User login
Postpartum urinary retention: Intermittent catheterization may be best
Intermittent catheterization every 6 hours in postpartum women with urinary retention may be a better strategy than extended catheterization over 24 hours, a new prospective, randomized, controlled study suggests.
Patients who were catheterized every 6 hours took significantly less time to reach full relief than those who were catheterized for at least 24 hours (mean 10.2 ± 11.8 hours vs. 26.5 ± 9.0 hours, P < .001, respectively), Israeli researchers found. Their research was released at the Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“There was no difference in hospital stay or in the rate of positive urine culture after catheter removal,” said ob.gyn. Dana Vitner, MD, of Rambam Health Care Campus in Haifa, Israel, in a presentation at the conference. “Our conclusion is that intermittent catheterization for postpartum urinary retention results in shorter time to resolution with a higher satisfaction rate and no additional complications.”
The true incidence of postpartum urinary retention is unclear, and estimates vary widely, said ob.gyn. and surgeon Lisa Hickman, MD, of the Ohio State University, Columbus, in an interview. “This is likely because many cases of covert urinary retention – when postpartum women are able to urinate but have incomplete emptying – go undiagnosed unless you are screening for it.”
According to Dr. Hickman, risk factors for postpartum urinary retention include operative vaginal births, having an epidural, obstetric anal sphincter injury, episiotomy, large newborns, first-time births, and prolonged induction of labor. Most cases resolve within 72 hours, she said, but they can lead to rare complications such as bladder injury.
For the new study, researchers defined urinary retention at the bladder holding least 150 mL more than 6 hours after vaginal delivery or removal of an in-dwelling catheter after cesarean delivery. “The treatment is catheterization,” Dr. Vitner said. “However, there is no standard protocol.”
From 2020 to 2022, researchers randomly assigned 73 women to the intermittent catheterization group and 74 to continuous catheterization. The average ages in the groups were 27.7 and 29.1 years, respectively (P = .11) and other characteristics such as body mass index, parity, infant birth weight, and mode of delivery were similar.
Most women in the intermittent catheterization group needed just one catheterization to reach resolution (75.3%); 93.2% had resolution after two, and 95.9% reached it after three. All resolved their urinary retention by 48 hours.
In the continuous catheterization group, 90.5% reached resolution at 24 hours, 97.3% at 48 hours, and 100% at 72 hours. Birth satisfaction scores were higher in the intermittent catheterization group (P < .001).
Dr. Hickman, who did not take part in the study, said the findings are helpful. Randomized, controlled trials are “important to get a better understanding of the natural history of this condition and ways to improve how we manage it clinically,” she said. Should intermittent catheterization become routine? “You need to have the staffing and the resources in order to do that, such as a bladder scanner and intermittent catheterization supplies,” Dr. Hickman said. “It can be time-intensive to continue to follow the patients to make sure they are voiding normally. And there may be many hospitals in the country that just don’t have the resources to do this, especially with all the current workforce issues.”
She added that some patients may not want the intermittent approach: “It can be uncomfortable for patients. They’ve just delivered a baby, they are likely experiencing discomfort from their delivery, and their anatomy can be distorted,” she said. “Some patients may say, ‘I would prefer you not insert a catheter into my bladder every few hours.’ They may just want to rest after having a baby.”
The best approach is to let patients make an informed choice, Dr. Hickman said. She recommended that clinicians say something like, “Because of your delivery, you are not able to empty your bladder all the way. This is typically a self-limited problem, meaning that it will likely resolve within a few days. But in the meantime, we need to let your bladder rest so that it can have time to start functioning on its own.” And then, she said, explain the catheterization options.
Dr. Vitner and Dr. Hickman have no disclosures.
Intermittent catheterization every 6 hours in postpartum women with urinary retention may be a better strategy than extended catheterization over 24 hours, a new prospective, randomized, controlled study suggests.
Patients who were catheterized every 6 hours took significantly less time to reach full relief than those who were catheterized for at least 24 hours (mean 10.2 ± 11.8 hours vs. 26.5 ± 9.0 hours, P < .001, respectively), Israeli researchers found. Their research was released at the Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“There was no difference in hospital stay or in the rate of positive urine culture after catheter removal,” said ob.gyn. Dana Vitner, MD, of Rambam Health Care Campus in Haifa, Israel, in a presentation at the conference. “Our conclusion is that intermittent catheterization for postpartum urinary retention results in shorter time to resolution with a higher satisfaction rate and no additional complications.”
The true incidence of postpartum urinary retention is unclear, and estimates vary widely, said ob.gyn. and surgeon Lisa Hickman, MD, of the Ohio State University, Columbus, in an interview. “This is likely because many cases of covert urinary retention – when postpartum women are able to urinate but have incomplete emptying – go undiagnosed unless you are screening for it.”
According to Dr. Hickman, risk factors for postpartum urinary retention include operative vaginal births, having an epidural, obstetric anal sphincter injury, episiotomy, large newborns, first-time births, and prolonged induction of labor. Most cases resolve within 72 hours, she said, but they can lead to rare complications such as bladder injury.
For the new study, researchers defined urinary retention at the bladder holding least 150 mL more than 6 hours after vaginal delivery or removal of an in-dwelling catheter after cesarean delivery. “The treatment is catheterization,” Dr. Vitner said. “However, there is no standard protocol.”
From 2020 to 2022, researchers randomly assigned 73 women to the intermittent catheterization group and 74 to continuous catheterization. The average ages in the groups were 27.7 and 29.1 years, respectively (P = .11) and other characteristics such as body mass index, parity, infant birth weight, and mode of delivery were similar.
Most women in the intermittent catheterization group needed just one catheterization to reach resolution (75.3%); 93.2% had resolution after two, and 95.9% reached it after three. All resolved their urinary retention by 48 hours.
In the continuous catheterization group, 90.5% reached resolution at 24 hours, 97.3% at 48 hours, and 100% at 72 hours. Birth satisfaction scores were higher in the intermittent catheterization group (P < .001).
Dr. Hickman, who did not take part in the study, said the findings are helpful. Randomized, controlled trials are “important to get a better understanding of the natural history of this condition and ways to improve how we manage it clinically,” she said. Should intermittent catheterization become routine? “You need to have the staffing and the resources in order to do that, such as a bladder scanner and intermittent catheterization supplies,” Dr. Hickman said. “It can be time-intensive to continue to follow the patients to make sure they are voiding normally. And there may be many hospitals in the country that just don’t have the resources to do this, especially with all the current workforce issues.”
She added that some patients may not want the intermittent approach: “It can be uncomfortable for patients. They’ve just delivered a baby, they are likely experiencing discomfort from their delivery, and their anatomy can be distorted,” she said. “Some patients may say, ‘I would prefer you not insert a catheter into my bladder every few hours.’ They may just want to rest after having a baby.”
The best approach is to let patients make an informed choice, Dr. Hickman said. She recommended that clinicians say something like, “Because of your delivery, you are not able to empty your bladder all the way. This is typically a self-limited problem, meaning that it will likely resolve within a few days. But in the meantime, we need to let your bladder rest so that it can have time to start functioning on its own.” And then, she said, explain the catheterization options.
Dr. Vitner and Dr. Hickman have no disclosures.
Intermittent catheterization every 6 hours in postpartum women with urinary retention may be a better strategy than extended catheterization over 24 hours, a new prospective, randomized, controlled study suggests.
Patients who were catheterized every 6 hours took significantly less time to reach full relief than those who were catheterized for at least 24 hours (mean 10.2 ± 11.8 hours vs. 26.5 ± 9.0 hours, P < .001, respectively), Israeli researchers found. Their research was released at the Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“There was no difference in hospital stay or in the rate of positive urine culture after catheter removal,” said ob.gyn. Dana Vitner, MD, of Rambam Health Care Campus in Haifa, Israel, in a presentation at the conference. “Our conclusion is that intermittent catheterization for postpartum urinary retention results in shorter time to resolution with a higher satisfaction rate and no additional complications.”
The true incidence of postpartum urinary retention is unclear, and estimates vary widely, said ob.gyn. and surgeon Lisa Hickman, MD, of the Ohio State University, Columbus, in an interview. “This is likely because many cases of covert urinary retention – when postpartum women are able to urinate but have incomplete emptying – go undiagnosed unless you are screening for it.”
According to Dr. Hickman, risk factors for postpartum urinary retention include operative vaginal births, having an epidural, obstetric anal sphincter injury, episiotomy, large newborns, first-time births, and prolonged induction of labor. Most cases resolve within 72 hours, she said, but they can lead to rare complications such as bladder injury.
For the new study, researchers defined urinary retention at the bladder holding least 150 mL more than 6 hours after vaginal delivery or removal of an in-dwelling catheter after cesarean delivery. “The treatment is catheterization,” Dr. Vitner said. “However, there is no standard protocol.”
From 2020 to 2022, researchers randomly assigned 73 women to the intermittent catheterization group and 74 to continuous catheterization. The average ages in the groups were 27.7 and 29.1 years, respectively (P = .11) and other characteristics such as body mass index, parity, infant birth weight, and mode of delivery were similar.
Most women in the intermittent catheterization group needed just one catheterization to reach resolution (75.3%); 93.2% had resolution after two, and 95.9% reached it after three. All resolved their urinary retention by 48 hours.
In the continuous catheterization group, 90.5% reached resolution at 24 hours, 97.3% at 48 hours, and 100% at 72 hours. Birth satisfaction scores were higher in the intermittent catheterization group (P < .001).
Dr. Hickman, who did not take part in the study, said the findings are helpful. Randomized, controlled trials are “important to get a better understanding of the natural history of this condition and ways to improve how we manage it clinically,” she said. Should intermittent catheterization become routine? “You need to have the staffing and the resources in order to do that, such as a bladder scanner and intermittent catheterization supplies,” Dr. Hickman said. “It can be time-intensive to continue to follow the patients to make sure they are voiding normally. And there may be many hospitals in the country that just don’t have the resources to do this, especially with all the current workforce issues.”
She added that some patients may not want the intermittent approach: “It can be uncomfortable for patients. They’ve just delivered a baby, they are likely experiencing discomfort from their delivery, and their anatomy can be distorted,” she said. “Some patients may say, ‘I would prefer you not insert a catheter into my bladder every few hours.’ They may just want to rest after having a baby.”
The best approach is to let patients make an informed choice, Dr. Hickman said. She recommended that clinicians say something like, “Because of your delivery, you are not able to empty your bladder all the way. This is typically a self-limited problem, meaning that it will likely resolve within a few days. But in the meantime, we need to let your bladder rest so that it can have time to start functioning on its own.” And then, she said, explain the catheterization options.
Dr. Vitner and Dr. Hickman have no disclosures.
FROM THE PREGNANCY MEETING
Meningococcal vaccine shows benefit in STI prevention
The latest study to show high efficacy of doxycycline post-exposure prophylaxis (Doxy PEP) in preventing sexually transmitted infections among men who have sex with men (MSM) adds a new twist, showing – for the first time – reductions in gonorrhea among those receiving the meningococcal B vaccine.
said first author Jean-Michel Molina, MD, PhD, in presenting the findings at the Conference on Retroviruses and Opportunistic Infections.
In addition, “two doses of the meningococcal B vaccine reduced the incidence of a first episode of gonorrhea by roughly 50% among men who have sex with men,” said Dr. Molina, a professor of infectious diseases at the University of Paris, and head of the Infectious Diseases Department at the Saint-Louis and Lariboisière Hospitals, Paris.
Whereas the advent of PrEP has been associated with significant reductions in HIV transmission, rates of STIs have conversely been on the rise among MSM, specifically among those receiving PrEP.
Post-exposure prophylaxis with Doxy PEP has been shown to reduce the incidence of chlamydia and syphilis by approximately 70%; however, effects on prevention of gonorrhea have been less clear.
Meningococcal B vaccination has, meanwhile, shown intriguing reductions of gonorrhea incidence of as much as 26%-46% in some observational studies.
Therefore, Dr. Molina and colleagues decided to further investigate Doxy PEP as well as the meningococcal B vaccine in prevention of STIs.
For the ANRS 174 DOXYVAC trial, they enrolled 546 MSM in the open-label, multicenter study between January 2021 and July 2022.
The men were randomly assigned to one of 4 groups: doxycycline postexposure prophylaxis (Doxy PEP: 200 mg; n = 332), no Doxy PEP (n = 170), two shots of meningococcal B vaccine (4CMenB vaccine; n = 257), or no 4CMenB vaccine (n = 245).
All participants were assigned to their groups within 72 hours of condomless sex.
The men, who had a median age of 39, had a median time of PrEP use of 42 months, a history of an STI in the past year, and their median number of sexual partners in the past 3 months was 10.
Their characteristics were well-balanced across the treatment groups. After discontinuations of 54 patients across the groups, the final analysis included 502 participants.
With a median follow-up of 9 months, the intent-to-treat analysis showed 13 subjects had a first episode of chlamydia or syphilis in the Doxy PEP group, versus 49 subjects infected in the no Doxy PEP arm, for an incidence of 5.6 versus 35.4 per 100 person-years, respectively (adjusted hazard ratio, 0.16; P < .0001).
Infection specifically with chlamydia occurred among 21 men with no Doxy PEP versus 5 receiving Dox PEP (19.3 vs. 2.1 per 100 person-years, respectively; HR, 0.11; P < .0001).
And infection with syphilis occurred in 18 men receiving no Doxy PEP versus 8 receiving the treatment (16.3 vs. 3.4 per 100 person-years, respectively; HR, 0.21; P < .001).
The corresponding rates for gonorrhea infection were an incidence 41.3 versus 20.5 per 100 person-years, in the no Doxy PEP versus Doxy PEP arms, respectively (adjusted HR, 0.49; P = .001), and 29.4 versus 16.8 per 100 person-years for Mycoplasma genitalium infection (aHR, 0.55; P = .015).
Throughout the study, about 80% of patients in the Doxy PEP group reported using the prophylaxis treatment after their most recent sexual intercourse, with subjects reporting taking a median of seven pills per month.
In the vaccine/no vaccine comparisons, 32 subjects in the no meningococcal vaccine group were infected with a first gonorrhea infection, compared with 17 in the vaccine group, representing an incidence of 19.7 versus 9.8 per 100 person-years, respectively (adjusted HR, 0.49; P = .016), which Dr. Molina called “highly significant.”
An analysis of the cumulative incidence of gonorrhea infection with the meningococcal vaccine showed rates in the no vaccine versus vaccine groups of 30.4 versus 20.1 per 100 person-years, respectively; however, statistical significance was not reached (aHR, 0.66; P = .052).
Importantly, there were no significant interactions in the results between those receiving Doxy PEP or the 4CMenB vaccine group, and there were no significant differences in drug-related serious adverse events between the groups.
Dr. Molina noted that the meningococcal B vaccine is known to contain key antigens that are shared between meningitis and gonorrhea, which could explain the benefits.
Although chlamydia and syphilis thus far appear to remain susceptible to Doxy PEP, resistances with gonorrhea remain a concern, hence the ability of the vaccine to provide some protection could be an added bonus.
“We know that [gonorrhea] is able to very quickly develop resistances to any antibiotics, so that was why we wanted to look beyond the antibiotic prophylaxis,” said Dr. Molina.
Among questions to explore looking ahead is the potential longevity of protection with the vaccine.
“We don’t know at this point how long the protection with the vaccine could last, or if [people] may need booster injections, for instance, but the literature suggests benefits for at least a year,” Dr. Molina said. “We are still monitoring the patients in the study to see what happens.”
He added that combination of the interventions may be of benefit.
“In the future, we think we may need to combine these approaches if we want to meet the WHO/UNAIDS targets to reduce the incidence of HIV and STIs by 90% by 2030.”
Commenting on the study, CROI vice-chair Landon Myer, MD, PhD, noted that “gonorrhea develops resistance quickly and can be hard to treat or prophylaxis, so the vaccine finding, which was hinted at by previous observational data, is really important.”
He agrees that “the duration of protective efficacy – a big thing in vaccines – is unknown.”
“Still, this is really significant,” Dr. Myer stressed. “An efficacious vaccine against a stubborn sexually transmitted infection.”
A version of this article first appeared on Medscape.com.
The latest study to show high efficacy of doxycycline post-exposure prophylaxis (Doxy PEP) in preventing sexually transmitted infections among men who have sex with men (MSM) adds a new twist, showing – for the first time – reductions in gonorrhea among those receiving the meningococcal B vaccine.
said first author Jean-Michel Molina, MD, PhD, in presenting the findings at the Conference on Retroviruses and Opportunistic Infections.
In addition, “two doses of the meningococcal B vaccine reduced the incidence of a first episode of gonorrhea by roughly 50% among men who have sex with men,” said Dr. Molina, a professor of infectious diseases at the University of Paris, and head of the Infectious Diseases Department at the Saint-Louis and Lariboisière Hospitals, Paris.
Whereas the advent of PrEP has been associated with significant reductions in HIV transmission, rates of STIs have conversely been on the rise among MSM, specifically among those receiving PrEP.
Post-exposure prophylaxis with Doxy PEP has been shown to reduce the incidence of chlamydia and syphilis by approximately 70%; however, effects on prevention of gonorrhea have been less clear.
Meningococcal B vaccination has, meanwhile, shown intriguing reductions of gonorrhea incidence of as much as 26%-46% in some observational studies.
Therefore, Dr. Molina and colleagues decided to further investigate Doxy PEP as well as the meningococcal B vaccine in prevention of STIs.
For the ANRS 174 DOXYVAC trial, they enrolled 546 MSM in the open-label, multicenter study between January 2021 and July 2022.
The men were randomly assigned to one of 4 groups: doxycycline postexposure prophylaxis (Doxy PEP: 200 mg; n = 332), no Doxy PEP (n = 170), two shots of meningococcal B vaccine (4CMenB vaccine; n = 257), or no 4CMenB vaccine (n = 245).
All participants were assigned to their groups within 72 hours of condomless sex.
The men, who had a median age of 39, had a median time of PrEP use of 42 months, a history of an STI in the past year, and their median number of sexual partners in the past 3 months was 10.
Their characteristics were well-balanced across the treatment groups. After discontinuations of 54 patients across the groups, the final analysis included 502 participants.
With a median follow-up of 9 months, the intent-to-treat analysis showed 13 subjects had a first episode of chlamydia or syphilis in the Doxy PEP group, versus 49 subjects infected in the no Doxy PEP arm, for an incidence of 5.6 versus 35.4 per 100 person-years, respectively (adjusted hazard ratio, 0.16; P < .0001).
Infection specifically with chlamydia occurred among 21 men with no Doxy PEP versus 5 receiving Dox PEP (19.3 vs. 2.1 per 100 person-years, respectively; HR, 0.11; P < .0001).
And infection with syphilis occurred in 18 men receiving no Doxy PEP versus 8 receiving the treatment (16.3 vs. 3.4 per 100 person-years, respectively; HR, 0.21; P < .001).
The corresponding rates for gonorrhea infection were an incidence 41.3 versus 20.5 per 100 person-years, in the no Doxy PEP versus Doxy PEP arms, respectively (adjusted HR, 0.49; P = .001), and 29.4 versus 16.8 per 100 person-years for Mycoplasma genitalium infection (aHR, 0.55; P = .015).
Throughout the study, about 80% of patients in the Doxy PEP group reported using the prophylaxis treatment after their most recent sexual intercourse, with subjects reporting taking a median of seven pills per month.
