
Ms. Lee, Dr. Kushner, and Dr. Sarkar report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE AMERICAN JOURNAL OF GASTROENTEROLOGY
RA causally associated with ischemic heart disease and myocardial infarction
Key clinical point: Rheumatoid arthritis (RA) is associated with a significant increase in the risk for ischemic heart disease (IHD) and myocardial infarction (MI), and managing RA activity may reduce the risk for cardiovascular diseases.
Major finding: RA is significantly associated with an increased risk for IHD (odds ratio [OR] 1.0006; P = .001551915) and MI (OR 1.0458; P = .001636), but not arrhythmia and atrial fibrillation.
Study details: Findings are from a two-sample Mendelian randomization study including patients and matched control individuals for RA (n = 14,361 and n = 43,923, respectively), MI (n = 12,801 and n = 187,840, respectively), IHD (n = 5861 and n = 457,149, respectively), atrial fibrillation (n = 60,620 and n = 970,216, respectively), and arrhythmia (n = 2545 and n = 460,388, respectively).
Disclosures: This study was supported by the Young Talent Development Plan of Changzhou Health Commission, China, and other sources. The authors declared no conflicts of interest.
Source: Wang M et al. Relationship between rheumatoid arthritis and cardiovascular comorbidity, causation or co-occurrence: A Mendelian randomization study. Front Cardiovasc Med. 2023;10:1099861 (Mar 17). Doi: 10.3389/fcvm.2023.1099861
Key clinical point: Rheumatoid arthritis (RA) is associated with a significant increase in the risk for ischemic heart disease (IHD) and myocardial infarction (MI), and managing RA activity may reduce the risk for cardiovascular diseases.
Major finding: RA is significantly associated with an increased risk for IHD (odds ratio [OR] 1.0006; P = .001551915) and MI (OR 1.0458; P = .001636), but not arrhythmia and atrial fibrillation.
Study details: Findings are from a two-sample Mendelian randomization study including patients and matched control individuals for RA (n = 14,361 and n = 43,923, respectively), MI (n = 12,801 and n = 187,840, respectively), IHD (n = 5861 and n = 457,149, respectively), atrial fibrillation (n = 60,620 and n = 970,216, respectively), and arrhythmia (n = 2545 and n = 460,388, respectively).
Disclosures: This study was supported by the Young Talent Development Plan of Changzhou Health Commission, China, and other sources. The authors declared no conflicts of interest.
Source: Wang M et al. Relationship between rheumatoid arthritis and cardiovascular comorbidity, causation or co-occurrence: A Mendelian randomization study. Front Cardiovasc Med. 2023;10:1099861 (Mar 17). Doi: 10.3389/fcvm.2023.1099861
Key clinical point: Rheumatoid arthritis (RA) is associated with a significant increase in the risk for ischemic heart disease (IHD) and myocardial infarction (MI), and managing RA activity may reduce the risk for cardiovascular diseases.
Major finding: RA is significantly associated with an increased risk for IHD (odds ratio [OR] 1.0006; P = .001551915) and MI (OR 1.0458; P = .001636), but not arrhythmia and atrial fibrillation.
Study details: Findings are from a two-sample Mendelian randomization study including patients and matched control individuals for RA (n = 14,361 and n = 43,923, respectively), MI (n = 12,801 and n = 187,840, respectively), IHD (n = 5861 and n = 457,149, respectively), atrial fibrillation (n = 60,620 and n = 970,216, respectively), and arrhythmia (n = 2545 and n = 460,388, respectively).
Disclosures: This study was supported by the Young Talent Development Plan of Changzhou Health Commission, China, and other sources. The authors declared no conflicts of interest.
Source: Wang M et al. Relationship between rheumatoid arthritis and cardiovascular comorbidity, causation or co-occurrence: A Mendelian randomization study. Front Cardiovasc Med. 2023;10:1099861 (Mar 17). Doi: 10.3389/fcvm.2023.1099861