In the vaccine/no vaccine comparisons, 32 subjects in the no meningococcal vaccine group were infected with a first gonorrhea infection, compared with 17 in the vaccine group, representing an incidence of 19.7 versus 9.8 per 100 person-years, respectively (adjusted HR, 0.49; P = .016), which Dr. Molina called “highly significant.”
An analysis of the cumulative incidence of gonorrhea infection with the meningococcal vaccine showed rates in the no vaccine versus vaccine groups of 30.4 versus 20.1 per 100 person-years, respectively; however, statistical significance was not reached (aHR, 0.66; P = .052).
Importantly, there were no significant interactions in the results between those receiving Doxy PEP or the 4CMenB vaccine group, and there were no significant differences in drug-related serious adverse events between the groups.
Dr. Molina noted that the meningococcal B vaccine is known to contain key antigens that are shared between meningitis and gonorrhea, which could explain the benefits.
Although chlamydia and syphilis thus far appear to remain susceptible to Doxy PEP, resistances with gonorrhea remain a concern, hence the ability of the vaccine to provide some protection could be an added bonus.
“We know that [gonorrhea] is able to very quickly develop resistances to any antibiotics, so that was why we wanted to look beyond the antibiotic prophylaxis,” said Dr. Molina.
Among questions to explore looking ahead is the potential longevity of protection with the vaccine.
“We don’t know at this point how long the protection with the vaccine could last, or if [people] may need booster injections, for instance, but the literature suggests benefits for at least a year,” Dr. Molina said. “We are still monitoring the patients in the study to see what happens.”
He added that combination of the interventions may be of benefit.
“In the future, we think we may need to combine these approaches if we want to meet the WHO/UNAIDS targets to reduce the incidence of HIV and STIs by 90% by 2030.”
Commenting on the study, CROI vice-chair Landon Myer, MD, PhD, noted that “gonorrhea develops resistance quickly and can be hard to treat or prophylaxis, so the vaccine finding, which was hinted at by previous observational data, is really important.”
He agrees that “the duration of protective efficacy – a big thing in vaccines – is unknown.”
“Still, this is really significant,” Dr. Myer stressed. “An efficacious vaccine against a stubborn sexually transmitted infection.”
A version of this article first appeared on Medscape.com.
The latest study to show high efficacy of doxycycline post-exposure prophylaxis (Doxy PEP) in preventing sexually transmitted infections among men who have sex with men (MSM) adds a new twist, showing – for the first time – reductions in gonorrhea among those receiving the meningococcal B vaccine.
said first author Jean-Michel Molina, MD, PhD, in presenting the findings at the Conference on Retroviruses and Opportunistic Infections.
In addition, “two doses of the meningococcal B vaccine reduced the incidence of a first episode of gonorrhea by roughly 50% among men who have sex with men,” said Dr. Molina, a professor of infectious diseases at the University of Paris, and head of the Infectious Diseases Department at the Saint-Louis and Lariboisière Hospitals, Paris.
Whereas the advent of PrEP has been associated with significant reductions in HIV transmission, rates of STIs have conversely been on the rise among MSM, specifically among those receiving PrEP.
Post-exposure prophylaxis with Doxy PEP has been shown to reduce the incidence of chlamydia and syphilis by approximately 70%; however, effects on prevention of gonorrhea have been less clear.
Meningococcal B vaccination has, meanwhile, shown intriguing reductions of gonorrhea incidence of as much as 26%-46% in some observational studies.
Therefore, Dr. Molina and colleagues decided to further investigate Doxy PEP as well as the meningococcal B vaccine in prevention of STIs.
For the ANRS 174 DOXYVAC trial, they enrolled 546 MSM in the open-label, multicenter study between January 2021 and July 2022.
The men were randomly assigned to one of 4 groups: doxycycline postexposure prophylaxis (Doxy PEP: 200 mg; n = 332), no Doxy PEP (n = 170), two shots of meningococcal B vaccine (4CMenB vaccine; n = 257), or no 4CMenB vaccine (n = 245).
All participants were assigned to their groups within 72 hours of condomless sex.
The men, who had a median age of 39, had a median time of PrEP use of 42 months, a history of an STI in the past year, and their median number of sexual partners in the past 3 months was 10.
Their characteristics were well-balanced across the treatment groups. After discontinuations of 54 patients across the groups, the final analysis included 502 participants.
With a median follow-up of 9 months, the intent-to-treat analysis showed 13 subjects had a first episode of chlamydia or syphilis in the Doxy PEP group, versus 49 subjects infected in the no Doxy PEP arm, for an incidence of 5.6 versus 35.4 per 100 person-years, respectively (adjusted hazard ratio, 0.16; P < .0001).
Infection specifically with chlamydia occurred among 21 men with no Doxy PEP versus 5 receiving Dox PEP (19.3 vs. 2.1 per 100 person-years, respectively; HR, 0.11; P < .0001).
And infection with syphilis occurred in 18 men receiving no Doxy PEP versus 8 receiving the treatment (16.3 vs. 3.4 per 100 person-years, respectively; HR, 0.21; P < .001).
The corresponding rates for gonorrhea infection were an incidence 41.3 versus 20.5 per 100 person-years, in the no Doxy PEP versus Doxy PEP arms, respectively (adjusted HR, 0.49; P = .001), and 29.4 versus 16.8 per 100 person-years for Mycoplasma genitalium infection (aHR, 0.55; P = .015).
Throughout the study, about 80% of patients in the Doxy PEP group reported using the prophylaxis treatment after their most recent sexual intercourse, with subjects reporting taking a median of seven pills per month.
In the vaccine/no vaccine comparisons, 32 subjects in the no meningococcal vaccine group were infected with a first gonorrhea infection, compared with 17 in the vaccine group, representing an incidence of 19.7 versus 9.8 per 100 person-years, respectively (adjusted HR, 0.49; P = .016), which Dr. Molina called “highly significant.”
An analysis of the cumulative incidence of gonorrhea infection with the meningococcal vaccine showed rates in the no vaccine versus vaccine groups of 30.4 versus 20.1 per 100 person-years, respectively; however, statistical significance was not reached (aHR, 0.66; P = .052).
Importantly, there were no significant interactions in the results between those receiving Doxy PEP or the 4CMenB vaccine group, and there were no significant differences in drug-related serious adverse events between the groups.
Dr. Molina noted that the meningococcal B vaccine is known to contain key antigens that are shared between meningitis and gonorrhea, which could explain the benefits.
Although chlamydia and syphilis thus far appear to remain susceptible to Doxy PEP, resistances with gonorrhea remain a concern, hence the ability of the vaccine to provide some protection could be an added bonus.
“We know that [gonorrhea] is able to very quickly develop resistances to any antibiotics, so that was why we wanted to look beyond the antibiotic prophylaxis,” said Dr. Molina.
Among questions to explore looking ahead is the potential longevity of protection with the vaccine.
“We don’t know at this point how long the protection with the vaccine could last, or if [people] may need booster injections, for instance, but the literature suggests benefits for at least a year,” Dr. Molina said. “We are still monitoring the patients in the study to see what happens.”
He added that combination of the interventions may be of benefit.
“In the future, we think we may need to combine these approaches if we want to meet the WHO/UNAIDS targets to reduce the incidence of HIV and STIs by 90% by 2030.”
Commenting on the study, CROI vice-chair Landon Myer, MD, PhD, noted that “gonorrhea develops resistance quickly and can be hard to treat or prophylaxis, so the vaccine finding, which was hinted at by previous observational data, is really important.”
He agrees that “the duration of protective efficacy – a big thing in vaccines – is unknown.”
“Still, this is really significant,” Dr. Myer stressed. “An efficacious vaccine against a stubborn sexually transmitted infection.”
A version of this article first appeared on Medscape.com.
FROM CROI 2023
Could your patients benefit? New trials in lung cancer
Untreated advanced non–small cell lung cancer (NSCLC). Adult patients with stage IIIB, IIIC, or IV disease without actionable genomic alterations can join a randomized, open-label, phase 3 study testing the survival advantage of datopotamab deruxtecan (Dato-DXd) (AstraZeneca/Daiichi Sankyo). Dato-DXd is one of a half dozen experimental antibody-drug conjugates that target TROP2, a transmembrane glycoprotein that is overexpressed in several solid tumors, including NSCLC. One group of participants will receive an intravenous (IV) infusion of Dato-DXd plus durvalumab (Imfinzi) for up to 4 years, and over the first 12 weeks, they will receive four rounds of IV carboplatin (Paraplatin). The other group will receive IV infusions of pembrolizumab (Keytruda) every 3 weeks plus a combination of standard IV chemotherapy appropriate for the patient’s histology (nonsquamous or squamous NSCLC). In the United States, centers in Arkansas, Nebraska, Ohio, and Texas started recruiting in December 2020; trial sites are planned in 16 other states and 23 other countries. The trialists plan to enroll 1,000 participants. Overall survival (OS) and progression-free survival (PFS) are the primary endpoints; quality of life (QoL) is not being tracked. More details at clinicaltrials.gov.
Untreated advanced or metastatic NSCLC. Adult patients in this clinical situation without actionable genomic alterations as well as those with a PD-L1 tumor proportion score (TPS) of < 50% are eligible to participate in a randomized, open-label, phase 3 trial of Dato-DXd in combination with pembrolizumab, with or without chemotherapy. One group of participants will receive IV Dato-DXd and pembrolizumab every 3 weeks. For the second group of patients, IV platinum chemotherapy will be added to the Dato-DXd and pembrolizumab for the first four rounds of treatment. The third group of individuals make up the comparator arm and will receive thrice-weekly IV pembrolizumab, pemetrexed (Alimta), plus platinum chemotherapy. All participants will be treated for approximately 2.5 years or until disease progression or death. The trial began recruiting 975 participants in Arizona, Florida, Maryland, and New Jersey, and in Japan in January 2023. The primary endpoints are OS and PFS; QoL will not be assessed. More details at clinicaltrials.gov.
Metastatic NSCLC. Individuals with this cancer who have a TPS of > 50% can also receive an antibody-drug conjugate targeting TROP2 in combination with pembrolizumab. This time, the product is sacituzumab govitecan (Trodelvy). The randomized, open-label phase 3 trial is testing whether the two drugs in combination improve survival and slow progression better than pembrolizumab alone. For approximately 2 years, one group of people in the trial will receive IV pembrolizumab every 3 weeks. The other group, in addition to the pembrolizumab, will receive IV sacituzumab govitecan weekly for 2 weeks then 1 week off until unacceptable toxicity, disease progression, withdrawal of consent, or death. Study sites in the states of Florida and Georgia, and in Australia, Taiwan, and Turkey, opened in February 2023 with the aim of recruiting 614 participants. Overall survival over 4 years and PFS are the primary outcomes. QoL is a secondary outcome. More details at clinicaltrials.gov.
Unresectable metastatic NSCLC. Individuals with this type of lung cancer are being recruited for a nonrandomized, phase 1/2 study to determine whether a combination of amivantamab (Rybrevant) and capmatinib (Tabrecta) is tolerable and more effective than either therapy alone. The two drugs inhibit different stages of mesenchymal-epithelial transition (MET), a step in cell development that is crucial for metastasis because it enhances cell mobility, invasion, and resistance to apoptosis. In the phase 1 study, participants will start with twice-daily tablets of capmatinib and IV amivantamab once weekly for 4 weeks then every 2 weeks. Doses will be adjusted on the basis of toxicities. In phase 2, a new group of participants will receive the refined doses for up to 2 years until progression or death. The study opened at the Oncology Institute of Hope and Innovation in Whittier, Calif., in December 2020 with the aim of recruiting 161 participants. Sites are gearing up in five more U.S. states and in Canada, Europe, and Asia. Objective response rate is the primary outcome of the phase 2 study, with OS and QoL as secondary endpoints. More details at clinicaltrials.gov.
Locally advanced or metastatic NSCLC with EGFR-exon-20 insertion mutations. Adults with this diagnosis who have not yet been treated and are not amenable to curative surgery or radiotherapy are sought for a randomized, open-label phase 3 trial testing whether investigational EGFR tyrosine-kinase inhibitor furmonertinib (from ArriVent) is more effective than chemotherapy for first-line treatment. Chemotherapy is currently standard of care in this indication with targeted therapies amivantamab-vmjw (Rybrevant) and mobocertinib succinate (Exkivity) as second-line options. Individuals in the trial will take daily tablets of furmonertinib or platinum-based IV chemotherapy for 32 months or until disease progression, whichever comes first. The study opened in December in sites across 15 U.S. states. Centers in a further nine states are gearing up, with the aim of enrolling a total of 375 people. The primary outcome is PFS. QoL and OS at 5 years are secondary outcomes. More details at clinicaltrials.gov.
NSCLC previously treated with at least one platinum chemotherapy and at least one targeted treatment. Adults aged 70 or younger with this type of lung cancer are eligible for a National Cancer Institute phase 2 investigation of autologous T-cell receptor (TCR) gene therapy. Unlike CAR T-cell therapy, which only reaches the 20% of cancer neoantigens that are expressed extracellularly, TCR technology can target the 80% of abnormal proteins that are expressed inside cancer cells. Participants will receive a single infusion of their own engineered T cells. They will attend follow-up visits every 3-6 months for 3 years, then join a long-term study in which they will be followed for 12 more years. The National Institutes of Health Clinical Center in Bethesda, Md., started recruiting for the trial’s 210 participants with one of a selection of solid cancers in February 2023. Response rate measured by objective tumor regression is the primary endpoint. OS and QoL will not be tracked. More details at clinicaltrials.gov.
All trial information is from the National Institutes of Health U.S. National Library of Medicine (online at clinicaltrials.gov).
A version of this article first appeared on Medscape.com.
Editor’s note: This article was changed on 24 February to remove an incorrect reference to osimertinib.
Untreated advanced non–small cell lung cancer (NSCLC). Adult patients with stage IIIB, IIIC, or IV disease without actionable genomic alterations can join a randomized, open-label, phase 3 study testing the survival advantage of datopotamab deruxtecan (Dato-DXd) (AstraZeneca/Daiichi Sankyo). Dato-DXd is one of a half dozen experimental antibody-drug conjugates that target TROP2, a transmembrane glycoprotein that is overexpressed in several solid tumors, including NSCLC. One group of participants will receive an intravenous (IV) infusion of Dato-DXd plus durvalumab (Imfinzi) for up to 4 years, and over the first 12 weeks, they will receive four rounds of IV carboplatin (Paraplatin). The other group will receive IV infusions of pembrolizumab (Keytruda) every 3 weeks plus a combination of standard IV chemotherapy appropriate for the patient’s histology (nonsquamous or squamous NSCLC). In the United States, centers in Arkansas, Nebraska, Ohio, and Texas started recruiting in December 2020; trial sites are planned in 16 other states and 23 other countries. The trialists plan to enroll 1,000 participants. Overall survival (OS) and progression-free survival (PFS) are the primary endpoints; quality of life (QoL) is not being tracked. More details at clinicaltrials.gov.
Untreated advanced or metastatic NSCLC. Adult patients in this clinical situation without actionable genomic alterations as well as those with a PD-L1 tumor proportion score (TPS) of < 50% are eligible to participate in a randomized, open-label, phase 3 trial of Dato-DXd in combination with pembrolizumab, with or without chemotherapy. One group of participants will receive IV Dato-DXd and pembrolizumab every 3 weeks. For the second group of patients, IV platinum chemotherapy will be added to the Dato-DXd and pembrolizumab for the first four rounds of treatment. The third group of individuals make up the comparator arm and will receive thrice-weekly IV pembrolizumab, pemetrexed (Alimta), plus platinum chemotherapy. All participants will be treated for approximately 2.5 years or until disease progression or death. The trial began recruiting 975 participants in Arizona, Florida, Maryland, and New Jersey, and in Japan in January 2023. The primary endpoints are OS and PFS; QoL will not be assessed. More details at clinicaltrials.gov.
Metastatic NSCLC. Individuals with this cancer who have a TPS of > 50% can also receive an antibody-drug conjugate targeting TROP2 in combination with pembrolizumab. This time, the product is sacituzumab govitecan (Trodelvy). The randomized, open-label phase 3 trial is testing whether the two drugs in combination improve survival and slow progression better than pembrolizumab alone. For approximately 2 years, one group of people in the trial will receive IV pembrolizumab every 3 weeks. The other group, in addition to the pembrolizumab, will receive IV sacituzumab govitecan weekly for 2 weeks then 1 week off until unacceptable toxicity, disease progression, withdrawal of consent, or death. Study sites in the states of Florida and Georgia, and in Australia, Taiwan, and Turkey, opened in February 2023 with the aim of recruiting 614 participants. Overall survival over 4 years and PFS are the primary outcomes. QoL is a secondary outcome. More details at clinicaltrials.gov.
Unresectable metastatic NSCLC. Individuals with this type of lung cancer are being recruited for a nonrandomized, phase 1/2 study to determine whether a combination of amivantamab (Rybrevant) and capmatinib (Tabrecta) is tolerable and more effective than either therapy alone. The two drugs inhibit different stages of mesenchymal-epithelial transition (MET), a step in cell development that is crucial for metastasis because it enhances cell mobility, invasion, and resistance to apoptosis. In the phase 1 study, participants will start with twice-daily tablets of capmatinib and IV amivantamab once weekly for 4 weeks then every 2 weeks. Doses will be adjusted on the basis of toxicities. In phase 2, a new group of participants will receive the refined doses for up to 2 years until progression or death. The study opened at the Oncology Institute of Hope and Innovation in Whittier, Calif., in December 2020 with the aim of recruiting 161 participants. Sites are gearing up in five more U.S. states and in Canada, Europe, and Asia. Objective response rate is the primary outcome of the phase 2 study, with OS and QoL as secondary endpoints. More details at clinicaltrials.gov.
Locally advanced or metastatic NSCLC with EGFR-exon-20 insertion mutations. Adults with this diagnosis who have not yet been treated and are not amenable to curative surgery or radiotherapy are sought for a randomized, open-label phase 3 trial testing whether investigational EGFR tyrosine-kinase inhibitor furmonertinib (from ArriVent) is more effective than chemotherapy for first-line treatment. Chemotherapy is currently standard of care in this indication with targeted therapies amivantamab-vmjw (Rybrevant) and mobocertinib succinate (Exkivity) as second-line options. Individuals in the trial will take daily tablets of furmonertinib or platinum-based IV chemotherapy for 32 months or until disease progression, whichever comes first. The study opened in December in sites across 15 U.S. states. Centers in a further nine states are gearing up, with the aim of enrolling a total of 375 people. The primary outcome is PFS. QoL and OS at 5 years are secondary outcomes. More details at clinicaltrials.gov.
NSCLC previously treated with at least one platinum chemotherapy and at least one targeted treatment. Adults aged 70 or younger with this type of lung cancer are eligible for a National Cancer Institute phase 2 investigation of autologous T-cell receptor (TCR) gene therapy. Unlike CAR T-cell therapy, which only reaches the 20% of cancer neoantigens that are expressed extracellularly, TCR technology can target the 80% of abnormal proteins that are expressed inside cancer cells. Participants will receive a single infusion of their own engineered T cells. They will attend follow-up visits every 3-6 months for 3 years, then join a long-term study in which they will be followed for 12 more years. The National Institutes of Health Clinical Center in Bethesda, Md., started recruiting for the trial’s 210 participants with one of a selection of solid cancers in February 2023. Response rate measured by objective tumor regression is the primary endpoint. OS and QoL will not be tracked. More details at clinicaltrials.gov.
All trial information is from the National Institutes of Health U.S. National Library of Medicine (online at clinicaltrials.gov).
A version of this article first appeared on Medscape.com.
Editor’s note: This article was changed on 24 February to remove an incorrect reference to osimertinib.
Untreated advanced non–small cell lung cancer (NSCLC). Adult patients with stage IIIB, IIIC, or IV disease without actionable genomic alterations can join a randomized, open-label, phase 3 study testing the survival advantage of datopotamab deruxtecan (Dato-DXd) (AstraZeneca/Daiichi Sankyo). Dato-DXd is one of a half dozen experimental antibody-drug conjugates that target TROP2, a transmembrane glycoprotein that is overexpressed in several solid tumors, including NSCLC. One group of participants will receive an intravenous (IV) infusion of Dato-DXd plus durvalumab (Imfinzi) for up to 4 years, and over the first 12 weeks, they will receive four rounds of IV carboplatin (Paraplatin). The other group will receive IV infusions of pembrolizumab (Keytruda) every 3 weeks plus a combination of standard IV chemotherapy appropriate for the patient’s histology (nonsquamous or squamous NSCLC). In the United States, centers in Arkansas, Nebraska, Ohio, and Texas started recruiting in December 2020; trial sites are planned in 16 other states and 23 other countries. The trialists plan to enroll 1,000 participants. Overall survival (OS) and progression-free survival (PFS) are the primary endpoints; quality of life (QoL) is not being tracked. More details at clinicaltrials.gov.
Untreated advanced or metastatic NSCLC. Adult patients in this clinical situation without actionable genomic alterations as well as those with a PD-L1 tumor proportion score (TPS) of < 50% are eligible to participate in a randomized, open-label, phase 3 trial of Dato-DXd in combination with pembrolizumab, with or without chemotherapy. One group of participants will receive IV Dato-DXd and pembrolizumab every 3 weeks. For the second group of patients, IV platinum chemotherapy will be added to the Dato-DXd and pembrolizumab for the first four rounds of treatment. The third group of individuals make up the comparator arm and will receive thrice-weekly IV pembrolizumab, pemetrexed (Alimta), plus platinum chemotherapy. All participants will be treated for approximately 2.5 years or until disease progression or death. The trial began recruiting 975 participants in Arizona, Florida, Maryland, and New Jersey, and in Japan in January 2023. The primary endpoints are OS and PFS; QoL will not be assessed. More details at clinicaltrials.gov.
Metastatic NSCLC. Individuals with this cancer who have a TPS of > 50% can also receive an antibody-drug conjugate targeting TROP2 in combination with pembrolizumab. This time, the product is sacituzumab govitecan (Trodelvy). The randomized, open-label phase 3 trial is testing whether the two drugs in combination improve survival and slow progression better than pembrolizumab alone. For approximately 2 years, one group of people in the trial will receive IV pembrolizumab every 3 weeks. The other group, in addition to the pembrolizumab, will receive IV sacituzumab govitecan weekly for 2 weeks then 1 week off until unacceptable toxicity, disease progression, withdrawal of consent, or death. Study sites in the states of Florida and Georgia, and in Australia, Taiwan, and Turkey, opened in February 2023 with the aim of recruiting 614 participants. Overall survival over 4 years and PFS are the primary outcomes. QoL is a secondary outcome. More details at clinicaltrials.gov.
Unresectable metastatic NSCLC. Individuals with this type of lung cancer are being recruited for a nonrandomized, phase 1/2 study to determine whether a combination of amivantamab (Rybrevant) and capmatinib (Tabrecta) is tolerable and more effective than either therapy alone. The two drugs inhibit different stages of mesenchymal-epithelial transition (MET), a step in cell development that is crucial for metastasis because it enhances cell mobility, invasion, and resistance to apoptosis. In the phase 1 study, participants will start with twice-daily tablets of capmatinib and IV amivantamab once weekly for 4 weeks then every 2 weeks. Doses will be adjusted on the basis of toxicities. In phase 2, a new group of participants will receive the refined doses for up to 2 years until progression or death. The study opened at the Oncology Institute of Hope and Innovation in Whittier, Calif., in December 2020 with the aim of recruiting 161 participants. Sites are gearing up in five more U.S. states and in Canada, Europe, and Asia. Objective response rate is the primary outcome of the phase 2 study, with OS and QoL as secondary endpoints. More details at clinicaltrials.gov.
Locally advanced or metastatic NSCLC with EGFR-exon-20 insertion mutations. Adults with this diagnosis who have not yet been treated and are not amenable to curative surgery or radiotherapy are sought for a randomized, open-label phase 3 trial testing whether investigational EGFR tyrosine-kinase inhibitor furmonertinib (from ArriVent) is more effective than chemotherapy for first-line treatment. Chemotherapy is currently standard of care in this indication with targeted therapies amivantamab-vmjw (Rybrevant) and mobocertinib succinate (Exkivity) as second-line options. Individuals in the trial will take daily tablets of furmonertinib or platinum-based IV chemotherapy for 32 months or until disease progression, whichever comes first. The study opened in December in sites across 15 U.S. states. Centers in a further nine states are gearing up, with the aim of enrolling a total of 375 people. The primary outcome is PFS. QoL and OS at 5 years are secondary outcomes. More details at clinicaltrials.gov.
NSCLC previously treated with at least one platinum chemotherapy and at least one targeted treatment. Adults aged 70 or younger with this type of lung cancer are eligible for a National Cancer Institute phase 2 investigation of autologous T-cell receptor (TCR) gene therapy. Unlike CAR T-cell therapy, which only reaches the 20% of cancer neoantigens that are expressed extracellularly, TCR technology can target the 80% of abnormal proteins that are expressed inside cancer cells. Participants will receive a single infusion of their own engineered T cells. They will attend follow-up visits every 3-6 months for 3 years, then join a long-term study in which they will be followed for 12 more years. The National Institutes of Health Clinical Center in Bethesda, Md., started recruiting for the trial’s 210 participants with one of a selection of solid cancers in February 2023. Response rate measured by objective tumor regression is the primary endpoint. OS and QoL will not be tracked. More details at clinicaltrials.gov.
All trial information is from the National Institutes of Health U.S. National Library of Medicine (online at clinicaltrials.gov).
A version of this article first appeared on Medscape.com.
Editor’s note: This article was changed on 24 February to remove an incorrect reference to osimertinib.
Physician group staffing down, expenses up, new reports show
Physician groups saw staff-to-physician ratios decline even as their workforce expenses rose between 2019 and 2021, according to recent reports from the American Medical Group Association (AMGA) and the Medical Group Management Association (MGMA).
As patients started to return to doctors’ offices as the pandemic eased in 2021, physician groups found it increasingly difficult to recruit and retain lower-level clinicians, including medical assistants and LPNs, officials from both associations told this news organization. Many clinics had to raise their pay scales to be competitive with employers in other fields, and some had to hire higher-priced RNs to keep their practices running.
The AMGA report was based largely on data from groups of over 500 physicians, mostly affiliated with health systems. According to a news release accompanying the report, the ratio between full-time equivalent (FTE) clinic staff and health care professionals in direct patient care dropped by 11.3% between 2019 and 2021. The ratio of medical assistants (MAs) to clinicians declined by a greater percentage.
In the MGMA report, which represented about 4,000 practices ranging from very small (two doctors) to very large groups, total support staff per FTE primary-care physician dropped by 18% from 2019 to 2021 in independent groups and by 13% in hospital-affiliated groups. The ratios decreased by smaller amounts in surgical practices.
In contrast, nonsurgical specialty groups under both types of ownership saw their staffing ratios rise slightly.
Although it’s unclear why medical specialties increased their staff while other types of specialties lost employees, Ron Holder, MHA, chief operating officer of MGMA, said that some specialists may have opened more ancillary facilities and hired new employees to recoup revenue lost during the pandemic.
Expenses rise sharply
The AMGA report found that staffing expenses for the surveyed groups increased by 15% between 2019 and 2021.
“We saw a decrease in staff and an increase in expenses during that time period, and there are a few reasons for that,” Rose Wagner, RN, chief operating officer of AMGA, said. “Groups increased salaries to maintain staff. We also saw lower-paid staff find other jobs outside of health care. For example, medical assistants and receptionists could find jobs outside of health care that paid more. [Open positions] got back-filled with other higher paid staff, such as RNs, doing lower skilled jobs.”
Mr. Holder added that rising wages in other sectors made leaving physician groups more attractive for employees.
“Three years ago, there weren’t many positions in a medical practice where you were competing with Chick-fil-A or Taco Bell,” he said. In Denver, where Mr. Holder is based, “every restaurant in town is now advertising $17-$19 [hourly] starting pay just to do fast food. That causes practices to either lose employees or pay more for the employees they have. So that raises per-employee expense significantly,” he said.
Mr. Holder noted that inflation also has driven up wages as employees demand higher pay to keep up with the cost of living.
Unusual exodus of employees
Fred Horton, MHA, president of AMGA Consulting, said he has never seen so many people leaving health care for other occupations.
Some exits resulted from practices laying people off early in the pandemic, but most staff members who left practices were seeking higher pay, he said. In addition, Ms. Wagner noted, some staff members didn’t want to be exposed to COVID at work.
“There was an exodus from health care that was different from what we’d experienced in the past,” Mr. Horton added. “It’s still extremely challenging to get up to the staffing levels that are appropriate.”
Mr. Holder, however, said that the situation is slowly improving. “Health care is fairly recession-proof, because people need it. So when you see companies in other industries closing shop or reducing their head count, that actually helps health care recruiting in some jobs. And people are coming back to the workplace who previously were worried about COVID or didn’t want to get the vaccine.”
Paying more for nurses
In 2021, groups adopted a variety of tactics to adapt to the pandemic and respond to patient demand, the AMGA survey shows. Forty percent of system-affiliated groups and 18% of independent practices changed registered nurses’ responsibilities, in many cases having them do the work of medical assistants who were in short supply.
Some practices hired RNs, who have historically been utilized less by primary care than by surgical specialties, Mr. Holder noted. Other clinics paid temp agencies to supply nurses at a steep cost.
“When you’re short staffed, you end up paying more overtime, you end up paying temporary agencies at higher dollars, and you hire higher skilled people to do lower-skilled work,” Ms. Wagner said.
Meanwhile, many physician groups tried to cope with the physician shortage by bringing on more advanced practice clinicians (APCs), including nurse practitioners (NPs) and physician assistants (PAs). Seventy percent of the AMGA groups used this strategy, the report revealed.
“The use of APCs has been steadily increasing as groups try to adopt a lower-cost care model in the midst of a nationwide physician shortage,” Ms. Wagner said in the press release.
Changes in patient care
About half of the groups in the AMGA survey said they changed their staff structure to allow APCs to carry their own patient panels. Although most of these clinicians were probably under physician supervision, nearly half of the states now allow NPs to practice autonomously.
Mr. Horton cautioned that APCs can’t fully substitute for physicians and require the same support staff that doctors do if they have their own panels. In primary care groups, Mr. Holder noted, the average salary of an APC “is continuing to rise, and there isn’t a huge difference between what they and doctors make.”
Nevertheless, he added, “there are more NPs and PAs being added to the marketplace all the time, whereas [physician] residency programs aren’t really growing. There are caps on the number of residency positions, and some physicians are retiring. So the clock is ticking to the point where someday doctors will be grossly outnumbered by NPs.”
A version of this article first appeared on Medscape.com.
Physician groups saw staff-to-physician ratios decline even as their workforce expenses rose between 2019 and 2021, according to recent reports from the American Medical Group Association (AMGA) and the Medical Group Management Association (MGMA).
As patients started to return to doctors’ offices as the pandemic eased in 2021, physician groups found it increasingly difficult to recruit and retain lower-level clinicians, including medical assistants and LPNs, officials from both associations told this news organization. Many clinics had to raise their pay scales to be competitive with employers in other fields, and some had to hire higher-priced RNs to keep their practices running.
The AMGA report was based largely on data from groups of over 500 physicians, mostly affiliated with health systems. According to a news release accompanying the report, the ratio between full-time equivalent (FTE) clinic staff and health care professionals in direct patient care dropped by 11.3% between 2019 and 2021. The ratio of medical assistants (MAs) to clinicians declined by a greater percentage.
In the MGMA report, which represented about 4,000 practices ranging from very small (two doctors) to very large groups, total support staff per FTE primary-care physician dropped by 18% from 2019 to 2021 in independent groups and by 13% in hospital-affiliated groups. The ratios decreased by smaller amounts in surgical practices.
In contrast, nonsurgical specialty groups under both types of ownership saw their staffing ratios rise slightly.
Although it’s unclear why medical specialties increased their staff while other types of specialties lost employees, Ron Holder, MHA, chief operating officer of MGMA, said that some specialists may have opened more ancillary facilities and hired new employees to recoup revenue lost during the pandemic.
Expenses rise sharply
The AMGA report found that staffing expenses for the surveyed groups increased by 15% between 2019 and 2021.
“We saw a decrease in staff and an increase in expenses during that time period, and there are a few reasons for that,” Rose Wagner, RN, chief operating officer of AMGA, said. “Groups increased salaries to maintain staff. We also saw lower-paid staff find other jobs outside of health care. For example, medical assistants and receptionists could find jobs outside of health care that paid more. [Open positions] got back-filled with other higher paid staff, such as RNs, doing lower skilled jobs.”
Mr. Holder added that rising wages in other sectors made leaving physician groups more attractive for employees.
“Three years ago, there weren’t many positions in a medical practice where you were competing with Chick-fil-A or Taco Bell,” he said. In Denver, where Mr. Holder is based, “every restaurant in town is now advertising $17-$19 [hourly] starting pay just to do fast food. That causes practices to either lose employees or pay more for the employees they have. So that raises per-employee expense significantly,” he said.
Mr. Holder noted that inflation also has driven up wages as employees demand higher pay to keep up with the cost of living.
Unusual exodus of employees
Fred Horton, MHA, president of AMGA Consulting, said he has never seen so many people leaving health care for other occupations.
Some exits resulted from practices laying people off early in the pandemic, but most staff members who left practices were seeking higher pay, he said. In addition, Ms. Wagner noted, some staff members didn’t want to be exposed to COVID at work.
“There was an exodus from health care that was different from what we’d experienced in the past,” Mr. Horton added. “It’s still extremely challenging to get up to the staffing levels that are appropriate.”
Mr. Holder, however, said that the situation is slowly improving. “Health care is fairly recession-proof, because people need it. So when you see companies in other industries closing shop or reducing their head count, that actually helps health care recruiting in some jobs. And people are coming back to the workplace who previously were worried about COVID or didn’t want to get the vaccine.”
Paying more for nurses
In 2021, groups adopted a variety of tactics to adapt to the pandemic and respond to patient demand, the AMGA survey shows. Forty percent of system-affiliated groups and 18% of independent practices changed registered nurses’ responsibilities, in many cases having them do the work of medical assistants who were in short supply.
Some practices hired RNs, who have historically been utilized less by primary care than by surgical specialties, Mr. Holder noted. Other clinics paid temp agencies to supply nurses at a steep cost.
“When you’re short staffed, you end up paying more overtime, you end up paying temporary agencies at higher dollars, and you hire higher skilled people to do lower-skilled work,” Ms. Wagner said.
Meanwhile, many physician groups tried to cope with the physician shortage by bringing on more advanced practice clinicians (APCs), including nurse practitioners (NPs) and physician assistants (PAs). Seventy percent of the AMGA groups used this strategy, the report revealed.
“The use of APCs has been steadily increasing as groups try to adopt a lower-cost care model in the midst of a nationwide physician shortage,” Ms. Wagner said in the press release.
Changes in patient care
About half of the groups in the AMGA survey said they changed their staff structure to allow APCs to carry their own patient panels. Although most of these clinicians were probably under physician supervision, nearly half of the states now allow NPs to practice autonomously.
Mr. Horton cautioned that APCs can’t fully substitute for physicians and require the same support staff that doctors do if they have their own panels. In primary care groups, Mr. Holder noted, the average salary of an APC “is continuing to rise, and there isn’t a huge difference between what they and doctors make.”
Nevertheless, he added, “there are more NPs and PAs being added to the marketplace all the time, whereas [physician] residency programs aren’t really growing. There are caps on the number of residency positions, and some physicians are retiring. So the clock is ticking to the point where someday doctors will be grossly outnumbered by NPs.”
A version of this article first appeared on Medscape.com.
Physician groups saw staff-to-physician ratios decline even as their workforce expenses rose between 2019 and 2021, according to recent reports from the American Medical Group Association (AMGA) and the Medical Group Management Association (MGMA).
As patients started to return to doctors’ offices as the pandemic eased in 2021, physician groups found it increasingly difficult to recruit and retain lower-level clinicians, including medical assistants and LPNs, officials from both associations told this news organization. Many clinics had to raise their pay scales to be competitive with employers in other fields, and some had to hire higher-priced RNs to keep their practices running.
The AMGA report was based largely on data from groups of over 500 physicians, mostly affiliated with health systems. According to a news release accompanying the report, the ratio between full-time equivalent (FTE) clinic staff and health care professionals in direct patient care dropped by 11.3% between 2019 and 2021. The ratio of medical assistants (MAs) to clinicians declined by a greater percentage.
In the MGMA report, which represented about 4,000 practices ranging from very small (two doctors) to very large groups, total support staff per FTE primary-care physician dropped by 18% from 2019 to 2021 in independent groups and by 13% in hospital-affiliated groups. The ratios decreased by smaller amounts in surgical practices.
In contrast, nonsurgical specialty groups under both types of ownership saw their staffing ratios rise slightly.
Although it’s unclear why medical specialties increased their staff while other types of specialties lost employees, Ron Holder, MHA, chief operating officer of MGMA, said that some specialists may have opened more ancillary facilities and hired new employees to recoup revenue lost during the pandemic.
Expenses rise sharply
The AMGA report found that staffing expenses for the surveyed groups increased by 15% between 2019 and 2021.
“We saw a decrease in staff and an increase in expenses during that time period, and there are a few reasons for that,” Rose Wagner, RN, chief operating officer of AMGA, said. “Groups increased salaries to maintain staff. We also saw lower-paid staff find other jobs outside of health care. For example, medical assistants and receptionists could find jobs outside of health care that paid more. [Open positions] got back-filled with other higher paid staff, such as RNs, doing lower skilled jobs.”
Mr. Holder added that rising wages in other sectors made leaving physician groups more attractive for employees.
“Three years ago, there weren’t many positions in a medical practice where you were competing with Chick-fil-A or Taco Bell,” he said. In Denver, where Mr. Holder is based, “every restaurant in town is now advertising $17-$19 [hourly] starting pay just to do fast food. That causes practices to either lose employees or pay more for the employees they have. So that raises per-employee expense significantly,” he said.
Mr. Holder noted that inflation also has driven up wages as employees demand higher pay to keep up with the cost of living.
Unusual exodus of employees
Fred Horton, MHA, president of AMGA Consulting, said he has never seen so many people leaving health care for other occupations.
Some exits resulted from practices laying people off early in the pandemic, but most staff members who left practices were seeking higher pay, he said. In addition, Ms. Wagner noted, some staff members didn’t want to be exposed to COVID at work.
“There was an exodus from health care that was different from what we’d experienced in the past,” Mr. Horton added. “It’s still extremely challenging to get up to the staffing levels that are appropriate.”
Mr. Holder, however, said that the situation is slowly improving. “Health care is fairly recession-proof, because people need it. So when you see companies in other industries closing shop or reducing their head count, that actually helps health care recruiting in some jobs. And people are coming back to the workplace who previously were worried about COVID or didn’t want to get the vaccine.”
Paying more for nurses
In 2021, groups adopted a variety of tactics to adapt to the pandemic and respond to patient demand, the AMGA survey shows. Forty percent of system-affiliated groups and 18% of independent practices changed registered nurses’ responsibilities, in many cases having them do the work of medical assistants who were in short supply.
Some practices hired RNs, who have historically been utilized less by primary care than by surgical specialties, Mr. Holder noted. Other clinics paid temp agencies to supply nurses at a steep cost.
“When you’re short staffed, you end up paying more overtime, you end up paying temporary agencies at higher dollars, and you hire higher skilled people to do lower-skilled work,” Ms. Wagner said.
Meanwhile, many physician groups tried to cope with the physician shortage by bringing on more advanced practice clinicians (APCs), including nurse practitioners (NPs) and physician assistants (PAs). Seventy percent of the AMGA groups used this strategy, the report revealed.
“The use of APCs has been steadily increasing as groups try to adopt a lower-cost care model in the midst of a nationwide physician shortage,” Ms. Wagner said in the press release.
Changes in patient care
About half of the groups in the AMGA survey said they changed their staff structure to allow APCs to carry their own patient panels. Although most of these clinicians were probably under physician supervision, nearly half of the states now allow NPs to practice autonomously.
Mr. Horton cautioned that APCs can’t fully substitute for physicians and require the same support staff that doctors do if they have their own panels. In primary care groups, Mr. Holder noted, the average salary of an APC “is continuing to rise, and there isn’t a huge difference between what they and doctors make.”
Nevertheless, he added, “there are more NPs and PAs being added to the marketplace all the time, whereas [physician] residency programs aren’t really growing. There are caps on the number of residency positions, and some physicians are retiring. So the clock is ticking to the point where someday doctors will be grossly outnumbered by NPs.”
A version of this article first appeared on Medscape.com.
Talazoparib add-on improves outcomes in metastatic prostate cancer
in the TALAPRO-2 trial.
As determined on the basis of imaging, PFS was 37% better for talazoparib plus enzalutamide than for enzalutamide monotherapy. Combination therapy proved superior regardless of homologous recombination repair (HRR) pathway status, noted the authors.
“Not only did the combination therapy delay disease progression, it also significantly delayed progression of PSA [prostate-specific antigen] readings and the time until chemotherapy was needed compared to the control group,” said lead study author Neeraj Agarwal, MD, professor of medicine and director of the genitourinary oncology program at the Huntsman Cancer Institute, University of Utah, Salt Lake City.
“This is important because advanced prostate cancer can be associated with pain, fractures, suffering, and death. The current standard of care treatments were approved almost a decade ago, leaving a huge, unmet need for novel drugs in this setting,” he said.
The new results could pave the way for a prostate cancer indication for talazoparib; the company has said that it will submit these data to regulatory authorities. At present, the drug is approved only for use in BRCA+ breast cancer, an indication that was approved in 2018.
The findings were presented at the 2023 ASCO Genitourinary Cancers Symposium.
Overall, talazoparib plus enzalutamide resulted in a statistically significant and clinically meaningful improvement in PFS over placebo plus enzalutamide. “Results from the primary analysis of the TALAPRO-2 trial support the use of talazoparib plus enzalutamide as a first-line treatment in patients with mCRPC regardless of HRR gene alteration status,” Dr. Agarwal and colleagues concluded.
However, one expert disagreed with the authors’ conclusion regarding HHR pathway status. On the basis of imaging, PFS was 54% better in HHR-deficient patients in the combination therapy group. It was 30% better for patients with HHR-nondeficient tumors or tumors without known HHR status based on imaging and 34% better based on tumor tissue testing.
“There was a huge magnitude in benefit based on HHR, and I think HRR status matters,” commented Elena Castro, MD, PhD, Instituto de Investigación Biomédica de Málaga (Spain), who served as the invited discussant.
“We need to understand the benefit of ARPi [androgen receptor pathway inhibition] and PARP inhibitors better,” she said. “The balance between side effects and benefit depends on HRR status.”
Dr. Castro also noted that the treatment landscape has changed. ARPi is now a standard of care for metastatic prostate cancer, both for hormone-sensitive and castration-resistant disease. “So the question is, does the addition of a PARP inhibitor induce responses after progression to an ARPi in HHR-nondeficient tumors?”
Study details
In the TALAPRO-2 trial, Dr. Agarwal and colleagues randomly assigned 805 patients to receive either talazoparib 0.5 mg or placebo. All patients in the cohort received enzalutamide 160 mg daily.
Participants had mCRPC and were unselected for genetic alterations in DNA damage repair pathways directly or indirectly involved with HRR. They were aged 36-91 years (median age, 71). The cohort was enrolled from 25 countries, including the United States, Canada, Europe, South America, and countries in the Asia-Pacific region.
The men were stratified on the basis of prior use of abiraterone or docetaxel for castration-sensitive prostate cancer and HRR gene alteration status. The study’s primary endpoint was imaging-based PFS (ibPFS) by blinded independent central review (BICR).
Overall, median ibPFS by BICR was significantly improved in the combination group in comparison with the patients who received placebo; it was not reached versus 21.9 months (hazard ratio, 0.63; P < .001). It was also significantly improved among the HRR-deficient subgroup (HR, 0.46; P < .001) as well as in the HRR-nondeficient or unknown (HR, 0.70; P = .004) and HRR-nondeficient patients by tumor tissue testing (HR, 0.66; P = .009).
Talazoparib plus enzalutamide was also favored with regard to other endpoints. Dr. Agarwal noted that, while overall survival data are as yet immature, objective response rates, PSA response of at least 50%, and time to PSA progression and use of subsequent cytotoxic chemotherapy and antineoplastic therapy significantly favored the talazoparib group.
The objective response rate was 61.7% versus 43.9% (P = .005), with 37.5% versus 18.2% complete responses.
“The higher rates of complete response suggest a cooperative effect of talazoparib plus enzalutamide treatment,” he explained.
High rate of adverse events
The rate of treatment-emergent adverse events was higher among patients who received talazoparib plus enzalutamide; 71.9% of the patients who received talazoparib plus enzalutamide experienced grade 3-4 TEAEs versus 40.6%. The most common grade 3 or greater TEAEs in the talazoparib group were anemia, low neutrophil counts, and low platelet counts. Hypertension, anemia, and fatigue were the most common in the placebo group. Talazoparib was discontinued in 19.1% of patients because of TEAEs. Enzalutamide was discontinued in 10.8% of patients in the combination group versus 11.0% in the placebo group.
Dr. Agarwal pointed out that there were TEAEs of special interest for talazoparib. “Myelodysplastic syndrome was reported in one patient during the safety reporting period, and acute myeloid leukemia was reported in one patient during the follow-up period,” he said.
Additionally, pulmonary embolism was reported in 10 (2.5%) patients (grade 3 in 9 patients) in the talazoparib arm and in 3 (0.7%) patients (all grade 3) in the placebo arm.
Results less relevant
Commenting on the study, Matthew Zibelman, MD, associate professor, department of hematology/oncology, Fox Chase Cancer Center, Philadelphia, noted that these results represent an “intriguing finding for men with mCRPC, particularly in conjunction with the previously reported PROPEL study results.
“However, given that many patients receive an androgen receptor inhibitor now for metastatic castration-sensitive prostate cancer, these results are less relevant to current practice,” Dr. Zibelman said.
“Demonstration of an overall survival benefit of the combination would be optimal to change standard of care vs potential sequential therapy.”
The study was sponsored by Pfizer, manufacturer of enzalutamide and talazoparib. Dr. Agarwal has relationships with numerous pharmaceutical companies. Dr. Castro has relationships with Astellas Pharma, AstraZeneca, Bayer, Clovis Oncology, Janssen-Cilag, Merck, MSD Oncology, Novartis and Pfizer, and Roche. Dr. Zibelman has relationships with Bristol-Myers Squibb, Exelixis, Pfizer, Jannsen, EMD Serono, and Blue Earth.
A version of this article first appeared on Medscape.com.
in the TALAPRO-2 trial.
As determined on the basis of imaging, PFS was 37% better for talazoparib plus enzalutamide than for enzalutamide monotherapy. Combination therapy proved superior regardless of homologous recombination repair (HRR) pathway status, noted the authors.
“Not only did the combination therapy delay disease progression, it also significantly delayed progression of PSA [prostate-specific antigen] readings and the time until chemotherapy was needed compared to the control group,” said lead study author Neeraj Agarwal, MD, professor of medicine and director of the genitourinary oncology program at the Huntsman Cancer Institute, University of Utah, Salt Lake City.
“This is important because advanced prostate cancer can be associated with pain, fractures, suffering, and death. The current standard of care treatments were approved almost a decade ago, leaving a huge, unmet need for novel drugs in this setting,” he said.
The new results could pave the way for a prostate cancer indication for talazoparib; the company has said that it will submit these data to regulatory authorities. At present, the drug is approved only for use in BRCA+ breast cancer, an indication that was approved in 2018.
The findings were presented at the 2023 ASCO Genitourinary Cancers Symposium.
Overall, talazoparib plus enzalutamide resulted in a statistically significant and clinically meaningful improvement in PFS over placebo plus enzalutamide. “Results from the primary analysis of the TALAPRO-2 trial support the use of talazoparib plus enzalutamide as a first-line treatment in patients with mCRPC regardless of HRR gene alteration status,” Dr. Agarwal and colleagues concluded.
However, one expert disagreed with the authors’ conclusion regarding HHR pathway status. On the basis of imaging, PFS was 54% better in HHR-deficient patients in the combination therapy group. It was 30% better for patients with HHR-nondeficient tumors or tumors without known HHR status based on imaging and 34% better based on tumor tissue testing.
“There was a huge magnitude in benefit based on HHR, and I think HRR status matters,” commented Elena Castro, MD, PhD, Instituto de Investigación Biomédica de Málaga (Spain), who served as the invited discussant.
“We need to understand the benefit of ARPi [androgen receptor pathway inhibition] and PARP inhibitors better,” she said. “The balance between side effects and benefit depends on HRR status.”
Dr. Castro also noted that the treatment landscape has changed. ARPi is now a standard of care for metastatic prostate cancer, both for hormone-sensitive and castration-resistant disease. “So the question is, does the addition of a PARP inhibitor induce responses after progression to an ARPi in HHR-nondeficient tumors?”
Study details
In the TALAPRO-2 trial, Dr. Agarwal and colleagues randomly assigned 805 patients to receive either talazoparib 0.5 mg or placebo. All patients in the cohort received enzalutamide 160 mg daily.
Participants had mCRPC and were unselected for genetic alterations in DNA damage repair pathways directly or indirectly involved with HRR. They were aged 36-91 years (median age, 71). The cohort was enrolled from 25 countries, including the United States, Canada, Europe, South America, and countries in the Asia-Pacific region.
The men were stratified on the basis of prior use of abiraterone or docetaxel for castration-sensitive prostate cancer and HRR gene alteration status. The study’s primary endpoint was imaging-based PFS (ibPFS) by blinded independent central review (BICR).
Overall, median ibPFS by BICR was significantly improved in the combination group in comparison with the patients who received placebo; it was not reached versus 21.9 months (hazard ratio, 0.63; P < .001). It was also significantly improved among the HRR-deficient subgroup (HR, 0.46; P < .001) as well as in the HRR-nondeficient or unknown (HR, 0.70; P = .004) and HRR-nondeficient patients by tumor tissue testing (HR, 0.66; P = .009).
Talazoparib plus enzalutamide was also favored with regard to other endpoints. Dr. Agarwal noted that, while overall survival data are as yet immature, objective response rates, PSA response of at least 50%, and time to PSA progression and use of subsequent cytotoxic chemotherapy and antineoplastic therapy significantly favored the talazoparib group.
The objective response rate was 61.7% versus 43.9% (P = .005), with 37.5% versus 18.2% complete responses.
“The higher rates of complete response suggest a cooperative effect of talazoparib plus enzalutamide treatment,” he explained.
High rate of adverse events
The rate of treatment-emergent adverse events was higher among patients who received talazoparib plus enzalutamide; 71.9% of the patients who received talazoparib plus enzalutamide experienced grade 3-4 TEAEs versus 40.6%. The most common grade 3 or greater TEAEs in the talazoparib group were anemia, low neutrophil counts, and low platelet counts. Hypertension, anemia, and fatigue were the most common in the placebo group. Talazoparib was discontinued in 19.1% of patients because of TEAEs. Enzalutamide was discontinued in 10.8% of patients in the combination group versus 11.0% in the placebo group.
Dr. Agarwal pointed out that there were TEAEs of special interest for talazoparib. “Myelodysplastic syndrome was reported in one patient during the safety reporting period, and acute myeloid leukemia was reported in one patient during the follow-up period,” he said.
Additionally, pulmonary embolism was reported in 10 (2.5%) patients (grade 3 in 9 patients) in the talazoparib arm and in 3 (0.7%) patients (all grade 3) in the placebo arm.
Results less relevant
Commenting on the study, Matthew Zibelman, MD, associate professor, department of hematology/oncology, Fox Chase Cancer Center, Philadelphia, noted that these results represent an “intriguing finding for men with mCRPC, particularly in conjunction with the previously reported PROPEL study results.
“However, given that many patients receive an androgen receptor inhibitor now for metastatic castration-sensitive prostate cancer, these results are less relevant to current practice,” Dr. Zibelman said.
“Demonstration of an overall survival benefit of the combination would be optimal to change standard of care vs potential sequential therapy.”
The study was sponsored by Pfizer, manufacturer of enzalutamide and talazoparib. Dr. Agarwal has relationships with numerous pharmaceutical companies. Dr. Castro has relationships with Astellas Pharma, AstraZeneca, Bayer, Clovis Oncology, Janssen-Cilag, Merck, MSD Oncology, Novartis and Pfizer, and Roche. Dr. Zibelman has relationships with Bristol-Myers Squibb, Exelixis, Pfizer, Jannsen, EMD Serono, and Blue Earth.
A version of this article first appeared on Medscape.com.
in the TALAPRO-2 trial.
As determined on the basis of imaging, PFS was 37% better for talazoparib plus enzalutamide than for enzalutamide monotherapy. Combination therapy proved superior regardless of homologous recombination repair (HRR) pathway status, noted the authors.
“Not only did the combination therapy delay disease progression, it also significantly delayed progression of PSA [prostate-specific antigen] readings and the time until chemotherapy was needed compared to the control group,” said lead study author Neeraj Agarwal, MD, professor of medicine and director of the genitourinary oncology program at the Huntsman Cancer Institute, University of Utah, Salt Lake City.
“This is important because advanced prostate cancer can be associated with pain, fractures, suffering, and death. The current standard of care treatments were approved almost a decade ago, leaving a huge, unmet need for novel drugs in this setting,” he said.
The new results could pave the way for a prostate cancer indication for talazoparib; the company has said that it will submit these data to regulatory authorities. At present, the drug is approved only for use in BRCA+ breast cancer, an indication that was approved in 2018.
The findings were presented at the 2023 ASCO Genitourinary Cancers Symposium.
Overall, talazoparib plus enzalutamide resulted in a statistically significant and clinically meaningful improvement in PFS over placebo plus enzalutamide. “Results from the primary analysis of the TALAPRO-2 trial support the use of talazoparib plus enzalutamide as a first-line treatment in patients with mCRPC regardless of HRR gene alteration status,” Dr. Agarwal and colleagues concluded.
However, one expert disagreed with the authors’ conclusion regarding HHR pathway status. On the basis of imaging, PFS was 54% better in HHR-deficient patients in the combination therapy group. It was 30% better for patients with HHR-nondeficient tumors or tumors without known HHR status based on imaging and 34% better based on tumor tissue testing.
“There was a huge magnitude in benefit based on HHR, and I think HRR status matters,” commented Elena Castro, MD, PhD, Instituto de Investigación Biomédica de Málaga (Spain), who served as the invited discussant.
“We need to understand the benefit of ARPi [androgen receptor pathway inhibition] and PARP inhibitors better,” she said. “The balance between side effects and benefit depends on HRR status.”
Dr. Castro also noted that the treatment landscape has changed. ARPi is now a standard of care for metastatic prostate cancer, both for hormone-sensitive and castration-resistant disease. “So the question is, does the addition of a PARP inhibitor induce responses after progression to an ARPi in HHR-nondeficient tumors?”
Study details
In the TALAPRO-2 trial, Dr. Agarwal and colleagues randomly assigned 805 patients to receive either talazoparib 0.5 mg or placebo. All patients in the cohort received enzalutamide 160 mg daily.
Participants had mCRPC and were unselected for genetic alterations in DNA damage repair pathways directly or indirectly involved with HRR. They were aged 36-91 years (median age, 71). The cohort was enrolled from 25 countries, including the United States, Canada, Europe, South America, and countries in the Asia-Pacific region.
The men were stratified on the basis of prior use of abiraterone or docetaxel for castration-sensitive prostate cancer and HRR gene alteration status. The study’s primary endpoint was imaging-based PFS (ibPFS) by blinded independent central review (BICR).
Overall, median ibPFS by BICR was significantly improved in the combination group in comparison with the patients who received placebo; it was not reached versus 21.9 months (hazard ratio, 0.63; P < .001). It was also significantly improved among the HRR-deficient subgroup (HR, 0.46; P < .001) as well as in the HRR-nondeficient or unknown (HR, 0.70; P = .004) and HRR-nondeficient patients by tumor tissue testing (HR, 0.66; P = .009).
Talazoparib plus enzalutamide was also favored with regard to other endpoints. Dr. Agarwal noted that, while overall survival data are as yet immature, objective response rates, PSA response of at least 50%, and time to PSA progression and use of subsequent cytotoxic chemotherapy and antineoplastic therapy significantly favored the talazoparib group.
The objective response rate was 61.7% versus 43.9% (P = .005), with 37.5% versus 18.2% complete responses.
“The higher rates of complete response suggest a cooperative effect of talazoparib plus enzalutamide treatment,” he explained.
High rate of adverse events
The rate of treatment-emergent adverse events was higher among patients who received talazoparib plus enzalutamide; 71.9% of the patients who received talazoparib plus enzalutamide experienced grade 3-4 TEAEs versus 40.6%. The most common grade 3 or greater TEAEs in the talazoparib group were anemia, low neutrophil counts, and low platelet counts. Hypertension, anemia, and fatigue were the most common in the placebo group. Talazoparib was discontinued in 19.1% of patients because of TEAEs. Enzalutamide was discontinued in 10.8% of patients in the combination group versus 11.0% in the placebo group.
Dr. Agarwal pointed out that there were TEAEs of special interest for talazoparib. “Myelodysplastic syndrome was reported in one patient during the safety reporting period, and acute myeloid leukemia was reported in one patient during the follow-up period,” he said.
Additionally, pulmonary embolism was reported in 10 (2.5%) patients (grade 3 in 9 patients) in the talazoparib arm and in 3 (0.7%) patients (all grade 3) in the placebo arm.
Results less relevant
Commenting on the study, Matthew Zibelman, MD, associate professor, department of hematology/oncology, Fox Chase Cancer Center, Philadelphia, noted that these results represent an “intriguing finding for men with mCRPC, particularly in conjunction with the previously reported PROPEL study results.
“However, given that many patients receive an androgen receptor inhibitor now for metastatic castration-sensitive prostate cancer, these results are less relevant to current practice,” Dr. Zibelman said.
“Demonstration of an overall survival benefit of the combination would be optimal to change standard of care vs potential sequential therapy.”
The study was sponsored by Pfizer, manufacturer of enzalutamide and talazoparib. Dr. Agarwal has relationships with numerous pharmaceutical companies. Dr. Castro has relationships with Astellas Pharma, AstraZeneca, Bayer, Clovis Oncology, Janssen-Cilag, Merck, MSD Oncology, Novartis and Pfizer, and Roche. Dr. Zibelman has relationships with Bristol-Myers Squibb, Exelixis, Pfizer, Jannsen, EMD Serono, and Blue Earth.
A version of this article first appeared on Medscape.com.
AT ASCO GU 2023
Adjuvant nivolumab as standard of care in resected bladder cancer
Extended follow-up data from the phase 3 CheckMate 274 trial continue to show that, compared with placebo, nivolumab improves disease-free survival, nonurothelial tract recurrence-free survival (NUTRFS), and distant metastasis-free survival (DMFS) in patients with high-risk, muscle-invasive urothelial cancer after undergoing radical surgery.
The benefit was observed in both in the intent-to-treat population (ITT) and in the subset of patients with programmed death–ligand 1 (PD-L1) expression of at least 1%.
“In the ITT population, median disease-free survival with nivolumab was doubled compared to placebo,” said lead author Matthew Galsky, MD, director of genitourinary medical oncology and codirector of the Center of Excellence for Bladder Cancer at Tisch Cancer Institute, New York. “For the patients with high PD-L1 expression, the median disease-free survival with nivolumab reached 52.6 months, more than six times that of the placebo arm.
“These results further support adjuvant nivolumab as a standard of care in high-risk muscle-invasive urothelial cancer after resection,” he concluded.
Dr. Galsky presented the findings at the 2023 ASCO Genitourinary Cancers Symposium.
Practice changing
The earlier results of this study have already led to an approval from the Food and Drug Administration. In August 2021, nivolumab became the first adjuvant immunotherapy for use in patients with urothelial carcinoma at high risk for recurrence after radical resection
“This is a practice-changing study,” said Scot Niglio, MD, medical oncologist, New York University Perlmutter Cancer Center, who was approached for an independent comment.
“For decades, there were limited to zero treatment options in the postsurgical setting for urothelial cancer patients with a high recurrence risk,” he said.
The standard of care for muscle-invasive urothelial carcinoma is surgery, which may include neoadjuvant cisplatin-based chemotherapy, but most patients will experience disease recurrence, he explained.
“When urothelial cancer recurs outside the urinary tract, the prognosis quickly changes from curable to incurable,” he said, “making this area of research paramount.”
Dr. Niglio emphasized that these updated results show continued benefit from nivolumab on disease-free survival, as well as nonurothelial tract recurrence-free survival and distant metastasis-free survival, supporting its use as standard of care therapy.
“Even though the overall survival data is still maturing, the current data remains promising,” he said. “Patients with urothelial cancer meeting the criteria for high risk now have a treatment option to mitigate the potential of distant recurrence.”
In his own practice, Dr. Niglio added that he will “continue to discuss adjuvant nivolumab as a potential treatment option with all patients who are eligible based on this study.”
Met all endpoints
The Checkmate 274 trial involved 353 patients (of whom 140 patients had PD-L1 ≥ 1%) randomly assigned to take nivolumab 240 mg every 2 weeks and 356 patients (with 142 patients with PD-L1 ≥ 1%) randomized to placebo. All patients had pathologic evidence of urothelial cancer at high risk of recurrence and Eastern Cooperative Oncology Group performance status (ECOG PS) of1 or less.
Previous results, at a median follow-up of about 20 months, show that the study met its primary endpoint, showing significant prolongation of disease-free survival in the intention-to-treat population, with nivolumab at 21 months versus placebo at 10.9 months (hazard ratio, 0.70; P < .001).
When the analysis considered only patients with tumors expressing PD-L1 of at least 1%, the median disease-free survival was even higher (not reached vs. 10.8 months; HR, 0.53; P < .001).
Nivolumab was also superior to placebo for NUTRFS, in both in the entire ITT population and in the subset with PD-L1–positive tumors.
The latest results come from a median follow-up of 36.1 months. The median disease-free survival was 22 months with nivolumab, compared with 10.9 months with placebo in ITT patients and 52.6 months on nivolumab versus 8.4 months in patients with PD-L1 of at least 1%.
Nivolumab was superior to placebo for secondary and exploratory endpoints, NUTRFS (ITT: HR, 0.72 and PD-L1 ≥ 1%: HR, 0.53) and DMFS (ITT: HR, 0.74; PD-L1 ≥ 1%: HR, 0.58). However, overall survival data remained immature and will be assessed as a future data cutoff, Dr. Galsky explained.
The updated analysis also included another exploratory endpoint, progression-free survival 2 (PFS2), defined as time from randomization to disease progression after subsequent next-line systemic therapy, start of second subsequent next-line systemic therapy, or death.
Median PFS2 was 61.2 months for all-patients who received nivolumab versus 47.1 months with placebo (HR, 0.79). In the PD-L1 of 1% or greater subgroup, median PFS2 was not reached with nivolumab versus 39.4 months with placebo (HR, 0.54).
Grade 3-4 treatment-related adverse events occurred in 18.2% and 7.2% of patients (nivolumab vs. placebo), and this was consistent with the primary analysis. “No new safety signals were identified,” said Dr. Galsky.
The CheckMate 274 trial was funded by Bristol-Myers Squibb, manufacturer of nivolumab. Dr. Galsky reported relationships with numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
Extended follow-up data from the phase 3 CheckMate 274 trial continue to show that, compared with placebo, nivolumab improves disease-free survival, nonurothelial tract recurrence-free survival (NUTRFS), and distant metastasis-free survival (DMFS) in patients with high-risk, muscle-invasive urothelial cancer after undergoing radical surgery.
The benefit was observed in both in the intent-to-treat population (ITT) and in the subset of patients with programmed death–ligand 1 (PD-L1) expression of at least 1%.
“In the ITT population, median disease-free survival with nivolumab was doubled compared to placebo,” said lead author Matthew Galsky, MD, director of genitourinary medical oncology and codirector of the Center of Excellence for Bladder Cancer at Tisch Cancer Institute, New York. “For the patients with high PD-L1 expression, the median disease-free survival with nivolumab reached 52.6 months, more than six times that of the placebo arm.
“These results further support adjuvant nivolumab as a standard of care in high-risk muscle-invasive urothelial cancer after resection,” he concluded.
Dr. Galsky presented the findings at the 2023 ASCO Genitourinary Cancers Symposium.
Practice changing
The earlier results of this study have already led to an approval from the Food and Drug Administration. In August 2021, nivolumab became the first adjuvant immunotherapy for use in patients with urothelial carcinoma at high risk for recurrence after radical resection
“This is a practice-changing study,” said Scot Niglio, MD, medical oncologist, New York University Perlmutter Cancer Center, who was approached for an independent comment.
“For decades, there were limited to zero treatment options in the postsurgical setting for urothelial cancer patients with a high recurrence risk,” he said.
The standard of care for muscle-invasive urothelial carcinoma is surgery, which may include neoadjuvant cisplatin-based chemotherapy, but most patients will experience disease recurrence, he explained.
“When urothelial cancer recurs outside the urinary tract, the prognosis quickly changes from curable to incurable,” he said, “making this area of research paramount.”
Dr. Niglio emphasized that these updated results show continued benefit from nivolumab on disease-free survival, as well as nonurothelial tract recurrence-free survival and distant metastasis-free survival, supporting its use as standard of care therapy.
“Even though the overall survival data is still maturing, the current data remains promising,” he said. “Patients with urothelial cancer meeting the criteria for high risk now have a treatment option to mitigate the potential of distant recurrence.”
In his own practice, Dr. Niglio added that he will “continue to discuss adjuvant nivolumab as a potential treatment option with all patients who are eligible based on this study.”
Met all endpoints
The Checkmate 274 trial involved 353 patients (of whom 140 patients had PD-L1 ≥ 1%) randomly assigned to take nivolumab 240 mg every 2 weeks and 356 patients (with 142 patients with PD-L1 ≥ 1%) randomized to placebo. All patients had pathologic evidence of urothelial cancer at high risk of recurrence and Eastern Cooperative Oncology Group performance status (ECOG PS) of1 or less.
Previous results, at a median follow-up of about 20 months, show that the study met its primary endpoint, showing significant prolongation of disease-free survival in the intention-to-treat population, with nivolumab at 21 months versus placebo at 10.9 months (hazard ratio, 0.70; P < .001).
When the analysis considered only patients with tumors expressing PD-L1 of at least 1%, the median disease-free survival was even higher (not reached vs. 10.8 months; HR, 0.53; P < .001).
Nivolumab was also superior to placebo for NUTRFS, in both in the entire ITT population and in the subset with PD-L1–positive tumors.
The latest results come from a median follow-up of 36.1 months. The median disease-free survival was 22 months with nivolumab, compared with 10.9 months with placebo in ITT patients and 52.6 months on nivolumab versus 8.4 months in patients with PD-L1 of at least 1%.
Nivolumab was superior to placebo for secondary and exploratory endpoints, NUTRFS (ITT: HR, 0.72 and PD-L1 ≥ 1%: HR, 0.53) and DMFS (ITT: HR, 0.74; PD-L1 ≥ 1%: HR, 0.58). However, overall survival data remained immature and will be assessed as a future data cutoff, Dr. Galsky explained.
The updated analysis also included another exploratory endpoint, progression-free survival 2 (PFS2), defined as time from randomization to disease progression after subsequent next-line systemic therapy, start of second subsequent next-line systemic therapy, or death.
Median PFS2 was 61.2 months for all-patients who received nivolumab versus 47.1 months with placebo (HR, 0.79). In the PD-L1 of 1% or greater subgroup, median PFS2 was not reached with nivolumab versus 39.4 months with placebo (HR, 0.54).
Grade 3-4 treatment-related adverse events occurred in 18.2% and 7.2% of patients (nivolumab vs. placebo), and this was consistent with the primary analysis. “No new safety signals were identified,” said Dr. Galsky.
The CheckMate 274 trial was funded by Bristol-Myers Squibb, manufacturer of nivolumab. Dr. Galsky reported relationships with numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
Extended follow-up data from the phase 3 CheckMate 274 trial continue to show that, compared with placebo, nivolumab improves disease-free survival, nonurothelial tract recurrence-free survival (NUTRFS), and distant metastasis-free survival (DMFS) in patients with high-risk, muscle-invasive urothelial cancer after undergoing radical surgery.
The benefit was observed in both in the intent-to-treat population (ITT) and in the subset of patients with programmed death–ligand 1 (PD-L1) expression of at least 1%.
“In the ITT population, median disease-free survival with nivolumab was doubled compared to placebo,” said lead author Matthew Galsky, MD, director of genitourinary medical oncology and codirector of the Center of Excellence for Bladder Cancer at Tisch Cancer Institute, New York. “For the patients with high PD-L1 expression, the median disease-free survival with nivolumab reached 52.6 months, more than six times that of the placebo arm.
“These results further support adjuvant nivolumab as a standard of care in high-risk muscle-invasive urothelial cancer after resection,” he concluded.
Dr. Galsky presented the findings at the 2023 ASCO Genitourinary Cancers Symposium.
Practice changing
The earlier results of this study have already led to an approval from the Food and Drug Administration. In August 2021, nivolumab became the first adjuvant immunotherapy for use in patients with urothelial carcinoma at high risk for recurrence after radical resection
“This is a practice-changing study,” said Scot Niglio, MD, medical oncologist, New York University Perlmutter Cancer Center, who was approached for an independent comment.
“For decades, there were limited to zero treatment options in the postsurgical setting for urothelial cancer patients with a high recurrence risk,” he said.
The standard of care for muscle-invasive urothelial carcinoma is surgery, which may include neoadjuvant cisplatin-based chemotherapy, but most patients will experience disease recurrence, he explained.
“When urothelial cancer recurs outside the urinary tract, the prognosis quickly changes from curable to incurable,” he said, “making this area of research paramount.”
Dr. Niglio emphasized that these updated results show continued benefit from nivolumab on disease-free survival, as well as nonurothelial tract recurrence-free survival and distant metastasis-free survival, supporting its use as standard of care therapy.
“Even though the overall survival data is still maturing, the current data remains promising,” he said. “Patients with urothelial cancer meeting the criteria for high risk now have a treatment option to mitigate the potential of distant recurrence.”
In his own practice, Dr. Niglio added that he will “continue to discuss adjuvant nivolumab as a potential treatment option with all patients who are eligible based on this study.”
Met all endpoints
The Checkmate 274 trial involved 353 patients (of whom 140 patients had PD-L1 ≥ 1%) randomly assigned to take nivolumab 240 mg every 2 weeks and 356 patients (with 142 patients with PD-L1 ≥ 1%) randomized to placebo. All patients had pathologic evidence of urothelial cancer at high risk of recurrence and Eastern Cooperative Oncology Group performance status (ECOG PS) of1 or less.
Previous results, at a median follow-up of about 20 months, show that the study met its primary endpoint, showing significant prolongation of disease-free survival in the intention-to-treat population, with nivolumab at 21 months versus placebo at 10.9 months (hazard ratio, 0.70; P < .001).
When the analysis considered only patients with tumors expressing PD-L1 of at least 1%, the median disease-free survival was even higher (not reached vs. 10.8 months; HR, 0.53; P < .001).
Nivolumab was also superior to placebo for NUTRFS, in both in the entire ITT population and in the subset with PD-L1–positive tumors.
The latest results come from a median follow-up of 36.1 months. The median disease-free survival was 22 months with nivolumab, compared with 10.9 months with placebo in ITT patients and 52.6 months on nivolumab versus 8.4 months in patients with PD-L1 of at least 1%.
Nivolumab was superior to placebo for secondary and exploratory endpoints, NUTRFS (ITT: HR, 0.72 and PD-L1 ≥ 1%: HR, 0.53) and DMFS (ITT: HR, 0.74; PD-L1 ≥ 1%: HR, 0.58). However, overall survival data remained immature and will be assessed as a future data cutoff, Dr. Galsky explained.
The updated analysis also included another exploratory endpoint, progression-free survival 2 (PFS2), defined as time from randomization to disease progression after subsequent next-line systemic therapy, start of second subsequent next-line systemic therapy, or death.
Median PFS2 was 61.2 months for all-patients who received nivolumab versus 47.1 months with placebo (HR, 0.79). In the PD-L1 of 1% or greater subgroup, median PFS2 was not reached with nivolumab versus 39.4 months with placebo (HR, 0.54).
Grade 3-4 treatment-related adverse events occurred in 18.2% and 7.2% of patients (nivolumab vs. placebo), and this was consistent with the primary analysis. “No new safety signals were identified,” said Dr. Galsky.
The CheckMate 274 trial was funded by Bristol-Myers Squibb, manufacturer of nivolumab. Dr. Galsky reported relationships with numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
AT ASCO GU 2023
‘Quick, affordable’ test helps predict CGRP response for migraine
new research suggests.
The ictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive massive nociceptive input from active meningeal nociceptors,” whereas the nonictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive no or subliminal nociceptive input from meningeal nociceptors,” investigators noted.
In an observational, open-label cohort study, pretreatment nonictal cephalic allodynia identified galcanezumab responders with nearly 80% accuracy, and it identified nonresponders with nearly 85% accuracy.
“Detection of nonictal allodynia with a simplified paradigm of Quantitative Sensory Testing (QST) may provide a quick, affordable, noninvasive, and patient-friendly way to prospectively distinguish between responders and nonresponders to the prophylactic treatment of chronic and high-frequency episodic migraine with drugs that reduce CGRP signaling,” Sait Ashina, MD, of Beth Israel Deaconess Medical Center and Harvard Medical School, both in Boston, and colleagues wrote.
The findings were published online in Cephalalgia.
Immediate clinical relevance
Investigator Rami Burstein, PhD, also with Beth Israel Deaconess Medical Center and Harvard Medical School, developed the concept of predicting response to anti-CGRP treatment by testing for the presence or absence of nonictal cephalic allodynia in collaboration with the company CGRP Diagnostics.
In 43 anti–CGRP-naive patients with migraine, the researchers used a simplified QST algorithm to determine the presence/absence of cephalic or extracephalic allodynia during the nonictal phase of migraine – defined as the period from less than 12 hours after a migraine attack to less than 12 hours before the next attack.
Patients were considered to have allodynia if heat pain thresholds were between 32° C and 40° C, if cold pain thresholds were between 32° C and 20° C, or if the mechanical pain was threshold was less than 60 g.
Using these strict criteria, pretreatment nonictal cephalic allodynia was a statistically significant predictor of response to anti-CGRP therapy. It was present in 84% of the 19 nonresponders and was absent in 79% of the 24 responders, for an overall accuracy rate of 86% (P < .0001).
Nonictal cephalic allodynia was “consistently” predictive of response for patients with chronic migraine as well as for those with high-frequency episodic migraine, the researchers reported.
In contrast, they noted that assessing nonictal extracephalic allodynia with QST missed nearly 50% of the patients with allodynia among the nonresponders (accuracy rate of 42%) and added little to the assessment of allodynia among the responders.
Mark Hasleton, PhD, CEO of CGRP Diagnostics, said in an interview that the study shows it’s possible to determine response to anti-CGRP therapy and to prescribe these medications to patients who are most likely to respond.
Dr. Hasleton, who was not personally involved with the current study, noted that pretreatment testing for nonictal cephalic allodynia may also allow for earlier prescription of anti-CGRP therapy and potentially dispense without the need for the current trial-and-error approach to prescribing. He noted that if one anti-CGRP fails the patient, it is highly likely that others will also fail.
Given the “very high correlation of the presence of nonictal cephalic allodynia in responders to galcanezumab, our recommendation would be to routinely pretest all potential anti-CGRP candidates prior to prescription,” he said.
End of trial-and-error prescribing
In a comment, Shaheen Lakhan, MD, a neurologist and researcher in Boston, said this research is “very noteworthy, moving us one step closer to predictive, precision medicine and away from the practice of trial-and-error prescribing.
“The trial-and-error approach to migraine management is daunting. These are very costly therapies, and when they don’t work, there is continued tremendous suffering and loss of quality of life for patients,” said Dr. Lakhan, who was not involved in the study.
He added that the failure of drugs to benefit individual patients “may lead to distrust of the health care provider” and to the system as a whole, which in turn could lead to less access to care for other conditions or for preventive measures.
“I envision a time when these predictive measures collectively (interictal allodynia, as in this study, plus biobehavioral data) will assist us neurologists in appropriately selecting migraine therapies,” Dr. Lakhan said.
“Beyond that, we will eventually test new therapies not in cells, animals, and even humans but in silico. In the very near future, we will have solutions tailored to not people suffering a disease but to you – an individual with a unique genetic, protein, physical, developmental, psychological, and behavioral makeup,” he added.
The study was funded in part by Eli Lilly, the National Institutes of Health, and the anesthesia department at Beth Israel Deaconess Medical Center. Galcanezumab was provided by Eli Lilly. Dr. Lakhan reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
new research suggests.
The ictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive massive nociceptive input from active meningeal nociceptors,” whereas the nonictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive no or subliminal nociceptive input from meningeal nociceptors,” investigators noted.
In an observational, open-label cohort study, pretreatment nonictal cephalic allodynia identified galcanezumab responders with nearly 80% accuracy, and it identified nonresponders with nearly 85% accuracy.
“Detection of nonictal allodynia with a simplified paradigm of Quantitative Sensory Testing (QST) may provide a quick, affordable, noninvasive, and patient-friendly way to prospectively distinguish between responders and nonresponders to the prophylactic treatment of chronic and high-frequency episodic migraine with drugs that reduce CGRP signaling,” Sait Ashina, MD, of Beth Israel Deaconess Medical Center and Harvard Medical School, both in Boston, and colleagues wrote.
The findings were published online in Cephalalgia.
Immediate clinical relevance
Investigator Rami Burstein, PhD, also with Beth Israel Deaconess Medical Center and Harvard Medical School, developed the concept of predicting response to anti-CGRP treatment by testing for the presence or absence of nonictal cephalic allodynia in collaboration with the company CGRP Diagnostics.
In 43 anti–CGRP-naive patients with migraine, the researchers used a simplified QST algorithm to determine the presence/absence of cephalic or extracephalic allodynia during the nonictal phase of migraine – defined as the period from less than 12 hours after a migraine attack to less than 12 hours before the next attack.
Patients were considered to have allodynia if heat pain thresholds were between 32° C and 40° C, if cold pain thresholds were between 32° C and 20° C, or if the mechanical pain was threshold was less than 60 g.
Using these strict criteria, pretreatment nonictal cephalic allodynia was a statistically significant predictor of response to anti-CGRP therapy. It was present in 84% of the 19 nonresponders and was absent in 79% of the 24 responders, for an overall accuracy rate of 86% (P < .0001).
Nonictal cephalic allodynia was “consistently” predictive of response for patients with chronic migraine as well as for those with high-frequency episodic migraine, the researchers reported.
In contrast, they noted that assessing nonictal extracephalic allodynia with QST missed nearly 50% of the patients with allodynia among the nonresponders (accuracy rate of 42%) and added little to the assessment of allodynia among the responders.
Mark Hasleton, PhD, CEO of CGRP Diagnostics, said in an interview that the study shows it’s possible to determine response to anti-CGRP therapy and to prescribe these medications to patients who are most likely to respond.
Dr. Hasleton, who was not personally involved with the current study, noted that pretreatment testing for nonictal cephalic allodynia may also allow for earlier prescription of anti-CGRP therapy and potentially dispense without the need for the current trial-and-error approach to prescribing. He noted that if one anti-CGRP fails the patient, it is highly likely that others will also fail.
Given the “very high correlation of the presence of nonictal cephalic allodynia in responders to galcanezumab, our recommendation would be to routinely pretest all potential anti-CGRP candidates prior to prescription,” he said.
End of trial-and-error prescribing
In a comment, Shaheen Lakhan, MD, a neurologist and researcher in Boston, said this research is “very noteworthy, moving us one step closer to predictive, precision medicine and away from the practice of trial-and-error prescribing.
“The trial-and-error approach to migraine management is daunting. These are very costly therapies, and when they don’t work, there is continued tremendous suffering and loss of quality of life for patients,” said Dr. Lakhan, who was not involved in the study.
He added that the failure of drugs to benefit individual patients “may lead to distrust of the health care provider” and to the system as a whole, which in turn could lead to less access to care for other conditions or for preventive measures.
“I envision a time when these predictive measures collectively (interictal allodynia, as in this study, plus biobehavioral data) will assist us neurologists in appropriately selecting migraine therapies,” Dr. Lakhan said.
“Beyond that, we will eventually test new therapies not in cells, animals, and even humans but in silico. In the very near future, we will have solutions tailored to not people suffering a disease but to you – an individual with a unique genetic, protein, physical, developmental, psychological, and behavioral makeup,” he added.
The study was funded in part by Eli Lilly, the National Institutes of Health, and the anesthesia department at Beth Israel Deaconess Medical Center. Galcanezumab was provided by Eli Lilly. Dr. Lakhan reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
new research suggests.
The ictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive massive nociceptive input from active meningeal nociceptors,” whereas the nonictal phase refers to “sensitization occurring during a time when central trigeminovascular neurons receive no or subliminal nociceptive input from meningeal nociceptors,” investigators noted.
In an observational, open-label cohort study, pretreatment nonictal cephalic allodynia identified galcanezumab responders with nearly 80% accuracy, and it identified nonresponders with nearly 85% accuracy.
“Detection of nonictal allodynia with a simplified paradigm of Quantitative Sensory Testing (QST) may provide a quick, affordable, noninvasive, and patient-friendly way to prospectively distinguish between responders and nonresponders to the prophylactic treatment of chronic and high-frequency episodic migraine with drugs that reduce CGRP signaling,” Sait Ashina, MD, of Beth Israel Deaconess Medical Center and Harvard Medical School, both in Boston, and colleagues wrote.
The findings were published online in Cephalalgia.
Immediate clinical relevance
Investigator Rami Burstein, PhD, also with Beth Israel Deaconess Medical Center and Harvard Medical School, developed the concept of predicting response to anti-CGRP treatment by testing for the presence or absence of nonictal cephalic allodynia in collaboration with the company CGRP Diagnostics.
In 43 anti–CGRP-naive patients with migraine, the researchers used a simplified QST algorithm to determine the presence/absence of cephalic or extracephalic allodynia during the nonictal phase of migraine – defined as the period from less than 12 hours after a migraine attack to less than 12 hours before the next attack.
Patients were considered to have allodynia if heat pain thresholds were between 32° C and 40° C, if cold pain thresholds were between 32° C and 20° C, or if the mechanical pain was threshold was less than 60 g.
Using these strict criteria, pretreatment nonictal cephalic allodynia was a statistically significant predictor of response to anti-CGRP therapy. It was present in 84% of the 19 nonresponders and was absent in 79% of the 24 responders, for an overall accuracy rate of 86% (P < .0001).
Nonictal cephalic allodynia was “consistently” predictive of response for patients with chronic migraine as well as for those with high-frequency episodic migraine, the researchers reported.
In contrast, they noted that assessing nonictal extracephalic allodynia with QST missed nearly 50% of the patients with allodynia among the nonresponders (accuracy rate of 42%) and added little to the assessment of allodynia among the responders.
Mark Hasleton, PhD, CEO of CGRP Diagnostics, said in an interview that the study shows it’s possible to determine response to anti-CGRP therapy and to prescribe these medications to patients who are most likely to respond.
Dr. Hasleton, who was not personally involved with the current study, noted that pretreatment testing for nonictal cephalic allodynia may also allow for earlier prescription of anti-CGRP therapy and potentially dispense without the need for the current trial-and-error approach to prescribing. He noted that if one anti-CGRP fails the patient, it is highly likely that others will also fail.
Given the “very high correlation of the presence of nonictal cephalic allodynia in responders to galcanezumab, our recommendation would be to routinely pretest all potential anti-CGRP candidates prior to prescription,” he said.
End of trial-and-error prescribing
In a comment, Shaheen Lakhan, MD, a neurologist and researcher in Boston, said this research is “very noteworthy, moving us one step closer to predictive, precision medicine and away from the practice of trial-and-error prescribing.
“The trial-and-error approach to migraine management is daunting. These are very costly therapies, and when they don’t work, there is continued tremendous suffering and loss of quality of life for patients,” said Dr. Lakhan, who was not involved in the study.
He added that the failure of drugs to benefit individual patients “may lead to distrust of the health care provider” and to the system as a whole, which in turn could lead to less access to care for other conditions or for preventive measures.
“I envision a time when these predictive measures collectively (interictal allodynia, as in this study, plus biobehavioral data) will assist us neurologists in appropriately selecting migraine therapies,” Dr. Lakhan said.
“Beyond that, we will eventually test new therapies not in cells, animals, and even humans but in silico. In the very near future, we will have solutions tailored to not people suffering a disease but to you – an individual with a unique genetic, protein, physical, developmental, psychological, and behavioral makeup,” he added.
The study was funded in part by Eli Lilly, the National Institutes of Health, and the anesthesia department at Beth Israel Deaconess Medical Center. Galcanezumab was provided by Eli Lilly. Dr. Lakhan reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM CEPHALALGIA
Ticking Time: Spreading Awareness About African Tick-Bite Fever
To the Editor:
One of the more common tick-borne infections seen in travelers returning from sub-Saharan Africa is caused by Rickettsia africae, which is the etiologic agent of African tick-bite fever (ATBF), the most common tick-borne bacterial zoonosis.1 There are 2 known tick vectors of disease: Amblyomma variegatum, found in sub-Saharan Africa and the West Indies, and Amblyomma hebraeum, found specifically in southern Africa.2,3
Unlike other disease-carrying ticks that passively wait on vegetation to be picked up by a host, A hebraeum uniquely attract other nearby ticks to the host. Studies have shown that male ticks feeding on a nonhuman host (usually cattle) can emit an aggression-attachment pheromone that attracts other ticks to the host. The presence of the pheromone allows unfed ticks to actively discriminate between hosts on which these parasites have fed successfully (ie, suitable hosts) and those on which they have not.4
The aggressive hunting nature of A hebraeum explains the clinical presentation of multiple eschars and why large groups of exposed travelers—such as soldiers, leisure safari tourists, game hunters, and foreign-aid workers—are affected.2
Another southern African spotted fever group, Rickettsia conorii is the causative agent of Mediterranean spotted fever (MSF). Ticks carrying R conorii exhibit a much less aggressive hunting stylethan A hebraeum; consequently, infected patients present with a single eschar site.5
Rickettsia africae is estimated to have very high prevalence (95.2%) in Amblyomma ticks and a fairly high prevalence (approximately 4.0% to 8.6%) in travelers coming from rural southern Africa,6,7 with an incubation period of 5 to 10 days after inoculation by an infected tick.8 Signs include fever, a generalized maculopapular or papulovesicular rash, and regional lymphadenopathy; symptoms include fatigue, headache, and myalgia.
The inoculation eschar—single or multiple—commonly presents on the legs and is accompanied by tender lymphadenopathy of draining nodes1,8 More severe findings, such as myocarditis and subacute neuropathy, have been reported in elderly patients.9
A 77-year-old man presented with a pruritic maculopapular and papulovesicular rash distributed over the upper and lower extremities of 3 weeks’ duration. The patient reported having been on a 12-day mission trip to Limpopo, South Africa, where he was constructing and installing safe toilets to replace dangerous toilet pits. He believed he had been bitten by 2 ticks, after which he noted a dark purple and black patch on the left lower leg by the third day of the trip. He developed a sudden persistent pruritic rash, first on the lower extremities and then spreading to the upper extremities. The patient was seen by an American physician in South Africa who gave him a 7-day course of oral doxycycline monohydrate 100 mg twice daily. He then returned to the United States.
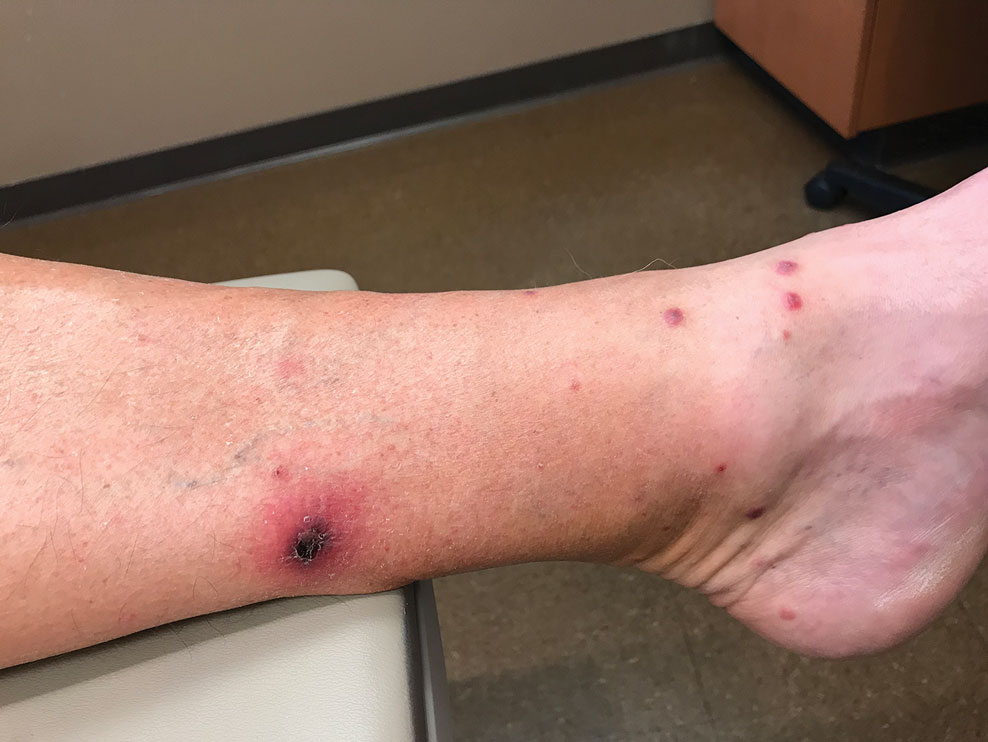
Sixteen days after being bitten by the ticks, the patient was examined in our dermatology office. Physical examination revealed an erythematous plaque with a central eschar over the medial aspect of the left leg (Figure 1) and multiple 3- to 6-mm, erythematous, dome-shaped papules scattered over the dorsal aspects of the feet and ankles (Figure 2). The examination was otherwise normal. Blood was drawn the same day for laboratory analysis; no abnormalities of platelets, red blood cells, or white blood cells were found. Results of a chemistry panel and liver enzyme tests were within reference range.
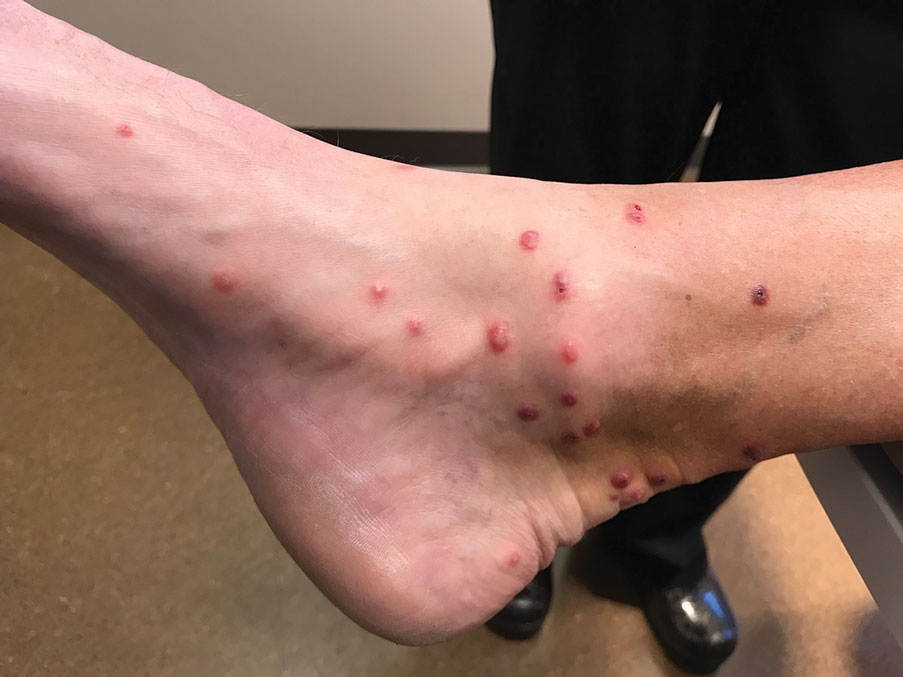
Skin biopsies were taken to elucidate the underlying pathology. Although an arthropod assault was suspected, there also was concern for deep vessel vasculitis because of the presence of considerable petechiae and purpura (Figure 3). Histologically, leukocytoclasia was seen in deep dermal blood vessels. A mild eosinophilic spongiosis with a mixed dermal infiltrate was identified—strengthening our suspicion of an arthropod assault. Bacterial cultures for aerobes and anaerobes using material taken from the right shin showed no growth.
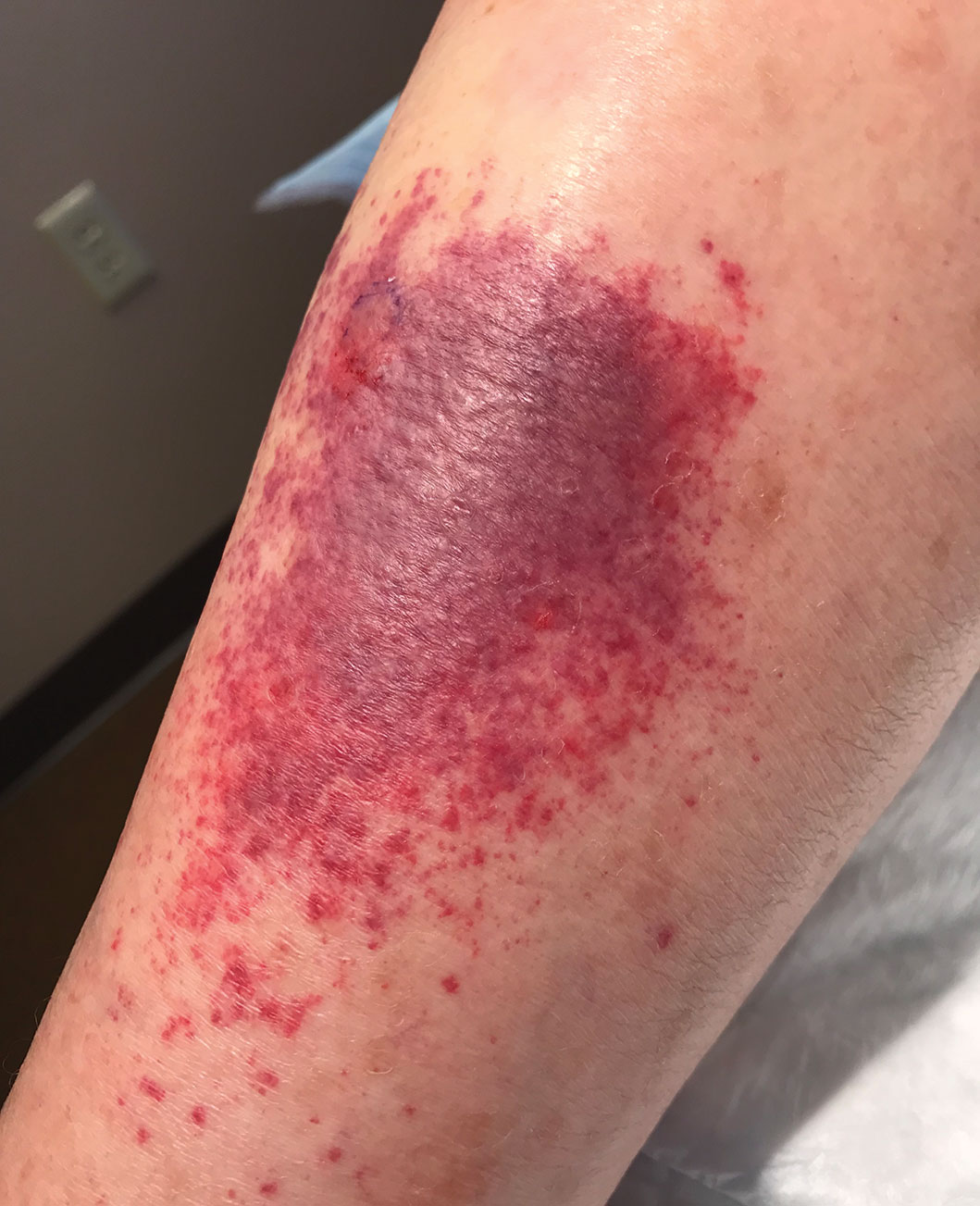
Ten days after the initial biopsies, serum specimens were drawn and swabs of eschar were collected and sent to the Centers for Disease Control and Prevention for further testing. Serum was tested by immunofluorescence assay (IFA) for spotted fever group IgG to detect Rocky Mountain spotted fever and ATBF antibodies; both tests were negative. Swab material from eschar was tested again by IFA for spotted fever group IgG (Rocky Mountain spotted fever) and antibodies to ATBF and with bacterial culture isolation and nucleic acid amplification; the culture and amplification came back positive for R africae.
Because the specialized tests confirmed infection with R africae, the patient was given triamcinolone cream 0.1% to apply twice daily to the pruritic lesions for as long as 4 weeks; an additional 14-day course of oral doxycycline monohydrate (100 mg twice daily) was given. At follow-up, the lesions had fully resolved without evident scarring.
Various diagnostic techniques can detect R africae. Bacterial culture and the polymerase chain reaction are specific and therefore diagnostic. In addition, the diagnosis of rickettsiosis can be made with serology testing, in which disease-specific antibodies are detected by indirect IFA using disease-specific antigens.
Antigens from R rickettsii (the agent of Rocky Mountain spotted fever), R conorii (Mediterranean spotted fever), and R africae (ATBF) are commercially available for making the diagnosis of rickettsiosis. However, antigens from R conorii exhibit cross-reactivity with R africae, which can confound the diagnosis.1,10 Serologic IFA tests have been shown to be less sensitive, especially when performed after antibacterial treatment has started.
In a study, 17 of 65 (26%) ATBF-confirmed patients were seronegative (acute and convalescent-phase sera) against R africae; 14 had received doxycycline during the first week of clinical signs. The current hypothesis is that R africae is highly sensitive to doxycycline and that early exposure to the drug prevented development of detectable titers of reactive antibodies, thus producing a negative serology test.11
Furthermore, it has been shown that seroconversion of IgG and IgM antibodies in R africae–infected sera is delayed compared to what is observed with R conorii–infected sera. Typically, seroconversion of R conorii–infected sera can be detected within 2 weeks; seroconversion in R africae–infected sera can take 4 weeks or longer.11
Our patient had a confirmed case of ATBF secondary to R africae infection, which was evident from tissue culture isolation and polymerase chain reaction analysis of swab material obtained from eschar sites, both of which yielded a positive result for R africae. The traveler’s negative serologic status might be due to his early exposure to doxycycline or to the 4-week delay in R africae seroconversion; his serum was collected only 3 weeks after the tick bites.
Clinical signs also aid in making the diagnosis of ATBF and distinguishing R conorii from R africae infection. Because of the aggressive hunting nature of the tick carrying R africae, they are associated with multiple eschars and tend to affect groups of multiple people, especially in rural areas.4,5 In contrast, ticks carrying R conorii yield a single eschar due to their passive style of infecting a host and because they favor a single host within urban areas.5 Both infections exhibit a maculopapular or papulovesicular rash and are accompanied by fatigue, headache, and myalgia, though ATBF tends to present with a milder rash than MSF.
Infection with either R conorii or R africae responds to tetracyclines, quinolones, and macrolides.10,12
African tick-bite fever is becoming more common, which should encourage clinicians to become familiar with the disease. Less than 2 decades ago, ATBF virtually was unknown outside of Zimbabwe, Botswana, Tanzania, Zambia, and Kenya, where it is endemic. However, after the abolition of apartheid in the 1990s, international tourism in southern Africa increased 6-fold.13 African tick-bite fever is now one of the most common rickettsial infections in Africa.7 In addition to diagnosing ATBF and managing infected patients, clinicians can help prevent ATBF in individuals who travel to endemic areas by recommending commercial topical insect repellents containing at least 19.5% N,N-diethyl-meta-toluamide (DEET).14
- Parola P, Paddock CD, Socolovschi C, et al. Update on tick-borne rickettsioses around the world: a geographic approach. Clin Microbiol Rev. 2013;26:657-702. doi:10.1128/CMR.00032-13
- Jensenius M, Fournier P-E, Vene S, et al; Norwegian African Tick Bite Fever Study Group. African tick bite fever in travelers to rural sub-equatorial Africa. Clin Infect Dis. 2003;36:1411-1417. doi:10.1086/375083
- Parola P, Jourdan J, Raoult D. Tick-borne infection caused by Rickettsia africae in the West Indies. N Engl J Med. 1998;338:1391-1392. doi:10.1056/NEJM199805073381918
- Norval RA, Andrew HR, Yunker CE. Pheromone-mediation of host-selection in bont ticks (Amblyomma hebraeum Koch). Science. 1989;243:364-365. doi:10.1126/science.2911745
- Parola P, Raoult D. Ticks and tickborne bacterial diseases in humans: an emerging infectious threat. Clin Infect Dis. 2001;32:897-928. doi:10.1086/319347
- Kelly PJ, Mason PR. Transmission of a spotted fever group rickettsia by Amblyomma hebraeum (Acari: Ixodidae). J Med Entomol. 1991;28:598-600. doi:10.1093/jmedent/28.5.598
- Maina AN, Jiang J, Omulo SA, et al. High prevalence of Rickettsia africae variants in Amblyomma variegatum ticks from domestic mammals in rural Western Kenya: implications for human health. Vector Borne Zoonotic Dis. 2014;14:693-702. doi:10.1089/vbz.2014.1578
- Jensenius M, Fournier P-E, Kelly P, et al. African tick bite fever. Lancet Infect Dis. 2003;3:557-564. doi:10.1016/s1473-3099(03)00739-4
- Roch N, Epaulard O, Pelloux I, et al. African tick bite fever in elderly patients: 8 cases in French tourists returning from South Africa. Clin Infect Dis. 2008;47:E28-E35. doi:10.1086/589868
- Palau L, Pankey GA. Mediterranean spotted fever in travelers from the United States. J Travel Med. 1997;4:179-182. doi:10.1111/j.1708-8305.1997.tb00816.x
- Fournier P-E, Jensenius M, Laferl H, et al. Kinetics of antibody responses in Rickettsia africae and Rickettsia conorii infections. Clin Diagn Lab Immunol. 2002;9:324-328. doi:10.1128/cdli.9.2.324-328.2002
- Brouqui P, Bacellar F, Baranton G, et al; ; . Guidelines for the diagnosis of tick-borne bacterial diseases in Europe. Clin Microbiol Infect. 2004;10:1108-1132. doi:10.1111/j.1469-0691.2004.01019.x
- Rolain JM, Jensenius M, Raoult D. Rickettsial infections—a threat to travelers? Curr Opin Infect Dis. 2004;17:433-437. doi:10.1097/00001432-200410000-00008
- Jensenius M, Pretorius AM, Clarke F, et al. Repellent efficacy of four commercial DEET lotions against Amblyomma hebraeum (Acari: Ixodidae), the principal vector of Rickettsia africae in southern Africa. Trans R Soc Trop Med Hyg. 2005;99:708-711. doi:10.1016/j.trstmh.2005.01.006
To the Editor:
One of the more common tick-borne infections seen in travelers returning from sub-Saharan Africa is caused by Rickettsia africae, which is the etiologic agent of African tick-bite fever (ATBF), the most common tick-borne bacterial zoonosis.1 There are 2 known tick vectors of disease: Amblyomma variegatum, found in sub-Saharan Africa and the West Indies, and Amblyomma hebraeum, found specifically in southern Africa.2,3
Unlike other disease-carrying ticks that passively wait on vegetation to be picked up by a host, A hebraeum uniquely attract other nearby ticks to the host. Studies have shown that male ticks feeding on a nonhuman host (usually cattle) can emit an aggression-attachment pheromone that attracts other ticks to the host. The presence of the pheromone allows unfed ticks to actively discriminate between hosts on which these parasites have fed successfully (ie, suitable hosts) and those on which they have not.4
The aggressive hunting nature of A hebraeum explains the clinical presentation of multiple eschars and why large groups of exposed travelers—such as soldiers, leisure safari tourists, game hunters, and foreign-aid workers—are affected.2
Another southern African spotted fever group, Rickettsia conorii is the causative agent of Mediterranean spotted fever (MSF). Ticks carrying R conorii exhibit a much less aggressive hunting stylethan A hebraeum; consequently, infected patients present with a single eschar site.5
Rickettsia africae is estimated to have very high prevalence (95.2%) in Amblyomma ticks and a fairly high prevalence (approximately 4.0% to 8.6%) in travelers coming from rural southern Africa,6,7 with an incubation period of 5 to 10 days after inoculation by an infected tick.8 Signs include fever, a generalized maculopapular or papulovesicular rash, and regional lymphadenopathy; symptoms include fatigue, headache, and myalgia.
The inoculation eschar—single or multiple—commonly presents on the legs and is accompanied by tender lymphadenopathy of draining nodes1,8 More severe findings, such as myocarditis and subacute neuropathy, have been reported in elderly patients.9
A 77-year-old man presented with a pruritic maculopapular and papulovesicular rash distributed over the upper and lower extremities of 3 weeks’ duration. The patient reported having been on a 12-day mission trip to Limpopo, South Africa, where he was constructing and installing safe toilets to replace dangerous toilet pits. He believed he had been bitten by 2 ticks, after which he noted a dark purple and black patch on the left lower leg by the third day of the trip. He developed a sudden persistent pruritic rash, first on the lower extremities and then spreading to the upper extremities. The patient was seen by an American physician in South Africa who gave him a 7-day course of oral doxycycline monohydrate 100 mg twice daily. He then returned to the United States.

Sixteen days after being bitten by the ticks, the patient was examined in our dermatology office. Physical examination revealed an erythematous plaque with a central eschar over the medial aspect of the left leg (Figure 1) and multiple 3- to 6-mm, erythematous, dome-shaped papules scattered over the dorsal aspects of the feet and ankles (Figure 2). The examination was otherwise normal. Blood was drawn the same day for laboratory analysis; no abnormalities of platelets, red blood cells, or white blood cells were found. Results of a chemistry panel and liver enzyme tests were within reference range.

Skin biopsies were taken to elucidate the underlying pathology. Although an arthropod assault was suspected, there also was concern for deep vessel vasculitis because of the presence of considerable petechiae and purpura (Figure 3). Histologically, leukocytoclasia was seen in deep dermal blood vessels. A mild eosinophilic spongiosis with a mixed dermal infiltrate was identified—strengthening our suspicion of an arthropod assault. Bacterial cultures for aerobes and anaerobes using material taken from the right shin showed no growth.

Ten days after the initial biopsies, serum specimens were drawn and swabs of eschar were collected and sent to the Centers for Disease Control and Prevention for further testing. Serum was tested by immunofluorescence assay (IFA) for spotted fever group IgG to detect Rocky Mountain spotted fever and ATBF antibodies; both tests were negative. Swab material from eschar was tested again by IFA for spotted fever group IgG (Rocky Mountain spotted fever) and antibodies to ATBF and with bacterial culture isolation and nucleic acid amplification; the culture and amplification came back positive for R africae.
Because the specialized tests confirmed infection with R africae, the patient was given triamcinolone cream 0.1% to apply twice daily to the pruritic lesions for as long as 4 weeks; an additional 14-day course of oral doxycycline monohydrate (100 mg twice daily) was given. At follow-up, the lesions had fully resolved without evident scarring.
Various diagnostic techniques can detect R africae. Bacterial culture and the polymerase chain reaction are specific and therefore diagnostic. In addition, the diagnosis of rickettsiosis can be made with serology testing, in which disease-specific antibodies are detected by indirect IFA using disease-specific antigens.
Antigens from R rickettsii (the agent of Rocky Mountain spotted fever), R conorii (Mediterranean spotted fever), and R africae (ATBF) are commercially available for making the diagnosis of rickettsiosis. However, antigens from R conorii exhibit cross-reactivity with R africae, which can confound the diagnosis.1,10 Serologic IFA tests have been shown to be less sensitive, especially when performed after antibacterial treatment has started.
In a study, 17 of 65 (26%) ATBF-confirmed patients were seronegative (acute and convalescent-phase sera) against R africae; 14 had received doxycycline during the first week of clinical signs. The current hypothesis is that R africae is highly sensitive to doxycycline and that early exposure to the drug prevented development of detectable titers of reactive antibodies, thus producing a negative serology test.11
Furthermore, it has been shown that seroconversion of IgG and IgM antibodies in R africae–infected sera is delayed compared to what is observed with R conorii–infected sera. Typically, seroconversion of R conorii–infected sera can be detected within 2 weeks; seroconversion in R africae–infected sera can take 4 weeks or longer.11
Our patient had a confirmed case of ATBF secondary to R africae infection, which was evident from tissue culture isolation and polymerase chain reaction analysis of swab material obtained from eschar sites, both of which yielded a positive result for R africae. The traveler’s negative serologic status might be due to his early exposure to doxycycline or to the 4-week delay in R africae seroconversion; his serum was collected only 3 weeks after the tick bites.
Clinical signs also aid in making the diagnosis of ATBF and distinguishing R conorii from R africae infection. Because of the aggressive hunting nature of the tick carrying R africae, they are associated with multiple eschars and tend to affect groups of multiple people, especially in rural areas.4,5 In contrast, ticks carrying R conorii yield a single eschar due to their passive style of infecting a host and because they favor a single host within urban areas.5 Both infections exhibit a maculopapular or papulovesicular rash and are accompanied by fatigue, headache, and myalgia, though ATBF tends to present with a milder rash than MSF.
Infection with either R conorii or R africae responds to tetracyclines, quinolones, and macrolides.10,12
African tick-bite fever is becoming more common, which should encourage clinicians to become familiar with the disease. Less than 2 decades ago, ATBF virtually was unknown outside of Zimbabwe, Botswana, Tanzania, Zambia, and Kenya, where it is endemic. However, after the abolition of apartheid in the 1990s, international tourism in southern Africa increased 6-fold.13 African tick-bite fever is now one of the most common rickettsial infections in Africa.7 In addition to diagnosing ATBF and managing infected patients, clinicians can help prevent ATBF in individuals who travel to endemic areas by recommending commercial topical insect repellents containing at least 19.5% N,N-diethyl-meta-toluamide (DEET).14
To the Editor:
One of the more common tick-borne infections seen in travelers returning from sub-Saharan Africa is caused by Rickettsia africae, which is the etiologic agent of African tick-bite fever (ATBF), the most common tick-borne bacterial zoonosis.1 There are 2 known tick vectors of disease: Amblyomma variegatum, found in sub-Saharan Africa and the West Indies, and Amblyomma hebraeum, found specifically in southern Africa.2,3
Unlike other disease-carrying ticks that passively wait on vegetation to be picked up by a host, A hebraeum uniquely attract other nearby ticks to the host. Studies have shown that male ticks feeding on a nonhuman host (usually cattle) can emit an aggression-attachment pheromone that attracts other ticks to the host. The presence of the pheromone allows unfed ticks to actively discriminate between hosts on which these parasites have fed successfully (ie, suitable hosts) and those on which they have not.4
The aggressive hunting nature of A hebraeum explains the clinical presentation of multiple eschars and why large groups of exposed travelers—such as soldiers, leisure safari tourists, game hunters, and foreign-aid workers—are affected.2
Another southern African spotted fever group, Rickettsia conorii is the causative agent of Mediterranean spotted fever (MSF). Ticks carrying R conorii exhibit a much less aggressive hunting stylethan A hebraeum; consequently, infected patients present with a single eschar site.5
Rickettsia africae is estimated to have very high prevalence (95.2%) in Amblyomma ticks and a fairly high prevalence (approximately 4.0% to 8.6%) in travelers coming from rural southern Africa,6,7 with an incubation period of 5 to 10 days after inoculation by an infected tick.8 Signs include fever, a generalized maculopapular or papulovesicular rash, and regional lymphadenopathy; symptoms include fatigue, headache, and myalgia.
The inoculation eschar—single or multiple—commonly presents on the legs and is accompanied by tender lymphadenopathy of draining nodes1,8 More severe findings, such as myocarditis and subacute neuropathy, have been reported in elderly patients.9
A 77-year-old man presented with a pruritic maculopapular and papulovesicular rash distributed over the upper and lower extremities of 3 weeks’ duration. The patient reported having been on a 12-day mission trip to Limpopo, South Africa, where he was constructing and installing safe toilets to replace dangerous toilet pits. He believed he had been bitten by 2 ticks, after which he noted a dark purple and black patch on the left lower leg by the third day of the trip. He developed a sudden persistent pruritic rash, first on the lower extremities and then spreading to the upper extremities. The patient was seen by an American physician in South Africa who gave him a 7-day course of oral doxycycline monohydrate 100 mg twice daily. He then returned to the United States.

Sixteen days after being bitten by the ticks, the patient was examined in our dermatology office. Physical examination revealed an erythematous plaque with a central eschar over the medial aspect of the left leg (Figure 1) and multiple 3- to 6-mm, erythematous, dome-shaped papules scattered over the dorsal aspects of the feet and ankles (Figure 2). The examination was otherwise normal. Blood was drawn the same day for laboratory analysis; no abnormalities of platelets, red blood cells, or white blood cells were found. Results of a chemistry panel and liver enzyme tests were within reference range.

Skin biopsies were taken to elucidate the underlying pathology. Although an arthropod assault was suspected, there also was concern for deep vessel vasculitis because of the presence of considerable petechiae and purpura (Figure 3). Histologically, leukocytoclasia was seen in deep dermal blood vessels. A mild eosinophilic spongiosis with a mixed dermal infiltrate was identified—strengthening our suspicion of an arthropod assault. Bacterial cultures for aerobes and anaerobes using material taken from the right shin showed no growth.

Ten days after the initial biopsies, serum specimens were drawn and swabs of eschar were collected and sent to the Centers for Disease Control and Prevention for further testing. Serum was tested by immunofluorescence assay (IFA) for spotted fever group IgG to detect Rocky Mountain spotted fever and ATBF antibodies; both tests were negative. Swab material from eschar was tested again by IFA for spotted fever group IgG (Rocky Mountain spotted fever) and antibodies to ATBF and with bacterial culture isolation and nucleic acid amplification; the culture and amplification came back positive for R africae.
Because the specialized tests confirmed infection with R africae, the patient was given triamcinolone cream 0.1% to apply twice daily to the pruritic lesions for as long as 4 weeks; an additional 14-day course of oral doxycycline monohydrate (100 mg twice daily) was given. At follow-up, the lesions had fully resolved without evident scarring.
Various diagnostic techniques can detect R africae. Bacterial culture and the polymerase chain reaction are specific and therefore diagnostic. In addition, the diagnosis of rickettsiosis can be made with serology testing, in which disease-specific antibodies are detected by indirect IFA using disease-specific antigens.
Antigens from R rickettsii (the agent of Rocky Mountain spotted fever), R conorii (Mediterranean spotted fever), and R africae (ATBF) are commercially available for making the diagnosis of rickettsiosis. However, antigens from R conorii exhibit cross-reactivity with R africae, which can confound the diagnosis.1,10 Serologic IFA tests have been shown to be less sensitive, especially when performed after antibacterial treatment has started.
In a study, 17 of 65 (26%) ATBF-confirmed patients were seronegative (acute and convalescent-phase sera) against R africae; 14 had received doxycycline during the first week of clinical signs. The current hypothesis is that R africae is highly sensitive to doxycycline and that early exposure to the drug prevented development of detectable titers of reactive antibodies, thus producing a negative serology test.11
Furthermore, it has been shown that seroconversion of IgG and IgM antibodies in R africae–infected sera is delayed compared to what is observed with R conorii–infected sera. Typically, seroconversion of R conorii–infected sera can be detected within 2 weeks; seroconversion in R africae–infected sera can take 4 weeks or longer.11
Our patient had a confirmed case of ATBF secondary to R africae infection, which was evident from tissue culture isolation and polymerase chain reaction analysis of swab material obtained from eschar sites, both of which yielded a positive result for R africae. The traveler’s negative serologic status might be due to his early exposure to doxycycline or to the 4-week delay in R africae seroconversion; his serum was collected only 3 weeks after the tick bites.
Clinical signs also aid in making the diagnosis of ATBF and distinguishing R conorii from R africae infection. Because of the aggressive hunting nature of the tick carrying R africae, they are associated with multiple eschars and tend to affect groups of multiple people, especially in rural areas.4,5 In contrast, ticks carrying R conorii yield a single eschar due to their passive style of infecting a host and because they favor a single host within urban areas.5 Both infections exhibit a maculopapular or papulovesicular rash and are accompanied by fatigue, headache, and myalgia, though ATBF tends to present with a milder rash than MSF.
Infection with either R conorii or R africae responds to tetracyclines, quinolones, and macrolides.10,12
African tick-bite fever is becoming more common, which should encourage clinicians to become familiar with the disease. Less than 2 decades ago, ATBF virtually was unknown outside of Zimbabwe, Botswana, Tanzania, Zambia, and Kenya, where it is endemic. However, after the abolition of apartheid in the 1990s, international tourism in southern Africa increased 6-fold.13 African tick-bite fever is now one of the most common rickettsial infections in Africa.7 In addition to diagnosing ATBF and managing infected patients, clinicians can help prevent ATBF in individuals who travel to endemic areas by recommending commercial topical insect repellents containing at least 19.5% N,N-diethyl-meta-toluamide (DEET).14
- Parola P, Paddock CD, Socolovschi C, et al. Update on tick-borne rickettsioses around the world: a geographic approach. Clin Microbiol Rev. 2013;26:657-702. doi:10.1128/CMR.00032-13
- Jensenius M, Fournier P-E, Vene S, et al; Norwegian African Tick Bite Fever Study Group. African tick bite fever in travelers to rural sub-equatorial Africa. Clin Infect Dis. 2003;36:1411-1417. doi:10.1086/375083
- Parola P, Jourdan J, Raoult D. Tick-borne infection caused by Rickettsia africae in the West Indies. N Engl J Med. 1998;338:1391-1392. doi:10.1056/NEJM199805073381918
- Norval RA, Andrew HR, Yunker CE. Pheromone-mediation of host-selection in bont ticks (Amblyomma hebraeum Koch). Science. 1989;243:364-365. doi:10.1126/science.2911745
- Parola P, Raoult D. Ticks and tickborne bacterial diseases in humans: an emerging infectious threat. Clin Infect Dis. 2001;32:897-928. doi:10.1086/319347
- Kelly PJ, Mason PR. Transmission of a spotted fever group rickettsia by Amblyomma hebraeum (Acari: Ixodidae). J Med Entomol. 1991;28:598-600. doi:10.1093/jmedent/28.5.598
- Maina AN, Jiang J, Omulo SA, et al. High prevalence of Rickettsia africae variants in Amblyomma variegatum ticks from domestic mammals in rural Western Kenya: implications for human health. Vector Borne Zoonotic Dis. 2014;14:693-702. doi:10.1089/vbz.2014.1578
- Jensenius M, Fournier P-E, Kelly P, et al. African tick bite fever. Lancet Infect Dis. 2003;3:557-564. doi:10.1016/s1473-3099(03)00739-4
- Roch N, Epaulard O, Pelloux I, et al. African tick bite fever in elderly patients: 8 cases in French tourists returning from South Africa. Clin Infect Dis. 2008;47:E28-E35. doi:10.1086/589868
- Palau L, Pankey GA. Mediterranean spotted fever in travelers from the United States. J Travel Med. 1997;4:179-182. doi:10.1111/j.1708-8305.1997.tb00816.x
- Fournier P-E, Jensenius M, Laferl H, et al. Kinetics of antibody responses in Rickettsia africae and Rickettsia conorii infections. Clin Diagn Lab Immunol. 2002;9:324-328. doi:10.1128/cdli.9.2.324-328.2002
- Brouqui P, Bacellar F, Baranton G, et al; ; . Guidelines for the diagnosis of tick-borne bacterial diseases in Europe. Clin Microbiol Infect. 2004;10:1108-1132. doi:10.1111/j.1469-0691.2004.01019.x
- Rolain JM, Jensenius M, Raoult D. Rickettsial infections—a threat to travelers? Curr Opin Infect Dis. 2004;17:433-437. doi:10.1097/00001432-200410000-00008
- Jensenius M, Pretorius AM, Clarke F, et al. Repellent efficacy of four commercial DEET lotions against Amblyomma hebraeum (Acari: Ixodidae), the principal vector of Rickettsia africae in southern Africa. Trans R Soc Trop Med Hyg. 2005;99:708-711. doi:10.1016/j.trstmh.2005.01.006
- Parola P, Paddock CD, Socolovschi C, et al. Update on tick-borne rickettsioses around the world: a geographic approach. Clin Microbiol Rev. 2013;26:657-702. doi:10.1128/CMR.00032-13
- Jensenius M, Fournier P-E, Vene S, et al; Norwegian African Tick Bite Fever Study Group. African tick bite fever in travelers to rural sub-equatorial Africa. Clin Infect Dis. 2003;36:1411-1417. doi:10.1086/375083
- Parola P, Jourdan J, Raoult D. Tick-borne infection caused by Rickettsia africae in the West Indies. N Engl J Med. 1998;338:1391-1392. doi:10.1056/NEJM199805073381918
- Norval RA, Andrew HR, Yunker CE. Pheromone-mediation of host-selection in bont ticks (Amblyomma hebraeum Koch). Science. 1989;243:364-365. doi:10.1126/science.2911745
- Parola P, Raoult D. Ticks and tickborne bacterial diseases in humans: an emerging infectious threat. Clin Infect Dis. 2001;32:897-928. doi:10.1086/319347
- Kelly PJ, Mason PR. Transmission of a spotted fever group rickettsia by Amblyomma hebraeum (Acari: Ixodidae). J Med Entomol. 1991;28:598-600. doi:10.1093/jmedent/28.5.598
- Maina AN, Jiang J, Omulo SA, et al. High prevalence of Rickettsia africae variants in Amblyomma variegatum ticks from domestic mammals in rural Western Kenya: implications for human health. Vector Borne Zoonotic Dis. 2014;14:693-702. doi:10.1089/vbz.2014.1578
- Jensenius M, Fournier P-E, Kelly P, et al. African tick bite fever. Lancet Infect Dis. 2003;3:557-564. doi:10.1016/s1473-3099(03)00739-4
- Roch N, Epaulard O, Pelloux I, et al. African tick bite fever in elderly patients: 8 cases in French tourists returning from South Africa. Clin Infect Dis. 2008;47:E28-E35. doi:10.1086/589868
- Palau L, Pankey GA. Mediterranean spotted fever in travelers from the United States. J Travel Med. 1997;4:179-182. doi:10.1111/j.1708-8305.1997.tb00816.x
- Fournier P-E, Jensenius M, Laferl H, et al. Kinetics of antibody responses in Rickettsia africae and Rickettsia conorii infections. Clin Diagn Lab Immunol. 2002;9:324-328. doi:10.1128/cdli.9.2.324-328.2002
- Brouqui P, Bacellar F, Baranton G, et al; ; . Guidelines for the diagnosis of tick-borne bacterial diseases in Europe. Clin Microbiol Infect. 2004;10:1108-1132. doi:10.1111/j.1469-0691.2004.01019.x
- Rolain JM, Jensenius M, Raoult D. Rickettsial infections—a threat to travelers? Curr Opin Infect Dis. 2004;17:433-437. doi:10.1097/00001432-200410000-00008
- Jensenius M, Pretorius AM, Clarke F, et al. Repellent efficacy of four commercial DEET lotions against Amblyomma hebraeum (Acari: Ixodidae), the principal vector of Rickettsia africae in southern Africa. Trans R Soc Trop Med Hyg. 2005;99:708-711. doi:10.1016/j.trstmh.2005.01.006
PRACTICE POINTS
- African tick-bite fever (ATBF) is one of the more common tick-borne bacterial zoonoses and should be considered in patients presenting with multiple eschar sites who have had exposure to rural areas of southern Africa in the preceding 2 weeks.
- Ticks carrying Rickettsia africae are unique, given their ability to actively be attracted to and hunt their nonhuman hosts via an aggression-attachment pheromone.
- Laboratory diagnosis of ATBF can be challenging due to the high cross-reactivity of Helvetica Neue LT StdR africae with Helvetica Neue LT StdRickettsia conorii in serologic testing and the delay in seroconversion in Helvetica Neue LT StdR africae infection.
Doctors and their families tend to ignore medical guidelines
according to a study by economic professors from the Massachusetts Institute of Technology, Cambridge; Stanford (Calif.) University; and the George Gund Professor of Economics and Business Administration at Harvard University, Boston.
What to know
- Doctors’ medical knowledge may influence them and their families to often ignore medical advice while the rest of the population adheres to general medication guidelines.
- Of the 63 guidelines used in the study, doctors and their families followed the standards less than a third of the time.
- The difference in adherence to guidelines between experts and nonexperts is largest with respect to antibiotics, in which doctors and their families are 5.2 percentage points less in compliance than everyone else.
- Doctors could be more likely to prescribe broader-spectrum antibiotics for themselves and their families, whereas most patients receive more narrow-spectrum antibiotics.
- Many members of the general public don’t understand medical guidelines, finding them too complex to follow, and many people don’t trust their doctors.
This is a summary of the article, “A Taste of Their Own Medicine: Guideline Adherence and Access to Expertise,” published in the American Economic Review: Insights on December 13, 2022. The full article can be found on aeaweb.org.
A version of this article first appeared on Medscape.com.
according to a study by economic professors from the Massachusetts Institute of Technology, Cambridge; Stanford (Calif.) University; and the George Gund Professor of Economics and Business Administration at Harvard University, Boston.
What to know
- Doctors’ medical knowledge may influence them and their families to often ignore medical advice while the rest of the population adheres to general medication guidelines.
- Of the 63 guidelines used in the study, doctors and their families followed the standards less than a third of the time.
- The difference in adherence to guidelines between experts and nonexperts is largest with respect to antibiotics, in which doctors and their families are 5.2 percentage points less in compliance than everyone else.
- Doctors could be more likely to prescribe broader-spectrum antibiotics for themselves and their families, whereas most patients receive more narrow-spectrum antibiotics.
- Many members of the general public don’t understand medical guidelines, finding them too complex to follow, and many people don’t trust their doctors.
This is a summary of the article, “A Taste of Their Own Medicine: Guideline Adherence and Access to Expertise,” published in the American Economic Review: Insights on December 13, 2022. The full article can be found on aeaweb.org.
A version of this article first appeared on Medscape.com.
according to a study by economic professors from the Massachusetts Institute of Technology, Cambridge; Stanford (Calif.) University; and the George Gund Professor of Economics and Business Administration at Harvard University, Boston.
What to know
- Doctors’ medical knowledge may influence them and their families to often ignore medical advice while the rest of the population adheres to general medication guidelines.
- Of the 63 guidelines used in the study, doctors and their families followed the standards less than a third of the time.
- The difference in adherence to guidelines between experts and nonexperts is largest with respect to antibiotics, in which doctors and their families are 5.2 percentage points less in compliance than everyone else.
- Doctors could be more likely to prescribe broader-spectrum antibiotics for themselves and their families, whereas most patients receive more narrow-spectrum antibiotics.
- Many members of the general public don’t understand medical guidelines, finding them too complex to follow, and many people don’t trust their doctors.
This is a summary of the article, “A Taste of Their Own Medicine: Guideline Adherence and Access to Expertise,” published in the American Economic Review: Insights on December 13, 2022. The full article can be found on aeaweb.org.
A version of this article first appeared on Medscape.com.
Docs with one paid malpractice claim are four times more likely to have another
In this retrospective case-control study, law and public health researchers from Georgetown University, the National Opinion Research Center, the University of Colorado, and Northwestern University analyzed paid malpractice claims for all licensed U.S. physicians.
The findings suggest that a single malpractice claim may not be a random stroke of bad luck but instead holds some predictive power into the risk for future paid claims.
“A four times increase in risk is huge, particularly since we observe a similar increase in both high-risk and lower-risk specialties,” David Hyman, JD, MD, professor of health law and policy at Georgetown University, Washington, and lead researcher on the study, told this news organization. “There are surely some false positives, but there must be lots of actual negligence too, or we would not see these results.”
For the 881,876 physicians analyzed, researchers looked at malpractice claims paid during two 5-year periods: 2009-2013 and 2014-2018. Nearly 96% of physicians had no paid malpractice claims between 2009 and 2013; 3% had one, and less than 1% had multiple claims. The proportion of physicians with paid claims between 2014 and 2018 was similar.
Compared with physicians with no 2009-2013 claims, a physician with just one paid claim in that time period had a 3.7 times higher risk for a future paid claim. Physicians with two paid claims were nearly 7 times more likely to have a future paid claim, and those with three or more paid claims were more than 11 times more likely to have one.
Approximately 3% of physicians with no paid claims between 2009 and 2013 had a future paid claim, growing to 12.4% of those with one paid claim during that time.
The study’s findings may have implications for medical licensing boards and hospitals granting staff privileges.
“After some number of paid claims, there should be an official response” from these entities, such as a hands-on assessment of technical skills or assignment of a peer mentor, said Dr. Hyman, who is also coauthor of a book titled “Medical Malpractice Litigation: How It Works, Why Tort Reform Hasn’t Helped.” A graduated set of interventions, whether voluntary or mandatory, can reduce future claim risk and patient harm, Dr. Hyman added.
Interventions may include error avoidance and post-error communication training, counseling to improve bedside skills, and encouragement to move into nonclinical practice. Either way, Dr. Hyman says a nuanced intervention strategy would be a welcome shift away from the current “all or nothing approach” that too often ends in the revocation of a physician’s medical license.
Although there are strategies to proactively identify physicians with excess risk for malpractice claims and implement preventive measures – like Vanderbilt University’s Patient Advocacy Reporting System, for example – most hospitals and physician groups fail to initiate even informal interventions after a malpractice settlement or verdict, which is a missed opportunity, Dr. Hyman said.
A version of this article first appeared on Medscape.com.
In this retrospective case-control study, law and public health researchers from Georgetown University, the National Opinion Research Center, the University of Colorado, and Northwestern University analyzed paid malpractice claims for all licensed U.S. physicians.
The findings suggest that a single malpractice claim may not be a random stroke of bad luck but instead holds some predictive power into the risk for future paid claims.
“A four times increase in risk is huge, particularly since we observe a similar increase in both high-risk and lower-risk specialties,” David Hyman, JD, MD, professor of health law and policy at Georgetown University, Washington, and lead researcher on the study, told this news organization. “There are surely some false positives, but there must be lots of actual negligence too, or we would not see these results.”
For the 881,876 physicians analyzed, researchers looked at malpractice claims paid during two 5-year periods: 2009-2013 and 2014-2018. Nearly 96% of physicians had no paid malpractice claims between 2009 and 2013; 3% had one, and less than 1% had multiple claims. The proportion of physicians with paid claims between 2014 and 2018 was similar.
Compared with physicians with no 2009-2013 claims, a physician with just one paid claim in that time period had a 3.7 times higher risk for a future paid claim. Physicians with two paid claims were nearly 7 times more likely to have a future paid claim, and those with three or more paid claims were more than 11 times more likely to have one.
Approximately 3% of physicians with no paid claims between 2009 and 2013 had a future paid claim, growing to 12.4% of those with one paid claim during that time.
The study’s findings may have implications for medical licensing boards and hospitals granting staff privileges.
“After some number of paid claims, there should be an official response” from these entities, such as a hands-on assessment of technical skills or assignment of a peer mentor, said Dr. Hyman, who is also coauthor of a book titled “Medical Malpractice Litigation: How It Works, Why Tort Reform Hasn’t Helped.” A graduated set of interventions, whether voluntary or mandatory, can reduce future claim risk and patient harm, Dr. Hyman added.
Interventions may include error avoidance and post-error communication training, counseling to improve bedside skills, and encouragement to move into nonclinical practice. Either way, Dr. Hyman says a nuanced intervention strategy would be a welcome shift away from the current “all or nothing approach” that too often ends in the revocation of a physician’s medical license.
Although there are strategies to proactively identify physicians with excess risk for malpractice claims and implement preventive measures – like Vanderbilt University’s Patient Advocacy Reporting System, for example – most hospitals and physician groups fail to initiate even informal interventions after a malpractice settlement or verdict, which is a missed opportunity, Dr. Hyman said.
A version of this article first appeared on Medscape.com.
In this retrospective case-control study, law and public health researchers from Georgetown University, the National Opinion Research Center, the University of Colorado, and Northwestern University analyzed paid malpractice claims for all licensed U.S. physicians.
The findings suggest that a single malpractice claim may not be a random stroke of bad luck but instead holds some predictive power into the risk for future paid claims.
“A four times increase in risk is huge, particularly since we observe a similar increase in both high-risk and lower-risk specialties,” David Hyman, JD, MD, professor of health law and policy at Georgetown University, Washington, and lead researcher on the study, told this news organization. “There are surely some false positives, but there must be lots of actual negligence too, or we would not see these results.”
For the 881,876 physicians analyzed, researchers looked at malpractice claims paid during two 5-year periods: 2009-2013 and 2014-2018. Nearly 96% of physicians had no paid malpractice claims between 2009 and 2013; 3% had one, and less than 1% had multiple claims. The proportion of physicians with paid claims between 2014 and 2018 was similar.
Compared with physicians with no 2009-2013 claims, a physician with just one paid claim in that time period had a 3.7 times higher risk for a future paid claim. Physicians with two paid claims were nearly 7 times more likely to have a future paid claim, and those with three or more paid claims were more than 11 times more likely to have one.
Approximately 3% of physicians with no paid claims between 2009 and 2013 had a future paid claim, growing to 12.4% of those with one paid claim during that time.
The study’s findings may have implications for medical licensing boards and hospitals granting staff privileges.
“After some number of paid claims, there should be an official response” from these entities, such as a hands-on assessment of technical skills or assignment of a peer mentor, said Dr. Hyman, who is also coauthor of a book titled “Medical Malpractice Litigation: How It Works, Why Tort Reform Hasn’t Helped.” A graduated set of interventions, whether voluntary or mandatory, can reduce future claim risk and patient harm, Dr. Hyman added.
Interventions may include error avoidance and post-error communication training, counseling to improve bedside skills, and encouragement to move into nonclinical practice. Either way, Dr. Hyman says a nuanced intervention strategy would be a welcome shift away from the current “all or nothing approach” that too often ends in the revocation of a physician’s medical license.
Although there are strategies to proactively identify physicians with excess risk for malpractice claims and implement preventive measures – like Vanderbilt University’s Patient Advocacy Reporting System, for example – most hospitals and physician groups fail to initiate even informal interventions after a malpractice settlement or verdict, which is a missed opportunity, Dr. Hyman said.
A version of this article first appeared on Medscape.com.
FROM JAMA